S A M P L E. Is Near. When Death. Logo A CAREGIVER S GUIDE
|
|
|
- Holly Caldwell
- 5 years ago
- Views:
Transcription
1 When Death Is Near A CAREGIVER S GUIDE Logo
2 Updated by Hospice of Santa Cruz County. This booklet (published as When Death is Near and When the Time Comes) was created by Hospice of Santa Cruz County, a community-based, not-for-profit organization in Scotts Valley, California, that serves Santa Cruz and North Monterey counties. All rights reserved. No part of this booklet may be reproduced without prior permission of the publisher. Printed in the United States of America. Published by Quality of Life Publishing Co. Naples, Florida Quality of Life Publishing Co. is an independent, mission-driven firm specializing in branded publications that help ease the way for those with serious illnesses and their families. Visit HOW TO ORDER BRANDED COPIES: Call Quality of Life Publishing Co. during regular business hours (Eastern Time) toll free at or info@qolpublishing.com. WDIN / WTTC Eng HL v1.3
3 The things that matter most in our lives are not fantastic or grand. They are the moments when we touch one another, when we are there in the most attentive or caring way. Jack Kornfield
4 Introduction Dying is a natural part of life. Yet many of us do not know how to care for someone at the end of life. It s normal to have a wide range of feelings or to be unsure of what to do. At times it may seem as if you re on a roller coaster. You may not know what will come next. This booklet will help you know what to expect when caring for someone in the final days of life. Family, friends, and caregivers can all play an important role. At the end of life, it is not so much what you say or do. Just being there can provide a sense of support and comfort. Each person s death is unique. No one can guess what it will be like or when it will happen. We hope this booklet helps to guide the way. Please contact us if you have questions. It is our goal to respect the sense of honor and self-esteem the dignity of each person by giving quality comfort care. Death is not extinguishing the light; it is only putting out the lamp because the dawn has come. Rabindranath Tagore 1
5 Table of Contents Introduction...1 Thoughts at the End of Life... 3 Withdrawal... 4 Changes in Eating... 5 Changes in Toileting... 6 Changes in Breathing... 7 Changes in Body Temperature... 8 Confusion... 9 Restlessness and Anxiety...11 Wave of Energy...13 Saying Goodbye...14 When Death Is Near...15 Moment of Death...17 Care for the Caregiver
6 Thoughts at the End of Life Source: Dr. Ira Byock Dr. Ira Byock is a well-known leader in end-of-life care. Below is his list of things people may think about as they near death. These thoughts put us in touch with the emotional and spiritual side of the dying process. Feeling love for one s self and for others. Having a sense of meaning about life. Being at peace about the finality of life. Having a sense of completion with life tasks. Having a sense of completion in relationships with others. Having a sense of a new self beyond personal loss. Giving in to the unknown being able to let go. The journey at the end of life may not be easy. But it can often be a time of growth and healing. We are here to help you and your loved ones along the way. 3
7 Withdrawal It is normal for people who are dying to begin to withdraw, or pull away, from the world around them. This might start as early as weeks before the death. They may stay in bed all day and spend more time asleep than awake. With withdrawal comes less of a need to talk. Touch and silence take on more meaning. People at this point may not respond or may look like they are in a coma. They may start to detach from surroundings and relationships. This may be their way of getting ready to let go. What you can do: Plan tasks and visits for the times of day when the person seems most alert. The person may be able to hear until the end. Speak to the person in your normal tone of voice. Do not say anything you would not say if they were awake. Say your name when you speak. Tell the person what you are going to do before you do it. For example: Bob, this is Karen. I m going to adjust your pillow now. One person caring about another represents life s greatest value. Jim Rohn 4
8 Changes in Eating Many people may no longer want food or drink at the end of life. Seeing a loved one who is not eating can be very hard for families to accept. Meals are how we spend time with family and feed our bodies. Often nothing tastes good to the person. Cravings will come and go. As the body slows down, it will no longer use food in the same way. Weight loss is normal. It does not mean that the person is hungry or being starved. What you can do: Do not force food or drink. Let the person be the guide. There may be times when the smell or a small taste of familiar foods is comforting. If the person asks for food or drink, check with the nurse to be sure it is safe. Liquids may be better than solid foods. Some people find thicker liquids easier to swallow. Small chips of ice or frozen juice may help if the person feels thirsty. Liquids may be given in small amounts by dropper. Ask the nurse for advice. Look for signs the person does not want to eat. Signs could be coughing, biting the spoon, clamping teeth closed, turning the head, or spitting food out. A person near death may appear thirsty but won t be able to drink water. Frequent mouth care can help. Use swabs to keep the mouth and lips moist. 5
9 Changes in Toileting The loss of bladder and bowel control (incontinence) can happen at the end of life. When the body weakens, muscles in the lower body will relax. These changes can be embarrassing. Make sure the person is kept clean, dry, and comfortable to protect their dignity. The amount of urine may lessen at this stage. The color may be darker than normal. It may also be cloudy or have a strong smell. This is a sign that the kidneys are slowing down. It is the normal response to drinking less liquids. Bowel movements that are hard, painful, or not regular (constipation) are also common. Pain medicine can slow the bowels even more. This can cause major discomfort at the end of life. What can help: The person must be checked often to be sure they are clean. Give privacy during personal care. Disposable briefs and bed pads may help. The nurse or home health aide can show you how to change these for someone who is in bed. The nurse may suggest certain creams to protect the skin. The nurse may place a tube (a catheter) into the bladder. This will keep the skin dry. There may be a little discomfort as the tube is placed. After that the person should not know it is there. Contact the nurse if the person has less than 3 stools per week or has trouble passing stools. Care teams will give laxatives or stool softeners with pain medicine to help. Only give treatments that are approved by the nurse. 6
10 Changes in Breathing Breathing patterns often change at the end of life. Breathing may slow down. There may be fast, shallow breaths with periods of no breathing. These periods can last from 5 seconds up to a full minute. This is not uncomfortable for the person. It is another normal response as the body weakens. Some people get so weak that they cannot swallow. Saliva will sit in the back of their throat and make a rattling sound. Suctioning will only make more saliva and cause more discomfort. The sound may be troubling to hear, but it does not mean the person is suffering. What you can do: Let the care team know if there are changes in breathing. They will check to see if oxygen might bring comfort. If the person is struggling to breathe, the care team may order medicine (such as morphine) to provide comfort. The person may breathe with their mouth open. This can make the mouth very dry. Routine mouth care is important. Moisten the mouth and lips often with swabs. Use lip balm to keep lips from chapping. If saliva gathers in the throat, gently turn the person on their side to help drain it. Raising the head of the bed may also help. Check with the nurse to see if medicine can be used to dry the saliva. 7
11 Changes in Body Temperature The brain will start to lose control of body temperature as the body weakens. This can cause a fever or cause the body to become cool. Sometimes the person may get sweaty. These changes are a natural part of the dying process. Blood flow will slow down. Feet, legs, hands, and arms might feel cool to the touch. Skin color may change. The person may look very pale. Hands and feet may turn slightly purple. Knees, ankles, and elbows may look blotchy. Lips and the skin under the fingernails may turn bluish. These changes to the skin do not cause any discomfort for the person. What can help if the person has a fever: Let the nurse know if the person has a fever. Put a cool washcloth on the forehead or remove blankets. The nurse may suggest pain medicine (like Tylenol) if the fever is high. The person might sweat a lot as the fever drops. Change the gown/pajamas and sheets as needed to provide comfort. Gently rearrange the person in bed. Consider using a fan or opening a window. If the person throws the covers off, remember that they may be warm even if you feel cool. What can help if the person becomes cold: Use a warm blanket, but not an electric blanket. Gentle massage may help increase blood flow. Check with the nurse before giving a massage. Some people may have skin that is too sensitive for massage. 8
12 Confusion People nearing the end of life may seem confused at times. They may not know what time it is or where they are. They may not recognize family or friends. They may say that they see things no one else can see. They may talk to people who are not there, or who have already died. People near the end of life will sometimes talk about travel. They may say things such as: I want to get my keys, I need to find my suitcase, or Where is the train/bus? This is known as symbolic language. It may be one of the ways people let us know that they are ready for death. They could be trying to tell us goodbye. Some people may think the medicine could be causing the confusion. But this is a normal part of the dying process. What you can do: Let the care team know if the person is confused. They will show you how to best support the person at this time. The care team will check to make sure the right medicine is being given at the right dose. Gently try to reorient the person. Remind them of who you are. Tell them what you are doing. Point out familiar things in the room. Provide comfort. Tell the person that you are there to take care of them. Let them know that they are safe. Limit visitors to help lessen confusion. 9
13 Let the person tell you what they are seeing, feeling, or hearing. Do not argue with them. These things are real to the person, even though they may not seem real to you. Listen carefully. There may be meaningful messages being shared in symbolic language. Consider writing down important things that happen. A journal may be a source of comfort to share with other loved ones later. We do not remember days, we remember moments. Cesare Pavese 10
14 Restlessness and Anxiety At times, the person may seem restless. They may pick at the sheets or make the same motions over and over again. This is common. Restlessness can be caused in part by a slowing of blood flow. This causes less oxygen to flow to the brain. Sometimes restlessness and anxiety can be a sign of discomfort or pain. Emotional or spiritual concerns may also cause anxiety. Having unfinished affairs may make the person feel uneasy or restless. What you can do: Let the nurse know if the person is restless or tense. They will check for pain or discomfort. Keep giving medicines as prescribed by the doctor. Ask the social worker or chaplain to talk with the person about emotional or spiritual matters. They can provide support if there are concerns. Try to help the person resolve issues. Offer to take over tasks that need to be finished. See if others can help complete tasks. Restraints, such as straps or belts, may cause more anxiety. Do not strap the person to the bed or hold them down. Instead, use bed rails or have someone sit with the person to keep them safe. Use a baby monitor when out of the room. Be calm and give comfort. Speak to the person in a slow and soothing tone of voice. Read something the person enjoys or play soft music. 11
15 Sharing memories can be comforting. Some people talk about special holidays, good times with loved ones, or favorite places. Keep the person s space quiet. Turn radios, TVs, and phone ringers down or off. It also may help to limit visitors. Bring comfort with a gentle touch or by holding hands. Among the best things we can give each other are good memories. Henri J.M. Nouwen 12
16 Wave of Energy Dying loved ones may show sudden, short-lived waves of energy. The person may become surprisingly alert and clear. They may ask to eat when they haven t had food for days. They may want to get up to visit when they haven t been out of bed for weeks. Waves of energy don t always happen in such dramatic ways. They can be more subtle, like the person being awake more often. It is easy to see how this might give false hope that the person is getting better. Sadly, this is not likely. It may be that the person is building up strength for their last full-body moments in this life. What you can do: Enjoy this special time for what it is. Use the time to share memories and say goodbye. Be together holding hands. In this life we cannot do great things. We can only do small things with great love. Mother Teresa 13
17 Saying Goodbye Family and friends may not be sure whether to say goodbye. Some worry that it might cause death sooner. Others may want to say goodbye, but do not know what to say. Some people wonder if they should say it is okay to let go. When and how to say goodbye is a personal choice. There is no right or wrong way to do it. Some people have a hard time saying goodbye. Many find that once it is done, it can be a gift. What you can do: Take time while the person is awake to say or do what you need to. Follow your heart. This time with your loved one is precious. Some people start with: What I love most about you... What I will always remember... What I will miss most about you... What I learned from you... What I hold close to my heart is... Some people may take this time to say, I am sorry, to forgive, or to let go of past anger. Some people use this time to give thanks. It may be helpful to hold your loved one, if possible. Or take their hand and say everything you need to say. Tears are a normal part of saying goodbye. Crying can be a healthy way to show how much you love the person. 14
18 When Death Is Near Below is a list of signs that may mean death will take place soon. Each person s dying process is unique. This is only a guide. Some people may not show all of these signs. Some may show signs at different times. 1 to 3 months: Withdraws from people and activities Talks less Eats and drinks less Sleeps more 1 to 2 weeks: Confused about place, time, or people Uses symbolic language ( Where is the train/bus? ) Talks to others who are not in the room Physical changes: Pulse speeds up or slows down Blood pressure drops Skin color changes Breathing is weak or uneven Body temperature turns hot or cold Does not eat, drinks little or no fluids 15
19 Days to hours: Sleeps most of the time Wave of energy Is restless Has a hard time swallowing Weak pulse Bigger drop in blood pressure More changes in skin color More changes in breathing (long pauses between breaths) Rattling sounds while breathing Less urine or no urine Eyelids do not close all the way Minutes: Short breaths with longer pauses Mouth open Does not respond 16
20 Moment of Death No one can tell when death will take place. Some people die when others are there. Some take their last breaths when they are alone. Talk to family, caregivers, and friends about what to do if they are there at the time of death. When the person has died, there will be no breathing or heartbeat. There will be no response to voice or touch. The eyes may be partly open. The pupils will not respond to light. The jaw will relax, and the mouth will open. There may be loss of bowel and bladder control. Death can feel like a shock even if it was expected. At the time of death, nothing needs to be done right away other than calling hospice. There is no need to call 911 or the police. What you can do: Please contact hospice. A nurse will visit. Other care team members may help as needed. You may want to call a friend or a family member to be with you at this time. When a nurse or care team member visits, they may: Confirm the death Remove any tubes Offer to bathe and prepare the body Give you guidance on what should be done with unused medicine Call the funeral home, if you wish Contact the doctor and the rest of the hospice team Arrange to have equipment removed Provide support 17
21 Some people want the funeral home to come right away. Others wait before calling. Some honor their loved ones by: Bathing and dressing the person in special clothes Telling stories Lighting a candle or putting flowers in the room Sharing a ritual from the person s spiritual beliefs Playing special music Let the funeral home know when you are ready for them to come. You can be there when they take the body or wait in another part of the house. The funeral home will help you make memorial plans, if you wish. Death ends a life, not a relationship. Mitch Albom, Tuesdays with Morrie 18
22 Care for the Caregiver Caring for someone who is at the end of life can be draining. It can leave caregivers weary in body, mind, and spirit. Caregivers often juggle other duties like work, caring for a family, or their own health concerns. Balancing another s care with your own needs can be a big challenge. What you can do: Find balance between your loved one s care and your own needs. It is important to take care of yourself too. Take a deep breath many times a day. Deep breathing can refresh body and mind. Rest when you can. Lie down or sit with your feet up in a quiet place for 20 minutes. Try an exercise routine. Take a walk outside. This can help lessen stress and boost energy. Drink plenty of water. Eat healthy meals at regular times. Decide if calls or visits will help. Limit visits if you need to. Give yourself time alone when you need it. Ask for help. People often want to help but don t know what you need. Keep a list of tasks to be done, such as shopping or walking the dog. Contact hospice. Trained volunteers can help with errands or sit with the person while you take a break. Share your feelings with a trusted friend, your spiritual counselor, or someone from the care team. Please be gentle with yourself. Take life one moment, one step at a time. Contact us if you need help. We are here for you. 19
23 Questions and Notes:
24 Provided by Organization Name Street Address City, State, Zip Toll Free: (000) Phone: (000) Fax: (000) Logo
May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way.
 May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way. Introduction Dying is a natural part of life, but many people do not have experience caring
May the longtime sun shine upon you, All love surround you, And the pure light within you Guide you on your way. Introduction Dying is a natural part of life, but many people do not have experience caring
Preparing for Approaching Death
 Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Preparing for Approaching Death Old Colony Hospice created this guide for our hospice family and caregivers by revising and adapting the following journal article: Hospice Techniques: Preparing for the
Palliative Care Victoria The Process of Dying Page 1. The Process of Dying. What to expect and how to help
 Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Palliative Care Victoria The Process of Dying Page 1 The Process of Dying What to expect and how to help Palliative Care Victoria The Process of Dying Page 2 About dying Dying is a natural part of life.
Physical/Emotional Symptoms and Appropriate Comfort Measures
 Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
Physical/Emotional Symptoms and Appropriate Comfort Measures A. Diminishing Appetite Page 2 B. Decreased Socialization Page 2 C. Sleeping Page 2 E. Changes in Pain Level Page 3 D. Incontinence Page 3 F.
ALONG THE FINAL JOURNEY
 ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
ALONG THE FINAL JOURNEY A Guide for families and caregivers TABLE OF CONTENTS STARTING THE JOURNEY...2 ALONG THE JOURNEY... 3 Physical/Emotional Symptoms and Appropriate Comfort Measures Diminishing Appetite...
Preparing for the Death of a Loved One. Information for Patients & Visitors
 Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
Preparing for the Death of a Loved One Information for Patients & Visitors This booklet is provided to help you know what to expect when your loved one is dying. It may help you to respond in ways that
What to expect in the last days and hours of life in the Intensive Care Unit (ICU)
 What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
What to expect in the last days and hours of life in the Intensive Care Unit (ICU) Information for patients and caregivers Please visit the UHN Patient Education website for more health information: www.uhnpatienteducation.ca
Preparing for Approaching Death By North Central Florida Hospice, Inc.
 Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
Preparing for Approaching Death By North Central Florida Hospice, Inc. When a person enters the final stage of the dying process, two different dynamics are at work which are closely interrelated and interdependent.
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 7 What can I do to help?... 7 Can friends and
What to expect in the last few days of life
 What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
What to expect in the last few days of life Contents Introduction... 3 What are the signs that someone is close to death?... 4 How long does death take?... 6 What can I do to help?... 7 Can friends and
Precious Moments. Giving comfort and support when someone you love is dying.
 Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Precious Moments Giving comfort and support when someone you love is dying www.stjoes.ca When someone you love is dying When someone you love is dying, you may want to know how you can provide comfort
Coping with dying. Information for families and carers
 Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
Coping with dying Information for families and carers This leaflet describes some of the physical changes that happen to people as they start to die. It also covers what will happen immediately following
S A M P L E. Your Pain. Managing. Logo A GUIDE TO PAIN MEDICATION USE
 Managing Your Pain A GUIDE TO PAIN MEDICATION USE Logo Revised 2019. 2015 by Quality of Life Publishing Co. All rights reserved. No part of this booklet may be reproduced without prior permission of the
Managing Your Pain A GUIDE TO PAIN MEDICATION USE Logo Revised 2019. 2015 by Quality of Life Publishing Co. All rights reserved. No part of this booklet may be reproduced without prior permission of the
Coach on Call. Letting Go of Stress. A healthier life is on the line for you! How Does Stress Affect Me?
 Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Coach on Call How Does Stress Affect Me? Over time, stress can affect the way you feel, think, and act. You need some time when you are free of stress. You need ways to get relief from stress. Without
Journey s End: What to Expect and What to Do When Giving Care at the End of Life
 Journey s End: What to Expect and What to Do When Giving Care at the End of Life 2009 Pathways Home Health & Hospice. All rights reserved. Journey s End: What to Expect and What to Do Just as our lives
Journey s End: What to Expect and What to Do When Giving Care at the End of Life 2009 Pathways Home Health & Hospice. All rights reserved. Journey s End: What to Expect and What to Do Just as our lives
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person
 Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
Preventing delirium while in hospital Tips for family, whānau, and friends who are supporting an older person This brochure shares some simple ways you can help our care staff to prevent delirium, recognize
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
Remember that preparing for a death can be difficult. We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect. While
When Someone Close To You Is Dying
 Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Remember that preparing for a death can be difficult We hope the information provided in this booklet may reduce the amount of stress you feel by giving you some information about what to expect While
Journey towards new life...
 Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
Journey towards new life... Dear Family, The staff of Maxville Manor accompanies you on this difficult journey. Our Residents are like family to us. In an effort to provide the support you need, we offer
Relaxation Techniques
 Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Relaxation is needed for good health. It gives your body and mind a chance to rest and recover from high-stress situations. Your heart rate slows down, blood pressure decreases and muscles relax. Relaxation
Palliative Care Asking the questions that matter to me
 Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
Palliative Care Asking the questions that matter to me THE PALLIATIVE HUB Adult This booklet has been developed by the Palliative Care Senior Nurses Network and adapted with permission from Palliative
for the grieving process How to cope as your loved one nears the end stages of IPF
 Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
Preparing yourself for the grieving process How to cope as your loved one nears the end stages of IPF 3 As your loved one nears the end stages of IPF, it s important that you be there for him or her as
and breathing Relaxation techniques East and North Hertfordshire NHS Trust Patient Information Series PI 83 a patient s guide
 Relaxation and breathing techniques Patient Information Series PI 83 East and North Hertfordshire NHS Trust 2 a patient s guide Relaxation and breathing techniques Contents Introduction 4 When and where
Relaxation and breathing techniques Patient Information Series PI 83 East and North Hertfordshire NHS Trust 2 a patient s guide Relaxation and breathing techniques Contents Introduction 4 When and where
Managing Other Medical Conditions
 Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Managing Other Medical Conditions When Dementia is Part of the Picture Terms You Will NEED to Know - Advanced directives - Living Will - DNR orders - Durable HC-POA - Palliative care - Hospice care - Comfort
Improving Your Sleep During Your Hospital Stay
 PATIENT & CAREGIVER EDUCATION Improving Your Sleep During Your Hospital Stay This information will help you improve your sleep during your hospital stay. Sleeping well at night can make you feel better
PATIENT & CAREGIVER EDUCATION Improving Your Sleep During Your Hospital Stay This information will help you improve your sleep during your hospital stay. Sleeping well at night can make you feel better
Be Fit for Life Series. Key Number Five Increase Metabolism
 Key #5 Increase Metabolism Page 1 of 9 Be Fit for Life Series Key Number Five Increase Metabolism Sit or lie in a safe and comfortable position I want you to close your eyes keep them closed until I ask
Key #5 Increase Metabolism Page 1 of 9 Be Fit for Life Series Key Number Five Increase Metabolism Sit or lie in a safe and comfortable position I want you to close your eyes keep them closed until I ask
GASTRECTOMY. Date of Surgery. Please bring this booklet the day of your surgery. QHC#34
 GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
GASTRECTOMY Date of Surgery Please bring this booklet the day of your surgery. QHC#34 What is a Gastrectomy? A Gastrectomy is the surgical removal of all or part of the stomach. The stomach is the digestion
Anterior Sphincter Repair Operation
 Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Anterior Sphincter Repair Operation How will the operation help me? The investigations that you have had indicate that your anal sphincter is damaged or very weak, and this is why you are having trouble
Hospice Journey. A guide of signs, symptoms and caregiving
 Hospice Journey A guide of signs, symptoms and caregiving 1 This book is a guide to help you through the dying journey a natural part of life. A variety of changes can be seen as a body prepares for death.
Hospice Journey A guide of signs, symptoms and caregiving 1 This book is a guide to help you through the dying journey a natural part of life. A variety of changes can be seen as a body prepares for death.
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION
 ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
ALZHEIMER S DISEASE, DEMENTIA & DEPRESSION Daily Activities/Tasks As Alzheimer's disease and dementia progresses, activities like dressing, bathing, eating, and toileting may become harder to manage. Each
Delirium: Information for Patients and Families
 health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
health information Delirium: Information for Patients and Families 605837 Alberta Health Services, (2016/11) Resources Delirium in the Older Person Family Guide: search delirium at viha.ca Go to myhealth.alberta.ca
Delirium A guide for caregivers
 Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
Delirium A guide for caregivers Disclaimer This is general information developed by The Ottawa Hospital. It is not intended to replace the advice of a qualified health-care provider. Please consult your
RELAXATION EXERCISES
 RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
RELAXATION EXERCISES Relaxation technique 1: Breathing meditation for stress relief With its focus on full, cleansing breaths, deep breathing is a simple, yet powerful, relaxation technique. It s easy
There For You. Your Compassionate Guide. World-Class Hospice Care Since 1979
 There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
There For You Your Compassionate Guide World-Class Hospice Care Since 1979 What Is Hospice? Hospice is a type of care designed to provide support during an advanced illness. Hospice care focuses on comfort
A Guide to Help New Mothers Stay Smoke-Free
 A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
A Guide to Help New Mothers Stay Smoke-Free 1 Welcome to motherhood! You have just been through a life-changing experience pregnancy and child birth. Having a plan to stay smoke-free is an important step.
- copyright
 Relaxation Exercises Let s start with breathing! Your breathing is often the first thing to be affected by stress. When we are anxious we tend to hunch up the shoulders and breathe in a more rapid and
Relaxation Exercises Let s start with breathing! Your breathing is often the first thing to be affected by stress. When we are anxious we tend to hunch up the shoulders and breathe in a more rapid and
information The Enhanced Recovery Programme for Total Hip Replacement (1 of 6) What will happen before I come into hospital?
 information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
information If you need this information in another language or medium (audio, large print, etc) please contact the Customer Care Team on 0800 374 208 email: customercare@ salisbury.nhs.uk. You are entitled
Ileal Conduit Diversion Surgery
 Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
Here are some words and pictures to help you understand this surgery: Bladder: the bladder stores urine that is made by the kidneys Bowels: the bowels are the parts of the body that digest food and fluids.
A Guide to Help You Reduce and Stop Using Tobacco
 Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Let s Talk Tobacco A Guide to Help You Reduce and Stop Using Tobacco Congratulations for taking this first step towards a healthier you! 1-866-710-QUIT (7848) albertaquits.ca It can be hard to stop using
Session 15: Mindful Eating, Mindful Movement
 Session 15: Mindful Eating, Mindful Movement Are there times when you realize that you are still eating and simply haven t noticed that you are not even hungry anymore? Do you ever get to the end of a
Session 15: Mindful Eating, Mindful Movement Are there times when you realize that you are still eating and simply haven t noticed that you are not even hungry anymore? Do you ever get to the end of a
UW MEDICINE PATIENT EDUCATION. Baby Blues and More DRAFT. Knowing About This in Advance Can Help
 UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
Understanding late stage dementia Understanding dementia
 Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Understanding late stage dementia About this factsheet This factsheet is for relatives of people diagnosed with dementia. It provides information about what to expect as dementia progresses to late stage.
Preparing for Death. A guide for families and caregivers as death approaches PALLIATIVE & END OF LIFE
 PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
PALLIATIVE & END OF LIFE Preparing for Death A guide for families and caregivers as death approaches In this booklet you will learn about: Things to consider when a loved one is seriously ill Checklist
CARING FOR YOUR CATHETER AT HOME
 CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
CARING FOR YOUR CATHETER AT HOME After surgery (radical prostatectomy) for prostate cancer you will have a urinary catheter for a short period of time and will need to go home with the catheter still in
keep track of other information like warning discuss with your doctor, and numbers of signs for relapse, things you want to
 Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
Helping you set your brain free from psychosis. www.heretohelp.bc.ca This book was written by Sophia Kelly and the BC Schizophrenia Society, for the BC Partners for Mental Health and Addictions Information.
SAFETYNET LEARNING TOOLS
 SAFETYNET LEARNING TOOLS Topic: Urinary Tract Infection Use the materials in this document to help others learn more about urinary tract infection. LEARNING TOOLS: 1. How to Say it Guide 2. Recognizing
SAFETYNET LEARNING TOOLS Topic: Urinary Tract Infection Use the materials in this document to help others learn more about urinary tract infection. LEARNING TOOLS: 1. How to Say it Guide 2. Recognizing
Keeping Home Safe WHAT CAN YOU DO?
 Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
Keeping Home Safe or dementia may have trouble knowing what is dangerous or making safe decisions. By helping him or her feel more relaxed and less confused at home, you can help stop accidents. trip because
CHEMOTHERAPY. What should I expect?
 CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
CHEMOTHERAPY What should I expect? WHAT IS CHEMOTHERAPY? Chemotherapy is treatment that uses drugs to stop the growth of cancer cells, either by killing the cells or by stopping them from dividing. Chemotherapy
Session 16: Manage Your Stress
 Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
Session 16: Manage Your Stress Stress is part of life. However, you can learn better ways to take care of yourself when faced with stress. Stress is not always bad. Some stress can make life interesting
Concussion & You. A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL
 Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
Concussion & You A Handbook for Parents and Kids DEVELOPED BY CONCUSSION EXPERTS AT HOLLAND BLOORVIEW KIDS REHABILITATION HOSPITAL Trusted experts in youth concussion www.hollandbloorview.ca/concussion
suicide Part of the Plainer Language Series
 Part of the Plainer Language Series www.heretohelp.bc.ca What is? Suicide means ending your own life. It is sometimes a way for people to escape pain or suffering. When someone ends their own life, we
Part of the Plainer Language Series www.heretohelp.bc.ca What is? Suicide means ending your own life. It is sometimes a way for people to escape pain or suffering. When someone ends their own life, we
Relaxing Exercises to Relieve Stress
 Relaxing Exercises to Relieve Stress UHN For patients and families Read this pamphlet to learn ways to relax to help you manage stress and lower anxiety. Ways to relax include: deep breathing relaxing
Relaxing Exercises to Relieve Stress UHN For patients and families Read this pamphlet to learn ways to relax to help you manage stress and lower anxiety. Ways to relax include: deep breathing relaxing
Controlling Worries and Habits
 THINK GOOD FEEL GOOD Controlling Worries and Habits We often have obsessional thoughts that go round and round in our heads. Sometimes these thoughts keep happening and are about worrying things like germs,
THINK GOOD FEEL GOOD Controlling Worries and Habits We often have obsessional thoughts that go round and round in our heads. Sometimes these thoughts keep happening and are about worrying things like germs,
The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions
 The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions Pain control is a key part of your care after surgery. It can help speed recovery and improve the results of your surgery. This handout
The 3 P s (Pain, Poop, Physical Therapy) for Post-Op Spinal Fusions Pain control is a key part of your care after surgery. It can help speed recovery and improve the results of your surgery. This handout
Smoking and Quitting Assessment
 Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
Smoking and Quitting Assessment A. Which of the following describes you? q I m not interested in trying to quit smoking. q I know I need to quit smoking, but I m not quite ready yet. q I m ready to quit
12 hours. Your body has eliminates all excess carbon monoxide and your blood oxygen levels become normal.
 Balance March 2018 What happens after the last cigarette? You know that smoking is one of the leading causes of preventable deaths but the process of quitting seems too daunting. After all, you ve tried
Balance March 2018 What happens after the last cigarette? You know that smoking is one of the leading causes of preventable deaths but the process of quitting seems too daunting. After all, you ve tried
Preventing delirium while in the hospital
 Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
Preventing delirium while in the hospital What is delirium? When an older person becomes ill and goes into the hospital, there is an increased risk of developing delirium and other problems. Delirium is
UW MEDICINE PATIENT EDUCATION. Baby Blues and More. Postpartum mood disorders DRAFT. Emotional Changes After Giving Birth
 UW MEDICINE PATIENT EDUCATION Baby Blues and More Postpartum mood disorders Some new mothers have baby blues or more serious postpartum mood disorders. This chapter gives ideas for things you can do to
UW MEDICINE PATIENT EDUCATION Baby Blues and More Postpartum mood disorders Some new mothers have baby blues or more serious postpartum mood disorders. This chapter gives ideas for things you can do to
When You re Having Surgery for a Fractured Hip
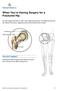 When You re Having Surgery for a Fractured Hip The hip includes the head or ball of the thigh bone (femur). The thigh bone fits into the socket of the pelvis. Ligaments and muscles hold the joint in place.
When You re Having Surgery for a Fractured Hip The hip includes the head or ball of the thigh bone (femur). The thigh bone fits into the socket of the pelvis. Ligaments and muscles hold the joint in place.
CARING FOR SICK PEOPLE AT HOME
 PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
PANDEMIC INFLUENZA CARING FOR SICK PEOPLE AT HOME What is pandemic flu? Pandemic flu means that a new strain of influenza has spread all over the world and is affecting a large number of people. During
ANESTHESIA. Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS
 ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
ANESTHESIA & YOU Planning Your Childbirth: Pain Relief During Labor and Delivery EACH WOMAN S LABOR IS UNIQUE T he amount of pain a woman feels during labor may differ from that felt by another woman.
Take Charge of Your Pain Program: Patient Booklet
 Take Charge of Your Pain Program: Patient Booklet TABLE OF CONTENTS ABOUT THIS BOOKLET... 3 THINGS TO KNOW ABOUT PAIN... 4 Pain Gate... 6 BECOMING MORE ACTIVE... 7 RELAXATION... 8 DEEP BREATHING... 9 IMAGERY...
Take Charge of Your Pain Program: Patient Booklet TABLE OF CONTENTS ABOUT THIS BOOKLET... 3 THINGS TO KNOW ABOUT PAIN... 4 Pain Gate... 6 BECOMING MORE ACTIVE... 7 RELAXATION... 8 DEEP BREATHING... 9 IMAGERY...
Beyond Cancer Moving On
 Beyond Cancer Moving On Today, people with cancer have a better chance at living a normal life than ever before in history. In fact, there are more than 10 million survivors people who have, or are living
Beyond Cancer Moving On Today, people with cancer have a better chance at living a normal life than ever before in history. In fact, there are more than 10 million survivors people who have, or are living
All Emotions Matter: for the Secondary Classroom
 All Emotions Matter: for the Secondary Classroom Mental Health Association in New York State, Inc. 1 The goal of this lesson is to: Validate feelings and emotions. Teach students to manage their response
All Emotions Matter: for the Secondary Classroom Mental Health Association in New York State, Inc. 1 The goal of this lesson is to: Validate feelings and emotions. Teach students to manage their response
Created by Support Plus, 2017 Sleep
 Created by Support Plus, 2017 Sleep You might want to look at this leaflet with someone you trust like a healthcare worker Sleep Contents Page Sleep Facts Page 3, 4 and 5 Sleep Problems Page 6 Why do people
Created by Support Plus, 2017 Sleep You might want to look at this leaflet with someone you trust like a healthcare worker Sleep Contents Page Sleep Facts Page 3, 4 and 5 Sleep Problems Page 6 Why do people
INFORMATION FOR PATIENTS, CARERS AND FAMILIES. Coping with dying
 INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
INFORMATION FOR PATIENTS, CARERS AND FAMILIES Coping with dying This leaflet describes some of the physical changes that happen to people as they start to die. It anticipates some of the questions you
Enhanced Recovery Programme Liver surgery
 Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Enhanced Recovery Programme Liver surgery General Surgery Patient information leaflet Introduction When you are admitted to hospital for your surgery you will be taking part in an enhanced recovery programme.
Sleeping Problems. Easy read information
 Sleeping Problems Easy read information A member of staff or a carer can support you to read this booklet. They will be able to answer any questions that you have. About this leaflet This leaflet is for
Sleeping Problems Easy read information A member of staff or a carer can support you to read this booklet. They will be able to answer any questions that you have. About this leaflet This leaflet is for
A Caregiver s Guide: Congestive Heart Failure
 A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
A Caregiver s Guide: Congestive Heart Failure This is a guide for family members, friends and other caregivers who are supporting someone who has congestive heart failure (CHF). This is a guide for family
Every day matters. To help you stay out of the hospital, you can: Live healthy with sickle cell disease
 Living with sickle cell disease (SCD) can be difficult. There can be severe pain and discomfort. AmeriHealth Caritas Louisiana wants to help you manage this life-threatening disease. To help you stay out
Living with sickle cell disease (SCD) can be difficult. There can be severe pain and discomfort. AmeriHealth Caritas Louisiana wants to help you manage this life-threatening disease. To help you stay out
Wellness along the Cancer Journey: Palliative Care Revised October 2015
 Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
Wellness along the Cancer Journey: Palliative Care Revised October 2015 Chapter 3: Addressing Cancer Pain as a part of Palliative Care Palliative Care Rev. 10.8.15 Page 360 Addressing Cancer Pain as Part
End-of-Life Care. Annual Education End-of-Life Care Mission Health System, Inc.
 Annual Education 2014 2013 Mission Health System, Inc. Why Cover This Subject? Patients who are near the end of their lives need to receive care that addresses their psychosocial, emotional, and spiritual
Annual Education 2014 2013 Mission Health System, Inc. Why Cover This Subject? Patients who are near the end of their lives need to receive care that addresses their psychosocial, emotional, and spiritual
wrha.mb.ca a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Healthcare Professional Guide
 a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
a conversation about tube feeding a guide for clients, families and friends healthcare professional guide Health Care Professional Guide Pamphlet Information Healthcare Professional Guide If you are reading
University of Oregon HEDCO Clinic Fluency Center. Diagnostic Intake Form for Adults Who Stutter
 University of Oregon HEDCO Clinic Fluency Center Phone 541-346-0923 Fax 541-346-6772 Physical Address: Mailing Address: HEDCO Education Complex HEDCO Clinic 1655 Alder Street, Eugene, OR 97403 5207 University
University of Oregon HEDCO Clinic Fluency Center Phone 541-346-0923 Fax 541-346-6772 Physical Address: Mailing Address: HEDCO Education Complex HEDCO Clinic 1655 Alder Street, Eugene, OR 97403 5207 University
Anal Atresia FACTS: There is no known cause for anal atresia. Children with anal atresia can lead very happy lives post surgery!
 Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
Anal Atresia FACTS: Anal atresia affects 1 in 5,000 births and is slightly more common in boys. There is no known cause for this condition. With anal atresia, any of the following can occur: The anal passage
5 Minute Strategies to Support Healthy Treatment and Recovery
 HPW-000030 TAKE FIVE 5 Minute Strategies to Support Healthy Treatment and Recovery Below you will find quick strategies, each related to one of 15 different moods commonly experienced by people coping
HPW-000030 TAKE FIVE 5 Minute Strategies to Support Healthy Treatment and Recovery Below you will find quick strategies, each related to one of 15 different moods commonly experienced by people coping
Total Hip Replacement: Your Guide to Preparation and Recovery
 Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Total Hip Replacement: Your Guide to Preparation and Recovery Table of Contents Preparing For Your Surgery...................... 1 During Your Hospital Stay...................... 6 After Surgery.............................
Ready to give up. Booklet 3
 Ready to give up Booklet 3 This booklet is written for people who have decided that they want to stop smoking. You can use this booklet on its own or go through it with the person who gave it to you. You
Ready to give up Booklet 3 This booklet is written for people who have decided that they want to stop smoking. You can use this booklet on its own or go through it with the person who gave it to you. You
General Symptoms. Cold Weather Symptoms TG-272
 General Symptoms Cold Weather Symptoms Cold weather injuries can range from mild chapped skin to life-threatening hypothermia. To avoid cold weather injuries, you must be prepared. Being prepared means
General Symptoms Cold Weather Symptoms Cold weather injuries can range from mild chapped skin to life-threatening hypothermia. To avoid cold weather injuries, you must be prepared. Being prepared means
Esophagectomy Surgery
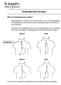 Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
Esophagectomy Surgery What is esophagectomy surgery? Esophagectomy surgery is the removal part, or all, of the esophagus. The esophagus is the tube that your food goes down on the way to your stomach.
NEW PATIENT HOME CARE PACKET
 NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
NEW PATIENT HOME CARE PACKET CORRECT POSTURE Correct posture is a very important component to your TMJ treatment and overall health. Poor posture can throw your head and spine off balance in relation to
Going home after breast surgery without drains
 Going home after breast surgery without drains Princess Margaret Information for patients and families Read this resource to learn: How to care for yourself when you go home What activities you can do
Going home after breast surgery without drains Princess Margaret Information for patients and families Read this resource to learn: How to care for yourself when you go home What activities you can do
Staying a non-smoker. Booklet 4
 Staying a non-smoker Booklet 4 Congratulations on giving up smoking! Use this booklet to help you stay a non-smoker. Now that you have stopped smoking you will be feeling healthier, and you will be breathing
Staying a non-smoker Booklet 4 Congratulations on giving up smoking! Use this booklet to help you stay a non-smoker. Now that you have stopped smoking you will be feeling healthier, and you will be breathing
Bowel Resection Surgery (Open Method)
 Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
Bowel Resection Surgery (Open Method) What is a bowel resection? A bowel resection is surgery to remove a part of the large or small intestine. These parts are shown on this diagram. small intestine large
Introduction. Today we hope to provide tips and resources to help balance the challenges of caregiving and ensure that everyone is being cared for.
 Caregiver Wellness Introduction Being a caregiver can be both rewarding and challenging. It s easy to forget to tend to your own needs while caring for your loved one, but it is incredibly important. Today
Caregiver Wellness Introduction Being a caregiver can be both rewarding and challenging. It s easy to forget to tend to your own needs while caring for your loved one, but it is incredibly important. Today
4/3/2014. Dame Cicely Sanders : Born in England Nursing Degree Social Work Degree Doctor Opened 1 st Stand Alone Hospice 1967
 Catherine Hausenfluke Independent Consultant 512-966-4955 Know More about Dying and Grief Come to Terms with Your Own Morality Understand Grief and What are the Rules Understand the Dying Process Relating
Catherine Hausenfluke Independent Consultant 512-966-4955 Know More about Dying and Grief Come to Terms with Your Own Morality Understand Grief and What are the Rules Understand the Dying Process Relating
Teaching Family and Friends in Your Community
 2 CHAPTER Teaching Family and Friends in Your Community 9 Old people can remember when there were fewer problems with teeth and gums. Children s teeth were stronger and adults kept their teeth longer.
2 CHAPTER Teaching Family and Friends in Your Community 9 Old people can remember when there were fewer problems with teeth and gums. Children s teeth were stronger and adults kept their teeth longer.
University Staff Counselling Service
 University Staff Counselling Service Anxiety and Panic What is anxiety? Anxiety is a normal emotional and physiological response to feeling threatened, ranging from mild uneasiness and worry to severe
University Staff Counselling Service Anxiety and Panic What is anxiety? Anxiety is a normal emotional and physiological response to feeling threatened, ranging from mild uneasiness and worry to severe
Lesson 9 Anxiety and Relaxation Techniques
 The following presentation was originally developed for individuals and families by Achieva (a Western PA service provider). Now offered as a webcast production, ODP is providing this valuable resource
The following presentation was originally developed for individuals and families by Achieva (a Western PA service provider). Now offered as a webcast production, ODP is providing this valuable resource
Radiotherapy to the Oesophagus
 The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow, G12 OYN Patient Information Sheet Radiotherapy to the Oesophagus This leaflet is for patients receiving radiotherapy for a cancer
The Beatson West of Scotland Cancer Centre 1053 Great Western Road, Glasgow, G12 OYN Patient Information Sheet Radiotherapy to the Oesophagus This leaflet is for patients receiving radiotherapy for a cancer
This patient guide will help you understand:
 How to Manage Your Shortness of Breath This patient guide will help you understand: What is cancer-related shortness of breath? pg 2 What causes shortness of breath? pg 4 What can I do to manage my shortness
How to Manage Your Shortness of Breath This patient guide will help you understand: What is cancer-related shortness of breath? pg 2 What causes shortness of breath? pg 4 What can I do to manage my shortness
UW MEDICINE PATIENT EDUCATION. Baby Blues and More. Knowing About This in Advance Can Help
 UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
UW MEDICINE PATIENT EDUCATION Baby Blues and More Recognizing and coping with postpartum mood disorders Some women have baby blues or more serious postpartum mood disorders. It helps to know about these
Approaching End of Life Some Thoughts... Information for Patients and Families
 Approaching End of Life Some Thoughts... Information for Patients and Families This pamphlet has been produced by the Cancer Care Program of North York General Hospital www.nygh.on.ca 4001 Leslie Street,
Approaching End of Life Some Thoughts... Information for Patients and Families This pamphlet has been produced by the Cancer Care Program of North York General Hospital www.nygh.on.ca 4001 Leslie Street,
FAMILY AND FRIENDS. are an important part of every woman s journey with ovarian cancer
 FAMILY AND FRIENDS are an important part of every woman s journey with ovarian cancer Going for a walk with me, taking me out of the house, just distracting me from my problems were good and talking about
FAMILY AND FRIENDS are an important part of every woman s journey with ovarian cancer Going for a walk with me, taking me out of the house, just distracting me from my problems were good and talking about
Pain Relief During Labor and Delivery
 Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
Pain Relief During Labor and Delivery Each woman's labor is unique. The amount of pain a woman feels during labor may differ from that felt by another woman. Pain depends on many factors, such as the size
How to Take Care of a Sick Person
 39 How to Take Care of a Sick Person Sickness weakens the body. To gain strength and get well quickly, special care is needed. The care a sick person receives is frequently the most important part of his
39 How to Take Care of a Sick Person Sickness weakens the body. To gain strength and get well quickly, special care is needed. The care a sick person receives is frequently the most important part of his
Intermittent Self-Catheterization. A Guide for Women
 Intermittent Self-Catheterization A Guide for Women 1986 2016 Contributors: Jennifer Skelly, Paula Eyles, Linda Hilts, Jane Worral, Linda Campbell & Janice North Artwork by: Elizabeth McMahon, Noah Fallis,
Intermittent Self-Catheterization A Guide for Women 1986 2016 Contributors: Jennifer Skelly, Paula Eyles, Linda Hilts, Jane Worral, Linda Campbell & Janice North Artwork by: Elizabeth McMahon, Noah Fallis,
Tips on How to Manage Stress and Sleep
 Tips on How to Manage Stress and Sleep Insomnia Everyone has had those times of watching the clock, noting with misery how slowly the night is passing. Insomnia is repeated difficulty in falling asleep,
Tips on How to Manage Stress and Sleep Insomnia Everyone has had those times of watching the clock, noting with misery how slowly the night is passing. Insomnia is repeated difficulty in falling asleep,
Intermittent Self-Catheterization. A Guide for Men and Women
 Intermittent Self-Catheterization A Guide for Men and Women 1986 2013 Contributors: Jennifer Skelly, Paula Eyles, Linda Hilts, Jane Worral, Linda Campbell & Janice North Artwork by: Elizabeth McMahon,
Intermittent Self-Catheterization A Guide for Men and Women 1986 2013 Contributors: Jennifer Skelly, Paula Eyles, Linda Hilts, Jane Worral, Linda Campbell & Janice North Artwork by: Elizabeth McMahon,
ORAL CHEMOTHERAPY EDUCATION
 Name of your medication Generic name letrozole (LEH-truh-zole) Brand name Femara (FEH-muh-ruh) Approved uses Letrozole is used in the treatment of certain types of hormone-dependent breast cancer in postmenopausal
Name of your medication Generic name letrozole (LEH-truh-zole) Brand name Femara (FEH-muh-ruh) Approved uses Letrozole is used in the treatment of certain types of hormone-dependent breast cancer in postmenopausal
