Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive Sleep Apnea Patients
|
|
|
- Byron Hall
- 5 years ago
- Views:
Transcription
1 The Laryngoscope Lippincott Williams & Wilkins, Inc The American Laryngological, Rhinological and Otological Society, Inc. Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive Sleep Apnea Patients Adriane I. Zonato, MD, PhD; Fernanda Louise Martinho, MD; Lia Rita Bittencourt, MD, PhD; Osíris de Oliveira Camponês do Brasil, MD, PhD; Luiz Carlos Gregório, MD, PhD; Sergio Tufik, MD, PhD Presented at the 7th World Congress in Sleep Apnea, Helsink, Finland, June 30 July 3, From the Otorhinolaryngology Discipline (F.L.M., O.D.O.C.D.B., L.C.G.), Universidade Federal de São Paulo, São Paulo, Brazil; and the Sleep Institute, Psychobiology Department (A.I.Z., L.R.B., S.T.), Universidade Federal de São Paulo, São Paulo, Brazil. Editor s Note: This Manuscript was accepted for publication February 18, Send Correspondence to Dr. Adriane I. Zonato, Rodovia Jornalista Manoel de Menezes, 2031 Casa 29, Cep: Florianópolis-SC, Brazil. aizonato@terra.com.br DOI: /01.MLG DC Study Objectives: The purpose of this study was to apply a systematic physical examination, used to evaluate obstructive sleep apnea (OSA) patients, in nonapneic patients. Design: Study was prospective. Setting: Patients were seen in the sleep laboratory and department of otorhinolaryngology. Patients or Participants: Nonapneic patients (n 100) were involved in the study. Interventions: Physical examination to evaluate facial skeleton, pharyngeal soft tissue, rhinoscopy, and body mass index. Data were compared with a previously published study (2003) on a group of OSA patients (n 223). Measurements and Results: Skeletal examination detected retrognathism in 6%, class II occlusion in 12%, and high-arched hard palate in 11%. The modified Mallampati classification showed 54% in class I to II and 46% in class III to IV. Only 1% of nonapneic patients had tonsils of degree III to IV. Oropharynx evaluation showed web palate in 38%, posterior palate in 19%, thick palate in 10%, thick uvula in 10%, long uvula 15%, voluminous lateral wall in 11%, and tongue edge crenations in 28%. Anterior rhinoscopy detected significant septal deviation in 1% and turbinate hypertrophy in 31% of patients. Conclusions: The head and neck physical examination, considering both skeletal and soft tissue alterations, illustrated significant differences between nonapneic and OSA patients. Body mass index, modified Mallampati classification, tonsils hypertrophy, and high-arched hard palate previously related to the presence of sleep apnea in the literature showed different outcomes in nonapneic patients. Nonapneic patients had less alterations in nasal anatomy (severe septal deviation and enlarged turbinate). Skeletal parameters, such as retropositioned mandible and angle class II occlusion, were less frequent in nonapneic patients. Key Words: Sleep apnea, physiopathology, physical examination, anatomical abnormalities, nasal obstruction. Laryngoscope, 115: , 2005 INTRODUCTION Although obstructive sleep apnea (OSA) has been described, a complete understanding of the physiopathology and upper airway (UAW) anatomic participation has yet to be reached. However, the scientific community has reached a consensus on how the occurrence of both anatomic abnormality and neuromuscular disorders can contribute to or facilitate the narrowing and closure of the pharynx during sleep. 1,2 Many authors have shown that relevant physical alterations (craniofacial, dental-bite, pharyngeal soft tissue, UAW size and shape, obesity) can easily be recognized in patients with OSA. 3 8 Despite such anatomic evidence, the relationship between anatomic abnormalities and the presence and severity of sleep apnea is unclear. Some physical aspects have been related to the presence or severity of OSA. These aspects are body mass index (BMI), modified Mallampati classification (MMC) (assesses palatal length and tongue size), tonsils size, low hyoid bone position, and high-arched hard palate. 6 9 None of the usual anatomic alterations seen in the soft palate (posterior placed, thick, or webbed) or in the uvula (thick or long) had any correlation to the presence or severity of sleep apnea. Zonato et al. 8 stated that at least one of the above cited soft-palate or uvula alterations were seen in 34% to 45% of the reviewed patients. Despite this, none of the palatal findings alone highlighted any correlation with the presence of sleep apnea. The authors observed that only pharyngeal abnormalities in combination (the presence of at least 3 of these 5 pharyngeal characteristics: tonsil size grade III or IV, abnormal palate, abnormal uvula, voluminous lateral wall, or web palate) were predictive of both presence and severity of OSA. 1030
2 Fig. 1. Modified Mallampati classification (the relative position of the palate and base of tongue inside the mouth). Class I: all the oropharynx including tonsils, pillars, soft palate, and the tip of uvula can be easily visible. Class II: tonsils upper polo and uvula are visible. Class III: part of the uvula and soft palate are visible. Class IV: just the hard palate and part of soft palate are visible. There is no consensus concerning the observed physical alterations that are important in patients with OSA or those that contribute to the physiopathology of sleep apnea. Only anthropometric measurements (BMI, neck and abdominal circumference) and MMC are seen to be the common denominators among the published studies so far. Furthermore, there are some patients with sleep apnea who do not present the most common physical abnormalities. As far as another group of patients without OSA is concerned, a question arises: would they present these most commonly described anatomic alterations? The objective of the present study was to apply a systematic head and neck physical examination in nonapneic patients to compare them with OSA patients. 8 MATERIALS AND METHODS Study Design We carried out a prospective study involving 100 patients from the Sleep Laboratory of Universidade Federal de São Paulo, during the period of April to September The patients were seen in the nonrespiratory sleep disturbance out-patient unit or on the evening before the polysomnography (PSG) study. Inclusion criteria comprised adult patients evaluated with an overnight standard PSG at the Sleep Institute, with an apneahypopnea index (AHI) of 5 or less events/hour, without habitual snoring. Exclusion criteria were patients with AHI greater than 5 events/hour, patients with AHI 5 or less events/hour with habitual snoring. Snoring was classified as habitual if it was present every night or almost every night. All subjects were questioned about past history of hypertension, cardiovascular diseases, diabetes mellitus, hypothyroidism, nasal obstruction, and rhinitis. PSG was performed for one full night using an SAC Oxford system containing 13 channels including electroencephalogram, electrocardiogram, oculogram, submental and anterior-tibialis electromyogram, nasal canula and oral airflow, thoracic and abdominal movements, body position, and oxygen saturation measured by pulse oximetry. The subjects underwent a specific otolaryngologic examination by the same ear, nose and throat investigator. All the physical characteristics of the nonapneic group (n 100) were compared with an OSA group of patients (n 223) whose results had already been published by our group. 8 Physical evaluation was assessed by a systematic head and neck examination, comprised of the following evaluation. 8 Facial Morphology Presence of mandible retrognathism is investigated. The patient is seated with the head in the Frankfort horizontal position, and a virtual vertical line is dropped from the vermilion border of the lower lip to the chin. If the anterior prominence of the chin (soft tissue pogonion) is greater than 2 mm behind this line, mandibular retro-displacement may be present. 10 Oral Cavity Oral cavity examination starts by looking for dental occlusion Angle Class II (possibility of mandibular retrognathism). By asking the patient to open his mouth with the tongue relaxed inside the mouth, the MMC is graded according to palatal length and tongue size as class I (all the oropharynx including tonsils, pillars, soft palate, and the tip of uvula can be easily visible), class II (tonsils upper polo and the uvula are visible), class III (part of the uvula and soft palate are visible), and class IV (just the hard palate and part of soft palate are visible) 7 (Fig. 1). The skeletal structure of the hard palate is inspected with attention to the presence of high and narrow arched palate (Fig. 2). The tongue inspection looks for the presence of edge crenations (consequence of teeth pressure) as a subjective sign of large tongue. Oropharynx In the oropharynx examination, soft palate is classified as posterior placed, thick (wide aspect of the tissue), and webbed (web palate caused by redundant posterior pillars); the lateral wall as voluminous with wrinkling pillars; and the uvula as thick (wide aspect of the tissue) and long (greater than 1 cm). Tonsils are classified as either degree I, II, III, or IV according to its hypertrophy (I: tonsils inside the tonsillar fossa lateral to posterior pillars; II: tonsils occupy 25% of oropharynx; III: tonsils occupy 50%; IV: tonsils occupy 75% or more, almost meeting in the midline) and as degree 0 (previous tonsillectomy). Nasal Examination Nasal examination by anterior rhinoscopy is used to detect septal deviation and turbinate hypertrophy. Fig. 2. High-arched hard palate. 1031
3 TABLE I. Nonapneic Patients and OSA Patients: Clinical Aspects. Nonapneic Patients (n 100) OSA Patients (n 223) P Value Male:Female (%) 46:54 64: Age BMI Hypertension (%) NS Diabetes mellitus (%) NS Cardiovascular disease (%) NS Hypothyroidism (%) NS Nasal obstruction (%) Rhinitis (%) NS OSA obstructive sleep apnea patients; BMI body mass index. Statistical Analysis Statistical differences between nonapneic and OSA patients were determined by the Mann-Whitney U test or the chi-square test, depending on the type of the variable. For all tests, the level of significance was set for P.05. Our data were analyzed using software Statistica for Windows release 5.1 (Statsoft, Inc., tulsa, OK). RESULTS One hundred patients were included in this analysis with a mean age of (range 18 70) years, with 46 (46%) men and 54 (54%) women and BMI of (range ) kg/m 2 (Table I). On clinical evaluation, hypertension was present in 22 (22%) patients, cardiovascular disease in 9 (9%), diabetes mellitus in 6 (6%), and hypothyroidism in 4 (4%) patients. In addition, nasal obstruction was seen in 42 (42%) patients and symptoms of rhinitis in 39 (39%) patients. All 100 patients were recorded by standard polysomnogram with a mean AHI of (range 0 5) events/hour (Table II). Facial skeletal examination detected retrognathism in six (6%) patients. Evaluation of dental occlusion showed that class II was observed in only 12 (12%) patients. Some patients (n 38) were totally or partially edentate, preventing a real evaluation of the occlusion. The MMC showed 20 patients (20%) in class I, 34 (34%) in class II, 31 (31%) in class III, and 15 (15%) in class IV. Classes III and IV of MMC, considered a sign of difficult tracheal intubation and small mouth, was observed in 46 (46%) patients. High-arched hard palate was observed in 11 (11%) patients and tongue edge crenations by teeth in 28 (28%). The oropharynx evaluation showed web palate in 38 patients (38%), posterior placed palate in 19 (19%), thick soft palate in 10 (10%), thick uvula in 10 (10%), long uvula 15 (15%), and voluminous lateral wall with wrinkling pillars in 11 (11%). The score of tonsils size was grade 0 24 (24%); grade I 53 (53%); grade II 22 (22%); and grade III 1 (1%), with no patient in grade IV. Taking patients with a low degree of tonsil hypertrophy (grades I and II) along with those who had previous tonsillectomy, we saw that they comprised almost the entire group (99%). Physical examination by anterior rhinoscopy detected some degree of septal deviation in 49 (49%) patients (degree I 22%; degree II 26%; degree III 1%) and turbinate hypertrophy in 31 (31%) patients. All the investigated physical variables were compared with the OSA group, and the findings with statistical significance are listed in Table III. DISCUSSION According to the literature, the anatomic abnormalities that have a correlation with sleep apnea are anthropometric measures (BMI, abdominal and neck circumference), MMC, high-arched hard palate, pharyngeal anatomic abnormalities in combination (presence of at least 3 abnormalities such as hypertrophied tonsils, abnormal palate, abnormal uvula, voluminous lateral wall, or web palate), low hyoid bone position (in this case, using complementary examination by cephalometric analysis), posterior wall redundancy, and endoscopy retropalatal size (analyzed by videotape endoscopy and lateral cephalometric radiograph). 4,6 9,11 13 In a previous paper, we observed that many of the anatomic parameters were frequently seen in OSA patients (retropositioned mandible was detected in 19.7%, class II occlusion in 26.3%, tongue edge crenation in 36.3%, web palate in 45.3%, posterior placed palate in 43%, thick palate in 35%, long uvula in 34.1%, thick uvula in 34.5%), but the statistical analyses failed to highlight any correlation between these parameters and AHI. According to MEDLINE data, we found only two studies that compared nonapneic individuals with OSA patients. Viner et al. 14 used a combination of history and physical examination as a screening for sleep apnea in 410 patients referred for suspected sleep apnea syndrome. All patients underwent clinical and physical examination with a subsequent PSG study, and the group was divided into patients with (AHI 10) and without sleep apnea. The UAW anatomic evaluation was limited; the only investigated parameter was the examination of the pharynx, which was considered as normal or abnormal if it appeared narrow and small; if the uvula were bulky, long, or rested on the base of tongue during phonation; or if the TABLE II. Nonapneic Patients and OSA Patients: Polysomnography Data. Sleep Efficiency AHI Sleep Stage 1 Sleep Stage 2 Sleep Stage 3/4 REM Sleep Lowest Oxygen Saturation Nonapneic patients 74.8% % 56.7% 19.6% 15.6% 89% OSA patients 79.4% % 58% 15.6% 15.9% 78% P value NS NS.003 NS.001 OSA obstructive sleep apnea patients; AHI apnea-hypopnea index; REM rapid eye movement. 1032
4 TABLE III. Comparison of Physical Examination Variables between Nonapneic Patients and OSA Patients. Nonapneic Patients (%) (n 100) OSA Patients (%) (n 223) P Value High-arched hard palate Retropositioned mandible Class II occlusion Total or partial edentate NS Tongue edge crenation NS Web palate NS Posterior palate Thick palate Long uvula Thick uvula Voluminous lateral wall MMC classes I and II MMC classes III and IV Previous tonsillectomy NS Tonsils degree I and II Tonsils degree III and IV Septal deviation degree I NS Septal deviation degree II NS Septal deviation degree III Turbinate hypertrophy OSA obstructive sleep apnea patients; MMC modified Malampatti classification. tonsils were big enough to fit the pharyngeal orifice. The authors observed a statistical difference between patients with and without sleep apnea: 78 of 218 patients without sleep apnea also presented an abnormal pharynx during examination, in contrast with 97 of 190 patients with sleep apnea. With sleep apnea clinical variables and pharyngeal examination to detect and differentiate patients with and without sleep apnea, the subjective impression had a sensitivity of 52% and a specificity of 70%. Deegan and McNicholas 15 carried out a study with 250 patients suspected of having sleep disordered breathing to evaluate the predictive value of clinical features to OSA. The clinical features were investigated by questionnaire, anthropometric measures (BMI, neck and abdominal circumference), and UAW examination. Only the pharynx described with redundant tissue or small, septal deviation and glossomegaly were assessed. For these three facial parameters, there was no statistical difference between the patients with and without OSA, but there was a correlation between the anthropometric measurements and the AHI. The authors considered as a non-osa group all patients with an AHI less than 15 events/hour. According to current classification, this would also comprise the mild apnea patients. This situation is also observed in Viner et al. s study, which considered patients without sleep apnea as those where AHI was 10 or greater. Neither of these previous studies had used a complete physical examination procedure for facial and UAW findings. In the present study, the majority of selected patients came from an insomnia clinic. Because of this fact, there was no prevalence of male over female patients and patients were not as obese as OSA patients commonly are. Our clinical investigation identified nasal obstruction as a clinical complaint that was more prevalent in OSA patients. In addition, we observed that the OSA group had more turbinate hypertrophy and septal deviation (only for deviation degree III, which represents the highest degree of deviation) than the nonapneic group. All the craniofacial characteristics (retropositioned mandible, class II occlusion, and high-arched hard palate) were less frequent in the nonapneic group. Despite this, our previous paper failed to observe any correlation between these skeletal parameters and AHI. The previous and actual papers data point to the fact that craniofacial evaluation appears to be relevant by presenting different expressions in OSA patients compared with nonapneic patients. We speculate that these deformities should not be ignored. The evaluation should be more precise, using objective parameters such as cephalometric measurements. All the soft tissue in the oropharynx, with the exception of web palate and tongue edge crenation, was found to be more predominant in the OSA group, with a very significant statistical value. The tongue edge crenation parameter, as an indirect sign of excessive tongue volume, was observed in both groups without any difference. This parameter is perhaps not the most adequate one to determine, subjectively, the tongue volume. The reference to the web palate was not a sound parameter. In fact, the web palate could be graduated whether the web mucosa was small or really large, with the mucosa insertion very close to the tip of uvula. Subsequently, we set out to quantify the web palate (small, moderate, and large web 1033
5 palate), in a new study, according to the point of mucosa insertion close to the base, middle, or the tip of uvula, and then repeated the examination in nonapneic and OSA patients. The anatomic parameters of tonsils size and oropharynx size were very interesting. The majority of nonapneic patients have tonsils of degrees I and II (75% of all group), only one patient had tonsil degree III, and none presented with severe hypertrophy. In our previous paper, we observed that just a few OSA patients had real hypertrophied tonsils (degree III or IV), in essence, less than 15% of them. In consideration of patients with previous tonsillectomy, nonapneic and OSA patients were similar. The III and IV scores MMC were present in most OSA patients (78.8%), indicating that most OSA patients may have a small oropharynx and a difficult endotracheal intubation. For our nonapenic patients, MMC class III or IV were observed in 46% of the group. This situation concurred with the data of our previous study and with Friedman et al. s 7 study where there was a correlation between the presence and severity of sleep apnea with MMC, and that this anatomic characteristic may be relevant in OSA patients. 8 For each of all other soft-tissue parameters, posterior or thick palate, long or thick uvula and voluminous lateral wall, the groups were different. Given the patient population of the present study, where the majority was referred to us by an insomnia clinic, the apneic and nonapneic groups were not well matched for sex, age, and obesity. Despite the imposed limitations of this present study, the results illustrated a real contrast in the common anatomic findings between apneic and nonapneic groups. CONCLUSION A systematic head and neck physical examination, which considered both skeletal and soft tissue alterations, illustrated significant differences between nonapneic and OSA groups. BMI, MMC, tonsil hypertrophy, and higharched hard palate arguably have different expressions in nonapneic patients. All skeletal alterations (high-arched hard palate, retroposition mandible, and class II occlusion) are less frequent in the nonapneic group. Nonapneic patients scarcely present enlarged tonsils (degree III and IV encompassed a mere 1% of patients), have fewer alterations in palate and uvula, and less nasal alterations (severe septal deviation and enlarged inferior turbinate). Significant anatomic differences were observed in the present study between apneic and nonapneic groups, but studies involving control matching clinical investigation are still needed for additional insights. The significance of anatomic findings in this field of study warrants further research and clinical investigation. BIBLIOGRAPHY 1. Isono S, Remmers JE. Anatomy and physiology of upper airway obstruction. In: Krygger MH, Roth T, Dement WC, eds. Principles and Practice of Sleep Medicine, 2nd ed. Philadelphia: W.B. Saunders, 1994: Sher AE. Obstructive sleep apnea syndrome: a complex disorder of the upper air way. Otolaryngol Clin North Am 1990;23: Woodson BT. Examination of the upper airway. Oral Maxillofac Surg Clin North Am 1995;7: Deegan PC, McNicholas WT. Predictive value of clinical features for the obstructive sleep apnoea syndrome. Eur Respir J 1996;9: Woodson BT. Predicting which patients will benefit from surgery for obstructive sleep apnea: the ENT exam. ENT J 1999;78: Woodson BT, Naganuma H. Comparison of methods of airway evaluation in obstructive sleep apnea syndrome. Otolaryngol Head Neck Surg 1999;120: Friedman M. Tanyeri H, La Rosa M, et al. Clinical predictors of obstructive sleep apnea. Laryngoscope 1999;109: Zonato AI, Bittencourt LRA, Martinho FL, et al. Association of systematic head and neck physical examination with severity of obstructive sleep apnea-hypopnea syndrome. Laryngoscope 2003;113: Petri N, Suadicani P, Wildschiodtz G, Bjorn-Jorgensen J. Predictive value of Müller maneuver, cephalometric and clinical features of the outcome of uvulopalatopharyngoplasty. Evaluation of predictive factors using discriminate analysis in 30 sleep apnea patients. Acta Otolaryngol (Stockh) 1994;114: Ridley MB. Aesthetic facial proportions. In: Papel ID, Nachlis NE, eds. Facial Plastic and Reconstructive Surgery. St. Louis: Mosby-Yearbook, 1992: Teculescu DB, Montaut-Verient B, Hannhart B, et al. Breathing pauses during sleep: can a non-invasive ENT examination help identify subjects at risk in epidemiological settings? Med Hypoth 2001;56: Roumbaux Ph, Bertrand B, Boudewyns A, et al. Standard ENT clinical evaluation of sleep-disordered breathing patient; a consensus report. Acta Otorhinolaryngol Belg 2002; 56: Tsai WH, Remmers JE, Brant R, et al. A decision rule for diagnostic testing in obstructive sleep apnea. Am J Crit Care Med 2003;167: Viner S, Szalai JP, Hoffstein V. Are history and physical examination a good screening test for sleep apnea? Ann Intern Med 1991;115: Deegan PC, McNicholas WT. Predictive value of clinical features for the obstructive sleep apnoea syndrome. Eur Respir J 1996;9:
Systematic head and neck physical examination as a predictor of obstructive sleep apnea in class III obese patients
 Brazilian ENT examination Journal of as Medical a predictor and Biological of OSAS in Research obese patients (2008) 41: 1093-1097 ISSN 0100-879X 1093 Systematic head and neck physical examination as a
Brazilian ENT examination Journal of as Medical a predictor and Biological of OSAS in Research obese patients (2008) 41: 1093-1097 ISSN 0100-879X 1093 Systematic head and neck physical examination as a
Obese obstructive sleep apnea patients with tonsil hypertrophy submitted to tonsillectomy
 Brazilian Journal of Medical and Biological Research (2006) 39: 1137-1142 Obese OSAHS patients submitted to tonsillectomy ISSN 0100-879X 1137 Obese obstructive sleep apnea patients with tonsil hypertrophy
Brazilian Journal of Medical and Biological Research (2006) 39: 1137-1142 Obese OSAHS patients submitted to tonsillectomy ISSN 0100-879X 1137 Obese obstructive sleep apnea patients with tonsil hypertrophy
Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
 Sleep Disorders Volume 2015, Article ID 749068, 4 pages http://dx.doi.org/10.1155/2015/749068 Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
Sleep Disorders Volume 2015, Article ID 749068, 4 pages http://dx.doi.org/10.1155/2015/749068 Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
New Insights on the Pathophysiology of Inspiratory Flow Limitation During Sleep
 Lung (2015) 193:387 392 DOI 10.1007/s00408-015-9714-x SLEEP APNEA New Insights on the Pathophysiology of Inspiratory Flow Limitation During Sleep Luciana B. M. de Godoy 1 Luciana O. Palombini 1 Fernanda
Lung (2015) 193:387 392 DOI 10.1007/s00408-015-9714-x SLEEP APNEA New Insights on the Pathophysiology of Inspiratory Flow Limitation During Sleep Luciana B. M. de Godoy 1 Luciana O. Palombini 1 Fernanda
Updated Friedman Staging System for Obstructive Sleep Apnea
 Updated Friedman Staging System for Obstructive Sleep Apnea Michael Friedman a, b Anna M. Salapatas b Lauren B. Bonzelaar c a Section of Sleep Surgery, Rush University Medical Center, and b Section of
Updated Friedman Staging System for Obstructive Sleep Apnea Michael Friedman a, b Anna M. Salapatas b Lauren B. Bonzelaar c a Section of Sleep Surgery, Rush University Medical Center, and b Section of
Alexandria Workshop on
 Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
New Perspectives on the Pathogenesis of OSA - Anatomic Perspective. New Perspectives on the Pathogenesis of OSA: Anatomic Perspective - Disclosures
 New Perspectives on the Pathogenesis of OSA - Anatomic Perspective Richard J. Schwab, M.D. Professor of Medicine Interim Chief, Division of Sleep Medicine Medical Director, Penn Sleep Centers University
New Perspectives on the Pathogenesis of OSA - Anatomic Perspective Richard J. Schwab, M.D. Professor of Medicine Interim Chief, Division of Sleep Medicine Medical Director, Penn Sleep Centers University
11/19/2012 ก! " Varies 5-86% in men 2-57% in women. Thailand 26.4% (Neruntarut et al, Sleep Breath (2011) 15: )
 Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
 SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
Association of Palatine Tonsil Size and Obstructive Sleep Apnea in Adults
 The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. Association of Palatine Tonsil Size and Obstructive Sleep Apnea in Adults Sebastian M. Jara, MD ; Edward
The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. Association of Palatine Tonsil Size and Obstructive Sleep Apnea in Adults Sebastian M. Jara, MD ; Edward
Persistent Obstructive Sleep Apnea After Tonsillectomy. Learning Objectives. Mary Frances Musso, DO Pediatric Otolaryngology
 Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty: A Single University Experience
 771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2
 Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2 CAUSES OF SNORING AND SLEEP APNEA We inhale air through our nose and mouth. From the nostrils, air flows
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2 CAUSES OF SNORING AND SLEEP APNEA We inhale air through our nose and mouth. From the nostrils, air flows
Pediatric Obstructive Sleep apnea An update What else is there to know?
 Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA
 SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
Clinical Predictors of Effective Continuous Positive Airway Pressure in Patients With Obstructive Sleep Apnea/Hypopnea Syndrome
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Clinical Predictors of Effective Continuous Positive Airway Pressure in Patients With Obstructive Sleep Apnea/Hypopnea
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Clinical Predictors of Effective Continuous Positive Airway Pressure in Patients With Obstructive Sleep Apnea/Hypopnea
Brian Palmer, D.D.S, Kansas City, Missouri, USA. April, 2001
 Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome
 ORIGINAL ARTICLE pissn 2093-9175 / eissn 2233-8853 http://dx.doi.org/10.17241/smr.2015.6.2.54 Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome Seung Hoon Lee, MD, PhD, In Sik Song, MD, Jae Woo
ORIGINAL ARTICLE pissn 2093-9175 / eissn 2233-8853 http://dx.doi.org/10.17241/smr.2015.6.2.54 Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome Seung Hoon Lee, MD, PhD, In Sik Song, MD, Jae Woo
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015
 Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
Obstructive Sleep Apnea Syndrome
 SMGr up Obstructive Sleep Apnea Syndrome Alper Dilci, Handan Koyuncu and Vural Fidan* Otorhinolaryngology Department, Yunus Emre Government Hospital, Turkey *Corresponding author: Vural Fidan, Otorhinolaryngology
SMGr up Obstructive Sleep Apnea Syndrome Alper Dilci, Handan Koyuncu and Vural Fidan* Otorhinolaryngology Department, Yunus Emre Government Hospital, Turkey *Corresponding author: Vural Fidan, Otorhinolaryngology
Sleep Disorders and the Metabolic Syndrome
 Sleep Disorders and the Metabolic Syndrome Tom V. Cloward, M.D. Intermountain Sleep Disorders Center LDS Hospital Objectives Describe how sleep disorders impact your daily medical practice Don Don t do
Sleep Disorders and the Metabolic Syndrome Tom V. Cloward, M.D. Intermountain Sleep Disorders Center LDS Hospital Objectives Describe how sleep disorders impact your daily medical practice Don Don t do
Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea
 European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
Snoring. Forty-five percent of normal adults snore at least occasionally and 25
 Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options
 Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
Obstructive Sleep Apnea- Hypopnea Syndrome and Snoring: Surgical Options Joshua L. Kessler, MD, FACS Boston ENT Associates Clinical Instructor, Otology and Laryngology Harvard Medical School Why Consider
Snoring: What Works?
 Snoring: What Works? Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Snoring: What Works? Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 6
 Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 6 MINIMALLY INVASIVE TREATMENTS OF SNORING AND SLEEP APNEA OVERVIEW The past decade has seen the rise of effective,
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 6 MINIMALLY INVASIVE TREATMENTS OF SNORING AND SLEEP APNEA OVERVIEW The past decade has seen the rise of effective,
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Influence of upper airways section area on oxygen blood saturation level in patients with obesity and sleep apnea syndrome
 Influence of upper airways section area on oxygen blood saturation level in patients with obesity and sleep apnea syndrome Poster No.: P-0028 Congress: ESCR 2015 Type: Scientific Poster Authors: E. Butorova,
Influence of upper airways section area on oxygen blood saturation level in patients with obesity and sleep apnea syndrome Poster No.: P-0028 Congress: ESCR 2015 Type: Scientific Poster Authors: E. Butorova,
Contemporary Snoring Management
 Contemporary Snoring Management Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Contemporary Snoring Management Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu Sleepsurgery.ucsf.edu
Brazilian Journal of OTORHINOLARYNGOLOGY. Obstructive sleep apnea and primary snoring: diagnosis. Objective.
 Braz J Otorhinolaryngol. 2014;80(1 Supl. 1):S1-S16 Brazilian Journal of OTORHINOLARYNGOLOGY www.bjorl.org.br GUIDELINE Obstructive sleep apnea and primary snoring: diagnosis Authors Associação Brasileira
Braz J Otorhinolaryngol. 2014;80(1 Supl. 1):S1-S16 Brazilian Journal of OTORHINOLARYNGOLOGY www.bjorl.org.br GUIDELINE Obstructive sleep apnea and primary snoring: diagnosis Authors Associação Brasileira
Lateral Pharyngoplasty Reduces Nocturnal Blood Pressure in Patients With Obstructive Sleep Apnea
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Lateral Pharyngoplasty Reduces Nocturnal Blood Pressure in Patients With Obstructive Sleep Apnea Carolina
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Lateral Pharyngoplasty Reduces Nocturnal Blood Pressure in Patients With Obstructive Sleep Apnea Carolina
Transsubmental tongue-base suspension in treating patients with severe obstructive sleep apnoea after failed uvulopalatopharyngoplasty:
 CORRESPONDENCE: OUR EXPERIENCE Transsubmental tongue-base suspension in treating patients with severe obstructive sleep apnoea after failed uvulopalatopharyngoplasty: Our Experience Huang, T.-W.,* Su,
CORRESPONDENCE: OUR EXPERIENCE Transsubmental tongue-base suspension in treating patients with severe obstructive sleep apnoea after failed uvulopalatopharyngoplasty: Our Experience Huang, T.-W.,* Su,
Snoring, obstructive sleep apnea (OSA), and upper. impact of basic research on tomorrow. Snoring Imaging* Could Bernoulli Explain It All?
 impact of basic research on tomorrow Snoring Imaging* Could Bernoulli Explain It All? Igor Fajdiga, MD, PhD Study objectives: To identify upper airway changes in snoring using CT scanning, to clarify the
impact of basic research on tomorrow Snoring Imaging* Could Bernoulli Explain It All? Igor Fajdiga, MD, PhD Study objectives: To identify upper airway changes in snoring using CT scanning, to clarify the
Disclosures. Learning Objectives. Obstructive sleep apnea and snoring 3/19/2014. None
 Obstructive sleep apnea and snoring Ashutosh Kacker, MD, FACS Professor of Clinical Otolaryngology Department of Otorhinolaryngology Weill Medical College of Cornell University New York Presbyterian Hospital
Obstructive sleep apnea and snoring Ashutosh Kacker, MD, FACS Professor of Clinical Otolaryngology Department of Otorhinolaryngology Weill Medical College of Cornell University New York Presbyterian Hospital
in China Shanghai Office Beijing Office (+86) (+86)
 SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea
 Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Sleep Diordered Breathing (Part 1)
 Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Upper Airway Obstruction
 Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
SLEEP DISORDERED BREATHING The Clinical Conditions
 SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
IEHP considers the treatment of obstructive sleep apnea (OSA) medically necessary according to the criteria outlined below:
 : Positive Airway Pressure, Oral Appliances, and Surgical Interventions Policy: Obstructive sleep apnea (OSA) is characterized by an interruption of breathing during sleep most commonly due to extra or
: Positive Airway Pressure, Oral Appliances, and Surgical Interventions Policy: Obstructive sleep apnea (OSA) is characterized by an interruption of breathing during sleep most commonly due to extra or
Obstructive sleep apnea (OSA)
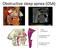 Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
Precision Sleep Medicine
 Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Precision Sleep Medicine Picking Winners Improves Outcomes and Avoids Side-Effects North American Dental Sleep Medicine Conference February 17-18, 2017 Clearwater Beach, FL John E. Remmers, MD Conflict
Sleep Apnea. Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa
 Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
Sleep Apnea Herbert A Berger, MD Pulmonary Division Department of Internal Medicine University of Iowa Disclosures No Relevant Financial Interests to Report Objectives Learn the history and physical examination
The most accurate predictors of arterial hypertension in patients with Obstructive Sleep Apnea Syndrome
 The most accurate predictors of arterial hypertension in patients with Obstructive Sleep Apnea Syndrome Natsios Georgios University Hospital of Larissa, Greece Definitions Obstructive Sleep Apnea (OSA)
The most accurate predictors of arterial hypertension in patients with Obstructive Sleep Apnea Syndrome Natsios Georgios University Hospital of Larissa, Greece Definitions Obstructive Sleep Apnea (OSA)
Treating OSA? Don't Forget the Tongue
 From: ENT Today, January 2008 Treating OSA? Don't Forget the Tongue by Pippa Wysong Although otolaryngologic surgeons commonly focus on the palate when treating patients with obstructive sleep apnea (OSA),
From: ENT Today, January 2008 Treating OSA? Don't Forget the Tongue by Pippa Wysong Although otolaryngologic surgeons commonly focus on the palate when treating patients with obstructive sleep apnea (OSA),
Overnight fluid shifts in subjects with and without obstructive sleep apnea
 Original Article Overnight fluid shifts in subjects with and without obstructive sleep apnea Ning Ding 1 *, Wei Lin 2 *, Xi-Long Zhang 1, Wen-Xiao Ding 1, Bing Gu 3, Bu-Qing Ni 4, Wei Zhang 4, Shi-Jiang
Original Article Overnight fluid shifts in subjects with and without obstructive sleep apnea Ning Ding 1 *, Wei Lin 2 *, Xi-Long Zhang 1, Wen-Xiao Ding 1, Bing Gu 3, Bu-Qing Ni 4, Wei Zhang 4, Shi-Jiang
Diagnostic Accuracy of the Multivariable Apnea Prediction (MAP) Index as a Screening Tool for Obstructive Sleep Apnea
 Original Article Diagnostic Accuracy of the Multivariable Apnea Prediction (MAP) Index as a Screening Tool for Obstructive Sleep Apnea Ahmad Khajeh-Mehrizi 1,2 and Omid Aminian 1 1. Occupational Sleep
Original Article Diagnostic Accuracy of the Multivariable Apnea Prediction (MAP) Index as a Screening Tool for Obstructive Sleep Apnea Ahmad Khajeh-Mehrizi 1,2 and Omid Aminian 1 1. Occupational Sleep
PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA)
 PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA) DEFINITION OSA Inspiratory airflow is either partly (hypopnea) or completely (apnea) occluded during sleep. The combination of sleep-disordered breathing with daytime
PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA) DEFINITION OSA Inspiratory airflow is either partly (hypopnea) or completely (apnea) occluded during sleep. The combination of sleep-disordered breathing with daytime
The Ear, Nose and Throat in MPS
 The Ear, Nose and Throat in MPS Annerose Keilmann Voice Care Center Bad Rappenau, Germany Preciptorship program on MPS Wiesbaden, November 2 nd 2015 Alterations of the outer and middle ear in MPS I narrowing
The Ear, Nose and Throat in MPS Annerose Keilmann Voice Care Center Bad Rappenau, Germany Preciptorship program on MPS Wiesbaden, November 2 nd 2015 Alterations of the outer and middle ear in MPS I narrowing
Sleep endoscopy with artificial induction of sleep and somnography in 385 snorers
 Sleep endoscopy with artificial induction of sleep and somnography in 385 snorers N.S. HESSEL, D.M. LAMAN, V.C.P.J. VAN AMMERS, N. DE VRIES, H. VAN DUIJN SINT LUCAS ANDREAS ZIEKENHUIS, LOCATIE SINT LUCAS,
Sleep endoscopy with artificial induction of sleep and somnography in 385 snorers N.S. HESSEL, D.M. LAMAN, V.C.P.J. VAN AMMERS, N. DE VRIES, H. VAN DUIJN SINT LUCAS ANDREAS ZIEKENHUIS, LOCATIE SINT LUCAS,
Outcomes of Upper Airway Surgery in Obstructive Sleep Apnea
 Original Research Outcomes of Upper Airway Surgery in Obstructive Sleep Apnea Hadiseh Hosseiny 1, Nafiseh Naeimabadi 1, Arezu Najafi 1 *, Reihaneh Heidari 1, Khosro Sadeghniiat-Haghighi 1 1. Occupational
Original Research Outcomes of Upper Airway Surgery in Obstructive Sleep Apnea Hadiseh Hosseiny 1, Nafiseh Naeimabadi 1, Arezu Najafi 1 *, Reihaneh Heidari 1, Khosro Sadeghniiat-Haghighi 1 1. Occupational
The morphometric model is a useful screening test to
 Rev Bras Otorrinolaringol 2006;72(4):541-8. ORIGINAL ARTICLE Application of the Kushida morphometric model in patients with sleep-disordered breathing Maria Claudia Mattos Soares 1, Lia Rita de Azeredo
Rev Bras Otorrinolaringol 2006;72(4):541-8. ORIGINAL ARTICLE Application of the Kushida morphometric model in patients with sleep-disordered breathing Maria Claudia Mattos Soares 1, Lia Rita de Azeredo
Prevalence of Snoring and High Risk of Obstructive Sleep Apnea Syndrome in Young Male Soldiers in Korea
 ORIGINAL ARTICLE Otorhinolaryngology http://dx.doi.org/10.3346/jkms.2013.28.9.1373 J Korean Med Sci 2013; 28: 1373-1377 Prevalence of Snoring and High Risk of Obstructive Sleep Apnea Syndrome in Young
ORIGINAL ARTICLE Otorhinolaryngology http://dx.doi.org/10.3346/jkms.2013.28.9.1373 J Korean Med Sci 2013; 28: 1373-1377 Prevalence of Snoring and High Risk of Obstructive Sleep Apnea Syndrome in Young
BTS sleep Course. Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith)
 BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
Does the dimple point represent the margin of soft palate musculature?
 Asian Biomedicine Vol. 2 No. 5 October 2008;397-401 Brief Communication Does the dimple point represent the margin of soft palate musculature? Department of Otolaryngology, Faculty of Medicine, Chulalongkorn
Asian Biomedicine Vol. 2 No. 5 October 2008;397-401 Brief Communication Does the dimple point represent the margin of soft palate musculature? Department of Otolaryngology, Faculty of Medicine, Chulalongkorn
SKUP 3 : 6 and 24 Months Follow-up of Changes in Respiration and Sleepiness After Modified UPPP
 The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. SKUP 3 : 6 and 24 Months Follow-up of Changes in Respiration and Sleepiness After Modified UPPP Nanna Browaldh,
The Laryngoscope VC 2017 The American Laryngological, Rhinological and Otological Society, Inc. SKUP 3 : 6 and 24 Months Follow-up of Changes in Respiration and Sleepiness After Modified UPPP Nanna Browaldh,
The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery
 432 Original Research THIEME The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery Francesco Lorusso 1 Francesco Dispenza 1 Domenico Michele Modica
432 Original Research THIEME The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery Francesco Lorusso 1 Francesco Dispenza 1 Domenico Michele Modica
Overview. Goal of Evaluation. DISE: Identifying the Sites of Obstruction in OSA. Characterize disorder to guide effective treatment.
 DISE: Identifying the Sites of Obstruction in OSA Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu
DISE: Identifying the Sites of Obstruction in OSA Eric J. Kezirian, MD, MPH Director, Division of Sleep Surgery Otolaryngology Head and Neck Surgery University of California, San Francisco ekezirian@ohns.ucsf.edu
Pang-Rotenberg Sign Snoring Surgery Prognosticator: A Prospective Clinical Trial of 153 Patients
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Pang-Rotenberg Sign Snoring Surgery Prognosticator: A Prospective Clinical Trial of 153 Patients Kenny P.
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. Pang-Rotenberg Sign Snoring Surgery Prognosticator: A Prospective Clinical Trial of 153 Patients Kenny P.
Questions: What tests are available to diagnose sleep disordered breathing? How do you calculate overall AHI vs obstructive AHI?
 Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012
 Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
Dr Alireza Yarahmadi and Dr Arvind Perathur Mercy Medical Center - Winter Retreat Des Moines February 2012 Why screen of OSA prior to surgery? What factors increase the risk? When due to anticipate problems?
Snoring And Sleep Apnea in the U.S. Definitions Apnea: Cessation of ventilation for > 10 seconds. Defining Severity of OSA
 Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
Treatment of Snoring. Useful Telephone Numbers. Information for Patients on. North Hampshire ENT Partnership Hampshire Clinic
 Useful Telephone Numbers North Hampshire ENT Partnership Hampshire Clinic - 01256 377733 The Hampshire Clinic Switchboard - 01256 357111 Lyde Ward - 01256 377773 Enbourne Ward - 01256 377772 Frimley Park
Useful Telephone Numbers North Hampshire ENT Partnership Hampshire Clinic - 01256 377733 The Hampshire Clinic Switchboard - 01256 357111 Lyde Ward - 01256 377773 Enbourne Ward - 01256 377772 Frimley Park
Learning Objectives. And it s getting worse. The Big Picture. Dr. Roger Roubal
 Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
Learning Objectives How to screen for sleep apnea; questions to ask your patients Industry treatment guidelines; when to consider an oral appliance vs. a CPAP What goals/thresholds to set for successful
NASAL OBSTRUCTION. Andy Whyte PERTH RADIOLOGICAL CLINIC UNIVERSITY OF MELBOURNE UNIVERSITY OF WA
 NASAL OBSTRUCTION Andy Whyte PERTH RADIOLOGICAL CLINIC UNIVERSITY OF MELBOURNE UNIVERSITY OF WA INTRODUCTION sinonasal imaging focuses on structural abnormalities of the POSTERIOR (BONY 3/4 ) of the nose
NASAL OBSTRUCTION Andy Whyte PERTH RADIOLOGICAL CLINIC UNIVERSITY OF MELBOURNE UNIVERSITY OF WA INTRODUCTION sinonasal imaging focuses on structural abnormalities of the POSTERIOR (BONY 3/4 ) of the nose
Ped e iat a r t i r c c S lee e p e A p A nea e a Surg r er e y
 Airway Imaging in Pediatric OSA Kasey Li, MD, DDS, FACS Stanford University Sleep Medicine Program The airway is smaller in children with OSA compared to controls The adenoid and tonsils are larger and
Airway Imaging in Pediatric OSA Kasey Li, MD, DDS, FACS Stanford University Sleep Medicine Program The airway is smaller in children with OSA compared to controls The adenoid and tonsils are larger and
Modified Uvulopalatopharyngoplasty: The Extended Uvulopalatal Flap
 Modified Uvulopalatopharyngoplasty: The Extended Uvulopalatal Flap Hseuh-Yu Li, MD,* Kasey K. Li, MD, DDS, Ning-Hung Chen, MD, and Pa-Chun Wang, MD Objective: To investigate the surgical outcomes of a
Modified Uvulopalatopharyngoplasty: The Extended Uvulopalatal Flap Hseuh-Yu Li, MD,* Kasey K. Li, MD, DDS, Ning-Hung Chen, MD, and Pa-Chun Wang, MD Objective: To investigate the surgical outcomes of a
Management of OSA. saurabh maji
 Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
An American Sleep Disorders Association Review
 Sleep, 19(2): 156--177 1996 American Sleep Disorders Association and Sleep Research Society An American Sleep Disorders Association Review The Efficacy of Surgical Modifications of the Upper Airway in
Sleep, 19(2): 156--177 1996 American Sleep Disorders Association and Sleep Research Society An American Sleep Disorders Association Review The Efficacy of Surgical Modifications of the Upper Airway in
NIH Public Access Author Manuscript Otolaryngol Head Neck Surg. Author manuscript; available in PMC 2010 May 1.
 NIH Public Access Author Manuscript Published in final edited form as: Otolaryngol Head Neck Surg. 2009 May ; 140(5): 646 651. doi:10.1016/j.otohns.2009.01.012. Test-retest reliability of drug-induced
NIH Public Access Author Manuscript Published in final edited form as: Otolaryngol Head Neck Surg. 2009 May ; 140(5): 646 651. doi:10.1016/j.otohns.2009.01.012. Test-retest reliability of drug-induced
Obstructive Sleep Apnea and COPD overlap syndrome. Financial Disclosures. Outline 11/1/2016
 Obstructive Sleep Apnea and COPD overlap syndrome Chitra Lal, MD, FCCP, FAASM Associate Professor of Medicine, Pulmonary, Critical Care, and Sleep, Medical University of South Carolina Financial Disclosures
Obstructive Sleep Apnea and COPD overlap syndrome Chitra Lal, MD, FCCP, FAASM Associate Professor of Medicine, Pulmonary, Critical Care, and Sleep, Medical University of South Carolina Financial Disclosures
Roles of Surgery in OSA MASM Annual Fall Conference 2017 October 14, 2017 Kathleen Yaremchuk, MD, MSA Chair, Department of Otolaryngology/Head and
 Roles of Surgery in OSA MASM Annual Fall Conference 2017 October 14, 2017 Kathleen Yaremchuk, MD, MSA Chair, Department of Otolaryngology/Head and Neck Surgery Senior Staff Sleep Medicine Henry Ford Hospital
Roles of Surgery in OSA MASM Annual Fall Conference 2017 October 14, 2017 Kathleen Yaremchuk, MD, MSA Chair, Department of Otolaryngology/Head and Neck Surgery Senior Staff Sleep Medicine Henry Ford Hospital
Inspiratory flow-volume curve in snoring patients with and without obstructive sleep apnea
 Brazilian Journal of Medical and Biological Research (1999) 32: 407-411 Flow-volume curve and obstructive sleep apnea ISSN 0100-879X 407 Inspiratory flow-volume curve in snoring patients with and without
Brazilian Journal of Medical and Biological Research (1999) 32: 407-411 Flow-volume curve and obstructive sleep apnea ISSN 0100-879X 407 Inspiratory flow-volume curve in snoring patients with and without
Morphological variations of soft palate and influence of age on it: A digital cephalometric study
 Original Research Article Morphological variations of soft palate and influence of age on it: A digital cephalometric study C. Vani 1*, T. Vinila Lakshmi 2, V. Dheeraj Roy 3 1 Professor, 2 Post graduate
Original Research Article Morphological variations of soft palate and influence of age on it: A digital cephalometric study C. Vani 1*, T. Vinila Lakshmi 2, V. Dheeraj Roy 3 1 Professor, 2 Post graduate
ORIGINAL ARTICLE. First-Choice Treatment in Mild to Moderate Obstructive Sleep Apnea
 ORIGINAL ARTICLE First-Choice Treatment in Mild to Moderate Obstructive Sleep Apnea Single-Stage, Multilevel, Temperature-Controlled Radiofrequency Tissue Volume Reduction or Nasal Continuous Positive
ORIGINAL ARTICLE First-Choice Treatment in Mild to Moderate Obstructive Sleep Apnea Single-Stage, Multilevel, Temperature-Controlled Radiofrequency Tissue Volume Reduction or Nasal Continuous Positive
Patients with upper airway resistance syndrome
 Two-Point Palatal Discrimination in Patients With Upper Airway Resistance Syndrome, Obstructive Sleep Apnea Syndrome, and Normal Control Subjects* Christian Guilleminault, MD, BiolD; Kasey Li, MD, DDS;
Two-Point Palatal Discrimination in Patients With Upper Airway Resistance Syndrome, Obstructive Sleep Apnea Syndrome, and Normal Control Subjects* Christian Guilleminault, MD, BiolD; Kasey Li, MD, DDS;
Treatment of Obstructive Sleep Apnea (OSA)
 MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
MP9239 Covered Service: Prior Authorization Required: Additional Information: Yes when meets criteria below Yes as shown below None Prevea360 Health Plan Medical Policy: 1.0 A continuous positive airway
THE PATIENT STRONGLY MOTIVATED TOWARDS THE TREATMENT? & ENT
 SNORING & OSAHS SURGERY International Workshop Preoperative Diagnostic Protocol < 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B.
SNORING & OSAHS SURGERY International Workshop Preoperative Diagnostic Protocol < 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B.
Corporate Medical Policy
 Corporate Medical Policy PALATOPHARYNGOPLASTY/UVULOPALATOPHARYGOPLASTY Description of Procedure or Service Palatopharyngoplasty refers to several surgical approaches for management of the upper airway,
Corporate Medical Policy PALATOPHARYNGOPLASTY/UVULOPALATOPHARYGOPLASTY Description of Procedure or Service Palatopharyngoplasty refers to several surgical approaches for management of the upper airway,
Sleep Apnoea. The Story of a Pause
 Sleep Apnoea The Story of a Pause There is almost zero awareness in India that many amongst us maybe living with Sleep Apnoea, which left untreated could be life threatening tomorrow. This largely undiagnosed
Sleep Apnoea The Story of a Pause There is almost zero awareness in India that many amongst us maybe living with Sleep Apnoea, which left untreated could be life threatening tomorrow. This largely undiagnosed
A Reversible Uvulopalatal Flap for Snoring and Sleep Apnea Syndrome
 Sleep, 19(7):593-599 1996 American Sleep Disorders Association and Sleep Research Society Short Report: Surgical Technique A Reversible Uvulopalatal Flap for Snoring and Sleep Apnea Syndrome Nelson Powell,
Sleep, 19(7):593-599 1996 American Sleep Disorders Association and Sleep Research Society Short Report: Surgical Technique A Reversible Uvulopalatal Flap for Snoring and Sleep Apnea Syndrome Nelson Powell,
Original Article. Chisato Iida-Kondo 1, Norio Yoshino 4, Tohru Kurabayashi 4, Shirou Mataki 2, Makoto Hasegawa 3 and Norimasa Kurosaki 1
 J Med Dent Sci 2006; 53: 119 126 Original Article Comparison of Tongue Volume/Oral Cavity Volume Ratio between Obstructive Sleep Apnea Syndrome Patients and Normal Adults Using Magnetic Resonance Imaging
J Med Dent Sci 2006; 53: 119 126 Original Article Comparison of Tongue Volume/Oral Cavity Volume Ratio between Obstructive Sleep Apnea Syndrome Patients and Normal Adults Using Magnetic Resonance Imaging
Anyone of any shape or size may snore, but there are certain features which significantly increase the chance of snoring.
 Snoring Snoring is a common sleep related problem affecting more than 20% of the population at some stage in their lives. Snoring occurs when various parts of the throat, including the soft palate, tonsils
Snoring Snoring is a common sleep related problem affecting more than 20% of the population at some stage in their lives. Snoring occurs when various parts of the throat, including the soft palate, tonsils
This pamphlet has been designed as
 This pamphlet has been designed as an educational resource for patients with Obstructive Sleep Apnea (OSA). The successful use of CPAP requires no further intervention; however, not every patient is able,
This pamphlet has been designed as an educational resource for patients with Obstructive Sleep Apnea (OSA). The successful use of CPAP requires no further intervention; however, not every patient is able,
The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea
 ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
ORIGINAL ARTICLE The Mandibular Advancement Device and Patient Selection in the Treatment of Obstructive Sleep Apnea Chul Hee Lee, MD; Ji-Hun Mo, MD; Ik-Joon Choi, MD; Hyun Jong Lee, MD; Beom Seok Seo,
Nasal Evaluation & Non-surgical Nasal Therapy in SDB
 Nasal Evaluation & Non-surgical Nasal Therapy in SDB Edward M. Weaver, MD, MPH Seattle VA Medical Center University of Washington Harborview Medical Center Acknowledgments This material is the result of
Nasal Evaluation & Non-surgical Nasal Therapy in SDB Edward M. Weaver, MD, MPH Seattle VA Medical Center University of Washington Harborview Medical Center Acknowledgments This material is the result of
CHALLENGES IN PEDIATRIC OBSTRUCTIVE SLEEP APNEA. Amy S. Whigham, MD Assistant Professor
 CHALLENGES IN PEDIATRIC OBSTRUCTIVE SLEEP APNEA Amy S. Whigham, MD Assistant Professor Disclosures I have nothing to disclose. Outline Epidemiology Diagnosis Adenotonsillectomy Failure Treatment of Refractory
CHALLENGES IN PEDIATRIC OBSTRUCTIVE SLEEP APNEA Amy S. Whigham, MD Assistant Professor Disclosures I have nothing to disclose. Outline Epidemiology Diagnosis Adenotonsillectomy Failure Treatment of Refractory
Using Questionnaire Tools to Predict Pediatric OSA outcomes. Vidya T. Raman, MD Nationwide Children s Hospital October 201
 Using Questionnaire Tools to Predict Pediatric OSA outcomes Vidya T. Raman, MD Nationwide Children s Hospital October 201 NCH Conflict of Interest SASM $10,000 Grant NCH intramural/interdepartmental $38,000
Using Questionnaire Tools to Predict Pediatric OSA outcomes Vidya T. Raman, MD Nationwide Children s Hospital October 201 NCH Conflict of Interest SASM $10,000 Grant NCH intramural/interdepartmental $38,000
JMSCR Vol 05 Issue 01 Page January 2017
 www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.161 Risk of Failure of Adenotonsillectomy
www.jmscr.igmpublication.org Impact Factor 5.84 Index Copernicus Value: 83.27 ISSN (e)-2347-176x ISSN (p) 2455-0450 DOI: https://dx.doi.org/10.18535/jmscr/v5i1.161 Risk of Failure of Adenotonsillectomy
4/28/2017. Adult Obesity Rates
 Adult Obesity Rates Prevalence of Obstructive Sleep Apnea Rising prevalence of sleep apnea in U.S. threatens public health DARIEN, IL Sept. 29, 2014 Public health and safety are threatened by the increasing
Adult Obesity Rates Prevalence of Obstructive Sleep Apnea Rising prevalence of sleep apnea in U.S. threatens public health DARIEN, IL Sept. 29, 2014 Public health and safety are threatened by the increasing
Initial Adherence to Autotitrating Positive Airway Pressure Therapy: Influence of Upper Airway Narrowing
 Clinical and Experimental Otorhinolaryngology Vol. 2, No. 4: 181-185, December 2009 DOI 10.3342/ceo.2009.2.4.181 Original Article Initial Adherence to Autotitrating Positive Airway Pressure Therapy: Influence
Clinical and Experimental Otorhinolaryngology Vol. 2, No. 4: 181-185, December 2009 DOI 10.3342/ceo.2009.2.4.181 Original Article Initial Adherence to Autotitrating Positive Airway Pressure Therapy: Influence
5, 2002 RESIDENT PHYSICIAN: W.
 TITLE: Adult and Pediatric Obstructive Sleep Apnea SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: June 5, 2002 RESIDENT PHYSICIAN: W. Kevin Katzenmeyer, MD FACULTY PHYSICIAN: Ronald
TITLE: Adult and Pediatric Obstructive Sleep Apnea SOURCE: Grand Rounds Presentation, UTMB, Dept. of Otolaryngology DATE: June 5, 2002 RESIDENT PHYSICIAN: W. Kevin Katzenmeyer, MD FACULTY PHYSICIAN: Ronald
The role of oral myofunctional therapy in managing patients with mild to moderate obstructive sleep apnea
 Hemmat Baz, et al. PAN Arab Journal of Rhinology, Vol. 2, No. 1, March, 2012 The role of oral myofunctional therapy in managing patients with mild to moderate obstructive sleep apnea Hemmat Baz, 1 Mohsen
Hemmat Baz, et al. PAN Arab Journal of Rhinology, Vol. 2, No. 1, March, 2012 The role of oral myofunctional therapy in managing patients with mild to moderate obstructive sleep apnea Hemmat Baz, 1 Mohsen
Polysomnography (PSG) (Sleep Studies), Sleep Center
 Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Policy Number: 1036 Policy History Approve Date: 07/09/2015 Effective Date: 07/09/2015 Preauthorization All Plans Benefit plans vary in coverage and some plans may not provide coverage for certain service(s)
Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome
 Oral Maxillofacial Surg Clin N Am 14 (2002) 371 376 Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome B. Tucker Woodson, MD, FACS, ABSM Department of Otolaryngology and Human Communication,
Oral Maxillofacial Surg Clin N Am 14 (2002) 371 376 Soft tissue hypopharyngeal surgery for obstructive sleep apnea syndrome B. Tucker Woodson, MD, FACS, ABSM Department of Otolaryngology and Human Communication,
The Effect of Uvula-Preserving Palatopharyngoplasty in Obstructive Sleep Apnea on Globus Sense and Positional Dependency
 Clinical and Experimental Otorhinolaryngology Vol. 3, No. 3: 141-146, September 2010 DOI 10.3342/ceo.2010.3.3.141 Original Article The Effect of Uvula-Preserving Palatopharyngoplasty in Obstructive Sleep
Clinical and Experimental Otorhinolaryngology Vol. 3, No. 3: 141-146, September 2010 DOI 10.3342/ceo.2010.3.3.141 Original Article The Effect of Uvula-Preserving Palatopharyngoplasty in Obstructive Sleep
An update on childhood sleep-disordered breathing
 An update on childhood sleep-disordered breathing แพทย หญ งวนพร อน นตเสร ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร มหาว ทยาล ยสงขลานคร นทร Sleep-disordered breathing Primary snoring Upper airway resistance syndrome
An update on childhood sleep-disordered breathing แพทย หญ งวนพร อน นตเสร ภาคว ชาก มารเวชศาสตร คณะแพทยศาสตร มหาว ทยาล ยสงขลานคร นทร Sleep-disordered breathing Primary snoring Upper airway resistance syndrome
