Postmenopausal women are at an increased risk
|
|
|
- Merryl French
- 5 years ago
- Views:
Transcription
1 AMERICAN ASSOCIATION FOR THE STUDY OFLIVERD I S E ASES HEPATOLOGY, VOL. 64, NO. 1, 2016 A Longer Duration of Estrogen Deficiency Increases Fibrosis Risk Among Postmenopausal Women With Nonalcoholic Fatty Liver Disease Jagpal Singh Klair, 1 Ju Dong Yang, 2 Manal F. Abdelmalek, 3 Cynthia D. Guy, 4 Ryan M. Gill, 5 Katherine Yates, 6 Aynur Unalp-Arida, 7 Joel E. Lavine, 8 Jeanne M. Clark, 9,10 Anna Mae Diehl, 3 and Ayako Suzuki, 3,11,12 for the Nonalcoholic Steatohepatitis Clinical Research Network Postmenopausal women with nonalcoholic steatohepatitis are at an increased risk of hepatic fibrosis compared with premenopausal women. Whether duration of estrogen deficiency in postmenopausal state dictates an individual s fibrosis risk remains uninvestigated. We assessed the associations of age at menopause and time from menopause with fibrosis severity in postmenopausal women with nonalcoholic fatty liver disease. Data from 488 postmenopausal women with (1) histologic diagnosis of nonalcoholic fatty liver disease and (2) self-reported information on age at menopause were analyzed. The associations of premature menopause (age at menopause of <40 years) and time from menopause (age at study enrollment - age at menopause, years) with fibrosis severity (stage 0-4) were assessed using multiple ordinal logistic regression models with and without adjusting for clinical confounders. Among the participants (age at menopause years), women with premature menopause (29.3%) were younger at enrollment (P < 0.001) and used hormone replacement therapy more often (P < 0.003). After adjusting for age at enrollment, race, waist circumference standardized by body mass index, current smoking, current alcohol use, hypertension, diabetes/impaired fasting glucose, homeostatic model assessment of insulin resistance, and hormone replacement therapy, premature menopause was associated with an increased likelihood of having more severe fibrosis (adjusted cumulative odds ratio 5 1.9, 95% confidence interval , P ), while time from menopause was directly associated with an increased likelihood of having more severe fibrosis (adjusted cumulative odds ratio for 5-year unit 5 1.2, 95% confidence interval , P ). Conclusion: Duration of estrogen deficiency in postmenopausal state confers fibrosis risk among postmenopausal women with nonalcoholic fatty liver disease. (HEPATOLOGY 2016;64:85-91) Postmenopausal women are at an increased risk of nonalcoholic fatty liver disease (NAFLD). Epidemiological studies have consistently reported that NAFLD risk increases after age of menopause. (1) This increased risk is likely explained by the loss of estrogen s protective effects after menopause; among postmenopausal women, those on hormone replacement therapy (HRT) were associated with a reduced risk of NAFLD defined by nonviral, nonalcoholic elevation of liver aminotransferases compared to Abbreviations: BMI, body mass index; CI, confidence interval; COR, cumulative odds ratio; HOMA-IR, homeostatic model assessment of insulin resistance; HRT, hormone replacement therapy; NAFLD, nonalcoholic fatty liver disease; NASH, nonalcoholic steatohepatitis; NASH CRN, Nonalcoholic Steatohepatitis Clinical Research Network. Received September 24, 2015; accepted February 24, Supported by the National Center for Advancing Translational Sciences in the conduct of Nonalcoholic Steatohepatitis Clinical Research Network studies (grants UL1TR000439, UL1TR000077, UL1TR000436, UL1TR000150, UL1TR000424, UL1TR000006, UL1TR000448, UL1TR000040, UL1TR000100, UL1TR000004, UL1TR000423, UL1TR000058, UL1TR000067, UL1TR000454). The Nonalcoholic Steatohepatitis Clinical Research Network is supported by the National Institute of Diabetes and Digestive and Kidney Diseases (grants U01DK061718, U01DK061728, U01DK061731, U01DK061732, U01DK061734, U01DK061737, U01DK061738, U01DK061730, U01DK061713). Copyright VC 2016 by the American Association for the Study of Liver Diseases. This article has been contributed to by U.S. Government employees and their work is in the public domain in the USA. View this article online at wileyonlinelibrary.com. DOI /hep Potential conflict of interest: Nothing to report. 85
2 KLAIR ET AL. HEPATOLOGY, July 2016 women not on HRT. (2) Postmenopausal women are also at increased risk of nonalcoholic steatohepatitis (NASH) fibrosis. We recently reported that postmenopausal women are at an increased risk of hepatic fibrosis compared to premenopausal women among patients with NASH. (3) This observation has been independently validated in nonobese, Japanese postmenopausal women. (4) The increased fibrosis risk in postmenopausal women was observed with adjustment for degrees of hepatocyte ballooning and portal inflammation, two strong histologic predictors for hepatic fibrosis, suggesting that the risk is likely attributed to fibrogenesis but not hepatocyte ballooning or portal inflammation. Estrogens are known to inhibit stellate cell activation and fibrogenesis in experimental models, which may mechanistically support the clinical observations. (5) Age at menopause significantly varies among women, depending on race/ethnicity, lifestyle factors, and genetic factors. (6) Most women experience menopause between 45 and 55 years of age. (6) However, some women experience premature menopause (age <40 years), due to either surgical procedures, chemotherapy, or other unknown causes. (7) Theoretically, a longer duration of estrogen deficiency may dictate a higher fibrosis risk among postmenopausal women with NAFLD. However, whether the duration of estrogen deficiency correlates with fibrosis severity among postmenopausal women with NAFLD remains unknown. In this study we investigated the associations of premature menopause and time from menopause with fibrosis severity among postmenopausal women with NAFLD, with adjustment for different sets of relevant clinical factors to interpret the associations. Materials and Methods STUDY DESIGN AND POPULATION This was a cross-sectional study designed to investigate the associations of premature menopause and time from menopause with the severity of fibrosis in postmenopausal women with NAFLD. Data from a NASH Clinical Research Network (CRN) database study, the Pioglitazone versus Vitamin E versus Placebo for the Treatment of Nondiabetic Patients with Nonalcoholic Steatohepatitis (PIVENS) trial at baseline, and the NASH CRN Adult Database 2 project (before November 2013) were used for our analysis. (8-10) First, postmenopausal women with a centrally reviewed liver biopsy within 6 months of enrollment in the above NASH CRN studies were identified (n 5 498). The definition of the postmenopausal state was based on self-reported menopause (more than 12 months amenorrhea) through the standardized NASH CRN questionnaire. (8-10) Per the NASH CRN study protocols, patients with serologic or histologic evidence of other forms of chronic liver diseases (viral hepatitis, primary biliary cirrhosis, primary sclerosing cholangitis, autoimmune hepatitis, hemochromatosis, Wilson s disease, alpha 1 -antitrypsin deficiency, hepatocellular carcinoma, or positive for human immunodeficiency virus) were excluded from the studies. (8-10) In the situation in which a participant had more than one study enrollment (i.e., follow-up enrollment), data from the first enrollment (baseline) were used for our analysis. Cases with reported alcohol intake of seven or more servings per week or those who did not meet histological criteria for ARTICLE INFORMATION: From the 1 Department of Medicine, University of Arkansas for Medical Sciences, Little Rock, AR; 2 Division of Gastroenterology and Hepatology, Mayo Clinic College of Medicine, Rochester, MN; 3 Gastroenterology and Hepatology and 4 Department of Pathology, Duke University, Durham, NC; 5 Department of Pathology, University of California San Francisco, San Francisco, CA; 6 Nonalcoholic Steatohepatitis Clinical Research Network Data Coordinating Center, Johns Hopkins Bloomberg School of Public Health, Baltimore, MD; 7 Division of Digestive Diseases and Nutrition, National Institute of Diabetes and Digestive and Kidney Diseases, National Institutes of Health, Bethesda, MD; 8 Department of Pediatrics, Columbia University, New York, NY; 9 Division of General Internal Medicine, Department of Medicine, The Johns Hopkins School of Medicine, and 10 Department of Epidemiology, The Johns Hopkins Bloomberg School of Public Health, Baltimore, MD; 11 Gastroenterology, Central Arkansas Veterans Healthcare System, and 12 Gastroenterology and Hepatology, University of Arkansas for Medical Sciences, Little Rock, AR ADDRESS CORRESPONDENCE AND REPRINT REQUESTS TO: Ayako Suzuki, M.D., Ph.D., M.Sc. Division of Gastroenterology Central Arkansas Veterans Healthcare System 111/HLR, Little Rock, AR ayako.suzuki@va.gov Tel: Fax:
3 HEPATOLOGY, Vol. 64, No. 1, 2016 KLAIR ET AL. NAFLD at the NASH CRN central pathology review were excluded from this analysis (n 5 3). Seven subjects who did not have information on age at menopause were also excluded from this analysis, resulting in a total of 488 subjects. The NASH CRN studies were approved by the institutional review boards at all sites. LIVER HISTOLOGY All liver biopsy specimens were stained with hematoxylin and eosin and Masson trichrome and reviewed and scored by the NASH CRN Pathology Committee in a consensus manner according to the NASH CRN scoring system. (11) STUDY VARIABLES The primary predictors of this study were premature menopause and time from menopause. Premature menopause was defined as self-reported age at menopause <40 years old. Time from menopause was calculated as age at study enrollment minus self-reported age at menopause (years). Surgical menopause was also considered as menopause. The primary outcome was fibrosis stage (stage 0-4). For the analysis, fibrosis stages 1a, 1b, and 1c were combined and treated as a single stage. Other variables taken into account in the analysis included age at enrollment (years), race (white versus other), waist circumference standardized by body mass index (BMI), current smoking (yes versus no), current alcohol use (yes versus no), diagnosis of hypertension, diagnosis of diabetes/impaired fasting glucose, homeostatic model assessment of insulin resistance (HOMA-IR), current use of HRT, and histologic grades of steatosis, lobular inflammation, portal inflammation, hepatocyte ballooning, and Mallory-Denk bodies. HOMA-IR was calculated from fasting insulin and glucose levels using the following formula: (fasting insulin [lu/l] 3 fasting glucose [mg/dl])/405. (12) All clinical information was collected at the time of study enrollment using the standardized questionnaires. (8-10) STATISTICAL ANALYSES Data were reported as mean 6 standard deviation or median and interquartile range for continuous variables and as a percentage for categorical variables. Clinical and histologic characteristics of the study population were compared in premature menopause versus others using Student t tests or Wilcoxon rank sum tests for continuous variables and chi-squared tests for categorical variables. Histologic scores, except for Mallory- Denk bodies (chi-squared test), were analyzed using Wilcoxon rank sum tests to compare the severity of histologic features between the groups. To assess the associations between the primary study predictors (premature menopause and time from menopause) and severity of NASH fibrosis, a multiple ordinal logistic regression model was developed. Age at enrollment, race, waist circumference standardized by BMI, current smoking, current alcohol use, hypertension, diabetes/impaired fasting glucose, HOMA- IR, and HRT were considered in the models as potential confounders. We also developed a model including grades of hepatocyte ballooning and portal inflammation in addition to the above model. Significance of the associations was determined using likelihood ratio tests. Magnitude of association was expressed as unadjusted or adjusted cumulative odds ratio (COR) and 95% confidence interval (CI). As a secondary analysis, we also developed the above-mentioned models including only subjects who had histologic diagnosis of borderline or definite NASH (n 5 396). Statistical analyses were performed using JMP statistical software, version 9.0 (SAS Institute, Cary, NC); and differences were considered statistically significant at P < All P values presented are two-sided. Results PATIENT CHARACTERISTICS Clinical characteristics of the 488 study participants are summarized in Table 1. Mean age 6 standard deviation at menopause was years, and 29.3% women had premature menopause. Women with premature menopause were younger at enrollment ( versus years, P < , t test) and used HRT more often (26.6% versus 13.9%, P , chi-squared test). Fibrosis stage was significantly different between premature menopause and others (Table 2). The other histologic variables were not statistically different, while grades of hepatocyte ballooning and portal inflammation tended to be higher in women with premature menopause versus others (Table 2). PREMATURE MENOPAUSE AND SEVERITY OF FIBROSIS Unadjusted and adjusted associations of premature menopause with hepatic fibrosis stage are shown in 87
4 KLAIR ET AL. HEPATOLOGY, July 2016 TABLE 1. Clinical Characteristics of the Study Population Premature Menopause (n 5 143) Others (n 5 345) P* Age of enrollment (years) <0.001 Age at menopause (years) <0.001 Race 0.98 White 111 (77.6%) 265 (77.3%) Others 32 (22.4%) 80 (22.7%) Ethnicity Hispanic 14 (9.7%) 29 (8.4%) 0.63 BMI (kg/m 2 ) Waist (cm) Diabetes/impaired glucose tolerance 78 (54.6%) 208 (60.3%) 0.24 HOMA-IR Hypertension 118 (82.5%) 274 (79.4%) 0.43 Current smokers 17 (11.9%) 28 (8.1%) 0.20 Alcohol consumption 55 (38.5%) 141 (40.9%) 0.62 Treatment with HRT 38 (26.6%) 48 (13.9%) *P values from chi-squared test, Student t test, or Wilcoxon rank sum test. Alcohol intake was defined as any reported alcohol consumption but fewer than seven drinks per week (alcohol consumption of seven or more drinks per week was exclusionary for the study enrollment and retention). Table 3. Premature menopause was associated with a 50% increased risk of more severe fibrosis when compared to others (1.5, 95% CI , P ). After adjusting for age at enrollment, race, waist circumference standardized by BMI, current smoking, current alcohol use, hypertension, diabetes/impaired fasting TABLE 2. Histologic Features of the Study Population Premature Menopause (n 5 143) Others (n 5 345) P Steatosis 0.34 Grade 0 7 (5%) 14 (4%) Grade 1 63 (44%) 140 (40.6%) Grade 2 43 (30%) 108 (31.4%) Grade 3 30 (21%) 83 (24%) Lobular inflammation 0.26 Grade 0 0 (0%) 1 (0.3%) Grade 1 74 (51.7%) 194 (56.2%) Grade 2 50 (35%) 115 (33.3%) Grade 3 19 (13.3%) 35 (10.2%) Hepatocyte ballooning 0.06 Grade 0 33 (23%) 106 (30.7%) Grade 1 35 (24.5%) 87 (25.2%) Grade 2 75 (52.5%) 152 (44.1%) Mallory-Denk body 0.17* No 82 (57.3%) 221 (64%) Yes 61 (42.7%) 124 (36%) Portal inflammation 0.10 Grade 0 10 (7%) 36 (10.4%) Grade 1 82 (57.3%) 210 (60.9%) Grade 2 50 (35%) 99 (28.7%) Fibrosis 0.03 Stage 0 22 (15.4%) 84 (24.4%) Stage 1 34 (23.8%) 84 (24.4%) Stage 2 32 (22.4%) 63 (18.3%) Stage 3 35 (24.4%) 78 (22.6%) Stage 4 20 (14%) 35 (10.1%) P values are from Wilcoxon rank sum tests except for *chi-squared test. glucose, HOMA-IR, and HRT (model 1), premature menopause was associated with a 90% increased risk of having more severe fibrosis (1.9, 95% CI , P ). Next, we added grades of hepatocyte ballooning and portal inflammation to model 1 (model 2) in order to assess the alteration of the association after adjusting for the levels of hepatocyte ballooning and portal inflammation. (3) The adjusted COR in model 2 was 1.5 (95% CI 1-2.3, P ), indicating a 44.4% reduction (from 90% to 50%) in the effect size. The above analysis was repeated after restricting the population to the subjects who had a histologic diagnosis of borderline or definite NASH. Premature menopause was associated with a 60% increased risk of having more severe fibrosis (1.6, 95% CI , P ) (Table 4). After adjusting for the levels of hepatocyte ballooning and portal inflammation, the effect size was reduced 30%. TIME FROM MENOPAUSE AND SEVERITY OF FIBROSIS Unadjusted and adjusted associations of time from menopause with hepatic fibrosis stage are shown in Table 3. In univariate analysis, time from menopause was associated with an increased risk of more severe fibrosis (COR for 5-year unit 5 1.2, 95% CI , P < ). After adjusting for age at enrollment, race, waist circumference standardized by BMI, current smoking, current alcohol use, hypertension, diabetes/impaired fasting glucose, HOMA-IR, and HRT (model 1), time from menopause was still associated with a similar increased risk of having more severe 88
5 HEPATOLOGY, Vol. 64, No. 1, 2016 KLAIR ET AL. TABLE 3. Premature Menopause, Time From Menopause, and Risk of Fibrosis Univariate Model 1 Model 2 Premature menopause No Yes 1.5 ( ), P ( ), P ( ), P Time from menopause, for 5 years 1.2 ( ), P < ( ), P ( ), P fibrosis (COR for 5-year unit 5 1.2, 95% CI , P ). After adding degrees of hepatocyte ballooning and portal inflammation to the model 1 (model 2), time from menopause remained associated with an increased risk (COR for 5-year unit 5 1.1, 95% CI , P ), with a 50% reduction in the effect size (10% reduction from 20%). After restricting the population to the subjects who had histologic diagnosis of borderline or definite NASH, the association between time from menopause and hepatic fibrosis stage remained the same (Table 4). Discussion In this study we showed that women who had menopause at an earlier age (<40 years or premature menopause) were at an increased likelihood of having more severe fibrosis compared with women who had menopause at a later age (40 years); women with premature menopause were associated with a 90% increased risk of more severe fibrosis after adjusting for age at enrollment, white race, waist circumference standardized by BMI, current smoking, current alcohol use, hypertension, diabetes/impaired fasting glucose, HOMA-IR, and HRT use. Interestingly, when adding grades of hepatocyte ballooning and portal inflammation to the model, the effect size was minimally reduced (44.4%). The time from menopause (years) was also directly associated with an increased likelihood of having more severe fibrosis. After restricting the population to subjects with a NASH diagnosis, the effect size of premature menopause was reduced by 30%. Our findings have clinical relevance. Fibrosis risk among patients with NAFLD determines not only liver outcomes (e.g., cirrhosis and hepatocellular carcinoma) but also overall outcomes. (13) Thus, risk stratification based on an individual s fibrosis risk is key to personalizing our care in NAFLD and allocating limited medical resources to the high-risk population. Our analysis suggests that women who experienced menopause at an earlier age (<40 years) are at an even higher risk of hepatic fibrosis and should be followed closely with more aggressive risk modification. The above-mentioned findings, together with previous reports, underscore the significance of reproductive information for risk stratification among women with NAFLD. (3,4) Not only menopausal status but also age at menopause and time from menopause appear to determine fibrosis risk among women with NAFLD. Our study suggests that the longer the time of estrogen depletion, the higher the risk of having more severe fibrosis among postmenopausal women. Postmenopausal women are known to be at an increased risk of NAFLD and metabolic features of insulin resistance; increased total as well as visceral adiposity in perimenopause and postmenopause are associated with an increased risk of insulin resistance, dyslipidemia, hypertension, diabetes, and cardiovascular disease. (1) Further, given the protective effects of estrogens against oxidative stress and fibrogenesis, postmenopausal women may be at an increased risk of portal inflammation, ballooning, and fibrosis at a given metabolic stress in a setting of NAFLD. (1) The observed association in this study remained significant (even TABLE 4. Premature Menopause, Time From Menopause, and Risk of Fibrosis: Subgroup Analysis in Patients With Borderline NASH or NASH Univariate Model 1 Model 2 Premature menopause No Yes 1.2 ( ), P ( ), P ( ), P Time from menopause, for 5 years 1.2 ( ), P < ( ), P ( ), P Model 1: adjusted for age at enrollment, race, waist circumference/bmi, current smoking/alcohol use, hypertension, diabetes/impaired fasting glucose, HOMA-IR, and HRT. Model 2: adjusted for the above covariates, hepatocyte ballooning grades, and portal inflammation grades. 89
6 KLAIR ET AL. HEPATOLOGY, July 2016 stronger) after adjusting for relevant clinical confounders such as visceral adiposity, metabolic features, and insulin resistance. Our secondary analysis in which we restricted the population to patients with NASH showed a 30% risk reduction (1.9 to 1.6 as adjusted COR). This may imply that one-third of the risk among postmenopausal women might be attributed to the risk of having NASH. Further, when we added grades of hepatocyte ballooning and portal inflammation to the model, the effect size was reduced by 44.4%. When we ran a logistic regression model with significant fibrosis (stage 2-4) as an outcome (an extended analysis), the results were basically same; premature menopause was associated with a 90% increased risk of having significant hepatic fibrosis versus others after adjusting for the same variable set, and the effect size was decreased by only 20% after adjusting for hepatocyte ballooning and portal inflammation (data not shown). These data suggest that the majority of the effect may be explained by fibrogenesis (or fibrosis regression), rather than insulin resistance or activity of ballooning or portal inflammation. Future prospective follow-up study is warranted to test the above hypothesis. Given estrogen s protective effect against fibrogenesis (5) and the clinical observations, (3,4) one may anticipate a protective effect of HRT on fibrogenesis. Our prior analysis showed a borderline beneficial effect of estrogen replacement therapy on fibrosis (50%). (3) In this study, our analysis did not show any beneficial effect of estrogen replacement therapy on fibrosis in any model or subgroup (premature menopause or others). Despite the theoretical beneficial effect of estrogens on fibrogenesis, whether estrogen replacement therapy with synthetic estrogens reduces fibrosis risk among postmenopausal women remains uncertain and inconclusive. Further analyses incorporating the information on age at initiation, dose, route of administration, and duration of estrogen replacement therapy would be helpful to better characterize the potential beneficial effect of estrogens on fibrosis among postmenopausal women with NAFLD and to determine whether or not the beneficial effect of estrogens is limited to a specific subgroup of postmenopausal women. This study has several limitations. The crosssectional study design precludes us from addressing causality. Our study population was enrolled at tertiary academic centers. Thus, there might be potential selection bias, and the findings should be interpreted with caution. Clinical and diagnostic information to discern whether or not patients with premature menopause met criteria for coexisting diagnosis of polycystic ovary syndrome (14) or obstructive sleep apnea are lacking. Whether the presence of polycystic ovary syndrome in patients with NAFLD and/or hyperandrogenemia contributes to our finding will require further investigation. Lastly, detailed information on HRT, such as age at initiation, dose, route of administration, and duration, was not available. Thus, as discussed above, the potential impact of HRT on fibrosis among postmenopausal women is still inconclusive, pending future investigation. Further extending our research question, one may ask whether number of pregnancies, duration of breast-feeding, or duration of oral contraceptive use may influence fibrosis risk among women. These questions could not be addressed in our analysis and await future investigation. In summary, our analysis revealed that not only menopausal status but also age at menopause and duration of estrogen depletion (time from menopause) appear to be significant fibrosis risk determinants among women with NAFLD. Our findings further emphasize the importance of reproductive history in risk stratification among female patients with NAFLD and in personalized medicine. Whether HRT is beneficial for the prevention of fibrosis progression among postmenopausal women remains uncertain. Further investigation is warranted to establish an effective prevention for this high-risk population. REFERENCES 1) Suzuki A, Abdelmalek MF. Nonalcoholic fatty liver disease in women. Womens Health (Lond Engl) 2009;5: ) Clark JM, Brancati FL, Diehl AM. Nonalcoholic fatty liver disease. Gastroenterology 2002;122: ) Yang JD, Abdelmalek MF, Pang H, Guy CD, Smith AD, Diehl AM, et al. Gender and menopause impact severity of fibrosis among patients with nonalcoholic steatohepatitis. HEPATOLOGY 2014;59: ) Yoneda M, Thomas E, Sumida Y, Eguchi Y, Schiff ER. The influence of menopause on the development of hepatic fibrosis in nonobese womenwithnonalcoholicfattyliverdisease.hepatology 2014;60: ) Yasuda M, Shimizu I, Shiba M, Ito S. Suppressive effects of estradiol on dimethylnitrosamine-induced fibrosis of the liver in rats. HEPATOLOGY 1999;29: ) Gold EB. The timing of the age at which natural menopause occurs. Obstet Gynecol Clin North Am 2011;38: ) Shuster LT, Rhodes DJ, Gostout BS, Grossardt BR, Rocca WA. Premature menopause or early menopause: long-term health consequences. Maturitas 2010;65: ) Chalasani NP, Sanyal AJ, Kowdley KV, Robuck PR, Hoofnagle J, Kleiner DE, et al. Pioglitazone versus vitamin E versus placebo for the treatment of non-diabetic patients with non-alcoholic steatohepatitis: PIVENS trial design. Contemp Clin Trials 2009;30: ) Nonalcoholic steatohepatitis clinical research network. HEPATO- LOGY 2003;37:
7 HEPATOLOGY, Vol. 64, No. 1, 2016 KLAIR ET AL. 10) Neuschwander-Tetri BA, Clark JM, Bass NM, Van Natta ML, Unalp-Arida A, Tonascia J, et al. Clinical, laboratory and histological associations in adults with nonalcoholic fatty liver disease. HEPATOLOGY 2010;52: ) Kleiner DE, Brunt EM, Van Natta M, Behling C, Contos MJ, Cummings OW, et al. Design and validation of a histological scoring system for nonalcoholic fatty liver disease. HEPATOLOGY 2005;41: ) Matthews DR, Hosker JP, Rudenski AS, Naylor BA, Treacher DF, Turner RC. Homeostasis model assessment: insulin resistance and beta-cell function from fasting plasma glucose and insulin concentrations in man. Diabetologia 1985;28: ) Ekstedt M, Hagstrom H, Nasr P, Fredrikson M, Stal P, Kechagias S, et al. Fibrosis stage is the strongest predictor for disease-specific mortality in NAFLD after up to 33 years of follow-up. HEPATOLOGY 2015;61: ) Baranova A, Tran TP, Birerdinc A, Younossi ZM. Systematic review: association of polycystic ovary syndrome with metabolic syndrome and non-alcoholic fatty liver disease. Aliment Pharmacol Ther 2011;33:
Challenges in the Diagnosis of Steatohepatitis
 The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
The Bugaboos of Fatty Liver Disease: Ballooning and Fibrosis Hans Popper Hepatopathology Society Companion Meeting San Antonio, Tx March, 2017 David Kleiner, M.D., Ph.D. NCI/Laboratory of Pathology Challenges
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health
 CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
CDHNF & NASPGHAN A Partnership for Research and Education for Children s Digestive and Nutritional Health Obesity and NAFLD Definitions: Nonalcoholic steatohepatitis (NASH) and nonalcoholic fatty liver
Nonalcoholic fatty liver disease (NAFLD) is a. Gender and Menopause Impact Severity of Fibrosis Among Patients With Nonalcoholic Steatohepatitis
 Gender and Menopause Impact Severity of Fibrosis Among Patients With Nonalcoholic Steatohepatitis Ju Dong Yang, 1 Manal F. Abdelmalek, 2 Herbert Pang, 3 Cynthia D. Guy, 4 Alastair D. Smith, 2 Anna Mae
Gender and Menopause Impact Severity of Fibrosis Among Patients With Nonalcoholic Steatohepatitis Ju Dong Yang, 1 Manal F. Abdelmalek, 2 Herbert Pang, 3 Cynthia D. Guy, 4 Alastair D. Smith, 2 Anna Mae
NONALCOHOLIC FATTY LIVER DISEASE. Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD. April 13, 2012
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Primary NAFLD Simple Steatosis Fatty hepatocytes Intracellular fat
Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup
 REVIEW REVIEW Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup Puneet Puri, M.B.B.S., M.D. and Arun J. Sanyal, M.B.B.S., M.D. Nonalcoholic fatty liver disease (NAFLD) is defined
REVIEW REVIEW Nonalcoholic Fatty Liver Disease: Definitions, Risk Factors, and Workup Puneet Puri, M.B.B.S., M.D. and Arun J. Sanyal, M.B.B.S., M.D. Nonalcoholic fatty liver disease (NAFLD) is defined
NONALCOHOLIC FATTY LIVER DISEASE
 NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
NONALCOHOLIC FATTY LIVER DISEASE Kiran Bambha, MD, MSc Hepatology and Liver Transplantation University of Colorado Denver April 13, 2012 Non-Alcoholic Fatty Liver Disease (NAFLD) Terminology Pathogenesis
Design and Validation of a Histological Scoring System for Nonalcoholic Fatty Liver Disease
 Design and Validation of a Histological Scoring System for Nonalcoholic Fatty Liver Disease David E. Kleiner, 1 Elizabeth M. Brunt, 2 Mark Van Natta, 3 Cynthia Behling, 4 Melissa J. Contos, 5 Oscar W.
Design and Validation of a Histological Scoring System for Nonalcoholic Fatty Liver Disease David E. Kleiner, 1 Elizabeth M. Brunt, 2 Mark Van Natta, 3 Cynthia Behling, 4 Melissa J. Contos, 5 Oscar W.
Liver Pathology in the 0bese
 Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
Liver Pathology in the 0bese Rob Goldin Centre for Pathology, Imperial College r.goldin@imperial.ac.uk Ludwig et al. Non-alcoholic steatohepatitis: Mayo Clinic experiences with a hitherto unnamed disease.
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE
 PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
PEDIATRIC FOIE GRAS: NON-ALCOHOLIC FATTY LIVER DISEASE Updates on New insights into NAFLD and NASH pathophysiology New AASLD/AGA/ACG guidelines for NAFLD and NASH, as pertains to pediatrics Evidence-based
Update on Nonalcoholic Fatty Liver Disease. Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic
 Update on Nonalcoholic Fatty Liver Disease Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic Outline Defining the phenotypes of nonalcoholic fatty liver disease NAFLD Diagnostics
Update on Nonalcoholic Fatty Liver Disease Kathleen E Corey, MD, MPH, MMSc Director, Mass General Fatty Liver Clinic Outline Defining the phenotypes of nonalcoholic fatty liver disease NAFLD Diagnostics
ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche,
 Supplemental Methods Analytical determinations ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche, Basel, Switzerland). Glucose, triglyceride, total
Supplemental Methods Analytical determinations ALT and aspartate aminotransferase (AST) levels were measured using the α-ketoglutarate reaction (Roche, Basel, Switzerland). Glucose, triglyceride, total
SAF score and mortality in NAFLD after up to 41 years of follow-up
 SAF score and mortality in NAFLD after up to 41 years of follow-up Hannes Hagström, Patrik Nasr, Mattias Ekstedt, Stergios Kechagias, Per Stal, Pierre Bedossa and Rolf Hultcrantz Journal Article N.B.:
SAF score and mortality in NAFLD after up to 41 years of follow-up Hannes Hagström, Patrik Nasr, Mattias Ekstedt, Stergios Kechagias, Per Stal, Pierre Bedossa and Rolf Hultcrantz Journal Article N.B.:
«STEATOSI EPATICA ED EPATOPATIE METABOLICHE» Ester Vanni Division of Gastroenterology University of Turin
 «STEATOSI EPATICA ED EPATOPATIE METABOLICHE» Ester Vanni Division of Gastroenterology University of Turin OUTLINE NAFLD overview NAFLD and menarche NAFLD and pregnancy NAFLD and menopause Other metabolic
«STEATOSI EPATICA ED EPATOPATIE METABOLICHE» Ester Vanni Division of Gastroenterology University of Turin OUTLINE NAFLD overview NAFLD and menarche NAFLD and pregnancy NAFLD and menopause Other metabolic
Association Between Puberty and Features of Nonalcoholic Fatty Liver Disease
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:786 794 Association Between Puberty and Features of Nonalcoholic Fatty Liver Disease AYAKO SUZUKI,* MANAL F. ABDELMALEK,* JEFFREY B. SCHWIMMER,, JOEL E.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:786 794 Association Between Puberty and Features of Nonalcoholic Fatty Liver Disease AYAKO SUZUKI,* MANAL F. ABDELMALEK,* JEFFREY B. SCHWIMMER,, JOEL E.
ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1062 1069 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Regional Anthropometric Measures and Hepatic Fibrosis in Patients With Nonalcoholic Fatty
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2010;8:1062 1069 ORIGINAL ARTICLES LIVER, PANCREAS, AND BILIARY TRACT Regional Anthropometric Measures and Hepatic Fibrosis in Patients With Nonalcoholic Fatty
Improving Access to Quality Medical Care Webinar Series
 Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Improving Access to Quality Medical Care Webinar Series Presented by The Arizona Telemedicine Program and the Southwest Telehealth Resource Center 2015 UA Board of Regents Welcome AZ, UT, CO, NM & NV FLEX
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016.
 Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
Early life determinants of Non-Alcoholic Fatty Liver Disease and NASH DR JULIANA MUIVA-GITOBU KENYA PAEDIATRIC ASSOCIATION CONFERENCE APRIL 2016. Outline Definition NAFLD and NASH Magnitude of the problem
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schauer PR, Kashyap SR, Wolski K, et al. Bariatric surgery
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Schauer PR, Kashyap SR, Wolski K, et al. Bariatric surgery
LIVER, PANCREAS, AND BILIARY TRACT
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1028 1033 LIVER, PANCREAS, AND BILIARY TRACT Prevalence and Indicators of Portal Hypertension in Patients With Nonalcoholic Fatty Liver Disease FLAVIA D.
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2012;10:1028 1033 LIVER, PANCREAS, AND BILIARY TRACT Prevalence and Indicators of Portal Hypertension in Patients With Nonalcoholic Fatty Liver Disease FLAVIA D.
The Absence of Obstructive Sleep Apnea May Protect against Non- Alcoholic Fatty Liver in Patients Undergoing Bariatric Surgery
 The Absence of Obstructive Sleep Apnea May Protect against Non- Alcoholic Fatty Liver in Patients Undergoing Bariatric Surgery The Harvard community has made this article openly available. Please share
The Absence of Obstructive Sleep Apnea May Protect against Non- Alcoholic Fatty Liver in Patients Undergoing Bariatric Surgery The Harvard community has made this article openly available. Please share
At Least 1 in 5 Patients in Your Practice Have Fatty Liver
 At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
At Least 1 in 5 Patients in Your Practice Have Fatty Liver What Can You Tell Your Patients Magnus McLeod MD FRCPC Assistant Professor Dalhousie University 30-NOV-2017 NAFLD Non-Alcoholic Fatty Liver Disease
Hepatocellular carcinoma is the most common liver-related complication in patients with histopathologically-confirmed NAFLD in Japan
 Akuta et al. BMC Gastroenterology (2018) 18:165 https://doi.org/10.1186/s12876-018-0900-1 RESEARCH ARTICLE Open Access Hepatocellular carcinoma is the most common liver-related complication in patients
Akuta et al. BMC Gastroenterology (2018) 18:165 https://doi.org/10.1186/s12876-018-0900-1 RESEARCH ARTICLE Open Access Hepatocellular carcinoma is the most common liver-related complication in patients
NON-ALCOHOLIC FATTY LIVER DISEASE:
 NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
NON-ALCOHOLIC FATTY LIVER DISEASE: ROLE OF THE PRIMARY PROVIDER Archita P. Desai, MD Assistant Professor of Medicine University of Arizona 25 th Annual Southwestern Conference on Medicine Outline Pathophysiology
Steatotic liver disease
 Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
Steatotic liver disease Fatty liver disease Prof. Dr. ANNE HOORENS Non-Neoplastic Liver Pathology December 8th 2018 Working Group of Digestive Pathology Belgian Society of Pathology OUTLINE NAFLD = Non-Alcoholic
Non-Alcoholic Fatty Liver Disease
 Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
Non-Alcoholic Fatty Liver Disease None Disclosures Arslan Kahloon M.D Chief, Division of Gastroenterology and Hepatology University of Tennessee College of Medicine Chattanooga Objectives Understand the
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
HHS Public Access Author manuscript Clin Gastroenterol Hepatol. Author manuscript; available in PMC 2016 April 13.
 Relationship between changes in serum keratin 18 and changes in liver histology in children and adults with nonalcoholic fatty liver disease Raj Vuppalanchi 1, Ajay K. Jain 2, Ross Deppe 1, Katherine Yates
Relationship between changes in serum keratin 18 and changes in liver histology in children and adults with nonalcoholic fatty liver disease Raj Vuppalanchi 1, Ajay K. Jain 2, Ross Deppe 1, Katherine Yates
Update on Non-Alcoholic Fatty Liver Disease. Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI
 Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
Update on Non-Alcoholic Fatty Liver Disease Timothy R. Morgan, MD Chief, Hepatology, VA Long Beach Professor of Medicine, UCI February 3, 2018 Disclosure Clinical trials: Genfit Speaker s Bureau: none
With the rise in obesity, nonalcoholic fatty. Hedgehog Pathway and Pediatric Nonalcoholic Fatty Liver Disease
 Hedgehog Pathway and Pediatric Nonalcoholic Fatty Liver Disease Marzena Swiderska-Syn, 1 Ayako Suzuki, 1 Cynthia D. Guy, 2 Jeffrey B. Schwimmer, 3 Manal F. Abdelmalek, 1 Joel E. Lavine, 4 and Anna Mae
Hedgehog Pathway and Pediatric Nonalcoholic Fatty Liver Disease Marzena Swiderska-Syn, 1 Ayako Suzuki, 1 Cynthia D. Guy, 2 Jeffrey B. Schwimmer, 3 Manal F. Abdelmalek, 1 Joel E. Lavine, 4 and Anna Mae
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
Despite the increasing incidence of nonalcoholic
 Relationship Between Adipose Tissue Insulin Resistance and Liver Histology in Nonalcoholic Steatohepatitis: A Pioglitazone Versus Vitamin E Versus Placebo for the Treatment of Nondiabetic Patients With
Relationship Between Adipose Tissue Insulin Resistance and Liver Histology in Nonalcoholic Steatohepatitis: A Pioglitazone Versus Vitamin E Versus Placebo for the Treatment of Nondiabetic Patients With
Accepted Manuscript. Nonalcoholic Fatty Liver Disease and Mortality. Norbert Stefan, MD
 Accepted Manuscript Nonalcoholic Fatty Liver Disease and Mortality Norbert Stefan, MD PII: S1542-3565(18)30161-7 DOI: 10.1016/j.cgh.2018.02.016 Reference: YJCGH 55704 To appear in: Clinical Gastroenterology
Accepted Manuscript Nonalcoholic Fatty Liver Disease and Mortality Norbert Stefan, MD PII: S1542-3565(18)30161-7 DOI: 10.1016/j.cgh.2018.02.016 Reference: YJCGH 55704 To appear in: Clinical Gastroenterology
Disclosure. Objectives. Smash the Nash: A practical approach to fatty liver disease
 Smash the Nash: A practical approach to fatty liver disease Bruce D. Askey, MS, ANP-BC Associate Lecturer North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology Guthrie Clinic
Smash the Nash: A practical approach to fatty liver disease Bruce D. Askey, MS, ANP-BC Associate Lecturer North Andover, MA Adult Nurse Practitioner Dept. of Hepatology/Gastroenterology Guthrie Clinic
NON-ALCOHOLIC FATTY LIVER DISEASE (NAFLD) NON-ALCOHOLIC STEATOHEPATITIS (NASH) ADDRESSING A GROWING SILENT EPIDEMIC
 NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
NON-ALCOHOLIC FATTY LIVER DISEASE () & NON-ALCOHOLIC STEATOHEPATITIS () ADDRESSING A GROWING SILENT EPIDEMIC PREVALENCE OF / USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology
Non alcoholic fatty liver disease and atherosclerosis Raul Santos, MD
 Non alcoholic fatty liver disease and atherosclerosis Raul Santos, MD Sao Paulo Medical School Hospital Sao Paulo, Brazil Disclosure Honoraria received for consult and/or speaker : Astra Zeneca, Amgen,
Non alcoholic fatty liver disease and atherosclerosis Raul Santos, MD Sao Paulo Medical School Hospital Sao Paulo, Brazil Disclosure Honoraria received for consult and/or speaker : Astra Zeneca, Amgen,
AAIM: GI Workshop Follow Up to Case Studies. Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease
 AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
AAIM: GI Workshop Follow Up to Case Studies Non-alcoholic Fatty Liver Disease Ulcerative Colitis Crohn s Disease Daniel Zimmerman, MD VP and Medical Director, RGA Global October 2015 Non-alcoholic Fatty
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES
 NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
NON-ALCOHOLIC STEATOHEPATITIS AND NON-ALCOHOLIC FATTY LIVER DISEASES Preface Zobair M. Younossi xiii Epidemiology and Natural History of NAFLD and NASH 1 Janus P. Ong and Zobair M. Younossi Understanding
Liver biopsy as the gold standard for diagnosis. Pierre BEDOSSA
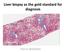 Liver biopsy as the gold standard for diagnosis Pierre BEDOSSA 1 PATHOLOGY OF NAFLD CONFLICTS OF INTEREST Grants and funding from Genfit, Intercept, Allergan, Inventiva, OWL, Echosens CEO and funding of
Liver biopsy as the gold standard for diagnosis Pierre BEDOSSA 1 PATHOLOGY OF NAFLD CONFLICTS OF INTEREST Grants and funding from Genfit, Intercept, Allergan, Inventiva, OWL, Echosens CEO and funding of
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse
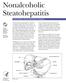 Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
Nonalcoholic Steatohepatitis National Digestive Diseases Information Clearinghouse National Institute of Diabetes and Digestive and Kidney Diseases NATIONAL INSTITUTES OF HEALTH Nonalcoholic steatohepatitis
Effect of Vitamin E or Metformin for Treatment of Nonalcoholic Fatty Liver Disease in Children and Adolescents JAMA. 2011;305(16):
 ORIGINAL CONTRIBUTION Effect of or for Treatment of Nonalcoholic Fatty Liver Disease in Children and Adolescents The TONIC Randomized Controlled Trial Joel E. Lavine, MD, PhD Jeffrey B. Schwimmer, MD Mark
ORIGINAL CONTRIBUTION Effect of or for Treatment of Nonalcoholic Fatty Liver Disease in Children and Adolescents The TONIC Randomized Controlled Trial Joel E. Lavine, MD, PhD Jeffrey B. Schwimmer, MD Mark
Effect of lifetime alcohol consumption on the histological severity of non-alcoholic fatty liver disease
 Liver International ISSN 1478-3223 METABOLIC AND STEATOHEPATITIS Effect of lifetime alcohol consumption on the histological severity of non-alcoholic fatty liver disease Hellan K. Kwon 1, Joel K. Greenson
Liver International ISSN 1478-3223 METABOLIC AND STEATOHEPATITIS Effect of lifetime alcohol consumption on the histological severity of non-alcoholic fatty liver disease Hellan K. Kwon 1, Joel K. Greenson
Original article J Bas Res Med Sci 2014; 1(1):50-55.
 The effect of pioglitazone and metformin on non-alcoholic fatty liver: A double blind clinical trial study Kourosh Sayehmiri 1, 2, Khairollah Asadollahi 1, 2*, Mariam Yaghubi 1, Ghobad Abangah 3, Hassan
The effect of pioglitazone and metformin on non-alcoholic fatty liver: A double blind clinical trial study Kourosh Sayehmiri 1, 2, Khairollah Asadollahi 1, 2*, Mariam Yaghubi 1, Ghobad Abangah 3, Hassan
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy
 Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
Fat, ballooning, plasma cells and a +ANA. Yikes! USCAP 2016 Evening Specialty Conference Cynthia Guy Goals Share an interesting case Important because it highlights a common problem that we re likely to
METABOLIC SYNDROME AND HCV: FROM HCV
 METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
METABOLIC SYNDROME AND HCV: FROM THEORY TO PRACTICE HCV Steatosis Insulin resistance Arun J Sanyal M.D. Chairman, Div. of Gastroenterology, Hepatology and Nutrition Virginia Commonwealth University Richmond,
Original Article. Significance of Hepatic Steatosis in Chronic Hepatitis B Infection INTRODUCTION
 Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Original Article Bhanthumkomol P, et al. THAI J GASTROENTEROL 2013 Vol. 14 No. 1 Jan. - Apr. 2013 29 Bhanthumkomol P 1 Charatcharoenwitthaya P 1 Pongpaiboon A 2 ABSTRACT Background: Significance of liver
Assessment of Liver Stiffness by Transient Elastography in Diabetics with Fatty Liver A Single Center Cross Sectional observational Study
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861.Volume 16, Issue 6 Ver. IV (June. 2017), PP 49-53 www.iosrjournals.org Assessment of Liver Stiffness by Transient
PREVALENCE OF NAFLD & NASH
 - - PREVALENCE OF & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology 2011; 140:124-31) Dallas Heart Study Prevalence Numbers (Browning et al., Hepatology 2004;40:1387-95)
- - PREVALENCE OF & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams et al., Gastroenterology 2011; 140:124-31) Dallas Heart Study Prevalence Numbers (Browning et al., Hepatology 2004;40:1387-95)
LEPTIN AS A NOVEL PREDICTOR OF DEPRESSION IN PATIENTS WITH THE METABOLIC SYNDROME
 LEPTIN AS A NOVEL PREDICTOR OF DEPRESSION IN PATIENTS WITH THE METABOLIC SYNDROME Diana A. Chirinos, Ronald Goldberg, Elias Querales-Mago, Miriam Gutt, Judith R. McCalla, Marc Gellman and Neil Schneiderman
LEPTIN AS A NOVEL PREDICTOR OF DEPRESSION IN PATIENTS WITH THE METABOLIC SYNDROME Diana A. Chirinos, Ronald Goldberg, Elias Querales-Mago, Miriam Gutt, Judith R. McCalla, Marc Gellman and Neil Schneiderman
EVALUATION OF ABNORMAL LIVER TESTS
 EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
EVALUATION OF ABNORMAL LIVER TESTS MIA MANABAT DO PGY6 MOA 119 TH ANNUAL SPRING SCIENTIFIC CONVENTION MAY 19, 2018 EVALUATION OF ABNORMAL LIVER TESTS Review of liver enzymes vs liver function tests Clinical
Non-Alcoholic Fatty Liver Disease (NAFLD)
 HEPATO-PANCREATO-BILIARY STOMACH CANCER PROGRAM Non-Alcoholic Fatty Liver Disease (NAFLD) Steatosis and Non-Alcoholic Steatohepatitis (NASH) Management Recommendations UCSF Fresno Department of Surgery
HEPATO-PANCREATO-BILIARY STOMACH CANCER PROGRAM Non-Alcoholic Fatty Liver Disease (NAFLD) Steatosis and Non-Alcoholic Steatohepatitis (NASH) Management Recommendations UCSF Fresno Department of Surgery
NAFLD & NASH: Russian perspective
 NAFLD & NASH: Russian perspective Vasily Isakov, MD, PhD Professor, Chief, Department Gastroenterology & Hepatology, Federal Research Center of nutrition, biotechnology and food safety Disclosures Received
NAFLD & NASH: Russian perspective Vasily Isakov, MD, PhD Professor, Chief, Department Gastroenterology & Hepatology, Federal Research Center of nutrition, biotechnology and food safety Disclosures Received
The classical metabolic work-up, approved by the Ethics Committee of the Antwerp
 SUPPLEMENTARY MATERIALS METHODS Metabolic work-up The classical metabolic work-up, approved by the Ethics Committee of the Antwerp University Hospital and requiring written informed consent, included a
SUPPLEMENTARY MATERIALS METHODS Metabolic work-up The classical metabolic work-up, approved by the Ethics Committee of the Antwerp University Hospital and requiring written informed consent, included a
CIRROSI E IPERTENSIONE PORTALE NELLA DONNA
 Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
Cagliari, 16 settembre 2017 CIRROSI E IPERTENSIONE PORTALE NELLA DONNA Vincenza Calvaruso, MD, PhD Ricercatore di Gastroenterologia Gastroenterologia & Epatologia, Di.Bi.M.I.S. Università degli Studi di
La sindrome metabolica e il suo impatto dopo la guarigione nel paziente HIV/HCV
 WORKSHOP HCV: la guarigione e il parallelismo tra risposta virologica sostenuta e outcome clinico Milano, 25 Ottobre 2018 Ospedale San Raffaele IRCCS - Sede Turro La sindrome metabolica e il suo impatto
WORKSHOP HCV: la guarigione e il parallelismo tra risposta virologica sostenuta e outcome clinico Milano, 25 Ottobre 2018 Ospedale San Raffaele IRCCS - Sede Turro La sindrome metabolica e il suo impatto
Nonalcoholic fatty liver disease (NAFLD) is the most common
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1249 1254 Cytokeratin 18 Fragment Levels as a Noninvasive Biomarker for Nonalcoholic Steatohepatitis in Bariatric Surgery Patients DIMA L. DIAB,* LISA YERIAN,
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2008;6:1249 1254 Cytokeratin 18 Fragment Levels as a Noninvasive Biomarker for Nonalcoholic Steatohepatitis in Bariatric Surgery Patients DIMA L. DIAB,* LISA YERIAN,
NAFLD: US GUIDELINES. US Guidelines for NAFLD
 NAFLD: US GUIDELINES Arun J Sanyal M.D. Charles Caravati Professor of Medicine Virginia Commonwealth University School of Medicine US Guidelines for NAFLD Represents consensus amongst AGA, AASLD and ACG
NAFLD: US GUIDELINES Arun J Sanyal M.D. Charles Caravati Professor of Medicine Virginia Commonwealth University School of Medicine US Guidelines for NAFLD Represents consensus amongst AGA, AASLD and ACG
NIH Public Access Author Manuscript Am J Med Sci. Author manuscript; available in PMC 2015 January 01.
 NIH Public Access Author Manuscript Published in final edited form as: Am J Med Sci. 2014 January ; 347(1):. doi:10.1097/maj.0b013e31828b25a5. Association Between Metabolic Syndrome and Its Individual
NIH Public Access Author Manuscript Published in final edited form as: Am J Med Sci. 2014 January ; 347(1):. doi:10.1097/maj.0b013e31828b25a5. Association Between Metabolic Syndrome and Its Individual
The diagnosis of nonalcoholic steatohepatitis
 Nonalcoholic Fatty Liver Disease (NAFLD) Activity Score and the Histopathologic Diagnosis in NAFLD: Distinct Clinicopathologic Meanings Elizabeth M. Brunt, 1 David E. Kleiner, 2 Laura A. Wilson, 3 Patricia
Nonalcoholic Fatty Liver Disease (NAFLD) Activity Score and the Histopathologic Diagnosis in NAFLD: Distinct Clinicopathologic Meanings Elizabeth M. Brunt, 1 David E. Kleiner, 2 Laura A. Wilson, 3 Patricia
Novel multiparametric magnetic resonance elastography (MRE) protocol accurately predicts NAS score for NASH diagnosis
 Novel multiparametric magnetic resonance elastography (MRE) protocol accurately predicts NAS score for NASH diagnosis Alina M. Allen, Meng Yin, Sudhakar K. Venkatesh, Taofic Mounajjed, Todd A. Kellogg,
Novel multiparametric magnetic resonance elastography (MRE) protocol accurately predicts NAS score for NASH diagnosis Alina M. Allen, Meng Yin, Sudhakar K. Venkatesh, Taofic Mounajjed, Todd A. Kellogg,
UMHS-PUHSC JOINT INSTITUTE
 Role of Visceral Adiposity in the Pathogenesis of Non-Alcoholic Fatty Liver Disease in Lean versus Obese Patients: A Comparative Study between Patients at UMHS versus PUHSC Lai WEI and Anna LOK W Zhang,
Role of Visceral Adiposity in the Pathogenesis of Non-Alcoholic Fatty Liver Disease in Lean versus Obese Patients: A Comparative Study between Patients at UMHS versus PUHSC Lai WEI and Anna LOK W Zhang,
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology
 Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
Linda Ferrell, MD Distinguished Professor Vice Chair Director of Surgical Pathology Dept of Pathology Nonalcoholic steatohepatitis and Fatty Liver Disease Liver manifestations of the obesity epidemic Changes
Non-alcoholic fatty liver disease (NAFLD) is a
 Original Article / Liver Hepatobiliary & Pancreatic Diseases International The association of non-alcoholic fatty liver disease and metabolic syndrome in a Chinese population Shou-Wu Lee, Teng-Yu Lee,
Original Article / Liver Hepatobiliary & Pancreatic Diseases International The association of non-alcoholic fatty liver disease and metabolic syndrome in a Chinese population Shou-Wu Lee, Teng-Yu Lee,
NASH Bench to Bedside
 NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
NASH Bench to Bedside October 2006 Anna Mae Diehl, M.D. Gastroenterology Division Duke University NonAlcoholic Fatty Liver Disease Common ~1/4-1/3 1/3 US adults Outcome highly variable Course indolent
Normal ALT for men 30 IU/L 36% US males abnormal. Abnl ALT. Assess alcohol use/meds. Recheck in 6-8 weeks. still pos
 Fatty liver disease Its not just for big boys anymore Ken Flora, MD, FAASLD, FACG, AGAF No disclosures Common situation Normal ALT for men 30 IU/L 36% US males abnormal Normal ALT for women 20 IU/L 28%
Fatty liver disease Its not just for big boys anymore Ken Flora, MD, FAASLD, FACG, AGAF No disclosures Common situation Normal ALT for men 30 IU/L 36% US males abnormal Normal ALT for women 20 IU/L 28%
Fatty Liver Disease A growing epidemic
 Fatty Liver Disease A growing epidemic Updates in GIM for Primary Care Don C. Rockey March 9 th, 2018 Disclosures 2018 Research Funding (all to MUSC) NIH/NIDDK Actelion Pharmaceuticals Gilead Sciences
Fatty Liver Disease A growing epidemic Updates in GIM for Primary Care Don C. Rockey March 9 th, 2018 Disclosures 2018 Research Funding (all to MUSC) NIH/NIDDK Actelion Pharmaceuticals Gilead Sciences
WORLDWIDE EPIDEMIOLOGY OF NASH
 WORLDWIDE EPIDEMIOLOGY OF NASH Stefano Bellentani, M.D., Ph.D. Chief of Gastroenterology and Hepatology Service Clinica Santa Chiara Locarno Switzerland & Fondazione Italiana Fegato (FIF), Bassovizza (Trieste),
WORLDWIDE EPIDEMIOLOGY OF NASH Stefano Bellentani, M.D., Ph.D. Chief of Gastroenterology and Hepatology Service Clinica Santa Chiara Locarno Switzerland & Fondazione Italiana Fegato (FIF), Bassovizza (Trieste),
Prognosis of NASH VII Workshop Intenracional de Actualizaçao em Hepatologia, Aug 29th 2014
 Prognosis of NASH VII Workshop Intenracional de Actualizaçao em Hepatologia, Aug 29th 2014 Vlad Ratziu, Université Pierre et Marie Curie, Hôpital Pitié Salpêtrière, Paris, France NASH : a severe hepatic
Prognosis of NASH VII Workshop Intenracional de Actualizaçao em Hepatologia, Aug 29th 2014 Vlad Ratziu, Université Pierre et Marie Curie, Hôpital Pitié Salpêtrière, Paris, France NASH : a severe hepatic
Fatty liver disease: What do we know?
 Fatty liver disease: What do we know? Prof. Dr. Claus Niederau Katholische Kliniken Oberhausen ggmbh St. Josef-Hospital Academic Teaching Hospital University of Duisburg-Essen NAFLD Non-Alcoholic Fatty
Fatty liver disease: What do we know? Prof. Dr. Claus Niederau Katholische Kliniken Oberhausen ggmbh St. Josef-Hospital Academic Teaching Hospital University of Duisburg-Essen NAFLD Non-Alcoholic Fatty
NICE guideline Published: 6 July 2016 nice.org.uk/guidance/ng49
 Non-alcoholic fatty liver disease (NAFLD): assessment and management NICE guideline Published: 6 July 20 nice.org.uk/guidance/ng49 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Non-alcoholic fatty liver disease (NAFLD): assessment and management NICE guideline Published: 6 July 20 nice.org.uk/guidance/ng49 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Diseases to Watch. Non-Alcoholic Fatty Liver Disease (NAFLD) and Non-alcoholic
 Diseases to Watch Non-Alcoholic Fatty Liver Disease (NAFLD) and Non-alcoholic steatohepatitis (NASH) - Prevalence and Symptoms - Risk Factors and Potential treatments - Target identification for NASH Robert
Diseases to Watch Non-Alcoholic Fatty Liver Disease (NAFLD) and Non-alcoholic steatohepatitis (NASH) - Prevalence and Symptoms - Risk Factors and Potential treatments - Target identification for NASH Robert
Pioglitazone, Vitamin E, or Placebo for Nonalcoholic Steatohepatitis
 original article,, or Placebo for Nonalcoholic Steatohepatitis Arun J. Sanyal, M.D., Naga Chalasani, M.B., B.S., Kris V. Kowdley, M.D., Arthur McCullough, M.D., Anna Mae Diehl, M.D., Nathan M. Bass, M.D.,
original article,, or Placebo for Nonalcoholic Steatohepatitis Arun J. Sanyal, M.D., Naga Chalasani, M.B., B.S., Kris V. Kowdley, M.D., Arthur McCullough, M.D., Anna Mae Diehl, M.D., Nathan M. Bass, M.D.,
Although nonalcoholic fatty liver disease (NAFLD) Decreased Survival of Subjects with Elevated Liver Function Tests During a 28-Year Follow-Up
 Decreased Survival of Subjects with Elevated Liver Function Tests During a 28-Year Follow-Up Cecilia Söderberg, 1 Per Stål, 2,3 Johan Askling, 1 Hans Glaumann, 3 Greger Lindberg, 3 Joel Marmur, 3 and Rolf
Decreased Survival of Subjects with Elevated Liver Function Tests During a 28-Year Follow-Up Cecilia Söderberg, 1 Per Stål, 2,3 Johan Askling, 1 Hans Glaumann, 3 Greger Lindberg, 3 Joel Marmur, 3 and Rolf
The Skinny On Non Alcoholic Fatty Liver Disease
 The Skinny On Non Alcoholic Fatty Liver Disease UCSF Advances in Internal Medicine Monika Sarkar, MD, MAS UCSF Division of GI/Hepatology June 24th, 2015 Non Alcoholic Fatty Liver Disease: Outline Pathogenesis
The Skinny On Non Alcoholic Fatty Liver Disease UCSF Advances in Internal Medicine Monika Sarkar, MD, MAS UCSF Division of GI/Hepatology June 24th, 2015 Non Alcoholic Fatty Liver Disease: Outline Pathogenesis
Role of Liver Biopsy. Role of Liver Biopsy 9/3/2009. Liver Biopsies in Viral Hepatitis: Beyond Grading and Staging
 Liver Biopsies in Viral Hepatitis: Beyond Grading and Staging for further reference: Liver biopsy assessment in chronic viral hepatitis: a personal, practical approach Neil Theise, MD. Depts of Pathology
Liver Biopsies in Viral Hepatitis: Beyond Grading and Staging for further reference: Liver biopsy assessment in chronic viral hepatitis: a personal, practical approach Neil Theise, MD. Depts of Pathology
ROKSANA KARIM, MBBS, PHD UNIVERSITY OF SOUTHERN CALIFORNIA LOS ANGELES, CA
 Gonadotropin and Sex Steroid Levels in HIVinfected Premenopausal Women and Their Association with Subclinical Atherosclerosis in HIVinfected and -uninfected Women in the Women s Interagency HIV Study (WIHS)
Gonadotropin and Sex Steroid Levels in HIVinfected Premenopausal Women and Their Association with Subclinical Atherosclerosis in HIVinfected and -uninfected Women in the Women s Interagency HIV Study (WIHS)
An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications
 REVIEW An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications Naim Alkhouri, M.D.,*, and Andrea Scott, B.S.* Nonalcoholic fatty liver disease (NAFLD)
REVIEW An Update on the Pharmacological Treatment of Nonalcoholic Fatty Liver Disease: Beyond Lifestyle Modifications Naim Alkhouri, M.D.,*, and Andrea Scott, B.S.* Nonalcoholic fatty liver disease (NAFLD)
FATTY LIVER DISEASE (NAFLD) (NASH) A GROWING
 NON ALCOHOLIC FATTY LIVER DISEASE () & NON ALCOHOLIC S T E ATO H E PAT I T I S () ADDRESSING A GROWING SILENT EPIDEMIC Prevalence of & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams
NON ALCOHOLIC FATTY LIVER DISEASE () & NON ALCOHOLIC S T E ATO H E PAT I T I S () ADDRESSING A GROWING SILENT EPIDEMIC Prevalence of & USA Prevalence in Middle Age Patients San Antonio, Texas (Williams
Laboratory analysis of the obese child recommendations and discussion. MacKenzi Hillard May 4, 2011
 Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
Laboratory analysis of the obese child recommendations and discussion MacKenzi Hillard May 4, 2011 aka: What to do with Fasting Labs The Obesity Epidemic The prevalence of obesity in adolescents has tripled
EASL EASD EASO Clinical practice guidelines for the management of nonalcoholic fatty liver disease.
 Commentary. EASL EASD EASO Clinical practice guidelines for the management of nonalcoholic fatty liver disease. Christopher D. Byrne 1,2, Giovanni Targher 3 1 Nutrition and Metabolism, Faculty of Medicine,
Commentary. EASL EASD EASO Clinical practice guidelines for the management of nonalcoholic fatty liver disease. Christopher D. Byrne 1,2, Giovanni Targher 3 1 Nutrition and Metabolism, Faculty of Medicine,
The relation between weight changes and alanine aminotransferase levels in a nonalcoholic population
 The relation between weight changes and alanine aminotransferase levels in a nonalcoholic population Ji Eun Yun Department of Public Health The Graduate School Yonsei University The relation between weight
The relation between weight changes and alanine aminotransferase levels in a nonalcoholic population Ji Eun Yun Department of Public Health The Graduate School Yonsei University The relation between weight
Fatty Liver Disease. Mark Thursz. Imperial College
 Fatty Liver Disease Mark Thursz Imperial College Non-Alcoholic Fatty Liver Disease UK adult obesity (BMI>30) 1980: 6% [M], 8% [F]. 1997: 17% [M], 20% [F]. By 2004, 23.6% of men and 23.8% of women were
Fatty Liver Disease Mark Thursz Imperial College Non-Alcoholic Fatty Liver Disease UK adult obesity (BMI>30) 1980: 6% [M], 8% [F]. 1997: 17% [M], 20% [F]. By 2004, 23.6% of men and 23.8% of women were
Case #1. Digital Slides 11/6/ year old woman presented with abnormal liver function tests. Liver Biopsy to r/o autoimmune hepatitis
 45 year old woman presented with abnormal liver function tests Liver Biopsy to r/o autoimmune hepatitis Further down. ANA 1: 160; ASMA 1:80 ANA 1: 160; ASMA 1:80 IgG = 14.5 g/l (upper normal range: 16)
45 year old woman presented with abnormal liver function tests Liver Biopsy to r/o autoimmune hepatitis Further down. ANA 1: 160; ASMA 1:80 ANA 1: 160; ASMA 1:80 IgG = 14.5 g/l (upper normal range: 16)
NAFLD & NASH. Naga Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology
 NAFLD & NASH Naga Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology Indiana University School of Medicine ACG Midwest Regional Course,
NAFLD & NASH Naga Chalasani, MD, FACG Professor of Medicine and Cellular & Integrative Physiology Director, Division of GI and Hepatology Indiana University School of Medicine ACG Midwest Regional Course,
PHC, Paris, 30th Jan 2017 PATHOLOGY OF NAFLD. Pierre Bedossa. Departement of Pathology Hôpital Beaujon University Paris-Diderot Paris - FRANCE
 PHC, Paris, 30th Jan 2017 PATHOLOGY OF NAFLD Pierre Bedossa Departement of Pathology Hôpital Beaujon University Paris-Diderot Paris - FRANCE 1 PATHOLOGY OF NAFLD NAFLD: a chronic liver disease with a wide
PHC, Paris, 30th Jan 2017 PATHOLOGY OF NAFLD Pierre Bedossa Departement of Pathology Hôpital Beaujon University Paris-Diderot Paris - FRANCE 1 PATHOLOGY OF NAFLD NAFLD: a chronic liver disease with a wide
Supplementary Online Content
 Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
Supplementary Online Content Larsen JR, Vedtofte L, Jakobsen MSL, et al. Effect of liraglutide treatment on prediabetes and overweight or obesity in clozapine- or olanzapine-treated patients with schizophrenia
Liver disease is a major cause of mortality and morbidity
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:524 530 Changes in the Prevalence of the Most Common Causes of Chronic Liver Diseases in the United States From 1988 to 2008 ZOBAIR M. YOUNOSSI,*, MARIA
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:524 530 Changes in the Prevalence of the Most Common Causes of Chronic Liver Diseases in the United States From 1988 to 2008 ZOBAIR M. YOUNOSSI,*, MARIA
NASH UPDATE ON DIAGNOSTICS AND THERAPY. Arun J Sanyal MBBS, MD Virginia Commonwealth University School of Medicine
 NASH UPDATE ON DIAGNOSTICS AND THERAPY Arun J Sanyal MBBS, MD Virginia Commonwealth University School of Medicine Conflicts of interest Salaried employee: of VCU Member of Board: McGuire VA Research Institute,
NASH UPDATE ON DIAGNOSTICS AND THERAPY Arun J Sanyal MBBS, MD Virginia Commonwealth University School of Medicine Conflicts of interest Salaried employee: of VCU Member of Board: McGuire VA Research Institute,
Keywords: NASH, insulin resistance, metformin, histopathology. William W. Shields, K.E. Thompson, G.A. Grice, S.A. Harrison and W.J.
 Therapeutic Advances in Gastroenterology Original Research The effect of metformin and standard therapy versus standard therapy alone in nondiabetic patients with insulin resistance and nonalcoholic steatohepatitis
Therapeutic Advances in Gastroenterology Original Research The effect of metformin and standard therapy versus standard therapy alone in nondiabetic patients with insulin resistance and nonalcoholic steatohepatitis
The effect of aerobic exercise on serum level of liver enzymes and liver echogenicity in patients with non-alcoholic fatty liver disease
 Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE The effect of aerobic exercise on serum level of liver enzymes
Gastroenterology and Hepatology From Bed to Bench. 2013 RIGLD, Research Institute for Gastroenterology and Liver Diseases ORIGINAL ARTICLE The effect of aerobic exercise on serum level of liver enzymes
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical
 Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
Nonalcoholic Fatty Liver Disease in Children: Typical and Atypical Disclosure Naim Alkhouri, MD discloses the following relationships with commercial companies: Membership in the Speakers Bureau for Alexion
One-Year Intense Nutritional Counseling Results in Histological Improvement in Patients with Nonalcoholic Steatohepatitis: A Pilot Study
 American Journal of Gastroenterology ISSN 0002-9270 C 2005 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2005.41334.x Published by Blackwell Publishing One-Year Intense Nutritional Counseling
American Journal of Gastroenterology ISSN 0002-9270 C 2005 by Am. Coll. of Gastroenterology doi: 10.1111/j.1572-0241.2005.41334.x Published by Blackwell Publishing One-Year Intense Nutritional Counseling
Downloaded from zjrms.ir at 3: on Monday February 25th 2019 NAFLD BMI. Kg/m2 NAFLD
 logistic regression Student s t-test P< BMI BMI P< ALT AST P< Email:mkhoshbaten@yahoo.com Kg/m2 NASH RUQ B C II Case-Control II Logistic Regression Chi-Square T-test P< Grade Model 1- A diffuse hyper echoic
logistic regression Student s t-test P< BMI BMI P< ALT AST P< Email:mkhoshbaten@yahoo.com Kg/m2 NASH RUQ B C II Case-Control II Logistic Regression Chi-Square T-test P< Grade Model 1- A diffuse hyper echoic
What is NAFLD?.NASH? Presenter Disclosure Information. Learning Objectives. Case 1: Rob. Questions Pertinent to Rob
 Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
Presenter Disclosure Information 5 6pm Nonalcoholic Fatty Liver Disease (NAFLD): Another Obesity-Related Epidemic SPEAKER Elliot Tapper, MD The following relationships exist related to this presentation:
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and
 Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
Dietary supplementation in treating non-alcoholic fatty liver disease Dr. Ahmad Saedi Associate Professor School of Nutritional Sciences and Dietetics Tehran University of Medical Sciences Honorary Academic
NAFLD/NASH. Definitions. Pathology NASH. Vicki Shah PA-C, MMS Rush University Hepatology
 NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
NAFLD/NASH Vicki Shah PA-C, MMS Rush University Hepatology Definitions NAFLD Evidence of hepatic steatosis by histology (5%) or imaging No causes for secondary fat accumulation EtOH, Drugs, hereditary
Recognition of Reversible Liver Disease: A Window of Opportunity in the Metabolic Syndrome Epidemic
 Recognition of Reversible Liver Disease: A Window of Opportunity in the Metabolic Syndrome Epidemic Harold T. Pretorius, M.D.,Ph.D,^ Alexander K. Antony, B.A. ^ Dennis E. Menke, A.A.,^ Nichole M. Richards,
Recognition of Reversible Liver Disease: A Window of Opportunity in the Metabolic Syndrome Epidemic Harold T. Pretorius, M.D.,Ph.D,^ Alexander K. Antony, B.A. ^ Dennis E. Menke, A.A.,^ Nichole M. Richards,
Understanding Liver Disease
 Visit us on the Web at: clevelandclinic.org/liver To make an appointment call: 888.410.1775, option 1 International patients call: 001.216.444.8184 WOULD YOU LIKE A SECOND OPINION? If you would like a
Visit us on the Web at: clevelandclinic.org/liver To make an appointment call: 888.410.1775, option 1 International patients call: 001.216.444.8184 WOULD YOU LIKE A SECOND OPINION? If you would like a
Steatosi epatica ed HCV
 Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
Steatosi epatica ed HCV Malattie delle vie biliari ed Epatologia Rho, Auditorium Padri Oblati, 11 Novembre 2006 Piero L. Almasio Università di Palermo HISTOPATHOLOGY Steatosis and accelerated fibrogenesis:
Non-alcoholic fatty liver disease: time to take note and manage. Philip Newsome Professor of Hepatology & Director of Centre for Liver Research
 Non-alcoholic fatty liver disease: time to take note and manage Philip Newsome Professor of Hepatology & Director of Centre for Liver Research Disclosures Consultancy, Co-ordinating Investigator roles
Non-alcoholic fatty liver disease: time to take note and manage Philip Newsome Professor of Hepatology & Director of Centre for Liver Research Disclosures Consultancy, Co-ordinating Investigator roles
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Neuschwander-Tetri BA, Loomba R, Sanyal AJ,
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Neuschwander-Tetri BA, Loomba R, Sanyal AJ,
