CARPAL TUNNEL SYNDROME
|
|
|
- Derrick Lindsey
- 6 years ago
- Views:
Transcription
1 ORIGINAL CONTRIBUTION vs in the Treatment of Carpal Tunnel Syndrome A Randomized Controlled Trial Annette A. M. Gerritsen, PhD Henrica C. W. de Vet, PhD Rob J. P. M. Scholten, MD, PhD Frits W. Bertelsmann, MD, PhD Marc C. T. F. M. de Krom, MD, PhD Lex M. Bouter, PhD CARPAL TUNNEL SYNDROME (CTS) is the most common entrapment neuropathy and is caused by compression of the median nerve at the wrist. The prevalence of electrophysiologically confirmed CTS in the adult general population in the Netherlands is 0.6% in men and 9.2% in women. 1 While CTS may be treated with conservative options such as wrist splints, injections with corticosteroids, or both, evidence for the efficacy of most conservative treatment options is limited. 2 A recent systematic review has shown that among the various available surgical techniques, open carpal tunnel release is the preferred method. 3 However, only 1 randomized controlled trial (RCT) has compared conservative treatment (splinting) with surgery, 4 but provided no information on comparability of the groups at baseline, cointerventions, compliance with the treatment, or blinding of the outcome assessor. Furthermore, only 1 follow-up assessment was performed after 1 year, showing that the 10 patients treated surgically had complete relief of See also p 1281 and Patient Page. Context Carpal tunnel syndrome (CTS) can be treated with nonsurgical or surgical options. However, there is no consensus on the most effective method of treatment. Objective To compare the short-term and long-term efficacy of splinting and surgery for relieving the symptoms of CTS. Design, Setting, and Patients A randomized controlled trial conducted from October 1998 to April 2000 at 13 neurological outpatient clinics in the Netherlands. A total of 176 patients with clinically and electrophysiologically confirmed idiopathic CTS were assigned to wrist splinting during the night for at least 6 weeks (89 patients) or open carpal tunnel release (87 patients); 147 patients (84%) completed the final follow-up assessment 18 months after randomization. Main Outcome Measures General improvement, number of nights waking up due to symptoms, and severity of symptoms. Results In the intention-to-treat analyses, surgery was more effective than splinting on all outcome measures. The success rates (based on general improvement) after 3 months were 80% for the surgery group (62/78 patients) vs 54% for the splinting group (46/86 patients), which is a difference of 26% (95% confidence interval [CI], 12%-40%; P.001). After 18 months, the success rates increased to 90% for the surgery group (61/68 patients) vs 75% for the splinting group (59/79 patients), which is a difference of 15% (95% CI, 3%-27%; P=.02). However, by that time 41% of patients (32/79) in the splint group had also received the surgery treatment. Conclusion Treatment with open carpal tunnel release surgery resulted in better outcomes than treatment with wrist splinting for patients with CTS. JAMA. 2002;288: symptoms while 2 of the 10 patients treated with a wrist splint had experienced relief only temporarily. Due to limited evidence, there is no consensus on the preferred method of treatment for CTS. Advocates of surgery refer to its safety and effectiveness for electrophysiologically confirmed cases with no underlying reversible disorder, 5 and point out that conservative treatment options generally offer only temporary symptom relief. Advocates of conservative options refer to the potential benefits and safety of these treatments and to the potential complications of surgery. 6 In the Netherlands, 40% of the neurologists reported to prefer conservative treatment options, 39% reported to prefer surgery, and 21% re- Author Affiliations: Institute for Research in Extramural Medicine, Vrije Universiteit Medical Center, Amsterdam, the Netherlands (Drs Gerritsen, de Vet, and Bouter); Dutch Cochrane Center/Department of Clinical Epidemiology and Biostatistics, Academic Medical Center, University of Amsterdam, Amsterdam, the Netherlands (Dr Scholten); Department of Neurology, Amstelveen Hospital, Amstelveen, the Netherlands (Dr Bertelsmann); and Department of Neurology, Maastricht University Hospital, Maastricht, the Netherlands (Dr de Krom). Corresponding Author: Annette A. M. Gerritsen, PhD, Institute for Research in Extramural Medicine, Vrije Universiteit Medical Center, Van der Boechorststraat 7, 1081 BT Amsterdam, the Netherlands ( aam.gerritsen.emgo@med.vu.nl) American Medical Association. All rights reserved. (Reprinted) JAMA, September 11, 2002 Vol 288, No
2 ported to have no preference. 7 was the preferred treatment of 26% of the neurologists and is the most common. The objective of this study was to compare the short-term and long-term efficacy of splinting and surgery for relieving the symptoms of CTS. METHODS The medical ethics committees of the 13 participating hospitals approved the study protocol of this multicenter RCT. A detailed description of the design of this RCT has been previously published. 8 Study Population All patients with clinically suspected CTS had been referred to one of the participating neurologists and were examined for eligibility to participate in the study. Inclusion criteria were (1) pain, paresthesia, and/or hypoesthesia in the hand in the area innervated by the median nerve 9 ; (2) electrophysiological confirmation of the diagnosis 8 (median nerve sensory conduction velocity of the index finger 41.9 m/s in patients 55 years or 37.3 m/s in patients 55 years, or median nerve distal sensory latency of the index finger 3.5 ms; or medianulnar distal sensory latency difference of the ring finger 0.4 ms; or median nerve distal motor latency 4.34 ms); (3) age of 18 years or older; and (4) ability to complete written questionnaires (in Dutch). Exclusion criteria were (1) previous treatment with splinting or surgery; (2) a history of wrist trauma (eg, fracture) or surgery; (3) a history suggesting underlying causes of CTS (eg, diabetes mellitus, pregnancy); (4) clinical signs or symptoms or electrophysiological findings suggesting conditions that could mimic CTS or interfere with its validation (eg, cervical radiculopathy, polyneuropathy); and (5) severe thenar muscle atrophy. Patients, who were eligible according to their neurologist and were interested in participation, were referred to one of the research physiotherapists in the same hospital, who verified that all selection criteria were met. After they had provided written informed consent, patients were included in the study. Subsequently, potential prognostic indicators and the baseline values of the outcome measures were assessed. Treatment Allocation Patients were randomly allocated to receive either splinting or surgery (FIGURE 1). If bilateral symptoms were present, the hand with the more severe symptoms (according to the patient) was treated. By preparing a list for each hospital, the randomization was stratified by center. Permuted blocks of 4 patients were formed to ensure near-equal distribution of patients over the 2 treatment groups in each hospital. 10 Despite the small block sizes, the potential for unmasking was considered to be low because the neurologists did not know the method of randomization and different neurologists selected patients in each hospital. Even if a neurologist were to know the allocation scheme, the chance was high that when he/she selected a patient, this patient would not be assigned the next treatment on the list because a patient selected by another neurologist has an earlier appointment for the trial. The random sequence of the permuted blocks was generated by using random number tables. The principal investigator (A.A.M.G.), who was not involved in the selection and allocation of patients, prepared, coded, and sealed opaque envelopes containing the treatment allocation. 11 After the baseline assessment, the next envelope was handed to the patient by the research assistant to ensure concealment of allocation. Blinding Attempts were made to keep the research physiotherapists unaware of the allocated treatment by encouraging the patients not to reveal any information regarding their treatment during the examination. Furthermore, before each examination, the research assistant placed a bandage over the wrist and palm of all patients to conceal the potential surgical scar. Afterward, the research physiotherapists were asked to indicate the type of treatment that they thought the patient had received and to give reasons for this assumption. 12 Treatment Depending on the usual procedures of the hospital, patients allocated to splinting received either a custom-made splint (made of soft cast) or a prefabricated splint (Tricodur, BSN Medical, Hamburg, Germany) that immobilized the wrist in a neutral position. 13 The patients were instructed to wear the splint during the night for at least 6 weeks, but could wear it during the day. No other types of treatment were permitted during the intervention period, except pain medication if necessary. After 6 weeks, the neurologist discussed with the patient whether any further treatment was necessary, including continued splinting, other conservative treatment options, or surgery. The decision to undergo surgery could also be made at a later stage. Patients allocated to surgery were referred to a general surgeon, neurosurgeon, plastic surgeon, or orthopedic surgeon, depending on the usual procedures of the hospital for an outpatient standard open carpal tunnel release. Because there are waiting lists for surgery in hospitals, efforts were made to make an appointment within 4 weeks after randomization. Before surgery, no other types of treatment were permitted, except pain medication. In all surgical cases, the transverse carpal ligament was released and no concomitant procedures were performed (eg, flexor tenosynovectomy, internal neurolysis, epineurotomy). Sutures were removed after 2 weeks. Patients were instructed to perform postoperative active range-ofmotion exercises and encouraged to use the hand as tolerated. None of the patients received a splint following the surgical procedure. No specific period off work was recommended. Outcome Assessment Patients completed questionnaires and were examined by a trained research physiotherapist in the hospital at baseline and 3, 6, and 12 months after randomization. Although different research physiotherapists assessed the outcomes, most patients were seen by the same therapist each time they vis JAMA, September 11, 2002 Vol 288, No. 10 (Reprinted) 2002 American Medical Association. All rights reserved.
3 ited the hospital. In the remaining months, and 18 months after randomization, questionnaires were mailed. General improvement was scored by the patient on a 6-point ordinal transition scale, ranging from completely recovered to much worse. 12 Treatment success was defined a priori as completely recovered or much improved. The 2 other outcome measures were number of nights that the patient awoke due to the symptoms during the past week and severity of the main complaint, pain, paresthesia, or hypoesthesia at night and during the day during the past week. Severity of the main complaint, pain, paresthesia, and hypoesthesia were scored by the patient on an 11-point numerical rating scale (with 0 equaling no symptoms and 10 equaling very severe symptoms used as anchors). 12 There were 3 secondary outcome measures used. Mean (SD) scores were collected using the Symptom Severity Scale (11 questions about symptoms experienced during the past 2 weeks with 1 equaling mildest and 5 equaling most severe) and the Functional Status Scale (8 items concerning difficulties in performing various activities of daily living during the past 2 weeks with 1 equaling no difficulty and 5 equaling cannot perform activity at all). 14 After a standardized history-taking and a physical examination, the overall severity of CTS complaints was scored by a research physiotherapist on an 11- point numerical rating scale with zero equaling no complaints and 10 equaling very severe complaints. 12 Results of nerve conduction studies after 12 months were also used. At each follow-up assessment, the patients were asked to record any treatment they had received and any adverse effects. Statistical Analysis The groups were primarily compared at 3, 6, and 12 months because all outcomes were assessed during the visits at the hospital. Furthermore, to obtain a clear picture of the short-term effects, the follow-up assessment time of 1 month was chosen. To determine the long-term effects, the assessment time of 18 months after randomization was chosen. Differences in success rates between the treatment groups along with 95% confidence intervals were calculated using 2 tests. Continuous outcomes were analyzed as change scores (difference between baseline assessment and each follow-up assessment). Subsequently, differences in improvement between the groups (mean change score in surgery group minus mean change score in splint group) along with 95% confidence intervals were calculated using t tests. Multivariate analyses (logistic or linear regression) were performed to adjust for the influence of eventual differences between the groups at baseline in prognostic indicators (age, sex, duration of current episode of CTS complaints, bilateral CTS complaints, dominant side more severely affected, previous episodes of CTS complaints, and patients preference for splinting or surgery). All analyses were performed according to the following intention-to-treat principle: the patients remained in the group to which they were allocated at baseline. 15 Two additional analyses were Figure 1. Progress of Patients Through Carpal Tunnel Syndrome (CTS) Trial 87 Assigned to Receive 14 Did Not Receive as Assigned 19 Withdrawals 8 Refused 1 Lack of Time 1 Death (Cancer) 2 Unable to Go to Hospital at 12 mo 5 Did Not Return Final Questionnaire 2 Other Follow-up and No. Included in Analyses 80 at 1 mo 78 at 3 mo 77 at 6 mo 73 at 12 mo 68 at 18 mo 326 Patients Examined for Eligibility by Neurologist 39 Not Eligible 5 No Electrophysiologically Confirmed CTS 9 Language Barrier 8 Prior Splint Treatment 4 Previous Wrist Trauma or 10 Underlying Causes of CTS 2 Polyneuropathy 1 Severe Thenar Muscle Atrophy 72 Refused Participation 23 Strongly Preferred 39 Strongly Preferred 10 Other 215 Examined for Eligibility by Research Physiotherapist 23 Not Eligible 1 No Electrophysiologically Confirmed CTS 1 Language Barrier 4 Prior Splint Treatment 6 Previous Wrist Trauma or 10 Underlying Causes of CTS 1 Severe Thenar Muscle Atrophy 16 Refused Participation 8 Strongly Preferred 6 Strongly Preferred 2 Other 176 Randomized 89 Assigned to Receive 13 Did Not Receive According to Protocol as Assigned 10 Withdrawals 3 Lack of Time 1 Not Satisfied With Treatment Result 1 Unable to Go to Hospital at 12 mo 4 Did Not Return Final Questionnaire 1 Other Follow-up and No. Included in Analyses 88 at 1 mo 86 at 3 mo 84 at 6 mo 83 at 12 mo 79 at 18 mo 2002 American Medical Association. All rights reserved. (Reprinted) JAMA, September 11, 2002 Vol 288, No
4 performed. In the first analysis, patients who received surgery after splinting were considered to be not improved. In the second analysis, patients in the splint group who had received surgery were compared with patients in the same group who had not. All patients who withdrew from the study were included in the analysis until the time of withdrawal. For patients who occasionally missed a follow-up assessment, the available data from completed assessments were included. Sample-size calculation was based on the ability to detect a clinically important difference in success rates of 20% or Table 1. Prognostic Indicators and Baseline Values of Outcomes* more 3 months after randomization. A total sample size of 190 patients was required (2-sided =.05, =.20). Values of P.05 were considered statistically significant. Data were analyzed using SPSS statistical software (Version 10.1; SPSS Inc, Chicago Ill). Prognostic Indicator (n = 87) (n = 89) Age, mean (SD), y 49 (11) 49 (12) Women, No. (%) 66 (76) 77 (87) Duration of current episode of CTS complaints, 40 (16-104) 52 (24-104) median (IQR), wk Bilateral CTS complaints, No. (%) 48 (55) 56 (63) Dominant side more severely affected, No. (%) 59 (68) 57 (64) Previous episodes of CTS complaints, No. (%) 29 (33) 24 (27) Patients preference for treatment, No. (%) 22 (25) 29 (33) 20 (23) 23 (26) No preference 46 (53) 37 (42) Primary Outcomes at Baseline, Median (IQR) No. of nights waking up due to symptoms (0-7) 4 (1-7) 4 (1-7) Severity of the main complaint 7 (6-8) 7 (5-8) Pain During day 4 (1-6) 4 (0-6) During night 5 (0-8) 4 (0-7) Paresthesia During day 6 (4-8) 6 (3-8) During night 6 (2-8) 6 (3-8) Hypoesthesia During day 4 (0-7) 3 (0.5-7) During night 5 (0-8) 5 (0-8) Secondary Outcomes at Baseline, Median (IQR) Symptom severity score (1-5) 2.5 ( ) 2.4 ( ) Functional status score (1-5) 2.3 ( ) 2.0 ( ) Severity of complaints rated by a research physiotherapist 6 (4-7) 7 (5-7) Nerve conduction studies, mean (SD), ms DSL (index finger) (n = 78) (n = 77) 4.2 (1.0) 4.1 (1.0) Median-ulnar DSL difference (ring finger) (n = 66) (n = 64) 1.7 (1.1) 1.8 (1.4) DML median nerve (n = 84) (n = 87) 5.6 (1.5) 5.7 (1.9) *CTS indicates carpal tunnel syndrome; IQR, interquartile range; DSL, distal sensory latency; and DML, distal motor latency. Range of scores is 0-10 (10 indicating severe complaints), unless otherwise indicated. The scores represent the status in the previous week, except for symptom severity and functional status scores, which represent the status in the previous 2 weeks. RESULTS Study Population During a period of 18 months (October 1998 to April 2000), 326 patients were examined for eligibility by the neurologists. There were 111 patients who were either ineligible or not interested in participation (Figure 1). The remaining 215 patients were referred to one of the research physiotherapists who verified that all selection criteria were met. Of these patients, 39 were not randomized for various reasons (Figure 1), and the remaining 176 were allocated to either splinting (89 patients) or surgery (87 patients). By October 2001, 147 patients had completed the follow-up assessment 18 months after randomization, resulting in a final follow-up rate of 84%. Reasons for withdrawal are presented in Figure 1. In both of the groups, some patients occasionally missed a follow-up assessment, but some of them completed the questionnaire at home. TABLE 1 shows the frequency of potential prognostic indicators and the baseline values of the outcome assessments for each group. There were small differences between the groups with regard to sex, duration of current episode of CTS complaints, and patients preference for treatment. Allocated Treatment All 89 patients allocated to splinting received a splint, either custom-made (28 patients [31%]) or prefabricated (61 patients [68%]), within a median period of 2 days after randomization (interquartile range, 0-5 days). However, 13 patients (15%) did not receive the treatment according to protocol: 2 received additional treatment, 1 received physiotherapy, 1 received Mensendieck (exercise) therapy, and 11 did not wear the splint every night for at least 6 weeks. Twenty-four patients (27%) indicated that they had also worn the splint during the day. Eleven patients (12%) used pain medication during the intervention period. Of the 87 patients allocated to surgery, 73 (84%) actually underwent this treatment within a median period of 35 days (interquartile range, days) after randomization. Of the patients who completed follow-up assessments, 36% had undergone surgery after 1 month (29/80), 80% after 3 months (62/78), and 92% after 6 (71/77), 12 (67/73), and 18 (63/68) months. Of the 14 patients who did not undergo carpal tunnel surgery, 9 did not receive any treatment and 1248 JAMA, September 11, 2002 Vol 288, No. 10 (Reprinted) 2002 American Medical Association. All rights reserved.
5 5 were treated differently. Two patients received physiotherapy, 2 received pain medication, and 1 received a splint. Seven patients (8%) used pain medication before surgery. Additional Treatment In the splint group, 74 (83%) of 89 patients continued to wear the splint after the intervention period for a varying period of time. Furthermore, 52 (58%) of 89 patients received 1 or more additional treatment options after 6 weeks. Twenty-nine patients received pain medication, 4 received physiotherapy, 1 received manual therapy, 2 received Mensendieck (exercise) therapy, 1 received occupational therapy, 5 received 1 or 2 local corticosteroid injections, and 35 received surgery. Of the patients who had completed follow-up assessment, 7% (6/86) received surgery after 3 months, 31% (26/84) after 6 months, 39% (32/83) after 12 months, and 41% (32/79) after 18 months. In the surgery group, 26 (30%) of 87 patients received 1 or more additional treatment options after surgery. Twentyfive patients received pain medication primarily to relieve pain caused by the operation, 2 received physiotherapy, 1 received occupational therapy, and 1 received a local corticosteroid injection and surgery to relieve pain caused by reflex sympathetic dystrophy. Treatment Efficacy Comparisons between the univariate and multivariate analyses showed that adjustment for potential prognostic indicators and the baseline values of the outcome measures minimally influenced the results. Therefore, only the unadjusted analyses are presented. Intention-to-Treat Analyses After 1 month, more patients in the splint group had improved than in the surgery group, but more patients in the surgery group improved after 3, 6, 12, and 18 months (TABLE 2 and FIGURE 2). The results of the other outcome measure assessments are also shown in Table 2 and TABLE 3. Scores for pain and hypoesthesia are not presented because the Table 2. Success Rates and Improvement in Primary Outcomes After 1, 3, 6, 12, and 18 Months (Intention-to-Treat Analyses)* Primary Outcome by Month Difference P Value Success rate, No./total (%) 1 23/80 (29) 37/88 (42) 13 ( 28 to 1) /78 (80) 46/86 (54) 26 (12 to 40) /77 (94) 57/84 (68) 26 (14 to 37) /73 (92) 60/83 (72) 20 (8 to 31) /68 (90) 59/79 (75) 15 (3 to 27).02 No. of nights waking up due to symptoms, mean (SD) (3.2) 2.0 (3.0) 1.2 ( 2.2 to 0.3) (3.5) 2.2 (3.1) 0.4 ( 0.7 to 1.4) (2.8) 2.6 (3.1) 1.0 (0.1 to 2.0) (2.9) 2.9 (3.0) 0.7 ( 0.2 to 1.7) (2.9) 3.2 (3.1) 0.4 ( 0.6 to 1.4).44 Severity of the main complaint, mean (SD) (2.9) 2.1 (2.2) 0.5 ( 1.3 to 0.3) (3.3) 3.2 (2.7) 1.9 (1.0 to 2.8) (2.4) 4.4 (3.2) 2.2 (1.4 to 3.1) (2.7) 5.1 (3.1) 1.3 (0.4 to 2.2) (2.8) 5.0 (3.3) 1.2 (0.2 to 2.3).02 Paresthesia during the day, mean (SD) (3.0) 1.4 (2.1) 0.1 ( 0.6 to 1.0) (3.2) 2.2 (3.2) 2.6 (1.6 to 3.6) (2.9) 3.7 (3.2) 1.8 (0.8 to 2.8) (2.9) 4.0 (3.4) 1.5 (0.5 to 2.5) (3.0) 4.0 (3.6) 1.3 (0.3 to 2.5).01 Paresthesia at night, mean (SD) (3.1) 2.5 (3.0) 1.2 ( 2.1 to 0.2) (3.8) 3.5 (3.3) 1.1 (0 to 2.2) (3.5) 4.1 (3.7) 1.3 (0.2 to 2.4) (3.6) 4.5 (3.4) 0.7 ( 0.4 to 1.8) (3.6) 4.4 (3.6) 0.6 ( 0.6 to 1.7).35 *Patient cohorts are presented in Figure 1. The values are expressed as the mean (SD) improvements from baseline unless otherwise indicated. Indicates the differences (surgery minus splint) in success rates and in the mean improvements from baseline (95% confidence interval). Figure 2. Success Rates at Each Follow-up Measurement Success Rate, % No. of Patients Time After Randomization, mo American Medical Association. All rights reserved. (Reprinted) JAMA, September 11, 2002 Vol 288, No
6 Table 3. Improvement in Secondary Outcomes After 3, 6, 12, and 18 Months (Intention-to-Treat Analyses)* Secondary Outcome by Month Difference P Value Symptom severity score (0.9) 0.6 (0.7) 0.4 (0.2 to 0.7) (0.8) 0.9 (0.8) 0.4 (0.2 to 0.7) (0.8) 0.9 (0.9) 0.4 (0.1 to 0.7) (0.8) 0.9 (0.9) 0.4 (0.1 to 0.6).02 Functional status score (0.9) 0.4 (0.7) 0.2 (0 to 0.5) (0.9) 0.5 (0.8) 0.5 (0.2 to 0.7) (0.9) 0.7 (0.8) 0.3 (0 to 0.6) (0.9) 0.7 (0.8) 0.2 ( 0.1 to 0.5).12 Severity of complaints rated by a research physiotherapist, mo 3 (n = 69) (n = 80) 3.5 (3.4) 2.2 (2.6) 1.3 (0.4 to 2.4) (n = 70) (n = 76) 5.4 (2.5) 3.3 (2.7) 2.1 (1.2 to 2.9) (n = 67) (n = 77) 5.3 (3.0) 3.7 (3.0) 1.6 (0.6 to 2.6).002 Nerve conduction studies at 12 mo, ms Distal sensory latency (index finger) (n = 56) (n = 59) 1.0 (1.0) 0.7 (0.8) 0.3 (0 to 0.7).04 Median-ulner distal sensory latency (n = 48) (n = 50) difference (ring finger) 1.1 (1.2) 0.7 (1.2) 0.4 (0 to 0.9).07 Distal motor latency median nerve (n = 63) (n = 70) 1.3 (1.5) 1.0 (1.5) 0.3 ( 0.2 to 0.8).25 *Patient cohorts are presented in Figure 1. The values are expressed as the mean (SD) improvements from baseline unless otherwise indicated. Indicates the differences (surgery minus splint) in success rates and in the mean improvements from baseline (95% confidence interval). Table 4. Adverse Effects Reported by the Patients During the Follow-up Period of 18 Months No. of Patients Who Reported (n = 87) (n = 89) Adverse effects, No. (%) 58 (67) 46 (52) Painful or hypertrophic scar Stiffness of the wrist, hand, or fingers Skin irritation 19 8 Wound hematoma 10 1 Wound infection 5 2 Discomfort caused by 0 6 pressure of the splint Swelling of the wrist, 0 4 hand, or fingers Severe pillar pain 2 0 Reflex sympathetic dystrophy 1 0 findings were similar to those for paresthesia. After 1 month, the differences in the primary outcome measures were mainly in favor of splinting. However, after 3, 6, 12, and 18 months, surgery was found to be more effective than splinting and with regard to the secondary outcomes. There was no difference in outcomes between patients in the splint group using a custom-made splint and those using a prefabricated splint. An additional analysis was performed for the outcome measure success rate, using last observation carried forward for the patients who withdrew from the study. When this was done for the 10 patients who withdrew from the splint group, the success rates for this group were 52% (46/ 89) after 3 months, 66% (59/89) after 6 months, 71% (63/89) after 12 months, and 72% (64/89) after 18 months. Four patients in the surgery group did not have any of the follow-up assessments taken and were regarded as not improved. In addition, in the analysis using the last observation carried forward for the other 15 patients who withdrew from the surgery group, the success rates were 26% (23/87) after 1 month, 74% (64/87) after 3 months, 87% (76/87) after 6 months, 86% (75/ 87) after 12 months, and 85% (74/87) after 18 months. Withdrawal was not related to general improvement. Of the 10 patients who withdrew from the splint group, 5 indicated to be much improved at the time of withdrawal, 2 indicated to be slightly improved, 1 indicated that no change had occurred, 1 indicated to be slightly worse, and 1 indicated to be much worse. Of the 19 patients who withdrew from the surgery group, 4 did not have any follow-up assessments, 10 indicated to be completely recovered at the time of withdrawal, 3 indicated to be much improved, 1 indicated to be slightly improved, and 1 indicated no change. In the first additional analysis, patients who received surgery after splinting were considered to be not improved. After 18 months, only 29 of 79 patients indicated to be improved by splinting alone, resulting in a final success rate of 37% for the splint group. In the second additional analysis, patients in the splint group who had received surgery were compared with patients in the same group who had not. After 18 months, the success rate in the group of patients who received surgery after splinting was 94% (30/32 patients) compared with 62% (29/47 patients) in the group who did not undergo surgical treatment. Also with regard to the other primary outcomes, the patients in the splint group who received surgery showed statistically significant more improvement after 18 months than the patients who did not have surgery. Adverse Effects TABLE 4 shows the frequency of adverse effects reported by the patients in each group during the 18 months of follow-up. Although many patients reported adverse effects, most of these were relatively mild and of short duration. However, 1 patient in the surgery group developed reflex sympathetic dystrophy. Success of Blinding The physiotherapists correctly indicated the treatment received 85% (139/ 164) of the time after 3 months, 71% (114/161) after 6 months, and 65% (101/ 156) after 12 months. Many patients inadvertently mentioned their treatment, 1250 JAMA, September 11, 2002 Vol 288, No. 10 (Reprinted) 2002 American Medical Association. All rights reserved.
7 and guesses were often based on the course of symptoms during the follow-up period and on the way patients reacted to the physical examinations. COMMENT This RCT compared the short-term and long-term efficacy of surgery and splinting for relieving the symptoms of CTS. Although only 176 patients were included, instead of the 190 originally planned, this did not reduce the power of the trial because the differences between the groups were large enough to be detected. Furthermore, although many outcomes were analyzed at different follow-up times, the results are not likely to be due to chance, as they all are in the same direction. The results of the intention-to-treat analyses showed that surgery was more effective than splinting after 3, 6, 12, and 18 months. These differences became smaller after 12 months, probably because a large proportion of patients in the splint group received additional surgery. The differences after 1 month were mainly in favor of splinting, which might have resulted from patients allocated to splinting having started their treatment almost immediately after randomization, in contrast to patients in the surgery group. Randomization was chosen as the reference point for the timing of the follow-up assessments, and not the actual start of the treatment because including the time waiting to undergo surgery reflects current clinical practice. However, as the median time to undergo surgery was 35 days, taking the actual start of the treatment as a reference point would result in a shift to the left (of 1 month) of the line of the surgery group in Figure 2. We believe the results of this trial are applicable to most patients with clinically and electrophysiologically confirmed idiopathic CTS. However, the least severe and the most severe cases were probably not included in this trial. These patients (or physicians) typically have a strong preference for splinting or surgery. This trial was mainly based on subjective, patient-reported outcomes because the perspective of the patient was considered to be the most important. As blinding of the patients for the allocated treatment was not possible, the results could be biased because patients tend to report greater effects from their preferred method of treatment. 16 However, subgroup analyses showed that treatment effects did not depend on the patients preference prior to randomization (data not shown). An attempt was made to include a more objective evaluation of outcome by involving blinded research physiotherapists who scored the overall severity of CTS complaints. However, blinding of the research physiotherapists was not successful in most cases. Treatment success was defined a priori as completely recovered or much improved. When analyzing the data, it was found that most of the successes in the surgery group were completely recovered, while patients in the splint group were only much improved. Thus, if success was solely defined as completely recovered, the differences between the groups would have been even more pronounced. The American Academy of Neurology recommends treatment of CTS with noninvasive options (eg, wrist splints) first, and open carpal tunnel release only if noninvasive treatment proves to be ineffective. 17 This RCT showed that treatment of CTS with surgery results in better outcomes. A splint might be used while a patient waits for surgery because the waiting period for open carpal tunnel release in practice is often longer than in this study, as efforts were made to make an appointment for the patients within 4 weeks after randomization. Patients not willing to undergo surgery could also be offered a splint. Another recently conducted RCT found that patients wearing a wrist splint showed more relief from symptoms than patients not receiving any treatment. 18 Author Contributions: Study concept and design: Gerritsen, Scholten, Bertelsmann, de Krom, Bouter. Acquisition of data: Gerritsen, Scholten, Bertelsmann. Analysis and interpretation of data: Gerritsen, de Vet, Scholten, Bertelsmann, de Krom, Bouter. Drafting of the manuscript: Gerritsen, de Vet. Critical revision of the manuscript for important intellectual content: de Vet, Scholten, Bertelsmann, de Krom, Bouter. Statistical expertise: Gerritsen, de Vet. Obtained funding: Scholten, Bouter. Administrative, technical, or material support: Gerritsen. Study supervision: de Vet, Scholten, Bertelsmann, de Krom, Bouter. Funding/Support: The research for this article was funded by grant OG from the Health Care Insurance Council of the Netherlands. Acknowledgment: We thank all participating neurologists, surgeons, and other hospital staff from the following hospitals: Boven I. J. Hospital (Amsterdam), Flevo Hospital (Almere), Hofpoort Hospital (Woerden), Lorentz Hospital (Zeist), Onze Lieve Vrouwe Gasthuis (Amsterdam), Rode Kruis Hospital (Beverwijk), Spaarne Hospital (Haarlem), Sint Lucas Andreas Hospital (Amsterdam), Waterland Hospital (Purmerend), Westfries Gasthuis (Hoorn), Amstelveen Hospital (Amstelveen), Bronovo Hospital (Den Haag), and Hilversum Hospital (Hilversum). REFERENCES 1. de Krom MC, Knipschild PG, Kester AD, et al. Carpal tunnel syndrome. J Clin Epidemiol. 1992;45: Gerritsen AA, de Krom MC, Struijs MA, et al. Conservative treatment options for carpal tunnel syndrome. J Neurol. 2002;249: Gerritsen AA, Uitdehaag BM, van Geldere D, Scholten RJ, de Vet HC, Bouter LM. Systematic review of randomized clinical trials of surgical treatment for carpal tunnel syndrome. Br J Surg. 2001;88: Garland H, Langworth EP, Taverner D, Clark JM. Surgical treatment for the carpal tunnel syndrome. Lancet. 1964;1: Wilson JR, Sumner AJ. Immediate surgery is the treatment of choice for carpal tunnel syndrome. Muscle Nerve. 1995;18: Johnson EW. Should immediate surgery be done for carpal tunnel syndrome? no! Muscle Nerve. 1995; 18: Scholten RJ, de Krom MC, Bertelsmann FW, Bouter LM. Variation in the treatment of carpal tunnel syndrome. Muscle Nerve. 1997;20: Gerritsen AA, Scholten RJ, Assendelft WJ, et al. or surgery for carpal tunnel syndrome? BMC Neurol. 2001;1:8. 9. D Arcy CA. McGee S. The rational clinical examination: does this patient have carpal tunnel syndrome? JAMA. 2000;283: Roberts C, Torgerson DJ. Randomization methods in controlled trials. BMJ. 1998;317: Torgerson DJ, Roberts C. Understanding controlled trials. BMJ. 1999;319: van der Windt DA, Koes BW, Deville W, et al. Effectiveness of corticosteroid injections versus physiotherapy for treatment of painful stiff shoulder in primary care. BMJ. 1998;317: BurkeDT,BurkeMM,StewartGW,CambreA. for carpal tunnel syndrome: in search of the optimal angle. Arch Phys Med Rehabil. 1994;75: Levine DW, Simmons BP, Koris MJ, et al. A selfadministered questionnaire for the assessment of severity of symptoms and functional status in carpal tunnel syndrome. J Bone Joint Surg Am. 1993;75: Lee YJ, Ellenberg JH, Hirtz DG, Nelson KB. Analysis of clinical trials by treatment actually received: is it really an option? Stat Med. 1991;10: Schulz KF, Chalmers I, Hayes RJ, Altman DG. Empirical evidence of bias. JAMA. 1995;273: American Academy of Neurology. Practice parameter for carpal tunnel syndrome (summary statement). Neurology. 1993;43: Manente G, Torrieri F, Di Blasio F, et al. An innovative hand brace for carpal tunnel syndrome. Muscle Nerve. 2001;24: American Medical Association. All rights reserved. (Reprinted) JAMA, September 11, 2002 Vol 288, No
How to write a scientific article?
 How to write a scientific article? Dr. A.A.M. Gerritsen, Epi Result 1 Overview lecture» Why a scientific format?» Sections of the article» Process of writing» Structure of a paragraph» Reporting and journal
How to write a scientific article? Dr. A.A.M. Gerritsen, Epi Result 1 Overview lecture» Why a scientific format?» Sections of the article» Process of writing» Structure of a paragraph» Reporting and journal
Acute Services Division. Information for patients. Carpal Tunnel. Physiotherapy Department Glasgow Royal Infirmary
 Acute Services Division Information for patients Carpal Tunnel Physiotherapy Department Glasgow Royal Infirmary Introduction Carpal tunnel syndrome (CTS) can cause the symptoms of pain, pins and needles
Acute Services Division Information for patients Carpal Tunnel Physiotherapy Department Glasgow Royal Infirmary Introduction Carpal tunnel syndrome (CTS) can cause the symptoms of pain, pins and needles
Surgical versus non-surgical treatment for carpal tunnel syndrome (Review)
 Surgical versus non-surgical treatment for carpal tunnel syndrome (Review) Verdugo RJ, Salinas RA, Castillo JL, Cea JG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
Surgical versus non-surgical treatment for carpal tunnel syndrome (Review) Verdugo RJ, Salinas RA, Castillo JL, Cea JG This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration
A Patient s Guide to Carpal Tunnel Syndrome
 A Patient s Guide to Carpal Tunnel Syndrome Concord Orthopaedics 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this
A Patient s Guide to Carpal Tunnel Syndrome Concord Orthopaedics 264 Pleasant Street Concord, NH 03301 Phone: 6032243368 Fax: 6032287268 marketing.copa@concordortho.com DISCLAIMER: The information in this
Disclosure. Carpal Tunnel Syndrome 11/9/15
 Michael S. Bednar, M.D. Chief, Hand Surgery Professor, Dept of Orthopaedic Surgery and Rehab Loyola University - Chicago Disclosure No conflicts for this talk Carpal Tunnel Syndrome AKA Corporal tunnel
Michael S. Bednar, M.D. Chief, Hand Surgery Professor, Dept of Orthopaedic Surgery and Rehab Loyola University - Chicago Disclosure No conflicts for this talk Carpal Tunnel Syndrome AKA Corporal tunnel
Referral Criteria: Carpal Tunnel Syndrome Feb
 Referral Criteria: Carpal Tunnel Syndrome Feb 2019 1 5.2. Carpal Tunnel Syndrome Background Carpal tunnel syndrome present with non-traumatic tingling of the fingers due to compression of the median nerve
Referral Criteria: Carpal Tunnel Syndrome Feb 2019 1 5.2. Carpal Tunnel Syndrome Background Carpal tunnel syndrome present with non-traumatic tingling of the fingers due to compression of the median nerve
Carpal Tunnel Release
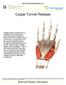 Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
Carpal Tunnel Release Carpal tunnel syndrome is a condition in the hand and wrist caused by excessive pressure on the median nerve in the wrist. Compression of the nerve typically causes numbness and tingling
NHS Fylde and Wyre Clinical Commissioning Group. Policies for the Commissioning of Healthcare. Policy for surgical treatment of carpal tunnel syndrome
 NHS Fylde and Wyre Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for surgical treatment of carpal tunnel syndrome 1 Introduction 1.1 This document is part of a suite
NHS Fylde and Wyre Clinical Commissioning Group Policies for the Commissioning of Healthcare Policy for surgical treatment of carpal tunnel syndrome 1 Introduction 1.1 This document is part of a suite
CARPAL TUNNEL SYNDROME (CTS) is a common
 ARTICLES Randomized Controlled Trial of Nocturnal Splinting for Active Workers With Symptoms of Carpal Tunnel Syndrome Robert A. Werner, MD, Alfred Franzblau, MD, Nancy Gell, MPH, PT 1 ABSTRACT. Werner
ARTICLES Randomized Controlled Trial of Nocturnal Splinting for Active Workers With Symptoms of Carpal Tunnel Syndrome Robert A. Werner, MD, Alfred Franzblau, MD, Nancy Gell, MPH, PT 1 ABSTRACT. Werner
Effect of age on subjective complaints and objective severity of carpal tunnel syndrome: prospective study
 RESEARCH Effect of age on subjective complaints and objective severity of carpal tunnel syndrome: prospective study B Povlsen 1 K Aggelakis 2 M Koutroumanidis 2 1 Department of Orthopaedics, Guy s, St
RESEARCH Effect of age on subjective complaints and objective severity of carpal tunnel syndrome: prospective study B Povlsen 1 K Aggelakis 2 M Koutroumanidis 2 1 Department of Orthopaedics, Guy s, St
Carpal Tunnel Syndrome Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Carpal Tunnel Syndrome Orthopaedic Department Patient Information Leaflet Page 1 Carpal Tunnel Syndrome Carpal tunnel syndrome (CTS) is a common problem which affects the hand and wrist. Symptoms are caused
Carpal Tunnel Syndrome Orthopaedic Department Patient Information Leaflet Page 1 Carpal Tunnel Syndrome Carpal tunnel syndrome (CTS) is a common problem which affects the hand and wrist. Symptoms are caused
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) Surgery is more cost-effective than splinting for carpal tunnel syndrome in the Netherlands: Results of an economic evaluation alongside a randomized controlled trial
UvA-DARE (Digital Academic Repository) Surgery is more cost-effective than splinting for carpal tunnel syndrome in the Netherlands: Results of an economic evaluation alongside a randomized controlled trial
A Patient s Guide to Carpal Tunnel Syndrome. William T. Grant, MD
 A Patient s Guide to Carpal Tunnel Syndrome Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
A Patient s Guide to Carpal Tunnel Syndrome Dr. Grant is a talented orthopedic surgeon with more than 30 years of experience helping people return to their quality of life. He and GM Pugh, PA-C pride themselves
Heecheon You Department of Industrial and Manufacturing Engineering The Pennsylvania State University, University Park, PA 16802
 PROCEEDINGS of ihe HUMAN FACTORS AND ERGONOMICS SOCIETY 42nd ANNUAL MEETING-1998 841 RELATIONSHIPS BETWEEN CLINICAL SCALES ON SEVERITY OF SYMPTOMS AND ELECTRODIAGNOSTIC MEASURES ON ABNORMALITY OF NERVE
PROCEEDINGS of ihe HUMAN FACTORS AND ERGONOMICS SOCIETY 42nd ANNUAL MEETING-1998 841 RELATIONSHIPS BETWEEN CLINICAL SCALES ON SEVERITY OF SYMPTOMS AND ELECTRODIAGNOSTIC MEASURES ON ABNORMALITY OF NERVE
A Patient s Guide to Carpal Tunnel Syndrome
 A Patient s Guide to Carpal Tunnel Syndrome 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Carpal Tunnel Syndrome 15195 Heathcote Blvd Suite 334 Haymarket, VA 20169 Phone: 703-369-9070 Fax: 703-369-9240 DISCLAIMER: The information in this booklet is compiled from a variety
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome)
 A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
A Patient s Guide to Ulnar Nerve Entrapment at the Wrist (Guyon s Canal Syndrome) Introduction The ulnar nerve is often called the funny bone at the elbow. However, there is little funny about injury to
OS05 Carpal Tunnel Release (under Local Anaesthetic)
 OS05 Carpal Tunnel Release (under Local Anaesthetic) What is carpal tunnel syndrome? Carpal tunnel syndrome is a condition where there is increased pressure on the nerve that crosses the front of your
OS05 Carpal Tunnel Release (under Local Anaesthetic) What is carpal tunnel syndrome? Carpal tunnel syndrome is a condition where there is increased pressure on the nerve that crosses the front of your
THE WRIST. At a glance. 1. Introduction
 THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
THE WRIST At a glance The wrist is possibly the most important of all joints in everyday and professional life. It is under strain not only in many blue collar trades, but also in sports and is therefore
S houlder problems are common, with up to 47% of adults
 156 EXTENDED REPORT Two pragmatic trials of treatment for shoulder disorders in primary care: generalisability, course, and prognostic indicators E Thomas, D A W M van der Windt, E M Hay, N Smidt, K Dziedzic,
156 EXTENDED REPORT Two pragmatic trials of treatment for shoulder disorders in primary care: generalisability, course, and prognostic indicators E Thomas, D A W M van der Windt, E M Hay, N Smidt, K Dziedzic,
CAN WE PREDICT SURGERY FOR SCIATICA?
 7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
7 CAN WE PREDICT SURGERY FOR SCIATICA? Improving prediction of inevitable surgery during non-surgical treatment of sciatica. Wilco C. Peul Ronald Brand Raph T.W.M. Thomeer Bart W. Koes Submitted for publication
There is substantial variation in
 Clin Orthop Relat Res (2016) 474:1770 1774 / DOI 10.1007/s11999-015-4183-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 18 February
Clin Orthop Relat Res (2016) 474:1770 1774 / DOI 10.1007/s11999-015-4183-3 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 18 February
)185( COPYRIGHT 2014 BY THE ARCHIVES OF BONE AND JOINT SURGERY
 )185( COPYRIGHT 2014 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Progression of Carpal Tunnel Syndrome According to Electrodiagnostic ing in Nonoperatively Treated Patients Mark van Suchtelen,
)185( COPYRIGHT 2014 BY THE ARCHIVES OF BONE AND JOINT SURGERY RESEARCH ARTICLE Progression of Carpal Tunnel Syndrome According to Electrodiagnostic ing in Nonoperatively Treated Patients Mark van Suchtelen,
Manual Therapy, Physical Therapy, or Continued Care by a General Practitioner for Patients with Neck Pain A Randomized, Controlled Trial
 Manual Therapy, Physical Therapy, or Continued Care by a General Practitioner for Patients with Neck Pain A Randomized, Controlled Trial Annals of Internal Medicine,, Vol. 136 No. 10, Pages 713-722 May
Manual Therapy, Physical Therapy, or Continued Care by a General Practitioner for Patients with Neck Pain A Randomized, Controlled Trial Annals of Internal Medicine,, Vol. 136 No. 10, Pages 713-722 May
What do we want? Cervicothoracic Workgroup. ICF Scheme. start with end in mind. What do consumers want?
 Cervicothoracic Workgroup Use of the International Classification of Functioning to Develop Evidence-Based Treatment Guidelines for the Management of Cervicothoracic Conditions John D. Childs, PT, PhD,
Cervicothoracic Workgroup Use of the International Classification of Functioning to Develop Evidence-Based Treatment Guidelines for the Management of Cervicothoracic Conditions John D. Childs, PT, PhD,
Does wrist immobilization following open carpal tunnel release improve functional outcome? A literature review
 Curr Rev Musculoskelet Med (2010) 3:11 17 DOI 10.1007/s12178-010-9060-9 Does wrist immobilization following open carpal tunnel release improve functional outcome? A literature review S. M. Isaac T. Okoro
Curr Rev Musculoskelet Med (2010) 3:11 17 DOI 10.1007/s12178-010-9060-9 Does wrist immobilization following open carpal tunnel release improve functional outcome? A literature review S. M. Isaac T. Okoro
Asymmetric Injury in Carpal Tunnel Syndrome. C. J. Zheng, MD, PhD. Department of Occupational and Environmental Medicine.
 Asymmetric Injury in Carpal Tunnel Syndrome C. J. Zheng, MD, PhD Department of Occupational and Environmental Medicine Regions Hospital University of Minnesota Saint Paul, Minnesota Tel: 65-54-3443 Pager:
Asymmetric Injury in Carpal Tunnel Syndrome C. J. Zheng, MD, PhD Department of Occupational and Environmental Medicine Regions Hospital University of Minnesota Saint Paul, Minnesota Tel: 65-54-3443 Pager:
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM
 TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
TECHNOLOGY AND HOW WE USE IT TO DAMAGE OURSELVES WILLIAM A. DELP, DO ASSISTANT PROFESSOR OF OMM GA PCOM OBJECTIVES Understand how we interact with technology new and old Understand how injury occurs Texting
Corticosteroid Injection vs. Nonsteroidal Antiinflammatory Drug and Splinting in Carpal Tunnel Syndrome
 Authors: Reyhan Çeliker, MD Şule Arslan, MD Fatma İnanıcı, MD Carpal Tunnel Syndrome Affiliations: From the Department of Physical Medicine and Rehabilitation, Hacettepe University School of Medicine,
Authors: Reyhan Çeliker, MD Şule Arslan, MD Fatma İnanıcı, MD Carpal Tunnel Syndrome Affiliations: From the Department of Physical Medicine and Rehabilitation, Hacettepe University School of Medicine,
carpal tunnel get back to life Patient information about Endoscopic Surgery for the treatment of Carpal Tunnel Syndrome
 carpal tunnel get back to life Patient information about Endoscopic Surgery for the treatment of Carpal Tunnel Syndrome what is carpal tunnel syndrome? Carpal Tunnel Syndrome (CTS) is a medical condition
carpal tunnel get back to life Patient information about Endoscopic Surgery for the treatment of Carpal Tunnel Syndrome what is carpal tunnel syndrome? Carpal Tunnel Syndrome (CTS) is a medical condition
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Horng, Y. S., Hsieh, S. F., Tu, Y. K., Lin, M. C., Horng, Y. S., & Wang, J. D. (2011). The comparative effectiveness of tendon and nerve gliding exercises in patients with
CRITICALLY APPRAISED PAPER (CAP) Horng, Y. S., Hsieh, S. F., Tu, Y. K., Lin, M. C., Horng, Y. S., & Wang, J. D. (2011). The comparative effectiveness of tendon and nerve gliding exercises in patients with
Measure #1a: Essential Components of Electrodiagnostic (EDX) Evaluation for Median Neuropathy at the Wrist
 Measure #1a: Essential Components of Electrodiagnostic (EDX) Evaluation for Median Neuropathy at the Wrist Measure Description Percentage of patients referred for EDX evaluation of CTS who had adequate
Measure #1a: Essential Components of Electrodiagnostic (EDX) Evaluation for Median Neuropathy at the Wrist Measure Description Percentage of patients referred for EDX evaluation of CTS who had adequate
Carpal Tunnel Syndrome
 Carpal Tunnel Syndrome Information for patients Therapy Services Phone no: 01625 661481 www.eastcheshire.nhs.uk @eastcheshirenhs Ref: 11437 Review: 06/2015 Revised review: 30/04/2018 Carpal Tunnel Syndrome
Carpal Tunnel Syndrome Information for patients Therapy Services Phone no: 01625 661481 www.eastcheshire.nhs.uk @eastcheshirenhs Ref: 11437 Review: 06/2015 Revised review: 30/04/2018 Carpal Tunnel Syndrome
Carpal Tunnel Syndrome. And Osteopathy. Kim C. Sanchez Aldana Camacho. National Academy of Osteopathy. DOMP Accelerated
 Running head: CARPAL TUNEL SYNDROME AND OSTEOPATHY 1 Carpal Tunnel Syndrome And Osteopathy Kim C. Sanchez Aldana Camacho National Academy of Osteopathy DOMP Accelerated CARPAL TUNNEL SYNDROME AND OSTEOPATHY
Running head: CARPAL TUNEL SYNDROME AND OSTEOPATHY 1 Carpal Tunnel Syndrome And Osteopathy Kim C. Sanchez Aldana Camacho National Academy of Osteopathy DOMP Accelerated CARPAL TUNNEL SYNDROME AND OSTEOPATHY
CARPAL TUNNEL RELEASE
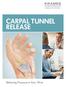 CARPAL TUNNEL RELEASE Relieving Pressure in Your Wrist What Is Carpal Tunnel Syndrome? Carpal tunnel syndrome (CTS) is a condition that affects nerves in the wrist and hand. CTS causes tingling and numbness
CARPAL TUNNEL RELEASE Relieving Pressure in Your Wrist What Is Carpal Tunnel Syndrome? Carpal tunnel syndrome (CTS) is a condition that affects nerves in the wrist and hand. CTS causes tingling and numbness
Shared Decision Making
 Deciding what to do about carpal This short decision aid is to help you decide what to do about your carpal. You can use it on your own, or with your doctor, to help you make a decision about what's right
Deciding what to do about carpal This short decision aid is to help you decide what to do about your carpal. You can use it on your own, or with your doctor, to help you make a decision about what's right
CUBITAL TUNNEL SYNDROME GUIDANCE
 CUBITAL TUNNEL SYNDROME GUIDANCE Author Louise Ross (Louise.Ross@ggc.scot.nhs.uk) Organisation NHS Greater Glasgow and Clyde Created 15/04/2016 15:32:54 Modified 26/10/2016 16:17:15 Modified By Louise
CUBITAL TUNNEL SYNDROME GUIDANCE Author Louise Ross (Louise.Ross@ggc.scot.nhs.uk) Organisation NHS Greater Glasgow and Clyde Created 15/04/2016 15:32:54 Modified 26/10/2016 16:17:15 Modified By Louise
Commissioning Policy Individual Funding Request
 Commissioning Policy Individual Funding Request Carpal Tunnel Syndrome Surgery Criteria Based Access Policy Date Adopted: 6 th February 2017 Version: 1617.1.02 Individual Funding Request Team Bristol,
Commissioning Policy Individual Funding Request Carpal Tunnel Syndrome Surgery Criteria Based Access Policy Date Adopted: 6 th February 2017 Version: 1617.1.02 Individual Funding Request Team Bristol,
British Journal of Rheumatology 1991; 30:
 British Journal of Rheumatology 1991; 30:468-470 CASE REPORT CARPAL TUNNEL SYNDROME COMPLICATED BY REFLEX SYMPATHETIC DYSTROPHY SYNDROME BY M.-A. FITZCHARLES AND J.M. ESDAILE Rheumatic Disease Unit, McGill
British Journal of Rheumatology 1991; 30:468-470 CASE REPORT CARPAL TUNNEL SYNDROME COMPLICATED BY REFLEX SYMPATHETIC DYSTROPHY SYNDROME BY M.-A. FITZCHARLES AND J.M. ESDAILE Rheumatic Disease Unit, McGill
CARPAL TUNNEL SYNDROME
 CARPAL TUNNEL SYNDROME Carpal tunnel syndrome results from the pinching or entrapping of the median nerve in the underside of the wrist. The actual pathology in most cases is due to either a decrease in
CARPAL TUNNEL SYNDROME Carpal tunnel syndrome results from the pinching or entrapping of the median nerve in the underside of the wrist. The actual pathology in most cases is due to either a decrease in
What you need to know about Carpal Tunnel Syndrome
 What you need to know about Carpal Tunnel Syndrome and Other Disorders of the Neck, Shoulder, Elbow, Wrist and Hands It is my mission to empower patients with knowledge and care so that they can enjoy
What you need to know about Carpal Tunnel Syndrome and Other Disorders of the Neck, Shoulder, Elbow, Wrist and Hands It is my mission to empower patients with knowledge and care so that they can enjoy
Carpal tunnel decompression advice
 Southend University Hospital NHS Foundation Trust Patient Information Service Carpal tunnel decompression advice SOU1277_120995_1018_V2.indd 1 28/11/2018 09:16 SOU1277_120995_1018_V2.indd 2 28/11/2018
Southend University Hospital NHS Foundation Trust Patient Information Service Carpal tunnel decompression advice SOU1277_120995_1018_V2.indd 1 28/11/2018 09:16 SOU1277_120995_1018_V2.indd 2 28/11/2018
Student Research Committee, International branch, Shiraz University of medical sciences, Shiraz, Iran
 Received: 22 July 2015 Accepted: 12 August 2015 Journal of Biology and Today's World ISSN 2322-3308 Journal home page: http://journals.lexispublisher.com/jbtw/ Short. C doi:10.15412/j.jbtw. 01040602 A
Received: 22 July 2015 Accepted: 12 August 2015 Journal of Biology and Today's World ISSN 2322-3308 Journal home page: http://journals.lexispublisher.com/jbtw/ Short. C doi:10.15412/j.jbtw. 01040602 A
Carpal Tunnel Syndrome
 Patient information Carpal Tunnel Syndrome i Important information for all patients having Carpal Tunnel surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
Patient information Carpal Tunnel Syndrome i Important information for all patients having Carpal Tunnel surgery. Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
A Patient s Guide to Elbow Dislocation 2 Introduction When the joint surfaces of an elbow are forced apart, the elbow is dislocated. The elbow is the second most commonly dislocated joint in adults (after
Dr David Ruttenberg MBChB.,MSc(Med).,FAFOEM
 Carpal Tunnel Syndrome Dr David Ruttenberg MBChB.,MSc(Med).,FAFOEM General Practitioners Outpatient Clinics Occupational Health Clinics 5-10% Prevalence in Community Is it common? Common Usually Females,
Carpal Tunnel Syndrome Dr David Ruttenberg MBChB.,MSc(Med).,FAFOEM General Practitioners Outpatient Clinics Occupational Health Clinics 5-10% Prevalence in Community Is it common? Common Usually Females,
Carpal Tunnel Syndrome: Background Information for HemaClear Product Specialists
 H E M A C L E A R P R E S S A u g u s t 2 0 1 2 P a g e 1 Carpal Tunnel Syndrome: Background Information for HemaClear Product Specialists Edith R. Gavriely Abstract Carpal Tunnel Syndrome (CTS) is the
H E M A C L E A R P R E S S A u g u s t 2 0 1 2 P a g e 1 Carpal Tunnel Syndrome: Background Information for HemaClear Product Specialists Edith R. Gavriely Abstract Carpal Tunnel Syndrome (CTS) is the
CUBITAL TUNNEL SYNDROME
 WHAT IS CUBITAL TUNNEL SYNDROME? SYMPTOMS Cubital tunnel syndrome is the second most commonly occurring nerve compression in the upper body It is caused by compression of the ulnar nerve at the elbow The
WHAT IS CUBITAL TUNNEL SYNDROME? SYMPTOMS Cubital tunnel syndrome is the second most commonly occurring nerve compression in the upper body It is caused by compression of the ulnar nerve at the elbow The
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION
 CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION The use of an othosis has been shown to decrease symptoms in carpal tunnel syndrome, but which type of orthosis (cock up or lumbrical) with which type
CRITICALLY APPRAISED PAPER (CAP) FOCUSED QUESTION The use of an othosis has been shown to decrease symptoms in carpal tunnel syndrome, but which type of orthosis (cock up or lumbrical) with which type
The Journal of Rheumatology Volume 33, no. 10. Lateral epicondylitis in general practice: course and prognostic indicators of outcome.
 The Journal of Rheumatology Volume 33, no. 10 Lateral epicondylitis in general practice: course and prognostic indicators of outcome. Nynke Smidt, Martyn Lewis, Daniëlle A W M VAN DER Windt, Elaine M Hay,
The Journal of Rheumatology Volume 33, no. 10 Lateral epicondylitis in general practice: course and prognostic indicators of outcome. Nynke Smidt, Martyn Lewis, Daniëlle A W M VAN DER Windt, Elaine M Hay,
Carpal Tunnel Syndrome/ Cubital Tunnel Syndrome. Nerve anatomy. Pathophysiology 6/14/2014. Most common compression neuropathies of the upper extremity
 Carpal Tunnel Syndrome/ Cubital Tunnel Syndrome Justin Arnold MD Family Medicine Update 2014 Most common compression neuropathies of the upper extremity Increasing prevalence CTS 50/1000 subjects Up to
Carpal Tunnel Syndrome/ Cubital Tunnel Syndrome Justin Arnold MD Family Medicine Update 2014 Most common compression neuropathies of the upper extremity Increasing prevalence CTS 50/1000 subjects Up to
Carpal tunnel syndrome (CTS) is a symptom com A PILOT STUDY COMPARING TWO MANUAL THERAPY INTERVENTIONS FOR CARPAL TUNNEL SYNDROME ABSTRACT
 A PILOT STUDY COMPARING TWO MANUAL THERAPY INTERVENTIONS FOR CARPAL TUNNEL SYNDROME Jeanmarie Burke, PhD, a, Dale J. Buchberger, DC, PT, b M. Terry Carey-Loghmani, MS, PT, c Paul E. Dougherty, DC, d Douglas
A PILOT STUDY COMPARING TWO MANUAL THERAPY INTERVENTIONS FOR CARPAL TUNNEL SYNDROME Jeanmarie Burke, PhD, a, Dale J. Buchberger, DC, PT, b M. Terry Carey-Loghmani, MS, PT, c Paul E. Dougherty, DC, d Douglas
Carpal Tunnel Syndrome
 Carpal Tunnel Syndrome Q: What is carpal tunnel syndrome (CTS)? A: Carpal tunnel syndrome (CTS) is the name for a group of problems that includes swelling, pain, tingling, and loss of strength in your
Carpal Tunnel Syndrome Q: What is carpal tunnel syndrome (CTS)? A: Carpal tunnel syndrome (CTS) is the name for a group of problems that includes swelling, pain, tingling, and loss of strength in your
Lowe Plastic Surgery (LPS)
 Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
Lowe Plastic Surgery (LPS) PATIENT EDUCATION FOR: CUMULATIVE TRAUMA DISORDER THE PROBLEM: There has been a remarkable increase in what is termed cumulative trauma disorder (CTD) in the last 20 years. Other
8 Recovering From HAND FRACTURE SURGERY
 8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
8 Recovering From HAND FRACTURE SURGERY Hand fractures are caused by trauma and result in breaking (fracturing) the phalanges or metacarpals. Surgery involves achieving acceptable alignment and providing
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity
 Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Current Developments in the Prevention and Treatment of Repetitive Motion Injuries of the Upper Extremity D. Mowry 1 Mowry, D. 1995. Current Development in the Prevention and Treatment of Repetitive Motion
Appendix. ECC Process We recommend carpal tunnel release as treatment for carpal tunnel syndrome (Grade A)
 Page 1 TABLE E-1 Upper Limb Quality Measures* Measure Number Source NQS Domain 1 CPG for diagnosis syndrome (2007) 2 CPG for treatment syndrome (2008) 3 CPG for treatment syndrome (2008) 4 CPG for treatment
Page 1 TABLE E-1 Upper Limb Quality Measures* Measure Number Source NQS Domain 1 CPG for diagnosis syndrome (2007) 2 CPG for treatment syndrome (2008) 3 CPG for treatment syndrome (2008) 4 CPG for treatment
Surgery for carpal tunnel syndrome
 Surgery for carpal tunnel syndrome This leaflet will help answer some of the questions you may have about having surgery to treat carpal tunnel syndrome. It should accompany the leaflet, Surgical Admissions
Surgery for carpal tunnel syndrome This leaflet will help answer some of the questions you may have about having surgery to treat carpal tunnel syndrome. It should accompany the leaflet, Surgical Admissions
Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb
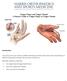 Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb Introduction Trigger finger and trigger thumb are conditions affecting the movement of the tendons as they bend the
Trigger Finger and Trigger Thumb A Patient's Guide to Trigger Finger & Trigger Thumb Introduction Trigger finger and trigger thumb are conditions affecting the movement of the tendons as they bend the
West Suffolk Hospital
 For staff use only: Patient Details: First names: Hospital no: (Use hospital identification label) West Suffolk Hospital Patient information leaflet Carpal Tunnel Syndrome 2-3 Patient agreement to investigation
For staff use only: Patient Details: First names: Hospital no: (Use hospital identification label) West Suffolk Hospital Patient information leaflet Carpal Tunnel Syndrome 2-3 Patient agreement to investigation
Arm Pain, Numbness, and Tingling: Etiologies and Treatment
 Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Arm Pain, Numbness, and Tingling: Etiologies and Treatment Steve Fowler MD Confluence Health Department of Physiatry Education Medical School: University of Utah Residency: Mayo Clinic Work Confluence
Dupuytrens disease. Exceptional healthcare, personally delivered
 Dupuytrens disease Exceptional healthcare, personally delivered Dupuytrens Disease Dupuytren s disease is a thickening of the tissue in the palm of the hand which may result in progressive flexion contractures
Dupuytrens disease Exceptional healthcare, personally delivered Dupuytrens Disease Dupuytren s disease is a thickening of the tissue in the palm of the hand which may result in progressive flexion contractures
Carpal tunnel syndrome in pregnancy. Information for patients MSK Outpatients - Women's Health (Therapy)
 Carpal tunnel syndrome in pregnancy Information for patients MSK Outpatients - Women's Health (Therapy) What is carpal tunnel syndrome in pregnancy? Carpal tunnel syndrome (CTS) is a common disorder of
Carpal tunnel syndrome in pregnancy Information for patients MSK Outpatients - Women's Health (Therapy) What is carpal tunnel syndrome in pregnancy? Carpal tunnel syndrome (CTS) is a common disorder of
 Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
Nerve Compression Syndromes Median Nerve Carpal Tunnel Syndrome Pronator Syndrome Ulnar Nerve Cubital Tunnel Syndrome Ulnar Tunnel Syndrome TOS www.fisiokinesiterapia.biz Carpal Tunnel Syndrome (CTS) Definition
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides
 IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
IAIABC 2003 Upper Extremity Impairment Guides Part 3 of the Supplemental Impairment Rating Guides Draft 11-03 IAIABC Executive Office 5610 Medical Circle, Suite 14 Madison, WI 53719 Phone: (608) 663-6355
INTRODUCTION Cubital Tunnel Syndrome
 INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
INTRODUCTION Cubital Tunnel Syndrome Diagram of the ulnar nerve supplying the muscles of forearm and hand Cubital Tunnel is a condition that refers to the ulnar nerve being compressed around the elbow.
Figure 1. Flowchart of literature review process (Questions 1 & 2)
 Figure 1. Flowchart of literature review process (Questions 1 & 2) Medline search (427 citations) Phase I Screening (abstracts) Papers retrieved (225) Phase II Screening (full-text) Preliminary included
Figure 1. Flowchart of literature review process (Questions 1 & 2) Medline search (427 citations) Phase I Screening (abstracts) Papers retrieved (225) Phase II Screening (full-text) Preliminary included
Platelet-Rich Plasma Compared With Other Common Injection Therapies in the Treatment of Chronic Lateral Epicondylitis
 Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
Journal of Sport Rehabilitation, 2016, 25, 77-82 http://dx.doi.org/10.1123/jsr.2014-0198 2016 Human Kinetics, Inc. CRITICALLY APPRAISED TOPIC Platelet-Rich Plasma Compared With Other Common Injection Therapies
Evaluating concomitant lateral epicondylitis and cervical radiculopathy
 Evaluating concomitant lateral epicondylitis and cervical radiculopathy March 06, 2010 This article describes a study of the prevalence of lateral epicondylitis or tennis elbow among patients with neck
Evaluating concomitant lateral epicondylitis and cervical radiculopathy March 06, 2010 This article describes a study of the prevalence of lateral epicondylitis or tennis elbow among patients with neck
Referral and pathways for surgically managed Carpal Tunnel Syndrome patients: guidelines and current practice
 Referral and pathways for surgically managed Carpal Tunnel Syndrome patients: guidelines and current practice A Report from the Musculoskeletal Audit on behalf of the Scottish Government The information
Referral and pathways for surgically managed Carpal Tunnel Syndrome patients: guidelines and current practice A Report from the Musculoskeletal Audit on behalf of the Scottish Government The information
* WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 84/07
 * WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 84/07 BEFORE: A. Suissa: Vice-Chair HEARING: January 12, 2007 at Toronto Written DATE OF DECISION: January 12, 2007 NEUTRAL CITATION: 2007
* WORKPLACE SAFETY AND INSURANCE APPEALS TRIBUNAL DECISION NO. 84/07 BEFORE: A. Suissa: Vice-Chair HEARING: January 12, 2007 at Toronto Written DATE OF DECISION: January 12, 2007 NEUTRAL CITATION: 2007
Cite this article as: BMJ, doi: /bmj f (published 15 June 2006)
 Cite this article as: BMJ, doi:10.1136/bmj.38863.632789.1f (published 15 June 2006) BMJ Outcomes of endoscopic surgery compared with open surgery for carpal tunnel syndrome among employed patients: randomised
Cite this article as: BMJ, doi:10.1136/bmj.38863.632789.1f (published 15 June 2006) BMJ Outcomes of endoscopic surgery compared with open surgery for carpal tunnel syndrome among employed patients: randomised
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training.
 Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
Effectiveness of passive and active knee joint mobilisation following total knee arthroplasty: Continuous passive motion vs. sling exercise training. Mau-Moeller, A. 1,2, Behrens, M. 2, Finze, S. 1, Lindner,
CARPAL TUNNEL CARPAL TUNNEL. A guide for patients and their family members
 If you have any concerns, contact your neurosurgeon or the hospital and ask for the neurosurgical registrar on-call: Prince of Wales Hospital & Community Services 9382 2222 St George Hospital & Community
If you have any concerns, contact your neurosurgeon or the hospital and ask for the neurosurgical registrar on-call: Prince of Wales Hospital & Community Services 9382 2222 St George Hospital & Community
A Patient s Guide to Elbow Dislocation
 A Patient s Guide to Elbow Dislocation 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
A Patient s Guide to Elbow Dislocation 20295 NE 29th Place, Ste 300 Aventura, FL 33180 Phone: (786) 629-0910 Fax: (786) 629-0920 admin@instituteofsports.com DISCLAIMER: The information in this booklet
Therapeutic ultrasound for carpal tunnel syndrome (Review)
 Page MJ, O Connor D, Pitt V, Massy-Westropp N This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2012, Issue 1 http://www.thecochranelibrary.com
Page MJ, O Connor D, Pitt V, Massy-Westropp N This is a reprint of a Cochrane review, prepared and maintained by The Cochrane Collaboration and published in The Cochrane Library 2012, Issue 1 http://www.thecochranelibrary.com
1. Common Health Problem/Condition: MSK Carpal Tunnel Syndrome (CTS)
 Midwifery Management Process for Common Health Problems 1. Common Health Problem/Condition: MSK Carpal Tunnel Syndrome (CTS) Definition: Carpal Tunnel Syndrome (CTS) is an upper extremity disability. It
Midwifery Management Process for Common Health Problems 1. Common Health Problem/Condition: MSK Carpal Tunnel Syndrome (CTS) Definition: Carpal Tunnel Syndrome (CTS) is an upper extremity disability. It
NHS Buckinghamshire Musculoskeletal Integrated Care Service (MusIC) Carpal tunnel syndrome
 NHS Buckinghamshire Musculoskeletal Integrated Care Service (MusIC) Carpal tunnel syndrome What is carpal tunnel? The carpal tunnel refers to an area at the base of the wrist which contains bones, nerves,
NHS Buckinghamshire Musculoskeletal Integrated Care Service (MusIC) Carpal tunnel syndrome What is carpal tunnel? The carpal tunnel refers to an area at the base of the wrist which contains bones, nerves,
Introduction to Neurosurgical Subspecialties:
 Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Introduction to Neurosurgical Subspecialties: Spine Neurosurgery Brian L. Hoh, MD 1 and Gregory J. Zipfel, MD 2 1 University of Florida, 2 Washington University Spine Neurosurgery Spine neurosurgeons treat
Official Definition. Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist.
 Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Mod 2 MMT Course Official Definition Carpal tunnel syndrome, the most common focal peripheral neuropathy, results from compression of the median nerve at the wrist. epidemiology Affects an estimated 3
Identification of Double Compression Lesion of Ulnar Nerve after Cubital Tunnel Release
 CASE REPORT pissn 1598-3889 eissn 2234-0998 J Korean Soc Surg Hand 2015;20(3):148-152. http://dx.doi.org/10.12790/jkssh.2015.20.3.148 JOURNAL OF THE KOREAN SOCIETY FOR SURGERY OF THE HAND Identification
CASE REPORT pissn 1598-3889 eissn 2234-0998 J Korean Soc Surg Hand 2015;20(3):148-152. http://dx.doi.org/10.12790/jkssh.2015.20.3.148 JOURNAL OF THE KOREAN SOCIETY FOR SURGERY OF THE HAND Identification
Motor and sensory nerve conduction studies
 3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
3 rd Congress of the European Academy of Neurology Amsterdam, The Netherlands, June 24 27, 2017 Hands-on Course 2 Assessment of peripheral nerves function and structure in suspected peripheral neuropathies
DOUBLE-CRUSH SYNDROME
 DOUBLE-CRUSH SYNDROME DOUBLE-CRUSH SYNDROME by Vladimir Golovchinsky M.D., Ph.D., D. Sei. SPRINGER SCIENCE+BUSINESS MEDIA, LLC Library of Congress Cataloging-in-Publication Data A c.i.p. Catalogue record
DOUBLE-CRUSH SYNDROME DOUBLE-CRUSH SYNDROME by Vladimir Golovchinsky M.D., Ph.D., D. Sei. SPRINGER SCIENCE+BUSINESS MEDIA, LLC Library of Congress Cataloging-in-Publication Data A c.i.p. Catalogue record
ORIGINAL ARTICLE. Department of Orthopedic Surgery, Mashad University of Medical Sciences, Mashad, Iran
 Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
Arch Iranian Med 2003; 6 (3): 196 199 ORIGINAL ARTICLE INJECTION OF METHYLPREDNISOLONE AND LIDOCAINE IN THE TREATMENT OF MEDIAL EPICONDYLITIS: A RANDOMIZED CLINICAL TRIAL Mahmood Bahari MD, Mohammad Gharehdaghi
Effects of Wrist Splinting for Carpal Tunnel Syndrome and Motor Nerve Conduction Measurements
 Upsala Journal of Medical Sciences ISSN: 0300-9734 (Print) 2000-1967 (Online) Journal homepage: http://www.tandfonline.com/loi/iups20 Effects of Wrist Splinting for Carpal Tunnel Syndrome and Motor Nerve
Upsala Journal of Medical Sciences ISSN: 0300-9734 (Print) 2000-1967 (Online) Journal homepage: http://www.tandfonline.com/loi/iups20 Effects of Wrist Splinting for Carpal Tunnel Syndrome and Motor Nerve
Conservative treatments for tennis elbow do subgroups of patients respond differently?
 Rheumatology 2007;46:1601 1605 doi:10.1093/rheumatology/kem192 Conservative treatments for tennis elbow do subgroups of patients respond differently? L. Bisset 1,2, N. Smidt 3,4, D. A. Van der Windt 5,6,
Rheumatology 2007;46:1601 1605 doi:10.1093/rheumatology/kem192 Conservative treatments for tennis elbow do subgroups of patients respond differently? L. Bisset 1,2, N. Smidt 3,4, D. A. Van der Windt 5,6,
JMSCR Vol 04 Issue 11 Page November 2016
 www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i11.82 Carpal Tunnel Syndrome: A Clinical and
www.jmscr.igmpublication.org Impact Factor 5.244 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v4i11.82 Carpal Tunnel Syndrome: A Clinical and
Clinical and Electrophysiological Study in Carpel Tunnel Syndrome
 IOSR Journal of Pharmacy and Biological Sciences (IOSR-JPBS) e-issn: 2278-3008, p-issn:2319-7676. Volume 10, Issue 3 Ver. IV (May - Jun. 2015), PP 32-37 www.iosrjournals.org Clinical and Electrophysiological
IOSR Journal of Pharmacy and Biological Sciences (IOSR-JPBS) e-issn: 2278-3008, p-issn:2319-7676. Volume 10, Issue 3 Ver. IV (May - Jun. 2015), PP 32-37 www.iosrjournals.org Clinical and Electrophysiological
Conservative treatments for tennis elbow: do subgroups of patients respond differently?
 Conservative treatments for tennis elbow: do subgroups of patients respond differently? Author Bisset, Leanne, Smidt, N., van der Windt, D., Bouter, L., Jull, G., Brooks, P., Vicenzino, B. Published 2007
Conservative treatments for tennis elbow: do subgroups of patients respond differently? Author Bisset, Leanne, Smidt, N., van der Windt, D., Bouter, L., Jull, G., Brooks, P., Vicenzino, B. Published 2007
Common Elbow Problems
 Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Common Elbow Problems Duncan Ferguson FRACS Knee and Shoulder Specialist Elbow Instability Common 10-25% of elbow injuries Median age 30 yrs Most simple dislocations are stable after reduction recurrence
Study of Long Term Effects of Laser Therapy Versus Local Corticosteroid Injection in Patients with Carpal Tunnel Syndrome
 Original Article Study of Long Term Effects of Laser Therapy Versus Local Corticosteroid Injection in Patients with Carpal Tunnel Syndrome Ahmad Raeissadat MD 1, Zara Reza Soltani MD 2 1Department of Physical
Original Article Study of Long Term Effects of Laser Therapy Versus Local Corticosteroid Injection in Patients with Carpal Tunnel Syndrome Ahmad Raeissadat MD 1, Zara Reza Soltani MD 2 1Department of Physical
CARPAL TUNNEL SYNDROME (CTS)
 CARPAL TUNNEL SYNDROME (CTS) CTS: why does it matter? Fairly prevalent Early detection may prevent permanent impairment 1 To review: Learning Objectives Signs/symptoms Causes Management prevention treatment
CARPAL TUNNEL SYNDROME (CTS) CTS: why does it matter? Fairly prevalent Early detection may prevent permanent impairment 1 To review: Learning Objectives Signs/symptoms Causes Management prevention treatment
Evaluation of Tingling and Numbness in the Upper Extremities
 Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Evaluation of Tingling and Numbness in the Upper Extremities DR. W. ANTHONY FRISELLA M.D. ADVANCED BONE & JOINT, ST CHARLES MO MONA 2018 Overview Polyneuropathy Compressive nerve lesions Carpal tunnel
Downloaded from armaghanj.yums.ac.ir at 16: on Friday March 8th 2019
 : : ) : ( ( ) SPSS : (p< / ) * ** * ** / / : / / : : emadm@sumsacir: : : () ( ) ( ) 1-Carpal Tunnel Syndrome 2-Entrapment 3-Median Nerve 4-Tinel 5-Phalen 6-Provocative test 7-Nerve conduction study 8-Bronson
: : ) : ( ( ) SPSS : (p< / ) * ** * ** / / : / / : : emadm@sumsacir: : : () ( ) ( ) 1-Carpal Tunnel Syndrome 2-Entrapment 3-Median Nerve 4-Tinel 5-Phalen 6-Provocative test 7-Nerve conduction study 8-Bronson
Carpal Tunnel Decompression Surgery. (Minor procedure in Primary Care)
 Carpal Tunnel Decompression Surgery (Minor procedure in Primary Care) Information for Patients Gateshead Upper Limb Unit Page 1 of 5 What is carpal tunnel syndrome? Carpal tunnel syndrome is a common condition
Carpal Tunnel Decompression Surgery (Minor procedure in Primary Care) Information for Patients Gateshead Upper Limb Unit Page 1 of 5 What is carpal tunnel syndrome? Carpal tunnel syndrome is a common condition
Carpal tunnel syndrome
 Carpal tunnel syndrome Patient Information Clinical Support Services Physiotherapy Median nerve Transverse carpal ligament Ulna Radius What is carpal tunnel syndrome? Carpal tunnel syndrome is a condition
Carpal tunnel syndrome Patient Information Clinical Support Services Physiotherapy Median nerve Transverse carpal ligament Ulna Radius What is carpal tunnel syndrome? Carpal tunnel syndrome is a condition
Case 1. Your diagnosis
 Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
Case 1 44-year-old midwife presented with intermittent pins and needles in the little and ring fingers with blanching. Symptoms were exacerbated by cold exposure. Your diagnosis Diagnosis Hypothenar syndrome
Citation: Talebi GA, Saadat P, Javadian Y, et al. Manual therapy in the treatment of carpal tunnel
 Original Article DOI: 10.22088/cjim.9.3.283 Manual therapy in the treatment of carpal tunnel syndrome in diabetic patients: A randomized clinical trial Ghadam Ali Talebi (PhD) 1 Payam Saadat (MD) 1, 2
Original Article DOI: 10.22088/cjim.9.3.283 Manual therapy in the treatment of carpal tunnel syndrome in diabetic patients: A randomized clinical trial Ghadam Ali Talebi (PhD) 1 Payam Saadat (MD) 1, 2
Jay Smith, M.D. Chief Medical Officer and Founder, Sonex Health LLC March 2018
 SX-One MicroKnife Ultrasound Guided Carpal Tunnel Release: Initial Clinical Experience Jay Smith, M.D. Chief Medical Officer and Founder, Sonex Health LLC March 2018 Introduction Carpal tunnel syndrome
SX-One MicroKnife Ultrasound Guided Carpal Tunnel Release: Initial Clinical Experience Jay Smith, M.D. Chief Medical Officer and Founder, Sonex Health LLC March 2018 Introduction Carpal tunnel syndrome
Complementary treatment options in carpal tunnel syndrome surgery; Prospective randomized controlled study
 Annals of Medical Research DOI: 10.5455/jtomc.2018.03.042 2018;25(2):236-40 Original Article Complementary treatment options in carpal tunnel syndrome surgery; Prospective randomized controlled study Yakup
Annals of Medical Research DOI: 10.5455/jtomc.2018.03.042 2018;25(2):236-40 Original Article Complementary treatment options in carpal tunnel syndrome surgery; Prospective randomized controlled study Yakup
Comparison of the results of open
 1131 Original Article Singapore Med.1 27; 48 (12) : Comparison of the results of open carpal tunnel release and KnifeLight carpal tunnel release Yeo K Q, Yeo E M N Yeo Orthopaedic Centre, Mount Elizabeth
1131 Original Article Singapore Med.1 27; 48 (12) : Comparison of the results of open carpal tunnel release and KnifeLight carpal tunnel release Yeo K Q, Yeo E M N Yeo Orthopaedic Centre, Mount Elizabeth
