Cue Cards for Counseling Adolescents on Contraception
|
|
|
- Johnathan Stafford
- 6 years ago
- Views:
Transcription
1 Cue Cards for Counseling Adolescents on Contraception About the Cue Cards This set of contraceptive counseling cue cards was developed to support a range of providers (such as facility-based providers, community health workers, pharmacists, outreach workers, counselors, and peer providers) in counseling young people on their contraceptive options. The cue cards provide information that is particularly relevant to adolescents (10 19 years), but can also be used with young people over age 19. The cards can be adapted to meet local circumstances and contexts. The cue cards cover the following methods: Implants Lactational Amenorrhea Method (LAM) Male Condom One side of the card serves to remind the provider of important information about the contraceptive method, such as the effectiveness, advantages, and disadvantages. The provider should use this information to educate an adolescent client about the full range of available methods and support the adolescent client in choosing a method that is right for her/him. After the client chooses a method, the provider can turn to the other side of the card to give the client specific instructions on her/his method of choice. This side of the card includes information that the provider should tell the adolescent client about how to use the method, possible side effects, and reasons to return to the provider. Intrauterine Device (IUD) DMPA (injectables) Combined Oral Contraceptives (COCs) Progestin-Only Pills (POPs) Female Condom Emergency Contraceptive Pills (ECPs) pathfinder international 2013
2 Cue Cards for Counseling Adolescents on Contraception Counseling Tips It is important to remember that adolescents regardless of age, relationship, marital, or childbearing status are eligible for the full range of contraceptive methods. The World Health Organization s (WHO) Medical Eligibility Criteria states that age alone is not a contraindication for any contraceptive method included in this set of cue cards, including long-acting methods. Providers have an obligation to provide adolescents with evidence-based and unbiased information about a full range of methods that might meet their needs. However, the provider should verify that the adolescent does not have any other condition that precludes use of a particular method per the WHO s Medical Eligibility Criteria. The cue cards can be used in any order based on the stated preferences and medical eligibility of the client. They are arranged in order of method effectiveness (from most effective to least effective) to encourage you to include method effectiveness as a key component of client counseling and to reinforce the fact that long-acting methods are an appropriate option for adolescents. Adolescent clients should have full information on a method, including potential side effects. This can help minimize an adolescent s concern if she/he does experience a side effect. However, adolescent clients also have more misinformation than adults about contraception and, as a result, often have greater fears about side effects. Therefore, when counseling adolescent clients on possible side effects, be sure to start by mentioning that most adolescent clients do not experience any side effects. Make sure to emphasize that only male and female condoms offer protection from sexually transmitted infections (STIs), HIV, and pregnancy. Therefore, if the client chooses a contraceptive method other than condoms, a condom must also be used to prevent pregnancy and STIs/HIV (dual method use). As you counsel adolescents remember to: ü Ensure privacy and confidentiality ü Be respectful of the client s choices, culture, religion, and sexuality ü Listen actively and show interest ü Be attentive to the client s questions and specific needs ü Use clear language the client can understand ü Avoid one-way communication and ask open-ended questions ü Avoid judgmental attitudes and behaviors don t lecture, scold, or tell the adolescent what he/she should do ü Provide unbiased, evidence-based information using the cue cards to ensure the adolescent has a choice of methods pathfinder international hq 9 Galen St., Suite 217, Watertown, MA USA TechnicalCommunications@pathfinder.org
3 Implants What are they? Implants are small flexible rods that contain the hormone progestin. The capsules are placed under the skin of a woman s upper arm and can prevent pregnancy for 3 5 years, depending on the type. There are several types of implants: Jadelle: 2 rods, effective for 5 years Implanon: 1 rod, effective for 3 years Sinoplant: 2 rods, effective for 5 years How effective are they? If 100 women use an implant, typically less than 1 becomes pregnant during the first year. Over the 3 5 years (depending on type), up to 1 pregnancy occurs per 100 women using an implant. How do implants work? Implants work by thickening cervical mucus, blocking sperm from meeting an egg, and by preventing the release of the egg from the ovary. Not recommended for adolescents who: Have unexplained vaginal bleeding (requires examination) Check medical eligibility criteria if adolescent has other serious health problems. Advantages Safe and effective Long lasting (3 5 years) and no daily action required Monthly bleeding becomes very light and often disappears after a year Can become pregnant again immediately after removing the implants Can be used while breastfeeding Doesn t interfere with sex May improve anemia Can be used discreetly Disadvantages Menstrual pattern will probably change Doesn t protect against STIs/HIV Requires a health provider to insert and remove
4 Implants Show the client the implants and explain the following: How to use implants The small rods or capsules are inserted under the skin of the client s upper arm. If implant is inserted within 7 days of the start of monthly bleeding, there is no need for a back-up method. If implant is inserted more than 7 days after the start of monthly bleeding (or more than 5 days for Implanon), the client will need a back-up method for the first 7 days. The implant will need to be removed after 3 5 years depending on implant type and client s weight. If a woman is heavier than 80 kg, advise her that Jadelle will become less effective after 4 years of use. Possible side effects may include: Changes in monthly bleeding: irregular spotting or prolonged light to moderate bleeding in the beginning. Later, bleeding is likely to be lighter, less frequent, or stop altogether. Weight gain, breast tenderness, headaches, dizziness, nausea, mood changes. Reasons to return to the provider Pus, heat, redness, or pain at the insertion site that worsens or does not go away (could indicate an infection at the site) Migraine headaches with blurred vision Implant seems to be coming out In the event of significant weight gain, as this may reduce the long-term effectiveness of the implant Any time there is a problem or if either partner has been exposed to an STI A resupply of condoms is needed (never run out before returning) Implants do not protect against STIs/HIV: To protect against pregnancy and STIs/HIV, use a condom every time you have sex. Have the client repeat this information back to you.
5 Intrauterine Device (IUD) (Information for the TCu 380A IUD) What is it? An IUD is a small plastic and copper device that is inserted into the uterus to prevent pregnancy. How effective is it? If 100 women use an IUD for 1 year, typically less than 1 woman becomes pregnant. How does the IUD work? The IUD works by preventing sperm from joining with the egg. Not recommended for adolescents who: Are 48 hours to 4 weeks postpartum Have postpartum sepsis or post-septic abortion Have unexplained vaginal bleeding (must do an examination before initiating method) Have active pelvic inflammatory disease, chlamydia, or gonorrhea (initiation only, continuation of method is acceptable) Have multiple sexual partners or whose partner has other sexual partners (at increased risk of STIs) Have AIDS and are not clinically well (initiation of IUD only) Check medical eligibility criteria if adolescent has other serious health problems. Advantages Safe, effective, and long-acting (up to 12 years) Easy to remove (by the provider) if the client wants to become pregnant No daily action required Doesn t interfere with sex Can be used discreetly no visible clues that it is used (occasionally a partner may feel the strings during sex) Can be inserted immediately postpartum Doesn t interfere with breastfeeding Can be used by young women, including those who have never been pregnant The copper IUD can also be used as emergency contraception to prevent pregnancy if inserted within 5 days of unprotected sex. Disadvantages Slight pain during the first few days after IUD insertion Heavier and/or longer periods, which normally decrease during the first and second years Doesn t protect against STIs/HIV Requires a health care provider to insert and remove
6 Intrauterine Device (IUD) (Information for the TCu 380A IUD) Show the client the IUD and explain the following: How to use the IUD The IUD is inserted by the provider once and can stay for up to 12 years. The client should come for a check-up 3 6 weeks after insertion, but no additional follow-up is required (unless there is a problem). Checking the strings is optional. The strings may be checked during the first few months and after monthly bleeding to see if the IUD is still in place. Explain how to check strings. Possible side effects may include: Heavier, longer, and/or irregular bleeding (usually decreases after first 3 6 months) More cramps and pain during monthly bleeding Increased vaginal discharge Possible infection Pain and cramping during insertion and the first few days after IUD insertion Reasons to return to provider Abnormal bleeding or discharge Pain (abdominal or pain with intercourse) Fever Strings are missing or you feel the hard plastic of an IUD that has partially come out. Any time there is a problem or if either partner has been exposed to an STI Any time a re-supply of condoms is needed (never run out completely before returning) The IUD does not protect against STIs/HIV: To protect against pregnancy and STIs/HIV, use a condom every time you have sex. Have the client repeat this information back to you.
7 DMPA: Injectable Contraceptive What is it? DMPA, sometimes known as the shot or Depo, is an injection containing the hormone progestin. The injection is given every 3 months. There are several types of injectable contraceptives. This card refers to DMPA, not NET-EN or monthly combined injectables. How effective is it? If 100 women use DMPA for 1 year, typically 3 become pregnant. How does DMPA work? DMPA works by preventing the release of the egg from the ovary. Without an egg, a woman cannot become pregnant. Not recommended for adolescents who: Have unexplained vaginal bleeding (before evaluation) Check medical eligibility criteria if adolescent has other serious health problems. Advantages Safe and effective Can be administered by non-physician health care workers Lasts for 3 months, no daily action required Discreet Monthly bleedings become very light and often disappear after a year of use Completely reversible can become pregnant again after stopping DMPA, but there might be a delay of several months Can be used while breastfeeding Doesn t interfere with sex May improve anemia Disadvantages Monthly bleeding pattern will probably change Increased appetite may cause weight gain On average, a 4-month longer delay in ability to get pregnant after stopping DMPA compared to other methods Doesn t protect against STIs/HIV
8 DMPA: Injectable Contraceptive Show the client the vial of DMPA and explain the following: How to use DMPA DMPA is given by injection every 3 months. Never be more than 4 weeks late for a repeat injection. Effective immediately if starting within 7 days after the start of monthly bleeding If starting more than 7 days after the first day of monthly bleeding, a back-up method (e.g., condoms) is needed for the first 7 days. Missed injection What to do Come immediately to get an injection and use a back-up method immediately until 7 days after the injection. If you can t come at the appointed time, but you can come earlier, it is possible to come up to 4 weeks early for your next injection. Possible side effects may include: Irregular spotting Prolonged light to moderate bleeding Bleeding is likely to become lighter, less frequent, or stop altogether. Possible weight gain, headaches, dizziness, mood changes Reasons to return to provider Heavy vaginal bleeding Excessive weight gain Extreme headaches with blurred vision Any time there is a problem or if either partner has been exposed to an STI Another 3-month injection or a resupply of condoms is needed (never run out completely before returning) DMPA does not protect against STIs/HIV: To protect against pregnancy and STIs/HIV, use a condom every time you have sex. Have the client repeat this information back to you.
9 Lactational Amenorrhea Method (LAM) What is it? The Lactational Amenorrhea Method (LAM) is the use of breastfeeding as a temporary contraceptive method. ( Lactational means related to breastfeeding and amenorrhea means not having menstrual bleeding.) How effective is it? If 100 women use LAM in the first 6 months after childbirth, typically 2 become pregnant. How does LAM work? LAM works by preventing ovulation because breastfeeding changes the rate of release of natural hormones. Advantages Effective in preventing pregnancy for at least 6 months Encourages the best breastfeeding patterns with health benefits for the mother and baby Can be used immediately after childbirth Doesn t interfere with sex No direct cost for contraception or for feeding the baby No supplies or procedures needed to prevent pregnancy Disadvantages Reduced effectiveness after 6 months Requires frequent breastfeeding (day and night), which may be difficult for some mothers Does not provide protection against STIs, including HIV If the mother has HIV there is a chance that breast milk will pass HIV to the baby. It is recommended for mothers to exclusively breastfeed to reduce this risk.
10 Lactational Amenorrhea Method (LAM) Explain the following to the client: LAM can be used if all the conditions below are met: Monthly bleeding has not returned. The baby is not receiving other food besides breast milk and does not go for long periods (more than 4 6 hours) without breastfeeding, either during the day or night. The baby is less than 6 months old. Note: A complementary form of contraception can also be used at any point. LAM cannot be used if any of the following conditions exist: Baby is 6 months of age or older Monthly bleeding begins Baby is receiving supplemental foods LAM does not protect against STIs/HIV: To protect against pregnancy and STIs/HIV, use a condom every time you have sex. How to make breastfeeding effective Breastfeed whenever the baby wants to be fed, day and night. Feed from both breasts. Avoid intervals of more than 4 hours between any daytime feeds and more than 6 hours between any nighttime feeds. Breastfeed for 6 months. Don t use pacifiers, nipples, or bottles. Express breast milk if separated from the baby. Don t give the baby water or teas. Reasons to return to provider No longer fully breastfeeding and need another contraceptive method Any time there is a problem or if either partner has been exposed to an STI A resupply of condoms is needed (never run out completely before returning) Have the client repeat this information back to you.
11 Combined Oral Contraceptives (COCs) What are they? COCs (also known as the pill ) are tablets containing the hormones estrogen and progestin. A woman takes 1 pill daily to prevent pregnancy. How effective are they? If 100 women use COCs for 1 year, typically 8 become pregnant. There is a higher failure rate for adolescents than for all other ages because adolescents have trouble remembering to take pills regularly. How do COCs work? COCs work by preventing the release of the egg from the ovary. Without releasing an egg, a woman cannot become pregnant. Not recommended for adolescents who: Gave birth less than 4 weeks ago (if not breastfeeding) Are breastfeeding a baby less than 6 months old Have migraine headaches with aura Have viral hepatitis with severe or acute flare-up Take Ritonavir-boosted protease inhibitor ARVs (If using any ARV, use COCs with at least 30 ug EE.) Take rifampicin or rifabutin for TB (If using rifampicin or rifabutin, use COCs with at least 30 ug EE.) Check medical eligibility criteria if adolescent has other serious health problems. Advantages Safe, effective, and easy to use Controlled by the woman Can be used before the onset of monthly bleeding Lighter, regular monthly bleeding with less cramping Possible to become pregnant again immediately after stopping COCs Don t interfere with sex May be beneficial for adolescents who have irregular or heavy monthly bleeding, severe cramping, or acne Decrease risk of cancer of the female reproductive organs Disadvantages Must be taken every day to be effective Not always discreet (someone could see the pills) Weight gain or unexpected bleeding/spotting in some adolescents Don t protect against STIs including HIV
12 Combined Oral Contraceptives (COCs) Show the client the pill packet and explain the following: How to use COCs Take first pill on the first day of monthly bleeding or any of the next 4 days. If taking the pill more than 5 days after the start of your monthly bleeding, use a back-up method for the first 7 days. Take 1 pill every day, at the same time of day. Keep the pills in a place that will help you remember, such as near where you wash at night. 28-day packet: After finishing the packet, begin next packet the following day. The last 7 pills do not contain hormones, but they are there to remind you to keep taking the pill. 21-day packet: After finishing the packet, wait 7 days and then begin the next packet. Missed pills What to do Missed pills may result in pregnancy. If you miss pills, ALWAYS take one as soon as you remember and continue to take the rest of the pills each day at the regular time. If you miss 3 or more pills, or start a pack more than 3 days late, continue taking the rest of the pills at the regular time and use a condom or avoid sex for the next 7 days. If you miss 3 or more pills in the third week of the pill packet, skip the inactive pills and start a new packet. Use a condom or avoid sex for the next 7 days. Possible side effects may include: Nausea, weight gain, breast tenderness, headaches, dizziness, mood changes Changes in monthly bleeding patterns, including unexpected bleeding or spotting Reasons to return to provider Severe headaches (including headaches with blurred vision) Severe, constant pain in belly, chest, or legs Jaundice or yellowing of the skin Brief loss of vision, seeing flashing lights or zigzag lines (with or without bad headaches) Brief trouble speaking or moving arms or legs Any time there is a problem or if either partner has been exposed to an STI When a resupply of COCs (always have at least 1 back-up pack) or condoms is needed COCs do not protect against STIs/HIV: To protect against pregnancy and STIs/HIV, use a condom every time you have sex. Have the client repeat this information back to you.
13 Progestin-only Pills (POPs) What are they? POPs (also known as the mini-pill ) are oral contraceptive pills containing only a very small amount of one hormone (a progestin). A woman takes 1 tablet daily to prevent pregnancy. How effective are they? POPs are very effective for breastfeeding women. If 100 breastfeeding women use POPs for 1 year, typically 1 becomes pregnant. As typically used, they are less effective for non-breastfeeding women. If 100 non-breastfeeding women use POPs for 1 year, typically 3 10 women become pregnant. There is a higher failure rate for adolescents since adolescents have trouble remembering to take pills regularly. How do POPs work? POPs work by thickening the cervical mucus, making it difficult for sperm to pass through, and by preventing the release of the egg from the ovary in about half of all menstrual cycles. Not recommended for adolescents who are: Taking ritonavir-boosted protease inhibitor ARVs Taking rifampicin or rifabutin therapy for TB Advantages Can be used while breastfeeding Good option for adolescents who can t use estrogen but want to use pills Can become pregnant again immediately after stopping Don t interfere with sex Disadvantages For adolescents (not breastfeeding), monthly bleeding patterns may change (including spotting and amenorrhea) Must be taken at the same time every day, which can be difficult for adolescents to remember a delay of 3 hours is similar to missing a pill Not always discreet (someone could see the pills) Don t protect against STIs/HIV
14 Progestin-only Pills (POPs) Show the client the pill packet and explain the following: How to use POPs If breastfeeding and monthly bleeding has not returned, can start POPs at any time without a back-up method. If monthly bleeding has returned, POPs can be started within the first 5 days after the start of monthly bleeding without a back-up method. If it has been more than 6 months since giving birth or if monthly bleeding has returned, but it is not within the first 5 days after the start of monthly bleeding, POPs can be started any time if you are reasonably certain you are not pregnant. But a back-up method, like a condom, should be used for the first 2 days. Take 1 pill every day, at the same time of day. When a packet finishes, start another pack the very next day. Don t miss a day or take the pill late. You may want to take the pill when you do something that you do every day, like washing your face or brushing your teeth. Missed pills What to do Take pill or pills as soon as you remember. You may take 2 pills at the same time or the same day. Continue taking the next pill at the usual time. Use a back-up method, like a condom, for the next 2 days. Possible side effects may include: Changes in monthly bleeding patterns, including amenorrhea, spotting, irregular or prolonged bleeding (for adolescents who are not breastfeeding) Breast tenderness, headaches, dizziness, mood changes, abdominal pain, nausea Breastfeeding adolescents may have a longer delay in return of monthly bleeding after childbirth. Reasons to return to provider Stopped breastfeeding and would like to switch methods Took a pill more than 3 hours late or missed one completely, and also had sex during this time, and want to consider ECPs (for women who have monthly bleeding) Severe headaches with blurred vision Any time there is a problem or if either partner has been exposed to an STI A resupply of POPs or condoms is needed (always have at least 1 back-up pack) POPs do not protect against STIs/HIV: To protect against pregnancy and STIs/HIV, use a condom every time you have sex. Have the client repeat this information back to you.
15 Male Condom What is it? The male condom is a thin sheath worn over the erect penis when a couple is having sex. How effective is it? If 100 couples use condoms for 1 year, typically 15 become pregnant. If used correctly with every act of intercourse, condoms are highly effective in protecting against most STIs (except herpes simplex and other genital ulcer diseases), including HIV. How do condoms work? The condom catches the man s sperm so that no sperm can enter the vagina. Not recommended for adolescents who: Have a severe allergy to latex rubber Advantages Safe Doesn t require a prescription or medical examination Effective and easy to use Protects against STIs/HIV Disadvantages Interrupts the sex act May decrease sexual sensitivity in some men and women Requires communication and consent from both partners A new condom must be used each time the couple has sex A supply of condoms must be available before sex occurs Note: Condoms are always recommended to prevent STIs/HIV. If the adolescent feels s/he may not always be able to negotiate condom use, it is recommended that s/he also use an additional contraceptive method.
16 Male Condom Show the client the condom and explain the following: How to use a condom 1. Check the expiration date on the condom package. 2. Open the package carefully so the condom doesn t tear. 3. Don t unroll the condom before putting it on. 4. Place the unrolled condom on the tip of the hard penis. 5. Hold the tip of the condom with the thumb and forefinger. 6. Unroll the condom until it covers the penis. 7. Leave enough space at the tip of the condom for the semen. 8. After ejaculation, hold the rim of the condom and pull the penis out of the vagina before it becomes soft. 9. Only use one condom at a time. 10. Always keep a supply of condoms readily available Care of condoms Don t apply oil-based lubricants (like baby oil, cooking oil, petroleum jelly/vaseline) because they can destroy the condom. It is safe to use clean water, saliva, or water-based lubricants. Store condoms in a cool, dry place. Don t carry them close to the body because heat can destroy them. Use each condom only once. Don t use a condom if the package is broken or if the condom is dry or sticky or the color has changed. Take care to dispose of used condoms properly. Possible side effects may include: A condom may break or come off during sex. A few men and women experience itching, burning, or swelling due to latex allergy. Reasons to return to provider Any time there is a problem (condom breaks or unhappy with method) A resupply is needed (never run out completely before returning) Either partner thinks s/he may have been exposed to an STI Have the client repeat this information back to you.
17 Female Condom What is it? The female condom is a thin lubricated sheath or lining made of a soft plastic film that fits loosely inside a woman s vagina. It has flexible rings at both ends. The ring at one end is closed and covers the cervix. A woman uses the female condom during intercourse to prevent pregnancy. How effective is it? If 100 women use the female condom for 1 year, typically 21 become pregnant. The female condom also effectively prevents many STIs including HIV when used correctly every time a woman and her partner have sexual intercourse. How does the female condom work? The condom catches the man s sperm so that no sperm can enter the vagina. Note: Condoms are always recommended to prevent STIs/HIV. If the adolescent feels s/he may not always be able to negotiate condom use, it is recommended that s/he also use an additional contraceptive method. Advantages Safe Effective Can be inserted up to 8 hours before sex Can be used with oil-based lubricants Can feel more natural during sex than male condoms Protects against STIs/HIV Reduces the chance of irritation or allergic reaction compared to latex condoms Disadvantages Costs more than the male condom May be noisy or awkward Is female initiated, but requires cooperation and consent of the male partner Can be difficult to insert
18 Female Condom Show the client the female condom and explain the following: How to use the female condom 1. Check the expiration date on the condom package. 2. Open the package carefully so the condom doesn t tear. 3. Find the inner ring, which is at the closed end of the condom. 4. Squeeze the inner ring together. 5. Put the inner ring in the vagina and push up into the vagina with the finger. (The outer ring stays outside the vagina.) 6. During sex, guide the penis through the outer ring. (If it is outside the ring, it will not offer protection from pregnancy or STIs/HIV.) 7. Remove condom immediately after sex, before standing up. 8. Squeeze and twist the outer ring to keep the sperm inside the pouch. 9. Pull the pouch out gently. 10. Burn or bury the condom do not put it down the toilet. Suggest that the client practice inserting and removing the condom before having sex with it for the first time and try different positions to see which way insertion is easiest Care of female condoms Store condoms in a cool, dry place. Don t carry them close to the body because heat can destroy them. Use each condom only once. Don t use a condom if the package is broken or if the condom is dry or sticky or the color has changed. Always keep a supply of condoms readily available. Possible side effects may include: Usually there are no side effects. Occasionally, a condom may break or slip out during intercourse. Very few adolescents may have itching, burning, or redness around the vagina (or partner s penis). Reasons to return to provider Any time there is a problem (condom breaks or unhappy with method) A resupply of condoms is needed (never run out completely) Either partner thinks s/he may have been exposed to an STI Have the client repeat this information back to you.
19 Emergency Contraceptive Pills (ECPs) What are they? ECPs are a hormonal method of contraception that can be used to prevent pregnancy up to 120 hours (5 days) following an act of unprotected sexual intercourse. How effective are they? If 100 women use progestin-only ECPs, typically 1 becomes pregnant. If 100 women use combined (estrogen and progestin) ECPs, typically 2 become pregnant. ECPs are most effective when used shortly after unprotected sex. How do ECPs work? ECPs prevent a pregnancy from occurring. They do not disrupt an implanted pregnancy. ECPs prevent the egg from leaving the ovary and may thicken cervical mucus to prevent the sperm from meeting the egg. ECPs only prevent pregnancy from unprotected sex that occurs before the pills are taken. They do not prevent pregnancy from sex that occurs after the ECPs are taken. Advantages Safe for women of all ages, including adolescents who may be less likely to prepare for a first sexual encounter Reduce risk of unintended pregnancy and need for abortion Appropriate for use after unprotected intercourse (including rape or contraceptive failure) Provide a bridge to the practice of regular contraception Drug exposure and side effects are of short duration Disadvantages Don t protect against STIs/HIV Don t provide ongoing protection against pregnancy Must be used with 120 hours after unprotected sex (and should be taken as soon as possible to be most effective) May change the time of the woman s next monthly bleeding Inappropriate for regular use (high cumulative pregnancy rate)
20 Emergency Contraceptive Pills (ECPs) Show the client the ECPs and explain the following: How to use ECPs For progestin-only ECP (dedicated product): When possible, take 2 pills at the same time within 120 hours of unprotected sex, or take 1 pill within 120 hours and 1 pill 12 hours later. For combined oral contraceptives (COCs): 1 dose of 0.1 mg ethinyl estradiol plus 0.5 mg levonorgestrel followed by a second identical dose 12 hours later. If vomiting occurs within 2 hours of taking ECPs, take another dose as soon as possible. If vomiting occurs after 2 hours, no additional dose is needed. To reduce nausea, take the tablets after eating or use anti-nausea medication. Do not to take any extra ECPs unless vomiting occurs. More pills will not decrease risk of pregnancy. Possible side effects may include:* Nausea and vomiting Headaches or dizziness Cramping/abdominal pain Breast tenderness Changes in monthly bleeding or slight irregular bleeding for 1 2 days after taking ECPs What to expect after using ECPs There will not be any immediate signs showing whether the ECPs worked. The next monthly bleeding should come on time (or a few days early or late). Reasons to return to provider If next monthly bleeding is more than 1 week later than expected Any time there is a problem or if either partner has been exposed to an STI Contraceptive methods after taking ECPs Now may be good time to begin a regular contraceptive method. COCs and POPs can be started the day after ECPs are taken. DMPA, IUD, and male and female condoms can be started on the same day as the ECP. For the implant, you must return after the next monthly bleeding. ECPs do not protect against STIs/HIV: To protect against pregnancy and STIs/HIV, use a condom every time you have sex. * Most do not last for more than 24 hours. Have the client repeat this information back to you.
The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings.
 The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings Counseling Cards Checklist to be reasonably sure a woman is not pregnant
The Balanced Counseling Strategy Plus: A Toolkit for Family Planning Service Providers Working in High STI/HIV Prevalence Settings Counseling Cards Checklist to be reasonably sure a woman is not pregnant
17. Preventing pregnancy
 17. Preventing pregnancy Objectives By the end of this session, group members will be able to: Define contraception. List ways young people can prevent pregnancy. Background notes What is contraception?
17. Preventing pregnancy Objectives By the end of this session, group members will be able to: Define contraception. List ways young people can prevent pregnancy. Background notes What is contraception?
The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that
 The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that may be used in the future Abstinence Choosing not to
The following lesson on contraception (birth control) is not intended to infer that you will be sexually active as a teen. This is information that may be used in the future Abstinence Choosing not to
100% Highly effective No cost No side effects
 effective? Advantages Disadvantages How do I get Cost Abstinence For some it can mean no sexual contact. For others it is no sexual intercourse or vaginal penetration. A permanent surgical procedure available
effective? Advantages Disadvantages How do I get Cost Abstinence For some it can mean no sexual contact. For others it is no sexual intercourse or vaginal penetration. A permanent surgical procedure available
Family Planning UNMET NEED. The Nurse Mildred Radio Talk Shows
 Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
Family Planning UNMET NEED The Nurse Mildred Radio Talk Shows TOPIC 9: IUD/COIL Guests FP counsellor from MSU, RHU& UHMG Nurse Mildred Nurse Betty Objectives of the programme: To inform listeners about
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system)
 FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
FDA-Approved Patient Labeling Patient Information Mirena (mur-ā-nah) (levonorgestrel-releasing intrauterine system) Mirena does not protect against HIV infection (AIDS) and other sexually transmitted infections
Information for Informed Consent for Insertion of a Mirena IUD
 Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
Information for Informed Consent for Insertion of a Mirena IUD What is an IUD (intrauterine Device)? An intrauterine device (IUD) is a plastic device that is placed into your uterus to prevent pregnancy.
WHAT ARE CONTRACEPTIVES?
 CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
CONTRACEPTION WHAT ARE CONTRACEPTIVES? Methods used to prevent fertilization *Also referred to as birth control methods With contraceptives, it is important to look at what works for you and your body.
Contraception Effective Methods of Birth Control
 Contraception Effective Methods of Birth Control Abstinence Means choosing NOT to have sex It is the ONLY method that is 100% effective It is your right to be in control of your body and say NO What are
Contraception Effective Methods of Birth Control Abstinence Means choosing NOT to have sex It is the ONLY method that is 100% effective It is your right to be in control of your body and say NO What are
Birth Control -- Especially for Teens
 AP112, June 2011 Birth Control -- Especially for Teens Making the decision whether to have sex can be difficult. You should make up your own mind when the time is right for you. If you are not ready for
AP112, June 2011 Birth Control -- Especially for Teens Making the decision whether to have sex can be difficult. You should make up your own mind when the time is right for you. If you are not ready for
Welcome to Mirena. The Mirena Handbook: A Personal Guide to Your New Mirena. mirena.com. Mirena is the #1 prescribed IUD * in the U.S.
 Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
Mirena is the #1 prescribed IUD * in the U.S. Welcome to Mirena The Mirena Handbook: A Personal Guide to Your New Mirena *Intrauterine Device Supported by 2015-2016 SHS data INDICATIONS FOR MIRENA Mirena
Birth Control Options Chart
 Hormonal Methods Birth control pills also known as mini-pills 91-99% A daily pill containing hormones that stops you from ovulating. There are combination estrogen or progestin-only (mini-pill) options.
Hormonal Methods Birth control pills also known as mini-pills 91-99% A daily pill containing hormones that stops you from ovulating. There are combination estrogen or progestin-only (mini-pill) options.
TRAINING PROGRAM CUPID FEMALE CONDOM
 CUPID LIMITED, INDIA WE HELP THE WORLD PLAY SAFE... Manufacturer and Supplier of Male Condoms, Female Condoms & Water based Lubricants. TRAINING PROGRAM CUPID FEMALE CONDOM Website:- http://www.cupidlimited.com
CUPID LIMITED, INDIA WE HELP THE WORLD PLAY SAFE... Manufacturer and Supplier of Male Condoms, Female Condoms & Water based Lubricants. TRAINING PROGRAM CUPID FEMALE CONDOM Website:- http://www.cupidlimited.com
Family Planning and Sexually Transmitted. Infections, including HIV
 Infections, including HIV Family Planning and Sexually Transmitted Introduction To protect themselves, people need correct information about sexually transmitted infections (STIs), including HIV. Women
Infections, including HIV Family Planning and Sexually Transmitted Introduction To protect themselves, people need correct information about sexually transmitted infections (STIs), including HIV. Women
Contraceptives. Kim Dawson October 2010
 Contraceptives Kim Dawson October 2010 Objectives: You will learn about: The about the different methods of birth control. How to use each method of birth control. Emergency contraception What are they?
Contraceptives Kim Dawson October 2010 Objectives: You will learn about: The about the different methods of birth control. How to use each method of birth control. Emergency contraception What are they?
Birth Control. Choosing the method that s right for you
 Birth Control Choosing the method that s right for you Contents Family planning services... 1 How to use this brochure... 2 Implant... 3 IUD/IUS... 5 Sterilization... 7 Depo-Provera : The shot...9 Pill/ring/patch...
Birth Control Choosing the method that s right for you Contents Family planning services... 1 How to use this brochure... 2 Implant... 3 IUD/IUS... 5 Sterilization... 7 Depo-Provera : The shot...9 Pill/ring/patch...
the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD the IUD your guide to
 your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
your guide to Helping you choose the method of contraception that s best for you IUD IUD the e IUD IU IUD the IUD 2 3 The intrauterine device (IUD) An IUD is a small plastic and copper device that s put
Preventing Sexually Transmitted Infections Storytelling Activity
 Preventing Sexually Transmitted Infections Storytelling Activity Trainer s Tips Make the context and characters in the story culturally relevant.» Choose culturally relevant girls and boys names for the
Preventing Sexually Transmitted Infections Storytelling Activity Trainer s Tips Make the context and characters in the story culturally relevant.» Choose culturally relevant girls and boys names for the
BIRTH CONTROL METHOD COMPARISON CHART
 BIRTH CONTROL METHOD COMPARISON CHART Abstinence 100% Yes Male latex condom 86%-95% Can increase to 98% by using with a contraceptive jelly Yes Highly effective No side effects, as with other methods No
BIRTH CONTROL METHOD COMPARISON CHART Abstinence 100% Yes Male latex condom 86%-95% Can increase to 98% by using with a contraceptive jelly Yes Highly effective No side effects, as with other methods No
Contraceptive Technology and Reproductive Health Series: Barrier Methods Post-test
 Contraceptive Technology and Reproductive Health Series: Barrier Methods Post-test Section I: Overview of Barrier Methods 1. The following are statements regarding all barrier methods. Please indicate
Contraceptive Technology and Reproductive Health Series: Barrier Methods Post-test Section I: Overview of Barrier Methods 1. The following are statements regarding all barrier methods. Please indicate
Positive health, dignity and prevention for women and their babies
 FLIPCHART Positive health, dignity and prevention for women and their babies A treatment literacy guide for pregnant women and mothers living with HIV Module 1: Human rights in healthcare settings 1 Knowing
FLIPCHART Positive health, dignity and prevention for women and their babies A treatment literacy guide for pregnant women and mothers living with HIV Module 1: Human rights in healthcare settings 1 Knowing
know!!! you gotta Tips, hints, and all the info you NEED to keep yourself safe from HIV/AIDS
 you gotta know!!! Tips, hints, and all the info you NEED to keep yourself safe from HIV/AIDS Latino HIV/AIDS Behavioral Science Center University Park, PCA 356 11200 SW 8th Street, Miami, Fl, 33199 lhabsc@fiu.edu
you gotta know!!! Tips, hints, and all the info you NEED to keep yourself safe from HIV/AIDS Latino HIV/AIDS Behavioral Science Center University Park, PCA 356 11200 SW 8th Street, Miami, Fl, 33199 lhabsc@fiu.edu
Power Point Use in EBPs. CAPP & PREP Learning Community May 15, 2018
 Power Point Use in EBPs CAPP & PREP Learning Community May 15, 2018 Objectives Best practices for power point use Why use power point for EBP delivery Examples: the Good, the Bad and the Ugly Recommendations
Power Point Use in EBPs CAPP & PREP Learning Community May 15, 2018 Objectives Best practices for power point use Why use power point for EBP delivery Examples: the Good, the Bad and the Ugly Recommendations
Informed Consent Flipchart. Version 1.0, 30 Jan 2018
 Informed Consent Flipchart Version 1.0, 30 Jan 2018 Knowledge is Power Did you know? Across the world, young women are at high risk of getting HIV. In Africa, more than half of people living with HIV are
Informed Consent Flipchart Version 1.0, 30 Jan 2018 Knowledge is Power Did you know? Across the world, young women are at high risk of getting HIV. In Africa, more than half of people living with HIV are
Introduction and Instructions
 Sexual and Reproductive Health Kit Introduction and Instructions The Sexual and Reproductive Health kit includes: Binder Introduction and Instructions for entire Sexual and Reproductive Health kit Pregnancy
Sexual and Reproductive Health Kit Introduction and Instructions The Sexual and Reproductive Health kit includes: Binder Introduction and Instructions for entire Sexual and Reproductive Health kit Pregnancy
WORTH A CLOSER LOOK.
 A birth control pill... WORTH A CLOSER LOOK. Ask your healthcare provider about. Please see Important Safety Information including Boxed Warning throughout this brochure and on pages 4 and 5. offers a
A birth control pill... WORTH A CLOSER LOOK. Ask your healthcare provider about. Please see Important Safety Information including Boxed Warning throughout this brochure and on pages 4 and 5. offers a
FAMILY PLANNING AND SEXUALLY TRANSMITTED INFECTIONS INCLUDING HIV. Unit 20. Learning Objectives. Teaching Resources in this Unit
 Unit 20 FAMILY PLANNING AND SEXUALLY TRANSMITTED INFECTIONS INCLUDING HIV Learning Objectives By the end of this unit, learners will be able to: Define sexually transmitted infections (STIs) Outline groups
Unit 20 FAMILY PLANNING AND SEXUALLY TRANSMITTED INFECTIONS INCLUDING HIV Learning Objectives By the end of this unit, learners will be able to: Define sexually transmitted infections (STIs) Outline groups
Fitting of an Intrauterine Device (IUD)
 PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an IUD? An IUD is a small T-shaped plastic and copper device that is put into
PLEASE PRINT WHOLE FORM DOUBLE SIDED ON YELLOW PAPER Patient Information to be retained by patient affix patient label What is an IUD? An IUD is a small T-shaped plastic and copper device that is put into
Quiz: Harm Reduction with Latex
 Quiz: Harm Reduction with Latex Name (first name only): Date: 1. HIV can be sexually-transmitted by exchanging which of the following body fluids: a. semen b. vaginal secretions c. blood d. all of the
Quiz: Harm Reduction with Latex Name (first name only): Date: 1. HIV can be sexually-transmitted by exchanging which of the following body fluids: a. semen b. vaginal secretions c. blood d. all of the
PMTCT Counseling Support Flipchart
 PMTCT Counseling Support Flipchart HOW TO USE THE COUNSELING CUE CARDS FLIPCHART The counseling cue cards flipchart was developed to support a range of providers (trained counselors, lay counselors, peer
PMTCT Counseling Support Flipchart HOW TO USE THE COUNSELING CUE CARDS FLIPCHART The counseling cue cards flipchart was developed to support a range of providers (trained counselors, lay counselors, peer
LARC. sample. ask brook about. Are any of them right for me? How effective is it? How long does it last? long acting reversible contraception
 72888_LARC:Layout 1 9/11/09 11:47 Page 1 Are any of them right for me? ask brook about LARC How effective is it? long acting reversible contraception How long does it last? 72888_LARC:Layout 1 9/11/09
72888_LARC:Layout 1 9/11/09 11:47 Page 1 Are any of them right for me? ask brook about LARC How effective is it? long acting reversible contraception How long does it last? 72888_LARC:Layout 1 9/11/09
Key Points for Providers and Clients
 CHAPTER 14 This chapter describes male latex condoms. Female condoms, which are inserted into a woman s vagina, are available in some areas (see Female Condoms, p. 261, and Comparing Condoms, p. 428).
CHAPTER 14 This chapter describes male latex condoms. Female condoms, which are inserted into a woman s vagina, are available in some areas (see Female Condoms, p. 261, and Comparing Condoms, p. 428).
Contraception for Women and Couples with HIV. Knowledge Test
 Contraception for Women and Couples with HIV Knowledge Test Instructions: For each question below, check/tick all responses that apply. 1. Which statements accurately describe the impact of HIV/AIDS in
Contraception for Women and Couples with HIV Knowledge Test Instructions: For each question below, check/tick all responses that apply. 1. Which statements accurately describe the impact of HIV/AIDS in
A Teacher s Guide Sexually
 sue 3. Grades 9-12 : Issue 3. milk. ed every year. ow stopthesilence TeenZine ol, even once, can Grades 9-12 : Issue 3. men who don't use me pregnant. s. chlamydia.,ghest can among 15 to Contraceptives
sue 3. Grades 9-12 : Issue 3. milk. ed every year. ow stopthesilence TeenZine ol, even once, can Grades 9-12 : Issue 3. men who don't use me pregnant. s. chlamydia.,ghest can among 15 to Contraceptives
Healthy Boys POWERFUL BOYS
 Healthy Boys are POWERFUL BOYS Your Sexual & Reproductive Health Education Booklet This book belongs to: Rise 2 Raise Mentoring Program By Robert Ingersoll 2 Introduction The more knowledge you have, the
Healthy Boys are POWERFUL BOYS Your Sexual & Reproductive Health Education Booklet This book belongs to: Rise 2 Raise Mentoring Program By Robert Ingersoll 2 Introduction The more knowledge you have, the
Notes to Teacher continued Contraceptive Considerations
 Abstinence a conscious decision to refrain from sexual intercourse 100% pregnancy will not occur if close contact between the penis and vagina does not take place. The risk of a number of STDs, including
Abstinence a conscious decision to refrain from sexual intercourse 100% pregnancy will not occur if close contact between the penis and vagina does not take place. The risk of a number of STDs, including
Emergency Contraception THE FACTS
 Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
Emergency Contraception Quick Facts What is it? Emergency contraception is birth control that you use after you have had unprotected sex--if you didn t use birth control or your regular birth control failed.
Taking Care of Your Sexual Health
 Sexual health is an important part of overall health. Taking responsibility for caring for their sexual health will help men and women stay healthy for a lifetime. Things for Everyone to Know Staying Clean
Sexual health is an important part of overall health. Taking responsibility for caring for their sexual health will help men and women stay healthy for a lifetime. Things for Everyone to Know Staying Clean
Sexually Transmitted Diseases: Overview
 Sexually Transmitted Diseases: Overview Q: What is a sexually transmitted disease (STD)? A: It is an infection or disease passed from person to person through sexual contact. Q: How many people have STDs?
Sexually Transmitted Diseases: Overview Q: What is a sexually transmitted disease (STD)? A: It is an infection or disease passed from person to person through sexual contact. Q: How many people have STDs?
Who s The Daddy? What You Should Know About OTC Contraception
 Who s The Daddy? What You Should Know About OTC Contraception By: Vona Broughton, BS Public Health & Kevin McCarthy, RPH This program has been brought to you by PharmCon PharmCon is accredited by the accreditation
Who s The Daddy? What You Should Know About OTC Contraception By: Vona Broughton, BS Public Health & Kevin McCarthy, RPH This program has been brought to you by PharmCon PharmCon is accredited by the accreditation
Acute Salpingitis. Fallopian Tubes. Uterus
 Acute Salpingitis Introduction Acute salpingitis is a type of infection that affects the Fallopian tubes. The Fallopian tubes carry eggs from the ovaries to the uterus. Acute salpingitis is one of the
Acute Salpingitis Introduction Acute salpingitis is a type of infection that affects the Fallopian tubes. The Fallopian tubes carry eggs from the ovaries to the uterus. Acute salpingitis is one of the
Contraception. Objectives. Unintended Pregnancy. Unintended Pregnancy in the US. What s the Impact? 10/7/2014
 Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
Contraception Tami Allen, RNC OB, MHA Robin Petersen, RN, MSN Perinatal Clinical Nurse Specialist Objectives Discuss the impact of unintended pregnancy in the United States Discuss the risks and benefits
Contraception. My Sexual Health: Objectives. Vocabulary. Standards Wisconsin Health Education Standards
 Contraception My Sexual Health: This lesson utilizes a game to review and explore the various forms of contraception. Abstinence is included as an option. Students will analyze scenarios to identify influences
Contraception My Sexual Health: This lesson utilizes a game to review and explore the various forms of contraception. Abstinence is included as an option. Students will analyze scenarios to identify influences
Package leaflet: Information for the user. Levonorgestrel 1.5 mg Tablet. levonorgestrel
 Package leaflet: Information for the user Levonorgestrel 1.5 mg Tablet levonorgestrel Read all of this leaflet carefully before you start taking this medicine because it contains important information
Package leaflet: Information for the user Levonorgestrel 1.5 mg Tablet levonorgestrel Read all of this leaflet carefully before you start taking this medicine because it contains important information
Unintended Pregnancy is Common LEARNING OBJECTIVES. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy And Contraceptive Use
 3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
3:45 4:30 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
LESSON 5. Counseling clients about DMPA and Sayana Press
 LESSON 5 Counseling clients about DMPA and Sayana Press 1 LESSON 5 Learning objectives List possible side effects of DMPA. Describe what to do if a client has concerns or is experiencing side effects.
LESSON 5 Counseling clients about DMPA and Sayana Press 1 LESSON 5 Learning objectives List possible side effects of DMPA. Describe what to do if a client has concerns or is experiencing side effects.
Patient Guide Levonorgestrel and Ethinyl Estradiol Tablets USP (0.1 mg/0.02 mg) and Ethinyl Estradiol Tablets USP (0.
 Patient Guide Levonorgestrel and Ethinyl Estradiol Tablets USP (0.1 mg/0.02 mg) and Ethinyl Estradiol Tablets USP (0.01 mg) Rx Only This product (like all oral contraceptives) is intended to prevent pregnancy.
Patient Guide Levonorgestrel and Ethinyl Estradiol Tablets USP (0.1 mg/0.02 mg) and Ethinyl Estradiol Tablets USP (0.01 mg) Rx Only This product (like all oral contraceptives) is intended to prevent pregnancy.
What do I need to know about HIV and sex? What are my responsibilities and choices?
 Patient and Family Education HIV: Teens and Sex This handout has information about sex and HIV. This handout answers common questions you might ask about sex. It is important for you to talk to your parents
Patient and Family Education HIV: Teens and Sex This handout has information about sex and HIV. This handout answers common questions you might ask about sex. It is important for you to talk to your parents
BOSLEER CONSUMER MEDICINE INFORMATION
 (Bosentan Film-coated Tablets 62.5 mg and 125 mg) Bosentan monohydrate Consumer Medicine Information What is in this leaflet This leaflet answers some common questions about. It does not contain all the
(Bosentan Film-coated Tablets 62.5 mg and 125 mg) Bosentan monohydrate Consumer Medicine Information What is in this leaflet This leaflet answers some common questions about. It does not contain all the
Family Planning and PMTCT Services for Adolescents
 Module 11 Family Planning and PMTCT Services for Adolescents Session 11.1: Session 11.2: Family Planning Counseling for ALHIV PMTCT Counseling for ALHIV Learning Objectives After completing this module,
Module 11 Family Planning and PMTCT Services for Adolescents Session 11.1: Session 11.2: Family Planning Counseling for ALHIV PMTCT Counseling for ALHIV Learning Objectives After completing this module,
and other sexually transmitted diseases can be prevented
 and other sexually transmitted diseases 1 Who should use a condom? 2 How do condoms protect against Aids and other sexually transmitted diseases? 3 What should we remember before using a condom? 4 How
and other sexually transmitted diseases 1 Who should use a condom? 2 How do condoms protect against Aids and other sexually transmitted diseases? 3 What should we remember before using a condom? 4 How
Transcervical Sterilization
 Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Q UESTIONS & ANSWERS A BOUT Transcervical Sterilization A New Choice in Permanent Birth Control Choosing a Birth Control Method Women and their partners now have more birth control choices than ever. How
Sexually Transmitted Diseases: Overview
 Sexually Transmitted Diseases: Overview frequent and more serious complications from STDs than men. Q: How do you get an STD? A: You can get and pass STDs through Q: What is a sexually transmitted vaginal,
Sexually Transmitted Diseases: Overview frequent and more serious complications from STDs than men. Q: How do you get an STD? A: You can get and pass STDs through Q: What is a sexually transmitted vaginal,
Unit 9 CONTRACEPTION LEARNING OBJECTIVES
 Unit 9 CONTRACEPTION LEARNING OBJECTIVES 1. Become aware of the magnitude of teen age sexual activity and pregnancy and some of the social and economic effects. 2. Learn about the various means of contraception,
Unit 9 CONTRACEPTION LEARNING OBJECTIVES 1. Become aware of the magnitude of teen age sexual activity and pregnancy and some of the social and economic effects. 2. Learn about the various means of contraception,
One daily pill can help prevent HIV. TRUVADA for PrEP, together with safer sex practices, can mean better protection.
 TRUVADA for PrEP is a prescription medicine that can help reduce the risk of getting HIV-1 through sex, when taken every day and used together with safer sex practices. TRUVADA for PrEP is only for people
TRUVADA for PrEP is a prescription medicine that can help reduce the risk of getting HIV-1 through sex, when taken every day and used together with safer sex practices. TRUVADA for PrEP is only for people
Birth Control Methods
 Birth Control Methods This guide provides useful information to help you and your partner consider pregnancy prevention options. Options are available through the CHS Pharmacy, Women s Health Clinic, and
Birth Control Methods This guide provides useful information to help you and your partner consider pregnancy prevention options. Options are available through the CHS Pharmacy, Women s Health Clinic, and
LEARNING OBJECTIVES. Beyond the Pill: Long Acting Contraception. Distribution Of Contraception Use By Women In The Us. Unintended Pregnancy is Common
 4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
4:15 5 pm Beyond the Pill: Long Acting Contraceptives and IUDs Presenter Disclosure Information The following relationships exist related to this presentation: Christine L. Curry, MD, PhD: No financial
FACT SHEET: Copper IUD
 FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
FACT SHEET: Copper IUD How does the copper IUD help me? The copper IUD is a hormone-free option. If you don t like the copper IUD or you decide to get pregnant, your health care provider can remove the
9p1 Identify the factors that contribute to positive relationships with others. 9p6 Describe the factors that lead to responsible sexual relationships
 Lesson Eight Title: Theme: Time: Materials: Wrapping up the Sexual Health Unit The 60 minutes * Sexuality Review-Quiz * Sexuality Review-Answer Sheet * Sexual Q & A -Laminated Game Cards * Sexual Q & A
Lesson Eight Title: Theme: Time: Materials: Wrapping up the Sexual Health Unit The 60 minutes * Sexuality Review-Quiz * Sexuality Review-Answer Sheet * Sexual Q & A -Laminated Game Cards * Sexual Q & A
Discover the birth control you ve been looking for. Highly reliable. Virtually hassle-free. Totally hormone-free.
 Discover the birth control you ve been looking for Highly reliable. Virtually hassle-free. Totally hormone-free. Over 70 million women worldwide use a nonhormonal IUC like ParaGard. Millions of women with
Discover the birth control you ve been looking for Highly reliable. Virtually hassle-free. Totally hormone-free. Over 70 million women worldwide use a nonhormonal IUC like ParaGard. Millions of women with
International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage:
 Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Review Article ISSN: 2319 9563 International Journal of Research in Pharmaceutical and Nano Sciences Journal homepage: www.ijrpns.com A REVIEW ON INTRAUTERINE DEVICES Boddu Venkata Komali* 1, M. Kalyani
Contraception Choices: An Evidence Based Approach Case Study Approach. Susan Hellier PhD, DNP, FNP-BC, CNE
 Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
Contraception Choices: An Evidence Based Approach Case Study Approach Susan Hellier PhD, DNP, FNP-BC, CNE Objectives Describe the U.S. Medical Eligibility Criteria for Contraceptive Use, 2016 (U.S. MEC)
LESSON 9. How to counsel clients on Sayana Press self-injection
 LESSON 9 How to counsel clients on Sayana Press self-injection 1 LESSON 9 Learning objectives In this session, you will learn how to advise clients on: Proper storage of Sayana Press. Proper disposal of
LESSON 9 How to counsel clients on Sayana Press self-injection 1 LESSON 9 Learning objectives In this session, you will learn how to advise clients on: Proper storage of Sayana Press. Proper disposal of
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION. DEPO-PROVERA Medroxyprogesterone acetate injectable suspension
 READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr DEPO-PROVERA Medroxyprogesterone acetate injectable suspension Read this carefully before you get your first injection
READ THIS FOR SAFE AND EFFECTIVE USE OF YOUR MEDICINE PATIENT MEDICATION INFORMATION Pr DEPO-PROVERA Medroxyprogesterone acetate injectable suspension Read this carefully before you get your first injection
Contraceptive case studies. Dr Christine Roke National Medical Advisor Family Planning June 2015
 Contraceptive case studies Dr Christine Roke National Medical Advisor Family Planning June 2015 Case 1 Mary is a 47 year old who has come in for a routine cervical smear. She asks when her Multiload IUD
Contraceptive case studies Dr Christine Roke National Medical Advisor Family Planning June 2015 Case 1 Mary is a 47 year old who has come in for a routine cervical smear. She asks when her Multiload IUD
Capecitabine. Other Names: Xeloda. About This Drug. Possible Side Effects. Warnings and Precautions
 Capecitabine Other Names: Xeloda About This Drug Capecitabine is used to treat cancer. It is given orally (by mouth). Possible Side Effects Tired and weakness Loose bowel movements (diarrhea) Nausea and
Capecitabine Other Names: Xeloda About This Drug Capecitabine is used to treat cancer. It is given orally (by mouth). Possible Side Effects Tired and weakness Loose bowel movements (diarrhea) Nausea and
PREVENTING PREGNANCY: TALKING ABOUT AND USING CONTRACEPTION
 PREVENTING PREGNANCY: TALKING ABOUT AND USING CONTRACEPTION Lesson 11 DIFFERING ABILITIES LEARNER OUTCOME Identify and describe basic types of contraceptives; i.e., abstinence, condom, foam, birth control
PREVENTING PREGNANCY: TALKING ABOUT AND USING CONTRACEPTION Lesson 11 DIFFERING ABILITIES LEARNER OUTCOME Identify and describe basic types of contraceptives; i.e., abstinence, condom, foam, birth control
What s New in Adolescent Contraception?
 What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
What s New in Adolescent Contraception? Abby Furukawa, MD Legacy Medical Group Portland Obstetrics and Gynecology April 29, 2017 Objectives Provide an update on contraception options for the adolescent
For the Patient: Lenalidomide Other names: REVLIMID
 For the Patient: Lenalidomide Other names: REVLIMID Lenalidomide (len a lid' oh mide) is a drug that is used to treat several types of cancer. It is a capsule that you take by mouth. Tell your doctor if
For the Patient: Lenalidomide Other names: REVLIMID Lenalidomide (len a lid' oh mide) is a drug that is used to treat several types of cancer. It is a capsule that you take by mouth. Tell your doctor if
SEX AND SEXUALLY TRANSMITTED INFECTIONS
 SEX AND SEXUALLY TRANSMITTED INFECTIONS Sex and STIs Be fully informed, Be safe! Prevent Pregnancy Practice abstinence Use effective birth control Use Emergency Contraception Prevent STI s Practice Abstinence
SEX AND SEXUALLY TRANSMITTED INFECTIONS Sex and STIs Be fully informed, Be safe! Prevent Pregnancy Practice abstinence Use effective birth control Use Emergency Contraception Prevent STI s Practice Abstinence
A Lesson Plan from Rights, Respect, Responsibility: A K-12 Curriculum
 Birth Control Basics A Lesson Plan from Rights, Respect, Responsibility: A K-12 Curriculum Fostering responsibility by respecting young people s rights to honest sexuality education. NSES ALIGNMENT: By
Birth Control Basics A Lesson Plan from Rights, Respect, Responsibility: A K-12 Curriculum Fostering responsibility by respecting young people s rights to honest sexuality education. NSES ALIGNMENT: By
STI Review. CALM: STI/HIV - Lesson One (Handout 3) Bacteria/ Transmission. Symptoms. Disease. Virus
 STI Review Bacteria/ Virus? Transmission Chlamydia Bacteria Unprotected vaginal or anal sex with a person who has Chlamydia Genital Herpes Virus By direct contact with the sores or blisters of an infected
STI Review Bacteria/ Virus? Transmission Chlamydia Bacteria Unprotected vaginal or anal sex with a person who has Chlamydia Genital Herpes Virus By direct contact with the sores or blisters of an infected
Sexual Health: 101 Sexual Health 101
 Sexual Health 101 An IC student s guide to birth control, STD s, sexuality, and relationships. Healthy relationships can be tricky to find, but don t give up! There are many genuine, caring people out
Sexual Health 101 An IC student s guide to birth control, STD s, sexuality, and relationships. Healthy relationships can be tricky to find, but don t give up! There are many genuine, caring people out
13: Condoms. Words of Wisdom. How to Use a Male Condom. Condom Line-Up Cards. Shopping Information Form. Condoms Dos & Don ts
 13: Condoms Words of Wisdom How to Use a Male Condom Condom Line-Up Cards Shopping Information Form Condoms Dos & Don ts Wishing cannot bring autumn glory nor cause winter to cease. Kiowa How to Use a
13: Condoms Words of Wisdom How to Use a Male Condom Condom Line-Up Cards Shopping Information Form Condoms Dos & Don ts Wishing cannot bring autumn glory nor cause winter to cease. Kiowa How to Use a
Sexuality/Reproduction CALM Summer 2015
 Female Reproduction Sexuality/Reproduction CALM Summer 2015 Male Reproduction Reproduction https://www.youtube.com/watch?v=_7rsh2loiy8 1 About Sex How to use a condom Set Limits Think about how far you
Female Reproduction Sexuality/Reproduction CALM Summer 2015 Male Reproduction Reproduction https://www.youtube.com/watch?v=_7rsh2loiy8 1 About Sex How to use a condom Set Limits Think about how far you
DEPO-PROVERA/DEPO-PROVERA-SC (medroxyprogesterone acetate) - Product Monograph Page 55 of 61
 PART III: CONSUMER INFORMATION DEPO-PROVERA DEPO-PROVERA-SC Medroxyprogesterone acetate Sterile Aqueous Suspension 50 mg/ml, 104 mg/0.65 ml and 150 mg/ml This leaflet is Part III of a three-part "Product
PART III: CONSUMER INFORMATION DEPO-PROVERA DEPO-PROVERA-SC Medroxyprogesterone acetate Sterile Aqueous Suspension 50 mg/ml, 104 mg/0.65 ml and 150 mg/ml This leaflet is Part III of a three-part "Product
Contraception for Adolescents: What s New?
 Contraception for Adolescents: What s New? US Medical Eligibility Criteria for Contraceptive Use Kathryn M. Curtis, PhD Division of Reproductive Health, CDC Expanding Our Experience and Expertise: Implementing
Contraception for Adolescents: What s New? US Medical Eligibility Criteria for Contraceptive Use Kathryn M. Curtis, PhD Division of Reproductive Health, CDC Expanding Our Experience and Expertise: Implementing
Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop.
 Dexamethasone Other Names: Decadron About This Drug Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop. Possible Side Effects (More Common) Increased
Dexamethasone Other Names: Decadron About This Drug Dexamethasone is used to treat cancer. This drug can be given in the vein (IV), by mouth, or as an eye drop. Possible Side Effects (More Common) Increased
For the Patient: Olaparib tablets Other names: LYNPARZA
 For the Patient: Olaparib tablets Other names: LYNPARZA Olaparib (oh lap' a rib) is a drug that is used to treat some types of cancer. It is a tablet that you take by mouth. Tell your doctor if you have
For the Patient: Olaparib tablets Other names: LYNPARZA Olaparib (oh lap' a rib) is a drug that is used to treat some types of cancer. It is a tablet that you take by mouth. Tell your doctor if you have
Detailed instructions for each learning activity may be found below. Here is an overview of learning activities for the instructor to choose from:
 Learning Activities Detailed instructions for each learning activity may be found below. Here is an overview of learning activities for the instructor to choose from: Number Name Methods Time 3.9.1 Knowing
Learning Activities Detailed instructions for each learning activity may be found below. Here is an overview of learning activities for the instructor to choose from: Number Name Methods Time 3.9.1 Knowing
Making Sense of HIV and Pregnancy. Day 2
 Making Sense of HIV and Pregnancy Day 2 Prenatal Class Day 2 What will be covered today? Labor Vaginal Delivery Cesarean Section Reproductive health care Sexually Transmitted Infections Signs and Symptoms
Making Sense of HIV and Pregnancy Day 2 Prenatal Class Day 2 What will be covered today? Labor Vaginal Delivery Cesarean Section Reproductive health care Sexually Transmitted Infections Signs and Symptoms
MYTHS OF STIs True or False
 MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
MYTHS OF STIs True or False 1. Most people with an STD experience painful symptoms. 2. Birth control pills prevent the spread of STDs. 3. Douching will cure and STD. 4. Abstinence is the best way to prevent
F REQUENTLY A SKED Q UESTIONS. fallopian tube instead of the uterus), constant pelvic pain, and other problems.
 PID can be treated and cured with Pelvic antibiotics. If left untreated, PID can lead to serious problems like infertility (not being able to get pregnant), ectopic pregnancy (pregnancy in the Inflammatory
PID can be treated and cured with Pelvic antibiotics. If left untreated, PID can lead to serious problems like infertility (not being able to get pregnant), ectopic pregnancy (pregnancy in the Inflammatory
Living Positively with HIV
 Living Positively with HIV Pregnancy and Planning a Family How do I avoid pregnancy and STI? What is this booklet for? This booklet gives basic information about planning a family if you are living with
Living Positively with HIV Pregnancy and Planning a Family How do I avoid pregnancy and STI? What is this booklet for? This booklet gives basic information about planning a family if you are living with
Sexually Transmitted
 CHAPTER 22 Infections, Including HIV Key Points for Providers and Clients People with sexually transmitted infections (STIs), including HIV, can use most family planning methods safely and effectively.
CHAPTER 22 Infections, Including HIV Key Points for Providers and Clients People with sexually transmitted infections (STIs), including HIV, can use most family planning methods safely and effectively.
Contraception: Common Problems Faced in Office Practice. Jane S. Sillman, MD Brigham and Women s Hospital
 Contraception: Common Problems Faced in Office Practice Jane S. Sillman, MD Brigham and Women s Hospital Disclosures I have no conflicts of interest Contraception: Common Problems How to discuss contraception
Contraception: Common Problems Faced in Office Practice Jane S. Sillman, MD Brigham and Women s Hospital Disclosures I have no conflicts of interest Contraception: Common Problems How to discuss contraception
Care of the HIV-Exposed Infant
 Care of the HIV-Exposed Infant Use of Flipchart To promote quality and consistency of counseling Why use the counseling flipchart? To improve HIV-exposed infant outcomes through high quality counseling.
Care of the HIV-Exposed Infant Use of Flipchart To promote quality and consistency of counseling Why use the counseling flipchart? To improve HIV-exposed infant outcomes through high quality counseling.
Quick Study: Sexually Transmitted Infections
 Quick Study: Sexually Transmitted Infections Gonorrhea What is it: A bacterial infection of the genitals, anus, or throat. How common: The CDC estimates 820,000 people in the United States get Gonorrhea
Quick Study: Sexually Transmitted Infections Gonorrhea What is it: A bacterial infection of the genitals, anus, or throat. How common: The CDC estimates 820,000 people in the United States get Gonorrhea
Can you imagine reversible birth control that s more than 99% effective and 100% hormone free, too?
 Can you imagine reversible birth control that s more than 99% effective and 100% hormone free, too? BIRTH CONTROL THAT FITS YOUR LIFE, NATURALLY. ParaGard is a registered trademark of Teva Women s Health,
Can you imagine reversible birth control that s more than 99% effective and 100% hormone free, too? BIRTH CONTROL THAT FITS YOUR LIFE, NATURALLY. ParaGard is a registered trademark of Teva Women s Health,
If you are sexually active, desire birth control or have other concerns, you should schedule a women s health h visit.
 If you are sexually active, desire birth control or have other concerns, you should schedule a women s health h visit. i Your appointment should not be made during your period. You should not have unprotected
If you are sexually active, desire birth control or have other concerns, you should schedule a women s health h visit. i Your appointment should not be made during your period. You should not have unprotected
Family Planning and Infertility
 Family Planning and Infertility Chapter 20 Objectives Discuss types of reversible contraception Natural methods Mechanical barrier methods Hormonal contraceptives Discuss types of permanent contraception
Family Planning and Infertility Chapter 20 Objectives Discuss types of reversible contraception Natural methods Mechanical barrier methods Hormonal contraceptives Discuss types of permanent contraception
STI s. (Sexually Transmitted Infections)
 STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
STI s (Sexually Transmitted Infections) Build Awareness In Canada and around the world, the trend is clear: sexually transmitted infections (STIs) are on the rise. One of the primary defenses in the fight
Instruction for the patient
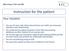 WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
WS 4 Case 3 STI and IUD Your situation Instruction for the patient You are 32 years old, divorced and have one child; you have just started a new relationship You underwent surgical resection of the left
Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur?
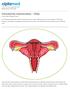 Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Published on: 8 Apr 2013 Intrauterine Insemination - FAQs Q. How Does Pregnancy Occur? A. The female reproductive system involves the uterus, ovaries, fallopian tubes, cervix and vagina. The female hormones,
Nivolumab. Other Names: Opdivo. About this Drug. Possible Side Effects (More Common) Warnings and Precautions
 Nivolumab Other Names: Opdivo About this Drug Nivolumab is used to treat cancer. It is given in the vein (IV). Possible Side Effects (More Common) Bone marrow depression. This is a decrease in the number
Nivolumab Other Names: Opdivo About this Drug Nivolumab is used to treat cancer. It is given in the vein (IV). Possible Side Effects (More Common) Bone marrow depression. This is a decrease in the number
Section 10 Counseling Considerations
 Section 10 Counseling Considerations 10.1 HIV Pre- /Post-Test Counseling... 10-1 10.2 HIV/STI Risk Reduction Counseling... 10-2 10.3 Contraceptive Counseling... 10-3 10.4 Product Use Instructions... 10-4
Section 10 Counseling Considerations 10.1 HIV Pre- /Post-Test Counseling... 10-1 10.2 HIV/STI Risk Reduction Counseling... 10-2 10.3 Contraceptive Counseling... 10-3 10.4 Product Use Instructions... 10-4
ZADITEN Eye Drops 1.0%
 ZADITEN Eye Drops 1.0% Ketotifen Consumer Medicine Information What is in this leaflet Please read this leaflet carefully before you use Zaditen Eye Drops. This leaflet answers some common questions about
ZADITEN Eye Drops 1.0% Ketotifen Consumer Medicine Information What is in this leaflet Please read this leaflet carefully before you use Zaditen Eye Drops. This leaflet answers some common questions about
PRECONCEPTION COUNSELING
 PRECONCEPTION COUNSELING A Counseling Guide for Healthcare Providers Preconception Care & Counseling 1 Introduction Pregnancy planning and preconception care are important in order to: 1. Ensure maternal
PRECONCEPTION COUNSELING A Counseling Guide for Healthcare Providers Preconception Care & Counseling 1 Introduction Pregnancy planning and preconception care are important in order to: 1. Ensure maternal
Medical Eligibility for Contraception Use
 Medical Eligibility for Contraception Use DIVISION OF REPRODUCTIVE HEALTH CENTERS FOR DISEASE CONTROL AND PREVENTION 2016 US Medical Eligibility Criteria for Contraceptive Use (US MEC) Purpose To assist
Medical Eligibility for Contraception Use DIVISION OF REPRODUCTIVE HEALTH CENTERS FOR DISEASE CONTROL AND PREVENTION 2016 US Medical Eligibility Criteria for Contraceptive Use (US MEC) Purpose To assist
