Anterior Stabilisation of the shoulder
|
|
|
- Rodney Green
- 6 years ago
- Views:
Transcription
1 Information for you after your operation Anterior Stabilisation of the shoulder If you require this leaflet in any other format, eg, large print, please telephone Leaflet No /09 16
2 This information booklet has been produced to help you gain the maximum benefit after your operation. It is not a substitute for professional medical care and should be used in association with treatment at the Orthopaedic Clinic. Individual variations requiring specific instructions not mentioned here may be required. Who to contact if you are worried or require further information For general enquiries about appointments, please phone: Mr Smibert s secretary on: Mr Chambler s secretary on: For enquiries regarding admission dates, please phone the Admissions Office on: This booklet was compiled by: Jane Moser (Senior Physiotherapist) Professor Andrew Carr (Orthopaedic Surgeon) Louise Le Good (Senior Occupational Therapist) At the Nuffield Orthopaedic Centre, Oxford. Help and feedback was given from people who have had shoulder stabilisation surgery If your wound changes in appearance, weeps fluid or pus, or you feel unwell with a high temperature, contact your GP. If you have a query about exercises or movements, contact the Physiotherapy department where you are having treatment if you have already started, or else the Yeovil Physiotherapy Department on For queries regarding self care (eg, dressing, bathing) contact the Occupational Therapy Department on Patients may be contacted by post and requested to complete and return a questionnaire. This is useful for the surgical team, for monitoring patients progress and may save an unnecessary visit to the hospital. We would like to thank the Nuffield Orthopaedic Centre (Upper Limb Clinic) for allowing us to re-produce the information in this leaflet. 2 15
3 Stand facing a wall. Keep arm close to side and elbow bent to 90. Push your fist into the wall but do not let arm move. Hold for 10 seconds. Repeat 30 times. The above section of exercises work the muscles without the joint moving. These can be progressed to using elastic exercise bands, so the muscles work with the joint moving. Kneeling on all fours. Gently rock forwards taking the weight of your body through your arms. Progress to lifting your unaffected arm up in the air (in different directions). Repeat times. Contents Page The Shoulder 4 Shoulder dislocation 4 About your shoulder stabilisation operation 5 The risks and complications 5 Common questions about a) pain 6 b) the sling 6 c) exercises 6 d) wound care 7 Press ups. Start by doing these against a wall. Keep back straight. Progress to doing from your knees. Keep your elbows under your body, rather than out to the side. Repeat times. e) returning to the hospital 7 f) things to avoid 8 g) how you may progress 8 h) return to work 10 i) return to driving 10 Phase 3 exercises (8-12 weeks after your operation) These will concentrate on increasing the strength and mobility around your shoulder. The exercise will be selected for your individual shoulder and lifestyle. j) leisure activities 10 Exercises 11 Contact points for further information
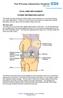
4 The shoulder The shoulder joint is a ball and socket joint. Most shoulder movements occur where the ball at the top of your arm bone ( humerus ) fits into the shallow socket ( glenoid ) which is part of the shoulder blade ( scapula ). The joint is designed to give a large amount of movement. This also means that it has a tendency to be too loose. There are various structures which help to keep the joint in position. The most important ones are: a) ligaments; which hold the bones together b) a rim of cartilage; which deepens the socket c) muscles; which keep the shoulder blade and joint in the correct position when moving or using the arm. Shoulder dislocation Most shoulders dislocate forwards and/or downwards (see diagram below). Sometimes the ball of the humerus bone only partly comes out of the socket of the shoulder blade (glenoid). This is known as subluxation. When the first dislocation or subluxation occurs, ligaments are often damaged at the front of the shoulder. 70% of people who have a shoulder dislocation have persistent symptoms of instability because the ligaments no longer keep the joint in position. This is particularly when the arm is lifted upwards and outwards. Right shoulder (from the front) Dislocated shoulder The top of the arm bone is now Normal Alignment in front of the socket Phase 2 exercises continued These additional exercises can be started 4 weeks after your operation. Stand with arm close to side and elbow bent. Push the palm of your hand into other hand but do not let it move. This can be done against a wall or door frame. Hold 10 seconds. Repeat 30 times. Standing with your operated arm against a wall. Bend your elbow. Push your hand into the wall but do not let arm move. Hold for 10 seconds. Repeat 30 times. Stand with your back against the wall. Keep arm close to side, elbow bent. Push the elbow back into the wall but do not let arm move. Hold for 10 seconds. Repeat 30 times. shoulder blade socket ( glenoid ) arm bone ( humerus ) 4 Stand sideways with operated arm against wall. Keep arm close to side, elbow bent. Push elbow into wall but do not let arm move. Hold 10 seconds. 13
5 Elbow exercise Standing or lying, straighten your elbow and then bend your elbow. Repeat 5 times. (Shown for left arm.) About your shoulder stabilisation operation The operation aims to tighten and/or repair the over-stretched and damaged ligaments, rim of cartilage and muscle. Different types of operation are done to achieve this, but normally it is the ligaments deep around the shoulder joint that are tightened up. Phase 2 Exercises Deep ligaments Start these as advised by the hospital doctor or physiotherapist. Normally about 3 weeks after the operation. Shoulder exercises Arm bone Stand. Lean forwards. Let your arm hang down. Swing arm forwards and backwards. Repeat 10 times. (Shown for the left shoulder.) Lying on your back. Support your operated arm with the other arm and lift it up overhead. Repeat 10 times. (Shown for the left shoulder.) Standing with arms behind your back. Grasp the wrist of your operated arm and gently stretch hand towards the opposite buttock. Then slide your hands up your back. Repeat 5 times. 12 What are the risks and complications? All operations involve an element of risk. We do not wish to over-emphasise them but feel that you should be aware of them before and after your operation. The risks include: a) complications relating to the anaesthetic b) infection. These are usually superficial wound problems. Occasionally deep infection may occur after the operation. c) unwanted stiffness and/or pain in (and around) the shoulder. d) damage to nerves and blood vessels around the shoulder. e) a need to re-do the surgery. The repair may fail and the shoulder become unstable again. This occurs in about 3-10% of cases. Please discuss these issues with the doctors if you would like further information. 5
6 Anaesthetic The operation is performed under a general anaesthetic. Usually the anaesthetist will administer a block of the shoulder and arm beforehand, by injecting local anaesthetic into the neck. This reduces pain after surgery and makes the whole operation smoother. The benefits of this method outweigh the small risk of complications associated with this technique. Questions that are often asked Will it be painful? It is quite normal for there to be pain initially after this operation. You will be given pain relief medication (either as tablets or injections) to help reduce the discomfort while you are in hospital. A prescription for continued pain medication will be given to you for your discharge home. If you require further medication after these are finished, please contact your general practitioner (GP). You may find ice packs over the area helpful. Use a packet of frozen peas, placing a piece of wet paper towel between your skin and the ice pack. Until it is healed, also use a plastic bag to protect the wound from getting wet. Leave on for minutes and you can repeat this several times a day. Do I need to wear a sling? Yes! Your arm will be immobilised in a sling for about 3 weeks. This is to protect the surgery during the early phases of healing and to make your arm more comfortable. You will be shown how to get your arm in and out of the sling by a nurse or physiotherapist. (A further information sheet on this is available if required.) You are advised to wear the body strap to keep your arm close to your body. Only take the sling off to wash, straighten your elbow or if sitting with your arm supported. You may find your armpit becomes uncomfortable whilst you are wearing the sling for long periods of time. Try using a dry pad or cloth to absorb the moisture. If you are lying on your back to sleep, you may find placing a thin pillow or rolled towel under your upper arm helpful. 6 Exercises Use pain relief medication and/or ice packs to reduce the pain before you exercise. It is normal for you to feel aching, discomfort or stretching sensations when doing these exercises. However, if you experience intense and lasting pain (eg, more than 30 minutes) reduce the exercises by doing them less forcefully or less often. If this does not help, discuss the problem with the physiotherapist. Certain exercises may be changed or added for your particular shoulder. Do short, frequent sessions (eg, 5-10 minutes, 4 times a day) rather than one long session. Gradually increase the number of repetitions you do. Aim for the repetitions that your therapist advises, the numbers stated here are rough guidelines. Get into the habit of doing them! Good luck. Please note: all pictures are shown for the right shoulder unless specified. Neck exercises Standing or sitting. Turn your head to one side. Repeat 5 times. Then turn your head to the other side and repeat 5 times. Twist your head towards one shoulder. Repeat 5 times. Repeat 5 times to the other side. 11
7 When can I return to work? You may be off work between 2-8 weeks, depending on the type of job you have, which arm has been operated on and if you need to drive. If you are involved in lifting, overhead activities or manual work you will not be able to do these for 8-12 weeks. Please discuss any queries with the physiotherapist or hospital doctor. When can I drive? This is likely to be 4-6 weeks after your operation. Check you can manage all the controls and it is advisable to start with short journeys. The seat-belt may be uncomfortable initially but your shoulder will not be harmed by it. In addition, check your insurance policy. You may need to inform the insurance company of your operation. When can I participate in my leisure activities? Your ability to start these will be dependent on the range of movement and strength that you have in your shoulder following the operation. Please discuss activities in which you may be interested with your physiotherapist or consultant. Start with short sessions, involving little effort and gradually increase. General examples are: Cycling 4 to 6 weeks Gentle swimming 8 to 12 weeks Light sports/racquet sports using non-operated arm 10 weeks Racquet sports using operated arm 12 weeks Contact sports 6 months Do I need to do exercises? For the first 3 weeks you will not be moving the shoulder joint. You will be shown exercises to maintain movement in your neck, elbow, wrist and hand and you need to continue with these at home. Out patient physiotherapy will be arranged to start about 3 weeks after your operation. You will start an exercise programme to gradually regain movements and to strengthen your shoulder. The exercises will be changed as you progress. You will need to get into the habit of doing regular daily exercises at home for several months. They will enable you to gain maximum benefit from your operation. Some of the early exercises are shown at the back of this booklet. What do I do about the wound and stitches? Keep the wound dry until it is healed. This is normally for 10 to 14 days. You can shower/wash and use ice packs but protect the wound with cling film or a plastic bag. Avoid using spray deodorants, talcum powder or perfumes near or on the scar. Normally your stitches or clips will be removed by the nurse at your GP surgery after 10 days. You will need to make an appointment to have this done. When do I return to the Orthopaedic Clinic at Yeovil District Hospital? This is usually arranged for approximately 6 weeks after your discharge from hospital to check how you are progressing. Please discuss any queries or worries you have at this time. Appointments are made after this as necessary. 10 7
8 Are there things I should avoid doing? In the first 3 weeks: Do not be tempted to remove your arm from the sling to use your arm for daily activities. For 6-8 weeks Avoid moving your arm out to the side and twisting it backwards, eg, when putting on a shirt or coat, put your operated arm in first. Try not to reach up and behind you (eg, seat belt in car). Do not force this movement for 12 weeks (3 months). These movements stretch the ligaments and muscles that have been tightened. Remember this operation has been done because you had too much movement in your shoulder. The ligaments and muscles need time to repair in their new, tightened position and it is advisable not to over-stretch them early on. They will benefit from gentle movements after 3 weeks. How am I likely to progress? This can be divided into 3 stages (phases). Phase 1 Sling on, no movement of the shoulder You will basically be one-handed, immediately after the operation for the first 3 weeks. This will affect your ability to do everyday activities, especially if your dominant hand (right if you are righthanded) is the side of the operation. Activities that are affected include dressing, shopping, eating, preparing meals and looking after small children. You will probably need someone else to help you. You may also find it easier to wear loose shirts and tops with front openings. Before you are discharged from hospital, the staff will help you plan for how you will manage when you leave. If you are having particular problems with aspects of self care, an occupational therapist can suggest ways to help you. In addition, we may be able to organise or suggest ways of getting help once you are discharged from hospital. Phase 2 Regaining everyday movements After 3 weeks you can gradually wean off using the sling and you will start out patient physiotherapy. You will be encouraged to use your arm in front of you, but not to take it out to the side and twist it backwards (see things to avoid on previous page). Exercises will help you regain muscle strength and control in your shoulder as the movement returns. The arm can now be used for daily activities, initially these will be possible at waist level but gradually you can return to light tasks with your arm away from your body. It may be 6-8 weeks after your operation before you can use your arm above shoulder height. Phase 3 Regaining strength with movement After 8-12 weeks you will be able to increase your activities, using your arm away from your body and for heavier tasks. You can start doing more vigorous activities but contact sports are restricted for at least 6 months (see leisure activities section). You should regain the movement and strength in your shoulder within 6-8 months. Research has shown that after 2-5 years, about 90% of people have a stable shoulder with few limitations. Vigorous sports or those involving overhead throwing may require adaptation for some people, although many return to previous levels of activity. 8 9
Sub-Acromial Decompression
 Who to contact if you are worried or require further information For general enquiries about appointments, please phone: Mr Smibert s secretary on: 01935 384597 Mr Chambler s secretary on: 01935 384779
Who to contact if you are worried or require further information For general enquiries about appointments, please phone: Mr Smibert s secretary on: 01935 384597 Mr Chambler s secretary on: 01935 384779
Rotator Cuff Repair. Information for you after your operation
 Who to contact if you are worried or require further information For general enquiries about appointments, please phone: Mr Smibert s secretary on: 01935 384597 Mr Chambler s secretary on: 01935 384779
Who to contact if you are worried or require further information For general enquiries about appointments, please phone: Mr Smibert s secretary on: 01935 384597 Mr Chambler s secretary on: 01935 384779
Shoulder Replacement. Information for you after your operation
 Who to contact if you are worried or require further information For general enquiries about appointments, please phone: Mr Smibert s secretary on: 01935 384597 Mr Chambler s secretary on: 01935 384779
Who to contact if you are worried or require further information For general enquiries about appointments, please phone: Mr Smibert s secretary on: 01935 384597 Mr Chambler s secretary on: 01935 384779
Elbow Replacement. Information for you after your operation
 Information for you after your operation Elbow Replacement We would like to thank the Nuffield Orthopaedic Centre (Upper Limb Clinic) for allowing us to re-produce the information If you require this leaflet
Information for you after your operation Elbow Replacement We would like to thank the Nuffield Orthopaedic Centre (Upper Limb Clinic) for allowing us to re-produce the information If you require this leaflet
Anterior stabilisation of the shoulder: open and arthroscopic (keyhole)
 Patient information Anterior stabilisation of the shoulder: open and arthroscopic (keyhole) This information has been produced to help you gain the maximum benefit and understanding of your operation.
Patient information Anterior stabilisation of the shoulder: open and arthroscopic (keyhole) This information has been produced to help you gain the maximum benefit and understanding of your operation.
Manipulation under anaesthetic (MUA) and arthroscopic capsular release (ACR)
 Patient information Manipulation under anaesthetic (MUA) and arthroscopic capsular release (ACR) This information has been produced to help you gain the maximum benefit and understanding of your operation.
Patient information Manipulation under anaesthetic (MUA) and arthroscopic capsular release (ACR) This information has been produced to help you gain the maximum benefit and understanding of your operation.
Shoulder distension. Orthopaedic department. yeovilhospital.nhs.uk
 Shoulder distension Orthopaedic department 01935 384 159 yeovilhospital.nhs.uk This information booklet has been produced to help you gain the maximum benefit after your operation. It is not a substitute
Shoulder distension Orthopaedic department 01935 384 159 yeovilhospital.nhs.uk This information booklet has been produced to help you gain the maximum benefit after your operation. It is not a substitute
Advice for patients following a Slap Repair
 Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Patient Advice and Liaison Service (PALS): 0151 430 1376 Advice for patients following a Slap Repair St Helens Hospital Marshall Cross
Shoulder Stabilisation Surgery. Patient Information
 Shoulder Stabilisation Surgery Patient Information Author ID: JW Leaflet Number: Musc 038 Version: 2 Name of Leaflet: Shoulder Stabilisation Surgery Date Produced: February 2017 Review Date: February 2019
Shoulder Stabilisation Surgery Patient Information Author ID: JW Leaflet Number: Musc 038 Version: 2 Name of Leaflet: Shoulder Stabilisation Surgery Date Produced: February 2017 Review Date: February 2019
Advice for patients following a Rotator Cuff Repair
 Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Advice for patients following a Rotator Cuff Repair Patient Advice and Liaison Service (PALS): 0151 430 1376 St Helens Hospital Marshall
Contact Information Acute Musculoskeletal Therapy Team: 0151 676 5519 Advice for patients following a Rotator Cuff Repair Patient Advice and Liaison Service (PALS): 0151 430 1376 St Helens Hospital Marshall
Exercises following arthroscopic (or open) anterior stabilisation
 Physiotherapy patient information Exercises following arthroscopic (or open) anterior stabilisation Introduction The shoulder joint is designed to give a large amount of movement, therefore support from
Physiotherapy patient information Exercises following arthroscopic (or open) anterior stabilisation Introduction The shoulder joint is designed to give a large amount of movement, therefore support from
Rehabilitation after shoulder dislocation
 Oxford University Hospitals NHS Trust Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your
Oxford University Hospitals NHS Trust Physiotherapy Department Rehabilitation after shoulder dislocation Information for patients This information leaflet gives you advice on rehabilitation after your
Your Stabilisation procedure Information for Patients
 Your Stabilisation procedure Information for Patients This leaflet will provide you with general information about the anterior stabilisation procedure. It will briefly explain the operation procedure
Your Stabilisation procedure Information for Patients This leaflet will provide you with general information about the anterior stabilisation procedure. It will briefly explain the operation procedure
It is most common in people between the age of 40 and 70 years and has been estimated to affect at least one person in 50 every year.
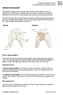 FROZEN SHOULDER The shoulder is designed to have a large amount of movement so that we can use our hands/arms in a wide variety of positions. Some movement occurs between the shoulder blade and chest wall.
FROZEN SHOULDER The shoulder is designed to have a large amount of movement so that we can use our hands/arms in a wide variety of positions. Some movement occurs between the shoulder blade and chest wall.
Posterior Shoulder Stabilisation
 Posterior Shoulder Stabilisation An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Posterior Shoulder Stabilisation An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Arthroscopic capsular release. Information for patients Orthopaedics - Upper Limb
 Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Arthroscopic capsular release Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
SHOULDER ACROMIOPLASTY
 ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY Please stick addressograph
ORTHOPAEDIC UNIT: 01-293 8687 /01-293 6602 UPMC BEACON CENTRE FOR ORTHOPAEDICS: 01-2937575 PHYSIOTHERAPY DEPARTMENT: 01-2936692 GUIDELINES FOR PATIENTS HAVING A SHOULDER ACROMIOPLASTY Please stick addressograph
SLAP repair. An information guide for patients. Delivering the best in care. UHB is a no smoking Trust
 SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
SLAP repair An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Information for Patients. SLAP Repair. One Health Group 131 Psalter Lane Sheffield S11 8UX T:
 Information for Patients SLAP Repair One Health Group 131 Psalter Lane Sheffield S11 8UX T: 0114 250 5510 enquiries@onehealth.co.uk SLAP Repair Introduction The Upper Limb Unit team would like you and
Information for Patients SLAP Repair One Health Group 131 Psalter Lane Sheffield S11 8UX T: 0114 250 5510 enquiries@onehealth.co.uk SLAP Repair Introduction The Upper Limb Unit team would like you and
Shoulder Capsular Release UHB is a no smoking Trust
 Shoulder Capsular Release UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Capsular release The shoulder complex
Shoulder Capsular Release UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Capsular release The shoulder complex
Biceps Tenodesis. An information guide for patients. UHB is a no smoking Trust
 Biceps Tenodesis An information guide for patients UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Biceps tenodesis
Biceps Tenodesis An information guide for patients UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Biceps tenodesis
Exercises following Copeland Surface Replacement Arthroplasty (CSRA)
 Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
Physiotherapy patient information Copeland Surface Replacement Arthroplasty Exercises following Copeland Surface Replacement Arthroplasty (CSRA) Introduction The Copeland Surface Replacement as it s name
LARS ligament stabilisation for the acromioclavicular joint
 Information and exercises LARS ligament stabilisation for the acromioclavicular joint Introduction Dislocation of the acromio-clavicular (AC) joint results in rupture of the ligaments which hold the clavicle
Information and exercises LARS ligament stabilisation for the acromioclavicular joint Introduction Dislocation of the acromio-clavicular (AC) joint results in rupture of the ligaments which hold the clavicle
Elbow Replacement Guide
 Elbow Replacement Guide IM-CNOH-12 Rev. 1 Issue Date: March 2011 Review Date: March 2012 Founded 1908 C A P PA G H N AT I O N A L O RT H O PA E D I C H O S P I TA L FINGLAS, DUBLIN 11. TEL: 01 814 0429
Elbow Replacement Guide IM-CNOH-12 Rev. 1 Issue Date: March 2011 Review Date: March 2012 Founded 1908 C A P PA G H N AT I O N A L O RT H O PA E D I C H O S P I TA L FINGLAS, DUBLIN 11. TEL: 01 814 0429
Anterior Shoulder Stabilisation UHB is a no smoking Trust
 Anterior Shoulder Stabilisation UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Shoulder anatomy The shoulder
Anterior Shoulder Stabilisation UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Shoulder anatomy The shoulder
Reverse Shoulder Replacement
 Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Reverse Shoulder Replacement An information guide for patients Delivering the best in care UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm
Shoulder Stabilisation A guide for patients Gateshead Upper Limb Unit Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy
 Shoulder Stabilisation A guide for patients Gateshead Upper Limb Unit Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 Shoulder Instability Your shoulder is a ball and socket joint
Shoulder Stabilisation A guide for patients Gateshead Upper Limb Unit Mr Andreas Hinsche Mr John Harrison Mr Jagannath Chakravarthy Page 1 of 7 Shoulder Instability Your shoulder is a ball and socket joint
Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients
 Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients This leaflet will provide you with general information about capsular release surgery. It will briefly explain the operation procedure
Your Arthroscopic Capsular Release (Arthrolysis) Information for Patients This leaflet will provide you with general information about capsular release surgery. It will briefly explain the operation procedure
Small and moderate rotator cuff repairs
 Information and exercises Small and moderate rotator cuff repairs Introduction The rotator cuff consists of four muscles and their tendons, which surround the ball (humeral head) of the shoulder joint.
Information and exercises Small and moderate rotator cuff repairs Introduction The rotator cuff consists of four muscles and their tendons, which surround the ball (humeral head) of the shoulder joint.
Acromio-Clavicular Joint Stabilisation UHB is a no smoking Trust
 Acromio-Clavicular Joint Stabilisation UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Acromio-Clavicular Joint
Acromio-Clavicular Joint Stabilisation UHB is a no smoking Trust To see all of our current patient information leaflets please visit www.uhb.nhs.uk/patient-information-leaflets.htm Acromio-Clavicular Joint
Exercises following stemmed hemiarthroplasty for trauma / fracture
 Physiotherapy patient information Stemmed hemiarthroplasty (Mr Malhas) Exercises following stemmed hemiarthroplasty for trauma / fracture Introduction A shoulder replacement is done following a fracture
Physiotherapy patient information Stemmed hemiarthroplasty (Mr Malhas) Exercises following stemmed hemiarthroplasty for trauma / fracture Introduction A shoulder replacement is done following a fracture
INFORMATION FOR PATIENTS. Reverse shoulder replacement operation
 INFORMATION FOR PATIENTS Reverse shoulder replacement operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
INFORMATION FOR PATIENTS Reverse shoulder replacement operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
Reverse geometry shoulder replacement
 Patient information Reverse geometry shoulder replacement Reverse geometry shoulder replacement This information has been produced to help you gain the maximum benefit and understanding of your operation.
Patient information Reverse geometry shoulder replacement Reverse geometry shoulder replacement This information has been produced to help you gain the maximum benefit and understanding of your operation.
INFORMATION FOR PATIENTS. Arthroscopic Bankart repair
 INFORMATION FOR PATIENTS Arthroscopic Bankart repair This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may have
INFORMATION FOR PATIENTS Arthroscopic Bankart repair This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may have
INFORMATION FOR PATIENTS. SLAP lesion repair operation
 INFORMATION FOR PATIENTS SLAP lesion repair operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions you may have
INFORMATION FOR PATIENTS SLAP lesion repair operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions you may have
Reversed geometry shoulder replacement
 Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
Information and exercises Reversed geometry shoulder replacement Introduction The reversed geometry total shoulder replacement is designed for use in shoulders that have a deficient rotator cuff, arthritis
INFORMATION FOR PATIENTS. Rotator cuff repair operation
 INFORMATION FOR PATIENTS Rotator cuff repair operation This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may
INFORMATION FOR PATIENTS Rotator cuff repair operation This booklet contains information about the shoulder surgery that you have been advised to have, and aims to answer some of the questions you may
Physiotherapy following shoulder surgery
 Trauma and Orthopaedic Therapy Services Physiotherapy following shoulder surgery Issued By: To:.. By Hand / By Post Date: Information 2 Shoulder Surgery Your surgery may have been done either open i.e.
Trauma and Orthopaedic Therapy Services Physiotherapy following shoulder surgery Issued By: To:.. By Hand / By Post Date: Information 2 Shoulder Surgery Your surgery may have been done either open i.e.
Shoulder Replacement Operation
 Shoulder Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact: Physiotherapy
Shoulder Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact: Physiotherapy
Exercises following rotator cuff repair (major tear: 3-5cm and massive tear: more than 5cm)
 Physiotherapy patient information Rotator cuff repair (major/massive tear) Exercises following rotator cuff repair (major tear: 3-5cm and massive tear: more than 5cm) Introduction The rotator cuff consists
Physiotherapy patient information Rotator cuff repair (major/massive tear) Exercises following rotator cuff repair (major tear: 3-5cm and massive tear: more than 5cm) Introduction The rotator cuff consists
Sub-acromial decompression surgery. Information for patients Orthopaedics - Upper Limb
 Sub-acromial decompression surgery Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Sub-acromial decompression surgery Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation
Reading Shoulder Unit
 Reading Shoulder Unit www.readingshoulderunit.com Patient information Impingement Syndrome / Acromioclavicular joint (AC Joint) arthritis Arthroscopic Subacromial Decompression/ Acromioclavicular joint
Reading Shoulder Unit www.readingshoulderunit.com Patient information Impingement Syndrome / Acromioclavicular joint (AC Joint) arthritis Arthroscopic Subacromial Decompression/ Acromioclavicular joint
Subacromial Impingement of Shoulder Orthopaedic Department Patient Information Leaflet
 Subacromial Impingement of Shoulder Orthopaedic Department Patient Information Leaflet Page 1 Subacromial Impingement of Shoulder About your shoulder The shoulder is a ball and socket joint formed by a
Subacromial Impingement of Shoulder Orthopaedic Department Patient Information Leaflet Page 1 Subacromial Impingement of Shoulder About your shoulder The shoulder is a ball and socket joint formed by a
Clavicle fracture - Open Reduction Internal Fixation (ORIF)
 Physiotherapy patient information Clavicle fracture ORIF Clavicle fracture - Open Reduction Internal Fixation (ORIF) Introduction Your clavicle (collarbone) is a long thin bone sitting between your shoulder
Physiotherapy patient information Clavicle fracture ORIF Clavicle fracture - Open Reduction Internal Fixation (ORIF) Introduction Your clavicle (collarbone) is a long thin bone sitting between your shoulder
OVERCOMING FROZEN SHOULDER
 OVERCOMING FROZEN SHOULDER Treatment to Relieve Pain and Regain Movement When You Have Frozen Shoulder Is your shoulder stiff and painful? If so, you may have frozen shoulder (sometimes called adhesive
OVERCOMING FROZEN SHOULDER Treatment to Relieve Pain and Regain Movement When You Have Frozen Shoulder Is your shoulder stiff and painful? If so, you may have frozen shoulder (sometimes called adhesive
Arthroscopic subacromial decompression of the shoulder
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Arthroscopic subacromial decompression of the shoulder Physiotherapy Department Information booklet for Name of Patient: Date:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Arthroscopic subacromial decompression of the shoulder Physiotherapy Department Information booklet for Name of Patient: Date:
Exercises following rotator cuff repair (minor tear: less than 1cm)
 Physiotherapy patient information Rotator cuff repair (minor tear) Exercises following rotator cuff repair (minor tear: less than 1cm) Introduction The rotator cuff consists of four muscles and their tendons,
Physiotherapy patient information Rotator cuff repair (minor tear) Exercises following rotator cuff repair (minor tear: less than 1cm) Introduction The rotator cuff consists of four muscles and their tendons,
INFORMATION FOR PATIENTS. Bristow-Latarjet operation
 INFORMATION FOR PATIENTS Bristow-Latarjet operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions you may have
INFORMATION FOR PATIENTS Bristow-Latarjet operation This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions you may have
Stabilisation of the shoulder joint
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Stabilisation of the shoulder joint Physiotherapy Department Information leaflet for Name of Patient: Date: Name of Physiotherapist:
POST OP CLOSED BANKART PROCEDURE
 POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
POST OP CLOSED BANKART PROCEDURE WEEKS 1-6 Do 1. Wear sling until advised otherwise 2. Keep dressing clean and dry 3. Do passive pendulum exercises to 90 degrees 4. Ice for 15 minutes after exercising
Reverse Shoulder Replacement Operation
 Reverse Shoulder Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact:
Reverse Shoulder Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact:
Exercises following arthroscopic subacromial decompression and/or acromioclavicular joint excision and/or excision of calcific deposits
 Physiotherapy patient information Exercises following arthroscopic subacromial decompression and/or acromioclavicular joint excision and/or excision of calcific deposits Introduction The subacromial area
Physiotherapy patient information Exercises following arthroscopic subacromial decompression and/or acromioclavicular joint excision and/or excision of calcific deposits Introduction The subacromial area
Subacromial Decompression
 PATIENT INFORMATION Subacromial Decompression You will be admitted for surgery to your shoulder as a result of a subacromial impingement syndrome. The subacromial impingement syndrome is a condition where
PATIENT INFORMATION Subacromial Decompression You will be admitted for surgery to your shoulder as a result of a subacromial impingement syndrome. The subacromial impingement syndrome is a condition where
INFORMATION FOR PATIENTS. Arthroscopic subacromial decompression
 INFORMATION FOR PATIENTS Arthroscopic subacromial decompression This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
INFORMATION FOR PATIENTS Arthroscopic subacromial decompression This booklet contains information about the shoulder surgery that you have been advised to have and aims to answer some of the questions
Manipulation under Anaesthetic (MUA) and Arthroscopic Release Operation
 Manipulation under Anaesthetic (MUA) and Arthroscopic Release Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats.
Manipulation under Anaesthetic (MUA) and Arthroscopic Release Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats.
Anterior Cruciate Ligament Reconstruction
 Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Anterior Cruciate Ligament Reconstruction Physiotherapy Department Patient information leaflet This patient information booklet is designed to provide you with information about the Anterior Cruciate Ligament
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement
 Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
Rehabilitation Program Following Shoulder Diagnostic Arthroscopy, Acromioplasty, Decompression, AC Resection, Debridement Richard Holtby Assistant professor, Department of Surgery University of Toronto
Coping with Osteoarthritis in the shoulder
 Coping with Osteoarthritis in the shoulder Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Coping with Osteoarthritis in the shoulder Other formats If you need this information in another format such as audio tape or computer disk, Braille, large print, high contrast, British Sign Language or
Northumbria Healthcare NHS Foundation Trust. Physiotherapy Exercises Following Shoulder Surgery. Issued by the Physiotherapy Department
 Northumbria Healthcare NHS Foundation Trust Physiotherapy Exercises Following Shoulder Surgery Issued by the Physiotherapy Department This leaflet aims to provide you with information following your shoulder
Northumbria Healthcare NHS Foundation Trust Physiotherapy Exercises Following Shoulder Surgery Issued by the Physiotherapy Department This leaflet aims to provide you with information following your shoulder
Total Elbow Replacement Operation
 Total Elbow Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact:
Total Elbow Replacement Operation Information for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact:
Looking After Your Shoulders
 A patient s guide to Looking After Your Shoulders Shoulder protection following a Spinal Cord Injury (SCI) This information, for patients with paraplegia, is a guide only and not prescriptive. Your therapist
A patient s guide to Looking After Your Shoulders Shoulder protection following a Spinal Cord Injury (SCI) This information, for patients with paraplegia, is a guide only and not prescriptive. Your therapist
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction
 Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
Physiotherapy Information following Anterior Cruciate Ligament (ACL) Reconstruction Name:... Surgery Date:... Graft:... Orthopaedic Outpatient Appointment Date: Time: Location: Contact Number: Contacting
 Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Latarjet Procedure (coracoid transfer) Shoulder Stabilisation Surgery Ms. Ruth Delaney Consultant Orthopaedic Surgeon
Specialists in Joint Replacement, Spinal Surgery, Orthopaedics and Sport Injuries The Latarjet Procedure (coracoid transfer) Shoulder Stabilisation Surgery Ms. Ruth Delaney Consultant Orthopaedic Surgeon
In Space Balloon. A guide for patients. The Nottingham Shoulder and Elbow Unit
 In Space Balloon A guide for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact: Physiotherapy Department
In Space Balloon A guide for patients The Nottingham Shoulder and Elbow Unit This document can be provided in different languages and formats. For more information please contact: Physiotherapy Department
ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An IPRS Guide to provide you with exercises and advice to ease your condition
 Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
Contents What causes an A/C joint sprain?..................................3 What treatment can I receive?.....................................4 YOUR GUIDE TO ACROMIO- CLAVICULAR (A/C) JOINT SPRAIN An
Total elbow replacement. Information for patients Orthopaedics - Upper Limb
 Total elbow replacement Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation you
Total elbow replacement Information for patients Orthopaedics - Upper Limb Introduction The Upper Limb Unit team would like you and your family to understand as much as possible about the operation you
Total Shoulder Replacement Rehabilitation Guidelines
 PH: 1300 746 853 Total Shoulder Replacement Rehabilitation Guidelines The following is a detailed outline of the rehabilitation regime for patients who have had a Total Shoulder Replacement by Dr. Macgroarty.
PH: 1300 746 853 Total Shoulder Replacement Rehabilitation Guidelines The following is a detailed outline of the rehabilitation regime for patients who have had a Total Shoulder Replacement by Dr. Macgroarty.
Urmston Physio Clinic
 Urmston Physio Clinic Patient Information Shoulder Instability Prepared for Mr B. Roy Consultant Orthopaedic Surgeon 102 Church Road, Urmston, Manchester, M41 9DB Tel: 0161 748 4100 Shoulder Instability
Urmston Physio Clinic Patient Information Shoulder Instability Prepared for Mr B. Roy Consultant Orthopaedic Surgeon 102 Church Road, Urmston, Manchester, M41 9DB Tel: 0161 748 4100 Shoulder Instability
Exercises and advice following your breast reconstruction surgery
 Exercises and advice following your breast reconstruction surgery This leaflet gives information to people who have had breast reconstructive surgery. It contains exercises that your physiotherapist would
Exercises and advice following your breast reconstruction surgery This leaflet gives information to people who have had breast reconstructive surgery. It contains exercises that your physiotherapist would
Traumatic Instability Understanding your shoulder injury and its repair
 Patient Education Traumatic Instability Understanding your shoulder injury and its repair Your upper arm bone popped out of the socket of your shoulder blade. When this happened, it tore your ligaments
Patient Education Traumatic Instability Understanding your shoulder injury and its repair Your upper arm bone popped out of the socket of your shoulder blade. When this happened, it tore your ligaments
Exercises After Shoulder Injury
 2011 Exercises After Shoulder Injury Shoulder Exercises Patient Information Your injury is now healed well enough that you can do the following exercises without any fear of hurting your shoulder again.
2011 Exercises After Shoulder Injury Shoulder Exercises Patient Information Your injury is now healed well enough that you can do the following exercises without any fear of hurting your shoulder again.
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS
 OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
OHIOHEALTH ORTHOPEDIC SURGEONS Dr. Nathaniel Long 614-566-8691 Sarah A. Domenicucci, PA-C POST OPERATIVE INSTRUCTIONS Shoulder Arthroscopy with Labral Repair (SLAP/Bankart/Posterior) Latarjet Procedure
Avon Office 2 Simsbury Rd. Avon, CT Office: (860) Fax: (860) REHABILITATION AFTER REVERSE SHOULDER ARTHROPLASTY
 Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Katherine J. Coyner, MD UCONN Musculoskeletal Institute Medical Arts & Research Building 263 Farmington Ave. Farmington, CT 06030 Office: (860) 679-6600 Fax: (860) 679-6649 www.drcoyner.com Avon Office
Latajet Rehabilitation Guidelines
 PH: 1300 746 853 Latajet Rehabilitation Guidelines The following is a detailed outline of the rehabilitation regime for patients who have had an Latajet Coracoid Process Transfer by Dr. Macgroarty. You
PH: 1300 746 853 Latajet Rehabilitation Guidelines The following is a detailed outline of the rehabilitation regime for patients who have had an Latajet Coracoid Process Transfer by Dr. Macgroarty. You
Physiotherapy following peri acetabular osteotomy (PAO) surgery
 Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
Physiotherapy following peri acetabular osteotomy (PAO) surgery This leaflet explains more about returning to your everyday activities after your peri acetabular osteotomy (PAO). It explains the exercises
The Leeds Teaching Hospitals NHS Trust Total Hip Replacement A guide to your Rehabilitation
 n The Leeds Teaching Hospitals NHS Trust Total Hip Replacement A guide to your Rehabilitation Information for patients Your questions answered What are hip precautions? There are precautions to follow
n The Leeds Teaching Hospitals NHS Trust Total Hip Replacement A guide to your Rehabilitation Information for patients Your questions answered What are hip precautions? There are precautions to follow
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection
 The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
The SUPPORT Trial: SUbacromial impingement syndrome and Pain: a randomised controlled trial Of exercise and injection SUPPORT Physiotherapy Intervention Training Manual Authors: Sue Jackson (SJ) Julie
Anterior Cruciate Ligament Reconstruction
 Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Patient information leaflet Royal Surrey County Hospital NHS Foundation Trust Anterior Cruciate Ligament Reconstruction Physiotherapy This patient information booklet is designed to provide you with information
Arthroscopy of the Knee
 Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
Arthroscopy of the Knee The information contained within this leaflet is only a guide and the timings and activities will depend upon your specific circumstances and Mr Hartley s individual instructions.
Proximal Humerus fracture Shoulder 7
 Proximal Humerus fracture Shoulder 7 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Proximal Humerus fracture Shoulder 7 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Rehabilitation programme after hemiarthroplasty surgery
 Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Rehabilitation programme after hemiarthroplasty surgery Information for patients at Princess Royal University Hospital This leaflet gives you advice about the things you can do after your operation both
Surgery for carpal tunnel syndrome
 Surgery for carpal tunnel syndrome This leaflet will help answer some of the questions you may have about having surgery to treat carpal tunnel syndrome. It should accompany the leaflet, Surgical Admissions
Surgery for carpal tunnel syndrome This leaflet will help answer some of the questions you may have about having surgery to treat carpal tunnel syndrome. It should accompany the leaflet, Surgical Admissions
ARTHROSCOPIC SHOULDER SURGERY
 Preoperative instructions ARTHROSCOPIC SHOULDER SURGERY Schedule surgery with the secretary in Dr.Gill s office. Within one month before surgery * Make an appointment for a preoperative office visit regarding
Preoperative instructions ARTHROSCOPIC SHOULDER SURGERY Schedule surgery with the secretary in Dr.Gill s office. Within one month before surgery * Make an appointment for a preoperative office visit regarding
Instability of the shoulder Orthopaedic Department Patient Information Leaflet. Under review. Page 1
 Instability of the shoulder Orthopaedic Department Patient Information Leaflet Page 1 Shoulder instability There is a balance between movements in the shoulder whilst maintaining stability. When the shoulder
Instability of the shoulder Orthopaedic Department Patient Information Leaflet Page 1 Shoulder instability There is a balance between movements in the shoulder whilst maintaining stability. When the shoulder
SHOULDER HEMIARTHROPLASTY PATIENT INFORMATION LEAFLET
 SHOULDER HEMIARTHROPLASTY PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your shoulder surgery. However if you still have any concerns or
SHOULDER HEMIARTHROPLASTY PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your shoulder surgery. However if you still have any concerns or
Physiotherapy advice and exercises following Breast Reconstruction using a Tissue Expander. Northumbria Healthcare NHS Foundation Trust
 Northumbria Healthcare NHS Foundation Trust Physiotherapy advice and exercises following Breast Reconstruction using a Tissue Expander Issued by the Physiotherapy Department How can Physiotherapy help
Northumbria Healthcare NHS Foundation Trust Physiotherapy advice and exercises following Breast Reconstruction using a Tissue Expander Issued by the Physiotherapy Department How can Physiotherapy help
Shoulder Arthroscopic Capsular Release Rehabilitation
 Shoulder Arthroscopic Capsular Release Rehabilitation Phase two: 3 to 6 weeks after surgery Goals: 1. Improve range of motion of the shoulder 2. Begin gentle strengthening Activities 1. Sling Your sling
Shoulder Arthroscopic Capsular Release Rehabilitation Phase two: 3 to 6 weeks after surgery Goals: 1. Improve range of motion of the shoulder 2. Begin gentle strengthening Activities 1. Sling Your sling
Shoulder Replacement Why do I need a shoulder replacement
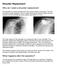 Shoulder Replacement Why do I need a shoulder replacement The shoulder is a ball and socket joint with a large range of movement. The joint sometimes needs replacing. This is usually when severe arthritis
Shoulder Replacement Why do I need a shoulder replacement The shoulder is a ball and socket joint with a large range of movement. The joint sometimes needs replacing. This is usually when severe arthritis
STERNO- CLAVICULAR (S/C) JOINT SPRAIN
 Contents What is a sprain?................................................3 What causes an S/C joint injury?...................................5 YOUR GUIDE TO STERNO- CLAVICULAR (S/C) JOINT SPRAIN An IPRS
Contents What is a sprain?................................................3 What causes an S/C joint injury?...................................5 YOUR GUIDE TO STERNO- CLAVICULAR (S/C) JOINT SPRAIN An IPRS
Therapy following a neck of femur fracture
 INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
INFORMATION FOR PATIENTS Therapy following a neck of femur fracture Name of patient: ffffffffffffffffffffffffffffffffffffffffffff Procedure: ffffffffffffffffffffffffffffffffffffffffffffffffffff Consultant:
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET
 TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
TOTAL KNEE REPLACEMENT PATIENT INFORMATION LEAFLET This leaflet has been produced to help answer some questions you may have following your knee replacement. However if you still have any concerns or queries
FROZEN SHOULDER REHABILITATION EXERCISES
 FROZEN SHOULDER REHABILITATION EXERCISES Exercise no. 1) Bend forward so that your torso is parallel to the ground, and lean on a stool or table with your healthy arm. Completely relax your sore arm, and
FROZEN SHOULDER REHABILITATION EXERCISES Exercise no. 1) Bend forward so that your torso is parallel to the ground, and lean on a stool or table with your healthy arm. Completely relax your sore arm, and
Greater Tuberosity Fracture Shoulder 6
 Greater Tuberosity Fracture Shoulder 6 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
Greater Tuberosity Fracture Shoulder 6 Fracture Care Team: Shared Care Plan Eastbourne - 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up your recent telephone
VERSO. Reverse Total Shoulder Replacement
 VERSO Reverse Total Shoulder Replacement Rotator cuff tear arthropathy is a problem that occurs when a patient has both shoulder arthritis and an irreparable rotator cuff tear. This condition results in
VERSO Reverse Total Shoulder Replacement Rotator cuff tear arthropathy is a problem that occurs when a patient has both shoulder arthritis and an irreparable rotator cuff tear. This condition results in
Shoulder Surgery YOUR GUIDE TO: SHOULDER SURGERY
 Shoulder Surgery YOUR GUIDE TO: SHOULDER SURGERY October 2017 1 NEJAC North East Joint Assessment Centre Table of Contents Introduction... 3 Shoulder Anatomy... 4 What to Expect... 5 Shoulder Surgery Patient
Shoulder Surgery YOUR GUIDE TO: SHOULDER SURGERY October 2017 1 NEJAC North East Joint Assessment Centre Table of Contents Introduction... 3 Shoulder Anatomy... 4 What to Expect... 5 Shoulder Surgery Patient
A FROZEN SHOULDER YOUR GUIDE TO. An IPRS Guide to provide you with exercises and advice to ease your condition
 YOUR GUIDE TO A FROZEN SHOULDER Contents Introduction................................................... 2 What is Frozen Shoulder?........................................ 3 What are the symptoms of Frozen
YOUR GUIDE TO A FROZEN SHOULDER Contents Introduction................................................... 2 What is Frozen Shoulder?........................................ 3 What are the symptoms of Frozen
Acromioclavicular Joint Injury (dislocation) Shoulder 3
 Acromioclavicular Joint Injury (dislocation) Shoulder 3 Fracture Care Team: Shared Care Plan Eastbourne 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up
Acromioclavicular Joint Injury (dislocation) Shoulder 3 Fracture Care Team: Shared Care Plan Eastbourne 01323 414928 Conquest - 01424 757576 Email - esht.vfc@nhs.net This information leaflet follows up
Rehabilitation Program Following Isolated Biceps Tenodesis
 Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
Rehabilitation Program Following Isolated Biceps Tenodesis Richard Holtby Assistant professor, Department of Surgery University of Toronto Biceps Groove Biceps tendon HOLLAND ORTHOPAEDIC & ARTHRITIC CENTRE
