Diabetic retinopathy
|
|
|
- Eunice Edwards
- 5 years ago
- Views:
Transcription
1 research Daniel Ting Jonathon Ng Nigel Morlet Joshua Yuen Antony Clark Hugh Taylor Jill Keefe David Preen Diabetic retinopathy Screening and management by Australian GPs Aim To describe current diabetic retinopathy (DR) screening and management practices among Australian general practitioners. Method A self administered questionnaire on DR management was mailed to 2000 rural and urban GPs across Australia in Results Only 29% of the GP respondents had read the National Health and Research Council guidelines at least once and 41% had a moderate to strong desire to screen for DR. A majority of GPs (74%) reported not routinely examining their diabetic patients for DR. Lack of confidence in detecting DR changes (86.4%) and time constraints (73.4%) were the two major barriers to GPs performing dilated fundoscopy on diabetic patients. Discussion Given that access to optometry is not evenly distributed across the country, and that ophthalmology is underresourced, GPs are the healthcare providers most able to manage and screen for DR in the community. Keywords: diabetes mellitus; diabetic retinopathy; mass screening; secondary prevention; general practice Diabetes mellitus is rising in prevalence within Australia and internationally, with estimates indicating that the global prevalence of diabetes will double by In Australia, the prevalence of diabetes is 8% in adult men and 6.5% in adult women; 2 of these, one in four will be diagnosed with diabetic retinopathy (DR). 3 Early detection and prompt treatment can prevent 98% of visual impairment. 4 Primary healthcare providers such as general practitioners and optometrists are at the front line of service provision and play a crucial role in screening for DR in the community. However, a 1994 survey of Victorian GPs found over half had little interest in DR screening and that most routinely examined less than half of their patients with diabetes for DR. 5 The National Health and Medical Research Council (NHMRC) released clinical practice guidelines for DR in 1997, 6 outlining evidence based DR management practices and encouraging physicians to increase the DR screening rate in order to reduce DR related visual impairment. Nonetheless, a subsequent Victorian survey reported that despite the NHMRC guidelines, 48% of GPs still had little or no desire to screen for DR. 7 This study is the first national survey of Australian GPs on DR management. The purpose is to investigate current Australian GPs management practices and attitudes towards DR and its management since the release of the 1997 NHMRC guidelines. Given the survey was started in late 2007, it can also serve as a baseline before the release of the most recent NHMRC guidelines in Method A random sample of 2000 currently practising Australian GPs selected from The Royal Australian College of General Practitioners (RACGP) membership database were surveyed. A package consisting of a self administered two page questionnaire, an information leaflet detailing the aim of the study and a reply paid return envelope was posted to selected GPs in December A repeat mailout of surveys to nonresponders was conducted after 3 months to maximise response. This study was approved by the University of Western Australia s Human Research Ethics Committee. The survey questions related to: general professional and practice details (eg. location of previous training, duration at and location of practices, rural or metropolitan practice) frequency of measurement of HbA1c, blood pressure, cholesterol, smoking status perceived barriers to DR screening (eg. time factors, patient refusal, fear of angle closure glaucoma, lack of confidence in detecting and managing DR and lack of dilating drops and ophthalmoscopes in practices) frequency of referral of diabetic patients to optometrists and ophthalmologists for DR screening eye examination routine (measurement of visual acuity, dilated or nondilated fundoscopy) GPs desire to undertake DR screening. The participants were also asked to respond to five case scenarios regarding the management of DR clinical signs: microaneurysms, retinal haemorrhages, cottonwool spots, new vessel formation and presence of hard exudates near Reprinted from Australian Family Physician Vol. 40, No. 4, April
2 research Diabetic retinopathy screening and management by Australian GPs the macula. A further seven hypothetical case scenarios involving patients that varied in age (7, 18 and 60 years of age), diabetic management (diet control, oral hypoglycaemic agents and insulin) and glycaemic control (poorly and well controlled) who had no signs of DR detected at baseline examination were also included. Analyses were performed using SPSS version 17 (SPSS, Chicago, IL, USA). Descriptive statistics (mean, standard deviation) were calculated for continuous variables. Relationships between categorical variables were explored using chi-square tests. Additionally, a multivariate logistic regression model was used to study the possible factors relating to GPs confidence in detecting DR clinical signs, such as their years in practice, previous training location and whether or not they had read the NHMRC guidelines. Results There were 429 (21%) respondents to the survey (Table 1). Almost half reported having received the 1997 NHMRC guidelines for DR management, however, of these only 29% had read the guidelines at least once. Apart from the NHMRC guidelines, GPs also reported using other resources such as RACGP guidelines, 9 Therapeutic guidelines: endocrinology, 10 National Prescribing Service Guidelines, 11 American Diabetic Association Guidelines, 12 various online websites, and diabetes focused peer reviewed journals. Almost all GPs reviewed their diabetic patients blood pressure (98.6%) and HbA1c (92.1%) at least every 6 months (Table 2). Assessment of lipid profile, smoking status and advice on diabetes complications were conducted less frequently by the respondent GPs (Table 2). Nearly 75% of GPs did not routinely examine their diabetic patients for DR; of those, 89% would refer their diabetic patients to see an ophthalmologist within 2 years of initial diabetes diagnosis. More GPs usually and always performed nondilated (61%) than dilated fundoscopy (13%) to detect DR signs and only 65% of GPs usually or always checked visual acuity. Only 21% of GPs responded that they were often or almost always confident in detecting DR changes. Lack of confidence in detecting Table 1. Demographics of GP respondents Demographic information Total (%) Australian GPs (%) 20 State or territory of practice New South Wales 101 (24%) 33.4 Victoria 122 (29%) 25.0 Queensland 74 (18%) 19.1 Western Australia 68 (16%) 9.2 South Australia 40 (9%) 8.5 Tasmania 11 (3%) 2.7 Australian Capital Territory 5 (1%) 1.5 Northern Territory 1 (<1%) 0.7 Years of practice 0 10 years 47 (11%) No comparison years 61 (14%) available years 136 (32%) >30 years 185 (43%) Locality of practice Metropolitan 279 (66%) 73.8 Rural 143 (34%) 26.2 Location of training Australia 343 (81%) 68.4 United Kingdom 39 (9%) India 12 (3%) New Zealand 6 (1%) Other 26 (6%) Overseas 31.6 DR changes (86%) and time constraints (73%) were the primary barriers to performing dilated fundoscopy on diabetic patients for GPs. Additional reported barriers included patient refusal, concern of angle closure glaucoma, lack of dilating drops and uncertainty surrounding DR management (Table 3). Less than half of GPs (41%) expressed moderate to strong desire to screen for DR in the community setting. Nearly all GPs (91%) referred diabetic patients to ophthalmologists every 1 2 years, while 68% referred their diabetic patients to optometrists in the first instance. One-fifth of GPs never referred any diabetic patients to see an optometrist, these GPs all preferred to refer their patients to see an ophthalmologist every 1 2 years. A small number of GPs (8%) would only refer their patients to an ophthalmologist or optometrist if visual symptoms were present. Nearly 80% of GPs felt their patients would see an ophthalmologist should it be necessary. Table 4 shows responses to the management of specific DR signs and hypothetical case scenarios. Most GPs (63%) would refer their patients with occasional microaneurysms with normal vision within 1 month to see an ophthalmologist while only 3% were confident to not refer these patients to the ophthalmologist. For patients with hard exudates near the macula and normal vision, 87% of GPs indicated that they would refer to an ophthalmologist within 1 month. Following the detection of peripheral microaneurysms and retinal haemorrhages, 95% of GPs would refer their patients to see an ophthalmologist within the recommended 234 Reprinted from Australian Family Physician Vol. 40, No. 4, April 2011
3 Diabetic retinopathy screening and management by Australian GPs research Table 2. Current GP management and attitudes to diabetes and diabetic retinopathy At diabetes follow up Never and rarely (%) Sometimes (%) Usually and always (%) Visual acuity measurement 30 (13.5%) 49 (22%) 144 (64.5%) Fundsocopy (undilated) 54 (25.1%) 29 (13.5%) 132 (61.4%) Dilated fundoscopy 155 (79.0%) 16 (8.2%) 25 (12.8%) Diabetic patients examined for diabetic retinopathy None 197 (46.4%) Some 119 (28%) All 109 (25.6%) Frequency with which diabetic patients Yearly or less More than yearly were reviewed 137 (57.3%) 102 (42.7%) Frequency of risk factor management Six monthly or less More than 6 monthly HbA1c 387 (92.1%) 33 (7.9%) Blood pressure 416 (98.6%) 6 (1.4%) Cholesterol 245 (58.2%) 176 (41.8%) Smoking 278 (65.9%) 144 (34.1%) Advice regarding complications 334 (79.7%) 85 (20.3%) timeframe. For new vessel formation, nearly all GPs would refer within 1 month to an ophthalmologist. A majority of GPs (82%) would (inappropriately) refer a child, 7 years of age, with diabetes and no signs of DR for regular eye screening while 18% would refer such patients in 5 years. As shown in Table 3, the majority of the GPs would refer patients of various ages (7, 18 and 60 years); diabetic management (diet control, oral hypoglycaemic and insulin); and glycaemic control (well and poorly controlled) elsewhere for regular eye screening even without any signs of DR rather than perform the review themselves. General practitioners desire to screen for DR in the community was strongly associated with having read the 1997 NHMRC guidelines at least once (χ 2 =17.64, p<0.001) and with reporting confidence in detecting DR clinical changes (χ 2 =28.5, p<0.001). In multivariate logistic regression analyses, GPs who reported confidence in detecting DR clinical signs were 3.31 times more likely to have a desire to screen for DR after controlling for reading the guidelines at least once, years of practice and previous training location (OR=3.31, SE=0.85, 95% CI: , p<0.001). However, the frequency of GPs performing visual acuity measurement and dilated fundoscopy as part of the routine eye examination for patients with diabetes was not associated with reading the NHMRC guidelines. General practitioners confidence in detecting DR changes was strongly associated with: GPs having read the guidelines at least once (χ 2 =7.48, p<0.01) GPs having been in practice for more than 15 years (χ 2 =7.71, p<0.01) being an Australian trained GP (χ 2 =3.88, p<0.05). When controlled for years of practice and previous training location, GPs who had read the guidelines at least once were 2.11 times more likely to report confidence in screening for DR (OR=2.11, SE=0.54, 95% CI: , p<0.005). The location of the GP practice (rural or metropolitan) was not associated with reported confidence in detecting DR changes, desire of DR screening or the frequency of referral to ophthalmologists or optometrists. Discussion Table 3. Barriers to GPs performing dilated fundoscopy Barrier In response to the World Health Assembly resolution on the elimination of avoidable blindness, the National Eye Health Framework was developed following the Australian Health Ministers Conference in It identified five potential key areas which may help prevent avoidable blindness and low vision. Two of these related to increasing early detection and improving access to eye healthcare services. 13 At the time of the release of the NHMRC guidelines on DR management in 1997, 6 the Victorian GP DR survey showed that half of GPs expressed a desire to regularly screen for DR in patients attending their practice. 7 Unfortunately, the authors found that since the last survey, even fewer GPs (41%) expressed a desire to screen No barrier or minor barrier (%) Moderate or major barrier (%) No confidence in detecting diabetic 55 (13.6%) 349 (86.4%) retinopathy signs Time consuming 109 (26.7%) 300 (73.3%) Patients refusal to dilation 145 (36.5%) 252 (63.5%) Worry of inducing angle closure glaucoma 223 (55.8%) 177 (44.2%) Lack of dilating drops 251 (62.4%) 151 (37.6%) Unsure of diabetic retinopathy management 328 (82.2%) 71 (17.8%) Lack of ophthalmoscopes 396 (97.8%) 9 (2.2%) Reprinted from Australian Family Physician Vol. 40, No. 4, April
4 Diabetic retinopathy screening and management by Australian GPs research Table 4. GP management of hypothetical clinical scenarios and specific signs of diabetic retinopathy Clinical scenario Appropriate referral (%) Inappropriate referral (%) Recommended referral time frame (2008)* Recommended referral time frame (1997)** Occasional microaneurysms with normal vision 101 (24.7%) 308 (75.3%) 1 year Nonurgent, routine referral Hard exudates near macula with normal vision 348 (86.6%) 54 (13.4%) 1 month or less Refer urgently Peripheral microaneurysms and retinal haemorrhages 384 (94.8%) 21 (5.2%) 6 months or less Refer urgently Extensive microaneurysms, retinal haemorrhages and 407 (99.5%) 2 (0.5%) 3 months or less Refer urgently cottonwool spots (all peripherally) New vessel formation 407 (99.8%) 1 (0.2%) 1 month or less Refer urgently If no signs of DR at baseline examination 7 year old newly diagnosed diabetic 338 (80.3%) 83 (19.7%) At puberty Refer in 5 years 18 year old newly diagnosed diabetic 351 (84.0%) 67 (16.0%) 1 to 2 years Yearly, no later than 2 yearly 60 year old with good HbA1c control diet # 284 (67.1%) 139 (32.9%) 2 years Yearly, no later than 2 yearly 60 year old, 10 years diabetes, commenced on OHA 361 (84.9%) 64 (15.1%) 1 to 2 years Yearly, no later than 2 yearly 60 year old, 10 years diabetes with good HbA1c 289 (68.5%) 133 (31.5%) 2 years Yearly, no later than 2 yearly on OHA # 60 year old, 10 years diabetes with good HbA1c 269 (63.4%) 155 (36.6%) 2 years Yearly, no later than 2 yearly on insulin # 60 year old, poorly controlled HbA1c despite insulin 306 (72.0%) 119 (28.0%) 1 year Yearly, no later than 2 yearly * Referral time frame recommended by 2008 NHMRC guidelines 8 ** Referral time frame recommended by 1997 NHMRC guidelines 6 Should HbA1c is unavailable, all diabetic patients should be referred within 1 2 years # Patients with good HbA1c control and no signs of DR are recommended to undergo 2 yearly fundus examination for DR OHA = oral hypoglycaemic agents; HbA1c = glycosylated haemoglobin for DR. This is of concern given that primary healthcare screening provides an excellent opportunity to differentiate those patients who require specialist ophthalmic care from those who can continue to be managed by their GP. We also found that similar to the previous Victorian study, 7 GPs perceived the lack of confidence in detecting clinical DR signs was the leading barrier to performing dilated fundoscopy. A fear of inducing angle closure glaucoma (a rare 1: event postdilation) 14 was perceived as another major barrier to performing dilated fundoscopy. Despite the low numbers of GPs who reported confidence in detecting DR clinical signs (21%), based on the hypothetical clinical scenarios in the survey most GPs were generally confident and proficient to manage DR once DR changes were detected. Given that the GPs who reported confidence in detecting DR clinical signs were three times more likely to have strong desire to screen for DR, more education needs to be directed toward detection of DR clinical signs to increase the DR screening rate in the Australian community. In this study, a great proportion of GPs (92%) reported that they review their patients HbA1c every 6 months or less. Nonetheless, numerous previous data based on Medicare data analysis showed that only 25 80% of GPs measured their patients HbA1c level at a 6 monthly interval. 15 This highlighted a gap between what GPs think they should do as opposed to what is done in reality on a routine basis. (However, those who completed the survey may have been more motivated to measure HbA1c than others.) Given that good HbA1c control significantly reduces the risk of microvascular and macrovascular complications, it is important to translate theoretical knowledge on diabetes management into routine clinical practices by checking their patients HbA1c every 6 months as per NHMRC guidelines. 8 In a similar survey of optometrists, the authors found that the optometric DR management was generally inferior to that of GPs. 18 Nearly 60% of optometrists would not refer patients with diabetic maculopathy to see an ophthalmologist and 10% would not refer patients with severe nonproliferative DR. Comparing these two surveys suggests that GPs may be the most proficient healthcare providers to manage and screen for DR in the community. From the 2009 study on optometrists, 18 the retinal cameras were shown to have increased optometrists confidence to detect DR changes such as microaneurysms, retinal haemorrhages, new vessel formation and macular oedema. It is unknown whether GPs would feel more confident with retinal photographic screening, however, a pilot study of photographic screening by GPs for DR found that they would be willing to expand their roles into DR screening if such infrastructure were readily accessible. 19 The study 19 also showed that GPs had good diagnostic accuracy (sensitivity 87%; specificity 95%) for DR. Given that this was a pilot study with a relatively small sample size, a larger study using cheaper, portable retinal cameras Reprinted from Australian Family Physician Vol. 40, No. 4, April
5 research Diabetic retinopathy screening and management by Australian GPs would provide more insight into the enthusiasm for, and effectiveness of, retinal photographic screening in primary care. The updated 2008 NHMRC guidelines suggest that mydriatic retinal photography is the most effective DR screening tool with a sensitivity of at least 80%. 8 Cheaper retinal cameras are now available and should be encouraged in primary healthcare, especially for large practices. Retinal photographs taken by staff could be instantly interpreted by the GP to determine the need for referrals to ophthalmologists during general diabetes consultations. The strength of this study is that it is the first nationwide GP DR survey. The study findings not only revealed the current management practices of Australian GPs on DR management but can be utilised as baseline findings for a future study to assess the impact of the 2008 NHMRC guidelines. 8 Additionally, the GPs demographics from this study, such as the distribution of respondent GPs and locality of practices, were comparable to the national demographics for GPs (age and gender were not enquired about in this survey). 20 On the other hand, the study findings were limited by several factors. Of the GPs practising in Australia (n=12 938), this study had a relatively small sample size (3.3%, n=429) which may affect the generalisability of results. 20 In addition, the study did not gather data regarding current use of retinal cameras among GPs, their previous education on eye training and the size of their practice, which could affect GPs confidence in screening for DR. Conclusion In conclusion, Australian GPs in general reported sound management of sight threatening DR. Given that the access to optometry is not evenly distributed across Australia and that ophthalmology is under-resourced, GPs may be the most proficient healthcare providers to manage and screen for DR in the community. In the absence of retinal photography, dilated ophthalmoscopy is still the most convenient and effective method to examine for DR and therefore, it is a basic clinical examination skill that should be encouraged for all GPs. Authors Daniel Ting MBBS, is a PhD student, University of Western Australia and Centre of Ophthalmology and Visual Science, Lions Eye Institute, University of Western Australia, Perth, Western Australia. daniel_ting45@hotmail.com Jonathon Ng MBBS, PhD, is an ophthalmology Nigel Morlet FRANZCO, is consultant ophthalmologist, Eye and Vision Epidemiology Research Group, Centre for Health Services Research, University of Western Australia Joshua Yuen MBBS, MPH, is an ophthalmology Antony Clark MBBS(Hons), is an ophthalmology Hugh Taylor AC, FRANZCO, is Harold Mitchell Chair of Indigenous Eye Health, School of Indigenous Health, University of Melbourne, Victoria Jill Keefe OAM, PhD, is Head, Centre of Eye Research Australia, School of Population Health, University of Melbourne, Victoria David Preen PhD, is Director, Centre for Health Services Research, University of Western Australia. Conflict of interest: none declared. References 1. Wild S, Roglic G, Green A, et al. Global prevalence of diabetes: estimates for the year 2000 and projections for Diabetes Care 2004;27: Dunstan DW, Zimmet PZ, Welborn TA, et al. The rising prevalence of diabetes and impaired glucose tolerance: the Australian Diabetes, Obesity and Lifestyle Study. Diabetes Care 2002;25: Tapp RJ, Shaw JE, Harper CA, et al. The prevalence of and factors associated with diabetic retinopathy in the Australian population. Diabetes Care 2003;26: Ferris FL, 3rd. How effective are treatments for diabetic retinopathy? JAMA 1993;269: Dickson PR, McCarty CA, Keeffe JE, et al. Diabetic retinopathy: examination practices and referral patterns of general practitioners. Med J Aust 1996;164: National Health and Medical Research Council. Clinical practice guidelines: management of diabetic retinopathy. Canberra: Commonwealth of Australia, Available at synopses/cp53covr.htm [Accessed 17 September 7. McCarty CA, Taylor KI, Keeffe JE. Management of diabetic retinopathy by general practitioners in Victoria. Clin Exp Ophthal 2001;29: National Health and Medical Research Council. Guidelines for the management of diabetic retinopathy. Canberra: Commonwealth of Australia, Available at synopses/di15syn.htm [Accessed 17 September 9. The Royal Australian College of General Practitioners. Management of diabetes mellitus 2010/ th edn. Canberra: Diabetes Australia, Available at diabetes [Accessed 17 September 10. Endocrinology Expert Group. Therapeutic guidelines: endocrinology. Diabetes: diagnosis and principles of management. 3rd edn. Therapeutic Guidelines Limited: North Melbourne, National Prescribing Service Limited. Diabetes drugs. Available at diabetes_drugs. [Accessed 3 December 12. American Diabetes Association. Management of diabetes mellitus. Available at [Accessed 20 September 13. Commonwealth of Australia. Eye health in Australia a background paper to the national framework for action to promote eye health and prevent avoidable blindness and vision loss. Canberra: Commonwealth of Australia, Talks SJ, Tsaloumas M, Mission GP, et al. Angle closure glaucoma and diagnostic mydriasis. Lancet 1993;342: National Health and Medical Research Council. Evidence-Practice Gaps Report Volume 1: a review of developments Available at www. nhmrc.gov.au/_files_nhmrc/file/nics/material_ resources/epgr_review_chapter_6.pdf. [Accessed 20 September 16. Selvin E, Marinopoulos S, Berkenblit G, et al. Meta-analysis: glycosylated hemoglobin and cardiovascular disease in diabetes mellitus. Ann Intern Med 2004;141: Stettler C, Allemann S, Juni P, et al. Glycemic control and macrovascular disease in types 1 and 2 diabetes mellitus: meta-analysis of randomized trials. Am Heart J 2006;152: Ting DSW, Yuen J, Clark A, et al. Australian Optometrists National Survey of Diabetic Retinopathy Management. Poster session presented at Annual General Meeting and Scientific Congress, November 2009, Brisbane, Australia. 19. Askew D, Schluter PJ, Spurling G, et al. Diabetic retinopathy screening in general practice: a pilot study. Aust Fam Physician 2009;38: Britt H, Miller GC, Charles J, et al. General practice activity in Australia Canberra: Australian Institute of Health and Welfare, Available at gep c03.pdf [Accessed 20 September 238 Reprinted from Australian Family Physician Vol. 40, No. 4, April 2011
RANZCO Screening and Referral Pathway for Diabetic Retinopathy #
 RANZCO Screening and Referral Pathway for Diabetic Retinopathy # Patient Presents a. Screen for Diabetic Retinopathy every 2 years b. Begin screening at diagnosis of Diabetes * Clinical Modifi ers Yearly
RANZCO Screening and Referral Pathway for Diabetic Retinopathy # Patient Presents a. Screen for Diabetic Retinopathy every 2 years b. Begin screening at diagnosis of Diabetes * Clinical Modifi ers Yearly
Use of eye care services by people with diabetes: the Melbourne Visual Impairment Project
 410 Department of Ophthalmology, University of Melbourne, Melbourne, Australia C A McCarty C W Lloyd-Smith P M Livingston Y L Stanislavsky H R Taylor Victorian WorkCover Authority, Melbourne, Australia
410 Department of Ophthalmology, University of Melbourne, Melbourne, Australia C A McCarty C W Lloyd-Smith P M Livingston Y L Stanislavsky H R Taylor Victorian WorkCover Authority, Melbourne, Australia
FINAL REPORT. as part of the National Visual Impairment Prevention Program. of the. Victorian Retinopathy Screening Development Project
 FINAL REPORT of the Victorian Retinopathy Screening Development Project as part of the National Visual Impairment Prevention Program Centre for Eye Research Australia July 2001 FINAL REPORT of the Victorian
FINAL REPORT of the Victorian Retinopathy Screening Development Project as part of the National Visual Impairment Prevention Program Centre for Eye Research Australia July 2001 FINAL REPORT of the Victorian
Use of Eye Care Services among Type 2 Diabetic Patients in Laguna
 Original Article Philippine Journal of OPHTHALMOLOGY Use of Eye Care Services among Type 2 Diabetic Patients in Laguna Glenn Carandang, MD, MPH, 1,2, Maria Victoria Rondaris, MD, MPH, 3, and Genejane Adarlo,
Original Article Philippine Journal of OPHTHALMOLOGY Use of Eye Care Services among Type 2 Diabetic Patients in Laguna Glenn Carandang, MD, MPH, 1,2, Maria Victoria Rondaris, MD, MPH, 3, and Genejane Adarlo,
Abstract. Introduction. Original paper. Comparison of screening for diabetic retinopathy by non-specialists and specialists
 Comparison of screening for diabetic retinopathy by non-specialists and specialists Effectiveness of screening for diabetic retinopathy by nonspecialist doctors: the importance of physician-ophthalmologist
Comparison of screening for diabetic retinopathy by non-specialists and specialists Effectiveness of screening for diabetic retinopathy by nonspecialist doctors: the importance of physician-ophthalmologist
Closing the Gap: Advancing Indigenous Eye Health Across Diverse Regions and Systems
 Closing the Gap: Advancing Indigenous Eye Health Across Diverse Regions and Systems Jatkar U, Anjou M, Schubert N, Roberts P, Taylor HR Uma Jatkar, Indigenous Eye Health National Rural Health Alliance
Closing the Gap: Advancing Indigenous Eye Health Across Diverse Regions and Systems Jatkar U, Anjou M, Schubert N, Roberts P, Taylor HR Uma Jatkar, Indigenous Eye Health National Rural Health Alliance
FRANZCO, MD, MBBS. Royal Darwin Hospital
 Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
Diabetes and Eye By Dr. Nishantha Wijesinghe FRANZCO, MD, MBBS Consultant Ophthalmologist Royal Darwin Hospital 98% of Diabetics do not need to suffer from severe visual loss Yet Diabetic eye disease is
The Cost to Close the Gap for Vision
 The to Close the Gap for Vision This report was prepared by Dr Ya-Seng (Arthur) Hsueh*, Mr Alex Brando*, Professor David Dunt, Mr Mitchell Anjou* and Professor Hugh Taylor of the Centre for Health Policy,
The to Close the Gap for Vision This report was prepared by Dr Ya-Seng (Arthur) Hsueh*, Mr Alex Brando*, Professor David Dunt, Mr Mitchell Anjou* and Professor Hugh Taylor of the Centre for Health Policy,
Enhancing eye health capacity in primary health care: closing the gap for vision
 Rural Health West Aboriginal Health Conference Perth 1 July 2017 Enhancing eye health capacity in primary health care: closing the gap for vision Anjou MD, Jatkar U, Gilden R, Schubert NS, Roberts PI,
Rural Health West Aboriginal Health Conference Perth 1 July 2017 Enhancing eye health capacity in primary health care: closing the gap for vision Anjou MD, Jatkar U, Gilden R, Schubert NS, Roberts PI,
Diabetic Retinopathy
 Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
Diabetic Retinopathy Overview This presentation covers the following topics: Definitions Epidemiology of diabetic retinopathy Evidence for public health approaches Screening for diabetic retinopathy Health
We are nearly there. Close the Gap for Vision
 We are nearly there Close the Gap for Vision Executive summary Australia is on the verge of closing the gap in Indigenous eye health Elimination of trachoma Sight restoration for ~4,000 Indigenous Australians
We are nearly there Close the Gap for Vision Executive summary Australia is on the verge of closing the gap in Indigenous eye health Elimination of trachoma Sight restoration for ~4,000 Indigenous Australians
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA
 Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
Diabetes and Eye Health more than meets the eye Vision Initiative - in association with PSA Vision 2020 Australia Vision Initiative RANZCO & OAA (Vic) Proud members of Vision 2020 Australia Outline Vision
Heart health CHD management gaps in general practice
 professional practice Nancy Huang MBBS, DipRACOG, MPH, is National Manager Clinical Programs, Heart Foundation, Melbourne, Victoria. nancy.huang@heartfoundation.org.au Marcus Daddo BSc(Hons), is Manager
professional practice Nancy Huang MBBS, DipRACOG, MPH, is National Manager Clinical Programs, Heart Foundation, Melbourne, Victoria. nancy.huang@heartfoundation.org.au Marcus Daddo BSc(Hons), is Manager
PRESCRIBING IN GLAUCOMA: GUIDELINES FOR NZ OPTOMETRISTS
 PRESCRIBING IN GLAUCOMA: GUIDELINES FOR NZ OPTOMETRISTS Introduction Independent prescribing relates to the capacity to use clinical judgement in respect of diagnosis and treatment. It does not mean working
PRESCRIBING IN GLAUCOMA: GUIDELINES FOR NZ OPTOMETRISTS Introduction Independent prescribing relates to the capacity to use clinical judgement in respect of diagnosis and treatment. It does not mean working
Diabetic Eye Disease
 Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Manchester Royal Eye Hospital Medical Retinal Services Information for Patients Diabetic Eye Disease This leaflet sets out to answer some of your questions about diabetic eye disease. You may wish to discuss
Locating advance care planning facilitators in general practice increases consumer participation
 RESEARCH Locating advance care planning facilitators in general practice increases consumer participation Jill Mann, Stephen D Gill, Lisa Mitchell, Margaret J Rogers, Peter Martin, Frances Quirk, Charlie
RESEARCH Locating advance care planning facilitators in general practice increases consumer participation Jill Mann, Stephen D Gill, Lisa Mitchell, Margaret J Rogers, Peter Martin, Frances Quirk, Charlie
Indigenous Eye Health Indicators
 Indigenous Eye Health Indicators This position paper frames pertinent Indigenous eye health indicators at the regional, jurisdictional, and national levels as recommended in the Roadmap to Close the Gap
Indigenous Eye Health Indicators This position paper frames pertinent Indigenous eye health indicators at the regional, jurisdictional, and national levels as recommended in the Roadmap to Close the Gap
Non mydriatic retinal photography
 Non mydriatic retinal photography A roundtable in preparation for new MBS items for people with diabetes Report Indigenous Eye Health Melbourne School of Population and Global Health 25 July 2016 TABLE
Non mydriatic retinal photography A roundtable in preparation for new MBS items for people with diabetes Report Indigenous Eye Health Melbourne School of Population and Global Health 25 July 2016 TABLE
Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic Retinopathy Screening Programme
 (2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
(2002) 16, 140 145 2002 Nature Publishing Group All rights reserved 1470-269X/02 $25.00 www.nature.com/eye CLINICAL STUDY Longitudinal study of a cohort of people with diabetes screened by the Exeter Diabetic
The first step to Getting Australia s Health on Track
 2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
2017 The first step to Getting Australia s Health on Track Heart Health is the sequential report to the policy roadmap Getting Australia s Health on Track and outlines a national implementation strategy
Diabetic retinopathy is the
 ORIGINAL ARTICLES Digital Retinal Imaging in a Residencybased Patient-centered Medical Home Robert Newman, MD; Doyle M. Cummings, PharmD; Lisa Doherty, MD, MPH; Nick R. Patel, MD BACKGROUND AND OBJECTIVES:
ORIGINAL ARTICLES Digital Retinal Imaging in a Residencybased Patient-centered Medical Home Robert Newman, MD; Doyle M. Cummings, PharmD; Lisa Doherty, MD, MPH; Nick R. Patel, MD BACKGROUND AND OBJECTIVES:
Diabetic retinopathy in Victoria, Australia: the Visual Impairment Project
 Br J Ophthalmol 2000;84:865 870 865 Centre for Eye Research Australia, University of Melbourne, Melbourne, Australia R McKay C A McCarty H R Taylor Correspondence to: Cathy McCarty, Centre for Eye Research
Br J Ophthalmol 2000;84:865 870 865 Centre for Eye Research Australia, University of Melbourne, Melbourne, Australia R McKay C A McCarty H R Taylor Correspondence to: Cathy McCarty, Centre for Eye Research
MANAGING DIABETIC RETINOPATHY. <Your Hospital Name> <Your Logo>
 MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
MANAGING DIABETIC RETINOPATHY It s difficult living with Diabetes Mellitus. Ask any diabetic... Their lives are centered around meal plans, glucose levels, and insulin
Diabetic Management beyond traditional risk factors and LDL-C control: Can we improve macro and microvascular risks?
 Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Retinopathy Diabetes has a negative effect on eyes in many ways, increasing the risk of cataracts for example, but the most common and serious ocular complication of diabetes is retinopathy. Diabetic retinopathy
Falls before and after cataract surgery: a prospective cohort study evaluating determinants of risk
 Falls before and after cataract surgery: a prospective cohort study evaluating determinants of risk Lisa Keay 1, Anna Palagyi 1, Kris Rogers 1, Lynn Meuleners 2, Peter McCluskey 3, Andrew White 3,4, Ecosse
Falls before and after cataract surgery: a prospective cohort study evaluating determinants of risk Lisa Keay 1, Anna Palagyi 1, Kris Rogers 1, Lynn Meuleners 2, Peter McCluskey 3, Andrew White 3,4, Ecosse
INTRODUCTION AND SYMPTOMS
 CHAPTER 1 INTRODUCTION AND SYMPTOMS Introduction of Diabetic Retinopathy Diabetic retinopathy (DR) is a potentially blinding complication of diabetes. It is defined as presence of one or more definite
CHAPTER 1 INTRODUCTION AND SYMPTOMS Introduction of Diabetic Retinopathy Diabetic retinopathy (DR) is a potentially blinding complication of diabetes. It is defined as presence of one or more definite
Building an eye care program with Aboriginal communities in Victoria a partnership approach
 Building an eye care program with Aboriginal communities in Victoria a partnership approach Genevieve Napper 1 and Cheryl Vickery 1 Kulan Barney 2, Jimi Peters 2, Mitchell Anjou 3, Tim Fricke 1,4, Jonathan
Building an eye care program with Aboriginal communities in Victoria a partnership approach Genevieve Napper 1 and Cheryl Vickery 1 Kulan Barney 2, Jimi Peters 2, Mitchell Anjou 3, Tim Fricke 1,4, Jonathan
Manual. Manual Welsh Eye Care Initiative. A Welsh Eye Care Initiative. Protocol. The Assessment and Management of Age-related Macular Degeneration
 A Protocol 1.0 Definitions The following terms are important in this text: Wet Macular Degeneration Condition caused by the growth of abnormal blood vessels under the retina. Symptoms appear suddenly and
A Protocol 1.0 Definitions The following terms are important in this text: Wet Macular Degeneration Condition caused by the growth of abnormal blood vessels under the retina. Symptoms appear suddenly and
On the move again. What is the AusDiab follow-up? AusDiab Partnership Meeting. Features: Newsletter of the AusDiab Study: September 2004
 Features: What is the AusDiab follow-up? AusDiab Partnership meeting Who is involved in running AusDiab? Participant Recruitment Strategies The Invitation Process Moving house how does it affect AusDiab?
Features: What is the AusDiab follow-up? AusDiab Partnership meeting Who is involved in running AusDiab? Participant Recruitment Strategies The Invitation Process Moving house how does it affect AusDiab?
Vision and eye healthcare study in residential aged care facilities
 Vision and eye healthcare study in residential aged care facilities Study report Report prepared by: Rob Cummins, Director, Research & Policy Julie Heraghty, Former Chief Executive Officer Macular Disease
Vision and eye healthcare study in residential aged care facilities Study report Report prepared by: Rob Cummins, Director, Research & Policy Julie Heraghty, Former Chief Executive Officer Macular Disease
The NGO has worked with the AMS and REHC to achieve the following:
 Providing eye care to remote Indigenous communities in the Northern Territory: a case study examining success factors and challenges from a collaborative approach between a NGO and AMS Tricia Keys 1, Maree
Providing eye care to remote Indigenous communities in the Northern Territory: a case study examining success factors and challenges from a collaborative approach between a NGO and AMS Tricia Keys 1, Maree
Identifying Problem Gamblers in Gambling Venues
 1 Identifying Problem Gamblers in Gambling Venues Commissioned for: The Ministerial Council on Gambling Prepared by: Dr. Paul Delfabbro Dr. Alexandra Osborn University of Adelaide Dr. Maurice Nevile Dr.
1 Identifying Problem Gamblers in Gambling Venues Commissioned for: The Ministerial Council on Gambling Prepared by: Dr. Paul Delfabbro Dr. Alexandra Osborn University of Adelaide Dr. Maurice Nevile Dr.
DR Screening In Singapore: Achievements & Future Challenges
 DR Screening In Singapore: Achievements & Future Challenges Ecosse Lamoureux Director, Population Research Platform Singapore Eye Research Institute (SERI) Background About 600,000 of Singaporeans aged
DR Screening In Singapore: Achievements & Future Challenges Ecosse Lamoureux Director, Population Research Platform Singapore Eye Research Institute (SERI) Background About 600,000 of Singaporeans aged
FREQUENCY OF DIABETIC RETINOPATHY IN A TERTIARY CARE HOSPITAL USING DIGITAL RETINAL IMAGING TECHNOLOGY
 ORIGINAL ARTICLE FREQUENCY OF DIABETIC RETINOPATHY IN A TERTIARY CARE HOSPITAL USING DIGITAL RETINAL IMAGING TECHNOLOGY INTRODUCTION As more and more people are being affected with diabetes and with poor
ORIGINAL ARTICLE FREQUENCY OF DIABETIC RETINOPATHY IN A TERTIARY CARE HOSPITAL USING DIGITAL RETINAL IMAGING TECHNOLOGY INTRODUCTION As more and more people are being affected with diabetes and with poor
Type 2 diabetes in Tuvalu: A drug use and chronic disease management evaluation. Prepared for the Ministry of Health, Tuvalu.
 Type 2 diabetes in Tuvalu: A drug use and chronic disease management evaluation Prepared for the Ministry of Health, Tuvalu. 2012 Investigator Alexander Bongers Intern pharmacist, Royal Melbourne Hospital,
Type 2 diabetes in Tuvalu: A drug use and chronic disease management evaluation Prepared for the Ministry of Health, Tuvalu. 2012 Investigator Alexander Bongers Intern pharmacist, Royal Melbourne Hospital,
Outline. Preventing & Treating Diabetes Related Blindness. Eye Care Center Doctors. Justin Kanoff, MD. Eye Care Center of Northern Colorado
 Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
Outline Preventing & Treating Diabetes Related Blindness Justin Kanoff, MD Eye Care Center of Northern Colorado 303 974 4302 Introduction to Eye Care Center of Northern Colorado How the eye works Eye problems
Diabetic and the Eye: An Introduction
 Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
Diabetic and the Eye: An Introduction Lawrence Iu FRCSEd (Ophth), FCOphthHK, FHKAM (Ophthalmology) Department of Ophthalmology, Grantham Hospital & Queen Mary Hospital Background Diabetes mellitus (DM)
 measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
measure of your overall performance. An isolated glucose test is helpful to let you know what your sugar level is at one moment, but it doesn t tell you whether or not your diabetes is under adequate control
OPHTHALMOLOGY DEPARTMENT Primary care referral guidelines
 OPHTHALMOLOGY DEPARTMENT Primary care referral guidelines Contents REFERRAL CATEGIES... 2 Emergency... 2 Urgent... 2 Semi urgent/routine... 2 Not accepted... 2 OPHTHALMOLOGY CONDITIONS NOT ACCEPTED...
OPHTHALMOLOGY DEPARTMENT Primary care referral guidelines Contents REFERRAL CATEGIES... 2 Emergency... 2 Urgent... 2 Semi urgent/routine... 2 Not accepted... 2 OPHTHALMOLOGY CONDITIONS NOT ACCEPTED...
Association of retinal vessel calibre with diabetic retinopathy in an urban Australian Indigenous population *
 Original Article Clinical Science Association of retinal vessel calibre with diabetic retinopathy in an urban Australian Indigenous population * Mohamed Dirani PhD, 1 Annie K McAuley BSc, 1 Louise Maple-Brown
Original Article Clinical Science Association of retinal vessel calibre with diabetic retinopathy in an urban Australian Indigenous population * Mohamed Dirani PhD, 1 Annie K McAuley BSc, 1 Louise Maple-Brown
Diagnosis and treatment of diabetic retinopathy. Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City
 Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diagnosis and treatment of diabetic retinopathy Blake Cooper MD Ophthalmologist Vitreoretinal Surgeon Retina Associates Kansas City Disclosures Consulted for Novo Nordisk 2017,2018. Will be discussing
Diabetic Eye Screening
 Diabetic Eye Screening Lorraine Lockwood Engagement Manager Health Intelligence Classification: Internal / Public 26/10/16 Who we are (EDESP) formed on 1 st April 2016 Who should be screened? All patients
Diabetic Eye Screening Lorraine Lockwood Engagement Manager Health Intelligence Classification: Internal / Public 26/10/16 Who we are (EDESP) formed on 1 st April 2016 Who should be screened? All patients
Diabetic Eye Disease Visual Recognition & Interpretation of Clinical Signs
 + Diabetic Eye Disease Visual Recognition & Interpretation of Clinical Signs Quiz created by CLEARVIEW Training Jane Macnaughton MCOptom & Peter Chapman MCOptom FBDO + CET Accreditation C 19106 2 CET Points
+ Diabetic Eye Disease Visual Recognition & Interpretation of Clinical Signs Quiz created by CLEARVIEW Training Jane Macnaughton MCOptom & Peter Chapman MCOptom FBDO + CET Accreditation C 19106 2 CET Points
 www.brisbaneeyeclinic.com.au Brisbane Eye Clinic is a modern ophthalmology practice focused on the provision of excellent medical eye care. The Clinic has two convenient consulting locations, our Wickham
www.brisbaneeyeclinic.com.au Brisbane Eye Clinic is a modern ophthalmology practice focused on the provision of excellent medical eye care. The Clinic has two convenient consulting locations, our Wickham
Clinical Policy Title: Retinal telescreening for diabetic retinopathy
 Clinical Policy Title: Retinal telescreening for diabetic retinopathy Clinical Policy Number: 10.01.01 Effective Date: July 1, 2016 Initial Review Date: April 27, 2016 Most Recent Review Date: May 19,
Clinical Policy Title: Retinal telescreening for diabetic retinopathy Clinical Policy Number: 10.01.01 Effective Date: July 1, 2016 Initial Review Date: April 27, 2016 Most Recent Review Date: May 19,
Tele-Eye Care and Eye Disease Risk Prediction Prof K Yogesan (Yogi)
 Tele-Eye Care and Eye Disease Risk Prediction Prof K Yogesan (Yogi) Australian of the Year in 2015 - WA Finalist Research Director, Australian E-Health Research Centre Visiting Scholar, Harvard University
Tele-Eye Care and Eye Disease Risk Prediction Prof K Yogesan (Yogi) Australian of the Year in 2015 - WA Finalist Research Director, Australian E-Health Research Centre Visiting Scholar, Harvard University
Eye health promotion by optometrists in rural Victoria
 Eye health promotion by optometrists in rural Victoria Lawrence Arnold, Ben Harris, Optometrists Association Victoria The Optometrists Association Victoria has been helping optometrists in rural Victoria
Eye health promotion by optometrists in rural Victoria Lawrence Arnold, Ben Harris, Optometrists Association Victoria The Optometrists Association Victoria has been helping optometrists in rural Victoria
The Future of Optometric Services in Primary Care in Wales
 IMPROVING HEALTH IN WALES The Future of Optometric Services in Primary Care in Wales a consultation document ISBN 0 7504 2968 2 Designed by CartoGraphic Services G/254/02-03 September 2002 INA - 15-02
IMPROVING HEALTH IN WALES The Future of Optometric Services in Primary Care in Wales a consultation document ISBN 0 7504 2968 2 Designed by CartoGraphic Services G/254/02-03 September 2002 INA - 15-02
DMEP Study Section 1 1
 DMEP Study Section 1 1 1. EXECUTIVE SUMMARY 1.1 Objectives The specific aims of the Diabetes Mellitus Education Program (DMEP) were to examine the role of the community pharmacist in the disease state
DMEP Study Section 1 1 1. EXECUTIVE SUMMARY 1.1 Objectives The specific aims of the Diabetes Mellitus Education Program (DMEP) were to examine the role of the community pharmacist in the disease state
Diabetic Retinopathy Screening: An Academic Practice Partnership
 Diabetic Retinopathy Screening: An Academic Practice Partnership Kristine D. Warner PhD MPH RN Cindy Wolff PhD MPA RD Dr. John McDonald, Optometrist Amber Genato BSN RN - Graduate Assistant California
Diabetic Retinopathy Screening: An Academic Practice Partnership Kristine D. Warner PhD MPH RN Cindy Wolff PhD MPA RD Dr. John McDonald, Optometrist Amber Genato BSN RN - Graduate Assistant California
Diabetic retinopathy (DR)
 Diabetic retinopathy screening in remote communities A futuristic outreach model Nicola Glasson Dr Lisa Crossland PhD, MPH&TM, BA (Hons) Professor Sarah Larkins MBBS, BMedSci, MPH&TM, FRACGP, FARGP, GradDip
Diabetic retinopathy screening in remote communities A futuristic outreach model Nicola Glasson Dr Lisa Crossland PhD, MPH&TM, BA (Hons) Professor Sarah Larkins MBBS, BMedSci, MPH&TM, FRACGP, FARGP, GradDip
PHYSIOTHERAPY AND DIABETES
 PHYSIOTHERAPY AND DIABETES March 2006 Executive Summary The Australian Physiotherapy Association (APA) strongly supports the use of multidisciplinary teams to provide evidence-based care to individuals
PHYSIOTHERAPY AND DIABETES March 2006 Executive Summary The Australian Physiotherapy Association (APA) strongly supports the use of multidisciplinary teams to provide evidence-based care to individuals
Vision 2020 Australia
 Vision 2020 Australia National Eye Health Initiative round two demonstration grants workshop outcomes 23 February 2011 National body working in partnership to prevent avoidable blindness and improve vision
Vision 2020 Australia National Eye Health Initiative round two demonstration grants workshop outcomes 23 February 2011 National body working in partnership to prevent avoidable blindness and improve vision
VisionNews. Artist asks; What does blindness look like?
 VisionNews WINTER 2012 Diabetic retinopathy affects 93 million worldwide Accomplished neuroscientist joins CERA Early treatment leads to better outcomes for common eye disease Global indicators for blindness
VisionNews WINTER 2012 Diabetic retinopathy affects 93 million worldwide Accomplished neuroscientist joins CERA Early treatment leads to better outcomes for common eye disease Global indicators for blindness
Evaluating the impact of optical coherence tomography in diabetic retinopathy screening for an Aboriginal population INTRODUCTION
 bs_bs_banner Clinical and Experimental Ophthalmology 2017; : doi: 10.1111/ceo.13018 Original Article Evaluating the impact of optical coherence tomography in diabetic retinopathy screening for an Aboriginal
bs_bs_banner Clinical and Experimental Ophthalmology 2017; : doi: 10.1111/ceo.13018 Original Article Evaluating the impact of optical coherence tomography in diabetic retinopathy screening for an Aboriginal
Improving Eye Health. Cardiff and Vale University Health Board
 Improving Eye Health Cardiff and Vale University Health Board Local Eye Care Plan 2013-2018 1. Introduction On the 18 th September 2013 the Welsh Government published Together for Health: Eye Health Care,
Improving Eye Health Cardiff and Vale University Health Board Local Eye Care Plan 2013-2018 1. Introduction On the 18 th September 2013 the Welsh Government published Together for Health: Eye Health Care,
Insight of adult health checks an approach to Aboriginal and Torres Strait Islander eye examinations. Prof Hugh Taylor and Mr Mitchell Anjou
 Insight of adult health checks an approach to Aboriginal and Torres Strait Islander eye examinations Prof Hugh Taylor and Mr Mitchell Anjou Insight of adult health checks An approach to Aboriginal and
Insight of adult health checks an approach to Aboriginal and Torres Strait Islander eye examinations Prof Hugh Taylor and Mr Mitchell Anjou Insight of adult health checks An approach to Aboriginal and
Diabetic Retinopathy. Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012
 Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Diabetic Retinopathy Barry Emara MD FRCS(C) Giovanni Caboto Club October 3, 2012 Outline Statistics Anatomy Categories Assessment Management Risk factors What do you need to do? Objectives Summarize the
Treatment of Diabetic Macular Edema without Intravitreal injections
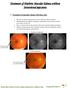 Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Treatment of Diabetic Macular Edema without Intravitreal injections 1. Treatment of macular edema with laser only This 60 year old female presented on 02-01-2007 for retinal evaluation. She had proliferative
Ophthalmology Unit Referral Guidelines
 Ophthalmology Unit Referral Guidelines Austin Health Ophthalmology Unit holds sub-specialty sessions to discuss and plan the treatment of patients with specific ocular conditions. General including cataract
Ophthalmology Unit Referral Guidelines Austin Health Ophthalmology Unit holds sub-specialty sessions to discuss and plan the treatment of patients with specific ocular conditions. General including cataract
Glaucoma screening. A global perspective. Contents. Introduction
 Glaucoma screening A global perspective Introduction Rather than referring to a single condition, glaucoma is a term used to describe a range of disorders affecting the optic nerve. This, combined with
Glaucoma screening A global perspective Introduction Rather than referring to a single condition, glaucoma is a term used to describe a range of disorders affecting the optic nerve. This, combined with
Sponsored by. Shared care and referral pathways. Part 2: diabetes screening leading from the front
 CET CONTINUING Sponsored by 1 CET POINT Shared care and referral pathways Part 2: diabetes screening leading from the front Chris Steele, BSc (Hons), FCOptom, DCLP, DipOC, DipTp(IP), FBCLA The alarming
CET CONTINUING Sponsored by 1 CET POINT Shared care and referral pathways Part 2: diabetes screening leading from the front Chris Steele, BSc (Hons), FCOptom, DCLP, DipOC, DipTp(IP), FBCLA The alarming
 www.brisbaneeyeclinic.com.au Brisbane Eye Clinic is a modern ophthalmology practice focused on the provision of excellent medical eye care. The Clinic has two convenient consulting locations, our Wickham
www.brisbaneeyeclinic.com.au Brisbane Eye Clinic is a modern ophthalmology practice focused on the provision of excellent medical eye care. The Clinic has two convenient consulting locations, our Wickham
Diabetic Retinopathy Screening in Hong Kong. Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong
 Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
Diabetic Retinopathy Screening in Hong Kong Dr. Rita Gangwani M.S, FRCS (Ophth), FCOphth(HK), FHKAM Eye Institute, The University of Hong Kong Co-Investigators Prof. David Wong Prof. Sarah McGhee Dr. Wico
Awareness of Diabetic Retinopathy in Rural Population in South Tamil Nadu
 Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/336 Awareness of Diabetic Retinopathy in Rural Population in South Tamil Nadu N Sharmila 1, K Kavitha 1, S Ganapathy
Original Article Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2016/336 Awareness of Diabetic Retinopathy in Rural Population in South Tamil Nadu N Sharmila 1, K Kavitha 1, S Ganapathy
MAGNITUDE OF DIABETIC EYE DISEASE IN INDIA
 Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Dear Doctor This booklet contains information about your role as a physician in preventing blindness in your diabetic patients. You are the first point of contact for your diabetic patients. You see them
Diabetic retinopathy (DR) was first PROCEEDINGS DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT
 DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT Diabetic retinopathy (DR) is characterized by the development of retinal microaneurysms, hemorrhages, deposits of leaked lipoproteins (hard exudates),
DIABETIC RETINOPATHY * Ronald Klein, MD, MPH ABSTRACT Diabetic retinopathy (DR) is characterized by the development of retinal microaneurysms, hemorrhages, deposits of leaked lipoproteins (hard exudates),
OAKLEIGH EYE CENTRE. THE EYE Before looking at diabetic retinopathy it is important to understand what the healthy eye looks like and how it works.
 ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
ABN: 80 836 359 971 Dr Mark Steiner 345 799X 135 Warrigal Road Dr Helen Steiner 292 419A OAKLEIGH VIC 3166 Tel: 03 9568 7706 Fax: 03 9568 4498 E-Mail: oakeye13@bigpond.com DIABETIC RETINOPATHY DIABETES
POSITION STATEMENT. Diabetic eye screening April Key points
 POSITION STATEMENT Title Date Diabetic eye screening April 2013 Key points Diabetic retinopathy is the most common cause of sight loss in the working age population (1) All people with any type of diabetes
POSITION STATEMENT Title Date Diabetic eye screening April 2013 Key points Diabetic retinopathy is the most common cause of sight loss in the working age population (1) All people with any type of diabetes
The Use of Complementary and Alternative Medicine in Australia Charlie Changli Xue, Lin Zhang, Vivian Lin and David F. Story
 The Use of Complementary and Alternative Medicine in Australia Charlie Changli Xue, Lin Zhang, Vivian Lin and David F. Story Despite apparent high usage of complementary and alterative medicine (CAM) and
The Use of Complementary and Alternative Medicine in Australia Charlie Changli Xue, Lin Zhang, Vivian Lin and David F. Story Despite apparent high usage of complementary and alterative medicine (CAM) and
The College of Optometrists - Learning outcomes for the Professional Certificate in Medical Retina
 Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
Learning outcomes for the Professional Certificate in Medical Retina, incorporating diabetic retinopathy screening and age related macular degeneration The professional certificate is a prerequisite to
DIABETIC RETINOPATHY
 THE UK GUIDE DIABETIC RETINOPATHY Everything you need to know about diabetic retinopathy Jaheed Khan BSc (Hons) MBBS MD FRCOphth Fellow of the Royal College of Ophthalmologists Association for Research
THE UK GUIDE DIABETIC RETINOPATHY Everything you need to know about diabetic retinopathy Jaheed Khan BSc (Hons) MBBS MD FRCOphth Fellow of the Royal College of Ophthalmologists Association for Research
SPEAKERS MARK ROTH STEPHEN LESLIE LAUREN AYTON
 SPEAKERS MARK ROTH SIMON CHEN Ophthalmologist specialising in vitreoretinal surgery, intravitreal anti-vegf therapy and laser cataract surgery. He is a principal investigator for numerous international
SPEAKERS MARK ROTH SIMON CHEN Ophthalmologist specialising in vitreoretinal surgery, intravitreal anti-vegf therapy and laser cataract surgery. He is a principal investigator for numerous international
PK Rani, R Raman, S Subramani, G Perumal, G Kumaramanickavel, T Sharma. Sankara Nethralaya, Nungambakam, Chennai, India
 O R I G I N A L R E S E A R C H Knowledge of diabetes and diabetic retinopathy among rural populations in India, and the influence of knowledge of diabetic retinopathy on attitude and practice PK Rani,
O R I G I N A L R E S E A R C H Knowledge of diabetes and diabetic retinopathy among rural populations in India, and the influence of knowledge of diabetic retinopathy on attitude and practice PK Rani,
Clinically Significant Macular Edema (CSME)
 Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
Clinically Significant Macular Edema (CSME) 1 Clinically Significant Macular Edema (CSME) Sadrina T. Shaw OMT I Student July 26, 2014 Advisor: Dr. Uwaydat Clinically Significant Macular Edema (CSME) 2
The RPS is the professional body for pharmacists in Wales and across Great Britain. We are the only body that represents all sectors of pharmacy.
 Royal Pharmaceutical Society 2 Ash Tree Court Woodsy Close Cardiff Gate Business Park Pontprennau Cardiff CF23 8RW Mr Mark Drakeford AM, Chair, Health and Social Care Committee National Assembly for Wales
Royal Pharmaceutical Society 2 Ash Tree Court Woodsy Close Cardiff Gate Business Park Pontprennau Cardiff CF23 8RW Mr Mark Drakeford AM, Chair, Health and Social Care Committee National Assembly for Wales
LOCSU Community Services. Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway. Issued by Local Optical Committee Support Unit May 2009
 LOCSU Community Services Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway Issued by Local Optical Committee Support Unit May 2009 [Revised November 2013] Contents Page Executive Summary...
LOCSU Community Services Glaucoma Repeat Readings & OHT Monitoring Community Service Pathway Issued by Local Optical Committee Support Unit May 2009 [Revised November 2013] Contents Page Executive Summary...
A Patient s Guide to Diabetic Retinopathy
 Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Diabetic Retinopathy A Patient s Guide to Diabetic Retinopathy 840 Walnut Street, Philadelphia PA 19107 www.willseye.org Diabetic Retinopathy 1. Definition Diabetic retinopathy is a complication of diabetes
Hydroxychloroquine and Chloroquine Retinopathy: Recommendations on Screening
 linical Guidelines Hydroxychloroquine and hloroquine Retinopathy: Recommendations on Screening February 2018 - Review date: February 2021 Executive Summary Recent data have highlighted that hydroxychloroquine
linical Guidelines Hydroxychloroquine and hloroquine Retinopathy: Recommendations on Screening February 2018 - Review date: February 2021 Executive Summary Recent data have highlighted that hydroxychloroquine
Diabetes Retinopathy Extension Dataset
 For reference only Do Not Use For more information contact: cdsis@nhs.net Diabetes Retinopathy Extension Dataset March 2006 National Clinical Dataset Development Programme (NCDDP) Support Team Information
For reference only Do Not Use For more information contact: cdsis@nhs.net Diabetes Retinopathy Extension Dataset March 2006 National Clinical Dataset Development Programme (NCDDP) Support Team Information
Specialist Eye Health Guidelines
 Specialist Eye Health Guidelines for use in Aboriginal and Torres Strait Islander Populations Cataract Diabetic Retinopathy Trachoma Commonwealth of Australia 2001 This work is copyright. It may be reproduced
Specialist Eye Health Guidelines for use in Aboriginal and Torres Strait Islander Populations Cataract Diabetic Retinopathy Trachoma Commonwealth of Australia 2001 This work is copyright. It may be reproduced
Stronger eye care systems in Aboriginal primary health care
 Stronger eye care systems in Aboriginal primary health care Anna Morse 1,2, Colina Waddell 1,2, Jenny Hunt 3, Fiona MacFarlane 4, Daniel Jackman 5, Christine Corby 6, Tricia Keys 1,2 1 Brien Holden Vision
Stronger eye care systems in Aboriginal primary health care Anna Morse 1,2, Colina Waddell 1,2, Jenny Hunt 3, Fiona MacFarlane 4, Daniel Jackman 5, Christine Corby 6, Tricia Keys 1,2 1 Brien Holden Vision
Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy
 European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
European Journal of Ophthalmology / Vol. 17 no. 1, 2007 / pp. 84-88 Clinical biomicroscopy versus fluorescein angiography: Effectiveness and sensitivity in detecting diabetic retinopathy S.S. KHALAF, M.D.
Champlain LHIN. Estimated that 55,563 people over age 18 live with diabetes
 Champlain LHIN Estimated that 55,563 people over age 18 live with diabetes Healthy, caring communities supported by health services of choice that achieve results- today and for the future Impact of Diabetes
Champlain LHIN Estimated that 55,563 people over age 18 live with diabetes Healthy, caring communities supported by health services of choice that achieve results- today and for the future Impact of Diabetes
Access to Health Services in Urban and Rural Australia: a Level Playing Field?
 Access to Health Services in Urban and Rural Australia: a Level Playing Field? Anne Young, Annette Dobson, Julie Byles Anne Young 6th National Rural Health Conference Canberra, Australian Capital Territory,
Access to Health Services in Urban and Rural Australia: a Level Playing Field? Anne Young, Annette Dobson, Julie Byles Anne Young 6th National Rural Health Conference Canberra, Australian Capital Territory,
D. Hilton. Keywords Epidemiological methods, aging, prevalence.
 Computational Methods in Official Statistics with an Example on Calculating and Predicting Diabetes Mellitus [DM] Prevalence in Different Age Groups within Australia in Future Years, in Light of the Aging
Computational Methods in Official Statistics with an Example on Calculating and Predicting Diabetes Mellitus [DM] Prevalence in Different Age Groups within Australia in Future Years, in Light of the Aging
Original Article. (This manuscript was submitted on 9 February Following blind peer review, it was accepted for publication on 6 June 2012)
 483331PED0Supp. 10.1177/1757975913483331D. Trouilloud and J. Regnier 013 Therapeutic education among adults with type diabetes: effects of a three-day intervention on perceived competence, self-management
483331PED0Supp. 10.1177/1757975913483331D. Trouilloud and J. Regnier 013 Therapeutic education among adults with type diabetes: effects of a three-day intervention on perceived competence, self-management
SCIENTIFIC STUDY REPORT
 PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
PAGE 1 18-NOV-2016 SCIENTIFIC STUDY REPORT Study Title: Real-Life Effectiveness and Care Patterns of Diabetes Management The RECAP-DM Study 1 EXECUTIVE SUMMARY Introduction: Despite the well-established
The Potential For Teleophthalmology in the Patient-Centered Medical Home Model
 The Potential For Teleophthalmology in the Patient-Centered Medical Home Model Christina Sheppler, PhD Legacy Research Institute Devers Eye Institute NRTRC Telemedicine Conference March 26, 2014 Disclosures
The Potential For Teleophthalmology in the Patient-Centered Medical Home Model Christina Sheppler, PhD Legacy Research Institute Devers Eye Institute NRTRC Telemedicine Conference March 26, 2014 Disclosures
What is the clinical problem?
 Team T2D: Empowering people living with Type 2 Diabetes Implementation and Evaluation of the Combined RBWH and QUT Health Clinics Model of Care for Patients with Type 2 Diabetes Adrienne Young: Research
Team T2D: Empowering people living with Type 2 Diabetes Implementation and Evaluation of the Combined RBWH and QUT Health Clinics Model of Care for Patients with Type 2 Diabetes Adrienne Young: Research
Teleretinal Screening for Diabetic Retinopathy: A Novel Approach to Reduce Screening Burden on the Healthcare Systems within Central Texas
 Teleretinal Screening for Diabetic Retinopathy: A Novel Approach to Reduce Screening Burden on the Healthcare Systems within Central Texas Robert W. Wong, MD; Maria Benson, BS; Jose A. Martinez, MD; Mark
Teleretinal Screening for Diabetic Retinopathy: A Novel Approach to Reduce Screening Burden on the Healthcare Systems within Central Texas Robert W. Wong, MD; Maria Benson, BS; Jose A. Martinez, MD; Mark
Diabetes Care 24: , 2001
 Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
Pathophysiology/Complications O R I G I N A L A R T I C L E Prevalence and Significance of Retinopathy in Subjects With Type 1 Diabetes of Less Than 5 Years Duration Screened for the Diabetes Control and
THE PREVALENCE OF CAUSES FOR DIABETIC RETINOPATHY USING MATHEMATICAL MODELS
 International Journal of Advanced Research in Engineering and Technology (IJARET) Volume 9, Issue 6, November-December 2018, pp. 167 171, Article ID: IJARET_09_06_017 Available online at http://www.iaeme.com/ijaret/issues.asp?jtype=ijaret&vtype=9&itype=6
International Journal of Advanced Research in Engineering and Technology (IJARET) Volume 9, Issue 6, November-December 2018, pp. 167 171, Article ID: IJARET_09_06_017 Available online at http://www.iaeme.com/ijaret/issues.asp?jtype=ijaret&vtype=9&itype=6
Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health
 Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health Pat Field National Director, Rural Remote and Indigenous Programs, Heart Foundation of Australia 5th National
Non-Government Organisations and a Collaborative Model for Rural, Remote and Indigenous Health Pat Field National Director, Rural Remote and Indigenous Programs, Heart Foundation of Australia 5th National
Aneurin Bevan University Health Board. Directorate of Ophthalmology. Action Plan Ophthalmology Thematic Review Final Version 2015/16 WET AMD
 Aneurin Bevan University Health Board Directorate of Ophthalmology Action Plan Ophthalmology Thematic Review Final Version 2015/16 WET AMD No. Item Action Responsible Person(s) Timeframe 1 Patient Referrals
Aneurin Bevan University Health Board Directorate of Ophthalmology Action Plan Ophthalmology Thematic Review Final Version 2015/16 WET AMD No. Item Action Responsible Person(s) Timeframe 1 Patient Referrals
Physical activity. Policy endorsed by the 50th RACGP Council 9 February 2008
 This paper provides a background to the Royal Australian College of General Practitioners (RACGP) current position on physical activity, as set out in the RACGP Guidelines for preventive activities in
This paper provides a background to the Royal Australian College of General Practitioners (RACGP) current position on physical activity, as set out in the RACGP Guidelines for preventive activities in
Progressing Aboriginal and Torres Strait Islander eye health and vision care. Policy and funding proposal
 Progressing Aboriginal and Torres Strait Islander eye health and vision care Policy and funding proposal March 2013 Contents 1 Executive Summary 1 1.1 Purpose 1 1.2 Key recommendations 2 1.3 Vision 2020
Progressing Aboriginal and Torres Strait Islander eye health and vision care Policy and funding proposal March 2013 Contents 1 Executive Summary 1 1.1 Purpose 1 1.2 Key recommendations 2 1.3 Vision 2020
Consumer Participation Strategy
 Consumer Participation Strategy Plan Implementation Period 2011-2013 Date: 24 December 2010 Developed by: NEMICS Directorate in consultation with Acknowledgements and thank you to: s, Dr Ian Roos (Cancer
Consumer Participation Strategy Plan Implementation Period 2011-2013 Date: 24 December 2010 Developed by: NEMICS Directorate in consultation with Acknowledgements and thank you to: s, Dr Ian Roos (Cancer
Health Technology Assessment Report 1. Organisation of services for diabetic retinopathy screening
 eé~äíü=qéåüåçäçöó=_ç~êç=ñçê=påçíä~åç Health Technology Assessment Report 1 Organisation of services for diabetic retinopathy screening Authors: Facey K, Cummins E, Macpherson K, Morris A, Reay L, Slattery
eé~äíü=qéåüåçäçöó=_ç~êç=ñçê=påçíä~åç Health Technology Assessment Report 1 Organisation of services for diabetic retinopathy screening Authors: Facey K, Cummins E, Macpherson K, Morris A, Reay L, Slattery
RISK FACTORS FOR DIABETIC RETINOPATHY PROGRESSION
 2015 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 22(2):159-165 doi: 10.1515/rjdnmd-2015-0020 RISK FACTORS FOR DIABETIC RETINOPATHY PROGRESSION Mónika
2015 ILEX PUBLISHING HOUSE, Bucharest, Roumania http://www.jrdiabet.ro Rom J Diabetes Nutr Metab Dis. 22(2):159-165 doi: 10.1515/rjdnmd-2015-0020 RISK FACTORS FOR DIABETIC RETINOPATHY PROGRESSION Mónika
