NATIONAL CONSENSUS PROJECT STAKEHOLDER STRATEGIC DIRECTIONS SUMMIT
|
|
|
- Bertram Garrett
- 6 years ago
- Views:
Transcription
1 NATIONAL CONSENSUS PROJECT STAKEHOLDER STRATEGIC DIRECTIONS SUMMIT Summary Report Special thank you to the Gordon and Betty Moore Foundation for their financial support Community-Based Palliative Care June 29-30, 2017 Chicago Marriott O Hare, Chicago, IL
2 Table of Contents I. Background and Purpose 1 II. Summit Objectives, Agenda, and Attendees 2 III. Key Themes and Considerations 5 IV. Summit Feedback 13 V. Next Steps and Project Timeline 15 VI. Appendix 17 A. Summit Participant Roster 18 B. Summit Discussion Worksheets Defining Community Stakeholder Perspective Domain Input 25
3 I. BACKGROUND AND PURPOSE In January 2017, the Gordon and Betty Moore Foundation awarded the National Coalition for Hospice and Palliative Care a two-year grant to support a stakeholder summit and the development, endorsement, dissemination and implementation of Community-based Palliative Care Guidelines. The Guidelines will be modeled on the success and strategies of the National Consensus Project (NCP) Clinical Practice Guidelines for Quality Palliative Care, 2013 and is scheduled for publication July (Read the press release.) To launch this effort, a NCP Stakeholder Strategic Directions Summit was held June 29-30, 2017 in Chicago IL, to bring together key national organizations to discuss and define essential elements of quality primary and specialty palliative care services in the community. The Summit was attended by 58 representatives from 43 national/regional organizations, that covered a broad range of care settings, provider associations, accrediting bodies, payers, and community services organizations. The Stakeholder Strategic Directions Summit was the first major step to solicit input for the 2018 NCP Clinical Practice Guidelines for Quality Palliative Care (4th edition). The NCP Steering Committee and Writing Workgroup will use the input from the Summit to refine and/or revise the current 2013 NCP Guidelines (3rd edition) to improve access to quality palliative care for all in need, regardless of setting, diagnosis, prognosis, or age. This Summary Report captures key themes, considerations, and ideas that were discussed during the Summit. Summit participants also provided an extensive amount of written input through small group discussions and worksheet exercises. That input combined with this report will be consolidated and synthesized, and made available for the NCP Steering Committee and Writing Workgroup to use over the course of this project. Summit participants having small group discussions to define community. From left to right: Stacie Sinclair and Tracy Schroepfer, NCP Writing Workgroup Co-Chairs; Martha Twaddle and Betty Ferrell, NCP Steering Committee Co-Chairs SUMMARY REPORT 1
4 II. Summit Attendees, Objectives, and Agenda Attendees Since community-based palliative care should be available to any patient with a serious illness in any care setting, the potential audience for the NCP Clinical Practices Guidelines for Quality Palliative Care includes health systems, small/rural hospitals, office practices, cancer centers, dialysis units, long-term care facilities, assisted living facilities, home health and hospice agencies, and other care providers as well as hospitals. Also, payers, accrediting organizations, and quality measurement organizations are seeking to support accountability standards for quality palliative care across settings. In addition, patient and family advocate organizations, social service agencies, and other community organizations serving individuals with palliative care needs are critical in ensuring the Guidelines align with and meet the needs of patients and family caregivers of those with serious illness. Therefore, significant efforts were taken to invite attendees that represented stakeholders outside of the hospice and palliative care field, and other organizations that also will be critical customers of the Guidelines. Of the 58 organizational representatives who attended the Summit: 75% were from organizations that are not members of the National Coalition for Hospice and Palliative Care; Over 50% did not previously have a formal role with the NCP project (i.e. not on the NCP Steering Committee or Writing Workgroup); and All represented a diverse range of stakeholder organizations (see table below). Attendees Organization Type Provider Organizations (e.g. American Health Care Association, National Association for Home Care and Hospice) Individual Professionals (e.g. Hospice and Palliative Care Nurses Association, HealthCare Chaplaincy Network) Patient and Family Caregivers (e.g. Alzheimer s Association, American Cancer Society, National Patient Advocate Foundation) Health Plans/Quality/Accreditations (e.g. Blue Shield of California, The Joint Commission, National Quality Forum) Other Stakeholders (e.g. The Pew Charitable Trusts, National Palliative Care Research Center, Coalition to Transform Advanced Care) % of Attendees 23% 35% 14% 14% 14% SUMMARY REPORT 2
5 A complete listing of attendees is included in Appendix A of this report and a listing of all organizations represented are listed on the website. Objectives To build a strong foundation for consensus over the course of the project, thoughtful consideration was made to the objectives and agenda for the Summit. The following objectives were used to guide the design of the Summit: 1. Build relationships among participants and across national stakeholder organizations 2. Provide a highly interactive forum for candid and creative discussion 3. Solicit input from all stakeholders to prioritize unique areas of focus and critical gaps for the project Agenda There was an intentional design of the Summit agenda to provide participants the opportunity to network and build relationships through general introductions, alternating table assignments, small group exercises, large group report outs, and informal networking throughout the Summit. In addition to the small and large group discussions, worksheets were provided for participants to provide individual input throughout the Summit (See Appendix B). These worksheets were collected at the end of each exercise so all the written input could be collated and synthesized. The Summit agenda included the following: DAY 1: Thursday, June 29, 5:00 8:00 PM 5:00 5:45 PM Registration & Networking 5:45 6:00 PM Welcome & Introductions (name, organization, where were you born, where do you live now?) 6:00 7:15 PM Small Group Discussion: Defining Community Why are community-based guidelines important to you and/or your organization? How do you define community? What are unique elements of community-based palliative care? 7:15 8:00 PM Networking SUMMARY REPORT 3
6 DAY 2: Friday, June 30, 7:30 AM 4:00 PM 7:30 8:15 AM Breakfast & Networking 8:15 8:45 AM Welcome & Day 2 Kick-off: Key Themes from Day 1 8:45 9:30 AM Why Are We Here? What Has Been Accomplished? 9:30 10:15 AM Panel: What s Unique About Community-based Palliative Care? 10:15 10:30 AM Break & Networking 10:30 11:30 AM Small Group Discussion: How will the NCP Guidelines be Used? (Stakeholder Perspectives) What is the value of incorporating community-based guidelines into the existing guidelines? What does the stakeholder need from this process? What are 2-3 opportunities and/or challenges in adopting community-based guidelines that the writers should consider? 11:30 12:00 PM Morning Recap / Key Insights 12:00 12:30 PM Lunch & Networking 12:30 1:45 PM Small Group Discussion: Incorporating Community into the Guidelines (Breakout by Domains PLUS one Wildcard Domain) How is this palliative care domain supporting community? What does not need to change? What is missing? How can this palliative care domain better incorporate community? 1:45 2:00 PM Break & Networking 2:00 3:00 PM Small Group Report Out 3:00 3:30 PM NCP Writing Workgroup 3:30 4:00 PM Final Reflections & Next Steps SUMMARY REPORT 4
7 III. Key Themes and Considerations A significant amount of ideas and perspectives were shared during the Summit during large and small group discussions, and collected through the worksheet exercises. (See Appendix B) Outlined below are the key themes that are representative of the input and discussions. The detailed information was collected through the corresponding worksheets of each key theme and will serve as the foundation for creating the 4th edition of the NCP Guidelines. The key themes and corresponding considerations outlined in this section are: A. Defining Community B. Stakeholder Perspectives (re: current and future use of the Guidelines) C. Domain Input A. Defining Community A significant amount of discussion occurred regarding how to define community, what is unique about the needs outside of hospitals and hospices, and whether it was important to define it. (Refer to Worksheet 1 in Appendix B) Some of the points raised included: Community should be defined by the person; however, needs can change based on the setting of care and other factors (e.g. in the ICU, home, etc.). It is helpful to define community as a lens through which people s needs can be assessed. Given current workforce limitations and access, the Guidelines should be inclusive of primary and specialty palliative care. Some define community as anything outside of large, academic hospitals while others define it to be any setting outside of any hospital. However community is defined, the Guidelines should be person-centric and not medicalized. The Guidelines need to be written in such a way as they can apply across all settings. If there are distinctions made as to settings or any other definitions, the Guidelines need to be able to be operationalized. It is important to have the Guidelines include family caregivers as part of community. Critical or unique elements to community-based palliative care include: 24/7 access, training, limited or no access to specialists, payment, caregiver support, and community-resource needs. SUMMARY REPORT 5
8 Guidelines should remain focused on clinical standards and not define operational standards given the variability in needs of populations, settings, and use (e.g. key is to make sure clinical elements are in place to ensure quality, but not try to define how a clinical standard is implemented). A distinction made was whether it was more important to define the community or a population. New models of care and organizations are quickly entering the market, creating both tension around the definition of quality and new, innovative approaches that may prove very effective. The graph below highlights the range of dimensions to define community. Geography Other... Setting Organization type COMMUNITY AS DEFINED BY THE PERSON Condition Age Ethnicity Disease Gender Considerations Based on the overall discussion of community and scope, the following are key considerations for the 2018 NCP Guidelines: Guidelines should be written such that they can be applied across settings wherever possible, preferably in one set of Guidelines. Guidelines should be written to incorporate both primary and specialty level palliative care. Careful consideration needs to be made to address access, particularly in remote or underserved geographies where specialty level palliative care may not be available. This includes achieving the appropriate balance on training or certification requirements. Careful consideration should be made to keep the Guidelines focused on clinical standards (the what ) and not be overly prescriptive on operational standards (the how). If the Clinical Guidelines are to be person-centric, they will need to accommodate a level of ambiguity as to how a person may define their needs based on multiple factors. SUMMARY REPORT 6
9 Given the pace of change and growth in need, the Guidelines should be flexible and adaptable over time as need grows and models evolve. B. Stakeholder Perspectives (re: current and future use of the Guidelines) The following are specific examples and perspectives that the Summit attendees shared for how the 2013 NCP Guidelines are currently being used and their expectations for the 2018 NCP Guidelines. (Refer to Worksheet 2 in Appendix B) Providers Provider practices, including accountable care organizations (ACOs) are using the Guidelines to design home-based and other community-based programs. A specific patient case example was provided by ProHEALTH, a provider practice, to demonstrate how they have designed their homebased palliative care program using the domains and standards in the Guidelines. Education Clinical Guidelines establish the expectations for the skills and knowledge needed to practice. End-of-Life Nursing Education Consortium (ELNEC) training incorporates the Guidelines. Curriculum for training oncology advanced practice nurses (APNs) is based on the domains and standards in the Guidelines. The Guidelines will serve as the foundation for new disciplines who are looking to offer specialized training programs and certifications (e.g. Physician Assistants). Measurement Guidelines are needed to establish a baseline for measuring where you are and then measuring change. The measurements are then incorporated into quality improvement initiatives, value-based payment models, and benchmarking programs. In 2006 the National Quality Forum (NQF) developed a palliative care measurement framework using the Guidelines. 38 preferred practices for palliative and end-of-life care were NQF endorsed using the Guidelines. NQF framework was recently updated to reflect community-based settings and will look to the revised Guidelines to further develop the framework. Accreditation The Guidelines have been used to define the care that should be expected for those with serious illness. Guidelines were used by the Accreditation Commission for Health Care (ACHC) to establish expectations for home health agencies delivering palliative care services. SUMMARY REPORT 7
10 The Joint Commission (TJC) used the Guidelines in 2003 to establish the Advanced Certification in Palliative Care standards for hospitals. TJC has started the certification process for non-hospital settings and is awaiting the release of new Guidelines. It was noted that the Guidelines have heavily influenced home health (serving over 17 million people a year) by requiring interdisciplinary teams (IDTs) and advance care planning (ACP). Health Plans and Payment The Guidelines are used to ensure health plans, working with providers in their networks, are responsive to the needs of their members with serious illness. Blue Shield of California shared the following examples of how they are using the Guidelines: Developing standards for payment (rolling out a state-wide payment bundle for serious illness) Using in medical policy to authorize services Including in member and consumer education materials Supporting regulatory and legislative efforts to improve access Incorporating the specific standards, word for word, into provider contracts Research The existence of the NCP Guidelines validates the level of importance and provides credibility to research. However, the challenge is that research is needed to create the evidence for the Guidelines, and the Guidelines are needed to establish credibility for the research. It was stated during the Summit to make sure that the Guidelines are evidence-based and should not outpace the evidence. Other Examples Physician Assistants (PA) representatives stated the Guidelines are important in defining skills and knowledge as their specialized training programs are developed. Pediatric representatives stated the need to establish Guidelines that are appropriate for the situation (e.g. appropriateness of an advance care discussion with parents of a new born with cystic fibrosis). Pharmacy representatives stated the Guidelines need to be trans-disciplinary and appropriately recognize the varying levels of involvement some professionals may have in the interdisciplinary team model. For example, need to strike a balance between highlighting pharmacy as a valuable team member, but realizing that we don t want to penalize programs that can t afford a dedicated pharmacist. Considerations Based on the overall discussion of the use of the Guidelines, the following are key considerations for the 2018 NCP Guidelines: Examples stated above demonstrate and validate the value of the 2013 Guidelines. SUMMARY REPORT 8
11 Expediting the next release of the 2018 Guidelines is important as organizations are holding off on implementing initiatives anticipating Guidelines that will incorporate community settings. Careful consideration will need to be made to any significant changes or additions to the existing domains since the current Guidelines are being used by providers, quality and accrediting organizations, research projects, and health plans. There is significant growth in the number of organizations providing some level of palliative care (both primary and specialty-level) and therefore it will be important to establish an appropriate balance that provides enough guidance to ensure quality (establish a floor ) without such specificity that unrealistic expectations are set that are not measurable or achievable. Careful consideration will need to be made in the wording and the level of specificity that is included in the Guidelines to establish benchmarks that can be incorporated into payment models, etc. The Guidelines need to be flexible enough to address varying needs and access across settings, age, etc. (e.g. what is needed for a newborn is different than a young child), and provider types. Including practical case studies was also recommended. C. Domain Input Specific attention (through small/large group discussion) was given to each of the following eight domains that are included in the 2013 Guidelines: 1. Structure and Processes for Care 2. Physical Aspects of Care 3. Psychological and Psychiatric Aspects of Care 4. Social Aspects of Care 5. Spiritual, Religious and Existential Aspects of Care 6. Cultural Aspects of Care 7. Care of the Patient at the End of Life 8. Ethical and Legal Aspects of Care In addition to the eight domains, a Wildcard small group discussion was held to brainstorm other domains that may need to be considered. (Refer to Worksheet 3 in Appendix B) Considerations Key themes re: the domains that emerged from the discussions included: Address how to integrate the palliative care specialist interdisciplinary team and the community resources Make the language consistent throughout the current Guidelines re: the interdisciplinary team SUMMARY REPORT 9
12 Expand family caregiver focus to include unit of care, assessment, and education Provide more on comprehensive assessment and integration of community services Address different populations, e.g. pediatrics and geriatrics Focus on a comprehensive approach to palliative care; avoid being too medicalized Incorporate culture, communication, coordination and transitions of care throughout all domains Include use of technology to improve patient and family care Maintain flexibility without compromising quality Recommendations for the structure of the Guidelines included: Provide flexibility in application of Guidelines based on resources, setting, etc. Make it practical! Include practical application examples and case studies as a means of illustrating application of Guidelines in different settings/communities Create a user-friendly electronic version and use hyperlinks Provide references and resources (e.g., sample assessment tools, particularly since this may vary in a community-based setting) Balance the tension between too general and too specific Add why this domain at the beginning of each domain Clarify the difference between clinical and operational guidelines in the Preface section Include a glossary Specific domain considerations included: Domain 1: Structure and Processes for Care Expand the focus, as it is highly medicalized and instead focus on the structures needed to care for the patient and family with serious illness Explore creative solutions so that 24/7 access to care is mandatory Incorporate community resources into the interdisciplinary team Emphasize workforce development Strengthen care transitions processes Focus on care coordination Identify triggers for palliative care referrals Domain 2: Physical Aspects of Care Focus on physical well-being and function as the framework, not pain and symptoms Emphasize comprehensive assessment and integration of community services Add information related to improving assessment and management of functional status Reframe opioids to solutions that are more long-term (patients living years with serious illness in the community) SUMMARY REPORT 10
13 Add anticipatory care to avoid pain and suffering Identify the patient s role in pain and symptom management Domain 3: Psychological and Psychiatric Aspects of Care Restructure to focus on screening, assessment, treatment, and education Add assessment of family caregiver Add information about capacity for decision making, including patients with developmental disabilities as well as caregiver capacity Emphasize PTSD, trauma, post-illness survivorship, post-illness psychosis, dual diagnosis, and behavioral disturbances/dementia Discuss scope of practice, safety of patient, caregiver and health care team Domain 4: Social Aspects of Care Revise interdisciplinary assessment so it isn t a medical model Define patient and family as the unit of care so that it s clear who the patient identifies as the caregiver and who is included as the identified family Add assessment of family caregiver Expand the domain to focus on community resources and social determinants of health Assess developmental needs of adults Domain 5: Spiritual, Religious and Existential Aspects of Care Describe the importance of incorporating community spiritual clergy (without implying that this is THE representative on the team) Define the roles of spiritual professionals Reorient the content upstream of end-of-life care Add age-appropriate spiritual care Make the language consistent spiritual/religious/existential Domain 6: Cultural Aspects of Care Broaden the definition of culture Incorporate language of disparities Ensure that all the domains describe how to serve traditionally underserved groups Describe culturally-inclusive care Add the importance of availability of education, training, and competencies of the professionals Emphasize the importance of a community needs assessment and cultural brokers Include a discussion on intersectionality Ensure that access to care is referenced in the Guidelines SUMMARY REPORT 11
14 Domain 7: Care of the Patient at the End of Life Describe end-of-life care when patients aren t eligible for or choose not to elect hospice Emphasize community-based care Ensure content focuses on pediatrics Add more information on assessment Add prognostication Rename this domain? Domain 8: Ethical and Legal Aspects of Care Describe ethical principles at the beginning Discuss importance of clinician education relative to legal treatment options Enhance proactive advance care planning process Reorient advance care planning to focus on maximizing the ability of the patient to achieve stated goals Describe how to access an ethics committee in the community Ensure that the team has a framework for processing emerging ethical dilemmas and issues Discuss the team conflict management process Identify current best practices related to advance care planning Add professional burnout as an ethical issue Identify the importance of assessing caregiver capacity Add financial issues to this domain Add references to professional position statements and other ethical resources Other suggested domains (from the Wildcard discussion group) Serious illness communication Practical aspects of daily living Caregiver assessment and care Coordination of care across settings Assessments/care plan Renewal/team care All recommendations for the eight domains plus any possible new domains will be consolidated and synthesized for the NCP Steering Committee and Writing Workgroup to use over the course of this project. SUMMARY REPORT 12
15 IV. Summit Feedback Of the 58 attendees, 39 (67%) completed the Summit evaluation that was distributed online immediately after the Summit. The evaluation included a rank order of specific features of the Summit plus open-ended questions to obtain individual comments. The overall results are provided in the table below. (Scale: 1 = strongly disagree to 5 = strongly agree) Summit Evaluation Statements I was provided with sufficient information and communication before the Summit. Rating 4.56 The Summit achieved its stated objectives The Summit was relevant to the work of my organization The design and facilitation of the Summit was effective The Summit increased my knowledge about Community-Based Palliative Care. I look forward to engaging my organization with the National Consensus Project Palliative Care Guidelines after the Summit Total Overall Rating 4.68 The following are some of the additional quotes from the evaluation: Re: attendee s experience of the Summit Î Î Î Î Î Î Î Î Î Î Organization and facilitation of summit was superb. It was an effective format to ensure all voices were included. Terrific stakeholder feedback process! This was a great event both in terms of the particular project at hand and in terms of building community across lots of stakeholders who are very seldom if ever in the same room. Very well planned and executed. Productive use of everyone s time. Objectives and expectations exceeded. Hearing about everyone s work and commitment was inspiring. Excellent and diverse group of people actually in the field doing palliative care which was great. Would have liked a few more academic voices in the room to challenge strong feelings about how teams should look for what should be required, especially if the data is lacking to support those recommendations. The care and planning that went into to preparing for this meeting was evident. Big thanks for your hard work! I felt that there wasn t nearly enough time - is there ever? - to leave you with a more robust set of proposals for the incorporation of SUMMARY REPORT 13
16 community into the Guidelines. But for the work that we did accomplish, there couldn t have been a more skilled, thoughtful and kind group of people. It was a pleasure working with this convened palliative care dedicated force. Re: key messages Summit attendees will share with their organization Î Î Î Î Î Î Î Î Î Î A thoughtful revision of the guidelines is in process that promises to further advance best practices in palliative care across all settings. There has been an ongoing movement toward community-based palliative care for a long time but it s finally coming to fruition with these guidelines that will hopefully broaden the reach and increase the impact of palliative care in the community. And with the shift from volume to value there s no better time! The 3rd edition is great; the 4th edition will be amazing. Now is the time to use these as a springboard for quality incentive discussions. It s not just about palliative care providers, but the many others in the community who are providing support and services to people with serious illness. The strategic support provided by Gordon and Betty Moore Foundation to advance quality improvement for all ages and all care settings to improve care for seriously ill patients and caregivers is remarkable, and the summit that captured input from across stakeholder populations was an essential step to change the game and draw on the momentum of value-based care reform to get this right. This project will help put people at the heart of healthcare reform. SUMMARY REPORT 14
17 V. Next Steps and Project Timeline Beginning July 2017, the NCP Steering Committee and Writing Workgroup will synthesize the input from this Summit and begin the drafting process of the 4th edition of the NCP Clinical Practice Guidelines for Quality Palliative Care that are scheduled to be published by July 1, Summit participants may be contacted to serve as subject matter experts as the Guidelines are being developed and revised. In addition, NCP staff will continue their outreach to other national stakeholder organizations that did not attend the Summit to engage for future endorsements of the 2018 NCP Guidelines. NCP Summit Ideas Domain Input Examples of Uses Ad Hoc Subject Matter Experts NCP Steering Committee Evidence NCP Writing Workgroup NCP Guidelines 4th edition SUMMARY REPORT 15
18 Below is an overall timeline for the project: Timeline/Details Q1 Q2 Q3 Q4 Q1 Q2 Q3 Q4 Project kick-off Summit prep and completion Synthesis and initial drafting DRAFT 1 Guidelines (1/31/18) DRAFT 2 Guidelines (2/28/18) Review by External Stakeholders Final Guidelines for endorsement Publish Guidelines (7/1/18) Disseminate Guidelines Updates and key milestones will periodically be published on the NCP web site at For more information about NCP, contact Gwynn Sullivan, NCP Project Director at gwynns@nationalcoalitionhpc.org. The National Coalition for Hospice and Palliative Care would like to thank Tom Gualtieri-Reed, MBA, for his invaluable guidance with the Summit design; expert facilitation of the Summit; and helpful drafting of this Summary Report. SUMMARY REPORT 16
19 VII. Appendix Appendix A: Summit Participant Roster SUMMARY REPORT 17
20 National Consensus Project Stakeholder Strategic Directions Summit Community-Based Palliative Care June 29-30, 2017 Chicago Marriott O Hare, Chicago, IL Participant Roster Academy of Integrative Pain Management Bob Twillman, PhD, FAPM Executive Director Accreditation Commission for Health Care Teresa Harbour, RN, MBA, MHA Director, Home Health, Hospice & Private Duty Alzheimer s Association Sam Fazio, PhD Director, Alzheimer s & Dementia Care American Academy of Home Care Medicine Carla Perissinotto, MD, MHS University of California San Francisco American Academy of Hospice and Palliative Medicine NCP Steering Committee Co-Chair Martha L. Twaddle, MD, FACP, FAAHPM, HMDC Senior Vice President, Education and Quality, Home Centered Care Institute Senior Medical Director, Aspire Health American Academy of Hospice and Palliative Medicine/National Coalition for Hospice and Palliative Care Executive Committee Steve Smith, MS, CAE Executive Director & Chief Executive Officer American Academy of Hospice and Palliative Medicine Joe Rotella, MD, MBA, HMDC, FAAHPM Chief Medical Officer American Academy of Hospice and Palliative Medicine Registries Collaborative Project Katherine Ast, MPH Director, Quality & Research American Cancer Society Lynne Padgett, PhD Strategic Director, Hospital Systems American Geriatrics Society Joseph Shega, MD Senior Vice President & National Medical Director VITAS Healthcare American Health Care Association Dianne Timmering, MBA, MFA, CNA Spirituality Co-Founder & Vice President, Legislative Affairs & Health Policy American Health Care Association Gail Sheridan, RN Chief Clinical Operations Officer American Medical Group Association David Introcaso, PhD Senior Director, Regulatory & Policy SUMMARY REPORT 18
21 American Medical Group Association Elizabeth Ciemins, PhD, MPH, MA Director, Research & Analytics Association of Professional Chaplains Margie Atkinson, DMin, BCC Director, Pastoral Care/Palliative Care & Ethics Morton Plant Mease/BayCare Health System Blue Shield of California Torrie Fields, MPH Senior Program Manager, Palliative Care Cambia Health Solutions Lee Spears Program Director, Personalized Care Support Regence Center to Advance Palliative Care Diane Meier, MD Director Center to Advance Palliative Care NCP Writing Workgroup Co-Chair Stacie Sinclair, MPP, LBSW Senior Policy Manager Coalition for Compassionate Care of California Judy (Citko) Thomas, JD Chief Executive Officer Coalition to Transform Advanced Care Marian Grant, DNP, ACNP-BC, ACHPN, FPCN, RN Policy Consultant College of Nursing, The University of Utah Lee Ellington, PhD Associate Professor Community Health Accreditation Partner Barbara McCann Interim President & CEO Discern Health Thomas Valuck, MD, JD Partner Duke University School of Medicine Kimberly Johnson, MD Associate Professor of Medicine Family Caregiver Alliance Leah Eskenazi, MSW Operations Director Gordon and Betty Moore Foundation Beth Berselli, MBA Program Officer Health Care Service Corporation Bruce Himelstein, MD Senior Medical Director, Government Programs HealthCare Chaplaincy Network Rev. George Handzo, BCC, CSSBB Director, Health Services Research & Quality HealthCare Chaplaincy Network Rev. Susan Wintz, MDiv, BCC Director, Professional & Community Education Hospice and Palliative Nurses Association NCP Steering Committee Co-Chair Betty Ferrell, PhD, RN, FAAN, FPCN, CHPN Director & Professor, Nursing Research & Education, City of Hope Hospice and Palliative Nurses Association Denise Stahl, MSN, ACHPN, FPCN Chief Clinical Officer Hospice and Palliative Nurses Foundation Sally Welsh, MSN, RN, NEA-BC Chief Executive Officer Leaders Engaged on Alzheimer s Disease Ian Kremer, JD Executive Director LeadingAge Janine Finck-Boyle, MBA/HCA, LNHA Director, Health Regulations & Policy SUMMARY REPORT 19
22 Long-Term Quality Alliance Larry Atkins, PhD Executive Director National Alliance for Caregiving Gail Gibson Hunt President & Chief Executive Officer National Association for Home Care and Hospice Andrea Devoti, MSN, MBA, RN Vice President, Policy & Education National Association for Home Care and Hospice John McIlvaine Senior Vice President National Association of Social Workers Carrie Dorn, LMSW, MPA Senior Practice Associate National Committee on Quality Assurance Maureen Henry, JD, PhD Research Scientist National Hospice and Palliative Care Organization John Mastrojohn III, RN, MSN, MBA Executive Vice President & Chief Operating Officer National Hospice and Palliative Care Organization Judi Lund Person, MPH, CHC Vice President, Regulatory & Compliance National Palliative Care Research Center Nathan Goldstein, MD Professor, Gerald J. and Dorothy R. Friedman Chair in Palliative Care Mount Sinai Medical Center National Patient Advocate Foundation Rebecca Kirch, JD Executive Vice President, Healthcare Quality & Value National Pediatric Hospice and Palliative Care Collaborative Tammy Kang, MD Co-Chair National Pediatric Hospice and Palliative Care Collaborative Kathie Kobler, MS, APN, PCNS-BC, CHPPN, FPCN Co-Chair National Quality Forum Karen Johnson Senior Director Oncology Nursing Society Michele Galioto, RN, MSN Assistant Chief Clinical Officer Physician Assistants in Hospice and Palliative Medicine Judy Knudson, PA-C Vice President Physician Assistants in Hospice and Palliative Medicine Richard Lamkin, MPH, MPAS, PA-C President ProHEALTH Care, an Optum Company Dana Lustbader, MD Chief, Department of Palliative Care Society of Palliative Care Pharmacists Rabia Atayee, PharmD, BCPS President Social Work Hospice and Palliative Care Network NCP Writing Workgroup Co-Chair Tracy Schroepfer, PhD Professor, School of Social Work University of Wisconsin-Madison Supportive Care Coalition Denise Hess, BCC Executive Director SUMMARY REPORT 20
23 The Joint Commission Kathy Clark, MSN, RN Associate Project Director Specialist, SBU Lead for Home Care & Palliative Care The Pew Charitable Trusts Katy Barnett Principle Associate, Improving End-of-Life Care Visiting Nurse Associations of American/ Elevating Home Danielle Pierotti, RN, PhD, CENP Vice President, Quality Staff National Coalition for Hospice and Palliative Care Amy Melnick, MPA, Executive Director Gwynn Sullivan, MSN, NCP Project Director Cozzie King, NCP Coordinator Kathy Brandt, MS, NCP Writer/Editor Summit Facilitator Thomas Gualtieri-Reed, MBA SUMMARY REPORT 21
24 Appendix Appendix B: Summit Discussion Worksheets 1. Defining Community 2. Stakeholder Perspective 3. Domain Input SUMMARY REPORT 22
25 National Consensus Project Stakeholder Strategic Directions Summit Community-Based Palliative Care WORKSHEET #1: Defining Community Name & Organization Purpose: To get input on how to define community and identify essential elements to consider in community-based palliative care 1. Why are community-based guidelines important to you and/or your organization? 2. How do you define community? 3. What are unique elements of community-based palliative care? What are 2 3 essential elements that are critical to incorporate? (e.g. transitions of care) SUMMARY REPORT 23
26 National Consensus Project Stakeholder Strategic Directions Summit Community-Based Palliative Care WORKSHEET #2: Stakeholder Perspective Name & Organization Stakeholder Organization Providers Individual Providers Quality/Accreditation/Health Plans Perspective Other Stakeholders People with serious illness /Family Caregivers (circle one) Purpose: To get input from key customers on how the guidelines will be used and what is important to consider when incorporating community-based guidelines 1. What is the value of incorporating community-based guidelines into the existing guidelines? How will they be used? 2. What does the stakeholder need from this process? 3. What are 2-3 opportunities and/or challenges in adopting community-based guidelines that the writers should consider (e.g. feasibility constraints)? SUMMARY REPORT 24
27 National Consensus Project Stakeholder Strategic Directions Summit Community-Based Palliative Care WORKSHEET #3: Domain Input Name & Organization Domain (circle one) 1. Structure and Process 6. Cultural 2. Physical 7. Care at End of Life 3. Psychological and Psychiatric 8. Ethical and Legal 4. Social 9. WILDCARD DOMAIN 5. Spiritual, Religious, Existential Purpose: To get input from key customers on how the guidelines will be used and what is important to consider when incorporating community-based guidelines How is this palliative care domain supporting community? What does not need to change? What is missing? How can this palliative care domain better incorporate community? Other comments or considerations: SUMMARY REPORT 25
28 NATIONAL CONSENSUS PROJECT STAKEHOLDER STRATEGIC DIRECTIONS SUMMIT Community-Based Palliative Care June 29 30, 2017 Chicago Marriott O Hare, Chicago, IL
Clinical Practice Guidelines for Quality Palliative Care, 4 th edition
 Welcome Clinical Practice Guidelines for Quality Palliative Care, 4 th edition Webinar December 17, 2:00 4:30 PM ET Webinar Host: www.nationalcoalitionhpc.org Moderator: Amy Melnick, MPA Executive Director
Welcome Clinical Practice Guidelines for Quality Palliative Care, 4 th edition Webinar December 17, 2:00 4:30 PM ET Webinar Host: www.nationalcoalitionhpc.org Moderator: Amy Melnick, MPA Executive Director
Disclosure. Clinical Practice Guidelines for Quality Palliative Care, 4 th edition
 Clinical Practice Guidelines for Quality Palliative Care, 4 th edition Lori Bishop, MHA, BSN, RN, CHPN, lbishop@nhpco.org Judi Lund Person, MPH, CHC, jlundperson@nhpco.org Gwynn Sullivan, MSN, gwynns@nationalcoalitionhpc.org
Clinical Practice Guidelines for Quality Palliative Care, 4 th edition Lori Bishop, MHA, BSN, RN, CHPN, lbishop@nhpco.org Judi Lund Person, MPH, CHC, jlundperson@nhpco.org Gwynn Sullivan, MSN, gwynns@nationalcoalitionhpc.org
NQF Serious Illness Initiative Quality Measurement Committee
 NQF Serious Illness Initiative Quality Measurement Committee Presentation for the C-TAC Summit October 3, 2018 This project is funded by the Gordon and Betty Moore Foundation. Background Serious Illness
NQF Serious Illness Initiative Quality Measurement Committee Presentation for the C-TAC Summit October 3, 2018 This project is funded by the Gordon and Betty Moore Foundation. Background Serious Illness
Center to Advance Palliative Care:
 Center to Advance Palliative Care: Transforming the Care of Serious Illness Diane E. Meier, MD 26 April 2018 Presentation to The Netherlands Palliative Care Quality Congress What is Palliative Care? A
Center to Advance Palliative Care: Transforming the Care of Serious Illness Diane E. Meier, MD 26 April 2018 Presentation to The Netherlands Palliative Care Quality Congress What is Palliative Care? A
Quality and Fiscal Metrics: What Proves Success?
 Quality and Fiscal Metrics: What Proves Success? 1 Quality and Fiscal Metrics: What Proves Success? Kathleen Kerr Kerr Healthcare Analytics Creating the Future of Palliative Care NHPCO Virtual Event February
Quality and Fiscal Metrics: What Proves Success? 1 Quality and Fiscal Metrics: What Proves Success? Kathleen Kerr Kerr Healthcare Analytics Creating the Future of Palliative Care NHPCO Virtual Event February
Cancer Policy Advocate Training (CPAT) June 25-26, 2015 Washington, DC Washington Court Hotel. Agenda
 Cancer Policy Advocate Training (CPAT) June 25-26, 2015 Washington, DC Washington Court Hotel Agenda Background Advances in cancer research have contributed to overall improvements in cancer survival rates,
Cancer Policy Advocate Training (CPAT) June 25-26, 2015 Washington, DC Washington Court Hotel Agenda Background Advances in cancer research have contributed to overall improvements in cancer survival rates,
TECHNICAL EXPERT PANEL COMPOSITION (MEMBERSHIP) LIST TEMPLATE
 TECHNICAL EPERT PANEL COMPOSITION (MEMBERSHIP) LIST TEMPLATE Project Title: Palliative Care Measures Project Dates: January 2019 August 2021 Project Overview: The Centers for Medicare & Medicaid Services
TECHNICAL EPERT PANEL COMPOSITION (MEMBERSHIP) LIST TEMPLATE Project Title: Palliative Care Measures Project Dates: January 2019 August 2021 Project Overview: The Centers for Medicare & Medicaid Services
Introduction and Purpose
 Proceedings Illinois Oral Health Summit September 11, 2001 Illinois Response to the Surgeon General s Report on Introduction and Purpose The landmark Illinois Oral Health Summit convened on September 11,
Proceedings Illinois Oral Health Summit September 11, 2001 Illinois Response to the Surgeon General s Report on Introduction and Purpose The landmark Illinois Oral Health Summit convened on September 11,
TECHNICAL EXPERT CLINICAL USER PATIENT PANEL/MEASURE SPECIFICATION PANEL (TECUPP/MSP) COMPOSITION (MEMBERSHIP) LIST
 TECHNICAL EXPERT CLINICAL USER PATIENT PANEL/MEASURE SPECIFICATION PANEL (TECUPP/MSP) COMPOSITION (MEMBERSHIP) LIST Project Title: Palliative Care Measures Project Meeting Dates: March 26, 2019, Virtual/Web
TECHNICAL EXPERT CLINICAL USER PATIENT PANEL/MEASURE SPECIFICATION PANEL (TECUPP/MSP) COMPOSITION (MEMBERSHIP) LIST Project Title: Palliative Care Measures Project Meeting Dates: March 26, 2019, Virtual/Web
SeniorMed Education Forum 2008 Piecing Together Today s Senior Healthcare Puzzle. May 1, Tampa Marriott Westshore
 SeniorMed Education Forum 2008 Piecing Together Today s Senior Healthcare Puzzle May 1, 2008 - Tampa Marriott Westshore SeniorMed Education Forum is a leading provider of pharmacy products and services
SeniorMed Education Forum 2008 Piecing Together Today s Senior Healthcare Puzzle May 1, 2008 - Tampa Marriott Westshore SeniorMed Education Forum is a leading provider of pharmacy products and services
RE: Draft CMS Quality Measure Development Plan: Supporting the Transition to the Merit-based Incentive Payment System and Alternative Payment Models
 March 1, 2016 Centers for Medicare & Medicaid Services Department of Health and Human Services P.O. Box 8016 Baltimore, MD 21244 Submitted electronically via MACRA-MDP@hsag.com. RE: Draft CMS Quality Measure
March 1, 2016 Centers for Medicare & Medicaid Services Department of Health and Human Services P.O. Box 8016 Baltimore, MD 21244 Submitted electronically via MACRA-MDP@hsag.com. RE: Draft CMS Quality Measure
Making your Measurement Matter: How Hospice and Palliative Care Answered the Call
 Making your Measurement Matter: How Hospice and Palliative Care Answered the Call Katherine Ast, MSW, LCSW Director, Quality and Research, AAHPM Marianne Matzo, PhD, APRN-CNP, FPCN, FAAN Director of Research,
Making your Measurement Matter: How Hospice and Palliative Care Answered the Call Katherine Ast, MSW, LCSW Director, Quality and Research, AAHPM Marianne Matzo, PhD, APRN-CNP, FPCN, FAAN Director of Research,
LeadingAge and Hospice Members: Partners in Providing Quality Care to Older Adults. January 2019
 LeadingAge and Hospice Members: Partners in Providing Quality Care to Older Adults January 2019 Hospice is a unique service delivery model providing holistic care to individuals at the end of their lives.
LeadingAge and Hospice Members: Partners in Providing Quality Care to Older Adults January 2019 Hospice is a unique service delivery model providing holistic care to individuals at the end of their lives.
2018 Via Hope Peer Services Implementation Learning Community Application Supplement
 2018 Via Hope Peer Services Implementation Learning Community Application Supplement About the Via Hope Recovery Institute The Via Hope Recovery Institute aims to promote mental health system transformation
2018 Via Hope Peer Services Implementation Learning Community Application Supplement About the Via Hope Recovery Institute The Via Hope Recovery Institute aims to promote mental health system transformation
PCPI Update Progress on Strategic Initiatives
 Convened by the American Medical Association The Physician Consortium for Performance Improvement PCPI Update Progress on Strategic Initiatives Kathleen Blake, MD, MPH Vice President, Performance Improvement
Convened by the American Medical Association The Physician Consortium for Performance Improvement PCPI Update Progress on Strategic Initiatives Kathleen Blake, MD, MPH Vice President, Performance Improvement
Submitted to the House Energy and Commerce Committee. Federal Efforts to Combat the Opioid Crisis
 STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
Insight. A message from the Director. In this issue
 Insight ACACIA s Mental Health Research Newsletter National Institute for Mental Health Research, Research School of Population Health In this issue A Message from the Director 1 Inaugural Forum for ACT
Insight ACACIA s Mental Health Research Newsletter National Institute for Mental Health Research, Research School of Population Health In this issue A Message from the Director 1 Inaugural Forum for ACT
OAMT ONCOLOGY ACCOUNT MANAGEMENT TRAINING. September 20 22, 2016 ARIA Resort & Casino, Las Vegas, NV. For the Life Sciences Industry
 OAMT ONCOLOGY ACCOUNT MANAGEMENT TRAINING For the Life Sciences Industry September 20 22, 2016 ARIA Resort & Casino, Las Vegas, NV Register at DecisionResourcesGroup.com/Events DEAR COLLEAGUE, Cancer affects
OAMT ONCOLOGY ACCOUNT MANAGEMENT TRAINING For the Life Sciences Industry September 20 22, 2016 ARIA Resort & Casino, Las Vegas, NV Register at DecisionResourcesGroup.com/Events DEAR COLLEAGUE, Cancer affects
Strategic Plan Executive Summary Society for Research on Nicotine and Tobacco
 Strategic Plan 2013 2017 Executive Summary Society for Research on Nicotine and Tobacco Prepared By: Corona Insights Corona Insights, 2012 CoronaInsights.com CONTENTS Introduction... 1 Background... 1
Strategic Plan 2013 2017 Executive Summary Society for Research on Nicotine and Tobacco Prepared By: Corona Insights Corona Insights, 2012 CoronaInsights.com CONTENTS Introduction... 1 Background... 1
The Quality and Value Proposition for Palliative Care in Home Care. Madeline Jacobs, MPA HCA Quality and Technology Symposium November 16, 2017
 The Quality and Value Proposition for Palliative Care in Home Care Madeline Jacobs, MPA HCA Quality and Technology Symposium November 16, 2017 Palliative Care Definition Palliative care is specialized
The Quality and Value Proposition for Palliative Care in Home Care Madeline Jacobs, MPA HCA Quality and Technology Symposium November 16, 2017 Palliative Care Definition Palliative care is specialized
The Neurocognitive and Psychosocial Impacts of Violence and Trauma: A Workshop July 31 August 1, 2017
 A WORKSHOP OF THE FORUM ON GLOBAL VIOLENCE PREVENTION: The Neurocognitive and Psychosocial Impacts of Violence and Trauma: A Workshop July 31 August 1, 2017 National Academies Building 2101 Constitution
A WORKSHOP OF THE FORUM ON GLOBAL VIOLENCE PREVENTION: The Neurocognitive and Psychosocial Impacts of Violence and Trauma: A Workshop July 31 August 1, 2017 National Academies Building 2101 Constitution
Symposium Program. #CLEARsymposium17. lean-healthcare-research-symposium/
 Symposium Program #CLEARsymposium17 www.clear.berkeley.edu/events/ lean-healthcare-research-symposium/ THANK YOU TO OUR SPONSORS WELCOME LETTER On behalf of the organizing committee we are delighted to
Symposium Program #CLEARsymposium17 www.clear.berkeley.edu/events/ lean-healthcare-research-symposium/ THANK YOU TO OUR SPONSORS WELCOME LETTER On behalf of the organizing committee we are delighted to
2018 Interprofessional Webinar Series in Palliative Care
 LIVE AND ON-DEMAND WEBINARS 2018 Interprofessional Webinar Series in Registration Now Open MJHSPalliativeInstitute.org/e-learning The MJHS Institute for Innovation in is pleased to offer our 2018 webinar
LIVE AND ON-DEMAND WEBINARS 2018 Interprofessional Webinar Series in Registration Now Open MJHSPalliativeInstitute.org/e-learning The MJHS Institute for Innovation in is pleased to offer our 2018 webinar
Strategies for Success: How to Achieve Palliative Care Certification
 Strategies for Success: How to Achieve Palliative Care Certification April 30, 2014 Michele M. Sacco, M.S. Executive Director Advanced Certification for Palliative Care Heather Miller, MSN, RN-BC, CPON
Strategies for Success: How to Achieve Palliative Care Certification April 30, 2014 Michele M. Sacco, M.S. Executive Director Advanced Certification for Palliative Care Heather Miller, MSN, RN-BC, CPON
Progress from the Patient-Centered Outcomes Research Institute (PCORI)
 Progress from the Patient-Centered Outcomes Research Institute (PCORI) Anne Beal, Chief Operating Officer of the Patient-Centered Outcomes Research Institute Sharon-Lise Normand, Vice Chair, Methodology
Progress from the Patient-Centered Outcomes Research Institute (PCORI) Anne Beal, Chief Operating Officer of the Patient-Centered Outcomes Research Institute Sharon-Lise Normand, Vice Chair, Methodology
Report by the Comptroller and. SesSIon January Improving Dementia Services in England an Interim Report
 Report by the Comptroller and Auditor General HC 82 SesSIon 2009 2010 14 January 2010 Improving Dementia Services in England an Interim Report 4 Summary Improving Dementia Services in England an Interim
Report by the Comptroller and Auditor General HC 82 SesSIon 2009 2010 14 January 2010 Improving Dementia Services in England an Interim Report 4 Summary Improving Dementia Services in England an Interim
GUIDE TO PROGRAM DESIGN
 GUIDE GUIDE Palliative Care in the Home A GUIDE TO PROGRAM DESIGN PALLIATIVE CARE IN THE HOME: A GUIDE TO PROGRAM DESIGN Table of Contents Section 1 Introduction A Letter from Diane E. Meier, MD B Key
GUIDE GUIDE Palliative Care in the Home A GUIDE TO PROGRAM DESIGN PALLIATIVE CARE IN THE HOME: A GUIDE TO PROGRAM DESIGN Table of Contents Section 1 Introduction A Letter from Diane E. Meier, MD B Key
NATIONAL QUALITY FORUM
 National Voluntary Consensus Standards for Patient Outcomes Summary of the Eye Care Technical Advisory Panel Conference Call March 25, 2010: 10:00-11:00PM Eastern Standard Time TAP members participating:
National Voluntary Consensus Standards for Patient Outcomes Summary of the Eye Care Technical Advisory Panel Conference Call March 25, 2010: 10:00-11:00PM Eastern Standard Time TAP members participating:
EHR Developer Code of Conduct Frequently Asked Questions
 EHR Developer Code of Conduct Frequently Asked Questions General What is the purpose of the EHR Developer Code of Conduct? EHR Association (the Association) members have a long tradition of working with
EHR Developer Code of Conduct Frequently Asked Questions General What is the purpose of the EHR Developer Code of Conduct? EHR Association (the Association) members have a long tradition of working with
Ministry of Health and Long-Term Care. Palliative Care. Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW
 Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
Chapter 1 Section 1.08 Ministry of Health and Long-Term Care Palliative Care Follow-Up on VFM Section 3.08, 2014 Annual Report RECOMMENDATION STATUS OVERVIEW # of Status of Actions Recommended Actions
October 4 6, 2017 The W Hotel, Chicago, IL
 October 4 6, 2017 The W Hotel, Chicago, IL Register for this and future events at https://drgconferences.com WELCOME Cancer affects us all. Some reading this have survived it. Many have watched loved ones
October 4 6, 2017 The W Hotel, Chicago, IL Register for this and future events at https://drgconferences.com WELCOME Cancer affects us all. Some reading this have survived it. Many have watched loved ones
A Decade of Data: Findings and Insights from the National Palliative Care Registry
 A Decade of Data: Findings and Insights from the National Palliative Care Registry Maggie Rogers, MPH Senior Research Manager, CAPC Rachael Heitner, MA, CHPCA Research Associate, CAPC July 19, 2018 at
A Decade of Data: Findings and Insights from the National Palliative Care Registry Maggie Rogers, MPH Senior Research Manager, CAPC Rachael Heitner, MA, CHPCA Research Associate, CAPC July 19, 2018 at
The Changing Landscape of Palliative Care
 The Changing Landscape of Palliative Care KAHPC 17th Annual Conference August 2015 Brian Jones Joe Rotella Elizabeth Wessels Turner West Kay Williams Why Home-based Palliative Care? Turner West, MPH, MTS
The Changing Landscape of Palliative Care KAHPC 17th Annual Conference August 2015 Brian Jones Joe Rotella Elizabeth Wessels Turner West Kay Williams Why Home-based Palliative Care? Turner West, MPH, MTS
AAHPM Member Guide Your guide to making the most of your membership in the only national medical specialty society for hospice and palliative medicine
 AAHPM Member Guide Your guide to making the most of your membership in the only national medical specialty society for hospice and palliative medicine NETWORK WITH YOUR PEERS Expanding your network with
AAHPM Member Guide Your guide to making the most of your membership in the only national medical specialty society for hospice and palliative medicine NETWORK WITH YOUR PEERS Expanding your network with
Georgia Aging and Disability Resource Connection (ADRC) Evaluation Report
 Georgia Aging and Disability Resource (ADRC) Evaluation Report Evaluation Report from Boston University March Prepared by: Bronwyn Keefe, MSW, MPH, PHD Associate Director, CADER Kathy Kuhn, MSW Director
Georgia Aging and Disability Resource (ADRC) Evaluation Report Evaluation Report from Boston University March Prepared by: Bronwyn Keefe, MSW, MPH, PHD Associate Director, CADER Kathy Kuhn, MSW Director
Introduction. Click here to access the following documents: 1. Application Supplement 2. Application Preview 3. Experiential Component
 Introduction The Via Hope Recovery Institute aims to promote mental health system transformation by helping organizations develop practices that support and expect recovery, and by promoting the voices
Introduction The Via Hope Recovery Institute aims to promote mental health system transformation by helping organizations develop practices that support and expect recovery, and by promoting the voices
IMPACT APA STRATEGIC PLAN
 IMPACT APA STRATEGIC PLAN I am very proud to be a psychologist. Most in psychology chose this field for the pursuit of knowledge and to make an impact, and I ve seen firsthand how psychology affects practically
IMPACT APA STRATEGIC PLAN I am very proud to be a psychologist. Most in psychology chose this field for the pursuit of knowledge and to make an impact, and I ve seen firsthand how psychology affects practically
Adding the Secret Sauce: Expanding the Role of Social Work in Hospice and Palliative Care Quality Initiatives
 Adding the Secret Sauce: Expanding the Role of Social Work in Hospice and Palliative Care Quality Initiatives Katherine Ast, MSW, LCSW Director, Quality and Research, AAHPM Joe Rotella, MD, MBA Chief Medical
Adding the Secret Sauce: Expanding the Role of Social Work in Hospice and Palliative Care Quality Initiatives Katherine Ast, MSW, LCSW Director, Quality and Research, AAHPM Joe Rotella, MD, MBA Chief Medical
Billing and Payment Models for Palliative Care
 Billing and Payment Models for Palliative Care Liz Fowler, MPH President and CEO Bluegrass Care Navigators October 15, 2017 Tom Gualtieri-Reed, MBA Partner, Spragens & Associates Consultant, Center to
Billing and Payment Models for Palliative Care Liz Fowler, MPH President and CEO Bluegrass Care Navigators October 15, 2017 Tom Gualtieri-Reed, MBA Partner, Spragens & Associates Consultant, Center to
CARE 4 Us: Promoting Improvements in Palliative Care in SE PA
 Compassion * Advocacy * Respect * Empowerment Building foundations for strong palliative care programs CARE 4 Us: Promoting Improvements in Palliative Care in SE PA Susan Choi, PhD, CPHQ March 19, 2014
Compassion * Advocacy * Respect * Empowerment Building foundations for strong palliative care programs CARE 4 Us: Promoting Improvements in Palliative Care in SE PA Susan Choi, PhD, CPHQ March 19, 2014
Population Health Management Accreditation Public Comment Overview
 For Public Comment March 5 April 3, 2018 Comments due 5:00 p.m. ET April 3, 2018 Population Health Management Accreditation Public Comment Overview PHM Accreditation 2018 Note: This publication is protected
For Public Comment March 5 April 3, 2018 Comments due 5:00 p.m. ET April 3, 2018 Population Health Management Accreditation Public Comment Overview PHM Accreditation 2018 Note: This publication is protected
Visit aahpm.org to learn more about these programs. We appreciate your continued support and look forward to serving you in the coming year.
 AAHPM Member Guide Your guide to making the most of your membership in the only national medical specialty society for hospice and palliative medicine. Thank you for your membership in AAHPM. This Member
AAHPM Member Guide Your guide to making the most of your membership in the only national medical specialty society for hospice and palliative medicine. Thank you for your membership in AAHPM. This Member
Washington State Collaborative Oral Health Improvement Plan
 Washington State Collaborative Oral Health Improvement Plan 2009-2014 Prioritization Criteria (non-financial): Strategic Area I: System Infrastructure (Partnerships, Funding, Technology) Goal 1: Mobilize
Washington State Collaborative Oral Health Improvement Plan 2009-2014 Prioritization Criteria (non-financial): Strategic Area I: System Infrastructure (Partnerships, Funding, Technology) Goal 1: Mobilize
c i r c l e o f l i f e a w a r d C I R C L E o f L I F E
 circle of life award 2017 The 2017 awards are supported, in part, by the California Health Care Foundation, based in Oakland, California, and Cambia Health Foundation, based in Portland, Oregon. Major
circle of life award 2017 The 2017 awards are supported, in part, by the California Health Care Foundation, based in Oakland, California, and Cambia Health Foundation, based in Portland, Oregon. Major
Please join us for Region VII Diabetes Summit. When Friday, November 18, :00 AM 4:00 PM
 Please join us for Region VII Diabetes Summit When Friday, November 18, 2016 8:00 AM 4:00 PM Location: John and Mary Pappajohn Education Center 1200 Grand Avenue, Des Moines, IA Purpose: The summit will
Please join us for Region VII Diabetes Summit When Friday, November 18, 2016 8:00 AM 4:00 PM Location: John and Mary Pappajohn Education Center 1200 Grand Avenue, Des Moines, IA Purpose: The summit will
The Researcher, Physician, Regulator, and Patient in an Age of Personalized Medicine
 Thursday, March 22, 2012 Breakfast 7:30 to 8:15 am Welcome and Introductions 8:15 to 8:30 am Session One 8:30 to 10:30 am NATIONAL COALITION FOR CANCER SURVIVORSHIP CANCER POLICY ROUNDTABLE March 22-23,
Thursday, March 22, 2012 Breakfast 7:30 to 8:15 am Welcome and Introductions 8:15 to 8:30 am Session One 8:30 to 10:30 am NATIONAL COALITION FOR CANCER SURVIVORSHIP CANCER POLICY ROUNDTABLE March 22-23,
Paul Glassman DDS, MA, MBA Professor and Director of Community Oral Health University of the Pacific School of Dentistry San Francisco, CA
 Paul Glassman DDS, MA, MBA Professor and Director of Community Oral Health University of the Pacific School of Dentistry San Francisco, CA 1 2 Purpose and Charge Develop a vision for the characteristics
Paul Glassman DDS, MA, MBA Professor and Director of Community Oral Health University of the Pacific School of Dentistry San Francisco, CA 1 2 Purpose and Charge Develop a vision for the characteristics
HEALTHSTREAM LIVING LABS IN ACTION
 HEALTHSTREAM LIVING LABS IN ACTION A CONVERSATION WITH: Mitchel T. Heflin MD, MHS Associate Professor of Medicine, Duke University School of Medicine Eleanor McConnell PhD, RN, GCNS-BC Associate Professor,
HEALTHSTREAM LIVING LABS IN ACTION A CONVERSATION WITH: Mitchel T. Heflin MD, MHS Associate Professor of Medicine, Duke University School of Medicine Eleanor McConnell PhD, RN, GCNS-BC Associate Professor,
PCC4U. Uptake of the PCC4U Resources. Funded by the Australian Government through the National Palliative Care Program
 Issue No. 19 July 2010 The Australian Government has committed to improving the quality of care provided to Australians at end of life, by supporting the inclusion of palliative care education as an integral
Issue No. 19 July 2010 The Australian Government has committed to improving the quality of care provided to Australians at end of life, by supporting the inclusion of palliative care education as an integral
March 31, Commissioner Barbara Leadholm Department of Mental Health 25 Staniford Street Boston, MA Dear Commissioner Leadholm:
 March 31, 2008 Commissioner Barbara Leadholm Department of Mental Health 25 Staniford Street Boston, MA 02114 Dear Commissioner Leadholm: The Massachusetts Transformation Committee (Transcom) and its Integrating
March 31, 2008 Commissioner Barbara Leadholm Department of Mental Health 25 Staniford Street Boston, MA 02114 Dear Commissioner Leadholm: The Massachusetts Transformation Committee (Transcom) and its Integrating
2018 Fall NAMD Meeting Washington Hilton 1919 Connecticut Avenue, NW Washington, DC November 12-14, 2018
 Preliminary DRAFT AGENDA 2018 Fall NAMD Meeting Washington Hilton 1919 Connecticut Avenue, NW Washington, DC 20009 November 12-14, 2018 Monday, November 12, 2018 State Only Day 8:00 AM - 5:00 PM Registration
Preliminary DRAFT AGENDA 2018 Fall NAMD Meeting Washington Hilton 1919 Connecticut Avenue, NW Washington, DC 20009 November 12-14, 2018 Monday, November 12, 2018 State Only Day 8:00 AM - 5:00 PM Registration
Essential Palliative Care Skills For Every Clinician
 Essential Palliative Care Skills For Every Clinician Tools for Assessment and Management of Serious Illness for Primary Care Providers Comprehensive Curriculum Self-Paced Fully Online 03012018 Online,
Essential Palliative Care Skills For Every Clinician Tools for Assessment and Management of Serious Illness for Primary Care Providers Comprehensive Curriculum Self-Paced Fully Online 03012018 Online,
Improving the Process
 University of Hawaii at Manoa John A. Burns School of Medicine Department of Geriatric Medicine Pacific Islands Geriatric Education Center Presents Improving the Process Intended Audience: physicians,
University of Hawaii at Manoa John A. Burns School of Medicine Department of Geriatric Medicine Pacific Islands Geriatric Education Center Presents Improving the Process Intended Audience: physicians,
Approved Care Model for Project 3gi: Integration of Palliative Care into the PCMH Model
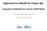 1 Approved Care Model for Project 3gi: Integration of Palliative Care into the PCMH Model OneCity Health Webinar January 13, 2016 Overview of presentation 2 Approach to care model development Project overview
1 Approved Care Model for Project 3gi: Integration of Palliative Care into the PCMH Model OneCity Health Webinar January 13, 2016 Overview of presentation 2 Approach to care model development Project overview
Advocacy Framework. St. Michael s Hospital Academic Family Health Team
 Advocacy Framework St. Michael s Hospital Academic Family Health Team Purpose To provide a framework by which the St. Michael s Hospital Academic Family Health Team (SMH AFHT) can expand its commitment
Advocacy Framework St. Michael s Hospital Academic Family Health Team Purpose To provide a framework by which the St. Michael s Hospital Academic Family Health Team (SMH AFHT) can expand its commitment
HealthCare Chaplaincy Network and The California State University Institute for Palliative Care and Palliative Care Chaplaincy Competencies
 HealthCare Chaplaincy Network and The California State University Institute for Palliative Care and Palliative Care Chaplaincy Competencies Competencies are the combination of knowledge, skills and attitudes
HealthCare Chaplaincy Network and The California State University Institute for Palliative Care and Palliative Care Chaplaincy Competencies Competencies are the combination of knowledge, skills and attitudes
Appendix 2 Good Relations Action Plan, Outcomes, Timescales
 Appendix 2 Appendix 2 Good Relations Action Plan, Outcomes, Timescales Theme 1 Increasing Visibility Develop a public statement on the Trust s commitment to challenging sectarianism and racism in all its
Appendix 2 Appendix 2 Good Relations Action Plan, Outcomes, Timescales Theme 1 Increasing Visibility Develop a public statement on the Trust s commitment to challenging sectarianism and racism in all its
SUNDAY, MARCH 24 TUESDAY, MARCH 26, 2019 THE MAYFLOWER HOTEL, WASHINGTON, DC 20 Y E A R S CELEBRATING 20 YEARS OF QUALITY
 SUNDAY, MARCH 24 TUESDAY, MARCH 26, 2019 THE MAYFLOWER HOTEL, WASHINGTON, DC 20 Y E A R S 1999-2019 CELEBRATING 20 YEARS OF QUALITY TOPICS AND THEMES FOR 2019 Behavioral Health and Improving Care for Serious
SUNDAY, MARCH 24 TUESDAY, MARCH 26, 2019 THE MAYFLOWER HOTEL, WASHINGTON, DC 20 Y E A R S 1999-2019 CELEBRATING 20 YEARS OF QUALITY TOPICS AND THEMES FOR 2019 Behavioral Health and Improving Care for Serious
Organ Donation and Transplantation Alliance impact report
 Organ Donation and Transplantation Alliance impact report Connecting OPOs, transplant centers and donor hospitals to education and best practice resources since 2006 Dear Organ Donation and Transplantation
Organ Donation and Transplantation Alliance impact report Connecting OPOs, transplant centers and donor hospitals to education and best practice resources since 2006 Dear Organ Donation and Transplantation
Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap
 Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap Avalere Health An Inovalon Company November 16, 2017 In Partnership with GSK Agenda 1 2 3 4 5 Welcome & Introductions Overview:
Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap Avalere Health An Inovalon Company November 16, 2017 In Partnership with GSK Agenda 1 2 3 4 5 Welcome & Introductions Overview:
Committee on Medication Assisted-Treatment for Opioid Use Disorder. October 29, Time Task/Objective Leader/Moderator
 Health and Medicine Division Board on Health Sciences Policy Committee on Medication Assisted-Treatment for Opioid Use Disorder October 29, 2018 Time Task/Objective Leader/Moderator OPEN SESSION 1:00pm
Health and Medicine Division Board on Health Sciences Policy Committee on Medication Assisted-Treatment for Opioid Use Disorder October 29, 2018 Time Task/Objective Leader/Moderator OPEN SESSION 1:00pm
Intensive Board Review Course. Faculty. August 9-11, 2018 Hyatt Regency Minneapolis Minneapolis, MN
 Intensive Board Review Course Faculty August 9-11, 2018 Hyatt Regency Minneapolis Minneapolis, MN Janet Bull, MD MBA FAAHPM Dr. Bull is the Chief Medical Officer at Four Seasons Compassion and holds a
Intensive Board Review Course Faculty August 9-11, 2018 Hyatt Regency Minneapolis Minneapolis, MN Janet Bull, MD MBA FAAHPM Dr. Bull is the Chief Medical Officer at Four Seasons Compassion and holds a
Coalition for Access and Opportunity Fast Track Medicaid for SNAP Participants. April 23, 2014
 Coalition for Access and Opportunity Fast Track Medicaid for SNAP Participants April 23, 2014 Center on Budget and Policy Priorities Our Plan For Today Description of the Option and why its important:
Coalition for Access and Opportunity Fast Track Medicaid for SNAP Participants April 23, 2014 Center on Budget and Policy Priorities Our Plan For Today Description of the Option and why its important:
Primary Palliative Care Skills
 Primary Palliative Care Skills Tools for Assessment and Management of Serious Illness for Primary Care Providers Comprehensive Curriculum Self-Paced Fully Online 03012018 Online, On-Demand Education for
Primary Palliative Care Skills Tools for Assessment and Management of Serious Illness for Primary Care Providers Comprehensive Curriculum Self-Paced Fully Online 03012018 Online, On-Demand Education for
The Way Ahead Our Three Year Strategic Plan EVERY MOMENT MATTERS
 The Way Ahead Our Three Year Strategic Plan 2017-2020 EVERY MOMENT MATTERS Every moment matters - that s what our logo says right next to our name John Taylor Hospice and for us the two are inseparable.
The Way Ahead Our Three Year Strategic Plan 2017-2020 EVERY MOMENT MATTERS Every moment matters - that s what our logo says right next to our name John Taylor Hospice and for us the two are inseparable.
RGP Operational Plan Approved by TC LHIN Updated Dec 22, 2017
 RGP Operational Plan 2017-2018 Approved by TC LHIN Updated Dec 22, 2017 1 Table of Contents Introduction... 1 Vision for the Future of Services for Frail Older Adults... 1 Transition Activities High Level
RGP Operational Plan 2017-2018 Approved by TC LHIN Updated Dec 22, 2017 1 Table of Contents Introduction... 1 Vision for the Future of Services for Frail Older Adults... 1 Transition Activities High Level
STATE ALZHEIMER S DISEASE PLANS: TRAINING
 STATE ALZHEIMER S DISEASE PLANS: TRAINING Recommendations to better equip health care professionals and others to deal with individuals with Alzheimer s Arkansas California Colorado Illinois Iowa Integrate
STATE ALZHEIMER S DISEASE PLANS: TRAINING Recommendations to better equip health care professionals and others to deal with individuals with Alzheimer s Arkansas California Colorado Illinois Iowa Integrate
Enhancing Quality of Life for Cancer Survivors in South Dakota. Outcomes from the South Dakota Cancer Survivorship Program
 Enhancing Quality of Life for Cancer Survivors in South Dakota Outcomes from the South Dakota Cancer Survivorship Program The South Dakota Survivorship Program was funded through cooperative agreement
Enhancing Quality of Life for Cancer Survivors in South Dakota Outcomes from the South Dakota Cancer Survivorship Program The South Dakota Survivorship Program was funded through cooperative agreement
MENTAL HEALTH AND WELLNESS OUTCOME OF THE TOWN HALL
 2017 2019 MENTAL HEALTH AND WELLNESS OUTCOME OF THE TOWN HALL INTRODUCTION The University of Guelph has committed to improving wellness of students, staff, and faculty on campus. In 2016, the University
2017 2019 MENTAL HEALTH AND WELLNESS OUTCOME OF THE TOWN HALL INTRODUCTION The University of Guelph has committed to improving wellness of students, staff, and faculty on campus. In 2016, the University
Physicians. Remote. Rural
 Physicians Remote Provincial Palliative and End-of-Life Care (PEOLC) Initiative: Collaborative model used to develop a resource guide for communities to enhance their palliative and end-of-life care: the
Physicians Remote Provincial Palliative and End-of-Life Care (PEOLC) Initiative: Collaborative model used to develop a resource guide for communities to enhance their palliative and end-of-life care: the
POLICY BRIEFING. Prime Minister s challenge on dementia 2020 implementation plan
 POLICY BRIEFING Prime Minister s challenge on dementia 2020 implementation plan Date: 14th March 2016 Author: Christine Heron LGiU associate Summary The Prime Minister s challenge on dementia contains
POLICY BRIEFING Prime Minister s challenge on dementia 2020 implementation plan Date: 14th March 2016 Author: Christine Heron LGiU associate Summary The Prime Minister s challenge on dementia contains
Palliative and End-of-Life Care
 Palliative and End-of-Life Care 2015-2016 TECHNICAL REPORT December 23, 2016 This report is funded by the Department of Health and Human Services under contract HHSM-500-2012-00009I Task Order HHSM-500-T0008
Palliative and End-of-Life Care 2015-2016 TECHNICAL REPORT December 23, 2016 This report is funded by the Department of Health and Human Services under contract HHSM-500-2012-00009I Task Order HHSM-500-T0008
ONCOLOGY MEDICAL HOME ACCREDITATION
 2015 Community Oncology Alliance 1 ONCOLOGY MEDICAL HOME ACCREDITATION Panel Moderator: Bo Gamble Director of Strategic Practice Initiatives, Community Oncology Alliance 1 ONCOLOGY MEDICAL HOME ACCREDITATION
2015 Community Oncology Alliance 1 ONCOLOGY MEDICAL HOME ACCREDITATION Panel Moderator: Bo Gamble Director of Strategic Practice Initiatives, Community Oncology Alliance 1 ONCOLOGY MEDICAL HOME ACCREDITATION
Port of Portland Hillsboro Airport Master Plan Update Planning Advisory Committee Charter
 Port of Portland Hillsboro Airport Master Plan Update Planning Advisory Committee Charter Charter Purpose The purpose of this charter is to define the role of the Planning Advisory Committee () within
Port of Portland Hillsboro Airport Master Plan Update Planning Advisory Committee Charter Charter Purpose The purpose of this charter is to define the role of the Planning Advisory Committee () within
Need to brush up on your hospice and palliative medicine knowledge?
 Need to brush up on your hospice and palliative medicine knowledge? LEARN FROM THE EXPERTS Enjoy the 2014 Intensive Board Review Course recordings (including synchronized PowerPoint presentations and MP3
Need to brush up on your hospice and palliative medicine knowledge? LEARN FROM THE EXPERTS Enjoy the 2014 Intensive Board Review Course recordings (including synchronized PowerPoint presentations and MP3
Become A Supporting Organization
 Become A Supporting Organization 2018 Otuska Pharmaceutical Development & Commercialization, Inc. May 2018 MRC2.CORP.X.02619 Contents 1.0 Table Of Contents 1.1-1.7 PsychU Overview 1.1-1.2 Overview 1.3
Become A Supporting Organization 2018 Otuska Pharmaceutical Development & Commercialization, Inc. May 2018 MRC2.CORP.X.02619 Contents 1.0 Table Of Contents 1.1-1.7 PsychU Overview 1.1-1.2 Overview 1.3
Spirituality in the Care Team:
 Spirituality in the Care Team: Fostering a Climate of Communication & A Dynamic of Caring Barbara Reville, DNP, CRNP, ACHPN Director, HUP Palliative Care Program 5 June 2013 1 To consider What is a palliative
Spirituality in the Care Team: Fostering a Climate of Communication & A Dynamic of Caring Barbara Reville, DNP, CRNP, ACHPN Director, HUP Palliative Care Program 5 June 2013 1 To consider What is a palliative
NP/PA Dementia Update
 FRIDAY, SEPTEMBER 23, 2011 Stoney Creek Inn, Rothschild, Wisconsin NP/PA Dementia Update JOINTLY SPONSORED BY: UNIVERSITY OF WISCONSIN SCHOOL OF MEDICINE AND PUBLIC HEALTH DEPARTMENT OF MEDICINE WISCONSIN
FRIDAY, SEPTEMBER 23, 2011 Stoney Creek Inn, Rothschild, Wisconsin NP/PA Dementia Update JOINTLY SPONSORED BY: UNIVERSITY OF WISCONSIN SCHOOL OF MEDICINE AND PUBLIC HEALTH DEPARTMENT OF MEDICINE WISCONSIN
Statewide Hospice & Palliative Care Summit
 Statewide Hospice & Palliative Care Summit The Future of End of Life Care Choice, Dignity and Compassion A Tribute to Florence Wald May 4, 2018 Hilton Garden Inn, Wallingford CT Western Connecticut Health
Statewide Hospice & Palliative Care Summit The Future of End of Life Care Choice, Dignity and Compassion A Tribute to Florence Wald May 4, 2018 Hilton Garden Inn, Wallingford CT Western Connecticut Health
2017 Executive Summary. The Conrad N. Hilton Foundation s Youth Substance Use Prevention and Early Intervention Strategic Initiative
 2017 Executive Summary The Conrad N. Hilton Foundation s Youth Substance Use Prevention and Early Intervention Strategic Initiative Executive Summary Youth substance use is a leading public health concern
2017 Executive Summary The Conrad N. Hilton Foundation s Youth Substance Use Prevention and Early Intervention Strategic Initiative Executive Summary Youth substance use is a leading public health concern
The NHS Cancer Plan: A Progress Report
 DEPARTMENT OF HEALTH The NHS Cancer Plan: A Progress Report LONDON: The Stationery Office 9.25 Ordered by the House of Commons to be printed on 7 March 2005 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL
DEPARTMENT OF HEALTH The NHS Cancer Plan: A Progress Report LONDON: The Stationery Office 9.25 Ordered by the House of Commons to be printed on 7 March 2005 REPORT BY THE COMPTROLLER AND AUDITOR GENERAL
Ruth McCorkle, PhD; Rebecca Kirch, JD; Kim Thiboldeaux; Julie Taylor; and Mark Gorman
 947 Journal of the National Comprehensive Cancer Network The Alliance for Quality Psychosocial Cancer Care: An Innovative Model for Disseminating and Improving Implementation of National Quality Care Recommendations
947 Journal of the National Comprehensive Cancer Network The Alliance for Quality Psychosocial Cancer Care: An Innovative Model for Disseminating and Improving Implementation of National Quality Care Recommendations
Strategic Plan
 2017-18 Strategic Plan 1 Strategic Planning Process The Summit County Opiate Task Force has made great strides in addressing the opiate crisis in the last few years. More than 100 Summit County citizens
2017-18 Strategic Plan 1 Strategic Planning Process The Summit County Opiate Task Force has made great strides in addressing the opiate crisis in the last few years. More than 100 Summit County citizens
Evidence as a Tactic to Advance Pediatric Palliative Care
 Evidence as a Tactic to Advance Pediatric Palliative Care Richard Goldstein, MD, Boston Children s Hospital-Harvard Medical School Maggie Rogers, MPH, Senior Research Associate, CAPC August 28, 2017 2017
Evidence as a Tactic to Advance Pediatric Palliative Care Richard Goldstein, MD, Boston Children s Hospital-Harvard Medical School Maggie Rogers, MPH, Senior Research Associate, CAPC August 28, 2017 2017
National Association of Catholic Chaplains Part Two, Section 600 Standards for Specialty Certification in Palliative Care and Hospice
 National Association of Catholic Chaplains Part Two, Section 600 Standards for Specialty Certification in Palliative Care and Hospice Those seeking NACC specialty certification in palliative care and hospice
National Association of Catholic Chaplains Part Two, Section 600 Standards for Specialty Certification in Palliative Care and Hospice Those seeking NACC specialty certification in palliative care and hospice
Palliative Care Quality Standard: Guiding Evidence-Based, High-Quality Palliative Care in Ontario Presented by: Lisa Ye, Lead, Quality Standards,
 Palliative Care Quality Standard: Guiding Evidence-Based, High-Quality Palliative Care in Ontario Presented by: Lisa Ye, Lead, Quality Standards, Health Quality Ontario Candace Tse, Specialist, Quality
Palliative Care Quality Standard: Guiding Evidence-Based, High-Quality Palliative Care in Ontario Presented by: Lisa Ye, Lead, Quality Standards, Health Quality Ontario Candace Tse, Specialist, Quality
The Honorable Tom Price, MD Secretary of the U.S. Department of Health and Human Services 200 Independence Avenue, SW Washington, DC 20201
 February 21, 2017 The Honorable Tom Price, MD Secretary of the U.S. Department of Health and Human Services 200 Independence Avenue, SW Washington, DC 20201 The Honorable David Shulkin, MD Secretary of
February 21, 2017 The Honorable Tom Price, MD Secretary of the U.S. Department of Health and Human Services 200 Independence Avenue, SW Washington, DC 20201 The Honorable David Shulkin, MD Secretary of
Over 425 Members Strong
 Quality Measurement 101: The Basics Camille Smith, MSW, MSPH Director, Member Education Karen Johnson, MS Senior Director, Quality Measurement October 8, 2015 2:00pm-3:00pm ET Over 425 Members Strong 2
Quality Measurement 101: The Basics Camille Smith, MSW, MSPH Director, Member Education Karen Johnson, MS Senior Director, Quality Measurement October 8, 2015 2:00pm-3:00pm ET Over 425 Members Strong 2
Section #3: Process of Change
 Section #3: Process of Change This module will: Describe a model of change that supported the development and implementation of a palliative care program in long term care. Describe strategies that assisted
Section #3: Process of Change This module will: Describe a model of change that supported the development and implementation of a palliative care program in long term care. Describe strategies that assisted
STRATEGIC DIRECTIONS AND FUTURE ACTIONS: Healthy Aging and Continuing Care in Alberta
 STRATEGIC DIRECTIONS AND FUTURE ACTIONS: Healthy Aging and Continuing Care in Alberta APRIL 2000 For additional copies of this document, or for further information, contact: Communications Branch Alberta
STRATEGIC DIRECTIONS AND FUTURE ACTIONS: Healthy Aging and Continuing Care in Alberta APRIL 2000 For additional copies of this document, or for further information, contact: Communications Branch Alberta
FACULTY OF REHABILITATION MEDICINE STATEMENT OF STRATEGIC INTENT
 FACULTY OF REHABILITATION MEDICINE STATEMENT OF STRATEGIC INTENT Tempo Strategies PO Box 4187 Manuka ACT 2603 (02) 6239 5766 MAY 2010 TABLE OF CONTENTS BACKGROUND AND PURPOSE 3 1. THE CURRENT POSITION
FACULTY OF REHABILITATION MEDICINE STATEMENT OF STRATEGIC INTENT Tempo Strategies PO Box 4187 Manuka ACT 2603 (02) 6239 5766 MAY 2010 TABLE OF CONTENTS BACKGROUND AND PURPOSE 3 1. THE CURRENT POSITION
SES Indicator. The. Issue No. 1, Spring In This Issue. A Publication of APA s Office on Socioeconomic Status. News CSES.
 A Publication of APA s Office on Socioeconomic Status The SES Indicator Newsletter Issue No. 1, Spring 2008 In This Issue - Welcome from the Director of APA s Office on SES News OSES Builds Communication
A Publication of APA s Office on Socioeconomic Status The SES Indicator Newsletter Issue No. 1, Spring 2008 In This Issue - Welcome from the Director of APA s Office on SES News OSES Builds Communication
Appendix 1. Cognitive Impairment and Dementia Service Elm Lodge 4a Marley Close Greenford Middlesex UB6 9UG
 Appendix 1 Mr Dwight McKenzie Scrutiny Review Officer Legal and Democratic Services Ealing Council Perceval House 14 16 Uxbridge Road Ealing London W5 2HL Cognitive Impairment and Dementia Service Elm
Appendix 1 Mr Dwight McKenzie Scrutiny Review Officer Legal and Democratic Services Ealing Council Perceval House 14 16 Uxbridge Road Ealing London W5 2HL Cognitive Impairment and Dementia Service Elm
Welcome to the Michigan Cancer Consortium (MCC) Marketing Toolkit An Easy to Use Resource to Promote the MCC.
 Phone: 877-588-6224 www.michigancancer.org Board of Directors: Anas Al-Janadi, MD Michigan State University Breslin Cancer Center Terrance Albrecht, PhD Barbara Ann Karmanos Cancer Institute/Wayne State
Phone: 877-588-6224 www.michigancancer.org Board of Directors: Anas Al-Janadi, MD Michigan State University Breslin Cancer Center Terrance Albrecht, PhD Barbara Ann Karmanos Cancer Institute/Wayne State
4/3/2018. Ed Ratner has nothing to disclose Julie Benson has nothing to disclose
 Ed Ratner, MD Associate Director, Education, Geriatrics Center, Minneapolis VAMC Julie Benson, MD Immediate Past President, MNHPC Member, Palliative Care Advisory Group Review the MN Commission on the
Ed Ratner, MD Associate Director, Education, Geriatrics Center, Minneapolis VAMC Julie Benson, MD Immediate Past President, MNHPC Member, Palliative Care Advisory Group Review the MN Commission on the
PARTNERS FOR A HUNGER-FREE OREGON STRATEGIC PLAN Learn. Connect. Advocate. Partners for a Hunger-Free Oregon. Ending hunger before it begins.
 Learn. Connect. Advocate. PARTNERS FOR A HUNGER-FREE OREGON STRATEGIC PLAN 2016-18 Partners for a Hunger-Free Oregon Ending hunger before it begins. Dear Partners, This has been a year of celebration,
Learn. Connect. Advocate. PARTNERS FOR A HUNGER-FREE OREGON STRATEGIC PLAN 2016-18 Partners for a Hunger-Free Oregon Ending hunger before it begins. Dear Partners, This has been a year of celebration,
Minnesota Cancer Alliance SUMMARY OF MEMBER INTERVIEWS REGARDING EVALUATION
 Minnesota Cancer Alliance SUMMARY OF MEMBER INTERVIEWS REGARDING EVALUATION Minnesota Cancer Alliance Comprehensive Cancer Control Program P.O. Box 64882 St. Paul, MN 55164 651-201-3661 lisa.gemlo@state.mn.us
Minnesota Cancer Alliance SUMMARY OF MEMBER INTERVIEWS REGARDING EVALUATION Minnesota Cancer Alliance Comprehensive Cancer Control Program P.O. Box 64882 St. Paul, MN 55164 651-201-3661 lisa.gemlo@state.mn.us
Competencies for Advanced Certification for Hospice Palliative Care
 Competencies for Advanced Certification for Hospice Palliative Care Part of the NACC Standards Re-Approved 2015-2021 United States Conference of Catholic Bishops Subcommittee on Certification for Ecclesial
Competencies for Advanced Certification for Hospice Palliative Care Part of the NACC Standards Re-Approved 2015-2021 United States Conference of Catholic Bishops Subcommittee on Certification for Ecclesial
Patient-Centered Measurement: Innovation Challenge Series
 Patient-Centered Measurement: Innovation Challenge Series Learning Collaborative 2018 Webinar Thursday, March 1, 2018 1 Hala Durrah, MTA Patient Family Engagement Consultant, Speaker & Advocate 3 2017-18
Patient-Centered Measurement: Innovation Challenge Series Learning Collaborative 2018 Webinar Thursday, March 1, 2018 1 Hala Durrah, MTA Patient Family Engagement Consultant, Speaker & Advocate 3 2017-18
QUESTIONS & ANSWERS: PRACTISING DENTAL HYGIENISTS and STUDENTS
 ENTRY-TO-PRACTICE COMPETENCIES AND STANDARDS FOR CANADIAN DENTAL HYGIENISTS QUESTIONS & ANSWERS: PRACTISING DENTAL HYGIENISTS and STUDENTS Canadian Dental Hygienists Association The ETPCS: Q&A attempts
ENTRY-TO-PRACTICE COMPETENCIES AND STANDARDS FOR CANADIAN DENTAL HYGIENISTS QUESTIONS & ANSWERS: PRACTISING DENTAL HYGIENISTS and STUDENTS Canadian Dental Hygienists Association The ETPCS: Q&A attempts
