Exercise Science and Sports Medicine
|
|
|
- Kristin Small
- 6 years ago
- Views:
Transcription
1 Unit 7 INJURY AND THE HEALING PROCESS Lecture notes I. Therapeutic Modalities can create an optimum environment for injury healing, while reducing pain and discomfort. The number of therapeutic modalities used in therapeutic environments is ever increasing. a. The selection of specific treatments or combinations of treatments is based on such factors as: i. Injury site, type, and severity. ii. Modality indications and contraindications. iii. The physician s prescription. iv. The athlete s willingness to accept treatment. b. A key point to remember is More is not better. c. Modalities are used to aid the athlete s tolerance to exercise, which is the ultimate modality. Misuse or overuse of modalities can often aggravate a condition, delaying rather than facilitating the athlete s return to play. d. Legal concerns: The use of therapeutic modalities in sports medicine must be performed with the greatest care possible. Modalities must be administered in accordance with local regulations. Documentation of all treatments should be maintained to ensure continuity and to help assess the efficacy of the treatment. II. Cryotherapy a. An umbrella term that describes multiple types of cold application. b. When applied intermittently for minutes every 1 _ waking hours, along with compression, elevation, and rest (RICE), it reduces many of the adverse conditions related to the inflammatory phase of an acute injury. c. Physical Principles i. When a cold object is applied to a warmer object, heat is abstracted. In terms of cryotherapy, the most common method for cold transfer to tissue is through conduction. ii. The extent to which tissue is cooled depends upon the cold medium that is being applied, the length of cold exposure, and the conductivity of the area being cooled. In most cases the longer the cold exposure is, the deeper the cooling. iii. Tissue that has previously been cooled takes longer to return to a normal temperature than that which has been heated. iv. Dept of cold penetration can reach up to 5 cm. d. Physiological Effects of Cold i. Decrease in tissue temperature. Once a muscle has been cooled through the subcutaneous fat layer, cold s effects last longer than heat because fat acts as an insulator against rewarming. The major problem is to penetrate the fat layer initially so that muscle cooling occurs. Unit 7 Therapeutic Modalities and Injury Rehabilitation 1 draft copy
2 ii. Decrease in blood flow. Vasoconstriction of the blood vessels in the area. This vasoconstriction is caused, in part, by the reflex action of smooth muscles. iii. Decrease in muscle spasms by slowing metabolism in the area, thus decreasing the waste products, which act as a muscle irritant and thus cause spasm, which may have accumulated in the area. iv. Decrease pain perception. Cold decreases free nerve ending excitability, as well as the excitability of peripheral nerves. Analgesia is caused by raising of the nerve s threshold. v. Decrease muscle fatigue and increase and maintain muscular contraction. vi. Decrease in metabolic rate. vii. Increase in collagen inelasticity. viii. Increase in joint stiffness. ix. Increase capillary permeability. e. Special Considerations i. Indications include acute soft tissue injuries such as sprains, strains, contusions, and muscle spasms. Cryotherapy is also indicated for chronic inflammatory conditions such as tendonitis, tenosynovitis, and fasciitis. ii. Contraindications include circulatory disturbances, hypersensitivity to cold, and prolonged application over superficial nerves. iii. Some individuals are allergic to cold, reacting with hives, and joint pain and swelling. iv. Raynaud s phenomenon is a condition that causes vasospasm of digital arteries lasting for minutes to hours, which could lead to tissue death. The early signs of Raynaud s are attacks of intermittent skin blanching or cyanosis of the fingers or toes, skin pallor followed by redness, and finally a return to normal color. Pain is uncommon, but numbness, tingling, or burning may occur during and shortly after an attack. v. Ice should never be applied longer than minutes at any one time. vi. If cold is continuously applied for minutes, an intermittent period of vasodilation occurs for 4-6 minutes. This period is known as the hunting response, a reaction against tissue damage from too much cold exposure. When the hunting response occurs, the tissue temperature does not return to pre-application levels. f. Stages of Cryotherapy i. Cold sensation (0-3 minutes after initiation). ii. Mild burning, aching (2-7 minutes after initiation). iii. Numbness; relative cutaneous anesthesia (5-12 minutes after initiation). Unit 7 Therapeutic Modalities and Injury Rehabilitation 2 draft copy
3 g. Cryotherapeutic Methods i. Ice Packs 1. Flaked or crushed ice can be encased in a towel or plastic bag and placed over the site of the injury. Crushed ice is more effective in conforming to the body s contours. The bag should not contain air, which acts to insulate the area. Wet ice packs provide the best cooling properties. 2. In acute conditions, ice packs are best combined with rest, compression and elevation (RICE). RICE is the standard treatment for most athletic injuries. Elevation of an injured extremity higher than the heart, as well as compression of the tissues with an elastic wrap applied distal to proximal, can minimize edema by decreasing blood flow and pressure to the area. ii. Ice Massage 1. A paper cup or specially made commercial cup filled with water is frozen to form an ice cylinder that can be rubbed or massaged directly onto the skin surface. The ice is rubbed gently over the site of the injury until the skin becomes a bright pink in color, usually 7-10 minutes for a 5-square-inch area. Ice massage is commonly used over a small area. iii. Cold Water Immersion 1. A whirlpool tank, bucket, or other similar container is filled with a mixture of water and ice. The water temperature should be maintained between F. Immersion of the injured part lasts for minutes. 2. Cold water immersion is extremely effective in delivering cryotherapy to highly contoured areas of the body such as the hands, feet, and ankles. iv. Vapocoolant Sprays 1. Cold sprays use rapid evaporation of chemicals, usually chloromethane or fluoromethane, sprayed on the surface of the skin to freeze it. The effects of such sprays are temporary and superficial. 2. Cold sprays are used for the treatment of myofascial pain and trigger points, and are sometimes combined with stretching techniques to help break the pain-spasm cycle of soft tissue injuries. III. Thermotherapy a. Heat application is typically used with sub-acute injuries to increase blood flow and promote healing in the injured area. b. Heat has the opposite effect of cryotherapy in that it produces an immediate increase in circulation. Vasodilation occurs as the body attempts to shunt cooler blood to the warmed area to dissipate the heat. Unit 7 Therapeutic Modalities and Injury Rehabilitation 3 draft copy
4 c. A safe guideline for the progression to thermotherapy is to avoid heat until the active inflammatory process has ceased. The injured area should have pain-free range of motion, not be acutely painful, and show no increased signs of heat or swelling prior to thermotherapy application. If any of these signs are present, the injured part is not yet ready for heat treatments. d. The transmission of heat energy is through conduction, convection, radiation, and conversion. e. Physical Principles i. Conduction 1. Occurs when heat is transferred from a warmer object to a cooler one. The ratio of this heat exchange is dependent on the temperature and the exposure time. 2. To avoid tissue damage the temperature should never exceed 116 F. 3. Examples of conductive therapeutic modalities are moist hot packs, paraffin baths, and electric heating pads. ii. Convection 1. Refers to the transference of heat through the movement of fluids or gases. 2. Factors that influence convection heating are temperature, speed of movement and the conductivity of the part. 3. The best example of thermotherapy through convection is the whirlpool bath. iii. Radiation 1. The process whereby heat energy is transmitted through empty space; in other words, heat is transferred from one object through space to another object. 2. Infrared heating and ultraviolet therapies are used in sports medicine as radiation therapies. Radiation will not be discussed further in this course. iv. Conversion 1. Refers to the generation of heat from another energy form such as sound, electricity, and chemical agents. 2. Examples of conversion modalities are ultrasound therapy, diathermy, and chemical agents such as liniments and balms. f. Physiological Effects of Heat i. The body s response to heat depends on the type of heat energy applied, the intensity of the heat energy, the duration of the application, and the unique tissue response to heat. ii. Decreased muscle spasms. iii. Decreased pain perception. Both heat and cold relieve pain, stimulating the free nerve endings and peripheral nerves by a gating mechanism or secretion of endorphins. iv. Increased blood flow; heat causes vasodilation. Unit 7 Therapeutic Modalities and Injury Rehabilitation 4 draft copy
5 v. Increased metabolic rate. vi. Decreased joint stiffness. vii. Increased extensibility of collagen tissues by use prior to stretching exercises. In this respect, heat can lead to increased range of motion. viii. Increased general relaxation. g. Special Considerations i. In general, superficial heating of the skin is a safe, therapeutic medium, assuming of course, that the heat is kept at a reasonable intensity and application is not for too long a period. ii. Contraindications: 1. Never apply heat when there is a loss of sensation. 2. Never apply heat immediately after an injury. 3. Never apply heat when there is decreased arterial circulation. 4. Never apply heat directly to the eyes or to the genitals. 5. Never heat the abdomen during pregnancy. 6. Never apply heat to a malignancy. iii. Carefully monitor heat when applied to either elderly patients or infants who cannot report their reactions. h. Thermotherapy Methods i. Moist Heat Packs 1. Commercial moist heat packs, sometimes called Hydrocollator packs, heat by conduction. 2. Moist heat packs contain silicate gel in a cotton pad, which is immersed in thermostatically controlled hot water at a temperature of 170 F. Each pad retains water and a constant heat level for minutes. 3. Layers of toweling are used between the packs and the skin to avoid burning. As packs cool, remove layers of toweling to continue the heating. 4. Treat the area for minutes. 5. Deeper tissues, including muscles, are usually not significantly heated with moist heat packs because the heat transfer from the skin surface into deeper tissues is inhibited by subcutaneous fat, which acts as a thermal insulator. 6. While receiving the treatment, the patient should be in a comfortable, supported position. 7. Patients should not lie on the hot pack because pressure from their body weight can impede the circulation necessary to dissipate the accumulated heat. ii. Whirlpool Bath 1. The whirlpool is essentially a tank and a turbine motor, which regulates the movement of water and air. The whirlpool can be used with the water at any temperature (cold - 55 F, neutral F, warm F, or hot F). Unit 7 Therapeutic Modalities and Injury Rehabilitation 5 draft copy
6 2. The whirlpool provides both conduction and convection. Conduction is achieved by the skin s contacting the higher water temperature. As the water swirls around the skin surface, convection occurs. The circulating water also provides a hydromassage effect on the body part. 3. This medium assists the body part in reducing swelling, muscle spasm, and pain. Because of the buoyancy of the water, active movement of the part is also assisted. 4. Once the tank has been filled with water at the desired temperature, the patient is comfortably positioned so that the part to be treated can be easily reached by the agitating water. In many cases it is best that the water jet is not placed directly on the part but to the side of the tank. 5. The maximum length of treatment time for acute injuries should not exceed 20 minutes. A duration of 20 minutes is usually recommended for the treatment of chronic injuries. 6. Whirlpool units and tanks must be kept clean. Frequent water changes and daily cleaning are essential. Whirlpool management of open wounds or abrasions should be handled cautiously, ensuring that contamination or spreading of the infection to others is prevented. iii. Contrast Baths 1. Contrasting hot and cold water is a popular therapy in sports medicine. It is primarily used in the treatment of the extremities. 2. The contrast bath technique requires the use of two containers or tanks, one to hold hot water at F and one to hold cold water at F. A whirlpool can be used for the hot container, and a basin or bucket can be used for the cold. 3. The goal behind the use of the contrast bath is alternately to produce vasodilation from the hot water and vasoconstriction from the cold water. The hypothesis is that this procedure will increase local circulation in the treated limb. 4. The limb is first placed in the warm water for 5 minutes and then is alternated to the cold water for 1 minute. After the initial cycle, the patient alternates 4 minutes warm water with 1 minute cold water. Cycles can be performed for up to 30 minutes. iv. Paraffin Baths 1. Paraffin baths are of particular use in providing superficial heat to angular, bony areas of the body (hands, feet, wrists), while allowing the part to remain elevated. 2. A mixture of paraffin and mineral oil is kept at F in a thermostatically controlled unit. Unit 7 Therapeutic Modalities and Injury Rehabilitation 6 draft copy
7 3. With its high melting point and low heat conductivity, paraffin can provide sustained heat, increasing circulation and decreasing pain in the affected area. 4. Before therapy, the part to be treated is thoroughly cleaned and dried. Then the patient dips the affected part into the paraffin bath and quickly pulls it out, allowing the accumulated wax to dry and form a solid covering. The process of dipping and withdrawing is repeated until the wax coating is _ to _ inch thick. v. Ultrasound Therapy 1. Ultrasound uses high frequency sound waves beyond the audible range. Sound energy causes molecules in the tissues to vibrate, thus producing heat and mechanical energy mhz is the frequency most commonly used in ultrasound therapy as it affords the best compromise between therapeutic heating and deep penetration. A 3.3 mhz unit can also be used for treating structures with minimal soft tissue coverage. 3. Nerve tissue is twice as sensitive to ultrasound as muscle. 4. The thermal and mechanical effects of ultrasound augment circulation and promote healing. Ultrasound is reported to raise tissue temperature 7-8 F up to 2 inches below the skin s surface, with little or no change in skin temperature. Along with the thermal benefits, the energy also provides a micromassaging action on the cells. 5. Ultrasound can be produced in a pulsed or continuous manner. a. Pulsed treatment produces primarily nonthermal effects due to interrupted flow and thus less total energy. It is used primarily in sub acute conditions, with wound healing and over bony areas. b. Continuous ultrasound provides both thermal and nonthermal responses. 6. Indications for ultrasound include: a. Post-acute soft tissue trauma b. Bursitis c. Tendinitis d. Fasciitis 7. Contraindications include: a. Treatment of acute inflammatory conditions with the continuous mode. b. Treatment over areas with limited vascularity or sensation. Unit 7 Therapeutic Modalities and Injury Rehabilitation 7 draft copy
8 c. Treatment over the ears, eyes, heart, reproductive organs, endocrine glands, central nervous system, or open epiphyses. 8. Because acoustic energy cannot travel through air and is reflected by the skin, there must be a coupling medium, such as lotion, gel, or water, applied to the skin. Treatment can also be given under water when the treatment surface is highly contoured. The purpose of a coupling medium is to provide an airtight contact with the skin and a slick, frictionproof surface to glide over. 9. The transducer (sound head) should be kept moving in small circles or longitudinal strokes at a speed of 1-2 inches per second. The sound head should be perpendicular to the body, and steady pressure should be applied. 10. Treatment time is 5 minutes for an area three to four times the size of the sound head. The intensity of the treatment is determined by the stage of injury, mode of transmission, and depth of the target tissues. 11. For underwater application, the body part is fully submerged in water; then the ultrasound head is submerged and positioned approximately _ -1 inch from the body part to be treated. The water medium provides an airtight coupling, allowing sound waves to travel at a constant velocity. The sound head is moved slowly in a circular or longitudinal pattern, while not actually coming in contact with the skin. vi. Phonophoresis 1. A method of driving molecules through the skin by ion transfer or by the mechanical vibration of the ultrasound. 2. It is designed to move an entire molecule of medication into injured tissues. Predominantly, hydrocortisone and an anesthetic are used with success in treating painful trigger points, tendonitis, and bursitis. 3. The medication should be massaged into the skin over the treatment area. The coupling gel is then spread over the medication and the ultrasound is applied. 4. Phonophoresis treatment is generally of lower intensity but longer duration than standard ultrasound therapy. IV. Electrotherapy a. In athletic injury care, the primary purposes of electrical stimulation are to control pain, exercise muscle tissue to decrease atrophy, encourage circulation, increase tissue temperature, encourage the breakdown of adhesions, and reeducate muscles. b. Physical Principles i. Electricity is a form of energy that displays magnetic, chemical, mechanical, and thermal effects on tissue. Unit 7 Therapeutic Modalities and Injury Rehabilitation 8 draft copy
9 ii. Instruments used for electrotherapy produce varying waveforms, depending on the capabilities of the generator. Waveform refers to the shape, direction, amplitude, and duration of a particular electrical current. 1. Direct current (DC) flows in one direction, with electrons moving from a negative to a positive pole. The first sensation the body experiences from direct current is one of tingling, followed by a feeling of warmth. Direct current is used to cause chemical reactions, increase blood flow and decrease swelling, spasm and pain. Muscle reeducation is also accomplished using direct current. 2. Alternating current (AC) refers to the flow of electrons that reverses direction once each cycle. iii. Special Considerations 1. Contraindications for electrical stimulation include: a. Pacemakers. b. Pregnancy. c. Never use electrotherapy when muscular contractions are not wanted, such as nonunited fractures, areas of active bleeding, and near malignancies. iv. Electrotherapy Methods 1. In electrotherapy, moist electrode pads are fixed directly to the skin. The smaller active pad, which brings current to the body, can range from very small to 4 inches square. The larger dispersal pad, from which electrons leave the body, should be as large as possible. 2. The closer the pads are, the shallower and more isolated the muscle contraction. The farther apart the pads are, the deeper and the more generalized the contraction. 3. Active exercising can be used while the muscles are being electrically stimulated. 4. Other therapies can be effectively combined with electrical stimulation such as ice pack treatments, cold water immersion or ultrasound. v. Iontophoresis 1. The process whereby chemical ions are transported through the intact skin by an electrical current. The polarity of the electrode used depends the polarity of the ion introduced. 2. The most commonly used medications for iontophoresis are hydrocortisone and salicylates. 3. The patient should not experience discomfort or a burning sensation while receiving the treatment. 4. Treatment times are minutes, once a day. Unit 7 Therapeutic Modalities and Injury Rehabilitation 9 draft copy
10 V. Mechanical Therapy a. Mechanical or manual therapies include the direct use of the provider s hands. b. Mechanical therapies are most often used in conjunction with, or as a supplement to, other methods of treatment. c. Massage i. One of the oldest modalities, massage is the systematic and scientific manipulation of the body s soft tissue. ii. Massage is most often used as an adjunct in treating post acute soft tissue trauma and strains. iii. The therapeutic effects of massage include 1. Stimulating cell metabolism. 2. Increasing venous flow and lymphatic drainage. 3. Increasing circulation and nutrition. 4. Stretching superficial scar tissue. 5. Relaxing muscle tissues. iv. Contraindications include 1. Areas of acute injuries, hemorrhaging, infection, thromboses, nerve damage, skin disease, and the possibility of calcification. v. Physiological Effects of Massage 1. The effects of massage are both mechanical and reflexive. 2. Mild stretching of scar and superficial tissue is its major mechanical effect. 3. Reflexive effects include stimulation and relaxation of the tissues. vi. Massage Methods 1. Basic massage techniques include a. Effleurage: superficial or deep stroking with the heels and palms of the hands gliding over the body. b. Pétrissage: kneading; a technique in which the soft tissue, held between the thumb and forefinger, is alternately rolled, lifted, and twisted to loosen tissue. c. Tapotement: consists of cupping, hacking, pincing, and percussive movements. d. Vibration: trembling, forward and backward movement; the rapid shaking of tissue by hand or using a machine vibrator. e. Friction: pressure across muscles or tendons; used successfully on joints and in areas in which there is little soft tissue. The fingers and thumbs move in circular patterns, stretching the underlying tissue and thus increasing circulation to the part. 2. Generally, lubricants such as oil, lanolin, lotion, or powder should be used during massage therapy. Unit 7 Therapeutic Modalities and Injury Rehabilitation 10 draft copy
11 3. Stroking toward the heart is also recommended to increase and promote venous return and to reduce swelling in the injured areas. 4. Proper positioning for massage is of great importance. The injured part must be made easily accessible; the athlete must be comfortable, and the part to be massaged must be relaxed. 5. Lack of confidence in the person doing the massage is easily transmitted through inexperienced hands. Every effort should be made to think out the procedure to be used and to present a confident appearance to the patient. d. Manipulation Therapy i. Also called manual therapy or joint mobilization, manipulation is the mobilization of joints and soft tissues to allow proper functioning of a body part. All movement is passive on the part of the patient. ii. Joint mobilization is based on the concepts of joint play the gliding and rolling of one joint surface on another that is necessary for normal joint function. iii. At no time should a provider attempt manipulation without education and practice under nonpathological conditions. VI. Rehabilitation is defined as restoration to a functional level for daily living and the return to an appropriate level of competitive fitness. a. Each rehab program must be individualized and influenced by: i. Severity of injury. ii. Stage of tissue healing. iii. Type of treatment (surgery precautions and restrictions). iv. Strength of the muscles of the limb. v. Pain on motion of the joint. vi. Joint swelling. vii. Other conditions within the joint. viii. Sport specific demands. b. Rules of rehabilitation i. Create an environment for optimal healing. ii. Do no harm. iii. Be as aggressive as you can without doing harm. iv. If it hurts, don t do it. c. Goals of rehabilitation i. Vigorous, intense, but controlled exercise allowing return to participation, ensuring that the injured part is as optimally conditioned as possible. ii. Restoration of function to the greatest possible degree in the shortest possible time. iii. Goals must be realistic and reachable: 1. Increase ROM. 2. Increase strength. Unit 7 Therapeutic Modalities and Injury Rehabilitation 11 draft copy
12 3. Increase joint mobility. 4. Increase endurance. 5. Encourage relaxation. 6. Enhance coordination and skill. 7. Decrease pain. 8. Improve function. 9. Minimize atrophy and deconditioning. 10. Improve technique, posture and mechanics. 11. Decrease inflammation and swelling. 12. Improve motor control. 13. Improve joint stability. 14. Prevent re-injury. d. Equipment i. There are many pieces of specialized equipment on the market that are very useful. ii. It is possible to use little or no equipment and still obtain adequate results if the program is carefully and knowledgably designed for a particular athlete s needs and if the athlete is adequately motivated and supervised. iii. Having the most expensive machinery will not guarantee results if there is an inadequate program, little motivation, or poor supervision. e. Psychology of rehabilitation i. Rehab is 75% psychological and 25% physical. ii. Rapport with athlete is critical (motivation and communication). iii. Help athlete deal with fear, anger, depression, self-doubt, motivation. iv. Use a wide variety of exercises to achieve the same results and avoid boredom. v. Involve injured athlete with team as much as possible including functions, meetings, and practice. f. Components of rehabilitation program i. Program must be progressive so that an increasing amount of work is performed at each session (as long as predetermined limits and limits of discomfort are not exceeded). ii. Correct form with each exercise should be constantly stressed in order to maximize the results and prevent injury. iii. Strength. iv. Speed. v. Endurance. vi. Flexibility. vii. Proprioception. viii. Sport specific skills (functional return to sport). Unit 7 Therapeutic Modalities and Injury Rehabilitation 12 draft copy
13 g. Common mistakes in rehabilitation i. Look for the culprit, not the victim. ii. Focused only on a single muscle group all muscles of the injured limb need to be exercised, concentrating on those that are weaker. iii. Seldom continued until the injured limb is equal or superior to the uninjured side. iv. Proprioception is often forgotten. v. Postural defects, anatomical malalignment and biomechanical imbalances are neglected. vi. Sport specific skills and the SAID principle are not incorporated. VII. Types of Exercises a. Isometric i. Does not result in any movement of the joint. ii. Often performed against a fixed resistance. iii. The least effective form of strength improvement. iv. Isometric exercise is said to be static since a definite force is exerted by no actual movement of the muscle involved. v. Examples wall press, stationary press. b. Isotonic i. A joint is moved through a range of motion against the resistance of a fixed weight. ii. The resistance is fixed and the speed is variable. iii. Isotonic exercise is said to be dynamic since definite and easily discerned movement takes place. 1. The greatest strength gain takes place in the initial movement of the muscle as it attempts to overcome the resistance. 2. The least gain is at the mid-point. iv. Examples bench press, arm curls, squats, heel raises. c. Isokinetic i. Exercise with accommodating variable resistance in which the speed of the motion is set and the resistance accommodates to match the force applied. ii. The maintenance of a constant velocity during a dynamic contraction. iii. An advantage is that visual readouts are possible which not only helps evaluate progress but also seems to act as a powerful psychological stimulus for the athlete. iv. Disadvantage is the cost of isokinetic machines. d. Plyometrics i. A variety of exercises that utilize explosive movements to increase athletic power. Unit 7 Therapeutic Modalities and Injury Rehabilitation 13 draft copy
14 ii. Plyometric exercise maximized the stretch reflex. By means of an eccentric (lengthening) contraction, the muscle is fully stretched ( on stretch ) immediately preceding the concentric (shortening) contraction. The greater the stretch put on the muscle from its resting length immediately before the concentric contraction, the greater the load the muscle can lift or overcome. The rate of stretch is more critical than the magnitude of the stretch. iii. Commonly performed plyometric exercises include power jumps, leaps or bounds, and throwing a weighted object such as a medicine ball or weighted baseball. iv. These exercises should not be performed on a daily basis but rather 2-3 days per week in order to allow proper muscular recovery from fatigue. v. Athletes who have a current injury should avoid plyometric exercises. Only after the athlete has attained strength adequate to perform such exercise with stability should plyometrics be added into the rehabilitation program. e. Manual Resistance i. A form of exercise in which the provider adjusts the speed of movement and resistance to that best suited to the athlete s needs at the particular moment, which will vary according to the stage of rehabilitation and the state of fatigue. f. Concentric Contraction i. Positive work. ii. Muscle shortens as the weight is lifted. g. Eccentric Contraction i. Negative work. ii. Muscle lengthens or is forcibly stretched while the weight is lowered. iii. Appears to effect a greater gain in strength but is also more stressful often resulting in muscle soreness. h. Open Chain i. Distal segment is not fixed and is freely moving in space. ii. Functional for upper extremity. iii. Examples: 1. Leg extension. 2. Leg flexion. 3. Abduction/Adduction exercise machines. 4. Functional activities throwing, jumping, etc. i. Closed Chain i. Distal segment is fixed. ii. Functional for lower extremity. iii. Examples: 1. Standing leg press with sport cord. 2. Lunges with or without a sport cord. 3. BAPS board. Unit 7 Therapeutic Modalities and Injury Rehabilitation 14 draft copy
15 4. Slide board. 5. Body blades. 6. Therapy balls. VIII. Phases of Rehabilitation a. Phase I Acute (first hours). i. Symptoms are redness, heat, swelling, pain, inflammation, loss of function. ii. Short term goals 1. Decrease pain. 2. Decrease swelling and inflammation. 3. Increase ROM. 4. Maintain cardiovascular conditioning. 5. Control pain. iii. Emphasis on cardiovascular fitness (ex: bike, rowing, stairclimber, treadmill not using affected limb). iv. Isometric contractions if joint is immobilized. v. Exercising the opposite unaffected limb may provide a cross-over reaction and maintain the muscles of the opposite limb. vi. Muscle stimulation. vii. RICE used to control swelling. b. Phase II Sub acute (72 hours to about 2 weeks). i. Inflammation is decreasing and tissue is being repaired. ii. Begins as soon as pain and swelling are controlled and complete immobilization is no longer necessary. iii. Short term goals 1. Reach full range of motion. 2. Increase muscle strength, power and endurance in all muscle groups. 3. Maintain cardiovascular endurance levels and pre-injury strength of all areas unaffected by the injury. 4. Begin proprioception training. iv. Warming up the area prior to attempting exercise and range of motion work will allow the tissues and muscles to respond more effectively. v. Ice the injured area after working it to prevent secondary swelling or effusion. vi. Amount of time needed for tissue repair is based on several factors 1. Degree and location of injury. 2. Presence of infection. 3. Age of athlete. 4. Athlete s nutritional status. 5. Medical problems such as diabetes. 6. Medications taken. 7. Use of corticosteroids. Unit 7 Therapeutic Modalities and Injury Rehabilitation 15 draft copy
16 c. Phase III Intermediate (up to six months). i. Tissue is repairing, changing and remodeling to restore function. ii. Prepare for specific functional exercises including open chain and closed chain work. iii. Ensure that the athlete s normal biomechanical function has been restored. iv. Restore balance and proprioception. v. Increasing intensity while decreasing frequency of exercise. d. Phase IV Return to Sport, Maturation (up to one year). i. Preparatory phase for returning the athlete to activity. ii. Analysis of sport technique, especially for the athlete who has sustained an overuse injury. iii. Correction of any biomechanical imbalances. iv. Evaluate for protective taping, bracing, padding, etc. These devices do not take the place of a maintenance rehabilitation program. IX. Example a. Ankle Sprain i. Rehabilitation following ankle sprains should emphasize strengthening the musculotendinous structures that surround the ligamentous injury. To regain normal function in an ankle that has been sprained, it is important to combine strengthening, flexibility, and proprioceptive activities. ii. Phase I 1. Modalities as appropriate. 2. Alphabet writing: Write the alphabet, using the big toe as the pen. Create the letters by using ankle motion rather than lower leg motion. 3. Towel stretches: Place a towel under the foot. Holding the ends of the towel to provide to assistance, perform the following movements: a. Pull the foot up into dorsiflexion. b. Push the foot down into plantar flexion. c. Pull the foot up and out into eversion. d. Pull the foot up and in to inversion. e. Do 3 sets of 10 for each movement. 4. Isometrics: Gentle strengthening can be accomplished through isometrics using the hand or uninjured foot to provide resistance. Make an isometric contraction by resisting the normal ankle movements of dorsiflexion, plantar flexion, eversion, and inversion. Hold each contraction for 10 seconds. Unit 7 Therapeutic Modalities and Injury Rehabilitation 16 draft copy
17 iii. Phase II 1. Modalities as appropriate. 2. Isotonics: Only perform when these exercises are not painful. These exercises can be done with surgical tubing, Theraband, an old bicycle tube, or an elastic bandage. Use the elastic as resistance as you move in all directions of normal ankle movements. Work up to 3 sets of 10 repetitions. The tubing should be taut and the heel should remain on the floor. The ankle is what moves not the entire lower leg. 3. Functional balancing: balance on one leg for 10 seconds with eyes open; repeat 10 times. Balance on one leg for 10 seconds with eyes closed; repeat 10 times. Walk heel to toe for 5 yards, 10 times with eyes open. Walk heel to toe for 5 yards, 10 times with eyes closed. 4. Calf raises: Stand on a flat surface, with weight evenly distributed. Raise your heels off the floor as high as possible, using your own body weight as resistance. Work up to 3 sets of 10 repetitions. Gradually shift weight to the injured foot, performing the calf raises on this leg only. Weight can be added to the shoulders to extend the effectiveness of this exercise. iv. Phases III & IV 1. The athlete should gradually work back into normal functional activities as well as sport specific activities. 2. It may be necessary, especially during athletic activities, for the athlete to wear protective equipment (taping or bracing) on the ankle for several months after injury. X. General Conditioning Principles a. The athlete who participates in a well-devised, scientifically based, and properly supervised athletic physical conditioning program should benefit in at least four areas: i. Enhanced athletic performance. ii. Decreased risk of injury. iii. Decreased severity should an injury occur. iv. Accelerated rehabilitation and return to activity after an injury. b. Overload i. To facilitate improvement, the system involved must be progressively and gradually challenged or placed under additional stress. Unit 7 Therapeutic Modalities and Injury Rehabilitation 17 draft copy
18 ii. Depending upon the component of conditioning being challenged, overload might be implemented by increasing the: 1. Resistance. 2. Repetitions or sets. 3. Rate (intensity) of work or exercise. 4. Duration of work or exercise. iii. A training load or a conditioning level should be used so that the workload is difficult enough that the final set is difficult to complete. c. SAID Principle (Specific Adaptations to Imposed Demands) i. Also known as specificity. ii. The effects of the conditioning program are specific to the type of stress applied and to the particular system of the body that is exercised. iii. If the body is placed under stress of varying intensities and durations, it attempts to overcome the stress by adapting specifically to the imposed demands (Allman, FL 1974). iv. While it is important to overload or place demands on the body so that improvement may occur, the stress should not be so severe as to prevent the body from being able to cope or adapt. XI. Joint Flexibility a. Flexibility is defined as the range of motion at a specific joint that is, the capacity of a muscle to lengthen or stretch. Abnormally tight muscles can alter form, thus reducing biomechanical efficiency and creating a climate for athletic injuries, particularly muscle strains and tendonitis. b. Appropriate stretching techniques increase the flexibility of tissues. c. Stretching techniques can be performed statically either actively or passively. i. Static stretch consists of stretching muscle tissue to a comfortable position and holding this position for a period of time. The effectiveness of static stretch depends on the intention and time of the actual stretch. 1. Each exercise should be taken to the point of tightness and slightly beyond. 2. For safety purposes, emphasis should be on proper form, and no motion should be forced. 3. All exercises should be held for 5 seconds (counting one thousand one, one thousand two, one thousand three, one thousand four, one thousand five ). 4. When in doubt, less tension and more time are best 1 to 2 minutes for each muscle group at 15 second intervals. 5. Normal breathing should take place during the stretch. ii. Active static stretch is performed without assistance from an outside force. Unit 7 Therapeutic Modalities and Injury Rehabilitation 18 draft copy
19 iii. Passive static stretch utilizes an outside force to assist in regaining full range of motion. Passive static stretch is performed in specific situations in the therapeutic environment with a trained provider. Caution and care must be taken by the provider when doing the actual stretch. d. Stretching should be performed after the athlete has warmed up. In colder climates, the warm-up period may need to be extended. e. Stretching exercises should also be repeated as the athlete cools down. f. The entire stretching program should take no longer than 10 minutes. g. Athletes, coaches and sports medicine professionals should choose specific stretching exercises that are not only comfortable and effective but also comprehensive in stretching each of the muscles groups. Unit 7 Therapeutic Modalities and Injury Rehabilitation 19 draft copy
Unit 9 MODALITIES AND REHABILITATION Lecture Guide
 Unit 9 MODALITIES AND REHABILITATION Lecture Guide Therapeutic Modalities What are they? Therapeutic= Modality= Many different modalities to choose from- selection is dependant on: Smaller, slower nerve
Unit 9 MODALITIES AND REHABILITATION Lecture Guide Therapeutic Modalities What are they? Therapeutic= Modality= Many different modalities to choose from- selection is dependant on: Smaller, slower nerve
Unit 9 MODALITIES AND REHABILITATION Lecture Notes
 Unit 9 MODALITIES AND REHABILITATION Lecture Notes THERAPEUTIC MODALITIES Objective 1: Explore Therapeutic Modalities I. Introduction A. Create an optimum environment for injury healing by reducing pain,
Unit 9 MODALITIES AND REHABILITATION Lecture Notes THERAPEUTIC MODALITIES Objective 1: Explore Therapeutic Modalities I. Introduction A. Create an optimum environment for injury healing by reducing pain,
Unit 9 MODALITIES AND REHABILITATION Mobility Worksheet
 Unit 9 MODALITIES AND REHABILITATION Mobility Worksheet Name Period The selection of specific treatments is based on a variety of factors list four: What is the protocol for RICE? What are the purposes
Unit 9 MODALITIES AND REHABILITATION Mobility Worksheet Name Period The selection of specific treatments is based on a variety of factors list four: What is the protocol for RICE? What are the purposes
Beginning Athletic Medicine. Non-Penetrating Therapy
 Beginning Athletic Medicine Non-Penetrating Therapy Therapeutic Modalities What are they? Therapeutic= something that promotes healing and injury repair Modality= the method of application of any therapeutic
Beginning Athletic Medicine Non-Penetrating Therapy Therapeutic Modalities What are they? Therapeutic= something that promotes healing and injury repair Modality= the method of application of any therapeutic
Chapter 23 Unit 28. Therapeutic Modalities
 Chapter 23 Unit 28 Therapeutic Modalities Chapter Objectives Discuss the purpose of therapeutic modalities Explain the legal implications associated with the use of therapeutic modalities List the different
Chapter 23 Unit 28 Therapeutic Modalities Chapter Objectives Discuss the purpose of therapeutic modalities Explain the legal implications associated with the use of therapeutic modalities List the different
Introduction to Physical Agents Part II: Principles of Heat for Thermotherapy
 Introduction to Physical Agents Part II: Principles of Heat for Thermotherapy Mohammed TA, Omar momarar@ksu.edu.sa Dr.taher_m@yahoo.com Mobile : 542115404 Office number: 2074 Objectives After studying
Introduction to Physical Agents Part II: Principles of Heat for Thermotherapy Mohammed TA, Omar momarar@ksu.edu.sa Dr.taher_m@yahoo.com Mobile : 542115404 Office number: 2074 Objectives After studying
FREE CPE OPPORTUNITY
 FREE CPE OPPORTUNITY Knowledge of Classical Massage Movements CHALLENGE Complete all Questions In the workbook exam paper attached Send in your Answers office@maa.org.au Collect 20 CPE Points for 90% -
FREE CPE OPPORTUNITY Knowledge of Classical Massage Movements CHALLENGE Complete all Questions In the workbook exam paper attached Send in your Answers office@maa.org.au Collect 20 CPE Points for 90% -
Caring For Your Lateral Ankle Middlebury College
 Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Hands on Sports Therapy KNOWLEDGE REVIEW QUESTIONS 2004 Thomson Learning. Q1: List 10 general but crucial safety factors relating to the use of
 CHAPTER 10 Knowledge Review Q1: List 10 general but crucial safety factors relating to the use of electrical therapy equipment. A1: Safety factors relating to the use of electrical therapy equipment include:
CHAPTER 10 Knowledge Review Q1: List 10 general but crucial safety factors relating to the use of electrical therapy equipment. A1: Safety factors relating to the use of electrical therapy equipment include:
Performance Enhancement. Strength Training
 Performance Enhancement Strength Training Muscle Fiber type & Performance Slow twitch More efficient using oxygen to generate fuel for continuous extended muscle contractions Contract slowly, but continue
Performance Enhancement Strength Training Muscle Fiber type & Performance Slow twitch More efficient using oxygen to generate fuel for continuous extended muscle contractions Contract slowly, but continue
Movements in massage. Effleurage. Effleurage To skim over Superficial Effleurage Deep effleurage
 Movements in massage Effleurage Effleurage To skim over Superficial Effleurage Deep effleurage The whole palm of the hands placed on the area being treated The fingers are close together It is a link movement.
Movements in massage Effleurage Effleurage To skim over Superficial Effleurage Deep effleurage The whole palm of the hands placed on the area being treated The fingers are close together It is a link movement.
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
CERVICAL STRAIN AND SPRAIN
 CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN (Whiplash)
 CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Ankle Rehabilitation with Wakefield Sports Clinic
 Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Manual Therapy Techniques
 Manual Therapy Techniques manual therapy: the use of hands-on techniques to evaluate, treat, and improve the status of neuromusculoskeletal conditions massage: the systematic and scientific manipulation
Manual Therapy Techniques manual therapy: the use of hands-on techniques to evaluate, treat, and improve the status of neuromusculoskeletal conditions massage: the systematic and scientific manipulation
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
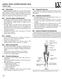 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
BICEPS TENDON TENDINITIS (PROXIMAL) AND TENOSYNOVITIS
 BICEPS TENDON TENDINITIS (PROXIMAL) AND TENOSYNOVITIS Description Proximal biceps tendon tendinitis and tenosynovitis is characterized by pain at the front of the shoulder and upper arm caused by inflammation
BICEPS TENDON TENDINITIS (PROXIMAL) AND TENOSYNOVITIS Description Proximal biceps tendon tendinitis and tenosynovitis is characterized by pain at the front of the shoulder and upper arm caused by inflammation
ANTERIOR ANKLE IMPINGEMENT
 ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
ANKLE SPRAIN, ACUTE. Description
 Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Suprascapular Nerve Entrapment
 Suprascapular Nerve Entrapment Suprascapular nerve entrapment is an uncommon nerve condition in the shoulder, causing pain and weakness. It involves compression of the suprascapular nerve at the top or
Suprascapular Nerve Entrapment Suprascapular nerve entrapment is an uncommon nerve condition in the shoulder, causing pain and weakness. It involves compression of the suprascapular nerve at the top or
When to Use Cold or Heat Therapy
 www.amazon.com/shops/reliablemedicalsupply When to Use Cold or Heat Therapy Instructions for Cold Therapy, also known as Cryotherapy For Acute Injuries, when you have sharp, stabbing or shooting pain,
www.amazon.com/shops/reliablemedicalsupply When to Use Cold or Heat Therapy Instructions for Cold Therapy, also known as Cryotherapy For Acute Injuries, when you have sharp, stabbing or shooting pain,
WRIST SPRAIN. Description
 WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
Dr. Abigail R. Hamilton, MD
 ACHILLES TENDINITIS Dr. Abigail R. Hamilton, MD ANATOMY The Achilles tendon is a strong tendon that connects the calf muscles to the heel. When the calf muscles contract, they pull on the Achilles tendon
ACHILLES TENDINITIS Dr. Abigail R. Hamilton, MD ANATOMY The Achilles tendon is a strong tendon that connects the calf muscles to the heel. When the calf muscles contract, they pull on the Achilles tendon
Source: Physical Agents in Rehabilitation from Research to Practice, 4 th edition, by Michelle Cameron.
 Online Continuing Education Courses AOTA Approved Provider #4023 www.onlinece.com Course Title: Therapeutic Modalities 101 Course Subtitle: Physical Agents in Rehabilitation Source: Physical Agents in
Online Continuing Education Courses AOTA Approved Provider #4023 www.onlinece.com Course Title: Therapeutic Modalities 101 Course Subtitle: Physical Agents in Rehabilitation Source: Physical Agents in
ANTERIOR KNEE PAIN. Explanation. Causes. Symptoms
 ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
ANTERIOR KNEE PAIN Explanation Anterior knee pain is most commonly caused by irritation and inflammation of the patellofemoral joint of the knee (where the patella/kneecap connects to the femur/thigh bone).
2006 Back to The Basics Strength and Conditioning Clinic. Warm Ups and Flexibility
 2006 Back to The Basics Strength and Conditioning Clinic Warm Ups and Flexibility Building the complete athlete Strength Training and Core Development Plyometric Training Speed and Agility Flexibility
2006 Back to The Basics Strength and Conditioning Clinic Warm Ups and Flexibility Building the complete athlete Strength Training and Core Development Plyometric Training Speed and Agility Flexibility
ANKLE SPRAINS. Explanation. Causes. Symptoms
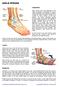 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
MENISCUS TEAR. Description
 MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
MENISCUS TEAR Description Expected Outcome The meniscus is a C-shaped cartilage structure in the knee that sits on top of the leg bone (tibia). Each knee has two menisci, an inner and outer meniscus. The
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS. Please check with the LCC bookstore for the required texts for this class.
 LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
LABETTE COMMUNITY COLLEGE BRIEF SYLLABUS SPECIAL NOTE: This brief syllabus is not intended to be a legal contract. A full syllabus will be distributed to students at the first class session. TEXT AND SUPPLEMENTARY
Everything. You Should Know. About Your Ankles
 Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Proximal Hamstring Tendon Repair
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Proximal Hamstring Tendon Repair The hamstrings are a group
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Proximal Hamstring Tendon Repair The hamstrings are a group
Treating the Ankle Sprain
 Treating the Ankle Sprain Ankle 'sprains' are very common injuries. Typically the ankle is rolled either inward (inversion sprain) or outward (eversion sprain). Inversion sprains cause pain along the outside
Treating the Ankle Sprain Ankle 'sprains' are very common injuries. Typically the ankle is rolled either inward (inversion sprain) or outward (eversion sprain). Inversion sprains cause pain along the outside
TIBIAL PLATEAU FRACTURE
 TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
TIBIAL PLATEAU FRACTURE Description Preventive Measures A tibial plateau fracture is a complete or incomplete break Appropriately warm up and stretch before practice or in the larger of the two leg bones
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN Tel: Fax:
 Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
What is arthroscopy? Normal knee anatomy
 What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
What is arthroscopy? Arthroscopy is a common surgical procedure for examining and repairing the inside of your knee. It is a minimally invasive surgical procedure which uses an Arthroscope and other specialized
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol:
 Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
RIB FRACTURE. Explanation. Causes. Symptoms. Diagnosis
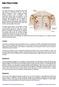 RIB FRACTURE Explanation The heart and lungs are encased by the chest wall, which is composed of the ribs. The ribs must be flexible in order to allow movement during expansion and contraction. This movement
RIB FRACTURE Explanation The heart and lungs are encased by the chest wall, which is composed of the ribs. The ribs must be flexible in order to allow movement during expansion and contraction. This movement
PDHPE HSC Enrichment Day 2011 Option 3
 PDHPE HSC Enrichment Day 2011 Option 3 Sports Medicine Rehabilitation Process Syllabus Focus Area From the Syllabus: Learn About: Learn To: rehabilitation procedures progressive mobilisation graduated
PDHPE HSC Enrichment Day 2011 Option 3 Sports Medicine Rehabilitation Process Syllabus Focus Area From the Syllabus: Learn About: Learn To: rehabilitation procedures progressive mobilisation graduated
WELLNESS UPDATE 2001, #1 THE PROPER TREATMENT OF ATHLETIC INJURIES
 WELLNESS UPDATE 2001, #1 THE PROPER TREATMENT OF ATHLETIC INJURIES There are three common errors coaches make in treating athletic injuries: 1) not referring the athlete to a physician or other health
WELLNESS UPDATE 2001, #1 THE PROPER TREATMENT OF ATHLETIC INJURIES There are three common errors coaches make in treating athletic injuries: 1) not referring the athlete to a physician or other health
72a Orthopedic Massage: Introduction!
 72a Orthopedic Massage: Introduction! 72a Orthopedic Massage: Introduction! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10 minutes Lecture: 25 minutes Lecture: 15 minutes Active
72a Orthopedic Massage: Introduction! 72a Orthopedic Massage: Introduction! Class Outline 5 minutes Attendance, Breath of Arrival, and Reminders 10 minutes Lecture: 25 minutes Lecture: 15 minutes Active
Effective Date: 01/01/2014 Revision Date: Administered by:
 ARBenefits Approval: Effective Date: 01/01/2014 Revision Date: Administered by: Medical Policy Title: Physical and Occupational Therapy Services Document: ARB0476 Public Statement: 1) Physical and occupational
ARBenefits Approval: Effective Date: 01/01/2014 Revision Date: Administered by: Medical Policy Title: Physical and Occupational Therapy Services Document: ARB0476 Public Statement: 1) Physical and occupational
August 2015 Newsletter
 1 August 2015 Newsletter www.coretherapy.co.uk CONTENTS: Stretch of the month Exercise of the month Education Section: Where have I been? STRETCH OF THE MONTH Overdeveloped and tight hip flexors can contribute
1 August 2015 Newsletter www.coretherapy.co.uk CONTENTS: Stretch of the month Exercise of the month Education Section: Where have I been? STRETCH OF THE MONTH Overdeveloped and tight hip flexors can contribute
HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY
 HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY EDMONTON BREWERY DISTRICT DOWNTOWN Edmonton s First Boutique Physiotherapy Clinic WHAT SETS US APART? NO ATHLETE IS TRULY TESTED UNTIL THEY VE STARED INJURY
HIGH PERFORMANCE CENTRE FOR SPORTS RECOVERY EDMONTON BREWERY DISTRICT DOWNTOWN Edmonton s First Boutique Physiotherapy Clinic WHAT SETS US APART? NO ATHLETE IS TRULY TESTED UNTIL THEY VE STARED INJURY
Foot and Ankle Conditioning Program
 Foot and Ankle Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Foot and Ankle Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle.
Modalities in physiotherapy
 Learning Guide Modalities in physiotherapy 27466 Apply modalities in physiotherapy as a health assistant Level 4 6 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved. Careerforce
Learning Guide Modalities in physiotherapy 27466 Apply modalities in physiotherapy as a health assistant Level 4 6 credits Name: Workplace: Issue 2.0 Copyright 2017 Careerforce All rights reserved. Careerforce
ILIOTIBIAL BAND SYNDROME
 Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Dr. S. Matthew Hollenbeck, MD Kansas Orthopaedic Center, PA 7550 West Village Circle, Wichita, KS 67205 2450 N Woodlawn, Wichita, KS 67220 Phone: (316) 838-2020 Fax: (316) 838-7574 Description ILIOTIBIAL
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Session 3 or 6: Being Active: A Way of Life.
 Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
Session 3 or 6: Being Active: A Way of Life. You can find the time to be active. Set aside one block of time every day to be active. When can you set aside 20 to 30 minutes to do an activity you like?
Iliotibial (IT) Band Syndrome
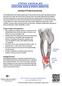 Iliotibial (IT) Band Syndrome The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon passes
Iliotibial (IT) Band Syndrome The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the front of the leg. Where the tendon passes
ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An IPRS Guide to provide you with exercises and advice to ease your condition
 Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
Post-op / Pre-op Page (ALREADY DONE)
 Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
Post-op / Pre-op Page (ALREADY DONE) We offer individualized treatment plans based on your physician's recommendations, our evaluations, and your feedback. Most post-operative and preoperative rehabilitation
NICHOLAS J. AVALLONE, M.D.
 NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
POSTERIOR TIBIAL TENDON RUPTURE
 POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
Shortwave Diathermy. Objectives. What is Shortwave Diathermy? What is Shortwave Diathermy? Physiological Responses
 Shortwave Diathermy http://www.rehaboutlet.com/images/me300.jpg Michael Banes Deep Bhavsar Ryan Machuca ATPE 414 11/6/05 http://www.btlnet.com/imgen/shortwave.jpg Objectives To learn what shortwave diathermy
Shortwave Diathermy http://www.rehaboutlet.com/images/me300.jpg Michael Banes Deep Bhavsar Ryan Machuca ATPE 414 11/6/05 http://www.btlnet.com/imgen/shortwave.jpg Objectives To learn what shortwave diathermy
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Does not print for diecut only
 Does not print for diecut only Treat Pain and Accelerate Healing with the Revolutionary ReBound Therapeutic Warming System. ReBound utilizes technology originally developed by the US Navy to warm SEAL
Does not print for diecut only Treat Pain and Accelerate Healing with the Revolutionary ReBound Therapeutic Warming System. ReBound utilizes technology originally developed by the US Navy to warm SEAL
leisure or sport skills living activities and other activities with vigor Ø Physical fitness: ability of the body to respond to physical demands
 LEARNING OBJECTIVES Ø Discuss benefits and guidelines of physical activity and exercise Ø Explain the components of health-related fitness Ø Explain how to improve health through moderate physical activity
LEARNING OBJECTIVES Ø Discuss benefits and guidelines of physical activity and exercise Ø Explain the components of health-related fitness Ø Explain how to improve health through moderate physical activity
Sky Ridge Medical Center, Aspen Building Ridgegate Pkwy., Suite 309 Lone Tree, Colorado Office: Fax:
 ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
Knee Conditioning Program
 Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
SUMMARY OF MEDICAL TREATMENT GUIDELINE FOR CARPAL TUNNEL SYNDROME AS IT RELATES TO PHYSICAL THERAPY
 SUMMARY OF MEDICAL TREATMENT GUIDELINE FOR CARPAL TUNNEL SYNDROME AS IT RELATES TO PHYSICAL THERAPY Effective March 1, 2013, the New York State Workers Compensation System will implement Medical Treatment
SUMMARY OF MEDICAL TREATMENT GUIDELINE FOR CARPAL TUNNEL SYNDROME AS IT RELATES TO PHYSICAL THERAPY Effective March 1, 2013, the New York State Workers Compensation System will implement Medical Treatment
Chapter 8: Muscular Strength & Endurance. ACE Personal Trainer Manual Third Edition
 Chapter 8: Muscular Strength & Endurance ACE Personal Trainer Manual Third Edition Introduction Muscles are unique in their ability to relax, contract, and produce force. In addition, this metabolically
Chapter 8: Muscular Strength & Endurance ACE Personal Trainer Manual Third Edition Introduction Muscles are unique in their ability to relax, contract, and produce force. In addition, this metabolically
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life
 Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Wellness 360 Online Nutrition Counseling* Session 6: Being Active A Way of Life. powered by WELLSTAR 360 Session 6: Overview Be Active It s Your Choice! This session focuses on how to become more physically
Foot and Ankle Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Bursitis. Other joints are found between the different bones of your fingers and toes. You also have joints that allow your vertebrae to move.
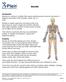 Bursitis Introduction Bursitis is a common condition that causes swelling around muscles and bones. It happens most often in the shoulder, elbow, hip, or knee. Bursitis is usually caused by overusing a
Bursitis Introduction Bursitis is a common condition that causes swelling around muscles and bones. It happens most often in the shoulder, elbow, hip, or knee. Bursitis is usually caused by overusing a
Back Safety Healthcare #09-066
 Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
Back Safety Healthcare Version #09-066 I. Introduction A. Scope of training This training program applies to healthcare employees whose job requires them to lift patients or other heavy objects. Lifting
Vermeulen, Liebenberg, Dippenaar en Louw Fisioterapeute
 Vermeulen, Liebenberg, Dippenaar en Louw Fisioterapeute In the Office Relaxation? Relaxation at work? Why doesn t my pain go away? Acute pain = Short term pain (Sprained ankle) Persistent/ Chronic
Vermeulen, Liebenberg, Dippenaar en Louw Fisioterapeute In the Office Relaxation? Relaxation at work? Why doesn t my pain go away? Acute pain = Short term pain (Sprained ankle) Persistent/ Chronic
Dr. Berkson offers a list of some of the most common exercise-related injuries:
 AS we get older, we become more vulnerable to injuries, in part because we are less agile than we used to be, and we have also lost some of our former bone and muscle mass, says the October 2013 issue
AS we get older, we become more vulnerable to injuries, in part because we are less agile than we used to be, and we have also lost some of our former bone and muscle mass, says the October 2013 issue
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
What Are Sports Injuries?
 What Should I Do if I Get Injured? Never try to "work through" the pain of a sports injury. Stop playing or exercising when you feel pain. Playing or exercising more only causes more harm. Some injuries
What Should I Do if I Get Injured? Never try to "work through" the pain of a sports injury. Stop playing or exercising when you feel pain. Playing or exercising more only causes more harm. Some injuries
Ankle Sprains. Treatment and Restoration of Motion
 Ankle Sprains Treatment and Restoration of Motion Ankle sprains Ankle anatomy The ankle is a complex joint made up of three bones: the tibia, the fibula and the talus. These three bones are connected by
Ankle Sprains Treatment and Restoration of Motion Ankle sprains Ankle anatomy The ankle is a complex joint made up of three bones: the tibia, the fibula and the talus. These three bones are connected by
DISCOID MENISCUS. Description
 DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
DISCOID MENISCUS Description For participation in jumping (basketball, volleyball) or The meniscus is a cartilage structure in the knee that sits on contact sports, protect the knee joint with supportive
Chapter 15: Using Therapeutic Modalities McGraw-Hill Higher Education. All rights reserved
 Chapter 15: Using Therapeutic Modalities Therapeutic modalities can be an effective adjunct to various techniques of therapeutic exercise Knowledge of the healing process is critical A variety of modalities
Chapter 15: Using Therapeutic Modalities Therapeutic modalities can be an effective adjunct to various techniques of therapeutic exercise Knowledge of the healing process is critical A variety of modalities
ILIOTIBIAL BAND SYNDROME
 ILIOTIBIAL BAND SYNDROME Description Maintain appropriate conditioning: The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the
ILIOTIBIAL BAND SYNDROME Description Maintain appropriate conditioning: The iliotibial band is the tendon attachment of hip muscles into the upper leg (tibia) just below the knee to the outer side of the
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
Hockey Canada. 8.0 Injury Prevention Techniques. 8.1 General Principles of Conditioning
 8.0 Injury Prevention Techniques 8.1 General Principles of Conditioning It is a well known fact that athletes are less likely to be injured when they are physically fit. In addition, well conditioned athletes
8.0 Injury Prevention Techniques 8.1 General Principles of Conditioning It is a well known fact that athletes are less likely to be injured when they are physically fit. In addition, well conditioned athletes
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
What Are Bursitis and Tendinitis?
 Shoulder Tendinitis, Bursitis, and Impingement Syndrome What Are Bursitis and Tendinitis? Two types of tendinitis can affect the shoulder. Biceps tendinitis causes pain in the front or side of the shoulder.
Shoulder Tendinitis, Bursitis, and Impingement Syndrome What Are Bursitis and Tendinitis? Two types of tendinitis can affect the shoulder. Biceps tendinitis causes pain in the front or side of the shoulder.
NATURAL DEVELOPMENT AND TRAINABILITY OF PLYOMETRIC ABILITY DURING CHILDHOOD BY KIRSTY QUERL SPORT SCIENTIST STRENGTH AND CONDITIONING COACH
 NATURAL DEVELOPMENT AND TRAINABILITY OF PLYOMETRIC ABILITY DURING CHILDHOOD BY KIRSTY QUERL SPORT SCIENTIST STRENGTH AND CONDITIONING COACH The truth... Youth are not as active as they used to be, Decline
NATURAL DEVELOPMENT AND TRAINABILITY OF PLYOMETRIC ABILITY DURING CHILDHOOD BY KIRSTY QUERL SPORT SCIENTIST STRENGTH AND CONDITIONING COACH The truth... Youth are not as active as they used to be, Decline
Lesson Plan: Sports Theory 2
 Sports Theory 2 Lesson Plan: Sports Theory 2 10 minutes: Breath of Arrival and Attendance 10 minutes: Kinesiology Pop Quiz 35 minutes: Lecture on Sports Massage Classroom Rules Punctuality- everybody's
Sports Theory 2 Lesson Plan: Sports Theory 2 10 minutes: Breath of Arrival and Attendance 10 minutes: Kinesiology Pop Quiz 35 minutes: Lecture on Sports Massage Classroom Rules Punctuality- everybody's
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS
 TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
TMD: CONSERVATIVE TREATMENT AND PHYSICAL THERAPY OPTIONS Massage: The temporalis on the side of the head is easy to locate. Press on it looking for painful nodules, massaging gently. Opening and closing
Knee Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
What Are Shoulder Problems?
 What Are the Parts of the Shoulder? The shoulder joint is made up of bones held in place by muscles, tendons, and ligaments. Tendons are tough cords of tissue that hold the shoulder muscles to bones. They
What Are the Parts of the Shoulder? The shoulder joint is made up of bones held in place by muscles, tendons, and ligaments. Tendons are tough cords of tissue that hold the shoulder muscles to bones. They
Cytology of Neoplasia An Essential Component of Diagnosis
 A Peer-Reviewed Journal Cytology of Neoplasia An Essential Component of Diagnosis September/October 2012 Volume 2, Issue 5 Internal MedIcIne Practice Pearls defeating ticks Preventing Tick-Borne Disease
A Peer-Reviewed Journal Cytology of Neoplasia An Essential Component of Diagnosis September/October 2012 Volume 2, Issue 5 Internal MedIcIne Practice Pearls defeating ticks Preventing Tick-Borne Disease
HEAT & COLD. Heat and cold applications applied to skin surface help treat certain conditions
 HEAT AND COLD HEAT & COLD Heat and cold applications applied to skin surface help treat certain conditions Heat and cold applications require a doctor s order when being used on a patient The body can
HEAT AND COLD HEAT & COLD Heat and cold applications applied to skin surface help treat certain conditions Heat and cold applications require a doctor s order when being used on a patient The body can
FITNESS, CONDITIONING AND HEALTH.
 FITNESS, CONDITIONING AND HEALTH. 1. CONCEPT. We understand FITNESS as the result of all the physical qualities, motor skills and healthy habits which are important in our daily life, during sports performance,
FITNESS, CONDITIONING AND HEALTH. 1. CONCEPT. We understand FITNESS as the result of all the physical qualities, motor skills and healthy habits which are important in our daily life, during sports performance,
Foot and Ankle Conditioning Program
 Foot and Ankle Conditioning Program Studies show, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. A program of this nature, focused
Foot and Ankle Conditioning Program Studies show, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. A program of this nature, focused
It is also important to make note of your function, as this may be your first indication of improvement.
 Back Pain 1 Management of Back Pain The resolution of pain involves gradually increasing the number of repetitions or resistance of the exercises performed. However, it is important to stay within a range
Back Pain 1 Management of Back Pain The resolution of pain involves gradually increasing the number of repetitions or resistance of the exercises performed. However, it is important to stay within a range
SEMIMEMBRANOSUS TENDINITIS
 SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
SEMIMEMBRANOSUS TENDINITIS Description Maintain appropriate conditioning: Semimembranosus tendinitis is characterized by inflammation and pain at the knee joint on the back part of the inner side of the
Introduction. Anatomy
 the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
the patella is called the quadriceps mechanism. Though we think of it as a single device, the quadriceps mechanism has two separate tendons, the quadriceps tendon on top of the patella and the patellar
Advice: After the Removal of a Lower Leg Cast
 Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Advice: After the Removal of a Lower Leg Cast The aim of this leaflet is to give you some understanding of the problems you have with your condition and to provide some advice on how to manage this. It
Therapeutic Ultrasound
 THERAPEUTIC ULTRASOUND Therapeutic is a form of MECHANICAL energy Mechanical vibration at increasing frequencies is known as sound energy. Below 16Hz, these vibrations are not recognizable as sound The
THERAPEUTIC ULTRASOUND Therapeutic is a form of MECHANICAL energy Mechanical vibration at increasing frequencies is known as sound energy. Below 16Hz, these vibrations are not recognizable as sound The
DISCOID MENISCUS. Description
 Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
Montefiore Pediatric Orthopedic and Scoliosis Center Children s Hospital at Montefiore Norman Otsuka MD Eric Fornari MD Jacob Schulz MD Jaime Gomez MD Christine Moloney PA 3400 Bainbridge Avenue, 6 th
EPICONDYLITIS, LATERAL (Tennis Elbow)
 EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
EPICONDYLITIS, LATERAL (Tennis Elbow) Description Expected Outcome Lateral epicondylitis (tennis elbow) is the most common painful condition of the elbow. Inflammation and pain occur on the outer side
INJURY PREVENTION TECHNIQUES
 Hockey Canada Safety Program Injury Prevention Techniques 8.1 General Principles of Conditioning INJURY PREVENTION TECHNIQUES It is a well known fact that athletes are less likely to be injured when they
Hockey Canada Safety Program Injury Prevention Techniques 8.1 General Principles of Conditioning INJURY PREVENTION TECHNIQUES It is a well known fact that athletes are less likely to be injured when they
