The process of pressure relief in a healthy
|
|
|
- Mercy Bailey
- 5 years ago
- Views:
Transcription
1 An holistic approach to turning patients Hawkins S, Stone K, Plummer L (1999) An holistic approach to turning patients. Nursing Standard. 14, 3, Date of acceptance: September Turning patients who are immobile is usually undertaken expressly to prevent pressure sores. Here the authors highlight some of the other factors that need to be taken into account when nursing dependent and/or immobile patients. Susan Hawkins MPH, BSc(Hons), MCSP, is Senior Physiotherapist in Acute Rehabilitation; Katharine Stone Grad Dip Phys, MCSP, is Senior Physiotherapist in Neurology; Lisa Plummer Grad Dip Phys, MCSP, is Senior Physiotherapist in Respiratory Care. key words Nursing care Mobility Pressure sores These key words are based on the subject headings from the British Nursing Index. This article has been subject to double-blind review. The process of pressure relief in a healthy individual can be considered a continuous dynamic activity, with a recognised chain of events. Pressure leads to tissue ischaemia which in turn leads to pain, as a consequence of which the individual moves to relieve the pressure, blood supply is restored and the ischaemic pain disappears (Collins 1998). On average, a healthy individual will alter his or her posture during sleep every 11.6 minutes (Keane 1978). For dependent patients, this process of moving to relieve pressure is not possible; they are reliant on health professionals to perform this movement for them. Traditionally this has been achieved with the two-hourly turn, but increasingly the use of devices such as alternating pressure air mattresses (APAMs) are fulfilling this movement requirement. The importance of turning Many papers stress how important it is to turn patients regularly for their pressure area care (Alexander et al 1992, Clarke 1997). Most healthcare professionals understand the benefits of two-hourly turns and could describe the physiological causes of pressure sores (Box 1). A paper by Helme (1994) shows that although staff had a high knowledge of turning protocols, they did not turn their patients as regularly as prescribed. The main reasons cited for not turning patients regularly include lack of time, lack of staff (Bliss 1990, Helme 1994, James and Fong 1996) and may include lack of access to, or knowledge about, handling equipment. As Dealey (1994) points out: Given the demands on their time, nurses are increasingly relying on pressurerelieving equipment instead of two-hourly turning to prevent pressure sores. Pressure sores develop as a result of two processes; occlusion of blood vessels by external pressure, and endothelial damage of arterioles and micro-circulation by application of friction and shearing forces (Collins 1998, McLeod 1997). Traditionally, the relief of pressure and promotion of circulation has been achieved by regular twohourly turning of patients (Maklebust and Sieggreen 1991). Now that we have a range of pressure-relieving mattresses, this dependence on turning for pressure area care has decreased. Some claim that APAMs take away the need to turn patients altogether (Collins 1998, Huntleigh Healthcare AIM 1995). Other reasons for turning Is pressure area care the only reason patients should be turned? Several months ago a physiotherapist came into the staff room complaining about the nursing care received by a patient on an acute ward. The patient had suffered a cerebrovascular event (CVE) and had developed what the physiotherapist considered to be a preventable chest infection. She discovered that the patient had been left lying supine for 24 hours a day since she had been admitted three days previously. When the physiotherapist enquired about the reasons for this, she was told: The patient did not need Box 1. Physiological causes of pressure sores INTRINSIC FACTORS EXTRINSIC FACTORS Malnutrition Medication Neurological deficit Moisture Reduced mobility/activity Pressure Increased age Shear Incontinence Friction Dehydration Mental status Skin condition Sepsis Medication october 6/vol14/no3/1999 nursing standard 51
2 turning because she was on an airflow mattress. For 72 hours this very ill, dependent patient had been moved for personal care and bedding changes only. She had been assessed using the Waterlow scale (1985) and had been deemed at high risk of developing pressure sores because of her level of dependence and fluctuating consciousness. Thereafter she was nursed on an alternating pressure air mattress (APAM), and subsequently had rarely been moved. This incident sparked debate among the physiotherapy staff from all specialties about the particular problems that they had encountered while treating patients who were nursed on APAMs. The various problems that were highlighted provoked us to take the issue further. A meeting was convened between nursing, therapy and tissue viability staff in the hospital, which led to stimulating, constructive, but ultimately non evidencebased discussion. This article aims to open out and continue this discussion, and perhaps stimulate research into reasons for turning patients, other than solely for pressure area care. In the example described above, the nursing staff had anticipated one of the problems associated with a high level of dependency, pressure area care, but had not taken into account other possible complications. Alternating pressure air mattresses APAMs work by temporarily removing compressive forces on the skin to restore perfusion. They reduce localised distortion of capillary beds by sequentially deflating cells. They may also aid metabolite clearance by stimulating a myogenic response that causes dilation of the microvascular and lymphatic systems (McLeod 1997). Evidence exists describing the effectiveness of these mattresses for both the prevention and treatment of pressure sores (Devine 1995, Exton- Smith et al 1982) and although there is little evidence assessing their cost effectiveness, they are now regularly used in the management of patients at risk of developing pressure sores (University of York and University of Leeds 1995). The literature Little evidence or information could be found in the literature specifically discussing the other advantages of turning patients. Papers that described the importance of turning for pressure area management did not describe other physiological or psychological benefits. Lack of information in the literature about these other effects may in part be to blame for the lack of knowledge among staff of the value of turning patients. This might mean that patients are not receiving the best standards of care that should be offered to them. Outlined below are some reasons to turn different case-mix groups, but many of the themes are common to all. Neurological factors Disease or damage to the central or peripheral nervous system can lead to temporary or even permanent physical, cognitive and psychological problems. If the person is unable to move, he or she is deprived of the physical benefits of movement including: Sensory-motor appreciation. Posture and balance control. Maintenance of joint and soft tissue range of movement (thus preventing contractures). Maximisation of functional independence. Minimisation of tonal changes, such as spasticity. From a psychological perspective, dependency can lead to behavioural problems such as withdrawal, and there is a need for regular contact and interaction to provide opportunities for orientation, socialisation, and communication (Table 1). In the unconscious patient, regular contact and stimulation is recommended to increase the patient s awareness of self and the environment. All healthcare professionals handling a dependent patient should, of course, explain their actions to them, so that an appropriate response can be stimulated. Effective postural management in the acute stage of any disease that challenges motor or postural ability, can enhance and reinforce recovery of function in those with the potential for this (Pope 1996). From an holistic perspective, the patient will benefit from regular turning and careful positioning. This will not only prevent secondary complications developing, but will also promote recovery (Edwards 1996). Importance of positioning Several papers caution against turning a patient to 90º because of the increased interface pressure that this puts onto the bony prominence of the greater trochanter (Colin et al 1996, Holmes 1997, Wind et al 1997). For many neurological patients, particularly those who have had a CVE, this is an important position for the control of muscle tone. If patients are well positioned, it allows them to feel support with their non-affected side and gives them visual cues from seeing themselves on a bed. It also gives them access to visual information about their upper limbs, as well as the ability to interact with visitors and to see what is happening on the ward around them. If patients are positioned safely and comfortably, they should be able to move with minimal effort. This will limit the stress of movement that can contribute to the development of spasticity. The person in Figure 1 has been positioned in forward lean side-lying which involves turning a patient to just forward of 90º. It requires careful attention to positioning, including weight forward off the greater trochanters and good supportive surfaces (for example pillows supporting anterior and posterior trunk, legs, and arms, as well as the head) to increase surface area in 52 nursing standard october 6/vol14/no3/1999
3 Table 1. Reasons to turn neurological patients PROBLEM REASONS TO TURN Sensory disturbance Altered muscle tone Promotes sensory awareness/appreciation including body image and perception (Grieve1993, Langdon 1996, Siev and Freistat 1986) Minimises spasticity by frequent change of posture and support (Davies 1994, Edwards 1998) Risk of aspiration Promotes safer swallowing with specific positioning (Ray 1985) Minimises respiratory complications (Hough 1984) Movement disturbance Bladder and bowel dysfunction Promotes effective movement with concurrent responses throughout the body and stimulates appropriate balance responses and function (Edwards 1996) Pressure care is maintained (Alexander et al 1992, Holmes 1997, The Stroke Association 1996) Functional posturing of the limbs promotes recovery and maintenance of joint and muscle length (Edwards 1998, Pope 1996) Essential for incontinent patients to prevent moisture accumulation which is a major contribution to the development of pressure sores (Clarke 1997, Grundy and Swain 1996) REFERENCES Alexander C et al (1992) Creating the optimal environment for pressure area care. British Journal of Nursing. 1, 15, Bliss M (1990) Geriatric medicine. In Bader DL (Ed) Pressure Sores: Clinical Practice and Scientific Approach. Basingstoke, Macmillan Press. Clarke G (1997) The problem of pressure sores and how to treat them. British Journal of Therapy and Rehabilitation. 4, 11, Closs SJ et al (1993) Pain in elderly orthopaedic patients. Journal of Clinical Nursing. 2, Colin D et al (1996) Comparison of 90º and 30º laterally inclined positions in the prevention of pressure ulcers using transcutaneous oxygen and carbon dioxide pressures. Advances in Wound Care. 9, 3, Collins F (1998) Seated Patients: Clinical Perspectives. Chertsey, Hayden Advertising. Davies P (1994) Starting Again. London, Springer Verlag. Dealey C (1994) A prevention and management aid: evaluation of the Nimbus II mattress. Professional Nurse. 9, 12, Dean E, Ross J (1992) Oxygen transport: the basis for contemporary cardiopulmonary physical therapy and its optimization with body positioning and mobilization. Physical Therapy Practice. 1, 4, Devine B (1995) Alternating pressure air mattresses in the management of established pressure sores. Journal of Tissue Viability. 5, 3, Edwards S (1998) Physiotherapy Management of Established Spasticity, Spasticity Rehabilitation. G Sheean, Churchill Communications Europe. Perceptual problems contact, thereby decreasing the interface pressure on the greater trochanter. This allows for the three main elements of positioning: safety, comfort and movement facilitation. Respiratory factors As well as for the management of patients with neurological conditions, a regular change of position is essential for patients at risk of developing pulmonary complications, or those already suffering from chest complaints. Regular turning enhances the reduction of the incidence of pulmonary infection and the development of sepsis (Gentilello et al 1988). The movement from the supine position to side-lying has numerous physiological advantages. Body position changes enhance oxygen transport due to the effect of gravity on the distribution of ventilation and perfusion throughout the lungs (Dean and Ross 1992). This alteration in the areas of dependent lung tissue has preventative and treatment advantages that help ensure that problematic lung areas do not develop. Altering chest position is thought to redistribute and mobilise mucus and interstitial fluid from dependent lung areas, which helps to prevent the development of atelectasis within these areas Stimulates orientation to the environment and body image awareness through the senses (Grieve 1993, Langdon 1996, Siev and Freistat 1986) Behaviour and cognitive Stimulates socialisation, memory, and appropriate behavioural problems responses (Grieve 1993, Langdon 1996, Siev and Freistat 1986) Stimulates language and communication skills through learned behavioural responses (Grieve 1993, Langdon 1996, Siev and Freistat 1986) Fig. 1. Pillow-supported forward lean lying (Dean and Ross 1992). Sepsis decreases the body s ability to withstand pressure insults by increasing metabolic demand. It increases systemic oxygen requirements, making the skin more susceptible to pressure by affecting oxygen supply to the skin (Colin et al 1996). A chest infection is a major cause of sepsis, so turning to prevent a pressure sore could also prevent a 54 nursing standard october 6/vol14/no3/1999
4 chest infection, which could also prevent a pressure sore. Pape et al (1998) studied patients at risk of developing adult respiratory distress syndrome (ARDS) following traumatic injury. Those patients receiving early positional changes on a regular basis showed a reduced incidence in the development of ARDS, improved systemic oxygenation and overall improved survival. The use of prone ventilation, where the patient is nursed face down, is a well known treatment in the management of ARDS. It has been shown to improve worsening hypoxia resulting from alveoli filled with watery exudate and increasingly noncompliant lungs. The alteration of body position allows the affected lung tissue to aerate because gravitational forces are altered. This has been demonstrated with CT scans before and after the initiation of prone ventilation (Gattinoni et al 1991). These findings reinforce the need for regular turning of dependent patients at risk of developing pulmonary complications. The cardiovascular system is also influenced by the effects of regular turning. Positioning serves as a treatment adjunct if mobilisation is not possible. Changing body position has a greater effect on the cardiovascular activity than maintaining a static position (Dean and Ross 1992). This exercises the cardiovascular system to benefit the patient at a later stage in recovery. Musculoskeletal factors Orthopaedic patients, particularly those who go on to have an operation, are at high risk of developing pressure sores. Versluysen (1986) found that 66 out of 100 patients developed pressure damage following fractured femur. Particular problems exist for those on traction or for whom turning jeopardises their operation site. These patients are at risk of developing complications such as: Osteoporosis. Homeostasis and dependent oedema which can lead to swollen limbs or deep vein thromboses. Deep vein thrombosis which can lead to embolic CVEs or pulmonary embolism, with associated risk of death. Other problems can include contractures and postural impairment, such as shortened Achilles tendons or joint fixed flexion deformities, which can lead to diminished proprioception and altered balance mechanisms (Nichols 1981). Discussion will be required with the orthopaedic surgeons, but any permitted position change will help diminish these risk factors. The Guide to Handling of Patients; Introducing a Safer Handling Policy (Holmes 1997) gives recommendations on how these patients can be safely moved. Pain is an important factor contributing to immobility in the post-operative period for patients allowed to mobilise. For these, effective analgesic management will enable early mobilisation, decrease risk factors and expedite discharge (Closs et al 1993, Hunt 1995). Patients immobilised following burns encounter similar problems. Vascular factors For patients with vascular problems, such as amputation, graft surgery or those confined to bed because of the pain of critical limb ischaemia, position changes are essential. They can prevent the development of contractures and assist in the control of oedema. Oedema management is essential for amputees and graft surgery patients to prevent wound breakdown or delayed healing, which can impede rehabilitation. This may result in muscle weakness, decreased tolerance of the upright position, poor balance, delayed use of the pneumatic post-amputation mobility (PAM) aid and delayed fitting of the prosthesis. This delay may lead to an increased length of stay, possibly poorer outcomes or poorer prognosis, and possible decreased quality of life (Engstrom and Van de Ven 1985). Manual handling Over the last decade there has been a shift towards a safer handling policy with the introduction of the Manual Handling Operations Regulations (Richmond 1997) and Health and Safety Executive Guidelines (HSE 1992). The legislation asserts the obligations of both the employee and the employer to ensure safe lifting and handling tasks. The Guide to the Handling of Patients (Holmes 1997) has a comprehensive approach to the manual handling of patients in bed, on differing mattress surfaces, and promotes regular turning of patients in the prevention of pressure sores. It explains that a risk assessment is required for all handling tasks and appropriate handling equipment, such as hoists and sliding aids, should be used to reduce the risk to the lowest level practicable. Clarke (1997) reinforces this in her paper stating: Accurate risk assessment, frequent repositioning and proper selection of equipment are essential in the prevention of pressure sore development The use of sliding sheets and low friction fabric rollers has revolutionised the way we handle dependent people. The technique allows the patient to be turned without any need to lift. They not only have the benefit of reducing risk of back injury, but have the significant effect of minimising friction and shearing one of the commonest causes of pressure sore development (Young et al 1998). Education and training in manual handling procedures and the use of equipment are essential Edwards S (1996) General Principles of Treatment: Neurological Physiotherapy: A Problem Solving Approach. London, Churchill Livingstone. Engstrom B, Van de Ven C (1985) Physiotherapy for Amputees: The Roehampton Approach. London, Churchill Livingstone. Exton-Smith AN et al (1982) Use of the Air Wave System to prevent pressure sores in hospital. Lancet. 2, Gattinoni L et al (1991) Body position changes redistribute lung computed tomographic density in patients with acute respiratory failure. Anesthesiology. 74, Gentilello L et al (1988) Effect of a rotating bed on the incidence of pulmonary complications in critically ill patients. Critical Care Medicine. 16, 783. Grieve J (1993) Neuropsychology for Occupational Therapists: Assessment of Perception and Cognition. London, Blackwell Scientific Publications. Grundy D, Swain A (1996) ABC of Spinal Cord Injury. Third edition. London, MMJ Publishing. Helme T (1994) Position changes for residents in long-term care. Advances in Wound Care. 7, 5, Holmes D (1997) Beds: how to move people in bed. In The Guide to Handling of Patients: Introducing a Safer Handling Policy. Fourth edition. RCN and NBPA. Hough A (1984) The effect of posture on lung function. Physiotherapy. 70, Health and Safety Executive (1992) Guidance on Manual Handling Regulations. L23. London, HMSO. Hunt K (1995) Perceptions of patients pain: a study assessing nurses attitudes. Nursing Standard. 10, 4, Huntleigh Healthcare AIM (1995) Prevention of Pressure Sores: Orthopaedics. Luton, Huntleigh Healthcare. october 6/vol14/no3/1999 nursing standard 55
5 Fig. 2. Spiral of dependence James H, Fong A (1996) Implementing and evaluating a pressure sore policy. Journal of Tissue Viability. 6, 2, Keane FX (1978) The minimum physiological movement required for a man supported on a soft surface. Paraplegia. 16, Langdon D (1996) Neuropsychological Problems and Solutions: Neurological Physiotherapy. London, Churchill Livingstone. Maklebust J, Sieggreen MY (1991) Pressure Ulcers: Guidelines for Prevention and Nursing Management. Illinois, S-N publications. McLeod AG (1997) Principles of alternating pressure surfaces. Advances in Wound Care. 10, 7, Nichols PJN (1981) Rehabilitation Medicine: The Management of Physical Disabilities. London, Butterworth. Pape HC et al (1998) Is early kinetic positioning beneficial for pulmonary function in multiple trauma patients? Injury. 29, 3, Pope P (1996) Postural management and special seating. In Edwards S (Ed) Neurological Physiotherapy: A Problem Solving Approach. London, Churchill Livingstone. Ray M (1985) Feeding problems in stroke. Nursing Mirror. 160, 9, Richmond H (1997) Legal and professional responsibilities. In RCN/NBPA The Guide to Handling of Patients; Introducing a Safer Handling Policy. Fourth edition. RCN/NBPA. Siev E, Freistat B (1986) Perceptual Dysfunction in the Adult Stroke Patient: Body Image Body Scheme Disorders. US, Slack Inc. The Stroke Association (1996) Stroke services and Research and Overview with Recommendations for Future Research. London, The Stroke Association. University of York, NHS Centre for Reviews and Dissemination; University of Leeds, Nuffield Institute for Health (1995) The prevention and treatment of pressure sores: how effective are pressure-relieving interventions and risk assessment for the prevention and treatment of pressure sores? Effective Health Care. 2, 1, Versluysen M (1986) How elderly patients with femoral fracture develop pressure sores in hospital. British Medical Journal. 292, Waterlow JA (1985) A risk assessment card. Nursing Times. 81, 49, Wind S et al (1997) Pressure ulcers: collaboration in wound care. Is there a reasonable approach? Ostomy/ Wound Management. 43, 4, Young T et al (1998) Nimbus 3 alternating-pressure replacement mattress. British Journal of Nursing. 7, 7, Delayed recovery or increased illness Spiral of independence Improved recovery for all those involved in the management of dependent patients. This should include how to move the patient to minimise the extrinsic factors associated with movement, shearing and friction to aid in pressure sore prevention. Patients should, within their own capacity, be encouraged to assist with position changes. This reinforces independence and aids in the prevention of secondary complications resulting from dependency. Conclusion Dependence Increasing dependence Complications Respiratory, eg, chest infection Musculoskelatal, eg, DVT Vascular, eg, wound breakdown Neuro, eg, increased spasticity pressure sores Increasing independence or improved prognosis Dependence Decreased complications No chest infection No DVT Good wound healing Maximised physical function Decreased incidence of pressure sores Inability to move TURN Inability to move Sufficient resources (including available equipment and staff) and ongoing education are vital in implementing proactive evidence-based practice. By anticipating all potential problems and encouraging a dynamic patient-centred approach, turning should be seen as an integral part in the holistic care of patients, breaking the spiral of dependence and putting them onto the spiral to independence (Fig. 2). Pressure sores are a serious but largely preventable complication of illness or disability, causing significant morbidity and mortality (Clarke 1997). Pressurerelieving and pressure-reducing equipment has contributed extensively to the prevention of such complications. This has resulted in a reduction of regular turning of patients (Dealey 1994). This can potentially lead to the development of other, nonpressure related complications. This article has outlined some of these potential complications and hopefully stimulated thought about reinstating regular turning in the management of immobile or dependent patients. Some evidence exists, from a variety of specialities, to encourage the use of regular changes of position for reasons beyond the prevention of pressure area problems. We possess the ability to prevent some of the respiratory, neurological and musculo-skeletal consequences of enforced immobility. The ultimate challenge for the carer is to prevent these secondary complications from occurring 56 nursing standard october 6/vol14/no3/1999
Pressure ulcer recognition and prevention. Mark Collier Tissue Viability Nurse Consultant United Lincoln Hospitals NHS Trust
 Pressure ulcer recognition and prevention Mark Collier Tissue Viability Nurse Consultant United Lincoln Hospitals NHS Trust PRESSURE ULCER RECOGNITION AND PREVENTION.. United Lincolnshire Hospitals NHS
Pressure ulcer recognition and prevention Mark Collier Tissue Viability Nurse Consultant United Lincoln Hospitals NHS Trust PRESSURE ULCER RECOGNITION AND PREVENTION.. United Lincolnshire Hospitals NHS
CARING FOR THE CLIENT ON COMPLETE BEDREST
 CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
CARING FOR THE CLIENT ON COMPLETE BEDREST INTRODUCTION The human body is designed to move. And just as the human body thrives on movement, it suffers when for one reason or another there is enforced immobility.
The Seated Patient 15 th Biennial Conference New Orleans
 The Seated Patient 15 th Biennial Conference New Orleans Track 1 March 11, 2017 Christine Berke MSN APRN-NP CWOCN-AP Nebraska Medicine cberke@nebraskamed.com 2017 National Pressure Ulcer Advisory Panel
The Seated Patient 15 th Biennial Conference New Orleans Track 1 March 11, 2017 Christine Berke MSN APRN-NP CWOCN-AP Nebraska Medicine cberke@nebraskamed.com 2017 National Pressure Ulcer Advisory Panel
COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery
 COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery Name Date 1. The systems involved with anesthesia, positioning and operative procedures are: a. b.
COMPLETION PROJECT POSITIONING THE PATIENT IN THE OR Source- Alexander s Care of the Patient in Surgery Name Date 1. The systems involved with anesthesia, positioning and operative procedures are: a. b.
Chapter 16 Moving and Positioning Patients
 Chapter 16 Moving and Positioning Patients Terminology Related to Movement Contractures Shortening and tightening of muscles due to disuse Dorsiflexion Bending of the foot in an upward direction Plantar
Chapter 16 Moving and Positioning Patients Terminology Related to Movement Contractures Shortening and tightening of muscles due to disuse Dorsiflexion Bending of the foot in an upward direction Plantar
ISS 34 Seating for Tone Management March
 SEATING FOR TONE MANAGEMENT JO-ANNE CHISHOLM AND JOANNE YIP ACCESS COMMUNITY THERAPISTS JO-ANNE CHISHOLM AND JOANNE YIP DO NOT HAVE AN AFFILIATION (FINANCIAL OR OTHERWISE) WITH AN EQUIPMENT, MEDICAL DEVICE
SEATING FOR TONE MANAGEMENT JO-ANNE CHISHOLM AND JOANNE YIP ACCESS COMMUNITY THERAPISTS JO-ANNE CHISHOLM AND JOANNE YIP DO NOT HAVE AN AFFILIATION (FINANCIAL OR OTHERWISE) WITH AN EQUIPMENT, MEDICAL DEVICE
Protect Your Skin. It s one of the most important things you can do!
 Protect Your Skin It s one of the most important things you can do! What is the skin? It s the largest organ in the body It protects you from the outside world It houses your sensory nerve endings It senses
Protect Your Skin It s one of the most important things you can do! What is the skin? It s the largest organ in the body It protects you from the outside world It houses your sensory nerve endings It senses
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment.
 24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
Appendix 3: Specialist Rehabilitation Prescription Proforma (example).
 Appendix 3: Specialist Rehabilitation Prescription Proforma (example). For patients with complex rehabilitation needs requiring Specialist (Level 1 or 2) Rehab services. The specialist rehabilitation Prescription
Appendix 3: Specialist Rehabilitation Prescription Proforma (example). For patients with complex rehabilitation needs requiring Specialist (Level 1 or 2) Rehab services. The specialist rehabilitation Prescription
Hip Fracture Orthopaedic Department Patient Information Leaflet
 riginator: Anne Flavall Professional Development Lead, Mr Marsh and Mr Quraishi Orthopaedic Consultant Surgeons Date: March 2012 Version: 2 Date for Review: March 2015 DGOH Ref No: DGOH/PIL/00611 Hip Fracture
riginator: Anne Flavall Professional Development Lead, Mr Marsh and Mr Quraishi Orthopaedic Consultant Surgeons Date: March 2012 Version: 2 Date for Review: March 2015 DGOH Ref No: DGOH/PIL/00611 Hip Fracture
Pressure Ulcers ecourse
 Pressure Ulcers ecourse Knowledge Checkup All Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Knowledge Checkup All Page
Pressure Ulcers ecourse Knowledge Checkup All Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Knowledge Checkup All Page
Expert Transfers in Rehabilitation: A Safety and Utilisation Review
 Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
Expert Transfers in Rehabilitation: A Safety and Utilisation Review Robert Mehan Meaghan Mackenzie Kim Brock Rehabilitation Care Centre NAHC 2007 - Hobart An important focus in stroke rehabilitation is
Managemen. Pressure Ulcer Prevention and Treatment. Guidance. Posture. Posture. Posture. Posture. Posture
 men menm Pressure Ulcer Prevention and Treatment Guidance Post ture Manag The reduction of the numbers of s is a high priority for Southern Health NHS Foundation Trust Purpose of this guidance is to help:
men menm Pressure Ulcer Prevention and Treatment Guidance Post ture Manag The reduction of the numbers of s is a high priority for Southern Health NHS Foundation Trust Purpose of this guidance is to help:
Pressure Injury Assessment Guide South West Regional Wound Care Program Last Updated October 31,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Reading: The Complications of Immobility Vocabulary
 Reading: The Complications of Immobility Vocabulary atrophy balance bed bound chairbound blood circulation bone bone loss bony prominence complication contracture deep vein thrombosis (DVT) deep vein thromboses
Reading: The Complications of Immobility Vocabulary atrophy balance bed bound chairbound blood circulation bone bone loss bony prominence complication contracture deep vein thrombosis (DVT) deep vein thromboses
The Shear Friction of pressure ulceration in aged care
 The Shear Friction of pressure ulceration in aged care Mr. Tal Ellis WoundHeal Australia, HWIG conference 2007 Introduction In Australia it is estimated that about 60,000 people have pressure ulcers (Porter&
The Shear Friction of pressure ulceration in aged care Mr. Tal Ellis WoundHeal Australia, HWIG conference 2007 Introduction In Australia it is estimated that about 60,000 people have pressure ulcers (Porter&
Body Mechanics and Safe Patient Handling
 Body Mechanics and Safe Patient Handling Body Mechanics means using the body in an efficient and careful way involves good posture, balance, and using your strongest and largest muscles for work good body
Body Mechanics and Safe Patient Handling Body Mechanics means using the body in an efficient and careful way involves good posture, balance, and using your strongest and largest muscles for work good body
Effective Seating Assessments
 Effective Seating Assessments Amy Barber @Yorkshire_Care #YORTRAINGOLD2017 www.yorkshirecareequipment.com Effective Seating Assessments A M Y B A R B E R O C C U PAT I O N A L T H E R A P I S T Y O RT
Effective Seating Assessments Amy Barber @Yorkshire_Care #YORTRAINGOLD2017 www.yorkshirecareequipment.com Effective Seating Assessments A M Y B A R B E R O C C U PAT I O N A L T H E R A P I S T Y O RT
CANCER REHABILITATION PATHWAY - HAEMATOLOGY
 CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
CANCER REHABILITATION PATHWAY - HAEMATOLOGY Statement: To be used in conjunction with Brain and CNS Rehabilitation Care Pathway as appropriate Diagnosis and Care Planning: The following symptom pathways
Pressure Ulcers Patient Information Leaflet
 Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet Shining a light on the future Introduction This leaflet is about pressure ulcers and includes information about what they are what can cause them and how they
Pressure Ulcers Patient Information Leaflet
 Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
Further information about the content, reference sources or production of this leaflet can be obtained from the Patient Information Centre. Pressure Ulcers Patient Information Leaflet This information
Presented By: Jennifer Birt, OT Reg(MB) Specialized Seating & Mobility Clinical Specialist
 Presented By: Jennifer Birt, OT Reg(MB) Specialized Seating & Mobility Clinical Specialist 2013 1. Define and understand the concept of practical pressure management and categorizing individuals at different
Presented By: Jennifer Birt, OT Reg(MB) Specialized Seating & Mobility Clinical Specialist 2013 1. Define and understand the concept of practical pressure management and categorizing individuals at different
CARE OF THE NEONATE: ITS ALL ABOUT THE SKIN. Katherine Kunkel, MSN, RNC-NIC, WCC
 CARE OF THE NEONATE: ITS ALL ABOUT THE SKIN Katherine Kunkel, MSN, RNC-NIC, WCC Learning Objectives Recognize what are risk factors for the neonate within the intensive care unit. Understand the physiology
CARE OF THE NEONATE: ITS ALL ABOUT THE SKIN Katherine Kunkel, MSN, RNC-NIC, WCC Learning Objectives Recognize what are risk factors for the neonate within the intensive care unit. Understand the physiology
Spinal cord compression: what it means and how it can be treated
 Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Spinal cord compression: what it means and how it can be treated Patient Information Oncology Department Author ID: Acute Oncology Nurse Specialist Leaflet Number: CC 036 Version: 2.1 Name of Leaflet:
Chapter 13. Body Mechanics. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 13 Body Mechanics Body Mechanics Body mechanics means using the body in an efficient and careful way. It involves good posture, balance, and using your strongest and largest muscles for work. 2
Chapter 13 Body Mechanics Body Mechanics Body mechanics means using the body in an efficient and careful way. It involves good posture, balance, and using your strongest and largest muscles for work. 2
PATIENT CARE MANUAL POLICY
 PATIENT CARE MANUAL POLICY NUMBER #VII-F-20 PAGE 1 OF 2 APPROVED BY: CATEGORY: Senior Vice President, Medicine and Chief of Staff; Vice President and Senior Operating Officer, Covenant Health, Rural Health
PATIENT CARE MANUAL POLICY NUMBER #VII-F-20 PAGE 1 OF 2 APPROVED BY: CATEGORY: Senior Vice President, Medicine and Chief of Staff; Vice President and Senior Operating Officer, Covenant Health, Rural Health
Prevention and management of Pressure ulcers
 Prevention and management of Pressure ulcers A guide for patients, carers and relatives What is a pressure ulcer? Pressure ulcers are an injury to the skin and/or underlying tissues. They are also known
Prevention and management of Pressure ulcers A guide for patients, carers and relatives What is a pressure ulcer? Pressure ulcers are an injury to the skin and/or underlying tissues. They are also known
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre.
 Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Spinal Cord Injury Info Sheet An information series produced by the Spinal Cord Program at GF Strong Rehab Centre. What does skin do? 1. It protects you. 2. It provides sensory information. 3. It helps
Ratified by: Care and Clinical Policies Date: 17 th February 2016
 Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Clinical Guideline Reference Number: 0803 Version 5 Title: Physiotherapy guidelines for the Management of People with Multiple Sclerosis Document Author: Henrieke Dimmendaal / Laura Shenton Date February
Presented by: Jennifer Birt, OT Reg(MB) Specialized Seating and Mobility Clinical Specialist Rehabilitation Day Program
 Pressure Management Assessment Tool (PMAT): Development and Implementation of a Comprehensive Clinical Evaluation for Managing Pressure from a 24 Hour Perspective Presented by: Jennifer Birt, OT Reg(MB)
Pressure Management Assessment Tool (PMAT): Development and Implementation of a Comprehensive Clinical Evaluation for Managing Pressure from a 24 Hour Perspective Presented by: Jennifer Birt, OT Reg(MB)
Pressure Ulcer Prevention and Management. Glenn Smith Clinical Nurse Specialist Nutrition and Tissue Viability
 Pressure Ulcer Prevention and Management Glenn Smith Clinical Nurse Specialist Nutrition and Tissue Viability Objectives An understanding of how pressure ulcers develop and what can be done to prevent
Pressure Ulcer Prevention and Management Glenn Smith Clinical Nurse Specialist Nutrition and Tissue Viability Objectives An understanding of how pressure ulcers develop and what can be done to prevent
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
Arthroscopic capsular release. Information for patients Orthopaedics - Upper Limb
 Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Skin matters Preventing Pressure Ulcers: a Guide for Patients and Carers
 Skin matters Preventing Pressure Ulcers: a Guide for Patients and Carers We recommend that you follow the advice within this leaflet and provided by your healthcare provider. However if anything changes
Skin matters Preventing Pressure Ulcers: a Guide for Patients and Carers We recommend that you follow the advice within this leaflet and provided by your healthcare provider. However if anything changes
Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders
 Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders Oedema, sometimes known as Lymphoedema or fluid retention is the build up of fluid and other elements
Supporting Information Leaflet (11): Managing Oedema and Circulatory Problems in Neuromuscular Disorders Oedema, sometimes known as Lymphoedema or fluid retention is the build up of fluid and other elements
North West London Trauma Network Spinal Pathway and Protocols
 North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
North West London Trauma Network Spinal Pathway and Protocols 1. Spinal Clearance in the Trauma Patient Inclusions: All trauma patients who are not alert and orientated, unable to cooperate (including
Pressure Ulcers ecourse
 Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
1/3/2008. Karen Burke Priscilla LeMone Elaine Mohn-Brown. Medical-Surgical Nursing Care, 2e Karen Burke, Priscilla LeMone, and Elaine Mohn-Brown
 Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
Medical-Surgical Nursing Care Second Edition Karen Burke Priscilla LeMone Elaine Mohn-Brown Chapter 42 Caring for Clients with Musculoskeletal Trauma Musculoskeletal Trauma Tissue is subjected to more
Prevention and management of pressure ulcers
 The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
Activity and Exercise
 Activity and Exercise Chapter 44 Ra'eda Almashaqba 1 Activity and Exercise refers to the persons rotten of exercise, activity, leisure, and recreation Include: 1. Activity of daily living 2. The type,
Activity and Exercise Chapter 44 Ra'eda Almashaqba 1 Activity and Exercise refers to the persons rotten of exercise, activity, leisure, and recreation Include: 1. Activity of daily living 2. The type,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery. By: Aun Lauriz E. Macuja SAC_SN4
 Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Nursing Management: Musculoskeletal Trauma and Orthopedic Surgery By: Aun Lauriz E. Macuja SAC_SN4 The most common cause of musculoskeletal injuries is a traumatic event resulting in fracture, dislocation,
Sara Combilizer. Multifunctional aid for early mobilization and ICU Rehabilitation. with people in mind
 Sara Combilizer Multifunctional aid for early mobilization and ICU Rehabilitation with people in mind Importance of mobilisation By counteracting the adverse effects of immobility and enhancing the function
Sara Combilizer Multifunctional aid for early mobilization and ICU Rehabilitation with people in mind Importance of mobilisation By counteracting the adverse effects of immobility and enhancing the function
Rehabilitation and Restorative Care
 170 25 Rehabilitation and Restorative Care 1. Define important words in this chapter 2. Discuss rehabilitation and restorative care 3. Describe the importance of promoting independence 4. Explain the complications
170 25 Rehabilitation and Restorative Care 1. Define important words in this chapter 2. Discuss rehabilitation and restorative care 3. Describe the importance of promoting independence 4. Explain the complications
11. Spinal cord injury
 11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
11. Spinal cord injury Introduction Always think spinal (vertebral) and/or spinal cord injury (SCI) in children with trauma. Remember SCIWORA cord injury may be present without abnormalities on routine
Course Information DPT 720 Professional Development (2 Credits) DPT 726 Evidenced-Based Practice in Physical Therapy I (1 Credit)
 Course Information DPT 720 Professional Development (2 Credits) This course introduces theories and experiences designed to develop professional socialization in students. Skills to accurately, sensitively
Course Information DPT 720 Professional Development (2 Credits) This course introduces theories and experiences designed to develop professional socialization in students. Skills to accurately, sensitively
What is Occupational Therapy? Introduction to Occupational Therapy. World Federation of Occupational Therapists 2012
 World Federation of Occupational Therapists 2012 Introduction to Occupational Therapy Suki HUI Occupational Therapist I Statement on Occupational Therapy Occupational therapy is a client-centred health
World Federation of Occupational Therapists 2012 Introduction to Occupational Therapy Suki HUI Occupational Therapist I Statement on Occupational Therapy Occupational therapy is a client-centred health
Sara Combilizer. Multifunctional aid for early mobilization and ICU rehabilitation. with people in mind
 Sara Combilizer Multifunctional aid for early mobilization and ICU rehabilitation with people in mind Importance of mobilization Enhancing the functionality of body mechanics from the beginning of a structured
Sara Combilizer Multifunctional aid for early mobilization and ICU rehabilitation with people in mind Importance of mobilization Enhancing the functionality of body mechanics from the beginning of a structured
Preventing pressure ulcers
 Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Golden Jubilee National Hospital NHS National Waiting Times Centre Preventing pressure ulcers Patient information guide for adults at risk of pressure ulcers Agamemnon Street Clydebank, G81 4DY (: 0141
Pressure ulcers can develop in a relatively short time, therefore it is important to prevent them or notice and recognise early signs of damage.
 Preventing Pressure Damage A Guide for Patients and Carers What is pressure damage? A pressure ulcer, (previously often referred to as a bed sore or pressure sore ) is a localised area of damage to the
Preventing Pressure Damage A Guide for Patients and Carers What is pressure damage? A pressure ulcer, (previously often referred to as a bed sore or pressure sore ) is a localised area of damage to the
National Cancer Action Team. Rehabilitation Care Pathway Poor Mobility and Loss of Function
 National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
National Cancer Action Team Rehabilitation Care Pathway Poor Mobility and Loss of Function Diagnosis & Care Planning Assess respiratory status especially in people with preexisting respiratory disease
Chapter 23 Body Mechanics, Positioning, and Moving
 Chapter 23 Body Mechanics, Positioning, and Moving Question Is the following statement true or false? Good body posture distributes gravity through the center of the body over a wide base of support. Answer
Chapter 23 Body Mechanics, Positioning, and Moving Question Is the following statement true or false? Good body posture distributes gravity through the center of the body over a wide base of support. Answer
Getting Comfortable with Managing Pain and Pressure Care in individuals with Motor Neuron Disease Stephanie Williams Occupational Therapist
 Getting Comfortable with Managing Pain and Pressure Care in individuals with Motor Neuron Disease Stephanie Williams Occupational Therapist State-wide Progressive Neurological Diseases Service Calvary
Getting Comfortable with Managing Pain and Pressure Care in individuals with Motor Neuron Disease Stephanie Williams Occupational Therapist State-wide Progressive Neurological Diseases Service Calvary
Fractures of the Thoracic and Lumbar Spine
 A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
A spinal fracture is a serious injury. Nader M. Hebela, MD Fellow of the American Academy of Orthopaedic Surgeons http://orthodoc.aaos.org/hebela Cleveland Clinic Abu Dhabi Cleveland Clinic Abu Dhabi Neurological
Nepal Spinal Cord Injury Working Group
 Nepal Spinal Cord Injury Working Group 19 June 2015 Overview by Fiona Stephenson Rehabilitation Cluster Meeting Aim of the Nepal SCI Working Group Ascertain numbers of patients with SCI Find key actors
Nepal Spinal Cord Injury Working Group 19 June 2015 Overview by Fiona Stephenson Rehabilitation Cluster Meeting Aim of the Nepal SCI Working Group Ascertain numbers of patients with SCI Find key actors
Posterior Lumbar Spinal Fusion
 Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
Posterior Lumbar Spinal Fusion Information to help patients prepare for a Posterior Lumbar Spinal Fusion Operation Directorates of Orthopaedic and Rheumatology, and Neurosciences Produced: February 2007
DEFINITION OF PRESSURE. Pressure = Force / Area
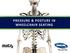 PRESSURE & POSTURE IN WHEELCHAIR SEATING DEFINITION OF PRESSURE Pressure = Force / Area ANATOMY OF THE SKIN Epidermis Dermis Subcutaneous Layer EFFECTS OF PRESSURE Occludes capillaries Restricts flow of
PRESSURE & POSTURE IN WHEELCHAIR SEATING DEFINITION OF PRESSURE Pressure = Force / Area ANATOMY OF THE SKIN Epidermis Dermis Subcutaneous Layer EFFECTS OF PRESSURE Occludes capillaries Restricts flow of
Information and exercises following a proximal femoral replacement
 Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Physiotherapy Department Information and exercises following a proximal femoral replacement Introduction The hip joint is a type known as a ball and socket joint. The cup side of the joint is known as
Hip Surgery and Mobility
 Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
Orthopedic Nursing, Part 1 Hip Surgery and Mobility Nursing Best Practice Guidelines Clinical Indications for Hip Surgery Selected fractures of the hip Unremitting pain and irreversible damaged joint from
The Seating Interface For The Individual With SCI: Minimizing Risk and Maximizing Function
 The Seating Interface For The Individual With SCI: Minimizing Risk and Maximizing Function Disclosure of PI- RRTC Grant James S. Krause, PhD, Holly Wise, PhD; PT, and Emily Johnson, MHA have disclosed
The Seating Interface For The Individual With SCI: Minimizing Risk and Maximizing Function Disclosure of PI- RRTC Grant James S. Krause, PhD, Holly Wise, PhD; PT, and Emily Johnson, MHA have disclosed
Preventing Pressure Ulcers
 Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Patient information Preventing Pressure Ulcers i Important information and care guide for patients at risk of pressure ulcers. Reproduced with kind permission from Healthcare Improvement Scotland Golden
Complex Limb Injury. Exceptional healthcare, personally delivered
 Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
Complex Limb Injury Exceptional healthcare, personally delivered Complex Limb Injuries Introduction This information booklet aims to help you to understand the nature, treatment and outcome of your limb
SUPPORT SURFACES AND POSITIONING
 SUPPORT SURFACES AND POSITIONING American Medical Technologies Irvine, CA 1 Disclaimer The information presented herein is provided for educational and informational purposes only and to promote the safeand-effective
SUPPORT SURFACES AND POSITIONING American Medical Technologies Irvine, CA 1 Disclaimer The information presented herein is provided for educational and informational purposes only and to promote the safeand-effective
Dynamic hip screw (sliding hip screw)
 Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Dynamic hip screw (sliding hip screw) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a dynamic hip screw, sometimes also known as a sliding hip
Sub-acromial decompression surgery. Information for patients Orthopaedics - Upper Limb
 Sub-acromial decompression surgery Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Sub-acromial decompression surgery Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Hip Fractures. Compliments of: Champlain Valley Orthopedics
 A Patient s Guide to Hip Fractures 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet is compiled from
A Patient s Guide to Hip Fractures 1436 Exchange Street Middlebury, VT 05753 Phone: 802-388-3194 Fax: 802-388-4881 cvo@champlainvalleyortho.com DISCLAIMER: The information in this booklet is compiled from
Pulmonary Rehabilitation in Acute Spinal Cord Injury. Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university
 Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Total Hip Replacement. Information and exercises for patients
 Total Hip Replacement Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy
Total Hip Replacement Information and exercises for patients The following guide is designed to help you understand more about your operation and the therapy you will receive Author: Orthopaedic Therapy
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after proximal tibial replacement Proximal tibial replacement surgery is usually carried out as part of treatment for
Total knee replacement: The enhanced recovery programme
 INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
INFORMATION FOR PATIENTS Total knee replacement: The enhanced recovery programme This leaflet aims to explain the enhanced recovery programme after total knee replacement surgery, to outline certain common
GLOSSARY. Active assisted movement: movement where the actions are assisted by an outside force.
 GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
GLOSSARY The technical words used in this guide are listed here in alphabetic order. The first time one of these words is used in the guide, it is written in italics. Sometimes there is reference to a
Surgery saved my life. Rehab is restoring my future.
 The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
The Best Way Back Baylor Institute for Rehabilitation offers care for the most challenging and medically complex patients, including those with traumatic brain injury, traumatic spinal cord injury and
Neuromuscular scoliosis
 Neuromuscular scoliosis By Mr Neil Upadhyay, Consultant Spinal Surgeon, North Bristol NHS Trust What is a scoliosis? Scoliosis is a medical condition that affects the spine. The term depicts a sideways
Neuromuscular scoliosis By Mr Neil Upadhyay, Consultant Spinal Surgeon, North Bristol NHS Trust What is a scoliosis? Scoliosis is a medical condition that affects the spine. The term depicts a sideways
Promoting Skin Integrity in End of Life Care. Part 1. Tracey McKenzie Head of Tissue Viability Services TSDFT
 Promoting Skin Integrity in End of Life Care Part 1 Tracey McKenzie Head of Tissue Viability Services TSDFT To Understand the Extrinsic Factors of Pressure Ulcer (PU) development To understand the Intrinsic
Promoting Skin Integrity in End of Life Care Part 1 Tracey McKenzie Head of Tissue Viability Services TSDFT To Understand the Extrinsic Factors of Pressure Ulcer (PU) development To understand the Intrinsic
MAJOR TRAUMA REHABILITATION PRESCRIPTION
 MAJOR TRAUMA REHABILITATION PRESCRIPTION Core Information Date Commenced: Time Commenced: Commenced By: GP: Date of Injury: Insert label or: Surname: First Name: MTC: Current Location: Date of Birth: Key
MAJOR TRAUMA REHABILITATION PRESCRIPTION Core Information Date Commenced: Time Commenced: Commenced By: GP: Date of Injury: Insert label or: Surname: First Name: MTC: Current Location: Date of Birth: Key
Pressure Ulcers ecourse
 Pressure Ulcers ecourse Knowledge Checkup Module 2 Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Knowledge Checkup Module
Pressure Ulcers ecourse Knowledge Checkup Module 2 Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Knowledge Checkup Module
Liability Risks for Physiatrists & Physical Therapists
 Liability Risks for Physiatrists & Physical Therapists Physiatrists and physical therapists work to improve and restore functionality to patients who have injuries and impairments affecting the musculoskeletal
Liability Risks for Physiatrists & Physical Therapists Physiatrists and physical therapists work to improve and restore functionality to patients who have injuries and impairments affecting the musculoskeletal
Hemiarthroplasty (half hip replacement)
 Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Hemiarthroplasty (half hip replacement) Trauma and Orthopaedics Patient Information Leaflet Introduction This leaflet is about an operation called a half hip replacement. It gives information about the
Bunion (hallux valgus deformity) surgery
 Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
Bunion (hallux valgus deformity) surgery Bunion surgery is generally reserved for bunions that are severe and impacting on function. There most frequent surgical procedure used involves a medial incision
CLPNA Pressure Ulcers ecourse: Module 4 Quiz II page 1
 CLPNA Pressure Ulcers ecourse: Module 4 Quiz II 1. When are good times to do a skin inspection of a patient or resident? a. Bathing b. Meal times c. Dressing d. Assisting e. Sleeping 2. For patients who
CLPNA Pressure Ulcers ecourse: Module 4 Quiz II 1. When are good times to do a skin inspection of a patient or resident? a. Bathing b. Meal times c. Dressing d. Assisting e. Sleeping 2. For patients who
Pressure Injury Prevention in the Hospitalised Elderly: A Medical Perspective
 Pressure Injury Prevention in the Hospitalised Elderly: A Medical Perspective Samuel TH Chew MB BCh BAO (NUI), MRCP (UK), CCT in Internal and Geriatric Medicine (UK), FAMS, FRCP
Pressure Injury Prevention in the Hospitalised Elderly: A Medical Perspective Samuel TH Chew MB BCh BAO (NUI), MRCP (UK), CCT in Internal and Geriatric Medicine (UK), FAMS, FRCP
Falls Prevention Awareness. Level 2
 Falls Prevention Awareness Level 2 LEVEL 2 CERTIFICATE IN FALLS PREVENTION AWARENESS About the Level 2 Certificate in Falls Prevention Awareness As people age they become more and more susceptible to falls,
Falls Prevention Awareness Level 2 LEVEL 2 CERTIFICATE IN FALLS PREVENTION AWARENESS About the Level 2 Certificate in Falls Prevention Awareness As people age they become more and more susceptible to falls,
Your Spasticity Management Service: Managing spasticity with Botulinum Toxin A in children with cerebral palsy
 Paediatric Unit information for parents and carers Your Spasticity Management Service: Managing spasticity with Botulinum Toxin A in children with cerebral palsy This leaflet is for children and young
Paediatric Unit information for parents and carers Your Spasticity Management Service: Managing spasticity with Botulinum Toxin A in children with cerebral palsy This leaflet is for children and young
Your Orthotics service is changing
 Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Your Orthotics service is changing Important for referrers on changes effective from January 2015 Why is the service changing? As demand for the orthotics service increases and budgets remain relatively
Femoral Neck (Hip) Fracture
 Patient Information Leaflet Femoral Neck (Hip) Fracture Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another
Patient Information Leaflet Femoral Neck (Hip) Fracture Produced By: Orthopaedic Department September 2013 Review due September 2016 1 If you require this leaflet in another language, large print or another
PRESSURE INJURIES WHAT S IN A NAME?
 PRESSURE INJURIES WHAT S IN A NAME? LINDA NORTON MScCH, PhD candidate, OT Reg.(ONT) Motion Specialties, University of Toronto and University of Western Ontario The term pressure ulcer has been replaced
PRESSURE INJURIES WHAT S IN A NAME? LINDA NORTON MScCH, PhD candidate, OT Reg.(ONT) Motion Specialties, University of Toronto and University of Western Ontario The term pressure ulcer has been replaced
Spinal Cord Injury. North American Spine Society Public Education Series
 Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Spinal Cord Injury North American Spine Society Public Education Series What Is a Spinal Cord Injury? A spinal cord injury is a condition that results from damage or trauma to the nerve tissue of the spine.
Rehabilitation/Geriatrics ADMISSION CRITERIA. Coordinated Entry System
 Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Guidelines for patients having. Achilles Tendon Repair. Achilles Tendon Repair
 Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Guidelines for patients having ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 Achilles Tendon Repair Please stick addressograph
Cervical Plating BACK PAIN
 BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge
 Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge What is a venous thromboembolism (VTE)? This is a medical term that describes a blood clot that develops in a deep vein
Reducing the risk of venous thrombo-embolism (VTE) in hospital and after discharge What is a venous thromboembolism (VTE)? This is a medical term that describes a blood clot that develops in a deep vein
Vascular dysfunction and vulnerable skin
 Vascular dysfunction and vulnerable skin Professor Peter Vowden Honorary Consultant Vascular Surgeon Clinical Director WoundTec HTC Bradford, UK 1 Exploring the clinical problem associated with the application
Vascular dysfunction and vulnerable skin Professor Peter Vowden Honorary Consultant Vascular Surgeon Clinical Director WoundTec HTC Bradford, UK 1 Exploring the clinical problem associated with the application
MMO 6000 Revolutionary Intelligence
 MMO 6000 Revolutionary Intelligence The Challenges of Immobility Immobility is a common pathway by which a host of diseases and problems in the elderly produce further disability. Patients who are chronically
MMO 6000 Revolutionary Intelligence The Challenges of Immobility Immobility is a common pathway by which a host of diseases and problems in the elderly produce further disability. Patients who are chronically
Ankle Fracture Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Ankle Fracture Orthopaedic Department Patient Information Leaflet Page 1 Ankle Fracture Welcome to the Dudley Group NHS Foundation Trust. This leaflet will provide you with information regarding the diagnosis
Foot and ankle fractures
 Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
Foot and ankle fractures Some fractures can be managed without surgery, but others require surgery to achieve the best possible outcome. Fractures and injuries to joints have a high risk of developing
North of England Bone and Soft Tissue Tumour Service
 North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
North of England Bone and Soft Tissue Tumour Service Guidelines for rehabilitation after replacement of the proximal femur Proximal femoral replacement surgery is usually carried out as part of treatment
South East Coast Operational Delivery Network. Critical Care Rehabilitation
 South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
South East Coast Operational Delivery Networks Hosted by Medway Foundation Trust South East Coast Operational Delivery Network Background Critical Care Rehabilitation The optimisation of recovery from
