Inpatient Pediatrics
|
|
|
- Gervase Robertson
- 5 years ago
- Views:
Transcription
1 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Inpatient Pediatrics 1. GOAL: Evaluate and manage common signs and symptoms associated with acute illness and hospitalization. 2. GOAL: Recognize and manage common childhood conditions presenting to the Inpatient Unit. 3. GOAL: Utilize common diagnostic tests and imaging studies appropriately in the inpatient setting. 4. GOAL: Understand how to use physiologic monitoring and special technology in the general inpatient setting, including issues specific to care of the chronically ill child. 5. GOAL: Demonstrate high standards of professional competence while working with patients on the Inpatient Service.
2 1. GOAL: Evaluate and manage common signs and symptoms associated with acute illness and hospitalization. A. Evaluate and manage, with consultation of indicated, patients with signs and symptoms that commonly present to the Inpatient Unit. 1. General: acute life-threatening event (ALTE), constitutional symptoms, hypothermia, excessive crying, failure to thrive, fatigue, fever without localizing signs, hypothermia, weight loss 2. Cardiorespiratory: apnea, chest pain, cough, cyanosis, dyspnea, heart murmur, hemoptysis, hypertension, hypotension, inadequate respiratory effort, rhythm disturbance, shock, shortness of breath, stridor, syncope, tachypnea, respiratory failure, wheezing 3. Dermatologic: ecchymoses, edema, petechiae, purpura, rashes, urticaria 4. EENT: acute visual changes, conjunctival injection, edema, epistaxis, hoarseness, nasal discharge, stridor, trauma 5. Endocrine: heat/cold intolerance, polydipsia, polyuria 6. GI/Nutrition/Fluids: abdominal masses or distention, abdominal pain, ascites, dehydration, diarrhea, dysphagia, hematemesis, inadequate intake, jaundice, melena, rectal bleeding, regurgitation, vomiting 7. Genitourinary/Renal: change in urine color, dysuria, edema, hematuria, oliguria, scrotal mass or edema 8. GYN: abnormal vaginal bleeding, pelvic pain, vaginal discharge 9. Hematologic/Oncologic: abnormal bleeding, bruising, hepatosplenomegaly, lymphadenopathy, masses, pallor 10. Musculoskeletal: arthritis/arthralgia, bone and soft tissue trauma, limb pain, limp 11. Neurologic: ataxia, coma, delirium, diplopia, headache, hypotonia, head trauma, lethargy, seizure, vertigo, weakness 12. Psychiatric/Psychosocial: acute psychosis, child abuse or neglect, conversion symptoms, depression, suicide attempt 2. GOAL: Recognize and manage common childhood conditions presenting to the Inpatient Unit. A. Evaluate and manage, with consultation as indicated, patients with conditions that commonly present to the Inpatient Unit. 1. General: failure to thrive, fever of unknown origin 2. Allergy/Immunology: acute drug allergies/reactions, anaphylaxis, immunodeficiencies, including graft vs. host disease, recurrent pneumonia, serum sickness, severe angioedema 3. Cardiovascular: bacterial endocarditis, cardiomyopathy, congenital heart disease, congestive heart failure, Kawasaki disease, myocarditis, rheumatic fever 4. Endocrine: diabetes (including diabetic ketoacidosis), electrolyte disturbances secondary to underlying endocrine disease 5. GI/Nutrition: appendicitis, bleeding, cholangitis, complications of inflammatory bowel disease, complications of liver transplantation, cystic fibrosis, gastroenteritis (with/without dehydration), gastroesophageal reflux, hepatic dysfunction (including alpha-1-antitrypson disease), bowel obstruction, pancreatitis, severe malnutrition
3 6. GU/Renal: electrolyte and acid-base disturbances, glomerulonephritis, hemolytic-uremic syndrome, nephrotic syndrome, urinary tract infection/pyelonephritis 7. Gynecologic: genital trauma, pelvic inflammatory disease, sexual assault 8. Hematologic/Oncologic: abdominal and mediastinal mass, common malignancies, fever and neutropenia, thrombocytopenia, severe anemia, tumor lysis syndrome, vaso-occlusive crises and other complications of sickle cell disease 9. Infectious Disease: cellulitis (including periorbital and orbital), cervical adenitis, dental abscess with complications, encephalitis, HIV, infections in immunocompromised hosts, laryngotracheobronchitis, late presentation of congenital infections (CMV, syphilis, tuberculosis, abscesses), line infection, meningitis (bacterial or viral), osteomyelitis, pneumonia (viral or bacterial), sepsis/bacteremia (including newborns), septic arthritis, tuberculosis 10. Pharmacology/Toxicology: common drug poisoning or overdose, dose adjustment for special conditions or serum drug levels 11. Neurology: acute neurologic conditions (acute cerebellar ataxia, Guillain Barre syndrome, movement disorders), developmental delay with acute medical conditions, seizures, shunt infections 12. Respiratory: airway obstruction, asthma exacerbation, bacterial tracheitis, bronchiolitis, croup, cystic fibrosis, epiglottitis 13. Rheumatologic: Henoch Schonlein purpura (HSP), juvenile rheumatoid arthritis (JRA), systemic lupus erythematosus (SLE) 14. Surgery: pre- and post-op consultation and evaluation of surgical patients (general, ENT, orthopedics, urology, neurosurgical, etc.), special needs of technology-dependent children (blocked trachea, gastric tube dysfunction) 3. GOAL: Utilize common diagnostic tests and imaging studies appropriately in the inpatient setting. A. Demonstrate an understanding of the common diagnostic tests and imaging studies used in the inpatient setting, by being able to: 1. Explain the indications for and limitations of each study. 2. Know or be able to locate age-appropriate normal ranges (lab studies). 3. Apply knowledge of diagnostic test properties, including the use of sensitivity, specificity, positive predictive value, negative predictive value, false-positive and negative results, likelihood ratios, and receiver operating characteristic curves, to assess the utility of tests in various clinical settings. 4. Recognize cost and utilization issues. 5. Interpret test results in the context of the specific patient. 6. Discuss therapeutic options for correction of abnormalities. B. Use common laboratory studies when indicated for patients in the inpatient setting. 1. CBC with differential, platelet count, RBC indices 2. Blood chemistries: electrolytes, glucose, calcium, magnesium, phosphate 3. Renal function tests 4. Tests of hepatic function (PT, albumin) and damage (liver enzymes, bilirubin) 5. Serologic tests for infection (e.g., hepatitis, HIV)
4 6. C-reactive protein, erythrocyte sedimentation rate 7. Therapeutic drug concentrations 8. Coagulation studies 9. Arterial, capillary, and venous blood gases 10. Detection of bacterial, viral, and fungal pathogens 11. Urinalysis 12. Cerebrospinal fluid analysis 13. Gram stain 14. Stool studies 15. Other fluid studies (e.g. pleural fluid, joint fluid) 16. Electrocardiogram C. Use common imaging or radiographic studies when indicated for patients on the inpatient unit. 1. Plain radiographs of the chest, extremities, abdomen, skull, sinuses 2. Other imaging techniques such as CT, MRI, angiography, ultrasound, nuclear scans, contrast studies (interpretation not expected) 3. Echocardiogram 4. GOAL: Understand how to use physiologic monitoring and special technology in the general inpatient setting, including issues specific to care of the chronically ill child. A. Demonstrate understanding of the monitoring techniques and special treatments commonly used in the inpatient setting, by being able to: 1. Discuss indications, contraindications and complications. 2. Demonstrate proper use of technique for children of varying ages. 3. Determine which patients need continuous monitoring or special monitoring (e.g., neurological checks). 4. Interpret and respond appropriately to results of monitoring based on method used, age and clinical situation. B. Use appropriate monitoring techniques in the inpatient setting. 1. Monitoring of temperature, blood pressure, heart rate, respirations 2. Cardiac monitoring 3. Pulse oximetry C. Use appropriately the treatments and techniques used in the inpatient setting. 1. Universal precautions 2. Nasogastric tube placement 3. Administration of nebulized medication 4. Injury, wound and burn care 5. Oxygen delivery systems 6. I.V. fluids 7. I.V. pharmacotherapy (antibiotics, antiepileptics, etc.) 8. Transfusion therapy D. Describe key issues in the inpatient and home management of the technologydependent child with the following care needs: 1. Tracheostomy
5 2. Chronic mechanical ventilation 3. Chronic parenteral nutrition (HAL) 4. Gastrostomy tube for feedings 5. Permanent central venous catheter E. Recognize normal and abnormal findings at tracheostomy, gastrostomy, or central venous catheter sites, and demonstrate appropriate intervention or referral for problems encountered. F. Demonstrate the skills for assessing and managing pain. 1. Use age-appropriate pain scales in assessment. 2. Describe indications for use and side effects of common narcotic and nonnarcotic analgesics. 3. Administer medications to control pain in appropriate dose, frequency and route. 4. Describe indications for and use of behavioral techniques and supportive care, and other non-pharmacologic methods of pain control. 5. GOAL: Demonstrate high standards of professional competence while working with patients on the Inpatient Service. A. Competency 1: Patient Care. Provide family-centered patient care that is development- and age-appropriate, compassionate, and effective for the treatment of health problems and the promotion of health. 1. Use a logical and appropriate clinical approach to the care of hospitalized patients, applying principles of evidence-based decision-making and problem-solving, demonstrating: a) Careful data collection and synthesis b) Appropriate orders for vital signs, I & Os, medications, nutrition, activity c) Well thought-out daily care plans d) Good clinical judgment and decision-making e) Careful discharge plans (orders, patient education, followup) 2. Provide sensitive support to patients with acute and chronic illnesses and to their families, and arrange for ongoing support and preventive services at discharge. B. Competency 2: Medical Knowledge. Understand the scope of established and evolving biomedical, clinical, epidemiological and social-behavioral knowledge needed by a pediatrician; demonstrate the ability to acquire, critically interpret and apply this knowledge in patient care. 1. Demonstrate a commitment to acquiring the base of knowledge needed to care for children in the inpatient setting. 2. Know and/or access medical information efficiently, evaluate it critically, and apply it to inpatient care appropriately. C. Competency 3: Interpersonal Skills and Communication. Demonstrate interpersonal and communication skills that result in information exchange and partnering with patients, their families and professional associates. 1. Provide effective patient education, including reassurance, for condition(s) commonly seen on the inpatient service.
6 2. Participate and communicate effectively as part of an interdisciplinary team, as both the primary provider and the consulting pediatrician (e.g., patient presentations, sign-out rounds, communication with consultants and primary care physicians of hospitalized patients). 3. Develop effective strategies for teaching students, colleagues, other professionals and laypersons. 4. Maintain accurate, legible, timely and legally appropriate medical records. D. Competency 4: Practice-based Learning and Improvement. Demonstrate knowledge, skills and attitudes needed for continuous self-assessment, using scientific methods and evidence to investigate, evaluate and improve one's patient care practice. 1. Use scientific methods and evidence to investigate, evaluate and improve one's patient care practice in the inpatient setting. 2. Identify personal learning needs, systematically organize relevant information resources for future reference, and plan for continuing acquisition of knowledge and skills. E. Competency 5: Professionalism. Demonstrate a commitment to carrying out professional responsibilities, adherence to ethical principles, and sensitivity to diversity. 1. Demonstrate personal accountability to the well being of patients (e.g., following-up on lab results, writing comprehensive notes, and seeking answers to patient care questions). 2. Demonstrate a commitment to professional behavior in interactions with staff and professional colleagues. 3. Adhere to ethical and legal principles, and sensitivity to diversity while providing care in the inpatient setting. F. Competency 6: Systems-Based Practice. Understand how to practice highquality health care and advocate for patients within the context of the health care system. 1. Identify key aspects of health care systems, cost control, billing and reimbursement in the hospital inpatient setting. 2. When providing care in the inpatient setting, consider cost and resource allocation without compromising quality of care. 3. Take steps to avoid medical errors by recognizing the limits of one's knowledge and expertise; work with the health care team to recognize and address systems errors. Procedures A. GOAL: Technical and therapeutic procedures. Describe the following procedures, including how they work and when they should be used; competently perform those commonly used by the pediatrician in practice. 1. Anesthesia/analgesia: pain management 2. Arterial puncture 3. Bladder: catherization 4. Central line: use/care 5. Chest physiotherapy 6. Gastric tube placement (OG/NG)
7 7. Gastrostomy tube replacement 8. Intravenous line placement 9. Lumbar puncture 10. Medication delivery: IM/SC/ID 11. Medication delivery: inhaled 12. Medication delivery: IV 13. Medication delivery: rectal 14. PPD: placement 15. Pulmonary function tests: peak flow meter 16. Pulmonary function tests: spirometry 17. Pulse oximeter: placement 18. Rectal swab 19. Sterile technique 20. Suctioning: nares 21. Suctioning: oral pharynx 22. Suctioning: tracheostomy 23. Tracheostomy tube: replacement 24. Venipuncture B. GOAL: Diagnostic and screening procedures. Describe the following tests or procedures, including how they work and when they should be used; competently perform those commonly used by the pediatrician in practice. 1. ECG: emergency interpretation 2. ECG: perform 3. Electroencephalogram (EEG) 4. ph probe (Tuttle test) 5. PPD: interpretation 6. Monitoring interpretation: cardiac 7. Monitoring interpretation: Holter 8. Monitoring interpretation: pulse oximetry 9. Monitoring interpretation: respiratory 10. Pulmonary function tests: interpretation 11. Radiologic interpretation: abdominal ultrasound 12. Radiologic interpretation: abdominal X-ray 13. Radiologic interpretation: chest X-ray 14. Radiologic interpretation: CT of head 15. Radiologic interpretation: extremity X-ray 16. Radiologic interpretation: GI contrast study 17. Radiologic interpretation: MRI of head 18. Radiologic interpretation: nuclear medicine GI scanning 19. Radiologic interpretation: renal ultrasound 20. Radiologic interpretation: skeletal X-ray (incl. abuse) 21. Radiologic interpretation: skull film for fracture 22. Radiologic interpretation: sinus films 23. Radiologic interpretation: voiding cystourethrogram
8 Adapted From Kittredge, D., Baldwin, C. D., Bar-on, M. E., Beach, P. S., Trimm, R. F. (Eds.). (2004). APA Educational Guidelines for Pediatric Residency. Ambulatory Pediatric Association Website. Available online:
Children s Hospital & Research Center Oakland Day Admit/Night Float
 Children s Hospital & Research Center Oakland Day Admit/Night Float Patient Care Provide family-centered patient care that is development- and ageappropriate, compassionate, and effective for the treatment
Children s Hospital & Research Center Oakland Day Admit/Night Float Patient Care Provide family-centered patient care that is development- and ageappropriate, compassionate, and effective for the treatment
Pediatric Critical Care
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pediatric Critical Care 1. GOAL: Recognize the critically ill patient and initiate appropriate stabilization and/or resuscitative
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pediatric Critical Care 1. GOAL: Recognize the critically ill patient and initiate appropriate stabilization and/or resuscitative
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Pulmonary
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Pulmonary 1. GOAL: Diagnose and manage patients with asthma. 2. GOAL: Understand the role of the pediatrician in preventing
Subspecialty Rotation: Anesthesia
 Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
Subspecialty Rotation: Anesthesia Faculty: John Heaton, M.D. GOAL: Maintenance of Airway Patency and Oxygenation. Recognize and manage upper airway obstruction and desaturation. Recognize and manage upper
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Neurology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Neurology 1. GOAL: Understand the role of the pediatrician in preventing neurological diseases, and in counseling and screening
Outpatient Pediatrics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Outpatient Pediatrics 1. GOAL: Evaluate and manage common signs and symptoms associated with the practice of pediatrics
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Outpatient Pediatrics 1. GOAL: Evaluate and manage common signs and symptoms associated with the practice of pediatrics
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Nephrology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Nephrology 1. GOAL: Understand the general pediatrician's role in diagnosis and management of hypertension in children.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Nephrology 1. GOAL: Understand the general pediatrician's role in diagnosis and management of hypertension in children.
Subspecialty Inpatient Rotation: Pediatric Oncology at Memorial Sloan Kettering Cancer Center Senior Resident
 Subspecialty Inpatient Rotation: Pediatric Oncology at Memorial Sloan Kettering Cancer Center Senior Resident Residents: Pediatric residents at the PL3 level Prerequisites: Successful completion or waiver
Subspecialty Inpatient Rotation: Pediatric Oncology at Memorial Sloan Kettering Cancer Center Senior Resident Residents: Pediatric residents at the PL3 level Prerequisites: Successful completion or waiver
Pediatric Residency Curriculum
 Pediatric Residency Curriculum Continuity Clinic: Goals and Objectives The goal of the longitudinal continuity clinic experience is to develop our residents ability to deliver high-quality primary care
Pediatric Residency Curriculum Continuity Clinic: Goals and Objectives The goal of the longitudinal continuity clinic experience is to develop our residents ability to deliver high-quality primary care
: Provide cardiovascular preventive counseling to parents and patients with specific cardiac diseases about:
 Children s Hospital & Research Center Oakland Cardiology Primary Goals for this Rotation 5.13 GOAL: Prevention, Counseling and Screening (Cardiovascular). Understand the role of the pediatrician in preventing
Children s Hospital & Research Center Oakland Cardiology Primary Goals for this Rotation 5.13 GOAL: Prevention, Counseling and Screening (Cardiovascular). Understand the role of the pediatrician in preventing
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Otolaryngology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Otolaryngology 1. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Otolaryngology 1. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Gastroenterology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Gastroenterology 1. GOAL: Understand the role of the general pediatrician in the assessment and management of patients with
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Gastroenterology 1. GOAL: Understand the role of the general pediatrician in the assessment and management of patients with
Emergency Medicine Scope of Practice
 Emergency Medicine Scope of Practice All Physician Assistants working in Emergency Medicine will encounter a wide variety of non acute, urgent and emergent patient complaints and conditions. Given the
Emergency Medicine Scope of Practice All Physician Assistants working in Emergency Medicine will encounter a wide variety of non acute, urgent and emergent patient complaints and conditions. Given the
Hematology/Oncology/BMT
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Hematology/Oncology/BMT 1. GOAL: Understand the role of the pediatrician in preventing hematologic or oncologic conditions,
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Hematology/Oncology/BMT 1. GOAL: Understand the role of the pediatrician in preventing hematologic or oncologic conditions,
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level
 Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
Subspecialty Rotation: Child Neurology at SUNY (KCHC and UHB) Residents: Pediatric residents at the PL1, PL2, PL3 level Prerequisites: Any prior pediatric rotations and experience Primary Goals for this
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Genetics
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Genetics 1. GOAL: Understand the role of the pediatrician in preventing genetic disease, and in counseling and screening
Provide specific counseling to parents and patients with neurological disorders, addressing:
 Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Neurology Description: The Pediatric Neurology elective will give the resident the opportunity to learn how to obtain an appropriate history and perform a complete neurologic exam. Four to five half days
Subspecialty Rotation: Otolaryngology
 Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Subspecialty Rotation: Otolaryngology Faculty: Evelyn Kluka, M.D. GOAL: Hearing Loss. Understand the morbidity of hearing loss, intervention strategies, and the pediatrician's and other specialists' roles
Orthopedics. 1. GOAL: Understand the pediatrician's role in preventing and screening for
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Orthopedics 1. GOAL: Understand the pediatrician's role in preventing and screening for orthopedic injury, disease and dysfunction.
PEDIATRICS 300A CORE TOPICS LIST
 PEDIATRICS 300A CORE TOPICS LIST Symptom, finding, or concern Heart findings Core Innocent murmurs Extended Congestive heart failure Myocarditis PDA Valvular defects Cyanotic congenital heart disease Acyanotic
PEDIATRICS 300A CORE TOPICS LIST Symptom, finding, or concern Heart findings Core Innocent murmurs Extended Congestive heart failure Myocarditis PDA Valvular defects Cyanotic congenital heart disease Acyanotic
Recognize the broad impact of hearing impairment on child and family, including social, psychological, educational and financial consequences.
 Otolaryngology Note: The goals and objectives described in detail below are not meant to be completed in a single one month block rotation but are meant to be cumulative, culminating in a thorough and
Otolaryngology Note: The goals and objectives described in detail below are not meant to be completed in a single one month block rotation but are meant to be cumulative, culminating in a thorough and
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Endocrinology
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Endocrinology 1. GOAL: Understand the role of the pediatrician in preventing endocrine dysfunction, and in counseling and
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Endocrinology 1. GOAL: Understand the role of the pediatrician in preventing endocrine dysfunction, and in counseling and
Table of Contents. Course CME Credits. General Principles Topic CME Credit(s)
 Table of Contents Course Course CME Credits Med-Challenger SPEX Comprehensive Review 266.0 CME Credits General Principles 21.0 CME Credit(s) Abdominal Pain 1.0 Acute Pelvic Pain in Women 1.0 Acute Vaginal
Table of Contents Course Course CME Credits Med-Challenger SPEX Comprehensive Review 266.0 CME Credits General Principles 21.0 CME Credit(s) Abdominal Pain 1.0 Acute Pelvic Pain in Women 1.0 Acute Vaginal
List of Chapters. 5. Care of the sick child Evidence-based pediatrics (page 77 to 80)
 Illustrated Textbook of Paediatrics, 4th Edition Tom Lissauer, and Graham Clayden, 2012 List of Chapters 1. The child in society 2. History and examination 3. Normal child development, hearing and vision
Illustrated Textbook of Paediatrics, 4th Edition Tom Lissauer, and Graham Clayden, 2012 List of Chapters 1. The child in society 2. History and examination 3. Normal child development, hearing and vision
PREAMBLE GENERAL DIAGNOSTIC RADIOLOGY
 PREAMBLE The General Diagnostic Radiology category is intended to cover the body of knowledge a practicing board certified Diagnostic Radiologist should know. Since the range of content relevant to the
PREAMBLE The General Diagnostic Radiology category is intended to cover the body of knowledge a practicing board certified Diagnostic Radiologist should know. Since the range of content relevant to the
Child Neurology Elective PL1 Rotation
 PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL1 Rotation The neurology elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
Pediatric GU Dysfunction
 Pediatric GU Dysfunction Assessment of pediatric renal function Signs and symptoms Laboratory tests Radiological tests Nursing considerations Psychosocial and developmental considerations GU Disorders
Pediatric GU Dysfunction Assessment of pediatric renal function Signs and symptoms Laboratory tests Radiological tests Nursing considerations Psychosocial and developmental considerations GU Disorders
Cardiology Competency Based Goals and Objectives
 Cardiology Competency Based Goals and Objectives COMPETENCY 1. Patient Care. Provide family centered patient care that is developmentally and age appropriate, compassionate, and effective for the treatment
Cardiology Competency Based Goals and Objectives COMPETENCY 1. Patient Care. Provide family centered patient care that is developmentally and age appropriate, compassionate, and effective for the treatment
4. Counsel patients and families regarding athletic participation, including:
 Sports Medicine Primary Goals for this Rotation GOAL: Prevention, Counseling and Screening. Understand the pediatrician's role in preventing sports-related injuries, disorders and dysfunction in children
Sports Medicine Primary Goals for this Rotation GOAL: Prevention, Counseling and Screening. Understand the pediatrician's role in preventing sports-related injuries, disorders and dysfunction in children
Pediatric Gastroenterology Referral Guidelines
 Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
Suggested Pre-Referral Workup This is a general suggestion of possible testing to confirm a suspected diagnosis. Although referrals will be accepted without the suggested work up being complete, to ensure
Rosen s Emergency Medicine 2018, 9/e Table of Contents
 Rosen s Emergency Medicine 2018, 9/e Table of Contents Dr.hamidmirjalili@gmail.com Telegram: @medup PART I : Fundamental Clinical Concepts Section One : CRITICAL MANAGEMENT PRINCIPLES 1. Arway >> page
Rosen s Emergency Medicine 2018, 9/e Table of Contents Dr.hamidmirjalili@gmail.com Telegram: @medup PART I : Fundamental Clinical Concepts Section One : CRITICAL MANAGEMENT PRINCIPLES 1. Arway >> page
Internal Medicine Certification Examination Blueprint
 Internal Medicine Certification Examination Blueprint What Does the Examination Cover? The exam is designed to evaluate the extent of the candidate s knowledge and clinical judgment in the areas in which
Internal Medicine Certification Examination Blueprint What Does the Examination Cover? The exam is designed to evaluate the extent of the candidate s knowledge and clinical judgment in the areas in which
APR-DRG Description Ave Charge
 Abdominal Pain 16,500.25 2.8 6,000.09 Acute & Subacute Endocarditis 15,339.30 3.0 5,113.10 Acute Myocardial Infarction 17,687.46 2.6 6,802.87 Alcohol Abuse & Dependence 19,126.64 4.2 4,553.96 Alcoholic
Abdominal Pain 16,500.25 2.8 6,000.09 Acute & Subacute Endocarditis 15,339.30 3.0 5,113.10 Acute Myocardial Infarction 17,687.46 2.6 6,802.87 Alcohol Abuse & Dependence 19,126.64 4.2 4,553.96 Alcoholic
Pulmonology Elective PL-1 Residents
 PL-1 Residents The Pulmonary elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
PL-1 Residents The Pulmonary elective is available to first year residents in either a 2 or 4 week block rotation. The experience will include performing inpatient consultations, attending outpatient clinics
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine
 Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
Specific Basic Standards for Osteopathic Fellowship Training in Pulmonary / Critical Care Medicine American Osteopathic Association and American College of Osteopathic Internists BOT Rev. 2/2011 These
Interpret clinical and laboratory tests to identify conditions that require surgical intervention, including:
 Pediatric Surgery Note: The goals and objectives described in detail below are not meant to be completed in a single one month block rotation but are meant to be cumulative, culminating in a thorough and
Pediatric Surgery Note: The goals and objectives described in detail below are not meant to be completed in a single one month block rotation but are meant to be cumulative, culminating in a thorough and
Fever. National Pediatric Nighttime Curriculum Written by Debbie Sakai, M.D. Institution: Lucile Packard Children s Hospital
 Fever National Pediatric Nighttime Curriculum Written by Debbie Sakai, M.D. Institution: Lucile Packard Children s Hospital Case 1 4-month-old well-appearing girl admitted for croup and respiratory distress.
Fever National Pediatric Nighttime Curriculum Written by Debbie Sakai, M.D. Institution: Lucile Packard Children s Hospital Case 1 4-month-old well-appearing girl admitted for croup and respiratory distress.
Episodes of Care Risk Adjustment
 Episodes of Care Risk Adjustment Episode Types Wave 1 Asthma Acute Exacerbation Perinatal Total Joint Replacement Wave 2 Acute Percutaneous Coronary Intervention COPD Acute Exacerbation Non-acute Percutaneous
Episodes of Care Risk Adjustment Episode Types Wave 1 Asthma Acute Exacerbation Perinatal Total Joint Replacement Wave 2 Acute Percutaneous Coronary Intervention COPD Acute Exacerbation Non-acute Percutaneous
Differentiate IgE-mediated food allergy from non-ige mediated food allergy. List the foods and formulas most commonly associated with food allergy.
 Gastroenterology Description: The resident will be exposed to various clinical symptoms and diseases of the gastrointestinal tract which are commonly seen by the gastroenterologist. The resident will be
Gastroenterology Description: The resident will be exposed to various clinical symptoms and diseases of the gastrointestinal tract which are commonly seen by the gastroenterologist. The resident will be
1. Adequate diet and iron intake to prevent iron deficiency 2. Signs and symptoms of malignant disease
 Hematology/Oncology Description: The pediatric hematology-oncology division sees a wide spectrum of pediatric disease including but not limited to leukemia, hemophilia, solid tumors, ITP, and other blood
Hematology/Oncology Description: The pediatric hematology-oncology division sees a wide spectrum of pediatric disease including but not limited to leukemia, hemophilia, solid tumors, ITP, and other blood
Legal aspects in accidents and neglect.
 Al-Al Bayt University Princess Salma Faculty of Nursing Adult Health nursing Course Title :Child Health Nursing Course Number :1001341 Credit Hours :3 Pre requisite :1001222 Placement : Instructor:,, Course
Al-Al Bayt University Princess Salma Faculty of Nursing Adult Health nursing Course Title :Child Health Nursing Course Number :1001341 Credit Hours :3 Pre requisite :1001222 Placement : Instructor:,, Course
PAEDIATRIC Point Prevalence Survey. Ward Form
 Appendix 1 PAEDIATRIC Point Prevalence Survey Ward Form Please fill in one form for each ward included in PPS Date of survey Person completing form (Auditor code) Hospital Name Department/Ward Paediatric
Appendix 1 PAEDIATRIC Point Prevalence Survey Ward Form Please fill in one form for each ward included in PPS Date of survey Person completing form (Auditor code) Hospital Name Department/Ward Paediatric
Scottish Surveillance of Healthcare Associated Infection Programme (SSHAIP) Health Protection Scotland (HPS) SSI Surveillance Protocol 7th Edition
 1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
1 Contents Female reproductive system operations (Abdominal hysterectomy and Caesarean section)... 3 Intra-abdominal infections... 3 Endometritis... 4 Other infections of the female reproductive tract...
Please list any treatments you have previously had for current illness. (Physical Therapy, Surgery, Radiation, etc.)
 Date: Patient Name: D.O.B Last First M.I History of Present Illness: What is the reason for your visit? Date symptom started? Please list any treatments you have previously had for current illness. (Physical
Date: Patient Name: D.O.B Last First M.I History of Present Illness: What is the reason for your visit? Date symptom started? Please list any treatments you have previously had for current illness. (Physical
Lahey Clinic Internal Medicine Residency Program: Curriculum for Infectious Disease
 Lahey Clinic Internal Medicine Residency Program: Curriculum for Infectious Disease Faculty representative: Eva Piessens, MD, MPH Resident representative: Karen Ganz, MD Revision date: February 1, 2006
Lahey Clinic Internal Medicine Residency Program: Curriculum for Infectious Disease Faculty representative: Eva Piessens, MD, MPH Resident representative: Karen Ganz, MD Revision date: February 1, 2006
Children s Hospital & Research Center Oakland. Endocrinology
 Children s Hospital & Research Center Oakland Endocrinology 5.22 GOAL: Prevention, Counseling and Screening (Endocrine). Understand the role of the pediatrician in preventing endocrine PC, MK, dysfunction,
Children s Hospital & Research Center Oakland Endocrinology 5.22 GOAL: Prevention, Counseling and Screening (Endocrine). Understand the role of the pediatrician in preventing endocrine PC, MK, dysfunction,
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C.
 NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
NORTHERN VIRGINIA PULMONARY AND CRITICAL CARE ASSOCIATES, P.C. Past Medical History AIDS/HIV disease Anemia Asthma Bronchitis Cancer Date of last Chest X-ray Diabetes Mellitus, Type I Diabetes Mellitus,
GOALS AND OBJECTIVES INFECTIOUS DISEASE
 GOALS AND OBJECTIVES INFECTIOUS DISEASE Infectious Disease and HIV Overview: The Infectious Diseases Program at the University of Southern California prepares trainees for the management of problems in
GOALS AND OBJECTIVES INFECTIOUS DISEASE Infectious Disease and HIV Overview: The Infectious Diseases Program at the University of Southern California prepares trainees for the management of problems in
NurseAchieve. CHAPTERS INCLUDED IN THE NURSEACHIEVE COMPREHENSIVE NCLEX REVIEW NURSING SKILLS AND FUNDAMENTALS:
 NurseAchieve www.nurseachieve.com CHAPTERS INCLUDED IN THE NURSEACHIEVE COMPREHENSIVE NCLEX REVIEW NCLEX TEST STRATEGIES: NCLEX EXAM OVERVIEW TEST TAKING STRATEGIES NURSING SKILLS AND FUNDAMENTALS: ADMINISTRATION
NurseAchieve www.nurseachieve.com CHAPTERS INCLUDED IN THE NURSEACHIEVE COMPREHENSIVE NCLEX REVIEW NCLEX TEST STRATEGIES: NCLEX EXAM OVERVIEW TEST TAKING STRATEGIES NURSING SKILLS AND FUNDAMENTALS: ADMINISTRATION
InterQual Level of Care 2018 Index
 InterQual Level of Care 2018 Index Long-Term Acute Care (LTAC) Criteria The Index is an alphabetical listing of conditions and/or diagnoses designed to guide the user to the criteria subset where a specific
InterQual Level of Care 2018 Index Long-Term Acute Care (LTAC) Criteria The Index is an alphabetical listing of conditions and/or diagnoses designed to guide the user to the criteria subset where a specific
Emergency Department Suite
 Emergency Department Suite This suite of Pediatric Learning Solutions (PLS) online courseware and curriculums provides 24/7 access to the foundational knowledge and just-in-time job aids clinicians working
Emergency Department Suite This suite of Pediatric Learning Solutions (PLS) online courseware and curriculums provides 24/7 access to the foundational knowledge and just-in-time job aids clinicians working
Product Catalog. Pediatric Learning Solutions. Listing of all current products (as of May, 2013) offered by Children's Hospital Association.
 Product Catalog Pediatric Learning Solutions Listing of all current products (as of May, 2013) offered by Children's Hospital Association. Acquired Heart Disease in Children WBT Acute Respiratory Distress
Product Catalog Pediatric Learning Solutions Listing of all current products (as of May, 2013) offered by Children's Hospital Association. Acquired Heart Disease in Children WBT Acute Respiratory Distress
Stepdown Skills Checklist
 Stepdown Skills Checklist This assessment is for determining your experience in the below outlined clinical areas. This checklist will not be used as a determining factor in accepting your application
Stepdown Skills Checklist This assessment is for determining your experience in the below outlined clinical areas. This checklist will not be used as a determining factor in accepting your application
RECOMMENDED COURSE ORDER
 Although you have the flexibility to view the videos in any order, we strongly recommend that you watch the videos in the order in which your dashboard presents them regardless of how many videos you view
Although you have the flexibility to view the videos in any order, we strongly recommend that you watch the videos in the order in which your dashboard presents them regardless of how many videos you view
High-Acuity Nursing. Global edition. Global edition. Kathleen Dorman Wagner Melanie G. Hardin-Pierce
 High-Acuity Nursing For these Global Editions, the editorial team at Pearson has collaborated with educators across the world to address a wide range of subjects and requirements, equipping students with
High-Acuity Nursing For these Global Editions, the editorial team at Pearson has collaborated with educators across the world to address a wide range of subjects and requirements, equipping students with
The University of Arizona Pediatric Residency Program. Primary Goals for Rotation. Surgery, Pediatric
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Surgery, Pediatric 1. GOAL: Anesthesia. Participate in the care and management of pediatric patients requiring general and
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Surgery, Pediatric 1. GOAL: Anesthesia. Participate in the care and management of pediatric patients requiring general and
Course Name: Internal medicine course for 6 th year medical students
 The University of Jordan Accreditation & Quality Assurance Center Course Syllabus Course Name: Internal medicine course for 6 th year medical students 1 Course title Internal Medicine for 6 th year medical
The University of Jordan Accreditation & Quality Assurance Center Course Syllabus Course Name: Internal medicine course for 6 th year medical students 1 Course title Internal Medicine for 6 th year medical
FEVER. What is fever?
 FEVER What is fever? Fever is defined as a rectal temperature 38 C (100.4 F), and a value >40 C (104 F) is called hyperpyrexia. Body temperature fluctuates in a defined normal range (36.6-37.9 C [97.9-100.2
FEVER What is fever? Fever is defined as a rectal temperature 38 C (100.4 F), and a value >40 C (104 F) is called hyperpyrexia. Body temperature fluctuates in a defined normal range (36.6-37.9 C [97.9-100.2
+ Color Change - + Hearing Loss - + Apnea - + Enuresis (urine - + Tremors - + Rash -
 Review of Systems: 0-1 year old Constitution neg Eyes neg GI neg Neurological neg + Activity Change - + Eye Discharge - + Reflux - + Facial Asymmetry - + Appetite Change - + Eye Redness - + Vomiting -
Review of Systems: 0-1 year old Constitution neg Eyes neg GI neg Neurological neg + Activity Change - + Eye Discharge - + Reflux - + Facial Asymmetry - + Appetite Change - + Eye Redness - + Vomiting -
EVALUATION OF A SICK CHILD WITH FEVER
 EVALUATION OF A SICK CHILD WITH FEVER Learning objectives At the conclusion of this learning activity, participants should be able to; Discuss the different etiologies of acute illness in a child Identify
EVALUATION OF A SICK CHILD WITH FEVER Learning objectives At the conclusion of this learning activity, participants should be able to; Discuss the different etiologies of acute illness in a child Identify
*Monitor for significant side effects, especially symptoms of neurological or cardiovascular events.
 Assessment Prior to administration: Obtain complete health history including allergies, drug history, and possible drug reactions Assess reason for drug administration such as presence/history of anemia
Assessment Prior to administration: Obtain complete health history including allergies, drug history, and possible drug reactions Assess reason for drug administration such as presence/history of anemia
M3 Pediatric Clerkship
 M3 Pediatric Clerkship The overall goals for the third year Pediatric Clerkship are to educate future physicians to provide competent, effective and compassionate care of patients by developing clinical
M3 Pediatric Clerkship The overall goals for the third year Pediatric Clerkship are to educate future physicians to provide competent, effective and compassionate care of patients by developing clinical
Welcome to the Acute/PAH Rotation
 Welcome to the Acute/PAH Rotation You are about to start your acute/pah rotation where you will get to see many infants, children and adolescents who present with a variety acute pediatric conditions.
Welcome to the Acute/PAH Rotation You are about to start your acute/pah rotation where you will get to see many infants, children and adolescents who present with a variety acute pediatric conditions.
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
By Your Sis: Ghada Odeh :)
 By Your Sis: Ghada Odeh :) Hx: Chest pain ACS. Hx.: Cough Bronchiectasis. Hx: Epigastric pain Peptic ulcer disease. Hx: Joints Pain SLE. Hx: Hematurea post-strep Glomerulonephritis. Hx: Jaundice Chronic
By Your Sis: Ghada Odeh :) Hx: Chest pain ACS. Hx.: Cough Bronchiectasis. Hx: Epigastric pain Peptic ulcer disease. Hx: Joints Pain SLE. Hx: Hematurea post-strep Glomerulonephritis. Hx: Jaundice Chronic
Infant Child and Adolescent Care
 Course Goals Goals 1. Gather a history and perform a complete physical exam on a pediatric patient. 2. Develop a prioritized differential diagnosis and select a working diagnosis following a patient encounter.
Course Goals Goals 1. Gather a history and perform a complete physical exam on a pediatric patient. 2. Develop a prioritized differential diagnosis and select a working diagnosis following a patient encounter.
CONTENTS 1. PUBLIC HEALTH ISSUES 2. SIGNS AND SYMPTOMS 3. DIAGNOSTIC TESTS 4. CARDIOVASCULAR DISEASES 5. RESPIRATORY DISEASES
 CONTENTS 1. PUBLIC HEALTH ISSUES 2. SIGNS AND SYMPTOMS 3. DIAGNOSTIC TESTS 4. CARDIOVASCULAR DISEASES 5. RESPIRATORY DISEASES 6. GASTROINTESTINAL DISEASES 7. UROGENITAL DISEASES 8. SEXUALLY TRANSMITTED
CONTENTS 1. PUBLIC HEALTH ISSUES 2. SIGNS AND SYMPTOMS 3. DIAGNOSTIC TESTS 4. CARDIOVASCULAR DISEASES 5. RESPIRATORY DISEASES 6. GASTROINTESTINAL DISEASES 7. UROGENITAL DISEASES 8. SEXUALLY TRANSMITTED
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University
 Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
Pediatric emergencies (SHOCK & COMA) Dr Mubarak Abdelrahman Assistant Professor Jazan University SHOCK Definition: Shock is a syndrome = inability to provide sufficient oxygenated blood to tissues. Oxygen
UCLA General Surgery Residency Program Rotation Educational Policy Goals and Objectives ROTATION: SURGICAL CRITICAL CARE AND TRANSPLANTATION SURGERY
 UPDATED: August 2009 UCLA General Surgery Residency Program ROTATION: SURGICAL CRITICAL CARE AND TRANSPLANTATION SURGERY ROTATION DIRECTOR: Gerald Lipshutz, M.D. SITE: UCLA Medical Center LEVEL OF TRAINEE:
UPDATED: August 2009 UCLA General Surgery Residency Program ROTATION: SURGICAL CRITICAL CARE AND TRANSPLANTATION SURGERY ROTATION DIRECTOR: Gerald Lipshutz, M.D. SITE: UCLA Medical Center LEVEL OF TRAINEE:
Salt Lake Orthopaedic Clinic Initial Visit Form
 Salt Lake Orthopaedic Clinic Initial Visit Form Name: Today s Date: Date of Birth: Age: Height: Weight: Handedness (R/L): Referring Physician: Primary Care Physician: Chief Complaint Why are you seeing
Salt Lake Orthopaedic Clinic Initial Visit Form Name: Today s Date: Date of Birth: Age: Height: Weight: Handedness (R/L): Referring Physician: Primary Care Physician: Chief Complaint Why are you seeing
Patient Intake Form for Allegany Ear, Nose, & Throat
 Patient Intake Form for Allegany Ear, se, & Throat Patient Name: What brings you to the office today? Who is your primary care doctor? Please list your current medications: Are you allergic to any medications?
Patient Intake Form for Allegany Ear, se, & Throat Patient Name: What brings you to the office today? Who is your primary care doctor? Please list your current medications: Are you allergic to any medications?
Allergy/Immunology Marshall University Pediatrics
 Allergy/Immunology Marshall University Pediatrics Description: This is a clinical rotation about the most common chronic diseases affecting both children and adults. Residents will be introduced to allergy,
Allergy/Immunology Marshall University Pediatrics Description: This is a clinical rotation about the most common chronic diseases affecting both children and adults. Residents will be introduced to allergy,
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING
 AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
AUTOIMMUNE DISORDERS IN THE ACUTE SETTING Diagnosis and Treatment Goals Aimee Borazanci, MD BNI Neuroimmunology Objectives Give an update on the causes for admission, clinical features, and outcomes of
Disclaimer. This is a broad survey and cannot cover all differential diagnoses or each condition in thorough detail
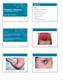 Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
Objectives Pediatric Infections: Differentiating Benign from Serious Eileen Klein, MD, MPH Rashes Infectious vs non-infectious Viral vs bacterial Respiratory and GI illnesses When do you treat When do
Cedars Sinai Medical Center Pediatric Electives
 PE 235.03 MEDICAL GENETICS COURSE CHAIR: John M. Graham, M.D., ScD.. By arrangement - Please contact the Student Coordinator 1. Counseling techniques and the approach to the patient and family with hereditary
PE 235.03 MEDICAL GENETICS COURSE CHAIR: John M. Graham, M.D., ScD.. By arrangement - Please contact the Student Coordinator 1. Counseling techniques and the approach to the patient and family with hereditary
Child Health Undergraduate Curriculum Editor: Dr Gardner-Medwin (Consultant Paediatric Rheumatologist)
 Child Health Undergraduate Curriculum Editor: Dr Gardner-Medwin (Consultant Paediatric Rheumatologist) This curriculum is supported by the Child Health Revision Guide For Medical Students at Glasgow University,
Child Health Undergraduate Curriculum Editor: Dr Gardner-Medwin (Consultant Paediatric Rheumatologist) This curriculum is supported by the Child Health Revision Guide For Medical Students at Glasgow University,
Northeast Ohio Urogynecology Patient History Intake Form. Last Name First Name Age. Date of Birth Race Referring Physician.
 Northeast Ohio Urogynecology Patient History Intake Form Last Name _First Name Age_ Date of Birth Race Referring Physician Reason for Visit: _ Allergies: Preferred Lab (circle): QUEST LABCARE PLUS LABCORP
Northeast Ohio Urogynecology Patient History Intake Form Last Name _First Name Age_ Date of Birth Race Referring Physician Reason for Visit: _ Allergies: Preferred Lab (circle): QUEST LABCARE PLUS LABCORP
Mayo Clinic Physician Assistant Board Review
 PHARMACOLOGY CONTENT Mayo Clinic Physician Assistant Board Review Select presentations will contain pharmacology content as noted in the program. Identified presentations represent approximately 11.75
PHARMACOLOGY CONTENT Mayo Clinic Physician Assistant Board Review Select presentations will contain pharmacology content as noted in the program. Identified presentations represent approximately 11.75
2017 ACCP/SCCM Critical Care Preparatory Review and Recertification Course Learning Objectives
 2017 ACCP/SCCM Critical Care Preparatory Review and Recertification Course Learning Objectives Shock Syndromes and Sepsis, Pulmonary Disorders, Hepatic Failure/GI/Endocrine Emergencies, Supportive and
2017 ACCP/SCCM Critical Care Preparatory Review and Recertification Course Learning Objectives Shock Syndromes and Sepsis, Pulmonary Disorders, Hepatic Failure/GI/Endocrine Emergencies, Supportive and
PLEASE COMPLETE ALL SECTIONS OF THIS FORM
 PLEASE COMPLETE ALL SECTIONS OF THIS FORM Patient Name: Date of Birth: Referring Doctor? (Name, telephone number and address) Chief Complaint: Why have you come here? How did it start? What are the symptoms?
PLEASE COMPLETE ALL SECTIONS OF THIS FORM Patient Name: Date of Birth: Referring Doctor? (Name, telephone number and address) Chief Complaint: Why have you come here? How did it start? What are the symptoms?
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES
 DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
DAYTON CHILDREN S HOSPITAL CLINICAL PRACTICE GUIDELINES DISCLAIMER: This Clinical Practice Guideline (CPG) generally describes a recommended course of treatment for patients with the identified health
Patient Name Date of Birth Page 1 of 6
 2545 W. Hillcrest Dr. #205 Thousand Oaks, CA 91320 Admissions: 888.822.8938 Fax: 805.273.5246 Dear Medical Professional, This patient is seeking care to address eating disorder behaviors. For the patient
2545 W. Hillcrest Dr. #205 Thousand Oaks, CA 91320 Admissions: 888.822.8938 Fax: 805.273.5246 Dear Medical Professional, This patient is seeking care to address eating disorder behaviors. For the patient
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Unit 4 Problems of Cardiac Output and Tissue Perfusion
 Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
Unit 4 Problems of Cardiac Output and Tissue Perfusion Lemone and Burke Ch 30-32 Objectives Review the anatomy and physiology of the cardiovascular system. Identify normal heart sounds and relate them
PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department
 PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department Overview Roles of the EMS in Pediatric Care Growth and Development Assessment Airway Adjuncts and Intravenous Access
PEDIATRIC EMERGENCIES Sandra Horning, MD Sacred Heart Medical Center Emergency Department Overview Roles of the EMS in Pediatric Care Growth and Development Assessment Airway Adjuncts and Intravenous Access
Emergency Room Skills Checklist
 _ XXX-XX- Print Name Last 4 of SS # Date Completed Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
_ XXX-XX- Print Name Last 4 of SS # Date Completed Directions Please circle a value for each question to provide us and the interested facilities with an assessment of your clinical experience. These values
Fever Without a Source Age: 0-28 Day Pathway - Emergency Department Evidence Based Outcome Center
 Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
Age: 0-28 Day Pathway - Emergency Department EXCLUSION CRITERIA Toxic appearing No fever Born < 37 weeks gestational age INCLUSION CRITERIA Non-toxic with temperature > 38 C (100.4 F) < 36 C (96.5 F) measured
LeMone & Burke Ch 30-32
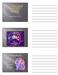 LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
LeMone & Burke Ch 30-32 2 Right side- Low oxygenation Low pressure Light workload Goes toward the lungs Left side High oxygenation Thick walled high pressure Heavier workload Carries oxygenation blood
Provide preventive counseling to parents and patients with specific endocrine conditions about:
 Endocrinology Description: The resident will become familiar with the diagnosis, management, and treatment of endocrine problems. The resident will evaluate patients with a multitude of endocrine problems,
Endocrinology Description: The resident will become familiar with the diagnosis, management, and treatment of endocrine problems. The resident will evaluate patients with a multitude of endocrine problems,
PALS Pulseless Arrest Algorithm.
 PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
PALS Pulseless Arrest Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Bradycardia Algorithm. Kleinman M E et al. Circulation 2010;122:S876-S908 PALS Tachycardia Algorithm. Kleinman M
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Clerkship Learning Activity Objectives
 Clerkship Learning Activity Objectives Inpatient Rotation 1. Conduct a pediatric history and physical examination appropriate to the nature of the visit (initial vs follow up) or complaint (complete vs
Clerkship Learning Activity Objectives Inpatient Rotation 1. Conduct a pediatric history and physical examination appropriate to the nature of the visit (initial vs follow up) or complaint (complete vs
CUMULATIVE ILLNESS RATING SCALE (CIRS)
 CUMULATIVE ILLNESS RATING SCALE (CIRS) The CIRS used in this protocol is designed to provide an assessment of recurrent or ongoing chronic comorbid conditions, classified by 14 organ systems. Using the
CUMULATIVE ILLNESS RATING SCALE (CIRS) The CIRS used in this protocol is designed to provide an assessment of recurrent or ongoing chronic comorbid conditions, classified by 14 organ systems. Using the
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating)
 Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
Appropriate Use Criteria for Initial Transthoracic Echocardiography in Outpatient Pediatric Cardiology (scores listed by Appropriate Use rating) Table 1: Appropriate indications (median score 7-9) Indication
Emergency Medicine. The University of Arizona Pediatric Residency Program. Primary Goals for Rotation
 The University of Arizona Pediatric Residency Program Primary Goals for Rotation Emergency Medicine 1. GOAL: Understand the basic principles and utilization of emergency medical services for children.
The University of Arizona Pediatric Residency Program Primary Goals for Rotation Emergency Medicine 1. GOAL: Understand the basic principles and utilization of emergency medical services for children.
Fever in the Newborn Period
 Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
Fever in the Newborn Period 1. Definitions 1 2. Overview 1 3. History and Physical Examination 2 4. Fever in Infants Less than 3 Months Old 2 a. Table 1: Rochester criteria for low risk infants 3 5. Fever
J. Van Lier Ribbink, M.D., F.A.C.S. Center for Endocrine and Pancreas Surgery at Honor Health
 J. Van Lier Ribbink, M.D., F.A.C.S. Center for Endocrine and Pancreas Surgery at Honor Health Patient Clinical Information Questionnaire 1.0 Date of Questionnaire Completion; / / 2.0 Patient Data 2.1 Name:
J. Van Lier Ribbink, M.D., F.A.C.S. Center for Endocrine and Pancreas Surgery at Honor Health Patient Clinical Information Questionnaire 1.0 Date of Questionnaire Completion; / / 2.0 Patient Data 2.1 Name:
Skills: Recall the incidence of seizures Recall the causes of seizures Describe types of seizures List signs and symptoms of seizure patients
 Medical 1 Resuscitation Describe the morbidity and mortality associated with sudden cardiac arrest List the chain of survival for sudden cardiac arrest as identified by the American Heart Association Discuss
Medical 1 Resuscitation Describe the morbidity and mortality associated with sudden cardiac arrest List the chain of survival for sudden cardiac arrest as identified by the American Heart Association Discuss
