Negative axillary sentinel node (SN) biopsy (SNB) Improved Sentinel Node Identification by SPECT/CT in Overweight Patients with Breast Cancer
|
|
|
- Barrie Patterson
- 5 years ago
- Views:
Transcription
1 Improved Sentinel Node Identification by SPECT/CT in Overweight Patients with Breast Cancer Hedva Lerman 1, Gennady Lievshitz 1, Osnat Zak 2, Ur Metser 1,3, Shlomo Schneebaum 3,4, and Einat Even-Sapir 1,3 1 Department of Nuclear Medicine, Tel-Aviv Sourasky Medical Center, Tel-Aviv, Israel; 2 GE Healthcare, Haifa, Israel; 3 Sackler Faculty of Medicine, Tel-Aviv University, Tel-Aviv, Israel; and 4 Department of Radio-Isotope Guided Surgery Unit of Surgery A, Tel-Aviv Sourasky Medical Center, Tel-Aviv, Israel Overweight has been reported as a cause for the nonvisualization of sentinel nodes (SNs) on preoperative planar lymphoscintigraphy in patients with breast cancer. The purpose of this study was to assess whether SPECT/CT may improve SN identification in overweight patients. Methods: Lymphoscintigraphy was performed in 220 consecutive patients with breast cancer. Body mass index (BMI) was calculated for each. A total of 122 patients were overweight or obese (BMI, $25). Planar images and SPECT/CT images were interpreted separately, and SN identification on each of the modalities was related to BMI and to findings at surgery. Results: Planar imaging identified SNs in 171 patients (78%) with a BMI (mean 6 SD) of kg/m 2 and failed to do so in 49 patients (22%) with a BMI of kg/m 2. In 29 of the latter patients (59%), SNs were identified on SPECT/CT. SPECT/CT detected hot nodes in 200 patients (91%) and failed to do so in 20 patients with a BMI of kg/m 2. For the 122 overweight or obese patients, planar assessment failed to identify SNs in 34 patients (28%) and SPECT/CT failed to do so in 13 patients (11%) (P, 0.001). For 116 patients, surgery took place in our hospital (Tel-Aviv Sourasky Medical Center). An intraoperative blue dye technique failed to detect SNs in 48 patients (41%) with a BMI of kg/m 2. SPECT/CT localized hot nodes in 36 (75%) of the latter patients, and planar imaging did so in 22 (46%) of those patients. Of 19 patients for whom scintigraphy failed, 6 (32%) had nodal metastatic involvement. Conclusion: The addition of SPECT/CT to lymphoscintigraphy improved SN identification in overweight patients with breast cancer. Moreover, SPECT/CT accurately identified SNs in 75% of patients for whom the identification of SNs by the intraoperative blue dye technique failed. Key Words: lymphoscintigraphy; sentinel node; SPECT/CT; breast; cancer J Nucl Med 2007; 48: Negative axillary sentinel node (SN) biopsy (SNB) offers patients with breast cancer minimally invasive surgery with reduced postsurgery morbidity. The incidence of Received Aug. 17, 2006; revision accepted Oct. 19, For correspondence or reprints contact: Hedva Lerman, MD, Department of Nuclear Medicine, Tel-Aviv Sourasky Medical Center, 6 Weizman St., Tel- Aviv, Israel. hedval@tasmc.health.gov.il COPYRIGHT ª 2007 by the Society of Nuclear Medicine, Inc. lymphedema after axillary lymph node (LN) dissection (ALND) ranges between 6% and 30% (1). Overweight is a major risk factor for the development of severe lymphedema after ALND (2). Intraoperative identification of SNs with the blue dye technique has been reported to be less successful in overweight patients (3). Using multivariate analysis, Nos et al. reported that body mass index (BMI) and breast size are the most significant factors affecting the rate of intraoperative SN identification (4). Nonobese patients and patients with small or medium breast sizes show better detection rates than do obese patients with large breast sizes and voluminous or fatty axillae. It is presumed that the decrease in the capacity of nodes to retain blue dye in obese patients is attributable to replacement of the normal nodal tissue by adipose tissue (4). In patients referred for SNB, particularly those for whom intraoperative techniques are suboptimal, the preoperative identification of SNs by lymphoscintigraphy is of clinical relevance. However, an increased BMI is associated with a high rate of failure of lymphoscintigraphic SN identification (5). We previously reported that the addition of SPECT/CT to planar imaging may improve the preoperative scintigraphic localization of draining nodes. SPECT/CT data allow the detection of hot nodes missed by planar imaging, exclude sites of false-positive nonnodal uptake, and accurately localize axillary and extraaxillary hot nodes (6,7). The purpose of this study was to assess whether the performance of SPECT/CT may improve SN identification in overweight patients with breast cancer. Our hypothesis was that the improved spatial resolution of SPECT and the better image quality achieved with the use of CT data for attenuation correction may improve the diagnostic accuracy of SN mapping in general and specifically in overweight patients. MATERIALS AND METHODS Patients Planar lymphoscintigraphy and SPECT/CT lymphoscintigraphy were performed in 220 consecutive women with invasive breast cancer (T02T2), with no clinical evidence of axillary LN metastases (N0), and with no remote metastases (M0). Their age (mean 6 SD) was y (range, 23283). These patients included 140 LYMPHOSCINTIGRAPHY AND OVERWEIGHT Lerman et al. 201
2 women with a palpable mass, 69 women with a nonpalpable mass, and 11 women after lumpectomy. Patients were interviewed by department nurses, and then height and weight measurements were obtained for BMI calculations. The BMI was calculated as the body weight in kilograms divided by the height in squared meters (kg/m 2 ). Patients with BMI values of 18.4 kg/m 2 and lower were considered to be underweight, those with BMI values of kg/m 2 were considered to be normal weight, those with BMI values of kg/m 2 were considered to be overweight, and those with BMI values of 30 kg/m 2 and over were considered obese. Of the study population, 122 patients were overweight or obese. Lymphoscintigraphic Techniques On the day before surgery, a dose of 74 MBq (2 mci) of 99m Tcrhenium colloid (TCK-17; CIS International), divided into 4 equal portions of 0.7 ml each, was injected. Women with palpable masses were injected at 4 peritumoral sites by a nuclear medicine physician, and patients after lumpectomy were injected at 4 sites along the border of the biopsy cavity. Patients with multifocal lesions or subareolar tumors were injected at 4 periareolar sites. All patients with nonpalpable masses were injected under mammographic guidance. After localization of the tumor and insertion of a Kopans wire (Cook), 1 intratumoral injection of 74 MBq (2 mci) of 99m Tc-rhenium colloid in 3 ml of saline solution was administered adjacent to the wire tip. The rhenium colloid preparation is characterized by a particle size of nm and contains gelatin. Therefore, it migrates slowly from the injection site and accumulates in SNs for a prolonged period of time. These characteristics permit a 2-d protocol; the scintigraphic study can be performed on the day before surgery, thus offering flexibility in scheduling surgery and a longer scintigraphic study time (8). Planar images, including anterior and lateral projections, were obtained immediately after injection for palpable masses and up to 60 min after injection during mammography for nonpalpable masses; imaging was continued until hot nodes were identified, up to 24 h after injection, if necessary. Planar images were obtained both before and after SPECT/CT, simulating the posture of the patient during surgery with the arm elevated to 110. In the anterior view, the patient was asked to remove the breast from the axillary field of view by using her contralateral hand, whereas in the lateral view, the breast was naturally removed from the axillary region. A 57 Co flood source was placed between the patient and the camera to define the body contour. The SPECT/CT study was performed with a hybrid system composed of a dual-head g-camera with a low-dose x-ray tube installed in the gantry. For 160 patients, we used a Hawkeye SPECT/CT system (GE Healthcare), which has been used and described in detail in earlier reports (6,7); for the other 60 patients, we used a novel SPECT/CT hybrid system, the Infinia/Hawkeye 4 (GE Healthcare). The latter system incorporates the Infinia dualhead camera with integrated low-dose, 4 5-mm-slice-thickness CT. The CT apparatus has a fixed anode oil-cooled x-ray tube and operates at 140 kv and up to 2.5 ma. The x-ray tube and detector array, located on the slip ring gantry of the g-camera, rotate together in a fixed geometry at 2.0 rpm for 90 L-mode scans. Multiple slices were obtained in the helical mode; 4 slices were acquired simultaneously with a beam coverage of 2 cm in each gantry rotation and reconstructed online to a image matrix. CT scans were acquired within 4.5 min. The acquisition time added by SPECT/CT was min. The radiation dose added to the breast tissue by the low-dose CTwas msv/ma (manufacturer data). Cross-sectional attenuation images in which each pixel represents the attenuation of the imaged tissue were generated. Fusion of the SPECT and CT images was performed on Xeleris workstations (GE Healthcare). On the basis of the scintigraphic findings from both planar imaging and SPECT/CT, the location of hot nodes was marked on the patient s skin. A compact disc with fused SPECT/CT images in 3 planes was given to the surgeon before surgery. Scintigraphic Interpretation The interpretation of lymphoscintigraphy data was performed by 2 nuclear medicine physicians in consensus. Planar images with and without the 57 Co flood source and SPECT/CT images were interpreted separately and in a masked fashion. The data for planar assessment included the number of hot nodes detected and whether they were axillary or internal mammary nodes. The locations of hot nodes on fused SPECT/CT images were categorized with the classification used by the surgeon into level I nodes, defined as nodes located lateral to the pectoralis minor muscle; level II nodes, defined as nodes located within the medial and lateral margins of the pectoralis minor muscle; and level III nodes, including nodes located in the axilla medial to the pectoralis minor muscle, interpectoral nodes located between the major and minor pectoralis muscles, intramammary nodes located within the breast tissue, internal mammary nodes, and nodes located in the supraclavicular area (9). Assessment of Impact of Attenuation Correction on Identification of Hot Nodes by SPECT/CT To assess the impact of attenuation correction on SN identification by SPECT/CT in an attempt to determine whether detection by SPECT/CT was attributable to the better spatial resolution of SPECT or to the attenuation correction with the CT maps, SPECT images of patients with negative planar study results and positive SPECT/CT study results were reconstructed twice, with and without attenuation correction. Each reconstructed image set was interpreted separately by 2 nuclear medicine physicians, who were unaware of the reconstruction mode. Correlation of BMI and Lymphoscintigraphic Findings The impact of BMI on the rate of detection of hot nodes by scintigraphy was assessed separately for planar images and for SPECT/CT images in the general study population as well as in the subgroup of 122 overweight and obese patients. Correlation of Intraoperative Blue Dye Detection of SNs, Lymphoscintigraphy, BMI, and Histology A total of 116 of the patients enrolled in this study underwent surgery at our hospital (Tel-Aviv Sourasky Medical Center), enabling access to surgical and pathologic reports. The identification of SNs by the intraoperative blue dye technique, preoperative planar imaging, and SPECT/CT was evaluated and was related to BMI and to the histologic diagnosis. Statistical Analysis The BMI values (mean 6 SD) in patients with positive and negative planar imaging or SPECT/CT SN detection results were calculated and compared. SN detection by planar imaging and SN detection by SPECT/CT were compared for the entire patient population as well as for separate BMI groups by use of the McNemar 202 THE JOURNAL OF NUCLEAR MEDICINE Vol. 48 No. 2 February 2007
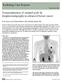
3 FIGURE 1. SPECT/CT identification of site of nonnodal uptake misinterpreted as hot node on planar images in 57-y-old obese patient (BMI, 33.2 kg/m 2 ) with nonpalpable mass. Labeled colloid injection was performed after insertion of guide wire during mammography. (A) Anterior and left lateral planar images of chest obtained with 57 Co flood. These images were interpreted as identifying hot node in left axilla (arrow). (B and C) Transaxial (B) and coronal (C) SPECT/CT images. CT, SPECT, and fused images are shown from left to right. Hot spot was found to be tip of guide wire and not node (arrows). No other hot nodes were detected, and lymphoscintigraphy results were interpreted as negative. Intraoperative techniques also failed to identify SN, and patient underwent ALND; results of ALND were negative for malignancy. test. A P value of less than 0.05 was considered statistically significant. RESULTS Data for General Study Population Hot nodes were detected by lymphoscintigraphy in 200 of the 220 study patients (91%). Planar imaging identified 337 hot sites suspected of being hot nodes. A total of 317 sites indeed represented nodal uptake in 171 patients (78% of the study cohort). The remaining 20 foci of uptake interpreted on planar images as hot nodes were found to be sites of falsepositive nonnodal uptake when further assessed on SPECT/ CT images and validated by surgery. Those sites represented contamination (n 5 4), skin folds (n 5 3), propagation from the injection site (n 5 4), leakage from the wire tract (n 5 5) (Fig. 1), sternoclavicular joint uptake (n 5 1), and mediastinal uptake in blood vessels (n 5 3). Eleven (3.5%) of the 317 hot nodes detected on planar images were masked when a cobalt flood was used to render the body contour. On SPECT/CT images, 402 hot nodes were detected in 200 patients (91%). In the remaining 20 patients (9%), SPECT/CT results were negative. In 29 of 49 patients with negative planar imaging results (59%), SPECT/CT identified hot nodes. No patients had negative SPECT/CT results and true hot nodes on planar assessment. The 85 hot nodes detected only by SPECT/CT included LNs obscured by the injection site (n 5 21), separated adjacent nodes (n 5 29), and nodes revealed by the better spatial resolution of TABLE 1 Identification of Hot Nodes by Planar Imaging and SPECT/CT in Patient-Based and Node-Based Analyses No. of nodes detected by: Planar imaging SPECT/CT Nodes Patient-based analysis Node-based analysis Patient-based analysis Node-based analysis Axillary Total Level I Level II Level III Internal mammary Others* Total *Others: intramammary, n 5 4; interpectoral, n 5 4; and supraclavicular, n 5 6. LYMPHOSCINTIGRAPHY AND OVERWEIGHT Lerman et al. 203
4 TABLE 2 Comparison of Detection of Hot Nodes on Attenuation- Corrected and Non Attenuation-Corrected SPECT Images Obtained for 29 Patients with Positive SPECT/CT and Negative Planar Imaging Results No. of patients whose results Attenuation were not attenuation corrected correction Positive Negative Yes 19 8 No 2 0 SPECT images (n 5 35). For the 220 study patients, the rates of SN detection by planar imaging and by SPECT/CT were 78% and 91%, respectively (P, 0.001). Table 1 summarizes the planar imaging and SPECT/CT results from patient-based and node-based analyses as well as the locations of the SNs determined with assistance from the anatomic landmarks provided by the CT data. Assessment of Impact of Attenuation Correction on Identification of Hot Nodes by SPECT/CT To determine whether the better detection of hot nodes by SPECT/CT than by planar imaging was attributable to better lesion detection by SPECT or to the improved image quality achieved with attenuation correction, SPECT images obtained for the 29 patients with positive SPECT and negative planar imaging results were interpreted separately, with and without attenuation correction. Both SPECT and attenuation correction were found to contribute to the better identification of hot nodes by SPECT/CT than by planar imaging (Table 2). Correlation of BMI and Lymphoscintigraphic Findings The BMI (mean 6 SD) of the 220 patients enrolled in this study was kg/m 2 (range, ). Planar imaging detected hot nodes in 171 patients (78%) with a BMI of kg/m 2 (range, ) and failed to do so in 49 patients (22%) with a BMI of kg/m 2 (range, ) (P, 0.001). SPECT/CT detected hot nodes in 220 patients (91%) with a BMI of kg/m 2 (range, ), including 29 patients (51%) with negative planar imaging results and a BMI of kg/m 2 (range, ). In 20 patients, both planar and SPECT/CT results were negative. The BMI of this subgroup was kg/m 2 (range, ). A total of 122 patients (55.5%) in the study population were found to have BMI values equal to or higher than 25 (mean 6 SD, kg/m 2 ; range, ). Among this subgroup of overweight and obese patients, planar imaging results were positive in 88 patients (72%) with a BMI of kg/m 2 (range, ) and negative in 34 patients with a BMI of kg/m 2 (range, ). SPECT/CT detected hot nodes in 109 overweight and obese patients (89%), including 18 of the 34 obese patients with negative planar imaging results (Fig. 2). The difference between SN detection by planar imaging and SN detection by SPECT/CT in overweight and obese patients was statistically significant (P, 0.001). The correlation of BMI and the detection of lymph nodes by planar imaging and by SPECT/CT is summarized in Table 3. This table illustrates the difference in the detection of hot nodes by planar imaging and the detection of hot nodes by SPECT/CT in patients with different BMI values. The superiority of SPECT/CT appears to be enhanced in overweight and obese patients. Although in planar imaging there is a progressively declining rate of detection as the BMI increases, the rate of detection by SPECT/CT is relatively stable. Correlation of Intraoperative Blue Dye Detection of SNs, Lymphoscintigraphy, BMI, and Histology A total of 116 study patients underwent surgery at our hospital. LNs were detected by the intraoperative blue dye technique in 68 patients (59%) with a BMI of kg/m 2 (range, ), and this technique failed in 48 patients with a BMI of kg/m 2 (range, ) (P, 0.01). Of the patients for whom the blue dye technique failed, SPECT/CT detected SNs in 36 patients (75%). FIGURE 2. Negative planar imaging and positive SPECT/CT identification of hot node in 64-y-old overweight patient (BMI, 29.1 kg/m 2 ). (A) Anterior and left lateral planar images of chest obtained with 57 Co flood. Except for uptake at injection site, no hot spot was identified. (B) SPECT/CT transaxial images. CT, SPECT, and fused images are shown from left to right. Hot node was detected at level I of left axilla (arrow), in keeping with SN. Increased uptake detected in left mediastinum appears to be nonnodal uptake in blood vessel. 204 THE JOURNAL OF NUCLEAR MEDICINE Vol. 48 No. 2 February 2007
5 BMI (kg/m 2 ) TABLE 3 Correlation of BMI and Detection of Hot Nodes in Patient-Based Analysis No. (%) of patients with the following results*: No. of Planar imaging SPECT/CT patients Negative Positive Negative Positive P (95% confidence interval) for comparison of planar imaging and SPECT/CT y, (100) 3 (100) (84) 7 88 (93),0.05 ( ) (82) 7 70 (92),0.05 ( ) (56) 6 39 (87),0.001 ( ) Total (78) (91),0.001 ( ) *Values in parentheses represent percentages of patients in each BMI group with positive detection of hot nodes. y McNemar analysis was used for comparison of detection of hot nodes by planar imaging and detection of hot nodes by SPECT/CT. Data for patients with BMI values of less than 18.4 and (normal weight) were analyzed together. The correlation of the blue dye technique, planar imaging, and SPECT/CT findings and BMI is summarized in Table 4. Lymphoscintigraphy, both planar and SPECT/CT, failed to identify hot nodes in 20 patients, 19 of whom underwent surgery at our hospital. In 12 patients (63%), intraoperative techniques, which included blue dye and g-probe assessments, also failed to identify SNs, and ALND was performed. On frozen sections from 5 of the latter patients, the SN was associated with metastatic involvement. Metastasis was found in another patient in whom the SN was detected by g-probe mapping; for this patient, lymphoscintigraphy and blue dye mapping results were negative. Thus, metastatic involvement of SNs was found in 6 of 19 patients (32%) for whom lymphoscintigraphy results were negative. The correlation of intraoperative mapping and histologic results in patients for whom lymphoscintigraphy results were negative is summarized in Table 5. DISCUSSION The assessment of LN involvement is a major prognostic factor in patients with breast cancer. Thus, early and accurate identification of LN involvement enables adequate therapeutic decisions. Incomplete SN resection may result in inaccurate staging and therapy. SNB is an alternative to axillary dissection as a surgical staging approach for patients with breast cancer, offering a minimally invasive surgical procedure with reduced morbidity. Furthermore, histologic sampling error can be reduced if only a few nodes, rather than a large number of excised nodes, are assessed extensively. Data on the value of preoperative lymphoscintigraphy for optimizing the SNB procedure are accumulating. During surgery, SN identification is achieved by injection of a blue dye, which makes the lymphatic vessels and the SN visible, and by the identification of the radioactive SN with a handheld g-probe (10). Intraoperative failure to identify SNs leads inevitably to ALND, which may be futile. Old age and overweight are reported to be associated with an increased incidence of failed SN identification during surgery. In a study of 1,356 patients, Cox et al. found that an increase of 1 BMI unit decreased the odds of SNB success by approximately 5%n (11). Consequently, patients with high BMI values are more likely to undergo ALND for axillary staging despite the fact that overweight carries a higher risk for postsurgery complications, mainly lymphedema. The identification and accurate localization of SNs in this selective group of patients is of major importance, as lymphedema is the most dreaded, refractory-to-treatment complication of ALND (12). As indicated by the results of the present study, the addition of SPECT/CT to the acquisition protocol for lymphoscintigraphy may improve the identification of hot nodes in overweight and obese patients. Such improvement is attributable to both the use of SPECT itself and the improved quality of SPECT images gained by use of CT maps for attenuation correction. SPECT data alone are, of course, not interpretable if they are not overlaid on CT anatomic landmarks. SPECT/CT identified hot nodes in 91% of the TABLE 4 Correlation of Scintigraphic Findings, Intraoperative Blue Dye Detection of SNs, and BMI Intraoperative blue dye technique result No. of patients with the following results: No. of Planar imaging SPECT/CT patients BMI (mean 6 SD kg/m 2 ) Negative Positive Negative Positive Positive Negative LYMPHOSCINTIGRAPHY AND OVERWEIGHT Lerman et al. 205
6 TABLE 5 Correlation of Intraoperative Mapping and Pathology for 19 Patients for Whom Both Planar Imaging and SPECT/CT Failed Intraoperative blue dye technique result Hand-held g-probe result No. of patients Malignancy Positive Positive 4 Negative Positive Negative 2 Negative Negative Positive 1 Positive (1 patient) Negative Negative 12 Positive (5 patients) study cohort, including 29 patients for whom planar imaging failed to detect hot nodes. SPECT/CT detected 85 hot nodes missed by planar images alone, including 14 nodes located in drainage sites, which are not routinely explored during surgery such as intramammary, interpectoral, and supraclavicular regions. SPECT/CT correctly identified 20 nonnodal hot spots, which were misinterpreted on planar images as SNs. Of note is the uptake at the edge of the wire inserted during mammography in patients with nonpalpable masses. It is valuable to identify the location of such a wire on data from the CT portion of SPECT/CT to avoid false-positive readings (Fig. 1). The rate of false-negative planar imaging results for 122 overweight and obese patients was 28%, higher than that for the general study population. The rate of false-negative SPECT/CT results for these 122 patients was also higher than that for the general study population, 11%; however, the latter modality identified hot nodes in 18 additional patients (53%) and had a statistically higher rate of detection of hot nodes in overweight patients. The superiority of SPECT/CT appears to be enhanced in overweight and obese patients. Although in planar imaging there is a progressively declining rate of detection as the BMI increases, the rate of detection by SPECT/CT is relatively stable. The advantage of SPECT/CT was particularly pronounced for 45 obese patients with BMI values of $30 kg/m 2 ; SPECT/CT identified hot nodes in 39 of these patients (87%), whereas planar imaging detected hot nodes in only 20 patients (44%). As previously reported by Nos et al., overweight was associated with a high failure rate for the intraoperative identification of hot nodes in the present study (4). Among 116 patients who underwent surgery at our hospital, the blue dye technique failed to identify draining nodes in 48 patients (41%) those with higher BMI values. Because SPECT/CT identified hot nodes in 36 (75%) of the latter patients (planar imaging did so in 26 patients), the surgeon actually performed surgery solely on the basis of the scintigraphic findings. In such a clinical scenario, the accurate localization of hot nodes is crucial, and the 3-dimensional data of fused SPECT/CT images have great clinical relevance. Six of 13 patients (50%) with negative lymphoscintigraphic and intraoperative SN identification had nodal metastatic involvement. It appears that even for overweight patients, in whom the nonvisualization of hot nodes may be a technical limitation, the nonvisualization of SNs by all techniques used for SN identification should raise the possibility of nodal metastatic involvement and should be approached with extreme caution. CONCLUSION The addition of SPECT/CT to the acquisition protocol for lymphoscintigraphy in overweight and obese patients with breast cancer improves the identification of hot nodes and avoids false-positive interpretations of sites of nonnodal uptake. It is of a particular value in overweight patients for whom the identification of draining nodes by intraoperative techniques has failed. ACKNOWLEDGMENTS The authors thank Tamar Geva and Maya Shacham for their contributions to this work. REFERENCES 1. Petrek JA, Heelan MC. Incidence of breast carcinoma-related lymphedema. Cancer. 1998;83: Petrek JA, Senie RT, Peters M, Rosen PP. Lymphedema in a cohort of breast carcinoma survivors 20 years after diagnosis. Cancer. 2001;92: Chakera AH, Friis E, Hesse U, Al-Suliman N, Zerahn B, Hesse B. Factors of importance for scintigraphic non-visualization of sentinel nodes in breast cancer. Eur J Nucl Med Mol Imaging. 2005;32: Nos C, Freneaux P, Guilbert S, Falcou MC, Salmon RJ, Clough KB. Sentinel lymph node detection for breast cancer: which patients are best suited for the patent blue dye only method of identification? Ann Surg Oncol. 2001;8: Derossis AM, Fey JV, Cody HS III, Borgen PI. Obesity influences outcome of sentinel lymph node biopsy in early-stage breast cancer. J Am Coll Surg. 2003; 197: Even-Sapir E, Lerman H, Lievshitz G, et al. Lymphoscintigraphy for sentinel node mapping using a hybrid SPECT/CT system. J Nucl Med. 2003;44: Lerman H, Metser U, Lievshitz G, Sperber F, Schneebaum S, Even-Sapir E. Lymphoscintigraphic sentinel node identification in patients with breast cancer: the roll of SPECT-CT. Eur J Nucl Med Mol Imaging. 2006;33: Schneebaum S, Stadler J, Cohen M, Yaniv D, Baron J, Skornick Y. Gamma probe-guided sentinel node biopsy: optimal timing for injection. Eur J Surg Oncol. 1998;24: Estourgie SH, Nieweg OE, Olmos RA, Rutgers EJ, Kroon BB. Lymphatic drainage patterns from the breast. Ann Surg. 2004;239: Schneebaum S, Even-Sapir E, Lerman H, Gat A, Brazovsky E, Lievshitz G. Clinical application of gamma detection probes: radio guided surgery. Eur J Nucl Med. 1999;26(suppl):S26 S Cox CE, Dupont E, Whitehead GF, et al. Age and body mass index may increase the chance of failure in sentinel lymph node biopsy for women with breast cancer. Breast J. 2002;8: Steering Committee on Clinical Practice Guidelines for the Care and Treatment of Breast Cancer. Can Med Assoc J. 1998;158(3 suppl):s22 S THE JOURNAL OF NUCLEAR MEDICINE Vol. 48 No. 2 February 2007
Radionuclide detection of sentinel lymph node
 Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
Radionuclide detection of sentinel lymph node Sophia I. Koukouraki Assoc. Professor Department of Nuclear Medicine Medicine School, University of Crete 1 BACKGROUND The prognosis of malignant disease is
SPECT/CT Imaging of the Sentinel Lymph Node
 IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
IAEA Regional Training Course on Hybrid Imaging SPECT/CT Imaging of the Sentinel Lymph Node Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa, Italy Vilnius,
The GOSTT concept. (radio)guided intraoperative Scintigraphic Tumor Targeting. Emmanuel Deshayes. GOSTT = Radioguided Surgery
 IAEA WorkShop, November 2017 Emmanuel Deshayes With the kind help of Pr Francesco Giammarile The GOSTT concept GOSTT = Radioguided Surgery (radio)guided intraoperative Scintigraphic Tumor Targeting 1 Radioguided
IAEA WorkShop, November 2017 Emmanuel Deshayes With the kind help of Pr Francesco Giammarile The GOSTT concept GOSTT = Radioguided Surgery (radio)guided intraoperative Scintigraphic Tumor Targeting 1 Radioguided
Practice of Axilla Surgery
 Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
Summer School of Breast Disease 2016 Practice of Axilla Surgery Axillary Lymph Node Dissection & Sentinel Lymph Node Biopsy 연세의대외과 박세호 Contents Anatomy of the axilla Axillary lymph node dissection (ALND)
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
Introduction. Mitsuru Koizumi 1 Masamichi Koyama 1
 https://doi.org/10.1007/s12149-018-1319-z ORIGINAL ARTICLE Comparison between single photon emission computed tomography with computed tomography and planar scintigraphy in sentinel node biopsy in breast
https://doi.org/10.1007/s12149-018-1319-z ORIGINAL ARTICLE Comparison between single photon emission computed tomography with computed tomography and planar scintigraphy in sentinel node biopsy in breast
Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer
 Radiology Case Reports Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer Volume 5, Issue 3, 2010 Brian Wosnitzer, MD; Rosna Mirtcheva, MD; and Munir Ghesani, MD Previous
Radiology Case Reports Nonvisualization of sentinel node by lymphoscintigraphy in advanced breast cancer Volume 5, Issue 3, 2010 Brian Wosnitzer, MD; Rosna Mirtcheva, MD; and Munir Ghesani, MD Previous
ENHANCED SENTINEL LYMPHOSCINTIGRAPHIC MAPPING IN BREAST TUMOR USING THE GRADED SHIELD TECHNIQUE
 ENHANCED SENTINEL LYMPHOSCINTIGRAPHIC MAPPING IN BREAST TUMOR USING THE GRADED SHIELD TECHNIQUE Yu-Wen Chen, Yung-Chang Lai, Chien-Chin Hsu, and Ming-Feng Hou 1 Departments of Nuclear Medicine and 1 Gastroenteric
ENHANCED SENTINEL LYMPHOSCINTIGRAPHIC MAPPING IN BREAST TUMOR USING THE GRADED SHIELD TECHNIQUE Yu-Wen Chen, Yung-Chang Lai, Chien-Chin Hsu, and Ming-Feng Hou 1 Departments of Nuclear Medicine and 1 Gastroenteric
Sentinel Node Localisation of Melanoma
 Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
Sentinel Node Localisation of Melanoma V Bongers, Diakonessenhuis, Utrecht 1. Introduction A melanoma is mostly a malignancy of the skin. The sentinel lymph node (SLN) concept of sequential progression
The Concept of GOSTT
 IAEA Regional Training Course on Sentinel Lymph Node Mapping and Radioguided Surgery The Concept of GOSTT Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa,
IAEA Regional Training Course on Sentinel Lymph Node Mapping and Radioguided Surgery The Concept of GOSTT Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa,
GOSTT General concept
 GOSTT General concept Francesco GIAMMARILE «Aut tace aut loquere meliora silentio» Presentation Outline Introduction: GOSTT and radioguided surgery The Sentinel Node Concept Latest technological knowledge
GOSTT General concept Francesco GIAMMARILE «Aut tace aut loquere meliora silentio» Presentation Outline Introduction: GOSTT and radioguided surgery The Sentinel Node Concept Latest technological knowledge
Sentinel Lymph Node Biopsy for Breast Cancer
 Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
Sentinel Lymph Node Biopsy for Breast Cancer Registrar Tutorial Adam Cichowitz Surgical Registrar The Royal Melbourne Hospital Sentinel Lymph Node Biopsy Axillary LN status important prognostic factor
DRAINAGE PATTERN OF THE UPPER MEDIAL QUADRANT OF THE BREAST IN YOUNG HEALTHY WOMEN AFTER SUBDERMAL INJECTION: A LYMPHSCINTIGRAPHIC STUDY
 197 Lymphology 38 (2005) 197-201 DRAINAGE PATTERN OF THE UPPER MEDIAL QUADRANT OF THE BREAST IN YOUNG HEALTHY WOMEN AFTER SUBDERMAL INJECTION: A LYMPHSCINTIGRAPHIC STUDY A. Tassenoy, P. van der Veen, P.
197 Lymphology 38 (2005) 197-201 DRAINAGE PATTERN OF THE UPPER MEDIAL QUADRANT OF THE BREAST IN YOUNG HEALTHY WOMEN AFTER SUBDERMAL INJECTION: A LYMPHSCINTIGRAPHIC STUDY A. Tassenoy, P. van der Veen, P.
BREAST CANCER SURGERY. Dr. John H. Donohue
 Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Dr. John H. Donohue HISTORY References to breast surgery in ancient Egypt (ca 3000 BCE) Mastectomy described in numerous medieval texts Petit formulated organized approach in 18 th Century Improvements
Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered])
![Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered]) Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered])](/thumbs/87/95258373.jpg) Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered]) Overview Indications The Lymphoscintigraphy Study demonstrates the flow of lymph from the
Austin Radiological Association Nuclear Medicine Procedure LYMPHOSCINTIGRAPHY (Tc-99m-Sulfur Colloid [Filtered]) Overview Indications The Lymphoscintigraphy Study demonstrates the flow of lymph from the
Sentinel Node Biopsy, Introduction and Application of the Technique in a Senology Unit of a District Hospital - Prospective Study.
 ISPUB.COM The Internet Journal of Surgery Volume 20 Number 2 Sentinel Node Biopsy, Introduction and Application of the Technique in a Senology Unit of a District Hospital - Prospective Study. Z Sidiropoulou,
ISPUB.COM The Internet Journal of Surgery Volume 20 Number 2 Sentinel Node Biopsy, Introduction and Application of the Technique in a Senology Unit of a District Hospital - Prospective Study. Z Sidiropoulou,
Breast Cancer. Most common cancer among women in the US. 2nd leading cause of death in women. Mortality rates though have declined
 Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women Mortality rates though have declined 1 in 8 women will develop breast cancer Breast Cancer Breast cancer increases
Breast Cancer. Saima Saeed MD
 Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
Breast Cancer Saima Saeed MD Breast Cancer Most common cancer among women in the US 2nd leading cause of death in women 1 in 8 women will develop breast cancer Incidence/mortality rates have declined Breast
16/09/2015. ACOSOG Z011 changing practice. Presentation outline. Nodal mets #1 prognostic tool. Less surgery no change in oncologic outcomes
 ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
ACOSOG Z011 changing practice The end of axillary US/FNA? Preoperative staging of the axilla in the era of Z011 Adena S Scheer MD MSc FRCSC Surgical Oncologist, St. Michael s Hospital Assistant Professor,
Sentinel Lymph Node Identification in Breast Cancer - Comparison of Planar Scintigraphy and SPECT/CT
 The Open Nuclear Medicine Journal, 2012, 4, 5-13 5 Open Access Sentinel Lymph Node Identification in Breast Cancer - Comparison of Planar Scintigraphy and SPECT/CT Otakar Kraft *,1,2 and Martin Havel 1
The Open Nuclear Medicine Journal, 2012, 4, 5-13 5 Open Access Sentinel Lymph Node Identification in Breast Cancer - Comparison of Planar Scintigraphy and SPECT/CT Otakar Kraft *,1,2 and Martin Havel 1
Eight false negative sentinel node procedures in breast cancer: what went wrong?
 EJSO 2003; 29: 336±340 doi:10.1053/ejso.2002.1379 Eight false negative sentinel node procedures in breast cancer: what went wrong? S. H. Estourgie*, O. E. Nieweg*, R. A. ValdeÂs Olmos², E. J. Th. Rutgers*,
EJSO 2003; 29: 336±340 doi:10.1053/ejso.2002.1379 Eight false negative sentinel node procedures in breast cancer: what went wrong? S. H. Estourgie*, O. E. Nieweg*, R. A. ValdeÂs Olmos², E. J. Th. Rutgers*,
Detection of sentinel lymph nodes by SPECT/CT and planar scintigraphy: The influence of age, gender and BMI
 ORIGINAL RESEARCH Detection of sentinel lymph nodes by SPECT/CT and planar scintigraphy: The influence of age, gender and BMI Otakar Kraft 1,2, Martin Havel 1 1. Clinic of Nuclear Medicine, University
ORIGINAL RESEARCH Detection of sentinel lymph nodes by SPECT/CT and planar scintigraphy: The influence of age, gender and BMI Otakar Kraft 1,2, Martin Havel 1 1. Clinic of Nuclear Medicine, University
ANNEX 1 OBJECTIVES. At the completion of the training period, the fellow should be able to:
 1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
1 ANNEX 1 OBJECTIVES At the completion of the training period, the fellow should be able to: 1. Breast Surgery Evaluate and manage common benign and malignant breast conditions. Assess the indications
UvA-DARE (Digital Academic Repository)
 UvADARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
UvADARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman
 Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Breast conservation surgery and sentinal node biopsy: Dr R Botha Moderator: Dr E Osman Breast anatomy: Breast conserving surgery: The aim of wide local excision is to remove all invasive and in situ
Citation for published version (APA): Vermeeren, L. (2011). Sentinel nodes in complex areas: innovating radioguided surgery
 UvA-DARE (Digital Academic Repository) Sentinel nodes in complex areas: innovating radioguided surgery Vermeeren, L. Link to publication Citation for published version (APA): Vermeeren, L. (2011). Sentinel
UvA-DARE (Digital Academic Repository) Sentinel nodes in complex areas: innovating radioguided surgery Vermeeren, L. Link to publication Citation for published version (APA): Vermeeren, L. (2011). Sentinel
Treatment Planning for Breast Cancer: Contouring Targets. Julia White MD Professor
 Treatment Planning for Breast Cancer: Contouring Targets Julia White MD Professor Outline 1. RTOG Breast Cancer Atlas 2. Target development on Clinical Trials Whole Breast Irradiation 2-D Radiotherapy
Treatment Planning for Breast Cancer: Contouring Targets Julia White MD Professor Outline 1. RTOG Breast Cancer Atlas 2. Target development on Clinical Trials Whole Breast Irradiation 2-D Radiotherapy
«Aut tace aut loquere meliora silentio» Francesco GIAMMARILE
 «Aut tace aut loquere meliora silentio» Francesco GIAMMARILE Presentation Outline Introduction: the GOSTT Concept The EANM Guideline in Melanoma Future trends and concluding remarks I sort of thought your
«Aut tace aut loquere meliora silentio» Francesco GIAMMARILE Presentation Outline Introduction: the GOSTT Concept The EANM Guideline in Melanoma Future trends and concluding remarks I sort of thought your
Is Sentinel Node Biopsy Practical?
 Breast Cancer Is Sentinel Node Biopsy Practical? Benefits and Limitations JMAJ 45(10): 444 448, 2002 Shigeru IMOTO *1, Satoshi EBIHARA *2 and Noriyuki MORIYAMA *3 *1 Breast Surgery Division, National Cancer
Breast Cancer Is Sentinel Node Biopsy Practical? Benefits and Limitations JMAJ 45(10): 444 448, 2002 Shigeru IMOTO *1, Satoshi EBIHARA *2 and Noriyuki MORIYAMA *3 *1 Breast Surgery Division, National Cancer
Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast.
 Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Relevant history 79-yr
Case 1: 79 yr-old woman with a lump in upper outer quadrant of left breast. Giuliano Mariani Regional Center of Nuclear Medicine, University of Pisa Medical School, Pisa (Italy) Relevant history 79-yr
Advances in Localized Breast Cancer
 Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Advances in Localized Breast Cancer Melissa Camp, MD, MPH and Fariba Asrari, MD June 18, 2018 Moderated by Elissa Bantug 1 Advances in Surgery for Breast Cancer Melissa Camp, MD June 18, 2018 2 Historical
Percutaneous Biopsy and Sentinel Lymphadenectomy: Minimally Invasive. he diagnosis and treatment of nonpalpable. Breast Cancer
 Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
Laura Liberman 1 Hiram S. Cody III 2 Received January 30, 2001; accepted after revision April 3, 2001. Supported by a grant from the New York State Department of Health (C015709). 1 Department of Radiology,
CLAUDIU PEŞTEAN 1,2, ELENA BĂRBUŞ 1,2, ANDRA PICIU 3,4, MARIA IULIA LARG 1,2, ALEXANDRINA SABO 1,5, CRISTINA MOISESCU-GOIA 1,5, DOINA PICIU 6,7
 Oncology DOI: 10.15386/cjmed-637 SENTINEL LYMPH NODE SCINTIGRAPHY IN CUTANEOUS MELANOMA USING A PLANAR CALIBRATION PHANTOM FILLED WITH TC-99M PERTECHNETATE SOLUTION FOR BODY CONTOURING CLAUDIU PEŞTEAN
Oncology DOI: 10.15386/cjmed-637 SENTINEL LYMPH NODE SCINTIGRAPHY IN CUTANEOUS MELANOMA USING A PLANAR CALIBRATION PHANTOM FILLED WITH TC-99M PERTECHNETATE SOLUTION FOR BODY CONTOURING CLAUDIU PEŞTEAN
Integrating new imaging modalities in breast cancer management Pouw, Bas
 UvA-DARE (Digital Academic Repository) Integrating new imaging modalities in breast cancer management Pouw, Bas Link to publication Citation for published version (APA): Pouw, B. (2016). Integrating new
UvA-DARE (Digital Academic Repository) Integrating new imaging modalities in breast cancer management Pouw, Bas Link to publication Citation for published version (APA): Pouw, B. (2016). Integrating new
COMPARATIVE ANALYSIS OF COLON AND RECTAL CANCERS IN SENTINEL LYMPH NODE MAPPING
 Trakia Journal of Sciences, Vol. 5, No. 1, pp 10-14, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution COMPARATIVE ANALYSIS OF COLON AND
Trakia Journal of Sciences, Vol. 5, No. 1, pp 10-14, 2007 Copyright 2007 Trakia University Available online at: http://www.uni-sz.bg ISSN 1312-1723 Original Contribution COMPARATIVE ANALYSIS OF COLON AND
A Snapshot on Nuclear Cardiac Imaging
 Editorial A Snapshot on Nuclear Cardiac Imaging Khalil, M. Department of Physics, Faculty of Science, Helwan University. There is no doubt that nuclear medicine scanning devices are essential tool in the
Editorial A Snapshot on Nuclear Cardiac Imaging Khalil, M. Department of Physics, Faculty of Science, Helwan University. There is no doubt that nuclear medicine scanning devices are essential tool in the
Lymphoseek (technetium Tc 99m tilmanocept) Injection
 Lymphoseek (technetium Tc 99m tilmanocept) Injection A Novel Receptor-Targeted Lymphatic Mapping Agent Karen B. Randall, B.S., CNMT Navidea Biopharmaceuticals Medical Science Liaison Lymphoseek (technetium
Lymphoseek (technetium Tc 99m tilmanocept) Injection A Novel Receptor-Targeted Lymphatic Mapping Agent Karen B. Randall, B.S., CNMT Navidea Biopharmaceuticals Medical Science Liaison Lymphoseek (technetium
3D Conformal Radiation Therapy for Mucinous Carcinoma of the Breast
 1 Angela Kempen February Case Study February 22, 2012 3D Conformal Radiation Therapy for Mucinous Carcinoma of the Breast History of Present Illness: JE is a 45 year-old Caucasian female who underwent
1 Angela Kempen February Case Study February 22, 2012 3D Conformal Radiation Therapy for Mucinous Carcinoma of the Breast History of Present Illness: JE is a 45 year-old Caucasian female who underwent
Breast Cancer: Management of the Axilla in Greg McKinnon MD FRCSC SON Vancouver Oct 2016
 Breast Cancer: Management of the Axilla in 2016 Greg McKinnon MD FRCSC SON Vancouver Oct 2016 No Disclosures Principle #1 There is no point talking about surgical therapy in isolation. From a patient
Breast Cancer: Management of the Axilla in 2016 Greg McKinnon MD FRCSC SON Vancouver Oct 2016 No Disclosures Principle #1 There is no point talking about surgical therapy in isolation. From a patient
EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY
 EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY AXILLARY LYMPH NODE METASTASIS Axillary lymph node metastasis is one of the most
EVALUATION OF AXILLARY LYMPH NODES AFTER NEOADJUVANT SYSTEMIC THERAPY KIM, MIN JUNG SEVERANCE HOSPITAL, YONSEI UNIVERSITY AXILLARY LYMPH NODE METASTASIS Axillary lymph node metastasis is one of the most
Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection
 456 Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection TOMOKO TAKAMARU 1, GORO KUTOMI 1, FUKINO SATOMI 1, HIROAKI
456 Use of the dye guided sentinel lymph node biopsy method alone for breast cancer metastasis to avoid unnecessary axillary lymph node dissection TOMOKO TAKAMARU 1, GORO KUTOMI 1, FUKINO SATOMI 1, HIROAKI
Breast Surgery When Less is More and More is Less. E MacIntosh, MD June 6, 2015
 Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Breast Surgery When Less is More and More is Less E MacIntosh, MD June 6, 2015 Presenter Disclosure Faculty: E. MacIntosh Relationships with commercial interests: None Mitigating Potential Bias Not applicable
Melanoma Surgery Update James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division
 Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Melanoma Surgery Update 2018 James R. Ouellette, DO FACS Premier Health Cancer Institute Wright State University Chief, Surgical Oncology Division Surgery for Melanoma Mainstay of treatment for potentially
Molecular Imaging and Breast Cancer
 Molecular Imaging and Breast Cancer Breast cancer forms in tissues of the breast usually in the ducts, tubes that carry milk to the nipple, and lobules, the glands that make milk. It occurs in both men
Molecular Imaging and Breast Cancer Breast cancer forms in tissues of the breast usually in the ducts, tubes that carry milk to the nipple, and lobules, the glands that make milk. It occurs in both men
I. Cancer staging problem
 Instrumentation Lab (Craig Levin) Angela Craig Peter Jin Frezghi Guillem Billie Garry Research interests (by imaging modality) I. High resolution radionuclide imaging : positron emission tomography (PET)
Instrumentation Lab (Craig Levin) Angela Craig Peter Jin Frezghi Guillem Billie Garry Research interests (by imaging modality) I. High resolution radionuclide imaging : positron emission tomography (PET)
SPECT/CT in Endocrine Diseases and Dosimetry
 SPECT/CT in Endocrine Diseases and Dosimetry Heather A. Jacene, MD Division of Nuclear Medicine Russell H. Morgan Dept. of Radiology and Radiological Science Johns Hopkins University Baltimore, MD Disclosures
SPECT/CT in Endocrine Diseases and Dosimetry Heather A. Jacene, MD Division of Nuclear Medicine Russell H. Morgan Dept. of Radiology and Radiological Science Johns Hopkins University Baltimore, MD Disclosures
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection
 The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
The Role of Sentinel Lymph Node Biopsy and Axillary Dissection Henry Mark Kuerer, MD, PhD, FACS Department of Surgical Oncology University of Texas MD Anderson Cancer Center SLN Biopsy Revolutionized surgical
Advances in Breast Surgery. Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015
 Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
Advances in Breast Surgery Catherine Campo, D.O. Breast Surgeon Meridian Health System April 17, 2015 Objectives Understand the surgical treatment of breast cancer Be able to determine when a lumpectomy
What you should know about Sentinel Lymph Node Biopsy
 What you should know about Sentinel Lymph Node Biopsy AFFILIATED WITH GENESIS MEDICAL CENTER 1228 East Rusholme Street, Suite 210 Davenport, Iowa 52803 (563) 421-7625 1-800-215-1444 www.genesishealth.com
What you should know about Sentinel Lymph Node Biopsy AFFILIATED WITH GENESIS MEDICAL CENTER 1228 East Rusholme Street, Suite 210 Davenport, Iowa 52803 (563) 421-7625 1-800-215-1444 www.genesishealth.com
SPECT/CT Fusion in the Diagnosis of Hyperparathyroidism
 SPECT/CT Fusion in the Diagnosis of Hyperparathyroidism Yoshio Monzen, Akihisa Tamura, Hajime Okazaki, Taichi Kurose, Masayuki Kobayashi, Masatsugu Kuraoka Department of Radiology, Hiroshima Prefectural
SPECT/CT Fusion in the Diagnosis of Hyperparathyroidism Yoshio Monzen, Akihisa Tamura, Hajime Okazaki, Taichi Kurose, Masayuki Kobayashi, Masatsugu Kuraoka Department of Radiology, Hiroshima Prefectural
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy
 Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
Clinical Outcome of Reconstruction With Tissue Expanders for Patients With Breast Cancer and Mastectomy Mitsui Memorial Hospital Department of Breast and Endocine surgery Daisuke Ota No financial support
The Role of Nuclear Medicine in the Preoparative Diagnostics of Malignant Breast Tumours
 PhD theses The Role of Nuclear Medicine in the Preoparative Diagnostics of Malignant Breast Tumours Erzsébet Schmidt M.D. Doctorial School leader: Program leader: Tutor: Prof. József Bódis M.D. Prof. István
PhD theses The Role of Nuclear Medicine in the Preoparative Diagnostics of Malignant Breast Tumours Erzsébet Schmidt M.D. Doctorial School leader: Program leader: Tutor: Prof. József Bódis M.D. Prof. István
Relevance. Axillary Node Recurrence. Purpose. Case Presentation: Is axillary staging required? Two trends have emerged:
 Axillary Node Recurrence N.L. Davis Associate Professor of Surgery, UBC Head of Surgical Oncology, BCCA Relevance In an attempt to minimize long term complications and to maximize cancer control, the management
Axillary Node Recurrence N.L. Davis Associate Professor of Surgery, UBC Head of Surgical Oncology, BCCA Relevance In an attempt to minimize long term complications and to maximize cancer control, the management
UvA-DARE (Digital Academic Repository)
 UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
UvA-DARE (Digital Academic Repository) In search of the sentinel node : validation and sophistication of lymphatic mapping and sentinel node biopsy in breast cancer and melanoma van der Ploeg, I.M.C. Link
LYMPHOSCINTIGRAPHY: WHY DO IT?
 OVERVIEW Lymphoscintigraphy refers to the scintigraphic visualization of lymphatic drainage of a specific body site following intradermal injection of a radiolabeled colloid. It is a valuable procedure
OVERVIEW Lymphoscintigraphy refers to the scintigraphic visualization of lymphatic drainage of a specific body site following intradermal injection of a radiolabeled colloid. It is a valuable procedure
Debate Axillary dissection - con. Prof. Dr. Rodica Anghel Institute of Oncology Bucharest
 Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Debate Axillary dissection - con Prof. Dr. Rodica Anghel Institute of Oncology Bucharest Summer School of Oncology, third edition Updated Oncology 2015: State of the Art News & Challenging Topics Bucharest,
Hybrid Imaging SPECT/CT PET/CT PET/MRI. SNMMI Southwest Chapter Aaron C. Jessop, MD
 Hybrid Imaging SPECT/CT PET/CT PET/MRI SNMMI Southwest Chapter 2014 Aaron C. Jessop, MD Assistant Professor, Department of Nuclear Medicine UT MD Anderson Cancer Center, Houston, Texas Complimentary role
Hybrid Imaging SPECT/CT PET/CT PET/MRI SNMMI Southwest Chapter 2014 Aaron C. Jessop, MD Assistant Professor, Department of Nuclear Medicine UT MD Anderson Cancer Center, Houston, Texas Complimentary role
New Visions in PET: Surgical Decision Making and PET/CT
 New Visions in PET: Surgical Decision Making and PET/CT Stanley J. Goldsmith, MD Director, Nuclear Medicine Professor, Radiology & Medicine New York Presbyterian Hospital- Weill Cornell Medical Center
New Visions in PET: Surgical Decision Making and PET/CT Stanley J. Goldsmith, MD Director, Nuclear Medicine Professor, Radiology & Medicine New York Presbyterian Hospital- Weill Cornell Medical Center
Sentinel lymph node (SLN) biopsy is a wellestablished
 ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
ORIGINAL ARTICLE DISCORDANT LYMPHATIC DRAINAGE PATTERNS REVEALED BY SERIAL LYMPHOSCINTIGRAPHY IN CUTANEOUS HEAD AND NECK MALIGNANCIES Alliric I. Willis, MD, John A. Ridge, MD, PhD Department of Surgical
Contributo della medicina nucleare nei tumori mammari: dal linfonodo sentinella alla IART
 Contributo della medicina nucleare nei tumori mammari: dal linfonodo sentinella alla IART Prof. Giovanni Paganelli Dipartimento delle procedure e tecnologie avanzate, IRST-IRCCS Meldola. Universita degli
Contributo della medicina nucleare nei tumori mammari: dal linfonodo sentinella alla IART Prof. Giovanni Paganelli Dipartimento delle procedure e tecnologie avanzate, IRST-IRCCS Meldola. Universita degli
STAGE CATEGORY DEFINITIONS
 CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX Tis Tis (DCIS) Tis (LCIS) Tis (Paget s) T1 T1mi T1a T1b T1c a b c
Is early dynamic lymphoscintigraphy for detection of sentinel lymph nodes always achievable in breast tumor?
 ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 20, No. 1, 45 50, 2006 Is early dynamic lymphoscintigraphy for detection of sentinel lymph nodes always achievable in breast tumor? Yu-Wen CHEN,* Ya-Wen
ORIGINAL ARTICLE Annals of Nuclear Medicine Vol. 20, No. 1, 45 50, 2006 Is early dynamic lymphoscintigraphy for detection of sentinel lymph nodes always achievable in breast tumor? Yu-Wen CHEN,* Ya-Wen
How can surgeons help the Radiation Oncologists?
 How can surgeons help the Radiation Oncologists? Lorna Weir BC Surgical Oncology fall breast cancer update Oct 24, 2009 Disclosure no conflict of interest Outline Introduction OR reports Marking of surgical
How can surgeons help the Radiation Oncologists? Lorna Weir BC Surgical Oncology fall breast cancer update Oct 24, 2009 Disclosure no conflict of interest Outline Introduction OR reports Marking of surgical
Technical Considerations. Imaging Considerations
 354 CUTANEOUS MALIGNANCY OF THE HEAD AND NECK desmoplastic melanomas are characterized by a uniform desmoplasia that is prominent throughout the entire tumor (termed pure desmoplastic melanoma), whereas
354 CUTANEOUS MALIGNANCY OF THE HEAD AND NECK desmoplastic melanomas are characterized by a uniform desmoplasia that is prominent throughout the entire tumor (termed pure desmoplastic melanoma), whereas
Donna Plecha, MD 1, Shiyu Bai, BS 2, Helen Patterson 3, Cheryl Thompson, PhD 4, and Robert Shenk, MD 5
 Ann Surg Oncol DOI 10.1245/s10434-015-4527-y ORIGINAL ARTICLE BREAST ONCOLOGY Improving the Accuracy of Axillary Lymph Node Surgery in Breast Cancer with Ultrasound-Guided Wire Localization of Biopsy Proven
Ann Surg Oncol DOI 10.1245/s10434-015-4527-y ORIGINAL ARTICLE BREAST ONCOLOGY Improving the Accuracy of Axillary Lymph Node Surgery in Breast Cancer with Ultrasound-Guided Wire Localization of Biopsy Proven
Results of the ACOSOG Z0011 Trial
 DCIS and Early Breast Cancer Symposium JUNE 15-17 2012 CAPPADOCIA Results of the ACOSOG Z0011 Trial Kelly K. Hunt, M.D. Professor of Surgery Axillary Node Dissection Staging, Regional control, Survival
DCIS and Early Breast Cancer Symposium JUNE 15-17 2012 CAPPADOCIA Results of the ACOSOG Z0011 Trial Kelly K. Hunt, M.D. Professor of Surgery Axillary Node Dissection Staging, Regional control, Survival
Keywords : SPECT/CT; sentinel lymph node, breast cancer. 10 Lebanese Medical Journal 2018 Volume 66 (1)
 ARTICLE ORIGINAL / ORIGINAL ARTICLE THE RoLE of SPECT/CT in DETECTion AnD LoCALizATion of SEnTinEL LyMPH node in BREAST CAnCER http://www.lebanesemedicaljournal.org/articles/66-/original2.pdf Mohamad haidar,
ARTICLE ORIGINAL / ORIGINAL ARTICLE THE RoLE of SPECT/CT in DETECTion AnD LoCALizATion of SEnTinEL LyMPH node in BREAST CAnCER http://www.lebanesemedicaljournal.org/articles/66-/original2.pdf Mohamad haidar,
Targeting Surgery for Known Axillary Disease. Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center
 Targeting Surgery for Known Axillary Disease Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center Nodal Ultrasound at Diagnosis Whole breast and draining lymphatic
Targeting Surgery for Known Axillary Disease Abigail Caudle, MD Henry Kuerer, MD PhD Dept. Surgical Oncology MD Anderson Cancer Center Nodal Ultrasound at Diagnosis Whole breast and draining lymphatic
Diagnosis and staging of breast cancer and multidisciplinary team working
 1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
1 Diagnosis and staging of breast cancer and multidisciplinary team working Common symptoms and signs Over 90% of breast cancers (BCs) are local or regional when first detected. At least 60% of patients
Scintimammography and Gamma Imaging of the Breast and Axilla
 Scintimammography and Gamma Imaging of the Breast and Axilla Policy Number: 6.01.18 Last Review: 9/2017 Origination: 9/2006 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Scintimammography and Gamma Imaging of the Breast and Axilla Policy Number: 6.01.18 Last Review: 9/2017 Origination: 9/2006 Next Review: 9/2018 Policy Blue Cross and Blue Shield of Kansas City (Blue KC)
Surgical Considerations in Breast Cancer treated with Neoadjuvant Therapy
 Surgical Considerations in Breast Cancer treated with Neoadjuvant Therapy Rebecca Warburton MD Department of Surgery, University of British Columbia Mount Saint Joseph Hospital, Providence Health Care
Surgical Considerations in Breast Cancer treated with Neoadjuvant Therapy Rebecca Warburton MD Department of Surgery, University of British Columbia Mount Saint Joseph Hospital, Providence Health Care
Whole Body MRI. Dr. Nina Tunariu. Prostate Cancer recurrence, progression and restaging
 Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Whole Body MRI Prostate Cancer recurrence, progression and restaging Dr. Nina Tunariu Consultant Radiology Drug Development Unit and Prostate Targeted Therapies Group 12-13 Janeiro 2018 Evolving Treatment
Table of contents. Page 2 of 40
 Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
Page 1 of 40 Table of contents Introduction... 4 1. Background Information... 6 1a: Referral source for the New Zealand episodes... 6 1b. Invasive and DCIS episodes by referral source... 7 1d. Age of the
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010
 Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Los Angeles Radiological Society 62 nd Annual Midwinter Radiology Conference January 31, 2010 Self Assessment Module on Nuclear Medicine and PET/CT Case Review FDG PET/CT IN LYMPHOMA AND MELANOMA Submitted
Radioactive Seed Localization of Nonpalpable Breast Lesions
 Subject: Radioactive Seed Localization of Page: 1 of 7 Last Review Status/Date: March 2017 Radioactive Seed Localization of Description Radioactive seed localization is used to detect nonpalpable breast
Subject: Radioactive Seed Localization of Page: 1 of 7 Last Review Status/Date: March 2017 Radioactive Seed Localization of Description Radioactive seed localization is used to detect nonpalpable breast
Cutaneous Melanoma: Epidemiology (USA) The Sentinel Node in Head and Neck Melanoma. Cutaneous Melanoma: Epidemiology (USA)
 The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
The Sentinel Node in Head and Neck Melanoma Cutaneous Melanoma: Epidemiology (USA) 6 th leading cause of cancer among men and women 68,720 new cases of invasive melanoma in 2009 8,650 deaths from melanoma
Molecular Breast Imaging: History and Recent Developments
 Molecular Breast Imaging: History and Recent Developments Associate Professor, Department of Imaging Physics The University of Texas MD Anderson Cancer Center, Houston, Texas Educational Objectives 1.
Molecular Breast Imaging: History and Recent Developments Associate Professor, Department of Imaging Physics The University of Texas MD Anderson Cancer Center, Houston, Texas Educational Objectives 1.
Breast Cancer Atlas for Radiation Therapy Planning: Consensus Definitions
 Breast Cancer Atlas for Radiation Therapy Planning: Consensus Definitions 1 Collaborators Julia White 1, An Tai 1, Douglas Arthur 2, Thomas Buchholz 3, Shannon MacDonald 4, Lawrence Marks 5, Lori Pierce
Breast Cancer Atlas for Radiation Therapy Planning: Consensus Definitions 1 Collaborators Julia White 1, An Tai 1, Douglas Arthur 2, Thomas Buchholz 3, Shannon MacDonald 4, Lawrence Marks 5, Lori Pierce
The Effects of DIBH on Liver Dose during Right-Breast Treatments Introduction
 1 The Effects of DIBH on Liver Dose during Right-Breast Treatments Megan E. Sullivan B.S.R.T.(T)., Patrick A. Melby, B.S. Ashley Hunzeker, M.S., CMD, Nishele Lenards, M.S., CMD Medical Dosimetry Program
1 The Effects of DIBH on Liver Dose during Right-Breast Treatments Megan E. Sullivan B.S.R.T.(T)., Patrick A. Melby, B.S. Ashley Hunzeker, M.S., CMD, Nishele Lenards, M.S., CMD Medical Dosimetry Program
Parathyroid Imaging: Current Concepts. Maria Gule-Monroe, M.D. Nancy Perrier, M.D.
 Parathyroid Imaging: Current Concepts Maria Gule-Monroe, M.D. Nancy Perrier, M.D. Disclosures None Objectives Ultrasound characteristics of parathyroid adenomas vs. lymph nodes 4D-CT evaluation of hyperparathyroidism
Parathyroid Imaging: Current Concepts Maria Gule-Monroe, M.D. Nancy Perrier, M.D. Disclosures None Objectives Ultrasound characteristics of parathyroid adenomas vs. lymph nodes 4D-CT evaluation of hyperparathyroidism
When do you need PET/CT or MRI in early breast cancer?
 When do you need PET/CT or MRI in early breast cancer? Elizabeth A. Morris MD FACR Chief, Breast Imaging Service Memorial Sloan-Kettering Cancer Center NY, NY Objectives What is the role of MRI in initial
When do you need PET/CT or MRI in early breast cancer? Elizabeth A. Morris MD FACR Chief, Breast Imaging Service Memorial Sloan-Kettering Cancer Center NY, NY Objectives What is the role of MRI in initial
declipse SPECT Imaging Probe Worldwide first registration-free ultrasound fusion with high-resolution 3D SPECT images
 declipse SPECT Imaging Probe Worldwide first registration-free ultrasound fusion with high-resolution 3D SPECT images high-resolution 3D SPECT live ultrasound realtime fusion of SPECT / ultrasound Hybrid
declipse SPECT Imaging Probe Worldwide first registration-free ultrasound fusion with high-resolution 3D SPECT images high-resolution 3D SPECT live ultrasound realtime fusion of SPECT / ultrasound Hybrid
Correspondence should be addressed to Donald R. Lannin;
 Hindawi Surgery Research and Practice Volume 2017, Article ID 5924802, 5 pages https://doi.org/10.1155/2017/5924802 Research Article Intraoperative Injection of Technetium-99m Sulfur Colloid for Sentinel
Hindawi Surgery Research and Practice Volume 2017, Article ID 5924802, 5 pages https://doi.org/10.1155/2017/5924802 Research Article Intraoperative Injection of Technetium-99m Sulfur Colloid for Sentinel
Surgery for Breast Cancer
 Surgery for Breast Cancer 1750 Mastectomy - Petit 1894 Radical mastectomy Halsted Extended, Super radical mastectomy 1948 Modified radical mastectomy Patey 1950-60 WLE & RT Baclesse, Mustakallio 1981-85
Surgery for Breast Cancer 1750 Mastectomy - Petit 1894 Radical mastectomy Halsted Extended, Super radical mastectomy 1948 Modified radical mastectomy Patey 1950-60 WLE & RT Baclesse, Mustakallio 1981-85
PET/CT in Breast Cancer
 PET/CT in Breast Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria Overview Introduction Locorregional
PET/CT in Breast Cancer Rodolfo Núñez Miller, M.D. Nuclear Medicine and Diagnostic Imaging Section Division of Human Health International Atomic Energy Agency Vienna, Austria Overview Introduction Locorregional
Melanoma Research 2007, 17: Received 1 April 2007 Accepted 24 August 2007
 Original article 365 Sentinel node-guided evaluation of drainage patterns for melanoma of the helix of the ear Thomas Shpitzer a, Haim Gutman b, Yoav Barnea d, Adam Steinmetz c, Dan Guttman a, Dean Ad-El
Original article 365 Sentinel node-guided evaluation of drainage patterns for melanoma of the helix of the ear Thomas Shpitzer a, Haim Gutman b, Yoav Barnea d, Adam Steinmetz c, Dan Guttman a, Dean Ad-El
Northumbria Healthcare NHS Foundation Trust. Breast Sentinel Lymph Node Biopsy. Issued by the Breast Team
 Northumbria Healthcare NHS Foundation Trust Breast Sentinel Lymph Node Biopsy Issued by the Breast Team Why do my Lymph Nodes require investigation? The lymphatic system is a pathway of lymph vessels and
Northumbria Healthcare NHS Foundation Trust Breast Sentinel Lymph Node Biopsy Issued by the Breast Team Why do my Lymph Nodes require investigation? The lymphatic system is a pathway of lymph vessels and
X-Ray & CT Physics / Clinical CT
 Computed Tomography-Basic Principles and Good Practice X-Ray & CT Physics / Clinical CT INSTRUCTORS: Dane Franklin, MBA, RT (R) (CT) Office hours will be Tuesdays from 5pm to 6pm CLASSROOM: TIME: REQUIRED
Computed Tomography-Basic Principles and Good Practice X-Ray & CT Physics / Clinical CT INSTRUCTORS: Dane Franklin, MBA, RT (R) (CT) Office hours will be Tuesdays from 5pm to 6pm CLASSROOM: TIME: REQUIRED
ACRIN 6666 Therapeutic Surgery Form
 S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
S1 ACRIN 6666 Therapeutic Surgery Form 6666 Instructions: Complete a separate S1 form for each separate area of each breast excised with the intent to treat a cancer (e.g. each lumpectomy or mastectomy).
Descriptor Definition Author s notes TNM descriptors Required only if applicable; select all that apply multiple foci of invasive carcinoma
 S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
S5.01 The tumour stage and stage grouping must be recorded to the extent possible, based on the AJCC Cancer Staging Manual (7 th Edition). 11 (See Tables S5.01a and S5.01b below.) Table S5.01a AJCC breast
Clinical outcomes after sentinel lymph node biopsy in clinically node-negative breast cancer patients
 Original Article Radiat Oncol J 4;():-7 http://dx.doi.org/.857/roj.4... pissn 4-9 eissn 4-56 Clinical outcomes after sentinel lymph node biopsy in clinically node-negative breast cancer patients Hee Ji
Original Article Radiat Oncol J 4;():-7 http://dx.doi.org/.857/roj.4... pissn 4-9 eissn 4-56 Clinical outcomes after sentinel lymph node biopsy in clinically node-negative breast cancer patients Hee Ji
Review Article SPECT/CT for Lymphatic Mapping of Sentinel Nodes in Early Squamous Cell Carcinoma of the Oral Cavity and Oropharynx
 International Molecular Imaging Volume 2011, Article ID 106068, 6 pages doi:10.1155/2011/106068 Review Article SPECT/CT for Lymphatic Mapping of Sentinel Nodes in Early Squamous Cell Carcinoma of the Oral
International Molecular Imaging Volume 2011, Article ID 106068, 6 pages doi:10.1155/2011/106068 Review Article SPECT/CT for Lymphatic Mapping of Sentinel Nodes in Early Squamous Cell Carcinoma of the Oral
Evaluation of the Axilla Post Z-0011 Trial New Paradigm
 Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Evaluation of the Axilla Post Z-0011 Trial New Paradigm Belinda Curpen, MD, FRCPC; Tetyana Dushenkovska; Mia Skarpathiotakis MD, FRCPC; Carrie Betel, MD, FRCPC; Kalesha Hack, MD, FRCPC; Lara Richmond,
Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study
 [ABS-0078] GBCC 2018 Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study Eun Young Kim 1, Kwan Ho Lee 1, Yong
[ABS-0078] GBCC 2018 Feasibility of Preoperative Axillary Lymph Node Marking with a Clip in Breast Cancer Patients before Neoadjuvant Chemotherapy: A Preliminary Study Eun Young Kim 1, Kwan Ho Lee 1, Yong
Appropriate Concept of Prevention of Lymphedema at the Initial Treatment
 Global Breast Cancer Conference 2018 Appropriate Concept of Prevention of Lymphedema at the Initial Treatment Zisun Kim Department of Surgery, Soonchunhyang University Bucheon Hospital, Soonchunhyang University
Global Breast Cancer Conference 2018 Appropriate Concept of Prevention of Lymphedema at the Initial Treatment Zisun Kim Department of Surgery, Soonchunhyang University Bucheon Hospital, Soonchunhyang University
PARATHYROID NUCLEAR MEDICINE IMAGING REVIEW DISCLOSURES
 PARATHYROID NUCLEAR MEDICINE IMAGING REVIEW Miguel Hernandez Pampaloni, M.D., Ph.D. Chief, Nuclear Medicine Assistant Professor of Radiology UCSF Department of Radiology and Biomedical Imaging DISCLOSURES
PARATHYROID NUCLEAR MEDICINE IMAGING REVIEW Miguel Hernandez Pampaloni, M.D., Ph.D. Chief, Nuclear Medicine Assistant Professor of Radiology UCSF Department of Radiology and Biomedical Imaging DISCLOSURES
PET/CT in lung cancer
 PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
PET/CT in lung cancer Andrei Šamarin North Estonia Medical Centre 3 rd Baltic Congress of Radiology 08.10.2010 Imaging in lung cancer Why do we need PET/CT? CT is routine imaging modality for staging of
Ultrasound or FNA for Predicting Node Positive in Breast Cancer
 Ultrasound or FNA for Predicting Node Positive in Breast Cancer Chiun Sheng Huang, MD, PhD, MPH Professor and Chairman Department of Surgery Director of Breast Care Center National Taiwan University Hospital
Ultrasound or FNA for Predicting Node Positive in Breast Cancer Chiun Sheng Huang, MD, PhD, MPH Professor and Chairman Department of Surgery Director of Breast Care Center National Taiwan University Hospital
Handheld Radiofrequency Spectroscopy for Intraoperative Assessment of Surgical Margins During Breast-Conserving Surgery
 Last Review Status/Date: December 2014 Page: 1 of 6 Intraoperative Assessment of Surgical Description Breast-conserving surgery as part of the treatment of localized breast cancer is optimally achieved
Last Review Status/Date: December 2014 Page: 1 of 6 Intraoperative Assessment of Surgical Description Breast-conserving surgery as part of the treatment of localized breast cancer is optimally achieved
Imaging in gastric cancer
 Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
Imaging in gastric cancer Gastric cancer remains a deadly disease because of late diagnosis. Adenocarcinoma represents 90% of malignant tumors. Diagnosis is based on endoscopic examination with biopsies.
