Rehabilitation. Friday, October 14, :00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA
|
|
|
- Isaac Ramsey
- 6 years ago
- Views:
Transcription
1 Rehabilitation Friday, October 14, :00 11:45am General Session Rehabilitation following FAI Surgery Mark Ryan, MS, ATC, CSCS USA Best Tip Srino Bharam, MD USA Best Tip Robroy Martin, PhD, PT USA Best Tip Per Hölmich, MD DENMARK Best Tip Rodrigo Mardones, MD CHILE
2 Slide 1 Hip Rehabilitation Following FAI Surgery Mark Ryan, MS ATC CSCS Rehabilitation Coordinator for Dr. Mark Philippon Howard Head Sports Medicine Steadman Philippon Research Institute Vail, Colorado Slide 2 OBJECTIVES Outline Initial ROM and Weightbearing restrictions General Philosophies Define Phases 1-4 and Goals of Each Slide 3 REHABILITATION PHASES
3 Slide 4 PHASE 1: PROTECTION & MOBILTIY Goals 1. Protect the integrity of the repaired tissues 2. Diminish pain and inflammation 3. Restore ROM within the restrictions 4. Preserve muscle function (glutes and stabilizers) Slide 5 PHASE 1: RESTRICTIONS/PROTECTION ROM Restrictions Capsular Protection: No ER x days, No extension x days Limit Flexion to 120 degrees x 14 days Limit Abduction to 45 degrees x 14 days Crutches 20# Flat Foot Weightbearing Non-McFx: 21 days, 50% BW x 7 days, then wean McFx: 6-8 Weeks, 50% BW x 7 days, then wean Hip Brace: 21 days Slide 6 PHASE 1: REDUCE INFLAMMATION Lymphatic Massage: Week 1 Cryotherapy: Game Ready Soft Tissue: Weeks 2-8 Scar Mobs IT Band Glute Med TFL
4 Slide 7 PHASE 1: EARLY MOBILITY: PROM Circumduction, Logs Rolls, CPM, Bike Slide 8 CPM Machine Used to reduce risk of adhesions and to promote post-op fluid movement Week 1: 4-6 hours/day 0-45 degrees Week 2: 4-6 hours/day 0-70 degrees Week 3: 4-6 hrs 0-80 degrees Week 4: 1-2 hrs 0-80 degrees Set machine at 10 degrees of Abduction Slide 9 PHASE 1: EARLY MOBILITY/ AROM AROM: Cat/Camel, Ab/ Adduction
5 Slide 10 PHASE 1: EARLY MOBOLITY AQUATICS BIKING Slide 11 PHASE 1: EARLY MUSCLE ACTIVATION ISOMETRICS: Glute Max, Quads, Transverse Abdominus, IR/ER Standing Abduction Slide 12 PHASE 2: EARLY STABILIZATION GOALS Wean off crutches GOLDEN RULE: No limping, use crutches as long as necessary until you can walk normally without them. Normalize Gait Continue Mobility Early Closed Chain Strengthening Stabilization
6 Slide 13 PHASE 2: NORMALIZE GAIT Aquatics Gait Training Slide 14 PHASE 2: CONTINUED MOBILITY Active Butterflies, FABER Slides Slide 15 8 WEEK MD FOLLOW UP Strength and ROM testing compared bilaterally, glute firing pattern evaluation Surgeon evaluates hip with physical exam, gait analysis Decision made to continue with Phase 2 rehab, or progress to Phase 3 and functional activities
7 Slide 16 PHASE 2: STABILIZATION Single leg stance, Resisted Stool Rotations, RDLs Slide 17 PHASE 2: EARLY CC STRENGTHENING Double knee bends Lunges Balance squats Pilates Slide 18 PHASE 3: GOALS Return to Functional Activity (Sport drills and skills) Strength and Stability: Bilaterally equal Pass Sport Test (SL Squats, Lateral Agility, Diagonal Agility, Lunges)
8 Slide 19 PHASE 3: Return to Sport Progressions 3 P s Pain-free Progressive Predictable to Performance Slide 20 Hip Sports Test Test Components Maximum score 1. Single leg squat (single knee bend) 3 min max 6 points 2. Lateral agility test 100s max 5 points 3. Diagonal agility test 100s max 5 points 4. Forward single leg lunges 2 min max 4 points Total 20 points Slide 21 Sports Test Single leg squat (single knee bend = 6pts): Time: 3 min Inadequate form: Trendelenburg Locked knee in extension Collapse of the leg in internal rotation and adduction Using the chair as support Lack of endurance: Inability to maintain rhythm Trembling
9 Slide 22 Lateral Agility (5 pts): Time: 100 seconds Inadequate form: Sports Test LACK OF ABSORPTION Trendelenburg Collapse of the leg in internal rotation and adduction Lack of endurance: Inability to maintain rhythm Trembling Slide 23 Sports Test Forward Bench Lunge (4 pts): Time: 2 min Inadequate form: Trendelenburg Avoidance of maximum flexion Lack of endurance: Inability to maintain rhythm Trembling
10 Srino Bharam, MD New York, NY, USA Introduction Rehabilitation Friday, October 14 th, rd Annual ISHA Meeting, Paris, France Is formal rehab necessary? Evolution of the postoperative rehab protocols Hip rehab in 2011 Surgeon s prospective Multidisciplinary approach Patient expectations Predictors of outcome Patient evaluation Symptoms Strength deficits ROM limitation FAI consideration Extra-articular soft tissue considerations Address before surgery? Surgical management Patient goals Initial postoperative rehab (week 0-4)- Phase 1 Weight bearing progression Passive motion concepts Rotational precautions Weeks (4-8)- Phase II Normalize gait
11 Hip joint mobs Progress hip strengthening Progress core strengthening Propioception activities S. Bharam Weeks (8-12)- Phase III Progressive ROM and strengthening Hip endurance exercises Dynamic balance exercises Week (12-16)- Phase IV Plyometrics Sport specific drills Avoiding postoperative complications Tendonitis Bursitis Scar tissue around portal sites Loss of motion Abnormal gait patterns My Best Tips
12 Rehabilitation After Arthroscopic Surgery to Correct Femoroacetabular Impingement Phase 1: 0-3 weeks Maximum Protection Phase 2: 3-6 weeks Moderate Protection Phase 3: 6-12 weeks Minimal Protection RobRoy L. Martin PhD, PT, CSCS Duquesne University Pittsburgh, PA UPMC Center for Sports Medicine 1 Phase 4: weeks Functional Progression Phase 5: weeks Sports Specific-Work Related Retraining 2 Phase 1 Phase 1 Pearls and Perils 0-3 weeks- Maximum Protection Goals: Maintain ROM- Quadruped Rocking Prevent muscular weakness and inhibition Protect repaired tissue Decrease pain Decrease inflammation Do enough BUT not to much Use pain to guide!! Do not forget exercises to target trunk/core 3 4 Phase weeks- Moderate Protection Goals: Increase ROM to near normal Use gentle distraction techniques General pain free status Increase strength Normalize gait with D/C of assistive device Phase 2 Pearls and Perils Make sure to include hip flexion combined with adduction and internal rotation Distraction allows to achieve more ROM Do not progress off assistive device to quickly Use cane if necessary Exercises and gait training can be done in water can include swimming with leg buoy No kicking aqua-suspended jogging Limit motion 5 6
13 Phase weeks- Minimal Protection Goals: ROM 100% normal Increase strength of trunk and entire LE to near normal Normal gait pattern Phase 3 Weight Bearing Status/Assistive Device: FWB no assistive device Any subtle deviations should be corrected with appropriate interventions: Stretching Mobilization Strengthening Stabilization Proprioceptive 7 8 Phase 3 Exercises: ROM should emphasize stretching. Joint mobilizations should be added to address any limitations particularly with flexion, internal rotation, and adduction. i.e. lateral distraction, long axis distraction, and posterior capsule mobilization General flexibility should be addressed as needed particularly the piriformis, gluteus medius, rectus, ITB, and hamstrings 9 Phase 3 Pearls and Perils Make sure the trunk-core muscle are encaged during exercises and gait Do not forget plantar flexors 85% of the forward propulsion Normalize motion Combine Hip adduction-flexion-internal rotation Correct subtle deviations Particularly hip internal rotation 10 Phase 3 tape Phase 3 Pearls and Perils S.E.R.F Hip Strap: DonJoy 11 12
14 Phase weeks- Functional Progression Goals: Strength of trunk and LE 100% normal Tolerate sport-job specific positions with proper lower extremity alignment Phase 4 Pearls and Perils Work on strengthening in functional positions Movements meaningful for the patients goals Do not progress to FAST 13 Monitor LE position Do not allow poor technique 14 Phase weeks- Sports Specific-Work Related Retraining Goals: Return to 100% normal sport and work activity level Phase 5 Pearls and Perils Be creative in program design Thank You 17
15 Lecture: Best Tip Per Hölmich, MD
16 Rehabilitation: Best Tip Rodrigo Mardones M.D. Rehabilitation is a process that starts right after hip arthroscopy or we should said during the surgery. Arthroscopic FAI treatment is a continuous process that begins with surgery and ends with full return to daily and sports activities. Achievement of this goal requires the completion of different steps, initiating with surgery, early and late rehabilitation period leading to re-activation up to normal muscle strength and pain-free full range of motion. Our rehabilitation protocol had dramatically changed over more than 850 procedures, leading to early sports return and less postoperative tendonitis. Step 1: Surgery Two factors that greatly affected our results were: 1. Reducing traction time 2. Use of a PRP clot over bony resection at the end of the surgery Step 2: Early rehabilitation period We think that best tips at this period are: 1. Start right after surgery with a the use of a CPM machine in order to avoid scar formation. 2. Ergonometric bicycle at 12 hours without any resistance 3. Full weight bearing with two crutches to avoid limping and pain. 4. Adding circumferential exercises from the beginning to your routine. Step 3: Late rehabilitation period During this period periarticular tendonitis appears mostly because suspension of rehabilitation and daily sports activity. Tips for this period are:
17 1. Strict follow-up with periodical controls 2. Follow specific activities (worksheet) 3. Specialized rehabilitation team 4. Constant evaluation to assess flexibility
Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement. Normalize gait pattern with brace (if indicated) and crutches
 General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
General Guidelines: Hip Arthroscopy Rehabilitation Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace (if indicated) and crutches Weight-bearing: 20 lbs foot flat
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
General Guidelines: Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic or Open Gluteus Medius Repair with or without Labral Debridement Normalize gait pattern with brace and crutches Weight-bearing:
Alejandro Verdugo, M.D.
 Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Alejandro Verdugo, M.D. Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Gluteus Medius Tear, Labral Tear, CAM / Pincer Procedure: Gluteus Medius Repair, CAM / Pincer Decompression, Labral refixation / Capsular Shift
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H This protocol provides appropriate guidelines for the rehabilitation of patients following
Travis G. - 1 Maak, - MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Travis G. - 1 Maak, - MD Rehabilitation for Arthroscopic Osteochondroplasty with or without Labral Repair/Debridement General Guidelines: Normalize gait pattern with brace and crutches Continuous Passive
Bryan T. Kelly, MD Center for Hip Pain and Preservation Hospital for Special Surgery
 Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
Hip Arthroscopy Rehabilitation Labral refixation with or without FAI Component General Guidelines: Limited external rotation to 20 degrees (2 weeks) No hyperextension (4 weeks) Normalize gait pattern with
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
Travis G. Maak, MD Sports Medicine University of Utah Orthopaedics 590 Wakara Way Salt Lake City, UT Tel: Fax:
 General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
General Guidelines: Hip Arthroscopy Rehabilitation Capsular Shift with or without FAI Labral Components No external rotation greater than 30 degrees for 4 weeks No hyperextension for 4 weeks Normalize
Precautions following Hip Arthroscopy/FAI: (Refixation/Osteochondroplasty)
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, CAM / Pincer Procedure: Labral Repair / Capsular Shift, CAM / Pincer Decompression RX: Evaluate / Treat, and follow attached protocol
Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component. Limited external rotation to 20 degrees (2 weeks)
 General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
General Guidelines: 4140 Centennial Hills Boulevard Casper, WY 82609 (307) 265-7205 Hip Arthroscopy Rehabilitation Labral Refixation with or without FAI Component Limited external rotation to 20 degrees
Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component. Normalize gait pattern with brace and crutches
 Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component General Guidelines: Normalize gait pattern with brace and crutches Weightbearing as per procedure performed Continuous Passive
Hip Arthroscopy Rehabilitation Labral Debridement with or without FAI Component General Guidelines: Normalize gait pattern with brace and crutches Weightbearing as per procedure performed Continuous Passive
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
ARTHROSCOPIC LABRAL REPAIR WITH CAPSULAR PLICATION PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use
Proximal Hamstring Rupture: Physical Therapy Protocol
 Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment.
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) Fax: (763)
 Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
Hip Arthroscopy Femoroacetabular Impingement (FAI) Ryan W. Hess, MD Tracey Pederson, PCC Office: (763) 302-2223 Fax: (763) 302-2401 GENERAL GUIDELINES: Despite the minimally invasive nature of hip arthroscopy,
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL
 ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
ARTHROSCOPIC GLUTEUS MEDIUS REPAIR PHYSICAL THERAPY PROTOCOL Jovan R. Laskovski, M.D. Hip Arthroscopy Sports Medicine & Orthopaedic Surgery Crystal Clinic Orthopaedic Center Please use appropriate clinical
Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer. Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement
 Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Physical Therapy Prescription: Hip Arthroscopy Diagnosis: Labral Tear, Internal Snapping Hip, CAM / Pincer Procedure: Partial Psoas Release with CAM / Pincer Decompression and Labral Debridement RX: Evaluate
Alejandro Verdugo m.d.
 Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Alejandro Verdugo m.d. Proximal Hamstring Rupture: Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Protocol G Arthroscopic Surgery: Therapist Information
 Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol G Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component
 Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Post Operative Hip Arthroscopy Rehabilitation Protocol Labral Repair With or Without FAI Component ROM Restrictions: -Perform PROM in patient s PAIN FREE Range FLEXION EXTENSION EXTERNAL ROTATION 90 degrees
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Labral Repair with a Microfracture
 Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Labral Repair with a Microfracture This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for
Hip Arthroscopy. Labral Repair/Debridement with Femoroplasty
 Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Precautions for weeks 1 4 post-op: Hip Arthroscopy Labral Repair/Debridement with Femoroplasty Patient Education o For 1 week, Assist the involved LE during all transfers o For 2 weeks, Do not sit with
Protocol D Arthroscopic Surgery: Therapist Information
 Protocol D Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol D Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol A Arthroscopic Surgery: Therapist Information
 Protocol A Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Protocol A Arthroscopic Surgery: Therapist Information Please read entire protocol prior to initiating therapy Please do not hesitate to contact Dr. Wolff with questions or concerns. Rest is a vital component
Abductor Repair (Gluteus Medius/Minimus Repair)
 (Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
(Gluteus Medius/Minimus Repair) This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for 8
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound
BENJAMIN G. DOMB, MD
 Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
Physical Therapy Protocol Partial or full thickness gluteus medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R
 S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
S p o r t s & O r t h o p a e d i c S p e c i a l i s t s D R. R Y A N F A D E R H I P A R T H R O S C O P Y W I T H L A B R A L R E P A I R P R O T O C O L This protocol provides appropriate guidelines
9180 KATY FREEWAY, STE. 200 (713)
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION Patella/Trochlea Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protection of healing tissue from load and shear forces - Decrease pain
9180 KATY FREEWAY, STE. 200 (713)
 AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
AUTOLOGOUS CHONDROCYTE IMPLANTATION Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Goals: - Protect healing tissue from load and shear forces - Decrease pain and effusion
JOHN M. REDMOND, M.D.
 Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Physical Therapy Protocol Gluteus Medius repair with or without labral repair The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as
Initial Exercises (Weeks 1-3)
 Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
Labral Repair This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Partial weight bearing (50%) (4 weeks). Encourage, but limit hip
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: - POD 1: Debulk dressing, TED Hose in place - POD 2: Change
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY AUTOLOGOUS CULTURED CHONDROCYTES FOR IMPLANTATION (CARTICEL ) POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair
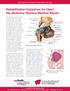 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Open Hip Abductor (Gluteus Medius) Repair The hip joint is composed of the femur (the thigh bone) and the acetabulum (the socket which is from
Microfracture. This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient.
 This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
This protocol should be used as a guideline for progression and should be tailored to the needs of the individual patient. Strict protective weight bearing status for two months (8-9 weeks). Allow to place
Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab Protocol
 Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
Matthew T. Mantell, MD 128 Medical Circle Winchester, VA 22601 Phone: 540-667-8975 Email: mattmantellmd@gmail.com Web: www.mattmantellmd.com Hip Arthroscopy with Labral Repair and Osteoplasties PT Rehab
Hip Labrum and FAI Post-Surgical Rehabilitation Guideline
 Hip Labrum and FAI Post-Surgical Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Hip Labrum and FAI Post-Surgical Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Rehabilitation Following Unilateral Patellar Tendon Repair
 Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Rehabilitation Following Unilateral Patellar Tendon Repair I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip. Joy Anderson PT, ATC, CSCS
 Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
Rehabilitation Considerations Following Surgical Arthroscopy of the Hip Joy Anderson PT, ATC, CSCS 1 Best Rehab Program? Review of the Evidence paucity of evidence surrounding post-operative rehabilitation
Femoral Condyle Rehabilitation Guidelines
 Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Femoral Condyle Rehabilitation Guidelines PHASE I - PROTECTION PHASE (WEEKS 0-6) Brace: Protect healing tissue from load and shear forces Decrease pain and effusion Restore full passive knee extension
Microfracture of Knee Joint
 Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
Microfracture of Knee Joint Post-op Precautions: The patient will ambulate with crutches for 4 weeks or more after surgery. The physician will base weightbearing status upon the location of the lesion.
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION
 OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
OSTEOCHONDRAL AUTOGRAFT TRANSPLANTATION FEMORAL CONDYLE REHABILITATION PROGRAM PHASE I - PROTECTION PHASE (WEEKS 0-6) Protection of healing tissue from load and shear forces Decrease pain and effusion
Dr Schock High Tibial Osteotomy
 Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Dr Schock High Tibial Osteotomy Goals for phase 1 Control pain Control edema Initiate ROM and quad strengthening Maintain WB restrictions Appropriate brace wear Criteria for progression to Phase 2 Edema
Hip Arthroscopy with CAM resection/labral Repair Protocol
 Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Hip Arthroscopy with CAM resection/labral Repair Protocol As tolerated should be understood to perform with safety for the reconstruction/repair. Pain, limp, swelling, or other undesirable factors are
Rehabilitation Following ACL with Semitendinosus Reconstruction
 Page 1 of 5 Rehabilitation Following ACL with Semitendinosus Reconstruction I. IMMEDIATE POSTOPERATIVE PHASE : Goals: 1) Protect ACL reconstruction 2) Reduce swelling & inflammation 3) Restore & maintain
Page 1 of 5 Rehabilitation Following ACL with Semitendinosus Reconstruction I. IMMEDIATE POSTOPERATIVE PHASE : Goals: 1) Protect ACL reconstruction 2) Reduce swelling & inflammation 3) Restore & maintain
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) Acetabuloplasty
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com This protocol
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com This protocol
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol
 REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
REHABILITATION PROTOCOL Criteria-Based Postoperative ACL Reconstruction Rehabilitation Protocol Phase I (Days 1 7) WEIGHTBEARING STATUS 1- Two crutches, weightbearing as tolerated. Exercises 1- Heel slides/wall
ARTHROSCOPIC MENISECTOMY PROTOCOL
 REHABILITATION PROGRESSION ARTHROSCOPIC MENISECTOMY PROTOCOL The following are guidelines for rehabilitation progression following menisectomy, loose body removed, or debridement etc. Progression through
REHABILITATION PROGRESSION ARTHROSCOPIC MENISECTOMY PROTOCOL The following are guidelines for rehabilitation progression following menisectomy, loose body removed, or debridement etc. Progression through
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ACUTE PROXIMAL HAMSTRING TENDON REPAIR BENJAMIN J. DAVIS, MD
 Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
Weeks 0-6 Goal: 1) Protection of the surgical repair Precautions: 1) Non-weight bearing with crutches for 6 weeks with foot flat or with knee Knee flexed to 90 degrees with sitting 2) No active hamstring
KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE
 PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
PHYSICAL THERAPY SECTION WILLIAM BEAUMONT ARMY MEDICAL CENTER 5005 N. PIEDRAS ST EL PASO, TEXAS 79920 KNEE DISLOCATION RECONSTRUCTION MCL and/or ACUTE Revised August 2008 Post-op Days 1 14 Dressing POD
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE
 HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
HIP ARTHROSCOPY CLINICAL PRACTICE GUIDELINE Progression is time and criterion-based, dependent on soft tissue healing, patient demographics and clinician evaluation. Contact Ohio State Sports Medicine
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
GALLAND/KIRBY ACL RECONSTRUCTION: BONE-TENDON- BONE AUTO / ALLOGRAFT POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing,
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GUIDELINES FOR REHABILITATION FOLLOWING SURGICAL RECONSTRUCTION
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 1/2018
Bone-Patellar tendon-bone Autograft ACL Recon. Date of Surgery: Patient Name:
 Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
Dx: o Right o Left Bone-Patellar tendon-bone Autograft ACL Recon Date of Surgery: Patient Name: PT/OT: Please evaluate and treat. Follow attached protocol. 2-3 x per week x 6 weeks. Signature/Date: GENERAL
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT. Brace E-Z Wrap locked at zero degree extension, sleep in Brace
 Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING A TWO TUNNEL GRAFT I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation Obtain Full Passive Knee Extension
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
GALLAND/KIRBY KNEE DISLOCATION RECONSTRUCTION LCL and/or CHRONIC POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
Routine Arthroscopic Procedure
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Patellar Tendon Debridement & Repair Rehabilitation Protocol
 Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
Patellar-quadriceps Tendon Repair Protocol
 Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
Patellar-quadriceps Tendon Repair Protocol Applicability: Physician Practice Date Effective: 3/2017 Department: Rehabilitation Services Supersedes: none Date Last Reviewed / or Date Last Revision: 3/2017
BENJAMIN G. DOMB, M.D.
 Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
Arthroscopic Hip Surgery Physical Therapy Protocol The intent of this protocol is to provide guidelines for your patient s therapy progression. It is not intended to serve as a recipe for treatment. We
CAPPAGH NATIONAL ORTHOPAEDIC HOSPITAL, FINGLAS, DUBLIN 11. The Sisters of Mercy. Hip Arthroscopy
 1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
1.0 Policy Statement... 2 2.0 Purpose... 2 3.0 Scope... 2 4.0 Health & Safety... 2 5.0 Responsibilities... 2 6.0 Definitions and Abbreviations... 3 7.0 Guideline... 3 7.1 Rehabilitation Phase 1 (Day 1
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals Precautions:
 Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Phase 1- Immediate Rehabilitation (1-3 weeks): Goals: Protection of the repaired tissue Prevent muscular inhibition and gait abnormalities Diminish pain and inflammation Precautions: 20 lb. flat-foot weight-bearing
Sports Rehabilitation & Performance Center Medial Patellofemoral Ligament Reconstruction Guidelines * Follow physician s modifications as prescribed
 The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
The following MPFL guidelines were developed by the Sports Rehabilitation and Performance Center team at Hospital for Special Surgery. Progression is based on healing constraints, functional progression
GUIDELINES FOR REHABILITATION Arthroscopic Meniscectomy/Loose Body Removal/Debridement
 GENERAL GUIDELINES Cryotherapy: Change ice packs or apply cryocuff every 4 hours while awake for first 72 hrs. GENERAL PROGRESSION OF ACTIVITIES OF DAILY LIVING Patients may begin the following activities
GENERAL GUIDELINES Cryotherapy: Change ice packs or apply cryocuff every 4 hours while awake for first 72 hrs. GENERAL PROGRESSION OF ACTIVITIES OF DAILY LIVING Patients may begin the following activities
TOTAL KNEE ARTHROPLASTY PROTOCOL
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 TOTAL KNEE ARTHROPLASTY PROTOCOL PHASE 1: IMMEDIATE
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 TOTAL KNEE ARTHROPLASTY PROTOCOL PHASE 1: IMMEDIATE
REHABILITATION PROTOCOL
 GEOFFREY S. VAN THIEL, MD/MBA Assistant Professor - Rush University Medical Center Team Physician - US National Soccer Teams Team Physician - Chicago Blackhawks Medical Network - Ice Hogs www.vanthielmd.com
GEOFFREY S. VAN THIEL, MD/MBA Assistant Professor - Rush University Medical Center Team Physician - US National Soccer Teams Team Physician - Chicago Blackhawks Medical Network - Ice Hogs www.vanthielmd.com
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ACL RECONSTRUCTION REVISION POST-SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft
 Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
Sports Medicine and Rehabilitation Center Therapist Phone REHABILITATION PROTOCOL FOLLOWING PCL RECONSTRUCTION USING Allograft I. IMMEDIATE POST-OPERATIVE PHASE (Week 1) Control Swelling and Inflammation
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction Hamstring Graft/PTG-Accelerated Rehabilitation
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol
 Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
Medial Patellofemoral Ligament Reconstruction Guidelines Brian Grawe Protocol Progression is based on healing constraints, functional progression specific to the patient. Phases and time frames are designed
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL
 GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
GALLAND/KIRBY ISOLATED MENISCAL REPAIR POST- SURGICAL REHABILITATION PROTOCOL POST-OP DAYS 1 14 Dressing: POD 1: Debulk dressing, TED Hose in place POD 2: Change dressing, keep wound covered, continue
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL REHABILITATION FOLLOWING UNILATERAL PETELLAR TENDON REPAIR BENJAMIN J.
 I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
Brennen Lucas, M.D. Advanced Orthopaedic Associates
 Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GENERAL GUIDELINES GUIDELINES FOR REHABILITATION FOLLOWING DISTAL
Brennen Lucas, M.D. Advanced Orthopaedic Associates 2778 N. Webb Rd. Wichita, KS 67226 316-631-1600 Fax: (316) 631-1674 1 (800) 362-0591 GENERAL GUIDELINES GUIDELINES FOR REHABILITATION FOLLOWING DISTAL
ACL REHABILITATION PROTOCOL
 Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Name: ID: Date Of Surgery :DD / MM / YYYY Procedure: ACL REHABILITATION PROTOCOL Note :If another procedure like meniscus repair or OATS (Osteochondralautograft transfer) has been done along with ACL reconstruction
Knee PCL Reconstruction Rehabilitation Program
 The Gundersen Health System Sports Medicine PCL Reconstruction Rehabilitation Program is an evidencebased and soft tissue healing dependent program allowing patients to progress to vocational and sports-related
The Gundersen Health System Sports Medicine PCL Reconstruction Rehabilitation Program is an evidencebased and soft tissue healing dependent program allowing patients to progress to vocational and sports-related
ACL Patella Tendon Autograft Reconstruction Protocol
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 ACL Patella Tendon Autograft Reconstruction Protocol The intent of this protocol is to provide the clinician
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL. WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches.
 REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
REHABILITATION FOLLOWING ACL RECONSTRUCTION PROTOCOL IMMEDIATE POST OPERATIVE PHASE Week 1: WEEK 1: Knee immobilizer locked in extension. WBAT with bilateral crutches. Ankle Pumps Passive knee extension
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Robert Klitzman
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Robert Klitzman This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Dr. Robert Klitzman This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction (HS graft/ptg/allograft)
Anterior Cruciate Ligament Reconstruction Delayed Rehab Protocol
 Anterior Cruciate Ligament Reconstruction Delayed Rehab Protocol Clarkstown Division This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction with other surgical
Anterior Cruciate Ligament Reconstruction Delayed Rehab Protocol Clarkstown Division This rehabilitation protocol has been designed for patients who have undergone an ACL reconstruction with other surgical
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Anterior Cruciate Ligament (ACL) Reconstruction- Delayed Rehabilitation Protocol
 Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction- Delayed Rehabilitation Protocol This rehabilitation
Robert K. Fullick, MD 6400 Fannin Street, Suite 1700 Houston, Texas 77030 Ph.: 713-486-7543 / Fx.: 713-486-5549 Anterior Cruciate Ligament (ACL) Reconstruction- Delayed Rehabilitation Protocol This rehabilitation
ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY
 WWW.MATTDRISCOLLMD.COM ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY ACL Reconstruction Rehab Protocol The intent of this protocol is to provide a general framework for ACL rehabilitation. Within
WWW.MATTDRISCOLLMD.COM ORTHOPEDIC SURGERY, SPORTS MEDICINE, AND ARTHROSCOPY ACL Reconstruction Rehab Protocol The intent of this protocol is to provide a general framework for ACL rehabilitation. Within
Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair
 Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
Page 1 of 7 Accelerated Rehabilitation Following ACL-PTG Reconstruction & PCL Reconstruction with Medial Collateral Ligament Repair PREOPERATIVE PHASE Goals: Diminish inflammation, swelling, and pain Restore
CENTER FOR ORTHOPAEDICS AND SPINE CARE PHYSICAL THERAPY PROTOCOL ORIF PATELLA BENJAMIN J. DAVIS, MD
 I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
I. Immediate Postoperative Phase (Days 1-7) Restore full passive knee extension Diminish pain and joint swelling Restore patellar mobility Initiate early controlled motion *Controlled forces on repair
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES
 APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
APPLICATION OF THE MOVEMENT SYSTEMS MODEL TO THE MANAGEMENT COMMON HIP PATHOLOGIES Tracy Porter, PT, DPT Des Moines University Department of Physical Therapy Objectives Review current literature related
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol
 Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
Anterior Cruciate Ligament Reconstruction Accelerated Rehabilitation Protocol Clarkstown Division This rehabilitation protocol has been designed for patients with ACL reconstruction who anticipate returning
