A s doctors who care for children, we have a
|
|
|
- Norah Norris
- 5 years ago
- Views:
Transcription
1 1163 PERSONAL PRACTICE The bleeding child; is it NAI? A E Thomas... As a paediatric haematologist, the question of whether a child has been abused or whether they might have a bleeding diathesis is a question that I am regularly asked. When I first became a consultant, I would often find that not enough information was available; for example, incomplete histories had been taken or investigations were incomplete and difficult to interpret. This inevitably led to delays in confirming the cause of the bleeding and meant that if parents or carers contested a diagnosis of abuse, excluding a bleeding disorder was extremely difficult. I was also aware that carers of several of my patients with haemophilia or other bleeding disorders had initially been under suspicion of abuse, most usually at the time of the first few presentations. By highlighting important questions in history taking, having a specific haematological screen for children being investigated for bleeding in the context of non-accidental injury, and encouraging discussion of abnormal results with a haematologist, these difficulties can, for the most part, be avoided Correspondence to: Dr A E Thomas, Department of Haematology, Royal Hospital for Sick Children, Edinburgh EH9 1LF, UK; angela.thomas@luht.scot. nhs.uk Accepted 6 April A s doctors who care for children, we have a responsibility to be aware of signs and symptoms suggestive of child abuse, including non-accidental injury. Equally however, we must also recognise that medical and physical conditions may simulate abuse and that appropriate measures need to be taken to rule out these conditions. Haemostatic abnormalities are manifest usually as bruising or other bleeding into the skin or mucosal membranes, and similarly cutaneous lesions are by far the most common presenting features of child abuse. 1 An incorrect diagnosis of child abuse can be devastating for the family and if a serious underlying blood disorder is later identified, regaining the trust of that family may be very difficult. Delay in diagnosis of a condition such as haemophilia will mean that no treatment can be offered which may lead to increased morbidity and even mortality. It is important to remember, however, that diagnosis of a bleeding disorder does not rule out abuse 2 and that these children will be at greater risk of bleeding secondary to abuse. CLINICAL HISTORY AND PRESENTATION When a child presents with bruising or bleeding, the main differential diagnoses are physiological or accidental bleeding, non-accidental injury, or a bleeding diathesis. Arch Dis Child 2004;89: doi: /adc Presenting complaint The history of the presenting complaint will include questions as to how the injury occurred and an assessment made as to whether this explains the injuries or bleeding seen. Guidance is given that abuse should be suspected if there is significant bruising or bleeding with no history of trauma or a history inconsistent with the severity of the injury, 3 but in a child with a bleeding diathesis, this may be precisely how the child presents. Where a child has bruising in a recognisable pattern such as a belt or hand, then suspected abuse must be reported regardless of the results of laboratory tests. 4 However, fingertip bruising can be seen in children with a bleeding diathesis from normal physical interaction. A drug history should also be elicited, particularly one of anticoagulant use. Past history Past history of bleeding and haemostatic challenges add important information and specific questions should be asked about birth; for example, whether there was a cephalhaematoma, unexpected bleeding from the umbilical stump, or bruising after intramuscular injections. Active children usually have bruises on their shins, but not normally on unexposed areas. Persistent mucocutaneous bleeding such as gum bleeding or epistaxis (often bilateral) in addition to bruising might indicate thrombocytopenia, a platelet disorder, or von Willebrand disease. Significant haemostatic challenges Significant haemostatic challenges will include operations such as circumcision, tonsillectomy, or removal of teeth. Bleeding response to injury such as a bitten tongue or a wound that requires stitching can yield useful information. In girls, menstrual loss may be an indicator of a bleeding diathesis. Bleeding may be due to other disease states that affect haemostasis such as hepatocellular dysfunction, renal disease, or malabsorption. Family history A family history of bleeding may be apparent and is more often seen in dominantly inherited or X- linked conditions such as haemophilia A or B. However, haemophilia A, the commonest type of haemophilia, arises as a result of spontaneous mutation in about 30% of cases and therefore family history will be lacking. 5 The sex of the patient and the age also help to distinguish between possible causes of bleeding. X-linked disorders such as haemophilia A and B usually occur in males. Such disorders may occur in girls but unless consanguinity or Turner s syndrome is present, the chances are very small. Extreme Lyonisation of the X chromosome can also result
2 1164 Thomas in girls being clinically affected; therefore, although such diagnoses are unlikely, they should be tested for as part of a full evaluation. The age at presentation influences the likelihood of a particular cause of a bleeding diathesis. A patient with a severe congenital bleeding diathesis is unlikely to present for the first time as an adolescent. It must also be remembered that the plasma concentration of many of the coagulation and fibrinolytic proteins are age dependent and therefore appropriate normal ranges must be used for interpretation. Ideally the laboratory should establish normal ranges for age using their reagents and methods for at least the more common parameters measured. Details of ethnic origin and consanguinity should be taken as certain disorders are more frequent in particular groups; for example, factor XI deficiency in those of Ashkenazy Jewish descent 6 and recessive disorders are more common in consanguineous families. Examination of the child When examining the child, the general health and state of the child should be assessed. Bruises If the child is presenting with bruising, particular note should be made of the distribution and size of the bruises. The age of a bruise is very difficult to ascertain with certainty and depends on the integrity of the coagulation system and vessels and the force and location of the injury. 7 Accompanying tissue swelling and abrasion may be present in more recent bruises. Bruises of different ages are seen both in abuse and in children with a bleeding diathesis. The pattern of bruising should be recorded, in particular if marks indicate use of an object such as a belt or flex. As has been noted above, fingertip bruising is not infrequently found in children with a bleeding diathesis. The distribution of bleeding may indicate a diagnosis of Henoch-Schönlein purpura, which presents as symmetrical bruising on extensor surfaces. It is due to a vasculitis rather than a coagulopathy, giving a normal coagulation screen and full blood count, and may be confused with non-accidental injury. 3 8 Neuroblastoma may present with bilateral black eyes due to tumour infiltration of the bone. However, the child is usually unwell with signs and symptoms of systemic disease. In contrast, comparatively minor injury may cause the same sign in a child with haemophilia who will be otherwise well. Petechial haemorrhages Presence or absence of petechial haemorrhages will help differentiate disorders associated with thrombocytopenia. Such haemorrhages however can occur in the distribution of the superior vena cava in association with a severe bout of coughing or vomiting in children without a bleeding diathesis or in cases of strangulation. Bleeding into joints A swollen, tender joint may indicate a bleed into that joint as is seen in haemophilia, but tender joints may also be seen in Henoch-Schönlein purpura, acute leukaemia, or neuroblastoma. Haematological investigation Haematological investigation of a bruised child is mandatory in all cases where the bruising is unexplained or implausible, and in cases where some explanation is given or found but the bleeding that results is disproportionate to the injury sustained. In a child who may have been abused, it is essential that the investigations are as atraumatic as possible and yield the maximum information. Initial screening and investigation are primarily aimed at the diagnosis of the commoner causes of bleeding and to exclude or confirm some of the rarer causes for the safety and management of the child. Further investigation might be needed if no explanation of the bleeding is found or no admission of nonaccidental injury is made. Venepuncture; reducing investigation artefact A set of screening investigations should be performed on blood taken from a single venepuncture, and analysed without delay by laboratories experienced in handling small samples. Artefact can significantly distort results and lead to misdiagnosis. The utmost care must be exerted in the way the specimens are taken and handled prior to processing. Ideally, they should be taken by a person experienced in paediatric phlebotomy, with the minimum of venous stasis and during core working hours. Pitfalls in specimen collection Common pitfalls in specimen collection and processing include poor venepuncture technique, whereby there is contamination by tissue fluid or air bubbles leading to activation of the sample in vitro which can result in both prolongation or shortening of clotting times as well as thrombocytopenia. If blood is taken from a cannula which has been heparinised, heparin contamination can occur, resulting in prolongation of the activated partial thromboplastin time (aptt). Over or under filling of the specimen tube will result in an altered ratio of the anticoagulant (citrate) to plasma, giving shortened or prolonged clotting times respectively. Prolonged clotting times may also be seen in severe polycythaemia where there is a reduced plasma volume. Inappropriate storage or transport of the specimen may result in activation of the sample or loss of factor activity. First line investigations Initial tests should include a coagulation screen consisting of a prothrombin time (PT), activated partial thromboplastin time (aptt), fibrinogen, and thrombin time (TT), plus a full blood count, platelet count, and blood film. A factor VIII, factor IX, and von Willebrand factor antigen and activity (Ristocetin cofactor) are also recommended in all cases of suspected non-accidental injury as a normal or marginally Table 1 Patterns of coagulation results; possible diagnoses Test results Prolonged aptt PT/fibrinogen/platelets normal Prolonged PT aptt/fibrinogen/platelets normal Prolonged PT and aptt Fibrinogen/platelets normal Prolonged PT and aptt Decreased fibrinogen Normal or low platelets Possible diagnosis von Willebrand disease* Factor VIII deficiency Factor IX deficiency Factor XI deficiency Warfarin ingestion Early vitamin K deficiency Early liver dysfunction Factor VII deficiency Over warfarinisation Severe vitamin K deficiency Over heparinisation Factor X, factor V, or prothrombin deficiency Acquired inhibitors Severe liver dysfunction Dysfibrinogenaemia/ afibrinogenaemia Disseminated intravascular coagulation (including meningococcal sepsis) *von Willebrand disease subtype 2B is associated with reduced platelets; aptt is not always prolonged.
3 The bleeding child 1165 prolonged aptt can be associated with a significant decrease in factor VIII or IX levels or with von Willebrand disease. If the blood is flowing well, a few millilitres extra can save a second venepuncture if an abnormality is found, for example a prolonged aptt, and further testing is required. It is important that results are compared against age specific ranges as test results and coagulation factor levels vary with age. 9 Platelet function is not tested in this screen, and although there are some screening tests none is completely satisfactory. A bleeding time is an invasive test requiring a small incision to be made in the forearm, and although it will show the integrity of the platelet vessel wall interaction, is unnecessary in the early stages of investigation and is highly operator dependent. An automated system, the PFA-100, measures both aggregation and the release reaction of platelets using small volumes of whole blood. This method is sensitive in detecting classical defects resulting in major platelet dysfunction, such as Bernard-Soulier syndrome and Glanzmann s thrombasthenia, and also von Willebrand disease. Apart from Glanzmann s thrombasthenia, which has a history highly suggestive of a severe bleeding disorder and is very rare, the other disorders can be detected by or suspected from the screening tests outlined above. False negative results occur in milder platelet defects such as storage pool disorder, and release defects which are not detectable by the routine laboratory tests, 10 and the test is not sensitive to vascular collagen disorders. Its use in identifying those who have a bleeding diathesis in cases of possible non-accidental injury has not been tested. It can be helpful to bleed parents, especially if results are equivocal or subsequent testing for clarification of any abnormality requires large volumes of blood. Identification of the child s natural parents, however, is not always certain, or they may not be available or locatable, and this approach may not be possible. Patterns of abnormal results The pattern of abnormalities obtained using first line tests along with the clinical presentation and history may well indicate or identify any underlying disorder (table 1). It is important to remember that some significant bleeding disorders give normal screen results (table 2) and that some abnormal results are not associated with bleeding. It is this latter category, if not properly investigated, that can cause confusion and misdiagnosis. The causes of bleeding in a well child can be subdivided into likely causes with or without normal results and unlikely causes with or without normal results (table 2). Table 2 Causes of bleeding in a well child Coagulation screen* or platelets Normal Likely causes of bleeding with a normal full blood count and coagulation screen include Henoch-Schönlein purpura and von Willebrand disease. Likely causes with an abnormal screen include idiopathic thrombocytopenic purpura where the platelet count is low but all other parameters are normal. Haemophilia A and B are the commonest, inherited causes of severe abnormal bleeding and both give an isolated, prolonged aptt, and low levels of factor VIII or IX respectively (table 3). Vitamin K deficiency or warfarin prolongs the PT with or without a prolonged aptt depending on the degree of deficiency or of warfarinisation (table 3). Heparin administration is suspected if both the aptt and thrombin time are prolonged (table 3) and can be confirmed by demonstration of a normal Reptilase time. In this test, fibrinogen is converted directly to fibrin, a reaction which is not inhibited by heparin. The thrombin time relies on activation of fibrinogen to fibrin by thrombin which is inhibited by heparin. Unlikely causes of bleeding in a child whose initial results are normal include both platelet disorders and factor deficiencies as well as vascular/collagen disorders (table 2). Factor XIII deficiency results in reduced clot stability and is associated with delayed haemorrhage and poor healing. There is delayed and repeated bleeding from superficial wounds and classically delayed separation by up to four weeks of the umbilical stump. Deficiency of a 2 antiplasmin gives a clinical picture similar to factor XIII deficiency, whereas deficiency of another of the anticoagulant proteins, plasminogen activator inhibitor-1, is associated with a less severe phenotype with bleeding usually after surgery or trauma. Vitamin C deficiency, resulting in perifollicular haemorrhages and bony changes, and Ehlers-Danlos syndrome are examples of collagen abnormalities that give rise to bleeding. However, all these causes are extremely rare, and apart from plasminogen activator inhibitor-1 deficiency, have a distinct clinical presentation. Rare causes of bleeding with an abnormal screen include both platelet disorders and factor deficiencies (table 1). Congenital platelet abnormalities (excluding Glanzmann s thrombasthenia) such as Bernard-Soulier or Wiskott Aldrich syndromes are associated with abnormal platelet numbers and morphology. Deficiencies of factors II (prothrombin), V, and X result in prolongation of the aptt or PT or both, depending on the reagents used, whereas factor VII deficiency gives an isolated, prolonged PT, and factor XI deficiency an isolated, prolonged aptt. Abnormalities of the PT or aptt should trigger appropriate factor assays (table 3). Dysfibrinogenaemias, hypoand afibrinogenaemias are picked up by a prolonged thrombin time and low or absent fibrinogen levels (table 3). Abnormal Common von Willebrand disease ITP Henoch-Schönlein purpura Haemophilia A or B Vitamin K deficiency Warfarin or heparin Uncommon Glanzmann s thrombasthenia Congenital platelet abnormality (excluding Glanzmann s) Platelet storage pool disorder Deficiencies of factors II, V, VII, X, XI Factor XIII deficiency Dysfibrinogenaemia PAI-1 deficiency Afibrinogenaemia a 2 antiplasmin deficiency Ehlers-Danlos Vitamin C deficiency ITP, idiopathic thrombocytopenic purpura; PAI-1, plasminogen activator inhibitor-1. *Excluding von Willebrand factor.
4 1166 Thomas Table 3 Initial and further investigations Initial Investigation Further investigation Consider PT Isolated prolongation Early warfarin therapy; early vitamin K deficiency, early liver disease. Possible factor VII deficiency aptt Isolated prolongation: 50:50 plasma mix Correction factor deficiency, measure levels No correction inhibitor Abnormal screening tests with no bleeding diathesis An abnormal screen does not necessarily indicate a bleeding diathesis; the two most common abnormalities giving rise to this are factor XII deficiency and the lupus anticoagulant, which is an inhibitor of in vitro coagulation. Both these conditions give rise to a prolonged aptt but do not result in a bleeding state (table 3). A factor deficiency can be differentiated from an inhibitor using mixing techniques. A 50:50 mix of patient plasma and normal plasma are incubated and the abnormal test repeated. Correction of the aptt by.50% indicates a deficiency, whereas lack of correction indicates an inhibitor. If the pattern of correction is one of a deficiency, factors VIII, IX, XI, and XII should be checked. Factors VIII and IX should have already been assayed as part of the screen, and once factor XI and XII are measured, if the only deficient factor is XII, then this is not associated with a bleeding state. Factor XII is only necessary for coagulation in vitro but does not have a role in vivo. If the pattern is one of an inhibitor, once heparin has been excluded (by a normal Reptilase time), further investigations to confirm a lupus anticoagulant can be performed. This should be possible without delay if enough blood is taken at the initial venepuncture. A lupus anticoagulant will prolong a dilute Russel viper venom time (DRVVT) but show correction with platelet neutralisation. Prolongation of the aptt in children secondary to a lupus anticoagulant is not an uncommon finding. The lupus anticoagulant only exerts its anticoagulant effect in vitro where it interferes with the exogenous phospholipids added to the test tube. In vivo, the phospholipid is provided by the platelet and is protected from the antiphospholipid effect of the lupus anticoagulant. It is usually a transient phenomenon and occurs secondary to infection resolving within about three months. Unless confirmed however, it may mislead clinicians into thinking a bleeding disorder is present. SPECIFIC DISORDERS Inherited disorders Von Willebrand disease Von Willebrand disease (vwd) is the commonest of the inherited bleeding disorders with a prevalence of 1 2%, 11 Factor VIII or factor IX deficiency von Willebrand disease Factor XI deficiency (rare) Factor XII deficiency (not associated with bleeding) Lupus anticoagulant; heparin contamination PT and APTT Both prolonged (fibrinogen normal) Warfarin, vitamin K deficiency, heparin Liver disease Rare factor deficiencies, e.g. II, V, X Fibrinogen Decreased Prolonged PT and aptt, decreased platelets If,0.8 g/l, PT and aptt will be prolonged Platelets normal Disseminated intravascular coagulation Severe liver disease Dys/afibrinogenaemia Thrombin time Prolonged reptilase time Normal Heparin Prolonged as for low fibrinogen Factor VIII Low levels,40% Haemophilia A Factor IX Low levels,40% Haemophilia B von Willebrand factor Low antigen and/or activity (ristocetin co-factor) levels von Willebrand disease whose typical presentation is one of mucocutaneous bleeding. It is inherited as an autosomal dominant but with marked variability of both phenotypic penetrance and expressivity, and thus a clear family history is not always elicited. Haemorrhagic tendency is variable and depends on the type and severity of the disease. Many in whom vwd is diagnosed have modestly reduced von Willebrand factor (vwf) levels that are associated with mild bleeding in some family members but not others. 12 Some cases are easy to diagnose, with the patient suffering from repeated and significant bleeding with exceptionally low vwf levels. However, many cases are not clear cut, despite repeated investigation and testing of family members. It is therefore important to include measurement of this protein and its activity routinely as recommended above, but to be cautious when attributing bruising in a child with suspected nonaccidental injury to low von Willebrand factor levels if identified. 2 Haemophilia Haemophilia A (factor VIII deficiency) and haemophilia B (factor IX deficiency), although rare, are the commonest inherited factor deficiencies associated with a bleeding diathesis. They are both X-linked conditions and the severe forms occur almost exclusively in males. The two types are indistinguishable from each other in their clinical presentation. Although an inherited disorder, approximately one third of cases arise as a result of a new mutation, and a positive history is only elicited in around 50% of cases. They are the commonest inherited bleeding disorders to present in the neonatal period, 13 and 90% of those with severe disease will have presented by the age of 1 year. After the immediate neonatal period, the infant is unlikely to bleed unless accidental injury, although generally trivial, occurs. Once the child begins to crawl and walk, soft tissue bleeding and haemarthroses occur more readily. Several reports describe children who have been misdiagnosed as victims of nonaccidental injury before full evaluation of the possible causes of bleeding has been undertaken A coagulation screen in haemophilia A or B will show an isolated prolongation of the aptt which will correct on 50:50 mixing with normal
5 The bleeding child 1167 plasma. Specific factor assays will identify the deficient factor. Moderate and mild haemophilia will present later, and in the case of mild haemophilia usually only after trauma. The aptt is not very sensitive to mildly reduced levels of factors VIII and IX, and therefore measurement of these factors is recommended in the routine screen as above. Haemophilia C Factor XI deficiency, haemophilia C, is a rare inherited bleeding disorder and is found mostly but not exclusively among the Ashkenazi Jewish population. It is inherited in an autosomal recessive manner and bleeding is usually mucocutaneous in nature. A coagulation screen shows an isolated, prolonged aptt. Rare coagulation deficiencies The rare coagulation deficiencies occur with a frequency of 1 in to 1 in 2 million, and include fibrinogen and prothrombin and factors V, VII, X, and XIII. Apart from factor XIII deficiency, all result in abnormalities of the coagulation screen (tables 1 and 2). Congenital platelet disorders The majority of the inherited platelet disorders that are associated with bleeding result in a degree of thrombocytopenia, for example, Bernard Soulier syndrome, Wiskott Aldrich syndrome, May Hegglin anomaly. Glanzmann s thrombasthenia is a severe condition where the patient s platelets lack the IIb-IIIa receptor essential for binding of fibrinogen and platelet aggregation. There is a positive history of bleeding from birth, with mucocutaneous bleeding, spontaneous bruising, and significant bleeding with minor trauma. It is inherited as an autosomal recessive condition and thus there is usually no family history. Diagnosis is made from platelet function tests. Platelet storage pool disorders are often associated with a mild bleeding phenotype and require platelet function tests for diagnosis. Again, the diagnosis of a platelet storage pool disorder does not rule out non-accidental injury, and the history and clinical findings are very important. Acquired disorders Reduced vitamin K dependent factors Vitamin K deficiency can occur in the neonatal period or early infancy. Early presentation may be secondary to maternal ingestion of vitamin K antagonists such as warfarin or anticonvulsants, or to lack of vitamin K prophylaxis at birth. Later presentation is commonly associated with exclusive breast feeding and either lack of vitamin K at birth or a single oral dose only. About 50% of babies who present late do so with intracranial haemorrhage, with high morbidity and mortality. Misdiagnosis of haemorrhagic disease of the newborn as child abuse has been reported. 14 The coagulation screen shows a prolonged PT, with a variably prolonged aptt dependent on the severity of the deficiency. Warfarin exerts its action by preventing carboxylation and thus activation of the vitamin K dependent factors. Again the PT is prolonged with variable prolongation of the aptt, dependent on how much warfarin has been taken. Warfarin can be administered therapeutically, accidentally, or nonaccidentally and can be tested for specifically. Heparin prolongs the aptt and thrombin time and is a common contaminant of blood taken from heparinised cannulae, even if a large discard sample has been taken. Occasionally children are given heparin therapeutically. The presence of heparin can be confirmed with this pattern of results and a normal Reptilase time. Thrombocytopenia This is easily identified from the full blood count. In a well child the most likely cause is idiopathic thrombocytopenic purpura (ITP), and under these circumstances the haemoglobin and white cell count is usually normal as is the coagulation screen. Other causes of acquired thrombocytopenia, such as bone marrow infiltration from malignant disease or leukaemia, or disseminated intravascular coagulation are associated with additional abnormalities of the blood count or coagulation screen, and are seen in an ill child. SUMMARY When trying to establish whether bleeding is due to a haematological disorder or to abuse, it is essential to take a pertinent personal and/or family history, investigate appropriately and without delay, and to limit the trauma to the child and the carers. Having a protocol for investigation of a possible bleeding diathesis allows laboratory investigation to proceed, including institution of some second line tests dependent on initial results, without unduly delaying the processes of investigation and reporting of suspected nonaccidental injury. Importantly, it also establishes involvement of a haematologist in interpretation of tests in the light of history and clinical findings. Initial screening tests should include a PT, aptt, thrombin time,and fibrinogen, a factor VIII and factor IX level, and von Willebrand factor antigen and activity. This set of tests is not comprehensive but will identify the majority of bleeding disorders or indicate which further tests are necessary. If there is a significant discrepancy between history and findings and the initial tests are normal, either there is a bleeding disorder which has not yet been identified or abuse has taken place. Discussion with parents or carers should take place at this stage and if discrepancies still exist, further investigation might include platelet function testing or specific factor assays such as factor XIII. If the case is likely to receive a formal legal challenge, even the rarest of causes may require exclusion. It is important to remember that diagnosis of a bleeding diathesis, especially if associated with a mild phenotype, does not exclude non-accidental injury, and where these are found concurrently, the child will be at even greater risk. REFERENCES 1 Stewart GM, Rosenberg NM. Conditions mistaken for child abuse: part II. Paediatr Emerg Care 1996;12: O Hare AE, Eden OB. Bleeding disorders and non-accidental injury. Arch Dis Child 1984;59: Daly KC, Siegel RM. Henoch-Schonlein purpura in a child at risk of abuse. Arch Pediatr Adolesc Med 1998;152: Harley JR. Disorders of coagulation misdiagnosed as nonaccidental bruising. Pediatr Emerg Care 1997;13: Giannelli F, Green PM. The molecular basis of haemophilia A and B. Baillieres Clin Haematol 1996;9: Bolton-Maggs PHB, Young Wa-Yin, McCraw AH, et al. Inheritance and bleeding in factor XI deficiency. Br J Haematol 1988;69: Stephenson T, Bialas Y. Estimation of the age of bruising. Arch Dis Child 1996;74: Menter A. Symmetrical purpura doesn t mirror child abuse. JAMA 1987;257: Andrew M, Vegh P, Johnston M, et al. Maturation of the hematopoietic system during childhood. Blood 1992;80: Harrison P, Robinson M, Leisner R, et al. The PFA-100: a potential rapid screening tool for the assessment of platelet dysfunction. Clin Lab Haematol 2002;24: Werner EJ, Broxson EH, Tucker EL, et al. Prevalence of von Willebrand disease in children: a multiethnic study. J Pediatr 1993;123: Sadler JE. Von Willebrand disease type 1: a diagnosis in search of a disease. Blood 2003;101: Smith PS. Congenital coagulation protein deficiencies in the perinatal period. Semin Perinatol 1990;14: Wheeler DM, Hobbs CJ. Mistakes in diagnosing non-accidental injury: 10 years experience. Med Pract 1988;296: Schiver W, Brueschke EE, Dent T. Family practice grand rounds: hemophilia. J Fam Pract 1982;14:661 4.
GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN. All children in whom there is concern regarding bruising / bleeding
 GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN Reference: Bruising / Bleeding / NAI Version No: 1 Applicable to All children in whom there is concern regarding bruising / bleeding Classification
GUIDELINE: ASSESSMENT OF BRUISING & BLEEDING IN CHILDREN Reference: Bruising / Bleeding / NAI Version No: 1 Applicable to All children in whom there is concern regarding bruising / bleeding Classification
Haemostasis & Coagulation disorders Objectives:
 Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
Haematology Lec. 1 د.ميسم مؤيد علوش Haemostasis & Coagulation disorders Objectives: - Define haemostasis and what are the major components involved in haemostasis? - How to assess the coagulation status?
Guidelines for Shared Care Centres and Community Staff
 Reference: CG1410 Written by: Dr Jeanette Payne Peer reviewer Dr Jenny Welch Approved: February 2016 Approved by D&TC: 8th January 2016 Review Due: February 2019 Intended Audience This document contains
Reference: CG1410 Written by: Dr Jeanette Payne Peer reviewer Dr Jenny Welch Approved: February 2016 Approved by D&TC: 8th January 2016 Review Due: February 2019 Intended Audience This document contains
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College
 Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Dr. Rai Muhammad Asghar Associate Professor Head of Pediatric Department Rawalpindi Medical College AN APPROACH TO BLEEDING DISORDERS NORMAL HEMOSTASIS After injury, 3 processes halt bleeding Vasoconstriction
Sysmex Educational Enhancement and Development No
 SEED Coagulation Sysmex Educational Enhancement and Development No 2 2016 An approach to the bleeding patient The purpose of this newsletter is to provide an overview of the approach to the bleeding patient
SEED Coagulation Sysmex Educational Enhancement and Development No 2 2016 An approach to the bleeding patient The purpose of this newsletter is to provide an overview of the approach to the bleeding patient
Coagulation Disorders. Dr. Muhammad Shamim Assistant Professor, BMU
 Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Coagulation Disorders Dr. Muhammad Shamim Assistant Professor, BMU 1 Introduction Local Vs. General Hematoma & Joint bleed Coagulation Skin/Mucosal Petechiae & Purpura PLT wound / surgical bleeding Immediate
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN
 Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
Dr. MUBARAK ABDELRAHMAN MD PEDIATRICS AND CHILD HEALTH Assistant Professor FACULTY OF MEDICINE -JAZAN The student should be able:» To identify the mechanism of homeostasis and the role of vessels, platelets
BLEEDING DISORDERS. JC Opperman 2012
 BLEEDING DISORDERS JC Opperman 2012 Primary and Secondary Clotting Laboratory Tests Routine screening tests Prothrombin time (PT) (INR) increased in neonates (12-18 sec) Partial thromboplastin time (PTT)
BLEEDING DISORDERS JC Opperman 2012 Primary and Secondary Clotting Laboratory Tests Routine screening tests Prothrombin time (PT) (INR) increased in neonates (12-18 sec) Partial thromboplastin time (PTT)
Easy Bleeding General Presentation
 Easy Bleeding General Presentation It is not uncommon for children to bleed and bruise after experiencing trauma. However, a child may also have an underlying coagulopathy, which results in easy and possibly
Easy Bleeding General Presentation It is not uncommon for children to bleed and bruise after experiencing trauma. However, a child may also have an underlying coagulopathy, which results in easy and possibly
BLEEDING (PLATELET) DISORDER. IAP UG Teaching slides
 BLEEDING (PLATELET) DISORDER 1 APPROACH The initial set of questions should establish the following: (1) the most common site and type of bleeding (e.g., mucocutaneous versus articular or deep muscle),
BLEEDING (PLATELET) DISORDER 1 APPROACH The initial set of questions should establish the following: (1) the most common site and type of bleeding (e.g., mucocutaneous versus articular or deep muscle),
The LaboratoryMatters
 Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
Laboratory Medicine Newsletter for clinicians, pathologists & clinical laboratory technologists. A Initiative. HEMOSTASIS AND THE LABORATORY This issue highlights: Primary Hemostasis Screening Tests Case
General approach to the investigation of haemostasis. Jan Gert Nel Dept. of Haematology University of Pretoria 2013
 General approach to the investigation of haemostasis Jan Gert Nel Dept. of Haematology University of Pretoria 2013 Clinical reasons to investigate haemostasis Investigating a clinically suspected bleeding
General approach to the investigation of haemostasis Jan Gert Nel Dept. of Haematology University of Pretoria 2013 Clinical reasons to investigate haemostasis Investigating a clinically suspected bleeding
Haemorrhagic Disorders. Dr. Bashar Department of Pathology Mosul Medical College
 Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
Haemorrhagic Disorders Dr. Bashar Department of Pathology Mosul Medical College Hemorrhagic Disorders These include Disorders of platelets. Disorders of blood vessels. Disorders of coagulation & fibrinolysis.
Bleeding disorders. Hemostatic failure: Inappropriate and excessive bleeding either spontaneous or in response to injury.
 1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
1 Bleeding disorders Objectives: 1. Discuss briefly the physiology of hemostasis. 2. Define the mechanisms of thrombocytopenia and the relative bleeding risk at any given platelet count. 3. Be able to
Bleeding Disorders. Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph
 Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
Bleeding Disorders Dr. Mazen Fawzi Done by Saja M. Al-Neaumy Noor A Mohammad Noor A Joseph Joseph Normal hemostasis The normal hemostatic response involves interactions among: The blood vessel wall (endothelium)
Routine preoperative coagulation tests: are they necessary?
 Routine preoperative coagulation tests: are they necessary? Dr Azzah Alzahrani MD Pediatrics Hematology /Oncology PSMMS Outline Introduction. Brief review of hemostatic mechanisms. A clinical aspect of
Routine preoperative coagulation tests: are they necessary? Dr Azzah Alzahrani MD Pediatrics Hematology /Oncology PSMMS Outline Introduction. Brief review of hemostatic mechanisms. A clinical aspect of
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche
 L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
L iter diagnostico di laboratorio nelle coagulopatie congenite emorragiche Armando Tripodi Angelo Bianchi Bonomi Hemophilia and Thrombosis Center Dept. of Clinical Sciences and Community Health University
Personal Practice. Screening for Bleeding Tendency in Suspected Child Abuse
 HK J Paediatr (new series) 2000;5:65-69 Personal Practice Screening for Bleeding Tendency in Suspected Child Abuse ACW LEE, ESK MA Abstract Key words Children who have been physically abused or victims
HK J Paediatr (new series) 2000;5:65-69 Personal Practice Screening for Bleeding Tendency in Suspected Child Abuse ACW LEE, ESK MA Abstract Key words Children who have been physically abused or victims
John Davidson Consultant in Intensive Care Medicine Freeman Hospital, Newcastle upon Tyne
 John Davidson Consultant in Intensive Care Medicine Freeman Hospital, Newcastle upon Tyne Overview of coagulation Testing coagulation Coagulopathy in ICU Incidence Causes Evaluation Management Coagulation
John Davidson Consultant in Intensive Care Medicine Freeman Hospital, Newcastle upon Tyne Overview of coagulation Testing coagulation Coagulopathy in ICU Incidence Causes Evaluation Management Coagulation
Easy bruising vs Coagulopathy
 Easy bruising vs Coagulopathy Sept. 19, 2015 Lakehead Summer School Chris Hillis, MD MSc FRCPC hillis@hhsc.ca @HemeHillis Aim & Objectives Aim: To increase comfort in detecting non-pathologic bleeding
Easy bruising vs Coagulopathy Sept. 19, 2015 Lakehead Summer School Chris Hillis, MD MSc FRCPC hillis@hhsc.ca @HemeHillis Aim & Objectives Aim: To increase comfort in detecting non-pathologic bleeding
Platelet Disorders. By : Saja Al-Oran
 Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
Platelet Disorders By : Saja Al-Oran Introduction The platelet arise from the fragmentation of the cytoplasm of megakaryocyte in the bone marrow. circulate in the blood as disc-shaped anucleate particles
Coagulation an Overview Dr.Abdolreza Abdolr Afrasiabi Thal assem a & Heamophili hilia G ene i tic R esearc C en er Shiraz Medical Medic University
 In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
In The Name God Coagulation an Overview Dr.Abdolreza Afrasiabi Thalassemia & Heamophilia Genetic Research hcenter Shiraz Medical University Bleeding Clotting Hemostasis Review of platelet function Platelets
HEME 10 Bleeding Disorders
 HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
HEME 10 Bleeding Disorders When injury occurs, three mechanisms occur Blood vessels Primary hemostasis Secondary hemostasis Diseases of the blood vessels Platelet disorders Thrombocytopenia Functional
Evaluating for Suspected Child Abuse: Conditions That Predispose to Bleeding
 FROM THE AMERICAN ACADEMY OF PEDIATRICS TECHNICAL REPORT Evaluating for Suspected Child Abuse: Conditions That Predispose to Bleeding Shannon L. Carpenter, MD, MS, Thomas C. Abshire, MD, James D. Anderst,
FROM THE AMERICAN ACADEMY OF PEDIATRICS TECHNICAL REPORT Evaluating for Suspected Child Abuse: Conditions That Predispose to Bleeding Shannon L. Carpenter, MD, MS, Thomas C. Abshire, MD, James D. Anderst,
Coagulation, Haemostasis and interpretation of Coagulation tests
 Coagulation, Haemostasis and interpretation of Coagulation tests Learning Outcomes Indicate the normal ranges for routine clotting screen and explain what each measurement means Recognise how to detect
Coagulation, Haemostasis and interpretation of Coagulation tests Learning Outcomes Indicate the normal ranges for routine clotting screen and explain what each measurement means Recognise how to detect
M B Garvey. University of Toronto
 Do I really need that test??? M B Garvey Professor Emeritus University of Toronto St Michael s Hospital No relevant conflicts of interest 1 HEMOSTASIS IS LIKE LOVE Everybody talks about it, nobody understands
Do I really need that test??? M B Garvey Professor Emeritus University of Toronto St Michael s Hospital No relevant conflicts of interest 1 HEMOSTASIS IS LIKE LOVE Everybody talks about it, nobody understands
When should I transfuse platelets and plasma for children? Dr Liz Chalmers. Consultant Paediatric Haematologist Royal Hospital for Children Glasgow
 When should I transfuse platelets and plasma for children? Dr Liz Chalmers Consultant Paediatric Haematologist Royal Hospital for Children Glasgow When should I transfuse platelets and plasma in children?
When should I transfuse platelets and plasma for children? Dr Liz Chalmers Consultant Paediatric Haematologist Royal Hospital for Children Glasgow When should I transfuse platelets and plasma in children?
There are two main causes of a low platelet count
 Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Thrombocytopenia Thrombocytopenia is a condition in which a person's blood has an unusually low level of platelets Platelets, also called thrombocytes, are found in a person's blood along with red blood
Approach To A Bleeding Patient
 ABDUL MAJEED, RAHUL RAJEEV REVIEW ARTICLE INTRODUCTION Hemostasis is the process of forming clots in the walls of damaged blood vessels and preventing blood loss while maintaining blood in a fluid state
ABDUL MAJEED, RAHUL RAJEEV REVIEW ARTICLE INTRODUCTION Hemostasis is the process of forming clots in the walls of damaged blood vessels and preventing blood loss while maintaining blood in a fluid state
BLEEDING DISORDERS Simple complement:
 BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
BLEEDING DISORDERS Simple complement: 1. Select the statement that describe the thrombocytopenia definition: A. Marked decrease of the Von Willebrandt factor B. Absence of antihemophilic factor A C. Disorder
CLINICAL FELLOWSHIP PROGRAM IN COAGULATION
 CLINICAL FELLOWSHIP PROGRAM IN COAGULATION The Department of Pathology and Laboratory Medicine University of Alberta, Faculty of Medicine and Dentistry and Alberta Health Services CLINICAL FELLOWSHIP IN
CLINICAL FELLOWSHIP PROGRAM IN COAGULATION The Department of Pathology and Laboratory Medicine University of Alberta, Faculty of Medicine and Dentistry and Alberta Health Services CLINICAL FELLOWSHIP IN
Bleeding history Recommendations of the working group on Perioperative Coagulation of the ÖGARI Gaps in the standard coagulation tests
 Bleeding history Recommendations of the working group on Perioperative Coagulation of the ÖGARI modified from the publication in: Anaesthesist 2007; 56: 604-11 The aim of the preoperative clarification
Bleeding history Recommendations of the working group on Perioperative Coagulation of the ÖGARI modified from the publication in: Anaesthesist 2007; 56: 604-11 The aim of the preoperative clarification
TRANSFUSION GUIDELINES FOR CARDIOTHORACIC UNIT 2006
 TRANSFUSION GUIDELINES FOR CARDIOTHORACIC UNIT 2006 CTU blood product transfusion guidelines 2006 1 Summary of guidelines RED CELLS (10-15ml/kg) This applies to ward patients / icu patients who are stable.
TRANSFUSION GUIDELINES FOR CARDIOTHORACIC UNIT 2006 CTU blood product transfusion guidelines 2006 1 Summary of guidelines RED CELLS (10-15ml/kg) This applies to ward patients / icu patients who are stable.
Approach to bleeding disorders &treatment. by RAJESH.N General medicine post graduate
 Approach to bleeding disorders &treatment by RAJESH.N General medicine post graduate 2 Approach to a patient of bleeding diathesis 1. Clinical evaluation: History, Clinical features 2. Laboratory approach:
Approach to bleeding disorders &treatment by RAJESH.N General medicine post graduate 2 Approach to a patient of bleeding diathesis 1. Clinical evaluation: History, Clinical features 2. Laboratory approach:
Blood coagulation and fibrinolysis. Blood clotting (HAP unit 5 th )
 Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Blood coagulation and fibrinolysis Blood clotting (HAP unit 5 th ) Vessel injury Antithrombogenic (Favors fluid blood) Thrombogenic (Favors clotting) 3 Major systems involved Vessel wall Endothelium ECM
Bleeding and Thrombotic Disorders. Kristine Krafts, M.D.
 Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
Bleeding and Thrombotic Disorders Kristine Krafts, M.D. Bleeding and Thrombotic Disorders Bleeding disorders von Willebrand disease Hemophilia A and B DIC TTP/HUS ITP Thrombotic disorders Factor V Leiden
TREATMENT & MANAGEMENT OF VON WILLEBRAND DISEASE
 TREATMENT & MANAGEMENT OF VON WILLEBRAND DISEASE Dr Susan Russell Director HTC Sydney Children s Hospital, Randwick HFA Meeting 2015 What is von Willebrand Factor? VWF is a large multimeric protein Two
TREATMENT & MANAGEMENT OF VON WILLEBRAND DISEASE Dr Susan Russell Director HTC Sydney Children s Hospital, Randwick HFA Meeting 2015 What is von Willebrand Factor? VWF is a large multimeric protein Two
Congenital bleeding disorders
 Congenital bleeding disorders Overview Factor VIII von Willebrand Factor Complex factor VIII von Willebrand factor (vwf) complex circulate as a complex + factor IX intrinsic pathway Platelets bind via
Congenital bleeding disorders Overview Factor VIII von Willebrand Factor Complex factor VIII von Willebrand factor (vwf) complex circulate as a complex + factor IX intrinsic pathway Platelets bind via
ACQUIRED COAGULATION ABNORMALITIES
 ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
ACQUIRED COAGULATION ABNORMALITIES ACQUIRED COAGULATION ABNORMALITIES - causes 1. Liver disease 2. Vitamin K deficiency 3. Increased consumption of the clotting factors (disseminated intravascular coagulation
Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012
 Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012 Clinical History Patient: 23-year-old female Clinical course: status-post cholecystectomy, complicated by retained common bile duct stones. Following three
Y. Helen Zhang, MD Andy Nguyen, MD 10/28/2012 Clinical History Patient: 23-year-old female Clinical course: status-post cholecystectomy, complicated by retained common bile duct stones. Following three
Thursday, February 26, :00 am. Regulation of Coagulation/Disseminated Intravascular Coagulation HEMOSTASIS/THROMBOSIS III
 REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
REGULATION OF COAGULATION Introduction HEMOSTASIS/THROMBOSIS III Regulation of Coagulation/Disseminated Coagulation necessary for maintenance of vascular integrity Enough fibrinogen to clot all vessels
Bleeding Disorders HOPE Maram Al-anbar
 Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
Bleeding Disorders HOPE Maram Al-anbar 9-9 - 2014 ^^ Attention Please ^^ We ( correction team of pediatric package^hope/2010^ ) had decided to make one lecture of bleeding disorders in place of the two
COAGULATIONS. Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin)
 COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
COAGULATIONS Dr. Hasan Fahmawi, MRCP(UK), FRCP(Edin) Haemostasis-blood must be maintained in a fluid state in order to function as a transport system, but must be able to solidify to form a clot following
Primary Exam Physiology lecture 5. Haemostasis
 Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
Primary Exam Physiology lecture 5 Haemostasis Haemostasis Body s response for the prevention and cessation of bleeding. Broadly consists of: Primary Haemostasis - vascular spasm and platlet plug formation
von Willebrand Disease
 von Willebrand Disease Jeremy Robertson Paediatric Haematologist Royal Children s s Hospital & Pathology Queensland Foglo,, April 1924: the journey begins Oskar and Augusta sail to Helsinki... ...to o
von Willebrand Disease Jeremy Robertson Paediatric Haematologist Royal Children s s Hospital & Pathology Queensland Foglo,, April 1924: the journey begins Oskar and Augusta sail to Helsinki... ...to o
Mohammadreza Tabatabaei IBTO COAG LAB
 Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Tests for the Evaluation of Lupus Anticoagulants t Mohammadreza Tabatabaei MSc Hematology blood bank MSc Hematology blood bank IBTO COAG LAB Lupus Anticoagulants General Background Lupus anticoagulants
Hemostasis. PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures
 Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Hemostasis PHYSIOLOGICAL BLOOD CLOTTING IN RESPONSE TO INJURY OR LEAK no disclosures Disorders of Hemostasis - Hemophilia - von Willebrand Disease HEMOPHILIA A defect in the thrombin propagation phase
Blood Transfusion Guidelines in Clinical Practice
 Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
Blood Transfusion Guidelines in Clinical Practice Salwa Hindawi Director of Blood Transfusion Services Associate Professor in Haematology and Transfusion Medicine King Abdalaziz University, Jeddah Saudi
EDUCATIONAL COMMENTARY PLATELET DISORDERS
 EDUCATIONAL COMMENTARY PLATELET DISORDERS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
EDUCATIONAL COMMENTARY PLATELET DISORDERS Educational commentary is provided through our affiliation with the American Society for Clinical Pathology (ASCP). To obtain FREE CME/CMLE credits click on Earn
Factor VII deficiency
 Factor VII deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 1 Factor VII deficiency (also known as Alexander s disease) is a type of clotting disorder.
Factor VII deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 1 Factor VII deficiency (also known as Alexander s disease) is a type of clotting disorder.
Determination of APTT factor sensitivity the misguiding guideline
 International Journal of Laboratory Hematology ORIGINAL ARTICLE The Official journal of the International Society for Laboratory Hematology INTERNATIONAL JOURNAL OF LABORATORY HEMATOLOGY Determination
International Journal of Laboratory Hematology ORIGINAL ARTICLE The Official journal of the International Society for Laboratory Hematology INTERNATIONAL JOURNAL OF LABORATORY HEMATOLOGY Determination
UNIT VI. Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav. Copyright 2011 by Saunders, an imprint of Elsevier Inc.
 UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
UNIT VI Chapter 37: Platelets Hemostasis and Blood Coagulation Presented by Dr. Diksha Yadav Hemostasis: Prevention of Blood Loss Vascular constriction Formation of a platelet plug Formation of a blood
Platelet disorders. Information for families. Great Ormond Street Hospital for Children NHS Foundation Trust
 Platelet disorders Information for families Great Ormond Street Hospital for Children NHS Foundation Trust Platelets are the cells responsible for making blood clot so platelet disorders mean that injured
Platelet disorders Information for families Great Ormond Street Hospital for Children NHS Foundation Trust Platelets are the cells responsible for making blood clot so platelet disorders mean that injured
Referrals for abnormal coagulation profiles are common
 A Practical Approach to Pediatric Patients Referred With an Abnormal Coagulation Profile Monica Acosta, MD; Rachel Edwards, BS; E. Ian Jaffe, MD; Donald L. Yee, MD; Donald H. Mahoney, MD; Jun Teruya, MD,
A Practical Approach to Pediatric Patients Referred With an Abnormal Coagulation Profile Monica Acosta, MD; Rachel Edwards, BS; E. Ian Jaffe, MD; Donald L. Yee, MD; Donald H. Mahoney, MD; Jun Teruya, MD,
Introduction to coagulation and laboratory tests
 Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
Introduction to coagulation and laboratory tests Marc Jacquemin Special Haemostasis Laboratory Center for Molecular and Vascular Biology University of Leuven Coagulation in a blood vessel: fibrin stabilises
INHERITED COAGULOPATHY
 Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
Disorder Etiology Pathophysiology and Presentation Lab Findings and Diagnosis Treatment INHERITED COAGULOPATHY HEMOPHILIA A and B Hemophilia A: deficiency in XIII (85%) Hemophilia B: deficiency in IX (15%)
HAEMORRHAGIA Bleeding
 HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechiae : 1-2 mm hemorrhages into skin, mucous membranes, or serosal surfaces increased
Factor XI deficiency. Information for families. Great Ormond Street Hospital for Children NHS Foundation Trust
 Factor XI deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Factor XI deficiency (also known as Haemophilia C, plasma thromboplastin antecedent deficiency
Factor XI deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Factor XI deficiency (also known as Haemophilia C, plasma thromboplastin antecedent deficiency
Hematologic Disorders. Assistant professor of anesthesia
 Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
Preoperative Evaluation Hematologic Disorders Dr M.Razavi Assistant professor of anesthesia Anemia Evaluation needs to consider the extent and type of surgery, the anticipated blood loss, and the patient's
HAEMORRHAGIA Bleeding
 HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechial rash (spot) : 1-2 mm hemorrhages into skin, mucous membranes, or serosal
HAEMORRHAGIA Bleeding Cassification Size Location pathomechanism Hematoma: external or may be enclosed within a tissue petechial rash (spot) : 1-2 mm hemorrhages into skin, mucous membranes, or serosal
Overview 5/8/2017. Management Strategies for Bleeding and Thrombocytopenia in the Neonate
 Management Strategies for Bleeding and Thrombocytopenia in the Neonate Kyle Annen, DO Medical Director Blood Bank, Transfusion Service and Hematology Mount Sinai Beth Israel Assistant Professor, Department
Management Strategies for Bleeding and Thrombocytopenia in the Neonate Kyle Annen, DO Medical Director Blood Bank, Transfusion Service and Hematology Mount Sinai Beth Israel Assistant Professor, Department
Idiopathic Thrombocytopenic Purpura
 Idiopathic Thrombocytopenic Purpura Title of Guideline Contact Name and Job Title (author) Directorate & Speciality Guideline for the management of idiopathic thrombocytopenic purpura Dr S Stokley, Consultant
Idiopathic Thrombocytopenic Purpura Title of Guideline Contact Name and Job Title (author) Directorate & Speciality Guideline for the management of idiopathic thrombocytopenic purpura Dr S Stokley, Consultant
Bleeding Disorders: (Hemorrhagic Diatheses) Tests used to evaluate different aspects of hemostasis are the following:
 Bleeding Disorders: (Hemorrhagic Diatheses) Excessive bleeding can result from: 1. Increased fragility of vessels. 2. Platelet deficiency or dysfunction. 3. Derangement of coagulation. 4. Combinations
Bleeding Disorders: (Hemorrhagic Diatheses) Excessive bleeding can result from: 1. Increased fragility of vessels. 2. Platelet deficiency or dysfunction. 3. Derangement of coagulation. 4. Combinations
HEMOSTASIS/THROMBOSIS II
 HEMOSTASIS/THROMBOSIS II Congenital/Acquired Hemorrhagic Disorders & Their Treatment COAGULATION TESTING!Bleeding time primary screening test for platelet function!if bleeding time abnormal!platelet Aggregation
HEMOSTASIS/THROMBOSIS II Congenital/Acquired Hemorrhagic Disorders & Their Treatment COAGULATION TESTING!Bleeding time primary screening test for platelet function!if bleeding time abnormal!platelet Aggregation
Clinical Guidance. Neonatal Manual Chapter 8: Haematology
 Clinical Guidance Neonatal Manual Chapter 8: Haematology Summary This manual contains clinical guidelines developed by the Neonatal Unit multidisciplinary team over recent years. This chapter contains
Clinical Guidance Neonatal Manual Chapter 8: Haematology Summary This manual contains clinical guidelines developed by the Neonatal Unit multidisciplinary team over recent years. This chapter contains
Factor X deficiency. Information for families. Great Ormond Street Hospital for Children NHS Foundation Trust
 Factor X deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 1 Factor X (previously known as the Stuart-Prower factor) deficiency is a type of clotting disorder.
Factor X deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 1 Factor X (previously known as the Stuart-Prower factor) deficiency is a type of clotting disorder.
FIGURE 1. Coagulation cascade. a = activated factor; Ca = calcium; PL = phospholipid. Adapted from Biochemistry, 2 with permission from American Chemi
 CONCISE REVIEW FOR CLINICIANS PROLONGED PT AND APTT How to Interpret and Pursue an Abnormal Prothrombin Time, Activated Partial Thromboplastin Time, and Bleeding Time in Adults ARIF H. KAMAL, MD; AYALEW
CONCISE REVIEW FOR CLINICIANS PROLONGED PT AND APTT How to Interpret and Pursue an Abnormal Prothrombin Time, Activated Partial Thromboplastin Time, and Bleeding Time in Adults ARIF H. KAMAL, MD; AYALEW
Pathologist-in-chief. Professor of Medicine and Pathology. School of Medicine
 Michael Laposata MD, PhD Pathologist-in-chief Vanderbilt University Hospital Professor of Medicine and Pathology Vanderbilt University School of Medicine Rosemary Jaromin Godmother of patient Jazmin Corinne
Michael Laposata MD, PhD Pathologist-in-chief Vanderbilt University Hospital Professor of Medicine and Pathology Vanderbilt University School of Medicine Rosemary Jaromin Godmother of patient Jazmin Corinne
Hemostatic System - general information
 PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
PLATELET DISORDERS Hemostatic System - general information Normal hemostatic system vessel wall circulating blood platelets blood coagulation and fibrynolysis Bleeding Diathesis inherited or acquired defects
Factor XIII deficiency
 Factor XIII deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Factor XIII deficiency is a type of clotting disorder. A specific protein is missing from
Factor XIII deficiency Information for families Great Ormond Street Hospital for Children NHS Foundation Trust 2 Factor XIII deficiency is a type of clotting disorder. A specific protein is missing from
Hemostasis Haemostasis means prevention of blood loss from blood vessels.
 ١ Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
١ Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
Pathology note 8 BLEEDING DISORDER
 Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
Pathology note 8 BLEEDING DISORDER Slide75 ( Types of clotting factors deficiency): Today we will talk about public public factor deficiency it could be acquired or inherited, acquired diseases are more
Recommendations for Celiac Disease Testing. IgA & ttg IgA
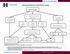 Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Recommendations for Celiac Disease Testing IgA & ttg IgA IgA Normal ttg IgA Negative IgA >10 mg/dl, but less than age matched range IgA
Evaluation for Bleeding Disorders in Suspected Child Abuse
 Guidance for the Clinician in Rendering Pediatric Care CLINICAL REPORT Evaluation for Bleeding Disorders in Suspected Child Abuse abstract Bruising or bleeding in a child can raise the concern for child
Guidance for the Clinician in Rendering Pediatric Care CLINICAL REPORT Evaluation for Bleeding Disorders in Suspected Child Abuse abstract Bruising or bleeding in a child can raise the concern for child
Approach to disseminated intravascular coagulation
 Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Approach to disseminated intravascular coagulation Khaire Ananta Shankarrao 1, Anil Burley 2, Deshmukh 3 1.MD Scholar, [kayachikitsa] 2.Professor,MD kayachikitsa. 3.Professor and HOD,Kayachikitsa. CSMSS
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89
 Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
Chapter 3 Diseases of the Blood and Bloodforming Organs and Certain Disorders Involving the Immune Mechanism D50-D89 Presented by Jennifer Kurkulonis 1 FOUR MAJOR TYPES OF BLOOD CELLS White blood cells
A Patient with a Prolonged Activated Partial Thromboplastin Time and a Deep Intracerebral Haemorrhage
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
WISKOTT-ALDRICH SYNDROME. An X-linked Primary Immunodeficiency
 WISKOTT-ALDRICH SYNDROME An X-linked Primary Immunodeficiency WHAT IS WISKOTT ALDRICH SYNDROME? Wiskott-Aldrich Syndrome (WAS) is a serious medical condition that causes problems both with the immune system
WISKOTT-ALDRICH SYNDROME An X-linked Primary Immunodeficiency WHAT IS WISKOTT ALDRICH SYNDROME? Wiskott-Aldrich Syndrome (WAS) is a serious medical condition that causes problems both with the immune system
The rare coagulation disorders review with guidelines for management from the United Kingdom Haemophilia Centre Doctors Organisation
 DOI: 10.1111/j.1365-2516.2004.00944.x GUIDELINES The rare coagulation disorders review with guidelines for management from the United Kingdom Haemophilia Centre Doctors Organisation P. H. B. BOLTON-MAGGS,*
DOI: 10.1111/j.1365-2516.2004.00944.x GUIDELINES The rare coagulation disorders review with guidelines for management from the United Kingdom Haemophilia Centre Doctors Organisation P. H. B. BOLTON-MAGGS,*
Approach to bleeding
 Approach to bleeding By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University The mechanism of
Approach to bleeding By Assoc. Prof. Darintr Sosothikul, MD Pediatric Hematology-Oncology division, King Chulalongkorn Memorial Hospital, Faculty of Medicine, Chulalongkorn University The mechanism of
Hemostasis and. Blood Coagulation
 Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
Hemostasis and Blood Coagulation Events in Hemostasis The term hemostasis means prevention of blood loss. Whenever a vessel is severed or ruptured, hemostasis is achieved by several mechanisms: (1) vascular
r). SUPPLEMENTARY/SECOND OPPORTUNITY EXAMINATION PAPER nnmlbih UNIVERSITY Sophia Blaauw INSTRUCTIONS FACULTY OF HEALTH AND APPLIED SCIENCES
 r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
r). nnmlbih UNIVERSITY OF SCIEFICE nnd TECHNOLOGY FACULTY OF HEALTH AND APPLIED SCIENCES DEPARTMENT OF HEALTH SCIENCES QUALIFICATION: BACHELOR OF MEDICAL LABORATORY SCIENCES QUALIFICATION CODE: 08BMLS
MANAGEMENT OF COAGULOPATHY AFTER TRAUMA OR MAJOR SURGERY
 MANAGEMENT OF COAGULOPATHY AFTER TRAUMA OR MAJOR SURGERY 19th ANNUAL CONTROVERSIES AND PROBLEMS IN SURGERY Thabo Mothabeng General Surgery: 1 Military Hospital HH Stone et al. Ann Surg. May 1983; 197(5):
MANAGEMENT OF COAGULOPATHY AFTER TRAUMA OR MAJOR SURGERY 19th ANNUAL CONTROVERSIES AND PROBLEMS IN SURGERY Thabo Mothabeng General Surgery: 1 Military Hospital HH Stone et al. Ann Surg. May 1983; 197(5):
Instruments smart solutions & service IGZ Instruments AG Räffelstrasse 32 CH 8045 Zürich
 ADP (Adenosine-5 -Diphosphate) 101312 3 x 0.5mL ADP is a lyophilized preparation of adenosine-5 -diphosphate. The working concentration of the reconstituted reagent is 2 x 10-4 M. ADP is for use in routine
ADP (Adenosine-5 -Diphosphate) 101312 3 x 0.5mL ADP is a lyophilized preparation of adenosine-5 -diphosphate. The working concentration of the reconstituted reagent is 2 x 10-4 M. ADP is for use in routine
Peri-operative strategy in patients with congenital disorders of haemostasis
 06RC1 - Filipescu Peri-operative strategy in patients with congenital disorders of haemostasis Daniela Filipescu Cardiac Anaesthesia and Intensive Care Medicine, Iliescu Emergency Cardiovascular Diseases
06RC1 - Filipescu Peri-operative strategy in patients with congenital disorders of haemostasis Daniela Filipescu Cardiac Anaesthesia and Intensive Care Medicine, Iliescu Emergency Cardiovascular Diseases
FELINE HEMATOLOGY Inherited and Acquired Bleeding Disorders Marjory Brooks DVM, D.ACVIM
 FELINE HEMATOLOGY Marjorie Brooks, D.V.M. Diplomate, A.C.V.I.M. Comparative Hematology Laboratory N.Y.S. Department of Health WCL&R P. O. Box 509 Albany, NY 12201 f / b - f / i 3 FELINE HEMATOLOGY Inherited
FELINE HEMATOLOGY Marjorie Brooks, D.V.M. Diplomate, A.C.V.I.M. Comparative Hematology Laboratory N.Y.S. Department of Health WCL&R P. O. Box 509 Albany, NY 12201 f / b - f / i 3 FELINE HEMATOLOGY Inherited
Review Article Sri Lanka Dental Journal 2016; 46(01) 05-13
 Review Article Sri Lanka Dental Journal 2016; 46(01) 05-13 The Importance of Knowing the Patient s Clotting Profile before Dental Treatment N.A. Alles, N.S. Soysa Introduction Patients having bleeding
Review Article Sri Lanka Dental Journal 2016; 46(01) 05-13 The Importance of Knowing the Patient s Clotting Profile before Dental Treatment N.A. Alles, N.S. Soysa Introduction Patients having bleeding
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust
 Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
Abnormal blood counts in children Dr Tina Biss Consultant Paediatric Haematologist Newcastle upon Tyne Hospitals NHS Foundation Trust Regional Paediatric Specialty Trainees teaching 4 th July 2017 Scope
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS
 QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
QUESTIONS OF HEMATOLOGY AND THEIR ANSWERS WHAT IS TRUE AND WHAT IS FALSE? Questions 1 Iron deficiency anemia a) Is usually associated with a raised MCV. b) The MCH is usually low. c) Is most commonly due
Hemostasis Haemostasis means prevention of blood loss from blood vessels.
 1 Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
1 Hemostasis Haemostasis means prevention of blood loss from blood vessels. Bleeding is stopped by several mechanisms, which are: 1. Local vasoconstriction 2. Formation of platelet plug 3. Blood coagulation
Commonly Encountered Hematologic Chief Complaints in the Pediatric Pa8ent Black Hills Pediatric Symposium 6/23/17 Sam Milanovich, MD Pediatric
 Commonly Encountered Hematologic Chief Complaints in the Pediatric Pa8ent Black Hills Pediatric Symposium 6/23/17 Sam Milanovich, MD Pediatric Hematology/Oncology Sanford Children s Specialty Clinic Sioux
Commonly Encountered Hematologic Chief Complaints in the Pediatric Pa8ent Black Hills Pediatric Symposium 6/23/17 Sam Milanovich, MD Pediatric Hematology/Oncology Sanford Children s Specialty Clinic Sioux
Common bleeding disorders affecting individuals with Hereditary Hemorrhagic Telangiectasia
 TRAINEE SECTION Jennifer LaBranche, BSc 1,2,4 Susan Nahirniak, MD, FRCPC 3 Dilini Vethanayagam, MD, FRCPC 1,4 1University of Alberta - Department of Medicine 2University of Alberta - Department of Biological
TRAINEE SECTION Jennifer LaBranche, BSc 1,2,4 Susan Nahirniak, MD, FRCPC 3 Dilini Vethanayagam, MD, FRCPC 1,4 1University of Alberta - Department of Medicine 2University of Alberta - Department of Biological
Managing Coagulopathy in Intensive Care Setting
 Managing Coagulopathy in Intensive Care Setting Dr Rock LEUNG Associate Consultant Division of Haematology, Department of Pathology & Clinical Biochemistry Queen Mary Hospital Normal Haemostasis Primary
Managing Coagulopathy in Intensive Care Setting Dr Rock LEUNG Associate Consultant Division of Haematology, Department of Pathology & Clinical Biochemistry Queen Mary Hospital Normal Haemostasis Primary
Familial Mediterranean Fever
 www.printo.it/pediatric-rheumatology/gb/intro Familial Mediterranean Fever Version of 2016 1. WHAT IS FMF 1.1 What is it? Familial Mediterranean Fever (FMF) is a genetically transmitted disease. Patients
www.printo.it/pediatric-rheumatology/gb/intro Familial Mediterranean Fever Version of 2016 1. WHAT IS FMF 1.1 What is it? Familial Mediterranean Fever (FMF) is a genetically transmitted disease. Patients
Pediatric Coagulation Disorders
 Pediatric Coagulation Disorders Vilmarie Rodriguez, MD,* Deepti Warad, MBBS* *Division of Pediatric Hematology-Oncology, Mayo Clinic Children s Center, Mayo Clinic Comprehensive Hemophilia Center, Mayo
Pediatric Coagulation Disorders Vilmarie Rodriguez, MD,* Deepti Warad, MBBS* *Division of Pediatric Hematology-Oncology, Mayo Clinic Children s Center, Mayo Clinic Comprehensive Hemophilia Center, Mayo
Appendix 3 PCC Warfarin Reversal
 Appendix 3 PCC Warfarin Reversal Reversal of Warfarin and Analogues 1. Principle of Procedure Guidelines for the Reversal of Oral-anticoagulation in the Event of Life Threatening Haemorrhage Prothrombin
Appendix 3 PCC Warfarin Reversal Reversal of Warfarin and Analogues 1. Principle of Procedure Guidelines for the Reversal of Oral-anticoagulation in the Event of Life Threatening Haemorrhage Prothrombin
The Clinical Features of Chinese Children with von Willebrand Disease: The Experience of a Tertiary Institute
 HK J Paediatr (new series) 2011;16:95-100 The Clinical Features of Chinese Children with von Willebrand Disease: The Experience of a Tertiary Institute ZQ ZHANG, GCF CHAN, CCK LAM, JCC SO, DKL CHEUK, AKS
HK J Paediatr (new series) 2011;16:95-100 The Clinical Features of Chinese Children with von Willebrand Disease: The Experience of a Tertiary Institute ZQ ZHANG, GCF CHAN, CCK LAM, JCC SO, DKL CHEUK, AKS
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion
 This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
This slide belongs to iron lecture and it is to clarify the iron cycle in the body and the effect of hypoxia on erythropoitein secretion Topics of today lectures: Hemostasis Meaning of hemostasis Mechanisms
Optimal Utilization of Thrombophilia Testing
 Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
Optimal Utilization of Thrombophilia Testing Rajiv K. Pruthi, MBBS Special Coagulation Laboratory & Comprehensive Hemophilia Center Division of Hematology/Internal Medicine Dept of Laboratory Medicine
GLANZMANN S THROMBASTHENIA. Stacey Shiovitz January 13, 2012
 GLANZMANN S THROMBASTHENIA Stacey Shiovitz January 13, 2012 HELP!! MY PATIENTHASGT DO YOU EVEN KNOW WHAT THAT IS? CASE 27yo woman presented tdto gynecology clinic i for menorrhagia x 10 days Bleeding started
GLANZMANN S THROMBASTHENIA Stacey Shiovitz January 13, 2012 HELP!! MY PATIENTHASGT DO YOU EVEN KNOW WHAT THAT IS? CASE 27yo woman presented tdto gynecology clinic i for menorrhagia x 10 days Bleeding started
