Population-Based Study on the Prevalence and Correlates of Orthostatic Hypotension/Hypertension and Orthostatic Dizziness
|
|
|
- Ashley Moore
- 6 years ago
- Views:
Transcription
1 897 Original Article Hypertens Res Vol.31 (2008) No.5 p Population-Based Study on the Prevalence and Correlates of Orthostatic Hypotension/Hypertension and Orthostatic Dizziness Jin-Shang WU 1),2), Yi-Ching YANG 1),2), Feng-Hwa LU 1),2), Chih-Hsing WU 2), and Chih-Jen CHANG 1),2) There are no epidemiological studies of orthostatic hypotension (OH)/ (OHT) and orthostatic dizziness (OD) in adults across all age groups. The aim of this study is to examine the prevalence and correlates of OH, OHT, and OD in community dwellers aged 20 years. OH was defined as a decline in systolic/ diastolic blood pressure of 20/10 mmhg when a person stood up from a supine position. OHT was a postural increase of 20 mmhg in systolic blood pressure. OD was dizziness, lightheadedness, or faintness as the person stood up. A total of 1,638 adults were included. Subjects were classified as normotensive, prehypertensive, or hypertensive. The prevalences of OH, OHT, and OD were 15.9, 1.1, and 4.8%, respectively. OD was associated with neither OH nor OHT. None of the subjects aged <40 had OHT; (p=0.030) and female gender (p<0.001) were the independent correlates of OH and OD, respectively, in that age range. For subjects aged 40 years, age (p=0.003), pre- (p=0.024), (p=0.008), and diabetes mellitus (p=0.036) were independently related to OH. Age (p<0.001) and supine systolic blood pressure (p=0.023) were the correlates of OHT. Female gender (p<0.001) and sedatives/hypnotics (p=0.040) were associated with OD. In conclusion, age, pre-,, and diabetes mellitus were important determinants of OH. OD was more prevalent in women and in subjects using sedatives/hypnotics. The risk of OHT increased with age and with supine systolic blood pressure in adults aged 40 years. OH and OHT cannot be determined solely from the presence of OD because of their dissociation. (Hypertens Res 2008; 31: ) Key Words: population-based study, orthostatic hypotension, orthostatic, orthostatic dizziness Introduction When a normotensive person stands up from a lying position, blood pressure (BP) is maintained by reflex vasoconstriction and an increase in heart rate and myocardial contractility (1). Any abnormality in BP homeostasis may result in orthostatic hypotension (OH) (2). Clinically, OH has been considered a potentially dangerous hypotensive response (2). OH is believed to be associated with age-related physiologic changes, medications, and pathological changes, such as diabetes mellitus,, and cardiovascular disease (2, 3). Because advancing age is often accompanied by an accumulation of diseases and medications that may be associated From the 1) Department of Family Medicine, College of Medicine, National Cheng Kung University, Tainan, Taiwan, ROC; and 2) Department of Family Medicine, National Cheng Kung University Hospital, Tainan, Taiwan, ROC. This study was supported by grants from the National Science Council, Taiwan, ROC (NSC B and NSC B ). Address for Reprints: Chih-Jen Chang, M.D., Department of Family Medicine, National Cheng Kung University Hospital, 138, Sheng Li Road, Tainan 70441, Taiwan, ROC. em75210@ .ncku.edu.tw Received July 2, 2007; Accepted in revised form December 19, 2007.
2 898 Hypertens Res Vol. 31, No. 5 (2008) with OH, the relative contributions of age, diseases, and medication are hard to separate (2, 4). Although OH is defined as a reduction in systolic or diastolic BP when the subject stands up from a supine position (2, 5, 6), some studies have also included symptoms of OH (7). Some people with minor falls in systemic BP developed dizziness or faintness on standing, whereas others with greater falls in BP have remained asymptomatic (8). Clinically, orthostatic dizziness (OD) is often perceived as being strongly associated with OH, but the evidence is conflicting (4, 6, 7). The prevalence of OH varied extremely, from 5 to 30%, depending on the selection of study subjects and diagnostic criteria (2, 4 6, 9 16). Most studies were confined to the elderly, except for two reports in which subjects were at least 40 and 55 years old, respectively (4, 16). The prevalence of OD was found to range from 2 to 19% in the elderly population (5 7), but figures for a younger population are not available. Orthostatic (OHT), indicated by an increase in BP with orthostatic change, has been associated with a greater risk for cardiovascular disease (17). Its definition remains inconclusive, and its clinical significance needs to be elucidated by more studies. Furthermore, the normal BP cutoffs have been revised to less than 120/80 mmhg (18), and the effects of pre- with BP of /80 89 mmhg on OH, OD, and even OHT are unclear. Because there is a lack of epidemiological studies on OH, OD, and OHT in adults across all age groups, the aim of this study is to examine the prevalences and correlates of OH, OD, and OHT in community dwellers aged 20 years from population-based data in Taiwan. Population Methods The subjects were recruited for a population-based study for chronic diseases conducted in Tainan, which is the oldest city in southern Taiwan and has a population of 700,000. A 3- stage sampling scheme was used to generate a stratified systemic cluster sample of households throughout the city. There were 2,416 eligible subjects under systematic sampling from 7 administrative districts. A total of 1,638 subjects aged 20 years old or more, representing a response rate of 67.8%, were included. Details of the study s sampling methods have been described elsewhere (19). Written consent was obtained from all participants, and the research committee of National Cheng Kung University Hospital, Taiwan, approved this study. Clinical Examination and Blood Pressure Measurement The participants were instructed not to consume alcohol, coffee, tea, or cigarettes on the day of the examination. Demographic characteristics, dietary habits, cigarette smoking, alcohol drinking, physical activity, medical history, and use of medications were assessed. All the subjects received a complete physical examination and measurement of seated BP, body weight, and height. The laboratory tests included blood biochemistry, urine examination, and ECG after an overnight fast of at least 10 h. Subjects without a history of diabetes mellitus received a 75 g oral glucose tolerance test after measurement of BP in the seated, supine, and standing positions. A blood sample was obtained 2 h after the subject drank a glucose solution. BP and heart rate were measured with a DINAMAP vital sign monitor (Model 1846SX; Critikon, Irvine, USA). Measurements were obtained in a fasting state. An appropriately sized cuff was wrapped around the right upper arm in a quiet room between 08:00 and 10:00 AM. Two readings of seated BP and heart rate were separated by at least 5-min intervals after the subject had rested for at least 15 min. Then, the subject lay down and rested in a supine position for at least 15 min. After supine BP and heart rate were each measured twice, the subject was asked to stand from the supine position with the entire forearm relaxed and supported at heart level (fourth intercostal space) on an adjustable table. BP and heart rate were measured twice again, after 1 and 3 min of standing. The subjects were asked about any feelings of dizziness, lightheadedness, or faintness as the person stood up and a positive or negative response was recorded to determine OD. Definition of Clinical Measurements OH was defined as a decline in systolic BP of at least 20 mmhg and/or a decline in diastolic BP of at least 10 mmhg after either 1 or 3 min of standing after the subject stood from a supine (20). The definition of OHT was a postural increase of at least 20 mmhg in systolic BP, which was calculated from the average of two BP readings of standing minus the average of two supine BP readings (17). OD was defined as dizziness, lightheadedness, or faintness as the person stood up with any change in systolic or diastolic BP (7). According to the JNC 7 report, the average of two seated readings of BP was classified as normotension (BP<120/80 mmhg without a history of ), pre- (BP of / mmhg without a history of ), or (BP 140/90 mmhg or a history of ) (18). Diabetes mellitus was diagnosed as fasting glucose 7.0 mmol/l, 2-h postload glucose 11.1 mmol/l, or a history of diabetes mellitus (21). Cerebrovascular disease was identified a previously documented stroke, the presence of hemiparesis, asymmetric hyperreflexia, or a positive Babinski reflex on physical examination. ECG with left bundle branch block or ischemic patterns included Q-QS abnormalities, ST segment depression, T wave changes, and left bundle branch block according to the Minnesota code (1.1 3; 4.1 3; 5.1 3; and 7.1) (22). Total physical activity, including work, walking, and leisure time, was assessed in metabolic equivalent hours
3 Wu et al: Orthostatic Hypotension/Hypertension and Dizziness 899 Table 1. Age-Specific Prevalence of Orthostatic Hypotension (OH), Orthostatic Hypertension (OHT), and Orthostatic Dizziness (OD) Age, years Number of subjects OH, n (%) OHT, n (%) OD, n (%) (7.6) 0 (0.0) 15 (4.4) (9.8) 0 (0.0) 12 (3.4) (16.9) 2 (0.5) 21 (5.3) (20.2) 5 (2.1) 12 (4.9) (25.8) 5 (2.6) 12 (6.2) (31.7) 6 (5.8) 6 (5.8) Total 1, (15.9)* 18 (1.1)* 78 (4.8) A test for trends among different age groups, *p< per week for the past year (23). Statistical Analysis Data analyses were performed using the Statistical Package for the Social Sciences version 10.0 (SPSS, Chicago, USA) for Windows. Age-stratified analyses were performed in subjects aged <40 years and 40 years. In univariate analysis, comparisons of categorical variables between groups were analyzed using the χ 2 test or Fisher s exact test for cells less than 5. A test for trends was used to compare the prevalence of OH, OD, and OHT among different age groups. Comparisons of continuous variables between the two groups were carried out using Student s t- or the Mann-Whitney test. ANOVA and the Bonferroni post hoc test were used to compare continuous variables among subjects with different statuses of orthostatic BP change, classified as orthostatic normotension (ON), OH, and OHT. The Kruskal-Wallis test was used to compare plasma triglyceride and physical activity levels among groups. Multivariate binary or multinomial logistic regression was used to assess the contributions of different clinical variables to orthostatic BP change and OD. The outcome variables were orthostatic BP change and OD. The predictor variables included age, gender, body mass index, pre-,, diabetes mellitus, physical activity level, current smoking, alcohol, antihypertensive agents, and sedative/ hypnotic use. Multinomial logistic regression was also used to examine the effect of supine BP as a continuous variable on the status of orthostatic BP change. p values of 0.05 or less were considered significant. Results Table 1 shows that the age-specific prevalences of OH, OHT, and OD were 15.9%, 1.1%, and 4.8%, respectively. The prevalence of OH increased with age (test for trend, p<0.001), but there was no significant difference in the prevalence of OD among the different age groups (p=0.483). OHT was absent in subjects aged <40 years, although the prevalence of OHT increased with age (test for trend, p<0.001). For the association between OH and OD in subjects aged <40 years, the prevalence of OD was not apparently different between those with OH and those without it (4.1 vs. 3.8%, p=0.713). For subjects aged 40 years, there was no significant difference in the prevalence of OD between those with different BP changes (ON:OH:OHT, 5.3:6.0:5.6%, p=0.916). Table 2 presents the clinical characteristics of subjects classified by orthostatic BP change and OD, respectively. Agestratified analyses were performed in two age groups: <40 years and 40 years. For subjects aged <40 years, those with OH had higher diastolic BP (p=0.014) but had lower systolic (p=0.002) and diastolic BP (p<0.001) during standing than did subjects without OH. Subjects aged <40 years with OD were younger (p=0.028) and more likely to be female (p<0.001) but were lower in body mass index (p=0.01), physical activity level (p=0.029), supine systolic (p<0.001) and diastolic BP (p=0.008), and standing systolic (p<0.001) and diastolic BP (p=0.007) compared to subjects aged <40 years without OD. For subjects aged 40 years with different orthostatic BP changes, there were significant differences in age (p<0.001), supine and standing systolic (p<0.001) and diastolic BP (p<0.001), and the prevalence of diabetes mellitus (p=0.015) and antihypertensive use (p=0.035) among subjects with ON, OH, and OHT. The OH group was older (p<0.001) and had higher supine systolic (p<0.001) and diastolic BP (p<0.001), but had lower standing systolic (p=0.021) and diastolic BP (p<0.001) than the ON group. Compared to the ON group, the OHT group was older (p<0.001) and had higher standing systolic BP (p<0.001). Univariate analysis in subjects aged 40 years with and without OD shows that subjects with OD were more likely to be female (p<0.001) and have sedative/hypnotic use (p=0.040); however, they also had lower supine (p=0.024) and standing diastolic BP (p=0.043) than did subjects without OD. Figure 1 shows the prevalences of OH, OHT, and OD in subjects with normotension, pre-, and. For subjects aged <40 years, there was a significant difference in the prevalence of OH (p=0.002) among those with normotension, pre-, and. However, the prevalence of OD was not apparently different among
4 900 Hypertens Res Vol. 31, No. 5 (2008) Table 2. Clinical Characteristics in Subjects Classified by Orthostatic Blood Pressure (BP) Change and Orthostatic Dizziness in Different Age Groups Age <40 years Age 40 years Orthostaitc BP change Orthostatic dizziness Orthostaitc BP change Orthostatic dizziness ON (n=639) OH (n=61) No (n=673) Yes (n=27) ON (n=721) OH (n=199) OHT (n=18) No (n=887) Yes (n=51) Age, years 29.5± ± ± ±5.7* 53.3± ± ± ± ±10.6 Female gender, % Body mass index, kg/m ± ± ± ±3.0* 24.5± ± ± ± ±3.7 Physical activity, met-h/week # 66.3± ± ± ±50.1* 55.9± ± ± ± ±39.8 Supine SBP, mmhg 109.8± ± ± ± ± ± ± ± ±23.1 Supine DBP, mmhg 67.1± ±8.1* 67.6± ± ± ± ± ± ±10.9* Standing SBP, mmhg 103.7± ± ± ± ± ±24.1* 149.9± ± ±25.4 Standing DBP, mmhg 66.1± ± ± ± ± ± ± ± ±12.0* Cholesterol, mmol/l 4.7± ± ± ± ± ± ± ± ±1.0 Triglyceride, mmol/l # 1.2± ± ± ± ± ± ± ± ±0.8 HDL-cholesterol, mmol/l 1.3± ± ± ± ± ± ± ± ±0.4 Cerebrovascular disease, % LBBB/ischemic ECG pattern, % Diabetes mellitus, % Antihypertensive use, % Sedative/hyponotics use, % * Antidepressant use, % Current smoking, % Current alcohol use, % ON, orthostatic normotension; OH, orthostatic hypotension; OHT, orthostatic ; SBP/DBP, average of two supine (standing) systolic/diastolic BPs; HDL, high-density lipoprotein; LBBB, left bundle branch block. *p<0.05, p<0.01, p<0.001 when compared to subjects with ON or absence of orthostatic dizziness; p<0.05, χ 2 test for the relationship between clinical variables and orthostatic BP change. # Mann-Whitney test or Kruskal-Wallis test. these three groups in subjects aged <40 years (p=0.257). For subjects aged 40 years, a significant difference in the prevalence of OH (p<0.001) existed among subjects with normotension, pre-, and, but the prevalences of OHT and OD were not significantly different among these three groups (OD, p=0.326; OHT, p=0.719). Table 3 shows multiple logistic regression analysis of the contributions of different clinical variables to orthostatic BP change and OD. In subjects aged <40 years, only (p=0.030) was independently associated with OH. The independent correlate of OD was female gender (p<0.001). In subjects aged 40 years, age (p=0.003), pre-
5 Wu et al: Orthostatic Hypotension/Hypertension and Dizziness 901 Fig. 1. Prevalences of orthostatic hypotension (OH), orthostatic (OHT), and orthostatic dizziness (OD) in subjects with normotension, pre-, and. Upper panel, age <40 years; lower panel, age 40 years. Table 3. Multiple Logistic Regression Analysis in the Contribution to Orthostatic Blood Pressure (BP) Change and Orthostatic Dizziness (OD) from Clinical Variables in Different Age Groups Age <40 years (n=700) Age 40 years (n=938) Orthostaitc BP Orthostaitc BP Variables change OD change OD OH OH OHT OR (95% CI) OR (95% CI) OR (95% CI) OR (95% CI) OR (95% CI) Age, years 0.96 ( ) 0.97 ( ) 1.08 ( ) 1.10 ( ) 1.02 ( ) Female vs. male 1.39 ( ) 5.05 ( ) 1.39 ( ) 0.81 ( ) 4.73 ( ) Pre- vs. normotension 1.74 ( ) 0.68 ( ) 2.86 ( )* 1.67 ( ) 0.72 ( ) Hypertension vs. normotension 2.20 ( )* 0.62 ( ) 4.38 ( ) 2.86 ( ) 1.05 ( ) Diabetes mellitus 1.51 ( ) 1.01 ( ) 1.85 ( )* 1.25 ( ) 0.70 ( ) Sedative/hypnotic use ( ) 1.11 ( ) 1.29 ( ) 2.25 ( )* OH, orthostatic hypotension; OHT, orthostatic ; OR, odds ratio; CI, confidence interval. Dependent variables: orthostatic BP change (including OH vs. orthostatic normotension and OHT vs. orthostatic normotension) and OD, respectively. OHT was absent in subjects aged <40 years. Independent variables: age, gender, body mass index, pre-,, diabetes mellitus, physical activity level, current smoking, alcohol, antihypertensive, and sedative/hypnotic use. *p<0.05, p<0.01, p< (p=0.024), (p=0.008), and diabetes mellitus (p=0.036) were independently related to OH. In contrast, age (p<0.001) was the independently associated factor in OHT. The independent correlates of OD were female gender (p<0.001) and sedative/hypnotic use (p=0.040) in subjects aged 40 years, after adjusting for other factors. We also evaluated the effect of supine BP on orthostatic BP change, including OH and OHT, by multiple logistic regression analysis (data not shown). For subjects aged 40 years, supine systolic BP was independently related to OH (p=0.003, odds ratio [OR]: 1.03, 95% confidence interval [CI]: ) and OHT (p=0.023, OR: 1.04, 95% CI: ). In addition, diastolic BP was also the independent correlate of OH (p=0.042, OR: 1.04, 95% CI: ), but not of OHT (p=0.404). For subjects aged <40 years, supine diastolic BP (p=0.020, OR: 1.03, 95% CI: ), but not systolic BP (p=0.087), was independently associated with OH. Discussion Our results showed the prevalence and correlates of OH and OD in community dwellers aged years. Although studies on the prevalence of OH in community dwellers aged <40
6 902 Hypertens Res Vol. 31, No. 5 (2008) years was lacking, a lower prevalence of OH was anticipated in younger adults. The prevalence of OH in our subjects aged <40 years was 8.7% with the criterion of a decline in BP of 20/10 mmhg from supine to standing BP. In Korean adults aged years, the prevalence of OH at 0 min after standing was 12.3% (16). In contrast 19.9% of our subjects aged had OH after either 1 or 3 min of standing. In other studies, the prevalences of OH at 1 min after standing were 16.2% and 30.0% in subjects aged 65 and 70 years, respectively (4, 11). The Korean study found a prevalence of 23.1% in adults aged years (16). Our results showed that the prevalences of OH were 26.5% and 31.7% in subjects aged 65 and 70 years, respectively. The variation in the prevalence of OH may be due to ethnicity, subject selection, and measurement bias (3). Studies have shown that is a risk factor for OH (4, 8, 16, 24), and our study demonstrated similar results. Our results also revealed that pre- with BP of /80 89 mmhg was independently associated with OH in subjects 40 years. The mechanism is related to impaired baroreflex sensitivity due to a decrease in vascular compliance and consequent diminution of baroreceptor stretch and relaxation during BP change (24). As BP increased, baroreflex sensitivity declined; this may be responsible, in part, for OH (3). Tilvis et al. demonstrated that supine systolic BP was associated with OH (5). Recently, basal systolic BP has been suggested as an important determinant of prone hypotension (25). We found that the higher the supine BP, the higher the prevalence of OH in subjects 40 years. This provides epidemiological evidence that subjects 40 years suffer a higher risk of OH and that the risk of OH increases with supine BP. However, the effect of supine systolic BP on OH was not apparent in subjects <40 years. The explanation for the insignificant association between antihypertensive medication use and OH in a cross-sectional study was an adjustment of the treatment regimen due to a side effect or related symptom, resulting in the underestimation of their relationship (15). Furthermore, the incidence of OH decreased significantly followed by decreasing or normalizing BP after use of antihypertensive agents (26). This may also be one of the explanations for the insignificant association between OH and antihypertensive medication use. OH is a clinical manifestation of diabetic autonomic neuropathy (27). Diabetes mellitus was an independently associated factor of OH in our study, which is consistent with the literature (27, 28). Regarding the mechanism of OH in diabetes mellitus, a neurogenic cause is usually associated with efferent involvement of the baroregulatory reflex arc with damaged sympathetic vasoconstrictor fibers in the splanchnic bed, muscle, and skin (28). In our study, diabetes mellitus, pre-, and were the independently associated factors for OH. Thus, diabetic subjects with, or even pre-, have a much higher risk of OH. Two studies (6, 9) on the elderly demonstrated that the prevalence of OH increased with age. One study on subjects aged years (16) showed a similar finding. Our results revealed that the prevalence of OH significantly increased with age in subjects 40 years but not in subjects <40 years, after adjusting for other clinical variables. The following agerelated physiologic changes are expected to favor the development of OH: declines in baroreflex sensitivity and in arterial and cardiac compliance, increased venous tortuosity, and decreased renal sodium conservation, plasma volume, renin, angiotensin, and aldosterone levels. Conversely, age-related changes such as increased plasma norepinephrine, diminished β-adrenergic responsiveness, and unaltered α-adrenergic sensitivity offer protection from OH (3). Age-related OH has been suggested to be predominantly associated with dysfunction in the afferent pathway of the baroreflex arc (29), although the precise mechanism of aged-related OH remains unknown. One study showed that 8.7% of community-dwelling elderly exhibited OHT (30), but data for the non-elderly population is not available. Our data adopted the same criterion as the previous study and revealed that the prevalence of OHT was 1.1% in study subjects aged years and 4.6% in elderly subjects. Although the mechanism of OHT is not well understood, it maybe involve excessive orthostatic venous pooling, which leads to decreased cardiac output, augmented sympathetic stimulation, and finally excessive arteriolar constriction (31). Further study is needed to determine whether or not the discrepancy in the prevalence of OHT is related to the difference in autonomic function due to ethnic effect. Although OHT may be associated with cerebrovascular disease,, and diabetes mellitus (17, 30, 32), our results showed that age and supine systolic BP were the independent correlates of OHT. The lower prevalence of OHT in our study may result in an insignificant association between OHT and the above chronic diseases due to a lower statistical power (33). Although a general decrease in sympathetic outflow and declining vagal modulation of heart rate (34) with advancing age may partially explain age-related OHT, the exact mechanism needs to be clarified. Clinically, OD is often thought to be associated with OH. Most population-based studies of the elderly showed a dissociation between OD and OH (4, 6), but only one report found that OD was related to OH (8). Our study, with a general population aged 20 years, provided further evidence for a dissociation between OD and OH. Reports have suggested that OH, cerebral ischemia, vestibular dysfunction, vision impairment, and disorders in the proprioceptive system may be involved in the mechanism of OD (8, 35 37). OH may be just one of the causes of OD, and they do not share all the same risk conditions (5). Therefore, a diagnosis of OH cannot be made just from the presence of OD in clinical practice, because of their dissociation. The prevalence of OD varied greatly, from 2 to 19%, in elderly population-based studies (5 7) and there are no reports covering a younger population. Our study revealed the preva-
7 Wu et al: Orthostatic Hypotension/Hypertension and Dizziness 903 lence of OD was 4.8% in adults aged 20 years. Our report and another study (7) showed that sedative/hypnotic use was a risk factor for OD. Although our results cannot clarify a cause and effect between OD and sedative/hypnotic use, they support the need to review the possible role of sedatives/hypnotics in subjects with OD. A report on the relationship between OD and gender is not available yet, although a study of community-dwelling elderly found that dizziness was more common in females than in males (37). Our study provides epidemiological evidence that female subjects have a higher risk of OD than male subjects, but further investigation is required to discover whether women are more sensitive to perceptions of postural change from a supine to an upright position. In conclusion, the overall prevalences of OH, OHT, and OD in adults 20 years were 15.9, 1.1, and 4.8%, respectively. No subjects <40 years had OHT. Hypertension and female gender were the independent correlates of OH and OD, respectively. For subjects 40 years, age, pre-,, and diabetes mellitus were important determinants of OH. The risk of OH increased as supine systolic/diastolic BP increased. OD was much more prevalent in women and subjects using sedatives/hypnotics. Age and supine systolic BP were independent correlates of OHT in subjects 40 years. OH and OHT cannot be determined solely from the presence of OD, because of their dissociation. References 1. Matalon SV, Farhi LE: Cardiopulmonary readjustment in passive tilt. J Appl Physiol 1979; 47: Lipsitz LA: Orthostatic hypotension in the elderly. N Engl J Med 1989; 321: Mader SL: Aging and postural hypotension: an update. J Am Geriatr Soc 1989; 37: Mader SL, Josephson KR, Rubenstein LZ: Low prevalence of postural hypotension among community-dwelling elderly. JAMA 1987; 258: Tilvis RS, Hakala SM, Valvanne J, Erkinjuntti T: Postural hypotension and dizziness in a general aged population: a four-year follow-up of the Helsinki Aging Study. J Am Geriatr Soc 1996; 44: Rutan GH, Hermanson B, Bild DE, Kittner SJ, LaBaw F, Tell GS: Orthostatic hypotension in older adults: the Cardiovascular Health Study. Hypertension 1992; 19: Ensrud KE, Nevitt MC, Yunis C, Hulley SB, Grimm RH, Cummings SR: Postural hypotension and postural dizziness in elderly women. The study of osteoporotic fractures. Arch Intern Med 1992; 152: Wollner L, McCarthy ST, Soper ND, Macy DJ: Failure of cerebral autoregulation as a cause of brain dysfunction in the elderly. BMJ 1979; 1: Masaki KH, Schatz IJ, Burchfiel CM, et al: Orthostatic hypotension predicts mortality in elderly men: the Honolulu Heart Program. Circulation 1998; 98: Davis BR, Langford HG, Blaufox MD, Curb JD, Polk BF, Shulman NB: The association of postural changes in systolic blood pressure and mortality in persons with : the Hypertension Detection and Follow-up Program experience. Circulation 1987; 75: Luukinen H, Koski K, Laippala P, Kivela SL: Prognosis of diastolic and systolic orthostatic hypotension in older persons. Arch Intern Med 1999; 159: Alli C, Avanzini F, Bettelli G, et al: Prevalence and variability of orthostatic hypotension in the elderly. Results of the Italian study on blood pressure in the elderly (SPAA). Eur Heart J 1992; 13: Harris T, Lipsitz LA, Kleinman JC, Cornoni-Huntley J: Postural change in blood pressure associated with age and systolic blood pressure. The National Health and Nutrition Examination Survey II. J Gerontol 1991; 46: M159 M Applegate WB, Davis BR, Black HR, Smith WM, Miller ST, Burlando AJ: Prevalence of postural hypotension at baseline in the Systolic Hypertension in the Elderly Program (SHEP) cohort. J Am Geriatr Soc 1991; 39: Strogatz DS, Keenan NL, Barnett EM, Wagner EH: Correlates of postural hypotension in a community sample of elderly blacks and whites. J Am Geriatr Soc 1991; 39: Shin C, Abbott RD, Lee H, Kim J, Kimm K: Prevalence and correlates of orthostatic hypotension in middle-aged men and women in Korea: the Korean Health and Genome Study. J Hum Hypertens 2004; 18: Kario K, Eguchi K, Hoshide S, et al: U-curve relationship between orthostatic blood pressure change and silent cerebrovascular disease in elderly hypertensives: orthostatic as a new cardiovascular risk factor. J Am Coll Cardiol 2002; 40: Chobanian AV, Bakris GL, Black HR, et al: The Seventh Report of the Joint National Committee on Prevention, Detection, Evaluation, and Treatment of High Blood Pressure: the JNC 7 report. JAMA 2003; 289: Lu FH, Yang YC, Wu JS, Wu CH, Chang CJ: A populationbased study of the prevalence and associated factors of diabetes mellitus in southern Taiwan. Diabet Med 1998; 15: The Consensus Committee of the American Autonomic Society and the American Academy of Neurology: Consensus statement on the definition of orthostatic hypotension, pure autonomic failure, and multiple system atrophy. Neurology 1996; 46: American Diabetes Association: Diagnosis and classification of diabetes mellitus. Diabetes Care 2004; 27: S5 S Blackburn H, Keys A: The electrocardiogram in population studies: a classification system. Circulation 1960; 21: Paffenbarger RS Jr, Blair SN, Lee IM, Hyde RT: Measurement of physical activity to assess health effects in free-living populations. Med Sci Sports Exerc 1993; 25: Lipsitz LA, Storch HA, Minaker KL, Rowe JW: Intra-individual variability in postural blood pressure in the elderly. Clin Sci 1985; 69: Tabara Y, Tachibana-Iimori R, Yamamoto M, et al: Hypotension associated with prone body position: a possible overlooked postural hypotension. Hypertens Res 2005; 28:
8 904 Hypertens Res Vol. 31, No. 5 (2008) 26. Masuo K, Mikami H, Ogihara T, Tuck ML: Changes in frequency of orthostatic hypotension in elderly hypertensive patients under medications. Am J Hypertens 1996; 9: Hilsted J, Low PA: Diabetic autonomic neuropathy, in Low PA (ed): Clinical Autonomic Disorder: Evaluation and Management, 2nd ed. Philadelphia, Lippincott-Raven Publishers, 1997, pp Ewing DJ, Campbell IW, Clarke BF: The natural history of diabetic autonomic neuropathy. Q J Med 1980; 49: Tonkin AL, Wing LM, Morris MJ, Kapoor V: Afferent baroreflex dysfunction and age-related orthostatic hypotension. Clin Sci 1991; 81: Matsubayashi K, Okumiya K, Wada T, et al: Postural dysregulation in systolic blood pressure is associated with worsened scoring on neurobehavioral function tests and leukoaraiosis in the older elderly living in a community. Stroke 1997; 28: Streeten DH, Auchincloss JH Jr, Anderson GH Jr, Richardson RL, Thomas FD, Miller JW: Orthostatic. Pathogenetic studies. Hypertension 1985; 7: Yoshinari M, Wakisaka M, Nakamura U, Yoshioka M, Uchizono Y, Iwase M: Orthostatic in patients with type 2 diabetes. Diabetes Care 2001; 24: Lang TA, Secic M: How to Report Statistics in Medicine. Philadelphia, Port City Press, 1997, p Goldstein DS: The Autonomic Nervous System in Health and Disease. New York, Marcel Dekker, 2001, pp Stark RJ, Wodak J: Primary orthostatic cerebral ischemia. J Neurol Neurosurg Psychiatry 1983; 46: Sloane PD, Baloh RW: Persistent dizziness in geriatric patients. J Am Geriatr Soc 1989; 37: Belal A Jr, Glorig A: Dysequilibrium of aging (presbyastasis). J Laryngol Otol 1986; 100:
ORIGINAL INVESTIGATION. Postural Hypotension and Postural Dizziness in Patients With Non Insulin-Dependent Diabetes
 ORIGINAL INVESTIGATION Postural Hypotension and Postural Dizziness in Patients With Non Insulin-Dependent Diabetes Jin-Shang Wu, MD; Feng-Hwa Lu, MD; Yi-Ching Yang, MD; Chih-Jen Chang, MD Background: Postural
ORIGINAL INVESTIGATION Postural Hypotension and Postural Dizziness in Patients With Non Insulin-Dependent Diabetes Jin-Shang Wu, MD; Feng-Hwa Lu, MD; Yi-Ching Yang, MD; Chih-Jen Chang, MD Background: Postural
Population-Based Study on the Prevalence and Risk Factors of Orthostatic Hypotension in Subjects With Pre-Diabetes and Diabetes
 Epidemiology/Health Services Research O R I G I N A L A R T I C L E Population-Based Study on the Prevalence and Risk Factors of Orthostatic Hypotension in Subjects With Pre-Diabetes and Diabetes JIN-SHANG
Epidemiology/Health Services Research O R I G I N A L A R T I C L E Population-Based Study on the Prevalence and Risk Factors of Orthostatic Hypotension in Subjects With Pre-Diabetes and Diabetes JIN-SHANG
Prevalence and correlates of orthostatic hypotension in middle-aged men and women in Korea: the Korean Health and Genome Study
 (2004) 18, 717 723 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Prevalence and correlates of orthostatic hypotension in middle-aged men and
(2004) 18, 717 723 & 2004 Nature Publishing Group All rights reserved 0950-9240/04 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Prevalence and correlates of orthostatic hypotension in middle-aged men and
ORIGINAL INVESTIGATION. Prognosis of Diastolic and Systolic Orthostatic Hypotension in Older Persons
 ORIGINAL INVESTIGATION Prognosis of Diastolic and Systolic Orthostatic Hypotension in Older Persons Heikki Luukinen, MD; Keijo Koski, MD; Pekka Laippala, PhD; Sirkka-Liisa Kivelä, MD Background: Orthostatic
ORIGINAL INVESTIGATION Prognosis of Diastolic and Systolic Orthostatic Hypotension in Older Persons Heikki Luukinen, MD; Keijo Koski, MD; Pekka Laippala, PhD; Sirkka-Liisa Kivelä, MD Background: Orthostatic
Risk Factors for Ischemic Stroke: Electrocardiographic Findings
 Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
Original Articles 232 Risk Factors for Ischemic Stroke: Electrocardiographic Findings Elley H.H. Chiu 1,2, Teng-Yeow Tan 1,3, Ku-Chou Chang 1,3, and Chia-Wei Liou 1,3 Abstract- Background: Standard 12-lead
droxidopa (Northera )
 Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Applies to all products administered or underwritten by Blue Cross and Blue Shield of Louisiana and its subsidiary, HMO Louisiana, Inc.(collectively referred to as the Company ), unless otherwise provided
Orthostatic hypotension is common in elderly people 1 4
 CLINICAL INVESTIGATIONS Orthostatic Hypotension and Risk of Cardiovascular Disease in Elderly People: The Rotterdam Study Germaine C. Verwoert, w Francesco U. S. Mattace-Raso, MD, PhD, w Albert Hofman,
CLINICAL INVESTIGATIONS Orthostatic Hypotension and Risk of Cardiovascular Disease in Elderly People: The Rotterdam Study Germaine C. Verwoert, w Francesco U. S. Mattace-Raso, MD, PhD, w Albert Hofman,
ORIGINAL INVESTIGATION. Orthostatic Hypotension in Acute Geriatric Ward
 Orthostatic Hypotension in Acute Geriatric Ward Is It a Consistent Finding? ORIGINAL INVESTIGATION Avraham Weiss, MD; Ehud Grossman, MD; Yichayaou Beloosesky, MD; Joseph Grinblat, MD Background: Orthostatic
Orthostatic Hypotension in Acute Geriatric Ward Is It a Consistent Finding? ORIGINAL INVESTIGATION Avraham Weiss, MD; Ehud Grossman, MD; Yichayaou Beloosesky, MD; Joseph Grinblat, MD Background: Orthostatic
Orthostatic hypotension, diabetes, and falling in older patients:
 Research Kornelis JJ van Hateren, Nanne Kleefstra, Marco H Blanker, Lielith J Ubink-Veltmaat, Klaas H Groenier, Sebastiaan T Houweling, Adriaan M Kamper, Klaas van der Meer and Henk JG Bilo Orthostatic
Research Kornelis JJ van Hateren, Nanne Kleefstra, Marco H Blanker, Lielith J Ubink-Veltmaat, Klaas H Groenier, Sebastiaan T Houweling, Adriaan M Kamper, Klaas van der Meer and Henk JG Bilo Orthostatic
Does Increased Arterial Stiffness Increase the Risk for Postural Hypotension?
 Original Paper Does Increased Arterial Stiffness Increase the Risk for Postural Hypotension? David Sengstock, MD, MS; Peter V. Vaitkevicius, MD; Mark A. Supiano, MD From the Department of Internal Medicine,
Original Paper Does Increased Arterial Stiffness Increase the Risk for Postural Hypotension? David Sengstock, MD, MS; Peter V. Vaitkevicius, MD; Mark A. Supiano, MD From the Department of Internal Medicine,
Wednesday September 20 th CMT Regional Study Day. Dr Colin Mason, Consultant DME, Addenbrooke s Hospital
 Wednesday September 20 th CMT Regional Study Day Dr Colin Mason, Consultant DME, Addenbrooke s Hospital Develop a structured approach to a patient presenting with a fall Risk stratify who can go home and
Wednesday September 20 th CMT Regional Study Day Dr Colin Mason, Consultant DME, Addenbrooke s Hospital Develop a structured approach to a patient presenting with a fall Risk stratify who can go home and
Responses to Changes in Posture QUESTIONS. Case PHYSIOLOGY CASES AND PROBLEMS
 64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
64 PHYSIOLOGY CASES AND PROBLEMS Case 12 Responses to Changes in Posture Joslin Chambers is a 27-year-old assistant manager at a discount department store. One morning, she awakened from a deep sleep and
Postural changes in blood pressure and the prevalence of orthostatic hypotension among home-dwelling elderly aged 75 years or older
 (2009) 23, 33 39 & 2009 Macmillan Publishers Limited All rights reserved 0950-9240/09 $32.00 www.nature.com/jhh ORIGINAL ARTICLE Postural changes in blood pressure and the prevalence of orthostatic hypotension
(2009) 23, 33 39 & 2009 Macmillan Publishers Limited All rights reserved 0950-9240/09 $32.00 www.nature.com/jhh ORIGINAL ARTICLE Postural changes in blood pressure and the prevalence of orthostatic hypotension
Comparison of the Assessment of Orthostatic Hypotension Using Peripheral and Central Blood Pressure Measurements
 Original Article J Clin Med Res. 2018;10(4):309-313 Comparison of the Assessment of Orthostatic Hypotension Using Peripheral and Central Blood Pressure Measurements Kannayiram Alagiakrishnan a, d, Ruojin
Original Article J Clin Med Res. 2018;10(4):309-313 Comparison of the Assessment of Orthostatic Hypotension Using Peripheral and Central Blood Pressure Measurements Kannayiram Alagiakrishnan a, d, Ruojin
:{ic0fp'16. Geriatric Medicine: Blood Pressure Monitoring in the Elderly. Terrie Ginsberg, DO, FACOI
 :{ic0fp'16 ACOFP 53 rd Annual Convention & Scientific Seminars Geriatric Medicine: Blood Pressure Monitoring in the Elderly Terrie Ginsberg, DO, FACOI Blood Pressure Management in the Elderly Terrie B.
:{ic0fp'16 ACOFP 53 rd Annual Convention & Scientific Seminars Geriatric Medicine: Blood Pressure Monitoring in the Elderly Terrie Ginsberg, DO, FACOI Blood Pressure Management in the Elderly Terrie B.
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide
 Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
Lab Period: Name: Physiology Chapter 14 Blood Flow and Blood Pressure, Plus Fun Review Study Guide Main Idea: The function of the circulatory system is to maintain adequate blood flow to all tissues. Clinical
HRV in Diabetes and Other Disorders
 HRV in Diabetes and Other Disorders Roy Freeman, MD Center for Autonomic and Peripheral Nerve Disorders Beth Israel Deaconess Medical Center Harvard Medical School Control Propranolol Atropine Wheeler
HRV in Diabetes and Other Disorders Roy Freeman, MD Center for Autonomic and Peripheral Nerve Disorders Beth Israel Deaconess Medical Center Harvard Medical School Control Propranolol Atropine Wheeler
Veins. VENOUS RETURN = PRELOAD = End Diastolic Volume= Blood returning to heart per cardiac cycle (EDV) or per minute (Venous Return)
 Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Veins Venous system transports blood back to heart (VENOUS RETURN) Capillaries drain into venules Venules converge to form small veins that exit organs Smaller veins merge to form larger vessels Veins
Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM
 Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM Faculty Disclosure I have no financial interest to disclose No off-label use of medications will be discussed FIFTH ANNUAL SYMPOSIUM Recognize changes between
Todd S. Perlstein, MD FIFTH ANNUAL SYMPOSIUM Faculty Disclosure I have no financial interest to disclose No off-label use of medications will be discussed FIFTH ANNUAL SYMPOSIUM Recognize changes between
Cardiac Pathophysiology
 Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Cardiac Pathophysiology Evaluation Components Medical history Physical examination Routine laboratory tests Optional tests Medical History Duration and classification of hypertension. Patient history of
Orthostatic hypotension (OH) is a major health problem
 Arterial Stiffness Is Associated with Orthostatic Hypotension in Elderly Subjects with History of Falls Jacques Boddaert, MD, w Hani Tamim, MD, Marc Verny, MD, w and Joël Belmin, MD OBJECTIVES: To test
Arterial Stiffness Is Associated with Orthostatic Hypotension in Elderly Subjects with History of Falls Jacques Boddaert, MD, w Hani Tamim, MD, Marc Verny, MD, w and Joël Belmin, MD OBJECTIVES: To test
Clinical Studies 129
 Clinical Studies 129 Syncope in migraine. The population-based CAMERA study Roland D. Thijs, 1* Mark C. Kruit, 2* Mark A. van Buchem, 2 Michel D. Ferrari, 1 Lenore J. Launer, 3,4 and J. Gert van Dijk
Clinical Studies 129 Syncope in migraine. The population-based CAMERA study Roland D. Thijs, 1* Mark C. Kruit, 2* Mark A. van Buchem, 2 Michel D. Ferrari, 1 Lenore J. Launer, 3,4 and J. Gert van Dijk
ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE
 Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 1 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE Emilia-Lidia
Rev. Med. Chir. Soc. Med. Nat., Iaşi 2014 vol. 118, no. 1 INTERNAL MEDICINE - PEDIATRICS ORIGINAL PAPERS ORTHOSTATIC INTOLERANCE AN EXPRESSION OF AUTONOMIC DISFUNCTION IN PARKINSON S DISEASE Emilia-Lidia
(D) (E) (F) 6. The extrasystolic beat would produce (A) increased pulse pressure because contractility. is increased. increased
 Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Review Test 1. A 53-year-old woman is found, by arteriography, to have 5% narrowing of her left renal artery. What is the expected change in blood flow through the stenotic artery? Decrease to 1 2 Decrease
Attenuated peripheral vasoconstriction during an orthostatic challenge in older men
 Age and Ageing 2008; 1 6 doi: 10.1093/ageing/afn195 Age and Ageing Advance Access published October 1, 2008 C The Author 2008. Published by Oxford University Press on behalf of the British Geriatrics Society.
Age and Ageing 2008; 1 6 doi: 10.1093/ageing/afn195 Age and Ageing Advance Access published October 1, 2008 C The Author 2008. Published by Oxford University Press on behalf of the British Geriatrics Society.
Impact of Physical Activity on Metabolic Change in Type 2 Diabetes Mellitus Patients
 2012 International Conference on Life Science and Engineering IPCBEE vol.45 (2012) (2012) IACSIT Press, Singapore DOI: 10.7763/IPCBEE. 2012. V45. 14 Impact of Physical Activity on Metabolic Change in Type
2012 International Conference on Life Science and Engineering IPCBEE vol.45 (2012) (2012) IACSIT Press, Singapore DOI: 10.7763/IPCBEE. 2012. V45. 14 Impact of Physical Activity on Metabolic Change in Type
Managing HTN in the Elderly: How Low to Go
 Managing HTN in the Elderly: How Low to Go Laxmi S. Mehta, MD, FACC The Ohio State University Medical Center Assistant Professor of Clinical Internal Medicine Clinical Director of the Women s Cardiovascular
Managing HTN in the Elderly: How Low to Go Laxmi S. Mehta, MD, FACC The Ohio State University Medical Center Assistant Professor of Clinical Internal Medicine Clinical Director of the Women s Cardiovascular
Hypertriglyceridemia and the Related Factors in Middle-aged Adults in Taiwan
 1 Hypertriglyceridemia and the Related Factors in Middle-aged Adults in Taiwan Cheng-Chieh Lin, Tsai-Chung Li 2, Shih-Wei Lai, Kim-Choy Ng 1, Kuo-Che Wang, Chiu-Shong Liu Department of Community Medicine,
1 Hypertriglyceridemia and the Related Factors in Middle-aged Adults in Taiwan Cheng-Chieh Lin, Tsai-Chung Li 2, Shih-Wei Lai, Kim-Choy Ng 1, Kuo-Che Wang, Chiu-Shong Liu Department of Community Medicine,
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to
 Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Hypertension The normal radial artery blood pressures in adults are: Systolic arterial pressure: 100 to 140 mmhg. Diastolic arterial pressure: 60 to 90 mmhg. These pressures are called Normal blood pressure
Contempo GIMSI Cosa cambia alla luce della letteratura in tema di terapia farmacologica
 Contempo GIMSI 2015-2017 Cosa cambia alla luce della letteratura in tema di terapia farmacologica Dott.ssa Diana Solari Centro Aritmologico e Sincope Unit, Lavagna www.gimsi.it POST 2 (Prevention of Syncope
Contempo GIMSI 2015-2017 Cosa cambia alla luce della letteratura in tema di terapia farmacologica Dott.ssa Diana Solari Centro Aritmologico e Sincope Unit, Lavagna www.gimsi.it POST 2 (Prevention of Syncope
I ngestion of water increases seated blood pressure (BP) in
 1737 PAPER The effects of water ingestion on orthostatic hypotension in two groups of chronic autonomic failure: multiple system atrophy and pure autonomic failure T M Young, C J Mathias... See end of
1737 PAPER The effects of water ingestion on orthostatic hypotension in two groups of chronic autonomic failure: multiple system atrophy and pure autonomic failure T M Young, C J Mathias... See end of
Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study
 Original Article DOI: 10.17354/ijss/2016/16 Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study M Usharani 1, K Chandini 2 1 Professor and Head, Department of Physiology,
Original Article DOI: 10.17354/ijss/2016/16 Autonomic Variation of Blood Pressure in Middle Aged Diabetics: A Prospective Study M Usharani 1, K Chandini 2 1 Professor and Head, Department of Physiology,
Blood Pressure Regulation. Faisal I. Mohammed, MD,PhD
 Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Blood Pressure Regulation Faisal I. Mohammed, MD,PhD 1 Objectives Outline the short term and long term regulators of BP Know how baroreceptors and chemoreceptors work Know function of the atrial reflex.
Hypertension in the Elderly. John Puxty Division of Geriatrics Center for Studies in Aging and Health, Providence Care
 Hypertension in the Elderly John Puxty Division of Geriatrics Center for Studies in Aging and Health, Providence Care Learning Objectives Review evidence for treatment of hypertension in elderly Consider
Hypertension in the Elderly John Puxty Division of Geriatrics Center for Studies in Aging and Health, Providence Care Learning Objectives Review evidence for treatment of hypertension in elderly Consider
CASE 13. What neural and humoral pathways regulate arterial pressure? What are two effects of angiotensin II?
 CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
CASE 13 A 57-year-old man with long-standing diabetes mellitus and newly diagnosed hypertension presents to his primary care physician for follow-up. The patient has been trying to alter his dietary habits
Central blood volume is abruptly reduced when one stands
 Epidemiology Orthostatic Hypotension Predicts Mortality in Middle-Aged Adults The Atherosclerosis Risk in Communities (ARIC) Study Kathryn M. Rose, PhD; Marsha L. Eigenbrodt, MD, MPH; Rebecca L. Biga,
Epidemiology Orthostatic Hypotension Predicts Mortality in Middle-Aged Adults The Atherosclerosis Risk in Communities (ARIC) Study Kathryn M. Rose, PhD; Marsha L. Eigenbrodt, MD, MPH; Rebecca L. Biga,
Stopping oral contraceptives: an effective blood pressure-lowering intervention in women with hypertension
 (2005) 19, 451 455 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Stopping oral contraceptives: an effective blood pressure-lowering intervention
(2005) 19, 451 455 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Stopping oral contraceptives: an effective blood pressure-lowering intervention
4/4/17 HYPERTENSION TARGETS: WHAT DO WE DO NOW? SET THE STAGE BP IN CLINICAL TRIALS?
 HYPERTENSION TARGETS: WHAT DO WE DO NOW? MICHAEL LEFEVRE, MD, MSPH PROFESSOR AND VICE CHAIR DEPARTMENT OF FAMILY AND COMMUNITY MEDICINE UNIVERSITY OF MISSOURI 4/4/17 DISCLOSURE: MEMBER OF THE JNC 8 PANEL
HYPERTENSION TARGETS: WHAT DO WE DO NOW? MICHAEL LEFEVRE, MD, MSPH PROFESSOR AND VICE CHAIR DEPARTMENT OF FAMILY AND COMMUNITY MEDICINE UNIVERSITY OF MISSOURI 4/4/17 DISCLOSURE: MEMBER OF THE JNC 8 PANEL
Influence of Age, Hypertension or Myocardial Infarction on Cardiovascular Responses to Changes in Body Position
 Influence of Age, Hypertension or Myocardial Infarction on Cardiovascular Responses to Changes in Body Position A population-based study in 30-, 50- and 60-year-old men BY ANNA HOFSTEN UPPSALA UNIVERSITY
Influence of Age, Hypertension or Myocardial Infarction on Cardiovascular Responses to Changes in Body Position A population-based study in 30-, 50- and 60-year-old men BY ANNA HOFSTEN UPPSALA UNIVERSITY
Diabetologia 9 Springer-Verlag 1991
 Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Diabetologia (1991) 34:590-594 0012186X91001685 Diabetologia 9 Springer-Verlag 1991 Risk factors for macrovascular disease in mellitus: the London follow-up to the WHO Multinational Study of Vascular Disease
Hypertension. Risk of cardiovascular disease beginning at 115/75 mmhg doubles with every 20/10mm Hg increase. (Grade B)
 Practice Guidelines and Principles: Guidelines and principles are intended to be flexible. They serve as reference points or recommendations, not rigid criteria. Guidelines and principles should be followed
Practice Guidelines and Principles: Guidelines and principles are intended to be flexible. They serve as reference points or recommendations, not rigid criteria. Guidelines and principles should be followed
AUTONOMIC FUNCTION IS A HIGH PRIORITY
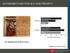 AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
DISCLOSURES OUTLINE OUTLINE 9/29/2014 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE
 ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
ANTI-HYPERTENSIVE MANAGEMENT OF CHRONIC KIDNEY DISEASE DISCLOSURES Editor-in-Chief- Nephrology- UpToDate- (Wolters Klewer) Richard J. Glassock, MD, MACP Geffen School of Medicine at UCLA 1 st Annual Internal
Joint Impact of Smoking and Hypertension on Cardiovascular Disease and All-Cause Mortality in Japan: NIPPON DATA80, a 19-Year Follow-Up
 1169 Original Article Hypertens Res Vol.30 (2007) No.12 p.1169-1175 Joint Impact of Smoking and Hypertension on Cardiovascular Disease and All-Cause Mortality in Japan: NIPPON DATA80, a 19-Year Follow-Up
1169 Original Article Hypertens Res Vol.30 (2007) No.12 p.1169-1175 Joint Impact of Smoking and Hypertension on Cardiovascular Disease and All-Cause Mortality in Japan: NIPPON DATA80, a 19-Year Follow-Up
Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction
 Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction David A. Low 1,2,3*, Ekawat Vichayanrat 2,3, Valeria Iodice 2,3 and Christopher J. Mathias 2,3 1 Research Institute of Sport and Exercise
Exercise hemodynamics in Parkinson s Disease and autonomic dysfunction David A. Low 1,2,3*, Ekawat Vichayanrat 2,3, Valeria Iodice 2,3 and Christopher J. Mathias 2,3 1 Research Institute of Sport and Exercise
Effect of Medicine Adherence on the Occurrence of Cerebrovascular Disorders in Diabetes Mellitus Patients
 Epidemiology and Health Epidemiology and Health Volume: 33, Article ID: e2011001, 6 pages DOI 10.4178/epih/e2011001 ORIGINAL ARTICLE Effect of Medicine Adherence on the Occurrence of Cerebrovascular Disorders
Epidemiology and Health Epidemiology and Health Volume: 33, Article ID: e2011001, 6 pages DOI 10.4178/epih/e2011001 ORIGINAL ARTICLE Effect of Medicine Adherence on the Occurrence of Cerebrovascular Disorders
Research Article Prevalence of Orthostatic Hypertension in Elderly Patients with Type 2 Diabetes
 International Endocrinology Volume 2015, Article ID 463487, 6 pages http://dx.doi.org/10.1155/2015/463487 Research Article Prevalence of Orthostatic Hypertension in Elderly Patients with Type 2 Diabetes
International Endocrinology Volume 2015, Article ID 463487, 6 pages http://dx.doi.org/10.1155/2015/463487 Research Article Prevalence of Orthostatic Hypertension in Elderly Patients with Type 2 Diabetes
Chapter 23. Media Directory. Cardiovascular Disease (CVD) Hypertension: Classified into Three Categories
 Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Chapter 23 Drugs for Hypertension Slide 37 Slide 41 Media Directory Nifedipine Animation Doxazosin Animation Upper Saddle River, New Jersey 07458 All rights reserved. Cardiovascular Disease (CVD) Includes
Clinical Recommendations: Patients with Periodontitis
 The American Journal of Cardiology and Journal of Periodontology Editors' Consensus: Periodontitis and Atherosclerotic Cardiovascular Disease. Friedewald VE, Kornman KS, Beck JD, et al. J Periodontol 2009;
The American Journal of Cardiology and Journal of Periodontology Editors' Consensus: Periodontitis and Atherosclerotic Cardiovascular Disease. Friedewald VE, Kornman KS, Beck JD, et al. J Periodontol 2009;
Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication
 41 Research Article Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication Amarjeet Singh*, Sudeep bhardwaj, Ashutosh aggarwal Department of Pharmacology, Seth
41 Research Article Risk Assessment of developing type 2 diabetes mellitus in patient on antihypertensive medication Amarjeet Singh*, Sudeep bhardwaj, Ashutosh aggarwal Department of Pharmacology, Seth
Blood Pressure Regulation. Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure
 Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Sheet physiology(18) Sunday 24-November Blood Pressure Regulation Slides 9-12 Mean Arterial Pressure (MAP) = 1/3 systolic pressure + 2/3 diastolic pressure MAP= Diastolic Pressure+1/3 Pulse Pressure CO=MAP/TPR
Analyzing diastolic and systolic blood pressure individually or jointly?
 Analyzing diastolic and systolic blood pressure individually or jointly? Chenglin Ye a, Gary Foster a, Lisa Dolovich b, Lehana Thabane a,c a. Department of Clinical Epidemiology and Biostatistics, McMaster
Analyzing diastolic and systolic blood pressure individually or jointly? Chenglin Ye a, Gary Foster a, Lisa Dolovich b, Lehana Thabane a,c a. Department of Clinical Epidemiology and Biostatistics, McMaster
Combination Therapy for Hypertension
 Combination Therapy for Hypertension Se-Joong Rim, MD Cardiology Division, Yonsei University College of Medicine, Seoul, Korea Goals of Therapy Reduce CVD and renal morbidity and mortality. Treat to BP
Combination Therapy for Hypertension Se-Joong Rim, MD Cardiology Division, Yonsei University College of Medicine, Seoul, Korea Goals of Therapy Reduce CVD and renal morbidity and mortality. Treat to BP
5.2 Key priorities for implementation
 5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
5.2 Key priorities for implementation From the full set of recommendations, the GDG selected ten key priorities for implementation. The criteria used for selecting these recommendations are listed in detail
Biostats Final Project Fall 2002 Dr. Chang Claire Pothier, Michael O'Connor, Carrie Longano, Jodi Zimmerman - CSU
 Biostats Final Project Fall 2002 Dr. Chang Claire Pothier, Michael O'Connor, Carrie Longano, Jodi Zimmerman - CSU Prevalence and Probability of Diabetes in Patients Referred for Stress Testing in Northeast
Biostats Final Project Fall 2002 Dr. Chang Claire Pothier, Michael O'Connor, Carrie Longano, Jodi Zimmerman - CSU Prevalence and Probability of Diabetes in Patients Referred for Stress Testing in Northeast
47 Hypertension in Elderly
 47 Hypertension in Elderly YOU DO NOT HEAL OLD AGE; YOU PROTECT IT; YOU PROMOTE IT; YOU EXTEND IT Sir James Sterling Ross Abstract: The prevalence of hypertension rises with age and the complications secondary
47 Hypertension in Elderly YOU DO NOT HEAL OLD AGE; YOU PROTECT IT; YOU PROMOTE IT; YOU EXTEND IT Sir James Sterling Ross Abstract: The prevalence of hypertension rises with age and the complications secondary
ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION*
 Progress in Clinical Medicine 1 ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION* Keishi ABE** Asian Med. J. 44(2): 83 90, 2001 Abstract: J-MUBA was a large-scale clinical
Progress in Clinical Medicine 1 ANTIHYPERTENSIVE DRUG THERAPY IN CONSIDERATION OF CIRCADIAN BLOOD PRESSURE VARIATION* Keishi ABE** Asian Med. J. 44(2): 83 90, 2001 Abstract: J-MUBA was a large-scale clinical
ΑΡΥΙΚΗ ΠΡΟΔΓΓΙΗ ΤΠΔΡΣΑΙΚΟΤ ΑΘΔΝΟΤ. Μ.Β.Παπαβαζιλείοσ Καρδιολόγος FESC - Γιεσθύνηρια ιζμανόγλειον ΓΝΑ Clinical Hypertension Specialist ESH
 ΑΡΥΙΚΗ ΠΡΟΔΓΓΙΗ ΤΠΔΡΣΑΙΚΟΤ ΑΘΔΝΟΤ Μ.Β.Παπαβαζιλείοσ Καρδιολόγος FESC - Γιεσθύνηρια ιζμανόγλειον ΓΝΑ Clinical Hypertension Specialist ESH Hypertension Co-Morbidities HTN Commonly Clusters with Other Risk
ΑΡΥΙΚΗ ΠΡΟΔΓΓΙΗ ΤΠΔΡΣΑΙΚΟΤ ΑΘΔΝΟΤ Μ.Β.Παπαβαζιλείοσ Καρδιολόγος FESC - Γιεσθύνηρια ιζμανόγλειον ΓΝΑ Clinical Hypertension Specialist ESH Hypertension Co-Morbidities HTN Commonly Clusters with Other Risk
Chronic kidney disease (CKD) has received
 Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
Participant Follow-up in the Kidney Early Evaluation Program (KEEP) After Initial Detection Allan J. Collins, MD, FACP, 1,2 Suying Li, PhD, 1 Shu-Cheng Chen, MS, 1 and Joseph A. Vassalotti, MD 3,4 Background:
HYPERTENSION: ARE WE GOING TOO LOW?
 HYPERTENSION: ARE WE GOING TOO LOW? George L. Bakris, M.D.,F.A.S.N.,F.A.S.H., F.A.H.A. Professor of Medicine Director, ASH Comprehensive Hypertension Center University of Chicago Medicine Chicago, IL USA
HYPERTENSION: ARE WE GOING TOO LOW? George L. Bakris, M.D.,F.A.S.N.,F.A.S.H., F.A.H.A. Professor of Medicine Director, ASH Comprehensive Hypertension Center University of Chicago Medicine Chicago, IL USA
Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure
 801 Original Article Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure Akira YAMASHINA, Hirofumi TOMIYAMA, Tomio ARAI, Yutaka KOJI, Minoru YAMBE, Hiroaki MOTOBE, Zydem
801 Original Article Nomogram of the Relation of Brachial-Ankle Pulse Wave Velocity with Blood Pressure Akira YAMASHINA, Hirofumi TOMIYAMA, Tomio ARAI, Yutaka KOJI, Minoru YAMBE, Hiroaki MOTOBE, Zydem
Chapter 08. Health Screening and Risk Classification
 Chapter 08 Health Screening and Risk Classification Preliminary Health Screening and Risk Classification Protocol: 1) Conduct a Preliminary Health Evaluation 2) Determine Health /Disease Risks 3) Determine
Chapter 08 Health Screening and Risk Classification Preliminary Health Screening and Risk Classification Protocol: 1) Conduct a Preliminary Health Evaluation 2) Determine Health /Disease Risks 3) Determine
Prevalence of orthostatic hypotension
 Clin Auton Res (2008) 18[Suppl 1]:8 13 DOI 10.1007/s10286-007-1001-3 ARTICLE Phillip A. Low Prevalence of orthostatic hypotension Received: 14 June 2007 Accepted: 30 June 2007 P.A. Low, MD Department of
Clin Auton Res (2008) 18[Suppl 1]:8 13 DOI 10.1007/s10286-007-1001-3 ARTICLE Phillip A. Low Prevalence of orthostatic hypotension Received: 14 June 2007 Accepted: 30 June 2007 P.A. Low, MD Department of
Hypertension in the very old. Objectives: Clinical Perspective
 Harvard Medical School Hypertension in the very old Ihab Hajjar, MD, MS, AGSF Associate Director, CV Research Lab Assistant Professor of Medicine, Harvard Medical School Objectives: Describe the clinical
Harvard Medical School Hypertension in the very old Ihab Hajjar, MD, MS, AGSF Associate Director, CV Research Lab Assistant Professor of Medicine, Harvard Medical School Objectives: Describe the clinical
High-dose monotherapy vs low-dose combination therapy of calcium channel blockers and angiotensin receptor blockers in mild to moderate hypertension
 (2005) 19, 491 496 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE High-dose monotherapy vs low-dose combination therapy of calcium channel blockers
(2005) 19, 491 496 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE High-dose monotherapy vs low-dose combination therapy of calcium channel blockers
Effects of exercise, diet and their combination on blood pressure
 (2005) 19, S20 S24 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Effects of exercise, diet and their combination on blood pressure Department
(2005) 19, S20 S24 & 2005 Nature Publishing Group All rights reserved 0950-9240/05 $30.00 www.nature.com/jhh ORIGINAL ARTICLE Effects of exercise, diet and their combination on blood pressure Department
Blood pressure. Formation of the blood pressure: Blood pressure. Formation of the blood pressure 5/1/12
 Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
Blood pressure Blood pressure Dr Badri Paudel www.badripaudel.com Ø Blood pressure means the force exerted by the blood against the vessel wall Ø ( or the force exerted by the blood against any unit area
290 Biomed Environ Sci, 2016; 29(4):
 290 Biomed Environ Sci, 2016; 29(4): 290-294 Letter to the Editor Prevalence and Predictors of Hypertension in the Labor Force Population in China: Results from a Cross-sectional Survey in Xinjiang Uygur
290 Biomed Environ Sci, 2016; 29(4): 290-294 Letter to the Editor Prevalence and Predictors of Hypertension in the Labor Force Population in China: Results from a Cross-sectional Survey in Xinjiang Uygur
Stroke A Journal of Cerebral Circulation
 Stroke A Journal of Cerebral Circulation JULY-AUGUST VOL. 7 1976 NO. 4 Components of Blood Pressure and Risk of Atherothrombotic Brain Infarction: The Framingham Study WILLIAM B. KANNEL, M.D., THOMAS R.
Stroke A Journal of Cerebral Circulation JULY-AUGUST VOL. 7 1976 NO. 4 Components of Blood Pressure and Risk of Atherothrombotic Brain Infarction: The Framingham Study WILLIAM B. KANNEL, M.D., THOMAS R.
T. Suithichaiyakul Cardiomed Chula
 T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
T. Suithichaiyakul Cardiomed Chula The cardiovascular (CV) continuum: role of risk factors Endothelial Dysfunction Atherosclerosis and left ventricular hypertrophy Myocardial infarction & stroke Endothelial
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES
 SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
SYMPATHETIC STRESSORS AND SYMPATHETIC FAILURES Any discussion of sympathetic involvement in circulation, and vasodilation, and vasoconstriction requires an understanding that there is no such thing as
Therefore MAP=CO x TPR = HR x SV x TPR
 Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Regulation of MAP Flow = pressure gradient resistance CO = MAP TPR Therefore MAP=CO x TPR = HR x SV x TPR TPR is the total peripheral resistance: this is the combined resistance of all blood vessels (remember
Awareness of Hypertension, Risk Factors and Complications among Attendants of a Primary Health Care Center In Jeddah, Saudi Arabia
 IOSR Journal of Nursing and Health Science (IOSR-JNHS e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 6, Issue 1 Ver. VIII (Jan. - Feb. 2017), PP 16-21 www.iosrjournals.org Awareness of Hypertension, Risk
IOSR Journal of Nursing and Health Science (IOSR-JNHS e-issn: 2320 1959.p- ISSN: 2320 1940 Volume 6, Issue 1 Ver. VIII (Jan. - Feb. 2017), PP 16-21 www.iosrjournals.org Awareness of Hypertension, Risk
BIOL 219 Spring Chapters 14&15 Cardiovascular System
 1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
1 BIOL 219 Spring 2013 Chapters 14&15 Cardiovascular System Outline: Components of the CV system Heart anatomy Layers of the heart wall Pericardium Heart chambers, valves, blood vessels, septum Atrioventricular
hypertension Head of prevention and control of CVD disease office Ministry of heath
 hypertension t. Samavat MD,Cadiologist,MPH Head of prevention and control of CVD disease office Ministry of heath RECOMMENDATIONS FOR HYPERTENSION DIAGNOSIS, ASSESSMENT, AND TREATMENT Definition of hypertension
hypertension t. Samavat MD,Cadiologist,MPH Head of prevention and control of CVD disease office Ministry of heath RECOMMENDATIONS FOR HYPERTENSION DIAGNOSIS, ASSESSMENT, AND TREATMENT Definition of hypertension
Blood Pressure Regulation -1
 CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
CVS Physiology Lecture 18 Blood Pressure Regulation -1 Please study the previous sheet before studying this one, even if the first part in this sheet is revision. In the previous lecture we were talking
Hypertension Management Controversies in the Elderly Patient
 Hypertension Management Controversies in the Elderly Patient Juan Bowen, MD Geriatric Update for the Primary Care Provider November 17, 2016 2016 MFMER slide-1 Disclosure No financial relationships No
Hypertension Management Controversies in the Elderly Patient Juan Bowen, MD Geriatric Update for the Primary Care Provider November 17, 2016 2016 MFMER slide-1 Disclosure No financial relationships No
The hypertensive effects of the renin-angiotensin
 Comparison of Telmisartan vs. Valsartan in the Treatment of Mild to Moderate Hypertension Using Ambulatory Blood Pressure Monitoring George Bakris, MD A prospective, randomized, open-label, blinded end-point
Comparison of Telmisartan vs. Valsartan in the Treatment of Mild to Moderate Hypertension Using Ambulatory Blood Pressure Monitoring George Bakris, MD A prospective, randomized, open-label, blinded end-point
Falls Assessment and Medication
 Falls Assessment and Medication Professor T.Masud President-Elect British Geriatrics Society Nottingham University Hospitals NHS Trust, UK Visiting Professor University of Southern Denmark Mrs GH is a
Falls Assessment and Medication Professor T.Masud President-Elect British Geriatrics Society Nottingham University Hospitals NHS Trust, UK Visiting Professor University of Southern Denmark Mrs GH is a
Cardiovascular Responses to Exercise
 CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
CARDIOVASCULAR PHYSIOLOGY 69 Case 13 Cardiovascular Responses to Exercise Cassandra Farias is a 34-year-old dietician at an academic medical center. She believes in the importance of a healthy lifestyle
Cedars Sinai Diabetes. Michael A. Weber
 Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
Cedars Sinai Diabetes Michael A. Weber Speaker Disclosures I disclose that I am a Consultant for: Ablative Solutions, Boston Scientific, Boehringer Ingelheim, Eli Lilly, Forest, Medtronics, Novartis, ReCor
김광일 서울대학교의과대학내과학교실 분당서울대학교병원내과
 치매예방을위한만성질환관리전략 김광일 서울대학교의과대학내과학교실 분당서울대학교병원내과 A sharp rise in the death rate from Alzheimer s disease Ivan Casserly & Eric Topol, Lancet 2004 Potential for primary prevention of Alzheimer s disease Alzheimer
치매예방을위한만성질환관리전략 김광일 서울대학교의과대학내과학교실 분당서울대학교병원내과 A sharp rise in the death rate from Alzheimer s disease Ivan Casserly & Eric Topol, Lancet 2004 Potential for primary prevention of Alzheimer s disease Alzheimer
Low fractional diastolic pressure in the ascending aorta increased the risk of coronary heart disease
 (2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
(2002) 16, 837 841 & 2002 Nature Publishing Group All rights reserved 0950-9240/02 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Low fractional diastolic pressure in the ascending aorta increased the risk
Relation between the angiotensinogen (AGT) M235T gene polymorphism and blood pressure in a large, homogeneous study population
 (2003) 17, 555 559 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Relation between the angiotensinogen (AGT) M235T gene polymorphism and blood
(2003) 17, 555 559 & 2003 Nature Publishing Group All rights reserved 0950-9240/03 $25.00 www.nature.com/jhh ORIGINAL ARTICLE Relation between the angiotensinogen (AGT) M235T gene polymorphism and blood
Hypertensive Crises. Controlling high blood pressure prevents disease. Recognition and Management of Acute Hypertensive Emergencies
 Controlling high blood pressure prevents disease Recognition and Management of Acute Hypertensive Emergencies David idweiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Functional Genomics
Controlling high blood pressure prevents disease Recognition and Management of Acute Hypertensive Emergencies David idweiner, M.D. Co-holder, C. Craig and Audrae Tisher Chair in Nephrology Functional Genomics
ORIGINAL INVESTIGATION. C-Reactive Protein Concentration and Incident Hypertension in Young Adults
 ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
ORIGINAL INVESTIGATION C-Reactive Protein Concentration and Incident Hypertension in Young Adults The CARDIA Study Susan G. Lakoski, MD, MS; David M. Herrington, MD, MHS; David M. Siscovick, MD, MPH; Stephen
International Journal of Current Research and Academic Review
 International Journal of Current Research and Academic Review ISSN: 2347-3215 (Online) Volume 6 Journal homepage: http://www.ijcrar.com Number 1 (January-2018) doi: https://doi.org/10.20546/ijcrar.2018.601.006
International Journal of Current Research and Academic Review ISSN: 2347-3215 (Online) Volume 6 Journal homepage: http://www.ijcrar.com Number 1 (January-2018) doi: https://doi.org/10.20546/ijcrar.2018.601.006
Note: At the end of the instructions, you will find a table which must be filled in to complete the exercise.
 Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
Autonomic Nervous System Theoretical foundations and instructions for conducting practical exercises carried out during the course List of practical exercises 1. Deep (controlled) breath test 2. Cold pressor
Hypertension and obesity. Dr Wilson Sugut Moi teaching and referral hospital
 Hypertension and obesity Dr Wilson Sugut Moi teaching and referral hospital No conflict of interests to declare Obesity Definition: excessive weight that may impair health BMI Categories Underweight BMI
Hypertension and obesity Dr Wilson Sugut Moi teaching and referral hospital No conflict of interests to declare Obesity Definition: excessive weight that may impair health BMI Categories Underweight BMI
Role of Minerals in Hypertension
 Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Role of Minerals in Hypertension Lecture objectives By the end of the lecture students will be able to Define primary and secondary hypertention and their risk factors. Relate role of minerals with hypertention.
Northera (droxidopa)
 Northera (droxidopa) Policy Number: 5.01.657 Last Review: 07/2018 Origination: 07/2018 Next Review: 07/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Northera
Northera (droxidopa) Policy Number: 5.01.657 Last Review: 07/2018 Origination: 07/2018 Next Review: 07/2019 Policy Blue Cross and Blue Shield of Kansas City (Blue KC) will provide coverage for Northera
A Study of relationship between frailty and physical performance in elderly women
 Original Article Journal of Exercise Rehabilitation 2015;11(4):215-219 A Study of relationship between frailty and physical performance in elderly women Bog Ja Jeoung 1, *, Yang Chool Lee 2 1 Department
Original Article Journal of Exercise Rehabilitation 2015;11(4):215-219 A Study of relationship between frailty and physical performance in elderly women Bog Ja Jeoung 1, *, Yang Chool Lee 2 1 Department
ORIGINAL INVESTIGATION. Effects of Prehypertension on Admissions and Deaths
 ORIGINAL INVESTIGATION Effects of Prehypertension on Admissions and Deaths A Simulation Louise B. Russell, PhD; Elmira Valiyeva, PhD; Jeffrey L. Carson, MD Background: The Joint National Committee on Prevention,
ORIGINAL INVESTIGATION Effects of Prehypertension on Admissions and Deaths A Simulation Louise B. Russell, PhD; Elmira Valiyeva, PhD; Jeffrey L. Carson, MD Background: The Joint National Committee on Prevention,
INCREASED PULSE PRESSURE AND SYSTOLIC x HEART RATE DOUBLE PRODUCT AND CARDIOVASCULAR AUTONOMIC NEUROPATHY IN TYPE 2 DIABETIC PATIENTS
 INCREASED PULSE PRESSURE AND SYSTOLIC x HEART RATE DOUBLE PRODUCT AND CARDIOVASCULAR AUTONOMIC NEUROPATHY IN TYPE 2 DIABETIC PATIENTS A.J. Scheen, J.C. Philips, M. Marchand Division of Diabetes, Nutrition
INCREASED PULSE PRESSURE AND SYSTOLIC x HEART RATE DOUBLE PRODUCT AND CARDIOVASCULAR AUTONOMIC NEUROPATHY IN TYPE 2 DIABETIC PATIENTS A.J. Scheen, J.C. Philips, M. Marchand Division of Diabetes, Nutrition
Table S1. Characteristics associated with frequency of nut consumption (full entire sample; Nn=4,416).
 Table S1. Characteristics associated with frequency of nut (full entire sample; Nn=4,416). Daily nut Nn= 212 Weekly nut Nn= 487 Monthly nut Nn= 1,276 Infrequent or never nut Nn= 2,441 Sex; n (%) men 52
Table S1. Characteristics associated with frequency of nut (full entire sample; Nn=4,416). Daily nut Nn= 212 Weekly nut Nn= 487 Monthly nut Nn= 1,276 Infrequent or never nut Nn= 2,441 Sex; n (%) men 52
Management of Hypertension. M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine
 Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
Management of Hypertension M Misra MD MRCP (UK) Division of Nephrology University of Missouri School of Medicine Disturbing Trends in Hypertension HTN awareness, treatment and control rates are decreasing
International Journal of Research and Review E-ISSN: ; P-ISSN:
 International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Short Communication Rate Pressure Product in Diabetic Cardiac Autonomic Neuropathy at Rest and Under
International Journal of Research and Review www.ijrrjournal.com E-ISSN: 2349-9788; P-ISSN: 2454-2237 Short Communication Rate Pressure Product in Diabetic Cardiac Autonomic Neuropathy at Rest and Under
Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts Future Cardiovascular Events
 Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Diabetes Care Publish Ahead of Print, published online May 28, 2008 Chronotropic response in patients with diabetes Impaired Chronotropic Response to Exercise Stress Testing in Patients with Diabetes Predicts
Hypertension awareness, treatment, and control
 O r i g i n a l P a p e r Prevalence of Self-Reported High Blood Pressure Awareness, Advice Received From Health Professionals, and Actions Taken to Reduce High Blood Pressure Among US Adults Healthstyles
O r i g i n a l P a p e r Prevalence of Self-Reported High Blood Pressure Awareness, Advice Received From Health Professionals, and Actions Taken to Reduce High Blood Pressure Among US Adults Healthstyles
Hypertension targets: sorting out the confusion. Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town
 Hypertension targets: sorting out the confusion Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town Historical Perspective The most famous casualty of this approach was the
Hypertension targets: sorting out the confusion Brian Rayner, Division of Nephrology and Hypertension, University of Cape Town Historical Perspective The most famous casualty of this approach was the
