In the rehabilitation of patients
|
|
|
- Lester Andrews
- 6 years ago
- Views:
Transcription
1 The Immediate Effects of Soft Tissue Mobilization With Proprioceptive Neuromuscular Facilitation on Glenohumeral External Rotation and Overhead Reach Joseph J. Godges, DPT, MA, OCS 1 Melodie Mattson-Bell, DPT, OCS 2 Donna Thorpe, PT, MS 3 Drashti Shah, MPT 4 Study Design: Randomized controlled 2-group, pretest-posttest, multivariate study of patients with shoulder musculoskeletal disorders. Objectives: The purpose of this study was to evaluate the immediate effect of soft tissue mobilization (STM) with proprioceptive neuromuscular facilitation (PNF) to increase glenohumeral external rotation at 45 of shoulder abduction and overhead reach. Background: It is postulated that limitation in, when measured at 45 of shoulder abduction, represents subscapularis muscle flexibility deficits and is associated with the inability to fully reach overhead. No research, however, is available to demonstrate whether intervention strategies intended to improve subscapularis flexibility and glenohumeral external rotation range of motion at 45 of shoulder abduction will improve a patient s ability to reach overhead. Methods and Measures: Twenty patients (10 males, 10 females; age range, years) with limited and overhead reach of 1 year duration or less served as subjects. The subjects were randomly assigned to a treatment group, which consisted of soft tissue mobilization to the subscapularis and proprioceptive neuromuscular facilitation to the shoulder rotators, or a control group. Goniometric measurements of at 45 abduction and overhead reach were taken preintervention and immediately postintervention for the treatment group or at prerest and postrest periods for the control group. Results: The treatment group improved by a mean of 16.4 (95% confidence interval [CI], ) of, as compared to less than a 1 gain (95% CI, ) in the control group (P.0005). Overhead reach in the treatment group improved by a mean of 9.6 cm (95% CI, cm) in comparison to a mean gain of 2.4 cm (95% CI, cm) for the control group (P =.009). Conclusion: These findings suggest that a single intervention session of STM and PNF was effective for producing immediate improvements in and overhead reach in patients with shoulder disorders. J Orthop Sports Phys Ther 2003;33: Key Words: manual therapy, proprioceptive neuromuscular facilitation, range of motion, shoulder, subscapularis 1 Assistant Professor, Department of Physical Therapy, School of Allied Health Professions, Loma Linda University, Loma Linda, CA; Coordinator, Kaiser Permanente Southern California, Physical Therapy Residency and Fellowship Programs, Los Angeles, CA. 2 Owner, High Desert Physical Rehabilitation Group, Twenty-Nine Palms, CA. 3 Assistant Professor, Department of Physical Therapy, School of Allied Health Professions, Loma Linda University, Loma Linda, CA. 4 Physical Therapist, High Desert Physical Rehabilitation Group, Twenty-Nine Palms, CA. This study was approved by the Institutional Review Board of Loma Linda University. Address correspondence to Joseph J. Godges, Kaiser Permanente Southern California, Physical Therapy Residency and Fellowship Programs, Los Angeles, CA Joseph.J.Godges@kp.org In the rehabilitation of patients with shoulder impairments, regaining adequate is believed to be essential for restoring the ability to reach overhead. 2 Identification of the structure, or structures, limiting may assist in planning the appropriate intervention for these patients. The common limiters of are the glenohumeral capsule and the shoulder internal rotators. 1,13 The investigators of this study have observed that glenohumeral external rotation is commonly more limited in the lower ranges of abduction, such as at 45 of abduction, when compared to the higher ranges of abduction, such as at 90 of abduction. Cadaver studies and outcomes of subscapular surgical releases suggest that subscapularis muscle flexibility deficits are responsible for limitations in the lower ranges of abduction. 9,13 A contrasting clinical and cadaver finding is where becomes more limited as the humerus moves toward 90 of abduction, suggestive of glen- RESEARCH REPORT Journal of Orthopaedic & Sports Physical Therapy 713
2 ohumeral capsular restrictions. 6,13 Thus, a patient who has greater limitation of glenohumeral external rotation at 45 of abduction, when compared to the available external rotation at 90 of abduction, may have a subscapularis muscle flexibility deficit rather than a glenohumeral capsular restriction. In this instance, an appropriate intervention may include procedures purported to improve muscle extensibility, such as soft tissue mobilization (STM) and proprioceptive neuromuscular facilitation (PNF). 3,5,7,8,10,11 This is in contrast to patients presumed to have a capsular restriction who would likely benefit from interventions that are intended to improve joint accessory motions, such as joint mobilization. 11,15 In this study, the investigators will presume that a patient who has less at 45 of abduction, when compared to the amount of external rotation at 90 of abduction, has a subscapularis muscle flexibility deficit. The investigators of this study hypothesized that STM and PNF procedures applied to the subscapularis would increase the available at 45 of abduction and would improve the ability to reach overhead. Soft tissue mobilization is the application of specific and progressive manual forces with the intent of promoting changes in the myofascia, allowing for elongation of shortened structures. 5 STM procedures are often combined with PNF procedures because they are both used to effect changes in myofascial length. Contract-relax PNF procedures have been shown to be effective in increasing range of motion (ROM). 3,10,16 It has been proposed that PNF methods, particularly those involving reciprocal activation of the agonist and antagonist to the desired motion, provide the greatest potential for muscle lengthening. 4 The immediate effects of combining STM and PNF interventions were demonstrated in a previous study using healthy subjects, where improvements were made in hip ROM utilizing midrange STM combined with PNF. 5 In a case series of 3 patients with shoulder impingement syndrome and accompanying limitations in shoulder abduction, myofascial massage and stretching of the subscapularis resulted in a return to full painless function in all 3 patients. 8 However, the immediate effects of STM and PNF to patients with shoulder motion limitations have not been examined in a randomized, controlled trial. Thus, the purpose of this study is to evaluate whether STM to the subscapularis combined with PNF procedures intended to increase shoulder external rotation will produce an immediate improvement in (1) when measured at 45 of abduction, and (2) overhead reach in subjects with shoulder pathology. METHODS Subjects Twenty subjects (10 males, 10 females) between the ages of 21 and 83 years, with shoulder pathology of 1 year or less, participated in the study. Subjects were patients referred to an outpatient physical therapy clinic for evaluation and interventions for the functional losses related to their shoulder pathology. Subjects were included in the study if they exhibited limitations in overhead reach as well as glenohumeral external rotation when measured at 45 of shoulder abduction. Limitations in overhead reach were operationally defined as inability to walk fingers up the side of a wall as high as the opposite (nonpathological) side. A subject was defined as having limitations in at 45 abduction if the amount of external rotation was less than 90 and the amount of external rotation increased when the limb was moved to 90 of abduction. Subjects whose available decreased as the humerus was abducted to 90 were presumed to have capsular restrictions and thus excluded from the study. Patients were also excluded if they had a surgical procedure to the shoulder less than 4 weeks prior to study enrollment, total shoulder arthroplasty, reflex sympathetic dystrophy and related syndromes, or rheumatoid arthritis. After they signed an informed consent to participate in the study, subjects were randomly assigned to a treatment or control group. A predetermined schedule of random assignments to treatment and control groups was followed. To develop the schedule, a random number table was used to assign the 20 enrollment numbers in blocks of 4. The protocol for this study was approved by the Institutional Review Board of Loma Linda University. Procedures Measurements of external rotation and overhead reach were made on all subjects before and after receiving either the experimental or control intervention. The same physical therapist investigator (D.S.), who was blinded to the group assignment, performed all measurements. Glenohumeral external rotation was measured with the subjects lying supine on a treatment table with a pillow under their knees. Stabilization of the scapula was achieved by depressing the shoulder girdle. Reference lines for abduction were drawn on the skin over the midline of the sternum and the anterior aspect of the midline of the humerus. A reference point was also drawn on the skin over the anterior aspect of the acromion. In addition, a reference line was drawn on the skin over the ulnar aspect of the 714 J Orthop Sports Phys Ther Volume 33 Number 12 December 2003
3 FIGURE 1. Measurement of at 45 of abduction. FIGURE 2. Measurement of overhead reach. on the forearm (see Figure 1), as described by Norkin and White. 12 Overhead reach was measured with the subjects in standing position facing a wall, with the tips of their toes aligned with a premarked line on the floor 30.5 cm from the wall. The subjects were asked to actively walk their fingers up the wall to reach as far as they could. Overhead reach was measured as the distance in cm from the floor to the tip of the middle finger using a tape measure (Figure 2). To establish intrarater reliability for measuring external rotation and overhead reach, the measurements taken before and after the control intervention on the 10 control subjects in the study were analyzed. The intraclass correlation (ICC 3,1 ) for the external rotation repeated measures was 0.96 (95% confidence interval [CI], ). The ICC 3,1 scores for the overhead reach was 0.97 (95% CI, ). Subjects in the treatment group received STM to the subscapularis, followed by PNF procedures. The subjects were positioned with the humerus abducted to approximately 45. With the elbow flexed to 90, the humerus was externally rotated to a midrange position, typically about 20 to 25 of external rotation. The subscapularis was palpated in the axilla to identify areas of myofascial mobility restrictions, taut bands, or trigger points. 14 Identified restrictions were treated with STM utilizing a combination of sustained manual pressure, and slow deep strokes to the subscapularis myofascia for 7 minutes (Figure 3). The STM was followed by contract-relax PNF to the subscapularis and other glenohumeral medial rotators, beginning in the same position used for the STM. The patients were instructed to perform maximal glenohumeral internal rotation against an opposing, isometric, manual resistance applied by the treating physical therapist for 7 seconds. Afterwards, the patient actively moved the humerus into full available external rotation. This position was main- RESEARCH REPORT forearm, with a reference point on the olecranon process. Using the line over the humerus and an imaginary line parallel to the line over the sternum as references, the shoulder was abducted to 45. Maintaining 45 of shoulder abduction and 90 of elbow flexion, the patient s arm was passively externally rotated through the available pain-free ROM. External rotation was measured with the stationary arm of the goniometer perpendicular to the ground and the moving arm in line with the reference line FIGURE 3. Soft tissue mobilization to the subscapularis region. J Orthop Sports Phys Ther Volume 33 Number 12 December
4 TABLE 1. Subjects medical diagnosis. Diagnosis n Impingement syndrome 6 Status post rotator cuff repair 5 Supraspinatus tendonitis 2 Humeral head fracture 2 Humeral neck fracture status post open reduction, 1 internal fixation Rotator cuff tear 1 Superior labral anterior-posterior lesion, status post 1 repair Shoulder posterior dislocation 1 Polymyalgia 1 Total 20 Journal of Orthopaedic & Sports Physical Therapy FIGURE 4. Proprioceptive neuromuscular facilitation of active shoulder flexion, abduction, and external rotation. tained for 15 seconds. This 7-second internal rotation contraction against resistance followed by full active external rotation was repeated 5 times. Subjects were then instructed to actively move through the PNF flexion-abduction external-rotation diagonal pattern 7 for 5 repetitions with manual facilitation (Figure 4). The same physical therapist investigator (M.M.B.) performed all of the STM and contract-relax PNF procedures. The total time for the described intervention was approximately 10 minutes. The control subjects lay supine on a treatment table with pillows under their knees and resting their hands on their abdomen for a period of 10 minutes. Data Analysis Independent t tests were used to determine whether there were differences of age, height, and days since onset of condition between the treatment and control groups. A chi-square test was used to determine gender difference between the groups. An individual mixed-model ANOVA, with the withinsubject factor being time and the between-subject factor being group, was used to test for significant changes in at 45 abduction and overhead reach. Because ANOVA results showed an interaction between time (premeasurements and postmeasurements) and treatment group for both variables, 1-way ANOVAs were used to test for differences initially and analyze the differences between premeasurements and postmeasurements for both variables. All statistical analyses were tested at the.05 level of significance. RESULTS Table 1 provides a summary of the medical diagnoses given to the subjects by their referring physi- TABLE 2. Baseline comparison of treatment (n = 10) and control (n = 10) groups on age, gender* and acuity of the condition. Treatment Group (mean ± SD) Control Group (mean ± SD) Significance Age (y) 60.8 ± ± 16.5 NS Height (cm) ± ± 12.8 NS Acuity (d) 86.2 ± ± 71.4 NS * There were 5 males and 5 females in each group. NS, nonsignificant results of independent t test (P.05) between groups. Acuity is the number of days between the onset of the dysfunction and the date of the study. cian. The majority of the subjects had shoulder dysfunctions relating to impingement syndrome or had had a rotator cuff repair. Table 2 compares the 2 groups at baseline for age, gender, height, and days since onset of condition. There were 5 males and 5 females in each group. Mean age was 60.8 years and 58.6 years for the treatment and control groups, respectively. The time since onset of the shoulder condition was approximately 3 months for the treatment group and 4 months for the control group. There were no significant differences between groups on any of these variables. The immediate effects of the STM and PNF treatment procedures were determined by comparing the postintervention gain in glenohumeral external ROM and overhead reach between the 2 groups. The groups were similar at baseline on these variables (Tables 3 and 4). Immediately after the intervention, the treatment group showed a gain of 16.4 of external rotation (95% CI, ), a significantly greater gain than the less than 1 gain (95% CI, ) in the control group (P.0005). Overhead reach improved by a mean gain of 9.6 cm (95% CI, cm) in comparison to a mean of 2.4 cm (95% CI, ) for the control group (P =.009). Tables 3 and 4 summarize the treatment and control group results. 716 J Orthop Sports Phys Ther Volume 33 Number 12 December 2003
5 TABLE 3. Glenohumeral external rotation (ER) range of motion (mean ± SD in degrees) at 45 of abduction before and after a single intervention session. Treatment Group (n = 10) Control Group (n = 10) P PreER 41.6 ± ± * PostER 58.0 ± ± 16.9 Change in ER 16.4 ± ± * No statistically significant difference between groups prior to treatment (1-way ANOVA). Statistically significant different change in range of motion between groups as a result of treatment (1-way ANOVA). TABLE 4. Comparison of overhead reach (OHR) (mean ± SD in cm) before and after a single intervention session. Treatment Group (n = 10) Control Group (n = 10) P PreOHR ± ± * PostOHR ± ± 24.9 Change in OHR 9.6 ± ± * No statistically significant difference between groups prior to treatment (1-way ANOVA). Statistically significant different change in overhead reach between groups as a result of treatment (1-way ANOVA). DISCUSSION The purpose of the study was to determine whether STM and PNF procedures are effective in producing an immediate improvement in at 45 of abduction and overhead reach in patients with shoulder disorders. The results showed that these procedures were able to produce a mean increase of 9.6 cm in overhead reach immediately following a single intervention sesssion. In addition, depending on the patient s stage of healing and intervention session tolerance, the procedures described in this study could be repeated during the same or subsequent intervention session to further improve the patient s ability to reach overhead. These results provide a useful treatment option where traditional end range stretching may cause discomfort, muscle guarding, or are contraindicated. These results also extend the findings of a previous study, where a combined STM and PNF intervention produced immediate improvements in hip mobility in a healthy population, 5 to patients with shoulder disorders. A noteworthy finding at the screening for initial inclusion into the research was that all subjects demonstrated greater limitations in glenohumeral external rotation at 45 than at 90 of abduction. It is also noteworthy that none of the subjects in this study received the medical diagnosis of adhesive capsulitis from their physician. Based on biomechanical studies that demonstrate more selective tension of the glenohumeral joint capsular-ligamentous structures than tensioning of the musculature surrounding the shoulder at 90 abduction, restrictions of external rotation at 45 of abduction are potentially caused by primarily muscular restriction rather than joint capsular restrictions. The results of this study suggest that examining the amount of glenohumeral external rotation at 45 of abduction may be useful in guiding a clinician s plan of care for patients with shoulder disorders. For example, initiating procedures intended to address subscapularis muscle flexibility deficits may be the intervention of choice for patients who exhibit less at 45 of abduction when compared to 90 of abduction. Assessing the comparative differences in external rotation range of motion at varying degrees of abduction on patients following surgical procedures that shorten the subscapularis (eg, in patients with recurring shoulder dislocation) may further examine the validity of this clinical test. This study used a single-intervention-session design. The design of the study does not allow for drawing conclusions regarding the effect of the intervention beyond a single visit. The design of this study also does not allow for comparison to a competing intervention program, such as active mobility exercises, passive stretching, or another manual therapy intervention. The possibility exists that any other intervention could have yielded similar or better results. The lack of a competing intervention group of similar duration and intensity is a limitation of the study. Future studies utilizing several repeated intervention sessions and additional outcome measures, such as self-report disability scales, are needed to determine the long-term efficacy of STM and PNF intervention versus a control or comparison group. CONCLUSION Soft tissue mobilization of the subscapularis for 7 minutes and 5 repetitions of contract-relax to the shoulder internal rotators, followed by 5 repetitions of PNF facilitating the flexion, abduction, and external rotation diagonal, was found to be effective in gaining during a single intervention session in patients with shoulder dysfunction. Additionally, patients treated with STM and PNF improved their ability to reach overhead. REFERENCES 1. DePalma AF. Loss of scapulohumeral motion (frozen shoulder). Ann Surg. 1952;135: Donatelli R, Greenfield B. Rehabilitation of a stiff and painful shoulder: a biomechanical approach. J Orthop Sports Phys Ther. 1984;9: RESEARCH REPORT J Orthop Sports Phys Ther Volume 33 Number 12 December
6 3. Etnyre BR, Abraham LD. Gains in range of ankle dorsiflexion using three popular stretching techniques. Am J Phys Med. 1986;65: Etnyre BR, Abraham LD. H-reflex changes during static stretching and two variations of proprioceptive neuromuscular facilitation techniques. Electroencephalogr Clin Neurophysiol. 1986;63: Godges J, MacRae H, Longdon C, Tinberg C, MacRae P. The effects of two stretching procedures on hip ROM and gait economy. J Orthop Sports Phys Ther. 1989;10: Gross J, Fetto J, Rosen E. Musculoskeletal Examination. Cambridge, MA: Blackwell Science; Ingber RS. Shoulder impingement in tennis/racquetball players treated with subscapularis myofascial treatments. Arch Phys Med Rehabil. 2000;81: Knott M, Voss D. Proprioceptive Neuromuscular Facilitation; Patterns and Techniques. New York, NY: Parker and Row; MacDonald PB, Hawkins RJ, Fowler PJ, Miniaci A. Release of the subscapularis for internal rotation contracture and pain after anterior repair for recurrent anterior dislocation of the shoulder. J Bone Joint Surg Am. 1992;74: Markos PD. Ipsilateral and contralateral effects of proprioceptive neuromuscular facilitation techniques on hip motion and electromyographic activity. Phys Ther. 1979;59: Nicholson GG. The effects of passive joint mobilization on pain and hypomobility associated with adhesive capsulitis of the shoulder. J Bone Joint Surg Am. 1985;6: Norkin C, White J. Measurements of joint ROM: A Guide to Goniometry. Philadelphia, PA: FA Davis Company; Ovesen J, Nielsen S. Stability of the shoulder joint. Cadaver study of stabilizing structures. Acta Orthop Scand. 1985;56: Travell J, Simons D. Myofascial Pain and Dysfunction: The Trigger Point Manual. Baltimore, MD: Williams and Wilkins; Vermeulen HM, Obermann WR, Burger BJ, Kok GJ, Rozing PM, van Den Ende CH. End-range mobilization techniques in adhesive capsulitis of the shoulder joint: A multiple-subject case report. Phys Ther. 2000;80: Wallin D, Ekblom B, Grahn R, Nordenborg T. Improvement of muscle flexibility. A comparison between two techniques. Am J Sports Med. 1985;13: J Orthop Sports Phys Ther Volume 33 Number 12 December 2003
Rehabilitation Guidelines for Labral/Bankert Repair
 Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Labral/Bankert Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Shoulder Mobility Deficits. ICD-9-CM codes: Adhesive capsulitis of the shoulder
 Shoulder Mobility Deficits ICD-9-CM codes: 726.0 Adhesive capsulitis of the shoulder ICF codes: Activities and Participation Domain codes: d4452 Reaching (Using the hands and arms to extend outwards and
Shoulder Mobility Deficits ICD-9-CM codes: 726.0 Adhesive capsulitis of the shoulder ICF codes: Activities and Participation Domain codes: d4452 Reaching (Using the hands and arms to extend outwards and
1-Apley scratch test.
 1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
1-Apley scratch test. The patient attempts to touch the opposite scapula to test range of motion of the shoulder. 1-Testing abduction and external rotation( +ve sign touch the opposite scapula, -ve sign
Phase I : Immediate Postoperative Phase- Protected Motion. (0-2 Weeks)
 Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Phase I : Immediate Postoperative Phase- Protected Motion (0-2 Weeks) Appointments Progression Criteria 2 weeks after surgery Rehabilitation appointments begin within 7-10 days of surgery, continue 1-2
Rehabilitation of Overhead Shoulder Injuries
 Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
Rehabilitation of Overhead Shoulder Injuries 16 th Annual Primary Care Orthopaedic & Sports Medicine Symposium January 29, 2016 Jeremy Sherman, PT, MPT Disclosures No financial disclosures to note. Jeremy
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol
 Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Total Shoulder Arthroplasty / Hemiarthroplasty Therapy Protocol The intent of this protocol is to provide the therapist with a guideline of the postoperative rehabilitation course of a patient that has
Effectiveness of Gong s Mobilization on shoulder abduction in adhesive capsulitis: A Case Study
 Case Report: Effectiveness of Gong s Mobilization on shoulder abduction in adhesive capsulitis: A Case Study Sunil G. Harsulkar 1, Keerthi Rao 2, Chandra Iyer 3, Khatri S.M. 4 1Post-graduate student of
Case Report: Effectiveness of Gong s Mobilization on shoulder abduction in adhesive capsulitis: A Case Study Sunil G. Harsulkar 1, Keerthi Rao 2, Chandra Iyer 3, Khatri S.M. 4 1Post-graduate student of
SHOULDER ARTHROSCOPY WITH ANTERIOR STABILIZATION / CAPSULORRHAPHY REHABILITATION PROTOCOL
 General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Shoulder Joint Examination. Shoulder Joint Examination. Inspection. Inspection Palpation Movement. Look Feel Move
 Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Shoulder Joint Examination History Cuff Examination Instability Examination AC Joint Examination Biceps Tendon Examination Superior Labrum Examination Shoulder Joint Examination Inspection Palpation Movement
Effectiveness of Scapular Proprioceptive Neuromuscular Facilitation (PNF) Techniques in Adhesive Capsulitis of the Shoulder Joint
 Research Article imedpub Journals www.imedpub.com Journal of Physiotherapy Research Effectiveness of Scapular Proprioceptive Neuromuscular Facilitation (PNF) Techniques in Adhesive Capsulitis of the Shoulder
Research Article imedpub Journals www.imedpub.com Journal of Physiotherapy Research Effectiveness of Scapular Proprioceptive Neuromuscular Facilitation (PNF) Techniques in Adhesive Capsulitis of the Shoulder
Joint Range of Motion Assessment Techniques. Presentation Created by Ken Baldwin, M.Ed Copyright
 Joint Range of Motion Assessment Techniques Presentation Created by Ken Baldwin, M.Ed Copyright 2001-2006 Objectives Understand how joint range of motion & goniometric assessment is an important component
Joint Range of Motion Assessment Techniques Presentation Created by Ken Baldwin, M.Ed Copyright 2001-2006 Objectives Understand how joint range of motion & goniometric assessment is an important component
Biceps Tenodesis Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Biceps Tenodesis Protocol The intent of this protocol is to provide the clinician with a
Physical Examination of the Shoulder
 General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
General setup Patient will be examined in both the seated and supine position so exam table needed 360 degree access to patient Expose neck and both shoulders (for comparison); female in gown or sports
A Comparison of the Immediate Effects of Eccentric Training vs Static Stretch on Hamstring Flexibility in Basketball Players Dr.
 A Comparison of the Immediate Effects of Eccentric Training vs Static Stretch on Hamstring Flexibility in Basketball Players Dr. Mandeep Thour* *Assistant Professor, Department of Physical Education SGGS
A Comparison of the Immediate Effects of Eccentric Training vs Static Stretch on Hamstring Flexibility in Basketball Players Dr. Mandeep Thour* *Assistant Professor, Department of Physical Education SGGS
RN(EC) ENC(C) GNC(C) MN ACNP *** MECHANISM OF INJURY.. MOST IMPORTANT ***
 HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
HISTORY *** MECHANISM OF INJURY.. MOST IMPORTANT *** Age - Certain conditions are more prevalent in particular age groups (i.e. Full rotator cuff tears are more common over the age of 45, traumatic injuries
Manual Therapy Techniques: Joint Mobilization and PNF Diagonal Patterns. Linda Gazzillo Diaz, Ed.D., ATC William Paterson University
 Manual Therapy Techniques: Joint Mobilization and PNF Diagonal Patterns Linda Gazzillo Diaz, Ed.D., ATC William Paterson University Assist in restoring joint motion by decreasing pain and stiffness Arthrokinematics
Manual Therapy Techniques: Joint Mobilization and PNF Diagonal Patterns Linda Gazzillo Diaz, Ed.D., ATC William Paterson University Assist in restoring joint motion by decreasing pain and stiffness Arthrokinematics
Manual Muscle Testing. Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department
 Manual Muscle Testing Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Manual Muscle Testing Evaluation of the function and strength of individual muscles and muscles
Manual Muscle Testing Yasser Moh. Aneis, PhD, MSc., PT. Lecturer of Physical Therapy Basic Sciences Department Manual Muscle Testing Evaluation of the function and strength of individual muscles and muscles
Hands on Sports Therapy KNOWLEDGE REVIEW QUESTIONS 2004 Thomson Learning. Q1:From the following list of acronyms, write down the full title of each
 CHAPTER 09 Knowledge Review Q1:From the following list of acronyms, write down the full title of each treatment technique: NMT; PRT; SCS; FT; MET; PNF; PIR; RI; CRAC; INIT; ICT; ICCT. A1: NMT: Neuromuscular
CHAPTER 09 Knowledge Review Q1:From the following list of acronyms, write down the full title of each treatment technique: NMT; PRT; SCS; FT; MET; PNF; PIR; RI; CRAC; INIT; ICT; ICCT. A1: NMT: Neuromuscular
Biceps Tenodesis Protocol
 Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Biceps Tenodesis Protocol A biceps tenodesis procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum and then anchoring the tendon along its anatomical
Page 2 of 13 Fig. E-2A Fig. E-2B Fig. E-2C Fig. E-2D Figs. E-2A through E-2D Treatment to relax the upper part of the trapezius muscle. Fig. E-2A Pati
 Page 1 of 13 Fig. E-1A Fig. E-1B Figs. E-1A through E-1C Correction of the sitting position to increase the patient s awareness for the correct sitting position and the interscapular muscles. Fig. E-1A
Page 1 of 13 Fig. E-1A Fig. E-1B Figs. E-1A through E-1C Correction of the sitting position to increase the patient s awareness for the correct sitting position and the interscapular muscles. Fig. E-1A
Biceps Tenotomy Protocol
 Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
Department of Rehabilitation Services Physical Therapy The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that has undergone
TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY
 Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Teodoro P. Nissen, M.D., Q.M.E. Fellowship Trained Board Certified Joseph M. Centeno, M.D. Fellowship Trained Board Certified TOTAL SHOULDER ARTHROPLASTY / HEMIARTHROPLASTY Protocol: The intent of this
Shoulder Arthroscopy with Posterior Labral Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Type II SLAP lesions are created when the biceps anchor has pulled away from the glenoid attachment.
 Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Arthroscopic Superior Labral (SLAP) Repair Protocol-Type II, IV, and Complex Tears The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of
Core deconditioning Smoking Outpatient Phase 1 ROM Other
 whereby the ball does not stay properly centered in the shoulder socket during shoulder movement. This condition may be associated with impingement of the rotator cuff on the acromion bone and coracoacromial
whereby the ball does not stay properly centered in the shoulder socket during shoulder movement. This condition may be associated with impingement of the rotator cuff on the acromion bone and coracoacromial
WEEKEND THREE HOMEWORK
 WEEKEND THREE HOMEWORK READING ASSIGNMENTS Salvo Massage Therapy Principles and Practice 4 th Edition Muscolino The Muscular System Manual Muscolino The Muscle and Bone Palpation Manual Ch. 19 Skeletal
WEEKEND THREE HOMEWORK READING ASSIGNMENTS Salvo Massage Therapy Principles and Practice 4 th Edition Muscolino The Muscular System Manual Muscolino The Muscle and Bone Palpation Manual Ch. 19 Skeletal
Rehabilitation Guidelines for Large Rotator Cuff Repair
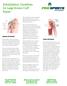 Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Rehabilitation Guidelines for Large Rotator Cuff Repair The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the
Active-Assisted Stretches
 1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
1 Active-Assisted Stretches Adequate flexibility is fundamental to a functional musculoskeletal system which represents the foundation of movement efficiency. Therefore a commitment toward appropriate
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations
 SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
SHOULDER DISLOCATION & INSTABILITY Rehabilitation Considerations Meagan Pehnke, MS, OTR/L, CHT, CLT March 1 st, 2019 Philadelphia Surgery & Rehabilitation of the Hand: Pediatric Pre-course OUTLINE Discuss
Arthroscopic Rotator Cuff Repair Protocol:
 Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Arthroscopic Rotator Cuff Repair Protocol: The intent of this protocol is to provide the therapist and patient with guidelines for the post-operative rehabilitation course after arthroscopic SLAP repair.
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer
 Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Rotator Cuff Repair Protocol for tear involving Subscapularis Tendon with or without Pectoralis Major Tendon Transfer D. WATTS, MD Precautions: BASIS Tendon healing back to bone is a slow process that
Conservative Massive Rotator Cuff Tear Protocol
 SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
SPORTS & ORTHOPAEDIC SPECIALISTS Conservative Massive Rotator Cuff Tear Protocol 3-4 visits over 4-6 weeks Emphasis is on AAROM and a high repetition, low weight free weight program Emphasize improved
PROM is not stretching!
 Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Dx: o Right o Left Shoulder Replacement/Hemiarthroplasty Rehab Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: The intent
Biceps Tenotomy Protocol
 Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Biceps Tenotomy Protocol A biceps tenotomy procedure involves cutting of the long head of the biceps just prior to its insertion on the superior labrum. A biceps tenotomy is typically done when there is
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD
 Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Shoulder and Elbow ORTHOPAEDIC SYPMPOSIUM APRIL 8, 2017 DANIEL DOTY MD Shoulder Articulations Glenohumeral Joint 2/3 total arc of motion Shallow Ball and Socket Joint Allows for excellent ROM Requires
Christopher K. Jones, MD Colorado Springs Orthopaedic Group
 Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Christopher K. Jones, MD Colorado Springs Orthopaedic Group 719-632-7669 Total Shoulder Replacement You have undergone a shoulder replacement procedure. The performance of the procedure is complete, but
Evidence- Based Examination of the Shoulder Presented by Eric Hegedus, PT, DPT, MHSC, OCS, CSCS Practice Sessions/Skill Check- offs
 Evidence- Based Examination of the Shoulder Practice Session & Skills Check- offs Evidence- Based Examination of the Shoulder Presented by Eric Hegedus, PT, DPT, MHSC, OCS, CSCS Practice Sessions/Skill
Evidence- Based Examination of the Shoulder Practice Session & Skills Check- offs Evidence- Based Examination of the Shoulder Presented by Eric Hegedus, PT, DPT, MHSC, OCS, CSCS Practice Sessions/Skill
Hemiplegic Shoulder Power Point for staff education sessions
 Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Appendix B Hemiplegic Shoulder Power Point for staff education sessions Jennifer Curry Physiotherapist, London Health Sciences Centre www.swostroke.ca Acknowledgements Maria Lung BSc (PT), MSc Train the
Latarjet Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
General Notes: As tolerated should be understood to include with safety for the reconstruction/repair; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing
APPENDIX: The Houston Astros Stretching Program
 Vol. 35, No. 4, 2007 Glenohumeral Internal Rotation Deficits 1 APPENDIX: The Houston Astros Stretching Program Our Flexibility program consists of 5 positions. Four of the 5 have 2 variations of each position.
Vol. 35, No. 4, 2007 Glenohumeral Internal Rotation Deficits 1 APPENDIX: The Houston Astros Stretching Program Our Flexibility program consists of 5 positions. Four of the 5 have 2 variations of each position.
Reverse Total Shoulder Arthroplasty Protocol
 General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
General Information: Reverse Total Shoulder Arthroplasty Protocol Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH) arthritis when it
Shoulder Arthroscopy with Rotator Cuff Repair Rehabilitation Protocol
 General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
General Notes: As tolerated should be understood to include with safety for the surgical procedure; a sudden increase in pain, swelling, or other undesirable factors are indicators that you are doing too
Neck Rehabilitation programme for Rugby players.
 Neck Rehabilitation programme for Rugby players. The programme consists of two parts, first the Therapeutic Exercise Programme to improve biomechanical function and secondly the Rehabilitation programme
Neck Rehabilitation programme for Rugby players. The programme consists of two parts, first the Therapeutic Exercise Programme to improve biomechanical function and secondly the Rehabilitation programme
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol
 Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol The following document is an evidence-based protocol for arthroscopic rotator cuff repair rehabilitation. The protocol is both chronologically
Harold Schock III, MD Rotator Cuff Repair Rehabilitation Protocol The following document is an evidence-based protocol for arthroscopic rotator cuff repair rehabilitation. The protocol is both chronologically
EFFECTIVENESS OF CONVENTIONAL EXERCISE REGIMEN FOR THE TREATMENT OF SHOULDER PAIN
 EFFECTIVENESS OF CONVENTIONAL EXERCISE REGIMEN FOR THE TREATMENT OF SHOULDER PAIN Dr.U.Ganapathy Sankar, Ph.D., Dean I/C,Faculty of Medical & Health Sciences, SRM College of Occupational Therapy, SRM University,Kattankulathur,
EFFECTIVENESS OF CONVENTIONAL EXERCISE REGIMEN FOR THE TREATMENT OF SHOULDER PAIN Dr.U.Ganapathy Sankar, Ph.D., Dean I/C,Faculty of Medical & Health Sciences, SRM College of Occupational Therapy, SRM University,Kattankulathur,
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT
 SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SHOULDER PROBLEMS & ARTHROSCOPIC MANAGEMENT DR.SHEKHAR SRIVASTAV Sr. Consultant-KNEE & SHOULDER Arthroscopy Sant Parmanand Hospital,Delhi Peculiarities of Shoulder Elegant piece of machinery It has the
SLAP LESION REPAIR PROTOCOL
 SLAP LESION REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
SLAP LESION REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of
 Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Review shoulder anatomy Review the physical exam of the shoulder Discuss some common causes of acute shoulder pain Discuss some common causes of chronic shoulder pain Review with some case questions Bones:
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines
 Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
Rehabilitation Protocol: Arthroscopic Anterior Capsulolabral Repair of the Shoulder - Bankart Repair Rehabilitation Guidelines Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington
UPPER EXTREMITY INJURIES. Recognizing common injuries to the upper extremity
 UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
UPPER EXTREMITY INJURIES Recognizing common injuries to the upper extremity ANATOMY BONES Clavicle Scapula Spine of the scapula Acromion process Glenoid fossa/cavity Humerus Epicondyles ANATOMY BONES Ulna
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT
 REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
REHABILITATION GUIDELINES FOR ARTHROSCOPIC CAPSULAR SHIFT The rehabilitation guidelines are presented in a criterion based progression. General time frames are given for reference to the average, but individual
SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE
 SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE The rotator cuff is responsible for stabilization and active movement of the glenohumeral joint. An acute or overuse injury may cause the rotator cuff to be injured
SMALL-MEDIUM ROTATOR CUFF REPAIR GUIDELINE The rotator cuff is responsible for stabilization and active movement of the glenohumeral joint. An acute or overuse injury may cause the rotator cuff to be injured
Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength in Patients with Shoulder Disorders: A Preliminary Report
 The University of Pennsylvania Orthopaedic Journal 16: 39 44, 2003 2003 The University of Pennsylvania Orthopaedic Journal Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength
The University of Pennsylvania Orthopaedic Journal 16: 39 44, 2003 2003 The University of Pennsylvania Orthopaedic Journal Relationship of the Penn Shoulder Score with Measures of Range of Motion and Strength
Tendinosis & Subacromial Impingement Syndrome. Gene Desepoli, LMT, D.C.
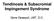 Tendinosis & Subacromial Impingement Syndrome Gene Desepoli, LMT, D.C. What is the shoulder joint? Shoulder joint or shoulder region? There is an interrelatedness of all moving parts of the shoulder and
Tendinosis & Subacromial Impingement Syndrome Gene Desepoli, LMT, D.C. What is the shoulder joint? Shoulder joint or shoulder region? There is an interrelatedness of all moving parts of the shoulder and
Shoulder Impingement Rehabilitation Recommendations
 Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Shoulder Impingement Rehabilitation Recommendations The following protocol can be utilized for conservative care of shoulder impingement as well as post- operative subacromial decompression (SAD) surgery.
Total Shoulder Arthroplasty / Hemiarthroplasty Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Shoulder Arthroplasty / Hemiarthroplasty Protocol The intent of this protocol is to provide the
Basics of Soft- Tissue Examination
 Basics of Soft- Tissue Examination Basics of Soft Tissue Exam For practitioners who primarily use their hands to treat the human structure: Examination must include functional tests to determine the type
Basics of Soft- Tissue Examination Basics of Soft Tissue Exam For practitioners who primarily use their hands to treat the human structure: Examination must include functional tests to determine the type
Reverse Total Shoulder Protocol
 Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Marion Herring, M.D. OrthoVirginia PH: (804) 270-1305 FX: (804) 273-9294 www.orthovirginia.com Reverse Total Shoulder Protocol General Information: Reverse Total Shoulder Arthroplasty (rtsa) is designed
Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD
 General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
General Information: Reverse Total Shoulder Arthroplasty Protocol Shawn Hennigan, MD Reverse or Inverse Total Shoulder Arthroplasty (rtsa) is designed specifically for the treatment of glenohumeral (GH)
Joint G*H. Joint S*C. Joint A*C. Labrum. Humerus. Sternum. Scapula. Clavicle. Thorax. Articulation. Scapulo- Thoracic
 A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
A*C Joint Scapulo- Thoracic Articulation Thorax Sternum Clavicle Scapula Humerus S*C Joint G*H Joint Labrum AC Ligaments SC Ligaments SC JOINT AC Coracoacromial GH GH Ligament Complex Coracoclavicular
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears:
 Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Arthroscopic Labral Repair Protocol-Type II, IV, and Complex Tears: The intent of this protocol is to provide the clinician with a guideline of the postoperative rehabilitation course of a patient that
Bradley C. Carofino, M.D. Shoulder Specialist 230 Clearfield Avenue, Suite 124 Virginia Beach, Virginia Phone
 Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Subpectoral Bicep Tenodesis Protocol (Spreadsheet) Weeks 1-2 Modalities Treatment Restrictions Goals No active elbow flexion (6weeks) Full PROM shoulder and elbow PROM: Shoulder, elbow, forearm No active
Anterior Labrum Repair Protocol
 Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Anterior Labrum Repair Protocol Stage I (0-4 weeks): Key Goals: Protect the newly repaired shoulder. Allow for decreased inflammation and healing. Maintain elbow, wrist and hand function. Maintain scapular
Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab
 1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair)
 Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Gregory N. Lervick, MD Andrew Anderson, PA-C 952-456-7111 POST-SURGICAL POSTERIOR GLENOHUMERAL STABILIZATION REHABILITATION PROTOCOL (Capsulolabral Repair) Open Arthroscopic Phase 1: Weeks 0-4 No shoulder
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
PNF STRETCHING It s Role in Rehabilitation LOWER BODY
 PNF STRETCHING It s Role in Rehabilitation LOWER BODY Paula Nutting RMT Dip of Rem Massage/BHSc MST. Reg Nurse III Certificate; Personal Trainer 2000-2005 Stretching any therapeutic manoeuvre designed
PNF STRETCHING It s Role in Rehabilitation LOWER BODY Paula Nutting RMT Dip of Rem Massage/BHSc MST. Reg Nurse III Certificate; Personal Trainer 2000-2005 Stretching any therapeutic manoeuvre designed
Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Anterior Shoulder Reconstruction with Arthroscopic Bankart Repair The anatomic configuration of the shoulder joint (glenohumeral joint) is
SLAP LESION REPAIR PROTOCOL Dr. Steven Flores
 SLAP LESION REPAIR PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
SLAP LESION REPAIR PROTOCOL Dr. Steven Flores This rehabilitation protocol has been developed for the patient following a SLAP (Superior Labrum Anterior Posterior) repair. It is extremely important to
Shoulder: Clinical Anatomy, Kinematics & Biomechanics
 Shoulder: Clinical Anatomy, Kinematics & Biomechanics Dr. Alex K C Poon Department of Orthopaedics & Traumatology Pamela Youde Nethersole Eastern Hospital Clinical Anatomy the application of anatomy to
Shoulder: Clinical Anatomy, Kinematics & Biomechanics Dr. Alex K C Poon Department of Orthopaedics & Traumatology Pamela Youde Nethersole Eastern Hospital Clinical Anatomy the application of anatomy to
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Stabilization of the Shoulder: Latarjet Protocol The intent of this protocol is
Rotator Cuff Repair Protocol
 Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rotator Cuff Repair Protocol Applicability: Physician Practices Date Effective: 11/2016 Department: Rehabilitation Services Supersedes: Rotator Cuff Repair (Beattie) Date Last Reviewed / or Date Last Revision:
Rehabilitation Guidelines for Shoulder Arthroscopy
 Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Rehabilitation Guidelines for Shoulder Arthroscopy The true shoulder joint is called the glenohumeral joint and consists humeral head and the glenoid. It is a ball and socket joint. Anatomy of the Shoulder
Exploring the Rotator Cuff
 Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Exploring the Rotator Cuff Improving one s performance in sports and daily activity is a factor of neuromuscular efficiency and metabolic enhancements. To attain proficiency, reaction force must be effectively
Orthopedic Surgery and Sports Medicine FL License:
 Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Reverse Shoulder Arthroplasty Protocol: The intent of this protocol is to provide the therapist with a guideline for the post-operative rehabilitation course of a patient that has undergone a Reverse Shoulder
Rehab protocol. Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits. Goals:
 Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
Reverse Total shoulder arthroplasty Rehab protocol Phase I: Immediate Post-Surgical Phase: Typically 0-4 weeks; 2 PT visits Allow healing of soft tissue Maintain integrity of replaced joint Gradually increase
BANKART REPAIR PROTOCOL
 BANKART REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following Bankart surgical procedure for anterior shoulder instability. The protocol is divided
BANKART REPAIR PROTOCOL Clarkstown Division This rehabilitation protocol has been developed for the patient following Bankart surgical procedure for anterior shoulder instability. The protocol is divided
Rotator Cuff Repair Protocol
 Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
Protocol This rehabilitation protocol has been developed for the patient following a rotator cuff surgical procedure. This protocol will vary in length and aggressiveness depending on factors such as:
REMINDER. Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns
 Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
Understanding Shoulder Dysfunction REMINDER Obtain medical clearance and physician s release prior to beginning an exercise program for clients with medical or orthopedic concerns What is a healthy shoulder?
OBJECTIVES. Therapists Management of Shoulder Instability SHOULDER STABILITY SHOULDER STABILITY WHAT IS SHOULDER INSTABILITY? SHOULDER INSTABILITY
 Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Therapists Management of Shoulder Instability Brian G. Leggin, PT, DPT, OCS Lead Therapist, Penn Therapy and Fitness at Valley Forge Adjunct Assistant Professor, Department of Orthopaedics, University
Anterior Stabilization of the Shoulder: Distal Tibial Allograft
 Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
Anterior Stabilization of the Shoulder: Distal Tibial Allograft Name: Diagnosis: Date: Date of Surgery: Phase I Immediate Post Surgical Phase (approximately Weeks 1-3) Minimize shoulder pain and inflammatory
WEEKEND 2 Shoulder. Shoulder Active Range of Motion Assessment
 Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Shoulder Shoulder Active Range of Motion Assessment - Patient Positioning: Standing, appropriately undressed so that
Virginia Orthopedic Manual Physical Therapy Institute - 2016 Technique Manual WEEKEND 2 Shoulder Shoulder Active Range of Motion Assessment - Patient Positioning: Standing, appropriately undressed so that
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery. Phase 1: Immediate postoperative period (weeks 0-6) Goals
 The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
The Four Phases of Healing During Rehabilitation Following Rotator Cuff Surgery Phase 1: Immediate postoperative period (weeks 0-6) Maintain/protect integrity of repair Gradually increase PROM Diminish
Rehabilitation after shoulder dislocation
 Oxford University Hospitals NHS Trust Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your
Oxford University Hospitals NHS Trust Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your
Jennifer L. Cook, MD Stephen A. Hanff, MD. Rotator Cuff Type I Repair (Small Large Tear)
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 Rotator Cuff Type I Repair (Small Large Tear) This
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood
 Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Nonoperative Treatment For Rotator Cuff Tendinitis/ Partial Thickness Tear Dr. Trueblood Relieving Pain Patients who present with SIS will have shoulder pain that is exacerbated with overhead activities.
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS
 Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
Ms. Ruth A. Delaney, MB BCh BAO, MMedSc, MRCS Consultant Orthopaedic Surgeon, Shoulder Specialist. +353 1 5262335 ruthdelaney@sportssurgeryclinic.com Modified from the protocol developed at Boston Shoulder
IP: Sling for 6 weeks Week 0-6: Immobilisation + Pendulum exercise Week 6-4 Months: Active ROM 4 Months-on: Strengthening exercises
 Supplemental material 5 Table 1. Summary of rehabilitation programs postoperative. Author (year) Early Rehabilitation Conservative Rehabilitation Arndt et al., 2012 [35] First day postoperative-week 6:
Supplemental material 5 Table 1. Summary of rehabilitation programs postoperative. Author (year) Early Rehabilitation Conservative Rehabilitation Arndt et al., 2012 [35] First day postoperative-week 6:
Anterior Stabilization of the Shoulder: Latarjet Protocol
 Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
Anterior Stabilization of the Shoulder: Latarjet Protocol Dr. Abigail R. Hamilton, M.D. Shoulder instability may be caused from congenital deformity, recurrent overuse activity, and/or traumatic dislocation.
ROTATOR CUFF REPAIR REHAB PROTOCOL
 Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Jayesh K. Patel, M.D. Trinity Clinic Orthopaedic and Sports Medicine 1327 Troup Hwy Tyler, TX 75701 (903) 510-8840 ROTATOR CUFF REPAIR REHAB PROTOCOL This rehabilitation protocol has been developed for
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair
 Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Rehabilitation Protocol: Massive Rotator Cuff Tear Repair Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650 Lahey Outpatient Center, Lexington 781-372-7020 Lahey
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211
Throwing Athlete Rehabilitation. Brett Schulz LAT/CMSS Sport and Spine Physical Therapy
 Throwing Athlete Rehabilitation Brett Schulz LAT/CMSS Sport and Spine Physical Therapy Disclosure No conflicts to disclose Throwing Athlete Dilemma The shoulder must have enough range of motion to allow
Throwing Athlete Rehabilitation Brett Schulz LAT/CMSS Sport and Spine Physical Therapy Disclosure No conflicts to disclose Throwing Athlete Dilemma The shoulder must have enough range of motion to allow
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
JMSCR Vol 05 Issue 01 Page January 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.61 Effectiveness of Proprioceptive Neuromuscular
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.61 Effectiveness of Proprioceptive Neuromuscular
Charlotte Shoulder Institute
 Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Charlotte Shoulder Institute Patient Centered. Research Driven. Outcome Maximized. James R. Romanowski, M.D. Gill Orthopaedic Midtown Medical Plaza 1918 Randolph Rd., Suite 700 Charlotte, NC 28211 704-342-3544
Shoulder Arthroscopy: Postop Instructions. Activites & Advice for in the Hospital and while at Home
 Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Dr. Mark Price MGH Sports Medicine Center 175 Cambridge Street, 4th floor Boston, MA 02114 www.massgeneral.org/ortho-sports-medicine/dr-price Shoulder Arthroscopy: Postop Instructions You will wake up
Assistant Professor, Harivandana Physiotherapy College, Munjaka, Rajkot, Gujarat, India. ABSTRACT
 Original Research Article EFFECT OF DIFFERENT SHOULDER POSITION ON EMG PARAMETER OF ROTATOR CUFF AND DELTOID MUSCLE DURING EXTERNAL ROTA- TION EXERCISE: A CROSS-SECTIONAL OBSERVATIONAL STUDY Radhika D.
Original Research Article EFFECT OF DIFFERENT SHOULDER POSITION ON EMG PARAMETER OF ROTATOR CUFF AND DELTOID MUSCLE DURING EXTERNAL ROTA- TION EXERCISE: A CROSS-SECTIONAL OBSERVATIONAL STUDY Radhika D.
