Case Report: Recognition and Diagnosis of Kinesiophobia in a Patient Following Calcaneal Fracture
|
|
|
- Ronald Dawson
- 6 years ago
- Views:
Transcription
1 Case Report: Recognition and Diagnosis of Kinesiophobia in a Patient Following Calcaneal Fracture Ross Jacques, SPT Garret Naze, DPT, OCS, FAAOMPT Carroll University Waukesha, WI Spring
2 Case Report: Recognition and Diagnosis of Kinesiophobia in a Patient Following Calcaneal Fracture AUTHORS/INSTITUTIONS: R. Jacques, Physical Therapy, Carroll University, Waukesha, WI; G. Naze, Physical Therapy, Carroll University, Waukesha, WI Abstract: Background and Purpose The intensity of a patient s fear of movement, or kinesiophobia, can occur independently from their current pain. Little discussion has been had regarding the patient who reports no pain yet demonstrates avoidant behaviors or movements. The purpose of this case report is to describe the presentation of catastrophization and kinesiophobia, to help clinicians appropriately diagnose, measure, and treat these conditions. Case Description The patient was a 71-year-old female who sustained a right anterior calcaneus fracture. At ten weeks from the date of injury, it was found that the patient had a mal-union calcaneal fracture. She was then casted and placed on non-weight bearing status for six weeks, followed by use of a walking boot for one week. Three weeks after discontinuation of the cast and boot the patient began outpatient physical therapy services. During pre-gait weight shifting activities and gait training she demonstrated abnormalities that appeared to be avoidance of right lower extremity weight bearing, despite no reports of pain. Outcomes The patient felt she had the progressed well and had the tools to continue to recover on her own and chose to discontinue therapy after 12 visits. She showed improved but persistent gait deviations, very slow gait velocity, decreased functional mobility scores, and elevated kinesiophobia scores. Discussion This patient demonstrated movement patterns and subjective information suggestive of kinesiophobia. Her Tampa Scale for Kinesiophobia scores were elevated from intake until discharge. The challenge for physical therapists is to begin to recognize, acknowledge, and treat this portion of the psychosocial domain to the best of their ability. Key Words: Kinesiophobia, Fear, TSK
3 A. Background and Purpose When a patient has pain, or the prospect of encountering pain, they must choose to confront (adaptive) or avoid (maladaptive) the daily activities that cause their pain. 1 Often there is a compromise or a combination of confrontation and avoidance based on the cost (pain) versus benefit (achieved task or fulfilled role). Long-term avoidance can lead to a disuse syndrome that may consist of heightened pain perception, psychological distress, and disability. 2 The decision to choose an avoidant behavior over confrontation can be influenced by a patient s pain catastrophization as well as the severity of a patient s pain. 3 Beck et al. describes catastrophizing as, dwelling on the worst possible outcome of any situation in which there is a possibility for an unpleasant outcome 4. It appears that the intensity of a patient s fear of movement, or kinesiophobia, can occur independently from their current visual analog scale (VAS) pain score. 5,6 Little discussion has been had regarding the patient who reports no pain, yet demonstrates avoidant behaviors and movement compensations, presumably to avoid an unpleasant outcome. 7 A model for the relationship between catastrophization and kinesiophobia has been made, describing the misinterpretation of innocuous stimuli leading to a fear of those movements causing those stimuli. 8 A clinician can use this model to help guide diagnosis of these conditions as well as intervention. According to the Guide to Physical Therapy Practice, pain is an impairment that may lead to subsequent functional limitations and disabilities. 9 When a patient experiences pain, there is often an element of fear or anxiety related to encountering, or the expectation of encountering, pain. It is also possible for a patient to present with pain-precipitated functional limitations long after they have experienced the related pain. 5 When this occurs, the treating physical therapist should address fear and avoidant behavior as the primary impairment, not the pain specifically. The purpose of this case report
4 is to describe a patient with kinesiophobia with low pain scores in order to appropriately diagnose, measure, and treat kinesiophobia. B. Case Description: Patient History and Systems Review The patient in this case report was referred by her podiatrist to outpatient physical therapy. The patient was a healthy, retired, 71-year-old female who sustained a right anterior calcaneus fracture after tripping and everting her ankle while playing basketball in her driveway with her grandson. She reports that she did not fall. The date of injury was twenty weeks prior to her initial physical therapy evaluation. Following the incident she went to urgent care for treatment of then present pain and swelling. A radiograph was ordered and the radiologist reported negative findings for a fracture. The following week, the patient was evaluated by her primary physician who ordered further imaging and diagnosed a right anterior calcaneus fracture. The physician prescribed a CAM walking boot which she was to wear during all weight bearing activities. Later that week, the physician contacted the patient stating there was not a fracture and he discontinued the CAM walking boot. For ten weeks from the date of injury, the patient ambulated without an assistive device or weight bearing precautions. However, she continued to have fluctuating levels of edema and pain and visited a local podiatrist for a second opinion. The podiatrist ordered magnetic resonance (MR) imaging and found that the patient had a right mal-union anterior calcaneal fracture. The podiatrist casted the patient s right foot in a non-weight bearing cast for six weeks, and then ordered a walking boot for one week. Three weeks after discontinuation of the cast and boot the patient began outpatient physical therapy services. At physical therapy evaluation, the patient reported using no prescription pain medications. The only medication she was taking daily was Atorvastatin and she reported no other comorbid health conditions. She reported that she had been using topical Voltaren (Diclofenac) gel on the right foot for
5 pain and inflammation with minimal effect. She also reported that she using an elastic wrap on the right foot to decreasing edema with moderate effect. The patient ambulated with bilateral axillary crutches and reported feeling pain and a burning sensation in the plantar surface of the foot that increased in intensity as the day progressed. At this time, she was medically cleared for full weight bearing by the referring podiatrist but she reported she was afraid to evenly weight bear. Functional limitations reported by the patient included an inability to ambulate without the use of two axillary crutches and an inability to ascend or descend stairs required for her to reach her bedroom, bathroom, and basement laundry. She stated she had been scooting on her backside to ascend and descend carpeted home stairs and she had discontinued going to the basement for laundry. She also reported being unable to complete cooking or cleaning tasks that requiring standing while using her hands as she was unable to let go of her crutches. Pain was rated as 0/10 (VAS) at rest and 5/10 at most when she was active and weight bearing. She reported 3/10 average foot pain on the day of the examination. Her pain was described as sharp and along the full length and width of the right plantar surface of the foot. Though did not plan to return to shooting hoops, her goal was to return to her prior level of function, which was very active and able to complete all activities of daily living and leisure. C. Clinical Impression The primary problem noted at the time of the examination was the limited weight bearing tolerated by the patient. Tests and measures such as gastrocnemius and soleus muscle testing and gait analysis would not be possible during the examination because of the patients unwillingness to stand without the majority of her weight being supported by her noninvolved leg and two axillary crutches. The subjective history was significant due to two critical items being present; the inconsistent, long, and painful process leading to the diagnosis and treatment of a right calcaneal fracture, and the mention of
6 being afraid of weight bearing on the right lower extremity despite being cleared for a full weight bearing status. At this point, it was important to determine what the patient feared about weight bearing on the involved extremity. The subjective history did not indicate confounding impairments or lack of healing at the tissue level, but instead possible concerns within the psychosocial domain. It was decided that this patient was a good candidate for a case report because more research is needed regarding early subjective reports of fear of movement in patients without significantly high pain reports. D. Examination Clinical observation was used to search for contributing factors that may explain why the patient had apprehension or fear related to weight bearing. The patient was a slender, light built woman. Gait and functional movement analysis showed that the patient had become efficient and comfortable ambulating, transferring, and negotiating the community with two axillary crutches. Further gait analysis was not possible as the patient was very apprehensive toward even 50% weight bearing on the affected foot. The patient also appeared apprehensive and showed a lack of weight shifting during all ambulation, standing, and sit-stand transfers. Closer observation showed that there was mild edema throughout the right ankle and foot, with a slight loss of contour and definition visible. Left and right figure-8 ankle anthropometrics were equal at 48.5 cm. The circumference at the left malleolus was 23 cm and the right was 24 cm. The circumference at the bases of the metatarsals on the left was 21.7 cm and on the right it was 22.1 cm. Palpation revealed slight tenderness in the plantar surface of the right foot near the calcaneus. Range of motion (ROM) goniometric measurements of the right ankle demonstrated limitations in inversion, dorsiflexion, and plantarflexion (Table 1). The patient also completed the Lower Extremity Functional Scale (LEFS) scoring a 35/80 (Figure 1). 10
7 E. Clinical Impression #2 The data gathered during the initial evaluation was limited, as more functional tests and measures were not assessable due to the patient s unwillingness to ambulate without axillary crutches. Her ankle range of motion was limited which was consistent with her prior immobilization. The gait and functional mobility observations appeared to be the most relevant piece of information related to upcoming procedural and educational intervention choice. On the day of the evaluation, it was noted by both the physical therapist and student physical therapist assessing the patient that there was fear of movement present, as the patient verbalized she had a sense of fear despite limited pain, as well as demonstrating it through limited weight bearing using the crutches for support. At the conclusion of the initial examination it was unclear to what extent the palpable tenderness present in the plantar surface of the right foot was contributing to her fear of weight shifting or ambulation. Following the examination and evaluation it was concluded that the patient s impairments and level of functional limitations warranted skilled physical therapy intervention. The patient was deemed to have a good rehabilitation potential due to the full union of her fracture, low pain level, and a previous high level of function. The treatment plan was for the patient to return to therapy two times per week for 6-8 weeks to resolve impairments such as loss of range of motion, strength, and pain as well as improve upon her functional mobility status, discontinuing the use of an assistive device, and improving her gait quality and speed. The treatment plan was to increase the active ROM of her right ankle to that of the left through strengthening, stretching, and possible joint mobilization. Follow-up treatments would also include functional movement and gait training. Depending on the behavior of her foot pain symptoms, future examination and treatment choice would be adjusted accordingly.
8 F. Intervention To reduce the impact of immobilization on the tissues of the foot and ankle, progressive resistive exercises for right ankle inversion, eversion, and plantarflexion were introduced and advanced as tolerated with resisted dorsiflexion being added later in the treatment plan. Cross friction massage was also implemented early to effectively decrease the irritability of the plantar surface of the foot. The primary focus of treatment was to increase the patient s awareness and confidence while weight shifting onto the affected foot. Treatment began with bipedal weight shifting activities progressing to static single-limb tasks and dynamic single-leg tasks. Exercises were performed between parallel bars to decrease the patient s anxiety and a mirror was used to increase sensorimotor feedback. Gait training began with the use of a single crutch and was progressed to a single point cane, and then to no assistive device. During gait training, the patient kept her leg in an abducted position during stance phase on the right to decrease the amount of weight shift to that side. Progress was delayed between the sixth and ninth visit as the patient was limited in weight bearing by 3/10 (VAS) medial knee pain, which was likely a result of the valgus stress she was applying while ambulating on an abducted right lower extremity. After this pain subsided with rest and ice, the patient was able to return to gait training, weight shift training, and single limb activities. G. Clinical Impression #3 Based on the patient s presentation in the first few visits, it was determined that focusing on the patient s lack of confidence, fear, and motor planning with weight bearing was a priority over aggressive strengthening or range of motion interventions. An early, significant development was an almost complete resolution of the pain in the plantar aspect of her right foot. She consistently reported 0/10 (VAS) pain rating in her foot during the first few follow-up visits. What also occurred was a progressive positive attitude about her perceived progress. She felt as though she was making improvements, but
9 also frequently reported that she did not want to push it too hard for fear of setting herself back. The patient was very slow to wean off of the use of an assistive device and never progressed past a single point can with daily activities. During follow-up visits, non-weight bearing ankle multi-planar resistance exercises were tolerated well, however, avoidance behaviors continued throughout weight bearing activity. For example, during pre-gait weight shifting activities or gait training she would occasionally quickly shift her weight away from the affected foot and onto the left lower extremity or support herself on a nearby object as if there was a sudden onset of sharp pain. However, subjective reports would deny the presence of pain and instead the patient would state the movement did not feel right for a moment. She would then assure the therapists that she felt no pain and proceed with the intervention. This presentation led to the use of the Tampa Scale for Kinesiophobia (TSK) to begin to track changes in the patient s fear of movement. 6 It also led treatment focus toward increasing body awareness and confidence to correct functional limitations more than impairments seen in ROM and strength. The patient completed the TSK, and a score of 41/68 was found. A score of 37 has been found to be indicative of a high degree of kinesiophobia. 6, 11 The individual answers were reviewed and statements such as 4. My accident has put my body at risk for the rest of my life and 13. Pain lets me know when to stop exercising so that I don t injure myself were recognized as the highest scored statements with Strongly Agree selected. This appeared to indicate that the patient felt her fracture was somewhat of a liability for further activity. While the patient arrived each day reporting she felt as though she was making great progress, feeling little discomfort, and reporting improvements in her level of function, she continued to demonstrate avoidance behaviors. In other words, there was a mismatch between her subjective report and her objective findings and outcome measures.
10 H. Outcome After a total of twelve visits the patient felt as though she was making consistent progress, was equipped with the tools to continue to progress, and had decided that she did not want to continue formal therapy. At the time of discharge her ankle inversion and eversion AROM measurements were equal from left to right. Her plantarflexion AROM was measured and showed 51 o on the left and 47 o on the right. Dorsiflexion was measured and showed 6 o on the left and 7 o on the right (Table 1). The patient was at this point still unable and/or unwilling to support all of her body weight during a right heel raise and therefore plantarflexor strength could not be accurately assessed. Gait velocity was measured and was.125 meters/second without the use of a gait aid. She reported 0/10 pain at all times, except for occasional right medial knee pain yielding a 1-3/10 (VAS). Gait analysis during ambulation without the use of an assistive device showed what had become a rather symmetrical hip drop of the contralateral hip during left and right stance phases, but this motion was more pronounced on the right and was likely in an attempt to cushion or slow the loading effect on the right side. The patient also demonstrated increased right ankle plantarflexion at initial contact and landed with a flat foot rather than using a heel strike. Notably, the patient was able to complete a right single leg stance 5-point star excursion drill two days before discharge. The LEFS was collected at intake, TSK initially at visit 4, both were collected at visit 6, and again at visit 12 (discharge) (Figures 1 and 2). I. Discussion This patient did arrive initially with a low level of pain in the plantar surface of her foot which quickly resolved. This resolution of symptoms led the treating therapists to attribute the patient s gait abnormalities to an abnormal motor plan driven by fear avoidant behavior. With this assessment it was decided that administering the TSK was the best way to track this patient s kinesiophobia. From there,
11 treatment was devoted to treating the patient s musculoskeletal impairments, as well as her psychological and neuromotor impairments. Her level of perceived functional limitation did improve by a clinically important margin from intake to discharge as reflected in the LEFS, but she had not returned to her prior level of function. One of the treatment goals was to decrease her kinesiophobia and thereby indirectly lessen her level of disability. Vlaeyen et al. proposed that pain catastrophizing can be a predisposing factor for patients to develop kinesiophobia, increasing the risk for disability and increased 5, 12 pain perception. It is within the scope of physical therapy practice to collect clinimetrics about the psychosocial and emotional domains, but rarely are these measures taken in clinical settings. 9, 13, 14, 15 The challenge for physical therapists and other clinicians is to interpret the TSK score and apply the gathered data in a clinically meaningful way. 7 When compared alongside the LEFS, the TSK showed a similar trend and change from intake to outcome, but making prognostic statements from this data was not possible. Most of the TSK s validation research has been done using subjects with spinal pain, making the application to a patient with a lower extremity condition less clear. 16 For physical therapists working with patients with various conditions and possible kinesiophobia, it is important for them to recognize, acknowledge, and treat this portion of the psychosocial domain to the best of their ability, and refer to mental health specialists when indicated. 7,9,12 Future research is needed for the prognostic interpretation and scope of use for both physical therapists and mental health professionals.
12 References: 1. Lethem J, Slade PD, Troup JDG, Bentley G. Outline of a fear-avoidance model of exaggerated pain perception I. Behav Res Ther. 1983;21(4): doi: / (83) Hirsh AT, George SZ, Bialosky JE, Robinson ME. Fear of pain, pain catastrophizing, and acute pain perception: Relative prediction and timing of assessment. The Journal of Pain. 2008;9(9): doi: /j.jpain Sullivan MJ, Thorn B, Haythornthwaite JA, et al. Theoretical perspectives on the relation between catastrophizing and pain. Clin J Pain. 2001;17(1): Beck AT, Emery G, Greenberg RL. Anxiety disorders and phobias. New York: Basic Books, Vlaeyen JWS, Kole-Snijders AMJ, Boeren RGB, van Eek H. Fear of movement/(re)injury in chronic low back pain and its relation to behavioral performance. Pain. 1995;62(3): doi: / (94)00279-N. 6. K.S. kori, R.P. miller, D.D. todd kinisophobia: A new view of chronic pain behaviour, pain manag, 3 (1990), pp Davenport TE. How should we interpret measures of patients' fear of movement, injury, or reinjury in physical therapist practice? Journal of Orthopaedic & Sports Physical Therapy. 2008;38(10): Picavet SJ, Vlaeyen JW, Schouten SA. Pain Catastrophizing and Kinesiophobia: Predictors of Chronic Low Back Pain. Am J Epidemiol. 2002; 156(11): Guide to physical therapist practice. 2nd ed. phys ther. 2001;81: Binkley JM, Stratford PW, Lott SA, Riddle DL, The North American Orthopaedic Rehabilitation Research Network. The lower extremity functional scale (LEFS): Scale development, measurement 16. properties, and clinical application. Physical Therapy. 1999;79(4): Lundberg, M.K.E., Styf, J., & Carlsson, S.G. (2004). A psychometric evaluation of the Tampa Scale for Kinesiophobia- from a physiotherapeutic perspective. Physiotherapy Theory and Practice. 20: , 12. Waddell G, Newton M, Henderson I, Somerville D, Main CJ. A fear-avoidance beliefs questionnaire (FABQ) and the role of fear-avoidance beliefs in chronic low back pain and disability. Pain. 1993;52(2): doi: / (93)90127-B. 13. Battie MC, Cherkin DC, Dunn R, Ciol MA, Wheeler KJ. Managing low back pain: Attitudes and treatment preferences of physical therapists. Phys Ther. 1994;74(3): Foster NE, Thompson KA, Baxter GD, Allen JM. Management of nonspecific low back pain by physiotherapists in britain and ireland. A descriptive questionnaire of current clinical practice. Spine (Phila Pa 1976). 1999;24(13):
13 15. Li LC, Bombardier C. Physical therapy management of low back pain: An exploratory survey of therapist approaches. Phys Ther. 2001;81(4): French DJ, France CR, Vigneau F, French JA, Evans RT. Fear of movement/(re)injury in chronic pain: A psychometric assessment of the original english version of the tampa scale for kinesiophobia (TSK). Pain. 2007;127(1 2): doi: /j.pain
14 Table 1: Ankle ROM Pre-/Post-Testing At Initial Examination At Discharge Ankle Motion Left Right Left Right Inversion Eversion Dorsiflexion Plantarflexion Figure 1: LEFS Scores LEFS Scores Intake 6 Weeks 12 Weeks *MCID = 9 points 10
15 Figure 2: TSK Scores TSK Scores Visit 4 Visit 6 Visit 12
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg)
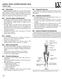 MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
MEDIAL HEAD GASTROCNEMIUS TEAR (Tennis Leg) Description Expected Outcome Medial head gastrocnemius tear is a strain of the inner part (medial head) of the major calf muscle (gastrocnemius muscle). Muscle
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon
 Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Mr Keith Winters MBChB, FRACS (Orth) Specialist Orthopaedic Surgeon Ph: (03) 9598 0691 Post op Instructions: Achilles Tendon Repair Recommended appliances for after your surgery: Crutches, walking frame
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol:
 Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Dr. Huff Modified Brostrom Repair Rehabilitation Protocol: The intent of this protocol is to provide the clinician with a guideline of the post-operative rehabilitation course of a patient who has undergone
Achilles Tendon Rupture
 43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
43 Thames Street, St Albans, Christchurch 8013 Phone: (03) 356 1353 Website: philip-bayliss.com Achilles Tendon Rupture Summary Achilles tendon ruptures commonly occur in athletic individuals in their
ACHILLES TENDON REPAIR REHAB GUIDELINES
 ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
ACHILLES TENDON REPAIR REHAB GUIDELINES Typically patients are discharged on the day of the operation or the next day. The leg is usually immobilized in a cast or hinged brace, ranging from 4-8 weeks.
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
ANKLE SPRAINS. Explanation. Causes. Symptoms
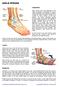 ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
ANKLE SPRAINS Explanation Ankle sprains occur when ligaments in the ankle are partially or completely torn due to sudden stretching, either laterally or medially, or when the ankle is suddenly twisted
METATARSAL FRACTURE (Including Jones and Dancer s Fractures)
 METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
METATARSAL FRACTURE (Including Jones and Dancer s Fractures) Description Possible Complications Metatarsal fracture is a broken bone (fracture) in the middle Nonunion (fracture does not heal, particularly
Everything. You Should Know. About Your Ankles
 Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Everything You Should Know About Your Ankles How Your Ankle Works The ankle joint is a hinge type joint that participates in movement and is involved in lower limb stability. There are 2 types of motions
Foot and ankle. Achilles tendon rupture repair. After surgery
 Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
Foot and ankle Achilles tendon rupture repair There is no agreed single best treatment for Achilles tendon ruptures. Similar results can be achieved with non-surgical and surgical treatments. There is
ANKLE SPRAIN, ACUTE. Description
 Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
Description ANKLE SPRAIN, ACUTE An acute ankle sprain involves the stretching and tearing of one or more ligaments in the ankle. A two-ligament sprain causes more disability than a single-ligament sprain.
High Ankle Sprain Rehabilitation Guideline
 High Ankle Sprain Rehabilitation Guideline This rehabilitation program is designed to return the individual to activity as quickly and safely as possible. It is designed for rehabilitation following high
High Ankle Sprain Rehabilitation Guideline This rehabilitation program is designed to return the individual to activity as quickly and safely as possible. It is designed for rehabilitation following high
Jennifer L. Cook, MD
 Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Jennifer L. Cook, MD Florida Joint Replacement and Sports Medicine Center 5243 Hanff Lane New Port Richey, FL 34652 Phone: (727)848-4249 Fax: (727) 841-8934 ANTERIOR CRUCIATE LIGAMENT RECONSTRUCTION POST-OPERATIVE
Total Hip Replacement Rehabilitation: Progression and Restrictions
 Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Total Hip Replacement Rehabilitation: Progression and Restrictions The success of total hip replacement (THR) is a result of predictable pain relief, improvements in quality of life, and restoration of
Rehabilitation Guidelines for Achilles Tendon Repair
 UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
UW HEALTH SPORTS REHABILITATION Rehabilitation Guidelines for Achilles Tendon Repair The Achilles tendon is the strongest and thickest tendon in the body. It attaches the calf muscles (soleus and gastrocnemius)
Mr. Siva Chandrasekaran Orthopaedic Surgeon MBBS MSpMed MPhil (surg) FRACS
 Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
Sprained Ankle An ankle sprain occurs when the strong ligaments that support the ankle stretch beyond their limits and tear. Ankle sprains are common injuries that occur among people of all ages. They
Gregory H. Tchejeyan, M.D. Orthopaedic Surgery of the Hip and Knee
 TOTAL KNEE REPLACEMENT (TKR) POST-OPERATIVE REHABILITATION PROTOCOL PRE-OPERATIVE PHYSICAL THERAPY The patient is seen for a pre-operative physical therapy session which includes: o Review of the TKR protocol.
TOTAL KNEE REPLACEMENT (TKR) POST-OPERATIVE REHABILITATION PROTOCOL PRE-OPERATIVE PHYSICAL THERAPY The patient is seen for a pre-operative physical therapy session which includes: o Review of the TKR protocol.
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol
 Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Anterior Cruciate Ligament Hamstring Rehabilitation Protocol Focus on exercise quality avoid overstressing the donor area while it heals. Typically, isolated hamstring strengthening begins after the 6
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
TOTAL KNEE ARTHROPLASTY PROTOCOL
 Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 TOTAL KNEE ARTHROPLASTY PROTOCOL PHASE 1: IMMEDIATE
Jennifer L. Cook, MD Stephen A. Hanff, MD Florida Joint Care Institute 2165 Little Road, Trinity, Florida 34655 PH: (727) 372 6637 FAX: (727) 375 5044 TOTAL KNEE ARTHROPLASTY PROTOCOL PHASE 1: IMMEDIATE
NICHOLAS J. AVALLONE, M.D.
 NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
NICHOLAS J. AVALLONE, M.D. www.dravallone.com ACHILLES TENDON REPAIR REHAB GUIDELINES DISCLAIMER: The intent of this protocol is to provide therapists with guidelines for rehabilitation based on a review
Stress Fracture Rehabilitation Guideline
 Stress Fracture Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation following
Stress Fracture Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation following
to a Patient Post Ankle Immobilization: A Case Report Catherine Schoob SPT* Anne Habeck DPT ** Kathleen Shields PT, MS***
 1 2 3 4 5 6 7 8 9 10 11 Application of the International Classification of Functioning, Disability and Health Model to a Patient Post Ankle Immobilization: A Case Report 12 13 14 15 16 17 Catherine Schoob
1 2 3 4 5 6 7 8 9 10 11 Application of the International Classification of Functioning, Disability and Health Model to a Patient Post Ankle Immobilization: A Case Report 12 13 14 15 16 17 Catherine Schoob
Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C
 Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C Department of Orthopaedic Surgery Sports Medicine and Shoulder Service Achilles Tendon Rupture Non-Operative
Christopher Kim, MD, Minh-Ha Hoang, DO, Scott G. Kaar, MD, William Mitchell, MD and Lauren Smith,PA-C Department of Orthopaedic Surgery Sports Medicine and Shoulder Service Achilles Tendon Rupture Non-Operative
Knee Replacement PROGRAM. Nightingale. Home Healthcare
 Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Knee Replacement PROGRAM TM Nightingale Home Healthcare With the help of Nightingale s experienced and professional rehabilitation team, you will be guided through a more complete and successful recovery
Leg and Ankle Problems in Primary Care.
 Leg and Ankle Problems in Primary Care www.fisiokinesiterapia.biz Leg and Ankle Presentations 4Trauma 4Pain Ankle Trauma 41. Twist and Fall--Fracture or Sprain 42. Patient hears/feels a pop--tendon or
Leg and Ankle Problems in Primary Care www.fisiokinesiterapia.biz Leg and Ankle Presentations 4Trauma 4Pain Ankle Trauma 41. Twist and Fall--Fracture or Sprain 42. Patient hears/feels a pop--tendon or
MEDIAL TIBIAL STRESS SYNDROME (Shin Splints)
 MEDIAL TIBIAL STRESS SYNDROME (Shin Splints) Description Expected Outcome Shin splints is a term broadly used to describe pain in the lower extremity brought on by exercise or athletic activity. Most commonly
MEDIAL TIBIAL STRESS SYNDROME (Shin Splints) Description Expected Outcome Shin splints is a term broadly used to describe pain in the lower extremity brought on by exercise or athletic activity. Most commonly
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS)
 Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Rehabilitation Protocol: Distal Femoral/Proximal Tibial Microfracture and Osteochondral Autograft Transplantation (OATS) Department of Orthopaedic Surgery Lahey Hospital & Medical Center, Burlington 781-744-8650
Ankle Rehabilitation with Wakefield Sports Clinic
 Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
Ankle Rehabilitation with Wakefield Sports Clinic With Michael Woodcock Adelaide 36ERS & Wakefield Sports Clinic Physiotherapist The ankle joint is one of the major weight bearing structures in the body.
MUSCULOSKELETAL PROGRAM OF CARE
 MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
MUSCULOSKELETAL PROGRAM OF CARE AUGUST 1, 2014 Table of contents Acknowledgements... 3 MSK POC Scope... 3 The Evidence... 3 Objectives.... 4 Target Population.... 4 Assessment of Flags and Barriers to
Ankle instability surgery
 Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Ankle instability surgery Ankle instability surgery is generally reserved for people with chronic ankle instability who have failed to respond to conservative treatment. The surgical technique used will
Physical & Occupational Therapy
 In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
In this section you will find our recommendations for exercises and everyday activities around your home. We hope that by following our guidelines your healing process will go faster and there will be
Home Exercise Program Progression and Components of the LTP Intervention. HEP Activities at Every Session Vital signs monitoring
 Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Home Exercise Program Progression and Components of the LTP Intervention HEP Activities at Every Session Vital signs monitoring Blood pressure, heart rate, Borg Rate of Perceived Exertion (RPE) and oxygen
Rehabilitation Protocol:
 Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Rehabilitation Protocol: Patellofemoral resurfacing: Osteochondral Autograft Transplantation (OATS), Autologous Chondrocyte Implantation (ACI) and Microfracture Department of Orthopaedic Surgery Lahey
Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme
 Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Chapter FOUR Exercise Therapy for Patients with Knee OA Knee Exercise Protocol Knee Home Exercise Programme Chris Higgs Cathy Chapple Daniel Pinto J. Haxby Abbott 99 n n 100 General Guidelines Knee Exercise
Rehabilitation and Return to Play Following Achilles Tendon Repair
 Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Rehabilitation and Return to Play Following Achilles Tendon Repair Monte Wong PT, DPT, SCS, ATC, CSCS Assistant Athletic Trainer/Physical Therapist Philadelphia Eagles Mechanism of Injury 1.) forceful
Ankle Sprain Recovery and Rehabilitation Protocol:
 Ankle Sprain Recovery and Rehabilitation Protocol: ***NOTE: Depending on the severity of your injury, you may be placed into a boot, brace, or similar type of supportive device for a brief period of time
Ankle Sprain Recovery and Rehabilitation Protocol: ***NOTE: Depending on the severity of your injury, you may be placed into a boot, brace, or similar type of supportive device for a brief period of time
Scar Engorged veins. Size of the foot [In clubfoot, small foot]
![Scar Engorged veins. Size of the foot [In clubfoot, small foot] Scar Engorged veins. Size of the foot [In clubfoot, small foot]](/thumbs/78/77722241.jpg) 6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
6. FOOT HISTORY Pain: Walking, Running Foot wear problem Swelling; tingly feeling Deformity Stiffness Disability: At work; recreation; night; walk; ADL, Sports Previous Rx Comorbidities Smoke, Sugar, Steroid
Post Operative Total Hip Replacement Protocol Brian J. White, MD
 Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Post Operative Total Hip Replacement Protocol Brian J. White, MD www.western-ortho.com The intent of this protocol is to provide guidelines for progression of rehabilitation. It is not intended to serve
Pain-Related Fear Contributes to Self-Reported Disability in Patients With Foot and Ankle Pathology
 557 ORIGINAL ARTICLE Pain-Related Fear Contributes to Self-Reported Disability in Patients With Foot and Ankle Pathology Trevor A. Lentz, PT, Zach Sutton, PT, DPT, Scott Greenberg, PT, DPT, Mark D. Bishop,
557 ORIGINAL ARTICLE Pain-Related Fear Contributes to Self-Reported Disability in Patients With Foot and Ankle Pathology Trevor A. Lentz, PT, Zach Sutton, PT, DPT, Scott Greenberg, PT, DPT, Mark D. Bishop,
Managing Tibialis Posterior Tendon Injuries
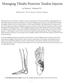 Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
Managing Tibialis Posterior Tendon Injuries by Thomas C. Michaud, DC Published April 1, 2015 by Dynamic Chiropractic Magazine Tibialis posterior is the deepest, strongest, and most central muscle of the
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: ACL RECONSTRUCTION +/- MENSICAL REPAIR 1. General Guidelines: Time lines in this rehabilitation protocol are
ACHILLES TENDON DISORDERS
 MUSCULOSKELETAL YOUR GUIDE TO ACHILLES TENDON DISORDERS An IPRS Guide to provide you with exercises and advice to ease your condition Contents What is the Achilles Tendon?.....................................
MUSCULOSKELETAL YOUR GUIDE TO ACHILLES TENDON DISORDERS An IPRS Guide to provide you with exercises and advice to ease your condition Contents What is the Achilles Tendon?.....................................
Review relevant anatomy of the foot and ankle. Learn the approach to examining the foot and ankle
 Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Objectives Review relevant anatomy of the foot and ankle Learn the approach to examining the foot and ankle Learn the basics of diagnosis and treatment of ankle sprains Overview of other common causes
Anterior Cruciate Ligament (ACL) Reconstruction Protocol
 Christopher M. Larson, MD Anterior Cruciate Ligament (ACL) Reconstruction Protocol **Please see the IMPORTANT NOTE for STRETCHING / KNEE EXTENSION on page 5** The intent of this protocol is to provide
Christopher M. Larson, MD Anterior Cruciate Ligament (ACL) Reconstruction Protocol **Please see the IMPORTANT NOTE for STRETCHING / KNEE EXTENSION on page 5** The intent of this protocol is to provide
Gait Analysis: Qualitative vs Quantitative What are the advantages and disadvantages of qualitative and quantitative gait analyses?
 Gait Analysis: Qualitative vs Quantitative What are the advantages and disadvantages of qualitative and quantitative gait analyses? Basics of Gait Analysis Gait cycle: heel strike to subsequent heel strike,
Gait Analysis: Qualitative vs Quantitative What are the advantages and disadvantages of qualitative and quantitative gait analyses? Basics of Gait Analysis Gait cycle: heel strike to subsequent heel strike,
Achilles Tendonitis and Tears
 Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
Achilles Tendonitis and Tears The Achilles tendon is an important structure for normal ankle motion and normal function, even for daily activities such as walking. Achilles tendonitis can occur in patients
NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY ( Program)
 Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
Therapist: Phone: NONOPERATIVE REHABILITATION FOLLOWING ACL INJURY (3-3-4-4 Program) IMMEDIATE INJURY PHASE (Day 1 to Day 7) Restore full passive knee extension Diminish joint swelling and pain Restore
THE EXTREMITY SCREEN MANUAL: A Guide to the Subjective and Objective Outcomes Assessment of the Upper and Lower Extremity
 THE EXTREMITY SCREEN MANUAL: A Guide to the Subjective and Objective Outcomes Assessment of the Upper and Lower Extremity Steven G. Yeomans, DC, FACO INTRODUCTION: Objective screen for the extremities
THE EXTREMITY SCREEN MANUAL: A Guide to the Subjective and Objective Outcomes Assessment of the Upper and Lower Extremity Steven G. Yeomans, DC, FACO INTRODUCTION: Objective screen for the extremities
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
ACL Reconstruction Rehabilitation Allograft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT 12+ weeks, no
Biokinesiology of the Ankle Complex
 Rehabilitation Considerations Following Ankle Fracture: Impact on Gait & Closed Kinetic Chain Function Disclosures David Nolan, PT, DPT, MS, OCS, SCS, CSCS I have no actual or potential conflict of interest
Rehabilitation Considerations Following Ankle Fracture: Impact on Gait & Closed Kinetic Chain Function Disclosures David Nolan, PT, DPT, MS, OCS, SCS, CSCS I have no actual or potential conflict of interest
ACHILLES TENDON RUPTURE
 ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
ACHILLES TENDON RUPTURE Description Expected Outcome Achilles tendon rupture is a complete tear of the Achilles tendon. This tendon, sometimes called the heel cord, is the tendon attachment of the calf
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN Tel: Fax:
 Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Jozef Murar, M.D. TCO Edina Crosstown 4010 W 65 th St, Edina, MN 55435 Tel: 952-456-7000 Fax: 952-832-0477 www.tcomn.com ACHILLES TENDON REHABILITATION PROTOCOL Pre-op: Gait training Post-op: Week 2 Post-op
Adam N. Whatley, M.D Main St., STE Zachary, LA Phone(225) Fax(225)
 Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
Adam N. Whatley, M.D. 6550 Main St., STE. 2300 Zachary, LA 70791 Phone(225)658-1808 Fax(225)658-5299 Total Knee Arthroplasty Protocol: The intent of this protocol is to provide the clinician with a guideline
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: PCL RECONSTRUCTION +/- ACL / MCL / LCL / POSTEROLATERAL CORNER 1. General Guidelines: Time lines in this rehabilitation
DR. GATCHEL HAS NO CONFLICTS OF INTEREST TO DISCLOSE. Gatchel
 Robert J. Gatchel, Ph.D., ABPP Nancy P. and John G. Penson Endowed Professor of Clinical Health Psychology Distinguished Professor of Psychology, College of Science Director, Center of Excellence for the
Robert J. Gatchel, Ph.D., ABPP Nancy P. and John G. Penson Endowed Professor of Clinical Health Psychology Distinguished Professor of Psychology, College of Science Director, Center of Excellence for the
Acute Ankle Injuries, Part 1: Office Evaluation and Management
 t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
t June 08, 2009 Obesity [1] Each acute ankle injury commonly seen in the office has associated with it a mechanism by which it can be injured, trademark symptoms that the patient experiences during the
Ankle Fracture Weber B Ankle 3
 Ankle Fracture Weber B Ankle 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Ankle Fracture Weber B Ankle 3 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
5 minutes: Attendance and Breath of Arrival. 50 minutes: Problem Solving Ankles and Feet
 5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Ankles and Feet Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here
5 minutes: Attendance and Breath of Arrival 50 minutes: Problem Solving Ankles and Feet Punctuality- everybody's time is precious: o o Be ready to learn by the start of class, we'll have you out of here
Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab
 1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
1 Physical Therapy for the Lower Extremity: What You and Your Patient Should Expect from Rehab Thomas Clennell, PT, DPT, SCS Physical Therapist UCSF Benioff Children s Hospital Oakland Sports Medicine
ANTERIOR ANKLE IMPINGEMENT
 ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
ANTERIOR ANKLE IMPINGEMENT Description Possible Complications Pinching of bone or soft tissue, including scar tissue, at the Frequent recurrence of symptoms, resulting in chronically front of the ankle
Hip Arthroscopy Protocol
 The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
The intent of this protocol is to provide guidelines for progression of rehabilitation, it is not intended to serve as a substitute for clinical decision making. Progression through each phase of rehabilitation
PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY
 Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
Exercises After Injury to the Anterior Cruciate Ligament (ACL) of the Knee Dr. Abigail R. Hamilton, M.D. PHASE ONE: THE FIRST SIX WEEKS AFTER INJURY Initially, the knee needs to be protected-use the knee
31b Passive Stretches:! Technique Demo and Practice - Lower Body
 31b Passive Stretches:! Technique Demo and Practice - Lower Body 31b Passive Stretches:! Technique Demo and Practice - Lower Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
31b Passive Stretches:! Technique Demo and Practice - Lower Body 31b Passive Stretches:! Technique Demo and Practice - Lower Body! Class Outline" 5 minutes" "Attendance, Breath of Arrival, and Reminders
LATERAL LIGAMENT SPRAIN OF THE ANKLE
 MUSCULOSKELETAL YOUR GUIDE TO LATERAL LIGAMENT SPRAIN OF THE ANKLE An IPRS Guide to provide you with exercises and advice to ease your condition Contents The ankle joint..................................................
MUSCULOSKELETAL YOUR GUIDE TO LATERAL LIGAMENT SPRAIN OF THE ANKLE An IPRS Guide to provide you with exercises and advice to ease your condition Contents The ankle joint..................................................
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD
 ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
ACL Reconstruction Rehabilitation Bone Patellar Tendon Bone Graft Kyle F. Chun, MD [ ] Meniscus Repair (If checked, WBAT in brace in full extension, ROM 0-90 x 6 wks; WBAT 0-90, ROM 0-120 weeks 7-12; WBAT/ROMAT
Lateral Collateral Ligament Sprain
 What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
What is lateral collateral ligament sprain? Lateral Collateral Ligament Sprain A sprain is a joint injury that causes a stretch or tear in a ligament, a strong band of tissue connecting one bone to another.
Avulsion Fracture of the Foot Foot 1
 Avulsion Fracture of the Foot Foot 1 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Avulsion Fracture of the Foot Foot 1 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Patellar Tendon Debridement & Repair Rehabilitation Protocol
 Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
Patellar Tendon Debridement & Repair Rehabilitation Protocol PREOPERATIVE PHASE Diminish inflammation, swelling, and pain Restore normal range of motion (especially knee extension) Restore voluntary muscle
POSTERIOR TIBIAL TENDON RUPTURE
 POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
POSTERIOR TIBIAL TENDON RUPTURE Description Expected Outcome Posterior tibial tendon rupture is a complete tear of the posterior tibial tendon. This structure is the tendon attachment of leg muscles (posterior
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline
 Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
Posterior/Direct Total Hip Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for
4 ACHILLES TENDONITIS
 4 ACHILLES TENDONITIS What is it? The Achilles tendon is a band of connective tissue that attaches your calf muscle (gastrocnemius and soleus) onto the back of your heel (calcaneus) and is the bodies largest
4 ACHILLES TENDONITIS What is it? The Achilles tendon is a band of connective tissue that attaches your calf muscle (gastrocnemius and soleus) onto the back of your heel (calcaneus) and is the bodies largest
A Patient s Guide to Ankle Sprain and Instability. Foot and Ankle Center of Massachusetts, P.C.
 A Patient s Guide to Ankle Sprain and Instability Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written
A Patient s Guide to Ankle Sprain and Instability Welcome to Foot and Ankle Center of Massachusetts, where we believe in accelerating your learning curve with educational materials that are clearly written
Soft tissue injury to ankle Information for patients Outpatient Fracture Care Team: Shared care plan
 Soft tissue injury to ankle Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108
Soft tissue injury to ankle Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108
King Khalid University Hospital
 King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
King Khalid University Hospital Rehabilitation Department Ortho Group Rehabilitation Protocol: MENISCAL REPAIR: 1. General Guidelines: Time lines in this rehabilitation protocol are approximate. If the
Caring For Your Lateral Ankle Middlebury College
 Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Caring For Your Lateral Ankle Sprain @ Middlebury College ** severe sprains or medial (inner side of ankle) sprains may require a different program Anatomy, Pathology, and Classification of Ankle Sprains
Sky Ridge Medical Center, Aspen Building Ridgegate Pkwy., Suite 309 Lone Tree, Colorado Office: Fax:
 ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
ANKLE SPRAIN What is the ATFL? The ankle joint is made up of the tibia, fibula (bones in the lower leg) and the talus (bone below the tibia and fibula). Ligaments in the ankle connect bone to bone and
AAP Boot Camp KNEE AND ANKLE EXAM
 AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
AAP Boot Camp KNEE AND ANKLE EXAM Disclosures I have no relevant financial relationships with the manufacturers of any commercial products and or providers of commercial services discussed in this CME
Internal Rotation (turning toes/knee toward other leg) 30 degree limit. limit
 Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Hip Arthroscopy Patient Education Use of Brace and Crutches: - Wear the brace all times of weight bearing for the first 3 weeks after surgery. This is done to protect your hip and motion into hip extension
Prevention and Management of Common Running Injuries. Presented by. Huub Habets (Sports Physiotherapist) Lynsey Ellis (Soft Tissue Therapist)
 Prevention and Management of Common Running Injuries Presented by Huub Habets (Sports Physiotherapist) Lynsey Ellis (Soft Tissue Therapist) Objectives DIALOGUE AND INTERACTION We are not here to preach,
Prevention and Management of Common Running Injuries Presented by Huub Habets (Sports Physiotherapist) Lynsey Ellis (Soft Tissue Therapist) Objectives DIALOGUE AND INTERACTION We are not here to preach,
Patellar Tendon Repair Rehabilitation Guideline
 Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Patellar Tendon Repair Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
ACL Reconstruction Rehabilitation Protocol
 ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
ACL Reconstruction Rehabilitation Protocol 1. Pre-OP Visit: a. Patient Education b. Exercises c. Gait Outline rehabilitation timeline. Discuss: Swelling/effusion control (PRICE). Quadriceps inhibition
Plantar Fasciitis. Equipment: Anti-inflammatory drugs: Night splints keep the plantar fascia from getting will relieve pain and reduce swelling.
 Plantar fasciitis is the most common cause of heel pain for which professional care is sought. This is caused by irritation of the plantar fascia a thickened fibrous band that runs from the heel to the
Plantar fasciitis is the most common cause of heel pain for which professional care is sought. This is caused by irritation of the plantar fascia a thickened fibrous band that runs from the heel to the
What are the symptoms of plantar fasciitis? The main symptoms of plantar fasciitis include: What causes plantar fasciitis?
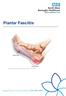 Plantar Fasciitis Plantar fasciitis is a condition which can cause heel pain. It happens when the strong band of tissue on the sole of your foot (fascia) becomes irritated, after repetitive use or due
Plantar Fasciitis Plantar fasciitis is a condition which can cause heel pain. It happens when the strong band of tissue on the sole of your foot (fascia) becomes irritated, after repetitive use or due
James R. Romanowski, M.D.
 James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
James R. Romanowski, M.D. Novant Health Perry & Cook Orthopedics and Sports Medicine 2826 Randolph Rd. Charlotte, NC 28211 704-358-0308 (Office) 704-358-0037 (Fax) www.charlotteshoulder.com DISCHARGE INSTRUCTIONS
Hip Arthroscopy Rehabilitation Protocol
 Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Hip Arthroscopy Rehabilitation Protocol 1. Concepts: a. Range of motion and weight bearing restrictions must be adhered to during the initial rehab process (4 total weeks of ROM and weight bearing restrictions)
Patient information. Forefoot surgery. Barts Health Physiotherapy Website:
 Patient information Forefoot surgery Barts Health Physiotherapy Website: www.bartshealth.nhs.uk/physiotherapy This booklet is for patients following surgery to the front of their foot. This may include
Patient information Forefoot surgery Barts Health Physiotherapy Website: www.bartshealth.nhs.uk/physiotherapy This booklet is for patients following surgery to the front of their foot. This may include
Calcaneal Fracture. Phase 1 Maximum Protection Phase (0-8 weeks)
 Phase 1 Maximum Protection Phase (0-8 ) Goals for Phase 1 Education of injury and surgical precautions Decrease edema Pain reduction Scar tissue mobility Increase ankle ROM Prevent muscular inhibition
Phase 1 Maximum Protection Phase (0-8 ) Goals for Phase 1 Education of injury and surgical precautions Decrease edema Pain reduction Scar tissue mobility Increase ankle ROM Prevent muscular inhibition
Total Knee Arthroplasty Rehabilitation Guideline
 Total Knee Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Total Knee Arthroplasty Rehabilitation Guideline This rehabilitation program is designed to return the individual to their activities as quickly and safely as possible. It is designed for rehabilitation
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan
 Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Weber B ankle fracture Information for patients Outpatient Fracture Care Team: Shared care plan Orthopaedic Department Tunbridge Wells Hospital Tonbridge Road Pembury TN2 4QJ Telephone: 07734370108 Email:
Prevention and Treatment of Injuries. Anatomy. Anatomy. Tibia: the second longest bone in the body
 Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Prevention and Treatment of Injuries The Ankle and Lower Leg Westfield High School Houston, Texas Anatomy Tibia: the second longest bone in the body Serves as the principle weight-bearing bone of the leg.
Exercise, Physical Therapy and Fall Prevention
 Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
Exercise, Physical Therapy and Fall Prevention University of Davis Medical Center Rosy Chow Neuro Clinical Specialist Physical Therapist Outline of Talk Role of Physical Therapy in care of people with
BORGinsole Measurement devices
 BORGinsole Measurement devices BORGinsole Angle-Finder Dorsal Flexion of the first Metatarsophalangeal joint - P. is sitting up on the examination table, with legs straight. - T. is sitting at the end
BORGinsole Measurement devices BORGinsole Angle-Finder Dorsal Flexion of the first Metatarsophalangeal joint - P. is sitting up on the examination table, with legs straight. - T. is sitting at the end
ANKLE FRACTURES. Contents The Ankle Joint... 3
 Contents The Ankle Joint................................................. 3 What is a fractured ankle?........................................ 4 YOUR GUIDE TO ANKLE FRACTURES What treatment can I receive?.....................................
Contents The Ankle Joint................................................. 3 What is a fractured ankle?........................................ 4 YOUR GUIDE TO ANKLE FRACTURES What treatment can I receive?.....................................
ACL Reconstruction Protocol (Allograft)
 ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACL Reconstruction Protocol (Allograft) Week one Week two Initial Evaluation Range of motion Joint hemarthrosis Ability to contract quad/vmo Gait (generally WBAT in brace) Patella Mobility Inspect for
ACHILLES RUPTURE YOUR GUIDE TO. An IPRS Guide to provide you with exercises and advice to ease your condition
 YOUR GUIDE TO ACHILLES RUPTURE Contents What is an Achilles Rupture?..................................... 3 What treatment can I receive?................................... 4 What exercises should I do?......................................
YOUR GUIDE TO ACHILLES RUPTURE Contents What is an Achilles Rupture?..................................... 3 What treatment can I receive?................................... 4 What exercises should I do?......................................
Tendo Achilles rupture
 Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
Tendo Achilles rupture Conservative and surgical management Therapy Department 01935 475 122 yeovilhospital.nhs.uk What is the Achilles tendon? The Achilles tendon is a large tendon at the back of the
Application of Motor Learning Principles in the Intervention of Patellofemoral Pain
 Application of Motor Learning Principles in the Intervention of Patellofemoral Pain Dorothy Beatty, SPT Virginia Commonwealth University September 29, 2016 Patient Introduction 22 y/o white female presenting
Application of Motor Learning Principles in the Intervention of Patellofemoral Pain Dorothy Beatty, SPT Virginia Commonwealth University September 29, 2016 Patient Introduction 22 y/o white female presenting
HIP REPLACEMENT SURGERY
 HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
HIP REPLACEMENT SURGERY HOW TO PREPARE FOR SURGERY AND REC0VERY Before surgery: Arrange for someone to help you around the house for a week or two after coming home from the hospital. Arrange for transportation
High Tibial Osteotomy (HTO) Rehabilitation Protocols
 High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
High Tibial Osteotomy (HTO) Rehabilitation Protocols Targets Upon Discharge from Hospital Protected weight-bearing (feather-weight -bearing) Ambulating with crutches Rehab brace without range of motion
