THE INTRA--UTERINE DEVICE
|
|
|
- Tamsyn Copeland
- 6 years ago
- Views:
Transcription
1 CANADIAN CONSENSUS CONFERENCE THE INTRA--UTERINE DEVICE WHY CONSIDER THIS METHOD? Use of an IUD should be considered for all women who seek a reversible, effective, coitally-independent method of contraception. It is particularly appropriate for family spacing or in women who are considering long-term contraception. HOW DOES IT WORK? The primary action of all IUDs is the induction of a foreign-body reaction within the endometrium. This sterile inflammatory process is toxic to gametes, primarily spermatozoa, and effectively prevents viable sperm from passing into the Fallopian tubes. The copperbearing devices have an independent toxic effect on spermatozoa. Only copper-bearing IUDs are marketed in Canada. The progesterone- and progestin-releasing devices produce a decidual reaction in the endometrium and promote glandular exhaustion, reducing the potential for implantation of a zygote. The progestin effect on cervical mucus reduces the penetrability of sperm. These devices are not currently marketed in Canada. WHAT ARE THE PROS AND CONS? The IUD is especially suited for: 1. women who seek a reversible, effective, coitallyindependent method of contraception; 2. women seeking a private form of contraception (this may require that the IUD strings are removed or cut short); 3. women who are concerned that they may not remember to use a daily method; 4. women who are considering sterilization; 5. following delivery or abortion; 6. women who are breastfeeding; 7. women who cannot use a hormonal method of contraception. The recognized contra-indications for use of an IUD are as follows: a) Absolute 1. Pregnancy or possible pregnancy. 2. Current pelvic inflammatory disease (PID), cervicitis, bacterial vaginosis, or chlamydial or gonococcal genital infection. 3. Lifestyle with increased risk of STD. 4. Known allergy to any constituent of the device. 5. Wilson's disease (copper devices). 6. Conditions leading to increased susceptibility to infection, especially AIDS, leukaemia, IV drug abuse. 7. Undiagnosed irregular genital tract bleeding. 8. Immunosuppressed individuals. b) Relative 1. Valvular heart disease. 2. Past history of PID. 3. Presence of a prosthesis potentially at risk with blood-borne infection (e.g. hip). 4. Abnormalities of the uterus resulting in a distorted cavity or a cavity that sounds to less than 6.0cm. FIGURE 1 IUDs-GYNE-T380 AND NOVA-T JOURNALSOGC 769 JULY 1998
2 TABLE! Device PERFORMANCE OF VARIOUS INTRA-UTERINE DEVICES Cumulative pregnancy Removal for bleeding rate at one year or pain at one year Cu-T % % Nova-T % % Levonorgestrel- 0.M.2% % releasing devices References History of ectopic pregnancy. 6. Severe primary dysmenorrhoea. 7. Menorrhagia_ 8. Cervical stenosis. 9. Uterine fibroids or congenital uterine anomaly. The risks currently associated with IUD use are as follows: a) Uterine perforation Perforation occurs, partially or completely, at the time the device is inserted. The perforation rates for devices available in Canada are approximately 0.6 incidents per 1,000 insertionsy Perforation is more likely to occur when the device is inserted post-partum. Postpartum insertion of an IUD should be performed cautiously, and preferably by an experienced inserter. An IUD which has partially or completely perforated the uterine wall must be removed. Even partial perforation will reduce the contraceptive effectiveness of the device. b) Pain and abnormal bleeding At one year after insertion, five to 15 percent ofiud users will have had the device removed because of increased menstrual pain or bleeding. 11,12 This combination of symptoms may be a physiological uterine response to the presence of the device, but may also indicate the presence of a pregnancy complication (ectopic pregnancy, spontaneous abortion), pelvic infection or malpositioning of the device, including perforation. Each of these possibilities must be considered. Measured blood loss in women with IUDs indicates that the volume of uterine bleeding is reduced in women using a progesterone- or progestin-releasing device, but in copper-bearing devices it will increase by 50 to 100 percent over non-users. 13 The increased blood loss typically occurs because of increased duration and heaviness of menstrual flow, but may also result from intermenstrual bleeding and spotting. c) Pelvic inflammatory disease Of the five risk factors for PID examined in the Women's Health Study in 1981,14 use of an IUD was the weakest, with an odds ratio of 1.6. More powerful risk factors were multiple sex partners, frequent coitus, young age (less than 25 years) and black race. Further analysis of the Women's Health Study data showed the significance of duration of use of the IUD in risk for PID.IS This analysis showed a statistically significant increase in risk for PID in women whose use of their current IUD was four months or less. The relative risk ofpid was 3.8 in the first month after insertion, reaching baseline risk after four months and remaining unchanged thereafter. Bacteriologic studies of the endometrial cavity showed that it was contaminated by the insertion of an IUD, but soon afterwards the cavity had sterilized itself. Whether or not the IUD had a string did not affect the probability of developingpid. A further reanalysis of the data from the Women's Health Study (1991) yielded a relative risk for PID of 1.02 for current IUD users, compared with women using no contraception; this study concluded that IUD use did not increase the risk of PID. 16 Continuation rate at one year % % % The recent findings can be summarized as follows: Pelvic inflammatory disease related to IUD use is limited to the first few months of use; IUD-related PID is rare beyond 20 days after insertion. IS 2. Exposure to STDs is responsible for an increased risk of PID, rather than the use of an IUD. Use of an IUD in low-risk women (particularly those in stable, mutually monogamous relationships) essentially carnes no added risk of PID. Colonization of an IUD with actinomycosis-like organisms is usually detected through cervical cytology. After five years of continuous use of an IUD, more than 20 percent of cervical smears may show evidence of the organism. 19 Frank actinomycotic infection is potentially life-threatening. Demonstration of the organism in the cervical smear of a woman with an IUD raises the possibility of serious pelvic infection, and usually warrants removal of the device and appropriate follow-up. d) Infertility Most women who discontinue use of an IUD in order to conceive do so at the same rate as women who JOURNALSOGC 770 JULY1998
3 have never used an IUD. However, the association between insertion of an IUD and increased risk of PID raises concerns about possible tubal factor infertility occurring after IUD use. It is unclear how often PID leads to tubal factor infertility. Cohort studies indicate that, of women discontinuing IUD use, 72 to 96 percent of women conceive within one year of IUD removal, and up to 51 percent actually deliver within one year of removapo Such rates are comparable to those in women who have never used contraception. e) Pregnancy complications When a pregnancy occurs with an IUD in situ, the risk of spontaneous abortion is increased. The 1989 study from the UK Family Planning Research Network 2l indicated that 75 percent of pregnancies aborted if the IUD remained in situ; this figure was significantly reduced if the IUD was removed, with 89 percent of these women having a live birth. A pregnant woman who retains an IUD has a two-fold to four-fold increase in the risk of delivering prematurely.22,23 There appears to be no increase in the rate of congenital anomalies in the offspring of women who continue through pregnancy with an IUD in situ. f ) Ectopic pregnancy International studies suggest that women using an IUD have between one-half and one-fifth of the risk of ectopic pregnancy faced by a woman using no contraception. 24 This translates into an incidence in IUD users of less than 1.5 ectopic pregnancies per 1,000 womanyears of use. 25 Nevertheless, a woman who conceives with an IUD in place should have a diagnosis of ectopic pregnancy excluded. WHAT ARE THE OPTIONS? There are three IUDs currently marketed in Canada. These are the Nova-T, the Oyne-T and the Oyne-T 380 Slimline. WHAT ARE THE PREREQUISITES FOR THE USE OF THIS METHOD? The woman who decides to use an IUD must first be screened for contra-indications and for suitability of the method. All candidates for IUD insertion ideally should be screened for STDs, particularly Chlamydia and bacterial vaginosis, at a previous visit, so that the results of such screening are known before the insertion is performed. If this is not possible or available, the cervix must be carefully inspected, and the uterus and adnexal regions palpated before undertaking IUD insertion. If there is any mucopurulent discharge or pelvic tenderness present, then cervical swabs should be taken for STD screening, and the insertion delayed until the results are known. Bimanual pelvic examination also serves to determine the size, position and regularity of the uterus. It is prudent also to sound the uterus before IUD insertion, to determine the depth of the endometrial cavity, the direction and patency of the canal and to rule out any major distortions within the cavity. TIMING OF INSERTION a) Post-partum Compared with interval insertion, the insertion of an IUD in post-partum women has been associated with higher rates of expulsion and uterine perforationy The optimal time for insertion after delivery remains unclear; insertion at any time after delivery of the placenta is an option, although devices are most commonly inserted at the four to six week post-partum check. b) Post-abortion An IUD can be safely inserted into the uterus following completion of a therapeutic abortion. c) Interval Insertion of an IUD can be done at any time in the menstrual cycle, as long as pregnancy is excluded. IMPLEMENTATION STEPS A vaginal speculum is inserted and the cervix visualized. Even if the cervix appears entirely clean and healthy, it must be vigorously cleansed, with the aim of removing mucus from the external os. A cotton-tip applicator soaked in an aqueous antiseptic solution should be used in the lower part of the cervical canal. Local anaesthetic (e.g. lidocaine 1 'Yo) is injected into the anterior lip of the cervix, prior to application of a tenaculum, and it can also be used to establish a paracervical block, particularly in nulliparous women. The tenaculum is applied to the anterior lip of the cervix, and gentle traction is applied to straighten the cervical canal. The uterus is sounded. The IUD is then loaded into the barrel of the inserter, using sterile technique and following the manufacturer's recommended method. The device is loaded only as far as needed to allow insertion. The strings on the tail of the device should trail down the JOURNALSOGC 771 JULY 1998
4 inside of the barrel and be accessible through the opposite end. The flange on the outside of the barrel is adjusted so it indicates the depth of the uterine cavity (measured by the sound) to which the IUD should be inserted. The long axis of the flange must correspond to the horizontal plane in which the arms of the device will open. Steady traction is applied to the tenaculum. The tip of the inserter barrel is directed into the cervical canal and passed gently to the fundus of the cavity. The flange should abut the cervix. The device is then expelled from the barrel using a "pull" or "push" technique; it is important to follow the directions of the package insert at this stage. The barrel is removed, leaving the IUD in the uterine cavity and allowing the strings to trail through the cervix. The strings are clipped at a distance of approximately 2.Scm from the external os, in order to facilitate removal of the device. The woman will be aware before the device is inserted that there may be cramping and some bleeding immediately after insertion. An initial visit should be scheduled for three months after insertion. This will allow for the exclusion of infection, an assessment of menstrual symptoms and a check of positioning of the device. The woman should be advised to seek medical attention thereafter if she has delayed menses (to rule out pregnancy), if she has unusual pelvic pain or bleeding (to rule out infection, ectopic pregnancy or a pregnancy complication), if her partner complains of pain during intercourse or if the device is expelled. There is ordinarily no need for her to check for the strings after each period or before intercourse. As for any sexually active woman, an IUD user should have at least annual pelvic examinations and Pap. smears. TROUBLESHOOTING a) Lost strings If the strings are not seen in the cervical os, the device may have been expelled or may have perforated the uterine wall. Alternatively, the strings may have been drawn up into the cervical canal. This can be caused by an intra-uterine pregnancy. The first step is to rule out pregnancy. If pregnancy is confirmed, management is directed towards this. Once pregnancy is excluded, the cervical canal should be explored (with Q-tip swab, Cytobrush, uterine dressing forcep or a similar instrument) to see if the strings can be found. If the strings are not found, a pelvic ultrasound should be done to identify whether the IUD is inside or outside the uterus. If the device is seen within the uterus, it can be left in situ. If the device is not identified within the uterus or in the pelvis, and there is no history to suggest expulsion, a plain X-ray of the abdomen will identify whether or not the device may have perforated the uterine wall and migrated within the abdomen. The devices are radio-opaque. b) Pregnancy with IUD in place The possibility of ectopic pregnancy must be excluded. The woman will be asked about her wishes for the pregnancy. If she wishes to terminate the pregnancy, the IUD can be removed or lefr in place until that procedure. If she wishes to continue with the pregnancy, she should be advised that there is an increased risk of miscarriage regardless of what is done, but that the risk is lower if the device is gently removed. If the strings are visible, gentle traction is applied to remove the device. If the strings are not visible, gentle exploration of the cervical canal is performed. If no strings are found, the possibility of perforation must be considered. This is best excluded by pelvic ultrasound. If the device remains in the uterus, ordinarily no attempt is made to remove it. Note must be made of its recovery at the time of delivery. c) Amenorrhoea or delayed period Pregnancy must be excluded. If the woman is not pregnant, her amenorrhoea should be managed as for a woman without an IUD. If she is post-menopausal, the device should be removed. d) Pain and abnormal bleeding If pain or abnormal bleeding persists after insertion of an IUD, it is usually best to remove the device. If the woman wants to leave the device in place, it is important to rule out infection and complications of pregnancy as underlying causes. If these are excluded, the use ofnsaids will reduce the volume of menstrual bleeding by up to 40 percenrl 6 and will reduce prostaglandin-induced pain. e) The IUD cannot be removed (traction on strings causes excessive discomfort, or strings pull off) If the woman wishes to conceive, she will need to have the device removed. This will usually require hysteroscopy and removal under direct vision. If she has no wish to conceive, and the device is inside the uterus, it can be left in place; but if it has perforated the uterine wall, it must be removed surgically. JOURNALSOGC 772 JULY1998
5 f) Chlamydial or gonococcal cervicitis identified with an IUD in situ. Antibiotic therapy for the woman and for any sexual contacts must be initiated immediately. If there is any suggestion of PID (pelvic tenderness), the device must be removed, and it should also be removed in any woman planning further pregnancies. Individual judgement can be applied regarding removal of the device in cases where a woman has completed her family. She should be counselled regarding the use of barrier contraceptive methods. g) Pap. smear demonstrates actinomyosis-like organisms As described above, there is potential for these organisms to cause PID. Optimal management is to remove the device, send it for culture and institute antibiotic treatment (usually penicillin). REFERENCES 1. Wilson, JC. A New Zealand randomized comparative study of three IUDs (Nova T, MLCu375, MLAgCu250): 1-, 2- and 3-year results. Adv Contracept 1992;8: World Health Organization. Special Programme of Research, Development and Research Training in Human Reproduction. A randomized multicentre trial of the Multiload 375 and TCu380A IUDs in parous women: threeyear results. Contraception 1994;49: Luukkainen T, Allonen H, Kaukkamaa M et a/. Effective contraception with the levonorgestrel-releasing intrauterine device: 12-month report of a European multicenter study. Contraception 1987;36: Cole LP, Potts DM, Aranda C, Behliliovic B, Etman S, Moreno J, Randic L. An evaluation of the T Cu380 Ag and the Multiload Cu375. Fertil SteriI1985;43: Indian Council of Medical Research, Task Force on IUD. Randomized clinical trial with intrauterine devices (Ievonorgestrel intrauterine device (LNG), CuT 380 Ag, CuT 220C and CuT 220B). Contraception 1989;39: Luukkainen T, Allonen H, Nielsen N-C, Nygren K-G, Pyorala T. Five years' experience of intrauterine contraception with the Nova-T and the Copper-T 200. Am J Obstet GynecoI1983;147: Sastrawinata S, Farr G, Prihadi SM, Hutapea H, Anwar M, Wahyudi I, Sunjoto, Kemara KP, Champion CB, Robbins M. A comparative clinical trial of the TCu 380 Ag, Lippes Loop D, and Multiload Cu 375 IUDs in Indonesia. Contraception 1991 ;44: Sivin I, Stern J. Long-acting, more effective Copper T IUDs: a summary of US experience, Stud Fam Plann 1979;10: Sivin I, Stern J, Diaz J. Two years of intrauterine contraception with levonorgestrel and with copper: a randomized comparison of the TCu 380 Ag and levonorgestrel 2 0 ~ g devices. / d a y Contraception 1987;35: World Health Organization. Special Programme of Research, Development and Research Training in Human Reproduction. The TCu 380 A IUD and the frameless IUD "the Flexigard:" interim three-year data from an international multicentre trial. Contraception 1995;52: World Health Organization (WHO). Mechanism of action safety and efficacy of intrauterine devices. Geneva, WHO, 1987 (Technical Report Series 753). 12. Rybo G, Andersson K. IUD use and endometrial bleedings. In: Bardin CW, Mishell DR Jr (Eds). Proceedings from the Fourth International Conference on IUDs. Boston, Mass: Butterworth-Heinemann;1994: Milsom I, Andersson K, Jonasson K, Linsted G, Rybo G. The influence of the Gyne-T 380S IUD on menstrual blood loss and iron status. Contraception 1995;52: Burkman RT and the Women's Health Study. Association between intrauterine devices and pelvic inflammatory disease. Obstet GynecoI1981;57: Lee NC, Rubin GL, Ory HW, Burkman RT. Type of intrauterine device and the risk of pelvic inflammatory disease. Obstet Gynecol 1983;62: Kronmal RA, Whitney CW, Mumford SD. The intrauterine device and pelvic inflammatory disease: the Women's Health Study reanalyzed. J Clin Epidemiol1991 ;44: Chi I-C. What we have learned from recent IUD studies: a researcher's perspective. Contraception 1993;48: Farley TMM, Rosenberg MJ, Rowe P, Chen J-H, Meirik O. Intrauterine devices and pelvic inflammatory disease: an international perspective. Lancet 1992;339: Guillebaud J. Contraception. Second Edition. London: Churchill Livingstone 1993: pp Population Information Program. Population Reports. The Johns Hopkins School of Public Health, Baltimore, 1995; Volume XXII, Series B, Number 6: p UK Family Planning Research Network. Pregnancy outcome associated with the use of IUDs. Br J Fam Plann 1989;15: Alvior GT Jr. Pregnancy outcome with removal of intrauterine device. Obstet Gynecol 1973;41 : Tatum HJ, Schmidt FH, Jain AK. Management and outcome of pregnancies associated with the Copper T intrauterine devices. Am J Obstet GynecoI1976;126: Sivin I, EI Mahgoub S, McCarthy T, Mishell DR, Shoupe D, Alvarez F, Brache V, Jimenez E, Diaz J, Faundes A. Diaz MM, Coutinho E, Mattos CER, Diaz SL, Pavez M, Stern J. Longterm contraception with the Levonorgestrel20 mcg/day (Lng 20) and the Copper T 380Ag intrauterine devices: a five-year randomized study. Contraception 1990;42: Population Information Program. Population Reports. The Johns Hopkins School of Public Health Baltimore 1995; Volume XXII, Series B, Number 6: p. {O. ' 26. Guillebaud J. Reduction by mefenamic acid of increased menstrual blood loss associated with intrauterine contraception. Br J Obstet Gynaecol 1978;85: JOURNALSOGC 773 JULY 1998
1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S.
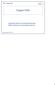 1 2 1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S. The contraceptive action of all IUDs is mainly in the uterine cavity. The major effect
1 2 1. Ortiz, M. E et al. Mechanisms of action of intrauterine devices. Obstet & Gynl Survey 1996; 51(12), 42S-51S. The contraceptive action of all IUDs is mainly in the uterine cavity. The major effect
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system)
 FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
Family Planning UNMET NEED. The Nurse Mildred Radio Talk Shows
 Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
What s New in Adolescent Contraception?
 What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage:
 Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Product Information. Confidence that lasts
 Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Confidence that lasts What is Mirena? Inhibition of sperm motility and function inside the uterus and the fallopian tubes, preventing fertilization (Videla-Rivero et al. 1987). Section of system Levonorgestrel
Information for Informed Consent for Insertion of a Mirena IUD
 Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Zurich Open Repository and Archive
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Partial and complete expulsion of the Multiload 375 IUD and the levonorgestrel-releasing
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Partial and complete expulsion of the Multiload 375 IUD and the levonorgestrel-releasing
Instruction for the patient
 WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
Contraception: I. Non-Hormonal Methods
 Contraception: I. Non-Hormonal Methods Prof. Karim Hassanein I. Abd- El-Maeboud OB/GYN Department Ain Shams University Family Planning A Branch of Reproductive Health Service (RHS). Def.: In advance regulation
Contraception: I. Non-Hormonal Methods Prof. Karim Hassanein I. Abd- El-Maeboud OB/GYN Department Ain Shams University Family Planning A Branch of Reproductive Health Service (RHS). Def.: In advance regulation
LONG-ACTING REVERSIBLE CONTRACEPTION. Summary Tables
 LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
LONG-ACTING REVERSIBLE CONTRACEPTION Summary Tables Bridging the Divide: A Project of the Jacobs Institute of Women s Health June 2016 Table 1. Summary of LARC Methods Available Years Since Effective Copper
Unintended Pregnancy is Common LEARNING OBJECTIVES. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy And Contraceptive Use
 3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
LEARNING OBJECTIVES. Beyond the Pill: Long Acting Contraception. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy is Common
 4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
INTRAUTERINE DEVICES AND INFECTIONS. Tips for Evaluation and Management
 INTRAUTERINE DEVICES AND INFECTIONS Tips for Evaluation and Management Objectives At the end of this presentation, the participant should be able to: 1. Diagnose infection after IUD placement 2. Provide
INTRAUTERINE DEVICES AND INFECTIONS Tips for Evaluation and Management Objectives At the end of this presentation, the participant should be able to: 1. Diagnose infection after IUD placement 2. Provide
the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD your guide to
 your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines
 Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines 1. Summary statement of the proposal for inclusion LNG-IUS is an effective contraceptive;
Application for inclusion of levonorgestrel - releasing IUD for contraception in the WHO Model List of Essential Medicines 1. Summary statement of the proposal for inclusion LNG-IUS is an effective contraceptive;
The use of long-acting reversible contraceptive
 Overcoming LARC complications: 7 case challenges The strings to your patient s intrauterine device (IUD) are missing. Clinical experience and ACOG direction guide the management plans for this and more
Overcoming LARC complications: 7 case challenges The strings to your patient s intrauterine device (IUD) are missing. Clinical experience and ACOG direction guide the management plans for this and more
Review of IUCD Complications: Lessons from CAT. Dr FG Mhlanga CAT Meeting 24 September 2016
 Review of IUCD Complications: Lessons from CAT Dr FG Mhlanga CAT Meeting 24 September 2016 INTRODUCTION The intrauterine device (IUD) is a reliable long term reversible, cost-effective,easy to use and
Review of IUCD Complications: Lessons from CAT Dr FG Mhlanga CAT Meeting 24 September 2016 INTRODUCTION The intrauterine device (IUD) is a reliable long term reversible, cost-effective,easy to use and
A systematic review of some of the side effects of copper T380 intrauterine contraceptive device
 A systematic review of some of the side effects of copper T380 intrauterine contraceptive device Ahmed Nehad Ahmed Hatem Askalani IAMANEH Scholarship Reproductive Health Research Course Geneva, 2006 Introduction
A systematic review of some of the side effects of copper T380 intrauterine contraceptive device Ahmed Nehad Ahmed Hatem Askalani IAMANEH Scholarship Reproductive Health Research Course Geneva, 2006 Introduction
ParaGard T 380A INTRAUTERINE COPPER CONTRACEPTIVE PRESCRIBING INFORMATION DESCRIPTION CLINICAL PHARMACOLOGY INDICATIONS AND USAGE CONTRAINDICATIONS
 % of Women Experiencing an Accidental Pregnancy within the First Year of Use % of Women Continuing Use at One Year Method (1) Typical Use 1 (2) Perfect Use 2 () (4) ParaGard T 80A INTRAUTERINE COPPER CONTRACEPTIVE
% of Women Experiencing an Accidental Pregnancy within the First Year of Use % of Women Continuing Use at One Year Method (1) Typical Use 1 (2) Perfect Use 2 () (4) ParaGard T 80A INTRAUTERINE COPPER CONTRACEPTIVE
Safety, Efficacy, and Patient Acceptability of the Copper T-380A Intrauterine Contraceptive Device
 Clinical Medicine Insights: Women s Health Review Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Safety, Efficacy, and Patient Acceptability of the Copper
Clinical Medicine Insights: Women s Health Review Open Access Full open access to this and thousands of other papers at http://www.la-press.com. Safety, Efficacy, and Patient Acceptability of the Copper
2
 1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
1 2 3 1. Usinger KM et al. Intrauterine contraception continuation in adolescents and young women: a systematic review. J Pediatr Adolesc Gynecol 2016; 29: 659 67. 2. Kost K et al. Estimates of contraceptive
Welcome to Mirena. The Mirena Handbook: A Personal Guide to Your New Mirena. mirena.com. Mirena is the #1 prescribed IUD * in the U.S.
 Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
Fitting of an Intrauterine Device (IUD)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an IUD? An IUD is a small T-shaped plastic and copper device that is put into
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an IUD? An IUD is a small T-shaped plastic and copper device that is put into
Can an iud cause back pain
 Can an iud cause back pain 3-11-2016 It can cause your periods to. Some women may also feel lightheaded from the pain. You can have most IUDs placed at any. "Intrauterine Device ( IUD )." Do not use this
Can an iud cause back pain 3-11-2016 It can cause your periods to. Some women may also feel lightheaded from the pain. You can have most IUDs placed at any. "Intrauterine Device ( IUD )." Do not use this
LIVE PLACEMENT TRAINING WEBCAST
 REGISTER FOR A LIVE PLACEMENT TRAINING WEBCAST Join us for a training webcast led by an expert speaker who brings extensive background in women s health. On this webcast, you can: Learn the steps for PARAGARD
REGISTER FOR A LIVE PLACEMENT TRAINING WEBCAST Join us for a training webcast led by an expert speaker who brings extensive background in women s health. On this webcast, you can: Learn the steps for PARAGARD
A PROSPECTIVE RANDOMIZED STUDY OF THE COPPER 7, MULTILOAD Cu 250 AND COPPER 220C IUDS IN SINGAPORE
 A PROSPECTIVE RANDOMIZED STUDY OF THE COPPER 7, MULTILOAD Cu 250 AND COPPER 220C IUDS IN SINGAPORE TG McCarthy LSLim S M M Karim S S Ratnam Department of Obstetrics and Gynaecology National University
A PROSPECTIVE RANDOMIZED STUDY OF THE COPPER 7, MULTILOAD Cu 250 AND COPPER 220C IUDS IN SINGAPORE TG McCarthy LSLim S M M Karim S S Ratnam Department of Obstetrics and Gynaecology National University
Levosert levonorgestrel 20mcg/24hour intrauterine device
 Levosert levonorgestrel 20mcg/24hour intrauterine device Verdict: Formulary inclusion: Formulary category: Restrictions: Reason for inclusion: Link to formulary: Link to medicine review summary: Levosert
Levosert levonorgestrel 20mcg/24hour intrauterine device Verdict: Formulary inclusion: Formulary category: Restrictions: Reason for inclusion: Link to formulary: Link to medicine review summary: Levosert
Levonorgestrel Intrauterine Device
 CHAPTER 11 Levonorgestrel Intrauterine Device Key Points for Providers and Clients y Long-term pregnancy protection. Very effective for 5 years, immediately reversible. yinserted into the uterus by a specifically
CHAPTER 11 Levonorgestrel Intrauterine Device Key Points for Providers and Clients y Long-term pregnancy protection. Very effective for 5 years, immediately reversible. yinserted into the uterus by a specifically
38 OBG Management August 2012 Vol. 24 No. 8 obgmanagement.com
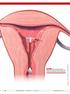 FIGURE 1 Copper intrauterine device displaced in the lower uterine segment with the left arm embedded in the myometrium. illustrations: craig zuckerman for obg management 38 OBG Management August 2012
FIGURE 1 Copper intrauterine device displaced in the lower uterine segment with the left arm embedded in the myometrium. illustrations: craig zuckerman for obg management 38 OBG Management August 2012
Carl Gustaf Nilsson, M.D. t:j: Hannu Allonen, M.D. Juan Diaz, M.D.II Tapani Luukkainen, M.D., Ph.D.t
 FERTILITY AND STERILITY Copyright 0 1983 The American Fertility Society Vol. 39, No.2, February 1983 Printed in U.8A. Two years' experience with two levonorgestrel-releasing intrauterine devices and one
FERTILITY AND STERILITY Copyright 0 1983 The American Fertility Society Vol. 39, No.2, February 1983 Printed in U.8A. Two years' experience with two levonorgestrel-releasing intrauterine devices and one
WHAT ARE CONTRACEPTIVES?
 CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
A Comparative Study between the Side Effects of Copper Intrauterine Device in Women with Non-scarred and Scarred Uterus
 Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 161-659 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ A Comparative Study between the Side Effects of Copper Intrauterine
Iraqi JMS Published by Al-Nahrain College of Medicine ISSN 161-659 Email: Iraqi_jms_alnahrain@yahoo.com http://www. colmed-nahrain.edu.iq/ A Comparative Study between the Side Effects of Copper Intrauterine
Contraceptives. Kim Dawson October 2010
 Contraceptives Kim Dawson October 2010 Objectives: You will learn about: The about the different methods of birth control. How to use each method of birth control. Emergency contraception What are they?
Contraceptives Kim Dawson October 2010 Objectives: You will learn about: The about the different methods of birth control. How to use each method of birth control. Emergency contraception What are they?
Jadelle Contraceptive Implants up to 5 years Insertion and Removal
 Contraceptive Implants up to 5 years Bayer AG Global HealthCare Programs Family Planning 13342 Berlin, Germany www.bayer.com September 2017 Global HealthCare Programs Family Planning Contraceptive Independence»»
Contraceptive Implants up to 5 years Bayer AG Global HealthCare Programs Family Planning 13342 Berlin, Germany www.bayer.com September 2017 Global HealthCare Programs Family Planning Contraceptive Independence»»
Primary Care Gynaecology Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
 Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
Primary Care Guidelines: HEAVY REGULAR MENSTRUAL BLEEDING
Gynaecology. Pelvic inflammatory disesase
 Gynaecology د.شيماءعبداألميرالجميلي Pelvic inflammatory disesase Pelvic inflammatory disease (PID) is usually the result of infection ascending from the endocervix causing endometritis, salpingitis, parametritis,
Gynaecology د.شيماءعبداألميرالجميلي Pelvic inflammatory disesase Pelvic inflammatory disease (PID) is usually the result of infection ascending from the endocervix causing endometritis, salpingitis, parametritis,
Examining Long-Acting Reversible Contraceptive Methods
 Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/examining-long-acting-reversible-contraceptivemethods/7078/
Transcript Details This is a transcript of an educational program accessible on the ReachMD network. Details about the program and additional media formats for the program are accessible by visiting: https://reachmd.com/programs/clinicians-roundtable/examining-long-acting-reversible-contraceptivemethods/7078/
Improving the Results Obtained with Current Intrauterine Contraceptive Devices
 Improving the Results Obtained with Current Intrauterine Contraceptive Devices MICHAEL S. BURNHILL, M.D., and CHARLES H. BIRNBERG, M.D. CAREFUL EXAMINATION of many of the clinical studies on the use of
Improving the Results Obtained with Current Intrauterine Contraceptive Devices MICHAEL S. BURNHILL, M.D., and CHARLES H. BIRNBERG, M.D. CAREFUL EXAMINATION of many of the clinical studies on the use of
Wendy Shen, MD, PhD Refresher Course for the Family Physician April 5, 2018 Coralville, Iowa
 Wendy Shen, MD, PhD Refresher Course for the Family Physician April 5, 2018 Coralville, Iowa Objectives Distinguish the different types of IUDs Understand the mechanism of action and selection of candidates
Wendy Shen, MD, PhD Refresher Course for the Family Physician April 5, 2018 Coralville, Iowa Objectives Distinguish the different types of IUDs Understand the mechanism of action and selection of candidates
Acute Salpingitis. Fallopian Tubes. Uterus
 Acute Salpingitis Introduction Acute salpingitis is a type of infection that affects the Fallopian tubes. The Fallopian tubes carry eggs from the ovaries to the uterus. Acute salpingitis is one of the
Acute Salpingitis Introduction Acute salpingitis is a type of infection that affects the Fallopian tubes. The Fallopian tubes carry eggs from the ovaries to the uterus. Acute salpingitis is one of the
Key words: Contraception, Copper T380A, Discontinuation.
 Discontinuation Rates among Women Using either the Combined Oral Contraceptive Pills or an Intrauterine Contraceptive Device for Contraception: A Comparative Study Ehab Al-Rayyan MD*, Zakarya Bani Meri
Discontinuation Rates among Women Using either the Combined Oral Contraceptive Pills or an Intrauterine Contraceptive Device for Contraception: A Comparative Study Ehab Al-Rayyan MD*, Zakarya Bani Meri
maybe it s time to With Your Current And move on to 100% hormone free, more than 99% effective Paragard (intrauterine copper contraceptive) IUD.
 maybe it s time to With Your Current And move on to 100% hormone free, more than 99% effective Paragard (intrauterine copper contraceptive) IUD. thinking about ParaGard (INTRAUTERINE COPPER CONTRACEPTIVE)?
maybe it s time to With Your Current And move on to 100% hormone free, more than 99% effective Paragard (intrauterine copper contraceptive) IUD. thinking about ParaGard (INTRAUTERINE COPPER CONTRACEPTIVE)?
Hysteroscopy. What you need to know. 139 Dumaresq Street Campbelltown Phone Fax
 Hysteroscopy What you need to know 139 Dumaresq Street Campbelltown Phone 4628 5292 Fax 4628 0349 www.nureva.com.au September 2015 HYSTEROSCOPY AND DILATATION & CURETTAGE OF THE UTERUS Introduction I have
Hysteroscopy What you need to know 139 Dumaresq Street Campbelltown Phone 4628 5292 Fax 4628 0349 www.nureva.com.au September 2015 HYSTEROSCOPY AND DILATATION & CURETTAGE OF THE UTERUS Introduction I have
Treatment of menorrhagia with a novel frameless intrauterine levonorgestrelreleasing drug delivery system: a pilot study
 European Journal of Contraception & Reproductive Health Care, 2001;6:93-101 Treatment of menorrhagia with a novel frameless intrauterine levonorgestrelreleasing drug delivery system: a pilot study D. Wildemeersch*,
European Journal of Contraception & Reproductive Health Care, 2001;6:93-101 Treatment of menorrhagia with a novel frameless intrauterine levonorgestrelreleasing drug delivery system: a pilot study D. Wildemeersch*,
IS PARAGARD RIGHT FOR YOU?
 IS PARAGARD RIGHT FOR YOU? Ask your doctor about the only reversible birth control that s more than % effective and 100% hormone free. What to Tell your Doctor How you feel about hormones How you feel
IS PARAGARD RIGHT FOR YOU? Ask your doctor about the only reversible birth control that s more than % effective and 100% hormone free. What to Tell your Doctor How you feel about hormones How you feel
Contraception and gynecological pathologies
 1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
1 Contraception and gynecological pathologies 18 years old, 2 CMI normal First menstruation at 14 years old Irregular (every 2/3 months), painful + She does not need contraception She is worried about
For more information, visit us online at PARAGARDAccessSolutions.com. To speak with a representative call PARAGARD ( ).
 Improve patient access with PARAGARD Access Solutions TM A comprehensive range of support services and resources designed to make access easier for your patients who choose PARAGARD. PARAGARD Direct is
Improve patient access with PARAGARD Access Solutions TM A comprehensive range of support services and resources designed to make access easier for your patients who choose PARAGARD. PARAGARD Direct is
Notes to Teacher continued Contraceptive Considerations
 Abstinence a conscious decision to refrain from sexual intercourse 100% pregnancy will not occur if close contact between the penis and vagina does not take place. The risk of a number of STDs, including
Abstinence a conscious decision to refrain from sexual intercourse 100% pregnancy will not occur if close contact between the penis and vagina does not take place. The risk of a number of STDs, including
Contraceptive Updates and Recommendations
 Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations
 Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Contraceptive Updates and Recommendations Emily M. Godfrey, MD MPH Associate Professor, Departments of Family Medicine and Obstetrics and Gynecology, University of Washington, Seattle WA Guest Researcher,
Chapter 7 Infertility, Contraception, and Abortion
 Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
Chapter 7 Infertility, Contraception, and Abortion Infertility Incidence Affects about 10% to 15% of reproductive-age population Subfertility: prolonged time to conceive Sterility: inability to conceive
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer
 levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
levonorgestrel 13.5mg intrauterine delivery system (Jaydess ) SMC No. (1036/15) Bayer 6 March 2015 The Scottish Medicines Consortium (SMC) has completed its assessment of the above product and advises
The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that
 The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that may be used in the future Abstinence Choosing not to
The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that may be used in the future Abstinence Choosing not to
Evaluation of the Infertile Couple
 Overview and Definition Infertility is defined as the inability of a couple to fall pregnant after one year of unprotected intercourse. Infertility is a very common condition as in any given year about
Overview and Definition Infertility is defined as the inability of a couple to fall pregnant after one year of unprotected intercourse. Infertility is a very common condition as in any given year about
Bursting Pelvic Inflammatory Disease.
 www.infertiltysolutionsng.info/blog Disclaimer The information in this book is provided for educational purposes only and is not intended to treat, diagnose or prevent any disease. The information in this
www.infertiltysolutionsng.info/blog Disclaimer The information in this book is provided for educational purposes only and is not intended to treat, diagnose or prevent any disease. The information in this
Quality of care in Copper T 380A services. A practical manual for service providers. Action Research & Training for Health (ARTH), Udaipur
 Quality of care in Copper T 380A services A practical manual for service providers Action Research & Training for Health (ARTH), Udaipur 2003 PART 1 COPPER-T: CLINICAL INFORMATION I. INTRODUCTION TO IUDS
Quality of care in Copper T 380A services A practical manual for service providers Action Research & Training for Health (ARTH), Udaipur 2003 PART 1 COPPER-T: CLINICAL INFORMATION I. INTRODUCTION TO IUDS
PRODUCT MONOGRAPH. Pr MIRENA. Levonorgestrel-releasing Intrauterine System (52 mg) to deliver. up to 20 mcg levonorgestrel per day.
 PRODUCT MONOGRAPH Pr MIRENA Levonorgestrel-releasing Intrauterine System (52 mg) to deliver up to 20 mcg levonorgestrel per day Progestogen Bayer Inc. 2920 Matheson Blvd East Mississauga, Ontario L4W 5R6
PRODUCT MONOGRAPH Pr MIRENA Levonorgestrel-releasing Intrauterine System (52 mg) to deliver up to 20 mcg levonorgestrel per day Progestogen Bayer Inc. 2920 Matheson Blvd East Mississauga, Ontario L4W 5R6
Subfertility B Y A L I S O N, B E N A N D J O H N
 Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
Subfertility B Y A L I S O N, B E N A N D J O H N Contents Definition Causes Male Female Hx & Ex Investigations Treatment Definition Failure to conceive after a year of frequent, unprotected communion.
CHAPTER 4 REPRODUCTIVE HEALTH POINTS TO REMEMBER
 CHAPTER 4 REPRODUCTIVE HEALTH POINTS TO REMEMBER Amniocentesis : Diagnostic technique to detect genetic disorder in the foetus. Infertility : Inability to produce children in spite of unprotected sexual
CHAPTER 4 REPRODUCTIVE HEALTH POINTS TO REMEMBER Amniocentesis : Diagnostic technique to detect genetic disorder in the foetus. Infertility : Inability to produce children in spite of unprotected sexual
Contraception. Objectives. Unintended Pregnancy. Unintended Pregnancy in the US. What s the Impact? 10/7/2014
 Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
Risk factors for IUD failure: results of a large multicentre case control study
 Human Reproduction Vol.21, No.10 pp. 2612 2616, 2006 Advance Access publication June 14, 2006. doi:10.1093/humrep/del208 Risk factors for IUD failure: results of a large multicentre case control study
Human Reproduction Vol.21, No.10 pp. 2612 2616, 2006 Advance Access publication June 14, 2006. doi:10.1093/humrep/del208 Risk factors for IUD failure: results of a large multicentre case control study
Essure By Mayo Clinic staff
 Page 1 of 5 Reprints A single copy of this article may be reprinted for personal, noncommercial use only. Essure By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/essure/my00999 Definition
Page 1 of 5 Reprints A single copy of this article may be reprinted for personal, noncommercial use only. Essure By Mayo Clinic staff Original Article: http://www.mayoclinic.com/health/essure/my00999 Definition
Bursting Pelvic Inflammatory Disease.
 www.infertiltysolutionsng.info/blog Disclaimer The information in this book is provided for educational purposes only and is not intended to treat, diagnose or prevent any disease. The information in this
www.infertiltysolutionsng.info/blog Disclaimer The information in this book is provided for educational purposes only and is not intended to treat, diagnose or prevent any disease. The information in this
New Patient Medical History
 New Patient Medical History MR #: Initial Appointment Date: / / Name: Birth Date: / / Address: City: State: Zip: Best Phone # to reach you: ( ) Second contact #: ( ) Email Address: Occupation: Marital
New Patient Medical History MR #: Initial Appointment Date: / / Name: Birth Date: / / Address: City: State: Zip: Best Phone # to reach you: ( ) Second contact #: ( ) Email Address: Occupation: Marital
Example Clinical Guideline for Immediate Postpartum LARC Insertion
 Example Clinical Guideline for Immediate Postpartum LARC Insertion RATIONALE Delay in contraceptive provision until the six week postpartum appointment can leave some women at risk for rapid repeat pregnancy.
Example Clinical Guideline for Immediate Postpartum LARC Insertion RATIONALE Delay in contraceptive provision until the six week postpartum appointment can leave some women at risk for rapid repeat pregnancy.
Nelson: Managing Side Effects and Complications Related to LARCs
 Managing Side Effects and Complications Related to LARCs Anita L. Nelson, MD Harbor-UCLA Medical Center Women s Health Update California Family Health Council San Francisco, CA - April 15-16, 2013 Conflict
Managing Side Effects and Complications Related to LARCs Anita L. Nelson, MD Harbor-UCLA Medical Center Women s Health Update California Family Health Council San Francisco, CA - April 15-16, 2013 Conflict
VCHIP LARC Needs Assessment Survey
 VCHIP LARC Needs Assessment Survey Demographics 1. How many have you been in practice (post-training)? Choose one of the following answers 0-5 6-10 11-15 16-20 21 or more 2. What are your professional
VCHIP LARC Needs Assessment Survey Demographics 1. How many have you been in practice (post-training)? Choose one of the following answers 0-5 6-10 11-15 16-20 21 or more 2. What are your professional
Long Acting Reversible Contraception: First Line Care for Adolescents. David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG
 Long Acting Reversible Contraception: First Line Care for Adolescents David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG Disclosures Melissa Kottke is a Nexplanon trainer for Merck Objectives Describe
Long Acting Reversible Contraception: First Line Care for Adolescents David A. Levine, MD, FAAP Melissa Kottke, MD, MPH, FACOG Disclosures Melissa Kottke is a Nexplanon trainer for Merck Objectives Describe
100% Highly effective No cost No side effects
 effective? Advantages Disadvantages How do I get Cost Abstinence For some it can mean no sexual contact. For others it is no sexual intercourse or vaginal penetration. A permanent surgical procedure available
effective? Advantages Disadvantages How do I get Cost Abstinence For some it can mean no sexual contact. For others it is no sexual intercourse or vaginal penetration. A permanent surgical procedure available
Zurich Open Repository and Archive
 University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Comparison of two procedures for routine IUD exchange in women with positive
University of Zurich Zurich Open Repository and Archive Winterthurerstr. 190 CH-8057 Zurich http://www.zora.uzh.ch Year: 2008 Comparison of two procedures for routine IUD exchange in women with positive
Example CLINICAL GUIDELINES for Postpartum IUD insertion
 Example CLINICAL GUIDELINES for Postpartum IUD insertion Postpartum Intrauterine Device Insertion 1.0 Indications: 1.1 Insertion of an intrauterine device (IUD) for long-acting reversible contraception
Example CLINICAL GUIDELINES for Postpartum IUD insertion Postpartum Intrauterine Device Insertion 1.0 Indications: 1.1 Insertion of an intrauterine device (IUD) for long-acting reversible contraception
Laparoscopy-Hysteroscopy
 Laparoscopy-Hysteroscopy Patient Information Laparoscopy The laparoscope, a surgical instrument similar to a telescope, is inserted through a small incision (cut) in the belly button during laparoscopy.
Laparoscopy-Hysteroscopy Patient Information Laparoscopy The laparoscope, a surgical instrument similar to a telescope, is inserted through a small incision (cut) in the belly button during laparoscopy.
Ardhanu Kusumanto Oktober Contraception methods for gyne cancer survivors
 Ardhanu Kusumanto Oktober 2017 Contraception methods for gyne cancer survivors Background cancer treatment Care of gyn cancer survivor Promotion of sexual, cardiovascular, bone, and brain health management
Ardhanu Kusumanto Oktober 2017 Contraception methods for gyne cancer survivors Background cancer treatment Care of gyn cancer survivor Promotion of sexual, cardiovascular, bone, and brain health management
Birth Control- an Overview. Keith Merritt, MD. Remember, all methods of birth control are safer and have fewer side effects than pregnancy
 Birth Control- an Overview Keith Merritt, MD Basics Remember, all methods of birth control are safer and have fewer side effects than pregnancy Even with perfect use, each method of birth control has a
Birth Control- an Overview Keith Merritt, MD Basics Remember, all methods of birth control are safer and have fewer side effects than pregnancy Even with perfect use, each method of birth control has a
Extended use of the intrauterine device: a literature review and recommendations for clinical practice,
 Contraception 89 (2014) 495 503 Review Extended use of the intrauterine device: a literature review and recommendations for clinical practice, Justine P. Wu, Sarah Pickle Department of Family Medicine
Contraception 89 (2014) 495 503 Review Extended use of the intrauterine device: a literature review and recommendations for clinical practice, Justine P. Wu, Sarah Pickle Department of Family Medicine
Postpartum LARC. (Long Acting Reversible Contraception) NURSING EDUCATION
 Postpartum LARC (Long Acting Reversible Contraception) NURSING EDUCATION What is LARC Long-acting reversible contraception (LARC) methods include the intrauterine device (IUD) and the birth control implant.
Postpartum LARC (Long Acting Reversible Contraception) NURSING EDUCATION What is LARC Long-acting reversible contraception (LARC) methods include the intrauterine device (IUD) and the birth control implant.
Birth Control Options Chart
 Hormonal Methods Birth control pills also known as mini-pills 91-99% A daily pill containing hormones that stops you from ovulating. There are combination estrogen or progestin-only (mini-pill) options.
Hormonal Methods Birth control pills also known as mini-pills 91-99% A daily pill containing hormones that stops you from ovulating. There are combination estrogen or progestin-only (mini-pill) options.
유일하게 100% 무호르몬인 IUD( 자궁내피임장치 ) 입니다!
 PARAGARD 사용을고려중이십니까? ( 동제자궁내피임장치 ) 유일하게 100% 무호르몬인 IUD( 자궁내피임장치 ) 입니다! PARAGARD 란? PARAGARD 는자궁내에삽입되어구리를배출함으로써최대 10 년까지임신을방지하는장치입니다. 이는자궁내장치 (Intrauterine Device,IUD) 라고도불리는피임방법입니다. PARAGARD 의작용방법 PARAGARD
PARAGARD 사용을고려중이십니까? ( 동제자궁내피임장치 ) 유일하게 100% 무호르몬인 IUD( 자궁내피임장치 ) 입니다! PARAGARD 란? PARAGARD 는자궁내에삽입되어구리를배출함으로써최대 10 년까지임신을방지하는장치입니다. 이는자궁내장치 (Intrauterine Device,IUD) 라고도불리는피임방법입니다. PARAGARD 의작용방법 PARAGARD
The number of women using long-acting reversible
 Long-acting reversible contraception: Who, what, when, and how This review provides practical tips and dispels some common misconceptions about these devices, which have higher rates of patient satisfaction
Long-acting reversible contraception: Who, what, when, and how This review provides practical tips and dispels some common misconceptions about these devices, which have higher rates of patient satisfaction
HYSTEROSALPINGOGRAPHY IN THE DIAGNOSIS OF INFERTILITY (STATISTICAL ANALYSIS OF 3437 CASES)
 FERTILITY AND STERIUTY Copyright 1972 by The Williams & Wilkins Co. Vol. 2:3, ~o. 11, November 1972 Printed in U.S.A. HYSTEROSALPINGOGRAPHY IN THE DIAGNOSIS OF INFERTILITY (STATISTICAL ANALYSIS OF 337
FERTILITY AND STERIUTY Copyright 1972 by The Williams & Wilkins Co. Vol. 2:3, ~o. 11, November 1972 Printed in U.S.A. HYSTEROSALPINGOGRAPHY IN THE DIAGNOSIS OF INFERTILITY (STATISTICAL ANALYSIS OF 337
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
The Doctor Is In. Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH
 The Doctor Is In Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH Contraception Resources from the CDC: 2016 U.S. Medical Eligibility Criteria
The Doctor Is In Brent N Davidson MD Vice Chair Women s Health Henry Ford Health System Medical Director Family Planning MDCH Contraception Resources from the CDC: 2016 U.S. Medical Eligibility Criteria
Chronic Pelvic Pain. AP099, December 2010
 AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
AP099, December 2010 Chronic Pelvic Pain Pain in the pelvic area that lasts for 6 months or longer is called chronic pelvic pain. An estimated 15 20% of women aged 18 50 years have chronic pelvic pain
INFERTILITY CAUSES. Basic evaluation of the female
 INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
Family Planning and Infertility
 Family Planning and Infertility Chapter 20 Objectives Discuss types of reversible contraception Natural methods Mechanical barrier methods Hormonal contraceptives Discuss types of permanent contraception
Family Planning and Infertility Chapter 20 Objectives Discuss types of reversible contraception Natural methods Mechanical barrier methods Hormonal contraceptives Discuss types of permanent contraception
Infertility F REQUENTLY A SKED Q UESTIONS. Q: Is infertility a common problem?
 Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Infertility (female factors). In another one third of cases, infertility is due to the man (male factors). The remaining cases are caused by a mixture of male and female factors or by unknown factors.
Guidelines for service providers on IUD insertion & removal
 Guidelines for service providers on IUD insertion & removal Family Health Bureau Ministry of Health SRI LANKA 0 1. INTRODUCTION Intra uterine contraceptive device (IUD) also called IUCD is the most commonly
Guidelines for service providers on IUD insertion & removal Family Health Bureau Ministry of Health SRI LANKA 0 1. INTRODUCTION Intra uterine contraceptive device (IUD) also called IUCD is the most commonly
Laparoscopy and Hysteroscopy
 AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
AMERICAN SOCIETY FOR REPRODUCTIVE MEDICINE Laparoscopy and Hysteroscopy A Guide for Patients PATIENT INFORMATION SERIES Published by the American Society for Reproductive Medicine under the direction of
The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings.
 The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings Counseling Cards Checklist to be reasonably sure a woman is not pregnant
The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings Counseling Cards Checklist to be reasonably sure a woman is not pregnant
Please fill out the following information and have it returned to our office prior to your consultation.
 Please fill out the following information and have it returned to our office prior to your consultation. Patient s Name Partner s Name Address: City: State: Zip: Phone (day#): ( ) (eve#) ( ) (cell) ( )
Please fill out the following information and have it returned to our office prior to your consultation. Patient s Name Partner s Name Address: City: State: Zip: Phone (day#): ( ) (eve#) ( ) (cell) ( )
1.Abstinence no sex (Abstinence only education has been proven ineffective in preventing unwanted pregnancies)
 REPRODUCTIVE SYSTEM Objectives: 1. Contraception 2. STDs 1. Ovary Transplants 2. Freezing Eggs 3. Choosing Gender 4. The Male Pill, parts 1&2 5. Male Birth Control: RISUG 6. Birth Control. 1.Abstinence
REPRODUCTIVE SYSTEM Objectives: 1. Contraception 2. STDs 1. Ovary Transplants 2. Freezing Eggs 3. Choosing Gender 4. The Male Pill, parts 1&2 5. Male Birth Control: RISUG 6. Birth Control. 1.Abstinence
FACT SHEET: Copper IUD
 FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
Contraception Choices: An Evidence Based Approach Case Study Approach. Susan Hellier PhD, DNP, FNP-BC, CNE
 Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Contraceptive case studies. Dr Christine Roke National Medical Advisor Family Planning June 2015
 Contraceptive case studies Dr Christine Roke National Medical Advisor Family Planning June 2015 Case 1 Mary is a 47 year old who has come in for a routine cervical smear. She asks when her Multiload IUD
Contraceptive case studies Dr Christine Roke National Medical Advisor Family Planning June 2015 Case 1 Mary is a 47 year old who has come in for a routine cervical smear. She asks when her Multiload IUD
1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7:
 1 2 1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7: 777 85. 3 1. Wu JP et al. Extended use of the intrauterine device: a
1 2 1. Attia AM et al. Role of the levonorgestrel intrauterine system in effective contraception. Patient Prefer Adherence 2013; 7: 777 85. 3 1. Wu JP et al. Extended use of the intrauterine device: a
Transcervical Sterilization
 Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
toe... Chlamydia - CDC Fact Sheet Appendix K - Part 2
 Appendix K - Part 2 Chlamydia - CDC Fact Sheet What is chlamydia? Chlamydia is a common STD that can infect both men and women. It can cause serious, permanent damage to a woman's reproductive system,
Appendix K - Part 2 Chlamydia - CDC Fact Sheet What is chlamydia? Chlamydia is a common STD that can infect both men and women. It can cause serious, permanent damage to a woman's reproductive system,
الحمد هلل رب العالمين والصالة والسالم علي محمد الصادق الوعد األمين اللهم أخرجنا من ظلمات الجهل والوهم إلى نور المعرفة والعلم..
 الحمد هلل رب العالمين والصالة والسالم علي محمد الصادق الوعد األمين اللهم أخرجنا من ظلمات الجهل والوهم إلى نور المعرفة والعلم.. سيدنا 11/6/2013 1 Goals of Family Planning services : 1- Enable women and
الحمد هلل رب العالمين والصالة والسالم علي محمد الصادق الوعد األمين اللهم أخرجنا من ظلمات الجهل والوهم إلى نور المعرفة والعلم.. سيدنا 11/6/2013 1 Goals of Family Planning services : 1- Enable women and
Reproductive health research at WHO
 Reproductive health research at WHO Paul F.A. Van Look, MD PhD Department of Reproductive Health and Research World Health Organization Geneva, 11 March 2004 PVL_GE_StudCourse_MAR04/1 Health is a state
Reproductive health research at WHO Paul F.A. Van Look, MD PhD Department of Reproductive Health and Research World Health Organization Geneva, 11 March 2004 PVL_GE_StudCourse_MAR04/1 Health is a state
