In today s healthcare arena, the prevention and treatment
|
|
|
- Charla Robinson
- 5 years ago
- Views:
Transcription
1 Constant Force Technology versus Low-Air-Loss Therapy in the Treatment of Pressure Ulcers Raquel Branom, RN, BSN, CWOCN, and Laurie M. Rappl, PT, CWS ABSTRACT Least costly but most effective has never been more important to healthcare delivery than in the current healthcare environment of changing reimbursement systems. In wound care, the high costs associated with renting advanced support surfaces may be an area where expenses can be decreased if similar outcomes can be attained by using more affordable mattresses. This article compares the healing rates and eventual outcomes of wounds among two groups of patients randomly assigned to one of two support surfaces. A commonly used low-air-loss mattress was compared with the study mattress, an advanced, nonpowered, air and foam surface. Subjects were patients admitted to either of two long-term healthcare settings for the treatment of wounds. The resulting two groups of patients each were evenly matched for average age and percentage of patients who were nutritionally deficient as indicated by albumin or pre-albumin levels. The presence of gastrointestinal tubes and ventilator dependency also was recorded. Consistent wound care protocols were used on both groups, including turning schedules, nutrition, topical medication, and dressings. The study period covered a maximum of 8 weeks; interest was centered on the rate of wound healing and progress toward a goal rather than the length of time to completely close a wound. After 8 weeks, or upon discharge from the study, pressure ulcers in the study mattress group closed at an average rate per week of 9.% ± 4.8 versus 5.% ±.7 in the low-air-loss mattress group. This study indicates that the study mattress can provide benefits to the wound healing process similar to or better than low-air-loss mattresses at a substantially reduced cost. Ostomy/Wound Management ;47(9):8 46 In today s healthcare arena, the prevention and treatment of pressure ulcers continues to present a challenging and costly focus for healthcare professionals. The most difficult task is to spread limited healthcare dollars over as large a patient base as possible; therefore, the least costly but most effective products must be utilized. The cornerstone of treating pressure ulcers is the removal or alleviation of pressure, the underlying cause of the condition. Powered specialty mattresses play an important role in this aspect of treatment. However, due to the confusing results of past studies, the role of specialty mattresses in the treatment of pressure ulcers remains controversial. Specialty mattresses usually are rented and costly to the entire healthcare system, but the question remains as to whether that expense is justified by wound healing that is faster than less expensive measures. Several studies have found the incidence of pressure ulcers to be between.7% and 9% in hospitals and from.9% to 8% in skilled nursing facilities and nursing homes. The impact of pressure ulcers can be seen both in human and economic terms. In human terms, the geriatric patient who develops a pressure ulcer has a fourfold increased risk of death. In economic terms, estimating the cost of healing pressure ulcers is difficult because of the complexity of individual treatment, including depth of wound, nutritional compromise, need for hospitalization, medications, modalities (eg, electrical At the time she wrote this manuscript, Ms. Branom was an enterostomal therapist with Vencor, San Diego, Calf. She is now the wound/ostomy/continence nurse consultant for Sharp Home Care, San Diego, Calf. Ms. Rappl is the Clinical Support Manager for Span-America Medical Systems Inc., Greenville, SC. Address correspondence to: Laurie M. Rappl, PT, CWS, P.O. Box 5, Greenville, SC 966; lrappl@spanamerica.com. 8 OstomyWound Management
2 stimulation or pulsed lavage), dressings, and equipment. Xakellis and Frantz 4 reported the mean cost to heal a Stage II pressure ulcer, including hospitalization, was $,9 ± $4,4. The mean cost to heal a Stage III or IV ulcer, including hospitalization, was $,85 ± $7,65. The mean cost to heal each ulcer in the Xakellis and Frantz study was $,7 ± $,84. The AHCPR s Clinical Practice Guidelinee Number : Pressure Ulcers in Adults: Prediction and Prevention 5 states any individual assessed to be at risk for developing pressure ulcers should be placed when lying in bed on a pressure-reducing device such as foam, static air, alternating air, gel, or water mattress. Medicare has divided mattresses into three distinct groups, each with clinical criteria the patient must meet to qualify for reimbursement. Basically, Group I surfaces include static surfaces that are provided for prevention and for the first line in intervention for pressure ulcers. Group III mattresses include airfluidized surfaces. This study concentrated on Group II surfaces. The majority of Group II surfaces are powered mattresses, usually either low-air-loss (LAL) or alternating air surfaces. Group II surfaces are used for those patients who meet one of the following criteria: multiple Stage II pressure ulcers on the trunk or pelvis comprehensive ulcer treatment for past days with Group I product ulcers have worsened or remained the same over the past month large or multiple Stage III or IV ulcers on pelvis or trunk recent myocutaneous flap or skin graft on trunk or pelvis and the patient has been on a Group II or III surface immediately prior to a recent discharge from a hospital or nursing facility. 6 Low-air-loss mattresses (designated Group II) were designed to reduce body interface pressure to below capillary closing pressure ( mm Hg), to distribute weight evenly (pressure relief), and to limit friction and shear. 7,8 In the literature, several researchers have attempted to prove the efficacy of LAL mattresses in the treatment of pressure ulcers. Some of these studies use interface pressure measurements. Others use reduction in KEY POINTS wound measurements rather than final patient outcome with complete wound closure. Some studies show no significant improvement in patient outcomes, such as pressure ulcer healing, when the patient is treated on an LAL mattress. 9 Often a study yields confusing results. For example, in a study conducted by Ferrell et al, an LAL mattress was compared to a 4-inch foam mattress overlay. The study results showed no significant difference in healing rates of deep wounds between the two surfaces, but the researchers did see improved healing of superficial ulcers in subjects treated on an LAL mattress. Mulder et al compared an LAL mattress to a foam overlay. They noted a significant increase in rate of healing among subjects treated on LAL as compared to subjects treated on the overlays. However, in the same study, the researchers found no significant difference in the percentage of wounds that healed completely between the two groups. Day and Leonard compared the healing rates of 87 patients on LAL versus a unique foam overlay, the Geo-Matt (Span-America Medical Systems, Inc., Greenville, SC). They found no significant difference in healing rates of pressure ulcers between these two groups. Goals The goal of this pilot study was to determine if costs could be decreased by purchasing a less expensive mattress than an LAL while maintaining or improving patient outcomes. In everyday practice, selecting a support surface goes beyond choosing what has worked before and what information is available in the literature. Today s clinician must weigh the individual needs of the Ostomy/Wound Management ;47(9):8 46 Because support surface rental costs can be substantial, many facilities are considering their purchase. However, few studies have been conducted to compare the effectiveness and efficacy of different support surfaces. To ascertain whether replacing currently used low-air-loss mattresses with nonpowered air and foam surfaces would affect outcomes, the authors conducted a pilot study involving patients with Stage III and IV pressure ulcers. Following randomization, outcomes in patients placed on the nonpowered surface were similar or better than those obtained in patients on the low-air-loss mattresses. Sample size limitations prohibited statistical analysis of the results obtained, but additional studies, involving a larger sample size, seem warranted, given the potential cost savings. September Vol. 47 Issue 9 9
3 patient, the drive for positive patient outcomes, the availability of cost-effective products, and the reimbursement for the chosen surface by third-party payors. More than types of pressure-reducing devices are available, ranging from the low-cost foam or static air overlays to the more expensive and widely used LAL mattresses to airfluidized beds. Rented LAL mattresses can be a great expense. The average rental cost billed to Medicare is approximately $7 per month. Some manufacturers will rent these surfaces for as little as $ per day or as much as $45 per day. When purchasing a specialty bed, the facility can expect to spend thousands of dollars per bed. Skyrocketing healthcare costs, recent changes in reimbursement to long-term care under PPS for Medicare patients under Part A, and further changes in Medicare guidelines that will effect reimbursement by third-party payors using the Medicare guidelines for guidance in criteria for payment make it essential for clinicians to evaluate new products that can provide superior pressure reduction and patient outcomes in the least costly manner. Long-term-care facilities can no longer rely on reimbursement from a third party. Under PPS regulations for long-term care, facilities now must pay out-of-pocket for durable medical equipment rental or purchase from a fixed rate they receive for the patient s total care. For many, purchase of equipment that was previously rented will make more financial sense in the long run. This financial investment must be made carefully and must be based on cost-effective outcomes. The two mattresses compared include a standard, wellknown, structurally comparable LAL surface and the PressureGuard CFT (Constant Force Technology) by Span-America Medical Systems Inc. (Greenville, SC), hereafter referred to as study mattress. This mattress is nonpowered and comprises a series of interconnected air tubes and elasticized air reservoirs with a Geo-Matt cut foam topper as the patient interface layer. The manufacturer s pressure mappings show that it equalizes pressure over the weight-bearing surface of the patient s body. Low-air-loss mattresses also equalize pressure but with air intake and outflow rather than movement within a fully enclosed system. The two measurable areas of patient outcomes were:. Meeting the goals of wound treatment as determined by the team. Goals included progressive closure, preparation for flap, and maintenance of condition. Maintenance of condition is frequently an appropriate goal if the patient s condition is deteriorating and other health concerns are more pressing than skin care. Each wound was rated achieved, not achieved, or exceeded. The goal of progressive closure was considered achieved if the wound showed progress toward closure.. The rate of wound healing over time, with a maximum of 8 weeks. The goal was to determine the rate of wound closure, expressed as a percentage of the original wound, rather than whether or not the wound fully closed during the study period. The author reports measurements at weeks and at exit from the study to determine if wound healing slowed or accelerated as the wound decreased in size. This helped determine if one mattress outperformed the other at an interim time point as well as at the end point a consistency that added confidence to the findings. If the study mattress matched the LAL surfaces in patient treatment, acquisition costs would save the participating facilities thousands of dollars in either rental or purchase of LAL in a very short time. Methodology This pilot study was set up as a prospective, randomized clinical trial involving patients who had Stage III or IV pressure ulcers on the trunk or pelvis. Inclusion criteria:. The patient was admitted as an inpatient to one of the two test sites.. The patient had pressure ulcer(s) at Stage III or IV on the trunk or pelvis.. The patient was bedridden, necessitating pressure distribution off of bony prominences and ulcer site(s). If a patient was admitted to the study with more than one pressure ulcer, only the deeper ulcer was followed in the study. Poor health status of a patient negatively affects wound healing on all of that patient s wounds. One patient with many wounds would have an unequally large effect on the results for that mattress, either positive or negative. Sites. Two facility sites were used. Vencor Hospital is a 7-bed, acute care hospital in San Diego, California specializing in ventilator-dependent patients and patients with extensive wound care needs. Horizon Health and 4 OstomyWound Management
4 Sub-Acute Center in Fresno, California, is a 5-bed long-term and subacute care center. These two sites have relatively homogenous patient profiles and lengths of stay, wound care protocols including use of LAL mattress replacements, and employ moist wound healing with nutrition intervention. Certified enterostomal therapy (ET) nurses direct their wound care programs and each facility has developed a reputation in their respective geographic area for excellence in wound care. Mattress assignment. For simplicity, each facility used a brand of LAL most familiar to its staff and equally approved as reimbursable, Group II surfaces under Medicare Guidelines. Each LAL surface vented air in the same manner and the capacity of the pumps to generate airflow through the mattresses (approximately L/minute) was nearly equal. The two brands are widely used in the United States. Patients who met the inclusion criteria were randomly assigned to one of the two groups, the study mattress or LAL, in an alternating pattern as they were admitted. The first patient admitted, who required a special support surface as part of ulcer treatment, was placed on the LAL, the second patient admitted was placed on the study mattress, the third patient on the LAL, and so on. Ten patients were placed on the study mattress and were placed on the LAL. Unfortunately, as often happens in patient-oriented research, two of the LAL patients were switched to the study mattress during their treatment upon physician s orders, despite inclusion in the study. Hence, the numbers of patients in the results show on the study mattress and only eight on LAL. The outcomes of these two patients are discussed separately in the results that follow; they are not included in the data analysis. Data collection. Data collected on each patient included: age, albumin or pre-albumin, g-tube, ventilator dependency, site and size of ulcer, presence of eschar, and the goal for wound healing. Albumin/pre-albumin. Albumin or pre-albumin determined nutritional status. A normal albumin range of. g/dl to 4.5 g/dl was used for this study. 7 An albumin level of less than.5 g/dl indicates the need for detailed nutritional assessment and possible intervention. 7 Albumin levels below. g/dl have been associated with poor wound healing outcomes. A normal pre-albumin range of g/dl to 4 g/dl was used for this study. 7 G-tube/ventilator dependency. These features were recorded because patients with g-tubes for enteral feedings or who are dependent on ventilators are more medically fragile. A concentration of these fragile patients in one of the two groups could negatively affect the comparison of outcomes. Wound measurements. Length, width, and depth, in centimeters, were taken at weeks and at end of the study and weekly as clinicians were able. The data were used to determine percent of wound healing that occurred over the initial -week time period and over the entire time the patient was in the study, up to the 8-week limit. The interim -week measurement was included to see if wound healing accelerated over time and to note if one mattress outperformed the other at an interim time point as well as at the end point. Goal for healing. Each subject was evaluated and the wound care team established a goal for wound healing progressive closure, maintenance, or preparation for flap surgery rather than completion of the wound healing process. The team included the patient and/or family, the ET nurse, nursing staff, and the patient s primary physician. These goals were established according to the patient s medical condition, prognosis, quality of life, age, and level of debilitation. At the end of the study, patients were rated as having achieved their goal, not having achieved their goal, or having exceeded their goal. For example, if the patient s condition made maintenance of the wound a reasonable goal, but the patient showed progress toward closure of the wound, the patient was scored as having exceeded his/her goal. Exit criteria. Eight weeks was the maximum time for participation in this study. Again, the goal was to determine differences in rate of wound closure and progress toward the stated goal. Therefore, a defined endpoint was necessary to calculate final size percentages. Other than the 8-week time limit, study exit criteria also included death, discharge from inpatient status, or flap surgery. Data for those patients who did not complete the full 8-week time period are calculated using the number of weeks they did participate. Topical wound care. The topical wound care protocols in each facility were similar. These protocols were based on the principals of moist wound healing, as described in the AHCPR Clinical Practice Guidelines for the Treatment of Pressure Ulcers, and the Clinicians Pocket Guide to Chronic Wound Repair (see Table for a description of the topical wound protocols). September Vol. 47 Issue 9 4
5 TABLE TOPICAL WOUND CARE PROTOCOLS Irrigate all wounds with cc of normal saline using a 5-cc syringe and -gauge anglocath. Apply appropriate topical dressing based on the following criteria: Superficial wounds with minimal amount of drainage Perform one of the following: Apply hydrogel to wound bed, cover with gauze Cover wound with thin foam dressing Cover wound with transparent film Wounds with depth or cavity with minimal amount of drainage Pack wound with hydrogel impregnated gauze and apply cover dressing Superficial wounds with moderate to large amount of drainage Cover with foam dressing, with or without calcium alginate Apply calcium alginate and cover with hydrocolloid dressing Wounds with depth or cavity with moderate to large amount of drainage Pack wound with calcium alginate, cover with gauze, foam dressing, or hydrocolloid The protocols also included patient positioning in bed, including positioning off of the ulcer site at all times if able, and employing the -degree, side-lying oblique position. This position provides pressure relief for the sacrum and both trochanters. 8 Position changes were performed at regular -hour intervals. Comparison of study groups. Upon admission to the study, the two groups were evenly matched in average age (see Table ).The two groups were also evenly matched in the percentage of patients who were nutritionally deficient as indicated by albumin or pre-albumin levels. The average albumin level, taken at the time of admission was.5, significantly below the.5 threshold cited above. The average pre-albumin was 4.7, significantly below the threshold of cited above. The two groups were also fairly evenly matched in the numbers of Number of patients Number of wounds Age range (years) Mean age (years) Albumin <.5 or pre-albumin < 8 G-tube Ventilator dependent Ulcer site Sacrum/coccyx Trochanter Ulcer stage III IV patients who used g-tubes seven of in the study mattress group and five of eight in the LAL group. The LAL group had more ventilator-dependent patients than the study mattress group five of eight (6%) versus four of (4%). Meeting wound treatment goal. Data gathered summarize the results, comparing goals, results, and average rate of wound closure of the two groups (see Table ). This chart includes data on the two patients who were switched from LAL to constant force technology. These data were not analyzed statistically as these patients are presented for added information only; they did not complete the study on the same mattress, but their results are of interest as case studies. Two wounds on one patient who switched surfaces are described in the results, although only one wound per patient was followed in the patients who started and completed the study on the same mattress. Under Goal for Wound, Achieved included those patients who fully met or were progressing toward meeting their established goal of progressive closure or maintenance, whether the wound was completely closed or not at the end of the 8-week study. Exceeded included those patients who had maintenance as their goal and TABLE PATIENT PROFILES Study Mattress (8%) 7 (7%) 4 (4%) 7 (7%) (%) (%) 7 (7%) LAL Remained on LAL (88%) 5 (6%) 5 (6%) 7 (88%) (%) (5%) 6 (75%) Switched from LAL to Study Mattress OstomyWound Management
6 TABLE RESULTS FOR WOUND TREATMENT AND RATE OF CLOSURE Number of wounds Goal for wound Progressive Closure Prepare for flap Maintenance Results Achieved Exceeded Not achieved Rate of wound closure as % over weeks Rate of wound closure as % at endpoint Study Mattress (7%) (%) 4.4% ±. 9.% ± 4.75 LAL Remained on LAL (5%) (%) (7%) 7.% ± % ±.7 Switched from LAL to Study Mattress Goal (Number of patients with this goal) Results: Achieved Exceeded Not achieved TABLE 4 GOALS FOR WOUND TREATMENT VS. RESULTS Study Mattress Progressive Closure Prepare Maintain for flap (4) () (5) 4 Progressive Closure (5) LAL Prepare for flap () Maintain () who progressed toward closure during the study. Not achieved included those patients who did not meet their goals for either progressive closure or maintenance. Table 4 compares the goals for wound healing with the results achieved for each of the two groups. In the study mattress group, the goal for four of the patients was progressive closure, five had maintenance as the goal, and one patient received wound care as preparation for flap surgery. In the LAL group, the goal for five of the eight patients was progressive closure, two had maintenance as their goal, and one received wound care in preparation for flap surgery. All patients on the study mattress (%) achieved or exceeded their goals during the study period. Five of the eight patients treated on the LAL achieved or exceeded their goals. Rate of wound healing. The rates of wound closure at weeks and at the end of the study are summarized in Table 5. These rates were determined by comparing the total change in wound volume in cm and in the percentage of change from the original wound. The author used wound volume rather than area, so length, width, and depth were recorded on each wound. In the following equations used as part of this process, X = either weeks or the number of weeks in the study (see Table 6). The number of weeks in the study was a maximum of 8-weeks as discussed earlier in this article (see Table 5). The resulting numbers in each group were averaged. At the end of weeks, wounds in each group had closed by nearly the same volume (7. cm and 7. cm respectively) and, therefore, at the same rate per week September Vol. 47 Issue 9 4
7 Study Mattress TABLE 5 COMPARISON OF WOUNDS, HEALING RATES,AND HEALING PERCENTAGES AT WEEKS AND 8 WEEKS Size at Start.5 Size at weeks 5.5 End of Weeks Amount Closed 7. 4 Rate of closure/ week % closed 4. 6 % closed/ week 4.4% ±. 7 Size at d/c from study 6.6 End of 8 Weeks or d/c from study 8 Amount Closed at d/c from study Rate of closure/ Week at d/c from study.5 % closed 6. % closed/ week 9.% ± 4.8 LAL 5.44 d/c = discharged % ± % ±.7 (5.7 cm ). However, as a percentage of the total wound closed in weeks, the study mattress group outperformed the LAL group 4% to.8%. At the end of the study period, the average volume closed was nearly equal (5.8 cm versus. cm ). However, the average rate of closure per week was higher on the study mattress (.5 versus.8) as was the average percentage closed (6% versus 9.6%). At weeks, the average rate of wound closure per week as a percentage of the original wound was 4.4% ±. on the study mattress and 7.% ± 7.6 on the LAL. At 8 weeks, or the end of the study (whichever came first for the individual patient) the average rate of wound closure per week as a percentage of the original wound was 9.% ± 4.8 on the study mattress, compared with 5.% ±.7 on the LAL. During the study, two of the subjects, whose wounds had reached a plateau in their healing, were switched from the LAL mattress to the study mattress at the insistence of their physicians. Data on two wounds on one patient and one wound on the other are included in the patient data tables to indicate the effects of each of the two surfaces. One patient s goal was for wound closure of both sites, and the other patient s wound was being prepared for myocutaneous flap surgery. On each of the two surfaces, Patient showed shortterm improvement, then reached a plateau. During each plateau period, the physician switched surfaces. Each change in surface resulted in a -cm reduction in wound depth; Patient showed no difference in healing between surfaces. It is believed that healing was impaired due to history of pelvic radiation. The patient subsequently had myocutanous flap surgery to close the wound. Patient had two Stage IV pressure ulcers. This patient was on LAL for approximately 5 weeks. During the first weeks, the ulcers closed by 5% (trochanter) and 86% (coccyx), respectively, then both stagnated in their closure process. No contributing factors such as significant change in health status, medications, or nutrition were observed to account for this occurrence. The physician ordered the switch to the study mattress. Progressive healing was again observed; after 4 weeks on the study mattress, the wounds closed by % and 7% of the size of the respective ulcer at the time the surface was switched to the study mattress. No patients developed new ulcers on either the study mattress or the LAL mattresses. Over the 8-week study period, the daily rental cost of the LAL mattresses was approximately $5./day, resulting in a total rental cost of $,96. per patient over the 8 weeks. In comparison, the purchase price (manufacturer s suggested retail price) of the study mattress is $,8., or approximately 5% of rental costs over 8 weeks. Over time, further savings will be realized because the study mattress will be available for future use. Discussion The goal of this study was to determine if the cost of an LAL mattress was justified in improved patient out- 44 OstomyWound Management
8 comes or whether similar or better outcomes can be achieved by using technology that was less costly. The results of the study showed that improved patient outcomes, as seen by improved healing rates, can be achieved when using an alternative pressure-reducing device, without incurring costly rental or purchasing bills. The study randomization yielded two groups that were evenly matched for nutritional deficiencies (low albumin or pre-albumin), nutritional source (enterally fed), and location of ulcers caused by pressure secondary to immobility. Although the majority of the subjects were elderly, each group had one relatively young subject (the study mattress group had one 6-year-old; the LAL group had one 49-year-old). Dressing changes at both facilities follow similar protocols based on the AHCPR guidelines and the principles of moist wound healing. Nursing care included routine turning and re-positioning every hours and nutritional supplementation when needed. Protocols guided the staff to keep the ulcer sites as free of pressure as possible with frequent turning and appropriate positioning. Without pressure testing each patient in every possible position on each weight-bearing bony prominence on both surfaces, making the generalized statement that surface X provides lower interface pressure than surface Y for all patients is impossible. From the results of this study, likewise, this conclusion cannot be reached because the author and her colleagues did not have access to pressure mapping or sensors that would accurately measure the interface pressures for the mattresses used. The small sample size is an acknowledged limitation of this study that may affect the conclusive results. Additional randomized controlled studies consisting of a larger patient sampling, comparison of support surfaces across surface categories, including the study mattress, and a longer period of study ending with full wound closure may prove to be of value. Another limitation of this study is the use of two different LAL mattresses, even though they are nearly identical in structure, method of venting air to the environment, and capacity of blowers to move air through the TABLE 6 EQUATIONS USED TO DETERMINE RATE OF WOUND CLOSURE Size (volume) Amount closed Rate of closure per week Percentage of wound closure Rate of wound closure per week (percentage) * X = weeks or the number of weeks in the study. Length x Width x Depth (cm) Size at Start Size at X * -weeks (Size at Start Size at X weeks) X (Size at Start Size at X-weeks) Size at Start Percentage of Wound Closure X mattresses (approximately L/minute). Using only one brand of LAL mattress would eliminate the possible factor of one LAL mattress performing differently from the other and negatively affecting all LAL results. Conclusion In relation to the two stated goals:. Meeting the goal of wound treatment: % of the subjects on the study mattress met or exceeded their goal for wound healing versus 6% of the LAL group.. Rate of wound healing over time: after weeks, pressure ulcers on subjects on the study mattress closed at an average rate per week of 4.4% ±., while the LAL subjects pressure ulcers closed at an average rate per week of 7.% ± 7.6. After 8 weeks, or upon discharge from the study, the pressure ulcers on subjects in the study mattress group closed at an average rate per week of 9.% ± 4.8, as opposed to 5.% ±.7 on the LAL. This study suggests that the study mattress is an effective and lower cost alternative to the LAL mattresses in positively affecting the rates of wound healing in patients with Stage III and IV pressure ulcers. - OWM Acknowledgment The mattresses used in the study were provided by Span-America Medical Systems Inc., Greenville, SC. September Vol. 47 Issue 9 45
9 References. Krasner D, Sibbald R. Interpretations for practice [sidebar]. Ostomy/Wound Management. 999;45(suppl A):75S.. Bergstrom N, Bennett MA, Carlson CE, et al. Clinical Practice Guideline Number 5: Treatment of Pressure Ulcers. Rockville, Md: US Department of Health and Human Services. Public Health Service, Agency for Health Care Policy and Research; 994 AHCPR Publication No Klein L, Boarini J, Burton C, et al. Pressure Ulcers: A Practical Nursing Reference for the Chronic Wound Care Environment. Sugar Land, Tex.: Dow Hickam Pharmaceuticals, Inc.; Xakellis G, Frantz R. The cost of healing pressure ulcers across multiple health care settings. Advances in Wound Care. 996;9(6):8. 5. Panel for the Prediction and Prevention of Pressure Ulcers in Adults. Clinical Practice Guideline Number : Pressure Ulcers in Adults: Prediction and Prevention. Rockville, Md: US Department of Health and Human Services. Public Health Service. Agency for Health Care Policy and Research; 99. AHCPR Publication No DMERC Region D Supply Manual, Bryant R. Acute and Chronic Wounds: Nursing Management. St. Louis, Mo.: Mosby Yearbook; Fowler E. Equipment and products used in management and treatment of pressure ulcers. Nurs Clin North Am. 987;(): Maklebust J. An update on horizontal patient support surfaces. Ostomy/Wound Management. 999;45(A suppl):7s 77S.. Ferrell BA, Osterweil D, Christensen P. A randomized trial of low-air-loss beds for treatment of pressure ulcers. JAMA. 99;69(4): Mulder GD, Seeley T. A study of pressure ulcer response to low-air-loss beds vs. conventional treatment. Journal of Geriatric Dermatology. 99;:87.. Day A, Leonard F. Seeing quality care for patients with pressure ulcers. Decubitus. 99;6(): 4. Mulder GD, Fairchild PA, Jeter, KF. Clinician s Pocket Guide to Chronic Wound Repair. Long Beach, Calf.: Wound Healing Institute Publications; OstomyWound Management
Durable Medical Equipment Providers
 August 2009 Provider Bulletin Number 974 Durable Medical Equipment Providers Vacuum Assisted Wound Closure Therapy Negative pressure wound therapy (NPWT) must be requested and supplied by an enrolled durable
August 2009 Provider Bulletin Number 974 Durable Medical Equipment Providers Vacuum Assisted Wound Closure Therapy Negative pressure wound therapy (NPWT) must be requested and supplied by an enrolled durable
Source of effectiveness data The effectiveness evidence was derived from a review of published studies.
 Cost and cost effectiveness of venous and pressure ulcer protocols of care Kerstein M D, Gemmen E, van Rijswijk L, Lyder C H, Phillips T, Xakellis G, Golden K, Harrington C Record Status This is a critical
Cost and cost effectiveness of venous and pressure ulcer protocols of care Kerstein M D, Gemmen E, van Rijswijk L, Lyder C H, Phillips T, Xakellis G, Golden K, Harrington C Record Status This is a critical
WOUND CARE. By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare
 WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
WOUND CARE By Laural Aiesi, RN, BSN Alina Kisiel RN, BSN Summit ElderCare PRESSURE ULCER DIABETIC FOOT ULCER VENOUS ULCER ARTERIAL WOUND NEW OR WORSENING INCONTINENCE CHANGE IN MENTAL STATUS DECLINE IN
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur
 VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
VACUUM ASSISTED CLOSURE (V.A.C.) THERAPY: Mr. Ismazizi Zaharudin Jabatan pembedahan Am Hospital Kuala Lumpur Learning Objectives Define Negative Pressure Wound Therapy (NPWT) Discuss guidelines for the
SUPPORT SURFACES AND POSITIONING
 SUPPORT SURFACES AND POSITIONING American Medical Technologies Irvine, CA 1 Disclaimer The information presented herein is provided for educational and informational purposes only and to promote the safeand-effective
SUPPORT SURFACES AND POSITIONING American Medical Technologies Irvine, CA 1 Disclaimer The information presented herein is provided for educational and informational purposes only and to promote the safeand-effective
DMEPOS: hospital beds, bed accessories, and pressurereducing
 ACTION: Final DATE: 07/02/2018 10:03 AM 5160-10-18 DMEPOS: hospital beds, bed accessories, and pressurereducing support surfaces. (A) Definitions and explanations. (1) "Group 1," "group 2," and "group
ACTION: Final DATE: 07/02/2018 10:03 AM 5160-10-18 DMEPOS: hospital beds, bed accessories, and pressurereducing support surfaces. (A) Definitions and explanations. (1) "Group 1," "group 2," and "group
Support Surfaces: Characteristics and Considerations
 Support Surfaces: Characteristics and Considerations Specialty Beds Air-fluidized bed (also known as a bead bed or sand bed ) Product Characteristics: This is a bed frame containing silicone-coated beads
Support Surfaces: Characteristics and Considerations Specialty Beds Air-fluidized bed (also known as a bead bed or sand bed ) Product Characteristics: This is a bed frame containing silicone-coated beads
Negative Pressure Wound Therapy (NPWT)
 Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
Negative Pressure Wound Therapy (NPWT) Policy Number: Original Effective Date: MM.01.005 11/19/1999 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 01/01/2015 Section: DME Place(s) of Service:
Bear of a Problem: Who should be sleeping in which bed?
 Bear of a Problem: Who should be sleeping in which bed? Dianne Mackey MSN, RN, CWOCN Wound/Skin Coordinator Kaiser Permanente San Diego California Evan Call MS, CSN (NRM) Adjunct Faculty Weber State University
Bear of a Problem: Who should be sleeping in which bed? Dianne Mackey MSN, RN, CWOCN Wound/Skin Coordinator Kaiser Permanente San Diego California Evan Call MS, CSN (NRM) Adjunct Faculty Weber State University
Topical Oxygen Wound Therapy (MEDICAID)
 Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
Topical Oxygen Wound Therapy (MEDICAID) Last Review Date: September 8, 2017 Number: MG.MM.DM.15C8v2 Medical Guideline Disclaimer Property of EmblemHealth. All rights reserved. The treating physician or
NPUAP Mission. Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries. npuap.org
 Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
Clinical Practice Guidelines: Wound Dressings for the Management of Pressure Injuries Margaret Goldberg, MSN, RN, CWOCN June 29, 2016 NPUAP Mission The National Pressure Ulcer Advisory Panel (NPUAP) serves
CASE 1: TYPE-II DIABETIC FOOT ULCER
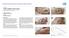 CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
CASE 1: TYPE-II DIABETIC FOOT ULCER DIABETIC FOOT ULCER 48 YEAR-OLD MALE Mr. C., was a 48-year old man with a history of Type-II diabetes over the past 6 years. The current foot ulcer with corresponding
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4
 A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
A GUIDE TO THE TREATMENT OF PRESSURE ULCERS FROM GRADE 1 GRADE 4 Gill Wicks, Nurse Consultant, Tissue Viability for Wiltshire Primary Care Trust and Lecturer at University of West England Pressure ulcers
Appropriate Dressing Selection For Treating Wounds
 Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
Appropriate Dressing Selection For Treating Wounds Criteria to Consider for an IDEAL DRESSING Exudate Management Be able to provide for moist wound healing by absorbing exudate or adding moisture Secure
TITLE: Australian Sheepskins for the Management of Pressure Ulcers: A Review of the Clinical-Effectiveness, Cost-Effectiveness, and Guidelines
 TITLE: Australian Sheepskins for the Management of Pressure Ulcers: A Review of the Clinical-Effectiveness, Cost-Effectiveness, and Guidelines DATE: 21 July 2009 CONTEXT AND POLICY ISSUES: Pressure ulcers,
TITLE: Australian Sheepskins for the Management of Pressure Ulcers: A Review of the Clinical-Effectiveness, Cost-Effectiveness, and Guidelines DATE: 21 July 2009 CONTEXT AND POLICY ISSUES: Pressure ulcers,
Afistula is an abnormal opening between two or. Colocutaneous Fistula Management in a Dehisced Wound: A Case Study FEATURE
 FEATURE Colocutaneous Fistula Management in a Dehisced Wound: A Case Study Terri Reed, BSN, WOCN; Diana Economon, RN, BSN, CWOCN; and Laurel Wiersema-Bryant, APRN, BC A fistula is an abnormal opening between
FEATURE Colocutaneous Fistula Management in a Dehisced Wound: A Case Study Terri Reed, BSN, WOCN; Diana Economon, RN, BSN, CWOCN; and Laurel Wiersema-Bryant, APRN, BC A fistula is an abnormal opening between
Beyond the Basics ImprovingYour Wound Care Knowledge. Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN
 Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Beyond the Basics ImprovingYour Wound Care Knowledge Berna Goldentyer RN, BSN, CWOCN Kathy Hugen RN, BSN, CWOCN Projects and Posters These resources were developed by creative VA nurses who had no special
Premier Health Plan considers Negative Pressure Wound Therapy (NPWT) in the home setting medically necessary for the following indications:
 Premier Health Plan POLICY AND PROCEDURE MANUAL PA.009.PH Negative Pressure Wound Therapy This policy applies to the following lines of business: Premier Commercial Premier Employee Premier Health Plan
Premier Health Plan POLICY AND PROCEDURE MANUAL PA.009.PH Negative Pressure Wound Therapy This policy applies to the following lines of business: Premier Commercial Premier Employee Premier Health Plan
Consider the possibility of pressure ulcer development
 Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
Douglas Fronzaglia II, DO, MS LECOM Institute for Successful Aging LECOM Institute for Advanced Wound Care and Hyperbaric Medicine Consider the possibility of pressure ulcer development 1 Identify ulcer
o Venous edema o Stasis ulcers o Varicose veins (not including spider veins) o Lipodermatosclerosis
 Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
Wound Care Equipment and Supply Benefits to Change for Texas Medicaid July 1, 2018 Effective for dates of service on or after July 1, 2018, wound care equipment and supply benefits will change for Texas
CARE OF THE NEONATE: ITS ALL ABOUT THE SKIN. Katherine Kunkel, MSN, RNC-NIC, WCC
 CARE OF THE NEONATE: ITS ALL ABOUT THE SKIN Katherine Kunkel, MSN, RNC-NIC, WCC Learning Objectives Recognize what are risk factors for the neonate within the intensive care unit. Understand the physiology
CARE OF THE NEONATE: ITS ALL ABOUT THE SKIN Katherine Kunkel, MSN, RNC-NIC, WCC Learning Objectives Recognize what are risk factors for the neonate within the intensive care unit. Understand the physiology
Pressure Ulcer Prevention Guidelines
 EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
EUROPEAN PRESSURE ULCER ADVISORY PANEL Pressure Ulcer Prevention Guidelines INTRODUCTION Pressure damage is common in many healthcare settings across Europe, affecting all age groups, and is costly both
Pressure Injury Assessment Guide South West Regional Wound Care Program Last Updated October 31,
 Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
Developed in collaboration with the Wound Care Champions, Wound Care Specialists, Enterostomal Nurses, and South West Regional Wound Care Program (SWRWCP) members from Long Term Care Homes, Hospitals,
NEGATIVE PRESURE WOUND THERAPY PROGRAM
 NEGATIVE PRESURE WOUND THERAPY PROGRAM WWW.USTOMWOUNDCARE.COM 866-802-0006/901-619-8897 SUPPORT@USTOM.COM TABLE OF CONTENTS 1. 2. 3. 4. To place an order: 1. Please visit our website 2. Please email to
NEGATIVE PRESURE WOUND THERAPY PROGRAM WWW.USTOMWOUNDCARE.COM 866-802-0006/901-619-8897 SUPPORT@USTOM.COM TABLE OF CONTENTS 1. 2. 3. 4. To place an order: 1. Please visit our website 2. Please email to
Negative Pressure Wound Therapy
 Origination: 6/29/04 Revised: 8/24/16 Annual Review: 11/10/16 Purpose: To provide Negative Pressure Wound Therapy (wound care treatment) guidelines for the Medical Department staff to reference when making
Origination: 6/29/04 Revised: 8/24/16 Annual Review: 11/10/16 Purpose: To provide Negative Pressure Wound Therapy (wound care treatment) guidelines for the Medical Department staff to reference when making
OF WOUNDS SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM. AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois
 1 THE WACKY WORLD OF WOUNDS ERIN RYDELL SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois www.ahia.org Carolinas HealthCare System 2 Carolinas
1 THE WACKY WORLD OF WOUNDS ERIN RYDELL SENIOR AUDITOR CAROLINAS HEALTHCARE SYSTEM AHIA 32 nd Annual Conference August 25-28, 2013 Chicago, Illinois www.ahia.org Carolinas HealthCare System 2 Carolinas
Acute and Chronic WOUND ASSESSMENT. Wound Assessment OBJECTIVES ITEMS TO CONSIDER
 WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
WOUND ASSESSMENT Acute and Chronic OBJECTIVES Discuss classification systems and testing methods for pressure ulcers, venous, arterial and diabetic wounds List at least five items to be assessed and documented
INTRODUCTION TO WOUND DRESSINGS
 WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
WOUND CARE INTRODUCTION TO WOUND DRESSINGS JEC 2017 Wound Care Successfully completed specialized skills training in Wound Management. WOUND CONDITIONS & SYMBOLS BY COLOURS Yellow Black Necrotic tissue
Genadyne A4 and foam to treat a postoperative debridment flank abscess
 Genadyne A4 and foam to treat a postoperative debridment flank abscess Michael S. DO, The Wound Healing Center Indianapolis, IN Cynthia Peebles RN D.O.N., Becky Beck RN Heartland at Prestwick NH Avon,
Genadyne A4 and foam to treat a postoperative debridment flank abscess Michael S. DO, The Wound Healing Center Indianapolis, IN Cynthia Peebles RN D.O.N., Becky Beck RN Heartland at Prestwick NH Avon,
Skin Deep. Agenda. Burns Wounds Debridement Evaluation and Management Services. Presented by: Mike Strong, SFM The Work Comp Experts.
 Presented by: Mike Strong, SFM The Work Comp Experts Agenda Wounds Debridement Evaluation and Management Services 2 1 Types of First Degree Second Degree Third Degree Rule of 9 Adults Infants Burn Coding
Presented by: Mike Strong, SFM The Work Comp Experts Agenda Wounds Debridement Evaluation and Management Services 2 1 Types of First Degree Second Degree Third Degree Rule of 9 Adults Infants Burn Coding
Negative Pressure Wound Therapy Overlay Technique With Collagen Dressings for Nonhealing Wounds
 J Wound Ostomy Continence Nurs. 2010;37(5):549-553. Published by Lippincott Williams & Wilkins CHALLENGES IN PRACTICE Negative Pressure Wound Therapy Overlay Technique With Collagen Dressings for Nonhealing
J Wound Ostomy Continence Nurs. 2010;37(5):549-553. Published by Lippincott Williams & Wilkins CHALLENGES IN PRACTICE Negative Pressure Wound Therapy Overlay Technique With Collagen Dressings for Nonhealing
Is noncontact normothermic wound therapy cost effective for the treatment of stages 3 and 4 pressure ulcers Macario A, Dexter F
 Is noncontact normothermic wound therapy cost effective for the treatment of stages 3 and 4 pressure ulcers Macario A, Dexter F Record Status This is a critical abstract of an economic evaluation that
Is noncontact normothermic wound therapy cost effective for the treatment of stages 3 and 4 pressure ulcers Macario A, Dexter F Record Status This is a critical abstract of an economic evaluation that
PRESSURE ULCERS SIMPLIFIED
 10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
10 PRESSURE ULCERS SIMPLIFIED This leaflet is intended to give you information and answers to some question you may have around pressure ulcers PRESSURE ULCERS SIMPLIFIED Pressure ulcer development has
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 7/1/2018 Section: DME Policy No: 377 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 10/13; 9/14: 9/15; 4/16 Medical Policy Committee Approved Date: 3/03;
Effective Date: 7/1/2018 Section: DME Policy No: 377 Medical Officer 7/1/18 Date Technology Assessment Committee Approved Date: 10/10; 10/13; 9/14: 9/15; 4/16 Medical Policy Committee Approved Date: 3/03;
DIABETES TEST STRIPS REIMBURSEMENT REDUCTIONS TO INDEPENDENT PHARMACIES WILL NEGATIVELY IMPACT MEDICARE PATIENTS
 DIABETES TEST STRIPS REIMBURSEMENT REDUCTIONS TO INDEPENDENT PHARMACIES WILL NEGATIVELY IMPACT MEDICARE PATIENTS NCPA Member Survey Results September 2012 CMS is considering cutting payments to pharmacies
DIABETES TEST STRIPS REIMBURSEMENT REDUCTIONS TO INDEPENDENT PHARMACIES WILL NEGATIVELY IMPACT MEDICARE PATIENTS NCPA Member Survey Results September 2012 CMS is considering cutting payments to pharmacies
Negative Pressure Wound Therapy Pumps
 Negative Pressure Wound Therapy Pumps Adopted from the National Government Services website. For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or The Health
Negative Pressure Wound Therapy Pumps Adopted from the National Government Services website. For any item to be covered by The Health Plan, it must: 1. Be eligible for a defined Medicare or The Health
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell
 Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
Uncovering the Pressure Ulcer Coverup Rhonda Kistler RN MS CWON Wound Care Concepts Gentell Objectives Identify the stages of pressure ulcer according to the depth of tissue destruction. Discuss the differences
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers
 A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
A Pilot Study of Oxygen Therapy for Acute Leg Ulcers Background: The concept of increasing the oxygen concentration in healing wounds developed originally with hyperbaric oxygen therapy and from the fact
Palliative Care. EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for. Treatment. Improving Quality of Care Based on CMS Guidelines 39
 Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Treatment EPUAP/NPUAP Publish New Pressure Ulcer Guidelines for Palliative Care Dealing with the end of a loved one s life is difficult enough, but when wound and skin care issues are involved, the decisions
Wound culture. (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center
 Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
Wound culture (Sampling methods) M. Rostami MSn.ICP Rajaei Heart Center Infection is a major impairment in delayed and nonhealing chronic wounds. Cultures of chronic wounds are not routinely performed
The VERSAJET II Hydrosurgery System
 Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
Precise Excision The VERSAJET II Hydrosurgery System The VERSAJET II Hydrosurgery System The VERSAJET II system enables a surgeon to precisely select, excise and evacuate nonviable tissue, bacteria and
PATIENT CARE MANUAL POLICY
 PATIENT CARE MANUAL POLICY NUMBER #VII-F-20 PAGE 1 OF 2 APPROVED BY: CATEGORY: Senior Vice President, Medicine and Chief of Staff; Vice President and Senior Operating Officer, Covenant Health, Rural Health
PATIENT CARE MANUAL POLICY NUMBER #VII-F-20 PAGE 1 OF 2 APPROVED BY: CATEGORY: Senior Vice President, Medicine and Chief of Staff; Vice President and Senior Operating Officer, Covenant Health, Rural Health
A A ~l~js AM f'ricj\n ACADBl\IY OF 0RTllOPAEDIC SURGEONS ~ J AMERICAN A SOCIATION OF ORTHOPAEDIC SURGEONS. Therapy billing for beginners
 Therapy billing for beginners http://www.aaos.org/news/aaosnow/nov10/managing1.asp 1 of 4 3/25/2014 2:56 PM A A ~l~js AM f'ricj\n ACADBl\IY OF 0RTllOPAEDIC SURGEONS ~ J AMERICAN A SOCIATION OF ORTHOPAEDIC
Therapy billing for beginners http://www.aaos.org/news/aaosnow/nov10/managing1.asp 1 of 4 3/25/2014 2:56 PM A A ~l~js AM f'ricj\n ACADBl\IY OF 0RTllOPAEDIC SURGEONS ~ J AMERICAN A SOCIATION OF ORTHOPAEDIC
Emerging Therapies. Laura E Edsberg PhD National Pressure Ulcer Advisory Panel
 Emerging Therapies Laura E Edsberg PhD Microclimate Local temperature and moisture at body/support surface interface Role in pressure ulcer etiology 2 1 Impact of Moisture Perspiration Drainage Incontinence
Emerging Therapies Laura E Edsberg PhD Microclimate Local temperature and moisture at body/support surface interface Role in pressure ulcer etiology 2 1 Impact of Moisture Perspiration Drainage Incontinence
Advanced Clinical Solutions. Pressure Ulcer. Carilex Medical Group 1
 Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
Advanced Clinical Solutions Pressure Ulcer Carilex Medical Group 1 Advanced Clinical Solutions Contents About Pressure Ulcer! 2 Stages of Pressure Ulcer! 5 Reference! 7 Carilex Medical Group 1 About Pressure
A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology
 A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology Farheen Walid, BA, Shrunjay R. Patel, BSc, Stephanie Wu, DPM, MS Center for Lower Extremity Ambulatory Research (CLEAR), Scholl College
A New Approach To Diabetic Foot Ulcers Using Keratin Gel Technology Farheen Walid, BA, Shrunjay R. Patel, BSc, Stephanie Wu, DPM, MS Center for Lower Extremity Ambulatory Research (CLEAR), Scholl College
PREVALENCE & INCIDENCE
 PREVALENCE & INCIDENCE Contents Prevalence.................................... 2 Point Prevalence...................................... 3 Period Prevalence..................................... 4 Incidence....................................
PREVALENCE & INCIDENCE Contents Prevalence.................................... 2 Point Prevalence...................................... 3 Period Prevalence..................................... 4 Incidence....................................
and Supplies Amended Date: November 1, 2016 Table of Contents
 Durable Medical Equipment and Supplies Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1... 1 1.2 Categories of... 1 2.0 Eligibility Requirements... 2 2.1 Provisions... 2
Durable Medical Equipment and Supplies Table of Contents 1.0 Description of the Procedure, Product, or Service... 1 1.1... 1 1.2 Categories of... 1 2.0 Eligibility Requirements... 2 2.1 Provisions... 2
Wound Assessment & Management
 Wound Assessment & Management Kim Krog, RN, BScN, CRN(C ) Contributors: Carol Thompson, RN, BScN, CRN(C ) Mary Scarlet, RN, BScN, CRN (C) Objectives Review: Anatomy and physiology of skin Enhance knowledge
Wound Assessment & Management Kim Krog, RN, BScN, CRN(C ) Contributors: Carol Thompson, RN, BScN, CRN(C ) Mary Scarlet, RN, BScN, CRN (C) Objectives Review: Anatomy and physiology of skin Enhance knowledge
Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types. Summary
 Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Dressing selection Agenda (45 minutes) Some questions for you. Which wound dressing? Dressing categories/types Summary Which wound dressing poster Ref: Which wound dressing? Practice Nursing, September
Clinical Policy Title: Vacuum assisted closure in surgical wounds
 Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Clinical Policy Title: Vacuum assisted closure in surgical wounds Clinical Policy Number: 17.03.00 Effective Date: September 1, 2015 Initial Review Date: June 16, 2013 Most Recent Review Date: August 17,
Managemen. Pressure Ulcer Prevention and Treatment. Guidance. Posture. Posture. Posture. Posture. Posture
 men menm Pressure Ulcer Prevention and Treatment Guidance Post ture Manag The reduction of the numbers of s is a high priority for Southern Health NHS Foundation Trust Purpose of this guidance is to help:
men menm Pressure Ulcer Prevention and Treatment Guidance Post ture Manag The reduction of the numbers of s is a high priority for Southern Health NHS Foundation Trust Purpose of this guidance is to help:
TOO MANY DRESSING CHOICES!!!! WOUND CARE MANAGEMENT AND PRODUCTS. Should Your Practice Dispense Wound Care Supplies? Pros:
 WOUND CARE MANAGEMENT AND PRODUCTS Animesh Bhatia DPM, CWS, FAPWCA Board Certified Wound Specialist Diplomate, American Academy of Wound Management Fellow, American Professional Wound Care Association
WOUND CARE MANAGEMENT AND PRODUCTS Animesh Bhatia DPM, CWS, FAPWCA Board Certified Wound Specialist Diplomate, American Academy of Wound Management Fellow, American Professional Wound Care Association
Managing Wounds. Esther White Tissue Viability Nurse
 Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
Managing Wounds Esther White Tissue Viability Nurse First things first.. Assess, measure and photograph Know what you re dealing with, look at anatomical position and the bigger picture to look for extra
2 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?)
 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Ann Rambusch, MSN, HCS D, HCS O, RN June 28, 2016 1 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Understanding NPUAP
Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Ann Rambusch, MSN, HCS D, HCS O, RN June 28, 2016 1 Pressure Ulcer or Pressure Injury? (Do you have skin in the game?) Understanding NPUAP
Lower Extremity Wound Evaluation and Treatment
 Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Lower Extremity Wound Evaluation and Treatment Boni-Jo Silbernagel, DPM Describe effective lower extremity wound evaluation and treatment. Discuss changes in theories of treatment in wound care and implications
Traditional Silicone Technology
 Innovative Non-Silicone Low Trauma Adhesives versus Traditional Silicone Technology A Review and Comparison Alan Neil Medical Industry Consultant Advanced Wound Care Lohmann Corporation 2016 Chronic wound
Innovative Non-Silicone Low Trauma Adhesives versus Traditional Silicone Technology A Review and Comparison Alan Neil Medical Industry Consultant Advanced Wound Care Lohmann Corporation 2016 Chronic wound
Dressings do not heal wounds properly selected dressings enhance the body s ability to heal the wound. Progression Towards Healing
 Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Dressings in Wound Care: They Do Matter John S. Steinberg, DPM FACFAS Associate Professor, Department of Plastic Surgery Georgetown University School of Medicine Dressings do not heal wounds properly selected
Wound Dressing. Choosing the Right Dressing
 Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Dressing Choosing the Right Dressing Benefits of using the correct Drsg Helps create the optimal wound environment Increases healing rates Reduces pain Decreases infection rates Cost effective Care
Wound Care for Hospice Patients
 Wound Care for Hospice Patients Kristen Lyn Brodrick, RN, BSN, CHPN,CWCN No financial disclosures. Unique Population Patients needing hospice/palliative care are often at risk for developing multiple skin
Wound Care for Hospice Patients Kristen Lyn Brodrick, RN, BSN, CHPN,CWCN No financial disclosures. Unique Population Patients needing hospice/palliative care are often at risk for developing multiple skin
The Shear Friction of pressure ulceration in aged care
 The Shear Friction of pressure ulceration in aged care Mr. Tal Ellis WoundHeal Australia, HWIG conference 2007 Introduction In Australia it is estimated that about 60,000 people have pressure ulcers (Porter&
The Shear Friction of pressure ulceration in aged care Mr. Tal Ellis WoundHeal Australia, HWIG conference 2007 Introduction In Australia it is estimated that about 60,000 people have pressure ulcers (Porter&
2. Advanced wound therapies... 4 (i) Maggots... 4 (ii) Negative Pressure Wound Therapy (NPWT)... 4
 Contents: Wound management Medicines Formulary 1. Interactive dressings... 2 (i) Hydrocolloid dressings... 2 (ii) Hydrogel dressings... 2 (iii) Alginate dressings... 2 (iv) Fibrous absorbent dressings...
Contents: Wound management Medicines Formulary 1. Interactive dressings... 2 (i) Hydrocolloid dressings... 2 (ii) Hydrogel dressings... 2 (iii) Alginate dressings... 2 (iv) Fibrous absorbent dressings...
THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant
 Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
Dysphagia THE POTENTIAL IMPACT OF VITALSTIM THERAPY ON HEALTHCARE COSTS: A White PaperVitalStim Therapy has significant Contents potential to dramatically impact the health care costs arising from oropharyngeal
The use of MEDIHONEY in Palliative Wound Care and the Advanced Aging Patient
 The use of MEDIHONEY in Palliative Wound Care and the Advanced Aging Patient Presenter: Angel Sutton, RN, MSN/Ed, CWCN, CFCN, CCCN Wound Care Nurse Consultant Click here to view detailed product descriptions
The use of MEDIHONEY in Palliative Wound Care and the Advanced Aging Patient Presenter: Angel Sutton, RN, MSN/Ed, CWCN, CFCN, CCCN Wound Care Nurse Consultant Click here to view detailed product descriptions
PRESSURE IQ EVOLVE NON-POWERED MATTRESS SOLUTION FOR THE PREVENTION AND TREATMENT OF STAGE I-IV PRESSURE ULCERS
 PRESSURE IQ EVOLVE NON-POWERED MATTRESS SOLUTION FOR THE PREVENTION AND TREATMENT OF STAGE I-IV PRESSURE ULCERS... with people in mind 10542_Arjo_EVOLVE_Brochurer_USA_215.9x279.4.indd 1 RAISING THE STANDARD
PRESSURE IQ EVOLVE NON-POWERED MATTRESS SOLUTION FOR THE PREVENTION AND TREATMENT OF STAGE I-IV PRESSURE ULCERS... with people in mind 10542_Arjo_EVOLVE_Brochurer_USA_215.9x279.4.indd 1 RAISING THE STANDARD
A film-dressing therapy [Open Wet-dressing Therapy (OWT)] for pressure ulcers. -a revolution of end of life care-
![A film-dressing therapy [Open Wet-dressing Therapy (OWT)] for pressure ulcers. -a revolution of end of life care- A film-dressing therapy [Open Wet-dressing Therapy (OWT)] for pressure ulcers. -a revolution of end of life care-](/thumbs/84/90807340.jpg) http://www.pressure-ulcer.net/ A film-dressing therapy [Open Wet-dressing Therapy (OWT)] for pressure ulcers. -a revolution of end of life care- Takeo SAIO (Fuji Toranomon Health Promotion Center) Shunichi
http://www.pressure-ulcer.net/ A film-dressing therapy [Open Wet-dressing Therapy (OWT)] for pressure ulcers. -a revolution of end of life care- Takeo SAIO (Fuji Toranomon Health Promotion Center) Shunichi
SLEEP SURFACES: INDICATIONS FOR USE (updated )
 SLEEP SURFACES: INDICATIONS FOR USE (updated 11.30.2016) TREATMENT LEVEL LOW NAME PHO IMAGE FEATURES WEIGHT LIMIT Low risk ambulatory patient. Multi-density foam for Group I 300 lbs pressure redistribution
SLEEP SURFACES: INDICATIONS FOR USE (updated 11.30.2016) TREATMENT LEVEL LOW NAME PHO IMAGE FEATURES WEIGHT LIMIT Low risk ambulatory patient. Multi-density foam for Group I 300 lbs pressure redistribution
HIGHLIGHTS OF THE 2017 PROPOSED MEDICARE PHYSICIAN FEE SCHEDULE RULE
 HIGHLIGHTS OF THE 2017 PROPOSED MEDICARE PHYSICIAN FEE SCHEDULE RULE July 13, 2016 INTRODUCTION The Medicare Physician Fee Schedule proposed rule released by the Centers for Medicare and Medicaid Services
HIGHLIGHTS OF THE 2017 PROPOSED MEDICARE PHYSICIAN FEE SCHEDULE RULE July 13, 2016 INTRODUCTION The Medicare Physician Fee Schedule proposed rule released by the Centers for Medicare and Medicaid Services
Pressure Ulcer Staging. Staging of Wounds are based on the deepest level of tissue damage
 Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Pressure Ulcer Staging Staging of Wounds are based on the deepest level of tissue damage Pressure Ulcer Staging New Pressure Ulcer Staging Stage I Stage II Stage III Stage IV Unstageable Suspected Deep
Skin Integrity and Wound Care
 Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Skin Integrity and Wound Care By Dr. Amer Hasanien & Dr. Ali Saleh Skin Integrity and Wound Care Skin integrity: the presence of normal Skin & Uninterrupted skin layers by wounds. Factors affecting appearance
Preventing Foot Ulcers in the Neuropathic Diabetic Foot. Glossary of Terms
 Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
Preventing Foot Ulcers in the Neuropathic Diabetic Foot Warren Woods, Certified Orthotist, Health Sciences Centre, Rehabilitation Engineering Department What you need to know Glossary of Terms Neuropathic
International Pressure Ulcer Guidelines Update Aamir Siddiqui, MD, FACS Division of Plastic Surgery Henry Ford Hospital Detroit MI
 International Pressure Ulcer Guidelines Update 2015 Aamir Siddiqui, MD, FACS Division of Plastic Surgery Henry Ford Hospital Detroit MI Disclosure Aamir Siddiqui has listed no financial interest/arrangement
International Pressure Ulcer Guidelines Update 2015 Aamir Siddiqui, MD, FACS Division of Plastic Surgery Henry Ford Hospital Detroit MI Disclosure Aamir Siddiqui has listed no financial interest/arrangement
The Use of the. in Clinical Practice
 The Use of the SNAP Therapy System in Clinical Practice It s an ultraportable, mechanically-powered disposable NPWT. By Animesh Bhatia, DPM, CWS This article is written exclusively for PM and appears courtesy
The Use of the SNAP Therapy System in Clinical Practice It s an ultraportable, mechanically-powered disposable NPWT. By Animesh Bhatia, DPM, CWS This article is written exclusively for PM and appears courtesy
Treatment options for diabetic neuropathic foot ulcers: a cost-effectiveness analysis Kantor J, Margolis D J
 Treatment options for diabetic neuropathic foot ulcers: a cost-effectiveness analysis Kantor J, Margolis D J Record Status This is a critical abstract of an economic evaluation that meets the criteria
Treatment options for diabetic neuropathic foot ulcers: a cost-effectiveness analysis Kantor J, Margolis D J Record Status This is a critical abstract of an economic evaluation that meets the criteria
Global Pulse Oximetry Project
 3.3 Introduction of new health technologies: lessons learned Over the past twenty years there have been a number of comprehensive public health projects which illustrate important lessons regarding the
3.3 Introduction of new health technologies: lessons learned Over the past twenty years there have been a number of comprehensive public health projects which illustrate important lessons regarding the
Water Works. The Value of Water
 Water Works The Value of Water The Value of Water Water Works Water is vital for the body Accounting for roughly 60% of body weight, water is the largest component of the human body and the major constituent
Water Works The Value of Water The Value of Water Water Works Water is vital for the body Accounting for roughly 60% of body weight, water is the largest component of the human body and the major constituent
Chapter 36 & 37. Types of wounds. Skin Tear
 Chapter 36 & 37 Wound Care and Pressure Ulcers Types of wounds A wound is a break in the skin d/t trauma, surgical incision, pressure sore, circulatory ulcers Abrasion, Contusion, Incision, Laceration,
Chapter 36 & 37 Wound Care and Pressure Ulcers Types of wounds A wound is a break in the skin d/t trauma, surgical incision, pressure sore, circulatory ulcers Abrasion, Contusion, Incision, Laceration,
Pressure Ulcers ecourse
 Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
Pressure Ulcers ecourse Module 4.1: Prevention of Pressure Ulcers Handout College of Licensed Practical Nurses of Alberta (Canada) CLPNA.com and StudywithCLPNA.com CLPNA Pressure Ulcers ecourse Module
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment.
 24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
24 Hour Positioning, Passive Movements, Shoulder pain, Splinting, Use of Assistive Technology, Early Mobilisation, and the Home Environment. Christine Hogg Physiotherapy Team Leader and Vicky Thomas Senior
Prevention and management of pressure ulcers
 The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
The Clatterbridge Cancer Centre NHS Foundation Trust Prevention and management of pressure ulcers Nursing A guide for patients and carers Contents What is a pressure ulcer?... 1 Who gets pressure ulcers?...
Update on Pressure Ulcers: Utilizing an Interdisciplinary Approach to Pressure Ulcer Prevention. Charlene A. Demers GNP-BC, CWOCN
 Update on Pressure Ulcers: Utilizing an Interdisciplinary Approach to Pressure Ulcer Prevention Charlene A. Demers GNP-BC, CWOCN Scope of the Issue Cost $9 billion to $11 billion $20,000-$150,000 per ulcer
Update on Pressure Ulcers: Utilizing an Interdisciplinary Approach to Pressure Ulcer Prevention Charlene A. Demers GNP-BC, CWOCN Scope of the Issue Cost $9 billion to $11 billion $20,000-$150,000 per ulcer
The Complex Rehab Technology Company. Focused on Providing Specialized Products and Related Services to People with Disabilities
 The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
The Complex Rehab Technology Company Focused on Providing Specialized Products and Related Services to People with Disabilities The Complex Rehab Technology Company What is Complex Rehab Technology and
V.A.C. Therapy Safety Information
 Bringing Safety Home V.A.C. Therapy Safety Information Bleeding Precautions Dressing Change Frequency Foam Removal Important Information 2 Prior to use of V.A.C. Therapy System it is important for the
Bringing Safety Home V.A.C. Therapy Safety Information Bleeding Precautions Dressing Change Frequency Foam Removal Important Information 2 Prior to use of V.A.C. Therapy System it is important for the
Vacuumed Assisted Closure
 Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
Vacuumed Assisted Closure Louise Morris Lead Nurse in Tissue Viability Jackie Stephen-Haynes Consultant Nurse and senior Lecturer in Tissue Viability 2009 Aims and Objectives To develop an awareness of
POLICIES AND PROCEDURE MANUAL
 POLICIES AND PROCEDURE MANUAL Policy: MP058 Section: Medical Benefit Policy Subject: Negative Pressure Wound Therapy I. Policy: Negative Pressure Wound Therapy II. Purpose/Objective: To provide a policy
POLICIES AND PROCEDURE MANUAL Policy: MP058 Section: Medical Benefit Policy Subject: Negative Pressure Wound Therapy I. Policy: Negative Pressure Wound Therapy II. Purpose/Objective: To provide a policy
Chronic Care. Coloplast Capital Market Day Jan Rolin Frederiksen, President Coloplast US. Coloplast Capital Market Day 2009
 Coloplast Capital Market Day 2009 Jan Rolin Frederiksen, President Coloplast US Page 1 Agenda Product Portfolio Ostomy Care Continence Care Wound and Skin Care Page 2 Portfolio covers four product-business
Coloplast Capital Market Day 2009 Jan Rolin Frederiksen, President Coloplast US Page 1 Agenda Product Portfolio Ostomy Care Continence Care Wound and Skin Care Page 2 Portfolio covers four product-business
Presented By: Jennifer Birt, OT Reg(MB) Specialized Seating & Mobility Clinical Specialist
 Presented By: Jennifer Birt, OT Reg(MB) Specialized Seating & Mobility Clinical Specialist 2013 1. Define and understand the concept of practical pressure management and categorizing individuals at different
Presented By: Jennifer Birt, OT Reg(MB) Specialized Seating & Mobility Clinical Specialist 2013 1. Define and understand the concept of practical pressure management and categorizing individuals at different
JAY J3 Cushion: Design Improvements for Enhanced Clinical Benefit
 A Sunrise Medical White Paper 7477 E. Dry Creek Parkway Longmont, CO 80503 www.sunrisemedical.com JAY J3 Cushion: Design Improvements for Enhanced Clinical Benefit By: JAY Design Team 5/7/2009 Contents
A Sunrise Medical White Paper 7477 E. Dry Creek Parkway Longmont, CO 80503 www.sunrisemedical.com JAY J3 Cushion: Design Improvements for Enhanced Clinical Benefit By: JAY Design Team 5/7/2009 Contents
7/2/2015 A.Shahrokhi 1
 7/2/2015 A.Shahrokhi 1 PRESSURE ULCER MANAGEMENT A.Shahrokhi,MSc Qazvin University of Medical Sciences 7/2/2015 A.Shahrokhi 3 Noticeable Facts Significant Prevalence 10% to 18% in acute care Cause of Death
7/2/2015 A.Shahrokhi 1 PRESSURE ULCER MANAGEMENT A.Shahrokhi,MSc Qazvin University of Medical Sciences 7/2/2015 A.Shahrokhi 3 Noticeable Facts Significant Prevalence 10% to 18% in acute care Cause of Death
PROTEX HEALTHCARE (UK) LIMITED PRODUCT QUESTIONS AND ANSWERS
 PROTEX HEALTHCARE (UK) LIMITED PRODUCT QUESTIONS AND ANSWERS Question What is Vacutex? How does Vacutex work? Does Vacutex prevent maceration to the surrounding skin? Does Vacutex adhere to the wound face?
PROTEX HEALTHCARE (UK) LIMITED PRODUCT QUESTIONS AND ANSWERS Question What is Vacutex? How does Vacutex work? Does Vacutex prevent maceration to the surrounding skin? Does Vacutex adhere to the wound face?
Pressure ulcer recognition and prevention. Mark Collier Tissue Viability Nurse Consultant United Lincoln Hospitals NHS Trust
 Pressure ulcer recognition and prevention Mark Collier Tissue Viability Nurse Consultant United Lincoln Hospitals NHS Trust PRESSURE ULCER RECOGNITION AND PREVENTION.. United Lincolnshire Hospitals NHS
Pressure ulcer recognition and prevention Mark Collier Tissue Viability Nurse Consultant United Lincoln Hospitals NHS Trust PRESSURE ULCER RECOGNITION AND PREVENTION.. United Lincolnshire Hospitals NHS
QUICK GUIDE SNAP THERAPY SYSTEM
 QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
QUICK GUIDE SNAP THERAPY SYSTEM Clinical Pathway to SNAP System Full holistic assessment of patient and wound Is the wound type indicated for NPWT use without contraindications 1? SNAP System is indicated
US Wound Dressing Market Size, Share, Growth, Industry Analysis, Competitive Strategies and Forescast to 2024 Hexa Research
 US Wound Dressing Market Size, Share, Growth, Industry Analysis, Competitive Strategies and Forescast to 2024 Hexa Research The U.S. wound dressing market size was valued at USD 3.18 billion in 2017. Increasing
US Wound Dressing Market Size, Share, Growth, Industry Analysis, Competitive Strategies and Forescast to 2024 Hexa Research The U.S. wound dressing market size was valued at USD 3.18 billion in 2017. Increasing
Simple, gentle and affordable. *smith&nephew V1STA Negative Pressure Wound Therapy
 Simple, gentle and affordable *smith&nephew V1STA Negative Pressure Wound Therapy Smith & Nephew s extensive presence and portfolio means that for every wound, at every stage, there is an appropriate solution.
Simple, gentle and affordable *smith&nephew V1STA Negative Pressure Wound Therapy Smith & Nephew s extensive presence and portfolio means that for every wound, at every stage, there is an appropriate solution.
Wound Care Program for Nursing Assistants-
 Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Wound Care Program for Nursing Assistants- Wound Cleansing,Types & Presentation Elizabeth DeFeo, RN, WCC, OMS, CWOCN Wound, Ostomy, & Continence Specialist ldefeo@cornerstonevna.org Outline/Agenda At completion
Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018
 Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018 Payment for Services Covered Services are reimbursed based on the Allowable Charge. Blue Cross
Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018 Payment for Services Covered Services are reimbursed based on the Allowable Charge. Blue Cross
Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018
 1 Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018 Payment for Services Covered Services are reimbursed based on the Allowable Charge. BlueCross
1 Schedule of Benefits Summary Group Name: Nebraska Bankers Association VEBA Effective Date: January 01, 2018 Payment for Services Covered Services are reimbursed based on the Allowable Charge. BlueCross
ד"ר בוריס פונצ' קי PRESSURE ULCERS
 ד"ר בוריס פונצ' קי 25.12.2013 PRESSURE ULCERS International EPUAP-NPUAP Pressure Ulcer Definition: (European Pressure Ulcer Advisory Panel and National Pressure Ulcer Advisory Panel, 2010).. is localized
ד"ר בוריס פונצ' קי 25.12.2013 PRESSURE ULCERS International EPUAP-NPUAP Pressure Ulcer Definition: (European Pressure Ulcer Advisory Panel and National Pressure Ulcer Advisory Panel, 2010).. is localized
