Managing Menstrual Disorders
|
|
|
- Clarissa Mitchell
- 6 years ago
- Views:
Transcription
1 Managing Menstrual Disorders David G. Weismiller, MD, ScM, FAAFP Professor Department of Family Medicine The Brody School of Medicine at East Carolina University Greenville, North Carolina Learning Objectives 1. Assess the etiologies of abnormal vaginal bleeding 2. Clarify the appropriate diagnostic strategies for evaluating abnormal bleeding 3. Review the major etiologies of dysfunctional uterine bleeding (DUB) 4. Discuss the various therapeutic interventions for the management of DUB and menorrhagia 5. Define a diagnostic and therapeutic approach to the patient with amenorrhea. 1. Which of the following is true regarding Dysfunctional Uterine Bleeding (DUB)? A. The diagnosis of DUB is associated with malignancies of the genitourinary tract B. Diagnosis is excluded if the bleeding is NOT controlled with estrogen and/or progestin C. A pregnancy test is typically NOT needed in the evaluation of DUB D. Hypothyroidism is a common cause of DUB 1. Which of the following is true regarding Dysfunctional Uterine Bleeding (DUB)? 18% 28% 6% 50% A. The diagnosis of DUB is associated with malignancies of the genitourinary tract B. Diagnosis is excluded if the bleeding is NOT controlled with estrogen and/or progestin C. A pregnancy test is typically NOT needed in the evaluation of DUB D. Hypothyroidism is a common cause of DUB Dysfunctional Uterine Bleeding (DUB) is ANOVULATORY Uterine Bleeding Absence of pathology or medical illness Diagnosis is excluded if the bleeding is NOT controlled with estrogen and/or progestin Search for other etiologies if hormones DO NOT correct the problem DUB Is a Diagnosis of Exclusion: Adolescence Perimenopause Rule out cancer PCOS (70%) Hypothalamic anovulation Anorexia (10%) Hyperprolactinemia Hypothyroidism Premature ovarian failure Iatrogenic Radiation, chemotherapy Hyperthyroidism Coagulation disorders Genital injury or foreign object Benign tumors (fibroids) and endometrial polyps Cancers of the reproductive tract Pregnancy and pregnancy-related disorders DUB is a diagnosis made AFTER exclusion of these conditions!
2 DUB Laboratory Evaluation Pregnancy test Pap smear CBC +/- CMP Platelets Coagulation studies UA Midluteal progesterone level (>3ng/mL) Prolactin TSH FSH LH Testosterone DHEA-S Next Endometrial Evaluation Endometrial Biopsy Exclude Endometrial Cancer Risk Factors History of Anovulatory cycles Obesity Nulliparity History of tamoxifen use Diabetes mellitus DUB Endometrial Biopsy Endometrial Axis Age > 35 or < 25 if risk factors (PCOS, obese) Best time is when patient is bleeding Combination of intrauterine lidocaine plus oral naproxen sodium significantly decreases pain with endometrium sampling (LOE=1b)» Dogan E. et al. Anesthetic effect of intrauterine lidocaine plus naproxen sodium in endometrial biopsy. Obstet Gynecol 2004;103: From: Wikipedia EMB Results Proliferative normal in the follicular phase When associated with abnormal bleeding, confirms anovulation and the effect of unopposed estrogen Secretory/Menstrual confirms ovulation has occurred Hyperplasia advanced effect of unopposed estrogen atypia = premalignant Atrophic seen in menopause or effect of OCPs, Depo-Provera, and continuous ERT 2. Which of the following is considered the first-line treatment of DUB? A. Dilation and Curettage B. Combined Oral Contraceptive Pill C. Danazol D. Cyclic estrogen for days per month
3 3% 2. Which of the following is considered the first-line treatment of DUB? 80% 2% 17% A. Dilation and Curettage B. Combined Oral Contraceptive Pill C. Danazol D. Cyclic estrogen for days per month DUB Therapeutic Agents Recommendations based on good evidence Treatment of choice for anovulatory bleeding (DUB) is medical therapy with OCPs Cyclic progestin is also effective Medroxyprogesterone acetate (MPA) 10 mg po for days each month Recommendations based on expert opinion IV Conjugated estrogen therapy for acute DUB is effective in controlling bleeding Oral estrogen + MPA or high-dose OCPs to stop bleeding - then cycle on combination OCPs. IV conjugated estrogen 25 mg q 4-6 hours IV route more costly, no advantage over oral route for speed or efficacy No mention of D&C ACOG Practice Bulletin -14 (2000) The Dilemma in Treatment Is the endometrium too Thick? Is the endometrium too Thin? Some patients can be managed with hormonal therapy before diagnostic testing Age < 35 When the Endometrium is too Thick Estrogen-stimulated withdrawal bleeding Continuous unopposed estrogen stimulation Endometrium attains an abnormally thick height and bleeding is common This is the issue with DUB! Too much estrogen stimulation No ovulation Lack of Progesterone luteal phase CANCER? Atypical endometrial hyperplasia Who Has THICK Endometrium? Women who: Are obese Have chronic anovulation Have PCOS Are taking unopposed estrogen (uncommon) Treatment of Thick Endometrium What is the therapy? Goal is to reduce the thickness of the endometrium Progestins or OCPs
4 DUB Emergency Management IV conjugated estrogen 25 mg q 4 hours until bleeding slows for 12 hours Isn t TOO much Estrogen what one is trying to correct? Why give MORE? Believed to be a stimulus for clotting at the capillary level Promotes rapid growth of endometrium to cover denuded endometrial surface and stop bleeding 75% will be controlled in 6 hours Oral conjugated estrogen 10 mg/day in four divided doses can be substituted for IV estrogen Start OCPs or 10 days of monthly progestin (cyclic) after bleeding stops to prevent recurrence DUB Non-Emergency Management One combined hormonal OCP for 7 days If the flow stops within12-24 hours, the diagnosis of DUB can be confidently made Stop combined OCPs for 7 days after one week of therapy Begin regular OCPs for the next 3-6 months Alternative Cyclic administration of progesterone for 3 months When the Endometrium is too Thin Because of Heavy Continuous Bleeding The endometrium is shed and minimal It may have previously been too thick Treatment Estrogen followed by progestin Endometrium Is too Thin Typically Associated with Endometrium has minimal estrogen stimulation High progestational OCP Lo/Ovral, Nordette Progestin-only contraception Depo-Provera, minipill, IUD Endometrium becomes thinner and potentially atrophic Treatment Add estrogen, change from minipill to combination OCP or change OCP General Rule: Using progestins when the endometrium is too thin makes a bad situation worse. Who Has THIN Endometrium? Women who: Have heavy continuous uterine bleeding Are using a progestin-dominant OCP, IUD, Depo-Provera, or minipill (progestin only) Are excessively thin or have low body fat may be hypoestrogenic Eating disorders Elite athletes Marathon runners, gymnasts, skaters 3. A 32 yo female presents to the office with a complaint of very heavy periods that occur at regular intervals. She complains, I soak a box of pads the first two days of my menses. Her past medical history is unremarkable and her physical exam reveals no abnormalities. The clinical presentation is most consistent with which of the following diagnoses? A. Metrorrhagia B. Menorrhagia C. Polymenorrhea D. Hypomenorrhea
5 0% 3. A 32 yo female presents to the office with a complaint of very heavy periods that occur at regular intervals. She complains, I soak a box of pads the first two days of my menses. Her past medical history is unremarkable and her physical exam reveals no abnormalities. The clinical presentation is most consistent with which of the following diagnoses? 17% 80% 5% A. Metrorrhagia B. Menorrhagia C. Polymenorrhea D. Hypomenorrhea Patterns of Bleeding Menorrhagia: Cyclic prolonged and/or excessive bleeding Metrorrhagia: Bleeding at irregular and frequent intervals Polymenorrhea: Cycles < 21 days Oligomenorrhea: Cycles > 35 days Amenorrhea: Absence of menses > 6 months Hypomenorrhea: Cyclic light flow So Where Are We We have been discussing anovulatory bleeding = DUB! Is there an entity related to ovulatory bleeding? Yes - Menorrhagia DUB with OVULATORY Cycles Much less common Physiologic: mid-cycle spotting result of small drop in estrogen prior to ovulation Shortened follicular phase or luteal phase (polymenorrhea) Abnormality in endometrial prostaglandin production leading to loss of endometrial hemostasis (Menorrhagia) What Is Menorrhagia? Prolonged or excessive menstrual bleeding that occurs at regular intervals (loss of > 80 ml or lasts more than 7 days). I soak a box of pads the first two days of menses. Consider uterine fibroids or endometrial polyps Consider coagulopathies (rare) Exclude endometrial cancer 4. Which of the following is considered a suitable medical treatment for menorrhagia? A. NSAIDs B. SSRIs C. Gabapentin D. Testosterone
6 8% 4. Which of the following is considered a suitable medical treatment for menorrhagia? 83% 10% 1% A. NSAIDs B. SSRIs C. Gabapentin D. Testosterone Treatment of Menorrhagia (Cochrane Review) Medical NSAIDs Danazol OCPs Continuous OCPs Oral continuous progestins (d 5-26) Levonorgestrel IUD Surgical Hysterectomy Ablation 1 st generation Resection» Laser» Rollerball 2 nd generation Cryoablation* Laser Intrauterine Thermotherapy Radiofrequency ablation* Thermal balloon ablation Microwave ablation* Alternate Medical Therapies NSAIDs: prostacyclin (platelet anti-aggregating vasodilator) Decrease blood flow 20-50% Mefenamic acid 500 mg po TID Danazol 200 mg po qd Anti-estrogen Decrease blood flow 50% Side effects limit use GnRH agonists limited by climacteric symptoms and osteoporosis Antifibrinolytic agents GI side effects,? Thrombosis LNG-IUS 80% decrease in blood loss Endometrial Ablation Methods Rule out preinvasive and invasive endometrial lesions before procedures Must have completed childbearing and tolerate some menstrual bleeding Treatment of Menorrhagia Cochrane 2005 Endometrial ablation significantly more effective with fewer side effects than medical therapies No significant differences between levonorgestrel IUD and any surgery in satisfaction rates or quality of life >64% of women scheduled for hysterectomy cancelled the surgery after Mirena Hysterectomy has high satisfaction rates but risks of major surgery 5. Which of the following statements is true when considering a patient with amenorrhea? A. Amenorrhea is rarely associated with PCOS B. It is unusual to find a positive pregnancy test in the patient presenting with amenorrhea C. The relative estrogen status can be evaluated with a progestin challenge test D. A TSH is not necessary in the evaluation
7 5. Which of the following statements is true when considering a patient with amenorrhea? 6% 4% 89% 1% A. Amenorrhea is rarely associated with PCOS B. It is unusual to find a positive pregnancy test in the patient presenting with amenorrhea C. The relative estrogen status can be evaluated with a progestin challenge test D. A TSH is not necessary in the evaluation Amenorrhea Systematic Approach Focus on the signs and symptoms that suggest an underlying cause Thyroid disease: Hypo- or Hyperthyroidism Estrogen deficiency: Menopause Androgen excess: Tumor, PCOS Pituitary tumors: Prolactinoma Step 1 Step 2 Step 3 - Steps in Evaluation Rule out pregnancy TSH to evaluate for hypo- or hyperthyroidism Prolactin to evaluate for pituitary tumor (fasting, no breast stimulation Determine the relative estrogen status Relative Estrogen Status Progestin Challenge Test 5-10 mg medroxyprogesterone acetate po q day x 10 days Any bleeding within 2-7 days is positive Elevated TSH or Prolactin Hypothyroidism Pituitary Disease Amenorrhea TSH Prolactin Progestin Challenge (+) withdrawal bleed Normal TSH and Prolactin Anovulation Anovulatory Amenorrhea Amenorrheic women with adequate estrogen [(+) Progestin challenge test] Anovulatory, frequently obese,+/- PCOS Progesterone is NOT being adequately produced in luteal phase Unopposed estrogen stimulation Risk of endometrial cancer is increased Treatment Progestin 10 mg q day 7-10 days every month or OCPs
8 Outflow Tract Obstruction (Asherman s, Mullerian agenesis) No withdrawal bleed Amenorrhea TSH (nl) Prolactin (nl) and Progestin Challenge (-) withdrawal bleed Estrogen and Progestin Challenge Test Low Hypothalamic amenorrhea Amenorrhea (+) withdrawal bleed following Estrogen and Progestin challenge Normal MRI Measure FSH and LH Normal High Ovarian Failure Hypothalamic Amenorrhea Hypogonadotropic Hypogonadism Low or normal FSH/LH, normal prolactin, low levels of endogenous estrogen, normal MRI of sella (+) withdrawal bleed following estrogenprogestin challenge test Usually diagnosed by exclusion of pituitary lesions Anorexia/bulimia, Kallmann s syndrome, stress, high-intensity exercise, chronic illness Hypothalamic Amenorrhea Amenorrheic Women with Inadequate Estrogen Risk of decreased bone density (10-20%) Cannot be completely overcome with supplemental calcium or weight-bearing exercise? Rate of fractures Although OCPs improve lumbar and total bone mineral, effect on fractures unknown Increase BMI > 20 to restore menses Decrease intensive exercising Ovarian Failure High FSH/LH Premature ovarian failure < 40 not always reversible Autoimmune, genetic, chemotherapy, mumps Postmenopausal ovarian failure Absence of secondary sex characteristics Gonadal dysgenesis Turner syndrome (most common form) 6. Which of the following statements is true regarding Polycystic Ovarian Syndrome? A. The serum FSH and LH are frequently abnormal B. Hyperandrogenism is an unusual finding with the syndrome C. It is one of the least common endocrinopathies seen in women D. Metformin is recommended as a first-line agent for anovulatory women with PCOS and Insulin resistance
9 3% 1% 0% 6. Which of the following statements is true regarding Polycystic Ovarian Syndrome? 97% A. The serum FSH and LH are frequently abnormal B. Hyperandrogenism is an unusual finding with the syndrome C. It is one of the least common endocrinopathies seen in women D. Metformin is recommended as a first-line agent for anovulatory women with PCOS and Insulin resistance What Is Polycystic Ovarian Syndrome? Consensus Infrequent or no ovulation; Infertility Oligomenorrhea or amenorrhea Hyperandrogenism Presence of hirsutism or biochemical hyperandrogenemia Polycystic ovaries on ultrasound Presence of one polycystic ovary is sufficient to provide diagnosis Appears between puberty and mid-20s Suggested Evaluation Physical BP BMI > 30 = obese Waist circumference to determine body fat distribution > 35 inches = abnormal Stigmata of hyperandrogenism and insulin resistance Acne, hirsutism, androgenic alopecia, acanthosis nigricans Pathophysiology Multiple genetic variants Environmental factors (diet, obesity, toxins) Excess LH secretion Deficient progesterone Increased free testosterone Functional androgen excess PCOS Diagnosis (AES 2009) Androgen excess (clinical and/or biochemical) Ovarian dysfunction (oligo-anovulation and/or polycystic ovarian morphology) Exclusion of other causes of androgen excess and ovulatory disorders Suggested Evaluation Laboratory/Imaging Documentation of biochemical hyperandrogenemia Total testosterone and sex hormone-binding globulin or Bioavailable and free testosterone Exclusion of other causes of hyperandrogenism TSH Prolactin 17-hydroxyprogesterone (nonclassical congenital adrenal hyperplasia due to 21 hydroxylase deficiency) Random normal level < 4ng/mL or Morning fasting level < 2ng/mL Consider screening for Cushing syndrome and other rare disorders such as acromegaly Transvaginal pelvic ultrasound
10 Suggested Evaluation Laboratory Evaluation for metabolic abnormalities 2-hour glucose tolerance test Fasting lipid and lipoprotein level Expected Values for PCOS FSH: Normal to mildly elevated LH: Generally moderately elevated Dependent on timing of sample to last menstrual period Prolactin: Normal to mildly elevated Testosterone: normal to moderately elevated Normal serum estradiol, increased serum estrone concentrations Hyperinsulinemia Insulin sensitivity DECREASES Insulin release and circulating insulin INCREASE; Normal glucose tolerance unless there is metabolic syndrome present 45% of PCOS patients will have impaired glucose tolerance of Type 2 DM Practical world: fasting glucose, Hgb A1c Insulin Resistance Insulin resistance stimulates ovarian androgen production leading to anovulation Prolonged anovulation can lead to development of enlarged ovaries with multiple cysts that were first seen on US thus the name of the syndrome Hyperinsulinemia and hyperandrogenemia interfere with the secretion of gonadotropins from the pituitary gland, resulting in changes to the mid-cycle LH surge and its diurnal variation Management of PCOS Oligomenorrhea and Amenorrhea OCPs # (Combination pill; low dose) Monthly progesterone Insulin Resistance Metformin # Cochrane 2007 * Farquhar et al. Cochrane 2004 ^ Farquhar et al. Cochrane 2005 Hirsutism OCP s Spironolactone * Finasteride Infertility Clomiphene ^ Metformin? Pioglitazone Key Points Improving insulin sensitivity with insulinsensitizing drugs is associated with decrease in circulating androgen levels, improved ovulation rate, and improved glucose tolerance Metformin or clomiphine alone or in combination are first-line treatment for ovulation induction No success add exogenous gonadotropins or laparoscopic ovarian surgery ACOG Practice Bulletin 108 Polycystic Ovary Syndrome. Obstet Gynecol. 2009;114(4): Radosh L. Drug treatments for PCOS. Am Fam Physician 2009;79(8):
11 7. Which of the following is a true statement regarding natural menopause? 7. Which of the following is a true statement regarding natural menopause? A. An FSH > 20 IU/mL is the most accurate biologic marker for menopause B. Postmenopause is defined as the period after menopause and begins following 6 months of spontaneous amenorrhea C. There appear to be no cultural differences in the reporting or experiencing of hot flashes D. Healthy women > 40 years of age who are nonsmokers can safely use combination estrogen-progestin contraceptives 24% 33% 7% 36% A. An FSH > 20 IU/mL is the most accurate biologic marker for menopause B. Postmenopause is defined as the period after menopause and begins following 6 months of spontaneous amenorrhea C. There appear to be no cultural differences in the reporting or experiencing of hot flashes D. Healthy women > 40 years of age who are nonsmokers can safely use combination estrogen-progestin contraceptives Vasomotor Instability Hot Flashes Probably hypothalamic origin Menopause Thyroid disease Panic or anxiety disorder Insulinoma Autoimmune disorders Pheochromocytoma Carcinoid syndrome Tamoxifen and raloxifene Influences on Hot Flashes Cultural More prevalent in black and Latin American women than in white women Less common in Chinese and Japanese women Other variables associated with increased reporting of hot flashes: Cigarette smoking Potential risk factors with inconsistent association: Maternal history Early age of menarche and menopause onset History of irregular menses Higher BMI Alcohol use Hot/humid weather Treatment of Hot Flashes All oral, transdermal, topical gel, and emulsions estrogen/testosterone preparations are FDA-approved Hot Flashes: Other Hormonal Therapies OCPs Highly effective Known contraindications Organization North American Menopause Society (NAMS) 2007 ACOG Cochrane 2006 AHRQ March 2005 Recommendation Treatment of moderate to severe hot flashes is the primary indication for oral estrogen therapy Primary indication for hormone therapy (HT) HT significantly reduces the frequency and severity (75%) of hot flashes Studies on reduction of vasomotor symptoms are conclusive ONLY for estrogen Androgen-estrogen therapy (Estratest) Custom hormone preparations (Compounding pharmacist) Approved for treatment of moderate to severe flashes not improved by estrogen alone Data are lacking Not adequately studied for any indication No data they are safer than conventional therapy
12 Atrophy of Vagina (Dryness) Suckling et al. Cochrane 2006 Local estrogens equally effective Vaginal estradiol ring (worn 90 days) preferred Vaginal estradiol tablets Vaginal cream (Premarin) More uterine bleeding, breast pain than tablets Significantly more endometrial stimulation than estradiol ring 8. Which of the following is true regarding combination estrogen-progesterone hormone therapy (HT)? A. HT reduces the risk of osteoporosis B. HT increases the risk of colon cancer C. HT decreases the risk of breast cancer D. HT has no effect on the risk of stroke 8. Which of the following is true regarding combination estrogen-progesterone hormone therapy (HT)? 85% 3% 8% 6% A. HT reduces the risk of osteoporosis B. HT increases the risk of colon cancer C. HT decreases the risk of breast cancer D. HT has no effect on the risk of stroke HRT Women s Health Initiative Study* Proven benefits Reduced risk of osteoporosis and related fractures (34%) Decreased colon cancer risk (37%) Improvement of vasomotor symptoms * Writing Group for the Women s Health Initiative. JAMA 2002;288: Increases the risk of the following Breast cancer (26%) CVA (41%) MI (29%) Venous thromboembolic events* Previous thromboembolic disease is the only ABSOLUTE contraindication to HRT. Heart disease, breast cancer and endometrial cancer Are RELATIVE contraindications USPSTF 2005: Chemoprevention for Combination HRT in Postmenopausal Women Recommends AGAINST routine use of combined HRT for prevention of chronic conditions in postmenopausal women Androgen Therapy The FDA has not approved any use of androgens alone for symptoms that may be attributable to androgen deficiency (which may also be attributable to estrogen deficiency): Low libido Decreased sexual response Decreased sense of well-being Poor concentration Fatigue Use of androgens is considered off-label Adverse effects with use at supraphysiologic levels Acne Hirsutism HDL
13 Testosterone Therapy Cochrane 2006 Addition of Testosterone to HT regimens improved sexual function scores in postmenopausal women Significant adverse effect: HDL reduction Conclusion: Limited number of trials cannot conclude efficacy and safety 9. A 52-year-old patient currently takes no prescribed or over-the-counter medications and declines estrogen replacement therapy Which one of the following would be most effective for relieving this patient s symptoms? A. Venlafaxine (Effexor) B. Black cohosh C. Soy protein D. Vitamin E 9. A 52-year-old patient currently takes no prescribed or over-the-counter medications and declines estrogen replacement therapy Which one of the following would be most effective for relieving this patient s symptoms? A. Venlafaxine (Effexor) B. Black cohosh C. Soy protein D. Vitamin E 56% 31% 11% 3% Hot Flashes Other Therapies Significant reduction Gabapentin 100 mg/d Clonidine mg/d Venlafaxine (SSRI) mg/d Some reduction Methyldopa 500 mg/d (frequent side effects) No better or only slightly better than placebo Vitamin E Soy protein Red clover Black cohosh Perimenopausal Postmenopausal Bleeding Perimenopausal Bleeding (Endometrial Biopsy First) Progestins Provera 5-10 mg for 12 days/month Prevents endometrial hyperplasia OCPs (agent of choice if nonsmoker Expert opinion) Regulate cycles and control bleeding, contraception Levonorgestrel IUD (Mirena) Induces amenorrhea, may cause atrophy HT sequential more effective than continuous Prevents hyperplasia but NO contraception
14 10. A 55 yo postmenopausal woman presents with two days of vaginal bleeding (spotting). She initiated hormone therapy 14 months ago because of significant nocturnal hot flashes. Which of the following statements is most accurate? 10. A 55 yo postmenopausal woman presents with two days of vaginal bleeding (spotting). She initiated hormone therapy 14 months ago because of significant nocturnal hot flashes. Which of the following statements is most accurate? A. Irregular bleeding is uncommon after HT is initiated B. Postmenopausal women on hormone therapy for > 6 months who experience bleeding require prompt evaluation C. Postmenopausal women on HT for <12 months who experience bleeding may be observed for one year before diagnosing abnormal uterine bleeding D. The sensitivity of endometrial biopsy for the detection of endometrial abnormalities is 50% 1% 74% 22% 4% A. Irregular bleeding is uncommon after HT is initiated B. Postmenopausal women on hormone therapy for > 6 months who experience bleeding require prompt evaluation C. Postmenopausal women on HT for <12 months who experience bleeding may be observed for one year before diagnosing abnormal uterine bleeding D. The sensitivity of endometrial biopsy for the detection of endometrial abnormalities is 50% Postmenopausal Bleeding Irregular bleeding is common after HT is initiated and improves within 6-12 months for most women Evaluate Cyclic HT, experience unusually prolonged or heavy bleeding that occurs near the end of the progestogen phase of the cycle, or breakthrough bleeding that occurs at any other time Continuous HT, experience bleeding that persists > 6-12 months or that occurs after amenorrhea has been established HT <12 months may be observed for 1 year before diagnosing abnormal uterine bleeding Postmenopausal on no HT or HT >12 months with bleeding Answers 1. B 2. B 3. B 4. A 5. C 6. D 7. D 8. A 9. A 10. C
Abnormal Uterine Bleeding Case Studies
 Case Study 1 Abnormal Uterine Bleeding Case Studies Abigail, a 24 year old female, presents to your office complaining that her menstrual cycles have become a problem. They are now lasting 6 7 days instead
Case Study 1 Abnormal Uterine Bleeding Case Studies Abigail, a 24 year old female, presents to your office complaining that her menstrual cycles have become a problem. They are now lasting 6 7 days instead
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018
 Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Polycystic Ovary Syndrome HEATHER BURKS, MD OU PHYSICIANS REPRODUCTIVE MEDICINE SEPTEMBER 21, 2018 Learning Objectives At the conclusion of this lecture, learners should: 1) Know the various diagnostic
Overview of Reproductive Endocrinology
 Overview of Reproductive Endocrinology I have no conflicts of interest to report. Maria Yialamas, MD Female Hypothalamic--Gonadal Axis 15 4 Hormone Secretion in the Normal Menstrual Cycle LH FSH E2, Progesterone,
Overview of Reproductive Endocrinology I have no conflicts of interest to report. Maria Yialamas, MD Female Hypothalamic--Gonadal Axis 15 4 Hormone Secretion in the Normal Menstrual Cycle LH FSH E2, Progesterone,
Conflicts 10/5/2016. Abnormal Uterine Bleeding. Objectives Review diagnosis and updated nomenclature. Management options for acute and chronic AUB.
 Abnormal Uterine Bleeding Barbara L. Keller, MD JD Naval Hospital Oak Harbor OB/GYN Physician Conflicts I have no conflicts or financial interests to disclose. Objectives Review diagnosis and updated nomenclature.
Abnormal Uterine Bleeding Barbara L. Keller, MD JD Naval Hospital Oak Harbor OB/GYN Physician Conflicts I have no conflicts or financial interests to disclose. Objectives Review diagnosis and updated nomenclature.
Frequency of menses. Duration of menses 3 days to 7 days. Flow/amount of menses Average blood loss with menstruation is 60-80cc.
 Frequency of menses 24 days (0.5%) to 35 days (0.9%) Age 25, 40% are between 25 and 28 days Age 25-35, 60% are between 25 and 28 days Teens and women over 40 s cycles may be longer apart Duration of menses
Frequency of menses 24 days (0.5%) to 35 days (0.9%) Age 25, 40% are between 25 and 28 days Age 25-35, 60% are between 25 and 28 days Teens and women over 40 s cycles may be longer apart Duration of menses
12/13/2017. Important references for PCOS. Polycystic Ovarian Syndrome (PCOS) for the Family Physician. 35 year old obese woman
 Polycystic Ovarian Syndrome (PCOS) for the Family Physician Barbara S. Apgar MD, MS Professor or Family Medicine University of Michigan Ann Arbor, Michigan Important references for PCOS Endocrine Society
Polycystic Ovarian Syndrome (PCOS) for the Family Physician Barbara S. Apgar MD, MS Professor or Family Medicine University of Michigan Ann Arbor, Michigan Important references for PCOS Endocrine Society
Cynthia Morris DO, FACOOG, FACOS Medical Director, Women s Wellness Center Fayette County Memorial Hospital
 Cynthia Morris DO, FACOOG, FACOS Medical Director, Women s Wellness Center Fayette County Memorial Hospital Touchdown to CME Eighth District Academy of Osteopathic Medicine & Surgery October 8. 2017 Goals
Cynthia Morris DO, FACOOG, FACOS Medical Director, Women s Wellness Center Fayette County Memorial Hospital Touchdown to CME Eighth District Academy of Osteopathic Medicine & Surgery October 8. 2017 Goals
Dr. Nancy Van Eyk Associate Professor, Dalhousie University Chief of Gynaecology, IWK Health Centre
 Dr. Nancy Van Eyk Associate Professor, Dalhousie University Chief of Gynaecology, IWK Health Centre AUB Outline Terminology Classification/Etiology Assessment Treatment Referral to Gynaecology U c pt 4
Dr. Nancy Van Eyk Associate Professor, Dalhousie University Chief of Gynaecology, IWK Health Centre AUB Outline Terminology Classification/Etiology Assessment Treatment Referral to Gynaecology U c pt 4
PCOS and Obesity DUB is better treated by OCPs
 PCOS and Obesity DUB is better treated by OCPs Dr. Ritu Joshi Senior consultant Fortis escorts Hospital, Jaipur Chairperson Family welfare com. FOGSI (20092012) Vice President FOGSI 2014 Introduction One
PCOS and Obesity DUB is better treated by OCPs Dr. Ritu Joshi Senior consultant Fortis escorts Hospital, Jaipur Chairperson Family welfare com. FOGSI (20092012) Vice President FOGSI 2014 Introduction One
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Definition: the diagnostic criteria Evidence of hyperandrogenism, biochemical &/or clinical (hirsutism, acne & male pattern baldness). Ovulatory dysfunction; amenorrhoea; oligomenorrhoea
Polycystic Ovary Syndrome Definition: the diagnostic criteria Evidence of hyperandrogenism, biochemical &/or clinical (hirsutism, acne & male pattern baldness). Ovulatory dysfunction; amenorrhoea; oligomenorrhoea
Abnormal Uterine Bleeding: Evaluation of Premenopausal Women. Vanessa Jacoby, MD, MAS Assistant Professor Ob, Gyn, & Reproductive Sciences UCSF
 Abnormal Uterine Bleeding: Evaluation of Premenopausal Women Vanessa Jacoby, MD, MAS Assistant Professor Ob, Gyn, & Reproductive Sciences UCSF Objectives Define normal and abnormal uterine bleeding Review
Abnormal Uterine Bleeding: Evaluation of Premenopausal Women Vanessa Jacoby, MD, MAS Assistant Professor Ob, Gyn, & Reproductive Sciences UCSF Objectives Define normal and abnormal uterine bleeding Review
Dysfunctional Uterine Bleeding (DUB) OB/GYN Hospital of Fudan University Weiwei Feng, MD,Ph D Tel:
 Dysfunctional Uterine Bleeding (DUB) OB/GYN Hospital of Fudan University Weiwei Feng, MD,Ph D Email: wfeng7347@aliyun.com Tel: 13918551061 2014-8-20 Contents DUB: definition, mechanism of normal menses,
Dysfunctional Uterine Bleeding (DUB) OB/GYN Hospital of Fudan University Weiwei Feng, MD,Ph D Email: wfeng7347@aliyun.com Tel: 13918551061 2014-8-20 Contents DUB: definition, mechanism of normal menses,
CASE 4- Toy et al. CASE FILES: Obstetrics & Gynecology
 CASE 4- Toy et al. CASE FILES: Obstetrics & Gynecology A 49-year-old woman complains of irregular menses over the past 6 months, feelings of inadequacy, vaginal dryness, difficulty sleeping, and episodes
CASE 4- Toy et al. CASE FILES: Obstetrics & Gynecology A 49-year-old woman complains of irregular menses over the past 6 months, feelings of inadequacy, vaginal dryness, difficulty sleeping, and episodes
Topics. Periods Menopause & HRT Contraception Vulva problems
 Girls stuff Topics Periods Menopause & HRT Contraception Vulva problems Menorrhagia Excessive menstrual loss occurring with regular or irregular cycles Ovulatory Anovulatory Usual blood loss 30-40ml per
Girls stuff Topics Periods Menopause & HRT Contraception Vulva problems Menorrhagia Excessive menstrual loss occurring with regular or irregular cycles Ovulatory Anovulatory Usual blood loss 30-40ml per
5/5/2010 FINANCIAL DISCLOSURE. Abnormal Uterine Bleeding. Is This A Problem? About me % of visits to gynecologist
 Abnormal Uterine FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology May 5, 2010 About
Abnormal Uterine FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology May 5, 2010 About
POTION OR POISON? MEDICAL TREATMENT ALTERNATIVES TO THE PILL. Lester Ruppersberger, D.O., FACOOG,CNFPI NFP only Gynecologist
 POTION OR POISON? MEDICAL TREATMENT ALTERNATIVES TO THE PILL Lester Ruppersberger, D.O., FACOOG,CNFPI NFP only Gynecologist THE PILL Released to US market in 1960 10-15 x dose of hormones in HRT Over 10-14
POTION OR POISON? MEDICAL TREATMENT ALTERNATIVES TO THE PILL Lester Ruppersberger, D.O., FACOOG,CNFPI NFP only Gynecologist THE PILL Released to US market in 1960 10-15 x dose of hormones in HRT Over 10-14
Learning Objectives. Peri menopause. Menopause Overview. Recommendation grading categories
 Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
Learning Objectives Identify common symptoms of the menopause transition Understand the risks and benefits of hormone replacement therapy (HRT) Be able to choose an appropriate hormone replacement regimen
UPDATE: Women s Health Issues
 UPDATE: Women s Health Issues Renee B. Alexis, MD, MBA, MPH, FACOG Associate Professor Department of OBGYN Kiran C. Patel College of Osteopathic Medicine Disclosure of Conflicts of Interest I have no financial
UPDATE: Women s Health Issues Renee B. Alexis, MD, MBA, MPH, FACOG Associate Professor Department of OBGYN Kiran C. Patel College of Osteopathic Medicine Disclosure of Conflicts of Interest I have no financial
Elaina Sexton, MD, MSc Obstetrics and Gynecology St. Vincent s Hospital. Objectives
 Elaina Sexton, MD, MSc Obstetrics and Gynecology St. Vincent s Hospital Objectives Definition of normal menstrual cycle and abnormal uterine bleeding (AUB) Evaluation of AUB Medical options for AUB Surgical
Elaina Sexton, MD, MSc Obstetrics and Gynecology St. Vincent s Hospital Objectives Definition of normal menstrual cycle and abnormal uterine bleeding (AUB) Evaluation of AUB Medical options for AUB Surgical
Index. Note: Page numbers of article titles are in boldface type.
 Index Note: Page numbers of article titles are in boldface type. A Abdominal myomectomy in leiomyoma management, 77 Abnormal uterine bleeding (AUB) described, 103 105 normal menstrual bleeding vs., 104
Index Note: Page numbers of article titles are in boldface type. A Abdominal myomectomy in leiomyoma management, 77 Abnormal uterine bleeding (AUB) described, 103 105 normal menstrual bleeding vs., 104
POLYCYSTIC OVARIAN SYNDROME Laura Tatpati, MD Reproductive Endocrinology and Infertility. Based on: ACOG No. 108 Oct 2009; reaffirmed 2015
 POLYCYSTIC OVARIAN SYNDROME Laura Tatpati, MD Reproductive Endocrinology and Infertility Based on: ACOG No. 108 Oct 2009; reaffirmed 2015 NO DISCLOSURES PATIENT 26 years old presents with complaint of
POLYCYSTIC OVARIAN SYNDROME Laura Tatpati, MD Reproductive Endocrinology and Infertility Based on: ACOG No. 108 Oct 2009; reaffirmed 2015 NO DISCLOSURES PATIENT 26 years old presents with complaint of
Perimenopausal DUB. Mary Anne Jamieson, MD Associate Professor, OB/GYN Queen s University Kingston, Ontario
 Perimenopausal DUB Mary Anne Jamieson, MD Associate Professor, OB/GYN Queen s University Kingston, Ontario Objectives Clinicians will: Make a confident diagnosis for Perimenopausal DUB (know how/when to
Perimenopausal DUB Mary Anne Jamieson, MD Associate Professor, OB/GYN Queen s University Kingston, Ontario Objectives Clinicians will: Make a confident diagnosis for Perimenopausal DUB (know how/when to
Reproductive Health and Pituitary Disease
 Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
Reproductive Health and Pituitary Disease Janet F. McLaren, MD Assistant Professor Division of Reproductive Endocrinology and Infertility Department of Obstetrics and Gynecology jmclaren@uabmc.edu Objectives
Polycystic Ovarian Syndrome. Heidi Hallonquist, MD Concord Hospital Concord Obstetrics and Gynecology
 Polycystic Ovarian Syndrome Heidi Hallonquist, MD Concord Hospital Concord Obstetrics and Gynecology Outline Definition Symptoms Causal factors Diagnosis Complications Treatment Why are we talking about
Polycystic Ovarian Syndrome Heidi Hallonquist, MD Concord Hospital Concord Obstetrics and Gynecology Outline Definition Symptoms Causal factors Diagnosis Complications Treatment Why are we talking about
The 6 th Scientific Meeting of the Asia Pacific Menopause Federation
 Abnormal uterine bleeding in the perimenopause Perimenopausal menstrual problems are among the most common causes for family practitioner and specialist referral. Often it is due to the hormone changes
Abnormal uterine bleeding in the perimenopause Perimenopausal menstrual problems are among the most common causes for family practitioner and specialist referral. Often it is due to the hormone changes
POLYCYSTIC OVARIAN SYNDROME WHERE WE ARE AT IN 2018
 POLYCYSTIC OVARIAN SYNDROME WHERE WE ARE AT IN 2018 PCOS: WHERE WE ARE AT IN 2018 Nancy Arquette, MD Premier Women s Health 6135 Trust Drive #114 Holland, OH 43528 February 3, 2018 Kalahari Resorts ME
POLYCYSTIC OVARIAN SYNDROME WHERE WE ARE AT IN 2018 PCOS: WHERE WE ARE AT IN 2018 Nancy Arquette, MD Premier Women s Health 6135 Trust Drive #114 Holland, OH 43528 February 3, 2018 Kalahari Resorts ME
Women s Health: Managing Menopause. Jane S. Sillman, MD Assistant Professor of Medicine Harvard Medical School
 Women s Health: Managing Menopause Jane S. Sillman, MD Assistant Professor of Medicine Harvard Medical School Disclosures I have no conflicts of interest. Learning Objectives 1. Apply strategies to help
Women s Health: Managing Menopause Jane S. Sillman, MD Assistant Professor of Medicine Harvard Medical School Disclosures I have no conflicts of interest. Learning Objectives 1. Apply strategies to help
Case Questions. Polycystic Ovarian Syndrome: Treatment Goals and Options. Differential Diagnosis of Hyperandrogenic Anovulation
 Polycystic Ovarian Syndrome: Treatment Goals and Options Marc Cornier, MD Division of Endocrinology, Metabolism and Diabetes Colorado Center for Health and Wellness University of Colorado School of Medicine
Polycystic Ovarian Syndrome: Treatment Goals and Options Marc Cornier, MD Division of Endocrinology, Metabolism and Diabetes Colorado Center for Health and Wellness University of Colorado School of Medicine
What is PCOS? PCOS THE CONQUER PCOS E-BOOK. You'll be amazed when you read this...
 PCOS What is PCOS? You'll be amazed when you read this... What is PCOS?. Who is at risk? How to get tested? What are the complications. Is there a cure? What are the right ways to eat? What lifestyle changes
PCOS What is PCOS? You'll be amazed when you read this... What is PCOS?. Who is at risk? How to get tested? What are the complications. Is there a cure? What are the right ways to eat? What lifestyle changes
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Kathleen Colleran, MD Professor of Medicine University of New Mexico HSC Presented for COMM-TC May 4, 2012 Objectives Understand the pathophysiology of PCOS Understand how to
Polycystic Ovary Syndrome Kathleen Colleran, MD Professor of Medicine University of New Mexico HSC Presented for COMM-TC May 4, 2012 Objectives Understand the pathophysiology of PCOS Understand how to
PERIMENOPAUSE. Objectives. Disclosure. The Perimenopause Perimenopause Menopause. Definitions of Menopausal Transition: STRAW.
 PERIMENOPAUSE Patricia J. Sulak, MD Founder, Living WELL Aware LLC Author, Should I Fire My Doctor? Author, Living WELL Aware: Eleven Essential Elements to Health and Happiness Endowed Professor Texas
PERIMENOPAUSE Patricia J. Sulak, MD Founder, Living WELL Aware LLC Author, Should I Fire My Doctor? Author, Living WELL Aware: Eleven Essential Elements to Health and Happiness Endowed Professor Texas
06-Mar-17. Premature menopause. Menopause. Premature menopause. Menstrual cycle oestradiol. Premature menopause. Prevalence ~1% Higher incidence:
 Menopause Dr Sonia Davison MBBS FRACP PhD Endocrinologist and Clinical Fellow, Jean Hailes for Women s Health Women s Health Research Program, Monash University = the last natural menstrual period depletion
Menopause Dr Sonia Davison MBBS FRACP PhD Endocrinologist and Clinical Fellow, Jean Hailes for Women s Health Women s Health Research Program, Monash University = the last natural menstrual period depletion
Polycystic Ovarian Syndrome (PCOS) LOGO
 Polycystic Ovarian Syndrome (PCOS) Ma qianhong Ob/Gyn Department LOGO Contents Epidemiology and Definition Pathophysiology, Endocrinological Features Diagnostic Criteria Treatment Prognosis Introduction
Polycystic Ovarian Syndrome (PCOS) Ma qianhong Ob/Gyn Department LOGO Contents Epidemiology and Definition Pathophysiology, Endocrinological Features Diagnostic Criteria Treatment Prognosis Introduction
Molly A. Brewer DVM, MD, MS Chair and Professor Department of Obstetrics and Gynecology University of Connecticut School of Medicine
 Molly A. Brewer DVM, MD, MS Chair and Professor Department of Obstetrics and Gynecology University of Connecticut School of Medicine Review causes of abnormal uterine bleeding: Adolescent Reproductive
Molly A. Brewer DVM, MD, MS Chair and Professor Department of Obstetrics and Gynecology University of Connecticut School of Medicine Review causes of abnormal uterine bleeding: Adolescent Reproductive
Polycystic Ovary Syndrome (PCOS):
 Polycystic Ovary Syndrome (PCOS): Current diagnosis and treatment Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the end of this presentation,
Polycystic Ovary Syndrome (PCOS): Current diagnosis and treatment Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the end of this presentation,
Dr Mary Birdsall. Fertility Associates Auckland
 Dr Mary Birdsall Fertility Associates Auckland Period Problems Mary Birdsall Medical Director Fertility Associates Auckland Period Problems Basic Physiology No Periods Irregular Periods Heavy Periods
Dr Mary Birdsall Fertility Associates Auckland Period Problems Mary Birdsall Medical Director Fertility Associates Auckland Period Problems Basic Physiology No Periods Irregular Periods Heavy Periods
Dysfunctional Uterine Bleeding
 Long term effects of PCOS Dysfunctional Uterine Bleeding Dr. Arulmozhi Ramarajan Church of South India Hospital, Bangalore Abnormal uterine bleeding Affects health-related QOL Causes social embarrasment
Long term effects of PCOS Dysfunctional Uterine Bleeding Dr. Arulmozhi Ramarajan Church of South India Hospital, Bangalore Abnormal uterine bleeding Affects health-related QOL Causes social embarrasment
MENOPAUSE. I have no disclosures 10/11/18 OBJECTIVES WHAT S NEW? WHAT S SAFE?
 MENOPAUSE WHAT S NEW? WHAT S SAFE? I have no disclosures Sara Whetstone, MD, MHS OBJECTIVES To describe risks of HT by age and menopause onset To recommend specific HT regimen for women who undergo early
MENOPAUSE WHAT S NEW? WHAT S SAFE? I have no disclosures Sara Whetstone, MD, MHS OBJECTIVES To describe risks of HT by age and menopause onset To recommend specific HT regimen for women who undergo early
Menstrual Disorders & Ambulatory Gynaecology
 Menstrual Disorders & Ambulatory Gynaecology Mr. Nagui Lewis Aziz M B, CH B, FRCOG Consultant Gynaecologist The Royal Oldham Hospital 01/09/2018 Heavy menstrual bleeding (HMB ) is a common problem responsible
Menstrual Disorders & Ambulatory Gynaecology Mr. Nagui Lewis Aziz M B, CH B, FRCOG Consultant Gynaecologist The Royal Oldham Hospital 01/09/2018 Heavy menstrual bleeding (HMB ) is a common problem responsible
Infertility DR. RAHUL BEVARA
 Infertility DR. RAHUL BEVARA Definitions Infertility is defined as the inability to conceive after one year of unprotected coitus. Affects 10-15% of couples Primary Infertility, that is inability to conceive
Infertility DR. RAHUL BEVARA Definitions Infertility is defined as the inability to conceive after one year of unprotected coitus. Affects 10-15% of couples Primary Infertility, that is inability to conceive
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU)
 ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
ROLE OF HORMONAL ASSAY IN DIAGNOSING PCOD DR GAANA SREENIVAS (JSS,MYSURU) In 1935, Stein and Leventhal described 7 women with bilateral enlarged PCO, amenorrhea or irregular menses, infertility and masculinizing
PCOS Awareness Symposium Atlanta September 24 th, Preventing Diabetes & Cardiovascular Disease in PCOS
 PCOS Awareness Symposium Atlanta September 24 th, 2016 Preventing Diabetes & Cardiovascular Disease in PCOS Katherine Sherif, MD Professor & Vice Chair, Department of Medicine Director, Jefferson Women
PCOS Awareness Symposium Atlanta September 24 th, 2016 Preventing Diabetes & Cardiovascular Disease in PCOS Katherine Sherif, MD Professor & Vice Chair, Department of Medicine Director, Jefferson Women
 Objectives 1. Be able to describe the classic presentation and diagnostic criteria 2. Be able to explain long-term health concerns associated with the diagnosis 3. Understand what basic treatment options
Objectives 1. Be able to describe the classic presentation and diagnostic criteria 2. Be able to explain long-term health concerns associated with the diagnosis 3. Understand what basic treatment options
Management of Abnormal Uterine Bleeding. Julie Strickland MD, MPH University of Missouri Kansas City Department of Obstetrics and Gynecology
 Management of Abnormal Uterine Bleeding Julie Strickland MD, MPH University of Missouri Kansas City Department of Obstetrics and Gynecology AUB Abnormal uterine bleeding (AUB): fairly broad term referring
Management of Abnormal Uterine Bleeding Julie Strickland MD, MPH University of Missouri Kansas City Department of Obstetrics and Gynecology AUB Abnormal uterine bleeding (AUB): fairly broad term referring
Premature Menopause : Diagnosis and Management
 Guideline Number 3 : August 2010 Premature Menopause : Diagnosis and Management Introduction : Premature menopause is a serious condition that affects young women and remains an enigma. The challenges
Guideline Number 3 : August 2010 Premature Menopause : Diagnosis and Management Introduction : Premature menopause is a serious condition that affects young women and remains an enigma. The challenges
Estrogens and progestogens
 Estrogens and progestogens Estradiol and Progesterone hormones produced by the gonads are necessary for: conception embryonic maturation development of primary and secondary sexual characteristics at puberty.
Estrogens and progestogens Estradiol and Progesterone hormones produced by the gonads are necessary for: conception embryonic maturation development of primary and secondary sexual characteristics at puberty.
Abnormal Uterine Bleeding
 Abnormal Uterine Bleeding Randy A. Fink, MD, FACOG Obstetrics & Gynecology A simplified approach for primary care Disclosures I have no relevant disclosures pertaining to this program. Learning Objectives
Abnormal Uterine Bleeding Randy A. Fink, MD, FACOG Obstetrics & Gynecology A simplified approach for primary care Disclosures I have no relevant disclosures pertaining to this program. Learning Objectives
Menopause Symptoms and Management: After Breast Cancer
 Menopause Symptoms and Management: After Breast Cancer An Educational Webinar for Patients and their Caregivers Wen Shen, MD, MPH Division of Gynecologic Specialties July 27, 2018 1 Disclosure I have a
Menopause Symptoms and Management: After Breast Cancer An Educational Webinar for Patients and their Caregivers Wen Shen, MD, MPH Division of Gynecologic Specialties July 27, 2018 1 Disclosure I have a
lactotrophs 120 min- FSH 60 min- LH Hypothalamus GnRH pituitary Estradiol +/- Progesterone _ FSH L H Ovary Uterus Ovulation Antral follicle >2mm
 lactotrophs Hypothalamus GnRH 120 min- 60 min- LH Progesterone _ pituitary L H + Ovary + Estradiol +/- Uterus Antral follicle >2mm Ovulation Preovulatory follicles atresia Follicular phase Luteal phase
lactotrophs Hypothalamus GnRH 120 min- 60 min- LH Progesterone _ pituitary L H + Ovary + Estradiol +/- Uterus Antral follicle >2mm Ovulation Preovulatory follicles atresia Follicular phase Luteal phase
Female Reproductive Endocrinology
 Female Reproductive Endocrinology Dr. Channa Jayasena PhD MRCP FRCPath Clinical Senior Lecturer & Consultant Endocrinologist Department of Gynaecology, Hammersmith Hospital Anovulation is a common cause
Female Reproductive Endocrinology Dr. Channa Jayasena PhD MRCP FRCPath Clinical Senior Lecturer & Consultant Endocrinologist Department of Gynaecology, Hammersmith Hospital Anovulation is a common cause
Approach to ovulation induction and superovulation in women with a history of infertility. Anatte E. Karmon, MD
 Approach to ovulation induction and superovulation in women with a history of infertility Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the
Approach to ovulation induction and superovulation in women with a history of infertility Anatte E. Karmon, MD Disclosures- Anatte Karmon, MD No financial relationships to disclose 2 Objectives At the
Managing menopause in Primary Care and recent advances in HRT
 Managing menopause in Primary Care and recent advances in HRT Raj Saha, MD, DMRT, FRCOG Consultant Gynaecologist Heart of England NHS Foundation Trust rajsaha1@yahoo.co.uk Content of today s talk Aims
Managing menopause in Primary Care and recent advances in HRT Raj Saha, MD, DMRT, FRCOG Consultant Gynaecologist Heart of England NHS Foundation Trust rajsaha1@yahoo.co.uk Content of today s talk Aims
MENOPAUSAL HORMONE THERAPY 2016
 MENOPAUSAL HORMONE THERAPY 2016 Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA NICE provides the National Health Service advice on effective, good value healthcare.
MENOPAUSAL HORMONE THERAPY 2016 Carolyn J. Crandall, MD, MS Professor of Medicine David Geffen School of Medicine at UCLA NICE provides the National Health Service advice on effective, good value healthcare.
Management of Menopausal Symptoms
 Management of Menopausal Symptoms Tammie Koehler DO, FACOG 1 Menopause Permanent cessation of menstruation that occurs after the loss of ovarian activity Determined to have occurred after 1 full year of
Management of Menopausal Symptoms Tammie Koehler DO, FACOG 1 Menopause Permanent cessation of menstruation that occurs after the loss of ovarian activity Determined to have occurred after 1 full year of
A Practitioner s Toolkit for the Management of the Menopause
 Medicine, Nursing and Health Sciences A Practitioner s Toolkit for the Management of the Menopause Developed by the Women s Health Research Program School of Public Health and Preventive Medicine Monash
Medicine, Nursing and Health Sciences A Practitioner s Toolkit for the Management of the Menopause Developed by the Women s Health Research Program School of Public Health and Preventive Medicine Monash
Sexual dysfunction of chronic kidney disease. Razieh salehian.md psychiatrist
 Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
Sexual dysfunction of chronic kidney disease Razieh salehian.md psychiatrist Disturbances in sexual function are a common feature of chronic renal failure. Sexual dysfunction is inversely associated with
12/27/2013. Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND
 Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND 7% of all women 18-45 Obesity 1/3 of all US women Incidence of PCOS is increasing with increase obesity Obesity Irregular
Kristen Cain, MD FACOG Reproductive Medicine Institute Sanford Health, Fargo ND 7% of all women 18-45 Obesity 1/3 of all US women Incidence of PCOS is increasing with increase obesity Obesity Irregular
Dr Stella Milsom. Endocrinologist Fertility Associates Auckland. 12:30-12:40 When Puberty is PCO
 Dr Stella Milsom Endocrinologist Fertility Associates Auckland 12:30-12:40 When Puberty is PCO Puberty or Polycystic Ovary Syndrome? Stella Milsom Endocrinologist Auckland DHB, University of Auckland,
Dr Stella Milsom Endocrinologist Fertility Associates Auckland 12:30-12:40 When Puberty is PCO Puberty or Polycystic Ovary Syndrome? Stella Milsom Endocrinologist Auckland DHB, University of Auckland,
Menopause management NICE Implementation
 Menopause management NICE Implementation Dr Paula Briggs Consultant in Sexual & Reproductive Health Southport and Ormskirk NHS Hospital Trust Why a NICE guideline (NG 23) Media reports about HRT have not
Menopause management NICE Implementation Dr Paula Briggs Consultant in Sexual & Reproductive Health Southport and Ormskirk NHS Hospital Trust Why a NICE guideline (NG 23) Media reports about HRT have not
Healthcare Education Research
 Healthcare Education Research Heavy menstrual bleeding: investigation, diagnosis & management An update for health professionals Assessment of heavy menstrual bleeding in primary care Dr Amanda Newman
Healthcare Education Research Heavy menstrual bleeding: investigation, diagnosis & management An update for health professionals Assessment of heavy menstrual bleeding in primary care Dr Amanda Newman
Estrogens & Antiestrogens
 Estrogens & Antiestrogens Menstrual cycle... Changes and hormonal events Natural estrogens: Estadiol >> Estrone > Estriol Ineffective orally Synthesis: From cholesterol ; role of aromatase enzyme in converting
Estrogens & Antiestrogens Menstrual cycle... Changes and hormonal events Natural estrogens: Estadiol >> Estrone > Estriol Ineffective orally Synthesis: From cholesterol ; role of aromatase enzyme in converting
Prof.Dr. Nabil Lymon Head of Internal Medicine Department
 By Prof.Dr. Nabil Lymon Head of Internal Medicine Department Definitions: Hirsutism: Is the presence of terminal hair in androgendependent sites where hair does not normally grow in women. This hair growth
By Prof.Dr. Nabil Lymon Head of Internal Medicine Department Definitions: Hirsutism: Is the presence of terminal hair in androgendependent sites where hair does not normally grow in women. This hair growth
 Non-contraceptive Uses of the Levonorgestrel Intrauterine Device Elena Gates, MD http://www.mirena-us.com/pvs1/pri/whatisframe.html Progestin levels with LNG- IUS Lower plasma levels Mirena 150-200 pg/ml
Non-contraceptive Uses of the Levonorgestrel Intrauterine Device Elena Gates, MD http://www.mirena-us.com/pvs1/pri/whatisframe.html Progestin levels with LNG- IUS Lower plasma levels Mirena 150-200 pg/ml
OB/GYN Update: Menopausal Management What Does The Evidence Show? Rebecca Levy-Gantt D.O. PremierObGyn Napa Inc.
 OB/GYN Update: Menopausal Management What Does The Evidence Show? Rebecca Levy-Gantt D.O. PremierObGyn Napa Inc. Napa, California IMPORTANT SAFETY INFORMATION ABOUT EVAMIST: WARNING: ENDOMETRIAL CANCER,
OB/GYN Update: Menopausal Management What Does The Evidence Show? Rebecca Levy-Gantt D.O. PremierObGyn Napa Inc. Napa, California IMPORTANT SAFETY INFORMATION ABOUT EVAMIST: WARNING: ENDOMETRIAL CANCER,
INFERTILITY CAUSES. Basic evaluation of the female
 INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
INFERTILITY Infertility is the inability to conceive after 12 months of unprotected intercourse. There are multiple causes of infertility and a systematic way to evaluate the condition. Let s look at some
OVERVIEW OF MENOPAUSE
 OVERVIEW OF MENOPAUSE Nicole Budrys, MD, MPH Reproductive Endocrinology Michigan Center for Fertility and Women s Health Presented at SEMCME March 13,2019 Objectives Define menopause Etiology of menopause
OVERVIEW OF MENOPAUSE Nicole Budrys, MD, MPH Reproductive Endocrinology Michigan Center for Fertility and Women s Health Presented at SEMCME March 13,2019 Objectives Define menopause Etiology of menopause
Chapter 100 Gynecologic Disorders
 Chapter 100 Gynecologic Disorders Episode Overview: 1. Describe the presentation and RF for Adnexal torsion 2. List the imaging findings of adnexal torsion (US vs CT) 3. What is the management of adnexal
Chapter 100 Gynecologic Disorders Episode Overview: 1. Describe the presentation and RF for Adnexal torsion 2. List the imaging findings of adnexal torsion (US vs CT) 3. What is the management of adnexal
Menopausal Management: What Has Changed?
 Menopausal Management: What Has Changed? Julia V. Johnson, M.D. Professor and Chair, OB/GYN University of Massachusetts Medical School UMass Memorial Medical Center Conflicts of Interest None Learning
Menopausal Management: What Has Changed? Julia V. Johnson, M.D. Professor and Chair, OB/GYN University of Massachusetts Medical School UMass Memorial Medical Center Conflicts of Interest None Learning
Amenorrhoea: polycystic ovary syndrome
 There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
There is so much we don't know in medicine that could make a difference, and often we focus on the big things, and the little things get forgotten. To highlight some smaller but important issues, we've
Therapeutic Cohort Results
 Patient: SAMPLE PATIENT DOB: Sex: MRN: Menopause Plus - Salivary Profile Therapeutic Cohort Results Hormone Average Result QUINTILE DISTRIBUTION 1st 2nd 3rd 4th 5th Therapeutic Range* Estradiol (E2) 8.7
Patient: SAMPLE PATIENT DOB: Sex: MRN: Menopause Plus - Salivary Profile Therapeutic Cohort Results Hormone Average Result QUINTILE DISTRIBUTION 1st 2nd 3rd 4th 5th Therapeutic Range* Estradiol (E2) 8.7
Menopause and HRT. John Smiddy and Alistair Ledsam
 Menopause and HRT John Smiddy and Alistair Ledsam Menopause The cessation of menstruation Diagnosed retrospectively after 1 year of amenorrhoea Average age 51 in the UK Normal physiology - Menstruation
Menopause and HRT John Smiddy and Alistair Ledsam Menopause The cessation of menstruation Diagnosed retrospectively after 1 year of amenorrhoea Average age 51 in the UK Normal physiology - Menstruation
WHI Estrogen--Progestin vs. Placebo (Women with intact uterus)
 HORMONE REPLACEMENT THERAPY In the historical period it was commonly held that estrogen had two principal benefits to postmenopausal women: 1) To alleviate the constitutional symptoms related to the climacteric
HORMONE REPLACEMENT THERAPY In the historical period it was commonly held that estrogen had two principal benefits to postmenopausal women: 1) To alleviate the constitutional symptoms related to the climacteric
CASE 41. What is the pathophysiologic cause of her amenorrhea? Which cells in the ovary secrete estrogen?
 CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
CASE 41 A 19-year-old woman presents to her gynecologist with complaints of not having had a period for 6 months. She reports having normal periods since menarche at age 12. She denies sexual activity,
16 YEAR-OLD OBESE FEMALE WITH OLIGOMENORRHEA
 16 YEAR-OLD OBESE FEMALE WITH OLIGOMENORRHEA Katie O Sullivan, MD Adult/Pediatric Endocrinology Fellow University of Chicago ENDORAMA Thursday, September 4th, 2014 Disclosures No financial interests. Will
16 YEAR-OLD OBESE FEMALE WITH OLIGOMENORRHEA Katie O Sullivan, MD Adult/Pediatric Endocrinology Fellow University of Chicago ENDORAMA Thursday, September 4th, 2014 Disclosures No financial interests. Will
Polycystic Ovary Syndrome: Cardiovascular Disease risk
 PCOS Challenge Atlanta September 16 th, 2017 Polycystic Ovary Syndrome: Cardiovascular Disease risk Katherine Sherif, MD Professor & Vice Chair, Department of Medicine Director, Jefferson Women s Primary
PCOS Challenge Atlanta September 16 th, 2017 Polycystic Ovary Syndrome: Cardiovascular Disease risk Katherine Sherif, MD Professor & Vice Chair, Department of Medicine Director, Jefferson Women s Primary
Women s Health: Take Home Messages
 Women s Health: Take Home Messages Caren Solomon, MD Associate Physician, BWH Associate Professor of Medicine, HMS Deputy Editor, NEJM No disclosures Contraception Contraceptive Effectiveness Rates of
Women s Health: Take Home Messages Caren Solomon, MD Associate Physician, BWH Associate Professor of Medicine, HMS Deputy Editor, NEJM No disclosures Contraception Contraceptive Effectiveness Rates of
New PCOS guidelines: What s relevant to general practice
 New PCOS guidelines: What s relevant to general practice Dr Michael Costello Fertility Specialist IVF Australia UNSW Royal Hospital for Women Sydney How do we know if something is new? Louvre Museum, Paris
New PCOS guidelines: What s relevant to general practice Dr Michael Costello Fertility Specialist IVF Australia UNSW Royal Hospital for Women Sydney How do we know if something is new? Louvre Museum, Paris
5/5/2010. Infertility FINANCIAL DISCLOSURE. Infertility Definition. Objectives. Normal Human Fertility. Normal Menstrual Cycle
 Infertility FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology I AM RECEIVING COMPENSATION
Infertility FINANCIAL DISCLOSURE I HAVE NO FINANCIAL INTEREST IN ANY OF THE PRODUCTS MENTIONED IN MY PRESENTATION Bryan K. Rone, M.D. University of Kentucky Obstetrics and Gynecology I AM RECEIVING COMPENSATION
Managing menopause in Primary Care and recent advances in HRT
 Managing menopause in Primary Care and recent advances in HRT Raj Saha, MD, DMRT, FRCOG PG Cert. Advanced Gynaecology Endoscopy Consultant Gynaecologist Heart of England NHS Foundation Trust Spire Parkway
Managing menopause in Primary Care and recent advances in HRT Raj Saha, MD, DMRT, FRCOG PG Cert. Advanced Gynaecology Endoscopy Consultant Gynaecologist Heart of England NHS Foundation Trust Spire Parkway
Hyperandrogenism. Dr Jack Biko. MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany)
 Hyperandrogenism Dr Jack Biko MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany) 2012 Hyperandrogenism Excessive production of androgens Adrenal glands main source
Hyperandrogenism Dr Jack Biko MB. BCh (Wits), MMED O & G (Pret), FCOG (SA), Dip Advanced Endoscopic Surgery(Kiel, Germany) 2012 Hyperandrogenism Excessive production of androgens Adrenal glands main source
Reproductive System. Testes. Accessory reproductive organs. gametogenesis hormones. Reproductive tract & Glands
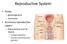 Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Reproductive System Testes gametogenesis hormones Accessory reproductive organs Reproductive tract & Glands transport gametes provide nourishment for gametes Hormonal regulation in men Hypothalamus - puberty
Infertility for the Primary Care Provider
 Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Infertility for the Primary Care Provider David A. Forstein, DO FACOOG Clinical Associate Professor Obstetrics and Gynecology University of South Carolina School of Medicine Greenville Disclosure I have
Abnormal Uterine Bleeding. Richard Dover Specialist gynaecologist
 Abnormal Uterine Bleeding Richard Dover Specialist gynaecologist A pragmatic guide. Wide topic range What s not coming up Precocious puberty Menorrhagia well maybe just a little Topics Adolescents IMB
Abnormal Uterine Bleeding Richard Dover Specialist gynaecologist A pragmatic guide. Wide topic range What s not coming up Precocious puberty Menorrhagia well maybe just a little Topics Adolescents IMB
Polycystic Ovary Syndrome
 What is the polycystic ovary syndrome? Polycystic Ovary Syndrome The polycystic ovary syndrome (PCOS) is a clinical diagnosis characterized by the presence of two or more of the following features: irregular
What is the polycystic ovary syndrome? Polycystic Ovary Syndrome The polycystic ovary syndrome (PCOS) is a clinical diagnosis characterized by the presence of two or more of the following features: irregular
HRT in Perimenopausal Women. Dr. Rubina Yasmin Asst. Prof. Medicine Dhaka Dental College
 HRT in Perimenopausal Women Dr. Rubina Yasmin Asst. Prof. Medicine Dhaka Dental College 1 This is the Change But the CHANGE is not a disease 2 Introduction With a marked increase in longevity, women now
HRT in Perimenopausal Women Dr. Rubina Yasmin Asst. Prof. Medicine Dhaka Dental College 1 This is the Change But the CHANGE is not a disease 2 Introduction With a marked increase in longevity, women now
22/09/2014. Menopause Management. Menopause. Menopause symptoms
 Menopause Management Dr Sonia Davison Jean Hailes for Women s Health Menopause Time of last menstrual period - average age 51 Premature Menopause: occurs before age 40 Perimenopause (menopause transition):
Menopause Management Dr Sonia Davison Jean Hailes for Women s Health Menopause Time of last menstrual period - average age 51 Premature Menopause: occurs before age 40 Perimenopause (menopause transition):
5 Mousa Al-Abbadi. Ola Al-juneidi & Obada Zalat. Ahmad Al-Tarefe
 5 Mousa Al-Abbadi Ola Al-juneidi & Obada Zalat Ahmad Al-Tarefe Abnormal Uterine Bleeding (AUB) AUB is a very common scenario or symptom where women complain of menorrhagia (heavy and/or for long periods),
5 Mousa Al-Abbadi Ola Al-juneidi & Obada Zalat Ahmad Al-Tarefe Abnormal Uterine Bleeding (AUB) AUB is a very common scenario or symptom where women complain of menorrhagia (heavy and/or for long periods),
Case. 24 year old female presented to your office complaining of excess hair growth on her face and abdomen. Questions?
 Hirsutism Case 24 year old female presented to your office complaining of excess hair growth on her face and abdomen Questions? Started around puberty with gradual progression Irregular menstrual cycle
Hirsutism Case 24 year old female presented to your office complaining of excess hair growth on her face and abdomen Questions? Started around puberty with gradual progression Irregular menstrual cycle
Reproductive Testing: Less is More G. Wright Bates, Jr., M.D. Professor and Director Reproductive Endocrinology and Infertility Objectives
 Reproductive Testing: Less is More G. Wright Bates, Jr., M.D. Professor and Director Reproductive Endocrinology and Infertility Objectives 1. Review definition of infertility and impact of age 2. Stress
Reproductive Testing: Less is More G. Wright Bates, Jr., M.D. Professor and Director Reproductive Endocrinology and Infertility Objectives 1. Review definition of infertility and impact of age 2. Stress
Ohio Northern University HealthWise. Authors: Alexis Dolin, Andrew Duska, Hannah Lamb, Eric Miller, Pharm D Candidates 2018 May 2018
 Women s Health Authors: Alexis Dolin, Andrew Duska, Hannah Lamb, Eric Miller, Pharm D Candidates 2018 May 2018 Let Your Body Empower You! National Women s Health Week Polycystic Ovary Syndrome Page 2 Breast
Women s Health Authors: Alexis Dolin, Andrew Duska, Hannah Lamb, Eric Miller, Pharm D Candidates 2018 May 2018 Let Your Body Empower You! National Women s Health Week Polycystic Ovary Syndrome Page 2 Breast
Appendix: Reference Table of HT Brand Names
 Appendix: Reference Table of HT Brand Names This is a full reference table in alphabetical order, of Brand Name drugs used in HT. It is the basis for prescription advice throughout this handbook. Drug
Appendix: Reference Table of HT Brand Names This is a full reference table in alphabetical order, of Brand Name drugs used in HT. It is the basis for prescription advice throughout this handbook. Drug
PCOS guidelines: What s relevant to general practice
 PCOS guidelines: What s relevant to general Dr David Molloy Medical Director, Queensland Fertility Group International evidence based PCOS guidelines 1st ever internationally endorsed & evidence based
PCOS guidelines: What s relevant to general Dr David Molloy Medical Director, Queensland Fertility Group International evidence based PCOS guidelines 1st ever internationally endorsed & evidence based
Gynecological Problems: Case Study Approach
 Gynecological Problems: Case Study Approach Joyce King, CNM, Ph.D. Disclosure Statement I have no real or perceived vested interests that relate to this presentation nor do I have any relationship with
Gynecological Problems: Case Study Approach Joyce King, CNM, Ph.D. Disclosure Statement I have no real or perceived vested interests that relate to this presentation nor do I have any relationship with
Achieving Pregnancy: Obesity and Infertility. Jordan Vaughan, MSN, APN, WHNP-BC Women s Health Nurse Practitioner Nashville Fertility Center
 Achieving Pregnancy: Obesity and Infertility Jordan Vaughan, MSN, APN, WHNP-BC Women s Health Nurse Practitioner Nashville Fertility Center Disclosures Speakers Bureau EMD Serono Board of Directors Nurse
Achieving Pregnancy: Obesity and Infertility Jordan Vaughan, MSN, APN, WHNP-BC Women s Health Nurse Practitioner Nashville Fertility Center Disclosures Speakers Bureau EMD Serono Board of Directors Nurse
Secondary amenorrhoea Dr.ASMAA AL SANJARY
 Secondary amenorrhoea Dr.ASMAA AL SANJARY The student at the end of this lecture should be able to: Define secondary amenorrhoea. Classify the causes of secondary amenorrhoea. Describe the commonest three
Secondary amenorrhoea Dr.ASMAA AL SANJARY The student at the end of this lecture should be able to: Define secondary amenorrhoea. Classify the causes of secondary amenorrhoea. Describe the commonest three
Polycystic ovary syndrome
 Polycystic ovary syndrome Overview Polycystic ovary syndrome (PCOS) is a condition most often characterized by irregular menstrual periods, excess hair growth and obesity, but it can affect women in a
Polycystic ovary syndrome Overview Polycystic ovary syndrome (PCOS) is a condition most often characterized by irregular menstrual periods, excess hair growth and obesity, but it can affect women in a
Polycystic Ovary Syndrome
 Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is common. It can cause period problems, reduced fertility, excess hair growth, and acne. Many women with PCOS are also overweight. Treatment
Polycystic Ovary Syndrome Polycystic ovary syndrome (PCOS) is common. It can cause period problems, reduced fertility, excess hair growth, and acne. Many women with PCOS are also overweight. Treatment
Contraception. Yolanda Evans MD MPH Assistant Professor of Pediatrics Division of Adolescent Medicine
 Contraception Yolanda Evans MD MPH Assistant Professor of Pediatrics Division of Adolescent Medicine Disclosures No financial relationships to disclose I have no commercial, financial, research ties to
Contraception Yolanda Evans MD MPH Assistant Professor of Pediatrics Division of Adolescent Medicine Disclosures No financial relationships to disclose I have no commercial, financial, research ties to
Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia
 Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
Precocious Puberty Laura Stewart, MD, FRCPC Clinical Associate Professor Division of Pediatric Endocrinology University of British Columbia Faculty Disclosure Faculty: Laura Stewart No relationships with
2017 Position Statement of Hormone Therapy of NAMS: overview SHELAGH LARSON, MS, RNC WHNP, NCMP ACCLAIM, JPS HEALTH NETWORK
 2017 Position Statement of Hormone Therapy of NAMS: overview SHELAGH LARSON, MS, RNC WHNP, NCMP ACCLAIM, JPS HEALTH NETWORK WHI the only large, long-term RCT of HT in women aged 50 to 79 years, Drug trail
2017 Position Statement of Hormone Therapy of NAMS: overview SHELAGH LARSON, MS, RNC WHNP, NCMP ACCLAIM, JPS HEALTH NETWORK WHI the only large, long-term RCT of HT in women aged 50 to 79 years, Drug trail
