2. The practitioner holds a current Wilderness Medical Associates International certification.
|
|
|
- Ronald Lindsey
- 6 years ago
- Views:
Transcription
1 Purpose These protocols have been developed for use by appropriately trained individuals working in remote, high risk, and low resource environments. They are based on the concepts and principles taught by Wilderness Medical Associates international, and address specific low risk medical procedures for the treatment of high risk problems. Authorization It is recommended that the integration of these procedures into the emergency response practices of agencies and programs be specifically authorized by the management of the agency or program, preferably with the guidance of a medical director or advisor familiar with field medicine and the area of operation. It is recommended that these protocols be authorized by certification level: Wilderness Advanced Life Support (WALS ), Wilderness Emergency Medical Technician (WEMT), and Wilderness First Responder (WFR) may use all protocols. Wilderness Advanced First Aid (WAFA) certified practitioners may only use protocols 1, 2, 3 and 4. Wilderness First Aid (WFA) certified practitioners may only use protocols 1 and 2. A careful review of the medical training program is recommended to ensure complete understanding of these protocols and their application. The following conditions for authorized use of these protocols are recommended: 1. The practitioner is on the job for the authorizing agency or program. 2. The practitioner holds a current certification. 3. The credentials and competence of the practitioner has been verified by agency or program management. 4. Application of the protocol will reduce risk, relieve pain, and improve outcome. Important Note This document is not designed to be used as a stand-alone reference. Practitioners should refer to their course textbook, lecture notes, and field guide for complete information on the use of these protocols. Rev Face any challenge, anywhere. Page 1
2 Protocol 1: Anaphylaxis Anaphylaxis is a systemic allergic reaction that has life-threatening effects on the circulatory and respiratory systems. Early recognition and prompt treatment with epinephrine is essential. 1. Inject 0.01 mg/kilogram (up to 0.5 mg) of 1 mg/ml solution of epinephrine intramuscularly into the lateral aspect of the thigh or upper arm. A dose of 0.3 to 0.5 mg is appropriate for the average adult and 0.15 mg for a child less than 30 kg. 2. Maintain an open airway and position of comfort. Initiate either positive pressure ventilations (PPV) or full cardiopulmonary resuscitation (CPR) as indicated, 3. Repeat epinephrine injections as soon as every 5 minutes if needed. 4. Administer an antihistamine by mouth (e.g.: mg of diphenhydramine every 4-6 hours for the average adult) 5. Consider prednisone 60 mg/day for an average adult or mg for a smaller person. 6. Evacuate to hospital care if safe to do so. Consider an advanced life support intercept. 7. If evacuation is not possible, monitor carefully for biphasic reaction. Repeat treatment per protocol as necessary. Note: The preferred concentration of epinephrine for IM injection is 1 mg/1 ml. Commercially available auto-injectors such as the EpiPen deliver either 0.3 mg or 0.5 mg as a standard adult dose or a 0.15 mg pediatric dose. The auto-injector is the most user-friendly technique, but also the most expensive. Epinephrine is also supplied in 1 ml ampules, and vials of various sizes, for a fraction of the cost. WMAI graduates at the WALS, WEMT, and WFR level are trained in the use of syringes, needles, vials, and ampules for this purpose. For patients weighing less than 66 lbs (30 kg), the doses are: epinephrine is 0.01 mg/kg; diphenhydramine is 1mg/kg; and prednisone is 1 2 mg/kg. Multiply the weight in pounds times 0.45 to get the weight in kilograms. The organization may need a prescription from a medical advisor to obtain the injectable epinephrine, syringes and prednisone used in the protocol. Antihistamines do not require a prescription in the United States and Canada. It is essential for prescribers and organizations to be familiar with state and provincial regulations that may address the prescribing of medication and the acceptable means of injecting epinephrine. Rev Face any challenge, anywhere. Page 2
3 The Anaphylaxis Protocol has been authorized for use by Wilderness Medical Associates International WALS, WEMT, WFR, WAFA, and WFA trained employees of the employer named on page one provided that they meet the requirements of the authorization criteria listed on page one. Rev Face any challenge, anywhere. Page 3
4 Protocol 2: Wound Cleaning and Debridement Control of severe bleeding is a higher priority than wound cleaning. Once bleeding has been controlled: OPEN WOUNDS 1. Cleaning a wound will involve a combination of the following procedures in an order that seems appropriate: a) Explore the wound and remove foreign material as completely as possible. b) Wash the surrounding skin with soap and water or other specified cleanser. c) Irrigate the wound with water clean enough to drink. Water preparation can be accomplished by filter, chemical, ultraviolet, or reverse osmosis. Water of questionable quality should be sterilized by creating a 1% povidone iodine solution. 2. High risk wounds (imbedded debris, devitalized tissue, bites, open fractures, deep structure involvement) should be irrigated with large amounts of water under pressure (e.g.: using a 30 or 60cc syringe with an 18 gauge catheter). If the wound cannot be completely cleansed of foreign material or the quantity of irrigation water is insufficient, rinse the wound with 1% povidone-iodine solution. DO NOT use pressure irrigation on puncture wounds where irrigation fluid cannot easily drain away. 3. Cover the wound with a sterile bandage, but allow for drainage. Splint or otherwise immobilize high-risk wounds if safe to do so. Do not close a high risk wound with sutures or tape. 4. Change the bandage and clean the wound at least daily. 5. If an infection develops (e.g., red, tender, swollen, drainage of pus), irrigate with clean water, allow for drainage, and apply warm compresses. Infected wounds should be evacuated to medical care promptly. 6. High-risk wounds require tetanus prophylaxis every five years, all others every ten. 7. Animal bite wounds require risk assessment for rabies exposure. The probability of rabies varies by geographic location. Check with state or local health agency for recommendations. Prophylaxis should be administered as soon as possible, but a period of several days between the bite and immunization is considered safe. Antibiotic prophylaxis may also be indicated. SHALLOW WOUNDS (ABRASIONS AND MINOR BURNS) 1. Clean the wound with drinking of quality water or a 1% povidone-iodine solution. 2. Apply an antibacterial ointment and cover with a clean dressing. 3. Inspect the wound and change the dressing as needed. IMPALED OBJECTS Impaled objects should be removed in the field and the wound cleaned as soon as practical. Exceptions include objects in the globe of the eye, and situations in which removal would result in significant tissue damage, intractable pain, or bleeding that cannot be controlled. Rev Face any challenge, anywhere. Page 4
5 Note: The should consider extending this protocol to include antibiotic use in settings where access to medical care will be delayed and the consequence of wound infection is high. The Wound Cleaning and Debridement protocol has been authorized for use by WALS, WEMT, WFR, WAFA, and WFA trained employees of the employer named on page one provided that they meet the requirements of the authorization criteria listed on page one. Rev Face any challenge, anywhere. Page 5
6 Protocol 3: Cardiopulmonary Resuscitation (CPR) teaches CPR according to current standards supported by the 2015 International Liaison Committee on Resuscitation (e.g., The American Heart Association, Heart and Stroke, European Resuscitation Council). This protocol amends those standards for remote and high risk situations. This protocol applies only to normothermic patients (core temperature > 90 F, 32 C). CPR should not be started, or may be discontinued at some point after initiation: 1. Cardiorespiratory arrest after submersion in water for more than one hour in the absence of a source of air such as SCUBA equipment or an air pocket. 2. Obvious lethal injury such as decapitation, exsanguination, or massive head injury. 3. Where cardiac arrest persists continuously for over 30 minutes of sustained CPR. 4. Where rescuers are at risk of injury or death. The CPR protocol has been authorized for use by Wilderness Medical Associates International WALS, WEMT, WFR, and WAFA trained employees of the employer named on page one provided that they meet the requirements of the authorization criteria listed on page one. Rev Face any challenge, anywhere. Page 6
7 Protocol 4: Spine Injuries Spine assessment criteria allow rescuers to determine the need and justification for spine stabilization or other protective measures in the presence of an uncertain or positive mechanism for spine injury. This evaluation focuses on patient reliability, signs of spinal column injury, and neurologic function. Adequate time must be allowed for the evaluation. An assessment that the spine is CLEAR means that there is no significant spine injury. 1. Assess the mechanism. If a positive or uncertain mechanism exists, protect the spine from further trauma by whatever method is feasible and available. 2. Do a thorough evaluation including a history and physical examination. To clear the spine, the patient must meet all of the following criteria: a) Patient must be reliable, cooperative, sober, and alert. b) Patient must be free of spine pain and tenderness. c) Patient must have normal motor/sensory function in all four extremities: Finger abduction or finger or wrist extension against resistance (check both hands) Foot plantar flexion/extension or great toe dorsiflexion (check both feet) No complaint of numbness and sensation intact to sharp and dull stimuli in all four extremities If reduced function in one particular extremity can be attributed with certainty to a specific extremity injury (e.g., unstable wrist injury), that deficit alone will not preclude ruling out a spine injury. 3. If the spine cannot be cleared, spine injury remains on the problem list and must be appropriately managed and followed up as part of patient care and evacuation. This may include stabilization and carry, assisted self extrication, or other means of reducing the risk of further injury pending medical evaluation and treatment. The Spine Assessment protocol has been authorized for use by Wilderness Medical Associates International WALS, WEMT, WFR, and WAFA trained employees of the employer named on page one provided that they meet the requirements of the authorization criteria listed on page one. Rev Face any challenge, anywhere. Page 7
8 Protocol 5: Joint Dislocations This protocol specifically applies to the reduction of dislocations of the shoulder, patella, and digits. These injuries are usually isolated, not accompanied by significant critical system injury, and caused by an indirect mechanism. All other dislocations should be treated as unstable joint injury and splinted in a position that maintains stability and neurovascular function while facilitating transport. SHOULDER Any manipulative technique that is performed slowly and gently on an awake and cooperative patient is generally safe. For the purposes of this protocol the Cunningham, External Rotation, Baseball, Hanging, and Scapular Manipulation are described. These techniques can be used in sequence or in combination as needed to achieve a successful reduction. Discontinue the procedure if pain significantly increases and/or if physical resistance is encountered. Neurovascular status is documented before and after reduction. Non-emergent medical evaluation is advised but may be delayed by up to 10 days if distal circulation and sensation has returned to normal. Cunningham: This technique encourages muscle relaxation which may allow the humeral head to return to normal position without additional manipulation. The patient is positioned sitting upright with the shoulders back and chest out facing the practitioner. The patients arm remains adducted (against the body) while the hand placed on the practitioner s shoulder (right dislocation, right hand on practitioner s left shoulder). The practitioner massages the trapezius, deltoid, and biceps muscles until reduction is achieved. External Rotation: This is essentially the same as the Cunningham technique with the addition of manipulation. The practitioner gently applies external rotation of the patient s arm with the elbow remaining adducted against the chest. Baseball : With the patient supine and while still sitting adjacent to the dislocated shoulder, apply gentle traction to the arm to overcome muscle spasm. Gradually abduct and externally rotate the arm until it is at a 90 degree angle to the patient s body. This is most easily achieved by keeping the elbow in the 90 degrees of flexion throughout the maneuver. Hold the arm in this position ( baseball throwing position ) and maintain traction until the dislocation has been reduced. Hanging Traction: Have the patient lie face down with the affected arm hanging unsupported. Secure approximately 3 5 kilograms to the patient s hand and allow the weight and gravity to fatigue the muscles until the shoulder is reduced. Scapular Manipulation: (This procedure may require 2 rescuers) Have the patient either lie face down (as above) or sit upright. Apply traction to the affected arm and bring it forward to shoulder level. While maintaining traction, stabilize the upper portion Rev Face any challenge, anywhere. Page 8
9 of the scapula with one hand and rotate the lower tip medially with the other hand. This technique is often an effective adjunct to the other techniques described. Note: If the patient cannot adduct the arm against the chest, techniques such as the baseball position, hanging traction, and scapular manipulation are more likely to be successful. PATELLA 1. Check and document distal neurovascular function. 2. Gently straighten the patient s knee and flex the hip. If the patella has not spontaneously reduced once the knee is fully extended, gently guide the displaced patella medially back into its normal anatomic position. Discontinue the procedure if pain significantly increases and/or if physical resistance is encountered. 3. Stabilize the patella with tape or an elastic wrap. 4. Reassess and document distal neurovascular status. 5. Arrange for non-emergent medical evaluation. Patients may walk out if pain is tolerable. DIGITS (FINGERS AND TOES, INCLUDING THUMB) 1. Check and document distal neurovascular function. 2. Apply axial traction distal and counter-traction proximal to the dislocated joint until the dislocation has been reduced. Discontinue the procedure if pain significantly increases and/or if physical resistance is encountered. 3. Splint in the anatomical position. 4. Reassess and document distal neurovascular status. 5. Arrange for non-emergent medical evaluation. The Dislocations Protocol has been authorized for use by Wilderness Medical Associates International WALS, WEMT, and WFR trained employees of the employer named on page one provided that they meet the requirements of the authorization criteria listed on page one. Rev Face any challenge, anywhere. Page 9
10 Protocol 6: Severe Asthma This protocol outlines the treatment of an asthma attack causing persistent respiratory distress not responding to the patient s use of a rescue inhaler. This is a high risk problem that can cause respiratory failure and death from respiratory arrest. Early recognition and prompt treatment is essential. 1. Inject 0.01 mg/kilogram (up to 0.5 mg) of 1 mg/ml solution of epinephrine intramuscularly into the lateral aspect of the thigh or deltoid. A dose of 0.3 to 0.5 mg is appropriate for the average adult and 0.15 mg for a child less than 30 kg. 2. Maintain an open airway and position of comfort. Initiate either positive pressure ventilations (PPV) or cardiopulmonary resuscitation (CPR) as indicated. 3. Repeat epinephrine injections as soon as every 5 minutes if needed. 4. Consider prednisone 60 mg/day for an average adult or mg for a smaller person. 5. Have the patient self-administer 6-10 puffs from the MDI/HFA. This may be repeated every 20 minutes for a total of three doses. 6. Evacuate to hospital care if safe to do so. Consider an advanced life support intercept en route (ALS). 7. If evacuation is not possible, monitor carefully and repeat treatment per protocol as necessary. Note: The preferred concentration of epinephrine for IM injection is 1 mg/1 ml. Commercially available auto-injectors such as the EpiPen deliver either 0.3 mg or 0.5 mg as a standard adult dose or a 0.15 mg pediatric dose. The auto-injector is the most user-friendly technique, but also the most expensive. Epinephrine is also supplied in 1 ml ampules, and vials of various sizes, for a fraction of the cost. WMAI graduates at the WALS, WEMT, and WFR level are trained in the use of syringes, needles, vials, and ampules for this purpose. For patients weighing less than 66 lbs (30 kg), the doses are: epinephrine is 0.01 mg/kg and prednisone is 1 2 mg/kg. Multiply the weight in pounds times 0.45 to get the weight in kilograms. The organization may need a prescription from a medical advisor to obtain the injectable epinephrine, syringes and prednisone used in the protocol. It is essential for prescribers and organizations to be familiar with state and provincial regulations that may address the prescribing of medication and the acceptable means of injecting epinephrine. Rev Face any challenge, anywhere. Page 10
11 The Asthma Protocol has been authorized for use by Wilderness Medical Associates International WALS, WEMT, and WFR trained employees of the employer named on page one provided that they meet the requirements of the authorization criteria listed on page one. Rev Face any challenge, anywhere. Page 11
Wilderness Medical Field Protocols
 Wilderness Medical Field Protocols The Center for Wilderness Safety Post Office Box 651324 Sterling, Virginia 20165 www.wildsafe.org (888) 945-3402 Copyright The Center for Wilderness Safety, Inc. 2011,
Wilderness Medical Field Protocols The Center for Wilderness Safety Post Office Box 651324 Sterling, Virginia 20165 www.wildsafe.org (888) 945-3402 Copyright The Center for Wilderness Safety, Inc. 2011,
Lesson 9: Bone & Joint Injuries. Emergency Reference Guide p
 Lesson 9: Bone & Joint Injuries Emergency Reference Guide p. 33-43 Objectives Define strain, sprain, fracture and dislocation List Signs & Symptoms of strain, sprain, fracture & dislocation Demonstrate
Lesson 9: Bone & Joint Injuries Emergency Reference Guide p. 33-43 Objectives Define strain, sprain, fracture and dislocation List Signs & Symptoms of strain, sprain, fracture & dislocation Demonstrate
ADMINISTRATIVE REQUIREMENT MANUAL EFFECTIVE DATE
 PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
PURPOSE: I. To establish the minimum requirements for a first responder training course in first aid, which all first responders must take, in order to meet the requirements of M.G.L. c. 111, 201 and 105
 International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
International Trauma Life Support for Prehospital Care Providers Sixth Edition Patricia M. Hicks, MS, NREMTP Roy Alson, PhD, MD, FACEP Donna Hastings, EMT-P John Emory Campbell, MD, FACEP and Alabama Chapter,
Emergency Care Progress Log
 Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Emergency Care Progress Log For further details on the National Occupational Competencies for EMRs, please visit www.paramedic.ca. Check off each skill once successfully demonstrated the Instructor. All
Medical First Responder Program Protocols
 Medical Scene Safety Protocol Verify Scene Safety with Police or Dispatch UNKWN Scene Safe? Enter Continue to Appropriate Protocol Possible to Make Safe Make Safe Then Continue Exit Area and Stage Outside
Medical Scene Safety Protocol Verify Scene Safety with Police or Dispatch UNKWN Scene Safe? Enter Continue to Appropriate Protocol Possible to Make Safe Make Safe Then Continue Exit Area and Stage Outside
Skill Evaluation Sheets
 Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
Skill Evaluation Sheets Skill Drill 2-: How to Remove Gloves Skill Drill 4-: Primary Check: RAP-CAB Skill Drill 4-2: Perform a Secondary Check Skill Drill 5-: Adult CPR Skill Drill 5-2: Child CPR Skill
Injuries to the Extremities
 Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
Injuries to the Extremities KNOWLEDGE OBJECTIVES 1. List seven signs and symptoms that suggest a serious extremity injury. 2. Describe how to care for injuries to the shoulder, upper arm, and elbow. 3.
RIB FRACTURE. Explanation. Causes. Symptoms. Diagnosis
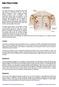 RIB FRACTURE Explanation The heart and lungs are encased by the chest wall, which is composed of the ribs. The ribs must be flexible in order to allow movement during expansion and contraction. This movement
RIB FRACTURE Explanation The heart and lungs are encased by the chest wall, which is composed of the ribs. The ribs must be flexible in order to allow movement during expansion and contraction. This movement
Rotator Cuff and Shoulder Conditioning Program
 Rotator Cuff and Shoulder Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy
Rotator Cuff and Shoulder Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy
Frontline First Aid 2012 Emergency Care Manual Treatments
 Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
Heart Attack/Angina (p. 132) 1. Recognize signals of a heart attack 2. Assist with Nitroglycerin 3. Assist with ASA 4. Rest and Comfort 6. More advanced medical care Breathing Emergencies (p. 105) Anaphylaxis
EMT OPTIONAL SKILL. Cell Phones and Pagers. Epinephrine Auto-injector. Course Outline 9/2017
 EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
EMT OPTIONAL SKILL Epinephrine Auto-injector Cell Phones and Pagers Be courteous to your classmates! Please set your cell phones and/or pagers to silent or turn them off. Course Outline Introduction and
Competency Log Professional Responder Courses
 Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Competency Log Professional Responder Courses Check off each competency once successfully demonstrated. This log may be used as a support tool when teaching a Professional Responder course. Refer to the
Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles
 1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
1 2 3 4 5 6 7 Chapter 29 Orthopaedic Injuries Principles of Splinting Types of Muscles Striated Skeletal Smooth Anatomy and Physiology of the Musculoskeletal System Skeletal System Skeletal System Functions
( PLUM BOROUGH SCHOOL DISTRICT
 No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
No. 209.1 ( PLUM BOROUGH SCHOOL DISTRICT SECTION: PUPILS TITLE: FIRST AID STANDING ORDERS ADOPTED: March 27,1990 REVISED: February 27, 2001 209.1. FIRST AID STANDING ORDERS 1. Guidelines When a student
Chapter 30 - Musculoskeletal_Trauma
 Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
Introduction to Emergency Medical Care 1 OBJECTIVES 30.1 Define key terms introduced in this chapter. Slides 11 12, 19 20, 22 23, 37 30.2 Describe the anatomy of elements of the musculoskeletal system.
GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE
 GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE POSTERIOR CAPSULAR STRETCH Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your elbow.
GOLFERS TEN PROGRAM 1. SELF STRETCHING OF THE SHOULDER CAPSULE POSTERIOR CAPSULAR STRETCH Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your elbow.
ARROW EZ-IO Intraosseous Vascular Access System Procedure Template
 ARROW EZ-IO Intraosseous Vascular Access System Procedure Template PURPOSE To provide procedural guidance for establishment of intraosseous vascular access using the ARROW EZ-IO Intraosseous Vascular Access
ARROW EZ-IO Intraosseous Vascular Access System Procedure Template PURPOSE To provide procedural guidance for establishment of intraosseous vascular access using the ARROW EZ-IO Intraosseous Vascular Access
Title: EZ-IO. Effective Date: January SOG Number: EMS Rescinds:
 S O G Title: EZ-IO Effective Date: January 2010 SOG Number: EMS - 25 Rescinds: Scope: Providers Authorized are AIC s in the following certifications EMT-I and EMT-P who have been trained and cleared by
S O G Title: EZ-IO Effective Date: January 2010 SOG Number: EMS - 25 Rescinds: Scope: Providers Authorized are AIC s in the following certifications EMT-I and EMT-P who have been trained and cleared by
SEMINOLE COUNTY EMS PROVISIONAL EMT SKILLS VERIFICATION
 The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
The following individual has completed the Seminole County EMS Provisional EMT Skills Verification check in the following areas: Oxygen, Airway and Ventilation Skills ALS Assistance Trauma Management Medical
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles. Striated Skeletal. Smooth
 1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
1 Chapter 29 Orthopaedic Injuries Principles of Splinting 2 Types of Muscles Striated Skeletal Smooth 3 Anatomy and Physiology of the Musculoskeletal System 4 Skeletal System 5 Skeletal System Functions
Osteoporosis Protocol
 PRODUCTS HELPING PEOPLE HELP THEMSELVES! Osteoporosis Protocol Rehabilitation using the Resistance Chair General Information Osteoporosis is a condition where bones gradually decrease in mass or density
PRODUCTS HELPING PEOPLE HELP THEMSELVES! Osteoporosis Protocol Rehabilitation using the Resistance Chair General Information Osteoporosis is a condition where bones gradually decrease in mass or density
Rotator Cuff and Shoulder Conditioning Program
 Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Prepared for: Prepared by: Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball
 1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball This is an example of Facilitating Combinations of Movements and Active Assist. Starting Position Have your patient sit
1 Pause and Practice: Facilitating Trunk and Shoulder Control with the Therapy Ball This is an example of Facilitating Combinations of Movements and Active Assist. Starting Position Have your patient sit
Prater Chiropractic Wellness Center 903 W. South St. Kalamazoo, MI PH: (269)
 Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following a well-structured conditioning
Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following a well-structured conditioning
The Golfers Ten Program. 1. Self Stretching of the Shoulder Capsule
 The Golfers Ten Program 1. Self Stretching of the Shoulder Capsule A. Posterior capsular stretch Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your
The Golfers Ten Program 1. Self Stretching of the Shoulder Capsule A. Posterior capsular stretch Bring your arm across your chest toward the opposite shoulder. With the opposite arm grasp your arm at your
MABEES. MFR & Basic EMT Epinephrine Study
 MABEES MFR & Basic EMT Epinephrine Study Acknowledgements This program is a State of Michigan approved special study designed by members of the Oakland County Medical Control Authority American CME developed
MABEES MFR & Basic EMT Epinephrine Study Acknowledgements This program is a State of Michigan approved special study designed by members of the Oakland County Medical Control Authority American CME developed
Injuries to Muscles, Bones and Joints. Emergency Medical Response
 Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Injuries to Muscles, Bones and Joints Lesson 33: Injuries to Muscles, Bones and Joints You Are the Emergency Medical Responder You are patrolling the state park where you are the emergency medical responder
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What is caused by overexerting or tearing of a muscle? p. 375 A.) Dislocation B.) Sprain C.) Fracture *D.)
ARTHROSCOPIC SHOULDER SURGERY
 Preoperative instructions ARTHROSCOPIC SHOULDER SURGERY Schedule surgery with the secretary in Dr.Gill s office. Within one month before surgery * Make an appointment for a preoperative office visit regarding
Preoperative instructions ARTHROSCOPIC SHOULDER SURGERY Schedule surgery with the secretary in Dr.Gill s office. Within one month before surgery * Make an appointment for a preoperative office visit regarding
CHAPTER 9. Shock National Safety Council
 CHAPTER 9 Shock Shock Dangerous condition: Not enough oxygen-rich blood reaching vital organs, such as brain and heart Caused by anything that significantly reduces blood flow Life-threatening emergency
CHAPTER 9 Shock Shock Dangerous condition: Not enough oxygen-rich blood reaching vital organs, such as brain and heart Caused by anything that significantly reduces blood flow Life-threatening emergency
Title Protocol for the Management of Shoulder Injuries in MIUs and WICs
 Document Control Title in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate, Logistics and Resilience Department Emergency Department Version Date Issued Status
Document Control Title in MIUs and WICs Author Author s job title Professional Lead, Minor Injuries Unit Directorate, Logistics and Resilience Department Emergency Department Version Date Issued Status
Orthopedics - Dr. Ahmad - Lecture 2 - Injuries of the Upper Limb
 The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
The shoulder and the upper arm Fractures of the clavicle 1. Fall on the shoulder. 2. Fall on outstretched hand. In mid shaft fractures, the outer fragment is pulled down by the weight of the arm and the
Surgical Care at the District Hospital. EMERGENCY & ESSENTIAL SURGICAL CARE
 Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
Surgical Care at the District Hospital 1 18 Orthopedic Trauma Key Points 2 18.1 Upper Extremity Injuries Clavicle Fractures Diagnose fractures from the history and by physical examination Treat with a
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
NOTE If it is necessary to perform abdominal thrusts, expose the abdominal area prior to pressing on the abdomen.
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
Physical Sense Activation Programme
 Flexion extension exercises for neck and upper back Sitting on stool Arms hanging by side Bend neck and upper back Breathe out Extend your neck and upper back Lift chest to ceiling Squeeze shoulder blades
Flexion extension exercises for neck and upper back Sitting on stool Arms hanging by side Bend neck and upper back Breathe out Extend your neck and upper back Lift chest to ceiling Squeeze shoulder blades
Standing Shoulder Internal Rotation with Anchored Resistance. Shoulder External Rotation Reactive Isometrics
 Standing Shoulder Row with Anchored Resistance Begin standing upright, holding both ends of a resistance band that is anchored in front of you at chest height, with your palms facing inward. Pull your
Standing Shoulder Row with Anchored Resistance Begin standing upright, holding both ends of a resistance band that is anchored in front of you at chest height, with your palms facing inward. Pull your
Basic First Aid. Sue Fisher Emergency Management Coordinator CSUF University Police
 Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
Basic First Aid Sue Fisher Emergency Management Coordinator CSUF University Police Information given for this lecture is not meant to replace any official training by the American Red Cross, or any other
McCann Technical School 70 Hodges Cross Road North Adams, MA Medical Assisting Program
 MA 104 MEDICAL SOCIAL SCIENCE 4 Credits Fall Semester Part IV FIRST RESPONDER Syllabus McCann Technical School 70 Hodges Cross Road North Adams, MA 01247 Medical Assisting Program INSTRUCTORS: Laurie Tuper,
MA 104 MEDICAL SOCIAL SCIENCE 4 Credits Fall Semester Part IV FIRST RESPONDER Syllabus McCann Technical School 70 Hodges Cross Road North Adams, MA 01247 Medical Assisting Program INSTRUCTORS: Laurie Tuper,
MASSACHUSETTS DEPARTMENT OF PUBLIC HEALTH OFFICE OF EMERGENCY MEDICAL SERVICES Basic EMT Practical Examination Cardiac Arrest Management
 Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Basic EMT Practical Examination 6.0 - Cardiac Arrest Management Station 1 RESUSCITATION & DEFIBRILLATION No Point WHILE FUNCTIONING AS FIRST RESCUER: Point 1. Verbalizes or takes body substance isolation
Pediatric Patients. BCFPD Paramedic Education Program. EMS Education Paramedic Level
 Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Pediatric Patients BCFPD Program Basic Considerations Much of the initial patient assessment can be done during visual examination of the scene. Involve the caregiver or parent as much as possible. Allow
Types of Body Movements
 Types of Body Movements Bởi: OpenStaxCollege Synovial joints allow the body a tremendous range of movements. Each movement at a synovial joint results from the contraction or relaxation of the muscles
Types of Body Movements Bởi: OpenStaxCollege Synovial joints allow the body a tremendous range of movements. Each movement at a synovial joint results from the contraction or relaxation of the muscles
OUTLINE SHEET 5.4 PRIMARY SURVEY
 ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
ENABLING OBJECTIVES: 4.7 List the procedures used in a primary survey. 4.8 Demonstrate primary survey procedures used in a mock trauma (moulage) scenario without injury to personnel or damage to equipment.
POST OP CLOSED BANKART PROCEDURE
 POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
PATELLAR DISLOCATION AND SUBLUXATION
 PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
PATELLAR DISLOCATION AND SUBLUXATION Description For jumping (basketball, volleyball) or contact sports, Patellar dislocation and subluxation are injuries to the protect the patella with supportive devices,
Movement Terminology. The language of movement is designed to allow us to describe how the body moves through space.
 Movement Terminology The language of movement is designed to allow us to describe how the body moves through space. In exercise it allows us to communicate with other movement professionals so we can describe
Movement Terminology The language of movement is designed to allow us to describe how the body moves through space. In exercise it allows us to communicate with other movement professionals so we can describe
Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, Page 1
 Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, 2014 Page 1 PROBLEM Billy is a maintenance person that has been conducting clean-up and service duties on the number one conveyor belt
Hatfield & McCoy Mine Safety Competition First-Aid Contest JULY 15, 2014 Page 1 PROBLEM Billy is a maintenance person that has been conducting clean-up and service duties on the number one conveyor belt
Principle Management of Wound and Fracture in Emergency Department
 Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
Principle Management of Wound and Fracture in Emergency Department Presented in Clinical Update Seminar January 15 th 2011 dr. Tedjo Rukmoyo, SpOT (K) Spine Initial Management ATLS Procedure A : airway
POST OPERATIVE ROTATOR CUFF REPAIR PROTOCOL. Home Program
 MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
MOON SHOULDER GROUP For information regarding the MOON Shoulder Group, speak to your surgeon or contact: Rosemary Sanders 4200 Medical Center East 1215 21st Avenue South Vanderbilt University Medical Center
OBJECTIVES. Unit 7:5 PROPERTIES OR CHARACTERISTICS OF MUSCLES. Introduction. 3 Kinds of Muscles. 3 Kinds of Muscles 4/17/2018 MUSCULAR SYSTEM
 OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
OBJECTIVES Unit 7:5 MUSCULAR SYSTEM Compare the three main kinds of muscles by describing the action of each Differentiate between voluntary and involuntary muscles List at least three functions of muscles
WRIST SPRAIN. Description
 WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
WRIST SPRAIN Description Other sports, such as skiing, bowling, pole vaulting Wrist sprain is a violent overstretching and tearing of one Poor physical conditioning (strength and flexibility) or more ligaments
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
GUIDELINES FOR REHABILITATION Arthroscopic Rotator Cuff Repair
 Indications: Tearing of the rotator cuff tendon(s) insertion on the humerus. Procedure: Arthroscopic repair: Tear Size: supraspinatus, infraspinatus, subscapularis tendons. biceps tenodesis or tenotomy
Indications: Tearing of the rotator cuff tendon(s) insertion on the humerus. Procedure: Arthroscopic repair: Tear Size: supraspinatus, infraspinatus, subscapularis tendons. biceps tenodesis or tenotomy
OMT Without An OMT Table Workshop. Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP
 OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
OMT Without An OMT Table Workshop Dennis Dowling, DO FAAO Ann Habenicht, DO FAAO FACOFP Cervical Somatic Dysfunction (C5 SR RR) - Seated 1. Patient position: seated. 2. Physician position: standing facing
Sick Call Screener Course
 Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
Sick Call Screener Course Musculoskeletal System Upper Extremities (2.7) 2.7-2-1 Enabling Objectives 1.46 Utilize the knowledge of musculoskeletal system anatomy while assessing a patient with a musculoskeletal
 55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
55-year-old male with 2nd and 3rd degree burns to face, chest, and arms on 25% of the body Respirations: 34 Pulse: 120 Mental Status: moans to painful stimulus Mucous membranes charred Stridor 10 cm scalp
Chapter 32. Injuries to the Spine by Pearson Education, Inc. Upper Saddle River, New Jersey
 Chapter Injuries to the Spine Topics Anatomy and physiology of the spine Spinal injuries Guidelines for immobilization Special considerations Enrichment Introduction Injuries to the spine are among the
Chapter Injuries to the Spine Topics Anatomy and physiology of the spine Spinal injuries Guidelines for immobilization Special considerations Enrichment Introduction Injuries to the spine are among the
Shoulder Dislocation. Explanation. Causes. Symptoms. Treatment. Diagnosis
 Shoulder Dislocation Explanation A dislocated shoulder occurs when the humerus separates from the scapula at the glenohumeral joint, or in simpler terms, the head of the upper arm bone (humerus) is dislodged
Shoulder Dislocation Explanation A dislocated shoulder occurs when the humerus separates from the scapula at the glenohumeral joint, or in simpler terms, the head of the upper arm bone (humerus) is dislodged
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Lifting and Moving Patients
 1. Which of the following factors should be considered before lifting any patient? a. The weight of the patient b. Your physical limitations c. Communications 2. When lifting a patient, a basic principle
1. Which of the following factors should be considered before lifting any patient? a. The weight of the patient b. Your physical limitations c. Communications 2. When lifting a patient, a basic principle
Air splint exercises. THINGS TO WATCH OUT FOR -Elevation of shoulder -Compensatory techniques throughout the body -Improper use of muscles -Breathing
 Air splint exercises Place arm in splint up until armpit, make sure that fingers are spread to start. Blow up splint until firm. This will stretch out the elbow. So if the elbow is tight, stretch out prior
Air splint exercises Place arm in splint up until armpit, make sure that fingers are spread to start. Blow up splint until firm. This will stretch out the elbow. So if the elbow is tight, stretch out prior
SPINAL IMMOBILIZATION
 Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
Spinal Immobilization Decision Assessment Recent studies have shown an increase in mortality for patients with isolated penetrating trauma who are spinally immobilized. Therefore spinal immobilization
NOTE: The first appearance of terms in bold in the body of this document (except titles) are defined terms please refer to the Definitions section.
 TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
TITLE SCOPE Provincial APPROVAL AUTHORITY Clinical Operations Executive Committee SPONSOR Pharmacy Services PARENT DOCUMENT TITLE, TYPE AND NUMBER Not applicable DOCUMENT # INITIAL EFFECTIVE DATE REVISION
Starting a Strength Training Program
 MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
MINTO PREVENTION & REHABILITATION CENTRE CENTRE DE PREVENTION ET DE READAPTATION MINTO Starting a Strength Training Program About This Kit The key to improving strength is applying resistance to the muscle
SHOULDER - ROTATOR CUFF REPAIR POSTOPERATIVE INSTRUCTIONS
 SHOULDER - ROTATOR CUFF REPAIR POSTOPERATIVE INSTRUCTIONS Phase One: the first week after surgery GOALS: 1. Control pain and swelling 2. Protect the rotator cuff repair 3. Protect wound healing 4. Begin
SHOULDER - ROTATOR CUFF REPAIR POSTOPERATIVE INSTRUCTIONS Phase One: the first week after surgery GOALS: 1. Control pain and swelling 2. Protect the rotator cuff repair 3. Protect wound healing 4. Begin
Range of motion and positioning
 Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Range of motion and positioning Learning guide Why is motion important? Most people take free, comfortable movement for granted. Motion is meant to be smooth and painless. The ligaments, tendons, muscles,
Disaster Medical Operations Part 2. CERT Basic Training Unit 4
 Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Disaster Medical Operations Part 2 Unit 4 Unit 3 Review 3 Killers Airway obstruction Excessive bleeding Shock 4-1 CERT Sizeup 1. Gather Facts 2. Assess Damage 3. Consider Probabilities 4. Assess Your Situation
Strength and Balance Exercises
 Strength and Balance Exercises LEG EXTENSIONS Purpose: Strengthen the thigh and leg muscles. Starting Position: Sit tall with your feet flat on floor, shoulderwidth apart. You may hold onto the sides of
Strength and Balance Exercises LEG EXTENSIONS Purpose: Strengthen the thigh and leg muscles. Starting Position: Sit tall with your feet flat on floor, shoulderwidth apart. You may hold onto the sides of
Resistance Training Program
 Name: Resistance Training Program How to do Resistance Training: Warm up for 5 minutes before resistance training e.g., walk or cycle slowly o Avoid stretching before resistance training Do all exercises
Name: Resistance Training Program How to do Resistance Training: Warm up for 5 minutes before resistance training e.g., walk or cycle slowly o Avoid stretching before resistance training Do all exercises
Resistance Training Program
 Name: Resistance Training Program How to do Resistance Training: Warm up for 5 minutes before resistance training e.g., walk or cycle slowly o Avoid stretching before resistance training Do all exercises
Name: Resistance Training Program How to do Resistance Training: Warm up for 5 minutes before resistance training e.g., walk or cycle slowly o Avoid stretching before resistance training Do all exercises
Frontline First Aid First Responder Session Quizzes
 Session 1 1. One of the 4 parts of the Patient Assessment Model is: a. Injury Survey b. Patient Survey c. Critical Survey d. Ongoing Survey 2. One of the Secondary responsibilities of the First Responder
Session 1 1. One of the 4 parts of the Patient Assessment Model is: a. Injury Survey b. Patient Survey c. Critical Survey d. Ongoing Survey 2. One of the Secondary responsibilities of the First Responder
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions
 Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
Caring for Muscle and Bone Injuries From Brady s First Responder (8 th Edition) 54 Questions 1. What do injuries to the shoulder often produce? p. 393 *A.) Anterior dislocation B.) Superior dislocation
SHOULDER PROCEDURE. Minimum Prerequisite BRM 2 (1-8) & BRM 3 (1-6)
 SHOULDER PROCEDURE Minimum Prerequisite BRM 2 (1-8) & BRM 3 (1-6) Shoulder Procedure (Solo) - SUMMARY With the client sitting, stand at the opposite side to the shoulder being worked on. Cradle the forearm
SHOULDER PROCEDURE Minimum Prerequisite BRM 2 (1-8) & BRM 3 (1-6) Shoulder Procedure (Solo) - SUMMARY With the client sitting, stand at the opposite side to the shoulder being worked on. Cradle the forearm
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS
 CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS PRACTICAL STATIONS CHANHASSEN FIRE DEPARTMENT MEDICAL / RESCUE SKILLS 1. CARDIAC ARREST MANAGEMENT 2. AIRWAY & RESPIRATORY MANAGEMENT 3. SPINAL IMMOBILIZATION
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
LESSON 2.1 Minor Wound Management Process
 LESSON 2.1 Minor Wound Management Process How do we make use of the four different kinds of first aid items such as gauze, melolin, padding (triangular bandage), and plaster to cover up the wounds? Cleaning
LESSON 2.1 Minor Wound Management Process How do we make use of the four different kinds of first aid items such as gauze, melolin, padding (triangular bandage), and plaster to cover up the wounds? Cleaning
Knee Conditioning Program
 Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
Knee Conditioning Program Purpose of Program After an injury or surgery, an exercise conditioning program will help you return to daily activities and enjoy a more active, healthy lifestyle. Following
CERVICAL STRAIN AND SPRAIN
 CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN Description Cervical strain/sprain is an injury to the neck caused when it is forcefully whipped or forced backward or forward. The structures involved are the muscles, ligaments,
CERVICAL STRAIN AND SPRAIN (Whiplash)
 CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
CERVICAL STRAIN AND SPRAIN (Whiplash) Description time and using proper technique decrease the frequency of Whiplash is an injury to the neck caused when it is forcefully whipped or forced backward or
MUSCULOSKELETAL INJURIES
 WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
WHAT ARE THEY They are injuries to muscles, nerves, tendons ligaments, joints, cartilage and spinal discs. WHAT KIND OF INJURIES ARE MUSCULOSKELETAL INJURIES 1. Fractures- -Open -Closed 2. Dislocations
Kinesiology Tape. Table of contents:
 1 Kinesiology Tape Welcome to the Anuva application center. These application guidelines and general use instructions are intended to be used with Anuve professional quality Kinesiology tape and if followed
1 Kinesiology Tape Welcome to the Anuva application center. These application guidelines and general use instructions are intended to be used with Anuve professional quality Kinesiology tape and if followed
Aviation Rescue Swimmer Course
 Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
Aviation Rescue Swimmer Course Primary Survey LT 5.4 December 2003 1 Objectives List the procedures used in a primary survey. Demonstrate primary survey procedures used in a mock trauma (moulage) scenario
4 inch laceration traversing down the front of forearm. Fracture of lower leg midway between knee and ankle
 2 inch wound on forehead 3 inch wound on top of shoulder islocated elbow in flexed position 4 inch laceration traversing down the front of forearm 3 inch wound on inner thigh Fracture of lower leg midway
2 inch wound on forehead 3 inch wound on top of shoulder islocated elbow in flexed position 4 inch laceration traversing down the front of forearm 3 inch wound on inner thigh Fracture of lower leg midway
OV United Soccer Club
 Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
Preventing disease transmission Place an effective barrier between you and the victim s blood when you give first aid. Examples of such barriers are: the victim s hand, a piece of plastic, clean folded
AMERICAN RED CROSS FIRST AID RESPONDING TO EMERGENCIES FOURTH EDITION Copyright 2006 by The American National Red Cross All rights reserved.
 Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Musculoskeletal injuries are most commonly caused by Mechanical forms of energy. Chemicals. Electrical energy. Heat Mechanical energy produces direct, indirect, twisting and contracting forces. Can be
Shoulder Arthroscopic Capsular Release Rehabilitation
 Shoulder Arthroscopic Capsular Release Rehabilitation Phase two: 3 to 6 weeks after surgery Goals: 1. Improve range of motion of the shoulder 2. Begin gentle strengthening Activities 1. Sling Your sling
Shoulder Arthroscopic Capsular Release Rehabilitation Phase two: 3 to 6 weeks after surgery Goals: 1. Improve range of motion of the shoulder 2. Begin gentle strengthening Activities 1. Sling Your sling
Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing
 1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
1 2 3 4 5 6 Chapter 8 Trauma Patient Assessment The Patient Assessment Process The Primary Assessment ABCDE s Airway, Breathing, Circulation while securing D-Disability Chief complaint and/or Mechanism
KNEE AND LEG EXERCISE PROGRAM
 KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
KNEE AND LEG EXERCISE PROGRAM These exercises are specifically designed to rehabilitate the muscles of the hip and knee by increasing the strength and flexibility of the involved leg. This exercise program
Lower Body. Exercise intensity moderate to high.
 Lower Body Lower Body Introduction This exercise routine is created for men and women with the goals of strengthening the lower body. Along with increasing strength of the leg muscles this workout will
Lower Body Lower Body Introduction This exercise routine is created for men and women with the goals of strengthening the lower body. Along with increasing strength of the leg muscles this workout will
Increase Strength, Flexibility, Range of Motion and Endurance. NeckXsystems Guidelines & Exercise. NeckX is Patent Pending
 Increase Strength, Flexibility, Range of Motion and Endurance NeckXsystems Guidelines & Exercise Instructions www.neckxsystems.com NeckX is Patent Pending Guidelines NeckX is an innovative neck exercise
Increase Strength, Flexibility, Range of Motion and Endurance NeckXsystems Guidelines & Exercise Instructions www.neckxsystems.com NeckX is Patent Pending Guidelines NeckX is an innovative neck exercise
Skin Anatomy and Physiology
 Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Skin Anatomy and Physiology Body s largest organ Three layers: Epidermis Dermis Subcutaneous tissue 1 2 Skin Anatomy and Physiology Complex system, variety of functions Sensation Control of water loss
Student Objectives. When you have completed the exercises in this chapter, you will have accomplished the following objectives:
 Student Objectives When you have completed the exercises in this chapter, you will have accomplished the following objectives: Classification of Joints 1. Define joint or articulation. 2. Classify joints
Student Objectives When you have completed the exercises in this chapter, you will have accomplished the following objectives: Classification of Joints 1. Define joint or articulation. 2. Classify joints
Proteus XR/f Patient positioning guide
 Proteus XR/f Patient positioning guide PROTEUS XR/F Now a single digital x-ray room accommodates nearly all your radiographic studies. With extended tube coverage and wireless detectors, Proteus XR/f gives
Proteus XR/f Patient positioning guide PROTEUS XR/F Now a single digital x-ray room accommodates nearly all your radiographic studies. With extended tube coverage and wireless detectors, Proteus XR/f gives
Medical Terminology. Unit 2
 Medical Terminology Unit 2 Students will apply medical terminology. Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how
Medical Terminology Unit 2 Students will apply medical terminology. Objective 1: Identify and utilize anatomical positions, planes, and directional terms. Demonstrate what anatomical position is and how
JOINT HEALTH. Joints are areas in the body where two or more bones meet. They have the following components:
 JOINT HEALTH Joints are areas in the body where two or more bones meet. They have the following components: Articular Cartilage: tissue covering the surface of a bone at a joint. Cartilage helps reduce
JOINT HEALTH Joints are areas in the body where two or more bones meet. They have the following components: Articular Cartilage: tissue covering the surface of a bone at a joint. Cartilage helps reduce
Note: This CareKit does not replace expert medical care. Be Prepared
 Note: This CareKit does not replace expert medical care. Be Prepared EMS #: 9-1-1 Poison Control #: 800.222.1222 Take a first aid course. Learn CPR and first aid for choking. Before you give first aid,
Note: This CareKit does not replace expert medical care. Be Prepared EMS #: 9-1-1 Poison Control #: 800.222.1222 Take a first aid course. Learn CPR and first aid for choking. Before you give first aid,
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES. Clavicle fractures Proximal head of humerus fractures
 REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
REHABILITATION FOR SHOULDER FRACTURES & SURGERIES Clavicle fractures Proximal head of humerus fractures By Dr. Mohamed Behiry Lecturer Department of physical therapy for Orthopaedic and its surgery. Delta
Snow Angels on Foam Roll
 Thoracic Mobilization on Foam Roll Lie on your back with a foam roller positioned horizontally across your mid back, and arms crossed in front of your body. Bend your knees so your feet are resting flat
Thoracic Mobilization on Foam Roll Lie on your back with a foam roller positioned horizontally across your mid back, and arms crossed in front of your body. Bend your knees so your feet are resting flat
