Vital Signs As Directional Signals by Charles Livesey edited by Julie Aberger
|
|
|
- Preston Wood
- 6 years ago
- Views:
Transcription
1 STATE JERSEY NEW The Gold Cross CONTINUING EDUCATION SERIES Vital Signs As Directional Signals by Charles Livesey edited by Julie Aberger EMT Objectives After reading this article, the EMT will be able to: define signs and symptoms and know the difference; define homeostasis and understand its relationship to vital signs; identify vital signs and their normal rates for adults, children and infants; define normal and abnormal qualities of respirations, pulse, blood pressure, skin condition, and mental status; understand the limitations of mechanical devices to monitor vital signs. Introduction In EMS we frequently discuss a patient s signs and symptoms. What are they and why are they important? A symptom is something the patient experiences and tells the EMT during the patient assessment: I feel dizzy. A sign is something the EMT discovers by inspection, palpation and auscultation during the patient assessment. The patient s skin is cold, sweaty and ashen. Like street signs, physical signs provide direction. If the patient says I feel dizzy and his skin is cold, wet and ashen, the EMT should promptly provide high-flow oxygen. The most important signs EMTs routinely assess are vital signs. Vital signs indicate the physiological direction the patient is headed. A thorough patient assessment includes taking baseline vital signs and reassessing them throughout the call. If you have more than one set of vitals, you will be able to chart your patient s progress. Such changes are referred to as trending and may indicate either an improvement or deterioration in the patient s condition. In this article we will discuss vital signs, review how they are determined, and explain what the measurements indicate. We ll focus on pulse, respirations, and blood pressure and also include a review of how to assess the patient s skin, and mental status. If you have more than one set of vitals, you will be able to chart your patient s progress. Such changes are referred to as trending. Keeping The Body In Check The human body seeks to maintain a relatively stable internal condition called homeostasis. It is a dynamic state of balance in which internal conditions vary, but always within a relatively narrow range. Nearly every organ participates in maintaining this constant balance. For instance, heart activity and blood pressure are constantly monitored and adjusted so that blood reaches all the body tissues and all the cells are adequately perfused. (Perfusion means that oxygen and nutrients are transported to the cells and waste products such as carbon dioxide CO 2 are eliminated.) Whenever conditions detour from what the brain considers a normal range, the body compensates to restore balance. For example, if there is an increase in the level of carbon dioxide ( CO 2) in the bloodstream, the body compensates by increasing its respiratory rate so as to blow-off the excessive CO 2. Vital signs reflect the body s juggling act to maintain homeostasis; they fluctuate moment-to-moment. When the body fails to keep its balance, such as when the patient is hemorrhaging and losing blood volume, vital signs reflect the insult. The heart rate first increases then decreases, the respiratory rate increases then decreases, and finally the blood pressure plummets. Not everyone shares the same normal vital signs. What may be required for one person to maintain homeostasis is not necessarily the same for another. For example, a systolic blood pressure of 90 mm Hg may be adequate for one patient, however, another would experience hypotension at this reading and present with signs of shock. Therefore, the EMT must continually monitor all the vital signs and assess them together to understand the patient s condition. The Big Picture consists of all the pieces of the assessment puzzle; each vital sign is merely one piece. Other essential pieces include age, medical history, medications, allergies, physical exam, and of course, history of the present illness or injury. 8 Winter 2015
2 STATE JERSEY NEW -continued from page 8 Adequate Breathing Adequate breathing ventilation and respiration is essential to maintaining homeostasis. Ventilation is the act of moving air into and out of the lungs. Respiration is the exchange of gases oxygen and carbon dioxide between the alveoli and bloodstream. The process of gas exchange is called diffusion. What causes us to breathe? The respiratory rate is regulated primarily by the autonomic nervous system that constantly monitors carbon dioxide levels in the blood. Increased levels of this cellular waste product cause the autonomic nervous system to stimulate an increase in the respiratory rate and volume to offload the excess CO 2. A second, back-up system exists which does not depend upon carbon dioxide levels in the bloodstream, but oxygen levels instead. This is called the hypoxic drive. For this type of patient, (typically a patient with chronic obstructive pulmonary disease or COPD), a decrease of Table 1: Normal Respiratory Rates Adults breaths per minute Children breaths per minute Infants breaths per minute oxygen in the bloodstream will stimulate breathing. Conversely, an increase in oxygen levels will cause the respiratory rate to slow. High volume oxygen delivery to a COPD patient who depends upon his hypoxic drive to stimulate breathing will eventually cause him to stop breathing. However, all patients in respiratory distress need high flow oxygen immediately regardless of their medical history. How do we know a patient is breathing adequately? The EMT must evaluate respiratory rate, rhythm, and quality. Rate: The range of normal respiratory rates for an adult is 12 to 20 breaths per minute (BPM). Children breathe at 15 to 30 times a minute. The newborn can even have a rate of up to 60 BPM. (See Table 1.) To determine respiratory rate the EMT counts the rise and fall of the patient s chest for thirty seconds and then multiplies by two. (Remember that the patient may become self-conscious and alter his breathing rate if he knows you are watching.) For a patient in distress, respirations less than ten per minute or greater than 24 per minute need to be supplemented For a patient in distress, respirations less than ten per minute or greater than 24 per minute need to be supplemented with high flow oxygen. with high flow oxygen. The EMT can also ventilate the patient with a positive pressure device to provide artificial respiration. (Positive pressure devices include pocket masks and bag-valve-masks or BVM.) Assessing a patient s respiratory rate is often overlooked by EMTs. But -continues on page 10 Winter
3 STATE JERSEY NEW -continued from page 9 it is essential information for the emergency department physicians especially if the patient is in respiratory distress. EMTs should assess and report a respiratory rate on every patient; make no exceptions! Rhythm: Rhythm refers to the tempo of breathing. This is assessed noting the time from the peak of one chest rise to the next. If consistent, the rhythm is considered regular. When you re awake, that rhythm can be affected by mood, exercise, and speech. When you sleep, the rhythm is more regular and even. An irregular breathing pattern is A traumatic brain injury with increased intracranial pressure can alter the regularity of breathing. caused by many conditions. For example, a traumatic brain injury with increased intracranial pressure can alter the regularity of breathing. As the pressure within the skull increases, the patient s breathing becomes more erratic with periods of deep, rapid breathing followed by slow, shallow breathing, followed by periods of apnea (absence of breathing). This pattern is called Cheyne- Stokes breathing and requires aggressive management of the patient s ventilations by the EMT. Irregular breathing patterns may also be caused by chronic illnesses (such as emphysema or asthma), fever, medication overdose, chest injuries, and hyperventilation. At the time of death, breathing patterns change. Breathing may simply stop, or slow down and become extremely shallow and then stop, or there can be a short series of great heaving gasps before the patient stops breathing entirely. The final respiratory effort is called agonal breathing. When breathing is inadequate, how does the brain compensate in an effort to maintain its equilibrium or homeostasis?» Initially it raises the body s respiratory rate and volume (amount) of air inhaled or exhaled. If the rate increases to over 30 BPM, however, the volume of air being inhaled decreases to the point where the total overall volume is inadequate. Abnormal rapid breathing is called tachypnea; the patient is breathing too rapidly to adequately refill the alveoli.» Once the body s compensatory mechanism ceases to function, the respiratory rate and volume both decrease. Suddenly the patient is breathing at ten BPM or less. (Abnormal slow breathing = bradypnea) The volume inhaled decreases and total overall volume becomes inadequate. The EMT should manage both conditions tachypnea and bradypnea by ventilating the patient with a bag-valve-mask device. Quality: Here the EMT assesses how labored the patient s breathing may be as well as any sounds that may be made during inhalation and exhalation. Quality falls into four categories: normal, shallow, labored or noisy. Let s first look at normal quality. A healthy person breathes with little effort. The diaphragm and the external intercostal muscles (those between the ribs) are the muscles primarily responsible for ventilation. No additional muscles of respiration Figure 1: Inspiration Muscles Accessory Sternocleidomastoid (elevates sternum) Scalenes (elevates upper ribs) Principal External intercostals (elevate ribs, increasing width of thoracic cavity) Diaphragm (domes descent, increasing vertical dimension of thoracic cavity; also elevates lower ribs) Muscles of Respiration (called accessory muscles) are used. (See Figure 1.) There is also a normal depth of respiration which gives rise to a steady rhythmic movement of the chest cage. However, the movement is minimal and can be almost imperceptible on a healthy, immobile patient. Finally, normal respirations make no noise; they are virtually silent. EMTs must assess each patient s respiratory effort by visual inspection (looking for equal chest rise and fall), auscultation (listening to the lungs with a stethoscope) and palpation (feeling for deformity or any other irregularity). Shallow breathing occurs when there is only a slight movement of the chest or abdomen. We see this often in the nursing home patient who has been bedridden for some time. Ventilation is poor; not enough oxygen and carbon dioxide are being moved in and out of the lungs to allow for proper diffusion. Labored breathing causes an increase in the amount of work that the body needs to do to exchange lung volume. The patient struggles to get air in and out. The EMT should be aware of signs of labored breathing:» How is your patient positioned? Is he sitting upright, leaning forward on his hands in a tripod position? Is he unable to lie down? Does he sleep with several pillows under his head and upper body? All of these signs point to respiratory distress. Inspiration Muscles Quiet Breathing Expiration results from passive recoil of lungs and rib cage Active Breathing Internal intercostals Abdominals (depress lower ribs, compress abdominal contents, pushes up diaphragm) 10 Winter 2015
4 NEW JERSEY STATE -continued from page 10» Do you see any accessory muscle usage when the patient breathes? Accessory muscles include those in the neck, clavicles, and abdomen. If the patient is breathing adequately, these muscles do not constrict. However, when respiration is inadequate, accessory muscles are used to increase the volume of air being moved. Severe respiratory distress causes these muscles to retract, creating depressions in the neck, above the shoulder blades, and between and below the ribs. If the patient is breathing adequately, accessory muscles do not constrict.» Does the pediatric patient present with nasal flaring? Are there sternal retractions, i.e., does the child s sternum pull inward when he inhales? If so, the pediatric patient is in severe respiratory distress. The EMT also evaluates breathing by listening to the patient speak. Does she have to interrupt the words in each sentence to take a breath? Is she gasping for air after a phrase or a few words? This is labored speech and is not normal. Finally, is the patient s breathing noisy? What do you hear without a stethoscope? Is there stridor, a high pitched sound on inspiration, or grunting on expiration? Is there an obstruction which is causing lack of sound altogether or a partial obstruction causing crowing or gurgling? What do you hear with a stethoscope? Breath sounds should be evaluated in three places both anteriorly and then posteriorly. Noisy breathing can further be described as:» Rales, fine crackling sounds, indicate fluid in the lungs.» Rhonchi, coarse sounds, indicate more significant fluid buildup or mucous accumulation.» Wheezing, a high-pitched (usually expiratory) sound, indicates lower airway narrowing and is prevalent in asthma.» No sound at all. If the respiratory sounds are not bilateral, the patient may have a pneumothorax or tension pneumothorax. The patient might also have had a lung removed. Wheezing, a highpitched (usually expiratory) sound, indicates lower airway narrowing and is prevalent in asthma. Heart Rate And Pulse Adequate circulation is also essential to maintaining homeostasis. As the heart beats, it sends a continuous wave of blood coursing through the body s arteries and veins. The EMT assesses the patient s circulation by taking two fingers and palpating (or feeling) for the heart beat at a point where an artery crosses between a bone and the skin s surface. The EMT assesses pulse rate, rhythm and quality. In the prehospital setting, we -continues on page 12 Winter
5 NEW JERSEY STATE -continued from page 11 commonly palpate the radial, brachial, carotid, dorsalis pedis and posterior tibial pulses. (See Figure 2.) During our initial assessment, if the adult patient has no radial pulse we immediately check for a carotid pulse. For an infant, the EMT first palpates the brachial pulse. Rate: To determine pulse rate the EMT should palpate the pulse for thirty seconds and then multiply by two. The average pulse rate for an adult at rest is 60 to 100 beats per minute. (See Table 2.) A palpable radial pulse generally indicates that the patient s organs have minimal perfusion. For an adult, a rate over 100 beats per minute is called tachycardia. A rate under 60 beats per minute is called bradycardia. A sustained rate under 50 or over 150 beats per minute for an adult usually indicates a serious condition and the patient should be transported as soon as possible. A rise in pulse rate of more than 15 beats per minute when the patient moves from supine to a seated position suggests significant blood loss, or hypovolemia. Pediatric patients have faster heart rates. A healthy child has a pulse rate of 80 to 120 beats per minute. The EMT should be aware that bradycardia in the pediatric patient is an ominous sign that signifies impending cardiac arrest. A newborn with a heart rate under 100 beats per minute requires immediate ventilation; a heart rate under 60 requires immediate cardiac compressions as well. Rhythm: The heart beats rhythmically to produce a regular pulse. Irregular pulse patterns, where the intervals between beats are not constant, may be caused when the atria (the top chambers of the heart) do not pump effectively. This condition, called atrial fibrillation, is common in the elderly patient. The atria normally provide a kick of blood into the ventricles. The loss of the atrial kick can Figure 2: Body Sites Where The Pulse Is Most Easily Palpated Common carotid artery Brachial artery Radial artery Femoral artery Popliteal artery Posterior tibial artery Dorsalis pedis artery Table 2: Normal Pulse Rate Ranges Adults beats per minute Children beats per minute Toddlers beats per minute Newborns beats per minute cause a 20% reduction in the amount of blood the heart pumps. This decreases the patient s ability to compensate to maintain homeostasis. Quality: Pulse quality is regulated by the heart s rhythm and force. The force of the pulse, or its strength, depends upon normal cardiac output. When you palpate the pulse, the wave should feel strong.» A weak, thready pulse that is difficult to palpate, means the patient may be in shock; he may be losing blood and/or blood pressure.» A bounding pulse that feels stronger than a normal pulse, indicates high blood pressure or perhaps head injury or heat stroke. Blood Pressure Blood must be kept constantly circulating in order to keep the body s cells perfused. The circulatory system does this job with its three components: the heart, the blood vessels and the blood, often referred to as the pump, the container and the volume.» The heart is a pump that pushes blood through the blood vessels to the cells for perfusion.» Blood vessels of the body form a closed delivery system, or sort of container, that begins and ends at the heart. The diameter of the blood vessels constricts or dilates (gets bigger or smaller) depending upon the pressure needed in the system. For example, if a patient is hemorrhag- 12 Winter 2015
6 NEW JERSEY STATE -continued from page 12 ing and losing a lot of blood or volume, the blood vessels will constrict in order to shunt the blood to the vital organs. The heart will also speed up to keep whatever volume is still in the system moving fast enough to keep the cells in the vital organs perfused.» Adequate blood pressure also depends on adequate blood volume. The average adult blood volume is about six liters; an eight-year old has about two liters, and an infant s blood volume almost fills a soda can (0.35 liters). Blood pressure is the pressure exerted against the inside walls of the arteries as the heart pumps and then relaxes. We measure two pressures: systolic and diastolic. Systolic pressure measures the maximum pressure within the arteries when the heart pumps. Diastolic pressure measures the minimum pressure within the arteries when the heart relaxes. The difference between the systolic and diastolic pressure is referred to as the pulse pressure. How To Take A Blood Pressure To determine a patient s blood pressure the EMT needs a properly sized blood pressure (BP) cuff. Adult cuffs should have a width of one-third to one-half the circumference of the limb. Pediatric cuffs should have a width of about two-thirds of the upper arm. Using a BP cuff that is too big gives a false low reading. Cuffs that are too small yield a false high reading. Auscultation: The blood pressure cuff should be placed on the patient s arm an inch or so above the elbow. Air is pumped into the bladder that inflates and temporarily halts arterial blood flow. The stethoscope is then placed over the patient s brachial artery. When the pressure in the cuff is released and falls below the internal systolic pressure, blood flow resumes and produces sounds. When the pressure in the cuff falls below the internal diastolic pressure, blood flow remains continuous and the sounds disappear completely. Pressure is measured in millimeters of mercury (mmhg). Palpation: An alternative method of determining blood pressure is by palpation. No stethoscope is needed. This method can be used if there is too much ambient noise to auscultate the pulse sounds, like in the back of an ambulance en route to the hospital. To palp a BP, the EMT locates a radial pulse with two fingers prior to pumping up the cuff. The cuff is then inflated until the pulse is no longer felt. The EMT should note the point on the gauge where this occurs and continue to inflate the cuff 30 mmhg The EMT should note the point on the gauge where the pulse is no longer felt and continue to inflate the cuff 30 mmhg beyond this point. beyond this point. The cuff should then be slowly deflated, and the EMT should note the reading at which the radial pulse returns, i.e., where it can be felt again. This results in a reading of about 10 mmhg lower than the systolic pressure determined by auscultation. Palpating a blood pressure has a disadvantage in that the diastolic pressure cannot be determined. Palpation should be used only when auscultation is not possible. High blood pressure is called hypertension. For an adult, this is usually defined as a systolic pressure that persists above 140 mmhg or a diastolic pressure that persists above 90 mmhg. Hypertension may be a sign of a possible illness (such as renal disease), injury (such as traumatic brain injury), exertion, anxiety, or even fright. Low blood pressure is called hypotension and causes poor perfusion to the cells. There must be an adequate pressure for oxygen and carbon dioxide exchange to occur between the capillaries and cells. A decreased blood pressure is a late sign of shock that occurs when the body can no longer compensate. Blood pressure varies among individuals. The accepted rule for normal systolic blood pressure for adults up to 40 years of age is the patient s age plus 100 for a male, and the patient s age plus 90 for a female. Thus a normal systolic BP for a 25- year old female would be approximately 115 mmhg. Children s normal systolic blood pressures are estimated with the formula: times the child s age. It is now advised that EMTs not take blood pressures on children under the age of three, (although some providers still believe it is important to practice). Although there has been controversy lately about ideal blood pressure numbers, the American Heart Association declared in October, 2015: A report published late in 2013 recommends healthcare providers take a new approach to treating high blood pressure for people older than 60. But based on the current research available, the American Heart Association recommends that healthcare providers continue to follow existing guidelines for treating high blood pressure. -continues on page 14 Winter
7 NEW JERSEY STATE -continued from page 13 We believe there s just not enough evidence at this point to justify such a major change in how we treat people with high blood pressure, American Heart Association Past President Mariell Jessup, M.D., said of the new opinion published in the Journal of the American Medical Association (JAMA). Asked At Convention: What are the best and worst parts of being a volunteer EMT? Being able to make a difference in someone s life. Doing everything you can for a patient and it not being enough. Kerry Walsh Lincoln Park EMS Helping our community. Dealing with Type-A personalities whose egos make it difficult to learn, thrive and succeed. Tal & Christel Jones Ringwood AC Helping the community and saving the taxpayers money. Insufficient communications within the squad. Duchess Lake Hopewell Fire Dept. EMU Everyone s really chill and I learn a lot from people of different backgrounds and professions. I love each individual s life stories. No respect from paid crew. Sandy Cheng Lyndhurst PES One in three American adults has high blood pressure, which is a reading of 140/90 millimeters of mercury or higher. The opinion published in JAMA advises treatment at 140/90 for adults from ages 30 to 59, but starting only at 150/90 for people 60 and older. The American Heart Association maintains its recommendation of initiating treatment starting with lifestyle changes and then medication if necessary at 140/90 until age 80, then at 150/90. The Importance Of Assessing Skin Condition One of the most overlooked signs of adequate or inadequate perfusion is the patient s skin. The color, temperature, and condition of the skin lead us to suspect the severity of illness or injury and therefore anticipate treatment. Color: The second layer of skin, the dermis, is richly embedded with blood vessels. Hemoglobin gives the skin its pinkish hue. Constriction of those vessels results in pale skin. This occurs as the body attempts to compensate for inadequate blood pressure (shock) or to conserve heat. In both cases, the body shunts its blood volume to the vital organs. In order for organs to function normally, the body must maintain an internal temperature within one or two degrees of 98.6 degrees. In Caucasians, the skin is pink. When the body is poorly oxygenated, that skin appears blue, a condition called cyanosis. In black or darkskinned individuals, cyanosis is apparent in the mucous membranes and nail beds. Jaundiced (yellow) skin is related to abnormalities of the liver. Temperature & Condition: Cool and clammy skin is a sign of shock. The skin loses its warmth as bloodflow is diverted from the skin to the vital organs. Patients in shock also experience diaphoresis or sweating caused by a surge of epinephrine (adrenaline) in the body. (Epinephrine also causes anxiety and agitation.) Cold dry skin results from exposure to a cold environment; heat loss has occurred. Conversely, hot, dry skin results from exposure to heat or fever. This can also be a serious sign that the body has exhausted its ability to compensate. Although skin temperature is important, EMTs do not take core temperatures in the field. Instead we use the back of our hands to assess whether the skin is cold, warm or hot. Testing capillary refill on adults is not a reliable indicator due to inaccuracies caused by cold environments or a history of poor circulation. Also, testing capillary refill on adults is not a reliable indicator due to inaccuracies caused by cold environments or a medical history of poor circulation. Responsiveness & Orientation Mental status is an important parameter for determining the stability of the patient. As you reassess the patient, be aware of any increase or decrease in responsiveness. An epidural bleed caused by intracranial bleeding presents with a patient who goes in and out of consciousness. The easiest way to determine mental status is by using the AVPU scale. There are several other scales that can be used, including the Glasgow Coma Scale. If you are familiar with these and use them often they work well. However don t delay your care and transport of the patient determining how to use them in the field. A = The patient is Alert and should be oriented to person (can tell you his name), place (within reason where he is), and time (date or day of week). Elderly and developmentally disabled patients may present a special challenge here. You may need to consult a caregiver to determine what is different about the patient s orientation today. You may also encounter the patient who used alcohol or other substances which makes the accurate assessment of orientation difficult. Do not automatically assume that alcohol is the cause of disorientation. -continues on page Winter 2015
8 -continued from page 14 V = The patient responds to Verbal stimuli. The most common patient in this category may be oriented, but lethargic and the EMT must repeatedly call her name before she responds. She may be awake, but has no recall of events before the incident. This is called retrograde amnesia. The patient who has no recall of events after the incident has antegrade amnesia. These patients may ask the same question over and over again, a condition called perseveration. This may be caused by traumatic brain injury or other organic disorder. P = The patient responds to Painful stimuli with either purposeful or non-purposeful movement. He moves to withdraw from your painful stimuli, e.g., a pinch. U = The patient is unresponsive to all stimuli. Some patients become combative or even experience seizures. While this is a serious sign, some motion of the limbs is better than none at all. The patient with no movement or muscle tone is said to be flaccid and has a poor chance of survival. Confusion, lethargy, agitation, stupor all may be caused by hypoxia, or insufficient oxygen in the brain. Confusion, lethargy, agitation, stupor all may be caused by hypoxia, or insufficient oxygen in the brain. Any patient with a mental status lower than Alert may have a life threatening injury or illness and should receive high flow oxygen using either a nonrebreather mask or a positive pressure device such as a bag-valve-mask. Shortcomings Of Mechanical Devices A word about mechanical devices now being used to take vital signs in the field as well as the hospital: A standard piece of equipment in the up-to-date EMS arsenal is the Figure 3: pulse oximeter. (See Figure 3.) This small, easy-to-use finger probe and its oximeter automatically measures the percentage of hemoglobin saturation in arterial blood. Healthy persons breathing room air have normal readings of 98% to 100%. Generally, a pulse ox reading of less than 96% in a nonsmoker may indicate hypoxemia. But the pulse ox has its flaws:» For patients with anemia or very low perfusion states (like shock), the pulse oximeter may not detect peripheral perfusion; you may not get a reading.» The pulse oximeter produces false oxygen saturation numbers in a patient with carbon monoxide poisoning as carbon monoxide has a greater affinity for hemoglobin than oxygen.» Dark nail polish or dirty fingers may also throw the results.» Patients with chronic respiratory illness have normal pulse oximetry readings that are low. Therefore, knowing the patient s medical history is essential. While pulse oximetry readings can provide valuable information about the patient s oxygenation, the EMT must consider its reading as one piece of the clinical picture. An overall clinical assessment must always be performed. EMS crews are now using automatic blood pressure gauges to monitor patient blood pressures. These digital cuffs use oscillometric measurements and electronic calculations rather than auscultation. They contain no mercury, are easy to operate and are effective in noisy environments. There is a growing concern, however, that they may not be as accurate as conventional mercury instruments and could lead to inappropriate patient care. An additional concern in the field is the lack of frequent calibration. While these automatic devices are Pulse Oximeter convenient, you must always observe the patient closely to ensure the Big Picture is consistent with the numbers you re reading. Rely on your clinical skills. Look at the entire patient, do a thorough patient assessment complete with SAMPLE history and vital signs. Put it all together. Anything that is inconsistent should be investigated. Summary Vital signs are needed for every patient. As part of the ongoing exam, vital signs should be repeated every 15 minutes for the stable patient and at least every five minutes for the unstable patient. Repeating and comparing vital signs permit you to chart your patient s progress, establish trends and treat appropriately. Is the patient s condition improving? Worsening? Vital signs will give you signals and provide compelling evidence, but they don t tell you all you need to know about your patient s condition. Keep a close eye on all your patient s signs and symptoms, and treat what s occurring at the moment. Charles Livezey, MICP, EMT Instructor, is the EMS Education Supervisor at MONOC. He is also a life member of the Englishtown Manalapan First Aid Squad. Julie Aberger is an EMT instructor and an active member of the Pennington First Aid Squad. Julie is also the editor emerita of The Gold Cross. The Gold Cross Magazine name and Logo, and the New Jersey State First Aid Council, Inc. name and Logo, are the property of the New Jersey State 15 First Aid Council. Articles from the Gold Cross Magazine reproduced on this Website are the property of Leonard Publications. None of such articles or any part thereof shall be reproduced, duplicated, copied, sold, resold, or otherwise exploited for any commercial purpose without the prior written consent.
Chapter 12 - Vital_Signs_and_Monitoring_Devices
 Introduction to Emergency Medical Care 1 OBJECTIVES 12.1 Define key terms introduced in this chapter. Slides 13 15, 17, 21 22, 26, 28, 30, 32 33, 35, 44, 47 48, 50, 55, 60 12.2 Identify the vital signs
Introduction to Emergency Medical Care 1 OBJECTIVES 12.1 Define key terms introduced in this chapter. Slides 13 15, 17, 21 22, 26, 28, 30, 32 33, 35, 44, 47 48, 50, 55, 60 12.2 Identify the vital signs
Topic: Baseline Vitals and Sample History Company Drill
 Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
Baseline Vitals and Sample History Company Drill Instructor Guide Session Reference: 1 Topic: Baseline Vitals and Sample History Company Drill Level of Instruction: 2 Time Required: Three Hours Materials
Overview. Baseline Vital Signs. Chapter 5. Baseline Vital Signs and SAMPLE History. Baseline Vital Signs. SAMPLE History
 Chapter 5 Baseline Vital Signs and SAMPLE History Slide 1 Baseline Vital Signs Breathing Skin Pupils Blood Pressure Overview Vital Sign Reassessment SAMPLE History Slide 2 Baseline Vital Signs Slide 3
Chapter 5 Baseline Vital Signs and SAMPLE History Slide 1 Baseline Vital Signs Breathing Skin Pupils Blood Pressure Overview Vital Sign Reassessment SAMPLE History Slide 2 Baseline Vital Signs Slide 3
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: ASSESSMENT Revised: 11/2013 DEFINITIONS General Impression - EMT develops a plan of action from the
Baseline Vital Signs and SAMPLE History. Chapter 5
 Baseline Vital Signs and SAMPLE History Chapter 5 Baseline Vital Signs and SAMPLE History Assessment is the most complex skill EMT-Bs learn. During assessment you will: Gather key information. Evaluate
Baseline Vital Signs and SAMPLE History Chapter 5 Baseline Vital Signs and SAMPLE History Assessment is the most complex skill EMT-Bs learn. During assessment you will: Gather key information. Evaluate
Aaron J. Katz, AEMT-P, CIC Outward signs of what is occurring inside the body
 Vital Signs Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Vital Signs Outward signs of what is occurring inside the body Also give valuable information about the patient s condition They are taken
Vital Signs Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Vital Signs Outward signs of what is occurring inside the body Also give valuable information about the patient s condition They are taken
Chapter 12. Vital Signs Assessment
 Chapter 12 Vital Signs Assessment Pre-Test 1. What are vital signs? 2. List as many vital signs as you know. Key Terms homeostasis: a state of equilibrium within the body maintained through the adaptation
Chapter 12 Vital Signs Assessment Pre-Test 1. What are vital signs? 2. List as many vital signs as you know. Key Terms homeostasis: a state of equilibrium within the body maintained through the adaptation
Chapter 15: Measuring Height, Weight, and Vital Signs. Copyright 2012 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 15: Measuring Height, Weight, and Vital Signs Height and Weight Weight Baseline measurement at patient s first visit Measured in kg or lbs Common types of scales Balance beam Dial Digital Height
Chapter 15: Measuring Height, Weight, and Vital Signs Height and Weight Weight Baseline measurement at patient s first visit Measured in kg or lbs Common types of scales Balance beam Dial Digital Height
7/12/2014. Patient History and SAMPLE. Vital Signs, History Taking and Mechanism Of Injury (Class 7)
 1 2 3 4 5 6 7 8 9 10 11 12 Vital Signs, History Taking and Mechanism Of Injury (Class 7) Patient History and SAMPLE General Information Chief complaint Why EMS assistance was requested Should always be
1 2 3 4 5 6 7 8 9 10 11 12 Vital Signs, History Taking and Mechanism Of Injury (Class 7) Patient History and SAMPLE General Information Chief complaint Why EMS assistance was requested Should always be
Chapter 9 Vital Signs and SAMPLE History DOT Directory
 Chapter 9 Vital Signs and SAMPLE History U.S. Objectives U.S. Objectives are covered and/or supported by the PowerPoint Slide Program and Notes for Emergency Care, 11th Ed. Please see the Chapter 9 correlation
Chapter 9 Vital Signs and SAMPLE History U.S. Objectives U.S. Objectives are covered and/or supported by the PowerPoint Slide Program and Notes for Emergency Care, 11th Ed. Please see the Chapter 9 correlation
Crucial Signs כל הזכויות שמורות למד"א מרחב ירושלים
 Crucial Signs Dan Drory, MDA Paramedic and Instructor, 2011 What are Signs? Sign Objective, measurable Symptom Subjective, evaluated by the patient ( Chest Pain, Difficulties Breathing, Headache ) Signs
Crucial Signs Dan Drory, MDA Paramedic and Instructor, 2011 What are Signs? Sign Objective, measurable Symptom Subjective, evaluated by the patient ( Chest Pain, Difficulties Breathing, Headache ) Signs
Vital Signs and SAMPLE History
 CHAPTER 9 Vital Signs and SAMPLE History Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
CHAPTER 9 Vital Signs and SAMPLE History Overall Assessment Scheme Scene Size-Up Initial Assessment Trauma Physical Exam Vital Signs & SAMPLE History Medical SAMPLE History Physical Exam & Vital Signs
Vital Signs. Vital Signs. Vital Signs
 Vital Signs Vital Signs Why do vital signs? Determine relative status of vital organs Establish baseline Monitor response to Rx, meds Observe trends Determine need for further evaluation, Rx, intervention
Vital Signs Vital Signs Why do vital signs? Determine relative status of vital organs Establish baseline Monitor response to Rx, meds Observe trends Determine need for further evaluation, Rx, intervention
Respiratory Emergencies
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons for
Pediatric Advanced Life Support
 Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Pediatric Advanced Life Support Pediatric Chain of Survival Berg M D et al. Circulation 2010;122:S862-S875 Prevention Early cardiopulmonary resuscitation (CPR) Prompt access to the emergency response system
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff
 Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
Physiological Measurements Training for Care/Nursing & LD Small Group Home Staff CONTENTS 1. The National Early Warning Score 2. Respiratory Rate 3. Oxygen Saturations 4. Temperature 5. Blood Pressure
Anatomy Review. Anatomy Review. Respiratory Emergencies CHAPTER 16
 CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
CHAPTER 16 Respiratory Emergencies Anatomy Review Anatomy Review 1 Pediatric Anatomy Airway structure differences Proportionally larger tongue Smaller, more flexible trachea Abdominal breathers Reasons
Measuring Vital Signs. Copyright 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved.
 Measuring Vital Signs Copyright 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Five Vital Signs Temperature, pulse, respiration, blood pressure, and pain Vital signs give indications
Measuring Vital Signs Copyright 2014, 2009 by Saunders, an imprint of Elsevier Inc. All rights reserved. Five Vital Signs Temperature, pulse, respiration, blood pressure, and pain Vital signs give indications
Appendix E Choose the sign or symptom that best indicates severe respiratory distress.
 Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Appendix E-2 1. In Kansas EMT-B may monitor pulse oximetry: a. after they complete the EMT-B course b. when the service purchases the state approved pulse oximeters c. when the service director receives
Airway and Ventilation. Emergency Medical Response
 Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Airway and Ventilation Lesson 14: Airway and Ventilation You Are the Emergency Medical Responder Your medical emergency response team has been called to the fitness center by building security on a report
Chapter 11. Objectives. Objectives 01/09/2013. Baseline Vital Signs, Monitoring Devices, and History Taking
 Chapter 11 Baseline Vital Signs, Monitoring Devices, and History Taking Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
Chapter 11 Baseline Vital Signs, Monitoring Devices, and History Taking Prehospital Emergency Care, Ninth Edition Joseph J. Mistovich Keith J. Karren Copyright 2010 by Pearson Education, Inc. All rights
Can be felt where an artery passes near the skin surface and over a
 1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
1 Chapter 14 Cardiovascular Emergencies 2 Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD) claimed
Appendix D An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires:
 Answer Key Appendix D-2 1. An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires: a. oxygen given via nasal cannula b. immediate transport to a medical facility c.
Answer Key Appendix D-2 1. An unresponsive patient with shallow, gasping breaths at a rate of six per minute requires: a. oxygen given via nasal cannula b. immediate transport to a medical facility c.
Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since.
 1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
1 2 3 4 5 Chapter 14 Cardiovascular Emergencies Cardiovascular Emergencies Cardiovascular disease has been leading killer of Americans since. Accounts for 1 of every 2.8 deaths Cardiovascular disease (CVD)
Chapter 24 Vital Signs. Copyright 2011 Wolters Kluwer Health Lippincott Williams & Wilkins
 Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
Chapter 24 Vital Signs Vital Signs Temperature Pulse Respiration Blood pressure When to Assess Vital Signs Upon admission to any healthcare agency Based on agency institutional policy and procedures Anytime
#6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure
 #6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure Objectives: Observe slide of artery and vein cross-section Auscultate heart sounds using a stethoscope Measure
#6 - Cardiovascular III Heart Sounds, Pulse Rate, Hemoglobin Saturation, and Blood Pressure Objectives: Observe slide of artery and vein cross-section Auscultate heart sounds using a stethoscope Measure
REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic. SMO: Pediatric Assessment Guidelines
 REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic SMO: Pediatric Assessment Guidelines Overview: Pediatric patients account for about 10% or less of
REGION 1 EMERGENCY MEDICAL SERVICES STANDING MEDICAL ORDERS EMT Basic, EMT Intermediate, EMT Paramedic SMO: Pediatric Assessment Guidelines Overview: Pediatric patients account for about 10% or less of
Respiratory Emergencies. Lesson Goal. Lesson Objectives 9/10/2012
 Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Respiratory Emergencies Lesson Goal Assess and provide timely treatment & transport to patients experiencing respiratory emergencies Lesson Objectives List parts of respiratory system and how they work
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of
 Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
Daniel A. Beals MD, FACS, FAAP Pediatric Surgery and Urology Community Medical Center Associate Professor of Surgery and Pediatrics University of Washington Seattle Children s Hospital Objectives Define
ALCO Regulations. Protocol pg. 47
 For the EMT-Basic Objectives Understand ALCO regulations relative to monitoring pulse oximetry by the EMT-B Review the signs and symptoms of respiratory compromise. Understand the importance of adequate
For the EMT-Basic Objectives Understand ALCO regulations relative to monitoring pulse oximetry by the EMT-B Review the signs and symptoms of respiratory compromise. Understand the importance of adequate
a central pulse located at the apex of the heart Apical pulse Apical-radial pulse a complete absence of respirations Apnea
 Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Afebrile absence of a fever Apical pulse a central pulse located at the apex of the heart Apical-radial pulse measurement of the apical beat and the radial pulse at the same time Apnea a complete absence
Respiratory Emergencies. Chapter 11
 Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Respiratory Emergencies Chapter 11 Respiratory System Anatomy and Function of the Lung Characteristics of Adequate Breathing Normal rate and depth Regular breathing pattern Good breath sounds on both sides
Vital Signs. Temperature. Pulse. Respirations. Blood Pressure. O2 Saturation
 Vital Signs Temperature Pulse Respirations Blood Pressure O2 Saturation Vital Signs Temperature, pulse, respiration, blood pressure (B/P) & oxygen saturation are the most frequent measurements taken by
Vital Signs Temperature Pulse Respirations Blood Pressure O2 Saturation Vital Signs Temperature, pulse, respiration, blood pressure (B/P) & oxygen saturation are the most frequent measurements taken by
Measuring and Recording Temperature
 Measuring and Recording Temperature Measurement of balance between heat lost and produced by the body. Lost through: Perspiration Respiration Excretion Produced by: Metabolism of food Muscle and gland
Measuring and Recording Temperature Measurement of balance between heat lost and produced by the body. Lost through: Perspiration Respiration Excretion Produced by: Metabolism of food Muscle and gland
VITAL SIGNS. Academic Success Center
 VITAL SIGNS Academic Success Center Because of the importance of these measurements they are referred to as Vital Signs. They are important indicators of the body s response to physical, environmental,
VITAL SIGNS Academic Success Center Because of the importance of these measurements they are referred to as Vital Signs. They are important indicators of the body s response to physical, environmental,
Appendix (i) The ABCDE approach to the sick patient
 Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Appendix (i) The ABCDE approach to the sick patient This appendix and the one following provide guidance on the initial approach and management of common medical emergencies which may arise in general
Techniques of Vital Signs. John Gazewood, MD, MSPH Department of Family Medicine
 Techniques of Vital Signs John Gazewood, MD, MSPH Department of Family Medicine Objectives Define normal in several ways. Describe correct technique of measuring vital signs. Describe correct technique
Techniques of Vital Signs John Gazewood, MD, MSPH Department of Family Medicine Objectives Define normal in several ways. Describe correct technique of measuring vital signs. Describe correct technique
ITLS Pediatric Provider Course Basic Pre-Test
 ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
ITLS Pediatric Provider Course Basic Pre-Test 1. You arrive at the scene of a motor vehicle collision and are directed to evaluate a child who was in one of the vehicles. The patient appears to be a child
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions
 Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Patient Assessment From Brady s First Responder (8th Edition) 83 Questions 1. Which question is important if your patient may be a candidate for surgery? p. 183 *A.) When did you last eat? B.) What is
Cardiac Emergencies. Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington
 Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
Cardiac Emergencies Jim Bennett Paramedic and Clinical Education Coordinator American Medical Response Spokane, Washington The Heart -------Aorta Pulmonary Veins---- Superior Vena Cava------ Right Atrium-----
VAO BASIC SUPPORT CLINICAL APPROACH TO THE PATIENT HANDOUT
 CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
CLINICAL APPROACH TO THE PATIENT HANDOUT 1 I am the most important part of patient care. How can you expect to treat a patient appropriately if you don t follow through on basic primary care? Remember:
Pediatric Assessment Lesson 3
 1 Pediatric Assessment Lesson 3 2 Pediatric Assessment Initial assessment methods used for adults are modified for children due to developmental and physiological considerations. 3 In this lesson, the
1 Pediatric Assessment Lesson 3 2 Pediatric Assessment Initial assessment methods used for adults are modified for children due to developmental and physiological considerations. 3 In this lesson, the
Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood
 1 2 3 Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood 4 5 6 7 8 9 10 Highlights: - A pulse consists of two phases: contraction
1 2 3 Pancreas: digestive enzymes Liver: bile-helps to digest fat, stored in gallblader; breaks down toxins, makes some parts of blood 4 5 6 7 8 9 10 Highlights: - A pulse consists of two phases: contraction
LEARNING OUTCOME The students will be able to elicit vital signs correctly on human volunteers/patients
 Vital signs (pulse, blood pressure, temperature, respiratory rate, pain) are physiological parameters that a healthcare professional requires when dealing with patients. Accurate measurement of vital signs
Vital signs (pulse, blood pressure, temperature, respiratory rate, pain) are physiological parameters that a healthcare professional requires when dealing with patients. Accurate measurement of vital signs
Vital Signs and Oxygen Administration
 Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Vital Signs and Oxygen Administration By Dr. Mohsen Dashti Patient Care and Management (202) May-9-2010 Vital Signs and Oxygen Administration What are the vital signs? Why do we need to know them? How
Chapter 29 1/8/2018. Vital Signs. Measuring and Reporting Vital Signs. Key Terms
 Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
Chapter 29 Vital Signs Key Terms Blood pressure Body temperature Diastolic pressure Hypertension Hypotension Pulse Pulse rate Respiration Sphygmomanometer Stethoscope Systolic pressure Vital signs Measuring
Chapter 29. Vital Signs
 Chapter 29 Vital Signs Vital Signs Temperature, pulse, respiratory rate, blood pressure Pain Oxygen saturation also frequently measured Vital signs are used to: Monitor patient s condition Identify problems
Chapter 29 Vital Signs Vital Signs Temperature, pulse, respiratory rate, blood pressure Pain Oxygen saturation also frequently measured Vital signs are used to: Monitor patient s condition Identify problems
Percussion These 4 techniques are the foundation of the physical exam. Respiration Blood pressure Body
 1 Chapter 11: Physical Exam Techniques 2 Introduction Although patient assessment formally starts with the, the physical examination actually begins when you first set eyes on your patient. The purpose
1 Chapter 11: Physical Exam Techniques 2 Introduction Although patient assessment formally starts with the, the physical examination actually begins when you first set eyes on your patient. The purpose
Pulse. Assess for the following:
 Vital Signs Overview LOC = AVPU Pulse Respiration's Blood Pressure Lung Sounds Skin: Color, Texture, Temperature Pupils = Equal, Reactive to Light with Accomodation Pulse Assess for the following: Rate
Vital Signs Overview LOC = AVPU Pulse Respiration's Blood Pressure Lung Sounds Skin: Color, Texture, Temperature Pupils = Equal, Reactive to Light with Accomodation Pulse Assess for the following: Rate
Chapter 11: Respiratory Emergencies
 29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
29698_CH11_ANS_p001_005 4/12/05 2:02 PM Page 1 Answer Key Chapter 11 1 Chapter 11: Respiratory Emergencies Matching 1. B (page 373) 8. E (page 370) 2. D (page 369) 9. M(page 389) 3. H (page 370) 10. A
Bronchoconstriction is also treated with medications that inhibit bronchiolar constriction such as: Ipratropium (Atrovent)
 Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Patients with difficulty breathing (dyspnea) may have problems with: Oxygenation due to alveolar problems Ventilation due to bronchiolar problems Oxygenation due to lung perfusion problems Combinations
Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations
 ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
ighapmlre33apg269_274 5/12/04 3:10 PM Page 269 impos03 302:bjighapmL:ighapmLrevshts:layouts: NAME Human Cardiovascular Physiology: Blood Pressure and Pulse Determinations LAB TIME/DATE REVIEW SHEET exercise
Bleeding and Shock *** CME Version *** Aaron J. Katz, AEMT-P, CIC
 Bleeding and Shock *** CME Version *** Aaron J. Katz, AEMT-P, CIC www.es26medic.net Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to
Bleeding and Shock *** CME Version *** Aaron J. Katz, AEMT-P, CIC www.es26medic.net Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to
PLANK 1 Direct Care Staff Trained in Accurate BP Measurement
 Direct Care Staff Trained in Accurate BP Measurement 1. 2. 3. 5. 22 to 26 cm Small adult (12X22 cm) 27 to 34 cm Adult (16X30 cm) 35 to 44 cm Large adult (16X36 cm) 45 to 52 cm Adult thigh (16X42 cm) widths
Direct Care Staff Trained in Accurate BP Measurement 1. 2. 3. 5. 22 to 26 cm Small adult (12X22 cm) 27 to 34 cm Adult (16X30 cm) 35 to 44 cm Large adult (16X36 cm) 45 to 52 cm Adult thigh (16X42 cm) widths
Pediatric Shock. Hypovolemia. Sepsis. Most common cause of pediatric shock Small blood volumes (80cc/kg)
 Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Critical Concepts: Shock Inadequate peripheral perfusion where oxygen delivery does not meet metabolic demand Adult vs Pediatric Shock - Same causes/different frequencies Pediatric Shock Hypovolemia Most
Firefighter Pre-Hospital Care Program Recruit Presentation. Respiratory Emergencies
 Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Firefighter Pre-Hospital Care Program Recruit Presentation Respiratory Emergencies The Respiratory System Anatomy Pharynx Nasopharynx Oropharynx Epiglottis Larynx Trachea Right main bronchus Left main
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013
 Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
Emergency Medical Training Services Emergency Medical Technician Basic Program Outlines Outline Topic: Shock Revised: 11/2013 DEFINITIONS Aerobic metabolism is energy using oxygen into cells. Anaerobic
How To Measure Vital Signs
 How To Measure Vital Signs How to Use This Tutorial This tutorial is intended for healthcare providers or students to teach basic vital signs skills Use the navigation buttons below to move through the
How To Measure Vital Signs How to Use This Tutorial This tutorial is intended for healthcare providers or students to teach basic vital signs skills Use the navigation buttons below to move through the
Introduction (1 of 3)
 Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Chapter 10 Shock Introduction (1 of 3) Shock (hypoperfusion) means a state of collapse and failure of the cardiovascular system. In the early stages, the body attempts to maintain homeostasis. As shock
Chapter 11 - The Primary Assessment
 Introduction to Emergency Medical Care 1 OBJECTIVES 11.1 Define key terms introduced in this chapter. Slides 11 12, 14, 19 21, 28 11.2 Explain the purpose of the primary assessment. Slides 11 13 OBJECTIVES
Introduction to Emergency Medical Care 1 OBJECTIVES 11.1 Define key terms introduced in this chapter. Slides 11 12, 14, 19 21, 28 11.2 Explain the purpose of the primary assessment. Slides 11 13 OBJECTIVES
Bayfield-Ashland Counties EMS Council Pediatric Protocol PP-001 PREHOSPITAL CARE GUIDELINE
 INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
INTRODUCTION: Pediatric emergencies may present a daunting challenge to prehospital care providers for a variety of reasons including: 1. The historical scarceness of primary training materials about the
WSCC EMT CLASS SEVIERVILLE EXAM 1 STUDY GUIDE 1. Describe what is needed for good eye protection. Are prescription eye glasses adequate?
 1. Describe what is needed for good eye protection. Are prescription eye glasses adequate? 2. What kind of report must be given to officially transfer patient care at the hospital? 3. What is subcutaneous
1. Describe what is needed for good eye protection. Are prescription eye glasses adequate? 2. What kind of report must be given to officially transfer patient care at the hospital? 3. What is subcutaneous
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be
 1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
1 Chapter 13 Respiratory Emergencies 2 Respiratory Distress Patients often complain about. Shortness of breath Symptom of many different Cause can be difficult to determine. Even for physician in hospital
Lesson 4-3: Cardiac Emergencies. CARDIAC EMERGENCIES Angina, AMI, CHF and AED
 Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Lesson 4-3: Cardiac Emergencies CARDIAC EMERGENCIES Angina, AMI, CHF and AED THREE FAMILIAR CARDIAC CONDITIONS Angina Pectoris Acute Myocardial Infarction Congestive Heart Failure ANGINA PECTORIS Chest
Objectives. Case Presentation. Respiratory Emergencies
 Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Respiratory Emergencies Objectives Describe how to assess airway and breathing, including interpreting information from the PAT and ABCDEs. Differentiate between respiratory distress, respiratory failure,
Human Circulation and Respiration Chapter 38
 Human Circulation and Respiration Chapter 38 Goals: 1. Compare closed and open circulatory systems. 2. Label the parts of the human heart. 3. Explain how blood travels through the heart; identify chambers
Human Circulation and Respiration Chapter 38 Goals: 1. Compare closed and open circulatory systems. 2. Label the parts of the human heart. 3. Explain how blood travels through the heart; identify chambers
PART I: HEART ANATOMY
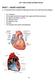 Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Lab 7: Heart Sounds and Blood Pressure PART I: HEART ANATOMY a) You should be able to identify the following structures on an adult human heart diagram. the 4 chambers the bicuspid (mitral) and tricuspid
Bleeding and Shock. Circulatory System
 Bleeding and Shock Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to body tissues Delivers
Bleeding and Shock Aaron J. Katz, AEMT-P, CIC www.es26medic.net 2013 Circulatory System Composed of heart, blood vessels and blood A closed system Pumps oxygenated blood and nutrients to body tissues Delivers
Chapter 21. Assisting With Assessment. Elsevier items and derived items 2014, 2010 by Mosby, an imprint of Elsevier Inc. All rights reserved.
 Chapter 21 Assisting With Assessment Vital Signs Vital signs reflect three body processes: Regulation of body temperature Breathing Heart function A person s vital signs: Vary within certain limits Are
Chapter 21 Assisting With Assessment Vital Signs Vital signs reflect three body processes: Regulation of body temperature Breathing Heart function A person s vital signs: Vary within certain limits Are
PEPP Course: PEPP BLS Pretest
 PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
PEPP Course: PEPP BLS Pretest 1. What is the best way to administer oxygen to a child in moderate respiratory distress? Nasal cannula Simple mask Nonrebreathing mask Bag-valve-mask device 2. A 2-year-old
Shock Kills! By the time you see it, it is probably too late! Contact Information. Overview
 Contact Information Tim Hillier, EMT-P Director of Professional Development M.D. Ambulance Saskatoon, SK (306) 975-8825 (Office) t.hillier@mdambulance.com Tim Hillier, EMT-P Shock Kills! By the time you
Contact Information Tim Hillier, EMT-P Director of Professional Development M.D. Ambulance Saskatoon, SK (306) 975-8825 (Office) t.hillier@mdambulance.com Tim Hillier, EMT-P Shock Kills! By the time you
CPAP. Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device. Charlottesville Albemarle Rescue Squad - CPAP
 CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CPAP Pre-Hospital Treatment Using The Respironics Whisperflow CPAP Device CPAP What Is It? C ontinuous P ositive A irway P ressure Anatomy Review Anatomy Review Anatomy Review Alveoli Anatomy Review Chest
CARDIOVASCULAR AND RESPIRATORY SYSTEMS
 CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
CARDIOVASCULAR AND RESPIRATORY SYSTEMS KEY TERMS: Cardiovascular System, cardio, vascular, blood vessels, valves, arteries, capillaries, veins, systemic circulation, pulmonary circulation Your Cardiovascular
ADVANCED ASSESSMENT Vital Signs
 ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Vital Signs 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Vital Signs AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager Grey-Bruce-Huron
ONTARIO BASE HOSPITAL GROUP QUIT ADVANCED ASSESSMENT Vital Signs 2007 Ontario Base Hospital Group ADVANCED ASSESSMENT Vital Signs AUTHORS Mike Muir AEMCA, ACP, BHSc Paramedic Program Manager Grey-Bruce-Huron
Michigan Pediatric Cardiac Protocols. Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS
 Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
Date: November 15, 2012 Page 1 of 1 TABLE OF CONTENTS Pediatric Asystole Section 4-1 Pediatric Bradycardia Section 4-2 Pediatric Cardiac Arrest General Section 4-3 Pediatric Narrow Complex Tachycardia
LAB 9: Metabolic Rates
 LAB 9: Metabolic Rates Introduction: The cardiovascular (circulatory) system functions to deliver oxygen and nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart pumps
LAB 9: Metabolic Rates Introduction: The cardiovascular (circulatory) system functions to deliver oxygen and nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart pumps
Capnography 101. James A Temple BA, NRP, CCP
 Capnography 101 James A Temple BA, NRP, CCP Expected Outcomes 1. Gain a working knowledge of the physiology and science behind End-Tidal CO2. 2.Relate End-Tidal CO2 to ventilation, perfusion, and metabolism.
Capnography 101 James A Temple BA, NRP, CCP Expected Outcomes 1. Gain a working knowledge of the physiology and science behind End-Tidal CO2. 2.Relate End-Tidal CO2 to ventilation, perfusion, and metabolism.
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium
 Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Written 01/09/17 Rewritten 3/29/17 for Interior Regional EMS Symposium MARIA E. MANDICH MD Fairbanks Memorial Hospital Emergency Department Attending Physician Interior Region EMS Council Medical Director
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials
 Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Trauma Life Support Pre-Hospital (TLS-P) Preparatory Materials 1 1. A high-risk bodily fluid for spreading infection is blood. 2. Items that can reduce the spread of infection include masks, gloves, and
Taking and recording blood pressure and pulse. City Gate Training Centre all rights reserved
 Taking and recording blood pressure and pulse City Gate Training Centre all rights reserved Course Content: Definition of Blood Pressure Normal Blood Pressure Readings Systolic and Diastolic Blood Pressure
Taking and recording blood pressure and pulse City Gate Training Centre all rights reserved Course Content: Definition of Blood Pressure Normal Blood Pressure Readings Systolic and Diastolic Blood Pressure
Chapter 19 - Respiratory_Emergencies
 Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
Introduction to Emergency Medical Care 1 OBJECTIVES 19.1 Define key terms introduced in this chapter. Slides 14 15, 41, 54 19.2 Describe the anatomy and physiology of respiration. Slides 13 15 19.3 Differentiate
The Pediatric Patient. Morgen Bernius, MD NCEMS Conference February 24, 2007
 The Pediatric Patient Morgen Bernius, MD NCEMS Conference February 24, 2007 Rule #1: Everyone Loves the Pediatric Patient Pediatrics in EMS Approximately 10% of all EMS treatment is for children younger
The Pediatric Patient Morgen Bernius, MD NCEMS Conference February 24, 2007 Rule #1: Everyone Loves the Pediatric Patient Pediatrics in EMS Approximately 10% of all EMS treatment is for children younger
PEDIATRIC INITIAL ASSESSMENT - ALS
 PEDIATRIC INITIAL ASSESSMENT - ALS I. SCENE SIZE-UP A. Protect from body substance through isolation (glasses, gloves, gown and mask). B. Assess the scene for safety and take appropriate steps. C. Determine
PEDIATRIC INITIAL ASSESSMENT - ALS I. SCENE SIZE-UP A. Protect from body substance through isolation (glasses, gloves, gown and mask). B. Assess the scene for safety and take appropriate steps. C. Determine
CRITERIA BASED DISPATCH (CBD)
 CRITERIA BASED DISPATCH (CBD) Key Concepts of CBD Critical/Non-Critical Criteria Based Dispatch (also referred to as CBD) is centered on two dimensions that characterize all pre-hospital emergency response.
CRITERIA BASED DISPATCH (CBD) Key Concepts of CBD Critical/Non-Critical Criteria Based Dispatch (also referred to as CBD) is centered on two dimensions that characterize all pre-hospital emergency response.
Vital Signs. 1. Define important words in this chapter. 2. Discuss the relationship of vital signs to health and well-being
 84 13 Vital Signs 1. Define important words in this chapter 2. Discuss the relationship of vital signs to health and well-being 3. Identify factors that affect body temperature 4. List guidelines for taking
84 13 Vital Signs 1. Define important words in this chapter 2. Discuss the relationship of vital signs to health and well-being 3. Identify factors that affect body temperature 4. List guidelines for taking
Patient Assessment. Chapter 8
 Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Patient Assessment Chapter 8 Patient Assessment Scene size-up Initial assessment Focused history and physical exam Vital signs History Detailed physical exam Ongoing assessment Patient Assessment Process
Introduction to Emergency Medical Care 1
 Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Introduction to Emergency Medical Care 1 OBJECTIVES 6.1 Define key terms introduced in this chapter. Slides 11, 15, 17, 26, 27, 31, 33, 37, 40 42, 44, 45, 51, 58 6.2 Describe the basic roles and structures
Resident At Risk. The National Early Warning Score (NEWS) and Monitoring Vital Signs
 Resident At Risk The National Early Warning Score (NEWS) and Monitoring Vital Signs Schein et al 64 consecutive ward patients requiring CPR 84% clinical deterioration 8 hours before arrest Pathophysiology
Resident At Risk The National Early Warning Score (NEWS) and Monitoring Vital Signs Schein et al 64 consecutive ward patients requiring CPR 84% clinical deterioration 8 hours before arrest Pathophysiology
Anatomy and Physiology
 Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
Anatomy and Physiology Respiratory Diagnostic Procedures 2004 Delmar Learning, a Division of Thomson Learning, Inc. Bell Work Complete cost of smoking exercise. We will go over this together! (Don t worry)!
How to Measure Vital Signs
 How to Measure Vital Signs Caregiving Series: Volume 10 Objectives Upon completion of this training, participants will understand: The definitions of temperature, pulse, respiration and blood pressure
How to Measure Vital Signs Caregiving Series: Volume 10 Objectives Upon completion of this training, participants will understand: The definitions of temperature, pulse, respiration and blood pressure
Chief Complaint lthe major sign and/or symptom reported by the patient lsymptoms Problems or a patient reports
 1 2 3 4 5 6 7 Chapter 8 Baseline Vital Signs and SAMPLE History Baseline Vital Signs and SAMPLE History lassessment is the most skill learn. lduring assessment you will: Gather key information. Evaluate
1 2 3 4 5 6 7 Chapter 8 Baseline Vital Signs and SAMPLE History Baseline Vital Signs and SAMPLE History lassessment is the most skill learn. lduring assessment you will: Gather key information. Evaluate
Cardiac Emergencies. A Review of Cardiac Compromise. Lawrence L. Lambert
 Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
Cardiac Emergencies A Review of Cardiac Compromise Lawrence L. Lambert 1 Cardiac Emergencies Objectives: Following successful completion of this training session, the student should be able to: 1. Describe
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE. MEASURING BLOOD PRESSURE - MANUAL (equ04)
 SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: MEASURING BLOOD PRESSURE - MANUAL Nursing DATE: REVIEWED: PAGES: 2/80 7/17 1 of 5 RESPONSIBILITY: RN, LPN, Patient Care Technician Multi-skilled
SARASOTA MEMORIAL HOSPITAL NURSING PROCEDURE TITLE: ISSUED FOR: MEASURING BLOOD PRESSURE - MANUAL Nursing DATE: REVIEWED: PAGES: 2/80 7/17 1 of 5 RESPONSIBILITY: RN, LPN, Patient Care Technician Multi-skilled
Physiology of the Circulatory System modified from
 Physiology of the Circulatory System modified from http://www.ekcsk12.org/science/aplabreview/aplab10.htm Introduction The circulatory system functions to deliver oxygen and nutrients to tissues for growth
Physiology of the Circulatory System modified from http://www.ekcsk12.org/science/aplabreview/aplab10.htm Introduction The circulatory system functions to deliver oxygen and nutrients to tissues for growth
MICHIGAN. State Protocols. Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.
 MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
MICHIGAN State Protocols Protocol Number Protocol Name Pediatric Cardiac Table of Contents 6.1 General Pediatric Cardiac Arrest 6.2 Bradycardia 6.3 Tachycardia PEDIATRIC CARDIAC PEDIATRIC CARDIAC ARREST
Clinical Research Coordinator Skills Program
 Clinical Research Coordinator Skills Program Vital Signs This Skill Requires Provider direction Standard Precautions Using purell before and after contact with the patient or the patient s environment
Clinical Research Coordinator Skills Program Vital Signs This Skill Requires Provider direction Standard Precautions Using purell before and after contact with the patient or the patient s environment
FIRST AID WRITTEN EXAM. Team Name: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. a. TRUE b. FALSE
 2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
2015 NEW IBERIA MINE RESCUE CONTEST FIRST AID WRITTEN EXAM Name: Date: 1. Participation in a critical incident stress debriefing (CISD) is mandatory. 2. The use of accessory muscles in the chest, abdomen
Chapter 11 The Respiratory System
 Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Biology 12 Name: Respiratory System Per: Date: Chapter 11 The Respiratory System Complete using BC Biology 12, page 342-371 11.1 The Respiratory System pages 346-350 1. Distinguish between A. ventilation:
Lab #10 Physiology of the Circulatory System
 Lab #10 Physiology of the Circulatory System Introduction The circulatory system functions to deliver oxygen an nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart
Lab #10 Physiology of the Circulatory System Introduction The circulatory system functions to deliver oxygen an nutrients to tissues for growth and metabolism, and to remove metabolic wastes. The heart
Shock. Perfusion. The cardiovascular system s circulation of blood and oxygen to all the cells in different tissues and organs of the body
 Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
Shock Chapter 10 Shock State of collapse and failure of the cardiovascular system Leads to inadequate circulation Without adequate blood flow, cells cannot get rid of metabolic wastes The result- hypoperfusion
