HammondCare Palliative Care
|
|
|
- Lesley Rich
- 5 years ago
- Views:
Transcription
1 HammondCare Palliative Care End of life flip chart
2 resource This flip chart forms part of the End of Life Palliative Care resource tool HammondCare Palliative Care End of life flip chart This resource has been designed by HammondCare for use in Residential Aged Care Homes (RACH) Who requires a Palliative Approach? Refer to the Surprise Question (page 1) and the SPICT Tool (page 2) Do you have the necessary equipment? Refer to the Equipment Stock List (page 4) and Personal Hygiene Stock List (page 5) in the End of life resource booklet Please refer to the Quick Links (page 6) in the End of life resource booklet and lanyard card to ensure you are aware who you can call upon to help you care for people in your RACH The End of Life Project is funded by the SNPHN (Sydney Northern Primary Health Network). If required please refer on to the Specialist Palliative Care Team. See the Palliative Care Referral Form on page 3 of the End of life resource booklet.
3 Depression anger sadness Illness and pain Not wanting to be in the nursing home Missing family members Symptoms especially pain Unfinished business How are you feeling? Are you depressed? You seem a little flat, are you ok? Ask the family what they think Complete a Cornell Depression Scale on ACFI and contact the GP using Handover using ISBAR Tool (page 7) Smile, offer reassurance Massage therapy Reminiscing Diversional activities Change of scenery, sitting in the sunshine Grief Depression anger sadness
4 Anxiety Long-term anxiety exacerbated by their illness Medication side effects Financial concerns Adjusting to their situation/illness/nursing home Fear of death How are you feeling? What makes it better? What makes it worse? Ask family about the person s history, have they been anxious in the past? Is the person short of breath? Contact GP using ISBAR Tool (page 7) and address any reversible causes Refer to the Palliative Care End of Life Medications Initial Suggested Doses (page 9) Find out what they enjoy doing Are they religious? Do they require Pastoral Care? Are there any spiritual or religious practices that may reduce anxiety? Offer reassurance and support Anxiety
5 Poor appetite or refusal to eat and drink The person s metabolism slowing down: the body is shutting down and not needing nourishment Nausea Are they not eating because of nausea or vomiting? If the cause is nausea contact the GP using the ISBAR Tool (page 7) and ensure an antiemetic is charted Refer to the Palliative Care End of Life Medications Initial Suggested Doses (page 9) If the person is hungrier early in the morning, offer breakfast as the main meal of day Open and honest communication with the family that this is normal when someone s condition is deteriorating Handover using ISBAR Tool (page 7) Supplement drinks and puddings as tolerated Good mouth care every 4 hours Reassure family and inform them of why subcutaneous or intravenous fluids are not recommended. Poor appetite or refusal to eat and drink
6 Nausea and vomiting Constipation Medication side effects Anxiety Brain tumour Liver & kidney disease Do you feel nauseas? What makes it worse: smell? seeing or thinking about food? eating? Are they vomiting how much and when? Contact the GP using Constant nausea requires a regular antiemetic. Occasional nausea requires a PRN antiemetic. Is it charted? Refer to the Palliative Care End of Life Medications Initial Suggested Doses (page 9) Visualisation and relaxation Fan in the room or open a window Wet sponge to the back of neck Close monitoring of bowels Nausea and vomiting
7 Profound weakness and fatigue Disease progression Weight loss Decreased food intake Organ failure Depression Are they very lethargic and wanting to remain in bed all of the time? Do they find it hard work to even have a shower? Reassure the person and family that this is common and that the person requires rest Ensure the person has allocated uninterrupted quiet time during the day Reassurance and support Limit activity Shower every second day or attend bed sponges only Ensure there is an air mattress on the bed Profound weakness and fatigue
8 End of life care Spirituality, religious and/or cultural needs Questions to ask What to do? Anger Get to know the person Despair What do I need to know about you to care for you best? Fear Are you at peace? Grief What spiritual or religious practices are important to you? Guilt Handover anything that will contribute to good care using ISBAR Tool (page 7) Loneliness Loss Regret Uncertainty Worry Spirituality, religious and/or cultural needs Non medical Sit with them and talk with them Offer reassurance and support Refer to pastoral care if available
9 Hallucinations vivid dreams delirium Infection Liver or kidney failure Medication side effects Lack of oxygen Blood disorders Vitamin deficiency Dementia and pain Excessive stimuli Are you seeing or hearing things that possibly aren t there? Are you having vivid dreams where you wake up and you are confused if the dream was real or not? What are you seeing? Is it bothering you? Check for infection Make sure the environment is safe Make sure you remove anything from the room that may be contributing to the hallucinations: marks on the wall, turn off talk back radio Handover using Reassurance and support Maintain a quiet and familiar environment Ask family to stay when person is restless or distressed Lower the bed and ensure crash mat is in place Contact GP using and address any reversible causes Hallucinations vivid dreams delirium
10 Shortness of breath Lung cancer Lung disease Fluid in the lungs Anxiety and fear Heart disease Terminal secretions What makes it worse: showering? walking short distances? getting dressed? going to the toilet? What makes it better? Is difficulty breathing making you feel panicked or anxious? Make sure the person has a Breathlessness Action Plan (page 12), and follow those instructions Have a room fan close to the person and make sure it is directed to their face Opioid for severe breathlessness as first line - dosing is the same as for pain - refer to the Palliative Care End of Life Medications Initial Suggested Doses (page 9) Open a window Make sure the fan is close and directed towards face Offer reassurance and support Relaxation exercises Positioning Handover using ISBAR Tool (page 7) Contact the GP using Does sublingual (under the tongue) medication need to be charted for anxiety related to breathlessness? Shortness of breath
11 Terminal restlessness agitation Pain Constipation Urinary retention UTI Insomnia Uncomfortable bed or environment Life regrets or unfinished business Medication side effects Is the person safe? Is there a possibility they could injure themselves? Is the cause of the agitation reversible? Maintain a safe environment: lower bed, crash mats Clear explanation to family that this can be a common problem when people are deteriorating and the cause is multifactorial Handover using Contact the GP using Quiet and familiar environment Re-positioning Address any pain concerns Limit interruptions or limit interaction Music Touch Reassurance and support Terminal secretions Does S/C medication need to be charted? Ask family members to stay Refer to the Palliative Care End of Life Medications Initial Suggested Doses (page 9) Terminal restlessness agitation
12 Constipation Dehydration Decreased mobility Unable go to the toilet themselves when needed Pain medication side effects Is the person emptying their bowels every three days, even if they are not eating much? See the Bristol Stool Chart (page 13) and Bowel Management Guidelines (page 14) Strict bowel charting Contact the GP using and ensure: Offer drinks frequently Ensure you give the person time and privacy in the bathroom Prune or pear juice regular stool softening medication is charted especially if someone taking pain medication if they are unable to swallow is a Microlax enema charted PRN Make sure stool softening medication is also charted PRN, and give if bowels are not opened for 2 days Constipation
13 Problems swallowing Deterioration in condition End-stage dementia Does the person cough when drinking or eating? Have you checked their swallowing reflex? (page 15) Is the person having problems swallowing tablets? How long does it take for the person to swallow their tablet/s? Make sure the person is alert and sitting upright before offering food or drinks If the person coughs, stop and try again later Explain to the family the risk of aspiration pneumonia and what that means Open and honest communication with family that problems with swallowing is normal when someone s condition is deteriorating Puréed diet and thickened fluids Only offer oral intake if it is safe If the person is not able to eat or drink, make sure you attend regular mouth care every 4 hours Show the family how to do mouth care and encourage them to do it if they want to GP to cease any nonessential oral medication Contact the GP using The GP will need to reassess all oral tablets and convert some medication to subcutaneous injections Problems swallowing
14 Respiratory moist secretions Inability to clear phlegm from the back of throat or chest Are the moist secretions causing a rattle or gurgling noise? Reposition the resident to help drain their secretions: from side to side Good mouth care every 4 hours or elevate head of bed Don t suction: it can be very uncomfortable it can cause distress for the patient it can cause further secretions to build up Reassure the family that this happens often at end of life and is not bothering the person, but it is not nice to hear Open and honest communication with the family that when this happens; it is likely the person is in the terminal phase of their illness and death is likely within days Try not to focus on the noise Handover using Respiratory moist secretions
15 Sore dry mouth and eyes Mouth: Mouth: Mouth: Mouth: Medication Mouth breathing Dehydration Weight loss Ill-fitting dentures Unable to brush own teeth Look in their mouth, is it: dry, cracked? discoloured? furry? Is there any food or medication left over in the mouth? Is the person constantly thirsty? Contact the GP using and request mouth care to be charted 4 times a day with: sodium bicarb mouth swabs oral balance gel lip balm If the resident has oral thrush (furry) ensure Nilstat is charted 4 times a day until it clears Make sure the mouth is cleaned well after meals Eyes: Dehydration Inability to clean their own eyes Infection Eyes: Are their eyes: dry and sticky? yellow discharge? Are they complaining of scratchy, itchy eyes? Eyes: Contact the GP using Ensure lubricating eye drops are charted twice a day If there is an infection, antibiotic eye drops are required Eyes: Saline-soaked gauze used as eye pads for 5 minutes to moisten and clean eyes Sore dry mouth and eyes
16 Sore Pain dry mouth and eyes Disease progression Mood disorders Pressure injuries Poor positioning Constipation Osteoarthritis Nerve pain Be creative if they deny pain ask are you uncomfortable / does anywhere feel tight? Where is the pain? What makes it worse? What makes it better? How would you describe the pain? Is it: sharp, dull, achy, shooting, feel like pins and needles? Can you score the pain out of ten? Is it worse when you move? Does it keep you awake at night? If the person can t tell you, use the Abbey Pain Scale (page 8) Record pain assessments 4/24 If results indicate pain give PRN analgesia Make sure you ask the family if they think the resident has pain? Handover using Contact the GP using the and request a review Does pain medication need to be charted? Constant pain requires regular medication. Occasional pain requires PRN medication. Explain to the family the results of the pain assessments and what you are doing about it. Refer to the Palliative Care End of Life Medications Initial Suggested Doses (page 9) Heat pack Reposition Diversional therapy Reassurance and support Gentle massage Pain
17 After death care What to do? Self care Inform the family (nominated person). If they were not present when the person died, ask the family if they would like to come in and spend time with the person and say goodbye Inform the GP Inform the funeral Director Follow any cultural or religious practices or beliefs Attend a full bed sponge and ensure the person looks as nice as possible. This image of the person will remain with loved ones forever Use the Gibbs Reflective Cycle Tool (page 31) to reflect on the persons death Use the After Death Audit Tool (page 33) in your next team meeting to debrief and learn from this experience and improve future care in your home Ensure the person is: laid flat on their back with the head of the bed slightly elevated which will assist with keeping the mouth closed close eyes hair combed clean, fresh clothes clean pillow case and sheets. Bedding is made so the persons arms and hands are available for loved ones to hold the persons hands if they would like to any religious symbols or significant ornaments are placed close to the person the room is cleared of any medical equipment or rubbish Ensure there is soft lighting, fresh water, chairs are by the bedside and tissues are available in the room Before moving the person include staff and family members in a bedside memorial using the Aboriginal Blessing (page 30) and share memories together of the person After death care
Precious Moments. Giving comfort and support when someone you love is dying.
 Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Preparing for Approaching Death
 Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Understanding and preventing delirium in older people
 Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
Understanding and preventing delirium in older people Tips for family, whānau, and friends As people get older, especially if they are unwell or living with a dementia, they have greater risk of developing
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
Preparing for the Death of a Loved One. Information for Patients & Visitors
 Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
Physical/Emotional Symptoms and Appropriate Comfort Measures
 Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Delirium: Information for Patients and Families
 health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
Delirium Information for patients and relatives. Delirium is common Delirium is treatable Relatives can stay to help us
 Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
Delirium Information for patients and relatives Delirium is common Delirium is treatable Relatives can stay to help us What is delirium? Delirium is caused by a disturbance of brain function. It is used
Recovering at home. How will I feel when I get home? How should I look after my wound?
 How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
How will I feel when I get home? Following your operation it is normal to have feelings of stress, anxiety or depression. Being affected emotionally is normal. It may help to talk about how you feel with
Mouth care for people with dementia. Delirium (Confusion) Understanding changes in behaviour in dementia
 Mouth care for people with dementia Delirium (Confusion) Understanding changes in behaviour in dementia 2 Dementia UK Delirium (confusion) A sudden change in a person s mental state is known as delirium.
Mouth care for people with dementia Delirium (Confusion) Understanding changes in behaviour in dementia 2 Dementia UK Delirium (confusion) A sudden change in a person s mental state is known as delirium.
Care in the Last Days of Life
 Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
Care in the Last Days of Life Introduction This guideline is an aid to clinical decision making and good practice in person-centred care for patients who are deteriorating and at risk of dying. The patient
Bowel Resection Surgery (Open Method)
 Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Preventing delirium while in the hospital
 Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Coping with dying. Information for families and carers
 Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Delirium A guide for caregivers
 Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
ALONG THE FINAL JOURNEY
 ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Renal Palliative Care Last Days of Life
 Renal Palliative Care Last Days of Life Introduction This guideline is an aid to clinical decision-making and good practice for patients with stage 4-5 chronic kidney disease (egfr
Renal Palliative Care Last Days of Life Introduction This guideline is an aid to clinical decision-making and good practice for patients with stage 4-5 chronic kidney disease (egfr
Enhanced Recovery Patient Diary
 Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
Enhanced Recovery Patient Diary I found the diary was helpful. I was able to chart my progress and see a difference. I was eating more each day and able to shower myself. I found it to be encouraging.
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS
 WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
WELCOME TO THE NORTHSHORE UNIVERSITY HEALTHSYSTEM SLEEP CENTERS Prior to your office visit, we request that you complete this questionnaire. It asks questions not only about your sleeping habits and behavior
LATE-STAGE CARE PROVIDING CARE AND COMFORT DURING THE LATE STAGE OF ALZHEIMER S DISEASE
 LATE-STAGE CARE PROVIDING CARE AND COMFORT DURING THE LATE STAGE OF ALZHEIMER S DISEASE 10 TIPS FOR LATE-STAGE CAREGIVING 1. Treat the person with compassion and respect. 2. Focus on what the person enjoys.
LATE-STAGE CARE PROVIDING CARE AND COMFORT DURING THE LATE STAGE OF ALZHEIMER S DISEASE 10 TIPS FOR LATE-STAGE CAREGIVING 1. Treat the person with compassion and respect. 2. Focus on what the person enjoys.
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Mouth care for people with dementia. Good habits for bedtime. Caring for someone with dementia
 Mouth care for people with dementia Good habits for bedtime Caring for someone with dementia 2 Dementia UK Looking after someone with dementia Caring for someone with dementia can be really difficult at
Mouth care for people with dementia Good habits for bedtime Caring for someone with dementia 2 Dementia UK Looking after someone with dementia Caring for someone with dementia can be really difficult at
Short-Term Side Effects from Head and Neck Radiation
 PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
PATIENT EDUCATION patienteducation.osumc.edu Short-Term Side Effects from Head and Neck Radiation Side effects are problems caused by radiation therapy. These problems are different for each person and
CLINICAL GUIDELINES FOR END OF LIFE CARE MEDICATIONS IN LONG TERM CARE HOMES
 CLINICAL GUIDELINES F END OF LIFE CARE MEDICATIONS IN LONG TERM CARE HOMES OPENING STATEMENT: Insert Facility Name is committed to providing effective end-of-life symptom management to all residents. Symptom
CLINICAL GUIDELINES F END OF LIFE CARE MEDICATIONS IN LONG TERM CARE HOMES OPENING STATEMENT: Insert Facility Name is committed to providing effective end-of-life symptom management to all residents. Symptom
Post Operative Instructions: Wisdom Teeth
 The removal of impacted teeth is a serious surgical procedure. Post-operative care is very important. Unnecessary pain and the complications of infection and swelling can be minimized if the instructions
The removal of impacted teeth is a serious surgical procedure. Post-operative care is very important. Unnecessary pain and the complications of infection and swelling can be minimized if the instructions
Delirium Information for relatives, carers and patients
 Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Delirium Information for relatives, carers and patients Contents Part A Introduction What is delirium? Quotes from relatives or carers showing what might happen to a patient suffering from delirium How
Total Knee Replacement: Your Guide to Preparation and Recovery
 Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Total Knee Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 5 After Surgery.............................
Progression LATE STAGE. What is Alzheimer s disease? The late stage - what to expect
 Progression LATE STAGE This document is one in a five-part series on the stages of Alzheimer s disease and is written for the person with the disease, their family 1 and caregivers. The late stage of the
Progression LATE STAGE This document is one in a five-part series on the stages of Alzheimer s disease and is written for the person with the disease, their family 1 and caregivers. The late stage of the
End of Life Care in Dementia. Sue Atkins Dignity in Care/Dementia/Learning Disabilities Clinical Nurse Specialist
 End of Life Care in Dementia Sue Atkins Dignity in Care/Dementia/Learning Disabilities Clinical Nurse Specialist Objectives Understanding the decline in people with dementia To recognise when patients
End of Life Care in Dementia Sue Atkins Dignity in Care/Dementia/Learning Disabilities Clinical Nurse Specialist Objectives Understanding the decline in people with dementia To recognise when patients
CENTRAL CARE POLICY SYMPTOMS OF ILLNESS. Policy: Consumers will be observed for symptoms of physical problems, distress, pain, or unusual behaviors.
 Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Page 1 of 5 CENTRAL CARE POLICY SYMPTOMS OF ILLNESS SUBJECT: SYMPTOMS OF ILLNESS ANNUAL REVIEW MONTH: June RESPONSIBLE FOR REVIEW: Director of Central Care LAST REVISION DATE: June 2009 Policy: Consumers
Pandemic FLU. What you need to know
 Pandemic FLU OR What you need to know Important note: Hygiene is the most important step in preventing the spread of flu. Pandemic Flu is it different to the normal flu? Yes it is a completely different
Pandemic FLU OR What you need to know Important note: Hygiene is the most important step in preventing the spread of flu. Pandemic Flu is it different to the normal flu? Yes it is a completely different
Your Spinal Anaesthetic Information for Patients
 Your Spinal Anaesthetic Information for Patients This leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients, patient representatives and
Your Spinal Anaesthetic Information for Patients This leaflet explains what to expect when you have an operation with a spinal anaesthetic. It has been written by patients, patient representatives and
S A M P L E. Is Near. When Death. Logo A CAREGIVER S GUIDE
 When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
When Death Is Near A CAREGIVER S GUIDE Logo Updated 2019. 2008 by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION
 ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
The Fresco Institute for Parkinson's and Movement Disorders
 The Fresco Institute for Parkinson's and Movement Disorders Follow Up Patient Questionnaire Name: Date: Accompanied by: Do you smoke? CURRENT PAST NEVER Which neurological symptom bothers you most right
The Fresco Institute for Parkinson's and Movement Disorders Follow Up Patient Questionnaire Name: Date: Accompanied by: Do you smoke? CURRENT PAST NEVER Which neurological symptom bothers you most right
Enhanced Recovery Programme
 Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
Enhanced Recovery Programme Enhanced Recovery Programme This leaflet should increase your understanding of the programme and how you can play an active part in your recovery. If there is anything you are
CHILDHOOD C 3 HANGE CARE TOOL: PROVIDER REPORT
 Date: / / Patient s Project ID# For use as-needed in clinic visits A SURVEY TO LEARN ABOUT A PATIENT S NEEDS AND ABILITIES: Health care providers of children and adolescents aged 5 to 2 How is this patient
Date: / / Patient s Project ID# For use as-needed in clinic visits A SURVEY TO LEARN ABOUT A PATIENT S NEEDS AND ABILITIES: Health care providers of children and adolescents aged 5 to 2 How is this patient
Preparing for Approaching Death By North Central Florida Hospice, Inc.
 Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
INFORMATION FOR PATIENTS, CARERS AND FAMILIES. Coping with dying
 INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
Surgical Instructions. Wisdom Tooth TREASURE VALLEY ORAL & FACIAL SURGERY
 TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
TREASURE VALLEY ORAL & FACIAL SURGERY Surgical Instructions Wisdom Tooth 1000 North Curtis Road, Suite 103 Boise, ID 83706 Phone: 208-343-0909 Fax: 208-343-6282 TREASURE VALLEY ORAL & FACIAL SURGERY AFTER
Nasogastric Tube Patient Passport
 Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
Nutrition and Dietetics Department Nasogastric Tube Patient Passport Please bring this booklet with you for all tube changes Patient Information If you need this information in another format or language
Swallowing problems. Patient information. Name: Date: Speech and Language Therapist: Reviewed: May 2016 Next review: June 2017 Version 1
 Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
Patient information Swallowing problems Name: Date: Speech and Language Therapist: Golden Jubilee National Hospital Agamemnon Street Clydebank, G81 4DY (: 0141 951 5000 www.nhsgoldenjubilee.co.uk Reviewed:
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life
 MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
MMG035 Symptom Management Guidelines for a Person thought to be in the Last Few Days and Hours of Life The following pages are guidelines for the management of common symptoms for a person thought to be
General Symptoms. Cold Weather Symptoms TG-272
 General Symptoms Cold Weather Symptoms Cold weather injuries can range from mild chapped skin to life-threatening hypothermia. To avoid cold weather injuries, you must be prepared. Being prepared means
General Symptoms Cold Weather Symptoms Cold weather injuries can range from mild chapped skin to life-threatening hypothermia. To avoid cold weather injuries, you must be prepared. Being prepared means
late-stage care Providing care and comfort during the late stage of Alzheimer s disease
 late-stage care Providing care and comfort during the late stage of Alzheimer s disease Caring for a person with late-stage Alzheimer s The journey to the late stage of Alzheimer s, sometimes referred
late-stage care Providing care and comfort during the late stage of Alzheimer s disease Caring for a person with late-stage Alzheimer s The journey to the late stage of Alzheimer s, sometimes referred
Esophagectomy Surgery
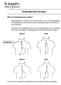 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
For the Patient: Everolimus tablets Other names: AFINITOR
 For the Patient: Everolimus tablets Other names: AFINITOR Everolimus (e'' ver oh' li mus) is a drug that is used to treat some types of cancer. It is a tablet that you take by mouth. Tell your doctor if
For the Patient: Everolimus tablets Other names: AFINITOR Everolimus (e'' ver oh' li mus) is a drug that is used to treat some types of cancer. It is a tablet that you take by mouth. Tell your doctor if
1/7/2013. An unstable or crucial time or state of affairs whose outcome will make a decisive difference for better or worse.
 B7 Responding to a Crisis Understanding a crisis Tools for assessing a crisis Understanding the phases of a crisis Understanding the types of crises Actions to take following a crisis Ways to cope with
B7 Responding to a Crisis Understanding a crisis Tools for assessing a crisis Understanding the phases of a crisis Understanding the types of crises Actions to take following a crisis Ways to cope with
Helpful tips for people with. Nausea and Vomiting
 Helpful tips for people with Nausea and Vomiting Nausea and vomiting are common side effects of certain cancer treatments. They may also be due to the illness itself. Poor health, admission to hospital
Helpful tips for people with Nausea and Vomiting Nausea and vomiting are common side effects of certain cancer treatments. They may also be due to the illness itself. Poor health, admission to hospital
Methadone for Pain Control
 Palliative Care Guidelines Methadone for Pain Control Information for patients, relatives and carers - 1 - Methadone for Pain Management Other names Methadone Hydrochloride Oral Solution: Metharose, Physeptone
Palliative Care Guidelines Methadone for Pain Control Information for patients, relatives and carers - 1 - Methadone for Pain Management Other names Methadone Hydrochloride Oral Solution: Metharose, Physeptone
Medical History. Instructions. My telephone number is: 1 Tools Medical History
 Medical History Instructions To do the best possible job with your pain, your doctor needs details about your history, including current and past medical problems, medications, health habits, and family
Medical History Instructions To do the best possible job with your pain, your doctor needs details about your history, including current and past medical problems, medications, health habits, and family
For the Patient: LUAVNP
 For the Patient: LUAVNP Other Names: Treatment of Advanced n-small Cell Lung Cancer with Cisplatin and Vinorelbine LU = LUng AV = AdVanced NP = Navelbine (Vinorelbine), cisplatin ABOUT THIS MEDICATION
For the Patient: LUAVNP Other Names: Treatment of Advanced n-small Cell Lung Cancer with Cisplatin and Vinorelbine LU = LUng AV = AdVanced NP = Navelbine (Vinorelbine), cisplatin ABOUT THIS MEDICATION
My Family-Hygiene Tips
 My Family-Hygiene Tips 1 Table of Contents Page 3 Hand washing Page 4 Showering, Bathing Hair washing Page 5 Oral Hygiene \fingernails Page 6 Haircuts 2 Hygiene How can I get my child to take a bath or
My Family-Hygiene Tips 1 Table of Contents Page 3 Hand washing Page 4 Showering, Bathing Hair washing Page 5 Oral Hygiene \fingernails Page 6 Haircuts 2 Hygiene How can I get my child to take a bath or
Symptom Management Guidelines for End of Life Care
 Symptom Management Guidelines for End of Life Care The following pages are guidelines for the management of common symptoms in the last few days of life. General principles: 1. Consider how symptoms can
Symptom Management Guidelines for End of Life Care The following pages are guidelines for the management of common symptoms in the last few days of life. General principles: 1. Consider how symptoms can
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division
 First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division TRUST Time the seizure Remove glasses and anything tight around the neck Use something soft under their head STAY CALM
First Aid Preparedness Patsy Ramey, RN, BSN Clinical Resource Nurse Epilepsy Division TRUST Time the seizure Remove glasses and anything tight around the neck Use something soft under their head STAY CALM
Dealing with Traumatic Experiences
 Dealing with Traumatic Experiences RECOGNIZING THE SIGNS POST INCIDENT STRESS AND HOW TO COPE WITH IT Some of the stress symptoms that individuals can experience after traumatic incidents are listed below.
Dealing with Traumatic Experiences RECOGNIZING THE SIGNS POST INCIDENT STRESS AND HOW TO COPE WITH IT Some of the stress symptoms that individuals can experience after traumatic incidents are listed below.
Chapter 20. Assisting With Nutrition and Fluids
 Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
Chapter 20 Assisting With Nutrition and Fluids Food and water: Are physical needs Basics of Nutrition Are necessary for life A poor diet and poor eating habits: Increase the risk for diseases and infection
For the Patient: ULUAVPMTN
 ABOUT THIS MEDICATION For the Patient: ULUAVPMTN Other Names: Maintenance Therapy of Advanced n-small Cell Lung Cancer (NSCLC) with Pemetrexed U = Undesignated (requires special approval) LU = LUng AV
ABOUT THIS MEDICATION For the Patient: ULUAVPMTN Other Names: Maintenance Therapy of Advanced n-small Cell Lung Cancer (NSCLC) with Pemetrexed U = Undesignated (requires special approval) LU = LUng AV
Care After Your Dental Treatment For Hospital Dentistry patients
 Patient Education Care After Your Dental Treatment For Hospital Dentistry patients Your surgeon today was Dr.. Please carefully follow the instructions in this handout. General Do not disturb the wound
Patient Education Care After Your Dental Treatment For Hospital Dentistry patients Your surgeon today was Dr.. Please carefully follow the instructions in this handout. General Do not disturb the wound
Keeping Home Safe WHAT CAN YOU DO?
 Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
risk factors for falling
 Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Resource # 10 Page 1 of 8 1. Dizziness- What Can Cause Dizziness? Not eating regularly Change in body position (e.g. from sitting to standing) Low blood pressure High blood pressure Medication side effects
Spinal Anaesthesia and Analgesia. Patient information Leaflet
 Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
Spinal Anaesthesia and Analgesia Patient information Leaflet February 2018 Introduction For many operations, patients receive a general anaesthetic and remain asleep during the operation. A spinal anaesthetic
CHEMOTHERAPY. What should I expect?
 CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
Every day matters. To help you stay out of the hospital, you can: Live healthy with sickle cell disease
 Living with sickle cell disease (SCD) can be difficult. There can be severe pain and discomfort. AmeriHealth Caritas Louisiana wants to help you manage this life-threatening disease. To help you stay out
Living with sickle cell disease (SCD) can be difficult. There can be severe pain and discomfort. AmeriHealth Caritas Louisiana wants to help you manage this life-threatening disease. To help you stay out
The last days of life in hospital and at home
 The last days of life in hospital and at home Beaumont Multi-disciplinary Palliative Care Study Day 28/9/2017 Dr Sarah McLean Consultant in Palliative Medicine St Francis Hospice Beaumont Hospital Overview
The last days of life in hospital and at home Beaumont Multi-disciplinary Palliative Care Study Day 28/9/2017 Dr Sarah McLean Consultant in Palliative Medicine St Francis Hospice Beaumont Hospital Overview
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
University Counselling Service
 Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
Bereavement The death of someone close can be devastating. There are no right or wrong reactions to death, the way you grieve will be unique to you. How you grieve will depend on many factors including
Your Spinal Anaesthetic
 Your Spinal Anaesthetic This leaflet is for anyone who may have a spinal anaesthetic. hope it will help you prepare and equip you to ask questions. Having a spinal anaesthetic for your operation. This
Your Spinal Anaesthetic This leaflet is for anyone who may have a spinal anaesthetic. hope it will help you prepare and equip you to ask questions. Having a spinal anaesthetic for your operation. This
A Caregiver s Guide: Congestive Heart Failure
 A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
Management of Chronic Obstructive Lung Disease
 Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
Management of Chronic Obstructive Lung Disease 慢性阻塞性肺病的治療與護理 Chapter Three Put Yourself in Control LEARNING HELPFUL WAYS TO BREATHE Learning helpful ways to breathe means learning to use your lungs smarter
UW MEDICINE PATIENT EDUCATION. Baby Blues and More DRAFT. Knowing About This in Advance Can Help
 UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
For the Patient: LUAVPG (Carboplatin Option)
 For the Patient: LUAVPG (Carboplatin Option) Other Names: Treatment of Advanced n-small Cell Lung Cancer with Carboplatin and Gemcitabine LU = LUng AV = AdVanced PG = CarboPlatin, Gemcitabine ABOUT THIS
For the Patient: LUAVPG (Carboplatin Option) Other Names: Treatment of Advanced n-small Cell Lung Cancer with Carboplatin and Gemcitabine LU = LUng AV = AdVanced PG = CarboPlatin, Gemcitabine ABOUT THIS
Your spinal anaesthetic
 Your spinal anaesthetic This booklet is for anyone who may have a spinal anaesthetic. We hope it will help you prepare and equip you to ask questions. This booklet explains what to expect when you have
Your spinal anaesthetic This booklet is for anyone who may have a spinal anaesthetic. We hope it will help you prepare and equip you to ask questions. This booklet explains what to expect when you have
Chemotherapy Questions and Concerns: General information about what to expect
 Chemotherapy Questions and Concerns: General information about what to expect Princess Margaret For patients who will get chemotherapy and their families Class Overview: What is chemotherapy Side effects
Chemotherapy Questions and Concerns: General information about what to expect Princess Margaret For patients who will get chemotherapy and their families Class Overview: What is chemotherapy Side effects
SLEEP HISTORY QUESTIONNAIRE
 Date of birth: Today s date: Dear Patient: SLEEP HISTORY QUESTIONNAIRE Thank you for taking the time to fill out a sleep history questionnaire. This will help our healthcare team to provide the best possible
Date of birth: Today s date: Dear Patient: SLEEP HISTORY QUESTIONNAIRE Thank you for taking the time to fill out a sleep history questionnaire. This will help our healthcare team to provide the best possible
Total Hip Replacement: Your Guide to Preparation and Recovery
 Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Managing Other Medical Conditions
 Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Chronic Obstructive Pulmonary Disease (COPD)
 James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
James Paget University Hospitals NHS Foundation Trust Great Yarmouth and Waveney Clinical Commissioning Group HealthEast Chronic Obstructive Pulmonary Disease (COPD) Information and Advice for Patients
For the Patient: GIAVPG Other Names: First-line palliative chemotherapy for advanced gallbladder and bile duct cancer using Gemcitabine and Cisplatin
 For the Patient: GIAVPG Other Names: First-line palliative chemotherapy for advanced gallbladder and bile duct cancer using Gemcitabine and Cisplatin GI = GastroIntestinal AV = Advanced PG = Cisplatin,
For the Patient: GIAVPG Other Names: First-line palliative chemotherapy for advanced gallbladder and bile duct cancer using Gemcitabine and Cisplatin GI = GastroIntestinal AV = Advanced PG = Cisplatin,
For the Patient: GDP-R Other names: LYGDPR
 1 For the Patient: GDP-R Other names: LYGDPR G Gemcitabine D Dexamethasone (taken by mouth) P cisplatin R Rituximab (also known as RITUXAN, RITUXAN SC) Uses: GDP-R is a drug treatment given for Non-Hodgkin
1 For the Patient: GDP-R Other names: LYGDPR G Gemcitabine D Dexamethasone (taken by mouth) P cisplatin R Rituximab (also known as RITUXAN, RITUXAN SC) Uses: GDP-R is a drug treatment given for Non-Hodgkin
End of Life with Dementia Sue Quist RN, CHPN
 End of Life with Dementia Sue Quist RN, CHPN Objectives: Describe the Medicare hospice benefit and services. Discuss the Medicare admission criteria for hospice patients with dementia due to Alzheimer
End of Life with Dementia Sue Quist RN, CHPN Objectives: Describe the Medicare hospice benefit and services. Discuss the Medicare admission criteria for hospice patients with dementia due to Alzheimer
Sleep History Questionnaire
 Sleep History Questionnaire Name: DOB: Phone: Date of Consultation: Consultation is requested by: Primary care provider: _ Preferred pharmacy: Chief complaint: Please tell us why you are here: How long
Sleep History Questionnaire Name: DOB: Phone: Date of Consultation: Consultation is requested by: Primary care provider: _ Preferred pharmacy: Chief complaint: Please tell us why you are here: How long
EATING WELL AND CANCER
 EATING WELL AND CANCER 2 Why is it important for people with cancer to eat well? If the person you care for has cancer, it is more important than ever that they eat well. Unfortunately, it is often at
EATING WELL AND CANCER 2 Why is it important for people with cancer to eat well? If the person you care for has cancer, it is more important than ever that they eat well. Unfortunately, it is often at
NUTRITION AT END-OF-LIFE HANDOUTS OBJECTIVES. Hospice Education Network. Nutrition at End-of-Life, by C. Andrew Martin, MS, RN, CHPN
 NUTRITION AT END-OF-LIFE C. Andrew Martin, MS RN CHPN Hospice Education Network camartin@hospiceonline.com HANDOUTS Pause the presentation Click on the link for the PowerPoint handouts and any supplemental
NUTRITION AT END-OF-LIFE C. Andrew Martin, MS RN CHPN Hospice Education Network camartin@hospiceonline.com HANDOUTS Pause the presentation Click on the link for the PowerPoint handouts and any supplemental
The Palliative Care Journey. By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home
 The Palliative Care Journey By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home Aims 1. To provide an overview of what palliative care involves. 2. Identify, at what stage should Dementia be acknowledged
The Palliative Care Journey By Sandra O Sullivan Clinical Nurse Manager 1 St Luke's home Aims 1. To provide an overview of what palliative care involves. 2. Identify, at what stage should Dementia be acknowledged
Your anaesthetic for major surgery
 Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Your anaesthetic for major surgery with planned high dependency care or intensive care afterwards Information for patients and families First Edition 2014 www.rcoa.ac.uk/patientinfo This leaflet is for
Your Anaesthetic Explained
 Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Your Anaesthetic Explained Patient Information Sheet Pre Admission Assessment Clinic Tel: 4920307 What is anaesthesia? The word anaesthesia means loss of sensation. If you have ever had a dental injection
Myeloma Haematology and Transplant Unit MPT
 MPT Myeloma Haematology and Transplant Unit MPT This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may reduce the risk of the
MPT Myeloma Haematology and Transplant Unit MPT This leaflet is offered as a guide to you and your family. The possible benefits of treatment vary; for some people chemotherapy may reduce the risk of the
Chapter 23. Nutrition Needs. Copyright 2019 by Elsevier, Inc. All rights reserved.
 Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Chapter 23 Nutrition Needs Copyright 2019 by Elsevier, Inc. All rights reserved. Lesson 23.1 Define the key terms and key abbreviations in this chapter. Explain the purpose and use of the MyPlate symbol.
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
PRE-VISIT QUESTIONNAIRE FOR NEW PATIENTS
 UF Health Senior Care PO Box 100383 Gainesville, FL 32608 352-265-0615 Fax 352-294-5803 PRE-VISIT QUESTIONNAIRE FOR NEW PATIENTS Please complete this questionnaire at home and bring it with you to the
UF Health Senior Care PO Box 100383 Gainesville, FL 32608 352-265-0615 Fax 352-294-5803 PRE-VISIT QUESTIONNAIRE FOR NEW PATIENTS Please complete this questionnaire at home and bring it with you to the
