The treatment of a tooth size-arch length discrepancy
|
|
|
- Jodie Manning
- 6 years ago
- Views:
Transcription
1 ORIGINAL ARTICLE A prospective long-term study on the effects of rapid maxillary expansion in the early mixed dentition Renée G. Geran, a James A. McNamara, Jr, b Tiziano Baccetti, c Lorenzo Franchi, d and Lainie M. Shapiro e Ann Arbor, South Lyon, and Commerce Township, Mich, and Florence, Italy Introduction: The aim of this prospective longitudinal clinical study was to evaluate the short-term and long-term changes in dental-arch dimensions in patients treated with the acrylic splint rapid maxillary expander in the early mixed dentition followed by fixed appliances in the permanent dentition. Methods: The dental casts of 51 consecutively treated patients (TG) were compared with those of 26 untreated controls (CG) at 3 different times: pretreatment (T1), after expansion and fixed appliance therapy (T2), and at long-term observation (T3). The mean ages for the TG were 8 years 10 months at T1, 13 years 10 months at T2, and 19 years 9 months at T3. Arch widths, arch depth, arch perimeter, and molar angulation were assessed in all subjects at all observation times. T1-T2, T2-T3, and T1-T3 changes were compared statistically in the TG with respect to the corresponding CG. Results: Treatment with an acrylic splint RME followed by fixed appliances produced significantly favorable short-term and long-term changes in almost all maxillary and mandibular arch measurements. The amount of change in both maxillary and mandibular intermolar and intercanine widths fully corrected the initial discrepancies. Approximately 4 mm of long-term relative increase in maxillary arch perimeter, and 2.5 mm additional maintenance of mandibular arch perimeter were observed in the TG compared with the CG. Conclusions: These results suggest that this protocol is effective and stable for the treatment of constricted maxillary arches, and can relieve modest deficiencies in arch perimeter. (Am J Orthod Dentofacial Orthop 2006;129:631-40) The treatment of a tooth size-arch length discrepancy by creating additional space in the dental arches is a task that many orthodontists undertake daily. In patients with mild ( 3 mm) or severe ( 6 mm) crowding, the choice of whether to extract teeth to gain space typically is obvious. In patients with moderate crowding, however, the choice is less clear. The use of an extraction or nonextraction approach to From the School of Dentistry, University of Michigan, Ann Arbor. a Graduate orthodontic program; private practice, South Lyon, Mich. b Thomas M. and Doris Graber Endowed Professor of dentistry, Department of Orthodontics and Pediatric Dentistry; professor of anatomy and cell biology, School of Medicine; research professor, Center for Human Growth and Development; private practice, Ann Arbor, Mich. c Thomas M. Graber Visiting Scholar, Department of Orthodontics and Pediatric Dentistry; assistant professor, Department of Orthodontics, University of Florence, Florence, Italy. d Thomas M. Graber Visiting Scholar, Department of Orthodontics and Pediatric Dentistry; research associate, Department of Orthodontics, Florence, Italy. e Graduate orthodontic program; private practice, Commerce Township, Mich. Supported in part by 2 grants from the American Association of Orthodontists Foundation and funds from the Thomas M. and Doris Graber Endowed Professorship, Department of Orthodontics and Pediatric Dentistry, University of Michigan. Reprint requests to: Dr James A. McNamara, Department of Orthodontics and Pediatric Dentistry, School of Dentistry, University of Michigan, Ann Arbor, MI ; , mcnamara@umich.edu. Submitted, July 2004; revised and accepted, October /$32.00 Copyright 2006 by the American Association of Orthodontists. doi: /j.ajodo treat these borderline patients has been a topic of controversy throughout the history of the orthodontic profession. Methods alternative to extractions aimed to relieve tooth size-arch length discrepancies include interproximal reduction of teeth or stripping, molar distalization, dental expansion, and orthopedic expansion of the maxilla. An orthodontist who decides to alleviate crowding without extractions might choose orthopedic expansion or a combination of these 3 alternatives. An important question then becomes whether the orthopedic expansion is stable in the long term. Unfortunately, few well-designed long-term studies address the stability of rapid maxillary expansion (RME). Most RME investigations give only short-term results, and many have shortcomings. 1-9 These limitations include the use of small sample sizes, the inclusion of older patients, inadequate descriptions of retention protocols, lack of control subjects, and lack of rigorous statistical analysis. One long-term study that addresses this issue is that of Moussa et al, 10 who evaluated 55 patients selected randomly from the practice of Andrew Haas, the developer of contemporary RME. The age range at the start of treatment was 8 to 19 years. Three time intervals were analyzed: pretreatment, posttreatment, 631
2 632 Geran et al American Journal of Orthodontics and Dentofacial Orthopedics May 2006 and postretention. The treatment included RME followed by fixed appliances. Retention protocols were explained in detail, and the time interval for postretention records was 8 to 10 years, or about 15 years postexpansion. The authors found good stability for maxillary intercanine width (75% maintained), maxillary and mandibular intermolar widths (81% and 100% maintained, respectively), and incisor irregularity. Small increases in arch perimeter and intercanine width still were present in the long term. No further increases in maxillary and mandibular arch lengths were reported at postretention. Moussa et al, 10 however, did not compare their results with data from untreated controls. This comparison is important because of the naturally occurring reduction in arch dimensions. 11,12 An adequate control group was included in the recent long-term study by McNamara et al, 13 who evaluated arch changes after Haas-type RME and fixed appliance therapy through age 20 years. Treatment with RME followed by fixed appliances induced stable favorable increases in the width of the dental arches and arch depth. Long-term increases of approximately 6 mm in maxillary arch perimeter (80% of initial deficiency) and 4.5 mm in mandibular arch perimeter (full correction of initial deficiency) were observed in patients when compared with untreated subjects. No studies are available on the long-term outcomes of bonded acrylic splint RME therapy. Evidence shows that the orthopedic effect of RME therapy is influenced by treatment timing. 5,14-16 Skeletal outcomes of greater magnitude and stability can be obtained when the expander is used before the pubertal growth spurt (eg, stages 1 to 3 of the cervical vertebral maturation (CVM) method 16 ), with transverse changes shifting to the dentoalveolar level when RME therapy is performed after the pubertal peak (stages 4 to 6 of the CVM method). 15 Unfortunately, little has been published on the effects of RME before the growth spurt or before the development of the permanent dentition. Spillane and McNamara 11 and Brust and Mc- Namara 12 conducted the first investigations of the effects of RME in the mixed dentition as part of an ongoing prospective clinical trial (Michigan Expansion Study). The initial study described the treatment effects and the short-term stability produced by the acrylic splint expander in the early mixed dentition. 11 Serial dental casts of 162 patients were analyzed to measure arch dimensions preexpansion, immediately postexpansion, and at yearly intervals until the eruption of the first premolars. The average increase in transpalatal width was 5 to 6 mm. At the end of the postexpansion observation period (2.4 years), 80% of the original expansion at the first permanent molars remained. In addition, maxillary dental arches that initially were narrow tended to display greater stability than those that initially were wider. Finally, maxillae with initially more lingually inclined molars tended to retain more expansion than maxillae with initially more buccally inclined molars. Brust and McNamara 12 continued the investigation of RME in the mixed dentition began by Spillane and McNamara. 11 Brust and McNamara 12 examined a larger sample of patients from the same private practice. Changes in arch width, arch perimeter, and molar angulation were evaluated immediately postexpansion, at first-premolar eruption, and before comprehensive orthodontic treatment. The changes were compared with those occurring over a similar time interval in a control group of 22 untreated subjects from the University of Michigan Elementary and Secondary School Growth Study. A significant amount of stable expansion was achieved in maxillary arches, but changes in the mandibular arches were less stable. Our investigation is an extension of this ongoing prospective clinical trial of the treatment effects of the acrylic splint RME in the mixed dentition, to assess the long-term stability of dental-arch changes of RME in the early mixed dentition followed by comprehensive orthodontic treatment (phase II). The final evaluation of the patients was an average of 6 years (minimum of 5 years) after phase II treatment, or approximately 10 years after the completion of RME. Serial dental casts of the maxillary and mandibular arches were compared with a control group (CG) of untreated subjects. SUBJECTS AND METHODS The patients examined were part of a prospective clinical investigation, the Michigan Expansion Study, of mixed dentition patients who underwent RME in a private faculty practice. A focus of that study is the short-term and long-term treatment effects of RME with acrylic splint expanders in the mixed dentition followed by fixed appliances in the permanent dentition. This study compared the long-term effects of this 2-phase treatment with an untreated group. Active expansion (eg, Schwarz appliance, lip bumper) of the mandibular dental arch was not undertaken during the first phase of treatment. The treated group (TG) consisted of consecutively treated patients from a group faculty practice; all patients were treated jointly by 3 practitioners. The decision to use RME therapy was based on at least 1 preexisting criterion: crowding, lingual crossbite, esthetics, or tendency toward Class II malocclusion. 17 The 51 patients (22 male, 29 female) in the TG
3 American Journal of Orthodontics and Dentofacial Orthopedics Volume 129, Number 5 Geran et al 633 underwent RME treatment with bonded acrylic splint appliances in the mixed dentition; they were 5 or more years out of phase II treatment. They had a consistent set of characteristics. Before treatment, the following teeth were present: erupted maxillary and mandibular first permanent molars, erupted maxillary and mandibular permanent central incisors, and deciduous second molars. Dental casts were obtained on all patients at 3 times: before treatment (T1), at the completion of phase II treatment (T2), and 5 years or more after the T2 records (T3). Lateral cephalograms at T1 showed stages 1 to 3 of the CVM method (prepeak skeletal maturity 16 ); lateral cephalograms at T3 showed stage 5 or 6 of the CVM method (completed or nearly completed active growth). The mean ages were 8 years 10 months at T1, 13 years 10 months at T2, and 19 years 9 months at T3. Serial dental casts of 26 untreated subjects (18 male, 8 female) were obtained from the longitudinal records of the University of Michigan Elementary and Secondary School Growth Study as the control group (CG). The dental casts were selected to resemble the treated group at each time that records were taken. The criteria for selection at T1 were based on dental development (early mixed dentition) and skeletal maturity (stages 1 to 3 of the CVM method) 16 ; T2 criteria were based on dental development and homogeneity of observation interval; T3 criteria were based on skeletal maturity (stage 5 or 6 of the CVM method), a chronological age of 16 years 6 months or older, and a minimum interval between T2 and T3 of 3 years. The mean ages were 8 years 9 months at T1, 14 years 2 months at T2, and 19 years 9 months at T3. The subjects selected from the University of Michigan Elementary and Secondary School Growth Study had predominantly Class I malocclusions; a few tended toward Class II malocclusion; no subject in the control group had a Class III relationship. The 51 patients underwent RME with bonded acrylic splints (Fig 1) that covered the maxillary first and second deciduous molars and the maxillary permanent first molars. 17 The midline expansion screw was attached to the appliance with a heavy (.045 in) wire framework and routinely was expanded a quarter turn per day until a buccal crossbite was approached. The transverse molar relationship obtained in most instances involved approximating the lingual cusps of the maxillary posterior teeth and the buccal cusps of the mandibular posterior teeth in the transverse dimension. After expansion, the bonded appliance usually remained in place for an additional 5 months, followed by stabilization with a simple palatal plate with posterior clasps bilaterally. The plate typically was worn full Fig 1. Acrylic splint RME. time for 12 months or more and then at night; in a few patients, however, the plate was discontinued after 1 year of retention. A transpalatal arch typically was placed before the loss of the second deciduous molars. In addition, over half of the patients had their maxillary incisors bracketed temporarily for alignment. After the eruption of the permanent teeth, the patients underwent comprehensive nonextraction orthodontic treatment with preadjusted edgewise appliances (phase II). The transpalatal arch was left in place for the duration of treatment in most patients. After phase II, a positioner usually was used to fine-detail the dentition for 3 weeks to 2 months. Then impressions for invisible retainers typically were taken; the patients were instructed to wear the retainers full time for a year. The patients then were advised to wear the invisible retainers at night for an additional year; then they were encouraged to wear them intermittently at night. Most patients were no longer wearing their retainers at the T3 records. The dental casts were measured with a digital imaging system (Bioscan OPTIMAS Imaging System, Seattle, Wash). This system was developed specifically for the acquisition, measurement, and storage of data obtained in the earlier study of Brust and McNamara. 12 The methods for image capture and landmark acquisition have been described extensively in previous articles ,18 Measurements on dental casts Arch width was measured at the following teeth: deciduous canines/permanent canines, deciduous first molars/first premolars, deciduous second molars/second premolars, and permanent first molars. Arch width was measured from the lingual point of a tooth to the like point on its antimere (Fig 2) and between the
4 634 Geran et al American Journal of Orthodontics and Dentofacial Orthopedics May 2006 Fig 2. Arch width was determined as distance between lingual landmarks on each posterior tooth. Lingual landmark on maxillary first molars was located at junction of lingual groove with palatal mucosa. Fig 4. Arch depth was determined by measuring length of perpendicular line constructed from contact point between mesial contact points of central incisors to line connecting contact points between second premolars and first molars. Fig 3. Location of centroid of each posterior tooth was found first by determining midpoint (A) of line connecting mesial and distal landmarks. Similar midpoint (B) was constructed midway between buccal and lingual landmarks of tooth. Centroid (C) was located midway between points A and B. Fig 5. Arch perimeter was determined by constructing line from mesial contact point of 1 molar through mesial and distal contact points of 6 anterior teeth to mesial contact point of opposite molar. centroids of a tooth and its antimere (Fig 3), as described by Moyers et al 19 and Brust and McNamara. 12 Arch depth was measured as the distance from a point midway between the facial surfaces of the central incisors to a line tangent to the mesial surfaces of the first molars (Fig 4). Arch perimeter was determined by summing the segments between contact points from the mesial surface of the first molar to the mesial surface of the opposite first molar (Fig 5). Molar angulation was calculated by measuring the angle of intersecting lines drawn tangent to the mesiofacial and mesiolingual cusp tips of the right and left maxillary and mandibular first molars (Fig 6). Angulation less than 180 indicated that the molars were tipped facially; values over 180 implied lingual tipping. The error of the method of the digital imaging system was described previously by several investigators. 12,18 In these studies, the error was relatively consistent and within acceptable limits for the analysis
5 American Journal of Orthodontics and Dentofacial Orthopedics Volume 129, Number 5 Geran et al 635 Table I. Comparison of starting forms of treated group (TG) and control group (CG) TG T1 (n 51) CG T1 (n 26) t test Measure (mm) Mean SD Mean SD P Fig 6. Angulation of maxillary and mandibular first molars was determined by measuring angle of intersection of lines passing through buccal and lingual cusps. Angulation less than 180 indicated that molars were tipped buccally; values over 180 implied lingual tipping. of serial dental casts. For example, the standard error for the measurement of maxillary intermolar width in these studies ranged from 0.03 to 0.13 mm. Comparisons between the TG and the CG were performed with the Student t test for independent samples. The following statistical comparisons were performed. Comparison of starting forms: TG at T1 vs CG at T1. Evaluation of treatment effect: T2-T1 changes in TG vs T2-T1 changes in CG. Evaluation of posttreatment changes: T3-T2 changes in TG vs T3-T2 changes in CG. Evaluation of overall changes: T3-T1 changes in TG vs T3-T1 changes in CG. Comparison of final forms: TG at T3 vs CG at T3. RESULTS Descriptive statistics for the measurements at T1 and T3, and for the changes T2-T1, T3-T2, and T3-T1, in both groups along with statistical comparisons are reported in Tables I through IV. At T1, both the maxillary and mandibular dental arches of the patients in the TG were significantly narrower than the corresponding dental arches of the subjects in the CG (Table I). All measurements for maxillary and mandibular arch width (except mandibular intercanine width) and arch perimeters were significantly smaller in the TG than in the CG. The maxillary permanent first molars also had a significantly greater buccal angulation in the TG than in the CG. The T2-T1 treatment changes with RME followed by fixed appliances produced significantly greater increments in all variables for maxillary and mandibular arch widths (Fig 4) when compared with the controls (Table II). Maxillary arch depth showed significantly greater decreases in the TG with respect to the CG. Significant differences in maxillary and mandibular Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Intermolar Interpremolar (2nd) * Interpremolar (1st) * Intercanine Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Manibular arch width Intermolar Interpremolar (2nd) * Interpremolar (1st) * Intercanine Maxillary arch depth 1st molar Mandibular arch depth 1st molar Maxillary arch perimeter * Mandibular arch perimeter Maxillary molar angulation * Mandibular molar angulation *P.05; P.01; P.001;, not significant. arch perimeters were found in the TG when compared with the CG. For example, maxillary arch perimeter increased 0.9 mm in the TG but decreased 1.8 mm in the CG. Mandibular arch perimeter decreased less in the TG ( 2.4 mm) than in the CG ( 4.4 mm). As for the changes in molar angulation (Fig 6), in the TG, the maxillary first permanent molars showed a significant tendency for more lingual inclination. For the T3-T2 changes in the TG vs the CG, no significant differences in the post-treatment changes were found with respect to the CG, except for maxillary first premolar widths (measured both at the centroid and lingually), which showed significantly greater decreases in the TG, and mandibular intermolar arch width (measured both at the centroid and lingually), which increased in the TG and decreased in the CG (Table II). measured at the
6 636 Geran et al American Journal of Orthodontics and Dentofacial Orthopedics May 2006 Table II. Comparisons of changes T2-T1, T2-T3, and T3-T1 between treated group (TG) and control group (CG) TG (n 51) CG (n 26) t test T2-T1 T3-T2 T3-T1 T2-T1 T3-T2 T3-T1 T2-T1 T3-T2 T3-T1 Measure (mm) Mean SD Mean SD Mean SD Mean SD Mean SD Mean SD P P P Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Intermolar * Interpremolar (2nd) Interpremolar (1st) Intercanine Maxillary arch depth 1st molar Mandibular arch depth 1st molar Maxillary arch perimeter Mandibular arch perimeter * Maxillary molar angulation * Mandibular molar angulation *P.05; P.01; P.001;, not significant. canines (lingually) showed significantly larger decreases in the TG. Significantly smaller decreases were recorded in the TG for changes in maxillary arch depth and maxillary arch perimeter when compared with the CG. The statistical comparison of the changes in the overall observation period from T1 to T3 in the TG vs the CG for the most part replicated the results of active treatment changes (T1-T2) (Table II). For example, by contrasting the overall change in maxillary arch perimeter in the TG (0.0 mm) with the same measurement decreases in the CG ( 3.8 mm), 3.8 mm more arch perimeter was recorded in the TG. In the mandibular arch, arch perimeter decreased 3.6 mm in the TG and 6.2 mm in the CG, leading to a difference of 2.8 mm more in the TG. No statistically significant difference was found between the final forms of the TG and the CG (Table III). The only exception was a slightly larger width in mandibular arch measured at the second premolars in the TG with respect to the CG. DISCUSSION The goal of this longitudinal prospective clinical study conducted in a private practice was to assess the changes in arch dimensions in mixed-dentition patients who were treated with RME followed by fixed appliances compared with those observed in an untreated CG. An original feature of this investigation was the use of acrylic splint RME in patients during the mixed-dentition phase. All subjects in the TG initially had significant constriction of the maxillary arch with respect to controls, associated with variable degrees of crowding. The TG required RME to improve the
7 American Journal of Orthodontics and Dentofacial Orthopedics Volume 129, Number 5 Geran et al 637 Table III. Comparison between treated group (TG) and control group (CG) at T3 Measure (mm) TG T1 (n 51) CG T1 (n 26) t test Mean SD Mean SD P Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Intermolar Interpremolar (2nd) * Interpremolar (1st) Intercanine Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Intermolar Interpremolar (2nd) Interpremolar (1st) Intercanine Maxillary arch depth 1st molar Mandibular arch depth 1st molar Maxillary arch perimeter Mandibular arch perimeter Maxillary molar angulation Mandibular molar angulation *P.05;, not significant. transverse arch dimension before fixed appliance treatment. No active expansion of the mandibular arch (eg, Schwarz appliance, lip bumper) occurred during the mixed dentition. The evaluation of the active treatment effects after RME and fixed appliance therapy showed significantly larger values in all arch dimensions relative to the CG. From T1 to T2, maxillary intermolar and intercanine widths demonstrated average increments of about 4 mm, whereas the increases in mandibular arch widths ranged between 1.0 and 1.5 mm. All subjects in both groups had their second deciduous molars at the beginning of the study. With regard to the actual change in arch perimeters, the 0.9-mm increase in maxillary arch perimeter was associated with a loss ( 2.4 mm) in mandibular arch perimeter at the end of phase II. By taking into account the normally occurring decreases in arch perimeter observed in the CG during the same time interval ( 1.8 and 4.4 mm for the maxillary and mandibular arches, respectively), maxillary arch perimeter in the TG was 2.7 mm larger relative to the CG at the end of fixed appliance therapy; mandibular arch perimeter was 2.0 mm larger in the TG as well. As for the changes in maxillary arch depth, a greater decrease in the TG was found with respect to the CG ( 2.5 vs 1.2 mm). During the posttreatment period, very slight changes occurred in arch width measurements in both the maxilla and the mandible of the TG. Furthermore, no relapse tendency was observed in arch perimeter after active treatment. On the contrary, significantly smaller decreases in maxillary arch perimeter were detected in the TG than in the CG, associated with significantly smaller decreases in maxillary arch depth in the TG. At the end of the overall observation period, the increase in maxillary intermolar width for the TG was 4.2 mm, which was 3.5 mm larger than in the CG (Table IV). Mandibular intermolar width showed an actual increase of 1.9 mm in the TG; this was 2.1 mm larger than the corresponding measurement in the CG. The relative change in arch perimeter in the TG vs the CG was 3.8 mm for the maxilla and 2.5 mm for the mandible. However, these apparent increases in arch perimeter were due in great part to the negative changes in the CG in the long term. In a time interval of 11 years that covers both the mixed and permanent dentitions, average decreases of 3.8 and.2 mm were observed in untreated subjects in maxillary and mandibular arch perimeters, respectively. The results of this study extend the information about modifications in arch perimeters in growing subjects analyzed previously by Spillane and McNamara 11 and Brust and McNamara. 12 Most obvious are the conspicuous losses that can be expected in both arches from childhood through young adulthood. The loss in arch perimeter, shown by the CG, must be ascribed mainly to the exfoliation of the second deciduous molars in both arches and their replacement with smaller second premolars. On a separate note, the behavior of arch depths in both the treated and untreated samples should be elucidated. Consistent losses in both maxillary and mandibular arch depths were recorded during active treatment and in the posttreatment periods. Interestingly, the amount of loss in maxillary arch depth in the TG was greater than that observed in the CG. Most of this difference occurred during the active treatment period when the loss in arch depth for the TG ( 2.5 mm) was more than twice that of the CG ( 1.2 mm). The active retraction of the anterior teeth by way of
8 638 Geran et al American Journal of Orthodontics and Dentofacial Orthopedics May 2006 Table IV. Net changes in treated group (TG) compared with control group (CG) Intermolar Intercanine Intermolar Intercanine Maxillary arch perimeter Mandibular arch perimeter TG (n 51) T1-T T2-T T1-T CG (n 26) T1-T T2-T T1-T Net changes T1-T T2-T T1-T fixed appliances probably accounted for most of this slight reduction in arch depth. At T3 (Table III), when all subjects in both samples had ended or nearly finished their active growth periods, the initial deficiencies in arch width and arch perimeter in the TG with respect to the CG were corrected completely. From a clinical standpoint, the amount of correction in maxillary intermolar and intercanine widths and in maxillary arch perimeter equaled the initial discrepancies. When analyzing the literature, a comparison of the outcomes of this study can be performed at least indirectly with the results of Moussa et al 10 and directly with those of McNamara et al, 13 who used a similar measurement protocol as that of our study. The latter group used the same measuring equipment (digital imaging system) and the same landmarks for analysis as we did. Moussa et al, 10 however, measured changes in dental-arch dimensions differently (a 2-pointed caliper was used to measure the dental casts directly), and the definitions of arch width, arch perimeter, and arch length included slightly different landmarks than those used here; thus a direct comparison between the 2 studies cannot be made. Both previous investigations evaluated treatment protocols that included a tooth/ tissue-borne device for RME (Haas expander), whereas our study evaluated an acrylic splint expander bonded to the teeth. The treated group of Moussa et al 10 showed a mean increase of 6.7 mm in maxillary intermolar width due to active intervention a value greater than that found in the study of McNamara et al 13 and in this study for the same measurement (4.4 mm in both studies). The increases in maxillary intercanine width in both previous studies were similar to the increase reported here (about 4.0 mm). As for the mandibular arch, Moussa et al 10 found an increase of about 2 mm for intermolar width, similar to the value reported here (1.7 mm) and in contrast to the value reported by McNamara et al 13 (1.0 mm). All 3 studies agreed on a 1.5-mm increase in mandibular intercanine width over the long term. Similar changes for the widths of both dental arches were assessed in the 3 studies for the overall observation period (T3-T1). As for the measurement for maxillary arch perimeter, in this study, the overall increase during active treatment was minimal (0.9 mm) when compared with the increases reported by Moussa et al 10 (4.1 mm) and McNamara et al 13 (6.3 mm). On the other hand, the significant decreases in maxillary arch perimeter during the posttreatment period in the previous studies ( 2.5 to 3.5 mm) were not observed in our study. In the overall observation period, although the previous articles indicated positive increases for maxillary arch perimeters, this study did not find a change for this measurement. Through the assessment of the loss in the CG ( 3.8 mm), the final outcome indicates actual maintenance of 3.8 mm in maxillary arch perimeter (Table IV), a value that is considerably less than that reported by Mc- Namara et al 13 (6.0 mm). The absence of untreated controls in the study by Moussa et al 10 does not allow a direct comparison with the other 2 investigations in terms of clinical significance of the values for changes in arch perimeters. The relatively smaller amount of increase in maxillary arch perimeter observed in this study with respect to the one by McNamara et al 13 can be explained by at least 2 clinical aspects. The first difference between the 2 studies (which might be of significant importance to the clinician) relates to the amount of activation of the expansion screw during the active treatment phase: 10.0 to 10.5 mm with the Haas-type of RME 13 and 7 to 8 mm (on average) in
9 American Journal of Orthodontics and Dentofacial Orthopedics Volume 129, Number 5 Geran et al 639 this study. It might be that more aggressive overcorrection of the transverse skeletal discrepancy in the mixed dentition is indicated, just as Haas suggested when using his appliance. The concept of overcorrection might be as important in RME therapy as it is in extraoral traction treatment for Class II malocclusion 17 or facial mask/rme therapy for Class III malocclusion. 20 A second explanation concerning the smaller amount of maxillary arch perimeter noted in the TG relative to the CG in this study is linked to the overall loss in maxillary arch depth that we observed ( 0.6 mm) in comparison with the actual increase in the same measurement in the study by McNamara et al 13 (2.9 mm). The net difference between the 2 studies is a lack of increase in maxillary arch depth of about 3.5 mm in subjects treated with the acrylic splint RME with respect to subjects treated with the Haas-type of RME. 13 The timing for RME, 5,14,15 however, more than the type of appliance probably accounted for different results for maxillary arch depth. The average age when expansion was performed in our study was 8 years 10 months, whereas it was 12 years 2 months in the sample analyzed by McNamara et al. 13 The use of RME in the early mixed dentition requires a significantly longer and more critical period of therapeutic management of space maintenance during the exfoliation of the posterior deciduous teeth. Mandibular arch perimeter decreased during active treatment in the TG, followed by a supplementary decrease during the posttreatment period; this produced a decrease in the overall observation period of 3.7 mm. This value apparently is much less promising with respect to those reported in previous investigations. Both Moussa et al 10 and McNamara et al 13 found substantial increases in mandibular arch perimeter during active treatment followed by decreases during the posttreatment period, with a final overall increase of about 1.5 mm in the study by McNamara et al 13 and a final overall decrease of about 0.5 mm in the sample of Moussa et al. 10 An obvious explanation lies in the stage of dental development of the subjects monitored in the 3 studies. All patients and subjects in our study were in the mixed dentition. Because the subjects in the other studies were on average 12 years of age at the time of initial records, many if not most of them were in the permanent dentition. The considerable amount of loss in mandibular arch perimeter in the CG during the overall observation period ( 6.2 mm) produced a maintenance of 2.5 mm in arch perimeter in the TG in this study (Table IV), an amount that is more than the half of the amount reported by McNamara et al 13 (4.5 mm). However, our patients did not undergo active orthodontic expansion in the mandibular arch in the mixed dentition (eg, Schwarz appliance, lip bumper), presumably because they were judged clinically to have sufficient arch perimeter in the mixed dentition to allow for the unimpeded eruption of the permanent mandibular teeth without active intervention in that arch. When compared with the only other study that includes observations on untreated controls in the long term, 13 the results of our study suggest that treatment with acrylic splint RME in the mixed dentition leads to less favorable amounts of relative increase in the perimeter of both arches in comparison with controls. Nevertheless, the relative increases in intermolar and intercanine widths in both the maxilla and the mandible were similar in the 2 studies, even with a considerably smaller amount of activation of the RME screw in the sample evaluated here in comparison with those treated with the Haas-type expander. 10,13 This favorable outcome in the transverse dimension of both arches probably should be ascribed to the different treatment timing of the expansion protocols (early mixed dentition in this study and late mixed dentition or early permanent dentition in the study by McNamara et al 13 ). It has been shown that when RME is performed during the early developmental phases, treatment outcomes are more skeletal and more stable over the long term. 15 RME in the early mixed dentition appears to be indicated for an effective and stable correction of transverse deficiencies of the dental arches, whereas the effectiveness of this treatment approach might be more critical if it aimed to increase arch perimeter. CONCLUSIO Therapy with an acrylic splint RME in the early mixed dentition followed by fixed appliances in the permanent dentition can be considered an effective treatment option to correct transverse deficiencies of both maxillary and mandibular arches when evaluated in the long term. No active expansion of the mandibular dental arch was undertaken during the mixed dentition. RME followed by fixed appliances can also be considered an option to relieve modest tooth size-arch length discrepancies. Approximately 4 mm of long-term relative increase in maxillary arch perimeter and 2.5 mm additional maintenance of mandibular arch perimeter were observed in the TG when compared with the CG. We thank Elvis L. Evans for modifying the digital imaging system for use in this study.
10 640 Geran et al American Journal of Orthodontics and Dentofacial Orthopedics May 2006 REFERENCES 1. Haas AJ. Rapid expansion of the maxillary dental arch and nasal cavity by opening the mid-palatal suture. Angle Orthod 1961;31: Krebs A. Midpalatal suture expansion studies by the implant method over a seven year period. Trans Eur Orthod Soc 1964;40: Wertz RA. Skeletal and dental changes accompanying rapid midpalatal suture opening. Am J Orthod 1970;58: Haas AJ. Palatal expansion: just the beginning of dentofacial orthopedics. Am J Orthod 1970;57: Wertz R, Dreskin M. Midpalatal suture opening: a normative study. Am J Orthod 1977;71: da Silva Filho OG, Montes LA, Torelly LF. Rapid maxillary expansion in the deciduous and mixed dentition evaluated through posteroanterior cephalometric analysis. Am J Orthod Dentofacial Orthop 1995;107: Haberson VA, Myers DR. Midpalatal suture opening during functional posterior crossbite correction. Am J Orthod 1978;74: Hesse KL, Årtun J, Joondeph DR, Kennedy DB. Changes in condylar position and occlusion associated with maxillary expansion for correction of functional unilateral posterior crossbite. Am J Orthod Dentofacial Orthop 1997;111: Adkins MD, Nanda RS, Currier GF. Arch perimeter changes on rapid palatal expansion. Am J Orthod Dentofacial Orthop 1990; 97: Moussa R, O Reilly MT, Close JM. Long-term stability of rapid palatal expander treatment and edgewise mechanotherapy. Am J Orthod Dentofacial Orthop 1995;108: Spillane LM, McNamara JA Jr. Maxillary adaptations following expansion in the mixed dentition. Semin Orthod 1995;1: Brust EW, McNamara JA Jr. Arch dimensional changes concurrent with expansion in mixed dentition patients. In: Trotman CA, McNamara JA Jr, editors. Orthodontic treatment: outcome and effectiveness. Monograph 30. Craniofacial Growth Series. Ann Arbor: Center for Human Growth and Development; University of Michigan; p McNamara JA Jr, Baccetti T, Franchi L, Herberger TA. Rapid maxillary expansion followed by fixed appliances: a long-term evaluation of changes in arch dimensions. Angle Orthod 2003; 73: Melsen B. Palatal growth studied on human autopsy material. A histologic microradiographic study. Am J Orthod 1975;68: Baccetti T, Franchi L, Cameron CG, McNamara JA Jr. Treatment timing for rapid maxillary expansion. Angle Orthod 2001; 71: Baccetti T, Franchi L, McNamara JA Jr. The cervical vertebral maturation (CVM) method for the assessment of optimal treatment timing in dentofacial orthopedics. Semin Orthod 2005;11: McNamara JA Jr, Brudon WL. Orthodontics and dentofacial orthopedics. Ann Arbor: Needham Press; Carter GA, McNamara JA Jr. Longitudinal dental arch changes in adults. Am J Orthod Dentofacial Orthop 1998;114: Moyers RE, van der Linden FPGM, Riolo ML, McNamara JA Jr. Standards of human occlusal development. Monograph 5. Craniofacial Growth Series. Ann Arbor: Center for Human Growth and Development; University of Michigan; Westwood PV, McNamara JA Jr, Baccetti T, Franchi L, Sarver DM. Long-term effects of early Class III treatment with rapid maxillary expansion and facial mask therapy. Am J Orthod Dentofacial Orthop 2003;123:
Extract or expand? Over the last 100 years, the
 ORIGINAL ARTICLE A long-term evaluation of the mandibular Schwarz appliance and the acrylic splint expander in early mixed dentition patients Paul W. O Grady, a James A. McNamara, Jr, b Tiziano Baccetti,
ORIGINAL ARTICLE A long-term evaluation of the mandibular Schwarz appliance and the acrylic splint expander in early mixed dentition patients Paul W. O Grady, a James A. McNamara, Jr, b Tiziano Baccetti,
Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction
 Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Case Report Case Report: Long-Term Outcome of Class II Division 1 Malocclusion Treated with Rapid Palatal Expansion and Cervical Traction Roberto M. A. Lima, DDS a ; Anna Leticia Lima, DDS b Abstract:
Aging in the Craniofacial Complex
 Original Article Aging in the Craniofacial Complex Longitudinal Dental Arch Changes Through the Sixth Decade Marcus M. Dager a ; James A. McNamara b ; Tiziano Baccetti c ; Lorenzo Franchi c ABSTRACT Objective:
Original Article Aging in the Craniofacial Complex Longitudinal Dental Arch Changes Through the Sixth Decade Marcus M. Dager a ; James A. McNamara b ; Tiziano Baccetti c ; Lorenzo Franchi c ABSTRACT Objective:
SPECIAL. The effects of eruption guidance and serial extraction on the developing dentition
 SPECIAL The effects of eruption guidance and serial extraction on the developing dentition Robert M. Little, DDS, MSD, PhD Clinical practice is a balance of our collective experience and intuitive clinical
SPECIAL The effects of eruption guidance and serial extraction on the developing dentition Robert M. Little, DDS, MSD, PhD Clinical practice is a balance of our collective experience and intuitive clinical
Changes of the Transverse Dental Arch Dimension, Overjet and Overbite after Rapid Maxillary Expansion (RME)
 Dental Journal Changes of the Transverse Dental Arch Dimension, Overjet and Overbite after Rapid Maxillary Expansion (RME) Department of Advanced General Dentistry Faculty of Dentistry, Mahidol University.
Dental Journal Changes of the Transverse Dental Arch Dimension, Overjet and Overbite after Rapid Maxillary Expansion (RME) Department of Advanced General Dentistry Faculty of Dentistry, Mahidol University.
Class II malocclusions are observed commonly in
 ORIGINAL ARTICLE Improving Class II malocclusion as a side-effect of rapid maxillary expansion: A prospective clinical study Susan S. Guest, a James A. McNamara, Jr., b Tiziano Baccetti, c and Lorenzo
ORIGINAL ARTICLE Improving Class II malocclusion as a side-effect of rapid maxillary expansion: A prospective clinical study Susan S. Guest, a James A. McNamara, Jr., b Tiziano Baccetti, c and Lorenzo
Instability of tooth alignment and occlusal relationships
 ORIGINAL ARTICLE Relapse revisited again Kenneth C. Dyer, a James L. Vaden, b and Edward F. Harris c Chattanooga, Cookeville, and Memphis, Tenn Introduction: Long-term changes in the dentitions of orthodontic
ORIGINAL ARTICLE Relapse revisited again Kenneth C. Dyer, a James L. Vaden, b and Edward F. Harris c Chattanooga, Cookeville, and Memphis, Tenn Introduction: Long-term changes in the dentitions of orthodontic
Interest in rapid maxillary expansion (RME) has
 ORIGINAL ARTICLE C E Long-term effects of rapid maxillary expansion: A posteroanterior cephalometric evaluation Christopher G. Cameron, DDS, MS, a Lorenzo Franchi, DDS, PhD, b Tiziano Baccetti, DDS, PhD,
ORIGINAL ARTICLE C E Long-term effects of rapid maxillary expansion: A posteroanterior cephalometric evaluation Christopher G. Cameron, DDS, MS, a Lorenzo Franchi, DDS, PhD, b Tiziano Baccetti, DDS, PhD,
The resolution of mandibular incisor
 CONTINUING EDUCATION ARTICLE The use of the lingual arch in the mixed dentition to resolve incisor crowding Mathew M. Brennan, DMD, a and Anthony A. Gianelly, DMD, PhD, MD b Boston, Mass In the mixed dentition,
CONTINUING EDUCATION ARTICLE The use of the lingual arch in the mixed dentition to resolve incisor crowding Mathew M. Brennan, DMD, a and Anthony A. Gianelly, DMD, PhD, MD b Boston, Mass In the mixed dentition,
EXPANSION. Effective Management of Transverse Problems in the Growing Patient: Evidence-based Approach
 Effective Management of Transverse Problems in the Growing Patient: Evidence-based Approach Lorenzo Franchi, DDS, PhD The transverse deficiency of the maxillary arch is the most common occlusal problem
Effective Management of Transverse Problems in the Growing Patient: Evidence-based Approach Lorenzo Franchi, DDS, PhD The transverse deficiency of the maxillary arch is the most common occlusal problem
Arch dimensional changes following orthodontic treatment with extraction of four first premolars
 Received: 14 June. 2015 Accepted: 7 Dec. 2015 Arch dimensional changes following orthodontic treatment with extraction of four first premolars Abstract Asghar Ebadifar DDS, MSc 1, Mohammad Hossien Shafazand
Received: 14 June. 2015 Accepted: 7 Dec. 2015 Arch dimensional changes following orthodontic treatment with extraction of four first premolars Abstract Asghar Ebadifar DDS, MSc 1, Mohammad Hossien Shafazand
Relapse of maxillary anterior crowding in Class I and Class II malocclusion treated orthodontically without extractions
 O r i g i n a l A r t i c l e Relapse of maxillary anterior crowding in Class I and Class II malocclusion treated orthodontically without extractions Willian J. G. Guirro*, Karina Maria Salvatore de Freitas**,
O r i g i n a l A r t i c l e Relapse of maxillary anterior crowding in Class I and Class II malocclusion treated orthodontically without extractions Willian J. G. Guirro*, Karina Maria Salvatore de Freitas**,
Palatal Depth and Arch Parameter in Class I Open Bite, Deep Bite and Normal Occlusion
 26 Iraqi Orthod J 1(2) 2005 Palatal Depth and Arch Parameter in Class I Open Bite, Deep Bite and Normal Occlusion Ahmad A. Abdulmawjood, a Mahmood K. Ahmed, a and Ne am R. Al-Saleem a Abstract: This study
26 Iraqi Orthod J 1(2) 2005 Palatal Depth and Arch Parameter in Class I Open Bite, Deep Bite and Normal Occlusion Ahmad A. Abdulmawjood, a Mahmood K. Ahmed, a and Ne am R. Al-Saleem a Abstract: This study
A comparative study of dental arch widths: extraction and non-extraction treatment
 European Journal of Orthodontics 27 (2005) 585 589 doi:10.1093/ejo/cji057 Advance Access publication 28 October 2005 The Author 2005. Published by Oxford University ss on behalf of the European Orthodontics
European Journal of Orthodontics 27 (2005) 585 589 doi:10.1093/ejo/cji057 Advance Access publication 28 October 2005 The Author 2005. Published by Oxford University ss on behalf of the European Orthodontics
ORTHODONTICS Treatment of malocclusion Assist.Lec.Kasem A.Abeas University of Babylon Faculty of Dentistry 5 th stage
 Lec: Treatment of class I malocclusion Class I occlusion can be defined by Angles, classification as the mesiobuccal cusp of the upper 1 st permanent molar occlude with the developmental groove of the
Lec: Treatment of class I malocclusion Class I occlusion can be defined by Angles, classification as the mesiobuccal cusp of the upper 1 st permanent molar occlude with the developmental groove of the
Dental tipping and rotation immediately after surgically assisted rapid palatal expansion
 European Journal of Orthodontics 25 (2003) 353 358 2003 European Orthodontic Society Dental tipping and rotation immediately after surgically assisted rapid palatal expansion Chun-Hsi Chung and Adena M.
European Journal of Orthodontics 25 (2003) 353 358 2003 European Orthodontic Society Dental tipping and rotation immediately after surgically assisted rapid palatal expansion Chun-Hsi Chung and Adena M.
Assessment of Archwidth Changes in Extraction and Non Extraction Patients. College of dental sciences, demotand, Hazaribagh, Jharkhand
 ISSN- O: 2458-868X, ISSN P: 2458-8687 International Journal of Medical Science and Innovative Research (IJMSIR) IJMSIR : A Medical Publication Hub Available Online at: www.ijmsir.com Volume 2, Issue 6,
ISSN- O: 2458-868X, ISSN P: 2458-8687 International Journal of Medical Science and Innovative Research (IJMSIR) IJMSIR : A Medical Publication Hub Available Online at: www.ijmsir.com Volume 2, Issue 6,
One of the greatest challenges in contemporary
 ORIGINAL ARTICLE Treatment and posttreatment craniofacial changes after rapid maxillary expansion and facemask therapy Tiziano Baccetti, DDS, PhD, a Lorenzo Franchi, DDS, PhD, b and James A. McNamara,
ORIGINAL ARTICLE Treatment and posttreatment craniofacial changes after rapid maxillary expansion and facemask therapy Tiziano Baccetti, DDS, PhD, a Lorenzo Franchi, DDS, PhD, b and James A. McNamara,
Self-ligating versus Invisalign: analysis of dento-alveolar effects
 Original article Self-ligating versus Invisalign: analysis of dento-alveolar effects Chiara Pavoni, DDS Roberta Lione, DDS Giuseppina Laganà, DDS, MS Paola Cozza, MD, DDS, MS University of Rome Tor Vergata,
Original article Self-ligating versus Invisalign: analysis of dento-alveolar effects Chiara Pavoni, DDS Roberta Lione, DDS Giuseppina Laganà, DDS, MS Paola Cozza, MD, DDS, MS University of Rome Tor Vergata,
Molar Changes with Cervical Headgear Alone or in Combination with Rapid Maxillary Expansion
 Original Article Molar Changes with Cervical Headgear Alone or in Combination with Rapid Maxillary Expansion Marcel Marchiori Farret a ; Eduardo Martinelli S. de Lima b ; Vanessa ereira Araújo c ; Susana
Original Article Molar Changes with Cervical Headgear Alone or in Combination with Rapid Maxillary Expansion Marcel Marchiori Farret a ; Eduardo Martinelli S. de Lima b ; Vanessa ereira Araújo c ; Susana
Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient
 Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
Case Report Maxillary Expansion and Protraction in Correction of Midface Retrusion in a Complete Unilateral Cleft Lip and Palate Patient Masayoshi Kawakami, DDS, PhD a ; Takakazu Yagi, DDS, PhD b ; Kenji
An RCT on treatment of palatally displaced canines with RME and/or a transpalatal arch
 European Journal of Orthodontics 33 (2011) 601 607 doi:10.1093/ejo/cjq139 Advance Access Publication 8 November 2010 The Author 2010. Published by Oxford University Press on behalf of the European Orthodontic
European Journal of Orthodontics 33 (2011) 601 607 doi:10.1093/ejo/cjq139 Advance Access Publication 8 November 2010 The Author 2010. Published by Oxford University Press on behalf of the European Orthodontic
Mandibular Cervical Headgear vs Rapid Maxillary Expander and Facemask for Orthopedic Treatment of Class III Malocclusion
 Original Article Mandibular Cervical Headgear vs Rapid Maxillary Expander and Facemask for Orthopedic Treatment of Class III Malocclusion Tiziano Baccetti a ; Diego Rey b ; David Angel c ; Giovanni Oberti
Original Article Mandibular Cervical Headgear vs Rapid Maxillary Expander and Facemask for Orthopedic Treatment of Class III Malocclusion Tiziano Baccetti a ; Diego Rey b ; David Angel c ; Giovanni Oberti
The ASE Example Case Report 2010
 The ASE Example Case Report 2010 The Requirements for Case Presentation in The Angle Society of Europe are specified in the Appendix I to the Bylaws. This example case report exemplifies how these requirements
The ASE Example Case Report 2010 The Requirements for Case Presentation in The Angle Society of Europe are specified in the Appendix I to the Bylaws. This example case report exemplifies how these requirements
RAPID PALATAL EXPANSION IN MIXED DENTITION STAGE WITH CUSTOM MADE MODIFIED EXPANSION DEVICE
 Pakistan Oral & Dent. Jr. 24 (2) Dec 2004 ABSTRACT RAPID PALATAL EXPANSION IN MIXED DENTITION STAGE WITH CUSTOM MADE MODIFIED EXPANSION DEVICE *FARHAT AMIN, MCPS (Oral Surg). FCPS-II. (Orth), Trainee **ABIDA
Pakistan Oral & Dent. Jr. 24 (2) Dec 2004 ABSTRACT RAPID PALATAL EXPANSION IN MIXED DENTITION STAGE WITH CUSTOM MADE MODIFIED EXPANSION DEVICE *FARHAT AMIN, MCPS (Oral Surg). FCPS-II. (Orth), Trainee **ABIDA
The Tip-Edge appliance and
 Figure 1: Internal surfaces of the edgewise archwire slot are modified to create the Tip-Edge archwire slot. Tipping surfaces (T) limit crown tipping during retraction. Uprighting surfaces (U) control
Figure 1: Internal surfaces of the edgewise archwire slot are modified to create the Tip-Edge archwire slot. Tipping surfaces (T) limit crown tipping during retraction. Uprighting surfaces (U) control
Skeletal changes of maxillary protraction without rapid maxillary expansion
 Original Article Skeletal changes of maxillary protraction without rapid maxillary expansion A comparison of the primary and mixed dentition Dong-Yul Lee a ; Eun-Soo Kim b ; Yong-Kyu Lim a ; Sug-Joon Ahn
Original Article Skeletal changes of maxillary protraction without rapid maxillary expansion A comparison of the primary and mixed dentition Dong-Yul Lee a ; Eun-Soo Kim b ; Yong-Kyu Lim a ; Sug-Joon Ahn
Lingual correction of a complex Class III malocclusion: Esthetic treatment without sacrificing quality results.
 SM 3M Health Care Academy Lingual correction of a complex Class III malocclusion: Esthetic treatment without sacrificing quality results. Christopher S. Riolo, DDS, M.S, Ph.D. Dr. Riolo received his DDS
SM 3M Health Care Academy Lingual correction of a complex Class III malocclusion: Esthetic treatment without sacrificing quality results. Christopher S. Riolo, DDS, M.S, Ph.D. Dr. Riolo received his DDS
Mixed Dentition Treatment and Habits Therapy
 Interception Mixed Dentition Treatment and Habits Therapy Anterior Crossbites Posterior Crossbites Interference s with Normal Eruption Habit Therapy Tsung-Ju Hsieh, DDS, MSD 1 2 Anterior Crossbites Anterior
Interception Mixed Dentition Treatment and Habits Therapy Anterior Crossbites Posterior Crossbites Interference s with Normal Eruption Habit Therapy Tsung-Ju Hsieh, DDS, MSD 1 2 Anterior Crossbites Anterior
Angle Class II, division 2 malocclusion with severe overbite and pronounced discrepancy*
 O C a s e R e p o r t ngle Class II, division 2 malocclusion with severe overbite and pronounced discrepancy* Daniela Kimaid Schroeder** bstract This article reports the treatment of a young patient at
O C a s e R e p o r t ngle Class II, division 2 malocclusion with severe overbite and pronounced discrepancy* Daniela Kimaid Schroeder** bstract This article reports the treatment of a young patient at
The treatment of patients with increased vertical
 ORIGINAL ARTICLE Treatment effects of bonded RME and verticalpull chincup followed by fixed appliance in patients with increased vertical dimension Scott O. Schulz, a James A. McNamara, Jr, b Tiziano Baccetti,
ORIGINAL ARTICLE Treatment effects of bonded RME and verticalpull chincup followed by fixed appliance in patients with increased vertical dimension Scott O. Schulz, a James A. McNamara, Jr, b Tiziano Baccetti,
Correction of Crowding using Conservative Treatment Approach
 Case Report Correction of Crowding using Conservative Treatment Approach Dr Tapan Shah, 1 Dr Tarulatha Shyagali, 2 Dr Kalyani Trivedi 3 1 Senior Lecturer, 2 Professor, Department of Orthodontics, Darshan
Case Report Correction of Crowding using Conservative Treatment Approach Dr Tapan Shah, 1 Dr Tarulatha Shyagali, 2 Dr Kalyani Trivedi 3 1 Senior Lecturer, 2 Professor, Department of Orthodontics, Darshan
Mesial Step Class I or Class III Dependent upon extent of step seen clinically and patient s growth pattern Refer for early evaluation (by 8 years)
 Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
Orthodontics and Dentofacial Development Overview Development of Dentition Treatment Retention and Relapse Growth of Naso-Maxillary Complex Develops postnatally entirely by intramenbranous ossification
An Effectiv Rapid Molar Derotation: Keles K
 An Effectiv ective e and Precise Method forf Rapid Molar Derotation: Keles K TPA Ahmet Keles, DDS, DMSc 1 /Sedef Impar, DDS 2 Most of the time, Class II molar relationships occur due to the mesiopalatal
An Effectiv ective e and Precise Method forf Rapid Molar Derotation: Keles K TPA Ahmet Keles, DDS, DMSc 1 /Sedef Impar, DDS 2 Most of the time, Class II molar relationships occur due to the mesiopalatal
Class III malocclusion occurs in less than 5%
 CDABO CASE REPORT Orthodontic correction of a Class III malocclusion in an adolescent patient with a bonded RPE and protraction face mask Steven W. Smith, DDS, a and Jeryl D. English, DDS, MS b Dallas,
CDABO CASE REPORT Orthodontic correction of a Class III malocclusion in an adolescent patient with a bonded RPE and protraction face mask Steven W. Smith, DDS, a and Jeryl D. English, DDS, MS b Dallas,
Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report
 Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
Case Report Print ISSN: 2321-6379 Online ISSN: 2321-595X DOI: 10.17354/ijss/2017/506 Class II Correction using Combined Twin Block and Fixed Orthodontic Appliances: A Case Report Ahmed Alassiry Assistant
A SIMPLE METHOD FOR CORRECTION OF BUCCAL CROSSBITE OF MAXILLARY SECOND MOLAR
 Short Communication International Journal of Dental and Health Sciences Volume 01,Issue 03 A SIMPLE METHOD FOR CORRECTION OF BUCCAL CROSSBITE OF MAXILLARY SECOND MOLAR Sumit Yadav 1,Davender Kumar 2,Achla
Short Communication International Journal of Dental and Health Sciences Volume 01,Issue 03 A SIMPLE METHOD FOR CORRECTION OF BUCCAL CROSSBITE OF MAXILLARY SECOND MOLAR Sumit Yadav 1,Davender Kumar 2,Achla
Case Report Unilateral Molar Distalization: A Nonextraction Therapy
 Case Reports in Dentistry Volume 2012, Article ID 846319, 4 pages doi:10.1155/2012/846319 Case Report Unilateral Molar Distalization: A Nonextraction Therapy M. Bhanu Prasad and S. Sreevalli Department
Case Reports in Dentistry Volume 2012, Article ID 846319, 4 pages doi:10.1155/2012/846319 Case Report Unilateral Molar Distalization: A Nonextraction Therapy M. Bhanu Prasad and S. Sreevalli Department
Angle Class II, division 2 malocclusion with deep overbite
 BBO Case Report Angle Class II, division 2 malocclusion with deep overbite Arno Locks 1 Angle Class II, division 2, malocclusion is characterized by a Class II molar relation associated with retroclined
BBO Case Report Angle Class II, division 2 malocclusion with deep overbite Arno Locks 1 Angle Class II, division 2, malocclusion is characterized by a Class II molar relation associated with retroclined
A SERIOUS CHALLENGE IN DENTOFACIAL ORTHOPEDICS
 New perspectives in the orthopedic approach to Class III treatment Lorenzo Franchi, DDS, PhD Department of Orthodontics, The University of Florence, Italy, and T.M. Graber Visiting Scholar Department of
New perspectives in the orthopedic approach to Class III treatment Lorenzo Franchi, DDS, PhD Department of Orthodontics, The University of Florence, Italy, and T.M. Graber Visiting Scholar Department of
The appraisal of the biological aspects of mandibular
 ORIGINAL ARTICLE Mandibular growth as related to cervical vertebral maturation and body height Lorenzo Franchi, DDS, PhD, a Tiziano Baccetti, DDS, PhD, a and James A. McNamara Jr, DDS, PhD b Florence,
ORIGINAL ARTICLE Mandibular growth as related to cervical vertebral maturation and body height Lorenzo Franchi, DDS, PhD, a Tiziano Baccetti, DDS, PhD, a and James A. McNamara Jr, DDS, PhD b Florence,
The fact that mandibular incisor irregularity
 CONTINUING EDUCATION Associations between initial, posttreatment, and postretention alignment of maxillary anterior teeth Burleigh T. Surbeck, BS, a Jon Årtun, DDS, DrOdont, b Natalie R. Hawkins, MS, c
CONTINUING EDUCATION Associations between initial, posttreatment, and postretention alignment of maxillary anterior teeth Burleigh T. Surbeck, BS, a Jon Årtun, DDS, DrOdont, b Natalie R. Hawkins, MS, c
The use of a rapid maxillary expander with a
 ORIGINAL ARTICLE Postpubertal assessment of treatment timing for maxillary expansion and protraction therapy followed by fixed appliances Lorenzo Franchi, DDS, PhD, a Tiziano Baccetti, DDS, PhD, b and
ORIGINAL ARTICLE Postpubertal assessment of treatment timing for maxillary expansion and protraction therapy followed by fixed appliances Lorenzo Franchi, DDS, PhD, a Tiziano Baccetti, DDS, PhD, b and
Class II Correction with Invisalign Molar rotation.
 Tips from your peers to help you treat with confidence. Class II Correction with Invisalign Molar rotation. Dr. Mazyar Moshiri. Class II Correction with Invisalign Molar Rotation. Dr. Mazyar Moshiri. Orthodontic
Tips from your peers to help you treat with confidence. Class II Correction with Invisalign Molar rotation. Dr. Mazyar Moshiri. Class II Correction with Invisalign Molar Rotation. Dr. Mazyar Moshiri. Orthodontic
THE USE OF VACCUM FORM RETAINERS FOR RELAPSE CORRECTION
 THE USE OF VACCUM FORM RETAINERS FOR RELAPSE CORRECTION Azrul Hafiz Abdul Aziz 1 and Haslinda Ramli 2 1,2 Islamic Science University of Malaysia, Faculty of Dentistry, Level 15, Tower B, Persiaran MPAJ,
THE USE OF VACCUM FORM RETAINERS FOR RELAPSE CORRECTION Azrul Hafiz Abdul Aziz 1 and Haslinda Ramli 2 1,2 Islamic Science University of Malaysia, Faculty of Dentistry, Level 15, Tower B, Persiaran MPAJ,
Nonsurgical Rapid Maxillary Expansion in Adults: Report on 47 Cases Using the Haas Expander
 Original Article Nonsurgical Rapid Maxillary Expansion in Adults: Report on 47 Cases Using the Haas Expander Chester S. Handelman, DMD a ; Lin Wang, DDS b ; Ellen A. BeGole, PhD c ; Andrew J. Haas, DDS,
Original Article Nonsurgical Rapid Maxillary Expansion in Adults: Report on 47 Cases Using the Haas Expander Chester S. Handelman, DMD a ; Lin Wang, DDS b ; Ellen A. BeGole, PhD c ; Andrew J. Haas, DDS,
The clinical management of malocclusions characterized
 ORIGINAL ARTICLE Treatment timing for an orthopedic approach to patients with increased vertical dimension Tiziano Baccetti, a Lorenzo Franchi, a Scott O. Schulz, b and James A. McNamara, Jr c Florence,
ORIGINAL ARTICLE Treatment timing for an orthopedic approach to patients with increased vertical dimension Tiziano Baccetti, a Lorenzo Franchi, a Scott O. Schulz, b and James A. McNamara, Jr c Florence,
ASSESSMENT OF MAXILLARY FIRST MOLAR ROTATION IN SKELETAL CLASS II, AND THEIR COMPARISON WITH CLASS I AND CLASS III SUBJECTS
 ORIGINAL ARTICLE ASSESSMENT OF MAXILLARY FIRST MOLAR ROTATION IN SKELETAL CLASS II, AND THEIR COMPARISON WITH CLASS I AND CLASS III SUBJECTS ABSTRACT FARHAT AMIN, BDS, MCPS, FCPS Mesial rotation of maxillary
ORIGINAL ARTICLE ASSESSMENT OF MAXILLARY FIRST MOLAR ROTATION IN SKELETAL CLASS II, AND THEIR COMPARISON WITH CLASS I AND CLASS III SUBJECTS ABSTRACT FARHAT AMIN, BDS, MCPS, FCPS Mesial rotation of maxillary
Interceptive Orthodontic Treatment: Efficient Early Correction of Malocclusions
 Interceptive Orthodontic Treatment: Efficient Early Correction of Malocclusions Cameron Mashouf, DDS, MS Kayhan L. Mashouf, DMD, MSD January 2014 www.interceptiveortho.com Introduction When deciding on
Interceptive Orthodontic Treatment: Efficient Early Correction of Malocclusions Cameron Mashouf, DDS, MS Kayhan L. Mashouf, DMD, MSD January 2014 www.interceptiveortho.com Introduction When deciding on
Nonsurgical Treatment of Adult Open Bite Using Edgewise Appliance Combined with High-Pull Headgear and Class III Elastics
 Case Report Nonsurgical Treatment of Adult Open Bite Using Edgewise Appliance Combined with High-Pull Headgear and Class III Elastics Isao Saito, DDS, PhD a ; Masaki Yamaki, DDS, PhD b ; Kooji Hanada,
Case Report Nonsurgical Treatment of Adult Open Bite Using Edgewise Appliance Combined with High-Pull Headgear and Class III Elastics Isao Saito, DDS, PhD a ; Masaki Yamaki, DDS, PhD b ; Kooji Hanada,
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER:44 CASE NUMBER: 2 Year: 2010 ESLO 01 RÉSUMÉ OF CASE 5 CASE CATEGORY: CLASS II DIVISION 1 MALOCCLUSION A MALOCCLUSION WITH SIGNIFICANT MANDIBULAR
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER:44 CASE NUMBER: 2 Year: 2010 ESLO 01 RÉSUMÉ OF CASE 5 CASE CATEGORY: CLASS II DIVISION 1 MALOCCLUSION A MALOCCLUSION WITH SIGNIFICANT MANDIBULAR
ADOLESCENT TREATMENT. Thomas J. Cangialosi. Stella S. Efstratiadis. CHAPTER 18 Pages CLASS II DIVISION 1 WHY NOW?
 ADOLESCENT By Thomas J. Cangialosi and Stella S. Efstratiadis From Riolo, M. and Avery, J. Eds., Essentials for Orthodontic Practice, EFOP Press of EFOP, LLC. Ann Arbor and Grand Haven, Michigan, U.S.A.,
ADOLESCENT By Thomas J. Cangialosi and Stella S. Efstratiadis From Riolo, M. and Avery, J. Eds., Essentials for Orthodontic Practice, EFOP Press of EFOP, LLC. Ann Arbor and Grand Haven, Michigan, U.S.A.,
Research methodology University of Turku, Finland
 Research methodology Prospective, controlled cohort study started in 1998 Treatment group: 167 children Treatment with eruption guidance appliance only Control group: 104 children No Keski-Nisula K; Keski-Nisula
Research methodology Prospective, controlled cohort study started in 1998 Treatment group: 167 children Treatment with eruption guidance appliance only Control group: 104 children No Keski-Nisula K; Keski-Nisula
The conservative treatment of Class I malocclusion with maxillary transverse deficiency and anterior teeth crowding
 B B O C a s e R e p o r t The conservative treatment of Class I malocclusion with maxillary transverse deficiency and anterior teeth crowding Lincoln I. Nojima* Abstract This report describes the treatment
B B O C a s e R e p o r t The conservative treatment of Class I malocclusion with maxillary transverse deficiency and anterior teeth crowding Lincoln I. Nojima* Abstract This report describes the treatment
ORTHOdontics SLIDING MECHANICS
 ORTHOdontics PGI/II SLIDING MECHANICS FOCUS ON TARGETED SPACE GAINING AND ITS APPLICATIONS, INCLUDING WITH RAPID PALATAL EXPANDIONS. ALSO INCLUDES RETENTION AND CLINICAL PEARLS FACULTY: Joseph Ghafari,
ORTHOdontics PGI/II SLIDING MECHANICS FOCUS ON TARGETED SPACE GAINING AND ITS APPLICATIONS, INCLUDING WITH RAPID PALATAL EXPANDIONS. ALSO INCLUDES RETENTION AND CLINICAL PEARLS FACULTY: Joseph Ghafari,
The Science Behind The System Clinical Abstracts, Volume 2
 The Science Behind The System Clinical Abstracts, Volume 2 Visit www.damonsystem.com for Damon product information, clinical procedures, seminar registrations and more! 1717 West Collins Avenue, Orange,
The Science Behind The System Clinical Abstracts, Volume 2 Visit www.damonsystem.com for Damon product information, clinical procedures, seminar registrations and more! 1717 West Collins Avenue, Orange,
The Modified Twin Block Appliance in the Treatment of Class II Division 2 Malocclusions
 Journal of Orthodontics/Vol. 28/2001/271 280 The Modified Twin Block Appliance in the Treatment of Class II Division 2 Malocclusions F. M. V. DYER H. F. MCKEOWN P. J. SANDLER Department of Orthodontics,
Journal of Orthodontics/Vol. 28/2001/271 280 The Modified Twin Block Appliance in the Treatment of Class II Division 2 Malocclusions F. M. V. DYER H. F. MCKEOWN P. J. SANDLER Department of Orthodontics,
Changes in Lip, Cheek, and Tongue Pressures After Rapid Maxillary Expansion Using a Diaphragm Pressure Transducer
 Original Article Changes in Lip, Cheek, and Tongue Pressures After Rapid Maxillary Expansion Using a Diaphragm Pressure Transducer Nazan Küçükkeleş, DDS, PhD a ; Cenk Ceylanoğlu, DDS b Abstract: The purpose
Original Article Changes in Lip, Cheek, and Tongue Pressures After Rapid Maxillary Expansion Using a Diaphragm Pressure Transducer Nazan Küçükkeleş, DDS, PhD a ; Cenk Ceylanoğlu, DDS b Abstract: The purpose
Correlation Between Naso Labial Angle and Effective Maxillary and Mandibular Lengths in Untreated Class II Patients
 9 International Journal of Interdisciplinary and Multidisciplinary Studies,2014,Vol 1,No.3,9-14. Available online at httt://www.ijims.com ISSN: 2348 0343 Correlation Between Naso Labial Angle and Effective
9 International Journal of Interdisciplinary and Multidisciplinary Studies,2014,Vol 1,No.3,9-14. Available online at httt://www.ijims.com ISSN: 2348 0343 Correlation Between Naso Labial Angle and Effective
Mandibular incisor extraction: indications and long-term evaluation
 European Journal of Orthodontics 18 (1996) 485-489 O 1996 European Orthodontic Society Mandibular incisor extraction: indications and long-term evaluation Jose-Antonio Canut University of Valencia, Spain
European Journal of Orthodontics 18 (1996) 485-489 O 1996 European Orthodontic Society Mandibular incisor extraction: indications and long-term evaluation Jose-Antonio Canut University of Valencia, Spain
A Clinical and Cephalometric Study of the Influence of Mandibular Third Molars on Mandibular Anterior Teeth
 10.5005/jp-journals-10021-1193 ORIGINAL ARTICLE Tara Ramprakash Kavra, Etika Kabra A Clinical and Cephalometric Study of the Influence of Mandibular Third Molars on Mandibular Anterior Teeth 1 Tara Ramprakash
10.5005/jp-journals-10021-1193 ORIGINAL ARTICLE Tara Ramprakash Kavra, Etika Kabra A Clinical and Cephalometric Study of the Influence of Mandibular Third Molars on Mandibular Anterior Teeth 1 Tara Ramprakash
Treatment of a Patient with Class I Malocclusion and Severe Tooth Crowding Using Invisalign and Fixed Appliances
 36 Dental Medicine Research 34 1 36 40, 2014 Case Report Treatment of a Patient with Class I Malocclusion and Severe Tooth Crowding Using Invisalign and Fixed Appliances Yumiko OGURA, Wakana YANAGISAWA,
36 Dental Medicine Research 34 1 36 40, 2014 Case Report Treatment of a Patient with Class I Malocclusion and Severe Tooth Crowding Using Invisalign and Fixed Appliances Yumiko OGURA, Wakana YANAGISAWA,
UNILATERAL UPPER MOLAR DISTALIZATION IN A SEVERE CASE OF CLASS II MALOCCLUSION. CASE PRESENTATION. 1*
 UNILATERAL UPPER MOLAR DISTALIZATION IN A SEVERE CASE OF CLASS II MALOCCLUSION. CASE PRESENTATION. 1* Department of Orthodontics and Pedodontics 1 Faculty of Dental Medicine, University of Medicine and
UNILATERAL UPPER MOLAR DISTALIZATION IN A SEVERE CASE OF CLASS II MALOCCLUSION. CASE PRESENTATION. 1* Department of Orthodontics and Pedodontics 1 Faculty of Dental Medicine, University of Medicine and
With judicious treatment planning, the clinical
 CLINICIAN S CORNER Selecting custom torque prescriptions for the straight-wire appliance Earl Johnson San Francisco, Calif Selecting custom torque prescriptions based on the treatment needs of each patient
CLINICIAN S CORNER Selecting custom torque prescriptions for the straight-wire appliance Earl Johnson San Francisco, Calif Selecting custom torque prescriptions based on the treatment needs of each patient
Developing Facial Symmetry Using an Intraoral Device: A Case Report
 Developing Facial Symmetry Using an Intraoral Device: A Case Report by Theodore R. Belfor, D.D.S.; and G. Dave Singh, D.D.Sc., Ph.D., B.D.S. Dr. Theodore Belfor graduated from New York University College
Developing Facial Symmetry Using an Intraoral Device: A Case Report by Theodore R. Belfor, D.D.S.; and G. Dave Singh, D.D.Sc., Ph.D., B.D.S. Dr. Theodore Belfor graduated from New York University College
Different Non Surgical Treatment Modalities for Class III Malocclusion
 IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 9, Issue 6 (Sep.- Oct. 2013), PP 48-52 Different Non Surgical Treatment Modalities for Class III Malocclusion
IOSR Journal of Dental and Medical Sciences (IOSR-JDMS) e-issn: 2279-0853, p-issn: 2279-0861. Volume 9, Issue 6 (Sep.- Oct. 2013), PP 48-52 Different Non Surgical Treatment Modalities for Class III Malocclusion
Sample Case #1. Disclaimer
 ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
ABO Sample Cases Disclaimer Sample Case #1 The following sample questions and answers were composed and vetted by a panel of experts in orthodontics and are intended to provide an example of the types
Attachment G. Orthodontic Criteria Index Form Comprehensive D8080. ABBREVIATIONS CRITERIA for Permanent Dentition YES NO
 First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
First Review IL HFS Dental Program Models Second Review Ortho cad Attachment G Orthodontic Criteria Index Form Comprehensive D8080 Ceph Film X-Rays Photos Narrative Patient Name: DOB: ABBREVIATIONS CRITERIA
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 RÉSUMÉ
EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 EUROPEAN SOCIETY OF LINGUAL ORTHODONTICS CANDIDATE NUMBER: Dr. Stefan Blasius Year: 2010 WBLO 01 RÉSUMÉ
The most common maxillary characteristics of
 ORIGINAL ARTICLE Treatment effects of the bionator and high-pull facebow combination followed by fixed appliances in patients with increased vertical dimensions Christopher S. Freeman, a James A. McNamara,
ORIGINAL ARTICLE Treatment effects of the bionator and high-pull facebow combination followed by fixed appliances in patients with increased vertical dimensions Christopher S. Freeman, a James A. McNamara,
ISW for the treatment of adult anterior crossbite with severe crowding combined facial asymmetry case
 International Research Journal of Medicine and Biomedical Sciences Vol.3 (2),pp. 15-29, November 2018 Available online at http://www.journalissues.org/irjmbs/ https://doi.org/10.15739/irjmbs.18.004 Copyright
International Research Journal of Medicine and Biomedical Sciences Vol.3 (2),pp. 15-29, November 2018 Available online at http://www.journalissues.org/irjmbs/ https://doi.org/10.15739/irjmbs.18.004 Copyright
One of the most common orthopedic treatment
 2011 JCO, Inc. May not be distributed without permission. www.jco-online.com Early Alt-RAMEC and Facial Mask Protocol in Class III Malocclusion LORENZO FRANCHI, DDS, PHD TIZIANO BACCETTI, DDS, PHD CATERINA
2011 JCO, Inc. May not be distributed without permission. www.jco-online.com Early Alt-RAMEC and Facial Mask Protocol in Class III Malocclusion LORENZO FRANCHI, DDS, PHD TIZIANO BACCETTI, DDS, PHD CATERINA
Chapter 2. Material and methods
 Chapter 2 Material and methods Material and methods Summary This chapter describes the subjects and methods being used in this study. Between 1986 and 1997 9 expeditions were undertaken in remote areas
Chapter 2 Material and methods Material and methods Summary This chapter describes the subjects and methods being used in this study. Between 1986 and 1997 9 expeditions were undertaken in remote areas
Management of Crowded Class 1 Malocclusion with Serial Extractions: Report of a Case
 Management of Crowded Class 1 Malocclusion with Serial Extractions: Report of a Case Hayder A. Hashim, BDS, MSc Abstract Aim: The purpose of this article is to show the value of serial extractions in a
Management of Crowded Class 1 Malocclusion with Serial Extractions: Report of a Case Hayder A. Hashim, BDS, MSc Abstract Aim: The purpose of this article is to show the value of serial extractions in a
The treatment options for nongrowing skeletal Class
 CASE REPORT Total distalization of the maxillary arch in a patient with skeletal Class II malocclusion Yoon Jeong Choi, a Jong-Suk Lee, b Jung-Yul Cha, c and Young-Chel Park d Seoul, Korea In nongrowing
CASE REPORT Total distalization of the maxillary arch in a patient with skeletal Class II malocclusion Yoon Jeong Choi, a Jong-Suk Lee, b Jung-Yul Cha, c and Young-Chel Park d Seoul, Korea In nongrowing
Class II. Bilateral Cleft Lip and Palate. Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Cleft Lip and Palate.
 Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
Bilateral Cleft Lip and Palate Clinician: Dr. Mike Mayhew, Boone, NC Patient: R.S. Class II Cleft Lip and Palate Pretreatment Diagnosis Class II dolichofacial female, age 22 years 11 months, presented
Background. review literature as topic, evidencebased dentistry, adolescent, growth and development. Accepted for publication 7 February 2016
 J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 543 564 Review Dental and skeletal effects of palatal expansion techniques: a systematic review of the current evidence from
J o u r n a l o f Oral Rehabilitation Journal of Oral Rehabilitation 2016 43; 543 564 Review Dental and skeletal effects of palatal expansion techniques: a systematic review of the current evidence from
Treatment planning of nonskeletal problems. in preadolescent children
 In the name of GOD Treatment planning of nonskeletal problems in preadolescent children Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 7 William R. Proffit,
In the name of GOD Treatment planning of nonskeletal problems in preadolescent children Presented by: Dr Somayeh Heidari Orthodontist Reference: Contemporary Orthodontics Chapter 7 William R. Proffit,
AAO / AAPD Scottsdale 2018
 AAO / AAPD Scottsdale 2018 Missing Premolars : What are the Options? David Kennedy Clinical Professor UBC Vancouver Canada drdavidkennedy@yahoo.ca At what age can you know second premolars are absent?
AAO / AAPD Scottsdale 2018 Missing Premolars : What are the Options? David Kennedy Clinical Professor UBC Vancouver Canada drdavidkennedy@yahoo.ca At what age can you know second premolars are absent?
Tooth Size Discrepancies and Arch Parameters among Different Malocclusions in a Jordanian Sample
 Original Article Size Discrepancies and Parameters among Different s in a Jordanian Sample Susan N. Al-Khateeb a ; Elham S. J. Abu Alhaija b Abstract: The objectives of this study were to determine the
Original Article Size Discrepancies and Parameters among Different s in a Jordanian Sample Susan N. Al-Khateeb a ; Elham S. J. Abu Alhaija b Abstract: The objectives of this study were to determine the
#45 Ortho-Tain, Inc PREVENTIVE ERUPTION GUIDANCE -- PREVENTIVE OCCLUSAL DEVELOPMENT
 #45 Ortho-Tain, Inc. 1-800-541-6612 PREVENTIVE ERUPTION GUIDANCE -- PREVENTIVE OCCLUSAL DEVELOPMENT Analysis and Diagnosis of Occlusion: The ideal child of 5 y ears of age that probably has the best chance
#45 Ortho-Tain, Inc. 1-800-541-6612 PREVENTIVE ERUPTION GUIDANCE -- PREVENTIVE OCCLUSAL DEVELOPMENT Analysis and Diagnosis of Occlusion: The ideal child of 5 y ears of age that probably has the best chance
Anterior Open Bite Correction with Invisalign Anterior Extrusion and Posterior Intrusion.
 Tips from your peers to help you treat with confidence. Anterior Open Bite Correction with Invisalign Anterior Extrusion and Posterior Intrusion. Dr. Linda Crawford DDS, MS, P.C. Anterior Open Bite Correction
Tips from your peers to help you treat with confidence. Anterior Open Bite Correction with Invisalign Anterior Extrusion and Posterior Intrusion. Dr. Linda Crawford DDS, MS, P.C. Anterior Open Bite Correction
Orthodontic Treatment Using The Dental VTO And MBT System
 Orthodontic Treatment Using The Dental VTO And MBT System by Dr. Hideyuki Iyano Dr. Hideyuki Iyano, Department of Orthodontics, Ohu University School of Dentistry, Japan. He is also a member of the Japan
Orthodontic Treatment Using The Dental VTO And MBT System by Dr. Hideyuki Iyano Dr. Hideyuki Iyano, Department of Orthodontics, Ohu University School of Dentistry, Japan. He is also a member of the Japan
Treatment of a severe class II division 1 malocclusion with twin-block appliance
 2018; 4(5): 167-171 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(5): 167-171 www.allresearchjournal.com Received: 27-03-2018 Accepted: 28-04-2018 Dr. Sheetal Bohra Resident
2018; 4(5): 167-171 ISSN Print: 2394-7500 ISSN Online: 2394-5869 Impact Factor: 5.2 IJAR 2018; 4(5): 167-171 www.allresearchjournal.com Received: 27-03-2018 Accepted: 28-04-2018 Dr. Sheetal Bohra Resident
Variation in arch shape and dynamics of shape change from infancy to early childhood
 University of Iowa Iowa Research Online Theses and Dissertations Spring 2017 Variation in arch shape and dynamics of shape change from infancy to early childhood Gisela Lilian Borget University of Iowa
University of Iowa Iowa Research Online Theses and Dissertations Spring 2017 Variation in arch shape and dynamics of shape change from infancy to early childhood Gisela Lilian Borget University of Iowa
Transverse malocclusion, posterior crossbite and severe discrepancy*
 O C a s e R e p o r t Transverse malocclusion, posterior crossbite and severe discrepancy* Roberto Carlos odart randão** bstract This article reports the orthodontic treatment of a 14 years and 2 months
O C a s e R e p o r t Transverse malocclusion, posterior crossbite and severe discrepancy* Roberto Carlos odart randão** bstract This article reports the orthodontic treatment of a 14 years and 2 months
Mx1 to NA = 34 & 10 mm. Md1 to NB = 21 & 3 mm.
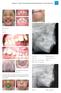 Chapter 16 Clinical cases: mixed dentition and adolescent, CLII non-extraction 219 Full CLII div I OJ = 15 OB = 8 SNA = 82 SNB = 75 Mx1 to NA = 34 & 10 mm. Md1 to NB = 21 & 3 mm. Md1 to A-pog = -2 GO-GN
Chapter 16 Clinical cases: mixed dentition and adolescent, CLII non-extraction 219 Full CLII div I OJ = 15 OB = 8 SNA = 82 SNB = 75 Mx1 to NA = 34 & 10 mm. Md1 to NB = 21 & 3 mm. Md1 to A-pog = -2 GO-GN
ALEXANDER DISCIPLINE
 The ALEXANDER DISCIPLINE Volume 2: Long-Term Stability R. G. Wick Alexander, DDS, MSD Clinical Professor of Orthodontics Baylor College of Dentistry Dallas, Texas University of Texas Dental Branch Houston,
The ALEXANDER DISCIPLINE Volume 2: Long-Term Stability R. G. Wick Alexander, DDS, MSD Clinical Professor of Orthodontics Baylor College of Dentistry Dallas, Texas University of Texas Dental Branch Houston,
Case Report Orthodontic Treatment of a Mandibular Incisor Extraction Case with Invisalign
 Case Reports in Dentistry, Article ID 657657, 4 pages http://dx.doi.org/10.1155/2014/657657 Case Report Orthodontic Treatment of a Mandibular Incisor Extraction Case with Invisalign Khalid H. Zawawi Department
Case Reports in Dentistry, Article ID 657657, 4 pages http://dx.doi.org/10.1155/2014/657657 Case Report Orthodontic Treatment of a Mandibular Incisor Extraction Case with Invisalign Khalid H. Zawawi Department
#60 Ortho-Tain, Inc TIMING FOR CROWDING CORRECTIONS WITH THE OCCLUS-O-GUIDE AND NITE-GUIDE APPLIANCES
 #60 Ortho-Tain, Inc. 1-800-541-6612 TIMING FOR CROWDING CORRECTIONS WITH THE OCCLUS-O-GUIDE AND NITE-GUIDE APPLIANCES Although timing is not as critical for the Occlus-o-Guide appliance as it is with the
#60 Ortho-Tain, Inc. 1-800-541-6612 TIMING FOR CROWDING CORRECTIONS WITH THE OCCLUS-O-GUIDE AND NITE-GUIDE APPLIANCES Although timing is not as critical for the Occlus-o-Guide appliance as it is with the
Contemporary Approaches to Orthodontic Retentionjerd_
 Contemporary Approaches to Orthodontic Retentionjerd_509 83..87 Guest Experts GAVIN C. HEYMANN, DDS, MS* DAN GRAUER, DDS, PhD Associate Editor EDWARD J. SWIFT, JR., DMD, MS Wouldn t it be nice if teeth
Contemporary Approaches to Orthodontic Retentionjerd_509 83..87 Guest Experts GAVIN C. HEYMANN, DDS, MS* DAN GRAUER, DDS, PhD Associate Editor EDWARD J. SWIFT, JR., DMD, MS Wouldn t it be nice if teeth
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS
 EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER: 44 CASE NUMBER: 1 Year: ESLO 01 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME: K.N BORN: 03/03/1980 SEX: Male PRE-TREATMENT RECORDS:
EUROPEAN SOCIETY OF LINGUAL ORTHODONTISTS CANDIDATE NUMBER: 44 CASE NUMBER: 1 Year: ESLO 01 RÉSUMÉ OF CASE 1 CASE CATEGORY: ADULT MALOCCLUSION NAME: K.N BORN: 03/03/1980 SEX: Male PRE-TREATMENT RECORDS:
Dr Robert Drummond. BChD, DipOdont Ortho, MChD(Ortho), FDC(SA) Ortho. Canad Inn Polo Park Winnipeg 2015
 Dr Robert Drummond BChD, DipOdont Ortho, MChD(Ortho), FDC(SA) Ortho Canad Inn Polo Park Winnipeg 2015 Severely compromised FPM with poor prognosis Children often present with a developing dentition affected
Dr Robert Drummond BChD, DipOdont Ortho, MChD(Ortho), FDC(SA) Ortho Canad Inn Polo Park Winnipeg 2015 Severely compromised FPM with poor prognosis Children often present with a developing dentition affected
Efficacy of Nickel-Titanium Palatal Expanders
 JIOS 10.5005/jp-journals-10021-1044 ORIGINAL ARTICLE 1 Rahul Paul, 2 Tapasya Juneja Kapoor, 3 Varun Malhotra, 4 US Krishna Nayak, 5 Shruti Bhatt ABSTRACT Objective: Timely treatment of narrow maxilla by
JIOS 10.5005/jp-journals-10021-1044 ORIGINAL ARTICLE 1 Rahul Paul, 2 Tapasya Juneja Kapoor, 3 Varun Malhotra, 4 US Krishna Nayak, 5 Shruti Bhatt ABSTRACT Objective: Timely treatment of narrow maxilla by
Skeletal Anchorage for Orthodontic Correction of Severe Maxillary Protrusion after Previous Orthodontic Treatment
 The Angle Orthodontist: Vol. 78, No. 1, pp. 181 188. Skeletal Anchorage for Orthodontic Correction of Severe Maxillary Protrusion after Previous Orthodontic Treatment Eiji Tanaka; a Akiko Nishi-Sasaki;
The Angle Orthodontist: Vol. 78, No. 1, pp. 181 188. Skeletal Anchorage for Orthodontic Correction of Severe Maxillary Protrusion after Previous Orthodontic Treatment Eiji Tanaka; a Akiko Nishi-Sasaki;
College & Hospital, DPU Vidyapeeth Pimpri, Pune, India. *Corresponding Author:
 Original Research Article DOI: 10.18231/2278-3784.2017.0001 Evaluation of changes in maxillary arch dimensions, Posterior Transverse Inter Arch Discrepancy (PTID), upper and lower incisor inclination in
Original Research Article DOI: 10.18231/2278-3784.2017.0001 Evaluation of changes in maxillary arch dimensions, Posterior Transverse Inter Arch Discrepancy (PTID), upper and lower incisor inclination in
The practice of orthodontics is faced with new
 CLINICIAN S CORNER A new approach to correction of crowding William Randol Womack, DDS, a Jae H. Ahn, DDS, MSD, b Zahra Ammari, DDS, MDSc, c and Anamaría Castillo, DDS, MS c Phoenix, Ariz, and Santa Clara,
CLINICIAN S CORNER A new approach to correction of crowding William Randol Womack, DDS, a Jae H. Ahn, DDS, MSD, b Zahra Ammari, DDS, MDSc, c and Anamaría Castillo, DDS, MS c Phoenix, Ariz, and Santa Clara,
Case Report: Early Correction of Class III Malocclusion with alternate Rapid Maxillary Expansion And Constriction (Alt-RAMEC) and Face Mask Therapy
 Case Report: Early Correction of Class III Malocclusion with alternate Rapid Maxillary Expansion And Constriction (Alt-RAMEC) and Face Mask Therapy Dr. Falguni Mehta 1, Dr. Shivam Mehta 2, Dr. Manop Agrawal
Case Report: Early Correction of Class III Malocclusion with alternate Rapid Maxillary Expansion And Constriction (Alt-RAMEC) and Face Mask Therapy Dr. Falguni Mehta 1, Dr. Shivam Mehta 2, Dr. Manop Agrawal
ISW for the Treatment of Bilateral Posterior Buccal Crossbite
 Journal of Dentistry and Oral Health Case report ISW for the Treatment of Bilateral Posterior Buccal Crossbite Chun-Shuo HUANG 1,2, Chien-Chih YU 3,*, Jian-Hong YU 1,2, and Yuan-Hou CHEN 1 1 Department
Journal of Dentistry and Oral Health Case report ISW for the Treatment of Bilateral Posterior Buccal Crossbite Chun-Shuo HUANG 1,2, Chien-Chih YU 3,*, Jian-Hong YU 1,2, and Yuan-Hou CHEN 1 1 Department
Invisalign technique in the treatment of adults with pre-restorative concerns
 Mampieri and Giancotti Progress in Orthodontics 2013, 14:40 REVIEW Open Access Invisalign technique in the treatment of adults with pre-restorative concerns Gianluca Mampieri * and Aldo Giancotti Abstract
Mampieri and Giancotti Progress in Orthodontics 2013, 14:40 REVIEW Open Access Invisalign technique in the treatment of adults with pre-restorative concerns Gianluca Mampieri * and Aldo Giancotti Abstract
