Pseudoachalasia: Still a Tough Clinical Challenge
|
|
|
- George Knight
- 5 years ago
- Views:
Transcription
1 ISSN DOI: /AJCR Received: Accepted: Published: : Still a Tough Clinical Challenge Authors Contribution: Study Design A Data Collection B Statistical Analysis C Data Interpretation D Manuscript Preparation E Literature Search F Funds Collection G ABCDEF ADEFG Yi Jia Richard W. McCallum Department of Internal Medicine, Texas Tech University Health Sciences Center, Paul L. Foster School of Medicine, El Paso, TX, U.S.A. Corresponding Author: Conflict of interest: Richard W. McCallum, richard.mccallum@ttuhsc.edu None declared Patient: Male, 81 Final Diagnosis: Symptoms: Dysphasia Medication: Clinical Procedure: Endoscopy ultrasound Specialty: Gastroenterology and Hepatology Objective: Background: Case Report: Conclusions: MeSH Keywords: Full-text PDF: Unusual clinical course Treatment of achalasia is focused on decreasing the resting lower esophageal sphincter by either pneumatic dilation or surgical myotomy. When patients symptomatically relapse after one or more pneumatic dilations, then one explanation is to consider the possibility of pseudoachalasia as the diagnosis. We present a rare case of an elderly patient with a presentation of chronic dysphagia and severe weight loss, who had diagnostic findings consistent with achalasia, and who also responded very well to a series of pneumatic dilations, but for only brief intervals. Further investigations finally uncovered esophageal adenocarcinoma, thus making our patient an example of the entity pseudoachalasia. secondary to an esophageal malignancy should be suspected when dysphagia progresses despite technically well-performed pneumatic dilations, and is particularly suspicious in the setting of an elderly patient with marked weight loss. Endoscopic ultrasound is a new diagnostic tool for detecting and staging malignancy by obtaining diagnostic tissue and allowing appropriate therapy to be planned. Endoscopy, Gastrointestinal Esophageal Achalasia Esophageal Neoplasms Gastric Dilatation
2 Background The patients with a presentation of dysphagia with or without noncardiac chest pain can have the diagnosis of achalasia. Treatment of achalasia can be accomplished by mechanical disruption of the muscle fibers of the lower esophageal sphincter (LES), by either pneumatic dilation (PD) or surgical myotomy. When patients symptomatically relapse after one or more PDs, then pseudoachalasia should be considered as another possibility diagnosis. Here, we present a rare case of a patient with a presentation of chronic dysphagia with an initial well documented diagnosis of achalasia and treated with PDs. However, further investigations were warranted in an elderly patient with marked weight loss when the PDs gave only a brief interval of relief. Esophageal adenocarcinoma was found and staged by Endoscopic ultrasound (EUS), thus making our patient an example of the entity pseudoachalasia. Case Report An 81-year-old Caucasian male was referred to the gastroenterology clinic with a 6 month history of progressive dysphagia. His referring physician had already made a diagnosis of achalasia and he had received a Botulinum toxin (Botox) injection into the LES through the endoscope about 3 weeks prior to his visit. He had responded well initially but then redeveloped dysphagia to both solids and liquids. He also has been having regurgitation of recently ingested food and in view of a more than 40 lbs weight loss history, he was admitted to hospital. In reviewing his history, he had been experience dysphagia for solids and liquids for 4 years as well as regurgitation of food, particularly old food at night. On review of systems, patient denied fever, weight loss, chest pain, cough or dyspnea. He did not report any neurological or respiratory symptoms. He had no medications at home. Pertinent history included colon cancer with colectomy 6 years ago without other further chemoradiation therapy. He was an active smoker for the past 20 years but denied any alcohol or illicit drug use. Upon physical examination, the patient was afebrile with stable vital signs. He weighed 68 Kg with a BMI of 25. On abdominal exam, there was a lower midline surgical scar from the colectomy; his abdomen was soft, non-distended and non-tender, no masses or organomegaly were palpable. Bowel sounds were present and normal. Other exam findings were unremarkable. His laboratory results indicated a normal comprehensive metabolic panel, but his complete blood count showed mild anemia with hemoglobin 11.5 g/dl, hematocrit of 38.9%, and MCV of 81 fl, more indicative of an anemia of chronic disease. Patient underwent a high resolution esophageal motility study which showed a classic achalasia pattern with resting LES Figure 1. A motility study can distinguish achalasia from other motility disorders. The presence of aperistalsis in the distal two-thirds of the esophagus and incomplete LES relaxation on esophageal manometry, defined as a mean four-second integrated relaxation pressure (IRP) >15 mmhg are the manometric criteria required for the achalasia. Our patient s outpatient high-resolution manometry results indicated a Type 2 classification. pressure of 36 mmhg (normal mmhg), integrated relaxation pressure (IRP) >15 mmhg, inadequate (25%) relaxation of the LES with wet swallows; aperistalsis with wet swallows with low amplitude contractions (<30 mmhg), consistent with type 2 Chicago classification for achalasia (Figure 1). The upper esophageal sphincter and striated muscle function were intact. Esophagogastroduodenoscopy (EGD) found patchy candidiasis in the lower third of the esophagus and a dilated, atonic esophagus. A hypertonic lower esophageal sphincter was found with resistance to endoscopic passage into the stomach. The Z-line was irregular and located 37 cm from the incisors with a 3 cm hiatus hernia. The therapy plan was to dilate the LES and improve esophageal emptying. Patient had pneumatic esophageal dilation using a Rigiflex 30 mm balloon dilator (90 French diameter). Post dilation, the esophagus was endoscopically examined and there was the usual mild mucosa trauma. An immediate post-dilation Gastrografin esophagram showed a long segment stricture of the distal esophagus with no evidence of leakage (Figure 2). No other complications were observed. He was able to tolerate a mechanical soft diet and discharged home. Three weeks later, patient presented to the ER with a chief complaint of the return of dysphagia to solids and liquids with decreased oral intake and received a second esophageal dilation, this time with a 35 mm pneumatic balloon dilator. Patient tolerated the esophageal dilation well and was able to be advanced to a regular diet before being discharged home. During his outpatient follow up, a chest CT was obtained that showed concentric mural thickening of the mid and distal esophagus 769
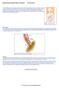
3 Figure 2. Gastrografin swallow of the esophagus immediately after pneumatic dilation showed long segment of stricture of the distal esophagus with suggestion of some irregularity without evidence of leakage. Figure 3. Follow up chest CT showed concentric mural thickening of the mid and distal esophagus which was out of proportion to that seen in a regular achalasia. which was out of proportion to the usual length of beaking present at the lower esophageal sphincter in regular achalasia (Figure 3). Six months later patient presented with return of dysphagia to both liquids and solids that had markedly progressed over the past month with about a 50 pounds weight loss over 3 months. Repeat EGD found moderately severe esophagitis, erosions, friability and a narrowing at 35 cm from the incisors 770
4 Figure 4. Endoscopic ultrasound (EUS) identified a hypoechoic mass in the lower third of the esophagus, encountered at 35 cm from the incisors and extended to 38 cm which was the furthest the echoendoscope could be advanced due to the stenosis. The endosonographic borders were irregular, and a T3 lesion with multiple benign-appearing lymph nodes was detected. EUS guided biopsies showed poorly differentiate adenocarcinoma. with granular irregular mucosa and moderate resistance to the passage of the endoscope. Pneumatic dilation was performed using a 40 mm balloon size over a guide wire for 5 total sessions. During the first 2 dilation attempts the balloon quickly migrated to the stomach. Hence extra attempts were required to ensure correct positioning. During the subsequent 3 dilations each of 1 minute duration, a lot of traction was required to keep the balloon in the lower esophageal sphincter and the impression was that the sphincter and distal esophagus were very tight and non-compliant. The post-procedure endoscopy and Gastrografin swallow confirmed no perforation and the patient was discharged home. Because of the endoscopic findings of irregular and inflamed tissue present proximal to the LES suggesting a mass effect together with the pneumatic dilation experience as well as the chest CT findings in the distal esophagus, an upper endoscopic ultrasound (EUS) was performed 2 weeks later, to rule out the possibility of underlying cancer of the esophagus that could explain his refractoriness to the dilations. EUS identified a hypoechoic mass in the lower third esophagus and several hypoechoic lymph nodes with poorly defined margins (Figure 4). The mass lesion was circumferential with irregular borders. There was one image that the mass appeared to protrude through the muscularis propria (layer 4) with intact interface between the mass and the adjacent structures. This was staged as T3 N0 Mx by endosonographic criteria. The biopsies of the mass indicated poorly differentiated adenocarcinoma. Tumor cells were diffusely positive for low molecular weight cytokeratin, focally positive for cytokeratin-7, and negative for high molecular weight cytokeratin, cytokeratin-20, P63, and leukocyte common antigen immunostains. This tumor is most compatible with poorly differentiated adenocarcinoma as the primary rather than metastatic tumor from the previous colon cancer. The adenocarcinoma was presumed to have developed in the setting of Barrett s esophagus. Patient had a PET scan which indicated no other metastasis. As a preventive measure to overcome any obstruction which could occur with the radiation therapy being planned preoperatively, the patient underwent esophageal stent placement and his nutrition status improved with ability to tolerate soft foods. He is currently being managed by the oncologist for his esophageal cancer with radiation and chemotherapy before surgery as the final goal. 771
5 Discussion In patients presenting with esophageal dysphagia, it is important to determine the types of food that produce symptoms (solids, liquids, or both) and whether there is the progression of symptoms from solids to liquids. Dysphagia for both solid and liquids from the onset of symptoms is most likely due to an esophageal motility disorder, such as achalasia and scleroderma. One the other hand, progressive dysphagia, beginning with dysphagia to solids evolving to liquids, is usually caused by a mechanical problem such as cancer or a peptic stricture or Schatzki ring [1]. The symptoms due to a malignancy usually progress rapidly, while the peptic strictures are more insidious [2]. However, patients with the motility disorders of achalasia or scleroderma, may also exhibit a worsening of their dysphagia when there is no treatment intervention. Achalasia results from the progressive degeneration of ganglion cells in the myenteric plexus in the lower esophageal sphincter and esophageal smooth muscle, leading to the loss of inhibitory innervation in the esophagus. Achalasia should be suspected in patients with dysphagia to solids and liquids with regurgitation of food from the esophagus, particularly occurring at night, sometimes accompanied by heartburn. Often this symptom triggers a trial of proton pump inhibitor (PPI) therapy because GERD is suspected by the primary care physicians. The heartburn accompanying the regurgitation is generally explained as the acidic ph of degraded food contents that have been retained in the esophagus [3]. Upper endoscopy indicates a dilated esophagus which appears to be atonic often with some retained food and a tight LES requiring pressure to push the endoscope into the stomach. A motility study is required to establish the diagnosis of achalasia and distinguish this entity from other motility disorders. The presence of aperistalsis following wet swallows in the distal two-thirds of the esophagus and incomplete LES relaxation on esophageal manometry, defined as a mean four-second integrated relaxation pressure (IRP) >15 mmhg in the setting of a normal to high pressure LES pressure are the manometric criteria required for the achalasia [3]. Other motility disorders, such as diffuse esophageal spasm and Jackhammer esophagus can also be detected in patients with nonstructural dysphagia [4]. Barium study is still helpful in confirming the classic beaking at the LES in achalasia. For our patient the beaking was more than 3 cm in length, exceeding the lower esophageal sphincter length, and somewhat asymmetric and irregular, all indicative that thus may not have been garden-variety achalasia. Treatment of achalasia is focused on decreasing the resting LES to facilitate emptying of esophageal contents. This can be accomplished by mechanical disruption of the muscle fibers of the LES (e.g., pneumatic dilation (PD) or surgical myotomy). Biochemical reduction in LES pressure (e.g., injection of botulinum toxin, or pharmacologically with oral nitrates, or calcium channel blockers) can be a short term initial therapy strategy [3]. Pneumatic dilation (PD) is the most cost-effective treatment for achalasia and has the advantage of being less invasive as compared with myotomy [5]. About 71-90% patients respond to PD initially. Approximately 50% of patients will relapse over a five-year period and will require additional dilation or surgery [6 9]. Type 1 and 2 achalasia by Chicago classification are the most appropriate for non-surgical intervention, while Type 3 is best managed by surgery, myotomy and a loose fundoplication. Hence in our patient with a Type 2 classification, we would have expected a better response from repeated PDs. The friable pattern of the mucosa with the barium contrast study in our patient could have been attributed to some irregularities and erosions due to leftover food retention and/or Candida infection. General rule is not to biopsy at the same time as a pneumatic dilation in fear of increased risk of perforation. Soon after the 3 rd dilation, abnormal CT and PD procedure findings led to EUS and defined the diagnosis of pseudoachalasia. is the term used when the manometric findings mimic classic idiopathic achalasia, but when some clinical characters are different and expected treatment outcomes are not achieved. has a number of possible contributing etiologies: Chagas disease (Trypanosoma cruzi parasite), adenocarcinoma of the gastric fundus or distal esophagus/ge junction, lymphoma, and metastatic malignancies from breast, pancreas, or lung [10]. in our patient is explained by adenocarcinoma of the lower esophagus involving the lower esophageal sphincter and microscopically infiltrating the myenteric plexus of the esophageal body and the LES [11]. The likelihood of pseudoachalasia in our patient was heightened by the following clinical characteristics: short duration of symptoms (in our patient the onset was less than six months); advanced age (our patient is over age 80); rapid and marked weight loss (our patient had a 50 pounds weight loss during 6 months); resistance to passing the endoscope through the gastroesophageal junction, and refractoriness to aggressive pneumatic dilation. In retrospect, our patient is atypical in that he had been experiencing dysphagia for up to 4 years. The biopsy might be done before or after pneumatic dilation. Pathology result is necessary to confirm the diagnosis of pseudoachalasia, especially since the patient had lost weight or anemia (probably due to iron deficiency, in old age, and disease did not last for long). Esophageal Biopsy is appropriate when abnormal or suspicious tissue to biopsy is identified. This was not apparent until the last pneumatic dilation in our patient as the atypical presentations and late onset of lost weight. 772
6 Hence, while the idiopathic achalasia may have been present initially the refractories, we witnessed was due to cancer occurring in underlying Barrett s esophagus. In such cases of refractories, a CT scan can be key to closely examine the esophagus and mediastinum. Endoscopic ultrasonography with fine-needle aspiration (EUS-FNA) is a new diagnostic tool to further investigate suspected etiologies of pseudoachalasia involving identifying and biopsying enlarged lymph nodes and masses [11]. In our patient, Barrett s esophagus was the underlying diagnosis with a history of GE reflux and predisposing to esophageal adenocarcinoma. References: 1. Boeckxstaens GE, Zaninotto G, Richter JE: Achalasia. Lancet, 2014; 383(9911): Lahbabi M, Ihssane M, Sidi Adil I, Dafr Allah B: secondary to metastatic breast carcinoma mimicking radiation stenosis. Clin Res Hepatol Gastroenterol, 2012; 36(6): e Vaezi MF, Pandolfino JE, Vela MF: ACG clinical guideline: diagnosis and management of achalasia. Am J Gastroenterol, 2013; 108(8): ; quiz Maradey-Romero C, Gabbard S, Fass R: Treatment of esophageal motility disorders based on the chicago classification. Curr Treat Options Gastroenterol, 2014; 12(4): Kostic S, Johnsson E, Kjellin A et al: Health economic evaluation of therapeutic strategies in patients with idiopathic achalasia: results of a randomized trial comparing pneumatic dilatation with laparoscopic cardiomyotomy. Surg Endosc, 2007; 21(7): Conclusions secondary to an esophageal malignancy should be suspected when dysphagia progresses despite technically well-performed pneumatic dilations, and endoscopic and imaging findings raise questions as to whether this is classic achalasia. EUS is a new diagnostic tool for staging the malignancy and obtaining diagnostic tissue. Disclosure of financial arrangements No financial disclosure for this article 6. Boeckxstaens GE, Annese V, des Varannes SB et al: Pneumatic dilation versus laparoscopic Heller s myotomy for idiopathic achalasia. N Engl J Med, 2011; 364(19): Eckardt VF, Gockel I, Bernhard G: Pneumatic dilation for achalasia: late results of a prospective follow up investigation. Gut, 2004; 53(5): Zerbib F, Thetiot V, Richy F et al: Repeated pneumatic dilations as longterm maintenance therapy for esophageal achalasia. Am J Gastroenterol, 2006; 101(4): Tabola R, Grabowski K, Lewandowski A et al: Achalasia balloon dilation or surgery? Med Sci Monit, 2013; 19: McCallum RW: Esophageal achalasia secondary to gastric carcinoma. Report of a case and a review of the literature. Am J Gastroenterol, 1979; 71(1): Tracey JP, Traube M: Difficulties in the diagnosis of pseudoachalasia. Am J Gastroenterol, 1994; 89(11):
A CURIOUS CASE OF HYPERTENSIVE LES. Erez Hasnis Department of Gastroenterology Rambam Health Care Campus
 A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
A CURIOUS CASE OF HYPERTENSIVE LES Erez Hasnis Department of Gastroenterology Rambam Health Care Campus CASE DESCRIPTION 63yo, F, single, attending nurse. PMH includes T2DM (Sitagliptin/Metformin), Hyperlipidemia
Achalasia: Inject, Dilate, or Surgery?
 Achalasia: Inject, Dilate, or Surgery? John E. Pandolfino, MD, MSCI, FACG Professor of Medicine Feinberg School of Medicine Northwestern University Chief, Division of Gastroenterology and Hepatology Northwestern
Achalasia: Inject, Dilate, or Surgery? John E. Pandolfino, MD, MSCI, FACG Professor of Medicine Feinberg School of Medicine Northwestern University Chief, Division of Gastroenterology and Hepatology Northwestern
9/18/2015. Disclosures. Objectives. Dysphagia Sherri Ekobena PA-C. I have no relevant financial interests to disclose I have no conflicts of interest
 Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Dysphagia Sherri Ekobena PA-C Disclosures I have no relevant financial interests to disclose I have no conflicts of interest Objectives Define what dysphagia is Define types of dysphagia Define studies
Oesophageal Disorders
 Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Oesophageal Disorders Anatomy Upper sphincter Oesophageal body Diaphragm Lower sphincter Gastric Cardia Symptoms Of Oesophageal Disorders Dysphagia Odynophagia Heartburn Atypical Chest Pain Regurgitation
Treating Achalasia. When to consider surgery and New options for therapy
 Treating Achalasia When to consider surgery and New options for therapy James B. Wooldridge,Jr., MD Ochsner Medical Center Senior Staff Surgeon General, Laparoscopic, and Bariatric Surgery Disclosures
Treating Achalasia When to consider surgery and New options for therapy James B. Wooldridge,Jr., MD Ochsner Medical Center Senior Staff Surgeon General, Laparoscopic, and Bariatric Surgery Disclosures
Gastroesophageal Reflux Disease, Paraesophageal Hernias &
 530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
530.81 553.3 & 530.00 43289, 43659 1043432842, MD Assistant Clinical Professor of Surgery, UH JABSOM Associate General Surgery Program Director Director of Minimally Invasive & Bariatric Surgery Programs
ESOPHAGEAL CANCER AND GERD. Prof Salman Guraya FRCS, Masters MedEd
 ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
ESOPHAGEAL CANCER AND GERD Prof Salman Guraya FRCS, Masters MedEd Learning objectives Esophagus anatomy and physiology Esophageal cancer Causes, presentations of esophageal cancer Diagnosis and management
Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD
 Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
Esophagus Anatomy/Physiology Gastroesophageal reflux disease Principles of GERD treatment Treatment of reflux diseases GERD Manometry Question 50 years old female with chest pain and dysphagia. Manometry
THORACIC SURGERY: Dysphagia. Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone. Thoracic Surgery Toronto East General Hospital
 THORACIC SURGERY: Dysphagia Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone Thoracic Surgery Toronto East General Hospital Objectives Definitions Common causes Investigations Treatment options Anatomy
THORACIC SURGERY: Dysphagia Dr. Robert Zeldin Dr. John Dickie Dr. Carmine Simone Thoracic Surgery Toronto East General Hospital Objectives Definitions Common causes Investigations Treatment options Anatomy
34th Annual Toronto Thoracic Surgery Refresher Course
 34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
34th Annual Toronto Thoracic Surgery Refresher Course TREATMENT OPTIONS FOR ACHALASIA Dr. Carmine Simone Director, Intensive Care Unit Head, Division of Critical Care Departments of Medicine and Surgery
Achalasia: Classic View
 Achalasia: Dilate, Botox, Knife or POEM Prateek Sharma, MD Kansas University School of Medicine Achalasia: Classic View 1 Diagnosis of Achalasia Endoscopy may be normal in as many as 44% Upper GI series
Achalasia: Dilate, Botox, Knife or POEM Prateek Sharma, MD Kansas University School of Medicine Achalasia: Classic View 1 Diagnosis of Achalasia Endoscopy may be normal in as many as 44% Upper GI series
Achalasia is a rare disease with an annual incidence estimated REVIEWS. Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2011;9:1020 1024 REVIEWS Erroneous Diagnosis of Gastroesophageal Reflux Disease in Achalasia BOUDEWIJN F. KESSING, ALBERT J. BREDENOORD, and ANDRÉ J. P. M. SMOUT
Chapter 14: Training in Radiology. DDSEP Chapter 1: Question 12
 DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
DDSEP Chapter 1: Question 12 A 52-year-old white male presents for evaluation of sudden onset of abdominal pain and shoulder pain. His past medical history is notable for a history of coronary artery disease,
Dysphagia. Conflicts of Interest
 Dysphagia Bob Kizer MD Assistant Professor of Medicine Creighton University School of Medicine August 25, 2018 Conflicts of Interest None 1 Which patient does not need an EGD as the first test? 1. 50 year
Dysphagia Bob Kizer MD Assistant Professor of Medicine Creighton University School of Medicine August 25, 2018 Conflicts of Interest None 1 Which patient does not need an EGD as the first test? 1. 50 year
Per-oral Endoscopic Myotomy
 POEM With the Flexible Scope as a Treatment for Achalasia and Zenker's Diverticulum Abraham Mathew, MD, MSc Professor of Medicine Penn State College of Medicine Penn State Hershey Medical Center Per-oral
POEM With the Flexible Scope as a Treatment for Achalasia and Zenker's Diverticulum Abraham Mathew, MD, MSc Professor of Medicine Penn State College of Medicine Penn State Hershey Medical Center Per-oral
Combined Experience of Two European Centers
 Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Minimally Invasive Surgery for Achalasia: Combined Experience of Two European Centers Garzi A, Valla JS*, Molinaro F, Amato G, Messina M. Unit of Pediatric Surgery, University of Siena (Italy) *Lenval
Case Scenario year-old white male presented to personal physician with dyspepsia with reflux.
 Case Scenario 1 57-year-old white male presented to personal physician with dyspepsia with reflux. 7/12 EGD: In the gastroesophageal junction we found an exophytic tumor. The tumor occupies approximately
Case Scenario 1 57-year-old white male presented to personal physician with dyspepsia with reflux. 7/12 EGD: In the gastroesophageal junction we found an exophytic tumor. The tumor occupies approximately
Steven Frachtman, M.D. Division of Gastroenterology/Hepatology August 18, 2011
 Steven Frachtman, M.D. Division of Gastroenterology/Hepatology August 18, 2011 Review normal esophageal anatomy and physiology Classifications of esophageal motility disorders Clinical features/diagnosis/management
Steven Frachtman, M.D. Division of Gastroenterology/Hepatology August 18, 2011 Review normal esophageal anatomy and physiology Classifications of esophageal motility disorders Clinical features/diagnosis/management
Case Scenario 1. The patient has now completed his neoadjuvant chemoradiation and has been cleared for surgery.
 Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
Case Scenario 1 July 10, 2010 A 67-year-old male with squamous cell carcinoma of the mid thoracic esophagus presents for surgical resection. The patient has completed preoperative chemoradiation. This
High Resolution Esophageal Manometry
 High Resolution Esophageal Manometry Dr. Geoffrey Turnbull MD, FRCPC Dalhousie University Dr. Yvonne Tse MD, FRCPC University of Toronto Name: Dr. Geoffrey Turnbull Conflict of Interest Disclosure (over
High Resolution Esophageal Manometry Dr. Geoffrey Turnbull MD, FRCPC Dalhousie University Dr. Yvonne Tse MD, FRCPC University of Toronto Name: Dr. Geoffrey Turnbull Conflict of Interest Disclosure (over
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 Final Pathology:
 Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Abstracting Upper GI Cancer Incidence and Treatment Data Quiz 1 Multiple Primary and Histologies Case 1 A 74 year old male with a history of GERD presents complaining of dysphagia. An esophagogastroduodenoscopy
Health-related quality of life and physiological measurements in achalasia
 Diseases of the Esophagus (2017) 30, 1 5 DOI: 10.1111/dote.12494 Original Article Health-related quality of life and physiological measurements in achalasia Daniel Ross, 1 Joel Richter, 2 Vic Velanovich
Diseases of the Esophagus (2017) 30, 1 5 DOI: 10.1111/dote.12494 Original Article Health-related quality of life and physiological measurements in achalasia Daniel Ross, 1 Joel Richter, 2 Vic Velanovich
A Multidisciplinary Approach to Esophageal Dysphagia: Role of the SLP. Darlene Graner, M.A., CCC-SLP, BRS-S Sharon Burton, M.D.
 A Multidisciplinary Approach to Esophageal Dysphagia: Role of the SLP Darlene Graner, M.A., CCC-SLP, BRS-S Sharon Burton, M.D. What is the role of the SLP? Historically SLPs the preferred providers for
A Multidisciplinary Approach to Esophageal Dysphagia: Role of the SLP Darlene Graner, M.A., CCC-SLP, BRS-S Sharon Burton, M.D. What is the role of the SLP? Historically SLPs the preferred providers for
Myogenic Control. Esophageal Motility. Enteric Nervous System. Alimentary Tract Motility. Determinants of GI Tract Motility.
 Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Myogenic Control Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Basic Electrical Rythym: intrinsic rhythmic fluctuation of smooth muscle membrane potential
Esophageal Motility. Alimentary Tract Motility
 Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
Esophageal Motility David Markowitz, MD Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions Mixing Allows for greater
David Markowitz, MD. Physicians and Surgeons
 Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Esophageal Motility David Markowitz, MD Columbia University, College of Columbia University, College of Physicians and Surgeons Alimentary Tract Motility Propulsion Movement of food and endogenous secretions
Surgical Evaluation for Benign Esophageal Disease. Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018
 Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
Surgical Evaluation for Benign Esophageal Disease Kimberly Howard, PA-C, MHS Duke University Medical Center April 7, 2018 Disclosures No disclosures relevant to this presentation. Objectives (for CME purposes)
ESOPHAGEAL MOTOR DISORDERS
 Medicine Dr. Taha Alkarbuli Lecture 1 (Esophageal & GIT Disorders) ESOPHAGEAL DISORDERS: - ESOPHAGEAL MOTOR DISORDERS. - GERD - ESOPHAGEAL TUMORS. ESOPHAGEAL MOTOR DISORDERS Present with chest pain, dysphagia,
Medicine Dr. Taha Alkarbuli Lecture 1 (Esophageal & GIT Disorders) ESOPHAGEAL DISORDERS: - ESOPHAGEAL MOTOR DISORDERS. - GERD - ESOPHAGEAL TUMORS. ESOPHAGEAL MOTOR DISORDERS Present with chest pain, dysphagia,
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL. September 17, Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous
 Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Duke Masters of Minimally Invasive Thoracic Surgery Orlando, FL September 17, 2016 Session VI: Minimally Invasive Thoracic Surgery: Miscellaneous NOTES and POEM James D. Luketich MD, FACS Henry T. Bahnson
Case 1- B.N. 66 yr old F with PMHx of breast cancer s/ p mastectomy, HTN, DM presented with dysphagia to solids and liquids.
 Case 1- B.N 66 yr old F with PMHx of breast cancer s/ p mastectomy, HTN, DM presented with dysphagia to solids and liquids. Reports retching to clear esophagus. Case 1- B.N EGD: Stricture in the distal
Case 1- B.N 66 yr old F with PMHx of breast cancer s/ p mastectomy, HTN, DM presented with dysphagia to solids and liquids. Reports retching to clear esophagus. Case 1- B.N EGD: Stricture in the distal
A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword?
 A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword? Pavlos Kaimakliotis, MD Department of Gastroenterology Lahey Hospital and Medical Center Assistant Professor of Medicine
A Novel Endoscopic Treatment for Achalasia Is the POEM mightier than the sword? Pavlos Kaimakliotis, MD Department of Gastroenterology Lahey Hospital and Medical Center Assistant Professor of Medicine
Surgical aspects of dysphagia
 Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Dysphagia Why is dysphagia important? Surgery Surgical aspects of dysphagia Adrian P. Ireland aireland@eircom.net Academic RCSI Department of Surgery, Beaumont Hospital Why important Definitons Swallowing
Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis.
 Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
Gut Online First, published on December 14, 2005 as 10.1136/gut.2005.085423 Clearance mechanisms of the aperistaltic esophagus. The pump-gun hypothesis. Radu Tutuian 1, Daniel Pohl 1, Donald O Castell
Esophageal Motility Disorders. Disclosures
 Esophageal Motility Disorders V. Raman Muthusamy, MD FACG Director of Endoscopy Clinical i l Professor of Medicine i David Geffen School of Medicine at UCLA UCLA Health System Disclosures I am an interventional
Esophageal Motility Disorders V. Raman Muthusamy, MD FACG Director of Endoscopy Clinical i l Professor of Medicine i David Geffen School of Medicine at UCLA UCLA Health System Disclosures I am an interventional
Esophageal Motor Abnormalities
 Esophageal Motor Abnormalities Brooks D. Cash, MD, FACP, AGAF, FACG, FASGE Professor of Medicine Gastroenterology Division University of South Alabama Mobile, AL High Resolution Manometry Late Ray Clouse,
Esophageal Motor Abnormalities Brooks D. Cash, MD, FACP, AGAF, FACG, FASGE Professor of Medicine Gastroenterology Division University of South Alabama Mobile, AL High Resolution Manometry Late Ray Clouse,
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease
 ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
ACG Clinical Guideline: Diagnosis and Management of Gastroesophageal Reflux Disease Philip O. Katz MD 1, Lauren B. Gerson MD, MSc 2 and Marcelo F. Vela MD, MSCR 3 1 Division of Gastroenterology, Einstein
Achalasia is a primary esophageal motility disorder of unknown
 Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Laparoscopic Heller Myotomy for Achalasia Andrew Pierre, MD, MSc Achalasia is a primary esophageal motility disorder of unknown etiology. Pathologically, it is characterized by loss of ganglion cells in
Post-Prandial Trouble! KPA 2017 Nutrition pre-congress case Presentation Dr. Esther Kimani. Facilitator- Dr. A. Laving. 25/04/2017
 Post-Prandial Trouble! KPA 2017 Nutrition pre-congress case Presentation Dr. Esther Kimani. Facilitator- Dr. A. Laving. 25/04/2017 Biodata. Name- I.M.M. Age-6 years Gender- female Referred to the Paediatric
Post-Prandial Trouble! KPA 2017 Nutrition pre-congress case Presentation Dr. Esther Kimani. Facilitator- Dr. A. Laving. 25/04/2017 Biodata. Name- I.M.M. Age-6 years Gender- female Referred to the Paediatric
Case Report Treatment Modalities for Achalasia Cardia: A Case Study and Literature Review
 IBIMA Publishing International Journal of Case Reports in Medicine http://www.ibimapublishing.com/journals/ijcrm/ijcrm.html Vol. 2013 (2013), Article ID 602167, 7 pages DOI: 10.5171/2013.602167 Case Report
IBIMA Publishing International Journal of Case Reports in Medicine http://www.ibimapublishing.com/journals/ijcrm/ijcrm.html Vol. 2013 (2013), Article ID 602167, 7 pages DOI: 10.5171/2013.602167 Case Report
Esophageal Manometry. John M. Wo, M.D. October 1, 2009
 Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
Esophageal Manometry John M. Wo, M.D. October 1, 2009 Esophageal Manometry Anatomy and physiology of the esophagus Conventional esophageal manometry High resolution esophageal manometry (Pressure Topography)
Diagnosis of Primary Versus Secondary Achalasia: Reassessment of Clinical and Radiographic Criteria
 Courtney A. Woodfield 1 Marc S. Levine Stephen E. Rubesin Curtis P. Langlotz Igor Laufer Received January 14, 2000; accepted after revision February 16, 2000. 1 All authors: Department of Radiology, Hospital
Courtney A. Woodfield 1 Marc S. Levine Stephen E. Rubesin Curtis P. Langlotz Igor Laufer Received January 14, 2000; accepted after revision February 16, 2000. 1 All authors: Department of Radiology, Hospital
What can you expect from the lab?
 Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
Role of the GI Motility Lab in the Diagnosis and Treatment of Esophageal Disorders Kenneth R. DeVault MD, FACG, FACP Professor and Chair Department of Medicine Mayo Clinic Florida What can you expect from
The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality
 Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Bahrain Medical Bulletin, Vol.22, No.4, December 2000 The Frequency of Gastroesophageal Reflux Disease in Nutcracker Esophagus and the Effect of Acid-Reduction Therapy on the Motor Abnormality Saleh Mohsen
Joel A. Ricci MD SUNY Downstate Medical Center Lutheran Medical Center Department of Surgery June 26, 2009
 Joel A. Ricci MD SUNY Downstate Medical Center Lutheran Medical Center Department of Surgery June 26, 2009 History Xx year old female with worsening dysphagia and solid food regurgitation for 2 days Other
Joel A. Ricci MD SUNY Downstate Medical Center Lutheran Medical Center Department of Surgery June 26, 2009 History Xx year old female with worsening dysphagia and solid food regurgitation for 2 days Other
Radiology. Gastrointestinal. Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact. Farooq P. Agha
 Gastrointest Radiol 9:9%103 (1984) Gastrointestinal Radiology 9 Springer-Verlag 1984 Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact Farooq P. Agha Department of Radiology,
Gastrointest Radiol 9:9%103 (1984) Gastrointestinal Radiology 9 Springer-Verlag 1984 Transient Intraluminal Diverticulum of the Esophagus: A Significant Flow Artifact Farooq P. Agha Department of Radiology,
Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine
 Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine none 32 yo male presents with a burning sensation in chest following most large meals for 2-3 months. He denies dysphagia,
Catherine Kerschen DO, FACOI Michigan State University College of Osteopathic Medicine none 32 yo male presents with a burning sensation in chest following most large meals for 2-3 months. He denies dysphagia,
Esophageal Motility Disorders
 GASTROENTEROLOGY BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, GROUP PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Becky Krumm, ELS ASSOCIATE EDITOR Lamont Williams ASSISTANT EDITOR
GASTROENTEROLOGY BOARD REVIEW MANUAL PUBLISHING STAFF PRESIDENT, GROUP PUBLISHER Bruce M. White EXECUTIVE EDITOR Debra Dreger SENIOR EDITOR Becky Krumm, ELS ASSOCIATE EDITOR Lamont Williams ASSISTANT EDITOR
EGD. John M. Wo, M.D. University of Louisville July 3, 2008
 EGD John M. Wo, M.D. University of Louisville July 3, 2008 Different Ways to do an EGD Which scope? Pediatric, regular, jumbo EGD endoscope or pediatric colonoscope Transnasal vs. transoral insertion Sedation
EGD John M. Wo, M.D. University of Louisville July 3, 2008 Different Ways to do an EGD Which scope? Pediatric, regular, jumbo EGD endoscope or pediatric colonoscope Transnasal vs. transoral insertion Sedation
Diagnosis and Management of Achalasia: Past, Present, & Future
 Diagnosis and Management of Achalasia: Past, Present, & Future Kyle A. Perry, MD, FACS Assistant Professor of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical
Diagnosis and Management of Achalasia: Past, Present, & Future Kyle A. Perry, MD, FACS Assistant Professor of Surgery Division of General & Gastrointestinal Surgery The Ohio State University Wexner Medical
Primary Squamous Cell Carcinoma of the Liver Initially Presenting with Pseudoachalasia
 Gut and Liver, Vol. 6, No. 2, April 2012, pp. 275-279 CASE REPORT Primary Squamous Cell Carcinoma of the Liver Initially Presenting with Pseudoachalasia Mun Ki Choi*, Gwang Ha Kim*, Geun Am Song*, Hyung
Gut and Liver, Vol. 6, No. 2, April 2012, pp. 275-279 CASE REPORT Primary Squamous Cell Carcinoma of the Liver Initially Presenting with Pseudoachalasia Mun Ki Choi*, Gwang Ha Kim*, Geun Am Song*, Hyung
Comparison of the Outcomes of Peroral Endoscopic Myotomy for Achalasia According to Manometric Subtype
 Gut and Liver, Vol. 11, No. 5, September 2017, pp. 642-647 ORiginal Article Comparison of the Outcomes of Peroral Endoscopic Myotomy for Achalasia According to Manometric Subtype Won Hee Kim 1, Joo Young
Gut and Liver, Vol. 11, No. 5, September 2017, pp. 642-647 ORiginal Article Comparison of the Outcomes of Peroral Endoscopic Myotomy for Achalasia According to Manometric Subtype Won Hee Kim 1, Joo Young
Slide 1. Slide 2. Slide 3 Pancreatic Cancer- Case #1. Endoscopic management of GI malignancy. Endoscopic approaches in GI malignancy- Agenda
 Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
Slide 1 A teaching hospital of Harvard Medical School Endoscopic management of GI malignancy Tyler Berzin MD, MS Center for Advanced Endoscopy Division of Gastroenterology Beth Israel Deaconess Medical
Gastrointestinal Tract Cancer
 Gastrointestinal Tract Cancer Tumors of the Stomach Gastric adenocarcinoma Incidence and Epidemiology Incidence mortality rates USA High incidence: Japan, China, Chile, Ireland risk lower socioeconomic
Gastrointestinal Tract Cancer Tumors of the Stomach Gastric adenocarcinoma Incidence and Epidemiology Incidence mortality rates USA High incidence: Japan, China, Chile, Ireland risk lower socioeconomic
Eosinophilic Esophagitis (EoE)
 Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
Eosinophilic Esophagitis (EoE) 01.06.2016 EoE: immune-mediated disorder food or environmental antigens => Th2 inflammatory response. Key cytokines: IL-4, IL-5, and IL-13 stimulate the production of eotaxin-3
THE CONNECTIVE TISSUE AND EPITHELIUM
 THE CONNECTIVE TISSUE AND EPITHELIUM The focus of this week s lab will be pathology of connective tissue and epithelium. The lab will introduce you to the four basic tissue types: epithelium, connective
THE CONNECTIVE TISSUE AND EPITHELIUM The focus of this week s lab will be pathology of connective tissue and epithelium. The lab will introduce you to the four basic tissue types: epithelium, connective
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012
 Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
Aliu Sanni MD SUNY Downstate Medical Center August 16, 2012 Case Presentation 60yr old AAF with PMH of CAD s/p PCI 1983, CVA, GERD, HTN presented with retrosternal chest pain on 06/12 Associated dysphagia
High Resolution Manometry: A new perspective on esophageal motility disorders. Chris Andrews & Bill Paterson
 High Resolution Manometry: A new perspective on esophageal motility disorders Chris Andrews & Bill Paterson CDDW/CASL Meeting Session: CanMEDS Roles Covered in this Session: Medical Expert (as Medical
High Resolution Manometry: A new perspective on esophageal motility disorders Chris Andrews & Bill Paterson CDDW/CASL Meeting Session: CanMEDS Roles Covered in this Session: Medical Expert (as Medical
Gastroesophageal Reflux Disease:
 Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
Gastroesophageal Reflux Disease: Introduction Gastroesophageal reflux is the involuntary movement of gastric contents to the esophagus. It is a common disease, occurring in one third of the population
01/26/2010 GENERAL SURGERY ABSITE ANATOMY ANATOMY. Yvonne M. Carter, MD Georgetown University Medical Center. Layers. mucosa. squamous epithelium
 GENERAL SURGERY ABSITE REVIEW: ESOPHAGUS Yvonne M. Carter, MD Georgetown University Medical Center ANATOMY Layers mucosa muscle squamous epithelium columnar epithelium (distal 2cm) inner = circular outer
GENERAL SURGERY ABSITE REVIEW: ESOPHAGUS Yvonne M. Carter, MD Georgetown University Medical Center ANATOMY Layers mucosa muscle squamous epithelium columnar epithelium (distal 2cm) inner = circular outer
Manometry Conundrums
 Manometry Conundrums Gastroenterology and Hepatology Symposium February 10, 2018 Reena V. Chokshi, MD Assistant Professor of Medicine Division of Gastroenterology, Hepatology, & Nutrition Department of
Manometry Conundrums Gastroenterology and Hepatology Symposium February 10, 2018 Reena V. Chokshi, MD Assistant Professor of Medicine Division of Gastroenterology, Hepatology, & Nutrition Department of
Achalasia Current Diagnosis and Management
 時間 :2017 年 9 月 16 日 14:45PM-17:50PM 地點 : 臺中榮民總醫院研究大樓一樓第二會場 Achalasia Current Diagnosis and Management 蔡成枝醫師 Seng-Kee Chuah, M.D. Professor of Medicine Division of Hepato-gastroenterology Department of
時間 :2017 年 9 月 16 日 14:45PM-17:50PM 地點 : 臺中榮民總醫院研究大樓一樓第二會場 Achalasia Current Diagnosis and Management 蔡成枝醫師 Seng-Kee Chuah, M.D. Professor of Medicine Division of Hepato-gastroenterology Department of
Hiatal Hernias and Barrett s esophagus. Dr Sajida Ahad Mercy General Surgery
 Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
Hiatal Hernias and Barrett s esophagus Dr Sajida Ahad Mercy General Surgery Objectives Identify the use of different diagnostic modalities for hiatal hernias List the different types of hiatal hernias
ACHALASIA ACHALASIA. Current Management of Achalasia
 Current Management of Achalasia Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ACHALASIA
Current Management of Achalasia Guilherme M Campos, MD, FACS Assistant Professor of Surgery Director G.I. Motility Center Director Bariatric Surgery Program University of California San Francisco ACHALASIA
University College Hospital. Achalasia. Gastrointestinal Services Division Physiology Unit
 University College Hospital Achalasia Gastrointestinal Services Division Physiology Unit Author: Dr Anton Emmanuel, Consultant Gastroenterologist First published: September 2012 Last review date: February
University College Hospital Achalasia Gastrointestinal Services Division Physiology Unit Author: Dr Anton Emmanuel, Consultant Gastroenterologist First published: September 2012 Last review date: February
B. Cystic Teratoma: Refer to virtual microscope slide p_223 ovary, teratoma and compare to normal virtual microscope slide 086 ovary.
 LAB 2: THE CONNECTIVE TISSUE AND EPITHELIUM The focus of this week s lab will be pathology of connective tissue and epithelium. The lab will introduce you to the four basic tissue types: epithelium, connective
LAB 2: THE CONNECTIVE TISSUE AND EPITHELIUM The focus of this week s lab will be pathology of connective tissue and epithelium. The lab will introduce you to the four basic tissue types: epithelium, connective
Esophagus: Spectrum of pathologies on Barium Swallow
 Esophagus: Spectrum of pathologies on Barium Swallow Poster No.: C-1426 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit E. Dhamija 1, D. Chandan 1, D. Srivastava 2 ; 1 New Delhi/IN,
Esophagus: Spectrum of pathologies on Barium Swallow Poster No.: C-1426 Congress: ECR 2013 Type: Authors: Keywords: DOI: Educational Exhibit E. Dhamija 1, D. Chandan 1, D. Srivastava 2 ; 1 New Delhi/IN,
Incidental discovery of oesophageal-gastric pathologies on chest X-ray.
 Incidental discovery of oesophageal-gastric pathologies on chest X-ray. Poster No.: C-0839 Congress: ECR 2012 Type: Educational Exhibit Authors: P. Giusti, M. Marchetti, U. tani, E. Fruzzetti, P. Bemi,
Incidental discovery of oesophageal-gastric pathologies on chest X-ray. Poster No.: C-0839 Congress: ECR 2012 Type: Educational Exhibit Authors: P. Giusti, M. Marchetti, U. tani, E. Fruzzetti, P. Bemi,
Imaging techniques in the diagnosis, staging and follow up of GI cancers. Moderators: Banke Agarwal, MD and Paul Schultz, MD
 Imaging techniques in the diagnosis, staging and follow up of GI cancers Moderators: Banke Agarwal, MD and Paul Schultz, MD Panelists Axel Grothey, MD Professor of Oncology Division of Medical Oncology
Imaging techniques in the diagnosis, staging and follow up of GI cancers Moderators: Banke Agarwal, MD and Paul Schultz, MD Panelists Axel Grothey, MD Professor of Oncology Division of Medical Oncology
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)?
 WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
WHAT IS GASTROESOPHAGEAL REFLUX DISEASE (GERD)? The term gastroesophageal reflux describes the movement (or reflux) of stomach contents back up into the esophagus, the muscular tube that extends from the
CASE REPORTS. Giant Esophagus. An Unusual Case of Massive Idiopathic Hypertrophy
 CASE REPORTS An Unusual Case of Massive Idiopathic Hypertrophy and Dilatation of the Esophagus and Proximal Stomach Mark H. Wall, M.D., Epifanio E. Espinas, M.D., Arthur W. Silver, M.D., and Francis X.
CASE REPORTS An Unusual Case of Massive Idiopathic Hypertrophy and Dilatation of the Esophagus and Proximal Stomach Mark H. Wall, M.D., Epifanio E. Espinas, M.D., Arthur W. Silver, M.D., and Francis X.
Departement of Surgery Faculty of Medicine University Sumatera Utara
 SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
SSS EESOPHAGEAL HPOSAGEAL DISORDERS IN SURGICAL PERSPECTIVE Departement of Surgery Faculty of Medicine University Sumatera Utara CONTENT 1. Esophageal Atresia 2. Achalasia 3. Esophageal Rupture 4. Tumor
Esophageal stricture causes and pattern of presentation at Ibn Sina Specialized Hospital Abstract Introduction: Methods: Results and discussion:
 bü z ÇtÄ TÜà väx causes and pattern of presentation at Ibn Sina Specialized Hospital Mohammed Osman El Hassan Gadour 1 and Hayder Hussein Elamin 2 Abstract Introduction: The aim of this study is to evaluate
bü z ÇtÄ TÜà väx causes and pattern of presentation at Ibn Sina Specialized Hospital Mohammed Osman El Hassan Gadour 1 and Hayder Hussein Elamin 2 Abstract Introduction: The aim of this study is to evaluate
Gender, medication use and other factors associated with esophageal motility disorders in non-obstructive dysphagia
 Gastroenterology Report, 6(3), 2018, 177 183 doi: 10.1093/gastro/goy018 Advance Access Publication Date: 2 June 2018 Original article ORIGINAL ARTICLE Gender, medication use and other factors associated
Gastroenterology Report, 6(3), 2018, 177 183 doi: 10.1093/gastro/goy018 Advance Access Publication Date: 2 June 2018 Original article ORIGINAL ARTICLE Gender, medication use and other factors associated
Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System
 Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System Used abbreviations BE: Barrett s esophagus EC: Early cancer ER: Endoscopic resection HGD:
Radiofrequency Ablation: Stepwise circumferential and focal RFA of Barrett s s esophagus using the HALO System Used abbreviations BE: Barrett s esophagus EC: Early cancer ER: Endoscopic resection HGD:
Surgical Treatment for Achalasia
 Surgical Treatment for Achalasia Date of Origin: 08/2015 Last Review Date: 08/23/2017 Effective Date: 08/23/2017 Dates Reviewed: 08/2016, 08/2017 Developed By: Medical Necessity Criteria Committee I. For
Surgical Treatment for Achalasia Date of Origin: 08/2015 Last Review Date: 08/23/2017 Effective Date: 08/23/2017 Dates Reviewed: 08/2016, 08/2017 Developed By: Medical Necessity Criteria Committee I. For
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS GASTROINTESTINAL (GI) PATHOLOGY LAB #1. January 06, 2012
 MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS GASTROINTESTINAL (GI) PATHOLOGY LAB #1 GOAL: January 06, 2012 Faculty Copy 1. Describe the basis morphologic and pathophysiologic changes which occur in
MECHANISMS OF HUMAN DISEASE: LABORATORY SESSIONS GASTROINTESTINAL (GI) PATHOLOGY LAB #1 GOAL: January 06, 2012 Faculty Copy 1. Describe the basis morphologic and pathophysiologic changes which occur in
Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India
 Indian J Gastroenterol 2010(January February):29(1):18 22 ORIGINAL ARTICLE Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India Asha Misra Dipti Chourasia
Indian J Gastroenterol 2010(January February):29(1):18 22 ORIGINAL ARTICLE Manometric and symptomatic spectrum of motor dysphagia in a tertiary referral center in northern India Asha Misra Dipti Chourasia
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: esophageal_ph_monitoring 4/2011 5/2017 5/2018 5/2017 Description of Procedure or Service Acid reflux is the
Accepted Manuscript. Classical features of Zollinger-Ellison syndrome, in images. Ali Alshati, MD, Toufic Kachaamy, MD
 Accepted Manuscript Classical features of Zollinger-Ellison syndrome, in images Ali Alshati, MD, Toufic Kachaamy, MD PII: S0016-5107(19)30069-0 DOI: https://doi.org/10.1016/j.gie.2019.01.026 Reference:
Accepted Manuscript Classical features of Zollinger-Ellison syndrome, in images Ali Alshati, MD, Toufic Kachaamy, MD PII: S0016-5107(19)30069-0 DOI: https://doi.org/10.1016/j.gie.2019.01.026 Reference:
Oro-pharyngeal and Esophageal Motility and Dysmotility John E. Pandolfino, MD, MSci
 Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
Oro-pharyngeal and Esophageal Department of Medicine Feinberg School of Medicine Northwestern University 1 Oro-pharyngeal and Esophageal Motility Function: Oropharynx Transfer food Prevent aspiration Breathing
Achalasia is diagnosed by showing dysfunction of lower
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:131 137 ALIMENTARY TRACT A Comparison of Symptom Severity and Bolus Retention With Chicago Classification Esophageal Pressure Topography Metrics in Patients
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2013;11:131 137 ALIMENTARY TRACT A Comparison of Symptom Severity and Bolus Retention With Chicago Classification Esophageal Pressure Topography Metrics in Patients
Laparoscopic Heller Myotomy for Achalasia: Changing Trend Toward True Day-Case Procedure
 JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 18, Number 6, 2008 Mary Ann Liebert, Inc. DOI: 10.1089/lap.2008.0057 Laparoscopic Heller Myotomy for Achalasia: Changing Trend Toward True
JOURNAL OF LAPAROENDOSCOPIC & ADVANCED SURGICAL TECHNIQUES Volume 18, Number 6, 2008 Mary Ann Liebert, Inc. DOI: 10.1089/lap.2008.0057 Laparoscopic Heller Myotomy for Achalasia: Changing Trend Toward True
Peptic ulcer disease Disorders of the esophagus
 Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Peptic ulcer disease Disorders of the esophagus Peptic ulcer disease Burning epigastric pain Exacerbated by fasting Improved with meals Ulcer: disruption of mucosal integrity >5 mm in size, with depth
Abstracting Hematopoietic Neoplasms
 CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
CASE 1: LYMPHOMA PHYSICAL EXAMINATION 43yo male with a history of lower gastrointestinal bleeding and melena undergoing colonoscopy and biopsy to rule out neoplasm versus inflammation. Patient had no other
Rings in the esophagus are not always eosinophilic esophagitis: Case series of ring forming lymphocytic esophagitis and review of the literature
 Rings in the esophagus are not always eosinophilic esophagitis: Case series of ring forming lymphocytic esophagitis and review of the literature Authors Julia L. Pleet 1,SofiaTaboada 2, Arvind Rishi 2,
Rings in the esophagus are not always eosinophilic esophagitis: Case series of ring forming lymphocytic esophagitis and review of the literature Authors Julia L. Pleet 1,SofiaTaboada 2, Arvind Rishi 2,
Gastrointestinal Imaging Clinical Observations
 Esophageal Motility Disorders After Laparoscopic Nissen Fundoplication Gastrointestinal Imaging Clinical Observations Natasha E. Wehrli 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer
Esophageal Motility Disorders After Laparoscopic Nissen Fundoplication Gastrointestinal Imaging Clinical Observations Natasha E. Wehrli 1 Marc S. Levine 1 Stephen E. Rubesin 1 David A. Katzka 2 Igor Laufer
Surgery for achalasia is an anachronism. John C. Dugal Jr. MD
 Surgery for achalasia is an anachronism. John C. Dugal Jr. MD Outline: Overview of achalasia Traditional surgical treatments Heller ±fundoplication Less invasive treatments Nitrates/Ca channel blockers
Surgery for achalasia is an anachronism. John C. Dugal Jr. MD Outline: Overview of achalasia Traditional surgical treatments Heller ±fundoplication Less invasive treatments Nitrates/Ca channel blockers
Understanding GERD. & Stretta Therapy. GERD (gĕrd): Gastroesophageal Reflux Disease
 Understanding GERD & Stretta Therapy GERD (gĕrd): Gastroesophageal Reflux Disease What is GERD? When the muscle between your stomach and esophagus is weak, stomach contents like acid or bile can reflux
Understanding GERD & Stretta Therapy GERD (gĕrd): Gastroesophageal Reflux Disease What is GERD? When the muscle between your stomach and esophagus is weak, stomach contents like acid or bile can reflux
Achalasia and Laparoscopic Heller Myotomy
 1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
1 Monterey County Surgical Associates 2 Upper Ragsdale Drive, Bldg B, Suite 230 Monterey, CA 93940 Phone: (831) 649-0808 Fax: (831) 649-8795 Mark Vierra, MD Achalasia and Laparoscopic Heller Myotomy Introduction
GERD DIAGNOSIS & TREATMENT DISCLOSURES 4/18/2018
 GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
GERD DIAGNOSIS & TREATMENT Subhash Chandra MBBS Assistant Professor CHI Health Clinic Gastroenterology Creighton University, School of Medicine April 28, 2018 DISCLOSURES None 1 OBJECTIVES Review update
4/24/2015. History of Reflux Surgery. Recent Innovations in the Surgical Treatment of Reflux
 Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Recent Innovations in the Surgical Treatment of Reflux Scott Carpenter, DO, FACOS, FACS Mercy Hospital Ardmore Ardmore, OK History of Reflux Surgery - 18 th century- first use of term heartburn - 1934-
Faculty Disclosure. Objectives. State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) 24/11/2014
 State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
State of the Art #3: Referrals for Gastroscopy (focus on common esophagus problems) Dr. Amy Morse November 2014 Faculty: Amy Morse Faculty Disclosure Relationships with commercial interests: Grants/Research
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation. Introduction. Predisposing factor. Introduction.
 Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Obesity Is Associated With Increased Transient Lower Esophageal Sphincter Relaxation Gastro Esophageal Reflux Disease (GERD) JUSTIN CHE-YUEN WU, et. al. The Chinese University of Hong Kong Gastroenterology,
Putting Chronic Heartburn On Ice
 Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Putting Chronic Heartburn On Ice Over the years, gastroesophageal reflux disease has proven to be one of the most common complaints facing family physicians. With quicker diagnosis, this pesky ailment
Barrett s Esophagus. Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI
 Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Barrett s Esophagus Abdul Sami Khan, M.D. Gastroenterologist Aurora Healthcare Burlington, Elkhorn, Lake Geneva, WI A 58 year-old, obese white man has had heartburn for more than 20 years. He read a magazine
Falk Symposium, , , Portorož. Physiology of Swallowing and Anti-Gastroesophageal. Reflux-Mechanisms. Mechanisms: C.
 Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Falk Symposium, 15.-16.6.07, 16.6.07, Portorož Physiology of Swallowing and Anti-Gastroesophageal Reflux-Mechanisms Mechanisms: Anything new from a radiologist s view? C.Kulinna-Cosentini Cosentini Medical
Predictors of Outcome of Pneumatic Dilation in Achalasia
 CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:389 394 Predictors of Outcome of Pneumatic Dilation in Achalasia KAVEH FARHOOMAND, JASON T. CONNOR, JOEL E. RICHTER, EDGAR ACHKAR, and MICHAEL F. VAEZI Department
CLINICAL GASTROENTEROLOGY AND HEPATOLOGY 2004;2:389 394 Predictors of Outcome of Pneumatic Dilation in Achalasia KAVEH FARHOOMAND, JASON T. CONNOR, JOEL E. RICHTER, EDGAR ACHKAR, and MICHAEL F. VAEZI Department
pissn: eissn: Journal of Neurogastroenterology and Motility
 JNM J Neurogastroenterol Motil, Vol. 24 No. 3 July, 2018 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/10.5056/jnm18038 Original Article 200 ml Rapid Drink Challenge During Highresolution Manometry
JNM J Neurogastroenterol Motil, Vol. 24 No. 3 July, 2018 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/10.5056/jnm18038 Original Article 200 ml Rapid Drink Challenge During Highresolution Manometry
Achalasia is a rare motility disorder of the esophagus
 GASTROENTEROLOGY 2013;144:718 725 CLINICAL ALIMENTARY TRACT Outcomes of Treatment for Achalasia Depend on Manometric Subtype WOUT O. ROHOF, 1, * RENATO SALVADOR, 2, * VITO ANNESE, 3 STANISLAS BRULEY DES
GASTROENTEROLOGY 2013;144:718 725 CLINICAL ALIMENTARY TRACT Outcomes of Treatment for Achalasia Depend on Manometric Subtype WOUT O. ROHOF, 1, * RENATO SALVADOR, 2, * VITO ANNESE, 3 STANISLAS BRULEY DES
performed to help sway the clinician in what the appropriate diagnosis is, which can substantially alter the treatment of management.
 Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
Hello, I am Maura Polansky at the University of Texas MD Anderson Cancer Center. I am a Physician Assistant in the Department of Gastrointestinal Medical Oncology and the Program Director for Physician
