The factors of deterioration in long-term clinical course of lumbar spinal canal stenosis after successful conservative treatment
|
|
|
- Anis Long
- 5 years ago
- Views:
Transcription
1 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 RESEARCH ARTICLE Open Access The factors of deterioration in long-term clinical course of lumbar spinal canal stenosis after successful conservative treatment Masanori Tsubosaka 1, Shuichi Kaneyama 1*, Tomonori Yano 2, Koichi Kasahara 1, Aritetsu Kanemura 1, Masato Takabatake 1, Hiroaki Hirata 1 and Masatoshi Sumi 1 Abstract Background: The treatment of lumbar spinal canal stenosis (LSS) depends on symptom severity. In the absence of severe symptoms such as severe motor disturbances or bowel and/or urinary dysfunction, conservative treatment is generally the first choice for the treatment of LSS. However, we experienced cases of worsening symptoms even after successful conservative treatment. The purpose of this study is to investigate the long-term clinical course of LSS following successful conservative treatment and analyze the prognostic factors associated with symptom deterioration. Methods: The study included 60 LSS patients (34 females and 26 males) whose symptoms were relieved by conservative treatment between April 2007 and March 2010 and who were followed up for 5 years or longer. The mean age at admission was 64.8 ± 8.5 years (range, years old), and the mean follow-up period was 7.3 years (range, years). We defined deterioration of symptoms as the shortening of intermittent claudication more than 50 m compared with those at discharge or the occurrence or progression of lower limb paralysis, and poor outcome as the deterioration within 5 years after discharge. The long-term outcome of conservative treatment for LSS was analyzed by Kaplan-Meier analysis. Furthermore, logistic regression analysis was performed to reveal the risk factors of poor outcome for clinical classification, severe intermittent claudication ( 100 m), lower limb muscle weakness, vertebral body slip ( 3 mm), scoliosis (Cobb angle 10 ), block on myelography, and redundant nerve roots of the cauda equina. Results: Thirty-four (56.7%) patients preserved their condition at discharge during the follow-up, whereas 26 patients (43.3%) showed deterioration. Sixteen patients had a decreased intermittent claudication distance, and 10 patients had newly developed or progressive paralysis. The probability of preservation was maintained at 68.3% at 5 years after discharge. Logistic regression analysis demonstrated that only severe intermittent claudication ( 100 m) was a significant risk factor of a poor outcome (p = 0.005, odds ratio = 6.665). Conclusions: The patients with severe intermittent claudication should be carefully followed up because those are the significant deterioration candidates despite the success in conservative treatment. Keywords: Lumbar spinal canal stenosis, Conservative treatment, Prognosis, Prognostic factors * Correspondence: syu1-k@kobeh.johas.go.jp 1 Department of Orthopaedic Surgery, Kobe Rosai Hospital, , Kagoike-dori, Chuo-ku, Kobe , Japan Full list of author information is available at the end of the article The Author(s) Open Access This article is distributed under the terms of the Creative Commons Attribution 4.0 International License ( which permits unrestricted use, distribution, and reproduction in any medium, provided you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons license, and indicate if changes were made. The Creative Commons Public Domain Dedication waiver ( applies to the data made available in this article, unless otherwise stated.
2 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 Page 2 of 8 Background Lumbar spinal canal stenosis (LSS) is a disease characterized by one or several symptoms such as low back pain, pain and/or numbness in the lower extremities, and neurogenic claudication that occurs secondary to spinal canal narrowing [1]. The treatment of LSS depends on symptom severity. The major indications for surgery are as follows: intolerable pain in daily activities despite adequate conservative treatment, progressively limited walking distance or standing endurance, and major neural deficits or evolving/progressive neural damage such as cauda equina syndrome, drop foot, and bowel and/or urinary dysfunction [2 6]. On the other hand, in the absence of severe symptoms such as severe motor disturbances or bowel and/or urinary dysfunction, conservative treatment is generally the first choice for the treatment of LSS [7 10]. Components of conservative treatment vary but generally include bed rest, medication or injection of anti-inflammatory analgesics, physical therapy or reduction of postural lordosis, and muscle weakness treatment with reportedly good outcomes [9, 11 13]. However, we experienced cases of worsening symptoms even after successful conservative treatment. Although there have been several reports regarding prognostic factors for the conservative treatment of LSS, studies with long-term follow-up have rarely been reported [9, 14, 15]. In addition, these reports did not describe the time course of the progress of symptom deterioration: when and how the symptom deteriorated in the patients with negative factors after successful conservative treatment in spite of its importance for decision-making around treatment. This study aimed to investigate the clinical course and prognosis of LSS after successful conservative treatment and identify the prognostic factors for predicting aggravation risk. Methods Study population All patients were examined by at least two physicians and diagnosed with LSS based on the symptoms (back, buttock, or leg pain and/or numbness; intermittent claudication or muscle weakness on legs), physical findings, and radiological findings demonstrating lumbar spinal canal stenosis of corresponding levels. We performed inpatient intensive conservative treatment described in the other sections if the patients had difficulty in normal daily activity in their home suffering from the symptoms which had prolonged despite outpatient conservative treatment including administration of nonsteroidal anti-inflammatory drugs, application of elastic lumbar orthosis and/or caudal block. This study was designed to include the patients who had achieved symptom relief with the inpatient intensive conservative treatment between April 2007 and March 2010 and were followed up for 5 years or longer, and excluded those who were diagnosed with lumbar disc herniation, had osteoarthritis of the knee or hip joint, had cerebrovascular diseases, or had undergone previous spinal surgery. Among 73 patients successively treated by inpatient intensive conservative treatment, 60 patients (34 females and 26 males) satisfied the criteria. The mean age at admission was 64.8 ± 8.5 years (range, years old), and the mean follow-up period was 7.3 years (range, years). The patients were clinically classified into three types as described by Miyamoto et al. [8] according to subjective symptoms and objective findings. The myelographic findings were taken into account in the objective findings. The myelographic findings were classified into three groups: completely blocked centrally (6 cases), centrally blocked but not completely (19 cases), and root defect (35 cases). Furthermore, the presence or absence of redundant nerve roots of the cauda equina was also considered (presence, 11 cases; absence, 49 cases). In consideration of these objective findings in addition to the subjective findings, the classification was carried out in three types as follows: radicular, 39 cases; cauda equina, 12 cases; and mixed, 9 cases. The hospital ethics committee approved the study protocol, and the patients provided informed consent for participation. Inpatient intensive conservative treatment Our protocol for inpatient conservative treatment consisted of pelvic traction, the application of a body cast, and an epidural steroid injection such as an epidural or selective nerve root block. Conservative treatment was performed in a phased manner from least invasive (pelvic traction) to most invasive (selective nerve root block) until the symptoms improved. Patients were normally admitted for 2 3 weeks. Pelvic traction was used 8 h a day to force patients into a jack-knife position and was applied for 2 3 days as a guide. The traction force was also applied one third of his/her weight. If pelvic traction was ineffective, a body cast was applied for 2 or 3 days to force the patient s lumbar spine into a slightly flexed position. The reason for adopting a slightly flexed position of the lumbar spine was that it was reported that the cross-sectional area of the spinal canal had been shown to decrease with extension and increase with flexion [16]. If the body cast was effective, a Williams corset was occasionally fitted after discharge. The patients were asked to wear a Williams corset mainly when going out during lifetime. An epidural block (10.0 ml of 1.0% xylocaine mixed with 10.0 mg of water-soluble predonine) was injected into the epidural space a maximum of two times. A selective nerve root block (1.5 ml of 1.0% xylocaine mixed with 10.0 mg of water-soluble predonine) was administered around the epiradicular membrane under
3 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 Page 3 of 8 fluoroscopy guidance for radicular pain a maximum of two times. Outcome evaluation The patients were routinely followed up with the physical or radiographic examination in the outpatient clinic after discharge. The physical or radiographic examination follow-up timings were 3, 6, and 12 months and every year after discharge. During follow-up, the symptoms were considered to deteriorate if the patient presented a shortening intermittent claudication distance more than 50 m and/or had a worse neurological defect than that at discharge (deterioration group). The neurological defect was defined as a drop of manual muscle test more than one grade. Symptoms were considered preserved if the patient showed no deterioration (preservation group). An outcome was defined as poor when the patient experienced deterioration by 5 years post-discharge. The long-term outcomes of conservative treatment for LSS were assessed by Kaplan-Meier analysis. The patients were stratified according to the following factors: age ( 65 years or > 65 years), severe intermittent claudication at the initial visit ( 100 m), clinical classification (radicular type or cauda equina and mixed type), lower limb muscle weakness, vertebral body slip ( 3 mm), scoliosis (Cobb angle 10 ), block on myelography, and redundant nerve roots of the cauda equina. The vertebral body slip was assessed on lateral radiographs of the lumbar spine and measured the sagittal distance of the slipped vertebral body. The redundant nerve root means the redundancy of cauda equina. Differences in outcomes were analyzed in each group by the log-rank test. Furthermore, the risk factors incurring a poor outcome even after successful conservative treatment for LSS were analyzed using logistic regression analysis of the factors listed above. Differences of age, sex, clinical LSS classification, the presence or absence of intermittent claudication, muscle weakness, vertebral body slip, scoliosis, block on myelography, and redundant nerve root between the preservation group and the deterioration group were also analyzed by the chi-square test. p values < 0.05 were considered statistically significant. Results Thirty-four patients (56.7%) preserved the conditions at discharge until the latest follow-up, while 26 patients (43.3%) showed deterioration during the follow-up period. The average age of the patients who showed deterioration during the follow-up period (67.8 ± 6.9 years) was significantly higher than that of the patients whose conditions at discharge were preserved (62.5 ± 8.8 years). Furthermore, the patients with severe intermittent claudication, muscle weakness, and redundant nerve root tend to be significantly worse of their symptoms. On the other hand, there were no significant differences in sex, clinical LSS classification and the presence of vertebral body slip, scoliosis, and block of myelography between the preservation group and deterioration group (Table 1). In the preservation group, 3 patients had no symptoms, 20 patients had minor symptoms such as slight low back pain or numbness of the lower extremities, and 11 patients needed only medication therapy at the latest follow-up. On the other hand, of the patients with deterioration, 16 patients had a decreased intermittent claudication distance more than 50 m and 10 patients had newly developed or progressive paralysis. Subsequently, 19 patients received surgical intervention. The patients who got worse of their symptoms after discharge and then were performed conservative treatment were 3 patients of 26 patients with deterioration. The inpatient conservative treatment also consisted of pelvic traction, the application of a body cast, and an epidural steroid injection such as an epidural or selective nerve root block as described before. All these 3 patients received conservative treatment only once; however, 2 patients of them received surgical intervention after the second conservative treatment. Although the probability of symptom preservation after the successful conservative treatment of LSS gradually decreased over time, it remained 68.3% at 5 years post-discharge and 57.2% at 7 years post-discharge (Fig. 1). The number of patients who were able to follow up was 39 to 7 years after discharge. The outcomes of conservative treatment were worse in patients with severe intermittent claudication at the initial visit ( 100 m), cauda equina or mixed-type LSS, lower limb muscle weakness, and block on myelography than those in patients with mild intermittent claudication (between 100 and 500 m) (p = 0.004), radicular-type LSS (p = 0.039), no muscle weakness (p = 0.049), and no block on myelography (p = 0.045), respectively (Fig. 2a d). The probability of symptom preservation at 5 years and median preservation expectancy in patients with severe intermittent claudication ( 100 m) were 38.9% and 4.1 years, respectively, whereas those in patients with mild intermittent claudication (between 100 and 500 m) were 81.1% and > 10 years. Similarly, in patients with the cauda equina and mixed types, the 5-year preservation probability and preservation expectancy were 52.4% and 5.8 years, respectively, whereas those in patients with the radicular type were 76.9% and 9.5 years. On the other hand, the 5-year preservation probabilities in patients with and without muscle weakness were 63.6% and 71.1%, although preservation expectancies were 5.8 years and > 10 years. In patients with and without block on myelography, the 5-year preservation probabilities were 60.0% and 74.3%, whereas preservation expectancies were 5.8 years and 9.5 years (Table 2). Age, vertebral body slip ( 3mm), scoliosis (Cobb angle 10 ), and redundant nerve roots of the cauda equina did not significantly influence symptom deterioration (Fig. 3a d). Logistic regression analysis
4 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 Page 4 of 8 Table 1 Patient population Preservation group Deterioration group p value No. of patients Age (years) 62.5 ± ± * Male/female 11/23 15/ Clinical classification Radicular type Cauda equina type 5 7 Mixed type 4 5 Intermittent claudication 0.005* Severe ( 100 m) 5 13 Mild (> 100 m) Muscle weakness 0.029* Presence 8 14 Absence Vertebral body slip ( 3 mm) Presence 17 9 Absence Scoliosis (Cobb angle 10 ) Presence 7 3 Absence Block on myelography Completely blocked Not completely blocked 8 11 Root defect 2 4 Redundant nerve roots 0.044* Presence 3 8 Absence *Statistically significant demonstrated that only severe intermittent claudication at the initial visit ( 100 m) was a significant risk factor incurring a poor outcome even after successful conservative treatment for LSS (p =0.005, odds ratio=6.665, correlation coefficient = 0.492) (Table 3). A post hoc power analysis demonstrated that the present study was enough powered with a power of to detect differences between the patients with poor prognosis and good prognosis and that required sample size was 16/38 patients for the patients with poor/good prognosis, respectively. Discussion Several reports have compared conservative and surgical treatments for LSS [14, 17, 18]. Amundsen et al. reported that the long-term results were better for surgery in a prospective 10-year follow-up study. However, more than half of the conservatively treated patients had a satisfactory outcome, and delaying surgery for some months did not worsen the prognosis. Therefore, a primarily conservative approach is recommended [14]. In their prospective 8- to 10-year follow-up study, Atlas et al. reported that low back pain relief, predominant symptom (either back or leg pain) improvement, and satisfaction were similar among patients who initially underwent surgery and those treated conservatively [17]. The randomized controlled trial study by Malmivaara et al. reported that patients treated both surgically and conservatively showed improved clinical outcomes in a 2-year follow-up [18]. Therefore, an initial conservative treatment approach seems advisable for appropriately selected patients. Actually, we showed 56.7% of LSS patients treated by inpatient intensive conservative treatment maintained their condition at discharge for at least 5 years, average 7.3 years follow-up. Although there have been differences in evaluation methods or primal symptom severity, the reported outcomes of conservative treatment for LSS are generally good [7 10]. Johnson et al. reported 32 LSS patients who had conservative treatment, and the mean Fig. 1 Long-term results of conservative treatment for LSS in this study. The probability of symptom preservation after the successful conservative treatment of LSS remained at 68.3% 5 years post-discharge and 57.2% 7 years post-discharge
5 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 Page 5 of 8 Fig. 2 a Comparison of symptom preservation in patients with severe versus mild intermittent claudication using Kaplan-Meier analysis. The outcomes of conservative treatment were worse in patients with severe intermittent claudication at the initial visit ( 100 m) than those in patients with mild intermittent claudication (between 100 and 500 m) (p = 0.004). b Comparison of symptom preservation in patients with radicular versus cauda equina or mixed type using Kaplan-Meier analysis. The outcomes of conservative treatment were worse in patients with cauda equina or mixed-type LSS than those in patients with radicular-type LSS (p = 0.039). c Comparison of symptom preservation in patients with versus without lower limb weakness using Kaplan-Meier analysis. The outcomes of conservative treatment were worse in patients with lower limb muscle weakness than those in patients with no muscle weakness (p =0.049).d Comparison of symptom preservation by absence or presence of block on myelography using Kaplan-Meier analysis. The outcomes of conservative treatment were worse in patients with block on myelography than those in patients with no block on myelography (p = 0.045) follow-up period was 4.1 years. Fifteen percent improved, 70% remained unchanged, and 15% deteriorated as assessed by the evaluation with the visual analog scale while 47% improved, 37% remained unchanged, and 16% deteriorated as assessed by the evaluation with their clinical examination [7]. Swezey reported 36 LSS patients who had conservative treatment by intermittent traction and/or epidural steroid injection, and the mean follow-up period was 5 years. Forty-three percent improved and 30% remained unchanged as assessed by a subjective assessment by using a telephone interview [10]. Miyamoto et al. reported 120 LSS patients who had conservative treatment by pelvic traction, application of body cast, and/or epidural steroid injection, and the mean follow-up period was 7.9 years. Forty-three percent improved, 17% remained unchanged, and 40% deteriorated as assessed by using a general evaluation with a modified JOA score [8]. Simotas et al. reported 49 LSS patients who had conservative treatment by exercise and analgesics and/or epidural steroid injection, and the mean follow-up period was 2.8 years. Forty-seven percent improved, 24% remained unchanged, and 29% deteriorated as assessed by using the pain/function score [9]. Our inpatient intensive conservative treatment was applied to the patients who failed to get satisfied with symptom relief by outpatient conservative treatment and demonstrated to be effective even for such persistent cases. Therefore, we believe Table 2 Five-year preservation probability and median preservation expectancy Factor 5-year preservation probability (%) Median preservation expectancy (years) Severe intermittent claudication Mild intermittent claudication 81.1 Over 10 Cauda equina and mixed type of LSS Radicular type of LSS Muscle weakness No muscle weakness 71.1 Over 10 Block on myelography No block on myelography
6 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 Page 6 of 8 Fig. 3 a Comparison of symptom preservation in patients 65 versus > 65 years of age using Kaplan-Meier analysis. Age did not significantly influence symptom deterioration. b Comparison of symptom preservation in patients with versus without vertebral body slip using Kaplan-Meier analysis. Vertebral body slip ( 3 mm) did not significantly influence symptom deterioration. c Comparison of symptom preservation in patients with versus without scoliosis using Kaplan-Meier analysis. Scoliosis (Cobb angle 10 ) did not significantly influence symptom deterioration. d Comparison of symptom preservation in patients with the presence or absence of redundant nerve roots of the cauda equina Kaplan-Meier analysis. Redundant nerve roots of the cauda equina did not significantly influence symptom deterioration that such inpatient conservative treatment should be positioned between outpatient conservative treatment and surgery. The predictive factors for the prognosis of conservative treatment for LSS have been investigated in several studies [8, 9, 14, 15]. Although Herno et al. [15] and Amundsen et al. [14] failed to identify any predictive factors, Simotas et al. referred to the presence of degenerative scoliosis and advanced age as negative factors for the outcomes of conservative treatment [9], and Miyamoto et al. cited degenerative scoliosis as a negative factor in outcomes and reported that radicular LSS was a positive factor for outcomes [8]. However, these reports described only the prognostic factors at final follow-up and lacked the information regarding the time course and risk factors of symptom deterioration. It is indispensable to know when and how many patients experienced symptom deterioration after successful conservative treatment for making a decision whether or not to have surgery without trying intensive conservative treatment. Our current study revealed prognostic factors and detailed clinical course of the symptom deterioration in LSS patients who once experienced symptom relief. Severe intermittent claudication at the initial visit ( 100 m), cauda equina or mixed type, lower limb muscle weakness, and block on myelography were identified as risk factors for symptom deterioration. Among them, severe intermittent claudication ( 100 m) was the only risk factor for symptom deterioration within 5 years post-discharge. In patients with severe intermittent claudication at the initial visit ( 100 m), deterioration was seen in 0.0% of patients by 3.6 years and increased to Table 3 Logistic regression analysis of prognostic factors Factor Regression coefficient Standard error Odds ratio p value 95% confidence interval 65 years or > 65 years Clinical classification Muscle weakness in lower limb Intermittent claudication at the initial visit (severe) * Vertebral body slip (3 mm or more) Scoliosis (Cobb angle 10 or greater) Block on myelography Redundant nerve roots of cauda equina *Statistically significant
7 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 Page 7 of % by 4.3 years after discharge. Hence, surgery may be considered for patients with severe intermittent claudication ( 100 m) since its symptoms are indicative of deterioration from an early stage after discharge even if they temporarily improved. Conversely, patients with mild claudication (between 100 and 500 m) should not require early surgical treatment since symptom preservation would be expected for 10 years post-discharge. Although the long-term outcomes of cauda equina and mixed LSS were worse than those of radicular LSS, cauda equina and mixed LSS were not identified as risk factors of a poor outcome. Actually, patients in cauda equina and mixed LSS were more likely to feature severe intermittent claudication (9 out of 21 patients, 42.9%) than those in radicular LSS (9 out of 39 patients, 23.1%) even though there was no statistical significance (p = 0.110). Therefore, it is considered that there was a potential confounder between the clinical classification and severity of LSS, and classification of LSS did not affect the long-term outcome after conservative treatment of LSS directly but had indirect influence through the severity of intermittent claudication. Interestingly, in patients with lower limb muscle weakness and block on myelography, there were relatively small differences in preservation probability from those of patients without these features until 5 years post-discharge despite significant differences in long-term outcomes. The differences in long-term outcomes between patients with and without muscle weakness or block on myelography should depend on symptom deterioration after 5 years of follow-up. Regular follow-up for > 5 years after discharge in these patients is important; otherwise, surgery can be considered for patients with a life expectancy > 5 years. Limitations The present study has some limitations. The largest limitation to this study is the relatively small sample size. We had only 60 patients followed longer than 5 years after successive conservative treatment of LSS. Although the power analysis showed strong statistical power, the sample size might be still insufficient to make conclusive statements. Therefore, our conclusion should be considered provisional and needs to be supported by a study with a larger patient population. Second, a mixed degree of symptom was included. The symptom at discharge after successful conservative treatment varied among patients because it depends a lot on the patients satisfaction, activity of daily life, or living environment. However, subjective evaluation by patients should be one of the most important outcomes. In the future study, it would be advisable to perform a survey using patient self-reporting measurement. Third, patients who had symptoms of LSS due to lumbar disc herniation may have been included,so the findings of these patients may be different. Lastly, more detailed radiological analysis such as lumbar canal diameters and quantification of the stenosis was not investigated. So, in the future, these factors should be investigated as prognostic factors of LSS after successful conservative treatment. Conclusions Here, we investigated the prognosis of patients with LSS after successful conservative treatment. Cauda equina or mixed type, severe intermittent claudication at the initial visit ( 100 m), lower limb muscle weakness, and the block on myelography were the prognostic factors predicting the risk of aggravation. Surgery should be considered for patients with severe intermittent claudication. Abbreviation LSS: Lumbar spinal canal stenosis Funding This research was supported by research funds to promote the hospital funding of Japan Organization of Occupational Health and Safety. Availability of data and materials Please contact the author for data requests. Authors contributions MTs investigated the parameters and also wrote the manuscript. SK designed the study, performed the statistical analysis and helped to revise the manuscript. TY participated in the design of the study and helped to collect patients data. KK collected the radiographs and patients data. AK performed the clinical examination of patients physical findings. MTa classified radiological findings. HH helped to collect patients radiological and physical data. MS conceived of the study and participated in its design and coordination and helped to draft the manuscript. All authors read and approved the final manuscript. Ethics approval and consent to participate The ethics committee of Kobe Rosai Hospital approved the study protocol, and the patients provided informed consent for participation. Consent for publication Not applicable. Competing interests The authors declare that they have no competing interests. Publisher s Note Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations. Author details 1 Department of Orthopaedic Surgery, Kobe Rosai Hospital, , Kagoike-dori, Chuo-ku, Kobe , Japan. 2 Department of Orthopaedic Surgery, Hyogo Rehabilitation Centre Central Hospital, 1070 Akebono-cho, Nishi-ku, Kobe , Japan. Received: 22 October 2017 Accepted: 10 September 2018 References 1. Arnoldi CC, Brodsky AE, Cauchoix J, Crock HV, Dommisse GF, Edgar MA, Gargano FP, Jacobson RE, Kirkaldy-Willis WH, Kurihara A, Langenskiold A, Macnab I, McIvor GW, Newman PH, Paine KW, Russin LA, Sheldon J, Tile M, Urist MR, Wilson WE, Wiltse LL. Lumbar spinal stenosis and nerve root entrapment syndromes. Definition and classification. Clin Orthop Relat Res. 1976;(115): Getty CJ. Lumbar spinal stenosis: the clinical spectrum and the results of operation. J Bone Joint Surg Br. 1980;62-b(4):481 5.
8 Tsubosaka et al. Journal of Orthopaedic Surgery and Research (2018) 13:239 Page 8 of 8 3. Grabias S. Current concepts review. The treatment of spinal stenosis. J Bone Joint Surg Am. 1980;62(2): Hutter CG. Spinal stenosis and posterior lumbar interbody fusion. Clin Orthop Relat Res. 1985;(193): Katz JN, Lipson SJ, Larson MG, McInnes JM, Fossel AH, Liang MH. The outcome of decompressive laminectomy for degenerative lumbar stenosis. J Bone Joint Surg Am. 1991;73(6): Wiltse LL, Kirkaldy-Willis WH, McIvor GW. The treatment of spinal stenosis. Clin Orthop Relat Res. 1976;(115): Johnsson KE, Rosen I, Uden A. The natural course of lumbar spinal stenosis. Clin Orthop Relat Res. 1992;279: Miyamoto H, Sumi M, Uno K, Tadokoro K, Mizuno K. Clinical outcome of nonoperative treatment for lumbar spinal stenosis, and predictive factors relating to prognosis, in a 5-year minimum follow-up. J Spinal Disord Tech. 2008;21(8): Simotas AC, Dorey FJ, Hansraj KK, Cammisa F Jr. Nonoperative treatment for lumbar spinal stenosis. Clinical and outcome results and a 3-year survivorship analysis. Spine (Phila Pa 1976). 2000;25(2): discussions Swezey RL. Outcomes for lumbar stenosis. J Clin Rheumatol. 1996;2(3): Kirkaldy-Willis WH, Paine KW, Cauchoix J, McIvor G. Lumbar spinal stenosis. Clin Orthop Relat Res. 1974;99: Kopp JR, Alexander AH, Turocy RH, Levrini MG, Lichtman DM. The use of lumbar extension in the evaluation and treatment of patients with acute herniated nucleus pulposus. A preliminary report. Clin Orthop Relat Res. 1986;(202): Porter RW, Hibbert C, Wellman P. Backache and the lumbar spinal canal. Spine (Phila Pa 1976). 1980;5(2): Amundsen T, Weber H, Nordal HJ, Magnaes B, Abdelnoor M, Lilleas F. Lumbar spinal stenosis: conservative or surgical management?: a prospective 10-year study. Spine (Phila Pa 1976). 2000;25(11): discussion Herno A, Airaksinen O, Saari T, Sihvonen T. Surgical results of lumbar spinal stenosis. A comparison of patients with or without previous back surgery. Spine (Phila Pa 1976). 1995;20(8): Ciricillo SF, Weinstein PR. Lumbar spinal stenosis. West J Med. 1993;158(2): Atlas SJ, Keller RB, Wu YA, Deyo RA, Singer DE. Long-term outcomes of surgical and nonsurgical management of lumbar spinal stenosis: 8 to 10 year results from the Maine Lumbar Spine Study. Spine (Phila Pa 1976). 2005;30(8): Malmivaara A, Slatis P, Heliovaara M, Sainio P, Kinnunen H, Kankare J, Dalin- Hirvonen N, Seitsalo S, Herno A, Kortekangas P, Niinimaki T, Ronty H, Tallroth K, Turunen V, Knekt P, Harkanen T, Hurri H. Surgical or nonoperative treatment for lumbar spinal stenosis? A randomized controlled trial. Spine (Phila Pa 1976). 2007;32(1):1 8.
QF-78. S. Tanaka 1, T.Yokoyama 1, K.Takeuchi 1, K.Wada 2, T. Tanaka 2, S.Abrakawa 2, G.Kumagai 2, T.Asari 2, A.Ono 2, Y.
 QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
QF-78 Patient-oriented outcomes after musclepreserving interlaminar decompression for patients with lumbar spinal canal stenosis: Multi-center study to identify risk factors for poor outcomes S. Tanaka
Evidence Table. Study Type: Randomized controlled trial. Study Aim: To evaluate the safety and efficacy of the X-Stop interspinous implant.
 Evidence Table Clinical Area: Reference: Spinal decompression device for lumbar spinal stenosis Zucherman JF et al. A prospective randomized multi-center study for the treatment of lumbar spinal stenosis
Evidence Table Clinical Area: Reference: Spinal decompression device for lumbar spinal stenosis Zucherman JF et al. A prospective randomized multi-center study for the treatment of lumbar spinal stenosis
Ioannis D. GELALIS, Christina ARNAOUTOGLOU, Giorgos CHRISTOFOROU, Marios G. LYKISSAS, Ioannis BATSILAS, Theodoros XENAKIS
 ACTA ORTHOPAEDICA et TRAUMATOLOGICA TURCICA Acta Orthop Traumatol Turc 2010;44(3):235-240 doi:10.3944/aott.2010.2278 Prospective analysis of surgical outcomes in patients undergoing decompressive laminectomy
ACTA ORTHOPAEDICA et TRAUMATOLOGICA TURCICA Acta Orthop Traumatol Turc 2010;44(3):235-240 doi:10.3944/aott.2010.2278 Prospective analysis of surgical outcomes in patients undergoing decompressive laminectomy
Lumbar spinal stenosis (LSS),
 Clin Orthop Relat Res (2017) 475:2632 2637 / DOI 10.1007/s11999-017-5452-0 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 28 July
Clin Orthop Relat Res (2017) 475:2632 2637 / DOI 10.1007/s11999-017-5452-0 Clinical Orthopaedics and Related Research A Publication of The Association of Bone and Joint Surgeons Published online: 28 July
Natural Evolution of Lumbar Spinal Stenosis
 Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
Natural Evolution of Lumbar Spinal Stenosis William R. Sears, MB BS FRACS Wentworth Spine Clinic, Sydney, Australia MUST KNOW An understanding of the natural evolution of lumbar spinal stenosis (LSS) is
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
LUMBAR SPINAL STENOSIS Always occurs in the mobile segment. Factors play role in Stenosis Pre existing congenital or developmental narrowing of the lumbar spinal canal Translation of one anatomic segment
The effect of duration of symptoms on standard outcome measures in the surgical treatment of spinal stenosis
 Eur Spine J (2007) 16: 199 206 DOI 10.1007/s00586-006-0078-z ORIGINAL ARTICLE Leslie C. L. Ng Suhayl Tafazal Philip Sell The effect of duration of symptoms on standard outcome measures in the surgical
Eur Spine J (2007) 16: 199 206 DOI 10.1007/s00586-006-0078-z ORIGINAL ARTICLE Leslie C. L. Ng Suhayl Tafazal Philip Sell The effect of duration of symptoms on standard outcome measures in the surgical
Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report
 ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
ISPUB.COM The Internet Journal of Neurosurgery Volume 5 Number 1 Bilateral Foot Drop Without Cauda Equinae Syndrome Due To L4-L5 Disc Prolapse: A Case Report R Ramnaryan, C Palinikumar Citation R Ramnaryan,
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Cover Page The handle http://hdl.handle.net/1887/29800 holds various files of this Leiden University dissertation. Author: Moojen, Wouter Anton Title: Introducing new implants and imaging techniques for
Changes in Spinal Canal Diameter and Vertebral Body Height with Age
 Original Article http://dx.doi.org/1.3349/ymj.213.54.6.1498 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 54(6):1498-154, 213 Changes in Spinal Canal Diameter and Vertebral Body Height with Age Kyung
Original Article http://dx.doi.org/1.3349/ymj.213.54.6.1498 pissn: 513-5796, eissn: 1976-2437 Yonsei Med J 54(6):1498-154, 213 Changes in Spinal Canal Diameter and Vertebral Body Height with Age Kyung
Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression and Fusion
 Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Egyptian Journal of Neurosurgery Volume 9 / No. 4 / October - December 014 51-56 Original Article Management of Single Level Lumbar Degenerative Spondylolisthesis: Decompression Alone or Decompression
Does functional evaluation and magnetic resonance imaging finding in a case of lumbar canal stenosis co-relate: a study of 50 cases
 International Journal of Research in Orthopaedics Hussain N et al. Int J Res Orthop. 2017 Jul;3(4):751-755 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20172543
International Journal of Research in Orthopaedics Hussain N et al. Int J Res Orthop. 2017 Jul;3(4):751-755 http://www.ijoro.org Original Research Article DOI: http://dx.doi.org/10.18203/issn.2455-4510.intjresorthop20172543
Peggers Super Summaries: The Aging Spine
 Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
Aging Spine: AGING PROCESS Osteopenia 10% of 50 year old males and 25% of 50 year females Disc dehydration Facet degeneration Soft tissue hypertrophy 2 0 deformity Leg pain worse than back pain from nerve
Dong-il Yuk, In-su Sung, Da-hyung Song, Min-jung Kim, Kown-eui Hong*
 ISSN 2093-6966 [Print], ISSN 2234-6856 [Online] Journal of Pharmacopuncture 2013;16[3]:046-051 DOI: http://dx.doi.org/10.3831/kpi.2013.16.017 Original article Clinical Study of Lumbar Spine Stenosis Treated
ISSN 2093-6966 [Print], ISSN 2234-6856 [Online] Journal of Pharmacopuncture 2013;16[3]:046-051 DOI: http://dx.doi.org/10.3831/kpi.2013.16.017 Original article Clinical Study of Lumbar Spine Stenosis Treated
Study of relationship between area of lumbar spinal canal and severity of symptoms in cases of lumbar canal stenosis
 Original article Study of relationship between area of lumbar spinal canal and severity of symptoms in cases of lumbar canal stenosis *Dr. Shashank Raut 1,Dr.Ajay Chandanwale 1, Dr.Ujjwal Wankhade 1, Dr.Rahul
Original article Study of relationship between area of lumbar spinal canal and severity of symptoms in cases of lumbar canal stenosis *Dr. Shashank Raut 1,Dr.Ajay Chandanwale 1, Dr.Ujjwal Wankhade 1, Dr.Rahul
Degenerative Disease of the Spine
 Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Degenerative Disease of the Spine Introduction: I. Anatomy Talk Overview II. Overview of Disease Processes: A. Spondylosis B. Intervertebral Disc Disease III. Diagnosis IV. Therapy Introduction: Myelopathy
Key words: Spinal Stenosis, Walking, Lumbar Region, Low Back Pain, Physiotherapy, Randomized Controlled Trial, Exercise Therapy, Back Pain
 Treadmill walking with body weight support is no more effective than cycling when added to an exercise program for lumbar spinal stenosis: a randomised controlled trial Yong-Hao Pua 1,2, Cong-Cong Cai
Treadmill walking with body weight support is no more effective than cycling when added to an exercise program for lumbar spinal stenosis: a randomised controlled trial Yong-Hao Pua 1,2, Cong-Cong Cai
Patient Selection and Lumbar Operative Interventions
 Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Patient Selection and Lumbar Operative Interventions John C France MD Professor of Orthopaedic & Neurosurgery West Virginia University Low back pain is a symptom not a diagnosis Epidemiology of LBP General
Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis
 Journal of Orthopaedic Surgery 2006;14(1):21-6 Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis DN Inamdar, M Alagappan, L Shyam, S Devadoss,
Journal of Orthopaedic Surgery 2006;14(1):21-6 Posterior lumbar interbody fusion versus intertransverse fusion in the treatment of lumbar spondylolisthesis DN Inamdar, M Alagappan, L Shyam, S Devadoss,
Cervical intervertebral disc disease Degenerative diseases F 04
 Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Cervical intervertebral disc disease Degenerative diseases F 04 How is a herniated cervical intervertebral disc treated? Conservative treatment is generally sufficient for mild symptoms not complicated
Lumbar Spinal Stenosis in Older Adults - Gender Differences
 Macedonian Journal of Medical Sciences. 2009 Sep 15; 2(3):200-204. doi:10.3889/mjms.1857-5773.2009.0062 Basic Science OPEN ACCESS Lumbar Spinal Stenosis in Older Adults - Gender Differences Niki Matveeva
Macedonian Journal of Medical Sciences. 2009 Sep 15; 2(3):200-204. doi:10.3889/mjms.1857-5773.2009.0062 Basic Science OPEN ACCESS Lumbar Spinal Stenosis in Older Adults - Gender Differences Niki Matveeva
Does Multilevel Lumbar Stenosis Lead to Poorer Outcomes?
 Does Multilevel Lumbar Lead to Poorer Outcomes? A Subanalysis of the Spine Patient Outcomes Research Trial (SPORT) Lumbar Study Daniel K. Park, MD,* Howard S. An, MD,* Jon D. Lurie, MD, MS, Wenyan Zhao,
Does Multilevel Lumbar Lead to Poorer Outcomes? A Subanalysis of the Spine Patient Outcomes Research Trial (SPORT) Lumbar Study Daniel K. Park, MD,* Howard S. An, MD,* Jon D. Lurie, MD, MS, Wenyan Zhao,
Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up
 Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Washington University School of Medicine Digital Commons@Becker Open Access Publications 8-1-2006 Nerve root blocks in the treatment of lumbar radicular pain: A minimum five-year follow-up K. Daniel Riew
Spinal Stenosis Surgical
 Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Spinal Stenosis Surgical Disclaimer This movie is an educational resource only and should not be used to make a decision on. All decisions about surgery must be made in conjunction with your surgeon or
Lumbar spinal canal stenosis Degenerative diseases F 08
 What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
What is lumbar spinal canal stenosis? This condition involves the narrowing of the spinal canal, and of the lateral recesses (recesssus laterales) and exit openings (foramina intervertebralia) for the
SpineFAQs. Lumbar Spondylolisthesis
 SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
SpineFAQs Lumbar Spondylolisthesis Normally, the bones of the spine (the vertebrae) stand neatly stacked on top of one another. The ligaments and joints support the spine. Spondylolisthesis alters the
Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with and without Instrumentation
 Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
Document heading doi: 10.21276/apjhs.2017.4.1.18 Research Article Comparative Analysis of outcome in patients of Lumbar Canal Stenosis undergoing decompression with without Instrumentation ABSTRACT Sanjay
The Comparison of the Result of Epiduroscopic Laser Neural Decompression between FBSS or Not
 Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Original Article Korean J Pain 2014 January; Vol. 27, No. 1: 63-67 pissn 2005-9159 eissn 2093-0569 http://dx.doi.org/10.3344/kjp.2014.27.1.63 The Comparison of the Result of Epiduroscopic Laser Neural
Corporate Medical Policy
 Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Corporate Medical Policy Epidural Steroid Injections for Back Pain File Name: Origination: Last CAP Review: Next CAP Review: Last Review: epidural_steroid_injections_for_back_pain 2/2016 4/2017 4/2018
Life can cause spinal stenosis. Take yours back with Superion.
 Indirect Decompression System Life can cause spinal stenosis. Take yours back with Superion. Superion can help you take back your life with a simple new procedure. What is spinal stenosis? Your spine is
Indirect Decompression System Life can cause spinal stenosis. Take yours back with Superion. Superion can help you take back your life with a simple new procedure. What is spinal stenosis? Your spine is
Jessica Jameson MD Post Falls, ID
 Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
Jessica Jameson MD Post Falls, ID Discuss the history of interventiona l pain Discuss previous tools to manage chronic pain Discuss current novel therapies to manage chronic pain and indications HISTORY
Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS NASS COVERAGE POLICY RECOMMENDATIONS TASKFORCE
 NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
NASS COVERAGE POLICY RECOMMENDATIONS Lumbar Laminotomy DEFINING APPROPRIATE COVERAGE POSITIONS North American Spine Society 7075 Veterans Blvd. Burr Ridge, IL 60527 TASKFORCE Introduction North American
The Efficacy of Physical Therapy and Physical Therapy Plus Calcitonin in the Treatment of Lumbar Spinal Stenosis
 Original Article DOI 10.3349/ymj.2009.50.5.683 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(5): 683-688, 2009 The Efficacy of Physical Therapy and Physical Therapy Plus Calcitonin in the Treatment
Original Article DOI 10.3349/ymj.2009.50.5.683 pissn: 0513-5796, eissn: 1976-2437 Yonsei Med J 50(5): 683-688, 2009 The Efficacy of Physical Therapy and Physical Therapy Plus Calcitonin in the Treatment
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽
 외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
외래에서흔히접하는 요통환자의진단과치료 울산의대서울아산병원가정의학과 R3 전승엽 Index Introduction Etiology & Type Assessment History taking & Physical examination Red flag sign Imaging Common disorder Management Reference Introduction Pain
Get back to: my life. Non-fusion treatment for lumbar spinal stenosis
 Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Get back to: my life Non-fusion treatment for lumbar spinal stenosis Do you have any of these symptoms? numbness, weakness or pain in the lower legs When any of these conditions occur, the spinal nerve,
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Low back pain
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: lumbar_spine_fusion_surgery 9/2010 5/2017 5/2018 5/2017 Description of Procedure or Service Low back pain
Wendy Field Advanced Physiotherapy Practitioner June 2018
 Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Wendy Field Advanced Physiotherapy Practitioner June 2018 Radiculopathy???? Lumbar radicular pain is where the clinician suspects the pain is coming from a lumbar nerve root. Essentially we are looking
Lumbar Spinal Stenosis
 Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Lumbar Spinal Stenosis This article is also available in Spanish: Estenosis de la columna lumbar (topic.cfm?topic=a00701). A common cause of low back and leg pain is lumbar spinal stenosis. As we age,
Myeloscopic observation of adhesive arachnoiditis in patients with lumbar spinal canal stenosis
 Spinal Cord (1996) 34, 403-410 1996 International Medical Society of Paraplegia All rights reserved 1362-4393/96 $12.00 Myeloscopic observation of adhesive arachnoiditis in patients with lumbar spinal
Spinal Cord (1996) 34, 403-410 1996 International Medical Society of Paraplegia All rights reserved 1362-4393/96 $12.00 Myeloscopic observation of adhesive arachnoiditis in patients with lumbar spinal
Lumbar Stenosis Rehabilitation Using the Resistance Chair
 PRODUCTS HELPING PEOPLE HELP THEMSELVES! Lumbar Stenosis Rehabilitation Using the Resistance Chair a. Description Lumbar spinal stenosis is a term used to describe a narrowing of the spinal canal. The
PRODUCTS HELPING PEOPLE HELP THEMSELVES! Lumbar Stenosis Rehabilitation Using the Resistance Chair a. Description Lumbar spinal stenosis is a term used to describe a narrowing of the spinal canal. The
Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report
 Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
Journal of Orthopaedic Surgery 2003: 11(2): 202 206 Degenerative spondylolisthesis at the L4 L5 in a 32-year-old female with previous fusion for idiopathic scoliosis: A case report RB Winter Clinical Professor,
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE
 CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
CERVICAL SPONDYLOSIS & CERVICAL DISC DISEASE Cervical spondylosis l Cervical osteophytosis l Most common progressive disease in the aging cervical spine l Seen in 95% of the people by 65 years Pathophysiology
Comprehension of the common spine disorder.
 Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
Objectives Comprehension of the common spine disorder. Disc degeneration/hernia. Spinal stenosis. Common spinal deformity (Spondylolisthesis, Scoliosis). Osteoporotic fracture. Anatomy Anatomy Anatomy
SWESPINE THE SWEDISH SPINE REGISTER 2010 REPORT
 SWESPINE THE SWEDISH SPINE REGISTER 21 REPORT SEPTEMBER 21 SWEDISH SOCIETY OF SPINAL SURGEONS Björn Strömqvist Peter Fritzell Olle Hägg Bo Jönsson ISBN 978-91-978553-8-9 Table of Contents 2 Introduction
SWESPINE THE SWEDISH SPINE REGISTER 21 REPORT SEPTEMBER 21 SWEDISH SOCIETY OF SPINAL SURGEONS Björn Strömqvist Peter Fritzell Olle Hägg Bo Jönsson ISBN 978-91-978553-8-9 Table of Contents 2 Introduction
Hailee Gibson, CCPA Neurosurgery Physician Assistant. Windsor Neurosurgery & Spine Associates. Windsor Regional Hospital Ouellette Campus
 Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
Hailee Gibson, CCPA Neurosurgery Physician Assistant Windsor Neurosurgery & Spine Associates Windsor Regional Hospital Ouellette Campus Disclosures I have no disclosures Learning Objectives Provide information
A Structural Service Plan: Towards Better and Safer Spine Surgeries. Department of Orthopaedics & Traumatology Tuen Mun Hospital
 A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
A Structural Service Plan: Towards Better and Safer Spine Surgeries Department of Orthopaedics & Traumatology Tuen Mun Hospital Cheung KK Wong CY Chan Andrew Tse Alfred Chow YY Department of Orthopaedics
Lumbar disc prolapse. Done by : Areej Al-Hadidi
 Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
Lumbar disc prolapse Done by : Areej Al-Hadidi Anatomy of IVD IVD is composed of two components: 1. anulus fibrosus : it is the outer fibrous layer (fibrocartilage ) **It is comressible &tough 2. nucleus
LUMBAR SPINAL STENOSIS
 LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
LUMBAR SPINAL STENOSIS North American Spine Society Public Education Series WHAT IS LUMBAR SPINAL STENOSIS? The vertebrae are the bones that make up the lumbar spine (low back). The spinal canal runs through
Lumbar Spinal Fusion Corporate Medical Policy
 Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Lumbar Spinal Fusion Corporate Medical Policy File name: Lumbar Spinal Fusion File code: UM.SURG.15 Origination: 09/01/2016 Last Review: 09/29/2016 Next Review: 09/29/2017 Effective Date: 01/01/2017 Populations
Same Segment Early Recurrence in Surgery of Lumbar Canal Stenosis- Role of Dissectomy
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. II (August. 2016), PP 34-40 www.iosrjournals.org Same Segment Early Recurrence in Surgery
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 15, Issue 8 Ver. II (August. 2016), PP 34-40 www.iosrjournals.org Same Segment Early Recurrence in Surgery
Original Date: October 2015 LUMBAR SPINAL FUSION FOR
 National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
National Imaging Associates, Inc. Clinical guidelines Original Date: October 2015 LUMBAR SPINAL FUSION FOR Page 1 of 9 INSTABILITY AND DEGENERATIVE DISC CONDITIONS FOR CMS (MEDICARE) MEMBERS ONLY CPT4
Comparison of Radiologic Signs and Clinical Symptoms of Spinal Stenosis
 SPINE Volume 31, Number 16, pp 1834 1840 2006, Lippincott Williams & Wilkins, Inc. Comparison of Radiologic Signs and Clinical Symptoms of Spinal Stenosis C. Martina Lohman, MD, PhD,* Kaj Tallroth, MD,
SPINE Volume 31, Number 16, pp 1834 1840 2006, Lippincott Williams & Wilkins, Inc. Comparison of Radiologic Signs and Clinical Symptoms of Spinal Stenosis C. Martina Lohman, MD, PhD,* Kaj Tallroth, MD,
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine..............................................
Outcome after laminectomy for lumbar spinal stenosis
 J Neurosurg 81:699 706, 1994 Outcome after laminectomy for lumbar spinal stenosis Part I: Clinical correlations GERALD F. TUITE, M.D., JOSEPH D. STERN, M.D., STEPHEN E. DORAN, M.D., STEPHEN M. PAPADOPOULOS,
J Neurosurg 81:699 706, 1994 Outcome after laminectomy for lumbar spinal stenosis Part I: Clinical correlations GERALD F. TUITE, M.D., JOSEPH D. STERN, M.D., STEPHEN E. DORAN, M.D., STEPHEN M. PAPADOPOULOS,
Patient Information MIS TLIF. Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques
 Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Patient Information MIS TLIF Transforaminal Lumbar Interbody Fusion Using Minimally Invasive Surgical Techniques MIS TLIF Table of Contents Anatomy of Spine...2 General Conditions of the Spine...4 6 MIS-TLIF
Lumbar spinal canal stenosis (LSS) is a common
 spine clinical article J Neurosurg Spine 23:49 54, 2015 The influence of preoperative spinal sagittal balance on clinical outcomes after microendoscopic laminotomy in patients with lumbar spinal canal
spine clinical article J Neurosurg Spine 23:49 54, 2015 The influence of preoperative spinal sagittal balance on clinical outcomes after microendoscopic laminotomy in patients with lumbar spinal canal
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy
 Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
Incidence and Risk Factors for Late Neurologic Deterioration after C3-6 Laminoplasty in Patients with Cervical Spondylotic Myelopathy Sakaura H, Miwa T, Kuroda Y, Ohwada T Dept. of Orthop. Surg., Kansai
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY
 PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
PREOPERATIVE RETROLISTHESIS IS A RISK FACTOR OF LUMBAR DISC HERNIATION AFTER FENESTRATION WITHOUT DISCECTOMY Shota Takenaka*, Noboru Hosono, Yoshihiro Mukai, Kosuke Tateishi, Takeshi Fuji Osaka Kosei-nenkin
Syddansk Universitet. Published in: Danish Medical Journal. Publication date: Document version Publisher's PDF, also known as Version of record
 Syddansk Universitet Patient are satisfied one year after decompression surgery for lumbar spinal stenosis Tendal Paulsen, Rune; Bouknaitir, Jamal Bech; Fruensgaard, Søren; Carreon, Leah Y; Andersen, Mikkel
Syddansk Universitet Patient are satisfied one year after decompression surgery for lumbar spinal stenosis Tendal Paulsen, Rune; Bouknaitir, Jamal Bech; Fruensgaard, Søren; Carreon, Leah Y; Andersen, Mikkel
DISORDERS OF THE SPINE TREATING PHYSICIAN DATA SHEET
 DISORDERS OF THE SPINE TREATING PHYSICIAN DATA SHEET Short form FOR REPRESENTATIVE USE ONLY REPRESENTATIVE S NAME AND ADDRESS REPRESENTATIVE S TELEPHONE REPRESENTATIVE S EMAIL PHYSICIAN S NAME AND ADDRESS
DISORDERS OF THE SPINE TREATING PHYSICIAN DATA SHEET Short form FOR REPRESENTATIVE USE ONLY REPRESENTATIVE S NAME AND ADDRESS REPRESENTATIVE S TELEPHONE REPRESENTATIVE S EMAIL PHYSICIAN S NAME AND ADDRESS
Lumbar Disc Prolapse. Dr. Ahmed Salah Eldin Hassan. Professor of Neurosurgery & Consultant spinal surgeon
 Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
Lumbar Disc Prolapse By Dr. Ahmed Salah Eldin Hassan Professor of Neurosurgery & Consultant spinal surgeon 1-What are the Functions of the Spine Structural support for upright posture Protection of Spinal
ProDisc-L Total Disc Replacement. IDE Clinical Study.
 ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
ProDisc-L Total Disc Replacement. IDE Clinical Study. A multi-center, prospective, randomized clinical trial. Instruments and implants approved by the AO Foundation Table of Contents Indications, Contraindications
Herniated Disk in the Lower Back
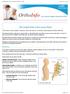 Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Herniated Disk in the Lower Back This article is also available in Spanish: Hernia de disco en la columna lumbar (topic.cfm?topic=a00730). Sometimes called a slipped or ruptured disk, a herniated disk
Paul Allan Regional Clinical Lead - South. Lumbar Spine. Assessment & Differential Diagnosis
 Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Paul Allan Regional Clinical Lead - South Lumbar Spine Assessment & Differential Diagnosis Aims Refresh lumbar spine anatomy Red flags Discuss common pathologies seen in general practice Subjective and
Common Thoraco- Lumbar Problems in the Mature Athlete
 Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Common Thoraco- Lumbar Problems in the Mature Athlete Diana Heiman, MD Associate Professor, Family Medicine Residency Director East Tennessee State University Objectives Review the pathophysiology of the
Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment
 Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
Tohoku J. Exp. Med., 2006, 209, 1-6 Cauda Equina Tumors 1 Clinical Features of Cauda Equina Tumors Requiring Surgical Treatment YOICHI SHIMADA, NAOHISA MIYAKOSHI, 1 YUJI KASUKAWA, 1 MICHIO HONGO, 1 SHIGERU
A Patient s Guide to Lumbar Spinal Stenosis
 A Patient s Guide to Lumbar Spinal Stenosis Glendale Adventist Medical Center 1500 E. Chevy Chase Drive, Suite 401B Glendale, CA 91206 Phone: (818) 863-4444 DISCLAIMER: The information in this booklet
A Patient s Guide to Lumbar Spinal Stenosis Glendale Adventist Medical Center 1500 E. Chevy Chase Drive, Suite 401B Glendale, CA 91206 Phone: (818) 863-4444 DISCLAIMER: The information in this booklet
Proof of Concept (POC) Studies for Chronic Low Back Pain
 Proof of Concept (POC) Studies for Chronic Low Back Pain REDACTED FOR WEBSITE Prepared for: ADEPT 3.25.2011 Southampton, Bermuda John Markman MD Associate Professor I University of Rochester School of
Proof of Concept (POC) Studies for Chronic Low Back Pain REDACTED FOR WEBSITE Prepared for: ADEPT 3.25.2011 Southampton, Bermuda John Markman MD Associate Professor I University of Rochester School of
North American Spine Society Public Education Series
 Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Herniated Lumbar Disc North American Spine Society Public Education Series What Is a Herniated Disc? The spine is made up of a series of connected bones called vertebrae. The disc is a combination of strong
Common Conditions. Visit our homepage for more info >> TABLE OF CONTENTS. Bulging/Herniated Disc... PAGE 2. Cervical (Neck) Pain...
 Common Conditions TABLE OF CONTENTS Bulging/Herniated Disc... PAGE 2 Cervical (Neck) Pain... PAGE 3 Degenerative Disc Disease... PAGE 4 Sciatica...PAGE 5 Spinal Stenosis... PAGE 6 Spondylolisthesis...
Common Conditions TABLE OF CONTENTS Bulging/Herniated Disc... PAGE 2 Cervical (Neck) Pain... PAGE 3 Degenerative Disc Disease... PAGE 4 Sciatica...PAGE 5 Spinal Stenosis... PAGE 6 Spondylolisthesis...
Spinal canal stenosis Degenerative diseases F 06
 What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
What is spinal canal stenosis? The condition known as spinal canal stenosis is a narrowing (stenosis) of the spinal canal that in most cases develops due to the degenerative (wear-induced) deformation
ACDF. Anterior Cervical Discectomy and Fusion. An introduction to
 An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
An introduction to ACDF Anterior Cervical Discectomy and Fusion This booklet provides general information on ACDF. It is not meant to replace any personal conversations that you might wish to have with
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018
 EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
EVALUATE, TREAT AND WHEN TO REFER RED FLAGS Mid Atlantic Occupational Regional Conference and Environmental Medicine October 6, 2018 Marc J. Levine, MD Rothman Institute Director Spine Surgery Program
Chronic Low Back Pain Seminar Patient Engagement. NHS North West London CCGs 6 th February 2017
 Chronic Low Back Pain Seminar Patient Engagement NHS North West London CCGs 6 th February 2017 Aims and Objectives Welcome and introductions Why are we here? To hear patient views as CCGs plan to adopt
Chronic Low Back Pain Seminar Patient Engagement NHS North West London CCGs 6 th February 2017 Aims and Objectives Welcome and introductions Why are we here? To hear patient views as CCGs plan to adopt
Current Spine Procedures
 SPINE BOOT CAMP: WHAT YOU DON T KNOW MAY COST YOU! David Abraham, M.D. The Reading Neck and Spine Center Reading, PA Current Spine Procedures Epidural/Transforaminal Injections Lumbar Procedures Laminectomy
SPINE BOOT CAMP: WHAT YOU DON T KNOW MAY COST YOU! David Abraham, M.D. The Reading Neck and Spine Center Reading, PA Current Spine Procedures Epidural/Transforaminal Injections Lumbar Procedures Laminectomy
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY
 Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
Lumbar Discectomy and Decompression INFORMATION FOR PATIENTS UNDERGOING SURGERY Informed consent is the process of the surgical team providing information to the patient and their carers to enable them
The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_
 Orthopaedic Surgery (2009), Volume 1, No. 3, 176 183 ORIGINAL ARTICLE The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_030 176..183 Wei Liu MD,
Orthopaedic Surgery (2009), Volume 1, No. 3, 176 183 ORIGINAL ARTICLE The clinical features and surgical treatment of degenerative lumbar scoliosis: A review of 112 patientsos4_030 176..183 Wei Liu MD,
Life can cause spinal stenosis. Take yours back with Superion.
 Indirect Decompression System Life can cause spinal stenosis. Take yours back with Superion. Superion can help you take back your life with a simple new procedure. What is spinal stenosis? Your spine is
Indirect Decompression System Life can cause spinal stenosis. Take yours back with Superion. Superion can help you take back your life with a simple new procedure. What is spinal stenosis? Your spine is
Use of pain drawing as an assessment tool of sciatica for patients with single level lumbar disc herniation
 DOI 10.1186/s40064-016-2981-z RESEARCH Open Access Use of pain drawing as an assessment tool of sciatica for patients with single level lumbar disc herniation Toshiya Tachibana *, Keishi Maruo, Shinichi
DOI 10.1186/s40064-016-2981-z RESEARCH Open Access Use of pain drawing as an assessment tool of sciatica for patients with single level lumbar disc herniation Toshiya Tachibana *, Keishi Maruo, Shinichi
Lumbar disc herniation
 Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Lumbar disc herniation Thomas Kishen Spine Surgeon Sparsh Hospital for Advanced Surgeries Bangalore Symptoms and Signs Radicular Pain in the distribution of the involved nerve Neurological deficit motor,
Correlation Between Severity of Lumbar Spinal Stenosis and Lumbar Epidural Steroid Injection
 bs_bs_banner Pain Medicine 2014; 15: 556 561 Wiley Periodicals, Inc. Correlation Between Severity of Lumbar Spinal Stenosis and Lumbar Epidural Steroid Injection Chan-Hong Park, MD, PhD,* and Sang-Ho Lee,
bs_bs_banner Pain Medicine 2014; 15: 556 561 Wiley Periodicals, Inc. Correlation Between Severity of Lumbar Spinal Stenosis and Lumbar Epidural Steroid Injection Chan-Hong Park, MD, PhD,* and Sang-Ho Lee,
Do you experience pain or numbness in your lower back when standing upright?
 is this you? Do you experience pain or numbness in your lower back when standing upright? Do you experience pain, numbness, or tingling in your legs or buttocks when you walk? Is your discomfort relieved
is this you? Do you experience pain or numbness in your lower back when standing upright? Do you experience pain, numbness, or tingling in your legs or buttocks when you walk? Is your discomfort relieved
Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine
 Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Neurol Med Chir (Tokyo) 51, 484 489, 2011 Radiculopathy Caused by Osteoporotic Vertebral Fractures in the Lumbar Spine Manabu SASAKI, 1 Masanori AOKI, 2 Kazuya NISHIOKA, 3 and Toshiki YOSHIMINE 4 1 Department
Cervical Plating BACK PAIN
 BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
BACK PAIN Back Pain Back pain is frequent complaint. It is the commonest cause of work-related absence in the world. Although back pain may be painful and uncomfortable, it is not usually serious. Even
University of Jordan. Professor Freih Abuhassan -
 Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
Freih Odeh Abu Hassan F.R.C.S.(Eng.), F.R.C.S.(Tr.& Orth.). Professor of Orthopedics University of Jordan 1 A. Sacroiliitis History Trauma is very common Repetitive LS motion--lumbar rotation or axial
PARADIGM SPINE. Patient Information. Treatment of a Narrow Lumbar Spinal Canal
 PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
PARADIGM SPINE Patient Information Treatment of a Narrow Lumbar Spinal Canal Dear Patient, This brochure is intended to inform you of a possible treatment option for narrowing of the spinal canal, often
d EFFECTIVE DATE: POLICY LAST UPDATED:
 Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Medical Coverage Policy Epidural Injections for Pain Management d EFFECTIVE DATE: 04 01 2018 POLICY LAST UPDATED: 03 20 2018 OVERVIEW Epidural injections are generally performed to treat pain arising from
Lumbar spinal stenosis is narrowing of the spinal canal that results in compression of the cauda
 1 CHAPTER 32: CLINICAL RESULTS OF THE IDE TRIAL OF X-STOP INTERSPINOUS SYSTEMS ELIZABETH YU AND JAMES ZUCHERMAN Lumbar spinal stenosis Lumbar spinal stenosis is narrowing of the spinal canal that results
1 CHAPTER 32: CLINICAL RESULTS OF THE IDE TRIAL OF X-STOP INTERSPINOUS SYSTEMS ELIZABETH YU AND JAMES ZUCHERMAN Lumbar spinal stenosis Lumbar spinal stenosis is narrowing of the spinal canal that results
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice
 The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
The NICE revised guidelines for the management of non-specific low back pain and; Implications for Practice David Walsh David.walsh@nottingham.ac.uk National Clinical Guideline Centre Commissioned by NICE
You Don t Understand This Stuff???
 SPINE SURGERY You Don t Understand This Stuff??? Welcome to the club Most PCP s don t understand what we do Half of other orthopods don t get it Sometimes we can t even explain it to each other Why would
SPINE SURGERY You Don t Understand This Stuff??? Welcome to the club Most PCP s don t understand what we do Half of other orthopods don t get it Sometimes we can t even explain it to each other Why would
University of Groningen. Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria
 University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
University of Groningen Thoracolumbar spinal fractures Leferink, Vincentius Johannes Maria IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from
Do you experience pain or numbness in your lower back when standing upright?
 is this you? Do you experience pain or numbness in your lower back when standing upright? Do you experience pain, numbness, or tingling in your legs or buttocks when you walk? Is your discomfort relieved
is this you? Do you experience pain or numbness in your lower back when standing upright? Do you experience pain, numbness, or tingling in your legs or buttocks when you walk? Is your discomfort relieved
WHAT IS SCIATICA? Apart from the compression of one of the nerves, there are other known causes of sciatica which include:
 WHAT IS SCIATICA? If you suffer from Sciatica, or you re close to someone who does, you already know that it is one of those conditions that can be quite overwhelming and incapacitating while causing a
WHAT IS SCIATICA? If you suffer from Sciatica, or you re close to someone who does, you already know that it is one of those conditions that can be quite overwhelming and incapacitating while causing a
Comparison of staged reconstruction with extreme lateral interbody fusion (XLIF) adult thoracolumbar kyphoscoliotic deformity
 Comparison of staged reconstruction with extreme lateral interbody fusion (XLIF) and multilevel corrective PLIF/TLIF for adult thoracolumbar kyphoscoliotic deformity Hidetoshi Yamaguchi, MD; Tokumi Kanemura,MD,
Comparison of staged reconstruction with extreme lateral interbody fusion (XLIF) and multilevel corrective PLIF/TLIF for adult thoracolumbar kyphoscoliotic deformity Hidetoshi Yamaguchi, MD; Tokumi Kanemura,MD,
MEDICAL HISTORY CHIRO PHYSICAL
 Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Overview of Spinal Injection Procedures Blake A. Johnson, MD, FACR 1 PATIENT MANAGEMENT EVALUATION TREATMENT P.T. MEDICAL CHIRO S SURGICAL Effective treatment requires a precise diagnosis! HISTORY PHYSICAL
Accuracy and reproducibility of a retrospective outcome assessment for lumbar spinal stenosis surgery
 Kuittinen et al. BMC Musculoskeletal Disorders 2012, 13:83 RESEARCH ARTICLE Open Access Accuracy and reproducibility of a retrospective outcome assessment for lumbar spinal stenosis surgery Pekka Kuittinen
Kuittinen et al. BMC Musculoskeletal Disorders 2012, 13:83 RESEARCH ARTICLE Open Access Accuracy and reproducibility of a retrospective outcome assessment for lumbar spinal stenosis surgery Pekka Kuittinen
Surgical Excision of the Lumbar Disc Herniation in Elementary School Age
 Asian Spine Journal Vol. 3, No. 1, pp 10~15, 2009 Surgical Excision of the Lumbar Disc Herniation in Elementary School Age Youn-Soo Kim*, Il-Jung Park*, Kee-Won Rhyu, Sang-Uk Lee*, Changhoon Jeong* *Department
Asian Spine Journal Vol. 3, No. 1, pp 10~15, 2009 Surgical Excision of the Lumbar Disc Herniation in Elementary School Age Youn-Soo Kim*, Il-Jung Park*, Kee-Won Rhyu, Sang-Uk Lee*, Changhoon Jeong* *Department
Luiz Claudio L Rodrigues 1 and Jamil Natour 2*
 Rodrigues and Natour Journal of Negative Results in BioMedicine 2014, 13:13 RESEARCH Open Access A double-blind, randomized controlled, prospective trial assessing the effectiveness of oral corticoids
Rodrigues and Natour Journal of Negative Results in BioMedicine 2014, 13:13 RESEARCH Open Access A double-blind, randomized controlled, prospective trial assessing the effectiveness of oral corticoids
The imaging features of spondylolisthesis : what the clinician needs to know
 The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
The imaging features of spondylolisthesis : what the clinician needs to know Poster No.: C-1018 Congress: ECR 2011 Type: Authors: Educational Exhibit D. Shah 1, C. J. Burke 1, A. C. andi 2, R. Houghton
The ABC s of LUMBAR SPINE DISEASE
 The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
The ABC s of LUMBAR SPINE DISEASE Susan O. Smith ANP-BC University of Rochester Department of Neurological Surgery Diagnosis/Imaging/Surgery of Lumbar Spine Disorders Objectives Identify the most common
