Ten Top Tips for the management of patients post-bariatric surgery in primary care
|
|
|
- Regina Curtis
- 5 years ago
- Views:
Transcription
1 Article Ten Top Tips for the management of patients post-bariatric surgery in primary care Helen Mary Parretti, Carly Anna Hughes, Mary O Kane, Sean Woodcock, Rachel Gillian Pryke Citation: Parretti HM, Hughes CA, O Kane M, Woodcock S, Pryke RG (2015) Ten Top Tips for the management of patients post-bariatric surgery in primary care. British Journal of Obesity 1: Article points 1. People who undergo bariatric surgery require lifelong followup of their comorbidities and nutritional status. 2. Currently, such individuals are monitored by the bariatric surgery team for the first 2 years and are then discharged back into primary care. 3. The Royal College of GPs Nutrition Group has developed this set of guidelines to assist non-specialist clinicians, dietitians and nurses in the management of these patients in primary care. Key words - Bariatric surgery - Primary care - RCGP Nutrition Group - Shared care Authors For author details, see the end of the article. There is a growing cohort of people undergoing bariatric surgery, and these patients require lifelong follow-up. Recent NICE guidelines recommend a shared care model for the long-term management of these individuals; therefore, GPs need guidance on how to appropriately monitor and manage them. Following a review of the current literature and discussions with experts in the field, guidance has been developed that will aid clinicians in providing high-quality shared care alongside Tier 3 or 4 specialist teams. Areas discussed include monitoring long-term associated conditions, potential nutritional deficiencies, nutritional supplements, changes to medications post-surgery, post-surgery contraception advice and criteria for re-referral to specialist services. In the UK, NICE recognises that bariatric surgery may be an appropriate and costeffective treatment for obesity. Following changes to the eligibility criteria to undergo bariatric surgery in the CG189 clinical guidelines (NICE, 2014), the number of procedures being performed per year is likely to increase. People who undergo such surgery require lifelong followup of their comorbidities and nutritional status. Guidance has been developed by the Royal College of GPs (RCGP) Nutrition Group in conjunction with the British Obesity and Metabolic Surgery Society (BOMSS) to aid GPs in providing high-quality shared care of these patients with Tier 3 or 4 teams. Ten Top Tips for the management of patients post-bariatric surgery in primary care Currently, according to the National Bariatric Surgery Registry (Welbourn et al, 2014), around 8500 procedures are performed in the UK each year. This is a complex cohort of patients, with an average of 3.4 comorbidities pre-surgery in women and 3.7 in men. This includes four or more comorbidities in 53.9% of men and 41.4% of women. While bariatric surgery has been reported to have significant benefits with regard to the improvement and remission of these comorbidities (Puzziferri et al, 2014; Sjöström et al, 2014; Welbourn et al, 2014), it also puts patients at risk of nutritional deficiencies (Aarts et al, 2011; Mechanick et al, 2013). People who undergo bariatric surgery require lifelong follow up of their comorbidities and monitoring of their nutritional status. CG189 suggests that after the first 2 years post-procedure, care should be carried out by primary care in a shared-care model with a named Tier 3 service or equivalent (NICE, 2014). This should include an annual review which, for many patients, will coincide with their annual comorbidity monitoring. In 2013, the American Association of Clinical Endocrinologists, The Obesity Society and the American Society for Metabolic and Bariatric Surgery published joint guidelines for the 68 British Journal of Obesity Volume 1 No
2 perioperative care of people undergoing bariatric surgery (Mechanick et al, 2013). However, currently, there are no comprehensive guidelines that focus on the long-term care of post-bariatric surgery patients within primary care. Therefore, the RCGP Nutrition Group has developed these guidelines in conjunction with BOMSS through review of the current literature and expert opinion. The guidance is specifically aimed at all non-specialist clinicians, dietitians and nurses to aid management of these people once they are discharged back to primary care, and also to aid management of any patients for whom follow-up guidance from the surgical team is not available. It is important to note that people who have moved to a different area or who undergo a private procedure are likely to have had less specialist follow-up and may need to be managed in primary care earlier post-procedure. In addition, any new concerns should always trigger referral to a Tier 3 weight management service (if available) or the local bariatric surgery team for further advice. Top Tip One Keep a register of bariatric surgery patients It is important to record the type of procedure in the register, as the different procedures have different risks of nutritional deficiencies. This is also essential information to include when liaising with specialist services. Top Tip Two Encourage patients to check their own weight regularly and to attend an annual BMI and diet review with a healthcare professional Do not assume that all patients are eating a wellbalanced diet. Some may have maladaptive eating patterns and poor nutritional intake. If BMI is increasing, consider referral to local weight management services to support and encourage lifelong weight maintenance. Top Tip Three Symptoms of continuous vomiting, dysphagia, intestinal obstruction (gastric bypass) or severe abdominal pain require emergency admission under the local surgical team Further details of both urgent and routine indications for referral back to specialist services are summarised in a printable at a glance poster that can be found on the RCGP nutrition web pages (available at: Top Tip Four Continue to review comorbidities postsurgery, including diabetes, hypertension, hypercholesterolaemia and obstructive sleep apnoea, as well as mental health Medication doses will need to be titrated in the postoperative period as weight loss occurs, but they may increase later if weight loss is not maintained. Studies have shown very positive results with regard to remission of diabetes post-surgery (Brethauer et al, 2013; Puzziferri et al, 2014; Sjöström et al, 2014), and people with diabetes need regular medication reviews, with treatment adjustments as required. However, longer-term studies have shown that some patients have a recurrence of diabetes (Brethauer et al, 2013; Sjöström et al, 2014). Therefore, people with diabetes should also continue to have routine diabetes follow-up (i.e. they should be kept on the Quality and Outcomes Framework diabetes register and receive annual retinopathy screening) even if their diabetes goes into remission. Whether or not weight loss occurs, cardiovascular and metabolic risk factors, such as blood pressure and cholesterol levels, must continue to be monitored, and treatments will need to be adjusted as required. Patients receiving continuous positive airway pressure should continue to use their machines until they have had a repeat sleep study performed post-surgery (Duke and Finer, 2012). It is worth noting that there is a higher rate of mental health problems in people with severe and complex obesity compared with the general population (Vaidya, 2006; Gundersen et al, 2011), and these problems may persist even after successful bariatric surgery. Therefore, mental health should be reviewed regularly following surgery. The psychological management of these people can be complex and, therefore, there should be a low threshold for referral to specialist mental health services. Top Tip Five Review the patient s regular medications The formulations may need adjusting post-surgery to allow for changes in bioavailability. This is Page points 1. Primary care practitioners should record their postsurgery patients in a register, complete with full details of the procedure, as different procedures have different risks of nutritional deficiencies. 2. Patients should monitor their own weight and attend yearly review of their BMI and diet. 3. Severe gastrointestinal signs require emergency readmission to surgery. 4. Comorbidities such as type 2 diabetes can improve rapidly after surgery as weight loss occurs, and thus they need long-term monitoring and treatment adjustment as appropriate. 5. There is a high rate of mental health problems in people with severe and complex obesity that may persist after the surgery, and long-term psychological monitoring may be required. British Journal of Obesity Volume 1 No
3 Box 1. Medication considerations post-bariatric surgery (Top Tip Five). Review comorbidity medications, such as antihypertensives, diabetes medications, etc., post-surgery. Requirements are likely to fall with postoperative weight loss, but may increase later if weight loss is not maintained. Consider pill size patients may need liquid formulations or syrups in the immediate postoperative period. However, usual medication formulations should be tolerated by around 6 weeks postoperatively. Replace extended-release formulations with immediate-release formulations. Psychiatric medications may need increased or divided doses. Use diuretics with caution due to the increased risk of hypokalaemia. Monitor anticoagulants carefully. Avoid non-steroidal anti-inflammatory drugs; if no alternative, use only with a proton pump inhibitor. Avoid bisphosphonates. Patients with gastric bands should avoid effervescent medications. Table 1. Recommended annual blood test monitoring (Top Tip Six). Blood test Surgical procedure Gastric bypass Sleeve gastrectomy Duodenal switch Liver function tests Yes Yes Yes Full blood count Yes Yes Yes Ferritin Yes Yes Yes Folate Yes Yes Yes Vitamin B12 Yes* Yes* Yes* Calcium Yes Yes Yes Vitamin D Yes Yes Yes Parathyroid hormone Yes Yes Yes Vitamin A Possibly No Yes Zinc, copper Yes Possibly Yes Selenium No No No *If the patient is having 3-monthly intramuscular injections of vitamin B12, there may be no need for annual checks. If the patient has had a long-limb bypass or has symptoms of steatorrhoea or night blindness. Measure when there are deficiency concerns (see Top Tip Seven). particularly relevant in people who undergo gastric bypass or duodenal switch. It is crucial that medications for comorbidities are closely monitored and adjusted as discussed in Top Tip Four. Other medication considerations are shown in Box 1 (Thomas and Taub, 2011). Top Tip Six Bariatric surgery patients require lifelong annual blood tests, including micronutrient monitoring Encourage patients to attend their annual blood tests. Use patient record reminders, where available, to prompt that annual blood testing is required, depending on practice computer systems. An annual audit of patient monitoring is recommended to ensure that correct follow-up is being performed. The recommended tests are shown in Table 1 (Heber et al, 2010; Mechanick et al, 2013; O Kane et al, 2014a; 2014b). Note that people who undergo gastric banding require annual full blood counts, urea and electrolyte tests, and liver function tests, but these should be carried out earlier if there are any concerns regarding the band. Top Tip Seven Be aware of potential nutritional deficiencies that may occur and their signs and symptoms Liaise with the local Tier 3 or 4 specialist unit regarding any deficiencies and their treatment. In particular, patients are at risk of anaemia and vitamin D deficiency, as well as protein malnutrition and other vitamin and micronutrient deficiencies. If a patient is deficient in one nutrient they are likely to be deficient in others as well, so it is advised to screen for these. Clinicians should be aware of the potential nutritional deficiencies listed in Table 2 (Heber et al, 2010; Mechanick et al, 2013; O Kane et al, 2014a; 2014b). Top Tip Eight Ensure the patient is taking the appropriate lifelong nutritional supplements as recommended by the bariatric centre Patients will need lifelong supplements, and guidance should have been given by the bariatric unit on discharge, as the supplementation required depends on both the procedure and the patient s individual requirements. Examples of the usual minimal supplements are listed in Table 3 for each type of procedure; however, see O Kane (2014b) for full guidance. If guidance on supplements has not been given on discharge, we would advise clinicians to always liaise with the Tier 4 bariatric unit in the first instance. 70 British Journal of Obesity Volume 1 No
4 Table 2. Potential nutritional deficiencies post-bariatric surgery (Top Tip Seven). Nutritional deficiency Protein malnutrition Anaemia Calcium and vitamin D deficiency Vitamin A deficiency Zinc, copper and selenium deficiency Notes May present as oedema several years post-surgery Needs urgent referral back to the bariatric team Iron deficiency (rule out and investigate other potential causes, such as blood loss) Folate deficiency Vitamin B12 deficiency Less common deficiencies such as zinc, copper and selenium are a potential cause of unexplained anaemia Some patients may need parenteral iron or blood transfusions if oral iron does not correct the deficiency May result in secondary hyperparathyroidism (it is recommended that vitamin D should be replaced as per National Osteoporosis Society guidance [Francis et al, 2013]) Suspect in patients with changes in night vision Patients with steatorrhoea or those who have had a duodenal switch are at high risk Unexplained anaemia, poor wound healing, hair loss, neutropenia, peripheral neuropathy and cardiomyopathy are potential symptoms Top Ten Tips at a glance 1. Keep a patient register. 2. Patients should check their weight regularly and attend an annual diet review. 3. Severe gastrointestinal signs require emergency readmission to surgery. 4. Continue to monitor obesity comorbidities and mental health. 5. Review medications. 6. Lifelong annual blood tests are required. 7. Be aware of the nutritional deficiencies that can occur. 8. Ensure that patients take the appropriate nutritional supplements. 9. Discuss contraception and try to avoid pregnancy in the first months. 10. Supplement regimens should be altered in cases of subsequent pregnancy. Ask about over-the-counter supplements and liaise with bariatric unit, as zinc supplements can induce copper deficiency and vice versa Thiamine deficiency Suspect in patients with poor intake, persistent regurgitation or vomiting This may be caused by anastomotic stricture in the early postoperative phase, food intolerances or an overtight band Start thiamine supplementation immediately and refer urgently to the local bariatric unit due to risk of Wernicke s encephalopathy Do not give sugary drinks as they may precipitate Wernicke s encephalopathy Top Tip Nine Discuss contraception ideally pregnancy should be avoided for at least months post-surgery A long-acting, reversible contraceptive of the patient s choice would be appropriate. Oral contraception and Depo-Provera are not recommended because of issues with absorption and weight gain, respectively. Top Tip Ten If a patient should plan or wish to become pregnant after bariatric surgery, alter their nutritional supplements to one suitable during pregnancy Additional monitoring and supplementation may be required. Inform the local bariatric unit (ideally prior to conception) so that the patient can be reviewed by a bariatric dietitian. In addition, people who undergo gastric band surgery may need their band adjusting on becoming pregnant to allow good nutritional intake and fetal growth. The obstetric team should also be informed of the patient s history of bariatric surgery as soon as possible, as there may be a higher rate of firsttrimester miscarriages in this cohort of patients (Guelinckx et al, 2009). Recommended changes to treatment before and during pregnancy are as follows (Duke and Finer, 2012; O Kane et al, 2014a; 2014b): l Change nutritional supplement to one that is appropriate in pregnancy, such as Pregnacare or Boots Pregnancy Support. British Journal of Obesity Volume 1 No
5 The long-term management of an increasing number of people who undergo bariatric surgery is likely to involve primary care clinicians, and guidance on how to manage these patients safely and appropriately within primary care is essential. Table 3. Typical minimal supplements required after bariatric surgery (Top Tip Eight). Bariatric procedure Gastric band Gastric bypass Recommendations Although no supplements should be needed for this group of patients, it is still recommended that they take a comprehensive multivitamin and mineral supplement, such as Sanatogen A Z or Forceval, once a day Multivitamin and mineral supplement (e.g. any over-the-counter comprehensive multivitamin preparation twice daily or Forceval once daily) Vitamin B12 injections every 3 months Calcium and vitamin D (e.g. Adcal D3 Forte, Calceos or Calcichew-D3 Forte) plus additional vitamin D as required Iron (start at 200 mg once daily and monitor as the dose may need to be increased), especially for women of menstruating age Sleeve gastrectomy Multivitamin and mineral supplement (e.g. any over-the-counter comprehensive multivitamin preparation twice daily or Forceval once daily) Vitamin B12 injections every 3 months Calcium and vitamin D (e.g. Adcal D3 Forte, Calceos or Calcichew-D3 Forte) plus additional vitamin D as required Possibly iron (start at 200 mg once daily and monitor as the dose may need to be increased), especially for women of menstruating age Duodenal switch As for gastric bypass, but additional fat-soluble vitamins (A, D, E and K) are also needed, as well as, possibly, zinc and copper; liaise with specialist local services for advice regarding these supplements l If a proton pump inhibitor is needed, omeprazole is recommended. l Continue vitamin D supplementation as indicated by vitamin D levels and as per National Osteoporosis Society guidance (Francis et al, 2013). l Continue vitamin B12 injections in those currently receiving them, or monitor levels in those not receiving them (for sleeve gastrectomy patients). l Once-daily iron 200 mg is recommended. l Once-daily folic acid 5 mg is recommended. Conclusions The long-term management of an increasing number of people who undergo bariatric surgery is likely to involve primary care clinicians, and guidance on how to manage these patients safely and appropriately within primary care is essential. Here, we have presented guidance for the followup of these people by non-specialist healthcare professionals working in primary care, and it is hoped that this guidance from the RCGP Nutrition Group will aid the shared care of these patients. n Acknowledgements The authors would like to thank Dr Rachel Batterham for her comments and advice during the development of this guidance. Further information The printable short leaflet and extended versions of the Ten Top Tips guidance are available on the RCGP nutrition web pages, together with the poster outlining referral criteria for post-surgery complications. The short leaflet is available at: The extended version is available at: The poster outlining both urgent and routine indications for referral back to specialist services is available at: 72 British Journal of Obesity Volume 1 No
6 Aarts EO, Janssen IM, Berends FJ (2011) The gastric sleeve: losing weight as fast as micronutrients? Obes Surg 21: Brethauer SA, Aminian A, Romero-Talamás H et al (2013) Can diabetes be surgically cured? Long-term metabolic effects of bariatric surgery in obese patients with type 2 diabetes mellitus. Ann Surg 258: Duke E, Finer N (2012) Bariatric Surgery: Pre-Operative and Post- Operative Care. Information for General Practitioners. UCLH Centre for Weight Loss, Metabolic and Endocrine Surgery, London. Francis R, Aspray T, Fraser W et al (2013) Vitamin D and Bone Health: A Practical Clinical Guideline for Patient Management. National Osteoporosis Society, Bath. Available at: (accessed ) Guelinckx I, Devlieger R, Vansant G (2009) Reproductive outcome after bariatric surgery: a critical review. Hum Reprod Update 15: Gundersen C, Mahatmya D, Garasky S, Lohman B (2011) Linking psychosocial stressors and childhood obesity. Obes Rev 12: e54 63 Heber D, Greenway FL, Kaplan LM et al (2010) Endocrine and nutritional management of the post-bariatric surgery patient: an Endocrine Society Clinical Practice Guideline. J Clin Endocrinol Metab 95: Mechanick JI, Youdim A, Jones DB (2013) Clinical practice guidelines for the perioperative nutritional, metabolic, and nonsurgical support of the bariatric surgery patient 2013 update: cosponsored by American Association of Clinical Endocrinologists, The Obesity Society, and American Society for Metabolic & Bariatric Surgery. Obesity (Silver Spring) 21(Suppl 1):1 27 NICE (2014) Obesity: Identification, Assessment and Management of Overweight and Obesity in Children, Young People and Adults (CG189). NICE, London. Available at: (accessed ) O Kane M, Pinkney J, Aasheim ET et al (2014a) GP Guidance: Management of Nutrition Following Bariatric Surgery. BOMSS, London. Available at: (accessed ) O Kane M, Pinkney J, Aasheim ET et al (2014b) BOMSS Guidelines on Peri-Operative and Postoperative Biochemical Monitoring and Micronutrient Replacement for Patients Undergoing Bariatric Surgery. BOMSS, London. Available at: (accessed ) Puzziferri N, Roshek TB, Mayo HG et al (2014) Long-term follow-up after bariatric surgery: a systematic review. JAMA 312: Sjöström L, Peltonen M, Jacobson P et al (2014) Association of bariatric surgery with long-term remission of type 2 diabetes and with microvascular and macrovascular complications. JAMA 311: Thomas CM, Taub LF (2011) Monitoring for and preventing the longterm sequelae of bariatric surgery. J Am Acad Nurse Pract 23: Vaidya V (2006) Psychosocial aspects of obesity. Adv Psychosom Med 27: Welbourn R, Small P, Finlay I et al (2014) The United Kingdom National Bariatric Surgery Registry. NBSR, London. Available at: (accessed ) Authors Helen Parretti is NIHR Clinical Lecturer, University of Birmingham; Carly Hughes is Clinical Lead, Fakenham Weight Management Service, and GP Research Fellow and Honorary Lecturer, University of East Anglia, Norwich; Mary O Kane is Consultant Dietitian (Adult Obesity), Leeds Teaching Hospitals NHS Trust; Sean Woodcock is Consultant Upper GI and Bariatric Surgeon, North Tyneside Hospital; Rachel Pryke is GP, Winyates Health Centre, Redditch, and Chair of the RCGP Nutrition Group. British Journal of Obesity Volume 1 No
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Guidelines for the follow-up of patients undergoing bariatric surgery O'Kane, Mary; Parretti, Helen; Hughes, Carly; Sharma, Manisha; Woodcock, Sean; Puplampu, Tamara; Blakemore, Alexandra; Clare, Kenneth;
Guidelines for the follow-up of patients undergoing bariatric surgery O'Kane, Mary; Parretti, Helen; Hughes, Carly; Sharma, Manisha; Woodcock, Sean; Puplampu, Tamara; Blakemore, Alexandra; Clare, Kenneth;
Practical recommendations for the post-bariatric surgery medical management
 Practical recommendations for the post-bariatric surgery medical management Dr L. Favre CHUV Sce Endocrinologie, diabétologie et métabolisme 26.04.2018 Bariatric surgery in Switzerland Multidisciplinary
Practical recommendations for the post-bariatric surgery medical management Dr L. Favre CHUV Sce Endocrinologie, diabétologie et métabolisme 26.04.2018 Bariatric surgery in Switzerland Multidisciplinary
Vitamin and Mineral Supplementation and Monitoring. Bariatric Surgery
 Vitamin and Mineral Supplementation and Monitoring Bariatric Surgery We put our patients first by working as one team; leading and listening, and striving for the best. Together, we make the difference.
Vitamin and Mineral Supplementation and Monitoring Bariatric Surgery We put our patients first by working as one team; leading and listening, and striving for the best. Together, we make the difference.
Metabolic Sequelaeof Bariatric Surgery. Roula BOU KHALIL Ass. Prof of Endocrinology SGHUMC Balamand University
 Metabolic Sequelaeof Bariatric Surgery Roula BOU KHALIL Ass. Prof of Endocrinology SGHUMC Balamand University OUTLINE Introduction Indications and metabolic benefits of bariatric surgery Obesity Paradox
Metabolic Sequelaeof Bariatric Surgery Roula BOU KHALIL Ass. Prof of Endocrinology SGHUMC Balamand University OUTLINE Introduction Indications and metabolic benefits of bariatric surgery Obesity Paradox
DEKAs after Bariatric Surgery*
 DEKAs after Bariatric Surgery* Once Daily All-in-one Multivitamin and Mineral Chewable Tablets with Enhanced Absorption for Dietary Management after Bariatric Surgery Roberto Jongejan, MD, PhD Gus Papas,
DEKAs after Bariatric Surgery* Once Daily All-in-one Multivitamin and Mineral Chewable Tablets with Enhanced Absorption for Dietary Management after Bariatric Surgery Roberto Jongejan, MD, PhD Gus Papas,
Long-Term Care Updates
 Long-Term Care Updates August 2017 By Alyson Lozicki, PharmD As the prevalence of obesity continues to rise, and with now over one-third (36.5%) of American adults considered obese, the number of weight
Long-Term Care Updates August 2017 By Alyson Lozicki, PharmD As the prevalence of obesity continues to rise, and with now over one-third (36.5%) of American adults considered obese, the number of weight
Bariatric Surgery Work Up, Patient Selection and Follow Up
 Bariatric Surgery Work Up, Patient Selection and Follow Up A/Professor Tania Markovic Metabolism & Obesity Services, RPAH Boden Institute of Obesity, Nutrition, Exercise & Eating Disorders SLHD Bariatric
Bariatric Surgery Work Up, Patient Selection and Follow Up A/Professor Tania Markovic Metabolism & Obesity Services, RPAH Boden Institute of Obesity, Nutrition, Exercise & Eating Disorders SLHD Bariatric
Having a Sleeve Gastrectomy
 University Teaching Trust Having a Sleeve Gastrectomy Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2016. Document for issue as handout. This booklet aims to describe: l What
University Teaching Trust Having a Sleeve Gastrectomy Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2016. Document for issue as handout. This booklet aims to describe: l What
10/16/2014. Normal Weight: BMI Overweight: BMI >25 Obese: BMI >30 Morbidly Obese: BMI >40 or >35 with 2 comorbidities
 Brinton Clark, MD, MPH Department of Medical Education Providence Portland Medical Center October 25 th, 2014 Oregon Society of Physician Assistants Fall Conference 45 yo woman with BMI=40kg/m2 (weight
Brinton Clark, MD, MPH Department of Medical Education Providence Portland Medical Center October 25 th, 2014 Oregon Society of Physician Assistants Fall Conference 45 yo woman with BMI=40kg/m2 (weight
Townhall: Assisting Patients Post Bariatric Surgery Katie McClendon, PharmD, BCPS, FCCP University of Mississippi School of Pharmacy
 Townhall: Assisting Patients Post Bariatric Surgery Katie McClendon, PharmD, BCPS, FCCP University of Mississippi School of Pharmacy Annual Meeting & Exposition Seattle, Washington March 22 25 Disclosures
Townhall: Assisting Patients Post Bariatric Surgery Katie McClendon, PharmD, BCPS, FCCP University of Mississippi School of Pharmacy Annual Meeting & Exposition Seattle, Washington March 22 25 Disclosures
Management of the Bariatric. Farah A. Husain MD, FACS, FASMBS Division Chief, Bariatric Services. Surgery Patient 2017
 Management of the Bariatric Farah A. Husain MD, FACS, FASMBS Division Chief, Bariatric Services Surgery Patient 2017 Financial Disclosures None Objectives Identify the most commonly performed bariatric
Management of the Bariatric Farah A. Husain MD, FACS, FASMBS Division Chief, Bariatric Services Surgery Patient 2017 Financial Disclosures None Objectives Identify the most commonly performed bariatric
Table Classification of body mass index (BMI) and risk of comorbidities in adults (WHO, 1998; WHO Expert Consultation,
 Table 7.13.1 Classification of body mass index (BMI) and risk of comorbidities in adults (WHO, 1998; WHO Expert Consultation, 2004) Classification BMI (kg/m 2 ) BMI (kg/ m 2 ) Asian origin Risk of comorbidities
Table 7.13.1 Classification of body mass index (BMI) and risk of comorbidities in adults (WHO, 1998; WHO Expert Consultation, 2004) Classification BMI (kg/m 2 ) BMI (kg/ m 2 ) Asian origin Risk of comorbidities
Complications from micronutrient deficiency following bariatric surgery
 Case Report Annals of Clinical Biochemistry 2014, Vol. 51(6) 705 709! The Author(s) 2014 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: 10.1177/0004563214535562 acb.sagepub.com Complications
Case Report Annals of Clinical Biochemistry 2014, Vol. 51(6) 705 709! The Author(s) 2014 Reprints and permissions: sagepub.co.uk/journalspermissions.nav DOI: 10.1177/0004563214535562 acb.sagepub.com Complications
Nutrients and Drugs Considerations after Bariatric Surgeries
 Nutrients and Drugs Considerations after Bariatric Surgeries Marwan Akel, Pharm D Clinical AssistantProfessor School of Pharmacy Lebanese International University Overweight and Obesity Prevalence 2013
Nutrients and Drugs Considerations after Bariatric Surgeries Marwan Akel, Pharm D Clinical AssistantProfessor School of Pharmacy Lebanese International University Overweight and Obesity Prevalence 2013
Weight Loss Surgery Program
 Weight Loss Surgery Program More than 500,000 Americans die prematurely each year from obesity-related complications, and it is one of the leading causes of preventable death. If you want to do something
Weight Loss Surgery Program More than 500,000 Americans die prematurely each year from obesity-related complications, and it is one of the leading causes of preventable death. If you want to do something
ENTRY CRITERIA: C. Approved Comorbidities: Diabetes
 KAISER PERMANENTE OHIO BARIATRIC SURGERY (GASTROPLASTY) Methodology: Expert Opinion Issue Date: 12-05 Champion: Surgery Review Date: 4-10, 4-12 Key Stakeholders: Surgery, IM Depts. Next Update: 4-14 RELEVANCE:
KAISER PERMANENTE OHIO BARIATRIC SURGERY (GASTROPLASTY) Methodology: Expert Opinion Issue Date: 12-05 Champion: Surgery Review Date: 4-10, 4-12 Key Stakeholders: Surgery, IM Depts. Next Update: 4-14 RELEVANCE:
Is mini bypass as mini as we think it is? Nutritional consequences
 Is mini bypass as mini as we think it is? Nutritional consequences Mini/ single loop bypass What is a mini bypass? Single loop One anastomosis Mini Prevalence Increasing Who is the single loop bypass for?
Is mini bypass as mini as we think it is? Nutritional consequences Mini/ single loop bypass What is a mini bypass? Single loop One anastomosis Mini Prevalence Increasing Who is the single loop bypass for?
Vitamin and mineral supplements after weight loss surgery. Information for patients Sheffield Dietetics
 Vitamin and mineral supplements after weight loss surgery Information for patients Sheffield Dietetics page 2 of 8 Why should I take multivitamin and minerals? After bariatric surgery, it becomes more
Vitamin and mineral supplements after weight loss surgery Information for patients Sheffield Dietetics page 2 of 8 Why should I take multivitamin and minerals? After bariatric surgery, it becomes more
Effect of Bariatric Surgery on Cardio-Metabolic Outcomes
 Effect of Bariatric Surgery on Cardio-Metabolic Outcomes Disclosure Research support from Bariatric Advantage (supplements donated for research study) Anne Schafer, MD Associate Professor of Medicine and
Effect of Bariatric Surgery on Cardio-Metabolic Outcomes Disclosure Research support from Bariatric Advantage (supplements donated for research study) Anne Schafer, MD Associate Professor of Medicine and
Policy Specific Section: April 14, 1970 June 28, 2013
 Medical Policy Bariatric Surgery Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date: April 14, 1970 June 28, 2013 Definitions
Medical Policy Bariatric Surgery Type: Medical Necessity and Investigational / Experimental Policy Specific Section: Surgery Original Policy Date: Effective Date: April 14, 1970 June 28, 2013 Definitions
VITAMIN AND MINERAL SUPPLEMENTATION AFTER BARIATRIC SURGERY. Adam Bryant, B.Sc, B.A.Sc, RD Bariatric Program St Joseph s Healthcare Hamilton
 VITAMIN AND MINERAL SUPPLEMENTATION AFTER BARIATRIC SURGERY Adam Bryant, B.Sc, B.A.Sc, RD Bariatric Program St Joseph s Healthcare Hamilton Disclosures I have no disclosures to make Overview Bariatric
VITAMIN AND MINERAL SUPPLEMENTATION AFTER BARIATRIC SURGERY Adam Bryant, B.Sc, B.A.Sc, RD Bariatric Program St Joseph s Healthcare Hamilton Disclosures I have no disclosures to make Overview Bariatric
BARIATRIC SURGERY. Weight Loss Surgery. A variety of surgical procedures to reduce weight performed on people who have obesity. Therapy Male & Female
 BARIATRIC SURGERY Weight Loss Surgery A variety of surgical procedures to reduce weight performed on people who have obesity. Therapy Male & Female About Bariatric surgery Bariatric surgery offers a treatment
BARIATRIC SURGERY Weight Loss Surgery A variety of surgical procedures to reduce weight performed on people who have obesity. Therapy Male & Female About Bariatric surgery Bariatric surgery offers a treatment
Benefits of Bariatric Surgery
 Benefits of Bariatric Surgery Dr Tan Bo Chuan Registrar, Department of Surgery GP Forum 27 May 2017 Improvements of Co-morbidities Type 2 diabetes mellitus Hypertension Hyperlipidemia Degenerative joint
Benefits of Bariatric Surgery Dr Tan Bo Chuan Registrar, Department of Surgery GP Forum 27 May 2017 Improvements of Co-morbidities Type 2 diabetes mellitus Hypertension Hyperlipidemia Degenerative joint
Obesity Who is suitable for surgery? Professor Rob Andrews University of Exeter / Taunton NHS trust
 Obesity Who is suitable for surgery? Professor Rob Andrews University of Exeter / Taunton NHS trust Investigator on BYBAND study Conflict of interest 3 Diet and Exercise studies (ACTID, EXTOD, STAMP2)
Obesity Who is suitable for surgery? Professor Rob Andrews University of Exeter / Taunton NHS trust Investigator on BYBAND study Conflict of interest 3 Diet and Exercise studies (ACTID, EXTOD, STAMP2)
Viriato Fiallo, MD Ursula McMillian, MD
 Viriato Fiallo, MD Ursula McMillian, MD Objectives Define obesity and effects on society and healthcare Define bariatric surgery Discuss recent medical management versus surgery research Evaluate different
Viriato Fiallo, MD Ursula McMillian, MD Objectives Define obesity and effects on society and healthcare Define bariatric surgery Discuss recent medical management versus surgery research Evaluate different
An Introduction to Bariatric Surgery
 An Introduction to Bariatric Surgery What is bariatric surgery? Bariatric surgery is a treatment used to help people with obesity manage their health and weight. Why use surgery to manage obesity? Obesity
An Introduction to Bariatric Surgery What is bariatric surgery? Bariatric surgery is a treatment used to help people with obesity manage their health and weight. Why use surgery to manage obesity? Obesity
EFFECTIVE SHARE CARE AGREEMENT. FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY
 Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
Specialist details Patient identifier Name Tel: EFFECTIVE SHARE CARE AGREEMENT FOR THE off license use of GLP1 mimetics in combination with insulin IN DUDLEY The aim of Effective Shared Care Guidelines
10/28/11. Bariatric Surgery: What the Primary Care Provider Should Know. Case Presentation: Rachelle
 Bariatric Surgery: What the Primary Care Provider Should Know 2,000 B.C. 2,000 A.D. Case Presentation: Rachelle 35 year-old woman with morbid obesity. 5 1 236 lbs BMI 44.5 PMHx: mild depression obstructive
Bariatric Surgery: What the Primary Care Provider Should Know 2,000 B.C. 2,000 A.D. Case Presentation: Rachelle 35 year-old woman with morbid obesity. 5 1 236 lbs BMI 44.5 PMHx: mild depression obstructive
Bariatric Surgery. Bariatric surgery could be your best option for living a healthy life. Let s find out together.
 Bariatric Surgery Bariatric surgery could be your best option for living a healthy life. Let s find out together. 1 What is obesity? Obesity is a complex health issue, characterized by an excessive amount
Bariatric Surgery Bariatric surgery could be your best option for living a healthy life. Let s find out together. 1 What is obesity? Obesity is a complex health issue, characterized by an excessive amount
Nutritional deficiencies & vitamins after surgery. What needs to be monitored? Ratna Pallapothu, MD, FACS, FASMBS
 Nutritional deficiencies & vitamins after surgery. What needs to be monitored? Ratna Pallapothu, MD, FACS, FASMBS Disclosures No financial disclosures Medical Director Bariatric program at Lourdes Types
Nutritional deficiencies & vitamins after surgery. What needs to be monitored? Ratna Pallapothu, MD, FACS, FASMBS Disclosures No financial disclosures Medical Director Bariatric program at Lourdes Types
Map 6: Percentage of people in the National Diabetes Audit (NDA) with Type 1 diabetes receiving all nine key care processes by PCT
 78 NHS ATLAS OF VARIATION ENDOCRINE, NUTRITIONAL AND METABOLIC PROBLEMS Map 6: Percentage of people in the National Diabetes Audit (NDA) with Type 1 diabetes receiving all nine key care processes by PCT
78 NHS ATLAS OF VARIATION ENDOCRINE, NUTRITIONAL AND METABOLIC PROBLEMS Map 6: Percentage of people in the National Diabetes Audit (NDA) with Type 1 diabetes receiving all nine key care processes by PCT
Obesity & Metabolic (Diabetes) Surgery
 Obesity & Metabolic (Diabetes) Surgery Sherif Awad PhD, FRCS Consultant Obesity Surgeon & Clinical Lead East-Midlands Bariatric & Metabolic Institute (EMBMI), Derby Teaching Hospitals BARS Conference,
Obesity & Metabolic (Diabetes) Surgery Sherif Awad PhD, FRCS Consultant Obesity Surgeon & Clinical Lead East-Midlands Bariatric & Metabolic Institute (EMBMI), Derby Teaching Hospitals BARS Conference,
Lecture Goals. Body Mass Index. Obesity Definitions. Bariatric Surgery What the PCP Needs to Know 11/17/2009. Indications for bariatric Surgeries
 Bariatric Surgery What the PCP Needs to Know Mouna Abouamara Assistant Professor Internal Medicine James H Quillen College Of Medicine Lecture Goals Indications for bariatric Surgeries Different types
Bariatric Surgery What the PCP Needs to Know Mouna Abouamara Assistant Professor Internal Medicine James H Quillen College Of Medicine Lecture Goals Indications for bariatric Surgeries Different types
Disclosures. Obesity and Its Challenges: Outline. Outline 5/2/2013. Lan Vu, MD Division of Pediatric Surgery Department of Surgery
 Obesity and Its Challenges: Bariatric Surgery: Why or Why Not I have nothing to disclose Disclosures Lan Vu, MD Division of Pediatric Surgery Department of Surgery Outline Growing obesity epidemic Not
Obesity and Its Challenges: Bariatric Surgery: Why or Why Not I have nothing to disclose Disclosures Lan Vu, MD Division of Pediatric Surgery Department of Surgery Outline Growing obesity epidemic Not
Bariatric surgery as a model for obesity research. Nick Finer BSc, FRCP, FAfN University College London UK
 Bariatric surgery as a model for obesity research Nick Finer BSc, FRCP, FAfN University College London UK Defining the problem - what do we know and what has been achieved (greatest achievements)? Obesity
Bariatric surgery as a model for obesity research Nick Finer BSc, FRCP, FAfN University College London UK Defining the problem - what do we know and what has been achieved (greatest achievements)? Obesity
3 Things To Know About Obesity Surgery
 3 Things To Know About Obesity Surgery Dr Jon Armstrong 1st Edition Introduction... 3 1. Am I A Candidate?... 4 2. What Are The Options?... 5 3. How Does It Work?... 6 Conclusion... 9 Follow me here...
3 Things To Know About Obesity Surgery Dr Jon Armstrong 1st Edition Introduction... 3 1. Am I A Candidate?... 4 2. What Are The Options?... 5 3. How Does It Work?... 6 Conclusion... 9 Follow me here...
Rajesh Jain MD Endorama
 50 F with history of duodenal switch presenting for low BMD Rajesh Jain MD Endorama HPI 50 F presenting with low BMD referred by PCP She has a history of malnutrition following duodenal switch procedure
50 F with history of duodenal switch presenting for low BMD Rajesh Jain MD Endorama HPI 50 F presenting with low BMD referred by PCP She has a history of malnutrition following duodenal switch procedure
Weight Loss Surgery. Outline 3/30/12. What Every GI Nurse Needs to Know. Define Morbid Obesity & its Medical Consequences. Treatments for Obesity
 3/30/12 Weight Loss Surgery What Every GI Nurse Needs to Know Kenneth A Cooper, D.O. March 31, 2012 Outline Define Morbid Obesity & its Medical Consequences Treatments for Obesity Bariatric (Weight-loss)
3/30/12 Weight Loss Surgery What Every GI Nurse Needs to Know Kenneth A Cooper, D.O. March 31, 2012 Outline Define Morbid Obesity & its Medical Consequences Treatments for Obesity Bariatric (Weight-loss)
Nutrition in obesity. Topic 23. Module Nutritional support after bariatric surgery. Copyright 2009 by ESPEN LLL Programme.
 Nutrition in obesity Topic 23 Module 23.5 Nutritional support after bariatric surgery Anders Thorell Learning Objectives To understand physiological and nutritional consequences of different bariatric
Nutrition in obesity Topic 23 Module 23.5 Nutritional support after bariatric surgery Anders Thorell Learning Objectives To understand physiological and nutritional consequences of different bariatric
Nutrition II: Long Term Post Op Care
 Nutrition II: Long Term Post Op Care Sherry Waroway, RD 2nd Annual Obesity Updates- For Healthcare Providers September 22 2018 Disclosures BSc. Nutrition and Food Science. Registered Dietitian, Edmonton
Nutrition II: Long Term Post Op Care Sherry Waroway, RD 2nd Annual Obesity Updates- For Healthcare Providers September 22 2018 Disclosures BSc. Nutrition and Food Science. Registered Dietitian, Edmonton
Update on Bariatric Surgery. Learning Objectives: At the end of this lecture you should be able to: Currently Available Options
 Update on Bariatric Surgery Dan Bessesen, MD Chief of Endocrinology; Denver Health Medical Center Professor of Medicine, University of Colorado School of Medicine Daniel.Bessesen@ucdenver.edu Learning
Update on Bariatric Surgery Dan Bessesen, MD Chief of Endocrinology; Denver Health Medical Center Professor of Medicine, University of Colorado School of Medicine Daniel.Bessesen@ucdenver.edu Learning
Not over when the surgery is done: surgical complications of obesity
 Not over when the surgery is done: surgical complications of obesity Gianluca Bonanomi, MD, FRCS Consultant Surgeon and Honorary Senior Lecturer Chelsea and Westminster Hospital London The Society for
Not over when the surgery is done: surgical complications of obesity Gianluca Bonanomi, MD, FRCS Consultant Surgeon and Honorary Senior Lecturer Chelsea and Westminster Hospital London The Society for
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease
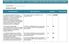 NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
NCEPOD - Measuring the Units; A review of patients who died with alcohol-related liver disease Hospital Number Admission to hospital 5. Trusts should ensure that medical patients are reviewed by a consultant
Bariatric Surgery Questionnaire
 Bariatric Surgery Questionnaire This guidance applies to N.H.S. England only. This sheet is to assist you in researching your weight loss surgery options. The National Health Service uses a Tier system
Bariatric Surgery Questionnaire This guidance applies to N.H.S. England only. This sheet is to assist you in researching your weight loss surgery options. The National Health Service uses a Tier system
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA
 GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
GASTROINTESTINAL SYSTEM MANAGEMENT OF DYSPEPSIA MANAGEMENT Dyspepsia refers to a spectrum of usually intermittent upper gastrointestinal symptoms, including epigastric pain and heartburn. For the majority
Chairman s Rounds, 02/15/2011
 Chairman s Rounds, 02/15/2011 Edward Lipkin, MD Associate Professor, Department of Medicine Division of Metabolism, Endocrinology and Nutrition University of Washington Predictive factors in patient s
Chairman s Rounds, 02/15/2011 Edward Lipkin, MD Associate Professor, Department of Medicine Division of Metabolism, Endocrinology and Nutrition University of Washington Predictive factors in patient s
Refeeding syndrome a practical approach
 Refeeding syndrome a practical approach PENG pre-bapen Conference Teaching Day Birmingham Monday 20 th November 2017 Rhys White Acting Clinical and Operational Lead Dietitian Guys and St Thomas NHS Foundation
Refeeding syndrome a practical approach PENG pre-bapen Conference Teaching Day Birmingham Monday 20 th November 2017 Rhys White Acting Clinical and Operational Lead Dietitian Guys and St Thomas NHS Foundation
GASTRIC BAND SURGERY THE FACTS THE QUESTIONS THE ANSWERS
 GASTRIC BAND SURGERY THE FACTS THE QUESTIONS THE ANSWERS A COMPANION E-BOOK FOR ANYONE CONSIDERING GASTRIC BAND, GASTRIC SLEEVE, OR GASTRIC BYPASS SURGERY www.gastricbandfrance.co.uk Tel: - 0033 686567031
GASTRIC BAND SURGERY THE FACTS THE QUESTIONS THE ANSWERS A COMPANION E-BOOK FOR ANYONE CONSIDERING GASTRIC BAND, GASTRIC SLEEVE, OR GASTRIC BYPASS SURGERY www.gastricbandfrance.co.uk Tel: - 0033 686567031
Nutrition Competency Framework (NCF) March 2016
 K1 SCIENCES understanding of the basic sciences in relation to nutrition Framework (NCF) March 2016 1. Describe the functions of essential nutrients, and the basis for the biochemical demand for energy
K1 SCIENCES understanding of the basic sciences in relation to nutrition Framework (NCF) March 2016 1. Describe the functions of essential nutrients, and the basis for the biochemical demand for energy
Outline. Types of Bariatric Surgery. Adjustable Gastric Band (LAP-BAND) Bariatric surgery
 Bariatric surgery Rona Osborne, Specialist Obesity Dietitian Glasgow and Clyde Weight Management Service November 2012- Weight Management Training Outline Types of Bariatric surgery Evidence Clinical Guidelines
Bariatric surgery Rona Osborne, Specialist Obesity Dietitian Glasgow and Clyde Weight Management Service November 2012- Weight Management Training Outline Types of Bariatric surgery Evidence Clinical Guidelines
Guideline for the management of Vitamin B12 deficiency (For adults)
 Guideline for the management of Vitamin B12 deficiency (For adults) Anaemia or Strong Clinical suspicion e.g Visual disturbance, memory loss, psychiatric abnormalities, loss of peripheral nerve function
Guideline for the management of Vitamin B12 deficiency (For adults) Anaemia or Strong Clinical suspicion e.g Visual disturbance, memory loss, psychiatric abnormalities, loss of peripheral nerve function
National Position Statement
 National Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes Background Approximately twenty five per cent (25%) of Australian
National Position Statement Weight Loss Surgery (Bariatric Surgery) and its Use in Treating Obesity or Treating and Preventing Diabetes Background Approximately twenty five per cent (25%) of Australian
Clinical Practice Guidelines for the Metabolic and Nonsurgical Support of the Bariatric Surgery Patient-2014 Update
 Clinical Practice Guidelines for the Metabolic and Nonsurgical Support of the Bariatric Surgery Patient-2014 Update 1.Introduction Obesity continues to be a major public health problem in Belgium, with
Clinical Practice Guidelines for the Metabolic and Nonsurgical Support of the Bariatric Surgery Patient-2014 Update 1.Introduction Obesity continues to be a major public health problem in Belgium, with
Cancer Genetics Unit Patient Information
 Chemoprevention for women at an increased risk of familial breast cancer Cancer Genetics Unit Patient Information What is chemoprevention? Chemoprevention describes drugs that are used to reduce the risk
Chemoprevention for women at an increased risk of familial breast cancer Cancer Genetics Unit Patient Information What is chemoprevention? Chemoprevention describes drugs that are used to reduce the risk
The Obesity Epidemic: Is There A Surgical Solution? Mr Roger Ackroyd Consultant Surgeon Northern General Hospital Sheffield UK
 The Obesity Epidemic: Is There A Surgical Solution? Mr Roger Ackroyd Consultant Surgeon Northern General Hospital Sheffield UK The right patient NICE Guidance (2002)Indications for surgery BMI >40
The Obesity Epidemic: Is There A Surgical Solution? Mr Roger Ackroyd Consultant Surgeon Northern General Hospital Sheffield UK The right patient NICE Guidance (2002)Indications for surgery BMI >40
FRESH START. Time For A BARIATRIC SURGERY! WHAT IS BARIATRIC SURGERY? UHS Medical Times EVERYTHING YOU NEED TO KNOW ABOUT علاج ال دانة وجراحة السمنة
 UHS Medical Times 1 Newsletter September 2018 علاج ال دانة وجراحة السمنة MINIMALLY INVASIVE Time For A FRESH START EVERYTHING YOU NEED TO KNOW ABOUT BARIATRIC SURGERY! While any surgical procedure carries
UHS Medical Times 1 Newsletter September 2018 علاج ال دانة وجراحة السمنة MINIMALLY INVASIVE Time For A FRESH START EVERYTHING YOU NEED TO KNOW ABOUT BARIATRIC SURGERY! While any surgical procedure carries
Having a Gastric Band
 University Teaching Trust Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2016. Document for issue as handout. This booklet aims to describe: l What is a gastric
University Teaching Trust Having a Gastric Band Hope Building Upper G.I. / Bariatrics 0161 206 5062 All Rights Reserved 2016. Document for issue as handout. This booklet aims to describe: l What is a gastric
Bariatric Patient Information Admission & Post Op Advice
 Bariatric Patient Information Admission & Post Op Advice 1 Pre-Operative Preparation Approximately 2 weeks before your operation you will receive your hospital admission documents and copies of the pre/post
Bariatric Patient Information Admission & Post Op Advice 1 Pre-Operative Preparation Approximately 2 weeks before your operation you will receive your hospital admission documents and copies of the pre/post
6/23/2011. Bariatric Surgery: What the Primary Care Provider Should Know. Case Presentation: Rachelle
 Bariatric Surgery: What the Primary Care Provider Should Know 2,000 B.C. 2,000 A.D. Case Presentation: Rachelle 35 year-old woman with morbid obesity. 5 1 236 lbs BMI 44.5 PMHx: mild depression obstructive
Bariatric Surgery: What the Primary Care Provider Should Know 2,000 B.C. 2,000 A.D. Case Presentation: Rachelle 35 year-old woman with morbid obesity. 5 1 236 lbs BMI 44.5 PMHx: mild depression obstructive
OBESITY AND WEIGHT LOSS SURGERY FOR THE PRIMARY CARE PHYSICIAN
 OBESITY AND WEIGHT LOSS SURGERY FOR THE PRIMARY CARE PHYSICIAN Nicole Basa, M.D., F.A.C.S., F.A.S.M.B.S Assistant Professor of Surgery Texas A&M Medical School Bariatric Medical Director- Cedar Park Regional
OBESITY AND WEIGHT LOSS SURGERY FOR THE PRIMARY CARE PHYSICIAN Nicole Basa, M.D., F.A.C.S., F.A.S.M.B.S Assistant Professor of Surgery Texas A&M Medical School Bariatric Medical Director- Cedar Park Regional
Guidelines for the Management of Dyspepsia and GORD. Gastroenterology/ Acute Adult Governance. Drugs and Therapeutics Committee
 Guidelines for the Management of Dyspepsia and GORD Document type: Version: 3.0 Author (name): Author (designation): Validated by Prescribing Dr. G. Lipscomb Date validated October 2015 Ratified by: Date
Guidelines for the Management of Dyspepsia and GORD Document type: Version: 3.0 Author (name): Author (designation): Validated by Prescribing Dr. G. Lipscomb Date validated October 2015 Ratified by: Date
The United Kingdom National Bariatric Surgery Registry
 The United Kingdom National Bariatric Surgery Registry First Registry Report to March 2010 Prepared by Richard Welbourn MD FRCS Alberic Fiennes MS FRCS on behalf of the NBSR Data Committee Robin Kinsman
The United Kingdom National Bariatric Surgery Registry First Registry Report to March 2010 Prepared by Richard Welbourn MD FRCS Alberic Fiennes MS FRCS on behalf of the NBSR Data Committee Robin Kinsman
Obesity and Weight Loss Surgery for the Primary Care Physician
 Saturday General Session Obesity and Weight Loss Surgery for the Primary Care Physician Nicole Basa, MD Bariatric and General Surgeon Cedar Park Surgeons, PA Cedar Park, Texas Educational Objectives By
Saturday General Session Obesity and Weight Loss Surgery for the Primary Care Physician Nicole Basa, MD Bariatric and General Surgeon Cedar Park Surgeons, PA Cedar Park, Texas Educational Objectives By
HOW CAN PRIMARY CARE CONTRIBUTE? INTEGRATING CARE & DEVELOPING PATIENT PATHWAYS Dr Carly Anna Hughes FRCGP
 HOW CAN PRIMARY CARE CONTRIBUTE? INTEGRATING CARE & DEVELOPING PATIENT PATHWAYS Dr Carly Anna Hughes FRCGP World Obesity SCOPE National Fellow Bariatric Physician Fakenham Weight Management Service Hon
HOW CAN PRIMARY CARE CONTRIBUTE? INTEGRATING CARE & DEVELOPING PATIENT PATHWAYS Dr Carly Anna Hughes FRCGP World Obesity SCOPE National Fellow Bariatric Physician Fakenham Weight Management Service Hon
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE SCOPE. Nutrition support in adults: oral supplements, enteral and parenteral feeding.
 NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
NATIONAL INSTITUTE FOR CLINICAL EXCELLENCE 1 Guideline title SCOPE Nutrition support in adults: oral supplements, enteral and parenteral feeding. 1.1 Short title Nutrition support 2 Background a) The National
Sleeve Gastrectomy Debate: Everyone Needs a Sleeve!!! Dana Portenier, MD Assistant Professor of Surgery Duke University Medical Center
 Sleeve Gastrectomy Debate: Everyone Needs a Sleeve!!! Dana Portenier, MD Assistant Professor of Surgery Duke University Medical Center 1. Safety Two Year Excess Weight Loss Two Year Weight Loss and Mortality
Sleeve Gastrectomy Debate: Everyone Needs a Sleeve!!! Dana Portenier, MD Assistant Professor of Surgery Duke University Medical Center 1. Safety Two Year Excess Weight Loss Two Year Weight Loss and Mortality
Surgery recommendations based on BMI and glycemic control
 Surgery recommendations based on BMI and glycemic control BMI (kg/m2) in type 2 diabetes patients Glycemic control Surgery guidelines 40+ (37.5+ in Asian Americans) Controlled or uncontrolled Recommended
Surgery recommendations based on BMI and glycemic control BMI (kg/m2) in type 2 diabetes patients Glycemic control Surgery guidelines 40+ (37.5+ in Asian Americans) Controlled or uncontrolled Recommended
Medical Task Force Peri Operative Recommendations
 Medical Task Force Peri Operative Recommendations Joseph Shaban, MD, FRCPC, FACE Endocrinology and Metabolism Adjunct Professor of Medicine, University of Western Ontario Medical Director, Windsor Regional
Medical Task Force Peri Operative Recommendations Joseph Shaban, MD, FRCPC, FACE Endocrinology and Metabolism Adjunct Professor of Medicine, University of Western Ontario Medical Director, Windsor Regional
Here are some types of gastric bypass surgery:
 Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
Gastric Bypass- Definition By Mayo Clinic staff Weight-loss (bariatric) surgeries change your digestive system, often limiting the amount of food you can eat. These surgeries help you lose weight and can
Bariatric Surgery Corporate Medical Policy
 Bariatric Surgery Corporate Medical Policy File name: Bariatric Surgery File code: UM.SURG.01 Origination: 07/2008 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018 Description/Summary
Bariatric Surgery Corporate Medical Policy File name: Bariatric Surgery File code: UM.SURG.01 Origination: 07/2008 Last Review: 06/2018 Next Review: 06/2019 Effective Date: 10/01/2018 Description/Summary
MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD)
 DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
DERBYSHIRE JOINT AREA PRESCRIBING COMMITTEE (JAPC) MANAGEMENT OF DYSPEPSIA AND GASTRO-OESOPHAGEAL REFLUX DISEASE (GORD) Routine endoscopic investigation of patients of any age, presenting with dyspepsia
Surgical Treatment of Obesity. 1. Understand who is an appropriate candidate for referral for surgical weight loss.
 Surgical Treatment of Obesity Learning Objectives: 1. Understand who is an appropriate candidate for referral for surgical weight loss. 2. Appreciate impact of operative weight reduction to improve co-morbid
Surgical Treatment of Obesity Learning Objectives: 1. Understand who is an appropriate candidate for referral for surgical weight loss. 2. Appreciate impact of operative weight reduction to improve co-morbid
The first 6 weeks after gastric band/bypass surgery
 Patient information The first 6 weeks after gastric band/bypass surgery Eating and drinking In the first 4-6 weeks after the operation it is vital that you keep to the diet that we have advised in order
Patient information The first 6 weeks after gastric band/bypass surgery Eating and drinking In the first 4-6 weeks after the operation it is vital that you keep to the diet that we have advised in order
PRE- AND POST-OPERATIVE MEDICAL CARE OF THE BARIATRIC SURGERY PATIENT
 Amanda G. Fontenot, MD, diplomate ABOM Obesity Medicine Specialist Bariatric Surgery Department Ochsner Medical Center PRE- AND POST-OPERATIVE MEDICAL CARE OF THE BARIATRIC SURGERY PATIENT Disclosures
Amanda G. Fontenot, MD, diplomate ABOM Obesity Medicine Specialist Bariatric Surgery Department Ochsner Medical Center PRE- AND POST-OPERATIVE MEDICAL CARE OF THE BARIATRIC SURGERY PATIENT Disclosures
Bariatric Surgery. Options & Outcomes
 Bariatric Surgery Options & Outcomes Obesity Obesity now leading cause of premature death & illness in Australia 67% of Australians are overweight or obese Australia 4 th fattest nation in OECD Obesity
Bariatric Surgery Options & Outcomes Obesity Obesity now leading cause of premature death & illness in Australia 67% of Australians are overweight or obese Australia 4 th fattest nation in OECD Obesity
NICE guideline Published: 2 September 2015 nice.org.uk/guidance/ng20
 Coeliac disease: recognition, assessment and management NICE guideline Published: 2 September 2015 nice.org.uk/guidance/ng20 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Coeliac disease: recognition, assessment and management NICE guideline Published: 2 September 2015 nice.org.uk/guidance/ng20 NICE 2017. All rights reserved. Subject to Notice of rights (https://www.nice.org.uk/terms-and-conditions#notice-ofrights).
Preparing for Surgery
 Preparing for Surgery Specialist Bariatric Surgery Dietitians Gail Pinnock Laura Carstairs Cleverly Fong Bariatric Nurse Specialist: Tamara Ramkalawan Cecilia Jones 1. 5 Golden Rules Objectives 2. Expected
Preparing for Surgery Specialist Bariatric Surgery Dietitians Gail Pinnock Laura Carstairs Cleverly Fong Bariatric Nurse Specialist: Tamara Ramkalawan Cecilia Jones 1. 5 Golden Rules Objectives 2. Expected
Specialised Services Commissioning Policy. CP29: Bariatric Surgery
 Specialised Services Commissioning Policy CP29: Bariatric Surgery Document Author: Specialist Planner, Cardiothoracic Executive Lead: Director of Planning Approved by: Management Group Issue Date: 12 June
Specialised Services Commissioning Policy CP29: Bariatric Surgery Document Author: Specialist Planner, Cardiothoracic Executive Lead: Director of Planning Approved by: Management Group Issue Date: 12 June
NHS Specialist Obesity Services
 NHS Specialist Obesity Services Teaching session for Trainee Doctors 5 th December 2017 Yvonne O Donnell, Obesity Specialist Nurse Andrea Maestre Guillen, Obesity Specialist Dietitian Outline Introduction
NHS Specialist Obesity Services Teaching session for Trainee Doctors 5 th December 2017 Yvonne O Donnell, Obesity Specialist Nurse Andrea Maestre Guillen, Obesity Specialist Dietitian Outline Introduction
SCHEDULE 2 THE SERVICES
 1 SCHEDULE 2 THE SERVICES A. Service Specifications Mandatory headings 1 4: mandatory but detail for local determination and agreement Optional headings 5-7: optional to use, detail for local determination
1 SCHEDULE 2 THE SERVICES A. Service Specifications Mandatory headings 1 4: mandatory but detail for local determination and agreement Optional headings 5-7: optional to use, detail for local determination
1. Adults; a. Risk factors. b. Who should be tested for vitamin D deficiency? c. Investigations. d. Who do we treat and how do we treat? 2.
 Vitamin D and Bone Health: A Practical Clinical Guideline for Patient Management For Adults and Children Adapted from existing local guidance, National Osteoporosis Society Practical Guides and from Royal
Vitamin D and Bone Health: A Practical Clinical Guideline for Patient Management For Adults and Children Adapted from existing local guidance, National Osteoporosis Society Practical Guides and from Royal
How Do I Eat Well when I have A Dry or Sore Mouth or Throat? /04/2018
 Patient Information Leaflets 1000 Iron Deficiency Anaemia 10 5.00 01/05/2017 1001 Bone Health 10 15.00 01/05/2017 1002 Curing Constipation Through Diet 10 5.00 01/05/2017 1005 Worried About Gaining Weight
Patient Information Leaflets 1000 Iron Deficiency Anaemia 10 5.00 01/05/2017 1001 Bone Health 10 15.00 01/05/2017 1002 Curing Constipation Through Diet 10 5.00 01/05/2017 1005 Worried About Gaining Weight
Management of dyspepsia and of Helicobacter pylori infection
 Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
Management of dyspepsia and of Helicobacter pylori infection The University of Nottingham John Atherton Wolfson Digestive Diseases Centre University of Nottingham, UK Community management of dyspepsia
JAWDA Bariatric Quality Performance Indicators. JAWDA Quarterly Guidelines for Bariatric Surgery (BS)
 JAWDA Guidelines for Bariatric Surgery (BS) January 2019 1 Table of Contents Executive Summary... 3 About this Guidance... 4 Bariatric Surgery Indicators... 5 Appendix A: Glossary... 19 Appendix B: Approved
JAWDA Guidelines for Bariatric Surgery (BS) January 2019 1 Table of Contents Executive Summary... 3 About this Guidance... 4 Bariatric Surgery Indicators... 5 Appendix A: Glossary... 19 Appendix B: Approved
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
Note: Page numbers of article titles are in boldface type. A Abdominal pain, enteral therapy in acute pancreatitis and, 812 Abscess(es), pancreatic, nutritional support for, 814 815 Acute Physiology and
GUIDELINES FOR MEDICINES MANAGEMENT FOLLOWING BARIATRIC SURGERY
 GUIDELINES FOR MEDICINES MANAGEMENT FOLLOWING BARIATRIC SURGERY This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances
GUIDELINES FOR MEDICINES MANAGEMENT FOLLOWING BARIATRIC SURGERY This guidance does not override the individual responsibility of health professionals to make appropriate decision according to the circumstances
Family Doctors Association July 2015 Weight Loss Surgery
 Family Doctors Association July 2015 Weight Loss Surgery Consultant Surgeon Salford Royal Hospital Introduction Definition BMI = weight (kg) height (m) 2 Classification: BMI (kg/m2) Description
Family Doctors Association July 2015 Weight Loss Surgery Consultant Surgeon Salford Royal Hospital Introduction Definition BMI = weight (kg) height (m) 2 Classification: BMI (kg/m2) Description
Prescribing Framework for Methotrexate for Immunosuppression in ADULTS
 Hull & East Riding Prescribing Committee Prescribing Framework for Methotrexate for Immunosuppression in ADULTS Patient s Name:.. NHS Number: Patient s Address:... (Use addressograph sticker) GP s Name:...
Hull & East Riding Prescribing Committee Prescribing Framework for Methotrexate for Immunosuppression in ADULTS Patient s Name:.. NHS Number: Patient s Address:... (Use addressograph sticker) GP s Name:...
Bariatric Surgery MM /11/2001. HMO; PPO; QUEST 05/01/2012 Section: Surgery Place(s) of Service: Outpatient; Inpatient
 Bariatric Surgery Policy Number: Original Effective Date: MM.06.003 09/11/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 05/01/2012 Section: Surgery Place(s) of Service: Outpatient;
Bariatric Surgery Policy Number: Original Effective Date: MM.06.003 09/11/2001 Line(s) of Business: Current Effective Date: HMO; PPO; QUEST 05/01/2012 Section: Surgery Place(s) of Service: Outpatient;
Module 1 An Overview of Nutrition. Module 2. Basics of Nutrition. Main Topics
 Module 1 An Overview of Nutrition Module 2 What is Nutrition? What Are Nutrients? Units of Energy Why we need energy? Maintaining energy balance Daily energy requirements Calorie Requirements for Different
Module 1 An Overview of Nutrition Module 2 What is Nutrition? What Are Nutrients? Units of Energy Why we need energy? Maintaining energy balance Daily energy requirements Calorie Requirements for Different
Bariatric Surgery Update
 Bariatric Surgery Update Alexander Perez, MD, FACS Professor of Surgery Chief, Division Minimally Invasive and Foregut Surgery Speaker Disclosure Dr. Perez has disclosed that the has no actual or potential
Bariatric Surgery Update Alexander Perez, MD, FACS Professor of Surgery Chief, Division Minimally Invasive and Foregut Surgery Speaker Disclosure Dr. Perez has disclosed that the has no actual or potential
Primary Outcome Results of DiRECT the Diabetes REmission Clinical Trial
 Finding a practical management solution for T2DM, in primary care Primary Outcome Results of DiRECT the Diabetes REmission Clinical Trial Mike Lean, Roy Taylor, and the DiRECT Team IDF Abu Dhabi, December
Finding a practical management solution for T2DM, in primary care Primary Outcome Results of DiRECT the Diabetes REmission Clinical Trial Mike Lean, Roy Taylor, and the DiRECT Team IDF Abu Dhabi, December
Prescribing Framework for Mycophenolate Mofetil or Mycophenolic Acid (Myfortic ) Post Solid Organ Transplant
 Hull & East Riding Prescribing Committee Prescribing Framework for Mycophenolate Mofetil or Mycophenolic Acid (Myfortic ) Post Solid Organ Transplant Patient s Name:.. NHS Number: Patient s Address:...
Hull & East Riding Prescribing Committee Prescribing Framework for Mycophenolate Mofetil or Mycophenolic Acid (Myfortic ) Post Solid Organ Transplant Patient s Name:.. NHS Number: Patient s Address:...
Allina Health Weight Management Weight Loss Surgery Online Post-test
 Allina Health Weight Management Weight Loss Surgery Online Post-test Name PRINT SAVE AS E-MAIL RESET Today s Date Email Address: This post-test is to be completed after viewing the on-line Informational
Allina Health Weight Management Weight Loss Surgery Online Post-test Name PRINT SAVE AS E-MAIL RESET Today s Date Email Address: This post-test is to be completed after viewing the on-line Informational
Guideline scope Neonatal parenteral nutrition
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Guideline scope Neonatal parenteral nutrition The Department of Health in England has asked NICE to develop a new guideline on parenteral nutrition in
Obesity and Bariatric Surgery Michel M. Murr, MD, FACS
 Obesity and Bariatric Surgery Michel M. Murr, MD, FACS Director of Bariatric Center Chief of Surgery, TGH Professor of Surgery, USF Disclosure Covidien: educational grants Obesity and Bariatric Surgery
Obesity and Bariatric Surgery Michel M. Murr, MD, FACS Director of Bariatric Center Chief of Surgery, TGH Professor of Surgery, USF Disclosure Covidien: educational grants Obesity and Bariatric Surgery
They are updated regularly as new NICE guidance is published. To view the latest version of this NICE Pathway see:
 bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
bring together everything NICE says on a topic in an interactive flowchart. are interactive and designed to be used online. They are updated regularly as new NICE guidance is published. To view the latest
Diabetes Head To Toe May 31, Obesity in Canada. Six million Canadians are living with obesity
 Medical & Surgical Options for the Bariatric Patient Michelle Mountain, RD, B.Sc Obesity in Canada 1 in 5 adults are obese Six million Canadians are living with obesity 1 in 10 children have clinical obesity
Medical & Surgical Options for the Bariatric Patient Michelle Mountain, RD, B.Sc Obesity in Canada 1 in 5 adults are obese Six million Canadians are living with obesity 1 in 10 children have clinical obesity
Review of Medical Nutrition Therapy In Surgical Treatment of Obesity. Bariatric Care Team Panel
 Review of Medical Nutrition Therapy In Surgical Treatment of Obesity Bariatric Care Team Panel Objectives 1. Identify surgical weight loss options 2. Identify key nutrition practice guidelines outlined
Review of Medical Nutrition Therapy In Surgical Treatment of Obesity Bariatric Care Team Panel Objectives 1. Identify surgical weight loss options 2. Identify key nutrition practice guidelines outlined
Physical health of children and adolescents
 Physical health of children and adolescents FR/CAP/02 What specialist child and adolescent psychiatrists need to know and do Faculty of Child and Adolescent Psychiatry, Royal College of Psychiatrists FACULTY
Physical health of children and adolescents FR/CAP/02 What specialist child and adolescent psychiatrists need to know and do Faculty of Child and Adolescent Psychiatry, Royal College of Psychiatrists FACULTY
