Chi Leung Liu, Chung Mau Lo, Sheung Tat Fan*
|
|
|
- Leon Evans
- 5 years ago
- Views:
Transcription
1 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) [13] Akabayashi A, Slingsby BT, Fujita M. The first donor death after living-related liver transplantation in Japan. Transplantation 2004;77: 634 (letter). [14] Marcos A, Ham J, Fisher R, Olzinski A, Posner M. Single-center analysis of the first forty living donor transplants using the right lobe. Liver Transpl 2000;6: [15] Pomfret EA, Pomposelli JJ, Gordon FD, Erbay N, Lyn Price L, Lewis WD, et al. Liver regeneration and surgical outcome in donors of right-lobe liver grafts. Transplantation 2003;76:5 10. [16] Marcos A, Ham JM, Fisher RA, Olzinski AT, Shiffman ML, Sanyal AJ, et al. Emergency adult-to-adult living donor liver transplantation for fulminant hepatic failure. Transplantation 2000; 69: [17] Marcos A, Killackey M, Orloff MS, Mieles L, Bozorgzadeh A, Tan HP. Hepatic arterial reconstruction in 95 adult right lobe living donor liver transplants: evolution of anastomotic technique. Liver Transpl 2003;9: [18] Tan HP, Marcos A. Hepatic arterial anatomy for right liver procurement from living donors. Liver Transpl 2004;10: [19] Testa G, Malago M, Nadalin S, Hertl M, Lang H, Frilling A, et al. Right-liver living donor transplantation for decompensated end-stage liver disease. Liver Transpl 2002;8: [20] New York State Health Department. New York State Committee on quality improvement in living liver donation [21] Marcos A, Ham JM, Fisher RA, Olzinski AT, Posner MP. Surgical management of anatomical variations of the right lobe in living donor liver transplantation. Ann Surg 2000;231: [22] Gondolesi GE, Varotti G, Florman S, Munoz L, Fishbein TM, Emre SH, et al. Biliary complications in 96 consecutive right lobe living donor transplant recipients. Transplantation 2004;77: [23] Lo CM, Fan ST, Liu CL, Yong BH, Wong Y, Lau GK, et al. Lessons learned from one hundred right lobe living donor liver transplants. Ann Surg 2004;240: [24] Brown Jr RS, Russo MW, Lai M, Shiffman ML, Richardson MC, Everhart JE, et al. A survey of liver transplantation from living adult donors in the United States. N Engl J Med 2003;348: [25] Todo S, Furukawa H. Japanese study group on organ transplantation. Living donor liver transplantation for adult patients with hepatocellular carcinoma: experience in Japan. Ann Surg 2004; 240: [26] Trotter JF. Living donor liver transplantation: is the hype over? J Hepatol 2005;42: [27] Garcia-Retortillo M, Forns X, Llovet JM, Navasa M, Feliu A, Massauer A, et al. Hepatitis C recurrence is more severe after living donor compared to cadaveric liver transplantation. Hepatology 2004; 40: [28] Sugawara Y, Makuuchi M. Should living donor liver transplantation be offered to patients with hepatitis C virus cirrhosis? J Hepatol 2005; in press. [29] Shiffman ML, Stravitz RT, Cantos MJ, Mills AS, Sterling RK, Luketic VA, et al. Histologic recurrence of chronic hepatitis C virus in patients after living donor and deceased donor liver transplantation. Liver Transpl 2004;10: [30] Russo MW, Shrestha R. Is severe recurrent hepatitis C more common after living donor liver transplantation? Hepatology 2004;40: [31] Bozorgzadeh A, Jain A, Ryan C, Ornt D, Zand M, Mantry P, et al. Impact of hepatitis C viral infection in primary cadaveric liver allograft versus primary living-donor allograft in 100 consecutive liver transplant recipients receiving tacrolimus. Transplantation 2004; 77: [32] Tan HP, Madeb R, Kovach SJ, Orloff M, Mieles L, Johnson LA, et al. Hypophosphatemia after 95 right-lobe living donor hepatectomies for liver trasplantation is not a significant source of morbidity. Trasplantation 2003;76: What is the best technique for right hemiliver living donor liver transplantation? With or without the middle hepatic vein? Duct-to-- duct biliary anastomosis or Roux-en-Y hepaticojejunostomy? Chi Leung Liu, Chung Mau Lo, Sheung Tat Fan* Department of Surgery, Centre for the Study of Liver Disease, Queen Mary Hospital, The University of Hong Kong, 102 Pokfulam Road, Pokfulam, Hong Kong, China Adult-to-adult right hemiliver living donor liver transplantation (LDLT) has become an accepted procedure in both Western and Eastern societies. It provides a realistic hope of new life for thousands of recipients worldwide who otherwise would have limited or delayed access to a cadaveric organ [1]. There is much variation in the surgical technique of LDLT in different transplant centers, and * Corresponding author. Tel.:C ; fax: C address: hrmsfst@hkucc.hku.hk (S.T. Fan). Abbreviations: LDLT, living donor liver transplantation; MHV, middle hepatic vein; RHV, right hepatic vein. controversies exist in the surgical management of the patients. The necessity of providing venous drainage to the right anterior sector of a right hemiliver graft in LDLT has been controversial. Inclusion of the middle hepatic vein (MHV) in the right hemiliver graft to ensure better early graft function is also under debate. Hepatico-jejunostomy has been the standard approach for biliary reconstruction since the first reported series of right hemiliver LDLT [2]. Duct-toduct biliary anastomosis has several theoretic advantages over hepatico-jejunostomy and has gained popularity in liver transplant centers worldwide. However, the incidence of /$30.00 q 2005 European Association for the Study of the Liver. Published by Elsevier B.V. All rights reserved. doi: /j.jhep
2 18 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) biliary complications remains high after LDLT. In this review, the current status of LDLT with reference to the venous drainage of the right anterior sector and biliary reconstruction of the right hemiliver graft is discussed. 1. Venous drainage of the anterior sector of the right hemiliver graft Although graft size is one of the important factors for the success of liver transplantation, the importance of a uniformly good venous drainage of the anterior sector of the right hemiliver graft as a crucial factor for the postoperative liver function in LDLT has been recognized [3]. Venous congestion of Couinaud s segments V and VIII of the right hemiliver graft is frequently observed if MHV tributaries from these segments are ligated and the MHV is not included in the liver graft. The consequences of compromised venous outflow can be evident in some cases after portal vein reperfusion. Segments V and VIII can become swollen and turgid, and have a dusky discoloration. Graft rupture has been reported in the situation of severe congestion of the anterior sector after reperfusion [4]. Recipients may also manifest a small-for-size graft syndrome characterized by prolonged cholestasis, coagulopathy, and persistent ascites because the right posterior sector may sustain damage by the increased blood flow. Furthermore, poor venous outflow increases the risk of hepatic artery thrombosis and impairs graft regeneration by elevating sinusoidal pressure and disrupting sinusoidal endothelium [5,6]. Although venous congestion can resolve when intrahepatic venous collaterals to the right hepatic vein (RHV) enlarge during the first postoperative week [7], it may persist and contribute to the development of graft dysfunction and failure. In order to have a good quality functional right hemiliver graft without venous congestion to the anterior sector and to ensure satisfactory operative outcomes of the recipients, different approaches have been adopted in various transplant centers, ranging from selective reconstruction of the venous drainage on the basis of criteria such as appearance of dusky area, result of hepatic artery or hepatic vein occlusion test [8], donor recipient body weight ratio, or presence of dominant segments V and VIII hepatic veins [9], to routine inclusion of the MHV in the graft [10]. Lee et al. reported the initial experience of five LDLTs without drainage of the right anterior sector in 2001 [11]. Two of the five recipients showed graft congestion, massive ascites, sepsis, or poor graft function, and one of them died 20 days after operation. It was suggested that preservation and reconstruction of the MHV tributaries are required to prevent congestion of the right hemiliver graft. Lee et al. advocated reconstruction of hepatic venous drainage of the segments V and VIII into the inferior vena cava using recipient s autogenous interposition vein graft including an external iliac vein or saphenous vein [12]. Using these modified right liver grafts, they reported a satisfactory survival outcome of the recipients [13]. Makuuchi et al. proposed to provide venous drainage to the right anterior sector in selected cases [8]. Instead of routine inclusion of the MHV in the graft, the prominent segments V and VIII hepatic vein branches are anastomosed to the recipient MHV and left hepatic vein using a homologous or cryo-preserved vein graft. Two tests were proposed to predict graft congestion and the need for the provision of venous drainage to the right anterior sector. The first test is to clamp the MHV at donor operation and observe the flow pattern in the right anterior sector portal vein by intraoperative ultrasonography. If reverse flow in the portal vein is seen, reconstruction of segments V and VIII branches is necessary [14]. The second test is to clamp the right hepatic artery and MHV at donor operation. If the right anterior sector is dusky, hepatic vein reconstruction is needed [8]. Among the 30 LDLT recipients reported by the Tokyo group [8], MHV tributaries were reconstructed according to the results of the tests described in 18 grafts. Plasty of recipient hepatic veins was performed in 15 patients. All patients survived the operation and regeneration of the anterior and posterior sectors of the right hemiliver grafts was equivalent on subsequent computed tomography. De Villa et al. proposed an algorithm based on donor recipient body weight ratio, right hemiliver-to-recipient standard liver volume estimation, and donor hepatic venous anatomy to determine whether the MHV should be included in the right hemiliver graft in LDLT [9]. The MHV is not included in the graft if the donor is bigger than the recipient. If the estimated graft volume by computed tomographic volumetry is greater than 50% of the standard liver volume after correction for steatosis, the RHV is large, and segments V and VIII hepatic veins are less than 5 mm in size, the MHV is also not included in the right hemiliver graft. Although various criteria have been adopted by different investigators for selective inclusion of the MHV in the liver graft or selective reconstruction of the segments V and VIII venous tributaries, there is no consensus on the indications for the selective approach on venous reconstruction. Moreover, the long-term patency of venous conduit draining segments V and VIII are not known. In order to obtain uniformly satisfactory operative outcomes of LDLT recipients with a uniformly good venous drainage of the liver graft, we recommend routine inclusion of the MHV with the grafts [10]. It is considered crucial in providing sufficient functioning liver volume with good venous drainage to meet the high metabolic demand of recipients with poor liver function reserve. In patients with fulminant hepatic failure or acute decompensation of chronic liver failure, this has resulted in favorable survival outcome [15]. Instead of separate end-to-end venous anastomoses of the donor RHV and MHV to recipient RHV and MHV, respectively, we proposed a technique of hepatic venoplasty [16]. The MHV is joined to the RHV in the right hemiliver graft at the back table to form a triangular common orifice.
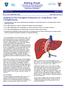
3 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) Fig. 1. (a, b) The orifice of the right hepatic vein in the recipient is enlarged to form a triangular opening to match the hepatic vein cuff of the graft. (c, d) The hepatic vein cuff is anastomosed to the caval opening using 5/0 polypropylene sutures. The septum in between the two hepatic veins is divided and sutured transversely to remove the ridge in between to create a large opening. The common orifice is anastomosed to a matched-size triangular opening in the recipient s vena cava (Fig. 1). Using this modification of the technique for venous anastomosis of the graft including the MHV, 1-year and 2-year graft survival rates of 100 and 96%, respectively, were reported [17]. Because of the perceived potential increase in surgical morbidity and mortality risk in the right hemiliver donor, controversies still exist concerning whether the MHV should be routinely included in the right hemiliver graft for LDLT. However, there are scarce data supporting the contention that inclusion of the MHV in the right hemiliver graft is associated with an increased postoperative complication rate in the donor [18]. Cattral et al. [19] reported a retrospective analysis on 56 right hemiliver donors, comparing the outcomes of the donors in whom the MHV was left intact (nz28) with those of the donors in whom the MHV was included in the graft (nz28). Operative time was significantly shorter in the group of donors who had the MHV included in the grafts. There was no difference in estimated blood loss, transfusion requirements, postoperative liver function, operative morbidity, and length of hospitalization. It was therefore concluded that including the MHV with the right hemiliver graft was not associated with an increase in operative risks of the donors. Similar observations on the operative and postoperative outcomes of liver donors with or without inclusion of the MHV in the right hemiliver grafts were also reported by Scatton et al. [20]. The operative outcomes were comparable in both groups of donors, except that liver function in terms of the prothrombin time ratio was significantly worse in the group with MHV included in the liver graft in the early postoperative period. However, the liver function was comparable in both groups of donors by the end of the first week after operation. The overall operative morbidity was comparable in both groups, and the donors remnant liver regeneration was similar as evaluated by computed tomography. The authors concluded that right hepatectomy including the MHV neither affects morbidity nor impairs early liver function and regeneration of the liver remnant in the donors for LDLT. However, it is undeniable that the segment IV is congested when the MHV is absent. The regeneration rate is reduced, but there is compensatory hypertrophy in segments II and III, resulting in the same amount of regeneration as segments II IV when the MHV is present [21]. In summary, there is an increasing trend of including the MHV in the right hemiliver graft in LDLT. Even without the MHV in the right hemiliver graft, increasing attention is paid to restore the venous drainage of segments V and VIII nowadays. 2. Biliary reconstruction in LDLT Biliary complication remains the Achilles s heel of LDLT and is the most common cause of postoperative morbidity [22]. The complication significantly affects the quality of life of the recipients and is occasionally the cause of graft and patient loss. Hepatico-jejunostomy was once the standard biliary reconstruction technique since the first reported series on adult-to-adult right hemiliver LDLT [2,23]. However, hepatico-jejunostomy has the disadvantages of requiring longer operation time, possible contamination due to opening of the jejunal loop, and delay in return of gastrointestinal function. In addition, the re-established bilio-enteric continuity is not physiological [24]. In contrast, duct-to-duct reconstruction, which is the technique of choice for biliary anastomosis in cadaveric liver transplantation [25], has the advantage of preserving the function of sphincter of Oddi as a defense against enteric reflux and ascending infection. Duct-to-duct biliary reconstruction has recently been advocated in LDLT [26, 27]. It is considered advantageous over hepatico-jejunostomy because it can minimize contamination by bowel content during transplantation, preserve physiological bilioenteric and bowel continuity, and result in early return of bowel function after transplantation. Without creation of mesenteric defects, duct-to-duct biliary anastomosis in LDLT can completely eliminate the risk of internal hernia of the small bowel [28]. Wachs et al. [26] in 1998 first reported the experience of duct-to-duct reconstruction for right hemiliver LDLT. However, biliary stricture developed 4 weeks later and the anastomosis was subsequently converted to a hepatico-jejunostomy. Thereafter, several studies reported the feasibility of duct-to-duct biliary anastomosis after right hemiliver LDLT [27,29 31]. Although duct-to-duct biliary reconstruction offers potential advantages over a
4 20 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) hepatico-jejunostomy, complications especially biliary strictures on long-term follow-up occur in about 30% of the LDLT recipients. It also remains controversial whether internal or external biliary drainage is beneficial in reducing the rate of biliary complications [32,33]. While there are obvious advantages of duct-to-duct biliary reconstruction over hepatico-jejunostomy, some investigators advocate routine hepatico-jejunostomy in adult-toadult LDLT, because of the possibility of increased risk of postoperative complications. In a retrospective analysis on 20 consecutive LDLT recipients reported by Kawachi et al. [34], biliary complication rate was observed in 60% among the 10 recipients who had a duct-to-duct anastomosis. These included biliary leakage (20%), biliary strictures (40%), and T-tube related biliary leakage (20%). All the 5 patients who received right hemiliver grafts developed biliary stricture. The incidence of biliary complication was only 20% in those patients who had hepatico-jejunostomy for biliary reconstruction. It was therefore suggested that duct-to-duct biliary reconstruction should be applied cautiously, especially in right hemiliver LDLT recipients. Other investigators suggested the use of duct-to-duct biliary anastomosis as the preferred technique as they did not observe an increased risk of morbidity. Gondolesi et al. reported biliary complications in 96 consecutive LDLT recipients [35], and failed to show significant differences in complications between the hepaticojejunostomy and duct-to-duct reconstruction groups. Regardless of the technique used, patients with more than one ductal opening had a higher incidence of bile leaks than those with only a single duct. In another retrospective study reported by Liu et al., the operative outcomes of 41 LDLT recipients who underwent duct-toduct biliary reconstruction were compared with those of 71 LDLT recipients who underwent hepatico-jejunostomy [33]. The overall biliary complication rate of the hepaticojejunostomy group was 31%, and was comparable to the figure of 24% observed in the duct-to-duct group. The postoperative intensive care unit stay (median: 3 days vs. 5 days, PZ0.01) and hospital stay (median, 19 days vs. 24 days, P!0.001) were significantly shorter in the ductto-duct group. Hospital mortality was also significantly lower in the duct-to-duct biliary reconstruction group (0 vs. 11%, PZ0.03). The overall biliary complication rate after duct-to-duct biliary reconstruction in LDLT remains high ranging from 24 to 67% in reported series (Table 1) [27,29,31 33,36]. Possible factors associated with an increased risk of postoperative biliary complication included multiple ductal openings [22] and a high preoperative model for end-stage liver disease score (R35) [33]. Ischiko et al. suggested that using continuous suture combined with an external stent might lower the biliary complication rate [32]. However, other investigators did not identify any significant factor associated with an increased risk of biliary complication after LDLT [35]. Nevertheless, complications related to biliary drainage tube including dislodgement and biliary leakage after removal of the tube have frequently been reported [35]. It was therefore controversial whether biliary drainage tube should be inserted after duct-to-duct biliary anastomosis in LDLT. The use of biliary drainage catheter or T-tube in cadaveric donor liver transplantation is still a topic for debate. In a multicenter prospective randomized trial, Scatton et al. [36] reported a significantly higher incidence of biliary complications in the T-tube group with a 10% incidence of biliary fistula. It was also found that T-tube did not provide a safer access to the biliary tract compared with the other available types of biliary exploration. Ben Ari et al. [37] also found that T-tube insertion after orthotopic liver transplantation was associated with a higher incidence of septic complications. It is still unknown whether the experience of T-tube drainage after cadaveric donor liver transplantation can be extrapolated to LDLT where the Table 1 Summary of reported series on duct-to-duct biliary reconstruction in living donor liver transplantation (LDLT) Author [Reference] Year No. of LDLT No. of Rt hemiliver LDLT Follow-up duration (months) Bile leakage Biliary stricture Shokouh-Amiri [31] (100%) MedianZ7.7, 4 (67%) 0 67 rangeznot available Grewal [27] (100%) Not available 2 (40%) 0 40 Malago [29] (100%) MedianZ11.6, 0 2 (40%) 40 rangez Kawachi [34] (50%) MeanZ20.3, 4 (40%) 4 (40%) 60 rangeznot available Ishiko [32] (100%) MedianZnot available, 5 (10%) 12 (23%) 31 rangez6 24 Liu [33] (100%) MedianZ13.3, 3 (7%) 10 (24%) 24 rangez Dulundu [35] (57%) MedianZ22.1, rangeznot available 12 (14%) 10 (12%) 32 Overall biliary complication rate (%)
5 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) right hepatic duct openings are usually small in caliber. The Kyoto group suggested that an external biliary stent is useful in patients undergoing LDLT with duct-to-duct biliary reconstruction [32]. However, the incidences of biliary complications in series with routine biliary drainage reported by the Kyoto group (31%) [32] and the Tokyo group (32%) [35] were similar to patients without biliary drainage (24%) as reported by the Hong Kong group [33] with a similar follow-up duration. Therefore, the controversy of whether biliary drainage or stent after LDLT with a duct-to-duct reconstruction is beneficial remains unsolved and should be further explored in prospective evaluations. Whatever the technique of biliary reconstruction, the prerequisite for success is good blood supply of stumps of the donor and recipient bile ducts. Steps to preserve arterial supply, venous drainage, and cautious handling of the ductal wall during suturing are essential [38]. Currently, many surgeons practice posterior continuous and anterior interrupted suturing without stenting. The long term outcome of such a technique awaits further evaluation. In conclusion, although routine inclusion of the MHV in the right hemiliver graft in LDLT is still controversial, the importance of providing venous drainage for the right anterior sector to ensure better early graft function has gained wide recognition. Different approaches have been adopted including routine inclusion of the MHV and a selective approach in the reconstruction of the venous drainage of segment V and VIII hepatic veins. Preservation of the MHV in the donor is intuitively considered important in reducing the donor risk. However, there are scarce data supporting the contention that the postoperative donor complication is related to the absence of the MHV in the left liver remnant. Hepatico-jejunostomy was once the standard biliary reconstruction technique in LDLT. Duct-to-duct biliary reconstruction has potential advantages becoming the preferred technique in several centers, recently. However, biliary complications such as biliary strictures on long-term follow-up occur in about 30% of the recipients. It also remains controversial whether internal or external biliary drainage is beneficial in reducing the biliary complication rate after duct-to-duct biliary anastomosis in LDLT. References [1] Trotter JF, Wachs M, Everson GT, Kam I. Adult-to-adult transplantation of the right hepatic lobe from a living donor. N Engl J Med 2002;346: [2] Lo CM, Fan ST, Liu CL, Wei WI, Lo RJ, Lai CL, et al. Adult-to-adult living donor liver transplantation using extended right lobe grafts. Ann Surg 1997;226: [3] Marcos A, Orloff M, Mieles L, Olzinski AT, Renz JF, Sitzmann JV. Functional venous anatomy for right-lobe grafting and techniques to optimize outflow. Liver Transpl 2001;7: [4] Marcos A, Fisher RA, Ham JM, Olzinski AT, Shiffman ML, Sanyal AJ, et al. Emergency portacaval shunt for control of hemorrhage from a parenchymal fracture after adult-to-adult living donor liver transplantation. Transplantation 2000;69: [5] Maetani Y, Itoh K, Egawa H, Shibata T, Ametani F, Kubo T, et al. Factors influencing liver regeneration following living-donor liver transplantation of the right hepatic lobe. Transplantation 2003;75: [6] Man K, Fan ST, Lo CM, Liu CL, Fung PC, Liang TB, et al. Graft injury in relation to graft size in right lobe live donor liver transplantation: a study of hepatic sinusoidal injury in correlation with portal hemodynamics and intragraft gene expression. Ann Surg 2003;237: [7] Kaneko T, Kaneko K, Sugimoto H, Inoue S, Hatsuno T, Sawada K, et al. Intrahepatic anastomosis formation between the hepatic veins in the graft liver of the living related liver transplantation: observation by Doppler ultrasonography. Transplantation 2000;70: [8] Sugawara Y, Makuuchi M, Sano K, Imamura H, Kaneko J, Ohkubo T, et al. Vein reconstruction in modified right liver graft for living donor liver transplantation. Ann Surg 2003;237: [9] de Villa VH, Chen CL, Chen YS, Wang CC, Lin CC, Cheng YF, et al. Right lobe living donor liver transplantation-addressing the middle hepatic vein controversy. Ann Surg 2003;238: [10] Lo CM, Fan ST, Liu CL, Yong BH, Wong Y, Lau GK, et al. Lessons learned from one hundred right lobe living donor liver transplants. Ann Surg 2004;240: [11] Lee S, Park K, Hwang S, Lee Y, Choi D, Kim K, et al. Congestion of right liver graft in living donor liver transplantation. Transplantation 2001;71: [12] Lee SG, Park KM, Hwang S, Kim KH, Choi DN, Joo SH, et al. Modified right liver graft from a living donor to prevent congestion. Transplantation 2002;74: [13] Lee SG, Park KM, Hwang S, Lee YJ, Kim KH, Ahn CS, et al. Adultto-adult living donor liver transplantation at the Asan Medical Center, Korea. Asian J Surg 2002;25: [14] Sano K, Makuuchi M, Miki K, Maema A, Sugawara Y, Imamura H, et al. Evaluation of hepatic venous congestion: proposed indication criteria for hepatic vein reconstruction. Ann Surg 2002;236: [15] Liu CL, Fan ST, Lo CM, Wei WI, Yong BH, Lai CL, et al. Live-donor liver transplantation for acute-on-chronic hepatitis B liver failure. Transplantation 2003;76: [16] Liu CL, Zhao Y, Lo CM, Fan ST. Hepatic venoplasty in right lobe live donor liver transplantation. Liver Transpl 2003;9: [17] Lo CM, Fan ST, Liu CL, Yong BH, Wong Y, Lau GK, et al. Lessons learned from one hundred right lobe living donor liver transplants. Ann Surg 2004;240: [18] Fan ST, Lo CM, Liu CL, Wang WX, Wong J. Safety and necessity of including the middle hepatic vein in the right lobe graft in adultto-adult live donor liver transplantation. Ann Surg 2003;238: [19] Cattral MS, Molinari M, Vollmer Jr CM, McGilvray I, Wei A, Walsh M, et al. Living-donor right hepatectomy with or without inclusion of middle hepatic vein: comparison of morbidity and outcome in 56 patients. Am J Transplant 2004;4: [20] Scatton O, Belghiti J, Dondero F, Goere D, Sommacale D, Plasse M, et al. Harvesting the middle hepatic vein with a right hepatectomy does not increase the risk for the donor. Liver Transpl 2004;10: [21] Hata S, Sugawara Y, Kishi Y, Niiya T, Kaneko J, Sano K, et al. Volume regeneration after right liver donation. Liver Transpl 2004; 10: [22] Gondolesi GE, Varotti G, Florman SS, Munoz L, Fishbein TM, Emre SH, et al. Biliary complications in 96 consecutive right lobe living donor transplant recipients. Transplantation 2004;77: [23] Marcos A, Fisher RA, Ham JM, Shiffman ML, Sanyal AJ, Luketic VA, et al. Right lobe living donor liver transplantation. Transplantation 1999;68:
6 22 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) [24] Calne RY. A new technique for biliary drainage in orthotopic liver transplantation utilizing the gall bladder as a pedicle graft conduit between the donor and recipient common bile ducts. Ann Surg 1976; 184: [25] Vallera RA, Cotton PB, Clavien PA. Biliary reconstruction for liver transplantation and management of biliary complications: overview and survey of current practices in the United States. Liver Transpl Surg 1995;1: [26] Wachs ME, Bak TE, Karrer FM, Everson GT, Shrestha R, Trouillot TE, et al. Adult living donor liver transplantation using a right hepatic lobe. Transplantation 1998;66: [27] Grewal HP, Shokouh-Amiri MH, Vera S, Stratta R, Bagous W, Gaber AO. Surgical technique for right lobe adult living donor liver transplantation without venovenous bypass or portocaval shunting and with duct-to-duct biliary reconstruction. Ann Surg 2001;233: [28] Liu CL, Lo CM, Chan SC, Fan ST, Wong J. Internal hernia of the small bowel after right-lobe live donor liver transplantation. Clin Transplant 2004;18: [29] Malago M, Testa G, Hertl M, Lang H, Paul A, Frilling A, et al. Biliary reconstruction following right adult living donor liver transplantation end-to-end or end-to-side duct-to-duct anastomosis. Langenbecks Arch Surg 2002;387: [30] Miller CM, Gondolesi GE, Florman S, Matsumoto C, Munoz L, Yoshizumi T, et al. One hundred nine living donor liver transplants in adults and children: a single-center experience. Ann Surg 2001;234: [31] Shokouh-Amiri MH, Grewal HP, Vera SR, Stratta RJ, Bagous W, Gaber AO. Duct-to-duct biliary reconstruction in right lobe adult living donor liver transplantation. J Am Coll Surg 2001;192: [32] Ishiko T, Egawa H, Kasahara M, Nakamura T, Oike F, Kaihara S, et al. Duct-to-duct biliary reconstruction in living donor liver transplantation utilizing right lobe graft. Ann Surg 2002;236: [33] Liu CL, Lo CM, Chan SC, Fan ST. Safety of duct-to-duct biliary reconstruction in right-lobe live-donor liver transplantation without biliary drainage. Transplantation 2004;77: [34] Kawachi S, Shimazu M, Wakabayashi G, Hoshino K, Tanabe M, Yoshida M, et al. Biliary complications in adult living donor liver transplantation with duct-to-duct hepaticocholedochostomy or Rouxen-Y hepaticojejunostomy biliary reconstruction. Surgery 2002;132: [35] Dulundu E, Sugawara Y, Sano K, Kishi Y, Akamatsu N, Kaneko J, et al. Duct-to-duct biliary reconstruction in adult living-donor liver transplantation. Transplantation 2004;78: [36] Scatton O, Meunier B, Cherqui D, Boillot O, Sauvanet A, Boudjema K, et al. Randomized trial of choledochocholedochostomy with or without a T tube in orthotopic liver transplantation. Ann Surg 2001;233: [37] Ben Ari Z, Neville L, Davidson B, Rolles K, Burroughs AK. Infection rates with and without T-tube splintage of common bile duct anastomosis in liver transplantation. Transpl Int 1998;11: [38] Fan ST, Lo CM, Liu CL, Tso WK, Wong J. Biliary reconstruction and complications of right lobe live donor liver transplantation. Ann Surg 2002;236: How to prevent and manage biliary complications in living donor liver transplantation? Satoru Todo*, Hiroyuki Furukawa, Toshiya Kamiyama The First Department of Surgery, Hokkaido University School of Medicine, N-15, W-7, Kita-ku, Sapporo , Japan Ever since the introduction of deceased donor (DD) liver transplantation, biliary complications have been the Achilles heel of the procedure [1]. Certain techniques used in early series (e.g. cholecysto-duodenostomy, cholecysto-jejunostomy) were associated with high complication rates of approximately 50%, and thus were rapidly abandoned. Currently, choledocho-jejunostomy or choledocho-choledochostomy are the standard methods for biliary reconstruction in liver transplantation, but complications still occur in 5 20% of recipients. For example, in 1792 consecutive liver transplantations at the University of Pittsburgh [2], 11.5% of the recipients suffered various biliary complications including strictures (42.8%), leaks * Corresponding author. Tel.: C ; fax: C address: stodo@med.hokudai.ac.jp (S. Todo). Abbreviations: DD; deceased donor; LDLT; living donor liver transplantation; HJ; hepatico-jejunostomy, duct-to-duct anastomosis; MRCP; magnetic resonance cholangio pancreaticography. (26.7%), ampullary dysfunction (6.6%), and obstruction (13.8%), leading to death in 21 patients. Although patient and graft survival rates after living donor liver transplantation (LDLT) have approached those after DD liver transplantation, biliary complications have been again identified as the Achilles heel of this newer procedure, affecting approximately 20 30% of recipients (Tables 1 and 2) (see previous article by CL Liu, CM Lo, and ST Fan in this forum). Initially, LDLT was undertaken to reduce mortality among children waiting for a cadaveric organ, by grafting the left lateral segment with a Roux-en Y hepatico-jejunostomy. Now, LDLT are mostly offered to adult recipients. The first adult recipient of a living donor graft successfully received the left hemiliver with a hepatico-jejunostomy reconstruction [3]. Currently, right hemiliver transplants are preferred in most centers often choosing a duct-to-duct biliary reconstruction in the hope of offering sufficient liver mass and preventing events associated with a hepatico-jejunostomy. Problems after /$30.00 q 2005 European Association for the Study of the Liver. Published by Elsevier B.V. All rights reserved. doi: /j.jhep
How to prevent and manage biliary complications in living donor liver transplantation?
 22 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) 13 37 [24] Calne RY. A new technique for biliary drainage in orthotopic liver transplantation utilizing the gall bladder as a pedicle
22 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) 13 37 [24] Calne RY. A new technique for biliary drainage in orthotopic liver transplantation utilizing the gall bladder as a pedicle
All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation
 DOI:10.1111/j.1477-2574.2012.00442.x HPB Technical Report All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation Chao-Long Chen*, Anthony
DOI:10.1111/j.1477-2574.2012.00442.x HPB Technical Report All-in-one sleeve patch graft venoplasty for multiple hepatic vein reconstruction in living donor liver transplantation Chao-Long Chen*, Anthony
Hepatic venous congestion (HVC) from deprivation
 Cryopreserved Iliac Artery is Indispensable Interposition Graft Material for Middle Hepatic Vein Reconstruction of Right Liver Grafts Shin Hwang, Sung-Gyu Lee, Chul-Soo Ahn, Kwang-Min Park, Ki-Hun Kim,
Cryopreserved Iliac Artery is Indispensable Interposition Graft Material for Middle Hepatic Vein Reconstruction of Right Liver Grafts Shin Hwang, Sung-Gyu Lee, Chul-Soo Ahn, Kwang-Min Park, Ki-Hun Kim,
Adult-to-adult living donor liver transplantation Triumphs and challenges
 Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Falk Symposium No. 163 on Chronic Inflammation of Liver and Gut Adult-to-adult living donor liver transplantation Triumphs and challenges ST Fan, MS, MD, PhD, DSc Professor Sun CY Chair of Hepatobiliary
Venous Outflow Reconstruction Using an Expanded Polytetrafluoroethylene Vascular Graft in Living-Donor Liver Transplant: A Single-Center Experience
 ARTICLe Venous Outflow Reconstruction Using an Expanded Polytetrafluoroethylene Vascular Graft in Living-Donor Liver Transplant: A Single-Center Experience Chia-Yu Lai, 1 Shao-Min Han, 2 Yi-Ju Chen, 1
ARTICLe Venous Outflow Reconstruction Using an Expanded Polytetrafluoroethylene Vascular Graft in Living-Donor Liver Transplant: A Single-Center Experience Chia-Yu Lai, 1 Shao-Min Han, 2 Yi-Ju Chen, 1
OPERATIVE TECHNIQUES AND HAZARDS
 OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
OPERATIVE TECHNIQUES AND HAZARDS CHRIS O SULLIVAN MD FRCSI CONSULTANT HBP AND LIVER TRANSPLANT SURGEON FREEMAN HOSPITAL, N-UPON-TYNE CAVAL RECONSTRUCTION IN ORTHOTOPIC LIVER TRANSPLANTATION RESECTION OF
Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation
 Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
Kasr El Aini Journal of Surgery VOL., 9, NO 3 January 2008 19 Variations in Surgical Anatomy of the Portal Vein in Living Donor Liver Transplantation A. Ayad ; W. Tobar; M.Hassan; A.Hosny; M.El Shazly;
An Artificial Vascular Graft Is a Useful Interpositional Material for Drainage of the Right Anterior Section in Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 13:1159-1167, 2007 ORIGINAL ARTICLE An Artificial Vascular Graft Is a Useful Interpositional Material for Drainage of the Right Anterior Section in Living Donor Liver Transplantation
LIVER TRANSPLANTATION 13:1159-1167, 2007 ORIGINAL ARTICLE An Artificial Vascular Graft Is a Useful Interpositional Material for Drainage of the Right Anterior Section in Living Donor Liver Transplantation
LEE AND OTHERS Annual LDLT (n) year Total Adult-to-adult Paedi
 ADULT-TO-ADULT LIVING DONOR LIVER TRANSPLANTATION Asian Journal of Surgery Excerpta Medica Asia Ltd Adult-to-Adult Living Donor Liver Transplantation at the Asan Medical Center, Korea S.G. Lee, 1 K.M.
ADULT-TO-ADULT LIVING DONOR LIVER TRANSPLANTATION Asian Journal of Surgery Excerpta Medica Asia Ltd Adult-to-Adult Living Donor Liver Transplantation at the Asan Medical Center, Korea S.G. Lee, 1 K.M.
The New England Journal of Medicine. Review Article 16,000 14,000 12,000. No. of Patients 10,000 8,000 6,000 4,000 2,000
 Review Article Medical Progress ADULT-TO-ADULT TRANSPLANTATION OF THE RIGHT HEPATIC LOBE FROM A LIVING DONOR JAMES F. TROTTER, M.D., MICHAEL WACHS, M.D., GREGORY T. EVERSON, M.D., AND IGAL KAM, M.D. TRANSPLANTATION
Review Article Medical Progress ADULT-TO-ADULT TRANSPLANTATION OF THE RIGHT HEPATIC LOBE FROM A LIVING DONOR JAMES F. TROTTER, M.D., MICHAEL WACHS, M.D., GREGORY T. EVERSON, M.D., AND IGAL KAM, M.D. TRANSPLANTATION
Split Graft Liver Transplant for Paediatric Patients in Hong Kong
 HK J Paediatr (new series) 2009;14:181-185 Split Graft Liver Transplant for Paediatric Patients in Hong Kong PHY CHUNG, KKY WONG, PKH TAM, KL CHAN, KKC NG, SC CHAN, TWC HUI, BH YONG, ST FAN, CM LO Abstract
HK J Paediatr (new series) 2009;14:181-185 Split Graft Liver Transplant for Paediatric Patients in Hong Kong PHY CHUNG, KKY WONG, PKH TAM, KL CHAN, KKC NG, SC CHAN, TWC HUI, BH YONG, ST FAN, CM LO Abstract
Synthetic Graft for Reconstruction of Middle Hepatic Vein Tributaries in Living-Donor Liver Transplant
 POSter PreSeNtAtION Synthetic Graft for Reconstruction of Middle Hepatic Vein Tributaries in Living-Donor Liver Transplant Refaat Kamel, 1 Yasser Hatata, 2 Karim Hosny, 3 Khaled Amer, 4 Mohamed Taha 5
POSter PreSeNtAtION Synthetic Graft for Reconstruction of Middle Hepatic Vein Tributaries in Living-Donor Liver Transplant Refaat Kamel, 1 Yasser Hatata, 2 Karim Hosny, 3 Khaled Amer, 4 Mohamed Taha 5
Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe. Patients
 Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe Yuji Soejima, Mitsuo Shimada, Taketoshi Suehiro, Shoji Hiroshige, Mizuki Ninomiya, Satoko Shiotani, Noboru Harada,
Outcome Analysis in Adult-to-Adult Living Donor Liver Transplantation Using the Left Lobe Yuji Soejima, Mitsuo Shimada, Taketoshi Suehiro, Shoji Hiroshige, Mizuki Ninomiya, Satoko Shiotani, Noboru Harada,
Anterior segment congestion of a right liver lobe graft in living-donor liver transplantation and strategy to prevent congestion
 J Hepatobiliary Pancreat Surg (2003) 10:16 25 DOI 10.1007/s10534-002-0789-5 Anterior segment congestion of a right liver lobe graft in living-donor liver transplantation and strategy to prevent congestion
J Hepatobiliary Pancreat Surg (2003) 10:16 25 DOI 10.1007/s10534-002-0789-5 Anterior segment congestion of a right liver lobe graft in living-donor liver transplantation and strategy to prevent congestion
One of the most important problems for patients
 Selection of Donors and Recipients for Living Donor Liver Transplantation Key Points 1. Living donor liver transplantation (LDLT) is increasingly used for adults with end-stage liver disease. 2. Standards
Selection of Donors and Recipients for Living Donor Liver Transplantation Key Points 1. Living donor liver transplantation (LDLT) is increasingly used for adults with end-stage liver disease. 2. Standards
pitfall Table 1 4 disorientation pitfall pitfall Table 1 Tel:
 11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
11 687 692 2002 pitfall 1078 29 17 9 1 2 3 dislocation outflow block 11 1 2 3 9 1 2 3 4 disorientation pitfall 11 687 692 2002 Tel: 075-751-3606 606-8507 54 2001 8 27 2002 10 31 29 4 pitfall 16 1078 Table
Simplifying Hepatic Venous Outflow Reconstruction in Sequential Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 15:1514-1518, 2009 ORIGINAL ARTICLE Simplifying Hepatic Venous Outflow Reconstruction in Sequential Living Donor Liver Transplantation See Ching Chan, Chung Mau Lo, Kelvin K. Ng,
LIVER TRANSPLANTATION 15:1514-1518, 2009 ORIGINAL ARTICLE Simplifying Hepatic Venous Outflow Reconstruction in Sequential Living Donor Liver Transplantation See Ching Chan, Chung Mau Lo, Kelvin K. Ng,
Biliary complications after right lobe living donor liver transplantation: a single-centre experience
 DOI:10.1111/j.1477-2574.2011.00401.x HPB ORIGINAL ARTICLE Biliary complications after right lobe living donor liver transplantation: a single-centre experience Onur Yaprak 1, Murat Dayangac 1, Murat Akyildiz
DOI:10.1111/j.1477-2574.2011.00401.x HPB ORIGINAL ARTICLE Biliary complications after right lobe living donor liver transplantation: a single-centre experience Onur Yaprak 1, Murat Dayangac 1, Murat Akyildiz
Biliary Anatomy in Living-related Liver Transplantation
 The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
The 5th IHPBA Congress - Istanbul Biliary Anatomy in Living-related Liver Transplantation biliary trees hilar plate Assessment for Vascular Anatomy 1. 3DCT portal vein hepatic vein hepatic artery 2. No
University College School of Medicine, Hampstead Campus, Pond Street, London NW3 2QG, UK
 HPB Surgery Volume 2013, Article ID 280857, 11 pages http://dx.doi.org/10.1155/2013/280857 Clinical Study Venous Outflow Reconstruction in Adult Living Donor Liver Transplant: Outcome of a Policy for Right
HPB Surgery Volume 2013, Article ID 280857, 11 pages http://dx.doi.org/10.1155/2013/280857 Clinical Study Venous Outflow Reconstruction in Adult Living Donor Liver Transplant: Outcome of a Policy for Right
Surgical Management of CBD Injury Jin Seok Heo
 Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
Surgical Management of CBD Injury Jin Seok Heo Department of Surgery, Samsung Medical Center Sungkyunkwan University School of Medicine, Seoul, Republic of Korea Bile duct injury (BDI) Introduction Incidence
HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein
 Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
Journal of Surgical Oncology 2006;93:338 342 HOW I DO IT Feasibility of Bisegmentectomy 7 8 is Independent of the Presence of a Large Inferior Right Hepatic Vein MARCEL AUTRAN C. MACHADO, MD, 1,2 * PAULO
University of Colorado Health Sciences Center, Denver Colorado ******************** ******************
 University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
University of Colorado Health Sciences Center, Denver Colorado ******************** 1988-2005 ****************** Disclosures No disclosures Case 53 M presents with sudden onset of upper abdominal pain
Living donor liver transplantation: Eastern experiences
 Living donor liver transplantation: Eastern experiences K Tanaka 1, Y Ogura 1, T Kiuchi 1, Y Inomata 2, S Uemoto 3 and H Furukawa 4 "Deportment of Transplantation and Immunology, Kyoto University Hospital,
Living donor liver transplantation: Eastern experiences K Tanaka 1, Y Ogura 1, T Kiuchi 1, Y Inomata 2, S Uemoto 3 and H Furukawa 4 "Deportment of Transplantation and Immunology, Kyoto University Hospital,
ORIGINAL ARTICLE. Characteristics of Liver Grafts in Living-Donor Adult Liver Transplantation
 ORIGINAL ARTICLE Characteristics of Liver Grafts in Living-Donor Adult Liver Transplantation Comparison Between Right- and Left-Lobe Grafts Mitsuo Shimada, MD, PhD; Satoko Shiotani, MD; Mizuki Ninomiya,
ORIGINAL ARTICLE Characteristics of Liver Grafts in Living-Donor Adult Liver Transplantation Comparison Between Right- and Left-Lobe Grafts Mitsuo Shimada, MD, PhD; Satoko Shiotani, MD; Mizuki Ninomiya,
Variations in portal and hepatic vein branching of the liver
 Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Yamagata Med J (ISSN 0288-030X)2015;33(2):115-121 DOI 10.15022/00003476 Variations in portal and hepatic vein branching of the liver Wataru Kimura, Tsuyoshi Fukumoto, Toshihiro Watanabe, Ichiro Hirai First
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center
 Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
Hepatic Artery Reconstruction in Living Donor Liver Transplant Experience at King Hussein Medical Center Khaldoun J. Haddadin MD FRCS (Eng)*, Nasser Q. Ahmad MD MRCSI*, Abdelhamid M. Aladwan MD ** ABSTRACT
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging
 Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Liver Transplantation in Children: Techniques and What the Surgeon Wants to Know from Imaging Jaimie D. Nathan, MD Associate Professor of Surgery and Pediatrics Associate Surgical Director, Liver Transplant
Since the first description of living-donor liver transplantation
 CLINICAL AND TRANSLATIONAL RESEARCH Endoscopic Management of Biliary Complications After Adult Living-Donor Versus Deceased-Donor Liver Transplantation Carlos Macías Gómez, 1,4 Jean-Marc Dumonceau, 2 Mariano
CLINICAL AND TRANSLATIONAL RESEARCH Endoscopic Management of Biliary Complications After Adult Living-Donor Versus Deceased-Donor Liver Transplantation Carlos Macías Gómez, 1,4 Jean-Marc Dumonceau, 2 Mariano
Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2003;1:183 188 Endoscopic Management of Postoperative Biliary Complications in Donors for Living Donor Liver Transplantation KAZUNORI HASEGAWA,* SHUJIRO YAZUMI,*
Liver retransplantation for adult recipients
 Korean J Hepatobiliary Pancreat Surg 2013;17:1-7 Review Article Liver retransplantation for adult recipients Shin Hwang, Chul-Soo Ahn, Ki-Hun Kim, Deok-Bog Moon, Tae-Yong Ha, Gi-Won Song, Dong-Hwan Jung,
Korean J Hepatobiliary Pancreat Surg 2013;17:1-7 Review Article Liver retransplantation for adult recipients Shin Hwang, Chul-Soo Ahn, Ki-Hun Kim, Deok-Bog Moon, Tae-Yong Ha, Gi-Won Song, Dong-Hwan Jung,
Endovascular Stent Placement for Interposed Middle Hepatic Vein Graft Occlusion after Living-Donor Liver Transplantation Using Right- Lobe Graft
 LIVER TRANSPLANTATION 12:269-276, 2006 ORIGINAL ARTICLE Endovascular Stent Placement for Interposed Middle Hepatic Vein Graft Occlusion after Living-Donor Liver Transplantation Using Right- Lobe Graft
LIVER TRANSPLANTATION 12:269-276, 2006 ORIGINAL ARTICLE Endovascular Stent Placement for Interposed Middle Hepatic Vein Graft Occlusion after Living-Donor Liver Transplantation Using Right- Lobe Graft
Current State of Living Donor Liver Transplantation
 REVIEW Current State of Living Donor Liver Transplantation Paige M. Porret, Kim M. Olthoff The discrepancy between the number of patients waiting for a liver and the available number of deceased donors
REVIEW Current State of Living Donor Liver Transplantation Paige M. Porret, Kim M. Olthoff The discrepancy between the number of patients waiting for a liver and the available number of deceased donors
Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation
 LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
LETTERS FROM THE FRONTLINE Successful Application of Supraceliac Aortohepatic Conduit Using Saphenous Venous Graft in Right Lobe Living Donor Liver Transplantation TO THE EDITOR: Hepatic artery (HA) reconstruction
Technique of Split-Liver Transplant for Two Adult Recipients
 F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
F'UJIUWA H.EAL,THCAREi, INC. PRESENTS IMAGES mljk?zr 3TUiVU?MAZ7ON Technique of Split-Liver Transplant for Two Adult Recipients Abhinuv Humur, KhuLid Khwuju> Timothy D. SieLu$'John R. Luke, und WiLLium
TIAN AND OTHERS common hepatic artery. For LDLT, a microvascular technique was employed to anastomose the donor artery to either the right or left hep
 Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
Original Article Treatment of Hepatic Artery Thrombosis After Orthotopic Liver Transplantation Ming Guo Tian, Wai Kuen Tso, 1 Chung Mau Lo, Chi Leung Liu and Sheung Tat Fan, Departments of Surgery and
Citation Transplantation Proceedings, 47(3),
 NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
NAOSITE: Nagasaki University's Ac Title Author(s) Hybrid Procedure in Living Donor Li Soyama, Akihiko; Takatsuki, Mitsuhi Tomohiko; Kitasato, Amane; Kinoshit Baimakhanov, Zhassulan; Kuroki, Tam Citation
Laparoscopic Liver Resection for Hepatocellular Carcinoma
 Original Article Laparoscopic Liver Resection for Hepatocellular Carcinoma Carmen D. Chung, Lydia L. Lau, Kwan Lung Ko, Andrew C. Wong, Shezam Wong, Albert C. Chan, Ronnie T. Poon, Chung Mau Lo and Sheung
Original Article Laparoscopic Liver Resection for Hepatocellular Carcinoma Carmen D. Chung, Lydia L. Lau, Kwan Lung Ko, Andrew C. Wong, Shezam Wong, Albert C. Chan, Ronnie T. Poon, Chung Mau Lo and Sheung
Current status of hepatic surgery in Korea
 Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Korean J Hepatol. 2009 Dec; 15(Suppl 6):S60 - S64. DOI: 10.3350/kjhep.2009.15.S6.S60 Current status of hepatic surgery in Korea Kyung Sik Kim Department of Surgery, Severance Hospital, Yonsei University
Living-donor liver transplantation European experiences
 Nephrol Dial Transplant (2004) 19 [Suppl 4]: iv16 iv21 doi:10.1093/ndt/gfh1036 Living-donor liver transplantation European experiences Utz Settmacher, Tom Theruvath, Andreas Pascher and Peter Neuhaus Department
Nephrol Dial Transplant (2004) 19 [Suppl 4]: iv16 iv21 doi:10.1093/ndt/gfh1036 Living-donor liver transplantation European experiences Utz Settmacher, Tom Theruvath, Andreas Pascher and Peter Neuhaus Department
Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy
 LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
LETTERS FROM THE FRONTLINE Optimal Bile Duct Division Using Real- Time Indocyanine Green Near-Infrared Fluorescence Cholangiography During Laparoscopic Donor Hepatectomy TO THE EDITOR: Despite advances
BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION 1,2
 004-33/8/430-004$02.00/0 TRANSPLANTATION Copyright (c) 98 by The Williams & Wilkins Co. Vol. 43, No. Printed in U.S.A. BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION,2 JAN LERUT,
004-33/8/430-004$02.00/0 TRANSPLANTATION Copyright (c) 98 by The Williams & Wilkins Co. Vol. 43, No. Printed in U.S.A. BILIARY TRACT COMPLICATIONS IN HUMAN ORTHOTOPIC LIVER TRANSPLANTATION,2 JAN LERUT,
Living Donor Liver Transplantation Wits Donald Gordon Medical Centre
 Living Donor Liver Transplantation Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, A Mahomed, B Bobat, S Rambarran, F van der Schyff et al The First 1963 C Henry Kempe presented
Living Donor Liver Transplantation Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, A Mahomed, B Bobat, S Rambarran, F van der Schyff et al The First 1963 C Henry Kempe presented
Sinusoidal Perfusion in the Veno-Occlusive Region of Living Liver Donors Evaluated by Indocyanine Green and Near-Infrared Spectroscopy
 LIVER TRANSPLANTATION 14:872 880, 2008 ORIGINAL ARTICLE Sinusoidal Perfusion in the Veno-Occlusive Region of Living Liver Donors Evaluated by Indocyanine Green and Near-Infrared Spectroscopy Takuya Hashimoto,
LIVER TRANSPLANTATION 14:872 880, 2008 ORIGINAL ARTICLE Sinusoidal Perfusion in the Veno-Occlusive Region of Living Liver Donors Evaluated by Indocyanine Green and Near-Infrared Spectroscopy Takuya Hashimoto,
Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology
 Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology Imaging for Pre-Transplant Evaluation of Living Donor Liver Transplantation Imaging plays a
Radiology Rounds A Newsletter for Referring Physicians Massachusetts General Hospital Department of Radiology Imaging for Pre-Transplant Evaluation of Living Donor Liver Transplantation Imaging plays a
Prevalence and Types of Main and Right Portal Vein Branching Variations on MDCT
 Atasoy and Özyürek Portal Vein MDCT Hepatobiliary Imaging Original Research A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:676 681 0361 803X/06/1873 676 American Roentgen Ray Society Y Çetin Atasoy
Atasoy and Özyürek Portal Vein MDCT Hepatobiliary Imaging Original Research A C M E D E N T U R I C A L I M A G I N G AJR 2006; 187:676 681 0361 803X/06/1873 676 American Roentgen Ray Society Y Çetin Atasoy
Should living donor liver transplantation be part of every liver transplant program?
 32 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) 13 37 [10] Markmann JF, Markmann JW, Markmann DA, Bacquerizo A, Singer J, Holt CD, et al. Preoperative factors associated with outcome
32 Forum on Liver Transplantation / Journal of Hepatology 43 (2005) 13 37 [10] Markmann JF, Markmann JW, Markmann DA, Bacquerizo A, Singer J, Holt CD, et al. Preoperative factors associated with outcome
A review of current status of living donor liver transplantation
 Review Article A review of current status of living donor liver transplantation Gil-Chun Park, Gi-Won Song, Deok-Bog Moon, Sung-Gyu Lee Division of Hepatobiliary Surgery and Liver Transplantation, Department
Review Article A review of current status of living donor liver transplantation Gil-Chun Park, Gi-Won Song, Deok-Bog Moon, Sung-Gyu Lee Division of Hepatobiliary Surgery and Liver Transplantation, Department
Soon after Starzl demonstrated the technical feasibility
 Review Article Simplifying living donor liver transplantation See Ching Chan, Chung Mau Lo and Sheung Tat Fan Hong Kong, China BACKGROUND: Living donor liver transplantation is a complex surgical operation.
Review Article Simplifying living donor liver transplantation See Ching Chan, Chung Mau Lo and Sheung Tat Fan Hong Kong, China BACKGROUND: Living donor liver transplantation is a complex surgical operation.
Living donor liver transplantation for patients with hepatocellular carcinoma in Japan
 Sugawara et al. Hepatoma Res 2018;4:33 DOI: 10.20517/2394-5079.2018.69 Hepatoma Research Review Open Access Living donor liver transplantation for patients with hepatocellular carcinoma in Japan Yasuhiko
Sugawara et al. Hepatoma Res 2018;4:33 DOI: 10.20517/2394-5079.2018.69 Hepatoma Research Review Open Access Living donor liver transplantation for patients with hepatocellular carcinoma in Japan Yasuhiko
One Hundred Nine Living Donor Liver Transplants in Adults and Children: A Single-Center Experience
 ANNALS OF SURGERY Vol. 234, No. 3, 301 312 2001 Lippincott Williams & Wilkins, Inc. One Hundred Nine Living Donor Liver Transplants in Adults and Children: A Single-Center Experience Charles M. Miller,
ANNALS OF SURGERY Vol. 234, No. 3, 301 312 2001 Lippincott Williams & Wilkins, Inc. One Hundred Nine Living Donor Liver Transplants in Adults and Children: A Single-Center Experience Charles M. Miller,
CHAPTER 46. The Liver Transplant Procedure
 CHAPTER 46 The Liver Transplant Procedure Bijan Eghtesad 1, Koji Hashimoto 1 and John Fung 2 1 Department of General Surgery, The Cleveland Clinic, Cleveland, OH, USA 2 Department of Surgery, The University
CHAPTER 46 The Liver Transplant Procedure Bijan Eghtesad 1, Koji Hashimoto 1 and John Fung 2 1 Department of General Surgery, The Cleveland Clinic, Cleveland, OH, USA 2 Department of Surgery, The University
Perpetuating proficiency in donor right hepatectomy for living donor liver transplantation
 Asian Journal of Surgery (2014) 37, 65e72 Available online at www.sciencedirect.com ScienceDirect journal homepage: www.e-asianjournalsurgery.com ORIGINAL ARTICLE Perpetuating proficiency in donor right
Asian Journal of Surgery (2014) 37, 65e72 Available online at www.sciencedirect.com ScienceDirect journal homepage: www.e-asianjournalsurgery.com ORIGINAL ARTICLE Perpetuating proficiency in donor right
Original article: new surgical approaches to the Klatskin tumour
 Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Alimentary Pharmacology & Therapeutics Original article: new surgical approaches to the Klatskin tumour T. M. VAN GULIK*, S. DINANT*, O. R. C. BUSCH*, E. A. J. RAUWS, H. OBERTOP* & D. J. GOUMA Departments
Case Report INTRODUCTION CASE REPORT
 Case Report J Korean Soc Transplant 2016;30:89-93 http://dx.doi.org/10.4285/jkstn.2016.30.2.89 Late Hepatic Venous Outflow Obstruction Following Inferior Vena Cava Stenting in Patient with Deceased Donor
Case Report J Korean Soc Transplant 2016;30:89-93 http://dx.doi.org/10.4285/jkstn.2016.30.2.89 Late Hepatic Venous Outflow Obstruction Following Inferior Vena Cava Stenting in Patient with Deceased Donor
Donor Safety and Remnant Liver Volume in Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 14:1174-1179, 2008 ORIGINAL ARTICLE Donor Safety and Remnant Liver Volume in Living Donor Liver Transplantation C. Burcin Taner, Murat Dayangac, Baris Akin, Deniz Balci, Suleyman
LIVER TRANSPLANTATION 14:1174-1179, 2008 ORIGINAL ARTICLE Donor Safety and Remnant Liver Volume in Living Donor Liver Transplantation C. Burcin Taner, Murat Dayangac, Baris Akin, Deniz Balci, Suleyman
Outcome of donor biliary complications following living donor liver transplantation
 ORIGINAL ARTICLE Korean J Intern Med 2018;33:705-715 Outcome of donor biliary complications following living donor liver transplantation Hyun Young Woo 1, In Seok Lee 2, Jae Hyuck Chang 2, Seung Bae Youn
ORIGINAL ARTICLE Korean J Intern Med 2018;33:705-715 Outcome of donor biliary complications following living donor liver transplantation Hyun Young Woo 1, In Seok Lee 2, Jae Hyuck Chang 2, Seung Bae Youn
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists. International authors and editors
 We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
We are IntechOpen, the world s leading publisher of Open Access books Built by scientists, for scientists 4,000 116,000 120M Open access books available International authors and editors Downloads Our
Working Up Donors for High-Urgency and Elective Adult-to-Adult Live Donor Liver Transplantation
 LIVER TRANSPLANTATION 13:509-515, 2007 ORIGINAL ARTICLE Working Up Donors for High-Urgency and Elective Adult-to-Adult Live Donor Liver Transplantation See Ching Chan, Sheung Tat Fan,* Chi Leung Liu, Chung
LIVER TRANSPLANTATION 13:509-515, 2007 ORIGINAL ARTICLE Working Up Donors for High-Urgency and Elective Adult-to-Adult Live Donor Liver Transplantation See Ching Chan, Sheung Tat Fan,* Chi Leung Liu, Chung
Management of Extensive Portal Vein Thrombosis
 Management of Extensive Portal Vein Thrombosis Deok-Bog Moon, Sung-Gyu Lee, Chul-Soo Ahn, Shin Hwang, Ki-Hun Kim, Gi-Won Song, Dong-Hwan Jung, Gil-Chun Park, Kyu-Bo Sung 1, Gi- Young Ko 1, Dong-Il Kweon
Management of Extensive Portal Vein Thrombosis Deok-Bog Moon, Sung-Gyu Lee, Chul-Soo Ahn, Shin Hwang, Ki-Hun Kim, Gi-Won Song, Dong-Hwan Jung, Gil-Chun Park, Kyu-Bo Sung 1, Gi- Young Ko 1, Dong-Il Kweon
Reconstruction of Inferior Right Hepatic Veins in Living Donor Liver Transplantation Using Right Liver Grafts
 LIVER TRANSPLANTATION 18:238-247, 2012 ORIGINAL ARTICLE Reconstruction of Inferior Right Hepatic Veins in Living Donor Liver Transplantation Using Right Liver Grafts Shin Hwang, 1 * Tae-Yong Ha, 1 * Chul-Soo
LIVER TRANSPLANTATION 18:238-247, 2012 ORIGINAL ARTICLE Reconstruction of Inferior Right Hepatic Veins in Living Donor Liver Transplantation Using Right Liver Grafts Shin Hwang, 1 * Tae-Yong Ha, 1 * Chul-Soo
Outcomes in partial liver transplantation: deceased donor split-liver vs. live donor liver transplantation
 DOI:10.1111/j.1477-2574.201360.x HPB ORIGINAL ARTICLE Outcomes in partial liver transplantation: deceased donor split-liver vs. live donor liver transplantation Reza F. Saidi, Nicolas Jabbour, YouFu Li,
DOI:10.1111/j.1477-2574.201360.x HPB ORIGINAL ARTICLE Outcomes in partial liver transplantation: deceased donor split-liver vs. live donor liver transplantation Reza F. Saidi, Nicolas Jabbour, YouFu Li,
Surgical anatomy of the biliary tract
 HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
HPB, 2008; 10: 7276 REVIEW ARTICLE Surgical anatomy of the biliary tract DENIS CASTAING Centre hépato-biliaire, Hôpital Paul Brousse, Assistance Publique- Hôpitaux de Paris, Université Paris XI, Paris,
Liver transplant for biliary atresia
 Jean de Ville de Goyet ISMETT Director of the Department for the Treatment and Study of Pediatric Abdominal Diseases and Abdominal Transplantation The first human liver transplant was performed on a pediatric
Jean de Ville de Goyet ISMETT Director of the Department for the Treatment and Study of Pediatric Abdominal Diseases and Abdominal Transplantation The first human liver transplant was performed on a pediatric
2 1999). The unceasing shortage of organs has led to development of other innovative techniques to maximize the donor organ access, namely LDLT, which
 Journal of Zhejiang University-SCIENCE B (Biomedicine & Biotechnology) ISSN 1673-1581 (Print); ISSN 1862-1783 (Online) www.zju.edu.cn/jzus; www.springerlink.com E-mail: jzus@zju.edu.cn Chen et al. / J
Journal of Zhejiang University-SCIENCE B (Biomedicine & Biotechnology) ISSN 1673-1581 (Print); ISSN 1862-1783 (Online) www.zju.edu.cn/jzus; www.springerlink.com E-mail: jzus@zju.edu.cn Chen et al. / J
Living Donor Liver Transplantation Adult Donor Outcomes: A Systematic Review
 LIVER TRANSPLANTATION 12:24 30, 2006 REVIEW Living Donor Liver Transplantation Adult Donor Outcomes: A Systematic Review Philippa F. Middleton, 1 Michael Duffield, 1 Stephen V. Lynch, 2 Robert T.A. Padbury,
LIVER TRANSPLANTATION 12:24 30, 2006 REVIEW Living Donor Liver Transplantation Adult Donor Outcomes: A Systematic Review Philippa F. Middleton, 1 Michael Duffield, 1 Stephen V. Lynch, 2 Robert T.A. Padbury,
A New Porcine Model of Autologous Living-donor Liver Transplantation
 Jichi Medical University Journal A New Porcine Model of Autologous Living-donor Liver Transplantation Nobuyuki Hojo, Toshimitsu Ishibashi, Toshihiko Yasuda, Yasunaru Sakuma, Taketo Fujiwara, Yoshikazu
Jichi Medical University Journal A New Porcine Model of Autologous Living-donor Liver Transplantation Nobuyuki Hojo, Toshimitsu Ishibashi, Toshihiko Yasuda, Yasunaru Sakuma, Taketo Fujiwara, Yoshikazu
Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre
 Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, S Rambarran, A Terblanche, C Kock, P Walabh, M Beretta, M Duncan et al 1817 reveal the
Paediatric Liver Transplant Programme Wits Donald Gordon Medical Centre J Loveland, J Botha, R Britz, B Strobele, S Rambarran, A Terblanche, C Kock, P Walabh, M Beretta, M Duncan et al 1817 reveal the
ORIGINAL ARTICLE. Safety of Donors in Live Donor Liver Transplantation Using Right Lobe Grafts
 ORIGINAL ARTICLE Safety of Donors in Live Donor Liver Transplantation Using Right Lobe Grafts Sheung-Tat Fan, MS, MD, FRCS(Glasg and Edin); Chung-Mau Lo, MS, FRACS, FRCS(Edin); Chi-Leung Liu, MBBS, FRCS(Edin);
ORIGINAL ARTICLE Safety of Donors in Live Donor Liver Transplantation Using Right Lobe Grafts Sheung-Tat Fan, MS, MD, FRCS(Glasg and Edin); Chung-Mau Lo, MS, FRACS, FRCS(Edin); Chi-Leung Liu, MBBS, FRCS(Edin);
Utility of Marginal Donors in Liver Transplantation
 Utility of Marginal Donors in Liver Transplantation HwanHyo, Lee Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Contents Review of Liver Transplantation(LT)
Utility of Marginal Donors in Liver Transplantation HwanHyo, Lee Department of Surgery, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Korea Contents Review of Liver Transplantation(LT)
Adult living donor versus deceased donor liver transplantation., 2009; 8 (4): At our center the waiting list mortality from 1994 to 1997 a
 298 Fisher RA, et al., 2009; 8 (4): 298-307 ORIGINAL ARTICLE October-December, Vol. 8 No.4, 2009: 298-307 Adult living donor versus deceased donor liver transplantation: A 10-year prospective single center
298 Fisher RA, et al., 2009; 8 (4): 298-307 ORIGINAL ARTICLE October-December, Vol. 8 No.4, 2009: 298-307 Adult living donor versus deceased donor liver transplantation: A 10-year prospective single center
[7] Greene, B. S., Loubeau, J. M., Peoples, J. B. and Elliott, D. W. (1991). Are pancreatoenteric anastomoses improved
![[7] Greene, B. S., Loubeau, J. M., Peoples, J. B. and Elliott, D. W. (1991). Are pancreatoenteric anastomoses improved [7] Greene, B. S., Loubeau, J. M., Peoples, J. B. and Elliott, D. W. (1991). Are pancreatoenteric anastomoses improved](/thumbs/82/86447000.jpg) 136 HPB INTERNATIONAL mosis. In our experience, roughly 10% of patients will have low volume amylase-rich fluid draining via the drains. Over 85% of these low volume pancreatic fistulas will heal with
136 HPB INTERNATIONAL mosis. In our experience, roughly 10% of patients will have low volume amylase-rich fluid draining via the drains. Over 85% of these low volume pancreatic fistulas will heal with
Living Donor Hepatectomy: The Importance of the Residual Liver Volume
 LIVER TRANSPLANTATION 17:1404-1411, 2011 ORIGINAL ARTICLE Living Donor Hepatectomy: The Importance of the Residual Liver Volume Trevor W. Reichman, Charbel Sandroussi, Solomon M. Azouz, Lesley Adcock,
LIVER TRANSPLANTATION 17:1404-1411, 2011 ORIGINAL ARTICLE Living Donor Hepatectomy: The Importance of the Residual Liver Volume Trevor W. Reichman, Charbel Sandroussi, Solomon M. Azouz, Lesley Adcock,
Biliary Reconstruction for Infantile Living Donor Liver Transplantation: Roux-en-Y Hepaticojejunostomy or Duct-to-Duct Choledochocholedochostomy?
 LIVER TRANSPLANTATION 14:1761-1765, 2008 ORIGINAL ARTICLE Biliary Reconstruction for Infantile Living Donor Liver Transplantation: Roux-en-Y Hepaticojejunostomy or Duct-to-Duct Choledochocholedochostomy?
LIVER TRANSPLANTATION 14:1761-1765, 2008 ORIGINAL ARTICLE Biliary Reconstruction for Infantile Living Donor Liver Transplantation: Roux-en-Y Hepaticojejunostomy or Duct-to-Duct Choledochocholedochostomy?
ORIGINAL ARTICLE ORIGINAL ARTICLE Liver Transplantation AASLD. Received April 25, 2017; accepted September 12, 2017.
 ORIGINAL ARTICLE BAKER ET AL. Biliary Reconstructive Techniques and Associated Anatomic Variants in Adult Living Donor Liver Transplantations: The Adult-to-Adult Living Donor Liver Transplantation Cohort
ORIGINAL ARTICLE BAKER ET AL. Biliary Reconstructive Techniques and Associated Anatomic Variants in Adult Living Donor Liver Transplantations: The Adult-to-Adult Living Donor Liver Transplantation Cohort
Adult to adult living donor liver transplantation: Operative techniques to optimize the recipient s outcome
 Review Article Adult to adult living donor liver transplantation: Operative techniques to optimize the recipient s outcome Peng Soon Koh, See Ching Chan 1 Department of Surgery, Faculty of Medicine, University
Review Article Adult to adult living donor liver transplantation: Operative techniques to optimize the recipient s outcome Peng Soon Koh, See Ching Chan 1 Department of Surgery, Faculty of Medicine, University
Living donor liver transplantation without the use of blood products. Liu, CL; Fan, ST; Lo, CM; Wei, WI; Yong, BH; Lai, CL; Wong, J
 Title Living donor liver transplantation without the use of blood products. Author(s) Liu, CL; Fan, ST; Lo, CM; Wei, WI; Yong, BH; Lai, CL; Wong, J Citation Hong Kong Medical Journal = Xianggang Yi Xue
Title Living donor liver transplantation without the use of blood products. Author(s) Liu, CL; Fan, ST; Lo, CM; Wei, WI; Yong, BH; Lai, CL; Wong, J Citation Hong Kong Medical Journal = Xianggang Yi Xue
The Whipple Operation Illustrations
 The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
The Whipple Operation Illustrations Fig. 1. Illustration of the sixstep pancreaticoduodenectomy (Whipple operation) as described in a number of recent text books by Dr. Evans. The operation is divided
Living donor liver transplantation
 Journal of Hepatology 38 (2003) S119 S135 www.elsevier.com/locate/jhep Living donor liver transplantation Dieter C. Broering, Martina Sterneck, Xavier Rogiers* Department of Hepatobiliary Surgery and Transplantation,
Journal of Hepatology 38 (2003) S119 S135 www.elsevier.com/locate/jhep Living donor liver transplantation Dieter C. Broering, Martina Sterneck, Xavier Rogiers* Department of Hepatobiliary Surgery and Transplantation,
Living donor liver transplantation (LDLT) is a
 Original Article / Transplantation Hepatobiliary & Pancreatic Diseases International Graft-to-recipient weight ratio lower to 0.7% is safe without portal pressure modulation in right-lobe living donor
Original Article / Transplantation Hepatobiliary & Pancreatic Diseases International Graft-to-recipient weight ratio lower to 0.7% is safe without portal pressure modulation in right-lobe living donor
Single-Center Experience and Long-Term Outcomes of Duct-to-Duct Biliary Reconstruction in Infantile Living Donor Liver Transplantation
 LIVER TRANSPLANTATION 20:347 354, 2014 ORIGINAL ARTICLE Single-Center Experience and Long-Term Outcomes of Duct-to-Duct Biliary Reconstruction in Infantile Living Donor Liver Transplantation Hidekazu Yamamoto,
LIVER TRANSPLANTATION 20:347 354, 2014 ORIGINAL ARTICLE Single-Center Experience and Long-Term Outcomes of Duct-to-Duct Biliary Reconstruction in Infantile Living Donor Liver Transplantation Hidekazu Yamamoto,
Liver transplantation is a gold standard of therapy. Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population
 Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population Hee Chul Yu, 1,2 Heecheon You, 3 Ho Lee, 4 Zhe-Wu Jin, 1 Jang Il Moon, 5 and Baik Hwan Cho 1,2 The standard liver
Estimation of Standard Liver Volume for Liver Transplantation in the Korean Population Hee Chul Yu, 1,2 Heecheon You, 3 Ho Lee, 4 Zhe-Wu Jin, 1 Jang Il Moon, 5 and Baik Hwan Cho 1,2 The standard liver
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES
 Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
Original article: SURGICAL TREATMENT FOR BENIGN BILIARY STRICTURES: SINGLE-CENTER EXPERIENCE ON 64 CASES Yunfeng Cui, Hongtao Zhang, Naiqiang Cui, Zhonglian Li* Department of Surgery, Tianjin Nankai Hospital,
Donor Postoperative Biliary Complications After Living-Donor Liver Transplant
 ARTICle Donor Postoperative Biliary Complications After Living-Donor Liver Transplant Abuzer Dirican, Cengiz Ara, Koray Kutluturk, Mustafa Ozsoy, Mustafa Ates, Adil Baskiran, Burak Isik, Sezai Yilmaz Abstract
ARTICle Donor Postoperative Biliary Complications After Living-Donor Liver Transplant Abuzer Dirican, Cengiz Ara, Koray Kutluturk, Mustafa Ozsoy, Mustafa Ates, Adil Baskiran, Burak Isik, Sezai Yilmaz Abstract
Bile Duct Injury during Lap Chole. Bile Duct Injury during cholecystectomy TOPICS. 1. Prevalence, mechanisms, prevention and diagnosis
 Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Bile Duct Injury during cholecystectomy Catherine HUBERT Jean-Fran François GIGOT Benoît t NAVEZ Division of Hepato-Biliary Biliary-Pancreatic Surgery Department of Abdominal Surgery and Transplantation
Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors?
 Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Original Article Living Donor Liver Transplantation for Hepatocellular Carcinoma: It Is All about Donors? R. F. Saidi 1 *, Y. Li 2, S. A. Shah 2, N. Jabbour 2 1 Division of Organ Transplantation, Department
Technical Considerations in Liver Transplantation. Luis S. Marsano, MD Professor of Medicine U. of Louisville & Louisville VAMC
 Technical Considerations in Liver Transplantation Luis S. Marsano, MD Professor of Medicine U. of Louisville & Louisville VAMC Types OLTX: Orthotopic liver Tx; placed in the anatomically correct position
Technical Considerations in Liver Transplantation Luis S. Marsano, MD Professor of Medicine U. of Louisville & Louisville VAMC Types OLTX: Orthotopic liver Tx; placed in the anatomically correct position
Renal Transplant Surgery
 Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
Renal Transplant Surgery Mr Somaiah Aroori MS MD EBS in HPB FRCS Consultant HPB & Renal Transplant Surgeon SWTC, Derriford Hospital, Plymouth Over next few minutes Aim to cover Details of Transplant procedure
CUAJ Techniques in Urology Techniques: Orthotopic kidney transplantation
 Techniques Orthotopic kidney transplantation in patients with diseased inferior vena cavas E. Chan 1 ; Alp Sener 1,2 ; Vivian C. McAlister 1,2, Patrick P. Luke 1,2 1 Western University Schulich School
Techniques Orthotopic kidney transplantation in patients with diseased inferior vena cavas E. Chan 1 ; Alp Sener 1,2 ; Vivian C. McAlister 1,2, Patrick P. Luke 1,2 1 Western University Schulich School
STUDY OF VASCULAR SEGMENTS OF LIVER IN DISSECTED CADAVERIC LIVER SPECIMEN
 Research Article International Journal of Bioassays ISSN: 2278-778X www.ijbio.com STUDY OF VASCULAR SEGMENTS OF LIVER IN DISSECTED CADAVERIC LIVER SPECIMEN Anju Balaji More Department of Anatomy, Sree
Research Article International Journal of Bioassays ISSN: 2278-778X www.ijbio.com STUDY OF VASCULAR SEGMENTS OF LIVER IN DISSECTED CADAVERIC LIVER SPECIMEN Anju Balaji More Department of Anatomy, Sree
Living Donor Liver Transplantation
 Trends in Transplantation Transplant. 2010;4:138-44 Living Donor Liver Transplantation Juan Carlos García-Valdecasas 1, Itxarone Bilbao Aguirre 2, Ramón Charco Torra 3, Constantino Fondevila Campo 4, Josep
Trends in Transplantation Transplant. 2010;4:138-44 Living Donor Liver Transplantation Juan Carlos García-Valdecasas 1, Itxarone Bilbao Aguirre 2, Ramón Charco Torra 3, Constantino Fondevila Campo 4, Josep
Liver Transplantation
 1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
1 Liver Transplantation Department of Surgery Yonsei University Wonju College of Medicine Kim Myoung Soo M.D. ysms91@wonju.yonsei.ac.kr http://gs.yonsei.ac.kr History Development of Liver transplantation
In-Hospital Mortality in Adult Recipients of Living Donor Liver Transplantation: Experience of 576 Consecutive Cases at a Single Center
 LIVER TRANSPLANTATION 15:1420-1425, 2009 ORIGINAL ARTICLE In-Hospital Mortality in Adult Recipients of Living Donor Liver Transplantation: Experience of 576 Consecutive Cases at a Single Center Toshimi
LIVER TRANSPLANTATION 15:1420-1425, 2009 ORIGINAL ARTICLE In-Hospital Mortality in Adult Recipients of Living Donor Liver Transplantation: Experience of 576 Consecutive Cases at a Single Center Toshimi
Impact Of Reconstructing A Single Hepatic Artery On Small-For-Size Grafts In Living Donor Liver Transplantation
 ISPUB.COM The Internet Journal of Surgery Volume 31 Number 2 Impact Of Reconstructing A Single Hepatic Artery On Small-For-Size Grafts In Living Donor Liver K, A, B, C Citation K, A, B, C.. The Internet
ISPUB.COM The Internet Journal of Surgery Volume 31 Number 2 Impact Of Reconstructing A Single Hepatic Artery On Small-For-Size Grafts In Living Donor Liver K, A, B, C Citation K, A, B, C.. The Internet
Case Report Life-Saving Super-Urgent Liver Transplantation with Replacement of Retrohepatic Vena Cava by Dacron Graft
 HPB Surgery Volume 2010, Article ID 828326, 4 pages doi:10.1155/2010/828326 Case Report Life-Saving Super-Urgent Liver Transplantation with Replacement of Retrohepatic Vena Cava by Dacron Graft Paolo Aseni,
HPB Surgery Volume 2010, Article ID 828326, 4 pages doi:10.1155/2010/828326 Case Report Life-Saving Super-Urgent Liver Transplantation with Replacement of Retrohepatic Vena Cava by Dacron Graft Paolo Aseni,
PRE-ASSESSMENT. Living Donor Liver Transplantation
 No. 24 Oct 2003 Before decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they are not extensive,
No. 24 Oct 2003 Before decides to undertake a health technology assessment, a pre-assessment of the literature is performed. Pre-assessments are based on a limited literature search; they are not extensive,
Early Outcome of Donors in Living-Donor Liver Transplantation at King Hussein Medical Center
 Early Outcome of Donors in Living-Donor Liver Transplantation at King Hussein Medical Center Salah Halasa MD*, Sahim Qusouss MD* ABSTRACT Objectives: To evaluate the safety and early outcome of donors
Early Outcome of Donors in Living-Donor Liver Transplantation at King Hussein Medical Center Salah Halasa MD*, Sahim Qusouss MD* ABSTRACT Objectives: To evaluate the safety and early outcome of donors
LiverGroup.org. Case Report Form (CRF) for STAGED procedures
 Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Case Report Form (CRF) for STAGED procedures Patient Characteristics Case number * Age * ( 18)y Gender * Male Female Race * Caucasian Asian African Other If other race, please specify Height * cm Weight
Value of CT and Doppler Sonography in the Evaluation of Hepatic Vein Stenosis After Dual-Graft Living Donor Liver Transplantation
 CT and Sonography After Liver Transplantation Hepatobiliary Imaging Original Research Seung Soo Lee 1 Kyoung Won Kim 1 Seong Ho Park 1 Yong Moon Shin 1 Pyo Nyun Kim 1 Sung Gyu Lee 2 Moon-Gyu Lee 1 Lee
CT and Sonography After Liver Transplantation Hepatobiliary Imaging Original Research Seung Soo Lee 1 Kyoung Won Kim 1 Seong Ho Park 1 Yong Moon Shin 1 Pyo Nyun Kim 1 Sung Gyu Lee 2 Moon-Gyu Lee 1 Lee
Proceedings S.Z.P.G.M.I. Vol: 32(1): pp , 2018.
 Proceedings S.Z.P.G.M.I. Vol: 32(1): pp. 50-55, 2018. PSZMC-670-32-1-2018 Choose Well, Cut Well and Get Well Living Donor Liver Transplants Sumbul Naz 1, Amer Latif 2, Tariq Ali Bangash 2, Asim Rana 2
Proceedings S.Z.P.G.M.I. Vol: 32(1): pp. 50-55, 2018. PSZMC-670-32-1-2018 Choose Well, Cut Well and Get Well Living Donor Liver Transplants Sumbul Naz 1, Amer Latif 2, Tariq Ali Bangash 2, Asim Rana 2
