Health outcomes improve and costs are lower when care is consistent with evidence-based treatments. Optum Symmetry EBM Connect
|
|
|
- Osborne Allen
- 5 years ago
- Views:
Transcription
1 Denit Optum audist Symmetry aut eostisciam EBM Connect nime Health care organizations recognize the need to measure and improve health care quality. According to a 2013 report from the U.S. Department of Health and Human Services (HHS), the quality of health care in America is fair. In 2010, Americans received on average only 70 percent of indicated health care services with substantial variation across types of care, geographic regions and patient populations. 1 Although some improvements have been made in recent years, gaps continue to exist between best possible care and services routinely delivered. 1,2 The Commonwealth Fund s 2014 national health system report places the United States last overall when comparing 11 countries on indicators of efficiency, equity and outcomes. 2 Health information technology provides tremendous opportunities for improvement. 2,3,4 Health outcomes improve and costs are lower when care is consistent with evidence-based treatments. High-quality health care at an affordable cost is a priority in the United States. As health care costs approach one-fifth of the U.S. economy, evidence suggests a significant portion of costs do not result in better health. 3 There is a welldocumented gap between current medical knowledge and actual health care practice. 5,6,7 Across geographic regions, there is significant variation in the use of medical services without any evidence of improved outcomes. 8 Studies have shown that outcomes improve and costs are lower when care is consistent with evidencebased treatments. 9,10,11,12
2 Historically, quality measurement efforts in the United States faced considerable challenges. These challenges included agreement on standards to measure care, determination of valid and available sources of data to support measurement, and tools that use robust and adaptable measurement criteria to assess compliance. Today, the industry is addressing these challenges head-on. Several national organizations, including the American Medical Association Physician Consortium for Performance Improvement (PCPI), CMS (Centers for Medicare & Medicaid Services), and the National Committee for Quality Assurance (NCQA), have dedicated programs that target quality measure development. Further, many physician specialty organizations and state programs have focused resources on quality initiatives. Beyond measure development and maintenance, the National Quality Forum (NQF) plays a significant role defining standards for quality measurement and endorsing actionable measures supported by evidence-based literature. The information, data sources and technology needed to support measurement have improved. Multiple sources such as clinical trials, peer-reviewed literature, specialty organization guidelines, and specifications from national organizations define standards of care and support measure development efforts. 13 Administrative data medical and pharmacy claims and laboratory results have increased in both availability and comprehensiveness, providing a rich and convenient information source from which organizations can evaluate health care services and outcomes. In addition, sophisticated tools and technology that encode standards of care provide an efficient and robust way to measure compliance and identify potential gaps in care. Quality measurement challenges Agreements on standards to measure care Valid and available sources of data to support measurement Tools that use robust and adaptable measurement criteria to assess compliance This paper describes Symmetry EBM Connect, a powerful Optum product that uses administrative data and laboratory results to measure health care quality. EBM Connect software identifies gaps between clinical evidence and health care practice with application for a variety of health care organizations. It captures substantial information about quality care measurement and compares actual, observed member care with care supported by sources such as clinical trials and national guidelines. Organizations use these findings to: Identify care opportunities, including gaps in care for members and populations Identify high-performing physicians as well as those where compliance with prescribed care is low relative to peer comparison groups or national benchmarks Identify unnecessary or potentially harmful diagnostic tests and treatment Identify members with suboptimal disease control or low adherence to prescribed medication regimens Identify potentially harmful drug-to-drug or drug-to-disease interactions EBM Connect software is part of the Symmetry Suite of information products from Optum, including Episode Treatment Groups (ETG ), Procedure Episode Groups (PEG ), Episode Risk Groups (ERG ), Pharmacy Risk Groups (PRG ) and Procedure Quality Measures (PQM). These products support a wide array of business needs, leveraging a single methodological platform. EBM Connect identifies gaps between clinical evidence and health care practice. This common platform means organizations can apply industry-accepted measurement and assessment standards across a number of dimensions, including cost of care, health risk, and quality of care. EBM Connect software, when run in conjunction with its companion product, Symmetry ETG, supports direct comparisons of quality and cost outcomes for a wide array of clinical conditions. Page 2
3 With more than 600 measures covering many important clinical conditions (see Appendix for condition list), the EBM Connect product provides a solid foundation for quality measurement. Organizations can choose which measures to use depending on their populations of interest and unique quality measurement needs. The next section of this paper provides detail about EBM Connect measure development, maintenance, testing and validation. The final section describes the types of measures, product transparency, features, outputs and clinical application. EBM Connect The Symmetry EBM Connect software is an application that uses administrative data and laboratory results to identify members with selected clinical conditions or with needs for preventive health care. The software identifies these members using criteria such as gender, age, diagnoses and patient s duration of medical and pharmacy coverage. Once the appropriate set of members are identified, the EBM Connect product assesses each one s medical care by applying a series of clinical rule-based measures that define whether the member s care was consistent with clinical guidelines and recommendations. The EBM Connect measure development and maintenance process National standard specifications from organizations such as the Pharmacy Quality Alliance, CMS, and NCQA HEDIS are the primary source for many EBM Connect measures, with priority given to any measure endorsed by the National Quality Forum (NQF). In addition to these national standard measures, the EBM Connect software contains two other types of measures. One type is derived from national standards but is enhanced with additional logic for more robust measures. An example is a measure that uses additional data sources (e.g., pharmacy prescriptions) to complement a measure dependent solely on CPT II or HCPCS codes. The second type consists of quality measures and care opportunities supported by clinical evidence where no national standard exists. EBM Connect uses administrative data and laboratory results to identify members with selected clinical conditions or with needs for preventive health care. Although the measure development and maintenance process is similar for all types of measures, there are some important differences. For national standard measures, or measures based on these standards, Optum obtains specifications and codes from the measure steward. Codes are loaded and validated to confirm proper entry. For non-national standard measures, including national standards for which the logic or coding is enhanced, the measure development process begins with a comprehensive review of existing literature, which might include guidelines from specialty and professional organizations and clearinghouses, published clinical trials and other relevant articles, and pharmaceutical manufacturer s recommendations. The EBM Connect team identifies potential measures, including code sets where needed, based on the supporting literature and the ability to adequately assess care using available data. Measures not solely based on national standards go through a clinical review process. This process involves an EBM Connect clinical expert panel that reviews and discusses the most current treatment guidelines and proposed measures. The expert panel includes physicians, advanced degree pharmacologists, coding experts and analysts with quality measurement expertise. The physician experts for each particular clinical condition are board-certified in their primary subspecialty and are currently practicing, most with more than 20 years of clinical experience. They work in a variety of health care settings including federal and state government-funded facilities, academic centers and private practice. After measure logic and code sets are defined, one analyst builds the measures and creates user documentation while another analyst reviews the work. The entire EBM Connect team, including a medical director, conducts a final review to confirm the logic matches the intent of the clinical expert panel. Page 3
4 EBM Connect testing and validation All measures undergo a testing and validation process. The first stage of testing involves a small dataset designed specifically for the demographic and diagnostic criteria of the measures. This allows the team to confirm the logic works correctly. During the second stage of testing, measures are run through a larger dataset containing claims from approximately one million members. This testing verifies the measure logic functions properly with a larger, more representative data set, and that results align with national rates and benchmarks, when that data is available, and are clinically reasonable. The third stage of testing results in national benchmarks using a geographically diverse population with no less than 12 million commercial members. An EBM Connect medical director reviews all results during every phase of testing and national benchmark results are reviewed with EBM Connect clinical expert panel members. For non-national standard measures, a clinician on the team creates a synopsis that summarizes the evidence for the measure. The synopsis provides rationale for the measurement criteria, citations for supporting research and guidelines, and any available strength of evidence ratings. The logic and detailed code sets of diagnosis, procedure, pharmacy, laboratory and other codes used to construct the measures within the EBM Connect product are similarly transparent. All measures undergo a testing and validation process and are reviewed every months. After measures are added to the product, they undergo maintenance on a regular basis. Measures authored by Optum are reviewed every months. This includes ensuring the measures reflect current literature and guidelines and reviewing measures with the expert panel. For national standard measures, the EBM Connect team reviews any specification update to see if the measures warrant changes. If changes are made to the measures, the testing process previously outlined is repeated. Clinical measures and application EBM Connect measures have been developed for clinical conditions (cases) that represent chronic diseases, new diagnoses, acute or self-limited medical conditions, or prevention screening. EBM Connect logic defines specific inclusion criteria and benefit coverage requirements for each clinical condition. In particular, the member must meet appropriate age and gender criteria; have defined medical and, if necessary, pharmacy benefit coverage; and, where applicable, confirmation of the relevant medical condition during the specified time period. Equally important is use of exclusion criteria where appropriate to avoid measuring members with certain contraindications or comorbidities. EBM Connect software applies intervention measures for a given clinical condition to all members of the population who meet these criteria. For some members, measures are identified as not applicable if further measurespecific criteria are not met. The EBM Connect product includes three broad types of conditions chronic, acute/episodic, and preventive. Examples in the following sections demonstrate the process and logic for each. Page 4
5 Chronic conditions For each chronic condition, EBM Connect logic uses member age, gender, eligibility, condition confirmation criteria, and exclusion criteria (if applicable) to identify the set of members to be measured. EBM Connect software identifies members for a chronic condition based on information from claims data, including the diagnoses assigned and services provided. Although most EBM Connect chronic conditions identify members with a specific diagnosis (e.g., coronary artery disease, diabetes, depression), a diagnosis is not required for some conditions (e.g., identifying high-risk medications used in the elderly). Capturing all relevant indicators is essential, as the greater the number of relevant indicators, the more reliable the confirmation of the condition and assessment of appropriate care. 14 In addition, for members identified through a disease or care management program, users can submit this information through a Disease Registry Input File. EBM Connect logic identifies the set of members that qualify for measurement. Once EBM Connect logic identifies the appropriate set of members, compliance is assessed for every measure within each given condition. A result flag is generated for each measure by applying available member data to the logic that defines each measure. There are numerous possible results for each clinical measure, as outlined in Table 1.This information is used to determine measure compliance. In some cases, there is insufficient information to assess measure compliance (e.g., absence of pharmacy coverage). In these situations, EBM Connect output notes this result and the specific data limitation. Table 1: Measure compliance Result flag value Yes No NRX Description The answer to the clinical question is yes. The answer to the clinical question is no. Indicates that the member did not have any pharmacy benefit during the reporting period. The NRX value is only applicable to certain measures that are pharmacy dependent. Q NA1 NA2 NA3 NA4 NA5 NA6 NA7 Indicates that the member has no claim record for the particular test or treatment during the time window of the measure, but the member did not have coverage throughout the time window or there was insufficient time range of input claims data, and hence, there may be data incompleteness. The Q value is applied only for certain measures and certain setup configurations. Member did not meet the age or gender criteria. Member was not currently taking the medication in question or had not taken it for the required Member was taking the medication, but a possession ratio could not be computed [less than two prescriptions during the measure time window]. Member did not meet the measure specific criteria [e.g., comorbidity, complexity (diagnosis and medication), intervention not warranted]. No lab result record or insufficient information. Member admitted to a hospital or long-term care facility which might cause data incompleteness. Member who did not receive treatment or medication had a contraindication or other justification. Page 5
6 Acute/episodic conditions The second type of condition acute or episodic typically represents medical diagnoses or interventions that are new, self-limited, or reflect an acute exacerbation of a chronic condition. Unlike a chronic condition, the logic used to define an acute/ episodic condition is anchored around a point in time (e.g., date of a procedure or diagnosis). EBM Connect software can identify single or multiple acute/episodic conditions, depending on the intent of the measure. One example is acute low back pain (LBP), an NCQA measure 15 that evaluates care associated with a single episode of LBP. The LBP measure determines if a member with uncomplicated acute LBP had an imaging study 28 days after the initial back pain claim, care not typically recommended. Figure 1 illustrates the steps that identify and confirm acute LBP. Similar to chronic conditions, EBM Connect logic assesses inclusion and exclusion criteria and the customer defines a common report period end date, which is used to define the claims processing window. In this example, the common report period end date is December 31. The claim review begins 28 days earlier, since the measure logic requires a review of all claims 28 days after the LBP episode begins. EBM Connect software locates a claim dated September 15, and applies subsequent measure. Figure 1: Identification and confirmation of low back pain User-defined Common report period end date 12/31/20xx MAR APR MAY JUN JUL AUG SEP OCT NOV DEC JAN Build event 3 Event start Set at 180 days before episode start: 3/19 Clear Window Patient selection: Patient age: at end date Patient gender: either Episode-specific coverage: continuous medical coverage through event (3/19-10/13) Patient exclusion: 1. Unclear window: Patient had claim of low back pain (HEDIS ) in 180 days prior to episode start (3/19-9/15) 2. Clinically appropriate: Imaging indicating recent trauma, intravenous drug abuse or neurological impairment 2 Episode start Date of earliest claim for low back pain: 9/15 4 Event end Set at 28 days after episode start: 10/13 1 Claim review Begins 28 days before end date: 12/3 Members with exclusion criteria, suggesting more complex causes or complications associated with their back pain (e.g., claims for cancer, drug abuse or neurological impairment), are removed from the LBP case. Since LBP can be a chronic problem, EBM Connect logic takes additional steps to ensure the recent episode of LBP is an acute, discrete event. For example, it searches for claims of LBP during the 180 days prior to the episode start. If no claims are identified, then the member satisfies the logic and likely the LBP is an acute event. Final logic is applied to determine measure compliance. Page 6
7 In addition to the single event approach used with LBP, EBM Connect logic can evaluate multiple distinct acute/episodic events. This approach is useful for conditions like acute sinusitis where identification of discrete recurrent events is possible and there is a desire to evaluate each separate event (e.g., use of an antibiotic). Preventive conditions Preventive conditions include screening for disease and immunizations. EBM Connect software uses different member selection criteria for preventive conditions than for chronic or acute/episodic conditions in that it includes all members meeting demographic criteria, not only those with claims, in the analysis. For example, the breast cancer screening condition identifies a screening mammogram among women of a specific age group. EBM Connect logic identifies females within a specific age range and searches for a breast cancer screening diagnosis or procedure during the prior 27 months. Exclusion criteria remove members for whom screening is unnecessary (e.g., bilateral mastectomy). Application and use of measures Output from EBM Connect software can support analysis at a payer, physician or member level. Reports of measure compliance can identify gaps in care, care opportunities, and changes associated with specific interventions. Measurement is a key step to focus resources and drive quality improvement efforts. The EBM Connect product provides the critical information needed to support a variety of measurement programs. At the payer level, reports identify the best opportunities for quality and cost improvement by highlighting areas of lowest measure compliance. Specific reports: Provide the prevalence of disease among the plan membership Reveal opportunities for intervention by identifying the rate of missed opportunities for care or insufficient compliance with care for each medical condition Health care organizations are continually challenged to identify ways to improve the quality of care delivered by physicians to members and populations. Evidence suggests that, on average, it takes 17 years for physicians to implement clinical research results in daily practice. 16 Payers who wish to improve compliance with evidence-based medicine require innovative ways to identify physicians who are not yet implementing or not yet aware of clinical developments. Physicians desire information about their quality measure performance and efficient identification of their patients with gaps in care or new medical problems. Results from EBM Connect software provide a powerful foundation to support these needs. EBM Connect Helps health care organizations identify high quality physicians Helps physicians gather information on their performance Identifies patients with gaps in care or new medical problems At the member level, the EBM Connect product can help case managers identify care opportunities, detect low medication adherence, and provide invaluable insight for member education. EBM Connect output indicates compliance or noncompliance with a clinical measure by a specific member with a specific condition. The EBM Connect software offers configuration options to override default coverage requirements. This feature can be used to increase the number of members identified with a condition. The software provides information to indicate when an apparent gap in a member s care could be the result of insufficient coverage during the measurement time period. Although the EBM Connect software is typically used to evaluate care provided in the past (retrospective measurement), customers can perform prospective measurement. With prospective measurement, the software is run with a customer identified end date that is in the future, or beyond the last date of the input claims. EBM Connect Page 7
8 logic modifies member eligibility for prospective measurement when appropriate to check that members have adequate eligibility during the prospective period. This allows customers to predict potential gaps in care as of the prospective end date. Customers can choose to run EBM Connect software in the traditional retrospective fashion only, prospective only, or both. As with the retrospective approach, customers can select which conditions, or cases, to run prospectively. Prospective measurement can be a powerful tool to identify members that could benefit from outreach, whether for care management or efforts to improve HEDIS reporting scores. Typically, clients use measure non-compliance to guide outreach to members who have gaps in care. However, clients may also have interest in compliant members to better understand when the services were last received. To this end, EBM Connect provides an output file, the Date of Last Service file, that provides the date a member last received a recommended service. These services align with many EBM Connect measures that evaluate if recommended care is given. Organizations can use information from the Date of Last Service file to individualize member notifications to remind members when services are next due. This file can support health plan, provider group, and care management programs designed to maximize quality reporting for national measure programs such as Medicare Stars. The Date of Last Service file can be used to individualize member notifications to remind members when services are next due. Physician attribution Often, it is important to assign a responsible physician(s) to a specific member when using data to examine care outcomes or find areas for improvement. The EBM Connect software identifies key data associated with member care, allowing customers to apply physician attribution algorithms tailored to their needs. Table 2 summarizes the EBM Connect methods implemented to support this objective. The output generated by these methods is not strictly limited to physicians but can include other health professionals such as nurse practitioners and physician assistants. Table 2: Supporting physician attribution components Component General Primary care provider (medical & gynecologic) A progressive multi-step process that identifies the physician or other health care provider who is serving as the primary care provider for a member. Medical imputation logic is applied to all members; gynecologic imputation is also performed for female members 12 years of age and older. Treating physician attribution A process that identifies all physicians involved in the care of a member s confirmed condition, as evidenced by a relevant diagnosis or procedure. Key data is computed for each treating physician, including number of visits, first and last visit date, and sum of visit costs. Treating physician identification is not performed for member preventive screenings and select chronic and episodic conditions Physician visits Logic that identifies for each member all physician visits in the 12 months preceding the report period end date. Visits include doctor office visits; evaluation and management (E&M) visits that occur in nursing homes, rest homes and other facilities; visits to outpatient facilities such as freestanding clinics and urgent care; and home visits. Key data is computed for each identified physician, including number of visits, first and last visit date and sum of visit costs. Physician visit logic is executed for all members regardless of enrollment and condition criteria. Page 8
9 EBM Connect output The EBM Connect product provides insight into members disease states, treatment intensity and adherence to treatment guidelines through various outputs. Users can link the output using common variables to produce data that meet their individual interests and requirements. Primary EBM Connect output includes essential information about members compliance with treatment guidelines. Additional outputs address aspects of health status or patient care, such as an unduplicated list of each member s clinical conditions, a list of all physicians who participated in the care of each member (by condition), and a list of all members identified as having each EBM Connect condition. Other output enables the user to drill down to the claims-level data, supporting the ability to audit results and understand findings. Summary statistics report the prevalence of patients identified with a particular condition and the observed compliance rate for each condition and measure. Summary Concerns about health care quality, safety and cost drive the need to measure, compare and improve health care performance. Research continues to point to major gaps between current medical knowledge and actual health care practice. Meanwhile, the U.S. health care system is the most expensive in the world, while it continues to underperform in many areas compared to other countries. A tremendous opportunity exists to improve clinical outcomes, decrease health care costs and positively impact member health and quality of life by improving compliance with evidence-based medicine and other standards. Valid and actionable approaches to measurement are critical to improve health care. Health care organizations can only make progress where they identify improvement opportunities, develop interventions to target those opportunities and gauge success using accurate metrics. EBM Connect software supports this process by efficiently using health care data to assess compliance to a robust set of quality measures. EBM Connect combines measures based on extensive clinical review and research findings with national standard measures offering a flexible, comprehensive information platform for health care quality measurement The EBM Connect product combines measures based on extensive clinical review and research findings with national standard measures to offer a flexible, comprehensive information platform for health care quality measurement. Results can identify key insights into performance and identify specific quality improvement opportunities at the member, physician and population level. Complete transparency around the methods and evidence basis for each measure promotes understanding by all stakeholders and actionable steps for improvement. Sources: 1. U.S. Department of Health and Human Services Agency for Healthcare Research and Quality National Healthcare Quality Report. AHRQ Publication No May Davis K, Stremikis K, Squires D, and Schoen C. Mirror, Mirror on the Wall: How the Performance of the U.S. Health Care System Compares Internationally, 2014 Update (New York:The Commonwealth Fund, June 2014). 3. President s Council of Advisors on Science and Technology. Report to the President Better Health Care and Lower Costs: Accelerating Improvements Through Systems Engineer- ing. The White House, May Virga PH, Jin B, Thomas J, Virodov S. Electronic health information technology as a tool for improving quality of care and health outcomes for HIV/AIDS patients. Int J Med Inform 2012;81(10):e39-e Crossing the Quality Chasm: A New Health System for the 21st Century. Institute of Medicine, Committee on Quality of Health Care in America. Academy Press, Institute of Medicine Committee on Quality of Health Care in America. To Err is Human: Building a Safer Health System. The National Academies Press; McGlynn EA, Asch SM, Adams J, Keesey J, Hicks J, DeCristofaro A, Kerr EA. The Quality of Health Care Delivered to Adults in the United States. N Engl J Med. 2003;348: Wennberg John E and Cooper MM, eds. The Dartmouth Atlas of Health Care in the United States. Chicago: American Hospital Publishing, Inc., Page 9
10 9 Diring Khan J. Non-compliance with proven treatments increases healthcare costs. Managed Healthcare Executive Osterberg L and Blaschke T. Adherence to medication. N Engl J Med. 2005;353: Ho PM, Bryson CL, Rumsfeld JS. Medication Adherence: its importance in cardiovascular outcomes. Circulation 2009;119(23): Roebuck MC, Liberman JN, Gemmill-Toyama M, Brennan TA. Medication adherence leads to lower health care use and costs despite increased drug spending. Health Aff 2011;30(1): Examples of these organizations include the National Committee for Quality Assurance, American Medical Association, Centers for Medicare & Medicaid Services, and commercial and academic entities. 14. Kerr EA, Hofer TP, Hayward RA, Adams JL, Hogan MM, McGlynn EA, and Asch SM. Quality by Any Other Name?: A Comparison of Three Profiling Systems for Assessing Health Quality. Health Services Research. 15. National Committee for Quality Assurance, Standards and Guidelines for the Certification of Physician and Hospital Quality, Washington, D.C.: National Committee for Quality Assurance, Balas EA, Boren SA. Managing Clinical Knowledge for Health Care Improvement.Yearbook of Medical Informatics 2000: Patient-centered Systems. Stuttgart, Germany: Schattauer, 2000: Appendix Conditions and screenings included in Symmetry EBM Connect 9.2 ADHD, Follow-Up Care for Children Prescribed ADHD Medication Adherence to Antipsychotic Medications for individuals with Schizophrenia Adolescent Well-Care Visits Adult BMI Assessment Adults' Access to Preventive/Ambulatory Health Services Annual Dental Visit Annual Monitoring for Patients on Persistent Medications Antidepressant Medication Management (National Antipsychotic Use in Persons with Dementia (National Asthma Asthma in Younger Adults: Hospitalization (National Asthma Medication Ratio Atrial Fibrillation Atrial Fibrillation and Atrial Flutter: Chronic Anticoagulation Therapy Bacterial Pneumonia: Hospitalization Body Mass Index (BMI) Screening and Follow-Up Breast Cancer Part 1 Breast Cancer Part 2 Breast Cancer Screening Bronchitis, Acute, Avoidance of Antibiotic Treatment in Adults Cardiac Surgery Cardiovascular Monitoring for People With Cardiovascular Disease and Schizophrenia Care for Older Adults Conditions and screenings included in Symmetry EBM Connect 9.2 Cerebral Vascular Accident & Transient Cerebral Ischemia Part 1 Cerebral Vascular Accident & Transient Cerebral Ischemia Part 2 Cerebral Vascular Accident & Transient Cerebral Ischemia Part 3 Cerebral Vascular Accident & Transient Cerebral Ischemia Part 4 Cervical Cancer Screening Cervical Dysplasia Childhood Immunizations Children and Adolescents' Access to Primary Care Practitioners Chlamydia Screening Chronic Kidney Disease Chronic Obstructive Pulmonary Disease Part 1 Chronic Obstructive Pulmonary Disease Part 2 Chronic Obstructive Pulmonary Disease (COPD) or Asthma in Older Adults: Hospitalization Colon Cancer Part 1 Colon Cancer Part 2 Colon Cancer Surveillance Colorectal Cancer Screening Congestive Heart Failure Controlling High Blood Pressure COPD Exacerbation, Pharmacotherapy Management COPD, Use of Spirometry Testing in Assessment and Diagnosis Coronary Artery Disease Coronary Artery Disease ACE and ARB Coronary Artery Disease (CAD): Antiplatelet Therapy Page 10
11 Conditions and screenings included in Symmetry EBM Connect 9.2 Dehydration: Hospitalization Depression Developmental Screening in the First Three Years of Life Diabetes (Biguanide-Containing Medication) Part D Medication Adherence Diabetes [Dipeptidyl-peptidase (DPP)-4-Containing Medication)] Part D Medication Adherence (National Diabetes (Sulfonylurea-Containing Medication) Part D Medication Adherence Diabetes (Thiazolidinedione-Containing Medication) Part D Medication Adherence Diabetes Care Extended Condition Confirmation Diabetes Care Diabetes Medications-Part D Medication Adherence Diabetes Mellitus Diabetes Mellitus: Diabetic Foot and Ankle Care, Ulcer Prevention Evaluation of Footwear Diabetes Monitoring for People With Diabetes and Schizophrenia Diabetes Screening for People With Schizophrenia or Bipolar Disorder Who Are Using Antipsychotic Medications Diabetes, Lower-extremity Amputation: Hospitalization Diabetes: Hospitalization Diabetic Retinopathy: Communication with the Physician Managing Ongoing Diabetes Care Disease-Modifying Anti-Rheumatic Drug Therapy for Rheumatoid Arthritis Drug Interactions Emergency Medicine Epilepsy Follow-Up After Emergency Department Visit for Alcohol and Other Drug Dependence Follow-Up After Emergency Department Visit for Mental Illness Heart Failure ACE and Acceptable Alternatives Heart Failure: Hospitalization Heart Failure: Hospital Discharge Heart Failure: Outpatient Setting Hepatitis C Conditions and screenings included in Symmetry EBM Connect 9.2 Hepatitis C: Screening for Hepatocellular Carcinoma (HCC) in Patients with Cirrhosis HIV/AIDS Hospice Indicator Hospitalization for Potentially Preventable Complications Part 1 Hospitalization for Potentially Preventable Complications Part 2 Hyperlipidemia Hypertension Hypertension: Hospitalization Immunizations for Adolescents Inflammatory Bowel Disease Inflammatory Bowel Disease (IBD) Influenza Immunization Influenza Immunization Initiation and Engagement of Alcohol and Other Drug Dependence Treatment Ischemic Vascular Disease (IVD): Use of Aspirin or Another Antithrombotic Lead Screening in Children Low Back Pain, Use of Imaging Studies Medication Management for People With Asthma (National Medication Reconciliation Post-Discharge (National Mental Illness, Follow-Up After Hospitalization (National Metabolic Monitoring for Children and Adolescents on Antipsychotics Migraine Headache Monitoring of Persistent Medicationsw Multiple Sclerosis Non-Recommended Cervical Cancer Screening in Adolescent Females Non-Recommended PSA-Based Screening in Older Men Obesity and Overweight Oncology: Medical and Radiation Pain Intensity Quantified One-Time Screening for Hepatitis C Virus (HCV) for Patients at Risk Optimal Diabetes Care Page 11
12 Conditions and screenings included in Symmetry EBM Connect 9.2 Osteoporosis Management Osteoporosis Management in Women Who Had a Fracture Osteoporosis Screening or Therapy in Women 65 Years and Older Otitis Externa, Acute Otitis Media, Acute Persistence of Beta-Blocker Treatment after a Heart Attack Pharyngitis, Appropriate Testing for Children (National Plan All-Cause Readmissions Part 1 Plan All-Cause Readmissions Part 2 Pneumonia Vaccination Status for Older Adults (National Pneumonia, Community-Acquired Bacterial (CAP) Post-fracture Care Potentially Harmful Drug-Disease Interactions in the Elderly Pregnancy Management Prenatal and Postpartum Care Prostate Cancer Prostate Cancer: Adjuvant Hormonal Therapy for High Risk or Very High Risk Prostate Cancer Renin Angiotensin System (RAS) Antagonists Part D Medication Adherence Conditions and screenings included in Symmetry EBM Connect 9.2 Rheumatoid Arthritis Sickle Cell Anemia Sinusitis, Acute Statin Therapy for Patients with Cardiovascular Disease Statin Therapy for Patients with Diabetes Statins Part D Medication Adherence Tobacco Use: Screening and Cessation Intervention Tonsillectomy Upper Respiratory Infection (URI), Appropriate Treatment for Children Urinary Tract Infection: Hospitalization Use of First-Line Psychosocial Care for Children and Adolescents on Antipsychotics Use of High-Risk Medications in the Elderly (National Use of High-Risk Medications in the Elderly Part D Use of Multiple Concurrent Antipsychotics in Children and Adolescents Weight Assessment and Counseling for Children/ Adolescents Well-Child Visits in the First 15 Months of Life (National Well-Child Visits in the Third, Fourth, Fifth and Sixth Years of Life Optum Circle, Eden Prairie, MN Optum is a registered trademark of Optum, Inc. in the U.S. and other jurisdictions. All other brand or product names are the property of their respective owners. Because we are continuously improving our products and services, Optum reserves the right to change specifications without prior notice. Optum is an equal opportunity employer Optum, Inc. All rights reserved. WF /17
2018 MIPS Reporting Family Medicine
 2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
2018 MIPS Reporting Family Medicine Quality Reporting Requirements: Report on 6 quality measures or a specialty measure set Include at least ONE outcome or high-priority measure Report on patients of All-Payers
SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES
 Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
Summary Table of Measures, Product Lines and Changes 1 SUMMARY TABLE OF MEASURES, PRODUCT LINES AND CHANGES General Guidelines for Data Collection and Reporting Guidelines for Calculations and Sampling
SUMMARY TABLE OF MEASURE CHANGES
 Summary Table of Measure 1 SUMMARY TABLE OF MEASURE CHANGES Guidelines for Physician Measurement Adult BMI Assessment Weight Assessment and Counseling for Nutrition and Physical Activity for Children/Adolescents
Summary Table of Measure 1 SUMMARY TABLE OF MEASURE CHANGES Guidelines for Physician Measurement Adult BMI Assessment Weight Assessment and Counseling for Nutrition and Physical Activity for Children/Adolescents
Changes for Physician Measurement 2018
 Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
Changes for Physician Measurement 2018 Measure Name Guidelines for Physician Measurement Effectiveness of Care Changes Revised the Systematic Sampling Methodology to require organizations to report using
th Street, NW Suite 1000 Washington, DC phone fax
 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Accreditation & Measures Policy DATE: May 15 2017 (Updated on October 18, 2017) RE: Measures for Accreditation Scoring in 2018
TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Accreditation & Measures Policy DATE: May 15 2017 (Updated on October 18, 2017) RE: Measures for Accreditation Scoring in 2018
2017 HEDIS Measures. PREVENTIVE SCREENING 2017 Measure Quality Indicator
 PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
PREVENTIVE SCREENING Childhood Immunization Children who turn 2 during the Adolescent Immunization Adolescents who turn 13 during the Lead Screening Children who turn 2 during the Breast Cancer Screening
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region December 2013 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
Commercial HMO/POS Effectiveness of Care Measure
 Commercial HMO/POS Effectiveness of Care Measure HEDIS 2017 NCQA Quality Compass National Average Adult BMI Assessment 91.85% 76.17% Weight Assessment and Counseling for Nutrition and Physical Activity
Commercial HMO/POS Effectiveness of Care Measure HEDIS 2017 NCQA Quality Compass National Average Adult BMI Assessment 91.85% 76.17% Weight Assessment and Counseling for Nutrition and Physical Activity
2016 PQRS Recommended Measures for: General/Family Practice
 Measures Groups Choose 1 Measures Group Report on a minimum of 20 eligible patients (at least 11 must be Medicare Part B FFS patients) #130: Documentation of Current Medications in the Medical Record #204:
Measures Groups Choose 1 Measures Group Report on a minimum of 20 eligible patients (at least 11 must be Medicare Part B FFS patients) #130: Documentation of Current Medications in the Medical Record #204:
2018 Commercial HMO/POS HEDIS 1 Results
 08 Commercial HMO/POS HEDIS Results Weight Assessment & Counseling for Nutrition & Physical Activity for Children/Adolescents HEDIS 06 CY 05 HEDIS 07 CY 06 HEDIS 08 CY 07 Compass BMI Percentile 70.47%
08 Commercial HMO/POS HEDIS Results Weight Assessment & Counseling for Nutrition & Physical Activity for Children/Adolescents HEDIS 06 CY 05 HEDIS 07 CY 06 HEDIS 08 CY 07 Compass BMI Percentile 70.47%
MEASURING CARE QUALITY
 MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
MEASURING CARE QUALITY Region November 2016 For Clinical Effectiveness of Care Measures of Performance From: Healthcare Effectiveness Data and Information Set (HEDIS ) HEDIS is a set of standardized performance
th Street, NW Suite 1000 Washington, DC phone fax
 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Accreditation & Measures Policy DATE: September 19, 2016 RE: Measures for Accreditation Scoring in 2017 This communication gives
TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Accreditation & Measures Policy DATE: September 19, 2016 RE: Measures for Accreditation Scoring in 2017 This communication gives
NCQA Health Insurance Plan Ratings Methodology October 2014
 NCQA Health Insurance Plan Ratings Methodology October 2014 REVISION CHART Date Published December 2013 April 2014 October 2014 Description Draft version Final version Updated measure list with 50% rule
NCQA Health Insurance Plan Ratings Methodology October 2014 REVISION CHART Date Published December 2013 April 2014 October 2014 Description Draft version Final version Updated measure list with 50% rule
Overview of Current Quality Measures that can be Impacted by Ambulatory Pharmacists
 Overview of Current Quality Measures that can be Impacted by Ambulatory Pharmacists Measure Name Measure Domain Measure Focus Comment/Explanation CMS Value-based Purchasing Program (CMS VBP) AMI 30-day
Overview of Current Quality Measures that can be Impacted by Ambulatory Pharmacists Measure Name Measure Domain Measure Focus Comment/Explanation CMS Value-based Purchasing Program (CMS VBP) AMI 30-day
Appendix 4: Summary of Recommended Changes to HEDIS/CAHPS Measure List
 Appendix 4: HEDIS/CAHPS List 1 Appendix 4: Summary of Recommended Changes to HEDIS/CAHPS List Add the following new measures for the commercial, Medicare and Medicaid product lines. Please refer to the
Appendix 4: HEDIS/CAHPS List 1 Appendix 4: Summary of Recommended Changes to HEDIS/CAHPS List Add the following new measures for the commercial, Medicare and Medicaid product lines. Please refer to the
The BlueCompare SM Physician Designation Program
 The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
The BlueCompare SM Physician Designation Program Continuing escalation of health care costs has driven premiums and medical expenses to higher and higher levels each year, motivating employers and consumers
Quality measures desktop reference for Medicaid providers
 Quality measures desktop reference for Medicaid providers providers.amerigroup.com Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance
Quality measures desktop reference for Medicaid providers providers.amerigroup.com Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance
B&T Format. New Measures. 2 CAHPS is a registered trademark of the Agency for Healthcare Research and Quality (AHRQ).
 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February 4, 2018 RE: 2018 Accreditation Benchmarks and Thresholds This document reports national benchmarks and
TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February 4, 2018 RE: 2018 Accreditation Benchmarks and Thresholds This document reports national benchmarks and
Quality measures desktop reference for Medicaid providers
 Quality measures desktop reference for Medicaid providers providers.amerigroup.com Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance
Quality measures desktop reference for Medicaid providers providers.amerigroup.com Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance
2016 Internal Medicine Preferred Specialty Measure Set
 1 0059 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the measurement period 5 0081 Registry, EHR, 9 0105
1 0059 Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients 18-75 years of age with diabetes who had hemoglobin A1c > 9.0% during the measurement period 5 0081 Registry, EHR, 9 0105
Quality measures desktop reference for Medicaid providers
 Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance given by the National Committee for Quality Assurance (NCQA), the Centers for
Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance given by the National Committee for Quality Assurance (NCQA), the Centers for
2015 PQRS Registry. Source Measure Title Measure Description CITIUS1
 1 CQ-IQ covers 65 CMS defined measures that Eligible Providers (EPs) have to report on to assess quality of care provided to the patients. Version Supported: PQRS Registry 2015 65 measures Reporting Period:
1 CQ-IQ covers 65 CMS defined measures that Eligible Providers (EPs) have to report on to assess quality of care provided to the patients. Version Supported: PQRS Registry 2015 65 measures Reporting Period:
2016 General Practice/Family Practice Preferred Specialty Measure Set
 1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
1 0059 5 0081 41 N/A 50 N/A 65 0069, EHR 66 0002, EHR Effective Clinical Care Effective Clinical Care Effective Clinical Care Diabetes: Hemoglobin A1c (HbA1c) Poor Control (>9%): Percentage of patients
B&T Format. New Measures. Better health care. Better choices. Better health.
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 13,
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 13,
Preferred Care Partners. HEDIS Technical Standards
 Preferred Care Partners HEDIS Technical Standards 1 HEDIS What is HEDIS HEDIS Overview Adults HEDIS Overview Pediatrics HEDIS is a registered trademark of the National Committee for Quality Assurance 2
Preferred Care Partners HEDIS Technical Standards 1 HEDIS What is HEDIS HEDIS Overview Adults HEDIS Overview Pediatrics HEDIS is a registered trademark of the National Committee for Quality Assurance 2
B&T Format. New Measures. Better health care. Better choices. Better health.
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: February
proposed set to a required subset of 3 to 5 measures based on the availability of electronic
 CMS-0033-P 143 proposed set to a required subset of 3 to 5 measures based on the availability of electronic measure specifications and comments received. We propose to require for 2011 and 2012 that EP's
CMS-0033-P 143 proposed set to a required subset of 3 to 5 measures based on the availability of electronic measure specifications and comments received. We propose to require for 2011 and 2012 that EP's
Meaningful Use Overview
 Eligibility Providers may be eligible for incentives from either Medicare or Medicaid, but not both. In addition, providers may not be hospital based. Medicare: A Medicare Eligible Professional (EP) is
Eligibility Providers may be eligible for incentives from either Medicare or Medicaid, but not both. In addition, providers may not be hospital based. Medicare: A Medicare Eligible Professional (EP) is
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights
 Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
Advances in Alignment, Measurement, and Performance MY 2017 Results Highlights Align. Measure. Perform. (AMP) Programs Launched in 2003, VBP4P is a statewide performance improvement program and one of
Certified Health IT Transparency and Disclosure Information 2014 Edition
 Certified Health IT Transparency and Disclosure Information 2014 Edition 2015 Edition Certified Health IT Transparency and Disclosure Information I. Disclaimer This Complete EHR is 2014 Edition compliant
Certified Health IT Transparency and Disclosure Information 2014 Edition 2015 Edition Certified Health IT Transparency and Disclosure Information I. Disclaimer This Complete EHR is 2014 Edition compliant
Quality measures a for measurement year 2016
 Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Quality measures a for measurement year 2016 Measure Description Eligible members Childhood immunizations b Adolescent immunizations b Children who turned 2 during the measurement and who were identified
Consensus Core Set: ACO and PCMH / Primary Care Measures Version 1.0
 Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Consensus Core Set: ACO and PCMH / Primary Care s 0018 Controlling High Blood Pressure patients 18 to 85 years of age who had a diagnosis of hypertension (HTN) and whose blood pressure (BP) was adequately
Improving Quality of Care for Medicare Patients: Accountable Care Organizations
 DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
DEPARTMENT OF HEALTH & HUMAN SERVICES Centers for Medicare & Medicaid Services Room 352-G 200 Independence Avenue, SW Washington, DC 20201 Office of Media Affairs MEDICARE FACT SHEET FOR IMMEDIATE RELEASE
QUALITY IMPROVEMENT Section 9
 Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
Quality Improvement Program The Plan s Quality Improvement Program serves to improve the health of its members through emphasis on health maintenance, education, diagnostic testing and treatment. The Quality
How pharmacy and retail health can support health and wellness. Nancy Gagliano Chief Medical Officer, MC September, 2014
 How pharmacy and retail health can support health and wellness Nancy Gagliano Chief Medical Officer, MC September, 2014 2 An important decision for public health Current Health Care Challenges The State
How pharmacy and retail health can support health and wellness Nancy Gagliano Chief Medical Officer, MC September, 2014 2 An important decision for public health Current Health Care Challenges The State
STARS SYSTEM 5 CATEGORIES
 TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
TMG STARS 2018 1 2 STARS Program Implemented in 2008 by CMS. Tool to inform beneficiaries of quality of various health plans 5-star rating system Used to adjust payments to health plans (bonus to plans
Jan Feb Mar Apr May Jun Jul Aug Sep X X X X X X X. Jan Feb Mar Apr May Jun Jul Aug Sep Oct Nov X X X X X X X X X X X X X
 Primary Prevention Breast Cancer Prevention Member: Mammography reminder letters to female members ages 51.5-74 who are overdue to get a mammogram Jan Feb Mar Apr May Jun Jul Aug Sep Oct Nov Providers:
Primary Prevention Breast Cancer Prevention Member: Mammography reminder letters to female members ages 51.5-74 who are overdue to get a mammogram Jan Feb Mar Apr May Jun Jul Aug Sep Oct Nov Providers:
Quality measures desktop reference for Medicaid providers
 Quality measures desktop reference for Medicaid providers Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance given by the National
Quality measures desktop reference for Medicaid providers Please note: The information provided is based on 2016 technical specifications and is subject to change based on guidance given by the National
Meaningful Use Simple Guide
 Meaningful Use Simple Guide 2011-2012 CORE Measures 1. CPOE for Medication Orders 2. Drug Interaction Checks * 3. Maintain Problem & Diagnosis List 4. eprescribing (erx) escripts 5. Active Medication List
Meaningful Use Simple Guide 2011-2012 CORE Measures 1. CPOE for Medication Orders 2. Drug Interaction Checks * 3. Maintain Problem & Diagnosis List 4. eprescribing (erx) escripts 5. Active Medication List
Adult HEDIS & STARs Measures
 HEDIS AND MEDICARE STAR DOCUMENTATION & CODING GUIDE Adult HEDIS & STARs Measures Adult BMI Assessment (ABA) 18 74-year-old Antidepressant Medication Management (AMM) Breast Cancer Screening (BCS) Cervical
HEDIS AND MEDICARE STAR DOCUMENTATION & CODING GUIDE Adult HEDIS & STARs Measures Adult BMI Assessment (ABA) 18 74-year-old Antidepressant Medication Management (AMM) Breast Cancer Screening (BCS) Cervical
QUALITY RATING SYSTEM: BACKGROUND
 QUALITY RATING SYSTEM: BACKGROUND Federally-required quality rating system Originally required for 2017, FFM delayed until 2018 in most states 5 states displaying QRS for 2017 2 FFM pilot states + CA,
QUALITY RATING SYSTEM: BACKGROUND Federally-required quality rating system Originally required for 2017, FFM delayed until 2018 in most states 5 states displaying QRS for 2017 2 FFM pilot states + CA,
NQF Measure Number & PQRI Implementation Number
 Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
Title NQF Steward s Adult Weight Screening and Follow-Up Hypertension: Blood Pressure ment Preventive Care and Screening Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention with a calculated
Condition/Procedure Measure Compliance Criteria Reference Attribution Method
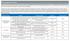 Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
Premium Specialty: Cardiology Credentialed Specialties include: Cardiac Diagnostic, Cardiology, Cardiovascular Disease, Clinical Cardiac Electrophysiology, and Interventional Cardiology This document is
MU - Selection & Configuration of Measures
 MU - Selection & Configuration of Measures Presenter: Christy Erickson October 14, 2011 Objectives Review the 15 Core Measures and highlight some findings from the field Discuss the MU Menu and Clinical
MU - Selection & Configuration of Measures Presenter: Christy Erickson October 14, 2011 Objectives Review the 15 Core Measures and highlight some findings from the field Discuss the MU Menu and Clinical
HEALTHCARE REFORM. September 2012
 HEALTHCARE REFORM Accountable Care Organizations: ACOs 101 September 2012 The enclosed slides are intended to provide you with a general overview of accountable care organizations (ACOs), created within
HEALTHCARE REFORM Accountable Care Organizations: ACOs 101 September 2012 The enclosed slides are intended to provide you with a general overview of accountable care organizations (ACOs), created within
TN Bundled Payment Initiative: Overview of Episode Risk Adjustment
 TN Bundled Payment Initiative: Overview of Episode Risk Adjustment United Healthcare, April 2014 The State of Tennessee has implemented an episode-based approach to reimburse providers for the care delivered
TN Bundled Payment Initiative: Overview of Episode Risk Adjustment United Healthcare, April 2014 The State of Tennessee has implemented an episode-based approach to reimburse providers for the care delivered
Colorado State Innovation Model (SIM) Clinical Quality Measures (CQMs) Reporting Schedules
 Colorado State Innovation Model (SIM) Clinical Quality Measures (CQMs) Reporting Schedules 1 SIM Clinical Quality Measure (CQM) Reporting Schedules: Cohort 3 Table of Contents Reporting Schedules... 3
Colorado State Innovation Model (SIM) Clinical Quality Measures (CQMs) Reporting Schedules 1 SIM Clinical Quality Measure (CQM) Reporting Schedules: Cohort 3 Table of Contents Reporting Schedules... 3
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual
 Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Arkansas Blue Cross and Blue Shield (ABCBS) Patient Centered Medical Home (PCMH) Specifications Manual 2017 This document is a guide to the 2017 Arkansas Blue Cross and Blue Shield Patient-Centered Medical
Modified Stage 2 Meaningful Use: Clinical Quality Measures (CQMs) Massachusetts Medicaid EHR Incentive Payment Program
 Modified Stage 2 Meaningful Use: Clinical Quality Measures (CQMs) Massachusetts Medicaid EHR Incentive Payment Program July 21, 2016 Today s presenter: Al Wroblewski, PCMH CCE, Client Services Relationship
Modified Stage 2 Meaningful Use: Clinical Quality Measures (CQMs) Massachusetts Medicaid EHR Incentive Payment Program July 21, 2016 Today s presenter: Al Wroblewski, PCMH CCE, Client Services Relationship
Submitted to the House Energy and Commerce Committee. Federal Efforts to Combat the Opioid Crisis
 STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
HEDIS/CAHPS 101 August 13, 2012 Minnesota Measurement and Reporting Workgroup
 HEDIS/CAHPS 101 Minnesota Measurement and Reporting Workgroup MNsure s Accessibility & Equal Opportunity (AEO) office can provide this information in accessible formats for individuals with disabilities.
HEDIS/CAHPS 101 Minnesota Measurement and Reporting Workgroup MNsure s Accessibility & Equal Opportunity (AEO) office can provide this information in accessible formats for individuals with disabilities.
Trending Determinations by Measure
 1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Parties FROM: Cindy Ottone, Director, Policy DATE: March 2019 RE: HEDIS 1 2019 Measure
1100 13th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org TO: Interested Parties FROM: Cindy Ottone, Director, Policy DATE: March 2019 RE: HEDIS 1 2019 Measure
HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING
 HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING ATTENTION-DEFICIT/HYPERACTIVITY DISORDER 1. Follow-up Care for Children Prescribed ADHD Medication (ADD) Percent children newly
HEDIS 2017 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING ATTENTION-DEFICIT/HYPERACTIVITY DISORDER 1. Follow-up Care for Children Prescribed ADHD Medication (ADD) Percent children newly
PCMH 2018 Enrollment and Update August 25, 2017
 PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
PCMH 2018 Enrollment and Update August 25, 2017 Enrollment Requirements Anne Santifer HealthCare Innovations Department of Human Services 2018 Enrollment Requirements A physician practice that is enrolled
CY 2017 MMA Performance Measure Scores HEDIS, Core Set, and Agency-defined measures
 Aetna Better Health Amerigroup Better Health Children's Medical Services Adherence to Antipsychotic Medications for Individuals with Schizophrenia 50% 60% 57% N/A 45% Adolescent Well Care Visits 62% 64%
Aetna Better Health Amerigroup Better Health Children's Medical Services Adherence to Antipsychotic Medications for Individuals with Schizophrenia 50% 60% 57% N/A 45% Adolescent Well Care Visits 62% 64%
Symmetry Episode Treatment Groups
 Symmetry Episode Treatment Groups Measuring Health Care with Meaningful Episodes of Care The information in this document is subject to change without notice. This documentation contains proprietary information,
Symmetry Episode Treatment Groups Measuring Health Care with Meaningful Episodes of Care The information in this document is subject to change without notice. This documentation contains proprietary information,
NCQA Health Insurance Plan Ratings Methodology March 2018
 00 3th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org NCQA Health Insurance Plan Ratings Methodology March 208 Better health care. Better choices. Better health.
00 3th Street NW, Third Floor Washington, DC 20005 phone 202.955.3500 fax 202.955.3599 www.ncqa.org NCQA Health Insurance Plan Ratings Methodology March 208 Better health care. Better choices. Better health.
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO
 The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
The table below includes the quality measures an ACO is required to submit to CMS as a participant in an MSSP Track 3 ACO ACO-1 ACO-2 Getting Timely Care, Appointments, and Information How Well Your Providers
PENNSYLVANIA MEDICAID AND MEDICARE Explanation of HEDIS Measures
 Each year, NCQA (National Committee for Quality Assurance) publishes HEDIS (Healthcare Effectiveness Data and Information Set), a set of standardized performance measures used in the managed care industry
Each year, NCQA (National Committee for Quality Assurance) publishes HEDIS (Healthcare Effectiveness Data and Information Set), a set of standardized performance measures used in the managed care industry
OCHSNER PHYSICIAN PARTNERS. PQRS Measures by Specialty (FINAL)
 OCHSNER PHYSICIAN PARTNERS PQRS Measures by Specialty (FINAL) Allergy and Immunology 2. Asthma: Pharmacologic Therapy for Persistent Asthma - Ambulatory Care Setting (PQRS 53) 3. Patients aged 18 years
OCHSNER PHYSICIAN PARTNERS PQRS Measures by Specialty (FINAL) Allergy and Immunology 2. Asthma: Pharmacologic Therapy for Persistent Asthma - Ambulatory Care Setting (PQRS 53) 3. Patients aged 18 years
COMMUNITY HEALTH GROUP HEDIS MEASURES (CY 2012) MEDICARE QUICK REFERENCE GUIDE FOR BILLING DEPARTMENT
 HEDIS MEASURES (CY ) MEDICARE QUICK REFERENCE GUIDE FOR BILLING DEPARTMENT Care for Older Adults Colorectal Cancer Screening Annual Monitoring for Patients on Persistent Medications COA COL MPM Age Description
HEDIS MEASURES (CY ) MEDICARE QUICK REFERENCE GUIDE FOR BILLING DEPARTMENT Care for Older Adults Colorectal Cancer Screening Annual Monitoring for Patients on Persistent Medications COA COL MPM Age Description
Care1st Health Plan Taking Quality to the Next Level REPORTING YEAR HEDIS Summary - MPL (Measurement Year 2012)
 Care1st Health Plan s Quality Improvement Department has been diligently working towards improving the Healthcare Effectiveness Data and Information Sets (HEDIS) results across all lines of business. HEDIS
Care1st Health Plan s Quality Improvement Department has been diligently working towards improving the Healthcare Effectiveness Data and Information Sets (HEDIS) results across all lines of business. HEDIS
Provider Perspective of Quality Measurement
 Provider Perspective of Quality Measurement The American Medical Group Association supports its members in enhancing population health and care for patients through integrated systems of care Improve
Provider Perspective of Quality Measurement The American Medical Group Association supports its members in enhancing population health and care for patients through integrated systems of care Improve
Clinical Quality Measures for Submission by Medicare or Medicaid EP/s for the 2011 and 2012 Payment Year
 1 NQF 0059 1 NQF 0064 2 NQF 0061 3 Title: Diabetes: Hemoglobin A1c Poor Control Description: Percentage of patients 18-75 years of age with diabetes (type 1 or type 2) who had hemoglobin A1c > 9.0%. Title:
1 NQF 0059 1 NQF 0064 2 NQF 0061 3 Title: Diabetes: Hemoglobin A1c Poor Control Description: Percentage of patients 18-75 years of age with diabetes (type 1 or type 2) who had hemoglobin A1c > 9.0%. Title:
Symmetry Episode Treatment Groups
 Symmetry Episode Treatment Groups Measuring health care with meaningful episodes of care Identifying clinical episodes of illness and the services involved in their diagnosis, management, and treatment
Symmetry Episode Treatment Groups Measuring health care with meaningful episodes of care Identifying clinical episodes of illness and the services involved in their diagnosis, management, and treatment
NCQA did not add new measures to Accreditation 2017 scoring.
 2017 Accreditation Benchmarks and Thresholds 1 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 2, 2017 RE: 2017 Accreditation Benchmarks and Thresholds
2017 Accreditation Benchmarks and Thresholds 1 TO: Interested Organizations FROM: Patrick Dahill, Assistant Vice President, Policy DATE: August 2, 2017 RE: 2017 Accreditation Benchmarks and Thresholds
Meaningful Use Clinical Quality Measures for Eligible Professionals
 Meaningful Use Clinical Quality Measures for Eligible Professionals Measure Type NQF ID CMS ID Description Title: Adult Weight Screening and Follow-Up 1 NQF 0421 PQRI 128 calculated BMI in the past six
Meaningful Use Clinical Quality Measures for Eligible Professionals Measure Type NQF ID CMS ID Description Title: Adult Weight Screening and Follow-Up 1 NQF 0421 PQRI 128 calculated BMI in the past six
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At Easy Choice, we
Disease Management. Measures At A Glance
 s At A Glance Updated: 11/2/2017 Page 1 of 7 Cross Cutting Mandatory s (4) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual
s At A Glance Updated: 11/2/2017 Page 1 of 7 Cross Cutting Mandatory s (4) Note: Mandatory measures are those measures that are a requirement of accreditation and must be reported to URAC on an annual
Fifth Annual National ACO Summit
 Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
Fifth Annual National ACO Summit June 18 20, 2014 Follow us on Twitter at @ACO_LN and use #ACOsummit The Engelberg Center for Health Care Reform at Brookings The Dartmouth Institute Track One: Performance
2017 Performance Recognition Program PROVIDER INCENTIVE PROGRAM FOR: BCN HMO SM Commercial BCN Advantage SM Blue Cross Medicare Plus Blue SM PPO
 Confidence comes with every card. 2017 Performance Recognition Program PROVIDER INCENTIVE PROGRAM FOR: BCN HMO SM Commercial BCN Advantage SM Blue Cross Medicare Plus Blue SM PPO Revised October 2017 CONTENTS
Confidence comes with every card. 2017 Performance Recognition Program PROVIDER INCENTIVE PROGRAM FOR: BCN HMO SM Commercial BCN Advantage SM Blue Cross Medicare Plus Blue SM PPO Revised October 2017 CONTENTS
LRE Executive Dashboard Integrated Care Delivery Platform (ICDP)
 Data in Report As Of: 2/17/2018 LRE Executive Dashboard Integrated Care Delivery Platform (ICDP) Key Performance Indicators (KPIs) Report Created by: Paige Horton LAKESHORE REGIONAL ENTITY Performance
Data in Report As Of: 2/17/2018 LRE Executive Dashboard Integrated Care Delivery Platform (ICDP) Key Performance Indicators (KPIs) Report Created by: Paige Horton LAKESHORE REGIONAL ENTITY Performance
Comprehensive ESRD Care (CEC) Model Proposed Quality Measures for Public Comment. Table of Contents
 Comprehensive ESRD Care (CEC) Model Proposed Quality s for Public Comment Table of Contents Page # Introduction 3 Summaries by Domain Technical Expert Panel Recommended CEC Quality s 4 s that were recommended
Comprehensive ESRD Care (CEC) Model Proposed Quality s for Public Comment Table of Contents Page # Introduction 3 Summaries by Domain Technical Expert Panel Recommended CEC Quality s 4 s that were recommended
PHPG. Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions
 PHPG The Pacific Health Policy Group Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions Prepared for: State of Oklahoma Oklahoma Health Care Authority April
PHPG The Pacific Health Policy Group Utilization and Expenditure Analysis for Dually Eligible SoonerCare Members with Chronic Conditions Prepared for: State of Oklahoma Oklahoma Health Care Authority April
HEDIS 2014 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING
 HEDIS 2014 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING DIABETES 1. Comprehensive Diabetes Care (CDC): Percentage of members 18-75 years of age with diabetes (type 1 and type 2) who had
HEDIS 2014 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING DIABETES 1. Comprehensive Diabetes Care (CDC): Percentage of members 18-75 years of age with diabetes (type 1 and type 2) who had
HealtheCNY Indicator List by Data Source
 American Community Survey 23 Adults with Health Insurance Children Living Below Poverty Level Children with Health Insurance Families Living Below Poverty Level Homeowner Vacancy Rate Homeownership Households
American Community Survey 23 Adults with Health Insurance Children Living Below Poverty Level Children with Health Insurance Families Living Below Poverty Level Homeowner Vacancy Rate Homeownership Households
2014 Clinical Quality Measures: Changes for the Medicaid EHR Incentive Program. Tracy McDonald Medicaid EHR Incentive Program Coordinator
 2014 Clinical Quality Measures: Changes for the Medicaid EHR Incentive Program Tracy McDonald Medicaid EHR Incentive Program Coordinator Agenda Why are Clinical Quality Measures important? Clinical Quality
2014 Clinical Quality Measures: Changes for the Medicaid EHR Incentive Program Tracy McDonald Medicaid EHR Incentive Program Coordinator Agenda Why are Clinical Quality Measures important? Clinical Quality
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 4 Episodes Attention deficit hyperactivity disorder (ADHD); Opposition defiance disorder (ODD); Coronary artery bypass
HEDIS 2016 results are in for our Anthem PPO and Anthem HealthKeepers products
 HEDIS 2016 results are in for our Anthem PPO and Anthem HealthKeepers products Anthem Blue Cross and Blue Shield thanks you for participating in the annual Healthcare Effectiveness Data and Information
HEDIS 2016 results are in for our Anthem PPO and Anthem HealthKeepers products Anthem Blue Cross and Blue Shield thanks you for participating in the annual Healthcare Effectiveness Data and Information
HEDIS 2015 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING
 HEDIS 2015 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING DIABETES 1. Comprehensive Diabetes Care (CDC): Percentage of members 18-75 years of age with diabetes (type 1 and type 2) who had
HEDIS 2015 MQIC MEASURES SUMMARY LISTING FOR ANNUAL PERFORMANCE REPORTING DIABETES 1. Comprehensive Diabetes Care (CDC): Percentage of members 18-75 years of age with diabetes (type 1 and type 2) who had
Audit Review Table Parkland Community Health Plan (Org ID: 19735, SubID: 11065, Medicaid, Spec Area: None, Spec Proj: None, Contract Number: None)
 Audit Review Table Parkland Community Health Plan (Org ID: 19735, SubID: 11065, Medicaid, Spec Area: one, Spec Proj: one, Contract umber: one) Measurement ear - 2017; Date & Timestamp - 6/27/2018 2:54:19
Audit Review Table Parkland Community Health Plan (Org ID: 19735, SubID: 11065, Medicaid, Spec Area: one, Spec Proj: one, Contract umber: one) Measurement ear - 2017; Date & Timestamp - 6/27/2018 2:54:19
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications
 HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
HEDIS Quick Reference Guide Updated to reflect NCQA HEDIS 2016 Technical Specifications Fidelis SecureCare strives to provide quality healthcare to our membership as measured through HEDIS quality metrics.
Capital Health Plan CMS Star Ratings Strategies for Improvement
 Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
Capital Health Plan CMS Star Ratings Strategies for Improvement ESTRELLITA REDMON, MD, MBA MEDICAL DIRECTOR The Ultimate Goal Outline Current 5 Star Plans CHP History Importance of Ratings Part C and Part
Evaluasi Mutu Pelayanan Kesehatan dalam Managed Care. Evaluating Quality of Healthcare Providers in Managed Care
 Evaluasi Mutu Pelayanan Kesehatan dalam Managed Care Evaluating Quality of Healthcare Providers in Managed Care Pokok bahasan Review indikator-indikator yang digunakan di negara lain Bagaimana dengan indikator-indikator
Evaluasi Mutu Pelayanan Kesehatan dalam Managed Care Evaluating Quality of Healthcare Providers in Managed Care Pokok bahasan Review indikator-indikator yang digunakan di negara lain Bagaimana dengan indikator-indikator
TN Bundled Payment Initiative: Overview of Episode Risk Adjustment
 TN Bundled Payment Initiative: Overview of Episode Risk Adjustment Amerigroup, April 2014 The State of Tennessee has implemented an episode-based approach to reimburse providers for the care delivered
TN Bundled Payment Initiative: Overview of Episode Risk Adjustment Amerigroup, April 2014 The State of Tennessee has implemented an episode-based approach to reimburse providers for the care delivered
HEDIS/QARR 2018 Quick Reference Guide ALL MEASURES
 2018 HEDIS Codes HEDIS/QARR 2018 Quick Reference Guide ALL MEASURES Code Age Band Denominator Event Numerator Requirement ADL AAB AAP ABA ADV Adolescent Preventive Care Avoidance of Antibiotic in Adults
2018 HEDIS Codes HEDIS/QARR 2018 Quick Reference Guide ALL MEASURES Code Age Band Denominator Event Numerator Requirement ADL AAB AAP ABA ADV Adolescent Preventive Care Avoidance of Antibiotic in Adults
Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings
 CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
CMS-1345-P 174 Table 1. Proposed Measures for Use in Establishing Quality Performance Standards that ACOs Must Meet for Shared Savings AIM: Better Care for Individuals 1. Patient/Care Giver Experience
Audit Review Table Parkland Community Health Plan (Org ID: 19735, SubID: 11066, Medicaid, Spec Area: None, Spec Proj: SCHIP, Contract Number: None)
 Audit Review Table Parkland Community Health Plan (Org ID: 19735, SubID: 11066, Medicaid, Spec Area: one, Spec Proj: SCHIP, Contract umber: one) Measurement ear - 2017; Date & Timestamp - 6/27/2018 2:55:12
Audit Review Table Parkland Community Health Plan (Org ID: 19735, SubID: 11066, Medicaid, Spec Area: one, Spec Proj: SCHIP, Contract umber: one) Measurement ear - 2017; Date & Timestamp - 6/27/2018 2:55:12
Star Measures At-A-Glance Guide
 Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
Star Measures At-A-Glance Guide This guide alerts you to important preventive care and services that you can provide to patients to help boost Star Ratings. ASSESSMENT AND SCREENING At WellCare, we value
Affordability AMGA - MIPS Webinar
 Affordability AMGA - MIPS Webinar Beth Averbeck, MD Senior Medical Director Primary Care, HealthPartners Consumer-governed, non-profit HealthPartners Medical Group Primary Care: 500,000 patients 29 locations
Affordability AMGA - MIPS Webinar Beth Averbeck, MD Senior Medical Director Primary Care, HealthPartners Consumer-governed, non-profit HealthPartners Medical Group Primary Care: 500,000 patients 29 locations
Multi-Specialty Quality Measure Information Sheet 2017
 Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
Prevention and Screening Adolescent Preventive Care Measures (APC) The percentage of adolescents 12-17 years of age who had at least one outpatient visit with a PCP or OB/ GYN practitioner during the measurement
MIPS: Quality Direct EHR Manual for Aprima Users
 MIPS: Quality Direct EHR Manual for Aprima Users CONTENTS QUALITY INTRODUCTION... 5 CMS 2: SCREENING FOR CLINICAL DEPRESSION AND FOLLOWUP PLAN....6 CMS 22: SCREENING FOR HIGH BLOOD PRESSURE AND FOLLOWUP
MIPS: Quality Direct EHR Manual for Aprima Users CONTENTS QUALITY INTRODUCTION... 5 CMS 2: SCREENING FOR CLINICAL DEPRESSION AND FOLLOWUP PLAN....6 CMS 22: SCREENING FOR HIGH BLOOD PRESSURE AND FOLLOWUP
For Electronic Measure Specification Information go to:
 Diabetes Recognition NQF 0421 PQRI 128 Title: Adult Weight Screening and Follow-Up Description: Percentage of patients aged 18 years and older with a calculated BMI in the past six months or during the
Diabetes Recognition NQF 0421 PQRI 128 Title: Adult Weight Screening and Follow-Up Description: Percentage of patients aged 18 years and older with a calculated BMI in the past six months or during the
Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper
 Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper For Health Care Professionals February 2016 Introduction... 2 Cigna Physician Quality and Cost-Efficiency
Cigna Care Designation and Physician Quality and Cost-Efficiency Displays 2016 Methodologies Whitepaper For Health Care Professionals February 2016 Introduction... 2 Cigna Physician Quality and Cost-Efficiency
WHO WE ARE WHAT WE DO
 WHO WE ARE In Virginia, the major community partners engaged in health reform -- health care providers, health systems, health plans, pharmaceutical manufacturers and laboratory companies, employers, consumers,
WHO WE ARE In Virginia, the major community partners engaged in health reform -- health care providers, health systems, health plans, pharmaceutical manufacturers and laboratory companies, employers, consumers,
Patient-Centered Primary Care Scorecard Measures
 Patient-Centered Primary Care Scorecard Measures Acute and Chronic Care Management Measures Medication Adherence Proportion of Days Covered (PDC): Oral Diabetes Identifies patients with at least two prescriptions
Patient-Centered Primary Care Scorecard Measures Acute and Chronic Care Management Measures Medication Adherence Proportion of Days Covered (PDC): Oral Diabetes Identifies patients with at least two prescriptions
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes
 TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
TENNCARE Bundled Payment Initiative: Description of Bundle Risk Adjustment for Wave 5 Episodes Mastectomy, Breast Cancer Medical Oncology, Breast Biopsy, Tonsillectomy, Otitis media, Anxiety, Non-emergent
Clinical Quality Measures
 Core Measures Preventive Care and Screening Measure Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention. Percentage of patients aged 18 years and older who have been seen for at least 2
Core Measures Preventive Care and Screening Measure Pair: a. Tobacco Use Assessment, b. Tobacco Cessation Intervention. Percentage of patients aged 18 years and older who have been seen for at least 2
Total Health Quality Indicators For Providers 2018
 Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2018 Adult- Preventive Z00.00 Report ALL components of an annual visit
Well Adult Well Visit 20 yrs > Yearly 99385-87, 99395-97, G0402, G0438, G0439, G0463 Total Health Quality Indicators For Providers 2018 Adult- Preventive Z00.00 Report ALL components of an annual visit
NCC Pediatrics Continuity Clinic Curriculum: Medical Home Module 2 Well Visits
 NCC Pediatrics Continuity Clinic Curriculum: Medical Home Module 2 Well Visits Overall Goal: To identify strategies for providing comprehensive care during a well visit. The provision of comprehensive
NCC Pediatrics Continuity Clinic Curriculum: Medical Home Module 2 Well Visits Overall Goal: To identify strategies for providing comprehensive care during a well visit. The provision of comprehensive
