New Insights on the Pathophysiology of Inspiratory Flow Limitation During Sleep
|
|
|
- Stephen Jones
- 5 years ago
- Views:
Transcription
1 Lung (2015) 193: DOI /s x SLEEP APNEA New Insights on the Pathophysiology of Inspiratory Flow Limitation During Sleep Luciana B. M. de Godoy 1 Luciana O. Palombini 1 Fernanda L. Martinho Haddad 1,2 David M. Rapoport 3 Tatiana de Aguiar Vidigal 1,2 Priscila Calixto Klichouvicz 1 Sergio Tufik 1 Sonia M. Togeiro 1 Received: 1 December 2014 / Accepted: 6 March 2015 / Published online: 1 April 2015 Ó Springer Science+Business Media New York 2015 Abstract Introduction Inspiratory flow limitation (IFL) is defined as a flattened shape of inspiratory airflow contour detected by nasal cannula pressure during sleep and can indicate increased upper airway resistance especially in mild sleeprelated breathing disorders (SRBD). The objective of this study was to investigate the association between upper airway abnormalities and IFL in patients with mild SRBD. Methods This study was derived from a general population study consisting of selected individuals with apnea hypopnea index (AHI) below 5 events/h of sleep, ( no obstructive sleep apnea group) and individuals with AHI between 5 and 15 events/h ( mild obstructive sleep apnea group). A total of 754 individuals were divided into four groups: group 1: AHI \5/h and \30 % of total sleep time (TST) with IFL (515 individuals), group 2: AHI \5/h and [30 % of (46 individuals), group 3: AHI: 5 15/h and\30 % of TST with IFL (168 individuals), and group 4: AHI: 5 15/h and [30 % of (25 individuals). Results Individuals with complains of oral breathing demonstrated a risk 2.7-fold larger of being group 4 compared with group 3. Abnormal nasal structure increased the chances of being in group fold in comparison to group 1. Individuals with voluminous lateral wall demonstrated a risk 4.2-fold larger of being group 4 compared with group 3. Conclusion More than 30 % of detected in sleep studies was associated with nasal and palatal anatomical abnormalities in mild SRBD patients. Keywords Flow limitation Nasal cannula Sleep apnea Upper airway & Sonia M. Togeiro togeiro.s.m@gmail.com Luciana B. M. de Godoy lu_bmg@yahoo.com.br Luciana O. Palombini luciana.palombini@sono.org.br Fernanda L. Martinho Haddad femartinho@uol.com.br David M. Rapoport david.rapoport@nyumc.org Tatiana de Aguiar Vidigal tatividigal@yahoo.com.br Priscila Calixto Klichouvicz calixto.priscila@gmail.com Sergio Tufik sergio.tufik@unifesp.br Disciplina de Medicina e Biologia do Sono, Departamento de Psicobiologia, Universidade Federal de Sao Paulo, Rua Napoleao de Barros 925, Sao Paulo , Brazil Departamento de Otorrinolaringologia e Cirurgia de Cabeça e Pescoço, Universidade Federal de Sao Paulo, Sao Paulo, Brazil Division of Pulmonary and Critical Care Medicine, New York University School of Medicine, NYC, New York, NY, USA
2 388 Lung (2015) 193: Introduction The diagnosis of sleep-related breathing disorders (SRBD) relies on a clinical history of snoring, gasping, nonrestorative sleep, excessive daytime sleepiness, or fatigue associated with an objective analysis of the obstructive respiratory events during sleep through polysomnography [1]. A sleep study can document the presence and severity of SRBD by recognizing apnea, hypopnea, and respiratory event-related arousal (RERA) [1]. The physiological consequences of apnea and hypopnea are similar and were well studied during the past decades. Individuals with mild SRBD present with less frequent apneas and with more frequent periods of partial upper airway obstruction and increased upper airway resistance. More subtle respiratory parameters indicating mild upper airway obstruction should be studied in order to better define mild SRBD. Inspiratory flow limitation (IFL) is a respiratory parameter that has been used to indicate increased upper airway resistance, based on flattening nasal cannula pressure signal [2]. IFL reflects upper airway collapsibility especially in mild SRBD. It is commonly caused by narrowing of a hypotonic upper airway in response to the negative intrathoracic pressure developed during inspiration [3]; however, the pathophysiology of IFL with no obstructive sleep apnea syndrome (OSAS) has not been described yet. Previous study has demonstrated that normal individuals can present up to 30 % of total sleep time (TST) with IFL [4]. The relationship between pharyngeal abnormalities and IFL seems complex, and the precise role played by these abnormalities in SRDB was not yet studied. The objective of this study was to investigate the association between upper airway anatomical abnormalities and IFL in patients with mild SRBD. Methods The study protocol was approved by the Ethics Committee for Research of the Universidade Federal de Sao Paulo/Hospital Sao Paulo (CEP:0593/06), Clinical Trials: NCT: This study was derived from a general population epidemiologic survey described in previous articles involving questionnaires, physical examination, and nocturnal polysomnography [5]. The cohort consisted of a representative sample of the inhabitants of Sao Paulo, Brazil according to gender, adult age (20 80 years old), and socioeconomic status, chosen with a three-stage cluster sampling technique. The sample consisted of 1101 individuals, which allowed for prevalence estimates with 3 % precision. Consenting subjects (1042 volunteers) underwent polysomnography. Methodological details of the Sao Paulo epidemiologic sleep study were described in previous studies [6]. A full-night, attended polysomnography was performed in each subject (EMBLA Ò S7000, Embla Systems, Inc., Broomfield, CO, USA) and sleep stages [7], arousals [8], and leg movements [8] were scored according to the standard criteria. OSAS was defined according to the International Classification of Sleep Disorders of the American Academy of Sleep Medicine criteria (2005) [9]. Apneas were scored following the recommended AASM rules [8]. Hypopneas were scored by the AASM alternative rules, i.e., when a [50 % reduction in airflow amplitude was observed on the nasal cannula signal lasting C10 s and accompanied by a decrease of C3 % in SpO 2 or an arousal [8]. We chose the alternative AASM rule in order to minimize the underestimation of obstructive sleep apnea (OSA) severity. Inspiratory flow limitation was scored manually and visually identified as a flattened shape of the inspiratory airflow contour at nasal cannula pressure from Embla system (square root of the flow signal), with no filters applied. At least four consecutive breaths with flattened shape were required to score IFL events [4, 10]. Those events should not meet the criteria for hypopnea. The percent of total sleep time (TST) during which the IFL was calculated. From the 1042 individuals of the epidemiologic sleep study [6], those selected were patients with apnea hypopnea index (AHI) below 5 events/h of sleep, considered as no OSA group and individuals with apnea hypopnea index between 5 and 15 events/h are considered as having mild OSA. Approximately 11 % of the polysomnographic records were excluded because their nasal cannula signal was not reliable. A total of 754 individuals were divided into four groups: group I (no OSA and no IFL group): AHI \5 events/h and\30 % of (515 individuals), group 2 (no OSA and with IFL group): AHI \5 events/h and [30 % of (46 individuals), group 3 (OSA and no IFL group): AHI: 5 15 events/h and \30 % of (168 individuals), and group 4 (OSA and with IFL group): AHI: 5 15 events/h and [30 % of TST with IFL (25 individuals). Upper airway physical examination was performed by six trained ear nose and throat physicians. Complaints were classified as present if individuals reported nasal obstruction, oral breathing, or habitual snoring. Body mass index (BMI) and neck circumference (NC) were measured at physical examination. NC was measured at the level of the cricothyroid membrane and was considered high when C43 cm in men or C38 cm in women. Physical examination consisted of facial inspection, oral and oropharynx examination, and anterior rhinoscopy [11]. During facial inspection, individual was seated in a horizontal Frankfurt position and the distance between a virtual vertical line tangential to the outer edge of lower lip and the most anterior part of chin was measured. If the
3 Lung (2015) 193: anterior prominence of the chin was two or more millimeters behind the virtual vertical line, individual was considered to have mandibular retrusion [12]. Oral cavity was evaluated for the presence of higharched palate and dental occlusions. Individuals were classified as class I (normal occlusion), class II (possibility of mandibular retrognathism), and class III (possibility of mandibular prognathism). Presence of class II dental occlusion, retrognathia, or high-arched palate was considered as unfavorable facial skeleton. Nasal septal deviation was evaluated through anterior rhinoscopy examination and was classified as Grade I (deviation did not touch the sidewall), Grade II (deviation touched the inferior turbinate), and Grade III (deviation touched and compressed the sidewall). Inferior turbinate was considered hypertrophic if at least one of them appeared swollen and touched by the nasal septum, significantly obstructing the nose [13]. The nasal structure was considered abnormal if one of the following conditions was present: Grade II or III septal deviation; an association of Grade I septal deviation with inferior turbinate hypertrophy or complaints of nasal obstruction, and inferior turbinate hypertrophy with complaints of nasal obstruction [13]. Soft palate characteristics were classified into three categories: posteriorly placed, thick (when rounded in size and swollen), and webbed (webbed palate due to redundant posterior pillars). The tonsillar pillars were considered voluminous if they were close to the midline of the oropharynx (voluminous lateral wall). Uvula was considered thick when swollen. Long uvula was defined as one that approached the base of the tongue [14, 15]. The tongue was considered voluminous if it has impression of teeth in the lingual border [14, 15]. Modified Mallampati scoring was conducted with the patient seated and asked to open the mouth to its maximum width and to maintain the tongue relaxed inside the oral cavity. It was classified as class I (the entire oropharynx was visible, including the soft palate, tonsillar pillars, tonsils, and tip of the uvula), class II (the upper pole of the tonsils and the uvula were visible), class III (part of the soft palate and the uvula were visible), and class IV (only the hard palate and part of the soft palate were visible) [16]. The palatine tonsils were classified as Grade I (intravelar), Grade II (extending beyond the anterior tonsillar pillar), Grade III (extending up to three quarters toward the midline), Grade IV (completely blocking the throat), and Grade 0 in tonsillectomized individuals [14, 16]. An oropharynx with at least three of the following observations was considered unfavorable: Grade III or IV palatine tonsils, an abnormal uvula (long and/or thick), an abnormal palate (posterior and/or thick), a webbed palate, and a voluminous lateral wall [14]. Statistical Analysis SPSS version 21.0 was used for the statistical analysis. Chi-squared tests (v 2 ) were conducted to identify associations between mild SRBD with/without IFL and upper airway abnormalities. Multivariate logistic regression models were used to analyze the adjusted associations and interactions among the SRBD groups and those upper airway abnormalities (abnormal nasal structure, abnormal oropharynx, unfavorable facial skeleton). BMI was used as covariate during multivariate logistic regression analysis. The level of significance set was 5 % (p \ 0.05). Results From the cohort of 1042 individuals, 754 were individuals with AHI \5 events/h ( no OSA group: 561 individuals) or mild OSA patients (193 individuals) that had the TST with IFL measured. There were 305 men (40.5 %) and 449 women (59.5 %). Mean age was 39.8 ± 13.4 years. Mean BMI was 26 ± 4.8 kg/m 2 and mean NC was 35.6 ± 5.6 cm. There were 515 individuals (68.3 %) in group I ( no OSA with \30 % of ), 46 individuals (6.1 %) in group 2 ( no OSA with [30 % of TST with IFL), 168 individuals (22.3 %) in group 3 (mild OSA with \30 % of ), and 25 individuals (3.3 %) in group 4 (mild OSA with [30 % of ). Multivariate logistic regression was used for upper airway abnormalities that had a significant statistical difference in the Chi-square test with adjusted residuals (Table 1 and 2). Oral breathing was associated with mild OSA with [30 % in comparison to mild OSA with \30 % of (p = 0.28). Habitual snoring increased 1.83-fold the chances of having OSA with \30 % of in comparison to normal group with \30 % of (p = 0.003). Abnormal nasal structure increased 3.2-fold the chances of having mild OSA with [30 % of TST with IFL and 1.84-fold the chances of having mild OSA with \30%ofTSTwithIFLincomparisonto noosa with \30 % of (p \ and p = 0.006, respectively). For those that had voluminous lateral wall, the odds of having mild OSA with [30 % of was 4.2- fold larger than the odds of having mild OSA with \30 % of (p = 0.025). Thick uvula increased fold the chances of having mild OSA with \30 % of TST with IFL in comparison to no OSA with \30 % of TST with IFL (p = 0.017).
4 390 Lung (2015) 193: Discussion For the best of our knowledge, this is the first study that investigates and demonstrates the role of nasal and palatal anatomical abnormalities in IFL during sleep in mild SRBD. The mechanisms of upper airway obstruction in OSAS are commonly interpreted in terms of the Starling resistor model [17]. Accordingly, the upper airway has a compliant wall that allows the air passage when the transmural pressure across the wall is positive. The intraluminal pressure must be greater than the external pressure to allow air passage. Inspiratory flow induces a negative intraluminal pressure. The degree of airway closure depends on the balance between the negative intraluminal pressure and the pressure at the external side of the airway wall. In patients with SRBD, the pressure applied by upper airway muscles is not sufficient to compensate the negative Table 1 Symptoms related to upper airway and upper airway abnormalities associated with mild SRBD and IFL (according to the X 2 test) (p \ 0.05) no OSA with \30 % (%) (N = 515) no OSA with [30 % (%) (N = 46) OSA with \30 % (%) (N = 168) OSA with [30 % (%) (N = 25) p Symptoms Nasal obstruction Dryness in the nose/mouth Habitual snoring \0.001* Oral breathing * Upper airway abnormalities Retrognathia High-arched palate Class II dental occlusion Unfavorable skeletal features Septal deviation Grade II or III Inferior turbinate * hypertrophy Abnormal nasal * structure Palate webbed Palate posterior Palate thick \0.001* Voluminous * lateral wall Long uvula Thick uvula \0.001* Palatine tonsils Grade III or IV Mallampati score * Grade III or IV Neck * circumference Abnormal oropharynx * OSA obstructive sleep apnea, TST total sleep time, IFL inspiratory flow limitation * p \ 0.05 (statistical significant)
5 Lung (2015) 193: Table 2 Multivariate logistic regression model for OSA with and without IFL adjusted for BMI Symptoms and upper airway abnormalities no OSA with \30 % TST no OSA with [30 % TST OSA with \30 % TST OSA with [30 % TST Oral breathing 1.61 ( ) 0.96 ( ) 2.74 ( )* 1 a Habitual snoring 1.98 ( ) 1.38 ( ) 1.06 ( ) 1 a Neck circunference b 1 a Inferior turbinate hypertrophy 0.98 ( ) 1.02 ( ) 2.18 ( ) 1 a Abnormal nasal structure 3.20 ( ) 2.66 ( ) 1.74 ( ) 1 a Palate thick 2.86 ( ) 2.46 ( ) 1.84 ( ) 1 a Voluminous lateral wall 2.55 ( ) 4.4 ( ) 4.25 ( )* 1 a Thick uvula 1.54 ( ) 0.72 ( ) 0.79 ( ) 1 a Mallampati score Grade III IV 1.74 ( ) 1.57 ( ) 1.29 ( ) 1 a Abnormal oropharynx 0.45 ( ) 0.58 ( ) 0.43 ( ) 1 a OSA obstructive sleep apnea, TST total sleep time, IFL inspiratory flow limitation * p \ 0.05 (statistical significant) a b Variable used as reference (OSA with [30 % ) Some numbers of patients with some variables were too small. There was not possible to calculate Odds ratio for neck circumference intraluminal pressure. Consequently, total occlusions (apnea) and/or partial collapse (hypopnea or IFL) of the upper airway occur [17]. It is important to perform a physical examination of the upper airway of patients with SRBD in order to detect areas that may collapse during sleep. The relationship between the nasal airway and the collapse of the upper airways is complex, and the precise role played by the nasal airway in SRDB is not yet completely known. But nasal obstruction forces the individual to breathe through the oral cavity. Oral breathing lengthens and narrows the upper airway and makes it more collapsible to inspiratory negative pressure [18]. IFL during sleep is a respiratory parameter that has been described and has been associated with consequences, however, the exact cut off point between healthy and disease is not well defined yet. Currently, AASM criteria considers IFL only if it is part of RERA event [8]. Isolated IFL is not recognized yet as an abnormal respiratory event. The clinical significance of IFL during sleep that includes insymptomatic (and non-symptomatic) individuals will be established after long-term studies associating different outcomes to this respiratory parameter. Palombini et al. [4] evaluated the distribution of IFL in a representative sample of the general population and found that normal individuals can present up to 30 % of the total sleep time with IFL. Some authors suggested that either isolated brief episodes or long periods of IFL can have clinical consequences [19, 20]. Calero et al. concluded after studying prolonged periods of IFL (lasting more than 10 min) induced by suboptimal nasal continuous positive airway pressure (ncpap), that they were associated with an increase in end tidal CO 2 and decrease in oxygen saturation [21]. Edwards et al. studied the presence of flow limitation in pre-eclamptic females and found that this respiratory parameter was common in this group of patients and that short-term relief of IFL by ncpap was associated with a reduction in nocturnal blood pressure (BP) levels [22]. We found that complain of oral breathing and presence of voluminous lateral wall were more frequent in individuals with mild OSA with IFL than in those with OSA without IFL. Abnormal nasal structure increased the chances of having mild OSA with IFL in comparison to mild OSA without IFL. These findings show that individuals with mild SRBD with more than 30 % of TST with IFL might have some upper airway anatomical differences in comparison to those without IFL. Our study demonstrates that IFL in OSA and non-osa individuals is associated with nasal and palatal abnormalities. This could indicate that having IFL as part of polysomnographic criterion in SRBD is associated with more significant disease. It could be suggested that as part of the treatment of these sleep breathing disorders, it should be aimed to decrease time with IFL, besides normalizing AHI. This study had some limitations. One of them is the fact that physical examination is a subjective task. The six otolaryngologists that evaluated the patients were well
6 392 Lung (2015) 193: trained, but we did not analyze their intra- and inter-rater agreement. The shape of the IFL as visualized during polysomnography is also subjective. Analyzing IFL using pneumotachograph flow measurement and esophageal manometry could solve this study limitation. However, Ayappa et al. showed that IFL, RERAs, and similar subtle respiratory events could be detected indirectly through the shape of the inspiratory flow curve on a nasal pressure cannula in place of esophageal manometry [23]. The nasal cannula is the most used tool for measuring airflow in sleep studies and is not invasive as esophageal manometry is, which is an important characteristic that allows its widespread clinical usage. Further studies addressing upper airway resistance of individuals with mild SRBD should be performed in order to better define the complete pathophysiology of IFL in this group with mild disease as well as the impact of these findings in clinical outcomes. Conclusion More than 30 % of TST (total sleep time) with IFL is associated with nasal and palatal anatomical abnormalities in mild SRBD patients. Acknowledgments The authors would like to thank for the support by Grants from Associaçao Fundo de Incentivo a Pesquisa (AFIP), Fundaçao de Amparo a Pesquisa do Estado de Sao Paulo (FAPESP), and Conselho Nacional de Desenvolvimento Cientifico e Tecnologico (CNPq). Conflict of interest References None. 1. American Academy of Sleep Medicine (2014) The International classification of sleep disorders, 3rd edn. American Academy of Sleep Medicine, Darien 2. Hosselet JJ, Norman RG, Ayappa I et al (1998) Detection of flow limitation with a nasal cannula/pressure transducer system. Am J Respir Crit Care Med 57: Remmers JE, DeGroot WJ, Sauerland EK (1978) Pathogenesis of upper airway occlusion during sleep. J Appl Physiol 44: Palombini LO, Tufik S, Rapoport DM et al (2013) Inspiratory flow limitation in a normal population of adults in São Paulo, Brazil. Sleep 36: Tufik S, Santos-Silva R, Taddei JA, Bittencourt LR (2010) Obstructive sleep apnea syndrome in the Sao Paulo epidemiologic sleep study. Sleep Med 11: Santos-Silva R, Tufik S, Conway SG et al (2009) Sao Paulo epidemiologic sleep study: rationale, design, sampling, and procedures. Sleep Med 10: Rechtschaffen A, Kales A (1968) A manual of standardized terminology: techniques and scoring system for sleep stages of human subjects. UCLA Brain Information Service/Brain Research Institute, Los Angeles 8. Iber C, Ancoli-Israel S, Chesson AL Jr et al (2007) The AASM manual for the scoring of sleep and associated events: rules, terminology and technical specifications. American Academy of Sleep Medicine, Westchester 9. American Academy of Sleep Medicine (2005) The International classification of sleep disorders: diagnostic & coding manual, 2nd edn. Academy of Sleep Medicine, Westchester 10. Bao G, Guilleminault C (2004) Upper airway resistance syndrome one decade later. Curr Opin Pulm Med 10: Bittencourt LR (2008) Diagnosis and treatment of sleep obstructive apnea syndrome (OSAS): practical guide. Bookstore Paulista Medical Publisher, São Paulo 12. Soares MC, Oliveira PW, Vidigal T et al (2010) Comparisons of the upper airway and facial skeleton of an adult population in the city of Sao Paulo with and without obstructive sleep apnoea. Sleep Res 19(Suppl 2): Ridley MB (1992) Aesthetic facial proportions. In: Papel ID, Nachlis NE (eds) Facial plastic and reconstructive surgery. St Louis, Mosby, p Zonato AI, Bittencourt LR, Martinho FL et al (2003) Association of systematic head and neck physical examination with severity of obstructive sleep apnea-hypopnea syndrome. Laryngoscope 113: Zonato AI, Martinho FL, Bittencourt LR et al (2005) Head and neck physical examination: comparison between nonapneic and obstructive sleep apnea patients. Laryngoscope 115: Friedman M, Tanyeri H, La Rosa M et al (1999) Clinical predictors of obstructive sleep apnea. Laryngoscope 109: Gold AR, Schwartz AR (1996) The pharyngeal critical pressure: the whys and hows of using nasal continuous positive airway pressure diagnostically. Chest 110: Lee SH, Choi JH, Shin C et al (2007) How does open-mouth breathing influence upper airway anatomy? Laryngoscope 117(6): Guilleminault C, Kirisoglu C, Poyares D et al (2006) Upper airway resistance syndrome: a long-term outcome study. J Psychiatr Res 40: Guilleminault C, Lopes MC, Hagen CC et al (2007) The cyclic alternating pattern demonstrates increased sleep instability and correlates with fatigue and sleepiness in adults with upper airway resistance syndrome. Sleep 30: Calero G, Farre R, Ballester E et al (2006) Physiological consequences of prolonged periods of flow limitation in patients with sleep apnea hypopnea syndrome. Respir Med 100: Edwards N, Blyton DM, Kirjavainen T et al (2000) Nasal continuous positive airway pressure reduces sleep-induced blood pressure increments in preeclampsia. Am J Respir Crit Care Med 162: Ayappa I, Norman RG, Krieger AC et al (2000) Non-Invasive detection of respiratory effort-related arousals (RERAs) by a nasal cannula/pressure transducer system. Sleep 23:
Systematic head and neck physical examination as a predictor of obstructive sleep apnea in class III obese patients
 Brazilian ENT examination Journal of as Medical a predictor and Biological of OSAS in Research obese patients (2008) 41: 1093-1097 ISSN 0100-879X 1093 Systematic head and neck physical examination as a
Brazilian ENT examination Journal of as Medical a predictor and Biological of OSAS in Research obese patients (2008) 41: 1093-1097 ISSN 0100-879X 1093 Systematic head and neck physical examination as a
Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive Sleep Apnea Patients
 The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive
The Laryngoscope Lippincott Williams & Wilkins, Inc. 2005 The American Laryngological, Rhinological and Otological Society, Inc. Head and Neck Physical Examination: Comparison Between Nonapneic and Obstructive
Inspiratory Flow Limitation in a Normal Population of Adults in São Paulo, Brazil
 INSPIRATORY FLOW LIMITATION IN A NORMAL POPULATION OF ADULTS http://dx.doi.org/10.5665/sleep.3122 Inspiratory Flow Limitation in a Normal Population of Adults in São Paulo, Brazil Luciana O. Palombini,
INSPIRATORY FLOW LIMITATION IN A NORMAL POPULATION OF ADULTS http://dx.doi.org/10.5665/sleep.3122 Inspiratory Flow Limitation in a Normal Population of Adults in São Paulo, Brazil Luciana O. Palombini,
Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
 Sleep Disorders Volume 2015, Article ID 749068, 4 pages http://dx.doi.org/10.1155/2015/749068 Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
Sleep Disorders Volume 2015, Article ID 749068, 4 pages http://dx.doi.org/10.1155/2015/749068 Research Article EK Sign: A Wrinkling of Uvula and the Base of Uvula in Obstructive Sleep Apnea-Hypopnea Syndrome
Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome
 ORIGINAL ARTICLE pissn 2093-9175 / eissn 2233-8853 http://dx.doi.org/10.17241/smr.2015.6.2.54 Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome Seung Hoon Lee, MD, PhD, In Sik Song, MD, Jae Woo
ORIGINAL ARTICLE pissn 2093-9175 / eissn 2233-8853 http://dx.doi.org/10.17241/smr.2015.6.2.54 Nasal Mass Presenting as Obstructive Sleep Apnea Syndrome Seung Hoon Lee, MD, PhD, In Sik Song, MD, Jae Woo
Alexandria Workshop on
 Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Alexandria Workshop on 1 Snoring & OSA Surgery Course Director: Yassin Bahgat MD Claudio Vicini MD Course Board: Filippo Montevecchi MD Pietro Canzi MD Snoring & Obstructive ti Sleep Apnea The basic information
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2
 Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2 CAUSES OF SNORING AND SLEEP APNEA We inhale air through our nose and mouth. From the nostrils, air flows
Snoring and Obstructive Sleep Apnea: Patient s Guide to Minimally Invasive Treatments Chapter 2 CAUSES OF SNORING AND SLEEP APNEA We inhale air through our nose and mouth. From the nostrils, air flows
The most accurate predictors of arterial hypertension in patients with Obstructive Sleep Apnea Syndrome
 The most accurate predictors of arterial hypertension in patients with Obstructive Sleep Apnea Syndrome Natsios Georgios University Hospital of Larissa, Greece Definitions Obstructive Sleep Apnea (OSA)
The most accurate predictors of arterial hypertension in patients with Obstructive Sleep Apnea Syndrome Natsios Georgios University Hospital of Larissa, Greece Definitions Obstructive Sleep Apnea (OSA)
Comparison of Nasal Prong Pressure and Thermistor Measurements for Detecting Respiratory Events during Sleep
 Clinical Investigations Respiration 2004;71:385 390 DOI: 10.1159/000079644 Received: August 25, 2003 Accepted after revision: March 16, 2004 Comparison of Nasal Prong Pressure and Thermistor Measurements
Clinical Investigations Respiration 2004;71:385 390 DOI: 10.1159/000079644 Received: August 25, 2003 Accepted after revision: March 16, 2004 Comparison of Nasal Prong Pressure and Thermistor Measurements
Obese obstructive sleep apnea patients with tonsil hypertrophy submitted to tonsillectomy
 Brazilian Journal of Medical and Biological Research (2006) 39: 1137-1142 Obese OSAHS patients submitted to tonsillectomy ISSN 0100-879X 1137 Obese obstructive sleep apnea patients with tonsil hypertrophy
Brazilian Journal of Medical and Biological Research (2006) 39: 1137-1142 Obese OSAHS patients submitted to tonsillectomy ISSN 0100-879X 1137 Obese obstructive sleep apnea patients with tonsil hypertrophy
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA
 SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
SURGERY FOR SNORING AND MILD OBSTRUCTIVE SLEEP APNOEA INTRODUCTION Snoring with or without excessive daytime somnolence, restless sleep and periods of apnoea are all manifestations of sleep disordered
Patients with upper airway resistance syndrome
 Two-Point Palatal Discrimination in Patients With Upper Airway Resistance Syndrome, Obstructive Sleep Apnea Syndrome, and Normal Control Subjects* Christian Guilleminault, MD, BiolD; Kasey Li, MD, DDS;
Two-Point Palatal Discrimination in Patients With Upper Airway Resistance Syndrome, Obstructive Sleep Apnea Syndrome, and Normal Control Subjects* Christian Guilleminault, MD, BiolD; Kasey Li, MD, DDS;
Sleep Diordered Breathing (Part 1)
 Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Sleep Diordered Breathing (Part 1) History (for more topics & presentations, visit ) Obstructive sleep apnea - first described by Charles Dickens in 1836 in Papers of the Pickwick Club, Dickens depicted
Diagnostic Accuracy of the Multivariable Apnea Prediction (MAP) Index as a Screening Tool for Obstructive Sleep Apnea
 Original Article Diagnostic Accuracy of the Multivariable Apnea Prediction (MAP) Index as a Screening Tool for Obstructive Sleep Apnea Ahmad Khajeh-Mehrizi 1,2 and Omid Aminian 1 1. Occupational Sleep
Original Article Diagnostic Accuracy of the Multivariable Apnea Prediction (MAP) Index as a Screening Tool for Obstructive Sleep Apnea Ahmad Khajeh-Mehrizi 1,2 and Omid Aminian 1 1. Occupational Sleep
Sleep Disorders and the Metabolic Syndrome
 Sleep Disorders and the Metabolic Syndrome Tom V. Cloward, M.D. Intermountain Sleep Disorders Center LDS Hospital Objectives Describe how sleep disorders impact your daily medical practice Don Don t do
Sleep Disorders and the Metabolic Syndrome Tom V. Cloward, M.D. Intermountain Sleep Disorders Center LDS Hospital Objectives Describe how sleep disorders impact your daily medical practice Don Don t do
Snoring, obstructive sleep apnea (OSA), and upper. impact of basic research on tomorrow. Snoring Imaging* Could Bernoulli Explain It All?
 impact of basic research on tomorrow Snoring Imaging* Could Bernoulli Explain It All? Igor Fajdiga, MD, PhD Study objectives: To identify upper airway changes in snoring using CT scanning, to clarify the
impact of basic research on tomorrow Snoring Imaging* Could Bernoulli Explain It All? Igor Fajdiga, MD, PhD Study objectives: To identify upper airway changes in snoring using CT scanning, to clarify the
(To be filled by the treating physician)
 CERTIFICATE OF MEDICAL NECESSITY TO BE ISSUED TO CGHS BENEFICIAREIS BEING PRESCRIBED BILEVEL CONTINUOUS POSITIVE AIRWAY PRESSURE (BI-LEVEL CPAP) / BI-LEVEL VENTILATORY SUPPORT SYSTEM Certification Type
CERTIFICATE OF MEDICAL NECESSITY TO BE ISSUED TO CGHS BENEFICIAREIS BEING PRESCRIBED BILEVEL CONTINUOUS POSITIVE AIRWAY PRESSURE (BI-LEVEL CPAP) / BI-LEVEL VENTILATORY SUPPORT SYSTEM Certification Type
Brian Palmer, D.D.S, Kansas City, Missouri, USA. April, 2001
 Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Brian Palmer, D.D.S, Kansas City, Missouri, USA A1 April, 2001 Disclaimer The information in this presentation is for basic information only and is not to be construed as a diagnosis or treatment for any
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015
 Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
Abdussalam Alahmari ENT Resident R2 KAUH 15/12/2015 Physiology of sleep Snoring mechanism, causes, sites, symptoms, and management. Sleep apnea definitions, pathophysiology, risk factors, evaluation of
11/19/2012 ก! " Varies 5-86% in men 2-57% in women. Thailand 26.4% (Neruntarut et al, Sleep Breath (2011) 15: )
 Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Snoring ก Respiratory sound generated in the upper airway during sleep that typically occurs during inspiration but may occur during expiration ICSD-2, 2005..... ก ก! Prevalence of snoring Varies 5-86%
Basics of Polysomnography. Chitra Lal, MD, FCCP, FAASM Assistant professor of Medicine, Pulmonary, Critical Care and Sleep, MUSC, Charleston, SC
 Basics of Polysomnography Chitra Lal, MD, FCCP, FAASM Assistant professor of Medicine, Pulmonary, Critical Care and Sleep, MUSC, Charleston, SC Basics of Polysomnography Continuous and simultaneous recording
Basics of Polysomnography Chitra Lal, MD, FCCP, FAASM Assistant professor of Medicine, Pulmonary, Critical Care and Sleep, MUSC, Charleston, SC Basics of Polysomnography Continuous and simultaneous recording
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update
 OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
OBSTRUCTIVE SLEEP APNEA and WORK Treatment Update David Claman, MD Professor of Medicine Director, UCSF Sleep Disorders Center 415-885-7886 Disclosures: None Chronic Sleep Deprivation (0 v 4 v 6 v 8 hrs)
A comparison of public and private obstructive sleep apnea clinics
 Brazilian Journal of Medical and Biological Research (2004) 37: 69-76 Public and private obstructive sleep apnea clinics ISSN 0100-879X 69 A comparison of public and private obstructive sleep apnea clinics
Brazilian Journal of Medical and Biological Research (2004) 37: 69-76 Public and private obstructive sleep apnea clinics ISSN 0100-879X 69 A comparison of public and private obstructive sleep apnea clinics
Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD
 A Physiologic Comparison of Nasal and Oral Positive Airway Pressure* Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD Study objectives: The effectiveness
A Physiologic Comparison of Nasal and Oral Positive Airway Pressure* Philip L. Smith, MD; Christopher P. O Donnell, PhD; Lawrence Allan, BS; and Alan R. Schwartz, MD Study objectives: The effectiveness
Nasal pressure recording in the diagnosis of sleep apnoea hypopnoea syndrome
 56 Unité de Recherche, Centre de Pneumologie de l Hôpital Laval, Université Laval, Québec, Canada F Sériès I Marc Correspondence to: Dr F Sériès, Centre de Pneumologie, 2725 Chemin Sainte Foy, Sainte Foy
56 Unité de Recherche, Centre de Pneumologie de l Hôpital Laval, Université Laval, Québec, Canada F Sériès I Marc Correspondence to: Dr F Sériès, Centre de Pneumologie, 2725 Chemin Sainte Foy, Sainte Foy
SLEEP DISORDERED BREATHING The Clinical Conditions
 SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
SLEEP DISORDERED BREATHING The Clinical Conditions Robert G. Hooper, M.D. In the previous portion of this paper, the definitions of the respiratory events that are the hallmarks of problems with breathing
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
New Perspectives on the Pathogenesis of OSA - Anatomic Perspective. New Perspectives on the Pathogenesis of OSA: Anatomic Perspective - Disclosures
 New Perspectives on the Pathogenesis of OSA - Anatomic Perspective Richard J. Schwab, M.D. Professor of Medicine Interim Chief, Division of Sleep Medicine Medical Director, Penn Sleep Centers University
New Perspectives on the Pathogenesis of OSA - Anatomic Perspective Richard J. Schwab, M.D. Professor of Medicine Interim Chief, Division of Sleep Medicine Medical Director, Penn Sleep Centers University
Myofunctional therapy improves adherence to continuous positive airway pressure treatment
 Myofunctional therapy improves adherence to continuous positive airway pressure treatment Giovana Diaféria, Rogerio Santos-Silva, Eveli Truksinas, Fernanda L. M. Haddad, Renata Santos, Silvana Bommarito,
Myofunctional therapy improves adherence to continuous positive airway pressure treatment Giovana Diaféria, Rogerio Santos-Silva, Eveli Truksinas, Fernanda L. M. Haddad, Renata Santos, Silvana Bommarito,
Obstructive sleep apnea (OSA)
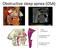 Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
Obstructive sleep apnea (OSA) In a healthy sleeping child, the mouth is typically closed, the oral cavity is collapsed, and the nasopharynx and hypopharynx are patent with minimal wall motion Obstructive
Medicare C/D Medical Coverage Policy
 Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Medicare C/D Medical Coverage Policy Surgical Treatment of Obstructive Sleep Apnea Origination: June 26, 2000 Review Date: January 18, 2017 Next Review January, 2019 DESCRIPTION OF PROCEDURE OR SERVICE
Snoring. Forty-five percent of normal adults snore at least occasionally and 25
 Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Snoring Insight into sleeping disorders and sleep apnea Forty-five percent of normal adults snore at least occasionally and 25 percent are habitual snorers. Problem snoring is more frequent in males and
Polycystic Ovarian Syndrome and Obstructive Sleep Apnea: Poor Bedpartners. M. Begay, MD UNM Sleep Medicine Fellow 01/31/2017
 Polycystic Ovarian Syndrome and Obstructive Sleep Apnea: Poor Bedpartners M. Begay, MD UNM Sleep Medicine Fellow 01/31/2017 Case of S.R. S.R. is a 39 year old female referred for suspected obstructive
Polycystic Ovarian Syndrome and Obstructive Sleep Apnea: Poor Bedpartners M. Begay, MD UNM Sleep Medicine Fellow 01/31/2017 Case of S.R. S.R. is a 39 year old female referred for suspected obstructive
BTS sleep Course. Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith)
 BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
BTS sleep Course Module 10 Therapies I: Mechanical Intervention Devices (Prepared by Debby Nicoll and Debbie Smith) S1: Overview of OSA Definition History Prevalence Pathophysiology Causes Consequences
Pharyngeal Critical Pressure in Patients with Obstructive Sleep Apnea Syndrome Clinical Implications
 Pharyngeal Critical Pressure in Patients with Obstructive Sleep Apnea Syndrome Clinical Implications EMILIA SFORZA, CHRISTOPHE PETIAU, THOMAS WEISS, ANNE THIBAULT, and JEAN KRIEGER Sleep Disorders Unit,
Pharyngeal Critical Pressure in Patients with Obstructive Sleep Apnea Syndrome Clinical Implications EMILIA SFORZA, CHRISTOPHE PETIAU, THOMAS WEISS, ANNE THIBAULT, and JEAN KRIEGER Sleep Disorders Unit,
Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea
 European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
European Journal of Orthodontics 20 (1998) 293 297 1998 European Orthodontic Society Effect of two types of mandibular advancement splints on snoring and obstructive sleep apnoea J. Lamont*, D. R. Baldwin**,
RESEARCH PACKET DENTAL SLEEP MEDICINE
 RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
RESEARCH PACKET DENTAL SLEEP MEDICINE American Academy of Dental Sleep Medicine Dental Sleep Medicine Research Packet Page 1 Table of Contents Research: Oral Appliance Therapy vs. Continuous Positive Airway
The diagnosis of obstructive sleep apnea syndrome. Combined Effects of a Nasal Dilator and Nasal Prongs on Nasal Airflow Resistance*
 Combined Effects of a Nasal Dilator and Nasal Prongs on Nasal Airflow Resistance* Anne Marie Lorino, PhD; Marie Pia d Ortho, MD; Estelle Dahan; Olivier Bignani; Carine Vastel; and Hubert Lorino, PhD Study
Combined Effects of a Nasal Dilator and Nasal Prongs on Nasal Airflow Resistance* Anne Marie Lorino, PhD; Marie Pia d Ortho, MD; Estelle Dahan; Olivier Bignani; Carine Vastel; and Hubert Lorino, PhD Study
Coding for Sleep Disorders Jennifer Rose V. Molano, MD
 Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
Practice Coding for Sleep Disorders Jennifer Rose V. Molano, MD Accurate coding is an important function of neurologic practice. This section of is part of an ongoing series that presents helpful coding
ORIGINAL ARTICLE. The Nasal Obstruction Symptom Evaluation. as a Screening Tool for Obstructive Sleep Apnea
 ORIGINAL ARTICLE The Nasal Obstruction Symptom Evaluation Survey as a Screening Tool for Obstructive Sleep Apnea Lisa Ishii, MD, MHS; Andres Godoy, MD; Stacey L. Ishman, MD, MPH; Christine G. Gourin, MD;
ORIGINAL ARTICLE The Nasal Obstruction Symptom Evaluation Survey as a Screening Tool for Obstructive Sleep Apnea Lisa Ishii, MD, MHS; Andres Godoy, MD; Stacey L. Ishman, MD, MPH; Christine G. Gourin, MD;
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea
 Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Surgical Options for the Successful Treatment of Obstructive Sleep Apnea Benjamin J. Teitelbaum, MD, FACS Otolaryngology Head and Neck Surgery Saint Agnes Medical Center Fresno, California Terms Apnea
Effects of continuous positive airway pressure on nasal and pharyngeal symptoms in patients with obstructive sleep apnea*
 Effects of continuous positive airway pressure on nasal and pharyngeal symptoms in patients with obstructive sleep apnea* ADELAIDE CRISTINA DE FIGUEIREDO, MARIA CECÍLIA LORENZI, SIMONE PREZZOTI (TESBPT),
Effects of continuous positive airway pressure on nasal and pharyngeal symptoms in patients with obstructive sleep apnea* ADELAIDE CRISTINA DE FIGUEIREDO, MARIA CECÍLIA LORENZI, SIMONE PREZZOTI (TESBPT),
Updated Friedman Staging System for Obstructive Sleep Apnea
 Updated Friedman Staging System for Obstructive Sleep Apnea Michael Friedman a, b Anna M. Salapatas b Lauren B. Bonzelaar c a Section of Sleep Surgery, Rush University Medical Center, and b Section of
Updated Friedman Staging System for Obstructive Sleep Apnea Michael Friedman a, b Anna M. Salapatas b Lauren B. Bonzelaar c a Section of Sleep Surgery, Rush University Medical Center, and b Section of
Physiological consequences of prolonged periods of flow limitation in patients with sleep apnea hypopnea syndrome
 Respiratory Medicine (2006) 100, 813 817 Physiological consequences of prolonged periods of flow limitation in patients with sleep apnea hypopnea syndrome Gabriel Calero, Ramon Farre, Eugeni Ballester,
Respiratory Medicine (2006) 100, 813 817 Physiological consequences of prolonged periods of flow limitation in patients with sleep apnea hypopnea syndrome Gabriel Calero, Ramon Farre, Eugeni Ballester,
PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA)
 PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA) DEFINITION OSA Inspiratory airflow is either partly (hypopnea) or completely (apnea) occluded during sleep. The combination of sleep-disordered breathing with daytime
PEDIATRIC OBSTRUCTIVE SLEEP APNEA (OSA) DEFINITION OSA Inspiratory airflow is either partly (hypopnea) or completely (apnea) occluded during sleep. The combination of sleep-disordered breathing with daytime
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
 SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
SLEEP APNOEA DR TAN KAH LEONG ALVIN CO-DIRECTOR SLEEP LABORATORY SITE CHIEF SDDC (SLEEP) DEPARTMENT OF OTORHINOLARYNGOLOGY, HEAD & NECK SURGERY
Ped e iat a r t i r c c S lee e p e A p A nea e a Surg r er e y
 Airway Imaging in Pediatric OSA Kasey Li, MD, DDS, FACS Stanford University Sleep Medicine Program The airway is smaller in children with OSA compared to controls The adenoid and tonsils are larger and
Airway Imaging in Pediatric OSA Kasey Li, MD, DDS, FACS Stanford University Sleep Medicine Program The airway is smaller in children with OSA compared to controls The adenoid and tonsils are larger and
Prefabricated Oral Appliances for Obstructive Sleep Apnea
 Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
Medical Policy Manual Allied Health, Policy No. 36 Prefabricated Oral Appliances for Obstructive Sleep Apnea Next Review: May 2019 Last Review: April 2018 Effective: May 1, 2018 IMPORTANT REMINDER Medical
Overnight fluid shifts in subjects with and without obstructive sleep apnea
 Original Article Overnight fluid shifts in subjects with and without obstructive sleep apnea Ning Ding 1 *, Wei Lin 2 *, Xi-Long Zhang 1, Wen-Xiao Ding 1, Bing Gu 3, Bu-Qing Ni 4, Wei Zhang 4, Shi-Jiang
Original Article Overnight fluid shifts in subjects with and without obstructive sleep apnea Ning Ding 1 *, Wei Lin 2 *, Xi-Long Zhang 1, Wen-Xiao Ding 1, Bing Gu 3, Bu-Qing Ni 4, Wei Zhang 4, Shi-Jiang
Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty: A Single University Experience
 771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
771395AORXXX10.1177/0003489418771395Annals of Otology, Rhinology & LaryngologyHuntley et al research-article2018 Original Article Comparing Upper Airway Stimulation to Expansion Sphincter Pharyngoplasty:
Sleep Apnoea. The Story of a Pause
 Sleep Apnoea The Story of a Pause There is almost zero awareness in India that many amongst us maybe living with Sleep Apnoea, which left untreated could be life threatening tomorrow. This largely undiagnosed
Sleep Apnoea The Story of a Pause There is almost zero awareness in India that many amongst us maybe living with Sleep Apnoea, which left untreated could be life threatening tomorrow. This largely undiagnosed
Is CPAP helpful in severe Asthma?
 Is CPAP helpful in severe Asthma? P RAP UN KI TTIVORAVITKUL, M.D. PULMONARY AND CRITICAL CARE DIVISION DEPARTMENT OF MEDICINE, PHRAMONGKUTKLAO HOSPITAL Outlines o Obstructive sleep apnea syndrome (OSAS)
Is CPAP helpful in severe Asthma? P RAP UN KI TTIVORAVITKUL, M.D. PULMONARY AND CRITICAL CARE DIVISION DEPARTMENT OF MEDICINE, PHRAMONGKUTKLAO HOSPITAL Outlines o Obstructive sleep apnea syndrome (OSAS)
Treatment of Snoring. Useful Telephone Numbers. Information for Patients on. North Hampshire ENT Partnership Hampshire Clinic
 Useful Telephone Numbers North Hampshire ENT Partnership Hampshire Clinic - 01256 377733 The Hampshire Clinic Switchboard - 01256 357111 Lyde Ward - 01256 377773 Enbourne Ward - 01256 377772 Frimley Park
Useful Telephone Numbers North Hampshire ENT Partnership Hampshire Clinic - 01256 377733 The Hampshire Clinic Switchboard - 01256 357111 Lyde Ward - 01256 377773 Enbourne Ward - 01256 377772 Frimley Park
Nasal Evaluation & Non-surgical Nasal Therapy in SDB
 Nasal Evaluation & Non-surgical Nasal Therapy in SDB Edward M. Weaver, MD, MPH Seattle VA Medical Center University of Washington Harborview Medical Center Acknowledgments This material is the result of
Nasal Evaluation & Non-surgical Nasal Therapy in SDB Edward M. Weaver, MD, MPH Seattle VA Medical Center University of Washington Harborview Medical Center Acknowledgments This material is the result of
Pediatric Obstructive Sleep apnea An update What else is there to know?
 Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Pediatric Obstructive Sleep apnea An update What else is there to know? Garani S. Nadaraja, MD, FAAP Medical Director BCH-Oakland Clinical Assistant Professor Division of Pediatric Otolaryngology UCSF
Index SLEEP MEDICINE CLINICS. Note: Page numbers of article titles are in boldface type.
 549 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2007) 549 553 Note: Page numbers of article titles are in boldface type. A Abdominal motion, in assessment of sleep-related breathing disorders, 452 454 Adherence,
549 SLEEP MEDICINE CLINICS Sleep Med Clin 1 (2007) 549 553 Note: Page numbers of article titles are in boldface type. A Abdominal motion, in assessment of sleep-related breathing disorders, 452 454 Adherence,
Upper Airway Obstruction
 Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Obstruction Adriaan Pentz Division of Otorhinolaryngology University of Stellenbosch and Tygerberg Hospital Stridor/Stertor Auditory manifestations of disordered respiratory function ie noisy
Upper Airway Stimulation for Obstructive Sleep Apnea
 Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Upper Airway Stimulation for Obstructive Sleep Apnea Background, Mechanism and Clinical Data Overview Seth Hollen RPSGT 21 May 2016 1 Conflicts of Interest Therapy Support Specialist, Inspire Medical Systems
Lateral Pharyngoplasty Reduces Nocturnal Blood Pressure in Patients With Obstructive Sleep Apnea
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Lateral Pharyngoplasty Reduces Nocturnal Blood Pressure in Patients With Obstructive Sleep Apnea Carolina
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. Lateral Pharyngoplasty Reduces Nocturnal Blood Pressure in Patients With Obstructive Sleep Apnea Carolina
Management of OSA. saurabh maji
 Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
Management of OSA saurabh maji INTRODUCTION Obstructive sleep apnea is a major public health problem Prevalence of OSAS in INDIA is 2.4% to 4.96% in men and 1% to 2 % in women In the rest of the world
4/28/2017. Adult Obesity Rates
 Adult Obesity Rates Prevalence of Obstructive Sleep Apnea Rising prevalence of sleep apnea in U.S. threatens public health DARIEN, IL Sept. 29, 2014 Public health and safety are threatened by the increasing
Adult Obesity Rates Prevalence of Obstructive Sleep Apnea Rising prevalence of sleep apnea in U.S. threatens public health DARIEN, IL Sept. 29, 2014 Public health and safety are threatened by the increasing
Sleep Disordered Breathing
 Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Sleep Disordered Breathing SDB SDB Is an Umbrella Term for Many Disorders characterized by a lack of drive to breathe Results n repetitive pauses in breathing with no effort Occurs for a minimum of 10
Brazilian Journal of OTORHINOLARYNGOLOGY. Obstructive sleep apnea and primary snoring: diagnosis. Objective.
 Braz J Otorhinolaryngol. 2014;80(1 Supl. 1):S1-S16 Brazilian Journal of OTORHINOLARYNGOLOGY www.bjorl.org.br GUIDELINE Obstructive sleep apnea and primary snoring: diagnosis Authors Associação Brasileira
Braz J Otorhinolaryngol. 2014;80(1 Supl. 1):S1-S16 Brazilian Journal of OTORHINOLARYNGOLOGY www.bjorl.org.br GUIDELINE Obstructive sleep apnea and primary snoring: diagnosis Authors Associação Brasileira
Apnoeic and obstructive nonapnoeic sleep respiratory events
 Eur Respir J 29; 34: 156 161 DOI: 1.1183/931936.1628 CopyrightßERS Journals Ltd 29 Apnoeic and obstructive nonapnoeic sleep respiratory events J.F. Masa*, **, J. Corral*, **, J. Teran #, **, M.J. Martin*,
Eur Respir J 29; 34: 156 161 DOI: 1.1183/931936.1628 CopyrightßERS Journals Ltd 29 Apnoeic and obstructive nonapnoeic sleep respiratory events J.F. Masa*, **, J. Corral*, **, J. Teran #, **, M.J. Martin*,
Influence of upper airways section area on oxygen blood saturation level in patients with obesity and sleep apnea syndrome
 Influence of upper airways section area on oxygen blood saturation level in patients with obesity and sleep apnea syndrome Poster No.: P-0028 Congress: ESCR 2015 Type: Scientific Poster Authors: E. Butorova,
Influence of upper airways section area on oxygen blood saturation level in patients with obesity and sleep apnea syndrome Poster No.: P-0028 Congress: ESCR 2015 Type: Scientific Poster Authors: E. Butorova,
Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions
 Jeff Rouse, DDS Txacad@aol.com 555 E. Basse #200 www.coredentistry.com San Antonio, TX 78209 210-828-3334 Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions CORE Concept Wear and
Jeff Rouse, DDS Txacad@aol.com 555 E. Basse #200 www.coredentistry.com San Antonio, TX 78209 210-828-3334 Bruxism: Revisiting an Old Problem with New Questions and Unique Solutions CORE Concept Wear and
Persistent Obstructive Sleep Apnea After Tonsillectomy. Learning Objectives. Mary Frances Musso, DO Pediatric Otolaryngology
 Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Persistent Obstructive Sleep Apnea After Tonsillectomy Mary Frances Musso, DO Pediatric Otolaryngology Learning Objectives Recognize indications for tonsillectomy List patients at risk for persistent OSA
Web-Based Home Sleep Testing
 Editorial Web-Based Home Sleep Testing Authors: Matthew Tarler, Ph.D., Sarah Weimer, Craig Frederick, Michael Papsidero M.D., Hani Kayyali Abstract: Study Objective: To assess the feasibility and accuracy
Editorial Web-Based Home Sleep Testing Authors: Matthew Tarler, Ph.D., Sarah Weimer, Craig Frederick, Michael Papsidero M.D., Hani Kayyali Abstract: Study Objective: To assess the feasibility and accuracy
Sleep Medicine. Paul Fredrickson, MD Director. Mayo Sleep Center Jacksonville, Florida.
 Sleep Medicine Paul Fredrickson, MD Director Mayo Sleep Center Jacksonville, Florida Fredrickson.Paul@mayo.edu DISCLOSURES No relevant conflicts to report. Obstructive Sleep Apnea The most common sleep
Sleep Medicine Paul Fredrickson, MD Director Mayo Sleep Center Jacksonville, Florida Fredrickson.Paul@mayo.edu DISCLOSURES No relevant conflicts to report. Obstructive Sleep Apnea The most common sleep
Tired of being tired?
 Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
Tired of being tired? Narval CC MRD ResMed.com/Narval Sleepiness and snoring are possible symptoms of sleep apnea. Did you know that one in every four adults has some form of sleep disordered-breathing
Questions: What tests are available to diagnose sleep disordered breathing? How do you calculate overall AHI vs obstructive AHI?
 Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Pediatric Obstructive Sleep Apnea Case Study : Margaret-Ann Carno PhD, CPNP, D,ABSM for the Sleep Education for Pulmonary Fellows and Practitioners, SRN ATS Committee April 2014. Facilitator s guide Part
Obstructive Sleep Apnea Syndrome
 SMGr up Obstructive Sleep Apnea Syndrome Alper Dilci, Handan Koyuncu and Vural Fidan* Otorhinolaryngology Department, Yunus Emre Government Hospital, Turkey *Corresponding author: Vural Fidan, Otorhinolaryngology
SMGr up Obstructive Sleep Apnea Syndrome Alper Dilci, Handan Koyuncu and Vural Fidan* Otorhinolaryngology Department, Yunus Emre Government Hospital, Turkey *Corresponding author: Vural Fidan, Otorhinolaryngology
THE PATIENT STRONGLY MOTIVATED TOWARDS THE TREATMENT? & ENT
 SNORING & OSAHS SURGERY International Workshop Preoperative Diagnostic Protocol < 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B.
SNORING & OSAHS SURGERY International Workshop Preoperative Diagnostic Protocol < 15 min Filippo Montevecchi M.D. Department of Special Surgery Head & Neck Surgery, Oral Surgery Unit (Head: C.Vicini) G.B.
Does AHI Value Enough for Evaluating the Obstructive Sleep Apnea Severity?
 DOI 10.1007/s12070-014-0722-6 ORIGINAL ARTICLE Does AHI Value Enough for Evaluating the Obstructive Sleep Apnea Severity? Yusuf Dündar Güleser Saylam Emel Çadallı Tatar Ali Özdek Hakan Korkmaz Hikmet Fırat
DOI 10.1007/s12070-014-0722-6 ORIGINAL ARTICLE Does AHI Value Enough for Evaluating the Obstructive Sleep Apnea Severity? Yusuf Dündar Güleser Saylam Emel Çadallı Tatar Ali Özdek Hakan Korkmaz Hikmet Fırat
Κλινικό Φροντιστήριο Αναγνώριση και καταγραφή αναπνευστικών επεισοδίων Λυκούργος Κολιλέκας Επιμελητής A ΕΣΥ 7η Πνευμονολογική Κλινική ΝΝΘΑ Η ΣΩΤΗΡΙΑ
 Κλινικό Φροντιστήριο Αναγνώριση και καταγραφή αναπνευστικών επεισοδίων Λυκούργος Κολιλέκας Επιμελητής A ΕΣΥ 7 η Πνευμονολογική Κλινική ΝΝΘΑ Η ΣΩΤΗΡΙΑ SCORING SLEEP -Rechtschaffen and Kales (1968) - AASM
Κλινικό Φροντιστήριο Αναγνώριση και καταγραφή αναπνευστικών επεισοδίων Λυκούργος Κολιλέκας Επιμελητής A ΕΣΥ 7 η Πνευμονολογική Κλινική ΝΝΘΑ Η ΣΩΤΗΡΙΑ SCORING SLEEP -Rechtschaffen and Kales (1968) - AASM
Pediatric Obstructive Sleep Apnea: A Short Review of Clinical Aspects
 Review Article Pediatric Obstructive Sleep Apnea: A Short Review of Clinical Aspects Christian Guilleminault 1, Yu Shu Huang 2 1 Division of Sleep Medicine, Stanford University, Redwood City, CA, USA,
Review Article Pediatric Obstructive Sleep Apnea: A Short Review of Clinical Aspects Christian Guilleminault 1, Yu Shu Huang 2 1 Division of Sleep Medicine, Stanford University, Redwood City, CA, USA,
Snoring And Sleep Apnea in the U.S. Definitions Apnea: Cessation of ventilation for > 10 seconds. Defining Severity of OSA
 Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
Snoring and Obstructive Sleep Apnea: Oral Appliance Therapy Management Midwest Society of Orthodontists October 16-17, 2009 Anthony J DiAngelis DMD, MPH Chief, Department of Dentistry, HCMC Professor,
Obstructive sleep apnoea How to identify?
 Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
Obstructive sleep apnoea How to identify? Walter McNicholas MD Newman Professor in Medicine, St. Vincent s University Hospital, University College Dublin, Ireland. Potential conflict of interest None Obstructive
Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease
 1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
1 Sleep and the Heart Reversing the Effects of Sleep Apnea to Better Manage Heart Disease Rami Khayat, MD Professor of Internal Medicine Director, OSU Sleep Heart Program Medical Director, Department of
PedsCases Podcast Scripts
 PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Obstructive Sleep Apnea These podcasts are designed to give medical students an overview of key topics in pediatrics.
PedsCases Podcast Scripts This is a text version of a podcast from Pedscases.com on Obstructive Sleep Apnea These podcasts are designed to give medical students an overview of key topics in pediatrics.
Sleep Apnea: Diagnosis & Treatment
 Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
Disclosure Sleep Apnea: Diagnosis & Treatment Lawrence J. Epstein, MD Sleep HealthCenters Harvard Medical School Chief Medical Officer for Sleep HealthCenters Sleep medicine specialty practice group Consultant
Effect of Smoking on Parameters of Polysomnography
 Original Research Effect of Smoking on Parameters of Polysomnography Amir Houshang Mehrparvar 1, Masoud Rahimian 2, Mahmoud Vakili 3, Behrouz Moghbelolhossain 1 *, Mohammad Javad Zare-Sakhvidi 4, Mojahedeh
Original Research Effect of Smoking on Parameters of Polysomnography Amir Houshang Mehrparvar 1, Masoud Rahimian 2, Mahmoud Vakili 3, Behrouz Moghbelolhossain 1 *, Mohammad Javad Zare-Sakhvidi 4, Mojahedeh
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea
 Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
Positive Airway Pressure and Oral Devices for the Treatment of Obstructive Sleep Apnea Policy Number: Original Effective Date: MM.01.009 11/01/2009 Line(s) of Business: Current Effective Date: HMO; PPO
Sleep-disordered breathing is a widespread disease 1. Breath-to-Breath Variability Correlates With Apnea-Hypopnea Index in Obstructive Sleep Apnea*
 Breath-to-Breath Variability Correlates With Apnea-Hypopnea Index in Obstructive Sleep Apnea* Peter Kowallik, MD; Ilka Jacobi, MD; Alexander Jirmann, MD; Malte Meesmann, MD; Michael Schmidt, MD; and Hubert
Breath-to-Breath Variability Correlates With Apnea-Hypopnea Index in Obstructive Sleep Apnea* Peter Kowallik, MD; Ilka Jacobi, MD; Alexander Jirmann, MD; Malte Meesmann, MD; Michael Schmidt, MD; and Hubert
Airway and Airflow Characteristics In OSAS
 Airway and Airflow Characteristics In OSAS 16 th Annual Advances in Diagnostics and Treatment of Sleep Apnea and Snoring February 12-13, 2010 San Francisco, CA Nelson B. Powell M.D., D.D.S. Adjunct Clinical
Airway and Airflow Characteristics In OSAS 16 th Annual Advances in Diagnostics and Treatment of Sleep Apnea and Snoring February 12-13, 2010 San Francisco, CA Nelson B. Powell M.D., D.D.S. Adjunct Clinical
The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery
 432 Original Research THIEME The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery Francesco Lorusso 1 Francesco Dispenza 1 Domenico Michele Modica
432 Original Research THIEME The Role of Modified Expansion Sphincter Pharyngoplasty in Multilevel Obstructive Sleep Apnea Syndrome Surgery Francesco Lorusso 1 Francesco Dispenza 1 Domenico Michele Modica
in China Shanghai Office Beijing Office (+86) (+86)
 SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
SLEEP Apnea in China Guide 2018-2019 Shanghai Office (+86) 21 2426 6400 Beijing Office (+86) 010 6464 0611 www.pacificprime.cn Follow us on WeChat t A comprehensive overview of sleep apnea Perhaps you
A new beginning in therapy for women
 A new beginning in therapy for women OSA in women Tailored solutions for Her AutoSet for Her algorithm ResMed.com Women and OSA OSA has traditionally been considered to be a male disease. However, recent
A new beginning in therapy for women OSA in women Tailored solutions for Her AutoSet for Her algorithm ResMed.com Women and OSA OSA has traditionally been considered to be a male disease. However, recent
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI
 DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
DOWNLOAD OR READ : TREATMENT FOR SNORING PROBLEMS PDF EBOOK EPUB MOBI Page 1 Page 2 treatment for snoring problems treatment for snoring problems pdf treatment for snoring problems problem, presenting
Efremidis George, Varela Katerina, Spyropoulou Maria, Beroukas Lambros, Nikoloutsou Konstantina, and Georgopoulos Dimitrios
 Sleep Disorders Volume 2012, Article ID 324635, 5 pages doi:10.1155/2012/324635 Clinical Study Clinical Features and Polysomnographic Findings in Greek Male Patients with Obstructive Sleep Apnea Syndrome:
Sleep Disorders Volume 2012, Article ID 324635, 5 pages doi:10.1155/2012/324635 Clinical Study Clinical Features and Polysomnographic Findings in Greek Male Patients with Obstructive Sleep Apnea Syndrome:
Sleep Apnea. What is sleep apnea? How does it occur? What are the symptoms?
 What is sleep apnea? Sleep Apnea Sleep apnea is a serious sleep problem. If you have it, you stop breathing for more than 10 seconds at a time many times while you sleep. Another term for this problem
What is sleep apnea? Sleep Apnea Sleep apnea is a serious sleep problem. If you have it, you stop breathing for more than 10 seconds at a time many times while you sleep. Another term for this problem
Step (2) Looked for correlations between baseline surrogates and postoperative AHI.
 Development of the PSG PLUS PHYIOLOGY model Step (1) Picked possible surrogates of the physiological traits (See Table 1 in the main text). Step (2) Looked for correlations between baseline surrogates
Development of the PSG PLUS PHYIOLOGY model Step (1) Picked possible surrogates of the physiological traits (See Table 1 in the main text). Step (2) Looked for correlations between baseline surrogates
Research Article Predictors of Nasal Obstruction: Quantification and Assessment Using Multiple Grading Scales
 Plastic Surgery International Volume 2016, Article ID 6945297, 9 pages http://dx.doi.org/10.1155/2016/6945297 Research Article Predictors of Nasal Obstruction: Quantification and Assessment Using Multiple
Plastic Surgery International Volume 2016, Article ID 6945297, 9 pages http://dx.doi.org/10.1155/2016/6945297 Research Article Predictors of Nasal Obstruction: Quantification and Assessment Using Multiple
Detection of Increased Upper Airway Resistance During Overnight Polysomnography
 Sleep Disordered 245.qxp 12/30/2004 8:49 AM Page 85 Detection of Increased Upper Airway Resistance During Overnight Polysomnography Pamela L Johnson, MSc 1 ; Natalie Edwards, PhD 1 ; Keith R Burgess, PhD
Sleep Disordered 245.qxp 12/30/2004 8:49 AM Page 85 Detection of Increased Upper Airway Resistance During Overnight Polysomnography Pamela L Johnson, MSc 1 ; Natalie Edwards, PhD 1 ; Keith R Burgess, PhD
Obstructive Sleep Apnea in Truck Drivers
 Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Rocky Mountain Academy of Occupational and Environmental Medicine Denver, Colorado February 6, 2010 Obstructive Sleep Apnea in Truck Drivers Philip D. Parks, MD, MPH, MOccH Medical Director, Lifespan Health
Home Video to Assess the Snoring Child
 Home Video to Assess the Snoring Child Federico Murillo-González Consider the following case: a 5 year-old child who snores and constantly wakesup every night, breathes through the mouth during the day,
Home Video to Assess the Snoring Child Federico Murillo-González Consider the following case: a 5 year-old child who snores and constantly wakesup every night, breathes through the mouth during the day,
The Ear, Nose and Throat in MPS
 The Ear, Nose and Throat in MPS Annerose Keilmann Voice Care Center Bad Rappenau, Germany Preciptorship program on MPS Wiesbaden, November 2 nd 2015 Alterations of the outer and middle ear in MPS I narrowing
The Ear, Nose and Throat in MPS Annerose Keilmann Voice Care Center Bad Rappenau, Germany Preciptorship program on MPS Wiesbaden, November 2 nd 2015 Alterations of the outer and middle ear in MPS I narrowing
Effects of Zolpidem CR on Sleep and Nocturnal Ventilation in Patients with Heart Failure
 pii: sp-00527-15 http://dx.doi.org/10.5665/sleep.6006 SLEEP-DISORDERED BREATHING Effects of Zolpidem CR on Sleep and Nocturnal Ventilation in Patients with Heart Failure Rodrigo C. Gatti 1 ; Patrick R.
pii: sp-00527-15 http://dx.doi.org/10.5665/sleep.6006 SLEEP-DISORDERED BREATHING Effects of Zolpidem CR on Sleep and Nocturnal Ventilation in Patients with Heart Failure Rodrigo C. Gatti 1 ; Patrick R.
A First Line Treatment for Sleep Disordered Breathing
 A First Line Treatment for Sleep Disordered Breathing Sleep Disordered Breathing Snoring & Obstructive Sleep Apnoea Snoring and Obstructive Sleep Apnoea (OSA) are caused by the airway narrowing or even
A First Line Treatment for Sleep Disordered Breathing Sleep Disordered Breathing Snoring & Obstructive Sleep Apnoea Snoring and Obstructive Sleep Apnoea (OSA) are caused by the airway narrowing or even
