Pan-London Haemato-Oncology Clinical Guidelines. Lymphoid Malignancies Part 3: Follicular Lymphoma
|
|
|
- Scot Walker
- 5 years ago
- Views:
Transcription
1 Pan-London Haemato-Oncology Clinical Guidelines Lymphoid Malignancies Part 3: Follicular Lymphoma September 2018
2 CONTENTS Contents 1 Introduction Early Diagnosis and Prevention Referral Pathways from Primary Care Presentation Referral Investigation and Diagnosis Diagnosis Staging and imaging Baseline investigations Prognosis Treatment Recommendations Follicular lymphoma: grades 1, 2 and 3a Follicular lymphoma: grade 3b Transformation Follow-up Arrangements Specific or Miscellaneous Considerations Follicular lymphoma in situ (FLIS) Primary cutaneous follicular cell lymphoma (PCFCL) Primary intestinal follicular lymphoma Irradiated cellular blood products Paediatric-type follicular lymphoma References
3 CONTENTS Lead authors: Dr Silvia Montoto, Barts Health NHS Trust Dr David Wrench, Guy s and St Thomas NHS Foundation Trust Disclaimer These guidelines should be read in conjunction with the latest NICE guidance, and all applicable national/international guidance. The prescribing information in these guidelines is for health professionals only. It is not intended to replace consultation with the Haematology Consultant at the patient s specialist centre. For information on cautions, contra-indications and side effects, refer to the up-to-date prescribing information. While great care has been taken to see that the information in these guidelines is accurate, the user is advised to check the doses and regimens carefully and if there is any uncertainty about the guidance provided, you should discuss your queries with a Haematology Consultant or Senior Pharmacist. No set of guidelines can cover all variations required for specific patient circumstances. It is the responsibility of the healthcare practitioners using them to adapt them for safe use within their institutions and for the individual needs of patients. Contact us The writing cycle for the guidelines will be from May-July each year. If you wish to be part of the writing group, please contact us through the following link: Pan London Blood Cancer (or via uclh.panlondonbloodcancer@nhs.net). If you wish to report errors or omissions that require urgent attention please contact us via the same addresses. RM Partners, South East London Accountable Cancer Network, ULCH Cancer Collaborative
4 INTRODUCTION 1 Introduction Follicular lymphoma (FL) is the most common form of indolent lymphoma and the second most common form of non-hodgkin lymphoma presenting in ~5/10,0000 population/year, with a median age of onset of around 60 years. It shows a slight male preponderance and the majority (~80 90%) have advanced (stage 3 or 4) disease at presentation, with at least half demonstrating bone marrow involvement. A proportion of limited stage FL cases may be considered cured after targeted radiotherapy but, for the vast majority of patients with FL, this remains an incurable disease with conventional therapy. While advanced stage disease may be managed by observation alone at least initially, and some cases never need treatment, most patients will require systemic treatment and FL may follow a pattern of relapsing and remitting disease over several years. Moreover, therapy resistant disease progression and transformation to aggressive lymphoma are common causes of death. However, overall survival (OS) has improved in recent years 1 in tandem with advances in both treatment and supportive care. Median survival is now expected to be in the region of two decades. 2 Early Diagnosis and Prevention While certain environmental factors, lifestyle influences and genetic loci are associated with the development of FL, no clear causative factor(s) exist for which screening or prevention of disease could be pursued. There is no known approach that may help prevent the development of FL and it has not been established that earlier diagnosis will impact the outcome of advanced stage FL. However, early clinical presentation might aid the diagnosis of FL when still at limited stage and enable treatment with just local radiotherapy. Moreover, FL commonly presents as a lump and early presentation by patients for medical review is encouraged as it is certainly the case that early diagnosis of other conditions presenting as a lump may benefit their clinical outcome. Local community engagement exercises to emphasise and raise awareness in the primary care setting regarding the potential presentation of lymphoma and when to refer for specialist review are encouraged, and all patients should be encouraged to adopt a healthy lifestyle. 3
5 REFERRAL PATHWAYS FROM PRIMARY CARE 3 Referral Pathways from Primary Care 3.1 Presentation Patients usually present with persistent lymph node enlargement. This may occasionally be accompanied by B symptoms (otherwise unexplained: temperature >38 C, drenching night sweats, loss of >10% body weight over 6 months). Unusual presentations may include the consequences of bone marrow suppression, skin lesions, bowel involvement, and other extra-nodal/organ site involvement. 3.2 Referral The typical trigger for referral is a persistent (>4 6 weeks) suspected enlarged lymph node. In work-up to referral it is recommended that the following blood tests are performed as a minimum in primary care: FBC LDH renal profile LFTs calcium/bone profile HIV. The urgent/2 week wait referral pathway should be utilised if lymphoma is suspected. Early direct contact is encouraged between the primary care referring team and the receiving lymphoma managing centre as appropriate, particularly in systemically unwell or complex cases. Similarly, specialist centres may receive internal referrals from other hospital teams (such as head and neck/ent, breast surgery, general surgery, HIV/infectious disease) regarding suspected or proven lymphoma and organisation specific pathways should be followed. 4
6 INVESTIGATION AND DIAGNOSIS 4 Investigation and Diagnosis 4.1 Diagnosis Definitive diagnosis requires examination of a tissue biopsy sample from an index lesion (most often an enlarged lymph node). If a tissue/excision biopsy is not possible, then needle core biopsy can be performed, acknowledging the limits this may impose on assessment of tissue architecture. Adequate material is essential and re-biopsy must be considered if samples are deemed insufficient. (Fine needle aspiration should not be performed as a diagnostic investigation for FL.) Biopsies should be transferred promptly for initial macroscopic examination and slicing by a histopathologist and immersed in formalin for fixation; where possible, separate fresh frozen storage of part of the biopsy is recommended. A diagnosis can typically be made through histological examination of adequate tissue samples stained with haematoxylin and eosin (H&E) supported by immuno-staining for: CD20 CD10 Bcl-2 CD5 CD3 (+/- Bcl-6, cyclin D1, CD43, κ and λ light chains). While not required in the majority of cases, fluorescent in situ hybridisation (FISH) or cytogenetic analyses may reveal evidence of the t(14;18)(q32;q21) that is present in the majority of FL. Molecular analysis using the polymerase chain reaction (PCR) may identify the corresponding IgH/Bcl-2 rearrangement. Occasionally, flow cytometry analysis of cellular samples may aid diagnosis while rarely a frozen section panel may be required. The diagnosis should be reported as per current WHO 2 requirements. 4.2 Staging and imaging A fundamental aspect of disease assessment is determining the anatomical extent (stage) of disease. This has direct implication on treatment selection and prognosis. The staging of FL using positron emission tomography (PET) with low dose computed tomography (CT), as PET/CT imaging, has been adopted as an international standard of care following consensus recommendations (Cheson, et al., ). Subsequent NICE guidance includes recommendations regarding the use of PET/CT imaging in FL (NICE guideline NG52). If standard CT imaging is performed as staging for FL then this should include the neck, chest, abdomen and pelvis, ideally with both oral and intravenous contrast, and a bone marrow biopsy should also be obtained. 5
7 INVESTIGATION AND DIAGNOSIS Staging has routinely been documented according to the Ann Arbor system. It is recommended that staging is recorded according to the recent updates to this approach detailed in the Revised Staging System for Primary Nodal Lymphomas 3 as indicated in Table 1. Table 1: Summary of Revised Staging System for Primary Nodal Lymphomas Stage^ Involved sites 1 One node or a group of adjacent nodes* 2 Two or more nodal groups on the same side of the diaphragm # 3 Nodes on both sides of the diaphragm; nodes above the diaphragm with spleen involvement 4 Additional non-contiguous extra-lymphatic involvement Staging is according to the modified Ann Arbor system. Notes: Tonsils, Waldeyer s ring, and spleen are considered nodal tissue. Bulk: ^2 bulky = as stage 2 above with bulky disease Extranodal (E) applies to stages 1 and 2 only: *1E = Single extra-nodal lesions without nodal involvement # 2E = Stage I or II by nodal extent with limited contiguous extra-nodal involvement 4.3 Baseline investigations Recommended as mandatory: Blood tests FBC, blood film, and consider peripheral blood immunophenotyping if lymphocytosis Renal profile LFTs Bone profile/calcium LDH ESR Immunoglobulins Serum protein electrophoresis Beta-2-microglobulin Virology: HIV/HCV/HBV sag + cab (and HBV DNA level if indicated) Bone marrow aspirate and trephine biopsy (if staging was not by PET/CT imaging or if there are other concerns regarding marrow) ECG CXR. Consider in specific cases: Cardiac function and left ventricular ejection fraction determination (for example in patients >65 70 years old +/- cardiac risk factors who are under consideration for anthracycline treatment and patients planned for myeloablative treatment) 6
8 INVESTIGATION AND DIAGNOSIS Targeted further organ assessment if indicated by patient review/past medical history/results of other investigations Fertility team review, counselling and preservation measures for those of reproductive age (and who meet NHS eligibility criteria) Formal ENT assessment Pleural fluid/ascitic fluid/csf for flow cytometry In young cases (aged years old): Teenage and Young Adult (TYA) review Psychology/talking therapy review Comprehensive geriatric assessment Independent mental capacity advocate. 4.4 Prognosis While the overall prognosis of FL has improved over recent years, it is also possible to risk stratify affected patients. Multiple clinical, radiological, haematological and biochemical aspects of FL correlate with outcome and these have been incorporated in various clinical risk models. The Follicular Lymphoma International Prognostic Indices (FLIPI and FLIPI2) each include five parameters, the presence or absence of which contribute to a score that can used to determine risk categories for progression-free and overall survival (Table 2). It is recommended that FLIPI scores are recorded at diagnosis as they may both inform patient discussion and influence first-line treatment options. Molecular aspects of both FL tumour cells and the surrounding micro-environment correlate with outcome but at present have no role in routine clinical management. Table 2: FLIPI and FLIPI2 prognostic systems FLIPI FLIPI2 Parameter Score = Total Risk OS Score = 1 Total Risk OS 1 score (%) score (%) 5y 10y 5y Age 60 Age >60 Stage 3 or low BM Involved 0 low 98 LDH >ULN 2 int B2M >ULN 1 2 int 88 Hb <120g/L 3 5 high Hb <120g/L 3 5 high 77 Nodal sites >4* Max node >6cm OS, overall survival; ULN, upper limit of normal range; LDH, lactate dehydrogenase; Hb, haemoglobin; Nodal sites, number of lymph node sites involved by lymphoma; int, intermediate; BM, bone marrow; B2M, beta-2- microglobulin; Max node, maximum diameter of largest involved lymph node. 7
9 INVESTIGATION AND DIAGNOSIS Figure 1: Nodal sites Reproduced with permission from: 8
10 TREATMENT RECOMMENDATIONS 5 Treatment Recommendations All patients with FL should be considered for entry to clinical trials appropriate to their aspect of disease management. If not available at the managing centre, then patients should be offered the opportunity to attend other centres where relevant trials may be open for accrual. For clinical trials in FL currently open to recruitment across London go to Ahead of any treatment, the informed consenting process, including completion of local consent forms, should be completed and documented in the patient s case-notes and communicated to their GP. Management is critically dependent on FL histological subtype and disease stage. National and international consensus recommendations for management should be consulted 5, 6 (NICE guideline NG52). 5.1 Follicular lymphoma: grades 1, 2 and 3a First-line management (a) Limited stage disease (Stage 1A or 2A non-bulky) FL is highly radiosensitive and the minority of cases presenting with limited stage 1 or 2 disease and no adverse factors may be considered for local radiotherapy utilising 24Gy over 12 fractions with curative potential. A lower radiation dose of 4Gy split over 2 fractions may be appropriate in cases where a palliative approach is pursued or radiation toxicity requires particular consideration. Expectant management ( watch and wait / watchful waiting ) may also be pursued in selected cases after taking into consideration patient preferences, the potential for spontaneous remissions in FL, and the sometimes waxing and waning nature of the disease. A progression-free survival (PFS) benefit has been demonstrated by the addition of rituximab with chemotherapy to radiotherapy. Such an approach is not recommended in this context due to the potential increased toxicity associated with chemotherapy. However, the addition of single agent rituximab to radiotherapy may yield additional benefit with a favourable toxicity profile. (b) Advanced stage disease The fundamental aspect of managing advanced disease is determining whether treatment is indicated. There is no overall survival benefit to initiation of anti-lymphoma therapy in advanced stage disease based solely on the presence of FL in the absence of other adverse factors. The presence of the following are indications for treatment: rapidly progressive disease vital organ compression/compromise significant bone marrow infiltration/disease mediated haematopoietic suppression (including haemoglobin <100g/L and/or neutrophils <1.0 x 10 9 /L and/or platelets <100 x 10 9 /L) 9
11 TREATMENT RECOMMENDATIONS ascites pleural effusion (but not if small and clinically insignificant) B symptoms bulky disease including multiple (>3LN sites each >3cm in diameter) or single (>7cm in diameter) sites. Reference should be made to treatment indicators from the EORTC and GELA (including the modified GELF criteria that consist of: high tumour burden (as evidenced by any of: bulky tumour with a greatest dimension of at least 7cm, splenomegaly with cranio-caudal dimension >20cm, 3 lymph node sites with a greatest dimension at each site of 3 cm in 3 distinct lymph node areas, organ compression, pleural effusion or ascites) B symptoms LDH level > ULN elevated beta-2-microglobulin level). In the absence of these signs/symptoms then watch and wait expectant management can safely be pursued, while treatment of patients with advanced stage, low-tumour burden FL with single agent rituximab is an alternative option that should be considered given its favourable impact on disease progression (however, it is acknowledged that there may not be commissioning arrangements in place for rituximab induction monotherapy). In contrast, some patients with bulky disease may be managed by watch and wait but are likely to have a shorter duration until progression that requires treatment. Moreover, patients without any clear indication for treatment may prefer to be treated. Such cases should be counselled carefully regarding the lack of evidence for an overall survival benefit to initiation of treatment in this situation and their understandable concerns or worries regarding the watch and wait approach addressed as far as possible. Similarly, patients with indications to recommend treatment may opt not to have treatment. They should be counselled and supported following their decision and closely monitored for evidence of disease progression. (c) Systemic treatment regimens Patients should be managed with combination immuno-chemotherapy. Immunotherapy options include: Obinutuzumab in combination with chemotherapy (for patients with FLIPI scores 2-5; NICE TA513) Rituximab in combination with chemotherapy (NICE TA243 8 ) for all patients with FLIPI scores 0-1 or for patients with FLIPI scores 2-5, including if obinutuzumab is not considered appropriate or declined by patient. No overall survival difference was demonstrated in the GALLIUM study that compared these two approaches, but a PFS improvement at 3 years was demonstrated in favour of obinutuzumab. 10
12 Chemotherapy options for use with either obinutuzumab or rituximab include: TREATMENT RECOMMENDATIONS Bendamustine Cyclophosphamide, doxorubicin (hydroxydaunorubicin), vincristine (oncovin), prednisolone (CHOP), which should particularly be considered for FL that demonstrates clinically aggressive behaviour (or where transformation is suspected but unable to be proven) Cyclophosphamide, vincristine, prednisolone (CVP) Other chemotherapy regimens are typically not used first-line and are not recommended here as standard first-line approaches. In frail patients, single agent rituximab or rituximab + chlorambucil are options. (d) Consolidation of response Maintenance options include: obinutuzumab following obinutuzumab-based induction treatment or rituximab following rituximab-based induction treatment. Both are given once every 2 months for 2 years and may be options if adequate response is achieved following respective first-line systemic therapy (NICE TA513 and TA226 9 ). It should be noted that the PRIMA study did not demonstrate an OS benefit for the addition of rituximab maintenance after first-line R-chemo (but did demonstrate a PFS improvement). Also, the GALLIUM study has since demonstrated no difference in OS between obinutuzumab and rituximab maintenance. So, having considered disease response and patient preferences, not pursuing maintenance may be appropriate. (e) Toxicity/co-morbidities/dose adjustments Although these regimens are typically well tolerated, particular attention should be paid to the potential for therapy-related toxicity regarding these or other regimens in this patient population who frequently have additional medical issues. Careful clinical and organ function assessment should be undertaken, dose modifications applied to the treatment regimen as necessary, and appropriate supportive therapy (such as primary prophylactic G-CSF in selected cases) administered. Reference should be made to the MHRA Drug Safety Alert regarding off-licence use of bendamustine published on 20 July Consideration should also be given to the safety aspects of the GALLIUM study, which included increased frequency of serious adverse events associated with obinutuzumab compared to rituximab, as well as a higher number of non-relapserelated fatal events associated with bendamustine compared to CHOP or CVP chemotherapy Second- (and subsequent) line management FL may relapse/progress and require (further) treatment. At progression or relapse, biopsy of index lesions is strongly recommended particularly to assess the possibility of disease transformation. If there is no evidence for transformation, there are multiple possible management approaches in FL in the second- (or subsequent) line setting. Important aspects to consider include: availability of clinical trials patient preference 11
13 TREATMENT RECOMMENDATIONS initial response duration previous treatment regimens toxicities patient fitness and co-morbidities emerging evidence supporting novel management approaches. The stage of disease helps guide management. In selected patients (particularly the less fit) with limited stage disease, a palliative approach with local radiotherapy as 4Gy split in 2 fractions may be appropriate. In advanced disease, particularly if low bulk and in the absence of other indications for treatment, selected patients may again be appropriate for watch and wait with close disease monitoring. If systemic treatment is indicated at relapse/progression following initial management, an important consideration is whether a patient is a candidate for consolidation of response to second-line treatment by either high-dose chemotherapy with autologous haematopoietic stem cell transplantation (HDT + Auto-HSCT) or allogeneic haematopoietic stem cell transplantation (Allo-HSCT). In fitter patients demonstrating a sufficient response to second-line therapy, Auto-HSCT should be considered to consolidate response. Rituximab administered following HDT + Auto-HSCT can improve PFS (Pettengell, et al., ). Occasionally, particularly in young, otherwise fit patients with rapidly progressive/early refractory disease, Allo-HSCT should be considered. Early liaison with the local transplantation centre is recommended. (a) Systemic treatment regimens The optimal systemic regimen at second- (or subsequent) line treatment is unknown and, where available, clinical trial enrolment should be considered. In the absence of a trial, determining the approach is particularly dependent on the preceding treatment regimen(s), response duration and patient fitness. At second-line, an alternative regimen should be considered (particularly if remission duration was less than months). Re-treatment with a previous regimen may be appropriate in selected cases who experienced good response duration and lack of significant toxicity, with appropriate consideration of fitness, co-morbidities and patient preference. Rituximab 11 may be used as treatment for relapsed disease (NICE TA137). Options for rituximab with chemotherapy at second- or subsequent line treatments include: BR RCHOP RCVP The purine analogue fludarabine and rituximab are efficacious in combination with cyclophosphamide (FCR), mitoxantrone (RFM), and cyclophosphamide + mitoxantrone (RFCM). These might be considered as possible alternative second-line regimens but may have significant toxicity (full courses are not recommended) 5, 7 and should be avoided where possible in Auto-HSCT candidates due to the potential adverse effect on haematopoietic stem cell harvesting. Rituximab monotherapy (NICE TA137) 11 or rituximab + chlorambucil may be appropriate in less fit cases. 12
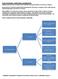
14 TREATMENT RECOMMENDATIONS Obinutuzumab with bendamustine may be used as treatment of patients who are refractory to rituximab-based first-line treatment (NICE TA472) (i.e. those who do not respond or progress within 6 months of treatment with rituximab). Other options to consider include early patient access schemes for emerging novel therapies. These typically require direct liaison with a pharmaceutical company. (b) Consolidation of response Maintenance of response may be considered with either: rituximab (NICE TA137) 11 given once every 3 months for 2 years if a complete or partial response is achieved following second-line systemic rituximab-based therapy; or obinutuzumab (NICE TA472) given once every 2 months for 2 years if disease responds to second-line systemic treatment with obinutuzumab with bendamustine. In certain cases, consolidation through a stem cell transplantation approach may be appropriate (as above). 5.2 Follicular lymphoma: grade 3b This should be managed as per diffuse large B-cell lymphoma (DLBCL) guidance. 5.3 Transformation FL has a risk of undergoing histological high-grade disease transformation 12 to aggressive lymphoma (typically DLBCL) at a rate of around 3% of cases per year. 13 If transformation is suspected, biopsy is recommended. Clinical indicators suggestive of possible transformation include: sudden rise in LDH to twice upper limit of normal rapid discordant localised nodal growth (detected clinically or by imaging) new involvement of unusual extra-nodal sites (e.g. liver, bone, muscle, brain) new B symptoms new hypercalcaemia. Transformation to DLBCL should initially be managed as per de novo DLBCL with the anthracycline containing RCHOP regimen. Consideration of enrolment in an appropriate clinical trial is encouraged. Previous treatment regimens represent a complicating issue and if transformation develops after anthracycline exposure then alternative regimens should be considered (such as platinum-based combination chemotherapy regimens) as indicated in Figure 2. Options for subsequent management of transformation to DLBCL that may be considered include: in previously treated patients, consolidation of response by HDT + Auto-HSCT in patients fit enough for this approach (early liaison with the local transplantation centre is recommended) in previously untreated patients (and in those in whom the disease is localised/limited stage), outcomes are usually better so HDT + Auto-HSCT may be avoided. 13
15 FOLLOW-UP ARRANGEMENTS Figure 2 Proposed treatment algorithm: W&W, watch and wait; RT, radiotherapy; CT, chemotherapy; HDT-ASCR, high-dose therapy and autologous stem cell rescue. Source: Silvia Montoto. Treatment of patients with transformed lymphoma. Hematology. 2015;2015(1): In the rare cases in which FL undergoes transformation to a different high-grade histology, treatment should be specific to the respective aggressive lymphoma, as appropriate. 6 Follow-up Arrangements The nature and frequency of follow-up review and investigations for patients will be somewhat tailored by their disease presentation, disease-related effects, co-morbidities, treatment type, treatment toxicities, and psycho-social factors. Follow-up clinical reviews should include history taking and physical examination with particular reference to eliciting any evidence of progression/recurrence of disease (or development of treatment-related toxicities). Blood tests performed at scheduled review visits should include FBC; while LDH, renal, liver and bone profile tests may be indicated. Given the long-term, ongoing risk of disease relapse, local pathways should be in place to ensure patients can promptly access their local lymphoma service for advice and review. Patients should be counselled as to when to re-present ahead of any scheduled review and should have a keyworker as a focal point of contact. Patients with early progression of disease within the first 2 years after diagnosis (termed progression of disease at 24 months; POD24) or treatment have inferior outcomes and relatively close follow-up is recommended during these periods (consider reviews 3 to 4 times a year). Subsequent follow-up will typically continue long-term at a frequency of 1 to 3 times a year. 14
16 7 Specific or Miscellaneous Considerations 7.1 Follicular lymphoma in situ (FLIS) SPECIFIC OR MISCELLANEOUS CONSIDERATIONS This may be identified in excised lymph nodes. While progression to FL is uncommon, it is recommended that patients with FLIS are assessed for evidence elsewhere of overt FL. 7.2 Primary cutaneous follicular cell lymphoma (PCFCL) PCFCL is a particularly indolent form of lymphoma that has excellent long-term survival and rarely disseminates from the skin. Localised disease can typically be managed by excision or radiotherapy with curative intent. For more extensive disease, observation may be appropriate particularly given the slow progression of this entity while radiation, intra-lesional steroids or topical agents may control disease; only rarely is systemic therapy indicated. 7.3 Primary intestinal follicular lymphoma This most commonly occurs in the small intestine and its clinical course may be particularly indolent. It may be managed with the watch and wait expectant management approach initially and treated only if disease is symptomatic or progresses; survival is very good even without any treatment. 7.4 Irradiated cellular blood products Patients treated with bendamustine and purine analogues (such as fludarabine) currently have a lifelong requirement to receive irradiated cellular blood products if such transfusions are ever needed. The proportion of patients this applies to will increase given the incorporation of bendamustine into first-and subsequent line treatment options for FL. Patients should be counselled and empowered to check and challenge regarding blood products if required and be provided with the NHSBT information booklet and wallet card, while the sticker is placed on any paper case-notes. Electronic case records should include notification of this requirement and blood bank systems should incorporate this information. Local and national policies and procedures regarding the notification, need for and administration of irradiated blood products should be followed when patients have received these agents or haematopoietic stem cell transplantation. 7.5 Paediatric-type follicular lymphoma Paediatric-type FL may occur in adults as well as children; is more common in males, lacks BCL2 rearrangements and demonstrates large, expansile, highly proliferative follicles. It typically presents as nodal disease of limited stage. Management may include excision alone followed by observation. It has a good prognosis with seemingly limited potential for progression. 15
17 REFERENCES References 1. Swenson WT, et al. Improved survival of follicular lymphoma patients in the United States. J Clin Oncol. 2005;23(22): Swerdlow, et al., (eds). WHO Classification Tumours of Haematopoeitic and Lymphoid Tissues (2008) IARC, Lyon. Blood 2016 Update. 2016;127(20): Cheson BD, Fisher RI, Barrington SF, et al. Recommendations for initial evaluation, staging, and response assessment of Hodgkin and non-hodgkin lymphoma: the Lugano classification. J Clin Oncol. 2014;32(27): Barrington SF, Mikhaeel NG, Kostakoglu L, et al. Role of imaging in the staging and response assessment of lymphoma: consensus of the International Conference on Malignant Lymphomas Imaging Working Group. J Clin Oncol. 2014;32(27): Ghielmini M, et al. ESMO Guidelines consensus conference on malignant lymphoma 2011 part 1: diffuse large B-cell lymphoma (DLBCL), follicular lymphoma (FL) and chronic lymphocytic leukemia (CLL). Ann Oncol. 2013;24(3): McNamara C, et al. Guidelines on the investigation and management of follicular lymphoma. Br J Haematol. 2012;156(4): Federico M, et al. R-CVP versus R-CHOP versus R-FM for the initial treatment of patients with advanced-stage follicular lymphoma: results of the FOLL05 trial conducted by the Fondazione Italiana Linfomi. J Clin Oncol. 2013;31(12): NICE technology appraisal guidance ; NICE. 9. NICE technology appraisal guidance ; NICE. 10. Pettengell R, et al. Rituximab purging and/or maintenance in patients undergoing autologous transplantation for relapsed follicular lymphoma: a prospective randomized trial from the lymphoma working party of the European group for blood and marrow transplantation. J Clin Oncol. 2013;31(13): NICE technology appraisal guidance ; NICE. 12. Montoto S, et al. Risk and clinical implications of transformation of follicular lymphoma to diffuse large B-cell lymphoma. J Clin Oncol. 2007;25(17): Al-Tourah AJ, et al. Population-based analysis of incidence and outcome of transformed non- Hodgkin's lymphoma. J Clin Oncol. 2008;26(32):
18 RM Partners, South East London Accountable Cancer Network, UCLH Cancer Collaborative th Floor Alliance House 12 Caxton Street London SW1H 0QS
Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma:
 1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
1 Lancashire and South Cumbria Haematology NSSG Guidelines for Follicular Lymphoma: 2018-19 1.1 Pretreatment evaluation The following tests should be performed: FBC, U&Es, creat, LFTs, calcium, LDH, Igs/serum
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
NON HODGKINS LYMPHOMA: INDOLENT Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and Dr.
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting?
 Indolent Lymphoma Workshop Bologna, Royal Hotel Carlton May 2017 FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting? Armando López-Guillermo Department of Hematology, Hospital
Indolent Lymphoma Workshop Bologna, Royal Hotel Carlton May 2017 FOLLICULAR LYMPHOMA: US vs. Europe: different approach on first relapse setting? Armando López-Guillermo Department of Hematology, Hospital
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center
 LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
LYMPHOMA Joginder Singh, MD Medical Oncologist, Mercy Cancer Center Lymphoma is cancer of the lymphatic system. The lymphatic system is made up of organs all over the body that make up and store cells
NICE guideline Published: 20 July 2016 nice.org.uk/guidance/ng52
 Non-Hodgkin s lymphoma: diagnosis and management NICE guideline Published: 20 July 2016 nice.org.uk/guidance/ng52 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Non-Hodgkin s lymphoma: diagnosis and management NICE guideline Published: 20 July 2016 nice.org.uk/guidance/ng52 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Indolent Lymphomas. Dr. Melissa Toupin The Ottawa Hospital
 Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Indolent Lymphomas Dr. Melissa Toupin The Ottawa Hospital What does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with
Indolent Lymphomas: Current. Dr. Laurie Sehn
 Indolent Lymphomas: Current Dr. Laurie Sehn Why does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with current standard
Indolent Lymphomas: Current Dr. Laurie Sehn Why does indolent mean? Slow growth Often asymptomatic Chronic disease with periods of relapse (long natural history possible) Incurable with current standard
Follicular Lymphoma. Michele Ghielmini. Oncology Institute of Southern Switzerland Bellinzona
 Follicular Lymphoma Michele Ghielmini Oncology Institute of Southern Switzerland Bellinzona Conflicts of interest Astra Zeneca Roche Cellgene Mundipharma Janssen Gilead Bayer Abbvie FL remains an incurable
Follicular Lymphoma Michele Ghielmini Oncology Institute of Southern Switzerland Bellinzona Conflicts of interest Astra Zeneca Roche Cellgene Mundipharma Janssen Gilead Bayer Abbvie FL remains an incurable
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL)
 Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
Guidelines for the Management of Chronic Lymphocytic Leukaemia (CLL) Version History Version Date Summary of Change/Process 2.0 08.05.08 Endorsed by the Governance Committee 2.1 16.02.11 Circulated at
How I approach newly diagnosed Follicular Lymphoma patients with advanced stage? Professeur Gilles SALLES
 How I approach newly diagnosed Follicular Lymphoma patients with advanced stage? Professeur Gilles SALLES How I Choose First Line Treatment in Follicular Lymphoma in 2017? 1. How do I take into account
How I approach newly diagnosed Follicular Lymphoma patients with advanced stage? Professeur Gilles SALLES How I Choose First Line Treatment in Follicular Lymphoma in 2017? 1. How do I take into account
Bendamustine for relapsed follicular lymphoma refractory to rituximab
 LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine for relapsed follicular lymphoma refractory to rituximab Bendamustine for relapsed follicular lymphoma refractory to rituximab Contents Summary 1
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Bendamustine for relapsed follicular lymphoma refractory to rituximab Bendamustine for relapsed follicular lymphoma refractory to rituximab Contents Summary 1
This is a controlled document and therefore must not be changed or photocopied L.80 - R-CHOP-21 / CHOP-21
 R- / INDICATION Lymphoma Histiocytosis Omit rituximab if CD20-negative. TREATMENT INTENT Disease modification or curative depending on clinical circumstances PRE-ASSESSMENT 1. Ensure histology is confirmed
R- / INDICATION Lymphoma Histiocytosis Omit rituximab if CD20-negative. TREATMENT INTENT Disease modification or curative depending on clinical circumstances PRE-ASSESSMENT 1. Ensure histology is confirmed
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary)
 NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
NON HODGKINS LYMPHOMA: AGGRESSIVE Updated June 2015 by Dr. Manna (PGY-5 Medical Oncology Resident, University of Calgary) Reviewed by Dr. Michelle Geddes (Staff Hematologist, University of Calgary) and
Rituximab for the first-line treatment of stage III-IV follicular lymphoma
 Rituximab for the first-line treatment of stage III-IV (review of guidance 110) Issued: January 2012 guidance.nice.org.uk/ta243 NICE has accredited the process used by the Centre for Health Technology
Rituximab for the first-line treatment of stage III-IV (review of guidance 110) Issued: January 2012 guidance.nice.org.uk/ta243 NICE has accredited the process used by the Centre for Health Technology
CLL & SLL: Current Management & Treatment. Dr. Isabelle Bence-Bruckler
 CLL & SLL: Current Management & Treatment Dr. Isabelle Bence-Bruckler Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of white blood cell B lymphocyte Lymphocytic Cancer
CLL & SLL: Current Management & Treatment Dr. Isabelle Bence-Bruckler Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of white blood cell B lymphocyte Lymphocytic Cancer
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113)
 Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Instructions for Chronic Lymphocytic Leukemia Post-HSCT Data (Form 2113) This section of the CIBMTR Forms Instruction Manual is intended to be a resource for completing the CLL Post-HSCT Data Form. E-mail
Non-Hodgkin lymphoma
 Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Non-Hodgkin lymphoma Non-Hodgkin s lymphoma Definition: - clonal tumours of mature and immature B cells, T cells or NK cells - highly heterogeneous, both histologically and clinically Non-Hodgkin lymphoma
Obinutuzumab in combination with bendamustine for treating rituximab-refractory follicular lymphoma
 Obinutuzumab in combination with bendamustine for treating rituximab-refractory follicular lymphoma 1 st Appraisal Committee meeting Background and Clinical Effectiveness Committee A Lead team John Watkins
Obinutuzumab in combination with bendamustine for treating rituximab-refractory follicular lymphoma 1 st Appraisal Committee meeting Background and Clinical Effectiveness Committee A Lead team John Watkins
Lugano classification: Role of PET-CT in lymphoma follow-up
 CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
CAR Educational Exhibit: ID 084 Lugano classification: Role of PET-CT in lymphoma follow-up Charles Nhan 4 Kevin Lian MD Charlotte J. Yong-Hing MD FRCPC Pete Tonseth 3 MD FRCPC Department of Diagnostic
Non-Hodgkin Lymphoma in Clinically Difficult Situations
 Winship Cancer Institute of Emory University Non-Hodgkin Lymphoma in Clinically Difficult Situations James Armitage, MD Professor, Department of Internal Medicine Joe Shapiro Distinguished Chair of Oncology
Winship Cancer Institute of Emory University Non-Hodgkin Lymphoma in Clinically Difficult Situations James Armitage, MD Professor, Department of Internal Medicine Joe Shapiro Distinguished Chair of Oncology
Acute Lymphoblastic Leukaemia Guidelines
 Acute Lymphoblastic Leukaemia Guidelines Approved by Pathway Board for Haematological Malignancies Coordinating author: Adele Fielding, Royal Free London NHS Trust Date of issue: 12.03.2015 Version number:
Acute Lymphoblastic Leukaemia Guidelines Approved by Pathway Board for Haematological Malignancies Coordinating author: Adele Fielding, Royal Free London NHS Trust Date of issue: 12.03.2015 Version number:
Clinical Commissioning Policy Proposition: Bendamustine with rituximab for relapsed indolent non-hodgkin s lymphoma (all ages)
 Clinical Commissioning Policy Proposition: Bendamustine with rituximab for relapsed indolent non-hodgkin s lymphoma (all ages) Reference: NHS England 1607 1 First published: TBC Prepared by NHS England
Clinical Commissioning Policy Proposition: Bendamustine with rituximab for relapsed indolent non-hodgkin s lymphoma (all ages) Reference: NHS England 1607 1 First published: TBC Prepared by NHS England
TRANSPARENCY COMMITTEE OPINION. 27 January 2010
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 January 2010 TORISEL 25 mg/ml, concentrate for solution and diluent for solution for infusion Box containing 1
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 27 January 2010 TORISEL 25 mg/ml, concentrate for solution and diluent for solution for infusion Box containing 1
Update: Non-Hodgkin s Lymphoma
 2008 Update: Non-Hodgkin s Lymphoma ICML 2008: Update on non-hodgkin s lymphoma Diffuse Large B-cell Lymphoma Improved outcome of elderly patients with poor-prognosis diffuse large B-cell lymphoma (DLBCL)
2008 Update: Non-Hodgkin s Lymphoma ICML 2008: Update on non-hodgkin s lymphoma Diffuse Large B-cell Lymphoma Improved outcome of elderly patients with poor-prognosis diffuse large B-cell lymphoma (DLBCL)
TRANSPARENCY COMMITTEE OPINION. 8 November 2006
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 8 November 2006 MABTHERA 100 mg, concentrate for solution for infusion (CIP 560 600-3) Pack of 2 MABTHERA 500 mg,
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 8 November 2006 MABTHERA 100 mg, concentrate for solution for infusion (CIP 560 600-3) Pack of 2 MABTHERA 500 mg,
Lymphoma: What You Need to Know. Richard van der Jagt MD, FRCPC
 Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
Lymphoma: What You Need to Know Richard van der Jagt MD, FRCPC Overview Concepts, classification, biology Epidemiology Clinical presentation Diagnosis Staging Three important types of lymphoma Conceptualizing
CLL: disease specific biology and current treatment. Dr. Nathalie Johnson
 CLL: disease specific biology and current treatment Dr. Nathalie Johnson Disclosures Consultant and Advisory boards Roche, Abbvie, Gilead, Jansson, Lundbeck,Merck Research funding Roche, Abbvie, Lundbeck
CLL: disease specific biology and current treatment Dr. Nathalie Johnson Disclosures Consultant and Advisory boards Roche, Abbvie, Gilead, Jansson, Lundbeck,Merck Research funding Roche, Abbvie, Lundbeck
Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL
 New Evidence reports on presentations given at ASH 2009 Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL From ASH 2009: Non-Hodgkin
New Evidence reports on presentations given at ASH 2009 Strategies for the Treatment of Elderly DLBCL Patients, New Combination Therapy in NHL, and Maintenance Rituximab Therapy in FL From ASH 2009: Non-Hodgkin
Note: There are other bendamustine protocols, ensure this is the correct one for a given patient.
 INDICATIONS 1 st line treatment for follicular lymphoma with FLIPI score 2 or higher: (NICE TA513- BLUETEQ required) Rituximab refractory follicular lymphoma (progression on R-chemo, R-maintenance or within
INDICATIONS 1 st line treatment for follicular lymphoma with FLIPI score 2 or higher: (NICE TA513- BLUETEQ required) Rituximab refractory follicular lymphoma (progression on R-chemo, R-maintenance or within
Large cell immunoblastic Diffuse histiocytic (DHL) Lymphoblastic lymphoma Diffuse lymphoblastic Small non cleaved cell Burkitt s Non- Burkitt s
 Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Non Hodgkin s Lymphoma Introduction 6th most common cause of cancer death in United States. Increasing in incidence and mortality. Since 1970, the incidence of has almost doubled. Overview The types of
Open questions in the treatment of Follicular Lymphoma. Prof. Michele Ghielmini Head Medical Oncology Dept Oncology Institute of Southern Switzerland
 Open questions in the treatment of Follicular Lymphoma Prof. Michele Ghielmini Head Medical Oncology Dept Oncology Institute of Southern Switzerland Survival of major lymphoma subtypes at IOSI 1.00 cause-specific
Open questions in the treatment of Follicular Lymphoma Prof. Michele Ghielmini Head Medical Oncology Dept Oncology Institute of Southern Switzerland Survival of major lymphoma subtypes at IOSI 1.00 cause-specific
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION. 18 July 2012
 The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 July 2012 MABTHERA 100 mg, concentrate for solution for infusion B/2 (CIP code: 560 600-3) MABTHERA 500 mg, concentrate
The legally binding text is the original French version TRANSPARENCY COMMITTEE OPINION 18 July 2012 MABTHERA 100 mg, concentrate for solution for infusion B/2 (CIP code: 560 600-3) MABTHERA 500 mg, concentrate
New Targets and Treatments for Follicular Lymphoma
 Winship Cancer Institute of Emory University New Targets and Treatments for Follicular Lymphoma Jonathon B. Cohen, MD, MS Assistant Professor Div of BMT, Emory University Intro/Outline Follicular lymphoma,
Winship Cancer Institute of Emory University New Targets and Treatments for Follicular Lymphoma Jonathon B. Cohen, MD, MS Assistant Professor Div of BMT, Emory University Intro/Outline Follicular lymphoma,
Scottish Medicines Consortium
 Scottish Medicines Consortium rituximab 10mg/ml concentrate for infusion (MabThera ) Roche (No.330/06) 10 November 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
Scottish Medicines Consortium rituximab 10mg/ml concentrate for infusion (MabThera ) Roche (No.330/06) 10 November 2006 The Scottish Medicines Consortium (SMC) has completed its assessment of the above
Technology appraisal guidance Published: 25 January 2012 nice.org.uk/guidance/ta243
 Rituximab for the first-line treatment of stage III-IV follicular lymphoma Technology appraisal guidance Published: 25 January 2012 nice.org.uk/guidance/ta243 NICE 2017. All rights reserved. Subject to
Rituximab for the first-line treatment of stage III-IV follicular lymphoma Technology appraisal guidance Published: 25 January 2012 nice.org.uk/guidance/ta243 NICE 2017. All rights reserved. Subject to
R-GDP: Rituximab, Gemcitabine, Dexamethasone &Cisplatin
 : Rituximab, &Cisplatin INDICATION Relapsed or refractory Hodgkin and non-hodgkin lymphoma. Omit Rituximab for patients with Hodgkin Lymphoma. TREATMENT INTENT Palliative or curative depending on context.
: Rituximab, &Cisplatin INDICATION Relapsed or refractory Hodgkin and non-hodgkin lymphoma. Omit Rituximab for patients with Hodgkin Lymphoma. TREATMENT INTENT Palliative or curative depending on context.
Patterns of Care in Medical Oncology. Follicular Lymphoma
 Patterns of Care in Medical Oncology Follicular Lymphoma CASE 1: A 72-year-old man with multiple comorbidities including COPD/asthma presents with slowly progressive cervical adenopathy. Bone marrow biopsy
Patterns of Care in Medical Oncology Follicular Lymphoma CASE 1: A 72-year-old man with multiple comorbidities including COPD/asthma presents with slowly progressive cervical adenopathy. Bone marrow biopsy
How to Refine Treatment Choice in Follicular Lymphoma: From Low-Tumor Burden to High-Risk Follicular Lymphoma
 How to Refine Treatment Choice in Follicular Lymphoma: From Low-Tumor Burden to High-Risk Follicular Lymphoma Peter A. Riedell, MD and Brad S. Kahl, MD Abstract Follicular lymphoma (FL) is the most common
How to Refine Treatment Choice in Follicular Lymphoma: From Low-Tumor Burden to High-Risk Follicular Lymphoma Peter A. Riedell, MD and Brad S. Kahl, MD Abstract Follicular lymphoma (FL) is the most common
B-cell lymphoma vaccine (BiovaxID) for follicular non-hodgkin s lymphoma
 B-cell lymphoma vaccine (BiovaxID) for follicular non-hodgkin s lymphoma May 2010 This technology summary is based on information available at the time of research and a limited literature search. It is
B-cell lymphoma vaccine (BiovaxID) for follicular non-hodgkin s lymphoma May 2010 This technology summary is based on information available at the time of research and a limited literature search. It is
1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes on the next page
 COME HOME Non-Hodgkin pathway development worksheet, v6 September 2014 1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes
COME HOME Non-Hodgkin pathway development worksheet, v6 September 2014 1. Please review the following table, make any changes you think are necessary and highlight those changes. Feel free to put notes
SEQUENCING FOLLICULAR LYMPHOMA
 SEQUENCING FOLLICULAR LYMPHOMA Thomas E. Witzig, MD October 24, 2015 Disclosures All presenters were independently selected by the organizing committee. Those presenters who disclosed affiliations or financial
SEQUENCING FOLLICULAR LYMPHOMA Thomas E. Witzig, MD October 24, 2015 Disclosures All presenters were independently selected by the organizing committee. Those presenters who disclosed affiliations or financial
DA-EPOCH-R (Etoposide/Inpatient)
 DA- (Etoposide/Inp) INDICATION High grade lymphoma. Omit rituximab if CD20 negative. PRE-ASSESSMENT 1. Ensure histology is confirmed prior to administration of chemotherapy and document in notes. 2. Record
DA- (Etoposide/Inp) INDICATION High grade lymphoma. Omit rituximab if CD20 negative. PRE-ASSESSMENT 1. Ensure histology is confirmed prior to administration of chemotherapy and document in notes. 2. Record
CLL: A Guide for Patients and Caregivers CHRONIC LYMPHOCYTIC LEUKEMIA
 CLL: A Guide for Patients and Caregivers LEUKEMIA LYMPHOMA CHRONIC LYMPHOCYTIC LEUKEMIA MYELOMA Introduction In the U.S. In 2006, about 91,000 people were living with CLL In 2007, more than 15,000 people
CLL: A Guide for Patients and Caregivers LEUKEMIA LYMPHOMA CHRONIC LYMPHOCYTIC LEUKEMIA MYELOMA Introduction In the U.S. In 2006, about 91,000 people were living with CLL In 2007, more than 15,000 people
A Phase II Clinical Trial of Fludarabine and Cyclophosphamide Followed by. Thalidomide for Angioimmunoblastic T-cell Lymphoma. An NCRI Clinical Trial.
 A Phase II Clinical Trial of Fludarabine and Cyclophosphamide Followed by Thalidomide for Angioimmunoblastic T-cell Lymphoma. An NCRI Clinical Trial. CRUK number C17050/A5320 William Townsend 1, Rod J
A Phase II Clinical Trial of Fludarabine and Cyclophosphamide Followed by Thalidomide for Angioimmunoblastic T-cell Lymphoma. An NCRI Clinical Trial. CRUK number C17050/A5320 William Townsend 1, Rod J
Treatment of Waldenström s Macroglobulinemia Mayo Consensus
 Treatment of Waldenström s Macroglobulinemia Mayo Consensus Scottsdale, Arizona Rochester, Minnesota Jacksonville, Florida Mayo Clinic College of Medicine Mayo Clinic Comprehensive Cancer Center Mayo Clinic
Treatment of Waldenström s Macroglobulinemia Mayo Consensus Scottsdale, Arizona Rochester, Minnesota Jacksonville, Florida Mayo Clinic College of Medicine Mayo Clinic Comprehensive Cancer Center Mayo Clinic
Lymphoma 101. Nathalie Johnson, MDPhD. Division of Hematology Jewish General Hospital Associate Professor of Medicine, McGill University
 Lymphoma 101 Nathalie Johnson, MDPhD Division of Hematology Jewish General Hospital Associate Professor of Medicine, McGill University Disclosures Consultant and Advisory boards for multiple companies
Lymphoma 101 Nathalie Johnson, MDPhD Division of Hematology Jewish General Hospital Associate Professor of Medicine, McGill University Disclosures Consultant and Advisory boards for multiple companies
NHS England. Evidence review: Bendamustine with Rituximab for relapsed low-grade Non- Hodgkin s Lymphoma
 NHS England Evidence review: Bendamustine with Rituximab for relapsed low-grade Non- Hodgkin s Lymphoma NHS England Evidence review: Bendamustine with Rituximab for relapsed low-grade Non- Hodgkin s Lymphoma
NHS England Evidence review: Bendamustine with Rituximab for relapsed low-grade Non- Hodgkin s Lymphoma NHS England Evidence review: Bendamustine with Rituximab for relapsed low-grade Non- Hodgkin s Lymphoma
Idelalisib treatment is associated with improved cytopenias in patients with relapsed/refractory inhl and CLL
 Idelalisib treatment is associated with improved cytopenias in patients with relapsed/refractory inhl and CLL Susan M O Brien, Andrew J Davies, Ian W Flinn, Ajay K Gopal, Thomas J Kipps, Gilles A Salles,
Idelalisib treatment is associated with improved cytopenias in patients with relapsed/refractory inhl and CLL Susan M O Brien, Andrew J Davies, Ian W Flinn, Ajay K Gopal, Thomas J Kipps, Gilles A Salles,
National Horizon Scanning Centre. Temsirolimus (Torisel) for mantle cell lymphoma - relapsed and/or refractory. January 2008
 Temsirolimus (Torisel) for mantle cell lymphoma - relapsed and/or refractory January 2008 This technology summary is based on information available at the time of research and a limited literature search.
Temsirolimus (Torisel) for mantle cell lymphoma - relapsed and/or refractory January 2008 This technology summary is based on information available at the time of research and a limited literature search.
Head and Neck: DLBCL
 Head and Neck: DLBCL Nikhil G. Thaker Chelsea C. Pinnix Valerie K. Reed Bouthaina S. Dabaja Department of Radiation Oncology MD Anderson Cancer Center Case 60 yo male Presented with right cervical LAD
Head and Neck: DLBCL Nikhil G. Thaker Chelsea C. Pinnix Valerie K. Reed Bouthaina S. Dabaja Department of Radiation Oncology MD Anderson Cancer Center Case 60 yo male Presented with right cervical LAD
Blood Cancers in the Community
 Over to you, mate Blood Cancers in the Community National Rural Health Conference NZ Rural General Practice Network April 7, 2018 Brian Grainger Haematology Registrar Auckland Acknowledgements Dr James
Over to you, mate Blood Cancers in the Community National Rural Health Conference NZ Rural General Practice Network April 7, 2018 Brian Grainger Haematology Registrar Auckland Acknowledgements Dr James
The treatment of DLBCL. Michele Ghielmini Medical Oncology Dept Oncology Institute of Southern Switzerland Bellinzona
 The treatment of DLBCL Michele Ghielmini Medical Oncology Dept Oncology Institute of Southern Switzerland Bellinzona NHL frequency at the IOSI Mantle Cell Lymphoma 6.5 % Diffuse Large B-cell Lymphoma 37%
The treatment of DLBCL Michele Ghielmini Medical Oncology Dept Oncology Institute of Southern Switzerland Bellinzona NHL frequency at the IOSI Mantle Cell Lymphoma 6.5 % Diffuse Large B-cell Lymphoma 37%
Is there a role of HDT ASCT as consolidation therapy for first relapse follicular lymphoma in the post Rituximab era? Yes
 Is there a role of HDT ASCT as consolidation therapy for first relapse follicular lymphoma in the post Rituximab era? Yes Bertrand Coiffier Service d Hématologie Hospices Civils de Lyon Equipe «Pathologie
Is there a role of HDT ASCT as consolidation therapy for first relapse follicular lymphoma in the post Rituximab era? Yes Bertrand Coiffier Service d Hématologie Hospices Civils de Lyon Equipe «Pathologie
2.07 Protocol Name: CHOP & Rituximab
 2.07 Protocol Name: CHOP & Rituximab Indication Intermediate and high grade, B-cell non-hodgkins lymphoma expressing CD20. Second or third line therapy for low grade, B cell non- Hodgkins lymphoma expressing
2.07 Protocol Name: CHOP & Rituximab Indication Intermediate and high grade, B-cell non-hodgkins lymphoma expressing CD20. Second or third line therapy for low grade, B cell non- Hodgkins lymphoma expressing
RADIOIMMUNOTHERAPY FOR TREATMENT OF NON- HODGKIN S LYMPHOMA
 RADIOIMMUNOTHERAPY FOR TREATMENT OF NON- HODGKIN S LYMPHOMA Pier Luigi Zinzani Institute of Hematology and Medical Oncology L. e A. Seràgnoli University of Bologna, Italy Slovenia, October 5 2007 Zevalin
RADIOIMMUNOTHERAPY FOR TREATMENT OF NON- HODGKIN S LYMPHOMA Pier Luigi Zinzani Institute of Hematology and Medical Oncology L. e A. Seràgnoli University of Bologna, Italy Slovenia, October 5 2007 Zevalin
Gazyva (obinutuzumab)
 Gazyva (obinutuzumab) Line(s) of Business: HMO; PPO; QUEST Integration Medicare Advantage Original Effective Date: 10/01/2015 Current Effective Date: 01/01/201807/01/2018 POLICY A. INDICATIONS The indications
Gazyva (obinutuzumab) Line(s) of Business: HMO; PPO; QUEST Integration Medicare Advantage Original Effective Date: 10/01/2015 Current Effective Date: 01/01/201807/01/2018 POLICY A. INDICATIONS The indications
Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies
![Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies](/thumbs/90/104309591.jpg) Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies UNCONTROLLED WHEN PRINTED Note: NOSCAN Haematology MCN has approved the information contained within this document to guide
Policy for Central Nervous System [CNS] Prophylaxis in Lymphoid Malignancies UNCONTROLLED WHEN PRINTED Note: NOSCAN Haematology MCN has approved the information contained within this document to guide
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL)
 Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
Non-Hodgkin lymphomas (NHLs) Hodgkin lymphoma )HL) Lymphoid Neoplasms: 1- non-hodgkin lymphomas (NHLs) 2- Hodgkin lymphoma 3- plasma cell neoplasms Non-Hodgkin lymphomas (NHLs) Acute Lymphoblastic Leukemia/Lymphoma
LEUKAEMIA and LYMPHOMA. Dr Mubarak Abdelrahman Assistant Professor Jazan University
 LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
LEUKAEMIA and LYMPHOMA Dr Mubarak Abdelrahman Assistant Professor Jazan University OBJECTIVES Identify etiology and epidemiology for leukemia and lymphoma. Discuss common types of leukemia. Distinguish
KTE-C19 for relapsed or refractory mantle cell lymphoma
 NIHR Innovation Observatory Evidence Briefing: July 2017 KTE-C19 for relapsed or refractory mantle cell lymphoma NIHRIO (HSRIC) ID: 11846 NICE ID: 9122 LAY SUMMARY Mantle cell lymphoma is an uncommon type
NIHR Innovation Observatory Evidence Briefing: July 2017 KTE-C19 for relapsed or refractory mantle cell lymphoma NIHRIO (HSRIC) ID: 11846 NICE ID: 9122 LAY SUMMARY Mantle cell lymphoma is an uncommon type
Clinical Policy: Obinutuzumab (Gazyva) Reference Number: CP.PHAR.305 Effective Date: Last Review Date: Line of Business: Medicaid
 Clinical Policy: (Gazyva) Reference Number: CP.PHAR.305 Effective Date: 02.01.17 Last Review Date: 11.17 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at the end of
Clinical Policy: (Gazyva) Reference Number: CP.PHAR.305 Effective Date: 02.01.17 Last Review Date: 11.17 Line of Business: Medicaid Coding Implications Revision Log See Important Reminder at the end of
The Clinical Characteristics and Treatment Response of Patients with Low Grade Non-Hodgkin Lymphoma
 The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (4), Page 789-796 The Clinical Characteristics and Treatment Response of Patients with Low Grade Non-Hodgkin Lymphoma Ahmed Yosry El-Agamawi,
The Egyptian Journal of Hospital Medicine (January 2019) Vol. 74 (4), Page 789-796 The Clinical Characteristics and Treatment Response of Patients with Low Grade Non-Hodgkin Lymphoma Ahmed Yosry El-Agamawi,
Clinical Commissioning Policy: Bendamustine with rituximab for relapsed and refractory mantle cell lymphoma (all ages)
 Clinical Commissioning Policy: Bendamustine with rituximab for relapsed and refractory mantle cell lymphoma (all ages) NHS England Reference: 170029P 1 NHS England INFORMATION READER BOX Directorate Medical
Clinical Commissioning Policy: Bendamustine with rituximab for relapsed and refractory mantle cell lymphoma (all ages) NHS England Reference: 170029P 1 NHS England INFORMATION READER BOX Directorate Medical
Clinical Commissioning Policy: Bendamustine with rituximab for relapsed and refractory mantle cell lymphoma (all ages) NHS England Reference: P
 Clinical Commissioning Policy: Bendamustine with rituximab for relapsed and refractory mantle cell lymphoma (all ages) NHS England Reference: 170054P 1 NHS England INFORMATION READER BOX Directorate Medical
Clinical Commissioning Policy: Bendamustine with rituximab for relapsed and refractory mantle cell lymphoma (all ages) NHS England Reference: 170054P 1 NHS England INFORMATION READER BOX Directorate Medical
Hodgkin's Lymphoma. Symptoms. Types
 Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
Hodgkin's lymphoma (Hodgkin's disease) usually develops in the lymphatic system, a part of the body's immune system. This system carries disease-fighting white blood cells throughout the body. Lymph tissue
CD20-positive high-grade non-hodgkin Lymphoma in patients in which R-CHOP is not indicated
 INDICATION CD20-positive high-grade non-hodgkin Lymphoma in patients in which R-CHOP is not indicated TREATMENT INTENT Curative or Disease Modification. PRE-ASSESSMENT 1. Ensure histology is confirmed
INDICATION CD20-positive high-grade non-hodgkin Lymphoma in patients in which R-CHOP is not indicated TREATMENT INTENT Curative or Disease Modification. PRE-ASSESSMENT 1. Ensure histology is confirmed
Aggressive Lymphomas - Current. Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre
 Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
Aggressive Lymphomas - Current Dr Kevin Imrie Physician-in-Chief, Sunnybrook Health Sciences Centre Conflicts of interest I have no conflicts of interest to declare Outline What does aggressive lymphoma
Blood Cancers. Blood Cells. Blood Cancers: Progress and Promise. Bone Marrow and Blood. Lymph Nodes and Spleen
 Blood Cancers: Progress and Promise Mike Barnett & Khaled Ramadan Division of Hematology Department of Medicine Providence Health Care & UBC Blood Cancers Significant health problem Arise from normal cells
Blood Cancers: Progress and Promise Mike Barnett & Khaled Ramadan Division of Hematology Department of Medicine Providence Health Care & UBC Blood Cancers Significant health problem Arise from normal cells
National Horizon Scanning Centre. Rituximab (MabThera) for chronic lymphocytic leukaemia. September 2007
 Rituximab (MabThera) for chronic lymphocytic leukaemia This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a definitive
Rituximab (MabThera) for chronic lymphocytic leukaemia This technology summary is based on information available at the time of research and a limited literature search. It is not intended to be a definitive
Lymphomas and multiple myeloma 12/23/2018 1
 60 Lymphomas and multiple myeloma 12/23/2018 1 Lymphomas Lymphoma is cancer of the lymphatic system. Lymphomas are subdivided into two main categories: Hodgkin's lymphoma (HL) and non- Hodgkin's lymphoma
60 Lymphomas and multiple myeloma 12/23/2018 1 Lymphomas Lymphoma is cancer of the lymphatic system. Lymphomas are subdivided into two main categories: Hodgkin's lymphoma (HL) and non- Hodgkin's lymphoma
2012 by American Society of Hematology
 2012 by American Society of Hematology Common Types of HIV-Associated Lymphomas DLBCL includes primary CNS lymphoma (PCNSL) Burkitt Lymphoma HIV-positive patients have a 60-200 fold increased incidence
2012 by American Society of Hematology Common Types of HIV-Associated Lymphomas DLBCL includes primary CNS lymphoma (PCNSL) Burkitt Lymphoma HIV-positive patients have a 60-200 fold increased incidence
R-GDP: Rituximab, Gemcitabine, Dexamethasone &Cisplatin
 : Rituximab, Gemcitabine, Dexamethasone &Cisplatin INDICATION Relapsed or refractory Hodgkin and non-hodgkin lymphoma. Omit Rituximab for patients with Hodgkin Lymphoma or high grade T cell non-hodgkin
: Rituximab, Gemcitabine, Dexamethasone &Cisplatin INDICATION Relapsed or refractory Hodgkin and non-hodgkin lymphoma. Omit Rituximab for patients with Hodgkin Lymphoma or high grade T cell non-hodgkin
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE. Single Technology Appraisal. Ibrutinib for treating chronic lymphocytic leukaemia.
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Ibrutinib for treating chronic lymphocytic leukaemia Final scope Remit/appraisal objective To appraise the clinical and cost
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Single Technology Appraisal Ibrutinib for treating chronic lymphocytic leukaemia Final scope Remit/appraisal objective To appraise the clinical and cost
Peripheral T-cell lymphoma. Matt Ahearne Clinical Lecturer, Leicester
 Peripheral T-cell lymphoma Matt Ahearne Clinical Lecturer, Leicester PTCL Objectives To understand the natural history of PTCL To appreciate the importance of accurate diagnosis of PTCL including recent
Peripheral T-cell lymphoma Matt Ahearne Clinical Lecturer, Leicester PTCL Objectives To understand the natural history of PTCL To appreciate the importance of accurate diagnosis of PTCL including recent
MEETING SUMMARY ASH 2018, San Diego, USA
 MEETING SUMMARY ASH 2018, San Diego, USA Prof. Stefano Luminari University of Modena and Reggio Emilia, Italy AN UPDATE ON PROGNOSTIC FACTORS IN INDOLENT LYMPHOMAS 2 DISCLAIMER Please note: The views expressed
MEETING SUMMARY ASH 2018, San Diego, USA Prof. Stefano Luminari University of Modena and Reggio Emilia, Italy AN UPDATE ON PROGNOSTIC FACTORS IN INDOLENT LYMPHOMAS 2 DISCLAIMER Please note: The views expressed
Maintenance rituximab following response to first-line therapy in mantle cell lymphoma
 LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Maintenance rituximab following response to first-line therapy in mantle cell lymphoma Maintenance rituximab following response to first-line therapy in mantle
LONDON CANCER NEW DRUGS GROUP RAPID REVIEW Maintenance rituximab following response to first-line therapy in mantle cell lymphoma Maintenance rituximab following response to first-line therapy in mantle
CLL Ireland Information Day Presentation
 CLL Ireland Information Day Presentation 5 May 2018 Professor Patrick Thornton Consultant Haematologist, Senior Lecturer RCSI, and Clinical Director Hermitage Medical Clinic Laboratory Chronic Lymphocytic
CLL Ireland Information Day Presentation 5 May 2018 Professor Patrick Thornton Consultant Haematologist, Senior Lecturer RCSI, and Clinical Director Hermitage Medical Clinic Laboratory Chronic Lymphocytic
Lymphoma/CLL 101: Know your Subtype. Dr. David Macdonald Hematologist, The Ottawa Hospital
 Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Lymphoma/CLL 101: Know your Subtype Dr. David Macdonald Hematologist, The Ottawa Hospital Function of the Lymph System Lymph Node Lymphocytes B-cells develop in the bone marrow and influence the immune
Rituximab in Lymphoma and Chronic Lymphocytic Leukemia: A Clinical Practice Guideline, Version 3
 A Quality Initiative of the Program in Evidence-based Care (PEBC), Cancer Care Ontario (CCO) Rituximab in Lymphoma and Chronic Lymphocytic Leukemia: A Clinical Practice Guideline, Version 3 A. Prica, F.
A Quality Initiative of the Program in Evidence-based Care (PEBC), Cancer Care Ontario (CCO) Rituximab in Lymphoma and Chronic Lymphocytic Leukemia: A Clinical Practice Guideline, Version 3 A. Prica, F.
Clinical Commissioning Policy: Bendamustine with rituximab for first line treatment of mantle cell lymphoma (all ages)
 Clinical Commissioning Policy: Bendamustine with rituximab for first line treatment of mantle cell lymphoma (all ages) NHS England Reference: 17088P NHS England INFORMATION READER BOX Directorate Medical
Clinical Commissioning Policy: Bendamustine with rituximab for first line treatment of mantle cell lymphoma (all ages) NHS England Reference: 17088P NHS England INFORMATION READER BOX Directorate Medical
The Lymphomas. An overview..
 The Lymphomas An overview.. Peter Anglin MD, FRCPC, MBA Stronach Regional Cancer Centre Newmarket, ON The lymphomas are an important part of the history of medicine 1666 Magpighi publishes first recorded
The Lymphomas An overview.. Peter Anglin MD, FRCPC, MBA Stronach Regional Cancer Centre Newmarket, ON The lymphomas are an important part of the history of medicine 1666 Magpighi publishes first recorded
O-CVP with maintenance Obinutuzumab
 with maintenance Obinutuzumab INDICATION Follicular Lymphoma: 1 st line treatment in advanced symptomatic patients (NICE TA513 for FLIPI score 2 or higher - BLUETEQ required) TREATMENT INTENT Disease modification.
with maintenance Obinutuzumab INDICATION Follicular Lymphoma: 1 st line treatment in advanced symptomatic patients (NICE TA513 for FLIPI score 2 or higher - BLUETEQ required) TREATMENT INTENT Disease modification.
National Optimal Lung Cancer Pathway
 National Optimal Lung Cancer Pathway This document was produced by the Lung Clinical Expert Group 2017 Document Title: National Optimal Lung Cancer Pathway and Implementation Guide Date of issue: August
National Optimal Lung Cancer Pathway This document was produced by the Lung Clinical Expert Group 2017 Document Title: National Optimal Lung Cancer Pathway and Implementation Guide Date of issue: August
Brad S Kahl, MD. Tracks 1-21
 I N T E R V I E W Brad S Kahl, MD Dr Kahl is Associate Professor and Director of the Lymphoma Service at the University of Wisconsin School of Medicine and Public Health and Associate Director for Clinical
I N T E R V I E W Brad S Kahl, MD Dr Kahl is Associate Professor and Director of the Lymphoma Service at the University of Wisconsin School of Medicine and Public Health and Associate Director for Clinical
Diffuse Large B-Cell Lymphoma (DLBCL)
 Diffuse Large B-Cell Lymphoma (DLBCL) DLBCL/MCL Dr. Anthea Peters, MD, FRCPC University of Alberta/Cross Cancer Institute Disclosures Honoraria from Janssen, Abbvie, Roche, Lundbeck, Seattle Genetics Objectives
Diffuse Large B-Cell Lymphoma (DLBCL) DLBCL/MCL Dr. Anthea Peters, MD, FRCPC University of Alberta/Cross Cancer Institute Disclosures Honoraria from Janssen, Abbvie, Roche, Lundbeck, Seattle Genetics Objectives
CLL & SLL: Current Management & Treatment. Dr. Peter Anglin
 CLL & SLL: Current Management & Treatment Dr. Peter Anglin Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of blood cell B lymphocyte Lymphocytic Cancer of white blood
CLL & SLL: Current Management & Treatment Dr. Peter Anglin Chronic Lymphocytic Leukemia Prolonged clinical course Chronic A particular type of blood cell B lymphocyte Lymphocytic Cancer of white blood
Corporate Medical Policy
 Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
Corporate Medical Policy Hematopoietic Cell Transplantation for CLL and SLL File Name: Origination: Last CAP Review: Next CAP Review: Last Review: hematopoietic_cell_transplantation_for_cll_and_sll 2/2001
pan-canadian Oncology Drug Review Initial Clinical Guidance Report Obinutuzumab (Gazyva) for Follicular Lymphoma August 30, 2018
 pan-canadian Oncology Drug Review Initial Clinical Guidance Report Obinutuzumab (Gazyva) for Follicular Lymphoma August 30, 2018 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
pan-canadian Oncology Drug Review Initial Clinical Guidance Report Obinutuzumab (Gazyva) for Follicular Lymphoma August 30, 2018 DISCLAIMER Not a Substitute for Professional Advice This report is primarily
PET-imaging: when can it be used to direct lymphoma treatment?
 PET-imaging: when can it be used to direct lymphoma treatment? Luca Ceriani Nuclear Medicine and PET-CT centre Oncology Institute of Southern Switzerland Bellinzona Disclosure slide I declare no conflict
PET-imaging: when can it be used to direct lymphoma treatment? Luca Ceriani Nuclear Medicine and PET-CT centre Oncology Institute of Southern Switzerland Bellinzona Disclosure slide I declare no conflict
Rituximab in the Treatment of NHL:
 New Evidence reports on presentations given at ASH 2010 Rituximab in the Treatment of NHL: Rituximab versus Watch and Wait in Asymptomatic FL, R-Maintenance Therapy in FL with Standard or Rapid Infusion,
New Evidence reports on presentations given at ASH 2010 Rituximab in the Treatment of NHL: Rituximab versus Watch and Wait in Asymptomatic FL, R-Maintenance Therapy in FL with Standard or Rapid Infusion,
NCCP Chemotherapy Regimen. Obinutuzumab Maintenance Therapy following O-Bendamustine therapy
 Obinutuzumab following O-Bendamustine therapy INDICATIONS FOR USE: INDICATION Obinutuzumab maintenance therapy is indicated in patients with follicular lymphoma (FL) who have responded to induction treatment
Obinutuzumab following O-Bendamustine therapy INDICATIONS FOR USE: INDICATION Obinutuzumab maintenance therapy is indicated in patients with follicular lymphoma (FL) who have responded to induction treatment
A CASE OF PRIMARY THYROID LYMPHOMA. Prof Dr.Dilek Gogas Yavuz Marmara University School of Medicine Endocrinology and Metabolism Istanbul, Turkey
 A CASE OF PRIMARY THYROID LYMPHOMA Prof Dr.Dilek Gogas Yavuz Marmara University School of Medicine Endocrinology and Metabolism Istanbul, Turkey 38 year old female She recognized a mass in her right neck
A CASE OF PRIMARY THYROID LYMPHOMA Prof Dr.Dilek Gogas Yavuz Marmara University School of Medicine Endocrinology and Metabolism Istanbul, Turkey 38 year old female She recognized a mass in her right neck
Challenges in the Treatment of Follicular Lymphoma
 Challenges in the Treatment of Follicular Lymphoma Prof. Michele Ghielmini Clinical Director Oncology Institute of Southern Switzerland Bellinzona ESMO guidelines 2014 (simplified) Low tumor burden High
Challenges in the Treatment of Follicular Lymphoma Prof. Michele Ghielmini Clinical Director Oncology Institute of Southern Switzerland Bellinzona ESMO guidelines 2014 (simplified) Low tumor burden High
New Evidence reports on presentations given at EHA/ICML Bendamustine in the Treatment of Lymphoproliferative Disorders
 New Evidence reports on presentations given at EHA/ICML 2011 Bendamustine in the Treatment of Lymphoproliferative Disorders Report on EHA/ICML 2011 presentations Efficacy and safety of bendamustine plus
New Evidence reports on presentations given at EHA/ICML 2011 Bendamustine in the Treatment of Lymphoproliferative Disorders Report on EHA/ICML 2011 presentations Efficacy and safety of bendamustine plus
(R) CHOEP. May be used for stage IA - IV Diffuse Large B Cell non-hodgkin lymphoma in combination with rituximab.
 (R) CHOEP Indication Treatment of stage IA - IV T cell non-hodgkin lymphoma as an alternative to CHOP in younger, fitter patients with normal LDH level. May be used for stage IA - IV Diffuse Large B Cell
(R) CHOEP Indication Treatment of stage IA - IV T cell non-hodgkin lymphoma as an alternative to CHOP in younger, fitter patients with normal LDH level. May be used for stage IA - IV Diffuse Large B Cell
LYMPHOMA DIAGNOSIS and PROGNOSIS. LC Lim Dept of Hematology Singapore General Hospital
 LYMPHOMA DIAGNOSIS and PROGNOSIS LC Lim Dept of Hematology Singapore General Hospital OUTLINE Accurate diagnosis Define subtype : WHO classification Staging : Defines extent of involvement Prognosis Determining
LYMPHOMA DIAGNOSIS and PROGNOSIS LC Lim Dept of Hematology Singapore General Hospital OUTLINE Accurate diagnosis Define subtype : WHO classification Staging : Defines extent of involvement Prognosis Determining
12 th Annual Hematology & Breast Cancer Update Update in Lymphoma
 12 th Annual Hematology & Breast Cancer Update Update in Lymphoma Craig Okada, MD, PhD Assistant Professor, Hematology January 14, 2010 Governors Hotel, Portland Oregon Initial Treatment of Indolent Lymphoma
12 th Annual Hematology & Breast Cancer Update Update in Lymphoma Craig Okada, MD, PhD Assistant Professor, Hematology January 14, 2010 Governors Hotel, Portland Oregon Initial Treatment of Indolent Lymphoma
What is a hematological malignancy? Hematology and Hematologic Malignancies. Etiology of hematological malignancies. Leukemias
 Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
Hematology and Hematologic Malignancies Cancer of the formed elements of the blood What is a hematological malignancy? A hematologic malignancy is a malignancy (or cancer) of any of the formed elements
