A National Blueprint for Disseminating and Implementing Evidence-Based Clinical and Community Strategies to Promote Tobacco-Use Cessation
|
|
|
- Marylou Gilbert
- 6 years ago
- Views:
Transcription
1 A National Blueprint for Disseminating and Implementing Evidence-Based Clinical and Community Strategies to Promote Tobacco-Use Cessation September 2002 Final Draft Document 1
2 A National Blueprint for Disseminating and Implementing Evidence-Based Clinical and Community Strategies to Promote Tobacco-Use Cessation September 2002 Goal The goal of this blueprint is to provide those interested in promoting tobacco-use cessation with objectives and strategies that will improve health and reduce tobaccorelated illness and death by implementing evidence-based clinical and community recommendations shown to be effective. Background Tobacco dependence is a chronic disease and treatment will require a commitment by a variety of groups and organizations, including but not limited to: clinicians, clinics, health systems, policymakers, insurers, health care purchasers, researchers, healthfunding organizations, consumers, and community leaders. In November 2000, the U.S. Department of Health and Human Services (DHHS) published the national health objectives for the year Healthy People 2010 (DHHS, 2000). There are 21 national health objectives related to tobacco use, covering tobacco use in population groups, cessation and treatment, exposure to secondhand smoke, and social and environmental changes. In addition, Healthy People 2010 has identified that reducing tobacco use is one of the 10 Leading Health Indicators for the Nation with a goal to improve the health of the U.S. population by reducing cigarette smoking by adults from 24 percent to 12 percent by Cessation efforts are an important part of a comprehensive approach to tobacco control. To reduce mortality related to tobacco use and achieve the Healthy People 2010 goals for the Nation, it is critical to help smokers quit. These national objectives on tobacco use for 2010 are a call to action. The need to increase cessation activities to accomplish these objectives has been supported by findings from multiple organizations: American Cancer Society (Byers et al., 1999) found that reducing cancer incidence by 25 percent and cancer mortality by 50 percent by the year 2015 would require redoubling efforts to reduce smoking and other known cancer risk factors by 2005; 2
3 Centers for Disease Control and Prevention (CDC, 1994) found that nearly 70 percent of smokers want to quit smoking; and Committee on Clinical Preventive Services Priorities (Coffield et al., 2001) found that tobacco cessation counseling was the highest-ranked preventive service for adults with the lowest delivery rate by clinicians. The likelihood of increasing cessation success has been improved by the recent publication of two sets of guidelines developed by DHHS that provide a roadmap of evidence-based strategies for tobacco cessation: 1. Treating Tobacco Use and Dependence. Clinical Practice Guideline, published by the U.S. Department of Health and Human Services, Public Health Service (Fiore et al., 2000). 2. Strategies for Reducing Exposure to Environmental Tobacco Smoke, Increasing Tobacco-Use Cessation, and Reducing Initiation in Communities and Health-Care Systems. A Report on Recommendations of the Task Force on Community Preventive Services, U.S. Department of Health and Human Services, Centers for Disease Control and Prevention (CDC, 2000). Each of these guidelines identifies effective cessation interventions and makes specific recommendations on how to use them. A remaining challenge is to promote the diffusion, dissemination, and implementation 1 of these recommendations and promote interventions that: encourage current tobacco users to quit; support individuals trying to quit; and protect from relapse individuals who have quit using tobacco. If the evidencebased recommendations in these guidelines are implemented widely, significant progress will be made towards a healthier future. Recognizing the unequal burden of tobacco-related diseases, particularly among low income and underserved populations, the blueprint goals and objectives encompass the overarching priority of eliminating smoking-related health disparities. Purpose The blueprint has been developed as a consensus document to: Help health plans and tobacco-use cessation programs build the strongest possible multilevel efforts to support cessation; Reflect common goals and objectives among concerned national, state, and local organizations and individuals that fund or support such efforts; and 1 In this document, diffusion is defined as a passive, unplanned spread of new ideas; dissemination is defined as a planned and active approach to the diffusion of new ideas; and implementation means putting the ideas that are diffused and disseminated into practice (Rogers, 1995). 3
4 Mobilize and guide concerted, coordinated action for funding and other activities related to tobacco-use cessation. The audience for this Blueprint is any individual, organization, or entity that seeks guidance on how to implement evidence-based tobacco-use cessation recommendations. The following agencies and organizations worked together to develop this blueprint: Agency for Healthcare Research and Quality American Cancer Society American Legacy Foundation Centers for Disease Control and Prevention Center for Medicare and Medicaid Services Health Resources and Services Administration National Cancer Institute National Heart Lung and Blood Institute The Robert Wood Johnson Foundation Substance Abuse and Mental Health Services Administration The agencies and organizations expect that additional partners will help implement these strategies and that the cessation collaboration will serve as a model in other areas of tobacco control, such as tobacco-use initiation and environmental tobacco smoke, and that these activities will be coordinated with other cessation activities, especially those outlined in the Youth Tobacco Cessation Collaborative s National Blueprint for Action and those planned by The National Partnership to Help Pregnant Smokers Quit. In addition, draft blueprint objectives were shared with tobacco control stakeholders, researchers, advocates, and clinicians through a concept mapping process (Trochim, 1989). This process solicited and ranked strategies to achieve the blueprint goals and objectives. Additional comments were also sought and obtained from individuals and organizations committed to tobacco dependence treatments. Guiding Principles Six key principles guide this national blueprint: 1. The blueprint uses the best scientific evidence currently available on clinical and community strategies to increase tobacco-use cessation in the United States. The knowledge bases for this blueprint are recommendations provided in the two DHHS guidelines. The guidelines represent the best currently available evidence. In the absence of specific findings for particular populations or settings, systems and clinicians are urged to incorporate the general guidelines recommendations as they develop population or setting-specific tools, strategies, and practices. Moreover, within this blueprint, clinicians is intended to include, but not be limited to, 4
5 physicians, nurses, psychologists, physical, occupational and respiratory therapists, substance abuse counselors, social workers, and other allied health professionals. Health care systems is intended to include, but not be limited to, clinics, hospitals, health care purchasers, community health programs, substance abuse treatment programs, and mental health delivery systems. The blueprint will evolve as the guidelines are updated and as blueprint outcomes are reassessed. 2. Coordinated efforts of multiple parties (public and private) will be needed to reach the blueprint s goal and objectives. The agencies and organizations that developed this blueprint are committed to working together and inviting others to join them. Successful implementation of the blueprint will necessitate engaging other stakeholders including, but not limited to: clinicians and clinic staff, health care systems, employers, health care purchasers, insurers, community leaders, policymakers, and consumers. Each partner should invest time and resources to implement the tobacco-use cessation strategies outlined in this blueprint. 3. Reaching the blueprint goal will require eliminating barriers and facilitating changes. Evidence suggests that individuals and systems fail to adopt recommendations due to internal and external barriers such as lack of awareness, fear of inefficacy, failure to identify sources of community and systematic support, a belief that the recommendations are not relevant, lack of time, and lack of funding (Cabana et al., 1999). To facilitate change, barriers relevant to the specific person or system must be identified, and appropriate strategies must be crafted to eliminate them. Success will require capitalizing on the demand that already exists for tobacco-use cessation interventions. Moreover, both individual behavior changes and system changes must be addressed through effective, multi-component strategies that are sustained over time. These changes should include addressing consumer barriers including social, cultural, and system characteristics that lead to health disparities. Finally, to best achieve the desired changes, strategies must be coordinated. 4. The best available dissemination techniques should be used to successfully implement the blueprint strategies. Implementing the blueprint s evidence-based tobacco-use cessation strategies will require understanding dissemination theory and science. Whenever possible this theory will guide efforts to refine and implement the strategies. For example: A review of efforts to disseminate clinical guidelines suggests that implementation is more likely to occur if messages are integrated and delivered at multiple times and in multiple ways (Davis and Taylor-Vaisey, 1997). 5
6 Strategies that have been shown to be consistently effective include two or more elements such as education, feedback, reminders (manual or computerized), local consensus processes, and marketing (Bero et al., 1998). Implementors should seek evidence of effectiveness of particular dissemination strategies or models, borrowing when necessary from a variety of disciplines including organizational theory, communication science, health services research, and policy research. 5. Implementation must be evaluated to ensure that blueprint objectives are met. Two types of evaluation are needed: evaluation of individually implemented blueprint strategies and evaluation of progress towards objectives. Program evaluation and evaluation research, where appropriate, should encompass standards of utility, feasibility, accuracy, and propriety. 6. Research to identify more effective tobacco-use cessation interventions, and methods for disseminating them, should be supported. This blueprint is based on the best scientific evidence currently available, but it will evolve with continued research. The collaborators should seek to increase the knowledge base of both tobacco-use cessation interventions and effective dissemination methods. Research to increase understanding of consumers (e.g., smokers and ex-smokers) and identify consumer preferences, needs and interests related to cessation is essential. In addition, research is needed on: the development of innovative interventions; how to best implement tobacco-use cessation interventions with underserved populations; and new ways to combine effective intervention components. Specific areas for future research are identified in the Public Health Service Clinical Practice Guideline Treating Tobacco Use and Dependence and the Report on Recommendations of the Task Force on Community Preventive Services Strategies for Reducing Exposure to Environmental Tobacco Smoke, Increasing Tobacco-Use Cessation, and Reducing Initiation in Communities and Health-Care Systems. Objectives and Strategies To guide dissemination and implementation and to facilitate evaluation, the blueprint has established a series of objectives and strategies for the year 2005 for four areas: 1. Clinicians 2. Systems 3. Consumers/Tobacco Users 4. Communities 6
7 When numerical objectives are used in the blueprint, the intent is to double the current state by the year 2005 to create sufficient change in order to achieve the Healthy People 2010 objectives. 7
8 Objectives and Clinicians Objective 1: Increase the utilization of the 5 A s (Ask, Advise, Assess, Assist, and Arrange) for treating tobacco dependence as defined in the U.S. Public Health Service (PHS) Clinical Practice Guideline (Fiore et al., 2000). Specifically: Increase to 100 percent the proportion of patients who are asked about their tobaccouse status and have it documented at every clinic visit. Increase to 90 percent the proportion of tobacco-using patients who are advised to quit and who are assessed for readiness to quit at every clinic visit. Increase to 75 percent the proportion of tobacco-using patients willing to make a quit attempt who are assisted (including counseling and medication) with that effort. Increase to 50 percent the proportion of tobacco-using patients attempting to quit for whom followup contact is arranged. Promote the implementation of clinical practices (inpatient and outpatient) that support and provide tobacco-use treatment. Promote the adoption of evidence-based reminder systems within clinical settings (inpatient and outpatient). Obtain buy-in from systems and insurers and their quality control organizations to encourage/support clinician or intake personnel identification of tobacco use. Promote curriculum changes in health care professional schools to provide clinicians-in-training with the skills necessary to deliver evidence-based tobacco dependence treatments. In combination with systems changes (such as reminder systems), provide and promote continuing educational programs to ensure that clinicians have the skills necessary to deliver and promote evidence-based tobacco dependence treatments. Provide clinician education on and promote the clinical use of appropriate tobacco dependence treatment and billing codes. Encourage clinicians to develop, within their clinical settings (inpatient and outpatient), systems that prompt and facilitate guidelines-based treatments for tobacco dependence at every patient visit. 8
9 Encourage clinicians to work collaboratively within the clinical setting (inpatient and outpatient) and across disciplines to coordinate the delivery of tobacco dependence treatments for smokers. Develop and disseminate evaluation measures to assess clinician provision of PHS recommended advice and assistance. Integrate clinical cessation services with community resources. Objective 2: Increase the use of evidence-based tobacco dependence counseling and medication in multiple settings. Specifically: Increase to 75 percent the proportion of clinical settings (inpatient and outpatient) that provide brief and comprehensive tobacco dependence counseling and medication. Work with publicly and privately funded entities to encourage the use of evidence-based tobacco dependence treatment tools and services as a part of routine care for those applying for funding to provide clinical services. Encourage publicly and privately funded clinical settings (inpatient and outpatient) to document the use of evidence-based cessation practices through quality evaluation techniques. Include tobacco dependence treatment as a performance measure (e.g., credentialing and accrediting) in clinical settings (inpatient and outpatient). Encourage clinicians to implement best practices by promoting achievable benchmarks for tobacco dependence treatment. Objective 3: Increase research into clinical strategies for treating tobacco dependence. Important topics of research include: Improving the effectiveness of current clinical treatment. Developing more effective clinical treatments for tobacco dependence. Promote requests for proposals and program announcements for research into improving current treatments for tobacco use, developing more effective treatments for tobacco use, and developing effective treatments for youth and special populations. 9
10 Promote requests for proposals and program demonstrations for research about cessation interventions in various clinical and nontraditional settings. Promote research to evaluate both the efficacy and effectiveness of interventions. Promote research into the cost-effectiveness of tobacco treatment implementation in a variety of settings. 10
11 Objectives and Systems Objective 1: Integrate evidence-based tobacco-use treatments into the regular health care delivery systems for all patients. Increase the use of reminder systems to identify and document tobacco use status for all patients at every clinic visit (except for adults who have never used tobacco or have not used tobacco for many years). Meet with leadership of large health care delivery systems to obtain buy-in and promote the use of reminder systems in clinical settings (inpatient and outpatient). Develop and disseminate effective models for integrating reminder systems into diverse health care systems. Provide mechanisms for skill building and sharing of information about integrating reminder systems into diverse health care systems. Promote the establishment of reminder systems in clinical settings (inpatient and outpatient) by obtaining buy-in from accrediting organizations (such as Joint Commission on Accreditation of Healthcare Organizations [JCAHO], National Committee for Quality Assurance [NCQA]), health care purchasers, and insurers. Increase to 75 percent the proportion of health care settings that provide evidencebased treatments for their patients who use tobacco. Develop and disseminate successful models and tools to create systems-level changes (such as best practice models including utilization of diverse staff for tobacco dependence treatments, provider feedback). Promote technical assistance to help managed care organizations implement systems changes to promote effective tobacco dependence treatment strategies (e.g., reimbursement, reminder systems, and the collection and dissemination of tobacco-related cost data). Implement an expanded measure to evaluate the provision of tobacco dependence treatments, including counseling and medication, delivered in the health care systems (e.g., NCQA sponsored Health Plan Employer Data and Information Set [HEDIS]). 11
12 Promote clinician reimbursement for the delivery of evidence-based tobacco dependence treatments and the inclusion of these treatments among the defined duties of clinicians in the following ways: Meet with leadership of large health care delivery systems to promote clinician reimbursement for tobacco dependence treatments. Disseminate successful models for clinician reimbursement. Provide mechanisms for skill building and sharing of ideas. Promote policies for inpatient and outpatient clinical settings that support and provide tobacco dependence treatments for all patients. Develop and disseminate successful models and tools for systems to promote the delivery of tobacco dependence treatments (e.g., using appropriate tobacco dependence treatment and billing codes on forms, entering them into administrative databases, and providing staff training). Develop and disseminate successful models for promoting tobacco dependence treatment policies in diverse health care systems. Collaborate with health professional organizations and academies to obtain their endorsement of evidence-based tobacco dependence treatments. Objective 2: Increase the proportion of health care delivery systems that make evidence-based tobacco dependence treatments delivered through multiple formats (individual, group, telephone-based counseling) readily available. Develop and disseminate models for promoting the use of multiple formats of delivering tobacco dependence treatments in various health care systems. Work to ensure that funding for tobacco dependence treatments in health care systems includes treatments delivered through a variety of evidence-based formats. Objective 3: Effectively integrate clinical tobacco dependence treatments with State and local cessation resources (e.g., quitlines, media campaigns, worksites). 12
13 Strategy: Develop and disseminate successful models for the integration of clinical tobacco dependence treatments and community resources, including quitlines. Objective 4: Decrease out-of-pocket costs for evidence-based tobacco dependence treatments (counseling and medication) for the insured and uninsured. Promote coverage of evidence-based tobacco dependence treatments in the private sector through the development and dissemination of successful models of coverage by working with professional organizations, trade organizations, labor unions, insurers, health care purchasers, and business coalitions. Promote coverage of evidence-based tobacco dependence treatments in the public sector through information sharing among systems and the development and dissemination of successful models of coverage. Promote the delivery of evidence-based tobacco dependence treatments for the uninsured and underinsured through innovative programs (e.g., quitlines, special funds, and grants). Promote models and strategies used by successful implementors in the private and public sectors. Identify key opinion leaders/stakeholders to work to obtain buy-in and promote comprehensive coverage for tobacco dependence treatments within the managed care, indemnity, Federal, and State health care systems. Monitor trends in the level of coverage for services nationwide. Develop and disseminate successful models to educate providers, purchasers, and consumers about the coverage options available to them. Objective 5: Increase research into systems strategies for treating tobacco dependence. Important topics of research include: Dissemination and implementation of evidence-based tobacco dependence treatments into health care delivery systems. Innovative evidence-based system strategies that promote the universal availability and utilization of tobacco dependence treatments. 13
14 Identification of systems and organizations that may promote the availability and utilization of tobacco dependence treatments to the uninsured. Impact of integrating multiple cessation services. Understanding the effects of individual system interventions. Promote requests for proposals and program announcements for research about insurance coverage for treating tobacco dependence and its impact on cessation and the impact of cessation on health care utilization. Promote requests for proposals and program announcements for research about clinician reimbursement for the delivery of tobacco dependence treatments and its impact on cessation. Promote requests for proposals and program announcements for research about consumer utilization of insurance coverage for tobacco dependence treatments. Promote research with and within State, community, and other systems to determine effective strategies for the dissemination, coverage, and implementation of tobacco dependence treatments. Promote research with and within the business community to determine the most effective strategies for dissemination and implementation of smoking cessation coverage for tobacco dependence treatments and the utilization of provided coverage/benefits. 14
15 Objectives and Consumers/Tobacco Users Objective 1: Increase to 40 percent annually the proportion of smokers who use evidence-based techniques while making a serious 2 quit attempt. Promote the use of evidence-based communication interventions (e.g., media campaigns proven to be effective in increasing consumer demand for evidencebased cessation) to increase smokers' motivation and self-efficacy related to quitting and to increase awareness of what products, techniques, and services have been shown to be effective or ineffective. Provide information about accessing effective methods. Motivate smokers who are willing to quit to ask their health care providers (and clinic, health care plan, employer/union benefits managers) for proven cessation services and benefits. Involve smokers/ex-smokers (including demographically and culturally diverse populations) in the design/redesign of cessation products and services to make them more acceptable and effective. Objective 2. Increase to 10 percent annually the number of smokers who are trying to quit who stay abstinent for a full year or longer. Increase the use of evidence-based cessation techniques proven to result in sustained cessation. See Objective 1 above. Work with health care systems to provide ongoing support for relapse prevention. Work to identify and implement policy and environmental changes that will support individuals in their cessation attempts. Related strategies can be found under Objectives and Communities. 2 Serious is defined as quitting for 24 hours or more. 15
16 Objective 3: Increase research into strategies for promoting tobacco-use cessation among consumers. Promote research that will: Support market analysis and evaluation to increase understanding of what creates barriers to seeking and using cessation services, how to empower smokers to seek proven cessation services and benefits (including destigmatizing cessation services), and how to develop culturally and linguistically appropriate strategies and materials. Identify ways to motivate consumers to become advocates for increasing the availability of proven cessation services and supportive policies by designing market research and exploring lessons learned from advocacy efforts in other fields, e.g., breast cancer. Consumers may include smokers, ex-smokers, victims of tobacco-caused disease, and their families. Update and refine statistical evidence of the proportion of smokers using evidence-based cessation methods. Identify and promote successful quitting maintenance/relapse prevention strategies. Identify the barriers ex-smokers encounter. These barriers may vary during different stages of maintenance and among different population groups. Explore the effectiveness of enhancing rewards and incentives for sustained abstinence, e.g., reduced insurance rates. Identify effective ways to harness the experience of ex-smokers to support smokers in their cessation attempts. Study the impact of potential reduced exposure products on cessation. 16
17 Objectives and Communities Objective 1: Objective to use evidence-based strategies to increase consumer cost consistent with Healthy People 2010 final language pending. Strategy: Evidence-based strategies to increase consumer cost consistent with Healthy People 2010 final language pending. Objective 2: Increase the proportion of States/territories implementing effective 3 mass media campaigns as part of multi-component tobacco control programs. Promote effective mass media campaigns as a component of comprehensive tobacco prevention and control programs, nationally and in States and territories. Promote the development and use of guidelines for developing effective mass media campaigns. Promote the use of mass media campaigns to increase consumer demand for evidence-based cessation resources. Identify mass media campaign models/campaign components (messages, materials, research, and evaluation reports) that have demonstrated their effectiveness in adult cessation and promote their use by States and territories. Promote mechanisms for counteradvertising campaign managers to build skills and share information. Promote the development and dissemination of standard evaluation measures for assessing media campaigns. 3 Effective is defined as paid counteradvertising campaigns that utilize messages developed through formative research and are sufficient in reach, frequency, and duration (6 months or longer). 17
18 Objective 3: Increase to 85 percent the proportion of the U.S. population having access to effective 4 telephone support (quitlines) for tobacco cessation. Identify models of effective quitlines and promote their use by States. Encourage quitline managers to incorporate evidence-based strategies into their initiatives. Promote the development, operation, and marketing of quitlines so that they are widely accessible across all socioeconomic, racial/ethnic, gender, disability and geographic groups. Promote the development of effective strategies for integrating quitline activities with other clinical and community tobacco dependence treatment initiatives. Promote the development and implementation of effective strategies to increase quitline use, particularly among States with existing quitlines. Encourage public/private partnerships to provide quitline access to residents of States that currently do not have quitline service. Promote the development and dissemination of standard evaluation measures for quitlines. Promote the evaluation of the effectiveness of quitlines through assessment of quitline reach (extent of use by specific populations), quit rates, quality control, and coordination with media campaigns. Encourage a mechanism for skill building and information sharing among quitline managers. Objective 4: Motivate insurers, health care purchasers, and employers to cover and reimburse effective cessation services as well as reduce or eliminate patient payments for effective cessation therapies. Further the education of policymakers, opinion leaders, and other stakeholders to promote the reduction or elimination of patient payments for effective cessation therapies. 4 Effective is defined as a comprehensive pro-active telephone program that is accessible to the population and includes the provision of patient cessation materials. 18
19 Encourage dialogue between successful implementors in public and private sectors and interested public and private agencies and organizations. Promote the development and dissemination of models for quality improvement and evaluation. Promote the creation of grassroots support for reimbursement of tobacco-use treatments. Objective 5: Increase research into community strategies to promote tobacco-use cessation. Promote research that will: Explore the salience of disseminating different types of data (e.g., cost elasticity between unit price increases and consumption) to inform policymakers, opinion leaders, and other stakeholders regarding increases in tobacco prices. Explore mass media approaches to adult cessation that could be effective among culturally diverse groups, e.g., family-focused approaches. Explore the use of mass media to increase consumer demand for access to cessation resources and services. Improve the effectiveness of behavioral and other interventions, including telephone and Internet cessation support systems. Explore the effects of the dissemination of cost, cost effectiveness, and return on investment data on cessation coverage and reimbursement decisions by insurers, employers, and health care purchasers. Explore the impact that worksite/employer interventions (e.g., smoke-free workplaces, worksite cessation programs) have on promoting tobacco use cessation. 19
20 Evaluation Rationale For this blueprint to be effective, evaluation must be an integral component of any initiatives, including whether the objectives are being met. If the objectives are not being met, changes in strategies may need to be considered, such as looking at the quality and effectiveness of the dissemination components, as well as encouraging health care systems to assess traditional measures of quality in health care--structures of the health care system, processes of care, and health care outcomes--as they relate to tobacco-use cessation. The evaluation will also provide timely feedback for continuous quality improvement. This will enable the collaborators, as well as each of the partners, to assess the performance of individual programs and to evaluate the impact of the blueprint as a whole. Stakeholders should design evaluations that document the effectiveness, outcomes, impact, and cost effectiveness of the various blueprint dissemination initiatives. Guiding Principles The evaluation must be: Feasible. It should be reasonable in scope and manageable. Clear on its intended use. It is intended to judge the effectiveness of the implementation process and to improve this process, not to provide accreditation to health care systems or to serve as a regulatory body. Cost-efficient. It should capitalize on efficiencies where possible; particularly evaluation measures, systems, and tools that are already in place. Multi-component. Because of the inherent complexity of the initiatives, no single evaluation approach can suffice. The partners must use multiple approaches: quantitative and qualitative; experimental and correlational; formative and summative. The emphasis should be on developing a plan that assesses the variety of initiative activities, products, and outcomes. Collaborative. The evaluation should be collaborative and incorporate the input of varied disciplines and perspectives. Development of an evaluation should itself be considered a central component of the various initiatives, and should embody the collaborative principles that are central to the blueprint. Rigorous. The quality of evaluation measures should be carefully assessed. 20
21 Flexible. The evaluation process and tools should be dynamic, and new methods, perspectives, tools, and targets should be continually incorporated into the process, as needed, and outmoded ones must be removed. Evaluation Strategies Strategy 1. Promote the implementation of an environmental scan to identify existing evaluation activities, methods, and tools; promote the implementation of a critical appraisal to identify best practice and identify need to develop new methods/tools. Strategy 2. Promote the creation of evaluation standards for use within the collaboration and by others involved in cessation-related activities, and promote their use. Strategy 3. Promote the creation and coordination of a network linking evaluation activities (community, State, Nation). Strategy 4. Promote the creation of an evaluation feedback and analysis system to evaluate progress toward blueprint goals and objectives and periodically reassess strategies and activities, including evaluation activities. Strategy 5. Promote the development of a national data management system that brings together existing and new summative data for analysis, provides access for all stakeholders for their own use, and provides systematic feedback to cessation programs. Building and Maintaining Collaboration Guiding Principles To promote the implementation of the blueprint objectives and strategies, a tobacco cessation collaboration should be created. The collaboration will be comprised of members who are experts in evidence-based tobacco-use cessation and are committed to the dissemination of those recommendations. The four guiding principles that follow provide a basis for building and maintaining the tobacco cessation collaboration, and the process by which the members of the collaboration can work towards the blueprint goal and objectives. 1. The members will promote shared actions many partners will be needed for the blueprint to succeed, and the members should invite participation. 2. The members will invite agencies willing to invest significant efforts and resources toward implementing blueprint strategies. 3. The members will work to build channels and strategies that integrate national, State, and local initiatives and roles. 21
22 4. The members will seek to include others at national, State, and local levels to achieve the blueprint objectives through public/private partnerships. Member Roles and Responsibilities 1. Within its own organization, each member will work to develop the commitment and resources required to support selected blueprint strategies. 2. Together, the members will, within the limits of their authority, develop a coordinated implementation plan. 3. The members will seek to partner with key stakeholders to achieve goals and objectives. 4. The members will work to provide leadership to identify resources that are commensurate with a realistic and achievable dissemination effort. 5. The members will make every effort to evaluate their own efforts towards building and maintaining the collaboration, achieving the blueprint s goal and objectives, and publicizing the successes. 22
23 References Bero, LA, Grilli, R, Grimshaw, JM, et al. Getting research findings into practice: Closing the gap between research and practice: an overview of systematic reviews of interventions to promote the implementation of research findings. BMJ 1998; 317, Byers, T, Mouchawa, J, Marks, J, et al. The American Cancer Society challenge goals: How far can cancer rates decline in the U.S. by the year 2015? Cancer 1999; 86, Cabana, MD, Rand CS, Powe, NR, et al., Why don't physicians follow clinical practice guidelines? A framework for improvement, JAMA 1999; 282, Centers for Disease Control and Prevention. Health objectives for the nation cigarette smoking among adults United States, MMWR 1994; 43(50), Centers for Disease Control and Prevention. Strategies for reducing exposure to environmental tobacco smoke, increasing tobacco-use cessation, and reducing initiation in communities and health-care systems. A report on recommendations of the Task Force on Community Preventive Services. MMWR 2000; 49(RR-12); Coffield, AB, Maciosek, MV, McGinnis, JM, et al. Priorities among recommended clinical preventive services. AmJPrevMed 2001; 21, 1-9. Davis, DA, Taylor-Vaisey, A. Translating guidelines into practice: A systematic review of theoretic concepts, practical experience and research evidence in the adoption of clinical practice guidelines. CMAJ 1997; 157, Fiore, MC, Bailey, WC, Cohen, SJ, et al. Treating Tobacco Use and Dependence. Clinical Practice Guideline. Rockville, MD: U.S. Department of Health and Human Services. Public Health Service. June Rogers, EM. Diffusion of innovations (4 th ed.). New York: The Free Press, Trochim, W. An introduction to concept mapping for planning and evaluation. Evaluation and program planning 1989; 12, U.S. Department of Health and Human Services. Healthy People 2010 (2 nd ed.) With Understanding and Improving Health and Objectives for Improving Health (2 vols.). Washington, DC, November
24 Glossary i Behavioral/counseling interventions. Refers to intervention strategies that are designed to increase tobacco abstinence rates due to psychological or social support mechanisms. Clinician. A professional directly providing services. This includes, but is not limited to, physicians, nurses, psychologists, physical, occupational, and respiratory therapists, substance abuse counselors, social workers, and other allied health professionals. Concept mapping. Concept mapping is an integrative mixed methods approach to developing a conceptual framework for a specific topic. Over the Web, participants brainstorm ideas to a specific focus and subsequently sort and rate them on one or more predefined dimensions (e.g., importance, feasibility). These data are analyzed with a sequence of multivariate statistical methods, the most prominent of which are multidimensional scaling and hierarchical cluster analysis. Participants interpret the results in a structured facilitated group meeting. Diffusion. A passive, unplanned spread of new ideas. Dissemination. A planned and active approach to the diffusion of new ideas. Effective mass media campaign. Paid counteradvertising campaigns that utilize messages developed through formative research and are sufficient in reach, frequency, and duration (6 months or longer). Effective telephone support. A comprehensive pro-active telephone program that is accessible to the population and includes the provision of patient cessation materials. Evidence-based. The process of systematically finding, appraising, and using contemporaneous research findings as the foundation for clinical and community treatments and programs. Evidence-based in this document refers to recommendations in the two DHHS guidelines. Health care purchaser. A corporation, company, Government agency, or other consortium that purchases health care benefits for a group of individuals. Health care systems. This includes, but is not limited to, clinics, hospitals, health care purchasers, community health programs, substance abuse treatment programs, and mental health delivery systems. Implementation. Putting the ideas that are diffused and disseminated into practice. Mass media campaigns. Multicomponent interventions which include long duration educational efforts using broadcast and print media for brief, recurring messages to inform and to motivate tobacco users to quit. 24
25 Proactive telephone support (quitlines). Treatment initiated by a clinician who telephones and counsels the patient over the telephone. Reminder system. System efforts (such as expanded vital signs, chart stickers) to identify tobacco-using patients, to prompt clinicians to discuss tobacco use with patients, to advise patients to quit, or to assist patients with a quit attempt. Serious quit attempt. Quitting for 24 hours or more. i More expansive glossaries can be found in Treating Tobacco Use and Dependence and Strategies for Reducing Exposure to Environmental Tobacco Smoke, Increasing Tobacco-Use Cessation, and Reducing Initiation in Communities and Health-Care Systems, the guidelines upon which this blueprint is based. 25
5. Expand access to proven, effective treatments for tobacco addiction
 National Tobacco Cessation Collaborative Tobacco Cessation Priorities for the Nation Partner Activities 5. Expand access to proven, effective treatments for tobacco addiction American Academy of Family
National Tobacco Cessation Collaborative Tobacco Cessation Priorities for the Nation Partner Activities 5. Expand access to proven, effective treatments for tobacco addiction American Academy of Family
NORTH CAROLINA CARDIOVASCULAR STATE PLAN I N T R O D U C T I O N S, G O A L S, O B J E C T I V E S A N D S T R A T E G I E S
 NORTH CAROLINA CARDIOVASCULAR STATE PLAN 2011-2016 I N T R O D U C T I O N S, G O A L S, O B J E C T I V E S A N D S T R A T E G I E S PRIMARY PREVENTION OF CARDIOVASCULAR DISEASE THROUGH HEALTHY LIVING
NORTH CAROLINA CARDIOVASCULAR STATE PLAN 2011-2016 I N T R O D U C T I O N S, G O A L S, O B J E C T I V E S A N D S T R A T E G I E S PRIMARY PREVENTION OF CARDIOVASCULAR DISEASE THROUGH HEALTHY LIVING
RHODE ISLAND CANCER PREVENTION AND CONTROL
 RHODE ISLAND CANCER PREVENTION AND CONTROL 2013 2018 STRATEGIC PLAN TABLE OF CONTENTS Purpose 1 The Partnership to Reduce Cancer 3 Prevention 4 Tobacco 4 Healthy Weight 6 Nutrition 6 Physical Activity
RHODE ISLAND CANCER PREVENTION AND CONTROL 2013 2018 STRATEGIC PLAN TABLE OF CONTENTS Purpose 1 The Partnership to Reduce Cancer 3 Prevention 4 Tobacco 4 Healthy Weight 6 Nutrition 6 Physical Activity
Priority Area: 1 Access to Oral Health Care
 If you are unable to attend one of the CHARTING THE COURSE: Developing the Roadmap to Advance Oral Health in New Hampshire meetings but would like to inform the Coalition of activities and services provided
If you are unable to attend one of the CHARTING THE COURSE: Developing the Roadmap to Advance Oral Health in New Hampshire meetings but would like to inform the Coalition of activities and services provided
Over the years the harmful effects of smoking have been well documented.
 Effective Tobacco-Control Interventions and the Health-Care System s Role Over the years the harmful effects of smoking have been well documented. Although great progress has been made, a challenging struggle
Effective Tobacco-Control Interventions and the Health-Care System s Role Over the years the harmful effects of smoking have been well documented. Although great progress has been made, a challenging struggle
QUALITY IMPROVEMENT TOOLS
 QUALITY IMPROVEMENT TOOLS QUALITY IMPROVEMENT TOOLS The goal of this section is to build the capacity of quality improvement staff to implement proven strategies and techniques within their health care
QUALITY IMPROVEMENT TOOLS QUALITY IMPROVEMENT TOOLS The goal of this section is to build the capacity of quality improvement staff to implement proven strategies and techniques within their health care
North Dakota Statewide Cancer Plan Evaluation
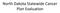 North Dakota Statewide Cancer Plan Evaluation Strategy Implementation Does your organization choose strategies to implement because they are suggested in the ND Cancer Control Plan? 72 28 Does your organization
North Dakota Statewide Cancer Plan Evaluation Strategy Implementation Does your organization choose strategies to implement because they are suggested in the ND Cancer Control Plan? 72 28 Does your organization
Centers for Disease Control and Prevention s Office on Smoking and Health
 Centers for Disease Control and Prevention s Office on Smoking and Health Tobacco use remains the leading cause of preventable death in the United States, killing more than 480,000 Americans every year,
Centers for Disease Control and Prevention s Office on Smoking and Health Tobacco use remains the leading cause of preventable death in the United States, killing more than 480,000 Americans every year,
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme
 Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Monitoring and Evaluation Framework for the Tackling Indigenous Smoking Programme 30 June 2016 Introduction... 3 Context the TIS programme... 4 2.1 TIS programme objectives... 5 2.2 The delivery of the
Washington State Collaborative Oral Health Improvement Plan
 Washington State Collaborative Oral Health Improvement Plan 2009-2014 Prioritization Criteria (non-financial): Strategic Area I: System Infrastructure (Partnerships, Funding, Technology) Goal 1: Mobilize
Washington State Collaborative Oral Health Improvement Plan 2009-2014 Prioritization Criteria (non-financial): Strategic Area I: System Infrastructure (Partnerships, Funding, Technology) Goal 1: Mobilize
The Global Network Aiming to deliver safe quality care in relation to tobacco for every service user, every time and everywhere
 The Global Network Aiming to deliver safe quality care in relation to tobacco for every service user, every time and everywhere STRATEGIC PLAN 2015 2018 Use of Terms For the purpose of Global Network the
The Global Network Aiming to deliver safe quality care in relation to tobacco for every service user, every time and everywhere STRATEGIC PLAN 2015 2018 Use of Terms For the purpose of Global Network the
Guidelines for implementation of Article 14
 Guidelines for implementation of Article 14 Demand reduction measures concerning tobacco dependence and cessation Adopted by the Conference of the Parties at its fourth session (decision FCTC/COP4(8))
Guidelines for implementation of Article 14 Demand reduction measures concerning tobacco dependence and cessation Adopted by the Conference of the Parties at its fourth session (decision FCTC/COP4(8))
Linking Public Interests to Ensure Sustainable Statewide Quitlines
 Linking Public Interests to Ensure Sustainable Statewide Quitlines Public health tobacco prevention and control programs (TCPs) find themselves working within evershifting financial and political landscapes,
Linking Public Interests to Ensure Sustainable Statewide Quitlines Public health tobacco prevention and control programs (TCPs) find themselves working within evershifting financial and political landscapes,
Building Capacity for Tobacco Dependence Treatment in Japan. Request for Proposals (RFP) - Background and Rationale
 Building Capacity for Tobacco Dependence Treatment in Japan Request for Proposals (RFP) - Background and Rationale Geographic Scope Japan Application process This application process has two steps: Letters
Building Capacity for Tobacco Dependence Treatment in Japan Request for Proposals (RFP) - Background and Rationale Geographic Scope Japan Application process This application process has two steps: Letters
TUPAC Five-Year Action Plan
 TUPAC Five-Year Action Plan 2015-2020 New Mexico Department of Health Tobacco Use Prevention and Control Program 5301 Central Avenue NE, Suite 800, Albuquerque, NM 87108 505.841.5845 nmtupac.com TUPAC
TUPAC Five-Year Action Plan 2015-2020 New Mexico Department of Health Tobacco Use Prevention and Control Program 5301 Central Avenue NE, Suite 800, Albuquerque, NM 87108 505.841.5845 nmtupac.com TUPAC
Dissemination and Implementation Research
 Dissemination and Implementation Research Catherine M. Stoney, Ph.D. National Heart, Lung, and Blood Institute March, 2013 Smoking rates in the US from 1965-2007 Smoking rates in the US from 1965-2007
Dissemination and Implementation Research Catherine M. Stoney, Ph.D. National Heart, Lung, and Blood Institute March, 2013 Smoking rates in the US from 1965-2007 Smoking rates in the US from 1965-2007
PREVENTION. Category: Initiation of Tobacco Use. Strategies to Reduce tobacco use initiation. used smokeless tobacco on one or more of the
 Goal 1: Reduce incidence and mortality from tobaccorelated cancers (lung, throat, mouth, pancreas, kidney, bladder and cervix) in all populations. Category: Initiation of Tobacco Use OBJECTIVE 1.1: By
Goal 1: Reduce incidence and mortality from tobaccorelated cancers (lung, throat, mouth, pancreas, kidney, bladder and cervix) in all populations. Category: Initiation of Tobacco Use OBJECTIVE 1.1: By
Executive Summary. Context. Guideline Origins
 Executive Summary Context In America today, tobacco stands out as the agent most responsible for avoidable illness and death. Millions of Americans consume this toxin on a daily basis. Its use brings premature
Executive Summary Context In America today, tobacco stands out as the agent most responsible for avoidable illness and death. Millions of Americans consume this toxin on a daily basis. Its use brings premature
Classes and Quitlines and Patches, Oh My! Tobacco Use Why it is Your Business. Deirdre Sullivan, Health Educator
 Classes and Quitlines and Patches, Oh My! Tobacco Use Why it is Your Business Deirdre Sullivan, Health Educator Why Tobacco? Smoking is the leading cause of preventable death and disability in the United
Classes and Quitlines and Patches, Oh My! Tobacco Use Why it is Your Business Deirdre Sullivan, Health Educator Why Tobacco? Smoking is the leading cause of preventable death and disability in the United
Guideline scope Smoking cessation interventions and services
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 Topic NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Smoking cessation interventions and services This guideline
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 Topic NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Smoking cessation interventions and services This guideline
Fax to Quit: A Model for Delivery of Tobacco Cessation Services to Wisconsin Residents
 Fax to Quit: A Model for Delivery of Tobacco Cessation Services to Wisconsin Residents Robin J. Perry, BS, CHES; Paula A. Keller, MPH; Dave Fraser, MS; Michael C. Fiore, MD, MPH ABSTRACT Research has shown
Fax to Quit: A Model for Delivery of Tobacco Cessation Services to Wisconsin Residents Robin J. Perry, BS, CHES; Paula A. Keller, MPH; Dave Fraser, MS; Michael C. Fiore, MD, MPH ABSTRACT Research has shown
Submitted to the House Energy and Commerce Committee. Federal Efforts to Combat the Opioid Crisis
 STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
STATEMENT FOR THE RECORD Submitted to the House Energy and Commerce Committee Federal Efforts to Combat the Opioid Crisis October 25, 2017 America s Health Insurance Plans 601 Pennsylvania Avenue, NW Suite
A systems approach to treating tobacco use and dependence
 A systems approach to treating tobacco use and dependence Ann Wendland, MSL Policy Analyst & Cessation Programs Manager NYSDOH Bureau of Tobacco Control ann.wendland@health.ny.gov A systems approach to
A systems approach to treating tobacco use and dependence Ann Wendland, MSL Policy Analyst & Cessation Programs Manager NYSDOH Bureau of Tobacco Control ann.wendland@health.ny.gov A systems approach to
BASIC SKILLS FOR WORKING WITH SMOKERS
 BASIC SKILLS FOR WORKING WITH SMOKERS Course Description Goals and Learning Objectives 368 Plantation Street, Worcester, MA 01605 www.umassmed.edu/tobacco 2018 Basic Skills for Working with Smokers 1 Table
BASIC SKILLS FOR WORKING WITH SMOKERS Course Description Goals and Learning Objectives 368 Plantation Street, Worcester, MA 01605 www.umassmed.edu/tobacco 2018 Basic Skills for Working with Smokers 1 Table
4.b.i Promote tobacco use cessation, especially among low SES populations and those with poor mental health (Focus Area 2; Goal #2.
 4.b.i Promote tobacco use cessation, especially among low SES populations and those with poor mental health (Focus Area 2; Goal #2.2) Project Objective: This project will promote tobacco use cessation,
4.b.i Promote tobacco use cessation, especially among low SES populations and those with poor mental health (Focus Area 2; Goal #2.2) Project Objective: This project will promote tobacco use cessation,
CHC TOBACCO CESSATION PROGRAM SCOPE OF WORK
 CHC TOBACCO CESSATION PROGRAM SCOPE OF WORK Goal 1: Develop a Tobacco Cessation Program focused on evidenced-based clinical guidelines that is seamlessly integrated in CHC's care processes. Strategy 1-1:
CHC TOBACCO CESSATION PROGRAM SCOPE OF WORK Goal 1: Develop a Tobacco Cessation Program focused on evidenced-based clinical guidelines that is seamlessly integrated in CHC's care processes. Strategy 1-1:
Collaborating to help Oregon tobacco users quit
 Collaborating to help Oregon tobacco users quit A health benefit plan (see ORS 743.730) must provide payment, coverage or reimbursement of at least $500 for a tobacco use cessation program for a person
Collaborating to help Oregon tobacco users quit A health benefit plan (see ORS 743.730) must provide payment, coverage or reimbursement of at least $500 for a tobacco use cessation program for a person
Message From the Minister
 May 2002 Message From the Minister A basic principle of the health and social services system is that people have a responsibility to maintain their own health. The Department of Health and Social Services
May 2002 Message From the Minister A basic principle of the health and social services system is that people have a responsibility to maintain their own health. The Department of Health and Social Services
Quick Reference: Logic Models for Goal Areas 1-4
 Quick Reference: Logic Models for Goal Areas - This document contains excerpts from: Starr G, Rogers T, Schooley M, Porter S, Wiesen E, Jamison N. Key Outcome Indicators for Evaluating Comprehensive Tobacco
Quick Reference: Logic Models for Goal Areas - This document contains excerpts from: Starr G, Rogers T, Schooley M, Porter S, Wiesen E, Jamison N. Key Outcome Indicators for Evaluating Comprehensive Tobacco
STRATEGIC PLAN
 STRATEGIC PLAN 2016 2020 Promoting and supporting excellence in research www.immunology.org BSI STRATEGY 2016 2020 EXECUTIVE SUMMARY OUR MISSION Our mission is to promote excellence in immunological research,
STRATEGIC PLAN 2016 2020 Promoting and supporting excellence in research www.immunology.org BSI STRATEGY 2016 2020 EXECUTIVE SUMMARY OUR MISSION Our mission is to promote excellence in immunological research,
Agenda. Illinois Diabetes Action Plan: What s In It for You? 10/27/2017
 Illinois Diabetes Action Plan: What s In It for You? AADE IL Coordinating Body 4th Annual Symposium Making Noise About Diabetes Bloomington, IL November 3, 2017 Agenda The Burden of Diabetes IL Diabetes
Illinois Diabetes Action Plan: What s In It for You? AADE IL Coordinating Body 4th Annual Symposium Making Noise About Diabetes Bloomington, IL November 3, 2017 Agenda The Burden of Diabetes IL Diabetes
June 1, Albert L. Siu, M.D., M.S.P.H Chair, United States Preventive Services Task Force 540 Gaither Road Rockville, MD Dear Dr.
 June 1, 2015 Albert L. Siu, M.D., M.S.P.H Chair, United States Preventive Services Task Force 540 Gaither Road Rockville, MD 20850 Dear Dr. Siu: The undersigned public health and medical organizations
June 1, 2015 Albert L. Siu, M.D., M.S.P.H Chair, United States Preventive Services Task Force 540 Gaither Road Rockville, MD 20850 Dear Dr. Siu: The undersigned public health and medical organizations
Centers for Disease Control and Prevention
 This document is scheduled to be published in the Federal Register on 12/11/2018 and available online at https://federalregister.gov/d/2018-26708, and on govinfo.gov Billing Code: 4163-18-P DEPARTMENT
This document is scheduled to be published in the Federal Register on 12/11/2018 and available online at https://federalregister.gov/d/2018-26708, and on govinfo.gov Billing Code: 4163-18-P DEPARTMENT
Community Benefit Strategic Implementation Plan. Better together.
 Community Benefit Strategic Implementation Plan 2016 2019 Better together. Table of Contents Introduction... 4 Priority 1: Community Health Infrastructure... 5 Objective 1.1: Focus resources strategically
Community Benefit Strategic Implementation Plan 2016 2019 Better together. Table of Contents Introduction... 4 Priority 1: Community Health Infrastructure... 5 Objective 1.1: Focus resources strategically
Ensuring Medicaid Coverage of Tobacco Cessation
 Ensuring Medicaid Coverage of Tobacco Cessation Why is Medicaid Coverage of Tobacco Cessation Important? In 2014, 32 percent of Medicaid enrollees were smokers, compared with 17 percent of the general
Ensuring Medicaid Coverage of Tobacco Cessation Why is Medicaid Coverage of Tobacco Cessation Important? In 2014, 32 percent of Medicaid enrollees were smokers, compared with 17 percent of the general
The Science and Practice of Perinatal Tobacco Use Cessation
 1 The Science and Practice of Perinatal Tobacco Use Cessation Erin McClain, MA, MPH Catherine Rohweder, DrPH Cathy Melvin, PhD, MPH erin_mcclain@unc.edu Prevention of Tobacco Use and Secondhand Smoke Exposure
1 The Science and Practice of Perinatal Tobacco Use Cessation Erin McClain, MA, MPH Catherine Rohweder, DrPH Cathy Melvin, PhD, MPH erin_mcclain@unc.edu Prevention of Tobacco Use and Secondhand Smoke Exposure
The National Public Health Initiative on Diabetes and Women s Health: An Overview
 The National Public Health Initiative on Diabetes and Women s Health: An Overview Michelle D. Owens-Gary, PhD Behavioral Scientist Division of Diabetes Translation NCCDPHP Presentation Outline Highlight
The National Public Health Initiative on Diabetes and Women s Health: An Overview Michelle D. Owens-Gary, PhD Behavioral Scientist Division of Diabetes Translation NCCDPHP Presentation Outline Highlight
C-Change Making the Business Case Questions & Answers
 C-Change Making the Business Case Questions & Answers How To Use This Document Following are a set of questions and answers about C-Change s multi-year Making the Business Case for cancer prevention and
C-Change Making the Business Case Questions & Answers How To Use This Document Following are a set of questions and answers about C-Change s multi-year Making the Business Case for cancer prevention and
You Can Make a Difference!
 You Can Make a Difference! How to help your clients become tobacco free What Does Smoking Cost Us? One study estimates that cost savings of between $1,142 and $1,358 per pregnancy can be achieved for each
You Can Make a Difference! How to help your clients become tobacco free What Does Smoking Cost Us? One study estimates that cost savings of between $1,142 and $1,358 per pregnancy can be achieved for each
WMC DSRIP PPS Project Plans Application Section 4
 4.b.i Promote tobacco use cessation, especially among low SES populations and those with poor mental health Project Response & Evaluation: Partnering with Entities Outside of the PPS for this Project Please
4.b.i Promote tobacco use cessation, especially among low SES populations and those with poor mental health Project Response & Evaluation: Partnering with Entities Outside of the PPS for this Project Please
Tobacco: A Critical Element in Addressing Cancer Disparities. Athena Ramos, PhD, MBA, MS, CPM
 Tobacco: A Critical Element in Addressing Cancer Disparities Athena Ramos, PhD, MBA, MS, CPM Learning Objectives 1. To discuss the impact of tobacco in Nebraska 2. To identify potential linkages between
Tobacco: A Critical Element in Addressing Cancer Disparities Athena Ramos, PhD, MBA, MS, CPM Learning Objectives 1. To discuss the impact of tobacco in Nebraska 2. To identify potential linkages between
Tools for Creating a Workplace Culture of Health. Cheryl Bettigole, MD, MPH Philadelphia Department of Public Health September, 2016
 Tools for Creating a Workplace Culture of Health Cheryl Bettigole, MD, MPH Philadelphia Department of Public Health September, 2016 CREATING A WORKPLACE CULTURE OF HEALTH Benefits of Choosing the Stairs
Tools for Creating a Workplace Culture of Health Cheryl Bettigole, MD, MPH Philadelphia Department of Public Health September, 2016 CREATING A WORKPLACE CULTURE OF HEALTH Benefits of Choosing the Stairs
Request for Applications. Mini-Grant: State Tobacco Programs Supporting Smoke-Free and Tobacco-Free Multi-Unit Housing
 Request for Applications Mini-Grant: State Tobacco Programs Supporting Smoke-Free and Tobacco-Free Multi-Unit Housing Total number of State Tobacco Prevention and Control Programs to be funded: A total
Request for Applications Mini-Grant: State Tobacco Programs Supporting Smoke-Free and Tobacco-Free Multi-Unit Housing Total number of State Tobacco Prevention and Control Programs to be funded: A total
Slide 1. Slide 2. Slide 3. Reducing Tobacco Use and Nicotine Dependence in Clinical Settings. Goals for Today
 Slide 1 UNIVERSITY OF HAWAI I CANCER CENTER Reducing Tobacco Use and Nicotine Dependence in Clinical Settings Pebbles Fagan, Ph.D., M.P.H. Associate Professor and Program Director Cancer Prevention and
Slide 1 UNIVERSITY OF HAWAI I CANCER CENTER Reducing Tobacco Use and Nicotine Dependence in Clinical Settings Pebbles Fagan, Ph.D., M.P.H. Associate Professor and Program Director Cancer Prevention and
EHR Developer Code of Conduct Frequently Asked Questions
 EHR Developer Code of Conduct Frequently Asked Questions General What is the purpose of the EHR Developer Code of Conduct? EHR Association (the Association) members have a long tradition of working with
EHR Developer Code of Conduct Frequently Asked Questions General What is the purpose of the EHR Developer Code of Conduct? EHR Association (the Association) members have a long tradition of working with
OCTOBER EOEA and the Alzheimer s Association have organized implementation of the plan around its five major recommendations:
 1 MASSACHUSETTS ALZHEIMER S DISEASE AND RELATED DISORDERS STATE PLAN RECOMMENDATIONS TWO-YEAR PROGRESS REPORT OCTOBER 2014 In February 2012, Massachusetts released a set of Alzheimer s Disease and Related
1 MASSACHUSETTS ALZHEIMER S DISEASE AND RELATED DISORDERS STATE PLAN RECOMMENDATIONS TWO-YEAR PROGRESS REPORT OCTOBER 2014 In February 2012, Massachusetts released a set of Alzheimer s Disease and Related
Measure #402: Tobacco Use and Help with Quitting Among Adolescents National Quality Strategy Domain: Community / Population Health
 Measure #402: Tobacco Use and Help with Quitting Among Adolescents National Quality Strategy Domain: Community / Population Health 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
Measure #402: Tobacco Use and Help with Quitting Among Adolescents National Quality Strategy Domain: Community / Population Health 2016 PQRS OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY DESCRIPTION:
Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap
 Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap Avalere Health An Inovalon Company November 16, 2017 In Partnership with GSK Agenda 1 2 3 4 5 Welcome & Introductions Overview:
Increasing Adult Immunization Rates in the US Through Data and Quality: A Roadmap Avalere Health An Inovalon Company November 16, 2017 In Partnership with GSK Agenda 1 2 3 4 5 Welcome & Introductions Overview:
Essentia Health East Improves Treatment of Tobacco Dependence
 Essentia Health East Improves Treatment of Tobacco Dependence Between October 2010 and June 2012, ClearWay Minnesota SM provided Essentia Health East s Duluth Heart and Vascular Center with funding and
Essentia Health East Improves Treatment of Tobacco Dependence Between October 2010 and June 2012, ClearWay Minnesota SM provided Essentia Health East s Duluth Heart and Vascular Center with funding and
10.4 Advocacy, Communication and Social Mobilization Working Group: summary strategic plan,
 10.4 Advocacy, Communication and Social Mobilization Working Group: summary strategic plan, 2006 2015 Introduction A significant scaling-up of advocacy, communication and social mobilization for TB will
10.4 Advocacy, Communication and Social Mobilization Working Group: summary strategic plan, 2006 2015 Introduction A significant scaling-up of advocacy, communication and social mobilization for TB will
Arizona Health Improvement Plan
 Arizona Health Improvement Plan Arizona Alliance for Community Health Centers February 4, 2015 Will Humble, MPH ADHS Director Leading Health Issues State Health Assessment Obesity Behavioral Health Services
Arizona Health Improvement Plan Arizona Alliance for Community Health Centers February 4, 2015 Will Humble, MPH ADHS Director Leading Health Issues State Health Assessment Obesity Behavioral Health Services
STATE AND COMMUNITY MODELS FOR IMPROVING ACCESS TO DENTAL CARE FOR THE UNDERSERVED
 American Dental Association STATE AND COMMUNITY MODELS FOR IMPROVING ACCESS TO DENTAL CARE FOR THE UNDERSERVED October 2004 Executive Summary American Dental Association. State and Community Models for
American Dental Association STATE AND COMMUNITY MODELS FOR IMPROVING ACCESS TO DENTAL CARE FOR THE UNDERSERVED October 2004 Executive Summary American Dental Association. State and Community Models for
Coalitions Linking Action & Science for Prevention (CLASP)
 Coalitions Linking Action & Science for Prevention (CLASP) Adapted from Jon F. Kerner, Ph.D. Chair-Primary Prevention Action Group Senior Scientific Advisor for Cancer Control & Knowledge Translation History
Coalitions Linking Action & Science for Prevention (CLASP) Adapted from Jon F. Kerner, Ph.D. Chair-Primary Prevention Action Group Senior Scientific Advisor for Cancer Control & Knowledge Translation History
The 5A's are practice guidelines on tobacco use prevention and cessation treatment (4):
 Smoking Cessation Module Tobacco use is the single greatest preventable cause of chronic diseases and premature deaths worldwide. The Canadian Cancer Society reports that tobacco product use is responsible
Smoking Cessation Module Tobacco use is the single greatest preventable cause of chronic diseases and premature deaths worldwide. The Canadian Cancer Society reports that tobacco product use is responsible
Common Diagnosis Codes and Tips for Coding Nicotine Use/
 ICD-10 Tobacco Billing Guide ICD-10 and Tobacco Common Diagnosis Codes and Tips for Coding Nicotine Use/ Dependence Tobacco use is the leading cause of preventable disease and death in the United States,
ICD-10 Tobacco Billing Guide ICD-10 and Tobacco Common Diagnosis Codes and Tips for Coding Nicotine Use/ Dependence Tobacco use is the leading cause of preventable disease and death in the United States,
Nebraska Diabetes Prevention Action Plan
 Nebraska Diabetes Prevention Action Plan 2016 2018 Promoting Awareness and Increasing Coverage to Support Scaling and Sustaining the National Diabetes Prevention Program in Nebraska. Table of Contents
Nebraska Diabetes Prevention Action Plan 2016 2018 Promoting Awareness and Increasing Coverage to Support Scaling and Sustaining the National Diabetes Prevention Program in Nebraska. Table of Contents
National Cancer Programme. Work Plan 2015/16
 National Cancer Programme Work Plan 2015/16 Citation: Ministry of Health. 2015. National Cancer Programme: Work plan 2015/16. Wellington: Ministry of Health. Published in October 2015 by the Ministry of
National Cancer Programme Work Plan 2015/16 Citation: Ministry of Health. 2015. National Cancer Programme: Work plan 2015/16. Wellington: Ministry of Health. Published in October 2015 by the Ministry of
Part Ⅰ- simplified version-a. Current situation of tobacco use and tobacco control in the country
 Part Ⅰ- simplified version-a Current situation of tobacco use and tobacco control in the country Brainstorming What is the prevalence of tobacco use in your country? What are the current tobacco control
Part Ⅰ- simplified version-a Current situation of tobacco use and tobacco control in the country Brainstorming What is the prevalence of tobacco use in your country? What are the current tobacco control
Epilepsy Across the Spectrum Promoting Health and Understanding
 RECOMMENDATIONS MARCH 2012 For more information visit www.iom.edu/epilepsy Epilepsy Across the Spectrum Promoting Health and Understanding Much can be done to improve the lives of people with epilepsy.
RECOMMENDATIONS MARCH 2012 For more information visit www.iom.edu/epilepsy Epilepsy Across the Spectrum Promoting Health and Understanding Much can be done to improve the lives of people with epilepsy.
Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care
 Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care New Futures mission is to advocate, educate, and collaborate to reduce alcohol and other drug problems in New Hampshire. Expanding
Include Substance Use Disorder Services in New Hampshire Medicaid Managed Care New Futures mission is to advocate, educate, and collaborate to reduce alcohol and other drug problems in New Hampshire. Expanding
Progress from the Patient-Centered Outcomes Research Institute (PCORI)
 Progress from the Patient-Centered Outcomes Research Institute (PCORI) Anne Beal, Chief Operating Officer of the Patient-Centered Outcomes Research Institute Sharon-Lise Normand, Vice Chair, Methodology
Progress from the Patient-Centered Outcomes Research Institute (PCORI) Anne Beal, Chief Operating Officer of the Patient-Centered Outcomes Research Institute Sharon-Lise Normand, Vice Chair, Methodology
Janine E. Janosky, Ph.D. Vice President and Head, Center for Community Health Improvement. June 2013
 Janine E. Janosky, Ph.D. Vice President and Head, Center for Community Health Improvement June 2013 ABIA: Unique Convergence Accountable Care Community (ACC) Vision To improve the health of the community.
Janine E. Janosky, Ph.D. Vice President and Head, Center for Community Health Improvement June 2013 ABIA: Unique Convergence Accountable Care Community (ACC) Vision To improve the health of the community.
A Perspective from the Co-Chairs of the: National Quality Forum Prevention Endorsement Maintenance Steering Committee
 A Perspective from the Co-Chairs of the: National Quality Forum Prevention Endorsement Maintenance Steering Committee Paul Jarris, MD, MBA Executive Director Association of State and Territorial Health
A Perspective from the Co-Chairs of the: National Quality Forum Prevention Endorsement Maintenance Steering Committee Paul Jarris, MD, MBA Executive Director Association of State and Territorial Health
Stop Delirium! A complex intervention for delirium in care homes for older people
 Stop Delirium! A complex intervention for delirium in care homes for older people Final report Summary September 2009 1 Contents Abstract...3 Lay Summary...4 1. Background...6 2. Objectives...6 3. Methods...7
Stop Delirium! A complex intervention for delirium in care homes for older people Final report Summary September 2009 1 Contents Abstract...3 Lay Summary...4 1. Background...6 2. Objectives...6 3. Methods...7
State of Rhode Island. Medicaid Dental Review. October 2010
 State of Rhode Island Medicaid Dental Review October 2010 EXECUTIVE SUMMARY The Centers for Medicare & Medicaid Services (CMS) is committed to improving pediatric dental care in the Medicaid program reflecting
State of Rhode Island Medicaid Dental Review October 2010 EXECUTIVE SUMMARY The Centers for Medicare & Medicaid Services (CMS) is committed to improving pediatric dental care in the Medicaid program reflecting
Patricia Bax, RN, MS August 17, Reaching New York State Tobacco Users through Opt-to-Quit
 Patricia Bax, RN, MS August 17, 2015 Reaching New York State Tobacco Users through Opt-to-Quit Good Afternoon! Welcome Roswell Park Cessation Services and Opt-to-Quit Overview Featured Site: Stony Brook
Patricia Bax, RN, MS August 17, 2015 Reaching New York State Tobacco Users through Opt-to-Quit Good Afternoon! Welcome Roswell Park Cessation Services and Opt-to-Quit Overview Featured Site: Stony Brook
Tobacco Prevention, Education & Cessation Grant Program. Tobacco Cessation Awareness Campaign and Web Hub
 Tobacco Prevention, Education & Cessation Grant Program Tobacco Cessation Awareness Campaign and Web Hub Request for Proposal #: SF-PSD13090412 CAMPAIGN I. Background, Overview and Goals The mission of
Tobacco Prevention, Education & Cessation Grant Program Tobacco Cessation Awareness Campaign and Web Hub Request for Proposal #: SF-PSD13090412 CAMPAIGN I. Background, Overview and Goals The mission of
WORKING WITH THE TRADES TO QUIT THE SMOKE BREAK. Heidi McKean,R.N.,B.Sc.N.,CCHN(C) John Atkinson, B.A. M.SW.
 WORKING WITH THE TRADES TO QUIT THE SMOKE BREAK Heidi McKean,R.N.,B.Sc.N.,CCHN(C) John Atkinson, B.A. M.SW. CONSTRUCTION CESSATION PROJECT An innovative public / private partnership Launched in 2012 funded
WORKING WITH THE TRADES TO QUIT THE SMOKE BREAK Heidi McKean,R.N.,B.Sc.N.,CCHN(C) John Atkinson, B.A. M.SW. CONSTRUCTION CESSATION PROJECT An innovative public / private partnership Launched in 2012 funded
It s All Acute to Me: Expanding Opportunities for Cessation Counseling Beyond Primary Care
 It s All Acute to Me: Expanding Opportunities for Cessation Counseling Beyond Primary Care Artwork by Keith J. 2013 American Academy of Pediatrics (AAP) Children's Art Contest. Support for the 2009, 2010,
It s All Acute to Me: Expanding Opportunities for Cessation Counseling Beyond Primary Care Artwork by Keith J. 2013 American Academy of Pediatrics (AAP) Children's Art Contest. Support for the 2009, 2010,
Oral Presentation to the H.E.L.P. Committee on February 14, 2012 Philip A. Pizzo, MD
 Oral Presentation to the H.E.L.P. Committee on February 14, 2012 Philip A. Pizzo, MD 1. I am Dr. Philip A Pizzo, Dean of the Stanford University School of Medicine as well as Professor of Pediatrics and
Oral Presentation to the H.E.L.P. Committee on February 14, 2012 Philip A. Pizzo, MD 1. I am Dr. Philip A Pizzo, Dean of the Stanford University School of Medicine as well as Professor of Pediatrics and
BASIC SKILLS FOR WORKING WITH SMOKERS
 BASIC SKILLS FOR WORKING WITH SMOKERS Course Description Goals and Learning Objectives 55 Lave Ave No, Worcester, MA 01655 www.umassmed.edu/tobacco 2016 Basic Skills for Working with Smokers 1 Table of
BASIC SKILLS FOR WORKING WITH SMOKERS Course Description Goals and Learning Objectives 55 Lave Ave No, Worcester, MA 01655 www.umassmed.edu/tobacco 2016 Basic Skills for Working with Smokers 1 Table of
Technical Assistance for Local Health Departments to Support, Leverage and Expand Use of CDC s Tips from Former Smokers Campaign
 [PROJECT REPORT] August 2017 Technical Assistance for Local Health Departments to Support, Leverage and Expand Use of CDC s Tips from Former Smokers Campaign Introduction In the United States, tobacco
[PROJECT REPORT] August 2017 Technical Assistance for Local Health Departments to Support, Leverage and Expand Use of CDC s Tips from Former Smokers Campaign Introduction In the United States, tobacco
PROMEDICA MONROE REGIONAL HOSPITAL 2016 COMMUNITY HEALTH NEEDS ASSESSMENT IMPLEMENTATION PLAN
 PROMEDICA MONROE REGIONAL HOSPITAL 2016 COMMUNITY HEALTH NEEDS ASSESSMENT IMPLEMENTATION PLAN 2017-2019 Approved and Adopted on December 19, 2016 PROMEDICA MONROE REGIONAL HOSPITAL 2016 COMMUNITY HEALTH
PROMEDICA MONROE REGIONAL HOSPITAL 2016 COMMUNITY HEALTH NEEDS ASSESSMENT IMPLEMENTATION PLAN 2017-2019 Approved and Adopted on December 19, 2016 PROMEDICA MONROE REGIONAL HOSPITAL 2016 COMMUNITY HEALTH
Healthy People A Resource for Promoting Health and Preventing Disease Throughout the Nation. Office of Disease Prevention and Health Promotion
 Healthy People 2020 A Resource for Promoting Health and Preventing Disease Throughout the Nation Office of Disease Prevention and Health Promotion Healthy People Background and History What Is Healthy
Healthy People 2020 A Resource for Promoting Health and Preventing Disease Throughout the Nation Office of Disease Prevention and Health Promotion Healthy People Background and History What Is Healthy
II. Transforming the Future through Dynamic Targeted Initiatives Reframing: Effective Communication for Creating Change
 II. Transforming the Future through Dynamic Targeted Initiatives Reframing: Effective Communication for Creating Change Definition and Purpose The prevention field recognizes that most of the current messages
II. Transforming the Future through Dynamic Targeted Initiatives Reframing: Effective Communication for Creating Change Definition and Purpose The prevention field recognizes that most of the current messages
Camden Citywide Diabetes Collaborative
 Camden Citywide Diabetes Collaborative The Camden Coalition of Healthcare Providers is an organization that seeks to improve the quality, capacity and accessibility of the health care system for vulnerable,
Camden Citywide Diabetes Collaborative The Camden Coalition of Healthcare Providers is an organization that seeks to improve the quality, capacity and accessibility of the health care system for vulnerable,
AIDS Foundation of Chicago Strategic Vision
 AIDS Foundation of Chicago Strategic Vision 2005-2007 Founded in 1985 by community activists and physicians, the AIDS Foundation of Chicago is a local and national leader in the fight against HIV/AIDS.
AIDS Foundation of Chicago Strategic Vision 2005-2007 Founded in 1985 by community activists and physicians, the AIDS Foundation of Chicago is a local and national leader in the fight against HIV/AIDS.
Achieving Quality and Value in Chronic Care Management
 The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
The Burden of Chronic Disease One of the greatest burdens on the US healthcare system is the rapidly growing rate of chronic disease. These statistics illustrate the scope of the problem: Nearly half of
Smoking Counselling and Cessation Service in Hospital Authority 7 May HA Convention 2014
 Smoking Counselling and Cessation Service in Hospital Authority 7 May 2014 - HA Convention 2014 On behalf of COC (Family Medicine) Dr Maria Leung Consultant, Department of Family Medicine New Territories
Smoking Counselling and Cessation Service in Hospital Authority 7 May 2014 - HA Convention 2014 On behalf of COC (Family Medicine) Dr Maria Leung Consultant, Department of Family Medicine New Territories
Dissemination and Implementation Research
 Dissemination and Implementation Research Catherine M. Stoney, Ph.D. National Heart, Lung, and Blood Institute March 2013 Smoking rates in the US from 1965-2007 Graph Graphic: Joe Camel Graphic: Woman
Dissemination and Implementation Research Catherine M. Stoney, Ph.D. National Heart, Lung, and Blood Institute March 2013 Smoking rates in the US from 1965-2007 Graph Graphic: Joe Camel Graphic: Woman
Tobacco-Control Policy Workshop:
 Tobacco-Control Policy Workshop: Goal: to introduce Mega-Country leaders to an effective policy framework for tobacco control and to develop skills to promote policy implementation. Objectives: As a result
Tobacco-Control Policy Workshop: Goal: to introduce Mega-Country leaders to an effective policy framework for tobacco control and to develop skills to promote policy implementation. Objectives: As a result
Meltdown : Investing in Prevention. October 7, 2008
 Averting a Health Care Meltdown : Investing in Prevention October 7, 2008 Agenda Introductory Remarks Featured Speakers Wendy E Braund, MD, MPH, MSEd, 11th Luther Terry Fellow & Senior Clinical Advisor
Averting a Health Care Meltdown : Investing in Prevention October 7, 2008 Agenda Introductory Remarks Featured Speakers Wendy E Braund, MD, MPH, MSEd, 11th Luther Terry Fellow & Senior Clinical Advisor
Readiness of Lung Cancer Screening Sites to Implement Smoking Cessation Treatment Services
 Readiness of Lung Cancer Screening Sites to Implement Smoking Cessation Treatment Services Jamie S. Ostroff, PhD Memorial Sloan Kettering Cancer Center June 20, 2016 Disclosures Research Consultant, New
Readiness of Lung Cancer Screening Sites to Implement Smoking Cessation Treatment Services Jamie S. Ostroff, PhD Memorial Sloan Kettering Cancer Center June 20, 2016 Disclosures Research Consultant, New
Chronic Disease and Injury Prevention (6210P)
 4-83 Program Locator County Health Heath Department Public Health and Environmental Protection Chronic Disease and Injury Prevention Disease Control and Prevention Headline Measures 50% 40% 30% 20% 10%
4-83 Program Locator County Health Heath Department Public Health and Environmental Protection Chronic Disease and Injury Prevention Disease Control and Prevention Headline Measures 50% 40% 30% 20% 10%
THE TEXAS CANCER PLAN KAREN TORGES CHAIR, CANCER ALLIANCE OF TEXAS
 THE TEXAS CANCER PLAN KAREN TORGES CHAIR, CANCER ALLIANCE OF TEXAS The Texas Cancer Plan Aims to reduce the cancer burden and improve lives of Texans. Identifies the challenges and issues and presents
THE TEXAS CANCER PLAN KAREN TORGES CHAIR, CANCER ALLIANCE OF TEXAS The Texas Cancer Plan Aims to reduce the cancer burden and improve lives of Texans. Identifies the challenges and issues and presents
Comprehensive Cancer Control Technical Assistance Training and Communication Plan. PI: Mandi Pratt-Chapman, MA. Cooperative Agreement #1U38DP
 Comprehensive Cancer Control Technical Assistance Training and Communication Plan PI: Mandi Pratt-Chapman, MA Cooperative Agreement #1U38DP004972-01 July 2014 Acknowledgement: This work was supported by
Comprehensive Cancer Control Technical Assistance Training and Communication Plan PI: Mandi Pratt-Chapman, MA Cooperative Agreement #1U38DP004972-01 July 2014 Acknowledgement: This work was supported by
Strategic Plan: Implementation Work Plan
 Healthy Eating Active Living New Hampshire Strategic Plan: Implementation Work Plan July 1, 2011 June 30, Adopted: July 28, 2011 Goal One: Increase the number and effectiveness of community coalitions
Healthy Eating Active Living New Hampshire Strategic Plan: Implementation Work Plan July 1, 2011 June 30, Adopted: July 28, 2011 Goal One: Increase the number and effectiveness of community coalitions
SICKLE CELL DISEASE TREATMENT DEMONSTRATION PROGRAM. CONGRESSIONAL REPORT Executive Summary
 SICKLE CELL DISEASE TREATMENT DEMONSTRATION PROGRAM CONGRESSIONAL REPORT Executive Summary OCTOBER 2014 The National Coordinating Center for the Sickle Cell Disease Treatment Demonstration Program was
SICKLE CELL DISEASE TREATMENT DEMONSTRATION PROGRAM CONGRESSIONAL REPORT Executive Summary OCTOBER 2014 The National Coordinating Center for the Sickle Cell Disease Treatment Demonstration Program was
New Jersey s Comprehensive Tobacco Control Program: Importance of Sustained Funding
 New Jersey s Comprehensive Tobacco Control Program: Importance of Sustained Funding History of Tobacco Control Funding Tobacco use is the leading preventable cause of death in the U.S., killing more than
New Jersey s Comprehensive Tobacco Control Program: Importance of Sustained Funding History of Tobacco Control Funding Tobacco use is the leading preventable cause of death in the U.S., killing more than
State of Behavioral Health. The Arizona Initiative for Tobacco Free Living in Individuals with Behavioral Health Disorders
 Helping People with Mental Health Issues Live Longer Lives without Tobacco The Arizona Initiative for Tobacco Free Living in Individuals with Behavioral Health Disorders Stephen S. Michael, MS Director,
Helping People with Mental Health Issues Live Longer Lives without Tobacco The Arizona Initiative for Tobacco Free Living in Individuals with Behavioral Health Disorders Stephen S. Michael, MS Director,
At the Intersection of Public Health and Health Care: CDC s National Asthma Control Program
 At the Intersection of Public Health and Health Care: CDC s National Asthma Control Program Shirl Ellis Odem Maureen Wilce Elizabeth Herman Asthma Initiative of Michigan Partnership Forum June 3, 2016
At the Intersection of Public Health and Health Care: CDC s National Asthma Control Program Shirl Ellis Odem Maureen Wilce Elizabeth Herman Asthma Initiative of Michigan Partnership Forum June 3, 2016
Suffolk Wide - Various locations (Ipswich, Bury St. Edmunds and Waveney) regular travel across Suffolk will be required
 Job Description Post: Location: Hours: Salary: Responsible to: Purpose of job: Key Relationships: Stop Smoking Service Liaison Officer Suffolk Wide - Various locations (Ipswich, Bury St. Edmunds and Waveney)
Job Description Post: Location: Hours: Salary: Responsible to: Purpose of job: Key Relationships: Stop Smoking Service Liaison Officer Suffolk Wide - Various locations (Ipswich, Bury St. Edmunds and Waveney)
Section #3: Process of Change
 Section #3: Process of Change This module will: Describe a model of change that supported the development and implementation of a palliative care program in long term care. Describe strategies that assisted
Section #3: Process of Change This module will: Describe a model of change that supported the development and implementation of a palliative care program in long term care. Describe strategies that assisted
Smokers & Their Workplaces
 Smokers & Their Workplaces Opportunities for Research & Intervention Peggy Hannon, PhD, MPH Collaborators Acknowledgements Jeff Harris, MD, MPH, MBA Courtney Hughes, PhD Emily Yette, MPHc This research
Smokers & Their Workplaces Opportunities for Research & Intervention Peggy Hannon, PhD, MPH Collaborators Acknowledgements Jeff Harris, MD, MPH, MBA Courtney Hughes, PhD Emily Yette, MPHc This research
Washington, D.C Washington, D.C
 May 24, 2018 The Honorable Roy Blunt The Honorable Patty Murray Chairman Ranking Member United States Senate United States Senate Washington, D.C. 20510 Washington, D.C. 20510 Dear Chairman Blunt and Ranking
May 24, 2018 The Honorable Roy Blunt The Honorable Patty Murray Chairman Ranking Member United States Senate United States Senate Washington, D.C. 20510 Washington, D.C. 20510 Dear Chairman Blunt and Ranking
Oregon Statewide Tobacco Control Plan. Taking Action for a Tobacco Free Oregon. Year 4/5 Operations Plan
 Oregon Statewide Tobacco Control Plan Taking Action for a Tobacco Free Oregon Year 4/5 Operations Plan 2008-2009 TABLE OF CONTENTS Goal 1: Eliminate Exposure to Tobacco Smoke 2 Goal 2: Prevent the Initiation
Oregon Statewide Tobacco Control Plan Taking Action for a Tobacco Free Oregon Year 4/5 Operations Plan 2008-2009 TABLE OF CONTENTS Goal 1: Eliminate Exposure to Tobacco Smoke 2 Goal 2: Prevent the Initiation
Nebraska Statewide Suicide Prevention Plan
 Nebraska Statewide Suicide Prevention Plan 2016-2020 This plan provides a framework to help Nebraskans work together to prevent suicide. It sets out shared strategies for suicide prevention and sets the
Nebraska Statewide Suicide Prevention Plan 2016-2020 This plan provides a framework to help Nebraskans work together to prevent suicide. It sets out shared strategies for suicide prevention and sets the
Sally Carter, MSW, LCSW Director of Statewide Initiatives Tobacco Use Prevention Service Oklahoma State Department of Health
 Making the Business Case for the State of Oklahoma to Provide Employee Cessation Benefits: A Collaborative Effort of the Oklahoma Tobacco Control Program Sally Carter, MSW, LCSW Director of Statewide Initiatives
Making the Business Case for the State of Oklahoma to Provide Employee Cessation Benefits: A Collaborative Effort of the Oklahoma Tobacco Control Program Sally Carter, MSW, LCSW Director of Statewide Initiatives
