Practitioners often encounter
|
|
|
- Jacob Freeman
- 5 years ago
- Views:
Transcription
1 Practical advice for treating newborns and toddlers. Making Lemonade out of Lyme Stan L. Block, MD, FAAP Practitioners often encounter peculiar round/oval rashes in pediatric patients, particularly during the warm-weather months. Most of these rashes are benign, and most are insect-related; but certain ones may be more ominous. In some regions of the country, tick bites are a year-round issue, but cases have been reported elsewhere in colder months, due to the frequent number of warm spells during the winter in which ticks may emerge. Besides, soon enough the warm months of lemonade-time and tick bites will be upon much of the rest of us. Thus I thought this presentation refreshing some aspects of particularly benign-looking rashes with especially problematic outcomes if left untreated would be worthwhile. As usual, these cases show that the synthesis of the history with the physical findings is critical. CASE ONE A previously healthy, white, 3-monthold girl presents to your office with a Stan L. Block, MD, FAAP, is Professor of Clinical Pediatrics, University of Louisville, and University of Kentucky, Lexington, KY; President, Kentucky Pediatric and Adult Research Inc.; and general pediatrician, Bardstown, KY. Address correspondence to Stan L. Block, MD, FAAP, via slblockmd@hotmail.com. Disclosure: Dr. Block has disclosed no relevant financial relationships. doi: / Figure 1. A 3-cm, faint, oval, maculopapular annular concentric lesion with some clearing in posterior axilla of 3-month-old girl. The small central papule, or punctum, was the site of tick bite. faint, concentric 3-cm ovoid rash in the posterior axillary area (see Figure 1) that started yesterday. During a 3-day family camping trip at a Kentucky state park the previous weekend, the mother noticed a small black dot under the baby s axilla, which she scraped off with much difficulty. The baby s immunizations are up to date, she has been healthy, and is growing well. There are no other symptoms such as pruritus, fever, cough, rhinorrhea, or fussiness. Her physical examination is otherwise unremarkable; there is no fever and the range of motion in her neck and joints is normal. The mother remarked that the day after the camping trip, she removed a lot of tiny little dark ticks from her 4-year-old son. Could a 3-month-old child develop an arthropodborne illness? CASE TWO A previously healthy, white, 4-yearold boy from central Kentucky comes to your office with a rash that has slowly progressed across his back since having a tiny tick removed. His mother reports the boy constantly plays outside on his family s farm and that the tick was on the boy s back for 7 days before it was removed 3 days prior to the office visit. Since the removal of the tick, the annular rash has enlarged to 5 cm in diameter with central clearing, a maculopapular border, and a central punctum bite (see Figure 2, page 58). The boy has been healthy recently and is fully vaccinated. He has no complaints of pruritus or pain with the rash, and also denies sore throat, other rashes, headache, fever, arthralgias, and gastrointestinal symptoms. All images courtesy of Stan L. Block, MD, FAAP. Reprinted with permission. PEDIATRIC ANNALS 42:2 FEBRUARY 2013 Healio.com/Pediatrics 57
2 The mother demands that her son be tested for Lyme disease. Is this rash alone significant enough to be diagnostic of an arthropod-borne illness? CASE THREE A previously healthy, white, 3-yearold boy from central Kentucky sustained a deer tick bite 8 days before coming to your office. When removed, the tiny tick was noted to be engorged and still barely visible. Six days later, an oval rash started on his left anterior chest region, which has now enlarged to 3 cm by 6 cm over 2 days (see Figure 3). The punctum area of the tick bite now has some mild papular urticaria as well. The rash has a mostly flat border, some central clearing, and has recently developed a tail of lymphangiitis spreading posterior-laterally. The rash is not painful and only slightly pruritic. The boy has been fully vaccinated. He denies any sore throat, arthralgias, headaches, neck stiffness, fever, other rash, or gastrointestinal symptoms. His physical examination is otherwise unremarkable. Does an arthropod-borne rash ever develop a mild lymphangiitis? Could there be two concomitant bacterial infections, such as a lymphangiitis from a concomitant staphylococcal infection? CASE FOUR A previously healthy, white, 16-yearold girl from central Kentucky frequently walks outside in the woods of her family s land. Twelve days earlier, she removed a deer tick from her left bicep area. Five days later she noticed the start of a small, red, slightly raised rash that was initially somewhat pruritic but never painful. It grew to about 5 cm by 5 cm by the time she presented to your office 2 days later. You prescribed amoxicillin 1 g twice daily for 14 days. Five days later, however, the rash had doubled in size (see Figure 4, page 59), and she now complained of arthralgias of her knees, elbows, and neck, along with mild headaches, malaise, and feeling slightly feverish. Although her initial physical examination 5 days earlier was normal, she now has some slight stiffness of her knees but no pain or redness of any joints. She is afebrile, her neck is supple, her retinal fundoscopic examination reveals no papilledema nor any blunting of the spontaneous venous pulsations, and the remainder of the examination is normal. You were not aware of any report of antibiotic resistance to amoxicillin for Borrelia, but you do know that doxycycline is the preferred antibiotic for patients aged older than 8 years because it may have a higher noncomparative cure rate than amoxicillin in adults (100% vs. 92%, respectively) and it covers anaplasmosis. 1 Because she has now developed some mild systemic symptoms but no true arthritis, you surmise that switching to doxycycline 100 mg twice daily for 14 days would be prudent. Within 48 hours, she is remarkably better, and her arthralgias and subjective fever had abated. LYME DISEASE Epidemiology Lyme disease, a zoonosis transmitted by the common deer tick (Ixodes scapularis in the East and Midwest, and Ixodes pacificus in the West), is caused by the bacterial spirochete, Borrelia burgdorferi. When ticks attach, they appear as a tiny, black or dark dot, similar to an elevated freckle on the skin. Of the 15,000 cases reported annually, 1 the mid-atlantic, northeastern, and north central areas of the United States account for 93% of all reports of Lyme disease. 2 Interestingly, Lyme disease is rarely reported south of Virginia because ticks in southeastern states and southwestern states feed mostly on reptiles rather than small mammals and deer. 2 Reptile blood is bacteriostatic for Borrelia, thus explaining the rare incidence of Lyme disease in the southern US. 1,3 However, the different species Figure 2. A white, 4-year-old boy with a 5-cm rash with concentric round rim of raised maculopapules surrounding a central punctum deer tick bite from 10 days earlier. Figure 3. A white 3-year-old boy with a 3-cm by 6-cm, oval, 2-day rash with slightly raised rim surrounding small raised papular-urticarial punctum deer tick bite from 8 days earlier. Note the faint 6-cm long, flat tail of redness spreading posteriorlaterally from rim of lesion. Slightly pruritic directly over the tick bite, the rash was not painful. of tick, Amblyomma americanum, can transmit a look-a-like spirochetal infection that can cause a similar solitary erythema migrans rash and a self-limited infection, known as southern tick-associated rash illness (STARI). 2,3 The etiology of this lesion is unknown. Kentucky is located on the same geographic latitude as Virginia, so in my opinion, all cases of solitary erythema migrans must unfortunately be considered as early Lyme disease in our region. Just like the other rarer arthropod-borne diseases, Rocky Mountain spotted fever and ehrlichiosis, the primary season for Lyme disease is April through October, with the peak during the summer months. 58 Healio.com/Pediatrics PEDIATRIC ANNALS 42:2 FEBRUARY 2013
3 The incubation period for Lyme disease is from 1 to 32 days, with a median of 11 days. Persons of any age can be infected, as we shall see in our discussion of Case One. Stages of Lyme Disease There are three distinct stages of Lyme disease. It is notable that these stages are similar to those of another rarer spirochetal infection, syphilis. 1 Stage one: early localized disease Early localized Lyme disease presents with a solitary lesion, erythema migrans, in 80% to 90% of cases. It usually starts as a central small punctum, or papule, where the tick bite originated. It then spreads centrifugally to form a large annular or sometimes ovoid lesion usually 5 cm or larger, often accompanied by central clearing. This lesion is usually painless and nonpruritic but not always. Erythema migrans can be differentiated from tick bite hypersensitivity. This usually occurs either while the tick is still attached or within 48 hours of detachment. The hypersensitivity rash typically begins to disappear within 1 to 2 days; is usually pruritic; and can sometimes become secondarily infected with Staphylococcus or Streptococcus bacteria, causing an abscess, cellulitis, lymphangiitis, or reactive lymphadenitis. Case Three is characteristic of a typical lymphangiitis from a tick bite. Lyme disease does not cause these types of skin manifestations by itself. The solitary erythema migrans rash of Lyme will typically begin to spread about 5 to 7 days after tick detachment or removal, and the untreated rash will last about 3 weeks. But be aware that about 65% of patients will also develop nonspecific virus-like symptoms, such as malaise, fatigue, neck pains, headache, migratory arthralgias, chills, and fever. 3 However, objective physical findings of frank arthritis are not present during stage one, when a diagnosis is made on clinical Figure 4. A rapidly spreading 10-cm, concentric, nonpruritic, round rash with raised maculopapular rash border, clearing around the punctum in a white, 16-year-old girl. The patient sustained a tick bite 12 days earlier. Despite amoxicillin therapy, the rash enlarged and the patient developed some systemic symptoms and arthralgias. grounds alone. Early treatment nearly always aborts the development of later stages of Lyme disease. Stage two: early disseminated disease If early Lyme disease is left untreated, as it is in about 10% to 20% of children, it will evolve into the secondary disseminated stage. 2,3 This stage most commonly manifests several weeks, or occasionally several days, after the tick bite as multiple lesions of smaller erythema migrans. Other rare findings during this stage include carditis manifested as mild to severe atrioventricular block, cranial nerve palsies (particularly of the 7th cranial nerve facial palsy), ophthalmic conditions, and a subacute lymphocytic meningitis. Systemic symptoms are also much more prevalent and intense at this stage, and include fever, headache, myalgia, arthralgia, and fatigue. 2,3 Stage three: late disease This very rarely observed stage is characterized most commonly by a large-joint, pauci-articular arthritis, usually in the knees. Peripheral neuropathy and central nervous system manifestations are rarely ever seen in children. 2 DIAGNOSTIC TESTS The early stage of Lyme disease is diagnosed strictly on the clinical observation of a solitary erythema migrans lesion of at least 5 cm, with or without a history of a deer tick attachment. Borrelia antibody titers are not detectable in most people within the first 4 weeks following the appearance of erythema migrans. 4 Once treated appropriately, most patients will never develop antibodies. The development of antibodies after the treatment of early stage Lyme disease, however, does not indicate therapy has failed. 5 The biopsy and culture of the skin lesion is not recommended due to the difficulty with growing the culture from the specimen. The diagnoses of early disseminated disease and late disease should be made on the basis of both clinical appearance PEDIATRIC ANNALS 42:2 FEBRUARY 2013 Healio.com/Pediatrics 59
4 and serologic confirmation. Nearly all patients with later stage Lyme disease will have detectable antibodies. This requires a two-step process for most laboratories. 1,2 The first test consists of either an enzyme immunoassay or an immunoflourescent antibody assay. Only if this test is positive or equivocal should a Western immunoblot test be performed for confirmation. TREATMENT OF EARLY STAGE LYME DISEASE Early Localized Disease According to the American Academy of Pediatrics (AAP) 2012 Red Book, Antimicrobial therapy for nonspecific symptoms or for asymptomatic seropositivity is discouraged. 2 Doxycycline is the preferred antibiotic for those older than 8 years; whereas amoxicillin is recommended for younger patients. Cefuroxime is recommended for those allergic to penicillin; note that first-generation cephalosporins are not effective for B. burgdorferi. Azithromycin is less effective and is not recommended as firstline therapy. Duration of beta-lactam and doxycycline therapy should be for at least 14 to 21 days. Erythema migrans usually resolves within a few days of antibiotic therapy, but other low-grade signs and symptoms may persist for weeks to months despite successful therapy. In fact, fatigue and arthralgias may persist for up to 3 months in 25% of adequately treated patients; 10% of adults do not respond to therapy. 3 For further specific antibiotic dosing regimens and for management of early disseminated disease and late disease, refer to the 2012 AAP Red Book. 2 DISCUSSION OF CASES Each of the four cases presented a peculiar diagnostic aspect of Lyme disease. All four cases were treated with appropriate doses (50 mg/kg/day to 90 mg/kg/ day, with a maximum dose of 1 g) of amoxicillin twice daily, and each patient responded rapidly and uneventfully to therapy except for Case Four. Case One You were perplexed by the very young age of this patient with an early erythema migrans lesion. But all other indicators pointed to the Lyme diagnosis, including the deer tick removal, the timing of the rash s appearance several days later and not immediately (tick hypersensitivity), the punctum, the central clearing, and the raised border. The down-side of nontreatment was too consequential because of high morbidity, and the risk of antibiotic treatment was miniscule. Case Two Despite your objections and clear explanations to the child s mother that serologic titers were unnecessary for early localized Lyme disease, at her insistence, you obtained the serology. The acute Borrelia titer results were negative, and the child did fine, with total resolution of the rash in a few days. Case Three Despite a fairly typical solitary ovoid erythema migrans lesion, this child most likely had a secondary bacterial infection of the tick bite with a mild ascending lymphangiitis from either a staphylococcal or streptococcal infection. In hindsight, amoxicillin clavulanate or cefuroxime may have been better choices because of their methicillin-sensitive Staphylococcus aureus coverage. The most important factor in atypical cases is the careful follow-up over the next several days. Case Four You initially thought that the continued spread and new onset of systemic symptoms 5 days into therapy most likely indicated a failure while on amoxicillin therapy. Up to 10% of adults do not respond to initial antibiotic therapy. However, one caveat: Could she have possibly experienced a Jarisch-Herxheimer like immunologic reaction from the lysis of the spirochetes treated with penicillin? This reaction is reported in 15% of patients. It typically consists of fever and chills within 24 hours of antibiotic therapy, and is associated with more intense systemic symptoms and an increase in size and intensity of erythema of the skin lesion. The rash will eventually resolve in 7 to 14 days. 2 Thus, in this case, a 10% antibiotic failure rate must be contrasted with a 15% Jarisch-Herxheimer reaction rate. Because this rash worsened despite 5 days of amoxicillin therapy, you surmise this patient was an antibiotic failure. For initial antibiotic failures with early stages of Lyme, a repeat course of a different appropriate oral antibiotic for 14 to 21 days is recommended. Finally, for early disseminated Lyme disease, appropriate oral antibiotics are still considered first-line therapy. Oral doxycycline for 21 days has been shown to be as comparably effective as intravenous ceftriaxone for the same duration. Hospitalization and intravenous therapy with ceftriaxone is only indicated for symptomatic patients with meningitis, carditis, second- or third-degree atrioventricular (AV) block, or first-degree AV block with a very prolonged PR interval ( 300 milliseconds). REFERENCES 1. Feigin RD, Cherry J, Demmler-Harrison GJ, Kaplan SL (eds). Feigin and Cherry s Textbook of Pediatric Infectious Diseases. 6th edition. Philadelphia, PA: Saunders Elsevier; AAP Committee on Infectious Diseases; Pickering LK, Baker CJ, Kimberlin DW, Long SS (eds). Red Book: Report of the Committee on Infectious Diseases (Red Book Report of the Committee on Infectious Diseases). 29th edition. Elk Grove Village, IL. American Academy of Pediatrics; Wormser GP. Lyme disease. In: Goldman L, Schafer AI (eds). Goldman s Cecil Medicine. 24th edition. Philadelphia, PA: Saunders Elsevier; Tibbles CD, Edlow JA. Does this patient have erythema migrans? JAMA. 2007;297: Steere AC, McHugh G, Damle N, Sikand VK. Prospective study of serologic tests for Lyme disease. Clin Infect Dis. 2008;47(2): Healio.com/Pediatrics PEDIATRIC ANNALS 42:2 FEBRUARY 2013
5 Reproduced with permission of the copyright owner. Further reproduction prohibited without permission.
LYME DISEASE Last revised May 30, 2012
 Wisconsin Department of Health Services Division of Public Health Communicable Disease Surveillance Guideline LYME DISEASE Last revised May 30, 2012 I. IDENTIFICATION A. CLINICAL DESCRIPTION: A multi-systemic
Wisconsin Department of Health Services Division of Public Health Communicable Disease Surveillance Guideline LYME DISEASE Last revised May 30, 2012 I. IDENTIFICATION A. CLINICAL DESCRIPTION: A multi-systemic
Update on Lyme Disease Surveillance in Wisconsin for Providers and Laboratories
 Update on Lyme Disease Surveillance in Wisconsin for Providers and Laboratories Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/14 Protecting and promoting the
Update on Lyme Disease Surveillance in Wisconsin for Providers and Laboratories Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/14 Protecting and promoting the
Lyme Disease, an Infectious Diseases Perspective
 Lyme Disease, an Infectious Diseases Perspective Lyme: Pretest 1. The pathognomonic finding of Lyme disease is: 1. An indurated lesion, measuring ~ 2 cm in diameter with a central, necrotic eschar. 2.
Lyme Disease, an Infectious Diseases Perspective Lyme: Pretest 1. The pathognomonic finding of Lyme disease is: 1. An indurated lesion, measuring ~ 2 cm in diameter with a central, necrotic eschar. 2.
Tick Talk: What s new in Lyme Disease. May 5 th, 2017 Cristina Baker, M.D., M.P.H.
 Tick Talk: What s new in Lyme Disease May 5 th, 2017 Cristina Baker, M.D., M.P.H. Dr. Baker indicated no potential conflict of interest to this presentation. She does not intend to discuss any unapproved/investigative
Tick Talk: What s new in Lyme Disease May 5 th, 2017 Cristina Baker, M.D., M.P.H. Dr. Baker indicated no potential conflict of interest to this presentation. She does not intend to discuss any unapproved/investigative
Lyme disease Overview
 Infectious Disease Epidemiology BMTRY 713 (A. Selassie, Dr.PH) Lecture 22 Lyme Disease Learning Objectives 1. Describe the agent and vector of Lyme Disease 2. Identify the geographic and temporal patterns
Infectious Disease Epidemiology BMTRY 713 (A. Selassie, Dr.PH) Lecture 22 Lyme Disease Learning Objectives 1. Describe the agent and vector of Lyme Disease 2. Identify the geographic and temporal patterns
Lyme Disease. 1. DISEASE REPORTING A. Purpose of Reporting and Surveillance
 1. DISEASE REPORTING A. Purpose of Reporting and Surveillance Lyme Disease 1. To determine the incidence of Lyme disease, the degree of endemicity, and potential risk of contracting Lyme disease in Washington
1. DISEASE REPORTING A. Purpose of Reporting and Surveillance Lyme Disease 1. To determine the incidence of Lyme disease, the degree of endemicity, and potential risk of contracting Lyme disease in Washington
STATEMENT FOR MANAGING LYME DISEASE IN NOVA SCOTIA
 INFECTIOUS DISEASES EXPERT GROUP (IDEG) DEPARTMENT OF HEALTH AND WELLNESS STATEMENT FOR MANAGING LYME DISEASE IN NOVA SCOTIA Executive Summary: In 2016, the Public Health Agency of Canada (PHAC) modified
INFECTIOUS DISEASES EXPERT GROUP (IDEG) DEPARTMENT OF HEALTH AND WELLNESS STATEMENT FOR MANAGING LYME DISEASE IN NOVA SCOTIA Executive Summary: In 2016, the Public Health Agency of Canada (PHAC) modified
Lyme disease Overview
 Infectious Disease Epidemiology BMTRY 713 (A. Selassie, DrPH) Lecture 21 Lyme Disease Learning Objectives 1. Describe the agent and vector of Lyme Disease 2. Identify the geographic and temporal patterns
Infectious Disease Epidemiology BMTRY 713 (A. Selassie, DrPH) Lecture 21 Lyme Disease Learning Objectives 1. Describe the agent and vector of Lyme Disease 2. Identify the geographic and temporal patterns
Technical Bulletin No. 121
 CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 121 January 31, 2014 Lyme Blot, IgG and IgM - Now Performed at CPAL Contact: J. Matthew Groeller, 717.851.1416 Operations Manager, Clinical
CPAL Central Pennsylvania Alliance Laboratory Technical Bulletin No. 121 January 31, 2014 Lyme Blot, IgG and IgM - Now Performed at CPAL Contact: J. Matthew Groeller, 717.851.1416 Operations Manager, Clinical
A Patient s Guide to Lyme Disease
 A Patient s Guide to Lyme Disease 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
A Patient s Guide to Lyme Disease 2350 Royal Boulevard Suite 200 Elgin, IL 60123 Phone: 847.931.5300 Fax: 847.931.9072 DISCLAIMER: The information in this booklet is compiled from a variety of sources.
Lyme Disease. By Farrah Jangda
 Lyme Disease By Farrah Jangda Disease Name: Lyme Disease Lyme disease is a common tick-borne bacterial infection transmitted from the bite of a tick in United States and Europe (2). It is caused by the
Lyme Disease By Farrah Jangda Disease Name: Lyme Disease Lyme disease is a common tick-borne bacterial infection transmitted from the bite of a tick in United States and Europe (2). It is caused by the
Infectious Diseases Expert Group (IDEG) Department of Health and Wellness. Statement for Managing Lyme Disease in Nova Scotia
 Infectious Diseases Expert Group (IDEG) Department of Health and Wellness Statement for Managing Lyme Disease in Nova Scotia 2018 Executive Summary: In 2016, the Public Health Agency of Canada (PHAC) modified
Infectious Diseases Expert Group (IDEG) Department of Health and Wellness Statement for Managing Lyme Disease in Nova Scotia 2018 Executive Summary: In 2016, the Public Health Agency of Canada (PHAC) modified
SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA. Lin Li, MD August, 2012
 SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA Lin Li, MD August, 2012 Case 1 32 year old male working in Arizona; on leave back in Singapore Presented to hospital A for fever x (7-10)
SELECTED INFECTIONS ACQUIRED DURING TRAVELLING IN NORTH AMERICA Lin Li, MD August, 2012 Case 1 32 year old male working in Arizona; on leave back in Singapore Presented to hospital A for fever x (7-10)
A Patient s Guide to Lyme Disease
 A Patient s Guide to Lyme Disease Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
A Patient s Guide to Lyme Disease Suite 11-13/14/15 Mount Elizabeth Medical Center 3 Mount Elizabeth Singapore, 228510 Phone: (65) 6738 2628 Fax: (65) 6738 2629 DISCLAIMER: The information in this booklet
Alabama Medicaid Pharmacist
 Published Quarterly by Health Information Designs, LLC, Summer 2013 edition A Service of Alabama Medicaid PDL Update Effective July 1, 2013, the Alabama Medicaid Agency will update the Preferred Drug List
Published Quarterly by Health Information Designs, LLC, Summer 2013 edition A Service of Alabama Medicaid PDL Update Effective July 1, 2013, the Alabama Medicaid Agency will update the Preferred Drug List
Lyme Disease Surveillance in Wisconsin Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/2014
 Lyme Disease Surveillance in Wisconsin Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/2014 Protecting and promoting the health and safety of the people of Wisconsin
Lyme Disease Surveillance in Wisconsin Christopher Steward Division of Public Health Wisconsin Department of Health Services 04/10/2014 Protecting and promoting the health and safety of the people of Wisconsin
My Case Study Solution
 My Case Study Solution By Chiara Corey Amy and John, recent newlyweds and hiking enthusiasts from California, completed a backpacking road trip across the United States for their honeymoon. They started
My Case Study Solution By Chiara Corey Amy and John, recent newlyweds and hiking enthusiasts from California, completed a backpacking road trip across the United States for their honeymoon. They started
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Feder HM Jr, Johnson BJB, O Connell S, et al. A critical appraisal
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Feder HM Jr, Johnson BJB, O Connell S, et al. A critical appraisal
Not currently the time of year, but spring is around the corner. Seems to be in the news every other week. Task forces being formed.
 1 2 3 Not currently the time of year, but spring is around the corner. Seems to be in the news every other week. Task forces being formed. Elizabeth May has been a big proponent. Avril Lavigne has come
1 2 3 Not currently the time of year, but spring is around the corner. Seems to be in the news every other week. Task forces being formed. Elizabeth May has been a big proponent. Avril Lavigne has come
Of Mice, Men and Mosquitoes
 Climate and Health Summit September 20, 2015 Of Mice, Men and Mosquitoes Vector-Borne Infections in a Changing Climate Samantha Ahdoot, MD, FAAP Assistant Professor of Pediatrics Virginia Commonwealth
Climate and Health Summit September 20, 2015 Of Mice, Men and Mosquitoes Vector-Borne Infections in a Changing Climate Samantha Ahdoot, MD, FAAP Assistant Professor of Pediatrics Virginia Commonwealth
During this current week of summer,
 Practical advice for treating newborns and toddlers. Spots and Lumps: Treacherous Tick-Borne Problems Stan L. Block, MD, FAAP During this current week of summer, you are seeing your fifth patient with
Practical advice for treating newborns and toddlers. Spots and Lumps: Treacherous Tick-Borne Problems Stan L. Block, MD, FAAP During this current week of summer, you are seeing your fifth patient with
Corporate Medical Policy
 Corporate Medical Policy Intravenous Antibiotic Therapy for Lyme Disease File Name: intravenous_antibiotic_therapy_for_lyme_disease Origination: 3/2006 Last CAP Review: 2/2017 Next CAP Review: 2/2018 Last
Corporate Medical Policy Intravenous Antibiotic Therapy for Lyme Disease File Name: intravenous_antibiotic_therapy_for_lyme_disease Origination: 3/2006 Last CAP Review: 2/2017 Next CAP Review: 2/2018 Last
Recognizing the Clinical and Laboratory Presentation of Human Granulocytic Anaplasmosis
 Recognizing the Clinical and Laboratory Presentation of Human Granulocytic Anaplasmosis NICOLE FENNIMORE, 3 RD YEAR MEDICAL STUDENT UNIVERSITY OF WISCONSIN SCHOOL OF MEDICINE AND PUBLIC HEALTH FRIDAY,
Recognizing the Clinical and Laboratory Presentation of Human Granulocytic Anaplasmosis NICOLE FENNIMORE, 3 RD YEAR MEDICAL STUDENT UNIVERSITY OF WISCONSIN SCHOOL OF MEDICINE AND PUBLIC HEALTH FRIDAY,
Tick-borne Infections
 Tick-borne Infections Wei Li Adeline Koay, MBBS, MSc, FAAP Attending, Infectious Diseases Children s National Medical Center, Washington DC Kari Simonsen, MD, FAAP Professor and Vice Chair of Pediatrics
Tick-borne Infections Wei Li Adeline Koay, MBBS, MSc, FAAP Attending, Infectious Diseases Children s National Medical Center, Washington DC Kari Simonsen, MD, FAAP Professor and Vice Chair of Pediatrics
Alberta Health Public Health Notifiable Disease Management Guidelines January 2013
 January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
January 2013 Rickettsial Infections Revision Dates Case Definition Reporting Requirements Remainder of the Guideline (i.e., Etiology to References sections inclusive) January 2013 January 2013 December
Lyme disease conference
 Lyme disease conference Epidemiology of Lyme in England and Wales Robert Smith, Public Health Wales 9 October 213 Lyme disease in England and Wales Dr Robert Smith Health Protection Division Public Health
Lyme disease conference Epidemiology of Lyme in England and Wales Robert Smith, Public Health Wales 9 October 213 Lyme disease in England and Wales Dr Robert Smith Health Protection Division Public Health
Lyme Disease. Abstract Lyme disease is a vector borne infection primarily transmitted by Ixodes ticks and. Special Issue
 Special Issue Lyme Disease Min Geol Lee, M.DYoung Hun Cho, M.D. Department of Dermatology Yonsei University College of Medicine, Severance Hospital Email : mglee@yumc.yonsei.ac.krsalute@yumc.yonsei.ac.kr
Special Issue Lyme Disease Min Geol Lee, M.DYoung Hun Cho, M.D. Department of Dermatology Yonsei University College of Medicine, Severance Hospital Email : mglee@yumc.yonsei.ac.krsalute@yumc.yonsei.ac.kr
Case Report Early Disseminated Lyme Disease with Carditis Complicated by Posttreatment Lyme Disease Syndrome
 Hindawi Case Reports in Infectious Diseases Volume 2017, Article ID 5847156, 4 pages https://doi.org/10.1155/2017/5847156 Case Report Early Disseminated Lyme Disease with Carditis Complicated by Posttreatment
Hindawi Case Reports in Infectious Diseases Volume 2017, Article ID 5847156, 4 pages https://doi.org/10.1155/2017/5847156 Case Report Early Disseminated Lyme Disease with Carditis Complicated by Posttreatment
Peter J. Weina, PhD, MD, FACP, FIDSA. Colonel, Medical Corps, US Army Deputy Commander Walter Reed Army Institute of Research
 Peter J. Weina, PhD, MD, FACP, FIDSA Colonel, Medical Corps, US Army Deputy Commander Walter Reed Army Institute of Research Background Most common vector-borne disease in U.S. First described in Lyme,
Peter J. Weina, PhD, MD, FACP, FIDSA Colonel, Medical Corps, US Army Deputy Commander Walter Reed Army Institute of Research Background Most common vector-borne disease in U.S. First described in Lyme,
Public Statement: Medical Policy Statement:
 Medical Policy Title: Lyme Disease, Intravenous Antibiotic Therapy ARBenefits Approval: 10/19/2011 and Associated Diagnostic Testing Effective Date: 01/01/2012 Document: ARB0235 Revision Date: Code(s):
Medical Policy Title: Lyme Disease, Intravenous Antibiotic Therapy ARBenefits Approval: 10/19/2011 and Associated Diagnostic Testing Effective Date: 01/01/2012 Document: ARB0235 Revision Date: Code(s):
Ticks & Tickborne Diseases of Minnesota. Vectorborne Diseases Unit Last Updated February 16, 2018
 Ticks & Tickborne Diseases of Minnesota Vectorborne Diseases Unit Last Updated February 16, 2018 What is a tickborne disease and why should you care about it? People can get a tickborne disease when they
Ticks & Tickborne Diseases of Minnesota Vectorborne Diseases Unit Last Updated February 16, 2018 What is a tickborne disease and why should you care about it? People can get a tickborne disease when they
Seroprevalence of Babesia microti in Individuals with Lyme Disease. Sabino R. Curcio, M.S, MLS(ASCP)
 Seroprevalence of Babesia microti in Individuals with Lyme Disease Sabino R. Curcio, M.S, MLS(ASCP) Lyme Disease Most common vectorborne illness in the United States Caused by the tick-transmitted spirochete
Seroprevalence of Babesia microti in Individuals with Lyme Disease Sabino R. Curcio, M.S, MLS(ASCP) Lyme Disease Most common vectorborne illness in the United States Caused by the tick-transmitted spirochete
THIS IS AN OFFICIAL NH HEALTH ALERT
 THIS IS AN OFFICIAL NH HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@dhhs.nh.gov June 01, 2017, 1100 EDT (11:00 AM EDT) NH-HAN 20170601 Emerging Tickborne Diseases in New Hampshire
THIS IS AN OFFICIAL NH HEALTH ALERT Distributed by the NH Health Alert Network Health.Alert@dhhs.nh.gov June 01, 2017, 1100 EDT (11:00 AM EDT) NH-HAN 20170601 Emerging Tickborne Diseases in New Hampshire
LYME DISEASE. Page. Lyme Disease: Medical Policy (Effective 10/01/2013)
 MEDICAL POLICY LYME DISEASE Policy Number: 2013T0351K Effective Date: October 1, 2013 Table of Contents COVERAGE RATIONALE... BENEFIT CONSIDERATIONS... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND
MEDICAL POLICY LYME DISEASE Policy Number: 2013T0351K Effective Date: October 1, 2013 Table of Contents COVERAGE RATIONALE... BENEFIT CONSIDERATIONS... BACKGROUND... CLINICAL EVIDENCE... U.S. FOOD AND
Unroofing a Rare Toddler Rash
 Practical advice for treating newborns and toddlers. Unroofing a Rare Toddler Rash Stan L. Block, MD, FAAP CASE SCENARIOS Case #1 A 24-month-old male presents with a history of a 2-day rash that his mother
Practical advice for treating newborns and toddlers. Unroofing a Rare Toddler Rash Stan L. Block, MD, FAAP CASE SCENARIOS Case #1 A 24-month-old male presents with a history of a 2-day rash that his mother
Rheumatic Fever And Post-streptococcal Reactive Arthritis
 www.printo.it/pediatric-rheumatology/gb/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 1. WHAT IS RHEUMATIC FEVER 1.1 What is it? Rheumatic fever is a disease caused by
www.printo.it/pediatric-rheumatology/gb/intro Rheumatic Fever And Post-streptococcal Reactive Arthritis Version of 2016 1. WHAT IS RHEUMATIC FEVER 1.1 What is it? Rheumatic fever is a disease caused by
Insect Bites and Stings Most are benign and require no medical intervention
 Insect Bites and Stings Most are benign and require no medical intervention Signs that a severe allergic reaction has occurred Swelling Difficulty swallowing or speaking Chest tightness, wheezing or difficulty
Insect Bites and Stings Most are benign and require no medical intervention Signs that a severe allergic reaction has occurred Swelling Difficulty swallowing or speaking Chest tightness, wheezing or difficulty
T H E F A C T S T H E C H A L L E N G E
 Lyme Disease THE FACTS THE CHALLENGE U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Institute of Allergy and Infectious Diseases National Institute of Arthritis and
Lyme Disease THE FACTS THE CHALLENGE U.S. DEPARTMENT OF HEALTH AND HUMAN SERVICES National Institutes of Health National Institute of Allergy and Infectious Diseases National Institute of Arthritis and
Dermclinic
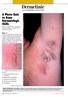 Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
Dermclinic /Dermclinic A Photo Quiz to Hone Dermatologic Skills DAVID L. KAPLAN, MD Series Editor University of Missouri Kansas City, University of Kansas Case 1: Upon his return from a summer visit to
Chlamydia-Mycoplasma-Legionella Groups
 Chlamydia-Mycoplasma-Legionella Groups Chlamydia group slide #4: Characteristics: A type of bacteria associated with respiratory tract infection obligate intracellular small pathogen (like viruses) more
Chlamydia-Mycoplasma-Legionella Groups Chlamydia group slide #4: Characteristics: A type of bacteria associated with respiratory tract infection obligate intracellular small pathogen (like viruses) more
Lyme disease is an uncommon, but not
 Continuing Medical Education Lyme Disease in Women: Recognition, Treatment, and Prevention Jonathan L. Temte, MD, PhD Lyme disease is easily treated, but the elusive symptoms require a high index of suspicion
Continuing Medical Education Lyme Disease in Women: Recognition, Treatment, and Prevention Jonathan L. Temte, MD, PhD Lyme disease is easily treated, but the elusive symptoms require a high index of suspicion
NO DISCLOSURES. Lyme Disease Convention and Controversies. Willie Burgdorfer, Ph.D. ( ) RM Lab in Hamilton, MT 1/20/2017
 Lyme Disease Convention and Controversies Richard A. Jacobs, M.D., PhD. NO DISCLOSURES Willie Burgdorfer, Ph.D. (1925 2014) RM Lab in Hamilton, MT Polly Murray who first reported an outbreak of arthritis
Lyme Disease Convention and Controversies Richard A. Jacobs, M.D., PhD. NO DISCLOSURES Willie Burgdorfer, Ph.D. (1925 2014) RM Lab in Hamilton, MT Polly Murray who first reported an outbreak of arthritis
Lyme Disease Diagnosis and Treatment
 Last Review Date: October 13, 2017 Number: MG.MM.ME.57a Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
Last Review Date: October 13, 2017 Number: MG.MM.ME.57a Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or primary care provider must submit to EmblemHealth
The new england journal of medicine. The Clinical Problem
 The new england journal of medicine clinical practice Caren G. Solomon, M.D., M.P.H., Editor Lyme Disease Eugene D. Shapiro, M.D. This Journal feature begins with a case vignette highlighting a common
The new england journal of medicine clinical practice Caren G. Solomon, M.D., M.P.H., Editor Lyme Disease Eugene D. Shapiro, M.D. This Journal feature begins with a case vignette highlighting a common
Tickborne Disease Case Investigations
 Massachusetts Department of Public Health Bureau of Infectious Disease and Laboratory Sciences Tickborne Disease Case Investigations Anthony Osinski, MPH May 31, 2018 Factors Associated with Increasing
Massachusetts Department of Public Health Bureau of Infectious Disease and Laboratory Sciences Tickborne Disease Case Investigations Anthony Osinski, MPH May 31, 2018 Factors Associated with Increasing
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Culex larvae found collecting in standing water Image by CDC/James Gathany - License: Public Domain. Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County Culex larvae found collecting in standing water Image by CDC/James Gathany - License: Public Domain. Maricopa County Department of Public Health Office of Epidemiology
Announcements. Please mute your phones and DO NOT place us on hold. Press *6 to mute your phone.
 Announcements Register for the Epi-Tech Trainings: 1. Log-on or Request log-on ID/password: https://tiny.army.mil/r/zb8a/cme 2. Register for Epi-Tech Surveillance Training: https://tiny.army.mil/r/dvrgo/epitechfy14
Announcements Register for the Epi-Tech Trainings: 1. Log-on or Request log-on ID/password: https://tiny.army.mil/r/zb8a/cme 2. Register for Epi-Tech Surveillance Training: https://tiny.army.mil/r/dvrgo/epitechfy14
The New England Journal of Medicine LYME DISEASE IN CHILDREN IN SOUTHEASTERN CONNECTICUT. Study Population
 LYME DISEASE IN CHILDREN IN SOUTHEASTERN CONNECTICUT MICHAEL A. GERBER, M.D., EUGENE D. SHAPIRO, M.D., GEORGINE S. BURKE, PH.D., VALERIE J. PARCELLS, R.N., AND GILLIAN L. BELL, B.L.T., FOR THE PEDIATRIC
LYME DISEASE IN CHILDREN IN SOUTHEASTERN CONNECTICUT MICHAEL A. GERBER, M.D., EUGENE D. SHAPIRO, M.D., GEORGINE S. BURKE, PH.D., VALERIE J. PARCELLS, R.N., AND GILLIAN L. BELL, B.L.T., FOR THE PEDIATRIC
ABACAVIR HYPERSENSITIVITY REACTION
 ABACAVIR HYPERSENSITIVITY REACTION Key Risk Minimisation Points: Abacavir Hypersensitivity Reaction (HSR) Abacavir is associated with a risk for hypersensitivity reactions (HSR) characterised by fever
ABACAVIR HYPERSENSITIVITY REACTION Key Risk Minimisation Points: Abacavir Hypersensitivity Reaction (HSR) Abacavir is associated with a risk for hypersensitivity reactions (HSR) characterised by fever
Lyme disease is a bacterial infection. Even if successfully treated, a person may become reinfected if bitten later by another infected tick.
 Wappingers Central School District Lyme Disease & Tick Awareness Lyme Disease Updated: October 2011 What is Lyme disease? Lyme disease is caused by bacteria transmitted by the deer tick (Ixodes scapularis).
Wappingers Central School District Lyme Disease & Tick Awareness Lyme Disease Updated: October 2011 What is Lyme disease? Lyme disease is caused by bacteria transmitted by the deer tick (Ixodes scapularis).
Persistence of Immunoglobulin M or Immunoglobulin G Antibody Responses to Borrelia burgdorferi Years after Active Lyme Disease
 MAJOR ARTICLE Persistence of Immunoglobulin M or Immunoglobulin G Antibody Responses to Borrelia burgdorferi 10 20 Years after Active Lyme Disease Robert A. Kalish, 1 Gail McHugh, 1 John Granquist, 1 Barry
MAJOR ARTICLE Persistence of Immunoglobulin M or Immunoglobulin G Antibody Responses to Borrelia burgdorferi 10 20 Years after Active Lyme Disease Robert A. Kalish, 1 Gail McHugh, 1 John Granquist, 1 Barry
Do you think you have Lyme Disease? Fill out The Horowitz MSIDS Questionnaire (HMQ)
 Do you think you have Lyme Disease? Fill out The Horowitz MSIDS Questionnaire (HMQ) Answer the following questions as honestly as possible. Think about how you have been feeling over the previous month
Do you think you have Lyme Disease? Fill out The Horowitz MSIDS Questionnaire (HMQ) Answer the following questions as honestly as possible. Think about how you have been feeling over the previous month
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 21 January 1, 29 December 31, 29 Commentary West Nile virus (WNV) is a mosquito-borne virus that
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
West Nile Virus in Maricopa County Maricopa County Department of Public Health Office of Epidemiology July 2009 January 1, 2008 December 31, 2008 Commentary West Nile virus (WNV) is a mosquito-borne virus
Tickborne Diseases: Challenges and Controversies
 Tickborne Diseases: Challenges and Controversies JENNIFER HANRAHAN, D.O. ASSOCIATE PROFESSOR, CWRU DIRECTOR OF INFECTION PREVENTION METROHEALTH MEDICAL CENTER Disclosures I have been on Advisory Boards
Tickborne Diseases: Challenges and Controversies JENNIFER HANRAHAN, D.O. ASSOCIATE PROFESSOR, CWRU DIRECTOR OF INFECTION PREVENTION METROHEALTH MEDICAL CENTER Disclosures I have been on Advisory Boards
RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS
 www.pediatric-rheumathology.printo.it RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS What is it? Rheumatic fever has been defined as a disease triggered by infection caused by streptococcus.
www.pediatric-rheumathology.printo.it RHEUMATIC FEVER AND POST-STREPTOCOCCAL REACTIVE ARTHRITIS What is it? Rheumatic fever has been defined as a disease triggered by infection caused by streptococcus.
Medical Review Criteria Lyme/Tick-Borne Diseases: Use of Parenteral Antibiotics
 Medical Review Criteria Lyme/Tick-Borne Diseases: Use of Parenteral Antibiotics Subject: Lyme/Tick-Borne Diseases: Use of Parenteral Antibiotics Authorization: Prior authorization is required for ALL parenteral
Medical Review Criteria Lyme/Tick-Borne Diseases: Use of Parenteral Antibiotics Subject: Lyme/Tick-Borne Diseases: Use of Parenteral Antibiotics Authorization: Prior authorization is required for ALL parenteral
West Nile Virus in Maricopa County
 West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
West Nile Virus in Maricopa County A Culex quinquefasciatus mosquito on a human finger. Image by James Gathany/ CDC gov/ public domain Maricopa County Department of Public Health Office of Epidemiology
WHAT WE KNOW ABOUT ANAPLASMOSIS AND BORRELIOSIS AND WHAT WE DO NOT A. Rick Alleman, DVM, PhD, DACVP, DABVP
 WHAT WE KNOW ABOUT ANAPLASMOSIS AND BORRELIOSIS AND WHAT WE DO NOT A. Rick Alleman, DVM, PhD, DACVP, DABVP Anaplasma phagocytophilum Anaplasma phagocytophilum is an intracellular, gram-negative bacterium
WHAT WE KNOW ABOUT ANAPLASMOSIS AND BORRELIOSIS AND WHAT WE DO NOT A. Rick Alleman, DVM, PhD, DACVP, DABVP Anaplasma phagocytophilum Anaplasma phagocytophilum is an intracellular, gram-negative bacterium
NO DISCLOSURES. Lyme Disease. Outline. Case. Case. Case 2/10/2014
 Lyme Disease Richard A. Jacobs, MD, PhD. NO DISCLOSURES Outline History of Lyme disease How the new disease was discovered How the etiology of the disease was discovered Clinical manifestations Diagnosis
Lyme Disease Richard A. Jacobs, MD, PhD. NO DISCLOSURES Outline History of Lyme disease How the new disease was discovered How the etiology of the disease was discovered Clinical manifestations Diagnosis
Monthly Safety Meeting
 Monthly Safety Meeting 26 June 2014 Please sign roster Before we begin Please sign the safety meeting roster Used to log safety currency in eservices Safety Officer logs currency Only other means (not
Monthly Safety Meeting 26 June 2014 Please sign roster Before we begin Please sign the safety meeting roster Used to log safety currency in eservices Safety Officer logs currency Only other means (not
Sickness and Illness Policy
 Sickness and Illness Policy Children should not be at nursery if they are unwell. If your child becomes unable to stay at nursery, a member of staff will contact the parent or carer, asking them to come
Sickness and Illness Policy Children should not be at nursery if they are unwell. If your child becomes unable to stay at nursery, a member of staff will contact the parent or carer, asking them to come
Diagnostic Dilemmas Between Viral and Bacterial Tonsillitis
 Diagnostic Dilemmas Between Viral and Bacterial Tonsillitis Round Table Moderator: Panelists: Edigar R. de Almeida Luiza Endo, Maria Helena Kiss, Renata di Francesco and Sílvio Luiz Zuquim Edigar R. de
Diagnostic Dilemmas Between Viral and Bacterial Tonsillitis Round Table Moderator: Panelists: Edigar R. de Almeida Luiza Endo, Maria Helena Kiss, Renata di Francesco and Sílvio Luiz Zuquim Edigar R. de
Necrotizing Granulomatous Hepatitis as an Unusual Manifestation of Lyme Disease
 Dig Dis Sci (2007) 52:2629 2632 DOI 10.1007/s10620-006-9405-9 Necrotizing Granulomatous Hepatitis as an Unusual Manifestation of Lyme Disease Antonela C. Zanchi Alan R. Gingold Neil D. Theise Albert D.
Dig Dis Sci (2007) 52:2629 2632 DOI 10.1007/s10620-006-9405-9 Necrotizing Granulomatous Hepatitis as an Unusual Manifestation of Lyme Disease Antonela C. Zanchi Alan R. Gingold Neil D. Theise Albert D.
Journal of Pediatric Sciences
 Journal of Pediatric Sciences Buccal Cellulitis in 3 Infants Martin W Stallings Journal of Pediatric Sciences 2016;8:e252 http://dx.doi.org/10.17334/jps.78460 How to cite this article: Stallings MW. Buccal
Journal of Pediatric Sciences Buccal Cellulitis in 3 Infants Martin W Stallings Journal of Pediatric Sciences 2016;8:e252 http://dx.doi.org/10.17334/jps.78460 How to cite this article: Stallings MW. Buccal
- Mycoplasma and Ureaplasma. - Rickettsia
 - Mycoplasma and Ureaplasma - Rickettsia Mycoplasma and Ureaplasma Family: Mycoplasmataceae Genus: Mycoplasma Species: M. pneumoniae Species: M. hominis Species: M. genitalium Genus: Ureaplasma Species:
- Mycoplasma and Ureaplasma - Rickettsia Mycoplasma and Ureaplasma Family: Mycoplasmataceae Genus: Mycoplasma Species: M. pneumoniae Species: M. hominis Species: M. genitalium Genus: Ureaplasma Species:
Lyme disease. Information for you. Follow us on Find us on Facebook at Visit our website:
 Lyme disease Information for you Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications are available in other formats What is
Lyme disease Information for you Follow us on Twitter @NHSaaa Find us on Facebook at www.facebook.com/nhsaaa Visit our website: www.nhsaaa.net All our publications are available in other formats What is
2/5/19. Lyme Disease: It s Complicated! Lyme Disease is Worldwide. Lyme Disease: An Immune Response initiated by Borrelia burgdoferi
 Lyme Disease: It s Complicated! Mark J. Soloski, Ph.D. Professor of Medicine Department of Medicine, Division of Rheumatology Co-Director for Basic Research, Lyme Disease Research Center Johns Hopkins
Lyme Disease: It s Complicated! Mark J. Soloski, Ph.D. Professor of Medicine Department of Medicine, Division of Rheumatology Co-Director for Basic Research, Lyme Disease Research Center Johns Hopkins
Chancroid Table of Contents
 Subsection: Chancroid Page 1 of 8 Chancroid Table of Contents Chancroid Fact Sheet Subsection: Chancroid Page 2 of 8 Chancroid (Haemophilus ducreyi) Overview (1,2) For a more complete description of chancroid,
Subsection: Chancroid Page 1 of 8 Chancroid Table of Contents Chancroid Fact Sheet Subsection: Chancroid Page 2 of 8 Chancroid (Haemophilus ducreyi) Overview (1,2) For a more complete description of chancroid,
Lyme Neuroborreliosis
 Lyme Neuroborreliosis Presenter: Elitza S. Theel, Ph.D., D(ABMM) Director of Infectious Diseases Serology Co-Director, Vector-Borne Diseases Service Line Department of Laboratory Medicine and Pathology
Lyme Neuroborreliosis Presenter: Elitza S. Theel, Ph.D., D(ABMM) Director of Infectious Diseases Serology Co-Director, Vector-Borne Diseases Service Line Department of Laboratory Medicine and Pathology
Ticks and Tick Borne Diseases
 Ticks & Lyme Disease Ticks and Tick Borne Diseases Bureau of Workers Compensation PA Training for Health & Safety (PATHS) 1 Topics Introduction to Problem Types Life Cycle Behavior Lyme Disease Signs &
Ticks & Lyme Disease Ticks and Tick Borne Diseases Bureau of Workers Compensation PA Training for Health & Safety (PATHS) 1 Topics Introduction to Problem Types Life Cycle Behavior Lyme Disease Signs &
Fatigue, persistence after Lyme borreliosis 196, 197 Francisella tularensis, see Tularemia
 Subject Index Acrodermatitis chronica atrophicans (ACA) antibiotic therapy 121, 122 Borrelia induction 13 clinical characteristics 64, 65, 82 diagnosis 65, 66 differential diagnosis 66 etiology 62 frequency
Subject Index Acrodermatitis chronica atrophicans (ACA) antibiotic therapy 121, 122 Borrelia induction 13 clinical characteristics 64, 65, 82 diagnosis 65, 66 differential diagnosis 66 etiology 62 frequency
NO DISCLOSURES. Lyme Disease. Outline. Case 4/16/2014. Richard A. Jacobs, MD, PhD.
 Lyme Disease Richard A. Jacobs, MD, PhD. NO DISCLOSURES Outline History of Lyme disease How the new disease was discovered How the etiology of the disease was discovered Clinical manifestations Diagnosis
Lyme Disease Richard A. Jacobs, MD, PhD. NO DISCLOSURES Outline History of Lyme disease How the new disease was discovered How the etiology of the disease was discovered Clinical manifestations Diagnosis
Massachusetts face to face with Lyme disease patient protection bill
 Massachusetts face to face with Lyme disease patient protection bill One of the most misunderstood and underdiagnosed diseases today is Lyme disease. Each year approximately 30,000 cases of Lyme disease
Massachusetts face to face with Lyme disease patient protection bill One of the most misunderstood and underdiagnosed diseases today is Lyme disease. Each year approximately 30,000 cases of Lyme disease
Diagnosis and Treatment of Respiratory Illness in Children and Adults
 Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Page 1 of 9 Main Algorithm Annotations 1. Patient Reports Some Combination of Symptoms Patients may present for an appointment, call into a provider to schedule an appointment or nurse line presenting
Health Council of the Netherlands. A closer look at Lyme disease. The Hague: Health Council of the Netherlands, 2013; publication no. 2013/12.
 Executive summary Health Council of the Netherlands. A closer look at Lyme disease. The Hague: Health Council of the Netherlands, 2013; publication no. 2013/12. A complex picture When diagnosed at an early
Executive summary Health Council of the Netherlands. A closer look at Lyme disease. The Hague: Health Council of the Netherlands, 2013; publication no. 2013/12. A complex picture When diagnosed at an early
LYME DISEASE: NEW OPTIONS FOR TREATMENT
 LYME DISEASE: NEW OPTIONS FOR TREATMENT Lyme disease prevalence is on the rise, arguably more now than any time in human history. Millions of people have been diagnosed with this debilitating illness,
LYME DISEASE: NEW OPTIONS FOR TREATMENT Lyme disease prevalence is on the rise, arguably more now than any time in human history. Millions of people have been diagnosed with this debilitating illness,
Lyme disease stakeholder scoping workshop
 1.1 Who is the focus: Groups that will be covered: Adults and children with a suspected or confirmed diagnosis of Lyme disease 1.2. Settings All setting where NHS care The group suggested that the following
1.1 Who is the focus: Groups that will be covered: Adults and children with a suspected or confirmed diagnosis of Lyme disease 1.2. Settings All setting where NHS care The group suggested that the following
the lyme diet 05C6AA30C457C5CC4F045DC84D04A422 The Lyme Diet 1 / 6
 The Lyme Diet 1 / 6 2 / 6 3 / 6 The Lyme Diet Lyme Disease resource providing news, Lyme Disease treatment information, medical abstracts and a support community for those coping with Lyme Disease. Lyme
The Lyme Diet 1 / 6 2 / 6 3 / 6 The Lyme Diet Lyme Disease resource providing news, Lyme Disease treatment information, medical abstracts and a support community for those coping with Lyme Disease. Lyme
Title: Public Health Reporting and National Notification for Lyme Disease
 10-ID-06 Committee: Infectious Disease Title: Public Health Reporting and National Notification for Lyme Disease I. tatement of the Problem: CTE position statement 07-EC-02 recognized the need to develop
10-ID-06 Committee: Infectious Disease Title: Public Health Reporting and National Notification for Lyme Disease I. tatement of the Problem: CTE position statement 07-EC-02 recognized the need to develop
Clue # 1: Before. After
 Clue # 1: Bacteria can be divided into two groups (gram positive and gram negative) based on their appearance after iodine staining. This method was developed in 1884 (OVER 100 YEARS AGO) but is still
Clue # 1: Bacteria can be divided into two groups (gram positive and gram negative) based on their appearance after iodine staining. This method was developed in 1884 (OVER 100 YEARS AGO) but is still
Lyme Disease: Prevention, Recognition & Treatment
 University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2017 Lyme Disease: Prevention, Recognition & Treatment Kristen J. Bartlett University of Vermont
University of Vermont ScholarWorks @ UVM Family Medicine Block Clerkship, Student Projects College of Medicine 2017 Lyme Disease: Prevention, Recognition & Treatment Kristen J. Bartlett University of Vermont
Sickness and Illness Policy
 Sickness and Illness Policy Children should not be at nursery if they are unwell. If your child becomes unable to stay at nursery, a member of staff will contact the parent or carer, asking them to come
Sickness and Illness Policy Children should not be at nursery if they are unwell. If your child becomes unable to stay at nursery, a member of staff will contact the parent or carer, asking them to come
Streptococcal Pharyngitis: Guidelines, Treatment Issues, and Sequelae
 This article has been amended to include factual corrections. Changes were made subsequent to its original printing. These changes were acknowledged on page 59, volume 43, issue 2. The online article and
This article has been amended to include factual corrections. Changes were made subsequent to its original printing. These changes were acknowledged on page 59, volume 43, issue 2. The online article and
Streptococcal Pharyngitis
 Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
Streptococcal Pharyngitis Guideline developed by JC Beavers, MD, in collaboration with the ANGELS Team. Last reviewed by JC Beavers, MD on November 2, 2016. Preface Streptococcal pharyngitis (ie, strep
WOMENCARE. Herpes. Source: PDR.net Page 1 of 8. A Healthy Woman is a Powerful Woman (407)
 WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
WOMENCARE A Healthy Woman is a Powerful Woman (407) 898-1500 Herpes Basics: Herpes is a common viral disease characterized by painful blisters of the mouth or genitals. The herpes simplex virus (HSV) causes
Department of Health. Year 8. vaccination program. Important information for parents and students
 Department of Health Year 8 vaccination program Important information for parents and students Contents Why immunise? 1 Vaccination program 1 Schedule of vaccinations 2 Vaccination records 2 Vaccine safety
Department of Health Year 8 vaccination program Important information for parents and students Contents Why immunise? 1 Vaccination program 1 Schedule of vaccinations 2 Vaccination records 2 Vaccine safety
Horowitz Lyme-MSlDS Questionnaire
 Horowitz Lyme-MSlDS Questionnaire The Horowitz Lyme-MSlDS Questionnaire is not intended to replace the advice of your own physician or other medical professional. You should consult a medical professional
Horowitz Lyme-MSlDS Questionnaire The Horowitz Lyme-MSlDS Questionnaire is not intended to replace the advice of your own physician or other medical professional. You should consult a medical professional
Controlling Communicable Diseases in the School Setting LCDR C. SCOTT LOVE, MD, MPH, FAAP DEPARTMENT HEAD, PEDIATRICS
 Controlling Communicable Diseases in the School Setting LCDR C. SCOTT LOVE, MD, MPH, FAAP DEPARTMENT HEAD, PEDIATRICS Disclosure There is no conflict of interest pertaining to this presentation, materials,
Controlling Communicable Diseases in the School Setting LCDR C. SCOTT LOVE, MD, MPH, FAAP DEPARTMENT HEAD, PEDIATRICS Disclosure There is no conflict of interest pertaining to this presentation, materials,
MCDB 3650 Lyme Disease. Team LTD Paige Hoffman, Victoria Schelkun, Madison Purdy, Evan Gallagher
 MCDB 3650 Lyme Disease Team LTD Paige Hoffman, Victoria Schelkun, Madison Purdy, Evan Gallagher Overview Review of lyme disease Current treatment options and their problems Chronic/persistent lyme disease
MCDB 3650 Lyme Disease Team LTD Paige Hoffman, Victoria Schelkun, Madison Purdy, Evan Gallagher Overview Review of lyme disease Current treatment options and their problems Chronic/persistent lyme disease
Using administrative medical claims data to estimate underreporting of infectious zoonotic diseases
 2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 40% Percentage of Yearly Cases 30% 25% 20% 15% 10% 5% 0% January Februar March April May June July August Septem October Novem Decem January Februar March
2000 2001 2002 2003 2004 2005 2006 2007 2008 2009 40% Percentage of Yearly Cases 30% 25% 20% 15% 10% 5% 0% January Februar March April May June July August Septem October Novem Decem January Februar March
MULTI-SYSTEMIC INFECTIOUS DISEASE SYNDROME SYMPTOM QUESTIONNAIRE
 MULTI-SYSTEMIC INFECTIOUS DISEASE SYNDROME SYMPTOM QUESTIONNAIRE SECTION 1: SYMPTOM FREQUENCY SCORE Select the frequency of each of the following symptoms. 0 = None 1 = Mild 2 = Moderate 3 = Severe 1.
MULTI-SYSTEMIC INFECTIOUS DISEASE SYNDROME SYMPTOM QUESTIONNAIRE SECTION 1: SYMPTOM FREQUENCY SCORE Select the frequency of each of the following symptoms. 0 = None 1 = Mild 2 = Moderate 3 = Severe 1.
8.L.1 Practice Questions
 Name: Date: 1. Why should antibiotics be given to a person who is ill with a bacterial disease like strep throat, but not to a person who has a viral disease like flu?. ntibiotics kill bacteria but not
Name: Date: 1. Why should antibiotics be given to a person who is ill with a bacterial disease like strep throat, but not to a person who has a viral disease like flu?. ntibiotics kill bacteria but not
Tickborne Disease in New Hampshire HEHNA Meeting Elliot Hospital September 27, 2017
 Tickborne Disease in New Hampshire HEHNA Meeting Elliot Hospital September 27, 2017 Carolyn Fredette, MPH Vectorborne Disease Surveillance Coordinator Division of Public Health Services, DHHS Infectious
Tickborne Disease in New Hampshire HEHNA Meeting Elliot Hospital September 27, 2017 Carolyn Fredette, MPH Vectorborne Disease Surveillance Coordinator Division of Public Health Services, DHHS Infectious
Prof Dr Najlaa Fawzi
 1 Prof Dr Najlaa Fawzi is an acute highly infectious disease, characterized by vesicular rash, mild fever and mild constitutional symptoms. is a local manifestation of reactivation of latent varicella
1 Prof Dr Najlaa Fawzi is an acute highly infectious disease, characterized by vesicular rash, mild fever and mild constitutional symptoms. is a local manifestation of reactivation of latent varicella
CLINICAL GUIDELINES. Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P.
 CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
CLINICAL GUIDELINES Summary of Literature and Recommendations Concerning Immunization and Steroid Injections Thomas J. Gilbert M.D., M.P.P. 11/2/15 Several practices routinely delay steroid injections
Community Acquired Pneumonia
 April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
April 2014 References: 1. Bradley JS, Byington CL, Shah SS, Alverson B, Carter ER, Harrison C, Kaplan SL Mace SE, McCracken Jr. GH, Moor MR, St. Peter SD, Stockwell JA, and Swanson JT. The Management of
Syphilis Treatment Protocol
 STD, HIV, AND TB SECTION Syphilis Treatment Protocol CLINICAL GUIDANCE FOR PRIMARY AND SECONDARY SYPHILIS AND LATENT SYPHILIS www.lekarzol.com (4/2016) Page 1 of 8 Table of Contents Description... 3 Stages
STD, HIV, AND TB SECTION Syphilis Treatment Protocol CLINICAL GUIDANCE FOR PRIMARY AND SECONDARY SYPHILIS AND LATENT SYPHILIS www.lekarzol.com (4/2016) Page 1 of 8 Table of Contents Description... 3 Stages
Future of Pediatrics: Blisters, Hives and Other Tales from the Emergency Room June 14 th, 2016
 A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
A. Yasmine Kirkorian MD Assistant Professor of Dermatology & Pediatrics Children s National Health System George Washington University School of Medicine & Health Sciences Future of Pediatrics: Blisters,
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults
 Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
Appropriate Use of Antibiotics for the Treatment of Acute Upper Respiratory Tract Infections in Adults Kyong Ran Peck, M.D. Division of Infectious Diseases Sungkyunkwan University School of Medicine, Samsung
