Impact of cholinesterase inhibitors on behavioral and psychological symptoms of Alzheimer s disease: A meta-analysis
|
|
|
- Valerie Dorothy Burns
- 5 years ago
- Views:
Transcription
1 ORIGINAL RESEARCH Impact of cholinesterase inhibitors on behavioral and psychological symptoms of Alzheimer s disease: A meta-analysis Noll Campbell 1 Amir Ayub 2 Malaz A Boustani 2 Chris Fox 3 Martin Farlow 4 Ian Maidment 3 Robert Howard 5 1 Wishard Health Services, Indianapolis, Indiana; 2 Indiana University Center for Aging Research, Regenstrief Institute, Inc., Indianapolis, Indiana; 3 University of Kent, Kent, United Kingdom; 4 Indiana University School of Medicine, Indianapolis, Indiana; 5 King s College, London, United Kingdom Objective: To determine the efficacy of cholinesterase inhibitors (ChEIs) in improving the behavioral and psychological symptoms of dementia (BPSD) in patients with Alzheimer s disease (AD). Data sources: We searched MEDLINE, Cochrane Registry, and the Cumulative Index to Nursing and Allied Health Literature (CINAHL) from 1966 to We limited our search to English Language, full text, published articles and human studies. Data extraction: We included randomized, double-blind, placebo-controlled trials evaluating the efficacy of donepezil, rivastigmine, or galantamine in managing BPSD displayed by AD patients. Using the United States Preventive Services Task Force (USPSTF) guidelines, we critically appraised all studies and included only those with an attrition rate of less than 40%, concealed measurement of the outcomes, and intention to treat analysis of the collected data. All data were imputed into pre-defined evidence based tables and were pooled using the Review Manager software for data synthesis. Results: We found 12 studies that met our inclusion criteria but only nine of them provided sufficient data for the meta-analysis. Among patients with mild to severe AD and in comparison to placebo, ChEIs as a class had a beneficial effects on reducing BPSD with a standard mean difference (SMD) of 0.10 (95% confidence interval [CI]; 0.18, 0.01) and a weighted mean difference (WMD) of 1.38 neuropsychiatry inventory point (95% CI; 2.30, 0.46). In studies with mild AD patients, the WMD was 1.92 (95% CI; 3.18, 0.66); and in studies with severe AD patients, the WMD was 0.06 (95% CI; 2.12, +0.57). Conclusion: Cholinesterase inhibitors lead to a statistical significant reduction in BPSD among patients with AD, yet the clinical relevance of this effect remains unclear. Keywords: Alzheimer s disease, dementia, cholinesterase inhibitors, behavioral and psychological symptoms Correspondence: Malaz A Boustani Regenstrief Institute, Inc., 410 West 10th Street, Suite 2000, Indianapolis, IN , USA Tel Fax mboustani@regenstrief.org Introduction The noncognitive behavioral and psychological symptoms of dementia (BPSD) displayed by patients suffering from Alzheimer disease (AD) include a heterogeneous spectrum of psychological reactions, psychiatric symptoms, and behaviors (Finkel et al 2000). More than 90% of AD patients will experience at least one BPSD at some point during the course of their illness (Tariot and Blazina 1994; Haupt et al 2000; Lyketsos et al 2000). A community-based epidemiological study found that 61% of AD patients exhibited one or more BPSD in the past month and 61% of those with no baseline BPSD developed at least one symptom within 18 months (Lyketsos et al 2000; Steinberg et al 2003). In a nursing home study a baseline prevalence of 76%, a two-year prevalence of 82%, and an annual incidence of 64% was detected (Ballard et al 2001). Clinical Interventions in Aging 2008:3(4) Campbell et al, publisher and licensee Dove Medical Press Ltd. This is an Open Access article which permits unrestricted noncommercial use, provided the original work is properly cited.
2 Campbell et al BPSD are a major problem for patients and their caregivers. They are considered one of the strongest predictors for institutionalization of demented patients (Colerick and George 1986; Steele et al 1990; O Donnell et al 1992; Haupt and Kurz 1993; Teresi and Weiner 1993; Swearer 1994); a prominent risk factor for caregiver burden and psychological morbidity (Kinney and Stephens 1989; Hamel et al 1990; Haupt and Kurz 1993; Morris et al 1996); a significant obstacle in achieving adequate medical management for other health conditions (Cohen-Mansfield 1995; Brodaty et al 2001); and a common cause of stress leading to staff burnout and subsequent turnover in institutional settings (Maslach and Jackson 1981). The traditional pharmacological management of BPSD has significant morbidity including extrapyramidal signs and symptoms, gait abnormalities, sedation, an increased risk of falls and fractures, incidence of delirium, cerebrovascular events, and death (Cummings 2000a; Cummings et al 2000, 2001; Boustani et al 2002). An agent specific for AD that can treat BPSD with fewer side effects is highly desirable. Currently ChEIs are the standard of care for the treatment of cognitive deficit in patients with AD (Doody et al 2001; Boustani et al 2002). Compared to alternatives, they are considered to have a more acceptable side effect profile (Boustani et al 2002). Over the past decade, their potential role as psychotropic agents has been investigated in a variety of basic and clinical studies, which have suggested that the central cholinergic deficit associated with AD may be causative for the cognitive deterioration and the neuropsychiatric manifestations of AD (Kaufer et al 1998; Cummings 2000a, 2000b; Cummings et al 2001; Chung and Cummings 2000). Previously, evaluating the use of ChEIs in managing BPSD has been reported in a meta-analysis by Trinh and colleagues (2003) which included published trials of ChEIs up to Trinh included patients with mild-moderate AD only and included studies which used metrifonate, which is no longer available for the treatment of AD. However, since the publication of Trinh meta-analysis, numerous new trials have been published that investigated further the role of ChEIs as a psychotherapeutic agent in AD. The aim of our study was to systematically review the available literature and examine the therapeutic role of the currently available ChEIs in decreasing the burden of BPSD among patients with any stage of AD living in any clinical setting. Methods Search strategies We searched MEDLINE from 1966 to 2007, Cochrane Collaboration Registry for Randomized Controlled Trials (RCT) from 1966 to 2007 and CINAHL from 1982 to 2007, using the following search terms: Alzheimer s disease, dementia, donepezil, rivastigmine, galantamine, cholinesterase inhibitors and behavioral and psychological symptoms. We limited our search to the English language, full text, published articles and human studies. We also retrieved relevant references of included studies for our search. Selection criteria The main goal of our systematic evidence review (SER) was to evaluate the efficacy of the currently available ChEIs in treating BPSD in patients with AD. Thus, we included only RCTs that evaluated the efficacy of any of the three FDA-approved and commonly used ChEIs (donepezil, rivastigmine, galantamine). We also included only studies that measured the BPSD with the Neuropsychiatric Inventory (NPI) among patients with any stage of AD living in any clinical setting. We selected NPI as the main outcome measure because it is considered by many investigators as the standard method to measure BPSD. The NPI is an informant-based structured interview with acceptable psychometric properties (Cummings et al 1994; Cummings and Kaufer 1996; Wood et al 2000; Schneider et al 2001). Higher scores indicate higher frequency and severity of BPSD and a positive change from baseline reflects worsening symptoms (Cummings et al 1994). We excluded pre and post studies and randomized controlled trials involving patients other than AD. Studies which were not placebo-controlled were also excluded from our SER. Critical appraisal Using the USPSTF critical appraisal method for quality assessment, we critically appraised the studies and included those with an attrition rate of less than 40%, a concealed measurement of the outcomes, and intention to treat analysis of the collected data. Data abstraction Three reviewers (AA, MB, NC) independently searched for the articles and abstracted data from each study that met our inclusion criteria into predefined evidence tables, that included: citation, total number of randomized patients, baseline demographic data (age, gender, educational level), mean Mini-Mental Status Examination score (MMSE), setting, duration of studies, drug used in studies, attrition rate, mean total NPI score, mean change from baseline of the total NPI score for both the treatment and placebo groups, and the level of significance for the mean difference in NPI between the two groups. 720 Clinical Interventions in Aging 2008:3(4)
3 The effi cacy of cheis (donepezil, rivastigmine, and galantamine) on BPSD in Alzheimer s disease Quantitative data synthesis We used Review Manager Software Version ( Plone Foundation, Houston, TX, USA) to calculate the effect size and confidence interval (CI) of each individual study and the combined results. The effect size is the difference in the change of the total NPI score from baseline between the treatment and the placebo groups divided by the pooled standard deviation. In addition, we were also interested in identifying any potential confounder for the effect of ChEIs on BPSD such as disease stage and specific drug. Thus, we conducted a series of sensitivity analyses that combined data from the studies using similar inclusion criteria and interventions. Authors were also contacted for the data not reported or missing in the studies. After testing the heterogeneity of included trials, we primarily used a random effect model to combine the results of included studies. Other factors which were considered when carrying out the meta- analysis were sources of variation, such as sample sizes, dosing regimens, differences between treatment durations and routes of administration. Confounding variables would be MMSE scores or stage of symptom and age of the patients. Variations such as these would impact effect sizes, but as long as these effect sizes are in the same direction, whether negative or positive, a reliable effect would be evident. Results Review fl ow Our search strategies yield a total of 105 potentially relevant RCTs for retrieval. sixteen studies were excluded as they were not placebo-controlled trials and 27 studies were further excluded as they were open label, subgroup analyses or duplicate studies. Out of remaining 62 studies, 50 studies were excluded as they failed to meet the inclusion criteria. Finally, 12 randomized controlled trials (RCTs) met the inclusion criteria for our SER (see Tables 1 and 2) and only nine studies provided complete data to conduct the meta-analysis. Study characteristics As demonstrated in Tables 1 and 2, the included studies were conducted among a heterogeneous group of participants with mild to severe cognitive deficits with a mean MMSE score ranging from 6.1 to 21. The mean difference of the primary outcome measure was not reported in three studies, which were therefore excluded from the meta-analysis. Five studies were conducted in outpatient settings, two in nursing homes, four in community and residential settings together, and one study did not report the clinical setting. Nine studies compared donepezil, two compared galantamine and one compared rivastigmine with placebos. The length of the studies varied from 3 to 12 months. The target dose of donepezil was 10 mg per day; that of galantamine varied from 16 to 24 mg daily; and rivastigmine was administered as either a capsule or a skin patch with target doses of 3 12 mg and 20 cm 2 patches per day, respectively. The mean age of the participants ranged from 72.5 to 85.7 years and the percentage of female participants ranged Table 1 Baseline variables of the included studies Study N Mean age % Female Education level (years) Mean MMSE Total NPI Score Tariot et al NR (10 items) Feldman et al NR (12 items) Rockwood et al NR (10 items) Tariot et al NR (12 items) NPI-NH Winblad et al NR (10 items) Gauthier et al NR (12 items) Nunez et al AD2000 et al NR Holmes et al NR (10 items) Winblad et al NR (12 items) Winblad et al (12 items) Howard et al NR (12 items) Abbreviations: N, total number of subjects included in the study; NPI, neuropsychiatric Inventory; NPI-NH, neuropsychiatric inventory-nursing home; NR, not reported. Clinical Interventions in Aging 2008:3(4) 721
4 Campbell et al from 56.5% to 84.5%. Education level was reported in only one study and was 9.9 years. NPI was used as primary outcome measure in only two studies (Tariot et al 2001; Holmes et al 2004) and the secondary outcome measure in nine studies for the assessment of BPSD. The mean baseline NPI score ranged from 9.20 to Two different versions of the NPI (10-item scale with score ranges from 0 to 120 points versus 12-item scale with score ranges from 0 to 144) were used. Baseline total NPI score was higher in the five studies that evaluated moderate to severe AD (15.1, 19.30, 19.55, 21.0 and 23.65) in comparison to the four studies which evaluated mild to moderate AD (9.2, 11.9, 13.05, 14.3). Quantitative data analyses The studies were not homogenous and therefore, we used the random effect model to combine their results and reported the standard mean difference (SMD). However, we have also reported the result from the fixed effect model and reported the weighted mean difference (WMD) for comparison with other reported meta-analyses (See Figure 1). Table 2 Evidence table for all included studies Study Countries Setting Drug Length (months) N Mean difference Intervention attrition rate, % Tariot et al 2000 USA Out-patient Galantamine SS Feldman et al 2001 Rockwood et al 2001 Canada, Australia, France USA, Canada, Britain, South Africa, Australia, New Zealand Tariot et al 2001 USA Nursing homes Winblad et al 2001 Gauthier et al 2002 Nunez et al 2003 AD2000 et al 2004 Holmes et al 2004 Winblad et al 2006 Winblad et al 2007 Howard et al 2007 Northern European countries Canada, Australia, France, USA Finland, Hungary, Denmark. UK Out-patient Donepezil SS Out-patient Galantamine NS Donepezil NS Out-patient Donepezil NS Community/ Residential Donepezil NR NR Donepezil NR NR NR Community/ Residential Donepezil NR 11 5 UK Out-patient Donepezil SS Sweden Sweden, USA, Germany, Switzerland United Kingdom Nursing Homes Community/ Residential Residential/ Community Donepezil NS Rivastigmine (20 cm-patch) (capsule) NS 0.50 NS Donepezil NS Abbreviations: MD, mean difference of change on total NPI score between placebo and treatment; NR, not reported; NS, not signifi cant; SS, statistically signifi cant. Note: Negative values indicate greater improvement in symptoms in the active treatment group Placebo attrition rate, % Clinical Interventions in Aging 2008:3(4)
5 The effi cacy of cheis (donepezil, rivastigmine, and galantamine) on BPSD in Alzheimer s disease Patients receiving ChEIs (donepezil, rivastigmine or galantamine) improved the total NPI score when compared to the placebo with a SMD between the two groups of 0.10 (95% CI: 0.18, 0.01) and a WMD of 1.38 (95% CI: 2.20, 0.46). Combining only the results of homogenous studies, for example, those conducted among patients with mild-moderate AD showed that the SMD between the two groups was 0.16 (95% CI: 0.28, 0.03) and the WMD was 1.92 (95% CI: 3.18, 0.66) (see Figure 2). When results of studies that included patients with moderate-severe AD were evaluated, the impact of ChEIs was not statistically significant anymore with a SMD of 0.06 (95% CI: 0.17, 0.05) and a WMD of 0.77(95% CI: 2.12, 0.57) (see Figure 3). Looking at the effect of each of the three ChEIs separately, we found that the SMD between galantamine and placebo (two studies) was 1.65 (95% CI: 3.10, 0.19), between donepezil and placebo (6 studies) was 1.76 (95% CI: 3.37, 0.15) and between rivastigmine and placebo (one study) was 0.55 (95% CI: 2.31, 1.21). Data on the individual domains of the NPI was not available to conduct a meta-analysis, but two studies (Feldman et al 2001; Tariot et al 2001) reported that donepezil significantly improved depression/dysphoria and apathy, but only anxiety symptoms were improved in one trial and only agitation/aggression in the other. Figure 1 The effects of ChEIs on BPSD among patients with mild to severe AD. Discussion Clinically relevant change in BPSD as measured by NPI Our meta-analysis found that in comparison to placebo, 3 to 12 months treatment with ChEIs had positive effects on global BPSD scores with an effect size (SMD) of 0.10 and WMD of 1.38 NPI points. The challenge, however, is to determine the clinical significance of this effect size and whether such an effect can be translated into reducing patients or caregivers burden. Various clinical investigators have used different total NPI points to determine the clinical meaning of NPI total change score. Kaufer and colleagues (1998) decided that a reduction or improvement of at least 50% in the average baseline NPI scores, approximately nine points difference on the total NPI score, is considered a clinically relevant change. We compared our results to a similar study published by Trinh and colleagues (2003). This study evaluated the impact of ChEIs on behavioral symptoms in patients with mild-moderate AD. The authors Clinical Interventions in Aging 2008:3(4) 723
6 Campbell et al Figure 2 The effects of ChEIs on BPSD among patients with mild to moderate AD. Figure 3 The effects of ChEIs on BPSD among patients with moderate to severe AD. 724 Clinical Interventions in Aging 2008:3(4)
7 The effi cacy of cheis (donepezil, rivastigmine, and galantamine) on BPSD in Alzheimer s disease found a WMD in improvement in NPI scores between all ChEIs (including metrifonate) and placebo of 1.72 (95% CI: ). By comparison, our study found similar results as the Trinh study when results for a similar population were evaluated (WMD 1.92 for patients in a mild-moderate stage of dementia). However, our results suggest this difference in NPI scores does not extend to the moderate-severe population (WMD of 0.77 with 95% CI of 2.12 to +0.57). The efficacy of ChEIs (galantamine and rivastigmine) on BPSD in other types of dementia such as vascular dementia and Lowy body dementia has been evaluated in two other studies (Erkinjuntti et al 2002; McKeith et al 2002). Both controlled trials had similar results as our study with a difference in mean change from baseline between treatment and placebo group of 2.3 points on the total NPI score for the vascular dementia trial (baseline total NPI score = 11.8) and 3.8 for trial including patients with Lewy body dementia (baseline total NPI score = 21.7). To further compare the clinical significance of our meta-analysis, we looked at the results of trials that used the NPI to evaluate the efficacy of an atypical antipsychotic (olanzapine) in reducing BPSD among AD nursing home residents who had clinically significant levels of behavioral and psychological symptoms at baseline with a total NPI score of at least 44 points (Street et al 2000). In comparison to placebo, the mean decline from baseline in total NPI score was 8.3 points among patients taking olanzapine for six weeks (Street et al 2000). Although the ChEIs trials did not specifically enroll patients with baseline behavioral and psychological symptoms, the difference in the NPI changes from baseline between olanzapine and placebo was much higher than what we detected in our meta-analysis. The natural history of the BPSD Before evaluating the efficacy of ChEIs on BPSD, one must examine their natural history as measured by a specific instrument such as the NPI. In a cross-sectional study, community dwelling elderly patients with dementia had a total NPI mean score of 7.11(SD = 10.9) as compared to 0.76 (SD = 2.89) points of those with no dementia. In addition, the total score increased as dementia-related disability worsened, individuals with mild dementia had a mean total score on the NPI of 5.80 (SD = 12.5), those with moderate dementia had a mean score of 8.8 (SD = 11.10), and those with severe dementia had a mean score of 10.6 (SD = 17.0) (Lyketsos et al 2002). The mean total NPI score increased dramatically, ie, 36.4 (SD = 24.5), among patients with moderate to severe dementia admitted to the hospital for the management of their disturbed behaviors (Iverson et al 2002). The prevalence data provide an idea of the total NPI score range but they do not explain the fluctuating nature of BPSD. During any specified period of time certain behaviors or symptoms will emerge, others will cease, some deteriorate, and others will improve (Levy et al 1996; Devanand et al 1997; Green et al 1999; Ballard et al 2001). This fluctuating pattern of BPSD must be accounted for when interpreting the efficacy of certain interventions. We are unaware of any study that tried to determine whether this fluctuating pattern occurred on daily, weekly, monthly, or yearly basis. Limitations Our study has some limitations. First, we restricted our review to BPSD measured by the NPI. We were concerned that including other measures would make it difficult to interpret the data. Nevertheless, the NPI is considered the current standard instrument to evaluate BPSD. We previously reviewed all RCTs of ChEIs that evaluated the efficacy of tacrine on BPSD and found similar results from trials using the Alzheimer s Disease Assessment Scale-Noncognitive symptoms (ADAS-noncog) (Cummings et al 2001). Secondly, we did not include individual domains of the NPI in our analysis, which may have truncated our findings. There is lack of published data on each of these 12 domains, although two included trials (Tariot et al 2000; Feldman et al 2001) reported the effect on individual domains but did not produce data that could be combined for meta-analysis (Tariot et al 2000; Feldman et al 2001). As the effect of ChEIs are likely to be greater on some BPSD than others, we believe that evaluating the effects of cholinesterase inhibitors on individual domains may carry more clinical meaning than using the global scale which sums all the BPSD in one score. The third limitation is related to being unable to identify the difference in the proportion of responders between placebo and treatment groups. One trial (Tariot et al 2001) with NPI as the primary outcome reported the difference in the percentage of patients who had worsening symptoms on the agitation domain (placebo 32%, donepezil 24%), but it only stated that no significant finding was detected in the other domains (Tariot et al 2001). We agree with Mulsant and colleagues (1997) in regard to the advantage of using comparisons based on the resolution of target BPSD domains or even the total score of NPI (categorical approach) rather than the use of an absolute or relative change in total score in interpreting the clinical value of certain interventions targeting BPSD. Finally, our review could not determine if the ChEI s effects were due to stability of BPSD among the treatment group Clinical Interventions in Aging 2008:3(4) 725
8 Campbell et al versus deterioration among the placebo group, or if their effects reflected a true improvement in treatment groups. Research need Our review found a statistically significant effect of ChEIs (donepezil, rivastigmine, and galantamine) on BPSD in AD patients. However, we could not interpret the clinical relevance of this finding. Given the heterogeneity of BPSD and the need to explore further the efficacy of ChEIs in managing BPSD, we need to have a more clinically focused evaluation method. This method could be accomplished by either conducting a new clinical trial (a very expensive and ethically challenging method because ChEIs are considered to be the current standard of care in AD) or a retrospective post-hoc analysis of individual data from the 12 clinical trials that we included in our meta-analysis. The analytic framework for the suggested study would stratify the participants into two groups based on their baseline NPI total score: the prevention strata; which would include individuals with low NPI scores ( 20) and crisis intervention strata; which would include individuals with high NPI scores ( 20). Although the NPI would still be the main assessment tool, the trial would evaluate the impact of ChEIs using the individual domain scores for the NPI and a categorical approach to identify responders. The primary outcome would be the proportion of responders after 3 to 6 months. The responders would be defined differently between the two strata: in the prevention strata, the responders would include any individual with at least a stable NPI domain score at the end of the study, whereas in the crisis strata, the responders would include any individual who had at least a 30% reduction in their domain score. The study might also include additional data from the two trials that tested rivastigmine efficacy in dementia with Lewy body and galantamine efficacy in vascular dementia. Using this methodology (categorical outcome and changes in domain score) would enable us to report the difference in proportion of items improved, worsened, emerged, and/or ceased between treatment and control groups, and thus, we would better understand the clinical meaning of positive effects. A detailed investigation of the effect of ChEIs on specific behaviors at different stages of illness may be beneficial. We await the results of an acute phase BPSD study using memantine (MAGD ISRCTN ) and studies on new drugs such as tarenflurbil (Wilcock et al 2008). Specific medical, supportive, social or psychological interventions in agitation require further evidence. Conclusions Cholinesterase inhibitors (donepezil, rivastigmine, and galantamine) have consistently shown a statistically significant improvement on BPSD as measured by the NPI. However, the existing clinical relevance of these findings is unclear and the use of this class of medications for BPSD does not appear to produce the necessary effect to be considered as monotherapy of behavioral or psychological symptoms in patients with dementia. Disclosure The authors report no conflicts of interest in this work. References AD2000 Collaborative Group Long-term donepezil treatment in 565 patients with Alzheimer s disease (AD2000): randomized double-blind trial. Lancet, 363: Ballard CG, Margallo-Lana M, Fossey J, et al A 1-year follow-up study of behavioral and psychological symptoms in dementia among people in care environments. J Clin Psychiatry, 62: Boustani M, Peterson B, Hanson L, et al Screening for Dementia. Systematic Evidence Review [online]. Accessed on Aug 29, URL: Rockville, MD: Agency for Healthcare Research and Quality. Brodaty H, Draper B, Saab D, et al Psychosis, depression, and behavioral disturbances in Sydney nursing home residents: prevalence and predictors. Int J Geriatr Psychiatry, 16: Chung JA, Cummings JL Neurobehavioral and neuropsychiatric symptoms in Alzheimer s disease: characteristics and treatment. Neurol Clinics, 18: Cohen-Mansfield J Assessment of disruptive behavior/agitation in the elderly: function, methods, and difficulties. J Geriatr Psychiatry Neurol, 8: Colerick EJ, George LK Predictors of institutionalization among caregivers of patients with Alzheimer s disease. J Am Geriatr Soc, 34: Cummings JL, Donohue JA, Brooks RL The relationship between donepezil and behavioral disturbances in patients with Alzheimer s disease. Am J Geriatr Psychiatry, 8: Cummings JL, Kaufer D Neuropsychiatric aspects of Alzheimer s disease: the cholinergic hypothesis revisited. Neurology, 47: Cummings JL, Mega M, Gray K, et al The Neuropsychiatric Inventory: comprehensive assessment of psychopathology in dementia. Neurology, 44: Cummings JL, Nadel A, Masterman D, et al Efficacy of metrifonate in improving the psychiatric and behavioral disturbances of patients with Alzheimer s disease. J Geriatr Psychiatry Neurol, 14: Cummings JL. 2000a. Cholinesterase inhibitors: a new class of psychotropic compounds. Am J Psychiatry, 157:4 15. Cummings JL. 2000b. Cognitive and behavioral heterogeneity in Alzheimer s disease: seeking the neurobiological basis. Neurobiol Aging, 21: Devanand DP, Jacobs DM, Tang MX, et al The course of psychopathological features in mild to moderate Alzheimer s disease. Arch Gen Psychiatry, 54: Doody RS, Stevens JC, Beck C, et al Practice parameter: management of dementia (an evidence-based review). Report of the Quality Standards Subcommittee of the American Academy of Neurology. Neurology, 56: Erkinjuntti T, Kurz A, Gauthier S, et al Efficacy of galantamine in probable vascular dementia and Alzheimer s disease combined with cerebrovascular disease: a randomized trial. Lancet, 359: Feldman H, Gauthier S, Hecker J, et al A 24-week, randomized, double-blind study of Donepezil in moderate to severe Alzheimer s disease. Neurology, 57: Clinical Interventions in Aging 2008:3(4)
9 The effi cacy of cheis (donepezil, rivastigmine, and galantamine) on BPSD in Alzheimer s disease Finkel SI, Burns A, Cohen GD Overview. Int Psychogeriatr, 12(Suppl):13 8. Gauthier S, Feldman H, Hecker J, et al Functional, cognitive and behavioral effects of donepezil in patients with moderate Alzheimer s disease. Curr Med Res Opin, 18: Green CR, Marin DB, Mohs RC, et al The impact of behavioral impairment on functional ability in Alzheimer s disease. Int J Geriatr Psychiatry, 14: Hamel M, Gold DP, Andres D, et al Predictors and consequences of aggressive behavior by community-based dementia patients. Gerontologist, 30: Haupt M, Kurz A, Janner M A 2-year follow-up of behavioral and psychological symptoms in Alzheimer s disease. Dement Geriatr Cogn Disord, 11: Haupt M, Kurz A Predictors of nursing home placement in patients with Alzheimer s disease. Int J Geriatr Psychiatr, 8: Holmes C, Wilkinson D, Dean C, et al The efficacy of donepezil in the treatment of neuropsychiatric symptoms in Alzheimer disease. Neurologyi, 63: Howard RJ, Juszczak E, Ballard CG, et al Donepezil for the treatment of agitation in Alzheimer s disease. N Engl J Med, 357: Iverson GL, Hopp GA, DeWolfe K, et al Measuring change in psychiatric symptoms using the Neuropsychiatric Inventory: Nursing Home version. Int J Geriatr Psychiatry, 17: Kaufer DI, Cummings JL, Christine D, et al Assessing the impact of neuropsychiatric symptoms in Alzheimer s disease: the Neuropsychiatric Inventory Caregiver Distress Scale. J Am Geriatr Soc, 46: Kinney JM, Stephens MA Caregiving Hassle Scale: assessment the daily hassles of caring for a family member with dementia. Gerontologist, 29: Levy ML, Cummings JL, Fairbanks LA, et al Longitudinal assessment of symptoms of depression, agitation, and psychosis in 181 patients with Alzheimer s disease. Am J Psychiatry, 153: Lyketsos CG, Lopez O, Jones B, et al Prevalence of neuropsychiatric symptoms in dementia and mild cognitive impairment: results from the cardiovascular health study. JAMA, 288: Lyketsos CG, Steinberg M, Tschanz JT, et al Mental and behavioral disturbances in dementia: findings from the Cache county study on memory in aging. Am J Psychiatry, 157: Maslach C, Jackson SE The measurement of experienced burnout. J Occup Behav, 2: McKeith I, Del Ser T, Spano P, et al Efficacy of rivastigmine in dementia with Lewy bodies: a randomized, double-blind, placebo-controlled international study. Lancet, 356: Morris PK, Rovner BW, German PS Factors contributing to nursing home admission because of disruptive behavior. Int J Geriatr Psychiatry, 11: Mulsant BH, Mazumdar S, Pollock BG, et al Methodological issues in characterizing treatment response in demented patients with behavioral disturbances. Int J Geriatr Psychiatry, 12: Nunez M, Jakab G, Jakobsen S, et al Donepezil-treated Alzheimer s disease patients initially rated as showing no apparent clinical benefit demonstrate significant benefits when therapy is continued [abstract]. AGS Annual Meeting, S99. O Donnell BF, Drachman DA, Barnes HJ, et al Incontinence and troublesome behaviors predict institutionalization in dementia. J Geriatr Psychiatry Neurol, 5: Rockwood K, Mintzer J, Truyen L, et al Effects of a flexible galantamine dose in Alzheimer s disease: a randomized, controlled trial. Neurol Neurosurg Psychiatry, 71: Schneider LS, Tariot PN, Lyketsos CG, et al National Institute of Mental Health Clinical Antipsychotic Trials of Intervention Effectiveness (CATIE): Alzheimer disease trial methodology. Am J Geriatr Psychiatr, 9: Steele C, Rovner B, Chase GA, et al Psychiatric symptoms and nursing home placement of patients with Alzheimer s disease. Am J Psychiatry, 147: Steinberg M, Sheppard JM, Tschanz J, et al The incidence of mental and behavioral disturbances in dementia: the cache county study. J Neuropsychiatry Clin Neurosci, 15: Street JS, Clark WS, Gannon KS, et al Olanzapine in the treatment of psychotic and behavioral symptoms in patients with Alzheimer s disease in nursing care facilities: a double-blind, randomized, placebo-controlled trial. The HGEU Study Group. Arch Gen Psychiatry, 57: Swearer JM Behavioral disturbances in dementia. In: Morris JC (ed). Handbook of Dementing Illnesses. New York: Marcel Dekker, pp Tariot PN, Blazina L The psychopathology of dementia. In: Morris JC (ed). Handbook of Dementing Illnesses. New York: Marcel Dekker, pp Tariot PN, Cummings JL, Katz IR, et al A randomized, double-blind, placebo-controlled study of the efficacy and safety of donepezil in patients with Alzheimer s disease in the nursing home setting. J Am Geriatr Soc, 49: Tariot PN, Solomon PR, Morris JC, et al A 5-month, randomized, placebo-controlled trial of galantamine in AD. The Galantamine USA-10 Study Group. Neurology, 54: Teresi JA, Weiner AS Respite care in the nursing home: predictors of length of stay. In: Tepper LM, Toner JA (eds). Respite Care: Programs, Problems and Solutions. Philadelphia: Charles Press, pp Trinh NH, Hoblyn J, Mohanty S, et al Efficacy of cholinesterase inhibitors in the treatment of neuropsychiatric symptoms and functional impairment in Alzheimer s Disease: A meta-analysis. JAMA, 289: Wilcock G, Black SE, Hendrix SB et al Efficacy and safety of tarenflurbil in mild to moderate Alzheimer s disease: a randomized phase 11 trial. Lancet Neurol, 7: Winblad B, Cummings J, Andreasen N, et al A six month double-blind, randomized, placebo-controlled study of a transdermal patch in Alzheimer s disease- Rivastigmine patch vs capsule. Int J Geriatr Psychiatry, 22: Winblad B, Engedal K, Soininen H, et al A 1-year, randomized, placebo-controlled study of donepezil in patients with mild to moderate AD. Neurology, 57: Winblad B, Kilander L, Eriksson S, et al Donepezil in patients with severe Alzheimer s disease: double blind, parallel-group, placebo-controlled study. Lancet, 367: Wood S, Cummings JL, Hsu MA, et al The use of the neuropsychiatric inventory in nursing home residents: characterization and measurement. Am J Geriatr Psychiatry, 8: Clinical Interventions in Aging 2008:3(4) 727
10 Campbell et al Flow chart Potentially relevant RCTs identifi ed and screened for retrieval: N = 105 RCTs retrieved for more detailed evaluation (n = 89) Potentially appropriate RCTs to be included in the meta-analyses (n = 62) RCTs included in meta-analysis: (n = 12) RCTs with usable information by outcome: (n = 9) RCTs excluded: N = 16 Not placebo-controlled trials RCTs excluded, with reasons (n = 27) Open label = 17 Sub-group analyses = 3 Duplicate = 7 RCTs excluded from the meta-analysis: (n = 50) Failed to meet inclusion criteria RCTs withdrawn by outcome (n = 3) Reasons: Data not reported Abbreviations: RCTs, randomized, controlled trials. 728 Clinical Interventions in Aging 2008:3(4)
Known as both a thief and murderer,
 &A Dementia Drugs: When Should They Be Stopped? Ron Keren, MD, FRCPC As presented at the University of Toronto s Primary Care Conference, Toronto, Ontario (May 25) Known as both a thief and murderer, Alzheimer
&A Dementia Drugs: When Should They Be Stopped? Ron Keren, MD, FRCPC As presented at the University of Toronto s Primary Care Conference, Toronto, Ontario (May 25) Known as both a thief and murderer, Alzheimer
Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias. Aaron H. Kaufman, MD
 Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, MD Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, M.D. Health Sciences
Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, MD Psychiatric and Behavioral Symptoms in Alzheimer s and Other Dementias Aaron H. Kaufman, M.D. Health Sciences
Management of the Acutely Agitated Long Term Care Patient
 Management of the Acutely Agitated Long Term Care Patient 80 60 Graying of the Population US Population Over Age 65 Millions of Persons 40 20 0 1900 1920 1940 1960 1980 1990 2010 2030 Year Defining Dementia
Management of the Acutely Agitated Long Term Care Patient 80 60 Graying of the Population US Population Over Age 65 Millions of Persons 40 20 0 1900 1920 1940 1960 1980 1990 2010 2030 Year Defining Dementia
Psychosis and Agitation in Dementia
 Psychosis and Agitation in Dementia Dilip V. Jeste, MD Estelle & Edgar Levi Chair in Aging, Director, Stein Institute for Research on Aging, Distinguished Professor of Psychiatry & Neurosciences, University
Psychosis and Agitation in Dementia Dilip V. Jeste, MD Estelle & Edgar Levi Chair in Aging, Director, Stein Institute for Research on Aging, Distinguished Professor of Psychiatry & Neurosciences, University
The course of neuropsychiatric symptoms in dementia. Part II: relationships among behavioural sub-syndromes and the influence of clinical variables
 INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2005; 20: 531 536. Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/gps.1317 The course of neuropsychiatric
INTERNATIONAL JOURNAL OF GERIATRIC PSYCHIATRY Int J Geriatr Psychiatry 2005; 20: 531 536. Published online in Wiley InterScience (www.interscience.wiley.com). DOI: 10.1002/gps.1317 The course of neuropsychiatric
Dementia of the Alzheimer Type: the Drug Treatment Debate
 Dementia of the Alzheimer Type: the Drug Treatment Debate I have no financial conflict of interest. Many years ago I was given a trip to San Fran and taught to use a slide set from the drug company. I
Dementia of the Alzheimer Type: the Drug Treatment Debate I have no financial conflict of interest. Many years ago I was given a trip to San Fran and taught to use a slide set from the drug company. I
Literature Scan: Alzheimer s Drugs
 Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Copyright 2012 Oregon State University. All Rights Reserved Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35 Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119
Behavioral and psychological symptoms of dementia characteristic of mild Alzheimer patients
 Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
Blackwell Science, LtdOxford, UKPCNPsychiatry and Clinical Neurosciences1323-13162005 Blackwell Publishing Pty Ltd593274279Original ArticleDementia and mild AlzheimersJ. Shimabukuro et al. Psychiatry and
NeuroPharmac Journal ISSN: Alzheimer s Disease: Pharmacotherapy of noncognitive symptoms Aslam Pathan; Abdulrahman M.
 ISSNISSN ISSN: 2456-3927 NeuroPharmac Journal Alzheimer s Disease: Pharmacotherapy of noncognitive symptoms Aslam Pathan; Abdulrahman M. Alshahrani www. neuropharmac.com Jan-April 2018, Volume 3, Issue
ISSNISSN ISSN: 2456-3927 NeuroPharmac Journal Alzheimer s Disease: Pharmacotherapy of noncognitive symptoms Aslam Pathan; Abdulrahman M. Alshahrani www. neuropharmac.com Jan-April 2018, Volume 3, Issue
Management of Agitation in Dementia. Kimberly Triplett Ferguson, MS4
 Management of Agitation in Dementia Kimberly Triplett Ferguson, MS4 Objectives 1. Review recommended evaluation of agitated patients with dementia. 2. Discuss evidence concerning nonpharmacologic management.
Management of Agitation in Dementia Kimberly Triplett Ferguson, MS4 Objectives 1. Review recommended evaluation of agitated patients with dementia. 2. Discuss evidence concerning nonpharmacologic management.
Clinical Trial Designs for RCTs focussing on the Treatment of Agitation in people with Alzheimer s disease
 Clinical Trial Designs for RCTs focussing on the Treatment of Agitation in people with Alzheimer s disease Professor Clive Ballard Dr Byron Creese University of Exeter, UK Guardian guide for 2018: Top
Clinical Trial Designs for RCTs focussing on the Treatment of Agitation in people with Alzheimer s disease Professor Clive Ballard Dr Byron Creese University of Exeter, UK Guardian guide for 2018: Top
Month/Year of Review: September 2013 Date of Last Review: February 2012
 Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119 Copyright 2012 Oregon State University. All Rights
Drug Use Research & Management Program Oregon State University, 500 Summer Street NE, E35, Salem, Oregon 97301-1079 Phone 503-947-5220 Fax 503-947-1119 Copyright 2012 Oregon State University. All Rights
Disclosure. Speaker Bureaus. Grant Support. Pfizer Forest Norvartis. Pan American Health Organization/WHO NIA HRSA
 Disclosure Speaker Bureaus Pfizer Forest Norvartis Grant Support Pan American Health Organization/WHO NIA HRSA How Common is Psychosis in Alzheimer s Disease? Review of 55 studies 41% of those with Alzheimer
Disclosure Speaker Bureaus Pfizer Forest Norvartis Grant Support Pan American Health Organization/WHO NIA HRSA How Common is Psychosis in Alzheimer s Disease? Review of 55 studies 41% of those with Alzheimer
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia
 Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
Screening and Management of Behavioral and Psychiatric Symptoms Associated with Dementia Measure Description Percentage of patients with dementia for whom there was a documented screening* for behavioral
Medications for treating people with dementia: summary of evidence on cost-effectiveness
 Medications for treating people with dementia: summary of evidence on cost-effectiveness Martin Knapp, A-La Park and Alistair Burns PSSRU, London School of Economics and Political Science v4 23 July 2017
Medications for treating people with dementia: summary of evidence on cost-effectiveness Martin Knapp, A-La Park and Alistair Burns PSSRU, London School of Economics and Political Science v4 23 July 2017
The place for treatments of associated neuropsychiatric and other symptoms
 The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
The place for treatments of associated neuropsychiatric and other symptoms Luca Pani dg@aifa.gov.it London, 25 th November 2014 Workshop on Alzheimer s Disease European Medicines Agency London, UK Public
An Evaluation of a Training Program in Restraint-Free Care for Individuals with Dementia Christina Garrison-Diehn, Clair Rummel, & Jane E.
 An Evaluation of a Training Program in Restraint-Free Care for Individuals with Dementia Christina Garrison-Diehn, Clair Rummel, & Jane E. Fisher Background Disease. (Xu, Kochanek & Tejada-Vera, 2009)
An Evaluation of a Training Program in Restraint-Free Care for Individuals with Dementia Christina Garrison-Diehn, Clair Rummel, & Jane E. Fisher Background Disease. (Xu, Kochanek & Tejada-Vera, 2009)
Supplementary Online Content
 Supplementary Online Content Atri A, Frölich L, Ballard C, et al. Effect of idalopirdine as adjunct to cholinesterase inhibitors on in cognition in patients with Alzheimer disease: three randomized clinical
Supplementary Online Content Atri A, Frölich L, Ballard C, et al. Effect of idalopirdine as adjunct to cholinesterase inhibitors on in cognition in patients with Alzheimer disease: three randomized clinical
Responsiveness of the QUALID to Improved Neuropsychiatric Symptoms in Patients with Alzheimer s Disease
 ORIGINAL RESEARCH Responsiveness of the QUALID to Improved Neuropsychiatric Symptoms in Patients with Alzheimer s Disease Hadas Benhabib 1, Krista L. Lanctôt, PhD 1,2,4, Goran M. Eryavec, MD, FRCPC 3,4,
ORIGINAL RESEARCH Responsiveness of the QUALID to Improved Neuropsychiatric Symptoms in Patients with Alzheimer s Disease Hadas Benhabib 1, Krista L. Lanctôt, PhD 1,2,4, Goran M. Eryavec, MD, FRCPC 3,4,
Neuropsychiatric Syndromes
 Neuropsychiatric Syndromes Susan Czapiewski,MD VAHCS December 10, 2015 Dr. Czapiewski has indicated no potential conflict of interest to this presentation. She does intend to discuss the off-label use
Neuropsychiatric Syndromes Susan Czapiewski,MD VAHCS December 10, 2015 Dr. Czapiewski has indicated no potential conflict of interest to this presentation. She does intend to discuss the off-label use
Dementia is a common neuropsychiatric disorder characterized by progressive impairment of
 Focused Issue of This Month Diagnosis and Treatment for Behavioral and Psychological Symptoms of Dementia Byoung Hoon Oh, MD Department of Psychiatry, Yonsei University College of Medicine E - mail : drobh@yuhs.ac
Focused Issue of This Month Diagnosis and Treatment for Behavioral and Psychological Symptoms of Dementia Byoung Hoon Oh, MD Department of Psychiatry, Yonsei University College of Medicine E - mail : drobh@yuhs.ac
USING ANTIPSYCHOTICS TO TREAT THE BEHAVIORAL AND PSYCHOLOGICAL SYMPTOMS OF DEMENTIA (BPSD)- WHAT IS THE EVIDENCE?
 USING ANTIPSYCHOTICS TO TREAT THE BEHAVIORAL AND PSYCHOLOGICAL SYMPTOMS OF DEMENTIA (BPSD)- WHAT IS THE EVIDENCE? Mugdha Thakur, MD Associate Professor of Psychiatry and Behavioral Sciences Duke University
USING ANTIPSYCHOTICS TO TREAT THE BEHAVIORAL AND PSYCHOLOGICAL SYMPTOMS OF DEMENTIA (BPSD)- WHAT IS THE EVIDENCE? Mugdha Thakur, MD Associate Professor of Psychiatry and Behavioral Sciences Duke University
Pharmacological Treatment of Aggression in the Elderly
 Pharmacological Treatment of Aggression in the Elderly Howard Fenn, MD Adjunct Clinical Associate Professor Department of Psychiatry and Behavioral Sciences Stanford University Self-Assessment Question
Pharmacological Treatment of Aggression in the Elderly Howard Fenn, MD Adjunct Clinical Associate Professor Department of Psychiatry and Behavioral Sciences Stanford University Self-Assessment Question
Neurocognitive Disorders Research to Emerging Therapies
 Neurocognitive Disorders Research to Emerging Therapies Edward Huey, MD Assistant Professor of Psychiatry and Neurology The Taub Institute for Research on Alzheimer s Disease and the Aging Brain Columbia
Neurocognitive Disorders Research to Emerging Therapies Edward Huey, MD Assistant Professor of Psychiatry and Neurology The Taub Institute for Research on Alzheimer s Disease and the Aging Brain Columbia
Ian McKeith MD, F Med Sci, Professor of Old Age Psychiatry, Newcastle University
 Ian McKeith MD, F Med Sci, Professor of Old Age Psychiatry, Newcastle University Design of trials in DLB and PDD What has been learnt from previous trials in these indications and other dementias? Overview
Ian McKeith MD, F Med Sci, Professor of Old Age Psychiatry, Newcastle University Design of trials in DLB and PDD What has been learnt from previous trials in these indications and other dementias? Overview
Rational Medication Use in Dementia
 Rational Medication Use in Dementia Stephen Thielke sthielke@u.washington.edu (206) 764 2815 I have no conflicts of interest to report. I am an employee of the federal government. The opinions in this
Rational Medication Use in Dementia Stephen Thielke sthielke@u.washington.edu (206) 764 2815 I have no conflicts of interest to report. I am an employee of the federal government. The opinions in this
LTC Research Influencing Practice
 LTC Research Influencing Practice David A. Nace, MD, MPH Division of Geriatric Medicine naceda@upmc.edu PGS Clinical Update April 6, 2017 Conflicts of Interest Dr. Nace does not have any current conflicts
LTC Research Influencing Practice David A. Nace, MD, MPH Division of Geriatric Medicine naceda@upmc.edu PGS Clinical Update April 6, 2017 Conflicts of Interest Dr. Nace does not have any current conflicts
CHCS. Multimorbidity Pattern Analyses and Clinical Opportunities: Dementia. Center for Health Care Strategies, Inc. FACES OF MEDICAID DATA SERIES
 CHCS Center for Health Care Strategies, Inc. FACES OF MEDICAID DATA SERIES Multimorbidity Pattern Analyses and Clinical Opportunities: Dementia December 2010 Cynthia Boyd, MD, MPH* Bruce Leff, MD* Carlos
CHCS Center for Health Care Strategies, Inc. FACES OF MEDICAID DATA SERIES Multimorbidity Pattern Analyses and Clinical Opportunities: Dementia December 2010 Cynthia Boyd, MD, MPH* Bruce Leff, MD* Carlos
11/11/2016. Disclosures. Natural history of BPSD. Objectives. Assessment of BPSD. Behavioral Management of Persons with Alzheimer s Disease
 Disclosures Behavioral Management of Persons with Alzheimer s Disease Wisconsin Association of Medical Directors November 17, 2016 Art Walaszek, M.D. Professor of Psychiatry UW School of Medicine & Public
Disclosures Behavioral Management of Persons with Alzheimer s Disease Wisconsin Association of Medical Directors November 17, 2016 Art Walaszek, M.D. Professor of Psychiatry UW School of Medicine & Public
Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic
 Original Articles 179 Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic Ching-Sen Shih 1, Sui-Hing Yan 2, Ying-Hoo Ho 1, Yuh-Te Lin 1, Jie-Yuan Li 1, and Yuk-Keung Lo 1 Abstract-
Original Articles 179 Psychiatric Morbidity in Dementia Patients in a Neurology-Based Memory Clinic Ching-Sen Shih 1, Sui-Hing Yan 2, Ying-Hoo Ho 1, Yuh-Te Lin 1, Jie-Yuan Li 1, and Yuk-Keung Lo 1 Abstract-
Acetylcholinesterase inhibitors: donepezil, rivastigmine, tacrine or galantamine for non-alzheimer s dementia
 STEER 2002; Vol 2: No.2 Acetylcholinesterase inhibitors: donepezil, rivastigmine, tacrine or galantamine for non-alzheimer s dementia Bunmi Fajemisin Evidence search date: November 2001 www.signpoststeer.org
STEER 2002; Vol 2: No.2 Acetylcholinesterase inhibitors: donepezil, rivastigmine, tacrine or galantamine for non-alzheimer s dementia Bunmi Fajemisin Evidence search date: November 2001 www.signpoststeer.org
Opinion statement. Introduction. Cognitive Disorders (M Geschwind, Section Editor)
 Current Treatment Options in Neurology DOI 10.1007/s11940-012-0166-9 Cognitive Disorders (M Geschwind, Section Editor) Treatment of Behavioral and Psychological Symptoms of Alzheimer s Disease Anne Corbett,
Current Treatment Options in Neurology DOI 10.1007/s11940-012-0166-9 Cognitive Disorders (M Geschwind, Section Editor) Treatment of Behavioral and Psychological Symptoms of Alzheimer s Disease Anne Corbett,
The prevalence of Alzheimer s disease
 GERIATRIC MEDICINE Maintaining Patients With Alzheimer s Disease in the Home Environment David S. Geldmacher, MD ABSTRACT The prevalence of the most common form of dementia, Alzheimer s disease (AD), is
GERIATRIC MEDICINE Maintaining Patients With Alzheimer s Disease in the Home Environment David S. Geldmacher, MD ABSTRACT The prevalence of the most common form of dementia, Alzheimer s disease (AD), is
Treatment of behavioral and psychological symptoms of dementia: a systematic review
 Psychiatr. Pol. 2016; 50(4): 679 715 PL ISSN 0033-2674 (PRINT), ISSN 2391-5854 (ONLINE) www.psychiatriapolska.pl DOI: http://dx.doi.org/10.12740/pp/64477 Treatment of behavioral and psychological symptoms
Psychiatr. Pol. 2016; 50(4): 679 715 PL ISSN 0033-2674 (PRINT), ISSN 2391-5854 (ONLINE) www.psychiatriapolska.pl DOI: http://dx.doi.org/10.12740/pp/64477 Treatment of behavioral and psychological symptoms
PRESCRIBING FOR PEOPLE WITH DEMENTIA; SELECTED FINDINGS FROM POMH-UK QUALITY IMPROVEMENT PROGRAMMES (QIPS)
 PRESCRIBING FOR PEOPLE WITH DEMENTIA; SELECTED FINDINGS FROM POMH-UK QUALITY IMPROVEMENT PROGRAMMES (QIPS) The Prescribing Observatory for Mental Health (POMH-UK) is a national initiative to improve the
PRESCRIBING FOR PEOPLE WITH DEMENTIA; SELECTED FINDINGS FROM POMH-UK QUALITY IMPROVEMENT PROGRAMMES (QIPS) The Prescribing Observatory for Mental Health (POMH-UK) is a national initiative to improve the
The efficacy of Rivastigmine in the management of the behavioral and psychological symptoms of lewy body dementia- a review of literature
 Review article: The efficacy of Rivastigmine in the management of the behavioral and psychological symptoms of lewy body dementia- a review of literature Dr. Ivan Netto 1, Aditya Iyer 2, Dr. Prathamesh
Review article: The efficacy of Rivastigmine in the management of the behavioral and psychological symptoms of lewy body dementia- a review of literature Dr. Ivan Netto 1, Aditya Iyer 2, Dr. Prathamesh
Optimal Management of Challenging Behaviours in Dementia: An Update on Pharmacologic and Non-Pharmacologic Approaches
 Optimal Management of Challenging Behaviours in Dementia: An Update on Pharmacologic and Non-Pharmacologic Approaches Andrea Iaboni, MD, DPhil, FRCPC Toronto Rehab Institute, UHN Learning objectives Recognize
Optimal Management of Challenging Behaviours in Dementia: An Update on Pharmacologic and Non-Pharmacologic Approaches Andrea Iaboni, MD, DPhil, FRCPC Toronto Rehab Institute, UHN Learning objectives Recognize
Parkinsonian Disorders with Dementia
 Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
Parkinsonian Disorders with Dementia George Tadros Consultant in Old Age Liaison Psychiatry, RAID, Heartlands Hospital Professor of Dementia and Liaison Psychiatry, Aston Medical School Aston University
TITLE: Memantine in Combination with Cholinesterase Inhibitors for Alzheimer s Disease: Clinical Effectiveness
 TITLE: Memantine in Combination with Cholinesterase Inhibitors for Alzheimer s Disease: Clinical Effectiveness DATE: 30 October 2008 RESEARCH QUESTION: What is the evidence for using memantine in combination
TITLE: Memantine in Combination with Cholinesterase Inhibitors for Alzheimer s Disease: Clinical Effectiveness DATE: 30 October 2008 RESEARCH QUESTION: What is the evidence for using memantine in combination
Combination therapy compared to monotherapy for moderate to severe Alzheimer's Disease. Summary
 Combination therapy compared to monotherapy for moderate to severe Alzheimer's Disease Summary Mai 17 th 2017 Background Alzheimer s disease is a serious neurocognitive disorder which is characterized
Combination therapy compared to monotherapy for moderate to severe Alzheimer's Disease Summary Mai 17 th 2017 Background Alzheimer s disease is a serious neurocognitive disorder which is characterized
November 16-18, 2017 Hotel Monteleone New Orleans, LA. Provided by
 November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Major Neurocognitive Disorder: The Beginning and the End. Making the Diagnosis and Addressing Distressing Behavior W. Vaughn McCall, MD,
November 16-18, 2017 Hotel Monteleone New Orleans, LA Provided by Major Neurocognitive Disorder: The Beginning and the End. Making the Diagnosis and Addressing Distressing Behavior W. Vaughn McCall, MD,
Assessing and Treating Agitation Associated with Alzheimer s Disease
 AXS-05 R&D Day April 24, 2018 Assessing and Treating Agitation Associated with Alzheimer s Disease Marc E. Agronin, MD VP, Behavioral Health and Clinical Research, Miami Jewish Health Affiliate Associate
AXS-05 R&D Day April 24, 2018 Assessing and Treating Agitation Associated with Alzheimer s Disease Marc E. Agronin, MD VP, Behavioral Health and Clinical Research, Miami Jewish Health Affiliate Associate
DOI: /
 Original Research Article This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the
Original Research Article This is an Open Access article licensed under the terms of the Creative Commons Attribution- NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the
Antipsychotic Medications
 TRAIL: Team Review of EVIDENCE REVIEW & RECOMMENDATIONS FOR LTC Behavioural and psychological symptoms of dementia (BPSD) refer to the non-cognitive symptoms of disturbed perception, thought content, mood
TRAIL: Team Review of EVIDENCE REVIEW & RECOMMENDATIONS FOR LTC Behavioural and psychological symptoms of dementia (BPSD) refer to the non-cognitive symptoms of disturbed perception, thought content, mood
Atypical Antipsychotics and the Risk of Diabetes in an Elderly Population in Long-Term Care: A Retrospective Nursing Home Chart Review Study
 Atypical Antipsychotics and the Risk of Diabetes in an Elderly Population in Long-Term Care: A Retrospective Nursing Home Chart Review Study Stewart G. Albert, MD, George T. Grossberg, MD, Papan J. Thaipisuttikul,
Atypical Antipsychotics and the Risk of Diabetes in an Elderly Population in Long-Term Care: A Retrospective Nursing Home Chart Review Study Stewart G. Albert, MD, George T. Grossberg, MD, Papan J. Thaipisuttikul,
Neuropsychiatric Inventory Nursing Home Version (NPI-NH)
 This is a Sample version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) The full version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) comes without sample watermark..
This is a Sample version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) The full version of the Neuropsychiatric Inventory Nursing Home Version (NPI-NH) comes without sample watermark..
Antipsychotic use in dementia: a systematic review of benefits and risks from metaanalyses
 658463TAJ0010.1177/2040622316658463Therapeutic Advances in Chronic DiseaseRR Tampi, DJ Tampi research-article2016 Therapeutic Advances in Chronic Disease Original Research Antipsychotic use in dementia:
658463TAJ0010.1177/2040622316658463Therapeutic Advances in Chronic DiseaseRR Tampi, DJ Tampi research-article2016 Therapeutic Advances in Chronic Disease Original Research Antipsychotic use in dementia:
Donepezil, galantamine, rivastigmine (review) and memantine for the treatment of Alzheimer s disease (amended)
 Issue date: November 2006 (amended September 2007) Review date: September 2009 Donepezil, galantamine, rivastigmine (review) and memantine for the treatment of Alzheimer s disease (amended) Includes a
Issue date: November 2006 (amended September 2007) Review date: September 2009 Donepezil, galantamine, rivastigmine (review) and memantine for the treatment of Alzheimer s disease (amended) Includes a
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA
 BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
BEHAVIOURAL AND PSYCHOLOGICAL SYMPTOMS IN DEMENTIA Unmet needs What might be your behavioural response to this experience? Content Definition What are BPSD? Prevalence How common are they? Aetiological
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE. Health Technology Appraisal
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Donepezil, galantamine, rivastigmine and memantine for the treatment of Alzheimer's disease (Review of TA 111) Appraisal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE Health Technology Appraisal Donepezil, galantamine, rivastigmine and memantine for the treatment of Alzheimer's disease (Review of TA 111) Appraisal
Multi-morbidity in Dementia: A 21st Century Challenge. Sube Banerjee. Professor of Dementia Brighton and Sussex Medical School
 Multi-morbidity in Dementia: A 21st Century Challenge Sube Banerjee Professor of Dementia Brighton and Sussex Medical School Most people of any age with any long term condition have multiple conditions
Multi-morbidity in Dementia: A 21st Century Challenge Sube Banerjee Professor of Dementia Brighton and Sussex Medical School Most people of any age with any long term condition have multiple conditions
ORIGINAL CONTRIBUTION. Response of Patients With Alzheimer Disease to Rivastigmine Treatment Is Predicted by the Rate of Disease Progression
 ORIGINAL CONTRIBUTION Response of Patients With Alzheimer Disease to Rivastigmine Treatment Is Predicted by the Rate of Disease Progression Martin R. Farlow, MD; Ann Hake, MD; John Messina, PharmD; Richard
ORIGINAL CONTRIBUTION Response of Patients With Alzheimer Disease to Rivastigmine Treatment Is Predicted by the Rate of Disease Progression Martin R. Farlow, MD; Ann Hake, MD; John Messina, PharmD; Richard
Alzheimer dementia: Starting, stopping drug therapy
 REVIEW LUKE D. KIM, MD, FACP, CMD Assistant Professor of Medicine, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University, Cleveland, OH; Center for Geriatric Medicine, Medicine
REVIEW LUKE D. KIM, MD, FACP, CMD Assistant Professor of Medicine, Cleveland Clinic Lerner College of Medicine of Case Western Reserve University, Cleveland, OH; Center for Geriatric Medicine, Medicine
Psychotropic Medication Use in Canadian Long-Term Care Patients Referred for Psychogeriatric Consultation
 Original Research Psychotropic Medication Use in Canadian Long-Term Care Patients Referred for Psychogeriatric Consultation Corinne E. Fischer, MD 1,2,3, Carole Cohen, MD 3,4, Lauren Forrest, BSc 3, Tom
Original Research Psychotropic Medication Use in Canadian Long-Term Care Patients Referred for Psychogeriatric Consultation Corinne E. Fischer, MD 1,2,3, Carole Cohen, MD 3,4, Lauren Forrest, BSc 3, Tom
Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia
 86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
86 Neuropsychiatric Manifestations in Vascular Cognitive Impairment Patients with and without Dementia Pai-Yi Chiu 1,3, Chung-Hsiang Liu 2, and Chon-Haw Tsai 2 Abstract- Background: Neuropsychiatric profile
NEUROPSYCHOMETRIC TESTS
 NEUROPSYCHOMETRIC TESTS CAMCOG It is the Cognitive section of Cambridge Examination for Mental Disorders of the Elderly (CAMDEX) The measure assesses orientation, language, memory, praxis, attention, abstract
NEUROPSYCHOMETRIC TESTS CAMCOG It is the Cognitive section of Cambridge Examination for Mental Disorders of the Elderly (CAMDEX) The measure assesses orientation, language, memory, praxis, attention, abstract
Trial clinici nell anziano: efficacy or effectiveness?
 LA SPERIMENTAZIONE FARMACOLOGICA CLINICA IN ETÀ GERIATRICA Trial clinici nell anziano: efficacy or effectiveness? Graziano Onder Fondazione Universitaria Policlinico A. Gemelli Università Cattolica del
LA SPERIMENTAZIONE FARMACOLOGICA CLINICA IN ETÀ GERIATRICA Trial clinici nell anziano: efficacy or effectiveness? Graziano Onder Fondazione Universitaria Policlinico A. Gemelli Università Cattolica del
Please Join Us. International Psychogeriatric Association. Dependency Ratio. Geriatric Psychiatry in the 21st Century: A Global Perspective
 International Psychogeriatric Association Please Join Us Geriatric Psychiatry in the 21st Century: A Global Perspective Jacobo Mintzer M.D. Executive Director Roper Saint Frances Clinical and Biotechnology
International Psychogeriatric Association Please Join Us Geriatric Psychiatry in the 21st Century: A Global Perspective Jacobo Mintzer M.D. Executive Director Roper Saint Frances Clinical and Biotechnology
Method. NeuRA Cholinesterase inhibitors August 2016
 Introduction A supplementary, or adjunctive, treatment is administered in conjunction with a patient s ongoing antipsychotic therapy. (ChEI), or anticholinesterase, have been proposed as an additional
Introduction A supplementary, or adjunctive, treatment is administered in conjunction with a patient s ongoing antipsychotic therapy. (ChEI), or anticholinesterase, have been proposed as an additional
Evidence-Based Interventions to Improve Caregiver and Patient Outcomes in Dementia
 Evidence-Based Interventions to Improve Caregiver and Patient Outcomes in Dementia Alan B. Stevens, PhD Professor, Department of Medicine Vernon D. Holleman-Lewis M. Rampy Centennial Chair in Gerontology
Evidence-Based Interventions to Improve Caregiver and Patient Outcomes in Dementia Alan B. Stevens, PhD Professor, Department of Medicine Vernon D. Holleman-Lewis M. Rampy Centennial Chair in Gerontology
Behaviour Units: Understanding what they can offer Older Patients with Dementia
 Behaviour Units: Understanding what they can offer Older Patients with Dementia David K. Conn Baycrest Centre and University of Toronto 2013 Mount Sinai Geriatrics institute Outline Alice s journey continues
Behaviour Units: Understanding what they can offer Older Patients with Dementia David K. Conn Baycrest Centre and University of Toronto 2013 Mount Sinai Geriatrics institute Outline Alice s journey continues
K. Kahle-Wrobleski 1, J.S. Andrews 1, M. Belger 2, S. Gauthier 3, Y. Stern 4, D.M. Rentz 5, D. Galasko 6
 The Journal of Prevention of Alzheimer s Disease - JPAD Volume 2, Number 2, 2015 Clinical and Economic Characteristics of Milestones along the Continuum of Alzheimer s Disease: Transforming Functional
The Journal of Prevention of Alzheimer s Disease - JPAD Volume 2, Number 2, 2015 Clinical and Economic Characteristics of Milestones along the Continuum of Alzheimer s Disease: Transforming Functional
The Long-term Prognosis of Delirium
 The Long-term Prognosis of Jane McCusker, MD, DrPH, Professor, Epidemiology and Biostatistics, McGill University; Head, Clinical Epidemiology and Community Studies, St. Mary s Hospital, Montreal, QC. Nine
The Long-term Prognosis of Jane McCusker, MD, DrPH, Professor, Epidemiology and Biostatistics, McGill University; Head, Clinical Epidemiology and Community Studies, St. Mary s Hospital, Montreal, QC. Nine
Acute Care Utilization by Dementia Caregivers Within Urban Primary Care Practices
 Acute Care Utilization by Dementia Caregivers Within Urban Primary Care Practices Cathy C. Schubert, MD 3, Malaz Boustani, MD, MPH 1,2,3, Christopher M. Callahan, MD 1,2,3, Anthony J. Perkins, MS 1,2,
Acute Care Utilization by Dementia Caregivers Within Urban Primary Care Practices Cathy C. Schubert, MD 3, Malaz Boustani, MD, MPH 1,2,3, Christopher M. Callahan, MD 1,2,3, Anthony J. Perkins, MS 1,2,
Donepezil, (R,S)-1-benzyl-4[(5,6 dimethoxy-1-indanon)- Update on Alzheimer Drugs (Donepezil) ORIGINAL ARTICLE. Rachelle Smith Doody, MD, PhD
 ORIGINAL ARTICLE Update on Alzheimer Drugs (Donepezil) Rachelle Smith Doody, MD, PhD Background: Several clinical trials have been conducted over a period of many years reporting the benefits of donepezil
ORIGINAL ARTICLE Update on Alzheimer Drugs (Donepezil) Rachelle Smith Doody, MD, PhD Background: Several clinical trials have been conducted over a period of many years reporting the benefits of donepezil
Organization: Sheppard Pratt Health System Solution Title: Lean Methodology: Appropriate Antipsychotic Use on an Inpatient Dementia Unit
 Organization: Sheppard Pratt Health System Solution Title: Lean Methodology: Appropriate Antipsychotic Use on an Inpatient Dementia Unit Problem: For dementia patients, antipsychotic medications are prescribed
Organization: Sheppard Pratt Health System Solution Title: Lean Methodology: Appropriate Antipsychotic Use on an Inpatient Dementia Unit Problem: For dementia patients, antipsychotic medications are prescribed
Pharmacological Treatment of Dementia
 Pharmacological Treatment of Dementia Measure Description Percentage of patients with dementia or their caregivers with whom available guideline-appropriate pharmacological treatment options and nonpharmacological
Pharmacological Treatment of Dementia Measure Description Percentage of patients with dementia or their caregivers with whom available guideline-appropriate pharmacological treatment options and nonpharmacological
Donepezil, galantamine, rivastigmine and memantine for the treatment of Alzheimer's disease (review of TA 111)
 National Institute for Health and Clinical Excellence Health Technology Appraisal Donepezil, galantamine, rivastigmine and memantine for the treatment of Alzheimer's disease (review of TA 111) Response
National Institute for Health and Clinical Excellence Health Technology Appraisal Donepezil, galantamine, rivastigmine and memantine for the treatment of Alzheimer's disease (review of TA 111) Response
MANAGEMENT OF NEUROPSYCHIATRIC SYMPTOMS OF DEMENTIA
 MANAGEMENT OF NEUROPSYCHIATRIC SYMPTOMS OF DEMENTIA Dr. Dallas Seitz MD PhD FRCPC Associate Professor and Division Chair, Division of Geriatric Psychiatry Department of Psychiatry, Queen s University President,
MANAGEMENT OF NEUROPSYCHIATRIC SYMPTOMS OF DEMENTIA Dr. Dallas Seitz MD PhD FRCPC Associate Professor and Division Chair, Division of Geriatric Psychiatry Department of Psychiatry, Queen s University President,
Hisanori Kobayashi, Takashi Ohnishi, Ryoko Nakagawa and Kazutake Yoshizawa
 RESEARCH ARTICLE The comparative efficacy and safety of cholinesterase inhibitors in patients with mild-to-moderate Alzheimer s disease: a Bayesian network meta-analysis Hisanori Kobayashi, Takashi Ohnishi,
RESEARCH ARTICLE The comparative efficacy and safety of cholinesterase inhibitors in patients with mild-to-moderate Alzheimer s disease: a Bayesian network meta-analysis Hisanori Kobayashi, Takashi Ohnishi,
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017.
 DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
DEMENTIA and BPSD in PARKINSON'S DISEASE. DR. T. JOHNSON. NOVEMBER 2017. Introduction. Parkinson's disease (PD) has been considered largely as a motor disorder. It has been increasingly recognized that
ANTIPSYCHOTICS IN LONG TERM CARE: Are We Doing More Harm than Good?
 ANTIPSYCHOTICS IN LONG TERM CARE: Are We Doing More Harm than Good? STEPHANIE M. OZALAS, PHARMD, BCPS, BCGP VA MARYLAND HEALTH CARE SYSTEM BALTIMORE, MD DISCLOSURES Off-label use of medications will be
ANTIPSYCHOTICS IN LONG TERM CARE: Are We Doing More Harm than Good? STEPHANIE M. OZALAS, PHARMD, BCPS, BCGP VA MARYLAND HEALTH CARE SYSTEM BALTIMORE, MD DISCLOSURES Off-label use of medications will be
Dementia and Fall Geriatric Interprofessional Training. Wael Hamade, MD, FAAFP
 Dementia and Fall Geriatric Interprofessional Training Wael Hamade, MD, FAAFP Prevalence of Dementia Age range 65-74 5% % affected 75-84 15-25% 85 and older 36-50% 5.4 Million American have AD Dementia
Dementia and Fall Geriatric Interprofessional Training Wael Hamade, MD, FAAFP Prevalence of Dementia Age range 65-74 5% % affected 75-84 15-25% 85 and older 36-50% 5.4 Million American have AD Dementia
SYNOPSIS. Risperidone-R064766: Clinical Study Report RIS-AUS-5 (FOR NATIONAL AUTHORITY USE ONLY)
 SYNOPSIS Protocol No.: RIS-AUS-5 Psychosis in Alzheimer s disease (PAD) analysis Title of Study: Risperidone in the treatment of behavioral and psychological symptoms in dementia: a multicenter, double-blind,
SYNOPSIS Protocol No.: RIS-AUS-5 Psychosis in Alzheimer s disease (PAD) analysis Title of Study: Risperidone in the treatment of behavioral and psychological symptoms in dementia: a multicenter, double-blind,
Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials
 Alzheimer s & Dementia 4 (2008) 390 394 Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials Donald J. Connor a, *, Marwan N. Sabbagh a, Jeffery L. Cummings b a Cleo
Alzheimer s & Dementia 4 (2008) 390 394 Comment on administration and scoring of the Neuropsychiatric Inventory in clinical trials Donald J. Connor a, *, Marwan N. Sabbagh a, Jeffery L. Cummings b a Cleo
MORTALITY ASSOCIATED WITH USE OF ANTIPSYCHOTICS IN DEMENTIA: REVIEWING THE EVIDENCE
 MORTALITY ASSOCIATED WITH USE OF ANTIPSYCHOTICS IN DEMENTIA: REVIEWING THE EVIDENCE KRISTA L. LANCTÔT, PHD PROFESSOR OF PSYCHIATRY AND PHARMACOLOGY, UNIVERSITY OF TORONTO; SENIOR SCIENTIST, HURVITZ BRAIN
MORTALITY ASSOCIATED WITH USE OF ANTIPSYCHOTICS IN DEMENTIA: REVIEWING THE EVIDENCE KRISTA L. LANCTÔT, PHD PROFESSOR OF PSYCHIATRY AND PHARMACOLOGY, UNIVERSITY OF TORONTO; SENIOR SCIENTIST, HURVITZ BRAIN
FROM THE ALZHEIMER S ASSOCIATION INTERNATIONAL CONFERENCE 2018 NEW RESEARCH FOCUSES ON TREATING NON-COGNITIVE SYMPTOMS OF PEOPLE WITH DEMENTIA
 CONTACT: Alzheimer s Association AAIC Press Office, 312-949-8710, aaicmedia@alz.org Niles Frantz, Alzheimer s Association, 312-335-5777, niles.frantz@alz.org FROM THE ALZHEIMER S ASSOCIATION INTERNATIONAL
CONTACT: Alzheimer s Association AAIC Press Office, 312-949-8710, aaicmedia@alz.org Niles Frantz, Alzheimer s Association, 312-335-5777, niles.frantz@alz.org FROM THE ALZHEIMER S ASSOCIATION INTERNATIONAL
Drugs for dementia: the first year
 The Ulster Medical Journal, Volume 69, No. 2, pp. 123-127, November 2000. Drugs for dementia: the first year An audit of prescribing practice G McGirr, S A Compton Accepted 12 September 2000 SUMMARY In
The Ulster Medical Journal, Volume 69, No. 2, pp. 123-127, November 2000. Drugs for dementia: the first year An audit of prescribing practice G McGirr, S A Compton Accepted 12 September 2000 SUMMARY In
C holinomimetic drugs constitute the first line of treatment
 310 PAPER Cholinesterase inhibitor treatment alters the natural history of Alzheimer s disease O L Lopez, J T Becker, S Wisniewski, J Saxton, D I Kaufer, S T DeKosky... See end of article for authors affiliations...
310 PAPER Cholinesterase inhibitor treatment alters the natural history of Alzheimer s disease O L Lopez, J T Becker, S Wisniewski, J Saxton, D I Kaufer, S T DeKosky... See end of article for authors affiliations...
Relapse Risk after Discontinuation of Risperidone in Alzheimer s Disease
 original article Relapse Risk after Discontinuation of Risperidone in Alzheimer s Disease D.P. Devanand, M.D., Jacobo Mintzer, M.D., M.B.A., Susan K. Schultz, M.D., Howard F. Andrews, Ph.D., David L. Sultzer,
original article Relapse Risk after Discontinuation of Risperidone in Alzheimer s Disease D.P. Devanand, M.D., Jacobo Mintzer, M.D., M.B.A., Susan K. Schultz, M.D., Howard F. Andrews, Ph.D., David L. Sultzer,
SYNOPSIS. Risperidone-R064766: Clinical Study Report RIS-USA-232 (FOR NATIONAL AUTHORITY USE ONLY)
 SYNOPSIS Protocol No.: RIS-USA-232 Title of Study: Efficacy and Safety of a Flexible Dose of Risperidone Versus Placebo in the Treatment of Psychosis of Alzheimer's Disease Principal Investigator: M.D.
SYNOPSIS Protocol No.: RIS-USA-232 Title of Study: Efficacy and Safety of a Flexible Dose of Risperidone Versus Placebo in the Treatment of Psychosis of Alzheimer's Disease Principal Investigator: M.D.
How I Treat Aggression in Outpatients With Dementia. C. Omelan MD, FRCP(C)
 How I Treat Aggression in Outpatients With Dementia C. Omelan MD, FRCP(C) Conflict of Interest I have no potential conflicts of interest to declare Overview Outline the prevalence of aggression Review
How I Treat Aggression in Outpatients With Dementia C. Omelan MD, FRCP(C) Conflict of Interest I have no potential conflicts of interest to declare Overview Outline the prevalence of aggression Review
Technology appraisal guidance Published: 23 March 2011 nice.org.uk/guidance/ta217
 Donepezil, galantamine, rivastigmine and memantine for the treatment of Alzheimer's disease Technology appraisal guidance Published: 23 March 2011 nice.org.uk/guidance/ta217 NICE 2017. All rights reserved.
Donepezil, galantamine, rivastigmine and memantine for the treatment of Alzheimer's disease Technology appraisal guidance Published: 23 March 2011 nice.org.uk/guidance/ta217 NICE 2017. All rights reserved.
Baseline Characteristics of Patients Attending the Memory Clinic Serving the South Shore of Boston
 Article ID: ISSN 2046-1690 Baseline Characteristics of Patients Attending the www.thealzcenter.org Memory Clinic Serving the South Shore of Boston Corresponding Author: Dr. Anil K Nair, Chief of Neurology,
Article ID: ISSN 2046-1690 Baseline Characteristics of Patients Attending the www.thealzcenter.org Memory Clinic Serving the South Shore of Boston Corresponding Author: Dr. Anil K Nair, Chief of Neurology,
An#psycho#c Medica#on in People with Demen#a
 An#psycho#c Medica#on in People with Demen#a GERARD BYRNE BSc (Med), MBBS (Hons), PhD, FRANZCP, MFPOA School of Medicine, University of Queensland Mental Health Service, Royal Brisbane & Women s Hospital
An#psycho#c Medica#on in People with Demen#a GERARD BYRNE BSc (Med), MBBS (Hons), PhD, FRANZCP, MFPOA School of Medicine, University of Queensland Mental Health Service, Royal Brisbane & Women s Hospital
RESEARCH AND PRACTICE IN ALZHEIMER S DISEASE VOL 10 EADC OVERVIEW B. VELLAS & E. REYNISH
 EADC BRUNO VELLAS 14/01/05 10:14 Page 1 EADC OVERVIEW B. VELLAS & E. REYNISH (Toulouse, France, EU) Bruno Vellas: The European Alzheimer's Disease Consortium is a European funded network of centres of
EADC BRUNO VELLAS 14/01/05 10:14 Page 1 EADC OVERVIEW B. VELLAS & E. REYNISH (Toulouse, France, EU) Bruno Vellas: The European Alzheimer's Disease Consortium is a European funded network of centres of
Appendix K: Evidence review flow charts
 K.1 Dementia diagnosis K.1.1 Dementia diagnosis What are the most effective methods of primary assessment to decide whether a person with suspected dementia should be referred to a dementia service? What
K.1 Dementia diagnosis K.1.1 Dementia diagnosis What are the most effective methods of primary assessment to decide whether a person with suspected dementia should be referred to a dementia service? What
MEDICATIONS IN MANAGING DIFFICULT BEHAVIORS
 MEDICATIONS IN MANAGING DIFFICULT BEHAVIORS A REALITY CHECK reality check Noun informal an occasion on which one is reminded of the state of things in the real world. ROBERT LACOSTE, MD MEDICAL DIRECTOR,
MEDICATIONS IN MANAGING DIFFICULT BEHAVIORS A REALITY CHECK reality check Noun informal an occasion on which one is reminded of the state of things in the real world. ROBERT LACOSTE, MD MEDICAL DIRECTOR,
NeuRA Obsessive-compulsive disorders October 2017
 Introduction (OCDs) involve persistent and intrusive thoughts (obsessions) and repetitive actions (compulsions). The DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition) defines
Introduction (OCDs) involve persistent and intrusive thoughts (obsessions) and repetitive actions (compulsions). The DSM-5 (Diagnostic and Statistical Manual of Mental Disorders, Fifth Edition) defines
Management of Alzheimer s Disease in the Managed Care Setting
 Management of Alzheimer s Disease in the Managed Care Setting Paul Stander, M.D. For a CME/CEU version of this article please go to http://www.namcp.org/cmeonline.htm, and then click the activity title.
Management of Alzheimer s Disease in the Managed Care Setting Paul Stander, M.D. For a CME/CEU version of this article please go to http://www.namcp.org/cmeonline.htm, and then click the activity title.
2006, Editrice Kurtis
 Aging Clinical and Experimental Research Pharmacological treatment of Alzheimer s Disease* Angelo Bianchetti 1, Piera Ranieri 1, Alessandro Margiotta 1, and Marco Trabucchi 2 1 Department of Medicine,
Aging Clinical and Experimental Research Pharmacological treatment of Alzheimer s Disease* Angelo Bianchetti 1, Piera Ranieri 1, Alessandro Margiotta 1, and Marco Trabucchi 2 1 Department of Medicine,
Drug Update. Treatments for Cognitive Impairment in the Older Adult. William Solan, M.D. Karen Sanders, Ph.D. Northwest Hospital Seattle
 Drug Update Treatments for Cognitive Impairment in the Older Adult William Solan, M.D. Karen Sanders, Ph.D. Northwest Hospital Seattle Current Drug Treatments for Alzheimer s Disease Cholinesterase Inhibitors:
Drug Update Treatments for Cognitive Impairment in the Older Adult William Solan, M.D. Karen Sanders, Ph.D. Northwest Hospital Seattle Current Drug Treatments for Alzheimer s Disease Cholinesterase Inhibitors:
Across the Spectrum of Dementia. Keys to Understanding Behaviours & Anticipating Needs
 Across the Spectrum of Dementia Keys to Understanding Behaviours & Anticipating Needs Outline Review current predictions for dementia prevalence, & the implications for future needs Discuss retrogenesis
Across the Spectrum of Dementia Keys to Understanding Behaviours & Anticipating Needs Outline Review current predictions for dementia prevalence, & the implications for future needs Discuss retrogenesis
A pan-european study on outcome measures for psychosocial intervention research in dementia
 A pan-european study on outcome measures for psychosocial intervention research in dementia CHATTAT Rabih, MONIZ-COOK Esme, WOODS Bob, and members of the INTERDEM JPND outcomes working group 26 th Alzheimer
A pan-european study on outcome measures for psychosocial intervention research in dementia CHATTAT Rabih, MONIZ-COOK Esme, WOODS Bob, and members of the INTERDEM JPND outcomes working group 26 th Alzheimer
NKR 55 demens og medicin PICO 2 seponering af antipsykotisk medicin versus forsat behandling Review information
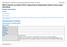 NKR 55 demens og medicin PICO 2 seponering af antipsykotisk medicin versus forsat behandling Review information Authors Sundhedsstyrelsen 1 1 [Empty affiliation] Citation example: S. NKR 55 demens og medicin
NKR 55 demens og medicin PICO 2 seponering af antipsykotisk medicin versus forsat behandling Review information Authors Sundhedsstyrelsen 1 1 [Empty affiliation] Citation example: S. NKR 55 demens og medicin
Coordinating Care Between Neurology and Psychiatry to Improve the Diagnosis and Treatment of Parkinson s Disease Psychosis
 Coordinating Care Between Neurology and Psychiatry to Improve the Diagnosis and Treatment of Parkinson s Disease Psychosis Jeff Gelblum, MD Senior Attending Neurologist Mt. Sinai Medical Center Miami,
Coordinating Care Between Neurology and Psychiatry to Improve the Diagnosis and Treatment of Parkinson s Disease Psychosis Jeff Gelblum, MD Senior Attending Neurologist Mt. Sinai Medical Center Miami,
Donepezil for the Treatment of Agitation in Alzheimer s Disease
 T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article for the Treatment of Agitation in Alzheimer s Disease Robert J. Howard, M.R.C.Psych., Edmund Juszczak, B.Sc., Clive G. Ballard, M.R.C.Psych.,
T h e n e w e ng l a nd j o u r na l o f m e dic i n e original article for the Treatment of Agitation in Alzheimer s Disease Robert J. Howard, M.R.C.Psych., Edmund Juszczak, B.Sc., Clive G. Ballard, M.R.C.Psych.,
A wide range of neuropsychiatric disturbances commonly
 36 PAPER Neuropsychiatric symptoms in patients with Parkinson s disease and dementia: frequency, profile and associated care giver stress D Aarsland, K Brønnick, U Ehrt, P P De Deyn, S Tekin, M Emre, J
36 PAPER Neuropsychiatric symptoms in patients with Parkinson s disease and dementia: frequency, profile and associated care giver stress D Aarsland, K Brønnick, U Ehrt, P P De Deyn, S Tekin, M Emre, J
ORIGINAL CONTRIBUTION. The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease
 ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
ORIGINAL CONTRIBUTION The Spectrum of Behavioral Responses to Cholinesterase Inhibitor Therapy in Alzheimer Disease Michael S. Mega, MD, PhD; Donna M. Masterman, MD; Susan M. O Connor, RNC; Terry R. Barclay,
Managing agitation in dementia using non-pharmacological therapies
 Managing agitation in dementia using non-pharmacological therapies Gill Livingston Lynsey Kelly, Elanor Lewis-Holmes, Gianluca Baio, Rumana Omar, Stephen Morris, Nishma Patel, Cornelius Katona, Claudia
Managing agitation in dementia using non-pharmacological therapies Gill Livingston Lynsey Kelly, Elanor Lewis-Holmes, Gianluca Baio, Rumana Omar, Stephen Morris, Nishma Patel, Cornelius Katona, Claudia
