Speech and Swallowing in Patients with Tracheostomy
|
|
|
- Linette Vivian Walton
- 5 years ago
- Views:
Transcription
1 ARTIFICIAL AIRWAYS AND ALTERED AIRWAYS: WHO, WHY, HOW AND WHAT NOW? DEBRA M. SUITER, PHD, CCC SLP, BCS S, FASHA TAMMY WIGGINTON; M.S., CCC/SLP BCS S UNIVERSITY OF KENTUCKY VOICE AND SWALLOW CLINIC Speech and Swallowing in Patients with Tracheostomy Normal Airflow for Phonation 1
2 Airflow Changes Airflow with a Trach Tube 2
3 Trach Related Changes 01 Open system 02 Decreased airflow through glottis 03 Increased secretions Anatomy of a Trach Tube 1. Faceplate 2. Hub 3. Outer Cannula 4. Pilot line/pilot balloon 5. Cuff Trach Tubes (cont.) Shiley Flex trach tubes Extended length trach tubes 3
4 Trach Tubes (cont.) Portex Plastic tube Clear or white faceplate Blue pilot balloon Trach Tubes (cont.) Bivona fomecuff (red pilot balloon) Used when unable to maintain seal with standard cuff Reduces risk of damage from over inflation of cuff Passive cuff inflation Cannot be used with speaking valves Trach Tubes (cont.) Extra length Used primarily with bariatric patients to ensure proper ventilation Made by most trach manufacturers 4
5 Trach Tubes Jackson (metal) Used for non vent patients Cuffless model only Communication Options Leak speech Speaking Valves Talking trach tubes Fenestrated trach tubes Digital trach tube occlusion Augmentative communication systems Electrolarynx Leak Speech For patients who are ventilator dependent Leak is created by a partially deflated trach tube cuff Must have medical clearance prior to attempting cuff deflation Concurrently with cuff deflation, changes in the ventilator that compensate for the loss of volume through the upper airway must be made. 5
6 Leak Speech Protocol for Cuff Deflation Obtain MD order for cuff deflation and vent modifications Suction patient through the trach tube, cuff inflated Slowly deflate cuff, 1 cc at a time RT makes adjustments in vent settings (e.g., tidal volume) SLP assesses patient s voice Monitor oxygen saturation and HR If patient is unable to voice adequately, review other vent settings (e.g., respiratory rate, inspiratory flow rate) Reassess patient s voicing Gradually increase length of time pt can tolerate cuff deflation Speaking Valves Patient can continue to breath in through the trach tube Exhalation is then redirected up through the trachea creating a closed system Promotes a more normal respiratory pattern for breathing and expelling secretions Passy Muir Valve 6
7 Passy Muir Benefits Along with allowing the patient to phonate, Passy Muir valves are also thought to: Expedite weaning from mechanical ventilation Restored positive airway pressure Reduce decannulation time Facilitate infection control Improve olfaction Improve quality of life Speaking Valve Candidacy Can be used with trach patients on and off the vent Pt should be awake, alert, and attempting to communicate Airway patency trach size/# of intubations Can be used for decannulation purposes in patients who are not communicative Contraindications for speaking valve use Inability to tolerate full cuff deflation End stage pulmonary disease Medical instability Foam filled tracheostomy tube cuff Thick, copious secretions Severe airway obstruction Total laryngectomy Laryngeal masses, stenosis, inadequate patency of upper airway Severe anxiety 7
8 Speaking Valve Assessment Preassessment Cognitive status Secretion management Ability to tolerate cuff deflation Airway patency Level of care/length of time post tracheotomy Ventilator Considerations The Passy Muir valve can be used with most conventional modes of ventilation Assist/control Synchronized Intermittent Mandatory Ventilation (SIMV) Pressure Support Continuous Positive Airway Pressure (CPAP) Positive End Expiratory Pressure (PEEP) Ventilator Considerations Valve placement may necessitate manipulation of the tracheostomy tube AND modifications of the ventilator. Work in collaboration with Respiratory Therapy. 8
9 Ventilator Considerations Prior to valve placement, record the following Mode of ventilation Tidal volume Rate : mechanical and spontaneous Fractional Inspired Oxygen Content (FiO2) PEEP Peak Inspiratory Pressure (PIP) Ventilator Considerations The ventilator is usually set to provide optimal ventilation to a patient with an inflated trach cuff. Cuff deflation creates a leak in that system. Changes of the ventilator that will compensate for the loss of volume through the upper airway must be made. Ventilator Considerations Tidal Volume Because of the leak created by cuff deflation, the patient does not receive the amount of air that was preset by the ventilator To compensate for the leak, the RT must increase the tidal volume setting on the ventilator If the amount of leakage is so great that ventilation cannot be maintained after an increase in tidal volume, tracheostomy tube size may need to be increased. 9
10 Ventilator Considerations Airway pressure Airway pressure may rise slightly with valve placement If peak pressures rise above allowable limits, remove valve PEEP requirements may be reduced Ventilator Considerations Sensitivity Setting Patients who are breathing spontaneously and who are on the assist mode of ventilation must inspire against the resistance provided by the speaking valve membrane. Respiratory effort may increase Patient may fatigue Decreasing the sensitivity at which a breath will be triggered from the ventilator will allow the patient to receive a breath after less inspiratory effort. Ventilator Considerations FiO2 Due to the effects of physiologic PEEP, FiO2 requirements may be reduced due to increased saturations. If there is significant desaturation, remove valve immediately. 10
11 Speaking Valve Assessment Assess size and type of tracheostomy tube Patients with Fome cuff trachs are not candidates for speaking valves secondary to passive inflation of cuff Larger diameter trachs may result in inadequate airflow through the upper airway (ideal size of trach is 2/3 size of tracheal lumen) Specialty trachs can be utilized for abnormal airways (e.g. extra length, double cuff, stoma cuff, TTS) Speaking Valve Assessment Assess size and type of tracheostomy tube Patients with Fome cuff trachs are not candidates for speaking valves secondary to passive inflation of cuff Larger diameter trachs may result in inadequate airflow through the upper airway (ideal size of trach is 2/3 size of tracheal lumen) Specialty trachs can be utilized for abnormal airways (e.g. extra length, double cuff, stoma cuff, TTS) Speaking Valve Assessment Verify and record baseline vital signs Slowly deflate cuff (~1cc at a time) and monitor pt s vitals and work of breathing Suction patient if necessary Verify voice by digital occlusion of trach Apply speaking valve and monitor for changes in voice, vitals, or work of breathing Advance time of use as tolerated 11
12 Speaking Valve Assessment Look at Oxygen saturation Vital signs Breath sounds Color Work of breathing Patient responsiveness Secretion status Swallowing and Trachs Phases of Swallowing 12
13 Swallow Apnea During the pharyngeal phase of swallowing, breathing stops briefly. This period usually corresponds to airway closure during the pharyngeal phase and cessation of chest wall movement Usually occurs midexpiration and is followed by expiration Usually lasts 0.3 s to 2.5 s Swallow Apnea Patients with dysphagia may interrupt inhalation to swallow, which may increase their risk of aspiration. Thought to be a result of its own neural mechanism Laryngectomy patients demonstrate SA (Hiss et al., 2003) 13
14 Respiration and Swallowing Breathing and swallowing are well coordinated in healthy adults This coordination is most evident at the level of the larynx. Protection of the airway during and around the time of swallowing is dependent upon the coordination of breathing and swallowing. Disruption of the ability to coordinate airway closure at the appropriate time in the swallow can lead to airway compromise. Respiration and Swallowing In healthy adults, there is a close coupling of respiration with swallowing. Physiologic conditions, including aging, neurologic disease, and head & neck cancer, disrupt this coupling. Respiration and Swallowing Respiratory patterns in young and elderly healthy individuals and in individuals with COPD Healthy young individuals Exhala on Swallow Exhala on Healthy elderly Inhala on Swallow Exhala on COPD exacerbation Inhala on Swallow Inhala on Shaker et al.,
15 Respiration and Swallowing Factors that affect airway protection in patients with pulmonary disease include: Alterations in timing of airway closure during the swallow Interruption of the normally well timed pattern of swallowing and breathing Diminished respiratory defenses (e.g., diminished cough, reduced airway clearance) Do Tracheostomy Tubes Affect Swallowing? Common thoughts Tracheostomy tubes cause aspiration and result in: Decreased hyolaryngeal excursion Decreased adductor vocal fold response Decreased subglottal air pressure Question: Do tracheostomy tubes cause aspiration? Reported incidence of aspiration in various patient populations with tracheostomy tubes ranges from 68 87%. 15
16 Question: Do tracheostomy tubes cause aspiration? Research indicates that tracheostomy tubes do not cause aspiration (Brady et al., 2009; Donzelli et al., 2005; Kang et al., 2012; Leder et al., 2005; Leder & Ross, 2000). Question: Do tracheotomy tubes limit hyolaryngeal excursion? Feldman, Deal, & Urquhart (1966) Fixation of the larynx by the tracheostomy might prevent normal elevation of the larynx [leading to] a disorder of swallowing produced by the tracheostomy. Question: Do tracheotomy tubes limit hyolaryngeal excursion? Bonnano (1971) Suggested that presence of a tracheotomy tube resulted in reduced laryngeal movement, presumably due to tethering of the larynx by the weight of the tracheotomy tube and/or the presence of an inflated tracheotomy tube cuff However, only 3 of 43 (7%) of participants in this study actually demonstrated this. 16
17 Question: Do tracheotomy tubes limit hyolaryngeal excursion? Yes No Ding & Logemann, 2005 Suiter, McCullough, & Powell, 2003 Terk, Leder, & Burell, 2007 Kang et al., 2012 Question: Do tracheotomy tubes affect vocal fold reflexes? Sasaki, Suzuki, Horiuchi, & Kirchner (1977) Examined the effects of tracheotomy on the protective laryngeal closure reflex in15 adult dogs Sensory threshold of the ipsilateral evoked adductor response was 0.5 volt in 4 dogs immediately posttracheotomy Sensory threshold of the ipsilateral adductor response was volts in 8 chronically tracheotomized dogs (2 8 months) Question: Do tracheotomy tubes affect vocal fold reflexes? Buckwalter & Sasaki (1984) Demonstrated in humans that threshold of adductor vocal fold reflex nearly doubles after a tracheotomy tube has been in place for 6 8 months 17
18 Question: Does loss of subglottal air pressure affect swallow safety? Eibling & Gross, 1996 Suggest that the loss of subglottic air pressure and glottic airflow are the active factors in predisposing individuals with tracheotomy to aspiration. Question: Does loss of subglottal air pressure affect swallow safety? Subglottal Pressure Theory (Diez Gross et al., 2003) Suggests that pressurized air during the swallow plays a roll in the neuroregulation of swallowing function by stimulating subglottic mechanoreceptors. Theory originated from observations of altered air pressure below the true vocal folds was modified depending on tube status (open vs. closed) Question: Does loss of subglottal air pressure affect swallow safety? Subglottal pressure theory (cont.) Suggests that the preferential timing of the normal swallow with exhalation is a mechanism that allows for stimulation of subglottic mechanoreceptors and the generation of subglottal air pressure. 18
19 Question: Does loss of subglottal air pressure affect swallow safety? Stretch receptors in the trachea have an inhibitory effect on the respiratory muscles, possible delaying inspiration until the end of expiration during normal respiration. These mechanoreceptors may also function during swallowing to interrupt inspiration. Question: Does loss of subglottal air pressure affect swallow safety? During normal swallowing, positive subglottic air pressure is likely present (Gross, Steinhauer, Zajac, & Weissler, 2006). The presence of a tracheotomy prevents the subglottic pressure rise associated with normal swallowing, and may reduce or eliminate the inhibitory effect of the stretch receptors This places the individual at increased risk for aspiration or dysphagia. Question: Does loss of subglottal air pressure affect swallow safety? Eibling & Gross, 1996 Measured subglottic air pressure and airflow through a tracheotomy during swallowing. Tube open: There was a minimal rise in pressure during a swallow, and there was significant expiratory airflow during the swallow. Patients aspirated. Passy Muir valve: Airflow ceased during the swallow There was a pressure peak that occurred at the time of the swallow, averaging 10 cm H2O. Patients did not aspirate. 19
20 Question: Does loss of subglottal air pressure affect swallow safety? Gross, Mahlmann, & Grayhack, 2003 Completed VFSS in 4 individuals with valve on vs. valve off Measured subglottal air pressure during the swallow with valve on vs. off Average air pressure with valve on = 8.5 cm H2O Average air pressure with valve off = 0 cm H2O Slower pharyngeal activity duration and bolus transit times were observed with valve off. Penetration aspiration scores increased (were worse) with the valve off. Question: Does tracheotomy tube occlusion affect swallow safety? Yes Maybe No Muz, Mathog, Nelson, & Jones, 1989 Muz, Hamlet, Mathog,& Farris, 1994 Logemann, Pauloski, & Coleangelo, 1998 Leder, Ross, Burrell, & Sasaki, 1998 Question: Does speaking valve placement affect swallow safety? Yes Dettelbach, Gross, Mahlmann, & Eibling, 1995 Stachler, Hamlet, Choi, & Fleming, 1996 Elpern, Okonek, Bacon, Gerstung, & Skrzynski, 2000 Gross, Mahlmann, & Grayhack, 2003 Suiter, McCullough, & Powell, 2003 No Leder, 1999 Leder, Joe, Hill, & Traube,
21 Question: Does speaking valve placement affect swallow safety? Overall, most reports in the literature indicate that the speaking valve placement improves swallow safety. Research is needed to further elucidate the specific effects of speaking valve placement on swallow function. Discussion: Cuff Deflation Cuff deflation did not reduce the incidence or severity of aspiration. Anatomical and functional separation of the respiratory and digestive tracts, such as occurs with tracheotomy, results in the loss of coordination between the protective and respiratory functions of the larynx. Cuff deflation may not fully restore pharyngeal and laryngeal sensation. Discussion: One Way Speaking Valve Speaking valve placement reduces the incidence and severity of aspiration of thin liquids. This may be due to restoration of subglottal air pressure or increased pharyngeal/laryngeal sensation. There was an increased incidence of penetration with speaking valve placement. 21
22 Conclusions Patients who are able to tolerate cuff deflation and speaking valve placement may benefit from eating with a valve in place. Specifically, patients with tracheotomy tubes who are unable to tolerate thin liquids may be able to safely take thin liquids when the valve is in place. Clinicians who complete swallow evaluations with patients with tracheotomy tubes should include several bolus presentations with the speaking valve in place before making any decisions regarding the use of the valve as a means to reduce aspiration. Bedside Swallow Evaluation Clinical bedside evaluation Modified Evans blue dye test Glucose oxidase strips Bedside Swallow Examination Components of a bedside swallow evaluation include Chart Review Medical diagnoses and complications How stable is the patient? Current and past respiratory details Trach size, type, cuff deflation, capping trials Weaning parameters, number and length of intubations, suctioning frequency, oxygen requirements Physical abilities Ambulation, sitting tolerance, self care 22
23 Bedside Swallow Examination Components (cont.) Patient observation Level of consciousness Secretion tolerance Suctioning frequency, spontaneous coughs, spontaneous swallows General bed/chair mobility Respiratory measures: Oxygen saturation levels, respiratory rate Bedside Swallow Examination Components (cont.) Oral mechanism examination Assess integrity of oral mucosa Assess oral hygiene, dentition Oral/tongue strength/range of motion Bedside Swallow Examination: Patients with Trachs Bolus presentation (if appropriate) Does the cuff need to be deflated in order for the patient to swallow safely? NO Cuff status did not impact hyolaryngeal excursion or aspiration status (Suiter et al., 2003, Terk, Leder, et al., 2007 Assess swallow function under condition in which patient is going to be eating. Deflating the cuff may allow better identification of aspiration if it occurs. 23
24 Bedside Swallow Examination: Patients with Trachs If cuff is to be deflated Need medical clearance Patient is suctioned prior to and immediately following deflation Note tolerance O2 sats, respiratory rate Digital occlusion during exhalation Can patient phonate? Bedside Swallow Examination: Patients with Trachs Is speaking valve placement necessary? Research on its benefits is equivocal Does eliminate aspiration for some individuals We re not sure why.» Necessitates cuff deflation» Restores airflow through glottis» Restores subglottic pressure If patient is a candidate for speaking valve placement, assess swallow function with valve on versus off. Bedside Swallow Examination: Patients with Trachs Speaking valve placement Cuff deflation Digital occlusion Speaking valve placement Secretion management Monitor O2 sats, respiratory rate, patient anxiety level Gradually increase length of time patient is to wear speaking valve 24
25 Bedside Swallow Examination Patients on mechanical ventilation Higher incidence of silent aspiration May not be able to tolerate cuff deflation and/or speaking valve placement If they are, BSE may still not be the best choice No evidence to suggest BSEs are accurate with this population Bedside Swallow Examination Patients on mechanical ventilation Can eat and drink safely, but we must consider Ventilator settings FiO2, Pressure Support, SIMV vs. spontaneous ventilation Cuff deflation Ability to tolerate speaking valve placement Instrumental assessment is preferential to clinical swallow evaluation Bedside Swallow Examinations (BSE) Evidence in the research indicates that bedside swallow evaluations are not accurate: Logemann, Lazarus, & Jenkins (1982) Splaingard et al. (1988) Aviv et al. (1996) Silent aspiration can occur in 40% to 70% of dysphagic patients who aspirate (Daniels et al., 2000) 25
26 BUT, There are some clinical predictors of aspiration that can be detected during BSE: Dysphonia Wet vocal quality Presence of a spontaneous cough during the swallow Overall estimate of the presence of aspiration Weak volitional cough Dysarthria Cough response may be diminished Most who aspirate do so silently Issues Specific to Individuals with Tracheotomy May be present due to history of intubation Dysphonia If unable to tolerate valve placement, may not be able to use. Difficult to assess hyolaryngeal excursion This isn t assessed accurately at bedside regardless of presence or absence of trach (Brates et al., 2017) Supplements to the Bedside Swallow Evaluation Modified Evans Blue Dye Test Glucose Oxidase Test Strips Pulse Oximetry Cervical Auscultation 26
27 Evans Blue Dye Test Original test (Cameron et al., 1973) Place 4 drops of a 1% solution of Evans blue dye on the tongue every 4 hours Tracheal suctioning at set intervals Aspiration assumed if blue dye is suctioned from the trach tube. Less expensive than instrumental assessment Advantages of Blue Dye Test Quick Easy to administer When done simultaneously with instrumental assessment, blue dye often fails to detect aspiration when it less than gross aspiration Brady et al. Blue dye test detected aspiration in 100% of cases in which aspiration was greater than trace. Blue dye test failed to identify 100% of those with trace aspiration. Most studies have similar results Acceptable specificity but low sensitivity Accuracy of the Blue Dye Test 27
28 The FDA has approved the use of Blue No. 1 for use in foods, drugs, and cosmetics. Blue dye is commonly found in candies, confections, and beverages. Is Blue Dye Safe? Is Blue Dye Safe? Maloney et al., 2000 Letter to the Editor in New England Journal of Medicine Reported 2 cases in which blue dye was added to enteral feedings. Both developed pneumonia with sepsis Both died of refractory hypotension and acidosis Their skin, serum, and urine turned green or blue. Autopsies revealed green or blue discoloration of the skin and internal organs. Is Blue Dye Safe? Maloney et al. (cont) Blue dye no. 1 is an inhibitor of mitochondrial respiration in vitro and reduces oxygen consumption by a factor of 8 in mitochondrial preparations in vitro. Maloney and colleagues hypothesized that the refractory hypotension and metabolic acidosis seen in the 2 patients was due to the known biochemical effects of the blue dye. 28
29 Is Blue Dye Safe? Other issues File, Tan, & Thomson (1995) described an outbreak of pseudomonas aeruginosa, a ventilator associated infection. 19/20 patients with this infection had received tube feedings that had been tinted from the same common use bottle of blue dye. When the hospital replaced the bottle with single use vials, the outbreak stopped. Is Blue Dye Safe? Knoll (1993) reported a study in which gram negative and grampositive rods (types of bacteria) were found, not only in an open bottle of dye, but also in two unopened bottles. Is Blue Dye Safe? Amount of dye SLPs use in MEBDT is typically quite small 5 10 cc Sterile vials of blue food dye are available, which might alleviate the concern over contamination (Novartis Nutrition, Freemont, MI). 29
30 Glucose Oxidase Testing Potts, Zaroukian, Guerrero, & Baker (1993) Evaluated the use of glucose oxidase strips to detect aspiration of enteral feedings. Based on the premise that enteral feedings contain glucose whereas tracheal secretions do not. Compared blue dye in tracheal secretions to glucose oxidase strips for detecting aspiration. Glucose oxidase strips proved to be better at detecting aspiration than blue dye. Pulse Oximetry Provides a non invasive method of testing Some have suggested that swallow associated declines in oxygen saturation (2% or more) correlates with aspiration events. Pulse Oximetry Some suggest that aspiration causes reflex bronchoconstriction and therefore ventilation perfusion imbalance, leading to hypoxia and desaturation (Zaidi et al., 1995). Others suggest that abnormal swallowing leads to poor breathing and ventilation perfusion mismatching because of reduced inspiratory volumes (Teramoto et al., 1996). 30
31 Pulse Oximetry Reports on sensitivity and specificity for pulse oximetry to detect aspiration have been variable: Sensitivity = 73 87% Specificity = 39% 87% (Ramsey & Smithard, 2003) Pulse Oximetry More recent reports have indicated that pulse oximetry, either alone or in combination with bedside swallow evaluation, does not have sufficient sensitivity or specificity to warrant its use for detection of aspiration (Ramsey, Smithard, & Kalra, 2006). Cervical Auscultation Involves the use of a stethoscope to listen to sounds associated with swallowing (clunks & bursts) Some say these sounds can be indicative of aspiration or penetration of material. 31
32 Cervical Auscultation Most reports indicate that cervical auscultation does not accurately detect aspiration (Leslie et al., 2007). May be useful in listening to breath sounds. Instrumental Assessment Videofluoroscopic Swallow Study (VFSS) Flexible Endoscopic Evaluation of Swallowing (FEES) Videofluoroscopy Allows for observation of interaction between three phases of swallowing Only exam that allows observation of esophageal phase Allows assessment of hyolaryngeal excursion, tongue base retraction 32
33 Videofluoroscopy Issues specific to patients with trachs or on mechanical ventilation Facility dependent Some will not allow patients in ICU to travel to fluoro suite Difficulty with positioning Patient fatigue Issues Specific to Individuals with Tracheotomy Cuff deflation Speaking valve placement Flexible Endoscopic Evaluation of Swallowing Involves the passage of a flexible endoscope transnasally to obtain a superior view of the pharynx, larynx, and trachea Allows the clinician to objectively evaluate the pharyngeal phase of the swallow 33
34 VFSS has disadvantages FEES has advantages, including: Portability Unlimited time for introduction of therapeutic strategies No radiation exposure Direct view of the anatomy Why FEES? What can we see with FEES? Actual structures moving Movement of the bolus Speed/duration of some movements Adequacy/completeness of velopharyngeal closure Epiglottal descent and return Airway status/closure before and at the onset of the swallow What can we see with FEES? Secretion management Murray et al., 1996 Endoscopically visible secretions located within the laryngeal vestibule were highly predictive of subsequent aspiration of food and liquid. Hospitalized patients swallowed less frequently than nonhospitalized patients. Donzelli et al., 2003 Patients with tracheotomy have more secretions Presence and amount of accumulated oropharyngeal secretions were predictive of aspiration of food and/or liquid. 34
35 Secretion Management Findings revealed better endoscopically Alterations in anatomy Effect of feeding tube on anatomy and swallowing Velopharyneal closure, nasal reflux Frequency of spontaneous or dry swallows Status of secretions, ability to sense, swallow, or clear secretions Findings revealed better endoscopically Amount, location of residue Patient response to residue Aspiration of residue after the swallow Fatigue over a meal Ability to hold breath volitionally or sustain breath holding 35
36 Treatment Traditional treatments Nothing specific to patients with trachs Super supraglottic swallow Shaker exercise Conclusions Evidence in the literature suggests there is no causal relationship between tracheotomy and aspiration status. Patients with tracheotomy often have accompanying medical diagnoses, e.g. pulmonary disease, that could predispose them to swallowing difficulty and aspiration. Conclusions Tracheotomy tube occlusion and/or speaking valve placement appear to improve aspiration status for some patients with some bolus types. Clinicians should evaluate swallowing with and without the tracheotomy tube occluded to determine if individual patients benefit. 36
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE?
 PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation David A. Muir Course Outline Physiology of Swallow
 Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes
 Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
Respiratory Compromise and Swallowing
 Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
What are the Challenges? Spreading the Word in NICU. Need for NICU Care: Impact. Baby Trachs: Use of the Passy Muir Valve in the NICU to
 What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP
 DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 13 Trachs, Tubes And Vents: Frequently Asked Questions 1:30-3:00pm
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 13 Trachs, Tubes And Vents: Frequently Asked Questions 1:30-3:00pm
Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor
 Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Mechanical Ventilation Prepared by : Bayan Kaddourah RN,MHM. GICU Clinical Instructor 1 Definition Is a supportive therapy to facilitate gas exchange. Most ventilatory support requires an artificial airway.
Assessment of Patients with Tracheostomy: Dispelling the Myths
 Assessment of Patients with Tracheostomy: Dispelling the Myths Stacey A. Skoretz, M.Sc., CCC-SLP University of Toronto James L. Coyle, M.A., CCC-SLP, BRS-S University of Pittsburgh Clinician Questions
Assessment of Patients with Tracheostomy: Dispelling the Myths Stacey A. Skoretz, M.Sc., CCC-SLP University of Toronto James L. Coyle, M.A., CCC-SLP, BRS-S University of Pittsburgh Clinician Questions
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS. Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis
 DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
DYSPHAGIA SCREENING and CLINICAL SWALLOW EVALUATIONS Debra M. Suiter, Ph.D., CCC-SLP, BRS-S VA Medical Center-Memphis Suiter, ASHA, 2012 Diagnostic Tests vs. Screening Diagnostic tests are used when a
Tracheostomy: Procedures, Timing and Tubes
 TRACHEOSTOMY: PROCEDURES, TIMING AND TUBES Gail M. Sudderth RRT Clinical Specialist Passy-Muir Inc. gsudderth@passy-muir.com (949) 833-8255 Objectives Explain how the timing of the tracheotomy and tube
TRACHEOSTOMY: PROCEDURES, TIMING AND TUBES Gail M. Sudderth RRT Clinical Specialist Passy-Muir Inc. gsudderth@passy-muir.com (949) 833-8255 Objectives Explain how the timing of the tracheotomy and tube
Where do we come from?
 Interdisciplinary Decision-Making with Patients Requiring Tracheostomy and Carrie Windhorst MS CCC-SLP Cheryl Wagoner MS CCC-SLP Ricque Harth MEd CCC-SLP Where do we come from? Welcome to Madonna Rehabilitation
Interdisciplinary Decision-Making with Patients Requiring Tracheostomy and Carrie Windhorst MS CCC-SLP Cheryl Wagoner MS CCC-SLP Ricque Harth MEd CCC-SLP Where do we come from? Welcome to Madonna Rehabilitation
Welcome to the Specialized Medical Services respiratory training webinar series!
 Welcome to the Specialized Medical Services respiratory training webinar series! SMS is your LTC facility single source for oxygen, medical equipment, respiratory care services and supplies nationwide.
Welcome to the Specialized Medical Services respiratory training webinar series! SMS is your LTC facility single source for oxygen, medical equipment, respiratory care services and supplies nationwide.
PMV 2020 (CLEAR) INSTRUCTION BOOKLET. Touching Lives and Advancing Patient Care Through Education. David A. Muir Inventor of the PMV
 PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE PMV 2020 (CLEAR) INSTRUCTION BOOKLET David A. Muir Inventor of the PMV PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE
PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE PMV 2020 (CLEAR) INSTRUCTION BOOKLET David A. Muir Inventor of the PMV PASSY-MUIR LOW PROFILE TRACHEOSTOMY SWALLOWING AND SPEAKING VALVE
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Passy-MuirInc. Passy-Muir Tracheostomy and. Ventilator Speaking Valve. Resource Guide. Passy-Muir Tracheostomy and Ventilator Speaking Valves
 Passy-Muir Tracheostomy and Ventilator Speaking Valve Resource Guide Touching Lives and Advancing Patient Care Through Education Passy-MuirInc. Passy-Muir Tracheostomy and Ventilator Speaking Valves TABLE
Passy-Muir Tracheostomy and Ventilator Speaking Valve Resource Guide Touching Lives and Advancing Patient Care Through Education Passy-MuirInc. Passy-Muir Tracheostomy and Ventilator Speaking Valves TABLE
TRACHEOSTOMY CARE. Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea.
 1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
1 TRACHEOSTOMY CARE Definitions: Trachea-Windpipe Tracheostomy- Surgically created hole that extends from the neck skin into the windpipe or trachea. Outer Cannula- The outer part of a trach tube. Usually
Waitin In The Wings. Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider
 Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
Waitin In The Wings Esophageal/Tracheal Double Lumen Airway (Combitube ) Indications and Use for the Pre-Hospital Provider 1 CombiTube Kit General Description The CombiTube is A double-lumen tube with
What is the next best step?
 Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
Noninvasive Ventilation William Janssen, M.D. Assistant Professor of Medicine National Jewish Health University of Colorado Denver Health Sciences Center What is the next best step? 65 year old female
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 9 Bedside Assessment: What Does It Tell You? 10:00 11:30 am Saturday,
Swallow-respiratory coordination. Liza Bergström, Leg. logoped.
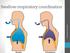 Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
Swallow-respiratory coordination Liza Bergström, Leg. logoped. Biological timeshare When we breathe, we don t swallow When we swallow, we don t breathe Body will always choose to breathe over anything
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR
 CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
CARING FOR THE TRACHEOSTOMISED PATIENT: WHAT TO LOOK OUT FOR DR MOHD NAZRI ALI Anaesthesiologist & Intensivist HRPZ II, Kota Bharu, Kelantan Tracheostomy The Enabling Disability Tracheostomy Are becoming
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Speech and Language Therapy. Kerrie McCarthy Senior Speech and Language Therapist
 Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
Speech and Language Therapy Kerrie McCarthy Senior Speech and Language Therapist Contents 1. Voice disorders 2. Swallow disorders 3. Videofluroscopy 4. Adult Acquired Communication Disorders 5. How to
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
SESSION 3 OXYGEN THERAPY
 SESSION 3 OXYGEN THERAPY Harith Eranga Yapa Department of Nursing Faculty of Health Sciences The Open University of Sri Lanka 1 Outline Methods of delivery Complications of oxygen therapy Artificial airways
SESSION 3 OXYGEN THERAPY Harith Eranga Yapa Department of Nursing Faculty of Health Sciences The Open University of Sri Lanka 1 Outline Methods of delivery Complications of oxygen therapy Artificial airways
Pediatric Modified Barium Swallow Studies. Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015
 Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
Pediatric Modified Barium Swallow Studies Presented by Jody Bousquet, MA, CCC- SLP Susan Shonbrun, MS, CCC- SLP November 7, 2015 Definition * Modified Barium Swallow Study * Assesses swallow functions
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
Respiratory Swallow Coordination in Healthy Individuals
 Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Cloud Publications International Journal of Advanced Speech and Hearing Research 2012, Volume 1, Issue 1, pp. 1-9, Article ID Med-03 Research Article Open Access Respiratory Swallow Coordination in Healthy
Policy x.xxx. Issued: Artificial Airways and Airway Care. ABC Home Medical Company Policy & Procedure Manual. A. Tracheostomy Tubes ( trach tubes)
 A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
A. Tracheostomy Tubes ( trach tubes) A tracheotomy is a surgical procedure whereby an opening is cut into the trachea of the patient for the purpose of inserting a tube (trach tube). The trach tube allows
1/22/2014. Disclosure. Course Outline. Course Objectives EARLY INTERVENTION IN PERSONS WITH MINIMALLY CONSCIOUS STATE & TRACHEOSTOMY
 Welcome to Passy-Muir s Event Webinar: Pediatric Candidacy for Speaking Valve Use: Journeys to Success If you have not registered for this event, go to the Education Portal to complete your registration.
Welcome to Passy-Muir s Event Webinar: Pediatric Candidacy for Speaking Valve Use: Journeys to Success If you have not registered for this event, go to the Education Portal to complete your registration.
Foundations of Critical Care Nursing Course. Tracheostomy Workbook
 Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
Foundations of Critical Care Nursing Course Tracheostomy Workbook 1 Key Reference: Dawson D (2014) Essential principles:trachepstomy care in the adult patient, Nursing in Critical Care, Vol 19, 2 p.63-72.
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA
 RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
RECOMMENDATIONS & UPDATES IN THE MANAGEMENT OF POST- STROKE DYSPHAGIA Feeding in the Acute Stroke Period: - Early initiation of feeding is beneficial w/c decreases the risk of infections, improve survival
Communication & The Mechanically Ventilated Patient. Megan Urban, MA, CCC-SLP Clinical Coordinator, Speech Pathology September 26, 2013
 Communication & The Mechanically Ventilated Patient Megan Urban, MA, CCC-SLP Clinical Coordinator, Speech Pathology September 26, 2013 Why is communication important? We had a young adult patient who sustained
Communication & The Mechanically Ventilated Patient Megan Urban, MA, CCC-SLP Clinical Coordinator, Speech Pathology September 26, 2013 Why is communication important? We had a young adult patient who sustained
Disclosures. Learning Objectives. Coeditor/author. Associate Science Editor, American Heart Association
 Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Tracheotomy Challenges for airway specialists Elizabeth H. Sinz, MD Professor of Anesthesiology & Neurosurgery Associate Dean for Clinical Simulation Disclosures Coeditor/author Associate Science Editor,
Passy-MuirInc. Clinical Inservice Outline. Touching Lives and Enhancing Patient Care Through Education
 Passy-MuirInc. Clinical Inservice Outline Touching Lives and Enhancing Patient Care Through Education Passy-Muir Tracheostomy & Ventilator Speaking Valves Clinical Inservice Outline I. Inventor, David
Passy-MuirInc. Clinical Inservice Outline Touching Lives and Enhancing Patient Care Through Education Passy-Muir Tracheostomy & Ventilator Speaking Valves Clinical Inservice Outline I. Inventor, David
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC
 Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Rota-Trach Double Lumen Tracheostomy Tube VITALTEC Contents INTRODUCTION HISTORY REVIEW ANATOMY & PHYSIOLOGY OPERATIVE PROCEDURE THE RANGE OF TRACHEOSTOMY TUBES ROTA-TRACH TRACHEOSTOMY TUBE INTRODUCTION
Tracheostomy management Kate Regan MRCP FRCA Katharine Hunt FRCA
 Kate Regan MRCP FRCA Katharine Hunt FRCA The use of tracheostomy has increased over recent years. Traditionally, it was confined to the emergency management of upper airway obstruction; more recently,
Kate Regan MRCP FRCA Katharine Hunt FRCA The use of tracheostomy has increased over recent years. Traditionally, it was confined to the emergency management of upper airway obstruction; more recently,
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR
 CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
CLINICAL CONSIDERATIONS FOR THE BUNNELL LIFE PULSE HIGH-FREQUENCY JET VENTILATOR 801-467-0800 Phone 800-800-HFJV (4358) Hotline TABLE OF CONTENTS Respiratory Care Considerations..3 Physician Considerations
Analysis of Trans-Tracheal Measurements in Children Wearing Speaking Valves during Sleep
 ISSN: 2250-0359 Research Article Volume 8 Issue : 66 208 Analysis of Trans-Tracheal Measurements in Children Wearing Speaking Valves during Sleep Melodi Pirzada *, John Bishara, Jessica Shaw 2, Joy Eribo
ISSN: 2250-0359 Research Article Volume 8 Issue : 66 208 Analysis of Trans-Tracheal Measurements in Children Wearing Speaking Valves during Sleep Melodi Pirzada *, John Bishara, Jessica Shaw 2, Joy Eribo
Developing a Speaking Valve Protocol in the NICU 5/17/2012
 Disclosures Developing a Speaking Valve Protocol in the NICU Melanie Stevens, MS-CCC/SLP Jen Finch, MA-CCC/SLP Leslie Justice, RN, MS, CPNP Erin Wishloff, BS/RRT-NPS Melanie Stevens, MS-CCC/SLP Disclosure:
Disclosures Developing a Speaking Valve Protocol in the NICU Melanie Stevens, MS-CCC/SLP Jen Finch, MA-CCC/SLP Leslie Justice, RN, MS, CPNP Erin Wishloff, BS/RRT-NPS Melanie Stevens, MS-CCC/SLP Disclosure:
*gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016
 *gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016 Learning objectives Describe the difference in anatomy between a tracheotomy and a laryngectomy Understand
*gurgle* *snore* *slaver* Tracheostomy Emergencies with Trachy Tracey Helen Lyall ACCP LUHT 03/06/2016 Learning objectives Describe the difference in anatomy between a tracheotomy and a laryngectomy Understand
Tracheostomy management
 BJA Education, 15 (3): 149 153 (2015) doi: 10.1093/bjaceaccp/mku008 Advance Access Publication Date: 25 April 2014 Matrix reference 1C02, 2A01, 3A01 Tracheostomy management Katharine Hunt MBBS FRCA 1,
BJA Education, 15 (3): 149 153 (2015) doi: 10.1093/bjaceaccp/mku008 Advance Access Publication Date: 25 April 2014 Matrix reference 1C02, 2A01, 3A01 Tracheostomy management Katharine Hunt MBBS FRCA 1,
Weaning from Mechanical Ventilation. Dr Azmin Huda Abdul Rahim
 Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Weaning from Mechanical Ventilation Dr Azmin Huda Abdul Rahim Content Definition Classification Weaning criteria Weaning methods Criteria for extubation Introduction Weaning comprises 40% of the duration
Problem-solving Respiratory Issues in Children With Neuromuscular Disease. December 13, 2018 Eliezer Be eri, M.D.
 Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
Problem-solving Respiratory Issues in Children With Neuromuscular Disease December 13, 2018 Eliezer Be eri, M.D. About Our Presenter Eliezer Be eri, M.D. Alyn Rehabilitation Hospital Jerusalem, Israel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device
 I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
I. Subject: Continuous Positive Airway Pressure CPAP by Continuous Flow Device II. Policy: Continuous Positive Airway Pressure CPAP by the Down's system will be instituted by Respiratory Therapy personnel
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy
 Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
Other methods for maintaining the airway (not definitive airway as still unprotected):
 Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Page 56 Where anaesthetic skills and drugs are available, endotracheal intubation is the preferred method of securing a definitive airway. This technique comprises: rapid sequence induction of anaesthesia
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube.
 Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency 1: General principles and equipment required to safely manage a patient with a tracheostomy tube. Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway.
 PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
PURPOSE This interdisciplinary clinical support document provides guidelines for the safe establishment of an artificial airway. POLICY STATEMENTS Endotracheal intubation will be performed by the Most
NON INVASIVE LIFE SAVERS. Non Invasive Ventilation (NIV)
 Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
Table 1. NIV: Mechanisms Of Action Decreases work of breathing Increases functional residual capacity Recruits collapsed alveoli Improves respiratory gas exchange Reverses hypoventilation Maintains upper
8/8/2013. Disclaimer. Tracheostomy Care in the Home. Polling Question 1. Upper Airway and Respiratory System
 Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff
 2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
2013 Medical Journal Tracheostomy and laryngectomy airway emergencies: an overview for medical and nursing staff Steven Lobaz 1 and Paul Bush 2 1 ST6 and 2 Consultant Department of Anaesthesia and Intensive
SWALLOWING DIFFICULTIES IN HD
 Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Nutrition, eating and swallowing needs, challenges and solutions Workshop SWALLOWING DIFFICULTIES IN HD Angela Nuzzi Speech and Language Pathologist (SLP) EHDN Language Coordinator - Italy The role of
Managing the Patient with Dysphagia
 Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
Managing the Patient with Dysphagia Patricia K. Lerner, MA, CCC, ASHA Fellow Board Certified Specialist in Swallowing & Swallowing Disorders Clinical Assistant Professor New York University School of Medicine
Weaning guidelines for Spinal Cord Injured patients in Critical Care Units
 RISCI Respiratory Information for Spinal Cord Injury UK Weaning guidelines for Spinal Cord Injured patients in Critical Care Units Introduction It is an unfortunate fact that Spinal Cord Injury Centres
RISCI Respiratory Information for Spinal Cord Injury UK Weaning guidelines for Spinal Cord Injured patients in Critical Care Units Introduction It is an unfortunate fact that Spinal Cord Injury Centres
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL
 AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
AFCH NEUROMUSCULAR DISORDERS (NMD) PROTOCOL A. Definition of Therapy: 1. Cough machine: 4 sets of 5 breaths with a goal of I:E pressures approximately the same of 30-40. Inhale time = 1 second, exhale
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
North Wales Critical Care Network
 North Wales Critical Care Network Weaning Guidelines for SPINAL CORD INJURED patients in North Wales Critical Care Units NWCCN Spinal Cord Injury Weaning Guidelines_APPROVED February 2014 Page 1 Weaning
North Wales Critical Care Network Weaning Guidelines for SPINAL CORD INJURED patients in North Wales Critical Care Units NWCCN Spinal Cord Injury Weaning Guidelines_APPROVED February 2014 Page 1 Weaning
The objectives of this presentation are to
 1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
1 The objectives of this presentation are to 1. Review the mechanics of airway clearance 2. Understand the difference between secretion mobilization and secretion clearance 3. Identify conditions that
Objectives. Apnea Definition and Pitfalls. Pathophysiology of Apnea. Apnea of Prematurity and hypoxemia episodes 5/18/2015
 Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
Apnea of Prematurity and hypoxemia episodes Deepak Jain MD Care of Sick Newborn Conference May 2015 Objectives Differentiating between apnea and hypoxemia episodes. Pathophysiology Diagnosis of apnea and
10/26/2017. Diagnostic Tests vs. Screening. Dysphagia Screening: What it is and what it is not
 Dysphagia Screening: What it is and what it is not Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director University of Kentucky Voice & Swallow Clinic Lexington, Kentucky ASHA's Preferred Practice Pattern on
Dysphagia Screening: What it is and what it is not Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director University of Kentucky Voice & Swallow Clinic Lexington, Kentucky ASHA's Preferred Practice Pattern on
STATE OF OKLAHOMA 2014 EMERGENCY MEDICAL SERVICES PROTOCOLS
 3K NON-INVASIVE POSITIVE PRESSURE VENTILATION (NIPPV) ADULT EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC Indications: 1. Dyspnea Uncertain Etiology Adult. 2. Dyspnea Asthma Adult. 3. Dyspnea Chronic
3K NON-INVASIVE POSITIVE PRESSURE VENTILATION (NIPPV) ADULT EMT EMT-INTERMEDIATE 85 ADVANCED EMT PARAMEDIC Indications: 1. Dyspnea Uncertain Etiology Adult. 2. Dyspnea Asthma Adult. 3. Dyspnea Chronic
Caring for Your TRACHEOSTOMY. Getting On with Your Life
 Caring for Your TRACHEOSTOMY Getting On with Your Life A New Pathway for Air Have you had a tracheostomy? Or, are you about to have one? If so, you may be wondering what the future holds for you. It s
Caring for Your TRACHEOSTOMY Getting On with Your Life A New Pathway for Air Have you had a tracheostomy? Or, are you about to have one? If so, you may be wondering what the future holds for you. It s
Competency Title: Continuous Positive Airway Pressure
 Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
Competency Title: Continuous Positive Airway Pressure Trainee Name: ------------------------------------------------------------- Title: ---------------------------------------------------------------
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
When Eating Becomes A Challenge Dysphagia
 When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
When Eating Becomes A Challenge Dysphagia 1. DYSPHAGIA, WHAT IS IT? 2. IMPLICATIONS 3. ASSESSMENT 4. COMPENSATORY SWALLOWING AND EXERCISES 5. DIET TEXTURE ADJUSTMENTS Swallowing Dysfunction = Dysphagia
Training. Continuous Positive Airway Pressure (CPAP)
 Training The training module will follow the national standard curriculum as it relates to the application and use of CPAP. The proposed curriculum will closely resemble the following algorithm utilizing
Training The training module will follow the national standard curriculum as it relates to the application and use of CPAP. The proposed curriculum will closely resemble the following algorithm utilizing
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด
 Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
Noninvasive Mechanical Ventilation in Children ศ.พญ.อร ณวรรณ พฤทธ พ นธ หน วยโรคระบบหายใจเด ก ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร โรงพยาบาลรามาธ บด Noninvasive Mechanical Ventilation Provide support without
1.40 Prevention of Nosocomial Pneumonia
 1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
1.40 Prevention of Nosocomial Pneumonia Purpose Audience Policy Statement: The guideline is designed to reduce the incidence of pneumonia and other acute lower respiratory tract infections. All UTMB healthcare
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the
 Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Neuromuscular diseases (NMDs) include both hereditary and acquired diseases of the peripheral neuromuscular system. They are diseases of the peripheral nerves (neuropathies and anterior horn cell diseases),
Dysphagic Patients with Tracheotomies: A Multidisciplinary Approach to Treatment and Decannulation Management
 Dysphagia 22:20 29 (2007) DOI: 10.1007/s00455-006-9036-5 Dysphagic Patients with Tracheotomies: A Multidisciplinary Approach to Treatment and Decannulation Management Ulrike Frank, MSc, 1 Mark Ma der,
Dysphagia 22:20 29 (2007) DOI: 10.1007/s00455-006-9036-5 Dysphagic Patients with Tracheotomies: A Multidisciplinary Approach to Treatment and Decannulation Management Ulrike Frank, MSc, 1 Mark Ma der,
NON-INVASIVE VENTILATION. Lijun Ding 23 Jan 2018
 NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
NON-INVASIVE VENTILATION Lijun Ding 23 Jan 2018 Learning objectives What is NIV The difference between CPAP and BiPAP The indication of the use of NIV Complication of NIV application Patient monitoring
I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP
 I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP II. Policy: PSV with BiPAP device/nasal CPAP will be initiated upon a physician's order by Respiratory Therapy personnel trained
I. Subject: Pressure Support Ventilation (PSV) with BiPAP Device/Nasal CPAP II. Policy: PSV with BiPAP device/nasal CPAP will be initiated upon a physician's order by Respiratory Therapy personnel trained
Basics of NIV. Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC. Consultant, Critical Care Medicine Medanta, The Medicity
 Basics of NIV Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Objectives: Definitions Advantages and Disadvantages Interfaces Indications Contraindications
Basics of NIV Dr Shrikanth Srinivasan MD,DNB,FNB,EDIC Consultant, Critical Care Medicine Medanta, The Medicity Objectives: Definitions Advantages and Disadvantages Interfaces Indications Contraindications
Mechanical Ventilation of the Patient with Neuromuscular Disease
 Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
Mechanical Ventilation of the Patient with Neuromuscular Disease Dean Hess PhD RRT Associate Professor of Anesthesia, Harvard Medical School Assistant Director of Respiratory Care, Massachusetts General
MULTIPLE reports have. Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer ORIGINAL ARTICLE
 ORIGINAL ARTICLE Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer Arie Rosen, MD; Thomas H. Rhee, MD; Rene Kaufman, MS, CCC-SLP Objectives: To determine
ORIGINAL ARTICLE Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer Arie Rosen, MD; Thomas H. Rhee, MD; Rene Kaufman, MS, CCC-SLP Objectives: To determine
Introducing the Fastrach-LMA. Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council
 Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
Introducing the Fastrach-LMA Prepared by Jim Medeiros, NREMT-P Regional Field Coordinator Lord Fairfax EMS Council Objectives Review Anatomy of the Upper Airway Review LFEMSC LMA Protocol Discuss Indications
RSPT Tracheal Aspiration. Tracheal Aspiration. RSPT 1410 Tracheal Aspiration
 1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
1 RSPT 1410 2 is the use of to facilitate the removal of secretions from the respiratory tract. Under normal circumstances, patients with normal coughing do not have difficulty in removing secretions.
RESPIRATORY COMPLICATIONS AFTER SCI
 SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
SHEPHERD.ORG RESPIRATORY COMPLICATIONS AFTER SCI NORMA I RIVERA, RRT, RCP RESPIRATORY EDUCATOR SHEPHERD CENTER 2020 Peachtree Road, NW, Atlanta, GA 30309-1465 404-352-2020 DISCLOSURE STATEMENT I have no
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol
 New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
New Evidence-Based Support of a 3 Ounce Water Swallow Challenge Protocol Steven B. Leder, Ph.D. Yale University School of Medicine New Haven, Connecticut Debra M. Suiter, Ph.D. VA Medical Center-Memphis
Small Volume Nebulizer Treatment (Hand-Held)
 Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Small Volume Aerosol Treatment Page 1 of 6 Purpose Policy Physician's Order Small Volume Nebulizer Treatment To standardize the delivery of inhalation aerosol drug therapy via small volume (hand-held)
Kapitex Healthcare. making things clearer for tracheostomy patients
 Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
Kapitex Healthcare making things clearer for tracheostomy patients preface In publishing this booklet, Kapitex Healthcare Ltd hopes to provide information and understanding for both the patient and carer
Respiratory Management of Facioscapulohumeral Muscular Dystrophy. Nicholas S. Hill, MD Tufts Medical Center Boston, MA
 Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
Respiratory Management of Facioscapulohumeral Muscular Dystrophy Nicholas S. Hill, MD Tufts Medical Center Boston, MA Respiratory Involvement in FSHD Very variable time of onset rate of progression Muscles
Bergen Community College Division of Health Professions Department of Respiratory Care Fundamentals of Respiratory Critical Care
 Bergen Community College Division of Health Professions Department of Respiratory Care Fundamentals of Respiratory Critical Care Date Revised: January 2015 Course Description Student Learning Objectives:
Bergen Community College Division of Health Professions Department of Respiratory Care Fundamentals of Respiratory Critical Care Date Revised: January 2015 Course Description Student Learning Objectives:
ALL orders are active unless: 1. Order is manually lined through to inactivate 2. Orders with check boxes ( ) are unchecked DRUG AND TREATMENT ORDERS
 DRUG AND TREATMENT Intubation Phase Notify Therapy for STAT intubation Medications SUB Rapid Sequence Induction (SUB)* ***Reminder: Order SUB Rapid Sequence Induction (SUB) on a separate form*** lidocaine
DRUG AND TREATMENT Intubation Phase Notify Therapy for STAT intubation Medications SUB Rapid Sequence Induction (SUB)* ***Reminder: Order SUB Rapid Sequence Induction (SUB) on a separate form*** lidocaine
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
AIRWAY MANAGEMENT AND VENTILATION
 AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
AIRWAY MANAGEMENT AND VENTILATION D1 AIRWAY MANAGEMENT AND VENTILATION Basic airway management and ventilation The laryngeal mask airway and Combitube Advanced techniques of airway management D2 Basic
Laryngeal Conservation
 Laryngeal Conservation Sarah Rodriguez, MD Faculty Advisor: Shawn Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngolgy Grand Rounds Presentation February 2005 Introduction
Laryngeal Conservation Sarah Rodriguez, MD Faculty Advisor: Shawn Newlands, MD, PhD The University of Texas Medical Branch Department of Otolaryngolgy Grand Rounds Presentation February 2005 Introduction
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
