CLINICAL SCIENCES. Metastatic Melanoma Death Rates by Anatomic Site After Proton Beam Irradiation for Uveal Melanoma
|
|
|
- Adelia Wade
- 5 years ago
- Views:
Transcription
1 CLINICAL SCIENCES Metastatic Melanoma Death Rates by Anatomic Site After Proton Beam Irradiation for Uveal Melanoma Wenjun Li, MS; Evangelos S. Gragoudas, MD; Kathleen M. Egan, ScD Background: Ciliary body location is an established prognostic factor for metastasis-related death from uveal melanoma. We evaluated alternative approaches for classifying this covariate when constructing predictive models of patient survival. Methods and Design: The analyses were based on a consecutive series of 1848 primary choroidal and/or ciliary body melanoma patients treated with proton beam irradiation (70 cobalt gray equivalent in 5 fractions) at the Harvard Cyclotron Laboratory, Boston, Mass, between July 1975 and December For each patient, the anatomic site of the tumor was classified according to an estimate of the proportion of the tumor base lying anterior to the ora serrata. Using proportional hazards regression, we estimated relative risk ratios and death rates from melanoma metastasis according to the extent of ciliary body involvement. All estimates were adjusted for other established prognostic factors. Results: Patients were followed up through April 30, 1998; none were lost to follow-up. Of 1848 patients analyzed, 378 died of melanoma metastasis. The median follow-up period among survivors was 9.5 years. Ciliary body origin ( 50% of tumor base anterior to the ora serrata) was positively associated with tumor pigmentation (P.001), tumor height (P.001), and extrascleral extension of the tumor (P.001). Compared with tumors involving only the choroid, melanoma-associated death rates increased with the proportion of the tumor base lying within the ciliary body (P=.006); the multivariateadjusted relative risk ratio for greater than 75% involvement was 2.30 (95% confidence interval [CI], ). The covariate-adjusted 5-year death rates for ciliary body origin and choroidal origin were 15.9% (95% CI, 11.3%- 21.2%) and 9.8% (95% CI, 8.3%-11.7%), respectively. Conclusion: Patients with melanomas of presumed ciliary body origin seem to be subject to a higher risk of death resulting from melanoma metastasis. Arch Ophthalmol. 2000;118: From the Retina Service, Massachusetts Eye and Ear Infirmary, Harvard Medical School, Boston (Drs Gragoudas and Egan and Mr Li); the Department of Biostatistics and Epidemiology, University of Massachusetts, Amherst (Mr Li); and the Department of Epidemiology, Harvard School of Public Health, Boston (Dr Egan). ANTERIOR TUMOR location is an adverse prognostic factor for patient survival after treatment for intraocular melanoma In past studies, tumor location has been classified according to the location of the most anterior margin, 1-14 presence or absence of ciliary body involvement, 15-20,31,32 anatomic location, or a combination of these. 13,14,25,26 The location of the most anterior margin has generally been classified as iris, ciliary body, or anterior or posterior to the equator. Recent cytogenetic and tumor vascular studies provided a biological explanation for the prognostic importance of tumor location. It has been shown that tumors involving the ciliary body have a predilection for 2 chromosomal abnormalities (monosomy 3 and multiple copies of 8q) 18,33-39 that are associated with a poor prognosis Tumors with ciliary body involvement also express vascular patterns 17,28,40 that are correlated with decreased patient survival. 17,27,28,31,40-43 If a single site of origin is assumed for ciliochoroidal tumors, the presumed anatomic site of origin determined by the proportion of the tumor base lying anterior to the ora serrata might better reflect a differential path of disease progression and clinical course of these tumors. In this article, we describe the importance of considering the extent of ciliary body involvement in prognostic models of metastasisfree survival in an analysis based on a large series of patients treated by proton beam irradiation. RESULTS There were no losses to follow-up. Of 1848 patients analyzed, 378 died of melanoma metastasis. The median follow-up among survivors was 9.5 years. The unadjusted 1066
2 SUBJECTS AND METHODS The subjects consisted of a consecutive series of 1848 patients treated with proton beam irradiation for uveal melanoma between 1975 and Patients were United States or Canadian citizens with unilateral tumors, having no evidence of metastasis at pretreatment examination. Irisonly melanomas were excluded from analysis. Most patients were treated with the standard therapeutic dose of 70 cobalt gray equivalents (CGE) (96.5%) (range, CGE [3.5%]) at the Harvard Cyclotron Laboratory, Boston, Mass. All patients were treated by the same physician (E.S.G.) and were followed up annually through April 30, The study protocol was approved by the Massachusetts Eye and Ear Infirmary Human Studies Committee, and written informed consent was obtained from all patients. In our analyses, tumor location was defined according to the extent of ciliary body involvement (Figure 1). 44,45 Tumors were classified into 6 groups according to the location of the tumor with respect to the equator. Ciliary body involved tumors were classified according to the proportion of the anteroposterior axis of the tumor base lying anterior to the ora serrata: (I) posterior to the equator, (II) anterior to the equator but posterior to the ora serrata, or (III) involving the ciliary body and anterior to the ora serrata by 1% to 25%, (IV) 26% to 50%, (V) 51% to 75%, or (VI) greater than 75% of the anteroposterior tumor diameter. Margins and anteroposterior diameter were obtained from surgical reports. For tumors extending posterior to the equator, distances between the anterior margin and limbus, posterior margin to limbus, and anteroposterior axial diameter of the tumor (APD) were recorded at the time of surgical placement of tantalum rings used for tumor localization during proton treatments. For ciliary body tumors treated without prior surgical localization, these distances were estimated by transillumination of the eye during pretreatment simulation. In both cases, the proportion of the tumor base lying within the ciliary body was estimated as the ratio between the anteroposterior axial length of the tumor lying anterior to ora serrata (LAO) and the APD: [proportion of the tumor base lying within the ciliary body]=[lao/apd] 100%. For tumors with the anterior margin posterior to the limbus, the LAO was approximated by subtracting the distance between the anterior margin and limbus from the length of ciliary body zone (LCB). For tumors with an anterior margin extending anterior to the limbus, the LAO was estimated as [APD distance between the posterior margin to limbus +LCB]. To control for variation in eye size, the LCB used for calculation was estimated for each patient using the following equation: LCB = Patient s Eye Diameter Eye Diameter of a Standard Eye (24.25 mm) LCB of a Standard Eye (6.5 mm) Ciliary body only and iridociliary tumors were classified as having 100% of the tumor base lying within the ciliary body. For analysis purposes, a tumor was considered to have a ciliary body origin if more than 50% of its anteroposterior axis fell anterior to the ora serrata. The end point in this study was death from melanoma metastasis after irradiation (documented by autopsy, biopsy, death certificates, or reported by physicians or next of kin). The prognostic value of anteroposterior tumor location was evaluated with multivariate Cox proportional hazards models 46 and adjusted for established prognostic factors, ie, sex, age at treatment, time from first visit to treatment, iris color, symptoms at first visit, tumor basal area, presence or absence of extrascleral extension, and tumor pigmentation. Interaction terms were evaluated using the procedures outlined by Hosmer and Lemeshow. 47 The proportional hazard assumption was examined via the Grambsch and Therneau 48 procedure. The covariateadjusted 5-, 10-, 15-, and 20-year death rates were computed using the modified risk score method, 47 and associated 95% confidence intervals (CIs) were constructed using bootstrap methods. 49 The baseline survivorship function was estimated for 60-year-old women with dark- or moderate-colored irises, no symptoms at first visit, and a time from first visit to treatment of 3 months, whose tumors had heavy tumor pigmentation, no extrascleral extension, and a tumor basal area of 125 mm 2. 5-, 10-, and 15-year metastatic death rates in the cohort were 14.9%, 23.9%, and 27.2%, respectively. Table 1 gives a comparison of patient and tumor characteristics according to presumed ciliary body origin ( 50% of tumor base). Ciliary body origin was associated with greater tumor pigmentation (P.01), female sex (P.04), larger tumor height (P.001), and extrascleral extension (P.001). Multivariate relative risk (RR) ratios for anterior location are given in Table 2. Compared with choroidonly tumors, the rate of metastatic death increased with the proportion of the tumor base lying within the ciliary body (P=.006, based on 4 categories of 0% of tumor base lying anterior to the ora serrata); the RR ratios for 51% to 75% and greater than 75% were 1.62 (95% CI, ) and 2.30 (95% CI, ), respectively. The RR for tumors with 100% ciliary body involvement (ciliary body only or iridociliary tumors; n=31) was 3.61 (95% CI, ). Patients with choroidal tumors having only peripheral involvement of the ciliary body ( 50%) had no greater risk for metastatic death (P.75) than patients with lesions confined to the posterior pole. The covariate-adjusted 5-, 10-, 15-, and 20-year death rates and associated 95% CIs for tumors with presumed ciliary body origin (n=145) and choroidal origin (n=1703) are listed in Table 3, and the covariate-adjusted cumulative failure function is shown in Figure 2. The relation of ciliary origin ( 50% of the tumor base within the ciliary body) to melanoma-free survival was similar across categories of other prognostic factors (data not shown). A comparison of 3 methods for classifying tumor location is given in Table 4. Most (77%) of 513 tumors with a margin anterior to the ora serrata likely arose from the choroid (eg, 50% of the tumor base resided in the ciliary body). The effect of such misclassification is bias to the null: the multivariate-adjusted RR ratios for any ciliary body involvement was only modestly and nonsignificantly elevated (RR, 1.16; 95% CI, ). 1067
3 24.6 mm Equator Ora Serrata Limbus 6.5 mm COMMENT Fovea Optic Disc Figure 1. Dimension of standard eye with 24.6-mm anteroposterior axial length Table 1. Patient and Tumor Characteristics by Presumed Anatomic Site of Tumor* Characteristics Choroidal Origin (n = 1703) Ciliary Body Origin (n = 145) P Patient Age, y 58.8 (14.3) 59.9 (15.8).18 Sex, No. (%) Female 857 (50.3) 86 (59.3).04 Male 846 (49.7) 59 (40.7) Symptoms at presentation, No. (%) Present 1264 (74.2) 99 (68.3).14 Absent 439 (25.8) 46 (31.7) Iris color Dark 327 (21.8) 38 (29.2).13 Medium 470 (31.3) 34 (26.2) Light 705 (46.9) 58 (44.6) Tumor Largest diameter, mm (3.73) (4.02).19 Perpendicular diameter, mm (3.36) (3.00).75 Height, mm 5.30 (2.82) 7.10 (2.86).001 Basal area, 100 mm (0.89) 1.43 (0.89).37 Extraocular extension, No. (%) Present 48 (2.8) 23 (15.9).001 Absent 1655 (97.2) 122 (84.1) Pigmentation, No. (%) Minimal 263 (23.2) 4 (4.0).001 Moderate 362 (32.0) 26 (26.0) Heavy 507 (44.8) 70 (70.0) *Values are given as mean (SD) except where indicated. Missing data not included. Originating site of the tumor was defined as choroidal origin ( 50% of tumor base lying anterior to ora serrata) and ciliary body origin ( 50% of tumor base lying anterior to ora serrata). Rank sum test. 2 Analysis. Patient had at least 1 of the following symptoms present at the time of treatment: decreased vision, loss of visual field, metamorphopsia, blurriness, pain, inflammation, photopsia, or floaters. Iris color and tumor pigmentation available on subset of 1632 and 1232 patients, respectively. In this article, we demonstrate that ciliochoroidal melanomas presumed to have arisen from the ciliary body exhibit more aggressive behavior (with respect to patient survival) than those arising from the choroid. Less quantitative approaches for classifying the anterior extent of Table 2. Adjusted Relative Risk Ratios for Metastatic Death by Presumed Anatomic Site of Tumor* Anatomic Site No. RR (95% CI) P Posterior to equator 897 Reference... Anterior to equator with no ciliary ( ).48 involvement Anterior to equator with ciliary body involvement (% of tumor base lying anterior to the ora serrata) 1%-25% ( ).70 26%-50% ( ).56 51%-75% ( ).03 76% ( ).01 *Test for trend (4 categories for 0% of tumor base lying anterior to ora serrata), P =.006. Ellipses indicate not applicable. Relative risk (RR) ratios adjusted for sex, age at treatment, time from first visit to treatment, iris color, symptoms at first visit, extraocular extension and tumor pigmentation, and tumor basal area. CI indicates confidence interval. the tumor will not adequately reflect this phenomenon, which in turn may lead to misclassification of prognosis. Based on these results, of 513 tumors involving the ciliary body to any extent, 368 (72%) with up to 50% of the tumor base anterior to the ora serrata carried no excess risk of metastatic death (RR, 0.93; 95% CI, ) compared with tumors posterior to the equator (Table 2). The overall RR for any ciliary body involvement, without regard to extent, was only modestly and nonsignificantly elevated (RR, 1.16; 95% CI, ). Increasing magnitude of excessive risk with the increasing proportion of the tumor base anterior to the ora serrata is consistent with progressively less misclassification of tumor origin and supports the inherently more aggressive clinical course of tumors originating in the ciliary body. Misclassification may have contributed to the null results in some previous studies 31,32,50 that found no excess risk for ciliary body location. McLean et al 6 noted the importance of the extent of ciliary body involvement. These authors reported that only tumors with angle or iris involvement had a significantly worse prognosis, which is consistent with our data showing a worsened prognosis confined to the most anterior tumors. Higher death rates specific to ciliary body origin are consistent with recent reports indicating that genetic defects in ciliary body tumors may be distinct from and carry a poorer prognosis than those giving rise to melanomas in the choroid. 33,34,37,38,51,52 In addition, microvascular networks linked to poor patient survival 17,28 tend to develop preferentially in the ciliary body relative to the choroid. 17,28,40 We excluded from analysis iris melanomas, which rarely if ever metastasize However, it is possible that some of the most anterior tumors may have originated in the iris. The fact that the RR ratios for ciliary body only melanoma (RR, 4.4; 95% CI, ; n=10) was substantially higher than the RR for iridociliary tumors (RR, 2.9; 95% CI, ; n=21) suggests that RR ratios for presumed ciliary body origin ( 50% of the tumor base) were attenuated by the inclusion of some tumors with low malignant potential. Sensitivity analysis, performed 1068
4 Table 3. Adjusted Metastatic Death 22p Rates and Their 95% Confidence Intervals (CIs)* by Presumed Anatomic Site of Tumor Choroid Ciliary Body No. of Years After Treatment Crude CI Covariate-Adjusted CI Crude CI Covariate-Adjusted CI ( ) 9.8 ( ) 25.2 ( ) 15.9 ( ) ( ) 17.1 ( ) 35.2 ( ) 27.0 ( ) ( ) 19.9 ( ) 39.7 ( ) 31.0 ( ) ( ) 21.7 ( ) ( ) *Death rates were computed using modified risk scores method and adjusted for sex, age at treatment, time between first visit and treatment, iris color, symptoms at first visit, extrascleral extension, tumor pigmentation, and tumor basal area. The 95% CIs were constructed using bootstrap methods and were bias-corrected. Originating site of the tumor was defined as choroidal origin ( 50% of tumor base lying anterior to ora serrata) and ciliary body origin ( 50% of tumor base lying anterior to ora serrata). Ellipses indicate not applicable. Probability of Death Tumors With Presumed Ciliary Body Origin (n = 145) Tumors With Presumed Choroidal Origin (n = 1703) No. at Risk: Relative Risk Ratio, 1.69 Wald Test, P = Years Since Treatment Figure 2. Covariate-adjusted metastatic death rates by anatomic site. 20 location and chromosome changes are intimately linked, 37 tumor location as classified here may provide a useful surrogate when cytogenetic parameters are not available. Accepted for publication February 12, This study was supported by the Melanoma Research Fund and by the Retina Research Foundation, Houston, Tex. Presented in part at the Association for Research in Vision and Ophthalmology 1999 Annual Meeting, Fort Lauderdale, Fla, May 9-14, Dr Gragoudas is a Research to Prevent Blindness Inc, New York, NY, senior scientific investigator. Corresponding author: Kathleen Egan, ScD, Retina Service, Massachusetts Eye and Ear Infirmary, Boston, MA ( kathleen.egan@channing.harvard.edu). Table 4. Presumed Anatomic Site by Anterior Margin and Area of Involvement of Tumor* Tumor Base Lying Anterior to Ora Serrata, % Site Total Anterior margin Choroid CB Iris Area of involvement Choroid only CB + Choroid Iris + CB + Choroid CB only Iris+CB Total *Ellipses indicate not applicable; CB, ciliary body. Tumors posterior to equator (n = 897) or anterior to equator with no involvement of ciliary body (n = 438). by varying reported cutoff points (25%, 50%, and 75%) from 1% to 5%, suggested that the reported estimates and trend of RR ratios for the 4 location categories were robust and not sensitive to slight changes in the cutoff points used. In summary, our results confirm recent findings indicating an excess risk for metastatic death in patients with ciliary body tumors linked to specific chromosomal alterations and/or vascular patterns. Since tumor REFERENCES 1. McLean MJ, Foster WD, Zimmerman LE. Prognostic factors in small malignant melanomas of choroid and ciliary body. Arch Ophthalmol. 1977;95: Kidd MN, Lyness RW, Patterson CC, Johnston PB, Archer DB. Prognostic factors in malignant melanoma of the choroid: a retrospective survey of cases occurring in Northern Ireland between 1965 and Trans Ophthalmol Soc U K. 1986;105: Gragoudas ES, Seddon JM, Egan KM, et al. Prognostic factors for metastasis following proton beam irradiation of uveal melanomas. Ophthalmology. 1986; 93: Gragoudas E, Seddon J, Egan K, et al. Metastasis from uveal melanoma after proton beam irradiation. Ophthalmology. 1988;95: Gragoudas E, Egan K, Seddon J, Walsh S, Munzenrider J. Intraocular recurrence of uveal melanoma after proton beam irradiation. Ophthalmology. 1992; 99: McLean IW, Ainbinder DJ, Gamel JW, McCurdy JB. Choroidal-ciliary body melanoma: a multivariate survival analysis of tumor location. Ophthalmology. 1995; 102: Collaborative Ocular Melanoma Study Group. Mortality in patients with small choroidal melanoma: COMS Report No. 4. Arch Ophthalmol. 1997;115: Harbour J, Char D, Kroll S, Quivey J, Castro J. Metastatic risk for distinct patterns of postirradiation local recurrence of posterior uveal melanoma. Ophthalmology. 1997;104: Augsburger JJ, Correa ZM, Freire J, Brady LW. Long-term survival in choroidal and ciliary body melanoma after enucleation versus plaque radiation therapy. Ophthalmology. 1998;105: Kroll S, Char DH, Quivey J, Castro J. A comparison of cause-specific melanoma mortality and all-cause mortality in survival analyses after radiation treatment for uveal melanoma. Ophthalmology. 1998;105: Egan K, Giovannucci E, Lane A, Gragoudas E. A prospective study of diet as a prognostic factor in choroidal melanoma [abstract]. Invest Ophthalmol Vis Sci. 1998;39(ARVO suppl):s Egan KM, Quinn JL, Gragoudas ES. Childbearing history associated with improved survival in choroidal melanoma. Arch Ophthalmol. 1999;117:
5 13. Char DH, Kroll SM, Castro J. Long-term follow-up after uveal melanoma charged particle therapy. Trans Am Ophthalmol Soc. 1997;95: Char DH, Kroll SM, Castro J. Ten-year follow-up of helium ion therapy for uveal melanoma. Am J Ophthalmol. 1998;125: Glynn R, Seddon J, Gragoudas E, Egan K, Hart L. Evaluation of tumor regression and other prognostic factors for early and late metastasis after proton irradiation of uveal melanoma. Ophthalmology. 1989;96: Decker M, Castro JR, Linstadt DE, et al. Ciliary body melanoma treated with helium particle irradiation. Int J Radiat Oncol Biol Phys. 1990;19: Rummelt V, Folberg R, Woolson RF, Hwang T, Pe er J. Relation between the microcirculation architecture and the aggressive behavior of ciliary body melanomas. Ophthalmology. 1995;102: Prescher G, Bornfeld N, Hirche H, Horsthemke B, Jockel KH, Becher R. Prognostic implications of monosomy 3 in uveal melanoma. Lancet. 1996;347: Castro JR, Char DH, Petti PL, et al. 15 years experience with helium ion radiotherapy for uveal melanoma. Int J Radiat Oncol Biol Phys. 1997;39: Daftari IK, Char DH, Verhey LJ, et al. Anterior segment sparing to reduce charged particle radiotherapy complications in uveal melanoma. Int J Radiat Oncol Biol Phys. 1997;39: Barr CC, McLean IW, Zimmerman LE. Uveal melanoma in children and adolescents. Arch Ophthalmol. 1981;99: Seddon JM, Albert DM, Lavin PT, Robinson N. A prognostic factor study of diseasefree interval and survival following enucleation for uveal melanoma. Arch Ophthalmol. 1983;101: Seddon JM, Gragoudas ES, Egan KM, et al. Relative survival rates after alternative therapies for uveal melanoma. Ophthalmology. 1990;97: Augsburger JJ, Gamel JW. Clinical prognostic factors in patients with posterior uveal malignant melanoma. Cancer. 1990;66: Augsburger JJ, Gamel JW, Sardi VF, Greenberg RA, Shields JA, Brady LW. Enucleation vs cobalt plaque radiotherapy for malignant melanomas of the choroid and ciliary body. Arch Ophthalmol. 1986;104: Summanen P, Immonen I, Heikkonen J, Tommila P, Laatikainen L, Tarkkanen A. Survival of patients and metastatic and local recurrent tumor growth in malignant melanoma of the uvea after ruthenium plaque radiotherapy. Ophthalmic Surg. 1993;24: Seregard S, Spangberg B, Juul C, Oskarsson M. Prognostic accuracy of the mean of the largest nucleoli, vascular patterns, and PC-10 in posterior uveal melanoma. Ophthalmology. 1998;105: Folberg R, Rummelt V, Parys-Van Ginderdeuren R, et al. The prognostic value of tumor blood vessel morphology in primary uveal melanoma. Ophthalmology. 1993;100: Seregard S, Kock E. Prognostic indicators following enucleation for posterior uveal melanoma: a multivariate analysis of long-term survival with minimized loss to follow-up. Acta Ophthalmol Scand. 1995;73: Foss AJ, Cree IA, Dolin PJ, Hungerford JL. Modelling uveal melanoma. Br J Ophthalmol. 1999;83: Foss AJ, Alexander RA, Jefferies LW, Hungerford JL, Harris AL, Lightman S. Microvessel count predicts survival in uveal melanoma. Cancer Res. 1996;56: Damato BE, Paul J, Foulds WS. Risk factors for metastatic uveal melanoma after trans-scleral local resection. Br J Ophthalmol. 1996;80: Sisley K, Rennie IG, Cottam DW, Potter AM, Potter CW, Rees RC. Cytogenetic findings in six posterior uveal melanomas: involvement of chromosomes 3, 6, and 8. Genes Chromosomes Cancer. 1990;2: Sisley K, Cottam DW, Rennie IG, et al. Non-random abnormalities of chromosomes 3, 6, and 8 associated with posterior uveal melanoma. Genes Chromosomes Cancer. 1992;5: Prescher G, Bornfeld N, Horsthemke B, Becher R. Chromosomal aberrations defining uveal melanoma of poor prognosis [letter]. Lancet. 1992;339: Horsman DE, White VA. Cytogenetic analysis of uveal melanoma: consistent occurrence of monosomy 3 and trisomy 8q. Cancer. 1993;71: Sisley K, Rennie IG, Parsons MA, et al. Abnormalities of chromosomes 3 and 8 in posterior uveal melanoma correlate with prognosis. Genes Chromosomes Cancer. 1997;19: Prescher G, Bornfeld N, Friedrichs W, Seeber S, Becher R. Cytogenetics of twelve cases of uveal melanoma and patterns of nonrandom anomalies and isochromosome formation. Cancer Genet Cytogenet. 1995;80: Singh AD, Boghosian-Sell L, Wary KK, et al. Cytogenetic findings in primary uveal melanoma. Cancer Genet Cytogenet. 1994;72: Rummelt V, Folberg R, Rummelt C, et al. Microcirculation architecture of melanocytic nevi and malignant melanomas of the ciliary body and choroid: a comparative histopathologic and ultrastructural study. Ophthalmology. 1994;101: Folberg R, Mehaffey M, Gardner LM, Meyer M, Rummelt V, Pe er J. The microcirculation of choroidal and ciliary body melanomas. Eye. 1997;11: Folberg R, Pe er J, Gruman LM, et al. The morphologic characteristics of tumor blood vessels as a marker of tumor progression in primary human uveal melanoma: a matched case-control study. Hum Pathol. 1992;23: Pe er J, Rummelt V, Mawn L, Hwang T, Woolson RF, Folberg R. Mean of the ten largest nucleoli, microcirculation architecture, and prognosis of ciliochoroidal melanomas. Ophthalmology. 1994;101: Olsen K, Curtin V. Enucleation and plaque treatment. In: Albert D, Jakobiec F, eds. Principles and Practice of Ophthalmology: Clinical Practice. Philadelphia, Pa: WB Saunders Co; 1994: Bron A, Tripathi R, Tripathi B. Wolff s Anatomy of the Eye and Orbit. 8th ed. London, England: Chapman & Hall Medical; Cox D. Regression models and life-tables. J Roy Stat Soc Ser. 1972;34: Hosmer D, Lemeshow S. Applied Survival Analysis: Regression Modeling of Time to Event. New York, NY: John Wiley & Sons Inc; Grambsch P, Therneau T. Proportional hazards tests and diagnostics based on weighted residuals. Biometrika. 1994;81: StataCorp. Bstrap: Bootstrap Sampling and Estimation: Stata Reference Manual: Release 6.0. College Station, Tex: Stata Press; 1999: Linstadt D, Castro J, Char D, et al. Long-term results of helium ion irradiation of uveal melanoma. Int J Radiat Oncol Biol Phys. 1990;19: Sisley K, Nichols C, Parsons MA, Farr R, Rees RC, Rennie IG. Clinical applications of chromosome analysis, from fine needle aspiration biopsies, of posterior uveal melanomas. Eye. 1998;12: Speicher MR, Prescher G, du Manoir S, et al. Chromosomal gains and losses in uveal melanomas detected by comparative genomic hybridization. Cancer Res. 1994;54: Davidorf FH. The melanoma controversy: a comparison of choroidal, cutaneous, and iris melanomas. Surv Ophthalmol. 1981;25: Geisse LJ, Roberston DM. Iris melanoma. Am J Ophthalmol. 1985;99: Jensen OA. Malignant melanoma of the iris: a 25-year analysis of Danish cases. Eur J Ophthalmol. 1993;3:
Gene Expression Profiling has been proposed as a method of risk stratification for uveal melanoma.
 Last Review Status/Date: September 2014 Description Page: 1 of 5 Gene Expression Profiling has been proposed as a method of risk stratification for uveal melanoma. Background Uveal melanoma Uveal melanoma,
Last Review Status/Date: September 2014 Description Page: 1 of 5 Gene Expression Profiling has been proposed as a method of risk stratification for uveal melanoma. Background Uveal melanoma Uveal melanoma,
Uveal melanoma (UM) is the most common primary intraocular
 A R T I C L E S Clinical and Cytogenetic Analyses in Uveal Melanoma Emine Kilic, 1 Walter van Gils, 1,2 Elisabeth Lodder, 2 H. Berna Beverloo, 2 Marjan E. van Til, 2 Cornelia M. Mooy, 3 Dion Paridaens,
A R T I C L E S Clinical and Cytogenetic Analyses in Uveal Melanoma Emine Kilic, 1 Walter van Gils, 1,2 Elisabeth Lodder, 2 H. Berna Beverloo, 2 Marjan E. van Til, 2 Cornelia M. Mooy, 3 Dion Paridaens,
Malignant melanoma of the uvea disseminates purely hematogenously, Very Long-Term Prognosis of Patients with Malignant Uveal Melanoma
 Very Long-Term Prognosis of Patients with Malignant Uveal Melanoma Emma Kujala, 1 Teemu Mäkitie, 2 and Tero Kivelä 1,2 From the 1 Ocular Oncology Service and 2 Ophthalmic Pathology Laboratory, Department
Very Long-Term Prognosis of Patients with Malignant Uveal Melanoma Emma Kujala, 1 Teemu Mäkitie, 2 and Tero Kivelä 1,2 From the 1 Ocular Oncology Service and 2 Ophthalmic Pathology Laboratory, Department
METHODS FOR coding the
 Assessment of Metastatic Disease Status at Death in 435 Patients With Large Choroidal Melanoma in the Collaborative Ocular Melanoma Study (COMS) COMS Report No. 15 The Collaborative Ocular Melanoma Study
Assessment of Metastatic Disease Status at Death in 435 Patients With Large Choroidal Melanoma in the Collaborative Ocular Melanoma Study (COMS) COMS Report No. 15 The Collaborative Ocular Melanoma Study
UCSF Uveal Melanoma Program: Outcomes with Proton Beam Radiation Therapy Kavita K. Mishra, M.D., M.P.H. UCSF Comprehensive Cancer Center
 Disclosures UCSF Uveal Melanoma Program: Outcomes with Proton Beam Radiation Therapy No disclosures Kavita K. Mishra, M.D., M.P.H. UCSF Comprehensive Cancer Center UCSF Uveal Melanoma Program: Ocular Melanoma
Disclosures UCSF Uveal Melanoma Program: Outcomes with Proton Beam Radiation Therapy No disclosures Kavita K. Mishra, M.D., M.P.H. UCSF Comprehensive Cancer Center UCSF Uveal Melanoma Program: Ocular Melanoma
Gender Differences in Clinical Presentation and Prognosis of Uveal Melanoma METHODS. Patients
 Anatomy and Pathology Gender Differences in Clinical Presentation and Prognosis of Uveal Melanoma Ofira Zloto, Jacob Pe er, and Shahar Frenkel PURPOSE. We examined the clinical differences in manifestation
Anatomy and Pathology Gender Differences in Clinical Presentation and Prognosis of Uveal Melanoma Ofira Zloto, Jacob Pe er, and Shahar Frenkel PURPOSE. We examined the clinical differences in manifestation
Transvitreal Fine Needle Aspiration Biopsy of Choroidal Melanoma via Pars Plana Vitrectomy
 Surgical Technique Is pars plana vitrectomy a safe method for performing fine needle aspiration biopsy of choroidal melanoma? What are the rates of complications? Clinical Characteristics Do tumor thickness
Surgical Technique Is pars plana vitrectomy a safe method for performing fine needle aspiration biopsy of choroidal melanoma? What are the rates of complications? Clinical Characteristics Do tumor thickness
Uveal melanoma is the most common primary intraocular
 Genetics Higher Percentage of FISH-Determined Monosomy 3 and 8q Amplification in Uveal Melanoma Cells relate to Poor Patient Prognosis Thomas van den Bosch, 1,2 Jackelien G. M. van Beek, 2,3 Jolanda Vaarwater,
Genetics Higher Percentage of FISH-Determined Monosomy 3 and 8q Amplification in Uveal Melanoma Cells relate to Poor Patient Prognosis Thomas van den Bosch, 1,2 Jackelien G. M. van Beek, 2,3 Jolanda Vaarwater,
This protocol is intended to assist pathologists in providing
 Protocol for the Examination of Specimens From Patients With Uveal Melanoma A Basis for Checklists Daniel Albert, MD; Nasreen Syed, MD; for the Members of the Cancer Committee, College of American Pathologists
Protocol for the Examination of Specimens From Patients With Uveal Melanoma A Basis for Checklists Daniel Albert, MD; Nasreen Syed, MD; for the Members of the Cancer Committee, College of American Pathologists
Iris-Ciliary Body Melanoma: 57-year-old female with iris lesion
 Iris-Ciliary Body Melanoma: 57-year-old female with iris lesion Gina M. Rogers, MD, Nasreen A. Syed, MD, Wallace L. M. Alward, MD, Juan Fernandez de Castro, MD, Lauren Jensen, BS Chief Complaint: Spot
Iris-Ciliary Body Melanoma: 57-year-old female with iris lesion Gina M. Rogers, MD, Nasreen A. Syed, MD, Wallace L. M. Alward, MD, Juan Fernandez de Castro, MD, Lauren Jensen, BS Chief Complaint: Spot
Tall, dark and.. Uh oh
 Tall, dark and.. Uh oh Jesse L. Berry, MD Arizona Ophthalmology Society 2017 Ocular Oncology Service USC Eye Institute Financial Disclosures Research Support: Bright Eyes Nautica Foundation Knights Templar
Tall, dark and.. Uh oh Jesse L. Berry, MD Arizona Ophthalmology Society 2017 Ocular Oncology Service USC Eye Institute Financial Disclosures Research Support: Bright Eyes Nautica Foundation Knights Templar
A study of iris melanoma in Northern Ireland
 British Journal of Ophthalmology, 1989, 73, 591-595 A study of iris melanoma in Northern Ireland J N McGALLIARD AND P B JOHNSTON From the Department of Ophthalmology, Royal Victoria Hospital, Grosvenor
British Journal of Ophthalmology, 1989, 73, 591-595 A study of iris melanoma in Northern Ireland J N McGALLIARD AND P B JOHNSTON From the Department of Ophthalmology, Royal Victoria Hospital, Grosvenor
Retina Center of Oklahoma Sam S. Dahr, M.D. Adult Intraocular Tumors
 Adult Intraocular Tumors Sam S. Dahr, M.D. Retina Center of Oklahoma www.retinacenteroklahoma.com www.rcoklahoma.com Table of Contents Posterior uveal malignant melanoma Uveal metastasis Uveal melanoma
Adult Intraocular Tumors Sam S. Dahr, M.D. Retina Center of Oklahoma www.retinacenteroklahoma.com www.rcoklahoma.com Table of Contents Posterior uveal malignant melanoma Uveal metastasis Uveal melanoma
Uveal Melanoma. Protocol applies to malignant melanoma of the uvea.
 Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Uveal Melanoma Protocol applies to malignant melanoma of the uvea. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Long-Term Survivors with Metastatic Uveal Melanoma
 The Open Ophthalmology Journal, 2012, 6, 49-53 49 Long-Term Survivors with Metastatic Uveal Melanoma Open Access Dominic M. Buzzacco,1, Mohamed H. Abdel-Rahman,1,2, Stanley Park 1, Frederick Davidorf 1,
The Open Ophthalmology Journal, 2012, 6, 49-53 49 Long-Term Survivors with Metastatic Uveal Melanoma Open Access Dominic M. Buzzacco,1, Mohamed H. Abdel-Rahman,1,2, Stanley Park 1, Frederick Davidorf 1,
Uveal melanoma (UM) is a deadly tumor associated with loss. Genomic Profile of 320 Uveal Melanoma Cases: Chromosome 8p-Loss and Metastatic Outcome
 Genetics Genomic Profile of 320 Uveal Melanoma Cases: Chromosome 8p-Loss and Metastatic Outcome Kathryn G. Ewens, 1 Peter A. Kanetsky, 2 Jennifer Richards-Yutz, 1 Saad Al-Dahmash, 3 Maria Carla De Luca,
Genetics Genomic Profile of 320 Uveal Melanoma Cases: Chromosome 8p-Loss and Metastatic Outcome Kathryn G. Ewens, 1 Peter A. Kanetsky, 2 Jennifer Richards-Yutz, 1 Saad Al-Dahmash, 3 Maria Carla De Luca,
Vitreoretinal surgical management In ocular oncology
 www.ophtalmique.ch Vitreoretinal surgical management In ocular oncology Pournaras Jean-Antoine C Vitreoretinal Surgery Unit 1. Surgical resection after proton beam therapy 2. Ocular Biopsy 3. RD in advanced
www.ophtalmique.ch Vitreoretinal surgical management In ocular oncology Pournaras Jean-Antoine C Vitreoretinal Surgery Unit 1. Surgical resection after proton beam therapy 2. Ocular Biopsy 3. RD in advanced
Prediction of prognosis in patients with uveal melanoma using fluorescence in situ hybridisation
 1440 Department of Surgical and Anaesthetic Sciences, Royal Hallamshire Hospital, SheYeld KAPatel Institute for Cancer Studies, University of SheYeld, SheYeld N D Edmondson Academic Unit of Ophthalmology
1440 Department of Surgical and Anaesthetic Sciences, Royal Hallamshire Hospital, SheYeld KAPatel Institute for Cancer Studies, University of SheYeld, SheYeld N D Edmondson Academic Unit of Ophthalmology
Uveal melanoma is the most common form of primary
 Concurrent Loss of Chromosome Arm 1p and Chromosome 3 Predicts a Decreased Disease-Free Survival in Uveal Melanoma Patients Emine Kilic, 1,2,3 Nicole C. Naus, 1,3 Walter van Gils, 2 Caroline C. Klaver,
Concurrent Loss of Chromosome Arm 1p and Chromosome 3 Predicts a Decreased Disease-Free Survival in Uveal Melanoma Patients Emine Kilic, 1,2,3 Nicole C. Naus, 1,3 Walter van Gils, 2 Caroline C. Klaver,
Development and validation of a patient based measure of outcome in ocular melanoma
 Br J Ophthalmol 2000;84:347 351 347 ORIGINAL ARTICLES Clinical science Queen s Medical Centre, University Hospital, Nottingham AJEFoss Health Services Research Unit, London School of Hygiene and Tropical
Br J Ophthalmol 2000;84:347 351 347 ORIGINAL ARTICLES Clinical science Queen s Medical Centre, University Hospital, Nottingham AJEFoss Health Services Research Unit, London School of Hygiene and Tropical
Routes of Extraocular Extension of Uveal Melanoma
 Routes of Extraocular Extension of Uveal Melanoma Risk Factors and Influence on Survival Probability Sarah E. Coupland, MBBS, PhD, 1 Ian Campbell, MD, FRCS, 2 Bertil Damato, MD, PhD 3 Purpose: To correlate
Routes of Extraocular Extension of Uveal Melanoma Risk Factors and Influence on Survival Probability Sarah E. Coupland, MBBS, PhD, 1 Ian Campbell, MD, FRCS, 2 Bertil Damato, MD, PhD 3 Purpose: To correlate
Uveal melanoma remains the most common primary intraocular. Monosomy 3 Predicts Death but Not Time until Death in Choroidal Melanoma
 Monosomy 3 Predicts Death but Not Time until Death in Choroidal Melanoma Maria T. Sandinha, 1 Maura A. Farquharson, 2 Ian C. McKay, 3 and Fiona Roberts 4 PURPOSE. To study whether monosomy 3 can predict
Monosomy 3 Predicts Death but Not Time until Death in Choroidal Melanoma Maria T. Sandinha, 1 Maura A. Farquharson, 2 Ian C. McKay, 3 and Fiona Roberts 4 PURPOSE. To study whether monosomy 3 can predict
Proton Radiation Therapy of Ocular Melanoma at PSI
 Proton Radiation Therapy of Ocular Melanoma at PSI G. Goitein*, A. Schalenbourg, J. Verwey*, A. Bolsi*, C. Ares*, L. Chamot, E. Hug*, L. Zografos *Paul Scherrer Institut, 5232 Villigen PSI; Hôpital Ophtalmique,
Proton Radiation Therapy of Ocular Melanoma at PSI G. Goitein*, A. Schalenbourg, J. Verwey*, A. Bolsi*, C. Ares*, L. Chamot, E. Hug*, L. Zografos *Paul Scherrer Institut, 5232 Villigen PSI; Hôpital Ophtalmique,
Protocol for the Examination of Specimens From Patients With Uveal Melanoma
 Protocol for the Examination of Specimens From Patients With Uveal Melanoma Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation
Protocol for the Examination of Specimens From Patients With Uveal Melanoma Version: Protocol Posting Date: June 2017 Includes ptnm requirements from the 8 th Edition, AJCC Staging Manual For accreditation
Microvascular Loops and Networks as Prognostic Indicators in Choroidal and Ciliary Body Melanomas
 Microvascular Loops and Networks as Prognostic Indicators in Choroidal and Ciliary Body Melanomas Teemu Mäkitie, Paula Summanen, Ahti Tarkkanen, Tero Kivelä Background: Malignant melanoma of the ciliary
Microvascular Loops and Networks as Prognostic Indicators in Choroidal and Ciliary Body Melanomas Teemu Mäkitie, Paula Summanen, Ahti Tarkkanen, Tero Kivelä Background: Malignant melanoma of the ciliary
Can Protons replace Eye Brachytherapy? 1 Department of Radiation Oncology
 Can Protons replace Eye Brachytherapy? Richard Pötter 1,2, Roman Dunavölgyi 3, Karin Dieckmann 1, Dietmar Georg 1,2 1 Department of Radiation Oncology 2 Christian Doppler Laboratory for Medical Radiation
Can Protons replace Eye Brachytherapy? Richard Pötter 1,2, Roman Dunavölgyi 3, Karin Dieckmann 1, Dietmar Georg 1,2 1 Department of Radiation Oncology 2 Christian Doppler Laboratory for Medical Radiation
Mesectodermal suprauveal iridociliary leiomyoma: Transscleral excision without postoperative iris defect
 4 Chapter Mesectodermal suprauveal iridociliary leiomyoma: Transscleral excision without postoperative iris defect Lubna Razzaq 1, Ekaterina A Semenova 2, Marina Marinkovic 1, Rob JW de Keizer 1, Sjoerd
4 Chapter Mesectodermal suprauveal iridociliary leiomyoma: Transscleral excision without postoperative iris defect Lubna Razzaq 1, Ekaterina A Semenova 2, Marina Marinkovic 1, Rob JW de Keizer 1, Sjoerd
Gene Expression Profiling for Melanoma
 Medical Policy Manual Genetic Testing, Policy No. 29 Gene Expression Profiling for Melanoma Next Review: April 2019 Last Review: April 2018 Effective: June 1, 2018 IMPORTANT REMINDER Medical Policies are
Medical Policy Manual Genetic Testing, Policy No. 29 Gene Expression Profiling for Melanoma Next Review: April 2019 Last Review: April 2018 Effective: June 1, 2018 IMPORTANT REMINDER Medical Policies are
FEP Medical Policy Manual
 FEP Medical Policy Manual Last Review: December 2016 Effective Date: January 15, 2017 Related Policies None Gene Expression Profiling for Uveal Melanoma Summary Uveal melanoma is associated with a high
FEP Medical Policy Manual Last Review: December 2016 Effective Date: January 15, 2017 Related Policies None Gene Expression Profiling for Uveal Melanoma Summary Uveal melanoma is associated with a high
UVEAL MELANOMA: THE PAST, THE PRESENT
 THE ASHTON LECTURE UVEAL MELANOMA: THE PAST, THE PRESENT AND THE FUTURE IAN G. RENNIE Sheffield Uveal melanomas are the most common primary intraocular neoplasm in adults. 1 In spite of this, most general
THE ASHTON LECTURE UVEAL MELANOMA: THE PAST, THE PRESENT AND THE FUTURE IAN G. RENNIE Sheffield Uveal melanomas are the most common primary intraocular neoplasm in adults. 1 In spite of this, most general
Enhancing survival prognostication in. integrating pathologic, clinical and genetic predictors of metastasis
 The Royal Liverpool and Broadgreen University Hospitals NHS Trust NHS Enhancing survival prognostication in patients with choroidal melanoma by integrating pathologic, clinical and genetic predictors of
The Royal Liverpool and Broadgreen University Hospitals NHS Trust NHS Enhancing survival prognostication in patients with choroidal melanoma by integrating pathologic, clinical and genetic predictors of
Management and Outcome of Uveal Melanoma in a Single Tertiary Cancer Center in Jordan
 Original Article doi:./tjpath.. Management and Outcome of Uveal Melanoma in a Single Tertiary Cancer Center in Jordan Ahmed Zewar, Ibrahim Nawaiseh, Imad Jaradat, Jakub Khzouz, Khaleel AlRawashdeh, Ghadeer
Original Article doi:./tjpath.. Management and Outcome of Uveal Melanoma in a Single Tertiary Cancer Center in Jordan Ahmed Zewar, Ibrahim Nawaiseh, Imad Jaradat, Jakub Khzouz, Khaleel AlRawashdeh, Ghadeer
National Guidelines for the management of uveal melanoma. Sponsored by Melanoma Focus
 National Guidelines for the management of uveal melanoma Sponsored by Melanoma Focus GDG Members Paul Nathan (Chair Oncologist Mt Vernon) Kieran McGuirk (Ocumel) Lesley Kirkpatrick (Ocumel) Kathryn Curtis
National Guidelines for the management of uveal melanoma Sponsored by Melanoma Focus GDG Members Paul Nathan (Chair Oncologist Mt Vernon) Kieran McGuirk (Ocumel) Lesley Kirkpatrick (Ocumel) Kathryn Curtis
Advances in Ocular Imaging
 Wide angle fundus imaging and Fuorescein angiography in evaluation and management of intraocular tumors Ihab Saad Othman, MD, FRCS Professor of Ophthalmology Cairo University Cairo, Egypt Advances in Ocular
Wide angle fundus imaging and Fuorescein angiography in evaluation and management of intraocular tumors Ihab Saad Othman, MD, FRCS Professor of Ophthalmology Cairo University Cairo, Egypt Advances in Ocular
The growth, progression, and metastasis of cancer depend
 Microvascular Density in redicting Survival of atients with Choroidal and Ciliary Body Melanoma Teemu Mäkitie, aula Summanen, Ahti Tarkkanen, and Tero Kivelä UROSE. Although malignant uveal melanoma disseminates
Microvascular Density in redicting Survival of atients with Choroidal and Ciliary Body Melanoma Teemu Mäkitie, aula Summanen, Ahti Tarkkanen, and Tero Kivelä UROSE. Although malignant uveal melanoma disseminates
M alignant melanoma of the uvea causes clinical metastases
 333 CLINICAL SCIENCE Mode of presentation and time to treatment of uveal melanoma in Finland S Eskelin, T Kivelä... See end of article for authors affiliations... Correspondence to: Sebastian Eskelin,
333 CLINICAL SCIENCE Mode of presentation and time to treatment of uveal melanoma in Finland S Eskelin, T Kivelä... See end of article for authors affiliations... Correspondence to: Sebastian Eskelin,
radiotherapy Treatment of non-resectable malignant iris tumours with custom designed plaque n551 cgy ORIGINAL ARTICLES - Clinical science
 306 British Journal of Ophthalmology 1995; 79: 306-312 ORIGINAL ARTICLES - Clinical science Ocular Oncology Service, Wills Eye Hospital, Thomas Jefferson University, Philadelphia, USA C L Shields J A Shields
306 British Journal of Ophthalmology 1995; 79: 306-312 ORIGINAL ARTICLES - Clinical science Ocular Oncology Service, Wills Eye Hospital, Thomas Jefferson University, Philadelphia, USA C L Shields J A Shields
Continuing Medical Education
 Continuing Medical Education The Department of Radiation Oncology offers free Continuing Medical Education credit to readers who read the designated CME article and successfully complete a follow-up test
Continuing Medical Education The Department of Radiation Oncology offers free Continuing Medical Education credit to readers who read the designated CME article and successfully complete a follow-up test
Ruthenium-106 plaque brachytherapy in the primary management of ocular medulloepithelioma
 Poon, DS; Reich, E; Smith, VM; Kingston, J; Reddy, MA; Hungerford, JL; Sagoo, MS; (2015) Ruthenium-106 Plaque Brachytherapy in the Primary Management of Ocular Medulloepithelioma. Ophthalmology, 122 (9)
Poon, DS; Reich, E; Smith, VM; Kingston, J; Reddy, MA; Hungerford, JL; Sagoo, MS; (2015) Ruthenium-106 Plaque Brachytherapy in the Primary Management of Ocular Medulloepithelioma. Ophthalmology, 122 (9)
ABOUT 50% OF PATIENTS
 CLINICAL SCIENCES Translating Uveal Melanoma Cytogenetics Into Clinical Care Bertil Damato, MD, PhD, FRCOphth; Sarah E. Coupland, MBBS, PhD, FRCPath Objective: To report our experience in translating uveal
CLINICAL SCIENCES Translating Uveal Melanoma Cytogenetics Into Clinical Care Bertil Damato, MD, PhD, FRCOphth; Sarah E. Coupland, MBBS, PhD, FRCPath Objective: To report our experience in translating uveal
Local Recurrence Significantly Increases the Risk of Metastatic Uveal Melanoma
 Local Recurrence Significantly Increases the Risk of Metastatic Uveal Melanoma The Ophthalmic Oncology Task Force Purpose: To assess of the effect of local recurrence of uveal melanoma on metastasis using
Local Recurrence Significantly Increases the Risk of Metastatic Uveal Melanoma The Ophthalmic Oncology Task Force Purpose: To assess of the effect of local recurrence of uveal melanoma on metastasis using
Case Study. Monocular Malignant Melanoma
 Case Study Monocular Malignant Melanoma Case History A 52 year old Caucasian female presented with a number of naevi on the skin and a right ciliary body malignant melanoma twelve years ago and had an
Case Study Monocular Malignant Melanoma Case History A 52 year old Caucasian female presented with a number of naevi on the skin and a right ciliary body malignant melanoma twelve years ago and had an
PROTON BEAM RADIOTHERAPY OF IRIS MELANOMA
 doi:10.1016/j.ijrobp.2005.01.050 Int. J. Radiation Oncology Biol. Phys., Vol. 63, No. 1, pp. 109 115, 2005 Copyright 2005 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/05/$ see front
doi:10.1016/j.ijrobp.2005.01.050 Int. J. Radiation Oncology Biol. Phys., Vol. 63, No. 1, pp. 109 115, 2005 Copyright 2005 Elsevier Inc. Printed in the USA. All rights reserved 0360-3016/05/$ see front
Systemic and ocular follow-up after conservative management of an intraocular tumor
 Systemic and ocular follow-up after conservative management of an intraocular tumor 7 th Thessaloniki international Vitreo Retinal Summer School,26.6-1.7.2017 L. Zografos MD Jules Gonin Eye Hospital Periodic
Systemic and ocular follow-up after conservative management of an intraocular tumor 7 th Thessaloniki international Vitreo Retinal Summer School,26.6-1.7.2017 L. Zografos MD Jules Gonin Eye Hospital Periodic
FEP Medical Policy Manual
 FEP Medical Policy Manual Effective Date: July 15, 2018 Related Policies: 8.01.10 Charged-Particle (Proton or Helium Ion) Radiotherapy for Neoplastic Conditions Gene Expression Profiling for Uveal Melanoma
FEP Medical Policy Manual Effective Date: July 15, 2018 Related Policies: 8.01.10 Charged-Particle (Proton or Helium Ion) Radiotherapy for Neoplastic Conditions Gene Expression Profiling for Uveal Melanoma
A Prognostic Model and Staging for Metastatic Uveal Melanoma. BACKGROUND. To identify factors that independently contribute to overall survival
 465 A Prognostic Model and Staging for Metastatic Uveal Melanoma Sebastian Eskelin, M.D. 1 Seppo Pyrhönen, M.D. 2 Marjo Hahka-Kemppinen, M.D. 3 Seppo Tuomaala, M.D. 1 Tero Kivelä, M.D. 1 1 Ophthalmic Oncology
465 A Prognostic Model and Staging for Metastatic Uveal Melanoma Sebastian Eskelin, M.D. 1 Seppo Pyrhönen, M.D. 2 Marjo Hahka-Kemppinen, M.D. 3 Seppo Tuomaala, M.D. 1 Tero Kivelä, M.D. 1 1 Ophthalmic Oncology
Corporate Medical Policy
 Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
Corporate Medical Policy File Name: Origination: Last CAP Review: Next CAP Review: Last Review: charged_particle_radiotherapy 3/12/96 5/2017 5/2018 5/2017 Description of Procedure or Service Charged-particle
Case Rep Oncol 2012;5: DOI: /
 This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
This is an Open Access article licensed under the terms of the Creative Commons Attribution-NonCommercial-NoDerivs 3.0 License (www.karger.com/oa-license), applicable to the online version of the article
Retinoblastoma. Protocol applies to retinoblastoma only.
 Retinoblastoma Protocol applies to retinoblastoma only. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
Retinoblastoma Protocol applies to retinoblastoma only. Protocol revision date: January 2005 Based on AJCC/UICC TNM, 6 th edition Procedures Cytology (No Accompanying Checklist) Biopsy (No Accompanying
CLINICAL SCIENCES. Three-Dimensional Ultrasound for the Measurement of Choroidal Melanomas
 CLINICAL SCIENCES Three-Dimensional Ultrasound for the Measurement of Choroidal Melanomas Juan M. Romero, MD; Paul T. Finger, MD; Richard B. Rosen, MD; Raymond Iezzi, MD Objective: To evaluate the reliability
CLINICAL SCIENCES Three-Dimensional Ultrasound for the Measurement of Choroidal Melanomas Juan M. Romero, MD; Paul T. Finger, MD; Richard B. Rosen, MD; Raymond Iezzi, MD Objective: To evaluate the reliability
M ALIGNANT MELANOMA OF THE UVEA STAGING FORM
 CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX T0 a a a d b c d a TUMOR SIZE: S TAGE C ATEGORY D EFINITIONS LATERALITY:
CLINICAL Extent of disease before any treatment y clinical staging completed after neoadjuvant therapy but before subsequent surgery TX T0 a a a d b c d a TUMOR SIZE: S TAGE C ATEGORY D EFINITIONS LATERALITY:
Genotypic Profiling of 452 Choroidal Melanomas with Multiplex Ligation-Dependent Probe Amplification
 Imaging, Diagnosis, Prognosis Clinical Cancer Research Genotypic Profiling of 452 Choroidal Melanomas with Multiplex Ligation-Dependent Probe Amplification Bertil Damato 1, Justyna A. Dopierala 2, and
Imaging, Diagnosis, Prognosis Clinical Cancer Research Genotypic Profiling of 452 Choroidal Melanomas with Multiplex Ligation-Dependent Probe Amplification Bertil Damato 1, Justyna A. Dopierala 2, and
Enhancing survival prognostication in patients with choroidal melanoma by integrating pathologic, clinical and genetic predictors of metastasis
 18 Int. J. Biomedical Engineering and Technology, Vol. 8, No. 1, 2012 Enhancing survival prognostication in patients with choroidal melanoma by integrating pathologic, clinical and genetic predictors of
18 Int. J. Biomedical Engineering and Technology, Vol. 8, No. 1, 2012 Enhancing survival prognostication in patients with choroidal melanoma by integrating pathologic, clinical and genetic predictors of
CLINICAL SCIENCES. Pretreatment Characteristics and Response to Plaque Radiation Therapy
 CLINICAL SCIENCES Subfoveal Choroidal Melanoma Pretreatment Characteristics and Response to Plaque Radiation Therapy Hadas Newman, MD; Kimberly J. Chin, OD; Paul T. Finger, MD Objective: To evaluate the
CLINICAL SCIENCES Subfoveal Choroidal Melanoma Pretreatment Characteristics and Response to Plaque Radiation Therapy Hadas Newman, MD; Kimberly J. Chin, OD; Paul T. Finger, MD Objective: To evaluate the
Characteristic Ultrasonographic Findings of Choroidal Tumors
 Characteristic Ultrasonographic Findings of Choroidal Tumors Tsung-Jen Wang, Chang-Hao Yang, Shu-Lang Liao, Tzyy-Chang Ho, Jen-Shang Huang, Chang-Ping Lin, Chung-May Yang, Muh-Shy Chen and Luke Long-Kuang
Characteristic Ultrasonographic Findings of Choroidal Tumors Tsung-Jen Wang, Chang-Hao Yang, Shu-Lang Liao, Tzyy-Chang Ho, Jen-Shang Huang, Chang-Ping Lin, Chung-May Yang, Muh-Shy Chen and Luke Long-Kuang
Outline. Brief history and principles of ophthalmic ultrasound. Types of ocular ultrasound. Examination techniques. Types of Ultrasound
 Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
Ultrasound and Intraocular Tumors 2015 Ophthalmic Photographers' Society Mid-Year Program Cagri G. Besirli MD, PhD Kellogg Eye Center University of Michigan Outline Brief history and principles of ophthalmic
Medical Policy An independent licensee of the Blue Cross Blue Shield Association
 Gene Expression Profiling for Uveal Melanoma Page 1 of 14 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Gene Expression Profiling for Uveal Melanoma Professional
Gene Expression Profiling for Uveal Melanoma Page 1 of 14 Medical Policy An independent licensee of the Blue Cross Blue Shield Association Title: Gene Expression Profiling for Uveal Melanoma Professional
Primary iris melanoma: diagnostic features and outcome of conservative surgical treatment
 848 Save Sight Institute and Department of Clinical Ophthalmology, University of Sydney, Sydney, Australia R M Conway W C-T Chua C Qureshi F A Billson Correspondence to: Dr Conway, Department of Clinical
848 Save Sight Institute and Department of Clinical Ophthalmology, University of Sydney, Sydney, Australia R M Conway W C-T Chua C Qureshi F A Billson Correspondence to: Dr Conway, Department of Clinical
Factory loaded, sterilized, ready to implant plaques:!
 in partnership with Factory loaded, sterilized, ready to implant plaques: Eye Physics plaques. 2 nd generation plaques (cast in 18K gold from hand carved wax prototypes). 3 rd generation plaques (cast
in partnership with Factory loaded, sterilized, ready to implant plaques: Eye Physics plaques. 2 nd generation plaques (cast in 18K gold from hand carved wax prototypes). 3 rd generation plaques (cast
An Interactive TreatmentPlanning System For Ophthalmic Plaque Radiotherapy
 An Interactive TreatmentPlanning System For Ophthalmic Plaque Radiotherapy Melvin A. Astrahan, PH.D.,¹ Gary Luxton, PH.D.,¹ Gabor Jozsef, PH.D.,¹ Thomas D. Kampp, PH.D.,¹ Peter E. Liggett, M.D.,² Michael
An Interactive TreatmentPlanning System For Ophthalmic Plaque Radiotherapy Melvin A. Astrahan, PH.D.,¹ Gary Luxton, PH.D.,¹ Gabor Jozsef, PH.D.,¹ Thomas D. Kampp, PH.D.,¹ Peter E. Liggett, M.D.,² Michael
Surveillance following treatment of primary ocular melanoma
 Surveillance following treatment of primary ocular melanoma Introduction 50% of UM patients relapse with predominantly liver metastases Risk of metastatic disease can be predicted relatively accurately
Surveillance following treatment of primary ocular melanoma Introduction 50% of UM patients relapse with predominantly liver metastases Risk of metastatic disease can be predicted relatively accurately
V.M.L. COHEN, S. DINAKARAN, M.A. PARSONS, I.G. RENNIE
 Transvitreal fine needle aspiration biopsy: the V.M.L. COHEN, S. DINAKARAN, M.A. PARSONS, I.G. RENNIE influence of intraocular lesion size on diagnostic biopsy resu It Abstract Purpose To detennine the
Transvitreal fine needle aspiration biopsy: the V.M.L. COHEN, S. DINAKARAN, M.A. PARSONS, I.G. RENNIE influence of intraocular lesion size on diagnostic biopsy resu It Abstract Purpose To detennine the
Does ocular treatment of uveal melanoma influence survival?
 British Journal of Cancer (2) 3, 285 29 All rights reserved 7 92/ www.bjcancer.com Minireview Does ocular treatment of uveal melanoma influence survival? *,1 1 Ocular Oncology Service, Royal Liverpool
British Journal of Cancer (2) 3, 285 29 All rights reserved 7 92/ www.bjcancer.com Minireview Does ocular treatment of uveal melanoma influence survival? *,1 1 Ocular Oncology Service, Royal Liverpool
ACTIVATED OR NOT? RETINAL CASE PRESENTATION Shorye Payne, MD Medical Retinal Specialist Robley Rex VA Eye Clinic
 ACTIVATED OR NOT? RETINAL CASE PRESENTATION Shorye Payne, MD Medical Retinal Specialist Robley Rex VA Eye Clinic C We anticipate that the future management of posterior uveal melanoma (PUM) will focus
ACTIVATED OR NOT? RETINAL CASE PRESENTATION Shorye Payne, MD Medical Retinal Specialist Robley Rex VA Eye Clinic C We anticipate that the future management of posterior uveal melanoma (PUM) will focus
Metastasis of choroidal melanoma to the contralateral
 British Journal of Ophthalmology, 1988, 72, 456-460 Metastasis of choroidal melanoma to the contralateral choroid, orbit, and eyelid* JERRY A SHIELDS,' CAROL L SHIELDS,' ERIC P SHAKIN,' AND LARRY E KOBETZ2
British Journal of Ophthalmology, 1988, 72, 456-460 Metastasis of choroidal melanoma to the contralateral choroid, orbit, and eyelid* JERRY A SHIELDS,' CAROL L SHIELDS,' ERIC P SHAKIN,' AND LARRY E KOBETZ2
Episcleral plaque brachytherapy has been proposed as an
 Effect of Radiation Dose on Ocular Complications after Iodine Brachytherapy for Large Uveal Melanoma: Empirical Data and Simulation of Collimating Plaques Ilkka Puusaari, 1 Jorma Heikkonen, 2 and Tero
Effect of Radiation Dose on Ocular Complications after Iodine Brachytherapy for Large Uveal Melanoma: Empirical Data and Simulation of Collimating Plaques Ilkka Puusaari, 1 Jorma Heikkonen, 2 and Tero
Survival from uveal melanoma in England and Wales 1986 to 2001
 This is an electronic version of an article published in Ophthalmic Epidemiology 2007;14(1):3-8. Ophthalmic Epidemiology is avialable online at: http://www.informaworld.com/smpp/content~content=a772114190~db=all~order=page
This is an electronic version of an article published in Ophthalmic Epidemiology 2007;14(1):3-8. Ophthalmic Epidemiology is avialable online at: http://www.informaworld.com/smpp/content~content=a772114190~db=all~order=page
Research Article Outcomes and Control Rates for I-125 Plaque Brachytherapy for Uveal Melanoma: A Community-Based Institutional Experience
 ISRN Ophthalmology, Article ID 95975, 7 pages http://dx.doi.org/1.1155/214/95975 Research Article Outcomes and Control Rates for I-125 Plaque Brachytherapy for Uveal Melanoma: A Community-Based Institutional
ISRN Ophthalmology, Article ID 95975, 7 pages http://dx.doi.org/1.1155/214/95975 Research Article Outcomes and Control Rates for I-125 Plaque Brachytherapy for Uveal Melanoma: A Community-Based Institutional
Size Overlap between Benign Melanocytic Choroidal Nevi and Choroidal Malignant Melanomas
 Size Overlap between Benign Melanocytic Choroidal Nevi and Choroidal Malignant Melanomas James J. Augsburger, Zélia M. Corrêa, Nikolaos Trichopoulos, and Adeel Shaikh PURPOSE. To estimate size overlap
Size Overlap between Benign Melanocytic Choroidal Nevi and Choroidal Malignant Melanomas James J. Augsburger, Zélia M. Corrêa, Nikolaos Trichopoulos, and Adeel Shaikh PURPOSE. To estimate size overlap
Ciliary Body Metastasis Masquerading as Scleritis. Brian J. Lee, MD 1. Careen Y. Lowder, MD, PhD 1. Charles Biscotti, MD 2. Lynn Schoenfield, MD 2
 Ciliary Body Metastasis Masquerading as Scleritis Brian J. Lee, MD 1 Careen Y. Lowder, MD, PhD 1 Charles Biscotti, MD 2 Lynn Schoenfield, MD 2 Arun D. Singh, MD 1 Cole Eye Institute 1 and Department of
Ciliary Body Metastasis Masquerading as Scleritis Brian J. Lee, MD 1 Careen Y. Lowder, MD, PhD 1 Charles Biscotti, MD 2 Lynn Schoenfield, MD 2 Arun D. Singh, MD 1 Cole Eye Institute 1 and Department of
C ancer cells require a great deal of sugar (glucose) for. PET/CT imaging: detection of choroidal melanoma SCIENTIFIC REPORT
 265 SCIENTIFIC REPORT PET/CT imaging: detection of choroidal melanoma S Reddy, M Kurli, L B Tena, P T Finger... Aim: To determine the size of untreated choroidal melanomas resolved by whole body positron
265 SCIENTIFIC REPORT PET/CT imaging: detection of choroidal melanoma S Reddy, M Kurli, L B Tena, P T Finger... Aim: To determine the size of untreated choroidal melanomas resolved by whole body positron
CHAPTER 4 PREDICTIVE VALUE OF EXFOLIATIVE CYTOL- OGY IN PIGMENTED CONJUNCTIVAL LESIONS
 CHAPTER 4 PREDICTIVE VALUE OF EXFOLIATIVE CYTOL- OGY IN PIGMENTED CONJUNCTIVAL LESIONS Acta Ophthalmologica Scandinavica 26;84:88-9. S. Keijser, C.M. van Luijk, G.S. Missotten, M. Veselic-Charvat, 2 D.
CHAPTER 4 PREDICTIVE VALUE OF EXFOLIATIVE CYTOL- OGY IN PIGMENTED CONJUNCTIVAL LESIONS Acta Ophthalmologica Scandinavica 26;84:88-9. S. Keijser, C.M. van Luijk, G.S. Missotten, M. Veselic-Charvat, 2 D.
Uveal melanoma: therapeutic consequences of doubling times and irradiation results; a review
 International Ophthalmology 16: 91-99, 1992. 9 1992 Kluwer Academic Publishers. Printed in the Netherlands. Uveal melanoma: therapeutic consequences of doubling times and irradiation results; a review
International Ophthalmology 16: 91-99, 1992. 9 1992 Kluwer Academic Publishers. Printed in the Netherlands. Uveal melanoma: therapeutic consequences of doubling times and irradiation results; a review
Exudative retinal detachment (RD) is detected clinically in
 Exudative Retinal Detachment from Malignant Uveal Melanoma: Predictors and Prognostic Significance Tero Kivelä, 1,2 Sebastian Eskelin, 1 Teemu Mäkitie, 2 and Paula Summanen 1 PURPOSE. To determine independent
Exudative Retinal Detachment from Malignant Uveal Melanoma: Predictors and Prognostic Significance Tero Kivelä, 1,2 Sebastian Eskelin, 1 Teemu Mäkitie, 2 and Paula Summanen 1 PURPOSE. To determine independent
Relationship of regression pattern to recurrence in retinoblastoma
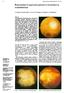 12 BritishJournal ofophthalmology 1993; 77: 12-16 Relationship of regression pattern to recurrence in retinoblastoma A D Singh, D Garway-Heath, S Love, P N Plowman, J Kingston, J L Hungerford Ophthalmology
12 BritishJournal ofophthalmology 1993; 77: 12-16 Relationship of regression pattern to recurrence in retinoblastoma A D Singh, D Garway-Heath, S Love, P N Plowman, J Kingston, J L Hungerford Ophthalmology
CLINICAL SCIENCES. Conclusions: A distinctive postbrachytherapy regression
 horoidal Melanomas With a ollar-utton onfiguration Response Pattern fter Iodine 125 rachytherapy Dennis M. Robertson, MD LINIL SIENES Objective: To describe a distinctive type of postbrachytherapy response
horoidal Melanomas With a ollar-utton onfiguration Response Pattern fter Iodine 125 rachytherapy Dennis M. Robertson, MD LINIL SIENES Objective: To describe a distinctive type of postbrachytherapy response
Progression of Cutaneous Vitiligo in a Patient with Large Posterior Choroidal Melanoma: A Case Report
 Received: November 27, 2014 Accepted after revision: January 28, 2015 Published online: April 1, 2015 2296 4681/15/0014 0241$39.50/0 Case Series and Brief Reports Progression of Cutaneous Vitiligo in a
Received: November 27, 2014 Accepted after revision: January 28, 2015 Published online: April 1, 2015 2296 4681/15/0014 0241$39.50/0 Case Series and Brief Reports Progression of Cutaneous Vitiligo in a
Standards and datasets for reporting cancers. December 2017
 Standards and datasets for reporting cancers Dataset for histopathological reporting of uveal melanoma December 2017 Authors: Dr Hardeep Singh Mudhar, Royal Hallamshire Hospital, Sheffield Professor Sarah
Standards and datasets for reporting cancers Dataset for histopathological reporting of uveal melanoma December 2017 Authors: Dr Hardeep Singh Mudhar, Royal Hallamshire Hospital, Sheffield Professor Sarah
Prognostication in UM
 Prognostication in UM Prognostication in UM 1. Is there a preferred prognostic tool? 2. What is the role of prognostic biopsy? Prognostic parameters in uveal melanoma Clinical Histomorphological Immunohistochemical
Prognostication in UM Prognostication in UM 1. Is there a preferred prognostic tool? 2. What is the role of prognostic biopsy? Prognostic parameters in uveal melanoma Clinical Histomorphological Immunohistochemical
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING
 PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
PEDIATRIC ORBITAL TUMORS RADIOTHERAPY PLANNING ANATOMY ANATOMY CONT ANATOMY CONT. ANATOMY CONT. EYE OF A CHILD Normal tissue tolerance doses (in conventional #) TD 5/5 TD 50/5 Endpoint Gy Gy Optic nerve
Asadi-Amoli et al Adenocarcinoma of RPE Iranian Journal of Ophthalmology - Volume 19, Number 4, 2007
 Adenocarcinoma of Retinal Pigment Epithelium Clinically Diagnosed as Malignant Melanoma; A Case Report with Unsystematic Review of Literature Fahimeh Asadi-Amoli, MD, 1 Hedyeh Moradi, MD 2 Mohammad-Taher
Adenocarcinoma of Retinal Pigment Epithelium Clinically Diagnosed as Malignant Melanoma; A Case Report with Unsystematic Review of Literature Fahimeh Asadi-Amoli, MD, 1 Hedyeh Moradi, MD 2 Mohammad-Taher
Supplementary appendix
 Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Callegaro D, Miceli R, Bonvalot S, et al. Development
Supplementary appendix This appendix formed part of the original submission and has been peer reviewed. We post it as supplied by the authors. Supplement to: Callegaro D, Miceli R, Bonvalot S, et al. Development
Radiotherapy of choroidal metastases 1
 Radiotherapy and Oncology 46 (1998) 263 268 Radiotherapy of choroidal metastases 1 Anna Rosset a, *, Leonidas Zografos b, Philippe Coucke a, May Monney a, René O. Mirimanoff a a Department of Radiation
Radiotherapy and Oncology 46 (1998) 263 268 Radiotherapy of choroidal metastases 1 Anna Rosset a, *, Leonidas Zografos b, Philippe Coucke a, May Monney a, René O. Mirimanoff a a Department of Radiation
Complicated Cataract to Intraocular Tumors, Beware of the unexpected
 Complicated Cataract to Intraocular Tumors, Beware of the unexpected Ihab Saad Othman, MD, FRCS Professor of Ophthalmology Cairo University In this part of the world: We Master Phakoemulsification 1 Intraoperative/Second
Complicated Cataract to Intraocular Tumors, Beware of the unexpected Ihab Saad Othman, MD, FRCS Professor of Ophthalmology Cairo University In this part of the world: We Master Phakoemulsification 1 Intraoperative/Second
DIAGNOSTIC TRANSVITREAL FINE-NEEDLE ASPIRATION BIOPSY OF SMALL MELANOCYTIC CHOROIDAL TUMORS IN NEVUS VERSUS MELANOMA CATEGORY
 DIAGNOSTIC TRANSVITREAL FINE-NEEDLE ASPIRATION BIOPSY OF SMALL MELANOCYTIC CHOROIDAL TUMORS IN NEVUS VERSUS MELANOMA CATEGORY BY James J. Augsburger, MD, Zélia M. Corrêa, MD (BY INVITATION), Susan Schneider,
DIAGNOSTIC TRANSVITREAL FINE-NEEDLE ASPIRATION BIOPSY OF SMALL MELANOCYTIC CHOROIDAL TUMORS IN NEVUS VERSUS MELANOMA CATEGORY BY James J. Augsburger, MD, Zélia M. Corrêa, MD (BY INVITATION), Susan Schneider,
J of Evolution of Med and Dent Sci/ eissn , pissn / Vol. 4/ Issue 55/ July 09, 2015 Page 9665
 RARE PRESENTATION OF BILATERAL CHOROIDAL METASTASIS FROM PRIMARY MUCO-EPIDERMOID CARCINOMA OF THE PAROTID GLAND: A G. Premalatha 1, Ramya Seetamraju 2 HOW TO CITE THIS ARTICLE: G. Premalatha, Ramya Seetamraju.
RARE PRESENTATION OF BILATERAL CHOROIDAL METASTASIS FROM PRIMARY MUCO-EPIDERMOID CARCINOMA OF THE PAROTID GLAND: A G. Premalatha 1, Ramya Seetamraju 2 HOW TO CITE THIS ARTICLE: G. Premalatha, Ramya Seetamraju.
Ocular Neoplasia What s Common? What s New? Richard R Dubielzig
 Ocular Neoplasia What s Common? What s New? Richard R Dubielzig Orbit 288 6% Tumors of the globe make up 3225 out of 6110 total neoplasms = 53%. Tumors of the conjunctiva make up 1192 out of 6110 total
Ocular Neoplasia What s Common? What s New? Richard R Dubielzig Orbit 288 6% Tumors of the globe make up 3225 out of 6110 total neoplasms = 53%. Tumors of the conjunctiva make up 1192 out of 6110 total
Confidence intervals for the interaction contrast ratio: A simple solution with SAS PROC NLMIXED and SAS PROC NLP
 Type of manuscript: Research Letter Confidence intervals for the interaction contrast ratio: A simple solution with SAS PROC NLMIXED and SAS PROC NLP Oliver Kuss 1, Andrea Schmidt-Pokrzywniak 2, Andreas
Type of manuscript: Research Letter Confidence intervals for the interaction contrast ratio: A simple solution with SAS PROC NLMIXED and SAS PROC NLP Oliver Kuss 1, Andrea Schmidt-Pokrzywniak 2, Andreas
Pseudohypopyon in Retinoblastoma. Choroidal Nevus. Masquerade Syndromes. Vision pathways. Flat with uniform color
 Primary Intraocular Tumors Thomas F. Freddo, O.D., Ph.D., F.A.A.O. Professor and Former Director School of Optometry University of Waterloo Masquerade Syndromes
Primary Intraocular Tumors Thomas F. Freddo, O.D., Ph.D., F.A.A.O. Professor and Former Director School of Optometry University of Waterloo Masquerade Syndromes
DECISIONDx BIOMARKER TESTS
 DECISIONDx BIOMARKER TESTS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
DECISIONDx BIOMARKER TESTS Non-Discrimination Statement and Multi-Language Interpreter Services information are located at the end of this document. Coverage for services, procedures, medical devices and
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience. Kevin Yiee MD, MPH Resident Physician
 Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
Sacral Chordoma: The Loma Linda University Radiation Medicine Experience Kevin Yiee MD, MPH Resident Physician What is a chordoma? 1 st chordoma discovered in clivus by Virchow and Luschka 1856 Rare tumor
points causes features therapy collaborative ocular melanoma study prognosis Choroid Nevus
 The Game of Uveal Melanoma Carol Shields MD Oncology Service Wills Eye Hospital Philadelphia PA USA www.fighteyecancer.com Oncology Service Wills Eye Institute points causes features therapy collaborative
The Game of Uveal Melanoma Carol Shields MD Oncology Service Wills Eye Hospital Philadelphia PA USA www.fighteyecancer.com Oncology Service Wills Eye Institute points causes features therapy collaborative
Gene Expression Profiling for Uveal Melanoma
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Continuing Medical Education: Primary photodynamic therapy with verteporfin for small pigmented posterior pole choroidal melanoma
 (2017) 31, 519 528 2017 Macmillan Publishers Limited, part of Springer Nature. All rights reserved 0950-222X/17 www.nature.com/eye Continuing Medical Education: Primary photodynamic therapy with verteporfin
(2017) 31, 519 528 2017 Macmillan Publishers Limited, part of Springer Nature. All rights reserved 0950-222X/17 www.nature.com/eye Continuing Medical Education: Primary photodynamic therapy with verteporfin
MATERIALS AND METHODS
 A R T I C L E S Detection of c-myc Amplification in Uveal Melanoma by Fluorescent In Situ Hybridization Paola Parrella, 1,2 Otavia L. Caballero, 2 David Sidransky, 2 and Shannath L. Merbs 3 PURPOSE. Genetic
A R T I C L E S Detection of c-myc Amplification in Uveal Melanoma by Fluorescent In Situ Hybridization Paola Parrella, 1,2 Otavia L. Caballero, 2 David Sidransky, 2 and Shannath L. Merbs 3 PURPOSE. Genetic
MATERIALS AND METHODS
 Incidence of Uveal Melanoma in Sweden from 1960 to 1998 Louise Bergman, 1 Stefan Seregard, 1 Bo Nilsson, 2 Ulrik Ringborg, 2 Göran Lundell, 2 and Boel Ragnarsson-Olding 2 PURPOSE. To investigate the incidence
Incidence of Uveal Melanoma in Sweden from 1960 to 1998 Louise Bergman, 1 Stefan Seregard, 1 Bo Nilsson, 2 Ulrik Ringborg, 2 Göran Lundell, 2 and Boel Ragnarsson-Olding 2 PURPOSE. To investigate the incidence
Visual Acuity, Contrast Sensitivity and Color Vision Three Years After Iodine-125 Brachytherapy for Choroidal and Ciliary Body Melanoma
 Send Orders for Reprints to reprints@benthamscience.ae The Open Ophthalmology Journal, 2015, 9, 131-135 131 Open Access Visual Acuity, Contrast Sensitivity and Color Vision Three Years After Iodine-125
Send Orders for Reprints to reprints@benthamscience.ae The Open Ophthalmology Journal, 2015, 9, 131-135 131 Open Access Visual Acuity, Contrast Sensitivity and Color Vision Three Years After Iodine-125
PC-10 as a Predictor of Prognosis After Antigen Retrieval in Posterior Uveal Melanoma
 PC-10 as a Predictor of Prognosis After Antigen Retrieval in Posterior Uveal Melanoma Stefan Seregard, Margareta Oskarsson, and Berit Spdngberg Purpose. The immunoexpression of the PC-10 monoclonal antibody
PC-10 as a Predictor of Prognosis After Antigen Retrieval in Posterior Uveal Melanoma Stefan Seregard, Margareta Oskarsson, and Berit Spdngberg Purpose. The immunoexpression of the PC-10 monoclonal antibody
Pigmented lesions of the
 Pigmented lesions of the choroid and retina are commonly encountered by optometrists in everyday practice. The increasing use of retinal imaging and indirect ophthalmoscopy among community optometrists
Pigmented lesions of the choroid and retina are commonly encountered by optometrists in everyday practice. The increasing use of retinal imaging and indirect ophthalmoscopy among community optometrists
Carlo Mosci. Ocular Oncology Service Galliera Hospital Genova Italy (www.galliera.it)
 RADIATION INDUCED Carlo Mosci Ocular Oncology Service Galliera Hospital Genova Italy (www.galliera.it) "Working Day - Radiation Side Effects" carlo.mosci@galliera.it RADIATION INDUCED Different treatment
RADIATION INDUCED Carlo Mosci Ocular Oncology Service Galliera Hospital Genova Italy (www.galliera.it) "Working Day - Radiation Side Effects" carlo.mosci@galliera.it RADIATION INDUCED Different treatment
