Distinct phenotypes of speech and voice disorders in Parkinson s disease after subthalamic nucleus deep brain stimulation
|
|
|
- Giles Allison
- 6 years ago
- Views:
Transcription
1 Downloaded from on March 5, Published by group.bmj.com JNNP Online First, published on October 3, 2014 as /jnnp Movement disorders RESEARCH PAPER Distinct phenotypes of speech and voice disorders in Parkinson s disease after subthalamic nucleus deep brain stimulation Takashi Tsuboi, 1 Hirohisa Watanabe, 1 Yasuhiro Tanaka, 1 Reiko Ohdake, 1 Noritaka Yoneyama, 1 Kazuhiro Hara, 1 Ryoichi Nakamura, 1 Hazuki Watanabe, 1 Jo Senda, 1 Naoki Atsuta, 1 Mizuki Ito, 1 Masaaki Hirayama, 1 Masahiko Yamamoto, 2 Yasushi Fujimoto, 3 Yasukazu Kajita, 4 Toshihiko Wakabayashi, 4 Gen Sobue 1 Additional material is published online only. To view please visit the journal online ( jnnp ). 1 Department of Neurology, Nagoya University Graduate School of Medicine, Nagoya, Japan 2 Faculty of Psychological and Physical Science, Aichi-Gakuin University, Aichi, Japan 3 Department of Otorhinolaryngology, Nagoya University Graduate School of Medicine, Nagoya, Japan 4 Department of Neurosurgery, Nagoya University Graduate School of Medicine, Nagoya, Japan Correspondence to Gen Sobue, Department of Neurology, Nagoya University Graduate School of Medicine, Showa-ku, Nagoya , Japan; sobueg@med.nagoya-u.ac.jp Received 5 March 2014 Accepted 11 September 2014 To cite: Tsuboi T, Watanabe H, Tanaka Y, et al. J Neurol Neurosurg Psychiatry Published Online First: [ please include Day Month Year] doi: / jnnp ABSTRACT Objectives To elucidate the phenotypes and pathophysiology of speech and voice disorders in Parkinson s disease (PD) with subthalamic nucleus deep brain stimulation (STN-DBS). Methods We conducted a cross-sectional study on 76 PD patients treated with bilateral STN-DBS (PD-DBS) and 33 medically treated PD patients (PD-Med). Speech and voice functions, electrode positions, motor function and cognitive function were comprehensively assessed. Moreover, speech and voice functions were compared between the on-stimulation and off-stimulation conditions in 42 PD-DBS patients. Results Speech and voice disorders in PD-DBS patients were significantly worse than those in PD-Med patients. Factor analysis and subsequent cluster analysis classified PD-DBS patients into five clusters: relatively good speech and voice function type, 25%; stuttering type, 24%; breathy voice type, 16%; strained voice type, 18%; and spastic dysarthria type, 17%. STN-DBS ameliorated voice tremor or low volume; however, it deteriorated the overall speech intelligibility in most patients. Breathy voice did not show significant changes and stuttering exhibited slight improvement after stopping stimulation. In contrast, patients with strained voice type or spastic dysarthria type showed a greater improvement after stopping stimulation. Spastic dysarthria type patients showed speech disorders similar to spastic dysarthria, which is associated with bilateral upper motor neuron involvement. Strained voice type and spastic dysarthria type appeared to be related to current diffusion to the corticobulbar fibres. Conclusions Stuttering and breathy voice can be aggravated by STN-DBS, but are mainly due to aging or PD itself. Strained voice and spastic dysarthria are considered corticobulbar side effects. INTRODUCTION Despite improved motor function after subthalamic nucleus deep brain stimulation (STN-DBS), Parkinson s disease (PD) patients sometimes develop speech and voice disorders, which reduce patient s quality of life. A systematic review of the literature reported that stimulation-related dysarthria was observed in 9.3% of PD patients with STN-DBS. 1 A prospective study focusing on speech function revealed that PD patients with STN-DBS showed a greater deterioration in speech intelligibility at 1 year after surgery than medically treated patients. 2 Current diffusion to the cerebellothalamic fibres 2 5 and corticobulbar fibres 6 9 is closely related to speech and voice disorders. Tripoliti et al 10 noted that after STN-DBS, voice could sometimes sound strained, strangled and breathless, resulting in a scanning, one-word-at-a-time speech. Tommasi et al 9 characterised dysarthria due to the corticobulbar side effect by hypophonic, slurred speech, rapid fatiguing and hesitation with frequent, long pauses. Stuttering worsened or relapsed after STN-DBS. Thus, STN-DBS can induce or aggravate widely different types of speech and voice disorders. However, there have been no reports that investigated the diverseness of speech and voice disorders in a large number of PD patients with STN-DBS. In this study, we assessed speech and voice functions in 76 PD patients with STN-DBS as well as 33 medically treated patients, and we aimed to divide patients with STN-DBS into several phenotypes by factor analysis and subsequent cluster analysis. Motor and cognitive functions and electrode positions were also evaluated to elucidate the underlying pathophysiology of speech and voice disorders. METHODS Subjects Patients with PD who had undergone bilateral STN-DBS were recruited in the Movement Disorders Clinic of the Nagoya University Hospital from 2005 to The inclusion criteria were as follows: (1) diagnosis of PD according to the UK Parkinson s Disease Society brain bank criteria, 13 (2) 6-month follow-up period after subthalamic implantation, (3) absence of further neurological disease, and (4) absence of severe cognitive impairment or psychiatric disorders that may hinder speech and voice assessment. A total of 76 eligible PD patients treated with STN-DBS participated in this study (PD-DBS group). Surgical procedures were performed as previously described. 14 PD-DBS patients were evaluated in the on-state under their usual optimised medication and STN-DBS. Age, sex, disease duration and motor and cognitive function matched those of 33 patients with medically Copyright Article author (or their employer) Produced by BMJ Publishing Group Ltd under licence. Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
2 Movement disorders Downloaded from on March 5, Published by group.bmj.com Table 1 Clinical background of PD-DBS and PD-Med groups PD-DBS PD-Med n=76 n=33 Age (years) 66.1± ±7.4 Sex (female, %) Disease duration (years) 14.8± ±4.7 Postsurgery period (years) 2.5±2.1 UPDRS-III 23.3± ±10.8 UPDRS-IV 4.7± ±2.8 MMSE 26.3± ±3.3 MoCA 21.1± ±5.0 Line orientation 14.5± ±3.4 Stroop color-word test 31.5± ±38 Verbal fluency (semantic) 10.2±3.7* 14.8±5.9 Verbal fluency (phonemic) 7.0±3.0* 8.7±3.4 Digit span test 10.5± ±2.4 LEDD (mg) 660.9±365.2* 949.3±451.7 Amplitude: left (V) 2.4±0.5 Frequency: left (Hz) 136.3±18.2 Pulse width: left (microseconds) 89.7±16.3 Amplitude: right (V) 2.4±0.5 Frequency: right (Hz) 134.7±23.9 Pulse width: right (microseconds) 91.5±18.6 Monopolar/Bipolar/Both monopolar and bipolar (n) 47/17/12 Values are mean±sd. Groups were compared using independent t tests or non-parametric Mann-Whitney U tests. p Value<0.05 was considered significant. *Significant difference between two groups. LEDD, levodopa equivalent daily dose; MMSE, Mini-Mental State Examination; MoCA, Montreal Cognitive Assessment; PD-DBS, patients treated with deep brain stimulation; PD-Med, medically treated patients; UPDRS, Unified Parkinson s Disease Rating Scale. treated PD were also included (PD-Med group). PD-Med patients were assessed in the on-state under continued medication. The sample characteristics are described in table 1. This study was approved by the ethics committee of the Nagoya University Graduate School of Medicine. All participants provided written informed consent. Speech and voice evaluation Sustained-vowels, reading task of a standard passage (The North Wind and the Sun) in Japanese, and short conversations were recorded using Computerised Speech Lab (Kay Elemetrics, Lincoln Park, New Jersey, USA) and a microphone (ECM-MS907; Sony, Tokyo, Japan) with a sampling rate of 44.1 khz in a sound-treated room. Speech disorders were perceptually evaluated using the Assessment of Motor Speech for Dysarthria (AMSD) which comprises analogous variables developed by Darley et al Voice disorders were perceptually evaluated using the Grade of dysphonia, Roughness, Breathiness, Asthenia and Strain (GRBAS) scale. 17 Three welltrained and certified speech pathologists independently and blindly rated recorded speech samples. The scores of the three raters were averaged subsequently. Inter-rater reliability was assessed using Cohen s κ coefficient (R, org/), which was According to the Landis and Koch classification, this fit was considered to be substantial. With regard to on-stimulation and off-stimulation assessment, changes in variables by 1.00 were considered as significant. The Stuttering Severity Instrument-3 (SSI-3) was used to assess the severity of stuttering. 18 Maximum phonation time (MPT) was determined by measuring the duration of the sustained vowel/a:/ after maximum inspiration. 19 A subjective self-assessment of speech and voice disorders was scored according to the Voice Handicap Index (VHI). 20 Definitions and interpretations of the variables used to evaluate speech and voice disorders are summarised in online supplementary table S1. Speech and voice assessment in the on-stimulation and off-stimulation conditions In 42 of 76 PD-DBS patients who agreed to stop stimulation temporarily, speech and voice functions were evaluated in the on-stimulation condition and 30 min after stopping stimulation. Clinical and radiological evaluations Motor function (the Unified Parkinson s Disease Rating Scale III (UPDRS-III) and UPDRS-IV) and cognitive function (the Mini-Mental State Examination (MMSE), Montreal Cognitive Assessment (MoCA), line orientation, Stroop color-word test, verbal fluency and digit span tests) were assessed. Levodopa equivalent daily dose (LEDD) was calculated as described previously. 21 Postoperative CTs (Asteion; Toshiba Medical Systems, Tochigi, Japan) with a slice thickness of 1 mm were obtained concurrently with clinical evaluations. Anatomical locations of DBS electrodes were identified by fusing the postoperative CT images with the preoperative MRI (iplan Stereotaxy; Brainlab, Munich, Germany). The lateral distance from the midline and the anteroposterior distance from the mid-commissural line to each electrode at the level of 3.5 mm below the AC PC line were calculated and plotted on the human brain atlas. 22 Statistical analysis The normal distribution of data was tested using the Shapiro-Wilk test. The clinical background and speech and voice functions of PD-DBS and PD-Med patients were compared using independent t tests or non-parametric Mann-Whitney U tests. Exploratory factor analysis (generalised least-squares method) was performed on the speech and voice variables of PD-DBS patients to extract factors, followed by Varimax rotation. Fits of the data for the final factor solution were examined using the Kaiser-Meyer-Olkin measure of sampling adequacy and Bartlett s test of sphericity. Components with eigenvalues >1 were selected. Subsequently, cluster analysis (Ward s method) on the basis of the factor scores classified PD-DBS patients into clusters according to the similarity of predominant speech and voice characteristics in each patient. Two-way ANOVA with post hoc tests (Tukey or Games-Howell) or nonparametric Kruskal-Wallis tests with post-hoc tests (Mann-Whitney) were used to examine the differences among the clusters and PD-Med patients. Speech and voice functions in the on-stimulation and off-stimulation conditions were compared using paired t tests or non-parametric Wilcoxon signed rank tests. p Values <0.05 were considered significant. Abovementioned statistical analyses were performed using the Predictive Analysis Software, V.18 (SPSS, Chicago, Illinois, USA). RESULTS Global population characteristics The clinical background was not significantly different between PD-DBS and PD-Med patients, except that semantic and phonemic verbal fluency were significantly worse in PD-DBS patients than those in PD-Med patients and that LEDD was significantly lower in PD-DBS patients than that in PD-Med patients (table 1). Several speech and voice variables were significantly 2 Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
3 Downloaded from on March 5, Published by group.bmj.com Movement disorders Table 2 Severity of speech and voice disorders in PD-DBS and PD-Med groups PD-DBS PD-Med n=76 n=33 AMSD Overall severity of speech disorders Intelligibility 2.7±1.0* 1.7±0.8 Naturalness 3.6±1.0* 2.4±1.0 Subparts Imprecise consonants 1.0±0.9* 0.4±0.4 Monoloudness 1.3± ±0.8 Monopitch 1.4± ±0.8 Low volume 1.5±0.9* 0.9±0.8 Short rushes of speech 1.0±1.0* 0.4±0.7 Voice tremor 0.4±0.5* 0.7±0.7 Sound repeated 0.7± ±0.6 Hypernasality 0.8±0.8* 0.3±0.5 Abnormal rate 1.1±0.8* 0.6±0.7 Variable rate 1.1± ±0.6 Excess loudness variation 1.1±0.7* 0.8±0.5 Abnormal pitch level 1.0±0.7* 0.5±0.5 Variable pitch 0.5±0.7* 0.1±0.2 GRBAS scale Overall severity of voice disorders Grade of dysphonia 2.0±0.7* 1.3±0.6 Subparts Roughness 1.3±0.7* 0.9±0.5 Breathiness 1.1± ±0.8 Asthenia 1.1±0.8* 0.7±0.8 Strain 1.0±0.8* 0.3±0.4 SSI-3 6.3± ±7.2 MPT (s) 18.7± ±8.8 VHI 52.5±27.9* 30.6±21.2 Values are means±sd. Groups were compared using independent t tests or non-parametric Mann-Whitney U tests. p Value<0.05 was considered significant. *Significant difference between two groups. AMSD, Assessment of Motor Speech for Dysarthria; GRBAS, Grade of dysphonia, Roughness, Breathiness, Asthenia and Strain; MPT, maximum phonation time; PD-DBS, patients treated with deep brain stimulation; PD-Med, medically treated patients; SSI-3, Stuttering Severity Instrument-3; VHI, Voice Handicap Index. worse in PD-DBS patients than in PD-Med patients; and voice tremor was significantly better in PD-DBS patients than in PD-Med patients (table 2). Factor analysis followed by cluster analysis Exploratory factor analysis was performed on all objective speech and voice variables (AMSD, GRBAS scale, SSI-3, and MPT) from PD-DBS patients. Intelligibility, naturalness and grade of dysphonia were dropped because of cross-loadings on several factors; abnormal rate and abnormal pitch level were dropped because they partially overlapped with variable rate and variable pitch, respectively; and voice tremor was dropped because its contribution to the overall instrument was of little importance. The final factor analysis extracted five factors with eigenvalues >1.092, which together, accounted for 74.4% of the total variation. The factor-loading matrix after Varimax rotation is shown in table 3. The Kaiser-Meyer-Olkin measure of the final factor solution was 0.654, and the result of Bartlett s test of sphericity was significant ( p<0.001), indicating the appropriateness of this factor analysis. Cluster analysis on the basis of the factor scores classified the 76 patients into five clusters. Table 3 rotation Factor loading matrix of the five factors after orthogonal Factor 1 Factor 2 Factor 3 Factor 4 Factor 5 Sound repeated SSI Variable rate Asthenia Low volume Breathiness Short rushes of speech Strain Roughness MPT Imprecise consonants Hypernasality Monopitch Monoloudness Excess loudness variation Variable pitch The generalised least-squares method was applied to extract factors, followed by orthogonal (Varimax) rotation. The highest factor loadings in each variable are written in bold characters. MPT, maximum phonation time; SSI-3, Stuttering Severity Instrument-3. Characterisation of the clusters The clinical background of the five clusters and PD-Med patients is summarised in online supplementary table S2. Cluster 5 had significantly longer postsurgery period and worse scores for UPDRS-III and MMSE than cluster 1. Clusters 2, 3, 4 and 5 showed significantly worse scores for semantic verbal fluency than PD-Med patients. LEDD in cluster 2 was significantly lower than that in PD-Med patients. Stimulation parameters were not significantly different among clusters. The characteristics of speech and voice disorders in the clusters and PD-Med patients are listed in table 4. Cluster 1 included 25% of PD-DBS patients, who showed generally better speech and voice functions than patients in the other clusters. Furthermore, voice tremor scores in cluster 1 were significantly better than those in PD-Med patients. We labelled cluster 1 as relatively good speech and voice function type. Cluster 2 included 24% patients and was characterised by the highest scores for sound repeated, abnormal rate and SSI-3. We labelled cluster 2 as stuttering type. Cluster 3 included 16% patients, and scores for low volume, grade of dysphonia, breathiness and asthenia were the highest among all clusters. We labelled cluster 3 as breathy voice type. Cluster 4 included 18% patients and was characterised by the highest scores for short rushes of speech, excess loudness variation, roughness and strain and the lowest scores for MPT. We labelled cluster 4 as strained voice type. Cluster 5 included 17% patients who had the highest scores for intelligibility and naturalness, imprecise consonants, monoloudness, monopitch, hypernasality and VHI. We labelled cluster 5 as spastic dysarthria type. The naming of the clusters will be discussed below. On-stimulation and off-stimulation assessment Forty-two PD-DBS patients consented to stopping stimulation temporarily. Since two patients became almost speechless due to severe akinesia and rigidity, speech and voice functions in 40 patients were compared between the on-stimulation and Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
4 Movement disorders Downloaded from on March 5, Published by group.bmj.com Table 4 Severity of speech and voice disorders in the five clusters and PD-Med patients Cluster 1 Cluster 2 Cluster 3 Cluster 4 Cluster 5 Relatively good speech and voice function type Stuttering type Breathy voice type Strained voice type Spastic dysarthria type PD-Med n=19 (25%) n=18 (24%) n=12 (16%) n=14 (18%) n=13 (17%) n=33 AMSD Overall severity of speech disorders Intelligibility 1.7±0.3* 2.4± ± ± ± ±0.8 Naturalness 2.3±0.5* 3.5± ± ± ± ±1.0 Subparts Imprecise consonants 0.4±0.5* 0.9±0.8* 0.6±0.4* 1.1± ± ±0.4 Monoloudness 0.4±0.5* 1.2±0.7* 1.9± ± ± ±0.8 Monopitch 0.5±0.4* 1.2± ± ± ± ±0.8 Low volume 0.9±0.5* 1.0±0.7* 2.3± ± ± ±0.8 Short rushes of speech 0.2±0.3* 0.5±0.5* 1.0± ± ± ±0.7 Voice tremor 0.2±0.4** 0.4± ± ± ± ±0.7 Sound repeated 0.3±0.4* 1.7± ±0.3* 0.5±0.5* 0.4±0.5* 0.6±0.6 Hypernasality 0.4±0.5* 0.7± ±0.5* 0.8± ± ±0.5 Abnormal rate 0.6±0.5* 1.5± ± ± ± ±0.7 Variable rate 0.8± ± ± ± ± ±0.6 Excess loudness variation 1.1± ± ± ± ± ±0.5 Abnormal pitch level 0.9± ± ± ± ± ±0.5 Variable pitch 0.4± ± ± ± ± ±0.2 GRBAS scale Overall severity of voice disorders Grade of dysphonia 1.2±0.4* 1.8± ± ± ± ±0.6 Subparts Roughness 0.9±0.6* 1.3± ± ± ± ±0.5 Breathiness 0.6±0.5* 1.0±0.7* 2.0± ± ± ±0.8 Asthenia 0.6±0.4* 0.9±0.8* 2.2± ±0.7* 1.5± ±0.8 Strain 0.5±0.4* 0.7±0.6* 0.6±0.6* 1.9± ± ±0.4 SSI-3 2.6±3.3* 13.4± ±5.4* 6.8± ±4.7* 5.0±6.9 MPT (s) 23.1±7.1* 22.0±9.3* 19.1± ± ± ±8.8 VHI 32.8±21.1* 49.9± ± ± ± ±21.2 Values are mean±sd. Groups were compared using two-way ANOVA with post hoc tests (Tukey or Games-Howell), or non-parametric Kruskal-Wallis tests with post hoc tests (Mann-Whitney). p Value <0.05 was considered significant. *Significantly better than other cluster groups. Significant difference between the clusters and PD-Med. Significantly worse than other cluster groups. AMSD, Assessment of Motor Speech for Dysarthria; GRBAS, Grade of dysphonia, Roughness, Breathiness, Asthenia, and Strain; MPT, maximum phonation time; PD-Med, medically treated patients; SSI-3, Stuttering Severity Instrument-3; VHI, Voice Handicap Index. off-stimulation conditions. The spider diagrams of the clusters and PD-Med patients are shown in figure 1, and the results of statistical analyses are included in online supplementary table S3. Speech and voice functions tended to improve in the off-stimulation condition, and statistically significant changes in several variables were observed between the on-stimulation and off-stimulation conditions. With regard to the representative speech or voice variable of each group, in cluster 2, the score for sound repeated improved significantly after stopping stimulation (p=0.010); in cluster 3, the score for breathiness tended to improve, albeit not significantly ( p=0.144); in cluster 4, the score for strain improved significantly ( p=0.018); and in cluster 5, the score for imprecise consonants improved significantly ( p=0.027). With regard to individual analyses, speech intelligibility significantly improved in eight patients (20%) after stopping stimulation, and significantly deteriorated in one patient (2.5%; figure 2A). With regard to low volume, significant improvement was observed in 11 patients (27.5%), and significant deterioration was observed in five patients (12.5%; figure 2B). In cluster 2, two of nine patients (22.2%) showed significant improvement in sound repeated after stopping stimulation (figure 2C). In cluster 3, one of four patients (25%) showed significant improvement in breathiness (figure 2D). In cluster 4, four of eight (50%) patients showed significant improvement in strain (figure 2E). Finally, in cluster 5, four of eight (50%) patients experienced significant improvement in imprecise consonants (figure 2F). Association between the clusters and electrode positions The electrode positions were available for 68 of 76 PD-DBS patients. Clusters 1, 4, and 5 tended to have a higher proportion of electrodes positioned laterally to STN than clusters 2 and 3 (figure 3). DISCUSSION In the present study, we comprehensively investigated the characteristics of speech and voice disorders in 76 PD-DBS patients and 33 PD-Med patients. The clinical background of PD-DBS and PD-Med patients were not significantly different with the exception of worse semantic and phonemic verbal fluency and lower LEDD in PD-DBS patients. This may be explained by the negative effects of STN-DBS on verbal fluency 23 and the effects of LEDD reduction of STN-DBS. 4 Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
5 Downloaded from on March 5, Published by group.bmj.com Movement disorders Figure 1 Spider diagrams of speech and voice variables in the five clusters and PD-Controls. Higher scores indicate worse condition. Cluster 1 (A); cluster 2 (B); cluster 3 (C); cluster 4 (D); cluster 5 (E); and PD-Med (F) are shown. With regard to the five clusters, spider diagrams of speech and voice disorders in the on and off stimulation conditions are indicated in blue and red, respectively. The overall grades of severity (intelligibility and naturalness) are shown above each spider diagram. The variables that changed significantly after stopping stimulation are marked in red. PD-DBS patients had significantly more severe speech and voice disorders than PD-Med patients. Voice tremor was the only variable that was significantly better in PD-DBS patients compared with that in PD-Med patients. Furthermore, speech intelligibility improved significantly in 20% and deteriorated significantly in 2.5% of patients after stopping stimulation. Low volume improved significantly in 27.5% and deteriorated significantly in 12.5% of patients. Reportedly, STN-DBS improves loudness or voice tremor presumably due to the ameliorating effect on hypokinesia, rigidity, and tremor in speech-related organs ; however, overall speech intelligibility remains unchanged24 26 or even worsens because of STN-DBS.2 6 Our findings are in agreement with these reports. Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
6 Movement disorders Downloaded from on March 5, Published by group.bmj.com Figure 2 Changes in speech intelligibility (A) and low volume (B) between the on and off stimulation conditions are shown for the 40 patients who underwent on and off stimulation evaluation. Sound repeated in cluster 2 (C); breathiness in cluster 3 (D); strain in cluster 4 (E); and imprecise consonants in cluster 5 (F) were also compared between the on and off stimulation conditions. The blue lines indicate significant improvement ( 1.00), red lines indicate significant worsening ( 1.00) and grey dotted lines represent no significant changes. Medically treated PD patients frequently have hypokinetic dysarthria, which predominantly consists of monoloudness, monopitch, reduced stress, short rushes of speech, imprecise consonants and breathy and harsh voice. 16 These variables were elevated to varying degrees in each cluster, in the on-stimulation and off-stimulation conditions, suggesting that PD-DBS patients have hypokinetic dysarthria. Factor analysis and subsequent cluster analysis classified PD-DBS patients into five clusters according to the phenotypes of their speech and voice disorders. These distinct phenotypes most likely resulted from the diversity in the mechanisms that underlie PD and in the influence of STN-DBS. Cluster 1: relatively good speech and voice function type Cluster 1 showed better speech and voice functions than the other clusters. Speech and voice functions in cluster 1 were roughly equal to those in PD-Med patients, with the exception of significantly better scores for voice tremor in cluster 1. Speech and voice functions tended to improve after stopping stimulation; however, their changes were relatively small in comparison with the other clusters. Therefore, we labelled cluster 1 as relatively good speech and voice function type. Cluster 2: stuttering type Cluster 2 patients were characteristically associated with stuttering. The score for sound repeated improved significantly after stopping stimulation; however, in individual analysis, only 22.2% of patients showed significant improvement after stopping stimulation. Stuttering is considered to be related to dysfunction of the basal ganglia-thalamocortical motor network 28 and is frequently observed in advanced PD patients. 29 Furthermore, some case reports have described improvement in stuttering and worsening of stuttering after STN-DBS. In conclusion, stuttering in cluster 2 patients was assumed to be primarily because of degeneration of the basal ganglia-thalamocortical motor network; STN-DBS can potentially affect stuttering. Cluster 3: breathy voice type Cluster 3 patients had the highest scores for grade of dysphonia, breathiness, asthenia and low volume, indicating laryngeal dysfunction. Previous laryngoscopic studies have demonstrated incomplete glottal closure in 60% 67% of PD patients, which is probably because of impaired control of laryngeal muscles or age-related vocal fold changes. Air leakage through the glottis is perceived as breathiness 17 and contributes to asthenia and low volume. Therefore, we labelled cluster 3 as breathy voice type. Cluster 3 patients showed a tendency for improvement (albeit not significant) in several variables after stopping stimulation. In individual analysis, breathiness was significantly improved in only one patient. In conclusion, cluster 3 patients appeared to have breathy voice mainly due to aging or PD itself; STN-DBS can potentially aggravate breathy voice. Cluster 4: strained voice type Voice in cluster 4 sounded strained, strangled and very effortful, which appeared to have contributed to high scores for short rushes of speech, excess loudness variation and short MPT. 6 Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
7 Downloaded from on March 5, Published by group.bmj.com Movement disorders Figure 3 Electrode positions in the five clusters are plotted on the axial view at the level of 3.5 mm below the AC PC line. Electrode positions are shown for 18 patients in cluster 1 (A); 17 patients in cluster 2 (B); 10 patients in cluster 3 (C); 10 patients in cluster 4 (D); and 13 patients in cluster 5. Therefore, we labelled cluster 4 as strained voice type. Cluster 4 exhibited the largest improvement after stopping stimulation among the clusters. In individual analysis, 50% of patients showed significant improvement in strain after stopping stimulation, and strain tended to improve in the remaining patients. Strained voice quality is uncommon in medically treated PD patients and is reportedly associated with hypertonicity of the laryngeal muscles. 33 Stimulation of the corticobulbar and corticospinal tracts induces a tonic muscle contraction that mimics fixed dystonia in the face and limbs and causes speech disorders. 9 Current diffusion to the corticobulbar fibres may cause abnormal tonic laryngeal muscle contraction, which resulted in strained voice quality. Cluster 5: spastic dysarthria type Cluster 5 patients showed the highest scores for imprecise consonants and hypernasality, which are common in spastic dysarthria. Therefore, we labelled cluster 5 as spastic dysarthria type. Spastic dysarthria is associated with bilateral upper motor neuron involvement. 16 A relationship between current diffusion to the corticobulbar fibres and speech and voice disorders has been mentioned. 6 9 Furthermore, in individual analysis, 50% of patients showed significant improvement in imprecise consonants after stopping stimulation. These results indicate that spastic dysarthria type is likely related to current diffusion to the corticobulbar fibres. Association between speech and voice disorders and electrode positions Given that clusters 4 and 5 tended to have a higher proportion of electrodes located laterally to STN than those in clusters 2 and 3, strained voice type and spastic dysarthria type were most likely related to current diffusion to the corticobulbar fibres. The corticobulbar fibres were believed to pass through the genu of the internal capsule. However, a recent study using diffusion tensor imaging has demonstrated that corticobulbar fibres pass through the posterior limb of the internal capsule, which is closer to the STN than the genu of the internal capsule. 34 With regard to strained voice type, STN-DBS may mainly affect the laryngeal muscles. In contrast, with regard to spastic dysarthria type, STN-DBS may mainly affect the lip, tongue and velum. This can be explained by individual differences in the corticobulbar tracts and electrical field generated by DBS. Interestingly, cluster 1 had relatively good speech and voice functions, and also tended to have a high proportion of laterally-located electrodes and had stimulation parameters similar to those of clusters 4 and 5. This finding suggests aetiologies other than electrode positions. Tripoliti et al 2 3 demonstrated that longer disease duration and a higher preoperative on-medication Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
8 Movement disorders Downloaded from on March 5, Published by group.bmj.com UPDRS-III score were predictive factors for postoperative deterioration of speech intelligibility. Additionally, speech and voice functions progressively deteriorate over time after implantation 35 probably due to both progression of brain degeneration and the stimulation effect. Longer disease duration, longer postsurgery period, and worse motor and cognitive functions may contribute to worse speech and voice functions in clusters 4 and 5 in comparison with cluster 1. Further prospective studies will be needed to elucidate this issue. Although we did not find an association between medially located electrodes and speech and voice disorders, some researchers have reported that medially located electrodes may lead to speech deterioration as a result of current diffusion to the cerebellothalamic fibres. 2 5 This can be another pathophysiological mechanism of stimulation-related speech and voice disorders. The relationship between electrode positions and speech and voice disorders in clusters 2 and 3 was not found. Additionally, most patients in clusters 2 and 3 did not experience significant improvement after stopping stimulation. These findings indicate that speech and voice disorders in clusters 2 and 3 are mainly due to PD itself. Therapies for speech and voice disorders after STN-DBS Our findings suggest that stuttering and breathy voice can be aggravated by STN-DBS, but are mainly due to PD itself, and that strained voice and spastic dysarthria, which are uncommon in medically treated PD patients, are related to current diffusion to the corticobulbar fibres. Moreover, the patients were thought to principally have hypokinetic dysarthria in common. One patient can combine more than two phenotypes (eg, a patient with hypokinetic dysarthria, stuttering and spastic dysarthria). This is an important point in determining how to treat patients speech and voice disorders. The Lee Silverman Voice Treatment (LSVT) is an efficacious treatment for hypokinetic dysarthria in medically treated PD patients. 36 However, patients treated with STN-DBS respond differently to the LSVT. 10 Before initiating the LSVT, stimulation parameters should be adjusted to eliminate the worsening effects of STN-DBS on speech and voice functions. Personalised programming approach (eg, individualised current-shaping with interleaving stimulation) or a new device (eg, directional stimulation) may reduce stimulation-related side effects without undermining the effects on the cardinal symptoms Patients with stuttering are thought to have difficulty in maintaining a precise rhythm of speech. Rhythm therapy such as a pacing board may be effective. 39 Based on the pathophysiology of speech and voice disorders, optimally balanced therapies comprising STN-DBS, medication, and rehabilitation are required to maximise patients quality of life. Methodological issues Several limitations of this study must be considered. First, because patients were not randomised prospectively to the PD-DBS and PD-Med groups, we could not determine whether both groups were completely equivalent. Second, this study aimed to elucidate the phenotypes of speech and voice disorders in PD patients with STN-DBS in the on-state under their usual treatment. No data under unilateral stimulation are available in this study. Therefore, we could not determine how much stimulation of each side was involved in speech and voice disorders. Additionally, the impact of medication on speech and voice functions was not assessed. Furthermore, healthy controls were not involved. Third, larger changes in speech and voice disorders may be obtained with a longer off-stimulation period. Further studies are required to determine the appropriate period to evaluate speech and voice functions in the off-stimulation condition. Fourth, there is controversy over the accuracy of electrode positions identified by fusing the postoperative CT with the preoperative MRI. 40 Additionally, we did not conduct statistical analyses on electrode positions. Ideally, the distance between the active contact and the corticobulbar fibres or cerebellothalamic fibres should be calculated using diffusion tensor imaging and the relationship between the distance and the stimulation parameters should be statistically analysed. Finally, changes in speech and voice disorders over time were unclear because of the cross-sectional nature of the study. Future longitudinal research is required to clarify changes in each phenotype of speech and voice disorders over time. Contributors TT, YT, RO, NY, KH, RN, HW, JS, NA, MI, MH, YF, YK were involved in data collection. TT, HW took part in analysis and interpretation of data and drafting of the manuscript. TT, HW, YT, RO, NY, KH, RN, HW, JS, NA, MI, MH, YF, YK, MY, TW and GS were involved in conceptualisation of the study and manuscript revision. Funding Part of this study represents the results of Integrated Research on Neuropsychiatric Disorders performed under the Strategic Research Programme for Brain Sciences by the Ministry of Education, Culture, Sports, Science and Technology of Japan. This study was also supported by Health and Labour Sciences Research grants for research on measures for intractable diseases and comprehensive research on aging and health from the Ministry of Health, Labour and Welfare, Japan. Competing interests None. Ethics approval Ethics committee of the Nagoya University Graduate School of Medicine. Provenance and peer review Not commissioned; externally peer reviewed. REFERENCES 1 Kleiner-Fisman G, Herzog J, Fisman DN, et al. Subthalamic nucleus deep brain stimulation: summary and meta-analysis of outcomes. Mov Disord 2006;21: S Tripoliti E, Zrinzo L, Martinez-Torres I, et al. Effects of subthalamic stimulation on speech of consecutive patients with Parkinson disease. Neurology 2011;76: Tripoliti E, Limousin P, Foltynie T, et al. Predictive factors of speech intelligibility following subthalamic nucleus stimulation in consecutive patients with Parkinson s disease. Mov Disord 2014;29: Paek SH, Lee JY, Kim HJ, et al. Electrode position and the clinical outcome after bilateral subthalamic nucleus stimulation. J Korean Med Sci 2011;26: Plaha P, Ben-Shlomo Y, Patel NK, et al. Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving contralateral parkinsonism. Brain 2006;129: Klostermann F, Ehlen F, Vesper J, et al. Effects of subthalamic deep brain stimulation on dysarthrophonia in Parkinson s disease. J Neurol Neurosurg Psychiatry 2008;79: Narayana S, Jacks A, Robin DA, et al. A noninvasive imaging approach to understanding speech changes following deep brain stimulation in Parkinson s disease. Am J Speech Lang Pathol 2009;18: Pinto S, Gentil M, Krack P, et al. Changes induced by levodopa and subthalamic nucleus stimulation on parkinsonian speech. Mov Disord 2005;20: Tommasi G, Krack P, Fraix V, et al. Pyramidal tract side effects induced by deep brain stimulation of the subthalamic nucleus. J Neurol Neurosurg Psychiatry 2008;79: Tripoliti E, Strong L, Hickey F, et al. Treatment of dysarthria following subthalamic nucleus deep brain stimulation for Parkinson s disease. Mov Disord 2011;26: Burghaus L, Hilker R, Thiel A, et al. Deep brain stimulation of the subthalamic nucleus reversibly deteriorates stuttering in advanced Parkinson s disease. J Neural Transm 2006;113: Toft M, Dietrichs E. Aggravated stuttering following subthalamic deep brain stimulation in Parkinson s disease two cases. BMC Neurol 2011;11: Hughes AJ, Daniel SE, Kilford L, et al. Accuracy of clinical diagnosis of idiopathic Parkinson s disease: a clinico-pathological study of 100 cases. J Neurol Neurosurg Psychiatry 1992;55: Tanei T, Kajita Y, Kaneoke Y, et al. Staged bilateral deep brain stimulation of the subthalamic nucleus for the treatment of Parkinson s disease. Acta Neurochir 2009;151: Nishio M. Assessment of motor speech for dysarthria. Tokyo: Interuna Publishers, Darley FL, Aronson AE, Brown JR. Differential diagnostic patterns of dysarthria. J Speech Hear Res 1969;12: Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
9 Downloaded from on March 5, Published by group.bmj.com Movement disorders 17 Hirano M. Clinical examination of voice. New York: Springer-Verlag, Riley G. The stuttering severity instrument for children and adults third edition (SSI-3). Austin: Pro-Ed, Speyer R, Bogaardt HC, Passos VL, et al. Maximum phonation time: variability and reliability. J Voice 2010;24: Jacobson BH, Johnson A, Grywalski C, et al. The voice handicap index (VHI): development and validation. Am J Speech-Lang Pathol 1997;6: Williams-Gray CH, Foltynie T, Brayne CE, et al. Evolution of cognitive dysfunction in an incident Parkinson s disease cohort. Brain 2007;130: Schaltenbrand G, Wahren W. Atlas for stereotaxy of the human brain. 2nd edn. Stuttgart: Thieme, Parsons TD, Rogers SA, Braaten AJ, et al. Cognitive sequelae of subthalamic nucleus deep brain stimulation in Parkinson s disease: a meta-analysis. Lancet Neurol 2006;5: D Alatri L, Paludetti G, Contarino M, et al. Effects of bilateral subthalamic nucleus stimulation and medication on parkinsonian speech impairment. J Voice 2008;22: Pinto S, Gentil M, Fraix V, et al. Bilateral subthalamic stimulation effects on oral force control in Parkinson s disease. J Neurol 2003;250: Dromey C, Kumar R, Lang AE, et al. An investigation of the effects of subthalamic nucleus stimulation on acoustic measures of voice. Mov Disord 2000;15: Skodda S, Grönheit W, Schlegel U, et al. Effect of subthalamic stimulation on voice and speech in Parkinson s disease: for the better or worse? Front Neurol 2014;4: Alm PA. Stuttering and the basal ganglia circuits: a critical review of possible relations. J Commun Disord 2004;37: Benke T, Hohenstein C, Poewe W, et al. Repetitive speech phenomena in Parkinson s disease. J Neurol Neurosurg Psychiatry 2000;69: Thiriez C, Roubeau B, Ouerchefani N, et al. Improvement in developmental stuttering following deep brain stimulation for Parkinson s disease. Park Relat Disord 2013;19: Smith ME, Ramig LO, Dromey C, et al. Intensive voice treatment in Parkinson disease: laryngostroboscopic findings. J Voice 1995;9: Midi I, Dogan M, Koseoglu M, et al. Voice abnormalities and their relation with motor dysfunction in Parkinson s disease. Acta Neurol Scand 2008;117: Boone D, McFarlane S, Von Berg S. The voice and voice therapy. 7th edn. Boston, MA: Pearson/Allyn & Bacon, Yim SH, Kim JH, Han ZA, et al. Distribution of the corticobulbar tract in the internal capsule. J Neurol Sci 2013;334: Fasano A, Romito LM, Daniele A, et al. Motor and cognitive outcome in patients with Parkinson s disease 8 years after subthalamic implants. Brain 2010;133: Ramig LO, Countryman S, O Brien C, et al. Intensive speech treatment for patients with Parkinson s disease Short-and long-term comparison of two techniques. Neurology 1996;47: Barbe MT, Dembek TA, Becker J, et al. Individualized current-shaping reduces DBS-induced dysarthria in patients with essential tremor. Neurology 2014;82: Pollo C, Kaelin-Lang A, Oertel MF, et al. Directional deep brain stimulation: an intraoperative double-blind pilot study. Brain 2014;137: Suzuki J, Tanaka Y, Watanabe H, et al. A case of Parkinson s disease treated effectively with a pacing board for repetitive speech phenomena after deep brain stimulation. Rinsho Shinkeigaku 2013;53: Lee JY, Kim JW, Lee JY, et al. Is MRI a reliable tool to locate the electrode after deep brain stimulation surgery? Comparison study of CT and MRI for the localization of electrodes after DBS. Acta Neurochir (Wien) 2010;152: Tsuboi T, et al. J Neurol Neurosurg Psychiatry 2014;0:1 9. doi: /jnnp
10 Downloaded from on March 5, Published by group.bmj.com Distinct phenotypes of speech and voice disorders in Parkinson's disease after subthalamic nucleus deep brain stimulation Takashi Tsuboi, Hirohisa Watanabe, Yasuhiro Tanaka, Reiko Ohdake, Noritaka Yoneyama, Kazuhiro Hara, Ryoichi Nakamura, Hazuki Watanabe, Jo Senda, Naoki Atsuta, Mizuki Ito, Masaaki Hirayama, Masahiko Yamamoto, Yasushi Fujimoto, Yasukazu Kajita, Toshihiko Wakabayashi and Gen Sobue J Neurol Neurosurg Psychiatry published online October 3, 2014 Updated information and services can be found at: Supplementary Material References alerting service These include: Supplementary material can be found at: html This article cites 35 articles, 8 of which you can access for free at: Receive free alerts when new articles cite this article. Sign up in the box at the top right corner of the online article. Topic Collections Articles on similar topics can be found in the following collections Ear, nose and throat/otolaryngology (202) Drugs: CNS (not psychiatric) (1850) Parkinson's disease (661) Notes To request permissions go to: To order reprints go to: To subscribe to BMJ go to:
 www.optimalsp.com.au What may happen to breathing, voice and swallow in PD? Muscles of breathing, voice and speech can be subject to the same disease processes as other muscle groups in PD Slowness, stiffness,
www.optimalsp.com.au What may happen to breathing, voice and swallow in PD? Muscles of breathing, voice and speech can be subject to the same disease processes as other muscle groups in PD Slowness, stiffness,
Linköping University Post Print. Patient-specific models and simulations of deep brain stimulation for postoperative follow-up
 inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
inköping University Post Print Patient-specific models and simulations of deep brain stimulation for postoperative follow-up Mattias Åström, Elina Tripoliti, Irene Martinez-Torres, udvic U. Zrinzo, Patricia
Critical Review: The Effects of Subthalamic Nucleus Deep Brain Stimulation on Speech Production in Parkinson s Disease
 Critical Review: The Effects of Subthalamic Nucleus Deep Brain Stimulation on Speech Production in Parkinson s Disease Marie McIntosh M.Cl.Sc SLP Candidate University of Western Ontario: School of Communication
Critical Review: The Effects of Subthalamic Nucleus Deep Brain Stimulation on Speech Production in Parkinson s Disease Marie McIntosh M.Cl.Sc SLP Candidate University of Western Ontario: School of Communication
Critical Review: Can sub-thalamic deep brain stimulation (STN-DBS) improve speech output in patients with Parkinson s Disease?
 Copyright 2007, Iulianella, I. Critical Review: Can sub-thalamic deep brain stimulation (STN-DBS) improve speech output in patients with Parkinson s Disease? Iulianella, I. M.Cl.Sc. (SLP) Candidate School
Copyright 2007, Iulianella, I. Critical Review: Can sub-thalamic deep brain stimulation (STN-DBS) improve speech output in patients with Parkinson s Disease? Iulianella, I. M.Cl.Sc. (SLP) Candidate School
DBS for Parkinson's Disease: Role of the Speech-Language Pathologist
 DBS for Parkinson's Disease: Role of the Speech-Language Pathologist Donna C. Tippett, M.P.H., M.A., CCC-SLP 1,2 Zoltan Mari, M.D. 3 Paul R. Rao, Ph.D., CCC-SLP, CPHQ, FACHE 4 Departments of Otolaryngology
DBS for Parkinson's Disease: Role of the Speech-Language Pathologist Donna C. Tippett, M.P.H., M.A., CCC-SLP 1,2 Zoltan Mari, M.D. 3 Paul R. Rao, Ph.D., CCC-SLP, CPHQ, FACHE 4 Departments of Otolaryngology
DBS surgery: The role of the Speech- Language Pathologist and Physical Therapist. Linda Bryans, MA, CCC-SLP Jennifer Wilhelm, PT, DPT, NCS
 DBS surgery: The role of the Speech- Language Pathologist and Physical Therapist Linda Bryans, MA, CCC-SLP Jennifer Wilhelm, PT, DPT, NCS DBS and Parkinson Disease Delivery of high frequency stimulation
DBS surgery: The role of the Speech- Language Pathologist and Physical Therapist Linda Bryans, MA, CCC-SLP Jennifer Wilhelm, PT, DPT, NCS DBS and Parkinson Disease Delivery of high frequency stimulation
Supplementary Online Content
 Supplementary Online Content Wang C-C, Chang M-H, Jiang R-S, et al. Laryngeal electromyography-guided hyaluronic acid vocal fold injection for unilateral vocal fold paralysis: a prospective long-term follow-up
Supplementary Online Content Wang C-C, Chang M-H, Jiang R-S, et al. Laryngeal electromyography-guided hyaluronic acid vocal fold injection for unilateral vocal fold paralysis: a prospective long-term follow-up
Introduction. Changes in speech as it relates to PD: Deep Brain Stimulation (DBS) and its impact on speech: Treatment for Speech Disturbance:
 Introduction Speech is one of the most fundamental means of connecting with others and expressing our wants and needs. Speech difficulties, then, can result in significant challenges when interacting with
Introduction Speech is one of the most fundamental means of connecting with others and expressing our wants and needs. Speech difficulties, then, can result in significant challenges when interacting with
Indications. DBS for Tremor. What is the PSA? 6/08/2014. Tremor. 1. Tremor. 2. Gait freezing/postural instability. 3. Motor fluctuations
 Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Indications Deep brain stimulation for Parkinson s disease A Tailored Approach 1. Tremor 2. Gait freezing/postural instability Wesley Thevathasan FRACP DPhil.Oxf 3. Motor fluctuations Consultant Neurologist,
Deep Brain Stimulation: Indications and Ethical Applications
 Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
Deep Brain Stimulation Overview Kara D. Beasley, DO, MBe, FACOS Boulder Neurosurgical and Spine Associates (303) 562-1372 Deep Brain Stimulation: Indications and Ethical Applications Instrument of Change
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD
 PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
PACEMAKERS ARE NOT JUST FOR THE HEART! Ab Siadati MD WHAT IS DEEP BRAIN STIMULATION? WHY SHOULD YOU CONSIDER DBS SURGERY FOR YOUR PATIENTS? HOW DOES DBS WORK? DBS electrical stimulation overrides abnormal
Troubleshooting algorithms for common DBS related problems in tremor and dystonia
 Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Troubleshooting algorithms for common DBS related problems in tremor and dystonia Elena Moro, MD, PhD, FEAN, FAAN Movement Disorder Center, CHU Grenoble, Grenoble Alpes University, INSERM U1216, Grenoble,
Basal ganglia motor circuit
 Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Parkinson s Disease Basal ganglia motor circuit 1 Direct pathway (gas pedal) 2 Indirect pathway (brake) To release or augment the tonic inhibition of GPi on thalamus Direct pathway There is a tonic inhibition
Treatment of Speech Impairments in Individuals with. Parkinson Disease
 Treatment of Speech Impairments in Individuals with : Principles of Motor Learning Jason A. Whitfield, Ph.D., CCC SLP Assistant Professor Communication Sciences and Disorders Bowling Green State University
Treatment of Speech Impairments in Individuals with : Principles of Motor Learning Jason A. Whitfield, Ph.D., CCC SLP Assistant Professor Communication Sciences and Disorders Bowling Green State University
Parkinson disease: Parkinson Disease
 Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
Surgical Surgical treatment treatment for for Parkinson disease: Parkinson Disease the Present and the Future the Present and the Future Olga Klepitskaya, MD Associate Professor of Neurology Co-Director,
SUPPLEMENTAL DIGITAL CONTENT
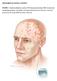 SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
SUPPLEMENTAL DIGITAL CONTENT FIGURE 1. Unilateral subthalamic nucleus (STN) deep brain stimulation (DBS) electrode and internal pulse generator. Copyright 2010 Oregon Health & Science University. Used
Surgical Treatment of Movement Disorders. Surgical Treatment of Movement Disorders. New Techniques: Procedure is safer and better
 Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Surgical Treatment of Movement Stephen Grill, MD, PHD Johns Hopkins University and Parkinson s and Movement Center of Maryland Surgical Treatment of Movement Historical Aspects Preoperative Issues Surgical
Deep Brain Stimulation: Surgical Process
 Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
Deep Brain Stimulation: Surgical Process Kia Shahlaie, MD, PhD Assistant Professor Bronte Endowed Chair in Epilepsy Research Director of Functional Neurosurgery Minimally Invasive Neurosurgery Department
A retrospective study of long-term treatment outcomes for reduced vocal intensity in hypokinetic dysarthria
 Watts BMC Ear, Nose and Throat Disorders (2016) 16:2 DOI 10.1186/s12901-016-0022-8 RESEARCH ARTICLE Open Access A retrospective study of long-term treatment outcomes for reduced vocal intensity in hypokinetic
Watts BMC Ear, Nose and Throat Disorders (2016) 16:2 DOI 10.1186/s12901-016-0022-8 RESEARCH ARTICLE Open Access A retrospective study of long-term treatment outcomes for reduced vocal intensity in hypokinetic
The Effects of LSVT LOUD and LSVT CLEAR on vowel production in STN-DBS Subjects with Idiopathic Parkinson's Disease
 University of Colorado, Boulder CU Scholar Speech, Language, and Hearing Sciences Graduate Theses & Dissertations Speech, Language and Hearing Sciences Spring 1-1-2011 The Effects of LSVT LOUD and LSVT
University of Colorado, Boulder CU Scholar Speech, Language, and Hearing Sciences Graduate Theses & Dissertations Speech, Language and Hearing Sciences Spring 1-1-2011 The Effects of LSVT LOUD and LSVT
Deep Brain Stimulation: Patient selection
 Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
Deep Brain Stimulation: Patient selection Halim Fadil, MD Movement Disorders Neurologist Kane Hall Barry Neurology Bedford/Keller, TX 1991: Thalamic (Vim) DBS for tremor Benabid AL, et al. Lancet. 1991;337(8738):403-406.
See Policy CPT/HCPCS CODE section below for any prior authorization requirements
 Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Effective Date: 1/1/2019 Section: SUR Policy No: 395 1/1/19 Medical Policy Committee Approved Date: 8/17; 2/18; 12/18 Medical Officer Date APPLIES TO: Medicare Only See Policy CPT/HCPCS CODE section below
Surgical Treatment for Movement Disorders
 Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Surgical Treatment for Movement Disorders Seth F Oliveria, MD PhD The Oregon Clinic Neurosurgery Director of Functional Neurosurgery: Providence Brain and Spine Institute Portland, OR Providence St Vincent
Long-term outcome of subthalamic nucleus deep brain stimulation for Parkinson s disease using an MRI-guided and MRI-verified approach
 RESEARCH PAPER Long-term outcome of subthalamic nucleus deep brain stimulation for Parkinson s disease using an MRI-guided and MRI-verified approach Iciar Aviles-Olmos, Zinovia Kefalopoulou, Elina Tripoliti,
RESEARCH PAPER Long-term outcome of subthalamic nucleus deep brain stimulation for Parkinson s disease using an MRI-guided and MRI-verified approach Iciar Aviles-Olmos, Zinovia Kefalopoulou, Elina Tripoliti,
Detection of Parkinson S Disease by Speech Analysis
 Detection of Parkinson S Disease by Speech Analysis Ch.Rajanikanth 1, A.Amardeep 2, B.Kishore 3, Shaik Azeez 4 Student, Department of ECE, Lendi Institute of Engineering And Technology, Vizianagaram, India
Detection of Parkinson S Disease by Speech Analysis Ch.Rajanikanth 1, A.Amardeep 2, B.Kishore 3, Shaik Azeez 4 Student, Department of ECE, Lendi Institute of Engineering And Technology, Vizianagaram, India
Rapid assessment of gait and speech after subthalamic deep brain stimulation
 SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
SNI: Stereotactic, a supplement to Surgical Neurology International OPEN ACCESS For entire Editorial Board visit : http://www.surgicalneurologyint.com Editor Antonio A. F. DeSalles, MD University of California,
Effect of Bilateral Stimulation of the Subthalamic Nucleus on Parkinsonian Voice
 Brain and Language 78, 233 240 (2001) doi:10.1006/brln.2001.2466, available online at http://www.idealibrary.com on Effect of Bilateral Stimulation of the Subthalamic Nucleus on Parkinsonian Voice M. Gentil,
Brain and Language 78, 233 240 (2001) doi:10.1006/brln.2001.2466, available online at http://www.idealibrary.com on Effect of Bilateral Stimulation of the Subthalamic Nucleus on Parkinsonian Voice M. Gentil,
ORIGINAL CONTRIBUTION. Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement
 ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
ORIGINAL CONTRIBUTION Improvement in Parkinson Disease by Subthalamic Nucleus Stimulation Based on Electrode Placement Effects of Reimplantation Mathieu Anheim, MD; Alina Batir, MD; Valérie Fraix, MD;
MULTI SYSTEM ATROPHY: REPORT OF TWO CASES Dipu Bhuyan 1, Rohit Kr. Chandak 2, Pankaj Kr. Patel 3, Sushant Agarwal 4, Debjanee Phukan 5
 MULTI SYSTEM ATROPHY: REPORT OF TWO CASES Dipu Bhuyan 1, Rohit Kr. Chandak 2, Pankaj Kr. Patel 3, Sushant Agarwal 4, Debjanee Phukan 5 HOW TO CITE THIS ARTICLE: Dipu Bhuyan, Rohit Kr. Chandak, Pankaj Kr.
MULTI SYSTEM ATROPHY: REPORT OF TWO CASES Dipu Bhuyan 1, Rohit Kr. Chandak 2, Pankaj Kr. Patel 3, Sushant Agarwal 4, Debjanee Phukan 5 HOW TO CITE THIS ARTICLE: Dipu Bhuyan, Rohit Kr. Chandak, Pankaj Kr.
Jitter, Shimmer, and Noise in Pathological Voice Quality Perception
 ISCA Archive VOQUAL'03, Geneva, August 27-29, 2003 Jitter, Shimmer, and Noise in Pathological Voice Quality Perception Jody Kreiman and Bruce R. Gerratt Division of Head and Neck Surgery, School of Medicine
ISCA Archive VOQUAL'03, Geneva, August 27-29, 2003 Jitter, Shimmer, and Noise in Pathological Voice Quality Perception Jody Kreiman and Bruce R. Gerratt Division of Head and Neck Surgery, School of Medicine
Review Article Effect of Deep Brain Stimulation on Speech Performance in Parkinson s Disease
 Parkinson s Disease Volume 2012, Article ID 850596, 10 pages doi:10.1155/2012/850596 Review Article Effect of Deep Brain Stimulation on Speech Performance in Parkinson s Disease Sabine Skodda Department
Parkinson s Disease Volume 2012, Article ID 850596, 10 pages doi:10.1155/2012/850596 Review Article Effect of Deep Brain Stimulation on Speech Performance in Parkinson s Disease Sabine Skodda Department
Effect of bilateral stimulation of the subthalamic nucleus on parkinsonian dysarthria
 Brain and Language 85 (2003) 190 196 www.elsevier.com/locate/b&l Effect of bilateral stimulation of the subthalamic nucleus on parkinsonian dysarthria Michele Gentil, * Serge Pinto, Pierre Pollak, and
Brain and Language 85 (2003) 190 196 www.elsevier.com/locate/b&l Effect of bilateral stimulation of the subthalamic nucleus on parkinsonian dysarthria Michele Gentil, * Serge Pinto, Pierre Pollak, and
SYLLABUS FOR PH.D ENTRANCE TEST IN SPEECH AND HEARING
 SYLLABUS FOR PH.D ENTRANCE TEST IN SPEECH AND HEARING 1) ADVANCES IN SPEECH SCIENCE. a) Life span changes in speech mechanism including developmental milestones b) Physiology of Speech production: Respiratory
SYLLABUS FOR PH.D ENTRANCE TEST IN SPEECH AND HEARING 1) ADVANCES IN SPEECH SCIENCE. a) Life span changes in speech mechanism including developmental milestones b) Physiology of Speech production: Respiratory
Lecture XIII. Brain Diseases I - Parkinsonism! Brain Diseases I!
 Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
Lecture XIII. Brain Diseases I - Parkinsonism! Bio 3411! Wednesday!! Lecture XIII. Brain Diseases - I.! 1! Brain Diseases I! NEUROSCIENCE 5 th ed! Page!!Figure!!Feature! 408 18.9 A!!Substantia Nigra in
The Effect of Pramipexole on Depressive Symptoms in Parkinson's Disease.
 Kobe J. Med. Sci., Vol. 56, No. 5, pp. E214-E219, 2010 The Effect of Pramipexole on Depressive Symptoms in Parkinson's Disease. NAOKO YASUI 1, KENJI SEKIGUCHI 1, HIROTOSHI HAMAGUCHI 1, and FUMIO KANDA
Kobe J. Med. Sci., Vol. 56, No. 5, pp. E214-E219, 2010 The Effect of Pramipexole on Depressive Symptoms in Parkinson's Disease. NAOKO YASUI 1, KENJI SEKIGUCHI 1, HIROTOSHI HAMAGUCHI 1, and FUMIO KANDA
Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving contralateral parkinsonism
 Brain Advance Access published May 23, 2006 doi:10.1093/brain/awl127 Brain (2006) Page 1 of 16 Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving
Brain Advance Access published May 23, 2006 doi:10.1093/brain/awl127 Brain (2006) Page 1 of 16 Stimulation of the caudal zona incerta is superior to stimulation of the subthalamic nucleus in improving
Clinical speech impairment in Parkinson s disease, progressive supranuclear palsy, and multiple system atrophy
 Ap proof done. OK Original Article Clinical speech impairment in Parkinson s disease, progressive supranuclear palsy, and multiple system atrophy S. Sachin, G. Shukla, V. Goyal, S. Singh, Vijay Aggarwal
Ap proof done. OK Original Article Clinical speech impairment in Parkinson s disease, progressive supranuclear palsy, and multiple system atrophy S. Sachin, G. Shukla, V. Goyal, S. Singh, Vijay Aggarwal
Non-motor subtypes of Early Parkinson Disease in the Parkinson s Progression Markers Initiative
 Non-motor subtypes of Early Parkinson Disease in the Parkinson s Progression Markers Initiative Samay Jain, MD MSc Seo Young Park, PhD University of Pittsburgh Department of Neurology and Center for Research
Non-motor subtypes of Early Parkinson Disease in the Parkinson s Progression Markers Initiative Samay Jain, MD MSc Seo Young Park, PhD University of Pittsburgh Department of Neurology and Center for Research
THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE
 11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
11 th Bienniel Speech Motor Control Conference, Colonial Williamsburg, Virginia, 2002. THE EFFECTS OF SUBTHALAMIC NUCLEUS DEEP BRAIN STIMULATION ON VOCAL TRACT DYNAMICS IN PARKINSON S DISEASE Steven Barlow,
Non-therapeutic and investigational uses of non-invasive brain stimulation
 Non-therapeutic and investigational uses of non-invasive brain stimulation Robert Chen, MA, MBBChir, MSc, FRCPC Catherine Manson Chair in Movement Disorders Professor of Medicine (Neurology), University
Non-therapeutic and investigational uses of non-invasive brain stimulation Robert Chen, MA, MBBChir, MSc, FRCPC Catherine Manson Chair in Movement Disorders Professor of Medicine (Neurology), University
The posterior subthalamic area (PSA) is a promising
 clinical article J Neurosurg 126:386 390, 2017 Dystonic tics induced by deep brain stimulation of the posterior subthalamic area for essential tremor Arjun S. Chandran, MBBS, 1 Stuti Joshi, MBBS, 2 Megan
clinical article J Neurosurg 126:386 390, 2017 Dystonic tics induced by deep brain stimulation of the posterior subthalamic area for essential tremor Arjun S. Chandran, MBBS, 1 Stuti Joshi, MBBS, 2 Megan
Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B.
 UvA-DARE (Digital Academic Repository) Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B. Link to publication Citation for published version (APA): Post, B. (2009). Clinimetrics,
UvA-DARE (Digital Academic Repository) Clinimetrics, clinical profile and prognosis in early Parkinson s disease Post, B. Link to publication Citation for published version (APA): Post, B. (2009). Clinimetrics,
Deep Brain Stimulation and Movement Disorders
 Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation and Movement Disorders Farrokh Farrokhi, MD Neurosurgery Maria Marsans, PA-C Neurosurgery Virginia Mason June 27, 2017 OBJECTIVES Understand the role of Deep Brain Stimulation (DBS)
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor
 Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Deep Brain Stimulation for Parkinson s Disease & Essential Tremor Albert Fenoy, MD Assistant Professor University of Texas at Houston, Health Science Center Current US Approvals Essential Tremor and Parkinsonian
Original Article. Clinical Archives of Communication Disorders / Vol. 2, No. 1:15-22 / April 2017 INTRODUCTION
 Original Article http://e-cacd.org/ eissn: 2287-903X Clinical Archives of Communication Disorders / Vol. 2, No. 1:15-22 / April 2017 https://doi.org/10.21849/cacd.2017.00024 Open Access Aerodynamic Parameters
Original Article http://e-cacd.org/ eissn: 2287-903X Clinical Archives of Communication Disorders / Vol. 2, No. 1:15-22 / April 2017 https://doi.org/10.21849/cacd.2017.00024 Open Access Aerodynamic Parameters
Ablative procedures for the treatment of Parkinson s disease
 Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
Ablative procedures for the treatment of Parkinson s disease Zeiad Y. Fayed MD Neurosurgery department Ain Shams University 1 2 Pallidotomy Pallidotomy Indications: Non tremor dominant PD Levodopa induced
years; baseline off-state Unified Parkinson s Disease Rating Scale (UPDRS) motor ratings 24.6 ± 6.8).
 Jourdain et al. 1 Supplemental Data Supplemental Methods Subjects We studied 28 PD subjects (20 men and 8 women; age 61.0 ± 9.6 (mean ± SD) years; duration 8.7 ± 9.6 years; baseline off-state Unified Parkinson
Jourdain et al. 1 Supplemental Data Supplemental Methods Subjects We studied 28 PD subjects (20 men and 8 women; age 61.0 ± 9.6 (mean ± SD) years; duration 8.7 ± 9.6 years; baseline off-state Unified Parkinson
Dysarthria and Dysphagia: a Neurology Perspective William Meador, MD Assistant Professor of Neurology, UAB
 Dysarthria and Dysphagia: a Neurology Perspective William Meador, MD Assistant Professor of Neurology, UAB 2.11.16 Disclosures I have no relevant conflicts or potential conflicts to disclose regarding
Dysarthria and Dysphagia: a Neurology Perspective William Meador, MD Assistant Professor of Neurology, UAB 2.11.16 Disclosures I have no relevant conflicts or potential conflicts to disclose regarding
Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease
 CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
CLINICAL ARTICLE Imaging alone versus microelectrode recording guided targeting of the STN in patients with Parkinson s disease Christopher S. Lozano, BSc, 1 Manish Ranjan, MBBS, 1 Alexandre Boutet, MD,
Tyler Phillips Levee M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
 Critical Review: Which Speech Symptoms Contribute Most to Reduced Intelligibility in Individuals with Ataxic Dysarthria Secondary to Friedreich s Disease? Tyler Phillips Levee M.Cl.Sc (SLP) Candidate University
Critical Review: Which Speech Symptoms Contribute Most to Reduced Intelligibility in Individuals with Ataxic Dysarthria Secondary to Friedreich s Disease? Tyler Phillips Levee M.Cl.Sc (SLP) Candidate University
Nonlinear signal processing and statistical machine learning techniques to remotely quantify Parkinson's disease symptom severity
 Nonlinear signal processing and statistical machine learning techniques to remotely quantify Parkinson's disease symptom severity A. Tsanas, M.A. Little, P.E. McSharry, L.O. Ramig 9 March 2011 Project
Nonlinear signal processing and statistical machine learning techniques to remotely quantify Parkinson's disease symptom severity A. Tsanas, M.A. Little, P.E. McSharry, L.O. Ramig 9 March 2011 Project
Sophia Neppel M.Cl.Sc (SLP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
 Critical Review: What is the evidence of the effectiveness of Lee Silverman Voice Treatment (LSVT) in increasing speech intensity in individuals with non-hypokinetic dysarthria?* Sophia Neppel M.Cl.Sc
Critical Review: What is the evidence of the effectiveness of Lee Silverman Voice Treatment (LSVT) in increasing speech intensity in individuals with non-hypokinetic dysarthria?* Sophia Neppel M.Cl.Sc
The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery
 Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
Welcome The webinar will begin momentarily. Tractography-based Targeting for Functional Neurosurgery Vibhor Krishna, MD, SM Assistant Professor, Center for Neuromoduation, Dept. of Neurosurgery and Dept.
doi: /brain/awq221 Brain 2010: 133;
 doi:10.1093/brain/awq221 Brain 2010: 133; 2664 2676 2664 BRAIN A JOURNAL OF NEUROLOGY Motor and cognitive outcome in patients with Parkinson s disease 8 years after subthalamic implants Alfonso Fasano,
doi:10.1093/brain/awq221 Brain 2010: 133; 2664 2676 2664 BRAIN A JOURNAL OF NEUROLOGY Motor and cognitive outcome in patients with Parkinson s disease 8 years after subthalamic implants Alfonso Fasano,
Speech Profile of Individuals with Dysarthria Following First Ever Stroke
 International Journal of Medical Research & Health Sciences Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2017, 6(9): 86-95 I J M R
International Journal of Medical Research & Health Sciences Available online at www.ijmrhs.com ISSN No: 2319-5886 International Journal of Medical Research & Health Sciences, 2017, 6(9): 86-95 I J M R
The motor regulator. 1) Basal ganglia/nucleus
 The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
The motor regulator 1) Basal ganglia/nucleus Neural structures involved in the control of movement Basal Ganglia - Components of the basal ganglia - Function of the basal ganglia - Connection and circuits
Parkinsonian rigidity
 J. Neurol. Neurosurg. Pyschiat., 1963, 26, 27 Studies on induced exacerbation of Parkinsonian rigidity The effect of contralateral voluntary activity KEIZO MATSUMOTO, FERDINAND ROSSMANN, TUNG HUI LIN,
J. Neurol. Neurosurg. Pyschiat., 1963, 26, 27 Studies on induced exacerbation of Parkinsonian rigidity The effect of contralateral voluntary activity KEIZO MATSUMOTO, FERDINAND ROSSMANN, TUNG HUI LIN,
Stuttering Research. Vincent Gracco, PhD Haskins Laboratories
 Stuttering Research Vincent Gracco, PhD Haskins Laboratories Stuttering Developmental disorder occurs in 5% of children Spontaneous remission in approximately 70% of cases Approximately 1% of adults with
Stuttering Research Vincent Gracco, PhD Haskins Laboratories Stuttering Developmental disorder occurs in 5% of children Spontaneous remission in approximately 70% of cases Approximately 1% of adults with
MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety
 MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety T Foltynie, L Zrinzo,,2 I Martinez-Torres, 3 E Tripoliti, E Petersen, 4 E Holl,,5 I Aviles-Olmos, M Jahanshahi,
MRI-guided STN DBS in Parkinson s disease without microelectrode recording: efficacy and safety T Foltynie, L Zrinzo,,2 I Martinez-Torres, 3 E Tripoliti, E Petersen, 4 E Holl,,5 I Aviles-Olmos, M Jahanshahi,
Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease
 CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
CLINICAL ARTICLE Outcomes following deep brain stimulation lead revision or reimplantation for Parkinson s disease Leonardo A. Frizon, MD, 1,2 Sean J. Nagel, MD, 1 Francis J. May, MS, 1 Jianning Shao,
A Review on Dysarthria speech disorder
 A Review on Dysarthria speech disorder Miss. Yogita S. Mahadik, Prof. S. U. Deoghare, 1 Student, Dept. of ENTC, Pimpri Chinchwad College of Engg Pune, Maharashtra, India 2 Professor, Dept. of ENTC, Pimpri
A Review on Dysarthria speech disorder Miss. Yogita S. Mahadik, Prof. S. U. Deoghare, 1 Student, Dept. of ENTC, Pimpri Chinchwad College of Engg Pune, Maharashtra, India 2 Professor, Dept. of ENTC, Pimpri
DEEP BRAIN STIMULATION
 DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
DEEP BRAIN STIMULATION Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs
Evaluating the Driving Ability in Patients with Parkinson s Disease Using a Driving Simulator
 ORIGINL RTICLE Evaluating the Driving bility in Patients with Parkinson s Disease Using a Driving Simulator Win Thiri Kyaw 1, Noriko Nishikawa 1, Takashi Moritoyo 2, Tomoaki Tsujii 1, Hirotaka Iwaki 1
ORIGINL RTICLE Evaluating the Driving bility in Patients with Parkinson s Disease Using a Driving Simulator Win Thiri Kyaw 1, Noriko Nishikawa 1, Takashi Moritoyo 2, Tomoaki Tsujii 1, Hirotaka Iwaki 1
Overweight after deep brain stimulation of the subthalamic nucleus in Parkinson disease: long term follow-up
 1 CHU Clermont-Ferrand, Department of Neurology, Gabriel Montpied Hospital, Clermont-Ferrand, France; 2 Univ Clermont 1, UFR Medecine, Clermont-Ferrand, France; 3 INRA, Centre Clermont-Ferrand Theix, Unite
1 CHU Clermont-Ferrand, Department of Neurology, Gabriel Montpied Hospital, Clermont-Ferrand, France; 2 Univ Clermont 1, UFR Medecine, Clermont-Ferrand, France; 3 INRA, Centre Clermont-Ferrand Theix, Unite
C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak, MD, PhD D.
 ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
ARTICLES STN-DBS frequency effects on freezing of gait in advanced Parkinson disease C. Moreau, MD L. Defebvre, MD, PhD A. Destée, MD, PhD S. Bleuse, PhD F. Clement, MD J.L. Blatt, MD, PhD P. Krystkowiak,
Deep brain stimulation (DBS) has been
 TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
TOPIC RESEARCH HUMAN CLINICAL STUDIES RESEARCH HUMAN CLINICAL STUDIES Do Stable Patients With a Premorbid Depression History Have a Worse Outcome After Deep Brain Stimulation for Parkinson Disease? Michael
The Direct Cost of Parkinson Disease at Juntendo Medical University Hospital, Japan
 ORIGINAL ARTICLE The Direct Cost of Parkinson Disease at Juntendo Medical University Hospital, Japan Asako Yoritaka 1,2, Jiro Fukae 3, Taku Hatano 2,EiseiOda 4 and Nobutaka Hattori 2 Abstract Objective
ORIGINAL ARTICLE The Direct Cost of Parkinson Disease at Juntendo Medical University Hospital, Japan Asako Yoritaka 1,2, Jiro Fukae 3, Taku Hatano 2,EiseiOda 4 and Nobutaka Hattori 2 Abstract Objective
COGNITIVE SCIENCE 107A. Motor Systems: Basal Ganglia. Jaime A. Pineda, Ph.D.
 COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
COGNITIVE SCIENCE 107A Motor Systems: Basal Ganglia Jaime A. Pineda, Ph.D. Two major descending s Pyramidal vs. extrapyramidal Motor cortex Pyramidal system Pathway for voluntary movement Most fibers originate
2012, Greenwood, L.
 Critical Review: How Accurate are Voice Accumulators for Measuring Vocal Behaviour? Lauren Greenwood M.Cl.Sc. (SLP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
Critical Review: How Accurate are Voice Accumulators for Measuring Vocal Behaviour? Lauren Greenwood M.Cl.Sc. (SLP) Candidate University of Western Ontario: School of Communication Sciences and Disorders
피대근절개에따른갑상선절제술후의음성변화. Voice Comparison between Strap Muscle Retraction and Cutting Technique in Thyroidectomy 김영모 1 조정일 1 김철호 1 박정선 1 최호순 3 하현령 2
 KISEP Head and Neck Korean J Otolaryngol 2000;43:985-91 피대근절개에따른갑상선절제술후의음성변화 김영모 1 조정일 1 김철호 1 박정선 1 최호순 3 하현령 2 Voice Comparison between Strap Muscle Retraction and Cutting Technique in Thyroidectomy
KISEP Head and Neck Korean J Otolaryngol 2000;43:985-91 피대근절개에따른갑상선절제술후의음성변화 김영모 1 조정일 1 김철호 1 박정선 1 최호순 3 하현령 2 Voice Comparison between Strap Muscle Retraction and Cutting Technique in Thyroidectomy
E ssential tremor is a commonly diagnosed movement
 684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
684 PAPER Bilateral thalamic deep brain stimulation: midline tremor control J D Putzke, R J Uitti, A A Obwegeser, Z K Wszolek, R E Wharen... See end of article for authors affiliations... Correspondence
Neurolaryngology and Neurogenic Voice Disorders. Introduction. If it walks like a duck.. Erin Guidera, MS, CCC-SLP 4/8/17
 Neurolaryngology and Neurogenic Voice Disorders Erin Guidera, MS, CCC-SLP 4/8/17 Introduction Changes in vocal quality and speech can be the presenting symptom of underlying neurological disorders (e.g.,
Neurolaryngology and Neurogenic Voice Disorders Erin Guidera, MS, CCC-SLP 4/8/17 Introduction Changes in vocal quality and speech can be the presenting symptom of underlying neurological disorders (e.g.,
A study of prosodic features of patients with idiopathic Parkinson s disease
 145 말소리와음성과학제권제1 호 (2011) pp 145~151 A study of prosodic features of patients with idiopathic Parkinson s disease ABSTRACT In view of the hypothesis that the effects of Parkinson's disease on voice production
145 말소리와음성과학제권제1 호 (2011) pp 145~151 A study of prosodic features of patients with idiopathic Parkinson s disease ABSTRACT In view of the hypothesis that the effects of Parkinson's disease on voice production
ORIGINAL CONTRIBUTION
 ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
ORIGINAL CONTRIBUTION Common Misdiagnosis of a Common Neurological Disorder How Are We Misdiagnosing Essential Tremor? Samay Jain, MD; Steven E. Lo, MD; Elan D. Louis, MD, MS Background: As a common neurological
Comparing Voice Self-Assessment with Auditory Perceptual Analysis in Patients with Multiple Sclerosis
 100 Original Research THIEME Comparing Voice Self-Assessment with Auditory Perceptual Analysis in Patients with Multiple Sclerosis Vladimir Bauer 1 Zorica Aleric 1 Ervin Jancic 2 1 Department of Otorhinolaryngology,
100 Original Research THIEME Comparing Voice Self-Assessment with Auditory Perceptual Analysis in Patients with Multiple Sclerosis Vladimir Bauer 1 Zorica Aleric 1 Ervin Jancic 2 1 Department of Otorhinolaryngology,
Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor
 Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor Karen L. Francis, PhD* Waneen W. Spirduso, EdD Tim Eakin, PhD Pamela Z.
Long-Term Effects of Thalamic Deep Brain Stimulation on Force Control in a Patient with Parkinson s Disease-Driven Action Tremor Karen L. Francis, PhD* Waneen W. Spirduso, EdD Tim Eakin, PhD Pamela Z.
DIFFERENTIAL DIAGNOSIS SARAH MARRINAN
 Parkinson s Academy Registrar Masterclass Sheffield DIFFERENTIAL DIAGNOSIS SARAH MARRINAN 17 th September 2014 Objectives Importance of age in diagnosis Diagnostic challenges Brain Bank criteria Differential
Parkinson s Academy Registrar Masterclass Sheffield DIFFERENTIAL DIAGNOSIS SARAH MARRINAN 17 th September 2014 Objectives Importance of age in diagnosis Diagnostic challenges Brain Bank criteria Differential
modulation of multiple brain networks.
 Neuroanatomy of Deep Brain Stimulation: modulation of multiple brain networks. Dr. med. Ettore A. Accolla Maladie de Parkinson: un diagnostic clinique 1. Bradykinésie 2. Tremblement de repos (4-6 Hz) 3.
Neuroanatomy of Deep Brain Stimulation: modulation of multiple brain networks. Dr. med. Ettore A. Accolla Maladie de Parkinson: un diagnostic clinique 1. Bradykinésie 2. Tremblement de repos (4-6 Hz) 3.
Parkinson s Disease in the Elderly A Physicians perspective. Dr John Coyle
 Parkinson s Disease in the Elderly A Physicians perspective Dr John Coyle Overview Introduction Epidemiology and aetiology Pathogenesis Diagnosis and clinical features Treatment Psychological issues/ non
Parkinson s Disease in the Elderly A Physicians perspective Dr John Coyle Overview Introduction Epidemiology and aetiology Pathogenesis Diagnosis and clinical features Treatment Psychological issues/ non
Idiopathic Parkinson s disease (IPD) affects as many as 10% of Americans. Speech Motor Stability in IPD: Effects of Rate and Loudness Manipulations
 Speech Motor Stability in IPD: Effects of Rate and Loudness Manipulations Jennifer Kleinow Anne Smith Department of Audiology and Speech Sciences Purdue University West Lafayette, IN Lorraine Olson Ramig
Speech Motor Stability in IPD: Effects of Rate and Loudness Manipulations Jennifer Kleinow Anne Smith Department of Audiology and Speech Sciences Purdue University West Lafayette, IN Lorraine Olson Ramig
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS)
 Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Subthalamic Nucleus Deep Brain Stimulation (STN-DBS) A Neurosurgical Treatment for Parkinson s Disease Parkinson s Disease Parkinson s disease is a common neurodegenerative disorder that affects about
Essential feature. Who are cochlear implants for? People with little or no hearing. substitute for faulty or missing inner hair
 Who are cochlear implants for? Essential feature People with little or no hearing and little conductive component to the loss who receive little or no benefit from a hearing aid. Implants seem to work
Who are cochlear implants for? Essential feature People with little or no hearing and little conductive component to the loss who receive little or no benefit from a hearing aid. Implants seem to work
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo
 Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
Supplementary Information for Decreased activity of single subthalamic nucleus neurons in Parkinson patients responding to placebo Fabrizio Benedetti, 1,2 Luana Colloca, 1,2 Elena Torre, 1 Michele Lanotte,
Combination of Bone-Conducted Speech with Air-Conducted Speech Changing Cut-Off Frequency
 Combination of Bone-Conducted Speech with Air-Conducted Speech Changing Cut-Off Frequency Tetsuya Shimamura and Fumiya Kato Graduate School of Science and Engineering Saitama University 255 Shimo-Okubo,
Combination of Bone-Conducted Speech with Air-Conducted Speech Changing Cut-Off Frequency Tetsuya Shimamura and Fumiya Kato Graduate School of Science and Engineering Saitama University 255 Shimo-Okubo,
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources
 COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
COMMUNICATION AND SWALLOWING DISORDERS IN PARKINSON S DISEASE Challenges, Treatments, and Resources Rosemary B. Loftin, M.S. CCC/SLP Supervisor of Speech Pathology Services Mayo Clinic Hospital Arizona
symptoms of Parkinson s disease EXCEPT.
 M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
M. Angele Theard, M.D Asst. Professor, Washington University, St. Louis, MO Quiz team; Shobana Rajan, M.D; Suneeta Gollapudy, MD; Verghese Cherian, M.D, M. Angele Theard, MD This quiz is being published
Voice Evaluation. Area of Concern:
 Name : Lilly Tulip File Number : 1002 Age : xx years D.O.B. : 9-9-1999 Address : 9999 9 th St NW D.O.E. : 11-30-2012 Minot, ND 59992 Referral : Dr. Andrew Hetland Phone : (701) 899-9999 Code : 784.40 Area
Name : Lilly Tulip File Number : 1002 Age : xx years D.O.B. : 9-9-1999 Address : 9999 9 th St NW D.O.E. : 11-30-2012 Minot, ND 59992 Referral : Dr. Andrew Hetland Phone : (701) 899-9999 Code : 784.40 Area
Who are cochlear implants for?
 Who are cochlear implants for? People with little or no hearing and little conductive component to the loss who receive little or no benefit from a hearing aid. Implants seem to work best in adults who
Who are cochlear implants for? People with little or no hearing and little conductive component to the loss who receive little or no benefit from a hearing aid. Implants seem to work best in adults who
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Value Units
 Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
Understand the New 2019 Neurostimulator Analysis-Programming CPT Coding Structure and Associated Relative Units The American Academy of Neurology (AAN) presents the following case studies to help you understand
MAXIMIZING FUNCTION IN PARKINSON S DISEASE
 1 MAXIMIZING FUNCTION IN PARKINSON S DISEASE September 13, 2016 End Falls This Falls Conference Jan Goldstein Elman One Step Ahead Mobility Toronto, Ontario Outline An overview of Parkinson s disease (PD):
1 MAXIMIZING FUNCTION IN PARKINSON S DISEASE September 13, 2016 End Falls This Falls Conference Jan Goldstein Elman One Step Ahead Mobility Toronto, Ontario Outline An overview of Parkinson s disease (PD):
Voice Pitch Control Using a Two-Dimensional Tactile Display
 NTUT Education of Disabilities 2012 Vol.10 Voice Pitch Control Using a Two-Dimensional Tactile Display Masatsugu SAKAJIRI 1, Shigeki MIYOSHI 2, Kenryu NAKAMURA 3, Satoshi FUKUSHIMA 3 and Tohru IFUKUBE
NTUT Education of Disabilities 2012 Vol.10 Voice Pitch Control Using a Two-Dimensional Tactile Display Masatsugu SAKAJIRI 1, Shigeki MIYOSHI 2, Kenryu NAKAMURA 3, Satoshi FUKUSHIMA 3 and Tohru IFUKUBE
Communication and Swallowing with PSP/CBD. Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist
 Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Communication and Swallowing with PSP/CBD Megan DePuy, MBA, MS, CCC-SLP Private Speech Pathologist A Speech Therapist? Why? Swallowing (Dysphagia) Speech (Dysarthria, Dysphonia) Language (Aphasia) An Experienced
Patient selection for surgery: Parkinson s disease
 Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Patient selection for surgery: Parkinson s disease Dr. María C. Rodríguez-Oroz Neurology and Neuroscience. University Hospital Donostia, Research Institute BioDonostia, Ikerbasque Senior Researcher San
Disclosures. Primary Methods for Treating UVP. Key Factors Influencing Treatment Planning. Guiding principle with Treatment Planning 2/4/2018
 Zen and art of vocal mechanics: Key Factors That Influence Unilateral Vocal Fold Paralysis (UVP) Treatment Decisions Julie Barkmeier Kraemer, Ph.D. Professor, Division of Otolaryngology Clinic Director,
Zen and art of vocal mechanics: Key Factors That Influence Unilateral Vocal Fold Paralysis (UVP) Treatment Decisions Julie Barkmeier Kraemer, Ph.D. Professor, Division of Otolaryngology Clinic Director,
Supplementary Information. Combined Diffusion Tensor Imaging and Arterial Spin Labeling as
 Supplementary Information Combined Diffusion Tensor Imaging and Arterial Spin Labeling as Markers of Early Parkinson s disease Xiaobo Wei MD 1, Ronghua Yan MD, Ph.D 2, Zhaoyu Chen MD 1, Ruihui Weng MD
Supplementary Information Combined Diffusion Tensor Imaging and Arterial Spin Labeling as Markers of Early Parkinson s disease Xiaobo Wei MD 1, Ronghua Yan MD, Ph.D 2, Zhaoyu Chen MD 1, Ruihui Weng MD
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
Deep brain stimulation for tremor resulting from acquired brain injury Sitsapesan, H A; Holland, P; Oliphant, Z; De Pennington, N; Brittain, John-Stuart; Jenkinson, Ned ; Joint, C; Aziz, T Z; Green, A
I n 1991 Benabid et al introduced deep brain stimulation
 PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
PAPER Multicentre European study of thalamic stimulation in essential tremor: a six year follow up O Sydow, S Thobois, F Alesch, J D Speelman, study collaborators... See Editorial Commentary, pp1361 2
ORIGINAL CONTRIBUTION. Subthalamic Stimulation in Parkinson Disease
 Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Subthalamic Stimulation in Parkinson Disease A Multidisciplinary Approach ORIGINAL CONTRIBUTION J. L. Houeto, MD; P. Damier, MD, PhD; P. B. Bejjani, MD; C. Staedler, MD; A. M. Bonnet, MD; I. Arnulf, MD;
Speech Intelligibility Measurements in Auditorium
 Vol. 118 (2010) ACTA PHYSICA POLONICA A No. 1 Acoustic and Biomedical Engineering Speech Intelligibility Measurements in Auditorium K. Leo Faculty of Physics and Applied Mathematics, Technical University
Vol. 118 (2010) ACTA PHYSICA POLONICA A No. 1 Acoustic and Biomedical Engineering Speech Intelligibility Measurements in Auditorium K. Leo Faculty of Physics and Applied Mathematics, Technical University
