The Spinal Cord Injury Rehab Program
|
|
|
- Augusta Morrison
- 5 years ago
- Views:
Transcription
1 The Spinal Cord Injury Rehab Program Wake Forest Baptist Medical Center s Spinal Cord Injury Program provides specialized, intensive rehabilitation for patients age 13 and older with spinal cord dysfunction due to trauma or disease resulting in paralysis (loss of strength), loss of sensation (feeling), and loss of control ove r body functions. The Program offers the expertise of a specialized interdisciplinary care team of rehab professionals who help patients cope with their injuries, relearn basic skills, maximize functional independence, and reintegrate back into their communities. The Program also provides patient and family training to prepare patients and their families for rehab discharge, to help coordinate equipment needs and home modifications, and to provide information on lifetime health and wellness resources. Philosophy of Care Each patient is unique, with specific needs, capabilities and potential. Therefore, each patient s treatment plan is individualized and modified as recovery progresses. The rehabilitation team, patient, and family/caregivers work together to set and achieve functional improvement goals. The Care Team The Program s success is attributed to its comprehensive, interdisciplinary team, which includes the patient, family members/caregivers, and professionals specializing in: Rehab Medicine Clinical Nutrition Social Work Rehabilitation Nursing Occupational Therapy Recreation Therapy Clinical Psychology Physical Therapy Assistive Technology* Neuropsychology Speech Language Pathology *These services are provided by team members who are not directly employed by WFBMC, but who work very collaboratively with the Wake Forest Baptist Medical Center Rehab Programs. Scope of Services Board-certified physicians specializing in Physical Medicine and Rehabilitation (PM&R) direct the patient s plan of care on a daily basis. Rehabilitation Nursing is provided 24 hours a day, 7 days a week Each patient receives a minimum of 15 hours of therapy each week, including a combination of physical therapy, occupational therapy, speech therapy, and/or orthotics/prosthetics training. The type of therapy, intensity of therapy, and schedule are tailored to the needs of each patient. Therapy services are provided between 7AM and 5PM Monday through Friday, and on Saturdays as needed. Recreation therapy, clinical psychology, neuropsychology, and assistive technology services are available 5 days a week, and are provided based on the needs of each patient. Each patient is assigned a Care Coordinator who acts as a liaison between patient, family/caregiver, rehabilitation professionals, and third party payers. Wake Forest Baptist Medical Center provides all ancillary services including, but not limited to, Diagnostic Imaging, Laboratory, Pharmacy, Spiritual Care, and Respiratory Therapy. Consulting physician services for other specialties are provided by Wake Forest Baptist, as needed. If services not available within the Wake Forest Baptist are needed, referrals or consultations are made for these services, which may include, but are not limited to: cognitive rehab, orthotics and prosthetics, durable medical equipment, caregiver/family services, substance abuse counseling, vocational rehabilitation, rehab engineering, and driver s assessment and education.
2 Treatment Goals and Common Interventions The ultimate goal is to return each patient to the highest level of independence possible, and in most cases, to return patient to home. Specific treatment goals are individualized for each patient and may include: Maximizing function in: o Mobility and balance o Activities of Daily Living (eating, grooming, dressing, bathing) o Communication and cognition o Bowel and bladder management Addressing sexuality and family issues Disability adjustment, counseling, and coping strategies Patient and family education for individualized needs Recommending healthy living practices for weight control and smoking cessation Optimizing community integration and life roles through community outings, recreation therapy and use of assistive technology Identifying additional services for families/support systems (e.g., support groups) Spinal Cord Injury The Program welcomes patients with spinal cord injury due to any etiology and for all levels of injury resulting in either paraplegia/para paresis or tetraplegia/tetra paresis as long as the patient no longer needs mechanical ventilator support (breathing machine). The following table describes the etiology, levels, and co-occurring conditions associated with Spinal Cord Injury. Includes, but not limited to: Levels of Cord Injury Effects Associated Deficits and Co- Occurring Conditions include, but are not limited to: Non-Traumatic Spinal Cord Injury Traumatic Spinal Cord Injury Intervertebral disco disorders with Anterior cord syndrome, Brown-Sequard myelopathy, intraspinal abscess, vascular Syndrome, cauda equine syndrome, central myelopathies cord syndrome, fracture of vertebral column with spinal cord injury, concussion and edema of spinal cord, posterior cord syndrome, nerve root Cervical (C1-C8) Cervical (C1-C8) Thoracic (T1-T12) Thoracic (T1-T12) Lumbar (L1-L5) Lumbar (L1-L5) Sacral region Sacral region Cauda equine Cauda equine Paraplegia, tetraplegia, no plegia, Paraplegia, tetraplegia, no plegia, complete, complete, incomplete incomplete Laterality: left, right, bilateral Acute vs sequalae (late effects) from initial injury Laterality: left, right, bilateral Bowel and bladder dysfunction, sexual dysfunction, blood pressure changes, bradykinesia (slowness in movement), clonus (involuntary muscle contraction and relaxation), depression, post-traumatic stress disorder, dysphagia (impaired swallowing), flaccidity, gait impairment, heterotrophic ossification, hyperreflexia, impaired balance, impaired motor control, orthostatic hypotension, postural instability, proprioception, respiratory dysfunction, spasticity, tremors, involuntary movements, muscle atrophy, pain, skin breakdown/pressure ulcers and changes in control of heart rate, body temperature, breathing rate, digestion, sensation
3 Demonstrated Excellence in Rehabilitation Wake Forest Baptist s Comprehensive Inpatient Rehabilitation Program has been awarded accreditation from the Commission on Accreditation of Rehabilitation Facilities. CARF Accreditation means that Wake Forest Baptist Medical Center s Rehab Program: is committed to excellence in rehabilitative care meets rigorous international standards of patient care and satisfaction is committed to helping each patient achieve their individualized rehabilitation goals constantly works to improve services and stays on the edge of rehabilitation techniques and technology surpasses communication expectations with referral and payer sources Admission Criteria and Referrals Patients admitted to the Spinal Cord Injury Rehab Program must have realistic rehabilitation goals that reflect the potential for gaining independence or achieving a higher functi on in self-care activities and mobility. Additionally, a patient must: Be 13 years of age or older Require and be able and willing to participate in intensive physical, occupational and/or speech therapy (if indicated) at least 3 hours a day Have the need for more than one type of rehab therapy and have potential for functional improvement. Be medically appropriate for an inpatient hospital environment and have stable vital signs. Have a supportive social system and a defined, expected discharge destination to home Have a cognitive level of three or higher on the Rancho Los Amigos scale. Be able to breath without the help of a mechanical ventilator at all times. Wake Forest Baptist Health accepts payment from all major private insurance plans, worker s compensation, Medicare and Medicaid. The Program evaluates and verifies insurance coverage for each patient prior to admission. If the patient does not have insurance coverage for the Rehabilitation Program, the patient and/or family/caregiver will be notified and alternate payment plans or treatment options will be discussed. Any estimated financial responsibilities will be communicated to the patient and/or family. The Program welcomes referrals from many sources, including, but not limited to, physicians, short term acute care hospitals, rehab hospitals, nursing facilities, long term acute care hospitals, and home health agencies. To make a referral, call (336) or (888) For additional information about the program, call (336) or Rehab4Life@wakehealth.edu. The Rehabilitation Programs at Wake Forest Baptist Medical Center do not discriminate against individuals of varying age, disability, race/ethnicity, religion, gender, or sexual preference and strive to understand and the be sensitive to these characteristics and to patient-specific preferences.
4 Spinal Cord Injury Program Patient Outcomes Program Patients Calendar Year 2017 Number of Patients: 98 Patients with Traumatic Spinal Cord Injuries: 36 Patients with Non Traumatic Spinal Cord Injuries: 62 76% were males 24% were females Average Days in Program: 22 Therapy Intensity (on average): 3.5 hours per day, 5 days per week Age Group Number of Patients Patient Outcomes Calendar Year 2017 Other 1% Home 75% Long Term Care 17% Acute Care 7% The ability to return home is a key outcome and expectation for most Program participants. During calendar year 2017, 75% of the Program s patients returned home. 7% of patients returned to their previous hospital setting, but often for just a short period prior to returning to Rehab. 17% of patients were discharged to a long term care setting for continued rehab and/or nursing care. Functional Improvement Goals % Patients with Improved Function between Admission and Discharge Traumatic Spinal Cord Injury Non-Traumatic Spinal Cord Injury Self-Care 94% 96% Bowel and Bladder 43% 61% Locomotion (Walking/Stairs) 100% 99% Bed, Toilet, & Chair Transfers 100% 99% Source: Uniform Data Systems for Medical Rehabilitation Function is measured, or scored, at admission, during the stay, and at discharge. The table to the left shows the percentage of patients who demonstrated improvement in function between admission and discharge from the Program. Patient/Family Satisfaction In 2017, Spinal Cord Injury Program participants completed a survey about their likelihood of recommending the Program to friends and family members. 95% gave a rating of 9 or 10 on a 10 point scale, indicating they are extremely likely to recommend the program.
5 What to Expect in Your Rehab Program The information below will give you an idea of what your rehab program may include. Please keep in mind that your rehab care team will complete a thorough evaluation after admission and develop a more detailed care plan based on your needs and your family s needs. Name Diagnosis Rehab Physician Location: Insurance Coverage: Expected Days in Program* Expected Discharge Rehab Intensity: Treatment will include a minimum of either three hours of therapy per day, five days per week, or fifteen hours of therapy over the seven day period. On average, patients in the Program receive 90 minutes physical therapy, 90 minutes occupational therapy, and 20 minutes of speech therapy per day, 5 days per week. Program Services Rehabilitation Physician Services Physical Therapy Occupational Therapy Speech Therapy Treatment Goals Manage your medical condition to ensure your safety and progress toward your goals. Nurse practitioners, physician s assistants, medical students, and residents may work in close collaboration with your rehab physician. During your stay, physician orders will be responded to, with results, within 24 hours, unless otherwise specified. Improve & maximize your mobility skills, safety, strength and endurance Improve your ability to complete activities of daily living such as eating, dressing, bathing, toileting and home management; address sexuality issues related to impairment Improve your swallowing, communication and cognitive skills Rehab Nursing Manage your bowel and bladder control, address family issues associated with impairment, educate on care needs, including health and wellness. Our team will be asking you to assume more responsibility and independence the closer you get to discharge. This will make you and your family better prepared for your activities of daily living and resuming home life. Nutrition Services Educate and ensure proper nutrition during treatment Clinical & Neuropsychology Recreation Therapy Care Coordination Orthotics Help you and your family members with emotional and mental health challenges associated with temporary or permanent disability Educate you and your family on how to adapt to community environment after discharge and how to enjoy recreational activities safely Coordinate services with the care team, you, and your family members to ensure needs are met prior to discharge Provide custom orthotic (if needed) to improve mobility and range of motion Other The Program is attentive to the specific cultural or other needs of each patient. Please let us know if you have any specific needs or requests.
6 What to Expect During Your Stay The following is a typical schedule for the first three days after admission to the Rehab Program. Day One Arrive on the 3rd floor of the Sticht Center at assigned room. Nurse assesses your condition and needs upon arrival to the rehabilitation unit. Meet with the physician, social worker and nurses within the first 24 hours. Receive an assigned wheelchair for the rehab stay. Receive a tentative schedule for each therapy. Throughout your stay, you will receive regular updates on the scheduled times for each therapy service identified for your care plan. Day Two Begin therapy evaluations and treatment, which could include physical therapy, occupational therapy, speech therapy and recreation therapy. You will participate approximately three hours of therapy each day and at least 15 hours per week. Day Three Working with you and your family, the Rehab team develops an individualized Plan of Care based on your condition and determines your functional status. The Plan of Care guides your treatment program. The rehab team reviews your progress toward your goals at least weekly. What to Expect During and After Discharge Your care coordinator will work with you, your care team, and your family/caregiver to coordinate the best discharge plan for your individual needs. Many activities must be completed prior to discharge. For example: Your care team will make recommendations for equipment you will need at home or modifications that you will need to make at home for your safety and continued recovery. Your Care Coordinator will arrange for delivery of equipment. Your care team will determine if you need assistance from a home health agency, which includes nursing and/or therapy at home. Another option is outpatient therapy after your discharge. If the best option for you is home health, your Care Coordinator will give you a list of agencies to choose from near your home and arrange Home Health visits. If outpatient therapy is the best option for you, the Care Coordinator will set up appointments for outpatient therapy. Your care team will review all discharge instructions with you. The unit secretary will schedule follow-up appointments with your physician. When your physician notifies you that you will be going home, please be aware that it may take several hours for the care team to complete all necessary items and ensure that you have a safe and successful discharge from the Program. After discharge from the Inpatient Rehabilitation Program: Your rehabilitation journey will continue, and you may need additional resources to assist with lifestyle changes. During your stay, we will provide information about additional resources that are tailored to your individual needs. If you have additional needs or questions about community resources, please contact Karen Lawrence at or Rehab4Life@wakehealth.edu. You will receive a Press-Ganey Survey in the mail to request feedback on your satisfaction with our services. Please note that you may receive 2 surveys one for your stay in the acute hospital and a second one for your stay in our Rehabilitation Program. Spinal Cord Resources for Your Continued Recovery
7 There are many other services within our health system and in your community that may assist in your recovery. The next two pages introduce some of the services and resources available through our organization, the local community, or national organizations. We encourage you to call or visit the website for these organizations. However, please do not hesitate to ask us for additional information on these services or for other providers or services in your community. The North Carolina Spinal Cord Injury Association (NCSCIA) works to enable people with spinal cord injury and disease to achieve their highest level of independence, health, and personal fulfillment by providing resources, services, and peer support. For more information: The National Spinal Cord Injury Association (NSCIA) provides active-lifestyle information, peer support and advocacy that empowers people living with spinal cord injuries and disorders (SCI/D) to achieve their highest potential. The NSCIA Resource Center connects you with information, resources, and access to an Ask Spinal Cord Central help center. Wake Forest Baptist Health is a member of NSCIA. For more information: info@spinalcord.org The National Institutes of Neurological Disorders and Stroke provides a wealth of information on treatment, prognosis, research, and rehabilitation for spinal cord injury. The Christopher Reeve Spinal Cord Injury and Paralysis Foundation is dedicated to curing spinal cord injury by funding innovative research, and improving the quality of life for people living with paralysis through grants, information and advocacy. For more information: Paralyzed Veterans of America offers resources and benefits to meet the needs of veterans who have experienced spinal cord injuries. For more information: Peer support services are designed to provide individuals and their families with an opportunity to me et and talk with others who are successfully coping with spinal cord injury. Peer Support services can be provided in informal one-on-one sessions or in small groups. During the inpatient stay, patients may also participate in an outing to participate in a local support group. To learn more, please notify your recreation therapist. After discharge, the following local spinal cord injury support groups are available. SpiNet of Winston-Salem, serving the Triad area. Contact: Celia Dixon, WFBH Spinal Cord Resources for Your Continued Recovery
8 WFBH s Club Independence (Club I) is an interactive Day Recreation Therapy Program that provides education, recreation, and overall health and wellness opportunities for individuals with disabling conditions, including spinal cord injury. Club I is the only program of its kind in the Triad and one of only two in North Carolina. Led by licensed recreation therapists, Club I addresses ways for members to enhance their quality of life and assists them in returning to the community and to recreational activities that they once enjoyed. Club I meets on Tuesdays and Thursdays from 9:00am to 4:00pm at Medical Plaza Miller. Members must be 18 years of age or older and independent with their activities of daily living and medical management. For more information: Wake Forest Baptist Health s Assistive Technology Center is a partnership with the North Carolina Assistive Technology Program (NCATP) and is a demonstration center for assistive technology devices (AT). Assistive Technology or AT is any piece of equipment or device that a person with a disability uses to make every day living easier, to be more productive in the workplace or to be more independent. Therapists, consumers/patients, and family members can visit the center at Medical Plaza Miller to look at devices, have them demonstrated, and try them out. Many of the devices can be loaned out for short periods of time to try out in the environment of choice. For more information: Contact: Paul Eklund BestHealth is the Piedmont Triad s trusted source for hands-on health knowledge, classes and screenings. BestHealth is presented by Wake Forest Baptist Health, one of America s top ranked hospitals. An optional membership is also available to individuals who wants to take a more active role in improving or managing t heir health. For more information: BEST ( ) The Winston-Salem Mayor s Council for Persons with Disability hosts free meetings at 11:30am, the second Tuesday of each month. For more information: The Inpatient Rehabilitation Programs are pleased to offer a Rehabilitation Resource Center on the Comprehensive Inpatient Rehabilitation Unit in the Sticht Center. Please visit the center and let us know what you think. If you need assistance finding additional resources in your community: Contact: Karen Lawrence, Rehabilitation Outreach Coordinator Rehab4Life@wakehealth.edu. Map and Driving Directions to the Sticht Center
9 The Rehabilitation Programs are located on the 3rd floor of the Sticht Center. Park in Patient/Visitor Deck A. From Interstate 40 East: Take Business 40 toward Winston Salem. Exit Cloverdale Avenue. At the bottom of the exit ramp, continue straight through the traffic light onto Medical Center Boulevard. Proceed up the hill and around the curve. Turn left into the Main Entrance to the Medical Center. Turn into the first drive on your left. And then right to park in Deck A. From Interstate 40 West: Take Business 40 toward Winston Salem. Exit Cloverdale Avenue. At the bottom of the exit ramp, turn right on Cloverdale Avenue. At the first traffic light, turn left onto Medical Center Boulevard and proceed up the hill and around the curve. Turn left into the Main Entrance to the Medical Center. Turn into the first drive on your left, and then right to park in Deck A.
10 Contact Numbers We want to provide the best possible care and service to you and your family. If you have a problem, concern, or unmet need related to your stay on the rehab unit, please speak to your nurse or care coordinator as soon as possible. We are here to help you each step of the way. Listed below are phone numbers that you may find helpful during your stay. Rehabilitation Units Acquired Brain Injury (ABI) Unit-3SA Rooms General Rehabilitation Unit-3SB Rooms Patient Rooms (room number) Rehabilitation Program Management Nurse Manager: Jamie Brown PT/OT Therapy Manager: Jennifer Brown Speech Therapy Manager: Brooke Johnson Administrative Director: Amy Crews Care Coordinator Joy Watson Katherine Conrad Auria Chamberlain Office of Patient Experience Billing and Insurance Billing or Financial Counselor After Discharge For Questions about community resources: Karen Lawrence, Outreach Coordinator Inpatient Rehabilitation Website: for all general inquires about rehab services: Rehab4Life@wakehealth.edu
Spinal Cord Injury Fact Sheet
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
2014 Report Card. 62 acute inpatient rehabilitation beds days
 Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
Surgery saved my life. Rehab is restoring my future.
 The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
2017 Report Card. 62 acute inpatient rehabilitation beds 13 DAYS
 Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
Lovelace UNM Rehabilitation Hospital is dedicated helping each patient overcome the effects of illness and injury through our comprehensive inpatient and outpatient programs. Our highly specialized physicians
National Stroke Association s Guide to Choosing Stroke. Rehabilitation Services
 National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
National Stroke Association s Guide to Choosing Stroke Rehabilitation Services Rehabilitation, often referred to as rehab, is an important part of stroke recovery. Through rehab, you: Re-learn basic skills
Specialty Rehabilitation Fact Sheet
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
Frequently Asked Questions: Riverview Rehabilitation Center
 Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab)
 Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab) TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted
Neurodegenerative Diseases, Debilitating Conditions and Multiple Trauma Program (Neuromuscular Rehab) TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
OUR BRAINS!!!!! Stroke Facts READY SET.
 HealthSouth Rehabilitation Hospital Huntington Dr. Timothy Saxe, Medical Director READY SET. OUR BRAINS!!!!! Stroke Facts 795,000 strokes each year- 600,000 new strokes 5.5 million stroke survivors Leading
HealthSouth Rehabilitation Hospital Huntington Dr. Timothy Saxe, Medical Director READY SET. OUR BRAINS!!!!! Stroke Facts 795,000 strokes each year- 600,000 new strokes 5.5 million stroke survivors Leading
Inpatient Acute Rehabilitation
 Inpatient Acute Rehabilitation A massive stroke. A major illness. A debilitating injury. At first, you can t imagine how life will ever be the same. Affiliated with the renowned Dignity Health Neurological
Inpatient Acute Rehabilitation A massive stroke. A major illness. A debilitating injury. At first, you can t imagine how life will ever be the same. Affiliated with the renowned Dignity Health Neurological
restoring hope rebuilding lives
 Spinal Cord Injury Brain Injury Stroke Neurologic Diseases Orthopedic Conditions Amputation Cancer Cardiac Recovery The patient experience: 2015 in review restoring hope rebuilding lives Advancing care
Spinal Cord Injury Brain Injury Stroke Neurologic Diseases Orthopedic Conditions Amputation Cancer Cardiac Recovery The patient experience: 2015 in review restoring hope rebuilding lives Advancing care
General Medical Rehabilitation
 General Medical Rehabilitation Outcomes Report 20 Rehabilitation Hospital is part of the Rehabilitation system of care, a post-acute provider of neuro-rehabilitation for over 45 years. Our 160-bed acute,
General Medical Rehabilitation Outcomes Report 20 Rehabilitation Hospital is part of the Rehabilitation system of care, a post-acute provider of neuro-rehabilitation for over 45 years. Our 160-bed acute,
We Have a Great Story to Tell
 We Have a Great Story to Tell Inpatient Outpatient Day Neuro Baylor Scott & White Institute for Rehabilitation Frisco is dedicated to helping patients find their way back from all types of injuries, illnesses,
We Have a Great Story to Tell Inpatient Outpatient Day Neuro Baylor Scott & White Institute for Rehabilitation Frisco is dedicated to helping patients find their way back from all types of injuries, illnesses,
Neurodegenerative diseases Includes multiple sclerosis, Parkinson s disease, postpolio syndrome, rheumatoid arthritis, lupus
 TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
TIRR Memorial Hermann is a nationally recognized rehabilitation hospital that returns lives interrupted by neurological illness, trauma or other debilitating conditions back to independence. Some of the
I tell my patients, If I can do it, you can do it. Lea Stewart
 I tell my patients, If I can do it, you can do it. Lea Stewart Baylor Institute for Rehabilitation Lea Stewart A traffic accident threw Lea Stewart around the back of a pick-up truck, leaving the life-long
I tell my patients, If I can do it, you can do it. Lea Stewart Baylor Institute for Rehabilitation Lea Stewart A traffic accident threw Lea Stewart around the back of a pick-up truck, leaving the life-long
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool Outpatient/ambulatory rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation
I tell my patients, If I can do it, you can do it. Lea Stewart
 I tell my patients, If I can do it, you can do it. Lea Stewart Baylor Institute for Rehabilitation Lea Stewart A traffic accident threw Lea Stewart around the back of a pick-up truck, leaving the life-long
I tell my patients, If I can do it, you can do it. Lea Stewart Baylor Institute for Rehabilitation Lea Stewart A traffic accident threw Lea Stewart around the back of a pick-up truck, leaving the life-long
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
NATIONAL REHABILITATION HOSPITAL SPINAL CORD SYSTEM OF CARE (SCSC) OUTPATIENT SCOPE OF SERVICE Introduction: The Spinal Cord System of Care (SCSC) at the National Rehabilitation Hospital (NRH) provides
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
Integrative Pain Treatment Center Programs Scope of Services
 Integrative Pain Treatment Center Programs Scope of Services The Integrative Pain Treatment Center at Marianjoy Rehabilitation Hospital, part of Northwestern Medicine, offers two specialized 21-day outpatient
Integrative Pain Treatment Center Programs Scope of Services The Integrative Pain Treatment Center at Marianjoy Rehabilitation Hospital, part of Northwestern Medicine, offers two specialized 21-day outpatient
Rehabilitation/Geriatrics ADMISSION CRITERIA. Coordinated Entry System
 Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Acute Rehabilitation. Giving Courage l Creating Hope l Building Strength
 Acute Rehabilitation Giving Courage l Creating Hope l Building Strength What is Acute Rehabilitation? Rehabilitation is a team of healthcare professionals working together to help people regain function
Acute Rehabilitation Giving Courage l Creating Hope l Building Strength What is Acute Rehabilitation? Rehabilitation is a team of healthcare professionals working together to help people regain function
More capacity for healing. More focus on you.
 REHABILITATION PROGRAM small means more. More capacity for healing. More focus on you. The Rehabilitation Center at Mt. Ascutney Hospital offering patient-centered rehabilitative care for your best possible
REHABILITATION PROGRAM small means more. More capacity for healing. More focus on you. The Rehabilitation Center at Mt. Ascutney Hospital offering patient-centered rehabilitative care for your best possible
LIFE-CHANGING CARE INPATIENT CARE
 LIFE-CHANGING CARE INPATIENT CARE Helping Patients Get the Most out of Rehab When a stroke, accident or other traumatic incident turns a person s world upside down, there s a place in Indiana where he
LIFE-CHANGING CARE INPATIENT CARE Helping Patients Get the Most out of Rehab When a stroke, accident or other traumatic incident turns a person s world upside down, there s a place in Indiana where he
Comprehensive Acute. Rehabilitation Unit
 Comprehensive Acute Rehabilitation Unit The Comprehensive Acute Rehabilitation Unit at Thomas Jefferson University Hospital has provided excellence in patient-focused acute rehabilitative care since 1963.
Comprehensive Acute Rehabilitation Unit The Comprehensive Acute Rehabilitation Unit at Thomas Jefferson University Hospital has provided excellence in patient-focused acute rehabilitative care since 1963.
The Complex Rehab Technology Company. Focused on Providing Specialized Products and Related Services to People with Disabilities
 The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
Northeast Rehabilitation Hospital Network
 Northeast Rehabilitation Hospital Network Rebuilding lives through hope, compassion and dedication to excellence NORTHEAST REHABILITATION HOSPITAL NETWORK www.northeastrehab.com Northeast Rehab Hospital
Northeast Rehabilitation Hospital Network Rebuilding lives through hope, compassion and dedication to excellence NORTHEAST REHABILITATION HOSPITAL NETWORK www.northeastrehab.com Northeast Rehab Hospital
FRAZIER REHAB INSTITUTE SCOPE OF THE BRAIN INJURY PROGRAM
 FRAZIER REHAB INSTITUTE SCOPE OF THE BRAIN INJURY PROGRAM Introduction to Frazier The Frazier Rehab Brain Injury Program provides comprehensive services to the individual who has experienced a brain injury
FRAZIER REHAB INSTITUTE SCOPE OF THE BRAIN INJURY PROGRAM Introduction to Frazier The Frazier Rehab Brain Injury Program provides comprehensive services to the individual who has experienced a brain injury
Stroke. Objectives: After you take this class, you will be able to:
 Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Stroke Objectives: After you take this class, you will be able to: 1. Describe the signs of a stroke and how a stroke happens. 2. Discuss stroke risk factors. 3. Detail the care and rehabilitation of a
Department of Physical Medicine and Rehabilitation
 For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
For enquiries and appointments, please contact us at: 物理醫學及復康科部 Department of Physical Medicine and Rehabilitation Department of Physical Medicine and Rehabilitation 5/F, Li Shu Pui Block, Hong Kong Sanatorium
Physical therapists also may be certified as clinical specialists through the American Board of Physical Therapy Specialists (ABPTS).
 GUIDELINES: PHYSICAL THERAPY CLAIMS REVIEW BOD G08-03-03-07 [Amended BOD 03-03- 13-29; BOD 02-02-22-31; BOD 03-01-16-52; BOD 03-00-22-56; BOD 03-99-16-50; Initial BOD 11-97- 16-54] [Guideline] The American
GUIDELINES: PHYSICAL THERAPY CLAIMS REVIEW BOD G08-03-03-07 [Amended BOD 03-03- 13-29; BOD 02-02-22-31; BOD 03-01-16-52; BOD 03-00-22-56; BOD 03-99-16-50; Initial BOD 11-97- 16-54] [Guideline] The American
2016 Rehabilitation Services. Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital
 2016 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
2016 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
The Department of Labor and Training is an equal opportunity employer/program; auxiliary aids and services are available on request to individuals
 Chief Judge Robert F. Arrigan Rehabilitation Center 249 Blackstone Boulevard Providence, RI 02906 (401) 243-1200 Fax (401) 222-3887 www.dlt.ri.gov/arrigan The Department of Labor and Training is an equal
Chief Judge Robert F. Arrigan Rehabilitation Center 249 Blackstone Boulevard Providence, RI 02906 (401) 243-1200 Fax (401) 222-3887 www.dlt.ri.gov/arrigan The Department of Labor and Training is an equal
WELCOME TO DUBOIS NURSING HOME
 For additional information or to schedule a tour, please contact our Admissions Coordinator at (814) 375-9100. WELCOME TO DUBOIS NURSING HOME We want your experience at our facility to be a pleasant one.
For additional information or to schedule a tour, please contact our Admissions Coordinator at (814) 375-9100. WELCOME TO DUBOIS NURSING HOME We want your experience at our facility to be a pleasant one.
2017 Rehabilitation Services. Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital
 2017 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
2017 Rehabilitation Services Rehabilitation Services Profile at The Ohio State University Wexner Medical Center Dodd Rehabilitation Hospital The Nation s Best Right Here in Central Ohio Accredited by CARF
Chapter 6. Hospice: A Team Approach to Care
 Chapter 6 Hospice: A Team Approach to Care Chapter 6: Hospice: A Team Approach to Care Comfort, Respect and Dignity in Dying Hospice care provides patients and family members with hope, comfort, respect,
Chapter 6 Hospice: A Team Approach to Care Chapter 6: Hospice: A Team Approach to Care Comfort, Respect and Dignity in Dying Hospice care provides patients and family members with hope, comfort, respect,
REHABILITATION UNIT ANNUAL OUTCOMES REPORT Prepared by
 REHABILITATION UNIT ANNUAL OUTCOMES Prepared by REPORT - 2014 Keir Ringquist, PT, PhD, GCS Rehabilitation Program Manager Director of Occupational and Physical Therapy DEMOGRAPHICS OF THE REHABILITATION
REHABILITATION UNIT ANNUAL OUTCOMES Prepared by REPORT - 2014 Keir Ringquist, PT, PhD, GCS Rehabilitation Program Manager Director of Occupational and Physical Therapy DEMOGRAPHICS OF THE REHABILITATION
Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit
 rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
rth & East GTA Stroke Network Stroke Rehab Definitions Framework Self-Assessment Tool Acute Integrated Stroke Unit Purpose of the Self-Assessment Tool: The GTA Rehab Network and the GTA regions of the
BRIGHAM AND WOMEN S FAULKNER HOSPITAL ADULT INPATIENT PSYCHIATRY ADVANCED PRACTICUM TRAINING PROGRAM
 BRIGHAM AND WOMEN S FAULKNER HOSPITAL ADULT INPATIENT PSYCHIATRY ADVANCED PRACTICUM TRAINING PROGRAM 2019-2020 Christopher AhnAllen, Ph.D. Director of Inpatient Psychology and Psychology Education 1153
BRIGHAM AND WOMEN S FAULKNER HOSPITAL ADULT INPATIENT PSYCHIATRY ADVANCED PRACTICUM TRAINING PROGRAM 2019-2020 Christopher AhnAllen, Ph.D. Director of Inpatient Psychology and Psychology Education 1153
Alcohol and chemical dependency Inpatient treatment programs
 Alcohol and chemical dependency Inpatient treatment programs Geisinger Marworth Treatment Center P.O. Box 3, Lily Lake Road Waverly, PA 18471-773 800-442-7722 marworth.org 84459-1-8/1-TPRA/DNFLD Geisinger
Alcohol and chemical dependency Inpatient treatment programs Geisinger Marworth Treatment Center P.O. Box 3, Lily Lake Road Waverly, PA 18471-773 800-442-7722 marworth.org 84459-1-8/1-TPRA/DNFLD Geisinger
Alcohol and Chemical Dependency Treatment Program for Healthcare Professionals
 Alcohol and Chemical Dependency Treatment Program for Healthcare Professionals Program Overview Recognized as a national leader in alcohol and chemical dependency treatment programs, Marworth s Healthcare
Alcohol and Chemical Dependency Treatment Program for Healthcare Professionals Program Overview Recognized as a national leader in alcohol and chemical dependency treatment programs, Marworth s Healthcare
THE RECOVERY CENTER AT MONTEFIORE NYACK HOSPITAL
 THE RECOVERY CENTER AT MONTEFIORE NYACK HOSPITAL THE RECOVERY CENTER AT MONTEFIORE NYACK HOSPITAL Our team of caring, licensed, and credentialed professionals includes physicians, nurses, psychiatrists,
THE RECOVERY CENTER AT MONTEFIORE NYACK HOSPITAL THE RECOVERY CENTER AT MONTEFIORE NYACK HOSPITAL Our team of caring, licensed, and credentialed professionals includes physicians, nurses, psychiatrists,
Spinal Injured patients getting adequate rehabilitation
 Starts on day one Requires specially trained staff and team effort Should be done according to the environment in which the patient has to return Major goal of rehabilitation is to reduce disability by
Starts on day one Requires specially trained staff and team effort Should be done according to the environment in which the patient has to return Major goal of rehabilitation is to reduce disability by
NATIONAL REHABILITATION HOSPITAL PROSTHETIC, ORTHOTIC & LIMB ABSENCE REHABILITATION PROGRAMME
 NATIONAL REHABILITATION HOSPITAL PROSTHETIC, ORTHOTIC & LIMB ABSENCE REHABILITATION PROGRAMME SCOPE OF SERVICE 1 Introduction: The Prosthetic, Orthotic & Limb Absence Rehabilitation Programme (POLAR) at
NATIONAL REHABILITATION HOSPITAL PROSTHETIC, ORTHOTIC & LIMB ABSENCE REHABILITATION PROGRAMME SCOPE OF SERVICE 1 Introduction: The Prosthetic, Orthotic & Limb Absence Rehabilitation Programme (POLAR) at
Hospice & Palliative Care
 Patient-centered Medical Neighborhood Hospice & Palliative Care Our Hospice of South Central Indiana 2626 East 17th Street Columbus, IN 47201 812-314-8089 Schneck Medical Center Hospice & Palliative Care
Patient-centered Medical Neighborhood Hospice & Palliative Care Our Hospice of South Central Indiana 2626 East 17th Street Columbus, IN 47201 812-314-8089 Schneck Medical Center Hospice & Palliative Care
FSBPT Supervised Clinical Practice Performance Evaluation Tool
 1. Practices in a manner that is safe for the patient 1.1. Responds appropriately in emergency situations 1.2. Recognizes and responds to unexpected changes in patient's physiological condition 1.3. Utilizes
1. Practices in a manner that is safe for the patient 1.1. Responds appropriately in emergency situations 1.2. Recognizes and responds to unexpected changes in patient's physiological condition 1.3. Utilizes
St. Mary s Acute Rehabilitation Center. Committed to getting you home.
 St. Mary s Acute Rehabilitation Center Committed to getting you home. Your road to recovery starts here If you have this booklet in your hands, it s likely to mean that your hospital care team believes
St. Mary s Acute Rehabilitation Center Committed to getting you home. Your road to recovery starts here If you have this booklet in your hands, it s likely to mean that your hospital care team believes
BURKE S ACUTE REHAB: PERSONALIZED FOR MAXIMUM RECOVERY
 WELCOME TO BURKE No one plans to experience a life-changing illness or traumatic injury. So it is comforting to know that for the past 100 years, Burke Rehabilitation Hospital has been a leader in rehabilitation
WELCOME TO BURKE No one plans to experience a life-changing illness or traumatic injury. So it is comforting to know that for the past 100 years, Burke Rehabilitation Hospital has been a leader in rehabilitation
*0055* Teaching & Instructions
 Department Plan for Providing Care / Services Patient Care Departments Department: Rehabilitation Services Scope of Service for Outpatient Rehabilitation and Therapy Center The Outpatient Therapy Center
Department Plan for Providing Care / Services Patient Care Departments Department: Rehabilitation Services Scope of Service for Outpatient Rehabilitation and Therapy Center The Outpatient Therapy Center
Elliot Senior Specialty Services. in Greater Manchester. 138 Webster Street Manchester NH
 Elliot Senior Specialty Services in Greater Manchester 138 Webster Street Manchester NH 03104 603-663-7000 Dedicated to helping seniors achieve their maximum quality of life ELLIOT SENIOR SPECIALTY SERVICES
Elliot Senior Specialty Services in Greater Manchester 138 Webster Street Manchester NH 03104 603-663-7000 Dedicated to helping seniors achieve their maximum quality of life ELLIOT SENIOR SPECIALTY SERVICES
Rehabilitation and Choosing a Rehab Center
 The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. https://www.christopherreeve.org/living-with-paralysis/rehabilitation/find-a-rehab-center
The following excerpt has been taken from the Christopher & Dana Reeve Foundation Paralysis Resource Center website. https://www.christopherreeve.org/living-with-paralysis/rehabilitation/find-a-rehab-center
Lucille Beck, PhD Chief Consultant, Rehabilitation and Prosthetic Services Veterans Health Administration Department of Veterans Affairs
 How to Facilitate Rehabilitation Care Lucille Beck, PhD Chief Consultant, Rehabilitation and Prosthetic Services Veterans Health Administration Department of Veterans Affairs The only victor in war is
How to Facilitate Rehabilitation Care Lucille Beck, PhD Chief Consultant, Rehabilitation and Prosthetic Services Veterans Health Administration Department of Veterans Affairs The only victor in war is
Mental Health Support
 Mental Health Support Services in Brown County Helping a Loved One with a Mental Health Condition Stylephotographs l Dreamstime.com ADRC of Brown County 920-448-4300 300 S. Adams Street Green Bay, WI 54301
Mental Health Support Services in Brown County Helping a Loved One with a Mental Health Condition Stylephotographs l Dreamstime.com ADRC of Brown County 920-448-4300 300 S. Adams Street Green Bay, WI 54301
Orthopaedic Therapy Service inpatient guide. Information for patients MSK Orthopaedic Inpatients (Therapy)
 Orthopaedic Therapy Service inpatient guide Information for patients MSK Orthopaedic Inpatients (Therapy) This leaflet is designed to answer any queries you may have about the Orthopaedic Therapy Service.
Orthopaedic Therapy Service inpatient guide Information for patients MSK Orthopaedic Inpatients (Therapy) This leaflet is designed to answer any queries you may have about the Orthopaedic Therapy Service.
Patient. and Family. programs and calendar Winter-Spring 2014
 Patient and Family support programs and calendar Winter-Spring 0 Living Well with Cancer Support to meet your individual needs At Vanderbilt-Ingram Cancer Center, we re committed to providing exceptional
Patient and Family support programs and calendar Winter-Spring 0 Living Well with Cancer Support to meet your individual needs At Vanderbilt-Ingram Cancer Center, we re committed to providing exceptional
PURPOSE OF THE SELF-ASSESSMENT TOOLS:
 Pulmonary Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Pulmonary Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different
Pulmonary Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Pulmonary Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different
The Road To Recovery: Bouncing Back From Injury with Rehabilitation. 1
 The Road To Recovery: Bouncing Back From Injury with Rehabilitation www.fletcherallen.org 1 PHYSIATRY From Greek physicos (physical) and iatreia (art of healing) Physical Medicine and Rehabilitation
The Road To Recovery: Bouncing Back From Injury with Rehabilitation www.fletcherallen.org 1 PHYSIATRY From Greek physicos (physical) and iatreia (art of healing) Physical Medicine and Rehabilitation
OUTCOMES AND DATA 2016
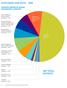 AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
CARE OF SPINAL CORD INJURY VICTIMS
 CARE OF SPINAL CORD INJURY VICTIMS Dr THIERRY ALBERT Centre de Rééducation et de Réadaptation pour Adulte de COUBERT Route de Liverdy, Coubert 77257 Brie comte robert, cedex talbert@ugecamif.fr Spinal
CARE OF SPINAL CORD INJURY VICTIMS Dr THIERRY ALBERT Centre de Rééducation et de Réadaptation pour Adulte de COUBERT Route de Liverdy, Coubert 77257 Brie comte robert, cedex talbert@ugecamif.fr Spinal
Bringing hope and lasting recovery to individuals and families since 1993.
 Bringing hope and lasting recovery to individuals and families since 1993. "What lies behind us and what lies before us are tiny matters compared to what lies within us." Ralph Waldo Emerson Our Statement
Bringing hope and lasting recovery to individuals and families since 1993. "What lies behind us and what lies before us are tiny matters compared to what lies within us." Ralph Waldo Emerson Our Statement
REHABILITATION SERVICES
 REHABILITATION SERVICES Rehabilitation is provided in a variety of ways, including inpatient services, physical therapy, occupational therapy, and other outpatient treatments. The resources listed in this
REHABILITATION SERVICES Rehabilitation is provided in a variety of ways, including inpatient services, physical therapy, occupational therapy, and other outpatient treatments. The resources listed in this
Integration How Can Behavioral Health And Health Care Be Better Coordinated?
 Integration How Can Behavioral Health And Health Care Be Better Coordinated? Mental Health America Annual Conference June 8, 2013 Harvey Rosenthal, NYAPRS New York Association of Psychiatric Rehabilitation
Integration How Can Behavioral Health And Health Care Be Better Coordinated? Mental Health America Annual Conference June 8, 2013 Harvey Rosenthal, NYAPRS New York Association of Psychiatric Rehabilitation
Occupational therapy after stroke
 Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
Call the Stroke Helpline: 0303 3033 100 or email: info@stroke.org.uk Occupational therapy after stroke This guide explains how occupational therapy can help your recovery and rehabilitation after a stroke.
New Zealand Spinal Cord Injury Registry. First Annual Report August 2016 to July 2017
 New Zealand Spinal Cord Injury Registry First Annual Report August 216 to July 217 2 The New Zealand Spinal Cord Injury Registry (NZSCIR) would like to acknowledge the spinal service clinicians and coordinators
New Zealand Spinal Cord Injury Registry First Annual Report August 216 to July 217 2 The New Zealand Spinal Cord Injury Registry (NZSCIR) would like to acknowledge the spinal service clinicians and coordinators
Case Review of Inpatient Rehabilitation Hospital Patients Not Suited for Intensive Therapy
 U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES OFFICE OF INSPECTOR GENERAL Case Review of Inpatient Rehabilitation Hospital Patients Not Suited for Intensive Therapy OEI-06-16-00360 DECEMBER 2016 SUZANNE MURRIN
U.S. DEPARTMENT OF HEALTH & HUMAN SERVICES OFFICE OF INSPECTOR GENERAL Case Review of Inpatient Rehabilitation Hospital Patients Not Suited for Intensive Therapy OEI-06-16-00360 DECEMBER 2016 SUZANNE MURRIN
The Role of Physiatry in the Care of Adults and Children with Hydrocephalus
 The Role of Physiatry in the Care of Adults and Children with Hydrocephalus Scott E. Brown, MD Chairman Department of Physical Medicine and Rehabilitation Sinai Hospital of Baltimore Who Are We? PHYSICAL
The Role of Physiatry in the Care of Adults and Children with Hydrocephalus Scott E. Brown, MD Chairman Department of Physical Medicine and Rehabilitation Sinai Hospital of Baltimore Who Are We? PHYSICAL
Using the AcuteFIM Instrument for Discharge Placement
 Using the AcuteFIM Instrument for Discharge Placement Paulette Niewczyk, MPH, PhD Manager of CFAR / Director of Research Center for Functional Assessment Research Uniform Data System for Medical Rehabilitation
Using the AcuteFIM Instrument for Discharge Placement Paulette Niewczyk, MPH, PhD Manager of CFAR / Director of Research Center for Functional Assessment Research Uniform Data System for Medical Rehabilitation
MEDICAL SCHEDULE OF BENEFITS
 MEDICAL SCHEDULE OF BENEFITS Plan(s) 011 (F) All health benefits shown on this Schedule of Benefits are subject to the following: Lifetime and annual maximums, Deductibles, Co-pays, Plan Participation
MEDICAL SCHEDULE OF BENEFITS Plan(s) 011 (F) All health benefits shown on this Schedule of Benefits are subject to the following: Lifetime and annual maximums, Deductibles, Co-pays, Plan Participation
CARF Specialty Standards for Stroke. Susan Ganson, RN, NHA CARF Washington, DC
 CARF Specialty Standards for Stroke Susan Ganson, RN, NHA CARF Washington, DC Presenter Disclosure Information FINANCIAL DISCLOSURE NONE GRANTS/Research support: None support: None UNLABELED/UNAPPROVED
CARF Specialty Standards for Stroke Susan Ganson, RN, NHA CARF Washington, DC Presenter Disclosure Information FINANCIAL DISCLOSURE NONE GRANTS/Research support: None support: None UNLABELED/UNAPPROVED
FAMILY & CHILDREN S SERVICES STRATEGIC PLAN
 2014-2019 FAMILY & CHILDREN S SERVICES STRATEGIC PLAN WHO WE ARE Family & Children s Services is a leading provider of behavioral health care and family services for people of all ages in Tulsa and surrounding
2014-2019 FAMILY & CHILDREN S SERVICES STRATEGIC PLAN WHO WE ARE Family & Children s Services is a leading provider of behavioral health care and family services for people of all ages in Tulsa and surrounding
AROC Intensity of Therapy Project. AFRM Conference 18 September 2013
 AROC Intensity of Therapy Project AFRM Conference 18 September 2013 What is AROC? AROC began as a joint initiative of the whole Australian rehabilitation sector (providers, payers, regulators and consumers)
AROC Intensity of Therapy Project AFRM Conference 18 September 2013 What is AROC? AROC began as a joint initiative of the whole Australian rehabilitation sector (providers, payers, regulators and consumers)
Pro Active Physical Therapy & Sports Medicine
 Pro Active Physical Therapy & Sports Medicine Consent and Statement of Financial Responsibility 1. CONSENT FOR TREATMENT: I consent to and authorize my physical therapist, occupational therapist and other
Pro Active Physical Therapy & Sports Medicine Consent and Statement of Financial Responsibility 1. CONSENT FOR TREATMENT: I consent to and authorize my physical therapist, occupational therapist and other
Physical Medicine & Rehabilitation: Maximum Combined Frequency per Day Policy
 Policy Number Physical Medicine & Rehabilitation: Maximum Combined Frequency per Day Policy 2017R0101E Annual Approval Date 7/13/2016 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT
Policy Number Physical Medicine & Rehabilitation: Maximum Combined Frequency per Day Policy 2017R0101E Annual Approval Date 7/13/2016 Approved By Payment Policy Oversight Committee IMPORTANT NOTE ABOUT
Please make sure that you complete a self-assessment survey for each type of rehab program that your organization provides.
 Oncology Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Oncology Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different settings
Oncology Rehab s Framework Self-Assessment Tool Inpatient Rehab Survey for Oncology Rehab INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered in many different settings
Patient Sticky Label. A Resource Guide for Stroke Survivors and their Caregivers
 A Resource Guide for Stroke Survivors and their Caregivers Patient Sticky Label An initiative of the Stroke Services Improvement (SSI) team in collaboration with all public hospitals in Singapore. Learning
A Resource Guide for Stroke Survivors and their Caregivers Patient Sticky Label An initiative of the Stroke Services Improvement (SSI) team in collaboration with all public hospitals in Singapore. Learning
Via Electronic Submission. March 13, 2017
 APTQI 20 F Street, NW Suite #700 Washington, DC 20001 Phone: 202-507-6354 www.aptqi.com Via Electronic Submission Centers for Medicare & Medicaid Services Department of Health & Human Services Attention:
APTQI 20 F Street, NW Suite #700 Washington, DC 20001 Phone: 202-507-6354 www.aptqi.com Via Electronic Submission Centers for Medicare & Medicaid Services Department of Health & Human Services Attention:
PREVIOUS EMPLOYMENT. Associate OT : CJ Occupational Therapy * Assessment and treatment for adults with neurological conditions
 CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
CURRICULUM VITAE Katie Hanagarth Green Owl Therapy Office 3, 36 Greenhill Street Stratford-upon-Avon CV37 6LE Tel: 01789 413960 / 07966 573317 Email: katie@greenowltherapy.co.uk - Web: www.greenowltherapy.co.uk
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
THE MULLER INSTITUTE FOR SENIOR HEALTH
 THE MULLER INSTITUTE FOR SENIOR HEALTH Rita Leinheiser, MA Social Gerontologist Elder Life Specialist OBJECTIVES 1. Discover the components of a comprehensive community wellness program for seniors and
THE MULLER INSTITUTE FOR SENIOR HEALTH Rita Leinheiser, MA Social Gerontologist Elder Life Specialist OBJECTIVES 1. Discover the components of a comprehensive community wellness program for seniors and
What You Need To Know About Palliative Care. Natalie Wu Moy, LCSW, MSPA RUHS Medical Center Hospital Social Services Director
 What You Need To Know About Palliative Care Natalie Wu Moy, LCSW, MSPA RUHS Medical Center Hospital Social Services Director None of the faculty, planners, speakers, providers, nor CME committee members
What You Need To Know About Palliative Care Natalie Wu Moy, LCSW, MSPA RUHS Medical Center Hospital Social Services Director None of the faculty, planners, speakers, providers, nor CME committee members
Exploring The Resources And Supports of the Paralysis Resource Center
 Exploring The Resources And Supports of the Paralysis Resource Center Today s Care. Tomorrow s Cure. The Christopher & Dana Reeve Foundation is dedicated to curing spinal cord injury by funding innovative
Exploring The Resources And Supports of the Paralysis Resource Center Today s Care. Tomorrow s Cure. The Christopher & Dana Reeve Foundation is dedicated to curing spinal cord injury by funding innovative
There For You. Your Compassionate Guide. World-Class Hospice Care Since 1979
 There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
Principal Benefits for Kaiser Permanente Senior Advantage (HMO) with Part D (7/1/18 6/30/19)
 Benefit Summary 35876D 35876 SCHOOLS INSURANCE GROUP #35876 Principal Benefits for Kaiser Permanente Senior Advantage (HMO) with Part D (7/1/18 6/30/19) Plan Out-of-Pocket Maximum For Services subject
Benefit Summary 35876D 35876 SCHOOLS INSURANCE GROUP #35876 Principal Benefits for Kaiser Permanente Senior Advantage (HMO) with Part D (7/1/18 6/30/19) Plan Out-of-Pocket Maximum For Services subject
CHRISTOPHER VENUS, PT, MPT, NCS. HOME: 209 Bernice Street Phone: (412) Pittsburgh, PA 15237
 CHRISTOPHER VENUS, PT, MPT, NCS HOME: 209 Bernice Street Phone: (412)780-7012 15237 BUSINESS: UPMC Centers for Rehab Services Phone: (412)586-6900 UPMC Mercy South Side 2000 Mary Street Suite 1218, First
CHRISTOPHER VENUS, PT, MPT, NCS HOME: 209 Bernice Street Phone: (412)780-7012 15237 BUSINESS: UPMC Centers for Rehab Services Phone: (412)586-6900 UPMC Mercy South Side 2000 Mary Street Suite 1218, First
Rehabilitation Programs
 Rehabilitation Programs Inpatient and Half-Day Rehabilitation Program Information and Referral Form WELCOME TO ST LUKE S CARE Thank you for choosing St Luke s Care for your rehabilitation. With an unwavering
Rehabilitation Programs Inpatient and Half-Day Rehabilitation Program Information and Referral Form WELCOME TO ST LUKE S CARE Thank you for choosing St Luke s Care for your rehabilitation. With an unwavering
INPATIENT CONSULT SERVICE
 INPATIENT CONSULT SERVICE Patient Care OBJECTIVES BEGINNER Obtain essential and accurate information and present it in a concise but thorough format Perform a rehabilitation medicine focused consultation
INPATIENT CONSULT SERVICE Patient Care OBJECTIVES BEGINNER Obtain essential and accurate information and present it in a concise but thorough format Perform a rehabilitation medicine focused consultation
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? How does the implant work?
 information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
information Sacral Anterior Root Stimulator (SARS) and Dorsal Rhizotomy (1 of 5) What is a sacral anterior root stimulator? If you need this information in another language or medium (audio, large print,
Social Worker on-site to provide initial counseling and community resources
 Cardiac Rehabilitation Welcome to our annual newsletter. As medical director of the OHSU Phase II Cardiac Rehabilitation program, I am happy to share some of the features that we have added over the last
Cardiac Rehabilitation Welcome to our annual newsletter. As medical director of the OHSU Phase II Cardiac Rehabilitation program, I am happy to share some of the features that we have added over the last
Rehabilitation and Metastatic Spinal Cord Compression
 Rehabilitation and Metastatic Spinal Cord Compression Pradeep Thumbikat MS, MSc, FRCS Consultant in Spinal Cord Injuries Sheffield Teaching Hospitals 1 Evidence for Rehabilitation Differences and similarities
Rehabilitation and Metastatic Spinal Cord Compression Pradeep Thumbikat MS, MSc, FRCS Consultant in Spinal Cord Injuries Sheffield Teaching Hospitals 1 Evidence for Rehabilitation Differences and similarities
MSK Rehab Definitions Framework - hip fractures Self assessment Survey Outpatient Rehab
 MSK Rehab Definitions Framework - hip fractures Self assessment Survey Outpatient Rehab In response to a changing rehab landscape in which rehabilitation is offered in many different settings with variations
MSK Rehab Definitions Framework - hip fractures Self assessment Survey Outpatient Rehab In response to a changing rehab landscape in which rehabilitation is offered in many different settings with variations
PTA 9 CLINICAL PRACTICUM II SYLLABUS AND COURSE INFORMATION PACKET SUMMER 2018
 Page 2 PTA 9 CLINICAL PRACTICUM II SYLLABUS AND COURSE INFORMATION PACKET SUMMER 2018 3 credits Dr. Michael Mattia, PT, DPT, MS, MHA Full Time Clinical Rotation Office: S128 Phone: 718-368-4818 email:
Page 2 PTA 9 CLINICAL PRACTICUM II SYLLABUS AND COURSE INFORMATION PACKET SUMMER 2018 3 credits Dr. Michael Mattia, PT, DPT, MS, MHA Full Time Clinical Rotation Office: S128 Phone: 718-368-4818 email:
Emerson Hospital Outpatient Services
 Emerson Hospital Outpatient Services A Growing Demand initiative to expand sports rehabilitation and specialty services 310 baker avenue, concord, massachusetts Our pediatric occupational therapy specialists
Emerson Hospital Outpatient Services A Growing Demand initiative to expand sports rehabilitation and specialty services 310 baker avenue, concord, massachusetts Our pediatric occupational therapy specialists
Day Programs. Information for patients, carers, family and support persons
 Day Programs Information for patients, carers, family and support persons Sometimes the smallest step in the right direction ends up being the biggest step of your life. Tip toe if you must, but take the
Day Programs Information for patients, carers, family and support persons Sometimes the smallest step in the right direction ends up being the biggest step of your life. Tip toe if you must, but take the
Troy Hillman Manager, Analytical Services Uniform Data System for Medical Rehabilitation
 Avoiding Confusion between Payment and Quality Items on the New IRF-PAI, Part II: Other Implications Troy Hillman Manager, Analytical Services Uniform Data System for Medical Rehabilitation 2016 Uniform
Avoiding Confusion between Payment and Quality Items on the New IRF-PAI, Part II: Other Implications Troy Hillman Manager, Analytical Services Uniform Data System for Medical Rehabilitation 2016 Uniform
Service Provider Department Phone Number
 Service Provider Department Phone Number A Activities of Daily Living Occupational Therapy Rehabilitation Services 734-593-5620 Adaptive Equipment - home Occupational Therapy Rehabilitation Services 734-593-5620
Service Provider Department Phone Number A Activities of Daily Living Occupational Therapy Rehabilitation Services 734-593-5620 Adaptive Equipment - home Occupational Therapy Rehabilitation Services 734-593-5620
2016 Report Card Gwen Neilsen Anderson Rehabilitation Center Inpatient Rehabilitation Unit. stlukesonline.org
 2016 Report Card Gwen Neilsen Anderson Rehabilitation Center Inpatient Rehabilitation Unit stlukesonline.org Why the Gwen Neilsen Anderson Rehabilitation Center? The Gwen Neilsen Anderson Rehabilitation
2016 Report Card Gwen Neilsen Anderson Rehabilitation Center Inpatient Rehabilitation Unit stlukesonline.org Why the Gwen Neilsen Anderson Rehabilitation Center? The Gwen Neilsen Anderson Rehabilitation
