Craniocervical Motion during Direct Laryngoscopy and Orotracheal Intubation with the Macintosh and Miller Blades
|
|
|
- Irma O’Neal’
- 5 years ago
- Views:
Transcription
1 Anesthesiology 2007; 107: Copyright 2007, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Craniocervical Motion during Direct Laryngoscopy and Orotracheal Intubation with the Macintosh and Miller Blades An In Vivo Cinefluoroscopic Study Scott A. LeGrand, M.D.,* Bradley J. Hindman, M.D., Franklin Dexter, M.D., Ph.D., Julie B. Weeks, M.P.T., Michael M. Todd, M.D. Background: Previous studies have characterized segmental craniocervical motion that occurs during direct laryngoscopy and intubation with a Macintosh laryngoscope blade. Comparable studies with the Miller blade have not been performed. The aim of this study was to compare maximal segmental craniocervical motion occurring during direct laryngoscopy and orotracheal intubation with Macintosh and Miller blades. Methods: Eleven anesthetized and pharmacologically paralyzed patients underwent two sequential orotracheal intubations, one with a Macintosh blade and another with a Miller in random order. During each intubation, segmental craniocervical motion from the occiput to the fifth cervical vertebra (C5) was recorded using continuous lateral cinefluoroscopy. Singleframe images corresponding to the point of maximal cervical motion for both blade types were compared with a preintubation image. Using image analysis software, angular change in the sagittal plane at each of five intervertebral segments was compared between the Macintosh and Miller blades. This article is accompanied by an Editorial View. Please see: Lanier WL: Developing and exercising the language of airway management. ANESTHESIOLOGY 2007; 107: Additional material related to this article can be found on the ANESTHESIOLOGY Web site. Go to click on Enhancements Index, and then scroll down to find the appropriate article and link. Supplementary material can also be accessed on the Web by clicking on the ArticlePlus link either in the Table of Contents or at the top of the Abstract or HTML version of the article. * Resident, Department of Anesthesia and Critical Care, Massachusetts General Hospital, Harvard Medical School, Boston, Massachusetts. Professor and Vice- Chair (Faculty Development), Professor, Research Assistant, Professor and Head, Department of Anesthesia, University of Iowa Roy J. and Lucille A. Carver College of Medicine. Received from the Department of Anesthesia, University of Iowa Roy J. and Lucille A. Carver College of Medicine, Iowa City, Iowa. Submitted for publication February 16, Accepted for publication June 12, Supported in part by a Doris Duke Clinical Research Fellowship for Medical Students, New York, New York (to Dr. LeGrand). Other support was provided by the Department of Anesthesia, The University of Iowa Roy J. and Lucille A. Carver College of Medicine, Iowa City, Iowa. Portions of this work were presented in abstract form at the Doris Duke Clinical Research Fellowship Meeting, Cold Spring Harbor, New York, June 24 26, This work was also presented in part at the Annual Meeting of the American Society of Anesthesiologists, Las Vegas, Nevada, October 13, 2003, and published in abstract form (LeGrand SA, Hindman BJ, Todd MM, Brian JE: The influence of straight versus curved laryngoscope blades on cervical spine motion during endotracheal intubation. ANESTHESIOLOGY 2003; 99:A353). Address correspondence to Dr. Hindman: Department of Anesthesia, University of Iowa Hospitals and Clinics, Iowa City, Iowa brad-hindman@uiowa.edu. Information on purchasing reprints may be found at or on the masthead page at the beginning of this issue. ANESTHESIOLOGY s articles are made freely accessible to all readers, for personal use only, 6 months from the cover date of the issue. Results: Extension at occiput C1 was greater with the Macintosh blade compared with the Miller ( vs , respectively; mean difference ; P 0.012). Total craniocervical extension (occiput C5) was also greater with the Macintosh blade compared with the Miller ( vs , respectively; mean difference ; P 0.008). Conclusions: Compared with the Macintosh, the Miller blade was associated with a statistically significant, but quantitatively small, decrease in cervical extension. This difference is likely too small to be important in routine practice. DURING direct laryngoscopy and orotracheal intubation, forces applied by the laryngoscope blade cause simultaneous displacement of the tongue and epiglottis and craniocervical extension, 1 creating a line of sight between the superior aspect of the oral cavity and the glottic inlet. Previous studies using a Macintosh laryngoscope blade have shown craniocervical extension during intubation is greatest between the occiput and first cervical vertebra (C1) and between C1 and C2, 1 3 with relatively little extension in subaxial segments. Subsequently, numerous studies have characterized craniocervical motion during intubation with alternative airway devices such as the Bullard laryngoscope, 2 4 intubating laryngeal mask, 4 6 light wand, 7 and other devices. 4,6 8 Surprisingly, despite the widespread use of the Miller laryngoscope blade, craniocervical motion during intubation with a Miller blade has not been well characterized. Previous studies have used only surrogate measures of spine motion, such as vertebral body displacement in the anterior posterior plane, 9 11 distance between spinous processes, 9,11 or external head/ neck extension angles 12 ; none have measured segmental craniocervical motion during intubation. Because of differing blade design and application of forces, there could be meaningful differences between the Macintosh and Miller blades in the location and/or magnitude of craniocervical motion that occurs during intubation. Therefore, the aim of this study was to measure and compare maximal segmental craniocervical motion occurring during direct laryngoscopy and orotracheal intubation with Macintosh and Miller blades. Materials and Methods Subjects This study was conducted in accordance with guidelines set forth by the University of Iowa Institutional 884
2 CERVICAL MOTION WITH MACINTOSH AND MILLER BLADES 885 Review Board for Human Subjects and Medical Radiation Protection Committee, Iowa City, Iowa. All patients gave written informed consent before participation. Previous studies had shown that intervertebral segmental motion (extension) during intubation with the Macintosh blade is greatest at occiput C1, approximately 10 5 (mean SD). 1 3 We hypothesized that a 40 50% difference in extension (i.e., 4 5 ) at this segment could be potentially clinically significant. Using paired data, approximately 12 patients were required to detect a 4 5 difference (two-sided test, 0.05, ). Of the initial 12 patients studied, data from three were rejected because of inadequate image quality (see Data Acquisition, Processing, and Image Analysis). Therefore, with institutional review board approval, an additional 2 patients were enrolled, for a total of 14 patients. Patients were adults (American Society of Anesthesiologists physical status I or II) scheduled to undergo elective spine surgery in which lateral fluoroscopy was to be used during the procedure (anterior cervical, n 13; posterior lumbar, n 1). All patients were free of myelopathic symptoms. Preoperative head and neck mobility were clinically unrestricted. Patients were excluded if they had (1) radiologic abnormalities of the cervical spine that precluded direct laryngoscopy (e.g., anatomic instability, severe stenosis, or severe immobility), (2) a body habitus that seemed likely to interfere with radiographic visualization of the cervical spine, and/or (3) any other contraindication to direct laryngoscopy. After consenting to participate, patients were assigned a study identification number. Thereafter, a sealed opaque envelope with a matching identification number was opened a few minutes before induction. The envelope contained a card indicating the randomized order of laryngoscope blades that were to be used during two sequential intubations. Either (1) the first intubation was to be performed with a Macintosh blade and the second was to be performed with a Miller or (2) the first intubation was to be performed with a Miller blade and the second was to be performed with a Macintosh. Intubation Protocol Each patient was supine on a flat operating table with the occiput resting on a 7-cm semicompressible pad. After initiation of standard respiratory and hemodynamic monitoring and preoxygenation, general anesthesia was induced with intravenous thiopental or propofol, and mask ventilation was established without the use of either oral or nasal airways. Patients lungs were ventilated with either isoflurane or sevoflurane in oxygen. Neuromuscular blockade was achieved by intravenous vecuronium or rocuronium. After an adequate depth of anesthesia was established and after disappearance of the fourth twitch of the trainof-four, lateral fluoroscopy was used to obtain a baseline still image of the cervical spine and occiput. This initial, preintubation, baseline image (baseline 1) was obtained after removing the ventilating mask and after allowing the head and neck to assume an unsupported midline resting position. After obtaining baseline image 1, the first of two direct laryngoscopies and oroendotracheal intubations were performed according to the assigned order. One intubation was performed with a Miller 2 blade, and the other intubation was performed with a Macintosh 3 (one patient required a Macintosh 4). After the first intubation (intubation 1), correct endotracheal tube position was verified, and the patient was ventilated with a volatile anesthetic in oxygen. If needed, anesthetic medications were administered and/or adjusted before the second intubation. When hemodynamically stable and when adequately oxygenated and ventilated, the patient was extubated, and mask ventilation was resumed. A second baseline image (baseline 2) was obtained after removal of the ventilating mask, again allowing the head and neck to assume an unsupported midline resting position. Thereafter, the second intubation was performed (intubation 2). After the second intubation, correct endotracheal tube position was verified, and the protocol was completed. Surgery then proceeded. In each patient, each of the two intubations was performed by the same faculty anesthesiologist. Four experienced anesthesiologists participated, all of whom were facile with both Macintosh and Miller blades. All intubations were performed without the use of any external airway manipulations such as cricoid pressure or laryngeal lift. Anesthesiologists were instructed to obtain glottic exposure that was sufficient to reliably insert the endotracheal tube. With the Macintosh blade, the distal tip of the laryngoscope blade was placed in the vallecula, followed by application of anterior- and slightly inferiordirected force to indirectly elevate the epiglottis and expose the glottis. With the Miller blade, the tip of the laryngoscope blade was placed posterior and slightly distal to the posterior surface of the epiglottis, followed by a largely anterior- and slightly superior-directed force so as to directly elevate the epiglottis and expose the glottis. After each intubation, the anesthesiologist rated the extent of glottic visualization using the four-point scale and diagram of Cormack and Lehane: 1 most of the glottis visible; 2 only the posterior aspect of the glottis visible (at least the arytenoids); 3 no part of the glottis seen, but epiglottis seen; 4 not even the epiglottis exposed. 13 During all intubations, the occiput remained in contact with the foam pad, but there was no other restriction of head or neck movement. Patients were intubated with either a 7.0- or 7.5-mm-ID wirereinforced endotracheal tube (Mallinckrodt Incorporated, St. Louis, Missouri) containing a removable inner wire stylet. Stylets and wire-reinforced tubes were used
3 886 LEGRAND ET AL. to aid visualization of the endotracheal tube on fluoroscopic images. Data Acquisition, Processing, and Image Analysis Each laryngoscopy and intubation sequence was monitored with continuous lateral fluoroscopy of the cervical spine (OEC models 9000 and 9800; OEC Diasonics, Salt Lake City, UT), affording visualization of the skull base, craniocervical junction, and cervical vertebrae through C5. Cervical vertebrae caudal to C5 could not be visualized in all patients because they were obscured by the shoulders. Exposure was adjusted to optimize visualization of the cervical spine with the autoexposure function of the fluoroscopy unit disabled to provide uniform exposure conditions. The fluoroscope was stationary throughout all imaging sessions. The tube-to-patient and patient-to-image intensifier distances were constant throughout all imaging sessions. Real-time analog fluoroscopic images were converted to digital format using a Dazzle Hollywood DV- Bridge (SCM Microsystems, Fremont, CA) and recorded on a laptop computer using digital video software (imovie; Apple Computer, Cupertino, CA). Additional information regarding this is available on the ANESTHESIOLOGY Web site at Because of incomplete roentgenographic visualization of the cervical spine (n 2) and poor image quality (n 1), images from 3 of 14 patients could not be analyzed. Digital cinefluoroscopic images were reviewed off-line by an investigator assigned to create masked and coded images for subsequent image analysis. First, this investigator reviewed the entire laryngoscopy and intubation sequence of each patient s two intubations. A previous study from our group showed that cervical spine movement during laryngoscopy and intubation was maximal during the interval from when the endotracheal tube was seen to enter the posterior oropharynx to the point of glottic intubation. 1 Accordingly, from each of the two intubation sequences, this investigator selected a single still image where endotracheal tube position corresponded to this point of maximal cervical spine motion, usually when the endotracheal tube was just superior to the glottic inlet. Thereafter, to conceal the laryngoscope blade and endotracheal tube on the image, this investigator digitally masked each of the four still images derived from each patient (baseline 1, intubation 1, baseline 2, intubation 2) (Photoshop; Adobe Systems, San Jose, CA). Masking was performed by overlaying an opaque white rectangle of uniform size over portions of the image that revealed the presence and/or type of laryngoscope blade. Because these regions were always in the anterior part of the image, masking did not obscure the occiput or cervical spine. For each patient, the four masked images were kept grouped together as a set, but, for subsequent image analysis, both patient identity and image sequence (i.e., whether the image corresponded to baseline 1, intubation 1, and so on) were coded. Using the masked and coded images, spine motion analysis was performed completely independently by two observers using image analysis software (Scion Image 4.02 Beta; Scion Corporation, Frederick, MD). In each set of four masked images, the position of each bony structure (occiput, C1, C2, C3, C4, and C5) in two dimensions (lateral view) was defined by a line formed between two anatomic reference points. As much as possible, each observer selected reference points that included points on the anterior and posterior aspect of each bony structure. Owing to variations in anatomy and image quality, the precise location of reference points varied between observers and among patients. However, care was taken to assure that, for each bony structure, identical reference points were selected on each of the four masked images of a given set. Therefore, each image had a total of six paired reference points corresponding to the occiput and C1 C5. After all reference points for an image set were selected, each observer measured the angle formed between the line connecting each pair of reference points and a horizontal line. The difference in this angle s value between that obtained at the initial preintubation baseline (baseline 1) and subsequent images (intubation 1, baseline 2, intubation 2) was equal to the angular rotation in the sagittal plane of each bony structure compared with the initial preintubation position (i.e., relative to baseline 1). Cephalad rotations were assigned a positive value, and caudal rotations were assigned a negative value. These angle changes constitute the absolute rotational movement of each bony structure in the sagittal plane, independent of the motion of adjacent vertebrae. Then, to calculate the degree of motion that occurred between adjacent bony structures (i.e., intervertebral angle changes), angular changes for adjacent levels were combined mathematically (the angular change of the cephalad structure minus the angular change of the caudad structure). Accordingly, positive values correspond to intervertebral extension, whereas negative values correspond to flexion. Therefore, for each of five intervertebral segments (occiput C1, C1 C2, and so on), as well as for the entire cervical spine (occiput C5), intervertebral motion relative to the initial preintubation baseline (baseline 1) was measured for each of the three subsequent images (intubation 1, baseline 2, intubation 2). Values for intervertebral motions derived from each of the two independent observers were combined to obtain mean values, which were used for subsequent statistical analysis. To quantify intraobserver measurement variation in intervertebral angle changes, images from 3 of the 11 patients were duplicated but were assigned different codes. Hence, each observer received a total of 14 sets of coded and masked images (8 patients with one image set per patient, and 3 patients with two image sets per patient). This process created a total of 45 intraobserver comparisons for
4 CERVICAL MOTION WITH MACINTOSH AND MILLER BLADES 887 each of the two observers (3 duplicated patients 5 intervertebral segments per patient 3 angle changes per segment 45 duplicated measurements). For each of the two observers, the difference between each of the 45 paired intervertebral angle changes was calculated. To quantify interobserver variation in intervertebral angle change measurement, the difference between the two observers in each of the 210 intervertebral angle changes was calculated (14 image sets 5 segments/set 3 angle changes/segment 210 measures). Statistical Analysis Interobserver Differences. Repeated-measures analysis of variance was used to determine whether interobserver differences (n 210) significantly varied with either experimental stage (e.g., Macintosh, Miller, baseline 2) or intervertebral segment (e.g., occiput C1, C1 C2, and so on). The dependence of interobserver differences on the magnitude of intervertebral angle changes was assessed by the Spearman rank correlation coefficient. Calculations were performed using Systat 10.0 (Systat Software; Inc., San Jose, CA). Intervertebral Angle Changes. At baseline 1, intervertebral angle changes were defined as 0. The Wilcoxon signed rank test was used to determine whether intervertebral angle changes at baseline 2 differed from those at baseline 1. Because we anticipated that the two baseline positions would be equivalent, our original analysis plan was to use baseline 1 as the reference position for intubation 1 and baseline 2 as the reference position for intubation 2. However, as shown in the Results section, cervical spine position at baseline 2 differed significantly from that at baseline 1. To compare craniocervical motion between the Macintosh and Miller blades, a common baseline reference position was needed. Therefore, changes in spine motion with both intubations were referenced to baseline 1. The Wilcoxon signed rank test was also used to determine whether intervertebral angle changes from baseline 1 significantly differed between Macintosh and Miller blades. The effect of order (Macintosh first or Miller first) on these differences was determined by use of the Wilcoxon Mann Whitney test. Analyses were performed using StatXact-6 (Cytel Software Corporation, Cambridge, MA). P values are two-sided and exact. P values of 0.05 or less were considered to be significant. All significant P values were also significant using corresponding parametric tests and vice versa. We report the more conservative distribution-free methods, because of our limited sample sizes and lack of previous knowledge of the statistical distributions. Results Table 1. Patient Demographics and Preoperative Airway Characteristics Age, yr 46 8 (44, 34 59) Sex, n Male 6 Female 5 Height, m (1.79, ) Weight, kg (80, ) Body mass index, kg/m (24.8, ) Mallampati class,* n I 10 II 0 III 0 IV 1 Interdental distance, cm (5.0, ) Thyromental distance, cm (6.0, ) Data are presented as mean SD (median, range) unless otherwise indicated. * Mallampati oropharyngeal classification as modified by Samsoon and Young. 14 All patients were intubated with both laryngoscope blades. There were no study-related complications. Because of incomplete roentgenographic visualization of the cervical spine (n 2) or poor image quality (n 1), images from 3 patients were excluded from cervical spine motion analysis. All 3 of these patients had body mass indices exceeding 30 kg/m 2, as compared with 2 of 11 patients in whom image analysis was feasible. Demographic and preoperative airway characteristics of the 11 patients for whom spine motion analysis was conducted are summarized in table 1. Five patients were first intubated with the Macintosh blade, and 6 were first intubated with the Miller. There was no significant difference in glottic visualization between the Macintosh and Miller blades (Macintosh: grade 1 (n 7), grade 2 (n 4); Miller: grade 1 (n 6), grade 2 (n 5); with 8 of 11 patients having the same glottic view with both blades, 2 patients with a better view with the Macintosh, and 1 patient with a better view with the Miller). Observer A had a mean intraobserver difference in intervertebral angle change equal to (median 0.3 ). Observer B had a mean intraobserver difference in intervertebral angle change equal to (median 0.1 ). The mean interobserver difference in intervertebral angle change equaled (median 0.2 ). Interobserver differences did not significantly vary with either the three experimental stages (e.g., Macintosh blade, Miller blade, baseline 2: F 2, , P 0.32) or the five segments being analyzed (e.g., occiput C1, C1 C2, and so on: F 4, , P 0.16). Interobserver variation differed over the range of intervertebral angle changes (P 0.001) but was so small as to be clinically irrelevant. For the lower quintile of angle changes (0 1.2, n 42), the interobserver difference was (median 1.3 ). For the upper quintile ( , n 43), the interobserver difference was (median 1.8 ). Cervical spine position at baseline 2 differed significantly from that at baseline 1, with a total of of extension from the occiput to C5 (P ). Individual intervertebral segments in which there was a significant
5 888 LEGRAND ET AL. Table 2. Intervertebral Angle Change Compared with Preintubation Baseline Position (Baseline 1) Experimental Stage Occiput C1 C1 C2 C2 C3 C3 C4 C4 C5 Occiput C5 Intubation Macintosh Intubation Miller Macintosh/Miller difference P value* Data are presented as mean SD, in degrees. * Two-sided Wilcoxon signed rank test. difference between baseline 1 and baseline 2 were occiput C1 ( of extension; P 0.010) and C1 C2 ( of extension; P 0.025). Therefore, cervical spine extension occurring during intubation 1 was not completely reversed by subsequent extubation and reestablishment of mask ventilation and head position before intubation 2. For this reason, all motion data were referenced to baseline 1. Intervertebral motion data, comparing Macintosh and Miller blades versus baseline 1, are summarized in table 2. With both blades, laryngoscopy and intubation resulted in extension at each of the five segments relative to baseline. Total craniocervical extension (occiput C5) was greater with the Macintosh blade compared with the Miller ( vs , respectively; mean difference ; P 0.008). The difference between Macintosh and Miller blades did not vary with the order of intubation (P 0.999). The occiput C1 segment was the only individual intervertebral segment in which there was a significant difference between Macintosh and Miller blades in the degree of extension ( vs , respectively; mean difference ; P 0.012). At occiput C1, the difference between Macintosh and Miller blades did not depend on order of intubation (P 1.000). Discussion Key Findings and Clinical Relevance This study is the first to characterize segmental craniocervical motion during intubation with the Miller blade and to compare it with that occurring with the Macintosh. Table 3 shows that our values for maximum craniocervical motion (extension) during intubation with the Macintosh blade are consistent with previous studies. In this study, the Miller blade was associated with a statistically significant but quantitatively small decrease in cervical extension when compared with the Macintosh, on average 2.7 at occiput C1 and 4.8 overall (occiput C5). In a previous study using an external angle finder, Table 3. Previous Studies Quantifying Intervertebral Angle Change Compared with Preintubation Baseline Position during Orotracheal Intubation with a Macintosh 3 Blade Study Patients, n Preintubation Head Position Glottic View Occiput C1 C1 C2 C2 C3 C3 C4 C4 C5 Occiput C5 Hastings 8 Occiput on board Best possible 12* 11* NM 31* et al. 2 Watts et al Occiput on board Grade 1 86%, grade 2 14% Sawin 10 Occiput on 3-cm et al. 1 pad Limited to that necessary to [intubate] under direct vision Rudolph 20 Occiput on table Grade 1 40%, et al. 8 grade 2 25%, grade 3 35% Turkstra et al Back on board, forehead taped to Mayfield horseshoe Current study 11 Occiput on 7-cm pad That providing a reasonable opportunity to intubate Grade 1 64%, grade 2 36% # 10 2** 10 3** 3 2** 5 3** NM 28 5 ** # Data are presented as mean SD, in degrees. * Only mean values reported in text. Values for C2 C3 and C3 C4 interpolated from data shown in figure 4 of the article. Value for occiput C4. Values for C2 C3, C3 C4, and C4 C5 not individually reported. Value for C2 C5 was Only mean values reported. # Value not reported. Value is sum of means. ** Numerical values not reported in text. Values are interpolated from figures 4 and 5 of the article. Numerical value not reported in text. Value is interpolated from figure 3 of the article. Values for C2 C3, C3 C4, and C4 C5 not individually reported. Value for C2 C5 was 7 5. NM not measured.
6 CERVICAL MOTION WITH MACINTOSH AND MILLER BLADES 889 Hastings et al. 12 observed that laryngoscopy with a Miller blade resulted in 3 less external head extension than a Macintosh blade. Our values are quantitatively similar to those of Hastings et al., but reveal the difference between blade types is largely accounted for by less extension at occiput C1 with the Miller blade. At each intervertebral segment, as well as overall, the difference between the Miller and Macintosh blades was less than the variation among patients. Therefore, in routine practice, the small difference between blades would be difficult to perceive against the background of normal interpatient variation. Because intubation with the Miller blade results in 15 20% less craniocervical extension to obtain the same glottic view as the Macintosh, it is possible that the Miller blade could be modestly advantageous in circumstances where neck mobility is less than normal and/or when minimization of craniocervical movement during intubation is desired. However, this potential advantage is entirely speculative because there are no randomized clinical trials showing the Miller blade to be superior to the Macintosh in either of these circumstances. In a cadaver model of a complete C5 C6 transection, Gerling et al. 15 reported that laryngoscopy with a Miller blade resulted in significantly less (1 2 mm) axial distraction at the unstable segment than with a Macintosh blade. However, in the same study, there were no differences between blades in anteroposterior subluxation or intervertebral extension at the unstable segment, although the study may have been underpowered. An accompanying editorial emphasized that the lesser cervical motion observed with the Miller blade was so small as to probably be clinically insignificant, even in the presence of an unstable spine. 16 Therefore, our study and others indicate that, although the Miller blade results in less craniocervical motion than the Macintosh, the difference is very small. When, if ever, such small differences might be clinically meaningful is not known. Mechanics of Direct Laryngoscopy and Tracheal Intubation All other factors being equal during laryngoscopy, the amount of craniocervical motion taking place will vary with how greatly preintubation head and neck position differs from that occurring with intubation. As an extreme example, suppose that, before intubation, the occiput and cervical spine were positioned in the same configuration as that occurring during intubation. In this circumstance, craniocervical motion during intubation would be zero. Therefore, the amount of spine motion that takes place during intubation necessarily depends on how the head, neck, and spine are initially positioned. Second, all other factors being equal, the degree of craniocervical extension required to create the line of sight varies, at least in part, with the degree of desired glottic visualization. This principle was demonstrated by Hastings et al., 17 who showed that, using a Macintosh blade, approximately 5 of greater head extension was necessary to visualize the entire glottis as opposed to only its posterior aspect. These two principles probably explain much of the variation present among previous studies that have quantified craniocervical motion during intubation with the Macintosh blade (table 3). However, these two principles do not explain the difference between the Macintosh and Miller blade observed in this study. First, in this study, preintubation head and neck position was radiographically defined (baseline 1) and was, for the purpose of measuring craniocervical motion, exactly the same for both intubations in each patient. Second, in this study, the degree of glottic visualization was equivalent between blade types; (see additional discussion in Limitations). Therefore, other mechanisms must be responsible for the lesser craniocervical extension associated with the Miller blade. Another principle of intubation mechanics is, all other factors being equal, when the glottic inlet is positioned in a relatively posterior and/or cephalad position in the neck, lesser degrees of tissue displacement and/or craniocervical extension are required to achieve a line of sight. This concept is supported by studies showing that external laryngeal manipulation causing posterior and cephalad movement of the glottis in the neck improves glottic visualization Therefore, it is conceivable that the lesser craniocervical extension observed during intubation with the Miller blade could be on the basis of a difference in glottic position at intubation as compared with the Macintosh blade with a relatively more posterior- and/or cephalad-oriented glottis with the Miller blade. To date, few studies have assessed how laryngoscopy and intubation change the position and anatomy of the larynx. Horton et al. 22 obtained lateral x-rays of the head and neck in conscious volunteers undergoing laryngoscopy with a Macintosh 3 blade. With laryngoscopy, the hyoid was displaced both anteriorly and caudad relative to the cervical spine. To explore the question of differential glottic position, we reviewed our cinefluoroscopy images. We observed that direct laryngoscopy resulted in an anterior and caudad displacement of the base of the epiglottis (vallecula) and hyoid relative to both the mandible and cervical spine in comparison with the preintubation (baseline 1) position. Because fluoroscopy exposure was set to optimize visualization of the cervical spine, in only a few patients was image quality sufficient to determine the position of the vallecula (n 5) and/or hyoid (n 3) throughout both intubation sequences relative to a fixed point on the mandible. However, in these patients, we observed that the vallecula was displaced more anteriorly (4 of 5; approximately cm) and more caudally (5 of 5; approximately cm) with the Macintosh blade compared with the Miller. The hyoid was also displaced more anteriorly (2 of 3; approximately cm) and
7 890 LEGRAND ET AL. Fig. 1. Still images for patient 13 at baseline 1 (A), intubation Miller (B), and intubation Macintosh (C). Compared with baseline, intervertebral motion (extension) with Miller and Macintosh blades was 2.7 and 7.0, respectively, at occiput C1; 0.4 and 2.2, respectively, at C1 C2; and 14.1 and 22.4, respectively, from the occiput to C5. The vallecula was displaced 1.4 cm more anteriorly and 1.7 cm more inferiorly with the Macintosh blade compared with the Miller. The hyoid was displaced 0.6 cm more anteriorly and 0.3 cm more inferiorly with the Macintosh compared with the Miller. more caudally (3 of 3; cm) with the Macintosh; an example is shown in figure 1. Therefore, these preliminary observations support but do not prove the hypothesis that laryngoscopy with Miller blade may result in a glottic position that is relatively less anterior and/or caudad than that which occurs with the Macintosh. Formal testing of this hypothesis deserves future study. If confirmed, this may explain, at least in part, why a lesser degree of craniocervical extension is required with the Miller blade. A fourth principle of intubation mechanics is, all other factors being equal, either more effective tissue displacement, or a lesser volume of tissue to displace, should require lesser degrees of craniocervical extension to create a line of sight. Because the width of the Miller blade is approximately 50 60% of the width of the Macintosh, it displaces a lesser volume of tissue (tongue) during laryngoscopy. Hastings et al. 12 observed that, in addition to less external head extension with the Miller blade, applied lifting forces were also significantly less (30%) with the Miller blade as compared with the Macintosh. A possible explanation for these observations is that, with the Miller blade, the smaller volume of displaced tongue is more readily accommodated in the submandibular space, such that less lifting force is required. If the Miller blade is more likely to be successful in tissue displacement than the Macintosh (because it requires less tissue displacement), it should, therefore, obtain a better view of the glottis and/or require less craniocervical extension to create a line of sight. In separate studies, both Benumof et al. 20 and Arino et al. 23 observed that glottic visualization was significantly better with the Miller blade. Although Arino et al. 23 found that glottic visualization was significantly better with the Miller blade, paradoxically, they found ease of intubation was greater with the Macintosh. Apparently, although the Miller blade more often displaced tissue sufficient to visualize the entire glottis, this visual pathway was often too small to introduce the endotracheal tube with ease. Finally, the preceding discussion of intubation mechanics has been based on the presumption that, with equivalent glottic position and visualization, the Macintosh and Miller blades would have precisely the same line of sight. However, that may not be the case. In a quantitative analysis of airway anatomy and laryngoscope design, Marks et al. 24 determined that, in the average adult, the line of sight along the Macintosh blade differs from the Miller by 2 4 in the posterior direction. In essence, the curvature of the Macintosh blade acts as a visual hill interrupting the line of sight. Therefore, to achieve the same glottic view with the Macintosh blade as with the Miller, either the tongue must be displaced slightly more into the submandibular space with the Macintosh or, if that cannot occur, an additional 2 4 of craniocervical extension from the occiput to C4 C5 (the level of the glottic inlet) would be required. Therefore, rather than differences in tongue displacement and/or glottic position, another explanation for our findings may simply be that the curvature of the Macintosh blade requires approximately 3 of extra craniocervical extension to obtain the same view of the glottis as that with the Miller. Limitations The findings of this study must be considered while keeping several limitations in mind. First, this is a small study, involving few patients and even fewer anesthesiologists. Therefore, whether our findings are applicable to the more general patient population and anesthesia community is unknown. Because of the differences in head, neck, and airway anatomy between adults and children, our findings cannot be applied to the pediatric population. Likewise, patients who have anatomically unstable spines cannot be expected to exhibit the same craniocervical motion in response to the forces of laryngoscopy as do patients with stable spines. Therefore, it would not be safe to assume that the lesser extension observed with the Miller blade in this study would necessarily also result in less extension in the presence of
8 CERVICAL MOTION WITH MACINTOSH AND MILLER BLADES 891 instability (e.g., patients with traumatic injury, trisomy 21, or rheumatoid arthritis). Another limitation of this study relates to how glottic visualization was quantified. Because the Cormack and Lehane scale is categorical rather than continuous, 13 it is possible for different degrees of glottic visualization to receive the same score. 25 For example, visualization of the posterior 30% of the glottis and visualization of the posterior 5% of the glottis would both be scored as Cormack and Lehane grade 2. Use of a continuous scale, such as the percentage of glottic opening scale, 26 would have increased our ability to detect any difference in glottic visualization between blades. In addition, glottic visualization was not independently assessed but, rather, was reported by the anesthesiologist, who was aware of the blade being used. Bias on the part of the anesthesiologist could have altered perceptions and/or reports of glottic view. Therefore, an independent assessment of glottic view, without knowledge of blade type, would have increased objectivity. Such assessments are now possible with the use of a head-mounted video system that aligns with the laryngoscopist s line of sight and records glottic exposure as visualized by the laryngoscopist. 27 A recent study shows good intrarater and interrater agreement in glottic visualization scores with such a system. 27 In summary, we observed that direct laryngoscopy and orotracheal intubation with a Miller blade resulted in 15 20% less craniocervical extension than with a Macintosh blade, on average approximately 3 less at occiput C1 and approximately 5 less from the occiput to C5. These small differences are less than interpatient variation and are not likely to be of importance in most circumstances. Compared with the Macintosh, lesser extension with the Miller blade could be on the basis of differences in glottic position, tongue displacement, and/or line of sight along the blade. Additional studies are needed to confirm these observations and hypotheses. The authors thank Luis Avila, M.D. (Wheaton Franciscan Hospital, Covenant Clinics Anesthesia, Waterloo, Iowa), Johnny E. Brian, M.D. (Anesthesia and Analgesia, P.C., Davenport, Iowa), and Robert From, D.O. (Associate Professor, University of Iowa Carver College of Medicine, Department of Anesthesia, Iowa City, Iowa), for their participation in this study. The authors also thank Koji Dairaku, M.D., Ph.D. (Physician, Yamaguchi University, Advanced Medical Emergency and Critical Care Center, Yamaguchi, Japan), for his translation of the article by Konishi et al., 11 and Thomas C. Smith, B.S. (Web Applications Developer, University of Iowa Carver College of Medicine, Department of Anesthesia, Iowa City, Iowa), for creating figure 1. References 1. Sawin PD, Todd MM, Traynelis VC, Farrell SB, Nader A, Sato Y, Clausen JD, Goel VK: Cervical spine motion with direct laryngoscopy and orotracheal intubation: An in vivo cinefluoroscopic study of subjects without cervical abnormality. ANESTHESIOLOGY 1996; 85: Hastings RH, Vigil AC, Hanna R, Yang B-Y, Sartoris DJ: Cervical spine movement during laryngoscopy with the Bullard, Macintosh, and Miller laryngoscopes. ANESTHESIOLOGY 1995; 82: Watts ADJ, Gelb AW, Bach DB, Pelz DM: Comparison of the Bullard and Macintosh laryngoscopes for endotracheal intubation of patients with a potential cervical spine injury. ANESTHESIOLOGY 1997; 87: Wahlen BM, Gercek E: Three-dimensional cervical spine movement during intubation using the Macintosh and Bullard laryngoscopes, the Bonfils fibrescope, and the intubating laryngeal mask airway. Eur J Anaesthesiol 2004; 21: Waltl B, Melischek M, Schusching C, Kabon B, Erlacher W, Nasel C, Fuchs M, Kapral S: Tracheal intubation and cervical spine excursion: Direct laryngoscopy versus intubating laryngeal mask. Anaesthesia 2001; 56: Sahin A, Salman MA, Erden A, Aypar U: Upper cervical vertebrae movement during intubating laryngeal mask, fibreoptic and direct laryngoscopy: A videofluoroscopic study. Eur J Anaesthesiol 2004; 21: Turkstra TP, Craen RA, Pelz DM, Gelb AW: Cervical spine motion: A fluoroscopic comparison during intubation with lighted stylet, GlideScope, and Macintosh laryngoscope. Anesth Analg 2005; 101: Rudolph C, Schneider JP, Wallenborn J, Schaffranietz L: Movement of the upper cervical spine during laryngoscopy: A comparison of the Bonfils intubation fibrescope and the Macintosh laryngoscope. Anaesthesia 2005; 60: Majernick TG, Bieniek R, Houston JB, Hughes HG: Cervical spine movement during orotracheal intubation. Ann Emerg Med 1986; 15: Hauswald M, Sklar DP, Tandberg D, Garcia JF: Cervical spine movement during airway management: Cinefluoroscopic appraisal in human cadavers. Am J Emerg Med 1991; 9: Konishi A, Sakai T, Nishiyama T, Higashizawa T, Bito H: Cervical spine movement during orotracheal intubation using the McCoy laryngoscope compared with the Macintosh and the Miller laryngoscopes [in Japanese]. Masui 1997; 46: Hastings RH, Hon ED, Nghiem C, Wahrenbrock EA: Force and torque vary between laryngoscopists and laryngoscope blades. Anesth Analg 1996; 82: Cormack RS, Lehane J: Difficult tracheal intubation in obstetrics. Anaesthesia 1984; 39: Samsoon GLT, Young JRB: Difficult tracheal intubation: a retrospective study. Anaesthesia 1987; 42: Gerling MC, Davis DP, Hamilton RS, Morris GF, Vilke GM, Garfin SR, Hayden SR: Effects of cervical spine immobilization technique and laryngoscope blade selection on an unstable cervical spine in a cadaver model of intubation. Ann Emerg Med 2000; 36: Grossman D, Schriger DL: Immobilization technique and blade choice in the endotracheal intubation of trauma patients: Miller time or much ado about nothing? (editorial). Ann Emerg Med 2000; 36: Hastings RH, Wood PR: Head extension and laryngeal view during laryngoscopy with cervical spine stabilization maneuvers. ANESTHESIOLOGY 1994; 80: Krantz MA, Poulos JG, Chaouki K, Adamek P: The laryngeal lift: A method to facilitate endotracheal intubation. J Clin Anesth 1993; 5: Knill RL: Difficult laryngoscopy made easy with a BURP. Can J Anaesth 1993; 40: Benumof JL, Cooper SD: Quantitative improvement in laryngoscopic view by optimal external laryngeal manipulation. J Clin Anesth 1996; 8: Takahata O, Kubota M, Mamiya K, Akama Y, Nozaka T, Matsumoto H, Ogawa H: The efficacy of the BURP maneuver during a difficult laryngoscopy. Anesth Analg 1997; 84: Horton WA, Fahy L, Charters P: Disposition of cervical vertebrae, atlantoaxial joint, hyoid, and mandible during x-ray laryngoscopy. Br J Anaesth 1989; 63: Arino JJ, Velasco JM, Gasco C, Lopez-Timoneda F: Straight blades improve visualization of the larynx while curved blades increase ease of intubation: A comparison of the Macintosh, Miller, McCoy, Belscope and Lee-Fiberview blades. Can J Anaesth 2003; 50: Marks RRD, Hancock R, Charters P: An analysis of laryngoscope blade shape and design: New criteria for laryngoscope evaluation. Can J Anaesth 1993; 40: Yentis SM, Lee DJH: Evaluation of an improved scoring system for the grading of direct laryngoscopy. Anaesthesia 1998; 53: Ochroch EA, Hollander JE, Kush S, Shofer FS, Levitan RM: Assessment of laryngeal view: percentage of glottic opening score versus Cormack and Lehane grading. Can J Anaesth 1999; 46: George RB, McKeen D, Law JA: Laryngoscopic evaluation with the Airway Cam laryngoscopy video system. Can J Anaesth 2006; 53:512 5
Cervical spine movement during laryngoscopy using the Airway Scope compared with the Macintosh laryngoscope
 doi:10.1111/j.1365-2044.2007.05188.x APPARATUS Cervical spine movement during laryngoscopy using the Airway Scope compared with the Macintosh laryngoscope Y. Hirabayashi, 1 A. Fujita, 2 N. Seo 1 and H.
doi:10.1111/j.1365-2044.2007.05188.x APPARATUS Cervical spine movement during laryngoscopy using the Airway Scope compared with the Macintosh laryngoscope Y. Hirabayashi, 1 A. Fujita, 2 N. Seo 1 and H.
Study of Comparison of Standard And English Macintosh Laryngoscope Blades in Patients Undergoing Surgery Under General Anaesthesia.
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. VIII (December. 2016), PP 111-118 www.iosrjournals.org Study of Comparison of Standard
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 12 Ver. VIII (December. 2016), PP 111-118 www.iosrjournals.org Study of Comparison of Standard
Cervical Spine Motion
 Anesthesiology 2009; 111:97 101 Cervical Spine Motion Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. A Fluoroscopic Comparison of the AirTraq Laryngoscope
Anesthesiology 2009; 111:97 101 Cervical Spine Motion Copyright 2009, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. A Fluoroscopic Comparison of the AirTraq Laryngoscope
CLINICAL INVESTIGATIONS. Materials and Methods
 CLINICAL INVESTIGATIONS Anesthesiology 2007; 107:875 83 Copyright 2007, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Dynamic Interaction of Craniofacial Structures
CLINICAL INVESTIGATIONS Anesthesiology 2007; 107:875 83 Copyright 2007, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Dynamic Interaction of Craniofacial Structures
Optimising tracheal intubation success rate using the Airtraq laryngoscope
 doi:10.1111/j.1365-2044.2008.05757.x APPARATUS Optimising tracheal intubation success rate using the Airtraq laryngoscope G. Dhonneur, 1 W. Abdi, 2 R. Amathieu, 2 S. Ndoko 2 and L. Tual 2 1 Professor,
doi:10.1111/j.1365-2044.2008.05757.x APPARATUS Optimising tracheal intubation success rate using the Airtraq laryngoscope G. Dhonneur, 1 W. Abdi, 2 R. Amathieu, 2 S. Ndoko 2 and L. Tual 2 1 Professor,
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Supplemental Digital Content 1
 Supplemental Digital Content 1 RESULTS Experiment 1: Primary Intubation Biomechanics In Experiment 1, cadavers were intubated twice (intubation Set 1) in random order: sequence 1 (Macintosh then Airtraq
Supplemental Digital Content 1 RESULTS Experiment 1: Primary Intubation Biomechanics In Experiment 1, cadavers were intubated twice (intubation Set 1) in random order: sequence 1 (Macintosh then Airtraq
British Journal of Anaesthesia 100 (4): (2008) doi: /bja/aen002 Advance Access publication January 31, 2008
 RESPIRATION AND THE AIRWAY Pentax-AWS, a new videolaryngoscope, is more effective than the Macintosh laryngoscope for tracheal intubation in patients with restricted neck movements: a randomized comparative
RESPIRATION AND THE AIRWAY Pentax-AWS, a new videolaryngoscope, is more effective than the Macintosh laryngoscope for tracheal intubation in patients with restricted neck movements: a randomized comparative
Airway Management & Safety Concerns Experience from Bariatric Surgery
 Airway Management & Safety Concerns Experience from Bariatric Surgery Issues of the Obese Critical Care Patient - Airway Srikantha Rao MBBS MS Associate Professor Department of Anesthesia Aug 2010 Objectives
Airway Management & Safety Concerns Experience from Bariatric Surgery Issues of the Obese Critical Care Patient - Airway Srikantha Rao MBBS MS Associate Professor Department of Anesthesia Aug 2010 Objectives
Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients.
 Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
Title Comparison of the Berman Intubating Airway and the Williams Airway Intubator for fibreoptic orotracheal intubation in anaesthetised patients Author(s) Greenland, KB; Ha, ID; Irwin, MG Citation Anaesthesia,
External Laryngeal Manipulation for Better Laryngeal View
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver. 2 March. (2018), PP 65-69 www.iosrjournals.org External Laryngeal Manipulation for Better
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 3 Ver. 2 March. (2018), PP 65-69 www.iosrjournals.org External Laryngeal Manipulation for Better
PREDICTORS OF DIFFICULT INTUBATION: STUDY IN KASHMIRI POPULATION
 Original article Pravara Med Rev 2009; 1(4) PREDICTORS OF DIFFICULT INTUBATION: STUDY IN KASHMIRI POPULATION Gupta A K, Ommid Mohamad, Nengroo Showkat, Naqash Imtiyaz, Mehta Anjali ABSTRACT Airway assessment
Original article Pravara Med Rev 2009; 1(4) PREDICTORS OF DIFFICULT INTUBATION: STUDY IN KASHMIRI POPULATION Gupta A K, Ommid Mohamad, Nengroo Showkat, Naqash Imtiyaz, Mehta Anjali ABSTRACT Airway assessment
Displacement of the epiglottis during intubation with the Pentax-AWS Airway Scope. Suzuki, Akihiro ; Katsumi, Norifumi ; Honda, Takashi ; Sasakawa,
 AMCoR Asahikawa Medical University Repository http://amcor.asahikawa-med.ac.jp/ Journal of Anesthesia (2010) 24(1): 124-127. Displacement of the epiglottis during intubation with the Pentax-AWS Airway
AMCoR Asahikawa Medical University Repository http://amcor.asahikawa-med.ac.jp/ Journal of Anesthesia (2010) 24(1): 124-127. Displacement of the epiglottis during intubation with the Pentax-AWS Airway
INFORMED CONSENT FOR publication of the present
 Acute Medicine & Surgery 2015; 2: 138 142 doi: 10.1002/ams2.88 Brief Communication Comparison of the conventional Macintosh laryngoscope, the Pentax Airwayscope, and the McGrath MAC video laryngoscope
Acute Medicine & Surgery 2015; 2: 138 142 doi: 10.1002/ams2.88 Brief Communication Comparison of the conventional Macintosh laryngoscope, the Pentax Airwayscope, and the McGrath MAC video laryngoscope
The Glidescope Ò system: a clinical assessment of performance
 Anaesthesia, 2005, 60, pages 60 64 APPARATUS The Glidescope Ò system: a clinical assessment of performance M. R. Rai, 1 A. Dering 1 and C. Verghese 2 1 Specialist Registrars, 2 Consultant, Department of
Anaesthesia, 2005, 60, pages 60 64 APPARATUS The Glidescope Ò system: a clinical assessment of performance M. R. Rai, 1 A. Dering 1 and C. Verghese 2 1 Specialist Registrars, 2 Consultant, Department of
Cervical spine motion: a fluoroscopic comparison of Shikani Optical Stylet vs Macintosh laryngoscope
 REPORTS OF ORIGINAL INVESTIGATIONS 441 Cervical spine motion: a fluoroscopic comparison of Shikani Optical Stylet vs Macintosh laryngoscope [Mouvement de la colonne cervicale : une comparaison fluoroscopique
REPORTS OF ORIGINAL INVESTIGATIONS 441 Cervical spine motion: a fluoroscopic comparison of Shikani Optical Stylet vs Macintosh laryngoscope [Mouvement de la colonne cervicale : une comparaison fluoroscopique
Omiros Chalkeidis*, Georgios Kotsovolis, Apostolos Kalakonas, Maria Filippidou, Christos Triantafyllou, Dimitris Vaikos, Epaminondas Koutsioumpas
 Acta Anaesthesiol Taiwan 2010;48(1):15 20 ORIGINAL ARTICLE A Comparison Between the Airtraq and Macintosh Laryngoscopes for Routine Airway Management by Experienced Anesthesiologists: A Randomized Clinical
Acta Anaesthesiol Taiwan 2010;48(1):15 20 ORIGINAL ARTICLE A Comparison Between the Airtraq and Macintosh Laryngoscopes for Routine Airway Management by Experienced Anesthesiologists: A Randomized Clinical
The reasons 13/11/ Cost 2. Availability 3. Comparison 4. Complications 5. Knowledge. Pulmonary and critical care medicine (PCCM) fellows.
 The reasons Why shouldn t we use videolaryngoscope for routine intubation? Wariya Sukhupragarn, MD Associate Professor Department of Anesthesiology Faculty of Medicine, Chiang Mai University 1. Cost 2.
The reasons Why shouldn t we use videolaryngoscope for routine intubation? Wariya Sukhupragarn, MD Associate Professor Department of Anesthesiology Faculty of Medicine, Chiang Mai University 1. Cost 2.
Clinical Study McGrath Video Laryngoscope May Take a Longer Intubation Time Than Macintosh Laryngoscope
 Anesthesiology Volume 2015, Article ID 901903, 4 pages http://dx.doi.org/10.1155/2015/901903 Clinical Study McGrath Video Laryngoscope May Take a Longer Intubation Time Than Macintosh Laryngoscope Prerana
Anesthesiology Volume 2015, Article ID 901903, 4 pages http://dx.doi.org/10.1155/2015/901903 Clinical Study McGrath Video Laryngoscope May Take a Longer Intubation Time Than Macintosh Laryngoscope Prerana
If you suspect airway problems, get a second opinion before you anaesthetise, not after!
 Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
Assessing the airway It is more important to be aware of the various methods of dealing with difficult laryngoscopy than to expect to be able to accurately identify the rare difficult patients without
ISPUB.COM. The Video-Intubating Laryngoscope. M Weiss THE LARYNGOSCOPE INTRODUCTION TECHNICAL DESCRIPTION
 ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 1 M Weiss Citation M Weiss.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 1. Abstract A Macintosh intubating laryngoscope
ISPUB.COM The Internet Journal of Anesthesiology Volume 3 Number 1 M Weiss Citation M Weiss.. The Internet Journal of Anesthesiology. 1998 Volume 3 Number 1. Abstract A Macintosh intubating laryngoscope
Cervical spine motion during flexible bronchoscopy compared with the Lo-Pro GlideScope w
 J dvance ccess published February 3, 29 ritish Journal of naesthesia Page 1 of 7 doi:.93/bja/aep2 Cervical spine motion during flexible bronchoscopy compared with the Lo-Pro GlideScope w D. M. Wong,. Prabhu
J dvance ccess published February 3, 29 ritish Journal of naesthesia Page 1 of 7 doi:.93/bja/aep2 Cervical spine motion during flexible bronchoscopy compared with the Lo-Pro GlideScope w D. M. Wong,. Prabhu
Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia
 DIFFICULT AIRWAY CANNOT VENTILATE, CANNOT INTUBATE. Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia Difficult airway According to AMERICAN SOCIETY OF ANAESTHESIOLOGISTS Difficult Airway is defined
DIFFICULT AIRWAY CANNOT VENTILATE, CANNOT INTUBATE. Dr.Bharghavi.M 2 nd year post graduate Dept of Anaesthesia Difficult airway According to AMERICAN SOCIETY OF ANAESTHESIOLOGISTS Difficult Airway is defined
Airway Workshop Lecture. University of Ottawa
 Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
[Les lames droites améliorent la visualisation du larynx tandis que les lames courbes facilitent
 CARDIOTHORACIC ANESTHESIA, RESPIRATION AND AIRWAY 501 Straight blades improve visualization of the larynx while curved blades increase ease of intubation: a comparison of the Macintosh, Miller, McCoy,
CARDIOTHORACIC ANESTHESIA, RESPIRATION AND AIRWAY 501 Straight blades improve visualization of the larynx while curved blades increase ease of intubation: a comparison of the Macintosh, Miller, McCoy,
Mouth opening with cervical collars Fig 1 Types of semi-rigid collar used (left to right): Stifneck (Laerdal Medical Corp.); Miami J (Jerome Medical);
 British Journal of Anaesthesia 95 (3): 344 8 (25) doi:1.193/bja/aei19 Advance Access publication July 8, 25 Reduction in mouth opening with semi-rigid cervical collars { C. M. Goutcher* and V. Lochhead
British Journal of Anaesthesia 95 (3): 344 8 (25) doi:1.193/bja/aei19 Advance Access publication July 8, 25 Reduction in mouth opening with semi-rigid cervical collars { C. M. Goutcher* and V. Lochhead
The LMA CTrach TM, a new laryngeal mask airway for endotracheal intubation under vision: evaluation in 100 patients
 British Journal of Anaesthesia 96 (3): 396 400 (2006) doi:10.1093/bja/ael001 Advance Access publication January 16, 2006 The LMA CTrach TM, a new laryngeal mask airway for endotracheal intubation under
British Journal of Anaesthesia 96 (3): 396 400 (2006) doi:10.1093/bja/ael001 Advance Access publication January 16, 2006 The LMA CTrach TM, a new laryngeal mask airway for endotracheal intubation under
Comparison of upper lip bite test with modified mallampati classification for prediction of difficult obstetric intubation
 ISPUB.COM The Internet Journal of Anesthesiology Volume 19 Number 1 Comparison of upper lip bite test with modified mallampati classification for prediction of difficult S Mishra, R Bhat, S K., M Nagappa,
ISPUB.COM The Internet Journal of Anesthesiology Volume 19 Number 1 Comparison of upper lip bite test with modified mallampati classification for prediction of difficult S Mishra, R Bhat, S K., M Nagappa,
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Airway/Breathing Chapter 5 Airway/Breathing Introduction Rapid assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur rapidly
Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway
 Case Report Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway Andrew Zura MD, D. John Doyle MD PhD FRCPC,
Case Report Use of the Aintree Intubation Catheter with the Laryngeal Mask Airway and a Fiberoptic Bronchoscope in a Patient with an Unexpected Difficult Airway Andrew Zura MD, D. John Doyle MD PhD FRCPC,
Hemodynamic responses to orotracheal intubation with a video laryngoscope. in infants: a comparison study
 Received: 30.5.2006 Accepted: 15.5.2007 Hemodynamic responses to orotracheal intubation with a video laryngoscope in infants: a comparison study Shahnaz Shayeghi*, Mehdi Ghasemi**, Afsaneh Sadeghi*, Sayed
Received: 30.5.2006 Accepted: 15.5.2007 Hemodynamic responses to orotracheal intubation with a video laryngoscope in infants: a comparison study Shahnaz Shayeghi*, Mehdi Ghasemi**, Afsaneh Sadeghi*, Sayed
Department of Anesthesia and Intensive Care, Vardhman Mahavir Medical College and Safdarjang Hospital, New Delhi , India 2
 Anesthesiology Research and Practice Volume 2011, Article ID 297913, 6 pages doi:10.1155/2011/297913 Clinical Study Comparative Evaluation of the Sniffing Position with Simple Head Extension for Laryngoscopic
Anesthesiology Research and Practice Volume 2011, Article ID 297913, 6 pages doi:10.1155/2011/297913 Clinical Study Comparative Evaluation of the Sniffing Position with Simple Head Extension for Laryngoscopic
A clinical evaluation of the Bonfils Intubation Fibrescope*
 APPARATUS A clinical evaluation of the Bonfils Intubation Fibrescope* M. Halligan and P. Charters Department of Anaesthesia, University Hospital Aintree, Lower Lane, Liverpool, L9 7AL, UK Summary The Bonfils
APPARATUS A clinical evaluation of the Bonfils Intubation Fibrescope* M. Halligan and P. Charters Department of Anaesthesia, University Hospital Aintree, Lower Lane, Liverpool, L9 7AL, UK Summary The Bonfils
Difficult Airway. Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.)
 Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
Difficult Airway Department of Anesthesiology University of Colorado Health Sciences Center (prepared by Brenda A. Bucklin, M.D.) Objectives Definition & incidence of the difficult airway Evaluation of
Original article Effect of Second Person Aid for Upward Displacement of Laryngoscope on Laryngeal View during Laryngoscopy
 Original article Effect of Second Person Aid for Upward Displacement of Laryngoscope on Laryngeal View during Laryngoscopy Seyd Hedayatallah Akhlagh1, Arash Farbood2, Seyed Mohammadreza Hadavi3, Reza Raeesi
Original article Effect of Second Person Aid for Upward Displacement of Laryngoscope on Laryngeal View during Laryngoscopy Seyd Hedayatallah Akhlagh1, Arash Farbood2, Seyed Mohammadreza Hadavi3, Reza Raeesi
Emergency Department/Trauma Adult Airway Management Protocol
 Emergency Department/Trauma Adult Airway Management Protocol Purpose: A standardized protocol for management of the airway in the setting of trauma in an academic center, with the goal of maximizing successful
Emergency Department/Trauma Adult Airway Management Protocol Purpose: A standardized protocol for management of the airway in the setting of trauma in an academic center, with the goal of maximizing successful
Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy
 Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy Amir Murad Khudad* Hoshyar Najeeb Karem** ABSTRACT Background and Objectives: The cardiovascular response
Haemodynamic response to orotracheal intubation: direct laryngoscopy versus fiberoptic bronchoscopy Amir Murad Khudad* Hoshyar Najeeb Karem** ABSTRACT Background and Objectives: The cardiovascular response
LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS. - Our Perspective.
 ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
ISSN: 2250-0359 Volume 3 Issue 4 2013 LEVITAN S FIBREOPTIC STYLET: BEYOND BARRIERS - Our Perspective. Justin Ebenezer Sargunaraj * Dr.Balasubramaniam Thiagarajan * *Stanley Medical College ABSTRACT: This
Materials and Methods. significance of respiratory problems in anesthetized patients. 1 This study laid the groundwork for the development
 Anesthesiology 2001; 95:1175 81 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating LMA-Fastrach in 254 Patients with Difficult-to-manage Airways
Anesthesiology 2001; 95:1175 81 2001 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating LMA-Fastrach in 254 Patients with Difficult-to-manage Airways
N. Jagannathan 1, *, J. Hajduk 1, L. Sohn 1, A. Huang 1, A. Sawardekar 1, B. Albers 1, S. Bienia 2 and G. S. De Oliveira 3.
 British Journal of Anaesthesia, 118 (6): 932 7 (2017) doi: 10.1093/bja/aex073 Respiration and the Airway RESPIRATION AND THE AIRWAY Randomized equivalence trial of the King Vision ablade videolaryngoscope
British Journal of Anaesthesia, 118 (6): 932 7 (2017) doi: 10.1093/bja/aex073 Respiration and the Airway RESPIRATION AND THE AIRWAY Randomized equivalence trial of the King Vision ablade videolaryngoscope
Cricoid pressure impedes placement of the laryngeal mask airway
 British Journal of Anaesthesia 995; 74: 52-525 impedes placement of the laryngeal mask airway T. ASAI, K. BARCLAY, I. POWER AND R. S. VAUGHAN Summary We have studied 22 patients to examine whether or not
British Journal of Anaesthesia 995; 74: 52-525 impedes placement of the laryngeal mask airway T. ASAI, K. BARCLAY, I. POWER AND R. S. VAUGHAN Summary We have studied 22 patients to examine whether or not
Airway/Breathing. Chapter 5
 Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Airway/Breathing Chapter 5 Airway/Breathing Introduction Skillful, rapid, assessment and management of airway and ventilation are critical to preventing morbidity and mortality. Airway compromise can occur
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Orotracheal Intubation
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e videos in clinical medicine Orotracheal Intubation Christopher Kabrhel, M.D., Todd W. Thomsen, M.D., Gary S. Setnik, M.D., and Ron M. Walls, M.D.
T h e n e w e ng l a nd j o u r na l o f m e dic i n e videos in clinical medicine Orotracheal Intubation Christopher Kabrhel, M.D., Todd W. Thomsen, M.D., Gary S. Setnik, M.D., and Ron M. Walls, M.D.
DIFFICULT AIRWAY MANAGMENT. Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr)
 DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
DIFFICULT AIRWAY MANAGMENT Dr.N.SANTHOSH KUMAR MD ANESTHESIA (2 nd Yr) AIRWAY MANAGEMENT AND MAINTAINING OXYGENATION ARE THE FUNDAMENTAL RESPONSIBILITIES OF ANY BASIC DOCTOR. TO MANAGE A DIFFICULT AIRWAY,
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Comparison of sniffing position and simple head extension for visualization of glottis during direct laryngoscopy.
 KATHMANDU UNIVERSITY MEDICAL JOURNAL Comparison of sniffing position and simple head extension for visualization of glottis during direct laryngoscopy. Bhattarai B, Shrestha SK, Kandel S Department of
KATHMANDU UNIVERSITY MEDICAL JOURNAL Comparison of sniffing position and simple head extension for visualization of glottis during direct laryngoscopy. Bhattarai B, Shrestha SK, Kandel S Department of
Brief report Failed Intubating Laryngeal Mask Airway-Guided Blind Endotracheal Intubation in a Severe Postburn Contractured Neck Patient.
 (Acta Anaesth. Belg., 2011, 62, 95-99) Brief report Failed Intubating Laryngeal Mask Airway-Guided Blind Endotracheal Intubation in a Severe Postburn Contractured Neck Patient. B. KUMAR (*), K. VADAJE
(Acta Anaesth. Belg., 2011, 62, 95-99) Brief report Failed Intubating Laryngeal Mask Airway-Guided Blind Endotracheal Intubation in a Severe Postburn Contractured Neck Patient. B. KUMAR (*), K. VADAJE
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Care Unit (FELLOW)
 Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Facilitating EndotracheaL Intubation by Laryngoscopy technique and Apneic Oxygenation Within the Intensive Data Analysis Plan: Apneic Oxygenation vs. No Apneic Oxygenation Background Critically ill patients
Use of the Intubating LMA-Fastrach in 254 Patients with Difficult-to-manage Airways
 Use of this content is subject to the Terms and Conditions Use of the Intubating LMA-Fastrach in 254 Patients with Difficult-to-manage Airways Anesthesiology - Volume 95, Issue 5 (November 2001) - Copyright
Use of this content is subject to the Terms and Conditions Use of the Intubating LMA-Fastrach in 254 Patients with Difficult-to-manage Airways Anesthesiology - Volume 95, Issue 5 (November 2001) - Copyright
British Journal of Anaesthesia 101 (6): (2008) doi: /bja/aen288 Advance Access publication October 3, 2008
 British Journal of Anaesthesia 101 (6): 863 9 (2008) doi:10.1093/bja/aen288 Advance Access publication October 3, 2008 RESPIRATION AND THE AIRWAY Airway Scope and gum elastic bougie with Macintosh laryngoscope
British Journal of Anaesthesia 101 (6): 863 9 (2008) doi:10.1093/bja/aen288 Advance Access publication October 3, 2008 RESPIRATION AND THE AIRWAY Airway Scope and gum elastic bougie with Macintosh laryngoscope
EUROANESTHESIA 2007 Munich, Germany, 9-12 June 2007
 LARYNGOSCOPY: PAST, PRESENT AND FUTURE EUROANESTHESIA 2007 Munich, Germany, 9-12 June 2007 EAMSRC1 JOHN HENDERSON Anaesthetic Department Gartnavel General Hospital Glasgow, UK Saturday Jun 9, 2007 15:00-15:45
LARYNGOSCOPY: PAST, PRESENT AND FUTURE EUROANESTHESIA 2007 Munich, Germany, 9-12 June 2007 EAMSRC1 JOHN HENDERSON Anaesthetic Department Gartnavel General Hospital Glasgow, UK Saturday Jun 9, 2007 15:00-15:45
Comparison of two methods of gum elastic bougie aided endotracheal intubation using Airtraq video laryngoscope
 Comparison of two methods of gum elastic bougie aided endotracheal intubation using Airtraq video laryngoscope S Muhamed 1, PK Narasimha 2, S Mathew 2*, A Nileshwar 3, AK Handigodu Duggappa 2, DC Nanjundegowda
Comparison of two methods of gum elastic bougie aided endotracheal intubation using Airtraq video laryngoscope S Muhamed 1, PK Narasimha 2, S Mathew 2*, A Nileshwar 3, AK Handigodu Duggappa 2, DC Nanjundegowda
Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital
 AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
AIRWAY MANAGEMENT Angkana Lurngnateetape,, MD. Department of Anesthesiology Siriraj Hospital Perhaps the most important responsibility of the anesthesiologist is management of the patient s airway Miller
Comparison. F Agro immobilization. to DL Trauma/SCI. GS experiences. to other. GS experiences. GS experiences. to DL.
 Page. Tracheal using a Macintosch The Cormack grading in 14 of the 15 patients laryngoscope or a GlideScope in 15 (93%) was reduced by one using the GlideScope. 1 patients with cervical spine The average
Page. Tracheal using a Macintosch The Cormack grading in 14 of the 15 patients laryngoscope or a GlideScope in 15 (93%) was reduced by one using the GlideScope. 1 patients with cervical spine The average
Fiberoptic bronchoscope and C-MAC video laryngoscope assisted nasal-oral tube exchange: two case reports
 Case Report pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2017;17(3):219-223 https://doi.org/10.17245/jdapm.2017.17.3.219 Fiberoptic bronchoscope and C-MAC video laryngoscope assisted nasal-oral
Case Report pissn 2383-9309 eissn 2383-9317 J Dent Anesth Pain Med 2017;17(3):219-223 https://doi.org/10.17245/jdapm.2017.17.3.219 Fiberoptic bronchoscope and C-MAC video laryngoscope assisted nasal-oral
Intubation techniques
 Operative Techniques in Otolaryngology (2005) 16, 166-170 FEATURE ARTICLES Intubation techniques Geoffrey Lane, MB, BChir, FRCA From the Department of Anesthesiology, The University of Colorado Health
Operative Techniques in Otolaryngology (2005) 16, 166-170 FEATURE ARTICLES Intubation techniques Geoffrey Lane, MB, BChir, FRCA From the Department of Anesthesiology, The University of Colorado Health
Pre anaesthetic evaluation of difficult tracheal intubation
 Pre anaesthetic evaluation of difficult tracheal intubation Dr. AL. Meenakshi Sundaram M.D., D.A., GC Member,ISA National Professor of Anesthesiology Thanjavur Medical College Thanjavur, TamilNadu Phone:
Pre anaesthetic evaluation of difficult tracheal intubation Dr. AL. Meenakshi Sundaram M.D., D.A., GC Member,ISA National Professor of Anesthesiology Thanjavur Medical College Thanjavur, TamilNadu Phone:
Does the Suggested Lightwand Bent Length Fit Every Patient?
 Anesthesiology 2003; 98:1070 6 2003 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Does the Suggested Lightwand Bent Length Fit Every Patient? The Relation between Bent
Anesthesiology 2003; 98:1070 6 2003 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Does the Suggested Lightwand Bent Length Fit Every Patient? The Relation between Bent
Exclusion Criteria 1. Operator or supervisor feels specific intra- procedural laryngoscopy device will be required.
 FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
FELLOW Study Data Analysis Plan Direct Laryngoscopy vs Video Laryngoscopy Background Respiratory failure requiring endotracheal intubation occurs in as many as 40% of critically ill patients. Procedural
Effects of Cervical Spine Immobilization Technique and Laryngoscope Blade Selection on an Unstable Cervical Spine in a Cadaver Model of Intubation
 LABORATORY INVESTIGATION Effects of Cervical Spine Immobilization Technique and Laryngoscope Blade Selection on an Unstable Cervical Spine in a Cadaver Model of Intubation From the University of California
LABORATORY INVESTIGATION Effects of Cervical Spine Immobilization Technique and Laryngoscope Blade Selection on an Unstable Cervical Spine in a Cadaver Model of Intubation From the University of California
Z.U.M.J.Vol.19; N.5; September; 2013
 COMPARISON OF THE EFFICACY AND SAFETY OF EACH OF LEVITAN AND SHIKANI OPTICAL STYLETS EITHER USED ALONE OR WITH DIRECT LARYNGOSCOPY FOR TRACHEAL INTUBATION Islam A. Eliwa, MD, Akmal Abd Elsamad, MD, Khalid
COMPARISON OF THE EFFICACY AND SAFETY OF EACH OF LEVITAN AND SHIKANI OPTICAL STYLETS EITHER USED ALONE OR WITH DIRECT LARYNGOSCOPY FOR TRACHEAL INTUBATION Islam A. Eliwa, MD, Akmal Abd Elsamad, MD, Khalid
The Mallampati Test versus the Upper Lip Bite Test in Predicting Difficult Intubation. Chance Buttars BSN, BA Bryan College of Health Sciences
 1 The Mallampati Test versus the Upper Lip Bite Test in Predicting ifficult Intubation Chance Buttars BSN, BA Bryan College of Health Sciences Keywords: Airway assessment, Mallampati test, upper lip bite
1 The Mallampati Test versus the Upper Lip Bite Test in Predicting ifficult Intubation Chance Buttars BSN, BA Bryan College of Health Sciences Keywords: Airway assessment, Mallampati test, upper lip bite
The Superiority Of Mcgrath Videolaryngoscope After Failed Conventional Laryngoscopy
 ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 The Superiority Of Mcgrath Videolaryngoscope After Failed Conventional Laryngoscopy S Karaman, S Arici, S Dogru, T Karaman, H Tapar,
ISPUB.COM The Internet Journal of Anesthesiology Volume 33 Number 1 The Superiority Of Mcgrath Videolaryngoscope After Failed Conventional Laryngoscopy S Karaman, S Arici, S Dogru, T Karaman, H Tapar,
A study to rank predictors of Preoperative Airway Assessment on the basis of accuracy of prediction while performing Laryngoscopy in Obese patients
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 4 Ver. 13 (April. 2018), PP 04-10 www.iosrjournals.org A study to rank predictors of Preoperative
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 17, Issue 4 Ver. 13 (April. 2018), PP 04-10 www.iosrjournals.org A study to rank predictors of Preoperative
Endotracheal intubation with airtraq W versus storz W videolaryngoscope in children younger than two years - a randomized pilot-study
 Sørensen and Holm-Knudsen BMC Anesthesiology 2012, 12:7 RESEARCH ARTICLE Open Access Endotracheal intubation with airtraq W versus storz W videolaryngoscope in children younger than two years - a randomized
Sørensen and Holm-Knudsen BMC Anesthesiology 2012, 12:7 RESEARCH ARTICLE Open Access Endotracheal intubation with airtraq W versus storz W videolaryngoscope in children younger than two years - a randomized
Use of the Intubating Laryngeal Mask Airway
 340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
340 Anesthesiology 2000; 93:340 5 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Use of the Intubating Laryngeal Mask Airway Are Muscle Relaxants Necessary? Janet
Cricoid pressure: useful or dangerous?
 Cricoid pressure: useful or dangerous? Francis VEYCKEMANS Cliniques Universitaires Saint Luc Bruxelles (2009) Controversial issue - Can J Anaesth 1997 JR Brimacombe - Pediatr Anesth 2002 JG Brock-Utne
Cricoid pressure: useful or dangerous? Francis VEYCKEMANS Cliniques Universitaires Saint Luc Bruxelles (2009) Controversial issue - Can J Anaesth 1997 JR Brimacombe - Pediatr Anesth 2002 JG Brock-Utne
British Journal of Anaesthesia 82 (5): (1999)
 British Journal of Anaesthesia 82 (5): 703 7 (1999) Laryngeal mask airway size selection in males and females: ease of insertion, oropharyngeal leak pressure, pharyngeal mucosal pressures and anatomical
British Journal of Anaesthesia 82 (5): 703 7 (1999) Laryngeal mask airway size selection in males and females: ease of insertion, oropharyngeal leak pressure, pharyngeal mucosal pressures and anatomical
Airway Management. Key points. Rapid Sequence Intubation. Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway
 Airway Management Prasha Ramanujam and Guy Shochat Department of Emergency Medicine UCSF Medical Center Key points Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway Rapid
Airway Management Prasha Ramanujam and Guy Shochat Department of Emergency Medicine UCSF Medical Center Key points Rapid Sequence Intubation Recognizing difficult airway Managing difficult airway Rapid
Video laryngoscopy in paediatric anaesthesia in South Africa
 Video laryngoscopy in paediatric anaesthesia in South Africa Abstract Nienaber LN, MBChB, MMed, FCA(SA) Department of Paediatric Anaesthesia Steve Biko Academic Hospital, University of Pretoria Correspondence
Video laryngoscopy in paediatric anaesthesia in South Africa Abstract Nienaber LN, MBChB, MMed, FCA(SA) Department of Paediatric Anaesthesia Steve Biko Academic Hospital, University of Pretoria Correspondence
Comparison between C-MAC video-laryngoscope and Macintosh direct laryngoscope during cervical spine immobilization
 Comparison between C-MAC video-laryngoscope and Macintosh direct laryngoscope during cervical spine immobilization Shahir HM Akbar * and Joanna SM Ooi ** Abstract Background: Video-laryngoscopes have gained
Comparison between C-MAC video-laryngoscope and Macintosh direct laryngoscope during cervical spine immobilization Shahir HM Akbar * and Joanna SM Ooi ** Abstract Background: Video-laryngoscopes have gained
Cronicon ANAESTHESIA. Khaled Mohammed Elnaghy 1 and Javier Yuste 2 * Abstract. Keywords: Intubation; Video laryngoscopes; GlideScope; LMA CTrach
 Cronicon OPEN ACCESS Khaled Mohammed Elnaghy 1 and Javier Yuste 2 * 1 Department of Anesthesia, sin Shams university Cairo, Egypt 1 Department of Anesthesia, Sulaiman Alhabib hospital, Riyadh, Saudi Arabia
Cronicon OPEN ACCESS Khaled Mohammed Elnaghy 1 and Javier Yuste 2 * 1 Department of Anesthesia, sin Shams university Cairo, Egypt 1 Department of Anesthesia, Sulaiman Alhabib hospital, Riyadh, Saudi Arabia
Is the Airtraq optical laryngoscope effective in tracheal intubation by novice personnel?
 Clinical Research Article Korean J Anesthesiol 21 July 59(1): 17-21 DOI: 1.497/kjae.21.59.1.17 Is the Airtraq optical laryngoscope effective in tracheal intubation by novice personnel? Sang-Jin Park, Won
Clinical Research Article Korean J Anesthesiol 21 July 59(1): 17-21 DOI: 1.497/kjae.21.59.1.17 Is the Airtraq optical laryngoscope effective in tracheal intubation by novice personnel? Sang-Jin Park, Won
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
Educational Session: Evaluation and Management of the Difficult Airway
 Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
Educational Session: Evaluation and Management of the Difficult Airway Diane M. Birnbaumer, MD, FACEP 3/24/2010 7:30 AM - 8:30 AM The Difficult Airway What s Up YOUR Sleeve? Diane M. Birnbaumer, M.D.,
Identification of the 2 Difficult and Failed Airway. Ron M. Walls Michael F. Murphy
 Identification of the 2 Difficult and Failed Airway Ron M. Walls Michael F. Murphy CHAPTER 2 THE DIFFICULT AND FAILED AIRWAY 9 DEFINITION OF THE DIFFICULT AND FAILED AIRWAY Although both difficult and
Identification of the 2 Difficult and Failed Airway Ron M. Walls Michael F. Murphy CHAPTER 2 THE DIFFICULT AND FAILED AIRWAY 9 DEFINITION OF THE DIFFICULT AND FAILED AIRWAY Although both difficult and
Pilot Study to Evaluate the Accuracy of Ultrasonography in Confirming Endotracheal Tube Placement
 AIRWAY/BRIEF RESEARCH REPORT Pilot Study to Evaluate the Accuracy of Ultrasonography in Confirming Endotracheal Tube Placement Sandra L. Werner, MD, RDMS Charles E. Smith, MD Jessica R. Goldstein, MD Robert
AIRWAY/BRIEF RESEARCH REPORT Pilot Study to Evaluate the Accuracy of Ultrasonography in Confirming Endotracheal Tube Placement Sandra L. Werner, MD, RDMS Charles E. Smith, MD Jessica R. Goldstein, MD Robert
Controversies in Management of Spinal Trauma. Associate Professor John Moloney The Alfred Monash University
 Controversies in Management of Spinal Trauma Associate Professor John Moloney The Alfred Monash University http://www.ncbi.nlm.nih.gov/pmc/articles/pmc2989268/table/tab1/ Management continuum from the
Controversies in Management of Spinal Trauma Associate Professor John Moloney The Alfred Monash University http://www.ncbi.nlm.nih.gov/pmc/articles/pmc2989268/table/tab1/ Management continuum from the
LARYNGOSCOPE IN MYASTHENIA GRAVIS PATIENTS
 TRACHEAL INTUBATION USING McGRATH VIDEO LARYNGOSCOPE IN MYASTHENIA GRAVIS PATIENTS Venkata Sesha Sai Krishna Manne, Madhavi Latha Marupudi 2, Surendranath Yelavarthy HOW TO CITE THIS ARTICLE: Venkata Sesha
TRACHEAL INTUBATION USING McGRATH VIDEO LARYNGOSCOPE IN MYASTHENIA GRAVIS PATIENTS Venkata Sesha Sai Krishna Manne, Madhavi Latha Marupudi 2, Surendranath Yelavarthy HOW TO CITE THIS ARTICLE: Venkata Sesha
Predictors of difficult intubation a simple approach
 ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 2 Predictors of difficult intubation a simple approach A Vasudevan, A Badhe Citation A Vasudevan, A Badhe. Predictors of difficult intubation
ISPUB.COM The Internet Journal of Anesthesiology Volume 20 Number 2 Predictors of difficult intubation a simple approach A Vasudevan, A Badhe Citation A Vasudevan, A Badhe. Predictors of difficult intubation
Difficult Intubation in Acromegalic Patients
 110 Anesthesiology 2000; 93:110 4 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Difficult Intubation in Acromegalic Patients Incidence and Predictability Hubert Schmitt,
110 Anesthesiology 2000; 93:110 4 2000 American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Difficult Intubation in Acromegalic Patients Incidence and Predictability Hubert Schmitt,
Diagnosis & Management of the Difficult Airway
 Diagnosis & Management of the Difficult Airway Dr. E. Rawlings Plymouth Anaesthetic Department Complications of Airway Management Medicolegal Serious morbidity Mortality Complications of Airway Management
Diagnosis & Management of the Difficult Airway Dr. E. Rawlings Plymouth Anaesthetic Department Complications of Airway Management Medicolegal Serious morbidity Mortality Complications of Airway Management
The implication of using dominant hand to perform laryngoscopy: an analysis of the laryngoscopic view and blade-tooth distance
 Anesth Pain Med 2018;13:207-213 https://doi.org/10.17085/apm.2018.13.2.207 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received October 20, 2017 Revised November 13, 2017 Accepted November 14,
Anesth Pain Med 2018;13:207-213 https://doi.org/10.17085/apm.2018.13.2.207 pissn 1975-5171 ㆍ eissn 2383-7977 Clinical Research Received October 20, 2017 Revised November 13, 2017 Accepted November 14,
In 2011 I received an unrestricted lecture honorarium from Ambu I have been loaned equipment by Intavent Direct (Teleflex) and Aircraft Medical As an
 Alistair McNarry In 2011 I received an unrestricted lecture honorarium from Ambu I have been loaned equipment by Intavent Direct (Teleflex) and Aircraft Medical As an organiser of airway workshops I have
Alistair McNarry In 2011 I received an unrestricted lecture honorarium from Ambu I have been loaned equipment by Intavent Direct (Teleflex) and Aircraft Medical As an organiser of airway workshops I have
British Journal of Anaesthesia 102 (4): (2009) doi: /bja/aep013 Advance Access publication February 20, 2009
 British Journal of Anaesthesia 12 (4): 546 5 (29) doi:1.193/bja/aep13 Advance Access publication February 2, 29 RESPIRATION AND THE AIRWAY Expected difficult tracheal intubation: a prospective comparison
British Journal of Anaesthesia 12 (4): 546 5 (29) doi:1.193/bja/aep13 Advance Access publication February 2, 29 RESPIRATION AND THE AIRWAY Expected difficult tracheal intubation: a prospective comparison
A study of the anatomy of the caudal space using magnetic resonance imaging
 British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
British Journal of Anaesthesia 1997; 78: 391 395 A study of the anatomy of the caudal space using magnetic resonance imaging I. M. CRIGHTON, B. P. BARRY AND G. J. HOBBS Summary We have studied, in 37 adult
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair. Krista Madden, MSNA. Westminster College
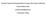 Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
Transient Lingual and Hypoglossal Nerve Damage After Rotator Cuff Repair Krista Madden, MSNA madden.krista@gmail.com Westminster College Abstract When providing anesthesia for patients in the sitting position,
Unanticipated difficult tracheal intubation - during routine induction of anaesthesia in an adult patient
 Unanticipated difficult tracheal intubation - during routine induction of anaesthesia in an adult patient Direct laryngoscopy Any problems Call for help Plan A: Initial tracheal intubation plan Direct
Unanticipated difficult tracheal intubation - during routine induction of anaesthesia in an adult patient Direct laryngoscopy Any problems Call for help Plan A: Initial tracheal intubation plan Direct
Comparison of the Airtraq to the Bonfils Fibroscope for Endotracheal Intubation in a Simulated Difficult Airway
 Med. J. Cairo Univ., Vol. 77, No. 4, June: 203-207, 2009 www.medicaljournalofcairouniversity.com Comparison of the Airtraq to the Bonfils Fibroscope for Endotracheal Intubation in a Simulated Difficult
Med. J. Cairo Univ., Vol. 77, No. 4, June: 203-207, 2009 www.medicaljournalofcairouniversity.com Comparison of the Airtraq to the Bonfils Fibroscope for Endotracheal Intubation in a Simulated Difficult
CAN DIFFICULT INTUBATION BE ACCURATELY PREDICTED USING UPPER LIP BITE TEST? ABSTRACT
 ORIGINAL ARTICLE CAN DIFFICULT INTUBATION BE ACCURATELY PREDICTED USING UPPER LIP BITE TEST? Azmat Ali Shah 1, Khalid Rafique 2, Mujahid Islam 3 1 Department of Anesthesia, Aga Khan Hospital, Dar es Salaam
ORIGINAL ARTICLE CAN DIFFICULT INTUBATION BE ACCURATELY PREDICTED USING UPPER LIP BITE TEST? Azmat Ali Shah 1, Khalid Rafique 2, Mujahid Islam 3 1 Department of Anesthesia, Aga Khan Hospital, Dar es Salaam
Estimation of Stellate Ganglion Block Injection Point Using the Cricoid Cartilage as Landmark Through X-ray Review
 Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
Original Article Korean J Pain 2011 September; Vol. 24, No. 3: 141-145 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2011.24.3.141 Estimation of Stellate Ganglion Block Injection Point
RESPIRATION AND THE AIRWAY. Key points. K. B. Greenland 1,2,3 *, M. J. Edwards 1, N. J. Hutton 1, V. J. Challis 4, M. G. Irwin 3 and J. W.
 British Journal of Anaesthesia 105 (5): 683 90 (2010) Advance Access publication 15 September 2010. doi:10.1093/bja/aeq239 RESPIRATION AND THE AIRWAY Changes in airway configuration with different head
British Journal of Anaesthesia 105 (5): 683 90 (2010) Advance Access publication 15 September 2010. doi:10.1093/bja/aeq239 RESPIRATION AND THE AIRWAY Changes in airway configuration with different head
Nicolette Mosinski MPAS, PA-C
 Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
Nicolette Mosinski MPAS, PA-C 1. Impaired respiratory effort 2. Airway obstruction Observe patient for detection Rate Pattern Depth Accessory muscle use Evidence of injury Noises Silent manifestations
How to Predict and Avoid Airway Disasters. Muhammad Umer Ihsan
 How to Predict and Avoid Airway Disasters Muhammad Umer Ihsan Four Key Aspect of Assessing a Difficult Airway Difficult Bag Mask Ventilation Difficult Direct Laryngoscopy Difficult Extra-glottic devices
How to Predict and Avoid Airway Disasters Muhammad Umer Ihsan Four Key Aspect of Assessing a Difficult Airway Difficult Bag Mask Ventilation Difficult Direct Laryngoscopy Difficult Extra-glottic devices
Fibreoptic assessment of laryngeal aperture in patients with difficult laryngoscopy
 226 REPORTS OF INVESTIGATION Fibreoptic assessment of laryngeal aperture in patients with difficult laryngoscopy Ichiro Takenaka MD, Kazuyoshi Aoyama MD, Tatsuo Kadoya MD, Takeyoshi Sata MD, Akio Shigematsu
226 REPORTS OF INVESTIGATION Fibreoptic assessment of laryngeal aperture in patients with difficult laryngoscopy Ichiro Takenaka MD, Kazuyoshi Aoyama MD, Tatsuo Kadoya MD, Takeyoshi Sata MD, Akio Shigematsu
Laryngoscopy: Time to broaden our horizon.
 Laryngoscopy: Time to broaden our horizon. Dr.Renu Devaprasath, D.N.B. (Anesthesia), Dept of Anesthesia, Dr.Jeyasekharan Medical Trust, Nagercoil, Abstract Failure to secure the airway & maintain oxygenation
Laryngoscopy: Time to broaden our horizon. Dr.Renu Devaprasath, D.N.B. (Anesthesia), Dept of Anesthesia, Dr.Jeyasekharan Medical Trust, Nagercoil, Abstract Failure to secure the airway & maintain oxygenation
Anesthesia Final Exam
 Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
Anesthesia Final Exam 1) For a patient who is chronically taking the following medications, which two should be withheld on the day of surgery? a) Lasix b) Metoprolol c) Glucophage d) Theodur 2) A 51 year
Success of Tracheal Intubation with Intubating Laryngeal Mask Airways
 Anesthesiology 2008; 108:621 6 Copyright 2008, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Success of Tracheal Intubation with Intubating Laryngeal Mask Airways
Anesthesiology 2008; 108:621 6 Copyright 2008, the American Society of Anesthesiologists, Inc. Lippincott Williams & Wilkins, Inc. Success of Tracheal Intubation with Intubating Laryngeal Mask Airways
Hong Kong Journal of Emergency Medicine. KL Tsui, CY Hung, CW Kam. t p= p=0.004
 Hong Kong Journal of Emergency Medicine A manikin study to compare video-optical intubation stylet versus Macintosh laryngoscope used by novice in normal and simulated difficult airway intubation KL Tsui,
Hong Kong Journal of Emergency Medicine A manikin study to compare video-optical intubation stylet versus Macintosh laryngoscope used by novice in normal and simulated difficult airway intubation KL Tsui,
