Alcohol-Related Consequences Mediating PTSD Symptoms and Mental Health Related Quality of Life in OEF/OIF Combat Veterans
|
|
|
- Heather Beasley
- 5 years ago
- Views:
Transcription
1 MILITARY MEDICINE, 180, 6:670, 2015 Alcohol-Related Consequences Mediating PTSD Symptoms and Mental Health Related Quality of Life in OEF/OIF Combat Veterans Abigail C. Angkaw, PhD* ; Moira Haller, PhD*; James O. E. Pittman, MSW* ; Sarah E. Nunnink, PhD* ; Sonya B. Norman, PhD* ; Jennifer A. Lemmer, PhD*; Robert N. McLay, MD, PhD ; Dewleen G. Baker, MD* ABSTRACT Veterans returning from Operation Enduring Freedom and Operation Iraqi Freedom (OEF/OIF) have been found to be at increased risk for post-traumatic stress disorder (PTSD) and alcohol use disorders, leading to negative mental health related quality of life (MHRQoL). The current study examined the unique impact of alcohol consumption levels versus alcohol-related consequences on the relationship between PTSD symptoms and MHRQoL in a sample of OEF/OIF combat veterans (N = 205, median age 29, 95% men). Mediation analyses indicated that the effect of PTSD symptoms on MHRQoL was explained only by alcohol-related consequences and not by alcohol consumption. Findings highlight the importance of including alcohol-related consequences in clinical assessment and intervention programs for OEF/OIF veterans. Additionally, this study enhances knowledge regarding the underlying mechanisms of functional impairment related to PTSD and alcohol use disorders. INTRODUCTION Post-traumatic stress disorder (PTSD) is highly comorbid with alcohol use disorders among Operation Enduring Freedom and Operation Iraqi Freedom (OEF/OIF) veterans seeking care through the Veterans Affairs (VA) healthcare system. In fact, research indicates that over 50% of men and 28% of women with PTSD reported concurrent alcohol abuse or dependence; 1 further, approximately 63% of OEF/OIF veterans with an alcohol use disorder meet criteria for PTSD. 2 A multimodal pathway to account for comorbid PTSD and alcohol use disorders has been posited, in which both selfmedication of PTSD symptoms and alcohol withdrawal induced increases in PTSD symptoms help to explain the continued maintenance of alcohol abuse. When compared to patients with either substance use disorder or PTSD alone, individuals with comorbid PTSD and substance use disorders present unique clinical challenges that can influence treatment outcome, including a more severe clinical profile and poorer social adjustment, which places them at a greater risk for premature termination of therapy, 3,4 as well as a common perception by clinicians that these comorbid patients are more difficult to treat. 5 Studies of both military and civilian cohorts have found that PTSD impacts health-related quality of life (HRQoL) across multiple domains of functioning For instance, both Vietnam era and OEF/OIF era veterans with PTSD are likely to experience poorer functioning and poorer objective *Veterans Affairs San Diego Healthcare System, 3350 La Jolla Village Drive, San Diego, CA Department of Psychiatry, University of California, San Diego, 9500 Gilman Drive (MC 0603), San Diego, CA Veterans Affairs Center of Excellence for Stress and Mental Health, 3350 La Jolla Village, Drive (MC 116A), San Diego, CA Naval Medical Center, San Diego, Bob Wilson Drive, San Diego, CA doi: /MILMED-D living conditions and lower satisfaction compared to those without PTSD. 7 Moreover, research suggests that individuals with comorbid PTSD and alcohol use disorders exhibit greater functional impairments in HRQoL than those with alcohol use disorder alone. 11 Problem drinking may partially mediate the relationship between PTSD and poor HRQoL. 12 McDevitt-Murphy et al 13 found that alcohol misuse significantly mediated the relationship between PTSD symptoms and mental HRQoL (MHRQoL), but not physical HRQoL. Given the high rates of comorbid substance use disorders among veterans with other psychiatric disorders 14 and the high prevalence of risky alcohol use in OEF/OIF veterans, 15 examining PTSD, alcohol misuse, and MHRQoL among newly returning OEF/ OIF combat veterans is important. 16 Although studies have explored the role of alcohol use as a mediator in the association between PTSD and HRQoL in OEF/OIF veterans, 12 no study to date has made a distinction between alcohol consumption levels versus consequences of alcohol use. Measuring multiple facets of problematic drinking behavior (i.e., overall hazardous drinking, alcohol consumption including quantity/frequency, and alcohol-related consequences) allows for a more comprehensive assessment of drinking behaviors and can help move the field toward a better understanding of mechanisms that link PTSD, problem drinking, and HRQoL. Highlighting the distinction between consumption and consequences, Mallett et al 17 pointed out that although much research has centered on predictors of alcohol consumption, fewer efforts have focused on predicting alcohol-related consequences, which are multidetermined in nature (may occur more frequently in the presence of certain intrapersonal, interpersonal, and environmental conditions) and may be independent of episodic drinking. Although correlated (greater consumption is associated with greater consequences 18 ), it is likely that these two constructs are still semi-independent and 670 MILITARY MEDICINE, Vol. 180, June 2015
2 worthy of individual consideration. This position is supported by Ray et al, 19 who directly address the divergent nature of consumption and consequences, stating that not all heavy drinkers experience alcohol-related problems and not all light drinkers avoid them. Furthermore, consequences of drinking may be a more clinically relevant indicator and examination of alcohol-related consequences may shed light on inconsistencies in intervention outcome data. In regard to screening for problematic alcohol use, assessing both consumption and adverse consequences has been recommended. 20 In fact, questions regarding alcoholrelated problems have been shown to be more sensitive indicators of problem drinking than items regarding consumption. 21 Additionally, alcohol-related problems (above and beyond alcohol-related consumption) have been associated with other negative outcomes, including maladaptive motivation. 22 Of concern, currently the Department of Defense and the Veterans Administration both use only measures of consumption (rather than consequences) in their initial screening of potential alcohol misuse (AUDIT consumption factor 19 ), potentially losing valuable information regarding those for whom alcohol might be problematic. The aim of the present study was to compare the role of alcohol consumption versus alcohol-related consequences in mediating the relationship between PTSD and MHRQoL in a cohort of OEF/OIF veterans. Because alcohol-related problems (consequences) appear to be as good as or better in predicting a host of outcomes as compared to consumption, 20,21 we hypothesized that alcohol-related consequences would be a stronger mediator than alcohol consumption in the relationship between PTSD and MHRQoL. METHOD Study Sample Participants were 205 OEF/OIF combat veterans (93% men; 43% active duty, 57% veteran; ages 19 52, median = 29, mean = 29.07, SD = 7.02) who were participating in a larger cross-sectional study of genetic factors underlying vulnerability for PTSD, which excluded participants with a self-reported Axis I disorder diagnosis before deployment (obtained at phone screen), current alcohol dependence, or current drug use participants self-identified ethnicity and race was 76% non-hispanic/latino, 24% Hispanic/Latino, 79% White, 8% Black, 7% Asian, 2% Native American, 1% Native Hawaiian/ Pacific Islander, and 4% Other. Utilizing clinical assessments and self-report measures, 49% of participants met PTSD diagnostic criteria, and 70% were identified as nonhazardous drinkers. Participants reported that they consumed 1 to 2 drinks (43%), 3 to 4 drinks (30%), 5 to 6 drinks (17%), 7 to 9 drinks (7%), or 10 or more (3%) drinks each drinking occasion. Recruitment efforts included posting flyers at VA medical centers and military bases and clinician referrals. Participant inclusion required having consumed at least one alcohol beverage in the last 30 days, at least lightmoderate combat exposure on the Combat Exposure Scale, 23 and a 6-month postdeployment interval to prevent the confounding effect of immediate postdeployment adjustment. The study received local institutional review board approval. All participants provided informed consent before being included in the study. Procedure Participants completed self-report questionnaires and a clinical interview to characterize the sample demographics and assess study-related constructs. All participants were treated in accordance with the Ethical Principles of Psychologists and Code of Conduct. 24 Measures PTSD Symptoms The total score of the Clinician Administered PTSD Scale (CAPS), 25 past month combined DSM-IV version, a structured interview corresponding to the diagnostic criteria for PTSD, provided a continuous measure of PTSD symptoms and PTSD diagnosis in the past month. CAPS assessments were indexed to any lifetime traumatic event meeting PTSD Criterion A endorsed by the participant as currently most distressing, ensuring the capture of maximum symptom burden. The CAPS assesses the frequency and intensity of PTSD symptoms that began or worsened following the Criterion A traumatic event, each rated on a Likert-type scale ranging from 0 ( Never or None ) to 4( Daily or almost daily or Extreme, incapacitating distress, cannot dismiss memories, unable to continue activities ). The CAPS has demonstrated good psychometric properties in numerous studies and is considered to be the gold standard in PTSD assessment with excellent inter-rater reliability for continuous scores (r = ) and internal consistency (α = ). The CAPS demonstrates high sensitivity and specificity, high test retest reliability, and strong convergence with other PTSD self-report measures. 26 The average total score on the CAPS was (SD = 31.77; range: ). In order to characterize the sample and determine if PTSD diagnostic criteria were met, the original rationally derived CAPS F1/I2 scoring rule (frequency 1, intensity 2) was used with DSM-IV criteria, which has 91% sensitivity, 71% specificity, and 82% efficiency, with a κ value of Drinking Behaviors Alcohol-related consequences and alcohol consumption over the past 12 months were measured utilizing the 10-item Alcohol Use Disorders Identification Test (AUDIT 19 ). The AUDIT demonstrates good reliability and validity in clinically identifying problem drinking behaviors. 19,27 To characterize the current study sample, AUDIT item scores ranging from 0 to 4 were summed to yield a composite score ranging from 1 to 30 with a cut-off score of 8 to identify hazardous MILITARY MEDICINE, Vol. 180, June
3 drinking. 26 The two-factor structure of alcohol consumption (items 1 3) and alcohol-related consequences (items 4 10), recommended over one- or three-factor structures, provided the potential hypothesized mediator variables. 28 The twofactor structure demonstrated adequate to good reliability in both alcohol consumption (Cronbach s α ranging from 0.83 to 0.92) and alcohol-related consequences (Cronbach s α ranging from 0.67 to 0.92). The average alcohol consumption score was 4.31 (SD = 2.47; range: ), and the average number of alcohol-related consequences was 2.48 (SD = 4.53; range: ). Mental Health Related Quality of Life The mental health component score of the 36-item Short- Form Health Survey (SF 36) 29 was used to provide a measure of mental health related quality of life (MHRQoL). The mental health component score (SF-36MCS) assesses the relative functional burden of mental health related problems. The SF-36 demonstrates high reliability, with internal consistency and test retest test statistics exceeding Additionally, the SF-36MCS has demonstrated validity in screening for psychiatric disorders with a sensitivity of 74% and specificity of 81%. 29 The average MHRQoL score was (SD = 14.89; range: ). Statistical Analysis All analyses were conducted using MPlus version There were no missing data. To examine preliminary hypothesized relationships among study variables, Pearson bivariate correlations were examined (described below). A path analysis framework was used for the primary analyses, in which both alcohol-related consequences and alcohol consumption were simultaneously examined as mediators of the relationship between PTSD symptoms and MHRQoL. Note that this approach controls for the effect of alcohol consumption on MHRQoL when examining whether alcoholrelated consequences significantly mediate the effect of PTSD symptoms on MHRQoL. The maximum likelihood estimator with robust standard errors was used in order to ensure robustness against heteroscedasticity, non-normality, and model misspecification. The residual covariance among alcohol-related consequences and consumption was specified. To test the significance of the indirect effects of PTSD symptoms on MHRQoL via alcohol-related consequences and alcohol consumption, we used 95% asymmetric confidence intervals based on the product of the coefficients approach to mediation. 32 To assess for potential confounding effects, a series of one-way analysis of variance were conducted in order to assess whether gender (93% male, 7% female), relationship status (40% married, 60% not married), ethnicity (57% non- Hispanic Caucasian, 43% other ethnicity), or education (28% no college, 57% some college, 15% college degree or higher) were associated with MHRQoL. We found no significant differences in MHRQoL between groups for any TABLE I. Pearson Bivariate Correlations and Descriptives for Study Variables Variable M SD 1. PTSD symptoms Alcohol Consumption Alcohol-Related Consequences 0.24*** 0.58*** Mental Health Related Quality of Life 0.75*** 0.18** 0.33*** **p 0.01 ***p PTSD, = Posttraumatic Stress Disorder. of these categorical demographic variables ( p >.05), and thus concluded that it was not necessary to include them as covariates in the data analysis. Likewise, age was not included as a covariate because a bivariate correlation indicated that it was not associated with MHRQoL. RESULTS Pearson bivariate correlations and descriptive statistics are reported in Table I. There were significant bivariate associations in the expected direction among PTSD symptoms, MHRQoL, and alcohol-related consequences ( p < 0.001). The association between alcohol consumption and MHRQoL was weak (r = 0.18, p = 0.010), and the association between alcohol consumption and PTSD symptoms was nonsignificant (r = 0.09, p = 0.203). Conversely, alcohol-related consequences were significantly associated with both MHRQoL (r = 0.33, p < 0.001) and PTSD symptoms (r = 0.24, p =0.001). Mediation Analyses Figure 1 presents results from the primary analyses (all coefficients are standardized). Higher levels of PTSD symptoms significantly increased risk for alcohol-related consequences FIGURE 1. Standardized regression coefficients for the relationship between PTSD and MHRQoL as mediated by alcohol-related consequences and alcohol consumption. 672 MILITARY MEDICINE, Vol. 180, June 2015
4 (B = 0.24, SE = 0.06, p < 0.001), which in turn significantly decreased MHRQoL (B = 0.13, SE = 0.05, p = 0.005). Moreover, alcohol-related consequences significantly mediated the effect of PTSD symptoms on MHRQoL while controlling for alcohol consumption (95% CI for the unstandardized indirect effect = [ 0.031, 0.003]). However, the direct effect of PTSD symptoms on MHRQoL was also significant (B = 0.71, SE = 0.03, p < 0.001), indicating that alcoholrelated consequences did not fully mediate the effect of PTSD symptoms on MHRQoL. Results also indicated that PTSD symptoms did not significantly influence risk for alcohol consumption (B = 0.09, SE = 0.07, p = 0.21), and that alcohol consumption did not significantly influence MHRQoL (B = 0.04, SE = 0.06, p = 0.52). Therefore, the effect of PTSD symptoms on MHRQoL was mediated only by alcohol-related consequences and not by alcohol consumption levels. DISCUSSION As hypothesized, results indicate that alcohol-related consequences partially mediate the association between PTSD symptoms and low MHRQoL (see Fig. 1) among OEF/OIF veterans, even when controlling for levels of alcohol consumption. Thus, one mechanism through which PTSD symptoms may decrease MHRQoL is by increasing alcoholrelated consequences, which in turn further decrease MHRQoL. However, the significant direct effect of PTSD symptoms on MHRQoL highlights the fact that PTSD symptoms directly decrease one s MHRQoL, independent of one s alcohol use or consequences. Bivariate correlations revealed that alcohol-related consequences were significantly related to PTSD symptoms, but alcohol consumption was not significantly associated with PTSD symptoms (see Table I). Further, alcohol consumption did not mediate the association between PTSD symptoms and MHRQoL. Study results with PTSD are similar to those of prior anxiety comorbidity studies, which have found alcoholrelated consequences to be more greatly associated with social anxiety and generalized anxiety than alcohol consumption levels. 33,34 Although a significant correlation was found between alcohol consumption and alcohol-related consequences, results indicated that the link between PTSD symptoms and poor MHRQoL among OEF/OIF veterans was partially explained by the negative consequences of alcohol use, rather than the volume or frequency of drinking. Findings highlight the need to routinely assess for alcohol-related consequences among OEF/OIF veterans in order to address an important mechanism through which PTSD symptoms may lead to poor MHRQoL. Results also lend additional support to existing research demonstrating the importance of addressing problematic drinking among OEF/OIF veterans presenting for PTSD treatment. Because functional impairments associated with mental health were found to be more strongly linked to alcoholrelated consequences than alcohol consumption, the development of prevention and intervention programs for OEF/ OIF veteran drinkers with PTSD symptoms should aim to assess and reduce the incidence of negative consequences related to drinking, rather than reducing alcohol consumption levels alone. Although, it is certainly possible that veterans who consume very large amounts of alcohol may eventually experience alcohol-related consequences, post hoc analysis of these data demonstrated that this is not always the case. Utilizing study standard deviations to create high, low (±1 SD), and moderate subgroups for alcohol consumption and consequences, post hoc analysis indicated that the majority of the cohort (42%) reported moderate consumption and low consequences, 4% reported high consumption but low consequences, and 3% reported moderate consumption but high consequences. General screens for problematic alcohol use, such as the AUDIT-C composed of only the three-item alcohol consumption subscale, often assess frequency and volume of drinking only. 35 However, study results support the importance of assessing for alcohol-related consequences, rather than only frequency and levels of alcohol consumption. A comprehensive assessment more accurately reflects potentially problematic drinking behaviors among OEF/OIF veterans with PTSD. Further, study results have important implications for addressing drinking among veterans endorsing PTSD symptoms. Young adult OEF/OIF veterans, especially those not meeting diagnostic criteria for alcohol dependence, may benefit from assessment of and intervention regarding problematic drinking behaviors. However, this veteran cohort is unlikely to embrace traditional abstinence-based alcohol treatments. 36,37 Intervention to reduce negative consequences of drinking may be more acceptable to this cohort than interventions to reduce quantity of drinking. Results of this study suggest that such intervention may in fact be the most clinically useful focus of treatment as well. Thus, future research explaining the link between PTSD and negative alcoholrelated consequences can be helpful. Alternative methods for addressing problematic drinking should be developed and incorporated into PTSD-focused treatments for OEF/OIF veterans who may be motivated to make changes to reduce the negative consequences of alcohol use. This study has several strengths including (1) exploring multiple rather than one-dimensional facets of problematic drinking; (2) use of both clinical and nonclinical participants (49% met PTSD criteria), which affords the possibility of improving the development of prevention and intervention programs; and (3) utilizing the gold standard in PTSD diagnosis, the Clinician-Administered PTSD Scale (CAPS). Although, this was the first study to examine PTSD, alcohol consumption versus alcohol-related problems, and MHRQoL among OEF/OIF veterans, results should be replicated in future studies and interpreted in light of study limitations, particularly the exclusion of veterans with current alcohol MILITARY MEDICINE, Vol. 180, June
5 dependence. Results may not fully generalize to a female veterans or a clinical sample of veterans with diagnosed PTSD or alcohol use disorders. Generalizability of findings should be considered in light of recent changes to PTSD and alcohol use disorder criteria in DSM-5. Additionally, results do not take into account likely comorbidities, such as depression or other substances. In a recent large-scale study, psychiatric diagnoses other than PTSD (especially bipolar disorder and schizophrenia) were most strongly associated with dual diagnosis in the OEF/OIF population. 13 Given the cross-sectional design of the study, alternative theoretical and directional models that may exist among study variables should be considered. Our cross-sectional data precluded us from testing temporal relations among study variables. A prospective study design would be beneficial in testing the causal effects over time among PTSD symptoms, alcohol behaviors, and MHRQoL. Following replication of results, future studies should also build upon the existing model to incorporate other mechanisms that may mediate or moderate the association between PTSD symptoms and MHRQoL among drinkers, such as coping motives, alcoholrelated expectancies, drinking refusal self-efficacy, 38 and other cognitive variables. ACKNOWLEDGMENTS The authors acknowledge Caroline Nievergelt for her support with data management for this project. REFERENCES 1. Kessler RC, Sonnega A, Broment E, Hughes M, Nelson CB: Posttraumatic stress disorder in the National Comorbidity Survey. Arch Gen Psychiatry 1995; 52: Seal KH, Cohen G, Waldrop A, Cohen BE, Maguen S, Ren L: Substance use disorders in Iraq and Afghanistan veterans in VA healthcare, : implications for screening, diagnosis and treatment. Drug Alcohol Depend 2011; 116: Najavits LM, Weiss RD, Shaw SR: The link between substance abuse and post-traumatic stress disorder in women: a research review. Am J Addict 1997; 6: Riggs DS, Rukstalis M, Volpicelli JR, Kalmanson D, Foa EB: Demographic and social adjustment characteristics of patients with comorbid post-traumatic stress disorder and alcohol dependence: potential pitfalls to PTSD treatment. Addict Behav 2003; 28: Najavits LM: Clinicians views on treating post-traumatic stress disorder and substance use disorder. J Subst Abuse Treat 2002; 22: Kuhn E, Blanchard EB, Hickling EJ: Post-traumatic stress disorder and psychosocial functioning within two samples of MVA survivors. Behav Res Ther 2003; 41: Pittman JO, Goldsmith AA, Lemmer JA, Kilmer MT, Baker DG: Posttraumatic stress disorder, depression, and health-related quality of life in OEF/OIF veterans. Qual Life Res 2012; 21: Schnurr PP, Lunney CA, Bovin MJ, Marx BP: Post-traumatic stress disorder and quality of life: extension of findings to veterans of the wars in Iraq and Afghanistan. Clin Psychol Rev 2009; 29: Schnurr PP, Hayes AF, Lunney CA, McFall M, Uddo M: Longitudinal analysis of the relationship between symptoms and quality of life in veterans treated for post-traumatic stress disorder. J Consult Clin Psychol 2006; 74: Stein MB, Walker JR, Hazen AL, Forde DR: Full and partial posttraumatic stress disorder: findings from a community survey. Am J Psychiatry 1997; 154: Evren C, Sar V, Dalbudak E, et al: Lifetime PTSD and quality of life among alcohol-dependent men: impact of childhood emotional abuse and dissociation. Psychiatry Res 2010; 186: Rheingold AA, Acierno R, Resnick H: Trauma, post-traumatic stress disorder, and health risk behaviors. In: Trauma and Health: Physical Health Consequences of Exposure to Extreme Stress, pp Edited by Schnurr PP, Green BL. Washington, DC, American Psychological Association, McDevitt-Murphy ME, Williams JL, Bracken KL, Fields JA, Monahan CJ, Murphy JG: PTSD symptoms, hazardous drinking, and health functioning among U.S. OEF and OIF veterans presenting to primary care. J Trauma Stress 2010; 23: Petrakis IL, Rosenheck R, Desai R: Substance use comorbidity among veterans with post-traumatic stress disroder and other psychiatric illness. Am J Addict 2011; 20: Calhoun PS, Elter JR, Jones ER, Kudler H, Straits-Tröster K: Hazardous alcohol use and receipt of risk-reduction counseling among US veterans of the wars in Iraq and Afghanistan. J Clin Psychiatry 2008; 69: Heltemes KJ, Dougherty AL, MacGregor AJ, Galarneau MR: Inpatient hospitalizations of U.S. military personnel medically evacuated from Iraq and Afghanistan with combat-related traumatic brain injury. Mil Med 2011; 176: Mallett KA, Varvil-Weld L, Turrisi R, Read A: An examination of college students willingness to experience consequences as a unique predictor of alcohol problems. Psychol Addict Behav 2011; 25: Cleveland MJ, Mallett KA, White HR, Turrisi R, Favero S: Patterns of alcohol use and related consequences in noncollege-attending emerging adults. J Stud Alcohol Drugs 2013; 74: Ray AE, Turrisi R, Abar BW, Peters KE: Social-cognitive correlates of protective drinking behaviors and alcohol-related consequences in college students. Addict Behav 2009; 34: Saunders JB, Aasland OG, Babor TF, De La Fuente JR, Grant M: Development of the alcohol use disorders identification test (AUDIT): WHO collaborative project on early detection of persons with harmful alcohol consumption-ii. Addiction 1993; 88: Ryder D, Lenton S, Harrison S, Dorricott J: Alcohol-related problems in a general hospital and general practice: screening and the preventative paradox. Med J Aust 1998; 149: Hosier SG, Cox WM: Personality and motivational correlates of alcohol consumption and alcohol-related problems among excessive drinking university students. Addict Behav 2011; 36: Keane TM, Fairbank JA, Caddell JM, Zimering RT, Taylor KL, Mora CA: Clinical evaluation of a measure to assess combat exposure. Psychol Assess 1989; 1: American Psychological Association: Ethical principles of psychologists and code of conduct. Am Psychol 2002; 57: Blake DD, Weathers FW, Nagy LM, et al: The development of a clinician-administered PTSD scale. J Trauma Stress 1995; 8: Weathers FW, Keane TM, Davidson JR: Clinician-administered PTSD scale: a review of the first ten years of research. Depress Anxiety 2001; 13: Allen JP, Litten RZ, Fertig JB, Babor TF: A review of research on the Alcohol Use Disorders Identification Test (AUDIT). Alcohol Clin Exp Res 1997; 21: Doyle SR, Donovan DM, Kivlahan DR: The factor structure of the alcohol use disorders identification test (AUDIT). J Stud Alcohol Drugs 2007; 68: Ware JE, Sherbourne CD: The MOS 36-item short-form health survey (SF-36): I. Conceptual framework and item selection. Med Care 1992; 30: Ware JE, Kosinski M, Keller SD: SF-36 Physical and Mental Health Summary scales: A User s Manual. Boston, MA, The Health Institute, MILITARY MEDICINE, Vol. 180, June 2015
6 31. Muthén BO, Muthén LK: Version 6.1, Computer Software and Manual. Los Angeles, CA, Muthén and Muthén, MacKinnon DP, Lockwood CM, Williams J: Confidence limits for the indirect effect: distribution of the product and resampling methods. Multivariate Behav Res 2004; 39: Buckner JD, Schmidt NB, Eggleston AM: Social anxiety and problematic alcohol consumption: the mediating role of drinking motives and situations. Behav Ther 2006; 37: Goldsmith AA, Thompson RD, Black JJ, Tran GQ, Smith JP: Drinking refusal self-efficacy and tension-reduction alcohol expectancies moderating the relationship between generalized anxiety and drinking behaviors in young adult drinkers. Psychol Addict Behav 2012; 26: Bush K, Kivlahan DR, McDonell MB, Fihn SD, Bradley KA: The AUDIT alcohol consumption questions (AUDIT-C): an effective brief screening test for problem drinking. Ambulatory Care Quality Improvement Project (ACQUIP). Arch Intern Med 1998; 158: Bernhardt A: Rising to the challenge of treating OEF/OIF veterans with co-occurring PTSD and substance abuse. Smith Coll Stud Soc Work 2009; 79: Norman SB, Wilkins KC, Tapert SF, Lang AJ, Najavits LM: A pilot study of seeking safety therapy with OEF/OIF veterans. J Psychoactive Drugs 2010; 42: Oei TPS, Morawska A: A cognitive model of binge drinking: the influence of alcohol expectancies and drinking refusal self-efficacy. Addict Behav 2004; 29: MILITARY MEDICINE, Vol. 180, June
Perceived Stigma and Barriers to Mental Health Care Utilization Among OEF-OIF Veterans
 Brief Reports Perceived Stigma and Barriers to Mental Health Care Utilization Among OEF-OIF Veterans Robert H. Pietrzak, Ph.D., M.P.H. Douglas C. Johnson, Ph.D. Marc B. Goldstein, Ph.D. James C. Malley,
Brief Reports Perceived Stigma and Barriers to Mental Health Care Utilization Among OEF-OIF Veterans Robert H. Pietrzak, Ph.D., M.P.H. Douglas C. Johnson, Ph.D. Marc B. Goldstein, Ph.D. James C. Malley,
Manual Supplement. Posttraumatic Stress Disorder Checklist (PCL)
 Manual Supplement V OLUME 1, I SSUE 1 N OVEMBER 18, 2014 Posttraumatic Stress Disorder Checklist (PCL) The Posttraumatic Stress Disorder Checklist (PCL) is one of the most frequently used standardized
Manual Supplement V OLUME 1, I SSUE 1 N OVEMBER 18, 2014 Posttraumatic Stress Disorder Checklist (PCL) The Posttraumatic Stress Disorder Checklist (PCL) is one of the most frequently used standardized
Traumatic Brain Injury, PTSD, and Current Suicidal Ideation Among Iraq and Afghanistan U.S. Veterans
 Journal of Traumatic Stress April 2014, 27, 244 248 BRIEF REPORT Traumatic Brain Injury, PTSD, and Current Suicidal Ideation Among Iraq and Afghanistan U.S. Veterans Blair E. Wisco, 1,2 Brian P. Marx,
Journal of Traumatic Stress April 2014, 27, 244 248 BRIEF REPORT Traumatic Brain Injury, PTSD, and Current Suicidal Ideation Among Iraq and Afghanistan U.S. Veterans Blair E. Wisco, 1,2 Brian P. Marx,
The Role of Emotional Numbing in Sexual Functioning Among Veterans of the Iraq and Afghanistan Wars
 MILITARY MEDICINE, 175, 6:424, 2010 The Role of Emotional Numbing in Sexual Functioning Among Veterans of the Iraq and Afghanistan Wars Sarah E. Nunnink * ; Gali Goldwaser ; Niloofar Afari* ; Caroline
MILITARY MEDICINE, 175, 6:424, 2010 The Role of Emotional Numbing in Sexual Functioning Among Veterans of the Iraq and Afghanistan Wars Sarah E. Nunnink * ; Gali Goldwaser ; Niloofar Afari* ; Caroline
Prevalence and Characteristics of Hazardous Drinkers: Results of the Greater Milwaukee Survey
 Prevalence and Characteristics of Hazardous Drinkers: Results of the Greater Milwaukee Survey Lisa K. Berger, PhD; Michael Fendrich, PhD; Adam Lippert, MA ABSTRACT Context: At-risk drinking is of particular
Prevalence and Characteristics of Hazardous Drinkers: Results of the Greater Milwaukee Survey Lisa K. Berger, PhD; Michael Fendrich, PhD; Adam Lippert, MA ABSTRACT Context: At-risk drinking is of particular
Primary Care Validation of a Single-Question Alcohol Screening Test
 JGIM ORIGINAL ARTICLES Primary Care Validation of a Single-Question Alcohol Screening Test Peter C. Smith, MD, MSc 1,5, Susan M. Schmidt 1, Donald Allensworth-Davies, MSc 2, and Richard Saitz, MD, MPH
JGIM ORIGINAL ARTICLES Primary Care Validation of a Single-Question Alcohol Screening Test Peter C. Smith, MD, MSc 1,5, Susan M. Schmidt 1, Donald Allensworth-Davies, MSc 2, and Richard Saitz, MD, MPH
Health Care Utilization by Veterans with Posttraumatic Stress Disorder: A Spouse/Intimate Partner Perspective By: Cassandra Buchanan, Nursing
 1 Health Care Utilization by Veterans with Posttraumatic Stress Disorder: A Spouse/Intimate Partner Perspective By: Cassandra Buchanan, Nursing 2 Introduction With Operation Iraqi Freedom (OIF) and Operation
1 Health Care Utilization by Veterans with Posttraumatic Stress Disorder: A Spouse/Intimate Partner Perspective By: Cassandra Buchanan, Nursing 2 Introduction With Operation Iraqi Freedom (OIF) and Operation
Reliability of the Deployment Resiliency Assessment
 BRIEF REPORTS MILITARY MEDICINE, 181, 7:638, 2016 Reliability of the Deployment Resiliency Assessment Samuel E. Simon, PhD*; Kate Stewart, PhD*; Michelle Kloc, PhD ; Thomas V. Williams, PhD ; MG Margaret
BRIEF REPORTS MILITARY MEDICINE, 181, 7:638, 2016 Reliability of the Deployment Resiliency Assessment Samuel E. Simon, PhD*; Kate Stewart, PhD*; Michelle Kloc, PhD ; Thomas V. Williams, PhD ; MG Margaret
WISAM 2018 Annual Conference Sept , PTSD and Substance Use Disorder in Veterans 9/28/2018. PTSD and SUD
 PTSD and Substance Use Disorder in Veterans Todd J Kammerzelt, MD General and Addiction Psychiatrist 9/28/2018 PTSD and SUD More than 1 in 4 veterans with PTSD also have SUD War Veterans with PTSD and
PTSD and Substance Use Disorder in Veterans Todd J Kammerzelt, MD General and Addiction Psychiatrist 9/28/2018 PTSD and SUD More than 1 in 4 veterans with PTSD also have SUD War Veterans with PTSD and
Sexual Harassment Experiences and Harmful Alcohol Use in a Military Sample: Differences in Gender and the Mediating Role of Depression
 University of South Carolina Scholar Commons Faculty Publications Psychology Department 5-2008 Sexual Harassment Experiences and Harmful Alcohol Use in a Military Sample: Differences in Gender and the
University of South Carolina Scholar Commons Faculty Publications Psychology Department 5-2008 Sexual Harassment Experiences and Harmful Alcohol Use in a Military Sample: Differences in Gender and the
Key words children; maternal posttraumatic stress symptoms; pediatric injury; posttraumatic
 Brief Report: The Impact of Maternal Posttraumatic Stress Disorder Symptoms and Child Gender on Risk for Persistent Posttraumatic Stress Disorder Symptoms in Child Trauma Victims Sarah A. Ostrowski, 1
Brief Report: The Impact of Maternal Posttraumatic Stress Disorder Symptoms and Child Gender on Risk for Persistent Posttraumatic Stress Disorder Symptoms in Child Trauma Victims Sarah A. Ostrowski, 1
APNA 30th Annual Conference Session 3037: October 21, 2016
 Erica Mumm, DNP, MSN, RN American Psychiatric Nurses Association 30 th Annual Conference October 19 th 22 nd, 2016 Disclosure This presenter has no conflict of interest to disclose. 2 OEF & OIF: A Different
Erica Mumm, DNP, MSN, RN American Psychiatric Nurses Association 30 th Annual Conference October 19 th 22 nd, 2016 Disclosure This presenter has no conflict of interest to disclose. 2 OEF & OIF: A Different
The Impact of Reported Direct and Indirect Killing on Mental Health Symptoms in Iraq War Veterans
 Journal of Traumatic Stress, Vol. 23, No. 1, February 2010, pp. 86 90 ( C 2010) The Impact of Reported Direct and Indirect Killing on Mental Health Symptoms in Iraq War Veterans Shira Maguen San Francisco
Journal of Traumatic Stress, Vol. 23, No. 1, February 2010, pp. 86 90 ( C 2010) The Impact of Reported Direct and Indirect Killing on Mental Health Symptoms in Iraq War Veterans Shira Maguen San Francisco
Derek Rutter Wake Forest University
 Derek Rutter Wake Forest University According to a 2008 Department of Veterans Affairs (VA) study cited by Albright and Thyer (2009), from 2002 until January of 2008, the VA diagnosed 40% of OEF (Operation
Derek Rutter Wake Forest University According to a 2008 Department of Veterans Affairs (VA) study cited by Albright and Thyer (2009), from 2002 until January of 2008, the VA diagnosed 40% of OEF (Operation
Alcohol Use and Alcohol-Related Problems Before and After Military Combat Deployment
 Alcohol Use and Alcohol-Related Problems Before and After Military Combat Deployment I. G. Jacobson M. A. K. Ryan, T. I. Hooper, T. C. Smith P. J. Amoroso, E. J. Boyko, G. D. Gackstetter T. S. Wells, N.
Alcohol Use and Alcohol-Related Problems Before and After Military Combat Deployment I. G. Jacobson M. A. K. Ryan, T. I. Hooper, T. C. Smith P. J. Amoroso, E. J. Boyko, G. D. Gackstetter T. S. Wells, N.
Smoking and hazardous alcohol
 Screening for Substance Abuse and Psychiatric Disorders Among Women Patients in a VA Health Care System Tania M. Davis, Ph.D. Kristen R. Bush, M.P.H. Daniel R. Kivlahan, Ph.D. Dorcas J. Dobie, M.D. Katharine
Screening for Substance Abuse and Psychiatric Disorders Among Women Patients in a VA Health Care System Tania M. Davis, Ph.D. Kristen R. Bush, M.P.H. Daniel R. Kivlahan, Ph.D. Dorcas J. Dobie, M.D. Katharine
Deployment Stressors, Coping, and. Psychological Well-Being Among Peacekeepers. Luigi Pastò, Ph.D., Don McCreary, Ph.D., Megan Thompson, Ph.D.
 Deployment Stressors, Coping, and Psychological Well-Being Among Peacekeepers Luigi Pastò, Ph.D., Don McCreary, Ph.D., Megan Thompson, Ph.D. Defence Research and Development Toronto 1133 Sheppard Avenue
Deployment Stressors, Coping, and Psychological Well-Being Among Peacekeepers Luigi Pastò, Ph.D., Don McCreary, Ph.D., Megan Thompson, Ph.D. Defence Research and Development Toronto 1133 Sheppard Avenue
To Reduce or Abstain? Substance Use Goals in the Treatment of Veterans With Substance Use Disorders and Comorbid PTSD
 The American Journal on Addictions, 24: 578 581, 2015 Copyright American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/ajad.12263 To Reduce or Abstain? Substance
The American Journal on Addictions, 24: 578 581, 2015 Copyright American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/ajad.12263 To Reduce or Abstain? Substance
Co-Occurring PTSD and Substance Abuse in Veterans
 Co-Occurring PTSD and Substance Abuse in Veterans Study of residential PTSD program: Substance abuse onset associated with onset of PTSD symptoms Increases in substance abuse paralleled increases in PTSD
Co-Occurring PTSD and Substance Abuse in Veterans Study of residential PTSD program: Substance abuse onset associated with onset of PTSD symptoms Increases in substance abuse paralleled increases in PTSD
Comorbidity With Substance Abuse P a g e 1
 Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
Comorbidity With Substance Abuse P a g e 1 Comorbidity With Substance Abuse Introduction This interesting session provided an overview of recent findings in the diagnosis and treatment of several psychiatric
SCREENING FOR SOCIAL ANXIETY DISORDER WITH THE SELF-REPORT VERSION OF THE LIEBOWITZ SOCIAL ANXIETY SCALE
 DEPRESSION AND ANXIETY 26:34 38 (2009) Research Article SCREENING FOR SOCIAL ANXIETY DISORDER WITH THE SELF-REPORT VERSION OF THE LIEBOWITZ SOCIAL ANXIETY SCALE Nina K. Rytwinski, M.A., 1 David M. Fresco,
DEPRESSION AND ANXIETY 26:34 38 (2009) Research Article SCREENING FOR SOCIAL ANXIETY DISORDER WITH THE SELF-REPORT VERSION OF THE LIEBOWITZ SOCIAL ANXIETY SCALE Nina K. Rytwinski, M.A., 1 David M. Fresco,
The Intersection of Post-Traumatic Stress and Substance Use Disorders. Implications for an emerging integrated treatment approach
 The Intersection of Post-Traumatic Stress and Substance Use Disorders Implications for an emerging integrated treatment approach Christal L. Badour, PhD Assistant Professor Department of Psychology Overview
The Intersection of Post-Traumatic Stress and Substance Use Disorders Implications for an emerging integrated treatment approach Christal L. Badour, PhD Assistant Professor Department of Psychology Overview
Screening and Brief Intervention for Risky Substance Use
 Screening and Brief Intervention for Risky Substance Use Trauma and Analgesia: Balancing Patient Comfort and Opioid-Related Risks Joe Glass, PhD MSW Assistant Scientific Investigator Group Health Research
Screening and Brief Intervention for Risky Substance Use Trauma and Analgesia: Balancing Patient Comfort and Opioid-Related Risks Joe Glass, PhD MSW Assistant Scientific Investigator Group Health Research
Readiness for Change Predicts VA Mental Healthcare Utilization Among Iraq and Afghanistan War Veterans
 Journal of Traumatic Stress February 2013, 26, 165 168 BRIEF REPORT Readiness for Change Predicts VA Mental Healthcare Utilization Among Iraq and Afghanistan War Veterans Matthew Jakupcak, 1,2 Katherine
Journal of Traumatic Stress February 2013, 26, 165 168 BRIEF REPORT Readiness for Change Predicts VA Mental Healthcare Utilization Among Iraq and Afghanistan War Veterans Matthew Jakupcak, 1,2 Katherine
Which Instruments Are Most Commonly Used to Assess Traumatic Event Exposure and Posttraumatic Effects?: A Survey of Traumatic Stress Professionals
 Journal of Traumatic Stress, Vol. 18, No. 5, October 2005, pp. 1 5 ( C 2005) Which Instruments Are Most Commonly Used to Assess Traumatic Event Exposure and Posttraumatic Effects?: A Survey of Traumatic
Journal of Traumatic Stress, Vol. 18, No. 5, October 2005, pp. 1 5 ( C 2005) Which Instruments Are Most Commonly Used to Assess Traumatic Event Exposure and Posttraumatic Effects?: A Survey of Traumatic
Chapter 7. Screening and Assessment
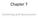 Chapter 7 Screening and Assessment Screening And Assessment Starting the dialogue and begin relationship Each are sizing each other up Information gathering Listening to their story Asking the questions
Chapter 7 Screening and Assessment Screening And Assessment Starting the dialogue and begin relationship Each are sizing each other up Information gathering Listening to their story Asking the questions
Psychology Research Institute, University of Ulster, Northland Road, Londonderry, BT48 7JL, UK
 Patterns of Alcohol Consumption and Related Behaviour in Great Britain: A Latent Class Analysis of the Alcohol Use Disorder Identification Test (AUDIT) Gillian W. Smith * and Mark Shevlin Psychology Research
Patterns of Alcohol Consumption and Related Behaviour in Great Britain: A Latent Class Analysis of the Alcohol Use Disorder Identification Test (AUDIT) Gillian W. Smith * and Mark Shevlin Psychology Research
Predictors of Employment and Productivity Among Returning National Guard Members
 Predictors of Employment and Productivity Among Returning National Guard Members Kara Zivin, Ph.D. VA National Serious Mental Illness Treatment Resource & Evaluation Center VA Ann Arbor HSR&D Center of
Predictors of Employment and Productivity Among Returning National Guard Members Kara Zivin, Ph.D. VA National Serious Mental Illness Treatment Resource & Evaluation Center VA Ann Arbor HSR&D Center of
Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes
 MILITARY MEDICINE, 178, 12:1328, 2013 Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes Meaghan O Donnell, PhD*; Tracey Varker, PhD*; Desmond Perry,
MILITARY MEDICINE, 178, 12:1328, 2013 Effect of Center-Based Counseling for Veterans and Veterans Families on Long-Term Mental Health Outcomes Meaghan O Donnell, PhD*; Tracey Varker, PhD*; Desmond Perry,
Mental Disorders Among OEF/OIF Veterans Using VA Health Care: Facts and Figures
 Mental Disorders Among OEF/OIF Veterans Using VA Health Care: Facts and Figures Erin Bagalman Analyst in Health Policy January 11, 2013 CRS Report for Congress Prepared for Members and Committees of Congress
Mental Disorders Among OEF/OIF Veterans Using VA Health Care: Facts and Figures Erin Bagalman Analyst in Health Policy January 11, 2013 CRS Report for Congress Prepared for Members and Committees of Congress
Angela E. Waldrop, PhD, 1,2 Beth E. Cohen, MD, MAS 1,2
 The American Journal on Addictions, 23: 53 61, 2014 Copyright American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/j.1521-0391.2013.12053.x Trauma Exposure Predicts
The American Journal on Addictions, 23: 53 61, 2014 Copyright American Academy of Addiction Psychiatry ISSN: 1055-0496 print / 1521-0391 online DOI: 10.1111/j.1521-0391.2013.12053.x Trauma Exposure Predicts
Cognitive-Behavioral Conjoint Therapy for PTSD: Initial Findings for Operations Enduring and Iraqi Freedom Male Combat Veterans and Their Partners
 The American Journal of Family Therapy, 41:277 287, 2013 Copyright Taylor & Francis Group, LLC ISSN: 0192-6187 print / 1521-0383 online DOI: 10.1080/01926187.2012.701592 Cognitive-Behavioral Conjoint Therapy
The American Journal of Family Therapy, 41:277 287, 2013 Copyright Taylor & Francis Group, LLC ISSN: 0192-6187 print / 1521-0383 online DOI: 10.1080/01926187.2012.701592 Cognitive-Behavioral Conjoint Therapy
Traumatic Brain Injury and Suicidal Ideation Among U.S. Operation Enduring Freedom and Operation Iraqi Freedom Veterans
 Journal of Traumatic Stress August 2015, 28, 361 365 BRIEF REPORT Traumatic Brain Injury and Suicidal Ideation Among U.S. Operation Enduring Freedom and Operation Iraqi Freedom Veterans Jaimie L. Gradus,
Journal of Traumatic Stress August 2015, 28, 361 365 BRIEF REPORT Traumatic Brain Injury and Suicidal Ideation Among U.S. Operation Enduring Freedom and Operation Iraqi Freedom Veterans Jaimie L. Gradus,
The potential for faking on the Mississippi Scale for Combat-Related PTSD
 The potential for faking on the Mississippi Scale for Combat-Related PTSD Lyons, J.A.; Caddell, J.M.; Pittman, R.L.; Rawls, R.; Perrin, Sean Published in: Journal of Traumatic Stress DOI: 10.1007/BF02102788
The potential for faking on the Mississippi Scale for Combat-Related PTSD Lyons, J.A.; Caddell, J.M.; Pittman, R.L.; Rawls, R.; Perrin, Sean Published in: Journal of Traumatic Stress DOI: 10.1007/BF02102788
Moral Injury and Stress Response Patterns in United States Military Veterans
 Modern Psychological Studies Volume 23 Number 1 2017 Moral Injury and Stress Response Patterns in United States Military Veterans Emily L. Ferrell Bowling Green State University, emilylf@bgsu.edu John
Modern Psychological Studies Volume 23 Number 1 2017 Moral Injury and Stress Response Patterns in United States Military Veterans Emily L. Ferrell Bowling Green State University, emilylf@bgsu.edu John
Traumatic Events and Suicide Attempts
 Traumatic Events and Suicide Attempts Findings from a large representative sample of Canadian military personnel Presenter: Shay-Lee Belik Co-Authors: Brian J Cox Gordon JG Asmundson Murray B Stein Jitender
Traumatic Events and Suicide Attempts Findings from a large representative sample of Canadian military personnel Presenter: Shay-Lee Belik Co-Authors: Brian J Cox Gordon JG Asmundson Murray B Stein Jitender
For surveillance purposes, a case of adjustment disorder is defined as:
 1 MH 12 ADJUSTMENT DISORDERS Does Not Include Acute Stress Reaction or Post Traumatic Stress Disorder (PTSD); For PTSD, See Post-Traumatic Stress Disorder Case Definition. Background This case definition
1 MH 12 ADJUSTMENT DISORDERS Does Not Include Acute Stress Reaction or Post Traumatic Stress Disorder (PTSD); For PTSD, See Post-Traumatic Stress Disorder Case Definition. Background This case definition
Chapter 7. Screening and Assessment
 Chapter 7 Screening and Assessment Screening And Assessment Starting the dialogue and begin relationship Each are sizing each other up Information gathering Listening to their story Asking the questions
Chapter 7 Screening and Assessment Screening And Assessment Starting the dialogue and begin relationship Each are sizing each other up Information gathering Listening to their story Asking the questions
Deployment, Readjustment & Restoration: The PTSD Family Workshop. Stratton VA Medical Center, Albany, NY
 Deployment, Readjustment & Restoration: The PTSD Family Workshop Stratton VA Medical Center, Albany, NY Homecoming With deployment comes change, knowing what to expect and how to deal with changes will
Deployment, Readjustment & Restoration: The PTSD Family Workshop Stratton VA Medical Center, Albany, NY Homecoming With deployment comes change, knowing what to expect and how to deal with changes will
The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders
 AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
AM. J. DRUG ALCOHOL ABUSE, 26(3), pp. 369 378 (2000) The Use of Collateral Reports for Patients with Bipolar and Substance Use Disorders Roger D. Weiss, M.D.* Shelly F. Greenfield, M.D., M.P.H. Margaret
Post-traumatic Growth
 Post-traumatic Growth By Jenna Van Slyke, M.S. Naval Center for Combat & Operational Stress Control The Impact of Trauma For centuries, man has pondered what sustains the human spirit in times of extreme
Post-traumatic Growth By Jenna Van Slyke, M.S. Naval Center for Combat & Operational Stress Control The Impact of Trauma For centuries, man has pondered what sustains the human spirit in times of extreme
Questionnaire on Anticipated Discrimination (QUAD)(1): is a self-complete measure comprising 14 items
 Online Supplement Data Supplement for Clement et al. (10.1176/appi.ps.201300448) Details of additional measures included in the analysis Questionnaire on Anticipated Discrimination (QUAD)(1): is a self-complete
Online Supplement Data Supplement for Clement et al. (10.1176/appi.ps.201300448) Details of additional measures included in the analysis Questionnaire on Anticipated Discrimination (QUAD)(1): is a self-complete
Addressing Mental Health in HIV Prevention and Treatment Research Kathleen J. Sikkema, Ph.D.
 Addressing Mental Health in HIV Prevention and Treatment Research Kathleen J. Sikkema, Ph.D. Professor of Psychology and Neuroscience, Global Health, and Psychiatry and Behavioral Sciences Director, Social
Addressing Mental Health in HIV Prevention and Treatment Research Kathleen J. Sikkema, Ph.D. Professor of Psychology and Neuroscience, Global Health, and Psychiatry and Behavioral Sciences Director, Social
Posttraumatic Stress Disorder and Suicidal Behavior: Current Understanding and Future Directions
 Posttraumatic Stress Disorder and Suicidal Behavior: Current Understanding and Future Directions Jaimie L. Gradus, DSc, MPH Epidemiologist, National Center for PTSD, VA Boston Healthcare System Associate
Posttraumatic Stress Disorder and Suicidal Behavior: Current Understanding and Future Directions Jaimie L. Gradus, DSc, MPH Epidemiologist, National Center for PTSD, VA Boston Healthcare System Associate
Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications
 MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
MWSUG 2017 - Paper DG02 Exploring the Relationship Between Substance Abuse and Dependence Disorders and Discharge Status: Results and Implications ABSTRACT Deanna Naomi Schreiber-Gregory, Henry M Jackson
CRITICALLY APPRAISED PAPER (CAP)
 CRITICALLY APPRAISED PAPER (CAP) Biggs, Q. M., Fullerton, C. S., McCarroll, J. E., Liu, X., Wang, L., Dacuyan, N. M.,... Ursano, R. J. (2016). Early intervention for post-traumatic stress disorder, depression,
CRITICALLY APPRAISED PAPER (CAP) Biggs, Q. M., Fullerton, C. S., McCarroll, J. E., Liu, X., Wang, L., Dacuyan, N. M.,... Ursano, R. J. (2016). Early intervention for post-traumatic stress disorder, depression,
Posttraumatic stress disorder (PTSD) is one of the most
 Article Medical Service Utilization by Veterans Seeking Help for Posttraumatic Stress Disorder Patrick S. Calhoun, Ph.D. Hayden B. Bosworth, Ph.D. Steven C. Grambow, Ph.D. Tara K. Dudley, M.Stat. Jean
Article Medical Service Utilization by Veterans Seeking Help for Posttraumatic Stress Disorder Patrick S. Calhoun, Ph.D. Hayden B. Bosworth, Ph.D. Steven C. Grambow, Ph.D. Tara K. Dudley, M.Stat. Jean
The traditional approach to. Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans
 Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans John A. Schinka, Ph.D. Roger J. Casey, Ph.D., M.S.W. Wesley Kasprow, Ph.D., M.P.H. Robert
Requiring Sobriety at Program Entry: Impact on Outcomes in Supported Transitional Housing for Homeless Veterans John A. Schinka, Ph.D. Roger J. Casey, Ph.D., M.S.W. Wesley Kasprow, Ph.D., M.P.H. Robert
Reliability. Internal Reliability
 32 Reliability T he reliability of assessments like the DECA-I/T is defined as, the consistency of scores obtained by the same person when reexamined with the same test on different occasions, or with
32 Reliability T he reliability of assessments like the DECA-I/T is defined as, the consistency of scores obtained by the same person when reexamined with the same test on different occasions, or with
EDRS. trends. bulletin. Alcohol use disorders amongst a group of regular ecstasy users. Key findings. july Introduction.
 ecstasy and related drug trends july 2011 bulletin Authors: Sheena Arora and Lucy Burns, National Drug and Alcohol Research Centre, University of New South Wales Suggested citation: Arora, S. & Burns,
ecstasy and related drug trends july 2011 bulletin Authors: Sheena Arora and Lucy Burns, National Drug and Alcohol Research Centre, University of New South Wales Suggested citation: Arora, S. & Burns,
A new scale (SES) to measure engagement with community mental health services
 Title A new scale (SES) to measure engagement with community mental health services Service engagement scale LYNDA TAIT 1, MAX BIRCHWOOD 2 & PETER TROWER 1 2 Early Intervention Service, Northern Birmingham
Title A new scale (SES) to measure engagement with community mental health services Service engagement scale LYNDA TAIT 1, MAX BIRCHWOOD 2 & PETER TROWER 1 2 Early Intervention Service, Northern Birmingham
Final Report. HOS/VA Comparison Project
 Final Report HOS/VA Comparison Project Part 2: Tests of Reliability and Validity at the Scale Level for the Medicare HOS MOS -SF-36 and the VA Veterans SF-36 Lewis E. Kazis, Austin F. Lee, Avron Spiro
Final Report HOS/VA Comparison Project Part 2: Tests of Reliability and Validity at the Scale Level for the Medicare HOS MOS -SF-36 and the VA Veterans SF-36 Lewis E. Kazis, Austin F. Lee, Avron Spiro
Do Homeless Veterans Have the Same Needs and Outcomes as Non-Veterans?
 MILITARY MEDICINE, 177, 1:27, 2012 Do Homeless Veterans Have the Same Needs and Outcomes as Non-Veterans? Jack Tsai, PhD * ; Alvin S. Mares, PhD ; Robert A. Rosenheck, MD * ABSTRACT Although veterans have
MILITARY MEDICINE, 177, 1:27, 2012 Do Homeless Veterans Have the Same Needs and Outcomes as Non-Veterans? Jack Tsai, PhD * ; Alvin S. Mares, PhD ; Robert A. Rosenheck, MD * ABSTRACT Although veterans have
Chronic Widespread Pain, Mental Health, and Physical Role Function in OEF/OIF Veteranspme_
 PAIN MEDICINE Volume 10 Number 7 2009 Chronic Widespread Pain, Mental Health, and Physical Role Function in OEF/OIF Veteranspme_723 1174..1182 Drew A. Helmer, MD, MS,* Helena K. Chandler, PhD, Karen S.
PAIN MEDICINE Volume 10 Number 7 2009 Chronic Widespread Pain, Mental Health, and Physical Role Function in OEF/OIF Veteranspme_723 1174..1182 Drew A. Helmer, MD, MS,* Helena K. Chandler, PhD, Karen S.
Working in post conflict zone is as stressful as working home
 IAMPS, Bucharest, May 10, 2018 Working in post conflict zone is as stressful as working home preliminary evidence from a multi sample PTSD screening Lt.col. Ştefan Liţă, PhD Psychological Services Section,
IAMPS, Bucharest, May 10, 2018 Working in post conflict zone is as stressful as working home preliminary evidence from a multi sample PTSD screening Lt.col. Ştefan Liţă, PhD Psychological Services Section,
Running head: RELIGIOUS STRENGTH AND PTG 1
 Running head: RELIGIOUS STRENGTH AND PTG 1 Religious Strength and Posttraumatic Growth: Examining the Effect of Alcohol Consumption in College Students Melissa Sawa and Valarie Pierson Faculty sponsor:
Running head: RELIGIOUS STRENGTH AND PTG 1 Religious Strength and Posttraumatic Growth: Examining the Effect of Alcohol Consumption in College Students Melissa Sawa and Valarie Pierson Faculty sponsor:
Trauma exposure is alarmingly high among the general
 ORIGINAL RESEARCH Posttraumatic Stress Symptoms and Cognitive-Based Smoking Processes Among Trauma-Exposed, Treatment-Seeking Smokers: The Role of Dysphoria Lorra Garey, BA, Jafar Bakhshaie, MD, Anka A.
ORIGINAL RESEARCH Posttraumatic Stress Symptoms and Cognitive-Based Smoking Processes Among Trauma-Exposed, Treatment-Seeking Smokers: The Role of Dysphoria Lorra Garey, BA, Jafar Bakhshaie, MD, Anka A.
Effects of PTSD with Family Members of Veterans. Dr. Barbara Anderson, DSW, MSW, BCD, MAC, LICSW
 Effects of PTSD with Family Members of Veterans Dr. Barbara Anderson, DSW, MSW, BCD, MAC, LICSW Learning Objectives: 1) Increased knowledge about Post-Traumatic Stress Disorder and the effects of Post-Traumatic
Effects of PTSD with Family Members of Veterans Dr. Barbara Anderson, DSW, MSW, BCD, MAC, LICSW Learning Objectives: 1) Increased knowledge about Post-Traumatic Stress Disorder and the effects of Post-Traumatic
Avoidant Coping Moderates the Association between Anxiety and Physical Functioning in Patients with Chronic Heart Failure
 Avoidant Coping Moderates the Association between Anxiety and Physical Functioning in Patients with Chronic Heart Failure Eisenberg SA 1, Shen BJ 1, Singh K 1, Schwarz ER 2, Mallon SM 3 1 University of
Avoidant Coping Moderates the Association between Anxiety and Physical Functioning in Patients with Chronic Heart Failure Eisenberg SA 1, Shen BJ 1, Singh K 1, Schwarz ER 2, Mallon SM 3 1 University of
Using the PTSD Checklist for DSM-5 (PCL-5)
 Using the PTSD Checklist for DSM-5 (PCL-5) www.ptsd.va.gov www.ptsd.va.gov Using the PTSD Checklist for DSM-5 NOTE: The PCL for DSM-IV was revised in accordance with DSM- 5 (PCL-5). Several important revisions
Using the PTSD Checklist for DSM-5 (PCL-5) www.ptsd.va.gov www.ptsd.va.gov Using the PTSD Checklist for DSM-5 NOTE: The PCL for DSM-IV was revised in accordance with DSM- 5 (PCL-5). Several important revisions
Perceived Behavioral Alcohol Norms Predict Drinking for College Students While Studying Abroad*
 924 JOURNAL OF STUDIES ON ALCOHOL and Drugs / NOVEMBER 2009 Perceived Behavioral Alcohol Norms Predict Drinking for College Students While Studying Abroad* ERIC R. PEDERSEN, m.a., JOSEPH W. LaBRIE, ph.d.,
924 JOURNAL OF STUDIES ON ALCOHOL and Drugs / NOVEMBER 2009 Perceived Behavioral Alcohol Norms Predict Drinking for College Students While Studying Abroad* ERIC R. PEDERSEN, m.a., JOSEPH W. LaBRIE, ph.d.,
Predicting Engagement in Psychotherapy, Pharmacotherapy, or Both Psychotherapy and Pharmacotherapy Among Returning Veterans Seeking PTSD Treatment
 Psychological Services 2016 American Psychological Association 2016, Vol. 13, No. 4, 341 348 1541-1559/16/$12.00 http://dx.doi.org/10.1037/ser0000093 Predicting Engagement in Psychotherapy, Pharmacotherapy,
Psychological Services 2016 American Psychological Association 2016, Vol. 13, No. 4, 341 348 1541-1559/16/$12.00 http://dx.doi.org/10.1037/ser0000093 Predicting Engagement in Psychotherapy, Pharmacotherapy,
Understanding the role of Acute Stress Disorder in trauma
 Understanding the role of Acute Stress Disorder in trauma Dr. Trina Hall Police Psychologist Dallas Police Department Lessons Learned: Unfolding the story of PTSD NAMI 2014 Fall Conference Trauma and
Understanding the role of Acute Stress Disorder in trauma Dr. Trina Hall Police Psychologist Dallas Police Department Lessons Learned: Unfolding the story of PTSD NAMI 2014 Fall Conference Trauma and
Center for the Study of Family Violence and Sexual Assault Military-Related Publications (chronological order)
 1 Center for the Study of Family Violence and Sexual Assault Military-Related Publications (chronological order) Note. In addition to this list of publicly available publications, there are several research
1 Center for the Study of Family Violence and Sexual Assault Military-Related Publications (chronological order) Note. In addition to this list of publicly available publications, there are several research
Trauma Centrality and PTSD Symptom Severity in Adult Survivors of Childhood Sexual Abuse
 Trauma Centrality and PTSD Symptom Severity in Adult Survivors of Childhood Sexual Abuse The Harvard community has made this article openly available. Please share how this access benefits you. Your story
Trauma Centrality and PTSD Symptom Severity in Adult Survivors of Childhood Sexual Abuse The Harvard community has made this article openly available. Please share how this access benefits you. Your story
Social Participation Among Veterans With SCI/D: The Impact of Post Traumatic Stress Disorder
 Social Participation Among Veterans With SCI/D: The Impact of Post Traumatic Stress Disorder Bella Etingen, PhD 1 ;Sara M. Locatelli, PhD 1 ;Scott Miskevics, BS 1 ; Sherri L. LaVela, PhD, MPH, MBA 1,2
Social Participation Among Veterans With SCI/D: The Impact of Post Traumatic Stress Disorder Bella Etingen, PhD 1 ;Sara M. Locatelli, PhD 1 ;Scott Miskevics, BS 1 ; Sherri L. LaVela, PhD, MPH, MBA 1,2
Mental Health Diagnoses and Utilization of VA Non-Mental Health Medical Services Among Returning Iraq and Afghanistan Veterans
 Mental Health Diagnoses and Utilization of VA Non-Mental Health Medical Services Among Returning Iraq and Afghanistan Veterans Beth E. Cohen, MD, MAS 1,2, Kris Gima, BA 1, Daniel Bertenthal, MPH 1,2,3,
Mental Health Diagnoses and Utilization of VA Non-Mental Health Medical Services Among Returning Iraq and Afghanistan Veterans Beth E. Cohen, MD, MAS 1,2, Kris Gima, BA 1, Daniel Bertenthal, MPH 1,2,3,
Reliability and Validity of the Pediatric Quality of Life Inventory Generic Core Scales, Multidimensional Fatigue Scale, and Cancer Module
 2090 The PedsQL in Pediatric Cancer Reliability and Validity of the Pediatric Quality of Life Inventory Generic Core Scales, Multidimensional Fatigue Scale, and Cancer Module James W. Varni, Ph.D. 1,2
2090 The PedsQL in Pediatric Cancer Reliability and Validity of the Pediatric Quality of Life Inventory Generic Core Scales, Multidimensional Fatigue Scale, and Cancer Module James W. Varni, Ph.D. 1,2
One important measure of the clinical relevance of a
 Article Five-Year Clinical Course Associated With DSM-IV Alcohol Abuse or Dependence in a Large Group of Men and Women Marc A. Schuckit, M.D. Tom L. Smith, Ph.D. George P. Danko, Ph.D. Kathleen K. Bucholz,
Article Five-Year Clinical Course Associated With DSM-IV Alcohol Abuse or Dependence in a Large Group of Men and Women Marc A. Schuckit, M.D. Tom L. Smith, Ph.D. George P. Danko, Ph.D. Kathleen K. Bucholz,
Acute Stabilization In A Trauma Program: A Pilot Study. Colin A. Ross, MD. Sean Burns, MA, LLP
 In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
In Press, Psychological Trauma Acute Stabilization In A Trauma Program: A Pilot Study Colin A. Ross, MD Sean Burns, MA, LLP Address correspondence to: Colin A. Ross, MD, 1701 Gateway, Suite 349, Richardson,
Treatment of PTSD in VA Facilities and Programs
 Treatment of PTSD in VA Facilities and Programs Alfonso R. Batres, Ph.D., M.S.S.W. Chief Officer Readjustment Counseling Service (15) Tuesday, January 16, 2007 The National Academy of Sciences Building
Treatment of PTSD in VA Facilities and Programs Alfonso R. Batres, Ph.D., M.S.S.W. Chief Officer Readjustment Counseling Service (15) Tuesday, January 16, 2007 The National Academy of Sciences Building
The lifesaving value and improved
 Cardiology Patient Page Coping With Trauma and Stressful Events as a Patient With an Implantable Cardioverter-Defibrillator Jessica Ford, MA; Samuel F. Sears, PhD; Julie B. Shea, MS, RNCS; John Cahill,
Cardiology Patient Page Coping With Trauma and Stressful Events as a Patient With an Implantable Cardioverter-Defibrillator Jessica Ford, MA; Samuel F. Sears, PhD; Julie B. Shea, MS, RNCS; John Cahill,
Setting Non-profit psychiatric hospital. The economic analysis was carried out in the USA.
 Inpatient alcohol treatment in a private healthcare setting: which patients benefit and at what cost? Pettinati H M, Meyers K, Evans B D, Ruetsch C R, Kaplan F N, Jensen J M, Hadley T R Record Status This
Inpatient alcohol treatment in a private healthcare setting: which patients benefit and at what cost? Pettinati H M, Meyers K, Evans B D, Ruetsch C R, Kaplan F N, Jensen J M, Hadley T R Record Status This
CHAPTER 2 CRITERION VALIDITY OF AN ATTENTION- DEFICIT/HYPERACTIVITY DISORDER (ADHD) SCREENING LIST FOR SCREENING ADHD IN OLDER ADULTS AGED YEARS
 CHAPTER 2 CRITERION VALIDITY OF AN ATTENTION- DEFICIT/HYPERACTIVITY DISORDER (ADHD) SCREENING LIST FOR SCREENING ADHD IN OLDER ADULTS AGED 60 94 YEARS AM. J. GERIATR. PSYCHIATRY. 2013;21(7):631 635 DOI:
CHAPTER 2 CRITERION VALIDITY OF AN ATTENTION- DEFICIT/HYPERACTIVITY DISORDER (ADHD) SCREENING LIST FOR SCREENING ADHD IN OLDER ADULTS AGED 60 94 YEARS AM. J. GERIATR. PSYCHIATRY. 2013;21(7):631 635 DOI:
Supplementary Methods
 Supplementary Materials for Suicidal Behavior During Lithium and Valproate Medication: A Withinindividual Eight Year Prospective Study of 50,000 Patients With Bipolar Disorder Supplementary Methods We
Supplementary Materials for Suicidal Behavior During Lithium and Valproate Medication: A Withinindividual Eight Year Prospective Study of 50,000 Patients With Bipolar Disorder Supplementary Methods We
A Validation Study of the Brief Alcohol Use Disorder Identification Test (AUDIT): A Brief Screening Tool Derived from the AUDIT
 Korean J Fam Med. 2013;34:11-18 http://dx.doi.org/10.4082/kjfm.2013.34.1.11 A Validation Study of the Brief Alcohol Use Disorder Identification Test (AUDIT): A Brief Screening Tool Derived from the AUDIT
Korean J Fam Med. 2013;34:11-18 http://dx.doi.org/10.4082/kjfm.2013.34.1.11 A Validation Study of the Brief Alcohol Use Disorder Identification Test (AUDIT): A Brief Screening Tool Derived from the AUDIT
Chapter 3. Psychometric Properties
 Chapter 3 Psychometric Properties Reliability The reliability of an assessment tool like the DECA-C is defined as, the consistency of scores obtained by the same person when reexamined with the same test
Chapter 3 Psychometric Properties Reliability The reliability of an assessment tool like the DECA-C is defined as, the consistency of scores obtained by the same person when reexamined with the same test
Trauma informed care. Prof. Edward Ogden PSM
 Trauma informed care Prof. Edward Ogden PSM Who Gets PTSD? It depends on: Severity Duration Proximity PTSD is mitigated or worsened by: Childhood experience Personality characteristics Family history Social
Trauma informed care Prof. Edward Ogden PSM Who Gets PTSD? It depends on: Severity Duration Proximity PTSD is mitigated or worsened by: Childhood experience Personality characteristics Family history Social
Supplemental Information
 Supplemental Information 1. Key Assessment Tools a. PTSD Checklist for DSM IV/V (PCL-5): A 20-item self-report measure that assesses the 20 DSM-IV/V. The PCL-5 serves to monitor symptoms change during
Supplemental Information 1. Key Assessment Tools a. PTSD Checklist for DSM IV/V (PCL-5): A 20-item self-report measure that assesses the 20 DSM-IV/V. The PCL-5 serves to monitor symptoms change during
Agrowing body of literature reveals. Service Utilization and Help Seeking in a National Sample of Female Rape Victims
 Service Utilization and Help Seeking in a National Sample of Female Rape Victims Ananda B. Amstadter, Ph.D. Jenna L. McCauley, Ph.D. Kenneth J. Ruggiero, Ph.D. Heidi S. Resnick, Ph.D. Dean G. Kilpatrick,
Service Utilization and Help Seeking in a National Sample of Female Rape Victims Ananda B. Amstadter, Ph.D. Jenna L. McCauley, Ph.D. Kenneth J. Ruggiero, Ph.D. Heidi S. Resnick, Ph.D. Dean G. Kilpatrick,
Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence
 Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
Journal of Affective Disorders 79 (2004) 279 283 Brief report Substance use and perceived symptom improvement among patients with bipolar disorder and substance dependence Roger D. Weiss a,b, *, Monika
Screening for Traumatic Stress among Re-deploying Soldiers
 R E S E A R C H R E P O R T # 2 0 0 4-0 0 1 US Army Medical Research Unit - Europe Walter Reed Army Institute of Research MAJ Paul Bliese (paul.bliese@us.army.mil) Dr. Kathleen Wright (kathleen.wright@us.army.mil)
R E S E A R C H R E P O R T # 2 0 0 4-0 0 1 US Army Medical Research Unit - Europe Walter Reed Army Institute of Research MAJ Paul Bliese (paul.bliese@us.army.mil) Dr. Kathleen Wright (kathleen.wright@us.army.mil)
The Many Presentations of Posttraumatic Stress Disorder: An Empirical Examination of Theoretical Possibilities
 480151SGOXXX10.1177/215824 4013480151SAGE OpenHickling et al. 2013 The Many Presentations of Posttraumatic Stress Disorder: An Empirical Examination of Theoretical Possibilities SAGE Open January-March
480151SGOXXX10.1177/215824 4013480151SAGE OpenHickling et al. 2013 The Many Presentations of Posttraumatic Stress Disorder: An Empirical Examination of Theoretical Possibilities SAGE Open January-March
THE LONG TERM PSYCHOLOGICAL EFFECTS OF DAILY SEDATIVE INTERRUPTION IN CRITICALLY ILL PATIENTS
 THE LONG TERM PSYCHOLOGICAL EFFECTS OF DAILY SEDATIVE INTERRUPTION IN CRITICALLY ILL PATIENTS John P. Kress, MD, Brian Gehlbach, MD, Maureen Lacy, PhD, Neil Pliskin, PhD, Anne S. Pohlman, RN, MSN, and
THE LONG TERM PSYCHOLOGICAL EFFECTS OF DAILY SEDATIVE INTERRUPTION IN CRITICALLY ILL PATIENTS John P. Kress, MD, Brian Gehlbach, MD, Maureen Lacy, PhD, Neil Pliskin, PhD, Anne S. Pohlman, RN, MSN, and
POSTTRAUMATIC GROWTH AND REDUCED PTSD FOR VETERANS THROUGH RECREATION
 1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 POSTTRAUMATIC GROWTH AND REDUCED PTSD FOR VETERANS THROUGH RECREATION Jessie
1 2 3 4 5 6 7 8 9 10 11 12 13 14 15 16 17 18 19 20 21 22 23 24 25 26 27 28 29 30 31 32 33 34 35 36 37 38 39 40 41 42 43 44 45 46 POSTTRAUMATIC GROWTH AND REDUCED PTSD FOR VETERANS THROUGH RECREATION Jessie
EMERGENCY ROOM AND PRIMARY CARE SERVICES UTILIZATION AND ASSOCIATED ALCOHOL AND DRUG USE IN THE UNITED STATES GENERAL POPULATION
 Alcohol & Alcoholism Vol. 34, No. 4, pp. 581 589, 1999 EMERGENCY ROOM AND PRIMARY CARE SERVICES UTILIZATION AND ASSOCIATED ALCOHOL AND DRUG USE IN THE UNITED STATES GENERAL POPULATION CHERYL J. CHERPITEL
Alcohol & Alcoholism Vol. 34, No. 4, pp. 581 589, 1999 EMERGENCY ROOM AND PRIMARY CARE SERVICES UTILIZATION AND ASSOCIATED ALCOHOL AND DRUG USE IN THE UNITED STATES GENERAL POPULATION CHERYL J. CHERPITEL
RESEARCH AND PRACTICE. Karen H. Seal, MD, MPH, Daniel Bertenthal, MPH, Shira Maguen, PhD, Kristian Gima, BA, Ann Chu, MS, and Charles R.
 Getting Beyond Don t Ask; Don t Tell : an Evaluation of US Veterans Administration Postdeployment Mental Health Screening of Veterans Returning From Iraq and Afghanistan Karen H. Seal, MD, MPH, Daniel
Getting Beyond Don t Ask; Don t Tell : an Evaluation of US Veterans Administration Postdeployment Mental Health Screening of Veterans Returning From Iraq and Afghanistan Karen H. Seal, MD, MPH, Daniel
PTSD and Other Invisible Wounds affecting our Service Members and Veterans. Alan Peterson, PhD, ABPP
 PTSD and Other Invisible Wounds affecting our Service Members and Veterans Alan Peterson, PhD, ABPP 1 Alan Peterson, PhD, ABPP Retired USAF Lt Col Clinical Health Psychologist Former Chair, Department
PTSD and Other Invisible Wounds affecting our Service Members and Veterans Alan Peterson, PhD, ABPP 1 Alan Peterson, PhD, ABPP Retired USAF Lt Col Clinical Health Psychologist Former Chair, Department
Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure (COPE): A Pilot Study in Alcohol-dependent Women
 ORIGINAL RESEARCH Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure (COPE): A Pilot Study in Alcohol-dependent Women Anna Persson, MSc, Sudie E. Back, PhD, Therese K. Killeen,
ORIGINAL RESEARCH Concurrent Treatment of PTSD and Substance Use Disorders Using Prolonged Exposure (COPE): A Pilot Study in Alcohol-dependent Women Anna Persson, MSc, Sudie E. Back, PhD, Therese K. Killeen,
b. Potentially harmful alcohol misuse remains a common behavioural problem, but has declined steadily from 16% in 2004/6 to 10% in 2014/16.
 THE MENTAL HEALTH OF THE UK ARMED FORCES (September 2018 version) This briefing note provides an outline of the current evidence on UK military mental health, including prevalence rates of mental health
THE MENTAL HEALTH OF THE UK ARMED FORCES (September 2018 version) This briefing note provides an outline of the current evidence on UK military mental health, including prevalence rates of mental health
Validation of the Chinese Juvenile Victimisation Questionnaire
 HK J Paediatr (new series) 2011;16:17-24 Validation of the Chinese Juvenile Victimisation Questionnaire KL CHAN, DYT FONG, E YAN, CB CHOW, P IP Abstract Key words Objective: The primary objective of this
HK J Paediatr (new series) 2011;16:17-24 Validation of the Chinese Juvenile Victimisation Questionnaire KL CHAN, DYT FONG, E YAN, CB CHOW, P IP Abstract Key words Objective: The primary objective of this
Prospective assessment of treatment use by patients with personality disorders
 Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
Wesleyan University From the SelectedWorks of Charles A. Sanislow, Ph.D. February, 2006 Prospective assessment of treatment use by Donna S. Bender Andrew E. Skodol Maria E. Pagano Ingrid R. Dyck Carlos
Trauma and Addiction
 Trauma and Addiction Martha T. Kane, PhD Clinical Director, Center for Addiction Medicine Clinical Director, Ambulatory Services Psychiatry Department Massachusetts General Hospital Disclosures Neither
Trauma and Addiction Martha T. Kane, PhD Clinical Director, Center for Addiction Medicine Clinical Director, Ambulatory Services Psychiatry Department Massachusetts General Hospital Disclosures Neither
Clinical Course of Alcohol Use in Veterans Following an AUDIT-C Positive Screen
 MILITARY MEDICINE, 179, 11:1198, 2014 Clinical Course of Alcohol Use in Veterans Following an AUDIT-C Positive Screen Jennifer S. Funderburk, PhD* ; Stephen A. Maisto, PhD* ; Michael J. Wade, MS*; Aileen
MILITARY MEDICINE, 179, 11:1198, 2014 Clinical Course of Alcohol Use in Veterans Following an AUDIT-C Positive Screen Jennifer S. Funderburk, PhD* ; Stephen A. Maisto, PhD* ; Michael J. Wade, MS*; Aileen
WOMEN VETERANS HEALTH: PSYCHOLOGICAL ASPECTS
 WOMEN VETERANS HEALTH: PSYCHOLOGICAL ASPECTS Carol OBrien, Ph.D. Chief, PTSD Programs Bay Pines VA Healthcare System Overview General issues in women s mental health Unique characteristics of women Veterans
WOMEN VETERANS HEALTH: PSYCHOLOGICAL ASPECTS Carol OBrien, Ph.D. Chief, PTSD Programs Bay Pines VA Healthcare System Overview General issues in women s mental health Unique characteristics of women Veterans
Self-reported problems: a comparison between PTSDdiagnosed veterans, their spouses, and clinicians
 Behaviour Research and Therapy 40 (2002) 853 865 www.elsevier.com/locate/brat Self-reported problems: a comparison between PTSDdiagnosed veterans, their spouses, and clinicians D. Biddle a, b,*, P. Elliott
Behaviour Research and Therapy 40 (2002) 853 865 www.elsevier.com/locate/brat Self-reported problems: a comparison between PTSDdiagnosed veterans, their spouses, and clinicians D. Biddle a, b,*, P. Elliott
Long-Term Effects of Military Service on Mental Health among Veterans of the Vietnam War Era
 MILITARY MEDICINE, 173, 6:570, 2008 Long-Term Effects of Military Service on Mental Health among Veterans of the Vietnam War Era Matthew S. Brooks, PhD*; Sarah B. Laditka, PhD ; James N. Laditka, DA PhD
MILITARY MEDICINE, 173, 6:570, 2008 Long-Term Effects of Military Service on Mental Health among Veterans of the Vietnam War Era Matthew S. Brooks, PhD*; Sarah B. Laditka, PhD ; James N. Laditka, DA PhD
Factor Analysis of Gulf War Illness: What Does It Add to Our Understanding of Possible Health Effects of Deployment?
 October 3, 2006 Factor Analysis Examples: Example 1: Factor Analysis of Gulf War Illness: What Does It Add to Our Understanding of Possible Health Effects of Deployment? 1 2 2 Susan E. Shapiro, Michael
October 3, 2006 Factor Analysis Examples: Example 1: Factor Analysis of Gulf War Illness: What Does It Add to Our Understanding of Possible Health Effects of Deployment? 1 2 2 Susan E. Shapiro, Michael
SHORT REPORT. Is Acute Stress Disorder the optimal means to identify child and adolescent trauma survivors. at risk for later PTSD?
 SHORT REPORT Is Acute Stress Disorder the optimal means to identify child and adolescent trauma survivors at risk for later PTSD? Tim Dalgleish PhD, Richard Meiser-Stedman PhD, Nancy Kassam-Adams PhD,
SHORT REPORT Is Acute Stress Disorder the optimal means to identify child and adolescent trauma survivors at risk for later PTSD? Tim Dalgleish PhD, Richard Meiser-Stedman PhD, Nancy Kassam-Adams PhD,
