Title: Post-transplant lymphoproliferative disease in liver transplant recipients
|
|
|
- Thomasine Rodgers
- 5 years ago
- Views:
Transcription
1 Title: Post-transplant lymphoproliferative disease in liver transplant recipients Authors: Mercedes Rubio-Manzanares Dorado, José María Álamo Martínez, Carmen Bernal Bellido, Luis Miguel Marín Gómez, Gonzalo Suárez Artacho, Carmen Cepeda Franco, Jize Wang, Miguel Ángel Gómez Bravo, Francisco Javier Padillo DOI: /reed /2016 Link: PubMed (Epub ahead of print) Please cite this article as: Rubio-Manzanares Dorado Mercedes, Álamo Martínez José María, Bernal Bellido Carmen, Marín Gómez Luis Miguel, Suárez Artacho Gonzalo, Cepeda Franco Carmen, Wang Jize, Gómez Bravo Miguel Ángel, Padillo Francisco Javier. Post-transplant lymphoproliferative disease in liver transplant recipients. Rev Esp Enferm Dig doi: /reed /2016. This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
2 OR 4228 inglés Post-transplant lymphoproliferative disease in liver transplant recipients Mercedes Rubio-Manzanares-Dorado, José María Álamo-Martínez, Carmen Bernal- Bellido, Luis Miguel Marín-Gómez, Gonzalo Suárez-Artacho, Carmen Cepeda-Franco, Jize Wang, Miquel Ángel Gómez-Bravo and Javier Padillo Unit of Hepatobiliary Surgery and Liver Transplantation. Hospital Universitario Virgen del Rocío. Sevilla, Spain Received: 03/02/2016 Accepted: 08/01/2017 Correspondence: Mercedes Rubio-Manzanares Dorado. Unit of Hepatobiliary Surgery and Liver Transplantation. Hospital Universitario Virgen del Rocío. Av. Manuel Siurot, s/n Sevilla, Spain ABSTRACT Introduction: Post-transplant lymphoproliferative syndrome (PTLD) is a rare and potentially life-threatening complication after liver transplantation. The aim of this study was to analyze the clinicopathologic features related to PTLD in a single institution after liver transplantation. Methods: Observational study where we have retrospectively analyzed 851 cases who underwent liver transplantation. Ten cases have developed PTLD. Their clinicalpathological characteristics and the treatment received have been analyzed. Results: PTLD incidence was 1.2% (10/851). The mean time from liver transplantation to PTLD diagnosis was 36 months (range 1.2 to 144 months). PTLD localization was extranodal in all cases, the most frequent location being intestinal. Seven cases showed a monomorphic lymphoma which in all cases was differentiated B cell lymphomas. Fifty per cent of the series were seropositive for Epstein-Barr virus. Five
3 patients were alive at the time of the review. Among these patients, we observed three cases of complete remission and two cases of disease stabilization. The death rate was higher in the first year after diagnosis of PTLD. Conclusion: PTLD is a rare complication after liver transplantation, but it may pose a threat to the life of a liver transplant recipient. It is essential to identify patients at risk, to establish an early diagnosis and treatment that can change the outcome of the disease. Key words: Post-transplant lymphoproliferative disease. Liver transplantation. Rituximab. INTRODUCTION During the past 20 years, liver transplantation programs have undergone a huge development. Advances in preoperative management, improvements in surgical techniques and progress in postoperative care have facilitated the improvement of liver transplant patient survival rates. The survival results published in European and American records exceed 85%, 75% and 60% at one, five and ten years respectively (1). However, long-term complications are a major cause overshadowing the prognosis of these patients. It has been observed that patients with solid organ transplantation are at increased risk of developing malignancies (2). Several factors have been described to contribute to the development of tumors. The reduction of immune surveillance mechanisms in the recipient, the activation of latent virus with oncological potential and the chronic use of immunosuppressive agents are the main factors for the appearance of cancer after a solid organ transplantation. In our country, the incidence of malignancies in liver transplantation is about 8%. The most common are skin tumors, followed by lymphoproliferative disorders (3). Post-transplant lymphoproliferative disease (PTLD) is a rare but also a serious complication in solid organ transplantation. In liver transplantation recipients, PTLD is reported in up to 1 to 2.8% of adults and 15% of children (4). It has been closely associated with exogenous immunosuppression and the Epstein-Barr virus (EBV); in fact, EBV is associated in up to 90% of cases. PTLD mortality has been estimated at
4 around 50%, although progress in treatment and chemotherapy regimens appear to have improved these results (5-9). Despite these different treatment options, mortality rates remain high. For this reason, early diagnosis is essential to facilitate prompt treatment. Relatively little is known about the incidence and outcome of PTLD in adults with a transplanted liver. The main objective of this study was to analyze the clinicalpathological characteristics of one of the most uncommon complications after liver transplantation. MATERIAL AND METHODS In this observational study, 851 cases who underwent liver transplantation in the Hospital Universitario Virgen del Rocío (Seville, Spain) from 1994 to 2011 were analyzed. Among the 851 cases analyzed, ten patients developed a PTLD that was diagnosed in all cases by biopsy of nodal or extranodal sites detected on imaging tests. Immunohistochemical markers were used to delineate the subtype of lymphoid proliferation, including CD20, CD79a, CD3, CD10 and bcl-6. Lymphomas were classified according to the World Health Organization (WHO) classification of PTLD (Table I). Inclusion and exclusion criteria We have included in this study all patients who received an isolated liver transplantation (not split or living donor) and developed PTLD. We have excluded from the study those who did not meet PTLD features according the WHO classification (Table I). Variables analysed The variables included in the study were as follows: age, gender, cause for liver transplantation, immunosuppressive agents used at the time of diagnosis, presence of acute rejection and need for treatment, lactate dehydrogenase (LDH) > 250 mg/dl before PTLD detection, PTLD histological classification, agents used after the PTLD diagnosis, chemotherapy used and use of rituximab.
5 EBV was diagnosed before the transplantation both in the donor and in the recipient by RNA in situ hybridization. Hepatitis C virus (HCV) recurrence was diagnosed by biopsy on the new liver graft prior to the development of PTLD, and confirmed by the HCV RNA detection. Immunosuppression was based on triple therapy, consisting of calcineurin inhibitor (tacrolimus [FK 506]/cyclosporin A [CyA]), steroids and mycophenolate mofetil/azathioprine. Corticosteroids were removed from the third month. We collected the cases that had a history of treated acute cellular rejection episodes. These cases were treated with 6-methylprednisolone intravenous bolus. In the same way, we have also collected patients who received induction therapy with OKT3 or anti-cd25 antibodies. Finally, we have analyzed those cases that converted from a calcineurin agent to mtor inhibitors (sirolimus/everolimus) after diagnosis of PTLD. Evaluation of response to treatment and survival Treatment response was assessed using follow-up computed tomographic (CT) scans. Restaging was performed following treatment. Complete remission was defined as the disappearance of all clinical evidence of active tumor for at least one month. Partial remission was defined as a minimum of 50% reduction in the measurement of detectable lesions for at least one month. Stable disease was considered when no objective modifications in the lesions were observed. Progressive disease was defined as the enlargement of tumor size or the occurrence of new lesions. Survival was defined as days survived from the date of diagnosis of PTLD to date of death or until the date of last revision. Statistical analysis Demographic characteristics, clinical presentation, histology and survival data were collected retrospectively in July 2013 in a SPSS 15.0 database (Tables II and III). A descriptive analysis was performed. For quantitative variables, data were expressed using means ± standard derivation, and percentage and counts were used for qualitative variables. For the analysis of two
6 qualitative variables in a sample of unequal size we used the Fisher s exact test. Statistical significance was considered if p < Finally, the Kaplan-Meier method was used to estimate survival following PTLD diagnosis. RESULTS During the study period ( ), the incidence of proven PTLD was 1.2% (10/851). Of the ten patients with histological PTLD, eight were male (80%) and two were women (20%). All patients studied were adults over 18 years of age. The mean age at disease presentation was 50 years (range 20-67). The causes underlying the liver transplantation included four patients with alcoholic cirrhosis, one case with hepatitis C cirrhosis, one case with hepatitis B cirrhosis and two cases of primary biliary cirrhosis. In addition, two patients had mixed alcohol cirrhosis and hepatitis C cirrhosis (Tables II and III). The timing from liver transplantation to first diagnosis of PTLD mean was two years and nine months (range 12 months to 12 years). In 50% of cases, PTLD was diagnosed during the first year after liver transplantation, whereas 30% presented a late onset, within three years after transplantation. Regarding clinical presentation, although symptoms were varied, the most common manifestations were fever and epigastric pain (30%). Other presentations were one case of intestinal obstruction, two cases of skin lesions, two cases of anemia, and one patient had chylous ascites. One case presented as a graft acute cellular rejection (Tables II and III). The most common manifestation in clinical examination and imaging tests was as a tumor mass. PTLD localization was extranodal in all cases, the most frequent location was intestinal. Among the four cases of intestinal localization, two were located in the stomach and two in the small intestine (one of these patients had both sites). Other sites include two retroperitoneal masses, one mediastinal mass and a cutaneous lymphoma. In two patients the PTLD was located on the liver graft, although no evidence of tumor mass in the previous image was detected.
7 Following the WHO classification of PTLD (Table I), one patient had early lesions showing plasmacytic hyperplasia features, two patients were polymorphic PTLD, whereas seven cases remained monomorphic. Among the latter, six patients were B cell lymphomas (five resembling diffuse large B cell lymphoma) and one patient was Hodgkin lymphoma. No patient had monomorphic T cell lymphoma. The status for the Epstein-Barr virus (EBV) receptor was performed in all cases by in situ RNA hybridization for EBV. Fifty per cent of patients were EBV positive and the remaining 50% were negative. All patients who had negative serology for EBV showed a monomorphic B cell lymphoma. Regarding the EBV status in the donor liver, 60% presented seropositivity for EBV. Among them, two grafts with positivity for EBV were implanted in recipients with negative EBV. In our series we found no significant difference among patients with EBV seronegativity who received a liver from a seropositive donor from those who received a negative EBV graft (Fisher s exact test p = 1). Concerning HCV recurrence in the graft after liver transplantation, two of the three patients transplanted for virus C cirrhosis had a recurrence of the disease in the graft. Lymphoma appearance was earlier in these cases. Both patients were monomorphic B cell lymphomas (Table III). LDH levels were determined prior to diagnosis of PTLD in eight cases, observing an elevation above 250 mg/dl in seven of them. Seven patients have been treated with tacrolimus as a basic immunosuppressive therapy. Among these cases, five patients developed a B cell lymphoma, one case was a Hodgkin lymphoma and another case was plasmocytic hyperplasia. Among the three patients who received cyclosporine, two developed a polymorphic lymphoma and one, a monomorphic B cell lymphoma. Although there is a tendency to use lower immunosuppressive levels in the latter years of the study, we have not seen a lower number of cases in this period. Fifty percent of the cases were diagnosed in the latter half of the study (Table III). Four patients required intravenous treatment with 6-methylprednisolone (6-MP) for acute rejection. Among them, three patients received OKT3. In these cases, PTLD developed earlier.
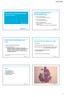
8 Three patients were diagnosed post mortem (30%) and they were not treated. The immunosuppression reduction without any other treatment allowed the achievement of complete remission of early lesions in one case and the stabilization of a cutaneous lymphoma in another. Three patients received rituximab as a first-line treatment and one patient as a second-line therapy. The latter received rituximab when current protocols for the administration of this drug were not established, thus receiving rituximab after chemotherapy. Immunosuppressive therapy of the three cases that received rituximab as first-line treatment was substituted for an mtor inhibitor after diagnosis of PTLD. Specifically, these patients received rapamycin (Sirolimus ) plus mycophenolate mofetil, among which a complete cure has been observed in two cases and disease stabilization in the remaining case. Two patients received chemotherapy. Among them, the patient who received rituximab as second-line treatment died. The other case was a Hodgkin lymphoma who received chemotherapy with ABVD regimen as first-line and CEP as second-line treatment with a resulting complete remission. The mortality in our series was 50%. The overall complete cure rate was 40%. One of the patients that had a complete remission died due to another cause not related with PTLD, specifically, he died due to a heart attack. We also observed a recurrence of 10%, resulting in death and rates of disease stabilization of 20%. The minimum followup time of patients from diagnosis of SLPT to the present time has been three years. It should be noted that since the use of rituximab (four patients) and calcineurin conversion to mtor inhibitors (three patients) the cure rate has been 66%, with one case of stabilization (33%). The latter patient had at the time of diagnosis a primary tumor in the stomach and a metastasis in the ocular nerve. After he received rituximab, the primary tumor completely disappeared but the metastasis still persisted. For this reason, he is waiting to receive radiotherapy. Survival mean was 71 ± 21 months and the actuarial survival at the time of the study was 50%. The overall survival at one, three and five years was 60%, 50% and 50%, respectively (Fig. 1). In three cases, the diagnosis of PTLD was made post mortem. In the remaining two cases, death occurred at eight and 25 months of diagnosis.
9 DISCUSION The incidence of PTLD after liver transplantation has been reported to vary from 2% to 5% (3,4). In our series, incidence was largely in accordance with the reference range in the literature, specifically, it was in up to 1.2% of cases. Although PTLD is a rare complication, it can be a threat to the patient s life due to its high mortality rate and rapid clinical progression. It is estimated that the mortality of PTLD is around 50% (5-9). In our series, the survival mean from diagnosis of PTLD to death or the last contact with the patient was 71 ± 21 months. We have observed that the survival rate after the first year of PTLD diagnosis was 60%. The death rate has been higher in the first year after diagnosis of PTLD. The median time for presentation was 36 months (range 1.2 to 144 months). In 70% of cases the diagnosis was made in the two years following liver transplantation. These findings are similar to those found in the literature, where the highest incidence of PTLD is observed at 18 months (10). Risk factors for PTLD development Risk factors for PTLD after liver transplant include EBV seronegativity, early age (especially children and adolescents), and high doses of immunosuppression and first year after transplant (11-13). In our case, 50% of recipients had EBV seronegativity prior to the liver transplant. Although multiple risk factors for the development of PTLD have been reported, the two main factors are EBV seronegativity of the recipient and the degree of immunosuppression. Recipients with EBV seronegativity who received a liver from a seropositive donor are at a particularly high risk due to the lack of specific immunity (cytotoxic T lymphocytes) to fight against infected B cells (14). In our series, no significant difference was observed, and this may be due to the limited number of receptors with seronegativity for EBV (Fisher s exact test p = 1). In the same way, the administration of high doses of steroids as a result of acute graft rejection has also been associated with an increased risk of PTLD (15). Immunosuppression after transplantation, leading to a decrease of the specific response function of cytotoxic T lymphocytes against EBV generates an uncontrolled proliferation mediated by the virus which culminates with the appearance of PTLD. In
10 our series, 40% of patients had acute liver graft rejection. As treatment, all patients received intravenous steroids. Among them three cases were also treated with OKT3. The latter may have had a greater predisposition to the development of PTLD due to the high degree of immunosuppression. Other risk factors that have been associated with PTLD are HCV recurrence on the graft, age older than 50 years, alcoholic cirrhosis and hepatitis C cirrhosis (16). In our series, all patients were of legal age, with an average age of presentation of 50 years (range years). The principal causes which motivated liver transplantation were alcohol and hepatitis C virus. Among patients with HCV, we have observed recurrence of hepatitis C virus on the graft in half of the cases. Immunosuppression received after liver transplantation suppress immunosurveillance mechanisms facilitating the activation of the virus with oncogenic potential that can lead to the development of tumors. PTLD diagnosis Clinical presentation often includes fever, lymphadenopathy, weight loss and splenomegaly. The disease can affect a single organ, graft or multiple organs. Bone marrow failure and central nervous system dysfunction is also common (6,17). Although in our series the most common clinical manifestations were fever along with epigastric pain (30%), in fact, the symptoms were varied. As noted, the first manifestations of PTLD are widely variable; for this reason, a high index of suspicion for early detection of PTLD is required. To resolve this, the measurement of EBV load by quantitative polymerase chain reaction can be an important weapon for monitoring and diagnosing patients with PTLD risk factors. Although a high load of EBV has a high sensitivity to predict PTLD, specificity in the liver transplant recipient is only around 50%. Due to the low specificity of EBV load for detecting PTLD, new biomarkers such as CD30 are being sought. In any case, an elevated EBV DNA in the peripheral blood should alert the physician to perform a physical examination and request imaging. If clinical suspicion is raised, an excisional biopsy should be done. Tissues should be submitted for EBV analysis and determination of CD20 expression, which are critical in determining treatment. If PTLD
11 is confirmed, it is necessary to perform a complete staging, including CT of the neck, chest, abdomen and pelvis, evaluation of the transplanted liver graft, an echocardiogram, and glomerular filtration rate. SPECT-CT is also useful, since it can detect areas infiltrated by lymphoma that had previously gone unnoticed (17). In our series, PTLD location was extranodal in all cases, the bowel being the most common site. These results do not agree with those obtained in other series where the most common localization were the lymph nodes followed by an intestinal location (18,19). On the other hand, the liver graft is a common site of presentation (up to 49% depending on the series) (19). In our case, although relatively frequent, the percentage is lower (20%). Early diagnosis of PTLD is essential to initiate treatment and prevent progression to a more aggressive variant. Thus, in 2008 the WHO introduced the PTLD classification, which establishes four categories according to their mode of presentation (Table I). Early lesions usually occur after the first year post-transplant. They have features of plasmocytic hyperplasia or mononucleosis primary infection (20). Lesions are usually polyclonal and they are more common in EBV seronegative recipients and in young patients. In our series, only one patient had early lesions such as plasmacytic hyperplasia. As in the literature, it occurred in the youngest patient in the series but this case was seropositive for EBV and debuted the first year after transplantation. Polymorphic PTLD, monomorphic PTLD and classic Hodgkin s lymphoma-type PTLD are usually monoclonal and they have a variable time of presentation after liver transplantation. Monomorphic B cell PTLD is the most frequent variant, especially diffuse large B cell lymphomas (21,22). In our cases, 60% of patients had monomorphic B cell lymphoma, of which 50% were diffuse large B cell variant. Lymphoproliferative syndromes are heterogeneous and EBV plays an important role in its pathogenesis. Eighty-five per cent of PTLD comes from the proliferation of B lymphocytes, and more than 80% of these are associated with EBV (21). Of the 15% that are of T-cell origin, 30% are associated with EBV (21). No monomorphic T cell PTLD was identified in our series; 100% of monomorphic lymphomas corresponded to B-cell lymphomas. These results are comparable with the revised data. However, in our series, only 20% of B cell lymphomas showed EBV seropositivity.
12 On the other hand, in our series, we observed a high mortality rate among patients who were EBV negative. Specifically, 80% of the deaths were EBV seronegative. The main prognostic factors for PTLD include high-grade lymphomas, EBV negativity on the recipient and an affected liver graft (6). This may explain the high mortality among patients with EBV negativity. As for the two patients who had liver involvement, both patients died and the diagnosis was made post mortem. PTLD located in the liver graft has a fulminant clinical course. Due to its similarity to acute rejection, it is essential to perform a liver biopsy to perform the diagnosis and start early treatment (23). PTLD treatment Current treatment for PTLD is based on an ascent therapy. It includes a reduction of immunosuppression, administration of monoclonal antibodies against specific biomarkers of B lymphocytes (anti-cd20) and chemotherapy. Surgery and radiation therapy may be useful when the disease is localized. It is estimated that reduction of immunosuppression can lead to regression of PTLD in up to 23-50% of cases (17). Immunosuppression should be decreased to the lowest tolerated levels, considering the risk of graft rejection. The liver is a resistant organ to reduction of immunosuppression, with a low rate of graft loss due to rejection. Liver transplantation has a better tolerance to immunosuppression reduction than other solid organ transplants. In our series, in two cases, reducing immunosuppression alone was sufficient to produce complete remission in one patient and stabilization in the other. None of these cases showed signs of acute or chronic rejection after decreasing immunosuppression. Although there is a tendency to use lower target levels of immunosuppressant in the second half of this study, this does not involves a trend towards a lower number of cases. Fifty percent of the cases were diagnosed in the latter half of the study (Table III). It is thought that the use of both CsA and FK506 per se increases the incidence of neoplasia with respect to common guidelines of this medication. Although the primary risk factor is the overall degree of immunosuppression, there is evidence to suggest that CsA and FK506 can promote tumor growth in immunosuppressed animals through
13 the release of tumor growth factor beta (24). When we have a suspicion or confirmation of PTLD, the first step should be to reduce or withdraw immunosuppressive medication if possible, adding drugs with antitumor effect. The use of immunosuppressive regimens that include an mtor inhibitor such as sirolimus or everolimus, which have an antitumor effect, could improve survival of these patients. However, although its effectiveness is recognized in patients with heart and kidney transplants, its efficacy in liver transplantation has not yet been established, so it is not advised as an initial immunosuppressive (25). In our series, immunosuppressive medication was replaced by an mtor inhibitor (sirolimus) in three cases. Among them, complete cure of the disease was observed in two cases and stabilization in the remaining case. New therapies with monoclonal antibodies against lymphocyte specific biomarkers have been a breakthrough in the treatment of lymphoproliferative syndrome. Rituximab therapy (an antibody against the CD20 receptor of B cells) seems to be effective in the management of PTLD cases, with a remission rate of 45-65% (17,26). In our study, 30% of patients received rituximab as first-line treatment, with a complete remission observed in 66% of these cases. Chemotherapy should be reserved for patients with high-grade lymphomas, disease progression after exhausting other therapeutic options or the occurrence of any organ failure. Generally, chemotherapies are based on anthracycline, which results in longer survival and disease free survival, although its benefits are overshadowed by its toxic effects (23). In our series, we observed the progression of the disease in the two patients who received chemotherapy, resulting in one death. CONCLUSION In summary, patients with suggestive symptoms of PTLD should undergo a liver biopsy and complementary imaging tests that allow early diagnosis. Our first action in PTLD treatment should be to reduce immunosuppression, always assessing the risk of acute liver graft rejection. Patients may also benefit from the replacement of a calcineurin inhibitor for an mtor inhibitor, specifically sirolimus.
14 Patient management should be based on histology, stage and location of the tumor. Patients with low-grade B cell lymphoma should be treated with rituximab monotherapy and the replacement of a calcineurin inhibitor for an mtor inhibitor. In the event of therapy failure, high grade lymphomas or organ failure, chemotherapy should be used. In conclusion, PTLD is a rare complication after liver transplantation that represents a threat to the patient s life. Due to the high mortality and therapeutic limitations, it is essential to identify patients at risk to obtain an early diagnosis and treatment that can change the outcome of the disease. REFERENCES 1. Adam R, Caillez V, Majno P, et al. intrinsic mortality risk in liver transplantation: European Liver Trasplant Registry study. Lancet 2000;356: DOI: /S (00) Engels EA, Pfeiffer RM, Fraumeni JF Jr, et al. Spectrum of cancer risk among US solid organ transplant recipients. JAMA 2011;306: DOI: /jama Bilbao Aguirre I, Lázaro Fernández L, Charco Torra R. Trasplante hepático. En: Parrrilla P, Landa JJ, editores. Cirugía AEC. 2º edición. Spain: Panamerica; p Taylor AL, Marcus R, Bradley JA. Post-transplant lymphoproliferative disorders (PTLD) after solid organ transplantation. Crit Rev Oncol Hematol 2005;56: DOI: /j.critrevonc Opelz G, Dohler B. Lymphomas after solid organ transplantation: A collaborative transplant study report. Am J Transplant 2004;4: DOI: /j x 6. Parker A, Bowles K, Bradley JA, et al. Management of post-transplant lymphoproliferative disorder in adult solid organ transplant recipients: BCSH and BTS Guidelines. Br J Haematol 2010;149: DOI: /j x 7. Evens AM, David KA, Helenowski I, et al. Multicenter analysis of 80 solid organ transplantation recipients with post-transplantation lymphoproliferative disease:
15 Outcomes and prognostic factors in the modern era. J Clin Oncol 2010;28: DOI: /JCO Kerkar N, Morotti RA, Madan RP, et al. The changing face of post-transplant lymphoproliferative disease in the era of molecular EBV monitoring. Pediatr Transplant 2010;14: DOI: /j x 9. Mukthinuthalapati PK, Gotur R, Ghabril M. Incidence, risk factors and outcomes of de novo malignancies post liver transplantation. World J Hepatol 2016;28: Kremers WK, Devarbhavi HC, Wiesner RH, et al. Post-transplant lymphoproliferative disorders following liver transplantation: Incidence, risk factors and survival. Am J Transplant 2006;6: DOI: /j x 11. Cockfield SM. Identifying the patient at risk for post-transplant lymphoproliferative disorder. Transpl Infect Dis 2001;3:70-8. DOI: /j x 12. Aucejo F, Rofaiel G, Miller C. Who is at risk for post-transplant lymphoproliferative disorders (PTLD) after liver transplantation? J Hepatol 2006;44: DOI: /j.jhep Mumtaz K, Faisal N, Márquez M, et al. Post-transplant lymphoproliferative disorder in liver transplant recipients: Characteristics, management and outcome from a single-centre experience with > 1,000 liver transplantations. Can J Gastroenterol Hepatol 2015;29: DOI: /2015/ Zimmermann T, Hoppe-Lotichius M, Tripkovic V, et al. Liver transplanted patients with preoperative autoimmune hepatitis and immunological disorders are at increased risk for post-transplant lymphoproliferative disease (PTLD). Eur J Intern Med 2010;21: DOI: /j.ejim Kamdara KY, Rooneya CM, Heslopa HE. Post-transplant lymphoproliferative disease following liver transplantation. Curr Opin Organ Transplant 2011;16: DOI: /MOT.0b013e McLaughlin K, Wajstaub S, Marotta P, et al. Increased risk for post-transplant lymphoproliferative disease in recipients of liver transplants with hepatitis C. Liver Transpl 2000;6: DOI: /jlts
16 17. Bakker NA, Van Imhoff GW, Verschuuren EA, et al. Presentation and early detection of posttransplant lymphoproliferative disorder after solid organ transplantation. Transpl Int 2007;20: DOI: /j x 18. Cheuk-lam Lo R, Chan SC, Chan KL, et al. Post-transplant lymphoproliferative disorders in liver transplant recipients: A clinicopathological study. J Clin Pathol 2013;66: DOI: /jclinpath Izadi M, Fazel M, Saadat SH, et al. Hepatic involvement by lymphoproliferative disorders post liver transplantation: PTLD. Int Survey Hepatol Int 2011;5: DOI: /s Swerdlow SH, Webber SA, Chadburn A, et al. Classification of tumours of haematopoietic and lymphoid tissues. 4 th ed. Lyon, France: International Agency for Research on Cancer; Koch DG, Christiansen L, Lazarchick J, et al. Post-transplantation lymphoproliferative disorder - The great mimic in liver transplantation: Appraisal of the clinicopathologic spectrum and the role of Epstein-Barr virus. Liver Transpl 2007;13: DOI: /lt Allen U, Alfieri C, Preiksaitis J, et al. Epstein-Barr virus infection in transplant recipients: Summary of a workshop on surveillance, prevention and treatment. Can J Infect Dis 2002;13: DOI: /2002/ Hoshida Y, Li T, Dong Z, et al. Lymphoproliferative disorders in renal transplant patients in Japan. Int J Cancer 2001;91: DOI: / (200002)9999:9999<::AID-IJC1125>3.0.CO;2-N 24. Hojo M, Morimoto T, Maluccio M, et al. Cyclosporine induce cancer progression by cell-autonomus mechanism. Nature 1999;397: DOI: / Andrassy J, Graeb C, Rentsch M, et al. mtor inhibition and its effect on cancer in trasplantation. Trasplantation 2005;80: DOI: /01.tp Mendizabal M, Marciano S, Dos Santos Schraiber L, et al. Post-transplant lymphoproliferative disorder in adult liver transplant recipients: A South American multicenter experience. Clin Transplant 2013:27: DOI: /ctr.12152
17 Table I WHO classification of post-transplant lymphoproliferative disease Category Clonality VEB status Early lesions (plasmacytic hyperplasia, infectious mononucleosis) Polymorphic PTLD Monomorphic PTLD B-cell lymphomas T-cell lymphomas Classic Hodgkin lymphomalike PTLD Polyclonal Monoclonal Monoclonal Monoclonal Monoclonal EBV positive EBV positive Frequently EBV positive Rarely EBV positive Frequently EBV positive Table II. Baseline characteristics Characteristics No. of cases (%) Age (years) 50 (± 13,24) Female gender 2 (20%) Etiology of liver disease Hepatitis C 1 (10%) Primary biliary cirrhosis 2 (20%) Alcohol 4 (40%) HCV + alcohol 2 (20%) Other 1 (10%) EBV serology recipient positive 5 (50%) EBV serology donor positive 6 (60%) Immunosuppression Cyclosporine-based 3 (30%) Tacrolimus-based 7 (70%) Corticosteroids 4 (40%) Mycophenolate 3 (30%)
18 Sirolimus 3 (30%) Azathioprine 6 (60%) Induction monoclonal 3 (30%) antibodies Acute rejection episode 4 (40%) Table III. Clinicopathological features of the ten PTLD cases
19 ACR* acute cellular rejection. Duration*: Duration from liver transplantation to first diagnosis of PTLD. Case Sex/Age Primary liver disease Year of diagnosis Immunosuppression Pre-PTLD ACR* Recurrence VHC Duration* (months) PTLD site Histological classification EBV donor EBV receptor Clinical outcome Rituximab mtor (sirolimus) 1 M/48 Alcoholic cirrhosis 1994 Cyclosporine Yes No 1.22 Hepatic graft Polymorphic - + Died No No 2 M/49 HCV cirrhosis 1998 FK506 Yes No 1.30 Hepatic graft Monomorphic, B cell - - Died No No 3 M/58 Alcoholic cirrhosis 2011 FK MMF No No 144 Stomach + ocular nerve Monomorphic, B cell + + Stabilization Yes Yes 4 F/46 Alcoholic and HCV cirrhosis 2001 FK506 No Yes 17 Retroperitoneum Monomorphic, B cell - - Died Yes No 5 M/44 HBV cirrhosis 2001 Cyclosporine No No 16 Cutaneous Polymorphic + + Stabilization No No 6 M/20 Primary biliary cirrhosis 2008 FK506 + MMF Yes No Intestinal Early lesions + + Complete remission No No 7 F/67 Primary biliary cirrhosis 2006 FK506 + MMF No No 47 Mediastinum Hodking lymphoma + + Complete remission No No 18
20 Fig. 1. Survival curve after PTLD diagnosis. 19
Nephrology Grand Rounds
 Nephrology Grand Rounds PTLD in Kidney Transplantation Charles Le University of Colorado 6/15/12 Objectives Background Pathogenesis Epidemiology and Clinical Manifestation Incidence Risk Factors CNS Lymphoma
Nephrology Grand Rounds PTLD in Kidney Transplantation Charles Le University of Colorado 6/15/12 Objectives Background Pathogenesis Epidemiology and Clinical Manifestation Incidence Risk Factors CNS Lymphoma
Title: Hepatocellular carcinoma in patients without advanced fibrosis after eradication of HCV with antiviral treatment
 Title: Hepatocellular carcinoma in patients without advanced fibrosis after eradication of HCV with antiviral treatment Authors: Yolanda Sánchez-Torrijos, Jara Eloísa Ternero Vega, Carmen Cepeda Franco
Title: Hepatocellular carcinoma in patients without advanced fibrosis after eradication of HCV with antiviral treatment Authors: Yolanda Sánchez-Torrijos, Jara Eloísa Ternero Vega, Carmen Cepeda Franco
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection. Masoud Mardani M.D,FIDSA
 Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Clinical Aspect and Application of Laboratory Test in Herpes Virus Infection Masoud Mardani M.D,FIDSA Shahidhid Bh BeheshtiMdi Medical lui Universityit Cytomegalovirus (CMV), Epstein Barr Virus(EBV), Herpes
Supplementary Appendix to manuscript submitted by Trappe, R.U. et al:
 Supplementary Appendix to manuscript submitted by Trappe, R.U. et al: Response to rituximab induction is a predictive marker in B-cell post-transplant lymphoproliferative disorder and allows successful
Supplementary Appendix to manuscript submitted by Trappe, R.U. et al: Response to rituximab induction is a predictive marker in B-cell post-transplant lymphoproliferative disorder and allows successful
European Risk Management Plan. Measures impairment. Retreatment after Discontinuation
 European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
European Risk Management Plan Table 6.1.4-1: Safety Concern 55024.1 Summary of Risk Minimization Measures Routine Risk Minimization Measures Additional Risk Minimization Measures impairment. Retreatment
Post Transplant Immunosuppression: Consideration for Primary Care. Sameh Abul-Ezz, M.D., Dr.P.H.
 Post Transplant Immunosuppression: Consideration for Primary Care Sameh Abul-Ezz, M.D., Dr.P.H. Objectives Discuss the commonly used immunosuppressive medications and what you need to know to care for
Post Transplant Immunosuppression: Consideration for Primary Care Sameh Abul-Ezz, M.D., Dr.P.H. Objectives Discuss the commonly used immunosuppressive medications and what you need to know to care for
Title: Painless jaundice as an initial presentation of lung adenocarcinoma
 Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Title: Painless jaundice as an initial presentation of lung adenocarcinoma Authors: Irene Andaluz García, Irene González Partida, Javier Lucas Ramos, Jorge Yebra Carmona DOI: 10.17235/reed.2018.5587/2018
Title: Linitis plastica of the colon due to metastases of invasive lobular breast carcinoma
 Title: Linitis plastica of the colon due to metastases of invasive lobular breast carcinoma Authors: David Viso Vidal, Rafael Villanueva Pavón, Francisco Jorquera Plaza DOI: 10.17235/reed.2019.6065/2018
Title: Linitis plastica of the colon due to metastases of invasive lobular breast carcinoma Authors: David Viso Vidal, Rafael Villanueva Pavón, Francisco Jorquera Plaza DOI: 10.17235/reed.2019.6065/2018
Overview of New Approaches to Immunosuppression in Renal Transplantation
 Overview of New Approaches to Immunosuppression in Renal Transplantation Ron Shapiro, M.D. Professor of Surgery Surgical Director, Kidney/Pancreas Transplant Program Recanati/Miller Transplantation Institute
Overview of New Approaches to Immunosuppression in Renal Transplantation Ron Shapiro, M.D. Professor of Surgery Surgical Director, Kidney/Pancreas Transplant Program Recanati/Miller Transplantation Institute
Leukaemia Section Short Communication
 Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL INIST-CNRS Leukaemia Section Short Communication Ding-Bao Chen Department of Pathology, Peking University People's Hospital,
Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL INIST-CNRS Leukaemia Section Short Communication Ding-Bao Chen Department of Pathology, Peking University People's Hospital,
Title: Post-transfusion hyperhemolysis syndrome following gastrointestinal bleeding secondary to prehepatic portal hypertension
 Title: Post-transfusion hyperhemolysis syndrome following gastrointestinal bleeding secondary to prehepatic portal hypertension Authors: María de los Ángeles Mejías Manzano, Álvaro Giráldez Gallego, Yolanda
Title: Post-transfusion hyperhemolysis syndrome following gastrointestinal bleeding secondary to prehepatic portal hypertension Authors: María de los Ángeles Mejías Manzano, Álvaro Giráldez Gallego, Yolanda
Methotrexate-associated Lymphoproliferative Disorders
 Methotrexate-associated Lymphoproliferative Disorders Definition A lymphoid proliferation or lymphoma in a patient immunosuppressed with methotrexate, typically for treatment of autoimmune disease (rheumatoid
Methotrexate-associated Lymphoproliferative Disorders Definition A lymphoid proliferation or lymphoma in a patient immunosuppressed with methotrexate, typically for treatment of autoimmune disease (rheumatoid
ORIGINAL ARTICLE. Adenotonsillar Enlargement in Pediatric Patients Following Solid Organ Transplantation. solid organ transplantation is increasingly
 Adenotonsillar Enlargement in Pediatric Patients Following Solid Organ Transplantation Robert Y. Huang, MD; Nina L. Shapiro, MD ORIGINAL ARTICLE Objective: To evaluate the management of adenotonsillar
Adenotonsillar Enlargement in Pediatric Patients Following Solid Organ Transplantation Robert Y. Huang, MD; Nina L. Shapiro, MD ORIGINAL ARTICLE Objective: To evaluate the management of adenotonsillar
2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA
 2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA SUSQUEHANNA HEALTH David B. Nagel, M.D. April 11, 2008 Hodgkin s lymphoma was first described by Thomas Hodgkin in 1832. It remained an incurable malignancy until
2007 ANNUAL SITE STUDY HODGKIN S LYMPHOMA SUSQUEHANNA HEALTH David B. Nagel, M.D. April 11, 2008 Hodgkin s lymphoma was first described by Thomas Hodgkin in 1832. It remained an incurable malignancy until
2017 CST-Astellas Canadian Transplant Fellows Symposium. EBV Post Transplantation Implications and Approach to Management
 2017 CST-Astellas Canadian Transplant Fellows Symposium EBV Post Transplantation Implications and Approach to Management Atul Humar, MD Atul Humar is a Professor in the Department of Medicine, University
2017 CST-Astellas Canadian Transplant Fellows Symposium EBV Post Transplantation Implications and Approach to Management Atul Humar, MD Atul Humar is a Professor in the Department of Medicine, University
Liver Transplant Pathology a general view
 Liver Transplant Pathology a general view Dr S E Davies Addenbrooke s Hospital Cambridge University Hospitals NHS Trust ACP/BSG Meeting Leeds 2012 Liver transplantation When and where? Who and why? How?
Liver Transplant Pathology a general view Dr S E Davies Addenbrooke s Hospital Cambridge University Hospitals NHS Trust ACP/BSG Meeting Leeds 2012 Liver transplantation When and where? Who and why? How?
Transplant Hepatology
 Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Transplant Hepatology Certification Examination Blueprint Purpose of the exam The exam is designed to evaluate the knowledge, diagnostic reasoning, and clinical judgment skills expected of the certified
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Limitations of EBV PCR monitoring to detect EBV associated post-transplant lymphoproliferative disorder
 Pediatr Transplantation 2003: 7: 223 227 Printed in UK. All rights reserved Copyright Ó 2003 Blackwell Munksgaard Pediatric Transplantation ISSN 1397-3142 Limitations of EBV PCR monitoring to detect EBV
Pediatr Transplantation 2003: 7: 223 227 Printed in UK. All rights reserved Copyright Ó 2003 Blackwell Munksgaard Pediatric Transplantation ISSN 1397-3142 Limitations of EBV PCR monitoring to detect EBV
Non-Hodgkin lymphoma
 Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Title: Utility of neoadjuvant therapy in rectal GIST. Authors: Víctor López-López, Juan Ángel Fernández, Pascual Parrilla
 Title: Utility of neoadjuvant therapy in rectal GIST Authors: Víctor López-López, Juan Ángel Fernández, Pascual Parrilla DOI: 10.17235/reed.2017.4751/2016 Link: PubMed (Epub ahead of print) Please cite
Title: Utility of neoadjuvant therapy in rectal GIST Authors: Víctor López-López, Juan Ángel Fernández, Pascual Parrilla DOI: 10.17235/reed.2017.4751/2016 Link: PubMed (Epub ahead of print) Please cite
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
Lymphoma co existing with Tuberculosis granulomatous
 Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
Available online at www.worldscientificnews.com WSN 90 (2017) 265-270 EISSN 2392-2192 SHORT COMMUNICATION Lymphoma co existing with Tuberculosis granulomatous Madeeha Subhan 1, *, Waleed Sadiq 2 1 Ayub
Title: Crohn s disease and cystic fibrosis: there is still a lot to learn
 Title: Crohn s disease and cystic fibrosis: there is still a lot to learn Authors: Claudio Trigo Salado, Eduardo Leo Carnerero, María Dolores de la Cruz Ramírez DOI: 10.17235/reed.2018.5725/2018 Link:
Title: Crohn s disease and cystic fibrosis: there is still a lot to learn Authors: Claudio Trigo Salado, Eduardo Leo Carnerero, María Dolores de la Cruz Ramírez DOI: 10.17235/reed.2018.5725/2018 Link:
11/2/2017. Immunodeficiencies. Joo Y. Song, MD Assistant Professor of Clinical Pathology. I have no financial disclosures.
 I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Transplant Autoimmunity Drugs T-cell dysfunction (Age,
I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Transplant Autoimmunity Drugs T-cell dysfunction (Age,
10/31/2017. Immunodeficiencies. Outline. Discuss EBV. Non-destructive Polymorphic Monomorphic Therapies Challenges
 I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Outline Transplant Congenital Autoimmunity T-cell/immune
I have no financial disclosures Joo Y. Song, MD Assistant Professor of Clinical Pathology City of Hope National Medical Center Immunodeficiencies Outline Transplant Congenital Autoimmunity T-cell/immune
Classical Hodgkin lymphoma type PTLD
 Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL AT INIST-CNRS Leukaemia Section Review Classical Hodgkin lymphoma type PTLD Ding-Bao Chen Department of Pathology, Peking
Atlas of Genetics and Cytogenetics in Oncology and Haematology OPEN ACCESS JOURNAL AT INIST-CNRS Leukaemia Section Review Classical Hodgkin lymphoma type PTLD Ding-Bao Chen Department of Pathology, Peking
Title: Lower gastrointestinal bleeding as a form of presentation in an adult case of Abernethy syndrome
 Title: Lower gastrointestinal bleeding as a form of presentation in an adult case of Abernethy syndrome Authors: Aida Suárez Sánchez, Lorena Solar García, Carmen María García Bernardo, Alberto Miyar de
Title: Lower gastrointestinal bleeding as a form of presentation in an adult case of Abernethy syndrome Authors: Aida Suárez Sánchez, Lorena Solar García, Carmen María García Bernardo, Alberto Miyar de
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Immunosuppressants. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Immunosuppressants Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Immunosuppressive Agents Very useful in minimizing the occurrence of exaggerated or inappropriate
Lymphatic System Disorders
 Lymphatic System Disorders Lymphomas Malignant neoplasms involving lymphocyte proliferation in lymph nodes Specific causes not identified // Higher risk in adults who received radiation during childhood
Lymphatic System Disorders Lymphomas Malignant neoplasms involving lymphocyte proliferation in lymph nodes Specific causes not identified // Higher risk in adults who received radiation during childhood
HAEMATOLOGICAL MALIGNANCY
 HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
HAEMATOLOGICAL MALIGNANCY Reference Compulsory reading Haematology at Glance 2 nd ed. Atul Mehta & Victor Hoffbrand Chapters: 20 to 31 Pages: 46 to 69 Pathogenesis of Haematological Malignancy Figure (a)
BK virus infection in renal transplant recipients: single centre experience. Dr Wong Lok Yan Ivy
 BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
BK virus infection in renal transplant recipients: single centre experience Dr Wong Lok Yan Ivy Background BK virus nephropathy (BKVN) has emerged as an important cause of renal graft dysfunction in recent
Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent
 Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
Int J Clin Exp Med 2014;7(1):307-311 www.ijcem.com /ISSN:1940-5901/IJCEM1311029 Case Report A case of EBV positive diffuse large B-cell lymphoma of the adolescent Qilin Ao 2, Ying Wang 1, Sanpeng Xu 2,
21/07/2017. Lymphoproliferations in immunodeficiency. IBD and EBV associated LPD in GIT Han van Krieken. Inflammatory bowel disease and cancer
 IBD and EBV associated LPD in GIT Han van Krieken Lymphoproliferations in immunodeficiency Primary immunodeficiencies Large variation in conditions and lesions Acquired immunodeficiencies HIV: changes
IBD and EBV associated LPD in GIT Han van Krieken Lymphoproliferations in immunodeficiency Primary immunodeficiencies Large variation in conditions and lesions Acquired immunodeficiencies HIV: changes
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
EBV in HSCT 2015 update of ECIL guidelines
 ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
ECIL-6 EBV in HSCT 2015 update of ECIL guidelines Jan Styczynski (Poland, chair), Walter van der Velden (Netherlands), Christopher Fox (United Kingdom), Dan Engelhard (Israel), Rafael de la Camara (Spain),
Transplantation in Australia and New Zealand
 Transplantation in Australia and New Zealand Matthew D. Jose MBBS (Adel), FRACP, FASN, PhD (Monash), AFRACMA Professor of Medicine, UTAS Renal Physician, Royal Hobart Hospital Overview CKD in Australia
Transplantation in Australia and New Zealand Matthew D. Jose MBBS (Adel), FRACP, FASN, PhD (Monash), AFRACMA Professor of Medicine, UTAS Renal Physician, Royal Hobart Hospital Overview CKD in Australia
Intruduction PSI MODE OF ACTION AND PHARMACOKINETICS
 Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
Multidisciplinary Insights on Clinical Guidance for the Use of Proliferation Signal Inhibitors in Heart Transplantation Andreas Zuckermann, MD et al. Department of Cardio-Thoracic Surgery, Medical University
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 30 November 2011
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 30 November 2011 NULOJIX 250 mg, powder for concentrate for solution for infusion B/1 (CIP code: 580 415-7) B/2 (CIP
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 30 November 2011 NULOJIX 250 mg, powder for concentrate for solution for infusion B/1 (CIP code: 580 415-7) B/2 (CIP
Vol. 29, pp.585 ~ 589, ml. 1.6 mg/dl 1 MRSA. Table 1 MRI
 Vol. 29, pp.585 ~ 589, 2001 8 13 10 22 8 7 1 14 49 26.1 6 2 ABO 7 1 400 800 ml 5 4 10 4 3 3 ABO 3 4 5 5 1 3 4 1 0.8 1.6 mg/dl 1 MRSA 10 7 1 10 7 22 40 8 CYA+ AZ+ MP 3 4 7 GSP 4 1 Table 1 23 1 15 11 5 Alport
Vol. 29, pp.585 ~ 589, 2001 8 13 10 22 8 7 1 14 49 26.1 6 2 ABO 7 1 400 800 ml 5 4 10 4 3 3 ABO 3 4 5 5 1 3 4 1 0.8 1.6 mg/dl 1 MRSA 10 7 1 10 7 22 40 8 CYA+ AZ+ MP 3 4 7 GSP 4 1 Table 1 23 1 15 11 5 Alport
Lugano classification: Role of PET-CT in lymphoma follow-up
 CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation
 LIVER TRANSPLANTATION 12:1210-1214, 2006 ORIGINAL ARTICLE Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation Ashesh Shah, 1 Avinash Agarwal, 1 Richard Mangus,
LIVER TRANSPLANTATION 12:1210-1214, 2006 ORIGINAL ARTICLE Induction Immunosuppression With Rabbit Antithymocyte Globulin in Pediatric Liver Transplantation Ashesh Shah, 1 Avinash Agarwal, 1 Richard Mangus,
Title: An intrahepatic cavoportal collateral pathway due to a liver hydatid cyst obstructing the inferior vena cava
 Title: An intrahepatic cavoportal collateral pathway due to a liver hydatid cyst obstructing the inferior vena cava Authors: Alba Manuel Vázquez, José Manuel Ramia Ángel, Luis Gijón, Roberto de la Plaza
Title: An intrahepatic cavoportal collateral pathway due to a liver hydatid cyst obstructing the inferior vena cava Authors: Alba Manuel Vázquez, José Manuel Ramia Ángel, Luis Gijón, Roberto de la Plaza
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
2012 by American Society of Hematology
 2012 by American Society of Hematology Common Types of HIV-Associated Lymphomas DLBCL includes primary CNS lymphoma (PCNSL) Burkitt Lymphoma HIV-positive patients have a 60-200 fold increased incidence
2012 by American Society of Hematology Common Types of HIV-Associated Lymphomas DLBCL includes primary CNS lymphoma (PCNSL) Burkitt Lymphoma HIV-positive patients have a 60-200 fold increased incidence
Epidemiology of Posttransplantation Lymphoproliferative Disorder in Adult Renal Transplant Recipients
 CLINICAL AND TRANSLATIONAL RESEARCH Epidemiology of Posttransplantation Lymphoproliferative Disorder in Adult Renal Transplant Recipients Muir Morton, 1 Beatrice Coupes, 1 Stephen A. Roberts, 2 Paul E.
CLINICAL AND TRANSLATIONAL RESEARCH Epidemiology of Posttransplantation Lymphoproliferative Disorder in Adult Renal Transplant Recipients Muir Morton, 1 Beatrice Coupes, 1 Stephen A. Roberts, 2 Paul E.
A Unique Case of Nasal NK/T Cell Lymphoma with Frequent Remission and Relapse Showing Different Histological Features During 12 Years of Follow Up
 J Clin Exp Hematopathol Vol. 50, No. 1, May 2010 Case Study A Unique Case of Nasal NK/T Cell Lymphoma with Frequent Remission and Relapse Showing Different Histological Features During 12 Years of Follow
J Clin Exp Hematopathol Vol. 50, No. 1, May 2010 Case Study A Unique Case of Nasal NK/T Cell Lymphoma with Frequent Remission and Relapse Showing Different Histological Features During 12 Years of Follow
SELECTED ABSTRACTS. All (n) % 3-year GS 88% 82% 86% 85% 88% 80% % 3-year DC-GS 95% 87% 94% 89% 96% 80%
 SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
SELECTED ABSTRACTS The following are summaries of selected posters presented at the American Transplant Congress on May 5 9, 2007, in San Humar A, Gillingham KJ, Payne WD, et al. Review of >1000 kidney
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia
 Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
Severe Viral Related Complications Following Allo-HCT for Severe Aplastic Anemia Liat Shragian Alon, MD Rabin Medical Center, ISRAEL #EBMT15 www.ebmt.org Patient: 25-year-old male No prior medical history
CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease
 CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease Maria Isabel Fiel, M.D. The Mount Sinai Medical Center New York, New York Case A 57 yo man, 7 months
CASE 1 Plasma Cell Infiltrates: Significance in post liver transplantation and in chronic liver disease Maria Isabel Fiel, M.D. The Mount Sinai Medical Center New York, New York Case A 57 yo man, 7 months
SKIN CANCER AFTER HSCT
 SKIN CANCER AFTER HSCT David Rice, PhD, MSN, RN, NP, NEA-BC Director, Education, Evidence-based Practice and Research City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES
SKIN CANCER AFTER HSCT David Rice, PhD, MSN, RN, NP, NEA-BC Director, Education, Evidence-based Practice and Research City of Hope National Medical Center HOW THE EXPERTS TREAT HEMATOLOGIC MALIGNANCIES
PUO in the Immunocompromised Host: CMV and beyond
 PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
PUO in the Immunocompromised Host: CMV and beyond PUO in the immunocompromised host: role of viral infections Nature of host defect T cell defects Underlying disease Treatment Nature of clinical presentation
Matched-pair analysis: identification of factors with independent influence on the development of PTLD after kidney or liver transplantation
 Rausch et al. Transplantation Research (2016) 5:6 DOI 10.1186/s13737-016-0036-1 RESEARCH Open Access Matched-pair analysis: identification of factors with independent influence on the development of PTLD
Rausch et al. Transplantation Research (2016) 5:6 DOI 10.1186/s13737-016-0036-1 RESEARCH Open Access Matched-pair analysis: identification of factors with independent influence on the development of PTLD
International Journal of Health Sciences and Research ISSN:
 International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Hodgkin s Lymphoma in Children Aged 6 Years Or Below- Long Term Follow Up Results Giri G V
International Journal of Health Sciences and Research www.ijhsr.org ISSN: 2249-9571 Original Research Article Hodgkin s Lymphoma in Children Aged 6 Years Or Below- Long Term Follow Up Results Giri G V
Literature Review: Transplantation July 2010-June 2011
 Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
Literature Review: Transplantation July 2010-June 2011 James Cooper, MD Assistant Professor, Kidney and Pancreas Transplant Program, Renal Division, UC Denver Kidney Transplant Top 10 List: July Kidney
Posttransplant Lymphoproliferative Disorders in Kidney Transplant Recipients An Iranian Multicenter Experience
 Transplantation Posttransplant Lymphoproliferative Disorders in Kidney Transplant Recipients An Iranian Multicenter Experience Behzad Einollahi, 1 Mahboob Lessan-Pezeshki, 2 Mohammad Hossein Nourbala,
Transplantation Posttransplant Lymphoproliferative Disorders in Kidney Transplant Recipients An Iranian Multicenter Experience Behzad Einollahi, 1 Mahboob Lessan-Pezeshki, 2 Mohammad Hossein Nourbala,
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
RAPID COMMUNICATION Preexisting malignancy is considered a relative contrain- dication to orthotopic liver transplantation (OLT) be-
 RAPID COMMUNICATION Successful Outcome of Orthotopic Liver Transplantation in s With Preexisting Malignant States Sanjiv Saigal, Suzanne Norris, Parthi Srinivasan, Paolo Muiesan, Mohamed Rela, Nigel Heaton,
RAPID COMMUNICATION Successful Outcome of Orthotopic Liver Transplantation in s With Preexisting Malignant States Sanjiv Saigal, Suzanne Norris, Parthi Srinivasan, Paolo Muiesan, Mohamed Rela, Nigel Heaton,
Long term liver transplant management
 Long term liver transplant management Dr Bill Griffiths Cambridge Liver Unit Royal College of Physicians 5.7.17 Success of Liver Transplantation Current survival, 1 st elective transplant: 1 yr survival
Long term liver transplant management Dr Bill Griffiths Cambridge Liver Unit Royal College of Physicians 5.7.17 Success of Liver Transplantation Current survival, 1 st elective transplant: 1 yr survival
Title: Aerophagia due to abdomino-phrenic dyssynergia in a 2-year-old child. Authors: Pablo Ercoli, Belinda García, Enrique del Campo, Sergio Pinillos
 Title: Aerophagia due to abdomino-phrenic dyssynergia in a 2-year-old child Authors: Pablo Ercoli, Belinda García, Enrique del Campo, Sergio Pinillos DOI: 10.17235/reed.2018.5444/2017 Link: PubMed (Epub
Title: Aerophagia due to abdomino-phrenic dyssynergia in a 2-year-old child Authors: Pablo Ercoli, Belinda García, Enrique del Campo, Sergio Pinillos DOI: 10.17235/reed.2018.5444/2017 Link: PubMed (Epub
Pathology of the indolent B-cell lymphomas Elias Campo
 Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Pathology of the indolent B-cell lymphomas Elias Campo Hospital Clinic, University of Barcelona Small B-cell lymphomas Antigen selection NAIVE -B LYMPHOCYTE MEMORY B-CELL MCL FL LPL MZL CLL Small cell
Lymphoma Read with the experts
 Lymphoma Read with the experts Marc Seltzer, MD Associate Professor of Radiology Geisel School of Medicine at Dartmouth Director, PET-CT Course American College of Radiology Learning Objectives Recognize
Lymphoma Read with the experts Marc Seltzer, MD Associate Professor of Radiology Geisel School of Medicine at Dartmouth Director, PET-CT Course American College of Radiology Learning Objectives Recognize
Risk factors for adenotonsillar hypertrophy in children following solid organ transplantation
 International Journal of Pediatric Otorhinolaryngology (2003) 67, 151 /155 www.elsevier.com/locate/ijporl Risk factors for adenotonsillar hypertrophy in children following solid organ transplantation Nina
International Journal of Pediatric Otorhinolaryngology (2003) 67, 151 /155 www.elsevier.com/locate/ijporl Risk factors for adenotonsillar hypertrophy in children following solid organ transplantation Nina
Int J Clin Exp Pathol 2014;7(1): /ISSN: /IJCEP
 Int J Clin Exp Pathol 2014;7(1):438-442 www.ijcep.com /ISSN:1936-2625/IJCEP1310053 Case Report Epstein-Barr virus-related post-transplant lymphoproliferative disorder occurring after bone marrow transplantation
Int J Clin Exp Pathol 2014;7(1):438-442 www.ijcep.com /ISSN:1936-2625/IJCEP1310053 Case Report Epstein-Barr virus-related post-transplant lymphoproliferative disorder occurring after bone marrow transplantation
What is a hematological malignancy? Hematology and Hematologic Malignancies. Etiology of hematological malignancies. Leukemias
 Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
Pediatric Kidney Transplantation
 Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Pediatric Kidney Transplantation Vikas Dharnidharka, MD, MPH Associate Professor Division of Pediatric Nephrology Conflict of Interest Disclosure Vikas Dharnidharka, MD, MPH Employer: University of Florida
Late effects, health status and quality of life after hemopoietic stem cell
 Late effects, health status and quality of life after hemopoietic stem cell transplantation (HSCT) THE 13th ESH-EBMT TRAINING COURSE ON BLOOD AND MARROW TRANSPLANTATION EBMT Slide template Barcelona 7
Late effects, health status and quality of life after hemopoietic stem cell transplantation (HSCT) THE 13th ESH-EBMT TRAINING COURSE ON BLOOD AND MARROW TRANSPLANTATION EBMT Slide template Barcelona 7
Indolent Lymphomas. Dr. Melissa Toupin The Ottawa Hospital
 Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant
 SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
SDC, Patients and Methods Complement-dependent lymphocytotoxic crossmatch test () Serum samples from recipients were obtained within 48 hours before transplantation. Pre-transplant donor-specific CXM was
Accepted Article. Granulomatous appendicitis as an uncommon cause of abdominal pain. Description of a case
 Accepted Article Granulomatous appendicitis as an uncommon cause of abdominal pain. Description of a case Carmen Salvia López Ramos, Ana Fuentes Coronel, Santiago Rodríguez Gómez DOI: 10.17235/reed.2015.3763/2015
Accepted Article Granulomatous appendicitis as an uncommon cause of abdominal pain. Description of a case Carmen Salvia López Ramos, Ana Fuentes Coronel, Santiago Rodríguez Gómez DOI: 10.17235/reed.2015.3763/2015
IBD-Related Lymphoma
 IBD-Related Lymphoma Larry Burgart MD Staff Pathologist, Allina Health and Minnesota Gastroenterology Clinical Professor of Pathology, University of Minnesota College of Medicine IBD-Related Lymphoma
IBD-Related Lymphoma Larry Burgart MD Staff Pathologist, Allina Health and Minnesota Gastroenterology Clinical Professor of Pathology, University of Minnesota College of Medicine IBD-Related Lymphoma
Immunopathology of T cell mediated rejection
 Immunopathology of T cell mediated rejection Ibrahim Batal MD Columbia University College of Physicians & Surgeons New York, NY, USA Overview Pathophysiology and grading of TCMR TCMR is still a significant
Immunopathology of T cell mediated rejection Ibrahim Batal MD Columbia University College of Physicians & Surgeons New York, NY, USA Overview Pathophysiology and grading of TCMR TCMR is still a significant
Doppler ultrasound of the abdomen and pelvis, and color Doppler
 - - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
- - - - - - - - - - - - - Testicular tumors are rare in children. They account for only 1% of all pediatric solid tumors and 3% of all testicular tumors [1,2]. The annual incidence of testicular tumors
Epstein Barr Virus Infection and Posttransplant Lymphoproliferative Disorder
 American Journal of Transplantation 2013; 13: 41 54 Wiley Periodicals Inc. Continuing Medical Education C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons
American Journal of Transplantation 2013; 13: 41 54 Wiley Periodicals Inc. Continuing Medical Education C Copyright 2013 The American Society of Transplantation and the American Society of Transplant Surgeons
Adenotonsillar Hypertrophy and Epstein-Barr Virus in Pediatric Organ Transplant Recipients
 The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. Adenotonsillar Hypertrophy and Epstein-Barr Virus in Pediatric
The Laryngoscope Lippincott Williams & Wilkins, Inc., Philadelphia 2001 The American Laryngological, Rhinological and Otological Society, Inc. Adenotonsillar Hypertrophy and Epstein-Barr Virus in Pediatric
Pediatric Oncology. Vlad Radulescu, MD
 Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Pediatric Oncology Vlad Radulescu, MD Objectives Review the epidemiology of childhood cancer Discuss the presenting signs and symptoms, general treatment principles and overall prognosis of the most common
Accepted Article. Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome
 Accepted Article Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome Aleix Martínez-Pérez, Ramón Trullenque-Juan, Sandra Santarrufina-Martínez,
Accepted Article Massive gastrointestinal pneumatosis in a patient with celiac disease and superior mesenteric artery syndrome Aleix Martínez-Pérez, Ramón Trullenque-Juan, Sandra Santarrufina-Martínez,
Date: 23 June Context and policy issues:
 Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
Title: Basiliximab for Immunosuppression During a Calcineurin Inhibitor Holiday in Renal Transplant Patients with Acute Renal Dysfunction: Guidelines for Use and a Clinical and Cost-Effectiveness Review
Title: unusual case report of inflammatory. fibrous polyps in the upper gastrointestinal tract. Authors: Baifang Wang, Guoqing Xiang, Jia Zhu
 Title: An unusual case report of inflammatory fibrous polyps in the upper gastrointestinal tract Authors: Baifang Wang, Guoqing Xiang, Jia Zhu DOI: 10.17235/reed.2018.5734/2018 Link: PubMed (Epub ahead
Title: An unusual case report of inflammatory fibrous polyps in the upper gastrointestinal tract Authors: Baifang Wang, Guoqing Xiang, Jia Zhu DOI: 10.17235/reed.2018.5734/2018 Link: PubMed (Epub ahead
clevelandclinic.org/transplant
 carolyn spiotta Pancreas/Kidney Transplant Recipient I feel so fortunate and thankful that I have received a second chance at life. Carolyn Spiotta, 44, Pittsburgh. Carolyn needed a new pancreas and kidney
carolyn spiotta Pancreas/Kidney Transplant Recipient I feel so fortunate and thankful that I have received a second chance at life. Carolyn Spiotta, 44, Pittsburgh. Carolyn needed a new pancreas and kidney
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation
 Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Increased Early Rejection Rate after Conversion from Tacrolimus in Kidney and Pancreas Transplantation Gary W Barone 1, Beverley L Ketel 1, Sameh R Abul-Ezz 2, Meredith L Lightfoot 1 1 Department of Surgery
Chapter 6: Transplantation
 Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
Chapter 6: Transplantation Introduction During calendar year 2012, 17,305 kidney transplants, including kidney-alone and kidney plus at least one additional organ, were performed in the United States.
POST TRANSPLANT OUTCOMES IN PSC
 POST TRANSPLANT OUTCOMES IN PSC Kidist K. Yimam, MD Medical Director, Autoimmune Liver Disease Program Division of Hepatology and Liver Transplantation California Pacific Medical Center (CPMC) PSC Partners
POST TRANSPLANT OUTCOMES IN PSC Kidist K. Yimam, MD Medical Director, Autoimmune Liver Disease Program Division of Hepatology and Liver Transplantation California Pacific Medical Center (CPMC) PSC Partners
Analysis of Circulating Tumor DNA: the Next Paradigm Shift in Detection and Treatment of Lung Cancer
 Accepted Manuscript Analysis of Circulating Tumor DNA: the Next Paradigm Shift in Detection and Treatment of Lung Cancer David S. Schrump, MD, MBA, Julie A. Hong, MS PII: S0022-5223(18)30295-2 DOI: 10.1016/j.jtcvs.2018.01.060
Accepted Manuscript Analysis of Circulating Tumor DNA: the Next Paradigm Shift in Detection and Treatment of Lung Cancer David S. Schrump, MD, MBA, Julie A. Hong, MS PII: S0022-5223(18)30295-2 DOI: 10.1016/j.jtcvs.2018.01.060
LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES
 LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES No conflict of interest Objectives Introduction Methods Results Conclusions Objectives Introduction Methods Results Conclusions
LIVER TRANSPLANTATION FOR OVERLAP SYNDROMES OF AUTOIMMUNE LIVER DISEASES No conflict of interest Objectives Introduction Methods Results Conclusions Objectives Introduction Methods Results Conclusions
Controversies in Renal Transplantation. The Controversial Questions. Patrick M. Klem, PharmD, BCPS University of Colorado Hospital
 Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
Controversies in Renal Transplantation Patrick M. Klem, PharmD, BCPS University of Colorado Hospital The Controversial Questions Are newer immunosuppressants improving patient outcomes? Are corticosteroids
Cellular Immunity to Epstein-Barr Virus in Liver Transplant Recipients Treated with Rituximab for Post-Transplant Lymphoproliferative Disease
 American Journal of Transplantation 5; 5: 566 572 Blackwell Munksgaard Copyright C Blackwell Munksgaard 4 doi:./j.6-643.4.693.x Cellular Immunity to Epstein-Barr Virus in Liver Transplant Recipients Treated
American Journal of Transplantation 5; 5: 566 572 Blackwell Munksgaard Copyright C Blackwell Munksgaard 4 doi:./j.6-643.4.693.x Cellular Immunity to Epstein-Barr Virus in Liver Transplant Recipients Treated
Title: Hepatitis E virus in neurological disorders: a case of Parsonage-Turner syndrome. Rev
 Title: Hepatitis E virus in neurological disorders: a case of Parsonage-Turner syndrome Authors: María Sánchez Azofra, Miriam Romero Portales, Lucia Tortajada Laureiro, Javier García-Samaniego, Pedro Mora
Title: Hepatitis E virus in neurological disorders: a case of Parsonage-Turner syndrome Authors: María Sánchez Azofra, Miriam Romero Portales, Lucia Tortajada Laureiro, Javier García-Samaniego, Pedro Mora
Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study
 NDT Plus (2010) 3 [Suppl 2]: ii32 ii36 doi: 10.1093/ndtplus/sfq064 Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study Miguel Gonzalez-Molina 1, Miguel Angel
NDT Plus (2010) 3 [Suppl 2]: ii32 ii36 doi: 10.1093/ndtplus/sfq064 Effect of long-term steroid withdrawal in renal transplant recipients: a retrospective cohort study Miguel Gonzalez-Molina 1, Miguel Angel
Hematologic Malignancies of the Liver : Spectrum of Disease. Zhou Jian
 Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Hematologic Malignancies of the Liver : Spectrum of Disease Zhou Jian 2015-7-8 Hematologic malignancies include a wide spectrum of lymphoproliferative and myeloproliferative disorders with nodal and extranodal
Disclosures. CMV and EBV Infection in Pediatric Transplantation. Goals. Common Aspects CMV (Cytomegalovirus) and EBV (Epstein-Barr virus)
 Disclosures I have financial relationships with the following companies: CMV and EBV Infection in Pediatric Transplantation Elekta Inc Lucence Diagnostics Spouse employed Spouse employed I will not discuss
Disclosures I have financial relationships with the following companies: CMV and EBV Infection in Pediatric Transplantation Elekta Inc Lucence Diagnostics Spouse employed Spouse employed I will not discuss
OBJECTIVES. Phases of Transplantation and Immunosuppression
 Transplant and Immunosuppression: Texas Transplant Center April 29, 2017 Regina L. Ramirez, Pharm.D., BCPS PGY1 Pharmacy Residency Program Director Clinical Practice Specialist Solid Organ Transplant and
Transplant and Immunosuppression: Texas Transplant Center April 29, 2017 Regina L. Ramirez, Pharm.D., BCPS PGY1 Pharmacy Residency Program Director Clinical Practice Specialist Solid Organ Transplant and
Cancer in kidney transplant recipients: epidemiology and prevention
 BTS 2018, Brighton Cancer in kidney transplant recipients: epidemiology and prevention Adnan Sharif Queen Elizabeth Hospital Birmingham Outline 1. The burden of cancer after kidney transplantation 2. Epidemiology
BTS 2018, Brighton Cancer in kidney transplant recipients: epidemiology and prevention Adnan Sharif Queen Elizabeth Hospital Birmingham Outline 1. The burden of cancer after kidney transplantation 2. Epidemiology
Lymphoma. Types of Lymphoma. Clinical signs
 Lymphoma Lymphoma is a tumour originating from lymphoid tissue, either nodal (lymph ) or extranodal (thymus, spleen, mucosa, conjunctiva, or skin-associated lymphoid tissue). It is one of the most common
Lymphoma Lymphoma is a tumour originating from lymphoid tissue, either nodal (lymph ) or extranodal (thymus, spleen, mucosa, conjunctiva, or skin-associated lymphoid tissue). It is one of the most common
Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies
![Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies](/thumbs/90/104309591.jpg) Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies UNCONTROLLED WHEN PRINTED Note: NOSCAN Haematology MCN has approved the information contained within this document to guide
Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies UNCONTROLLED WHEN PRINTED Note: NOSCAN Haematology MCN has approved the information contained within this document to guide
Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients
 Accepted Manuscript Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients George Cholankeril, MD, Andrew A. Li, MD, Brittany B. Dennis, PhD, Alice E. Toll, MS, Donghee
Accepted Manuscript Increasing Trends in Transplantation of HCV-positive Livers into Uninfected Recipients George Cholankeril, MD, Andrew A. Li, MD, Brittany B. Dennis, PhD, Alice E. Toll, MS, Donghee
Heart Transplantation ACC Middle East Conference Dubai UAE October 21, 2017
 Heart Transplantation ACC Middle East Conference Dubai UAE October 21, 2017 Randall C Starling MD MPH FACC FAHA FESC FHFSA Professor of Medicine Kaufman Center for Heart Failure Department of Cardiovascular
Heart Transplantation ACC Middle East Conference Dubai UAE October 21, 2017 Randall C Starling MD MPH FACC FAHA FESC FHFSA Professor of Medicine Kaufman Center for Heart Failure Department of Cardiovascular
