Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis
|
|
|
- Lesley Patterson
- 5 years ago
- Views:
Transcription
1 Chapter 10 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis Abiramy Jeyabalan and Andrew RL Medford Additional information is available at the end of the chapter 1. Introduction Endobronchial ultrasound-guided transbronchial needle aspiration (EBUS-TBNA) is a minimally invasive mediastinal sampling technique which combines the use of ultrasound with conventional bronchoscopy in order to visualise and sample structures adjacent to the tracheo-bronchial tree such as mediastinal and hilar lymph nodes. The technique is commonly used in the staging and diagnosis of lung cancers but can also be used for the diagnosis of benign conditions affecting the mediastinum including sarcoidosis. In asymptomatic stage I sarcoidosis (bilateral hilar adenopathy) with evidence of arthritis and erythema nodosum (Lofgren s syndrome) it may be possible to make a presumptive diagnosis based on clinical and radiological findings however in symptomatic patients and particularly where immunosuppressive therapy is being considered or exclusion of other causes of mediastinal lymphadenopathy is required (e.g. tuberculosis, histoplasmosis, silicosis or lymphoma) a tissue diagnosis may be sought. A diagnosis of sarcoidosis can be made in the presence of pathological evidence demonstrating non-caseating granulomata, in the absence of positive mycobacterial and fungal cultures and with supporting clinical and radiological evidence. Tissue for diagnosis should be obtained from the most accessible involved organ. Since pulmonary sarcoidosis is the most frequent form, bronchoscopic techniques are often the first line investigation. Conventional flexible bronchoscopy is frequently performed in the diagnosis of sarcoidosis but is of limited use when central or peripheral airways are not affected. Endobronchial biopsy (EBB) where there is evidence of disease affecting the airways may assist with the diagnosis. Transbronchial lung biopsy (TBLB) can be performed where there is evidence of parenchymal disease however this technique carries a risk of bleeding and pneumothorax. Transbronchial needle aspiration (TBNA) can be useful in the context of mediastinal lymphadenopathy however this is a blind technique and as such diagnostic accuracy is variable and further 2013 Jeyabalan and Medford; licensee InTech. This is an open access article distributed under the terms of the Creative Commons Attribution License ( which permits unrestricted use, distribution, and reproduction in any medium, provided the original work is properly cited.
2 240 Sarcoidosis more there is risk of bleeding and damage to vascular structures. There are also limitations in terms of which nodes can be sampled using conventional TBNA. Mediastinoscopy remains the gold standard approach for sampling the mediastinal glands, particularly when other sampling techniques are non-diagnostic however this is an invasive procedure which requires a general anesthetic and is associated with morbidity. Many of the limitations associated with the aforementioned techniques can be overcome by the use of EBUS-TBNA. The following chapter describes the technique, its application in the diagnosis of sarcoidosis and the advantages of EBUS-TBNA over alternative mediastinal sampling techniques. 2. EBUS TBNA - Technical issues 2.1. The EBUS scope There are two probes available. The radial probe was initially developed in This is a high frequency probe (20-30MHz) which achieves a high resolution image but has limited depth penetration (4-5cm) and provides a 360 degree view. The radial probe is particularly useful for imaging of the airway wall however it does not allow real time identification of structures during sampling (table 1). The convex or linear probe EBUS scope integrates a convex transducer probe at the tip of a flexible bronchoscope (figure 1). The transducer has a frequency of 7.5 MHz and scans through the airway wall in a plane which is parallel to the insertion direction of the bronchoscope. Although images using the convex probe are of lower resolution there is improved depth of penetration (up to 9cm) and most importantly this probe enables real time imaging of the EBUS-TBNA needle throughout the sampling process thus reducing the risk of damage to vascular structures. The endoscopic image is viewed at an angle of 30 degrees forward oblique and the operator needs to compensate accordingly. The ultrasonic image is viewed at an angle of 90 degrees to the bronchoscope. The ultrasonic image of mediastinal structures is obtained by making direct contact between the probe and the airway wall. Improved image quality can be achieved by increasing the contact between the transducer and the airway wall using a balloon attached to the tip of the ultrasound which is filled with normal saline. The ultrasound image is processed and visualized with the conventional bronchoscopic image, on the same monitor (figure 2). The ultrasonic image can be frozen and the size of lesions or nodes can be measured in two dimensions. The use of colour flow and power Doppler also allows accurate identification of vascular structures adjacent to or within the area of interest. The linear probe is most commonly used in the sampling of mediastinal lymph nodes. Unless specified, the term EBUS in this chapter refers to linear probe EBUS. Radial Probe Convex Probe Frequency 20-30MHz 7.5MHz Penetration (cm) Applications Assessment of airway wall Sampling of mediastinal lesions e.g. Sampling of peripheral lesions lymph nodes Table 1. Comparison of radial probe vs convex probe
3 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis Figure 1. Linear EBUS probe Figure 2. EBUS Scope Processor and Monitor
4 242 Sarcoidosis EBUS-TBNA is sometimes performed at the same time as flexible bronchoscopy which may be necessary when more detailed examination of the distal tracheobronchial tree or endobronchial biopsies are required. The external diameter of the EBUS-TBNA scope is wider than a conventional bronchoscope (6.9mm compared with 5-6mm) however endobronchial biopsies of more proximal airways can be carried out via the EBUS bronchoscope. As with flexible bronchoscopy, EBUS-TBNA procedure is commonly performed under light conscious sedation using intravenous midazolam and fentanyl as well as topical anaesthesia however some centres prefer to use deep sedation with propofol or a remifentanil infusion with a laryngeal mask airway in order to minimize coughing. Typically the procedure is carried out as a day case. Adequate sedation is essential as EBUS-TBNA takes longer than a flexible bronchoscopy, particularly if multiple nodal stations are sampled. The patient is positioned in a supine position and the bronchoscopist stands behind the patient. In view of the wider diameter of the EBUS-TBNA scope, oral intubation is preferred. As described above the endoscopic view is 30 degrees forward oblique, therefore the bronchoscope needs to be flexed down in order to obtain a straight view. In order to pass the bronchoscope through the vocal cords the anterior angle of the glottis should be visualized with the bronchoscope in the neutral position. The mediastinal lymph nodes are examined by positioning the bronchoscope in the correct anatomical position and then by flexing and pressing the ultrasound probe onto the airway wall. The bronchoscope is adjusted so that the area for sampling is viewed in its maximum diameter at the centre of the ultrasound image. The Doppler mode is used to visualize vascular landmarks and can be used to identify vessels within lymph nodes. The size of the lymph node is measured using the calipers The sampling technique For a more detailed review of this aspect, the reader is directed to other sources [1]. Sampling using the dedicated single use TBNA needle is ideally performed by two operators however it is possible for the technique to be carried out with a single operator. Currently 2 sizes of dedicated EBUS-TBNA sampling needles (21-gauge and 22-gauge) are available. The needle is housed within a sheath which is inserted into the 2.0mm working channel of the EBUS bronchoscope. The sampling needle has multiple small dimples along its shaft in order to increase the echogenicity and screen visualisation. 21 gauge needles are often preferred for suspected granulomatous disease as there is evidence to suggest that the histological structure of specimens is better preserved using the larger needle [2, 3]. Following intubation, lymph nodes are identified according to the International Staging System [4] with the aid of vascular landmarks and the Doppler mode. Mediastinal lymph nodes at stations 2-4, 7, 10 and 11 can be accessed for EBUS-TBNA (figure 3). The EBUS-TBNA sampling needle is inserted through the working channel and is positioned so that the tip of the needle sheath is just visible on the endoscopic image. This is extremely important in order to avoid damage to the bronchoscope channel when the needle exits. The needle is locked on to the working channel and the internal stylet is withdrawn slightly. The depth for sampling is determined (0.5-4 cm) and this distance is set using the safety calibrator (figure 4). Holding the bronchoscope against the airway wall the needle is then inserted using a jabbing
5 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis movement. The needle exits the working channel at angle of 20 degrees to the sheath of the insertion tube (figure 5). Following insertion of the needle the internal stylet is advanced and withdrawn within the needle lumen to clear any airway wall debris before it is completely removed. A 3-way vacuum syringe is attached to the needle and sampling commences by advancing and withdrawing the needle approximately 15 times within the node under direct vision (figure 6). Once sampling is complete the 3-way syringe is disconnected and then the needle is removed from the working channel. The internal stylet is used to expel the histological core tissue sample from the needle lumen onto a specimen collecting system. The stylet is removed and cleaned with saline and air is injected though the needle lumen to remove any remaining particles. The same node is usually sampled 2 to 3 times assuming a good sample is obtained at each pass. For benign disease such as granulomatous disease it may be preferable to do a limited number of passes in a greater number of lymph nodes in order to limit the total length of the procedure if conscious sedation is being used rather than general anaesthesia [5]. Figure 3. Diagrammatic representation of lymph node stations accessed via EBUS-TBNA/ EUS-FNA. EUS-FNA = endoscopic ultrasound-guided fine needle aspiration.
6 244 Sarcoidosis Figure 4. Sampling Needle inserted into working channel of EBUS scope Figure 5. Tip of EBUS scope with balloon inflated and TBNA needle exiting
7 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis Figure 6. Ultrasound image of lymph node with EBUS-TBNA sampling needle in situ Figure 7. Histological sample obtained using EBUS-TBNA showing non-caseating granuloma
8 246 Sarcoidosis 2.3. The specimen The handling of the histological and cytological samples is extremely important. The diagnosis of sarcoidosis is established when clinical and radiological findings are supported by histological or cytological evidence of non-caseating epithelioid cell granulomas. Granulomas are defined by loose collections of non-pigmented epithelioid or spindle cell histiocytes with lymphocytes, necrotic material and neutrophils. In sarcoidosis numerous granulomas can be seen in FNA samples without evidence of necrosis [7]. It is important to exclude local sarcoidlike reactions and infective causes. Many centres choose to utilise rapid on-site evaluation (ROSE) of cytology samples in order to confirm the adequacy of specimens however resources and cost are limiting factors. ROSE of specimens has been shown to increase diagnostic yield in some circumstances, however a recent meta-analysis examining the use of ROSE in cases of suspected sarcoidosis did not demonstrate a statistically significant increase (p = 0.66) in yield in studies where ROSE was carried out (165/206; 80.1% vs 282/347; 81.3%) [6]. ROSE allows a smaller number of passes to be carried per node. Once a diagnosis of granulomatous disease or malignancy is reached sampling of that particular node can be stopped. In order to minimize the number of false negative results, if no malignancy or granulomatous inflammation is seen, further sampling should be performed. Gross examination of the specimen can be helpful as adequate samples often appear creamy (rather than bloody, watery or mucoid) or may be black as a result of anthracosis [7]. Typically the EBUS-TBNA samples are smeared on to glass slides and air dried then fixed however some centres prefer to use liquid cytology bottles. Tissue cores are fixed in formalin or saline depending on whether culture for Mycobacterial disease is required. It has recently been reported that cell block analysis in addition to the Diff-Quick smear examination can reduce the false negative rate by 33%. Furthermore, Wang et al [8], found that of 37 patients who had EBUS-TBNA carried out, 100% of cell blocks contained non-necrotizing granulomas compared to 27% of smears. This may be because smearing samples between two slides disrupts the epithelioid groups in FNA samples which does not tend to occur during cell block preparation. There is debate regarding the definition of an adequate tissue sample. In the absence of malignant cells or granulomatous cells it is clearly important to confirm that an adequate amount of lymphoid tissue is present in the sample. The negative predictive value of samples is far superior when lymphocytes are detected. Attempts have been made to quantify the number of cells required to define the adequacy of a sample. For example, [see 7] state that a sample containing at least 40 benign-appearing lymphocytes in a high-power field in the areas of highest cellularity of the smear constitutes an adequate sample. Likewise the identification of large numbers of anthracotic pigment and macrophages or large clusters of admixed lymphocytes and pigmented macrophages may further indicate an adequacy. If malignancy or granulomatous disease is seen with small numbers of lymphocytes this can also be considered to be adequate. The interpretation of adequacy is somewhat subjective and development of a standardised approach may help to reduce the number of false negative or positive results.
9 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis Sarcoid-like granulomata may be visualized in the context of malignancy such as non-small cell lung cancer, lymphoid and germ cell neoplasms and are thought to be a result of a local T cell-mediated immune reaction. It is therefore important to continue to attempt to exclude malignancy even if granulomatous inflammation is seen. Similarly granulomatous inflammation can be seen as a result of fungal or mycobacterial infections particularly in immunosuppressed patients and appropriate culture should be considered. The implication of EBUS- TBNA detection of granulomatous inflammation in patients with previously treated cancer and new mediastinal lymphadenopathy has been examined [9]. In this study, 17/153 (11%) of patients referred for EBUS-TBNA were found to have non-caseating granuloma. A subgroup of patients had a previous history of cancer and presented with mediastinal lymphadenopathy suspicious of cancer recurrence. All these patients had granulomatous inflammation confirmed via EBUS-TBNA and remained clinically stable during follow-up. The study highlights the importance of obtaining a tissue diagnosis in this subgroup of patients and supports the utility of EBUS-TBNA as a diagnostic tool in this circumstance. The differentiation between true sarcoidosis and sarcoid-like reaction must be made through clinical and radiological correlation Diagnostic yield of EBUS-TBNA The diagnostic yield of EBUS-TBNA in sarcoid has been reported between 80-90% [10]. It is important to note that the highest sensitivity (92%) of EBUS-TBNA has been demonstrated in patients with stage I and II disease with nodes of >10mm however even in patients with nodes of <10mm and all stages of sarcoidosis the sensitivity is still adequate (85%) [11,12]. A recent meta-analysis of 15 studies of EBUS-TBNA in sarcoidosis described a yield between 54-93% with a pooled diagnostic accuracy of 79% (95% CI, 71-86%) however there was heterogeneity between studies included. There was also variability regarding the experience of the operators in these studies [6] Contraindications EBUS-TBNA is a well tolerated procedure. Patients should be fit enough to undergo flexible bronchoscopy in accordance with local guidelines [13]. Biopsies should not be carried out in patients who are currently taking warfarin and the international normalized ratio (INR) should be less than 1.4. Clopidogrel is normally withheld at least one week prior to the procedure although a small series of patients who had EBUS-TBNA whilst still taking clopidogrel (and a significant proportion also taking aspirin) did not report any bleeding complications [14]. The procedure should be avoided for 6 weeks after myocardial infarction and should not carried out in patients with arrhythmia or severe hypoxaemia at rest [15] Complications EBUS-TBNA has been shown to be a safe, minimally invasive technique. Only 5 minor complications (minimal pneumothorax, minor bleeding, airway oedema/hypoxaemia, prolonged coughing) were reported in a recent systematic review of 532 patients undergoing EBUS-TBNA for suspected sarcoidosis [6]. Compared to mediastinoscopy which carries a 0.5%
10 248 Sarcoidosis risk of major complications and % risk of significant complications the risk of complications with EBUS-TBNA is lower [15]. Routine chest radiograph is not required following the procedure unless the patient reports specific symptoms (e.g. chest pain) during or after the procedure although some centres do a chest radiograph after sampling the hilar stations routinely [16] Costs The main costs of setting up an EBUS-TBNA service are due to equipment costs such as the EBUS bronchoscope, ultrasound processor and also the disposable EBUS needles (which are more expensive than conventional TBNA needles) and accessories (approximately ). As the procedure takes longer than a conventional flexible bronchoscopy, the cost of additional staff time must be considered. If ROSE is required this is a further cost. Repair and servicing of the EBUS bronchoscope is more expensive than a flexible bronchoscope. Similar to conventional TBNA there is a risk of damage to the biopsy channel of the bronchoscope if the sheath of the EBUS-TBNA needle is not positioned correctly when the needle is advanced. Having taken into account the additional costs of EBUS-TBNA, since the technique has a higher sensitivity than conventional TBNA (particularly where distal or smaller node sampling is required, the overall cost saving potential from avoiding a mediastinoscopy is likely to be greater with this technique than with conventional TBNA [15] Training and learning curve EBUS-TBNA can be performed by pulmonologists. Training requires the operator to have had sufficient experience in all standard bronchoscopic techniques, including conventional TBNA. Experience with the interpretation of ultrasound is also useful e.g. thoracic ultrasound. Training of nursing staff is also required. The American College of Chest Physicians (ACCP) recommends that in order to achieve competence in EBUS-TBNA, 50 supervised procedures must be carried out. Furthermore in order to maintain competence it is recommended that a minimum of 20 procedures per year are carried out [17]. The learning curve and the number of procedures required to produce optimal results is high [18]. In fact a recent prospective study has demonstrated improving results up to 120 procedures [19]. 3. Other diagnostic bronchoscopic techniques 3.1. Conventional TBNA The use of TBNA in the diagnosis of sarcoidosis has been described since the 1980 s. The technique of sampling lymph nodes using this method is a blind technique and diagnostic accuracy is likely to be dependant on the skill of the operator. The reported sensitivity of TBNA is variable, ranging from 46-90% [3]. It is also a technique which is underutilised by pulmonologists (10-30% uptake) because of concerns regarding diagnostic yield and fear of vascular injury [10]. There is also a belief that it is not useful (reported by 30% pulmonologists in one
11 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis study) and concerns about performing the technique without onsite pathology support [20].. EBUS-TBNA carries a lower risk of complications compared with conventional TBNA. Several studies have directly compared EBUS-TBNA with conventional TBNA. In one, small prospective study of patients with suspected sarcoidosis EBUS-TBNA was followed by conventional TBNA. The two techniques were found to be of similar efficacy with a positive diagnosis established in 93% of patients using EBUS-TBNA and/ or conventional TBNA [3]. Only one randomised controlled trial has directly compared EBUS-TBNA with conventional TBNA. This study demonstrated a superior diagnostic yield with EBUS-TBNA compared to conventional TBNA (using a 19-gauge needle) in patients with suspected sarcoidosis. An absolute increase in yield of 29.5% was demonstrated with EBUS-TBNA (p <0.05; 95% confidence interval 8.6 to 55.4%). Sensitivity and specificity in the conventional TBNA group was 60.9% and 100% respectively compared with 83.3% and 100% in the EBUS-TBNA group. Of note, more lymph nodes were sampled in the EBUS-TBNA group but more passes were required in the TBNA group [21] Bronchoalveolar Lavage (BAL) BAL is a safe, minimally invasive and low cost technique which can be performed during flexible bronchoscopy but can also be performed via the EBUS bronchoscope. BAL samples can be used to support a diagnosis of sarcoidosis if a characteristic cytological predominance of lymphocytes is seen. A CD4+/CD8+ ratio of greater than 3.5 in the lymphocyte population has a high specificity (94%) for sarcoidosis. However a low ratio cannot be used to exclude a diagnosis of sarcoidosis [22]. BAL is also of use for microbiological testing particularly where mycobacterial disease is suspected Endobronchial and transbronchial lung biopsy In patients with suspected sarcoidosis with evidence of parenchymal disease transbronchial lung biopsy (TBLB) can be used to obtain a diagnosis however the reported diagnostic yield is variable (44-90%) dependent on the number of sites sampled and the extent of the parenchymal disease [23]. TBLB has limited value in stage I disease and unlike EBUS-TBNA, TBLB carries a risk of pneumothorax and a higher risk of bleeding. Endobronchial biopsy (EBB) can be carried out where there is evidence of airway involvement and even if the airways do not appear grossly abnormal EBB can further increase the yield with a 30% yield even in normal airways [24]. In practice EBB is typically performed when macroscopic disease is visible. EBUS-TBNA has been demonstrated to have superior diagnostic utility when compared with TBLB and endobronchial biopsy [3,25,26] Endoscopic ultrasound-guided fine needle aspiration (EUS-FNA) Transoesophageal EUS-FNA was first introduced in the early 1990s and was most commonly used by gastroenterologists to obtain tissue from pancreatic lesions. Subsequently this technique has been applied in the diagnosis of both intrabdominal and intrathoracic lesions. EUS-FNA enables access to lymph node stations 2L, 4L and most importantly
12 250 Sarcoidosis the lower mediastinum (7, 8, and 9). Nodes in the aortopulmonary window (5) and paraaortic nodes (6) can be visualized however sampling is limited by the proximity of vascular structures. The left adrenal gland and the left lobe of the liver can also be sampled. The accuracy of EUS-FNA is greater with ROSE. The technique can be combined with EBUS- TBNA and pulmonologists can train to carry out both procedures or (if appropriately trained) alternatively intubate the oesophagus with the EBUS bronchoscope, as described in some centres, EUS-B-FNA [27, 28]. The disadvantage of EUS-FNA without EBUS- TBNA is the range of nodes which can be accessed is more limited and it is not possible to sample hilar nodes. This is of particular relevance in sarcoidosis as hilar nodes and nodes anterolateral to the trachea are more commonly involved [7]. Diagnostic yield is high with EUS-FNA and has been reported as 82%, sensitivity 89% and specificity 96% [29]. When combined with EBUS-TBNA the yield is improved further and the range of nodes which can be sampled is greater Mediastinoscopy Mediastinoscopy has been considered to be the gold standard mediastinal sampling method of choice particularly if other techniques such as TBLB are non-contributory. Mediastinoscopy is an invasive technique which requires a general anaesthetic and an overnight hospital stay. There are several approaches which allow access to different nodal stations and areas of the mediastinum. Cervical mediastinoscopy (via an incision at the suprasternal notch) allows access to the pretracheal, upper paratracheal (2R, 2L), lower paratracheal (4R, 4L), subcarinal (7) and hilar (10) nodes. The extended cervical mediastinoscopy also allows access to the anterior mediastinum including pre-aortic (6) and aortopulmonary window (5) nodes. There are currently no studies comparing EBUS-TBNA with mediastinoscopy in suspected sarcoidosis. Successful diagnosis with EBUS-TBNA may obviate the need for mediastinoscopy. This is not only likely to be more preferable to patients who may avoid an invasive procedure but there are also cost saving benefits as discussed previously Peripheral lymph node biopsy Sarcoidosis involving peripheral lymph nodes is frequently asymptomatic. The incidence of peripheral lymph node involvement has been reported between 2-25%. High diagnostic yield with sampling of peripheral lymph nodes has been reported. In one study, at least one enlarged peripheral lymph node was found in 14.5% (79/546) of patients with a diagnosis of sarcoidosis [30]. The diagnostic yield of peripheral lymph node biopsy in these patients was 93% with no associated complications and significantly a lower cost compared to other techniques. The most common sites of involvement were the cervical nodes (31.3%) and supraclavicular nodes (29.9%). Ultrasound guided peripheral lymph node biopsy may be an option in patients who have contraindications to mediastinal sampling techniques. The advantages and disadvantages of all these techniques are summarised in table 2.
13 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis Technique Advantages over EBUS-TBNA Disadvantages over EBUS-TBNA Lower cost Risk of complications/ injury ( blind technique) Conventional TBNA More commonly performed by Shorter needle throw therefore smaller pulmonologists tissue core Shorter procedure time Lower diagnostic yield Less extensive range of node sampling EBB Performed by pulmonologists Lower cost Lower diagnostic yield Risk of complications Performed by pulmonologists TBLB Less useful in the absence of Lower cost parenchymal disease Unable to access hilar nodes Improved access to some lymph node EUS-FNA More commonly performed by stations gastroenterologists /radiologists Invasive procedure with risk of significant complications Generally performed by thoracic Larger histological tissue sample obtained Mediastinoscopy surgeons High negative predictive value Requires general anaesthetic and overnight hospital stay Higher cost Low cost (especially if ultrasound-guided Peripheral lymph node Small proportion of patients with without theatre) biopsy enlarged nodes Low complication rate Table 2. Pros and cons of other non-ebus sampling techniques in sarcoidosis involving mediastinum/nodal tissue and/or lung 4. Advantages and disadvantages of EBUS-TBNA 4.1. Compared to conventional TBNA Unlike conventional TBNA, EBUS-TBNA allows access to a wider range of lymph nodes stations (2-4,7, 10 and 11) and therefore provides access to more distal locations. This is of particular relevance in granulomatous disease where sampling of multiple nodal stations can further increase diagnostic yield. This advantage is augmented further by combining EBUS- TBNA with EUS-FNA thereby enabling access to even more lymph node stations. Conventional TBNA is a blind technique and therefore carries a risk of bleeding through potential damage to vascular structures. EBUS-TBNA carries a lower bleeding risk as it is performed under real time ultrasound guidance. The use of Doppler mode imaging allows accurate visualisation of vessels prior to sampling. Furthermore because sampling is carried out under direct vision it is possible for the EBUS-TBNA needle to be inserted further into the
14 252 Sarcoidosis sampling area with each pass compared with sampling during conventional TBNA. Larger cores of tissue can therefore be obtained compared with conventional TBNA. Once again this is particularly important in granulomatous disease. The cost of equipment and additional staff time required in order to carry out EBUS-TBNA makes it a more expensive technique when compared with conventional TBNA, however as discussed earlier the overall cost saving gained from avoiding the need for mediastinoscopy is likely to be greater for EBUS-TBNA than with conventional TBNA Compared to mediastinoscopy Mediastinoscopy has been considered to be the gold standard mediastinal sampling method of choice particularly if other techniques such as TBLB are non-contributory. Mediastinoscopy is an invasive technique which requires a general anaesthetic and an overnight hospital stay unlike EBUS-TBNA which is typically carried out under light conscious sedation as a day case procedure. Clearly there are financial advantages to a less invasive approach and it is likely to be more preferable to patients. Mediastinoscopy carries a risk of major complications (0.5%) and % risk of significant complications such as supraventricular arrhythmias. It also results in a neck scar and the development of adhesions following mediastinoscopy may hinder future attempts at lymph node sampling [16]. Previous neck surgery is a relative contraindication to mediastinoscopy. As discussed previously, the risk of complications with EBUS-TBNA is lower than with mediastinoscopy. The range of nodes which are accessible via EBUS-TBNA is greater than with mediastinoscopy particularly the hilar nodes. This is of relevance in granulomatous disease as the hilar nodes are frequently affected. Smaller tissue samples are obtained with EBUS-TBNA compared to mediastinoscopy and as discussed earlier this can affect the adequacy of tissue samples obtained. For this reason the negative predictive value of EBUS-TBNA is lower. This is particularly relevant when sampling for malignancy. If there is concern that malignancy such as lymphoma is a possible cause for lymphadenopathy, mediastinoscopy should be the sampling technique of choice. Alternatively, a non-diagnostic EBUS-TBNA result should be considered for further investigation with mediastinoscopy. In experienced centres where adequate tissue samples are obtained through EBUS-TBNA the technique may be an alternative option for patients who have been deemed not fit for invasive mediastinoscopy. 5. Comparative studies of EBUS-TBNA with other mediastinal sampling techniques Combining EBUS-TBNA with standard bronchoscopic techniques has been shown to improve diagnostic yield further. This is important as improved accuracy in non-invasive techniques may obviate the need for mediastinoscopy. A number of studies have evaluated combining EBUS-TBNA.
15 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis A prospective study carried out in an experienced centre examining the safety and efficacy of combining EBUS-TBNA with TBLB and EBB for the diagnosis of sarcoidosis in an unselected group of patients [26] demonstrate a sensitivity of standard bronchoscopic techniques (TBLB and EBB) of 35% (P<0.001) compared with 85% with EBUS-TBNA. Combining the two techniques resulted in a diagnostic yield of 93% (P<0.0001). In this study the relatively low sensitivity with TBLB and EBB was attributed to the fact that the majority of patients had stage I sarcoidosis without evidence of parenchymal disease. Another study in which patients with clinical and radiological evidence of sarcoidosis underwent EBUS-TBNA, TBLB and BAL also supports a combined approach. The diagnostic accuracy was superior with EBUS-TBNA compared with TBLB (p<0.001). Analysis of BAL samples demonstrated that the CD4/CD8 ratio was >3.5 in 65.7% of patients with a final diagnosis of sarcoidosis. The diagnostic yield for all modalities of sampling was very high (100%) in patients with stage II sarcoidosis, however EBUS-TBNA was superior to all other modalities for stage I disease. Of note, all patients underwent cross sectional imaging prior to the procedure and had nodes measuring >10mm diameter. ROSE was also utilized [31]. There is evidence to support the use of combined flexible bronchoscopy and EUS-FNA +/- EBUS-TBNA in order to increase diagnostic yield. Tournoy et al, confirmed this in a study of patients with suspected sarcoidosis who did not have a definite diagnosis following standard bronchoscopic techniques (TBNA, TBLB and EBB) [32]. These patients were sent for EBUS- TBNA and/ or EUS-FNA. A definite diagnosis of sarcoidosis was established in 45% patients following standard flexible bronchoscopic procedures. However diagnostic yield increased by a further 39% with the addition of EBUS-TBNA and/ or EUS-FNA Newer techniques EBUS-guided forceps or transbronchial needle forceps are currently under evaluation. This sampling tool is a combination of a needle and forceps which can be passed through the working channel of the EBUS scope. These forceps can potentially allow larger histological cores of tissue to be obtained. An initial pilot study has shown this tool to be safe and specific diagnosis was established in 86% of patients [33]. 6. Conclusion EBUS-TBNA is a safe, well tolerated and effective mediastinal sampling tool which can be used in the diagnosis of suspected sarcoidosis. As with all mediastinal sampling techniques, histological samples should be interpreted in the context of clinical and radiological findings. EBUS-TBNA has been shown to have a higher diagnostic yield compared to conventional bronchoscopic techniques such as EBB, TBLB and TBNA. Combining EBUS-TBNA with other modalities such as EUS-FNA may further increase diagnostic yield as may the use of newer sampling tools such as the transbronchial needle forceps. Improved accuracy and yield with this technique may obviate the need for further invasive sampling attempts such as mediastinoscopy. This consequently reduces the overall cost compared to other techniques and
16 254 Sarcoidosis importantly reduces the potential for procedure related complications. Future studies are required to further evaluate this technique in sarcoidosis as compared to existing sampling techniques. Author details Abiramy Jeyabalan and Andrew RL Medford * *Address all correspondence to: andrewmedford@hotmail.com North Bristol Lung Centre, Southmead Hospital, Westbury-on-Trym, Bristol, UK References [1] Medford AR. Convex probe endobronchial ultrasound: pitfalls, training and service issues. Br J Hosp Med (Lond). 2011;72(6):312 [2] Nakajima T, Yasufuku K, Takahashi, Shingyoji M, Hirata T, Itami M, Matsui Y, Itakura M, Ilzasa T, Kimura H. Comparison of 21-gauge and 22-gauge aspiration needle during endobronchial ultrasound-guided transbronchial needle aspiration. Respirology 2011;16: [3] Oki M, Saka H, Kitagawa C, Kogure Y, Murata N, Ichihara, Mortamni S, Ando M. Randomized study of 21-gauge versus 22-gauge endobronchial ultrasound-guided transbronchial aspiration needles for sampling histology specimens. J Bronchol Intervent Pulmonol 2011;18: [4] Mountain CF, Dresler CM. Regional lymph node classification for lung cancer staging. Chest 1997; 111: [5] Tremblay A, Stather DR, MacEachern P, Khalil M, Field S. A randomized controlled trial of standard vs endobronchial ultrasonography-guide transbronchial needle aspiration in patients with suspected sarcoidosis. Chest 2009;136(2): [6] Agrawal R, Srinivasan, A, Aggarwal AN, Gupta D. Efficacy and safety of convex probe EBUS-TBNA in sarcoidosis: A systematic review and meta-analysis. Respiratory Medicine 2012;106: [7] Cameron SHE, Andrade RS, Pambuccian. Endobronchial ultrasound-guided transbronchial needle aspiration cytology: a state of the art review. Cytopathology 2010; 21:6-26 [8] Wang H, Rao A, Lafranco A, Vachani A, Haas A, Gupta P. Cell block examination is critical for sarcoidosis diagnosis by endobronchial ultrasound-guided mediastinal
17 Endobronchial Ultrasound in the Diagnostic Evaluation of Sarcoidosis lymph node fine needle aspiration. North American Journal of Medicine and Science 2012;5(4): [9] Kennedy MP, Jimenez CA, Mhatre AD, Morice RC, Eapen GA. Clinical implications of granulomatous inflammation detected by endobronchial ultrasound transbronchial needle aspiration on patients with suspected cancer recurrence in the mediastinum. Journal of Cardiothoracic Surgery 2008;3:8 [10] Fielding D, Bashirzadeh F, Nguyen P, Hodgson A, James, D. Review of the role of EBUS-TBNA for the pulmonologist including lung cancer staging. Thoracic Cancer 2010 doi: /j x [11] Wong M, Yasufuku K, Nakajima T, Herth FJ, Sekine Y, Shibuya K et al. Endobronchial ultrasound: a new insight for the diagnosis of sarcoidosis. Eur Respir J 2007;29: [12] Garwood S, Judson MA, Silvestri G, Hoda R, Fraid M, Doelken P. Endobronchial ultrasound for the diagnosis of pulmonary sarcoidosis. Chest 2007; 132: [13] British Thoracic Society Bronchoscopy Guidelines Committee, a Subcommittee of the Standards of Care Committee of the British Thoracic Society. Thorax (2001);56:(suppl I) i1 i21 British Thoracic Society guidelines on diagnostic flexible bronchoscopy [14] Stather DR, MacEachern P, Chee A, Tremblay A. Safety of endobronchial ultrasoundguided transbronchial needle aspiration in patients taking clopidogrel: a report of 12 consecutive cases. Respiration 2012; 83(4):330-4 [15] Medford ARL, Bennett JA, Free CM and Agrawal S. Endobronchial ultrasound guided transbronchial needle aspiration. Postgrad Med J 2010; 86: [16] Pillai A and Medford ARL. Upcoming endoscopic techniques: endobronchial ultrasound-guided transbronchial needle aspiration. Minerva Pneumol 2011;50:67-82 [17] Ernst A, Silvestri GA, Johnstone D. American College of Chest Physicians. Interventional pulmonary procedures: Guidelines from the American College of Chest Physicians. Chest 2003; 123: [18] Medford AR. Learning curve for endobronchial ultrasound-guided transbronchial needle aspiration. Chest 2012;141(6): [19] Fernandez-Villar A, Leiro-Fernandez V, Botana-Rial M, Represas-Represas C, Nunez- Delgado M. The endobronchial ultrasound-guided transbronchial needle biopsy learning curve for mediastinal and hilar lymph node diagnosis. Chest 2012; 1411: [20] Haponik EF, Shure D. Underutilization of transbronchial needle aspiration: experiences of current pulmonary fellows. Chest. 1997;112(1):251 [21] Tremblay A, Stather DR, MacEachern P, Khalil M, Field SK. A randomized controlled trial of standard vs endobronchial ultrasonography-guided transbronchial needle aspiration in patients with suspected sarcoidosis. Chest 2009;136(2):
18 256 Sarcoidosis [22] Costabel U. CD4/CD8 ratios in bronchoalveolar lavage fluid: of value for diagnosing sarcoidosis (comment). Eur Respir J 1997;10: [23] de Boer S, Wilsher M. Sarcoidosis. Chronic respiratory disease 2010;7(4): [24] Shorr AF, Torrington KG, Hnatiuk OW. Endobronchial biopsy for sarcoidosis: a prospective study. Chest 2001;120(1): [25] Plit M, Perason R, Da Costa J, Glanville AR. The diagnostic utility of endobronchial ultrasound-guided transbronchial needle aspiration compared to transbronchial and endobronchial biopsy for suspected sarcoidosis. Internal Medicine Journal 2011;42(4): [26] Navani N, Booth HL, Kocjan G, Falzon M, Capitanio A, Brown JM et al. Combination of endobronchial ultrasound guided transbronchial needle aspiration with standard bronchoscopic techniques for the diagnosis of stage I and stage II pulmonary sarcoidosis. Respirology 2011;16(3): [27] Medford AR, Agrawal S. Single bronchoscope combined endoscopic-endobronchial ultrasound guided fine-needle aspiration for tuberculous mediastinal nodes. Chest 2010;138(5):1274 [28] Hwangbo B, Lee GK, Lee HS, Lim KY, Lee SH, Kim HY, Lee HS, Kim MS, Lee JM, Nam BH, Zo JL. Transbronchial and transoesophageal fine-needle aspiration using an ultrasound bronchoscope in mediastinal staging of potentially operable lung cancer. Chest 2010;138(4): [29] Wildi SM, Judson MA, Friag M, Fickling E, Schmulewitz N, Varadarajulu S, Roberts SS, Prasad P, Hawes RH, Wallace MB, Hoffman BJ. Is endosonography guided fine needle aspiration (EUS-FNA) for sarcoidosis as good as we think. Thorax 2004; 59: [30] Yanardag H, Caner M, Papila I, Uygun S, Demirci S, Karayel T. Diagnostic value of peripheral lymph node biopsy in sarcoidosis: A report of 67 cases. Can Respir J 2007; 14(4): [31] Nakajima T, Yasufuku K, Kurisu K, Takiguchi Y, Fugiwara T, Chiyo M, Shibuya K, Hiroshima K, Nakatani Y, Yoshino I. The role of EBUS-TBNA for the diagnosis of sarcoidosis comparisons with other bronchoscopic diagnostic modalities. Respiratory Medicine 2009;103: [32] Tournoy KG, Bolly A, Aerts JG, Pierard P, De Pauw R, Leduc D et al. The value of endoscopic ultrasound after bronchoscopy to diagnose thoracic sarcoidosis. Eur Respir J 2010; 35(6): [33] Herth H, Gompelmann D, Kahn N, Gasparini S, Ernst A, Schuhmann M, Eberhardt R. Endobronchial ultrasound-guided lymph node biopsy with transbronchial needle forceps: a pilot study. Eur Respir J 2012;39(2): 373-7
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis)
 Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Diagnostic Value of EBUS-TBNA in Various Lung Diseases (Lymphoma, Tuberculosis, Sarcoidosis) Sevda Sener Cömert, MD, FCCP. SBU, Kartal Dr.Lütfi Kırdar Training and Research Hospital Department of Pulmonary
Use of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration (EBUS- TBNA) in the Diagnosis of Granulomatous Mediastinal Lymphadenopathy
 Original Article 250 Use of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration (EBUS- TBNA) in the Diagnosis of Granulomatous Mediastinal Lymphadenopathy Su Ying Low, 1 BMBCh, Mariko S Koh,
Original Article 250 Use of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration (EBUS- TBNA) in the Diagnosis of Granulomatous Mediastinal Lymphadenopathy Su Ying Low, 1 BMBCh, Mariko S Koh,
Abhishek Biswas 1, John P. Wynne 2, Divya Patel 1, Michelle Weber 3, Shaleen Thakur 4, P. S. Sriram 1
 Letter to the Editor Comparison of the yield of 19-G excelon core needle to a 21-G EUS needle during endobronchial ultrasound guided transbronchial needle aspiration of mediastinal lymph nodes for the
Letter to the Editor Comparison of the yield of 19-G excelon core needle to a 21-G EUS needle during endobronchial ultrasound guided transbronchial needle aspiration of mediastinal lymph nodes for the
Endobronchial ultrasound-guided lymph node biopsy with transbronchial needle forceps: a pilot study
 Eur Respir J 2012; 39: 373 377 DOI: 10.1183/09031936.00033311 CopyrightßERS 2012 Endobronchial ultrasound-guided lymph node biopsy with transbronchial needle forceps: a pilot study F.J.F. Herth*, H. Schuler*,
Eur Respir J 2012; 39: 373 377 DOI: 10.1183/09031936.00033311 CopyrightßERS 2012 Endobronchial ultrasound-guided lymph node biopsy with transbronchial needle forceps: a pilot study F.J.F. Herth*, H. Schuler*,
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE
 NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
NATIONAL INSTITUTE FOR HEALTH AND CLINICAL EXCELLENCE INTERVENTIONAL PROCEDURES PROGRAMME Interventional procedure overview of endobronchial ultrasound-guided transbronchial needle aspiration for mediastinal
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL
 The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
The Various Methods to Biopsy the Lung PROF SHITRIT DAVID HEAD, PULMONARY DEPARTMENT MEIR MEDICAL CENTER, ISRAEL Conflict of Interest This presentation is supported by AstraZeneca Two main steps before
Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases
 Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases Akintayo Sokunbi, M.D MidMichigan Hospital Midland, Michigan Objectives Discuss EBUS guided biopsy principles
Utilizing EBUS (Endobronchial Ultrasound) for Diagnosis of Lung Cancer and other Pulmonary Diseases Akintayo Sokunbi, M.D MidMichigan Hospital Midland, Michigan Objectives Discuss EBUS guided biopsy principles
Endoscopy. Pulmonary Endoscopy
 Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Pulmonary 1 Direct visualization of TB tree Developed in 1890 s to remove foreign bodies - rigid metal tube Advances added light system, Sx Flexible fiberoptic scopes introduced in early 1960 s 2 Used
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/1887/44702 holds various files of this Leiden University dissertation. Author: Von Bartheld, M.B. Title: Advancements in pulmonary endosonography : the new standard
Cover Page The handle http://hdl.handle.net/1887/44702 holds various files of this Leiden University dissertation. Author: Von Bartheld, M.B. Title: Advancements in pulmonary endosonography : the new standard
General Thoracic Surgery
 General Thoracic Surgery Oki et al Prospective study of endobronchial ultrasound guided transbronchial needle aspiration of lymph nodes versus transbronchial lung biopsy of lung tissue for diagnosis of
General Thoracic Surgery Oki et al Prospective study of endobronchial ultrasound guided transbronchial needle aspiration of lymph nodes versus transbronchial lung biopsy of lung tissue for diagnosis of
endoscopic ultrasound-guided fine-needle aspiration
 Original article 213 Endoscopic ultrasound-guided fine-needle aspiration for the diagnosis of sarcoidosis Authors M. B. von Bartheld 1, M. Veseliç-Charvat 2, K. F. Rabe 1, J. T. Annema 1 Institutions 1
Original article 213 Endoscopic ultrasound-guided fine-needle aspiration for the diagnosis of sarcoidosis Authors M. B. von Bartheld 1, M. Veseliç-Charvat 2, K. F. Rabe 1, J. T. Annema 1 Institutions 1
ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM
 ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM This competency-based curriculum has been designed by a task force of interventional pulmonology specialists to underline the learning outcomes
ENDOBRONCHIAL ULTRASOUND (EBUS) TRAINING PROGRAMME CURRICULUM This competency-based curriculum has been designed by a task force of interventional pulmonology specialists to underline the learning outcomes
Endobronchial ultrasound: what is it and when should it be used?
 CLINICAL PRACTICE Clinical Medicine 2010, Vol 10, No 5: 458 63 Endobronchial ultrasound: what is it and when should it be used? ARL Medford ABSTRACT Endobronchial ultrasound has become increasingly used
CLINICAL PRACTICE Clinical Medicine 2010, Vol 10, No 5: 458 63 Endobronchial ultrasound: what is it and when should it be used? ARL Medford ABSTRACT Endobronchial ultrasound has become increasingly used
Introduction to Interventional Pulmonology
 Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
Introduction to Interventional Pulmonology Alexander Chen, M.D. Director, Interventional Pulmonology Assistant Professor of Medicine and Surgery Divisions of Pulmonary and Critical Care Medicine and Cardiothoracic
EBUS-TBNA in PET-positive lymphadenopathies in treated cancer patients
 ORIGINAL ARTICLE LUNG IMAGING EBUS-TBNA in PET-positive lymphadenopathies in treated cancer patients Juliana Guarize 1, Monica Casiraghi 1, Stefano Donghi 1, Chiara Casadio 2, Cristina Diotti 1, Niccolò
ORIGINAL ARTICLE LUNG IMAGING EBUS-TBNA in PET-positive lymphadenopathies in treated cancer patients Juliana Guarize 1, Monica Casiraghi 1, Stefano Donghi 1, Chiara Casadio 2, Cristina Diotti 1, Niccolò
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP Lead Lung Cancer Clinician, Consultant Respiratory Physician & Speciality Director Manchester University NHS
The diagnostic efficacy and safety of endobronchial ultrasound-guided transbronchial needle aspiration as an initial diagnostic tool
 ORIGINAL ARTICLE Korean J Intern Med 2013;28.660-667 The diagnostic efficacy and safety of endobronchial ultrasound-guided transbronchial needle aspiration as an initial diagnostic tool Young Rak Choi
ORIGINAL ARTICLE Korean J Intern Med 2013;28.660-667 The diagnostic efficacy and safety of endobronchial ultrasound-guided transbronchial needle aspiration as an initial diagnostic tool Young Rak Choi
Endoscopic ultrasound-guided needle aspiration in lung cancer
 ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
ORIGINAL ARTICLE Artur Szlubowski 1, Marcin Zieliński 1, Joanna Figura 1, Jolanta Hauer 1, Witold Sośnicki 1, Juliusz Pankowski 2, Anna Obrochta 2, Magdalena Jakubiak 2 1 Department of Thoracic Surgery
The Role of Endobronchial Biopsy in the Diagnosis of Pulmonary Sarcoidosis
 DOI: 10.5578/ttj.17.1.004 ORIGINAL INVESTIGATION The Role of Endobronchial Biopsy in the Diagnosis of Pulmonary Sarcoidosis Tuğba Göktalay 1, Pınar Çelik 1, Aylin Özgen Alpaydın 2, Yavuz Havlucu 1, Ayşın
DOI: 10.5578/ttj.17.1.004 ORIGINAL INVESTIGATION The Role of Endobronchial Biopsy in the Diagnosis of Pulmonary Sarcoidosis Tuğba Göktalay 1, Pınar Çelik 1, Aylin Özgen Alpaydın 2, Yavuz Havlucu 1, Ayşın
Endobronchial Ultrasound and Lymphoproliferative Disorders: A Retrospective Study
 Endobronchial Ultrasound and Lymphoproliferative Disorders: A Retrospective Study Seher Iqbal, MD,* Zachary S. DePew, MD,* Paul J. Kurtin, MD, Anne-Marie G. Sykes, MD, Geoffrey B. Johnson, MD, Eric S.
Endobronchial Ultrasound and Lymphoproliferative Disorders: A Retrospective Study Seher Iqbal, MD,* Zachary S. DePew, MD,* Paul J. Kurtin, MD, Anne-Marie G. Sykes, MD, Geoffrey B. Johnson, MD, Eric S.
Mediastinal Mysteries: What can be solved with EBUS?
 Mediastinal Mysteries: What can be solved with EBUS? W. Graham Carlos MD Pulmonary & Critical Care Fellow Indiana University School of Medicine Disclosures None Objectives Introduce you to the technique
Mediastinal Mysteries: What can be solved with EBUS? W. Graham Carlos MD Pulmonary & Critical Care Fellow Indiana University School of Medicine Disclosures None Objectives Introduce you to the technique
A Standard Endobronchial Ultrasound Image Classification System
 CHEST Original Research INTERVENTIONAL PULMONOLOGY The Utility of Sonographic Features During Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for Lymph Node Staging in Patients With Lung
CHEST Original Research INTERVENTIONAL PULMONOLOGY The Utility of Sonographic Features During Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for Lymph Node Staging in Patients With Lung
Mediastinal lymphadenopathy is a common finding in
 ORIGINAL ARTICLE Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for the Diagnosis of Intrathoracic Lymphadenopathy in Patients with Extrathoracic Malignancy A Multicenter Study Neal Navani,
ORIGINAL ARTICLE Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for the Diagnosis of Intrathoracic Lymphadenopathy in Patients with Extrathoracic Malignancy A Multicenter Study Neal Navani,
Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules
 Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Original article Electromagnetic navigational bronchoscopy in patients with solitary pulmonary nodules Samuel Copeland MD, Shrinivas Kambali MD, Gilbert Berdine MD, Raed Alalawi MD Abstract Background:
Endobronchial Ultrasound Guided Transbronchial Needle Aspiration in the Diagnosis of Lymphoma.
 Thorax Online First, published on October 26, 200 as 10.1136/thx.200.08409 Title Page Endobronchial Ultrasound Guided Transbronchial Needle Aspiration in the Diagnosis of. Marcus P Kennedy MD 1, Carlos
Thorax Online First, published on October 26, 200 as 10.1136/thx.200.08409 Title Page Endobronchial Ultrasound Guided Transbronchial Needle Aspiration in the Diagnosis of. Marcus P Kennedy MD 1, Carlos
Endobronchial ultrasound-guided transbronchial needle aspiration in the diagnosis of lymphoma
 1 Department of Pulmonary Medicine, University of Texas MD 2 Department of Radiology, 3 Department of Statistics, 4 Department of Leukemia, 5 Department of Pathology, Houston, Texas, USA Correspondence
1 Department of Pulmonary Medicine, University of Texas MD 2 Department of Radiology, 3 Department of Statistics, 4 Department of Leukemia, 5 Department of Pathology, Houston, Texas, USA Correspondence
MEDIASTINAL STAGING surgical pro
 MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
MEDIASTINAL STAGING surgical pro Paul E. Van Schil, MD, PhD Department of Thoracic and Vascular Surgery University of Antwerp, Belgium Mediastinal staging Invasive techniques lymph node mapping cervical
Chest radiograph of an. asymptomatic man. Case report. Case history
 Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Eleftheria Chaini 1, Niki Giannakou 2, Dimitra Haini 3, Anna Maria Athanassiadou 4, Angelos Tsipis 4, Nikolaos D. Hainis 5 elhaini@otenet.gr 1 Pulmonary Dept, Corfu General Hospital, Kontokali, Greece.
Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire. V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique
 Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique 1 Invasive Mediastinal Staging Purpose : to exclude Involvement
Les techniques invasives et minimalement invasives dans le staging du cancer bronchopulmonaire V. Ninane, Hôpital Saint-Pierre, Bruxelles, Belgique 1 Invasive Mediastinal Staging Purpose : to exclude Involvement
Bronchoscopy and endobronchial ultrasound for diagnosis and staging of lung cancer
 FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
FRANCISCO AÉCIO ALMEIDA, MD, MS, FCCP Associate Staff Member, Director, Interventional Pulmonary Medicine Fellowship Program, Respiratory Institute, Cleveland Clinic, Cleveland, OH Bronchoscopy and endobronchial
Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration vs Conventional Transbronchial Needle Aspiration in the Diagnosis of Sarcoidosis
 [ Original Research Pulmonary Procedures ] Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration vs Conventional Transbronchial Needle Aspiration in the Diagnosis of Sarcoidosis Dheeraj Gupta,
[ Original Research Pulmonary Procedures ] Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration vs Conventional Transbronchial Needle Aspiration in the Diagnosis of Sarcoidosis Dheeraj Gupta,
Looking beyond the bronchial wall.
 10th anniversary of scientific study ON EBUS-TBNA A review Looking beyond the bronchial wall. Am J Respir Crit Care Med Eur Respir J Endoscopy Chest JAMA Thorax J Bronchol J Clin Oncol J Thorac Oncol Ann
10th anniversary of scientific study ON EBUS-TBNA A review Looking beyond the bronchial wall. Am J Respir Crit Care Med Eur Respir J Endoscopy Chest JAMA Thorax J Bronchol J Clin Oncol J Thorac Oncol Ann
Accurate mediastinal staging is a critical component
 Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Endobronchial Ultrasound for Lung Cancer Staging: How Many Stations Should Be Sampled? Mark I. Block, MD Thoracic Surgery, Memorial Healthcare System, Hollywood, Florida Background. No guidelines exist
Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions
 Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions Original Effective Date: 8/25/14 Policy Number: MCP-206 Revision Date(s): Review
Subject: Virtual Bronchoscopy and Electromagnetic Navigational Bronchoscopy for Evaluation of Peripheral Pulmonary Lesions Original Effective Date: 8/25/14 Policy Number: MCP-206 Revision Date(s): Review
REVIEW ARTICLES. Aslam Khan, Shahid Jamal, Jawad Khaliq Ansari, Arshad Naseem
 REVIEW ARTICLES A REVIEW OF ENDOBRONCHIAL ULTRASOUND GUIDED TRANSBRONCHIAL NEEDLE ASPIRATE (EBUS-TBNA) Aslam Khan, Shahid Jamal, Jawad Khaliq Ansari, Arshad Naseem Army Medical College & National University
REVIEW ARTICLES A REVIEW OF ENDOBRONCHIAL ULTRASOUND GUIDED TRANSBRONCHIAL NEEDLE ASPIRATE (EBUS-TBNA) Aslam Khan, Shahid Jamal, Jawad Khaliq Ansari, Arshad Naseem Army Medical College & National University
Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer
 Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Original Article on Transbronchial Needle Aspiration (TBNA) Standardized transbronchial needle aspiration procedure for intrathoracic lymph node staging of non-small cell lung cancer Xu-Ru Jin 1 *, Min
Mediastinal Staging. Samer Kanaan, M.D.
 Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Mediastinal Staging Samer Kanaan, M.D. Overview Importance of accurate nodal staging Accuracy of radiographic staging Mediastinoscopy EUS EBUS Staging TNM Definitions T Stage Size of the Primary Tumor
Role of EBUS in mediastinal staging of lung cancer. -Dr. Nandakishore Baikunje
 Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
Role of EBUS in mediastinal staging of lung cancer -Dr. Nandakishore Baikunje Overview of the seminar Introduction Endosonography to stage the mediastinum Technical aspects of EBUS-TBNA for mediastinal
RESPIRATORY CARE Paper in Press. Published on March 10, 2015 as DOI: /respcare.03779
 Utility and Safety of Endoscopic Ultrasound With Bronchoscope- Guided Fine-Needle Aspiration in Mediastinal Lymph Node Sampling: Systematic Review and Meta-Analysis Sahajal Dhooria MD DM, Ashutosh N Aggarwal
Utility and Safety of Endoscopic Ultrasound With Bronchoscope- Guided Fine-Needle Aspiration in Mediastinal Lymph Node Sampling: Systematic Review and Meta-Analysis Sahajal Dhooria MD DM, Ashutosh N Aggarwal
A Guide to Endobronchial and Endoscopic Ultrasound (EBUS and EUS) for Thoracic Radiologists.
 A Guide to Endobronchial and Endoscopic Ultrasound (EBUS and EUS) for Thoracic Radiologists. AP Barker 1, S Karia 1, NR Carroll 1,2, RC Rintoul 2, J Herre 1, EM Godfrey 1, S Ramasundara 1, JL Babar 1 ;
A Guide to Endobronchial and Endoscopic Ultrasound (EBUS and EUS) for Thoracic Radiologists. AP Barker 1, S Karia 1, NR Carroll 1,2, RC Rintoul 2, J Herre 1, EM Godfrey 1, S Ramasundara 1, JL Babar 1 ;
Transbronchial fine needle aspiration
 Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
Thorax 1982;37 :270-274 Transbronchial fine needle aspiration J LEMER, E MALBERGER, R KONIG-NATIV From the Departments of Cardio-thoracic Surgery and Cytology, Rambam Medical Center, Haifa, Israel ABSTRACT
Endobronchial ultrasound-guided transbronchial needle aspiration for staging of non-small cell lung cancer
 Surgical Technique on Thoracic Surgery Page 1 of 6 Endobronchial ultrasound-guided transbronchial needle aspiration for staging of non-small cell lung cancer Habiba Hashimi 1, David T. Cooke 1, Elizabeth
Surgical Technique on Thoracic Surgery Page 1 of 6 Endobronchial ultrasound-guided transbronchial needle aspiration for staging of non-small cell lung cancer Habiba Hashimi 1, David T. Cooke 1, Elizabeth
Chapter 8. Other Important Tests and Procedures. Mosby items and derived items 2011, 2006 by Mosby, Inc., an affiliate of Elsevier Inc.
 Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
Chapter 8 Other Important Tests and Procedures 1 Introduction Additional important diagnostic studies include: Sputum examination Skin tests Endoscopic examination Lung biopsy Thoracentesis Hematology,
INTRODUCTION. Jpn J Clin Oncol 2013;43(11) doi: /jjco/hyt123 Advance Access Publication 29 August 2013
 Jpn J Clin Oncol 2013;43(11)1110 1114 doi:10.1093/jjco/hyt123 Advance Access Publication 29 August 2013 Usefulness of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration in Distinguishing
Jpn J Clin Oncol 2013;43(11)1110 1114 doi:10.1093/jjco/hyt123 Advance Access Publication 29 August 2013 Usefulness of Endobronchial Ultrasound-guided Transbronchial Needle Aspiration in Distinguishing
Electromagnetic Navigation Bronchoscopy
 Medical Policy Manual Surgery, Policy No. 179 Electromagnetic Navigation Bronchoscopy Next Review: March 2018 Last Review: March 2017 Effective: May 1, 2017 IMPORTANT REMINDER Medical Policies are developed
Medical Policy Manual Surgery, Policy No. 179 Electromagnetic Navigation Bronchoscopy Next Review: March 2018 Last Review: March 2017 Effective: May 1, 2017 IMPORTANT REMINDER Medical Policies are developed
Endobronchial ultrasound-guided transbronchial needle aspiration for staging of lung cancer: a concise review
 Review Article Endobronchial ultrasound-guided transbronchial needle aspiration for staging of lung cancer: a concise review Fahad Aziz Department of Internal Medicine, Section on Hospital Medicine, Wake
Review Article Endobronchial ultrasound-guided transbronchial needle aspiration for staging of lung cancer: a concise review Fahad Aziz Department of Internal Medicine, Section on Hospital Medicine, Wake
The value of endoscopic ultrasound after bronchoscopy to diagnose thoracic sarcoidosis
 Eur Respir J 2010; 35: 1329 1335 DOI: 10.1183/09031936.00111509 CopyrightßERS 2010 The value of endoscopic ultrasound after bronchoscopy to diagnose thoracic sarcoidosis K.G. Tournoy, A. Bolly, J.G. Aerts,
Eur Respir J 2010; 35: 1329 1335 DOI: 10.1183/09031936.00111509 CopyrightßERS 2010 The value of endoscopic ultrasound after bronchoscopy to diagnose thoracic sarcoidosis K.G. Tournoy, A. Bolly, J.G. Aerts,
Transbronchial fine needle aspiration cytology in the diagnosis of mediastinal/hilar sarcoidosis
 DOI:10.1111/j.1365-2303.2006.00336.x Transbronchial fine needle aspiration cytology in the diagnosis of mediastinal/hilar sarcoidosis S. Smojver-Ježek*, T. Peroš-Golubičić, J. Tekavec-Trkanjec, I. Mažuranić
DOI:10.1111/j.1365-2303.2006.00336.x Transbronchial fine needle aspiration cytology in the diagnosis of mediastinal/hilar sarcoidosis S. Smojver-Ježek*, T. Peroš-Golubičić, J. Tekavec-Trkanjec, I. Mažuranić
Multicentric study of endobronchial ultrasound-transbronchial needle aspiration for lung cancer staging in Italy
 Original Article Multicentric study of endobronchial ultrasound-transbronchial needle aspiration for lung cancer staging in Italy Nicola Rotolo 1, Andrea Imperatori 1, Mario Nosotti 2, Luigi Santambrogio
Original Article Multicentric study of endobronchial ultrasound-transbronchial needle aspiration for lung cancer staging in Italy Nicola Rotolo 1, Andrea Imperatori 1, Mario Nosotti 2, Luigi Santambrogio
Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis
 1 Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis Optimal management of Cancer Histological diagnosis & accurate staging at presentation Molecular analysis of primary tumour
1 Assessing the lung and mediastinum in cancer-is tissue the issue? George Santis Optimal management of Cancer Histological diagnosis & accurate staging at presentation Molecular analysis of primary tumour
Endosonography guided fine needle aspiration in the diagnosis of sarcoidosis: a randomized study
 ORIGINAL ARTICLE Endosonography guided fine needle aspiration in the diagnosis of sarcoidosis: a randomized study Piotr Kocoń 1, Artur Szlubowski 2, Jarosław Kużdżał 1, Lucyna Rudnicka Sosin 3, Adam Ćmiel
ORIGINAL ARTICLE Endosonography guided fine needle aspiration in the diagnosis of sarcoidosis: a randomized study Piotr Kocoń 1, Artur Szlubowski 2, Jarosław Kużdżał 1, Lucyna Rudnicka Sosin 3, Adam Ćmiel
The value of endoscopic ultrasound after bronchoscopy to diagnose thoracic sarcoidosis
 ERJ Express. Published on November 6, 2009 as doi: 10.1183/09031936.00111509 The value of endoscopic ultrasound after bronchoscopy to diagnose thoracic sarcoidosis K.G. Tournoy 1, A. Bolly 2, J.G. Aerts
ERJ Express. Published on November 6, 2009 as doi: 10.1183/09031936.00111509 The value of endoscopic ultrasound after bronchoscopy to diagnose thoracic sarcoidosis K.G. Tournoy 1, A. Bolly 2, J.G. Aerts
Corporate Medical Policy Electromagnetic Navigation Bronchoscopy
 Corporate Medical Policy Electromagnetic Navigation Bronchoscopy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: electromagnetic_navigation_bronchoscopy 1/2010 3/2017 3/2018 9/2017
Corporate Medical Policy Electromagnetic Navigation Bronchoscopy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: electromagnetic_navigation_bronchoscopy 1/2010 3/2017 3/2018 9/2017
EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE. Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University
 EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University Objectives Brief overview of EBUS-FNA Strategies to optimize
EBUS-FNAB: HOW TO OPTIMIZE YOUR CYTOLOGY SAMPLES, LHSC EXPERIENCE Dr. Mariamma Joseph Division Head of Cytopathology LHSC and Western University Objectives Brief overview of EBUS-FNA Strategies to optimize
Lung biopsy (mucosal/transbronchial/open lung)
 Lung biopsy (mucosal/transbronchial/open lung) Ernst Eber, MD Respiratory and Allergic Disease Division, Paediatric Department, Medical University of Graz, Austria ERS Task Force. Eur Respir J 2003;22:698-708.
Lung biopsy (mucosal/transbronchial/open lung) Ernst Eber, MD Respiratory and Allergic Disease Division, Paediatric Department, Medical University of Graz, Austria ERS Task Force. Eur Respir J 2003;22:698-708.
Endoscopic and Endobronchial Ultrasound Staging for Lung Cancer. Michael B. Wallace, MD, MPH Professor of Medicine Mayo Clinic, Jacksonville
 Endoscopic and Endobronchial Ultrasound Staging for Lung Cancer Michael B. Wallace, MD, MPH Professor of Medicine Mayo Clinic, Jacksonville Background: Lung Cancer 170,000 cases/yr in U.S. (# 1 cancer)
Endoscopic and Endobronchial Ultrasound Staging for Lung Cancer Michael B. Wallace, MD, MPH Professor of Medicine Mayo Clinic, Jacksonville Background: Lung Cancer 170,000 cases/yr in U.S. (# 1 cancer)
Larry Tan, MD Thoracic Surgery, HSC. Community Cancer Care Educational Conference October 27, 2017
 Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Larry Tan, MD Thoracic Surgery, HSC Community Cancer Care Educational Conference October 27, 2017 To describe patient referral & triage for the patient with suspected lung cancer To describe the initial
Owing to the recent attention given to lung cancer
 Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
Electromagnetic : A Surgeon s Perspective Todd S. Weiser, MD, Kevin Hyman, MD, Jaime Yun, MD, Virginia Litle, MD, Cythinia Chin, MD, and Scott J. Swanson, MD Department of Cardiothoracic Surgery, Mount
Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C.
 Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Research Grants: Disclosures
Endoscopic UltraSound (EUS) Endoscopic Mucosal Resection (EMR) Moishe Liberman Director C.E.T.O.C. Division of Thoracic Surgery Centre Hospitalier de l Université de Montréal Research Grants: Disclosures
Endoscopic ultrasound-guided fine-needle aspiration for the diagnosis of sarcoidosis
 Eur Respir J 2005; 25: 405 409 DOI: 10.1183/09031936.05.00098404 CopyrightßERS Journals Ltd 2005 Endoscopic ultrasound-guided fine-needle aspiration for the diagnosis of sarcoidosis J.T. Annema*, M. Veseliç
Eur Respir J 2005; 25: 405 409 DOI: 10.1183/09031936.05.00098404 CopyrightßERS Journals Ltd 2005 Endoscopic ultrasound-guided fine-needle aspiration for the diagnosis of sarcoidosis J.T. Annema*, M. Veseliç
ORIGINAL ARTICLE Oncology & Hematology INTRODUCTION MATERIALS AND METHODS
 ORIGINAL ARTICLE Oncology & Hematology http://dx.doi.org/10.3346/jkms.2013.28.4.550 J Korean Med Sci 2013; 28: 550-554 Clinical Implication of Microscopic Anthracotic Pigment in Mediastinal Staging of
ORIGINAL ARTICLE Oncology & Hematology http://dx.doi.org/10.3346/jkms.2013.28.4.550 J Korean Med Sci 2013; 28: 550-554 Clinical Implication of Microscopic Anthracotic Pigment in Mediastinal Staging of
Specimen Processing Techniques for Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration
 Specimen Processing Techniques for Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration Jennifer W. Toth, MD, Konstantin Zubelevitskiy, MD, Jennifer A. Strow, DO, Jussuf T. Kaifi, MD, PhD,
Specimen Processing Techniques for Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration Jennifer W. Toth, MD, Konstantin Zubelevitskiy, MD, Jennifer A. Strow, DO, Jussuf T. Kaifi, MD, PhD,
Cervical Lymph Nodes
 Cervical Lymph Nodes Diana Gaitini, MD Unit of Ultrasound, Department of Medical Imaging Rambam Medical Center and Faculty of Medicine Technion, Israel Institute of Technology Haifa, Israel Learning Targets
Cervical Lymph Nodes Diana Gaitini, MD Unit of Ultrasound, Department of Medical Imaging Rambam Medical Center and Faculty of Medicine Technion, Israel Institute of Technology Haifa, Israel Learning Targets
Patient Satisfaction During Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration Performed Under Conscious Sedation
 Patient Satisfaction During Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration Performed Under Conscious Sedation Daniel P Steinfort MBBS FRACP and Louis B Irving MBBS FRACP BACKGROUND: Mediastinal
Patient Satisfaction During Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration Performed Under Conscious Sedation Daniel P Steinfort MBBS FRACP and Louis B Irving MBBS FRACP BACKGROUND: Mediastinal
Felix J. F. Herth, MD, FCCP; Ralf Eberhardt, MD; Mark Krasnik, MD; and Armin Ernst, MD, FCCP
 Original Research INTERVENTIONAL PULMONOLOGY Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration of Lymph Nodes in the Radiologically and Positron Emission Tomography-Normal Mediastinum in
Original Research INTERVENTIONAL PULMONOLOGY Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration of Lymph Nodes in the Radiologically and Positron Emission Tomography-Normal Mediastinum in
Respiratory Interactive Session. Elaine Borg
 Respiratory Interactive Session Elaine Borg Case 1 Respiratory Cytology 55 year old gentleman Anterior mediastinal mass EBUS FNA Case 1 Respiratory Cytology 55 year old gentleman with anterior mediastinal
Respiratory Interactive Session Elaine Borg Case 1 Respiratory Cytology 55 year old gentleman Anterior mediastinal mass EBUS FNA Case 1 Respiratory Cytology 55 year old gentleman with anterior mediastinal
Središnja medicinska knjižnica.
 Središnja medicinska knjižnica Smojver-Ježek, S., Peroš-Golubičić, T., Tekavec-Trkanjec, J., Mažuranić, I., Alilović, M. (2007) Transbronchial fine needle aspiration cytology in the diagnosis of mediastinal/hilar
Središnja medicinska knjižnica Smojver-Ježek, S., Peroš-Golubičić, T., Tekavec-Trkanjec, J., Mažuranić, I., Alilović, M. (2007) Transbronchial fine needle aspiration cytology in the diagnosis of mediastinal/hilar
Electromagnetic Navigation Bronchoscopy
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Endobronchial Ultrasound for Diagnosis and Staging of Lung Cancer
 Endobronchial Ultrasound for Diagnosis and Staging of Lung Cancer Policy Number: 6.01.58 Last Review: 08/2017 Origination: 08/2015 Next Review: 08/2018 Policy Blue Cross and Blue Shield of Kansas City
Endobronchial Ultrasound for Diagnosis and Staging of Lung Cancer Policy Number: 6.01.58 Last Review: 08/2017 Origination: 08/2015 Next Review: 08/2018 Policy Blue Cross and Blue Shield of Kansas City
Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis
 CHEST Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis Carlos G. Micames, MD; Douglas C. McCrory, MD; Darren A. Pavey, MD;
CHEST Endoscopic Ultrasound-Guided Fine- Needle Aspiration for Non-small Cell Lung Cancer Staging* A Systematic Review and Metaanalysis Carlos G. Micames, MD; Douglas C. McCrory, MD; Darren A. Pavey, MD;
GENERAL THORACIC SURGERY
 GENERAL THORACIC SURGERY A prospective controlled trial of endobronchial ultrasound-guided transbronchial needle aspiration compared with mediastinoscopy for mediastinal lymph node staging of lung cancer
GENERAL THORACIC SURGERY A prospective controlled trial of endobronchial ultrasound-guided transbronchial needle aspiration compared with mediastinoscopy for mediastinal lymph node staging of lung cancer
Combined endobronchial and oesophageal endosonography for the diagnosis and staging of lung cancer
 TASK FORCE REPORT ESGE/ERS/ESTS GUIDELINES Combined endobronchial and oesophageal endosonography for the diagnosis and staging of lung cancer European Society of Gastrointestinal Endoscopy (ESGE) Guideline,
TASK FORCE REPORT ESGE/ERS/ESTS GUIDELINES Combined endobronchial and oesophageal endosonography for the diagnosis and staging of lung cancer European Society of Gastrointestinal Endoscopy (ESGE) Guideline,
Pulmonary Sarcoidosis - Radiological Evaluation
 Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
Original Research Article Pulmonary Sarcoidosis - Radiological Evaluation Jayesh Shah 1, Darshan Shah 2*, C. Raychaudhuri 3 1 Associate Professor, 2 1 st Year Resident, 3 Professor and HOD Radiology Department,
FLEXIBLE BRONCHOSCOPY INSPECTION, BAL, BX AND TBLB
 FLEXIBLE BRONCHOSCOPY INSPECTION, BAL, BX AND TBLB Bronchoscopy Education Project Assessment Tools Scoring Recommendations for Bronchoscopy Assessment Tools (BSTAT, BSTAT-TBLB/TBNA, BSAT) The goal of these
FLEXIBLE BRONCHOSCOPY INSPECTION, BAL, BX AND TBLB Bronchoscopy Education Project Assessment Tools Scoring Recommendations for Bronchoscopy Assessment Tools (BSTAT, BSTAT-TBLB/TBNA, BSAT) The goal of these
BRONCHOSCOPY AND ASSOCIATED PROCEDURE CODING IN ICD-10-PCS AND CPT
 BRONCHOSCOPY AND ASSOCIATED PROCEDURE CODING IN ICD-10-PCS AND CPT WHY AND HOW IS A BRONCHOSCOPY PERFORMED? A bronchoscopy is a test to view the airways and diagnose lung disease. It may also be used during
BRONCHOSCOPY AND ASSOCIATED PROCEDURE CODING IN ICD-10-PCS AND CPT WHY AND HOW IS A BRONCHOSCOPY PERFORMED? A bronchoscopy is a test to view the airways and diagnose lung disease. It may also be used during
Endobronchial ultrasound-guided transbronchial needle aspiration
 ORIGINAL ARTICLE Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for the Evaluation of Suspected Lymphoma Daniel P. Steinfort, MBBS, FRACP,* Matthew Conron, MBBS, FRACP, Alpha Tsui, MBBS,
ORIGINAL ARTICLE Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration for the Evaluation of Suspected Lymphoma Daniel P. Steinfort, MBBS, FRACP,* Matthew Conron, MBBS, FRACP, Alpha Tsui, MBBS,
All bedside percutaneously placed tracheostomies
 Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
Page 1 of 5 Scope: All bedside percutaneously placed tracheostomies Population: All ICU personnel Outcomes: To standardize and outline the steps necessary to safely perform a percutaneous tracheostomy
UNDERSTANDING SERIES LUNG CANCER BIOPSIES LungCancerAlliance.org
 UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
UNDERSTANDING SERIES LUNG CANCER BIOPSIES 1-800-298-2436 LungCancerAlliance.org CONTENTS What is a Biopsy?...2 Non-Surgical Biopsies...3 Surgical Biopsies...5 Biopsy Risks...6 Biopsy Results...6 Questions
Interventional Pulmonology
 Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Interventional Pulmonology The Division of Thoracic Surgery Department of Cardiothoracic Surgery New York Presbyterian/Weill Cornell Medical College p: 212-746-6275 f: 212-746-8223 https://weillcornell.org/eshostak
Thorax Online First, published on August 3, 2011 as /thoraxjnl Tuberculosis
 Thorax Online First, published on August 3, 2011 as 10.1136/thoraxjnl-2011-200063 Tuberculosis 1 Centre for Respiratory Research, University College London, 2 Respiratory Medicine, Imperial College Healthcare
Thorax Online First, published on August 3, 2011 as 10.1136/thoraxjnl-2011-200063 Tuberculosis 1 Centre for Respiratory Research, University College London, 2 Respiratory Medicine, Imperial College Healthcare
State of the art lecture: EUS and EBUS in pulmonary medicine
 State of the art lecture: EUS and EBUS in pulmonary medicine J. T. Annema 1, K. F. Rabe 1 1 Division of Pulmonary Medicine, Leiden University Medical Center, Leiden, The Netherlands Introduction The development
State of the art lecture: EUS and EBUS in pulmonary medicine J. T. Annema 1, K. F. Rabe 1 1 Division of Pulmonary Medicine, Leiden University Medical Center, Leiden, The Netherlands Introduction The development
Subhash Chandra MD, Mahendra Nehra MD, Dipti Agarwal MD, and Anant Mohan MD
 Diagnostic Accuracy of Endobronchial Ultrasound-Guided Transbronchial Needle Biopsy in Mediastinal Lymphadenopathy: A Systematic Review and Meta-analysis Subhash Chandra MD, Mahendra Nehra MD, Dipti Agarwal
Diagnostic Accuracy of Endobronchial Ultrasound-Guided Transbronchial Needle Biopsy in Mediastinal Lymphadenopathy: A Systematic Review and Meta-analysis Subhash Chandra MD, Mahendra Nehra MD, Dipti Agarwal
Sectional Anatomy Quiz II
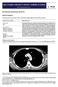 Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Sectional Anatomy II Rashid Hashmi Rural Clinical School, University of New South Wales, Wagga Wagga, New South Wales, Australia A R T I C L E I N F O Article type: Article history: Received: 3 Aug 2017
Imaging Guided Biopsy. Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer
 Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Imaging Guided Biopsy Edited & Presented by ; Hussien A.B ALI DINAR. Msc Lecturer,Reporting Sonographer Objective By the End of this lessons you should : Define what biopsy Justify Aim to perform biopsy
Mediastinal Incidentalomas
 ORIGINAL ARTICLE Jos A. Stigt, MD,* James E. Boers, MD, PhD, Ad H. Oostdijk, MD, Jan-Willem K. van den Berg, MD, PhD,* and Harry J. M. Groen, MD, PhD Introduction: Incidental mediastinal lymphadenopathy
ORIGINAL ARTICLE Jos A. Stigt, MD,* James E. Boers, MD, PhD, Ad H. Oostdijk, MD, Jan-Willem K. van den Berg, MD, PhD,* and Harry J. M. Groen, MD, PhD Introduction: Incidental mediastinal lymphadenopathy
Abstract. Introduction. Salah Abobaker Ali
 Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Sensitivity and specificity of combined fine needle aspiration cytology and cell block biopsy versus needle core biopsy in the diagnosis of sonographically detected abdominal masses Salah Abobaker Ali
Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture
 Cronicon OPEN ACCESS EC PULMONOLOGY AND RESPIRATORY MEDICINE Case Report Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture Swan Lee 1 and Rolando Sanchez Sanchez
Cronicon OPEN ACCESS EC PULMONOLOGY AND RESPIRATORY MEDICINE Case Report Lung Cancer Screening in the Midwest of the US: When Histoplasmosis Complicates the Picture Swan Lee 1 and Rolando Sanchez Sanchez
Section: Radiology Effective Date: July 15, 2016 Subsection: Original Policy Date: March 20, 2015 Subject:
 Last Review Status/Date: June 2016 Page: 1 of 14 Endobronchial Ultrasound for Diagnosis and Summary Endobronchial ultrasound (EBUS) is a technique that enhances standard flexible bronchoscopy by providing
Last Review Status/Date: June 2016 Page: 1 of 14 Endobronchial Ultrasound for Diagnosis and Summary Endobronchial ultrasound (EBUS) is a technique that enhances standard flexible bronchoscopy by providing
PET CT for Staging Lung Cancer
 PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
PET CT for Staging Lung Cancer Rohit Kochhar Consultant Radiologist Disclosures Neither I nor my immediate family members have financial relationships with commercial organizations that may have a direct
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer
 Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP ESMO-Christie Lung Cancer Course Manchester 2017 Overview What is Endobronchial Ultrasound? Why & When Do We
Endobronchial Ultrasound in the Diagnosis & Staging of Lung Cancer Dr Richard Booton PhD FRCP ESMO-Christie Lung Cancer Course Manchester 2017 Overview What is Endobronchial Ultrasound? Why & When Do We
Recommendations 1 For mediastinal nodal staging in patients with suspected or proven non-small-cell lung cancer
 Guideline 545 Combined endobronchial and esophageal endosonography for the diagnosis and staging of lung cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline, in cooperation with the
Guideline 545 Combined endobronchial and esophageal endosonography for the diagnosis and staging of lung cancer: European Society of Gastrointestinal Endoscopy (ESGE) Guideline, in cooperation with the
Received: 23 February 2018; Accepted: 4 April 2018; Published: 18 April 2018
 medicina Article Diagnostic Yield of Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration Cytological Smears and Cell Blocks: A Single-Institution Experience Marius Žemaitis 1, *, Greta Musteikienė
medicina Article Diagnostic Yield of Endobronchial Ultrasound-Guided Transbronchial Needle Aspiration Cytological Smears and Cell Blocks: A Single-Institution Experience Marius Žemaitis 1, *, Greta Musteikienė
JMSCR Vol 06 Issue 03 Page March 2018
 www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
www.jmscr.igmpublication.org Impact Factor (SJIF): 6.379 Index Copernicus Value: 71.58 ISSN (e)-2347-176x ISSN (p) 2455-4 DOI: https://dx.doi.org/.18535/jmscr/v6i3.63 Diagnostic Role of FOB in Radiological
GUIDELINE RECOMMENDATIONS
 European Journal of Cardio-Thoracic Surgery 48 (2015) 1 15 doi:10.1093/ejcts/ezv194 Cite this article as: Vilmann P, Frost Clementsen P, Colella S, Siemsen M, De Leyn P, Dumonceau J-M et al. Combined endobronchial
European Journal of Cardio-Thoracic Surgery 48 (2015) 1 15 doi:10.1093/ejcts/ezv194 Cite this article as: Vilmann P, Frost Clementsen P, Colella S, Siemsen M, De Leyn P, Dumonceau J-M et al. Combined endobronchial
PET/CT in lung cancer
 PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
The Itracacies of Staging Patients with Suspected Lung Cancer
 The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
The Itracacies of Staging Patients with Suspected Lung Cancer Gerard A. Silvestri, MD,MS, FCCP Professor of Medicine Medical University of South Carolina Charleston, SC silvestri@musc.edu Staging Lung
Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit
 Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Page1 Original Article NJR 2011;1(1):1 7;Available online at www.nranepal.org Diagnostic and Complication Rate of Image-guided Lung Biopsies in Raigmore Hospital, Inverness: A Retrospective Re-audit S
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Electromagnetic Navigation Bronchoscopy
 Electromagnetic Navigation Bronchoscopy Policy Number: 7.01.122 Last Review: 9/2017 Origination: 1/2010 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
Electromagnetic Navigation Bronchoscopy Policy Number: 7.01.122 Last Review: 9/2017 Origination: 1/2010 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will not provide coverage
ADVANCED LUNG DIAGNOSTICS
 ADVANCED LUNG DIAGNOSTICS SAMIR S. MAKANI, MD, FCCP DIRECTOR INTERVENTIONAL PULMONARY AND BROCHOSCOPY UNIVERSITY OF CALIFORNIA SAN DIEGO MEDICAL CENTER SAN DIEGO, CA Dr. Samir Makani is an Associate professor
ADVANCED LUNG DIAGNOSTICS SAMIR S. MAKANI, MD, FCCP DIRECTOR INTERVENTIONAL PULMONARY AND BROCHOSCOPY UNIVERSITY OF CALIFORNIA SAN DIEGO MEDICAL CENTER SAN DIEGO, CA Dr. Samir Makani is an Associate professor
