46 Chest Examination PETER G. TUTEUR. Definition. Technique
|
|
|
- Irene Perry
- 6 years ago
- Views:
Transcription
1 46 Chest Examination PETER G. TUTEUR Definition The patient's history determines the scope and intensity of the chest. When the history elicits suspicion of the presence of a chest problem, the physical of the thorax must be expanded beyond a minimal screening to determine the nature of the problem so that a diagnosis can be made. Technique The setting for the chest must be environmentally comfortable for both clinician and patient. The physical begins with the commencement of history taking. The examiner extends a hand in greeting, asks about the symptoms that initiated the visit, and begins physical inspection, noting body position, assessing degree of comfort, inspecting and palpating the hands, and noting grip strength. The history determines the format. Experienced clinicians exploit the history to help them "look" for specific physical findings to answer questions posed by the totality of data collected previously. When using this process, it is unusual for two consecutive chest s to be identical. By the time the physical is complete, even before laboratory evaluations are initiated, the diagnosis should be reasonably certain. The pulmonary consists of inspection, palpation, percussion, and auscultation. The inspection process initiates and continues throughout the patient encounter. Palpation, confirmed by percussion, assesses for tenderness and degree of chest expansion. Auscultation, a more sensitive process, confirms earlier findings and may help to identify specific pathologic processes not previously recognized. nspection nspection (Table 46.1) is an active process. t is done with the eyes and the intellect. t begins with the initial greeting and continues uninterruptedly during the entire data collection process. Even as the first serious question of the fully dressed patient is asked, the inspection begins through active observation. Specifically, one must note the dynamics of the patient's facial expression in relationship to physiologic activities (inspiration and expiration) and to the questions asked by the examiner. Similarly, active observation skills are used to search for the use of pursed lips during expiration, the activity and development of the sternocleidomastoid muscles, the use of other accessory muscles of ventilation, the presence of shoulder girdle fixation in relationship to the use of these accessory muscles, the flaring of the nasal alae, the presence of jugular venous distention, the degree of comfort, and, as discussed in previous chapters, the presence of cyanosis and clubbing. Not only may a voluntary smile be helpful in assessing neurologic function, but also inspection of the teeth at that time (even though you are just starting to take the history) may reveal extensive pyorrhea that serves to alert the clinician to a dental problem that has a potential as a bacterial source for necrotizing pneumonia. As the interview continues, assessment of the level of consciousness and the appropriateness of behavior may lead one to suspect a primary pulmonary process that secondarily produces alterations of central nervous system function. Two examples are respiratory acidosis and cerebral metastases from primary carcinoma of the lung. Dress, too, may give a clue to occupation or hobby, grooming may be related to the conscientiousness with which the patient may follow a health care plan, and a bulging shirt pocket may be stuffed with an open package of cigarettes, an important clue to the possibility of a chest problem. The inspection continues even though the patient remains fully clothed and the "formal" physical has not yet begun. t is often helpful to make an initial assessment of the ventilatory pattern early in the data collection process. Specifically, one should be concerned about rate, rhythm, breath volume, and the apparent effort associated with breathing. ost resting adults breathe about 12 times per minute, not the customary 20 often noted in medical records. Tidal volumes range around 600 ml. Except for an occasional sigh, the normal ventilatory pattern is regular and effortless. n disease this pattern may change. The assessment of ventilatory pattern during the history does not give the patient an opportunity to alter breathing involuntarily and confound the data. t also allows one to process data earlier and to increase efficiency. When the "formal" physical does begin, the setting is changed. nspection continues, but with the patient undressed from the waist up, either entirely or sequentially, as drapes are changed to expose only those areas being actively observed. A chaperon should be present when it would make either the patient or the examiner more comfortable. First, one should observe for thoracic cage deformity (pectus excavatum, pectus carinatum, scoliosis, kyphosis, surgical or traumatic scars, thoracoplasty, gynecomastia, and so-called barrel chest deformity). The presence of some skin lesions may reflect intrathoracic pathology. These are "static" observations. Even more useful information can be obtained as the patient breathes, both quietly and deeply. Such "dynamic" observations include the search for supraclavicular or intercostal retraction, paradoxical movement of the abdomen, any degree of asymmetry or asynchrony of chest expansion, muscle wasting or hypertrophy, and reproducible grimaces of discomfort at a given point in the ventilatory cycle. Other nonmanually elicited data such as audible musical breath sounds-wheezes-strongly influence the decision-making process. 239
2 THE PULONARY SYSTE Table 46.1 nspection inimal Hemoptysis smoke Environmental Other organ disease Facial expression : Nasal alae Pursed lips Pyorrhea Sternocleido- mastoid Jugular venous Right-sided heart distention failure Posture : Fixed shoulder girdle Diaphoresis Splinting ntraabdominal process Breathing pattern : Rate Rhythm Cerebral Breath volume metabolic acidosis Degree of effort Chest configuration Static : Pectus excavatum Spine contour Surgical scars Gynecomastia Barrel chest (T A-P in adult diameter) Dynamic : Expansion Retraction Paradoxical movement uscles Grimaces Audible wheezes No clinical significance Neuromuscular disorders Skin : Spider heman- Liver giomas Fibroma Neurofibromatosis Acanthosis nigri- alignancy cans Acne + striae Cushing's disease/ syndrome Upper airway obstruction = indicated ; = mandatory. Palpation Palpation (Table 46.2) is the next stage of the. With the patient disrobed, place the entire palm of each hand first on the superior portion of both hemithoraces and then, gently though firmly, move the hand inferiorly to just below the twelfth rib. Repeat the process moving laterally and subsequently anteriorly ; search for rib deformities, nodules, and areas of tenderness. n the face of a history of chest discomfort, ask the patient to point to the area(s) of greatest discomfort. Palpate the area with increasing firmness in an attempt to elicit tenderness and to assess if this maneuver reproduces the patient's symptoms. Pay particular attention to the costochondral junctions in patients reporting anterior chest pain to evaluate the possibility of costochondritis. Palpation is also important in the assessment of ventilation. One can sensitively assess the symmetry, synchrony, and volume of each breath. This is done by examining the patient posteriorly, placing the examiner's thumbs together at the midline at the level of the tenth rib with hands grasping the lateral rib cage ; both visual and tactile observations are made both during tidal volume breathing and during deep forceful inhalation. With the latter, thumbs typically separate by approximately 2 to 3 cm. A part of the palpatory portion of the chest is to assess the position of the trachea. This is accomplished best with the examiner stationed behind the patient, palpating the anterior inferior neck just above the jugular notch by gently pressing the fingertips between the lateral tracheal wall and the medial portion of the sternocleidomastoid mus-
3 46. CHEST EXANATON 241 Table 46.2 Palpation inimal Hemoptysis smoke Environmental Other organ disease Palpation for cutaneous or subcutaneous nodules Soft Hard Palpation for tenderness : Costochondral junction Other Assess ventilatory excursion : Symmetry Synchrony Expansion Assess observed abnormalities : Gynecomastia Spider hemangiomas Position of trachea Neurofibromatoses Chest pain () Chest pain () Liver () = indicated ; = mandatory. cle. Comparing one side to the other, an assessment is made of the position of the trachea : midline or deviation away from the centrist position. Tactile appreciation of vibrations transmitted to the surface of the thorax as upper airways sounds are generated by breathing or speaking is a traditional though insensitive maneuver referred to as tactile or vocal fremitus. Egophony is both more specific and sensitive. t is discussed under auscultation. Percussion The purpose of percussion (Table 46.3) is to determine if the area under the percussed finger is air filled (sounding resonant like a drum), fluid filled (a dull sound) or solid (a flat sound). To make this interpretation it is important not only to listen for the sound produced but also to feel the intensity and frequency of vibrations produced by this maneuver. The technique of percussion is best accomplished by the following approach : 1. Press the distal phalanx of the middle finger firmly on the area to be percussed and raise the second and fourth fingers off the chest surface ; otherwise, both sound and tactile vibrations will be blunted. 2. Use a quick, sharp wrist motion (like a catcher throwing a baseball to second base) to strike the finger in contact with the chest wall with the tip of the third finger of the other hand. The best percussion site is between the proximal and distal interphalangeal joints. The novice quickly learns to trim the fingernail to prevent personal discomfort of minor abrasions and lacerations. 3. f the sound and the vibrations produced seem suboptimal, make sure that the finger placed directly on the thorax is making very firm direct contact with the chest wall. f not, few vibrations and little sound will be produced. Table 46.3 Percussion inimal Hemoptysis smoke Environmental Other organ diseases General percussion : Note over thorax dentification of Lymphoma focal changes Diaphragmatic : ovement yasthemia and other Asymmetry neuromuscular Asynchrony disorders = indicated ; = mandatory.
4 THE PULONARY SYSTE 4. Percuss the posterior, lateral, and anterior chest wall in such a manner that the long axis of the percussed finger is roughly parallel to the ribs. Compare one side to the other. 5. Over each area, begin percussion superiorly and extend inferiorly to identify the level of the diaphragm during quiet (tidal volume) breathing. Note the position of the diaphragm. Then ask the patient to inhale fully and "hold it" ; continue to percuss inferiorly to determine the new level of the diaphragm, now during forced maximal inspiration. Then, don't forget to tell the patient to "breathe normally." The difference between the two levels is known as diaphragmatic excursion and should equal 2 to 3 cm. Auscultation Auscultation of the chest (Table 46.4) is part of every chest but it is the data collected during inspection, palpation, and percussion that alert the clinician what to listen for during auscultation in order to identify the correct diagnosis most effectively. The stethoscope is an instrument that does not significantly amplify sound, but, more important, acts as a selective filter of sound. Briefly, the bell filters high-frequency sounds greater than 1500 cycles per second and therefore should be used to detect low-frequency sounds. On the other hand, the diaphragm selectively filters low-frequency sounds. Since sounds produced by breathing tend to be of relatively high pitch, the chest is ausculted with the diaphragm. Auscultation of the chest ideally is performed in a quiet room with the patient either sitting or standing. When the posterior thorax is examined, the patient's arms should be crossed anteriorly to move the scapulas laterally as much as possible. Comparing one side to the other is a helpful maneuver to identify the patient's "normal." Auscultation should be performed during tidal ventilation, deep forceful inspiration, and forceful expiration. t is not only intuitively obvious but rigorously proved that the intensity of breath sounds is related to flow rates ; that is, the louder the sound, the greater the flow rate, all other things being equal. Basic Science The primary structure of the chest is designed to facilitate ventilation, which can be accomplished only by increasing the intrathoracic volume. This increase is due to elevation of the ribs, contraction of the scalene and intercostal muscles, and descent of the diaphragm. Because of the structure of the ribs, the scalenus muscles elevate the first rib and the sternum anteriorly. This causes slight increase in the anteroposterior (A-P) diameter of the chest. The lower ribs (T6-T 12) expand laterally by contraction of the intercostal muscles. The diaphragm, by contracting, elevates the lower ribs superiorly and laterally as well as increases the intrathoracic volume. Any deviation from the normal anatomical relationship of the skeletal system and the associated muscles would be expected to cause some abnormality in the inspiratory cycle of ventilation. During ventilation, the movement of gas produces sound audible with a stethoscope. Generally, the velocity of gas movement is proportional to the intensity of the sound. Qualitatively, there are three types of "normal" breath sounds : vesicular, bronchovesicular, and bronchial. The three sounds are clearly differentiated by the characteristics of duration, pitch, and intensity (see Table 46.4). Vesicular sounds are thought to be produced by gas movement through the distalmost portions of lung units. They are low in pitch, predominantly inspiratory in timing, and have a breezy character. Bronchial or tracheal sounds are produced high in the upper airways and trachea. They are often loud and high pitched. The expiratory phase is longer than inspiration and follows a "silent gap." Bronchovesicular sounds are intermediate between the two. Under normal circumstances, air-filled lung units act as high-frequency filters so that the bronchial breath sounds generated in the upper airways are poorly transmitted through airfilled lung. On the other hand, when there is little air-filled lung between airways and the stethoscope, or when lung units are filled with liquid rather than gas, bronchial breath sounds are heard clearly. As a result, bronchial breath sounds are heard normally over the trachea, the upper sternum, and paraspinal areas of the upper thoracic vertebrae. As Table 46.4 Auscultation inimal Hemoptysis smoke Environmental Other organ diseases Breath sounds : General nappropriate : Location of bronchial breath sounds Abnormal breath sounds : Wheezes : General Local Crackles Early inspiratory Late inspiratory "Collagen vascular diseases" ; congestive heart failure Gurgles Pulmonary edema = indicated ; = mandatory.
5 46. CHEST EXANATON one moves peripherally and more air-filled lung is found between the airways and the stethoscope, breath sounds first become bronchovesicular in quality and eventually vesicular. As stated above, the intensity of sound is a function of airflow. Careful of upper lung fields reveals greater intensity of breath sounds early during the inspiratory phase compared to the sounds generated during inspiration over lower lung fields where the intensity peaks rather late. This is a reflection of the normal physiologic phenomenon that as one inhales from residual volume, the initial bolus of gas enters upper lobe alveoli ; and only when these lung units are nearly filled is there bulk movement of gas to the lower lung fields. When there is obstruction to the airways of the upper lobes, this pattern is no longer present. There are three types of abnormal breath sounds. Frequently, they are collectively referred to as adventitious breath sounds. The most easily recognized abnormal breath sound is the wheeze, a continuous musical sound produced when a critical velocity of gas flow passes through a slitlike opening. The pitch of sound is a function of the compliance of the material producing the slitlike opening, not the original size of the obstructed tube. One may appreciate wheezing over the entire thorax or locally. The other two abnormal breath sounds are noncontinuous in nature. The crackle, often called "rale," sounds like the rubbing of a lock of hair over the ear. n vivo, this sound is produced by the snapping open of previously collapsed lung structures, either airways or alveoli. The timing of crackles, which invariably occur during inspiration, should be noted. This is done by asking the patient to exhale fully and then noting the timing of crackles during the subsequent full inspiratory maneuver. When crackles are heard during the initiation of inspiration, they are called early inspiratory crackles. When they occur toward the terminal portion of the inspiratory maneuver, they are referred to as late inspiratory crackles. At times, crackling sounds can be heard throughout the inspiratory phase and are called paninspiratory crackles. The final abnormal breath sound is called a gurgle. t is similar to the sound produced when one exhales through a straw placed in a glass of water. Gurgles are produced by airflow through liquid of varying viscosities in the airways. Since some clinicians use the term rhonchus to mean lowpitched wheeze and others use this same term to mean gurgle, it is recommended that confusion be minimized by not using the term rhonchus. nspection The respiratory rate may increase with the presence of an interstitial pulmonary process or chest wall restriction, but tidal volume typically remains unchanged. The presence of slow, gasping ventilatory maneuvers is an ominous sign suggesting cerebral hypoxemia. Dysrhythmic breathing is typified by Cheyne-Stokes respiration. This eponym refers to a periodic pattern of alternating hyperpnea and apnea. Though, at times, it is a normal phenomenon seen in infants, the elderly, and during ascent to altitude, more often it is a reflection of significant cardiac and/or pleural nervous system dysfunction. Breath volumes are increased without substantial modification of rate as a compensatory mechanism to blunt the effects of a metabolic acidosis such as occurs with uncontrolled diabetes. When this occurs, the effort associated with this Kussmaul breathing seems to be minimal. The configuration of the chest may aid in the diagnostic process. Typically, pectus excavatum (funnel chest) or its counterpart pectus carinatum (pigeon breast) are associated with unequivocal physical findings but rarely have an adverse impact on pulmonary function. Scars identify previous surgery or trauma and alert the clinician to the need for a complete history of the event. The so-called barrel chest deformity, sometimes referred to as increased A-P diameter, often erroneously is interpreted as associated with the presence of pulmonary emphysema. Several studies have proved that this description is not necessarily associated with underlying pulmonary disease but regularly is a function of weight loss and mild kyphosis, a function of the aging process. During breathing, assessment of changing chest shape can be more helpful. The presence of intercostal retraction, pursued-lip breathing, and use of accessory muscles suggest airways obstruction. Paradoxical movement of chest and abdominal muscles should alert the clinician to the possible usefulness of pulmonary physiotherapy to improve ventilatory efficiency. Grimaces or other expressions of discomfort occurring at the same point in each ventilatory cycle should influence the examiner to identify the origin of that discomfort more precisely. Finally, wheezing heard by the examiner during tidal volume breathing or exaggerated breathing may be a reflection of upper airway obstruction (stridor) or severe lower airway narrowing. The search for dermatologic abnormalities also may lead one to the identification of other systemic or pulmonary processes. Clinical Significance Physical findings must be interpreted in light of all previously collected data. The general scheme is to develop a postulate and test it with further history, additional observations or maneuvers on physical s, and laboratory tests. For example, a 60-year-old pipefitter with known exposure to airborne asbestos material who never smoked cigarettes and presents with increasing dyspnea and cough would most likely have asbestosis (interstitial fibrosis caused by the asbestos inhalation) if one observed dry, nonproductive cough following every moderate to deep breath ; if the same initial data differed because of cigarettes in his pocket and an intermittent cough associated with the expectoration of blood, carcinoma of the lung might head the differential diagnosis list. Palpation Palpation is used both as a screening technique and as a means to confirm a specific diagnosis. Light palpation over the entire thorax posteriorly, laterally, and anteriorly will aid in the identification of cutaneous and subcutaneous nodules and the site of previously unsuspected tenderness. Nodules that are firm and freely moveable suggest a focal benign inflammatory or clinically insignificant problem. Those that are hard, fixed, and multiple suggest metastatic malignancy. Fleshy nodules may be indicative of a systemic disease such as neurofibromatosis. Tenderness may be elicited during this same maneuver. At times, it is unsuspected by both the patient and the examiner. Under other circumstances, it is used to aid in a diagnosis of the complaint of chest pain. Localizing a rib
6 244. THE PULONARY SYSTE fracture, either traumatic or pathologic, or reproducing the chest pain of costochondritis by firm palpation of an inflamed costochondral junction may be most helpful in planning further management. Tenderness over an inflamed or infarcted area of lung may also aid in the localization of the disease process. Assessment of ventilatory excursion includes evaluation of the synchrony of expansion and the degree of chest expansion associated with a deep forceful inspiration from residual volume. Asymmetrical expansion invariably implies decreased ventilation to one side. This may be due to thoracic wall abnormalities, particularly those that are either associated with structural immobility or defect (thoracoplasty) or pain (rib fracture). Similarly, the problem may be caused by an inflamed, fibrosed, or malignantly infiltrated pleura, a unilateral pleural effusion, an interstitial pulmonary process, or a complete obstruction of an airway or airways on the ipsilateral side. Functional severing of the phrenic nerve or intraabdominal process causing paralysis of the ipsilateral hemidiaphragm may be responsible for asymmetrical expansion. Asynchronous expansion may occur secondary to these processes but usually occurs with functional diaphragmatic impairment or pain. Palpation is used to assess further abnormalities ; gynec omastia suspected because of observed breast enlargement is confirmed by the palpation of breast tissue. Similarly, spider hemangiomas are confirmed when the central arterial supply is seen to feed the spider's radicals following manual occlusion. Finally, deviation of the trachea to one side can mean that a process is either pulling the trachea to one side, such as occurs with lung volume loss (lobar collapse, atelectasis, pneumothorax), or pushing the trachea away, such as might occur with either a tumor or an inflammatory mass. Spontaneous movement of the trachea in synchrony with the pulse suggests the presence of an aortic aneurysm. Percussion Percussion is a major aid in the assessment of ventilatory exertion, the assessment of hyperinflation, and the presence of focal thoracic disease. The general percussion over a hemithorax can give a clue as to the presence or absence of a pulmonary process. When the percussion note is hyperresonant, one can postulate that the lungs are hyperinflated, such as may occur with emphysema or during so-called air trapping seen in patients with acute asthma. This may also occur in patients with an acute spontaneous pneumothorax. Dullness to percussion, particularly associated with the presence of a high, poorly moving diaphragm, is likely to be associated with a restrictive ventilatory defect if the findings are bilaterally symmetrical. Usually this is associated with an interstitial pulmonary process that can be further evaluated by the presence or absence of late inspiratory crackles on auscultation. Flatness to percussion suggests the virtual absence of air directly beneath the percussed finger and may reflect either fluid in the pleural space (pleural effusion, empyema), solid material in the pleural space (fibrothorax, mesothelioma), or atelectases. Auscultation breath sounds are normally heard, one can imply that the airways to the lung units are open but that the lung units themselves are filled with liquid-like material. When this occurs without pleural fluid, the bronchial breath sounds are loud ; when consolidation is associated with a pleural effusion, the bronchial breath sounds are present but often quite decreased in intensity. Confirmation of the presence of bronchial breath sounds can be obtained by listening for egophony ("E to A" sound). This sound is elicited by asking the patient to say the letter "E" as one listens over the suspicious area with the stethoscope. When consolidation is present, the spoken "E" sound is converted to an ausculted "A" sound, similar to that produced by a bleating goat. n addition to assessing the quality of breath sounds, it is also important to assess the duration of the expiratory phase. Timing the duration of expiratory sound while listening with the diaphragm over the trachea during a forced expiratory volume maneuver is used to identify airways obstruction. Expiratory sound should terminate within 6 seconds. f the sound is prolonged, airways obstruction manifested by an FEV, of less than 1.5 liters can be assumed. Auscultatory wheezes imply the presence of slitlike openings through which a critical velocity of gas is passing. When wheezes are local, one must consider external compression of an airway. Enlarged lymph nodes and tumors do this. A lesion within the airway, such as an endobronchial malignancy or foreign body, also can produce a localized wheeze. Diffuse wheezing is present in inflammatory processes such as bronchitis (both acute or chronic), contraction of hypertrophied bronchial smooth muscle as seen in asthma, inspissated thick secretions of pneumonia, and airway collapse associated with the dynamic compression of pulmonary emphysema. Crackles imply the snapping open of airways or alveoli. Since larger airways open first as inhalation progresses from residual volume, early inspiratory crackles imply large airways disease while late inspiratory crackles either mean small airways problems (less than 2 mm) or poorly compliant alveoli walls such as seen in congestive heart failure, pulmonary fibrosis, or other interstitial pulmonary processes. Gurgles suggest fluid in the airways. This may be produced by excessive serous secretion in alveolar cell carcinoma, infected purulent secretion of acute or chronic bronchitis or bronchiectasis, or transudated fluid entering the airways from the alveoli as occurs in pulmonary edema. References Forgacs P. Functional significance of clinical signs in diffuse airway obstruction. Brit J Dis Chest 1971 ;65 :170. Kilburn KH, et al. Anterior-posterior chest diameter in emphysema. Arch nt ed 1969 ;123 :379. Leblanc P, et al. Breath sounds and distribution of pulmonary ventilation. Amer Rev Resp Dis 1970 ;102 :10. Lehrer S. Understanding lung sounds, Philadelphia : W.B. Saunders, Nath AR, Capel LH. nspiratory crackles-early and late. Thorax 1974 ;29 :223. Pierce JA, Ebert RB. The barrel deformity of the chest, the senile lung and obstructive pulmonary emphysema. Amer J ed 1958 ;25 :13. Rales, rhonchi, and Laennec, recorded by A. John Robertson, after an evening with Robert Coope. Lancet 1957 ;2 :417. Bronchial breath sounds may be either normal or abnormal. When they are heard on the periphery, where vesicular
LESSON ASSIGNMENT. Physical Assessment of the Respiratory System. After completing this lesson, you should be able to:
 LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
LESSON ASSIGNMENT LESSON 2 Physical Assessment of the Respiratory System. LESSON ASSIGNMENT Paragraphs 2-1 through 2-8. LESSON OBJECTIVES After completing this lesson, you should be able to: 2-1. Perform
Respiratory Assessment
 Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
Module Four Physical examination of Respiratory Assessment 1 THORACIC CAGE: Anterior thoracic cage Posterior thoracic cage 2 Reference lines: Anterior vertical lines Lateral vertical line Posterior vertical
BIOE221. Session 5. Examination of Thorax- Respiratory system. Bioscience Department. Endeavour College of Natural Health endeavour.edu.
 BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
BIOE221 Session 5 Examination of Thorax- Respiratory system Bioscience Department Session Objectives Understand the structure of the thorax and the organs contained in this cavity Understand the importance
Examination of the Respiratory System
 Examination of the Respiratory System Wash your hands & Introduce the exam to your patient Positioning & Draping while seated or standing, the patient should be exposed to the waist? patients can be uncovered
Examination of the Respiratory System Wash your hands & Introduce the exam to your patient Positioning & Draping while seated or standing, the patient should be exposed to the waist? patients can be uncovered
Techniques of examination of the thorax and lungs. Dr. Szathmári Miklós Semmelweis University First Department of Medicine 24. Sept
 Techniques of examination of the thorax and lungs Dr. Szathmári Miklós Semmelweis University First Department of Medicine 24. Sept. 2013. Inspection of the thorax Observe: the shape of chest Deformities
Techniques of examination of the thorax and lungs Dr. Szathmári Miklós Semmelweis University First Department of Medicine 24. Sept. 2013. Inspection of the thorax Observe: the shape of chest Deformities
d) Always ensure patient comfort. Be considerate and warm the diaphragm of your stethoscope with your hand before auscultation.
 Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Auscultation Auscultation is perhaps the most important and effective clinical technique you will ever learn for evaluating a patient s respiratory function. Before you begin, there are certain things
Percussion, auscultation. Dr. Szathmári Miklós Semmelweis University First Department of Medicine 23. Sept. 2013
 Percussion, auscultation Dr. Szathmári Miklós Semmelweis University First Department of Medicine 23. Sept. 2013 The physical principles of the percussion Percussion sets the body surface (chest wall) and
Percussion, auscultation Dr. Szathmári Miklós Semmelweis University First Department of Medicine 23. Sept. 2013 The physical principles of the percussion Percussion sets the body surface (chest wall) and
VITAL SIGNS AND PHYSICAL EXAMINATION OF THE CHEST Eve Bargmann, MD 9/22/03
 VITAL SIGNS AND PHYSICAL EXAMINATION OF THE CHEST Eve Bargmann, MD 9/22/03 Objectives: 1. To understand normal 2. To introduce examination of vital signs, pulses and the chest 3. To relate anatomy to physical
VITAL SIGNS AND PHYSICAL EXAMINATION OF THE CHEST Eve Bargmann, MD 9/22/03 Objectives: 1. To understand normal 2. To introduce examination of vital signs, pulses and the chest 3. To relate anatomy to physical
RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE
 RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE What does respiratory assessment involve? Subjective Assessment Objective Assessment Inspection, palpation, percussion and auscultation
RESPIRATORY ASSESSMENT JENNY CASEY RESPIRATORY SERVICES LEAD ACE What does respiratory assessment involve? Subjective Assessment Objective Assessment Inspection, palpation, percussion and auscultation
The Goal of the Respiratory Assessment. Two Parts of the Respiratory Assessment
 The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
The Respiratory System Respiratory Assessment of the Adult Patient Mary Douglas, MSN, RN Nurse Educator Minneapolis VA Health Care System Respiratory system: moves oxygen into the body and carbon dioxide
Wash your hands, introduce yourself, obtain consent.
 Introduction At the start: Wash your hands, introduce yourself, obtain consent. Patient position: Sitting upright (45 o ) & adequately exposed (undress to waist). NB: if you have a female patient, the
Introduction At the start: Wash your hands, introduce yourself, obtain consent. Patient position: Sitting upright (45 o ) & adequately exposed (undress to waist). NB: if you have a female patient, the
Landmarks. Lung Examination for the Chiropractor 8/16/2016. ChiroCredit.com Presents. Physical Diagnosis 153. Anatomy and Physiology
 ChiroCredit.com Presents Physical Diagnosis 153 Lung Examination for the Chiropractor Presented by: Jennifer Illes, DC, MS 1 Lung Examination for the Chiropractor Anatomy and Physiology The Chest Wall
ChiroCredit.com Presents Physical Diagnosis 153 Lung Examination for the Chiropractor Presented by: Jennifer Illes, DC, MS 1 Lung Examination for the Chiropractor Anatomy and Physiology The Chest Wall
Auscultation of the lung
 Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
Auscultation of the lung Auscultation of the lung by the stethoscope. *Compositions of the stethoscope: 1-chest piece 2-Ear piece 3-Rubber tubs *Auscultation area of the lung(triangle of auscultation).
NEO 111 Melanie Jorgenson, RN, BSN
 NEO 111 Melanie Jorgenson, RN, BSN Inspection: performing deliberate, purposeful observations in a systematic manner Palpation: using the sense of touch Percussion: striking one object against another
NEO 111 Melanie Jorgenson, RN, BSN Inspection: performing deliberate, purposeful observations in a systematic manner Palpation: using the sense of touch Percussion: striking one object against another
Tracheal normal sound heard over trachea loud tubular quality high-pitched expiration equal to or slightly longer than inspiration
 = listening for sounds produced in the body over chest to ID normal & abnormal lung sounds all BS made by turbulent flow in the airways useful in making initial D & evaluating effects of R 4 characteristics
= listening for sounds produced in the body over chest to ID normal & abnormal lung sounds all BS made by turbulent flow in the airways useful in making initial D & evaluating effects of R 4 characteristics
Breath Sounds. It gives you an opportunity to listen to both normal and abnormal breath sounds, as well as explaining their clinical relevance.
 Breath Sounds Introduction This tutorial is an introduction to Breath Sounds. It gives you an opportunity to listen to both normal and abnormal breath sounds, as well as explaining their clinical relevance.
Breath Sounds Introduction This tutorial is an introduction to Breath Sounds. It gives you an opportunity to listen to both normal and abnormal breath sounds, as well as explaining their clinical relevance.
Percussion These 4 techniques are the foundation of the physical exam. Respiration Blood pressure Body
 1 Chapter 11: Physical Exam Techniques 2 Introduction Although patient assessment formally starts with the, the physical examination actually begins when you first set eyes on your patient. The purpose
1 Chapter 11: Physical Exam Techniques 2 Introduction Although patient assessment formally starts with the, the physical examination actually begins when you first set eyes on your patient. The purpose
NURS 2240: Review A&P of respiratory system
 NURS 2240: Review A&P of respiratory system Objetives: Identify landmarks used in assessment of respiratory system Complete a focused history in the lab using specific examples of respiratory problems
NURS 2240: Review A&P of respiratory system Objetives: Identify landmarks used in assessment of respiratory system Complete a focused history in the lab using specific examples of respiratory problems
Chapter 10 The Respiratory System
 Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Chapter 10 The Respiratory System Biology 2201 Why do we breathe? Cells carry out the reactions of cellular respiration in order to produce ATP. ATP is used by the cells for energy. All organisms need
Problem Based Learning Session. Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days.
 Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
Problem Based Learning Session Mr Robinson is a 67 year old man. He visits the GP as he has had a cough and fever for 5 days. The GP takes a history from him and examines his chest. Over the left base
HEALTH ASSESSMENT. Afnan Tunsi BSN, RN, MSc.
 HEALTH ASSESSMENT Afnan Tunsi BSN, RN, MSc. Learning Outcomes 2 After completion of this lecture, the student will be able to: Describe suggested sequencing to conduct a thorax and lungs physical health
HEALTH ASSESSMENT Afnan Tunsi BSN, RN, MSc. Learning Outcomes 2 After completion of this lecture, the student will be able to: Describe suggested sequencing to conduct a thorax and lungs physical health
Abdominal Examination Benchmarks
 Abdominal Examination Benchmarks Preparation and Positioning: Stand on the right side of the patient. The patient should be supine and double draped so only the abdomen is exposed o To relax the abdominal
Abdominal Examination Benchmarks Preparation and Positioning: Stand on the right side of the patient. The patient should be supine and double draped so only the abdomen is exposed o To relax the abdominal
Respiratory Assessment 2; More key skills to improve care
 Respiratory Assessment 2; More key skills to improve care Author Meredith, Tara, Massey, Debbie Published 2011 Journal Title British Journal of Cardiac Nursing Copyright Statement 2011 Mark Allen Healthcare
Respiratory Assessment 2; More key skills to improve care Author Meredith, Tara, Massey, Debbie Published 2011 Journal Title British Journal of Cardiac Nursing Copyright Statement 2011 Mark Allen Healthcare
Respiratory Medicine
 Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
Respiratory Medicine This document is based on the handout from the Medicine for Finals course. The notes provided here summarise key aspects, focusing on areas that are popular in clinical examinations.
RESPIRATORY REHABILITATION
 RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
RESPIRATORY REHABILITATION By: Dr. Fatima Makee AL-Hakak University of kerbala College of nursing CHEST PHYSIOTHERAPY Chest physiotherapy (CPT) includes: 1.Postural drainage. 2.Chest percussion and vibration.
Sick Call Screener Course. Respiratory System (2.2)
 Sick Call Screener Course Respiratory System (2.2) 2.2-2-1 Enabling Objectives 1.17 Utilize the knowledge of respiratory system anatomy while assessing a patient with a respiratory complaint 1.18 Utilize
Sick Call Screener Course Respiratory System (2.2) 2.2-2-1 Enabling Objectives 1.17 Utilize the knowledge of respiratory system anatomy while assessing a patient with a respiratory complaint 1.18 Utilize
SMALL GROUP SESSION 18A January 17th or January 19th. Groups 1-12: VS and Chest Exam and Harvey Stethophone Session
 SMALL GROUP SESSION 18A January 17th or January 19th Groups 1-12: VS and Chest Exam and Harvey Stethophone Session Readings: Complete the cardiac examination web module. Mosby s Physical Examination, 4
SMALL GROUP SESSION 18A January 17th or January 19th Groups 1-12: VS and Chest Exam and Harvey Stethophone Session Readings: Complete the cardiac examination web module. Mosby s Physical Examination, 4
SMALL GROUP SESSION 13 December 1 st or December 3 rd
 SMALL GROUP SESSION 13 December 1 st or December 3 rd Vital Signs/Chest Exam & Clinical Case Discussion Suggested Readings: Complete online physical examination module and quiz. Review Mosby s Guide to
SMALL GROUP SESSION 13 December 1 st or December 3 rd Vital Signs/Chest Exam & Clinical Case Discussion Suggested Readings: Complete online physical examination module and quiz. Review Mosby s Guide to
Chapter 39 Oxygenation. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 39 Oxygenation Factors Essential to Normal Functioning of the Respiratory System Integrity of the airway system to transport air to and from lungs Properly functioning alveolar system in lungs
Chapter 39 Oxygenation Factors Essential to Normal Functioning of the Respiratory System Integrity of the airway system to transport air to and from lungs Properly functioning alveolar system in lungs
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM
 CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
CHAPTER 7.1 STRUCTURES OF THE RESPIRATORY SYSTEM Pages 244-247 DO NOW What structures, do you think, are active participating in the breathing process? 2 WHAT ARE WE DOING IN TODAY S CLASS Finishing Digestion
RESPIRATORY PHYSIOLOGY Pre-Lab Guide
 RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
RESPIRATORY PHYSIOLOGY Pre-Lab Guide NOTE: A very useful Study Guide! This Pre-lab guide takes you through the important concepts that where discussed in the lab videos. There will be some conceptual questions
Pulmonary Pathophysiology
 Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Pulmonary Pathophysiology 1 Reduction of Pulmonary Function 1. Inadequate blood flow to the lungs hypoperfusion 2. Inadequate air flow to the alveoli - hypoventilation 2 Signs and Symptoms of Pulmonary
Respiratory System Overview for RN CM/DNs. Debra Ward Goldberg, RN, MSN DDA SMRO August 2013
 Respiratory System Overview for RN CM/DNs Debra Ward Goldberg, RN, MSN DDA SMRO August 2013 A comprehensive nursing assessment includes an assessment of each system. The purpose of this training is to
Respiratory System Overview for RN CM/DNs Debra Ward Goldberg, RN, MSN DDA SMRO August 2013 A comprehensive nursing assessment includes an assessment of each system. The purpose of this training is to
Northwest Community EMS System Continuing Education Class Credit Questions Respiratory Assessment January 2012
 Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
Name (PRINT): Date submitted: Affiliation: Rating: [ ] Complete [ ] Incomplete Reminder: You must schedule to take the class post-test with your assigned hospital EMS Coordinator/educator or their designee
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC
 Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Chest X-ray (CXR) Interpretation Brent Burbridge, MD, FRCPC An approach to reviewing a chest x-ray will create a foundation that will facilitate the detection of abnormalities. You should create your own
Anatomy & Physiology 2 Canale. Respiratory System: Exchange of Gases
 Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Anatomy & Physiology 2 Canale Respiratory System: Exchange of Gases Why is it so hard to hold your breath for Discuss! : ) a long time? Every year carbon monoxide poisoning kills 500 people and sends another
Physical Assessment of the Respiratory System. Hajinezhad, Mohammad Esmaiel
 Physical Assessment of the Respiratory System بررسي دستگاه تنفس History Physical problems Function problems Life style Smoking Family Hx Occupation hx Allergens / environment Recreational exposure Anxiety
Physical Assessment of the Respiratory System بررسي دستگاه تنفس History Physical problems Function problems Life style Smoking Family Hx Occupation hx Allergens / environment Recreational exposure Anxiety
Coexistence of confirmed obstruction in spirometry and restriction in body plethysmography, e.g.: COPD + pulmonary fibrosis
 Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
Volumes: IRV inspiratory reserve volume Vt tidal volume ERV expiratory reserve volume RV residual volume Marcin Grabicki Department of Pulmonology, Allergology and Respiratory Oncology Poznań University
4/16/2017. Learning Objectives. Interpretation of the Chest Radiograph. Components. Production of the Radiograph. Density & Appearance
 Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Interpretation of the Arthur Jones, EdD, RRT Learning Objectives Identify technical defects in chest radiographs Identify common radiographic abnormalities This Presentation is Approved for 1 CRCE Credit
Unconscious exchange of air between lungs and the external environment Breathing
 Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Respiration Unconscious exchange of air between lungs and the external environment Breathing Two types External Exchange of carbon dioxide and oxygen between the environment and the organism Internal Exchange
Paramedic Rounds. Pre-Hospital Continuous Positive Airway Pressure (CPAP)
 Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Paramedic Rounds Pre-Hospital Continuous Positive Airway Pressure (CPAP) Morgan Hillier MD Class of 2011 Dr. Mike Peddle Assistant Medical Director SWORBHP Objectives Outline evidence for pre-hospital
Pulmonary Techniques. Chest Physical Therapy
 Pulmonary Techniques Chest Physical Therapy Review Last Lecture CPM stands for CPM provides what kind of motion? CPM does what 2 things? Contraindications for CPM use are Anatomy Review Respiratory System
Pulmonary Techniques Chest Physical Therapy Review Last Lecture CPM stands for CPM provides what kind of motion? CPM does what 2 things? Contraindications for CPM use are Anatomy Review Respiratory System
MENNONITE COLLEGE OF NURSING AT ILLINOIS STATE UNIVERSITY Diagnostic Reasoning for Advanced Practice Nursing 431
 MENNONITE COLLEGE OF NURSING AT ILLINOIS STATE UNIVERSITY Diagnostic Reasoning for Advanced Practice Nursing 431 MODULE: THORAX AND LUNGS OBJECTIVES: Upon completion of this module, the student will be
MENNONITE COLLEGE OF NURSING AT ILLINOIS STATE UNIVERSITY Diagnostic Reasoning for Advanced Practice Nursing 431 MODULE: THORAX AND LUNGS OBJECTIVES: Upon completion of this module, the student will be
1997, 1999, 2003, 2010, 2016 by Bob Page, M.Ed, NRP, CCP. By the end of this session, participants will be able to:
 An interactive and informative session designed to enhance your knowledge and understanding of the use of your stethoscope, while identifying common and critical lung, heart, and voice sounds in the emergency
An interactive and informative session designed to enhance your knowledge and understanding of the use of your stethoscope, while identifying common and critical lung, heart, and voice sounds in the emergency
Chapter 10. The Respiratory System Exchange of Gases. Copyright 2009 Pearson Education, Inc.
 Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Chapter 10 The Respiratory System Exchange of Gases http://www.encognitive.com/images/respiratory-system.jpg Human Respiratory System UPPER RESPIRATORY TRACT LOWER RESPIRATORY TRACT Nose Passageway for
Assessment. Respiratory System. The health exam is an opportunity to explore. of the 1.5
 .5 HOURS Continuing Education This article on respiratory system assessment is the first of a four-part series. Future articles will include instructions on focused examinations of the cardiac, gastrointestinal,
.5 HOURS Continuing Education This article on respiratory system assessment is the first of a four-part series. Future articles will include instructions on focused examinations of the cardiac, gastrointestinal,
Inspiratory crackles-early and late
 Inspiratory crackles-early and late A. R. NATH and L. H. CAPEL The London Chest Hospital, Bonner Road, London E2 Thorax (1974), 29, 223. Nath, A. R. and Capel, L. H. (1974). Thorax, 29, 223-227. Inspiratory
Inspiratory crackles-early and late A. R. NATH and L. H. CAPEL The London Chest Hospital, Bonner Road, London E2 Thorax (1974), 29, 223. Nath, A. R. and Capel, L. H. (1974). Thorax, 29, 223-227. Inspiratory
Objectives. Pulmonary Assessment 12/13/2017
 Pulmonary Assessment Reid Blackwelder, MD, FAAFP Professor and Chair, Family Medicine Quillen Colege of Medicine, ETSU Objectives Understand anatomy and physiology of pulmonary assessment techniques Remember
Pulmonary Assessment Reid Blackwelder, MD, FAAFP Professor and Chair, Family Medicine Quillen Colege of Medicine, ETSU Objectives Understand anatomy and physiology of pulmonary assessment techniques Remember
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days
 Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Semiology of respiratory system in children Simple choice 1. Mark the intrauterine age of lung development onset from the gut: a) 1 week b) 24 days c) 6 weeks d) 12 weeks e) 35 weeks 2. Stridor is not
Examination Of The Respiratory System
 Examination Of The Respiratory System by Dr. Rosie C Taylor 1. General Introduce yourself to the patient. Explain to the patient what you are going to do by asking them I would like to examine your chest,
Examination Of The Respiratory System by Dr. Rosie C Taylor 1. General Introduce yourself to the patient. Explain to the patient what you are going to do by asking them I would like to examine your chest,
Respiratory system. Applied Anatomy &Physiology
 Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Respiratory system Applied Anatomy &Physiology Anatomy The respiratory system consists of 1)The Upper airway : Nose, mouth and larynx 2)The Lower airways Trachea and the two lungs. Within the lungs,
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Basic mechanisms disturbing lung function and gas exchange
 Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Basic mechanisms disturbing lung function and gas exchange Blagoi Marinov, MD, PhD Pathophysiology Department, Medical University of Plovdiv Respiratory system 1 Control of breathing Structure of the lungs
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Levine Children s Hospital. at Carolinas Medical Center. Respiratory Care Department
 Page 1 of 7 at Carolinas Medical Center 02.04 Pediatric Patient-Centered Respiratory Care Protocol Application of Chest Physical Therapy Created: 1/98 Reviewed: 4/03, 1/05, 6/08 Revised: Purpose: To describe
Page 1 of 7 at Carolinas Medical Center 02.04 Pediatric Patient-Centered Respiratory Care Protocol Application of Chest Physical Therapy Created: 1/98 Reviewed: 4/03, 1/05, 6/08 Revised: Purpose: To describe
Respiratory Disease. Dr Amal Damrah consultant Neonatologist and Paediatrician
 Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Respiratory Disease Dr Amal Damrah consultant Neonatologist and Paediatrician Signs and Symptoms of Respiratory Diseases Cardinal Symptoms Cough Sputum Hemoptysis Dyspnea Wheezes Chest pain Signs and Symptoms
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations
 Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
Chest XRay interpretation INTERPRETATIONS Identifications: Name & Date Technical evaluation Basic Interpretations TECHNICAL EVALUATION 1. Projection: AP/PA view To differentiate between AP & PA films,
GOALS AND INSTRUCTIONAL OBJECTIVES
 October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
October 4-7, 2004 Respiratory GOALS: GOALS AND INSTRUCTIONAL OBJECTIVES By the end of the week, the first quarter student will have an in-depth understanding of the diagnoses listed under Primary Diagnoses
The Respiratory System
 130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
130 20 The Respiratory System 1. Define important words in this chapter 2. Explain the structure and function of the respiratory system 3. Discuss changes in the respiratory system due to aging 4. Discuss
Protocol for performing chest clearance techniques by nursing staff
 Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
Protocol for performing chest clearance techniques by nursing staff Rationale The main indications for performing chest clearance techniques (CCT) are to assist in the removal of thick, tenacious secretions
The External Anatomy of the Lungs. Prof Oluwadiya KS
 The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
The External Anatomy of the Lungs Prof Oluwadiya KS www.oluwadiya.com Introduction The lungs are the vital organs of respiration Their main function is to oxygenate the blood by bringing inspired air into
Respiratory Diseases and Disorders
 Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 9 Respiratory Diseases and Disorders Anatomy and Physiology Chest, lungs, and conducting airways Two parts: Upper respiratory system consists of nose, mouth, sinuses, pharynx, and larynx Lower
Chapter 3: Thorax. Thorax
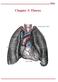 Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
Chapter 3: Thorax Thorax Thoracic Cage I. Thoracic Cage Osteology A. Thoracic Vertebrae Basic structure: vertebral body, pedicles, laminae, spinous processes and transverse processes Natural kyphotic shape,
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Chronic obstructive lung disease. Dr/Rehab F.Gwada
 Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Chronic obstructive lung disease Dr/Rehab F.Gwada Obstructive lung diseases Problem is in the expiratory phase Lung disease Restrictive lung disease Restriction may be with, or within the chest wall Problem
Respiratory Physiology
 Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Respiratory Physiology Dr. Aida Korish Associate Prof. Physiology KSU The main goal of respiration is to 1-Provide oxygen to tissues 2- Remove CO2 from the body. Respiratory system consists of: Passages
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Right lung. -fissures:
 -Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
-Right lung is shorter and wider because it is compressed by the right copula of the diaphragm by the live.. 2 fissure, 3 lobes.. hilum : 2 bronchi ( ep-arterial, hyp-arterial ), one artery mediastinal
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
3. Identify the importance in the prehospital setting for the administration of nebulized bronchodilator.
 TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
TERMINAL OBJECTIVE At the end of this lesson, the EMT-Basic will be able to utilize the assessment findings to formulate a field impression of bronchospasm and understand the administration of nebulized
Approach to CXR. Terminology. 1.Identification. Greg Blecher SCH Respir Fellow. Correct patient Correct date and time Correct examination
 Approach to CXR Greg Blecher SCH Respir Fellow From Rob Posteraro http://home.earthlink.net/~rhpos/cxr_interpret.txt.html ; http://home.earthlink.net/~rhpos/cxr_main.txt.html) Approach to viewing Chest
Approach to CXR Greg Blecher SCH Respir Fellow From Rob Posteraro http://home.earthlink.net/~rhpos/cxr_interpret.txt.html ; http://home.earthlink.net/~rhpos/cxr_main.txt.html) Approach to viewing Chest
Pulmonary Rehabilitation in Acute Spinal Cord Injury. Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university
 Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
Pulmonary Rehabilitation in Acute Spinal Cord Injury Jatuporn Jatutawanit Physical therapist, Physical therapy unit, Prince of songkla university Causes of spinal cord injury Traumatic injury Motor vehicle
SMALL GROUP SESSION 19 January 30 th or February 1st. Groups 1-12: Cardiac Case and Cardiac Exam Workshop
 SMALL GROUP SESSION 19 January 30 th or February 1st Groups 1-12: Cardiac Case and Cardiac Exam Workshop Readings: Complete the cardiac examination tutorial on the POM1 web site. Optional: http://medicine.ucsd.edu/clinicalmed/heart.htm
SMALL GROUP SESSION 19 January 30 th or February 1st Groups 1-12: Cardiac Case and Cardiac Exam Workshop Readings: Complete the cardiac examination tutorial on the POM1 web site. Optional: http://medicine.ucsd.edu/clinicalmed/heart.htm
FOREIGN BODY ASPIRATION in children. Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital
 FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
FOREIGN BODY ASPIRATION in children Dr. Xayyavong Bouathongthip, M.D Emergency department, children s hospital How common is choking? About 3,000 people die/year from choking Figure remained unchanged
Chest X-ray Interpretation
 Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
Chest X-ray Interpretation Introduction Routinely obtained Pulmonary specialist consultation Inherent physical exam limitations Chest x-ray limitations Physical exam and chest x-ray provide compliment
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
SMALL GROUP SESSION 8 October 21st or October 23 rd. Narratives Discussion/ OSCE Practice
 SMALL GROUP SESSION 8 October 21st or October 23 rd Narratives Discussion/ OSCE Practice Readings: Review your upper extremity, blood pressure and chest/lung OSCEs; Read Rita Charon s Narrative Medicine:
SMALL GROUP SESSION 8 October 21st or October 23 rd Narratives Discussion/ OSCE Practice Readings: Review your upper extremity, blood pressure and chest/lung OSCEs; Read Rita Charon s Narrative Medicine:
AUSCULTATION AS METHOD OF PHYSICAL EXAMINATION OF THE LUNGS. AUSCULTATION OF THE LUNGS TECHNIQUE. THE MAIN RESPIRATORY SOUNDS
 Ministry of Health of Ukraine Kharkiv National Medical University AUSCULTATION AS METHOD OF PHYSICAL EXAMINATION OF THE LUNGS. AUSCULTATION OF THE LUNGS TECHNIQUE. THE MAIN RESPIRATORY SOUNDS Methodical
Ministry of Health of Ukraine Kharkiv National Medical University AUSCULTATION AS METHOD OF PHYSICAL EXAMINATION OF THE LUNGS. AUSCULTATION OF THE LUNGS TECHNIQUE. THE MAIN RESPIRATORY SOUNDS Methodical
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Now, we will move onto the objective data collection of this physical examination. I will be first examining the posterior chest.
 FOCUSED EXAMINATION OBJECTIVE DATA THORAX AND LUNGS Now, we will move onto the objective data collection of this physical examination. I will be first examining the posterior chest. I would like to kindly
FOCUSED EXAMINATION OBJECTIVE DATA THORAX AND LUNGS Now, we will move onto the objective data collection of this physical examination. I will be first examining the posterior chest. I would like to kindly
PLEURAE and PLEURAL RECESSES
 PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
PLEURAE and PLEURAL RECESSES By Dr Farooq Aman Ullah Khan PMC 26 th April 2018 Introduction When sectioned transversely, it is apparent that the thoracic cavity is kidney shaped: a transversely ovoid space
Critical Care Monitoring. Indications. Pleural Space. Chest Drainage. Chest Drainage. Potential space. Contains fluid lubricant
 Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
Critical Care Monitoring Indications 1-2- 2 Pleural Space Potential space Contains fluid lubricant Can fill with air, blood, plasma, serum, lymph, pus 3 1 Pleural Space Problems when contain abnormal substances:
PULMONARY FUNCTION TESTS
 Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 4 PULMONARY FUNCTION TESTS M.G.Rajanandh, Department of Pharmacy Practice, SRM College of Pharmacy, SRM University. OBJECTIVES Review basic pulmonary anatomy and physiology. Understand the reasons
Chapter 19 - Respiratory_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Lung Cancer - Suspected
 Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Lung Cancer - Suspected Shared Decision Making Lung Cancer: http://www.enhertsccg.nhs.uk/ Patient presents with abnormal CXR Lung cancer - clinical presentation History and Examination Incidental finding
Foundation in Critical Care Nursing. Airway / Respiratory / Workbook
 Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Foundation in Critical Care Nursing Airway / Respiratory / Workbook Airway Anatomy: Please label the following: Tongue Larynx Epiglottis Pharynx Trachea Vertebrae Oesophagus Where is the ET (endotracheal)
Chest X rays and Case Studies. No disclosures. Outline 5/31/2018. Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital
 Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Chest X rays and Case Studies Carlo Manalo, M.D. Department of Radiology Loma Linda University Children s Hospital No disclosures. Outline Importance of history Densities delineated on radiography An approach
Pulmonary Manifestations of Ankylosing Spondylitis
 Pulmonary Manifestations of Ankylosing Spondylitis PULMONARY MEDICINE. DR. R. ADITYAVADAN FINAL YEAR PG, DEPT. OF ETIOLOGY AS is a chronic multisystem disease characterized by inflammation of the spine,
Pulmonary Manifestations of Ankylosing Spondylitis PULMONARY MEDICINE. DR. R. ADITYAVADAN FINAL YEAR PG, DEPT. OF ETIOLOGY AS is a chronic multisystem disease characterized by inflammation of the spine,
LUNGS. Requirements of a Respiratory System
 Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Respiratory System Requirements of a Respiratory System Gas exchange is the physical method that organisms use to obtain oxygen from their surroundings and remove carbon dioxide. Oxygen is needed for aerobic
Ventilation 7/28/2013. Clarification of Terminology. Osteology of Ventilation
 Ventilation Clarification of Terminology Ventilation: the mechanical process by which air is inhaled and exhaled through the lungs. It describes only the movement of air. Respiration: a term used to describe
Ventilation Clarification of Terminology Ventilation: the mechanical process by which air is inhaled and exhaled through the lungs. It describes only the movement of air. Respiration: a term used to describe
Lecture Notes. Chapter 3: Asthma
 Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
Lecture Notes Chapter 3: Asthma Objectives Define asthma and status asthmaticus List the potential causes of asthma attacks Describe the effect of asthma attacks on lung function List the clinical features
October Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE
 October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
October 2017 Paediatric Respiratory Workbook APCP RESPIRATORY COMMITTEE This workbook is designed to introduce to you the difference between paediatric and adult anatomy and physiology. It will also give
Respiration & Trunk control The Great Connection. Brief Review of Normal Development of the Rib Cage
 Respiration & Trunk control The Great Connection. are part of a complex combination of interactive systems. Muscles of respiration are part of the musculature of dynamic postural control. First 3 Years
Respiration & Trunk control The Great Connection. are part of a complex combination of interactive systems. Muscles of respiration are part of the musculature of dynamic postural control. First 3 Years
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010
 Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Bony Thorax. Anatomy and Procedures of the Bony Thorax Edited by M. Rhodes
 Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
Bony Thorax Anatomy and Procedures of the Bony Thorax 10-526-191 Edited by M. Rhodes Anatomy Review Bony Thorax Formed by Sternum 12 pairs of ribs 12 thoracic vertebrae Conical in shape Narrow at top Posterior
The Respiratory System
 Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 13 The Respiratory System Slides 13.1 13.30 Lecture Slides in PowerPoint by Jerry L. Cook Copyright 2003 Pearson Education,
Essentials of Human Anatomy & Physiology Elaine N. Marieb Seventh Edition Chapter 13 The Respiratory System Slides 13.1 13.30 Lecture Slides in PowerPoint by Jerry L. Cook Copyright 2003 Pearson Education,
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA
 DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA INTRODUCTION In this lecture we will discuss atelectasis which is a complication of several medical and surgical
DISEASES OF THE RESPIRATORY SYSTEM 2018 DR HEYAM AWAD LECTURE 2: ATELECTASIS AND EMPHYSEMA INTRODUCTION In this lecture we will discuss atelectasis which is a complication of several medical and surgical
RESPIRATORY SYSTEM. A. Upper respiratory tract (Fig. 23.1) Use the half-head models.
 RESPIRATORY SYSTEM I. OVERVIEW OF THE RESPIRATORY SYSTEM AND THORAX A. Upper respiratory tract (Fig. 23.1) Use the half-head models. Nasal cavity Pharynx (fare-rinks) B. Lower respiratory tract (Fig. 23.1)
RESPIRATORY SYSTEM I. OVERVIEW OF THE RESPIRATORY SYSTEM AND THORAX A. Upper respiratory tract (Fig. 23.1) Use the half-head models. Nasal cavity Pharynx (fare-rinks) B. Lower respiratory tract (Fig. 23.1)
THE RESPIRATORY SYSTEM. Pages and
 THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
THE RESPIRATORY SYSTEM Pages 103-105 and 146-150 1 When the respiratory system is mentioned, people generally think of breathing, but breathing is only one of the activities of the respiratory system.
