Arrhythmias in Children
|
|
|
- Melina Miles
- 6 years ago
- Views:
Transcription
1 DOI /s x SYMPOSIUM ON PICU PROTOCOLS OF AIIMS Arrhythmias in Children Kana Ram Jat & Rakesh Lodha & Sushil K. Kabra Received: 23 August 2010 / Accepted: 12 October 2010 # Dr. K C Chaudhuri Foundation 2010 Abstract Arrhythmias in children can be classified according to their effect on central pulse: Fast pulse rate tachyarrhythmia; Slow pulse rate bradyarrhythmia; and Absent pulse is pulseless arrest (cardiac arrest). Tachyarrythmia may be narrow complex tachycardia (QRS duration 0.08 s): sinus tachycardia (ST), supraventricular tachycardia (SVT), atrial flutter or Wide-complex tachycardia (QRS duration >0.08 s): ventricular tachycardia (VT), SVT with aberrant intraventricular conduction. The choice of therapy depends on the patient s degree of hemodynamic instability. Attempt vagal stimulation, if patient is stable and if it does not unduly delay chemical or electrical cardioversion. Bradyarrhythmias include: sinus bradycardia, sinus node arrest with atrial, junctional and idioventricular escape rhythms and AV block. The emergency treatment of bradycardia depends on its hemodynamic consequences. If heart rate is <60 beats per minute with poor perfusion despite effective ventilation with oxygen, it may be treated with chest compressions, epinephrine through IV or endotracheal tube. If bradycardia persists or responds only transiently, consider a continuous infusion of epinephrine or isoproterenol and plan for emergency transcutaneous pacing. If bradycardia is due to vagal stimulation or primary A-V block, giving atropine may be beneficial. Keywords Bradyarrythmia. Tachyarrythmia. Cardioversion. Heart block K. R. Jat : R. Lodha (*) : S. K. Kabra Department of Pediatrics, All India Institute of Medical Sciences, Ansari Nagar, New Delhi , India rakesh_lodha@hotmail.com Rhythm disturbances (arrhythmias) are not uncommon in sick children admitted in pediatric intensive care unit. These occur as a result of abnormalities in, or insults to, the cardiac conduction system or heart tissues. A rhythm disturbance in a child should be treated as life threatening emergency. Normal Electrocardiogram (ECG) The ECG is a graphic representation of the sequence of myocardial depolarization and re-polarization with each normal cardiac cycle consisting of a P, QRS and a T wave (Fig. 1). Electrical depolarization begins in sinuatrial node at the junction of superior vena cava and right atrium and advances via atrial tissue and the intermodal pathways to the atrioventricular junctional tissue. It then progresses via bundle of His and its divisions to depolarize the ventricular myocardium. Approach to a Child with Arrhythmia The two most important considerations in evaluating the rhythm disturbance in a child are: 1. Child s typical heart rate and rhythm 2. Child s clinical condition, especially hemodynamic status. Arrhythmias in children can be classified according to their effect on central pulse: 1. Fast pulse rate = tachyarrhythmia; 2. Slow pulse rate = bradyarrhythmia; and 3. Absent pulse = pulseless arrest (cardiac arrest).
2 Fig. 1 Normal electrocardiogram Tachyarrhythmias Tachyarrhythmias represent a variety of fast abnormal rhythms originating either in the atria or the ventricles of heart. Tachycardia is defined as a heart rate that is fast compared with normal heart rate for the patient s age. Normal heart rate by age is given in Table 1. If there is tachycardia, look for hemodynamic stability and QRS complex in ECG. The rhythm is unstable if it causes signs or symptoms of poor tissue perfusion (weak pulses, shock with hypotension, respiratory distress, and altered consciousness). Tachyarrhythmias may be classified according to width of the QRS complex: & & Narrow complex tachycardia (QRS duration 0.08 s): sinus tachycardia (ST), supraventricular tachycardia (SVT), atrial flutter, or Wide-complex tachycardia (QRS duration >0.08 s): ventricular tachycardia (VT), SVT with aberrant intraventricular conduction. Sinus Tachycardia (ST) Sinus tachycardia is defined as a rate of sinus node discharge faster than normal for patient s age (Table 1). ST typically develops in response to body s need for increased cardiac output or oxygen delivery. Evaluation of a 12-lead ECG and the patient s clinical presentation should help differentiate sinus tachycardia from supraventricular tachycardia (SVT) (Table 2). Common causes of ST include tissue hypoxia, hypovolemia, fever, metabolic stress, injury, pain, anxiety, toxins, and anemia. Less common causes include cardiac tamponade, tension pneumothorax, and thromboembolism. If the rhythm is ST, search for and treat causes. Table 1 Normal heart rate by age [1] Age Heart rate (per min) Mean (per min) Newborn to 3 months months to 2 years years to 10 years >10 years Supraventricular Tachycardia (SVT) SVT [previously known as paroxysmal atrial tachycardia (PAT) and paroxysmal supraventricular tachycardia (PSVT)] is an abnormally fast rhythm originating above the ventricles. SVT is the most common tachyarrhythmia producing cardiovascular compromise during infancy. Three groups of tachycardia are included in SVT [2]: 1) AV re-entrant (or reciprocating) tachycardia is not only the most common mechanism of SVT but also the most common tachyarrhythmia seen in the pediatric age group. In SVT caused by re-entry, two pathways are involved; at least one of these is the AV node, and the other is an accessory pathway. Patients with accessory pathways frequently have Wolff-Parkinson-White (WPW) pre-excitation (producing a delta wave on ECG). 2) Ectopic (or nonreciprocating) atrial tachycardia is a rare mechanism of SVT in which rapid firing of a single focus in the atrium is responsible for the tachycardia. Table 2 Differentiation between sinus tachycardia and supraventricular tachycardia Parameter Sinus tachycardia SVT Heart rate Infants Usually <220/min Usually 220/min Children Usually <180/min Usually 180/min History Gradual onset, compatible with known cause e.g. fever, pain, volume loss. Abrupt onset, vague, non-specific history, symptoms of CHF. P-wave Present/normal (upright in I/aVF) Absent/abnormal (negative in leads II/III/aVF) R-R interval Variable with level Not variable of activity P-R interval Constant Variable Chest Radiograph Usually small heart and clear lungs unless pneumonia or underlying heart disease. Signs of CHF (e.g. cardiomegaly, pulmonary edema) may present.
3 3) Nodal (or AV junctional) tachycardia may superficially resemble atrial tachycardia because the P wave is buried in the T waves of the preceding beat and becomes invisible, but the rate of nodal tachycardia is relatively slower (120 to 200 beats/min) than the rate of ectopic atrial tachycardia. Causes of SVT 1. Idiopathic in about 50% and this type more commonly in young infants than in older children. 2. WPW pre-excitation is present in 10% to 20%. 3. Some congenital heart defects (e.g., Ebstein s anomaly, single ventricle, congenitally corrected transposition of the great arteries) are more susceptible to this arrhythmia. 4. Following cardiac surgeries. Clinical Features of SVT Many infants tolerate SVT well. If the tachycardia is sustained for 6 to 12 h, signs of CHF (irritability, tachypnea, poor feeding, and pallor) usually develop. Older children may complain of chest pain, palpitation, shortness of breath, lightheadedness, and fatigue. History and ECG characteristics are helpful in differentiating SVT from ST (Table 2, Fig. 2). Management of SVT The choice of therapy depends on the patient s degree of hemodynamic instability. Attempt vagal stimulation, if patient is stable and if it does not unduly delay chemical or electrical cardioversion [3]. In infants and young children, apply ice to the face without occluding the airway [4]. In older children, carotid sinus massage or Valsalva maneuvers are safe [5]. One method of a Valsalva maneuver is to have the child blow through an obstructed straw [6]. Do not apply pressure to the eye because this can damage the retina. Adenosine is the drug of choice for SVT. If IV access is readily available administer adenosine 0.1 mg/kg (maximum first dose 6 mg) using 2 syringes connected to a T-connector or stopcock; give adenosine rapidly with one syringe and immediately flush with 5 ml of normal saline with the other. If there is no reversal, then double the first dose (maximum second dose 12 mg) once. If the patient is very unstable or IV access is not readily available, provide electrical (synchronized) cardioversion. Start with a dose of 0.5 to 1 J/kg. If unsuccessful, repeat using a dose of 2 J/kg. If a second shock is unsuccessful or the tachycardia recurs quickly, consider antiarrhythmic therapy amiodarone (5 mg/kg over 20 to 60 min) or procainamide (15 mg/kg over min) before a third shock. Use extreme caution when administering more than one drug that causes QT prolongation (e.g., amiodarone and procainamide). If there is no effect and there are no signs of toxicity, give additional doses; amiodarone upto 15 mg/kg (maximum 300 mg). Intravenously administered propranolol has been commonly used to treat SVT in the presence of WPW syndrome. Esmolol, other β- adrenergic blockers, verapamil and digoxin have also been used with some success. Do not use verapamil in infants below 1 year because it may cause refractory hypotension and cardiac arrest, and use with caution in children because it may cause hypotension and myocardial depression [7]. Radiofrequency catheter ablation or surgical interruption of accessory pathways should be considered if medical management fails or frequent recurrences occur. Atrial Flutter (Intra-Atrial Re-entrant Tachycardia) It is characterized by re-entry circuit within the atria that allows a wave of depolarization to travel in a circle within the atria. There is an atrial rate (F wave with sawtooth configuration) of about 300 (range 250 to 400) beats/min, a ventricular response with varying degrees of block (e.g., 2:1, 3:1, 4:1), and normal QRS complexes (Fig. 3). The ventricular rate determines eventual cardiac output; a toorapid ventricular rate may decrease cardiac output. Thrombus formation may lead to embolic events. Uncontrolled atrial flutter may precipitate heart failure. The flutter may be associated with syncope, presyncope, or chest pain. Causes include structural heart disease with dilated atria, acute infectious illness, myocarditis or pericarditis, previous surgery involving atria (the Senning procedure, Fontan operation, or atrial septal defect repair), digitalis toxicity, and thyrotoxicosis. Fig. 2 Electrocardiogram showing supraventricular tachycardia
4 Fig. 3 Atrial flutter Management Immediate synchronized DC cardioversion is the treatment of choice for atrial flutter of short duration, if the infant or child is in severe CHF. In some cases, IV amiodarone or IV procainamide may be effective. For chronic cases: anticoagulation with warfarin (with International Normalized Ratio target of between 2.0 and 3.0) is started and cardioversion is delayed for 2 to 3 weeks. After conversion to sinus rhythm, anticoagulation is continued for an additional 3 to 4 weeks. Atrial Fibrillation Atrial fibrillation is less common than atrial flutter in children. The atrial excitation is chaotic and more rapid ( beats/min) producing an irregularly irregular ventricular response and pulse with normal QRS complexes (Fig. 4). Causes include structural heart diseases with dilated atria, such as seen with rheumatic heart disease, Ebstein s anomaly, tricuspid atresia, atrial septal defect, AV valve regurgitation, previous intra-atrial surgery, thyrotoxicosis, pulmonary emboli, and pericarditis. If atrial fibrillation has been present for more than 48 h, anticoagulation with warfarin for 2 to 3 weeks is recommended to prevent systemic embolization of atrial thrombus, if the conversion can be delayed. Anticoagulation is continued for 3 to 4 weeks after the restoration of sinus rhythm. Propranolol, digoxin, quinidine, procainamide or amiodarone may be used to slow the ventricular rate. Ventricular Tachycardia Ventricular tachycardia (VT) is a wide-complex tachyarrhythmia generated within the ventricles. Rapid ventricular rate often compromise stroke volume and cardiac output, and they may deteriorate into pulseless VT or Ventricular Fibrillation (VF). Causes include underlying heart disease (or post cardiac surgery), prolonged QT syndrome, myocarditis/cardiomyopathy, electrolyte disturbances (e.g. hyperkalemia, hypocalcemia, hypomagnesemia) and drug toxicity (e.g. tricyclic antidepressants, cocaine). In VT, ventricular rate is at least 120/min and regular, QRS complex is wide (>0.08 s), P waves are often not identifiable; when present there is AV dissociation and T wave are typically opposite in polarity from QRS (Fig. 5). Management of VT If hemodynamically stable, give an infusion of amiodarone 5 mg/kg slowly while you monitor the ECG and blood pressure. If there is no effect and there are no signs of toxicity, give additional doses up to 15 mg/kg (max. 300 mg). If amiodarone is not available, consider giving procainamide 15 mg/kg slowly (over 30 to 60 min) or lidocaine 1 mg/kg bolus followed by infusion μg/kg/min. If there is poor perfusion, treat with synchronized electrical cardioversion (0.5 J to 1 J/kg). Repeat with 2 J/kg, if no response. If it does not delay cardioversion, try a dose of adenosine first to determine if the rhythm is SVT with aberrant conduction. If second shock is unsuccessful or if the tachycardia recurs quickly, consider antiarrhythmic therapy (amiodarone or procainamide) before a third shock. If at any time the patient develops pulseless arrest, start CPR. Torsades de Pointes This polymorphic VT is seen in patients with hypomagnesemia, long QT interval, which may be congenital or may Fig. 4 Atrial fibrillation
5 Fig. 5 Electrocardiogram showing ventricular tachycardia result from toxicity with type IA antiarrhythmics (e.g., procainamide, quinidine, and disopyramide) or type III antiarrhythmics (e.g., sotalol and amiodarone), tricyclic antidepressants, digitalis, or drug interactions [8]. In torsades the QRS complexes change in polarity and amplitude, appearing to rotate around the ECG iso-electric line (Fig. 6). Regardless of the cause, treat torsades de pointes with IV infusion of magnesium sulfate mg/kg over min. While managing tachyarrhythmia, look for and treat possible contributing factors which can be remembered as Hs and Ts [1]: Hs hypovolemia, hypoxia/ventilation problem, hydrogen ion (acidosis), hypo-/hyperkalemia, hypoglycemia, hypothermia and Ts toxins, tamponade (cardiac), tension pneumothorax, thrombosis (coronary or pulmonary) and trauma (hypovolemia). Bradyarrhythmias Bradycardia is defined as a heart rate that is slow compared with normal heart rates for patient s age. Clinically significant bradycardia is defined as a heart rate less than normal for patient s age associated with poor systemic perfusion. Bradyarrhythmias are the most common prearrest rhythm in children. They are often associated with conditions such as hypoxia, hypotension, and acidosis. Examples of bradyarrhythmias include: sinus bradycardia, sinus node arrest with atrial, junctional and idioventricular escape rhythms and AV block. Sinus Bradycardia It is usually an incidental finding in otherwise healthy persons, particularly in young adults, sleeping patients, and wellconditioned athletes. Pathologic causes of sinus bradycardia include hypoxia (most common), poisoning, electrolyte disorders, infection, sleep apnea, drug effects, hypoglycemia, hypothyroidism, and increased intracranial pressure. Sinus Node Arrest It is characterized by absent pacemaker activity in the sinus node and a subsidiary pacemaker in atrium, AV junction or ventricles initiating cardiac depolarization with following rhythms: 1. Atrial escape rhythm Impulse arises from a subsidiary nonsinus atrial pacemaker. There is late P wave of different morphology. 2. Junctional escape rhythm Impulse originates in AV node and produces a slow, uniform, narrow QRS complex because the ventricles are depolarized through normal conduction system. Retrograde P wave may or may not be present. 3. Idioventricular escape rhythm Impulse originates in ventricles when there is significant bradycardia or high grades AV block and produce slow (usually between 30 40/min) wide complex. AV Block It is a disturbance of electrical conduction through the AV node. It is classified as following (Fig. 7): 1. First degree Characterized by a prolonged PR interval representing a slow conduction through AV node. Causes include intrinsic AV nodal disease, myocarditis, electrolyte disturbance (hyperkalemia), drugs (digoxin, β-blockers, calcium channel blockers), acute rheumatic fever and may also in healthy persons. It is usually asymptomatic. Fig. 6 ECG showing torsades de pointes
6 Fig. 7 Conduction blocks 2. Second degree Some but not all atrial impulses are conducted to ventricles. It is of two types: a. Mobitz type I block (Wenckebach phenomenon): Block occurs at AV node and there is progressive prolongation of PR interval until an atrial impulse is not conducted to ventricles. As a result, one P is not followed by a QRS complex. Causes include drugs (digoxin, β-blockers, calcium channel blockers), any condition that stimulates parasympathic tone. It rarely causes dizziness. b. Mobitz type II: Block occurs below AV node and it is characterized by consistent inhibition of a specific proportion of atrial impulses, 2:1 or 3:1 atrial to ventricular rate. It typically results from organic lesion in the conduction pathway or acute coronary syndrome. It may cause faintness or lightheadedness. 3. Third degree It is complete heart block and none of the atrial impulse is conducted to ventricles. There is no relationship between P waves and QRS complex. Ventricular rhythm is maintained by subsidiary pacemaker. Causes include extensive conduction system disease or injury (post surgery), congenital block, myocarditis, myocardial infarction, toxic drug effects. Symptom may include fatigue, syncope. Management of Bradyarrhythmias The emergency treatment of bradycardia depends on its hemodynamic consequences. If at any time the patient develops pulseless arrest, start CPR. If bradycardia is causing cardiorespiratory compromise, support airway, breathing, and circulation as needed, administer oxygen, and attach a monitor/defibrillator. Reassess; if pulses, perfusion, and respirations are normal, no emergency treatment is necessary. Monitor and proceed with evaluation. If heart rate is <60 beats per min with poor perfusion despite effective ventilation with oxygen, start chest compressions. Continue to support airway, ventilation, oxygenation (and provide compressions as needed) and give epinephrine 0.01 mg/kg IV/IO (1:10,000; 0.1 ml/kg) or 0.1 mg/kg through endotracheal tube (1:1,000; 0.1 ml/kg) and repeat every 3 5 min. If bradycardia persists or responds only transiently, consider a continuous infusion of epinephrine ( μg/kg/min) or isoproterenol. If bradycardia is due to vagal stimulation or primary A-V block, give atropine 0.02 mg/kg IV/IO (minimum dose 0.1 mg; maximum single dose 0.5 mg for child and 1 mg for adolescent) or 0.04 to 0.06 mg/kg through endotracheal tube. Repeat dose in 5 min, if no response (maximum total dose, 1 mg for child and 2 mg for adolescent). Emergency transcutaneous pacing may be lifesaving if the bradycardia is due to complete heart block or sinus node dysfunction unresponsive to ventilation, oxygenation, chest compressions, and medications, especially if it is associated with congenital or acquired heart disease [9]. Pacing is not useful for asystole or bradycardia due to post-arrest hypoxic/ischemic myocardial insult or respiratory failure. While managing bradyarrhythmia, look for and treat possible
7 contributing factors which can be remembered as Hs and Ts (see above). Cardiac Arrest It, also called cardiopulmonary arrest or pulseless arrest, is the cessation of circulation of blood as a result of absent or ineffective cardiac mechanical activity. Clinically, the patient is unresponsive, apneic, with no detectable pulse. In children, cardiac arrest is more often caused by progression of respiratory distress, respiratory failure, or shock than primary cardiac arrhythmias [10]. Two presentations of cardiac arrest in children are: hypoxic/asphyxial arrest (common) and sudden cardiac arrest (uncommon, usually associated with VF or pulseless VT). Asystole and bradycardia with a wide QRS complex are most common in asphyxial cardiac arrest [10]. Cardiac arrest is associated with one of the following rhythm, also known as arrest rhythm: 1. Asystole 2. Pulseless electrical activity (PEA) 3. Ventricular Fibrillation (VF) 4. Pulseless VT (including torsades de pointes) Management of Cardiac Arrest If there is cardiac arrest, support ABC and start high quality CPR immediately (start with chest compressions, push hard and push fast, minimize interruptions of chest compressions with a ratio of 15 compressions to 2 breaths. Once an advanced airway is secured, give continuous chest compressions at a rate of 100 per min without pauses for ventilation, that is, at a rate of 8 12/min. Rotate the compressor role, approximately every 2 min to prevent compressor fatigue and deterioration in quality and rate of chest compressions). Give supplementary oxygen and attach ECG monitor/defibrillator. Determine the rhythm whether it is shockable (i.e., VF or pulseless VT) or notshockable (i.e., asystole or PEA). Shockable Rhythm : Ventricular Fibrillation (VF)/ Pulseless VT VF is a chaotic, disorganized series of depolarization that results in a quering myocardium without organized contractions (Fig. 8). VF occurs in 5% to 15% of all pediatric victims of out-of hospital cardiac arrest and is reported in up to 20% of pediatric in-hospital arrests at some point during the resuscitation [11]. Defibrillation is the definitive treatment for VF with an overall survival rate of 17% to 20% [11]. Use a dose of 2 J/kg for the first attempt and 4 J/kg for subsequent attempts. Give 1 shock (2 J/kg) as quickly as possible and immediately resume CPR. Give 5 cycles of CPR in 2 min. Check the rhythm. If a shockable rhythm persists, give 1 shock (4 J/kg), resume CPR immediately. Give a dose of epinephrine. Use a standard dose of epinephrine for the first and subsequent doses. Repeat epinephrine about every 3 to 5 min during cardiac arrest. After 5 cycles of CPR, check the rhythm. If the rhythm continues to be shockable, deliver a shock (4 J/kg), resume CPR immediately, and give amiodarone (5 mg/kg) or lidocaine (1 mg/kg). Continue CPR for 5 cycles before again checking the rhythm and attempting to defibrillate if needed with 4 J/kg. If there is an organized rhythm at any time, check for a pulse and if pulse present, begin post-resuscitation care. If defibrillation is successful but VF recurs, continue CPR while you give another bolus of amiodarone before you try to defibrillate with the previously successful shock dose. Search for and treat reversible causes. Nonshockable Rhythm : Asystole/PEA The most common ECG findings in infants and children in cardiac arrest are asystole and PEA. PEA is organized electrical activity most commonly slow, wide QRS complexes without palpable pulses. This subcategory (formerly known as electromechanical dissociation [EMD]) is more likely to be treatable. For asystole and PEA: resume CPR and continue with as few interruptions in chest compressions as possible. A second rescuer gives epinephrine while the first continues CPR. Use a standard dose for the first and subsequent doses. Search for and treat reversible causes. Fig. 8 Ventricular fibrillation
8 References 1. American Heart Association. Pediatric assessment: In: Pediatric Advanced Life Support (PALS) provider manual Park MK. Cardiac arrhythmia. In: Park MK, editor. Pediatric cardiology for practitioners. 5th ed. Philadelphia: Mosby Elsevier; p American Heart Association in collaboration with International Liaison Committee on Resuscitation. Guidelines 2005 for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care: International Consensus on Science, Part 6: Pediatric Basic and Advanced Life Support. Circulation. 2005;112:III Aydin M, Baysal K, Kucukoduk S, Cetinkaya F, Yaman S. Application of ice water to the face in initial treatment of supraventricular tachycardia. Turk J Pediatr. 1995;37: Lim SH, Anantharaman V, Teo WS, Goh PP, Tan AT. Comparison of treatment of supraventricular tachycardia by Valsalva maneuver and carotid sinus massage. Ann Emerg Med. 1998;31: Wen ZC, Chen SA, Tai CT, Chiang CE, Chiou CW, Chang MS. Electrophysiological mechanisms and determinants of vagal maneuvers for termination of paroxysmal supraventricular tachycardia. Circulation. 1998;98: Rankin AC, Rae AP, Oldroyd KG, Cobbe SM. Verapamil or adenosine for the immediate treatment of supraventricular tachycardia. Q J Med. 1990;74: Ray WA, Murray KT, Meredith S, Narasimhulu SS, Hall K, Stein CM. Oral erythromycin and the risk of sudden death from cardiac causes. N Engl J Med. 2004;351: Beland MJ, Hesslein PS, Finlay CD, Faerron-Angel JE, Williams WG, Rowe RD. Noninvasive transcutaneous cardiac pacing in children. Pacing Clin Electrophysiol. 1987;10: Young KD, Seidel JS. Pediatric cardiopulmonary resuscitation: a collective review. Ann Emerg Med. 1999;33: Mogayzel C, Quan L, Graves JR, Tiedeman D, Fahrenbruch C, Herndon P. Out-of-hospital ventricular fibrillation in children and adolescents: causes and outcomes. Ann Emerg Med. 1995;25:
CSI Skills Lab #5: Arrhythmia Interpretation and Treatment
 CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
CSI 202 - Skills Lab #5: Arrhythmia Interpretation and Treatment Origins of the ACLS Approach: CSI 202 - Skills Lab 5 Notes ACLS training originated in Nebraska in the early 1970 s. Its purpose was to
PEDIATRIC CARDIAC RHYTHM DISTURBANCES. -Jason Haag, CCEMT-P
 PEDIATRIC CARDIAC RHYTHM DISTURBANCES -Jason Haag, CCEMT-P General: CARDIAC RHYTHM DISTURBANCES - More often the result and not the cause of acute cardiovascular emergencies - Typically the end result
PEDIATRIC CARDIAC RHYTHM DISTURBANCES -Jason Haag, CCEMT-P General: CARDIAC RHYTHM DISTURBANCES - More often the result and not the cause of acute cardiovascular emergencies - Typically the end result
Chapter 9. Learning Objectives. Learning Objectives 9/11/2012. Cardiac Arrhythmias. Define electrical therapy
 Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Chapter 9 Cardiac Arrhythmias Learning Objectives Define electrical therapy Explain why electrical therapy is preferred initial therapy over drug administration for cardiac arrest and some arrhythmias
Emergency treatment to SVT Evidence-based Approach. Tran Thao Giang
 Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
Emergency treatment to SVT Evidence-based Approach Tran Thao Giang Description ECG manifestations: HR is extremely rapid and regular (240bpm ± 40) P wave is: usually invisible When visible: anormal P axis,
PEDIATRIC SVT MANAGEMENT
 PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
PEDIATRIC SVT MANAGEMENT 1 INTRODUCTION Supraventricular tachycardia (SVT) can be defined as an abnormally rapid heart rhythm originating above the ventricles, often (but not always) with a narrow QRS
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
European Resuscitation Council
 European Resuscitation Council Objectives To know basic elements to evaluate patients with rythm disturbance To know advanced treatment of paediatric cardiac arrest To know emergency treatment of most
European Resuscitation Council Objectives To know basic elements to evaluate patients with rythm disturbance To know advanced treatment of paediatric cardiac arrest To know emergency treatment of most
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Anti arrhythmic drugs. Hilal Al Saffar College of medicine Baghdad University
 Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
Anti arrhythmic drugs Hilal Al Saffar College of medicine Baghdad University Mechanism of Arrhythmia Abnormal heart pulse formation Abnormal heart pulse conduction Classification of Arrhythmia Abnormal
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material
 1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
1 Cardiology Acute Care Day 22 April 2013 Arrhythmia Tutorial Course Material Arrhythmia recognition This tutorial builds on the ECG lecture and provides a framework for approaching any ECG to allow the
Preparing for your upcoming PALS course
 IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
IU Health PALS Study Guide Preparing for your upcoming PALS course UPDATED November 2016 Course Curriculum: 2015 American Heart Association (AHA) Guidelines for Pediatric Advanced Life Support (PALS) AHA
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif
 2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
2) Heart Arrhythmias 2 - Dr. Abdullah Sharif Rhythms from the Sinus Node Sinus Tachycardia: HR > 100 b/m Causes: o Withdrawal of vagal tone & Sympathetic stimulation (exercise, fight or flight) o Fever
ACLS Review. Pulse Oximetry to be between 94 99% to avoid hyperoxia (high oxygen tension can lead to tissue death
 ACLS Review BLS CPR BLS CPR changed in 2010. The primary change is from the ABC format to CAB. After establishing unresponsiveness and calling for a code, check for a pulse less than 10 seconds then begin
ACLS Review BLS CPR BLS CPR changed in 2010. The primary change is from the ABC format to CAB. After establishing unresponsiveness and calling for a code, check for a pulse less than 10 seconds then begin
Review Packet EKG Competency This packet is a review of the information you will need to know for the proctored EKG competency test.
 Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
Review Packet EKG Competency 2015 This packet is a review of the information you will need to know for the proctored EKG competency test. Normal Sinus Rhythm Rhythm: Regular Ventricular Rate: 60-100 bpm
CRC 431 ECG Basics. Bill Pruitt, MBA, RRT, CPFT, AE-C
 CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
CRC 431 ECG Basics Bill Pruitt, MBA, RRT, CPFT, AE-C Resources White s 5 th ed. Ch 6 Electrocardiography Einthoven s Triangle Chest leads and limb leads Egan s 10 th ed. Ch 17 Interpreting the Electrocardiogram
Update of CPR AHA Guidelines
 Update of CPR AHA Guidelines Donald Hal Shaffner Course objective is to have an updated understanding of the American Heart Association s treatment algorithms for the management of cardiac decompensation
Update of CPR AHA Guidelines Donald Hal Shaffner Course objective is to have an updated understanding of the American Heart Association s treatment algorithms for the management of cardiac decompensation
national CPR committee Saudi Heart Association (SHA). International Liason Commission Of Resuscitation (ILCOR)
 2 It is our pleasure to present to you this work as a result of team work of the national CPR committee at the Saudi Heart Association (SHA). We adapted the 2010 guidelines as per International Liason
2 It is our pleasure to present to you this work as a result of team work of the national CPR committee at the Saudi Heart Association (SHA). We adapted the 2010 guidelines as per International Liason
Arrhythmic Complications of MI. Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine
 Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Arrhythmic Complications of MI Teferi Mitiku, MD Assistant Clinical Professor of Medicine University of California Irvine Objectives Brief overview -Pathophysiology of Arrhythmia ECG review of typical
Pediatrics. Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment. Overview
 Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
Pediatrics Arrhythmias in Children: Bradycardia and Tachycardia Diagnosis and Treatment See online here The most common form of cardiac arrhythmia in children is sinus tachycardia which can be caused by
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
4/14/15 HTEC 91. Topics for Today. Guess That Rhythm. Premature Ventricular Contractions (PVCs) Ventricular Rhythms
 4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
4/14/15 Topics for Today HTEC 91 Medical Office Diagnostic Tests Week 5 Ventricular Rhythms PVCs: Premature Ventricular Contractions VT: Ventricular Tachycardia VF: Ventricular Fibrillation Asystole Study
3. AV Block 1. First-degree AV block 1. Delay in AV node 2. Long PR interval 3. QRS complex follows each P wave 4. Benign, no tx
 1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
1. Rhythms & arrhythmias SA nodal rhythms Sinus rhythm Sinus tachycardia Sinus bradycardia Sinus arrhythmia Sick sinus syndrome SA block Sinus arrest AV blocks First-degree Second-degree Mobitz Type I
Pediatrics ECG Monitoring. Pediatric Intensive Care Unit Emergency Division
 Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
Pediatrics ECG Monitoring Pediatric Intensive Care Unit Emergency Division 1 Conditions Leading to Pediatric Cardiology Consultation 12.7% of annual consultation Is arrhythmias problems Geggel. Pediatrics.
CORONARY ARTERIES. LAD Anterior wall of the left vent Lateral wall of left vent Anterior 2/3 of interventricluar septum R & L bundle branches
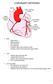 CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
CORONARY ARTERIES RCA Right atrium Right ventricle SA node 55% AV node 90% Posterior wall of left ventricle in 90% Posterior third of interventricular septum 90% LAD Anterior wall of the left vent Lateral
Core Content In Urgent Care Medicine
 Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Palpitations/Arrhythmias Ebrahim Barkoudah, MD Clinical Instructor in Internal Medicine Harvard Medical School Assistant in Internal Medicine & Pediatrics Massachusetts General Hospital MGH Chelsea Chelsea,
Step by step approach to EKG rhythm interpretation:
 Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
Sinus Rhythms Normal sinus arrhythmia Small, slow variation of the R-R interval i.e. variation of the normal sinus heart rate with respiration, etc. Sinus Tachycardia Defined as sinus rhythm with a rate
The ABCs of EKGs/ECGs for HCPs. Al Heuer, PhD, MBA, RRT, RPFT Professor, Rutgers School of Health Related Professions
 The ABCs of EKGs/ECGs for HCPs Al Heuer, PhD, MBA, RRT, RPFT Professor, Rutgers School of Health Related Professions Learning Objectives Review the basic anatomy of the heart Describe the cardiac conducting
The ABCs of EKGs/ECGs for HCPs Al Heuer, PhD, MBA, RRT, RPFT Professor, Rutgers School of Health Related Professions Learning Objectives Review the basic anatomy of the heart Describe the cardiac conducting
Cardiac arrhythmias. Janusz Witowski. Department of Pathophysiology Poznan University of Medical Sciences. J. Witowski
 Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
Cardiac arrhythmias Janusz Witowski Department of Pathophysiology Poznan University of Medical Sciences A 68-year old man presents to the emergency department late one evening complaining of increasing
UNDERSTANDING YOUR ECG: A REVIEW
 UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
UNDERSTANDING YOUR ECG: A REVIEW Health professionals use the electrocardiograph (ECG) rhythm strip to systematically analyse the cardiac rhythm. Before the systematic process of ECG analysis is described
DYSRHYTHMIAS. D. Assess whether or not it is the arrhythmia that is making the patient unstable or symptomatic
 DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
DYSRHYTHMIAS GENERAL CONSIDERATIONS A. The 2015 American Heart Association Guidelines were referred to for this protocol development. Evidence-based science was implemented in those areas where the AHA
Adult Basic Life Support
 Adult Basic Life Support UNRESPONSIVE? Shout for help Open airway NOT BREATHING NORMALLY? Call 112* 30 chest compressions 2 rescue breaths 30 compressions *or national emergency number Fig 1.2_Adult BLS
Adult Basic Life Support UNRESPONSIVE? Shout for help Open airway NOT BREATHING NORMALLY? Call 112* 30 chest compressions 2 rescue breaths 30 compressions *or national emergency number Fig 1.2_Adult BLS
Chapter 16: Arrhythmias and Conduction Disturbances
 Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Complete the following. Chapter 16: Arrhythmias and Conduction Disturbances 1. Cardiac arrhythmias result from abnormal impulse, abnormal impulse, or both mechanisms together. 2. is the ability of certain
Rhythm ECG Characteristics Example. Normal Sinus Rhythm (NSR)
 Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Substances
Normal Sinus Rhythm (NSR) Rate: 60-100 per minute Rhythm: R- R = P waves: Upright, similar P-R: 0.12-0.20 second & consistent P:qRs: 1P:1qRs Sinus Tachycardia Exercise Hypovolemia Medications Fever Substances
Course Objectives. Proper Lead Placements. Review the ECG print paper. Review the mechanics of the Myocardium. Review basics of ECG Rhythms
 ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
ECG Interpretations Course Objectives Proper Lead Placements Review the ECG print paper Review the mechanics of the Myocardium Review basics of ECG Rhythms How Leads Work The ECG Leads we use are Bipolar
Chapter 03: Sinus Mechanisms Test Bank MULTIPLE CHOICE
 Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
Instant download and all chapters Tesst Bank ECGs Made Easy 5th Edition Barbara J Aehlert https://testbanklab.com/download/tesst-bank-ecgs-made-easy-5th-edition-barbara-jaehlert/ Chapter 03: Sinus Mechanisms
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University. OBHG Education Subcommittee
 -RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
-RHYTHM PRACTICE- By Dr.moanes Msc.cardiology Assistant Lecturer of Cardiology Al Azhar University The Normal Conduction System Sinus Node Normal Sinus Rhythm (NSR) Sinus Bradycardia Sinus Tachycardia
PALS Case Scenario Testing Checklist Respiratory Case Scenario 1 Upper Airway Obstruction
 Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
Respiratory Case Scenario 1 Upper Airway Obstruction Directs administration of 100% oxygen or supplementary oxygen as needed to support oxygenation Identifies signs and symptoms of upper airway obstruction
1. Normal sinus rhythm 2. SINUS BRADYCARDIA
 1. Normal sinus rhythm 2. SINUS BRADYCARDIA No signs and symptoms observe There are severe signs or symptoms o What are the signs and symptom Hypotension
1. Normal sinus rhythm 2. SINUS BRADYCARDIA No signs and symptoms observe There are severe signs or symptoms o What are the signs and symptom Hypotension
The most common. hospitalized patients. hypotension due to. filling time Rate control in ICU patients may be difficult as many drugs cause hypotension
 Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Arrhythmias in the critically ill ICU patients: Approach for rapid recognition & management Objectives Be able to identify and manage: Atrial fibrillation with a rapid ventricular response Atrial flutter
Advanced Cardiac Life Support ACLS
 Essential Medical Training, LLC Providing Quality, Professional Training Advanced Cardiac Life Support ACLS Course Study Guide and Agenda 772-781-9249 office 772-382-0607 fax Email: treasurecoastcpr@gmail.com
Essential Medical Training, LLC Providing Quality, Professional Training Advanced Cardiac Life Support ACLS Course Study Guide and Agenda 772-781-9249 office 772-382-0607 fax Email: treasurecoastcpr@gmail.com
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD
 Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Nathan Cade, MD Brandon Fainstad, MD Andrew Prouse, MD OBJECTIVES 1. Identify the basic electrophysiology of the four causes of wide complex tachycardia. 2. Develop a simple framework for acute management
Adult Advanced Cardiovascular Life Support 2015 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular
 Adult Advanced Cardiovascular Life Support 2015 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care 1 DR. Alireza Abootalebi Assistant Professor Of
Adult Advanced Cardiovascular Life Support 2015 American Heart Association Guidelines for Cardiopulmonary Resuscitation and Emergency Cardiovascular Care 1 DR. Alireza Abootalebi Assistant Professor Of
INSTITUTE FOR MEDICAL SIMULATION & EDUCATION ACLS PRACTICAL SCENARIOS
 Practical Teaching for Respiratory Arrest with a Pulse (Case 1) You are a medical officer doing a pre-operative round when 60-year old patient started coughing violently and becomes unconscious. Fortunately
Practical Teaching for Respiratory Arrest with a Pulse (Case 1) You are a medical officer doing a pre-operative round when 60-year old patient started coughing violently and becomes unconscious. Fortunately
Final Written Exam ASHI ACLS
 Final Written Exam ASHI ACLS Instructions: Identify the choice that best completes the statement or answers the question. Questions 1 and 2 pertain to the following scenario: A 54-year-old man has experienced
Final Written Exam ASHI ACLS Instructions: Identify the choice that best completes the statement or answers the question. Questions 1 and 2 pertain to the following scenario: A 54-year-old man has experienced
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment
 Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Intraoperative and Postoperative Arrhythmias: Diagnosis and Treatment Karen L. Booth, MD, Lucile Packard Children s Hospital Arrhythmias are common after congenital heart surgery [1]. Postoperative electrolyte
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Emergency Medical Training Services Emergency Medical Technician Paramedic Program Outlines Outline Topic: WPW Revised: 11/2013 Wolff-Parkinson-White syndrome (WPW) is a syndrome of pre-excitation of the
Cardiac Arrhythmias & Drugs used in Advanced Life Support and Cardiac Emergencies
 Cardiac Arrhythmias & Drugs used in Advanced Life Support and Cardiac Emergencies CNHE Ballarat Health Services Valid from 1 st March 2016 to 31 st June 2018 1 Supraventricular Tachycardia (SVT) An atrial
Cardiac Arrhythmias & Drugs used in Advanced Life Support and Cardiac Emergencies CNHE Ballarat Health Services Valid from 1 st March 2016 to 31 st June 2018 1 Supraventricular Tachycardia (SVT) An atrial
1 Pediatric Advanced Life Support Science Update What s New for 2010? 3 CPR. 4 4 Steps of BLS Survey 5 CPR 6 CPR.
 1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
1 Pediatric Advanced Life Support Science Update 2010 2 What s New for 2010? 3 CPR Take no longer than seconds for pulse check Rate at least on per minute (instead of around 100 per minute ) Depth change:
TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT
 Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
Link download full: http://testbankair.com/download/test-bank-for-ecgs-made-easy-5thedition-by-aehlert/ TEST BANK FOR ECGS MADE EASY 5TH EDITION BY AEHLERT Chapter 5 TRUE/FALSE 1. The AV junction consists
TACHYARRHYTHMIAS IN INFANTS AND CHILDREN
 Principles of Management SVT Algorithm VT Algorithm Interpretations of ECG Supra-ventricular Tachycardia (SVT) background SVT Management SVT Ongoing Care Ventricular Tachycardia (VT) References Principles
Principles of Management SVT Algorithm VT Algorithm Interpretations of ECG Supra-ventricular Tachycardia (SVT) background SVT Management SVT Ongoing Care Ventricular Tachycardia (VT) References Principles
EKG Abnormalities. Adapted from:
 EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
EKG Abnormalities Adapted from: http://www.bem.fi/book/19/19.htm Some key terms: Arrhythmia-an abnormal rhythm or sequence of events in the EKG Flutter-rapid depolarizations (and therefore contractions)
ACLS Study Guide for Precourse Self-Assessment
 20 rhythm strips on Precourse Self-Assessment with the following matching choices: Agonal Rhythm/Asystole Atrial Fibrillation Flutter Ventricular Fibrillation Monomorphic Ventricular Normal Sinus Rhythm
20 rhythm strips on Precourse Self-Assessment with the following matching choices: Agonal Rhythm/Asystole Atrial Fibrillation Flutter Ventricular Fibrillation Monomorphic Ventricular Normal Sinus Rhythm
APPROACH TO TACHYARRYTHMIAS
 APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
APPROACH TO TACHYARRYTHMIAS PROF.DR.MD.ZAKIR HOSSAIN PROFESSOR AND HEAD DEPARTMENT OF MEDICINE SZMCH TACHYARRYTHMIA Cardiac arrythmia is a disturbance of electrical rhythm of heart. Cardac arrythmia with
Pediatric advanced life support. Management of decreased conscious level in children. Virgi ija Žili skaitė 2017
 Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
Pediatric advanced life support. Management of decreased conscious level in children Virgi ija Žili skaitė 2017 Life threatening conditions: primary assessment, differential diagnostics and emergency care.
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology)
 ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
ECG Interpretation Cat Williams, DVM DACVIM (Cardiology) Providing the best quality care and service for the patient, the client, and the referring veterinarian. GOAL: Reduce Anxiety about ECGs Back to
Advanced Resuscitation - Child
 C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
C02C Resuscitation 2017-03-23 1 up to 10 years Office of the Medical Director Advanced Resuscitation - Child Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
Requirements to successfully complete PALS:
 The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. The new AHA Handbook of Emergency Cardiac Care (ECC) contains these 2010 Guidelines.The 2010
The American Heart Association released new resuscitation science and treatment guidelines on October 19, 2010. The new AHA Handbook of Emergency Cardiac Care (ECC) contains these 2010 Guidelines.The 2010
Antiarrhythmic Drugs
 Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Antiarrhythmic Drugs DR ATIF ALQUBBANY A S S I S T A N T P R O F E S S O R O F M E D I C I N E / C A R D I O L O G Y C O N S U L T A N T C A R D I O L O G Y & I N T E R V E N T I O N A L E P A C H D /
Paramedic Rounds. Tachyarrhythmia's. Sean Sutton Dallas Wood
 Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Paramedic Rounds Tachyarrhythmia's Sean Sutton Dallas Wood Objectives At the end of this session, the paramedic will be able to: State the key components of the cardiac conduction pathway, along with the
Patient Examination. Objectives for Presentation RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS 9/8/2016
 RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
RECOGNITION OF COMMON ARRHYTHMIAS THEIR CAUSES AND TREATMENT OPTIONS Ryan Fries, DVM, DACVIM (Cardiology) Clinical Assistant Professor University of Illinois Department of Clinical Veterinary Medicine
CARDIAC ARRHYTHMIAS IN NEONATE
 Introduction: CARDIAC ARRHYTHMIAS IN NEONATE DR. PANKAJ SAKHUJA Neonatologist Average heart rate in a healthy newborn is 120-160 beats/min and the range is from 80-230 beats/min. A normal (sinus) rhythm
Introduction: CARDIAC ARRHYTHMIAS IN NEONATE DR. PANKAJ SAKHUJA Neonatologist Average heart rate in a healthy newborn is 120-160 beats/min and the range is from 80-230 beats/min. A normal (sinus) rhythm
Practical Approach to Arrhythmias
 Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Outline Practical Approach to Arrhythmias Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Conduction System ECG Acquisition ECG Interpretation Heart rate Rhythm Arrhythmias Tachyarrhythmias Supraventricular
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition
 Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
Cardiovascular Nursing Practice: A Comprehensive Resource Manual and Study Guide for Clinical Nurses 2 nd Edition Table of Contents Volume 1 Chapter 1: Cardiovascular Anatomy and Physiology Basic Cardiac
EKG Rhythm Interpretation Exam
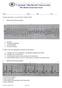 as EKG Rhythm Interpretation Exam Name: Date: ID# Unit Assume each strip is a 6 second strip. Passing is 80%. 1. Identify the following rhythm: a. Asystole b. Ventricular fibrillation c. Atrial fibrillation
as EKG Rhythm Interpretation Exam Name: Date: ID# Unit Assume each strip is a 6 second strip. Passing is 80%. 1. Identify the following rhythm: a. Asystole b. Ventricular fibrillation c. Atrial fibrillation
ARRHYTHMIAS IN THE INTENSIVE CARE UNIT
 ARRHYTHMIAS IN THE INTENSIVE CARE UNIT Nicole Van Israël, DVM, CESOpht, CertSAM, CertVC, DECVIM-CA (Cardiology), MSc, MRCVS European Specialist in Veterinary Cardiology Animal CardioPulmonary Consultancy
ARRHYTHMIAS IN THE INTENSIVE CARE UNIT Nicole Van Israël, DVM, CESOpht, CertSAM, CertVC, DECVIM-CA (Cardiology), MSc, MRCVS European Specialist in Veterinary Cardiology Animal CardioPulmonary Consultancy
Supraventricular Tachycardia: From Fetus to Adult. Mohamed Hamdan, MD
 Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
Supraventricular Tachycardia: From Fetus to Adult Mohamed Hamdan, MD Learning Objectives Define type of SVT by age Describe clinical approach Describe prenatal and postnatal management of SVT 2 SVT Across
BEDSIDE ECG INTERPRETATION
 BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
BEDSIDE ECG INTERPRETATION Presented by: Ryan Dean, RN, MSN, CCRN, CCNS, CFRN Flight Nurse 2017 Based on presentations originally by Gennifer DePaoli, RN Objectives Hospital policies Electrical conduction
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014
 Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Rhythm Control: Is There a Role for the PCP? Blake Norris, MD, FACC BHHI Primary Care Symposium February 28, 2014 Financial disclosures Consultant Medtronic 3 reasons to evaluate and treat arrhythmias
Arrhythmia 341. Ahmad Hersi Professor of Cardiology KSU
 Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
Arrhythmia 341 Ahmad Hersi Professor of Cardiology KSU Objectives Epidemiology and Mechanisms of AF Evaluation of AF patients Classification of AF Treatment and Risk stratification of AF Identify other
table of contents pediatric treatment guidelines
 table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
table of contents pediatric treatment guidelines P1 PEDIATRIC PATIENT CARE...70 P2 APPARENT LIFE-THREATENING EVENT (ALTE)...71 P3 CARDIAC ARREST INITIAL CARE AND CPR...72 73 P4 NEONATAL CARE AND RESUSCITATION...74
Cardiology Flash Cards
 Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
Cardiology Flash Cards EKG in a nut shell www.brain101.info Conduction System www.brain101.info 2 Analyzing EKG Step by step Steps in Analyzing ECG'S 1. Rhythm: - Regular _ Sinus, Junctional or Ventricular.
COUNTY OF SACRAMENTO EMERGENCY MEDICAL SERVICES AGENCY
 COUNTY OF SACRAMENTO EMERGENCY MEDICAL SERVICES AGENCY Document # 8024.31 PROGRAM DOCUMENT: Initial Date: 10/26/94 Cardiac Dysrhythmias Last Approval Date: 11/01/16 Effective Date: 11/01/18 Next Review
COUNTY OF SACRAMENTO EMERGENCY MEDICAL SERVICES AGENCY Document # 8024.31 PROGRAM DOCUMENT: Initial Date: 10/26/94 Cardiac Dysrhythmias Last Approval Date: 11/01/16 Effective Date: 11/01/18 Next Review
Acute Arrhythmias in the Hospitalized Patient
 Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
Acute Arrhythmias in the Hospitalized Patient Gregory M Marcus, MD, MAS Associate Professor of Medicine Division of Cardiology University of California, San Francisc Disclosures Medtronic: Research Support
Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/AV Blocks Connie J. Mattera, M.S., R.N., EMT-P
 Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/ Connie J. Mattera, M.S., R.N., EMT-P Reading assignments: Bledsoe Vol. 3: pp. 88-93; 120-121 (atropine, norepinephrine,
Northwest Community Healthcare Paramedic Education Program AV Conduction Defects/ Connie J. Mattera, M.S., R.N., EMT-P Reading assignments: Bledsoe Vol. 3: pp. 88-93; 120-121 (atropine, norepinephrine,
ARRHYTHMIAS IN THE ICU
 ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
ARRHYTHMIAS IN THE ICU Nora Goldschlager, MD MACP, FACC, FAHA, FHRS SFGH Division of Cardiology UCSF IDENTIFIED VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar) Electrolyte imbalance Proarrhythmia
Pediatric Advanced Life Support Overview Judy Haluka BS, RCIS, EMT-P
 Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Pediatric Advanced Life Support Overview 2006 Judy Haluka BS, RCIS, EMT-P General Our Database is lacking in pediatrics Pediatrics are DIFFERENT than Adults not just smaller The same procedure may require
Atrial fibrillation in the ICU
 Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Atrial fibrillation in the ICU Atrial fibrillation Preexisting or incident (new onset) among nearly one in three critically ill patients Formation of arrhythogenic substrate usually fibrosis (CHF, hypertension,
Arrhythmias. Sarah B. Murthi Department of Surgery University of Maryland Medical School R. Adams Cowley Shock Trauma Center
 Arrhythmias Sarah B. Murthi Department of Surgery University of Maryland Medical School R. Adams Cowley Shock Trauma Center 2012 Clinical Congress Presenter Disclosure Slide American College of Surgeons
Arrhythmias Sarah B. Murthi Department of Surgery University of Maryland Medical School R. Adams Cowley Shock Trauma Center 2012 Clinical Congress Presenter Disclosure Slide American College of Surgeons
ACLS Prep. Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep.
 November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
November, 2013 ACLS Prep Preparation is key to a successful ACLS experience. Please complete the ACLS Pretest and Please complete this ACLS Prep. ACLS Prep Preparation is key to a successful ACLS experience.
Paroxysmal Supraventricular Tachycardia PSVT.
 Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Atrial Tachycardia; is the name for an arrhythmia caused by a disorder of the impulse generation in the atrium or the AV node. An area in the atrium sends out rapid signals, which are faster than those
Case #1. 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136
 Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Tachycardias Case #1 73 y/o man with h/o HTN and CHF admitted with dizziness and SOB Treated for CHF exacerbation with Lasix Now HR 136 Initial Assessment Check Telemetry screen if pt on tele Telemetry
Atrial Fibrillation 10/2/2018. Depolarization & ECG. Atrial Fibrillation. Hemodynamic Consequences
 Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Depolarization & ECG Atrial Fibrillation How to make ORDER out of CHAOS Julia Shih, VMD, DACVIM (Cardiology) October 27, 2018 Depolarization & ECG Depolarization & ECG Atrial Fibrillation Hemodynamic Consequences
Unstable: Hypotension/Shock, Fever, Altered Mental Status, Chest discomfort, Acute Heart Failure Saturation <94%, Systolic BP < 90mmHg
 Bradycardia Heart Rate less than 50/min Stable: Monitor Seek expert help Treat Reversible Causes Unstable Signs and Symptoms: chest pain, shortness of breath, altered mental status, weak, Hypotension,
Bradycardia Heart Rate less than 50/min Stable: Monitor Seek expert help Treat Reversible Causes Unstable Signs and Symptoms: chest pain, shortness of breath, altered mental status, weak, Hypotension,
HigHligHts of the 2018 Focused In 2015 Updates to the American Heart Association Guidelines for CPR and ECC: Advanced Cardiovascular Life
 Highlights of the 2018 Focused Updates to the American Heart Association Guidelines for CPR and ECC: Advanced Cardiovascular Life Support and Pediatric Advanced Life Support - Heart and Stroke Foundation
Highlights of the 2018 Focused Updates to the American Heart Association Guidelines for CPR and ECC: Advanced Cardiovascular Life Support and Pediatric Advanced Life Support - Heart and Stroke Foundation
Adenosine. poison/drug induced. flushing, chest pain, transient asystole. Precautions: tachycardia. fibrillation, atrial flutter. Indications: or VT
 Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Adenosine Indications: 1. Narrow complex PSVT 2. Does not convert atrial fibrillation, atrial flutter or VT 1. Side effects include flushing, chest pain, transient asystole 2. May deteriorate widecomplex
Dysrhythmias 11/7/2017. Disclosures. 3 reasons to evaluate and treat dysrhythmias. None. Eliminate symptoms and improve hemodynamics
 Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Dysrhythmias CYDNEY STEWART MD, FACC NOVEMBER 3, 2017 Disclosures None 3 reasons to evaluate and treat dysrhythmias Eliminate symptoms and improve hemodynamics Prevent imminent death/hemodynamic compromise
Chapter 26. Media Directory. Dysrhythmias. Diagnosis/Treatment of Dysrhythmias. Frequency in Population Difficult to Predict
 Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Chapter 26 Drugs for Dysrythmias Slide 33 Slide 35 Media Directory Propranolol Animation Amiodarone Animation Upper Saddle River, New Jersey 07458 All rights reserved. Dysrhythmias Abnormalities of electrical
Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines
 Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines www.circ.ahajournals.org Elham Pishbin. M.D Assistant Professor of Emergency Medicine MUMS C H E S Advanced Life Support
Management of Cardiac Arrest Based on : 2010 American Heart Association Guidelines www.circ.ahajournals.org Elham Pishbin. M.D Assistant Professor of Emergency Medicine MUMS C H E S Advanced Life Support
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT
 ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
ARRHYTHMIAS IN THE ICU: DIAGNOSIS AND PRINCIPLES OF MANAGEMENT Nora Goldschlager, M.D. MACP, FACC, FAHA, FHRS SFGH Division of Cardiogy UCSF CLINICAL VARIABLES IN ARRHYTHMOGENESIS Ischemia/infarction (scar)
PALS Review 2015 Guidelines
 PALS Review 2015 Guidelines BLS CPR BLS CPR changed in 2010. The primary change is from the ABC format to CAB. 1. Scene Safety 2. Establish Unresponsiveness 3. Check for breathing if absent or agonal (No
PALS Review 2015 Guidelines BLS CPR BLS CPR changed in 2010. The primary change is from the ABC format to CAB. 1. Scene Safety 2. Establish Unresponsiveness 3. Check for breathing if absent or agonal (No
Treatment of Arrhythmias in the Emergency Setting
 Treatment of Arrhythmias in the Emergency Setting Zian H. Tseng, M.D. Assistant Professor of Medicine Cardiac Electrophysiology Section Cardiology Division University of California, San Francisco There
Treatment of Arrhythmias in the Emergency Setting Zian H. Tseng, M.D. Assistant Professor of Medicine Cardiac Electrophysiology Section Cardiology Division University of California, San Francisco There
Ventricular tachycardia Ventricular fibrillation and ICD
 EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
EKG Conference Ventricular tachycardia Ventricular fibrillation and ICD Samsung Medical Center CCU D.I. Hur Ji Won 2006.05.20 Ventricular tachyarrhythmia ventricular tachycardia ventricular fibrillation
HTEC 91. Performing ECGs: Procedure. Normal Sinus Rhythm (NSR) Topic for Today: Sinus Rhythms. Characteristics of NSR. Conduction Pathway
 HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
HTEC 91 Medical Office Diagnostic Tests Week 3 Performing ECGs: Procedure o ECG protocol: you may NOT do ECG if you have not signed up! If you are signed up and the room is occupied with people who did
Advanced Resuscitation - Adolescent
 C02B Resuscitation 2017-03-23 10 up to 17 years Office of the Medical Director Advanced Resuscitation - Adolescent Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia
C02B Resuscitation 2017-03-23 10 up to 17 years Office of the Medical Director Advanced Resuscitation - Adolescent Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia
Advanced Cardiac Life Support G 2010
 Advanced Cardiac Life Support G 2010 Produced by the Advanced Cardiac Life Support Council of the Irish Heart Foundation March 2012 Introduction: The Arrhythmia and ACLS Councils of the Irish Heart Foundation
Advanced Cardiac Life Support G 2010 Produced by the Advanced Cardiac Life Support Council of the Irish Heart Foundation March 2012 Introduction: The Arrhythmia and ACLS Councils of the Irish Heart Foundation
Arrhythmias. 1. beat too slowly (sinus bradycardia). Like in heart block
 Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Arrhythmias It is a simple-dysfunction caused by abnormalities in impulse formation and conduction in the myocardium. The heart is designed in such a way that allows it to generate from the SA node electrical
Electrocardiography for Healthcare Professionals
 Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Electrocardiography for Healthcare Professionals Kathryn A. Booth Thomas O Brien Chapter 5: Rhythm Strip Interpretation and Sinus Rhythms Learning Outcomes 5.1 Explain the process of evaluating ECG tracings
Dysrhythmias that every Learn how to recognize an abnormal cardiac rhythm and intervene appropriately. By AnneMarie Palatnik, RN, APN-BC, MSN
 Too fast, too slow, too ugly: Dysrhythmias that every Learn how to recognize an abnormal cardiac rhythm and intervene appropriately. By AnneMarie Palatnik, RN, APN-BC, MSN 2.5 ANCC CONTACT HOURS CONTINUOUS
Too fast, too slow, too ugly: Dysrhythmias that every Learn how to recognize an abnormal cardiac rhythm and intervene appropriately. By AnneMarie Palatnik, RN, APN-BC, MSN 2.5 ANCC CONTACT HOURS CONTINUOUS
Advanced Resuscitation - Adult
 C02A Resuscitation 2017-03-23 17 years & older Office of the Medical Director Advanced Resuscitation - Adult Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
C02A Resuscitation 2017-03-23 17 years & older Office of the Medical Director Advanced Resuscitation - Adult Intermediate Advanced Critical From PRIMARY ASSESSMENT Known or suspected hypothermia Algorithm
Arrhythmias_for_6_c..docx. Олена Костянтинівна Редько
 Arrhythmias_for_6_c..docx Олена Костянтинівна Редько 2015 Ключові терміни: 3 Зміст Ключові терміни: Arrhythmias 3 3 Ключові терміни: 4 Arrhythmias Ключові терміни: An irregular heart rhythm, Atrial flutter,
Arrhythmias_for_6_c..docx Олена Костянтинівна Редько 2015 Ключові терміни: 3 Зміст Ключові терміни: Arrhythmias 3 3 Ключові терміни: 4 Arrhythmias Ключові терміни: An irregular heart rhythm, Atrial flutter,
