PHAR 7632 Chapter 16
|
|
|
- Angelina Mills
- 6 years ago
- Views:
Transcription
1 PHAR 7632 Chapter 16 Routes of Excretion Routes of Excretion Student Objectives for this Chapter After completing the material in this chapter each student should:- be able to describe the various routes by which a drug may be excreted from the body understand the parameter renal clearance and its relationship with the excretion processes in the kidney understand the influence of renal disease on drug elimination be able to calculate suitable drug dosage regimen for patients with impaired renal function based on a or a Cp min /Cp max approach The major routes of drug excretion described in this Chapter are renal, biliary, pulmonary and salivary. This page was last modified: Saturday 31 Dec 2005 at 03:57 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne (david@boomer.org) Page 1 of 23
2 PHAR 7632 Chapter 16 Routes of Excretion Renal Excretion The major organ for the excretion of drugs is the KIDNEY. The functional unit of the kidney is the nephron and components of the nephron include Bowman's capsule, Proximal Tubule, Loop of Henle, Distal Tubule and the Collecting Duct. Low molecular weight molecules are filtered in Bowman's capsule. Active secretion of weak electrolyte drugs (acids) and reabsorption of water occurs in the proximal tubules. Additional reabsorption of water occurs in the Loop of Henle. Passive reabsorption of water and lipid soluble drugs occur in the distal tubule. There are three major renal excretion processes to consider; 1) glomerular filtration; 2) tubular secretion; and 3) tubular re-absorption Glomerular Filtration Figure One Nephron of the Kidney In the glomerular all molecules of low molecular weight (< 60,000 Dalton) are filtered out of the blood. Most drugs are readily filtered from the blood unless they are tightly bound to large molecules such as plasma protein or have been incorporated into red blood cells. The glomerular filtration rate varies from individual to individual but in healthy individuals the normal range is 110 to 130 ml/min ( 180 L/day). About 10% of the blood which enters the glomerular is filtered. This filtration rate is often measured by determining the renal clearance of inulin. Inulin is readily filtered in the glomerular, and is not subject to tubular secretion or re-absorption. Thus inulin clearance is equal to the glomerular filtration rate. Again, most drugs are filtered from blood in the glomerular, the overall renal excretion however is controlled by what happens in the tubules. More than 90% of the filtrate is reabsorbed. 120 ml/min is 173 L/day. Normal urine output as you may realize is much less than this, about 1 to 2 liter per day. Tubular secretion In the proximal tubule there is re-absorption of water and active secretion of some weak electrolyte but especially weak acids. As this process is an active secretion it requires a carrier and a supply of energy. This may be a significant pathway for some compounds such Page 2 of 23
3 as penicillins. Because tubular secretion is an active process there may be competitive inhibition of the secretion of one compound by another. A common example of this phenomena is the inhibition of penicillin excretion by competition with probenecid. When penicillin was first used it was expensive and in short supply, thus probenecid was used to reduce the excretion of the penicillin and thereby prolong penicillin plasma concentrations (PDR). Since then it has been shown that probenecid also alters the distribution of penicillins to various tissues causing more drug to distribute out of plasma, causing even less to be eliminated. This could also be used to reduce the excretion of cephalosporins. Drugs or compounds which are extensively secreted, such as p-aminohippuric acid (PAH), may have clearance values approaching the renal plasma flow rate of 425 to 650 ml/min, and are used clinically to measure this physiological parameter (see Documenta Geigy). Tubular re-absorption In the distal tubule there is passive excretion and re-absorption of lipid soluble drugs. Drugs which are present in the glomerular filtrate can be reabsorbed in the tubules. The membrane is readily permeable to lipids so filtered lipid soluble substances are extensively reabsorbed. A reason for this is that much of the water, in the filtrate, has been reabsorbed and therefore the concentration gradient is now in the direction of re-absorption. Thus if a drug is non-ionized or in the unionized form it maybe readily reabsorbed. Many drugs are either weak bases or acids and therefore the ph of the filtrate can greatly influence the extent of tubular re-absorption for many drugs. When urine is acidic weak acid drugs tend to be reabsorbed. Alternatively when urine is more alkaline, weak bases are more extensively reabsorbed. Making the urine more acidic can cause less reabsorption of weak bases or enhanced excretion. These changes can be quite significant as urine ph can vary from 4.5 to 8.0 depending on the diet (e.g. meat can cause a more acidic urine) or drugs (which can increase or decrease urine ph). In the case of a drug overdose it is possible to increase the excretion of some drugs by suitable adjustment of urine ph. For example, in the case of pentobarbital (a weak acid) overdose it may be possible to increase drug excretion by making the urine more alkaline with sodium bicarbonate injection. Figure Pentobarbital Ionization This method is quite effective if the drug is extensively excreted as the unchanged drug (i.e. fe approaches 1). If the drug is Page 3 of 23
4 extensively metabolized then alteration of kidney excretion will not alter the overall drug metabolism all that much. The effect of ph change on tubular re-absorption can be predicted by consideration of drug pka according to the Henderson- Hesselbalch equation. Renal clearance One method of quantitatively describing the renal excretion of drugs is by means of the renal clearance value for the drug. Renal clearance relates the rate of excretion, Δ U/Δ t, to drug concentration. Units are ml/min. Equation Rate of Excretion Remember that renal clearance can be calculated as part of the total body clearance for a particular drug. Renal clearance can be used to investigate the mechanism of drug excretion. If the drug is filtered but not secreted or reabsorbed the renal clearance will be about 120 ml/min in normal subjects. If the renal clearance is less than 120 ml/min then we can assume that at least two processes are in operation, glomerular filtration and tubular re-absorption. If the renal clearance is greater than 120 ml/min then tubular secretion must be contributing to the elimination process. It is also possible that all three processes are occurring simultaneously. The drug renal clearance value can be compared with physiologically significant values, e.g. glomerular filtration rate (GFR) of approximately 120 ml/min or renal plasma flow of about 650 ml/min. Renal clearance is then: Equation Renal Clearance Renal clearance values can range from 0 ml/min, the normal value for glucose which is usually completely reabsorbed to a value equal to the renal plasma flow of about 650 ml/min for compounds like p-aminohippuric acid. We can calculate renal clearance using the pharmacokinetic parameters ke and V. Thus CL renal = ke V. Renal clearance can also be determined as U /AUC. We can calculate renal clearance by measuring the total amount of drug excreted over some time interval and dividing by the plasma concentration measured at the midpoint of the time interval. (This was part of a laboratory experiments- -first beaker experiment). Equation Renal Clearance Equation Renal Clearance Page 4 of 23
5 To continue we can briefly look at some other routes of drug excretion. We will then return to the topic of renal excretion by considering drug dosage adjustments in patients with reduced renal function. References How the Kidney Works by Stephen Z. Fadem, M.D., FACP The Kidney at Wikipedia This page was last modified: Tuesday 03 Jan 2006 at 02:08 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne Page 5 of 23
6 PHAR 7632 Chapter 16 Routes of Excretion Hemodialysis Hemodialysis or 'artificial kidney' therapy is used in renal failure to remove toxic waste material normally removed by the kidneys, from the patient's blood. In the procedure blood is diverted externally and allowed to flow across a semi-permeable membrane that is bathed with an aqueous isotonic solution. Small molecules including nitrogenous waste products and some drugs will diffuse from the blood, thus these compounds will be eliminated. Therefore in patients with kidney failure, hemodialysis may be an important route of drug elimination. This technique is particularly important with drugs which: 1. are smaller (< 500) molecular weight; and 2. are not tightly bound to plasma protein; 3. have a small apparent volume of distribution. 4. have good water solubility; Conversely drugs which are tightly bound or extensively stored or distributed into tissues are only poorly removed by this route, or process. A simulation of drug concentration with and without dialysis is shown in Figure Figure Drug Concentration before, during and after Low Flux Dialysis Click on the figure to view the Java Applet window Java Applet as a Linear Plot Low flux hemodialysis will readily remove molecules smaller than 500 Dalton. As the molecular weight increases to approximately 1000 Dalton the amount removed steadily decreases to insignificant. Thus clearance by hemodialysis falls from a maximum of about 4 L/hr to near zero with higher molecular weight compounds. Hemodialysis clearance is converted to a rate constant by dividing by the apparent volume distribution. This rate constant is added to the patient's elimination rate constant to give the increased, apparent rate constant during hemodialysis. As can be seen in Figure this can cause an increased removal of a drug. This can be useful in Page 6 of 23
7 cases where the concentration is too high but it can also complicate the maintenance of therapeutic concentrations. In Chapter 14 and 15 drug dosage regimens were calculated using elimination rate constant and volume of distriubtion. Hemodialysis can mean a significant increase in the amount of drug removed during the dialysis period. An additional dose maybe required. Later in this chapter we will adjust dosage regimens for reduced renal function according to Cp average or Cp min /Cp max requirements Item 1. Hemodialysis may contribute significantly to the elimination of some drugs in patients with poor renal function. Explore the effect of molecular weight, protein binding and apparent volume of distribution on dialysis and explore the need for a post-dialysis dose. Explore the problem as a Linear Plot - Java Applet References Shargel, L. and Yu, A.B.C "Applied Biopharmaceutics and Pharmacokinetics", 4th ed., Appleton-Century-Crofts, Norwalk, CT, page 556, table 18.6 This page was last modified: Saturday 31 Dec 2005 at 03:57 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne (david@boomer.org) Page 7 of 23
8 PHAR 7632 Chapter 16 Routes of Excretion Biliary Excretion The liver secretes 0.25 to 1 liter of bile each day. Some drugs and/or their metabolites are excreted by the liver into bile. Anions, cations, and non-ionized molecules containing both polar and lipophilic groups are excreted into the bile provided that the molecular weight is greater than about 300 Dalton. Molecular weights around 500 Dalton appears optimal for biliary excretion in humans. Lower molecular weight compounds are reabsorbed before being excreted from the bile duct. Conjugates, glucuronides (drug metabolites) are often of sufficient molecular weight for biliary excretion. This can lead to biliary recycling. Indomethacin is one compound which undergoes this form of recycling. Figure Enteroheptic Recycling Page 8 of 23
9 Figure Cp versus Time showing a Second Peak Figure illustrate plasma concentration versus time curve which may result from extensive enterohepatic recycling. Note, the presence of the second peak shortly after the dumping of bile into the small intestine in response to the presence of food. Other compounds extensively excreted in bile include cromoglycate (unchanged drug), morphine, and chloramphenicol (as glucuronide). At least part of the biliary secretion is active since bile/plasma concentrations maybe as high as 50/1. There can also be competition between compounds. The efficiency of this biliary excretion system can be assessed by use of a test substance, such as Bromsulphalein. This page was last modified: Saturday 31 Dec 2005 at 03:57 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne (david@boomer.org) Page 9 of 23
10 PHAR 7632 Chapter 16 Routes of Excretion Pulmonary Excretion The lung is the major organ of excretion for gaseous and volatile substances. Most of the gaseous anesthetics are extensively eliminated in expired air. The breathalyzer test is based on a quantitative pulmonary excretion of ethanol. How a Breathalyzer works This page was last modified: Saturday 31 Dec 2005 at 03:57 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne (david@boomer.org) Page 10 of 23
11 PHAR 7632 Chapter 16 Routes of Excretion Salivary Excretion Saliva volume is typically one to two liters per day with flow rates ranging from 0.5 ml/min to more than 10 times that in the presence or thought of food. Saliva ph commonly ranges between 7.4 and 6.2 although lower values are possible. Saliva also contains a number of enzymes including amylase, ptylin, lipase, and esterases. Salivary excretion is not really a method of drug excretion as the drug will usually be swallowed and reabsorbed, thus a form of 'salivary recycling'. Drug excretion into saliva appears to be dependent on ph partition and protein binding. In many cases salivary concentration represents the free drug concentration in plasma. This mechanism appears attractive in terms of drug monitoring, that is determining drug concentration to assist in drug dosage adjustment. For some drugs, the saliva/free plasma ratio is fairly constant. Therefore drug concentrations in saliva could be a good indication of drug concentration in plasma. For some drugs localized side effects maybe due to salivary excretion of the drug. Pharmacokinetic studies in special populations may be more feasible using saliva concentrations. References Washington, N., Washington C. and Wilson, C.G Physiological Pharmaceutics, Barriers to Drug Absorption, Taylor and Francis, Inc., New York, NY ISBN This page ( was last modified: Saturday 31 Dec 2005 at 03:57 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne (david@boomer.org) Page 11 of 23
12 PHAR 7632 Chapter 16 Routes of Excretion Renal Disease Considerations Getting back to the renal excretion of drugs. If a drug is extensively excreted unchanged into urine (i.e. fe closer to 1), alteration of renal function will extensively alter the drug elimination rate. Fortunately creatinine or inulin clearance can be used as a measure of renal function. For most drugs which are excreted extensively as unchanged drug it has been found that there is a good correlation between creatinine or inulin clearance and drug clearance or observed renal clearance and elimination rate (since V is usually unchanged). Dose adjustment Creatinine clearance Creatinine is produced in the body by muscle metabolism from creatine phosphate. Creatinine production is dependent on the age, weight, and sex of the patient. Elimination of creatinine is mainly by glomerular filtration (> 90%) with a small percentage by active secretion. With the patient in stable condition the production is like a continuous infusion to steady state with the infusion rate controlled by muscle metabolism and the elimination controlled by renal function. Thus as renal function is reduced serum creatinine concentrations increases. Other compounds such as inulin are also used for GFR measurement. Although inulin GFR values are probably more accurate they involve administration of inulin and careful collection of urine for inulin determination. The major advantage of creatinine is that its formation is endogenous. Determination of creatinine clearance consists of collection of total urine and a plasma/serum determination at the mid-point time. Thus: Equation Creatinine Clearance with serum creatinine expressed as mg/100 ml and creatinine clearance as ml/min. Normal inulin clearance values are 124 ml/min for men and 109 ml/min for women (Documenta Geigy, 1970). Because of some small renal secretion of creatinine, normal values of creatinine clearance are slightly higher than GFR measured with inulin. Thus, normal creatinine clearance values are about 120 to 130 ml/min. Various investigators have developed equations which allow calculation of creatinine clearance using serum creatinine values. Thus a single serum level may used when renal condition is stable. One commonly used equation is that of Cockcroft and Gault. Males: Equation Creatinine Clearance Females: Use 85% of the value calculated for males. Cr is the serum creatinine concentration in mg/dl. The original authors of this Page 12 of 23
13 equation used actual body weight in Equation More recently it has been recommended that ideal body (IBW) be used in this equation unless the actual body weight (ABW) is less (Murphy, 2001). Generally use lean body weight in this equation as creatinine is formed in muscle (Shargel and Yu, 1985). Estimation of kel in a patient The relationship between creatinine clearance and overall drug elimination can be easily seen by looking at plots of kel observed versus creatinine clearance. These are often called Dettli plots. Figure Plot of kel versus CLCR (Dettli Plot) Figure shows the situation with considerable excretion as unchanged drug. i.e. fe between 0.3 and 0.7. Figure Dettli Plot (fe = 1) In Figure drug is excreted entirely as unchanged drug. i.e. fe = 1 Page 13 of 23
14 Figure Dettli Plot (fe = 0) In Figure drug is excretion only as metabolized drug. i.e. fe = 0 We can use this information to calculate initial dosage regimens for patients taking drugs with high (> 0.25) fe values. The first step is to estimate the creatinine clearance in the patient from their serum creatinine value. From a Dettli plot (kel versus CLcr) constructed from previous studies with this drug we can estimate the elimination rate constant in this patient. We can therefore calculate an optimum dose and dosing interval to achieve the desired average drug concentration or maximum or minimum drug concentrations. The Dettli plot may be built into a computer program or nomogram. Figure Dettli Plot Showing kel Observed versus CL cr This is the plot shown before. In the references shown below there is information useful for calculating kel in patients with impaired renal function. Page 14 of 23
15 Table Some Example Values (Wagner, 1975) knr Kanamycin Sulfadiazine Tetracycline As an example these data could be used to calculate the kel for a patient with a CLcr of 10 ml/min compared a subject with normal renal function of 120 ml/min For kanamycin kel patient = knr + b CLcr = x 10 = = hr -1 Compare this with the value for the normal subject: kel = x 120 = hr -1 For sulfadiazine kel patient = x 10 = = hr -1 Compare this with the value for the normal subject: kel = x 120 = 0.09 hr -1 For tetracycline kel patient = x 10 = = hr -1 Compare this with the value for the normal subject: kel = x 120 = hr -1 b References Documenta Geigy, Scientific Tables. 7th ed., Geigy Pharmaceuticals, 1970, p531 Shargel, L. and Yu, A.B.C Applied Biopharmaceutics and Pharmacokinetics, 2nd ed., Appleton-Century-Crofts, Norwalk, CT, page 312 Murphy, J.E Clinical Pharmacokinetics, 2nd ed., ASHP, Bethesda, MD Wagner, J.G Fundamentals of Clinical Pharmacokinetics, Drug Intelligence Publications, Inc., Hamilton, IL Dettli, Clin.P'col. 16, 274 (1974) Chow, J.Clin.P'col. 15, 405 (1975) Welling, Clin.P'col. 18, 45 (1975) Bennett, Annals Int.Med. 754 (1977) This page was last modified: Tuesday 03 Jan 2006 at 02:09 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne (david@boomer.org) Page 15 of 23
16 PHAR 7632 Chapter 16 Routes of Excretion Cp average Calculations For patients with poor renal function taking drugs with high fe values, dosage regimen adjustment is essential. Drugs that are eliminated via the kidneys will have reduced elimination in patients with impaired renal function. Steady state and average drug concentration will rise dangerously unless the dosage regimen is adjusted. One way to make this adjustment is to adjust the dose or dosing interval to maintain a required average drug concentration. For example consider the drug kanamycin. A patient of 70 kg with normal kidney function may receive 250 mg IM every six hours (about 3 half-lives; t 1/2 = 2.3 hours). If F = 1.0 and V = 13.3 liter, kel = 0.693/2.3 = 0.30 hr -1. Then If we assume that ka >> kel then Equation Average Drug Concentration where R = e -0.3 * 6 = Thus, Cp min = 3.7 mg/l These are the results you should expect in a patient with a normal creatinine clearance value. However in a patient with a creatinine clearance of only 10 ml/min the elimination rate constant will be quite different and if the same dosage regimen were used quite different plasma concentrations would be achieved (see Figure ). The elimination rate constant for this patient would be hr -1 (t 1/2 = 20 hr). Using the same dosing regimen: This average plasma concentration is well above the maximum recommended value of 35 mg/l which should be avoided (in the PDR 89 p740). Clearly some dosage adjustment should be made to the dosage regimen. Page 16 of 23
17 Figure Linear Plot of Cp versus Time We could consider a) changing the dose b) changing the dosing interval or c) changing both the dose and the dosing interval. We can make these alterations easily using the equation. Equation Average Drug Concentration Equation From this we can see that decreasing the dose or increasing the dosing interval will have the desired response. Altered dose Assuming that a Cp of 10.4 mg/l (the value obtained in the normal patient on a normal dosage regimen) is satisfactory we can calculate a dose to achieve this value as: = Assuming ka >> kel, R = and Cpmin = 9.3 mg/l Thus this new dosing regimen of 28 mg every 6 hours should work Page 17 of 23
18 Altered dose interval = Therefore giving 250 mg every 53 hours should achieve a satisfactory plasma concentration profile. R = 0.165; Cpmin = 3.7 mg/l We would expect greater fluctuations with this method and dosing every 53 hours is not all that convenient. Every 6 hours is not all that great either if a longer dosing interval would work. We might consider dosing every 24 hours. Altered dose and interval Using t = 24 hours = = 113 mg every 24 hours (maybe 100 mg every 24 hours) R = 0.442; Cpmin = 6.7 mg/l. Figure Plot of Cp versus Time The lines in Figure were calculated to achieve a of 10.4 mg/l using 28 mg q6h, 250 mg q54h, pr 113 mg q24h. Page 18 of 23
19 Calculator Calculations Using the Cp average Equation Drug Information Enter Drug Name Kanamycin Enter required Cbar mg/l? Enter required F 1 Enter Dose 250 mg? Enter V 13.3 L Enter kel 0.3 hr -1 Enter tau 6 hr? Calculate missing Value This page ( was last modified: Tuesday 03 Jan 2006 at 02:53 PM Material on this website should only be used for Educational or Self-Study Purposes Copyright David W. A. Bourne (david@boomer.org) Page 19 of 23
20 PHAR 7632 Chapter 16 Routes of Excretion Cp max /Cp min Calculations Another apprach is to use the desired Cp max and C pmin to define the dosing regimen. The steps to be taken for this approach include: a. Define Cpmin/Cpmax. From information on the drug with reference to the patient's clinical requirements. For example the normal upper limit for gentamicin peak concentrations might be 6 mg/l, however in case of life-threatening infection higher levels may be approached. Initial calculation might be based on a peak of 6 mg/l and a trough below 1 mg/l. (Use 1 mg/l as the trough and extend the interval when making the adjustment in τ. b. Determine CLcr. Probably from serum creatinine levels using the Cockcroft-Gault equation. c. Determine kel. Using the equation kel = km + b CLCr with km and b values from the literature d. Calculate Tau. Since and we know Cpmin, Cpmax, and kel we can calculate tau, τ. Typically this will be some uneven time value. e. Round Tau. A more usual dosing interval should now be chosen. For example a tau of 7.8 or 6.7 hour could be rounded to 8 hours, thus dosing three times a day. f. Recalculate R. A new value of tau results in a new value of R. g. Calculate Maintenance Dose. The maintenance dose can be calculated from the minimum or the maximum plasma concentration. Thus Maintenance dose = Cpmax V (1 - R) OR = Cpmin V (1 - R)/R h. Calculate Loading DOSE. The loading dose can be calculated directly (for an IV bolus) by equating Cp 0 and the Cpmax value. Thus, Loading dose = Cpmax V Example: A 75 kg, 65 year old male patient, serum creatinine concentration of 2.3 mg/100 ml, is to be given gentamicin IV to achieve a peak plasma concentration of 6 mg/l and trough concentration below 1 mg/l. The apparent volume of distribution is reported to be 0.28 L/kg. From Table 3-9 (Wagner, 1975 p161), km and b values are 0.02 and , respectively. a. Cpmax = 6 mg/l and Cpmin = 1 mg/l b. CLcr = c. kel = km + b CLcr = x 34 = hr -1 Page 20 of 23
21 d. R = ln (0.1667) = = x τ τ = 15.6 hour e. Since a longer dosing interval is needed to keep the trough level below 1 mg/l use a tau value of 18 hours. f. New R value. R = e x 18 = g. Calculate maintenance dose using Cpmax = 6 mg/l as reference point. Thus Maintenance dose = Cpmax V (1 - R) = 6 x 75 x 0.28 x ( ) = 110 mg Thus use 100 mg iv every 18 hours Cpmin = Cpmax R = 5.45 x = 0.69 mg/l h. The loading dose can be calculated as:- Loading dose = Cpmax V = 6 x 75 x 0.28 = 126 mg. Using 125 mg would give a Cpmax = = 5.95 mg/l. Thus a loading dose of 125 mg followed by 100 mg every 18 hours should be satisfactory. Comparison with PDR recommendation. Usual dose for 75 kg patient is 75 mg q8h. With serum creatinine 2.3 mg/100 ml give 40 percent of 75 mg q8h. That is 30 mg q8h (R = 0.399) giving 2.38 and 0.95 for Cpmax and Cpmin, respectively. Page 21 of 23
22 Calculator Calculator Using Cp max and Cp min Criteria Drug Information Patient Information Click for a new Problem or Enter your own Data Enter required Cpmax 6 mg/l Enter required Cpmin 1 mg/l Enter V 0.28 L/kg Enter km or knr value 0.02 hr -1 Enter Dettli slope value min.ml -1.hr -1 Enter Patient Weight 75 kg Age 65 years Sex Male Female Enter Patient Serum Creatinine level 2.3 mg/100 ml Calculate CLcr, kel and Tau Creatine Clearance ml/min Elimination Rate constant hr -1 R is Exact Tau hr Now enter a rounded value of Tau below Enter Rounded Tau value hr Calculate Maintenance and Loading Dose New R value Maintenance Dose mg every hr and Loading Dose mg Practice calculating a patient's elimination rate constant from creatinine clearance References Wagner, J.G Fundamentals of Clinical Pharmacokinetics, Drug Intelligence Publications, Inc., Hamilton, IL Student Objectives for this Chapter This page ( was last modified: Saturday 31 Dec 2005 at 03:57 PM Material on this website should only be used for Educational or Self-Study Purposes Page 22 of 23
23 Copyright David W. A. Bourne Page 23 of 23
Excretion of Drugs. Prof. Hanan Hagar Pharmacology Unit Medical College
 Excretion of Drugs Prof. Hanan Hagar Pharmacology Unit Medical College Excretion of Drugs By the end of this lecture, students should be able to! Identify main and minor routes of excretion including renal
Excretion of Drugs Prof. Hanan Hagar Pharmacology Unit Medical College Excretion of Drugs By the end of this lecture, students should be able to! Identify main and minor routes of excretion including renal
Renal Excretion of Drugs
 Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Renal Excretion of Drugs 3 1 Objectives : 1 Identify main and minor routes of Excretion including renal elimination and biliary excretion 2 Describe its consequences on duration of drugs. For better understanding:
Unit 2b: EXCRETION OF DRUGS. Ms.M.Gayathri Mpharm (PhD) Department of Pharmaceutics Krishna Teja Pharmacy college Subject code: 15R00603 (BPPK)
 Unit 2b: EXCRETION OF DRUGS By Ms.M.Gayathri Mpharm (PhD) Department of Pharmaceutics Krishna Teja Pharmacy college Subject code: 15R00603 (BPPK) Excretion, along with metabolism and tissue redistribution,
Unit 2b: EXCRETION OF DRUGS By Ms.M.Gayathri Mpharm (PhD) Department of Pharmaceutics Krishna Teja Pharmacy college Subject code: 15R00603 (BPPK) Excretion, along with metabolism and tissue redistribution,
Renal Function. 1. Glomerular filtration 2. Active tubular secretion 3. Passive tubular reabsorption 4. Excretion
 59-291 Section 1, Lecture 5 Drug Excretion -most drugs are excreted in urine either as unchanged or drug metabolites Renal Function 1. Glomerular filtration 2. Active tubular secretion 3. Passive tubular
59-291 Section 1, Lecture 5 Drug Excretion -most drugs are excreted in urine either as unchanged or drug metabolites Renal Function 1. Glomerular filtration 2. Active tubular secretion 3. Passive tubular
PHA Final Exam Fall 2006
 PHA 5127 Final Exam Fall 2006 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Please transfer the answers onto the bubble sheet. The question number refers
PHA 5127 Final Exam Fall 2006 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Please transfer the answers onto the bubble sheet. The question number refers
PHA Second Exam Fall On my honor, I have neither given nor received unauthorized aid in doing this assignment.
 PHA 5127 Second Exam Fall 2013 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question/Points Set I 20 pts Set II 20 pts Set III 20 pts Set IV 20 pts Set
PHA 5127 Second Exam Fall 2013 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question/Points Set I 20 pts Set II 20 pts Set III 20 pts Set IV 20 pts Set
ADME Review. Dr. Joe Ritter Associate Professor of Pharmacology
 ADME Review Dr. Joe Ritter Associate Professor of Pharmacology 828-1022 jkritter@vcu.edu What percent of a weak base (pka = 7.5) and weak acid (pka = 3.5) will be respectively ionized in urine of ph 5.5?
ADME Review Dr. Joe Ritter Associate Professor of Pharmacology 828-1022 jkritter@vcu.edu What percent of a weak base (pka = 7.5) and weak acid (pka = 3.5) will be respectively ionized in urine of ph 5.5?
DRUG ELIMINATION II BILIARY EXCRETION MAMMARY, SALIVARY AND PULMONARY EXCRETION
 DRUG ELIMINATION II BILIARY EXCRETION MAMMARY, SALIVARY AND PULMONARY EXCRETION ROUTE OF DRUG ADMINISTRATION AND EXTRAHEPATIC DRUG METABOLISM The decline in plasma concentration after drug administration
DRUG ELIMINATION II BILIARY EXCRETION MAMMARY, SALIVARY AND PULMONARY EXCRETION ROUTE OF DRUG ADMINISTRATION AND EXTRAHEPATIC DRUG METABOLISM The decline in plasma concentration after drug administration
PHA Final Exam. Fall On my honor, I have neither given nor received unauthorized aid in doing this assignment.
 PHA 5127 Final Exam Fall 2010 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Please transfer the answers onto the bubble sheet. The question number refers
PHA 5127 Final Exam Fall 2010 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Please transfer the answers onto the bubble sheet. The question number refers
BASIC PHARMACOKINETICS
 BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
BASIC PHARMACOKINETICS MOHSEN A. HEDAYA CRC Press Taylor & Francis Croup Boca Raton London New York CRC Press is an imprint of the Taylor & Francis Group, an informa business Table of Contents Chapter
PHA Second Exam. Fall On my honor, I have neither given nor received unauthorized aid in doing this assignment.
 PHA 5127 Second Exam Fall 2011 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Put all answers on the bubble sheet TOTAL /200 pts 1 Question Set I (True or
PHA 5127 Second Exam Fall 2011 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Put all answers on the bubble sheet TOTAL /200 pts 1 Question Set I (True or
Drug Dosing in Renal Insufficiency. Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila
 Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
Drug Dosing in Renal Insufficiency Coralie Therese D. Dimacali, MD College of Medicine University of the Philippines Manila Declaration of Conflict of Interest For today s lecture on Drug Dosing in Renal
Renal Disease and PK/PD. Anjay Rastogi MD PhD Division of Nephrology
 Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
Renal Disease and PK/PD Anjay Rastogi MD PhD Division of Nephrology Drugs and Kidneys Kidney is one of the major organ of drug elimination from the human body Renal disease and dialysis alters the pharmacokinetics
PHA5128 Dose Optimization II Case Study I Spring 2013
 Silsamicin is an investigational compound being evaluated for its antimicrobial effect. The route of administration for this drug is via intravenous bolus. Approximately 99.9% of this drug is eliminated
Silsamicin is an investigational compound being evaluated for its antimicrobial effect. The route of administration for this drug is via intravenous bolus. Approximately 99.9% of this drug is eliminated
TDM of Aminoglycoside Antibiotics
 TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
TDM Lecture 3 5 th Stage TDM of Aminoglycoside Antibiotics The aminoglycoside antibiotics are widely used for the treatment of gram-negative infections, often in combination with a β-lactam antibiotic
PHA Final Exam. Fall On my honor, I have neither given nor received unauthorized aid in doing this assignment.
 PHA 5127 Final Exam Fall 2012 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Please transfer the answers onto the bubble sheet. The question number refers
PHA 5127 Final Exam Fall 2012 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Please transfer the answers onto the bubble sheet. The question number refers
PHAR 7633 Chapter 20 Non Compartmental Analysis
 Student Objectives for this Chapter PHAR 7633 Chapter 20 Non Compartmental Analysis To understand and use the non compartmental approach to parameter estimation be able to define, use, and calculate the
Student Objectives for this Chapter PHAR 7633 Chapter 20 Non Compartmental Analysis To understand and use the non compartmental approach to parameter estimation be able to define, use, and calculate the
The principal functions of the kidneys
 Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
Renal physiology The principal functions of the kidneys Formation and excretion of urine Excretion of waste products, drugs, and toxins Regulation of body water and mineral content of the body Maintenance
You should know the T max for any substance that you use and for PAH ; T max = mg / min
 Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
Tubular function - What is clearance? o clearance referred to the theoretical volume of plasma from which a substance is cleared ( cleaned ) over a period of time and so its unit would be ((ml/min)) -
PHA Spring First Exam. 8 Aminoglycosides (5 points)
 PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
PHA 5128 Spring 2012 First Exam 1 Aminoglycosides (5 points) 2 Aminoglycosides (10 points) 3 Basic Principles (5 points) 4 Basic Principles (5 points) 5 Bioavailability (5 points) 6 Vancomycin (5 points)
General Principles of Pharmacology and Toxicology
 General Principles of Pharmacology and Toxicology Parisa Gazerani, Pharm D, PhD Assistant Professor Center for Sensory-Motor Interaction (SMI) Department of Health Science and Technology Aalborg University
General Principles of Pharmacology and Toxicology Parisa Gazerani, Pharm D, PhD Assistant Professor Center for Sensory-Motor Interaction (SMI) Department of Health Science and Technology Aalborg University
Ch 19: The Kidneys. Functional unit of kidneys:?? Developed by John Gallagher, MS, DVM
 Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Ch 19: The Kidneys Homeostatic regulation of ECF volume and BP Osmolarity 290 mosm Ion balance Na+ and K+, etc. ph (acid-base balance Excretion of wastes & foreign substances Hormone production EPO Renin
Assessing Renal Function: What you Didn t Know You Didn t Know
 Assessing Renal Function: What you Didn t Know You Didn t Know Presented By Tom Wadsworth PharmD, BCPS Associate Clinical Professor UAA/ISU Doctor of Pharmacy Program Idaho State University College of
Assessing Renal Function: What you Didn t Know You Didn t Know Presented By Tom Wadsworth PharmD, BCPS Associate Clinical Professor UAA/ISU Doctor of Pharmacy Program Idaho State University College of
Drug elimination and Hepatic clearance Chapter 6
 Drug elimination and Hepatic clearance Chapter 6 DRUG ELIMINATION Drugs are removed from the body by various elimination processes. Drug elimination refers to the irreversible removal of drug from the
Drug elimination and Hepatic clearance Chapter 6 DRUG ELIMINATION Drugs are removed from the body by various elimination processes. Drug elimination refers to the irreversible removal of drug from the
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D.
 RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
RENAL SYSTEM 2 TRANSPORT PROPERTIES OF NEPHRON SEGMENTS Emma Jakoi, Ph.D. Learning Objectives 1. Identify the region of the renal tubule in which reabsorption and secretion occur. 2. Describe the cellular
Excretion Chapter 29. The Mammalian Excretory System consists of. The Kidney. The Nephron: the basic unit of the kidney.
 Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
Excretion Chapter 29 The Mammalian Excretory System consists of The Kidney 1. Vertebrate kidneys perform A. Ion balance B. Osmotic balance C. Blood pressure D. ph balance E. Excretion F. Hormone production
KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin
![KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin KD02 [Mar96] [Feb12] Which has the greatest renal clearance? A. PAH B. Glucose C. Urea D. Water E. Inulin](/thumbs/87/96174332.jpg) Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
Renal Physiology MCQ KD01 [Mar96] [Apr01] Renal blood flow is dependent on: A. Juxtaglomerular apparatus B. [Na+] at macula densa C. Afferent vasodilatation D. Arterial pressure (poorly worded/recalled
PHA Second Exam. Fall On my honor, I have neither given nor received unauthorized aid in doing this assignment.
 PHA 5127 Second Exam Fall 2012 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Put all answers on the bubble sheet TOTAL /150 pts 1 Question Set I (True or
PHA 5127 Second Exam Fall 2012 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Put all answers on the bubble sheet TOTAL /150 pts 1 Question Set I (True or
Basic Pharmacokinetic Principles Stephen P. Roush, Pharm.D. Clinical Coordinator, Department of Pharmacy
 Basic Pharmacokinetic Principles Stephen P. Roush, Pharm.D. Clinical Coordinator, Department of Pharmacy I. General principles Applied pharmacokinetics - the process of using drug concentrations, pharmaco-kinetic
Basic Pharmacokinetic Principles Stephen P. Roush, Pharm.D. Clinical Coordinator, Department of Pharmacy I. General principles Applied pharmacokinetics - the process of using drug concentrations, pharmaco-kinetic
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology
 Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Human Physiology - Problem Drill 17: The Kidneys and Nephronal Physiology Question No. 1 of 10 Instructions: (1) Read the problem statement and answer choices carefully, (2) Work the problems on paper
Renal Physiology. April, J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine.
 Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Renal Physiology April, 2011 J. Mohan, PhD. Lecturer, Physiology Unit, Faculty of Medical Sciences, U.W.I., St Augustine. Office : Room 105, Physiology Unit. References: Koeppen B.E. & Stanton B.A. (2010).
Pharmacokinetics of Drugs. Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia
 Pharmacokinetics of Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Absorption Is the transfer of a drug from its site of administration to the bloodstream.
Pharmacokinetics of Drugs Assistant Prof. Dr. Najlaa Saadi PhD Pharmacology Faculty of Pharmacy University of Philadelphia Absorption Is the transfer of a drug from its site of administration to the bloodstream.
1. remove: waste products: urea, creatinine, and uric acid foreign chemicals: drugs, water soluble vitamins, and food additives, etc.
 Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Making Water! OR is it really Just Water Just Ask the Nephron!! Author: Patricia L. Ostlund ostlundp@faytechcc.edu (910) 678-9892 Fayetteville Technical Community College Fayetteville, NC 28303 Its just
Nephron Function and Urine Formation. Ms. Kula December 1, 2014 Biology 30S
 Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Nephron Function and Urine Formation Ms. Kula December 1, 2014 Biology 30S The Role of the Nephron In order for the body to properly function and maintain homeostasis, the amount of dissolved substances
Tamer Barakat. Abdul Aziz ALShamali. Abdul Aziz ALShamali
 10 Tamer Barakat Abdul Aziz ALShamali Abdul Aziz ALShamali Dr. Alia Elimination: Refampin is used to treat TB not malaria (Quinacrine is used for malaria) It s the opposite process of absorption. It's
10 Tamer Barakat Abdul Aziz ALShamali Abdul Aziz ALShamali Dr. Alia Elimination: Refampin is used to treat TB not malaria (Quinacrine is used for malaria) It s the opposite process of absorption. It's
Industrial Toxicology
 Industrial Toxicology Learning Objectives Know the assumptions of the doseresponse and time-course curves Be able to define and label key points of a curve Know the difference between potency and efficacy
Industrial Toxicology Learning Objectives Know the assumptions of the doseresponse and time-course curves Be able to define and label key points of a curve Know the difference between potency and efficacy
Rational Dose Prediction. Pharmacology. φαρμακον. What does this mean? pharmakon. Medicine Poison Magic Spell
 1 Rational Dose Prediction Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand 2 Pharmacology Pharmacology is derived from a Greek word (pharmakon). The Greeks used
1 Rational Dose Prediction Nick Holford Dept Pharmacology & Clinical Pharmacology University of Auckland, New Zealand 2 Pharmacology Pharmacology is derived from a Greek word (pharmakon). The Greeks used
Introduction to the kidney: regulation of sodium & glucose. Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health
 Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Introduction to the kidney: regulation of sodium & glucose Dr Nick Ashton Senior Lecturer in Renal Physiology Faculty of Biology, Medicine & Health Objectives Overview of kidney structure & function Glomerular
Ch 17 Physiology of the Kidneys
 Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
Ch 17 Physiology of the Kidneys Review Anatomy on your own SLOs List and describe the 4 major functions of the kidneys. List and explain the 4 processes of the urinary system. Diagram the filtration barriers
PHA First Exam Fall 2003
 PHA 5127 First Exam Fall 2003 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question/Points 1. /14 pts 2. /6 pts 3. /15 pts 4. /12 pts 5. /20 pts 6. /10pts
PHA 5127 First Exam Fall 2003 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question/Points 1. /14 pts 2. /6 pts 3. /15 pts 4. /12 pts 5. /20 pts 6. /10pts
Introduction to. Pharmacokinetics. University of Hawai i Hilo Pre-Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D
 Introduction to 1 Pharmacokinetics University of Hawai i Hilo Pre-Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 2 Learning objectives Understand compartment models and how they effects
Introduction to 1 Pharmacokinetics University of Hawai i Hilo Pre-Nursing Program NURS 203 General Pharmacology Danita Narciso Pharm D 2 Learning objectives Understand compartment models and how they effects
PRESCRIBING IN LIVER AND RENAL DISEASE
 THERAPEUTICS FOR INDEPENDENT PRESCRIBERS PRESCRIBING IN LIVER AND RENAL DISEASE Number 6 in a series of 15 articles on Therapeutics Aims and Objectives To outline the pathophysiological changes that occur
THERAPEUTICS FOR INDEPENDENT PRESCRIBERS PRESCRIBING IN LIVER AND RENAL DISEASE Number 6 in a series of 15 articles on Therapeutics Aims and Objectives To outline the pathophysiological changes that occur
The kidneys are excretory and regulatory organs. By
 exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
exercise 9 Renal System Physiology Objectives 1. To define nephron, renal corpuscle, renal tubule, afferent arteriole, glomerular filtration, efferent arteriole, aldosterone, ADH, and reabsorption 2. To
Filtration and Reabsorption Amount Filter/d
 Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
Renal Physiology 2011 Lisa M. Harrison-Bernard, PhD Contact me at lharris@lsuhsc.edu Renal Physiology Lecture 3 Renal Clearance and Glomerular Filtration Filtration and Reabsorption Amount Filter/d Amount
PHA First Exam. Fall 2004
 PHA 5127 First Exam Fall 2004 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Put all answers on the bubble sheet. If you need to comment or question a problem
PHA 5127 First Exam Fall 2004 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Put all answers on the bubble sheet. If you need to comment or question a problem
Basic Concepts in Pharmacokinetics. Leon Aarons Manchester Pharmacy School University of Manchester
 Basic Concepts in Pharmacokinetics Leon Aarons Manchester Pharmacy School University of Manchester Objectives 1. Define pharmacokinetics 2. Describe absorption 3. Describe distribution 4. Describe elimination
Basic Concepts in Pharmacokinetics Leon Aarons Manchester Pharmacy School University of Manchester Objectives 1. Define pharmacokinetics 2. Describe absorption 3. Describe distribution 4. Describe elimination
Kidney Physiology. Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed
 Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Kidney Physiology Mechanisms of Urine Formation TUBULAR SECRETION Eunise A. Foster Shalonda Reed The purpose of tubular secrection To dispose of certain substances that are bound to plasma proteins. To
Lecture-2 Review of the previous lecture:
 Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
Lecture-2 Review of the previous lecture: -Kidney s function is to clean the blood by the removing of the waste plus adding some valuable substances -kidney failure will lead to death for many reasons,
Functional morphology of kidneys Clearance
 Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Functional morphology of kidneys Clearance Assoc. Prof. MUDr. Markéta Bébarová, Ph.D. Department of Physiology Faculty of Medicine, Masaryk University This presentation includes only the most important
Renal Clearance. Dr. Eman El Eter
 Renal Clearance Dr. Eman El Eter Concept of clearance Clearance is the volume of plasma that is completely cleared of a substance each minute. Example: Renal clearance of Substance X is defined as the
Renal Clearance Dr. Eman El Eter Concept of clearance Clearance is the volume of plasma that is completely cleared of a substance each minute. Example: Renal clearance of Substance X is defined as the
Homeostatic Regulation
 Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Homeostatic Regulation A hormone is :a Water-soluble hormones: Composed of amino acids and bind a receptor protein on the of the target cell. This starts a signal cascade inside the cell and the signal
Renal System Physiology
 M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
M58_MARI0000_00_SE_EX09.qxd 7/18/11 2:37 PM Page 399 E X E R C I S E 9 Renal System Physiology Advance Preparation/Comments 1. Prior to the lab, suggest to the students that they become familiar with the
Name: UFID: PHA Exam 2. Spring 2013
 PHA 5128 Exam 2 Spring 2013 1 Carbamazepine (5 points) 2 Theophylline (10 points) 3 Gentamicin (10 points) 4 Drug-drug interaction (5 points) 5 Lidocaine (5 points) 6 Cyclosporine (5 points) 7 Phenobarbital
PHA 5128 Exam 2 Spring 2013 1 Carbamazepine (5 points) 2 Theophylline (10 points) 3 Gentamicin (10 points) 4 Drug-drug interaction (5 points) 5 Lidocaine (5 points) 6 Cyclosporine (5 points) 7 Phenobarbital
Pharmacokinetics in Drug Development. Edward P. Acosta, PharmD Professor & Director Division of Clinical Pharmacology Director, CCC PK/PD Core
 Pharmacokinetics in Drug Development Edward P. Acosta, PharmD Professor & Director Division of Clinical Pharmacology Director, CCC PK/PD Core Finding new drugs: A crap shoot Clinical Development Phase
Pharmacokinetics in Drug Development Edward P. Acosta, PharmD Professor & Director Division of Clinical Pharmacology Director, CCC PK/PD Core Finding new drugs: A crap shoot Clinical Development Phase
Renal-Related Questions
 Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
Renal-Related Questions 1) List the major segments of the nephron and for each segment describe in a single sentence what happens to sodium there. (10 points). 2) a) Describe the handling by the nephron
INTRODUCTION TO PHARMACOKINETICS
 INTRODUCTION TO PHARMACOKINETICS 1 http://www.biology.iupui.edu/biocourses/biol540/4pipeline2css.html 2 PHARMACOKINETICS 1. ABSORPTION 2. DISTRIBUTION 3. METABOLISM 4. EXCRETION ALL THESE PROCESSES ARE
INTRODUCTION TO PHARMACOKINETICS 1 http://www.biology.iupui.edu/biocourses/biol540/4pipeline2css.html 2 PHARMACOKINETICS 1. ABSORPTION 2. DISTRIBUTION 3. METABOLISM 4. EXCRETION ALL THESE PROCESSES ARE
UNIVERSITY OF THE WEST INDIES, ST AUGUSTINE
 UNIVERSITY OF THE WEST INDIES, ST AUGUSTINE FACULTY OF MEDICAL SCIENCES SCHOOL OF PHARMACY BACHELOR OF SCIENCE IN PHARMACY DEGREE COURSE SYLLABUS COURSE TITLE: COURSE CODE: BIOPHARMACEUTICS, NEW DRUG DELIVERY
UNIVERSITY OF THE WEST INDIES, ST AUGUSTINE FACULTY OF MEDICAL SCIENCES SCHOOL OF PHARMACY BACHELOR OF SCIENCE IN PHARMACY DEGREE COURSE SYLLABUS COURSE TITLE: COURSE CODE: BIOPHARMACEUTICS, NEW DRUG DELIVERY
BCH 450 Biochemistry of Specialized Tissues
 BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BCH 450 Biochemistry of Specialized Tissues VII. Renal Structure, Function & Regulation Kidney Function 1. Regulate Extracellular fluid (ECF) (plasma and interstitial fluid) through formation of urine.
BIOL 2402 Renal Function
 BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOL 2402 Renal Function Dr. Chris Doumen Collin County Community College 1 Renal Clearance and GFR Refers to the volume of blood plasma from which a component is completely removed in one minute by all
BIOPHARMACEUTICS and CLINICAL PHARMACY
 11 years papers covered BIOPHARMACEUTICS and CLINICAL PHARMACY IV B.Pharm II Semester, Andhra University Topics: Absorption Distribution Protein binding Metabolism Excretion Bioavailability Drug Interactions
11 years papers covered BIOPHARMACEUTICS and CLINICAL PHARMACY IV B.Pharm II Semester, Andhra University Topics: Absorption Distribution Protein binding Metabolism Excretion Bioavailability Drug Interactions
It the process by which a drug reversibly leaves blood and enter interstitium (extracellular fluid) and/ or cells of tissues.
 It the process by which a drug reversibly leaves blood and enter interstitium (extracellular fluid) and/ or cells of tissues. Primarily depends on: 1.Regional blood flow. 2.Capillary permeability. 3.Protein
It the process by which a drug reversibly leaves blood and enter interstitium (extracellular fluid) and/ or cells of tissues. Primarily depends on: 1.Regional blood flow. 2.Capillary permeability. 3.Protein
Physiology questions review
 Physiology questions review 1- The consumption of O2 by the kidney: a- decrease as blood flow increases b- regulated by erythropoiten c- remains constant as blood flow increase d- direct reflects the level
Physiology questions review 1- The consumption of O2 by the kidney: a- decrease as blood flow increases b- regulated by erythropoiten c- remains constant as blood flow increase d- direct reflects the level
The Excretory System. Biology 20
 The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
The Excretory System Biology 20 Introduction Follow along on page 376 What dangers exist if your body is unable to regulate the fluid balance of your tissues? What challenged would the body have to respond
1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- renal cortex - X- renal medulla Y- renal pelvis collecting center of urine and then
Pharmacokinetics I. Dr. M.Mothilal Assistant professor
 Pharmacokinetics I Dr. M.Mothilal Assistant professor DRUG TRANSPORT For a drug to produce a therapeutic effect, it must reach to its target and it must accumulate at that site to reach to the minimum
Pharmacokinetics I Dr. M.Mothilal Assistant professor DRUG TRANSPORT For a drug to produce a therapeutic effect, it must reach to its target and it must accumulate at that site to reach to the minimum
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University
 Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Renal System Dr. Naim Kittana Department of Biomedical Sciences Faculty of Medicine & Health Sciences An-Najah National University Declaration The content and the figures of this seminar were directly
Urinary System. consists of the kidneys, ureters, urinary bladder and urethra
 Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
Urinary System 1 Urinary System consists of the kidneys, ureters, urinary bladder and urethra 2 Location of Kidneys The kidneys which are positioned retroperitoneally lie on either side of the vertebral
The kidney. (Pseudo) Practical questions. The kidneys are all about keeping the body s homeostasis. for questions Ella
 The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
The kidney (Pseudo) Practical questions for questions Ella (striemit@gmail.com) The kidneys are all about keeping the body s homeostasis Ingestion Product of metabolism H 2 O Ca ++ Cl - K + Na + H 2 O
Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations
 Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations Rosenbaum, Sara E. ISBN-13: 9780470569061 Table of Contents 1 Introduction to Pharmacokinetics and Pharmacodynamics.
Basic Pharmacokinetics and Pharmacodynamics: An Integrated Textbook with Computer Simulations Rosenbaum, Sara E. ISBN-13: 9780470569061 Table of Contents 1 Introduction to Pharmacokinetics and Pharmacodynamics.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1
 BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
BIPN100 F15 Human Physiology (Kristan) Problem Set #8 Solutions p. 1 1. a. Proximal tubule. b. Proximal tubule. c. Glomerular endothelial fenestrae, filtration slits between podocytes of Bowman's capsule.
12/7/10. Excretory System. The basic function of the excretory system is to regulate the volume and composition of body fluids by:
 Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Excretory System The basic function of the excretory system is to regulate the volume and composition of body fluids by: o o removing wastes returning needed substances to the body for reuse Body systems
Chapter 23. Composition and Properties of Urine
 Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Chapter 23 Composition and Properties of Urine Composition and Properties of Urine (1 of 2) urinalysis the examination of the physical and chemical properties of urine appearance - clear, almost colorless
Excretory Lecture Test Questions Set 1
 Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Excretory Lecture Test Questions Set 1 1. The separation and ejection of metabolic wastes, usually in aqueous solution, is: a. reabsorption b. secretion c. filtration d. excretion e. endocrinology 2. Besides
Lecture 4. Use of clearance methods to quantify kidney functions:
 Lecture 4 Why does the colloid osmotic pressure increase throughout the glomeruar capillaries whereas it doesn t increase significantly throughout any other systemic capillary? The cardiac output equals
Lecture 4 Why does the colloid osmotic pressure increase throughout the glomeruar capillaries whereas it doesn t increase significantly throughout any other systemic capillary? The cardiac output equals
Excretory System Workbook
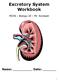 Excretory System Workbook MCHS Biology 20 Mr. Korotash Name: Date: 1 Study the diagram above. Name the structures and indicate their functions by completing the following table: Structure 1. Function 2.
Excretory System Workbook MCHS Biology 20 Mr. Korotash Name: Date: 1 Study the diagram above. Name the structures and indicate their functions by completing the following table: Structure 1. Function 2.
Excretory System 1. a)label the parts indicated above and give one function for structures Y and Z
 Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Excretory System 1 1. Excretory System a)label the parts indicated above and give one function for structures Y and Z W- X- Y- Z- b) Which of the following is not a function of the organ shown? A. to produce
Renal Physiology II Tubular functions
 Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
Renal Physiology II Tubular functions LO. 42, 43 Dr. Kékesi Gabriella Basic points of renal physiology 1. Glomerular filtration (GF) a) Ultrafiltration 2. Tubular functions active and passive a) Reabsorption
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION
 LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
LECTURE 25: FILTRATION AND CLEARANCE NEPHRON FILTRATION 1. Everything in the plasma is filtered except large proteins and red blood cells. The filtrate in Bowman s capsule is an isosmotic fluid that is
General Principles of Pharmacology and Toxicology
 General Principles of Pharmacology and Toxicology Parisa Gazerani, Pharm D, PhD Assistant Professor Center for Sensory-Motor Interaction (SMI) Department of Health Science and Technology Aalborg University
General Principles of Pharmacology and Toxicology Parisa Gazerani, Pharm D, PhD Assistant Professor Center for Sensory-Motor Interaction (SMI) Department of Health Science and Technology Aalborg University
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS
 RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
RENAL PHYSIOLOGY, HOMEOSTASIS OF FLUID COMPARTMENTS (2) Dr. Attila Nagy 2017 TUBULAR FUNCTIONS (Learning objectives 54-57) 1 Tubular Transport About 99% of filtrated water and more than 90% of the filtrated
Osmoregulation and the Excretory System
 Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Honors Biology Study Guide Chapter 25.4 25.10 Name Osmoregulation and the Excretory System FUNCTIONS OF THE EXCRETORY SYSTEM OSMOREGULATION Freshwater: Marine: Land Animals: Sources of Nitrogenous Wastes?
Click to edit Master title style
 A Short Course in Pharmacokinetics Chris Town Research Pharmacokinetics Outline Pharmacokinetics - Definition Ideal Pharmacokinetic Parameters of a New Drug How do we optimize PK for new compounds Why
A Short Course in Pharmacokinetics Chris Town Research Pharmacokinetics Outline Pharmacokinetics - Definition Ideal Pharmacokinetic Parameters of a New Drug How do we optimize PK for new compounds Why
PHA 4120 Second Exam Key Fall On my honor, I have neither given nor received unauthorized aid in doing this assignment.
 PHA 4120 Second Exam Key Fall 1997 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question Points 1. /10 ponts 2. /20 points 3. /10 points 4. /10 points
PHA 4120 Second Exam Key Fall 1997 On my honor, I have neither given nor received unauthorized aid in doing this assignment. Name Question Points 1. /10 ponts 2. /20 points 3. /10 points 4. /10 points
Effects of Renal Disease on Pharmacokinetics
 Effects of Renal Disease on Pharmacokinetics Juan J. L. Lertora, M.D., Ph.D. Director Clinical Pharmacology Program October 14, 2010 Office of Clinical Research Training and Medical Education National
Effects of Renal Disease on Pharmacokinetics Juan J. L. Lertora, M.D., Ph.D. Director Clinical Pharmacology Program October 14, 2010 Office of Clinical Research Training and Medical Education National
Osnove farmakokinetike. Aleš Mrhar. Prirejeno po. A First Course in Pharmacokinetics and Biopharmaceutics by David Bourne,
 Osnove farmakokinetike Aleš Mrhar Prirejeno po A First Course in Pharmacokinetics and Biopharmaceutics by David Bourne, College of Pharmacy, University of Oklahoma Pharmacokinetics/Pharmacodynamics Pharmacodynamics
Osnove farmakokinetike Aleš Mrhar Prirejeno po A First Course in Pharmacokinetics and Biopharmaceutics by David Bourne, College of Pharmacy, University of Oklahoma Pharmacokinetics/Pharmacodynamics Pharmacodynamics
Nephron Structure inside Kidney:
 In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
In-Depth on Kidney Nephron Structure inside Kidney: - Each nephron has two capillary regions in close proximity to the nephron tubule, the first capillary bed for fluid exchange is called the glomerulus,
April 08, biology 2201 ch 11.3 excretion.notebook. Biology The Excretory System. Apr 13 9:14 PM EXCRETORY SYSTEM.
 Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Biology 2201 11.3 The Excretory System EXCRETORY SYSTEM 1 Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid base concentrations and metabolite concentrations
Human Urogenital System 26-1
 Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Human Urogenital System 26-1 Urogenital System Functions Filtering of blood, Removal of wastes and metabolites Regulation of blood volume and composition concentration of blood solutes ph of extracellular
Nephron Anatomy Nephron Anatomy
 Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
Kidney Functions: (Eckert 14-17) Mammalian Kidney -Paired -1% body mass -20% blood flow (Eckert 14-17) -Osmoregulation -Blood volume regulation -Maintain proper ion concentrations -Dispose of metabolic
1. If the MTC is 100 ng/ml and the MEC is 0.12 ng/ml, which of the following dosing regimen(s) are in the therapeutic window?
 Page 1 PHAR 750: Biopharmaceutics/Pharmacokinetics October 23, 2009 - Form 1 Name: Total 100 points Please choose the BEST answer of those provided. For numerical answers, choose none of the above if your
Page 1 PHAR 750: Biopharmaceutics/Pharmacokinetics October 23, 2009 - Form 1 Name: Total 100 points Please choose the BEST answer of those provided. For numerical answers, choose none of the above if your
HIHIM 409 7/26/2009. Kidney and Nephron. Fermamdo Vega, M.D. 1
 Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Function of the Kidneys Nephrology Fernando Vega, M.D. Seattle Healing Arts Center Remove Wastes Regulate Blood Pressure Regulate Blood Volume Regulates Electrolytes Converts Vitamin D to active form Produces
Physiology Lecture 2. What controls GFR?
 Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Physiology Lecture 2 Too much blood is received by the glomerular capillaries, this blood contains plasma, once this plasma enters the glomerular capillaries it will be filtered to bowman s space. The
Renal Reabsorption & Secretion
 Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
Renal Reabsorption & Secretion Topics for today: Nephron processing of filtrate Control of glomerular filtration Reabsorption and secretion Examples of solute clearance rates Hormones affecting kidney
CREATININE: is another nitrogenous waste. Creatinine comes from creatinine phosphate in muscle metabolism (a Phosphate-storage molecule)
 BIOLOGY 12 - EXCRETION: CHAPTER NOTES Your cells are constantly carrying out chemical reactions to maintain homeostasis. Many of these chemical reactions produce wastes that must be removed from cells
BIOLOGY 12 - EXCRETION: CHAPTER NOTES Your cells are constantly carrying out chemical reactions to maintain homeostasis. Many of these chemical reactions produce wastes that must be removed from cells
014 Chapter 14 Created: 9:25:14 PM CST
 014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
014 Chapter 14 Created: 9:25:14 PM CST Student: 1. Functions of the kidneys include A. the regulation of body salt and water balance. B. hydrogen ion homeostasis. C. the regulation of blood glucose concentration.
PARTS OF THE URINARY SYSTEM
 EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETORY SYSTEM Excretory System How does the excretory system maintain homeostasis? It regulates heat, water, salt, acid-base concentrations and metabolite concentrations 1 ORGANS OF EXCRETION Skin and
EXCRETION QUESTIONS. Use the following information to answer the next two questions.
 EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
EXCRETION QUESTIONS Use the following information to answer the next two questions. 1. Filtration occurs at the area labeled A. V B. X C. Y D. Z 2. The antidiuretic hormone (vasopressin) acts on the area
Renal System and Excretion
 Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
Renal System and Excretion Biology 105 Lecture 19 Chapter 16 Outline Renal System I. Functions II. Organs of the renal system III. Kidneys 1. Structure 2. Function IV. Nephron 1. Structure 2. Function
PHA5128 Dose Optimization II Case Study 3 Spring 2013
 Use the vancomycin dosing nomogram table below: A female patient, 57 years of age, 5 6 in height and 100 in weight had an infection requiring vancomycin treatment. Her serum creatinine was 0.8 mg/d. What
Use the vancomycin dosing nomogram table below: A female patient, 57 years of age, 5 6 in height and 100 in weight had an infection requiring vancomycin treatment. Her serum creatinine was 0.8 mg/d. What
Adult Institutional Pharmacokinetics Protocol
 Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
Adult Institutional Pharmacokinetics Protocol Policy Title: Clinical Pharmacokinetics (PK) Service Policy Policy Statement: It is the policy of UMHC that PK consult orders (for vancomycin or aminoglycosides)
