Evaluation of Salivary Aspiration in Brain- Injured Patients With Tracheostomy Yujeong Kang, MD, Min Ho Chun, MD, Sook Joung Lee, MD
|
|
|
- Annabella Atkinson
- 6 years ago
- Views:
Transcription
1 Original Article Ann Rehabil Med 2013;37(1): pissn: eissn: Annals of Rehabilitation Medicine Evaluation of Salivary Aspiration in Brain- Injured Patients With Tracheostomy Yujeong Kang, MD, Min Ho Chun, MD, Sook Joung Lee, MD Department of Rehabilitation Medicine, Asan Medical Center, University of Ulsan College of Medicine, Seoul, Korea Objective To determine the useful tool for evaluating salivary aspiration in brain-injured patients with tracheostomy. Methods Radionuclide salivagram and laryngoscopy was done in 27 brain-injured patients with tracheostomy. During salivagram, 99m Tc sulfur colloid was placed sublingually in the supine position, and 50-minute dynamic images and 2-hour delayed images were obtained. Salivary aspiration was detected when the tracer was entered into the major airways or lung parenchyma. Laryngoscopy was done by otolaryngologists, and saliva aspiration, saliva pooling, and vocal cord palsy were evaluated. Videofluoroscopic swallowing study was done in patients who were able to undergo the test. Results The detection rate of salivary aspiration was 44.4% with salivagram, and 29.6% with laryngoscopy. The correlation of the two tests was 70.4%. Of the laryngoscopy findings, salivary pooling had significant correlation with positive salivagram results (p=0.04). Frequent need of suction correlated with salivary aspiration in both salivagram (p=0.01) and laryngoscopy (p=0.01). Patients with negative results in salivagram or laryngoscopy had higher rates of progressing to oral feeding or tapering tracheostomy. Two patients developed aspiration pneumonia, and both patients only showed aspiration in salivagram. Conclusion Brain-injured patients with tracheostomy have a high risk of salivary aspiration. Evaluation of salivary aspiration is important, as it may predict aspiration pneumonia and aids in clinical decisions of oral feeding or tracheostomy removal. Salivagram is more sensitive than laryngoscopy, but laryngoscopy may be useful for evaluating structural abnormalities or for follow-up examinations to assess the changes. Keywords Radionuclide imaging, Laryngoscopy, Respiratory aspiration, Aspiration pneumonia INTRODUCTION Received June 12, 2012; Accepted August 29, 2012 Corresponding author: Min Ho Chun Department of Rehabilitation Medicine, Asan Medical Center, University of Ulsan College of Medicine, 88 Olympic-ro 43-gil, Songpa-gu, Seoul , Korea Tel: , Fax: , mhchun@amc. seoul.kr This is an open-access article distributed under the terms of the Creative Commons Attribution Non-Commercial License ( org/licenses/by-nc/3.0) which permits unrestricted noncommercial use, distribution, and reproduction in any medium, provided the original work is properly cited. Copyright 2013 by Korean Academy of Rehabilitation Medicine Pulmonary aspiration is a common problem in patients with brain injury, and it can cause purulent sputum and pneumonia. Causes of pulmonary aspiration include aspiration due to swallowing dysfunction, aspiration from gastroesophageal reflux, and salivary aspiration. The last of these is the least commonly recognized form of aspiration, but can result in recurrent pneumonia from pathogenic bacteria and yeast in the oral cavity [1]. Risk factors of salivary aspiration include swallowing incoor-
2 Salivary Aspiration in Brain-Injured Patients dination, absent laryngeal sensation, excess production of saliva, and vocal cord paresis. Videofluroscopic swallowing studies (VFSS), scintigraphic swallowing studies, and fiberoptic endoscopic evaluation of swallowing are used to assess food aspiration. For salivary aspiration, radionuclide salivagram and laryngoscopy (fiberoptic endoscopy) can be used, but a standard test has not been established [2]. Heyman and Respondek [3] and Heyman [4] first described radionuclide salivagrams in 1989; a small dose of radiotracer is injected into the patient s mouth, and serial images are recorded. Salivary aspiration is diagnosed when tracheal or bronchial activity is detected. Previous studies claim that salivagrams are the most sensitive test for saliva aspiration [5]. However, it is used mostly in children, and there are few studies that have assessed its utility in adults. Laryngoscopy can be used to evaluate salivary aspiration or pooling, vocal cord abnormality, and other relevant structures. Pooled oral secretions may predict aspiration, but the study is done in a short period of time and may lack sensitivity [6]. Patients with tracheostomy are at a high risk for aspiration, which can occur for various reasons, such as pharyngeal pooling of secretions above the airway cuff, decreased laryngeal elevation, desensitization of the larynx, and loss of protective reflexes. The incidence of aspiration in adults with tracheostomy is reported to be 30% to 50%, and the risk of aspiration is directly related to the amount of oropharyngeal secretion [7,8]. Also, pneumonia rates were higher even in tube feeding patients, whom food aspiration is less likely to occur, indicating a possibility of pneumonia from salivary aspiration [8]. These findings underscore the need to evaluate salivary aspiration in patients with tracheostomy, followed with appropriate management to prevent pneumonia in high risk patients. The goal of this study is to compare the two tools salivagram and laryngoscopy, for evaluating salivary aspiration, and also to explore the clinical significance by investigating the frequency and associated factors of salivary aspiration in brain-injured patients with tracheostomy. MATERIALS AND METHODS Subjects A total of 27 brain-injured patients with tracheostomy tubes, who were transferred or admitted to the rehabilitation department between April 2011 and December 2011, were included in the study. We enrolled only patients who required suction of sputum or saliva. Radionuclide salivagram and laryngoscopy were conducted with an interval of less than 3 days. Patients who were medically unstable or unable to follow simple one step commands were excluded. Assessment For radionuclide salivagram, all patients fasted for 2 hours before the test. The patient was placed in a supine position under a gamma camera fitted with a low-energy high-resolution collimator and received a sublingual drooping of 0.5 ml saline with 0.5 mci Tc-99m diethylene triamine pentaacetic acid (18.5 MBq). Dynamic images of the mouth to the upper abdomen were recorded for 50 minutes, and after, anteroposterior and lateral static chest images were also obtained. Any suggestive findings of positive radionuclide salivagram from these images were an indication of ending the test. In case of negative Fig. 1. (A) Example of a positive salivagram image shows radiotracer present in the right trachea. (B) Laryngoscopic image shows direct view of aspirated saliva in the trachea. ANT, anterior; POST, posterior. 97
3 Yujeong Kang, et al. or inconclusive findings on the initial 50-minute test, delayed anteroposterior and lateral static chest images were acquired after 2 hours. Interpretation of the images was performed by two expertise nuclear medicine physicians. Salivary aspiration was indicated by detection of positive radioactivity in dynamic and/or static images on tracheobronchial tree, either side of both lung fields or site of tracheostomy (Fig. 1A). Fiberoptic laryngoscopy was performed by an otolaryngologist through the tracheostomy. During the procedure, salivary aspiration, pooling of secretions in the valleculae or pyrifrom sinuses, vocal cord gap and mobility, and other airway structures were evaluated. Salivary aspiration was assessed when saliva in the trachea or active aspiration was visualized (Fig. 1B). Structures evaluated included the vallecula, epiglottis, arytenoids, true and false vocal cords, and the oral and nasal cavity. Disease duration, history of pneumonia, cooperation level, and feeding method were assessed. Cooperation level was evaluated by the ability to participate in a Mini- Mental Status Examination-Korean version. VFSS was done in patients who were able to perform the protocol. The clinical course of the patients was followed until the patient was discharged from the hospital. Data analysis was performed using SPSS ver (SPSS Inc., Chicago, IL, USA) correlation between variables were determined by χ 2 analysis with the Fisher s exact test. Significance was defined as p<0.05. The study was approved by the Institutional Review Board. Table 1. Demographic characteristics of patients Characteristic Value No. of patients 27 Sex (male:female) 18:9 Age (yr), mean±sd 52.2±17.8 Brain injury Stroke 15 Traumatic brain injury 5 Hypoxic brain injury 4 Brain abscess 1 Encephalopathy/encephalitis 2 Disease duration (mo), mean±sd (range) 6.3±7.5 (1 30) History of pneumonia 6 Methods of feeding (oral:tube) 6:21 Cooperation (good:poor) 15:12 SD, standard deviation. RESULTS Twenty-seven patients who were enrolled completed the evaluations, and their demographic data are presented in Table 1. All patients who were able to follow simple commands were evaluated with both laryngoscopy and salivagram. The studies were conducted within intervals of 3 days, and all patients were medically stable at the time of the study. Salivary aspiration was detected in 12 out of 27 patients with salivagram. On laryngoscopy, 8 out of 27 patients showed salivary aspiration. Among the 8 patients who showed aspiration, 6 patients also had aspiration in the salivagram (Table 2). The frequency of salivary aspiration among patients was 44.4% with salivagram and 29.6% with laryngoscopy, and the correlation between the two studies was 70.4% (p=0.09 by Fisher s exact test). The association between laryngoscopy findings and salivagram results are shown in Table 3. There was a significant association between any abnormality, including saliva pooling, saliva aspiration, or vocal cord abnormality, and salivary pooling observed by laryngoscopy with salivary aspiration on salivagram. Salivary aspiration or vocal cord abnormality seen on a laryngoscopy did not show significant association with salivary aspiration on Table 2. Comparison of salivagram and laryngoscopy results Laryngoscopy Salivagram No aspiration Aspiration Total No aspiration Aspiration Total Table 3. Association between laryngoscopy findings and salivagram results P:N p-value Laryngoscopy Any abnormality 17: * (n=27) Saliva pooling 16: * Saliva aspiration 8: Vocal cord abnormality 7: p-values are associated with salivagram. P, positive; N, negative. *p<0.05 by chi-square test. 98
4 Salivary Aspiration in Brain-Injured Patients salivagram. The association of clinical characteristics with salivagram and laryngoscopy is presented in Table 4. Of the clinical characteristics, frequent manual suction of secretions (more than ten times per day) was significantly associated with salivary aspiration seen on both salivagram and laryngoscopy. Among the 27 patients, only 15 patients could be evaluated by VFSS; the others were unable or unwilling to cooperate. Of the 15 patients who completed the study, five showed aspiration, five showed penetration, and five had no abnormalities. We compared the salivagram results with those of VFSS and found that of the 12 patients who were diagnosed with salivary aspiration by salivagram, 4 patients also had aspiration in VFSS, 2 patients had penetration, and the other 6 patients failed the study or could not be evaluated. In comparing the laryngoscopy and VFSS results, of the 8 patients who had aspiration as assessed by laryngoscopy, 4 also had aspiration in VFSS, 2 had penetration, and the others could not be tested. Table 5 shows the clinical course of patients according to the findings on salivagram or laryngoscopy. The follow-up period of patients ranged from 1 to 3 months (mean, 1.7 months). Of the 12 patients who showed aspiration on salivagram, only 2 were able to progress to oral feeding, compared to 6 in patients without aspiration. None of the patients with aspiration on salivagram were able to remove tracheostomy, while four patients without aspiration had their tracheostomy closed. Similar results were seen in patients with positive laryngoscopy results. Two patients developed aspiration pneumonia, and these patients both showed aspiration on salivagram, whereas in laryngoscopy, one showed only salivary pooling, and one had no abnormality. DISCUSSION In this study, we found that the frequency of salivary aspiration in brain-injured patients with tracheostomy was as high as 44.4% by salivagram. However, the frequency was lower when evaluated with laryngoscopy, which demonstrated salivary aspiration in 29.6% of patients. Both tests were used to evaluate salivary aspiration in patients who were unable to cooperate during VFSS. This is the first study to evaluate salivary aspiration using both laryngoscopy and salivagram. To date, salivagram is most commonly used in children who cannot cooperate during VFSS to evaluate aspira- Table 4. Association of clinical characteristics with salivagram and laryngoscopy No. Clinical characteristic Onset duration Cooperation Suction frequency History of pneumonia Salivagram * 0.46 Laryngoscopy 27 Any abnormality Saliva pooling Saliva aspiration * 0.63 Vocal cord abnormality p-values are associated with salivagram or laryngoscopy and clinical characteristics. *p<0.05 by chi-square test. Table 5. Clinical course of patients according to test results Laryngoscopy Salivagram (Aspiration) No. Aspiration Salivary pooling Negative Positive Negative Positive Negative Positive Aspiration pneumonia 2 0 (0) 2 (16.7) 2 (10.5) 0 (0) 1 (9.1) 1 (6.3) Oral feeding 8 6 (40.0) 2 (16.7) 6 (31.6) 2 (25.0) 6 (54.5) 2 (12.5) Tracheostomy removal 4 4 (26.7) 0 (0) 4 (21.1) 0 (0) 3 (27.3) 1 (6.3) Values are presented as number of patients (%). 99
5 Yujeong Kang, et al. tion. Since Heyman and Respondek [3] and Heyman [4] first proposed the use of salivagram for detecting aspiration in children, previous studies have mostly involved children. In a study that compared salivagram in severe cerebral palsy (CP), who are at high risk of aspiration with able-bodied adult volunteers, the frequency of aspiration was 56% in children with CP compared to 0% in young adults, showing that salivagram is a useful tool for the demonstration of aspiration [9]. Other studies have reported the frequency of positive salivagram in high risk children as 26% to 28% [10,11]. The difference in the rate of aspiration can be explained by the different infusion method; the former study used a continuous infusion method for 1 hour, whereas the latter studies used the sublingual dose method, as in our study. When Kang et al. [2] studied bedridden patients with brain lesions, the frequency of positive response was 22%. Silver and Van Nostrand [12] reported a case series of patients evaluated with salivagram, in which one patient had tracheostomy. These are the only studies to our knowledge that evaluated adults at risk of aspiration with salivagram. The frequency of salivary aspiration, detected by salivagram in our study, was higher than the previous studies. This may imply that tracheostomy further increases the risk of salivary aspiration in addition to deficits of pharyngeal or laryngeal control caused by brain lesions. It is not clear yet whether positive salivagram results predict more frequent episodes of acute aspiration or lung disease. However, Bar-Sever et al. [10] demonstrated the utility of salivagram in assessing children with unexplained lung disease or recurrent pneumonias. Twentysix percent showed salivary aspiration, suggesting aspiration of oral contents as a contributing factor [10]. Cook et al. [13] suggested salivagram as a tool for identifying candidates for laryngotracheal separation as a definitive mean of eliminating aspiration. Few studies have compared salivagram with other tools for evaluating aspiration. In a study by Baikie et al. [5], positive results for aspiration in CP patients were most frequent in salivagram, compared to that of VFSS and milk scans. One explanation for this result is that aspiration is an intermittent event, and because salivagram has the longest monitoring time, it is more likely to detect aspiration. Laryngoscopy is useful for evaluating the pharyngeal structures and can directly observe aspiration. This method can also be used to assess laryngeal sensation or to evaluate the swallowing process, as in fiberoptic endoscopic evaluation of swallowing. Other advantages of laryngoscopic evaluation includes that it can be performed bedside, it does not require fluoroscopic equipments, the patient is not exposed to radiation, and minimal positioning or cooperation of the patient is needed. It can also be repeated over time to assess the changes in a patient s swallowing function [14]. Oropharyngeal secretions, frequency of spontaneous swallows, and laryngopharyngeal sensation were highly predictive of aspiration in a study by Murray et al. [6]. Here, we focused on the detection of salivary pooling, aspiration, and structural problems. Sixty-three percent of the patients had abnormality detected by laryngoscopy. Salivary pooling was the most common problem, occurring in 59.3%. The lower rate of salivary aspiration in laryngoscopy compared to salivagram can be explained by the shorter evaluation time. Another possible reason is patient positioning during the tests. During the salivagram, patients are supine, whereas laryngoscopy is done in an upright position, and this may increase the aspiration rate in salivagram. The results demonstrate that salivary pooling should also be considered as an important predictor for aspiration, as it showed significant association with a positive salivagram. When this is considered, laryngoscopy may be useful for assessing changes in follow-up studies, as it is more simple and convenient than salivagram. Patients with positive salivagram results showed either aspiration or penetration on VFSS, but only half of the patients could undergo the latter study. Patients only need to follow simple commands in order to undergo salivagram, whereas more level of cooperation is needed to participate in VFSS. In those that only show penetration on VFSS who are being considered for oral feeding or removal of tracheostomy, salivagram may provide additional information to evaluate aspiration risk. Clinical factors related to positive salivagram results in previous studies include recurrent pneumonia and gastroesophageal reflux in children and anterior drooling, and cooperation in brain-injured adults [2,15]. Our results demonstrated a significant association between frequent suction of secretions and salivary aspiration. This can easily be explained since patients who lack control and/or have copious oral secretions will need frequent manual suction, either orally or through their tracheos
6 Salivary Aspiration in Brain-Injured Patients tomy, and this also increases the risk of aspirating secretions. The possible clinical applications of the two tests evaluating salivary aspiration can be inferred from the clinical courses of patients. Both salivagram and laryngoscopy correlated well with the progression to oral feeding and removal of tracheostomy. Negative results on salivagram and laryngoscopy may be useful for informing decisions on feeding or tracheostomy tapering. Salivagram appeared to be more helpful in predicting pneumonia, as two patients who developed aspiration pneumonia only had positive results on salivagram. The strength of this study includes that it is the first study to evaluate salivary aspiration with both salivagram and laryngoscopy, and compare the findings. Also, we selected a homogeneous high risk group, brain-injured patients with tracheostomy, and demonstrated the frequency and clinical implications of salivary aspiration. There are also a few limitations to our study. The duration of observation of the clinical course was limited to the inpatient rehabilitation period, and the sample size was small. Also, only a part of the subjects were evaluated by VFSS, therefore, comparison with VFSS results is limited. Further studies with larger sample size and longer follow-up period will be required to ascertain the results of our study. In conclusion, the rate of salivary aspiration in braininjured patients with tracheostomy as evaluated by salivagram was 44.4%. Salivagram was more sensitive than laryngoscopy in detecting aspiration. Evaluating salivary aspiration is important in brain-injured patients with tracheostomy, especially in patients with salivary pooling or frequent need of suction, and appropriate interventions should be considered according to the results. CONFLICT OF INTEREST No potential conflict of interest relevant to this article was reported. REFERENCES 1. Boesch RP, Daines C, Willging JP, Kaul A, Cohen AP, Wood RE, et al. Advances in the diagnosis and management of chronic pulmonary aspiration in children. Eur Respir J 2006;28: Kang IS, Kwon JG, Lee SU, Lee ZI, Park GY, Park HW. Detection of saliva aspiration using salivagram in bedridden patients with brain lesion. J Korean Acad Rehabil Med 2010;34: Heyman S, Respondek M. Detection of pulmonary aspiration in children by radionuclide salivagram. J Nucl Med 1989;30: Heyman S. The radionuclide salivagram for detecting the pulmonary aspiration of saliva in an infant. Pediatr Radiol 1989;19: Baikie G, South MJ, Reddihough DS, Cook DJ, Cameron DJ, Olinsky A, et al. Agreement of aspiration tests using barium videofluoroscopy, salivagram, and milk scan in children with cerebral palsy. Dev Med Child Neurol 2005;47: Murray J, Langmore SE, Ginsberg S, Dostie A. The significance of accumulated oropharyngeal secretions and swallowing frequency in predicting aspiration. Dysphagia 1996;11: Elpern EH, Jacobs ER, Bone RC. Incidence of aspiration in tracheally intubated adults. Heart Lung 1987;16: Donzelli J, Brady S, Wesling M, Theisen M. Secretions, occlusion status, and swallowing in patients with a tracheotomy tube: a descriptive study. Ear Nose Throat J 2006;85: Baikie G, Reddihough DS, South M, Cook DJ. The salivagram in severe cerebral palsy and able-bodied adults. J Paediatr Child Health 2009;45: Bar-Sever Z, Connolly LP, Treves ST. The radionuclide salivagram in children with pulmonary disease and a high risk of aspiration. Pediatr Radiol 1995;25 Suppl 1:S Levin K, Colon A, DiPalma J, Fitzpatrick S. Using the radionuclide salivagram to detect pulmonary aspiration and esophageal dysmotility. Clin Nucl Med 1993;18: Silver KH, Van Nostrand D. Scintigraphic detection of salivary aspiration: description of a new diagnostic technique and case reports. Dysphagia 1992;7: Cook SP, Lawless S, Mandell GA, Reilly JS. The use of the salivagram in the evaluation of severe and chronic aspiration. Int J Pediatr Otorhinolaryngol 1997;41: Kaye GM, Zorowitz RD, Baredes S. Role of flexible laryngoscopy in evaluating aspiration. Ann Otol Rhinol 101
7 Yujeong Kang, et al. Laryngol 1997;106: Simons JP, Rubinstein EN, Mandell DL. Clinical predictors of aspiration on radionuclide salivagrams in children. Arch Otolaryngol Head Neck Surg 2008;134:
Detection of salivary aspiration using radionuclide salivagram SPECT/CT in patients with COPD exacerbation: a preliminary study
 Original Article Detection of salivary aspiration using radionuclide salivagram SPECT/CT in patients with COPD exacerbation: a preliminary study Peng Hou 1 *, Huaifu Deng 1 *, Zhida Wu 2, Haiping Liu 1,
Original Article Detection of salivary aspiration using radionuclide salivagram SPECT/CT in patients with COPD exacerbation: a preliminary study Peng Hou 1 *, Huaifu Deng 1 *, Zhida Wu 2, Haiping Liu 1,
Utility of Salivagram in Pulmonary Aspiration in Pediatric Patients: Comparison of Salivagram and Chest Radiography
 Pediatric Imaging Original Research Drubach et al. Salivagram in Pulmonary Aspiration Pediatric Imaging Original Research Laura A. Drubach 1 David Zurakowski 2 Edwin L. Palmer, III 3 Donald A. Tracy 4
Pediatric Imaging Original Research Drubach et al. Salivagram in Pulmonary Aspiration Pediatric Imaging Original Research Laura A. Drubach 1 David Zurakowski 2 Edwin L. Palmer, III 3 Donald A. Tracy 4
Endoscopic Examination in Postmortem Examination
 Korean J Leg Med 2017;41:94-99 Original Article Endoscopic Examination in Postmortem Examination Joo-Young Na 1, Ji Hye Park 2 1 Biomedical Research Institute, Chonnam National University Hospital, Gwangju,
Korean J Leg Med 2017;41:94-99 Original Article Endoscopic Examination in Postmortem Examination Joo-Young Na 1, Ji Hye Park 2 1 Biomedical Research Institute, Chonnam National University Hospital, Gwangju,
Department of Pediatric Otolarygnology. ENT Specialty Programs
 Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Department of Pediatric Otolarygnology ENT Specialty Programs Staffed by fellowship-trained otolaryngologists, assisted by pediatric nurse practitioners, ENT (Otolaryngology) at Nationwide Children s Hospital
Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy
 Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
Page 1 of 9 Guideline of Videofluoroscopic Swallowing Study (VFSS) in Speech Therapy Version 1.0 Effective Date Document Number HKIST-C-VFG-v1 Author HKAST AR Sub-committee Custodian Chairperson of HKIST
Factors Associated With Compliance With Viscosity-Modified Diet Among Dysphagic Patients Jae Seong Shim, MD, Byung-Mo Oh, MD, Tai Ryoon Han, MD
 Original Article Ann Rehabil Med 2013;37(5):628-632 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.628 Annals of Rehabilitation Medicine Factors Associated With Compliance With
Original Article Ann Rehabil Med 2013;37(5):628-632 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.628 Annals of Rehabilitation Medicine Factors Associated With Compliance With
Feeding and Swallowing Problems in the Child with Special Needs
 Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Feeding and Swallowing Problems in the Child with Special Needs Joan Surfus, OTR/L, SWC Amy Lynch, MS, OTR/L Misericordia University This presentation is made possible, in part, by the support of the American
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล
 Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
Swallowing Screen Why? How? and So What? พญ.พวงแก ว ธ ต สก ลช ย ภาคว ชาเวชศาสตร ฟ นฟ คณะแพทยศาสตร ศ ร ราชพยาบาล Dysphagia in Stroke The incidence of dysphagia after stroke ranging from 23-50% 1 Location
ORIGINAL ARTICLE. Synchronous Airway Lesions and Outcomes in Infants With Severe Laryngomalacia Requiring Supraglottoplasty
 ORIGINAL ARTICLE Synchronous Airway Lesions and Outcomes in Infants With Severe Laryngomalacia Requiring Supraglottoplasty James W. Schroeder Jr, MD; Naveen D. Bhandarkar, MD; Lauren D. Holinger, MD Objective:
ORIGINAL ARTICLE Synchronous Airway Lesions and Outcomes in Infants With Severe Laryngomalacia Requiring Supraglottoplasty James W. Schroeder Jr, MD; Naveen D. Bhandarkar, MD; Lauren D. Holinger, MD Objective:
COMMUNICATION. Communication and Swallowing post Tracheostomy. Role of SLT. Impact of Tracheostomy. Normal Speech. Facilitating Communication
 Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
Communication and Swallowing post Tracheostomy. Role of SLT 1. 2. 3. Management of communication needs. Management of swallowing issues. Working with the multidisciplinary team to facilitate weaning. Impact
The Role of the Speech Language Pathologist & Spinal Cord Injury
 The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
The Role of the Speech Language Pathologist & Spinal Cord Injury Facts According to the National Spinal Cord Injury Statistical Center (NSCISC) there are approxiamtely 12,000 new spinal cord injuries (SCI)
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes
 Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
Evidence-Based Swallowing Related Issues in Patients with Tracheotomy Tubes Steven B. Leder, Ph.D. Yale University School of Medicine Debra M. Suiter,, Ph.D. University of Memphis Impetus Swallowing Rx
Understanding your child s videofluoroscopic swallow study report
 Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Understanding your child s videofluoroscopic swallow study report This leaflet is given to you during your child s appointment in order to explain some of the words used by the speech and language therapist
Symptoms such as heartburn, pyrosis, and acid regurgitation
 CLINICAL INVESTIGATIONS 99m Tc-Sulfur Colloid Gastroesophageal Scintigraphy with Late Lung Imaging to Evaluate Patients with Posterior Laryngitis Alberto Bestetti, Federica Carola, PierMarziano Carnevali-Ricci,
CLINICAL INVESTIGATIONS 99m Tc-Sulfur Colloid Gastroesophageal Scintigraphy with Late Lung Imaging to Evaluate Patients with Posterior Laryngitis Alberto Bestetti, Federica Carola, PierMarziano Carnevali-Ricci,
Tracheostomy in pediatric. Tran Quoc Huy, MD ENT department
 Tracheostomy in pediatric Tran Quoc Huy, MD ENT department 1. History 2. Indication 3. Tracheostomy vs Tracheal intubation 4. A systematic review 5. Decannulation 6. Swallowing 7. Communication concerns
Tracheostomy in pediatric Tran Quoc Huy, MD ENT department 1. History 2. Indication 3. Tracheostomy vs Tracheal intubation 4. A systematic review 5. Decannulation 6. Swallowing 7. Communication concerns
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant. Tara Brennan, MD 2,3
 Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Multilevel airway obstruction including rare tongue base mass presenting as severe croup in an infant Tara Brennan, MD 2,3 Jeffrey C. Rastatter, MD, FAAP 1,2 1 Department of Otolaryngology, Northwestern
Neonatal Airway Disorders, Treatments, and Outcomes. Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center
 Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
Neonatal Airway Disorders, Treatments, and Outcomes Steven Goudy, MD Pediatric Otolaryngology Emory University Medical Center Disclosure I have nothing to disclose Neonatal and Pediatric Tracheostomy Tracheostomy
MULTIPLE reports have. Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer ORIGINAL ARTICLE
 ORIGINAL ARTICLE Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer Arie Rosen, MD; Thomas H. Rhee, MD; Rene Kaufman, MS, CCC-SLP Objectives: To determine
ORIGINAL ARTICLE Prediction of Aspiration in Patients With Newly Diagnosed Untreated Advanced Head and Neck Cancer Arie Rosen, MD; Thomas H. Rhee, MD; Rene Kaufman, MS, CCC-SLP Objectives: To determine
Respiratory Compromise and Swallowing
 Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Speech Pathology and Respiratory Care April 11, 2013 By Angela Parcaro-Tucker, MA, CCC-SLP, LSVT How can Speech Therapy help? 1 Respiratory Compromise and Swallowing Swallowing is a complex sequence of
Postoperative Assessment of Laryngopharyngeal Dysfunction in Neonates After Norwood Operation
 ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
ORIGINAL ARTICLES: SURGERY: The Annals of Thoracic Surgery CME Program is located online at http://cme.ctsnetjournals.org. To take the CME activity related to this article, you must have either an STS
Oral care & swallowing
 Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Oral care & swallowing Oral care is important as it has a role to play in preventing healthcare associated infections. Dental plaque and the oropharynx can become colonized by bacteria and a biofilm can
Min Hur, Eun-Hee Kim, In-Kyung Song, Ji-Hyun Lee, Hee-Soo Kim, and Jin Tae Kim INTRODUCTION. Clinical Research
 Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Anesth Pain Med 2016; 11: 375-379 https://doi.org/10.17085/apm.2016.11.4.375 Clinical Research http://crossmark.crossref.org/dialog/?doi=10.17085/apm.2016.11.4.375&domain=pdf&date_stamp=2016-10-25 pissn
Applied physiology. 7- Apr- 15 Swallowing Course/ Anatomy and Physiology
 Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
Applied physiology Temporal measures: Oral Transit Time (OTT) Pharyngeal Delay Time (PDT) Pharyngeal Transit Time (PTT) Oropharyngeal Swallowing Efficiency Score (OPSE score) 7- Apr- 15 Swallowing Course/
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY
 SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
SWALLOW PHYSIOLOGY IN PATIENTS WITH TRACH CUFF INFLATED OR DEFLATED: A RETROSPECTIVE STUDY Ruiying Ding, PhD, 1 Jeri A. Logemann, PhD 2 1 University of Wisconsin-Whitewater, Department of Communicative
Department of Occupational Therapy, Graduate School of Yonsei University, Wonju, Korea
 Original Article Ann Rehabil Med 2014;38(5):612-619 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.5.612 Annals of Rehabilitation Medicine Cutoff Value of Pharyngeal Residue in
Original Article Ann Rehabil Med 2014;38(5):612-619 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2014.38.5.612 Annals of Rehabilitation Medicine Cutoff Value of Pharyngeal Residue in
Department of Rehabilitation Medicine, CHA Bundang Medical Center, CHA University, Seongnam, Korea
 Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
Original Article Ann Rehabil Med 2015;39(4):624-629 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.4.624 Annals of Rehabilitation Medicine Gross Motor Function Outcome After Intensive
What are the Challenges? Spreading the Word in NICU. Need for NICU Care: Impact. Baby Trachs: Use of the Passy Muir Valve in the NICU to
 What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
What are the Challenges? Baby Trachs: Use of the Passy Muir Valve in the NICU to Optimize Swallowing and Feeding Catherine S Shaker, MS/CCC SLP, BRS S and Cari Mutnick, MS/CCC SLP Florida Hospital for
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation David A. Muir Course Outline Physiology of Swallow
 Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
Swallow Function: Passy-Muir Valve Use for Evaluation & Rehabilitation Mary Spremulli, MA, CCC-SLP Passy-Muir Clinical Consultant spre713@hotmail.com (949) 833-8255 David A. Muir 23 year-old ventilator
The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effect of a Speaking Valve on Laryngeal Aspiration and Penetration in Children With Tracheotomies Julina
The Ability of the Eating Assessment Tool-10 to Detect Aspiration in Patients With Neurological Disorders
 JNM J Neurogastroenterol Motil, Vol. 23 No. 4 October, 2017 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/10.5056/jnm16165 Original Article The Ability of the Eating Assessment Tool-10 to Detect Aspiration
JNM J Neurogastroenterol Motil, Vol. 23 No. 4 October, 2017 pissn: 2093-0879 eissn: 2093-0887 https://doi.org/10.5056/jnm16165 Original Article The Ability of the Eating Assessment Tool-10 to Detect Aspiration
ORIGINAL ARTICLE. Correlation of Findings at Direct Laryngoscopy and Bronchoscopy With Gastroesophageal Reflux Disease in Children
 Correlation of Findings at Direct Laryngoscopy and Bronchoscopy With Gastroesophageal Reflux Disease in Children A Prospective Study ORIGINAL ARTICLE Michele M. Carr, DDS, MD, MEd, FRCSC; Mark L. Nagy,
Correlation of Findings at Direct Laryngoscopy and Bronchoscopy With Gastroesophageal Reflux Disease in Children A Prospective Study ORIGINAL ARTICLE Michele M. Carr, DDS, MD, MEd, FRCSC; Mark L. Nagy,
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA
 TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
TREATMENT OF DYSPHAGIA IN PATIENTS AFTER STROKE IN ESTONIA ANNE URIKO SPORTS MEDICINE AND REHABILITATION CLINIG OF TARTU UNIVERSITY HOSPITAL 17.09.2010 DYSPHAGIA DIFFICULTY MOVING FOOD FROM MOUTH TO STOMACH
Dysphagia in Tongue Cancer Patients Yu Ri Son, MD, Kyoung Hyo Choi, MD, PhD, Tae Gyun Kim, MD
 Original Article Ann Rehabil Med 2015;39(2):210-217 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.2.210 Annals of Rehabilitation Medicine Dysphagia in Tongue Cancer Patients Yu
Original Article Ann Rehabil Med 2015;39(2):210-217 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2015.39.2.210 Annals of Rehabilitation Medicine Dysphagia in Tongue Cancer Patients Yu
Mapping Regional Laryngopharyngeal Mechanoreceptor Response
 Original Article Clinical and Experimental Otorhinolaryngology Vol. 7, No. 4: 319-323, December 2014 http://dx.doi.org/10.3342/ceo.2014.7.4.319 pissn 1976-8710 eissn 2005-0720 Mapping Regional Laryngopharyngeal
Original Article Clinical and Experimental Otorhinolaryngology Vol. 7, No. 4: 319-323, December 2014 http://dx.doi.org/10.3342/ceo.2014.7.4.319 pissn 1976-8710 eissn 2005-0720 Mapping Regional Laryngopharyngeal
Relation between the Peripherofacial Psoriasis and Scalp Psoriasis
 pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
pissn 1013-9087ㆍeISSN 2005-3894 Ann Dermatol Vol. 28, No. 4, 2016 http://dx.doi.org/10.5021/ad.2016.28.4.422 ORIGINAL ARTICLE Relation between the Peripherofacial Psoriasis and Scalp Psoriasis Kyung Ho
copyrighted material by PRO-ED, Inc.
 CONTENTS Preface xi Chapter 1 Introduction: Definitions and Basic Principles of Evaluation and Treatment of Swallowing Disorders Signs and Symptoms of Dysphagia Screening: Identifying the Patient at High
CONTENTS Preface xi Chapter 1 Introduction: Definitions and Basic Principles of Evaluation and Treatment of Swallowing Disorders Signs and Symptoms of Dysphagia Screening: Identifying the Patient at High
Aerodigestive Disorders in the NICU. Dawn Simon, M.D Associate Professor in Pediatrics Attending in Pediatric Pulmonary Medicine
 Aerodigestive Disorders in the NICU Dawn Simon, M.D. 2016 Associate Professor in Pediatrics Attending in Pediatric Pulmonary Medicine Dawn M. Simon, M.D. Personal/Professional Financial Relationships with
Aerodigestive Disorders in the NICU Dawn Simon, M.D. 2016 Associate Professor in Pediatrics Attending in Pediatric Pulmonary Medicine Dawn M. Simon, M.D. Personal/Professional Financial Relationships with
Case Presentation Topic: Difficult to Ventilate Difficult to Intubate
 Case Presentation Topic: Difficult to Ventilate Difficult to Intubate Dr. K. Shruthi Jeevan 1 st Year Post Graduate Department of Anaesthesiology CASE SCENARIO : 1 A 65 years old female patient, resident
Case Presentation Topic: Difficult to Ventilate Difficult to Intubate Dr. K. Shruthi Jeevan 1 st Year Post Graduate Department of Anaesthesiology CASE SCENARIO : 1 A 65 years old female patient, resident
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP
 DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
DYSPHAGIA MANAGEMENT IN ACUTE CARE AMANDA HEREFORD, MA, CCC- SLP OVERVIEW Decision making re: swallowing in the medically compromised patient Swallow evaluation vs. Nursing Swallow Screening Instrumental
Airway Management in the ICU
 Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
Airway Management in the ICU New developments in management of epistaxis. April 28, 2008 Methods of airway control Non surgical BIPAP CPAP Mask ventilation Laryngeal Mask Intubation Surgical Cricothyrotomy
15/11/2011. Swallowing
 Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Swallowing Swallowing starts from placement of the food in the mouth and continues until food enters the stomach. Dysphagia: any difficulty in moving food from mouth to stomach. Pharynx is shared for both
Domino KB: Closed Malpractice Claims for Airway Trauma During Anesthesia. ASA Newsletter 62(6):10-11, 1998.
 Citation Domino KB: Closed Malpractice Claims for Airway Trauma During Anesthesia. ASA Newsletter 62(6):1-11, 18. Full Text As experts in airway management, anesthesiologists are at risk for liability
Citation Domino KB: Closed Malpractice Claims for Airway Trauma During Anesthesia. ASA Newsletter 62(6):1-11, 18. Full Text As experts in airway management, anesthesiologists are at risk for liability
THE COMPLEX PUZZLE OF MANAGING THE ELDERLY BURN PATIENT:
 THE COMPLEX PUZZLE OF MANAGING THE ELDERLY BURN PATIENT: BURN LOCATION IS IRRELEVANT TO RISK FOR DYSPHAGIA AND ITS COMPLICATIONS IN PATIENTS OVER 75 YEARS Nicola Clayton 1,2,3, Caroline Nicholls 2,4, Karen
THE COMPLEX PUZZLE OF MANAGING THE ELDERLY BURN PATIENT: BURN LOCATION IS IRRELEVANT TO RISK FOR DYSPHAGIA AND ITS COMPLICATIONS IN PATIENTS OVER 75 YEARS Nicola Clayton 1,2,3, Caroline Nicholls 2,4, Karen
Case Report. Annals of Rehabilitation Medicine INTRODUCTION
 Case Report Ann Rehabil Med 2013;37(3):438-442 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.3.438 Annals of Rehabilitation Medicine Traumatic Atlanto-Occipital Dislocation Presenting
Case Report Ann Rehabil Med 2013;37(3):438-442 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.3.438 Annals of Rehabilitation Medicine Traumatic Atlanto-Occipital Dislocation Presenting
2013 Charleston Swallowing Conference
 Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 13 Trachs, Tubes And Vents: Frequently Asked Questions 1:30-3:00pm
Providing Quality Affordable Continuing Education and Treatment Materials for over 30 years. 2013 Charleston Swallowing Conference Session 13 Trachs, Tubes And Vents: Frequently Asked Questions 1:30-3:00pm
Issues in Enteral Feeding: Aspiration
 Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
Issues in Enteral Feeding: Aspiration A webinar for HealthTrust Members February 11, 2019 Co-sponsored by HealthTrust and V NOS Continuing Education Provider Presented by: Kathleen Stoessel, RN, BSN, MS
Unilateral Supraglottoplasty for Severe Laryngomalacia in Children. Nasser A Fageeh, MD, FRCSC, FACS*
 Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
Bahrain Medical Bulletin, Vol. 37, No. 1, March 2015 Unilateral Supraglottoplasty for Severe Laryngomalacia in Children Nasser A Fageeh, MD, FRCSC, FACS* Objective: To study the efficacy of Unilateral
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA
 AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
AIRWAY MANAGEMENT SUZANNE BROWN, CRNA OBJECTIVE OF LECTURE Non Anesthesia Sedation Providers Review for CRNA s Informal Questions encouraged 2 AIRWAY MANAGEMENT AWARENESS BASICS OF ANATOMY EQUIPMENT 3
Supplementary Motor Area Syndrome and Flexor Synergy of the Lower Extremities Ju Seok Ryu, MD 1, Min Ho Chun, MD 2, Dae Sang You, MD 2
 Case Report Ann Rehabil Med 2013;37(5):735-739 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.735 Annals of Rehabilitation Medicine Supplementary Motor Area Syndrome and Flexor
Case Report Ann Rehabil Med 2013;37(5):735-739 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.5.735 Annals of Rehabilitation Medicine Supplementary Motor Area Syndrome and Flexor
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy
 Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Tracheostomy and Ventilator Education Program Module 2: Respiratory Anatomy Disclaimer This material is intended for use by trained family members and caregivers of children with tracheostomies who are
Postoperative swallowing function after posterior fossa tumor resection in pediatric patients
 Childs Nerv Syst (2006) 22: 1296 1300 DOI 10.1007/s00381-006-0065-z ORIGINAL PAPER Lisa A. Newman Frederick A. Boop Robert A. Sanford Jerome W. Thompson Carrie K. Temple Christopher D. Duntsch Postoperative
Childs Nerv Syst (2006) 22: 1296 1300 DOI 10.1007/s00381-006-0065-z ORIGINAL PAPER Lisa A. Newman Frederick A. Boop Robert A. Sanford Jerome W. Thompson Carrie K. Temple Christopher D. Duntsch Postoperative
Airway Workshop Lecture. University of Ottawa
 Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
Airway Workshop Lecture Department of Anesthesiology University of Ottawa Overview Ventilation Airway assessment Difficult airways Airway management equipment aids Intubation/Improving Intubation Success
Implementing Cough Reflex Testing in a clinical pathway for acute stroke: A pragmatic randomised control trial
 Implementing Cough Reflex Testing in a clinical pathway for acute stroke: A pragmatic randomised control trial Makaela Field 1, Rachel Wenke 1,2, Arman Sabet 1, Melissa Lawrie 1,2, Elizabeth Cardell 2
Implementing Cough Reflex Testing in a clinical pathway for acute stroke: A pragmatic randomised control trial Makaela Field 1, Rachel Wenke 1,2, Arman Sabet 1, Melissa Lawrie 1,2, Elizabeth Cardell 2
Validation of the Yale Swallow Protocol: A Prospective Double-Blinded Videofluoroscopic Study
 Dysphagia (2014) 29:199 203 DOI 10.1007/s00455-013-9488-3 ORIGINAL ARTICLE Validation of the Yale Swallow Protocol: A Prospective Double-Blinded Videofluoroscopic Study Debra M. Suiter JoAnna Sloggy Steven
Dysphagia (2014) 29:199 203 DOI 10.1007/s00455-013-9488-3 ORIGINAL ARTICLE Validation of the Yale Swallow Protocol: A Prospective Double-Blinded Videofluoroscopic Study Debra M. Suiter JoAnna Sloggy Steven
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE?
 PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
PMV ON OR OFF WITH SWALLOWING DOES IT MAKE A DIFFERENCE? 1 Tedd Masiongale, MA, CCC-SLP Lorry Lewis, MS, CCC-SLP REASON FOR STUDY After several years of working with trach and ventilator dependent patients,
Advanced Airway Management. University of Colorado Medical School Rural Track
 Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Advanced Airway Management University of Colorado Medical School Rural Track Advanced Airway Management Basic Airway Management Airway Suctioning Oxygen Delivery Methods Laryngeal Mask Airway ET Intubation
Pediatric Fiberoptic Endoscopic Evaluation of Swallowing (FEES) When, Where, How, & Who?
 Pediatric Fiberoptic Endoscopic Evaluation of Swallowing (FEES) When, Where, How, & Who? Claire Kane Miller, PhD CCC/SLP, BRS-S J. Paul Willging, MD Professor, Pediatric Otolaryngology, Head and Neck Surgery
Pediatric Fiberoptic Endoscopic Evaluation of Swallowing (FEES) When, Where, How, & Who? Claire Kane Miller, PhD CCC/SLP, BRS-S J. Paul Willging, MD Professor, Pediatric Otolaryngology, Head and Neck Surgery
Evaluation of oropharyngeal dysphagia: which diagnostic tool is superior? Susan E. Langmore
 Evaluation of oropharyngeal dysphagia: which diagnostic tool is superior? Susan E. Langmore Purpose of review As flexible endoscopic examinations of swallowing become more widely used to evaluate patients
Evaluation of oropharyngeal dysphagia: which diagnostic tool is superior? Susan E. Langmore Purpose of review As flexible endoscopic examinations of swallowing become more widely used to evaluate patients
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital.
 Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
Risk Factors of Early Complications of Tracheostomy at Kenyatta National Hospital. G. Karuga 1, H. Oburra 2, C. Muriithi 3. 1 Resident Ear Nose & Throat (ENT) Head & Neck Department. University of Nairobi
Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia
 NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
NATIONAL INSTITUTE FOR HEALTH AND CARE EXCELLENCE Interventional procedure consultation document Endoscopic carbon dioxide laser cricopharyngeal myotomy for relief of oropharyngeal dysphagia Difficulty
ORIGINAL ARTICLE. Use of Rigid and Flexible Bronchoscopy Among Pediatric Otolaryngologists. widely used in the diagnosis and treatment of disorders
 ORIGINAL ARTICLE Use of Rigid and Flexible Among Pediatric Otolaryngologists Seth Cohen, MPH, MD; Harold Pine, MD; Amelia Drake, MD Objective: To explore how rigid and flexible bronchoscopy are used in
ORIGINAL ARTICLE Use of Rigid and Flexible Among Pediatric Otolaryngologists Seth Cohen, MPH, MD; Harold Pine, MD; Amelia Drake, MD Objective: To explore how rigid and flexible bronchoscopy are used in
Clearing the air.. How to assist and rescue neck breathing patients. Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA
 Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
Clearing the air.. How to assist and rescue neck breathing patients Presented by: Don Hall MCD, CCC/SLP Sarah Markel RRT, MHA Learning Objectives Define common terms identified with total (laryngectomy)
The Effects of Topical Anesthetic on Swallowing During Nasoendoscopy
 The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effects of Topical Anesthetic on Swallowing During Nasoendoscopy Scott Lester, BS; Susan E. Langmore,
The Laryngoscope VC 2013 The American Laryngological, Rhinological and Otological Society, Inc. The Effects of Topical Anesthetic on Swallowing During Nasoendoscopy Scott Lester, BS; Susan E. Langmore,
Analyzing Swallow Studies in Pediatrics
 Analyzing Swallow Studies in Pediatrics About the Speaker Robert Beecher, M.S., CCC-SLP was formerly senior speech-language pahologist at the Children's Hospital of Wisconsin in Milwaukee. He is specialized
Analyzing Swallow Studies in Pediatrics About the Speaker Robert Beecher, M.S., CCC-SLP was formerly senior speech-language pahologist at the Children's Hospital of Wisconsin in Milwaukee. He is specialized
Complex Decision Making in Pediatric Dysphagia
 Complex Decision Making in Pediatric Dysphagia Alana Lowry, MS, CCC-SLP Fletcher Allen Health Care Kara Fletcher Larson, MS, CCC-SLP Jennifer Miller, MS, CCC-SLP Children s s Hospital Boston ASHA November
Complex Decision Making in Pediatric Dysphagia Alana Lowry, MS, CCC-SLP Fletcher Allen Health Care Kara Fletcher Larson, MS, CCC-SLP Jennifer Miller, MS, CCC-SLP Children s s Hospital Boston ASHA November
Review of dysphagia in poststroke
 Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Review of dysphagia in poststroke patients Danielle Thompson, Speech and Language Therapist Northwick Park Hospital With acknowledgement to Mary McFarlane, Principal Speech and Language Therapist, Acute
Extraesophageal Manifestations of GERD in Children
 Extraesophageal Manifestations of GERD in Children Jose Luis Martinez, M.D. Associate Professor University of California San Francisco Director Endoscopy Unit Children s Hospital Central California Overview
Extraesophageal Manifestations of GERD in Children Jose Luis Martinez, M.D. Associate Professor University of California San Francisco Director Endoscopy Unit Children s Hospital Central California Overview
Anatomy and Physiology. The airways can be divided in to parts namely: The upper airway. The lower airway.
 Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Airway management Anatomy and Physiology The airways can be divided in to parts namely: The upper airway. The lower airway. Non-instrumental airway management Head Tilt and Chin Lift Jaw Thrust Advanced
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Afferent nerves, interactions of, in cough, 20 21 Airway, eosinophilic inflammation of, 124 narrowing of, in asthma, 126 protection of, terms
Note: Page numbers of article titles are in boldface type. A Afferent nerves, interactions of, in cough, 20 21 Airway, eosinophilic inflammation of, 124 narrowing of, in asthma, 126 protection of, terms
Acquired pediatric esophageal diseases Imaging approaches and findings. M. Mearadji International Foundation for Pediatric Imaging Aid
 Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Acquired pediatric esophageal diseases Imaging approaches and findings M. Mearadji International Foundation for Pediatric Imaging Aid Acquired pediatric esophageal diseases The clinical signs of acquired
Accuracy of Fiberoptic Nasopharyngoscopy in the Diagnosis of Pharyngolaryngeal Diseases
 FIBEROPTIC THE IRAQI POSTGRADUATE NASOPHARYNGOSCOPY MEDICAL JOURNAL Accuracy of Fiberoptic Nasopharyngoscopy in the Diagnosis of Pharyngolaryngeal Diseases Ragheed Turky Miteab ABSTRACT: BACKGROUND: In
FIBEROPTIC THE IRAQI POSTGRADUATE NASOPHARYNGOSCOPY MEDICAL JOURNAL Accuracy of Fiberoptic Nasopharyngoscopy in the Diagnosis of Pharyngolaryngeal Diseases Ragheed Turky Miteab ABSTRACT: BACKGROUND: In
8/8/2013. Disclaimer. Tracheostomy Care in the Home. Polling Question 1. Upper Airway and Respiratory System
 Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Disclaimer Appendix 3 Declaration of Vested Interest Form Name of presenter: Heather Murgatroyd RRT RPSGT Name of employer: DeVilbiss Healthcare Tracheostomy Care in the Home Heather Murgatroyd, RRT, RPSGT
Reluctance or refusal to feed or eat. Understanding Feeding Aversion in a City Full of Foodies. Presentation Outline. Learning Objectives
 Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
Understanding Feeding Aversion in a City Full of Foodies Amy Houtrow, MD, MPH Pediatric Physical Medicine & Rehabilitation UCSF Department of Pediatrics June 2, 2007 Learning Objectives Learners will be
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS
 SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
SUPER-SUPRAGLOTTIC SWALLOW IN IRRADIATED HEAD AND NECK CANCER PATIENTS Jeri A. Logemann, PhD, 1 Barbara Roa Pauloski, PhD, 1 Alfred W. Rademaker, PhD, 2 Laura A. Colangelo, MS 2 1 Department of Communication
FLEXIBLE FIBREOPTIC BRONCHOSCOPY IN 582 CHILDREN-VALUE OF ROUTE, SEDATION AND LOCAL ANESTHETIC
 FLEXIBLE FIBREOPTIC BRONCHOSCOPY IN 582 CHILDREN-VALUE OF ROUTE, SEDATION AND LOCAL ANESTHETIC N. Somu D. Vijayasekaran T.P. Ashok A. Balachandran L. Subramanyam ABSTRACT The value of route, sedation and
FLEXIBLE FIBREOPTIC BRONCHOSCOPY IN 582 CHILDREN-VALUE OF ROUTE, SEDATION AND LOCAL ANESTHETIC N. Somu D. Vijayasekaran T.P. Ashok A. Balachandran L. Subramanyam ABSTRACT The value of route, sedation and
Interesting Case Series. Pulmonary Injury Secondary to Feeding Tube Misplacement
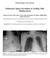 Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Interesting Case Series Pulmonary Injury Secondary to Feeding Tube Misplacement Thomas R. Resch, MD, Leigh A. Price, MD, and Stephen M. Milner, MBBS, BDS, FRCS (Ed), FACS Johns Hopkins Burn Center, The
Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori
 Gut and Liver, Vol. 6, No. 2, April 2012, pp. 270-274 CASE REPORT Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori Soo-Kyung Park, Hwoon-Yong Jung, Do Hoon Kim,
Gut and Liver, Vol. 6, No. 2, April 2012, pp. 270-274 CASE REPORT Regression of Advanced Gastric MALT Lymphoma after the Eradication of Helicobacter pylori Soo-Kyung Park, Hwoon-Yong Jung, Do Hoon Kim,
Laryngomalacia and Swallowing Function in Children
 The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Laryngomalacia and Swallowing Function in Children Jeffrey P. Simons,
The Laryngoscope VC 2015 The American Laryngological, Rhinological and Otological Society, Inc. TRIOLOGICAL SOCIETY CANDIDATE THESIS Laryngomalacia and Swallowing Function in Children Jeffrey P. Simons,
Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010
 Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Original Article Endocrinol Metab 2014;29:530-535 http://dx.doi.org/10.3803/enm.2014.29.4.530 pissn 2093-596X eissn 2093-5978 Standardized Thyroid Cancer Mortality in Korea between 1985 and 2010 Yun Mi
Prior Authorization Review Panel MCO Policy Submission
 Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
Prior Authorization Review Panel MCO Policy Submission A separate copy of this form must accompany each policy submitted for review. Policies submitted without this form will not be considered for review.
The Clinical Swallow Evaluation: What it can and cannot tell us. Introduction
 The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
The Clinical Swallow Evaluation: What it can and cannot tell us Debra M. Suiter, Ph.D., CCC-SLP, BCS-S Director, Voice & Swallow Clinic Associate Professor, Division of Communication Sciences & Disorders
Randall J. Amis *, Deepak Gupta *, Jayme R. Dowdall **, Abstract. Introduction
 Ultrasound assessment of Vocal Fold Paresis: A Correlation Case Series with Flexible Fiberoptic Laryngoscopy and Adding the Third Dimension (3-D) to Vocal Fold Mobility Assessment Randall J. Amis *, Deepak
Ultrasound assessment of Vocal Fold Paresis: A Correlation Case Series with Flexible Fiberoptic Laryngoscopy and Adding the Third Dimension (3-D) to Vocal Fold Mobility Assessment Randall J. Amis *, Deepak
Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal and Anterior Mediastinal Abscess
 Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
Hindawi Case Reports in Pediatrics Volume 2017, Article ID 1848945, 4 pages https://doi.org/10.1155/2017/1848945 Case Report Complete Obstruction of Endotracheal Tube in an Infant with a Retropharyngeal
Subject Index. Bacterial infection, see Suppurative lung disease, Tuberculosis
 Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Subject Index Abscess, virtual 107 Adenoidal hypertrophy, features 123 Airway bleeding, technique 49, 50 Airway stenosis, see Stenosis, airway Anaesthesia biopsy 47 complications 27, 28 flexible 23 26
Original Article. Annals of Rehabilitation Medicine INTRODUCTION
 Original Article Ann Rehabil Med 2013;37(2):183-190 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.2.183 Annals of Rehabilitation Medicine The Cervical Range of Motion as a Factor
Original Article Ann Rehabil Med 2013;37(2):183-190 pissn: 2234-0645 eissn: 2234-0653 http://dx.doi.org/10.5535/arm.2013.37.2.183 Annals of Rehabilitation Medicine The Cervical Range of Motion as a Factor
Objectives. Module A2: Upper Airway Anatomy & Physiology. Function of the Lungs/Heart. The lung is for gas exchange. Failure of the Lungs/Heart
 Module A2: Upper Airway Anatomy & Physiology Objectives Classify epithelial tissue based on cell type and tissue layers. Identify location of tissue epithelium in the respiratory system. Describe the major
Module A2: Upper Airway Anatomy & Physiology Objectives Classify epithelial tissue based on cell type and tissue layers. Identify location of tissue epithelium in the respiratory system. Describe the major
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010
 Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Compliance Department ELEMENTS OF EAR, NOSE AND THROAT EXAMINATION 11/2010 System/ Body Area Constitutional Measurement of any three of the following seven vital signs: 1) sitting or standing blood pressure,
Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10
 GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
GBMC Stroboscopy Rounds October 12, 2007 Case Presentation JC: 65 y/o retired plumber CC: Hoarseness HPI: Admitted to a local hospital on May 30 for severe pneumonia. Intubated in ICU for 10 days, total
Dysphagia and Swallowing. Jan Adams, DNP, MPA, RN and Karen Kern
 Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Dysphagia and Swallowing Jan Adams, DNP, MPA, RN and Karen Kern Scope of the Problem and Incidence 15 million people in the US have some form of Dysphagia. Every year, 1 million people are diagnosed with
Endoscopic Posterior Cricoid Split with Costal Cartilage Graft: A Fifteen Year Experience
 1 Endoscopic Posterior Cricoid Split with Costal Cartilage Graft: A Fifteen Year Experience John P. Dahl, MD, PhD, MBA 1,2, *, Patricia L. Purcell, MD 1, MPH, Sanjay R. Parikh, MD, FACS 1, and Andrew F.
1 Endoscopic Posterior Cricoid Split with Costal Cartilage Graft: A Fifteen Year Experience John P. Dahl, MD, PhD, MBA 1,2, *, Patricia L. Purcell, MD 1, MPH, Sanjay R. Parikh, MD, FACS 1, and Andrew F.
IVOR LEWIS Esophagogastrectomy
 IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
IVOR LEWIS Esophagogastrectomy SPEECH-LANGUAGE PATHOLOGY S ROLE MAGGIE BOYD, MS, CCC/SLP Biography Maggie Boyd, MS, CCC-SLP is a dysphagia clinical specialist at UAB hospital. She has 14 years clinical
Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis
 Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
Otolaryngology Head and Neck Surgery (2006) 135, 318-322 ORIGINAL RESEARCH Pediatric partial cricotracheal resection: A new technique for the posterior cricoid anastomosis Mark E. Boseley, MD, and Christopher
TRACHEOSTOMY. Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion
 TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
TRACHEOSTOMY Definition Tracheostomy means creation an artificial opening in the trachea with tracheostomy tube insertion Indications for tracheostomy 1-upper airway obstruction with stridor, air hunger,
VIDEOFLUOROSCOPIC SWALLOWING EXAM
 VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
VIDEOFLUOROSCOPIC SWALLOWING EXAM INDENTIFYING INFORMATION May include the following: Name, ID/medical record number, date of birth, date of exam, referred by, reason for referral HISTORY/SUBJECTIVE INFORMATION
Infant Videofluoroscopic Swallow Study Testing, Swallowing Interventions, and Future Acute Respiratory Illness
 RESEARCH ARTICLE Infant Videofluoroscopic Swallow Study Testing, Swallowing Interventions, and Future Acute Respiratory Illness Eric R. Coon, MD, MSCI, a Rajendu Srivastava, MD, FRCPC, MPH, a,b Gregory
RESEARCH ARTICLE Infant Videofluoroscopic Swallow Study Testing, Swallowing Interventions, and Future Acute Respiratory Illness Eric R. Coon, MD, MSCI, a Rajendu Srivastava, MD, FRCPC, MPH, a,b Gregory
Airway Anatomy. Soft palate. Hard palate. Nasopharynx. Tongue. Oropharynx. Hypopharynx. Thyroid cartilage
 Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
Airway Anatomy Hard palate Soft palate Tongue Nasopharynx Oropharynx Hypopharynx Thyroid cartilage Airway Anatomy Hyoid bone Thyroid cartilage Cricoid cartilage Trachea Cricothyroid membrane Airway Anatomy
The surgical management of subglottic stenosis (SGS)
 Original Research Pediatric Otolaryngology Short- versus Long-term Stenting in Children with Subglottic Stenosis Undergoing Laryngotracheal Reconstruction Otolaryngology Head and Neck Surgery 2018, Vol.
Original Research Pediatric Otolaryngology Short- versus Long-term Stenting in Children with Subglottic Stenosis Undergoing Laryngotracheal Reconstruction Otolaryngology Head and Neck Surgery 2018, Vol.
Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
 National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
National Multiple Sclerosis Society 733 Third Avenue New York, NY 10017-3288 Clinical Bulletin Information for Health Professionals Swallowing Disorders and Their Management in Patients with Multiple Sclerosis
Audra Fuller MD, Mark Sigler MD, Shrinivas Kambali MD, Raed Alalawi MD
 Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Clinical Series Successful treatment of post-intubation tracheal stenosis with balloon dilation, argon plasma coagulation, electrocautery and application of mitomycin C Audra Fuller MD, Mark Sigler MD,
Safety of flexible endoscopic biopsy of the pharynx and larynx under topical anesthesia
 Eur Arch Otorhinolaryngol (2017) 274:3471 3476 DOI 10.1007/s00405-017-4647-z HEAD AND NECK Safety of flexible endoscopic biopsy of the pharynx and larynx under topical anesthesia David J. Wellenstein 1
Eur Arch Otorhinolaryngol (2017) 274:3471 3476 DOI 10.1007/s00405-017-4647-z HEAD AND NECK Safety of flexible endoscopic biopsy of the pharynx and larynx under topical anesthesia David J. Wellenstein 1
