Chapter Four. The principles of combined movement assessment. Chris McCarthy
|
|
|
- Erika Daniels
- 5 years ago
- Views:
Transcription
1 Chapter Four 4 c0020 The principles of combined movement assessment Chris McCarthy CHAPTER CONTENTS u0010 Subjective examination u0015 Physical examination u0020 Observation...54 u0025 Functional u0030 Active movements...56 u0035 Degree of symptom reproduction deemed acceptable...57 u0040 Prime movement and prime combination. 57 u0045 Muscle assessment...59 u0050 Passive movement and mini-treatments. 59 u0055 Assessing for the suitability of manipulative thrust techniques...60 u0060 Cervical spine case study u0065 Lumbar spine case study p0070 The purpose of clinical examination is not simply to gather as much information as is possible in the time available. Often the inexperienced clinician can spend an entire examination gathering data with little evaluation of its clinical relevance. As manual therapists we provide our patients with incredibly sensitive examinations. The volume and sophistication of our examination procedures is immense. However, we may occasionally fail to grasp the problem of specificity. We must find a balance between gathering enough information to prioritize the patient s most significant dysfunction whilst not being distracted by the less relevant dysfunctions we discover. p0075 We are essentially searching for the patient s predominant dysfunction or fault in order to direct our intervention towards it. The process of ranking the importance of our findings requires that we test the hypothesis of predominant dysfunction throughout our interaction with our patients. In short, during the examination of patients we are considering if our hypothesis will guide treatment more effectively than the next most likely hypothesis. In addition, during treatment we should be continually considering if our chosen intervention is in fact more effective than the next most likely intervention. This process of analytical assessment is not new and was advocated by Maitland (1986) and Grieve (1988, 1991) over 30 years ago. Simply gathering huge quantities of information that is neither discriminatory nor influential in management represents a failure in our duty of care to our patients. The purpose of clinical examination is to evaluate valid information that will facilitate the prioritization of likely diagnoses and strategies of management. In other words, our duty to our patients is to ensure we are identifying their predominant dysfunction/fault and to continually ensure that we are providing the most effective management strategy at the time. Ensuring we adhere to this principle will ensure we are facilitating recovery as quickly as possible. It could be argued that the primary objective of manual therapy is to facilitate recovery as quickly as possible. On the whole, the conservative management of most musculoskeletal dysfunctions will facilitate recovery. Manual therapy s role is in the acceleration of this process. Thus, ensuring our treatment choice is making more difference, more quickly than the next most likely choice of treatment is a crucial responsibility. p0080 ã 2010, Elsevier Ltd.
2 SECTION ONE Combined Movement Theory s0010 Subjective examination p0085 During the initial consultation the therapist will begin to form an impression of the patient based on verbal and non-verbal communication. Expert clinicians form an impression regarding diagnosis, management and expectations of the patient very quickly. Mixed methods of clinical reasoning are utilized in this process as outlined in Chapter 3. p0090 The diverse nature of musculoskeletal dysfunction rarely allows the definitive identification of definitive patterns of presentation. The clinician is frequently required to make reasoned judgements as to the predominant dysfunction from several alternatives. Some of the typical judgements required are listed below. This is by no means an exhaustive list. The process of establishing that one treatment approach is superior to another begins during the initial consultation with the patient. Early in the initial interview with a patient, the therapist should look for answers to the following questions. s0030 Is this patient s presentation suitable for a manual therapy approach? u0070 Is this patient presentation sounding like I should explore further with an assessment of biomechanical dysfunction? u0075 Does this patient s presentation suggest that a more psychosocial approach may elicit effective treatment strategies? s0035 Which patterns of presentation does this presentation match with? u0080 Does the presentation fit a pattern of presentation I have encountered before? u0085 If so, what is it that makes this patient s presentation fit this pattern better than the next most likely pattern? u0090 What questions and tests do I need to use to test this hypothesis? s0040 Does the functional fault have a directional quality? u0095 In what combination of positions are symptoms reproduced? u0100 In what combination of positions are symptoms reduced? s0045 What is the likely source of the directional fault? u0105 Does the presentation have predominantly arthrogenic features? Does the presentation have predominantly myogenic features? Does the presentation have predominantly neurodynamic features? Is this predominantly a control or impairment fault? Does the presentation suggest a dysfunction in control of movement? Does the presentation suggest a dysfunction associated with limitation (or impairment) of movement? Is it acceptable to reproduce symptoms are they severe? Is the faulty position producing severe pain? Is positioning in the faulty position likely to cause a latent or long-term exacerbation of symptoms? Is there a position that will allow examination and treatment whilst avoiding unacceptable symptom reproduction? Is it likely that caution needs to be taken due to a patho-anatomical reason that would make the use of combined movement theory (CMT) unwise? See the contraindications to manual therapy in the box below. What is the predominant pain mechanism? Is the patient s predominant pain mechanism: nociceptive, peripheral neurogenic, central sensitivity, autonomic or affective? A proforma planning sheet can be found on the CD. See Figure 4.1. Prior to the conduct of a physical examination using the CMT approach the patient should be informed of your plans and the risks and benefits of the approach against other approaches. By examining the expectations of the patient the suitability of utilizing a CMT approach can be established. If the patient s expectations of treatment are radically different to the therapist s, a discussion of future management should ensue. A detailed biomechanical assessment of spinal dysfunction may be unwarranted if the patient is expecting and consenting only to generic advice and exercise. u0110 u0115 s0050 u0120 u0125 s0055 u0130 u0135 u0140 u0145 s0060 u0150 b0010 p0215 p0370 p
3 The principles of combined movement assessment CHAPTER 4 b0015 b0015 Clinical point Contraindications to spinal passive movement that takes a joint to the end of passive range or thrust techniques s0065 Bone p0220 Any pathology that has led to significant bone weakening: u0155 Tumour, e.g. metastatic deposits u0160 Infection, e.g. tuberculosis u0165 Metabolic, e.g. osteomalacia u0170 Congenital, e.g. dysplasias u0175 Iatrogenic, e.g. long-term corticosteroid medication u0180 Inflammatory, e.g. severe rheumatoid arthritis u0185 Traumatic, e.g. fracture s0070 Neurological u0190 Spinal cord compression u0195 Cauda equina compression u0200 Nerve root compression with increasing neurological deficit s0075 Vascular u0205 Aortic aneurysm u0210 Bleeding into joints, e.g. severe haemophilia u0215 Cervical artery dysfunction (Kerry et al, 2008a, 2008b) s0080 Relative contraindications p0300 Special consideration should be given prior to the use of spinal manipulative thrust techniques in the following circumstances: u0220 Adverse reactions to previous manual therapy u0225 Disc herniation or prolapse u0230 Inflammatory arthritides u0235 Pregnancy u0240 Spondylolysis u0245 Spondylolisthesis u0250 Osteoporosis u0255 Anticoagulant or long-term corticosteroid use u0260 Advanced degenerative joint disease and spondylosis u0265 Psychological dependence upon spinal manipulative thrust techniques u0270 Ligamentous laxity u0275 Arterial calcification u0280 Hypertension (diastolic >95)incervicalmanualtherapy (See Gibbons & Tehan, 2001a,b; Grieve, 1991.) s0085 Is the patient suitable for a biomechanical assessment of their movement fault? p0380 Patient presentations suggestive of a predominant mechanical influence on symptoms are suitable for detailed biomechanical assessment and treatment. Presentations that do not feature mechanical/movement influences on symptomology suggest that specific positions and movements may not be the predominant influences to be addressed during examination and treatment. Thus, patients who have constant symptoms, regardless of positioning, will be unlikely to benefit from management with a positional bias. Patients with central sensitization or inflammatory neurogenic pathology ( irritable patients (Maitland, 1985) have no mechanical predominance. How acceptable is it to reproduce symptoms? Patients, seeking manual therapy, present with pain and largely judge their improvement by an amelioration of their pain. In the process of assessing the effect of testing and treatment, changes in pain are assessed. However, in cases where pain is severe, it is unacceptable to reproduce pain and inappropriate to treat an underlying mechanical dysfunction whilst reproducing pain. Thus, prior to any physical testing the therapist must be clear regarding the degree to which pain is to be reproduced during their interaction with the patient. In certain presentations it may be deemed acceptable to fully reproduce the minor discomfort the patient is seeking help for, in order to fully relieve it. However, in situations where pain is severe this is unacceptable. Using positions that can reduce the likelihood of reproducing severe pain is one of the key advantages of CMT. Clinical relevance If it is not acceptable to reproduce symptoms, the condition is severe. If it is acceptable it is not. Use a nominal (yes/no) approach to this decision and your clinical reasoning will be decisive and more reasonable. What is the functional of the positional fault? Patient presentations, suggestive of the suitability of a CMT approach, have symptoms predominantly influenced by specific positions or movements. Patients can often demonstrate these movements or positions and reproduce them in the course of replicating a functional activity. For example, patients with anterior stretch patterns of the mid cervical spine often relate symptom reproduction with activities inducing ipsilateral lateral flexion and rotation, e.g. reversing the car. The monitoring of change in the functional, during examination and treatment is a crucial monitor of treatment effectiveness. Again, the concept of a functional is a long- s0090 p0385 b0020 p0390 s0095 p
4 SECTION ONE Combined Movement Theory established tenet of the Maitland concept (Maitland, 1986) and at the heart of CMT. s0100 What is the region of the spine that is likely to be faulty? p0400 The biomechanical interpretation of patient presentation can allow the therapist to judge the location of regions of dysfunction. Careful questioning can elicit functional activities that influence specific regions of the spine. For example, the influence of breathing on thoracic movement can provide valuable inference towards spinal or rib dysfunctions. s0105 What is the predominant hypothesis for the source and mechanism of symptom production and the next most likely hypothesis that will be tested against it? p0405 It is crucial to form hypotheses regarding the underlying source and mechanism of symptom production as you recognize presentation patterns. As a pattern of presentation begins to emerge the use of follow-up questions will establish a good fit with this pattern. Having identified a match with a recognizable pattern, the manual therapist should test the assumption that this hypothesis is predominant by comparing the match with the next most likely pattern. For example, having established that a patient s presentation matched an arthrogenic presentation, one would expect the presentation to be less well matched with a myogenic presentation. In order to facilitate this process it can be useful to develop a library of stock questions and tests for common presentations. p0410 The use of these strategies will facilitate the therapist s reasoning regarding the appropriateness of using CMT, the most likely hypotheses for aetiology of symptoms, the extent and direction of movements to be included in the examination and most importantly the starting positions in which assessment and treatment will be undertaken. p0415 Figure 4.1 shows a suggested planning sheet for use in clinical reasoning during the CMT examination. s0110 Physical examination p0420 The objective examination will follow the subjective examination and is conducted in light of the considerations and clinical reasoning process outlined in this book. The object of the physical examination is not to form a long list of impairments with little evidence of their relative contribution to the patient s dysfunction. The physical examination should allow the hypotheses, generated following the subjective examination, to be tested. Thus, the examination should be structured to allow this process to occur. In order to assess the influence of the testing procedures themselves on a patient s dysfunction the physical examination should be split into components. The order in which components of the examination are conducted will be guided by the subjective examination. A clinician may hypothesize that the predominant mechanism of symptom production is related to a restriction in articular mobility rather than, e.g. a restriction in overlying muscle mobility. In this case, the examination would be structured to examine the articular system, assess its influence on the fault, and then assess the muscular influence and reassess that system s influence on the fault. In this way, in addition to gathering information from each component of the examination the relative influence of the components can be evaluated. Each component begins with an assessment of movement fault (using the patient s functional ), testing procedures and a subsequent reassessment of functional. See Figure 4.2. Observation Observation of static posture can give valuable insight into the likely mechanical presentation of symptoms with movement. A number of static features will help in the interpretation of active movement. A deep skin crease may suggest hypermobility at the level whilst flat sections with reduced muscle bulk may suggest hypomobility. Defined muscle borders may indicate hypertonicity whilst unilateral atrophy may indicate local neuropraxia or trophic change. See Figure 4.3. Functional The functional is the term given to the combination of plane movements that the patient has identified to take them into their most aggravating position. This position identifies the movement fault, whilst the quality, range and speed of movement from neutral into this position and return, should be analyzed in depth. The combination of physiological movements that constitute the functional will provide invaluable information about the starting position that should be adopted for passive movement assessment and treatment. In addition, the three-dimensional components of this position will identify the movements p0425 p0430 s0115 p0435 s0120 p
5 The principles of combined movement assessment CHAPTER 4 OBJECTIVE EXAMINATION PLAN List your hypotheses for the nature of the condition Which two hypotheses will you test against each other in the initial physical examination? Primary... Secondary... Is the nature of the condition severe? Yes No Is the nature of the condition irritable? Yes No To what point are you allowing movement to occur? Before pain To pain To end What is your functional /re-test marker?... What is the primary pain mechanism of this patient s condition? Nociceptive Peripheral neurogenic Central Autonomic Affective To what extent will you perform a neurological exam? None required Local peripheral Lower motor neuron, upper motor neuron, limbs Lower motor neuron, upper motor neuron, limbs and cranial What is the weighting of the following components of the problem? % Radar plot Arthrogenic Arthrogenic Myogenic 100 Neurogenic Osteogenic Myogenic Inflammagenic 50 Psychogenic Viscerogenic Neurogenic 0 Sociogenic Pathogenic Pathogenic Inflammagenic Viscerogenic Osteogenic Sociogenic Psychogenic Likely first treatment: In:... Will:... Comments/cautions: f0010 Figure 4.1 Clinical reasoning form. 55
6 SECTION ONE Combined Movement Theory First hypothesis Arthrogenic Functional Posterior stretch Second hypothesis Myogenic Figure 4.2 A flow chart showing the suggested compartmentalization of the physical examination. The functional is at the head of the differentiation. Two common differentiations are displayed: primary arthrogenic versus primary myogenic. f0015 Observation Observation Hypomobile mid cx Hypertonic muscles ipsilaterally Active movement Active movement Prime movement Prime combination Passive movement In the correct starting position Palpation Passive movement Starting position Palpation Muscle stretch Reassess functional PPIVMS Reassess functional PAIVMS Reassess functional Muscle contraction Reassess functional that should be examined in isolation. Change in the range of movement and pain experienced in the functional position will most accurately reflect overall improvement in the patient s impairment. Active movements s0125 f0020 Figure 4.3 Active extension, right rotation, showing hypomobility of L5, L4, with movement (and skin crease) at L3. IN: standing; DID: active extension of lumbar spine. Segmental restriction of L4/L5 demonstrated. Active movements should be carefully controlled by the therapist. It is important that the patient moves to a point in range that is appropriate for their severity and nature. Simply asking a patient to extend their back will not give adequate guidance about how acceptable it is to reproduce their pain. A patient with very severe pain may be eager to please the therapist and extend beyond the onset of pain causing an exacerbation, or alternatively, may be fearful of p
7 The principles of combined movement assessment CHAPTER 4 s0130 movement and not move to the point that reproduces symptoms. Variability on interpretation of incomplete commands will lead to difficulties with the reliability of testing. Thus, clear commands regarding how far to move in relation to reproduction of symptoms should be included in the commands. A decision about how acceptable it is to reproduce symptoms will need to have been made prior to undertaking this section of the examination. Degree of symptom reproduction deemed acceptable p0450 Having agreed on this the therapist must use clear commands to instruct the movement conducted: u0285 If the agreed degree of symptom reproduction is nil, then at the completion of a combination of movements, the therapist s command should state clearly stop before the pain starts. u0290 If the agreed degree of symptom reproduction is full, then at the completion of a combination of movements, the therapist s command should be move as far as you possibly can. u0295 If the agreed degree of symptom reproduction is partial then at the completion of a combination of movements, the therapist s command should be stop when the pain starts. p0470 Good control of symptom reproduction will enable the combination of movements needed to fully assess the patient s movement dysfunction. Disregard of this important control will lead to situations where the patient s symptoms are exacerbated or under-evaluated. hypomobile section of the spine. The patient can find it difficult to move the hypomobile segments as they move at areas presenting the least resistance to movement and move only at the hyper-mobile segments. This can lead to a situation where symptoms are not reproduced as the symptomatic levels are not being tested, during the test movement. False negatives can occur unless this error in clinical reasoning is considered. Consequently, it is important to guide patients to move at regions you consider likely to be symptomatic during active movement testing. See Figures 4.4, 4.5 and 4.6. The active movement examination is structured to examine the movements most relevant for the patient s impairment. The functional will have provided the examiner with evidence that certain movements are more important in reproducing the dysfunction than others. The functional position will justify a detailed examination of the three movements that constitute it. The next stage in examining the biomechanical features of the impairment is to examine each of the three components of the position to establish which p0485 b0025 p0475 Clinical point If the patient has severe pain at rest the examination will be aimed at finding the movement and position that most reduces pain and it will typically involve finding starting positions for assessment and treatment in the quadrant opposite to the dysfunctional quadrant. s0135 Prime movement and prime combination p0480 Whilst observing active movements, particular attention should be paid to ensuring that the patient moves areas of the spine that are impaired. Very often a patient will have developed hypermobility above a Figure 4.4 Active movement of the lumbar spine. Here, movement of the stiff L4/L5, L5/S1 segment is facilitated by fixing the sacrum with one hand whilst guiding movement to the low lumbar spine. IN: Standing, bed edge support, lumbar extension; DID: active right lateral flexion, range assessment. Note the wide stance required to ensure balance. f
8 SECTION ONE Combined Movement Theory Neutral Right rotation Extension Right rotation Sensitized nociceptors C5 C6 f0030 f0035 p0490 p0495 Figure 4.5 Active movement of the low thoracic spine. Here, movement of the stiff T10/T11 segment is facilitated by fixing the lumbar spine with one hand whilst guiding movement to the low thoracic spine. IN: sitting, lumbar neutral; DID: active left rotation, low thoracic range assessment. Figure 4.6 Active, guided low cervical flexion. IN: sitting, cervical flexion; DID: active assisted left rotation of the low cervical spine. The patient is given feedback on where to move. two movements are the most important, and within these two movements, which is of primary importance or prime movement. The primary movement has an importance within CMT in both the classification of syndromes and in selection of starting positions for treatment. The movement itself is defined as being the movement that either reproduces the patient s signs and/or symptoms most completely (when it is appropriate to do so) or most completely relieves symptoms when the condition is too severe to reproduce symptoms. Having established the prime movement in one plane it should be explored by repeating the movement when combined with another movement, in Figure 4.7 The illustration shows the selective tension of articular and peri-articular tissue with progressive addition of three planes of movement. A progressive increase in anterior stretch is observed with the addition of extension to right rotation (right rotation being coupled with right lateral flexion). another plane, which will move one side of the motion segment in the same direction. In a simplified model of spinal biomechanics extension, ipsilateral rotation and ipsilateral lateral flexion will cause the superior joint facet to move down the inferior segment s joint facet (see Fig. 4.7). Flexion, contralateral flexion and contralateral rotation will cause the superior facet to move up the inferior segment s joint facet. For example, right rotation is the patient s prime movement, reproducing right-sided neck pain. Exploring this movement by examining right rotation in extension and extension in right rotation will elicit which combination is the primary combination. The prime combination will closely resemble the patient s functional. The primary combination holds a crucial place in CMT as it is the starting position where passive movement assessment is conducted. By positioning the spine in the position of dysfunction the addition of passive movements will be more influential in reproducing symptoms and more likely to alter movement dysfunction than if conducted in a neutral position. Passive movement conducted in neutral will rarely be sufficient to reproduce symptoms adequately. When performed in a position related to dysfunction, the application of passive movement or muscle contraction will provide valuable information on, not only the quality and control of movement, but also the effect of the test on the dysfunction. Finding the primary combination is the process by which the clinician can be sure that passive movement testing will be the most informative and that treatment in this position will have the quickest effect on dysfunction. A two-dimensional equivalent would be the need to assess and treat a patient with a 10 loss of elbow extension at this f0040 p0500 p0505 p
9 The principles of combined movement assessment CHAPTER 4 s0140 position, not at 90 of elbow flexion (the equivalent of assessing in neutral). Muscle assessment p0515 The assessment of muscular influences on the spinal dysfunction should involve an assessment of muscular activity (tone) in the primary combination starting position. The degree and location of hypertonicity can be readily palpated in local, deep paraspinal muscles and the overlaying, superficial, musculature (see Figs 4.8 and 4.9). At this point an assessment for trigger points (Travell & Simmons, 1998) can be Table 4.1 Listing the musculature that becomes over or under-active in common spinal pain syndromes (Chaitow, 2006) Short/facilitated/over recruited Occipital extensors Sternocleidomastoid Scalenes Upper trapezius Long/inhibited/under recruited Upper cervical flexors (rectus capitis anterior) Deep cervical flexors (longus colli) Low cervical extensors (iliocostalis) Lower/middle fibres of trapezius t0010 Levator scapulae Rhomboids Subscapularis Serratus anterior Pectoralis minor Pectoralis major Latissimus dorsi Iliopsoas Tensor fascia latae Gluteal muscles Abdominal muscles Quadratus lumborum f0045 Figure 4.8 Palpation of anterior paraspinal muscles, fascia and neurovasular structures. IN: supine, neutral; DID: palpation of anterior low cervical musculature. Special care must be taken to ensure that the flat of the thumb is used to avoid painful pressure. conducted, followed by an assessment of extensibility (Chaitow, 2006) of the superficial phasic muscles that have a tendency to become hypertonic in the presence of spinal pain. See Table 4.1. During this process, hypertonic muscles are passively lengthened either locally, globally or both and a temporary reflexogenic reduction in muscular activity can be induced. Consequently, these tests are effectively mini-treatments of the muscular system. The effect of this mini-treatment on the patient s functional can be immediately assessed. In this way the relative contribution of the myogenic system can be assessed against the arthrogenic system by mini-treating first one system and then another. See Figures 4.10 and p0520 p0525 f0050 Figure 4.9 Palpation of upper thoracic soft tissue tone. IN: prone, neutral; DID: soft tissue tension palpation, upper thoracic spine. Firm pressure will be needed to pick and work through the superficial musculature. Bands of resistance to movement will be palpated. Passive movement and mini-treatments Having established the optimal position to induce passive movement at the motion segments moving dysfunctionally, an assessment is made to determine which passive movement will be the most effective s0145 p
10 SECTION ONE Combined Movement Theory f0055 Figure 4.10 Post-isometric relaxation technique for the right, posterior paraspinals. IN: sitting, thoracic flexion; DID: isometric contraction resisting left rotation of T1 on T2. The patient is told to Don t let me win as the neck is moved towards more flexion and rotation. The patient will contract the extensors and right rotators. An isometric contraction can be held for 6 10 seconds. requires a degree of skill to perform. Whilst the treatment is of a short duration, in order to fit into the assessment process without becoming too time consuming, it must be enough of a dose of treatment to evoke a change in muscle activity and/or joint mobility. Thus, the examiner needs the palpatory skill to be able to tell when these features have subtly changed. With practice the skilled manual therapist can be as confident in discriminating this change in mobility as they have in their ability to discriminate between a normal or hypomobile joint on initial assessment. If we really are striving to provide treatment that is the most efficacious option we must prove that the specific treatment we are proposing is indeed more effective at reducing the dysfunction than the next most likely option. Testing one treatment against another is something we do whilst treating patients, however, the incorporation of this principle during the assessment process is of particular importance with the CMT approach. p0535 p0540 Assessing for the suitability of manipulative thrust techniques s0150 f0060 Figure 4.11 Post-isometric relaxation technique for the right, anterior paraspinal muscles. IN: supine, neutral extension; DID: isometric contraction resisting extension and right rotation. The patient performs an isometric contraction in response to AP pressure. Contraction of the right anterior musculature is produced. See video clip number 4 at reducing the dysfunction. This will involve deciding between accessory and physiological passive movement and between particular combinations of both. One method of deciding between two likely treatment options is to compare the immediate effectiveness of using the treatments. Even a short period of treatment, if applied in the correct starting position, will have an immediate effect on movement dysfunction. The patient will be able to discriminate between the treatment effects and tell you which treatment to use! Local movement impairment, specific to one or two spinal segments, can present with hypomobility in the contralateral side glide that accompanies ipsilateral lateral flexion and rotation. Acute muscle spasm or long-standing movement impairment can lead to a perceptible change in the passive range of contralateral side glide during ipsilateral lateral flexion. When visualizing the quality of resistance to passive movement the movement diagram, developed by Maitland (1986) is useful. When passively inducing lateral flexion at one spinal segment a perception of the profile of resistance to movement can be drawn. Profiles of resistance that are short in range represent a crisp end feel, whilst a long range of resistance profile will feel bouncy. Finally a movement that has no range of resistance and comes to a complete stop immediately resistance is felt, will feel solid. See Figure Segments that do not have this crisp profile do not generally cavitate in response to a high velocity thrust. Thus, unless the therapist assesses lateral flexion and its associated contralateral side glide the rationale for choosing a manipulation technique over a mobilization technique is less clear. The assessment of accessory glides does not afford the information to make this judgement. The assessment of p0545 p
11 The principles of combined movement assessment CHAPTER 4 R2 IV- R1 R2 III+ Figure 4.13 Assessment of the contralateral glide with right lateral flexion of the lumbar spine. IN: supine, cervical extension, left rotation, right lateral flexion; DID: passive right lateral flexion, Grade IV thrust of the C4 segment on C5. Thrust starts before the beginning of resistance and stops just after the beginning of resistance. f0070 R1 R2 R1 f0065 Figure 4.12 This illustration shows the profiles of resistance to segmental movement that can be detected with passive intervertebral movement testing. The top diagram represents a crisp profile of resistance, the middle a bouncy feel and the bottom figure a solid feel. Only the top profile signifies that a manipulative thrust will be successful in inducing cavitation. Figure 4.14 Assessment of contralateral lateral glide with ipsilateral lateral flexion in a combined starting position, prior to application of a IV thrust technique. IN: sitting, thoracic extension; DID: right lateral flexion of T12 on L1. As the upper segment is ipsilaterally side-flexed the motion segment is contralaterally side glided. f0075 segmental lateral flexion can be conducted in combined starting positions in order to fully examine for the presence of this crisp profile of resistance. See Figures 4.12, 4.13, 4.14, 4.15 and In the following case studies there are two worked examples of the practical application of CMT approach during initial assessment, with one example from the cervical spine and one from the lumbar spine. p
12 SECTION ONE Combined Movement Theory f0080 Figure 4.15 Assessment of the contralateral glide associated with ipsilateral flexion of the low lumbar spine. IN: left side-lying, flexion; DID: right lateral flexion with left side glide at the motion segment. As the lumbar spine is laterally flexed, firm pressure is applied towards the bed. Figure 4.16 Assessment of resistance profile of contralateral glide in a combined position used to induce cavitation. IN: flexion, left lateral flexion, right rotation; DID: right rotation combined with contralateral glide downwards. The combined starting position for a Grade IV rotation, thrust technique. f0085 b0030 s0155 s0160 p0560 s0165 p0565 s0170 p0570 s0175 p0575 s0180 p0580 CERVICAL SPINE CASE STUDY INITIAL INTERVIEW Symptomology A 22-year-old female sought treatment for pain in the right cervical spine and right shoulder. The pain was located in the lower cervical spine and referred into the right shoulder across the right supra-scapula fossa (Fig. 4.17). The pain was not radicular in quality but severe (8/10). There was no suggestion of an upper motor neuron lesion and no indication of other red flags. There were no features suggestive of segmental cervical instability or shoulder derangement. There was no history of cervical locking, catching or weakness. There was no headache. Relevant history Symptoms developed over a 6-day period following a mild, rear shunt whiplash injury, a week previously. Behaviour of symptoms Pain was reproduced with low cervical flexion and left lateral flexion. Sitting with the neck in this position reproduced symptoms within 2 minutes. The symptoms were eased immediately, by positioning the lower cervical spine in extension and right lateral flexion. No latent pain was exhibited. Diurnal pattern There was no stiffness in the cervical spine in the morning. Shoulder pain developed in the evening. Sleep was not disturbed. Special questions The patient s general health was good. There was no weight loss, no dizziness, no dysphagia, no dysarthria, Figure 4.17 Cervical spine case study pain chart. no diplopia, no raised blood pressure, and no symptoms of cervical artery dysfunction. Radiographs of the cervical spine were normal. The patient was not currently taking any anticoagulant or steroid therapy and had received no benefit from anti-inflammatory medication. There was no history of locking, clunking or giving way of the shoulder, with no history of trauma. See the completed planning sheet in Figure f0090 p
13 The principles of combined movement assessment CHAPTER 4 OBJECTIVE EXAMINATION PLAN List your hypotheses for the nature of the condition Posterior facet capsule sprain Posterior paraspinal strain Posterior annular disc sprain... Which two hypotheses will you test against each other in the initial physical examination? Primary... Articular predominance... Secondary... Myogenic predominance... Is the nature of the condition severe? Yes No Is the nature of the condition irritable? Yes No To what point are you allowing movement to occur? Before pain To pain To limit What is the functional /primary re-test marker?... Flexion contralateral, lateral flexion quadrant... What is the primary pain mechanism of this patient s condition? Nociceptive Peripheral neurogenic Central Autonomic Affective To what extent will you perform a neurological exam? None required Local peripheral Lower motor neuron, upper motor neuron, limbs Lower motor neuron, upper motor neuron, limbs and cranial What is the weighting of the following components of the problem? % Radar plot Arthrogenic 50 Arthrogenic Myogenic Neurogenic 1 Osteogenic Myogenic Inflammagenic 2 50 Psychogenic 1 Viscerogenic Neurogenic 0 Sociogenic 1 Pathogenic 1 Pathogenic Inflammagenic Viscerogenic 1 Osteogenic 3 Sociogenic Psychogenic Likely first treatment: In: Extension, right lateral flexion quadrant... Will: Anterior capsular stretch, large amplitude movement, in resistance (Grade III)... Comments/cautions: Pain relief approach, progressing to a stretch of the tissues driving the nociceptive pattern of presentation f0095 Figure 4.18 Objective examination plan for the cervical spine. 63
14 SECTION ONE Combined Movement Theory Prime movement = left lateral flexion Prime combination = left lateral flexion followed by flexion. 3 /4 full range Right-sided cervical and shoulder pain Severe PHYSICAL EXAMINATION Observation There was no atrophy of the cervical musculature. There was an increase in muscle tone of the right sternocleidomastoid, upper fibres of trapezius and levator scapula and right scalenes. Active movement Pain was reproduced earliest in range with left lateral flexion. Restriction to flexion was apparent at the C5/C6 level. Pain was reproduced further into range with flexion than with left lateral flexion. Restriction to movement was most obvious in the mid cervical region. See Figure s0185 s0190 p0590 s0195 p0595 f0100 Figure 4.19 Box diagram showing the prime combination for the patient. Functional Flexion, left lat flex Figure 4.20 Flow chart of differential examination for the cervical spine. f0105 First hypothesis Posterior facet capsule sprain Second hypothesis Posterior musculature strain Observation Postural positioning malalignment Observation Muscle atrophy Hypertrophy Hypotonicity Hypertonicity Active movement Prime movement Prime combination Active movement Control and timing of muscles during movement Passive movement Starting position Palpation Passive movement Starting position Palpation Local stretch Effect on functional 0% PPIVMS Effect on functional 10% PAIVMS Effect on functional 40% Muscle contraction Effect on functional 10% The technique that alters movement and muscle tone most with mini-treatment is the initial treatment choice 64
15 The principles of combined movement assessment CHAPTER 4 s0200 p0600 s0205 p0610 Passive physiological intervertebral movement (PPIVMS) Due to the severity, the examination was undertaken in right lateral flexion and extension (posterior structures off stretch) to establish the movement that most reduced pain and dysfunction. Right lateral flexion induced the greatest increase in movement and reduction in muscle tone. A short passive treatment, using this right lateral flexion of C5 on C6 reduced the pain produced by the functional by 10%. Passive accessory intervertebral movement (PAIVMS) Due to the severity, examination was undertaken in right lateral flexion and extension (posterior structures off stretch) to establish the movement that most reduced pain and dysfunction. Anterior pressure (AP) on C5 induced the greatest increase in movement and reduction in muscle tone (greater than induced by AP movement of C4 or C6). A short passive treatment, using this accessory movement reduced the pain produced by the functional by 40%. Muscular assessment In right lateral flexion and extension due to severity of pain, palpation of musculature revealed hypertonicity of deep paraspinals (C4 to C6) and hypertonicity of the region s phasic muscles. No trigger points were detected. Palpation and length assessment of the levator scapulae, scalenes, upper fibres of trapezius and sternocleidomastoid did not alter the functional. See Figure s0210 p0620 p0630 b0035 LUMBAR SPINE CASE STUDY s0215 s0220 p0635 INITIAL INTERVIEW Symptomology A 45-year-old male sought treatment for pain in the right back and buttock (Fig. 4.21). The pain was not radicular in quality and not severe (4/10). There was no suggestion of an upper motor neuron lesion and no indication of other red flags. There were no features suggestive of segmental lumbar instability or disc derangement. There was no history of lumbar locking, catching or weakness and there was no cauda equina syndrome. Relevant history Symptoms developed over a 6-month-period with no history of trauma. Behaviour of symptoms Pain was reproduced with low lumbar extension and right lateral flexion (whilst arching his back to put on his coat). Standing reproduced symptoms within 20 minutes. Walking reproduced symptoms in 30 minutes. The symptoms were eased, immediately, by positioning the back in flexion, either by sitting or leaning over in standing. Pain was also eased by crossing the right leg over the left, in sitting. No latent pain was exhibited. Pain was also experienced whilst turning over in bed. s0225 p0640 s0230 p0645 Diurnal pattern There was less than 30 minutes of stiffness in the back in the morning. Buttock pain developed in the evening. Sleep was not disturbed. s0235 p0650 Special questions His general health was good. There was no weight loss, no night sweats or fever, no constant night pain (worse than during the day), no raised blood pressure, no symptoms of vascular stenosis or peripheral vascular disease. No history of cancer. The patient was not currently taking any anticoagulant or steroid therapy and had received no benefit from anti-inflammatory medication. s0240 p0655 f0110 Figure 4.21 Lumbar spine case study pain chart. See the completed planning sheet in Figure p
16 SECTION ONE Combined Movement Theory OBJECTIVE EXAMINATION PLAN List your hypotheses for the nature of the condition Superior facet capsule source Sacro-iliac joint source Anterior paraspinal muscle source... Which two hypotheses will you test against each other in the initial physical examination? Primary... Lumbar articular drive (75%)... Secondary... Sacro-iliac articular drive (25%)... Is the nature of the condition severe? Yes No Is the nature of the condition irritable? Yes No To what point are you allowing movement to occur? Before pain To pain To limit What is the functional /primary re-test marker?... Extension, ipsilateral lateral flexion quadrant... What is the primary pain mechanism of this patient s condition? Nociceptive Peripheral neurogenic Central Autonomic Affective To what extent will you perform a neurological exam? None required Local peripheral Lower motor neuron, upper motor neuron, limbs Lower motor neuron, upper motor neuron, limbs and cranial What is the weighting of the following components of the problem? % Radar plot Arthrogenic 70 Arthrogenic Myogenic Neurogenic 1 Osteogenic Myogenic Inflammagenic 4 50 Psychogenic 1 Viscerogenic Neurogenic 0 Sociogenic 1 Pathogenic 1 Pathogenic Inflammagenic Viscerogenic 1 Osteogenic 1 Sociogenic Psychogenic Likely first treatment: In: Extension, right lateral flexion quadrant... Will: Superior capsular stretch, large amplitude movement, in resistance (Grade III)... Comments/cautions: Pain relieving mobilization, combined with a stretch of the tissues driving the nociceptive pattern of presentation... f0115 Figure 4.22 Objective examination plan for the lumbar spine. 66
17 The principles of combined movement assessment CHAPTER 4 s0245 s0250 p0665 PHYSICAL EXAMINATION Observation There was no atrophy of the lumbar musculature. There was an increase in muscle tone of the right erectore spinae, quadratus lumborum and piriformis. s0255 Active movement p0670 Pain was reproduced earliest in range with right lateral flexion. Restriction to extension was apparent at the L4/L5 level. Pain was reproduced further into range with extension than with right lateral flexion. See Figure s0260 p0675 s0265 p0685 Passive physiological intervertebral movement (PPIVMS) Right lateral flexion, in extension of L4 on L5, induced the greatest increase in movement and reduction in muscle tone, when compared with movement at L3/L4 and L5/S1. A short passive treatment, using this right lateral flexion of L4 on L5 reduced the pain produced by the functional by 50%. Passive accessory intervertebral movement (PAIVMS) In right lateral flexion and extension, posterior pressure (unilateral posterior-anterior angled caudad) on L4 induced the greatest increase in movement and reduction in muscle tone, when compared to the same accessory movement appliedtol3orl5. Passive movement of the sacroiliac joint (SIJ) In right lateral flexion and extension PA pressure on the right apex of the sacrum (encouraging nutation) reproduced symptoms and was the most restricted sacral glide, when compared to the response of moving the other three corners of the sacrum. A short passive treatment, using this passive movement reduced the pain produced by the functional by 10%. See Figure First hypothesis Superior facet capsule sprain Observation Postural positioning malalignment Active movement Prime movement Prime combination Functional Extension, right lat flex Second hypothesis Restricted nutation of the right SIJ Observation Postural positioning malalignment Active movement Same Prime movement Prime combination s0270 p0695 p0705 A short passive treatment, using this accessory movement reduced the pain produced by the functional by 20%. Passive movement Starting position Palpation Passive movement Same Starting position Palpation SIJ passive movement Effect on functional 10% Right-sided lumbar and buttock pain Not severe PPIVMS Effect on functional 50% PAIVMS Effect on functional 20% Prime movement = right lateral flexion Prime combination = right lateral flexion followed by extension. 3 /4 full range The technique that most alters movement and pain response with mini-treatment is the initial treatment choice f0120 Figure 4.23 Box diagram showing the prime combination for the patient. Figure 4.24 Flow chart of differential examination for the lumbar spine. f
18 SECTION ONE Combined Movement Theory References Chaitow, L., Muscle energy techniques. Elsevier Health Sciences, Oxford. Gibbons, P., Tehan, P., 2001a. Patient positioning and spinal locking for lumbar spine rotation manipulation. Man. Ther. 6 (3), Gibbons, P., Tehan, P., 2001b. Spinal manipulation: indications, risks and benefits. Journal of Bodywork & Movement Therapies 5 (2), Grieve, G.P., Common vertebral joint problems. Churchill Livingstone, New York, pp Grieve, G.P., Mobilization of the spine. A Primary handbook of Clinical Method. Churchill Livingstone, Edinburgh. Kerry, R., Taylor, A.J., Mitchell, J., et al., 2008a. Manual therapy and cervical arterial dysfunction, directions for the future: a clinical perspective. The Journal of Manual & Manipulative Therapy 16 (1), Kerry, R., Taylor, A.J., Mitchell, J., et al., 2008b. Cervical arterial dysfunction and manual therapy: a critical literature review to inform professional practice. Man. Ther. 13 (4), Maitland, G., Vertebral manipulation. Elsevier Health Sciences, Sydney. Travell, Simmons, Travell Simons myofascial pain and dysfunction: the trigger point manual, second ed. Lippincott Williams & Wilkins, San Francisco. 68
WEEKEND 1 CERVICAL SPINE
 Virginia Orthopedic Manual Physical Therapy Institute - Technique Manual WEEKEND 1 CERVICAL SPINE Cervical Active Range of Motion Testing Rotation CT Flexion Mid Cervical Flexion Extension Side-Bending
Virginia Orthopedic Manual Physical Therapy Institute - Technique Manual WEEKEND 1 CERVICAL SPINE Cervical Active Range of Motion Testing Rotation CT Flexion Mid Cervical Flexion Extension Side-Bending
Active-Assisted Stretches
 1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
10/8/2015. FACTORS IN BACK PAIN introduction 27% Framing the Discussion from a Clinical and Anatomical Perspective
 FACTORS IN BACK PAIN Framing the Discussion from a Clinical and Anatomical Perspective A B M P B a ck Pa i n S u m m i t With Clint Chandler FACTORS IN BACK PAIN introduction Back pain affects 8 out of
FACTORS IN BACK PAIN Framing the Discussion from a Clinical and Anatomical Perspective A B M P B a ck Pa i n S u m m i t With Clint Chandler FACTORS IN BACK PAIN introduction Back pain affects 8 out of
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner
 Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
Cervical Spine Exercise and Manual Therapy for the Autonomous Practitioner Eric Chaconas PT, PhD, DPT, FAAOMPT Assistant Professor and Assistant Program Director Doctor of Physical Therapy Program Eric
VIRGINIA ORTHOPEDIC MANUAL PHYSICAL THERAPY INSTITUTE TECHNIQUE MANUAL
 VIRGINIA ORTHOPEDIC MANUAL PHYSICAL THERAPY INSTITUTE TECHNIQUE MANUAL Lumbar and Thoracic Spine Lumbar AROM Assessment -Patient Positioning: Standing, appropriately undressed so that the lumbar and thoracic
VIRGINIA ORTHOPEDIC MANUAL PHYSICAL THERAPY INSTITUTE TECHNIQUE MANUAL Lumbar and Thoracic Spine Lumbar AROM Assessment -Patient Positioning: Standing, appropriately undressed so that the lumbar and thoracic
The Back. Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa
 The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
The Back Anatomy RHS 241 Lecture 9 Dr. Einas Al-Eisa The spine has to meet 2 functions Strength Mobility Stability of the vertebral column is provided by: Deep intrinsic muscles of the back Ligaments
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK
 ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
ACE s Essentials of Exercise Science for Fitness Professionals TRUNK Posture and Balance Posture refers to the biomechanical alignment of the individual body parts and the orientation of the body to the
Passive Intervertebral Mobilization
 Passive Intervertebral Mobilization Terry Rose DPT, FAAOMPT, Cert, MDT Guide to Physical Therapy Practice Section 4D-Impairment/Connective Tissue Dysfunction Section 4E,4F,4G,4H,4I,4J Impaired Joint Mobility
Passive Intervertebral Mobilization Terry Rose DPT, FAAOMPT, Cert, MDT Guide to Physical Therapy Practice Section 4D-Impairment/Connective Tissue Dysfunction Section 4E,4F,4G,4H,4I,4J Impaired Joint Mobility
CERVICAL SPINE TIPS A
 CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
CERVICAL SPINE TIPS A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of
Rotational Forces. : Their impact; our treatments
 Rotational Forces : Their impact; our treatments Lee Stang, LMT, LMBT, BCTMB NCBTMB Provider: 450217-06 bridgestohealthseminars.com bthseminars@gmail.com 860.985.5834 Facebook.com/BridgesToHealthSeminars
Rotational Forces : Their impact; our treatments Lee Stang, LMT, LMBT, BCTMB NCBTMB Provider: 450217-06 bridgestohealthseminars.com bthseminars@gmail.com 860.985.5834 Facebook.com/BridgesToHealthSeminars
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem-Solving: Back
 Low Back Pain 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: Back Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of
Low Back Pain 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem-Solving: Back Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of
9/4/10. James J. Lehman, DC, MBA, DABCO. Why is posture important to you, the chiropractic physician?
 James J. Lehman, DC, MBA, DABCO The posture of homo sapiens is a complex biomechanical continuum, which involves the function of muscles, ligaments, fascia, nerves, osseous structures, neuromuscular control,
James J. Lehman, DC, MBA, DABCO The posture of homo sapiens is a complex biomechanical continuum, which involves the function of muscles, ligaments, fascia, nerves, osseous structures, neuromuscular control,
Clinical examination of the shoulder girdle
 Clinical of the shoulder girdle CHAPTER CONTENTS Symptoms referred to the shoulder girdle........ e72 Symptoms referred from the shoulder girdle...... e72 History........................... e72 Inspection.........................
Clinical of the shoulder girdle CHAPTER CONTENTS Symptoms referred to the shoulder girdle........ e72 Symptoms referred from the shoulder girdle...... e72 History........................... e72 Inspection.........................
Cervical Spine: Pearls and Pitfalls
 Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
Cervical Spine: Pearls and Pitfalls Presenters Dr. Rob Donkin Functional Anatomy Current research Cervical Radiculopathy Dr. Gert Ferreira Red flags Case Study Kinesio Taping Chris Neethling Gonstead adjusting
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Examination of the lumbosacral spine. Dr Lucy Holtzhausen Rotorua GP CME June 2015
 Examination of the lumbosacral spine Dr Lucy Holtzhausen Rotorua GP CME June 2015 Diagnostic Algorithm Presenting symptoms Diagnostic decisions Diagnostic triage LOW BACK PAIN Mechanical NON-SPECIFIC LBP
Examination of the lumbosacral spine Dr Lucy Holtzhausen Rotorua GP CME June 2015 Diagnostic Algorithm Presenting symptoms Diagnostic decisions Diagnostic triage LOW BACK PAIN Mechanical NON-SPECIFIC LBP
Planning the Objective Exam. Objective Examination of the Cervical Spine. Clearing Tests. Observation. Functional Demonstration.
 Objective Examination of the Cervical Spine Taking the complaint and identifying the damaged structure Planning the Objective Exam With a clear picture from the subjective exam, the objective exam should
Objective Examination of the Cervical Spine Taking the complaint and identifying the damaged structure Planning the Objective Exam With a clear picture from the subjective exam, the objective exam should
Main Menu. Trunk and Spinal Column click here. The Power is in Your Hands
 1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
1 The Trunk and Spinal Column click here Main Menu K.9 http://www.handsonlineeducation.com/classes/k9/k9entry.htm[3/27/18, 2:00:55 PM] The Trunk and Spinal Column Vertebral column complex 24 intricate
Thoracic Spine Mobilization for Shoulder Pain. Scott Tauferner PT, ATC
 Thoracic Spine Mobilization for Shoulder Pain Scott Tauferner PT, ATC Conflicts of Interest None 1 2 3 Participants will be able to select thoracic mobilization strategies in patients with shoulder pain.
Thoracic Spine Mobilization for Shoulder Pain Scott Tauferner PT, ATC Conflicts of Interest None 1 2 3 Participants will be able to select thoracic mobilization strategies in patients with shoulder pain.
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age of patient - Certain conditions are more prevalent in particular age groups (Hip pain in children may refer to the knee from Legg-Calve-Perthes
Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives
 1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
1 2 Thoracolumbar Anatomy Eric Shamus Catherine Patla Objectives List the muscular and ligamentous attachments of the thoracic and lumbar spine Describe how the muscles affect the spine and upper extremity
Exercise for Reducing Neck Pain and Enhancing Dynamic Stability.
 Exercise for Reducing Neck Pain and Enhancing Dynamic Stability www.fisiokinesiterapia.biz Presentation Outline Compare/Contrast Lumbar Exercise Literature to Cervical Spine Discuss Neck Musculature and
Exercise for Reducing Neck Pain and Enhancing Dynamic Stability www.fisiokinesiterapia.biz Presentation Outline Compare/Contrast Lumbar Exercise Literature to Cervical Spine Discuss Neck Musculature and
LUMBAR SPINE CASE 3. Property of VOMPTI, LLC. For Use of Participants Only. No Use or Reproduction Without Consent 1. L4-5, 5-S1 disc, facet (somatic)
 LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE 3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Richmond 2018-2019 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014
 Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
Upper Cross Syndrome: Assessment & Management in Family Practice HKDU Symposium Dec 2014 Dr. Ngai Ho Yin Allen Family Medicine Specialist PGDipMusculoskeletal Medicine MBBS(HK), DCH(London), DFM(CUHK),
A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT
 LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
LUMBAR SPINE CASE #3 A.J. Lievre, PT, DPT, OCS, CMPT Aaron Hartstein, PT, DPT, OCS, FAAOMPT Orthopaedic Manual Physical Therapy Series Charlottesville 2017-2018 L4-5, 5-S1 disc, facet (somatic) L5/S1 Radiculopathy
Overuse Injuries. Overuse injury defined. Overuse Injuries
 Overuse Injuries Lisa DeStefano, DO Associate Professor and Chair Department of Osteopathic Manipulative Medicine College of Osteopathic Medicine Michigan State University Overuse injury defined Overuse
Overuse Injuries Lisa DeStefano, DO Associate Professor and Chair Department of Osteopathic Manipulative Medicine College of Osteopathic Medicine Michigan State University Overuse injury defined Overuse
Clinical Guidelines for Spinal Manipulation in Naturopathic Practice
 QUALITY ASSURANCE REPORT ON NATUROPATHIC MANIPULATION Clinical Guidelines for Spinal Manipulation in Naturopathic Practice Executive Summary April 19, 2005 Clinical guidelines are designed to assist clinicians
QUALITY ASSURANCE REPORT ON NATUROPATHIC MANIPULATION Clinical Guidelines for Spinal Manipulation in Naturopathic Practice Executive Summary April 19, 2005 Clinical guidelines are designed to assist clinicians
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain
 Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
Session 4: Exercise Prescription for Musculoskeletal Disorders: Low Back Pain Course: Designing Exercise Prescriptions for Normal/Special Populations Presentation Created by Ken Baldwin, M.ED, ACSM-H/FI
72a Orthopedic Massage: Introduction!
 72a Orthopedic Massage: Introduction! 72a Orthopedic Massage: Introduction! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10 minutes Lecture: 25 minutes Lecture: 15 minutes Active
72a Orthopedic Massage: Introduction! 72a Orthopedic Massage: Introduction! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10 minutes Lecture: 25 minutes Lecture: 15 minutes Active
Specific muscle strengthening for a pain-free back
 Medical Strengthening Therapy (MST) Specific muscle strengthening for a pain-free back For an active life without back pain. MST an aetiological therapy against dorsal pain Today, diseases and malfunctions
Medical Strengthening Therapy (MST) Specific muscle strengthening for a pain-free back For an active life without back pain. MST an aetiological therapy against dorsal pain Today, diseases and malfunctions
CLINICAL NOTES. Aust. J. Physiother. 26:5, October,
 CLINICAL NOTES COMBINED MOVEMENTS IN THE CERVICAL SPINE (C2-7) THEIR VALUE IN EXAMINATION AND TECHNIQUE CHOICE Brian C. Edwards Private Practitioner Lecturer in Manipulative Therapy, Western Australian
CLINICAL NOTES COMBINED MOVEMENTS IN THE CERVICAL SPINE (C2-7) THEIR VALUE IN EXAMINATION AND TECHNIQUE CHOICE Brian C. Edwards Private Practitioner Lecturer in Manipulative Therapy, Western Australian
An Osteopathic Approach to Low Back Pain. Ryan Seals DO Interim Chair of Family Medicine and OMM
 An Osteopathic Approach to Low Back Pain Ryan Seals DO Interim Chair of Family Medicine and OMM Objectives Review Osteopathic Philosophy and Principles Discuss how somatic dysfunction influences low back
An Osteopathic Approach to Low Back Pain Ryan Seals DO Interim Chair of Family Medicine and OMM Objectives Review Osteopathic Philosophy and Principles Discuss how somatic dysfunction influences low back
OMT FOR THE PERFORMING ARTIST
 OMT FOR THE PERFORMING ARTIST Sajid A. Surve, DO Associate Professor, UNTHSC-TCOM Co-Director, UNT Texas Center for Performing Arts Health http://tcpah.unt.edu Occupation History for the Performer Pertinent
OMT FOR THE PERFORMING ARTIST Sajid A. Surve, DO Associate Professor, UNTHSC-TCOM Co-Director, UNT Texas Center for Performing Arts Health http://tcpah.unt.edu Occupation History for the Performer Pertinent
Information within the handout. Brief Introduction Anatomy & Biomechanics Assessment & Diagnosis Treatment through Muscle Energy
 Manual Medicine Diagnosis and Treatment for Somatic Dysfunction of the Pelvis Through Muscle Energy Greenman s Priciples of Manual Medicine (5 th Ed.)- Lisa DeStefano,DO Speaker disclosure I declare I
Manual Medicine Diagnosis and Treatment for Somatic Dysfunction of the Pelvis Through Muscle Energy Greenman s Priciples of Manual Medicine (5 th Ed.)- Lisa DeStefano,DO Speaker disclosure I declare I
External Obliques Abdominal muscles that attaches at the lower ribs, pelvis, and abdominal fascia.
 The Core The core is where most of the body s power is derived. It provides the foundation for all movements of the arms and legs. The core must be strong, have dynamic flexibility, and function synergistically
The Core The core is where most of the body s power is derived. It provides the foundation for all movements of the arms and legs. The core must be strong, have dynamic flexibility, and function synergistically
3 Movements of the Trunk. Flexion Rotation Extension
 3 Movements of the Trunk Flexion Rotation Extension 1 TRUNK FLEXION 2 TRUNK FLEXION: Rectus Abdominalis O: Crest of Pubis & ligaments covering front of symphysis pubis. I: By «3 portions into cartilages
3 Movements of the Trunk Flexion Rotation Extension 1 TRUNK FLEXION 2 TRUNK FLEXION: Rectus Abdominalis O: Crest of Pubis & ligaments covering front of symphysis pubis. I: By «3 portions into cartilages
Institute of Holistic Healthcare. Certificate in Orthopaedic Manipulative Therapy PROSPECTUS
 Institute of Holistic Healthcare Certificate in Orthopaedic Manipulative Therapy PROSPECTUS 2019 Contents Contents... 1 Aims:... 2 Objectives:... 2 Format of the Program:... 3 Program... 3 Continuing Professional
Institute of Holistic Healthcare Certificate in Orthopaedic Manipulative Therapy PROSPECTUS 2019 Contents Contents... 1 Aims:... 2 Objectives:... 2 Format of the Program:... 3 Program... 3 Continuing Professional
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms
 Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Clarification of Terms The Spine, Spinal Column, and Vertebral Column are synonymous terms referring to the bony components housing the spinal cord Spinal Cord = made of nervous tissue Facet = a small,
Chiropractic Glossary
 Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
Chiropractic Glossary Anatomy Articulation: A joint formed where two or more bones in the body meet. Your foot bone, for example, forms an articulation with your leg bone. You call that articulation an
Subluxation and Muscle Patterns for the Lower Thoracics Marc Heller, DC
 Subluxation and Muscle Patterns for the Lower Thoracics Marc Heller, DC An extremely common subluxation pattern is a lack of extension, with restricted lateral bending and rotation to one side in the lower
Subluxation and Muscle Patterns for the Lower Thoracics Marc Heller, DC An extremely common subluxation pattern is a lack of extension, with restricted lateral bending and rotation to one side in the lower
10/5/2017. Cervical Manual Evaluation and Mobilizations. Upper Cervical Stability Testing Alar Ligament
 Cervical Manual Evaluation and Mobilizations Upper Cervical Stability Testing Alar Ligament Upper Cervical Stability Testing Transverse Ligament 1 Upper Cervical Stability Testing Transverse Plane Positive
Cervical Manual Evaluation and Mobilizations Upper Cervical Stability Testing Alar Ligament Upper Cervical Stability Testing Transverse Ligament 1 Upper Cervical Stability Testing Transverse Plane Positive
Wake me when this makes sense. Today s Objectives. Quote from Maitland. Quote from Maitland 8/4/2012
 Wake me when this makes sense Today s Objectives Selection of techniques Order of efficacy of techniques Ground the theory in reality Application of techniques How do you do what you should do Quote from
Wake me when this makes sense Today s Objectives Selection of techniques Order of efficacy of techniques Ground the theory in reality Application of techniques How do you do what you should do Quote from
Structure and Function of the Vertebral Column
 Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
Structure and Function of the Vertebral Column Posture Vertebral Alignment Does it really matter? Yes it does! Postural Curves The vertebral column has a series of counterbalancing curves posterior anterior
ESSENTIALPRINCIPLES. Part II. Cervical Injuries
 ESSENTIALPRINCIPLES Part II Cervical Injuries By Ben E. Benjamin 86 MASSAGE & BODYWORK AUGUST/SEPTEMBER 2005 In the last article, we took a broad look at cervical injuries, discussing the anatomy of this
ESSENTIALPRINCIPLES Part II Cervical Injuries By Ben E. Benjamin 86 MASSAGE & BODYWORK AUGUST/SEPTEMBER 2005 In the last article, we took a broad look at cervical injuries, discussing the anatomy of this
The Biomechanics of the Human Spine. Basic Biomechanics, 6 th edition By Susan J. Hall, Ph.D.
 Chapter 9 The Biomechanics of the Human Spine Structure of the Spine The spine is a curved stack of 33 vertebrae structurally divided into five regions: cervical region - 7 vertebrae thoracic region -
Chapter 9 The Biomechanics of the Human Spine Structure of the Spine The spine is a curved stack of 33 vertebrae structurally divided into five regions: cervical region - 7 vertebrae thoracic region -
Journal of Orthopaedic & Sports Physical Therapy. January 2012; Volume 42; Number 1; pp. 5-18
 1 Upper Cervical and Upper Thoracic Thrust Manipulation Versus Nonthrust Mobilization in Patients With Mechanical Neck Pain: A Multicenter Randomized Clinical Trial Journal of Orthopaedic & Sports Physical
1 Upper Cervical and Upper Thoracic Thrust Manipulation Versus Nonthrust Mobilization in Patients With Mechanical Neck Pain: A Multicenter Randomized Clinical Trial Journal of Orthopaedic & Sports Physical
Location of Pain/Symptoms Where do you feel the pain/symptoms? Can you point with one finger to location of pain? Is the pain general or localized?
 Injury Evaluation History A complete and accurate medical history is one of the most important and useful parts of the clinical examination. A complete history consists of past history and a history of
Injury Evaluation History A complete and accurate medical history is one of the most important and useful parts of the clinical examination. A complete history consists of past history and a history of
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education Objectives Discuss concepts relevant to pathophysiology and differential diagnosis for lumbar radiculopathy
7) True/False: Rigid motor strategies are the most effective way to handle high forces
 The Sacro-Iliac Joint 1) Which of the following make up part of the SIJ provocative physical examination? A. Gaenslen s, FABERS, stork, joint distraction B. Fortin finger test, joint compression, thigh
The Sacro-Iliac Joint 1) Which of the following make up part of the SIJ provocative physical examination? A. Gaenslen s, FABERS, stork, joint distraction B. Fortin finger test, joint compression, thigh
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Tel# Department of Physical Therapy King Saud University
 1 RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Tel# 4693601 Department of Physical Therapy King Saud University 2 The scapulae lie against the thorax approximately
1 RHS 221 Manual Muscle Testing Theory 1 hour practical 2 hours Dr. Ali Aldali, MS, PT Tel# 4693601 Department of Physical Therapy King Saud University 2 The scapulae lie against the thorax approximately
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
82a Orthopedic Massage! Introduction - Thoracic Outlet"
 82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
82a Orthopedic Massage! Introduction - Thoracic Outlet" 82a Orthopedic Massage! Introduction - Thoracic Outlet! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders " 10 minutes "Lecture:"
30b Passive Stretches:! Technique Demo and Practice - Upper Body
 30b Passive Stretches:! Technique Demo and Practice - Upper Body 30b Passive Stretches:! Technique Demo and Practice - Upper Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
30b Passive Stretches:! Technique Demo and Practice - Upper Body 30b Passive Stretches:! Technique Demo and Practice - Upper Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
Regional Review of Musculoskeletal System: Head, Neck, and Cervical Spine Presented by Michael L. Fink, PT, DSc, SCS, OCS Pre- Chapter Case Study
 Regional Review of Musculoskeletal System: Presented by Michael L. Fink, PT, DSc, SCS, OCS (20 minutes CEU Time) Subjective A 43-year-old male, reported a sudden onset of left-sided neck and upper extremity
Regional Review of Musculoskeletal System: Presented by Michael L. Fink, PT, DSc, SCS, OCS (20 minutes CEU Time) Subjective A 43-year-old male, reported a sudden onset of left-sided neck and upper extremity
Lumbar Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT
 Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Lumbar Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education 1 Objectives Apply key concepts from the cervical anatomy/kinesiology self-study to aid
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D.
 Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Chest cavity, vertebral column and back muscles. Respiratory muscles. Sándor Katz M.D., Ph.D. Chest cavity - bony structures Chest cavity- bony structures Sternum Ribs True ribs: first seven pairs connect
Documentation and Billing For Myofacial Disruption Treatment
 Documentation and Billing For Myofacial Disruption Treatment Page 1 of 7 Documentation Requirements The following information comes directly from the American Medical Association CPT coding Committee:
Documentation and Billing For Myofacial Disruption Treatment Page 1 of 7 Documentation Requirements The following information comes directly from the American Medical Association CPT coding Committee:
BASIC ORTHOPEDIC ASSESSMENT Muscle and Joint Testing
 BASIC ORTHOPEDIC ASSESSMENT Muscle and Joint Testing The following tests are for the purpose of determining relative shortening, restriction or bind of muscle tissues. In this context the term bind in
BASIC ORTHOPEDIC ASSESSMENT Muscle and Joint Testing The following tests are for the purpose of determining relative shortening, restriction or bind of muscle tissues. In this context the term bind in
Muscle Energy Technique
 PRACTICE SESSION: Muscle Energy Technique BE AN ARTIST and work out the best way for you to use the Muscle Energy Technique (MET). This technique works best when muscles are shortened. If you try MET on
PRACTICE SESSION: Muscle Energy Technique BE AN ARTIST and work out the best way for you to use the Muscle Energy Technique (MET). This technique works best when muscles are shortened. If you try MET on
SPINAL JOINT MOBILIZATION. Dr. Asif Islam PT,SMC,UOS.
 SPINAL JOINT MOBILIZATION Dr. Asif Islam PT,SMC,UOS. Effects of Mobilization Neurophysiological effects: Restoration of neurodynamics Stimulates mechanoreceptors Decrease muscle spasm & muscle guarding
SPINAL JOINT MOBILIZATION Dr. Asif Islam PT,SMC,UOS. Effects of Mobilization Neurophysiological effects: Restoration of neurodynamics Stimulates mechanoreceptors Decrease muscle spasm & muscle guarding
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology
 Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
Physical Therapy Diagnostic and Treatment Approach to the Active Patient with Complex Spine Pathology Scott Behjani, DPT, OCS Introduction Prevalence 1-year incidence of first-episode LBP ranges from
NECK PAIN WORKSHOP A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide
 NECK PAIN WORKSHOP A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of neck
NECK PAIN WORKSHOP A Musculoskeletal Approach to managing Neck Pain An ALGORITHM, as a management guide Rick Bernau & Ian Wallbridge June 2010 THE PROCESS An interactive approach to the management of neck
86b Orthopedic Massage:! Technique Review and Practice - Neck Pain
 86b Orthopedic Massage:! Technique Review and Practice - Neck Pain 86b Orthopedic Massage:! Technique Review and Practice - Neck Pain! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
86b Orthopedic Massage:! Technique Review and Practice - Neck Pain 86b Orthopedic Massage:! Technique Review and Practice - Neck Pain! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders
The theory and practice of getting fitter and stronger
 The theory and practice of getting fitter and stronger David Docherty, PhD, Professor Emeritus School of Exercise Science, Physical and Health Education University of Victoria All the presentations are
The theory and practice of getting fitter and stronger David Docherty, PhD, Professor Emeritus School of Exercise Science, Physical and Health Education University of Victoria All the presentations are
85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain"
 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain" 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain" 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
DPT 772 Spine Notebook Matt Kubalski, SPT
 DPT 772 Spine Notebook Matt Kubalski, SPT Table of Contents: IMPAIRMENTS/CLASSIFICATIONS PAGES Neck Pain with Mobility Deficit: Cervicalgia, Pain in thoracic spine - JOSPT 3-6 Neck Pain with Headache:
DPT 772 Spine Notebook Matt Kubalski, SPT Table of Contents: IMPAIRMENTS/CLASSIFICATIONS PAGES Neck Pain with Mobility Deficit: Cervicalgia, Pain in thoracic spine - JOSPT 3-6 Neck Pain with Headache:
Strain-Counterstrain. Harmon Myers, DO and Julie Jernberg, MD
 Strain-Counterstrain Harmon Myers, DO and Julie Jernberg, MD Origin of Counterstrain Lawrence Jones, DO Original Patient: 4 Months of lower back pain, sleep deprivation and high velocity therapy Jones
Strain-Counterstrain Harmon Myers, DO and Julie Jernberg, MD Origin of Counterstrain Lawrence Jones, DO Original Patient: 4 Months of lower back pain, sleep deprivation and high velocity therapy Jones
Algorithm #1 Lumbo-Pelvic Region Examination
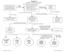 Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
Red Screen for Potentially Serious Conditions (i.e., Red Flags) including Neurologic when indicated Positive Findings Algorithm #1 Lumbo-Pelvic Region Clinical Prediction Rule Screening: Duration of symptoms
INTRODUCTION. Objectives
 Objectives Functional Anatomy for Fitness Professionals focuses on functional anatomy, with an emphasis on weight training. Through the emphasis on biomechanics, neurology, and muscle physiology, participants
Objectives Functional Anatomy for Fitness Professionals focuses on functional anatomy, with an emphasis on weight training. Through the emphasis on biomechanics, neurology, and muscle physiology, participants
Spinal manipulative thrust technique using combined movement theory
 Manual Therapy (2001) 6(4), 197 204 doi:10.1054/math.2001.0409, available online at http://www.idealibrary.com on Masterclass Spinal manipulative thrust technique using combined movement theory C. J. McCarthy
Manual Therapy (2001) 6(4), 197 204 doi:10.1054/math.2001.0409, available online at http://www.idealibrary.com on Masterclass Spinal manipulative thrust technique using combined movement theory C. J. McCarthy
Epidemiology of Low back pain
 Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Low Back Pain Definition Pain felt in your lower back may come from the spine, muscles, nerves, or other structures in that region. It may also radiate from other areas like the mid or upper back, a inguinal
Evaluating the Athlete Questionnaire
 Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
Evaluating the Athlete Questionnaire Prior to developing the strength and conditioning training plan the coach should first evaluate factors from the athlete s questionnaire that may impact the strength
38b Body Mobilization Techniques:! Technique Demo and Practice Prone
 38b Body Mobilization Techniques:! Technique Demo and Practice Prone 38b Body Mobilization Techniques:! Technique Demo and Practice - Prone! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
38b Body Mobilization Techniques:! Technique Demo and Practice Prone 38b Body Mobilization Techniques:! Technique Demo and Practice - Prone! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and
The Hip Joint: Myofascial and Joint Patterns
 The Hip Joint: Myofascial and Joint Patterns Marc Heller, DC, practices in Ashland, Ore. He can be contacted at mheller@marchellerdc.com or www.marchellerdc.com. For more information, including a brief
The Hip Joint: Myofascial and Joint Patterns Marc Heller, DC, practices in Ashland, Ore. He can be contacted at mheller@marchellerdc.com or www.marchellerdc.com. For more information, including a brief
NECK AND BACK PAIN AN INTRODUCTION TO
 AN INTRODUCTION TO NECK AND BACK PAIN This booklet provides general information on neck and back pain. It is not meant to replace any personal conversations that you might wish to have with your physician
AN INTRODUCTION TO NECK AND BACK PAIN This booklet provides general information on neck and back pain. It is not meant to replace any personal conversations that you might wish to have with your physician
Manual Muscle Testing. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Manual Muscle Testing Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Manual Muscle Testing Evaluation of the function and strength of individual muscles and muscles
Manual Muscle Testing Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Manual Muscle Testing Evaluation of the function and strength of individual muscles and muscles
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 1 Handout
 Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 1 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
Solving Today s Pain and Injury Puzzle with Erik Dalton An Online Workshop for ABMP Members Session 1 Handout Please Note: Erik Dalton teaches his Myoskeletal Alignment Techniques with the expectation
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain
 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10
85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain 85b Orthopedic Massage:! Technique Demo and Practice - Neck Pain! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Torso
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Torso Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here on time
Thoracic Spine Applied Anatomy. Jason Zafereo, PT, OCS, FAAOMPT
 Thoracic Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education Objectives Discuss concepts relevant to thoracic pain of red flag origin Discuss concepts
Thoracic Spine Applied Anatomy Jason Zafereo, PT, OCS, FAAOMPT Clinical i l Orthopedic Rehabilitation ti Education Objectives Discuss concepts relevant to thoracic pain of red flag origin Discuss concepts
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM
 TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
Self Myofascial Release
 Adductor Stretch Adductor Stretch 1. Extend the thigh and place foam roll in the groin region with body prone on the floor. 2. Be cautious when rolling near the adductor complex origins at the pelvis.
Adductor Stretch Adductor Stretch 1. Extend the thigh and place foam roll in the groin region with body prone on the floor. 2. Be cautious when rolling near the adductor complex origins at the pelvis.
Lumbar Stenosis Rehabilitation Using the Resistance Chair
 PRODUCTS HELPING PEOPLE HELP THEMSELVES! Lumbar Stenosis Rehabilitation Using the Resistance Chair a. Description Lumbar spinal stenosis is a term used to describe a narrowing of the spinal canal. The
PRODUCTS HELPING PEOPLE HELP THEMSELVES! Lumbar Stenosis Rehabilitation Using the Resistance Chair a. Description Lumbar spinal stenosis is a term used to describe a narrowing of the spinal canal. The
Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS AND PAIN
 Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
Cox Technic Case Report #100 published at www.coxtechnic.com (sent October 2011 on 10/11/11 ) 1 Case Report: CASE REPORT OF FACET ARTHROPATHY INDUCED NERVE ROOT COMPRESSION RESULTING IN MOTOR WEAKNESS
The Swimmer s Shoulder: An Osteopathic Approach
 The Swimmer s Shoulder: An Osteopathic Approach Mary Solomon, D.O. Rainbow Babies and Children s Hospital Cleveland, OH 440-914-7865 1 I have no relevant relationships/affiliations with any proprietary
The Swimmer s Shoulder: An Osteopathic Approach Mary Solomon, D.O. Rainbow Babies and Children s Hospital Cleveland, OH 440-914-7865 1 I have no relevant relationships/affiliations with any proprietary
A Simple Guide to Stretching By Lenny Parracino Date Released : 01 Sep 2001
 Page 1 of 6 close A Simple Guide to ing By Lenny Parracino Date Released : 01 Sep 2001 We all know that flexibility is a critical component to our health, but do we know which stretches are the best or
Page 1 of 6 close A Simple Guide to ing By Lenny Parracino Date Released : 01 Sep 2001 We all know that flexibility is a critical component to our health, but do we know which stretches are the best or
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
Objectives. Objectives HEADACHE. Pathophysiology of Headache. Pathophysiology of Headache. Cervical Spine Applied Anatomy
 Cervical Spine Applied Anatomy Objectives Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education diagnosis for headache diagnosis for cervical radiculopathy Objectives diagnosis for
Cervical Spine Applied Anatomy Objectives Jason Zafereo, PT, OCS, FAAOMPT Clinical Orthopedic Rehabilitation Education diagnosis for headache diagnosis for cervical radiculopathy Objectives diagnosis for
Scapula Spine Lateral edge of clavicle. Medial border Scapula. Medial border of Scapula, between superior angle and root of spine. Scapula.
 Muscle attachments and actions answer sheet Muscle Origins insertions Movements Joints crossed Trapezius Base of skull Spinous process of C7 Thoracic Spine Lateral edge of clavicle Elevation Retraction
Muscle attachments and actions answer sheet Muscle Origins insertions Movements Joints crossed Trapezius Base of skull Spinous process of C7 Thoracic Spine Lateral edge of clavicle Elevation Retraction
Mid-Thoracic Dysfunction: A Key Perpetuating Factor of Pain in the Locomotor System
 Mid-Thoracic Dysfunction: A Key Perpetuating Factor of Pain in the Locomotor System Dysfunction involving excessive T4-T8 kyphosis is common. Symptoms arising from regions at a distance to the mid-thoracic
Mid-Thoracic Dysfunction: A Key Perpetuating Factor of Pain in the Locomotor System Dysfunction involving excessive T4-T8 kyphosis is common. Symptoms arising from regions at a distance to the mid-thoracic
Michael, J./ Gyer, G./ Davis, R. Osteopathic and Chiropractic Techniques for Manual Therapists
 Michael, J./ Gyer, G./ Davis, R. Osteopathic and Chiropractic Techniques for Manual Therapists zum Bestellen hier klicken by naturmed Fachbuchvertrieb Aidenbachstr. 78, 81379 München Tel.: + 49 89 7499-156,
Michael, J./ Gyer, G./ Davis, R. Osteopathic and Chiropractic Techniques for Manual Therapists zum Bestellen hier klicken by naturmed Fachbuchvertrieb Aidenbachstr. 78, 81379 München Tel.: + 49 89 7499-156,
The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University
 The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University The Trunk and Spinal Column Vertebral column 24 articulating vertebrae 31 pairs of spinal nerves Abdominal muscles some
The Trunk and Spinal Column Kinesiology Cuneyt Mirzanli Istanbul Gelisim University The Trunk and Spinal Column Vertebral column 24 articulating vertebrae 31 pairs of spinal nerves Abdominal muscles some
Core Stabilization Training in Rehabilitation
 Core Stabilization Training in Rehabilitation Assistant professor of Sports Medicine Department of Sports Medicine Tehran university of Medical Sciences Introduction To develop a comprehensive functional
Core Stabilization Training in Rehabilitation Assistant professor of Sports Medicine Department of Sports Medicine Tehran university of Medical Sciences Introduction To develop a comprehensive functional
Chapter 20: The Spine The McGraw-Hill Companies, Inc. All rights reserved.
 Chapter 20: The Spine Anatomy of the Spine Prevention of Injuries to the Spine Cervical Spine Muscle Strengthening Muscles of the neck resist hyperflexion, hyperextension and rotational forces Prior
Chapter 20: The Spine Anatomy of the Spine Prevention of Injuries to the Spine Cervical Spine Muscle Strengthening Muscles of the neck resist hyperflexion, hyperextension and rotational forces Prior
