COMPLICATIONS FOLLOWING SPINAL CORD INJURY: OCCURRENCE AND RISK FACTORS IN A LONGITUDINAL STUDY DURING AND AFTER INPATIENT REHABILITATION
|
|
|
- Hubert Cox
- 6 years ago
- Views:
Transcription
1 J Rehabil Med 2007; 39: ORIGINAL REPORT COMPLICATIONS FOLLOWING SPINAL CORD INJURY: OCCURRENCE AND RISK FACTORS IN A LONGITUDINAL STUDY DURING AND AFTER INPATIENT REHABILITATION Janneke A. Haisma, MD 1, Lucas H. van der Woude, PhD 2,3, Henk J. Stam, MD, PhD, FRCP 1, Michael P. Bergen, MD, PhD 4, Tebbe A. Sluis, MD 4, Marcel W. Post, PhD 5 and Johannes B. Bussmann, PhD 1 From the 1 Department of Rehabilitation Medicine, Erasmus MC, University Medical Center Rotterdam, 2 Institute for Fundamental and Clinical Human Movement Sciences, Faculty of Human Movement Sciences, Vrije Universiteit Amsterdam, 3 Rehabilitation Center Amsterdam, 4 Rijndam Rehabilitation Center, Rotterdam and 5 Rehabilitation Center de Hoogstraat, Utrecht, The Netherlands Objective: To assess the occurrence and risk factors for complications following spinal cord injury during and after inpatient rehabilitation. Design: Multicentre longitudinal study. Subjects: A total of 212 persons with a spinal cord injury admitted to specialized rehabilitation centres. Methods: Assessments at the start of active rehabilitation (n = 212), 3 months later (n = 143), at discharge (n = 191) and 1 year after discharge (n = 143). Results: Multi-level random coefficient analyses revealed that complications were common following spinal cord injury. Most subjects reported neurogenic and musculoskeletal pain, or had spasticity at each assessment. During the year after discharge, complications remained common: urinary tract infections and pressure sores affected 49% and 36% of the population, respectively. The degree of pain decreased, whereas the degree of spasticity increased significantly during inpatient rehabilitation. Overall, increased age, increased body mass index, traumatic lesion, tetraplegia, and complete lesion all increased the risk of complications. Conclusion: Complications are common following spinal cord injury. They need specific attention after discharge from inpatient rehabilitation and within subpopulations. Key words: spinal cord injury, complications, risk factors, rehabilitation. J Rehabil Med 2007; 39: Correspondence address: Janneke A. Haisma, Department of Rehabilitation Medicine, Erasmus MC, University Medical Center Rotterdam, PO Box 2040, 3000 CA Rotterdam, The Netherlands. j.haisma@erasmusmc.nl Submitted July 3, 2006; accepted January 12, 2007 Introduction 2007 Foundation of Rehabilitation Information. ISSN DOI: / Spinal cord injury (SCI) is often followed by complications, which add to the detrimental effect that loss of motor, sensory and autonomic function have on a person s health, social participation and quality of life (1 4). There is some debate about the operational definition of complications, about whether complications are strictly causally related to the SCI, and on how to distinguish complications from co-morbidity (5). However, a condition may only be defined as being a complication if it has a chronological relation with the SCI, i.e. the SCI needs to precede the condition. Additionally, although this condition may also occur in the general population, one assumes those with SCI to be at increased risk (5). The range of conditions following SCI can be categorized into neurological consequences and secondary complications. Neurological consequences result from the injury itself, following interruption and decentralization of the nervous system, and may be regarded as sequelae to the injury (6). Examples are neurogenic pain or spasticity; the latter being part of the upper motor neurone syndrome (7, 8). Secondary complications follow the ensuing loss of pulmonary function, loss of bladder control or reduced mobility. Examples are pulmonary infections and pressure sores (1, 9, 10). Neurological consequences and secondary complications behave similarly; they often require, and react to, treatment, and they affect the rehabilitation process. Therefore, we refer to them all as complications of SCI. Complications have a considerable impact on those with SCI. A high incidence of complications is associated with a lower level of health-related aspects, such as physical capacity, activities and functional outcome (1, 3, 4, 11). Complications may interfere with the start of active rehabilitation, can form a disappointing set-back during rehabilitation, and frequently lead to re-hospitalization (7, 12, 13). Additionally, complications are an important cause of mortality following SCI (5, 14). In order to optimize the individual rehabilitation process and outcome, it is important to predict and prevent complications or to recognize and treat them (5). Previous studies have investigated complications following SCI and their risk factors. They have illustrated the association between subject and lesion characteristics and the occurrence of complications (1, 8, 15, 16). They have also showed that the diversity and occurrence of complications change over time (1, 9, 10, 17). However, these studies have limitations. Firstly, most studies were cross-sectional in design, whereas a longitudinal study in which data are collected prospectively
2 394 J. A. Haisma et al. could better establish which factors actually lead to complications. Secondly, in most studies only one or a few complications were assessed, whereas the simultaneous investigation of a range of complications will give insight into their diversity, and into how their occurrence compares. Therefore, we have formulated the following 3 research questions: What is the occurrence of complications (pain, spasticity, hypotension, autonomic dysreflexia, pressure sores, urinary tract infections, pulmonary infections, venous thromboembolism, oedema, heterotopic ossification, other cardiovascular disease and other musculoskeletal complaints) in subjects with SCI during and after inpatient rehabilitation? What is the degree of pain and spasticity and does this change during and after inpatient rehabilitation? What are the risk factors for these complications? MethodS The present study was part of the Dutch research program on the restoration of mobility in persons with SCI. Subjects admitted to one of the 8 participating rehabilitation centres between May 2000 and September 2003 were included if they met the eligibility criteria. During their first period of inpatient rehabilitation, they were eligible for inclusion if they were between 18 and 65 years of age, were wheelchair-dependent, had sufficient comprehension of the Dutch language to understand the purpose of the study, and did not have a progressive or psychiatric condition that would interfere with constructive participation. Design Subjects were assessed according to a standardized protocol at 4 assessment times: at the start of active inpatient rehabilitation, defined as the moment when the subject was able to sit in a wheelchair for 3 hours (t1), 3 months later (t2), at discharge (t3), and one year after discharge from inpatient rehabilitation (t4). If the subject was discharged within one month after t2, the assessment at t2 was considered a "discharge" assessment, and was included in the analyses of t3. The protocol was approved by the Medical Ethics Committee and prior to participation all subjects gave their written informed consent. Complications Based on the subject s history and medical chart, the physicians registered each complication on a standardized list. At t1, complications then present or that had occurred since admission to rehabilitation were registered. At t2 and t3, complications then present or that had occurred since t1 and t2, respectively, were registered. At t4, complications then present or that had occurred since discharge were registered. The occurrence of a complication was registered as follows: 0 = no complication; 1 = presence or history of this complication. Other cardiovascular disease and musculoskeletal complaints were grouped, and included conditions such as myocardial disease and bursitis occurring after the lesion, respectively. If the subject reported having pain, the research assistants completed a standardized list addressing the nature of the pain. Musculoskeletal pain was defined as nociceptive pain originating from bone, joint or muscle structures following trauma or overuse (7). Thirteen locations (on the upper and lower limbs, the neck and the back) were assigned severity scores with a 5-point Likert scale (1 5: ranging from not severe to very severe ), and frequency scores (1 3: ranging from once a week or less to more than 3 times a week ). Neurogenic pain was defined as at-level or below-level pain originating from spinal cord ischaemia or trauma (7). Hence, 9 neurogenic pain characteristics (other pain, numbness, itching, tingling, cold, warm, perspiration, girdle zone pain and phantom feeling) were assigned frequency and severity scores. A sum score was made for the product (severity frequency) of these locations or pain characteristics. Therefore, sum scores ranging from 1 to 195, or from 1 to 135 could be attained for musculoskeletal or neurogenic pain, respectively. Additionally, the research assistant determined the presence of spasticity, defined as the velocity dependent increase in muscle tone combined with exaggerated reflexes, through a direct standardized examination (7). The left and right hip adductors, knee flexors and extensors, ankle extensors, and elbow flexors and extensors were examined. In the presence of spasticity, each muscle group was assigned severity scores ranging from 1 to 3 (1: catch; 2: clonus < 5 beats; 3: clonus 5 beats). These scores were summated, which gave a sum score ranging from 1 to 36. Risk factors The associations with the following potential risk factors were assessed: age, gender, smoking status (smoker vs non-smoker), body mass index (BMI: body mass in kilograms divided by height in metres squared; kg/m 2 ), the cause (traumatic vs non-traumatic), the level and the completeness of the lesion. Although some smokers refrained from smoking during inpatient rehabilitation, nearly all resumed smoking after discharge. Therefore, subjects were defined as being a smoker if they smoked prior to the injury. Tetraplegia was defined as a lesion at or above the first thoracic segment, and paraplegia as a lesion below the first thoracic segment. A complete lesion was diagnosed in the absence of sensory or motor function in the sacral segments, i.e. American Spinal Injury Association (ASIA) category A. An incomplete lesion was defined as ASIA categories B, C or D (18). Statistics Random coefficient analyses (MlwiN version 1.1; Centre for Multilevel Modelling, Institute of Education, London, UK) were used to estimate the occurrence of complications, the change in the degree of pain and spasticity, and the association with risk factors (19, 20). The longitudinal aspect of the study is enhanced by the fact that the analyses can be done with missing values and varying group composition. Therefore, all assessments can be included in the analyses, which gives a more accurate description, compared with repeated measurements analysis of variance, for example, of complications and their risk factors at each assessment. Analysis of complications. A logistic random coefficient model was made for the occurrence of each complication. Time was included in the model as a set of 3 dummy variables (each with their own regression coefficient). The discharge assessment was chosen as their reference and was estimated by the intercept. The occurrence of a complication during the other intervals was estimated as follows: 1/ {1 + exp[ (intercept + regression coefficient)]} (19). The sum scores for pain and spasticity were estimated with similar models for continuous outcome variables. Again, time was modelled as 3 dummy variables, and the score at discharge was estimated by the intercept. The sum scores at the other assessments were calculated by adding the intercept to the regression coefficient of the dummy variable. Analysis of risk factors. All risk factors were simultaneously added to the previously described models. With these multivariate models, the contribution of each risk factor was corrected for. The regression coefficients for the risk factors were converted to odds ratios (ORs); OR = exp[regression coefficient]. An OR of 1 indicated that there was no association with this particular variable, whereas an OR < 1 indicated a decreased risk, and an OR > 1 indicated an increased risk of this complication in the presence of the risk factor. For the continuous outcome variables, the regression coefficient indicated the difference in the sum score associated with the difference in the risk factor of 1 unit. Results Table I gives the descriptive characteristics of the subjects. Subjects were lost to follow-up for several reasons: 9 died, 5
3 Complications following spinal cord injury 395 Table I. Descriptive subject characteristics. Start 3 months Discharge 1 year after discharge Subjects (n) Age (years) mean (SD) 40 (14) 41 (14) 41 (14) 41 (14) Gender (% male) Body mass index 22.7 (3.8) 23.1 (4.0) 23.4 (4.0) 24.5 (4.5) (kg/m 2 ) mean (SD) Smoker (% smoker) Days since previous 49 (44) 103 (33) 162 (125) 397 (57) assessment* mean (SD) Cause (% traumatic) Level (% tetraplegia) Completeness (% complete) *For the start of active rehabilitation, days since admission are given. moved abroad, 26 refused further participation, 7 developed a psychiatric or progressive condition, 5 were untraceable and 3 dropped out for unknown reasons. Forty-four subjects were discharged within one month after t2, and therefore, no data were included for them at t2. The mean (SD) duration between injury and admission to rehabilitation was 44 (43) days. Complications Fig. 1 shows the estimated occurrence of a complication during each interval. All data are derived from random coefficient analyses. Most subjects reported neurogenic and musculoskeletal pain, or had spasticity at each assessment. Common secondary complications were urinary tract infections and pressure sores, reported by 47% and 36% of the population at t1, respectively. Like most complications, they remained common during the year after discharge, occurring in 49% and 36% of the population at t4, respectively. Additionally, Fig. 1 shows the estimated degree of pain and spasticity at each assessment. The degree of pain decreased, whereas the degree of spasticity increased significantly during inpatient rehabilitation. Risk factors Table II gives the ORs for the association between the risk factors and the occurrence of a complication. An increase in age, tetraplegia and completeness of the lesion were the most frequently identified risk factors. Those with a high BMI and those with a traumatic lesion were at increased risk of several complications; the largest effect was seen for cardiovascular disease. The risk associated with gender or smoking varied for different complications. Table III gives the regression coefficients for the association between the degree of pain or spasticity and the risk factors. Overall, an increase in age was associated with an increase in pain. Men and those with a traumatic lesion had a higher degree of spasticity. Those with a tetraplegia and those with an incomplete lesion reported more musculoskeletal pain and showed a higher degree of spasticity. Fig. 1. The estimated occurrence of a complication during each interval and the sum scores for pain or spasticity at 4 assessment times: random coefficient modelling. * Significant difference (p 0.05) between the sum score at t1 and that at t3. Sum scores determined in those subjects who reported pain or who had spasticity at examination, expressed as a percentage of the maximum obtainable score. Complications Discussion The present study showed that the occurrence of a range of complications was high both during and after inpatient rehabilitation. Most of our findings coincided with previous studies, but inconsistencies may be attributed to the variation in both the selected population and the design. Excluding those with progressive disease or those over the age of 65 years, for example, will have influenced the findings. Complications
4 396 J. A. Haisma et al. Table II. Odds ratios for the association with potential risk factors: multivariate logistic random coefficient modelling. Age (years) Gender* Smoking* Neurogenic pain (0.99; 1.05) (0.23; 1.21) (0.63; 2.27) Spasticity (0.96; 0.99) (1.60; 3.98) (0.93; 2.16) Hypotension (0.97; 1.02) (0.43; 1.54) (0.41; 1.29) Autonomic dysreflexia (0.95; 1.00) (0.81; 3.52) (0.68; 2.15) Pressure sore (1.00; 1.03) (0.72; 1.63) (0.93; 1.93) Urinary tract infection (0.99; 1.02) (0.60; 1.28) (0.56; 1.11) Pulmonary infection (1.02; 1.08) (0.51; 2.07) (0.79; 2.80) Thromboembolism (0.97; 1.06) (0.22; 2.12) (0.72; 6.11) Oedema (1.03; 1.06) (0.53; 1.24) (1.09; 2.41) Heterotopic ossification (0.96; 1.01) (2.74; 47.32) (0.27; 0.91) Cardiovascular disease (1.01; 1.10) (0.24; 2.13) (0.41; 3.96) Musculoskeletal pain (0.98; 1.02) (0.40; 0.99) (0.53; 1.14) Other musculoskeletal complaints (1.00; 1.05) (0.56; 2.19) (0.58; 1.93) Body mass index (kg/m 2 ) Cause* Level* Completeness* (0.91; 1.08) (0.41; 2.41) (0.44; 1.70) (0.29; 1.11) (1.04; 1.18) (0.64; 1.79) (0.08; 0.23) (0.61; 1.48) (0.90; 1.04) (0.59; 3.25) (0.05; 0.18) (1.32; 4.52) (0.99; 1.15) (0.40; 2.21) (0.07; 0.27) (1.26; 4.42) (0.93; 1.03) (0.67; 1.74) (0.36; 0.78) (1.17; 2.56) (0.93; 1.02) (1.02; 2.47) (0.36; 0.75) (1.26; 2.60) (0.85; 1.01) (0.45; 2.42) (0.13; 0.53) (1.74; 7.17) (0.79; 1.08) (0.42; 4.32) (0.59; 5.74) (1.04; 1.16) (1.23; 3.43) (0.72; 1.65) (0.97; 2.21) (0.93; 1.09) (0.35; 1.78) (0.42; 1.49) (1.29; 4.67) (1.11; 1.46) (1.25; 20.46) (0.31; 2.63) (0.19; 1.94) (1.01; 1.13) 0.96 (0.89; 1.04) (1.17; 3.15) 1.33 (0.60; 2.96) (0.43; 1.00) 0.86 (0.45; 1.64) (0.48; 1.09) 1.53 (0.81; 2.89) Odds ratios (and 95% confidence intervals) are given; significant associations (p 0.05) are printed in bold. *Gender: men = 1, women = 0; Smoking: smoker = 1, non-smoker = 0; Cause: traumatic = 1, non-traumatic = 0; Level: paraplegia = 1, tetraplegia = 0; Completeness: complete = 1, incomplete = 0. As an example is given that an increase in age of one year was associated with a 1.05 times larger risk of a pulmonary infection; those with a complete lesion were 3.53 times more at risk of a pulmonary infection, than those with an incomplete lesion. Cause could not be modelled; in this population all subjects with thromboembolism had a traumatic lesion. were registered based on clinical symptoms often confirmed by additional examination, whereas some others searched for pathology in the absence of clinical symptoms. Furthermore, the longitudinal design will have revealed different information on the association with risk factors than did previous cross-sectional data. Although pain and spasticity were common, understanding their impact remains challenging. The reported degree of pain is influenced by both psychosocial and physical factors, which interfere with the interpretation of changes over time and the associations with risk factors (21, 22). It remains to say, that when pain is experienced, it does often necessitate intervention. Besides increased stretch reflexes, spasticity encompasses increased muscle tone, involuntary movements and primitive reflexes. Lack of effective measurement techniques makes the quantification of all components of spasticity difficult (7). Furthermore, in contrast to pain, the degree of spasticity is not necessarily related to individual functional complaints Table III. Regression coefficients for the association between risk factors and the degree of pain or spasticity: multivariate random coefficient modelling. Neurogenic pain 0.12 (0.01; 0.23) Spasticity 0.00 ( 0.03; 0.03) Musculoskeletal pain 0.14 (0.01; 0.28) Age Gender* Smoking* 2.20 ( 5.30; 0.89) 1.02 (0.13; 1.90) 2.33 ( 6.08; 1.43) 2.29 ( 5.10; 0.52) 0.64 ( 0.11; 1.38) 2.13 ( 5.58; 1.32) Body mass index (kg/m 2 ) Cause* Level* Completeness* 0.27 ( 0.11; 0.64) 0.02 ( 0.09; 0.12) 0.06 ( 0.39; 0.50) 1.28 ( 4.86; 2.30) 2.33 (1.35; 3.32) 1.24 ( 5.76; 3.27) 9.84 ( 12.81; 6.88) 2.86 ( 0.10; 5.82) ( 1.86; 0.28) ( 3.02; 1.39) ( 13.61; 6.44) ( 8.26; 0.94) Regression coefficients (and 95% confidence intervals) are given; significant associations (p 0.05) are printed in bold. *Gender: men = 1, women = 0; Smoking: smoker = 1, non-smoker = 0; Cause: traumatic = 1, non-traumatic = 0; Level: paraplegia = 1, tetraplegia = 0; Completeness: complete = 1, incomplete = 0. As an example is given that the sum score for musculoskeletal pain was points lower for those with paraplegia than for those with tetraplegia.
5 Complications following spinal cord injury 397 or to the required treatment. Because pain and spasticity are common sequelae to SCI, which may require intervention, it is important to reach consensus on how to monitor their clinical impact. Several mechanisms may explain why complications are common after discharge from inpatient rehabilitation (9, 10, 12). After discharge, both the demanding activities of daily living (ADLs) and the reduction in structured training, could make subjects susceptible to complications associated with overuse (1). Additionally, many subjects have less guidance or peer-control in self-care (23). The higher demands of ADLs, together with reduced feedback, could make subjects less conscientious towards preventive measures, such as skin checks and bladder management. The active involvement of the spouse may contribute to the prevention of complications, and further analyses of our data showed a tendency for those living alone to be at increased risk. Although the interval evaluated after discharge is long compared with the intervals during rehabilitation, complications remain a common problem. This should warrant decision-makers investing in effective followup programs (3, 12, 23). Persons with SCI have an increasing life expectancy, and it is important for rehabilitation medicine to strive for the long-term prevention of complications. Risk factors This study indicated subpopulations inherently at risk of complications. The level and completeness of the lesion determine the extent of pareses and loss of respiratory and autonomic function (1, 24, 25), which are inevitably associated with the risk of complications (1, 10, 22). The physiological age-related decline in cardio-respiratory function and mobility leave the elderly susceptible to complications (9, 26). Concurrent extraspinal injury may be an additional risk factor (27). Although concurrent injury was poorly registered in the present study, further investigation revealed that it was more common in traumatic lesions. This may partly explain why those with a traumatic lesion were at risk of some complications. However, a standardized registration of concurrent injury is needed to establish these correlations. The unexplained predisposition of men for heterotropic ossification has been described before (13). It could be that in men symptoms were more apparent, or more often attributed to heterotopic ossification. Although type of lesion, age and gender cannot be influenced, their identification as important risk factors allows us to target screening and prevention programs. Besides these unchangeable risk factors, the effect of some lifestyle risks was investigated. An increase in BMI increased the risk of several complications. However, the interpretation of the BMI is difficult in those with SCI, especially during the early phase of rehabilitation (28). Changes in body weight may be attributed to an increase in upper body muscle mass, a decrease in muscle mass of the lower limbs, the accumulation of extra-vascular fluids and an increase in fat mass (28). The associations with other modifiable lifestyle risks, such as alcohol consumption and inactivity, remain ambiguous (29, 30). We anticipate that the cumulative damaging effect of smoking, alcohol consumption, dietary intake and inactivity will become more evident at a later phase post-injury. Therefore, the correlation between lifestyle exposure and complications needs to be investigated in a longitudinal study with a longer follow-up period. Limitations The present study design needs some consideration. One should bear in mind that the study investigated medical complications, whereas SCI also has psychosocial complications beyond the scope of this investigation. In general, data on the occurrence of complications during a time interval do not inform us about their severity or duration. Because the occurrence of a complication may have delayed discharge, the population assessed 3 months into active inpatient rehabilitation was probably more prone to complications. The assessed population and the varying intervals should be considered when interpreting results. However, random coefficient analyses has allowed us to include all present subjects at each assessment point and this has provided more realistic data on the occurrence of complications during each interval. Our longitudinal design provided insight into the timing of complications, and contributed to the understanding of the nature of risk factors during different phases of rehabilitation. In conclusion, complications are common following SCI and subpopulations are at increased risk. Educational programs for patients and their families need to focus on the prevention and early recognition of complications. Structural follow-up visits after inpatient rehabilitation need to be implemented at specialized rehabilitation centres. Besides addressing functional outcome and social participation, these visits also need to focus on complications. Only through the timely prevention, surveillance and treatment of complications can their impact be reduced, and can the individual rehabilitation outcome be optimized. Acknowledgements This article was presented in part at the 8th International Neurotrauma Symposium, May 2006, Rotterdam, The Netherlands, and at the 45th ISCoS Annual Scientific Meeting, June 2006, Boston, USA. This study was supported by the Health Research and Development Council of The Netherlands (grants ; ). References 1. Noreau L, Proulx P, Gagnon L, Drolet M, Laramee MT. Secondary impairments after spinal cord injury: a population-based study. Am J Phys Med Rehabil 2000; 79: Westgren N, Levi R. Quality of life and traumatic spinal cord injury. Arch Phys Med Rehabil 1998; 79: Bloemen-Vrencken JH, Post MW, Hendriks JM, De Reus EC, De Witte LP. Health problems of persons with spinal cord injury living in the Netherlands. Disabil Rehabil 2005; 27: Valtonen K, Karlsson AK, Alaranta H, Viikari-Juntura E. Work participation among persons with traumatic spinal cord injury and meningomyelocele1. J Rehabil Med 2006; 38:
6 398 J. A. Haisma et al. 5. Meyers AR, Andresen EM, Hagglund KJ. A model of outcomes research: spinal cord injury. Arch Phys Med Rehabil 2000; 81: S81 S Kirschblum S, Campagnolo DI, DeLisa JA, editors. Spinal cord medicine. Philadelphia: Lippincott Williams & Wilkins; Burchiel KJ, Hsu FP. Pain and spasticity after spinal cord injury: mechanisms and treatment. Spine 2001; 26: S146 S Werhagen L, Budh CN, Hultling C, Molander C. Neuropathic pain after traumatic spinal cord injury relations to gender, spinal level, completeness, and age at the time of injury. Spinal Cord 2004; 42: McKinley WO, Jackson AB, Cardenas DD, DeVivo MJ. Longterm medical complications after traumatic spinal cord injury: a regional model systems analysis. Arch Phys Med Rehabil 1999; 80: Chen Y, Devivo MJ, Jackson AB. Pressure ulcer prevalence in people with spinal cord injury: age-period-duration effects. Arch Phys Med Rehabil 2005; 86: Post MW, Dallmeijer AJ, Angenot EL, van Asbeck FW, van der Woude LH. Duration and functional outcome of spinal cord injury rehabilitation in the Netherlands. J Rehabil Res Dev 2005; 42: Cardenas DD, Hoffman JM, Kirshblum S, McKinley W. Etiology and incidence of rehospitalization after traumatic spinal cord injury: a multicenter analysis. Arch Phys Med Rehabil 2004; 85: Vanden Bossche L, Vanderstraeten G. Heterotopic ossification: a review. J Rehabil Med 2005; 37: DeVivo MJ, Krause JS, Lammertse DP. Recent trends in mortality and causes of death among persons with spinal cord injury. Arch Phys Med Rehabil 1999; 80: Aito S. Complications during the acute phase of traumatic spinal cord lesions. Spinal Cord 2003; 41: New P, Rawicki HB, Bailey MJ. Nontraumatic spinal cord injury rehabilitation: pressure ulcer pattern, prediction and impact. Arch Phys Med Rehabil 2004; 85: Chen D, Apple DF Jr., Hudson LM, Bode R. Medical complications during acute rehabilitation following spinal cord injury current experience of the model systems. Arch Phys Med Rehabil 1999; 80: Maynard FM Jr., Bracken MB, Creasey G, Ditunno JF Jr., Donovan WH, Ducker TB, et al. International standards for neurological and functional classification of spinal cord injury. American Spinal Injury Association. Spinal Cord 1997; 35: Twisk JW. Applied longitudinal data analysis for epidemiology; a practical guide. Cambridge: Cambridge University Press; Rasbash J, Browne W, Goldstein H, Yang M, Plewis I, Healy M, et al. A user s guide to MLwiN. London: University of London: Siddall PJ, Loeser JD. Pain following spinal cord injury. Spinal Cord 2001; 39: van Drongelen S, de Groot S, Veeger HE, Angenot EL, Dallmeijer AJ, Post MW, et al. Upper extremity musculoskeletal pain during and after rehabilitation in wheelchair-using persons with a spinal cord injury. Spinal Cord 2006; 44: Bloemen-Vrencken JH, de Witte LP. Post-discharge nursing problems of spinal cord injured patients: on which fields can nurses contribute to rehabilitation? Clin Rehabil 2003; 17: Winslow C, Rozovsky J. Effect of spinal cord injury on the respiratory system. Am J Phys Med Rehabil 2003; 82: Haisma JA, Bussmann JB, Stam HJ, Sluis TA, Bergen MP, Dallmeijer AJ, et al. Changes in physical capacity during and after inpatient rehabilitation in subjects with a spinal cord injury. Arch Phys Med Rehabil 2006; 87: DeVivo MJ, Kartus PL, Rutt RD, Stover SL, Fine PR. The influence of age at time of spinal cord injury on rehabilitation outcome. Arch Neurol 1990; 47: van Asbeck FW, Post MW, Pangalila RF. An epidemiological description of spinal cord injuries in The Netherlands in Spinal Cord 2000; 38: Buchholz AC, Bugaresti JM. A review of body mass index and waist circumference as markers of obesity and coronary heart disease risk in persons with chronic spinal cord injury. Spinal Cord 2005; 43: Janssen TW, van Oers CA, van Kamp GJ, TenVoorde BJ, van der Woude LH, Hollander AP. Coronary heart disease risk indicators, aerobic power, and physical activity in men with spinal cord injuries. Arch Phys Med Rehabil 1997; 78: Tate DG, Forchheimer MB, Krause JS, Meade MA, Bombardier CH. Patterns of alcohol and substance use and abuse in persons with spinal cord injury: risk factors and correlates. Arch Phys Med Rehabil 2004; 85:
ORIGINAL REPORT. J Rehabil Med 2013 Epub ahead of print
 J Rehabil Med 2013 Epub ahead of print ORIGINAL REPORT in persons with spinal cord injury: a longitudinal study from One to Five Years postdischarge Jacinthe J. E. Adriaansen, MD 1, Marcel W. M. Post,
J Rehabil Med 2013 Epub ahead of print ORIGINAL REPORT in persons with spinal cord injury: a longitudinal study from One to Five Years postdischarge Jacinthe J. E. Adriaansen, MD 1, Marcel W. M. Post,
Inge E. Eriks-Hoogland, MD 1, Sonja de Groot, PhD 2,4, Marcel W. M. Post, PhD 2,3 and Lucas H. V. van der Woude, PhD 4,5
 J Rehabil Med 2011; 43: 210 215 ORIGINAL REPORT CoRrelation of shoulder range of motion limitations at discharge WITH limitations in activities and participation one year later in persons with spinal cord
J Rehabil Med 2011; 43: 210 215 ORIGINAL REPORT CoRrelation of shoulder range of motion limitations at discharge WITH limitations in activities and participation one year later in persons with spinal cord
Erasmus Medical Center, Dept. of Rehabilitation Medicine and Physical Therapy
 A more active lifestyle in persons with a recent spinal cord injury benefits physical fitness and health Running head: SCI and the importance of physical activity Carla F.J. Nooijen, MSc 1, Sonja de Groot,
A more active lifestyle in persons with a recent spinal cord injury benefits physical fitness and health Running head: SCI and the importance of physical activity Carla F.J. Nooijen, MSc 1, Sonja de Groot,
Morbidity Aspects in Spinal Cord Injury Patients: Experience of the Spinal Unit at King Hussein Medical Center
 Morbidity Aspects in Spinal Cord Injury Patients: Experience of the Spinal Unit at King Hussein Medical Center Ali H. Otom MD, D. Med Rehab (RCP)* ABSTRACT Objectives: To investigate the frequency of medical
Morbidity Aspects in Spinal Cord Injury Patients: Experience of the Spinal Unit at King Hussein Medical Center Ali H. Otom MD, D. Med Rehab (RCP)* ABSTRACT Objectives: To investigate the frequency of medical
University of Groningen
 University of Groningen Longitudinal association between lifestyle and coronary heart disease risk factors among individuals with spinal cord injury de Groot, Sonja; Post, Marcel W.M.; Snoek, G. J.; Schuitemaker,
University of Groningen Longitudinal association between lifestyle and coronary heart disease risk factors among individuals with spinal cord injury de Groot, Sonja; Post, Marcel W.M.; Snoek, G. J.; Schuitemaker,
SOCIAL SUPPORT AND LIFE SATISFACTION IN SPINAL CORD INJURY DURING AND UP TO ONE YEAR AFTER INPATIENT REHABILITATION
 J Rehabil Med 2010; 42: 265 271 ORIGINAL REPORT SOCIAL SUPPORT AND LIFE SATISFACTION IN SPINAL CORD INJURY DURING AND UP TO ONE YEAR AFTER INPATIENT REHABILITATION Christel M. C. van Leeuwen, MSc 1, Marcel
J Rehabil Med 2010; 42: 265 271 ORIGINAL REPORT SOCIAL SUPPORT AND LIFE SATISFACTION IN SPINAL CORD INJURY DURING AND UP TO ONE YEAR AFTER INPATIENT REHABILITATION Christel M. C. van Leeuwen, MSc 1, Marcel
Ageing with Spinal Cord Injury
 Ageing with Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review Date October 2016 This document has been developed to provide health service
Ageing with Spinal Cord Injury A Resource for Health Service Providers WA State Spinal Injury Unit Version 1 October 2013 Review Date October 2016 This document has been developed to provide health service
SIMILAR TO THE GENERAL population, cardiovascular
 ORIGINAL ARTICLE Prospective Analysis of Lipid Profiles in Persons With a Spinal Cord Injury During and 1 Year After Inpatient Rehabilitation Sonja de Groot, PhD, Annet J. Dallmeijer, PhD, Marcel W. Post,
ORIGINAL ARTICLE Prospective Analysis of Lipid Profiles in Persons With a Spinal Cord Injury During and 1 Year After Inpatient Rehabilitation Sonja de Groot, PhD, Annet J. Dallmeijer, PhD, Marcel W. Post,
Functional outcome of patients with spinal cord injury: rehabilitation outcome study
 Clinical Rehabilitation 1999; 13: 457 463 Functional outcome of patients with spinal cord injury: rehabilitation outcome study MC Schönherr Rehabilitation Centre Beatrixoord, Haren and Department of Rehabilitation,
Clinical Rehabilitation 1999; 13: 457 463 Functional outcome of patients with spinal cord injury: rehabilitation outcome study MC Schönherr Rehabilitation Centre Beatrixoord, Haren and Department of Rehabilitation,
SEVERAL STUDIES ON spinal cord injury (SCI) recovery. Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study
 512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
512 Early Versus Delayed Inpatient Spinal Cord Injury Rehabilitation: An Italian Study Giorgio Scivoletto, MD, Barbara Morganti, PT, Marco Molinari, MD, PhD ABSTRACT. Scivoletto G, Morganti B, Molinari
University of Groningen
 University of Groningen Return to work five years after spinal cord injury inpatient rehabilitation van Velzen, Judith M.; van Leeuwen, Caroline; de Groot, Sonja; van der Woude, L. H. V.; Faber, Willemijn
University of Groningen Return to work five years after spinal cord injury inpatient rehabilitation van Velzen, Judith M.; van Leeuwen, Caroline; de Groot, Sonja; van der Woude, L. H. V.; Faber, Willemijn
This is a published version of a paper published in Journal of Rehabilitation Medicine. Access to the published version may require subscription.
 Umeå University This is a published version of a paper published in Journal of Rehabilitation Medicine. Citation for the published paper: Flank, P., Wahman, K., Levi, R., Fahlström, M. (2012) "Prevalence
Umeå University This is a published version of a paper published in Journal of Rehabilitation Medicine. Citation for the published paper: Flank, P., Wahman, K., Levi, R., Fahlström, M. (2012) "Prevalence
Bryan Andresen MD Advances in Clinical Neuroscience Practice /2/11
 Bryan Andresen MD Advances in Clinical Neuroscience Practice 2011 5/2/11 Intro/History Definition Differential Diagnosis Clinical Characteristics Exam Findings Treatment Outcomes 46 yo female admitted
Bryan Andresen MD Advances in Clinical Neuroscience Practice 2011 5/2/11 Intro/History Definition Differential Diagnosis Clinical Characteristics Exam Findings Treatment Outcomes 46 yo female admitted
American Board of Physical Medicine & Rehabilitation. Part I Curriculum & Weights
 American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
American Board of Physical Medicine & Rehabilitation Part I Curriculum & Weights Neurologic Disorders 30% Stroke Spinal Cord Injury Traumatic Brain Injury Neuropathies a) Mononeuropathies b) Polyneuropathies
University of Groningen. Functional outcome after spinal cord injury Schonherr, Marleen C.
 University of Groningen Functional outcome after spinal cord injury Schonherr, Marleen C. IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
University of Groningen Functional outcome after spinal cord injury Schonherr, Marleen C. IMPORTANT NOTE: You are advised to consult the publisher's version (publisher's PDF) if you wish to cite from it.
AUTONOMIC FUNCTION IS A HIGH PRIORITY
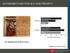 AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
AUTONOMIC FUNCTION IS A HIGH PRIORITY 1 Bladder-Bowel-AD Tetraplegia Sexual function Walking Bladder-Bowel-AD Paraplegia Sexual function Walking 0 10 20 30 40 50 Percentage of respondents an ailment not
Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the patient
 () 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
() 8, 8 ± ã International Medical Society of Paraplegia All rights reserved ± / $. www.nature.com/sc Prediction of functional outcome after spinal cord injury: a task for the rehabilitation team and the
THE COMPLICATIONS OF traumatic spinal cord injury
 87 Nontraumatic Spinal Cord Injury Rehabilitation: Pressure Ulcer Patterns, Prediction, and Impact Peter W. New, MBBS, FAFRM (RACP), H. Barry Rawicki, MBBS, FACRM, FAFRM (RACP), Michael J. Bailey, MSc
87 Nontraumatic Spinal Cord Injury Rehabilitation: Pressure Ulcer Patterns, Prediction, and Impact Peter W. New, MBBS, FAFRM (RACP), H. Barry Rawicki, MBBS, FACRM, FAFRM (RACP), Michael J. Bailey, MSc
Changes in lipid, lipoprotein and apolipoprotein pro les in persons with spinal cord injuries during the rst 2 years post-injury
 Spinal Cord (999) 37, 96 0 ã 999 International Medical Society of Paraplegia All rights reserved 36 4393/99 $.00 http://www.stockton-press.co.uk/sc Changes in lipid, lipoprotein and apolipoprotein pro
Spinal Cord (999) 37, 96 0 ã 999 International Medical Society of Paraplegia All rights reserved 36 4393/99 $.00 http://www.stockton-press.co.uk/sc Changes in lipid, lipoprotein and apolipoprotein pro
Rehabilitation and Metastatic Spinal Cord Compression
 Rehabilitation and Metastatic Spinal Cord Compression Pradeep Thumbikat MS, MSc, FRCS Consultant in Spinal Cord Injuries Sheffield Teaching Hospitals 1 Evidence for Rehabilitation Differences and similarities
Rehabilitation and Metastatic Spinal Cord Compression Pradeep Thumbikat MS, MSc, FRCS Consultant in Spinal Cord Injuries Sheffield Teaching Hospitals 1 Evidence for Rehabilitation Differences and similarities
ORIGINAL ARTICLE Good validity of the international spinal cord injury quality of life basic data set
 (2016) 54, 314 318 & 2016 International Society All rights reserved 1362-4393/16 www.nature.com/sc ORIGINAL ARTICLE Good validity of the international spinal cord injury quality of life basic data set
(2016) 54, 314 318 & 2016 International Society All rights reserved 1362-4393/16 www.nature.com/sc ORIGINAL ARTICLE Good validity of the international spinal cord injury quality of life basic data set
SURGICAL SPINE INTERVENTION after traumatic spinal
 1818 Outcomes of Early Surgical Management Versus Late or No Surgical Intervention After Acute Spinal Cord Injury William McKinley, MD, Michelle A. Meade, PhD, Steven Kirshblum, MD, Barbara Barnard, DO
1818 Outcomes of Early Surgical Management Versus Late or No Surgical Intervention After Acute Spinal Cord Injury William McKinley, MD, Michelle A. Meade, PhD, Steven Kirshblum, MD, Barbara Barnard, DO
Inter-rater reliability of the 1992 international standards for neurological and functional classi cation of incomplete spinal cord injury
 (2000) 38, 675 ± 679 ã 2000 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/00 $15.00 www.nature.com/sc Inter-rater reliability of the 1992 international standards for neurological
(2000) 38, 675 ± 679 ã 2000 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/00 $15.00 www.nature.com/sc Inter-rater reliability of the 1992 international standards for neurological
Ageing. Organs declining at approximately 1% per year. Spinal cord injury - ageing commences at injury
 Ageing Ageing begins at 25 years old Organs declining at approximately 1% per year. Spinal cord injury - ageing commences at injury > 25 at injury - may influence functional outcomes Impact of Long Term
Ageing Ageing begins at 25 years old Organs declining at approximately 1% per year. Spinal cord injury - ageing commences at injury > 25 at injury - may influence functional outcomes Impact of Long Term
WORKING MECHANISMS OF A BEHAVIOURAL INTERVENTION PROMOTING PHYSICAL ACTIVITY IN PERSONS WITH SUBACUTE SPINAL CORD INJURY
 J Rehabil Med 2016; 48: 583 588 ORIGINAL REPORT WORKING MECHANISMS OF A BEHAVIOURAL INTERVENTION PROMOTING PHYSICAL ACTIVITY IN PERSONS WITH SUBACUTE SPINAL CORD INJURY Carla F. J. Nooijen, PhD 1, Henk
J Rehabil Med 2016; 48: 583 588 ORIGINAL REPORT WORKING MECHANISMS OF A BEHAVIOURAL INTERVENTION PROMOTING PHYSICAL ACTIVITY IN PERSONS WITH SUBACUTE SPINAL CORD INJURY Carla F. J. Nooijen, PhD 1, Henk
Promoting Physical Activity in Persons with Subacute Spinal Cord Injury
 Promoting Physical Activity in Persons with Subacute Spinal Cord Injury Carla Nooijen Promoting Physical Activity in Persons with Subacute Spinal Cord Injury Carla Nooijen The research described in this
Promoting Physical Activity in Persons with Subacute Spinal Cord Injury Carla Nooijen Promoting Physical Activity in Persons with Subacute Spinal Cord Injury Carla Nooijen The research described in this
CARE OF SPINAL CORD INJURY VICTIMS
 CARE OF SPINAL CORD INJURY VICTIMS Dr THIERRY ALBERT Centre de Rééducation et de Réadaptation pour Adulte de COUBERT Route de Liverdy, Coubert 77257 Brie comte robert, cedex talbert@ugecamif.fr Spinal
CARE OF SPINAL CORD INJURY VICTIMS Dr THIERRY ALBERT Centre de Rééducation et de Réadaptation pour Adulte de COUBERT Route de Liverdy, Coubert 77257 Brie comte robert, cedex talbert@ugecamif.fr Spinal
Paraplegia: Exercise and Health Considerations. By: Juli and Trina
 Paraplegia: Exercise and Health Considerations By: Juli and Trina What is paraplegia? Paraplegia is impairment of motor and/or sensory function to the lower extremities, and sometimes the lower trunk Complete
Paraplegia: Exercise and Health Considerations By: Juli and Trina What is paraplegia? Paraplegia is impairment of motor and/or sensory function to the lower extremities, and sometimes the lower trunk Complete
REHABILITATION AIMS TO improve participation and ultimately
 82 ORIGINAL ARTICLE Relationships Between Activities, Participation, Personal Factors, Mental Health, and Life Satisfaction in Persons With Spinal Cord Injury Christel M. van Leeuwen, MSc, Marcel W. Post,
82 ORIGINAL ARTICLE Relationships Between Activities, Participation, Personal Factors, Mental Health, and Life Satisfaction in Persons With Spinal Cord Injury Christel M. van Leeuwen, MSc, Marcel W. Post,
The validation of the Dutch SF-Qualiveen, a questionnaire on urinary-specific quality of life, in spinal cord injury patients
 Reuvers et al. BMC Urology (2017) 17:88 DOI 10.1186/s12894-017-0280-9 RESEARCH ARTICLE The validation of the Dutch SF-Qualiveen, a questionnaire on urinary-specific quality of life, in spinal cord injury
Reuvers et al. BMC Urology (2017) 17:88 DOI 10.1186/s12894-017-0280-9 RESEARCH ARTICLE The validation of the Dutch SF-Qualiveen, a questionnaire on urinary-specific quality of life, in spinal cord injury
ORIGINAL ARTICLE The International Spinal Cord Injury Pain Basic Data Set (version 2.0)
 (2014) 52, 282 286 & 2014 International Society All rights reserved 1362-4393/14 www.nature.com/sc ORIGINAL ARTICLE The International Injury Pain Basic Data Set (version 2.0) E Widerström-Noga 1,2, F Biering-Sørensen
(2014) 52, 282 286 & 2014 International Society All rights reserved 1362-4393/14 www.nature.com/sc ORIGINAL ARTICLE The International Injury Pain Basic Data Set (version 2.0) E Widerström-Noga 1,2, F Biering-Sørensen
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE
 NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
NATIONAL REHABILITATION HOSPITAL (NRH) THE SPINAL CORD SYSTEM OF CARE (SCSC) PROGRAMME INPATIENT SCOPE OF SERVICE NATIONAL REHABILITATION HOSPITAL SCOPE OF SERVICE FOR THE SPINAL CORD SYSTEM OF CARE PROGRAMME
New Zealand Spinal Cord Injury Registry. First Annual Report August 2016 to July 2017
 New Zealand Spinal Cord Injury Registry First Annual Report August 216 to July 217 2 The New Zealand Spinal Cord Injury Registry (NZSCIR) would like to acknowledge the spinal service clinicians and coordinators
New Zealand Spinal Cord Injury Registry First Annual Report August 216 to July 217 2 The New Zealand Spinal Cord Injury Registry (NZSCIR) would like to acknowledge the spinal service clinicians and coordinators
University of Groningen
 University of Groningen Time-courses of lung function and respiratory muscle pressure generating capacity after spinal cord injury Mueller, Gabi; de Groot, Sonja; van der Woude, Lucas; Hopman, Maria T
University of Groningen Time-courses of lung function and respiratory muscle pressure generating capacity after spinal cord injury Mueller, Gabi; de Groot, Sonja; van der Woude, Lucas; Hopman, Maria T
Evaluation of Pain and Its Effect on Quality of Life and Functioning in Men with Spinal Cord Injury
 Original Article Korean J Pain 2015 April; Vol. 28,. 2: 129136 pissn 20059159 eissn 20930569 http://dx.doi.org/10.3344/kjp.2015.28.2.129 Evaluation of Pain and Its Effect on Quality of Life and Functioning
Original Article Korean J Pain 2015 April; Vol. 28,. 2: 129136 pissn 20059159 eissn 20930569 http://dx.doi.org/10.3344/kjp.2015.28.2.129 Evaluation of Pain and Its Effect on Quality of Life and Functioning
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc. Copyright 2014, 2011, 2006 by Saunders, an imprint of Elsevier, Inc.
 Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Spinal Cord Injury Transection Injury, Spinal Shock, and Hermiated Disc 1 Spinal Cord Injury Results from fracture and/or dislocation of vertebrae // Compresses, stretches, or tears spinal cord Cervical
Effect of Surface Spinal Stimulation (SSS) on H-reflex in Normal Individuals Narkeesh 1, A., Navroop kaur 2, N. & Sharma 3, S.
 Effect of Surface Spinal (SSS) on H-reflex in Normal Individuals Narkeesh 1, A., Navroop kaur 2, N. & Sharma 3, S. 1 Associate Professor, Email: narkeesh@gmail.com, 2 & 3 Post Graduate Students, Department
Effect of Surface Spinal (SSS) on H-reflex in Normal Individuals Narkeesh 1, A., Navroop kaur 2, N. & Sharma 3, S. 1 Associate Professor, Email: narkeesh@gmail.com, 2 & 3 Post Graduate Students, Department
Exoskeleton. Information for patients Spinal Injuries
 Exoskeleton Information for patients Spinal Injuries What is Ekso GT? Ekso GT is a robotic human-assisted exoskeleton that is designed as an assisted walking device for individuals with impaired walking
Exoskeleton Information for patients Spinal Injuries What is Ekso GT? Ekso GT is a robotic human-assisted exoskeleton that is designed as an assisted walking device for individuals with impaired walking
THE NEUROLOGIC LEVEL after spinal cord injury (SCI)
 389 Recovery of Upper-Extremity Strength in Complete and Incomplete Tetraplegia: A Multicenter Study John F. Ditunno, Jr., MD, Michelle E. Cohen, PhD, Walter W. Hauck, PhD, Amie B. Jackson, MD, Marca L.
389 Recovery of Upper-Extremity Strength in Complete and Incomplete Tetraplegia: A Multicenter Study John F. Ditunno, Jr., MD, Michelle E. Cohen, PhD, Walter W. Hauck, PhD, Amie B. Jackson, MD, Marca L.
Spinal Trauma. General Rehabilitation of Patient with Spinal Trauma. Common Spinal Injuries. Important Anatomical Structures at each Vertebral Level
 Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Asian Association for Dynamic Osteosynthesis Workshop on Management of Spinal Trauma 22 April 2007 (Sunday) Orthopaedic Learning Centre, PWH, Shatin, Hong Kong General Rehabilitation of Patient with Spinal
Normative values and determinants of physical capacity in individuals with spinal cord injury
 Journal of Rehabilitation Research and Development Vol. 39 No. 1, January/February 2002 Pages 29 39 Normative values and determinants of physical capacity in individuals with spinal cord injury Thomas
Journal of Rehabilitation Research and Development Vol. 39 No. 1, January/February 2002 Pages 29 39 Normative values and determinants of physical capacity in individuals with spinal cord injury Thomas
Neurologic improvement after thoracic, thoracolumbar, and lumbar spinal cord (conus medullaris) injuries
 Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 1-2011 Neurologic improvement after thoracic, thoracolumbar, and
Thomas Jefferson University Jefferson Digital Commons Department of Orthopaedic Surgery Faculty Papers Department of Orthopaedic Surgery 1-2011 Neurologic improvement after thoracic, thoracolumbar, and
Complex regional pain syndrome in adults: concise guidance
 CONCISE GUIDANCE Clinical Medicine 2011, Vol 11, No 6: 596 600 Complex regional pain syndrome in adults: concise guidance Lynne Turner-Stokes and Andreas Goebel on behalf of the guideline development group
CONCISE GUIDANCE Clinical Medicine 2011, Vol 11, No 6: 596 600 Complex regional pain syndrome in adults: concise guidance Lynne Turner-Stokes and Andreas Goebel on behalf of the guideline development group
Health-related outcomes of people with spinal cord injury - a 10 year longitudinal study
 Health-related outcomes of people with spinal cord injury - a 10 year longitudinal study Author Dorsett, Pat, Geragthy, T Published 2008 Journal Title Spinal Cord DOI https://doi.org/10.1038/sj.sc.3102159
Health-related outcomes of people with spinal cord injury - a 10 year longitudinal study Author Dorsett, Pat, Geragthy, T Published 2008 Journal Title Spinal Cord DOI https://doi.org/10.1038/sj.sc.3102159
Haemodynamic and Respiratory Responses to Abdominal Muscle FES A Pilot Study
 Haemodynamic and Respiratory Responses to Abdominal Muscle FES A Pilot Study H Rischbieth 1 *, J Clark 1, S Donohoe 1, J Strayer 1,2, M Jelbart 1, K Stiller 3, T McDonald 3, R Marshall 1,2. FES Clinic,
Haemodynamic and Respiratory Responses to Abdominal Muscle FES A Pilot Study H Rischbieth 1 *, J Clark 1, S Donohoe 1, J Strayer 1,2, M Jelbart 1, K Stiller 3, T McDonald 3, R Marshall 1,2. FES Clinic,
Chapter 2 Published as:
 The effects of hybrid cycle training in inactive people with long-term spinal cord injury: design of a multicenter randomized controlled trial Published as: Bakkum AJ, de Groot S, van der Woude LH, Janssen
The effects of hybrid cycle training in inactive people with long-term spinal cord injury: design of a multicenter randomized controlled trial Published as: Bakkum AJ, de Groot S, van der Woude LH, Janssen
Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury. Original Policy Date
 MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
MP 7.01.58 Stimulation of the Sacral Anterior Root Combined with Posterior Sacral Rhizotomy in Patients with Spinal Cord Injury Medical Policy Section Issue 12:2013 Original Policy Date 12:2013 Last Review
ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS
 CHAPTER 5 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS J. AM. GERIATR. SOC. 2013;61(6):882 887 DOI: 10.1111/JGS.12261 61 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER,
CHAPTER 5 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER, PHYSICAL HEALTH, AND LIFESTYLE IN OLDER ADULTS J. AM. GERIATR. SOC. 2013;61(6):882 887 DOI: 10.1111/JGS.12261 61 ATTENTION-DEFICIT/HYPERACTIVITY DISORDER,
Central Cord Syndrome: Does early surgical intervention improve neurological outcome
 Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Central Cord Syndrome: Does early surgical intervention improve neurological outcome Ciara Stevenson, Jonathan Warnock, Suzanne Maguire, Niall Eames Department of Trauma and Orthopaedic Surgery, Royal
Life Care Plan. Eric Henderson Potential Complications For Information Purposes Only. No Prediction of Frequency of Occurrence Available.
 Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
ANXIETY AND DEPRESSION LEVEL AND RELATED FACTORS IN PATIENTS WITH SPINAL CORD INJURY
 Acta Medica Mediterranea, 2014, 30: 291 ANXIETY AND DEPRESSION LEVEL AND RELATED FACTORS IN PATIENTS WITH SPINAL CORD INJURY İRFAN KOCA 1, MEHMET UÇAR 2, AHMET UNAL 3, AHMET TUTOĞLU 4, AHMET BOYACI 4,
Acta Medica Mediterranea, 2014, 30: 291 ANXIETY AND DEPRESSION LEVEL AND RELATED FACTORS IN PATIENTS WITH SPINAL CORD INJURY İRFAN KOCA 1, MEHMET UÇAR 2, AHMET UNAL 3, AHMET TUTOĞLU 4, AHMET BOYACI 4,
Life Care Plan. Hannah Sayne Potential Complications For Information Purposes Only. No Prediction of Frequency of Occurrence Available.
 Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Cost of Potential s Arthritis Greater risk for developing arthritis due to orthopedic injuries. Arthroplasty $26,800 - $29,000 Replacement of hip joint due to bone disease. Autonomic Dysreflexia (exaggerated
Chapter V Depression and Women with Spinal Cord Injury
 1 Chapter V Depression and Women with Spinal Cord Injury L ike all women with disabilities, women with spinal cord injury (SCI) may be at an elevated risk for depression due to the double jeopardy of being
1 Chapter V Depression and Women with Spinal Cord Injury L ike all women with disabilities, women with spinal cord injury (SCI) may be at an elevated risk for depression due to the double jeopardy of being
3/3/2016. International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI)
 International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI) American Spinal Injury Association International Spinal Cord Society Presented by Adam Stein, MD Chairman and Professor
International Standards for the Neurologic Classification of Spinal Cord Injury (ISNCSCI) American Spinal Injury Association International Spinal Cord Society Presented by Adam Stein, MD Chairman and Professor
AS THE NUMBER OF interventions proposed for study in
 ORIGINAL ARTICLE Upper- and Lower-Extremity Motor Recovery After Traumatic Cervical Spinal Cord Injury: An Update From the National Spinal Cord Injury Database Ralph J. Marino, MD, Stephen Burns, MD, Daniel
ORIGINAL ARTICLE Upper- and Lower-Extremity Motor Recovery After Traumatic Cervical Spinal Cord Injury: An Update From the National Spinal Cord Injury Database Ralph J. Marino, MD, Stephen Burns, MD, Daniel
, and HR peak. were lowest in those with cervical and high thoracic lesions. SAP and DAP increased with age; HR peak
 504542NNRXXX10.1177/1545968313504542Neurorehabilitation and Neural RepairRavensbergen et al research-article2013 Clinical Research Article Cardiovascular Function After Spinal Cord Injury: Prevalence and
504542NNRXXX10.1177/1545968313504542Neurorehabilitation and Neural RepairRavensbergen et al research-article2013 Clinical Research Article Cardiovascular Function After Spinal Cord Injury: Prevalence and
Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1, Raisa Deber, PhD 3, Junlang Yin, MSc 1 and Hwan Kim, PhD candidate 1
 J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
J Rehabil Med 2011; 43: 311 315 ORIGINAL REPORT Differential Profiles for Patients with Traumatic and Non- Traumatic Brain Injury Angela Colantonio, PhD 1, Gary Gerber, PhD 2, Mark Bayley, MD, FRCPC 1,
SPINAL CORD INJURY. Sci. A damage of the spinal cord that causes changes in its function, either temporary or permanent. Risk factor Male & Female
 SPINAL CORD INJURY Sci A damage of the spinal cord that causes changes in its function, either temporary or permanent. Risk factor Male & Female About Spinal cord injury Spinal cord injury is any damage
SPINAL CORD INJURY Sci A damage of the spinal cord that causes changes in its function, either temporary or permanent. Risk factor Male & Female About Spinal cord injury Spinal cord injury is any damage
Diagnostic coding accuracy for traumatic spinal cord injuries
 (2009) 47, 367 371 & 2009 International Society All rights reserved 1362-4393/09 $32.00 www.nature.com/sc ORIGINAL ARTICLE Diagnostic coding accuracy for traumatic spinal cord injuries EM Hagen 1,2, T
(2009) 47, 367 371 & 2009 International Society All rights reserved 1362-4393/09 $32.00 www.nature.com/sc ORIGINAL ARTICLE Diagnostic coding accuracy for traumatic spinal cord injuries EM Hagen 1,2, T
A test of the 1992 International Standards for Neurological and Functional Classi cation of Spinal Cord Injury
 Spinal Cord (1998) 36, 554 ± 560 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc A test of the 1992 International Standards
Spinal Cord (1998) 36, 554 ± 560 1998 International Medical Society of Paraplegia All rights reserved 1362 ± 4393/98 $12.00 http://www.stockton-press.co.uk/sc A test of the 1992 International Standards
A New Health Strategy to Prevent Pressure Ulcer Formation in Paraplegics using Computer and Sensory Substitution via the Tongue
 A New Health Strategy to Prevent Pressure Ulcer Formation in Paraplegics using Computer and Sensory Substitution via the Tongue Alexandre MOREAU-GAUDRY a,c,1, Anne PRINCE b, Jacques DEMONGEOT a,c and Yohan
A New Health Strategy to Prevent Pressure Ulcer Formation in Paraplegics using Computer and Sensory Substitution via the Tongue Alexandre MOREAU-GAUDRY a,c,1, Anne PRINCE b, Jacques DEMONGEOT a,c and Yohan
Physical Therapist Assistant Principles of Neuromuscular Rehabilitation
 Western Technical College 10524144 Physical Therapist Assistant Principles of Neuromuscular Rehabilitation Course Outcome Summary Course Information Description Career Cluster Instructional Level Total
Western Technical College 10524144 Physical Therapist Assistant Principles of Neuromuscular Rehabilitation Course Outcome Summary Course Information Description Career Cluster Instructional Level Total
Background (1) The CONECSI trial. Background (2) Intervention (2) Intervention (1)
 Background (1) The CONECSI trial: an RCT of a multidisciplinary cognitive behavioral program for coping with chronic neuropathic SCI pain Matagne Heutink Minisymposium, September 23, 2011 Adelante, Hoensbroek
Background (1) The CONECSI trial: an RCT of a multidisciplinary cognitive behavioral program for coping with chronic neuropathic SCI pain Matagne Heutink Minisymposium, September 23, 2011 Adelante, Hoensbroek
Impact of comorbidity and lifestyle related factors on functioning in aging polio survivors
 Impact of comorbidity and lifestyle related factors on functioning in aging polio survivors Irene Tersteeg Janneke Stolwijk Anita Beelen Frans Nollet Department of Rehabilitation, University of Amsterdam,
Impact of comorbidity and lifestyle related factors on functioning in aging polio survivors Irene Tersteeg Janneke Stolwijk Anita Beelen Frans Nollet Department of Rehabilitation, University of Amsterdam,
Definition of Complete Spinal Cord Injury
 29 (1991) 573--581 1991 International Medical Society of Definition of Complete Spinal Cord Injury R. L. Waters, MD,i R. H. Adkins, PhD,2 J. S. Yakura, MS, PT3 1 Clinical Professor of Orthopedic Surgery,
29 (1991) 573--581 1991 International Medical Society of Definition of Complete Spinal Cord Injury R. L. Waters, MD,i R. H. Adkins, PhD,2 J. S. Yakura, MS, PT3 1 Clinical Professor of Orthopedic Surgery,
Disclosure. Esquenazi
 Learning Objectives At the conclusion of this activity, the participant will be able to: A. Understand the purpose and function of the ReWalk exoskeletal orthotic device. B. Understand the variation in
Learning Objectives At the conclusion of this activity, the participant will be able to: A. Understand the purpose and function of the ReWalk exoskeletal orthotic device. B. Understand the variation in
Spinal Cord (2017) 55, & 2017 International Spinal Cord Society All rights reserved /17
 (2017) 55, 47 51 & 2017 International Society All rights reserved 1362-4393/17 www.nature.com/sc ORIGINAL ARTICLE Associations between disability-management self-efficacy, participation and life satisfaction
(2017) 55, 47 51 & 2017 International Society All rights reserved 1362-4393/17 www.nature.com/sc ORIGINAL ARTICLE Associations between disability-management self-efficacy, participation and life satisfaction
Obesity and Inpatient Rehabilitation Outcomes for Patients With a Traumatic Spinal Cord Injury
 384 ORIGINAL ARTICLE Obesity and Inpatient Rehabilitation Outcomes for Patients With a Traumatic Spinal Cord Injury Katherine W. Stenson, MD, Anne Deutsch, RN, PhD, CRRN, Allen W. Heinemann, PhD, David
384 ORIGINAL ARTICLE Obesity and Inpatient Rehabilitation Outcomes for Patients With a Traumatic Spinal Cord Injury Katherine W. Stenson, MD, Anne Deutsch, RN, PhD, CRRN, Allen W. Heinemann, PhD, David
NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE. Measure Information Form Collected For: CMS Outcome Measures (Claims Based)
 Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Last Updated: Version 4.3 NQF-ENDORSED VOLUNTARY CONSENSUS STANDARD FOR HOSPITAL CARE Measure Information Form Collected For: CMS Outcome Measures (Claims Based) Measure Set: CMS Readmission Measures Set
Survival rates in dysvascular lower limb amputees
 International Journal of Surgery (26) 4, 217e221 journal homepage: www.int-journal-surgery.com Survival rates in dysvascular lower limb amputees J. Kulkarni*, S. Pande, J. Morris Rehabilitation Medicine,
International Journal of Surgery (26) 4, 217e221 journal homepage: www.int-journal-surgery.com Survival rates in dysvascular lower limb amputees J. Kulkarni*, S. Pande, J. Morris Rehabilitation Medicine,
NUMEROUS STUDIES HAVE addressed the incidence of
 332 ORIGINAL ARTICLE Trends in New Injuries, Prevalent Cases, and Aging With Spinal Cord Injury Michael J. DeVivo, DrPH, Yuying Chen, MD, PhD ABSTRACT. DeVivo MJ, Chen Y. Trends in new injuries, prevalent
332 ORIGINAL ARTICLE Trends in New Injuries, Prevalent Cases, and Aging With Spinal Cord Injury Michael J. DeVivo, DrPH, Yuying Chen, MD, PhD ABSTRACT. DeVivo MJ, Chen Y. Trends in new injuries, prevalent
AROC Outcome Targets Report Inpatient Pathway 3
 AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
AROC Outcome Targets Report Inpatient Pathway 3 Anywhere Hospital January 2013 December 2013 Australasian Faculty of Rehabilitation Medicine AROC impairment specific benchmarking process...3 Introducing
Factors that influence functional ability in individuals with spinal cord injury. Bronwyn Meloney Hastings
 Factors that influence functional ability in individuals with spinal cord injury. Bronwyn Meloney Hastings A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand,
Factors that influence functional ability in individuals with spinal cord injury. Bronwyn Meloney Hastings A research report submitted to the Faculty of Health Sciences, University of the Witwatersrand,
Rehabilitation/Geriatrics ADMISSION CRITERIA. Coordinated Entry System
 Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
Rehabilitation/Geriatrics ADMISSION CRITERIA Coordinated Entry System Table of Contents Rehabilitation and Geriatric Service Sites 3 Overview of Coordinated Entry System...4 Geriatric Rehabilitation Service
OUTCOMES AND DATA 2016
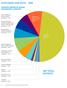 AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
AND DATA 2016 SERVED BY REHAB IMPAIRMENT CATEGORY 20 patients 5.1% MAJOR MULTIPLE TRAUMA W/BRAIN OR SPINAL CORD INJURY 24 patients 6.2% TRAUMATIC 39 patients 10.0% AMPUTATION LOWER EXTREMITY 26 patients
Research in Physical Medicine and Rehabilitation
 Research in Physical Medicine and Rehabilitation IV. Some Practical Designs in Applied Research RICHARD P. REILLY, PHD AND THOMAS W. FINDLEY, MD, PHD The randomized controlled trial is often difficult,
Research in Physical Medicine and Rehabilitation IV. Some Practical Designs in Applied Research RICHARD P. REILLY, PHD AND THOMAS W. FINDLEY, MD, PHD The randomized controlled trial is often difficult,
HIGH LEVEL - Science
 Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Learning Outcomes HIGH LEVEL - Science Describe the structure and function of the back and spine (8a) Outline the functional anatomy and physiology of the spinal cord and peripheral nerves (8a) Describe
Neurological and Trauma Impairment Set Version 10
 Neurological and Trauma Impairment Set Version 10 Admission/Discharge - Neurological + Trauma Impairment Set Version 10 (Please circle reason for assessment) Name: Severity scores - extent to which deficit
Neurological and Trauma Impairment Set Version 10 Admission/Discharge - Neurological + Trauma Impairment Set Version 10 (Please circle reason for assessment) Name: Severity scores - extent to which deficit
Nutrition status and its relationship with health status in individuals with spinal cord injury: a scoping review
 Nutrition status and its relationship with health status in individuals with spinal cord injury: a scoping review Jia Li, Devin Drummer, Thomas Hoover, Christian Sidebottom, Rachel Cowan, John-Paul Tortorich,
Nutrition status and its relationship with health status in individuals with spinal cord injury: a scoping review Jia Li, Devin Drummer, Thomas Hoover, Christian Sidebottom, Rachel Cowan, John-Paul Tortorich,
Lecture 6 Fitness Fitness 1. What is Fitness? 2. Cardiorespiratory Fitness 3. Muscular Fitness 4. Flexibility 5. Body Composition
 Lecture 6 Fitness 1 Fitness 1. What is Fitness? 2. Cardiorespiratory Fitness 3. Muscular Fitness 4. Flexibility 5. Body Composition 2 1 Americans (on average) are not a healthy bunch 3 Sitting is the new
Lecture 6 Fitness 1 Fitness 1. What is Fitness? 2. Cardiorespiratory Fitness 3. Muscular Fitness 4. Flexibility 5. Body Composition 2 1 Americans (on average) are not a healthy bunch 3 Sitting is the new
Downloaded from ijwph.ir at 19: on Friday September 21st
 * Downloaded from ijwph.ir at 9:30 +0430 on Friday September st 8 0978770 : 7 : : * Email:Pegah.rahmani87@gmail.com : 40 ( ) 40. :. ( ). ) (r=0.99) WUSPI ( ). (. (p 0.05) t 90. 70 80 :. 77.(p 0.05).(p
* Downloaded from ijwph.ir at 9:30 +0430 on Friday September st 8 0978770 : 7 : : * Email:Pegah.rahmani87@gmail.com : 40 ( ) 40. :. ( ). ) (r=0.99) WUSPI ( ). (. (p 0.05) t 90. 70 80 :. 77.(p 0.05).(p
Line Murtnes Hagestande
 Line Murtnes Hagestande The relation between leisure time physical exercise, physical and psychosocial work demands, and risk of fibromyalgia in working women; The Nord-Trøndelag Health Study BEV3901,
Line Murtnes Hagestande The relation between leisure time physical exercise, physical and psychosocial work demands, and risk of fibromyalgia in working women; The Nord-Trøndelag Health Study BEV3901,
SPINAL CORD INJURY Rehab Definitions Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI)
 SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
SPINAL CORD INJURY Rehab s Framework Self-Assessment Tool inpatient rehab Survey for Spinal Cord Injury (SCI) INTRODUCTION: In response to a changing rehab landscape in which rehabilitation is offered
What to expect following spinal cord injury. Information for patients Therapy Services
 What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
What to expect following spinal cord injury Information for patients Therapy Services Introduction This leaflet aims to explain what spinal cord injury is and what to expect over the next few months. What
RICHMOND PARK SCHOOL LIFESTYLE SCREENING REPORT Carmarthenshire County Council
 RICHMOND PARK SCHOOL LIFESTYLE SCREENING REPORT 2016 Carmarthenshire County Council WHY LEAD A HEALTHY LIFESTYLE? A nutritious, well-balanced diet along with physical activity and refraining from smoking
RICHMOND PARK SCHOOL LIFESTYLE SCREENING REPORT 2016 Carmarthenshire County Council WHY LEAD A HEALTHY LIFESTYLE? A nutritious, well-balanced diet along with physical activity and refraining from smoking
Frequently Asked Questions: Riverview Rehabilitation Center
 Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Frequently Asked Questions: Riverview Rehabilitation Center WHAT SERVICES ARE PROVIDED? Riverview Rehabilitation Center provides a comprehensive, interdisciplinary and functionally based treatment program
Last Updated: July 20, 2016 Articles up-to-date as of: July 2015
 Reviewer ID: Christie Chan, John Zhu, Jeremy Mak, Kyle Diab Type of Outcome Measure: 10 Meter Walk Test (10MWT) Total articles: 21 Author ID Year Amatachaya Datta 2009 Ditunno et al. 2007 Duffell 2015
Reviewer ID: Christie Chan, John Zhu, Jeremy Mak, Kyle Diab Type of Outcome Measure: 10 Meter Walk Test (10MWT) Total articles: 21 Author ID Year Amatachaya Datta 2009 Ditunno et al. 2007 Duffell 2015
ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE
 ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE Title: BACLOFEN PUMP PROGRAM (INTRATHECAL) Issued by: Physical Medicine and Outpatient Therapy Date: 6/99 Reviewed: 2/17 Revision: 2/11 Page: 1 of
ALTRU HEALTH SYSTEM Grand Forks, ND STANDARD GUIDELINE Title: BACLOFEN PUMP PROGRAM (INTRATHECAL) Issued by: Physical Medicine and Outpatient Therapy Date: 6/99 Reviewed: 2/17 Revision: 2/11 Page: 1 of
Spinal injury. Structure of the spine
 Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Spinal injury Structure of the spine Some understanding of the structure of the spine (spinal column) and the spinal cord is important as it helps your Neurosurgeon explain about the part of the spine
Index. Note: Page numbers of article titles are in boldface type.
 Note: Page numbers of article titles are in boldface type. A Absorption of drugs in the elderly, 278 Abuse substance in patient with cognitive impairment safety concerns related to, 323, 325, 329 330 ADEs.
Note: Page numbers of article titles are in boldface type. A Absorption of drugs in the elderly, 278 Abuse substance in patient with cognitive impairment safety concerns related to, 323, 325, 329 330 ADEs.
Effect of Spinal Stimulation on Monosynaptic Reflex by Medium Frequency Current
 Effect of Spinal Stimulation on Monosynaptic Reflex by Medium Frequency Current Nidhi et al Effect of Spinal Stimulation on Monosynaptic Reflex by Medium Frequency Current Nidhi 1, B., Narkeesh 2, A. &
Effect of Spinal Stimulation on Monosynaptic Reflex by Medium Frequency Current Nidhi et al Effect of Spinal Stimulation on Monosynaptic Reflex by Medium Frequency Current Nidhi 1, B., Narkeesh 2, A. &
3/5/2014. Rehabilitation Technology versus Research Technology: Where/What is the Value?
 Technology Applied to SCI: The Value of Assistive Devices During SCI Recovery and While Living with SCI Mark S. Nash, Ph.D., FACSM Departments of Neurological Surgery and Rehabilitation Medicine Principal
Technology Applied to SCI: The Value of Assistive Devices During SCI Recovery and While Living with SCI Mark S. Nash, Ph.D., FACSM Departments of Neurological Surgery and Rehabilitation Medicine Principal
DEPARTMENT OF PHYSICAL MEDICINE AND REHABILITATION P.G. TEACHING SCHEDULE FOR THE MONTH JUNE -2018
 DEPARTMENT OF PHYSICAL MEDICINE AND REHABILITATION P.G. TEACHING SCHEDULE FOR THE MONTH JUNE -2018 THEORY (TIME: 3 PM) DATE TOPIC FACULTY 1/06/2018 NEUROLOGIC LEVEL OF INJURY DR.RAVI 4/06/2018 CERVICAL
DEPARTMENT OF PHYSICAL MEDICINE AND REHABILITATION P.G. TEACHING SCHEDULE FOR THE MONTH JUNE -2018 THEORY (TIME: 3 PM) DATE TOPIC FACULTY 1/06/2018 NEUROLOGIC LEVEL OF INJURY DR.RAVI 4/06/2018 CERVICAL
E-Poster P 117 Does Spinal Cord Decompression Reduces Spasticity in Patients with Spinal Cord Injury and Residual Compression?
 E-Poster P 117 Does Spinal Cord Decompression Reduces Spasticity in Patients with Spinal Cord Injury and Residual Compression? R Yurac, S Ramírez, S Mandiola, M Lecaros, JJ Zamorano, C Tapia, F Ilabaca,
E-Poster P 117 Does Spinal Cord Decompression Reduces Spasticity in Patients with Spinal Cord Injury and Residual Compression? R Yurac, S Ramírez, S Mandiola, M Lecaros, JJ Zamorano, C Tapia, F Ilabaca,
Slide 1. Slide 2. Slide 3. Introduction CHAPTER 10:CLIENTS WITH SPINAL CORD INJURY PART I. Introduction - page 252(pathophysiology)
 Slide 1 CHAPTER 10:CLIENTS WITH SPINAL CORD INJURY PART I PT 151 Slide 2 Introduction - page 252(pathophysiology) Traumatic SCI occurs when an external force, such as fracture of the vertebrae or penetration
Slide 1 CHAPTER 10:CLIENTS WITH SPINAL CORD INJURY PART I PT 151 Slide 2 Introduction - page 252(pathophysiology) Traumatic SCI occurs when an external force, such as fracture of the vertebrae or penetration
REX REX Clinical Assessment Guide
 REX Clinical Assessment Guide All product names and brand names in this document are trademarks or registered trademarks of their respective holders. Copyright Rex Bionics Ltd 2016. All rights reserved.
REX Clinical Assessment Guide All product names and brand names in this document are trademarks or registered trademarks of their respective holders. Copyright Rex Bionics Ltd 2016. All rights reserved.
Brake. About this report
 Best practice guidance Providing effective support following spinal injury Produced by: Brake About this report This report is produced by Brake,. It aims to raise awareness and understanding of the devastation
Best practice guidance Providing effective support following spinal injury Produced by: Brake About this report This report is produced by Brake,. It aims to raise awareness and understanding of the devastation
Reliability and validity of the International Spinal Cord Injury Basic Pain Data Set items as self-report measures
 (2010) 48, 230 238 & 2010 International Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc ORIGINAL ARTICLE Reliability and validity of the International Injury Basic Pain Data Set items
(2010) 48, 230 238 & 2010 International Society All rights reserved 1362-4393/10 $32.00 www.nature.com/sc ORIGINAL ARTICLE Reliability and validity of the International Injury Basic Pain Data Set items
Bladder Management. A guide for patients. Key points
 Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
Bladder Management A guide for patients Key points Urinary issues remain one of the highest causes of readmission to hospital following Spinal Cord Injury (SCI). Following SCI most patients experience
EFFECTIVENESS OF PHONE AND LIFE- STYLE COUNSELING FOR LONG TERM WEIGHT CONTROL AMONG OVERWEIGHT EMPLOYEES
 CHAPTER 5: EFFECTIVENESS OF PHONE AND E-MAIL LIFE- STYLE COUNSELING FOR LONG TERM WEIGHT CONTROL AMONG OVERWEIGHT EMPLOYEES Marieke F. van Wier, J. Caroline Dekkers, Ingrid J.M. Hendriksen, Martijn W.
CHAPTER 5: EFFECTIVENESS OF PHONE AND E-MAIL LIFE- STYLE COUNSELING FOR LONG TERM WEIGHT CONTROL AMONG OVERWEIGHT EMPLOYEES Marieke F. van Wier, J. Caroline Dekkers, Ingrid J.M. Hendriksen, Martijn W.
