Vitamin D Supplementation in Allo-HSCT Patients
|
|
|
- Arabella Banks
- 5 years ago
- Views:
Transcription
1 University of Nebraska Medical Center Theses & Dissertations Graduate Studies Spring Vitamin D Supplementation in Allo-HSCT Patients Bailey Nelson University of Nebraska Medical Center Follow this and additional works at: Part of the Dietetics and Clinical Nutrition Commons, Medical Nutrition Commons, and the Oncology Commons Recommended Citation Nelson, Bailey, "Vitamin D Supplementation in Allo-HSCT Patients" (2017). Theses & Dissertations This Thesis is brought to you for free and open access by the Graduate Studies at DigitalCommons@UNMC. It has been accepted for inclusion in Theses & Dissertations by an authorized administrator of DigitalCommons@UNMC. For more information, please contact digitalcommons@unmc.edu.
2 Vitamin D Supplementation in Allo-HSCT Patients By Bailey Nelson RD, LMNT A THESIS Presented to the Faculty of The Graduate College of the University of Nebraska Medical Center In Partial Fulfillment of Requirements for the Degree of Master of Science in Medical Nutrition Medical Sciences Interdepartmental Area Graduate Program Medical Nutrition Under the Supervision of Dr. Corrine Hanson University of Nebraska Medical Center Omaha, NE April 2017 Advisory Committee: Ann Anderson-Berry, Nicole Spurgeon, Glenda Woscyna
3 ii DEDICATION I dedicate my thesis work to my parents Kim and Brad, my sister Alex and brother-in-law Matt, and my fiancé Sam. Thank you for the laughter, support, and truly knowing what this means to me.
4 iii ACKNOWLEDGEMENTS Thank you to my committee members, Corri, Nikki, Ann, and Glenda. Your patience, guidance, expertise, and valuable time was an integral part in helping me achieve my goal.
5 iv Vitamin D Supplementation in Allo-HSCT Patients By Bailey Nelson RD, LMNT University of Nebraska Medical Center, 2017 ABSTRACT BACKGROUND: Bone health is a serious concern for long-term survivors of Allo-HSCT due to multiple risk factors including steroids, chemotherapy, immunosuppressive drugs, and poor nutrition status 1. Steroids have been long proven to have negative impact on bone health and the National Osteoporosis Foundation (NOF) lists steroids as a contributing factor to osteoporosis and fractures. NOF guidelines recommend providing adequate daily vitamin D as a safe and inexpensive way to help reduce fracture risk 1. Therefore, proper supplementation of vitamin D may increase the quality of life for patients post Allo-HSCT. PURPOSE: The purpose of this study is to determine if Allo-HSCT patients who receive steroids as part of their treatment at Nebraska Medicine are being supplemented with vitamin D. METHODS: A retrospective review of electronic medical records was used to determine if vitamin D supplementation was prescribed to patients who received steroids after undergoing Allo-HSCT and whether this had an impact on their bone health, including serum 25(OH)D levels, incidence of fractures/falls, DEXA scan results, and GVHD
6 v diagnosis. Inclusion criteria included adults who received Allo-HSCT from January 1, 2013 to December 31, RESULTS: Out of 99 patients who underwent Allo-HSCT, 59 percent were prescribed steroids of > 5 mg/day of prednisone or equivalent for > 3 months, compared to 41 percent who were not. Vitamin D supplementation was significantly different between the two groups with 71 percent of the steroid group receiving vitamin D supplementation compared to 40 percent of the non-steroid group (p=0.004). Diagnosis of GVHD was also found to be statistically significant between groups with 90 percent of the steroid group compared to 71 percent of the non-steroid group (p=0.016). Mortality was found to be significantly higher in the non-steroid group compared to the steroid group (p=0.005). CONCLUSION: This study found 71 percent of patients who received steroids of > 5 mg/day of prednisone or equivalent for > 3 months, received vitamin D supplementation. However, adequacy of vitamin D supplementation is still uncertain in this patient population.
7 vi TABLE OF CONTENTS DEDICATION ii ACKKNOWLEDGEMENTS..iii ABSTRACT iv TABLE OF CONTENTS..vi LIST OF FIGURES/TABLES vii LIST OF ABBREVIATIONS viii CHAPTER1: INTRODUCTION 1 CHAPTER 2: LITERATURE REVIEW.. 2 CHAPTER 3: METHODS.11 CHAPTER 4: RESULTS.16 CHAPTER 5: DISCUSSION...20 CHAPTER 6: CONCLUSION BIBILIOGRAPHY....27
8 vii LIST OF FIGURES/TABLES Figure 1: Pathophysiologic pathways from vitamin D deficiency to osteoporosis, osteomalacia, falls and fractures 3 Figure 2: Pathophysiology of corticosteroid-induced osteoporosis 8 Table 1: Steroid Groups.. 16 Table 2: Continuous Variables Comparing Steroid Groups..17 Table 3: Categorical Variables Comparing Steroid Groups.17 Table 4: Results of the Logistic Regression Model 18 Table 5: Serum 25(OH)D in Supplemented vs. Not Supplemented Patients.19 Table 6: Re-Categorized Steroid Groups.19
9 viii LIST OF ABBREVIATIONS ACR: American College of Rheumatology Allo-HSCT: Allogenic Hematopoietic Stem Cell Transplant BMD: Bone mineral density cgvhd: Chronic graft-versus-host-disease DEXA: Dual-energy X-ray absorptiometry GVHD: Graft-versus-host-disease HR: Hazard ratio LASA: Longitudinal Aging Study Amsterdam NOF: National Osteoporosis Foundation OR: Odds ratio PTH: Parathyroid hormone RR: Risk ratio Serum 25(OH)D: Serum 25-hydroxyvitamin D VDD: Vitamin D deficiency
10 1 CHAPTER 1: INTRODUCTION Allogeneic hematopoietic stem-cell transplantation (Allo-HSCT) is a proven treatment for those suffering from malignant hematologic diseases of the blood or bone marrow such as acute myeloid leukemia or myelodysplastic syndrome. Allo-HSCT involves the transfer of stem cells from the donor to recipient, after their immune systems have been wiped out by chemotherapy, radiation, or a combination of both. The most significant risk of undergoing Allo-HSCT is the development of graft-versushost disease (GVHD). Studies have been conducted to evaluate supplementation of vitamin D and improved survival rate of certain cancers and decreased risk of developing GVHD 2,3. However, there are few studies which evaluate supplementation of vitamin D related to the use of steroids during Allo-HSCT. Steroids are proven to have negative effects on the metabolism vitamin D, including inhibition of osteoblast function, enhancement of bone resorption, inhibition of gastrointestinal calcium absorption, and increase in urine calcium loss. To treat vitamin D deficiency, NOF recommends adults be treated with 50,000 IU of vitamin D once a week or the equivalent daily dose (7,000 IU vitamin D2 or vitamin D3 daily) for 8-12 weeks to achieve normal (> 30 ng/ml) serum 25(OH)D concentrations 1. Overall, the nutrition status of patients who undergo Allo-HSCT is extremely complex and unstable. For those patients who are treated with steroids, it is important to prevent further deterioration of their health and functional status by adequately supplementing vitamin D to ensure adequate 25(OH)D levels.
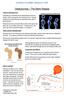
11 2 CHAPTER 2: LITERATURE REVIEW Vitamin D Vitamin D is often categorized as a fat-soluble vitamin; however, it is not an essential dietary factor as humans can produce it endogenously 4. More accurately, vitamin D is closely related to a steroid hormone due to its molecular structure. Vitamin D consists of two bioequivalent forms (ergocalciferol and cholecalciferol) both of which are biologically inert until metabolized in the body 5. Ergocalciferol (vitamin D2) is obtained from dietary vegetable sources and oral supplements. Cholecalciferol (vitamin D3) is obtained in fortified foods and oral supplements, but primarily through skin exposure to ultraviolet B radiation in sunlight 5. The skin produces vitamin D3 photochemically from 7-dehydrocholesterol, which is then metabolized in the liver to produce 25-hydroxycholecalciferol (25[OH]D). Within the kidneys, 25(OH)D serves as a substrate for 1-alpha-hydroxylase to make 1,25-dihydroxycholecalciferaol (1,25[OH]2D), the biologically active form 4. The biologically active form then has a significant role in bone health. 1,25(OH)2D stimulates the absorption of calcium and phosphate from the gut by opening calcium channels and stimulating the formation of calcium binding proteins 6. If 1,25(OH)2D concentrations drop due to deficiencies, less calcium is available for bone mineralization. Parathyroid hormone (PTH) will then increase, stimulating the hydroxylation of 25(OH)D in the kidney to produce more 1,25(OH)2D. This increase in PTH stimulates bone turnover and loss 6. Therefore, vitamin D deficiency is known to cause high bone turnover leading to osteoporosis, osteomalacia, falls and fractures. (Figure 1)
12 3 Figure 1: Pathophysiologic pathways from vitamin D deficiency to osteoporosis, osteomalacia, falls and fractures. 6 In the Longitudinal Aging Study Amsterdam (LASA) study which looked at serum 25(OH)D influences on serum PTH and parameters of bone health, serum osteocalcin (maker for bone formation) and urinary deoxypyridinolin excretion (marker of bone resorption), were shown to be elevated when serum 25(OHD) was low. Both markers were shown to decrease with a rise in serum 25(OH)D levels up to 40 nmol/l (16.03 ng/dl) 7. A placebo-controlled trial of 330 older women found a serum 25(OH)D level of 10 nmol/l (4 ng/ml) resulted in a risk ratio (RR) of hip fracture of In a global study of 7,441 postmenopausal women with osteoporosis there was a significant positive relationship between serum 25(OH)D and bone mineral density (BMD) in the trochanteric area of the hip, threshold below 50 nmol/l 9.
13 4 High bone turnover can then lead to increased risk of falls and fractures. Epidemiological studies show a relationship between vitamin D deficiency and fractures. In the LASA study incidence of fractures was higher when serum 25(OH)D was lower than 30 nmol/l (12.01 ng/ml), and the lowest percentage of fractures was found with serum 25(OH)D above 75 nmol/l (30 ng/ml) 10. In the Women s Health Initiative study, all women were treated with 1500mg/day of calcium citrate and 1000 IU/day of vitamin D3 for 6 weeks 11. The purpose of this study was to examine the effect of short term calcium and vitamin D supplementation on biochemical markers of bone turnover. Their analysis showed a significant decrease of hip fracture incidence and hip bone density was found to be 1.06 percent higher in the calcium plus vitamin D group than in the placebo (p<0.01) 11. Assessing Vitamin D To determine vitamin D levels within the body, serum 25(OH)D concentrations are assessed as the active form of vitamin D is physiologically regulated. 25(OH)D is the key substrate for 1-alpha-hydroxylase to produce 1,25(OH)2D. Therefore, production of 1,25(OH)2D is directly dependent on the absolute concentrations of 25(OH)D. Currently there is debate among research regarding adequate levels of serum 25(OH)D levels. According to the Institute of Medicine, serum 25(OH)D levels of 20 ng/ml is considered adequate for most individuals 9. However, the Endocrine Society, International Osteoporosis Foundation, American Geriatric Society, and NOF suggest a minimum level of 30 ng/ml 1, The debate regarding adequate serum 25(OH)D concentrations is
14 5 based on adequate suppression of PTH concentrations to ensure intestinal absorption of calcium does not lead to a decrease in serum calcium. In a prospective study of serum 25(OH)D level it was found baseline 25(OH)D levels were inversely associated with allcause mortality risk (adjusted hazard ratio [HR] = 0.95, 95% CI= , per 10 nmol/l [4 ng/ml] of 25[0H]D) 16. Vitamin D Supplementation Vitamin D supplementation comes in two forms, ergocalciferol (vitamin D2) and cholecalciferol (Vitamin D3). Vitamin D3 is the most efficient form of supplementation as it has greater affinity for the vitamin D-binding protein and has a longer half-life (~3 weeks) compared to that of vitamin D2, therefore less frequent dosing may be required 18. In a meta-analysis of seven randomized control trials evaluating serum 25(OH)D concentrations after supplementation with vitamin D3 versus vitamin D2, vitamin D3 was shown to increase serum 25(OH)D levels more efficiently (p=0.001) 19. However, at this time the NOF recommends either form of supplementation to reach adequate serum 25(OH)D levels. The NOF recommends vitamin D intake for adults age 50 and older of IU per day, including supplementation if necessary 1. If a patient is diagnosed with vitamin D deficiency (VDD) the NOF recommends adults be treated with 50,000 IU of vitamin D once a week or the equivalent daily dose (7,000 IU vitamin D2 or vitamin D3 daily) for 8-12 weeks to achieve serum 25(OH)D level of 30 ng/ml 1. After this level is reached NOF recommends maintenance therapy to preserve those concentrations 1. However, determining adequate dosing should be individualized based on a multitude of factors such as baseline serum 25(OH)D, absorptive capacity,
15 6 and ability of liver to convert metabolites 20. Therefore, Allo-HSCT patients likely require higher dosages due to their multiple risk factors and complex health status. Regardless of specific units of vitamin D supplementation, NOF and ACR guidelines, recommend supplementing enough vitamin D to maintain adequate serum 25(OH)D levels, whatever amount that may be 1,17. Although severe vitamin D deficiencies are uncommon, the NHANES study reported subclinical vitamin D deficiencies (defined as < 20 ng/ml) in 41.6% of their adult participants 21. For generalized healthy adults, VDD may not have any severe signs and symptoms, but for those who are undergoing treatment for cancer, VDD may have more of an effect on their overall outcomes. Vitamin D and Cancer Research regarding vitamin D status and cancer has become of more interest in recent years, with the potential role of vitamin D as an easily modifiable mediator of a broad array of pathologic conditions, including cancer 22. In a prospective study which looked at vitamin D status and cancer incidence in men, an increment of 25nmol/L (10 ng/ml) in predicted 25(OH)D level was associated with a 17% reduction in total cancer incident (RR=0.83, 95% CI ), a 29% reduction in total cancer mortality (RR=0.71, 95% CI ), and a 45% reduction in digestive-system cancer mortality (RR=0.55, 95% CI ) 23. Another study looked at association between total average annual sunlight and age-adjust breast cancer mortality rates in 87 regions of the U.S. Risk of fatal breast cancer in the major urban areas of the U.S. was inversely proportional to intensity of local sunlight (r=0.82, p=0.0001) 24. In addition, a study which looked to determine how many types of cancer are affected by solar radiation found the annual
16 7 number of premature deaths ( ) from cancer due to lower UV-B exposures was 21,7000 (95% CI 20,400-23,400) for white Americans, 1400 (95% CI ) for black Americans and 500 (95% CI, ) for Asian Americans and other mortalities 25. Vitamin D and GVHD Significant research has also been completed looking at vitamin D supplementation and its effect on GHVD, as GVHD is considered one of the most significant complications of Allo-HSCT with detrimental impact on transplant related mortality, overall survival, and patient quality of life 25. According to research, Grade II-IV acute GVHD in patients range from 20-50% and chronic GVHD from 40-50% after Allo- HSCT 26,27. In a retrospective cohort analysis, fifty-three patients serum 25(OH)D levels were looked at prior to Allo-HSCT to determine correlation with risk of GVHD 27. They found the cumulative incidence of chronic GVHD at 2 years in patients with serum 25(OH)D levels <25 ng/ml was 63.8% compared to 23.8% in patients with levels >25 ng/ml (p=0.009) 27. Additionally, in another retrospective analysis of 166 patients which evaluated 25(OH)D levels before allo-hsct found through multivariate analysis, vitamin D level before transplant to be a significant independent risk factor for development of chronic GVHD (cgvhd) (p=0.04) 28. The RR of cgvhd at two years after transplant was measure at 2.66 (95% CI ) for 25(OH)D below 60 nmol/l compared with above 60 nmol/l (24 ng/ml) before transplant 28. Steroids and Allo-HSCT Steroids, specifically glucocorticoids are often prescribed to patients undergoing Allo-HSCT as they have an inhibitory effect on specific immune responses as well as
17 8 suppressive effects which allow for management of inflammation or autoimmune disorders 29. While they have many benefits for those undergoing Allo-HSCT, they have been proven to negatively impact bone health, causing decreased bone formation and bone loss, reduce bone quality, and disrupt microarchitectural integrity 1. (Figure 2) Figure 2. Pathophysiology of corticosteroid-induced osteoporosis 31. Glucocorticoid-induced osteoporosis is the most common form of secondary osteoporosis, and needs to be considered in patients who receive Allo-HSCT due to their fragile and complex health status 30. Bone density declines rapidly at the beginning stages of using steroids and then more slowly and steadily as steroid use continues 30. Therefore, appropriate supplementation at the beginning of steroid use is critical. The NOF lists glucocorticoids use of > 5 mg/d of prednisone or equivalent for > 3 months as a risk factor for developing osteoporosis and fractures, as well as the point to which supplementation of vitamin D should be initiated 1. The American College of
18 9 Rheumatology (ACR) recommends stricter guidelines, recommending patients taking glucocorticoids at any dose or duration should receive vitamin D supplementation 17. In this patient population in which steroids are often a standard form of treatment, it would be important to take swift action in providing proper supplementation early on in Allo-HSCT treatment. A prospective study of 146 patients who received Allo-HSCT found that at two months after transplant, more than 50% of the patients had DEXA detected osteoporosis, showing that subclinical bone abnormalities appear early post-hsct 32. The same study found that duration of steroid use was a significant risk factor for developing clinical bone complications as well (Hazards Ration [HR]: 1.06/month; 95% CI ; p=0.038) 32. Bone Mineral Density Assessment To better assess patient s bone mineral density and risk of fracture, dual energy x-ray absorptiometry (DEXA) is considered the gold standard when determining bone mineral density of the lumbar spine and hip. DEXA measurements of the hip and spine is most often used to confirm a diagnosis of osteoporosis or predict future fracture risk 1. Peak bone mass is achieved in early adulthood, followed by a declined which is accelerated in women at menopause 1. NOF recommends BMD testing be performed in women age 65 and older and men age 70 and older. NOF continues to recommend BMD testing by DEXA scan in post-menopausal women and men > 50 years of age if prescribed short or long term glucocorticoid treatment 1. Although there is no consensus for optimal frequency of monitoring BMD, NOF guidelines suggest one to two year BMD testing after initiating medical therapy for treatment of osteoporosis and
19 10 every two years thereafter 1. A study in 2001 assessed bone mineral density of 67 adult patients who received stem cell transplants. Of those patients 49% were found to have osteopenia and osteoporosis prior to transplant. There was also significant decrease in T-score when comparing bone mineral density before transplant and at six months post- HSCT ( compared to ) (p<0.001) 3. This study proposed the demand for vitamin D is increased after Allo-HSCT, likely due to the multiple risk factors this patient population carries, and supplementation of both calcium and vitamin D not being prescribed outpatient 3. As a result, this study encourages measurement of BMD prior to transplant for baseline measurements.
20 11 CHAPTER 3: METHODS Participants and Study Design This study was a retrospective chart review of data collect from the electronic medical record. Inclusion criteria included age of 19 years or older and receiving an Allo- HSCT at Nebraska Medicine from January 1, 2013 to December 31, Exclusion criteria included children (less than 19 years of age) and those who received Auto-HSCT. The Study protocol was approved by the Institutional Review Board at the University of Nebraska Medical Center in Omaha, Nebraska. Ninety-nine patients were eligible for this study. Data Collection Patients were identified with help of the Oncology/Hematology Transplant Data Office at the University of Nebraska Medical Center. All data was collected between two time points. The first time point, time of transplant, was defined as the day the patient underwent Allo-HSCT (this included up to 30 days prior to transplant if labs or information was gathered prior to the exact date of transplant). The second time point was at the one year follow up appointment after receiving their transplant (this included up to 15 months after their transplant as scheduling conflicts could have impacted their one year follow-up). Baseline characteristics were gathered at time of transplant and included age, sex, and race. Additional data was gathered between the time of transplant and one year follow-up, this included: steroids prescribed, vitamin D supplementation, serum 25(OH)D levels, documented falls/fractures, DEXA results, LOS, and, mortality.
21 12 Steroids Prescribed steroids were gathered by review of the medications tab and a keyword search of the term steroid within the medical record. The first classification of steroid use was based on the NOF criterial for vitamin D supplementation which specifies > 5 mg of prednisone or equivalent for >3 months for inclusion in the steroid group. Patients did not have to be prescribed steroids consecutively to meet requirements for duration of > 3 months. For example, if the patient was prescribed > 5 mg for six non-consecutive two week periods, they met criteria to be included in the steroid group. All patients not meeting this criteria were placed in the non-steroid groups. Therefore, if a patient received high dose steroids for one month they did not meet criteria and were placed in the non-steroid group. Steroid groups were later re-categorized based on ACR recommendations for when vitamin D supplementation should be started. The steroid group was re-defined as those who received any dose/duration of steroid during the first year following transplant. Therefore, the patient who received high dose steroids for one month would be included in the steroid group. The non-steroid group consisted of those who never received any steroid between time of transplant and one year follow-up. Vitamin D Supplementation The primary outcome of the study was vitamin D supplementation. Supplementation was found via the medications tab along with keyword search for vitamin D in the medical chart. Use of a multivitamin was not considered as supplemental vitamin D. Vitamin D supplementation was categorized into yes/no
22 13 groups. Any dose or duration of vitamin D supplementation was placed in the yes group. The no group consisted of those who did not receive any vitamin D supplementation during time of transplant and one year follow-up. Serum 25(OH)D Serum 25(OH)D levels were collected from the results review tab within the medical record, which is the location of all laboratory results in the electronic medical record. All serum 25(OH)D levels were collected that occurred between date of transplant and one year follow-up. Therefore, if a patient had five serum 25(OH)D levels drawn during our study time points, all were recorded. However only the first serum 25(OH)D level was used in the analysis. Serum 25(OH)D levels were collected as continuous variables and also categorized as adequate and inadequate. Adequate was defined as > 30 ng/ml and inadequate was defined as < 30 ng/ml. GVHD Diagnosis of GVHD was found through keyword search in the medical chart. Criteria for a diagnosis of GVHD was the documentation of diagnosis within a physician s note. GVHD diagnosis was categorized into yes/no groups. The yes group included acute and chronic GVHD and any specified type (i.e. skin, liver, gut). Those without diagnosis of GVHD within a physician s note were placed in the no group. Falls/Fractures Documented falls and fractures were found through key word search in the medical record. Only falls/fractures documented in physician or nursing notes during the defined time period were gathered. Severity of fall/fracture was not collected and
23 14 there was no differentiation if a patient had more than one fall/fracture. To meet criteria for the yes group there needed to be at least one documentation in a physician or nurse note stating the patient had a fall/fracture. Those who did not have documentation of either were placed in the no group. DEXA scan Results DEXA results were collected between date of transplant and one year follow-up. Results were found within the results review tab where non-laboratory tests are reported. All DEXA results were collected between our two time-points. However, only initial DEXA scans were used for analysis. DEXA results were categorized based on the stated report within each scan. DEXA results at Nebraska Medicine describe bone health in two ways: increased risk of fracture and low risk for fracture. Therefore, these were the two categories used for the classification of patients in this study. Risk of fracture was only categorized if patient underwent DEXA scanning. Therefore, if the patient had documentation in the medical record of osteoporosis or osteopenia but did not have a DEXA scan during our time of data collection, they were categorized as missing data from our analysis. Mortality Mortality was collected between time of transplant and one year follow-up and categorized a yes/no. Length of Stay Length of stay was defined as the length in days during the hospitalization to undergo Allo-HSCT. This number was taken from day of admittance to day of discharge.
24 15 This information was provided by the Oncology/Hematology Transplant Data Office. Data Analysis Descriptive statistics were calculated for all variables. Continuous variables were represented by means and standard deviations and categorical variables were represented as counts and percentages. The difference in means of the steroid vs. the non-steroid groups were tested using Independent Sample T-Test. The difference in proportion between steroid vs. the non-steroid group were evaluated with the Chi- Square Test or the Fischer s Exact Test, as appropriate. Multivariate analysis was preformed using Logistic Regression for those variables found to be significant through the univariate analysis. Logistic regression established an odds ratio (OR) for select variables of interest to determine if statistical significance remained independent of all other variables. A Chi-squared test was used to compare the proportion of vitamin D supplementation in both groups after re-categorizing steroid groups based on the ACR guidelines. Data analysis was preformed using IBM SPSS Statistics 23 software and p- values of < 0.05 were considered significant.
25 16 CHAPTER 4: RESULTS Ninety-nine patients were included in the study. Forty-five were female and 54 were male, ranging in age from 19 to 71 years of age, with a mean age of 49.7 years. The majority of patients were Caucasian, compiling 94.5% of the population. Fifty-eight met criteria for the steroid group while 41 were placed in the non-steroid group as seen in Table 1. Table 1: Steroid Groups Steroid vs. Non-Steroid N(%) Steroid (>5 mg for > 3 months) 58 (59) Non-Steroid 41 (41) Total Patients 99 Baseline and clinical characteristics can be seen in Table 3 and 4 based. There was no significant difference between steroid groups in age, sex, and race. When assessing clinical characteristics based on steroid groups there was a statistically larger percentage of vitamin D supplementation in the steroid group compared to the non-steroid group (71% vs 41% respectively, p=0.04). GVHD diagnosis was significantly different between the groups as well; with 90% in the steroid group and 71% in the non-steroid group (p=0.016). Mortality was found to be statistically significant between groups with 51% of the non-steroid group compared to only 24% of those in the steroid group (p=0.005). Documented falls/fractures had a close trend to significance with a p-value of 0.08, with 41% of the steroid group compared to 24% of the non-steroid group having a documented falls or fracture. Serum 25(OH)D levels and DEXA results did not have p-values of significance.
26 17 Table 3: Continuous Variables Comparing Steroid Groups Groups Steroid (N=58) Non-Steroid (N=41) Variables (N) P N Mean (S.D.) N Mean (S. D.) value Age, years (13.26) (13.69) Serum 25(OH)D, ng/ml (16.32) (18.05) Length of Stay, days (5.66) (6.47) Table 4: Categorical Variables Comparing Steroid Groups Groups Steroid (N=58) Non-steroid (N= 41) Variable N % N % P Value Gender Male Female Race Caucasian Other Vitamin D Supplementation Yes No (OH)D Adequate (> 30 ng/ml) Inadequate (< 30 ng/ml) GVHD Diagnosis Yes No Falls/Fractures Yes No DEXA Results Increased Risk for Fracture Low Risk for Fracture Mortality Yes No
27 18 Logistic regression was used to compare the two steroid groups and the variables that were found to be significant through univariate analysis. Those found to be significant include vitamin D supplementation, GVHD, and mortality. When controlling for GVHD and mortality the odds of patients in the steroid group receiving vitamin D supplementation are times higher than the non-steroid group (p=0.019; 95% CI: ). The odds of individuals being diagnosed with GVHD are 4.26 times higher in the steroid group (p=0.014; 95% CI ( ) when vitamin D supplementation and mortality are controlled. Mortality was times more likely to occur in the non-steroid group comparatively when controlling for vitamin D supplementation and GVHD (p=0.020; 95% CI ( ) (Table 5). Table 5: Results of the Logistic Regression Model Variable(s) p-value OR 95% Confidence Interval (CI) Vitamin D Supplementation GVHD Mortality Additionally, an analysis was done to compare serum 25(OH)D levels between patients who were supplemented vitamin D and those who were not supplemented vitamin D. Out of 99 patients, 40 received vitamin D supplementation compared to 18 who did not. Overall there was no significant difference found between mean serum 25(OH)D levels between those who were supplemented and those who were not supplemented.
28 19 Table 6: Serum 25(OH)D Levels in Supplemented vs. Not Supplemented Patients Variables (N) Supplemented (N=45) Groups Non-Supplemented (N=23) N Mean (S.D.) N Mean (S. D.) P value Serum 25(OH)D (ng/ml) (17.06) (16.56) One final analysis was done in which steroid groups were re-categorized based upon ACR recommendations for vitamin D supplementation. Using these redefined groups, 93 individuals met criteria for the steroid group, leaving 6 in the non-steroid group. Of those 93 patients in the steroid group, 60% received vitamin D supplementation while 40% did not. Using a Fischer s Exact test due to large discrepancy in group sizes, no statistical significance was found between groups (p=0.228). Table 7: Steroid groups categorized according to the ACR guidelines Steroid (N=93) Groups Non-steroid (N=6) Variable (Total N) N % N % Vitamin D Supplementation Yes No P Value 0.228
29 20 CHAPTER 5: DISCUSSION The primary outcome of this research was to determine if Allo-HSCT patients who received steroids > 5mg of prednisone or equivalent for > 3 months were supplemented with vitamin D. We found that a significantly higher proportion of those in the steroid group were supplemented with vitamin D compared to the non-steroid group. Based on this, we can speculate that clinicians at Nebraska Medicine are aware of the implications of steroid use in the Allo-HSCT population and are starting a significant proportion of those patients on vitamin D supplementation as a result. However, nearly a quarter of patients remained unsupplemented. This study did not quantify the dose or duration of vitamin D supplementation which would have been beneficial to determine if patients were receiving adequate amounts during and after their transplant, which may be of relevance for future studies in this patient population. As discussed in the literature review, standard prophylactic measurements for bone health may not be enough to protect this patient population 3. To gather more information on vitamin D supplementation according to steroid regimen in our population, we re-categorized groups based on ACR guidelines. Using these redefined groups, which recommend vitamin D supplementation with any dose/duration of steroid, it was found there was no statistical significance in vitamin D supplementation between the steroid and non-steroid groups. Therefore, the same proportion of patients were supplemented regardless of steroid use. The sample sizes of these two groups were highly skewed with 93 patients in the steroid group and only 6 in the non-steroid group. Therefore, 94% of our population received some dose/duration of steroid
30 21 between our defined time points, further demonstrating the need for vitamin D supplementation. Allo-HSCT have increased need for vitamin D supplementation based on multiple factors including steroid use, previous chemotherapy, lack of sun exposure, and poor nutrition status 1,20. While those in the non-steroid group were likely appropriate for supplementation, it shows that patients who did not meet criteria for > 5mg of prednisone or equivalent for > 3 months were not being supplemented with vitamin D. Therefore, if a patient received high dose steroids for one month they would have likely not been prescribed vitamin D supplementation. A study by Petropoulou, et al. found that at two months post-transplant more than 50% of patients had DEXA detected osteoporosis, showing how critical early intervention is 32. Our secondary aim was to determine what clinical outcomes were associated with steroid use of > 5mg of prednisone or equivalent for > 3 months. Based on review of literature, we hypothesized that a significant proportion Allo-HSCT patients who received steroids would also have inadequate serum 25(OH)D levels, documented falls/fractures, DEXA results demonstrating increased risk for fracture, and diagnosis of GVHD. There was no statistical difference in proportions of patients with inadequate serum 25(OH)D levels compared between steroid groups. There was also no significant difference in mean serum 25(OH)D levels when compared between steroid and nonsteroid groups ( vs , p=0.799). This could be explained by the fact there was a significant portion of patients in the steroid group who were supplemented with vitamin D, likely maintaining serum 25(OH)D levels or at least
31 22 preventing a decrease. Both of our mean serum 25(OH)D levels were very similar and met criteria for > 30 ng/ml. With that being said, out of 99 patients only 68 had initial serum 25(OH)D levels drawn. Of those assessed, 50% had levels categorized as inadequate. Overall, 33% of our patient population were never assessed for serum 25(OH)D levels, making it difficult to accurately evaluate differences between steroid groups. Knowing the extensive risk factors Allo-HSCT patients carry, in the future it would beneficial to have more consistent testing of serum 25(OH)D levels. We also assessed mean serum 25(OH)D compared between supplemented and non-supplemented groups, as supplementation of vitamin D is a better indicator of serum 25(OH)D. Through this analysis, we found there was no significant difference between supplemented and non-supplemented groups ( vs , p=0.927). Urbain, et al. found baseline 25(OH)D levels were ng/ml in HSCT patients 33. Although our levels were not collected at baseline, they do show adequate serum 25(OH)D levels between our two time points. It should also be noted the study population of Allo-HSCT patients was predominately Caucasian, thus potentially impacting our results as Caucasian individuals are at less risk for vitamin D deficiency when compared to those with darker skin tones, such as African American or Hispanic individuals 1. Falls and fractures between steroid groups were not found significant, however did trend in that direction (p=0.08). This finding is of interest, given our small sample size and the self-reported nature of this variable. Of the 34 documented falls or fractures, 71% were in the steroid group compared to only 39% in the non-steroid
32 23 group. The LASA study found incidence of fracture was higher when serum 25(OH)D was lower than 30 nmol/l (12.01 ng/ml) 10. They also found the lowest percentage of fractures occurred with serum 25(OH)D levels were above 75 nmol/l (30 ng/ml) 10. Knowing our mean serum 25(OH)D level for the steroid group was above 30 ng/ml ( ) and there was still a trend towards significance for falls and fractures, we could propose our patient population may benefit from having serum 25(OH)D levels above adequate. When assessing DEXA screening between groups, 72% of those in the steroid group underwent DEXA screening compared to 41% of the non-steroid group. Of those patient s in the steroid group, 55% were deemed to be at increased risk for fracture compared to only 15% in the non-steroid group (p=0.176). This finding is similar to Massenkeil, et al. which found 49% of HSCT patients to have osteopenia and osteoporosis prior to transplant 3. Out of the total 99 patients who received Allo-HSCT, only 60% underwent DEXA scanning, leaving 40% of the population without an accurate look at their bone density health. These findings suggest there is need for more consistency when evaluating patients bone health. Massenkeil, et al. states it may be beneficial for Allo-HSCT patients to receive DEXA scans prior to transplant and one year after treatment has been started 3. While NOF recommends BMD follow-up one year after initiating treatment for osteoporosis 1. In this patient population, we have room for improvement with assessing and treating risk factors for decreased bone health. Although there was a significant portion of those in the steroid group being supplemented with vitamin D, there was also a trend towards significant for
33 24 falls/fractures suggesting supplementation was not adequate to raise their 25(OH)D levels to sufficient amounts. The lack of consistency in testing 25(OH)D levels and DEXA scans as well made it difficult to find meaningful results. GVHD diagnosis was statistically significant between steroid groups with 90% of the steroid group being diagnosed with GVHD compared to 71% of the non-steroid group (p=0.016). This can be explained as steroids are a common treatment for GHVD disease. Therefore, these patients were likely diagnosed with GVHD and then started on steroids. As we know pre-transplant 25(OH)D, specifically levels under <25 ng/ml, are associate with increased risk of chronic GVHD 27,28. Therefore, it may be beneficial to start assessing serum 25(OH)D levels prior to transplant and have their levels adequate before starting transplant 27. Mortality was not a variable we had predicted to have statistical significance when beginning our research. However, mortality was found to be significantly higher in the non-steroid group compared to the steroid group, with 51% of the non-steroid group compared to 24% of the steroid group (p=0.005). Initially, this finding seems inconsistent from the information gathered from the literature review. It would have seemed more likely that those in the steroid group would have a higher proportion of mortality as they were likely being treated for complications from Allo-HSCT such as GVHD. However, this finding could be explained by the fact these patients who died may not have lived long enough to meet our requirements of the steroid group.
34 25 Limitations Inherently, this study has limitations. As it is a retrospective chart review, bias may have occurred due to misclassification errors. The small sample size could have shown less strength in association compared with a broader sample size. Another large limitation to the study was the lack of consistency in drawing 25(OH)D levels along with DEXA scanning. More consistent information regarding these outcomes could have given us more detailed information to draw conclusions. Applications for Clinical Practice Development of this study came from clinical judgement regarding the risk factors for decreased bone health in Allo-HSCT patients. It became apparent through daily observation and clinical experience that these patients had multiple factors putting their bone health at risk. Therefore, this study was developed in hopes to encourage use of vitamin D supplementation. The results from this study are to show that while many Allo-HSCT patients are being supplemented with vitamin D, there are inconsistencies in dosage and objective testing to determine if supplementation is enough to prevent a decline in bone health.
35 26 CHAPTER 6: CONCLUSION In conclusion, our study reports that 71% of patients who received steroids according to NOF guidelines received vitamin D supplementation. Overall, it is encouraging that over half of the patient population received vitamin D supplementation. However, we do not know if supplementation was adequate for this complex patient population due to the lack of consistency when treating and assessing bone health. Further research should be completed to identify adequate amounts of vitamin D supplementation in Allo-HSCT to maintain adequate serum 25(OH)D levels and prevent deteriorating bone health in this complex patient population.
36 27 BIBLIOGRAPHY 1. Clinician s guide to prevention and treatment of osteoporosis. (2014). Washington, DC: National Osteoporosis Foundation. 2. Robien, K., Strayer, L., Majhail, N., Lazovich,D., Baker, K., Smith, A.,... Burns, L. (2011). Vitamin D status among long-term survivors of hematopoietic cell transplantation. Bone Marrow Transplantation, Massenkeil G, Fiene C, Rosen O, Michael R, Reisinger W, Arnold R. Loss of bone mass and vitamin D deficiency after hematopoietic stem cell transplantation: standard prophylactic measures fail to prevent osteoporosis. Leukemia. 2001;15: Norman AW. From vitamin D to hormone D: fundamentals of the vitamin D endocrine system essential for good health. Am J Clin Nutr. 2008;88(2):491S- 499S. 5. Kennel KA, Drake MT, Hurley DL. Vitamin D deficiency in adults: when to test and how to treat. Mayo Clin Proc. 2010;85: Lips P., van Schoor N.M. The effect of vitamin d on bone and osteoporosis. Best Pract. Res. Clin. Endocrinol. Metab. 2011;25: Kuchuk NO, Pluijm SM, van Schoor NM et al. Relationships of serum 25- hydroxyvitamin D to bone mineral density and serum parathyroid hormone and markers of bone turnover in older persons. Journal of Clinical Endocrinology and Metabolism 2009; 94: Ooms ME, Roos JC, Bezemer PD et al. Prevention of bone loss by vitamin D supplementation in elderly women: a randomized double-blind trial. Journal of Clinical Endocrinology and Metabolism 1995; 80: Kuchuk NO, van Schoor NM, Pluijm SM et al. Vitamin D status, parathyroid function, bone turnover, and BMD in post- menopausal women with osteoporosis: global perspective. Journal of Bone and Mineral Research 2009; 24: van Schoor NM, Visser M, Pluijm SM et al. Vitamin D deficiency as a risk factor for osteoporotic fractures. Bone 2008; 42: Jackson RD, LaCroix AZ, Gass M et al. Calcium plus vitamin D supplementation and the risk of fractures. The New England Journal of Medicine 2006; 354: 669
37 (Accessed on Feb 2017). 13. M.F. Holick, N.C. Binkley, H.A. Bischoff-Ferrari, et al. Evaluation, treatment, and prevention of vitamin D deficiency: an Endocrine Society clinical practice guideline. J Clin Endocrinol Metab, 96 (2011), pp Dawson-Hughes B, Mithal A, Bonjour JP, Boonen S, Burckhardt P, Fuleihan GE. et al. IOF position statement: vitamin D recommendations for older adults. Osteoporos Int. 2010;21: Judge J, Birge S, Gloth F, Heaney R, Hollis B, Kenny A, et al. Recommendations abstracted from the American geriatrics society consensus statement on vitamin D for prevention of falls and their consequences. J Am Geriatr Soc. 2014;62(1): Ginde AA, Scragg R, Schwartz RS, Camargo CA Jr. Prospective study of serum 25- hydroxyvitamin d level, cardiovascular disease mortality, and all- cause mortality in older U.S. Adults. J Am Geriatr Soc. 2009;57: Grossman JM, Gordon R, Ranganath VK, et al. American College of Rheumatology 2010 recommendations for the prevention and treatment of glucocorticoidinduced osteoporosis. Arthritis Care Res (Hoboken) 2010; 62: Armas LA, Hollis BW, Heaney RP. Vitamin D2 is much less effective than vitamin D3 in humans. J Clin Endocrinol Metab. 2004;89: Tripkovic L, Lambert H, Hart K, et al. Comparison of vitamin D2 and vitamin D3 supplementation in raising serum 25-hydroxyvitamin D status: a systematic review and meta-analysis. Am J Clin Nutr 2012; 95: Dawson-Hughes, B. (2017). Vitamin D deficiency in adults: Definition, clinical manifestations, and treatment. In J. E. Mulder (Ed), UpToDate. Retrieved from Forrest, K. Y., & Stuhldreher, W. L. (2011). Prevalence and correlates of vitamin D deficiency in US adults. Nutrition research, 31(1), Kennel KA, Drake MT. Vitamin D in the cancer patient. Curr Opin Support Palliat Care (2013) 7: Giovannucci E, Liu Y, Rimm EB, Hollis BW, Fuchs CS, Stampfer MJ, Willett WC. Prospective study of predictors of vitamin D status and cancer incidence and mortality in men. J Natl Cancer Inst. 2006;98(7): Garland FC, Garland CF, Gorham ED, Young JF. Geographic variation in breast cancer mortality in the United States: a hypothesis involving exposure to solar radiation. Prev Med. 1990; 19(6): Grant WB. An estimate of premature cancer mortality in the US due to inadequate doses of solar ultraviolet B radiation. Cancer. 2002;94(6):
38 26. Benrashid, M., Moyers, K., Mohty, M., & Savani, B. (n.d.). Vitamin D deficiency, autoimmunity, and graft-versus-host-disease risk: Implication for preventive therapy. Experimental Hematology, Glotzbecker, B., Ho, V. T., Aldridge, J., Kim, H. T., Horowitz, G., Ritz, J.,... & Rosenblatt, J. (2013). Low levels of 25-hydroxyvitamin D before allogeneic hematopoietic SCT correlate with the development of chronic GVHD. Bone marrow transplantation, 48(4), von Bahr L, Blennow O, Alm J, Björklund A, Malmberg KJ, Mougiakakos D, et al. Increased incidence of chronic GvHD and CMV disease in patients with vitamin D deficiency before allogeneic stem cell transplantation. Bone Marrow Transplant. 2015;50: Van Staa TP, Leufkens HG, Cooper C. The epidemiology of corticosteroid-induced osteoporosis: a meta-analysis. Osteoporos Int 2002; 13: Canalis, E., Mazziotti, G., Giustina, A. et al. Osteoporosis Int (2007) 18: W.P. Olszynski, J.D. Adachi, D.A. Hanley, D.L. Kendler, A.B. Hodsman, K.G. Siminoski, et al.management of corticosteroid-induced osteoporosissemin Arthritis Rheum, 29 (4) (2000), pp Petropoulou AD, Porcher R, Herr AL, et al. Prospective assessment of bone turnover and clinical bone diseases after allogeneic hematopoietic stem-cell transplantation. Transplantation. 2010;89: Urbain, P., Ihorst, G., Biesalski, HK. et al. course of serum 25-hydroxyvitamin D3 status and its influencing factors in adults undergoing allogeneic hematopoietic cell transplantation. Ann Hematol (2012) 91:
FOR CONSUMERS AND PATIENTS
 AVAILABILITY OF VITAMIN D FOR CONSUMERS AND PATIENTS Prof. Heike A. Bischoff-Ferrari, MD, DrPH Centre on Aging and Mobility, University of Zurich Dept. of Rheumatology, University Hospital Zurich Overview
AVAILABILITY OF VITAMIN D FOR CONSUMERS AND PATIENTS Prof. Heike A. Bischoff-Ferrari, MD, DrPH Centre on Aging and Mobility, University of Zurich Dept. of Rheumatology, University Hospital Zurich Overview
Vitamin D. Vitamin functioning as hormone. Todd A Fearer, MD FACP
 Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
Vitamin D Vitamin functioning as hormone Todd A Fearer, MD FACP Vitamin overview Vitamins are organic compounds that are essential in small amounts for normal metabolism They are different from minerals
AMERICAN COLLEGE OF RHEUMATOLOGY POSITION STATEMENT. Committee on Rheumatologic Care
 AMERICAN COLLEGE OF RHEUMATOLOGY POSITION STATEMENT SUBJECT: PRESENTED BY: FOR DISTRIBUTION TO: Bone Mineral Density Measurement and the Role of Rheumatologists in the Management of Osteoporosis Committee
AMERICAN COLLEGE OF RHEUMATOLOGY POSITION STATEMENT SUBJECT: PRESENTED BY: FOR DISTRIBUTION TO: Bone Mineral Density Measurement and the Role of Rheumatologists in the Management of Osteoporosis Committee
Elecsys bone marker panel. Optimal patient management starts in the laboratory
 bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
bone marker panel Optimal patient management starts in the laboratory Complete solution for osteoporosis The most complete bone metabolism panel on a single platform bone marker assays are important diagnostic
BAD TO THE BONE. Peter Jones, Rheumatologist QE Health, Rotorua. GP CME Conference Rotorua, June 2008
 BAD TO THE BONE Peter Jones, Rheumatologist QE Health, Rotorua GP CME Conference Rotorua, June 2008 Agenda Osteoporosis in Men Vitamin D and Calcium Long-term treatment with Bisphosphonates Pathophysiology
BAD TO THE BONE Peter Jones, Rheumatologist QE Health, Rotorua GP CME Conference Rotorua, June 2008 Agenda Osteoporosis in Men Vitamin D and Calcium Long-term treatment with Bisphosphonates Pathophysiology
Vitamin D Replacement ROCKY MOUNTAIN MEETING NOV 2013 BANFF W.COKE UNIVERSITY OF TORONTO
 Vitamin D Replacement ROCKY MOUNTAIN MEETING NOV 2013 BANFF W.COKE UNIVERSITY OF TORONTO Disclosures: (Academic Mea Culpa) No financial conflicts I have no expertise re: Vitamin D. OBJECTIVES: 1) Review
Vitamin D Replacement ROCKY MOUNTAIN MEETING NOV 2013 BANFF W.COKE UNIVERSITY OF TORONTO Disclosures: (Academic Mea Culpa) No financial conflicts I have no expertise re: Vitamin D. OBJECTIVES: 1) Review
Update on vitamin D. J Chris Gallagher Professor of Medicine and Endocrinology Creighton University Omaha,Nebraska USA
 Update on vitamin D J Chris Gallagher Professor of Medicine and Endocrinology Creighton University Omaha,Nebraska 68131 USA Cali, Colombia 2016 definitions DRIs are the recommended dietary reference intakes
Update on vitamin D J Chris Gallagher Professor of Medicine and Endocrinology Creighton University Omaha,Nebraska 68131 USA Cali, Colombia 2016 definitions DRIs are the recommended dietary reference intakes
Vitamin D, Sunlight Exposure, and Bone Density in Elderly African American Females of Low Socioeconomic Status
 Vol. 42, No. 1 47 Clinical Research and Methods Vitamin D, Sunlight Exposure, and Bone Density in Elderly African American Females of Low Socioeconomic Status Sally P. Weaver, PhD, MD; Cindy Passmore,
Vol. 42, No. 1 47 Clinical Research and Methods Vitamin D, Sunlight Exposure, and Bone Density in Elderly African American Females of Low Socioeconomic Status Sally P. Weaver, PhD, MD; Cindy Passmore,
Skeletal Manifestations
 Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Skeletal Manifestations of Metabolic Bone Disease Mishaela R. Rubin, MD February 21, 2008 The Three Ages of Women Gustav Klimt 1905 1 Lecture Outline Osteoporosis epidemiology diagnosis secondary causes
Description of Study Protocol. Data Collection Summary
 AND Evidence Analysis Worksheet Citation Kostoglou-athanassiou I, AthanassiouP, Lyraki A, Raftakis I, Antoniadis C. Vitamin D and rheumatoid arthritis. Ther Adv Endocrinol Metab. 2012; 3(6):181-7. Study
AND Evidence Analysis Worksheet Citation Kostoglou-athanassiou I, AthanassiouP, Lyraki A, Raftakis I, Antoniadis C. Vitamin D and rheumatoid arthritis. Ther Adv Endocrinol Metab. 2012; 3(6):181-7. Study
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 9/29/2017 If the member s subscriber contract excludes coverage
BMD: A Continuum of Risk WHO Bone Density Criteria
 Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
Pathogenesis of Osteoporosis Osteoporosis Diagnosis: BMD, FRAX and Assessment of Secondary Osteoporosis AGING MENOPAUSE OTHER RISK FACTORS RESORPTION > FORMATION Bone Loss LOW PEAK BONE MASS Steven T Harris
JOURNAL OF INTERNATIONAL ACADEMIC RESEARCH FOR MULTIDISCIPLINARY Impact Factor 1.393, ISSN: , Volume 2, Issue 7, August 2014
 HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
HYPOVITAMINOSIS D IN INDIAN FEMALES WITH POSTMENOPAUSAL OSTEOPOROSIS DR. SHAH WALIULLAH 1 DR. VINEET SHARMA 2 DR. R N SRIVASTAVA 3 DR. YASHODHARA PRADEEP 4 DR. A A MAHDI 5 DR. SANTOSH KUMAR 6 1 Research
Pharmacy Management Drug Policy
 SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
SUBJECT: - Forteo (teriparatide), Prolia (denosumab), Tymlos (abaloparatide), Boniva injection (Ibandronate) POLICY NUMBER: Pharmacy-35 EFFECTIVE DATE: 9/07 LAST REVIEW DATE: 10/15/2018 If the member s
Vitamin D and Calcium Therapy: how much is enough
 Vitamin D and Calcium Therapy: how much is enough Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco DISCLOSURE Nothing to disclose 1 RECOMMENDATIONS
Vitamin D and Calcium Therapy: how much is enough Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco DISCLOSURE Nothing to disclose 1 RECOMMENDATIONS
V t i amin i n D a nd n d Calc l iu i m u : Rol o e l in i n Pr P eve v nt n io i n and n d Tr T eatment n of o Fr F actur u es and n d Fa F ll l s
 Vitamin D and Calcium: Role in Prevention and Treatment of Fractures and Falls Osteoporosis 21: New Insights In Research, Diagnosis, and Clinical Care Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic
Vitamin D and Calcium: Role in Prevention and Treatment of Fractures and Falls Osteoporosis 21: New Insights In Research, Diagnosis, and Clinical Care Deborah Sellmeyer, MD Director, Johns Hopkins Metabolic
The Endocrine Society Guidelines
 Vitamin D and Calcium Therapy: how much is enough DISCLOSURE Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco Nothing to disclose RECOMMENDATIONS
Vitamin D and Calcium Therapy: how much is enough DISCLOSURE Daniel D Bikle, MD, PhD Professor of Medicine VA Medical Center and University of California San Francisco Nothing to disclose RECOMMENDATIONS
The Skeletal Response to Aging: There s No Bones About It!
 The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
The Skeletal Response to Aging: There s No Bones About It! April 7, 2001 Joseph E. Zerwekh, Ph.D. Interrelationship of Intestinal, Skeletal, and Renal Systems to the Overall Maintenance of Normal Calcium
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Osteoporosis- Do We Need to Think Beyond Bone Mineral Density? Dr Preeti Soni 1, Dr Shipra
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Osteoporosis- Do We Need to Think Beyond Bone Mineral Density? Dr Preeti Soni 1, Dr Shipra
AETNA BETTER HEALTH Prior Authorization guideline for Injectable Osteoporosis Agents
 AETNA BETTER HEALTH Prior Authorization guideline for Injectable Osteoporosis Agents Injectable Osteoporosis Agents Forteo (teriparatide); zoledronic acid Prolia (denosumab)] Authorization guidelines For
AETNA BETTER HEALTH Prior Authorization guideline for Injectable Osteoporosis Agents Injectable Osteoporosis Agents Forteo (teriparatide); zoledronic acid Prolia (denosumab)] Authorization guidelines For
8/6/2018. Glucocorticoid induced osteoporosis: overlooked and undertreated? Disclosure. Objectives. Overview
 Disclosure Glucocorticoid induced osteoporosis: overlooked and undertreated? I have no financial disclosure relevant to this presentation Tasma Harindhanavudhi, MD Division of Diabetes and Endocrinology
Disclosure Glucocorticoid induced osteoporosis: overlooked and undertreated? I have no financial disclosure relevant to this presentation Tasma Harindhanavudhi, MD Division of Diabetes and Endocrinology
Vitamin D Deficiency. Micol Rothman, MD Assistant Professor of Medicine Clinical Director Metabolic Bone Program University of CO-Denver
 Vitamin D Deficiency Micol Rothman, MD Assistant Professor of Medicine Clinical Director Metabolic Bone Program University of CO-Denver 50 yo woman referred for osteoporosis What is striking about her
Vitamin D Deficiency Micol Rothman, MD Assistant Professor of Medicine Clinical Director Metabolic Bone Program University of CO-Denver 50 yo woman referred for osteoporosis What is striking about her
Vitamin D Deficiency. Decreases renal calcium excretion. Increases intestinal absorption Calcium. Increases bone resorption of calcium
 Vitamin D Deficiency Deborah Gordish, MD Assistant Professor of Clinical Internal Medicine Lead Physician Lewis Center Primary Care Associate Division Director General Internal Medicine The Ohio State
Vitamin D Deficiency Deborah Gordish, MD Assistant Professor of Clinical Internal Medicine Lead Physician Lewis Center Primary Care Associate Division Director General Internal Medicine The Ohio State
Aamir Hussain MD Maya D. Srivastava MD Michael Moore MD
 Assessment of Bone Health in patients with Eosinophilic Esophagitis Aamir Hussain MD Maya D. Srivastava MD Michael Moore MD Background Eosinophilic esophagitis is defined as a chronic, immune/antigen mediated,
Assessment of Bone Health in patients with Eosinophilic Esophagitis Aamir Hussain MD Maya D. Srivastava MD Michael Moore MD Background Eosinophilic esophagitis is defined as a chronic, immune/antigen mediated,
The Vitamin D Gap. Vitamin D intake guidelines were established to prevent. Estimating an adequate intake of vitamin D. FEATURE VITAMIN D GAP
 The Vitamin D Gap Estimating an adequate intake of vitamin D. By Laurence Montgomery, ND and George Tardik, ND Vitamin D intake guidelines were established to prevent rickets in children and osteomalacia
The Vitamin D Gap Estimating an adequate intake of vitamin D. By Laurence Montgomery, ND and George Tardik, ND Vitamin D intake guidelines were established to prevent rickets in children and osteomalacia
Vitamin D: Conflict of Interest Statement Corporate. Outline 7/5/2016
 Vitamin D: What s New and Not? Clifford J Rosen MD Maine Medical Center Research Institute rosenc@mmc.org Conflict of Interest Statement Corporate NO STOCKS or EQUITY Editor UpToDate, New England Journal
Vitamin D: What s New and Not? Clifford J Rosen MD Maine Medical Center Research Institute rosenc@mmc.org Conflict of Interest Statement Corporate NO STOCKS or EQUITY Editor UpToDate, New England Journal
Vitamin D and Inflammation
 Vitamin D and Inflammation Susan Harris, D.Sc. Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University Boston, MA Vitamin D Liver 25(OH)D storage form nmol/l=ng/ml x 2.5 Renal 1,25(OH)
Vitamin D and Inflammation Susan Harris, D.Sc. Jean Mayer USDA Human Nutrition Research Center on Aging at Tufts University Boston, MA Vitamin D Liver 25(OH)D storage form nmol/l=ng/ml x 2.5 Renal 1,25(OH)
nogg Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK
 nogg NATIONAL OSTEOPOROSIS GUIDELINE GROUP Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK Produced by J Compston, A Cooper,
nogg NATIONAL OSTEOPOROSIS GUIDELINE GROUP Guideline for the diagnosis and management of osteoporosis in postmenopausal women and men from the age of 50 years in the UK Produced by J Compston, A Cooper,
Vitamin D for the Prevention of Osteoporotic Fractures
 TITLE: Vitamin D for the Prevention of Osteoporotic Fractures AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine University of California
TITLE: Vitamin D for the Prevention of Osteoporotic Fractures AUTHOR: Jeffrey A. Tice, MD Assistant Professor of Medicine Division of General Internal Medicine Department of Medicine University of California
9/26/2016. The Impact of Dietary Protein on the Musculoskeletal System. Research in dietary protein, musculoskeletal health and calcium economy
 The Impact of Dietary Protein on the Musculoskeletal System Outline A. The musculoskeletal system and associated disorders Jessica D Bihuniak, PhD, RD Assistant Professor of Clinical Nutrition Department
The Impact of Dietary Protein on the Musculoskeletal System Outline A. The musculoskeletal system and associated disorders Jessica D Bihuniak, PhD, RD Assistant Professor of Clinical Nutrition Department
Additional Research is Needed to Determine the Effects of Soy Protein on Calcium Binding and Absorption NDFS 435 3/26/2015. Dr.
 Additional Research is Needed to Determine the Effects of Soy Protein on Calcium Binding and Absorption NDFS 435 3/26/2015 Dr. Tessem Osteoporosis is a public health problem in all stages of life. Many
Additional Research is Needed to Determine the Effects of Soy Protein on Calcium Binding and Absorption NDFS 435 3/26/2015 Dr. Tessem Osteoporosis is a public health problem in all stages of life. Many
Osteoporosis/Fracture Prevention
 Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Osteoporosis/Fracture Prevention NATIONAL GUIDELINE SUMMARY This guideline was developed using an evidence-based methodology by the KP National Osteoporosis/Fracture Prevention Guideline Development Team
Clinician s Guide to Prevention and Treatment of Osteoporosis
 Clinician s Guide to Prevention and Treatment of Osteoporosis Published: 15 August 2014 committee of the National Osteoporosis Foundation (NOF) Tipawan khiemsontia,md outline Basic pathophysiology screening
Clinician s Guide to Prevention and Treatment of Osteoporosis Published: 15 August 2014 committee of the National Osteoporosis Foundation (NOF) Tipawan khiemsontia,md outline Basic pathophysiology screening
The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome
 CRC IRB Proposal Matthew Champion PGY-1 8/29/12 The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome Study Purpose
CRC IRB Proposal Matthew Champion PGY-1 8/29/12 The effect of supplementation with vitamin D on recurrent ischemic events and sudden cardiac death in patients with acute coronary syndrome Study Purpose
Coordinator of Post Professional Programs Texas Woman's University 1
 OSTEOPOROSIS Update 2007-2008 April 26, 2008 How much of our BMD is under our control (vs. genetics)? 1 2 Genetic effects on bone loss: longitudinal twin study (Makovey, 2007) Peak BMD is under genetic
OSTEOPOROSIS Update 2007-2008 April 26, 2008 How much of our BMD is under our control (vs. genetics)? 1 2 Genetic effects on bone loss: longitudinal twin study (Makovey, 2007) Peak BMD is under genetic
Interpreting DEXA Scan and. the New Fracture Risk. Assessment. Algorithm
 Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Interpreting DEXA Scan and the New Fracture Risk Assessment Algorithm Prof. Samir Elbadawy *Osteoporosis affect 30%-40% of women in western countries and almost 15% of men after the age of 50 years. Osteoporosis
Nutritional Aspects of Osteoporosis Care and Treatment Cynthia Smith, FNP-BC, RN, MSN, CCD Pars Osteoporosis Clinic, Belpre, Ohio
 Osteoporosis 1 Nutritional Aspects of Osteoporosis Care and Treatment Cynthia Smith, FNP-BC, RN, MSN, CCD Pars Osteoporosis Clinic, Belpre, Ohio 1) Objectives: a) To understand bone growth and development
Osteoporosis 1 Nutritional Aspects of Osteoporosis Care and Treatment Cynthia Smith, FNP-BC, RN, MSN, CCD Pars Osteoporosis Clinic, Belpre, Ohio 1) Objectives: a) To understand bone growth and development
VITAMIN D AND THE ATHLETE
 VITAMIN D AND THE ATHLETE CONSIDERATIONS FOR THE PRACTITIONER Written by Bruce Hamilton, Qatar Vitamin D is a steroid hormone that has previously been given little attention, partially as a result of its
VITAMIN D AND THE ATHLETE CONSIDERATIONS FOR THE PRACTITIONER Written by Bruce Hamilton, Qatar Vitamin D is a steroid hormone that has previously been given little attention, partially as a result of its
Vitamin D and Calcium
 Vitamin D and Calcium American Association of Clinical Endocrinologists Marina Del Rey, CA September 15, 2018 Albert Shieh, MD MS Assistant Clinical Professor Department of Medicine Division of Endocrinology
Vitamin D and Calcium American Association of Clinical Endocrinologists Marina Del Rey, CA September 15, 2018 Albert Shieh, MD MS Assistant Clinical Professor Department of Medicine Division of Endocrinology
VITAMIN D IN HEALTH AND DISEASE
 VITAMIN D IN HEALTH AND DISEASE Margus Lember University of Tartu, Estonia ESIM, Saas Fee, January 16, 2014 l It`s most healthy to live on the southern side of a mountain l Hippokrates of Kos 460-370 BC
VITAMIN D IN HEALTH AND DISEASE Margus Lember University of Tartu, Estonia ESIM, Saas Fee, January 16, 2014 l It`s most healthy to live on the southern side of a mountain l Hippokrates of Kos 460-370 BC
original Se Hwa Kim 1), Tae Ho Kim 1) and Soo-Kyung Kim 2)
 Endocrine Journal 2014, 61 (12), 1197-1204 original Effect of high parathyroid hormone level on bone mineral density in a vitamin D-sufficient population: Korea National Health and Nutrition Examination
Endocrine Journal 2014, 61 (12), 1197-1204 original Effect of high parathyroid hormone level on bone mineral density in a vitamin D-sufficient population: Korea National Health and Nutrition Examination
Fragile Bones and how to recognise them. Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey
 Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
Fragile Bones and how to recognise them Rod Hughes Consultant physician and rheumatologist St Peter s hospital Chertsey Osteoporosis Osteoporosis is a skeletal disorder characterised by compromised bone
Osteoporosis: A Tale of 3 Task Forces!
 Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Osteoporosis: A Tale of 3 Task Forces! Robert A. Adler, MD McGuire Veterans Affairs Medical Center Virginia Commonwealth University Richmond, Virginia, USA Disclosures The opinions are those of the speaker
Osteoporosis: An Overview. Carolyn J. Crandall, MD, MS
 Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Objectives Review osteoporosis
Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Osteoporosis: An Overview Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA Objectives Review osteoporosis
Vitamin D Supplementation for Pain
 Vitamin D Supplementation for Pain Christan M. Thomas, PharmD; Peter Campbell, PharmD US Pharmacist. 2015;40(3):43 46. www.medscape.com Abstract and Introduction Abstract Vitamin D, a fat soluble vitamin
Vitamin D Supplementation for Pain Christan M. Thomas, PharmD; Peter Campbell, PharmD US Pharmacist. 2015;40(3):43 46. www.medscape.com Abstract and Introduction Abstract Vitamin D, a fat soluble vitamin
Zeenat Ali, PGY3 Joseph Grisanti, MD June 7 th, 2012
 A Randomized Open Label Trial to Evaluate the Efficacy of Different Dosage Forms of Vitamin D in Patients with Vitamin D Deficiency, and the Effect of Food on Vitamin D Absorption. Zeenat Ali, PGY3 Joseph
A Randomized Open Label Trial to Evaluate the Efficacy of Different Dosage Forms of Vitamin D in Patients with Vitamin D Deficiency, and the Effect of Food on Vitamin D Absorption. Zeenat Ali, PGY3 Joseph
Osteoporosis. Overview
 v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
v2 Osteoporosis Overview Osteoporosis is defined as compromised bone strength that increases risk of fracture (NIH Consensus Conference, 2000). Bone strength is characterized by bone mineral density (BMD)
Prophylactic treatment for osteoporosis: Student EBM Presentation
 Prophylactic treatment for osteoporosis: Student EBM Presentation Callum Harris & Ealish Swift University of Oxford October 2015 Example patient JS is a 67 year old lady who needs to start taking long-term
Prophylactic treatment for osteoporosis: Student EBM Presentation Callum Harris & Ealish Swift University of Oxford October 2015 Example patient JS is a 67 year old lady who needs to start taking long-term
Efficacy of risedronate in men with primary and secondary osteoporosis: results of a 1-year study
 Rheumatol Int (2006) 26: 427 431 DOI 10.1007/s00296-005-0004-4 ORIGINAL ARTICLE J. D. Ringe Æ H. Faber Æ P. Farahmand Æ A. Dorst Efficacy of risedronate in men with primary and secondary osteoporosis:
Rheumatol Int (2006) 26: 427 431 DOI 10.1007/s00296-005-0004-4 ORIGINAL ARTICLE J. D. Ringe Æ H. Faber Æ P. Farahmand Æ A. Dorst Efficacy of risedronate in men with primary and secondary osteoporosis:
Vitamin D and Systemic Lupus Erythematosus: Bones, Muscles, and Joints
 Curr Rheumatol Rep (2010) 12:259 263 DOI 10.1007/s11926-010-0106-1 Vitamin D and Systemic Lupus Erythematosus: Bones, Muscles, and Joints Nancy E. Lane Published online: 29 April 2010 # The Author(s) 2010.
Curr Rheumatol Rep (2010) 12:259 263 DOI 10.1007/s11926-010-0106-1 Vitamin D and Systemic Lupus Erythematosus: Bones, Muscles, and Joints Nancy E. Lane Published online: 29 April 2010 # The Author(s) 2010.
Men and Osteoporosis So you think that it can t happen to you
 Men and Osteoporosis So you think that it can t happen to you Jonathan D. Adachi MD, FRCPC Alliance for Better Bone Health Chair in Rheumatology Professor, Department of Medicine Michael G. DeGroote School
Men and Osteoporosis So you think that it can t happen to you Jonathan D. Adachi MD, FRCPC Alliance for Better Bone Health Chair in Rheumatology Professor, Department of Medicine Michael G. DeGroote School
Dr Seeta Durvasula.
 Dr Seeta Durvasula seeta.durvasula@sydney.edu.au 1 Avoid sun skin cancer risk Australia has highest rates of skin cancer in the world Epidemic of Vitamin D deficiency Lack of Vitamin D increases risk of
Dr Seeta Durvasula seeta.durvasula@sydney.edu.au 1 Avoid sun skin cancer risk Australia has highest rates of skin cancer in the world Epidemic of Vitamin D deficiency Lack of Vitamin D increases risk of
Osteoporosis The Silent Disease
 Joel Johnson, Yr, Subtask, Biology ER., 7/9/5 Osteoporosis The Silent Disease What is Osteoporosis? Osteoporosis is a disease which causes bones to become brittle, which increases the risk of broken bones.
Joel Johnson, Yr, Subtask, Biology ER., 7/9/5 Osteoporosis The Silent Disease What is Osteoporosis? Osteoporosis is a disease which causes bones to become brittle, which increases the risk of broken bones.
BONE HEALTH Dr. Tia Lillie. Exercise, Physical Activity and Osteoporosis
 BONE HEALTH Dr. Tia Lillie Exercise, Physical Activity and Osteoporosis Food for thought... How old would you be if you didn t know how old you were? DEFINITION: Osteoporosis Osteoporosis (OP) is a disease
BONE HEALTH Dr. Tia Lillie Exercise, Physical Activity and Osteoporosis Food for thought... How old would you be if you didn t know how old you were? DEFINITION: Osteoporosis Osteoporosis (OP) is a disease
The discovery of Vitamin D and the elimination of rickets has been considered as one of Medicine s Greatest Achievements.
 The discovery of Vitamin D and the elimination of rickets has been considered as one of Medicine s Greatest Achievements. SIR EDWARD MELLANBY 1 8 8 4-1 9 5 5 A D I E T C H A R A C T E R I S T I C O F S
The discovery of Vitamin D and the elimination of rickets has been considered as one of Medicine s Greatest Achievements. SIR EDWARD MELLANBY 1 8 8 4-1 9 5 5 A D I E T C H A R A C T E R I S T I C O F S
CASE 1 WHY IS IT IMPORTANT TO TREAT? FACTS CONCERNS
 4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
4:30-5:15pm Ask the Expert: Osteoporosis SPEAKERS Silvina Levis, MD OSTEOPOROSIS - FACTS 1:3 older women and 1:5 older men will have a fragility fracture after age 50 After 3 years of treatment, depending
New York State County Comparison of Fall-related Hip Fractures of Older Adults and Number of Dual-X-ray Absorptiometry Machines
 New York State County Comparison of Fall-related Hip Fractures of Older Adults and Number of Dual-X-ray Absorptiometry Machines Michael Bauer New York State Department of Health Bureau of Occupational
New York State County Comparison of Fall-related Hip Fractures of Older Adults and Number of Dual-X-ray Absorptiometry Machines Michael Bauer New York State Department of Health Bureau of Occupational
Helpful information about bone health & osteoporosis Patient Resource
 Helpful information about bone health & osteoporosis Patient Resource Every year In the United States, 2.5 million fractures occur due to osteoporosis. Out of these, 330,000 are hip fractures, and half
Helpful information about bone health & osteoporosis Patient Resource Every year In the United States, 2.5 million fractures occur due to osteoporosis. Out of these, 330,000 are hip fractures, and half
The Prevalence of Vitamin D Deficiency in Benghazi Population
 IOSR Journal of Pharmacy and Biological Sciences (IOSR-JPBS) e-issn:2278-3008, p-issn:2319-7676. Volume 13, Issue 4 Ver. I (Jul Aug 2018), PP 36-42 www.iosrjournals.org The Prevalence of Vitamin D Deficiency
IOSR Journal of Pharmacy and Biological Sciences (IOSR-JPBS) e-issn:2278-3008, p-issn:2319-7676. Volume 13, Issue 4 Ver. I (Jul Aug 2018), PP 36-42 www.iosrjournals.org The Prevalence of Vitamin D Deficiency
Study of the Association between Serum Vitamin D 25(OH) D levels, Muscle Strength and fall among Elderly.
 DOI: 10.21276/aimdr.2017.3.2.ME7 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Study of the Association between Serum Vitamin D 25(OH) D levels, Muscle Strength and fall among Elderly. Karthik
DOI: 10.21276/aimdr.2017.3.2.ME7 Original Article ISSN (O):2395-2822; ISSN (P):2395-2814 Study of the Association between Serum Vitamin D 25(OH) D levels, Muscle Strength and fall among Elderly. Karthik
To understand bone growth and development across the lifespan. To develop a better understanding of osteoporosis.
 Nutrition Aspects of Osteoporosis Care and Treatment t Cynthia Smith, FNP-BC, RN, MSN, CCD Pars Osteoporosis Clinic, Belpre, OH. Objectives To understand bone growth and development across the lifespan.
Nutrition Aspects of Osteoporosis Care and Treatment t Cynthia Smith, FNP-BC, RN, MSN, CCD Pars Osteoporosis Clinic, Belpre, OH. Objectives To understand bone growth and development across the lifespan.
Osteoporosis and Lupus. Andrew Ruthberg, MD University Rheumatologists
 Osteoporosis and Lupus Andrew Ruthberg, MD University Rheumatologists 1 Forget the medical terminology (osteoporosis, osteopenia, low bone mass, DEXA, DXA, T score etc) The bottom line is that you don
Osteoporosis and Lupus Andrew Ruthberg, MD University Rheumatologists 1 Forget the medical terminology (osteoporosis, osteopenia, low bone mass, DEXA, DXA, T score etc) The bottom line is that you don
Original Article The epidemic investigation of serum 25-hydroxy vitamin D levels in the adults in Qujing area of Yunnan province in China
 Int J Clin Exp Pathol 2015;8(8):9597-9601 www.ijcep.com /ISSN:1936-2625/IJCEP0013259 Original Article The epidemic investigation of serum 25-hydroxy vitamin D levels in the adults in Qujing area of Yunnan
Int J Clin Exp Pathol 2015;8(8):9597-9601 www.ijcep.com /ISSN:1936-2625/IJCEP0013259 Original Article The epidemic investigation of serum 25-hydroxy vitamin D levels in the adults in Qujing area of Yunnan
A Review of Vitamin D Supplementation in the Adult Patient ACPE UAN: H01-P
 A Review of Vitamin D Supplementation in the Adult Patient ACPE UAN: 0171-9999-15-053-H01-P Joshua Hirschhorn, PharmD Candidate, Class of 2015. South Carolina College of Pharmacy, MUSC Campus. Kristy L.
A Review of Vitamin D Supplementation in the Adult Patient ACPE UAN: 0171-9999-15-053-H01-P Joshua Hirschhorn, PharmD Candidate, Class of 2015. South Carolina College of Pharmacy, MUSC Campus. Kristy L.
Shon E. Meek, M.D., Ph.D. Assistant Professor of Medicine
 Shon E. Meek, M.D., Ph.D. Assistant Professor of Medicine meek.shon@mayo.edu 2016 MFMER 3561772-1 Update on Vitamin D Shon Meek MD, PhD 20 th Annual Endocrine Update January 30-Feb 3, 2017 Disclosure Relevant
Shon E. Meek, M.D., Ph.D. Assistant Professor of Medicine meek.shon@mayo.edu 2016 MFMER 3561772-1 Update on Vitamin D Shon Meek MD, PhD 20 th Annual Endocrine Update January 30-Feb 3, 2017 Disclosure Relevant
LOVE YOUR BONES Protect your future
 www.worldosteoporosisday.org LOVE YOUR BONES Protect your future Know your risk for osteoporosis www.iofbonehealth.org Osteoporosis is a problem worldwide, and in many countries, up to one in three women
www.worldosteoporosisday.org LOVE YOUR BONES Protect your future Know your risk for osteoporosis www.iofbonehealth.org Osteoporosis is a problem worldwide, and in many countries, up to one in three women
Vitamin D Deficiency in Patients presented in Medical OPD with Fibromyalgia Muhammad Arif Mahmood, Muhammad Arshad Qureshi, Ijaz-Ul-Haque Taseer
 Original Article Vitamin D Deficiency in Patients presented in Medical OPD with Fibromyalgia Muhammad Arif Mahmood, Muhammad Arshad Qureshi, Ijaz-Ul-Haque Taseer ABSTRACT Objectives: To determine the prevalence
Original Article Vitamin D Deficiency in Patients presented in Medical OPD with Fibromyalgia Muhammad Arif Mahmood, Muhammad Arshad Qureshi, Ijaz-Ul-Haque Taseer ABSTRACT Objectives: To determine the prevalence
Benefits of Vitamin D for Cancer and Pregnancy/Birth Outcomes. William B. Grant, PhD Sunlight, Nutrition and Health Research Center, San Francisco
 Benefits of Vitamin D for Cancer and Pregnancy/Birth Outcomes William B. Grant, PhD Sunlight, Nutrition and Health Research Center, San Francisco Disclosure I receive funding from Bio Tech Pharmacal, Inc.
Benefits of Vitamin D for Cancer and Pregnancy/Birth Outcomes William B. Grant, PhD Sunlight, Nutrition and Health Research Center, San Francisco Disclosure I receive funding from Bio Tech Pharmacal, Inc.
Forteo (teriparatide) Prior Authorization Program Summary
 Forteo (teriparatide) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1 FDA Indication 1 : Forteo (teriparatide) is indicated for: the treatment of postmenopausal women with osteoporosis
Forteo (teriparatide) Prior Authorization Program Summary FDA APPROVED INDICATIONS DOSAGE 1 FDA Indication 1 : Forteo (teriparatide) is indicated for: the treatment of postmenopausal women with osteoporosis
Correlation between Thyroid Function and Bone Mineral Density in Elderly People
 IBBJ Spring 2016, Vol 2, No 2 Original Article Correlation between Thyroid Function and Bone Mineral Density in Elderly People Ali Mirzapour 1, Fatemeh Shahnavazi 2, Ahmad Karkhah 3, Seyed Reza Hosseini
IBBJ Spring 2016, Vol 2, No 2 Original Article Correlation between Thyroid Function and Bone Mineral Density in Elderly People Ali Mirzapour 1, Fatemeh Shahnavazi 2, Ahmad Karkhah 3, Seyed Reza Hosseini
Pharmacy Management Drug Policy
 Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
Clinical criteria used to make utilization review decisions are based on credible scientific evidence published in peer reviewed medical literature generally recognized by the medical community. Guidelines
Index. B BMC. See Bone mineral content BMD. See Bone mineral density Bone anabolic impact, Bone mass acquisition
 A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
A Acid base balance dietary protein detrimental effects of, 19 Acid base balance bicarbonate effects, 176 in bone human studies, 174 mechanisms, 173 174 in muscle aging, 174 175 alkali supplementation
Chapter 39: Exercise prescription in those with osteoporosis
 Chapter 39: Exercise prescription in those with osteoporosis American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Chapter 39: Exercise prescription in those with osteoporosis American College of Sports Medicine. (2010). ACSM's resource manual for guidelines for exercise testing and prescription (6th ed.). New York:
Using the FRAX Tool. Osteoporosis Definition
 How long will your bones remain standing? Using the FRAX Tool Gary Salzman M.D. Director Banner Good Samaritan/ Hayden VAMC Internal Medicine Geriatric Fellowship Program Phoenix, Arizona Using the FRAX
How long will your bones remain standing? Using the FRAX Tool Gary Salzman M.D. Director Banner Good Samaritan/ Hayden VAMC Internal Medicine Geriatric Fellowship Program Phoenix, Arizona Using the FRAX
NIH Public Access Author Manuscript Osteoporos Int. Author manuscript; available in PMC 2011 January 8.
 NIH Public Access Author Manuscript Published in final edited form as: Osteoporos Int. 2011 January ; 22(1): 345 349. doi:10.1007/s00198-010-1179-4. Does Dietary Protein Reduce Hip Fracture Risk in Elders?
NIH Public Access Author Manuscript Published in final edited form as: Osteoporos Int. 2011 January ; 22(1): 345 349. doi:10.1007/s00198-010-1179-4. Does Dietary Protein Reduce Hip Fracture Risk in Elders?
Hellenic Endocrine Society position statement: Clinical management of Vitamin D Deficiency. Spyridon Karras MD, Phd Endocrinologist
 Hellenic Endocrine Society position statement: Clinical management of Vitamin D Deficiency Spyridon Karras MD, Phd Endocrinologist Pregnancy We recommend a minimum intake of 600 international units of
Hellenic Endocrine Society position statement: Clinical management of Vitamin D Deficiency Spyridon Karras MD, Phd Endocrinologist Pregnancy We recommend a minimum intake of 600 international units of
Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors
 University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
University of Massachusetts Amherst ScholarWorks@UMass Amherst Masters Theses 1911 - February 2014 2013 Perceived Recurrence Risk and Health Behavior Change Among Breast Cancer Survivors E Konieczny University
[If no, skip to question 10.] Y N. 2. Does the member have a diagnosis of Paget s disease of bone? Y N. [If no, skip to question 4.
![[If no, skip to question 10.] Y N. 2. Does the member have a diagnosis of Paget s disease of bone? Y N. [If no, skip to question 4. [If no, skip to question 10.] Y N. 2. Does the member have a diagnosis of Paget s disease of bone? Y N. [If no, skip to question 4.](/thumbs/86/94943423.jpg) Pharmacy Prior Authorization AETA BETTER HEALTH EW JERSE (MEDICAID) Zoledronic Acid (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Pharmacy Prior Authorization AETA BETTER HEALTH EW JERSE (MEDICAID) Zoledronic Acid (Medicaid) This fax machine is located in a secure location as required by HIPAA regulations. Complete/review information,
Keeping old bones from breaking: The diagnosis, prevention, and treatment of osteoporosis
 Keeping old bones from breaking: The diagnosis, prevention, and treatment of osteoporosis Balanced data about medications www.rxfacts.org Copyright 2010 by The Alosa Foundation. All rights reserved. www.rxfacts.org
Keeping old bones from breaking: The diagnosis, prevention, and treatment of osteoporosis Balanced data about medications www.rxfacts.org Copyright 2010 by The Alosa Foundation. All rights reserved. www.rxfacts.org
Vitamin D physiology
 Progress in Biophysics and Molecular Biology 92 (2006) 4 8 Review Vitamin D physiology P. Lips www.elsevier.com/locate/pbiomolbio Department of Endocrinology, VU University Medical Center, P.O. Box 7057,
Progress in Biophysics and Molecular Biology 92 (2006) 4 8 Review Vitamin D physiology P. Lips www.elsevier.com/locate/pbiomolbio Department of Endocrinology, VU University Medical Center, P.O. Box 7057,
The Relationship Between Serum 25(OH)D and Parathyroid Hormone Levels
 CLINICAL RESEARCH STUDY The Relationship Between Serum 25(OH)D and Parathyroid Hormone Levels Walid Saliba, MD, MPH, a Ofra Barnett, PhD, a Hedy S. Rennert, MPH, a Idit Lavi, MA, a Gad Rennert, MD, PhD
CLINICAL RESEARCH STUDY The Relationship Between Serum 25(OH)D and Parathyroid Hormone Levels Walid Saliba, MD, MPH, a Ofra Barnett, PhD, a Hedy S. Rennert, MPH, a Idit Lavi, MA, a Gad Rennert, MD, PhD
Bisphosphonates in the Management of. Myeloma Bone Disease
 Bisphosphonates in the Management of Myeloma Bone Disease James R. Berenson, MD Medical & Scientific Director Institute for Myeloma & Bone Cancer Research Los Angeles, CA Myeloma Bone Disease Myeloma cells
Bisphosphonates in the Management of Myeloma Bone Disease James R. Berenson, MD Medical & Scientific Director Institute for Myeloma & Bone Cancer Research Los Angeles, CA Myeloma Bone Disease Myeloma cells
TREATMENT OF OSTEOPOROSIS
 TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
TREATMENT OF OSTEOPOROSIS Summary Prevention is the key issue in the management of osteoporosis. HRT is the agent of choice for prevention of postmenopausal osteoporosis. Bisphosphonates and Calcitonin
ESPEN Congress Prague 2007
 ESPEN Congress Prague 2007 Key papers in the field of nutrition Dietitian Geila S Rozen Key Papers in the field of Nutrition ESPEN 2007 Prague Geila S Rozen Clinical Nutrition Dep. Rambam health campus
ESPEN Congress Prague 2007 Key papers in the field of nutrition Dietitian Geila S Rozen Key Papers in the field of Nutrition ESPEN 2007 Prague Geila S Rozen Clinical Nutrition Dep. Rambam health campus
The Role of the Laboratory in Metabolic Bone Disease
 The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
The Role of the Laboratory in Metabolic Bone Disease Howard Morris PhD, FAACB, FFSc(RCPA) President, IFCC Professor of Medical Sciences, University of South Australia, Clinical Scientist, SA Pathology
Calcium Nephrolithiasis and Bone Health. Noah S. Schenkman, MD
 Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Calcium Nephrolithiasis and Bone Health Noah S. Schenkman, MD Associate Professor of Urology and Residency Program Director, University of Virginia Health System; Charlottesville, Virginia Objectives:
Osteoporosis. Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective. Old Definition of Osteoporosis
 Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective Dr Dicky T.K. Choy Physician Jockey Club Centre for Osteoporosis Care and Control, CUHK Osteoporosis Global public health
Current Trend in Osteoporosis Management for Elderly in HK- Medical Perspective Dr Dicky T.K. Choy Physician Jockey Club Centre for Osteoporosis Care and Control, CUHK Osteoporosis Global public health
Calcium and Vitamin D Supplementation is an Ineffective Strategy for the Prevention of Fractures in Older People
 Calcium and Vitamin D Supplementation is an Ineffective Strategy for the Prevention of Fractures in Older People For the Motion: Professor Roger Francis, Institute for Ageing and Health, Newcastle University,
Calcium and Vitamin D Supplementation is an Ineffective Strategy for the Prevention of Fractures in Older People For the Motion: Professor Roger Francis, Institute for Ageing and Health, Newcastle University,
OSTEOPOROSIS: PREVENTION AND MANAGEMENT
 OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
OSTEOPOROSIS: OVERVIEW OSTEOPOROSIS: PREVENTION AND MANAGEMENT Judith Walsh, MD, MPH Departments of Medicine and Epidemiology and Biostatistics UCSF Definitions Key Risk factors Screening and Monitoring
Body Mass Index as Predictor of Bone Mineral Density in Postmenopausal Women in India
 International Journal of Public Health Science (IJPHS) Vol.3, No.4, December 2014, pp. 276 ~ 280 ISSN: 2252-8806 276 Body Mass Index as Predictor of Bone Mineral Density in Postmenopausal Women in India
International Journal of Public Health Science (IJPHS) Vol.3, No.4, December 2014, pp. 276 ~ 280 ISSN: 2252-8806 276 Body Mass Index as Predictor of Bone Mineral Density in Postmenopausal Women in India
Bone Health in Celiac Disease. Partha S. Sinha MD, PhD October 29 th, 2017
 Bone Health in Celiac Disease Partha S. Sinha MD, PhD October 29 th, 2017 No Disclosures Objectives Recognize the mechanisms by which celiac disease can affect bone health Review what diagnostic tests
Bone Health in Celiac Disease Partha S. Sinha MD, PhD October 29 th, 2017 No Disclosures Objectives Recognize the mechanisms by which celiac disease can affect bone health Review what diagnostic tests
Horizon Scanning Centre March Denosumab for glucocorticoidinduced SUMMARY NIHR HSC ID: 6329
 Horizon Scanning Centre March 2014 Denosumab for glucocorticoidinduced osteoporosis SUMMARY NIHR HSC ID: 6329 This briefing is based on information available at the time of research and a limited literature
Horizon Scanning Centre March 2014 Denosumab for glucocorticoidinduced osteoporosis SUMMARY NIHR HSC ID: 6329 This briefing is based on information available at the time of research and a limited literature
Differentiating Pharmacological Therapies for Osteoporosis
 Differentiating Pharmacological Therapies for Osteoporosis Socrates E Papapoulos Department of Endocrinology & Metabolic Diseases Leiden University Medical Center The Netherlands Competing interests: consulting/speaking
Differentiating Pharmacological Therapies for Osteoporosis Socrates E Papapoulos Department of Endocrinology & Metabolic Diseases Leiden University Medical Center The Netherlands Competing interests: consulting/speaking
Continuing Education for Pharmacy Technicians Dietary Supplements: Calcium and Vitamin D
 1 Continuing Education for Pharmacy Technicians Dietary Supplements: Calcium and Vitamin D Ashley Elliott, PharmD candidate Julie N. Bosler, PharmD McWhorter School of Pharmacy Birmingham, AL Objectives:
1 Continuing Education for Pharmacy Technicians Dietary Supplements: Calcium and Vitamin D Ashley Elliott, PharmD candidate Julie N. Bosler, PharmD McWhorter School of Pharmacy Birmingham, AL Objectives:
Aromatase Inhibitors & Osteoporosis
 Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
Aromatase Inhibitors & Osteoporosis Miss Sarah Horn Consultant Oncoplastic Breast Surgeon April 2018 Aims Role of Aromatase Inhibitors (AI) in breast cancer treatment AI s effects on bone health Bone health
Advances in Nutrition for Bone Health
 Advances in Nutrition for Bone Health IOF INTERNATIONAL OSTEOPOROSIS FOUNDATION Dominique D Pierroz, PhD, Science Manager, IOF www.iofbonehealth.org MEMBERSHIP STRUCTURE CSA Committee of Scientific Advisors
Advances in Nutrition for Bone Health IOF INTERNATIONAL OSTEOPOROSIS FOUNDATION Dominique D Pierroz, PhD, Science Manager, IOF www.iofbonehealth.org MEMBERSHIP STRUCTURE CSA Committee of Scientific Advisors
Name of Active Ingredient: Fully human monoclonal antibody to receptor activator for nuclear factor-κb ligand
 Page 2 of 1765 2. SYNOPSIS Name of Sponsor: Amgen Inc. Name of Finished Product: Denosumab (AMG 162) Name of Active Ingredient: Fully human monoclonal antibody to receptor activator for nuclear factor-κb
Page 2 of 1765 2. SYNOPSIS Name of Sponsor: Amgen Inc. Name of Finished Product: Denosumab (AMG 162) Name of Active Ingredient: Fully human monoclonal antibody to receptor activator for nuclear factor-κb
Importance of Vitamin D in Healthy Ageing. Peter Liu, B Pharmacy Market Development Manager DSM Nutritional Products Asia Pacific 11 th November 2014
 Importance of Vitamin D in Healthy Ageing Peter Liu, B Pharmacy Market Development Manager DSM Nutritional Products Asia Pacific 11 th November 2014 Healthy life expectancy the challenge! Life expectancy
Importance of Vitamin D in Healthy Ageing Peter Liu, B Pharmacy Market Development Manager DSM Nutritional Products Asia Pacific 11 th November 2014 Healthy life expectancy the challenge! Life expectancy
VITAMIN D TESTING CLINICAL GUIDELINES. Policy Number: PDS Effective Date: January 1, Table of Contents
 CLINICAL GUIDELINES VITAMIN D TESTING Policy Number: PDS - 010 Effective Date: January 1, 2013 Table of Contents Page Guidelines 1 BACKGROUND 3 CLINICAL EVIDENCE 5 U.S. FOOD AND DRUG ADMINISTRATION (FDA)
CLINICAL GUIDELINES VITAMIN D TESTING Policy Number: PDS - 010 Effective Date: January 1, 2013 Table of Contents Page Guidelines 1 BACKGROUND 3 CLINICAL EVIDENCE 5 U.S. FOOD AND DRUG ADMINISTRATION (FDA)
