Document Version Version created as part of publication process; publisher's layout; not normally made publicly available
|
|
|
- Erin Palmer
- 5 years ago
- Views:
Transcription
1 Aalborg Universitet Venous thromboembolic complications to hysterectomy for benign disease Kahr, Henriette Strøm; Thorlacius-Ussing, Ole; Christiansen, Ole Bjarne; Skals, Regitze Kuhr; Torp-Pedersen, Christian; Knudsen, Aage Published in: Journal of Minimally Invasive Gynecology DOI (link to publication from Publisher): /j.jmig Publication date: 2018 Document Version Version created as part of publication process; publisher's layout; not normally made publicly available Link to publication from Aalborg University Citation for published version (APA): Kahr, H. S., Thorlacius-Ussing, O., Christiansen, O. B., Skals, R. K., Torp-Pedersen, C., & Knudsen, A. (2018). Venous thromboembolic complications to hysterectomy for benign disease: a nationwide cohort study. Journal of Minimally Invasive Gynecology, 25(4), e2. General rights Copyright and moral rights for the publications made accessible in the public portal are retained by the authors and/or other copyright owners and it is a condition of accessing publications that users recognise and abide by the legal requirements associated with these rights.? Users may download and print one copy of any publication from the public portal for the purpose of private study or research.? You may not further distribute the material or use it for any profit-making activity or commercial gain? You may freely distribute the URL identifying the publication in the public portal? Take down policy If you believe that this document breaches copyright please contact us at vbn@aub.aau.dk providing details, and we will remove access to the work immediately and investigate your claim. Downloaded from vbn.aau.dk on: november 28, 2018
2 Accepted Manuscript Title: Venous Thromboembolic Complications to Hysterectomy for Benign Disease. a Nationwide Cohort Study Author: Henriette Strøm Kahr, Ole Thorlacius-Ussing, Ole Bjarne Christiansen, Regitze Kuhr Skals, Christian Torp-Pedersen, Aage Knudsen PII: S (17) DOI: Reference: JMIG 3355 To appear in: The Journal of Minimally Invasive Gynecology Received date: Revised date: Accepted date: Please cite this article as: Henriette Strøm Kahr, Ole Thorlacius-Ussing, Ole Bjarne Christiansen, Regitze Kuhr Skals, Christian Torp-Pedersen, Aage Knudsen, Venous Thromboembolic Complications to Hysterectomy for Benign Disease. a Nationwide Cohort Study, The Journal of Minimally Invasive Gynecology (2017), This is a PDF file of an unedited manuscript that has been accepted for publication. As a service to our customers we are providing this early version of the manuscript. The manuscript will undergo copyediting, typesetting, and review of the resulting proof before it is published in its final form. Please note that during the production process errors may be discovered which could affect the content, and all legal disclaimers that apply to the journal pertain.
3 Venous thromboembolic complications to hysterectomy for benign disease. A nationwide cohort study. Henriette Strøm Kahr, MD, Ole Thorlacius-Ussing, MD DMSC, Ole Bjarne Christiansen, MD DMSC, Regitze Kuhr Skals, MSc, Christian Torp-Pedersen, MD DMSC FACC FESC, Aage Knudsen, MD DMSC From the Department of Gynecology and Obstetrics, Aalborg University Hospital, Aalborg, Denmark (Drs Kahr, Christiansen, Knudsen), Department of Surgical Gastroenterology, Aalborg University Hospital, Aalborg, Denmark (Drs Kahr, Thorlacius-Ussing), Department of Clinical Medicine, Aalborg University, Aalborg, Denmark (Drs Kahr, Thorlacius-Ussing, Christiansen, Torp- Pedersen, Knudsen), Fertility Clinic 4071, Rigshospitalet, University of Copenhagen, Copenhagen, Denmark (Dr Christiansen), Department of Cardiology, Aalborg University Hospital, Aalborg, Denmark (Dr Torp-Pedersen), Unit of Epidemiology and Biostatistics, Aalborg University Hospital, Aalborg, Denmark (Drs Skals, Torp-Pedersen), Department of Health Science and Technology, Aalborg University, Aalborg, Denmark (Dr Torp-Pedersen). Corresponding author Henriette Strøm Kahr, Department of Gynecology and Obstetrics, Aalborg University Hospital, 9000 Aalborg, Denmark. henristrom@gmail.com. Phone: Source of the study A nationwide cohort study using The Danish National Patient Register. Disclosure statements The authors have no conflicts of interests to declare. Henriette Strøm Kahr received financial support from Aalborg University, Department of Clinical Medicine and the Danish Cancer Research Fund during her Ph D study. Prior Presentation This work has not been presented before. Word count 2,809 (Title page, abstract, précis and references not included) Short title Venous thromboembolism after hysterectomy Précis The risk of venous thromboembolism after hysterectomy for benign disease is generally low, highest with an abdominal procedure, and particularly low after laparoscopic and vaginal procedures. 45 Venous thromboembolism after hysterectomy 1 Page 1 of 23
4 46 Abstract Study Objective: To estimate the risk of venous thromboembolic complications following abdominal, laparoscopic and vaginal hysterectomy when performed for benign disorders. 49 Design: Nationwide cohort study (Canadian Task Force Classification II-2) Setting: Data from Danish national registers on all women undergoing hysterectomy for benign conditions in the period Patients: Women aged 18 and above who underwent hysterectomy for benign disease were stratified into 3 groups according to hysterectomy approach: abdominal, laparoscopic or vaginal. 54 Intervention: Hysterectomy Measurements and Main Results: 89,931 women met the inclusion criteria. Venous thromboembolism (VTE) as a diagnosis or cause of death was identified. Risk of postoperative VTE was examined with Cox proportional hazard models adjusting for age, surgical approach and relevant comorbidities. Mean age was 49.9, 47.9 and 54.3 years for women with abdominal, laparoscopic and vaginal hysterectomy, respectively. Crude incidences of VTE within 30 days after hysterectomy were 0.24% (n=142), 0.13% (n=12) and 0.10% (n=21). The most important predictors of VTE were approach to hysterectomy and a history of thromboembolic disease. In the multivariable analysis risk of VTE was significantly reduced with laparoscopic hysterectomy (HR 0.51; 95% CI , P=.03) and vaginal hysterectomy (HR 0.39; 95% CI , P<.001) when compared to the abdominal procedure. Data on postoperative heparin thromboprophylaxis were available in 53,566 patients and adjusted HR was 0.63 (95 % CI , P=.03) in patients receiving heparin thromboprophylaxis Conclusions: The 30-day cumulative incidence of VTE after hysterectomy for benign conditions was low overall (0.19%). Laparoscopic and vaginal hysterectomy carry a lower risk than the Venous thromboembolism after hysterectomy 2 Page 2 of 23
5 69 70 abdominal procedure. Postoperative heparin thromboprophylaxis significantly reduces risk of VTE and should be considered especially if risk factors are present Keywords: Deep venous thrombosis; hysterectomy; pulmonary embolism; thromboprophylaxis Venous thromboembolism after hysterectomy 3 Page 3 of 23
6 Introduction Postoperative venous thromboembolism (VTE) is the second-most common medical complication to general surgery and results in excess morbidity and mortality[1]. The most feared consequence, pulmonary embolism (PE), is the most common preventable cause of hospital death[1]. Deep vein thrombosis (DVT) and PE are preventable with proper thromboprophylaxis as demonstrated in clinical trials[2]. One of the most common gynecologic procedures is hysterectomy with ,000 procedures per year in the United States[3,4]. Few studies have focused on the incidence of VTE in women undergoing hysterectomy for benign conditions. There are three different approaches to hysterectomy: abdominal, laparoscopic and vaginal. In 2015, 20 % were performed as abdominal, 64 % as laparoscopic assisted (including robotic-assisted surgery) and 16 % as vaginal hysterectomies in Denmark[5]. The risk of postoperative DVT and PE, in patients undergoing surgery for benign conditions, is presumed to be low in general[6,7], and in particular when performed laparoscopically[8]. This is probably the reason, why pharmacologic VTE prophylaxis has not been used systematically. Despite being the recommendation in most clinical guidelines, the proportion of patients actually receiving thromboprophylaxis after hysterectomy may be as low as 11.9%[6]. Danish guidelines recommend postoperative venous thromboprophylaxis with low molecular weight heparin administered 4-12 hours following hysterectomy in prophylactic dose once daily until discharge from hospital, this can optionally be supplemented with graduated elastic compression stockings[9]. Few studies have focused on VTE in benign gynecologic surgery and recommendations on thromboprophylaxis have mostly been based on the experience from abdominal surgery and study populations with a broad variation of risk factors[10]. The striking difference between clinical practice and guidelines calls for a more precise estimation of risk of VTE after hysterectomy for benign conditions Venous thromboembolism after hysterectomy 4 Page 4 of 23
7 Materials and Methods Data-sources This study is based on data from national Danish administrative registries. In Denmark, every resident is at the time of birth or immigration assigned a unique and permanent civil registration number, which enables linkage between nationwide administrative registers on the individual level. The Danish National Patient Register (DNPR) was established in 1977 and holds data on all hospitalizations in Denmark[11]. Each admission is registered at discharge with one primary and if appropriate one or more secondary diagnoses according to the International Classification of Diseases, the 10 th revision (ICD-10). Surgical procedures are registered according to the Nordic Medico-statistical Committee s Classification of Surgical Procedures[12], together with the indication for the procedure. There could be multiple indications for hysterectomy. We retrieved information on hormone substitution and anticoagulant treatment from The Danish Register of Medicinal Product Statistics where all prescription based pharmacy dispensings are stored. The National Population Register and the National Causes of Death Register hold information on vital status, date of birth and death including cause of death. Study population All patients who underwent hysterectomy from January 1 st 1996 until December 31 st 2015 were identified. The patients were separated into three groups according to the surgical approach: abdominal (subtotal or total abdominal hysterectomy comprised the codes KLCD00, KLCD96, KLCC10), laparoscopic (total, subtotal, vaginal and robotic assisted laparoscopic hysterectomy comprised the codes KLCD01, KLCD04, KLCC11, KLCD11, KLCD97) or vaginal (total or subtotal comprised the codes KLCD10, KLCC20, colpoperineoplasty and vaginal hysterectomy KLEF13). Patients diagnosed with any type of cancer within 1 month prior to surgery or two months following the surgical procedure were excluded (ICD10 codes DC00-96). Radical hysterectomies (KLCD30, KLCD31, KLCD40) were excluded because these procedures are only performed in the case of gynecologic malignancy. We did not include hysterectomies performed at the same time as cesarean section or hysterectomy performed at the same time as cystectomy in the case of urine Venous thromboembolism after hysterectomy 5 Page 5 of 23
8 bladder malignancy. Patients were excluded if the specific date of surgery was not defined. Outcome VTE comprised the following ICD-10 codes: I80.1 (phlebitis or thrombophlebitis in the femoral vein), I80.2 (deep phlebitis or thrombophlebitis in other veins in lower extremities), I80.3 (deep phlebitis or thrombophlebitis in other veins in lower extremities without specification), I80.8 (phlebitis or thrombophlebitis at other locations), I80.9 (phlebitis or thrombophlebitis without specification) and I26 (pulmonary embolism). If one of these codes occurred prior to the date of hysterectomy it was registered as a previous VTE. If the code was assigned to a patient within one month after hysterectomy it was registered as a postoperative VTE. Confounders Use of hormones or antithrombotic agents prior to surgery was defined as at least one claimed prescription within 180 days before surgery of the following agents: oral contraceptives with estrogen in combination with progesterone (Anatomical Therapeutic Chemical Classification G03A, G03HB01) or hormone therapy (estrogen as monotherapy or in combination with progesterone, both orally and transdermal administrated G03F, G03CX, G03CA and G03CB; low dose estrogen vagitories were excluded by product number). Antithrombotic agents were defined including antiplatelet drugs (B01AC) and anticoagulant drugs (B01 except B01AC). Co-morbidities were defined as one of the following ICD-10 codes if the code was used at discharge within 365 days prior to the hysterectomy date: ischemic heart disease (I20, I23, I24, I25), cerebral vascular disease (I60-69), acute myocardial infarction (I21), varices of the lower extremities (I83), thrombophilia (D68), heart failure ((I50), chronic obstructive lung disease (J44). Two time periods were compared as the Danish Board of Health in 2003 published a national guideline for benign hysterectomy including recommendations on postoperative VTE prophylaxis with heparin injections and graduated elastic compression stockings during hospitalization[13]. A Danish national hysterectomy database was established in October 2003 and one of the clinical Venous thromboembolism after hysterectomy 6 Page 6 of 23
9 indicators is the use of VTE prophylaxis which is registered in the DNPR by the clinicians (BOHA03C). Information on Body Mass Index (BMI) was obtained from the Danish Anesthesia Database (DAD). This information was not available for all patients since the database was established in 2004 and it does not cover all departments in Denmark. Data are reported in accordance with the STROBE statement[14] Statistics Cumulative incidence was calculated for the competing risks VTE and death after abdominal, laparoscopic and vaginal hysterectomy respectively. Time to event was calculated from the date of surgery, follow-up time was 30 days and data were analyzed using univariable and multivariable Cox proportional hazard regression. Hazard ratios (HRs) of VTE after abdominal, laparoscopic and vaginal hysterectomy were hence estimated and presented with 95% confidence intervals (95% CI). A P-value less than 0.05 was considered statistically significant. Plots of Schoenfeld Residuals were used to examine the proportional hazard assumption. Linearity between the continuous variable age and outcome was tested. Interaction between approach to hysterectomy and presence of uterine fibroids was tested using analysis of variance. Calculations were performed using SAS V.9.4 (SAS Institute, Cary, North Carolina, USA) and R version (R Core Team (2014))[15] Ethics The study was approved by The Danish Data Protection Agency (Re: , int.ref: GEH ). Permission from the ethics committee is not required for retrospective register studies in Denmark Results Venous thromboembolism after hysterectomy 7 Page 7 of 23
10 We identified 89,931 patients who underwent hysterectomy for benign conditions in the period January 1 st 1996 until December 31 st Patients were divided into three groups according to the route of hysterectomy: Abdominal (n=59,231), laparoscopic (n=9,198) and vaginal (n=21,502) (figure 1). Table 1 shows the demographic data of the cohort according to age at surgery, length of stay, body mass index (BMI), concomitant disease, use of medicine before surgery, the indication for hysterectomy and postoperative pharmacologic VTE prophylaxis. Women undergoing vaginal hysterectomy were older and more likely to have comorbidities, although the general incidence of comorbidity was low in the total cohort. The indication for hysterectomy was uterine prolapse in more than 50 % of cases within the vaginal hysterectomy group. In the abdominal and laparoscopic hysterectomy groups, uterine fibroids and abnormal uterine bleeding were the dominant causes. Comparing the two time periods before and after January 1 st, 2004 showed that the proportion of minimally invasive hysterectomy was increasing during the study period with 29,060 abdominal approaches in 36,365 hysterectomies before 2004 ~80 %. After January 1 st, % of hysterectomies were performed as laparoscopic and vaginal procedures. During 30-day follow up after surgery we observed 175 cases of VTE with 100 cases of PE. There were 109 deaths in the abdominal hysterectomy group compared to one in the laparoscopic and 12 in the vaginal hysterectomy group. Competing risk analysis of the cumulative incidence of VTE showed higher incidence with open surgery compared to the two minimally invasive methods. Cumulative incidence of mortality showed the highest incidence with open surgery compared to the two minimally invasive methods. (Figures S1 and S2 are provided in supplemental material). Unadjusted HRs in different exposure groups are provided in table 2. The indication for hysterectomy could be strongly correlated to the choice of surgery approach as surgeons might prefer to perform abdominal hysterectomy in the presence of uterine and ovarian neoplasms. Statistical testing showed no evidence of interaction between hysterectomy approach and uterine fibroids (P=0.35). Venous thromboembolism after hysterectomy 8 Page 8 of 23
11 Length of stay was associated with surgical approach (table 1) with median value highest in the abdominal hysterectomy group and univariable analysis (table 2) shows that it is significantly associated with HR of VTE. Adjusting for age, time period, ovarian and uterine neoplasms, relevant drugs and concomitant disease, the laparoscopic (HR 0.51; 95% CI , P=.03) and vaginal (HR 0.39; 95% CI , P<.001) procedures are correlated with a significantly reduced HR of VTE when compared to abdominal hysterectomy (figure 2). The use of oral hormonal contraceptives or hormone therapy did not influence on the HR of VTE in women undergoing hysterectomy (figure 2 and 3). In contrast, anticoagulant drugs, previous acute myocardial infarction (AMI) and previous VTE significantly increase the HR of VTE (figure 2 and 3). Usage of postoperative heparin as VTE prophylaxis has been registered in the DNPR since There is no change in the impact of the different factors included in the first model (figure 2) when performing the same multivariable analysis on hysterectomies performed after 2003 including VTE prophylaxis instead of time period (figure 3). This subgroup analysis shows a reduced HR (0.63; 95% CI , P=.03) for VTE in patients receiving pharmacologic VTE prophylaxis. Data on BMI were available in 11,177 patients with overall mean BMI 26.1 (SD 5.0) and 19 VTE events (table 1). We found no difference in risk of VTE between BMI groups in a univariable Cox proportional hazard regression analysis. Because of the smaller number of events we did not attempt of multivariable analysis including BMI Discussion This study demonstrates that the 30-day incidence of postoperative VTE after hysterectomy for any benign condition is low. The rate of VTE was lowest in patients treated with laparoscopic and vaginal hysterectomy compared to the abdominal approach. A Cochrane review (2009) comparing the complication rates between different procedures concluded that vaginal hysterectomy was superior to abdominal on almost all outcome measures Venous thromboembolism after hysterectomy 9 Page 9 of 23
12 and recommended laparoscopic surgery in cases where vaginal hysterectomy could not be performed[17]. However, there was no apparent difference in the VTE incidence according to surgical approach, probably due to limited power. Barber et al (2014) found an overall incidence of VTE at 0.35 % in 44,167 women undergoing hysterectomy for benign conditions and showed abdominal hysterectomy to be associated with higher risk of VTE compared to minimally invasive surgery (OR 2.45; CI )[18]. Swenson et al (2015) registered 110 VTE events (0.5%) during 30 days of follow-up in 20,496 women with hysterectomy for benign, malignant and obstetric indications. Prominent risk factors were abdominal approach, cancer, BMI>35 and increased surgical time[19]. The frequency of VTE in these studies is consistent with our findings. The association between BMI and VTE is debated and experience from bariatric surgery suggests that it has been overestimated[20]. We found no association between BMI and VTE in a subgroup of the cohort; due to missing data, we could not include BMI in the multivariable analysis. White et al (2003) showed, that the incidence of first-time VTE increases exponentially with age with a dramatically increase after the age of 60[21]. Ritch et al (2011) identified age as a significant risk factor of VTE after hysterectomy[6]. In accordance with these studies we found the crude HR of VTE increasing with age in the unadjusted model. This association could not be reproduced in the multivariable models, indicating a stronger association between VTE and approach to hysterectomy. Several studies have reported an increased risk of VTE with hormone therapy (HT) [22]. In the present study we found no difference in HR between women on HT or oral contraceptives containing estrogen compared to women not exposed. A benign pelvic mass might compress the iliac veins leading to venous stasis and subsequent thrombosis. Fletcher et al. (2009) found an increased risk of VTE (OR 3.75; CI , P<.001) among women with uterine fibroids with and without surgery when compared to the expected rate in hospitalized women[23]. Shiota et al. (2011) found an overall incidence of preoperative asymptomatic DVT at 3.7 % (31/843) in patients with benign ovarian tumors[24]. Our analysis Venous thromboembolism after hysterectomy 10 Page 10 of 23
13 indicated no correlation between any benign indication for hysterectomy and risk of postoperative symptomatic VTE. Our dataset did not contain neoplastic size, therefore, the possible impact of large tumors on VTE risk cannot be assessed. It must be emphasized that we can only report cases of symptomatic VTE s. The incidence would probably be higher with more sensitive methods as demonstrated in randomized controlled trials[2]. In Denmark, thromboprophylaxis is administered by the hospital and was not registered in the DNPR before Hansen et al. (2008) reported an increase in heparin thromboprophylaxis administered following hysterectomy from 20 % in 2004 to more than 90 % of patients undergoing hysterectomy for benign disease in 2006[25]. Surgeons were probably paying more attention to VTE prophylaxis after the establishment of the Danish Hysterectomy and Hysteroscopy Database and implementation of recommendations on postoperative VTE prophylaxis. Our results indicate a significant reduction in risk of VTE following hysterectomy for benign conditions when pharmacologic VTE prophylaxis was administered during hospital stay after surgery. The ACOG Practice Bulletin (2007) recommends initiation of venous thromboprophylaxis with graduated compression stockings or pneumatic compression devices before surgery as VTE begins in the perioperative period[10]. Our results show a decrease in HR of VTE in patients receiving postoperative heparin which is supported by Hansen et al. (2008) who found preoperative administration associated with higher risk of bleeding complications compared to postoperative administration and no apparent difference in risk of VTE.[26] From our study we cannot draw any conclusions on the timing of VTE prophylaxis. Not all patients received prophylaxis, it is likely that patients within a fast track regimen undergoing MIS are discharged before heparin administration. Increasing length of stay increased the HR of VTE in a univariable analysis (table 2), despite this finding we did not include it in the multivariable analysis as we believe the variable is not a confounder because it is on the causal pathway between main exposure and outcome[27]. Talec et al (2016) suggest individual evaluation of thromboprophylaxis in each patient based on patient- Venous thromboembolism after hysterectomy 11 Page 11 of 23
14 related risk factors, type of surgery including length of operation and duration to mobilization[28]. Our results support this approach to the planning of VTE prophylaxis. The strength of epidemiologic research using national registries is the availability of a large patient cohort. Through our study, we found an important association between the risk of VTE and the approaches to hysterectomy. Groups were considered highly comparable according to baseline characteristics. The vaginal approach was used more often in case of pelvic organ prolapse and the abdominal approach in the presence of benign neoplasms, consistent with available gynecologic guidelines[29,30]. Bias could arise from misclassification of diseases and treatments. We calculated cumulative incidence of VTE considering mortality as a competing risk to illustrate how mortality affect the probability of a VTE event to occur. As mortality was highest in the abdominal hysterectomy group we found no reason to think mortality precluded the occurrence of VTE in the laparoscopic and vaginal hysterectomy groups. The coding of co-morbidity and coexisting diseases in DNPR is validated by Thygesen et al. (2011), with a positive predictive value ranging from 82 to 100 %.[31]. The validity of VTE discharge diagnoses in DNPR was investigated by Severinsen et al. (2010) who found a positive predictive value of 75% for diagnoses coded at wards[32]. Confounding by indication could arise if the indication for hysterectomy carries a risk of developing VTE. Most other studies included patients with both benign and malignant diseases[6,19]. We chose to exclude patients with malignant disease and also obstetric patients, as these conditions are recognized risk factors for VTE[33,34] Conclusion: The risk of postoperative VTE in the first 30 days after hysterectomy is low (0.19 %). Laparoscopic and vaginal approach to hysterectomy significantly reduce the risk of VTE when compared to abdominal approach and adjusted for age and relevant risk factors. Our results indicate that postsurgical use of pharmacologic thromboprophylaxis reduce the risk of VTE. If heparin prophylaxis is not routinely used we suggest individual evaluation in each patient considering Venous thromboembolism after hysterectomy 12 Page 12 of 23
15 335 approach to surgery, concomitant disease and previous thromboembolic events Acknowledgements Danish Anesthesia Database (DAD) is acknowledged References 1 Geerts William H, Bergqvist David, Pineo Graham F, et al. Prevention of venous thromboembolism: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines (8th Edition). Chest. 2008;133(6 Suppl):381S 453S. 2 Gould Michael K, Garcia David a, Wren Sherry M, et al. Prevention of VTE in nonorthopedic surgical patients: Antithrombotic Therapy and Prevention of Thrombosis, 9th ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest. 2012;141(2 Suppl):e227S 77S. 3 Clarke-Pearson Daniel L, Geller Elizabeth J. Complications of hysterectomy. Obstet Gynecol. 2013;121(3): Wallace Sumer K, Fazzari Melissa J, Chen Hui, Cliby William A, Chalas Eva. Outcomes and Postoperative Complications After Hysterectomies Performed for Benign Compared With Malignant Indications. Obstet Gynecol. 2016;128(3): Settnes Annette. Dansk Hysterektomi og Hysteroskopi Database National Årsrapport : Ritch Jessica MB, Kim Jin Hee, Lewin Sharyn N, et al. Venous thromboembolism and use of prophylaxis among women undergoing laparoscopic hysterectomy. Obstet Gynecol. 2011;117(6): Ageno W, Manfredi E, Dentali F, et al. The incidence of venous thromboembolism following gynecologic laparoscopy: a multicenter, prospective cohort study. J Thromb Haemost. 2007;5(3): Venous thromboembolism after hysterectomy 13 Page 13 of 23
16 Nguyen Ninh T, Hinojosa Marcelo W, Fayad Christine, et al. Laparoscopic surgery is associated with a lower incidence of venous thromboembolism compared with open surgery. Ann Surg. 2007;246(6): Dansk Hysterektomi og Hysteroskopi Database ACOG practice bulletin no 84. Prevention of Deep Vein Thrombosis and Pulmonary Embolism. Obtetrics Gynecol. 2007;110(2): n.d. 12 Nordic Medico-statistical Committee. NOMESCO Classification of Surgical Procedures n.d. 13 Knudsen UB. Referenceprogram for Hysterektomi på benign indikation. [Reference programme for hysterectomy for benign disease] von Elm Erik, Altman Douglas G, Egger Matthias, Pocock Stuart J, Gøtzsche Peter C, Vandenbroucke Jan P. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol. 2008;61(4): R Core Team (2014). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria Heit John A, Spencer Frederick A, White Richard H. The epidemiology of venous thromboembolism. J Thromb Thrombolysis. 2016;41(1): Nieboer TE, Johnson N, Lethaby A, et al. Surgical approach to hysterectomy for benign gynaecological disease ( Review ). Cochrane Database Syst Rev. 2009;(3). 18 Barber Emma L, Neubauer Nikki L, Gossett Dana R. Risk of venous thromboembolism in abdominal versus minimally invasive hysterectomy for benign conditions. Am J Obstet Gynecol. 2014: Swenson Carolyn W, Berger Mitchell B, Kamdar Neil S, Campbell Darrell a, Morgan Daniel M. Risk Factors for Venous Thromboembolism After Hysterectomy. Obstet Gynecol. 2015;125(5): Venous thromboembolism after hysterectomy 14 Page 14 of 23
17 Westling Agneta, Bergqvist David, Boström Annika, Karacagil Sadettin, Gustavsson Sven. Incidence of deep venous thrombosis in patients undergoing obesity surgery. World J Surg. 2002;26(4): White Richard H. The epidemiology of venous thromboembolism. Circulation. 2003;107(23 Suppl 1):I Rossouw JE, Anderson GL, Prentice RL. Risks and Benefits of Estrogen Plus Progestin in Healthy Postmenopausal Women. JAMA. 2002;288(3): Fletcher H, Wharfe G, Williams NP, Gordon-Strachan G, Pedican M, Brooks A. Venous thromboembolism as a complication of uterine fibroids: a retrospective descriptive study. J Obstet Gynaecol. 2009;29(8): M Shiota, Y Kotani M Umemoto. Risk Factors for Deep-Vein Thrombosis and Pulmonary Thromboembolism in Benign Ovarian Tumor. Tohuku J Exp Med. 2011;225: Hansen Charlotte T, Møller Charlotte, Daugbjerg Signe, Utzon Jan, Kehlet Henrik, Ottesen Bent. Establishment of a national Danish hysterectomy database: preliminary report on the first 13,425 hysterectomies. Acta Obstet Gynecol Scand. 2008;87(5): Hansen Charlotte T, Kehlet Henrik, Møller Charlotte, Mørch Lina, Utzon Jan, Ottesen Bent. Timing of heparin prophylaxis and bleeding complications in hysterectomy a nationwide prospective cohort study of 9,949 Danish women. Acta Obstet Gynecol Scand. 2008;87(10): Greenland Sander, Pearl Judea, Robins James M. Causal Diagrams for Epidemiologic Research. Epidemiology. 1999;10(1): Talec P, Gaujoux S, Samama CM. Early ambulation and prevention of post-operative thrombo-embolic risk. J Visc Surg. 2016;153:S Sundhedsstyrelsen. Referenceprogram for hysterektomi på benign indikation American College of Obstetricians and Gynecologists Committee on Gynecologic Practice. Choosing the Route of Hysterectomy for Benign Disease. Commitee Opin ACOG. 2009;114(5): Venous thromboembolism after hysterectomy 15 Page 15 of 23
18 Thygesen Sandra K, Christiansen Christian F, Christensen Steffen, Lash Timothy L, Sørensen Henrik T. The predictive value of ICD-10 diagnostic coding used to assess Charlson comorbidity index conditions in the population-based Danish National Registry of Patients. BMC Med Res Methodol. 2011;11(1): Severinsen Marianne Tang, Kristensen Søren Risom, Overvad Kim, Dethlefsen Claus, Tjønneland Anne, Johnsen Søren Paaske. Venous thromboembolism discharge diagnoses in the Danish National Patient Registry should be used with caution. J Clin Epidemiol. 2010;63(2): Wun Ted, White Richard H. Epidemiology of cancer-related venous thromboembolism. Best Pract Res Clin Haematol. 2009;22(1): Greer Ian A. Epidemiology, risk factors and prophylaxis of venous thrombo-embolism in obstetrics and gynaecology. Baillieres Clin Obstet Gynaecol. 1997;11: Figure 1. Flowchart presenting the patient selection using Danish National Registries Figure 2. Multivariable Cox proportional Hazards Regression analysis presenting hazard ratios of venous thromboembolism associated with the approach to hysterectomy, adjusted for age, time period, ovarian and uterine neoplasm, use of sex hormones, a history of acute myocardial infarction (AMI) and previous venous thromboembolism (VTE). Abdominal hysterectomy is used as reference in the main exposure group, among categorical variables in the confounder group exposed individuals are compared to non-exposed Figure 3. Multivariable Cox proportional Hazards Regression analysis presenting hazard ratios of venous thromboembolism associated with the approach to hysterectomy, adjusted for age, use of postoperative thromboprophylaxis, ovarian and uterine neoplasm, use of sex hormones and a history of acute myocardial infarction (AMI) and previous venous thromboembolism (VTE). Venous thromboembolism after hysterectomy 16 Page 16 of 23
19 Stratified for period, showing results after Abdominal hysterectomy is used as reference in the main exposure group, among categorical variables in the confounder group exposed individuals are compared to non-exposed Figure S1. Cumulative incidence of venous thromboembolism 30 days following hysterectomy Figure S2. Cumulative incidence of death 30 days following hysterectomy Venous thromboembolism after hysterectomy 17 Page 17 of 23
20 453 Table 1. Baseline characteristics and variables related to treatment Variable* Abdominal hysterectomy N=59,231 Laparoscopic hysterectomy N=9,198 Vaginal hysterectomy N=21,502 Totals N=89,93 1 Mean age, years Median length of stay, days (interquartile range) 3 (2,5) 1 (1,2) 2 (1,2) 3 (2,4) Length of stay data missing Body Mass Index (BMI) BMI missing 52,706 8,394 17,654 78,754 Anticoagulant drugs 631 (1.1) 110 (1.2) 177 (0.8) 918 (1.0) 4,235 Antiplatelet drugs 2,243 (3.8) 359 (3.9) 1,633 (7.6) (4.7) Hormonal contraception 4,422 (7.5) 894 (9.7) 1,280 (6.0) 6,596 (7.3) Hormone therapy 7,183 (12.1) 927 (10.1) 4,821 (22.4) 12,931 (14.4) Hysterectomy before ,060 (49.1) 2,166 (23.5) 5,139 (23.9) 36,363 (40.4) Hysterectomy after ,171 (50.9) 7,032 (76.5) 16,363 (76,1) 53,566 (59.6) Indication for hysterectomy Abnormal uterine bleeding 21,187 (35.8) 4,389 (47.7) 7,806 (36.3) 33,382 (37.1) Benign ovarian neoplasm 4,910 (8.3) 292 (3.2) 189 (0.9) 5,391(6.0 ) Uterine fibroids 34,849 (58.8) 3,314 (36.0) 4,888 (22.7) 43,051 (47.9) Pelvic organ prolapse 1,209 (2.0) 319 (3.5) 10,935 (50.9) 12,463 (13.9) Pelvic pain 8,536 (14.4) 2,061 (22.4) 3,115 (14.5) 13,712 (15.2) Endometriosis 5,161 (8.7) 1,192 (13.0) 1,191 (5.5) 7,544 (8.4) Cervical intraepithelial neoplasia 1,958 (3.3) 624 (6.8) 872 (4.1) 3,454 (3.8) Endometrial hyperplasia 485 (0.8) 123 (1.3) 184 (0.9) 792 (0.9) 1,282 Urinary incontinence 628 (1.1) 66 (0.7) 588 (2.7) (1.4) Cancer predisposition 100 (0.2) 91 (1.0) 8 (0.04) 199 (0.2) Concomitant diseases Ischemic heart disease 1,498 (2.5) 329 (3.6) 902 (4.2) 2,729 (3.0) Cardiovascular disease 873 (1.5) 176 (1.9) 419 (1.9) 1,468 (1.6) History of acute myocardial infarction 320 (0.5) 67 (0.7) 186 (0.9) 573 (0.6) Thrombophilia 266 (0.4) 68 (0.7) 120 (0.6) 454 (0.5) 3,354 Varicose disease 1,838 (3.1) 350 (3.8) 1,166 (5.4) (3.7) Heart failure 345 (0.6) 53 (0.6) 158 (0.7) 556 (0.6) Chronic obstructive lung disease 720 (1.2) 136 (1.5) 337 (1.6) 1,193 Venous thromboembolism after hysterectomy 18 Page 18 of 23
21 Previous VTE 1,026 (1.7) 182 (2.0) 332 (1.5) Postoperative VTE prophylaxis N=30,171 N=7,032 N=16,363 No prophylaxis 13,755 (45.6) 2,797 (39.8) 5,623 (34.4) VTE prophylaxis 16,416 (54.4) 4,235 (60.2) 10,740 (65.6) * Data are expressed as N (column %), mean SD. There could be more than one indication for hysterectomy. Only registered in patients undergoing surgery after (1.3) 1,540 (1.7) N=53, ,175 (41.4) 31,391 (58.6) Venous thromboembolism after hysterectomy 19 Page 19 of 23
22 Table 2. Unadjusted hazard ratios (HRs) of venous thromboembolism (VTE) in different exposure groups VTE events/n HR 95 % CI P value total Age (by decade) 175/89, Age<60 years 129/72, (reference) Age 60 years 46/ Length of stay (LOS), days* 175/89, <.001 Abdominal hysterectomy 142/59, (reference) Laparoscopic hysterectomy 12/9, Vaginal hysterectomy 21/21, <.001 Previous VTE 67/1, <.001 Previous acute myocardial infarction 6/ <.001 Benign ovarian neoplasm 11/5, Uterine fibroids 76/43, Abnormal uterine bleeding 55/33, Hormone therapy 24/12, Contraceptives 13/6, Anticoagulant drugs 31/ <.001 Surgery after 2003 After implementation of VTE prophylaxis 105/53, VTE prophylaxis registered 43/31, <.001 *354 patients with missing data on LOS or LOS exceeding follow-up time of 30 days were excluded from the analysis. There were no cases of VTE within this group Venous thromboembolism after hysterectomy 20 Page 20 of 23
23 467 Figure Women 18 years of age undergoing hysterectomy in the period from January 1996 until December 2015 N = 109,280 Missing data on date of surgery (N = 310) One-month follow-up data not available due to surgery in December 2015 (N = 204) Hysterectomies with one month of follow-up N = 108,766 Hysterectomies for benign disease N = 89,931 Excluded diagnoses (N = 17,784): Patients diagnosed with any type of cancer within one month prior to or two months after hysterectomy (DC00-DC96) Radical hysterectomies (N = 1,051) Hysterectomies sorted by approach Abdominal hysterectomies (N = 59,231) Laparoscopic hysterectomies (N = 9,198) Vaginal hysterectomies (N = 21,502) Venous thromboembolism after hysterectomy 21 Page 21 of 23
24 Figure S1_bestsetConverted.png 474 Venous thromboembolism after hysterectomy 22 Page 22 of 23
25 Figure S2_bestsetConverted.png Venous thromboembolism after hysterectomy 23 Page 23 of 23
Where a licence is displayed above, please note the terms and conditions of the licence govern your use of this document.
 Using the CHA2DS2-VASc score for stroke prevention in atrial fibrillation Nielsen, Peter Brønnum; Skjøth, Flemming; Rasmussen, Lars Hvilsted; Larsen, Torben Bjerregaard; Lip, Gregory DOI: 10.1016/j.cjca.2015.01.034
Using the CHA2DS2-VASc score for stroke prevention in atrial fibrillation Nielsen, Peter Brønnum; Skjøth, Flemming; Rasmussen, Lars Hvilsted; Larsen, Torben Bjerregaard; Lip, Gregory DOI: 10.1016/j.cjca.2015.01.034
General. Recommendations. Guideline Title. Bibliographic Source(s) Guideline Status. Major Recommendations
 General Guideline Title Prevention of deep vein thrombosis and pulmonary embolism. Bibliographic Source(s) American College of Obstetricians and Gynecologists (ACOG). Prevention of deep vein thrombosis
General Guideline Title Prevention of deep vein thrombosis and pulmonary embolism. Bibliographic Source(s) American College of Obstetricians and Gynecologists (ACOG). Prevention of deep vein thrombosis
Use of vaginal hysterectomy in Denmark: rates, indications and patient characteristics
 A C TA Obstetricia et Gynecologica MAIN RESEARCH ARTICLE Use of vaginal hysterectomy in Denmark: rates, indications and patient characteristics SIDSEL LYKKE NIELSEN 1, SIGNE B. DAUGBJERG 2,3,4, HELGA GIMBEL
A C TA Obstetricia et Gynecologica MAIN RESEARCH ARTICLE Use of vaginal hysterectomy in Denmark: rates, indications and patient characteristics SIDSEL LYKKE NIELSEN 1, SIGNE B. DAUGBJERG 2,3,4, HELGA GIMBEL
VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies
 VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies VTE in Surgical Patients: Recognizing the Patients at Risk Pathogenesis of thrombosis: Virchow s triad and VTE Risk Hypercoagulability
VTE Management in Surgical Patients: Optimizing Prophylaxis Strategies VTE in Surgical Patients: Recognizing the Patients at Risk Pathogenesis of thrombosis: Virchow s triad and VTE Risk Hypercoagulability
Anticoagulation for prevention of venous thromboembolism
 Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Anticoagulation for prevention of venous thromboembolism Original article by: Michael Tam Note: updated in June 2009 with the eighth edition (from the seventh) evidence-based clinical practice guidelines
Protocol. Postsurgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Postsurgical Outpatient Use of Limb Compression Devices for (10128) (Formerly Outpatient Use of Limb Pneumatic Compression Devices for ) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15
Postsurgical Outpatient Use of Limb Compression Devices for (10128) (Formerly Outpatient Use of Limb Pneumatic Compression Devices for ) Medical Benefit Effective Date: 07/01/14 Next Review Date: 03/15
Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement. Marilyn Szekendi, PhD, RN
 Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement Marilyn Szekendi, PhD, RN ANA 7 th Annual Nursing Quality Conference, February 2013 Research Team Banafsheh Sadeghi,
Early Ambulation Reduces the Risk of Venous Thromboembolism After Total Knee Replacement Marilyn Szekendi, PhD, RN ANA 7 th Annual Nursing Quality Conference, February 2013 Research Team Banafsheh Sadeghi,
Bath, Philip M.W. and England, Timothy J. (2009) Thighlength compression stockings and DVT after stroke. Lancet. ISSN (In Press)
 Bath, Philip M.W. and England, Timothy J. (2009) Thighlength compression stockings and DVT after stroke. Lancet. ISSN 0140-6736 (In Press) Access from the University of Nottingham repository: http://eprints.nottingham.ac.uk/1087/1/lancet_clots_1_20090522_4.pdf
Bath, Philip M.W. and England, Timothy J. (2009) Thighlength compression stockings and DVT after stroke. Lancet. ISSN 0140-6736 (In Press) Access from the University of Nottingham repository: http://eprints.nottingham.ac.uk/1087/1/lancet_clots_1_20090522_4.pdf
Aalborg Universitet. Statistical analysis plan Riis, Allan; Karran, E. L. ; Jørgensen, Anette; Holst, S.; Rolving, N. Publication date: 2017
 Aalborg Universitet Statistical analysis plan Riis, Allan; Karran, E. L. ; Jørgensen, Anette; Holst, S.; Rolving, N. Publication date: 2017 Document Version Publisher's PDF, also known as Version of record
Aalborg Universitet Statistical analysis plan Riis, Allan; Karran, E. L. ; Jørgensen, Anette; Holst, S.; Rolving, N. Publication date: 2017 Document Version Publisher's PDF, also known as Version of record
*Corresponding Author:
 Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
Audit of venous thromboembolism prophylaxis administered to general surgical patients undergoing elective and emergency operations at National Hospital, Sri Lanka *Migara Seneviratne 1, Asanka Hemachandra
Clinical Policy: Dalteparin (Fragmin) Reference Number: ERX.SPA.207 Effective Date:
 Clinical Policy: (Fragmin) Reference Number: ERX.SPA.207 Effective Date: 01.11.17 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Fragmin) Reference Number: ERX.SPA.207 Effective Date: 01.11.17 Last Review Date: 11.17 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms
 TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
TITLE: Acetylsalicylic Acid for Venous Thromboembolism Prophylaxis: A Review of Clinical Evidence, Benefits and Harms DATE: 23 August 2011 CONTEXT AND POLICY ISSUES: Thromboembolism occurs when a blood
Society of Trauma Nurses TraumaCon 03/22/2018
 Prophylaxis Against Venous Thromboemblism (VTE) in Pediatric Trauma Society of Trauma Nurses TraumaCon 03/22/2018 Arash Mahajerin, MD, MSCr Hematology, CHOC Children s Specialists Orange, CA Disclosure
Prophylaxis Against Venous Thromboemblism (VTE) in Pediatric Trauma Society of Trauma Nurses TraumaCon 03/22/2018 Arash Mahajerin, MD, MSCr Hematology, CHOC Children s Specialists Orange, CA Disclosure
Gynecologic Quality Measures. David M. Jaspan, DO FACOOG Chairman The Department of Obstetrics and Gynecology The Einstein Healthcare Network
 Gynecologic Quality Measures David M. Jaspan, DO FACOOG Chairman The Department of Obstetrics and Gynecology The Einstein Healthcare Network Presenter Disclosure No Conflict of Interest to disclose No
Gynecologic Quality Measures David M. Jaspan, DO FACOOG Chairman The Department of Obstetrics and Gynecology The Einstein Healthcare Network Presenter Disclosure No Conflict of Interest to disclose No
1. SCOPE of GUIDELINE:
 Page 1 of 35 CLINICAL PRACTICE GUIDELINE: Venous Thromboembolism (VTE) Prevention Guideline: Thromboprophylaxis AUTHORIZATION: VP, Medicine Date Approved: May 17, 2012 Date Revised: Vancouver Coastal Health
Page 1 of 35 CLINICAL PRACTICE GUIDELINE: Venous Thromboembolism (VTE) Prevention Guideline: Thromboprophylaxis AUTHORIZATION: VP, Medicine Date Approved: May 17, 2012 Date Revised: Vancouver Coastal Health
LIMB COMPRESSION DEVICES FOR VENOUS THROMBOEMBOLISM PROPHYLAXIS
 PROPHYLAXIS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
PROPHYLAXIS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and drugs are dependent
Facing Gynecologic Surgery?
 Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
Facing Gynecologic Surgery? Domenico Vitobello, MD Domenico Vitobello is the medical director of the Gynecologic Unit at the Humanitas Clinical and Research Center since 2009. He has developed a comprehensive
HYSTERECTOMY FOR BENIGN CONDITIONS
 HYSTERECTOMY FOR BENIGN CONDITIONS UnitedHealthcare Oxford Clinical Policy Policy Number: SURGERY 104.7 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
HYSTERECTOMY FOR BENIGN CONDITIONS UnitedHealthcare Oxford Clinical Policy Policy Number: SURGERY 104.7 T2 Effective Date: April 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 CONDITIONS OF COVERAGE...
SUBJECT: LIMB PNEUMATIC COMPRESSION EFFECTIVE DATE: 06/27/13 DEVICES FOR VENOUS REVISED DATE: 06/26/14 THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases, medical
Update on the risk of DVT during air travel - does the economy class syndrome really exist?
 Update on the risk of DVT during air travel - does the economy class syndrome really exist? Thomas HW Stadlbauer Department of Vascular and Endovascular Surgery, Klinikum rechts der Isar, Technical University
Update on the risk of DVT during air travel - does the economy class syndrome really exist? Thomas HW Stadlbauer Department of Vascular and Endovascular Surgery, Klinikum rechts der Isar, Technical University
HYSTERECTOMY FOR BENIGN CONDITIONS
 UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
UnitedHealthcare Commercial Medical Policy HYSTERECTOMY FOR BENIGN CONDITIONS Policy Number: 2018T0572G Effective Date: September 1, 2018 Table of Contents Page INSTRUCTIONS FOR USE... 1 BENEFIT CONSIDERATIONS...
Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Clinical Position Statement Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Effective: October 2017 Next Review: September 2018 CLINICAL POSITION STATEMENT Postsurgical
Clinical Position Statement Postsurgical Home Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Effective: October 2017 Next Review: September 2018 CLINICAL POSITION STATEMENT Postsurgical
Linas Venclauskas, Juan V. Llau, Jean-Yves Jenny, Per Kjaersgaard-Andersen and Øivind Jans, for the ESA VTE Guidelines Task Force PROOF
 GUIDELINES European guidelines on perioperative venous thromboembolism prophylaxis Day surgery and fast-track surgery Linas Venclauskas, Juan V. Llau, Jean-Yves Jenny, Per Kjaersgaard-Andersen and Øivind
GUIDELINES European guidelines on perioperative venous thromboembolism prophylaxis Day surgery and fast-track surgery Linas Venclauskas, Juan V. Llau, Jean-Yves Jenny, Per Kjaersgaard-Andersen and Øivind
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE)
 DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
DVT PROPHYLAXIS IN HOSPITALIZED MEDICAL PATIENTS SAURABH MAJI SR (PULMONARY,MEDICINE) Introduction VTE (DVT/PE) is an important complication in hospitalized patients Hospitalization for acute medical illness
Corporate Medical Policy
 Corporate Medical Policy Postsurgical Home Use of Limb Compression Devices for Venous File Name: Origination: Last CAP Review: Next CAP Review: Last Review: postsurgical_home_use_of_limb_ compression_devices_for_vte_prophylaxis
Corporate Medical Policy Postsurgical Home Use of Limb Compression Devices for Venous File Name: Origination: Last CAP Review: Next CAP Review: Last Review: postsurgical_home_use_of_limb_ compression_devices_for_vte_prophylaxis
INDICATIONS FOR THROMBO-PROPHYLAXIS AND WHEN TO STOP ANTICOAGULATION BEFORE ELECTIVE SURGERY
 INDICATIONS FOR THROMBO-PROPHYLAXIS AND WHEN TO STOP ANTICOAGULATION BEFORE ELECTIVE SURGERY N.E. Pearce INTRODUCTION Preventable death Cause of morbidity and mortality Risk factors Pulmonary embolism
INDICATIONS FOR THROMBO-PROPHYLAXIS AND WHEN TO STOP ANTICOAGULATION BEFORE ELECTIVE SURGERY N.E. Pearce INTRODUCTION Preventable death Cause of morbidity and mortality Risk factors Pulmonary embolism
Abdominal versus laparoscopic hysterectomies for benign diseases: evaluation of morbidity and mortality among 465,798 cases
 Gynecol Surg (2013) 10:117 122 DOI 10.1007/s10397-013-0781-9 ORIGINAL ARTICLE Abdominal versus laparoscopic hysterectomies for benign diseases: evaluation of morbidity and mortality among 465,798 cases
Gynecol Surg (2013) 10:117 122 DOI 10.1007/s10397-013-0781-9 ORIGINAL ARTICLE Abdominal versus laparoscopic hysterectomies for benign diseases: evaluation of morbidity and mortality among 465,798 cases
Innie Chen MD, Sarka Lisonkova MD PhD, Catherine Allaire MD, Christina Williams MD, Paul Yong MD PhD, K.S. Joseph MD PhD
 Routes of hysterectomy in women with benign uterine disease in the Vancouver Coastal Health and Providence Health Care regions: a retrospective cohort analysis Innie Chen MD, Sarka Lisonkova MD PhD, Catherine
Routes of hysterectomy in women with benign uterine disease in the Vancouver Coastal Health and Providence Health Care regions: a retrospective cohort analysis Innie Chen MD, Sarka Lisonkova MD PhD, Catherine
Duration of Anticoagulant Therapy. Linda R. Kelly PharmD, PhC, CACP September 17, 2016
 Duration of Anticoagulant Therapy Linda R. Kelly PharmD, PhC, CACP September 17, 2016 Conflicts of Interest No conflicts of interest to report Objectives At the end of the program participants will be
Duration of Anticoagulant Therapy Linda R. Kelly PharmD, PhC, CACP September 17, 2016 Conflicts of Interest No conflicts of interest to report Objectives At the end of the program participants will be
Getting Started Kit VENOUS THROMBOEMBOLISM PREVENTION. Section 2: Evidence-Based Appropriate VTE Prophylaxis
 Reducing Harm Improving Healthcare Protecting Canadians VENOUS THROMBOEMBOLISM PREVENTION Getting Started Kit Section 2: Evidence-Based Appropriate VTE Prophylaxis January 2017 www.patientsafetyinstitute.ca
Reducing Harm Improving Healthcare Protecting Canadians VENOUS THROMBOEMBOLISM PREVENTION Getting Started Kit Section 2: Evidence-Based Appropriate VTE Prophylaxis January 2017 www.patientsafetyinstitute.ca
NICE Guidance: Venous thromboembolism (deep vein thrombosis and pulmonary embolism) in patients admitted to hospital 1
 The College of Emergency Medicine Patron: HRH The Princess Royal Churchill House Tel +44 (0)207 404 1999 35 Red Lion Square Fax +44 (0)207 067 1267 London WC1R 4SG www.collemergencymed.ac.uk CLINICAL EFFECTIVENESS
The College of Emergency Medicine Patron: HRH The Princess Royal Churchill House Tel +44 (0)207 404 1999 35 Red Lion Square Fax +44 (0)207 067 1267 London WC1R 4SG www.collemergencymed.ac.uk CLINICAL EFFECTIVENESS
Risk of venous thromboembolism and benefits of prophylaxis use in hospitalized medically ill US patients up to 180 days post-hospital discharge
 ORIGINAL CLINICAL INVESTIGATION Open Access Risk of venous thromboembolism and benefits of prophylaxis use in hospitalized medically ill US patients up to 180 days post-hospital discharge Li Wang 1, Nishan
ORIGINAL CLINICAL INVESTIGATION Open Access Risk of venous thromboembolism and benefits of prophylaxis use in hospitalized medically ill US patients up to 180 days post-hospital discharge Li Wang 1, Nishan
American Journal of Obstetrics and Gynecology
 American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
American Journal of Obstetrics and Gynecology 1 2 3 Recurrence of vaginal prolapse after total vaginal hysterectomy with concurrent vaginal uterosacral ligament suspension: comparison between normal-weight
Predicting Venous Thromboembolic Complications following Neurosurgical Procedures
 1 Predicting Venous Thromboembolic Complications following Neurosurgical Procedures David Dornbos III, Varun Shah, Blake Priddy, Victoria Schunemann, Ciarán Powers Venous Thromboembolic (VTE) Complications
1 Predicting Venous Thromboembolic Complications following Neurosurgical Procedures David Dornbos III, Varun Shah, Blake Priddy, Victoria Schunemann, Ciarán Powers Venous Thromboembolic (VTE) Complications
Venous Thromboembolism Prophylaxis - Why Should We Care? Harry Gibbs FRACP FCSANZ Vascular Physician The Alfred Hospital
 Venous Thromboembolism Prophylaxis - Why Should We Care? Harry Gibbs FRACP FCSANZ Vascular Physician The Alfred Hospital VTE is common and dangerous 5 VTE is Common VTE Incidence: 1.5 / 1000 per year
Venous Thromboembolism Prophylaxis - Why Should We Care? Harry Gibbs FRACP FCSANZ Vascular Physician The Alfred Hospital VTE is common and dangerous 5 VTE is Common VTE Incidence: 1.5 / 1000 per year
OUTCOMES OF ROBOTIC, LAPAROSCOPIC AND OPEN ABDOMINAL HYSTERECTOMY FOR BENING CONDITIONS IN OBESE PATIENTS
 OUTCOMES OF ROBOTIC, LAPAROSCOPIC AND OPEN ABDOMINAL HYSTERECTOMY FOR BENING CONDITIONS IN OBESE PATIENTS Omer L. Tapisiz, Tufan Oge, Ibrahim Alanbay, Mostafa Borahay, Gokhan S. Kilic Department of Obstetrics
OUTCOMES OF ROBOTIC, LAPAROSCOPIC AND OPEN ABDOMINAL HYSTERECTOMY FOR BENING CONDITIONS IN OBESE PATIENTS Omer L. Tapisiz, Tufan Oge, Ibrahim Alanbay, Mostafa Borahay, Gokhan S. Kilic Department of Obstetrics
Alcohol intake and risk of venous thromboembolism
 Blood Coagulation, Fibrinolysis and Cellular Haemostasis 39 Alcohol intake and risk of venous thromboembolism A Danish follow-up study Freja Stoltze Gaborit 1 ; Kim Overvad 2, 3 ; Mette Nørgaard 1 ; Søren
Blood Coagulation, Fibrinolysis and Cellular Haemostasis 39 Alcohol intake and risk of venous thromboembolism A Danish follow-up study Freja Stoltze Gaborit 1 ; Kim Overvad 2, 3 ; Mette Nørgaard 1 ; Søren
Symptomatic Venous Thromboembolism after Total Hip/Knee Replacement: A Population-based Taiwan Study
 IMPROVING PATIENT SAFETY Preventing & Managing Venous Thromboembolism Session 8 Data Driving Strategies for VTE Prevention and Management 3/30/2012; 15.35-15.55 Symptomatic Venous Thromboembolism after
IMPROVING PATIENT SAFETY Preventing & Managing Venous Thromboembolism Session 8 Data Driving Strategies for VTE Prevention and Management 3/30/2012; 15.35-15.55 Symptomatic Venous Thromboembolism after
Danish population-based registries in cancer pharmacoepidemiology. Cancer Pharmacoepidemiology Meeting Dublin September 2013
 Danish population-based registries in cancer pharmacoepidemiology Deirdre Cronin Fenton dc@dce.au.dk Cancer Pharmacoepidemiology Meeting Dublin September 2013 Frank L. Science 2003 The Danish Cohort The
Danish population-based registries in cancer pharmacoepidemiology Deirdre Cronin Fenton dc@dce.au.dk Cancer Pharmacoepidemiology Meeting Dublin September 2013 Frank L. Science 2003 The Danish Cohort The
AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS
 The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
The West London Medical Journal 2010 Vol 2 No 4 pp 19-24 AN AUDIT: THROMBOPROPHYLAXIS FOR TOTAL HIP REPLACEMENT PATIENTS AT NORTHWICK PARK AND CENTRAL MIDDLESEX HOSPITALS Soneji ND Agni NR Acharya MN Anjari
Clinical Policy: Dalteparin (Fragmin) Reference Number: ERX.SPA.207 Effective Date:
 Clinical Policy: (Fragmin) Reference Number: ERX.SPA.207 Effective Date: 01.11.17 Last Review Date: 02.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
Clinical Policy: (Fragmin) Reference Number: ERX.SPA.207 Effective Date: 01.11.17 Last Review Date: 02.18 Revision Log See Important Reminder at the end of this policy for important regulatory and legal
SUBJECT: LIMB PNEUMATIC COMPRESSION EFFECTIVE DATE: 06/27/13 DEVICES FOR VENOUS REVISED DATE: 06/26/14, 09/15/15,09/21/17. THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY REVISED DATE: 06/26/14, 09/15/15,09/21/17. PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
MEDICAL POLICY REVISED DATE: 06/26/14, 09/15/15,09/21/17. PAGE: 1 OF: 5 If the member's subscriber contract excludes coverage for a specific service it is not covered under that contract. In such cases,
Anus,Rectum and Colon
 JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp ORIGINAL RESEARCH ARTICLE Risk factors for bleeding in patients receiving fondaparinux after colorectal cancer surgery Jongsung Pak, Masataka
JOURNAL OF THE Anus,Rectum and Colon http://journal-arc.jp ORIGINAL RESEARCH ARTICLE Risk factors for bleeding in patients receiving fondaparinux after colorectal cancer surgery Jongsung Pak, Masataka
Page: 1 of 13. Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Last Review Status/Date: March 2014 Page: 1 of 13 Compression Devices for Venous Description Patients undergoing major orthopedic surgery are at increased risk for venous thromboembolism (VTE). Patients
Last Review Status/Date: March 2014 Page: 1 of 13 Compression Devices for Venous Description Patients undergoing major orthopedic surgery are at increased risk for venous thromboembolism (VTE). Patients
Venous Thromboembolism Prophylaxis in Gynecologic Surgery A Systematic Review
 Venous Thromboembolism Prophylaxis in Gynecologic Surgery A Systematic Review David D. Rahn, MD, Mamta M. Mamik, MD, Tatiana V. D. Sanses, MD, Kristen A. Matteson, MD, MPH, Sarit O. Aschkenazi, MD, MS,
Venous Thromboembolism Prophylaxis in Gynecologic Surgery A Systematic Review David D. Rahn, MD, Mamta M. Mamik, MD, Tatiana V. D. Sanses, MD, Kristen A. Matteson, MD, MPH, Sarit O. Aschkenazi, MD, MS,
ABSTRACT. KEY WORDS antibiotics; prophylaxis; hysterectomy
 Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Infectious Diseases in Obstetrics and Gynecology 8:230-234 (2000) (C) 2000 Wiley-Liss, Inc. Wound Infection in Gynecologic Surgery Aparna A. Kamat,* Leo Brancazio, and Mark Gibson Department of Obstetrics
Cover Page. The handle holds various files of this Leiden University dissertation.
 Cover Page The handle http://hdl.handle.net/188/20915 holds various files of this Leiden University dissertation. Author: Flinterman, Linda Elisabeth Title: Risk factors for a first and recurrent venous
Cover Page The handle http://hdl.handle.net/188/20915 holds various files of this Leiden University dissertation. Author: Flinterman, Linda Elisabeth Title: Risk factors for a first and recurrent venous
What is the risk of venous thromboembolism (VTE) in patients treated by an Outpatient Parenteral Antimicrobial Therapy (OPAT) Service?
 What is the risk of venous thromboembolism (VTE) in patients treated by an Outpatient Parenteral Antimicrobial Therapy (OPAT) Service? David A. Barr; Sharon Irvine; Neil D. Ritchie; Jay McCutcheon; R.
What is the risk of venous thromboembolism (VTE) in patients treated by an Outpatient Parenteral Antimicrobial Therapy (OPAT) Service? David A. Barr; Sharon Irvine; Neil D. Ritchie; Jay McCutcheon; R.
Venous Thromboembolism Prophylaxis: Checked!
 Venous Thromboembolism Prophylaxis: Checked! William Geerts, MD, FRCPC Director, Thromboembolism Program, Sunnybrook HSC Professor of Medicine, University of Toronto National Lead, VTE Prevention, Safer
Venous Thromboembolism Prophylaxis: Checked! William Geerts, MD, FRCPC Director, Thromboembolism Program, Sunnybrook HSC Professor of Medicine, University of Toronto National Lead, VTE Prevention, Safer
Venous Thromboembolism. Prevention
 Venous Thromboembolism Prevention August 2010 Venous Thromboembloism Prevention 1 1 Expected Practice Assess all patients upon admission to the ICU for risk factors of venous thromboembolism (VTE) and
Venous Thromboembolism Prevention August 2010 Venous Thromboembloism Prevention 1 1 Expected Practice Assess all patients upon admission to the ICU for risk factors of venous thromboembolism (VTE) and
VENOUS THROMBOEMBOLISM: DURATION OF TREATMENT
 VENOUS THROMBOEMBOLISM: DURATION OF TREATMENT OBJECTIVE: To provide guidance on the recommended duration of anticoagulant therapy for venous thromboembolism (VTE). BACKGROUND: Recurrent episodes of VTE
VENOUS THROMBOEMBOLISM: DURATION OF TREATMENT OBJECTIVE: To provide guidance on the recommended duration of anticoagulant therapy for venous thromboembolism (VTE). BACKGROUND: Recurrent episodes of VTE
Venous Thrombosis in Asia
 Venous Thrombosis in Asia Pantep Angchaisuksiri, M.D. Professor of Medicine, Mahidol University, Thailand Adjunct Associate Professor, University of North Carolina, Chapel Hill, USA Venous Thromboembolism
Venous Thrombosis in Asia Pantep Angchaisuksiri, M.D. Professor of Medicine, Mahidol University, Thailand Adjunct Associate Professor, University of North Carolina, Chapel Hill, USA Venous Thromboembolism
ACS-NSQIP 2015 Julietta Chang MD, Ali Aminian MD, Stacy A Brethauer MD, Philip R Schauer MD Bariatric and Metabolic Institute
 ACS-NSQIP 2015 Julietta Chang MD, Ali Aminian MD, Stacy A Brethauer MD, Philip R Schauer MD Bariatric and Metabolic Institute Disclosures Authors: No disclosures ACS-NSQIP Disclaimer: The American College
ACS-NSQIP 2015 Julietta Chang MD, Ali Aminian MD, Stacy A Brethauer MD, Philip R Schauer MD Bariatric and Metabolic Institute Disclosures Authors: No disclosures ACS-NSQIP Disclaimer: The American College
Supplementary Online Content
 Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Supplementary Online Content Pincus D, Ravi B, Wasserstein D. Association between wait time and 30-day mortality in adults undergoing hip fracture surgery. JAMA. doi: 10.1001/jama.2017.17606 eappendix
Page: 1 of 14. Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Subject: Post-Surgical Outpatient Use of Limb Page: 1 of 14 Last Review Status/Date: March 2015 Post-Surgical Outpatient Use of Limb Compression Devices for Venous Description Patients undergoing major
Subject: Post-Surgical Outpatient Use of Limb Page: 1 of 14 Last Review Status/Date: March 2015 Post-Surgical Outpatient Use of Limb Compression Devices for Venous Description Patients undergoing major
2018 OPTIONS FOR INDIVIDUAL MEASURES: REGISTRY ONLY. MEASURE TYPE: Process
 Quality ID #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Quality ID #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2018 OPTIONS FOR INDIVIDUAL MEASURES:
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H
 Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
Deep vein thrombosis and its prevention in critically ill adults Attia J, Ray J G, Cook D J, Douketis J, Ginsberg J S, Geerts W H Authors' objectives To systematically review the incidence of deep vein
GYNECOLOGY UPDATE IN. & Minimally Invasive Surgery. 6th Annual Collaborative Symposium
 Mayo Clinic School of Continuous Professional Development 6th Annual Collaborative Symposium UPDATE IN GYNECOLOGY & Minimally Invasive Surgery In collaboration with BRIGHAM AND WOMEN S HOSPITAL Florida
Mayo Clinic School of Continuous Professional Development 6th Annual Collaborative Symposium UPDATE IN GYNECOLOGY & Minimally Invasive Surgery In collaboration with BRIGHAM AND WOMEN S HOSPITAL Florida
Nielsen, Jane Hyldgård; Rotevatn, Torill Alise; Peven, Kimberly; Melendez-Torres, G. J.; Sørensen, Erik Elgaard; Overgaard, Charlotte
 Aalborg Universitet A realist review of the use of reminder systems for follow-up screening and early detection of type 2 diabetes in women with previous gestational diabetes Nielsen, Jane Hyldgård; Rotevatn,
Aalborg Universitet A realist review of the use of reminder systems for follow-up screening and early detection of type 2 diabetes in women with previous gestational diabetes Nielsen, Jane Hyldgård; Rotevatn,
Venous Thromboembolism (VTE) Prevention
 Venous Thromboembolism (VTE) Prevention 7 VTE Risk Assessment: General Patient Population Assess VTE risk at admission, post-op, and transfer See page 2 for VTE risk assessment among Obstetrical (OB) patients
Venous Thromboembolism (VTE) Prevention 7 VTE Risk Assessment: General Patient Population Assess VTE risk at admission, post-op, and transfer See page 2 for VTE risk assessment among Obstetrical (OB) patients
Boston Experience: Benchmark for the Nation
 Boston Experience: Benchmark for the Nation NSQIP Surgeon Champion Call January 22, 2015 David McAneny MD, FACS Vice Chair, Department of Surgery I have no relevant financial relationships or conflicts
Boston Experience: Benchmark for the Nation NSQIP Surgeon Champion Call January 22, 2015 David McAneny MD, FACS Vice Chair, Department of Surgery I have no relevant financial relationships or conflicts
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION DEVICES FOR VENOUS THROMBOEMBOLISM PROPHYLAXIS
 MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION REVISED DATE: 06/26/14, 10/15/15, 06/16/16, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria
MEDICAL POLICY SUBJECT: LIMB PNEUMATIC COMPRESSION REVISED DATE: 06/26/14, 10/15/15, 06/16/16, PAGE: 1 OF: 5 If a product excludes coverage for a service, it is not covered, and medical policy criteria
Hysterectomy : A Clinicopathologic Correlation
 Bahrain Medical Bulletin, Vol. 28, No.2, June 2006 Hysterectomy : A Clinicopathologic Correlation Layla S Abdullah, FRCPC* Objective : To study the most common pathologies identified in hysterectomy specimens
Bahrain Medical Bulletin, Vol. 28, No.2, June 2006 Hysterectomy : A Clinicopathologic Correlation Layla S Abdullah, FRCPC* Objective : To study the most common pathologies identified in hysterectomy specimens
Comparison of Venothromboembolism Prophylaxis Practices in a Winnipeg Tertiary Care Hospital to Chest Guidelines: A Quality Improvement Project
 Comparison of Venothromboembolism Prophylaxis Practices in a Winnipeg Tertiary Care Hospital to Chest Guidelines: A Quality Improvement Project Dr. Jonathan Laxton, FRCPC, R5 GIM University of Manitoba
Comparison of Venothromboembolism Prophylaxis Practices in a Winnipeg Tertiary Care Hospital to Chest Guidelines: A Quality Improvement Project Dr. Jonathan Laxton, FRCPC, R5 GIM University of Manitoba
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Svanström H, Pasternak B, Hviid A. Use of azithromycin and
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Svanström H, Pasternak B, Hviid A. Use of azithromycin and
CPT only copyright 2014 American Medical Association. All rights reserved. 12/23/2014 Page 66 of 593
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2015 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2015 PQRS OPTIONS FOR INDIVIDUAL MEASURES:
Supplementary Appendix
 Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Olesen JB, Lip GYH, Kamper A-L, et al. Stroke and bleeding
Supplementary Appendix This appendix has been provided by the authors to give readers additional information about their work. Supplement to: Olesen JB, Lip GYH, Kamper A-L, et al. Stroke and bleeding
Article begins on next page
 Association of cervical microglandular hyperplasia with exogenous progestin exposure Rutgers University has made this article freely available. Please share how this access benefits you. Your story matters.
Association of cervical microglandular hyperplasia with exogenous progestin exposure Rutgers University has made this article freely available. Please share how this access benefits you. Your story matters.
Research Article Comparison of Chemical and Mechanical Prophylaxis of Venous Thromboembolism in Nonsurgical Mechanically Ventilated Patients
 rombosis Volume 2015, Article ID 849142, 6 pages http://dx.doi.org/10.1155/2015/849142 Research Article Comparison of Chemical and Mechanical Prophylaxis of Venous Thromboembolism in Nonsurgical Mechanically
rombosis Volume 2015, Article ID 849142, 6 pages http://dx.doi.org/10.1155/2015/849142 Research Article Comparison of Chemical and Mechanical Prophylaxis of Venous Thromboembolism in Nonsurgical Mechanically
EXTENDING VTE PROPHYLAXIS IN ACUTELY ILL MEDICAL PATIENTS
 EXTENDING VTE PROPHYLAXIS IN ACUTELY ILL MEDICAL PATIENTS Samuel Z. Goldhaber, MD Director, VTE Research Group Cardiovascular Division Brigham and Women s Hospital Professor of Medicine Harvard Medical
EXTENDING VTE PROPHYLAXIS IN ACUTELY ILL MEDICAL PATIENTS Samuel Z. Goldhaber, MD Director, VTE Research Group Cardiovascular Division Brigham and Women s Hospital Professor of Medicine Harvard Medical
improved with an MIS approach. This clinical benefit for American women has been demonstrated with Level I evidence. Hysterectomy is one of the most
 Statement of the Society of Gynecologic Oncology to the Food and Drug Administration s Obstetrics and Gynecology Medical Devices Advisory Committee Concerning Safety of Laparoscopic Power Morcellation
Statement of the Society of Gynecologic Oncology to the Food and Drug Administration s Obstetrics and Gynecology Medical Devices Advisory Committee Concerning Safety of Laparoscopic Power Morcellation
Japanese Deep Vein Thrombosis
 Japanese Deep Vein Thrombosis and Pulmonary Embolism after Total Knee Arthroplasty Artificial joint and cartilage implantation center, Kitasato institute hospital, Kitasato university Yasunori Tsukimura
Japanese Deep Vein Thrombosis and Pulmonary Embolism after Total Knee Arthroplasty Artificial joint and cartilage implantation center, Kitasato institute hospital, Kitasato university Yasunori Tsukimura
OBSTETRIC ADMISSION ORDERS 1 of 4
 OBSTETRIC ADMISSION 1 of 4 Actual Estimated Weight kg Actual Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART ADMIT TO: Labor and Delivery ( ) Check, circle and/or fill in all orders
OBSTETRIC ADMISSION 1 of 4 Actual Estimated Weight kg Actual Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART ADMIT TO: Labor and Delivery ( ) Check, circle and/or fill in all orders
BSO, HRT, and ERT. No relevant financial disclosures
 BSO, HRT, and ERT Jubilee Brown, MD Professor & Associate Director, Gynecologic Oncology Levine Cancer Institute at the Carolinas HealthCare System Charlotte, North Carolina No relevant financial disclosures
BSO, HRT, and ERT Jubilee Brown, MD Professor & Associate Director, Gynecologic Oncology Levine Cancer Institute at the Carolinas HealthCare System Charlotte, North Carolina No relevant financial disclosures
MY APPROACH to the use of NOACs for stroke prevention in patients with atrial fibrillation Lip, Gregory
 MY APPROACH to the use of NOACs for stroke prevention in patients with atrial fibrillation Lip, Gregory DOI: 10.1016/j.tcm.2014.05.012 License: Other (please specify with Rights Statement) Document Version
MY APPROACH to the use of NOACs for stroke prevention in patients with atrial fibrillation Lip, Gregory DOI: 10.1016/j.tcm.2014.05.012 License: Other (please specify with Rights Statement) Document Version
Title: Low Molecular Weight Heparins (LMWH), fondaparinux (Arixtra)
 Origination: 03/29/05 Revised: 09/01/10 Annual Review: 11/20/13 Purpose: To provide guidelines and criteria for the review and decision determination of requests for medications that requires prior authorization.
Origination: 03/29/05 Revised: 09/01/10 Annual Review: 11/20/13 Purpose: To provide guidelines and criteria for the review and decision determination of requests for medications that requires prior authorization.
Prevention of Venous Thromboembolism
 Prevention of Venous Thromboembolism Surgical Care Improvement Project Dale W. Bratzler, DO, MPH President and CEO Dale W. Bratzler, DO, MPH Oklahoma Foundation for Medical Quality QIOSC Medical Director
Prevention of Venous Thromboembolism Surgical Care Improvement Project Dale W. Bratzler, DO, MPH President and CEO Dale W. Bratzler, DO, MPH Oklahoma Foundation for Medical Quality QIOSC Medical Director
Understanding thrombosis in venous thromboembolism. João Morais Head of Cardiology Division and Research Centre Leiria Hospital Centre Portugal
 Understanding thrombosis in venous thromboembolism João Morais Head of Cardiology Division and Research Centre Leiria Hospital Centre Portugal Disclosures João Morais On the last year JM received honoraria
Understanding thrombosis in venous thromboembolism João Morais Head of Cardiology Division and Research Centre Leiria Hospital Centre Portugal Disclosures João Morais On the last year JM received honoraria
Venous Thromboembolism (VTE) Prophylaxis Guideline
 Guideline Venous Thromboembolism (VTE) Prophylaxis Guideline 1. Purpose This guideline outlines the requirement for risk assessment, prescribing, administration and monitoring of venous thromboembolism
Guideline Venous Thromboembolism (VTE) Prophylaxis Guideline 1. Purpose This guideline outlines the requirement for risk assessment, prescribing, administration and monitoring of venous thromboembolism
Surgical Interruption of Pelvic Nerve Pathways for Primary and Secondary Dysmenorrhea
 Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
Page: 1 of 7 Last Review Status/Date: June 2015 for Primary and Secondary Dysmenorrhea Description Two laparoscopic surgical approaches are proposed as adjuncts to conservative surgical therapy for the
Two-thirds of the almost one-half million
 Minimally Invasive Surgery New data and the guidance of our professional societies are bringing us closer to clarity in understanding the superiority of minimally invasive techniques of hysterectomy Amy
Minimally Invasive Surgery New data and the guidance of our professional societies are bringing us closer to clarity in understanding the superiority of minimally invasive techniques of hysterectomy Amy
Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis
 29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
29 29 33 Incidence of deep vein thrombosis after major spine surgeries with no mechanical or chemical prophylaxis Author Institution Sreedharan Namboothiri Kovai Medical Center and Hospitals, Coimbatore,
COMPARATIVE EFFECTIVENESS RESEARCH IN GYNECOLOGY: OPPORTUNITIES AND CHALLENGES IN USING BIG DATA
 COMPARATIVE EFFECTIVENESS RESEARCH IN GYNECOLOGY: OPPORTUNITIES AND CHALLENGES IN USING BIG DATA Jason D. Wright, M.D. Columbia University College of Physicians and Surgeons Disclosures I have no relevant
COMPARATIVE EFFECTIVENESS RESEARCH IN GYNECOLOGY: OPPORTUNITIES AND CHALLENGES IN USING BIG DATA Jason D. Wright, M.D. Columbia University College of Physicians and Surgeons Disclosures I have no relevant
High diagnostic value of general practitioners' presumptive diagnosis for pyelonephritis, meningitis and pancreatitis
 Syddansk Universitet High diagnostic value of general practitioners' presumptive diagnosis for pyelonephritis, meningitis and pancreatitis Sriskandarajah, Srishamanthi; Carter-Storch, Rasmus ; Frydkjær-Olsen,
Syddansk Universitet High diagnostic value of general practitioners' presumptive diagnosis for pyelonephritis, meningitis and pancreatitis Sriskandarajah, Srishamanthi; Carter-Storch, Rasmus ; Frydkjær-Olsen,
Status Update on the National Cardiovascular Prevention Guidelines - JNC 8, ATP 4, and Obesity 2
 TABLE OF CONTENTS Status Update on the National Cardiovascular Prevention Guidelines 1 Drosperinone-Containing Oral Contraceptives and Venous Thromboembolism Risk 1-4 P&T Committee Formulary Action 5 Status
TABLE OF CONTENTS Status Update on the National Cardiovascular Prevention Guidelines 1 Drosperinone-Containing Oral Contraceptives and Venous Thromboembolism Risk 1-4 P&T Committee Formulary Action 5 Status
Use of combined oral contraceptives and risk of venous thromboembolism: nested case-control studies using the QResearch and CPRD databases
 open access Use of combined oral contraceptives and risk of venous thromboembolism: nested case-control studies using the and databases Yana Vinogradova, Carol Coupland, Julia Hippisley-Cox Division of
open access Use of combined oral contraceptives and risk of venous thromboembolism: nested case-control studies using the and databases Yana Vinogradova, Carol Coupland, Julia Hippisley-Cox Division of
Medical Patients: A Population at Risk
 Case Vignette A 68-year-old woman with obesity was admitted to the Medical Service with COPD and pneumonia and was treated with oral corticosteroids, bronchodilators, and antibiotics. She responded well
Case Vignette A 68-year-old woman with obesity was admitted to the Medical Service with COPD and pneumonia and was treated with oral corticosteroids, bronchodilators, and antibiotics. She responded well
Drug Class Review Newer Oral Anticoagulant Drugs
 Drug Class Review Newer Oral Anticoagulant Drugs Final Original Report May 2016 The purpose of reports is to make available information regarding the comparative clinical effectiveness and harms of different
Drug Class Review Newer Oral Anticoagulant Drugs Final Original Report May 2016 The purpose of reports is to make available information regarding the comparative clinical effectiveness and harms of different
Menopausal Hormone Therapy & Haemostasis
 Menopausal Hormone Therapy & Haemostasis The Haematologist Perspective Dr. Batia Roth-Yelinek Coagulation unit Hadassah MC Menopausal Hormone Therapy & Hemostasis Hemostatic mechanism Mechanism of estrogen
Menopausal Hormone Therapy & Haemostasis The Haematologist Perspective Dr. Batia Roth-Yelinek Coagulation unit Hadassah MC Menopausal Hormone Therapy & Hemostasis Hemostatic mechanism Mechanism of estrogen
Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis
 Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Post-Surgical Outpatient Use of Limb Compression Devices for Venous Thromboembolism Prophylaxis Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary,
Extent of lymphadenectomy for esophageal squamous cell cancer: interpreting the post-hoc analysis of a randomized trial
 Accepted Manuscript Extent of lymphadenectomy for esophageal squamous cell cancer: interpreting the post-hoc analysis of a randomized trial Vaibhav Gupta, MD PII: S0022-5223(18)33169-6 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.055
Accepted Manuscript Extent of lymphadenectomy for esophageal squamous cell cancer: interpreting the post-hoc analysis of a randomized trial Vaibhav Gupta, MD PII: S0022-5223(18)33169-6 DOI: https://doi.org/10.1016/j.jtcvs.2018.11.055
Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism
 Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
Agency for Healthcare Research and Quality Evidence Report/Technology Assessment Diagnosis and Treatment of Deep Venous Thrombosis and Pulmonary Embolism Summary Number 68 Overview Venous thromboembolism
THROMBOSIS RISK FACTOR ASSESSMENT
 Name: Procedure: Doctor: Date: THROMBOSIS RISK FACTOR ASSESSMENT CHOOSE ALL THAT APPLY EACH RISK FACTOR REPRESENTS 1 POINT Age 41 60 years Minor Surgery Planned History of Prior Major Surgery (< 1 month)
Name: Procedure: Doctor: Date: THROMBOSIS RISK FACTOR ASSESSMENT CHOOSE ALL THAT APPLY EACH RISK FACTOR REPRESENTS 1 POINT Age 41 60 years Minor Surgery Planned History of Prior Major Surgery (< 1 month)
THROMBOEMBOLIC EVENTS AFTER IVC FILTER PLACEMENT IN TRAUMA PATIENTS. Lidie Lajoie, MD SUNY Downstate Department of Surgery December 20, 2012
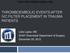 THROMBOEMBOLIC EVENTS AFTER IVC FILTER PLACEMENT IN TRAUMA PATIENTS Lidie Lajoie, MD SUNY Downstate Department of Surgery December 20, 2012 Background Trauma Patients at High Risk for VTE Spain, D.A.,
THROMBOEMBOLIC EVENTS AFTER IVC FILTER PLACEMENT IN TRAUMA PATIENTS Lidie Lajoie, MD SUNY Downstate Department of Surgery December 20, 2012 Background Trauma Patients at High Risk for VTE Spain, D.A.,
North American Menopause Society (NAMS)
 North American Menopause Society (NAMS) 2012 Hormone Therapy Position Statement Cynthia B. Evans, MD Assistant Professor-Clinical Department of Obstetrics and Gynecology The Ohio State University College
North American Menopause Society (NAMS) 2012 Hormone Therapy Position Statement Cynthia B. Evans, MD Assistant Professor-Clinical Department of Obstetrics and Gynecology The Ohio State University College
Recent Trends in Clinical Outcomes and Resource Utilization for Pulmonary Embolism in the United States. Findings From the Nationwide Inpatient Sample
 CHEST Recent Trends in Clinical Outcomes and Resource Utilization for Pulmonary Embolism in the United States Findings From the Nationwide Inpatient Sample Brian Park, MD; Louis Messina, MD; Phong Dargon,
CHEST Recent Trends in Clinical Outcomes and Resource Utilization for Pulmonary Embolism in the United States Findings From the Nationwide Inpatient Sample Brian Park, MD; Louis Messina, MD; Phong Dargon,
Is laparoscopic sleeve gastrectomy safer than laparoscopic gastric bypass?
 Is laparoscopic sleeve gastrectomy safer than laparoscopic gastric bypass? A comparison of 30-day complications using the MBSAQIP data registry Sandhya B. Kumar MD, Barbara C. Hamilton MD, Soren Jonzzon,
Is laparoscopic sleeve gastrectomy safer than laparoscopic gastric bypass? A comparison of 30-day complications using the MBSAQIP data registry Sandhya B. Kumar MD, Barbara C. Hamilton MD, Soren Jonzzon,
DENOMINATOR: All surgical patients aged 18 years and older undergoing procedures for which VTE prophylaxis is indicated in all patients
 Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
Measure #23 (NQF 0239): Perioperative Care: Venous Thromboembolism (VTE) Prophylaxis (When Indicated in ALL Patients) National Quality Strategy Domain: Patient Safety 2017 OPTIONS FOR INDIVIDUAL MEASURES:
ADULT TRANSCATHETER AORTIC VALVE REPLACEMENT (TAVR) TELEMETRY BED TRANSFER ORDERS 1 of 4
 TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Transfer to: 10 South Attending Physician: Diagnosis:
TELEMETRY BED TRANSFER 1 of 4 9 Actual 9 Estimated Patient ID Area Weight kg 9 Actual 9 Estimated Height cm ALLERGIES: REFER TO ALLERGY PROFILE/ POWERCHART Transfer to: 10 South Attending Physician: Diagnosis:
THROMBOPROPHYLAXIS: NON-ORTHOPEDIC SURGERY
 THROMBOPROPHYLAXIS: NON-ORTHOPEDIC SURGERY OBJECTIVE: To outline a practical approach for the prevention of venous thromboembolism (VTE) in patients undergoing non-orthopedic surgery. BACKGROUND: VTE is
THROMBOPROPHYLAXIS: NON-ORTHOPEDIC SURGERY OBJECTIVE: To outline a practical approach for the prevention of venous thromboembolism (VTE) in patients undergoing non-orthopedic surgery. BACKGROUND: VTE is
